WTA 2012 PLENARY PAPER
|
|
|
- Silas Green
- 6 years ago
- Views:
Transcription
1 WTA 2012 PLENARY PAPER Efficacy of anatomic and physiologic indicators versus mechanism of injury criteria for trauma activation in pediatric emergencies Andrew R. Krieger, Hale E. Wills, MD, MS, Mary Christine Green, APN, Ana L. Gleisner, MD, PhD, and Dennis W. Vane, MD, MBA, St. Louis, Missouri BACKGROUND: In pediatric trauma patients, adult triage criteria that use mechanism of injury (MOI) have been shown to result in overactivation of trauma teams. Anatomy- and physiology-based (APB) triage criteria have been recommended to improve the accuracy of trauma activations. At our Level 1 academic tertiary pediatric trauma referral center, we recently changed our triage criteria by emphasizing APB criteria and de-emphasizing MOI. This study was conducted to analyze the resulting change in accuracy of activations. METHODS: This was a criterion standard, cohort-controlled retrospective study comparing patients triaged by MOI criteria (January 2006 to March 2009) to those triaged by APB criteria (April 2009 to June 2010). Patients were subdivided according to trauma activation level as major (TMaj), minor (TMin), or consult (TC). Demographic, vital sign, injury pattern, trauma activation level, and emergency department disposition data were collected. Triage criteria were retrospectively applied to the patients according to the criteria that were in effect when they arrived. Patients were assigned to either high-risk (HR) or low-risk (LR) groups based on the need for urgent intervention (emergency department procedure, emergent operation, or blood transfusion), admission to intensive care unit, Injury Severity Score [ISS] of greater than 12, or death. Sensitivity and specificity of major activations were calculated using the following groups: true positive, trauma activation and HR; false positive, trauma activation and LR, false negative, no trauma activation and HR; true negative, no trauma activation and LR. Comparisons were then made between the MOI to the APB patients. RESULTS: The MOI and APB patients were similar in race (p = 0.201), sex (p = 0.639), and age (p = 0.643). The APB criteria resulted in 14% TMaj, 35% TMin, and 51% TC, compared with 41%, 23%, and 36%, respectively, for MOI. Median ISS in the APB group was 16 for TMaj, 5 for TMin, and 4 for TC compared with 8, 4, and 4, respectively, for MOI. Sensitivity for trauma activation of HR patients was 89.2% versus 89.1% (equivalent), while specificity increased from 45.8% to 65.8% for MOI versus APB, respectively. CONCLUSION: For pediatric trauma patients, the emphasis on APB triage criteria and de-emphasis on MOI results in selection of higher-acuity patients for major activation while maintaining acceptable undertriage and overtriage rates overall. This improved accuracy of major activation results in a more cost-efficient resource use and fewer unnecessary disruptions for the surgeon, operating room, and other staff while maintaining appropriate capture and evaluation of trauma patients. The low sensitivity noted in both the MOI and APB groups is largely caused by the broad definition of HR patients used in this study. We recommend the use of APB criteria for pediatric trauma triage. (. 2012;73: 1471Y1477. Copyright * 2012 by Lippincott Williams & Wilkins) LEVEL OF EVIDENCE: Therapeutic study, level IV. KEY WORDS: Pediatric trauma; triage; health care costs; anatomy- and physiology-based triage; mechanism of injury. In treating pediatric trauma, the activation of a trauma team is essential to provide rapid assessment and treatment of injured patients; however, trauma team activations involve numerous health care providers and consume a large quantity of hospital resources. While a certain amount of overtriage is essential to minimize the potential of missing life-threatening injuries, frequent overactivation leads to the disruption of hospital and Submitted: April 13, 2012, Revised: August 8, 2012, Accepted: August 15, From the School of Medicine (A.R.K.), Saint Louis University (H.E.W., A.L.G., D.W.V.); Cardinal Glennon Children s Medical Center (H.E.W., M.C.G., D.W.V.), St. Louis, Missouri. This study was presented at the 42nd annual meeting of the Western Trauma Association, February 26YMarch 2, 2012, in Vail, Colorado. This was presented as part of the Earl Young Resident Competition. Address for reprints: Dennis Vane, MD, MBA, Department of Pediatric Surgery, Cardinal Glennon Children s Medical Center 1465 S. Grand Blvd, St. Louis, MO 63104; dvane@slu.edu. DOI: /TA.0b013e practitioner activities, practitioner burn out from unnecessary participation, and increased costs in providing this essential service. We hypothesized that the use of adult triage and mechanism of injury (MOI)Ybased criteria for trauma activations leads to inappropriate trauma team activations for pediatric trauma patients and that anatomy- and physiology-based (APB) criteria were more accurate for children and reduced unnecessary trauma activations. At our hospital, the trauma guidelines were recently modified to emphasize anatomic and physiologic indicators of injury severity (airway integrity, open wounds, neurologic status, hemodynamics, skeletal integrity, and contusions to the head and/or torso) and to de-emphasize MOI criteria. The goal of this study was to compare the sensitivity and specificity of current APB activation guidelines in identifying significant injury with the previous MOI-based guidelines and, if necessary, modify them to attain optimal levels of overtriage and undertriage with our trauma activations. 1471
2 Krieger et al. Figure 1. Trauma activation criteria for MOI-based protocol. This study was approved by the institutional review board of Saint Louis University (IRB # 16827). PATIENTS AND METHODS This was a criterion standard, cohort-controlled retrospective study comparing patients triaged by MOI criteria (January 2006 to March 2009, Fig. 1) with those triaged by APB criteria (April 2009 to June 2010, Fig. 2). All data had been prospectively entered into our trauma registry contemporaneously. The trauma registry contained the records of all trauma activations, trauma consults, and admissions for traumatic injury. Demographic data, vital signs, injury pattern, 1472 trauma activation level, and emergency department disposition data were collected. All patients younger than 19 years were included. Patients seen for ingestions, bites, stings, asphyxiation, and near drowning were excluded from the analysis. Consultations for nonaccidental trauma were also excluded because these patients often have acute and chronic injury and commonly present in a delayed time frame relative to their injury. In addition, readmissions and direct admissions were not considered. Patients were placed into either MOI or APB groups by their date of arrival. When the prospectively generated activation data on our patients was reviewed, it was found that many activations were inappropriate or justification for the activation level was incomplete. Therefore, trauma activation * 2012 Lippincott Williams & Wilkins
3 Krieger et al. level (major [TMaj], minor [TMin], or consult [TC]) was retrospectively assigned to each patient according to the criteria that were in effect when they arrived. Patients were classified into either a high-risk category (injury warrants trauma team activation) or a low-risk category (injuries could successfully be evaluated and managed Figure 2. Trauma activation criteria for APB protocol. * 2012 Lippincott Williams & Wilkins 1473
4 Krieger et al. TABLE 1. Criteria for High-Risk and Low-Risk Classification High risk ISS 9 12 Emergent operative intervention from the ED Admission to the ICU Endotracheal intubation on arrival Chest tube placement Intracranial pressure monitoring Blood product administration Diagnostic peritoneal lavage Mortality related to the trauma Low risk ISS G 12 No need for urgent intervention No outcome of mortality by the emergency department staff without morbidity or detriment to outcome). Patients were classified as high risk if they had an Injury Severity Score (ISS) of greater than 12, need for urgent intervention related to the trauma, admission to the intensive care unit (ICU) or transitional care unit (TCU), emergent operative intervention, endotracheal intubation on arrival, chest tube placement, intracranial pressure monitoring, blood product administration, diagnostic peritoneal lavage in the first 24 hours of admission, or mortality (Table 1). Patients were considered low risk if they exhibited an ISS of less than 12, no need for urgent intervention, and no outcome of mortality. Of note, emergent operative intervention included only those procedures considered life threatening or limb and/ or organ sparing. Those patients who were taken directly to the operating room from the emergency department at surgeon convenience (i.e., minor fracture stabilization or who were otherwise stable enough for floor admission) were considered low risk. Patients were considered overtriaged if any trauma activation occurred but they were identified as low risk. Patients were considered undertriaged if they were found to be high risk but no trauma team activation occurred. All high-risk patients for whom trauma activation occurred were considered appropriate activations. Sensitivity and specificity of all trauma activations were calculated (major and minor together) using the following groups: true positive, any trauma activation and high risk; false positive, any trauma activation and low risk; false negative, no trauma activation and high risk; true negative, no trauma activation and low risk. We then compared the MOI with the APB patients. We also reviewed the records of all patients with false-negative (undertriaged) activations to identify injuries that were missed by the triage criteria. In addition, a cost analysis using hospital-billed costs and charges provided by the hospital financial services department was calculated. The cost values used were derived from 2010 financial reports for major and minor trauma activations. Direct and indirect costs were combined to ascertain the cost for each of these activations. Charges were taken from a preassigned fee for major and minor trauma activations added to each patient s bill when one of these activations is determined. Savings were calculated for both charges and costs by calculating the changes in the relative proportions of patients activated as trauma major or minor, then determining the per patient differences that were realized. Statistical Analysis W 2 test was used when comparing proportions or frequencies and Fisher s exact test when indicated. Student s t test was used for continuous variables with normal distribution and Mann-Whitney U-test for continuous variables lacking a normal distribution. W 2 test was used to calculate the statistical significance of sensitivity and specificity ratings clinically and by protocol for both the MOI-based and APB criteria. RESULTS A total of 3,967 charts were included in the trauma registry for the study period. Four were excluded from the Figure 3. Flow chart of study population. After removal of patients with nontrauma diagnoses, nonaccidental trauma victims, direct admissions and readmissions, 3,626 patients remained in the study population, 2,538 in the MOI-based protocol group and 1,088 in the APB protocol group TABLE 2. Comparison of Demographics for MOI and APB Groups Demographic Age mean (SD), y 8.77 (5.6) 8.86 (5.5) Female, n (%) 852 (33.6) 374 (34.4) Race, n (%) White 1,605 (63.2) 712 (65.4) Nonwhite 933 (36.8) 376 (36.6) ISS, median (range) 4 (1Y75) 4 (1Y75) * 2012 Lippincott Williams & Wilkins
5 Krieger et al. TABLE 3. Sensitivity and Specificity of MOI and APB Protocols Sensitivity, % Specificity, % G0.001 Undertriage Overtriage G0.001 TABLE 5. Percent Classification as TMaj, TMin, and TC for MOI and APB Groups and Proportion of High-Risk Patients Within Those Classifications TMaj, n (%) 1,044 (41.1) 151 (13.9) G0.001 TMin, n (%) 581 (22.9) 383 (35.2) TC, n (%) 913 (36.0) 554 (50.9) study as readmissions and 95 as direct admissions from other facilities. Another 149 were removed from the analysis for diagnoses that we excluded from our review (ingestions, 67; drowning/near drowning, 35; bites/stings, 24; not otherwise classified, 11; strangulation/hanging, 6; smoke inhalation, 4; and asphyxiation, 2). An additional 93 patients were removed from analysis because they were consults for nonaccidental trauma. This left 3,626 children in our review (Fig. 3). The MOI and APB cohorts were compared based on age, sex, race, and ISS. There were 2,538 patients triaged by MOI criteria (January 2006 to March 2009) and 1,088 by APB criteria (April 2009 to June 2010, Fig. 3) The MOI and APB patients were similar in age (mean, 8.77 years vs years, respectively; p = 0.643), sex (33.6% vs. 34.4% female; p = 0.639), race (63.2% vs. 65.4% white; p = 0.201) and ISS (median, 4 for each group; p = 0.576; Table 2). When the performance of the MOI and APB triage criteria were compared looking at any activation (TMaj + TMin) versus TC, sensitivity for the MOI and APB protocols in correctly triaged low- and high-risk children was found to be similar (89.1% and 89.2%, respectively, p = 0.93). Specificity for this same analysis was 45.8% for the MOI group but increased significantly in the APB group to 65.4 (p G 0.001). This corresponds to an undertriage rate of 10.9% and 10.8%, and overtriage rate of 54.2% and 34.6%, respectively, for our MOI and APB criteria (Table 3). The APB criteria resulted in a lower proportion of trauma patients being seen as trauma activations (either TMaj or TMin) with 49.1% of cases being trauma activations compared with 64.0% of the MOI cases (p G 0.001, Table 4). When TMaj and TMin activations were analyzed separately, the APB protocol activated a smaller proportion to the TMaj category and larger proportion to TMin (13.9% and 35.2%, respectively), as compared with the MOI protocol (41.1% and 22.9%, respectively; Table 5). When the relative acuity of patients (high risk vs. low risk) was examined, the APB protocol identified a higher percentage of high-risk patients to the activation categories (76.2% TMaj and 37.1%TMin) than did the MOI protocol (47.6% TMaj and 24.3%TMin, Table 6) The median ISS of the APB group (16 TMaj and 5 TMin) was also higher than that in the MOI group (8 TMaj and 4 TMin, Table 7). TABLE 4. Proportion of Activations for MOI and APB Groups Not activated, n (%) 913 (36.0) 554 (50.9) G0.001 Any activation, n (%) 1,625 (64.0) 534 (49.1) Review of the patients with false-negative activations (undertriaged) identified only one patient in the MOI group who did not meet trauma activation criteria yet did require urgent surgery. This patient presented with an isolated tibiofibular fracture and neurovascularly intact leg yet developed compartment syndrome shortly after arrival in the emergency department and was taken for emergent fixation and decompression. There were no trauma consult patients in the APB who underwent emergency operation. There were no deaths in any patient who did not meet trauma activation criteria in either the MOI or APB groups. The remaining patients with falsenegative activations were those who did not meet trauma activation criteria but either required nonfloor admission (TCU or ICU) or had ISS of greater than 12. The 2010 cost for a trauma major activation was /5,084 (direct cost, /2,180; indirect cost, /2,904). The cost for a minor activation was /3,340 (direct cost, /1,411; indirect cost, /1,928). The charge for major trauma activation was /9,332 and was /5,599 for minor activation. When APB and MOI criteria were compared, the APB criteria resulted in a decrease of TMaj activations from 411 to 138 per 1,000 trauma patients, an increase of TMin activations from 229 to 352 per 1,000 patients, and an increase in TC activations (i.e., no added activation costs or charges incurred) from 360 to 510 per 1,000 patients. The APB criteria resulted in a net savings in charges of /1,858,959 and savings in total costs of /977,385 per 1,000 trauma patients (/6,740,585 charges: /3,543,998 costs for this patient cohort, Table 8). DISCUSSION In some cases, pediatric trauma teams are activated based solely on MOI information, which have been historically used for fear of missing injuries. 1,2 Several studies have demonstrated that trauma team activation based solely on MOI criteria has led to overuse of trauma activations and likely resulted in an unnecessary consumption of resources. 3Y5 In response to this, some authors have investigated more sensitive and specific trauma activation guidelines. To date, however, no criterion standard has been established. 6,7 It has also been shown that TABLE 6. Proportion High Risk Patients Within TMaj, TMin and TC Classifications for MOI and APB Protocols High risk patients in: MOI APB p Trauma Major, n (%) 497 (47.6) 115 (76.2) G0.001 Trauma Minor, n (%) 141 (24.3) 142 (37.1) G0.001 Trauma Consult, n (%) 79 (8.7) 31 (5.6) G0.04 * 2012 Lippincott Williams & Wilkins 1475
6 Krieger et al. TABLE 7. Comparison of Median ISS Between MOI and APB Criteria TMaj 8 (1Y75) 16 (1Y75) G0.001 TMin 4 (1Y30) 5 (1Y34) G0.001 TC 4 (1Y25) 4 (1Y25) adult trauma activation guidelines do not translate well to pediatric patients, lending to a movement to establish separate criteria for pediatric patients. 8 Simon et al. 2 developed a modified pediatric trauma score for the triage of pediatric cases in the emergency department. It determines the necessity for trauma team activation based on 5 physiologic indicators (airway integrity, open wounds, neurologic status, hemodynamics, and skeletal integrity) with good sensitivity and specificity and with an acceptable level of overtriage. In a further study, Nasr et al. 9 applied this score to a different population and found it necessary to add two more indicators (history of loss of consciousness and contusions to the head and/or torso) to the scoring to reach this same safety level. These criteria however are overly complex and have not proven realistic for field triage. At our facility, the trauma guidelines were modified on April 1, 2009, to include physiologic indicators (airway integrity, open wounds, neurologic status, hemodynamics, gross skeletal integrity, and contusions to the head and/or torso). We think that these criteria were simple and easily evaluated in the field by basic life support prepared responders. The primary goal of this study was to assure that these physiologic and more easily identifiable criteria would not miss any significant injuries and compromise the safety of our patients while still allowing for appropriate evaluation in the field. We evaluated this efficacy by comparing the sensitivity and specificity of our new APB trauma activation guidelines with the previous MOI-based method. Our findings demonstrate that the emphasis on APB triage criteria for pediatric patients and de-emphasis on MOI results in no loss of sensitivity for high-risk patients while improving the specificity. The new criteria also resulted in the appropriate selection of higheracuity patients for both categories of trauma team activation. These APB criteria also maintained acceptable undertraige and overtriage rates. This improved accuracy of trauma activation results in more cost-efficient resource use and fewer unnecessary disruptions for the surgeon, operating room, and other staff while maintaining appropriate capture and evaluation of significantly injured children. A recent cost analysis study of pediatric trauma activations found that overactivation at the trauma major level (TMaj) resulted in increased charges during the first 24 hours of trauma management of $4,700 and increased costs of $800 for each overactivation. 6 Our study found that the APB criteria shifted the overall burden of trauma patients from activation to trauma consult. While we noted an increase in the proportion of minor activations overall, the net effect of shifting the balance from major activation to minor activation and consult resulted in a savings in emergency department charges of $1,859 and emergency department costs of $977 per activation. Furthermore, for every 1,000 trauma patients, we noted a decrease of 273 major activations with no detriment to patient safety. This study has several limitations. First is the retrospective design. Although the data on each patient were prospectively generated, we found in our pilot study that a review of the appropriateness of each activation as it was initially assigned was incomplete and often inaccurate. To improve the accuracy, we retrospectively reviewed each chart and rigidly applied the appropriate triage criteria. While this approach provided consistency to the evaluation of each triage scheme, it could be argued that this risks introduction of observer bias. Second, the definition of high risk used was quite broad to effectively capture all patients whose acuity warrants activation. ISS of greater than 12 and the inclusion of TCU admissions in the ICU admission groups may falsely augment the size of our high-risk population. We feel this resulted in our low sensitivity in both the MOI and APB groups as compared with recommendations from the American College of Surgeons Committee on Trauma. 10 They recommend a 0% to 5% undertriage rate and a 25% to 50% overtriage rate. Their criteria translate to a 95% sensitivity and 50% to 75% specificity. Our study identified an undertriage rate of 11% for both the MOI and APB criteria, but the overtriage rate dropped from 54.2% to 34.2%. The results of this study show that APB criteria increases specificity without a concomitant decrease in sensitivity. Investigation of the undertriaged patients identified only one child who did not meet major or minor activation criteria TABLE 8. Cost Comparison Between MOI and BP Criteria Criteria Trauma MOI APB Activation n Direct Costs, $ Indirect Costs, $ Total Costs, $ Charges, $ n Direct Costs, $ Indirect Costs, $ Total Costs, $ Charges, $ TMaj ,980 1,193,544 2,089,935 3,835, , , ,730 1,287,816 TMin , , ,860 1,282, , ,656 1,175,680 1,970,848 All 640 1,219,328 1,653,056 2,854,795 5,117, ,864 1,079,408 1,877,410 3,258,664 Savings in ED direct costs, $ 421,464 Savings in ED indirect costs, $ 555,648 Savings in ED total costs, $ 977,385 Savings in ED charges, $ 1,858, * 2012 Lippincott Williams & Wilkins
7 Krieger et al. yet required urgent intervention. There were no deaths among the undertriaged patients. The remaining undertriaged patients were considered high risk based either on their eventual admission to our TCU or ICU or an ISS of greater than 12. While this latter group does potentially represent seriously injured patients, none of these children seemed to necessitate the immediate presence of a trauma surgery attending physician upon their arrival at the emergency department or the accompanying resource use of a trauma activation. Third, we excluded consultations for nonaccidental trauma because these patients generally present with conflicting histories, vague and not trauma-related complaints, and in a delayed manner. Many have subacute, chronic, or acute on chronic injuries. Most nonaccidental trauma patients are hemodynamically stable, and their injuries are not immediately life threatening. Those that do present with hemodynamic instability most commonly present with nontrauma-related complaints, which are found only later on examination to be related to injuries. Their injury patterns often give them high ISSs. This would have made these patients high risk in our study and give the appearance of significant undertriage because almost all of these patients are referred after being worked up for a medical condition. For this reason, they were excluded them from our analysis a priori. In conclusion, our study supports the safe use of APB criteria in determining trauma activations in this pediatric population. Our findings also demonstrate that the de-emphasis of MOI for trauma activations results in a decrease in overactivations and a selection of higher-acuity patients for all levels of trauma activation. These criteria create better use of resources and reduce overuse of physician time and hospital resources. AUTHORSHIP A.R.K. contributed in the literature search, study design, data collection, data analysis, data interpretation, article preparation, and figures. H.E.W. contributed in the study design, statistical analysis, data interpretation, article preparation, and figures. M.C.G. contributed in the literature search and data collection. A.L.G. performed the statistical analysis. D.W.V. contributed in the study design, data interpretation, and article preparation. DISCLOSURE This study was internally funded by Cardinal Glennon Children s Hospital. REFERENCES 1. Haller JA Jr., Shorter N, Miller D, Colombani P, Hall J, Buck J. Organization and function of a regional pediatric trauma center: does a system of management improve outcome? J Trauma. 1983;23:691Y Simon B, Gabor R, Letourneau P. Secondary triage of the injured pediatric patient within the trauma center: support for a selective resource-sparing two-stage system. Pediatr Emerg Care. 2004;20:5Y Dowd MD, McAneney C, Lacher M, Ruddy RM. Maximizing the sensitivity and specificity of pediatric trauma team activation criteria. Acad Emerg Med. 2000;7:1119Y Boyle MJ. Is mechanism of injury alone in the prehospital setting a predictor of major traumava review of the literature. J Trauma Manag Outcomes. 2007;1:4. 5. Shatney CH, Sensaki K. Trauma team activation for mechanism of injury blunt trauma victims: time for a change? J Trauma. 1994;37:275Y281; discussion 281Y Mukherjee K, Rimer M, McConnell MD, Miller RS, Morrow SE. Physiologically focused triage criteria improve utilization of pediatric surgeondirected trauma teams and reduce costs. J Pediatr Surg. 2010;45: 1315Y Furnival RA, Schunk JE. ABCs of scoring systems for pediatric trauma. Pediatr Emerg Care. 1999;15:215Y Phillips S, Rond PC 3rd, Kelly SM, Swartz PD. The need for pediatricspecific triage criteria: results from the Florida Trauma Triage Study. Pediatr Emerg Care. 1996;12:394Y Nasr A, Mikrogianakis A, McDowall D, Wales P. External validation and modification of a pediatric trauma triage tool. J Trauma. 2007;62:606Y American College of Surgeons. Resources for Optimal Care of the Injured Patient Chicago: American College of Surgeons; EDITORIAL CRITIQUE The development of pediatric-specific management practices in traumatic injury has lagged within the larger framework of the evolution of pediatric surgery as a discipline, related yet distinct from general surgery. A major reason is likely differential volume due to age with pediatric trauma representing a fraction of the overall trauma statistic in this country, as well as age related differences in at risk behavior leading to injury. While application of trauma management principles across age groups has advantages related to larger experience, children can benefit from age specific management with improved outcomes. This paper addresses the utility of triage emphasis on anatomic derangement and physiologic response in allocating precious hospital resources in response to pediatric injury; many pediatric trauma surgeons would agree it is best to let the child s status tell us what is wrong. Mechanism of injury is deemphasized and, while that raises the historical concern of missed injury, acceptable under- and over-triage rates were maintained. The recognition that vital signs or anatomic indicators in a child may be more indicative of injury than mechanism is not a new concept, but one that has been slow to develop in the literature, making this paper a welcome addition. Caveats on this paper might include broad applicability of the suggested criteria. These findings are from an urban Level l pediatric trauma center. While such centers are well experienced with the acutely injured child, low volume, non-specialty centers may do well to apply broader trauma alert criteria. Additionally, the study included data on patients under 19 years of age. The older adolescent arriving in a pediatric trauma center acts physiologically and often behaviorally as an adult. The argument to separate these triage criteria out as pediatric may be better served by analyzing a younger subset of the study group. This is a needed contribution to the continued refinement of pediatric injury management. Jeffrey H. Haynes, MD Professor of Surgery and Pediatrics Director Children s Trauma Center Children s Hospital of Richmond VCU Health System * 2012 Lippincott Williams & Wilkins 1477
Pediatric Trauma Systems: Critical Distinctions
 J Trauma 1999 September Supplement;47(3):S85-S89. Copyright 1999 Lippincott WilliamPage... 1 of 6 Previous Full Text References (22) Next Full Text Pediatric Trauma Systems: Critical Distinctions Frieda
J Trauma 1999 September Supplement;47(3):S85-S89. Copyright 1999 Lippincott WilliamPage... 1 of 6 Previous Full Text References (22) Next Full Text Pediatric Trauma Systems: Critical Distinctions Frieda
Chapter 2 Triage. Introduction. The Trauma Team
 Chapter 2 Triage Chapter 2 Triage Introduction Existing trauma courses focus on a vertical or horizontal approach to the ABCDE assessment of an injured patient: A - Airway B - Breathing C - Circulation
Chapter 2 Triage Chapter 2 Triage Introduction Existing trauma courses focus on a vertical or horizontal approach to the ABCDE assessment of an injured patient: A - Airway B - Breathing C - Circulation
Effect of post-intubation hypotension on outcomes in major trauma patients
 Effect of post-intubation hypotension on outcomes in major trauma patients Dr. Robert S. Green Professor, Emergency Medicine and Critical Care Dalhousie University Medical Director, Trauma Nova Scotia
Effect of post-intubation hypotension on outcomes in major trauma patients Dr. Robert S. Green Professor, Emergency Medicine and Critical Care Dalhousie University Medical Director, Trauma Nova Scotia
ARTICLE IN PRESS. doi: /j.jemermed TRAUMA PATIENTS CAN SAFELY BE EXTUBATED IN THE EMERGENCY DEPARTMENT
 doi:10.1016/j.jemermed.2009.05.033 The Journal of Emergency Medicine, Vol. xx, No. x, pp. xxx, 2009 Copyright 2009 Elsevier Inc. Printed in the USA. All rights reserved 0736-4679/09 $ see front matter
doi:10.1016/j.jemermed.2009.05.033 The Journal of Emergency Medicine, Vol. xx, No. x, pp. xxx, 2009 Copyright 2009 Elsevier Inc. Printed in the USA. All rights reserved 0736-4679/09 $ see front matter
HOW TO START ASSALTING YOUR TRIAGE SCHEMES - SORTING THE DIFFERENT TRIAGE SCHEMES
 HOW TO START ASSALTING YOUR TRIAGE SCHEMES - SORTING THE DIFFERENT TRIAGE SCHEMES W. Scott Gilmore, MD, EMT-P, FACEP Medical Director, St. Louis Fire Department Disclosures I have no significant financial
HOW TO START ASSALTING YOUR TRIAGE SCHEMES - SORTING THE DIFFERENT TRIAGE SCHEMES W. Scott Gilmore, MD, EMT-P, FACEP Medical Director, St. Louis Fire Department Disclosures I have no significant financial
Use Of The Pediatric Trauma Score To Triage Severity Of Childhood Injury
 Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine January 2014 Use Of The Pediatric Trauma Score To Triage Severity
Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine January 2014 Use Of The Pediatric Trauma Score To Triage Severity
Original Article. Emergency Department Evaluation of Ventricular Shunt Malfunction. Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH
 Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Use of CT in minor traumatic brain injury. Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD
 Use of CT in minor traumatic brain injury Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD No financial or other conflicts of interest Epidemiology of traumatic brain injury (TBI) Risks associated
Use of CT in minor traumatic brain injury Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD No financial or other conflicts of interest Epidemiology of traumatic brain injury (TBI) Risks associated
Imaging in the Trauma Patient
 Imaging in the Trauma Patient David A. Spain, MD Department of Surgery Stanford University Pan Scan Instead of Clinical Exam? 1 Granted, some patients don t need CT scan Platinum Package Stanford Special
Imaging in the Trauma Patient David A. Spain, MD Department of Surgery Stanford University Pan Scan Instead of Clinical Exam? 1 Granted, some patients don t need CT scan Platinum Package Stanford Special
Trauma Registry Documentation December 16, 2014
 Trauma Registry Documentation December 16, 2014 The State of Florida now requires ALL Acute Care hospitals to submit data to the statetrauma Registry. Although Baptist Health hospitals are NOT Trauma Centers
Trauma Registry Documentation December 16, 2014 The State of Florida now requires ALL Acute Care hospitals to submit data to the statetrauma Registry. Although Baptist Health hospitals are NOT Trauma Centers
journal ORIGINAL RESEARCH
 texas orthopaedic journal ORIGINAL RESEARCH Mortality with Circumferential Pelvic Compression for Pelvic Ring Disruption in Polytraumatized Patients: A Retrospective Analysis of 1,639 Pelvic Ring Injuries
texas orthopaedic journal ORIGINAL RESEARCH Mortality with Circumferential Pelvic Compression for Pelvic Ring Disruption in Polytraumatized Patients: A Retrospective Analysis of 1,639 Pelvic Ring Injuries
SPEED ISN'T EVERYTHING: IDENTIFYING PATIENTS WHO MAY BENEFIT FROM HELICOPTER TRANSPORT DESPITE FASTER GROUND TRANSPORT
 SPEED ISN'T EVERYTHING: IDENTIFYING PATIENTS WHO MAY BENEFIT FROM HELICOPTER TRANSPORT DESPITE FASTER GROUND TRANSPORT Joshua B. Brown MD, MSc, Mark L. Gestring* MD, Matthew R. Rosengart* MD,MPH, Timothy
SPEED ISN'T EVERYTHING: IDENTIFYING PATIENTS WHO MAY BENEFIT FROM HELICOPTER TRANSPORT DESPITE FASTER GROUND TRANSPORT Joshua B. Brown MD, MSc, Mark L. Gestring* MD, Matthew R. Rosengart* MD,MPH, Timothy
APR-DRG and the Trauma Registry. Jodi Hackworth, MPH Johanna Askegard-Giesmann, MD Thomas Rouse, MD Brian Benneyworth, MD, MS
 APR-DRG and the Trauma Registry Jodi Hackworth, MPH Johanna Askegard-Giesmann, MD Thomas Rouse, MD Brian Benneyworth, MD, MS November 2015 Conflict of Interests Disclosures Jodi Hackworth and her co-authors
APR-DRG and the Trauma Registry Jodi Hackworth, MPH Johanna Askegard-Giesmann, MD Thomas Rouse, MD Brian Benneyworth, MD, MS November 2015 Conflict of Interests Disclosures Jodi Hackworth and her co-authors
Midlands Silver Trauma Group.
 Midlands Silver Trauma Group. The Silver Safety Net A Proposal for a Regional Trauma Desk Response to Triage Older People with Injuries Raven D, Hall R, Chamberlain H, Roberts S, Littleson S, Graham S
Midlands Silver Trauma Group. The Silver Safety Net A Proposal for a Regional Trauma Desk Response to Triage Older People with Injuries Raven D, Hall R, Chamberlain H, Roberts S, Littleson S, Graham S
UNDERTRIAGE and OVERTRIAGE
 UNDERTRIAGE and OVERTRIAGE Alison Wilson, MD, FACS Professor Skewes Family Chair in Trauma Director, Critical Care and Trauma Institute TRIAGE 18 TH century French: Trier = to separate out Minimal use
UNDERTRIAGE and OVERTRIAGE Alison Wilson, MD, FACS Professor Skewes Family Chair in Trauma Director, Critical Care and Trauma Institute TRIAGE 18 TH century French: Trier = to separate out Minimal use
Daniel W. Spaite, MD Uwe Stolz, PhD, MPH Bentley J. Bobrow, MD Vatsal Chikani, MPH Duane Sherrill, PhD Michael Sotelo, BS Bruce Barnhart, RN, CEP
 Daniel W. Spaite, MD Uwe Stolz, PhD, MPH Bentley J. Bobrow, MD Vatsal Chikani, MPH Duane Sherrill, PhD Michael Sotelo, BS Bruce Barnhart, RN, CEP Joshua B. Gaither, MD Terry Mullins, MBA Will Humble, MPH
Daniel W. Spaite, MD Uwe Stolz, PhD, MPH Bentley J. Bobrow, MD Vatsal Chikani, MPH Duane Sherrill, PhD Michael Sotelo, BS Bruce Barnhart, RN, CEP Joshua B. Gaither, MD Terry Mullins, MBA Will Humble, MPH
New tools to reduce and standardize the triage review process
 New tools to reduce and standardize the triage review process JW Roden-Foreman, BA NR Rapier, MSN L Yelverton, RN ML Foreman, MD Baylor University Medical Center, Level I Trauma Center Dallas, Texas None
New tools to reduce and standardize the triage review process JW Roden-Foreman, BA NR Rapier, MSN L Yelverton, RN ML Foreman, MD Baylor University Medical Center, Level I Trauma Center Dallas, Texas None
Paramedic Trauma
 Western Technical College 10531920 Paramedic Trauma Course Outcome Summary Course Information Description Career Cluster Instructional Level Total Credits 3.00 Total Hours 72.00 This course teaches the
Western Technical College 10531920 Paramedic Trauma Course Outcome Summary Course Information Description Career Cluster Instructional Level Total Credits 3.00 Total Hours 72.00 This course teaches the
The effect of early versus delayed radiation therapy on length of hospital stay in the palliative setting
 Original Article on Palliative Radiotherapy The effect of early versus delayed radiation therapy on length of hospital stay in the palliative setting Taylor R. Cushman 1, Shervin Shirvani 2, Mohamed Khan
Original Article on Palliative Radiotherapy The effect of early versus delayed radiation therapy on length of hospital stay in the palliative setting Taylor R. Cushman 1, Shervin Shirvani 2, Mohamed Khan
SIERRA-SACRAMENTO VALLEY EMS AGENCY PROGRAM POLICY
 SIERRA-SACRAMENTO VALLEY EMS AGENCY PROGRAM POLICY PURPOSE: To identify those patients who are at greatest risk for severe injury and determine the most appropriate facility to transport persons with different
SIERRA-SACRAMENTO VALLEY EMS AGENCY PROGRAM POLICY PURPOSE: To identify those patients who are at greatest risk for severe injury and determine the most appropriate facility to transport persons with different
Case Presentation. The Failure to Diagnose Sepsis. chills. pain out of proportion to mechanism. low-grade fever. tachycardia that does not make sense
 Case Presentation The Failure to Diagnose Sepsis Sepsis is a regular visitor in the news as cases of flesh-eating bacteria and the dramatic speed with which victims deteriorate hit the headlines. The failure
Case Presentation The Failure to Diagnose Sepsis Sepsis is a regular visitor in the news as cases of flesh-eating bacteria and the dramatic speed with which victims deteriorate hit the headlines. The failure
1 Emergency Medicine Academic Group, Department of Cardiovascular Sciences, University of Leicester, UK.
 Title: A week of pain in the Emergency Department Authors: Thornton HS 1, Reynolds J 1, Coats TJ 1 1 Emergency Medicine Academic Group, Department of Cardiovascular Sciences, University of Leicester, UK.
Title: A week of pain in the Emergency Department Authors: Thornton HS 1, Reynolds J 1, Coats TJ 1 1 Emergency Medicine Academic Group, Department of Cardiovascular Sciences, University of Leicester, UK.
Cover Page. The handle holds various files of this Leiden University dissertation
 Cover Page The handle http://hdl.handle.net/1887/22997 holds various files of this Leiden University dissertation Author: Wilden, Gwendolyn M. van der Title: The value of surgical treatment in abdominal
Cover Page The handle http://hdl.handle.net/1887/22997 holds various files of this Leiden University dissertation Author: Wilden, Gwendolyn M. van der Title: The value of surgical treatment in abdominal
TRAUMA in the pediatric age group remains a
 Prehospital Triage in the Injured Pediatric Patient By S.A. Engum, M.K. Mitchell, L.R. Scherer, G. Gomez, L. Jacobson, K. Solotkin, and J.L. Grosfeld Indianapolis, Indiana Background/Purpose: Identifying
Prehospital Triage in the Injured Pediatric Patient By S.A. Engum, M.K. Mitchell, L.R. Scherer, G. Gomez, L. Jacobson, K. Solotkin, and J.L. Grosfeld Indianapolis, Indiana Background/Purpose: Identifying
Criteria for cancelling Helicopter Emergency Medical Services (HEMS) - dispatches
 Criteria for cancelling Helicopter Emergency Medical Services (HEMS) - dispatches G.F. Giannakopoulos, F.W. Bloemers, W.D. Lubbers, H.M.T. Christiaans, P. van Exter, E.S.M. de Lange - de Klerk, W.P. Zuidema,
Criteria for cancelling Helicopter Emergency Medical Services (HEMS) - dispatches G.F. Giannakopoulos, F.W. Bloemers, W.D. Lubbers, H.M.T. Christiaans, P. van Exter, E.S.M. de Lange - de Klerk, W.P. Zuidema,
Time Equals Neurons - Spinal Cord Injury Management in the first 4 Hours
 Time Equals Neurons - Spinal Cord Injury Management in the first 4 Hours William D. Whetstone M.D. Clinical Professor UCSF Department of Emergency Medicine SFGH ED Center for Neuro-Critical Emergencies
Time Equals Neurons - Spinal Cord Injury Management in the first 4 Hours William D. Whetstone M.D. Clinical Professor UCSF Department of Emergency Medicine SFGH ED Center for Neuro-Critical Emergencies
SAN LUIS OBISPO COUNTY EMERGENCY MEDICAL SERVICES AGENCY PREHOSPITAL POLICY
 SAN LUIS OBISPO COUNTY EMERGENCY MEDICAL SERVICES AGENCY PREHOSPITAL POLICY Policy Reference No: 153 [01/08/2013] Formerly Policy No: 201.3 Effective Date: 11/01/2012 Review Date: 03/01/2014 TRAUMA PATIENT
SAN LUIS OBISPO COUNTY EMERGENCY MEDICAL SERVICES AGENCY PREHOSPITAL POLICY Policy Reference No: 153 [01/08/2013] Formerly Policy No: 201.3 Effective Date: 11/01/2012 Review Date: 03/01/2014 TRAUMA PATIENT
Geriatric Emergency Management PLUS Program Costing Analysis at the Ottawa Hospital
 Geriatric Emergency Management PLUS Program Costing Analysis at the Ottawa Hospital Regional Geriatric Program of Eastern Ontario March 2015 Geriatric Emergency Management PLUS Program - Costing Analysis
Geriatric Emergency Management PLUS Program Costing Analysis at the Ottawa Hospital Regional Geriatric Program of Eastern Ontario March 2015 Geriatric Emergency Management PLUS Program - Costing Analysis
Massive Transfusion in Pediatric Trauma: Analysis of the National Trauma Databank
 Massive Transfusion in Pediatric Trauma: Analysis of the National Trauma Databank Michelle Shroyer, MPH, Russell Griffin, PhD, Vincent Mortellaro, MD, and Rob Russell MD, MPH Introduction Hemorrhage is
Massive Transfusion in Pediatric Trauma: Analysis of the National Trauma Databank Michelle Shroyer, MPH, Russell Griffin, PhD, Vincent Mortellaro, MD, and Rob Russell MD, MPH Introduction Hemorrhage is
Resource Utilization in Helicopter Transport of Head-Injured Children
 Resource Utilization in Helicopter Transport of Head-Injured Children Clay M. Elswick MD, Deidre Wyrick MD, Lori Gurien MD, Mallik Rettiganti PhD, Marie Saylors MS, Ambre Pownall APRN, Diaa Bahgat MD,
Resource Utilization in Helicopter Transport of Head-Injured Children Clay M. Elswick MD, Deidre Wyrick MD, Lori Gurien MD, Mallik Rettiganti PhD, Marie Saylors MS, Ambre Pownall APRN, Diaa Bahgat MD,
D. Pre-Hospital Trauma Triage and Bypass Algorithm
 D. Pre-Hospital Trauma Triage and Bypass Algorithm Hospital bypass is defined as transporting the patient to the nearest hospital that has the appropriate level of care for the patient s suspected severity
D. Pre-Hospital Trauma Triage and Bypass Algorithm Hospital bypass is defined as transporting the patient to the nearest hospital that has the appropriate level of care for the patient s suspected severity
Journal reading. Introduction. Introduction. Ottawa Ankle Rules. Method
 Journal reading Presenter: PGY 林聖傑 Supervisor: Dr. 林俊龍 102.12.23 The accuracy of ultrasound evaluation in foot and ankle trauma Salih Ekinci, MD American Journal of Emergency Medicine 31 (2013) 1551 1555
Journal reading Presenter: PGY 林聖傑 Supervisor: Dr. 林俊龍 102.12.23 The accuracy of ultrasound evaluation in foot and ankle trauma Salih Ekinci, MD American Journal of Emergency Medicine 31 (2013) 1551 1555
Risk Factors Predicting Mortality in Spinal Cord Injury in Nigeria
 Article ID: WMC00807 ISSN 2046690 Risk Factors Predicting Mortality in Spinal Cord Injury in Nigeria Corresponding Author: Dr. Ahidjo Kawu, Consultant Surgeon, Dept of Orthopaedics, UATH, Gwagwalada Abuja
Article ID: WMC00807 ISSN 2046690 Risk Factors Predicting Mortality in Spinal Cord Injury in Nigeria Corresponding Author: Dr. Ahidjo Kawu, Consultant Surgeon, Dept of Orthopaedics, UATH, Gwagwalada Abuja
Efficacy of the Motor Component of the Glasgow Coma Scale in Trauma Triage
 Page 1 of 7 Journals A-Z > Journal of Trauma-Injury... > 45(1) July 1998 > Efficacy of the... The Journal of Trauma: Injury, Infection, and Critical Care Issue: Volume 45(1), July 1998, pp 42-44 Copyright:
Page 1 of 7 Journals A-Z > Journal of Trauma-Injury... > 45(1) July 1998 > Efficacy of the... The Journal of Trauma: Injury, Infection, and Critical Care Issue: Volume 45(1), July 1998, pp 42-44 Copyright:
Complex evaluation of polytrauma in intensive care with multiple severity scores
 UNIVERSITY OF MEDICINE AND PHARMACY CRAIOVA DOCTORAL SCHOOL PhD THESIS Complex evaluation of polytrauma in intensive care with multiple severity scores Superviser Coordinator Prof. Univ. Dr. Florea Purcaru
UNIVERSITY OF MEDICINE AND PHARMACY CRAIOVA DOCTORAL SCHOOL PhD THESIS Complex evaluation of polytrauma in intensive care with multiple severity scores Superviser Coordinator Prof. Univ. Dr. Florea Purcaru
Presented at 2015 TQIP conference. Developed by a panel of experts. Evidence based with expert opinion as needed
 Presented at 2015 TQIP conference Developed by a panel of experts Evidence based with expert opinion as needed Orthopaedic Trauma Best Practice Guidelines (BPG) Goals Offer guidance on what is practical
Presented at 2015 TQIP conference Developed by a panel of experts Evidence based with expert opinion as needed Orthopaedic Trauma Best Practice Guidelines (BPG) Goals Offer guidance on what is practical
ACUTE CLINICAL MANAGEMENT OF TRAUMA Tina Gaarder, MD, PhD
 ACUTE CLINICAL MANAGEMENT OF TRAUMA Tina Gaarder, MD, PhD Trauma represents a leading cause of disability and preventable death and is mainly affecting people between 15 and 40 years of age, accounting
ACUTE CLINICAL MANAGEMENT OF TRAUMA Tina Gaarder, MD, PhD Trauma represents a leading cause of disability and preventable death and is mainly affecting people between 15 and 40 years of age, accounting
EmergencyKT: Management of Thermal Injury in Adult Patients
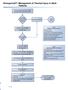 EmergencyKT: Management of Thermal Injury in Adult Patients Remove patient from source of injury, including burned clothing and jewelry Does patient appear to have minor burns? (See Box A) No Notify Burn
EmergencyKT: Management of Thermal Injury in Adult Patients Remove patient from source of injury, including burned clothing and jewelry Does patient appear to have minor burns? (See Box A) No Notify Burn
Daniel W. Spaite, MD Vatsal Chikani, MPH Bentley J. Bobrow, MD Michael Sotelo, BS Bruce Barnhart, RN, CEP Kurt R. Denninghoff, MD Joshua B.
 Daniel W. Spaite, MD Vatsal Chikani, MPH Bentley J. Bobrow, MD Michael Sotelo, BS Bruce Barnhart, RN, CEP Kurt R. Denninghoff, MD Joshua B. Gaither, MD Chad Viscusi, MD David P. Adelson, MD Duane Sherrill,
Daniel W. Spaite, MD Vatsal Chikani, MPH Bentley J. Bobrow, MD Michael Sotelo, BS Bruce Barnhart, RN, CEP Kurt R. Denninghoff, MD Joshua B. Gaither, MD Chad Viscusi, MD David P. Adelson, MD Duane Sherrill,
Episode 66 Backboard and Collar Nightmares from EMU Conference. The Risks Associated with Backboard & Collar
 However, backboards and collars are not without risk: Episode 66 Backboard and Collar Nightmares from EMU Conference With Dr. Kylie Bosman Prepared by Dr., edited by Dr. Kylie Bosman & Anton Helman, May
However, backboards and collars are not without risk: Episode 66 Backboard and Collar Nightmares from EMU Conference With Dr. Kylie Bosman Prepared by Dr., edited by Dr. Kylie Bosman & Anton Helman, May
TRAUMA ALERT: THE OLDER ADULT TRAUMA PATIENT - FIX ME QUICK
 TRAUMA ALERT: THE OLDER ADULT TRAUMA PATIENT - FIX ME QUICK Alicia Mangram, MD, FACS HonorHealth John C. Lincoln Medical Center Learning Objectives: Prevalence of geriatric trauma. New management strategies.
TRAUMA ALERT: THE OLDER ADULT TRAUMA PATIENT - FIX ME QUICK Alicia Mangram, MD, FACS HonorHealth John C. Lincoln Medical Center Learning Objectives: Prevalence of geriatric trauma. New management strategies.
Guidelines for Field Triage of Injured Patients Recommendations of the National Expert Panel on Field Triage
 Recommendations and Reports January 23, 2009 / 58(RR01);1-35 Guidelines for Field Triage of Injured Patients Recommendations of the National Expert Panel on Field Triage Prepared by Scott M. Sasser, MD
Recommendations and Reports January 23, 2009 / 58(RR01);1-35 Guidelines for Field Triage of Injured Patients Recommendations of the National Expert Panel on Field Triage Prepared by Scott M. Sasser, MD
Objectives. Central MA EMS Corp. Field Triage Decision Scheme: The National Trauma Triage Protocol 5/27/2011
 Course GOAL Central MA EMS Corp. Region II Trauma Point-of-Entry Plan Region II Trauma Point-of-Entry Plan This presentation is designed to help you do your job as EMS providers more effectively by helping
Course GOAL Central MA EMS Corp. Region II Trauma Point-of-Entry Plan Region II Trauma Point-of-Entry Plan This presentation is designed to help you do your job as EMS providers more effectively by helping
The Sydney paediatric trauma system and the effect of the discontinuation of the HIRT case identification process
 The Sydney paediatric trauma system and the effect of the discontinuation of the HIRT case identification process Alan Garner CareFlight 20 th Aug 2015 1 2 3 The Sydney paediatric trauma system Background
The Sydney paediatric trauma system and the effect of the discontinuation of the HIRT case identification process Alan Garner CareFlight 20 th Aug 2015 1 2 3 The Sydney paediatric trauma system Background
Neurovascular Observations Nursing Clinical Guideline
 Reference (include title, Patel, k., & McCann, P. A. (2012). The emergent assessment of supracondylar fractures of the paediatric humerus. Hand Surgery, 17(2), 161-165. From Medline Evidence level (I-)
Reference (include title, Patel, k., & McCann, P. A. (2012). The emergent assessment of supracondylar fractures of the paediatric humerus. Hand Surgery, 17(2), 161-165. From Medline Evidence level (I-)
Exclusion Criteria 1. Operator or supervisor feels specific intra- procedural laryngoscopy device will be required.
 FELLOW Study Data Analysis Plan Direct Laryngoscopy vs Video Laryngoscopy Background Respiratory failure requiring endotracheal intubation occurs in as many as 40% of critically ill patients. Procedural
FELLOW Study Data Analysis Plan Direct Laryngoscopy vs Video Laryngoscopy Background Respiratory failure requiring endotracheal intubation occurs in as many as 40% of critically ill patients. Procedural
: Undifferentiated Patient
 INTRODUCTION Though many patients in the pre-hospital setting have specific complaints such as my belly hurts or I m having chest pain, there are numerous situations in which the patient complains of symptoms
INTRODUCTION Though many patients in the pre-hospital setting have specific complaints such as my belly hurts or I m having chest pain, there are numerous situations in which the patient complains of symptoms
Controversies in Spinal Immobilization
 Controversies in Spinal Immobilization Ken Berumen, BSN, MD, FACEP Medical Director El Paso Fire Department Medical Director Emergency Services District #1 Network Director EM Sierra Providence Health
Controversies in Spinal Immobilization Ken Berumen, BSN, MD, FACEP Medical Director El Paso Fire Department Medical Director Emergency Services District #1 Network Director EM Sierra Providence Health
DATA COLLECTION AND MANAGEMENT
 DATA COLLECTION AND MANAGEMENT PURPOSE To specify the components of the data collection and management processes. RELATED POLICIES Patient Care Record, # 8115; Quality Improvement and System Evaluation,
DATA COLLECTION AND MANAGEMENT PURPOSE To specify the components of the data collection and management processes. RELATED POLICIES Patient Care Record, # 8115; Quality Improvement and System Evaluation,
Traumatic Cardiac Arrest Protocol
 Traumatic Cardiac Arrest Protocol Background: Major Trauma continues to be the leading worldwide cause of death in young adults. Mortality remains high but there are reports of good neurological outcomes
Traumatic Cardiac Arrest Protocol Background: Major Trauma continues to be the leading worldwide cause of death in young adults. Mortality remains high but there are reports of good neurological outcomes
Hospice and Palliative Care An Essential Component of the Aging Services Network
 Hospice and Palliative Care An Essential Component of the Aging Services Network Howard Tuch, MD, MS American Academy of Hospice and Palliative Medicine Physician Advocate, American Academy of Hospice
Hospice and Palliative Care An Essential Component of the Aging Services Network Howard Tuch, MD, MS American Academy of Hospice and Palliative Medicine Physician Advocate, American Academy of Hospice
Injury caused by an object breaking the skin and entering the body. immediate intervention to repair internal
 1 Chapter 16: Trauma & Trauma Systems 2 Trauma Leading killer of persons under in US. -150,000 Deaths annually -44,000 MVC -28,000 GSW Most medical problem in terms of lost wages, initial care, rehabilitation,
1 Chapter 16: Trauma & Trauma Systems 2 Trauma Leading killer of persons under in US. -150,000 Deaths annually -44,000 MVC -28,000 GSW Most medical problem in terms of lost wages, initial care, rehabilitation,
Pediatric Aspects of Advanced Trauma Life Support: Transition from EMS to the Trauma Room PEDIATRIC TRAUMA DIRECTOR, HASBRO CHILDREN S HOSPITAL
 Pediatric Aspects of Advanced Trauma Life Support: Transition from EMS to the Trauma Room HALE WILLS, MD PEDIATRIC TRAUMA DIRECTOR, HASBRO CHILDREN S HOSPITAL Objectives 1. Identify the critical components
Pediatric Aspects of Advanced Trauma Life Support: Transition from EMS to the Trauma Room HALE WILLS, MD PEDIATRIC TRAUMA DIRECTOR, HASBRO CHILDREN S HOSPITAL Objectives 1. Identify the critical components
Just like Adults? Evaluating the Impact of Fluid Resuscitation in Pediatric Trauma
 Just like Adults? Evaluating the Impact of Fluid Resuscitation in Pediatric Trauma Abbas PI 1,2, Carpenter K 2, Sheikh F 1,2, Peterson ML 1,2, Kljajic M 1, Naik-Mathuria B 1,2 1 Texas Children s Hospital
Just like Adults? Evaluating the Impact of Fluid Resuscitation in Pediatric Trauma Abbas PI 1,2, Carpenter K 2, Sheikh F 1,2, Peterson ML 1,2, Kljajic M 1, Naik-Mathuria B 1,2 1 Texas Children s Hospital
PALLIATIVE CARE FOR THE HEART AND STROKE PATIENT December 8, 2017
 PALLIATIVE CARE FOR THE HEART AND STROKE PATIENT December 8, 2017 1 Faculty Disclosure Faculty: Jeff Myers, MD, MSEd, CCFP (PC) Associate Professor, University of Toronto Palliative Care Physician, Sinai
PALLIATIVE CARE FOR THE HEART AND STROKE PATIENT December 8, 2017 1 Faculty Disclosure Faculty: Jeff Myers, MD, MSEd, CCFP (PC) Associate Professor, University of Toronto Palliative Care Physician, Sinai
INJURY IN HEAD TRAUMA
 The Journal ol Emergency Medfane, Vol 6, pp 203-207, 1988 Punted in the USA l Copyright K 1988 Pergamon Press plc CERVICAL INJURY IN HEAD TRAUMA Gary L. Neifeld, MD*, John G. Keene, MD, * George Hevesy,
The Journal ol Emergency Medfane, Vol 6, pp 203-207, 1988 Punted in the USA l Copyright K 1988 Pergamon Press plc CERVICAL INJURY IN HEAD TRAUMA Gary L. Neifeld, MD*, John G. Keene, MD, * George Hevesy,
Does a Blush on CT following Blunt Abdominal Injury Necessitate an Invasive Intervention?
 Does a Blush on CT following Blunt Abdominal Injury Necessitate an Invasive Intervention? Ragavan V Siddharthan, MD, Martha-Conley Ingram, BS., Andrew Morris, MD, Curtis Travers, MPH, Courtney McCracken,
Does a Blush on CT following Blunt Abdominal Injury Necessitate an Invasive Intervention? Ragavan V Siddharthan, MD, Martha-Conley Ingram, BS., Andrew Morris, MD, Curtis Travers, MPH, Courtney McCracken,
They re not little adults, but they are little humans. Pearls for your next pediatric trauma patient. Children are little humans
 They re not little adults, but they are little humans Pearls for your next pediatric trauma patient Alisa McQueen MD, FAAP, FACEP Associate Professor of Pediatrics The University of Chicago Alisa McQueen
They re not little adults, but they are little humans Pearls for your next pediatric trauma patient Alisa McQueen MD, FAAP, FACEP Associate Professor of Pediatrics The University of Chicago Alisa McQueen
ESCAMBIA COUNTY TRAUMA TRANSPORT
 TRAUMA ALERT CRITERIA are established state mandated criteria. ADULT TRAUMA ALERT CRITERIA (Physical and anatomical characteristics of a person 16 years of age or older) Any 1 of the following: 1. Airway:
TRAUMA ALERT CRITERIA are established state mandated criteria. ADULT TRAUMA ALERT CRITERIA (Physical and anatomical characteristics of a person 16 years of age or older) Any 1 of the following: 1. Airway:
Trauma CT Scanning Protocol
 Northern Trauma Network Trauma CT Scanning Protocol Background Whole body CT (WBCT) has assumed a pivotal position in trauma management. UK trauma is typically described as blunt and blind i.e. blunt trauma
Northern Trauma Network Trauma CT Scanning Protocol Background Whole body CT (WBCT) has assumed a pivotal position in trauma management. UK trauma is typically described as blunt and blind i.e. blunt trauma
Objectives 9/23/2014. Field Triage for Trauma Patients: What s the Evidence? EMS in Trauma Systems
 Field Triage for Trauma Patients: What s the Evidence? Craig D. Newgard, MD, MPH Center for Policy and Research in Emergency Medicine Department of Emergency Medicine Oregon Health & Science University
Field Triage for Trauma Patients: What s the Evidence? Craig D. Newgard, MD, MPH Center for Policy and Research in Emergency Medicine Department of Emergency Medicine Oregon Health & Science University
External Validation of the Clinical Dehydration Scale for Children With Acute Gastroenteritis
 CLINICAL INVESTIGATION External Validation of the Clinical Dehydration Scale for Children With Acute Gastroenteritis Benoit Bailey, MD, MSc, Jocelyn Gravel, MD, MSc, Ran D. Goldman, MD, Jeremy N. Friedman,
CLINICAL INVESTIGATION External Validation of the Clinical Dehydration Scale for Children With Acute Gastroenteritis Benoit Bailey, MD, MSc, Jocelyn Gravel, MD, MSc, Ran D. Goldman, MD, Jeremy N. Friedman,
The Geriatric Trauma Institute (GTI) The Efficacy of a Dedicated Geriatric Trauma Service: A Pilot Study
 The Geriatric Trauma Institute (GTI) The Efficacy of a Dedicated Geriatric Trauma Service: A Pilot Study Connie DeLa O MD, Anthony Miller MD, Aurelio Rodriguez MD, Russell Dumire MD, Jami Zipf RN,BSN Conemaugh
The Geriatric Trauma Institute (GTI) The Efficacy of a Dedicated Geriatric Trauma Service: A Pilot Study Connie DeLa O MD, Anthony Miller MD, Aurelio Rodriguez MD, Russell Dumire MD, Jami Zipf RN,BSN Conemaugh
Critical care resources are often provided to the too well and as well as. to the too sick. The former include the patients admitted to an ICU
 Literature Review Critical care resources are often provided to the too well and as well as to the too sick. The former include the patients admitted to an ICU following major elective surgery for overnight
Literature Review Critical care resources are often provided to the too well and as well as to the too sick. The former include the patients admitted to an ICU following major elective surgery for overnight
Protocol Development: The Guiding Light of Any Clinical Study
 Protocol Development: The Guiding Light of Any Clinical Study Susan G. Fisher, Ph.D. Chair, Department of Clinical Sciences 1 Introduction Importance/ relevance/ gaps in knowledge Specific purpose of the
Protocol Development: The Guiding Light of Any Clinical Study Susan G. Fisher, Ph.D. Chair, Department of Clinical Sciences 1 Introduction Importance/ relevance/ gaps in knowledge Specific purpose of the
Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Care Unit (FELLOW)
 Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Data Analysis Plan: Apneic Oxygenation vs. No Apneic Oxygenation Background Critically ill patients
Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Data Analysis Plan: Apneic Oxygenation vs. No Apneic Oxygenation Background Critically ill patients
Title: Post traumatic Diaphragmatic hernia in children: Diagnostic Dilemmas and lessons learned. Type: Original article
 Title: Post traumatic Diaphragmatic hernia in children: Diagnostic Dilemmas and lessons learned. Type: Original article Authors: Dr Vaibhav Pandey 1*, Dr. Pranay Panigrahi 2 Srivastav 4 & Dr Rakesh Kumar
Title: Post traumatic Diaphragmatic hernia in children: Diagnostic Dilemmas and lessons learned. Type: Original article Authors: Dr Vaibhav Pandey 1*, Dr. Pranay Panigrahi 2 Srivastav 4 & Dr Rakesh Kumar
Trauma Patients What do we really know?
 Patients What do we really know? Dan Talbert MHS, EMT-P, FP-C TraumaOne / UF Health Jacksonville Objectives Introduction to trauma Overview of the trauma system Overview of the traumatic injury Case review
Patients What do we really know? Dan Talbert MHS, EMT-P, FP-C TraumaOne / UF Health Jacksonville Objectives Introduction to trauma Overview of the trauma system Overview of the traumatic injury Case review
Geriatric Trauma Resuscitation: Lessons from a Geriatric Trauma Surgeon
 Geriatric Trauma Resuscitation: Lessons from a Geriatric Trauma Surgeon Aurelio Rodriguez, M.D., FACS Conemaugh Memorial Medical Center Trauma Center Johnstown, PA Demographics The fastest growing age
Geriatric Trauma Resuscitation: Lessons from a Geriatric Trauma Surgeon Aurelio Rodriguez, M.D., FACS Conemaugh Memorial Medical Center Trauma Center Johnstown, PA Demographics The fastest growing age
The ABC s of Chest Trauma
 The ABC s of Chest Trauma J Bradley Pickhardt MD, FACS Providence St Patrick Hospital What s the Problem? 2/3 of trauma patients have chest trauma Responsible for 25% of all trauma deaths Most injuries
The ABC s of Chest Trauma J Bradley Pickhardt MD, FACS Providence St Patrick Hospital What s the Problem? 2/3 of trauma patients have chest trauma Responsible for 25% of all trauma deaths Most injuries
Can we abolish skull x-rays for head injury?
 ADC Online First, published on April 25, 2005 as 10.1136/adc.2004.053603 Can we abolish skull x-rays for head injury? Matthew J Reed, Jen G Browning, A. Graham Wilkinson & Tom Beattie Corresponding author:
ADC Online First, published on April 25, 2005 as 10.1136/adc.2004.053603 Can we abolish skull x-rays for head injury? Matthew J Reed, Jen G Browning, A. Graham Wilkinson & Tom Beattie Corresponding author:
Risk Factors of Early Complications of Tracheostomy at Kenyatta National Hospital.
 Risk Factors of Early Complications of Tracheostomy at Kenyatta National Hospital. G. Karuga 1, H. Oburra 2, C. Muriithi 3. 1 Resident Ear Nose & Throat (ENT) Head & Neck Department. University of Nairobi
Risk Factors of Early Complications of Tracheostomy at Kenyatta National Hospital. G. Karuga 1, H. Oburra 2, C. Muriithi 3. 1 Resident Ear Nose & Throat (ENT) Head & Neck Department. University of Nairobi
CURRICULUM VITAE THOMAS JOHN OTTO, M.D.
 CURRICULUM VITAE THOMAS JOHN OTTO, M.D. PERSONAL INFORMATION: Birth date: February 27, 1951 Citizenship: United States of America EDUCATION: Saint Louis University St. Louis, Missouri B.A. (Chemistry),
CURRICULUM VITAE THOMAS JOHN OTTO, M.D. PERSONAL INFORMATION: Birth date: February 27, 1951 Citizenship: United States of America EDUCATION: Saint Louis University St. Louis, Missouri B.A. (Chemistry),
Fri., 10/17/14 Polytrauma, PAPER #74, 4:00 pm OTA 2014
 Fri., 10/17/14 Polytrauma, PAPER #74, 4:00 pm OTA 2014 Clinical Indications for CT Angiography in Lower Extremity Trauma Joseph T. Patterson, MD 1 ; Thomas Fishler, MD 2 ; Daniel D. Bohl, MPH 3 ; Michael
Fri., 10/17/14 Polytrauma, PAPER #74, 4:00 pm OTA 2014 Clinical Indications for CT Angiography in Lower Extremity Trauma Joseph T. Patterson, MD 1 ; Thomas Fishler, MD 2 ; Daniel D. Bohl, MPH 3 ; Michael
ADENIYI MOFOLUWAKE MPH APPLIED EPIDEMIOLOGY WEEK 5 CASE STUDY ASSIGNMENT APRIL
 ADENIYI MOFOLUWAKE MPH 510 - APPLIED EPIDEMIOLOGY WEEK 5 CASE STUDY ASSIGNMENT APRIL 4 2013 Question 1: What makes the first study a case-control study? The first case study is a case-control study because
ADENIYI MOFOLUWAKE MPH 510 - APPLIED EPIDEMIOLOGY WEEK 5 CASE STUDY ASSIGNMENT APRIL 4 2013 Question 1: What makes the first study a case-control study? The first case study is a case-control study because
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 17 Orthopedic Techniques Key Points 2 17.1 Traction Use an appropriate method of traction to treat fractures of the extremities and cervical spine Apply extremity
Surgical Care at the District Hospital 1 17 Orthopedic Techniques Key Points 2 17.1 Traction Use an appropriate method of traction to treat fractures of the extremities and cervical spine Apply extremity
What the s wrong with this person?
 Ketamine for Prehospital Management of Excited Delirium Syndrome: Is it all just a bunch of hype?!? Financial Disclosure Asa M. Margolis, DO, MPH, MS, FACEP Assistant Professor Division of Special Operation
Ketamine for Prehospital Management of Excited Delirium Syndrome: Is it all just a bunch of hype?!? Financial Disclosure Asa M. Margolis, DO, MPH, MS, FACEP Assistant Professor Division of Special Operation
Goals. Geriatric Trauma. What s the impact Erlanger Trauma Symposium
 Geriatric Trauma William S. Havron III MD Assistant Professor of Surgery University of Oklahoma Goals Realize the impact of injuries in the ageing population Identify the pitfalls associated with geriatric
Geriatric Trauma William S. Havron III MD Assistant Professor of Surgery University of Oklahoma Goals Realize the impact of injuries in the ageing population Identify the pitfalls associated with geriatric
CLINICAL MANUAL. Trauma System Activation Trauma Code Criteria
 CLINICAL MANUAL Policy Number: CM T-28 Approved by: Nursing Congress, Management Forum Issue Date: 09/1999 Applies to: Downtown Value(s): Respect, Integrity, Innovation Page(s): 1 of 4 Trauma System Activation
CLINICAL MANUAL Policy Number: CM T-28 Approved by: Nursing Congress, Management Forum Issue Date: 09/1999 Applies to: Downtown Value(s): Respect, Integrity, Innovation Page(s): 1 of 4 Trauma System Activation
Children diagnosed with skull fractures are often. Transfer of children with isolated linear skull fractures: is it worth the cost?
 clinical article J Neurosurg Pediatr 17:602 606, 2016 Transfer of children with isolated linear skull fractures: is it worth the cost? Ian K. White, MD, 1 Ecaterina Pestereva, BS, 1 Kashif A. Shaikh, MD,
clinical article J Neurosurg Pediatr 17:602 606, 2016 Transfer of children with isolated linear skull fractures: is it worth the cost? Ian K. White, MD, 1 Ecaterina Pestereva, BS, 1 Kashif A. Shaikh, MD,
Scoring of anatomic injury after trauma: AIS 98 versus AIS 90 do the changes affect overall severity assessment?
 Injury, Int. J. Care Injured (2007) 38, 84 90 www.elsevier.com/locate/injury Scoring of anatomic injury after trauma: AIS 98 versus AIS 90 do the changes affect overall severity assessment? Nils O. Skaga
Injury, Int. J. Care Injured (2007) 38, 84 90 www.elsevier.com/locate/injury Scoring of anatomic injury after trauma: AIS 98 versus AIS 90 do the changes affect overall severity assessment? Nils O. Skaga
Improved IPGM: Demonstrating the Value to both Patients and Hospitals
 Improved IPGM: Demonstrating the Value to both Patients and Hospitals Osama Hamdy, MD, PhD, FACE Medical Director, Inpatient Diabetes Program Joslin Diabetes Center Harvard Medical School, Boston, MA Cost
Improved IPGM: Demonstrating the Value to both Patients and Hospitals Osama Hamdy, MD, PhD, FACE Medical Director, Inpatient Diabetes Program Joslin Diabetes Center Harvard Medical School, Boston, MA Cost
Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of
 Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of Washington Seattle Children s Hospital Objectives Define
Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of Washington Seattle Children s Hospital Objectives Define
Displaced Supracondylar Humerus Fractures in Children Are They All Identical?
 Doi: http://dx.doi.org/10.5704/moj.1707.017 Displaced Supracondylar Humerus Fractures in Children Are They All Identical? Gera SK, MS Orth, Tan MCH, MBBS, Lim YG, MRCS Ed, Lim KBL, FRCSEd Orth Department
Doi: http://dx.doi.org/10.5704/moj.1707.017 Displaced Supracondylar Humerus Fractures in Children Are They All Identical? Gera SK, MS Orth, Tan MCH, MBBS, Lim YG, MRCS Ed, Lim KBL, FRCSEd Orth Department
EMS System for Metropolitan Oklahoma City and Tulsa 2018 Medical Control Board Treatment Protocols
 EMERGENCY MEDICAL RESPONDER EMT EMT-INTERMEDIATE 85 ADVANCED EMT PARAMEDIC 14G PATIENT PRIORITIZATION While each patient will receive the best possible EMS care in a humane and ethical manner, proper patient
EMERGENCY MEDICAL RESPONDER EMT EMT-INTERMEDIATE 85 ADVANCED EMT PARAMEDIC 14G PATIENT PRIORITIZATION While each patient will receive the best possible EMS care in a humane and ethical manner, proper patient
Regulatory Realities Redefining Benefit of Lung Transplant in the Current Era
 Regulatory Realities Redefining Benefit of Lung Transplant in the Current Era Gundeep S Dhillon, MD, MPH Associate Professor of Medicine Medical Director, Lung & Heart-Lung Transplantation Program Stanford
Regulatory Realities Redefining Benefit of Lung Transplant in the Current Era Gundeep S Dhillon, MD, MPH Associate Professor of Medicine Medical Director, Lung & Heart-Lung Transplantation Program Stanford
Pediatric Trauma Cases
 Pediatric Trauma Cases QPEM 2018 Barbara Blackie, MD, MEd, FRCPC DISCLOSURE I do not have any relevant financial relationship with commercial interest to disclose. Learning Objectives -Manage interactive
Pediatric Trauma Cases QPEM 2018 Barbara Blackie, MD, MEd, FRCPC DISCLOSURE I do not have any relevant financial relationship with commercial interest to disclose. Learning Objectives -Manage interactive
CHILDHOOD MOTOCROSS TRUNCAL INJURIES: HIGH VELOCITY, FOCAL FORCE TO THE CHEST AND ABDOMEN: A Cohort Study For peer review only
 CHILDHOOD MOTOCROSS TRUNCAL INJURIES: HIGH VELOCITY, FOCAL FORCE TO THE CHEST AND ABDOMEN: A Cohort Study Journal: Manuscript ID: bmjopen-0-00 Article Type: Research Date Submitted by the Author: -Jul-0
CHILDHOOD MOTOCROSS TRUNCAL INJURIES: HIGH VELOCITY, FOCAL FORCE TO THE CHEST AND ABDOMEN: A Cohort Study Journal: Manuscript ID: bmjopen-0-00 Article Type: Research Date Submitted by the Author: -Jul-0
Physician specialty and the outcomes and cost of admissions for end-stage liver disease Ko C W, Kelley K, Meyer K E
 Physician specialty and the outcomes and cost of admissions for end-stage liver disease Ko C W, Kelley K, Meyer K E Record Status This is a critical abstract of an economic evaluation that meets the criteria
Physician specialty and the outcomes and cost of admissions for end-stage liver disease Ko C W, Kelley K, Meyer K E Record Status This is a critical abstract of an economic evaluation that meets the criteria
Asthma Disease Management Demonstration Project:
 Asthma Disease Management Demonstration Project: Using EMS Health Coaches May Decrease Emergency Department Revisits, Length of Hospital Admissions and Costs Michael T. Hilton, MD Jan 13, 2012 NAEMSP Annual
Asthma Disease Management Demonstration Project: Using EMS Health Coaches May Decrease Emergency Department Revisits, Length of Hospital Admissions and Costs Michael T. Hilton, MD Jan 13, 2012 NAEMSP Annual
General Goals and Objectives for the Orthopaedic Surgery Resident McGill Orthopaedic Trauma (MGH)
 General Goals and Objectives for the Orthopaedic Surgery Resident McGill Orthopaedic Trauma (MGH) The resident must show appropriate-for-level mastering of the CanMed qualifications of medical expert,
General Goals and Objectives for the Orthopaedic Surgery Resident McGill Orthopaedic Trauma (MGH) The resident must show appropriate-for-level mastering of the CanMed qualifications of medical expert,
Clinical and financial analyses of laparoscopically assisted vaginal hysterectomy versus abdominal hysterectomy Hidlebaugh D, O'Mara P, Conboy E
 Clinical and financial analyses of laparoscopically assisted vaginal hysterectomy versus abdominal hysterectomy Hidlebaugh D, O'Mara P, Conboy E Record Status This is a critical abstract of an economic
Clinical and financial analyses of laparoscopically assisted vaginal hysterectomy versus abdominal hysterectomy Hidlebaugh D, O'Mara P, Conboy E Record Status This is a critical abstract of an economic
The found down patient: A diagnostic dilemma
 ORIGINAL ARTICLE The found down patient: A diagnostic dilemma Lucy Z. Kornblith, MD, Matthew E. Kutcher, MD, Abigail E. Evans, BA, Brittney J. Redick, BA, Alicia Privette, MD, William P. Schecter, MD,
ORIGINAL ARTICLE The found down patient: A diagnostic dilemma Lucy Z. Kornblith, MD, Matthew E. Kutcher, MD, Abigail E. Evans, BA, Brittney J. Redick, BA, Alicia Privette, MD, William P. Schecter, MD,
Head trauma is a common chief complaint among children visiting
 Discussions in Surgery Validation of the Sainte-Justine Head Trauma Pathway for children younger than two years of age Sarah Spénard Serge Gouin, MDCM Marianne Beaudin, MD Jocelyn Gravel, MD, MSc Partial
Discussions in Surgery Validation of the Sainte-Justine Head Trauma Pathway for children younger than two years of age Sarah Spénard Serge Gouin, MDCM Marianne Beaudin, MD Jocelyn Gravel, MD, MSc Partial
vel 2 Level 2 3,034 c-spine evaluations with CSR Level 3 detected injury only 53% of the time. Level 3 False (-) rate 47%
 Objectives Blunt and Penetrating Neck Trauma Julie Mayglothling, MD, FACEP Virginia Commonwealth University Richmond, VA Summit to Sound, May 20 th, 2011 Blunt Neck Trauma Evaluation of the low mechanism,
Objectives Blunt and Penetrating Neck Trauma Julie Mayglothling, MD, FACEP Virginia Commonwealth University Richmond, VA Summit to Sound, May 20 th, 2011 Blunt Neck Trauma Evaluation of the low mechanism,
Avoidable Imaging Learning Collaborative: 2008 Mild Traumatic Brain Injury Clinical Policy Success Story BWH Head and PE CTs with Clinical Decision
 Avoidable Imaging Learning Collaborative: 2008 Mild Traumatic Brain Injury Clinical Policy Success Story BWH Head and PE CTs with Clinical Decision Support Using the Canadian CT Head Rule to Reduce Unnecessary
Avoidable Imaging Learning Collaborative: 2008 Mild Traumatic Brain Injury Clinical Policy Success Story BWH Head and PE CTs with Clinical Decision Support Using the Canadian CT Head Rule to Reduce Unnecessary
England & Wales 2 YEARS OF SEVERE INJURY IN CHILDREN
 England & Wales 2 YEARS OF SEVERE INJURY IN CHILDREN January 2013-December 2014 THE TRAUMA AUDIT AND RESEARCH NETWORK The TARNlet Committee Mr Ross Fisher Co-chairman of TARNlet Consultant in Paediatric
England & Wales 2 YEARS OF SEVERE INJURY IN CHILDREN January 2013-December 2014 THE TRAUMA AUDIT AND RESEARCH NETWORK The TARNlet Committee Mr Ross Fisher Co-chairman of TARNlet Consultant in Paediatric
Research Article Demographic Analysis of Emergency Department Patients at the Ruijin Hospital, Shanghai
 Emergency Medicine International Volume 2011, Article ID 748274, 5 pages doi:10.1155/2011/748274 Research Article Demographic Analysis of Emergency Department Patients at the Ruijin Hospital, Shanghai
Emergency Medicine International Volume 2011, Article ID 748274, 5 pages doi:10.1155/2011/748274 Research Article Demographic Analysis of Emergency Department Patients at the Ruijin Hospital, Shanghai
Low Tolerance Long Duration (LTLD) Stroke Demonstration Project
 Low Tolerance Long Duration (LTLD) Stroke Demonstration Project Interim Summary Report October 25 Table of Contents 1. INTRODUCTION 3 1.1 Background.. 3 2. APPROACH 4 2.1 LTLD Stroke Demonstration Project
Low Tolerance Long Duration (LTLD) Stroke Demonstration Project Interim Summary Report October 25 Table of Contents 1. INTRODUCTION 3 1.1 Background.. 3 2. APPROACH 4 2.1 LTLD Stroke Demonstration Project
Neurologic improvement after thoracic, thoracolumbar, and lumbar spinal cord (conus medullaris) injuries
 Thomas Jefferson University Jefferson Digital Commons Department of Orthopaedic Surgery Faculty Papers Department of Orthopaedic Surgery 1-2011 Neurologic improvement after thoracic, thoracolumbar, and
Thomas Jefferson University Jefferson Digital Commons Department of Orthopaedic Surgery Faculty Papers Department of Orthopaedic Surgery 1-2011 Neurologic improvement after thoracic, thoracolumbar, and
