Multiple sclerosis (MS) is the most frequent chronic. ActiGait implantable drop foot stimulator in multiple sclerosis: a new indication
|
|
|
- Harriet Crawford
- 5 years ago
- Views:
Transcription
1 CLINICAL ARTICLE J Neurosurg 126: , 2017 ActiGait implantable drop foot stimulator in multiple sclerosis: a new indication *K. Daniel Martin, MD, 1 Witold H. Polanski, MD, 1 Anne-Kathrin Schulz, 1 Michael Jöbges, MD, PhD, 2 Tjalf Ziemssen, MD, PhD, 3 Gabriele Schackert, MD, PhD, 1 Thomas Pinzer, MD, 1 and Stephan B. Sobottka, MD 1 1 Department of Neurosurgery and 3 Center of Clinical Neuroscience, Department of Neurology, University Hospital Carl-Gustav-Carus, Technical University of Dresden; and 2 Neurologic Rehabilitation Centre, Brandenburg Klinik, Bernau-Waldsiedlung, Germany OBJECTIVE Direct stimulation of the peroneal nerve by the ActiGait implantable drop foot stimulator is a potent therapy that was described previously for stroke-related drop foot. The authors report here successful long-term application of the ActiGait implantable drop foot stimulator in patients with multiple sclerosis (MS). METHODS Six patients with MS and 2 years of persisting central leg paresis received an implantable ActiGait drop foot stimulator after successful surface test stimulation. Ten weeks and 1 year after surgery, their gait speed, endurance, and safety were evaluated. Patient satisfaction was assessed with a questionnaire. RESULTS In the 20-m gait test, stimulation with the ActiGait stimulator significantly reduced the time needed, on average, by approximately 23.6% 10 weeks after surgery, and the time improved further by 36.3% after 1 year. The median distance covered by patients with the stimulator after 6 minutes of walking increased significantly from 217 m to 321 m and remained stable for 1 year; the distance covered by patients after surface stimulation was 264 m. Patients with an implanted ActiGait stimulator noticed pronounced improvement in their mobility, social participation, and quality of life. CONCLUSIONS The ActiGait implantable drop foot stimulator improved gait speed, endurance, and quality of life in all patients over a period of 1 year. It may serve as a new therapeutic option for patients with MS-related drop foot. KEY WORDS ActiGait; multiple sclerosis; neuromodulation; peripheral nerve; drop foot; functional neurosurgery Multiple sclerosis (MS) is the most frequent chronic inflammatory disorder of the central nervous system. During the later phases of the disease, it may result in central paresis of the lower limbs with a drop foot, which can lead to an increased risk of falls, 8 limited mobility, and a reduction in social participation and quality of life. Until now, using an ankle foot orthosis and surface stimulation of the peroneal nerve have been the only therapeutic options. However, increased walking speed and improved ankle and knee kinematics that led to improved quality of life 1 were described recently after surface stimulation of the peroneal nerve. 11,12,15,17 In 12 months of follow-up, this therapeutic effect was reported to be significant, 16 and there is evidence that chronic use of the surface stimulator strengthens activation of the motor cortex and the descending connections. 5 This might lead to an improvement in gait after long-term use, 5 even when the stimulator is off. Direct stimulation of the peroneal nerve by an implantable device was described recently as a new therapeutic option for patients with stroke-related drop foot, and it resulted in improved ankle joint kinematics and increased walking speed. 2 4,10 The advantage of this system is the more specific stimulation. 3 Patients who used this device also reported a better therapeutic effect and easier operability than patients who underwent surface stimulation. 3 ABBREVIATIONS MS = multiple sclerosis. SUBMITTED January 8, ACCEPTED April 7, INCLUDE WHEN CITING Published online July 1, 2016; DOI: / JNS1660. * Drs. Martin and Polanski contributed equally to this work. AANS, 2017 J Neurosurg Volume 126 May
2 K. D. Martin et al. In addition, direct 4-channel nerve stimulation in 2 patients with MS-dependent drop foot was reported to result in improvements in walking speed in a follow-up time of 3 months. 6 Although in patients after stroke and patients with MS, the resulting drop foot is caused by a central lesion, the therapeutic effects of nerve stimulation can differ over time, because MS may be progressive. In contrast, patients with MS tend to be younger and suffer less morbidity than patients after stroke, and they might experience a greater benefit from nerve stimulation and improvement in their quality of life. In this study, we report the first, to our knowledge, successful long-term benefit of the ActiGait (Neurodan) implantable drop foot stimulator in 6 patients with MSrelated drop foot. Methods Patient Screening Six patients with at least 1 year of stable MS and 2 years of persisting spastic paresis of the leg with a drop foot were offered a new therapeutic option via an implantable drop foot stimulator (patient characteristics are listed in Table 1). The drop foot was diagnosed according to features described by Perry et al., 13 including a dragging foot during the swing phase. The possible benefit of an implantable stimulator was tested preoperatively by external functional surface stimulation of the peroneal nerve (CE- FAR Step II [Compex Scandinavia AB], SN , output 60 ma, frequency Hz) with dorsiflexion of the ankle. This observational study was approved by the Technical University of Dresden ethics committee. The trial did not involve experimental medication, surgical products, or techniques. Gait Tests To evaluate possible changes in walking speed, patients were asked to walk 20 m, and the time needed was documented. This test was performed preoperatively without walking aids, with an ankle orthosis, and with a surface stimulator and 10 weeks and 1 year after implantation of the ActiGait system. In each case, the patient was asked to perform the test at normal walking speed ( pleasant gait) and as fast as possible ( maximal gait). In addition, walking endurance was tested by having the patient walk for 6 minutes continuously before and after surgery. Finally, to assess the risk of falls, the time needed to stand up from a chair, walk 3 m, and go back and be seated again was measured (Timed Up and Go test). 14 All 3 tests were performed without any medical aids, with an ankle foot orthosis (tested only in the 20-m gait test), and with surface stimulation before the operation and with the activated ActiGait stimulator 10 weeks and 1 year after the operation. In addition, patient satisfaction was assessed with a subjective quality-of-life questionnaire (Table 2). Surgery For this study, the patients underwent implantation of the ActiGait system, which consists of an implantable 4-channel drop foot stimulator, an external control unit, a footswitch, and a clinical station 2 4,9,10 (Fig. 1). MRI of TABLE 1. Patient characteristics and stimulation parameters of 6 patients with MS who underwent implantation of an ActiGait drop foot stimulator 20-m Gait Test/Walking Speed (sec) 6-min Walking Test (m) Timed Up & Go Test (sec) w/ Stimulation w/ Stimulation w/ Stimulation Stimulation Parameters 1 yr 10 wks w/o Stimulation 1 yr 10 wks w/o Stimulation 1 yr 10 wks w/o Stimulation Muscle Strength of Foot Elevation* Duration of Drop Foot (yrs) Age (yrs) Side of Hemiplegia Pt No. Sex 1 M Lt / Channels 1 & 4 active; 1 ma; 30 Hz; optimal impulse duration 70 μsec; heel switch, ipsilat 2 F Rt / Channel 1 active; 1 ma; 20 Hz; optimal impulse duration 70 μsec; heel switch, ipsilat 3 F Lt / Channel 4 active; 1 ma; 20 Hz; optimal impulse duration 70 μsec; heel switch, ipsilat 4 M Rt / Channel 4 active; 20 Hz; optimal impulse duration 60 μsec; heel switch, ipsilat 5 F Rt / Channels 1 and 4 active; 25 Hz; optimal impulse duration 65 μsec; heel switch, ipsilat 6 F Lt / Channel 4 active; 25 Hz; optimal impulse duration 70 μsec; heel switch, ipsilat Pt = patient. * Scores based on the Janda Classification J Neurosurg Volume 126 May 2017
3 Implantable drop foot stimulator for patients with MS TABLE 2. Subjective quality-of-life survey from 6 patients with MS 1 year after implantation of an ActiGait drop foot stimulator Pt No. Have You Noticed Changes in Mobility in Daily Living? (go for a walk, shopping, public transit)* Have You Noticed Changes in Interpersonal Contacts & Social Participation? Would You Recommend the Operation? Have You Noticed Changes in Your Quality Of Life? * 1 = worsening; 0 = no changes; 1 = only minor improvement; 2 = marked improvement; 3 = pronounced improvement, complete return to normal (life). 1 = less social interaction; 0 = no changes; 1 = only minor improvement; 2 = marked improvement; 3 = pronounced improvement, complete return to normal (life). 1 = no; 0 = unsure; 1 = yes. 1 = worsening; 0 = no changes; 1 = only minor improvement; 2 = marked improvement; 3 = pronounced improvement, complete return to normal (life). the leg was performed preoperatively to determine the anatomical localization of the bifurcation of the sensible branch of the common peroneal nerve for proper electrode positioning. The operation was performed with the patient under general anesthesia, as described by Martin et al. 9 In brief, the common peroneal nerve was exposed above the knee for 4 cm, and dorsiflexion was tested using a nerve stimulator (GN 015). ward, the electrode cuff was closed around the nerve, and the stimulator body was fixed to the lateral femoral fascia. Finally, the correct positions of the cuff and the stimulator were controlled visually in maximal flexion and extension of the knee to ensure free gliding of the cuff. 60 minutes. Each patient described the handling of the ActiGait system in daily living as being uncomplicated and easy. Walking Speed (20-m Gait Test) The mean time to walk 20 m at normal walking speed was significantly (p = 0.003) decreased from 25.9 (± 4.4) seconds preoperatively without walking aids to 19.8 (± 2.9) seconds with ActiGait stimulation 10 weeks after sur- Postoperative Care and Programming of the Stimulator For the first 4 weeks after surgery, the patients had to restrict the movement of the leg on which surgery was performed to a maximal knee flexion of 30. To avoid contractures during this time period, the Achilles tendon was stretched passively. ward, every channel was tested for the best dorsiflexion, and the stimulator was activated with 1 ma, Hz, and an optimal impulse duration of 70 μsec (Table 1). Patients were able to readjust the impulse intensity with a programmer. Gait evaluation was performed after 10 weeks to measure gait speed and walking endurance, and the Timed Up and Go test was repeated. In addition, a subjective quality-of-life survey was given. All tests were repeated 1 year after surgery. Statistics The results of the gait tests are expressed as mean ± SEM. The significance level was calculated with a Mann- Whitney U-test in Excel 2010 software. Results Surgery and Postoperative Care Implantation of the ActiGait system in 6 patients with MS resulted in no technical or surgical complications. The implantable device did not appear bulky but was palpable in every patient. Programming of the ActiGait stimulator, as described above, was uncomplicated for all 6 patients. The programming time demand ranged between 45 and FIG. 1. Schematic illustration of the implantable and nonimplantable components of the ActiGait drop foot stimulator. The system consists of an external control unit (1) with a transmission coil (antenna) (2), which receives signals from the external footswitch (5) via a wireless radiofrequency signal. It enables precise activation depending on the gait cycle and allows for the adjustment of the stimulation parameters. The subcutaneously implanted stimulator (3) is connected to the 4-channel cuff (4), which is placed around the peroneal nerve. The stimulator communicates via a wireless radio frequency signal with the antenna and transmits the stimulation signals. Copyright Klaus Daniel Martin. Published with permission. J Neurosurg Volume 126 May
4 K. D. Martin et al. FIG. 2. Evaluation of mean walking speeds in the 20-m gait test at pleasant and maximal walking speeds preoperatively and 10 weeks and 1 year after ActiGait implantation in 6 patients with MS. *p < 0.05 compared with no stimulation; #p < 0.05 compared with use of ankle orthosis; p < 0.05 compared with surface stimulation. gery and decreased further to 16.5 (± 2) seconds 1 year after implantation. Surface stimulation also resulted in a significant (p < 0.05) reduction in the mean time needed (to 21.4 ± 2.3 seconds). Ten weeks after surgery, there were no significant differences between ActiGait stimulation and surface stimulation. However, after 1 year, the Acti- Gait stimulator resulted in significant improvement over surface stimulation (p < 0.05). In contrast, the use of an ankle orthosis resulted in no significant change in walking speed over that with no walking aids. Similar results were observed under maximal gait-speed conditions (Fig. 2). Video 1 exemplarily shows Patient 2 without walking aids and with ActiGait stimulation 1 year after surgery. VIDEO 1. Clip showing walking speed of a patient with an activated ActiGait drop foot stimulator and no walking aids 1 year after surgery. Copyright Klaus Daniel Martin. Published with permission. Click here to view. 6-Minute Walking Test Gait endurance was examined by measuring the distances that the patients walked within 6 minutes. Before stimulation, the patients walked, on average, 215 ± 15.6 m in 6 minutes. With surface stimulation, the mean distance increased significantly (p < 0.05) to 261 ± 16 m. the patients underwent ActiGait implantation, their mean covered distance increased even further to 315 ± 9.5 m 10 weeks after surgery and remained stable at 325 ± 8 m 1 year after implantation (Fig. 3). This result, compared with those for patients without walking aids (p < 0.05) and with surface stimulation (p < 0.05), is significant. Timed Up and Go Test To assess activation time and the risk of falls, the Timed Up and Go test was performed without walking aids, with surface stimulation, and with ActiGait stimulation. The time needed for the test without walking aids was 19.5 ± 6.8 seconds, which indicates mild mobility impairment (> 10 seconds needed). surface stimulation, the time was reduced significantly to 13.2 ± 3.3 seconds. ActiGait stimulation 10 weeks after implantation led to a further reduction of the time needed to 9.29 ± 1.2 seconds, which was significant compared with surface stimulation, and a slight increase to ± 2.4 seconds 1 year after surgery (Fig. 4). Subjective Quality-of-Life Survey For subjective changes in daily living after implantation of the ActiGait stimulator, the patients were asked to answer a short quality-of-life survey (Table 2). Four patients noticed an improvement in their mobility in daily living up to normal, in quality of life, and in social participation; 2 patients stated that they had a marked improvement. All of the patients said that they would recommend the surgical procedure. Discussion The aim of this study was to elucidate whether the ActiGait implantable drop foot stimulator can provide longterm improvements in gait speed and endurance and re- FIG. 3. Mean covered distances after 6 minutes of walking by 6 patients with MS with an ActiGait drop foot stimulator 10 weeks and 1 year after implantation. *p < 0.05 compared with no stimulation; #p < 0.05 compared with surface stimulation J Neurosurg Volume 126 May 2017
5 Implantable drop foot stimulator for patients with MS FIG. 4. Mean times needed to complete the Timed Up and Go tests by 6 patients with MS 10 weeks and 1 year after implantation of an ActiGait drop foot stimulator. *p < 0.05 compared with no stimulation; #p < 0.05 compared with surface stimulation. duce the risk of falls in patients with MS-related drop foot, because its efficacy and superiority over surface stimulation in patients after stroke were reported recently. 10,16 In this study, no adverse events were observed. Until now, only rare complications, such as hematoma and lymphedema (both in 1 of 5 patients), 16 wound-healing deficit (1 of 15 patients) and infections (2 of 15 patients), 3 and injury to the peroneal nerve (2 of 27 patients), 10 have been reported. The surgery and postoperative care were easy and uncomplicated. The patients had no problems using the ActiGait stimulator in daily living. In addition, recent reports have shown that the implantable device is easier to use than the surface stimulator. 3 Gait evaluations revealed that walking speed was increased significantly by 30.8% 10 weeks after using the ActiGait system and increased more significantly by 57.0% 1 year after surgery. These results are comparable with recent findings in patients after stroke, in which ActiGait stimulation resulted in improvements of 19% 4 and 25% 10 in a 10-m gait test and 47% 10 in a 20-m gait test. In our study, the implantable stimulator was superior to an ankle foot orthosis (p = ) and to surface stimulation after 10 weeks, but the difference was not significant (p = ). However, after 1 year, a significant improvement in gait over that with surface stimulation (p = ) and with the foot orthosis (p = ) was found. In addition, gait endurance was improved significantly by 47% 10 weeks after surgery and increased further to 52% improvement after 1 year. Compared with surface stimulation, which had already improved gait endurance, ActiGait stimulation resulted in a pronounced and significant increase in the distance covered by our patients in the 6-minute walking test, and the therapeutic effect was stable over a period of 1 year. This result confirms the superiority of the implantable stimulator over surface stimulation. These findings might be explained by the fact that an implantable stimulator provides more specific stimulation with finer adjustability of stimulation parameters than does surface stimulation, and it produces a considerable orthotic effect with more physiological kinematics in the lower limb. 16 Furthermore, in the Timed Up and Go test 10 weeks after surgery, a nonsignificant improvement of 47% was measured for patients with the ActiGait stimulator as a result of a safer gait. One year after implantation, this effect decreased to 43% but remained higher than the improvement with surface stimulation (29% improvement compared with no walking aids). In this test, a normal gait without increased risk of falls is determined by a time needed of less than 10 seconds. 14 Only with ActiGait stimulation was this criterion reached, with 9.3 (± 0.9) seconds needed to finish the test. Finally, all 6 patients noticed at least a marked improvement of mobility in daily living, in quality of life, and in social participation, and they had no regrets about the implantation. Conclusions The ActiGait implantable drop foot stimulator is a safe and simple device for drop foot caused by a lesion of the central nervous system. It improved gait speed and endurance and quality of life and reduced the risk of falls in all 6 patients with MS. In addition, these results were stable and even improved further over a period of 1 year. These results are comparable with recent reported improvements in patients after stroke. Acknowledgments We thank Andrei Patriciu for excellent technical help during the surgical procedures and programming of the ActiGait stimulator and Prof. Jens Haase for scientific discussions. References 1. Barrett C, Taylor P: The effects of the Odstock drop foot stimulator on perceived quality of life for people with stroke and multiple sclerosis. Neuromodulation 13:58 64, Burridge JH, Haugland M, Larsen B, Pickering RM, Svaneborg N, Iversen HK, et al: Phase II trial to evaluate the ActiGait implanted drop-foot stimulator in established hemiplegia. J Rehabil Med 39: , Burridge JH, Haugland M, Larsen B, Svaneborg N, Iversen HK, Christensen PB, et al: Patients perceptions of the benefits and problems of using the ActiGait implanted drop-foot stimulator. J Rehabil Med 40: , Ernst J, Grundey J, Hewitt M, von Lewinski F, Kaus J, Schmalz T, et al: Towards physiological ankle movements with the ActiGait implantable drop foot stimulator in chronic stroke. Restor Neurol Neurosci 31: , Everaert DG, Thompson AK, Chong SL, Stein RB: Does functional electrical stimulation for foot drop strengthen corticospinal connections? Neurorehabil Neural Repair 24: , Hausmann J, Sweeney-Reed CM, Sobieray U, Matzke M, Heinze HJ, Voges J, et al: Functional electrical stimulation through direct 4-channel nerve stimulation to improve gait in multiple sclerosis: a feasibility study. J Neuroeng Rehabil 12:100, Janda DH, Geiringer SR, Hankin FM, Barry DT: Objective evaluation of grip strength. J Occup Med 29: , 1987 J Neurosurg Volume 126 May
6 K. D. Martin et al. 8. Luukinen H, Koski K, Laippala P, Kivelä SL: Predictors for recurrent falls among the home-dwelling elderly. Scand J Prim Health Care 13: , Martin KD, Polanski W, Schackert G, Sobottka SB: New therapeutic option for drop foot with the ActiGait peroneal nerve stimulator a technical note. World Neurosurg 84: , Martin KD, Polanski WH, Schulz AK, Jöbges M, Hoff H, Schackert G, et al: Restoration of ankle movements with the ActiGait implantable drop foot stimulator: a safe and reliable treatment option for permanent central leg palsy. J Neurosurg 124:70 76, Miller L, Rafferty D, Paul L, Mattison P: A comparison of the orthotic effect of the Odstock dropped foot stimulator and the Walkaide functional electrical stimulation systems on energy cost and speed of walking in multiple sclerosis. Disabil Rehabil Assist Technol 10: , Paul L, Rafferty D, Young S, Miller L, Mattison P, McFadyen A: The effect of functional electrical stimulation on the physiological cost of gait in people with multiple sclerosis. Mult Scler 14: , Perry J, Garrett M, Gronley JK, Mulroy SJ: Classification of walking handicap in the stroke population. Stroke 26: , Podsiadlo D, Richardson S: The timed Up & Go : a test of basic functional mobility for frail elderly persons. J Am Geriatr Soc 39: , Scott SM, van der Linden ML, Hooper JE, Cowan P, Mercer TH: Quantification of gait kinematics and walking ability of people with multiple sclerosis who are new users of functional electrical stimulation. J Rehabil Med 45: , Stein RB, Everaert DG, Thompson AK, Chong SL, Whittaker M, Robertson J, et al: Long-term therapeutic and orthotic effects of a foot drop stimulator on walking performance in progressive and nonprogressive neurological disorders. Neurorehabil Neural Repair 24: , Taylor P, Barrett C, Mann G, Wareham W, Swain I: A feasibility study to investigate the effect of functional electrical stimulation and physiotherapy exercise on the quality of gait of people with multiple sclerosis. Neuromodulation 17:75 84, 2014 Disclosures The authors report no conflict of interest concerning the materials or methods used in this study or the findings specified in this paper. Author Contributions Conception and design: Martin, Polanski. Acquisition of data: Martin, Polanski, Schulz. Analysis and interpretation of data: Martin, Polanski, Schulz, Jöbges. Drafting the article: Martin, Polanski, Sobottka. Critically revising the article: Polanski, Ziemssen, Schackert, Pinzer, Sobottka, Jöbges. Reviewed submitted version of manuscript: Martin, Polanski, Schackert, Pinzer. Approved the final version of the manuscript on behalf of all authors: Martin. Statistical analysis: Polanski. Administrative/ technical/material support: Martin, Ziemssen, Schackert. Study supervision: Sobottka. Supplemental Information Videos Video 1. Correspondence K. Daniel Martin, Department of Neurological Surgery, Carl- Gustav-Carus University Hospital of the Technical University of Dresden, Fetscherstrasse 74, Dresden 01307, Germany. kontakt@dr-daniel-martin.com J Neurosurg Volume 126 May 2017
A preliminary non-randomised study to evaluate the safety and performance of the ActiGait implanted drop-foot stimulator in established hemiplegia
 A preliminary non-randomised study to evaluate the safety and performance of the ActiGait implanted drop-foot stimulator in established hemiplegia Haugland M, Larsen B, Burridge J, Svaneborg N, Iversen
A preliminary non-randomised study to evaluate the safety and performance of the ActiGait implanted drop-foot stimulator in established hemiplegia Haugland M, Larsen B, Burridge J, Svaneborg N, Iversen
Medical Coverage Policy Functional Neuromuscular Electrical Stimulation EFFECTIVE DATE: 10/16/212 POLICY LAST UPDATED: 09/11/2014
 Medical Coverage Policy Functional Neuromuscular Electrical Stimulation EFFECTIVE DATE: 10/16/212 POLICY LAST UPDATED: 09/11/2014 OVERVIEW Neuromuscular Electrical Stimulation, (NMES), involves the use
Medical Coverage Policy Functional Neuromuscular Electrical Stimulation EFFECTIVE DATE: 10/16/212 POLICY LAST UPDATED: 09/11/2014 OVERVIEW Neuromuscular Electrical Stimulation, (NMES), involves the use
Configure for Diverse
 Configure for Diverse Clinical Needs Foot Drop Lower Cuff Foot Drop & Knee Instability Lower & Thigh Cuffs Pediatric Foot Drop Small Lower Cuff Foot Sensor: required for gait Knee Instability & Thigh Weakness
Configure for Diverse Clinical Needs Foot Drop Lower Cuff Foot Drop & Knee Instability Lower & Thigh Cuffs Pediatric Foot Drop Small Lower Cuff Foot Sensor: required for gait Knee Instability & Thigh Weakness
Protocol. Functional Neuromuscular Electrical Stimulation
 Protocol Functional Neuromuscular Electrical Stimulation (80301) Medical Benefit Effective Date: 04/01/10 Next Review Date: 01/13 Preauthorization* Yes Review Dates: 03/07, 05/08, 05/09, 01/10, 01/11,
Protocol Functional Neuromuscular Electrical Stimulation (80301) Medical Benefit Effective Date: 04/01/10 Next Review Date: 01/13 Preauthorization* Yes Review Dates: 03/07, 05/08, 05/09, 01/10, 01/11,
Precise Pulses Optimised Support
 Precise Pulses Optimised Support The Functional Electrical Stimulation (FES) MyGait system for drop foot and gait rehabilitation Information for clinical specialists MyGait Ottobock 1 2 Ottobock MyGait
Precise Pulses Optimised Support The Functional Electrical Stimulation (FES) MyGait system for drop foot and gait rehabilitation Information for clinical specialists MyGait Ottobock 1 2 Ottobock MyGait
Lack of muscle control (Stroke, bladder control, neurological disorders) Mechanical movement therapist assisted
 By Lisa Rosenberg Electrical Current Stimulates muscles and nerves Produces movement Helps Individuals with Disabilities Lack of muscle control (Stroke, bladder control, neurological disorders) Passive
By Lisa Rosenberg Electrical Current Stimulates muscles and nerves Produces movement Helps Individuals with Disabilities Lack of muscle control (Stroke, bladder control, neurological disorders) Passive
Toe walking gives rise to parental concern. Therefore, toe-walkers are often referred at the 3 years of age.
 IDIOPATHIC TOE WALKING Toe walking is a common feature in immature gait and is considered normal up to 3 years of age. As walking ability improves, initial contact is made with the heel. Toe walking gives
IDIOPATHIC TOE WALKING Toe walking is a common feature in immature gait and is considered normal up to 3 years of age. As walking ability improves, initial contact is made with the heel. Toe walking gives
III. Based upon our criteria and review of the peer-reviewed literature, NMES has not been proven to be effective and is
 MEDICAL POLICY SUBJECT: NEUROMUSCULAR ELECTRICAL PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
MEDICAL POLICY SUBJECT: NEUROMUSCULAR ELECTRICAL PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
Created in January 2005 Duration: approx. 20 minutes
 1 1 The Timed Up and Go Test Created in January 2005 Duration: approx. 20 minutes 2 Credits 2005 Stein Gerontological Institute. All rights reserved. Principal medical contributors: Alan Katz, MD Francois
1 1 The Timed Up and Go Test Created in January 2005 Duration: approx. 20 minutes 2 Credits 2005 Stein Gerontological Institute. All rights reserved. Principal medical contributors: Alan Katz, MD Francois
Effectiveness of a home-based rehabilitation programme on lower limb functions after stroke
 HEALTH SERVICES RESEARCH FUND CWY Hui-Chan 許陳雲影 SSM Ng 伍尚美 MKY Mak 麥潔儀 Effectiveness of a home-based rehabilitation programme on lower limb functions after stroke Key Messages 1. Home-based rehabilitation
HEALTH SERVICES RESEARCH FUND CWY Hui-Chan 許陳雲影 SSM Ng 伍尚美 MKY Mak 麥潔儀 Effectiveness of a home-based rehabilitation programme on lower limb functions after stroke Key Messages 1. Home-based rehabilitation
Functional Ability Screening Tools for the Clinic
 Functional Ability Screening Tools for the Clinic Shelley Hockensmith,, P.T., NCS Objectives Review screening tools for physical or functional ability including Five Times Sit to Stand, Walking Speed,
Functional Ability Screening Tools for the Clinic Shelley Hockensmith,, P.T., NCS Objectives Review screening tools for physical or functional ability including Five Times Sit to Stand, Walking Speed,
NeuroOrthopaedics upper extremities
 NeuroOrthopaedics upper extremities Medical devices for deficiencies in the arm-shoulder-hand region Information for practitioners Effectively supporting rehabilitation of the hand and shoulder Strokes
NeuroOrthopaedics upper extremities Medical devices for deficiencies in the arm-shoulder-hand region Information for practitioners Effectively supporting rehabilitation of the hand and shoulder Strokes
2/24/2014. Outline. Anterior Orthotic Management for the Chronic Post Stroke Patient. Terminology. Terminology ROM. Physical Evaluation
 Outline Anterior Orthotic Management for the Chronic Post Stroke Patient Physical Evaluation Design Considerations Orthotic Design Jason M. Jennings CPO, LPO, FAAOP jajennings@hanger.com Primary patterning
Outline Anterior Orthotic Management for the Chronic Post Stroke Patient Physical Evaluation Design Considerations Orthotic Design Jason M. Jennings CPO, LPO, FAAOP jajennings@hanger.com Primary patterning
2 Gait Laboratory, Queen Mary's Hospital, London, UK. 3 One Small Step Gait Laboratory, Guy's Hospital London, UK
 Upper and Lower Limb Electrical Stimulation in Paediatrics Held at Queen Mary's Hospital, Roehampton, London Thursday, 13th June 2002 The aim of the workshop was to promote discussion and the exchange
Upper and Lower Limb Electrical Stimulation in Paediatrics Held at Queen Mary's Hospital, Roehampton, London Thursday, 13th June 2002 The aim of the workshop was to promote discussion and the exchange
Functional Electrical Stimulation for foot drop in Multiple Sclerosis: A. Systematic Review and Meta-Analysis of the impact on gait speed.
 1 2 3 4 Functional Electrical Stimulation for foot drop in Multiple Sclerosis: A Systematic Review and Meta-Analysis of the impact on gait speed. Miller L, MPhil 1, 2, McFadyen A, PhD 3, Lord AC, MSc 1,
1 2 3 4 Functional Electrical Stimulation for foot drop in Multiple Sclerosis: A Systematic Review and Meta-Analysis of the impact on gait speed. Miller L, MPhil 1, 2, McFadyen A, PhD 3, Lord AC, MSc 1,
Functional Neuromuscular Electrical Stimulation. Description
 Subject: Functional Neuromuscular Electrical Stimulation Page: 1 of 16 Last Review Status/Date: June 2015 Functional Neuromuscular Electrical Stimulation Description Functional neuromuscular electrical
Subject: Functional Neuromuscular Electrical Stimulation Page: 1 of 16 Last Review Status/Date: June 2015 Functional Neuromuscular Electrical Stimulation Description Functional neuromuscular electrical
Sunshine Prosthetics & Orthotics, LLC 1700 Rt. 23 N Ste 180 Wayne NJ Functional electrical stimulation (FES)
 Functional electrical stimulation (FES) We hope you find the information in this factsheet helpful. If you would like to speak with someone about any aspect of MS, contact the MS Trust information team
Functional electrical stimulation (FES) We hope you find the information in this factsheet helpful. If you would like to speak with someone about any aspect of MS, contact the MS Trust information team
ii. Reduction of tone in upper limb Lycra arm splints improve movement fluency in children with cerebral palsy.
 Guidelines for the Provision of Dynamic Compression for people diagnosed with Multiple Sclerosis The use of Lycra garments in patients with the diagnosis of Multiple Sclerosis has been initiated with very
Guidelines for the Provision of Dynamic Compression for people diagnosed with Multiple Sclerosis The use of Lycra garments in patients with the diagnosis of Multiple Sclerosis has been initiated with very
Patient Details Front Sheet
 Name DOB/ PID ODSTOCK MEDICAL LIMITED National Clinical FES Centre - Salisbury Quality Form QF/020 Clinical Care Pathway; ODFS Patient Details Front Sheet Address Contact telephone numbers; Home Work Mobile..
Name DOB/ PID ODSTOCK MEDICAL LIMITED National Clinical FES Centre - Salisbury Quality Form QF/020 Clinical Care Pathway; ODFS Patient Details Front Sheet Address Contact telephone numbers; Home Work Mobile..
Ratified by: Care and Clinical Policies Date: 17 th February 2016
 Clinical Guideline Reference Number: 0803 Version 5 Title: Physiotherapy guidelines for the Management of People with Multiple Sclerosis Document Author: Henrieke Dimmendaal / Laura Shenton Date February
Clinical Guideline Reference Number: 0803 Version 5 Title: Physiotherapy guidelines for the Management of People with Multiple Sclerosis Document Author: Henrieke Dimmendaal / Laura Shenton Date February
Clinical Laboratory of Experimental Neurorehabilitation, I.R.C.C.S., Santa Lucia Foundation, Via Ardeatina 306, Rome, Italy 2
 Stroke Research and Treatment Volume 2012, Article ID 523564, 5 pages doi:10.1155/2012/523564 Clinical Study Walking Training with Foot Drop Stimulator Controlled by a Tilt Sensor to Improve Walking Outcomes:
Stroke Research and Treatment Volume 2012, Article ID 523564, 5 pages doi:10.1155/2012/523564 Clinical Study Walking Training with Foot Drop Stimulator Controlled by a Tilt Sensor to Improve Walking Outcomes:
A Measurement of Lower Limb Angles Using Wireless Inertial Sensors during FES Assisted Foot Drop Correction with and without Voluntary Effort
 A Measurement of Lower Limb Angles Using Wireless Inertial Sensors during FES Assisted Foot Drop Correction with and without Voluntary Effort Takashi Watanabe, Shun Endo, Katsunori Murakami, Yoshimi Kumagai,
A Measurement of Lower Limb Angles Using Wireless Inertial Sensors during FES Assisted Foot Drop Correction with and without Voluntary Effort Takashi Watanabe, Shun Endo, Katsunori Murakami, Yoshimi Kumagai,
Department of Physical Medicine and Rehabilitation
 For enquiries and appointments, please contact us at: 物理醫學及復康科部 Department of Physical Medicine and Rehabilitation Department of Physical Medicine and Rehabilitation 5/F, Li Shu Pui Block, Hong Kong Sanatorium
For enquiries and appointments, please contact us at: 物理醫學及復康科部 Department of Physical Medicine and Rehabilitation Department of Physical Medicine and Rehabilitation 5/F, Li Shu Pui Block, Hong Kong Sanatorium
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: neurostimulation_electrical 4/2004 10/2017 10/2018 10/2017 Description of Procedure or Service Neuromuscular
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: neurostimulation_electrical 4/2004 10/2017 10/2018 10/2017 Description of Procedure or Service Neuromuscular
Rehabilitation and Return to Play Following Achilles Tendon Repair
 Rehabilitation and Return to Play Following Achilles Tendon Repair Monte Wong PT, DPT, SCS, ATC, CSCS Assistant Athletic Trainer/Physical Therapist Philadelphia Eagles Mechanism of Injury 1.) forceful
Rehabilitation and Return to Play Following Achilles Tendon Repair Monte Wong PT, DPT, SCS, ATC, CSCS Assistant Athletic Trainer/Physical Therapist Philadelphia Eagles Mechanism of Injury 1.) forceful
Vibramoov NEUROREHABILITATION OF THE LOCOMOTOR SYSTEM THROUGH FUNCTIONAL PROPRIOCEPTIVE STIMULATION
 Vibramoov NEUROREHABILITATION OF THE LOCOMOTOR SYSTEM THROUGH FUNCTIONAL PROPRIOCEPTIVE STIMULATION Principe of action BRAIN ACTIVATION VIBRAMOOV REVOLUTIONIZES FUNCTIONAL MOVEMENT THERAPY One of the main
Vibramoov NEUROREHABILITATION OF THE LOCOMOTOR SYSTEM THROUGH FUNCTIONAL PROPRIOCEPTIVE STIMULATION Principe of action BRAIN ACTIVATION VIBRAMOOV REVOLUTIONIZES FUNCTIONAL MOVEMENT THERAPY One of the main
Subject: Functional Neuromuscular Stimulation
 09-E0000-54 Original Effective Date: 04/15/02 Reviewed: 08/23/18 Revised: 09/15/18 Subject: Functional Neuromuscular Stimulation THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION, CERTIFICATION,
09-E0000-54 Original Effective Date: 04/15/02 Reviewed: 08/23/18 Revised: 09/15/18 Subject: Functional Neuromuscular Stimulation THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION, CERTIFICATION,
Salisbury FES User Day Friday, 22 nd February 2013
 Salisbury FES User Day Friday, 22 nd February 2013 RCP Guidelines The fourth addition of the Royal College of Physicians National Clinical Guideline for Stroke has been published. The guidelines have been
Salisbury FES User Day Friday, 22 nd February 2013 RCP Guidelines The fourth addition of the Royal College of Physicians National Clinical Guideline for Stroke has been published. The guidelines have been
Total Hip Replacement Rehabilitation: Progression and Restrictions
 Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
Protocols for Posterior Tibial Tendon Dysfunction & Achilles Tendinosis. Tara Bries, PT
 Protocols for Posterior Tibial Tendon Dysfunction & Achilles Tendinosis Tara Bries, PT Non-Operative Protocol for Posterior Tibialis Tendon Dysfunction Based on research by Alvarez et al. (2006) entitled
Protocols for Posterior Tibial Tendon Dysfunction & Achilles Tendinosis Tara Bries, PT Non-Operative Protocol for Posterior Tibialis Tendon Dysfunction Based on research by Alvarez et al. (2006) entitled
Adam N. Whatley, M.D Main St., STE Zachary, LA Phone(225) Fax(225)
 Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Knee Arthroplasty Protocol: The intent of this protocol is to provide the clinician with a guideline
Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Knee Arthroplasty Protocol: The intent of this protocol is to provide the clinician with a guideline
ACHILLES TENDON REPAIR REHAB GUIDELINES
 ACHILLES TENDON REPAIR REHAB GUIDELINES Typically patients are discharged on the day of the operation or the next day. The leg is usually immobilized in a cast or hinged brace, ranging from 4-8 weeks.
ACHILLES TENDON REPAIR REHAB GUIDELINES Typically patients are discharged on the day of the operation or the next day. The leg is usually immobilized in a cast or hinged brace, ranging from 4-8 weeks.
Omo and Manu Neurexa plus
 Omo and Manu Neurexa plus Promote movement. Stay independent. Information for specialists Omo and Manu Neurexa plus Effectively supporting rehabilitation of the hand and shoulder The devices in the Neurexa
Omo and Manu Neurexa plus Promote movement. Stay independent. Information for specialists Omo and Manu Neurexa plus Effectively supporting rehabilitation of the hand and shoulder The devices in the Neurexa
are: Standard of care are: are:
 Protocol Functional Neuromuscular Electrical Stimulation (80301) Medical Benefit Effective Date: 07/01/16 Next Review Date: 05/19 Preauthorization Yes Review Dates: 03/07, 05/08, 05/09, 01/10, 01/11, 01/12,
Protocol Functional Neuromuscular Electrical Stimulation (80301) Medical Benefit Effective Date: 07/01/16 Next Review Date: 05/19 Preauthorization Yes Review Dates: 03/07, 05/08, 05/09, 01/10, 01/11, 01/12,
How Biodex programs give UHS Pruitt the clinical advantage BIODEX
 CASESTUDY How Biodex programs give UHS Pruitt the clinical advantage UHS Pruitt Corporation BIODEX Biodex Medical Systems, Inc. 20 Ramsey Road, Shirley, New York, 11967-4704, Tel: 800-224-6339 (Int l 631-924-9000),
CASESTUDY How Biodex programs give UHS Pruitt the clinical advantage UHS Pruitt Corporation BIODEX Biodex Medical Systems, Inc. 20 Ramsey Road, Shirley, New York, 11967-4704, Tel: 800-224-6339 (Int l 631-924-9000),
Selective Motor Control Assessment of the Lower Extremity in Patients with Spastic Cerebral Palsy
 Overview Selective Motor Control Assessment of the Lower Extremity in Patients with Spastic Cerebral Palsy Marcia Greenberg MS, PT* Loretta Staudt MS, PT* Eileen Fowler PT, PhD Selective Motor Control
Overview Selective Motor Control Assessment of the Lower Extremity in Patients with Spastic Cerebral Palsy Marcia Greenberg MS, PT* Loretta Staudt MS, PT* Eileen Fowler PT, PhD Selective Motor Control
Are randomised controlled trials telling us what rehabilitation interventions work?
 Are randomised controlled trials telling us what rehabilitation interventions work? Focus on stroke Jane Burridge March 6 th 2014 Neurorehabilitation: facts, fears and the future Overview Stroke recovery
Are randomised controlled trials telling us what rehabilitation interventions work? Focus on stroke Jane Burridge March 6 th 2014 Neurorehabilitation: facts, fears and the future Overview Stroke recovery
WHY THE HEEL? Sharon Lucich, PT, CWS. By the end of this session, the learner will be able to:
 WHY THE HEEL? Sharon Lucich, PT, CWS Objectives By the end of this session, the learner will be able to: 1. Describe the unique anatomical features that contribute to the development of heel pressure ulcers
WHY THE HEEL? Sharon Lucich, PT, CWS Objectives By the end of this session, the learner will be able to: 1. Describe the unique anatomical features that contribute to the development of heel pressure ulcers
A new model of plastic ankle foot orthosis (FAFO (II)) against spastic foot and genu recurvatum
 Prosthetics and Orthotics International, 1992,16,104-108 A new model of plastic ankle foot orthosis (FAFO (II)) against spastic foot and genu recurvatum *S. OHSAWA, S. IKEDA, S. TANAKA, T. TAKAHASHI, +
Prosthetics and Orthotics International, 1992,16,104-108 A new model of plastic ankle foot orthosis (FAFO (II)) against spastic foot and genu recurvatum *S. OHSAWA, S. IKEDA, S. TANAKA, T. TAKAHASHI, +
1-Apley scratch test.
 1-Apley scratch test. The patient attempts to touch the opposite scapula to test range of motion of the shoulder. 1-Testing abduction and external rotation( +ve sign touch the opposite scapula, -ve sign
1-Apley scratch test. The patient attempts to touch the opposite scapula to test range of motion of the shoulder. 1-Testing abduction and external rotation( +ve sign touch the opposite scapula, -ve sign
William C Miller, PhD, FCAOT Professor Occupational Science & Occupational Therapy University of British Columbia Vancouver, BC, Canada
 William C Miller, PhD, FCAOT Professor Occupational Science & Occupational Therapy University of British Columbia Vancouver, BC, Canada THE L TEST MANUAL Version: November 2014 Table of Contents Introduction...
William C Miller, PhD, FCAOT Professor Occupational Science & Occupational Therapy University of British Columbia Vancouver, BC, Canada THE L TEST MANUAL Version: November 2014 Table of Contents Introduction...
MUSCULOSKELETAL AND NEUROLOGICAL DISORDERS
 MUSCULOSKELETAL AND NEUROLOGICAL DISORDERS There are a wide variety of Neurologic and Musculoskeletal disorders which can impact driving safety. Impairment may be the result of altered muscular, skeletal,
MUSCULOSKELETAL AND NEUROLOGICAL DISORDERS There are a wide variety of Neurologic and Musculoskeletal disorders which can impact driving safety. Impairment may be the result of altered muscular, skeletal,
Erigo User Script 1. Erigo Background Information. 2. Intended use and indications
 Erigo User Script 1. Erigo Background Information The Erigo was developed in collaboration with the Spinal Cord Injury Center at the Balgrist University Hospital in Zurich, Switzerland and the Orthopaedic
Erigo User Script 1. Erigo Background Information The Erigo was developed in collaboration with the Spinal Cord Injury Center at the Balgrist University Hospital in Zurich, Switzerland and the Orthopaedic
Neuromuscular Electrical Stimulator (NMES) Corporate Medical Policy
 Neuromuscular Electrical Stimulator (NMES) Corporate Medical Policy File name: Neuromuscular Electrical Stimulator (NMES) File Code: UM.NS.04 Origination: 05/01/2007 Last Review: 06/2018 Next Review: 06/2019
Neuromuscular Electrical Stimulator (NMES) Corporate Medical Policy File name: Neuromuscular Electrical Stimulator (NMES) File Code: UM.NS.04 Origination: 05/01/2007 Last Review: 06/2018 Next Review: 06/2019
Functional Electrical Stimulation
 Functional Electrical Stimulation www.proffessa.co.za Mr. Deon Bührs 22/04/2002 What is Functional Electrical Stimulation 4 The Odstock Dropped Foot Stimulator 4 Development 4 Approvals and recommendations
Functional Electrical Stimulation www.proffessa.co.za Mr. Deon Bührs 22/04/2002 What is Functional Electrical Stimulation 4 The Odstock Dropped Foot Stimulator 4 Development 4 Approvals and recommendations
Fascial Turn-Down Flap Repair of Chronic Achilles Tendon Rupture
 19 Fascial Turn-Down Flap Repair of Chronic Achilles Tendon Rupture S. Ghosh, P. Laing, and Nicola Maffulli Introduction Fascial turn-down flaps can be used for an anatomic repair of chronic Achilles tendon
19 Fascial Turn-Down Flap Repair of Chronic Achilles Tendon Rupture S. Ghosh, P. Laing, and Nicola Maffulli Introduction Fascial turn-down flaps can be used for an anatomic repair of chronic Achilles tendon
Gait analysis and medical treatment strategy
 Gait analysis and medical treatment strategy Sylvain Brochard Olivier Rémy-néris, Mathieu Lempereur CHU and Pediatric Rehabilitation Centre Brest Course for European PRM trainees Mulhouse, October 22,
Gait analysis and medical treatment strategy Sylvain Brochard Olivier Rémy-néris, Mathieu Lempereur CHU and Pediatric Rehabilitation Centre Brest Course for European PRM trainees Mulhouse, October 22,
Management of knee flexion contractures in patients with Cerebral Palsy
 Management of knee flexion contractures in patients with Cerebral Palsy Emmanouil Morakis Orthopaedic Consultant Royal Manchester Children s Hospital 1. Introduction 2. Natural history 3. Pathophysiology
Management of knee flexion contractures in patients with Cerebral Palsy Emmanouil Morakis Orthopaedic Consultant Royal Manchester Children s Hospital 1. Introduction 2. Natural history 3. Pathophysiology
Orthotic Management for Children with Cerebral Palsy
 Orthotic Management for Children with Cerebral Palsy Brian Emling, MSPO, CPO, LPO Brian.emling@choa.org Karl Barner, CPO, LPO karl.barner@choa.org Learning Objectives Inform audience of the general services
Orthotic Management for Children with Cerebral Palsy Brian Emling, MSPO, CPO, LPO Brian.emling@choa.org Karl Barner, CPO, LPO karl.barner@choa.org Learning Objectives Inform audience of the general services
Int J Physiother.Vol1 (2), 40-45, June (2014) ISSN:
 Int J Physiother.Vol1 (2), 40-45, June (2014) ISSN: 2348-8336 Sandesh Rayamajhi 1 Dipika Khanal 2 Mallikarjunaiah H S 3 ABSTRACT Background: Stroke has been considered to be the most common cause of neurological
Int J Physiother.Vol1 (2), 40-45, June (2014) ISSN: 2348-8336 Sandesh Rayamajhi 1 Dipika Khanal 2 Mallikarjunaiah H S 3 ABSTRACT Background: Stroke has been considered to be the most common cause of neurological
MOTION DIAGNOSTIC IMAGING (CMDI)/ GAIT ANALYSIS
 Page: 1 of 5 MEDICAL POLICY MEDICAL POLICY DETAILS Medical Policy Title COMPUTERIZED MOTION DIAGNOSTIC IMAGING (CMDI)/ GAIT ANALYSIS Policy Number 2.01.13 Category Technology Assessment Effective Date
Page: 1 of 5 MEDICAL POLICY MEDICAL POLICY DETAILS Medical Policy Title COMPUTERIZED MOTION DIAGNOSTIC IMAGING (CMDI)/ GAIT ANALYSIS Policy Number 2.01.13 Category Technology Assessment Effective Date
Typical Patient. Clinical Guidelines AAOS: Tx of Achilles Tendon Rupture. Key to Rehab
 Typical Patient Melanie McNeal, PT melanie.mcneal2@memorialhermann.org Male Middle aged Active in recreational sports Weekend warrior Key to Rehab Strengthen healing tendon while maintaining integrity
Typical Patient Melanie McNeal, PT melanie.mcneal2@memorialhermann.org Male Middle aged Active in recreational sports Weekend warrior Key to Rehab Strengthen healing tendon while maintaining integrity
10/26/2017. Comprehensive & Coordinated Orthopaedic Management of Children with CP. Objectives. It s all about function. Robert Bruce, MD Sayan De, MD
 Comprehensive & Coordinated Orthopaedic Management of Children with CP Robert Bruce, MD Sayan De, MD Objectives Understand varying levels of intervention are available to optimize function of children
Comprehensive & Coordinated Orthopaedic Management of Children with CP Robert Bruce, MD Sayan De, MD Objectives Understand varying levels of intervention are available to optimize function of children
ANATOMIC ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL
 ANATOMIC ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL PREOPERATIVE: If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain
ANATOMIC ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL PREOPERATIVE: If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain
E-MAG Active. More dynamic in everyday life. Information for Practitioners NOW BILATERAL UP TO 100 KG (220 LBS) OR UNILATERAL UP TO 85 KG (180 LBS)
 E-MAG Active More dynamic in everyday life NOW BILATERAL UP TO 100 KG (220 LBS) OR UNILATERAL UP TO 85 KG (180 LBS) Information for Practitioners 2 Ottobock E-MAG Active E-MAG Active The E-MAG Active is
E-MAG Active More dynamic in everyday life NOW BILATERAL UP TO 100 KG (220 LBS) OR UNILATERAL UP TO 85 KG (180 LBS) Information for Practitioners 2 Ottobock E-MAG Active E-MAG Active The E-MAG Active is
WalkOn Family of AFOs
 WalkOn Family of AFOs Product Information NeW Lightweight, Low Profile, Durable Stabilization WalkOn Ankle Foot Orthoses are fabricated from advanced prepreg carbon composite material and help users with
WalkOn Family of AFOs Product Information NeW Lightweight, Low Profile, Durable Stabilization WalkOn Ankle Foot Orthoses are fabricated from advanced prepreg carbon composite material and help users with
Total ankle replacement
 Total ankle replacement Initial rehabilitation phase 0-4 weeks To be safely and independently mobile with appropriate walking aid, adhering to weight bearing status To be independent with home exercise
Total ankle replacement Initial rehabilitation phase 0-4 weeks To be safely and independently mobile with appropriate walking aid, adhering to weight bearing status To be independent with home exercise
Anterior Cruciate Ligament Hamstring Rehabilitation Protocol
 Anterior Cruciate Ligament Hamstring Rehabilitation Protocol Focus on exercise quality avoid overstressing the donor area while it heals. Typically, isolated hamstring strengthening begins after the 6
Anterior Cruciate Ligament Hamstring Rehabilitation Protocol Focus on exercise quality avoid overstressing the donor area while it heals. Typically, isolated hamstring strengthening begins after the 6
Foot and ankle. Achilles tendon rupture repair. After surgery
 Foot and ankle Achilles tendon rupture repair There is no agreed single best treatment for Achilles tendon ruptures. Similar results can be achieved with non-surgical and surgical treatments. There is
Foot and ankle Achilles tendon rupture repair There is no agreed single best treatment for Achilles tendon ruptures. Similar results can be achieved with non-surgical and surgical treatments. There is
Patellar Tendon Debridement & Repair Rehabilitation Protocol
 Patellar Tendon Debridement & Repair Rehabilitation Protocol PREOPERATIVE PHASE Diminish inflammation, swelling, and pain Restore normal range of motion (especially knee extension) Restore voluntary muscle
Patellar Tendon Debridement & Repair Rehabilitation Protocol PREOPERATIVE PHASE Diminish inflammation, swelling, and pain Restore normal range of motion (especially knee extension) Restore voluntary muscle
ODSTOCK MEDICAL LIMITED National Clinical FES Centre - Salisbury Quality Form August 2010 Clinical Care Pathway; O2CHS Patient Details Front Sheet
 ODSTOCK MEDICAL LIMITED National Clinical FES Centre - Salisbury Quality Form August 2010 Clinical Care Pathway; O2CHS Patient Details Front Sheet Name. Address DOB Contact telephone numbers; Home Work..
ODSTOCK MEDICAL LIMITED National Clinical FES Centre - Salisbury Quality Form August 2010 Clinical Care Pathway; O2CHS Patient Details Front Sheet Name. Address DOB Contact telephone numbers; Home Work..
Week 1 Orthotics- 1. Knee brace locked in full extension at all times except for rehab exercises 2. Elastic bandage as needed to control swelling
 General Principles: This protocol was designed to provide the rehabilitation professional with a guideline of postoperative care. It should be stressed that this is only a protocol and should not be a
General Principles: This protocol was designed to provide the rehabilitation professional with a guideline of postoperative care. It should be stressed that this is only a protocol and should not be a
Bone-Patellar tendon-bone Autograft ACL Recon. Date of Surgery: Patient Name:
 Dx: o Right o Left Bone-Patellar tendon-bone Autograft ACL Recon Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: GENERAL
Dx: o Right o Left Bone-Patellar tendon-bone Autograft ACL Recon Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: GENERAL
PHYSICAL THERAPY. RC K PART 1 Florence Kendall's Muscle testing Trunk and hip muscles (length tests)
 PHYSICAL THERAPY RC 925.7.K46 1987 PART 1 Trunk and hip muscles (length tests) RC 925.7.K46 1987 PART 2 Trunk and hip (strength tests) RC 925.7.K46 1987 PART 3 Shoulder joint and shoulder girdle muscles
PHYSICAL THERAPY RC 925.7.K46 1987 PART 1 Trunk and hip muscles (length tests) RC 925.7.K46 1987 PART 2 Trunk and hip (strength tests) RC 925.7.K46 1987 PART 3 Shoulder joint and shoulder girdle muscles
Microlight. Kinetic Therapies: Microcurrents with Motion. Electro-Acupuncture. Darren Starwynn, O.M.D., Dipl. Ac., L.Ac.
 Microlight Electro-Acupuncture Kinetic Therapies: Microcurrents with Motion Darren Starwynn, O.M.D., Dipl. Ac., L.Ac. Your Instructor Darren Starwynn, O.M.D., Tiburon, California is a licensed acupuncturist,
Microlight Electro-Acupuncture Kinetic Therapies: Microcurrents with Motion Darren Starwynn, O.M.D., Dipl. Ac., L.Ac. Your Instructor Darren Starwynn, O.M.D., Tiburon, California is a licensed acupuncturist,
Novel Treatments in Stroke Rehabilitation Electrical Stimulation 2012 International Stroke Conference New Orleans, LA
 Novel Treatments in Stroke Rehabilitation Electrical Stimulation 2012 International Stroke Conference New Orleans, LA John Chae, MD Physical Medicine and Rehabilitation Biomedical Engineering Cleveland
Novel Treatments in Stroke Rehabilitation Electrical Stimulation 2012 International Stroke Conference New Orleans, LA John Chae, MD Physical Medicine and Rehabilitation Biomedical Engineering Cleveland
Meniscus Repair Rehabilitation Protocol
 Meniscus Repair Rehabilitation Protocol GENERAL GUIDELINES - Use the cryotherapy cuff continuously for the first 72 hours, then as needed thereafter - Ensure that the cuff never contacts the skin directly
Meniscus Repair Rehabilitation Protocol GENERAL GUIDELINES - Use the cryotherapy cuff continuously for the first 72 hours, then as needed thereafter - Ensure that the cuff never contacts the skin directly
Anterior Tibialis Tendon Rupture: The Other Cause of Foot Drop. Alicia Rozario, DPM PGY-3 DVA Puget Sound Healthcare System
 Anterior Tibialis Tendon Rupture: The Other Cause of Foot Drop Alicia Rozario, DPM PGY-3 DVA Puget Sound Healthcare System Disclosures Nothing to Disclose. ANATOMY https://osteopathysingapore.files.wordpress.com/2015/05/tibialis-anterior-muscle1.png
Anterior Tibialis Tendon Rupture: The Other Cause of Foot Drop Alicia Rozario, DPM PGY-3 DVA Puget Sound Healthcare System Disclosures Nothing to Disclose. ANATOMY https://osteopathysingapore.files.wordpress.com/2015/05/tibialis-anterior-muscle1.png
Supplementary Motor Area Syndrome and Flexor Synergy of the Lower Extremities Ju Seok Ryu, MD 1, Min Ho Chun, MD 2, Dae Sang You, MD 2
 Case Report Ann Rehabil Med 2013;37(5):735-739 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2013.37.5.735 Annals of Rehabilitation Medicine Supplementary Motor Area Syndrome and Flexor
Case Report Ann Rehabil Med 2013;37(5):735-739 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2013.37.5.735 Annals of Rehabilitation Medicine Supplementary Motor Area Syndrome and Flexor
Dr. Gene Desepoli Anterolateral Shin Splints Summary Treatment Sheet
 Dr. Gene Desepoli Anterolateral Shin Splints Summary Treatment Sheet Pathology: Anterolateral shin splints results from strain to the tibialis anterior muscle from eccentric overuse, running on hard ground
Dr. Gene Desepoli Anterolateral Shin Splints Summary Treatment Sheet Pathology: Anterolateral shin splints results from strain to the tibialis anterior muscle from eccentric overuse, running on hard ground
Rehabilitation. Walking after Total Knee Replacement. Continuous Passive Motion Device
 Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
Gait analysis in children and adolescents with spinal cord injuries.
 gfedcb 1: J Spinal Cord Med. 2004;27 Suppl 1:S44-9. Gait analysis in children and adolescents with spinal cord injuries. Smith PA, Hassani S, Reiners K, Vogel LC, Harris GF. Motion Analysis Laboratory,
gfedcb 1: J Spinal Cord Med. 2004;27 Suppl 1:S44-9. Gait analysis in children and adolescents with spinal cord injuries. Smith PA, Hassani S, Reiners K, Vogel LC, Harris GF. Motion Analysis Laboratory,
What is an ACL Tear?...2. Treatment Options...3. Surgical Techniques...4. Preoperative Care...5. Preoperative Requirements...6
 Table of Contents What is an ACL Tear?....2 Treatment Options...3 Surgical Techniques...4 Preoperative Care...5 Preoperative Requirements...6 Postoperative Care...................... 7 Crutch use...8 Initial
Table of Contents What is an ACL Tear?....2 Treatment Options...3 Surgical Techniques...4 Preoperative Care...5 Preoperative Requirements...6 Postoperative Care...................... 7 Crutch use...8 Initial
ODFS Pace Patient Handling Profile Date:
 ODFS Pace Patient Handling Profile Date: Handling Considerations Height: Cognition: Impairment: Mild, Moderate, Severe Pain: Weight: Balance: Impairment: Mild, Moderate, Severe Eyesight: Impairment: Mild,
ODFS Pace Patient Handling Profile Date: Handling Considerations Height: Cognition: Impairment: Mild, Moderate, Severe Pain: Weight: Balance: Impairment: Mild, Moderate, Severe Eyesight: Impairment: Mild,
Effectiveness of Qualitative Therapeutic Exercises on Junior Handball Injured by Achilles tendon Tear (First-degree)
 1 Effectiveness of Qualitative Therapeutic Exercises on Junior Handball Injured by Achilles tendon Tear (First) Prof. Dr. Mohammed kadry Bakry 1 Dr. Ashraf Abdulsalam Alabasy 2 Introduction The rupture
1 Effectiveness of Qualitative Therapeutic Exercises on Junior Handball Injured by Achilles tendon Tear (First) Prof. Dr. Mohammed kadry Bakry 1 Dr. Ashraf Abdulsalam Alabasy 2 Introduction The rupture
King Khalid University Hospital
 King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: ACL RECONSTRUCTION +/- MENSICAL REPAIR 1. General Guidelines: Time lines in this rehabilitation protocol are
King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: ACL RECONSTRUCTION +/- MENSICAL REPAIR 1. General Guidelines: Time lines in this rehabilitation protocol are
Post Operative ACL Reconstruction Protocol Brian J. White, MD
 Post Operative ACL Reconstruction Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve as
Post Operative ACL Reconstruction Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve as
The causes of OA of the knee are multiple and include aging (wear and tear), obesity, and previous knee trauma or surgery. OA affects usually the
 The Arthritic Knee The causes of OA of the knee are multiple and include aging (wear and tear), obesity, and previous knee trauma or surgery. OA affects usually the medial compartment of the knee, and
The Arthritic Knee The causes of OA of the knee are multiple and include aging (wear and tear), obesity, and previous knee trauma or surgery. OA affects usually the medial compartment of the knee, and
Retrospective Analysis of coflex : Long-term Cohort in 240 Patients
 Retrospective Analysis of coflex : Long-term Cohort in 24 Patients Dieter Adelt Damp, Germany Degenerative Spinal Stenosis Disease of Facet Joints! Damaged Cartilage Synovitis / Synovial Cysts Osteophyte
Retrospective Analysis of coflex : Long-term Cohort in 24 Patients Dieter Adelt Damp, Germany Degenerative Spinal Stenosis Disease of Facet Joints! Damaged Cartilage Synovitis / Synovial Cysts Osteophyte
EXERCISE PRESCRIPTION PART 1
 EXERCISE PRESCRIPTION PART 1 Michael McMurray, PT, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 What is MET? An active rehabilitation system based in the biopsychosocial
EXERCISE PRESCRIPTION PART 1 Michael McMurray, PT, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 What is MET? An active rehabilitation system based in the biopsychosocial
Preventative Exercises for the Achilles
 Preventative Exercises for the Achilles Outline 1. Toe walk x 15 each foot 2. Feet out walk x 15 each foot 3. Feet in walk x 15 each foot 4. Ankle in walk x 10 each foot 5. Ankle out walk x 10 each foot
Preventative Exercises for the Achilles Outline 1. Toe walk x 15 each foot 2. Feet out walk x 15 each foot 3. Feet in walk x 15 each foot 4. Ankle in walk x 10 each foot 5. Ankle out walk x 10 each foot
The Deconditioned Elderly Patient: Have We Been Getting it Wrong? By: Ernest Roy PT, DPT
 The Deconditioned Elderly Patient: Have We Been Getting it Wrong? By: Ernest Roy PT, DPT The Debilitated Patient A review of outcomes for > 84,000 patients over 65 y/o revealed: Rate of functional recovery
The Deconditioned Elderly Patient: Have We Been Getting it Wrong? By: Ernest Roy PT, DPT The Debilitated Patient A review of outcomes for > 84,000 patients over 65 y/o revealed: Rate of functional recovery
CORE MEASURE: CORE MEASURE: BERG BALANCE SCALE (BBS)
 OVERVIEW NUMBER OF TEST ITEMS SCORING EQUIPMENT TIME (NEW CLINICIAN) TIME (EXPERIENCED CLINICIAN) COST o The BBS is a widely-used, clinician-rated scale used to assess sitting and standing, static and
OVERVIEW NUMBER OF TEST ITEMS SCORING EQUIPMENT TIME (NEW CLINICIAN) TIME (EXPERIENCED CLINICIAN) COST o The BBS is a widely-used, clinician-rated scale used to assess sitting and standing, static and
Rehabilitation. Walkers, Crutches, Canes
 Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
FES courses from Salisbury District Hospital
 FES courses from Salisbury District Hospital The purpose of the course is to give an introduction to practical clinical FES as practised in the clinical service at Salisbury District Hospital. The techniques
FES courses from Salisbury District Hospital The purpose of the course is to give an introduction to practical clinical FES as practised in the clinical service at Salisbury District Hospital. The techniques
Intended purpose of using the medical device including indication:
 Intended purpose of using the medical device including indication: SunBall is a medical device that is used as an interactive rehabilitation tool that works on the principle of biological feedback and
Intended purpose of using the medical device including indication: SunBall is a medical device that is used as an interactive rehabilitation tool that works on the principle of biological feedback and
Total Hip Replacement Exercise Guide
 Total Hip Replacement Exercise Guide Regular exercise to restore strength and mobility to your hip and a gradual return to everyday activities are important for your full recovery after hip replacement.
Total Hip Replacement Exercise Guide Regular exercise to restore strength and mobility to your hip and a gradual return to everyday activities are important for your full recovery after hip replacement.
Jozef Murar, M.D. TCO Edina Crosstown 4010 W 65 th St, Edina, MN Tel: Fax:
 Jozef Murar, M.D. TCO Edina Crosstown 4010 W 65 th St, Edina, MN 55435 Tel: 952-456-7000 Fax: 952-832-0477 www.tcomn.com ACHILLES TENDON REHABILITATION PROTOCOL Pre-op: Gait training Post-op: Week 2 Post-op
Jozef Murar, M.D. TCO Edina Crosstown 4010 W 65 th St, Edina, MN 55435 Tel: 952-456-7000 Fax: 952-832-0477 www.tcomn.com ACHILLES TENDON REHABILITATION PROTOCOL Pre-op: Gait training Post-op: Week 2 Post-op
A PHYSIATRIC APPROACH TO PATIENTS WITH FACIOSCAPULOHUMERAL MUSCULAR DYSTROPHY
 A PHYSIATRIC APPROACH TO PATIENTS WITH FACIOSCAPULOHUMERAL MUSCULAR DYSTROPHY SUSAN KEESHIN M.D. MEDICAL DIRECTOR DAY REHAB THE SHIRLEY RYAN ABILITY LAB (FORMERLY KNOWN AS RIC) WHAT IS A PHYSIATRIST AND
A PHYSIATRIC APPROACH TO PATIENTS WITH FACIOSCAPULOHUMERAL MUSCULAR DYSTROPHY SUSAN KEESHIN M.D. MEDICAL DIRECTOR DAY REHAB THE SHIRLEY RYAN ABILITY LAB (FORMERLY KNOWN AS RIC) WHAT IS A PHYSIATRIST AND
COMMON PERONEAL NERVE INJURIES: GUIDELINES FOR SURGICAL TREATMENT IN OUR EXPERIENCE
 COMMON PERONEAL NERVE INJURIES: GUIDELINES FOR SURGICAL TREATMENT IN OUR EXPERIENCE Debora Garozzo Brachial Plexus and Peripheral Nerve Surgery Unit Neurospinal Hospital Dubai, United Arab Emirates Common
COMMON PERONEAL NERVE INJURIES: GUIDELINES FOR SURGICAL TREATMENT IN OUR EXPERIENCE Debora Garozzo Brachial Plexus and Peripheral Nerve Surgery Unit Neurospinal Hospital Dubai, United Arab Emirates Common
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction
 Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Bilateral Foot Drop Without Cauda Equinae Syndrome Due To L4-L5 Disc Prolapse: A Case Report
 ISPUB.COM The Internet Journal of Neurosurgery Volume 5 Number 1 Bilateral Foot Drop Without Cauda Equinae Syndrome Due To L4-L5 Disc Prolapse: A Case Report R Ramnaryan, C Palinikumar Citation R Ramnaryan,
ISPUB.COM The Internet Journal of Neurosurgery Volume 5 Number 1 Bilateral Foot Drop Without Cauda Equinae Syndrome Due To L4-L5 Disc Prolapse: A Case Report R Ramnaryan, C Palinikumar Citation R Ramnaryan,
GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction
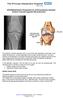 GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction Femur ACL Graft Fibula Tibia The Anterior Cruciate Ligament (ACL) is one of the main ligaments in the
GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction Femur ACL Graft Fibula Tibia The Anterior Cruciate Ligament (ACL) is one of the main ligaments in the
Effectiveness of passive and active knee joint mobilisation following total knee arthroplasty: Continuous passive motion vs. sling exercise training.
 Effectiveness of passive and active knee joint mobilisation following total knee arthroplasty: Continuous passive motion vs. sling exercise training. Mau-Moeller, A. 1,2, Behrens, M. 2, Finze, S. 1, Lindner,
Effectiveness of passive and active knee joint mobilisation following total knee arthroplasty: Continuous passive motion vs. sling exercise training. Mau-Moeller, A. 1,2, Behrens, M. 2, Finze, S. 1, Lindner,
Neurological Examination
 Neurological Examination Charles University in Prague 1st Medical Faculty and General University Hospital Neurological examination: Why important? clinical history taking and bedside examination: classical
Neurological Examination Charles University in Prague 1st Medical Faculty and General University Hospital Neurological examination: Why important? clinical history taking and bedside examination: classical
Knee Capsular Disorder. ICD-9-CM: Stiffness in joint of lower leg, not elsewhere classified
 1 Knee Capsular Disorder "Knee Capsulitis" ICD-9-CM: 719.56 Stiffness in joint of lower leg, not elsewhere classified Diagnostic Criteria History: Physical Exam: Stiffness Aching with prolonged weight
1 Knee Capsular Disorder "Knee Capsulitis" ICD-9-CM: 719.56 Stiffness in joint of lower leg, not elsewhere classified Diagnostic Criteria History: Physical Exam: Stiffness Aching with prolonged weight
North of England Bone and Soft Tissue Tumour Service
 North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after replacement of the proximal femur Proximal femoral replacement surgery is usually carried out as part of treatment
North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after replacement of the proximal femur Proximal femoral replacement surgery is usually carried out as part of treatment
Clinical Use of the Odstock Dropped Foot Stimulator: Its Effect ion the Speed and Effort of Walking
 1577 Clinical Use of the Odstock Dropped Foot Stimulator: Its Effect ion the Speed and Effort of Walking Paul N. Taylor, MSc, Jane H. Burridge, Phi), Anna L. Dunkerley, MSc, Duncan E. Wood, PhD, Jonathan
1577 Clinical Use of the Odstock Dropped Foot Stimulator: Its Effect ion the Speed and Effort of Walking Paul N. Taylor, MSc, Jane H. Burridge, Phi), Anna L. Dunkerley, MSc, Duncan E. Wood, PhD, Jonathan
IMPROVING CHRONIC PAIN PATIENTS QUALITY OF LIFE WITH CUTTING EDGE TECHNOLOGY. Jacqueline Weisbein, DO Napa Valley Orthopaedic Medical Group
 IMPROVING CHRONIC PAIN PATIENTS QUALITY OF LIFE WITH CUTTING EDGE TECHNOLOGY Jacqueline Weisbein, DO Napa Valley Orthopaedic Medical Group Who Am I? Avid equestrian Trained in Physical Medicine & Rehabilitation
IMPROVING CHRONIC PAIN PATIENTS QUALITY OF LIFE WITH CUTTING EDGE TECHNOLOGY Jacqueline Weisbein, DO Napa Valley Orthopaedic Medical Group Who Am I? Avid equestrian Trained in Physical Medicine & Rehabilitation
