Kelsey Renwick. Clinical Case Report Competition. West Coast College of Massage Therapy Victoria Part-Time. Third Place Winner
|
|
|
- Maximilian Todd
- 6 years ago
- Views:
Transcription
1 Registered Massage Therapists of British Columbia Clinical Case Report Competition West Coast College of Massage Therapy Victoria Part-Time April 2014 Third Place Winner Kelsey Renwick The effects of massage therapy and decreasing thoracic outlet syndrome symptoms P: F: massagetherapy.bc.ca RMTBC 2014
2 Conflict of Interest The author and patient were previously acquainted before the start of the case study. Although previously acquainted, there was no conflict of interest and a therapeutic relationship was developed throughout the course of the case study. The patient committed to the study and was informed of procedures prior to commencing, and was aware her identity would be kept confidential. Acknowledgments I would like to thank my case advisor Dean Robertson for his advice and ideas as well as the rest of the supervisors for their input and motivation. I would also like to thank my patient, who volunteered her time, effort, and positive attitude. Without her this case study would not have been possible.
3 Table of Contents Title Page....1 Acknowledgments 2 Conflict of Interest....2 Abstract Introduction...6 Methods and Procedures...8 Client History...8 Assessment Treatment Reassessment Results Discussion Conclusion References Appendix A: Orthopedic Tests Appendix B: Initial and Final Assessment Pictures Appendix C: Treatment Breakdown Appendix D: Anatomy Pictures Patient Consent Form Clinic Notes
4 Abstract Objective: The objective of this case study was to determine if massage therapy is an effective choice when there is a compression of the brachial plexus, causing Thoracic Outlet Syndrome (TOS) symptoms. The main choice of techniques used was myofascial release, and General Swedish Massage (GSM) techniques. Background: TOS is a common disorder, occurring mainly in athletes who play over hand sports, or workers who do lots of overhead work. The brachial plexus is often compressed due to constant overhead movements, resulting in numbness and tingling down the arm and into the 4 th and 5 th metacarpal joints. The patient being a twenty-year old female, complained of numbness and tingling bilaterally in both her hands and arms. Methods: A total of thirteen hands on treatments were conducted over an eight-week period, focusing on decreasing hyper tonicity bilaterally in the and Pectoralis Minor muscles to relieve neurological symptoms. A postural assessment using a plumb line was used for the initial and final assessment, cervical spine ranges of motion and a selection of orthopedic tests. Myofascial and GSM techniques were preformed each treatment, predominantly focusing on the cervical spine, anterior chest, and forearm musculature. Results: The patient s neurological symptoms decreased immensely, and she was able to perform certain actions (abduction, external rotation and extension) with no feeling of numbness or tingling at all. Most orthopedic tests that were strongly positive prior to massage intervention became negative during the final assessment.
5 Conclusion: Massage therapy was found to be an effective modality in decreasing neurological symptoms due to a compression of the brachial plexus. Keywords: Thoracic Outlet Syndrome, compression, brachial plexus, impingement, neurological symptoms, myofascial release, General Swedish Massage, upper extremity, bilateral Introduction Thoracic Outlet Syndrome (TOS) is a compression disorder of the brachial plexus and potentially the subclavian vasculature (Rattray, 2000). The brachial plexus arises from the cervical spine, traveling through various musculatures, below the clavicle towards the axilla,
6 down the arm, and terminating at the phalanges see Figure 10 in appendix D. Compression occurs because of increased pressure on structures in the thoracic outlet, which consists of muscles, nerves, bones and vasculature. The lower trunks of the brachial plexus, C8-T1 nerve roots, are the most commonly affected, which leads to pain and numbness in the posterior neck, shoulder, medial arm, forearm, and radiates into the ulnarly innervated digits of the hand (Goodman, 2009). TOS causes neuropraxia, which results in the loss of conduction at the compression spot, resulting with no axonal degeneration (Rattray, 2000). When a nerve is compressed most people report paresthesias and pain in the arm (Goodman, 2009). There are three major locations that are prone to impingement: the intrascalene triangle (Anterior Scalene, Middle Scalene and the first rib), costoclavicular space (clavicle and first rib), and the coracopectoral space (under the coracoid process of the scapula and the Pectoralis Minor muscle) please see Figure 11 in appendix D. The trunks of the brachial plexus pass through the intrascalene triangle, and impingement occurs if this space is narrowed, leading to potential neurological or vascular symptoms (Rattray, 2000). Impingement of the Costoclavicular space leads to the vascular symptoms of TOS. The subclavian artery and vein are more susceptible to impingement as the space varies in size due to the position of the shoulder and possible anatomical abnormalities (Rattray, 2000). As the neurovascular bundle passes through the coracopectoral space it can be compressed during certain movements, such as Glenohumeral joint (GH) abduction and maximal extension. There are many contributing factors associated with TOS. Postural variations and stress are most commonly found to be the cause (Goodman, 2009). Postural variations such as anteriorly rounded shoulders, and head forward carriage can cause shortening of Scalene, Levator
7 Scapulae, Subscapularis and Pectoralis Minor muscles, which leads to a decrease of space in the thoracic outlet please see Figure 9 in appendix D. If there is increased pressure on the shoulder girdle such as carrying a heavy bag with a strap, which could result in pressure on the thoracic outlet or potential traction to the brachial plexus (Kisner, 2012). Hypertrophy of the can be caused from over usage of the respiratory muscles due to bronchitis, pneumonia, asthma and emphysema; paradoxical breathing is often present (Rattray, 2000). Injuries resulting with scar tissue formation, inflammation, adhesions or fractures to the clavicle can result in a decrease of motility to the nerves and potential damage to the plexus and surrounding vessels (Kisner, 2009). Congenital factors associated with compression of the brachial plexus involve, a cervical rib or a long transverse process of the C7 vertebra (Kisner, 2012). Overhead sports (such as racquet sports, volleyball etc.) and heavy lifting aggravate and produce symptoms in the upper plexus (Goodman, 2009). Nerve compressions can be treated manually or surgically, with massage therapy playing a key role in the manual aspect. In relation to nerve compression, the use and effectiveness of massage therapy to help relieve symptoms would be beneficial to the profession as this is a common disorder that occurs in the population. This case study was conducted to demonstrate that myofascial release techniques, with integrated GSM techniques, would benefit and over all decrease the bilateral symptoms of Thoracic Outlet Syndrome. Methods and Procedures Client History The patient of this study is a 20-year-old female student, who has bilateral neurological symptoms involving compression of her brachial plexus. The neurological symptoms are felt
8 when the patient externally rotates and extends her GH, or abducts the GH joint; symptoms increase when wrist is extended. With extension and external rotation the patient feels the symptoms on the palmer aspect of her second, fourth, and fifth phalanges. Abduction results in symptoms appearing in the axilla, Triceps, and Biceps Brachii, as well the fourth and fifth phalanges. The symptoms were described by the patient as a heaviness as well as numbness and sharp, shooting tingling ranging from a seven to eight out of ten on the pain scale see appendix A. It was noted that the patient s sleeping position was having the left hand under the pillow with the right leg hip hiked, and occasionally would experience neural symptoms at night due to the fact that the left shoulder was overstretched. The patient had no previous injuries to her cervical spine (C/S), or her GH joint, but has had chronic recurring pain and stiffness bilaterally in her cervical spine, mainly the right side. On palpation it was noted that the Scalene and Sternoclediomastiod (SCM) muscles were hypertoned and the patient felt that she had limited range of motion of her C/S. The patient has no known cervical ribs, although presented with a family history of her grandmother having two. The patient reported that she had headaches rarely, approximately five times a year, mostly stemming from the sub-occipital muscles and were usually stress induced tension headaches. The patient visits a Registered Massage Therapist once a month for maintenance treatments on her neck, as well as recently getting treatment from a Chiropractor twice a week (the patient was instructed to withhold treatments throughout the duration of this case study, although had eight treatments, most pertaining to the lumbar spine). The patient was diagnosed in 1998 with exercise-induced asthma, which is also triggered with sickness or allergies. The asthma does not occur day to day, and the patient has an inhaler (Salbutamol) for when needed. Attacks are often experienced at random. She has noticed that she
9 tends to breathe more from her chest and not so much with her Diaphragm, as she finds it uncomfortable due to her asthma. The patient also mentioned she has undiagnosed Raynaud s Disease, which is cold weather induced. Her hands experience cyanosis bilaterally, usually occurring in all five phalanges as well as the entire hands. Sometimes the patient experiences this in her feet as well. The patient has a family history of cardiovascular problems such as valve replacements and stints, but she has not been diagnosed with any of these at this time. There has been no history of smoking. Assessment The initial assessment took place on September 12 th, In the postural scan the patient showed bilateral anterior rotated shoulders with the left shoulder slightly more superior then the right. Both knees showed hyperextension with a slight valgus angle. It was also observed that there was approximately 9.5 centimeters of head forward carriage projected from the plumb line please see Figure 5 and 7 in appendix B. The patient complained of tightness and stiffness in the C/S, this was assessed using a verbal analogue using the pain scale please see appendix A. A gonimometer (see appendix A) was used on the initial assessment to measure range of motion of the GH and C/S please see appendix A for normal ranges. The patient had neural symptoms in flexion, abduction, internal and external rotation, in the right GH joint and external rotation and abduction in the left GH joint all amounting to seven-eight out of ten on the neural pain scale. Minimal ranges were also seen in flexion, abduction, extension and adduction in both the right and left GH. C/S range of motion showed minimal ranges in all motions, with bilateral rotations and side flexion having the most limitations. C/S presented with no neural symptoms but with pain, which was assessed by using the verbal pain scale.
10 Orthopedic tests were performed to determine what was causing the neural symptoms. These tests included Adson s Maneuver, Wrights Hyperabduction, and Allen s test, which are common TOS tests. Median, radial, and ulnar Upper Limb Tension tests were performed to determine which nerve roots were affected. Other orthopedic tests performed included Costoclavicular Syndrome and Halstead to check for neural symptoms. Capillary Refill and Roo s were performed in order to see if the patient had any vascular symptoms as well as any neural symptoms see appendix A for orthopedic testing results. A series of manual muscle tests were performed as well to indicate which muscles were weak, or which were associated with the pain in the C/S. Over the course of the 13 hands on treatments Adson s and Allen s were used approximately every treatment. After the seventh treatment, all of the Upper Limb Tension tests were performed pre and post treatment. Progress was seen as early as the third hands on treatment. Charts of the orthopedic testing results can be found in appendix 1. Treatments Thirteen sixty-minute hands on treatments took place twice a week for the first ten treatments and then progressed to once a week for the last three treatments. There were two, 70 minute assessments that took place initially and for the final fifteenth session. All thirteen treatments were in the supine position working on the C/S, anterior chest, and bilateral arms. Treatments two to four, twelve, and thirteen included Pectoralis Minor and Major work. Treatments five to thirteen included work on bilateral arms and forearms. All treatments were otherwise the same. Treatments would start with myofascial release (MFR) techniques to the C/S, including a sub-occipital release in order to relax the body and C/S musculature. This technique would be
11 held for approximately one to three minutes depending on when the release was felt. Next, the Scalene muscles would be palpated and the subject would be instructed to place her hands on her stomach and take five deep diaphragmatic breaths, pushing the air into her hands, while still maintaining the hold on the, all the while waiting for a release. GSM techniques were used on the C/S in order to flush out the area, and decrease the hyper tonicity in the SCM and Scalene musculature. A series of thumb, fingertip, and knuckle kneading and stroking were applied. A muscle squeeze was applied to the SCM in order for the musculature to release, therefore gaining better access to the. Contract-relax and isolytic release techniques for the Scalene muscles were introduced in treatments nine to thirteen. The patient was to actively side flex and rotate to the ipsilateral side as far as they could and then resist the pressure of the therapist for five seconds, rest for seven seconds, and repeat twice with the last resting period being held for thirty seconds. This would occur bilaterally. The isolytic release was done passively and actively for three times each, bilaterally. The patient s head would be passively held, and laterally flexed to the opposite side while doing a downward strip of the Scalene musculature, mainly the anterior Scalene. This would be done in the same manner only getting the patient to actively do the side flexion motion. Multiple MFR techniques were applied in order to open up the anterior chest and promote a posterior rotation of the GH joints. An arm pull traction technique was used, with one hand on the Pectoralis musculature and the other applying traction at the mid-humerus, creating a myofascial pull. This would be held for approximately one hundred and twenty seconds or until a release was felt and would be performed bilaterally. Next, the MFR technique used was called reshaping, and would be performed on the Pectoralis Minor muscle by inserting both thumbs into
12 the axilla and then grabbing the rest of the muscle on the anterior chest, applying pressure and holding. With this technique the sheering moved inferiorly down the muscle and applying a slight bend in it as well, creating space around the corocoid process, which is the attachment point of the Pectoralis Minor. Micro-sheering was performed on the Pectoralis Major, by using the middle and index fingers of both hands and applying a MFR sheer. GSM was used to flush as well as to break down adhesions found in the Pectoralis musculature and Subclavius mainly using the muscle stripping techniques. During the treatments that involved the arms and forearms, MFR techniques were used such as sheering, cross-hands and v-stroking to break up adhesions and decrease potential entrapment of the nerves in the forearm. Applying pressure on the tendons and having the patient actively flex and extend her wrist applied Isolytic release to the common flexor and extensor tendons. GSM techniques such as knuckle and forearm stroking and kneading were used. Passive range of motion of wrist, elbow and GH joint and traction to the wrist were applied. This was all performed bilaterally on both arms. In six of the treatments the Diaphragm was worked on with MFR techniques. One hand was placed under her back, in line with where the diaphragm sits, and the other resting inferiorly to the ribs on top of the diaphragm, and held for three to five minutes, waiting for a release or movement. Muscle stripping was also used to break down multiple adhesions in the diaphragm. This was preformed in hopes of taking pressure off the Scalene muscles, as they are a part of the muscles of inspiration see appendix C for treatment breakdown. The patient was given a homecare regime, which included hydrotherapy and remedial exercises to do on a daily basis, in correlation with the massage treatments. Contrast using hot and cold were to be applied to the forearms and the. Starting with heat for three minutes,
13 and then cold for one minute repeating this for three cycles and making sure to end with cold. Heat was given to the patient to apply to the Pectoralis muscles once a day, for a maximum of 20 minutes. The patient was given two stretches after the first treatment, the first was for the Pectoralis muscles, using a doorway or wall, having the elbow bent at ninety degrees with the forearm on the door frame, and turning the torso to the opposite side, feeling a stretch in the anterior chest. The second stretch was for the SCM muscle, stabilizing by holding the chair with one hand, and then extending the C/S, side bend the head to the opposite shoulder, and then rotate the head back the midline, and bringing the chin in towards the chest. A Scalene stretch was added, stabilizing on a chair with the opposite hand, other hand on head, side flexion to that side, and then bring chin into chest slightly to increase the stretch. All stretches were to be held for thirty seconds, twice a day with no pain. The patient was also given the exercise called neural flossing. The arm is to be abducted and slightly extended, or until neural symptoms are felt, and then the wrist is to be flexed and extended. The flossing was to be done for a total of thirty seconds, twice a day, and to be done with no pain. Diaphragmatic breathing was given to the patient to do once a day, for five breaths. The patient was encouraged to place hands on stomach, ribs and back in order to practice breathing into those areas. Reassessment The final assessment took place on November 7 th, Ranges of motion for the GH and the C/S were taken again using the Goniometer. All previous orthopedic testing was repeated in order to find out what the final results were, and if the symptoms had decreased throughout the thirteen treatments. The patient was also put into the positions and preformed the motions that
14 previously brought on the neural symptoms, and it was recorded what the outcome was. Overall the patient was asked if they felt their symptoms had decreased or if they had improved. Results The patient s symptoms had decreased immensely by the end of the thirteen hands on treatments. The Scalene and Pectoralis muscles had decreased hyper tonicity, and the overall tissue quality felt more moveable. The TOS symptoms were decreasing as early as the third treatment as the Adson s test had been negative in the post treatment of the right side. The Upper Limb Tension test for the Ulnar nerve decreased during the ninth treatment, and Allen s started to see negative results on the tenth treatment. Overall GH and C/S range of motion improved greatly. C/S ranges were brought to the maximum range, with no pain. Tension in the C/S has decreased but subject described the C/S as still being stiff. GH ranges improved considerably, all neural symptoms disappeared, only abduction on both sides had a minimal amount (one out of ten on the pain scale). (See appendix A for full results) The patient stated that neural symptoms were minimal, and was now able to hold the GH extension, external rotation, and wrist extension position without discomfort. The patient remarked that the symptoms on the left side were almost gone, where as the right still has more, but very minimal symptoms. Neural symptoms were no longer felt in axilla or the phalanges with external rotation and extension but the patient could feel very minimal fuzzy symptoms in the forearm and upper arm. With abduction symptoms were only occurring minimally in the Biceps Brachaii and Triceps. The final postural scan showed an improvement, the shoulders were now more posteriorly rotated, with the chest looking more open. The head forward carriage has decreased by.5 of a centimeter, resulting in 9 centimeters of head forward carriage please see Figure 6 and 8 in
15 appendix B. By the tenth treatment, the patient was able to go from two treatments a week, down to once a week and did not break the pain tension cycle. Discussion The results of this study indicate that the use of MFR and GSM techniques are beneficial in releasing the compression of the brachial plexus in a TOS subject. By using MFR techniques the patients anteriorly rotated shoulders became more posteriorly rotated, which allowed more space for the brachial plexus, and thus relieving compression. Notably, a correction of posture played a role in relieving symptoms and for further improvement it would be advisable for the patient to do strengthening exercises for the back and continue stretching the anterior chest in order to prevent a kyphotic posture and future compression. The patient was compliant following the homecare given specific to the neural symptoms, which was the neural flossing technique, but was unsuccessful with the other homecare exercises provided to her. The patient was asked prior to each treatment how the homecare regime was going and by the eighth interview it was reported that the subject was not keeping up with the SCM stretch and Pectoralis stretch as much as the neural flossing and Scalene stretches. If the patient had been more proactive with the homecare, there could have been more room for potentially better results. The patient was also advised to withhold getting treatments from her Chiropractor and RMT for the duration of this case study in order to keep the variables as low as possible. However, the patient continued to see her chiropractor for a total of eight treatments. In the regards to changing the treatments, spending more time on the Diaphragm, with MFR and strengthening exercises would have been beneficial to the patient due to her asthma. Strengthening her diaphragm could potentially aid in decreasing the extra stress put on the Scalene and Pectoralis muscles as it would encourage the subject to breath into her abdomen and
16 not consistently into her chest. With a decrease of stress on her and Pectoralis Minor muscle, the hyper tonicity would potentially decrease, causing less compression symptoms. It would be advisable for the patient to continue getting massage therapy treatment once a week, and paying attention to strengthening her Diaphragm and continue to maintain the muscles of respiration. Conclusion This case study proved that using MFR and GSM techniques could decrease neurological symptoms due to compression of the brachial plexus. Performing myofascial techniques beginning at the C/S and following the nerve path down the arm provided a positive result in relieving symptoms, decreasing pain and tension in the C/S and anterior chest. The main focus was to decrease the tension in the and Pectoralis Minor muscles and progress was seen by the fourth treatment, when the patient extended her GH joints, neurological symptoms had decreased since the first initial assessment. By treatment seven, the patient could extend the GH joints with no symptoms except with wrist extension, and by the thirteenth treatment neurological symptoms were minimal to none. It would be advised to explore the idea of further studies on the impacts and effects of massage therapy on compression syndromes of the brachial plexus. References Goodman, C. C., & Fuller, K. S. (2009). The Peripheral Nervous System. Pathology: Implications for the Physical Therapist (3rd ed., pp ). Philadelphia: Saunders. Hertling, D., & Kessler, R. M. (2006). Shoulder and Shoulder Girdle. Management of Common Musculoskeletal Disorders: Physical Therapy Principles and Methods (4 th ed., pp. 317-
17 319). Philadelphia: J.B. Lippincott. Kisner, C., & Colby, L. A. (2012). Peripheral Nerve Disorders and Management. Therapeutic Exercise: Foundations and Techniques (6 th ed., pp ). Philadelphia: F.A. Davis. Lowe, S. (2013). Musculoskeletal Anatomy & Kinesiology Lab 2: Manual Muscle Testing Magee, D. J. (2008). Shoulder. Orthopedic Physical Assessment (5 th ed., pp ). St. Louis, Mo.: Saunders Elsevier. Morphopedics. (n.d.). Thoracic Outlet Syndrome -. Retrieved December 22, 2013, from Rattray, F. S., & Ludwig, L. (2000). Thoracic Outlet Syndrome. Clinical Massage Therapy: Understanding, Assessing and Treating Over 70 Conditions (pp ). Toronto: Talus Inc.. "Repetitive Strain Injuries (RSI)." Repetitive Strain Injuries (RSI) Carpal Tunnel Syndrome Symptoms Treatment COEN Baltimore Neurology Maryland COEN Center for Occupational and Environmental Neurology. N.p., n.d. Web. 22 Dec < TOS - Thoracic Outlet Syndrome. (n.d.). TOS - Thoracic Outlet Syndrome. Retrieved December 22, 2013, from
18 Appendix A: Orthopedic Testing Verbal analogue of the pain scale Zero being no pain and ten being the worst pain you ve felt Goniometer A device used to measure angles; visual of how much movement is at a joint. Table 1.0: Cervical Spine Normal Range of Motion (Magee, 2007) Flexion Extension Right side bend side bend Right rotation rotation
19 Table 2.0: Glenohumeral Joint Normal Range of Motion (Magee, 2007) Flexion Extension Abduction Adduction Internal Rotation External Rotation Table 3.0: GH Active Range of Motion First Assessment Range of Motion Right GH GH Flexion 165 7/10 neural 170 Extension Abduction 175 8/10 neural 170 8/10 neural Adduction Internal Rotation 85 7/10 neural 85 External Rotation 80 7/10 neural 80 7/10 neural Table 4.0 GH Active Range of Motion Final Assessment Range of Motion Right GH GH Flexion Extension Abduction 180 1/10 neural 180 1/10 neural Adduction Internal Rotation External Rotation Table 5.0: Cervical Spine Active Range of Motion: * Initial and final assessments were preformed with the use of a Goniometer
20 Treatment Flexion Extension Right Side flex Side flex Right Rotation Rotation Pre Post Pre Post Pre Post Pre Post Pre Post Pre Post 1 Assessment / / / / / / / / / / / / / Assessment / Manual Muscle Test
21 Grade 5 Normal 100% = range of motion against gravity, max resistance Grade 4 Good 75% = Complete range of motion against gravity, moderate resistance Grade 3 Fair 50% = Complete range of motion against gravity Grade 2 Poor 25% = Complete range of motion, gravity eliminated Grade 1 Poor trace = slight contraction, no joint movement Grade 0 Zero = no contraction palpable Table 6.0: First Assessment Muscle Side Grade Pain Sternocleidomastoid Right 4 1/ Levator Scapulae Right 5 1/ Right Pectoralis Major Right Pectoralis Minor Right Triceps Right Biceps Right Upper Trapezius Right Rhomboids Right Table 7.0: Final Assessment Muscle Side Grade Pain Sternocleidomastoid Right Levator Scapulae Right Right Pectoralis Major Right Pectoralis Minor Right Triceps Right Biceps Right Upper Trapezius Right Rhomboids Right
22 Table 8.0: Wrights Test Side Test Results First Assessment Right Positive - pulse instantly disappeared Positive pulse instantly disappeared Final Assessment Right Negative pulse still palpable Negative pulse still palpable Table 9.0: Capillary Refill Test Side Test Results First Assessment Right Positive 5+ seconds for refill to occur Positive 5+ seconds for refill to occur Final Assessment Right 0.98 seconds for refill 1.56 seconds for refill Table 10.0: Costoclavicular Syndrome Test Side Test Results First Assessment Right Positive pulse instantly disappeared Positive pulse instantly disappeared Final Assessment Right Negative 1/10 neural in middle finger Negative 1/10 neural in middle finger Table 11.0: Halstead Test Side Test Results First Assessment Right Positive pulse decreased, 7/10 Positive pulse decreased, 7/10 Final Assessment Right Negative Negative Table 12.0: Roo s Test Side Test Results First Assessment Right Positive Positive, fatigued faster Final Assessment Right Positive, less symptoms, equal fatigue, same color in hands Positive, less symptoms, equal fatigue, same color in hands.
23 Table 13.0: Median Nerve Upper Limb Tension Test Side Test Results Pre Treatment Post Treatment First Assessment Right Positive into fingers/hand Positive into fingers/hand Treatment 8 Right Positive, Positive, symptoms decreased symptoms decreased Positive, Positive, symptoms decreased symptoms decreased Treatment 9 Right Positive into Positive into elbow elbow only Positive into wrist and elbow Positive into wrist and elbow Treatment 10 Right Positive into palm Positive into palm Positive into elbow and fingers Positive into elbow and fingers Treatment 12 Right Positive into Positive into elbow elbow Positive into Positive into elbow elbow Treatment 13 Right Positive into Positive into elbow elbow Positive into Positive into elbow elbow Final Assessment Right Positive into elbow Positive into elbow Table 14.0: Radial Nerve Upper Limb Tension Test Treatment Side Test Results Pre Treatment Post Treatment First Assessment Right Positive Positive Treatment 8 Right Positive, symptoms decreased Positive, symptoms decreased Positive, symptoms decreased Positive, symptoms decreased Treatment 9 Right Positive into forearm extensors Positive into forearm extensors Positive into forearm Positive into forearm
24 extensors extensors Treatment 10 Right Positive into extensors Positive into forearm extensors Positive into extensors Positive into forearm extensors Treatment 12 Right Positive into extensors Positive into forearm extensors Positive into extensors Positive into forearm extensors Treatment 13 Right Positive into extensors Positive into forearm extensors Positive into extensors Positive into forearm extensors Final Assessment Right Positive into extensors Positive into extensors Table 15.0: Ulnar Upper Limb Tension Test Treatment Side Test Results: Pre treatment Post Treatment First Assessment Right Positive Positive Treatment 8 Right Positive Decreased symptoms Positive Decreased symptoms Treatment 9 Right Positive, decreased Decreased symptoms since last treatment Positive, decreased Decreased symptoms since last treatment Treatment 10 Right Positive, minimal Negative Positive, minimal Negative Treatment 12 Right Negative Negative Negative Negative Treatment 13 Right Negative Negative Negative Negative Final Assessment Right Negative Negative Table 16.0: Phalens Test Side Test Results First Assessment Right Negative Negative Final Assessment Right Negative Negative Table 17.0: Reverse Phalens Test
25 Side Test Results First Assessment Right Negative Negative Final Assessment Right Negative Negative Table 18.0: Tinells Test Side Test Results First Assessment Right Negative Negative Final Assessment Right Negative Negative Table 19.0: Allen s Test Treatment number Side Result Pre Treatment First Assessment Right Positive Post Treatment Positive Treatment 3 Right Positive Positive Positive Positive Treatment 4 Right Positive Positive Positive Positive Treatment 5 Right Positive Positive Positive Positive Treatment 6 Right Positive Positive Positive Positive Treatment 7 Right Positive Positive Positive Positive Treatment 9 Right Positive Positive Positive Positive Treatment 10 Right Positive Positive Positive Positive Treatment 11 Right Positive Negative Positive Positive Treatment 12 Right Positive Positive Negative Negative Treatment 13 Right Positive Negative Negative Negative Treatment 14 Right Negative Negative Negative Negative Final Assessment Right Negative Negative Table 20.0: Adson s Test
26 Treatment Number Side Result Pre Treatment Post Treatment First Assessment Right Positive pulse disappeared Positive pulse decreased Treatment 3 Right Positive Positive Positive Positive Treatment 4 Right Positive pulse Negative decreased Positive pulse disappeared Positive pulse disappeared Treatment 5 Right Negative Negative Negative Negative Treatment 6 Right Negative Negative Negative Negative Final Assessment Right Negative Negative Appendix B: Initial and Final Pictures
27 Figure 2: Initial Anterior View Figure 1: Final Anterior View Figure 3: Initial Posterior View Figure 4: Final Posterior View
28 27 ure 6: Initial Assessment Right Figure 5: Final Assessment Right w View Figure 8: Initial Assessment View Figure 7: Final Assessment View Appendix C: Treatment
29 28 Table 21.0: Treatment breakdown Treatment Areas Worked Techniques Used 1 Assessment Only 2 September 13 th, September 16 th, September 19 th, th September 24 th, 2013 Sub occipitals SCM Pectoralis Minor and Major Subclavius Suboccipitals SCM Pectoralis Minor and Major Subclavius Suboccipitals Pectoralis Minor and Major Biceps Deltoids Suboccipitals Biceps Deltoids Forearm Extensors Forearm Flexors Sub occipital release C/S ROM Scalene release Fascial traction Reshaping Cervical diaphragm Subclavius grab Muscle squeeze to SCM Pincher Grip to SCM Trigger point release GSM Subocciptal release C/S ROM Scalene release Fascial traction Reshaping Cervical diaphragm Subclavius grab Muscle squeeze to SCM Pincher Grip to SCM Trigger point release GSM Subocciptal release C/S and GH ROM Scalene release Fascial traction Reshaping Bear claw Cervical diaphragm Arm pull Trigger point release Scalene stretch MFR sheering GSM Subocciptal release C/S and GH ROM Scalene release MFR: Cross hands Sheering Wrist traction Isolytic release to forearm
30 29 6th September 26 th, th October 1 st, th October 3 rd, th October 8 th, 2013 Suboccipitals Forearm Extensors Forearm Flexors Diaphragm Suboccipitals Forearm Extensors Forearm Flexors Diaphragm Suboccipitals Forearm Extensors Forearm Flexors Pectoralis Minor and Major Diaphragm Suboccipitals Forearm Extensors Forearm Flexors extensors GSM Subocciptal release C/S and GH ROM Scalene release MFR: cross hands Shearing Skin rolling to forearms Diaphragm release (to diaphragm Wrist traction Isolytic release to forearm flexors GSM Subocciptal release C/S and GH ROM MFR: Cross hands Sheering Skin rolling to forearms Diaphragm release Wrist traction Isolytic release to forearm flexors GSM Subocciptal release C/S and GH ROM Scalene release Arm pull MFR: cross hands Sheering Skin rolling to forearms Diaphragm release Wrist traction Isolytic release to forearm flexors GSM Subocciptal release C/S and GH ROM Scalene release MFR: cross hands Shearing Skin rolling Diaphragm release Wrist traction Isolytic release to forearm
31 30 10 th October 10 th, th October 15 th, th October 23 rd, th October 31 st, 2013 Suboccipitals Forearm Extensors Forearm Flexors Diaphragm Suboccipitals Forearm Extensors Forearm Flexors Diaphragm Suboccipitals Forearm Extensors Forearm Flexors Deltoids Biceps Pectoralis minor and major Suboccipitals Forearm Extensors Forearm Flexors flexors, extensors and Contract relax to GSM Subocciptal release C/S and GH ROM Arm pull MFR: cross hands Shearing Skin rolling V stroking Diaphragm release Wrist traction Isolytic release to forearm flexors, extensors and Contract relax to GSM Subocciptal release C/S and GH ROM MFR: cross hands Shearing Skin rolling V stroking Diaphragm release Wrist traction Isolytic release to forearm flexors, extensors and Contract relax to GSM Subocciptal release C/S and GH ROM Arm pull Skin rolling V stroking Wrist traction Isolytic release to forearm flexors, extensors and Contract relax to GSM Subocciptal release C/S and GH ROM Fascial traction Reshaping
32 31 14 th November 6 th, November 7 th, 2013 Deltoids Biceps Pectoralis minor and major Suboccipitals Forearm Extensors Forearm Flexors Deltoids Biceps Pectoralis minor and major Assessment Only Arm pull Wrist traction Isolytic release to forearm flexors, extensors and Contract relax to Scalene stretch GSM Subocciptal release C/S and GH ROM Fascial traction Reshaping Arm pull Wrist traction Isolytic release to forearm flexors, extensors and Contract relax to Scalene stretch GSM
33 32 Appendix D: Anatomy Pictures Figure 9. Postural abnormalities in relation to TOS Retrieved from: Figure 10. Brachial plexus anatomy Retrieved from: Figure 11. Brachial plexus compression areas Retrieved from:
82a Orthopedic Massage! Introduction - Thoracic Outlet"
 82a Orthopedic Massage! Introduction - Thoracic Outlet" 82a Orthopedic Massage! Introduction - Thoracic Outlet! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and Reminders " 10 minutes "Lecture:"
82a Orthopedic Massage! Introduction - Thoracic Outlet" 82a Orthopedic Massage! Introduction - Thoracic Outlet! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and Reminders " 10 minutes "Lecture:"
5 minutes: Attendance and Breath of Arrival. 50 minutes: Problem Solving Torso
 5 minutes: Attendance and Breath of Arrival 50 minutes: Problem Solving Torso Punctuality- everybody's time is precious: o o Be ready to learn by the start of class, we'll have you out of here on time
5 minutes: Attendance and Breath of Arrival 50 minutes: Problem Solving Torso Punctuality- everybody's time is precious: o o Be ready to learn by the start of class, we'll have you out of here on time
79b Orthopedic Massage: Technique Demo and Practice! Rotator Cuff and Carpal Tunnel!
 79b Orthopedic Massage: Technique Demo and Practice! Rotator Cuff and Carpal Tunnel! 79b Orthopedic Massage: Technique Demo and Practice! Rotator Cuff and Carpal Tunnel! Class Outline" 5 minutes" "Attendance,
79b Orthopedic Massage: Technique Demo and Practice! Rotator Cuff and Carpal Tunnel! 79b Orthopedic Massage: Technique Demo and Practice! Rotator Cuff and Carpal Tunnel! Class Outline" 5 minutes" "Attendance,
Official Definition. Carpal tunnel syndrome, the most common focal peripheral neuropathy, results from compression of the median nerve at the wrist.
 Mod 2 MMT Course Official Definition Carpal tunnel syndrome, the most common focal peripheral neuropathy, results from compression of the median nerve at the wrist. epidemiology Affects an estimated 3
Mod 2 MMT Course Official Definition Carpal tunnel syndrome, the most common focal peripheral neuropathy, results from compression of the median nerve at the wrist. epidemiology Affects an estimated 3
Richard Dobrusin DO FACOFP
 Richard Dobrusin DO FACOFP Define Thoracic Outlet Syndrome (TOS) Describe the Mechanisms of Dysfunction List Diagnostic tests for (TOS) Understand (TOS) referral patterns Discuss Treatment Options Definition:
Richard Dobrusin DO FACOFP Define Thoracic Outlet Syndrome (TOS) Describe the Mechanisms of Dysfunction List Diagnostic tests for (TOS) Understand (TOS) referral patterns Discuss Treatment Options Definition:
80b Orthopedic Massage: Technique Review and Practice! Rotator Cuff and Carpal Tunnel!
 80b Orthopedic Massage: Technique Review and Practice! Rotator Cuff and Carpal Tunnel! 80b Orthopedic Massage: Technique Review and Practice! Rotator Cuff and Carpal Tunnel! Class Outline 5 minutes Attendance,
80b Orthopedic Massage: Technique Review and Practice! Rotator Cuff and Carpal Tunnel! 80b Orthopedic Massage: Technique Review and Practice! Rotator Cuff and Carpal Tunnel! Class Outline 5 minutes Attendance,
The Brachial Plexus and Thoracic Outlet Syndrome
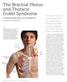 The Brachial Plexus and Thoracic Outlet Syndrome Understanding Signs and Symptoms By Joseph E. Muscolino, DC The brachial plexus of nerves and the subclavian/axillary artery and vein comprise a neurovascular
The Brachial Plexus and Thoracic Outlet Syndrome Understanding Signs and Symptoms By Joseph E. Muscolino, DC The brachial plexus of nerves and the subclavian/axillary artery and vein comprise a neurovascular
Symptoms and Referred Pain from Myofascial Trigger Points in the Anterior Scalene Muscle or Scalenus Anterior
 Symptoms and Referred Pain from Myofascial Trigger Points in the Anterior Scalene Muscle or Scalenus Anterior picture Symptoms and signs Aching or throbbing in the lateral forearm extending to thumb and
Symptoms and Referred Pain from Myofascial Trigger Points in the Anterior Scalene Muscle or Scalenus Anterior picture Symptoms and signs Aching or throbbing in the lateral forearm extending to thumb and
Unit 3 -- Relieve the Burden of Shoulder Dysfunction. Upper Torso & Shoulder Unit Study Guide
 Unit 3 -- Relieve the Burden of Shoulder Dysfunction Upper Torso & Shoulder Unit Study Guide This unit identifies problems of the shoulder joint and thoracic regions. Module 1 Module 2 Module 3 Module
Unit 3 -- Relieve the Burden of Shoulder Dysfunction Upper Torso & Shoulder Unit Study Guide This unit identifies problems of the shoulder joint and thoracic regions. Module 1 Module 2 Module 3 Module
Pain Assessment Patient Interview (location/nature of symptoms), Body Diagram. Observation and Examination: Tests and Measures
 Examination of Upper Quarter Neurogenic Pain Jane Fedorczyk, PT, PhD, CHT Thomas Jefferson University, Philadelphia, PA Center of Excellence for Hand and Upper Limb Rehabilitation I. History Mechanism
Examination of Upper Quarter Neurogenic Pain Jane Fedorczyk, PT, PhD, CHT Thomas Jefferson University, Philadelphia, PA Center of Excellence for Hand and Upper Limb Rehabilitation I. History Mechanism
When Technology Strikes Back!
 When Technology Strikes Back! Suffering from thumb or wrist pain from chronic texting? Many tech-savvy individuals have felt the side-effects of texting, typing, or web browsing. This is the pain you get
When Technology Strikes Back! Suffering from thumb or wrist pain from chronic texting? Many tech-savvy individuals have felt the side-effects of texting, typing, or web browsing. This is the pain you get
The Upper Limb III. The Brachial Plexus. Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa
 The Upper Limb III The Brachial Plexus Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa Brachial plexus Network of nerves supplying the upper limb Compression of the plexus results in motor & sensory changes
The Upper Limb III The Brachial Plexus Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa Brachial plexus Network of nerves supplying the upper limb Compression of the plexus results in motor & sensory changes
Physical Examination of the Shoulder
 General setup Patient will be examined in both the seated and supine position so exam table needed 360 degree access to patient Expose neck and both shoulders (for comparison); female in gown or sports
General setup Patient will be examined in both the seated and supine position so exam table needed 360 degree access to patient Expose neck and both shoulders (for comparison); female in gown or sports
Julia Perkins. Clinical Case Report Competition. Utopia Academy. Second Place Winner. Fall 2009
 Massage Therapists Association of British Columbia Clinical Case Report Competition Utopia Academy Fall 2009 Second Place Winner Julia Perkins The role of massage therapy in reducing anxiety related to
Massage Therapists Association of British Columbia Clinical Case Report Competition Utopia Academy Fall 2009 Second Place Winner Julia Perkins The role of massage therapy in reducing anxiety related to
Heather L. Muir. Clinical Case Report Competition. Utopia Academy. First Place Winner. Massage Therapists Association of British Columbia
 Massage Therapists Association of British Columbia Clinical Case Report Competition Utopia Academy December 2013 First Place Winner Heather L. Muir The effects of massage therapy on a professional opera
Massage Therapists Association of British Columbia Clinical Case Report Competition Utopia Academy December 2013 First Place Winner Heather L. Muir The effects of massage therapy on a professional opera
Please Note: This is an Example Case Study Not to Be Reproduced, Copied or Shared
 Please Note: This is an Example Case Study Not to Be Reproduced, Copied or Shared Your Name Workshops Name and date Case Study For Level 3 FST History: a) Torn labrum R shoulder 2009 Complete rupture/tear
Please Note: This is an Example Case Study Not to Be Reproduced, Copied or Shared Your Name Workshops Name and date Case Study For Level 3 FST History: a) Torn labrum R shoulder 2009 Complete rupture/tear
Alex Mayr-Landrecht. Clinical Case Report Competition. West Coast College of Massage Therapy, Victoria Campus. First Place Winner
 Massage Therapists Association of British Columbia Clinical Case Report Competition West Coast College of Massage Therapy, Victoria Campus April 2012 First Place Winner Alex Mayr-Landrecht The efficacy
Massage Therapists Association of British Columbia Clinical Case Report Competition West Coast College of Massage Therapy, Victoria Campus April 2012 First Place Winner Alex Mayr-Landrecht The efficacy
General Information - Exercise
 General Information - Exercise To maximize the potential for prevention and recovery, it is important to make a commitment to daily stretching and cardiovascular exercise and to perform strengthening exercises
General Information - Exercise To maximize the potential for prevention and recovery, it is important to make a commitment to daily stretching and cardiovascular exercise and to perform strengthening exercises
Darya Lyubar. Clinical Case Report Competition. Utopia Academy. Second Place Winner. Massage Therapists Association of British Columbia.
 Massage Therapists Association of British Columbia Clinical Case Report Competition Utopia Academy April 2012 Second Place Winner Darya Lyubar The effects of massage therapy techniques on restoring pain
Massage Therapists Association of British Columbia Clinical Case Report Competition Utopia Academy April 2012 Second Place Winner Darya Lyubar The effects of massage therapy techniques on restoring pain
MLT Muscle(s) Patient Position Therapist position Stabilization Limb Position Picture Put biceps on slack by bending elbow.
 MLT Muscle(s) Patient Position Therapist position Stabilization Limb Position Picture Put biceps on slack by bending elbow. Pectoralis Minor Supine, arm at side, elbows extended, supinated Head of Table
MLT Muscle(s) Patient Position Therapist position Stabilization Limb Position Picture Put biceps on slack by bending elbow. Pectoralis Minor Supine, arm at side, elbows extended, supinated Head of Table
Active-Assisted Stretches
 1 Active-Assisted Stretches Adequate flexibility is fundamental to a functional musculoskeletal system which represents the foundation of movement efficiency. Therefore a commitment toward appropriate
1 Active-Assisted Stretches Adequate flexibility is fundamental to a functional musculoskeletal system which represents the foundation of movement efficiency. Therefore a commitment toward appropriate
Postural Correction for Neck and Back
 Dr. Bradley Gueldner Dr. Dana Gueldner Dr. Morgan Gueldner 101-32630 George Ferguson Way. Abbotsford, British Columbia. V2T 4V6. Tel: 604.852.1820 Purpose of Program: Postural Correction for Neck and Back
Dr. Bradley Gueldner Dr. Dana Gueldner Dr. Morgan Gueldner 101-32630 George Ferguson Way. Abbotsford, British Columbia. V2T 4V6. Tel: 604.852.1820 Purpose of Program: Postural Correction for Neck and Back
Osteopathic Considerations in Shoulder Pain. Kristen Brusky DO February 22, 2018
 Osteopathic Considerations in Shoulder Pain Kristen Brusky DO February 22, 2018 Overview Importance of pectoral girdle Ligaments, ligaments tensegrity Bones, joints, muscles Neurovasculature Innervation
Osteopathic Considerations in Shoulder Pain Kristen Brusky DO February 22, 2018 Overview Importance of pectoral girdle Ligaments, ligaments tensegrity Bones, joints, muscles Neurovasculature Innervation
The SUPPORT Trial: SUbacromial impingement syndrome and Pain: a randomised controlled trial Of exercise and injection
 The SUPPORT Trial: SUbacromial impingement syndrome and Pain: a randomised controlled trial Of exercise and injection SUPPORT Physiotherapy Intervention Training Manual Authors: Sue Jackson (SJ) Julie
The SUPPORT Trial: SUbacromial impingement syndrome and Pain: a randomised controlled trial Of exercise and injection SUPPORT Physiotherapy Intervention Training Manual Authors: Sue Jackson (SJ) Julie
OBJECTIVES. Unit 7:5 PROPERTIES OR CHARACTERISTICS OF MUSCLES. Introduction. 3 Kinds of Muscles. 3 Kinds of Muscles 4/17/2018 MUSCULAR SYSTEM
 OBJECTIVES Unit 7:5 MUSCULAR SYSTEM Compare the three main kinds of muscles by describing the action of each Differentiate between voluntary and involuntary muscles List at least three functions of muscles
OBJECTIVES Unit 7:5 MUSCULAR SYSTEM Compare the three main kinds of muscles by describing the action of each Differentiate between voluntary and involuntary muscles List at least three functions of muscles
Postural Correction for Neck and Back
 Dr. Bradley Gueldner Dr. Dana Gueldner Dr. Morgan Gueldner 101-32630 George Ferguson Way. Abbotsford, British Columbia. V2T 4V6. Tel: 604.852.1820 Purpose of Program: Postural Correction for Neck and Back
Dr. Bradley Gueldner Dr. Dana Gueldner Dr. Morgan Gueldner 101-32630 George Ferguson Way. Abbotsford, British Columbia. V2T 4V6. Tel: 604.852.1820 Purpose of Program: Postural Correction for Neck and Back
Lowe Plastic Surgery (LPS)
 Lowe Plastic Surgery (LPS) PATIENT EDUCATION FOR: CUMULATIVE TRAUMA DISORDER THE PROBLEM: There has been a remarkable increase in what is termed cumulative trauma disorder (CTD) in the last 20 years. Other
Lowe Plastic Surgery (LPS) PATIENT EDUCATION FOR: CUMULATIVE TRAUMA DISORDER THE PROBLEM: There has been a remarkable increase in what is termed cumulative trauma disorder (CTD) in the last 20 years. Other
INSTRUCTION MANUAL FOR THE FLEXTEND AC Exercise System for The Acromioclavicular (AC) / Shoulder Joint
 INSTRUCTION MANUAL FOR THE FLEXTEND AC Exercise System for The Acromioclavicular (AC) / Shoulder Joint FLEXTEND -AC: Congratulations! You have chosen to use the FLEXTEND -AC Upper Extremity Training System,
INSTRUCTION MANUAL FOR THE FLEXTEND AC Exercise System for The Acromioclavicular (AC) / Shoulder Joint FLEXTEND -AC: Congratulations! You have chosen to use the FLEXTEND -AC Upper Extremity Training System,
Lab Workbook. ANATOMY Manual Muscle Testing Lower Trapezius Patient: prone
 ANATOMY Manual Muscle Testing Lower Trapezius Patient: prone Lab Workbook Fixation: place on hand below the scapula on the opposite side Test: adduction and depression of the scapula with lateral rotation
ANATOMY Manual Muscle Testing Lower Trapezius Patient: prone Lab Workbook Fixation: place on hand below the scapula on the opposite side Test: adduction and depression of the scapula with lateral rotation
Work Related Musculoskeletal Disorders
 Work Related Musculoskeletal Disorders Upper Extremity Disorders Carpel tunnel syndrome Cubital tunnel syndrome Thoracic outlet syndrome Raynaud s syndrome (white finger) Rotator cuff syndrome DeQuervain
Work Related Musculoskeletal Disorders Upper Extremity Disorders Carpel tunnel syndrome Cubital tunnel syndrome Thoracic outlet syndrome Raynaud s syndrome (white finger) Rotator cuff syndrome DeQuervain
Sick Call Screener Course
 Sick Call Screener Course Musculoskeletal System Upper Extremities (2.7) 2.7-2-1 Enabling Objectives 1.46 Utilize the knowledge of musculoskeletal system anatomy while assessing a patient with a musculoskeletal
Sick Call Screener Course Musculoskeletal System Upper Extremities (2.7) 2.7-2-1 Enabling Objectives 1.46 Utilize the knowledge of musculoskeletal system anatomy while assessing a patient with a musculoskeletal
OMT Without An OMT Table Workshop. Dennis Dowling, DO FAAO Ann Habenicht, DO FAAO FACOFP
 OMT Without An OMT Table Workshop Dennis Dowling, DO FAAO Ann Habenicht, DO FAAO FACOFP Cervical Somatic Dysfunction (C5 SR RR) - Seated 1. Patient position: seated. 2. Physician position: standing facing
OMT Without An OMT Table Workshop Dennis Dowling, DO FAAO Ann Habenicht, DO FAAO FACOFP Cervical Somatic Dysfunction (C5 SR RR) - Seated 1. Patient position: seated. 2. Physician position: standing facing
Muscles in the Shoulder, Chest, Arm, Stomach, and Back
 Muscles in the Shoulder, Chest, Arm, Stomach, and Back Shoulder Muscles Deltoid Supraspinatus Infraspinatus Teres Major Teres Minor Subscapularis Deltoid (Delts) Function: Raises the upper arm Origin:
Muscles in the Shoulder, Chest, Arm, Stomach, and Back Shoulder Muscles Deltoid Supraspinatus Infraspinatus Teres Major Teres Minor Subscapularis Deltoid (Delts) Function: Raises the upper arm Origin:
TECHNOLOGY AND HOW WE USE IT TO DAMAGE OURSELVES WILLIAM A. DELP, DO ASSISTANT PROFESSOR OF OMM GA PCOM
 TECHNOLOGY AND HOW WE USE IT TO DAMAGE OURSELVES WILLIAM A. DELP, DO ASSISTANT PROFESSOR OF OMM GA PCOM OBJECTIVES Understand how we interact with technology new and old Understand how injury occurs Texting
TECHNOLOGY AND HOW WE USE IT TO DAMAGE OURSELVES WILLIAM A. DELP, DO ASSISTANT PROFESSOR OF OMM GA PCOM OBJECTIVES Understand how we interact with technology new and old Understand how injury occurs Texting
BASIC ORTHOPEDIC ASSESSMENT Muscle and Joint Testing
 BASIC ORTHOPEDIC ASSESSMENT Muscle and Joint Testing The following tests are for the purpose of determining relative shortening, restriction or bind of muscle tissues. In this context the term bind in
BASIC ORTHOPEDIC ASSESSMENT Muscle and Joint Testing The following tests are for the purpose of determining relative shortening, restriction or bind of muscle tissues. In this context the term bind in
Dynamic Neuromobilization for the Treatment of Thoracic Outlet Syndrome Courtney Convey and Dr. Erickson
 Dynamic Neuromobilization for the Treatment of Thoracic Outlet Syndrome Courtney Convey and Dr. Erickson Abstract Title: Dynamic Neuromobilization for the Treatment of Thoracic Outlet Syndrome Background:
Dynamic Neuromobilization for the Treatment of Thoracic Outlet Syndrome Courtney Convey and Dr. Erickson Abstract Title: Dynamic Neuromobilization for the Treatment of Thoracic Outlet Syndrome Background:
RHS 221 Manual Muscle Testing Theory 1 hour practical 2 hours Dr. Ali Aldali, MS, PT Tel# Department of Physical Therapy King Saud University
 1 RHS 221 Manual Muscle Testing Theory 1 hour practical 2 hours Dr. Ali Aldali, MS, PT Tel# 4693601 Department of Physical Therapy King Saud University 2 The scapulae lie against the thorax approximately
1 RHS 221 Manual Muscle Testing Theory 1 hour practical 2 hours Dr. Ali Aldali, MS, PT Tel# 4693601 Department of Physical Therapy King Saud University 2 The scapulae lie against the thorax approximately
G24: Shoulder and Axilla
 G24: Shoulder and Axilla Syllabus - Pg. 2 ANAT 6010- Medical Gross Anatomy David A. Morton, Ph.D. Objectives Upper limb Systemically: Bones (joints) Muscles Nerves Vessels (arteries/veins) Fascial compartments
G24: Shoulder and Axilla Syllabus - Pg. 2 ANAT 6010- Medical Gross Anatomy David A. Morton, Ph.D. Objectives Upper limb Systemically: Bones (joints) Muscles Nerves Vessels (arteries/veins) Fascial compartments
Thoracic Outlet Syndrome
 Thoracic Outlet Syndrome Part 1: The Scalene Triangle TOS: Vascular Symptom Presentation Venous persistent/intermittent edema heaviness and fatigue deep pain in neck/shoulder increased pain at night warm
Thoracic Outlet Syndrome Part 1: The Scalene Triangle TOS: Vascular Symptom Presentation Venous persistent/intermittent edema heaviness and fatigue deep pain in neck/shoulder increased pain at night warm
Muscle Energy Technique
 PRACTICE SESSION: Muscle Energy Technique BE AN ARTIST and work out the best way for you to use the Muscle Energy Technique (MET). This technique works best when muscles are shortened. If you try MET on
PRACTICE SESSION: Muscle Energy Technique BE AN ARTIST and work out the best way for you to use the Muscle Energy Technique (MET). This technique works best when muscles are shortened. If you try MET on
Shoulder Joint Examination. Shoulder Joint Examination. Inspection. Inspection Palpation Movement. Look Feel Move
 Shoulder Joint Examination History Cuff Examination Instability Examination AC Joint Examination Biceps Tendon Examination Superior Labrum Examination Shoulder Joint Examination Inspection Palpation Movement
Shoulder Joint Examination History Cuff Examination Instability Examination AC Joint Examination Biceps Tendon Examination Superior Labrum Examination Shoulder Joint Examination Inspection Palpation Movement
Physical Sense Activation Programme
 Flexion extension exercises for neck and upper back Sitting on stool Arms hanging by side Bend neck and upper back Breathe out Extend your neck and upper back Lift chest to ceiling Squeeze shoulder blades
Flexion extension exercises for neck and upper back Sitting on stool Arms hanging by side Bend neck and upper back Breathe out Extend your neck and upper back Lift chest to ceiling Squeeze shoulder blades
Grace Wu. Clinical Case Report Competition. Utopia Academy. Second Place Winner. Massage Therapists Association of British Columbia.
 Massage Therapists Association of British Columbia Clinical Case Report Competition Utopia Academy November 2013 Second Place Winner Grace Wu Therapy for the therapist: the effects of myofascial release
Massage Therapists Association of British Columbia Clinical Case Report Competition Utopia Academy November 2013 Second Place Winner Grace Wu Therapy for the therapist: the effects of myofascial release
Rotator Cuff Strain and Carpal Tunnel Syndrome
 Rotator Cuff Strain and Carpal Tunnel Syndrome 5 minutes: Attendance and Breath of Arrival 50 minutes: Problem-Solving: SG, Arms, and Hands Punctuality- everybody's time is precious: o o Be ready to learn
Rotator Cuff Strain and Carpal Tunnel Syndrome 5 minutes: Attendance and Breath of Arrival 50 minutes: Problem-Solving: SG, Arms, and Hands Punctuality- everybody's time is precious: o o Be ready to learn
RN(EC) ENC(C) GNC(C) MN ACNP *** MECHANISM OF INJURY.. MOST IMPORTANT ***
 HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age - Certain conditions are more prevalent in particular age groups (i.e. Full rotator cuff tears are more common over the age of 45, traumatic injuries
HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age - Certain conditions are more prevalent in particular age groups (i.e. Full rotator cuff tears are more common over the age of 45, traumatic injuries
Clinical Case Report Competition
 Massage Therapists Association of B.C. Clinical Case Report Competition West Coast College of Massage Therapy June, 2009 Honourable Mention Janet Lee The Effects of Massage Therapy in Pain Management of
Massage Therapists Association of B.C. Clinical Case Report Competition West Coast College of Massage Therapy June, 2009 Honourable Mention Janet Lee The Effects of Massage Therapy in Pain Management of
Certified Personal Trainer Re-Certification Manual
 Certified Personal Trainer Re-Certification Manual Section II 1 Anatomy & Physiology Terms Anatomy and physiology are closely related fields of study: anatomy is the study of form, and physiology is the
Certified Personal Trainer Re-Certification Manual Section II 1 Anatomy & Physiology Terms Anatomy and physiology are closely related fields of study: anatomy is the study of form, and physiology is the
Upledger Institute Case Study CranioSacral Therapy Pain/Numbness/Limited Mobility By Amy Sanders, O.T.R., LMT, CST T
 Upledger Institute Case Study CranioSacral Therapy Pain/Numbness/Limited Mobility By Amy Sanders, O.T.R., LMT, CST T The purpose of this case report is to describe treatment for a client with cervical
Upledger Institute Case Study CranioSacral Therapy Pain/Numbness/Limited Mobility By Amy Sanders, O.T.R., LMT, CST T The purpose of this case report is to describe treatment for a client with cervical
1-Apley scratch test.
 1-Apley scratch test. The patient attempts to touch the opposite scapula to test range of motion of the shoulder. 1-Testing abduction and external rotation( +ve sign touch the opposite scapula, -ve sign
1-Apley scratch test. The patient attempts to touch the opposite scapula to test range of motion of the shoulder. 1-Testing abduction and external rotation( +ve sign touch the opposite scapula, -ve sign
3 Mohammad Al-Mohtasib Areej Mosleh
 3 Mohammad Al-Mohtasib Areej Mosleh ***Muscles Connecting the Upper Limb to the Vertebral Column 1.Trapezius Muscle ***The first muscle on the back is trapezius muscle, it s called so according
3 Mohammad Al-Mohtasib Areej Mosleh ***Muscles Connecting the Upper Limb to the Vertebral Column 1.Trapezius Muscle ***The first muscle on the back is trapezius muscle, it s called so according
Role Of The Fitness Professional. Causes of Fitness Related Injuries. The Assessments. Screening & Assessing: A Holistic Approach 2/9/2016
 Screening & Assessing: A Holistic Approach Role Of The Fitness Professional Fitness professionals must assess clientele, but need to understand the difference between medical diagnosis vs fitness limitations.
Screening & Assessing: A Holistic Approach Role Of The Fitness Professional Fitness professionals must assess clientele, but need to understand the difference between medical diagnosis vs fitness limitations.
Nerve Injury. 1) Upper Lesions of the Brachial Plexus called Erb- Duchene Palsy or syndrome.
 Nerve Injury - Every nerve goes to muscle or skin so if the nerve is injured this will cause paralysis in the muscle supplied from that nerve (paralysis means loss of function) then other muscles and other
Nerve Injury - Every nerve goes to muscle or skin so if the nerve is injured this will cause paralysis in the muscle supplied from that nerve (paralysis means loss of function) then other muscles and other
9/4/10. James J. Lehman, DC, MBA, DABCO. Why is posture important to you, the chiropractic physician?
 James J. Lehman, DC, MBA, DABCO The posture of homo sapiens is a complex biomechanical continuum, which involves the function of muscles, ligaments, fascia, nerves, osseous structures, neuromuscular control,
James J. Lehman, DC, MBA, DABCO The posture of homo sapiens is a complex biomechanical continuum, which involves the function of muscles, ligaments, fascia, nerves, osseous structures, neuromuscular control,
SHOULDER PROCEDURE. Minimum Prerequisite BRM 2 (1-8) & BRM 3 (1-6)
 SHOULDER PROCEDURE Minimum Prerequisite BRM 2 (1-8) & BRM 3 (1-6) Shoulder Procedure (Solo) - SUMMARY With the client sitting, stand at the opposite side to the shoulder being worked on. Cradle the forearm
SHOULDER PROCEDURE Minimum Prerequisite BRM 2 (1-8) & BRM 3 (1-6) Shoulder Procedure (Solo) - SUMMARY With the client sitting, stand at the opposite side to the shoulder being worked on. Cradle the forearm
Upper Limb Muscles Muscles of Axilla & Arm
 Done By : Saleh Salahat Upper Limb Muscles Muscles of Axilla & Arm 1) Muscles around the axilla A- Muscles connecting the upper to thoracic wall (4) 1- pectoralis major Origin:- from the medial half of
Done By : Saleh Salahat Upper Limb Muscles Muscles of Axilla & Arm 1) Muscles around the axilla A- Muscles connecting the upper to thoracic wall (4) 1- pectoralis major Origin:- from the medial half of
1. Which branch of the brachial plexus is most commonly involved in thoracic outlet syndrome compression?
 1 1. Which branch of the brachial plexus is most commonly involved in thoracic outlet syndrome compression? a. Musculocutaneous nerve b. Radial nerve c. Ulnar nerve d. Median nerve 2. Sensory symptoms
1 1. Which branch of the brachial plexus is most commonly involved in thoracic outlet syndrome compression? a. Musculocutaneous nerve b. Radial nerve c. Ulnar nerve d. Median nerve 2. Sensory symptoms
60b Chair Massage: Technique Review and Practice
 60b Chair Massage: Technique Review and Practice 60b Chair Massage: Technique Review and Practice! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and Reminders " 10 minutes "Lecture:" 25 minutes
60b Chair Massage: Technique Review and Practice 60b Chair Massage: Technique Review and Practice! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and Reminders " 10 minutes "Lecture:" 25 minutes
Upper Cross Syndrome: Assessment & Management in Family Practice HKDU Symposium Dec 2014
 Upper Cross Syndrome: Assessment & Management in Family Practice HKDU Symposium Dec 2014 Dr. Ngai Ho Yin Allen Family Medicine Specialist PGDipMusculoskeletal Medicine MBBS(HK), DCH(London), DFM(CUHK),
Upper Cross Syndrome: Assessment & Management in Family Practice HKDU Symposium Dec 2014 Dr. Ngai Ho Yin Allen Family Medicine Specialist PGDipMusculoskeletal Medicine MBBS(HK), DCH(London), DFM(CUHK),
EVALUATION AND MEASUREMENTS. I. Devreux
 EVALUATION AND MEASUREMENTS I. Devreux To determine the extent and degree of muscular weakness resulting from disease, injury or disuse. The records obtained from these tests provide a base for planning
EVALUATION AND MEASUREMENTS I. Devreux To determine the extent and degree of muscular weakness resulting from disease, injury or disuse. The records obtained from these tests provide a base for planning
79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel!
 79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel! 79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and
79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel! 79a Orthopedic Massage: Introduction! Rotator Cuff and Carpal Tunnel! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and
Joint G*H. Joint S*C. Joint A*C. Labrum. Humerus. Sternum. Scapula. Clavicle. Thorax. Articulation. Scapulo- Thoracic
 A*C Joint Scapulo- Thoracic Articulation Thorax Sternum Clavicle Scapula Humerus S*C Joint G*H Joint Labrum AC Ligaments SC Ligaments SC JOINT AC Coracoacromial GH GH Ligament Complex Coracoclavicular
A*C Joint Scapulo- Thoracic Articulation Thorax Sternum Clavicle Scapula Humerus S*C Joint G*H Joint Labrum AC Ligaments SC Ligaments SC JOINT AC Coracoacromial GH GH Ligament Complex Coracoclavicular
72a Orthopedic Massage: Introduction!
 72a Orthopedic Massage: Introduction! 72a Orthopedic Massage: Introduction! Class Outline 5 minutes Attendance, Breath of Arrival, and Reminders 10 minutes Lecture: 25 minutes Lecture: 15 minutes Active
72a Orthopedic Massage: Introduction! 72a Orthopedic Massage: Introduction! Class Outline 5 minutes Attendance, Breath of Arrival, and Reminders 10 minutes Lecture: 25 minutes Lecture: 15 minutes Active
Frozen Shoulder Syndrome Rehabilitation Using the Resistance Chair
 Frozen Shoulder Syndrome Rehabilitation Using the Resistance Chair General Information Frozen shoulder is a condition where the shoulder joint (glenohumeral joint) gradually becomes stiff, resulting in
Frozen Shoulder Syndrome Rehabilitation Using the Resistance Chair General Information Frozen shoulder is a condition where the shoulder joint (glenohumeral joint) gradually becomes stiff, resulting in
Exercises to restore range of movement: Rotation
 Exercises to restore range of movement: Rotation Start position: Sitting upright with your back supported in a chair. Position your head so it is evenly balanced, looking forward. Avoid allowing your head
Exercises to restore range of movement: Rotation Start position: Sitting upright with your back supported in a chair. Position your head so it is evenly balanced, looking forward. Avoid allowing your head
REMINDER. Obtain medical clearance and physician s release prior to beginning an exercise program for clients with medical or orthopedic concerns
 Understanding Shoulder Dysfunction REMINDER Obtain medical clearance and physician s release prior to beginning an exercise program for clients with medical or orthopedic concerns What is a healthy shoulder?
Understanding Shoulder Dysfunction REMINDER Obtain medical clearance and physician s release prior to beginning an exercise program for clients with medical or orthopedic concerns What is a healthy shoulder?
Clinical Case Report Competition
 Massage Therapists Association of B.C. Clinical Case Report Competition Okanagan Valley College of Massage Therapy Spring 2009 3rd Place Winner Kathryn H. Blundell A Combination of Modalities Constitutes
Massage Therapists Association of B.C. Clinical Case Report Competition Okanagan Valley College of Massage Therapy Spring 2009 3rd Place Winner Kathryn H. Blundell A Combination of Modalities Constitutes
ACTIVE AGING.
 Shoulder Pain Rehabilitation Protocol Rotator Cuff Syndrome Shoulder impingement The Resistance Chair Solution Shoulder Impingement a. Shoulder impingement is one of the most common causes of shoulder
Shoulder Pain Rehabilitation Protocol Rotator Cuff Syndrome Shoulder impingement The Resistance Chair Solution Shoulder Impingement a. Shoulder impingement is one of the most common causes of shoulder
GOLFERS TEN PROGRAM 1. SELF STRETCHING OF THE SHOULDER CAPSULE
 GOLFERS TEN PROGRAM 1. SELF STRETCHING OF THE SHOULDER CAPSULE POSTERIOR CAPSULAR STRETCH Bring your arm across your chest toward the opposite shoulder. With the opposite arm grasp your arm at your elbow.
GOLFERS TEN PROGRAM 1. SELF STRETCHING OF THE SHOULDER CAPSULE POSTERIOR CAPSULAR STRETCH Bring your arm across your chest toward the opposite shoulder. With the opposite arm grasp your arm at your elbow.
The Golfers Ten Program. 1. Self Stretching of the Shoulder Capsule
 The Golfers Ten Program 1. Self Stretching of the Shoulder Capsule A. Posterior capsular stretch Bring your arm across your chest toward the opposite shoulder. With the opposite arm grasp your arm at your
The Golfers Ten Program 1. Self Stretching of the Shoulder Capsule A. Posterior capsular stretch Bring your arm across your chest toward the opposite shoulder. With the opposite arm grasp your arm at your
Sports Medicine Part II : ANATOMY OF THE SPINE, ABDOMEN AND SHOULDER COMPLEX
 Sports Medicine 25 1.1 Part II : ANATOMY OF THE SPINE, ABDOMEN AND SHOULDER COMPLEX c.w.p. Wagner High School, Sports Medicine, A. Morgan, T. Morgan & A. Eastlake, 2008 Muscles of the Upper Limbs In this
Sports Medicine 25 1.1 Part II : ANATOMY OF THE SPINE, ABDOMEN AND SHOULDER COMPLEX c.w.p. Wagner High School, Sports Medicine, A. Morgan, T. Morgan & A. Eastlake, 2008 Muscles of the Upper Limbs In this
Hemiplegic Shoulder Power Point for staff education sessions
 Appendix B Hemiplegic Shoulder Power Point for staff education sessions Jennifer Curry Physiotherapist, London Health Sciences Centre www.swostroke.ca Acknowledgements Maria Lung BSc (PT), MSc Train the
Appendix B Hemiplegic Shoulder Power Point for staff education sessions Jennifer Curry Physiotherapist, London Health Sciences Centre www.swostroke.ca Acknowledgements Maria Lung BSc (PT), MSc Train the
GENERAL EXERCISES SHOULDER BMW MANUFACTURING CO. PZ-AM-G-US I July 2017
 GENERAL EXERCISES SHOULDER BMW MANUFACTURING CO. PZ-AM-G-US I July 2017 Disclosure: The exercises, stretches, and mobilizations provided in this presentation are for educational purposes only are not to
GENERAL EXERCISES SHOULDER BMW MANUFACTURING CO. PZ-AM-G-US I July 2017 Disclosure: The exercises, stretches, and mobilizations provided in this presentation are for educational purposes only are not to
SHOULDER PAIN. A Real Pain in the Neck. Michael Wolk, MD Northeastern Rehabilitation Associates October 31, 2017
 SHOULDER PAIN A Real Pain in the Neck Michael Wolk, MD Northeastern Rehabilitation Associates October 31, 2017 THE SHOULDER JOINT (S) 1. glenohumeral 2. suprahumeral 3. acromioclavicular 4. scapulocostal
SHOULDER PAIN A Real Pain in the Neck Michael Wolk, MD Northeastern Rehabilitation Associates October 31, 2017 THE SHOULDER JOINT (S) 1. glenohumeral 2. suprahumeral 3. acromioclavicular 4. scapulocostal
BRACHIAL PLEXUS. DORSAL SCAPULAR NERVE (C5) supraclavicular branch innervates rhomboids (major and minor) and levator scapulae
 THE BRACHIAL PLEXUS DORSAL SCAPULAR NERVE (C5) supraclavicular branch innervates rhomboids (major and minor) and levator scapulae SCHEMA OF THE BRACHIAL PLEXUS THE BRACHIAL PLEXUS PHRENIC NERVE supraclavicular
THE BRACHIAL PLEXUS DORSAL SCAPULAR NERVE (C5) supraclavicular branch innervates rhomboids (major and minor) and levator scapulae SCHEMA OF THE BRACHIAL PLEXUS THE BRACHIAL PLEXUS PHRENIC NERVE supraclavicular
Whit Truong. Clinical Case Report Competition. West Coast College of Massage Therapy. New Westminster. Second Place Winner
 Massage Therapists Association of British Columbia Clinical Case Report Competition West Coast College of Massage Therapy New Westminster July 2013 Second Place Winner Whit Truong The effects of myofascial
Massage Therapists Association of British Columbia Clinical Case Report Competition West Coast College of Massage Therapy New Westminster July 2013 Second Place Winner Whit Truong The effects of myofascial
INSTRUCTOR INFORMATION
 Course Listing: Thoracic Outlet Syndrome: Treatment of Brachial Neuralgia Dates & Times: Saturday, October 15, 2016, 9am - 5pm Venue: TBA, Vancouver, BC Notes for Participants: sheets, large towel, pillow,
Course Listing: Thoracic Outlet Syndrome: Treatment of Brachial Neuralgia Dates & Times: Saturday, October 15, 2016, 9am - 5pm Venue: TBA, Vancouver, BC Notes for Participants: sheets, large towel, pillow,
For Our Loved Ones. First Aid Massage
 For Our Loved Ones First Aid Massage First Aid Massage Introduction Communication Anatomy Basics Care: First Aid Massage Communication Where Ask where the pain is. Determine the anatomical location. What
For Our Loved Ones First Aid Massage First Aid Massage Introduction Communication Anatomy Basics Care: First Aid Massage Communication Where Ask where the pain is. Determine the anatomical location. What
Chiropractic Glossary
 Chiropractic Glossary Anatomy Articulation: A joint formed where two or more bones in the body meet. Your foot bone, for example, forms an articulation with your leg bone. You call that articulation an
Chiropractic Glossary Anatomy Articulation: A joint formed where two or more bones in the body meet. Your foot bone, for example, forms an articulation with your leg bone. You call that articulation an
Exercises for Thoracic Outlet Syndrome
 Exercises for Thoracic Outlet Syndrome Information for patients who have been diagnosed with Thoracic Outlet Syndrome Read this pamphlet to learn more about: Thoracic Outlet Syndrome Treatment options
Exercises for Thoracic Outlet Syndrome Information for patients who have been diagnosed with Thoracic Outlet Syndrome Read this pamphlet to learn more about: Thoracic Outlet Syndrome Treatment options
Evaluating the Athlete Questionnaire
 Evaluating the Athlete Questionnaire Prior to developing the strength and conditioning training plan the coach should first evaluate factors from the athlete s questionnaire that may impact the strength
Evaluating the Athlete Questionnaire Prior to developing the strength and conditioning training plan the coach should first evaluate factors from the athlete s questionnaire that may impact the strength
Rotator Cuff and Shoulder Conditioning Program
 Rotator Cuff and Shoulder Conditioning Program Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy
Rotator Cuff and Shoulder Conditioning Program Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5. September 30, 2011
 STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 September 30, 2011 PART l. Answer in the space provided. (12 pts) 1. Identify the structures. (2 pts) EXAM NUMBER A. Suprascapular nerve B. Axillary nerve
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 September 30, 2011 PART l. Answer in the space provided. (12 pts) 1. Identify the structures. (2 pts) EXAM NUMBER A. Suprascapular nerve B. Axillary nerve
The Massage Routine. Start with your client lying face down - Prone Position. Clean YOUR HANDS and CLIENTS FEET using antibacterial wipes
 The Massage Routine Start with your client lying face down - Prone Position Clean YOUR HANDS and CLIENTS FEET using antibacterial wipes!!!! GROUNDING FOR 3 BREATHS TUNE YOUR BREATHING WITH THE CLIENTS!!!
The Massage Routine Start with your client lying face down - Prone Position Clean YOUR HANDS and CLIENTS FEET using antibacterial wipes!!!! GROUNDING FOR 3 BREATHS TUNE YOUR BREATHING WITH THE CLIENTS!!!
Palpation Assessment
 Palpation Assessment by Joe Muscolino Never treat without an ASSESSMENT There is an old adage in the world of medicine - never treat without a diagnosis. A similar principle can be articulated in the world
Palpation Assessment by Joe Muscolino Never treat without an ASSESSMENT There is an old adage in the world of medicine - never treat without a diagnosis. A similar principle can be articulated in the world
Do the same as above, but turn your head TOWARDS the side that you re holding on to the chair.
 Stretch 4-6 times per day and hold each stretch for a minimum of 30 seconds. Perform the stretch gently without bouncing. Discuss any problems with your Chiropractor. Sit upright with your head and shoulder
Stretch 4-6 times per day and hold each stretch for a minimum of 30 seconds. Perform the stretch gently without bouncing. Discuss any problems with your Chiropractor. Sit upright with your head and shoulder
WEEKEND THREE HOMEWORK
 WEEKEND THREE HOMEWORK READING ASSIGNMENTS Salvo Massage Therapy Principles and Practice 4 th Edition Muscolino The Muscular System Manual Muscolino The Muscle and Bone Palpation Manual Ch. 19 Skeletal
WEEKEND THREE HOMEWORK READING ASSIGNMENTS Salvo Massage Therapy Principles and Practice 4 th Edition Muscolino The Muscular System Manual Muscolino The Muscle and Bone Palpation Manual Ch. 19 Skeletal
Chiropractic Technician Class
 Chiropractic Technician Class Presentation By: Dr. Kay Miller. The Role of Exercise as it Relates to Our Musculoskeletal System Introduction to the topic and Preliminary Physical exam Musculoskeletal anatomy:
Chiropractic Technician Class Presentation By: Dr. Kay Miller. The Role of Exercise as it Relates to Our Musculoskeletal System Introduction to the topic and Preliminary Physical exam Musculoskeletal anatomy:
Neck Class. Kaiser Permanente Fremont Physical Therapy
 Kaiser Permanente Fremont How Body Reacts to Injury and Pain Postural Muscles (Core) become Weak. Deep Neck Muscles Shoulder Blade Muscles Movement Muscles become Tight. Long Neck Muscles Sub-occipital
Kaiser Permanente Fremont How Body Reacts to Injury and Pain Postural Muscles (Core) become Weak. Deep Neck Muscles Shoulder Blade Muscles Movement Muscles become Tight. Long Neck Muscles Sub-occipital
BLUE SKY SCHOOL OF PROFESSIONAL MASSAGE AND THERAPEUTIC BODYWORK. Musculoskeletal Anatomy & Kinesiology MUSCLES, MOVEMENTS & BIOMECHANICS
 BLUE SKY SCHOOL OF PROFESSIONAL MASSAGE AND THERAPEUTIC BODYWORK Musculoskeletal Anatomy & Kinesiology MUSCLES, MOVEMENTS & BIOMECHANICS MSAK101-I Session 7 Learning Objectives: 1. List the three types
BLUE SKY SCHOOL OF PROFESSIONAL MASSAGE AND THERAPEUTIC BODYWORK Musculoskeletal Anatomy & Kinesiology MUSCLES, MOVEMENTS & BIOMECHANICS MSAK101-I Session 7 Learning Objectives: 1. List the three types
Muscle Action Origin Insertion Nerve Innervation Chapter Page. Deltoid. Trapezius. Latissimus Dorsi
 Muscle Action Origin Insertion Nerve Innervation Chapter Page All Fibers Abduct the shoulder (glenohumeral joint) Deltoid Anterior Fibers Flex the shoulder (G/H joint) Horizontally adduct the shoulder
Muscle Action Origin Insertion Nerve Innervation Chapter Page All Fibers Abduct the shoulder (glenohumeral joint) Deltoid Anterior Fibers Flex the shoulder (G/H joint) Horizontally adduct the shoulder
85b Orthopedic Massage:! Technique Demo and Practice - Neck Pain"
 85b Orthopedic Massage:! Technique Demo and Practice - Neck Pain" 85b Orthopedic Massage:! Technique Demo and Practice - Neck Pain! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and Reminders
85b Orthopedic Massage:! Technique Demo and Practice - Neck Pain" 85b Orthopedic Massage:! Technique Demo and Practice - Neck Pain! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and Reminders
Region of upper limb attachment to the trunk Proximal segment of limb overlaps parts of the trunk (thorax and back) and lower lateral neck.
 Region of upper limb attachment to the trunk Proximal segment of limb overlaps parts of the trunk (thorax and back) and lower lateral neck. includes Pectoral Scapular Deltoid regions of the upper limb
Region of upper limb attachment to the trunk Proximal segment of limb overlaps parts of the trunk (thorax and back) and lower lateral neck. includes Pectoral Scapular Deltoid regions of the upper limb
THE SHOULDER JOINT T H E G L E N O H U M E R A L ( G H ) J O I N T
 THE SHOULDER JOINT T H E G L E N O H U M E R A L ( G H ) J O I N T CLARIFICATION OF TERMS Shoulder girdle = scapula and clavicle Shoulder joint (glenohumeral joint) = scapula and humerus Lippert, p115
THE SHOULDER JOINT T H E G L E N O H U M E R A L ( G H ) J O I N T CLARIFICATION OF TERMS Shoulder girdle = scapula and clavicle Shoulder joint (glenohumeral joint) = scapula and humerus Lippert, p115
Rotator Cuff and Shoulder Conditioning Program
 Prepared for: Prepared by: Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
Prepared for: Prepared by: Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
Upper limb Arm & Cubital region 黃敏銓
 Upper limb Arm & Cubital region 黃敏銓 1 Arm Lateral intermuscular septum Anterior (flexor) compartment: stronger Medial intermuscular septum Posterior (extensor) compartment 2 Coracobrachialis Origin: coracoid
Upper limb Arm & Cubital region 黃敏銓 1 Arm Lateral intermuscular septum Anterior (flexor) compartment: stronger Medial intermuscular septum Posterior (extensor) compartment 2 Coracobrachialis Origin: coracoid
Tracy Crawford. Clinical Case Report Competition. West Coast College of Massage Therapy, Victoria Campus. Third Place Winner
 Massage Therapists Association of British Columbia Clinical Case Report Competition West Coast College of Massage Therapy, Victoria Campus April 2012 Third Place Winner Tracy Crawford Decreasing symptoms
Massage Therapists Association of British Columbia Clinical Case Report Competition West Coast College of Massage Therapy, Victoria Campus April 2012 Third Place Winner Tracy Crawford Decreasing symptoms
Physical Capability Exam Testing Protocol
 Test Duration: ~ min Physical Capability Exam Testing Protocol Pinch Gauge Grip Dynamometer Inclinometer Stop Watch Lift Box Table Weight Plates (5 lbs., lbs., lbs., 50 lbs., 0 lbs.) Physical Capability
Test Duration: ~ min Physical Capability Exam Testing Protocol Pinch Gauge Grip Dynamometer Inclinometer Stop Watch Lift Box Table Weight Plates (5 lbs., lbs., lbs., 50 lbs., 0 lbs.) Physical Capability
Prime movers provide the major force for producing a specific movement Antagonists oppose or reverse a particular movement Synergists
 Dr. Gary Mumaugh Prime movers provide the major force for producing a specific movement Antagonists oppose or reverse a particular movement Synergists Add force to a movement Reduce undesirable or unnecessary
Dr. Gary Mumaugh Prime movers provide the major force for producing a specific movement Antagonists oppose or reverse a particular movement Synergists Add force to a movement Reduce undesirable or unnecessary
Nonoperative Treatment For Rotator Cuff Tendinitis/ Partial Thickness Tear Dr. Trueblood
 Nonoperative Treatment For Rotator Cuff Tendinitis/ Partial Thickness Tear Dr. Trueblood Relieving Pain Patients who present with SIS will have shoulder pain that is exacerbated with overhead activities.
Nonoperative Treatment For Rotator Cuff Tendinitis/ Partial Thickness Tear Dr. Trueblood Relieving Pain Patients who present with SIS will have shoulder pain that is exacerbated with overhead activities.
