Reasons why patients referred to physiotherapy with continence or pelvic floor dysfunction fail to complete treatment
|
|
|
- Sabrina Crystal Marshall
- 5 years ago
- Views:
Transcription
1 Journal of the Association of Chartered Physiotherapists in Women s Health, Autumn 2009, 105, CLINICAL PAPER Reasons why patients referred to physiotherapy with continence or pelvic floor dysfunction fail to complete treatment F. J. Lennard Physiotherapy Department, Ipswich Hospital National Health Service Trust, Ipswich, UK Abstract The aim of this study was to identify why patients with continence or pelvic floor dysfunction (PFD) fail to complete their treatment. A postal questionnaire was sent to patients who had attended for, but failed to complete, treatment within a physiotherapy department for continence or PFD during a specific year. In 2006, 112 patients (27%) with continence or pelvic floor disorders failed to complete their courses of treatment. Questionnaires were mailed to the 109 surviving patients and 60 (55%) of these were returned. Various reasons were given by subjects for not completing treatment: 34% cited difficulty attending appointments; 27% stated that they were better ; 20% mentioned other health problems that took precedence; 18% reported that they either did not wish to be referred to physiotherapy or did not think that physiotherapy would benefit them; and 10% stated that they had undergone surgery for the problem (although 33% of this group reported that the surgery had been unsuccessful). Following the audit and in combination with the 18-week waiting initiative, the department gained more staff, which reduced the waiting times and allowed early-morning and lunchtime appointments to be offered. A patient information leaflet was produced that gave comprehensive explanations of conditions and treatments, and details of self-help groups. Extra emphasis was placed on pelvic floor exercises for all pregnant and postnatal women seen by the physiotherapists. In 2008, when the service was re-audited for patients seen in 2007, the percentage of patients who failed to complete treatment had reduced to 21.2%. Physiotherapists need to be aware of the barriers and costs faced by patients seeking treatment. Physiotherapy practice needs to continue to change to reduce these barriers and costs in order to maximize the benefits that physiotherapy can offer patients, and increase the effectiveness and efficiency of the physiotherapy services available to healthcare providers and users. Keywords: failure to complete treatment, incontinence, pelvic floor dysfunction, physiotherapy. Introduction A number of studies have focused on the percentage of outpatients with both musculoskeletal and pelvic floor dysfunction (PFD) who fail to complete physiotherapy treatment, and figures varying from 24% to 59% have been reported (O Brien et al. 1991; Holdsworth et al. 2006). Correspondence: F. J. Lennard, Finn Clinic, Physiotherapy Department, 9th Floor, Maternity Block, Ipswich Hospital NHS Trust, Heath Road, Ipswich, Suffolk IP4 5PD, UK ( fiona.lennard@ipswichhospital.nhs.uk). These figures have cost implications for both physiotherapy services and the UK National Health Service (NHS) as a whole because they have a negative impact on the efficiency of services and waiting lists. In 2006, 685 patients with continence or PFD were referred to the Continence and Pelvic Floor Physiotherapy Department, Ipswich Hospital NHS Trust, Ipswich, UK. A total of 411 individuals were seen and discharged in the same period. Of those, 299 patients completed treat Association of Chartered Physiotherapists in Women s Health
2 Failure to complete physiotherapy treatment Table 1. Outcomes of treatment for patients who completed treatment Condition Number of patients Percentage of patients cured (90 100%) Percentage of patients improved (50 89%) Average number of treatments Average length of treatment (months) Stress incontinence 43 (14%) 28.0% 53.5% Mixed incontinence 76 (25%) 25.0% 41.0% Urge incontinence 17 (5%) 18.0% 65.0% Faecal incontinence 13 (4%) 8.0% 61.0% Male incontinence 17 (5%) 47.0% 36.0% Prolapse 31 (10%) 29.0% 48.0% Dyspareunia 12 (4%) 33.5% 50.0% Multiple problems 90 (30%) 23.0% 51.0% ment. At discharge, the patients are asked by what percentage they feel they have improved following treatment, and this is combined with objective measures of improvement (e.g. frequency and severity of symptoms at discharge compared to time of initial assessment, and pad usage, if relevant) and quality of life questionnaire scores. Their outcomes of treatment are collated in Table 1. The remaining 112 (27%) patients who were assessed either failed to return or failed to complete treatment. This resulted in at least 56 h of physiotherapy time being wasted. The superintendent physiotherapist audits the outcomes of the Ipswich Hospital NHS Trust continence service each year and distributes the results to all services users. However, it is only possible to collate the outcomes of those patients who complete treatment since the outcomes for those who fail to return are unknown. In 2006, the urogynaecologist consultant at Ipswich Hospital requested the outcomes for those who had failed to complete treatment. The superintendent physiotherapist decided to send a postal questionnaire to those patients who had not completed treatment in an effort to establish the reasons for this. Background Urinary incontinence is one of the most common chronic diseases. It has been estimated to affect 8.5% of women aged between 15 and 65 years, and this figure rises to 57% of women aged between 45 and 65 years (Miner 2004). While the incidence of incontinence is higher in women than men, a survey of adults aged over 40 years in Leicester, UK, found that 8.9% of men reported being incontinent several times a month (Perry et al. 2000). Faecal incontinence appears to increase with age, with the incidence varying from 1% to 16% in healthy women to 50% in female residents of nursing homes (Jackson et al. 1997). The incidence of pelvic organ prolapse varies depending on the population studied and the diagnostic criteria, ranging from 30% to 93% (Samuelsson et al. 1999). Incontinence is a condition that impacts on all areas of life, from the ability to get a good night s sleep to the ability to travel. It affects the sufferer s physical, emotional and sexual health, reducing or removing the ability to take part in physical exercise and social activities. It commonly causes depression, embarrassment and anxiety, and may result in withdrawal from sexual relationships (Kelleher 2001). In a survey of community residents aged over 65 years, Rockwood et al. (1999) found that subjects with urinary incontinence, but without cognitive impairment or significant physical disability, were 70% more likely to be admitted to an institution and 20% more likely to die within 5 years than those who were continent. The lifetime medical costs of women with stress urinary incontinence are 1.8 times higher than those of women without the condition (Birnbaum et al. 2003). Pelvic floor muscle exercises (PFMEs) and bladder training have been shown to be simple, low-cost and effective methods of treating incontinence (Melton 2002; Bond et al. 2004; Dorey et al. 2006). However, it has been found that most people with clinically significant symptoms do not find these bothersome, with only 3.8% of those affected reporting that they would like help (Perry et al. 2000). A number of reasons have been cited that explain why people do not seek help for continence problems. Davis & Kumar (2003) reported that women with PFD do not seek help immediately unless their symptoms are severe and have a negative impact on their quality of life. Facione et al. (2000) found that some women view symptoms of PFD as normal and, indeed, inevitable after childbirth. Others may fear what 2009 Association of Chartered Physiotherapists in Women s Health 57
3 F. J. Lennard investigation and treatment involves, and therefore, hope that the symptoms will improve on their own (Norton et al. 1988). A significant number of women are embarrassed by their condition, and as a result, do not, or cannot, talk about it to anyone, including health professionals (Holst & Wilson 1988). The Health Belief Model proposes that, for someone to seek medical help, they need to believe that illness can have a negative impact on their life and that taking action will successfully avoid the possible negative consequences (Holm et al. 1999). Shaw et al. (2001) reported that fear of a serious disease, such as cancer, actively promotes help-seeking. Women with vaginal prolapse often present with a lump in the vagina and many are concerned this may be of a sinister nature. If their fears of cancer are allayed, they may then drop out of a treatment programme if they no longer see their condition as a threat to their health and lifestyle. If someone perceives they have a high quality of life, they are less likely to recognize that they have a health problem (Shaw et al. 2001). Cognitive and motor activities are employed by a person suffering from illness in order to preserve bodily function and cope with the effects of the illness (Lipowski 1970). In the case of incontinence, this may involve the use of pads, toilet mapping, carrying a change of clothes and avoiding activities such as exercise that result in leakage. Women have been found to use more strategies than men to cope, and therefore, they minimize the impact of disease (Sutherland & Jenson 2000). However, if their symptoms become worse and the coping strategies no longer work, individuals may recognize that the illness is a threat to their well-being and seek help. Holm et al. (1999) reported that women either expect that health outcomes are the result of their own actions (i.e. the internal locus of control) or the actions of others (i.e. the external locus of control). In its treatment of incontinence, physiotherapy requires patients to take an active role in their treatment, which involves undertaking some lifestyle changes and individual home exercise programmes. Therefore, women with an internal locus of control may respond better to physiotherapy than those with an external locus of control, who may prefer surgical or pharmaceutical options. It has been reported that individuals who intend to seek help may fail to do so following a cost benefit analysis of the implications of carrying out the behaviour. If the perceived benefits of seeking help are outweighed by costs or other barriers to seeking help, then no action is taken (Oh & Park 2004). If a further trigger occurs, then the individual may start the process again. Several barriers or perceived barriers to healthcare have been described. Moss (2002) reported that transport issues may prevent individuals from receiving treatment. The time of day when a service is provided can also impact on a person s ability to access healthcare (Currie & Wiesenberg 2003). Economic constraints were reported in women with breast cancer (Facione et al. 2000), and low expectations (Horrocks et al. 2004) have also been reported to be barriers to seeking help. Subjects and methods A tick-box questionnaire (see Appendix 1 ) was devised by the superintendent that listed common reasons given by the patients who did contact the department to cancel appointments. However, the questionnaire also allowed patients an opportunity to give other reasons and relevant details. It was also felt to be a good opportunity to discover this group of patients experiences of the department and how the service could be improved. The superintendent felt that giving patients a range of options to tick would make completion of the questionnaire quick and easy. However, in the area of patient experience of the service, no suggestions were given, and therefore, patients completed this section in their own words without prompts. One possible failing of the audit was that the questionnaire was neither validated nor piloted. Each questionnaire was numbered corresponding to a patient s set of notes, so it was possible to identify who had returned the questionnaire. Before sending out the questionnaire and covering letter (see Appendix 1 ) to each patient who failed to complete treatment, the hospital database was checked to see if any patients had passed away. It was found that three (2.6%) patients had died. Because of the financial status of the Trust, the 109 questionnaires with a stamped addressed envelope were not sent out until May Of the 112 patients who had not completed their treatments, 49 (43%) had only attended the initial assessment and the other 63 (57%) patients had failed to return at various points during their therapy Association of Chartered Physiotherapists in Women s Health
4 Failure to complete physiotherapy treatment Table 2. Diagnoses of patients who returned the questionnaire following failure to complete treatment Table 3. Reasons reported for not completing treatment: (DNA) did not attend Condition Results Number of patients Stress incontinence 10 (16%) 2 (20%) Mixed incontinence 14 (23%) 2 (14%) Urge incontinence 4 (6%) 0 (0%) Faecal incontinence 1 (1.6%) 1 (100%) Male incontinence 1 (1.6%) 1 (100%) Prolapse 6 (10%) 3 (50%) Multiple problems 24 (40%) 7 (29%) Number of patients who reported that they were better A total of 60 (55%) questionnaires were returned to the department. Although this response rate is slightly below the ideal return rate of 65% stated by editor of the journal of Physiotherapy, it was a higher response rate than the present author expected in view of the fact that these patients had failed to complete treatment and had not contacted the department to cancel their appointments. There was found to be minimal bias among the respondents, with 25 (42%) having only attended for the initial assessment, and the other 35 (58%) having attended between two and 13 appointments (average number of appointments=4.5). In addition, when comparing the initial diagnosis of the respondents with the initial diagnosis of those patients who did complete their treatment, the percentages were very similar (see Tables 1 & 2). Therefore, it was felt that the results were representative of the group. Diagnosis of patients who returned the questionnaire The average number of treatments for those patients who reported that they had got better was five treatments (Table 2). Reasons reported for not completing treatment Sixteen patients stated more than one reason for not completing their treatment, with 15 giving two reasons and one patient giving three reasons (Table 3). Ten of the patients who returned the questionnaires stated that they wished to return to physiotherapy. These patients were contacted by a letter explaining that, since they had not attended without contacting the department, in line with hospital policy, they had been discharged, but that we would be happy to see them again if they were to be re-referred by their Reason reported for DNA Number of patients Got better 16 (27%) Other health problems 12 (20%) Didn t wish to be referred 9 (15%) Didn t think physiotherapist would help 2 (3%) Family commitments 8 (13%) Work commitments 6 (10%) Had surgery for the problem 6 (10%) Car parking too expensive/stressful 5 (8%) Moved out of the area 4 (6%) Difficulty getting to hospital 2 (3%) Appointment cancelled hadn t rebooked 2 (3%) Referred back to consultant 1 (1.5%) Done own experiments hadn t worked 1 (1.5%) Other reasons (no details given) 1 (1.5%) Table 4. Comments on the service Comment on service Very good 15 (43%) Excellent 6 (17%) Good 3 (8%) Information received was helpful 6 (17%) Staff were kind 5 (14%) Staff were sympathetic 3 (8%) Physiotherapist was very professional 1 (2%) Area was very clean 1 (2%) Number of patients general practitioner (GP), six of these patients subsequently returned for further treatment. Comments on the service The questionnaire asked patients to comment on the physiotherapy service as they had found it and 35 (58%) patients responded to this. The majority of comments on the service that were received were positive and are broken down in Table 4. In addition, one patient said, Thank you for sending me this letter. It shows you are concerned about your patients. Five patients gave negative feedback. The following criticisms were made: + I was really happy with the treatment until it ended without a follow-up. + Didn t tell me anything that I didn t already know. (This patient was seen by a junior physiotherapist.) + It was OK, but I couldn t do the exercises and work. + I was not able to have a vaginal examination on my first appointment due to a senior member of staff not being available. I arrived 2009 Association of Chartered Physiotherapists in Women s Health 59
5 F. J. Lennard for my second appointment after the appointment time had finished and was told I had to rebook I found it all too stressful. + Dreadful dirty area. (This lady attended the department for her appointment a few days after the Trust had been on the national news following a high-profile case of methicillinresistant Staphylococcus aureus (MRSA). She declined a vaginal examination at her assessment, stating that she did not wish to contract MRSA. The department is cleaned daily, and all therapists adhere to local and national infection control policies and guidelines. This demonstrates the importance of trusts reducing infection rates in order to regain public confidence.) Patients comments on how the service could be improved Twenty-six (43%) respondents made comments and/or suggestions. Five of the 26 patients (19%) said that the service could not be improved further. Three (11%) felt that the service needed to meet people s expectations. (These patients indicated that they wanted surgery, not exercises.) Three (11%) stated that the department needed more staff. Two (7%) said that the waiting time for appointments should be less. Because of the financial status of the Trust, we had not been able to recruit when our band 6 physiotherapist had left or to have cover for our band 7 while she was on maternity leave. This resulted in our waiting list, which normally runs at between 8 and 12 weeks, growing to 9 months at its peak. Two respondents (7%) commented that they did not like having to leave a message on the telephone answering machine. Two (7%) said that they would like to book follow-up appointments at each visit, rather than having to call to make an appointment. (This was something that the department trialled for a short time in order to make the diary more flexible. However, it was found that the system did not work because patients forgot to call or the diary was already booked up, and thus, it was difficult to find available slots within a week of them calling. Therefore, we went back to the system of booking their next appointment face-to-face after their consultation.) One patient (3.5%) felt that postnatal women should be given more advice on PFMEs because she hadn t been taught these exercises after she had delivered her children. Almost all women who deliver at the Trust are seen by a physiotherapist since ward cover is provided 7 days a week. All postnatal women are verbally taught PFMEs on the ward, and are able to self-refer up to 6 weeks postnatally if they experience any PFD. They are given a patient information booklet, and following the audit, the pelvic floor section was revised with the exercises being printed in bold and the Knack was added. One (3.5%) suggested that a newsletter with self-help advice should be sent to all patients referred to the department. One (3.5%) requested more treatment rooms away from the office area, which would allow for more privacy and a more-relaxed atmosphere. One (3.5%) said that car parking should be free. One (3.5%) proposed a telephone advisory service. One (3.5%) said that the service should be provided on a more local basis. The department does have one satellite clinic in the community that is very popular and the superintendent has continually strived to set up other satellite clinics; however, to date, this has proved to be unsuccessful because of charges for rooms. One (3.5%) commented that she would like to be able to self-refer because having to see her GP was too stressful. Because of the tariff system for pregnancy care, the department has been able to accept self-referral for pregnant women or for women up to 6 weeks postnatally; however, as a result of payment by referral, all other patient groups currently have to be referred by a doctor. One (3.5%) thought the area was dirty (see Comments on the service above). One respondent (3.5%) said that she would like to see the same physiotherapist each time she attended the department. (Patients usually see the same physiotherapist at each session unless rotational staff rotate out of the department, or if staff are on long-term sick or maternity leave.) Discussion Difficulty attending appointments as a result of time constraints and/or expense was the commonest reason given for not completing treatment (with 13% citing family commitments, 10% mentioning work, 8% stating that car parking was too expensive/stressful and 3% finding it difficult to get to the hospital), accounting for a total of 34% of patients in the present sample. Physiotherapy has historically been a Monday Friday, 9:00 5:00 service, and although there have been recent moves in some areas to change this, it is clear that this issue needs to be Association of Chartered Physiotherapists in Women s Health
6 addressed globally in order to meet the needs of clients. The second commonest reason for patients not completing treatment was that they reported that they were better and no longer felt that treatment was needed (27%). It is not known whether these respondents were actually better, or if their trigger factor had resolved and their symptoms had been reduced to a level with which they could cope. A further 20% of patients reported that they had other health problems that had taken precedence over their course of treatment. It is unknown whether these problems were related directly or indirectly to their continence problem, or were totally unrelated. However, Thom et al. (1997) reported that the risk of hospitalization was 30% higher in women and 50% higher in men following a diagnosis of incontinence. It was found that a total of 18% of patients had either not wanted to be referred to physiotherapy or felt that physiotherapy would not be beneficial to them, which suggests that referrers need to ensure that individuals are aware of what physiotherapy can offer and that they wish to try that treatment option before referral takes place. Therapists should endeavour to ascertain that physiotherapy is the patient s preferred course of treatment, and that she is not just attending to please the doctor or family member who has pressed her into seeking treatment. Alternatively, a move to a system that allows selfreferral would ensure that only patients who want physiotherapy would present for treatment. Holdsworth et al. (2006) reported that, [S]elf-referring patients attended more reliably than patients referred by their GP, with a greater proportion of self-referring patients completing their full course of treatment, particularly when compared with patients referred at the suggestion of their GP (76% versus 69%). The present study found that the diagnosis is not a good indicator of those patients who are unlikely to complete treatment because the percentage of individuals who failed to complete their therapy was very similar to the percentages of patients with each condition who did complete treatment (see Tables 1 & 2). The literature suggests that subjects with stress incontinence may be more likely to drop out of treatment if their trigger factor resolves. Women with vaginal prolapse were also thought to be likely to drop out of treatment once they were reassured that their condition was not of a sinister nature. Failure to complete physiotherapy treatment However, these two groups may make up a significant number of the patients who fail to attend their initial assessment, an area that was not investigated in the present study. Changes made to clinical practice following the outcomes of the audit Because of the 18-Week Wait Initiative, the department was able to increase the level of staffing with the addition of an extra whole-time equivalent (WTE) band 5 and WTE band 6 physiotherapist, which enabled early-morning and lunch-time appointments to be offered to patients. Previously, outpatient appointments had only been offered between the hours of 10:30 4:30 because the three established WTE staff covered the wards first thing in the morning. A detailed subjective and objective assessment, including a vaginal/rectal examination with consent, is routinely performed on the first visit. The negative comment received regarding this highlighted to the staff the importance of ensuring that this standard was met as much as possible. All treatment choices (including medical and surgical options) and contraindications/risks are now explained on the first visit and the patient s preferred appropriate treatment programme is then initiated. Previously, surgical and medical options were only explained to those patients who openly expressed an interest, or to those whom it was felt, following assessment, would not respond favourably to physiotherapy. Following the audit, a patient information booklet was compiled that contained descriptions of pelvic anatomy, bladder and pelvic floor function, types of vaginal prolapse and incontinence, how to perform pelvic floor exercises, voiding, and defer the urge techniques. The booklet also includes details of support groups. Patients are given the option of returning for a follow-up appointment, having a consultation over the telephone or being placed on SOS, where their notes are kept for up to 6 months, so if they wish to return for another appointment, they can do so without a new referral. If muscle stimulation is indicated, patients are given the option of attending the department or purchasing a home stimulator. Prior to the audit, advice on purchasing a home stimulator was only given to those patients who openly expressed an interest. Following the audit, all patients for whom stimulation was indicated were given information on purchasing their own machine as well as the option to attend for stimulation within the department Association of Chartered Physiotherapists in Women s Health 61
7 F. J. Lennard It was hoped that there would be a reduction in the percentage of patients who failed to complete treatment when the service was audited again at the beginning of At the beginning of 2008, it was found that, during 2007, a total of 366 patients completed treatment for incontinence and PFD, with a further 99 patients (21.2%) failing to complete treatment. A further questionnaire was not sent out to these patients since it was not thought to be of additional benefit to the service. Conclusions Physiotherapy has been shown to be an effective, low-risk and inexpensive treatment for incontinence and PFD. Patients should be encouraged to access the treatment options that are offered by physiotherapy. However, physiotherapists need to be aware of the personal barriers, both perceived and actual, that are faced by individuals who present for treatment, and be able to address these so as to ensure that every patient receives the maximum benefit from the therapies available at the minimum cost to themselves and their health service providers. References Birnbaum H., Leong S. & Kabra A. (2003) Lifetime medical costs for women: cardiovascular disease, diabetes and stress urinary incontinence. Women s Health Issues 13 (6), Bond E., Dorey G., Eckford S. & McDonnell K. (2004) The role of pelvic muscle exercises in reducing surgical management of women with stress incontinence: a clinical audit. Journal of the Association of Chartered Physiotherapists in Women s Health 95 (Autumn), Currie D. H. & Wiesenberg S. E. (2003) Promoting women s health-seeking behaviour: research and the empowerment of women. Health Care for Women International 24 (10), Davis K. & Kumar D. (2003) Pelvic floor dysfunction: a conceptual framework for collaborative patient-centred care. Journal of Advanced Nursing 43 (6), Dorey G., Sultan H., Eckford S. D., Parker J. & Lowe D. (2006) Pelvic floor muscle exercises and urge suppression techniques in women with urge urinary incontinence: a retrospective study from a dedicated urogynaecology clinic. Journal of the Association of Chartered Physiotherapists in Women s Health 99 (Autumn), Facione N. C., Giancarlo C. & Chan L. (2000) Perceived risk and help-seeking behaviour for breast cancer: a Chinese-American perspective. Cancer Nursing 23 (4), Holdsworth L. K., Webster V. S. & McFadyen A. K. (2006) Self-referral to physiotherapy: deprivation and geographical setting: is there a relationship? Results of a national trial. Physiotherapy 92 (1), Holm C. J., Frank D. I. & Curtin J. (1999) Health beliefs, health locus of control, and women s mammography behaviour. Cancer Nursing 22 (2), Holst K. & Wilson P. D. (1988) The prevalence of female urinary incontinence and reasons for not seeking treatment. New Zealand Medical Journal 101 (857), Horrocks S., Somerset M., Stoddart H. & Peters T. J. (2004) What prevents older people from seeking treatment for urinary incontinence? A qualitative exploration of barriers to the use of community continence services. Family Practice 21 (6), Jackson S. L., Weber A. M., Hull T. L., Mitchinson A. R. & Walters M. D. (1997) Fecal incontinence in women with urinary incontinence and pelvic organ prolapse. Obstetrics and Gynecology 89 (3) Kelleher C. (2001) Quality of life and urinary incontinence. In: Textbook of Female Urology and Urogynaecology (eds L. Cardozo & D. Staskin), pp Taylor & Francis, London. Lipowski Z. J. (1970) Physical illness, the individual, and the coping process. Psychiatry in Medicine 1 (2), Melton L. (2002) Targeted treatment for incontinence beckons. Lancet 359 (9303), 326. Miner P. B., Jr (2004) Economic and personal impact of fecal and urinary incontinence. Gastroenterology 126 (Suppl. 1), S8 S13. Moss D. (2002) The circle of the soul: the role of spirituality in health care. Applied Psychophysiology and Biofeedback 27 (4), Norton P. A., MacDonald L. D., Sedgwick P. M. & Stanton S. L. (1988) Distress and delay associated with urinary incontinence, frequency and urgency in women. British Medical Journal 297 (6657), O Brien J., Austin M., Sethi P. & O Boyle P. (1991) Urinary incontinence: prevalence, need for treatment, and effectiveness of intervention by nurse. British Medical Journal 303 (6813), Oh H. S. & Park H. A. (2004) Decision tree model of the treatment-seeking behaviours among Korean cancer patients. Cancer Nursing 27 (4), Perry S., Shaw C., Assassa P., et al. (2000) An epidemiological study to establish the prevalence of urinary symptoms and felt need in the community: the Leicestershire MRC incontinence study. Journal of Public Health Medicine 22 (3), Rockwood K., Stadnyk K., MacKnight C., et al. (1999) A brief clinical instrument to classify frailty in elderly people. Lancet 353 (9148), Samuelsson E. C., Victor F. T. A., Tibblin G. & Svärdsudd K. F. (1999) Signs of genital prolapse in a Swedish population of women 20 to 59 years of age and possible related factors. American Journal of Obstetrics and Gynecology 180 (2, Pt 1), Shaw C., Tansey R., Jackson C., Hyde C. & Allan R. (2001) Barriers to help seeking in people with urinary symptoms. Family Practice 18 (1), Sutherland B. & Jensen L. (2000) Living with change: elderly women s perceptions of having a myocardial infarction. Qualitative Health Research 10 (5), Thom D. H., Haan M. N. & van den Eeden S. K. (1997) Medically recognized urinary incontinence and risks of hospitalization, nursing home admission and mortality. Age and Ageing 26 (5), Association of Chartered Physiotherapists in Women s Health
8 Failure to complete physiotherapy treatment Fiona Lennard qualified from Guy s Hospital in During her training, she spent 3 weeks with the great Margie Polden, who inspired her to develop an interest in women s health. This interest was further nurtured by Linda Maude, the superintendent of women s health at Ipswich Hospital. Fiona gained her Postgraduate Certificate in Health Studies: Continence from the University of East London in She is now the clinical specialist in women s health at Ipswich Hospital. Appendix 1 Continence Specialist Physiotherapy Department Ipswich Hospital NHS Trust Patient Questionnaire Please tick the appropriate box/boxes. I did not return to physiotherapy because: I did not wish to be referred to physiotherapy. I had other health concerns. Family commitments made it di$cult. Work commitments made it di$cult. Car parking/travel to the hospital was too stressful/expensive/di$cult. I did not feel physiotherapy would benefit me. Personality clash with the physiotherapist. I got better. Other reasons please give details. Please give comments on the service as you experienced it. How could we improve the service? Many thanks for your help. Covering letter Dear The Ipswich Hospital NHS Trust Directorate of Nursing and Patient Services Continence Specialist Physiotherapy Department The Ipswich Hospital Heath Road Ipswich Suffolk IP4 5PD The physiotherapists working in continence care at Ipswich Hospital are committed to providing the best possible care to all their patients and improving the standards of care provided. Our records show that you were referred to the department, and that you attended for an assessment session and started treatment, but did not return for any further treatment sessions. It would help us a great deal if you would fill out and return the enclosed questionnaire in order that we might address any issues and improve the quality of care we provide. I enclose a SAE and thank you for your time. Yours sincerely Fiona Lennard Superintendent Physiotherapist 2009 Association of Chartered Physiotherapists in Women s Health 63
Women's physiotherapy
 The women s health physiotherapy outpatient team treats a variety of conditions affecting women: chronic pelvic pain urinary incontinence birth-related perineal trauma antenatal and postnatal musculoskeletal
The women s health physiotherapy outpatient team treats a variety of conditions affecting women: chronic pelvic pain urinary incontinence birth-related perineal trauma antenatal and postnatal musculoskeletal
Keeping control What you should expect from your NHS bladder and bowel service
 Keeping control What you should expect from your NHS bladder and bowel service Based on findings from the national audit of continence care 2010 National audit funded by: Report authors Dr Danielle Harari
Keeping control What you should expect from your NHS bladder and bowel service Based on findings from the national audit of continence care 2010 National audit funded by: Report authors Dr Danielle Harari
Tension-free Vaginal Tape (TVT)
 Page 1 of 7 Tension-free Vaginal Tape (TVT) Introduction This leaflet will provide you with basic information about the Tension--free Vaginal Tape (TVT) procedure. What is a TVT? TVT is an operation to
Page 1 of 7 Tension-free Vaginal Tape (TVT) Introduction This leaflet will provide you with basic information about the Tension--free Vaginal Tape (TVT) procedure. What is a TVT? TVT is an operation to
Pessary for Prolapse Priority Setting Partnership (PSP) interim ranking survey
 Pessary for Prolapse Priority Setting Partnership (PSP) interim ranking survey Background: Prolapse is a very common problem affecting many women. Pessaries are commonly used as a treatment for prolapse.
Pessary for Prolapse Priority Setting Partnership (PSP) interim ranking survey Background: Prolapse is a very common problem affecting many women. Pessaries are commonly used as a treatment for prolapse.
Integrated Continence Service Policy. January SafeCare Council January Carol Giffin, Continence Advisor
 Policy No: OP51 Version: 1.0 Name of Policy: Integrated Continence Service Policy Effective From: January 2008 Approved by: SafeCare Council January 2008 Next Review Date: January 2010 Reviewed by: Carol
Policy No: OP51 Version: 1.0 Name of Policy: Integrated Continence Service Policy Effective From: January 2008 Approved by: SafeCare Council January 2008 Next Review Date: January 2010 Reviewed by: Carol
ADHD clinic for adults Feedback on services for attention deficit hyperactivity disorder
 ADHD clinic for adults Feedback on services for attention deficit hyperactivity disorder Healthwatch Islington Healthwatch Islington is an independent organisation led by volunteers from the local community.
ADHD clinic for adults Feedback on services for attention deficit hyperactivity disorder Healthwatch Islington Healthwatch Islington is an independent organisation led by volunteers from the local community.
Guidelines for referring patients to Physiotherapy for the treatment of Pelvic Floor Dysfunction
 Guidelines for referring patients to Physiotherapy for the treatment of Pelvic Floor Dysfunction N.B. Staff should be discouraged from printing this document. This is to avoid the risk of out of date printed
Guidelines for referring patients to Physiotherapy for the treatment of Pelvic Floor Dysfunction N.B. Staff should be discouraged from printing this document. This is to avoid the risk of out of date printed
Lomond & Argyll Advocacy Service Client Satisfaction Survey
 Lomond & Argyll Advocacy Service Client Satisfaction Survey 2010 2017 Client Satisfaction Survey Lomond & Argyll Advocacy Service is keen to hear the views of people who use our service and other stakeholders.
Lomond & Argyll Advocacy Service Client Satisfaction Survey 2010 2017 Client Satisfaction Survey Lomond & Argyll Advocacy Service is keen to hear the views of people who use our service and other stakeholders.
Urinary incontinence. Urology Department. Patient Information Leaflet
 Urinary incontinence Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been diagnosed with urinary incontinence. It contains information about the bladder,
Urinary incontinence Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been diagnosed with urinary incontinence. It contains information about the bladder,
2010 National Survey. University College London Hospitals NHS Foundation Trust
 National Cancer Patient Experience Programme 2010 National Survey University College London Hospitals NHS Foundation Trust Published January 2011 The National Cancer Patient Experience Survey Programme
National Cancer Patient Experience Programme 2010 National Survey University College London Hospitals NHS Foundation Trust Published January 2011 The National Cancer Patient Experience Survey Programme
University College Hospital
 University College Hospital Haematology Psychology and Counselling Service (for patients with blood cancer, red cell disorders and other non-cancer conditions) 1 If you would like this document in another
University College Hospital Haematology Psychology and Counselling Service (for patients with blood cancer, red cell disorders and other non-cancer conditions) 1 If you would like this document in another
International Urogynecological Association (IUGA) Observership Grant. Final Report
 International Urogynecological Association (IUGA) 2009-10 Observership Grant Final Report Observership Grant Recipient: Renato Silva Martins 5 th Year Obstetrics and Gynaecology Resident at Coimbra s University
International Urogynecological Association (IUGA) 2009-10 Observership Grant Final Report Observership Grant Recipient: Renato Silva Martins 5 th Year Obstetrics and Gynaecology Resident at Coimbra s University
2010 National Survey. East Kent Hospitals University NHS Trust
 National Cancer Patient Experience Programme 2010 National Survey Published January 2011 The National Cancer Patient Experience Survey Programme is being undertaken by Quality Health on behalf of the Department
National Cancer Patient Experience Programme 2010 National Survey Published January 2011 The National Cancer Patient Experience Survey Programme is being undertaken by Quality Health on behalf of the Department
2010 National Survey. The North West London Hospitals NHS Trust
 National Cancer Patient Experience Programme 2010 National Survey Published January 2011 The National Cancer Patient Experience Survey Programme is being undertaken by Quality Health on behalf of the Department
National Cancer Patient Experience Programme 2010 National Survey Published January 2011 The National Cancer Patient Experience Survey Programme is being undertaken by Quality Health on behalf of the Department
2010 National Survey. Royal National Orthopaedic Hospital NHS Trust
 National Cancer Patient Experience Programme 2010 National Survey Published January 2011 The National Cancer Patient Experience Survey Programme is being undertaken by Quality Health on behalf of the Department
National Cancer Patient Experience Programme 2010 National Survey Published January 2011 The National Cancer Patient Experience Survey Programme is being undertaken by Quality Health on behalf of the Department
2010 National Survey. The Leeds Teaching Hospitals NHS Trust
 National Cancer Patient Experience Programme 2010 National Survey Published January 2011 The National Cancer Patient Experience Survey Programme is being undertaken by Quality Health on behalf of the Department
National Cancer Patient Experience Programme 2010 National Survey Published January 2011 The National Cancer Patient Experience Survey Programme is being undertaken by Quality Health on behalf of the Department
Joint Mental Health Commissioning Strategy for Adults
 Joint Mental Health Commissioning Strategy for Adults 2014-2019 Summary Developed in partnership with: NHS Ipswich and East Suffolk CCG, NHS West Suffolk CCG, Suffolk Constabulary and Suffolk County Council
Joint Mental Health Commissioning Strategy for Adults 2014-2019 Summary Developed in partnership with: NHS Ipswich and East Suffolk CCG, NHS West Suffolk CCG, Suffolk Constabulary and Suffolk County Council
2010 National Survey. Northern Lincolnshire and Goole Hospitals NHS Foundation Trust
 National Cancer Patient Experience Programme 2010 National Survey Northern Lincolnshire and Goole Hospitals NHS Foundation Trust Published January 2011 The National Cancer Patient Experience Survey Programme
National Cancer Patient Experience Programme 2010 National Survey Northern Lincolnshire and Goole Hospitals NHS Foundation Trust Published January 2011 The National Cancer Patient Experience Survey Programme
The symptom recognition and help- seeking experiences of men in Australia with testicular cancer: A qualitative study
 The symptom recognition and help- seeking experiences of men in Australia with testicular cancer: A qualitative study Stephen Carbone,, Susan Burney, Fiona Newton & Gordon A. Walker Monash University gordon.walker@med.monash.edu.au
The symptom recognition and help- seeking experiences of men in Australia with testicular cancer: A qualitative study Stephen Carbone,, Susan Burney, Fiona Newton & Gordon A. Walker Monash University gordon.walker@med.monash.edu.au
Pain Management Programme
 Pain Management Programme 1 2 History of Pain Management Programme The Walton Centre Pain Management Programme (PMP) is a leading pain management service in the UK and delivers a variety of pain management
Pain Management Programme 1 2 History of Pain Management Programme The Walton Centre Pain Management Programme (PMP) is a leading pain management service in the UK and delivers a variety of pain management
Promoting Continence with Physiotherapy
 A Common problem for Men and women Promoting Continence with Physiotherapy This leaflet contains information about physiotherapy advice and treatment for anyone with bladder and bowel problems. This may
A Common problem for Men and women Promoting Continence with Physiotherapy This leaflet contains information about physiotherapy advice and treatment for anyone with bladder and bowel problems. This may
AVELEY MEDICAL CENTRE & THE BLUEBELL SURGERY
 AVELEY MEDICAL CENTRE & THE BLUEBELL SURGERY Drs Leighton, Ahrin, Beroiz, Munro, Saluja, Ruiz-Gutierrez and George Aveley Medical Centre, 22 High Street, Aveley, Essex, RM15 4AD The Bluebell Surgery, Darenth
AVELEY MEDICAL CENTRE & THE BLUEBELL SURGERY Drs Leighton, Ahrin, Beroiz, Munro, Saluja, Ruiz-Gutierrez and George Aveley Medical Centre, 22 High Street, Aveley, Essex, RM15 4AD The Bluebell Surgery, Darenth
Oral Medicine Psychology Service
 Oral Medicine Psychology Service Information for patients Introduction The team in Oral Medicine includes oral medicine consultants, clinical fellows, clinical psychologists, specialist nurses and pain
Oral Medicine Psychology Service Information for patients Introduction The team in Oral Medicine includes oral medicine consultants, clinical fellows, clinical psychologists, specialist nurses and pain
National Cancer Patient Experience Programme. 2012/13 National Survey. James Paget University Hospitals NHS Foundation Trust. Published August 2013
 National Cancer Patient Experience Programme 2012/13 National Survey Published August 2013 The National Cancer Patient Experience Survey Programme is being undertaken by Quality Health on behalf of NHS
National Cancer Patient Experience Programme 2012/13 National Survey Published August 2013 The National Cancer Patient Experience Survey Programme is being undertaken by Quality Health on behalf of NHS
National Cancer Patient Experience Programme. 2012/13 National Survey. Milton Keynes Hospital NHS Foundation Trust. Published August 2013
 National Cancer Patient Experience Programme 2012/13 National Survey Published August 2013 The National Cancer Patient Experience Survey Programme is being undertaken by Quality Health on behalf of NHS
National Cancer Patient Experience Programme 2012/13 National Survey Published August 2013 The National Cancer Patient Experience Survey Programme is being undertaken by Quality Health on behalf of NHS
The Obstetrics and Gynaecology Health Psychology Service
 Northumbria Healthcare NHS Foundation Trust The Obstetrics and Gynaecology Health Psychology Service Issued by the Obstetrics and Gynaecology Department Psychological therapy Everyone has different strategies
Northumbria Healthcare NHS Foundation Trust The Obstetrics and Gynaecology Health Psychology Service Issued by the Obstetrics and Gynaecology Department Psychological therapy Everyone has different strategies
CASY Counselling Services for Schools
 CASY Counselling Services for Schools Registered Charity Number 1092938 A Company Limited by Guarantee in England and Wales. Registered number 4310724 16 London Rd, Newark, Nottinghamshire NG24 1TW T:
CASY Counselling Services for Schools Registered Charity Number 1092938 A Company Limited by Guarantee in England and Wales. Registered number 4310724 16 London Rd, Newark, Nottinghamshire NG24 1TW T:
National Cancer Patient Experience Programme. 2012/13 National Survey. East Kent Hospitals University NHS Foundation Trust. Published August 2013
 National Cancer Patient Experience Programme 2012/13 National Survey Published August 2013 The National Cancer Patient Experience Survey Programme is being undertaken by Quality Health on behalf of NHS
National Cancer Patient Experience Programme 2012/13 National Survey Published August 2013 The National Cancer Patient Experience Survey Programme is being undertaken by Quality Health on behalf of NHS
Employee Feedback Form
 Employee Feedback Form The following physiotherapy service questionnaire was handed to those new patients who were seen over a 3 month period (December February 7). There were 15 new patients seen, of
Employee Feedback Form The following physiotherapy service questionnaire was handed to those new patients who were seen over a 3 month period (December February 7). There were 15 new patients seen, of
National Cancer Patient Experience Programme National Survey. Royal National Orthopaedic Hospital NHS Trust. Published September 2014
 National Cancer Patient Experience Programme 2014 National Survey Royal National Orthopaedic Hospital NHS Trust Published September 2014 The National Cancer Patient Experience Survey Programme is undertaken
National Cancer Patient Experience Programme 2014 National Survey Royal National Orthopaedic Hospital NHS Trust Published September 2014 The National Cancer Patient Experience Survey Programme is undertaken
Hearing Voices Group. Introduction. And. Background information. David DddddFreemanvvvvvvvvv
 Hearing Voices Group Introduction And Background information David DddddFreemanvvvvvvvvv Contents Hearing Voices Group Rationale Inclusion criteria for hearing voices group Structure of Group Process The
Hearing Voices Group Introduction And Background information David DddddFreemanvvvvvvvvv Contents Hearing Voices Group Rationale Inclusion criteria for hearing voices group Structure of Group Process The
Chemotherapy Suite: Ward [Mon - Fri 2pm - 4pm] Your oncologist s secretary:...
![Chemotherapy Suite: Ward [Mon - Fri 2pm - 4pm] Your oncologist s secretary:... Chemotherapy Suite: Ward [Mon - Fri 2pm - 4pm] Your oncologist s secretary:...](/thumbs/85/92602023.jpg) Coping, now your chemotherapy is finishing [ovarian cancer] Patient Information Series PI 41a East and North Hertfordshire NHS Trust 2 Contacts Chemotherapy Suite:... 020 3826 2236 [Mon - Fri, 8.00am -
Coping, now your chemotherapy is finishing [ovarian cancer] Patient Information Series PI 41a East and North Hertfordshire NHS Trust 2 Contacts Chemotherapy Suite:... 020 3826 2236 [Mon - Fri, 8.00am -
Telford and Wrekin Clinical Commissioning Group
 Telford and Wrekin Clinical Commissioning Group Agenda Item 9.2 CLINICAL COMMISSIONING GROUP GOVERNANCE BOARD EXECUTIVE SUMMARY DATE: 9 th April 2013 TITLE OF PAPER: Continence pathway and Referral letter
Telford and Wrekin Clinical Commissioning Group Agenda Item 9.2 CLINICAL COMMISSIONING GROUP GOVERNANCE BOARD EXECUTIVE SUMMARY DATE: 9 th April 2013 TITLE OF PAPER: Continence pathway and Referral letter
National Cancer Patient Experience Programme National Survey. South Tees Hospitals NHS Foundation Trust. Published September 2014
 National Cancer Patient Experience Programme 2014 National Survey South Tees Hospitals NHS Foundation Trust Published September 2014 The National Cancer Patient Experience Survey Programme is undertaken
National Cancer Patient Experience Programme 2014 National Survey South Tees Hospitals NHS Foundation Trust Published September 2014 The National Cancer Patient Experience Survey Programme is undertaken
Scottish Parliament Region: North East Scotland. Case : Tayside NHS Board. Summary of Investigation
 Scottish Parliament Region: North East Scotland Case 201104213: Tayside NHS Board Summary of Investigation Category Health: General Surgical; communication Overview The complainant (Mrs C) raised concerns
Scottish Parliament Region: North East Scotland Case 201104213: Tayside NHS Board Summary of Investigation Category Health: General Surgical; communication Overview The complainant (Mrs C) raised concerns
Bladder retraining - treatment for urgency and urge incontinence
 Bladder retraining - treatment for urgency and urge incontinence This leaflet explains what urge incontinence is and how we can help to reduce and relieve your symptoms. If you have any questions or concerns,
Bladder retraining - treatment for urgency and urge incontinence This leaflet explains what urge incontinence is and how we can help to reduce and relieve your symptoms. If you have any questions or concerns,
Palliative Care Asking the questions that matter to me
 Palliative Care Asking the questions that matter to me THE PALLIATIVE HUB Adult This booklet has been developed by the Palliative Care Senior Nurses Network and adapted with permission from Palliative
Palliative Care Asking the questions that matter to me THE PALLIATIVE HUB Adult This booklet has been developed by the Palliative Care Senior Nurses Network and adapted with permission from Palliative
Vaginal Tapes to Treat Stress Incontinence. Patient Information
 Vaginal Tapes to Treat Stress Incontinence Patient Information Author ID: JD Leaflet Number: Gyn 044 Version: 6 Name of Leaflet: Vaginal Tapes to Treat Stress Incontinence Date Produced: May 2017 Review
Vaginal Tapes to Treat Stress Incontinence Patient Information Author ID: JD Leaflet Number: Gyn 044 Version: 6 Name of Leaflet: Vaginal Tapes to Treat Stress Incontinence Date Produced: May 2017 Review
One-off assessments within a community mental health team
 Primary Care Mental Health 2007;4:00 00 # 2007 Radcliffe Publishing International research One-off assessments within a community mental health team Linda Heaney Consultant Psychiatrist, Avon and Wiltshire
Primary Care Mental Health 2007;4:00 00 # 2007 Radcliffe Publishing International research One-off assessments within a community mental health team Linda Heaney Consultant Psychiatrist, Avon and Wiltshire
Patient Information Leaflet
 Patient Information Leaflet MID-URETHRAL SLING OPERATION TENSION-FREE VAGINAL TAPE (TVT) TRANSOBTURATOR TAPE (TOT, TVT-O) This information leaflet has been developed to help your understanding of what
Patient Information Leaflet MID-URETHRAL SLING OPERATION TENSION-FREE VAGINAL TAPE (TVT) TRANSOBTURATOR TAPE (TOT, TVT-O) This information leaflet has been developed to help your understanding of what
Patient Information. Basic Information on Overactive Bladder Symptoms. pubic bone. urethra. scrotum. bladder. vaginal canal
 Patient Information English Basic Information on Overactive Bladder Symptoms The underlined terms are listed in the glossary. What is the bladder? pubic bone bladder seminal vesicles prostate rectum The
Patient Information English Basic Information on Overactive Bladder Symptoms The underlined terms are listed in the glossary. What is the bladder? pubic bone bladder seminal vesicles prostate rectum The
Defining quality in ovarian cancer services: the patient perspective
 Defining quality in ovarian cancer services: the patient perspective 1 Contents Introduction... 3 Awareness and early diagnosis... 4 Information and support... 5 Treatment and care... 6 Living with and
Defining quality in ovarian cancer services: the patient perspective 1 Contents Introduction... 3 Awareness and early diagnosis... 4 Information and support... 5 Treatment and care... 6 Living with and
Update of C/YEL/cm/iii v1.0. Keith Shaw, Chaplain Kenny Laing, Deputy Director of Nursing. Policy and Procedures Committee Date: 19/01/2017
 Clinical Spirituality, Religion and Pastoral Care Policy & SOP Document Control Summary Status: Update of C/YEL/cm/iii v1.0 Version: v1.1 Date: 16-01-17 Author/Owner: Keith Shaw, Chaplain Kenny Laing,
Clinical Spirituality, Religion and Pastoral Care Policy & SOP Document Control Summary Status: Update of C/YEL/cm/iii v1.0 Version: v1.1 Date: 16-01-17 Author/Owner: Keith Shaw, Chaplain Kenny Laing,
IAPT for SMI: Findings from the evaluation of service user experiences. Julie Billsborough & Lisa Couperthwaite, Researchers at the McPin Foundation
 IAPT for SMI: Findings from the evaluation of service user experiences Julie Billsborough & Lisa Couperthwaite, Researchers at the McPin Foundation About us A small, specialist mental health research charity
IAPT for SMI: Findings from the evaluation of service user experiences Julie Billsborough & Lisa Couperthwaite, Researchers at the McPin Foundation About us A small, specialist mental health research charity
Pelvic Floor Exercises
 Pelvic Floor Exercises Physiotherapy Department Patient information leaflet Up to a third of women experience a problem with their pelvic floor muscles at some point during their life. The muscles can
Pelvic Floor Exercises Physiotherapy Department Patient information leaflet Up to a third of women experience a problem with their pelvic floor muscles at some point during their life. The muscles can
Bulkamid. Patient Information. Obstetrics & Gynaecology Department
 Bulkamid Patient Information Obstetrics & Gynaecology Department Author ID: JD Leaflet Number: Gyn 050 Version: 5 Name of Leaflet: Bulkamid Date Produced: November 2017 Review Date: November 2019 Bulkamid
Bulkamid Patient Information Obstetrics & Gynaecology Department Author ID: JD Leaflet Number: Gyn 050 Version: 5 Name of Leaflet: Bulkamid Date Produced: November 2017 Review Date: November 2019 Bulkamid
This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request.
 Information for patients This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request. This leaflet tells you about acupuncture
Information for patients This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request. This leaflet tells you about acupuncture
PSYCHOLOGIST-PATIENT SERVICES
 PSYCHOLOGIST-PATIENT SERVICES PSYCHOLOGICAL SERVICES Welcome to my practice. Because you will be putting a good deal of time and energy into therapy, you should choose a psychologist carefully. I strongly
PSYCHOLOGIST-PATIENT SERVICES PSYCHOLOGICAL SERVICES Welcome to my practice. Because you will be putting a good deal of time and energy into therapy, you should choose a psychologist carefully. I strongly
Centre for Specialist Psychological Treatments of Anxiety and Related Problems
 Centre for Specialist Psychological Treatments of Anxiety and Related Problems Information for people interested in accessing treatment at the Centre and those who already have a referral Welcome Welcome
Centre for Specialist Psychological Treatments of Anxiety and Related Problems Information for people interested in accessing treatment at the Centre and those who already have a referral Welcome Welcome
Psychological Services
 Psychological Services Acute Inpatient Care Alnmouth, Warkworth and Embleton St George s Park Hospital Patient information leaflet Shining a light on the future Introduction This leaflet provides information
Psychological Services Acute Inpatient Care Alnmouth, Warkworth and Embleton St George s Park Hospital Patient information leaflet Shining a light on the future Introduction This leaflet provides information
Programme. April - July
 Programme April - July 2018 Mindplymouth @Plymouth_Mind www.plymouthmind.com Contents Welcome.. 2 How to Register 3 Counselling Service 4 Courses..5 Listening Support Service..7 Workshops..8 Peer Support
Programme April - July 2018 Mindplymouth @Plymouth_Mind www.plymouthmind.com Contents Welcome.. 2 How to Register 3 Counselling Service 4 Courses..5 Listening Support Service..7 Workshops..8 Peer Support
Pain management programme. Information for patients Pain Management Service
 Pain management programme Information for patients Pain Management Service page 2 of 8 What is a Pain Management Programme? Pain Management Programmes are group-based courses that usually run over nine
Pain management programme Information for patients Pain Management Service page 2 of 8 What is a Pain Management Programme? Pain Management Programmes are group-based courses that usually run over nine
Renal counselling at the Sussex Kidney Unit
 Renal counselling at the Sussex Kidney Unit Patient Information There are four specialist renal counsellors working at the Sussex Kidney Unit. We are fully qualified to post graduate level and accredited
Renal counselling at the Sussex Kidney Unit Patient Information There are four specialist renal counsellors working at the Sussex Kidney Unit. We are fully qualified to post graduate level and accredited
2017 Dentist Schedule: Sharing Smiles Orthodontics
 2017 Dentist Schedule: Sharing Smiles Orthodontics 1 Contents 1. Introduction 1.1 Details of visit 1.2 Acknowledgments 1.3 Disclaimer 2. What is Enter and View? 2.1 Purpose of visit 2.2 Strategic drivers
2017 Dentist Schedule: Sharing Smiles Orthodontics 1 Contents 1. Introduction 1.1 Details of visit 1.2 Acknowledgments 1.3 Disclaimer 2. What is Enter and View? 2.1 Purpose of visit 2.2 Strategic drivers
Pinderfields. Macmillan Information centre report. Quarter 2
 Pinderfields Macmillan Information centre report Quarter 2 1 July-September 2017 The Mid Yorkshire Hospitals NHS Trust provides care to the communities of Wakefield, Pontefract and North Kirklees, a population
Pinderfields Macmillan Information centre report Quarter 2 1 July-September 2017 The Mid Yorkshire Hospitals NHS Trust provides care to the communities of Wakefield, Pontefract and North Kirklees, a population
Mental Health Strategy. Easy Read
 Mental Health Strategy Easy Read Mental Health Strategy Easy Read The Scottish Government, Edinburgh 2012 Crown copyright 2012 You may re-use this information (excluding logos and images) free of charge
Mental Health Strategy Easy Read Mental Health Strategy Easy Read The Scottish Government, Edinburgh 2012 Crown copyright 2012 You may re-use this information (excluding logos and images) free of charge
Patient Survey Report Spring 2013
 Patient Survey Report Spring 2013 We invited the original group of Patients from last year s PPG to become part of a Virtual Forum once again this year and also sent text messages to all out patients inviting
Patient Survey Report Spring 2013 We invited the original group of Patients from last year s PPG to become part of a Virtual Forum once again this year and also sent text messages to all out patients inviting
6. PATIENT RECRUITMENT
 6. PATIENT RECRUITMENT 6.1 Suitable patient criteria Not all patients will benefit from a DAFNE course. At this stage we do not have evidence to help us decide who would and who would not benefit from
6. PATIENT RECRUITMENT 6.1 Suitable patient criteria Not all patients will benefit from a DAFNE course. At this stage we do not have evidence to help us decide who would and who would not benefit from
Bowel health and screening: carers guide. A booklet for carers of people who use easy read materials
 Bowel health and screening: carers guide A booklet for carers of people who use easy read materials Contents About this booklet Page 3: Page 4: Page 5: Page 6: Page 6: Page 7: Page 8: Page 10: Page 10:
Bowel health and screening: carers guide A booklet for carers of people who use easy read materials Contents About this booklet Page 3: Page 4: Page 5: Page 6: Page 6: Page 7: Page 8: Page 10: Page 10:
Case Study. Salus. May 2010
 Case Study Salus May 2010 Background Based within Coatbridge, Salus consists of one of the largest NHS based multidisciplinary teams in Scotland. Through its various services Salus Case Management Services
Case Study Salus May 2010 Background Based within Coatbridge, Salus consists of one of the largest NHS based multidisciplinary teams in Scotland. Through its various services Salus Case Management Services
Advanced Practice in Women s Health and Continence Physiotherapy Project. Robyn Brennen Grade 4 Physiotherapist, Monash Health
 Advanced Practice in Women s Health and Continence Physiotherapy Project Robyn Brennen Grade 4 Physiotherapist, Monash Health Acknowledgements Desiree Terrill, Wendy Davis, Duncan Baulch Sarah Cleaver,
Advanced Practice in Women s Health and Continence Physiotherapy Project Robyn Brennen Grade 4 Physiotherapist, Monash Health Acknowledgements Desiree Terrill, Wendy Davis, Duncan Baulch Sarah Cleaver,
Patient information leaflet. Royal Surrey County Hospital. NHS Foundation Trust. CT Scanning. Radiology
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust CT Scanning Radiology This leaflet tells you about having a Computerised Tomography (CT) Scan. It explains what is involved
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust CT Scanning Radiology This leaflet tells you about having a Computerised Tomography (CT) Scan. It explains what is involved
Report on the data collected by Healthwatch Oldham at our Low Mood, Anxiety and Depression Forum held in January 2017
 Report on the data collected by Healthwatch Oldham at our Low Mood, Anxiety and Depression Forum held in January 17 Healthwatch Oldham 1 Manchester Chambers, West Street, Oldham, Lancashire, OL1 1LF. Tel:
Report on the data collected by Healthwatch Oldham at our Low Mood, Anxiety and Depression Forum held in January 17 Healthwatch Oldham 1 Manchester Chambers, West Street, Oldham, Lancashire, OL1 1LF. Tel:
Family & Individual Support Program - Handbook
 Family & Individual Support Program - Handbook Welcome to the Simon Fraser Society for Community Living (SFSCL). The SFSCL is an accredited not-for-profit, charitable organization that has been serving
Family & Individual Support Program - Handbook Welcome to the Simon Fraser Society for Community Living (SFSCL). The SFSCL is an accredited not-for-profit, charitable organization that has been serving
The audit is managed by the Royal College of Psychiatrists in partnership with:
 Background The National Audit of Dementia (NAD) care in general hospitals is commissioned by the Healthcare Quality Improvement Partnership on behalf of NHS England and the Welsh Government, as part of
Background The National Audit of Dementia (NAD) care in general hospitals is commissioned by the Healthcare Quality Improvement Partnership on behalf of NHS England and the Welsh Government, as part of
Using Physiotherapy to Manage Urinary Incontinence in Women
 Using Physiotherapy to Manage Urinary Incontinence in Women Bladder control problems are common, and affect people of all ages, genders and backgrounds. These problems are referred to as urinary incontinence
Using Physiotherapy to Manage Urinary Incontinence in Women Bladder control problems are common, and affect people of all ages, genders and backgrounds. These problems are referred to as urinary incontinence
Wales Cancer Patient Experience. Survey Aneurin Bevan University Health Board. Published January 2014
 Wales Cancer Patient Experience Survey 2013 Aneurin Bevan University Health Published January 2014 The Wales Cancer Patient Experience Survey was undertaken by Quality Health on behalf of the Welsh Government
Wales Cancer Patient Experience Survey 2013 Aneurin Bevan University Health Published January 2014 The Wales Cancer Patient Experience Survey was undertaken by Quality Health on behalf of the Welsh Government
The Colorectal (bowel) Family History Clinic. Information for patients Endoscopy
 The Colorectal (bowel) Family History Clinic Information for patients Endoscopy What does the Colorectal Family History Clinic provide? The Family History Clinic provides a chance for you to talk about
The Colorectal (bowel) Family History Clinic Information for patients Endoscopy What does the Colorectal Family History Clinic provide? The Family History Clinic provides a chance for you to talk about
Young Healthwatch pilot
 Young Healthwatch pilot Sefton CVS were commissioned to carry out a pilot project to ascertain what children and young people locally thought about the health care services they receive. Between April
Young Healthwatch pilot Sefton CVS were commissioned to carry out a pilot project to ascertain what children and young people locally thought about the health care services they receive. Between April
Uterus (Womb) Rectum. Another problem could be the sensation of something coming down at the birth canal or back passage (prolapse).
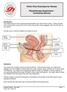 Pelvic Floor Exercises for Women Physiotherapy Department Continence Service Introduction This leaflet tells you how to exercise and strengthen your pelvic floor muscles. These muscles form a broad sling
Pelvic Floor Exercises for Women Physiotherapy Department Continence Service Introduction This leaflet tells you how to exercise and strengthen your pelvic floor muscles. These muscles form a broad sling
Audiology Patient Satisfaction Survey April 2015
 Introduction Audiology Patient Satisfaction Survey April 2015 This report contains the results of the Adult Audiology patient satisfaction survey. A self completion questionnaire was handed out to patients
Introduction Audiology Patient Satisfaction Survey April 2015 This report contains the results of the Adult Audiology patient satisfaction survey. A self completion questionnaire was handed out to patients
Worcestershire Health and Care NHS Trust. Autism Assessment. The Umbrella Pathway
 Worcestershire Health and Care NHS Trust Autism Assessment The Umbrella Pathway www.hacw.nhs.uk Working together Autism for outstanding Assessment care 1 After a child s referral to the Umbrella Pathway
Worcestershire Health and Care NHS Trust Autism Assessment The Umbrella Pathway www.hacw.nhs.uk Working together Autism for outstanding Assessment care 1 After a child s referral to the Umbrella Pathway
Cardiovascular rehabilitation programme
 Cardiovascular rehabilitation programme Name Hospital number Consultant Welcome to the cardiovascular rehabilitation programme Aim of the programme The cardiovascular rehabilitation programme is designed
Cardiovascular rehabilitation programme Name Hospital number Consultant Welcome to the cardiovascular rehabilitation programme Aim of the programme The cardiovascular rehabilitation programme is designed
Information for Patients. Overactive bladder syndrome (OAB) English
 Information for Patients Overactive bladder syndrome (OAB) English Table of contents What is the bladder?... 3 What are overactive bladder symptoms?... 3 What causes overactive bladder symptoms?... 3 Diagnosis
Information for Patients Overactive bladder syndrome (OAB) English Table of contents What is the bladder?... 3 What are overactive bladder symptoms?... 3 What causes overactive bladder symptoms?... 3 Diagnosis
Dclin Psych Open Day October 2017
 Doctorate in Clinical Psychology Open Day 20 October 2017 Selection and Admission Dr. Gundi Kiemle Academic Director & Admissions Tutor National numbers for NHS funded courses 15% of applicants succeeded
Doctorate in Clinical Psychology Open Day 20 October 2017 Selection and Admission Dr. Gundi Kiemle Academic Director & Admissions Tutor National numbers for NHS funded courses 15% of applicants succeeded
Mon - Fri: 8.30am 4.30pm If you have any questions or concerns at all about this. 24 hour Acute Oncology Service
 Radium-223 therapy Patient Information Series PI 79 East and North Hertfordshire NHS Trust 2 Contacts Who can I contact about this treatment? If you have any questions or concerns at all about this treatment
Radium-223 therapy Patient Information Series PI 79 East and North Hertfordshire NHS Trust 2 Contacts Who can I contact about this treatment? If you have any questions or concerns at all about this treatment
DIABETES NEWS SPRING 2018
 DIABETES NEWS SPRING 2018 Local News from the Children s and Young People s Diabetes Clinic at the Oxford Children s & Horton Hospitals CLINIC STAFFING NEWS Management News There has been a new opportunity
DIABETES NEWS SPRING 2018 Local News from the Children s and Young People s Diabetes Clinic at the Oxford Children s & Horton Hospitals CLINIC STAFFING NEWS Management News There has been a new opportunity
Information on Physical Therapy For Urogynecologic Problems
 Information on Physical Therapy For Urogynecologic Problems You have scheduled an appointment for evaluation and treatment of a urogynecologic problem. Following, you will find a pelvic floor questionnaire
Information on Physical Therapy For Urogynecologic Problems You have scheduled an appointment for evaluation and treatment of a urogynecologic problem. Following, you will find a pelvic floor questionnaire
PATIENT PROCEDURE INFORMATION LEAFLET
 PATIENT PROCEDURE INFORMATION LEAFLET BIOFEEDBACK CLINIC 1 Introduction You have been referred by your consultant for a course of biofeedback (bowel retraining) with the physiologist. Following your recent
PATIENT PROCEDURE INFORMATION LEAFLET BIOFEEDBACK CLINIC 1 Introduction You have been referred by your consultant for a course of biofeedback (bowel retraining) with the physiologist. Following your recent
Improving Access to Psychological Therapies. Guidance for faith and community groups
 Improving Access to Psychological Therapies Guidance for faith and community groups 1 The aims of this resource This document aims to improve faith communities understanding of the professional treatments
Improving Access to Psychological Therapies Guidance for faith and community groups 1 The aims of this resource This document aims to improve faith communities understanding of the professional treatments
Bedfordshire Mental Health Crisis Care
 Bedfordshire Mental Health Crisis Care BCCG is asking patients and the public to think about the following questions when considering the crisis response in Bedfordshire:- What do you need when in crisis?
Bedfordshire Mental Health Crisis Care BCCG is asking patients and the public to think about the following questions when considering the crisis response in Bedfordshire:- What do you need when in crisis?
Perinatal Community Mental Health Team Patient Information Leaflet
 Perinatal Community Mental Health Team Patient Information Leaflet Shining a light on the future What is the Perinatal Community Mental Health Team? The Perinatal Team provides a community service to support
Perinatal Community Mental Health Team Patient Information Leaflet Shining a light on the future What is the Perinatal Community Mental Health Team? The Perinatal Team provides a community service to support
Pelvic Floor Muscle Exercises
 INFORMATION FOR WOMEN OF ALL AGES Pelvic Floor Muscle Exercises How to exercise and strengthen your pelvic floor muscles ASSOCIATION OF CHARTERED PHYSIOTHERAPISTS IN WOMEN S HEALTH This leaflet is supported
INFORMATION FOR WOMEN OF ALL AGES Pelvic Floor Muscle Exercises How to exercise and strengthen your pelvic floor muscles ASSOCIATION OF CHARTERED PHYSIOTHERAPISTS IN WOMEN S HEALTH This leaflet is supported
Patient Information Series PI 79. Look Good...Feel Better. Relaxation classes. beauty workshops The Way Ahead
 a patient s guide Lynda Jackson Macmillan Centre... supporting people affected by cancer... Drop-in centre for support and information Telephone helpline Complementary therapies* Counselling* Benefits
a patient s guide Lynda Jackson Macmillan Centre... supporting people affected by cancer... Drop-in centre for support and information Telephone helpline Complementary therapies* Counselling* Benefits
Physiotherapy Tender Questions and Answers
 Physiotherapy Tender Questions and Answers Background 1. Q. Why has Bupa conducted a review of physiotherapy? A. Over the last year, we have been reviewing orthopaedic care to see whether there are opportunities
Physiotherapy Tender Questions and Answers Background 1. Q. Why has Bupa conducted a review of physiotherapy? A. Over the last year, we have been reviewing orthopaedic care to see whether there are opportunities
Trust Board Meeting in Public: Wednesday 13 January 2016 TB
 Trust Board Meeting in Public: Wednesday 13 January 2016 Title Ms P - Patient Story Status History For information Patient stories are regularly presented to Trust Board and Quality Committee Board Lead(s)
Trust Board Meeting in Public: Wednesday 13 January 2016 Title Ms P - Patient Story Status History For information Patient stories are regularly presented to Trust Board and Quality Committee Board Lead(s)
SCHEDULE 2 THE SERVICES. A. Service Specifications
 SCHEDULE 2 THE SERVICES A. Service Specifications Service Specification No. 04/MSKT/0013 Service PAN DORSET FRACTURE LIAISON SERVICE Commissioner Lead CCP for Musculoskeletal & Trauma Provider Lead Deputy
SCHEDULE 2 THE SERVICES A. Service Specifications Service Specification No. 04/MSKT/0013 Service PAN DORSET FRACTURE LIAISON SERVICE Commissioner Lead CCP for Musculoskeletal & Trauma Provider Lead Deputy
Bowel health and screening: carers guide. A booklet for carers of people who use easy read materials
 Bowel health and screening: carers guide A booklet for carers of people who use easy read materials Contents Page 3: About this booklet Page 4: What is the bowel? Page 5: Helping someone to have good bowel
Bowel health and screening: carers guide A booklet for carers of people who use easy read materials Contents Page 3: About this booklet Page 4: What is the bowel? Page 5: Helping someone to have good bowel
Ultrasound scan of abdomen and pelvis followed by transvaginal scan
 Ultrasound scan of abdomen and pelvis followed by transvaginal scan Radiology Department Patient information leaflet This leaflet has been produced in order to let you know what to expect and how to prepare
Ultrasound scan of abdomen and pelvis followed by transvaginal scan Radiology Department Patient information leaflet This leaflet has been produced in order to let you know what to expect and how to prepare
The Mind Your Memory Group: A supported self management group for individuals with dementia
 The Mind Your Memory Group: A supported self management group for individuals with dementia January 0 Angela Smith, Specialist Occupational Therapist, Old Age Psychiatry, Royal Cornhill Hospital, Aberdeen
The Mind Your Memory Group: A supported self management group for individuals with dementia January 0 Angela Smith, Specialist Occupational Therapist, Old Age Psychiatry, Royal Cornhill Hospital, Aberdeen
Having a Flexible Cystoscopy
 ENDOSCOPY DEPARTMENT Patient Information Having a Flexible Cystoscopy Endoscopy Unit North Wing Entrance 1 Dorset County Hospital Williams Avenue Dorchester DT1 2JY If you need this information in large
ENDOSCOPY DEPARTMENT Patient Information Having a Flexible Cystoscopy Endoscopy Unit North Wing Entrance 1 Dorset County Hospital Williams Avenue Dorchester DT1 2JY If you need this information in large
Hysteroscopy Clinic. Patient Information. Women and Children - Gynaecology
 8 Hysteroscopy Clinic Patient Information Women and Children - Gynaecology When a woman is first told that she has a gynaecological condition that requires further investigation at a specialised hospital
8 Hysteroscopy Clinic Patient Information Women and Children - Gynaecology When a woman is first told that she has a gynaecological condition that requires further investigation at a specialised hospital
Community Sleep Studies Hub and Spoke service Community first attends (schedule 1) and Community follow-ups (schedule 2)
 Community Sleep Studies Hub and Spoke service 2018-2019 Community first attends (schedule 1) and Community follow-ups (schedule 2) 1. Purpose of Agreement This local service agreement is for patients with
Community Sleep Studies Hub and Spoke service 2018-2019 Community first attends (schedule 1) and Community follow-ups (schedule 2) 1. Purpose of Agreement This local service agreement is for patients with
CYSTOSCOPY AND URETHRAL BULKING INJECTIONS INFORMATION FOR PATIENTS
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk CYSTOSCOPY
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk CYSTOSCOPY
Caring for someone who has self-harmed or had suicidal thoughts. A family guide
 Caring for someone who has self-harmed or had suicidal thoughts A family guide This booklet is aimed at the families/carers of people who have self-harmed or had suicidal thoughts. It will be provided
Caring for someone who has self-harmed or had suicidal thoughts A family guide This booklet is aimed at the families/carers of people who have self-harmed or had suicidal thoughts. It will be provided
Intermittent Self-Catheterisation / Catheterisation Continence Advisory Service Community & Therapy Services North Lincolnshire
 Intermittent Self-Catheterisation / Catheterisation Continence Advisory Service Community & Therapy Services North Lincolnshire This leaflet has been designed to give you important information about Intermittent
Intermittent Self-Catheterisation / Catheterisation Continence Advisory Service Community & Therapy Services North Lincolnshire This leaflet has been designed to give you important information about Intermittent
My hip fracture care: 12 questions to ask A guide for patients, their families and carers
 My hip fracture care: 12 questions to ask A guide for patients, their families and carers About this guide This guide is aimed at patients who have a hip fracture, and their families and carers. It explains
My hip fracture care: 12 questions to ask A guide for patients, their families and carers About this guide This guide is aimed at patients who have a hip fracture, and their families and carers. It explains
PELVIC PHYSIOTHERAPY EDUCATION GUIDELINE
 PELVIC PHYSIOTHERAPY EDUCATION GUIDELINE Initiated at the International Continence Society (ICS) Annual Meeting in San Francisco 2009 Initially Adopted by the ICS Physiotherapy Committee September 2010
PELVIC PHYSIOTHERAPY EDUCATION GUIDELINE Initiated at the International Continence Society (ICS) Annual Meeting in San Francisco 2009 Initially Adopted by the ICS Physiotherapy Committee September 2010
Women s & Children s Directorate The TVT Operation - a guide for patients
 Women s & Children s Directorate The TVT Operation - a guide for patients This leaflet was written for women who are considering having a TVT operation. If you have any questions that aren't answered by
Women s & Children s Directorate The TVT Operation - a guide for patients This leaflet was written for women who are considering having a TVT operation. If you have any questions that aren't answered by
