Thorax Online First, published on February 14, 2008 as /thx Title page
|
|
|
- Jeremy Watson
- 6 years ago
- Views:
Transcription
1 Thorax Online First, published on February 14, 2008 as /thx Title page Title of the article: Chest physical therapy for children hospitalized with acute pneumonia: a randomized controlled trial Names and degrees of the authors: Cistina Paludo, BSc, Universidade Federal do Rio Grande Linjie Zhang, M.D, Ph.D, Universidade Federal do Rio Grande Carla S. Lincho, M.D, Universidade Federal do Rio Grande Daniel V. Lemos, M.D, Universidade Federal do Rio Grande Gustavo G. Real, M.D, Universidade Federal do Rio Grande Jorge A. Bergamin, M.D, Universidade Federal do Rio Grande Department and institution in which the work was done: Department of Maternal and Child Health Universidade Federal do Rio Grande, Rio Grande, RS, Brazil Name and address of the corresponding author: Linjie Zhang Rua Barao de Santa Tecla 884, 202 A Centro, Pelotas, RS, Brazil Telephone/fax: (55) zhanglinjie63@yahoo.com.br Word count: 1997 words Key words: Chest physical therapy. Pneumonia. Children. Randomized controlled trial. Effectiveness. 1 Copyright Article author (or their employer) Produced by BMJ Publishing Group Ltd (& BTS) under licence.
2 Declaration As the corresponding author, I declare that I have the right to grant on behalf of all authors and do grant on behalf of all authors, an exclusive licence on a worldwide basis to the BMJ Publishing Group Ltd and its Licensees to permit this article to be published in [THORAX] editions and any other BMJPG Ltd products to exploit all subsidiary rights, as set out in the licence ( There is no competing interest related to this manuscript. Sincerely yours, Linjie Zhang 2
3 3 ABSTRACT Background: The indication of chest physical therapy as an adjunct to treatment of children hospitalized with acute pneumonia remains controversial and there is lack of robust scientific evidence on effectiveness of this modality in these patients. Methods: A randomized controlled trial was conducted in two tertiary hospitals in southern Brazil. Children aged 29 days to 12 years, hospitalized with pneumonia between February and October of 2006 were recruited. Fifty-one patients were randomly allocated to the intervention group (chest physical therapy plus standard treatment for pneumonia) and 47 to the control group (standard treatment for pneumonia alone). The primary outcome was time to clinical resolution. The secondary outcomes were length of hospitalization and duration of respiratory symptoms and signs. Results: There were no significant differences in terms of median time to clinical resolution (4.0 vs 4.0 days, p=0.84) and median length of hospital stay (6.0 vs 6.0 days, p=0.76) between the intervention and control groups. The intervention group had longer median duration of coughing (5.0 vs 4.0 days, p=0.04) and of rhonchi in lung auscultation (2.0 vs 0.5 days, p=0.03) than the control group. Conclusions: Chest physical therapy as adjunct to the standard treatment does not hasten clinical resolution of children hospitalized with acute pneumonia and may prolong duration of coughing and rhonchi.
4 4 Main text Introduction The indication of chest physical therapy as an adjunct to treatment of children hospitalized with acute pneumonia remains controversial. On the one hand, chest physical therapy has been and continues to be widely applied to these patients in pediatric practice, based on beliefs of the potential benefits of this modality on evacuating inflammatory exudates and tracheobronchial secretion, removing airway obstruction, reducing airway resistance, enhancing gas exchange and reducing the work of breathing.[1-3] On the other hand, there is lack of robust scientific evidence on effectiveness of chest physical therapy in children hospitalized with pneumonia. The British Thoracic Society guidelines for managing pneumonia in childhood recommend that chest physical therapy is not beneficial and should not be performed in children with pneumonia,[4] however, these recommendations are based mainly on the results of two randomized controlled trials, one in adults and another in children.[5, 6] Moreover, the validity of this old clinical trial in children is questionable due to small sample size, exclusion of patients with pneumonia of presumed bacterial origin and inadequate randomization and blinding.[6] Therefore, more data from high quality randomized trials are needed to make a more precise decision on the indication of chest physical therapy for acute pneumonia in childhood. This randomized controlled trial was conducted to assess the effectiveness of chest physical therapy in children hospitalized with acute pneumonia. We hypothesized that chest physical therapy as adjunct to standard treatment could hasten clinical resolution of children hospitalized with acute pneumonia. Methods Study setting This study was conducted in the pediatric wards of two tertiary hospitals: 30-bed teaching hospital of Federal University of Rio Grande and 30-bed hospital da Santa Casa de Rio Grande. These are two unique hospitals in the city of Rio Grande in southern Brazil, covering a population of approximately 200,000. The ethic committee of the Federal University of Rio Grande (Rio Grande, RS, Brazil) and the ethic committee of the hospital da Santa Casa de Rio Grande (Rio Grande, RS, Brazil) approved the study. Participants Children aged 29 days to 12 years old, hospitalized with a diagnosis of acute pneumonia, were assessed for eligibility for this study. The patients were included in the study if they met all of the following clinical and radiological diagnosis criteria for pneumonia:[4, 7] (1) presence of coughing and/or fever; (2) tachypnea, defined as respiratory rate above age-dependent upper limits: <2 months: 60 breaths per minute (bpm); 2 12 months: 50 bpm; >1 5 years: 40 bpm; >5 years: 30 bpm; (3) consolidations and/or infiltrates, associated or not with other findings compatible with pneumonia on chest X-ray. All chest radiographs were interpreted routinely in the Department of Radiology and reviewed by a senior pediatric pulmologist (Z.L). Any disagreement was resolved by discussion with a reference radiologist. We excluded patients who needed a chest drain, who had haemodynamic instability, bone fragility or rib fractures, and any other contraindication to chest physical therapy.[1] The recruitment of participants occurred between February and October of The parents or legal guardians of each child gave written informed consent before enrollment. Study design and protocol This study was a randomized and controlled clinical trial. Simple randomization was performed from a table of random numbers. The recruited participants were randomly allocated to the intervention group or the control group. The intervention group received chest
5 physical therapy twice daily plus standard treatment for pneumonia until discharge and the control group received standard treatment for pneumonia alone. Each session of chest physical therapy took about 30 minutes, consisted of postural drainage, thoracic squeezing, chest percussion, vibration, cough stimulation and aspiration of secretions (if necessary).[1, 5, 6] The positions for postural drainage were guided by chest X-ray to allow more effective drainage of tracheobronchial secretion and inflammatory exudates in the most affected areas. [1, 6] The same certified physiotherapist (C.P) administered chest physical therapy to all patients. The standard treatment for pneumonia in each patient was administered by the attending pediatricians, based on the recommendations of Brazilian guidelines for diagnosis and treatment of pneumonia.[7] It included antibiotic therapy, fluid therapy and oxygen therapy if needed. The decision of hospital discharge was also made by the attending pediatricians. All attending pediatricians were blinded to group assignment and study protocol. The patients were assessed at enrollment and every afternoon between 5:00 and 6:00pm by one of 4 investigators, using a pre-codified questionnaire. The same investigator was responsible for assessment of each patient from enrollment to discharge. Patient s assessment included respiratory symptoms, respiratory signs (respiratory rate, chest indrawing, nasal flaring, cyanosis and lung auscultation) and arterial oxygen saturation measured by pulse oximetry. All 4 investigators received adequate training in assessment of the patient, specially in measuring respiratory rate and arterial oxygen saturation, in observing chest in-drawing and in lung auscultation. The standard technique for measurement of respiratory rate and arterial oxygen saturation was same as previously reported.[8] The definition of adventitious sounds in lung auscultation was based on the recommendations of 1985 International Symposium on Lung Sounds.[9] The inter-observer agreement between 4 investigators and a senior pediatric pulmologist (Z.L) regarding observation of respiratory signs (tachypnea, chest in-drawing, rhonchus, wheezes, fine crackles and coarse crackles) was evaluated and Kappa indexes were 0.53, 0.63, 0.48, 0.70, 0.60 and 0.47 respectively. Daily maximum body temperature was noted by the investigators based on patient s nursing record. The patient s axillary temperature was measured by the attending nurses every 3 hours throughout the hospital stay. All investigators and nurses were blinded to group assignment and study protocol. The different schedules were arranged for investigators and physiotherapist to avoid their chance encounter at patient s bedside. Outcome measures The primary outcome was time to clinical resolution, being defined as the number of days needed for patient to present with the following clinical parameters: afebrile (daily maximum body temperature<37.5c 0 ), absence of signs of the severity (chest in-drawing, nasal flaring and cyanosis), normal respiratory rate and arterial oxygen saturation equal to or higher than 95%. Secondary outcomes were length (days) of hospital stay and persistence (days) of respiratory symptoms and signs (fever, cough, wheezing, tachypnea, chest indrawing, adventitious sounds in lung auscultation and arterial oxygen saturation below 95%). Sample size The Sample size was determined on the assumption that mean time to clinical resolution (mean SD) in the control group were days. [6] To detect a clinicallyrelevant reduction of one day in the time to clinical resolution, we needed 47 participants in each group (two-sided alpha of 5% and power of 90%). Statistical analysis Statistical analysis was performed using STATA 8.0 program (Stata Corporation, Texas, USA, 2003). The χ 2 test was used for analysis of dichotomous data. Unpaired Student s t-test or Mann-Whitney rank-sum test were used for analysis of continuous data as appropriate. Analyses were based on the intention-to treat principle. In the additional analysis, we excluded the possible cases of acute bronchiolitis, that is, patients who were younger than 2 years old and presented with wheezes in lung auscultation at enrollment. The explanatory 5
6 analysis was also performed to verify the potential changes in the results. Two-tailed P value <0.05 was considered as statistically significant. Results One hundred and ten children were assessed for eligibility during the study period and 98 were included for the trial (Figure 1). Of 98 recruited patients, 51 were randomly allocated to the intervention group and 47 to the control group. Table 1 summarizes characteristics of all 98 patients at enrollment and randomization. There were not significant differences between the intervention and control groups in terms of the baseline characteristics. Table 1. Characteristics of 89 patients at enrollment and randomization Characteristic Intervention group Control group P value (n = 47) (n = 42) Age (months) 44.0 ( ) 32.2 ( ) 0.14 Male sex 29 (61.7) 24 (57.1) 0.66 Low birthweight (<2500g) 5 (10.6) 4 (9.5) 0.86 Prematurity (<37 weeks) 8 (17.0) 6 (14.2) 0.72 Maternal smoking 17 (36.1) 17 (40.4) 0.67 Respiratory symptoms and signs Coughing 46 (97.8) 38 (92.6) 0.24 Fever 45 (95.7) 37 (90.2) 0.30 Parent s reported wheezing 31 (65.9) 24 (58.5) 0.47 Respiratory rate (bpm) 45.0 ( ) 45.8 ( ) 0.78 Chest in-drawing 24 (51.0) 22 (53.6) 0.80 Fine crackles 16 (34.0) 11 (26.8) 0.46 Coarse crackles 17 (36.1) 19 (46.3) 0.33 Rhonchi 9 (19.2) 6 (14.6) 0.57 Wheezes 13 (27.6) 5 (12.2) 0.07 Chest x-ray findings Consolidation 39/45 (86.7) 35/39 (89.7) 0.66 Hyperinflation 6/45 (13.3) 5/39 (12.8) 0.95 Pleural effusion 5/45 (11.1) 6/39 (15.4) 0.56 Arterial oxygen saturation 95.0 ( ) 95.7 ( ) 0.15 Antibiotic therapy 47 (100.0) 42 (100.0) 1.00 Values expressed as mean (IC 95%) or N (%) Table 2 compares clinical evolution between the intervention group and the control group. The intervention group had longer median duration of coughing (5.0 vs 4.0 days, p=0.04) and of rhonchi in lung auscultation (2.0 vs 0.5 days, p=0.03) than the control group. There were no significant differences between the two groups in terms of other parameters of the clinical evolution. No significant changes were observed in the results when additional analysis (excluding 12 patients who were younger than 2 years old and presented with wheezes at enrollment) and explanatory analysis (excluding 7 patients in the control group who received chest physical therapy indicated by attending pediatricians) were performed. Discussion This randomized trial failed to confirm that chest physical therapy as adjunct to standard treatment could hasten clinical resolution of children hospitalized with acute pneumonia. The time to clinical resolution and the length of hospital stay were similar between the intervention group and the control group. Moreover, this study showed that the patients who received chest physical therapy had had prolonged duration of coughing and 6
7 rhonchi in lung auscultation. However, the persistence of these respiratory symptoms and signs may not necessarily represent a unfavorable clinical evolution. Coughing might be induced by physiotherapist since it was an essential component of chest physical therapy. Rhonchus, a typical secretion sound in lung auscultation might be prolonged by chest physical therapy as this modality could dislodge tracheobronchial secretion and produce this adventitious sound. In this sense, chest physical therapy might effectively mobilize tracheobronchial secretion in this group of children, but failed to modify the clinical evolution of acute pneumonia assessed by time to clinical resolution, length of hospital stay, and persistence of other individual clinical parameter like fever, respiratory rate, chest in-drawing and arterial oxygen saturation. Table 2. Effects of chest physical therapy on clinical evolution of children hospitalized with acute pneumonia Outcomes Intervention group Control group P value (n = 47) (n = 42) Time to clinical resolution 4.0 ( ) 4.0 ( ) 0.84 Length of hospital stay 6.0 ( ) 6.0 ( ) 0.76 Time to normal respiratory rate 3.0 (0-7.0) 3.0 ( ) 0.75 Time to normal arterial oxygen 1.0 (0-2.0) 0.5 (0-2.0) 0.98 saturation ( 95%) Time to normal lung 4.0 ( ) 4.0 ( ) 0.28 auscultation Duration of fever 2.0 (0-2.0) 1.0 (0-3.0) 0.78 Duration of coughing 5.0 ( ) 4.0 ( ) 0.04 Duration of parent s reported 1.5 (0-5.0) 1.0 (0-3.5) 0.29 wheezing Duration of fine crackles 0 (0-2.0) 0 (0-2.0) 0.72 Duration of coarse crackles 2.0 (0-4.0) 1.0 (0-3.0) 0.83 Duration of wheezes 0 (0-5.0) 0 (0-4.0) 0.62 Duration of rhonchi 2.0 (0-4.0) 0.5 (0-2.0) 0.03 Duration of chest in-drawing 2.0 (0-3.0) 2.0 (0-3.0) 0.75 Number of days expressed as median (interquartile range) No beneficial effect of chest physical therapy in children hospitalized with viral pneumonia has been reported by one clinical trial, in spite of serious methodological limitations mentioned previously.[6] Moreover, prolonged fever was observed in the intervention group. The similar finding was also reported by the other randomized trial in adults with primary pneumonia.[5] The spread of the infiltrates and physical activity associated with chest physical therapy were speculated to explain prolonged fever in the patients who received this modality. In the present trial, the intervention group had longer median duration of fever than the control group (2.0 vs 1.0 days), however, this difference was not statistically significant (p=0.78). The data derived from this randomized trial support the recommendations of the British Thoracic Society guidelines regarding the indication of chest physical therapy in children with acute pneumonia,[4] that is, chest physical therapy is not beneficial and should not be performed in these patients. However, these recommendations may not be suitable for special groups of children with acute pneumonia, like those who have impaired mucociliary clearance and who have complications such as atelectasis and pleural effusion needing a chest drain. Future randomized trials should focus on these special groups of patients. Some methodological aspects of this trial deserve special comments. Firstly, no placebo is available to blind those involved in a trial of physical therapy and it may be the source of performance and observation bias.[10] To minimize these potential bias, all 7
8 investigators who assessed the patients and all attending pediatricians and nurses were blinded to group assignment and study protocol. Secondly, no standard protocol of physical therapy is well defined for special respiratory disease and the art of this modality may introduce a number of personal and uncontrollable factors. In this trial, the protocol of physical therapy was defined a priori, based on the experiences of the previous studies and on the potential benefits of each component on acute pneumonia.[1, 5, 6, 11] To avoid inter-individual variation caused by art of physical therapy, the same physiotherapist administered this modality to all patients. Thirdly, the outcomes currently used to assess the effectiveness of chest physical therapy, such as radiolabelled aerosols, chest x-ray, sputum volume, oxygen saturation and pulmonary function testing, are considered unreliable or impractical, specially in pediatric population.[2] We used the time to clinical resolution as the primary outcome since we expected that chest physical therapy could hasten clinical evolution of children hospitalized with acute pneumonia. This variable consists of various relevant and relatively accurate signs which reflect the severity and evolution of pneumonia.[4, 7, 12] Therefore, this outcome may be more reliable and objective than the length of hospital stay or duration of any individual symptom or sign to represent clinical evolution of acute pneumonia in childhood. Acknowledgements Cristina Paludo, Carla S. Lincho and Jorge A. Bergamin received grants from the following Brazilian government research support agencies: the Coordination for the Improvement of Higher Education Personnel (CAPES), the National Council for the Scientific and Technologic Development (CNPq) and the Research Assistance Fund of Rio Grande do Sul (FAPERGS). The authors thank Raúl Mendoza-Sassi for advice on statistical analysis. 8
9 References 1 Balachandran A, Shivbalan S, Thangavelu S. Chest Physiotherapy in Pediatric Practice. Indian Pediatrics 2005;42: Wallis C, Prasad A. Who needs chest physiotherapy? Moving from anecdote to evidence. Arch Dis Child 1999;80: Chalumeau M, Foix-L Helias L, Schinmann P, et al. Rib fractures after chest physiotherapy for bronchiolitis or pneumonia in infants. Pediatr Radiol 2002;32: British Thoracic Society Standards of Care Committee. BTS guidelines for the management of community acquired pneumonia in childhood. Thorax 2002;57(suppl 1):i1-i24. 5 Britton S, Bejstedt M, Vedin L. Chest physiotherapy in primary pneumonia. BMJ 1985; 290: Levine A. Chest physical therapy for children with pneumonia. J Am Osteopath Assoc 1978; 78: Sociedade Brasileira de Pneumologia e Tisologia. I Consenso brasileiro de pneumonias. J Pneumol 1998;24: Zhang L, Ferruzzi E, Bonfanti T, et al. Long and short-term effect of prednisolone in hospitalized infants with acute bronchiolitis. J Paediatr Child Health 2003;39: Mikami R, Murao M, Cugell DW, et al. International symposium on lung sounds. Synopsis of preceedings. Chest 1987;92: Greenhalgh T. Assessing the methodological quality of published papers. BMJ 1997;315: Oberwaldner B. Physiotherapy for airway clearance in paediatrics. Eur Respir J 2000;15: Palafox M, Guiscafré H, Reyes H, et al. Diagnostic value of tachypnoea in pneumonia defined radiologically. Arch Dis Child 2000;82:
10 Figures Figure 1. Flow diagram of the trial Intervention group (n=51) Patients assessed for eligibility (n=110) Randomization (n=98) 4 were withdrawn, with incomplete follow-up data 2 had hospital discharge/ transfer before the second assessment 2 met an exclusion criterion Control group (n=47) 12 excluded 10 did not meet inclusion criteria 2 met an exclusion criterion 7 patients received chest physical therapy indicated by attending pediatricians 5 were withdrawn, with incomplete follow-up data 2 had hospital discharge before the second assessment 3 met an exclusion criterion 47 were analysed 42 were analysed 1
Protocol for performing chest clearance techniques by nursing staff
 Protocol for performing chest clearance techniques by nursing staff Rationale The main indications for performing chest clearance techniques (CCT) are to assist in the removal of thick, tenacious secretions
Protocol for performing chest clearance techniques by nursing staff Rationale The main indications for performing chest clearance techniques (CCT) are to assist in the removal of thick, tenacious secretions
Sorting the sheep from the goats
 Sorting the sheep from the goats How do we improve the diagnosis of pediatric respiratory diseases under low-resource conditions? Pediatric Grand Rounds February 27, 2015 It doesn t matter. refugee camp
Sorting the sheep from the goats How do we improve the diagnosis of pediatric respiratory diseases under low-resource conditions? Pediatric Grand Rounds February 27, 2015 It doesn t matter. refugee camp
Respiratory Diseases and Disorders
 Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
Accuracy of Parental and Child s Reports of Changes in Symptoms of Childhood Asthma
 7. Cecka JM, Gjertson DW, Terasaki PI. Pediatric renal transplantation - a review of the UNOS data. Pediatr Transplant 1997; 1: 55-64. 8. Alexander SR. Pediatric end stage renal disease. Am J Kidney Dis
7. Cecka JM, Gjertson DW, Terasaki PI. Pediatric renal transplantation - a review of the UNOS data. Pediatr Transplant 1997; 1: 55-64. 8. Alexander SR. Pediatric end stage renal disease. Am J Kidney Dis
Characteristics of Radiographically Diagnosed Pneumonia in Under-5 Children in Salvador, Brazil
 R E S E A R C H P A P E R Characteristics of Radiographically Diagnosed Pneumonia in Under-5 Children in Salvador, Brazil NK KEY, *CA ARAÚJO-NETO, $ M-RA CARDOSO AND CM NASCIMENTO-CARVALHO From the Departments
R E S E A R C H P A P E R Characteristics of Radiographically Diagnosed Pneumonia in Under-5 Children in Salvador, Brazil NK KEY, *CA ARAÚJO-NETO, $ M-RA CARDOSO AND CM NASCIMENTO-CARVALHO From the Departments
The McMaster at night Pediatric Curriculum
 The McMaster at night Pediatric Curriculum Community Acquired Pneumonia Based on CPS Practice Point Pneumonia in healthy Canadian children and youth and the British Thoracic Society Guidelines on CAP Objectives
The McMaster at night Pediatric Curriculum Community Acquired Pneumonia Based on CPS Practice Point Pneumonia in healthy Canadian children and youth and the British Thoracic Society Guidelines on CAP Objectives
GOALS AND INSTRUCTIONAL OBJECTIVES
 October 4-7, 2004 Respiratory GOALS: GOALS AND INSTRUCTIONAL OBJECTIVES By the end of the week, the first quarter student will have an in-depth understanding of the diagnoses listed under Primary Diagnoses
October 4-7, 2004 Respiratory GOALS: GOALS AND INSTRUCTIONAL OBJECTIVES By the end of the week, the first quarter student will have an in-depth understanding of the diagnoses listed under Primary Diagnoses
Is follow up chest X-ray required in children with round pneumonia?
 Is follow up chest X-ray required in children with round pneumonia? McCrossan, P., McNaughten, B., Shields, M., & Thompson, A. (2017). Is follow up chest X-ray required in children with round pneumonia?
Is follow up chest X-ray required in children with round pneumonia? McCrossan, P., McNaughten, B., Shields, M., & Thompson, A. (2017). Is follow up chest X-ray required in children with round pneumonia?
Epiglottitis. Bronchitis. Bronchiolitis. Pneumonia. Croup syndrome. Miss. kamlah 2
 Miss. kamlah 1 Epiglottitis. Bronchitis. Bronchiolitis. Pneumonia. Croup syndrome. Miss. kamlah 2 Acute Epiglottitis Is an infection of the epiglottis, the long narrow structure that closes off the glottis
Miss. kamlah 1 Epiglottitis. Bronchitis. Bronchiolitis. Pneumonia. Croup syndrome. Miss. kamlah 2 Acute Epiglottitis Is an infection of the epiglottis, the long narrow structure that closes off the glottis
Problem Based Learning Session. Mr Robinson is a 67 year old man. He visits the GP as he has had a cough and fever for 5 days.
 Problem Based Learning Session Mr Robinson is a 67 year old man. He visits the GP as he has had a cough and fever for 5 days. The GP takes a history from him and examines his chest. Over the left base
Problem Based Learning Session Mr Robinson is a 67 year old man. He visits the GP as he has had a cough and fever for 5 days. The GP takes a history from him and examines his chest. Over the left base
Antimicrobial Stewardship in Community Acquired Pneumonia
 Antimicrobial Stewardship in Community Acquired Pneumonia Medicine Review Course 2018 Dr Lee Tau Hong Consultant Department of Infectious Diseases National Centre for Infectious Diseases Scope 1. Diagnosis
Antimicrobial Stewardship in Community Acquired Pneumonia Medicine Review Course 2018 Dr Lee Tau Hong Consultant Department of Infectious Diseases National Centre for Infectious Diseases Scope 1. Diagnosis
Chronic Obstructive Pulmonary Disease
 Chronic Obstructive Pulmonary Disease 07 Contributor Dr David Tan Hsien Yung Definition, Diagnosis and Risk Factors for (COPD) Differential Diagnoses Goals of Management Management of COPD THERAPY AT EACH
Chronic Obstructive Pulmonary Disease 07 Contributor Dr David Tan Hsien Yung Definition, Diagnosis and Risk Factors for (COPD) Differential Diagnoses Goals of Management Management of COPD THERAPY AT EACH
Levine Children s Hospital. at Carolinas Medical Center. Respiratory Care Department
 Page 1 of 7 at Carolinas Medical Center 02.04 Pediatric Patient-Centered Respiratory Care Protocol Application of Chest Physical Therapy Created: 1/98 Reviewed: 4/03, 1/05, 6/08 Revised: Purpose: To describe
Page 1 of 7 at Carolinas Medical Center 02.04 Pediatric Patient-Centered Respiratory Care Protocol Application of Chest Physical Therapy Created: 1/98 Reviewed: 4/03, 1/05, 6/08 Revised: Purpose: To describe
 PHYSIOTHERAPY IN INTENSIVE CARE: how the evidence has changed since 2000 Kathy Stiller Physiotherapy Department Royal Adelaide Hospital Adelaide South Australia Kathy.Stiller@health.sa.gov.au Aim review
PHYSIOTHERAPY IN INTENSIVE CARE: how the evidence has changed since 2000 Kathy Stiller Physiotherapy Department Royal Adelaide Hospital Adelaide South Australia Kathy.Stiller@health.sa.gov.au Aim review
Lecture Notes. Chapter 16: Bacterial Pneumonia
 Lecture Notes Chapter 16: Bacterial Pneumonia Objectives Explain the epidemiology Identify the common causes Explain the pathological changes in the lung Identify clinical features Explain the treatment
Lecture Notes Chapter 16: Bacterial Pneumonia Objectives Explain the epidemiology Identify the common causes Explain the pathological changes in the lung Identify clinical features Explain the treatment
Chapter 16. Lung Abscess. Mosby items and derived items 2011, 2006 by Mosby, Inc., an affiliate of Elsevier Inc.
 Chapter 16 Lung Abscess 1 EDA PM C AFC RB A B Figure 16-1. Lung abscess. A, Cross-sectional view of lung abscess. B, Consolidation and (C) excessive bronchial secretions are common secondary anatomic alterations
Chapter 16 Lung Abscess 1 EDA PM C AFC RB A B Figure 16-1. Lung abscess. A, Cross-sectional view of lung abscess. B, Consolidation and (C) excessive bronchial secretions are common secondary anatomic alterations
Differential diagnosis
 Differential diagnosis The onset of COPD is insidious. Pathological changes may begin years before symptoms appear. The major differential diagnosis is asthma, and in some cases, a clear distinction between
Differential diagnosis The onset of COPD is insidious. Pathological changes may begin years before symptoms appear. The major differential diagnosis is asthma, and in some cases, a clear distinction between
CYSTIC FIBROSIS INPATIENT PROTOCOL PURPOSE POLICY STATEMENTS SITE APPLICABILITY PRACTICE LEVEL/COMPETENCIES DEFINITIONS EQUIPMENT
 PURPOSE Physiotherapy role for inpatients with cystic fibrosis. POLICY STATEMENTS On admission to hospital all patients will be assessed by the physiotherapist within 24 hours. Physiotherapists have standing
PURPOSE Physiotherapy role for inpatients with cystic fibrosis. POLICY STATEMENTS On admission to hospital all patients will be assessed by the physiotherapist within 24 hours. Physiotherapists have standing
BRONCHIOLITIS. See also the PSNZ guideline - Wheeze & Chest Infections in infants under 1 year (www.paediatrics.org.nz)
 Definition What is Bronchiolitis? Assessment Management Flow Chart Admission Guidelines Investigations Management Use of Bronchodilators Other treatments Discharge Planning Bronchiolitis & Asthma References
Definition What is Bronchiolitis? Assessment Management Flow Chart Admission Guidelines Investigations Management Use of Bronchodilators Other treatments Discharge Planning Bronchiolitis & Asthma References
Early Rehabilitation in the ICU: Do We Still Need Chest Physiotherapy?
 Early Rehabilitation in the ICU: Do We Still Need Chest Physiotherapy? Michelle Kho, PT, PhD Assistant Professor, School of Rehabilitation Science, McMaster University Adjunct Assistant Professor, Department
Early Rehabilitation in the ICU: Do We Still Need Chest Physiotherapy? Michelle Kho, PT, PhD Assistant Professor, School of Rehabilitation Science, McMaster University Adjunct Assistant Professor, Department
British Thoracic Society Paediatric Pneumonia Audit National Audit Period: 1 November January 2017 Dr Julian Legg and Dr Charlotte Rampton
 British Thoracic Society Paediatric Pneumonia Audit National Audit Period: 1 November 2016 31 January 2017 Dr Julian Legg and Dr Charlotte Rampton Number of records submitted: 7302 Number of participants:
British Thoracic Society Paediatric Pneumonia Audit National Audit Period: 1 November 2016 31 January 2017 Dr Julian Legg and Dr Charlotte Rampton Number of records submitted: 7302 Number of participants:
Unconscious exchange of air between lungs and the external environment Breathing
 Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
Management of Common Respiratory Disorders in Children. Whitney Pressler, MD Pediatric Brown Bag Series Webinar June 14, 2016
 Management of Common Respiratory Disorders in Children Whitney Pressler, MD Pediatric Brown Bag Series Webinar June 14, 2016 Disclosures I have no financial relationships to disclose I will not be discussing
Management of Common Respiratory Disorders in Children Whitney Pressler, MD Pediatric Brown Bag Series Webinar June 14, 2016 Disclosures I have no financial relationships to disclose I will not be discussing
Management of Common Respiratory Disorders in Children. Disclosures. Roadmap 6/10/2016
 Management of Common Respiratory Disorders in Children Whitney Pressler, MD Pediatric Brown Bag Series Webinar June 14, 2016 Disclosures I have no financial relationships to disclose I will not be discussing
Management of Common Respiratory Disorders in Children Whitney Pressler, MD Pediatric Brown Bag Series Webinar June 14, 2016 Disclosures I have no financial relationships to disclose I will not be discussing
RESPIRATORY ASSESSMENT JENNY CASEY RESPIRATORY SERVICES LEAD ACE
 RESPIRATORY ASSESSMENT JENNY CASEY RESPIRATORY SERVICES LEAD ACE What does respiratory assessment involve? Subjective Assessment Objective Assessment Inspection, palpation, percussion and auscultation
RESPIRATORY ASSESSMENT JENNY CASEY RESPIRATORY SERVICES LEAD ACE What does respiratory assessment involve? Subjective Assessment Objective Assessment Inspection, palpation, percussion and auscultation
Multicenter Osteopathic Pneumonia Study in the Elderly (MOPSE) The Primary Outcomes
 Multicenter Osteopathic Pneumonia Study in the Elderly (MOPSE) The Primary Outcomes BACKGROUND MOPSE A registered study at www.clinicaltrials.gov Conducted between March 2004 and April 2007 Protocol Paper:
Multicenter Osteopathic Pneumonia Study in the Elderly (MOPSE) The Primary Outcomes BACKGROUND MOPSE A registered study at www.clinicaltrials.gov Conducted between March 2004 and April 2007 Protocol Paper:
BIOE221. Session 5. Examination of Thorax- Respiratory system. Bioscience Department. Endeavour College of Natural Health endeavour.edu.
 BIOE221 Session 5 Examination of Thorax- Respiratory system Bioscience Department Session Objectives Understand the structure of the thorax and the organs contained in this cavity Understand the importance
BIOE221 Session 5 Examination of Thorax- Respiratory system Bioscience Department Session Objectives Understand the structure of the thorax and the organs contained in this cavity Understand the importance
Non-Invasive PCO 2 Monitoring in Infants Hospitalized with Viral Bronchiolitis
 Non-Invasive PCO 2 Monitoring in Infants Hospitalized with Viral Bronchiolitis Gal S, Riskin A, Chistyakov I, Shifman N, Srugo I, and Kugelman A Pediatric Department and Pediatric Pulmonary Unit Bnai Zion
Non-Invasive PCO 2 Monitoring in Infants Hospitalized with Viral Bronchiolitis Gal S, Riskin A, Chistyakov I, Shifman N, Srugo I, and Kugelman A Pediatric Department and Pediatric Pulmonary Unit Bnai Zion
Pulmonology Elective PL-1 Residents
 PL-1 Residents The Pulmonary elective is available to first year residents in either a 2 or 4 week block rotation. The experience will include performing inpatient consultations, attending outpatient clinics
PL-1 Residents The Pulmonary elective is available to first year residents in either a 2 or 4 week block rotation. The experience will include performing inpatient consultations, attending outpatient clinics
Diffusion: Oxygen in the alveoli move into capillaries to go to the body, and carbon
 1 2 Oxygenation and Perfusion Alina Ruiz, MSN-Ed., RN Anatomy and Physiology of Oxygenation What does the respiratory system do? 3 4 5 6 7 Lungs: Ventilation vs Respiration vs Perfusion Ventilation is
1 2 Oxygenation and Perfusion Alina Ruiz, MSN-Ed., RN Anatomy and Physiology of Oxygenation What does the respiratory system do? 3 4 5 6 7 Lungs: Ventilation vs Respiration vs Perfusion Ventilation is
Quick Literature Searches
 Quick Literature Searches National Pediatric Nighttime Curriculum Written by Leticia Shanley, MD, FAAP Institution: University of Texas Southwestern Medical Center Case 1 It s 1:00am and you have just
Quick Literature Searches National Pediatric Nighttime Curriculum Written by Leticia Shanley, MD, FAAP Institution: University of Texas Southwestern Medical Center Case 1 It s 1:00am and you have just
Bronchiolitis Update. Key reviewer: Dr Philip Pattemore, Associate Professor of Paediatrics, University of Otago, Christchurch.
 www.bpac.org.nz keyword: bronchiolitis Bronchiolitis Update Key reviewer: Dr Philip Pattemore, Associate Professor of Paediatrics, University of Otago, Christchurch Key Points: Bronchiolitis is the most
www.bpac.org.nz keyword: bronchiolitis Bronchiolitis Update Key reviewer: Dr Philip Pattemore, Associate Professor of Paediatrics, University of Otago, Christchurch Key Points: Bronchiolitis is the most
Acute Respiratory Disorders. and How to Assess them: Diagnostics
 Acute Respiratory Disorders and How to Assess them: Diagnostics Objectives Discuss 6 diagnostic tests or procedures used to assess lung disorders Name the parts of a focused assessment of a patient with
Acute Respiratory Disorders and How to Assess them: Diagnostics Objectives Discuss 6 diagnostic tests or procedures used to assess lung disorders Name the parts of a focused assessment of a patient with
Author's response to reviews
 Author's response to reviews Title:Differences upon admission and in hospital course of children hospitalized pneumonia: a retrospective cohort study Authors: Raquel Simbalista (r.simbalista@terra.com.br)
Author's response to reviews Title:Differences upon admission and in hospital course of children hospitalized pneumonia: a retrospective cohort study Authors: Raquel Simbalista (r.simbalista@terra.com.br)
PAEDIATRIC RESPIRATORY MEDICINE- LOGBOOK 1
 PAEDIATRIC RESPIRATORY MEDICINE- LOGBOOK 1 Module A1 In-patient management of acute respiratory illness 1. Record of a total of 50 cases in 24 36 months to reflect competencies outlined in curriculum Bronchiolitis
PAEDIATRIC RESPIRATORY MEDICINE- LOGBOOK 1 Module A1 In-patient management of acute respiratory illness 1. Record of a total of 50 cases in 24 36 months to reflect competencies outlined in curriculum Bronchiolitis
Is Physiotherapy routinely required following video-assisted thoracoscopic surgery (VATS)?
 Is Physiotherapy routinely required following video-assisted thoracoscopic surgery (VATS)? SCTS Forum presentation #938 March 27 th 2015 P Agostini, K Massey, M Kalkat, PB Rajesh, RS Steyn, B Naidu, E
Is Physiotherapy routinely required following video-assisted thoracoscopic surgery (VATS)? SCTS Forum presentation #938 March 27 th 2015 P Agostini, K Massey, M Kalkat, PB Rajesh, RS Steyn, B Naidu, E
Chapter 24. Kyphoscoliosis. Mosby items and derived items 2011, 2006 by Mosby, Inc., an affiliate of Elsevier Inc.
 Chapter 24 Kyphoscoliosis 1 A Figure 24-1. Kyphoscoliosis. Posterior and lateral curvature of the spine causing lung compression. Excessive bronchial secretions (A) and atelectasis (B) are common secondary
Chapter 24 Kyphoscoliosis 1 A Figure 24-1. Kyphoscoliosis. Posterior and lateral curvature of the spine causing lung compression. Excessive bronchial secretions (A) and atelectasis (B) are common secondary
RESPIRATORY REHABILITATION
 RESPIRATORY REHABILITATION By: Dr. Fatima Makee AL-Hakak University of kerbala College of nursing CHEST PHYSIOTHERAPY Chest physiotherapy (CPT) includes: 1.Postural drainage. 2.Chest percussion and vibration.
RESPIRATORY REHABILITATION By: Dr. Fatima Makee AL-Hakak University of kerbala College of nursing CHEST PHYSIOTHERAPY Chest physiotherapy (CPT) includes: 1.Postural drainage. 2.Chest percussion and vibration.
Community Acquired Pneumonia
 April 2014 References: 1. Bradley JS, Byington CL, Shah SS, Alverson B, Carter ER, Harrison C, Kaplan SL Mace SE, McCracken Jr. GH, Moor MR, St. Peter SD, Stockwell JA, and Swanson JT. The Management of
April 2014 References: 1. Bradley JS, Byington CL, Shah SS, Alverson B, Carter ER, Harrison C, Kaplan SL Mace SE, McCracken Jr. GH, Moor MR, St. Peter SD, Stockwell JA, and Swanson JT. The Management of
Active Cycle of Breathing Technique
 Active Cycle of Breathing Technique Full Title of Guideline: Author (include email and role): Division & Speciality: Version: 3 Ratified by: Scope (Target audience, state if Trust wide): Review date (when
Active Cycle of Breathing Technique Full Title of Guideline: Author (include email and role): Division & Speciality: Version: 3 Ratified by: Scope (Target audience, state if Trust wide): Review date (when
EMPYEMA. Catheter Based Treatment vs. VATS. UCHSC Department of Surgery Grand Rounds August 27 th, Jeremy Hedges, M.D.
 EMPYEMA Catheter Based Treatment vs. VATS UCHSC Department of Surgery Grand Rounds August 27 th, 2007 Jeremy Hedges, M.D. OVERVIEW Empyema Pathogenesis Treatment Catheter based treatment Fibrinolytics
EMPYEMA Catheter Based Treatment vs. VATS UCHSC Department of Surgery Grand Rounds August 27 th, 2007 Jeremy Hedges, M.D. OVERVIEW Empyema Pathogenesis Treatment Catheter based treatment Fibrinolytics
Chronic obstructive pulmonary disease
 Chronic obstructive pulmonary disease By: Dr. Fatima Makee AL-Hakak () University of kerbala College of nursing Out lines What is the? Overview Causes of Symptoms of What's the difference between and asthma?
Chronic obstructive pulmonary disease By: Dr. Fatima Makee AL-Hakak () University of kerbala College of nursing Out lines What is the? Overview Causes of Symptoms of What's the difference between and asthma?
Clinical signs of pneumonia in infants under
 Archives of Disease in Childhood 1994; 70: 413-417 Postgraduate Institute of Medical Education and Research, Chandigarh, India, Department of Paediatrics Sunit Singhi Anil Dhawan B N S Walia Department
Archives of Disease in Childhood 1994; 70: 413-417 Postgraduate Institute of Medical Education and Research, Chandigarh, India, Department of Paediatrics Sunit Singhi Anil Dhawan B N S Walia Department
Chronic Obstructive Pulmonary Disease (COPD) Copyright 2014 by Mosby, an imprint of Elsevier Inc.
 Chronic Obstructive Pulmonary Disease () 8.18.18 Copyright 2014 by Mosby, an imprint of Elsevier Inc. Description Airflow limitation not fully reversible progressive Abnormal inflammatory response of lungs
Chronic Obstructive Pulmonary Disease () 8.18.18 Copyright 2014 by Mosby, an imprint of Elsevier Inc. Description Airflow limitation not fully reversible progressive Abnormal inflammatory response of lungs
Setting The setting was outpatient departments of referral hospitals. The economic analysis was conducted in India.
 Three day versus five day treatment with amoxicillin for non-severe pneumonia in young children: a multicentre randomised controlled trial ISCAP study group Record Status This is a critical abstract of
Three day versus five day treatment with amoxicillin for non-severe pneumonia in young children: a multicentre randomised controlled trial ISCAP study group Record Status This is a critical abstract of
Chronic Lung Disease in vertically HIV infected children. Dr B O Hare Senior Lecturer in Paediatrics and Child Health, COM, Blantyre
 Chronic Lung Disease in vertically HIV infected children Dr B O Hare Senior Lecturer in Paediatrics and Child Health, COM, Blantyre Natural history of HIV in vertically infected children without and with
Chronic Lung Disease in vertically HIV infected children Dr B O Hare Senior Lecturer in Paediatrics and Child Health, COM, Blantyre Natural history of HIV in vertically infected children without and with
Repeated Pneumonia Severity Index Measurement After Admission Increases its Predictive Value for Mortality in Severe Community-acquired Pneumonia
 ORIGINAL ARTICLE Repeated Pneumonia Severity Index Measurement After Admission Increases its Predictive Value for Mortality in Severe Community-acquired Pneumonia Chiung-Zuei Chen, 1 Po-Sheng Fan, 2 Chien-Chung
ORIGINAL ARTICLE Repeated Pneumonia Severity Index Measurement After Admission Increases its Predictive Value for Mortality in Severe Community-acquired Pneumonia Chiung-Zuei Chen, 1 Po-Sheng Fan, 2 Chien-Chung
The Use of Active Cycle of Breathing Technique (ACBT) In Pulmonary Physiotherapy: A Critical Review of the Literature Lauro G. Villegas Jr.
 The Use of Active Cycle of Breathing Technique (ACBT) In Pulmonary Physiotherapy: A Critical Review of the Literature Lauro G. Villegas Jr., PTRP Keywords: Active Cycle of Breathing Technique (ACBT), Pulmonary
The Use of Active Cycle of Breathing Technique (ACBT) In Pulmonary Physiotherapy: A Critical Review of the Literature Lauro G. Villegas Jr., PTRP Keywords: Active Cycle of Breathing Technique (ACBT), Pulmonary
CHEST PHYSIOTHERAPY IN NICU PURPOSE POLICY STATEMENTS SITE APPLICABILITY PRACTICE LEVEL/COMPETENCIES. The role of chest physiotherapy in the NICU
 PURPOSE The role of chest physiotherapy in the NICU POLICY STATEMENTS In principle chest physiotherapy should be limited to those infants considered most likely to benefit with significant respiratory
PURPOSE The role of chest physiotherapy in the NICU POLICY STATEMENTS In principle chest physiotherapy should be limited to those infants considered most likely to benefit with significant respiratory
Community-Acquired Pneumonia OBSOLETE 2
 Community-Acquired Pneumonia OBSOLETE 2 Clinical practice guidelines serve as an educational reference, and do not supersede the clinical judgment of the treating physician with respect to appropriate
Community-Acquired Pneumonia OBSOLETE 2 Clinical practice guidelines serve as an educational reference, and do not supersede the clinical judgment of the treating physician with respect to appropriate
AFCH NEUROMUSCULAR DISORDERS (NMD) PROTOCOL
 AFCH NEUROMUSCULAR DISORDERS (NMD) PROTOCOL A. Definition of Therapy: 1. Cough machine: 4 sets of 5 breaths with a goal of I:E pressures approximately the same of 30-40. Inhale time = 1 second, exhale
AFCH NEUROMUSCULAR DISORDERS (NMD) PROTOCOL A. Definition of Therapy: 1. Cough machine: 4 sets of 5 breaths with a goal of I:E pressures approximately the same of 30-40. Inhale time = 1 second, exhale
Respiratory Emergencies. Chapter 11
 Respiratory Emergencies Chapter 11 Respiratory System Anatomy and Function of the Lung Characteristics of Adequate Breathing Normal rate and depth Regular breathing pattern Good breath sounds on both sides
Respiratory Emergencies Chapter 11 Respiratory System Anatomy and Function of the Lung Characteristics of Adequate Breathing Normal rate and depth Regular breathing pattern Good breath sounds on both sides
PRE-HOSPITAL EMERGENCY CARE COURSE.
 PRE-HOSPITAL EMERGENCY CARE COURSE www.basics.org.uk Chest Assessment & Management BASICS Education March 2016 Objectives To understand the importance of oxygenation and ventilation To be able to describe
PRE-HOSPITAL EMERGENCY CARE COURSE www.basics.org.uk Chest Assessment & Management BASICS Education March 2016 Objectives To understand the importance of oxygenation and ventilation To be able to describe
Moving from VAP to VAC
 Moving from VAP to VAC Cindy Munro, PhD, RN, ANP-BC, FAANP, FAAN Associate Dean of Research and Innovation Professor College of Nursing Conflict of interest: No relationships with pharmaceutical companies,
Moving from VAP to VAC Cindy Munro, PhD, RN, ANP-BC, FAANP, FAAN Associate Dean of Research and Innovation Professor College of Nursing Conflict of interest: No relationships with pharmaceutical companies,
Frequency of Positive Radiological Findings in Clinically Diagnosed Cases of Pneumonia in Children
 Proceeding S.Z.P.G.M.I. Vol: 30(2): pp. 89-93, 2016. Frequency of Positive Radiological Findings in Clinically Diagnosed Cases of Pneumonia in Children Hajira Umer, 1 Uzma Jabeen, 2 Sara Saeed Malik 1
Proceeding S.Z.P.G.M.I. Vol: 30(2): pp. 89-93, 2016. Frequency of Positive Radiological Findings in Clinically Diagnosed Cases of Pneumonia in Children Hajira Umer, 1 Uzma Jabeen, 2 Sara Saeed Malik 1
Semiology of respiratory system in children Simple choice 1. Mark the intrauterine age of lung development onset from the gut: a) 1 week b) 24 days
 Semiology of respiratory system in children Simple choice 1. Mark the intrauterine age of lung development onset from the gut: a) 1 week b) 24 days c) 6 weeks d) 12 weeks e) 35 weeks 2. Stridor is not
Semiology of respiratory system in children Simple choice 1. Mark the intrauterine age of lung development onset from the gut: a) 1 week b) 24 days c) 6 weeks d) 12 weeks e) 35 weeks 2. Stridor is not
Original Article Zinc supplementation for the treatment of severe pneumonia in hospitalized children: A randomized controlled trial
 Original Article Zinc supplementation for the treatment of severe pneumonia in hospitalized children: A randomized controlled trial Nazia Shehzad (1), Muhammd Irfan Anwar (2), Tahira Muqaddas (1) (1) Lahore
Original Article Zinc supplementation for the treatment of severe pneumonia in hospitalized children: A randomized controlled trial Nazia Shehzad (1), Muhammd Irfan Anwar (2), Tahira Muqaddas (1) (1) Lahore
Shifting Atelectasis: A sign of foreign body aspiration in a pediatric patient
 Shifting Atelectasis: A sign of foreign body aspiration in a pediatric patient Diana L Mark, RRT Pediatric Clinical Specialist Respiratory Care Wesley Children s Hospital Discuss when foreign body aspiration
Shifting Atelectasis: A sign of foreign body aspiration in a pediatric patient Diana L Mark, RRT Pediatric Clinical Specialist Respiratory Care Wesley Children s Hospital Discuss when foreign body aspiration
Guideline for the Management of Acute Chest Syndrome in Children with Sickle Cell Disease
 Guideline for the Management of Acute Chest Syndrome in Children with Sickle Cell Disease Definition Acute chest syndrome (ACS) is defined as an acute illness characterized by fever and/or respiratory
Guideline for the Management of Acute Chest Syndrome in Children with Sickle Cell Disease Definition Acute chest syndrome (ACS) is defined as an acute illness characterized by fever and/or respiratory
Safety, feasibility and efficacy of outpatient management of moderate pneumonia at Port Moresby General Hospital: a prospective study
 Safety, feasibility and efficacy of outpatient management of moderate pneumonia at Port Moresby General Hospital: a prospective study Dr Rose Morre Master of Medicine research project, 2017 Aim To trial
Safety, feasibility and efficacy of outpatient management of moderate pneumonia at Port Moresby General Hospital: a prospective study Dr Rose Morre Master of Medicine research project, 2017 Aim To trial
Chapter 21. Flail Chest. Mosby items and derived items 2011, 2006 by Mosby, Inc., an affiliate of Elsevier Inc.
 Chapter 21 Flail Chest 1 Figure 21-1. Flail chest. Double fractures of three or more adjacent ribs produce instability of the chest wall and paradoxical motion of the thorax. Inset, Atelectasis, a common
Chapter 21 Flail Chest 1 Figure 21-1. Flail chest. Double fractures of three or more adjacent ribs produce instability of the chest wall and paradoxical motion of the thorax. Inset, Atelectasis, a common
Management of acute asthma in children in emergency department. Moderate asthma
 152 Moderate asthma SpO2 92% No clinical features of severe asthma NB: If a patient has signs and symptoms across categories, always treat according to their most severe features agonist 2-10 puffs via
152 Moderate asthma SpO2 92% No clinical features of severe asthma NB: If a patient has signs and symptoms across categories, always treat according to their most severe features agonist 2-10 puffs via
Auscultation of the lung
 Auscultation of the lung Auscultation of the lung by the stethoscope. *Compositions of the stethoscope: 1-chest piece 2-Ear piece 3-Rubber tubs *Auscultation area of the lung(triangle of auscultation).
Auscultation of the lung Auscultation of the lung by the stethoscope. *Compositions of the stethoscope: 1-chest piece 2-Ear piece 3-Rubber tubs *Auscultation area of the lung(triangle of auscultation).
Competency Title: Continuous Positive Airway Pressure
 Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Welcome To Journal Club
 Welcome To Journal Club Presented By Dr. Md. Al-Amin Mridha Registrar, Paediatrics ICMH, Matuail, Dhaka. Evaluation of Hospitalized Infant and Young Children with Bronchiolitisa multi-centre study Kabir
Welcome To Journal Club Presented By Dr. Md. Al-Amin Mridha Registrar, Paediatrics ICMH, Matuail, Dhaka. Evaluation of Hospitalized Infant and Young Children with Bronchiolitisa multi-centre study Kabir
Respiratory Assessment
 Module Four Physical examination of Respiratory Assessment 1 THORACIC CAGE: Anterior thoracic cage Posterior thoracic cage 2 Reference lines: Anterior vertical lines Lateral vertical line Posterior vertical
Module Four Physical examination of Respiratory Assessment 1 THORACIC CAGE: Anterior thoracic cage Posterior thoracic cage 2 Reference lines: Anterior vertical lines Lateral vertical line Posterior vertical
Original article. Abstract. Anil Raj A*, B V Kathyayani.
 Original article Abstract Raj AA, et al: Breathing exercises for pulmonary complications Pre-operative breathing exercise using instructional demonstrationin preventing post-operative pulmonary complications
Original article Abstract Raj AA, et al: Breathing exercises for pulmonary complications Pre-operative breathing exercise using instructional demonstrationin preventing post-operative pulmonary complications
SIMLPE PREDICTORS TO DIFFERENTIATE ACUTE ASTHMA FROM ARI IN CHILDREN : IMPLICATIONS FOR REFINING CASE MANAGEMENT IN THE ARI CONTROL PROGRAMME
 SIMLPE PREDICTORS TO DIFFERENTIATE ACUTE ASTHMA FROM ARI IN CHILDREN : IMPLICATIONS FOR REFINING CASE MANAGEMENT IN THE ARI CONTROL PROGRAMME H.P.S. Sachdev B. Vasanthi L. Satyanarayana R.K. Puri ABSTRACT
SIMLPE PREDICTORS TO DIFFERENTIATE ACUTE ASTHMA FROM ARI IN CHILDREN : IMPLICATIONS FOR REFINING CASE MANAGEMENT IN THE ARI CONTROL PROGRAMME H.P.S. Sachdev B. Vasanthi L. Satyanarayana R.K. Puri ABSTRACT
Top Tips for Pleural Disease in 2012
 Top Tips for Pleural Disease in 2012 The unilateral pleural effusion on the Post Take Ward Round Pleural Effusion on CXR Bedside ultrasound + Pleural aspirate Empyema Nil evidence infection Admit IV antibiotics
Top Tips for Pleural Disease in 2012 The unilateral pleural effusion on the Post Take Ward Round Pleural Effusion on CXR Bedside ultrasound + Pleural aspirate Empyema Nil evidence infection Admit IV antibiotics
Bacterial pneumonia with associated pleural empyema pleural effusion
 EMPYEMA Synonyms : - Parapneumonic effusion - Empyema thoracis - Bacterial pneumonia - Pleural empyema, pleural effusion - Lung abscess - Complicated parapneumonic effusions (CPE) 1 Bacterial pneumonia
EMPYEMA Synonyms : - Parapneumonic effusion - Empyema thoracis - Bacterial pneumonia - Pleural empyema, pleural effusion - Lung abscess - Complicated parapneumonic effusions (CPE) 1 Bacterial pneumonia
H: Respiratory Care. Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79
 H: Respiratory Care Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79 Competency: H-1 Airway Management H-1-1 H-1-2 H-1-3 H-1-4 H-1-5 Demonstrate knowledge
H: Respiratory Care Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79 Competency: H-1 Airway Management H-1-1 H-1-2 H-1-3 H-1-4 H-1-5 Demonstrate knowledge
IPV INTRAPULMONARY PERCUSSIVE VENTILATION IPV 23/03/2013 IPV INTRAPULMONARY PERCUSSIVE VENTILATION
 INTRAPULMONARY PERCUSSIVE VENTILATION INTRAPULMONARY PERCUSSIVE VENTILATION FT Vilma Donizetti Valduce Hospital FT Vilma Donizetti Rehabilitation Center Villa Beretta Costa Masnaga, Lecco (I) It s a ventilatory
INTRAPULMONARY PERCUSSIVE VENTILATION INTRAPULMONARY PERCUSSIVE VENTILATION FT Vilma Donizetti Valduce Hospital FT Vilma Donizetti Rehabilitation Center Villa Beretta Costa Masnaga, Lecco (I) It s a ventilatory
Learning Objectives: continued
 Learning Objectives: Describe the importance of a comprehensive assessment of a critically ill patient Describe how to assess the efficacy of breathing, work of breathing and adequacy of ventilation Discuss
Learning Objectives: Describe the importance of a comprehensive assessment of a critically ill patient Describe how to assess the efficacy of breathing, work of breathing and adequacy of ventilation Discuss
Over the last several years various national and
 Recommendations for the Management of COPD* Gary T. Ferguson, MD, FCCP Three sets of guidelines for the management of COPD that are widely recognized (from the European Respiratory Society [ERS], American
Recommendations for the Management of COPD* Gary T. Ferguson, MD, FCCP Three sets of guidelines for the management of COPD that are widely recognized (from the European Respiratory Society [ERS], American
PERIODIC ASBESTOS MEDICAL QUESTIONNAIRE
 Date: / / PERIODIC ASBESTOS MEDICAL QUESTIONNAIRE NAME: SS#: - - COMPANY: 1. OCCUPATIONAL HISTORY A. Have you ever worked full time (30 hours per week or more) for 6 months or more? IF YES, TO 1B: B. Have
Date: / / PERIODIC ASBESTOS MEDICAL QUESTIONNAIRE NAME: SS#: - - COMPANY: 1. OCCUPATIONAL HISTORY A. Have you ever worked full time (30 hours per week or more) for 6 months or more? IF YES, TO 1B: B. Have
Respiratory Failure in the Pediatric Patient
 Respiratory Failure in the Pediatric Patient Ndidi Musa M.D. Associate Professor of Pediatrics Medical College of Wisconsin Pediatric Cardiac Intensivist Children s Hospital of Wisconsin Objectives Recognize
Respiratory Failure in the Pediatric Patient Ndidi Musa M.D. Associate Professor of Pediatrics Medical College of Wisconsin Pediatric Cardiac Intensivist Children s Hospital of Wisconsin Objectives Recognize
JOINT CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD) MANAGEMENT GUIDELINES
 JOINT CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD) MANAGEMENT GUIDELINES Authors Dr Ian Benton Respiratory Consultant COCH Penny Rideal Respiratory Nurse COCH Kirti Burgul Respiratory Pharmacist COCH Pam
JOINT CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD) MANAGEMENT GUIDELINES Authors Dr Ian Benton Respiratory Consultant COCH Penny Rideal Respiratory Nurse COCH Kirti Burgul Respiratory Pharmacist COCH Pam
Master of Physical Therapy Program: Year 2 CARDIORESPIRATORY COURSE OUTLINES SUMMARY
 Master of Physical Therapy Program: Year 2 CARDIORESPIRATORY COURSE OUTLINES SUMMARY Course: PT 6124 Physical Therapy and Hospital based Care Through lecture, tutorial and laboratory sessions, students
Master of Physical Therapy Program: Year 2 CARDIORESPIRATORY COURSE OUTLINES SUMMARY Course: PT 6124 Physical Therapy and Hospital based Care Through lecture, tutorial and laboratory sessions, students
Respiratory Physio Protocol for Paediatric Patients on BIPAP via a tracheotomy (uncuffed tube)
 This is an official Northern Trust policy and should not be edited in any way Respiratory Physio Protocol for Paediatric Patients on BIPAP via a tracheotomy (uncuffed tube) Reference Number: NHSCT/12/547
This is an official Northern Trust policy and should not be edited in any way Respiratory Physio Protocol for Paediatric Patients on BIPAP via a tracheotomy (uncuffed tube) Reference Number: NHSCT/12/547
PATIENT CHARACTERISTICS AND PREOPERATIVE DATA (ecrf 1).
 PATIENT CHARACTERISTICS AND PREOPERATIVE DATA (ecrf 1). 1 Inform Consent Date: / / dd / Mmm / yyyy 2 Patient identifier: Please enter the 6 digit Patient identification number from your site patient log
PATIENT CHARACTERISTICS AND PREOPERATIVE DATA (ecrf 1). 1 Inform Consent Date: / / dd / Mmm / yyyy 2 Patient identifier: Please enter the 6 digit Patient identification number from your site patient log
Viruses, bacteria, fungus, parasites (in rare cases) or other organisms can cause pneumonia.
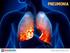 1 Pneumonia Pneumonia is an infection which inflames the air sacs either in one or both of the lungs. The air sacs are generally filled with fluid or pus, causing cough along with phlegm or pus, fever,
1 Pneumonia Pneumonia is an infection which inflames the air sacs either in one or both of the lungs. The air sacs are generally filled with fluid or pus, causing cough along with phlegm or pus, fever,
Care of the Patient with a Respiratory Disorder
 Care of the Patient with a Respiratory Disorder 1 Slide 1 Overview of Anatomy and Physiology External respiration Exchange of oxygen and carbon dioxide between the lung and the environment Internal respiration
Care of the Patient with a Respiratory Disorder 1 Slide 1 Overview of Anatomy and Physiology External respiration Exchange of oxygen and carbon dioxide between the lung and the environment Internal respiration
Bronchiolitis: when to reassure and monitor, and when to refer
 CHILD health Respiratory conditions Bronchiolitis: when to reassure and monitor, and when to refer Key practice points: Bronchiolitis should be diagnosed clinically; blood tests, analysis of sputum, testing
CHILD health Respiratory conditions Bronchiolitis: when to reassure and monitor, and when to refer Key practice points: Bronchiolitis should be diagnosed clinically; blood tests, analysis of sputum, testing
Critical Care Therapy and Respiratory Care Section
 Critical Care Therapy and Respiratory Care Section Category: Clinical Section: Bronchial Hygiene Title: Chest Physiotherapy Policy #: 01 Revised: 03/00 1.0 DESCRIPTION 1.1 Definition Chest physiotherapy
Critical Care Therapy and Respiratory Care Section Category: Clinical Section: Bronchial Hygiene Title: Chest Physiotherapy Policy #: 01 Revised: 03/00 1.0 DESCRIPTION 1.1 Definition Chest physiotherapy
and localized ground glass opacities, or bronchiolar focal or multifocal micronodules;
 E1 Chest CT scan and Pneumoniae_YE Claessens et al- Supplementary methods Level of CAP probability according to CT scan - definite CAP: systematic alveolar condensation, or alveolar condensation with peripheral
E1 Chest CT scan and Pneumoniae_YE Claessens et al- Supplementary methods Level of CAP probability according to CT scan - definite CAP: systematic alveolar condensation, or alveolar condensation with peripheral
REFERRAL GUIDELINES RESPIRATORY
 REFERRAL GUIDELINES RESPIRATORY Referral Form: The GP Referral Template is the preferred referral tool (previously known as the Victorian Statewide Referral Form) GP Referral Template This tool is housed
REFERRAL GUIDELINES RESPIRATORY Referral Form: The GP Referral Template is the preferred referral tool (previously known as the Victorian Statewide Referral Form) GP Referral Template This tool is housed
Management of Bronchiolitis in Infants
 Co-issued by Paediatric Medicine and the Division of Paediatric Emergency Medicine. 1.0 Introduction Bronchiolitis is an acute inflammatory disease of the lower respiratory tract, resulting from obstruction
Co-issued by Paediatric Medicine and the Division of Paediatric Emergency Medicine. 1.0 Introduction Bronchiolitis is an acute inflammatory disease of the lower respiratory tract, resulting from obstruction
Nebulized Hypertonic Saline for Acute Bronchiolitis: A Systematic Review
 Nebulized Hypertonic Saline for Acute Bronchiolitis: A Systematic Review Linjie Zhang, MD, PhD a, Raúl A. Mendoza-Sassi, MD, PhD a, Terry P. Klassen, MD b, Claire Wainwright, MD c BACKGROUND AND OBJECTIVE:
Nebulized Hypertonic Saline for Acute Bronchiolitis: A Systematic Review Linjie Zhang, MD, PhD a, Raúl A. Mendoza-Sassi, MD, PhD a, Terry P. Klassen, MD b, Claire Wainwright, MD c BACKGROUND AND OBJECTIVE:
DOI: /peds The online version of this article, along with updated information and services, is located on the World Wide Web at:
 Clinical Predictors of Pneumonia Among Children With Wheezing Bonnie Mathews, Sonal Shah, Robert H. Cleveland, Edward Y. Lee, Richard G. Bachur and Mark I. Neuman Pediatrics 2009;124;e29 DOI: 10.1542/peds.2008-2062
Clinical Predictors of Pneumonia Among Children With Wheezing Bonnie Mathews, Sonal Shah, Robert H. Cleveland, Edward Y. Lee, Richard G. Bachur and Mark I. Neuman Pediatrics 2009;124;e29 DOI: 10.1542/peds.2008-2062
pneumonia 2015;6:48 56
 pneumonia 2015 Aug 21;6:48 56 pneumonia Brief Report Anne B Chang a,b, Heidi Smith-Vaughan a,c, Theo P Sloots f, Patricia C Valery a, David Whiley f, Jemima Beissbarth a, Paul J Torzillo d,e a Menzies
pneumonia 2015 Aug 21;6:48 56 pneumonia Brief Report Anne B Chang a,b, Heidi Smith-Vaughan a,c, Theo P Sloots f, Patricia C Valery a, David Whiley f, Jemima Beissbarth a, Paul J Torzillo d,e a Menzies
The Respiratory System
 130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Pulmonary
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Pulmonary 1. GOAL: Diagnose and manage patients with asthma. 2. GOAL: Understand the role of the pediatrician in preventing
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Pulmonary 1. GOAL: Diagnose and manage patients with asthma. 2. GOAL: Understand the role of the pediatrician in preventing
Carole Wegner RN, MSN And Lori Leiser CRT
 Airway Clearance Carole Wegner RN, MSN And Lori Leiser CRT Topics Suctioning and suctioning equipment Medications to facilitate t airway clearance Bronchial hygiene modalities Preparing for suctioning
Airway Clearance Carole Wegner RN, MSN And Lori Leiser CRT Topics Suctioning and suctioning equipment Medications to facilitate t airway clearance Bronchial hygiene modalities Preparing for suctioning
Chronic obstructive lung disease. Dr/Rehab F.Gwada
 Chronic obstructive lung disease Dr/Rehab F.Gwada Obstructive lung diseases Problem is in the expiratory phase Lung disease Restrictive lung disease Restriction may be with, or within the chest wall Problem
Chronic obstructive lung disease Dr/Rehab F.Gwada Obstructive lung diseases Problem is in the expiratory phase Lung disease Restrictive lung disease Restriction may be with, or within the chest wall Problem
Exam 1 Review. Cardiopulmonary Symptoms Physical Examination Clinical Laboratory Studies
 Exam 1 Review Cardiopulmonary Symptoms Physical Examination Clinical Laboratory Studies WBC Count Differential A patient had been admitted to the hospital for acute shortness of breath. A CXR examination
Exam 1 Review Cardiopulmonary Symptoms Physical Examination Clinical Laboratory Studies WBC Count Differential A patient had been admitted to the hospital for acute shortness of breath. A CXR examination
The RESPIRATORY System. Unit 3 Transportation Systems
 The RESPIRATORY System Unit 3 Transportation Systems Functions of the Respiratory System Warm, moisten, and filter incoming air Resonating chambers for speech and sound production Oxygen and Carbon Dioxide
The RESPIRATORY System Unit 3 Transportation Systems Functions of the Respiratory System Warm, moisten, and filter incoming air Resonating chambers for speech and sound production Oxygen and Carbon Dioxide
Community Acquired Pneumonia. Abdullah Alharbi, MD, FCCP
 Community Acquired Pneumonia Abdullah Alharbi, MD, FCCP A 68 y/ male presented to the ED with SOB and productive coughing for 2 days. Reports poor oral intake since onset due to nausea and intermittent
Community Acquired Pneumonia Abdullah Alharbi, MD, FCCP A 68 y/ male presented to the ED with SOB and productive coughing for 2 days. Reports poor oral intake since onset due to nausea and intermittent
Respiratory Management in Pediatrics
 Respiratory Management in Pediatrics Children s Hospital Omaha Critical Care Transport Sue Holmer RN, C-NPT Objectives Examine the differences between the pediatric and adults airways. Recognize respiratory
Respiratory Management in Pediatrics Children s Hospital Omaha Critical Care Transport Sue Holmer RN, C-NPT Objectives Examine the differences between the pediatric and adults airways. Recognize respiratory
National Horizon Scanning Centre. Mannitol dry powder for inhalation (Bronchitol) for cystic fibrosis. April 2008
 Mannitol dry powder for inhalation (Bronchitol) for cystic fibrosis April 2008 This technology summary is based on information available at the time of research and a limited literature search. It is not
Mannitol dry powder for inhalation (Bronchitol) for cystic fibrosis April 2008 This technology summary is based on information available at the time of research and a limited literature search. It is not
