Purpose/goal: To provide nurses with information on how they can best care for patients receiving therapeutic hypothermia.
|
|
|
- Elwin Johnson
- 6 years ago
- Views:
Transcription
1 CNE: Temp management ANT, June 2014 Therapeutic hypothermia after cardiac arrest By Julie M. Waters RN MS CCRN Continuing Nursing Education Learning objectives 1. Describe therapeutic hypothermia (TH). 2. Compare cooling methods used for TH. 3. Discuss clinical management of patients receiving TH. Purpose/goal: To provide nurses with information on how they can best care for patients receiving therapeutic hypothermia. The authors and planners of this CNE activity have disclosed no relevant financial relationships with any commercial companies pertaining to this activity. See the end of this article to learn how to earn 1.4 CNE credit. Expiration: 6/1/17 Dr. Mary Smith*, age 56, is the picture of health a vegetarian and an avid runner who logs about 50 to 60 miles each week. She s also an accomplished researcher, traveling the country to present her findings. One morning at home she has a seizure. She and her husband, a cardiologist, decide to go to the hospital to have her checked out. On the way there, Mary goes into cardiac arrest. Her husband calls 911 and begins cardiopulmonary resuscitation (CPR) at the roadside. In about 20 minutes, the ambulance arrives. When the emergency medical technicians deliver two shocks with the defibrillator, Mary regains spontaneous circulation. When she arrives at the hospital, she s still unresponsive, so her husband and the emergency department physicians decide to begin therapeutic hypothermia (TH). According to the American Heart Association (AHA), nearly 383,000 out-of-hospital sudden cardiac arrests occur each year. Neurologic injury is the most common cause of death after these events. Recent recommendations by the AHA and the International Liaison Committee on Resuscitation (ILCOR) recommend inducing mild hypothermia (32 to 34 C [89.6 to 93.2 F]) for 12 to 24 hours after out-ofhospital cardiac arrests followed by return of spontaneous circulation (ROSC) in adults who are unresponsive on admission. The goal of TH is to improve survival and neurologic function. This treatment should begin within 6 hours of ROSC. Studies show the sooner it starts, the greater the benefit. Renewed interest and unanswered questions In 2002, clinicians took a new look at TH after two trials showed it brought significant improvements in neurologic function and survival. But much remains unknown about this therapy. For instance: What s the best cooling method? What s the optimal cooling temperature? How long should optimal temperature be maintained? How soon should patients be brought to target temperature after achieving ROSC? Can TH help other patients, such as those who ve had in-hospital arrests and those who are conscious but not at their baseline neurologic status after ROSC?
2 A recent study found mild cooling (36 C [96.8 F]) is as effective as deeper cooling (33 C (91.4 F]) in achieving a good outcome. The use of mild cooling is currently under debate and has led some hospitals to use targeted temperature management (36 c [96.8 f]) in place of TH. Despite the unanswered questions, bedside nurses have seen TH bring amazing recoveries. And although we may not be sure why it works, we re convinced it s making a difference. How cooling affects the brain After cardiac arrest, neurologic injury may manifest as coma and a decreased state of arousal, seizures, neurocognitive dysfunction, and brain death. Brain injury occurs during cardiac arrest and continues even as blood flow is reestablished. This response stems from multiple complex processes, such as inflammation and posthypoxic release of toxic substances that interfere with normal cell function. Cooling the brain decreases cellular metabolism by 5% to 7% for every 1 C drop in body temperature. Early and aggressive implementation of therapeutic hypothermia has been shown to protect against temperature-dependent mechanisms, such as fever. Patient selection All patients who remain unresponsive after cardiac arrest should be evaluated to determine if they re good candidates for TH. Original trials excluded pregnant women and hemodynamically unstable patients. But since then, positive outcomes in these patients have been reported. The only absolute contraindications to TH are active noncompressible bleeding and do-not-resuscitate orders. Cooling methods Typical hospital protocols for TH call for multiple simultaneous interventions to achieve target temperature. Each intervention has advantages and disadvantages. Cooling can be accomplished with noninvasive or invasive methods, or a combination. Clinicians should use the method that s most readily available and familiar to them. Noninvasive cooling methods Noninvasive methods include the use of ice packs, fans, alcohol or cool-water baths, and cooling blankets not connected to a thermostatically controlled device. These low-cost, readily available methods have proven to be extremely effective in decreasing body temperature. On the other hand, they are laborintensive, may not reduce core temperature rapidly enough, may not maintain target temperature, and may cause overcooling or lead to too-rapid rewarming. Technologies used in TH continue to advance, helping to reduce labor intensity for nurses, decrease patient risk, and speed the time to target temperature. Initially, some clinicians may choose to give up to 30 ml/kg or 2 L of cold (4 C [39.2 F) isotonic saline solution I.V. over 30 minutes to help drop the core temperature quickly. But recent evidence suggests this increases pulmonary edema and may cause negative hemodynamic effects, so it should be used cautiously on a case-by-case basis. Thermostatically controlled devices. Although cooling can be initiated with ice packs and fans, it s best to use a thermostatically controlled device to provide the most precise minute-to-minute temperature regulation. While expensive, these devices prevent excessive hypothermia and temperature fluctuations, which can harm the patient. Also, they can be used to promote controlled rewarming. Noninvasive water-circulating systems, which use water-filled blankets or pads and hydrogel-coated pads, are placed on the patient s skin. Along with a patient temperature source, the blankets or pads are connected to a console that automatically adjusts circulating water temperature to achieve and maintain
3 target temperature. A water-circulating system can be started immediately with a nurse-driven protocol, with no need for direct physician intervention. Be aware that it may cause skin injury with prolonged and intense surface cooling, although this risk appears low and can be reduced with frequent skin assessments and monitoring of water temperature. Invasive cooling methods Endovascular cooling systems use a specialized heat-exchange catheter that s inserted into a central vein and connected to an external temperature-control module. Cold water circulates through a balloon on the catheter tip to cool the patient. A sensor provides feedback on the patient s temperature and makes adjustments to maintain the programmed target temperature. With this system, the catheter can be used for central venous access, allowing medication administration, central venous pressure monitoring, and blood sampling. As a major disadvantage, it requires a specially trained practitioner to place the catheter, which may delay initiation of cooling. Also, it carries the risk of catheter-related injury and infection, although this risk appears similar to that of other central catheters. (See the box below.) //START BOX// Comparing invasive and noninvasive cooling methods METHOD BENEFITS AND DRAWBACKS Noninvasive methods Fans Inexpensive Easy to use Slow for induction phase Lack a feedback mechanism to maintain desired target temperature May spread microbes, which can cause infection Ice packs Inexpensive Easy to apply Cool at moderate rate Lack a feedback mechanism to maintain desired target temperature Labor intensive May cause skin breakdown Water-circulating cooling blankets and pads Invasive methods Expensive Easy for nurse to apply and maintain Achieve effective cooling rate Has feedback mechanism that maintains target temperature and controlled rewarming rate May cause skin breakdown Cold (4 C) crystalloid infusion Inexpensive Causes rapid induction rate Easy to use Some patients may not tolerate rapid volume infusion May overshoot target temperature Doesn t maintain target temperature
4 Endovascular catheter //END BOX// Involves large fluid volumes, which can harm patients with heart failure May compromise renal function or cause pulmonary edema Expensive Causes rapid induction rate Has feedback mechanism that maintains target temperature and controlled rewarming rate Requires trained clinician for insertion Carries risk of complications associated with central catheters Patient monitoring Regardless of the cooling method used, accurate temperature monitoring throughout TH is crucial. The patient s core temperature must be monitored closely via an esophageal, bladder, or pulmonary artery catheter (PAC) or a rectal temperature probe. For optimal safety, two monitoring methods should be used. Although PACs are the gold standard for core temperature monitoring, most patients don t require one. Monitor patients with a temperature-sensing Foley catheter for adequate urine output to ensure accurate readings. When positioned correctly, esophageal probes rapidly and accurately detect temperature changes. Rectal probes are easy to insert but are more likely to become dislodged; also, they have a longer lag time in detecting temperature changes. Hypothermia induces physiologic changes in virtually every organ, so vigilant monitoring is required to keep the patient safe. Initially, you may note an increase in the patient s heart rate, but as the patient cools, bradycardia commonly occurs. Due to the decreased metabolic demand during TH, bradycardia rarely requires intervention as long as blood pressure is stable. Patients may become hypotensive from sedation or loss of cardiac function, which might warrant volume replacement or vasopressors. In addition, cold diuresis may occur, possibly leading to hypovolemia and electrolyte loss. Be sure to monitor laboratory results, especially electrolyte levels. During TH, potassium, magnesium, and phosphate shift into the intracellular space, resulting in low levels. As needed and ordered, replace electrolytes and stay alert for arrhythmias. Know that metabolic effects of cooling may alter arterial blood gases, causing increased PaO 2, decreased CO 2, and acidosis. These reactions can be controlled primarily with ventilator setting changes. Hyperglycemia is common during TH and linked to poor outcomes in critically ill patients. During cooling, insulin sensitivity decreases, so patients may need high insulin doses to keep blood glucose levels within the range of 140 to 180 mg/dl. Also, gut motility decreases, so enteral feedings may be needed once the patient is rewarmed. TH decreases liver metabolism of drugs; thus, boluses are recommended instead of continuous infusions or short-acting agents when possible. Infection and bleeding risk TH may lead to infection and bleeding. Hypothermia impairs leukocyte function, which may increase the risk of infection (especially in wounds) and pneumonia. Keep in mind that hypothermia masks an increased body temperature a key sign of infection. Also, body temperatures below 35 C (95 F) depress clotting enzyme reactions and impair platelet function. Mild coagulopathy may increase bleeding risk in some patients, although this risk is comparable to that in patients who remain normothermic after cardiac arrest. Three phases of TH TH occurs in three phases cooling (induction), maintenance, and rewarming. (See the box below.)
5 //START BOX //END BOX// Phases of therapeutic hypothermia Induction: unstable period during which the patient s core temperature is reduced quickly to target temperature Maintenance: more stable period during which the patient is maintained at target temperature for 12 to 24 hours Rewarming: relatively unstable period during which the patient is returned to normothermia over the course of 12 to16 hours Induction phase The induction phase usually is the most unstable period, so clinicians should try to get patients through it as quickly as possible. Once core temperature drops to approximately 33.5 C (92.3 F), patients typically become more stable. Most evidence suggests target temperature should be achieved within 6 hours of ROSC. Before therapy begins, all patients must be intubated and mechanically ventilated and an indwelling urinary catheter, adequate venous access, and two core temperature-sensing devices must be placed. Shivering is a major complication of TH. Vasoconstriction and shivering are normal thermoregulatory responses to cooling as the body attempts to maintain normothermia. Shivering typically raises the basal metabolic rate two to five times the normal rate. Linked to increased heat production, oxygen consumption, and CO 2 production, shivering impedes the ability to cool the patient and may negate the possible neuroprotective effects of TH. (See the box below.)
6 //START BOX// /Title/The dangers of shivering during TH Studies show more than 60% of patients experience shivering during therapeutic hypothermia (TH). Young males and patients with magnesium levels below 1.7 mg/dl are at increased risk. Monitor patients closely for signs of shivering to promote early intervention and prevent negative consequences. One of the first signs is piloerection (goose bumps) as the body tries to prevent heat loss. Initially, shivering may not be visible; you ll need to palpate the patient s mandible for vibrations. Monitor the electrocardiogram for artifact caused by skeletal muscle movement. Resistance to cooling or inability to achieve target temperature despite multiple interventions may indicate heat production from shivering. Using an objective tool, such as the Bedside Shivering Assessment Scale (BSAS), helps quantify shivering in adults. With this validated tool (shown below), increased shivering intensity correlates with increased metabolic consumption. The goal is 0 (no shivering). Bedside Shivering Assessment Scale Score Degree of Description shivering 0 None No shivering present 1 Mild Shivering localized to neck and thorax only 2 Moderate Involves gross movement of upper extremities (plus neck and thorax) 3 Severe Involves gross movements of trunk and upper and lower extremities Based on data from Badjatia N, Strongilis E, Gordon E, et al. Metabolic impact of shivering during therapeutic temperature modulation: the Bedside Shivering Assessment Scale. Stroke. 2008;39(12): Treatment of shivering commonly starts with the least invasive method but may need to proceed quickly to more aggressive means. An effective plan may involve multiple interventions and medications. Nonpharmacologic interventions include use of surface counterwarming devices, which blow warm air onto the patient s skin at 40 to 43 C (104 to F); this blunts the shivering response by countering the feedback loop from the skin temperature to the hypothalamus. Surface counterwarming tricks the brain into thinking the body is warm. Another nonpharmacologic method is to wrap the patient s arms and legs in towels. Pharmacologic interventions aim to develop the patient s thermal tolerance, helping the body eliminate a cooling-related stress response through pharmacologic impairment. Various agents may be used in combination to reduce toxicities from high doses of any one drug. Sedation should be titrated to shivering suppression, not standard sedation scales, which frequently require high doses and aren t applicable if neuromuscular blocking agents are used. Continually monitor the patient s response to interventions aimed at eliminating shivering so you can assess their effectiveness. Be aware that patients who generate a strong shivering response have a better chance for a neurologically intact recovery. //END BOX//
7 All patients undergoing TH should receive sedation to decrease metabolic demand, oxygen consumption, and the shivering threshold as well as to help maintain neuroprotective benefits of TH. The most commonly used sedatives are propofol, midazolam, and dexmedetomidine. Continuous propofol and fentanyl infusions are highly effective during TH. Also, propofol has antiseizure properties at high doses. Some clinicians may start with propofol, increase the dosage, and add fentanyl if needed. Be aware that propofol has no analgesic effects, so if you think your patient on propofol is in pain, start fentanyl as ordered. Hypotensive patients may require midazolam instead of propofol; be aware, though, that midazolam accumulation may complicate subsequent neurologic examination because it can take days to clear the body. Meperidine is one of the most beneficial agents in reducing the shivering threshold. However, some clinicians are reluctant to use it because of its proconvulsant effects in an already vulnerable patient population. Buspirone helps prevent shivering but is available only in oral form, takes 1 hour to reach peak plasma concentrations, and depends on a functioning gut for absorption. Magnesium sulfate may promote the cooling process through its effects on peripheral vasodilation and thus decrease the time to target temperature. With low magnesium levels linked to an increased shivering risk, maintaining magnesium levels of 2.5 to 3.5mg/dL appears to be a reasonable goal. Inducing paralysis with neuromuscular blocking agents (NMBAs) is highly effective at suppressing shivering. But remember that although the muscles stop moving, the brain is still working and trying to generate a shivering response. This makes sedation crucial. NMBAs are the quickest way to stop shivering and don t cause hypotension. But they mask seizures, which have been reported in more than one-third of post-cardiac arrest patients. So patients receiving paralytic agents should undergo continuous electroencephalographic (EEG) monitoring to detect seizures. Once target temperature is achieved, paralytic drugs usually can be withdrawn during the maintenance phase, as most patients can t mount a shivering response at that point. NMBAs may need to be restarted during rewarming as the patient passes through the shivering threshold again. (See the box below.) //START BOX// DRUGS USED IN THERAPEUTIC HYPOTHERMIA Sedatives and analgesics Advantages Disadvantages Dexmedetomidine Brief-acting Relatively expensive May cause hypotension and bradycardia Fentanyl Rapid onset Decreased drug metabolism Mild hypotensive effect Midazolam Low risk of hypotension Takes longer to clear the body, which may delay neurologic evaluation Propofol Highly effective May cause hypotension Rapidly metabolized Has antiseizure properties Drugs that reduce shivering Buspirone Works well in combination with other agents Available by oral route only Takes 1 hour to peak onset Requires functioning gut for
8 Magnesium sulfate Promotes faster cooling Decreases shivering risk Provides neuroprotection Meperidine Highly effective absorption May cause hypotension with rapid administration May cause seizures Rapid onset of action Neuromuscular blocking agents 100% effective Doesn t affect neurologic triggers for shivering Masks seizures //END BOX// Maintenance phase Once target temperature is achieved, it needs to be maintained for a certain period typically 12 to 24 hours. During this phase, monitor the patient s vital signs, fluid status, and laboratory tests and intervene as needed. Provide supportive care to ensure skin integrity, especially if you re using a water-circulating device on the skin s surface. Also perform basic critical-care interventions, such as venous thromboembolism prophylaxis, measures to prevent ventilator-associated pneumonia, and eye care for patients receiving paralytics. Rewarming phase Rewarming must be done in a slow, controlled manner. Rapid rewarming can cause electrolyte abnormalities, cerebral edema, seizures, and other problems that negate the benefits of TH. The patient s temperature should be increased no more than 0.5 C per hour; many clinicians prefer 0.25 C per hour. It may take 12 to 16 hours to get the patient back to a temperature of about 36.5 C (97.7 F). Use of thermostatically controlled devices allows controlled temperature management through all hypothermia phases, especially rewarming. As patients begin to rewarm, they pass through the shivering threshold again; as needed, reinstate interventions used previously to prevent shivering. Stop administering potassium-containing infusions several hours before rewarming starts; potassium shifts out of the cell during rewarming, putting the patient at risk for hyperkalemia. Glucose levels start to normalize, so monitor the patient s glucose level closely and adjust the insulin drip as necessary. Once the patient reaches a core temperature of 36 C (96.8 F), discontinue any paralytic agents that were restarted during rewarming. Start weaning the patient off sedatives so a complete neurologic evaluation can be completed. Evidence suggests clinicians should prevent posthypothermia fever, which may be associated with increased mortality or worse neurologic outcomes. To do this, leave the cooling device in place for 24 to 36 hours after the patient has been rewarmed and maintain normothermia for the duration of the rewarming period. Assessing neurologic status after TH Evaluating the patient s neurologic status after TH can be challenging. Drugs used for sedation and shivering suppression may make clinical assessment unreliable. Diagnostic tests used to evaluate the patient s neurologic status may include magnetic resonance imaging, EEG, and somatosensory evoked potentials. AHA and ILCOR recommend delaying neurologic prognostication for at least 72 hours after the patient has been rewarmed. Signs of poor clinical prognosis include absent corneal, pupillary, and motor responses and extensor posturing after rewarming.
9 Keep in mind that TH can be a difficult time for the patient s family as they wait to see if and how well their loved one will recover. You can play an important role in providing support, answering questions, and providing honest but sensitive communication about the patient s condition. Dr. Smith s outcome The team works hard to ensure they re doing everything they can to implement and follow the hypothermia protocol, to provide the best chance for Mary Smith s complete recovery. They know that just surviving this event won t be enough for her; she loves her research and they are sure she ll want to be able to continue it. The team initiates cooling per hospital protocol, using iced saline and watercirculating cooling pads to reach target temperature in 3.5 hours. When Kathleen experiences minor shivering, they administer fentanyl and propofol for sedation and to manage shivering. Her potassium levels remain below normal; the team monitors these levels closely and administers replacement potassium. After being maintained at target temperature for 18 hours, they rewarm Mary over the next 16 hours. The day after she is rewarmed, she is extubated; she looks at her husband and calls him by name. Although her recovery takes some time, she eventually returns to her practice and has several articles published again in prominent medical journals. Julie M. Waters is a clinical nurse educator for critical care at Providence Sacred Heart Medical Center in Spokane, Washington. Selected references Arrich J, Holzer M, Herkner H, et al. Hypothermia for neuroprotection in adults after cardiopulmonary resuscitation. Cochrane Database Syst Rev. 2012;(4):CD Badjatia N, Strongilis E, Gordon E, et al. Metabolic impact of shivering during therapeutic temperature modulation: the Bedside Shivering Assessment Scale. Stroke. 2008;39(12): Bro-Jeppesen J, Hassager C, Wanscher M, et al. Post-hypothermia fever is associated with increased mortality after out-of-hospital cardiac arrest. Resuscitation. 2013;84(12): Hazinski MF, Nolan JP, Billi JE, et al. Part 1 Executive summary: 2010 International Consensus on Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Science With Treatment Recommendations. Circulation. 2010;122(16 Suppl 2):S Neumar RW, Nolan JP, Adrie, C, et al. ILCOR Consensus Statement: Post-Cardiac Arrest Syndrome. Epidemiology, Pathophysiology, Treatment, and Prognostication. A consensus statement from the International Liaison Committee on Resuscitation (American Heart Association, Australian and New Zealand Council on Resuscitation, European Resuscitation Council, Heart and Stroke Foundation of Canada, InterAmerican Heart Foundation, Resuscitation Council of Asia, and the Resuscitation Council of Southern Africa); the American Heart Association Emergency Cardiovascular Care Committee; the Council on Cardiovascular Surgery and Anesthesia; the Council on Cardiopulmonary, Perioperative, and Critical Care; the Council on Clinical Cardiology; and the Stroke Council. Circulation. 2008; 118(23): Nielsen N, Wetterslev J, Cronberg T, et al. Targeted temperature management at 33 C versus 36 C after cardiac arrest. N Engl J Med. 2013;369(23):
10 Olson DM, Grissom JL, Williamson RA, et al. Interrater reliability of the bedside shivering assessment scale. Am J Crit Care. 2013;22(1):70-4. Polderman KH, Herold I. Therapeutic hypothermia and controlled normothermia in the intensive care unit: practical considerations, side effects, and cooling methods. Crit Care Med. 2009;37(3): Rittenberger JC, Callaway CW. Post cardiac arrest management in adults. UpToDate. Last updated January 9, Accessed April 10, *Name is fictitious. CNE Instructions To take the post-test for this article and earn contact hour credit, please click here. Simply use your Visa or MasterCard to pay the processing fee. (ANA members $15; nonmembers $20.) Once you ve successfully passed the post-test and completed the evaluation form, you ll be able to print out your certificate immediately. Provider accreditation The American Nurses Association s Center for Continuing Education and Professional Development is accredited as a provider of continuing nursing education by the American Nurses Credentialing Center s Commission on Accreditation. ANCC Provider Number Contact hours: 1.4 ANA s Center for Continuing Education and Professional Development is approved by the California Board of Registered Nursing, Provider Number CEP6178 for 1.6 contact hours. Post-test passing score is 75%. Expiration: 4/8/17 ANA Center for Continuing Education and Professional Development s accredited provider status refers only to CNE activities and does not imply that there is real or implied endorsement of any product, service, or company referred to in this activity nor of any company subsidizing costs related to the activity. The planners and author of this CNE activity have disclosed no relevant financial relationships with any commercial companies pertaining to this CNE.
Case Presentation. Cooling. Case Presentation. New Developments in Cardiopulmonary Arrest: Therapeutic Hypothermia in Resuscitation
 New Developments in Cardiopulmonary Arrest: Therapeutic Hypothermia in Resuscitation Michael Sayre, MD Emergency Medicine and LeRoy Essig, MD Pulmonary/Critical Care Medicine Case Presentation 3:40 (+
New Developments in Cardiopulmonary Arrest: Therapeutic Hypothermia in Resuscitation Michael Sayre, MD Emergency Medicine and LeRoy Essig, MD Pulmonary/Critical Care Medicine Case Presentation 3:40 (+
Pathophysiology and Cardiac Insights for Targeted Temperature Management in Emergency Medicine and Critical Care
 Pathophysiology and Cardiac Insights for Targeted Temperature Management in Emergency Medicine and Critical Care LINDSAY LEWIS BSN, RN, CCCC Faculty Disclosure I AM CURRENTLY EMPLOYED AS A CLINICAL MANAGER
Pathophysiology and Cardiac Insights for Targeted Temperature Management in Emergency Medicine and Critical Care LINDSAY LEWIS BSN, RN, CCCC Faculty Disclosure I AM CURRENTLY EMPLOYED AS A CLINICAL MANAGER
INDUCED HYPOTHERMIA. F. Ben Housel, M.D.
 INDUCED HYPOTHERMIA F. Ben Housel, M.D. Historical Use of Induced Hypothermia 1950 s - Moderate hypothermia (30-32º C) in open heart surgery to protect brain against global ischemia 1960-1980 s - Use of
INDUCED HYPOTHERMIA F. Ben Housel, M.D. Historical Use of Induced Hypothermia 1950 s - Moderate hypothermia (30-32º C) in open heart surgery to protect brain against global ischemia 1960-1980 s - Use of
Post-Resuscitation Care: Optimizing & Improving Outcomes after Cardiac Arrest. Objectives: U.S. stats
 Post-Resuscitation Care: Optimizing & Improving Outcomes after Cardiac Arrest Nicole L. Kupchik RN, MN, CCNS CCRN-CMC Clinical Nurse Specialist Harborview Medical Center Seattle, WA Objectives: At the
Post-Resuscitation Care: Optimizing & Improving Outcomes after Cardiac Arrest Nicole L. Kupchik RN, MN, CCNS CCRN-CMC Clinical Nurse Specialist Harborview Medical Center Seattle, WA Objectives: At the
CHILL OUT! Induced Hypothermia: Challenges & Successes in the
 CHILL OUT! Induced Hypothermia: Challenges & Successes in the ICU Colleen Bell RN, BS, CCRN, Donna Brault RN, BSN, CCRN, Cathy Patnode RN, BSN, CCRN Champlain Valley Physician Hospital November 2012 Objectives
CHILL OUT! Induced Hypothermia: Challenges & Successes in the ICU Colleen Bell RN, BS, CCRN, Donna Brault RN, BSN, CCRN, Cathy Patnode RN, BSN, CCRN Champlain Valley Physician Hospital November 2012 Objectives
INDUCED HYPOTHERMIA A Hot Topic. R. Darrell Nelson, MD, FACEP Emergency Medicine Wake Forest University Health Sciences
 INDUCED HYPOTHERMIA A Hot Topic R. Darrell Nelson, MD, FACEP Emergency Medicine Wake Forest University Health Sciences Conflicts of Interest Sadly, we have no financial or industrial conflicts of interest
INDUCED HYPOTHERMIA A Hot Topic R. Darrell Nelson, MD, FACEP Emergency Medicine Wake Forest University Health Sciences Conflicts of Interest Sadly, we have no financial or industrial conflicts of interest
Therapeutic Hypothermia after Resuscitated Cardiac Arrest
 Therapeutic Hypothermia after Resuscitated Cardiac Arrest The purpose of this protocol is to improve the neurologic outcomes of patients who have experienced cardiac arrest and have been successfully resuscitated.
Therapeutic Hypothermia after Resuscitated Cardiac Arrest The purpose of this protocol is to improve the neurologic outcomes of patients who have experienced cardiac arrest and have been successfully resuscitated.
SYSTEM-WIDE POLICY & PROCEDURE MANUAL. Policy Title: Hypothermia Post Cardiac Arrest Policy Number: PC-124. President & CEO Page 1 of 9
 Approved By: President & CEO Date Page 1 of 9 POLICY: PURPOSE: To define and describe the implementation of induced hypothermia post cardiac arrest and the nursing assessment and interventions required
Approved By: President & CEO Date Page 1 of 9 POLICY: PURPOSE: To define and describe the implementation of induced hypothermia post cardiac arrest and the nursing assessment and interventions required
Hypothermia Induction Methods
 Hypothermia Induction Methods Advantages and Disadvantages Xia Luo, M.D. Vice President, Clinical Education ZOLL Corporation Targeted Temperature Management (TTM) Temperature is one of the four vital signs
Hypothermia Induction Methods Advantages and Disadvantages Xia Luo, M.D. Vice President, Clinical Education ZOLL Corporation Targeted Temperature Management (TTM) Temperature is one of the four vital signs
Post-Cardiac Arrest Syndrome. MICU Lecture Series
 Post-Cardiac Arrest Syndrome MICU Lecture Series Case 58 y/o female collapses at home, family attempts CPR, EMS arrives and notes VF, defibrillation x 3 with return of spontaneous circulation, brought
Post-Cardiac Arrest Syndrome MICU Lecture Series Case 58 y/o female collapses at home, family attempts CPR, EMS arrives and notes VF, defibrillation x 3 with return of spontaneous circulation, brought
Patient Case. Post cardiac arrest pathophysiology 10/19/2017. Disclosure. Objectives. Patient Case-TM
 Disclosure TARGETED TEMPERATURE MANAGEMENT POST CARDIAC ARREST I have nothing to disclose concerning possible financial or personal relationships with commercial entities that may have a direct or indirect
Disclosure TARGETED TEMPERATURE MANAGEMENT POST CARDIAC ARREST I have nothing to disclose concerning possible financial or personal relationships with commercial entities that may have a direct or indirect
Curricullum Vitae. Dr. Isman Firdaus, SpJP (K), FIHA
 Curricullum Vitae Dr. Isman Firdaus, SpJP (K), FIHA Email: ismanf@yahoo.com Qualification : o GP 2001 (FKUI) o Cardiologist 2007 (FKUI) o Cardiovascular Intensivist 2010 - present o Cardiovascular Intervensionist
Curricullum Vitae Dr. Isman Firdaus, SpJP (K), FIHA Email: ismanf@yahoo.com Qualification : o GP 2001 (FKUI) o Cardiologist 2007 (FKUI) o Cardiovascular Intensivist 2010 - present o Cardiovascular Intervensionist
Therapeutic Hypothermia and Pharmacologic Considerations. Genelle Butz, PharmD Director of Pharmacy CarolinaEast Medical Center August 6, 2013
 Therapeutic Hypothermia and Pharmacologic Considerations Genelle Butz, PharmD Director of Pharmacy CarolinaEast Medical Center August 6, 2013 Disclosures Disclosure tatement: I have no financial or personal
Therapeutic Hypothermia and Pharmacologic Considerations Genelle Butz, PharmD Director of Pharmacy CarolinaEast Medical Center August 6, 2013 Disclosures Disclosure tatement: I have no financial or personal
POST-CARDIAC ARREST CARE: WHAT HAPPENS AFTER ROSC MATTERS! Emergency Nurses Association
 POST-CARDIAC ARREST CARE: WHAT HAPPENS AFTER ROSC MATTERS! Emergency Nurses Association - 2016 Nicole Kupchik MN, RN, CCNS, CCRN, PCCN, CMC Objectives Discuss the 2015 AHA Guideline Updates for Post- Arrest
POST-CARDIAC ARREST CARE: WHAT HAPPENS AFTER ROSC MATTERS! Emergency Nurses Association - 2016 Nicole Kupchik MN, RN, CCNS, CCRN, PCCN, CMC Objectives Discuss the 2015 AHA Guideline Updates for Post- Arrest
Induced Hypothermia for Cardiac Arrest. Heather Hand RN,CCRN,CNRN,ATCN,LNC
 Induced Hypothermia for Cardiac Arrest Heather Hand RN,CCRN,CNRN,ATCN,LNC Cardiac Arrest Epidemiology 400,000 arrests / year in U.S.A 3 / 4 Out-of-hospital 1 / 4 In-hospital survival to hospital 1-5% discharge
Induced Hypothermia for Cardiac Arrest Heather Hand RN,CCRN,CNRN,ATCN,LNC Cardiac Arrest Epidemiology 400,000 arrests / year in U.S.A 3 / 4 Out-of-hospital 1 / 4 In-hospital survival to hospital 1-5% discharge
PATIENT CARE MANUAL. Guideline For Managing Shivering In Neurocritical Care Patients Undergoing Therapeutic Temperature Modulation
 PATIENT CARE MANUAL MANUAL CODE: SUBJECT: Guideline For Managing Shivering In Neurocritical Care Patients Undergoing Therapeutic Temperature Modulation DATE ISSUED: DATE REVISED: SUPERSEDES: CROSS REFERENCES:
PATIENT CARE MANUAL MANUAL CODE: SUBJECT: Guideline For Managing Shivering In Neurocritical Care Patients Undergoing Therapeutic Temperature Modulation DATE ISSUED: DATE REVISED: SUPERSEDES: CROSS REFERENCES:
Therapeutic Hypothermia
 Objectives Overview Therapeutic Hypothermia Nerissa U. Ko, MD, MAS UCSF Department of Neurology Critical Care Medicine and Trauma June 4, 2011 Hypothermia as a neuroprotectant Proven indications: Adult
Objectives Overview Therapeutic Hypothermia Nerissa U. Ko, MD, MAS UCSF Department of Neurology Critical Care Medicine and Trauma June 4, 2011 Hypothermia as a neuroprotectant Proven indications: Adult
CrackCast Episode 8 Brain Resuscitation
 CrackCast Episode 8 Brain Resuscitation Episode Overview: 1) Describe 6 therapeutic interventions for the post-arrest brain 2) List 5 techniques for initiating therapeutic hypothermia 3) List 4 mechanisms
CrackCast Episode 8 Brain Resuscitation Episode Overview: 1) Describe 6 therapeutic interventions for the post-arrest brain 2) List 5 techniques for initiating therapeutic hypothermia 3) List 4 mechanisms
H Alex Choi, MD MSc Assistant Professor of Neurology and Neurosurgery The University of Texas Health Science Center Mischer Neuroscience Institute
 H Alex Choi, MD MSc Assistant Professor of Neurology and Neurosurgery The University of Texas Health Science Center Mischer Neuroscience Institute Memorial Hermann- Texas Medical Center Learning Objectives
H Alex Choi, MD MSc Assistant Professor of Neurology and Neurosurgery The University of Texas Health Science Center Mischer Neuroscience Institute Memorial Hermann- Texas Medical Center Learning Objectives
Targeted Temperature Management: Normothermia for Neuroprotection
 Targeted Temperature Management: Normothermia for Neuroprotection I. Rationale Elevated body temperature is associated with increased cerebral metabolic rate and associated metabolic demand, which can
Targeted Temperature Management: Normothermia for Neuroprotection I. Rationale Elevated body temperature is associated with increased cerebral metabolic rate and associated metabolic demand, which can
Please consult package insert for more detailed safety information and instructions for use. BMD/AS50/0516/0115
 Indications for Use: The ARCTIC SUN Temperature Management System is a thermal regulating system, indicated for monitoring and controlling patient temperature in adult and pediatric patients of all ages.
Indications for Use: The ARCTIC SUN Temperature Management System is a thermal regulating system, indicated for monitoring and controlling patient temperature in adult and pediatric patients of all ages.
Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC
 Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC Objectives 1. Define Hypoxic-Ischemic Encephalopathy (HIE) 2. Identify the criteria used to determine if an infant qualifies for therapeutic
Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC Objectives 1. Define Hypoxic-Ischemic Encephalopathy (HIE) 2. Identify the criteria used to determine if an infant qualifies for therapeutic
The Evidence Base. Stephan A. Mayer, MD. Columbia University New York, NY
 Hypothermic for Cardiac Arrest The Evidence Base Stephan A. Mayer, MD Director, Neuro-ICU Columbia University New York, NY Disclosures Columbia University Clinical Trials Pilot Award Radiant Medical, Inc.
Hypothermic for Cardiac Arrest The Evidence Base Stephan A. Mayer, MD Director, Neuro-ICU Columbia University New York, NY Disclosures Columbia University Clinical Trials Pilot Award Radiant Medical, Inc.
Module 2. Troubleshooting / Case Studies
 Module 2 Troubleshooting / Case Studies Alarms / Alerts If an alarm or alert occurs, the Arctic Sun will produce both an audible and visual cue The screen will appear that displays: alarm or alert number,
Module 2 Troubleshooting / Case Studies Alarms / Alerts If an alarm or alert occurs, the Arctic Sun will produce both an audible and visual cue The screen will appear that displays: alarm or alert number,
Objectives. Trends in Resuscitation POST-CARDIAC ARREST CARE: WHAT S THE EVIDENCE?
 POST-CARDIAC ARREST CARE: WHAT S THE EVIDENCE? Nicole Kupchik RN, MN, CCNS, CCRN, PCCN, CMC Objectives Discuss the 2015 AHA Guideline Updates for Post- Arrest Care Discuss oxygenation & hemodynamic taregts
POST-CARDIAC ARREST CARE: WHAT S THE EVIDENCE? Nicole Kupchik RN, MN, CCNS, CCRN, PCCN, CMC Objectives Discuss the 2015 AHA Guideline Updates for Post- Arrest Care Discuss oxygenation & hemodynamic taregts
In-hospital Care of the Post-Cardiac Arrest Patient. David A. Pearson, MD, FACEP, FAAEM Associate Program Director Department of Emergency Medicine
 In-hospital Care of the Post-Cardiac Arrest Patient David A. Pearson, MD, FACEP, FAAEM Associate Program Director Department of Emergency Medicine Disclosures I have no financial interest, arrangement,
In-hospital Care of the Post-Cardiac Arrest Patient David A. Pearson, MD, FACEP, FAAEM Associate Program Director Department of Emergency Medicine Disclosures I have no financial interest, arrangement,
Hypothermia: The Science and Recommendations (In-hospital and Out)
 Hypothermia: The Science and Recommendations (In-hospital and Out) L. Kristin Newby, MD, MHS Professor of Medicine Duke University Medical Center Chair, Council on Clinical Cardiology, AHA President, Society
Hypothermia: The Science and Recommendations (In-hospital and Out) L. Kristin Newby, MD, MHS Professor of Medicine Duke University Medical Center Chair, Council on Clinical Cardiology, AHA President, Society
Therapeutic Hypothermia for Post Cardiac Arrest Plan Initial Orders
 Arrest Plan Initial Orders Weight Allergies Therapeutic Hypothermia Guidelines ***Required to continue with ordering Plan.*** Strict Intake and Output q1h, throughout cooling and re warming. Set Up for
Arrest Plan Initial Orders Weight Allergies Therapeutic Hypothermia Guidelines ***Required to continue with ordering Plan.*** Strict Intake and Output q1h, throughout cooling and re warming. Set Up for
New Therapeutic Hypothermia Techniques
 New Therapeutic Hypothermia Techniques Joseph P. Ornato, MD, FACP, FACC, FACEP Professor & Chairman, Emergency Medicine Virginia Commonwealth University Health System Richmond, VA Medical Director Richmond
New Therapeutic Hypothermia Techniques Joseph P. Ornato, MD, FACP, FACC, FACEP Professor & Chairman, Emergency Medicine Virginia Commonwealth University Health System Richmond, VA Medical Director Richmond
Post-Cardiac Arrest Syndrome Henry L. Green, MD, FACC Clinical Professor of Medicine, Wayne State University December 11, 2016
 Post-Cardiac Arrest Syndrome Henry L. Green, MD, FACC Clinical Professor of Medicine, Wayne State University December 11, 2016 Introduction Advanced cardiac life support training focuses on restoration
Post-Cardiac Arrest Syndrome Henry L. Green, MD, FACC Clinical Professor of Medicine, Wayne State University December 11, 2016 Introduction Advanced cardiac life support training focuses on restoration
Targeted Temperature Management: An Evolving Therapy for Cardiac Arrest
 Targeted Temperature Management: An Evolving Therapy for Cardiac Arrest By Meagan Dunn, BScN, MSc,, RN, CNE NP Forum April 8, 2016 Objectives To understand: What Therapeutic Temperature Management (TTM)
Targeted Temperature Management: An Evolving Therapy for Cardiac Arrest By Meagan Dunn, BScN, MSc,, RN, CNE NP Forum April 8, 2016 Objectives To understand: What Therapeutic Temperature Management (TTM)
CARES Targeted Temperature Management (TTM) Module
 CARES Targeted Temperature Management (TTM) Module OHCA Data Dictionary June 2014 1 CASE NUMBER This is the number assigned to the patient by the hospital. The case number is the number the hospital assigns
CARES Targeted Temperature Management (TTM) Module OHCA Data Dictionary June 2014 1 CASE NUMBER This is the number assigned to the patient by the hospital. The case number is the number the hospital assigns
Therapeutic hypothermia
 INDUCED HYPOTHERMIA Dr. Attilla Kiss M.D. Acting Medical Director Emergency Services EMS Medical Director St. John Medical Center OBJECTIVES Define and explain Induced Hypothermia Discuss both pre-hospital
INDUCED HYPOTHERMIA Dr. Attilla Kiss M.D. Acting Medical Director Emergency Services EMS Medical Director St. John Medical Center OBJECTIVES Define and explain Induced Hypothermia Discuss both pre-hospital
Page 1 of 9 PATIENT PRESENTATION COOLING. See Page 2 for Re-Warming Phase. Patient not eligible for TTM protocol. Yes
 1 Page 1 of 9 PATIENT PRESENTATION Cardiac arrest PEA Asystole Ventricular fibrillation Pulseless ventricular tachycardia Sustained ROSC greater than 20 consecutive minutes? PEA = pulseless electrical
1 Page 1 of 9 PATIENT PRESENTATION Cardiac arrest PEA Asystole Ventricular fibrillation Pulseless ventricular tachycardia Sustained ROSC greater than 20 consecutive minutes? PEA = pulseless electrical
Post Cardiac Arrest Care 2015 American Heart Association Guideline Update for CPR and Emergency Cardiovascular Care
 Post Cardiac Arrest Care 2015 American Heart Association Guideline Update for CPR and Emergency Cardiovascular Care รศ.ดร.พญ.ต นหยง พ พานเมฆาภรณ ภาคว ชาว ส ญญ ว ทยา คณะแพทยศาสตร มหาว ทยาล ยเช ยงใหม System
Post Cardiac Arrest Care 2015 American Heart Association Guideline Update for CPR and Emergency Cardiovascular Care รศ.ดร.พญ.ต นหยง พ พานเมฆาภรณ ภาคว ชาว ส ญญ ว ทยา คณะแพทยศาสตร มหาว ทยาล ยเช ยงใหม System
Update on Sudden Cardiac Death and Resuscitation
 Update on Sudden Cardiac Death and Resuscitation Ashish R. Panchal, MD, PhD Medical Director Center for Emergency Medical Services Assistant Professor Clinical Department of Emergency Medicine The Ohio
Update on Sudden Cardiac Death and Resuscitation Ashish R. Panchal, MD, PhD Medical Director Center for Emergency Medical Services Assistant Professor Clinical Department of Emergency Medicine The Ohio
(31189) Hypothermia Initiation Phase One
 Hypothermia Initiation Phase One Diagnosis Allergies For hypothermia tracking purposes only. Please do not uncheck.- Required Cardiac Emergency Tracking For hypothermia tracking purposes only. Consults
Hypothermia Initiation Phase One Diagnosis Allergies For hypothermia tracking purposes only. Please do not uncheck.- Required Cardiac Emergency Tracking For hypothermia tracking purposes only. Consults
Post-Arrest Care: Beyond Hypothermia
 Post-Arrest Care: Beyond Hypothermia Damon Scales MD PhD Department of Critical Care Medicine Sunnybrook Health Sciences Centre University of Toronto Disclosures CIHR Physicians Services Incorporated Main
Post-Arrest Care: Beyond Hypothermia Damon Scales MD PhD Department of Critical Care Medicine Sunnybrook Health Sciences Centre University of Toronto Disclosures CIHR Physicians Services Incorporated Main
State of Florida Hypothermia Protocol. Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology
 State of Florida Hypothermia Protocol Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology I. Entry Criteria 1. Gestational Age greater than or equal to 35 weeks gestation
State of Florida Hypothermia Protocol Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology I. Entry Criteria 1. Gestational Age greater than or equal to 35 weeks gestation
Targeted temperature management after post-anoxic brain insult: where do we stand?
 Targeted temperature management after post-anoxic brain insult: where do we stand? Alain Cariou Intensive Care Unit Cochin University Hospital Paris Descartes University INSERM U970 (France) COI Disclosure
Targeted temperature management after post-anoxic brain insult: where do we stand? Alain Cariou Intensive Care Unit Cochin University Hospital Paris Descartes University INSERM U970 (France) COI Disclosure
Post Cardiac Arrest Care. From : 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care
 Post Cardiac Arrest Care From : 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Initial Objectives of Post cardiac Arrest Care Optimize cardiopulmonary
Post Cardiac Arrest Care From : 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Initial Objectives of Post cardiac Arrest Care Optimize cardiopulmonary
Stayin Alive: Pediatric Advanced Life Support (PALS) Updated Guidelines
 Stayin Alive: Pediatric Advanced Life Support (PALS) Updated Guidelines Margaret Oates, PharmD, BCPPS Pediatric Critical Care Specialist GSHP Summer Meeting July 16, 2016 Disclosures I have nothing to
Stayin Alive: Pediatric Advanced Life Support (PALS) Updated Guidelines Margaret Oates, PharmD, BCPPS Pediatric Critical Care Specialist GSHP Summer Meeting July 16, 2016 Disclosures I have nothing to
3/6/2017. Endovascular Selective Cerebral Hypothermia First-in-Human Experience
 Endovascular Selective Cerebral Hypothermia First-in-Human Experience Ronald Jay Solar, Ph.D. San Diego, CA 32 nd Annual Snowmass Symposium March 5-10, 2017 Introduction Major limitations in acute ischemic
Endovascular Selective Cerebral Hypothermia First-in-Human Experience Ronald Jay Solar, Ph.D. San Diego, CA 32 nd Annual Snowmass Symposium March 5-10, 2017 Introduction Major limitations in acute ischemic
Module 3 Troubleshooting/Case Studies
 Module 3 Troubleshooting/Case Studies If an alarm or alert occurs, the ARCTIC SUN Temperature Management System will produce both an audible and visual cue A screen will appear that displays: alarm or
Module 3 Troubleshooting/Case Studies If an alarm or alert occurs, the ARCTIC SUN Temperature Management System will produce both an audible and visual cue A screen will appear that displays: alarm or
Neurotrauma: The Place for Cooling
 Neurotrauma: The Place for Cooling Cooling: to achieve hypothermia History, evidence, open questions Cooling: to achieve normothermia Evidence, open questions Cooling: Practical Aspects Hypothermia: History
Neurotrauma: The Place for Cooling Cooling: to achieve hypothermia History, evidence, open questions Cooling: to achieve normothermia Evidence, open questions Cooling: Practical Aspects Hypothermia: History
THERAPEUTIC HYPOTHERMIA POST CARDIAC ARREST
 THERAPEUTIC HYPOTHERMIA POST CARDIAC ARREST Heather Harrington RN, BScN, CNCC(c) Clinical Nurse Educator Sunnybrook Health Sciences Centre Objectives Define Therapeutic Hypothermia (TH) Describe current
THERAPEUTIC HYPOTHERMIA POST CARDIAC ARREST Heather Harrington RN, BScN, CNCC(c) Clinical Nurse Educator Sunnybrook Health Sciences Centre Objectives Define Therapeutic Hypothermia (TH) Describe current
1) According to ILCOR guidelines, to what temperature should patients be cooled? a ºC b ºC c ºC d ºC
 MANAGEMENT OF OUT-OF-HOSPITAL CARDIAC ARRESTS WITH INDUCED HYPOTHERMIA ANAESTHESIA TUTORIAL OF THE WEEK 206 22 ND NOVEMBER 2010 Dr Clare Attwood, Specialist Trainee in Anaesthesia Royal Devon and Exeter
MANAGEMENT OF OUT-OF-HOSPITAL CARDIAC ARRESTS WITH INDUCED HYPOTHERMIA ANAESTHESIA TUTORIAL OF THE WEEK 206 22 ND NOVEMBER 2010 Dr Clare Attwood, Specialist Trainee in Anaesthesia Royal Devon and Exeter
Therapeutic Hypothermia After Cardiac Arrest: Best Practices 2014
 Therapeutic Hypothermia After Cardiac Arrest: Best Practices 2014 Deborah Klein, RN, MSN, ACNS-BC, CCRN, CHFN, FAHA Clinical Nurse Specialist Coronary ICU, Heart Failure ICU, and Cardiac Short Stay/PACU/CARU
Therapeutic Hypothermia After Cardiac Arrest: Best Practices 2014 Deborah Klein, RN, MSN, ACNS-BC, CCRN, CHFN, FAHA Clinical Nurse Specialist Coronary ICU, Heart Failure ICU, and Cardiac Short Stay/PACU/CARU
In the past decade, two large randomized
 Mild therapeutic hypothermia improves outcomes compared with normothermia in cardiac-arrest patients a retrospective chart review* David Hörburger, MD; Christoph Testori, MD; Fritz Sterz, MD; Harald Herkner,
Mild therapeutic hypothermia improves outcomes compared with normothermia in cardiac-arrest patients a retrospective chart review* David Hörburger, MD; Christoph Testori, MD; Fritz Sterz, MD; Harald Herkner,
Unrestricted. Dr ppooransari fellowship of perenatalogy
 Unrestricted Dr ppooransari fellowship of perenatalogy Assessment of severity of hemorrhage Significant drops in blood pressure are generally not manifested until substantial bleeding has occurred, and
Unrestricted Dr ppooransari fellowship of perenatalogy Assessment of severity of hemorrhage Significant drops in blood pressure are generally not manifested until substantial bleeding has occurred, and
Cardiopulmonary Resuscitation in Adults
 Cardiopulmonary Resuscitation in Adults Fatma Özdemir, MD Emergency Deparment of Uludag University Faculty of Medicine OVERVIEW Introduction Pathophysiology BLS algorithm ALS algorithm Post resuscitation
Cardiopulmonary Resuscitation in Adults Fatma Özdemir, MD Emergency Deparment of Uludag University Faculty of Medicine OVERVIEW Introduction Pathophysiology BLS algorithm ALS algorithm Post resuscitation
Hypothermic Resuscitation 1 st Intercontinental Emergency Medicine Congress, Belek-Antalya 2014
 Hypothermic Resuscitation 1 st Intercontinental Emergency Medicine Congress, Belek-Antalya 2014 Jasmin Arrich Department of Emergency Medicine Medical University of Vienna jasmin.arrich@meduniwien.ac.at
Hypothermic Resuscitation 1 st Intercontinental Emergency Medicine Congress, Belek-Antalya 2014 Jasmin Arrich Department of Emergency Medicine Medical University of Vienna jasmin.arrich@meduniwien.ac.at
Update in Critical Care Medicine
 Update in Critical Care Medicine Michael A. Gropper, MD, PhD Professor and Executive Vice Chair Department of Anesthesia and Perioperative Care Director, Critical Care Medicine UCSF Disclosure None Update
Update in Critical Care Medicine Michael A. Gropper, MD, PhD Professor and Executive Vice Chair Department of Anesthesia and Perioperative Care Director, Critical Care Medicine UCSF Disclosure None Update
Hypothermia Presentation
 Hypothermia Presentation Thermoregulation Thermal regulation is a balance between heat production and heat loss. Despite marked changes in skin temperature, the body s homeostatic mechanisms are able to
Hypothermia Presentation Thermoregulation Thermal regulation is a balance between heat production and heat loss. Despite marked changes in skin temperature, the body s homeostatic mechanisms are able to
Therapeutic Hypothermia. Jonas Cooper, MD MPH
 Therapeutic Hypothermia Jonas Cooper, MD MPH Hypothermia in Cardiology Early cardiac surgery included cooling to 15 C and stopping all blood flow for one hour while surgery proceeded Belsey RH et al. Profound
Therapeutic Hypothermia Jonas Cooper, MD MPH Hypothermia in Cardiology Early cardiac surgery included cooling to 15 C and stopping all blood flow for one hour while surgery proceeded Belsey RH et al. Profound
Therapeutic Hypothermia: 2011 Research Update. Richard R. Riker MD, FCCM Chest Medicine Associates South Portland, Maine
 Therapeutic Hypothermia: 2011 Research Update Richard R. Riker MD, FCCM Chest Medicine Associates South Portland, Maine Agenda NMBA, Sedation, and Shivering Seizures Prognostication Early = Staging Late
Therapeutic Hypothermia: 2011 Research Update Richard R. Riker MD, FCCM Chest Medicine Associates South Portland, Maine Agenda NMBA, Sedation, and Shivering Seizures Prognostication Early = Staging Late
Ac#ve, ECMO or locally available alterna#ves. invasive warming. Ini#ally: Ac#ve noninvasive or minimally
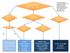 Suspected Hypothermia Temp
Suspected Hypothermia Temp
CLINICAL POLICY AND PROCEDURES
 SUPERSEDES POLICY: PAGE: 1 OF 16 POLICY STATEMENT: Patients undergoing post-cardiac arrest resuscitation and therapeutic hypothermia (TH) will have nursing care provided according to the following policy.
SUPERSEDES POLICY: PAGE: 1 OF 16 POLICY STATEMENT: Patients undergoing post-cardiac arrest resuscitation and therapeutic hypothermia (TH) will have nursing care provided according to the following policy.
HEAT STROKE. Lindsay VaughLindsay Vaughn, DVM, DACVECCDVM, DACVECC
 HEAT STROKE Lindsay VaughLindsay Vaughn, DVM, DACVECCDVM, DACVECC Heat Stroke More Preventable Than Treatable Heat Stroke A form of hyperthermia associated with a systemic inflammatory response leading
HEAT STROKE Lindsay VaughLindsay Vaughn, DVM, DACVECCDVM, DACVECC Heat Stroke More Preventable Than Treatable Heat Stroke A form of hyperthermia associated with a systemic inflammatory response leading
Hypothermia Short Set-Critical Care HYPOTHERMIA SS- CRITICAL CARE
 Hypothermia Short Set-Critical Care HYPOTHERMIA SS- CRITICAL CARE Inclusion Criteria all must be present Cardiac arrest with return of spontaneous circulation (ROSC) ROSC within 60 mins of witnessed arrest;
Hypothermia Short Set-Critical Care HYPOTHERMIA SS- CRITICAL CARE Inclusion Criteria all must be present Cardiac arrest with return of spontaneous circulation (ROSC) ROSC within 60 mins of witnessed arrest;
Accidental Hypothermia
 Accidental Hypothermia Gordon G. Giesbrecht, Ph.D., Professor Health Leisure and Human Performance Research Institute University of Manitoba, Winnipeg, Manitoba, Canada, R3T 2N2 Learning Objectives: 1)
Accidental Hypothermia Gordon G. Giesbrecht, Ph.D., Professor Health Leisure and Human Performance Research Institute University of Manitoba, Winnipeg, Manitoba, Canada, R3T 2N2 Learning Objectives: 1)
Therapeutic hypothermia following cardiac arrest
 TITLE: Therapeutic hypothermia following cardiac arrest AUTHOR: Jeffrey A. Tice, MD Assistant Professor of Medicine Division of General Internal Medicine Department of Medicine University of California
TITLE: Therapeutic hypothermia following cardiac arrest AUTHOR: Jeffrey A. Tice, MD Assistant Professor of Medicine Division of General Internal Medicine Department of Medicine University of California
Targeted Temperature Management in Post Cardiac Arrest Patients
 Targeted Temperature Management in Post Cardiac Arrest Patients Treesa Joseph, PharmD PGY-1 Pharmacy Resident Atlantic Health System Continuing Education Presentation June 15 th, 2017 Objectives Explain
Targeted Temperature Management in Post Cardiac Arrest Patients Treesa Joseph, PharmD PGY-1 Pharmacy Resident Atlantic Health System Continuing Education Presentation June 15 th, 2017 Objectives Explain
Algorithm Focus. Emergency Cardiovascular Care: EMT-Intermediate Treatment Algorithms. Perspective regarding the EMT- Intermediate algorithms
 Emergency Cardiovascular Care: EMT-Intermediate Treatment Algorithms Algorithms for the Conscious Patient Prehospital Medication Profiles Algorithm Focus Bradycardia Acute Pulmonary Edema and Shock Hypothermia
Emergency Cardiovascular Care: EMT-Intermediate Treatment Algorithms Algorithms for the Conscious Patient Prehospital Medication Profiles Algorithm Focus Bradycardia Acute Pulmonary Edema and Shock Hypothermia
Mild. Moderate. Severe. 32 to to and below
 Mohamud Daya MD, MS Mild 32 to 34 Moderate 28 to 32 Severe 28 and below Jon Rittenberger Shervin Ayati Protocol Development Committee Hypothermia Working Group Lynn Wittwer Jon Jui John Stouffer Scott
Mohamud Daya MD, MS Mild 32 to 34 Moderate 28 to 32 Severe 28 and below Jon Rittenberger Shervin Ayati Protocol Development Committee Hypothermia Working Group Lynn Wittwer Jon Jui John Stouffer Scott
The ALS Algorithm and Post Resuscitation Care
 The ALS Algorithm and Post Resuscitation Care CET - Ballarat Health Services Valid from 1 st July 2018 to 30 th June 2020 2 Defibrillation Produces simultaneous mass depolarisation of myocardial cells
The ALS Algorithm and Post Resuscitation Care CET - Ballarat Health Services Valid from 1 st July 2018 to 30 th June 2020 2 Defibrillation Produces simultaneous mass depolarisation of myocardial cells
Standardize comprehensive care of the patient with severe traumatic brain injury
 Trauma Center Practice Management Guideline Iowa Methodist Medical Center Des Moines Management of Patients with Severe Traumatic Brain Injury (GCS < 9) ADULT Practice Management Guideline Contact: Trauma
Trauma Center Practice Management Guideline Iowa Methodist Medical Center Des Moines Management of Patients with Severe Traumatic Brain Injury (GCS < 9) ADULT Practice Management Guideline Contact: Trauma
Admission of patient CVICU and hemodynamic monitoring
 Admission of patient CVICU and hemodynamic monitoring Prepared by: Rami AL-Khatib King Fahad Medical City Pi Prince Salman Heart tcentre CVICU-RN Admission patient to CVICU Introduction All the patients
Admission of patient CVICU and hemodynamic monitoring Prepared by: Rami AL-Khatib King Fahad Medical City Pi Prince Salman Heart tcentre CVICU-RN Admission patient to CVICU Introduction All the patients
Capnography: The Most Vital of Vital Signs. Tom Ahrens, PhD, RN, FAAN Research Scientist, Barnes-Jewish Hospital, St. Louis, MO May, 2017
 Capnography: The Most Vital of Vital Signs Tom Ahrens, PhD, RN, FAAN Research Scientist, Barnes-Jewish Hospital, St. Louis, MO May, 2017 Assessing Ventilation and Blood Flow with Capnography Capnography
Capnography: The Most Vital of Vital Signs Tom Ahrens, PhD, RN, FAAN Research Scientist, Barnes-Jewish Hospital, St. Louis, MO May, 2017 Assessing Ventilation and Blood Flow with Capnography Capnography
Update on Sudden Cardiac Death and Resuscitation
 Update on Sudden Cardiac Death and Resuscitation Ashish R. Panchal, MD, PhD Medical Director Center for Emergency Medical Services Assistant Professor Clinical Department of Emergency Medicine The Ohio
Update on Sudden Cardiac Death and Resuscitation Ashish R. Panchal, MD, PhD Medical Director Center for Emergency Medical Services Assistant Professor Clinical Department of Emergency Medicine The Ohio
NURSING DEPARTMENT CRITICAL CARE POLICY MANUAL CRITICAL CARE PROTOCOL USE OF PROPOFOL (DIPRIVAN) FOR VENTILATOR MANAGEMENT
 NURSING DEPARTMENT CRITICAL CARE POLICY MANUAL CRITICAL CARE PROTOCOL I. PURPOSE: To provide guidelines for the administration of Propofol, which is an anesthetic agent, indicated for the continuous intravenous
NURSING DEPARTMENT CRITICAL CARE POLICY MANUAL CRITICAL CARE PROTOCOL I. PURPOSE: To provide guidelines for the administration of Propofol, which is an anesthetic agent, indicated for the continuous intravenous
Introduction1. Introduction2. Introduction3. Thermoregulation2. Thermoregulation1
 Introduction1 Pharmacologic Options for Reducing the Shivering Response to Therapeutic Hypothermia Cerebral ischemia occurs when there is inadequate blood flow to the brain for more than 5 minutes. As
Introduction1 Pharmacologic Options for Reducing the Shivering Response to Therapeutic Hypothermia Cerebral ischemia occurs when there is inadequate blood flow to the brain for more than 5 minutes. As
Outcomes of Therapeutic Hypothermia in Cardiac Arrest. Saad Mohammed Shariff, MBBS Aravind Herle, MD, FACC
 Outcomes of Therapeutic Hypothermia in Cardiac Arrest Saad Mohammed Shariff, MBBS Aravind Herle, MD, FACC https://my.americanheart.org/idc/groups/ahamah-public/@wcm/@sop/@scon/documents/downloadable/ucm_427331.pdf
Outcomes of Therapeutic Hypothermia in Cardiac Arrest Saad Mohammed Shariff, MBBS Aravind Herle, MD, FACC https://my.americanheart.org/idc/groups/ahamah-public/@wcm/@sop/@scon/documents/downloadable/ucm_427331.pdf
Thermoregulation 2015 WMA
 1 Structure: Temperature sensors Endocrine system Muscles Skin Function: Maintain body core at 37 C Problem: Too little heat Too much heat 2 Normal Body Compensation Heat Response: Vasodilation Sweat Cold
1 Structure: Temperature sensors Endocrine system Muscles Skin Function: Maintain body core at 37 C Problem: Too little heat Too much heat 2 Normal Body Compensation Heat Response: Vasodilation Sweat Cold
Instituting preventive warming measures for patients who are normothermic. A variety of measures may be used, unless contraindicated.
 Patient Warmer Perioperative Hypothermia specifies that a preoperative patient management assessment should include: Identification of a patient s risk factors for unplanned perioperative hypothermia Measurement
Patient Warmer Perioperative Hypothermia specifies that a preoperative patient management assessment should include: Identification of a patient s risk factors for unplanned perioperative hypothermia Measurement
INFORMAL COPY WHEN PRINTED
 Doc Control Ref: TEM-003 Version 2.0 (Admin use only) Version no: (Admin use only) Effective Date: (Admin use only) 1. Principle Post-return of spontaneous circulation (ROSC) management is an important
Doc Control Ref: TEM-003 Version 2.0 (Admin use only) Version no: (Admin use only) Effective Date: (Admin use only) 1. Principle Post-return of spontaneous circulation (ROSC) management is an important
Applicable to. Team Members Performing MD House Staff APRN/PA RN LPN
 Protocol: Adult Burn Fluid Resuscitation Category Clinical Practice Protocol Number Approval Date vember 1, 2016 Due for review vember 1, 2018 Applicable to VUH Children s DOT VMG Off-site locations VMG
Protocol: Adult Burn Fluid Resuscitation Category Clinical Practice Protocol Number Approval Date vember 1, 2016 Due for review vember 1, 2018 Applicable to VUH Children s DOT VMG Off-site locations VMG
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 13 Resuscitation and Preparation for Anesthesia & Surgery Key Points 2 13.1 Management of Emergencies and Cardiopulmonary Resuscitation The emergency measures that
Surgical Care at the District Hospital 1 13 Resuscitation and Preparation for Anesthesia & Surgery Key Points 2 13.1 Management of Emergencies and Cardiopulmonary Resuscitation The emergency measures that
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials
 Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
Enhancing 5 th Chain TTM after Cardiac Arrest
 Enhancing 5 th Chain TTM after Cardiac Arrest Seoul St. Mary s Hospital Department of Emergency Medicine Chun Song Youn Agenda Past Current Future First study, 1958 2002, Two landmark paper HACA Trial
Enhancing 5 th Chain TTM after Cardiac Arrest Seoul St. Mary s Hospital Department of Emergency Medicine Chun Song Youn Agenda Past Current Future First study, 1958 2002, Two landmark paper HACA Trial
Post-Resuscitation Care. Prof. Wilhelm Behringer Center of Emergency Medicine University of Jena
 Post-Resuscitation Care Prof. Wilhelm Behringer Center of Emergency Medicine University of Jena Conflict of interest Emcools Shareholder and founder, honoraria Zoll: honoraria Bard: honoraria, nephew works
Post-Resuscitation Care Prof. Wilhelm Behringer Center of Emergency Medicine University of Jena Conflict of interest Emcools Shareholder and founder, honoraria Zoll: honoraria Bard: honoraria, nephew works
Neurological Prognosis after Cardiac Arrest Guideline
 Neurological Prognosis after Cardiac Arrest Guideline I. Associated Guidelines and Appendices 1. Therapeutic Hypothermia after Cardiac Arrest 2. Hypothermia after Cardiac Arrest Algorithm II. Rationale
Neurological Prognosis after Cardiac Arrest Guideline I. Associated Guidelines and Appendices 1. Therapeutic Hypothermia after Cardiac Arrest 2. Hypothermia after Cardiac Arrest Algorithm II. Rationale
Ipotermia terapeutica controversie e TTM 2 Trial Iole Brunetti
 Ipotermia terapeutica controversie e TTM 2 Trial Iole Brunetti U.O.C Anestesia e Terapia Intensiva Policlinico San Martino - GENOVA Natural Course of Neurological Recovery Following Cardiac Arrest Cardiac
Ipotermia terapeutica controversie e TTM 2 Trial Iole Brunetti U.O.C Anestesia e Terapia Intensiva Policlinico San Martino - GENOVA Natural Course of Neurological Recovery Following Cardiac Arrest Cardiac
Hypothermia After Cardiac Arrest: Where Are We Now?
 Hypothermia After Cardiac Arrest: Where Are We Now? David A. Pearson, MD, MS Associate Professor Director of Cardiac Arrest Resuscitation Carolinas HealthCare System Disclosures I have no financial interest,
Hypothermia After Cardiac Arrest: Where Are We Now? David A. Pearson, MD, MS Associate Professor Director of Cardiac Arrest Resuscitation Carolinas HealthCare System Disclosures I have no financial interest,
Post-resuscitation care for adults. Jerry Nolan Royal United Hospital Bath
 Post-resuscitation care for adults Jerry Nolan Royal United Hospital Bath Post-resuscitation care for adults Titration of inspired oxygen concentration after ROSC Urgent coronary catheterisation and percutaneous
Post-resuscitation care for adults Jerry Nolan Royal United Hospital Bath Post-resuscitation care for adults Titration of inspired oxygen concentration after ROSC Urgent coronary catheterisation and percutaneous
Cardiac Critical Care Lance Cohen, MD MBBCh FCCP
 Cardiac Critical Care 2011 Lance Cohen, MD MBBCh FCCP Open Heart Surgery Program Lance Cohen, MD MBBCh FCCP Medical Director - HSU Open Heart Surgery Program Team Cardiac Surgeons Richard Perryman, MD
Cardiac Critical Care 2011 Lance Cohen, MD MBBCh FCCP Open Heart Surgery Program Lance Cohen, MD MBBCh FCCP Medical Director - HSU Open Heart Surgery Program Team Cardiac Surgeons Richard Perryman, MD
Chapter 8 ADMINISTRATION OF BLOOD COMPONENTS
 Chapter 8 ADMINISTRATION OF BLOOD COMPONENTS PRACTICE POINTS Give the right blood product to the right patient at the right time. Failure to correctly check the patient or the pack can be fatal. At the
Chapter 8 ADMINISTRATION OF BLOOD COMPONENTS PRACTICE POINTS Give the right blood product to the right patient at the right time. Failure to correctly check the patient or the pack can be fatal. At the
Intensive Care Paramedic
 Doc Control Ref: TEM-003 Version 2.0 (Admin use only) Version no: (Admin use only) Effective Date: (Admin use only) 1. Principle Post-return of spontaneous circulation (ROSC) management is an important
Doc Control Ref: TEM-003 Version 2.0 (Admin use only) Version no: (Admin use only) Effective Date: (Admin use only) 1. Principle Post-return of spontaneous circulation (ROSC) management is an important
University of Wisconsin - Madison Cardiovascular Medicine Fellowship Program UW CICU Rotation Goals and Objectives
 Background: The field of critical care cardiology has evolved considerably over the past 2 decades. Contemporary critical care cardiology is increasingly focused on the management of patients with advanced
Background: The field of critical care cardiology has evolved considerably over the past 2 decades. Contemporary critical care cardiology is increasingly focused on the management of patients with advanced
Update in Therapeutic Hypothermia Post Cardiac Arrest
 Learning Objectives Update in Therapeutic Hypothermia Post Cardiac Arrest Allison Forni, PharmD, BCPS Clinical Pharmacy Specialist UMass Memorial Medical Center, Worcester MA Learning Objective 1: Describe
Learning Objectives Update in Therapeutic Hypothermia Post Cardiac Arrest Allison Forni, PharmD, BCPS Clinical Pharmacy Specialist UMass Memorial Medical Center, Worcester MA Learning Objective 1: Describe
Update on Guidelines for Traumatic Brain Injury
 Update on Guidelines for Traumatic Brain Injury Current TBI Guidelines Shirley I. Stiver MD, PhD Department of Neurosurgery Guidelines for the management of traumatic brain injury Journal of Neurotrauma
Update on Guidelines for Traumatic Brain Injury Current TBI Guidelines Shirley I. Stiver MD, PhD Department of Neurosurgery Guidelines for the management of traumatic brain injury Journal of Neurotrauma
Disclosures. Pediatrician Financial: none Volunteer :
 Brain Resuscitation Neurocritical Care Monitoring & Therapies CCCF November 2, 2016 Anne-Marie Guerguerian Critical Care Medicine, The Hospital for Sick Children University of Toronto Disclosures Pediatrician
Brain Resuscitation Neurocritical Care Monitoring & Therapies CCCF November 2, 2016 Anne-Marie Guerguerian Critical Care Medicine, The Hospital for Sick Children University of Toronto Disclosures Pediatrician
ADVOCATING FOR COMPREHENSIVE POST-RESUSCITATION CARE. Heather Harrington RN, BScN, CCNC(c)
 ADVOCATING FOR COMPREHENSIVE POST-RESUSCITATION CARE Heather Harrington RN, BScN, CCNC(c) Objectives Define Post-Resuscitation Syndrome Discuss the American Heart Association (AHA) 2010 Guidelines: i.
ADVOCATING FOR COMPREHENSIVE POST-RESUSCITATION CARE Heather Harrington RN, BScN, CCNC(c) Objectives Define Post-Resuscitation Syndrome Discuss the American Heart Association (AHA) 2010 Guidelines: i.
Surviving Sepsis Campaign. Guidelines for Management of Severe Sepsis/Septic Shock. An Overview
 Surviving Sepsis Campaign Guidelines for Management of Severe Sepsis/Septic Shock An Overview Mechanical Ventilation of Sepsis-Induced ALI/ARDS ARDSnet Mechanical Ventilation Protocol Results: Mortality
Surviving Sepsis Campaign Guidelines for Management of Severe Sepsis/Septic Shock An Overview Mechanical Ventilation of Sepsis-Induced ALI/ARDS ARDSnet Mechanical Ventilation Protocol Results: Mortality
Post-resuscitation Therapy in Adult Advanced Life Support. ARC and NZRC Guideline 2010
 Emergency Medicine Australasia (2011) 23, 292 296 doi: 10.1111/j.1742-6723.2011.01422_15.x POST-RESUSCITATION THERAPY Post-resuscitation Therapy in Adult Advanced Life Support. ARC and NZRC Guideline 2010
Emergency Medicine Australasia (2011) 23, 292 296 doi: 10.1111/j.1742-6723.2011.01422_15.x POST-RESUSCITATION THERAPY Post-resuscitation Therapy in Adult Advanced Life Support. ARC and NZRC Guideline 2010
CRS Center for Resuscitation Science
 Therapeutic hypothermia after cardiac arrest and in critical care Speaker disclosures Research Funding: NIH NHLBI Philips Healthcare Doris Duke Foundation American Heart Association CRS Center for Resuscitation
Therapeutic hypothermia after cardiac arrest and in critical care Speaker disclosures Research Funding: NIH NHLBI Philips Healthcare Doris Duke Foundation American Heart Association CRS Center for Resuscitation
SARASOTA MEMORIAL HOSPITAL. INITIATION AND MAINTAINANCE OF Normothermia/Temperature Managment
 SARASOTA MEMORIAL HOSPITAL TITLE: NURSING PROCEDURE Temperature Management ThermoGard XP or Arctic Sun (crc26) DATE: REVIEWED: PAGES: 5/15 5/18 1 of 8 PS1094 ISSUED FOR: Nursing RESPONSIBILITY: Critical
SARASOTA MEMORIAL HOSPITAL TITLE: NURSING PROCEDURE Temperature Management ThermoGard XP or Arctic Sun (crc26) DATE: REVIEWED: PAGES: 5/15 5/18 1 of 8 PS1094 ISSUED FOR: Nursing RESPONSIBILITY: Critical
Beyond the Golden Hour: Caring for the ICU Boarder
 Beyond the Golden Hour: Caring for the ICU Boarder Kami M. Hu, MD Dept. of Emergency Medicine Dept. of Pulmonology & Critical Care University of Maryland SOM I have no relevant financial relationships
Beyond the Golden Hour: Caring for the ICU Boarder Kami M. Hu, MD Dept. of Emergency Medicine Dept. of Pulmonology & Critical Care University of Maryland SOM I have no relevant financial relationships
Introduction to Organ Systems & Homeostasis. Packet #2
 Introduction to Organ Systems & Homeostasis Packet #2 Properties of Life Order All living things maintain a high degree of order and complexity Even the smallest living thing a cell Regulate Use of Energy
Introduction to Organ Systems & Homeostasis Packet #2 Properties of Life Order All living things maintain a high degree of order and complexity Even the smallest living thing a cell Regulate Use of Energy
-Blood Warming- A Hot topic?
 -Blood Warming- A Hot topic? Blaine Kent, MD, FRCPC Associate Professor of Anesthesia Director, Peri-Operative Blood Management Chief, Cardiac Anesthesia Objectives To learn / review the deleterious systemic
-Blood Warming- A Hot topic? Blaine Kent, MD, FRCPC Associate Professor of Anesthesia Director, Peri-Operative Blood Management Chief, Cardiac Anesthesia Objectives To learn / review the deleterious systemic
