Cervical Spine Clearance in Australian Intensive Care Units
|
|
|
- Dorcas Fisher
- 6 years ago
- Views:
Transcription
1 Original articles Cervical Spine Clearance in Australian Intensive Care Units D. LIEN, T. JACQUES, K. POWELL Intensive Care Unit, The St. George Hospital, Sydney, NEW SOUTH WALES ABSTRACT Objective: Rigid or semi-rigid collar and spine board related complications may be causes of significant morbidity in intubated polytraumatised patients. As the process quantifying cervical spine injuries is controversial, exclusion of cervical spinal injuries (cervical spine clearance) can be delayed, thereby increasing complications associated with spinal cord immobilisation. We examined current practices in Australian ICU s by survey. Methods: The intensive care unit or trauma services director and the senior nursing unit manager from 17 units within designated Australian trauma centres were surveyed separately by telephone. The presence of a written protocol for cervical spine clearance including radiological and clinical criteria, time goals for clearance, immobilisation methods and formal surveillance of collar related complications were assessed using a standardised questionnaire. Results: All states and territories were represented. Of those services surveyed, only 50% had a written protocol, 50% had no specific time goal for cervical spinal clearance and the method of clearance ranged from plain cervical spine X-rays only to routine use of MRI. Immobilisation methods also varied, including use of rigid (hard) or soft collars with 71% having no formal surveillance of collar-related complications. Despite these results, 65% were satisfied with their approach to cervical spine clearance. Conclusions: There is no standardised approach to the clearance of the cervical spine in intubated trauma patients in Australian intensive care units. In addition, morbidity from current practices and the true incidence of cervical spine injuries remains unknown. We recommend use of a written protocol and formal documentation of collar related complications. A standardised approach to radiological and clinical clearance of cervical spine injuries, which is practical, yet safe, remains a subject for future riskbenefit analysis. (Critical Care and Resuscitation 2003; 5: 91-96) Key words: Cervical spine, trauma, ligamentous, injury Cervical spine clearance in intubated, polytraumatised patients presents unique problems to the intensive care specialist. These patients are usually obtunded due to an associated head injury or drugs (recreational or medically administered) and haemodynamic instability or airway problems often confound the assessment. In addition, spinal immobilisation related complications of decubitus and pressure ulcers can occur within 30 minutes of spinal immobilisation. 1 Even when the cervical spine has been cleared of bony injury, the possibility of ligamentous, soft tissue, or non-bony cervical spine injury is difficult to exclude. This may result in a further delay and an increase complications associated with collar and spinal board use. The current practice of cervical spine clearance in Australian intensive care units was examined. METHODS A standardised questionnaire was devised to investigate the following issues: Correspondence to: Dr. D. Lien, Intensive Care Unit, The St. George Hospital, Kogarah, New South Wales
2 D. LIEN, ET AL Critical Care and Resuscitation 2003; 5: the presence of written cervical spine clearance protocols, radiological and clinical techniques used to assess cervical spine injury, established time goals for achieving cervical spine clearance, methods of immobilisation used in uncleared patients and, surveillance and documentation of complications related to collar and board use. The survey was undertaken over a 2 week period in 16 major hospitals throughout Australia using a standard questionnaire (appendix 1). The institutions were contacted by telephone and the director of the intensive care unit (ICU) was invited to answer each question. If the director was not readily available, the director of trauma was asked to participate. To provide insight into the nursing perspective, the senior nursing unit manager was also asked to complete the same questionnaire. Only intensive care units from hospitals with trauma centre status were asked to participate. In the majority of cases both the medical and nursing participants from the same centre were taken through the questionnaire by the same investigator (either D. Lien or K. Powell). If one of the participants was not available, a follow-up call was made by either investigator. The responses of all participants were entered on separate questionnaire sheets and, for the purposes of analysis, were recorded on an Excel spreadsheet. RESULTS A total of 16 centres participated. One hospital had a separate neurosurgical ICU, bringing the total to 17 intensive care units surveyed. All states and territories were represented (Table1). The majority of participants were staff from an intensive care unit (i.e. 75% ICU directors, 25% directors of trauma and 94% ICU senior nursing unit managers). Table 1. State of origin and number of participating intensive care units State NSW VIC QLD SA WA ACT NT TAS No ICU s No ICUs = Number of intensive care units There was a recurring difference between the responses from the directors and senior nursing unit managers (NUMs), suggesting that procedures or knowledge of agreed unit procedures in many institutions were not clearly understood (Table 2). Many units did not have a written cervical spine clearance protocol and did not use time-goals in the clearance of cervical spine injuries (Table 2). While the ICU staff were usually involved in the management of cervical spine clearance in intubated trauma patients (e.g. from protocol development through to final arbitration on clearance of the cervical spine), the neurosurgical, orthopaedic and spinal teams often had a significant input (Table 2). Table 3 shows that the most common initial films ordered in assessing cervical spine injury were static 3 view cervical vertebra series (e.g. anteroposterior, lateral and open-mouth or odontoid views), or a 3-view series plus a CT, either of the upper and lower cervical spine or of poorly visualised regions. A significant number of units equated radiological clearance with clinical clearance, making no attempt to rule out ligamentous or soft-tissue injuries prior to removal of a cervical spine immobiliser. Some units managed patients as though radiological clearance equated to clinical clearance unless patients were likely to be assessable within 24 hours, in which case the cervical spine immobilisation was left in place. Some units used more than one technique for cervical spine clearance. Alternatively, a large number of units left the cervical spine immobilisation in place, in some cases for the full duration of intubation and ventilation, and then assessed patients either radiologically or clinically when the patient was more cooperative. A third of the intensive care units monitored patients for pressure sores from collar and board use, and of those that did not regularly monitor for decubitus or pressure sores, less than 25% felt that this practice was necessary (Table 2). DISCUSSION After inconsistencies of cervical spine clearance were identified in our own practice we conducted a national audit in an attempt to review the current Australian practice and to standardise our own practice. In our study, a major discrepancy often existed between the responses of the ICU or trauma directors and the senior nursing unit managers, indicating that clinical practice within many units was unclear. This lack of consistency has also been reported in a British study by Gupta and Clancy who found in a survey of 25 units, that cervical spine clearance was based on normal plain static radiology of the cervical spine in patients with no focal neurological signs in 19 units, and on the combined clinical examination (when the patients were awake) with a normal cervical spine X-ray, in 6 units. In only 4 of the 19 units lateral, anteroposterior and odontoid views of the cervical spine were required for clearance, and in 16 units a lateral cervical spine view only was required. Fifteen units had no guidelines in place. 2 92
3 Critical Care and Resuscitation 2003; 5: D. LIEN, ET AL Table 2. Cervical spine clearance protocols according to the directors and senior nursing unit managers of the intensive care units % of directors % of NUM Protocol for cervical spine clearance Written protocol Verbal protocol 25 7 Unknown 0 13 Specialty involved in developing the protocol Intensive care staff Joint effort Radiology 0 10 Time goals and range in hours Goals established None or ASAP Time goals in hours Specialist involved in final say on clearance Intensivist Neurosurgeon Radiology Orthopaedic surgeon Spinal team 6 11 Emergency medicine 6 0 Immobilisation techniques used in uncleared patients Hard collar Soft collar 5 6 Philadelphia collar Jordan frame 10 6 Log roll Sedation 5 0 Paralysis 0 0 Sandbags Modified log roll 5 0 Supine nursing Surveillance of complications related to collar and board use Formal surveillance Formal surveillance unnecessary Satisfied with current practice NUM = senior nursing unit manager, Verbal protocol = an undocumented common clinical pathway or accepted practice agreed between the intensive care staff and other relevant specialties, Joint effort = a cooperative effort between several specialties, usually neurosurgery and orthopaedics, ASAP = as soon as possible. A common approach to cervical spine clearance in intubated or sedated polytraumatised patients involves radiological clearance after a normal three static filmseries (e.g. lateral, anteroposterior and odontoid views) has been confirmed. A former ATLS chairman cites a 1990 study of 7500 trauma patients where 470 patients were identified with acute cervical spine injuries and claimed that No obtunded patient with adequate three view screening examination correctly interpreted by the senior trauma surgeon and an experienced radiolo- Table 3. Initial radiological imaging ordered (in percent) by directors for cervical-spine clearance Anteroposterior/lateral/odontoid views 25 3-view series with CT 57 Anteroposterior/odontiod/oblique views 6 Anteroposterior/lateral views 6 Anteroposterior/lateral/oblique views 6 93
4 D. LIEN, ET AL Critical Care and Resuscitation 2003; 5: gist was subsequently identified as having an unstable cervical fracture or if the three views are inadequate a non-contrast CT of the relevant cervical spine portions is sufficient. 1 With the exclusion of a cervical spine bony injury, the concern of the possibility of cervical spine ligamentous injury, which usually has an incidence of < 1% of all major trauma patients, lingers. 3 Therefore, three questions remain: should radiologically cleared patients have no collar, a soft collar, Philadelphia (semi-rigid) collar or hard collar applied?, Should strict log rolling still be enforced? and Should one attempt to clear the cervical spine of ligamentous injury as early as possible or wait until the patient is cooperative to assess the disorder either radiologically with flexion/extension films or clinically? Polytraumatised patients often emerge from sedation in an agitated state. In such cases strict immobilisation is usually unrealistic. It is our practice, where the clinical suspicion of a cervical spine injury is low, to place a radiologically cleared patient in a soft collar if an endotracheal tube is in situ, or a Philadelphia collar in the case of a tracheostomised patient. Flexion/extension views are then arranged when the patient is extubated and oriented, with the soft collar serving as a reminder to minimise extreme neck movements. To reduce the nursing load on these patients, we move these patients using a modified log roll (appendix 2). Limitations of both soft and hard collars have been described. A soft collar prevents about 30% of the cervical spine movement, compared with up to 70% for the hard collar. 4 It has been suggested that as the hard collar fails to immobilise the cervical spine completely 5 it may even worsen cervical spine instability for the mobile patient, especially to the upper and lower cervical spine junctions, where the majority of injuries are located. Moreover, some of the methods commonly used to immobilise the cervical spine may cause venous occlusion and hence raise intracranial pressure. Figure 1 illustrates the dramatic reduction of intracranial pressure with removal of a hard collar from a head injured patient managed in our ICU. Other adverse effects of prolonged hard collar application include pressure sores (a Philadelphia collar may reduce this risk), tracheostomy delay, hindrance of central line insertion, hypersensitivity and skin rashes. It is recognised that it is impossible to clear the cervical spine of all injury despite normal radiographs. In one review of 29 studies, 16% of cervical spine fractures were missed in patients with normal cervical spine lateral, anteroposterior and odontoid views, in contrast with the classical teaching of 1-2%. 6 Adding two oblique views does not change this outcome and Figure 1. Effect on the intracranial pressure in a polytrauma patient with the removal of a cervical spine hard collar. the swimmers view is considered by many to also be of minimal benefit. 7 Neck CT scans also fail to detect ligamentous injury, 3 unless there is a significant associated haematoma. An Australian study involving routine use of fine-cut helical CTs with reconstruction claimed to eliminate the need for dynamic functional X-rays to clear the cervical spine. 8 Two studies from United States of America claim that three static plain films with a cervical spine CT, as an adjunct, can clear the cervical spine, although no mention of the risk of ligamentous injury was made, and the numbers in both these studies were 179 and 204 respectively. 9,10 The role of MRI is less well defined. It is thought to be sensitive for the detection of haemorrhage, contusion, cord or nerve root compression. Its disadvantages include difficulty in performing in the intubated patient, cost, poor definition of bony injury and need to be interpreted in the presence of a CT (thus mandating both in any trauma patient where one is suspicious of a cervical spine injury). 11 Passive flexion and extension views may exclude significant cervical spine instability where MRI, CT and plain films cannot. 3 However, the safety of such a technique has been called into question. 12 Davis et al, performed a prospective study reviewing the safety of dynamic fluoroscopy, using 116 patients with normal plain X-rays. They used full range of motion and found there were no neurological complications. They also quoted a 44% decubitus ulcer rate in patients, with cervical collars that remained on for more than 5 days. 5 An Australian study found that only 1 in 48 patients had an unstable cervical spine injury which was detected on dynamic testing, with no deleterious effects from neck manipulation. The guidelines in for clearing the cervical spine in unconscious or intoxicated patients recommend anteroposterior, lateral and CT scan of the occiput to C 3 rather than odontoid views of the cervical spine and 2 mm axial CT scanning on specific bone windows with sagittal and coronal reconstruction 94
5 Critical Care and Resuscitation 2003; 5: D. LIEN, ET AL to evaluate abnormal or poorly visualised areas on plane radiology. However, to exclude ligamentous 2. Gupta KJ, Clancy M. Discontinuation of cervical spine immobilisation in unconscious patients with trauma in injury they recommend continuous cervical immobilisation until the patient is fully conscious in patients who intensive care units telephone survey of South and West region. BMJ 1997;314: Ajani AE, Cooper DJ, Scheinkestel J, Laidlaw J, are expected to regain consciousness within hrs Tuxen DV. Optimal assessment of cervical spine and then clinically exclude significant ligamentous trauma in critically ill patients: a prospective injury (e.g. no neck pain and no abnormal neurological evaluation. Anaesth Intensive Care 1998;26: signs or symptoms). Otherwise, a CT scan, MRI of the 4. Injuries of the Lower Cervical Spine. whole of the cervical spine or dynamic 5. Davis JW, Parks SN, Detlefs CL, Williams GG, flexion/extension under image intensifier control for patients unlikely to regain consciousness in less than Williams JL, Smith RW. Clearing the cervical spine in obtunded patients: the use of dynamic fluoroscopy. J 48 hours. 13 Trauma 1995;39: Collier AM. Discontinuation of cervical spine In our study the three most common approaches in immobilisation: Immobilisation should not be Australian intensive care units in patients who are discontinued in unconscious patients. BMJ radiologically clear but not clinically clear are: 1997;315: a) accept the risk and remove the hard-collar (around 7. Streitwieser DR, Knopp R, Wales LR, Williams JL, 30-45% of units surveyed), Tonnemacher K. Accuracy of standard radiographic b) leave the collar (hard or Philadelphia) in place and perform clinical or radiological testing when conscious (5-23% of units surveyed); or, 8. views in detecting c-spine fractures. Ann Emerg Med 1983;12: Padayachee LL, Irons SS, Cooper DJ. Evaluation of an c) attempt to exclude ligamentous injury through improved ICU cervical spine screening protocol for unconscious patients with traumatic brain injury. flexion/extension films or use of fine-cut helical Abstracts; 27 th Australian and New Zealand Annual CT and sagittal and coronal reconstruction (up to Scientific Meeting on Intensive Care. Oct % of units). 9. Borock EC, Gabram SG, Jacobs LM, Murphy MA. A CONCLUSION Our survey revealed lack of a standardised approach to the clearance of the cervical spine in intubated and sedated polytraumatised patients in major Australian intensive care units. In addition, there was a lack of written protocols and no routine surveillance for spinal board or collar morbidity. Thus, the true incidence of spinal board and collar morbidity was unclear. A significant number of intensive care units make little or no attempt to exclude ligamentous injury in intubated polytraumatised patients. We recommend formal written protocols to achieve consistency within and between units and surveillance for complications such as pressure area surveillance, collar related intracranial pressure changes, and missed neck injuries. Further studies should be undertaken to assess risk benefit analysis of clinical clearance techniques, which may also allow us to identify a specific group of head injured patients at risk of ligamentous cervical spine injury. Received: 12 March 2003 Accepted: 7 May 2003 REFERENCES 1. Bell RM. Professor of Surgery, University of South Carolina, Chairman ATLS Clearing the cervical spine. ICU Registrar Manual. prospective analysis of a two year experience using computed tomography as an adjunct for cervical clearance. J Trauma 1991;31: Ross SE, Schwab CW, David ET, Delong WG, Born CT. Clearing the cervical spine: initial radiological evaluation. J Trauma 1987; 27: Chiles B, Cooper PR. Current Concepts: Acute Spinal Injury. N Engl J Med 1996;334: Ross SE, Schwab CM, Born CT, et al. Clearing the cervical spine: Initial radiological evaluation. J Trauma 1987;27: Guidelines for Evaluation of the Cervical Spine. APPENDIX 1 QUESTIONNAIRE In your unit, 1. Do you have a protocol for cervical spine clearance in sedated, unconscious or intubated multi-trauma patients. If so, who developed and who ratified it? 2. Is there a specific time frame for cervical spine clearance, and if so what is it? 3. Who has final say on cervical spine clearance? (e.g. intensivist, neurosurgeon, orthopaedic surgeon). 4. How do you clear the cervical spine? (if no response, ask) 95
6 D. LIEN, ET AL Critical Care and Resuscitation 2003; 5: a) How is radiological clearance undertaken? (e.g. plain anteroposterior, lateral and odontoid views, swimmers, oblique views, CT with or without 2mm axial cuts and sagittal and coronal reconstruction, MRI) b) Clinical clearance (e.g. assessing dynamic flexion/extension, passive flexion/extension, awake flexion/extension) c) What is the usual method of cervical spine immobilisation in the uncleared patient? (e.g. hard collar, soft collar, sandbags, none, Philadelphia collar, Halo and jacket). What other precautions are taken? (e.g. log roll, Jordan frame, sedation/paralysis, head straps) d) Do you survey for collar related adverse events (eg pressure sores)? If not, do you think there needs to be? 5. Do you find cervical spine clearance a problem in your intensive care patients, or are you satisfied with the approach used in your unit? Thank you for participating in this survey. We hope that the results may help contribute to a higher quality of care in intensive care units in Australia. APPENDIX 2 ST GEORGE HOSPITAL INTENSIVE CARE UNIT SPINAL PROTECTION MOBILISATION PROTOCOL 1. Log roll To be used for all patents who have a suspected or definite spinal injury. Requires 4 people 1 person - maintaining the axial alignment of head & neck 3 people - maintaining body alignment - one holding the shoulder and lower chest - one holding the lower chest and hip - one holding the upper thigh and ankle A rigid cervical collar must be used. 2. Modified log roll To be used for patents who have had their spine cleared radiologically, but are awaiting soft tissue (e.g. ligamentous) clearance. Requires 2 people (may require a 3 rd person if patient tall or obese) 1 person - maintaining the axial alignment of the head and neck 1 person - maintaining body alignment (holding the shoulder and hip) May use a soft collar or Philadelphia collar if the patient has a tracheostomy. 96
Evaluation for spinal injuries among unconscious victims of blunt polytrauma: a management guideline for intensive care
 Evaluation for spinal injuries among unconscious victims of blunt polytrauma: a management guideline for intensive care Background 1.0 There is lack of consistency among clinicians when managing critically
Evaluation for spinal injuries among unconscious victims of blunt polytrauma: a management guideline for intensive care Background 1.0 There is lack of consistency among clinicians when managing critically
Determination of Cervical Spine Stability in Trauma Patients (Update of the 1997 EAST Cervical Spine Clearance Document)
 1 Determination of Cervical Spine Stability in Trauma Patients (Update of the 1997 EAST Cervical Spine Clearance Document) Cervical Spine Clearance Committee Donald Marion Robert Domeier C. Michael Dunham
1 Determination of Cervical Spine Stability in Trauma Patients (Update of the 1997 EAST Cervical Spine Clearance Document) Cervical Spine Clearance Committee Donald Marion Robert Domeier C. Michael Dunham
CERVICAL SPINE CLEARANCE
 DISCLAIMER: These guidelines were prepared by the Department of Surgical Education, Orlando Regional Medical Center. They are intended to serve as a general statement regarding appropriate patient care
DISCLAIMER: These guidelines were prepared by the Department of Surgical Education, Orlando Regional Medical Center. They are intended to serve as a general statement regarding appropriate patient care
Indications for cervical spine immobilisation: -
 Paediatric Trauma Cervical Spine Guidelines UHW Traumatic injuries of the cervical spine (C-spine) are uncommon in children. However, it is safer assume there is a cervical spine injury until examination
Paediatric Trauma Cervical Spine Guidelines UHW Traumatic injuries of the cervical spine (C-spine) are uncommon in children. However, it is safer assume there is a cervical spine injury until examination
North West London Trauma Network Spinal Pathway and Protocols
 North West London Trauma Network Spinal Pathway and Protocols 1. Spinal Clearance in the Trauma Patient Inclusions: All trauma patients who are not alert and orientated, unable to cooperate (including
North West London Trauma Network Spinal Pathway and Protocols 1. Spinal Clearance in the Trauma Patient Inclusions: All trauma patients who are not alert and orientated, unable to cooperate (including
TALK TRAUMA Clearing the C-Spine. David Ouellette
 TALK TRAUMA 2011 Clearing the C-Spine David Ouellette Case #1 - Mother / Daughter MVC 34 y/o female Dangerous mechanism CHI Mumbling incoherently Femur # - distracting injury ETOH - 22 9 y/o female Dangerous
TALK TRAUMA 2011 Clearing the C-Spine David Ouellette Case #1 - Mother / Daughter MVC 34 y/o female Dangerous mechanism CHI Mumbling incoherently Femur # - distracting injury ETOH - 22 9 y/o female Dangerous
THE ALFRED SPINAL CLEARANCE MANAGEMENT PROTOCOL (Updated: November, 2009)
 THE ALFRED SPINAL CLEARANCE MANAGEMENT PROTOCOL (Updated: November, 2009) Notice to staff at centres other than The Alfred Hospital: There is no obligation to utilise this document. However, should the
THE ALFRED SPINAL CLEARANCE MANAGEMENT PROTOCOL (Updated: November, 2009) Notice to staff at centres other than The Alfred Hospital: There is no obligation to utilise this document. However, should the
Spinal Cord Injuries: The Basics. Kadre Sneddon POS Rounds October 1, 2003
 Spinal Cord Injuries: The Basics Kadre Sneddon POS Rounds October 1, 2003 Anatomy Dorsal columntouch, vibration Corticospinal tract- UMN Anterior horn-lmn Spinothalamic tractpain, temperature (contralateral)
Spinal Cord Injuries: The Basics Kadre Sneddon POS Rounds October 1, 2003 Anatomy Dorsal columntouch, vibration Corticospinal tract- UMN Anterior horn-lmn Spinothalamic tractpain, temperature (contralateral)
Evaluation and Initial Management of Potential Traumatic Spinal Injuries
 Evaluation and Initial Management of Potential Traumatic Spinal Injuries Reference Number: NHSCT/10/268 Responsible Directorate: Acute Hospital Services Replaces (if appropriate): N/A Policy Author/Team:
Evaluation and Initial Management of Potential Traumatic Spinal Injuries Reference Number: NHSCT/10/268 Responsible Directorate: Acute Hospital Services Replaces (if appropriate): N/A Policy Author/Team:
Acute spinal cord injury
 Acute spinal cord injury Thakul Oearsakul Songklanagarind hospital Hat Yai Songkhla Introduction New SCI 10000-12000 cases Approximately 4.0-5.3 per 100000 population Common causes of traumatic SCI :Motor
Acute spinal cord injury Thakul Oearsakul Songklanagarind hospital Hat Yai Songkhla Introduction New SCI 10000-12000 cases Approximately 4.0-5.3 per 100000 population Common causes of traumatic SCI :Motor
Competency Statement: Manoeuvring an In-Patient with a Spinal or Suspected Spinal Injury.
 Competency Statement: Manoeuvring an In-Patient with a Spinal or Suspected Spinal Injury. 1 st Level 2 nd Level 3 rd level 4 th level Competently participate as part of the manoeuvring team; To turn (Log
Competency Statement: Manoeuvring an In-Patient with a Spinal or Suspected Spinal Injury. 1 st Level 2 nd Level 3 rd level 4 th level Competently participate as part of the manoeuvring team; To turn (Log
Cervical Collar Policy 2010
 Cervical Collar Policy 2010 Version 1 For implementation in 2011 1 P a g e Introduction The Australian Rugby League is committed in providing the best possible care for all players who play the game of
Cervical Collar Policy 2010 Version 1 For implementation in 2011 1 P a g e Introduction The Australian Rugby League is committed in providing the best possible care for all players who play the game of
Clearing the C-spine in Obtunded Trauma Patients Based on Admission CT: A Prospective Randomized Tria l
 Clearing the C-spine in Obtunded Trauma Patients Based on Admission CT: A Prospective Randomized Tria l Cervical Spine Research Society e-poster 45 December 3-5, 2015 Chris O Boynick MD, Tim Lonergan MD,
Clearing the C-spine in Obtunded Trauma Patients Based on Admission CT: A Prospective Randomized Tria l Cervical Spine Research Society e-poster 45 December 3-5, 2015 Chris O Boynick MD, Tim Lonergan MD,
Subaxial Cervical Spine Trauma. Introduction. Anatomic Considerations 7/23/2018
 Subaxial Cervical Spine Trauma Sheyan J. Armaghani, MD Florida Orthopedic Institute Assistant Professor USF Dept of Orthopedics Introduction Trauma to the cervical spine accounts for 5 of all spine injuries
Subaxial Cervical Spine Trauma Sheyan J. Armaghani, MD Florida Orthopedic Institute Assistant Professor USF Dept of Orthopedics Introduction Trauma to the cervical spine accounts for 5 of all spine injuries
Introduction. Objectives C-Spine: Where Are We Now? NAEMSP Medical Director Course 1/9/2013
 NAEMSP Medical Director Course 1/9/2013 Objectives C-Spine: Where Are We Now? Robert M. Domeier, MD EMS Medical Director Washtenaw/Livingston Medical Control Authority Department of Emergency Medicine
NAEMSP Medical Director Course 1/9/2013 Objectives C-Spine: Where Are We Now? Robert M. Domeier, MD EMS Medical Director Washtenaw/Livingston Medical Control Authority Department of Emergency Medicine
SPINE EVALUATION AND CLEARANCE Basic Principles
 SPINE EVALUATION AND CLEARANCE Basic Principles General 1. Entire spine is immobilized during primary survey. 2. Radiographic clearance of the spine is not required before emergent surgical procedures.
SPINE EVALUATION AND CLEARANCE Basic Principles General 1. Entire spine is immobilized during primary survey. 2. Radiographic clearance of the spine is not required before emergent surgical procedures.
Subaxial Cervical Spine Trauma
 Subaxial Cervical Spine Trauma Pooria Salari, MD Assistant Professor Of Orthopaedics Department of Orthopaedic Surgery St. Louis University School of Medicine St. Louis, Missouri, USA Initial Evaluation
Subaxial Cervical Spine Trauma Pooria Salari, MD Assistant Professor Of Orthopaedics Department of Orthopaedic Surgery St. Louis University School of Medicine St. Louis, Missouri, USA Initial Evaluation
ISPUB.COM. Fracture Through the Body of the Axis. B Johnson, N Jayasekera CASE REPORT
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 8 Number 1 B Johnson, N Jayasekera Citation B Johnson, N Jayasekera.. The Internet Journal of Orthopedic Surgery. 2007 Volume 8 Number 1. Abstract
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 8 Number 1 B Johnson, N Jayasekera Citation B Johnson, N Jayasekera.. The Internet Journal of Orthopedic Surgery. 2007 Volume 8 Number 1. Abstract
Upper Cervical Spine - Occult Injury and Trigger for CT Exam
 Upper Cervical Spine - Occult Injury and Trigger for CT Exam Main Menu Introduction Clinical clearance of C-SpineC Radiographic evaluation Norms for C-spineC Triggers for CT exam: Odontoid Lateral view
Upper Cervical Spine - Occult Injury and Trigger for CT Exam Main Menu Introduction Clinical clearance of C-SpineC Radiographic evaluation Norms for C-spineC Triggers for CT exam: Odontoid Lateral view
Spine and Spinal Cord Injury in Children
 Spine and Spinal Cord Injury in Children S. Danielle Brown, MS, RN, CNRN, SCRN Director, Research Coordination and Education Barrow Neurological Institute at Phoenix Children s Hospital Introduction Trauma
Spine and Spinal Cord Injury in Children S. Danielle Brown, MS, RN, CNRN, SCRN Director, Research Coordination and Education Barrow Neurological Institute at Phoenix Children s Hospital Introduction Trauma
Evaluation and Stabilization of the Athlete with Possible Spine Injury
 Evaluation and Stabilization of the Athlete with Possible Spine Injury Jeffrey H. Bohmer, MD, FACEP Emergency Physician Northwestern Medicine Central DuPage Hospital June 12, 2015 Introduction Goals: 1.
Evaluation and Stabilization of the Athlete with Possible Spine Injury Jeffrey H. Bohmer, MD, FACEP Emergency Physician Northwestern Medicine Central DuPage Hospital June 12, 2015 Introduction Goals: 1.
Joint Theater Trauma System Clinical Practice Guideline
 CERVICAL SPINE EVALUATION & N-SURGICAL MANAGEMENT Original Release/Approval: 1 March 2010 Note: This CPG requires an annual review Reviewed: Feb 2012 Approved: 19 Mar 2012 Supersedes: Cervical Spine Evaluation,
CERVICAL SPINE EVALUATION & N-SURGICAL MANAGEMENT Original Release/Approval: 1 March 2010 Note: This CPG requires an annual review Reviewed: Feb 2012 Approved: 19 Mar 2012 Supersedes: Cervical Spine Evaluation,
Heidi Lako-Adamson, MD, NRP, FAEMS FM Ambulance and Sanford EMS Education Medical Director
 Heidi Lako-Adamson, MD, NRP, FAEMS FM Ambulance and Sanford EMS Education Medical Director Spinal cord injury statistics. Definition of spinal motion restriction. Difference between spinal motion restriction
Heidi Lako-Adamson, MD, NRP, FAEMS FM Ambulance and Sanford EMS Education Medical Director Spinal cord injury statistics. Definition of spinal motion restriction. Difference between spinal motion restriction
11. Spinal cord injury
 11. Spinal cord injury Introduction Always think spinal (vertebral) and/or spinal cord injury (SCI) in children with trauma. Remember SCIWORA cord injury may be present without abnormalities on routine
11. Spinal cord injury Introduction Always think spinal (vertebral) and/or spinal cord injury (SCI) in children with trauma. Remember SCIWORA cord injury may be present without abnormalities on routine
Imaging of Cervical Spine Trauma
 Imaging of Cervical Spine Trauma C Craig Blackmore, MD, MPH Professor of Radiology and Adjunct Professor of Health Services University of Washington, Harborview Medical Center Salary support: AHRQ grant
Imaging of Cervical Spine Trauma C Craig Blackmore, MD, MPH Professor of Radiology and Adjunct Professor of Health Services University of Washington, Harborview Medical Center Salary support: AHRQ grant
Episode 66 Backboard and Collar Nightmares from EMU Conference. The Risks Associated with Backboard & Collar
 However, backboards and collars are not without risk: Episode 66 Backboard and Collar Nightmares from EMU Conference With Dr. Kylie Bosman Prepared by Dr., edited by Dr. Kylie Bosman & Anton Helman, May
However, backboards and collars are not without risk: Episode 66 Backboard and Collar Nightmares from EMU Conference With Dr. Kylie Bosman Prepared by Dr., edited by Dr. Kylie Bosman & Anton Helman, May
CP80 Version: V01. Acute Oncology Management Service Date approved: 8 th May 2015 Date ratified: 1 st June 2015 Review date: 1 st June 2017
 STANDARD OPERATING PROCEDURE (SOP) AND PATHWAY FOR THE MANAGEMENT OF PATIENTS WITH METASTATIC SPINAL CORD COMPRESSION (MSCC) WITHIN THE CHRISTIE (Refer to the Manchester Cancer Network MSCC Pathway flowchart)
STANDARD OPERATING PROCEDURE (SOP) AND PATHWAY FOR THE MANAGEMENT OF PATIENTS WITH METASTATIC SPINAL CORD COMPRESSION (MSCC) WITHIN THE CHRISTIE (Refer to the Manchester Cancer Network MSCC Pathway flowchart)
Cervical Spine Injury Guidelines
 6/15/2018 Cervical Spine Injury Guidelines Benjamin Oshlag, MD, CAQSM Assistant Professor of Emergency Medicine Assistant Professor of Sports Medicine Columbia University Medical Center Nothing to Disclose
6/15/2018 Cervical Spine Injury Guidelines Benjamin Oshlag, MD, CAQSM Assistant Professor of Emergency Medicine Assistant Professor of Sports Medicine Columbia University Medical Center Nothing to Disclose
Incidence And Radiography Of Upper Cervical Spine Injury In Blunt Head Injury In A Rural Hospital Setting
 ISPUB.COM The Internet Journal of Radiology Volume 9 Number 1 Incidence And Radiography Of Upper Cervical Spine Injury In Blunt Head Injury In A Rural Hospital N Mohd, M Ansari, I Shuaib, E Mohd, H Hashim
ISPUB.COM The Internet Journal of Radiology Volume 9 Number 1 Incidence And Radiography Of Upper Cervical Spine Injury In Blunt Head Injury In A Rural Hospital N Mohd, M Ansari, I Shuaib, E Mohd, H Hashim
4/19/2017. Prehospital Spinal Care: Then. Prehospital Spinal Care: Then. Prehospital Spinal Care: Then. Prehospital Spinal Care: Then. Why Immobilize?
 Management of Cervical Spine Injuries and Athletic Equipment Removal Gianluca Del Rossi, PhD, ATC Prehospital Spinal Care: Then While the exact origins of backboards in EMS are unclear, noted trauma surgeon
Management of Cervical Spine Injuries and Athletic Equipment Removal Gianluca Del Rossi, PhD, ATC Prehospital Spinal Care: Then While the exact origins of backboards in EMS are unclear, noted trauma surgeon
Spinal Trauma. Dr T G Kruger
 Spinal Trauma Dr T G Kruger Epidemiology Spine injury in 6% of trauma patients Multiple levels involved in 20% of cases 80% of spinal cord injury patients have concurrent other system injuries 41% have
Spinal Trauma Dr T G Kruger Epidemiology Spine injury in 6% of trauma patients Multiple levels involved in 20% of cases 80% of spinal cord injury patients have concurrent other system injuries 41% have
Spinal injury. Structure of the spine
 Spinal injury Structure of the spine Some understanding of the structure of the spine (spinal column) and the spinal cord is important as it helps your Neurosurgeon explain about the part of the spine
Spinal injury Structure of the spine Some understanding of the structure of the spine (spinal column) and the spinal cord is important as it helps your Neurosurgeon explain about the part of the spine
Management of Severe Traumatic Brain Injury
 Guideline for North Bristol Trust Management of Severe Traumatic Brain Injury This guideline describes the following: Initial assessment and management of the patient with head injury Indications for CT
Guideline for North Bristol Trust Management of Severe Traumatic Brain Injury This guideline describes the following: Initial assessment and management of the patient with head injury Indications for CT
Fractures of the Thoracic and Lumbar Spine
 A spinal fracture is a serious injury. Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological
A spinal fracture is a serious injury. Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological
EMS Spinal Assessment and Precautions
 EMS Spinal Assessment and Precautions Adapted from a presentation prepared by Chelsea C. White IV, MD, NREMT-P Medical Director, Bernalillo County Fire Department Robert M. Domeier, MD, EMS Medical Director,
EMS Spinal Assessment and Precautions Adapted from a presentation prepared by Chelsea C. White IV, MD, NREMT-P Medical Director, Bernalillo County Fire Department Robert M. Domeier, MD, EMS Medical Director,
CORE STANDARDS STANDARDS USED IN TARN REPORTS
 CORE STANDARDS Time to CT Scan BEST PRACTICE TARIFF SECTION 4.10 MAJOR TRAUMA 7 If the patient is admitted directly to the MTC or transferred as an emergency, the patient must be received by a trauma team
CORE STANDARDS Time to CT Scan BEST PRACTICE TARIFF SECTION 4.10 MAJOR TRAUMA 7 If the patient is admitted directly to the MTC or transferred as an emergency, the patient must be received by a trauma team
Subaxial Cervical Spine Trauma Dr Hesarikia BUMS
 Subaxial Cervical Spine Trauma Dr. Hesarikia BUMS Subaxial Cervical Spine From C3-C7 ROM Majority of cervical flexion Lateral bending Approximately 50% rotation Ligamentous Anatomy Anterior ALL, PLL, intervertebral
Subaxial Cervical Spine Trauma Dr. Hesarikia BUMS Subaxial Cervical Spine From C3-C7 ROM Majority of cervical flexion Lateral bending Approximately 50% rotation Ligamentous Anatomy Anterior ALL, PLL, intervertebral
MEDICAL CONTROL POLICY STATEMENT/ADVISORY. Re: Spinal Injury Assessment & Spinal Precautions Procedure
 MEDICAL CONTROL POLICY STATEMENT/ADVISORY No. 2015-01 Date: January 20, 2015 Re: Spinal Injury Assessment & Spinal Precautions Procedure Office of the Medical Director Noel Wagner, MD, NREMT-P 1000 Houghton
MEDICAL CONTROL POLICY STATEMENT/ADVISORY No. 2015-01 Date: January 20, 2015 Re: Spinal Injury Assessment & Spinal Precautions Procedure Office of the Medical Director Noel Wagner, MD, NREMT-P 1000 Houghton
Cervical Spine Clearance in Critical Care!
 Academic Department of Critical Care Queen Alexandra Hospital Portsmouth Cervical Spine Clearance in Critical Care! Aim To provide guidance on the management of proven or suspected cervical spine (c-spine)
Academic Department of Critical Care Queen Alexandra Hospital Portsmouth Cervical Spine Clearance in Critical Care! Aim To provide guidance on the management of proven or suspected cervical spine (c-spine)
Oral and Maxillofacial Surgeons and the seriously injured patient. Barts and The London NHS Trust
 Oral and Maxillofacial Surgeons and the seriously injured patient Barts and The London NHS Trust How do you assess this? Primary Survey A B C D E Airway & Cervical Spine Breathing & Ventilation Circulation
Oral and Maxillofacial Surgeons and the seriously injured patient Barts and The London NHS Trust How do you assess this? Primary Survey A B C D E Airway & Cervical Spine Breathing & Ventilation Circulation
Pelvic Fractures. AOCP National Course Belfast City Hospital. 11 th June D Swain BSc; FRCSI; FRCS (Orth.)
 Pelvic Fractures AOCP National Course Belfast City Hospital 11 th June 2010 Who s this bloke? Consultant orthopaedic surgeon RVH Trained in Belfast, England and Toronto Interests - pelvic and acetabular
Pelvic Fractures AOCP National Course Belfast City Hospital 11 th June 2010 Who s this bloke? Consultant orthopaedic surgeon RVH Trained in Belfast, England and Toronto Interests - pelvic and acetabular
Controversies in Spinal Immobilization
 Controversies in Spinal Immobilization Ken Berumen, BSN, MD, FACEP Medical Director El Paso Fire Department Medical Director Emergency Services District #1 Network Director EM Sierra Providence Health
Controversies in Spinal Immobilization Ken Berumen, BSN, MD, FACEP Medical Director El Paso Fire Department Medical Director Emergency Services District #1 Network Director EM Sierra Providence Health
SPINAL CORD INJURIES DR. F. DE V. THERON MUELMED/PAH HOSPITAL SPINAL UNIT 2012
 SPINAL CORD INJURIES DR. F. DE V. THERON MUELMED/PAH HOSPITAL SPINAL UNIT 2012 INTRODUCTION Mortal condition recognised since antiquity First described in the Edwin Smith papyrus 2500BC An ailment not
SPINAL CORD INJURIES DR. F. DE V. THERON MUELMED/PAH HOSPITAL SPINAL UNIT 2012 INTRODUCTION Mortal condition recognised since antiquity First described in the Edwin Smith papyrus 2500BC An ailment not
Neurosurgery (Orthopaedic PGY-1) Goals. Objectives
 Neurosurgery (Orthopaedic PGY-1) Length: 1 month of PGY-1 (Orthopaedic Designated Residents) or 1 month of PGY-2, -3, or -4 year Location: The Queen's Medical Center Primary Supervisor: William Obana,
Neurosurgery (Orthopaedic PGY-1) Length: 1 month of PGY-1 (Orthopaedic Designated Residents) or 1 month of PGY-2, -3, or -4 year Location: The Queen's Medical Center Primary Supervisor: William Obana,
Universally accepted guidelines for clearance of the cervical
 ORIGINAL ARTICLE Are rmal Multidetector Computed Tomographic Scans Sufficient to Allow Collar Removal in the Trauma Patient? Josef B. Simon, MD, Andrew J. Schoenfeld, MD, Jeffrey N. Katz, MD, MS, Atul
ORIGINAL ARTICLE Are rmal Multidetector Computed Tomographic Scans Sufficient to Allow Collar Removal in the Trauma Patient? Josef B. Simon, MD, Andrew J. Schoenfeld, MD, Jeffrey N. Katz, MD, MS, Atul
Physical and Radiographic Examination of the Spine
 Physical and Radiographic Examination of the Spine Christopher M. Bono, MD Assistant Professor, Department of Orthopaedic Surgery Boston University School of Medicine, Boston Medical Center, Boston, MA
Physical and Radiographic Examination of the Spine Christopher M. Bono, MD Assistant Professor, Department of Orthopaedic Surgery Boston University School of Medicine, Boston Medical Center, Boston, MA
Time Equals Neurons - Spinal Cord Injury Management in the first 4 Hours
 Time Equals Neurons - Spinal Cord Injury Management in the first 4 Hours William D. Whetstone M.D. Clinical Professor UCSF Department of Emergency Medicine SFGH ED Center for Neuro-Critical Emergencies
Time Equals Neurons - Spinal Cord Injury Management in the first 4 Hours William D. Whetstone M.D. Clinical Professor UCSF Department of Emergency Medicine SFGH ED Center for Neuro-Critical Emergencies
Fall-related hip fracture in NSW Epidemiology, evidence, practice and the future
 Fall-related hip fracture in NSW Epidemiology, evidence, practice and the future Jacqueline CT Close Orthogeriatrician, Prince of Wales Hospital Director - Falls and Injury Prevention Group Neuroscience
Fall-related hip fracture in NSW Epidemiology, evidence, practice and the future Jacqueline CT Close Orthogeriatrician, Prince of Wales Hospital Director - Falls and Injury Prevention Group Neuroscience
Pre-hospital Response to Trauma and Brain Injury. Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center
 Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
17. Imaging and interventional radiology
 17. Imaging and interventional radiology These guidelines have been adapted from the Leeds Major Trauma Centre Imaging in Paediatric Major Trauma guidelines Written by Dr Annmarie Jeanes (Consultant Paediatric
17. Imaging and interventional radiology These guidelines have been adapted from the Leeds Major Trauma Centre Imaging in Paediatric Major Trauma guidelines Written by Dr Annmarie Jeanes (Consultant Paediatric
Spinal or Suspected Spinal, Injury: Logrolling Technique with C- Spine Precautions
 Approved by: Spinal or Suspected Spinal, Injury: Logrolling Technique with C- Spine Precautions Vice President and Chief Medical Officer; and Vice President and Chief Operating Officer Corporate Policy
Approved by: Spinal or Suspected Spinal, Injury: Logrolling Technique with C- Spine Precautions Vice President and Chief Medical Officer; and Vice President and Chief Operating Officer Corporate Policy
Kinematic Cervical Spine Magnetic Resonance Imaging in Low-Impact Trauma Assessment
 Kinematic Cervical Spine Magnetic Resonance Imaging in Low-Impact Trauma Assessment 1 Seminars in Ultrasound, CT, and MRI June 2009; Volume 30; Number 3; pp. 168-173 Vincenzo Giuliano, MD, Antonio Pinto,
Kinematic Cervical Spine Magnetic Resonance Imaging in Low-Impact Trauma Assessment 1 Seminars in Ultrasound, CT, and MRI June 2009; Volume 30; Number 3; pp. 168-173 Vincenzo Giuliano, MD, Antonio Pinto,
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 17 Orthopedic Techniques Key Points 2 17.1 Traction Use an appropriate method of traction to treat fractures of the extremities and cervical spine Apply extremity
Surgical Care at the District Hospital 1 17 Orthopedic Techniques Key Points 2 17.1 Traction Use an appropriate method of traction to treat fractures of the extremities and cervical spine Apply extremity
A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint
 J Orthop Sci (2012) 17:189 193 DOI 10.1007/s00776-011-0082-y CASE REPORT A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint Kei Shinohara Shigeru Soshi
J Orthop Sci (2012) 17:189 193 DOI 10.1007/s00776-011-0082-y CASE REPORT A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint Kei Shinohara Shigeru Soshi
SPINAL IMMOBILIZATION
 Spinal Immobilization Decision Assessment Recent studies have shown an increase in mortality for patients with isolated penetrating trauma who are spinally immobilized. Therefore spinal immobilization
Spinal Immobilization Decision Assessment Recent studies have shown an increase in mortality for patients with isolated penetrating trauma who are spinally immobilized. Therefore spinal immobilization
Update on Management of Malignant Spinal Cord Compression. Heino Hugel Consultant in Palliative Medicine University Hospital Aintree
 Update on Management of Malignant Spinal Cord Compression Heino Hugel Consultant in Palliative Medicine University Hospital Aintree Current Guidelines The symptoms of MSCC may be subtle and therefore careful
Update on Management of Malignant Spinal Cord Compression Heino Hugel Consultant in Palliative Medicine University Hospital Aintree Current Guidelines The symptoms of MSCC may be subtle and therefore careful
Expert Group Meeting-Trauma
 Why was Trauma Summit needed? There are no clear guidelines/algorithms to assist acute management of trauma patients in the Indian setting. One of our visions is to assist young doctors in acute care medicine
Why was Trauma Summit needed? There are no clear guidelines/algorithms to assist acute management of trauma patients in the Indian setting. One of our visions is to assist young doctors in acute care medicine
Selective Spine Assessment & Spinal Motion Restriction
 Selective Spine Assessment & Spinal Motion Restriction Supersedes: 02-09-15 Effective: 10-20-15 Spinal cord injury may be the result of direct blunt and/or penetrating trauma, compression forces (axial
Selective Spine Assessment & Spinal Motion Restriction Supersedes: 02-09-15 Effective: 10-20-15 Spinal cord injury may be the result of direct blunt and/or penetrating trauma, compression forces (axial
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT
 SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
Trauma resuscitation in the Elderlyfrom a physiological perspective
 6 November 2017 Trauma resuscitation in the Elderlyfrom a physiological perspective Joseph Mathew Consultant, Emergency/ 6 November 2017 2 http://www.who.int/ageing/publications/global_health.pdf 6 November
6 November 2017 Trauma resuscitation in the Elderlyfrom a physiological perspective Joseph Mathew Consultant, Emergency/ 6 November 2017 2 http://www.who.int/ageing/publications/global_health.pdf 6 November
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedures overview of direct C1 lateral mass screw procedure for cervical spine stabilisation Introduction
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedures overview of direct C1 lateral mass screw procedure for cervical spine stabilisation Introduction
Regions Hospital Delineation of Privileges Orthopaedic Surgery
 Regions Hospital Delineation of Orthopaedic Surgery Applicant s Last First M. Instructions: Place a check-mark where indicated for each core group you are requesting. Review education and basic formal
Regions Hospital Delineation of Orthopaedic Surgery Applicant s Last First M. Instructions: Place a check-mark where indicated for each core group you are requesting. Review education and basic formal
Activity Three: Where s the Bleeding?
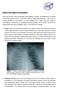 Activity Three: Where s the Bleeding? There are five main sites of potentially fatal bleeding in trauma, remembered by the phrase on the floor and four more. On the floor refers to losing blood externally
Activity Three: Where s the Bleeding? There are five main sites of potentially fatal bleeding in trauma, remembered by the phrase on the floor and four more. On the floor refers to losing blood externally
Rheumatoid Arthritis and the Cervical Spine. Radiology Rounds November 21, 2006 Derek Haaland
 Rheumatoid Arthritis and the Cervical Spine Radiology Rounds November 21, 2006 Derek Haaland Laiho et al. Semin Arthritis Rheum. 2004:34;267. Laiho et al. Semin Arthritis Rheum. 2004:34;267. *Shen et al.
Rheumatoid Arthritis and the Cervical Spine Radiology Rounds November 21, 2006 Derek Haaland Laiho et al. Semin Arthritis Rheum. 2004:34;267. Laiho et al. Semin Arthritis Rheum. 2004:34;267. *Shen et al.
VAriation. Orthotics and Me (?surgeons) Greg Etherington Spine Surgeon. Orthopaedic & Neurosurgery backgrounds. Subspeciality training
 Orthotics and Me (?surgeons) Greg Etherington Spine Surgeon Orthopaedic & Neurosurgery backgrounds Subspeciality training spine, upper limb, trauma, pelvis. What do you do in spine? Lumbar Cervical Trauma
Orthotics and Me (?surgeons) Greg Etherington Spine Surgeon Orthopaedic & Neurosurgery backgrounds Subspeciality training spine, upper limb, trauma, pelvis. What do you do in spine? Lumbar Cervical Trauma
Other methods for maintaining the airway (not definitive airway as still unprotected):
 Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Overview. Background. Table of Contents
 Trauma Service Guidelines Title: Cervical Spine Guidelines Developed by: P. Page, R. Judson, K. Gumm, M. Kennedy, D. McDonald & Advisory Committee on Trauma Created: Version 1.0 October 2005, Revised:
Trauma Service Guidelines Title: Cervical Spine Guidelines Developed by: P. Page, R. Judson, K. Gumm, M. Kennedy, D. McDonald & Advisory Committee on Trauma Created: Version 1.0 October 2005, Revised:
Spinal, or Suspected Spinal Injury
 Approved by: Spinal, or Suspected Spinal Injury Vice President and Chief Medical Officer; and Vice President and Chief Operating Officer Corporate Policy & Procedures Manual Number: VII-B-150 Date Approved
Approved by: Spinal, or Suspected Spinal Injury Vice President and Chief Medical Officer; and Vice President and Chief Operating Officer Corporate Policy & Procedures Manual Number: VII-B-150 Date Approved
Each year, approximately 12,000 people in the US
 J Neurosurg Spine 14:341 347, 2011 The role of flexion and extension computed tomography with reconstruction in clearing the cervical spine in trauma patients: a pilot study Clinical article Rishi Wadhwa,
J Neurosurg Spine 14:341 347, 2011 The role of flexion and extension computed tomography with reconstruction in clearing the cervical spine in trauma patients: a pilot study Clinical article Rishi Wadhwa,
X-ray (Radiography) - Bone
 Scan for mobile link. X-ray (Radiography) - Bone Bone x-ray uses a very small dose of ionizing radiation to produce pictures of any bone in the body. It is commonly used to diagnose fractured bones or
Scan for mobile link. X-ray (Radiography) - Bone Bone x-ray uses a very small dose of ionizing radiation to produce pictures of any bone in the body. It is commonly used to diagnose fractured bones or
Cervical laminectomy for spinal cord compression. Information for patients Neurosurgery
 Cervical laminectomy for spinal cord compression Information for patients Neurosurgery What is a compression of the spinal cord and how has it been caused? The bones in our back are called vertebras and
Cervical laminectomy for spinal cord compression Information for patients Neurosurgery What is a compression of the spinal cord and how has it been caused? The bones in our back are called vertebras and
All bedside percutaneously placed tracheostomies
 Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
Major Trauma Scenarios. Ballarat Health Services Emergency Medicine Training Hub
 Major Trauma Scenarios Ballarat Health Services Emergency Medicine Training Hub Trauma Scenario 1 You receive a phone call from the ambulance service. They have a 27 yr old male involved in a MCA, he is
Major Trauma Scenarios Ballarat Health Services Emergency Medicine Training Hub Trauma Scenario 1 You receive a phone call from the ambulance service. They have a 27 yr old male involved in a MCA, he is
Head injuries. Severity of head injuries
 Head injuries ED Teaching day 23 rd October Severity of head injuries Minor GCS 14-15 Must not have any of the following: Amnesia 10min Neurological sign or symptom Skull fracture (clinically or radiologically)
Head injuries ED Teaching day 23 rd October Severity of head injuries Minor GCS 14-15 Must not have any of the following: Amnesia 10min Neurological sign or symptom Skull fracture (clinically or radiologically)
3/10/17 Spinal a Injury 1
 Spinal Injury 1 'Paralysed' Watmough vows he'll have the backbone for Game Two after treatment for neck injury Watmough will have cortisone injected into his spine this morning to speed up the recovery
Spinal Injury 1 'Paralysed' Watmough vows he'll have the backbone for Game Two after treatment for neck injury Watmough will have cortisone injected into his spine this morning to speed up the recovery
Outline. Epidemiology Indications for C-spine imaging Modalities Interpretation Types of fractures
 C-Spine Plain Films Outline Epidemiology Indications for C-spine imaging Modalities Interpretation Types of fractures Epidemiology 7000-10000 c-spine injuries treated each year Additional 5000 die at the
C-Spine Plain Films Outline Epidemiology Indications for C-spine imaging Modalities Interpretation Types of fractures Epidemiology 7000-10000 c-spine injuries treated each year Additional 5000 die at the
CERVICAL SPINE INJURY. Narain Chotirosniramit MD. Trauma and critical care unit Department of surgery Faculty of medicine Chiangmai University
 CERVICAL SPINE INJURY Narain Chotirosniramit MD. Trauma and critical care unit Department of surgery Faculty of medicine Chiangmai University NEUROLOGICAL ASSESSMENT AIRWAY MANEUVERS ON C-SPINE MOVEMENT
CERVICAL SPINE INJURY Narain Chotirosniramit MD. Trauma and critical care unit Department of surgery Faculty of medicine Chiangmai University NEUROLOGICAL ASSESSMENT AIRWAY MANEUVERS ON C-SPINE MOVEMENT
Radiology. General radiology department. X-ray
 The radiology directorate provides a diagnostic, interventional and therapeutic service for its local population, and a tertiary service for the region. It also provides support to some national work such
The radiology directorate provides a diagnostic, interventional and therapeutic service for its local population, and a tertiary service for the region. It also provides support to some national work such
CERVICAL SPINE INJURIES IN THE ELDERLY
 CERVICAL SPINE INJURIES IN THE ELDERLY ISADOR H. LIEBERMAN, JOHN K. WEBB From University Hospital, Queen s Medical Centre, Nottingham, England We reviewed 41 patients over the age of 65 years (mean 76.5)
CERVICAL SPINE INJURIES IN THE ELDERLY ISADOR H. LIEBERMAN, JOHN K. WEBB From University Hospital, Queen s Medical Centre, Nottingham, England We reviewed 41 patients over the age of 65 years (mean 76.5)
Injuries to the cervical spine occur in 2.0 to 6.6% of blunt
 Review Article The Journal of TRAUMA Injury, Infection, and Critical Care Magnetic Resonance Imaging for Clearing the Cervical Spine in Unconscious Intensive Care Trauma Patients Helen M. Ackland, MHSc,
Review Article The Journal of TRAUMA Injury, Infection, and Critical Care Magnetic Resonance Imaging for Clearing the Cervical Spine in Unconscious Intensive Care Trauma Patients Helen M. Ackland, MHSc,
Posterior cervical fusion in children
 Posterior cervical fusion in children JOE M. MCWHORTER, M.D., EBEN ALEXANDER, JR., M.D., COURTLAND H. DAVIS, JR., M.D., AND DAVID L. KELLY, JR., M.D. Section on Neurosurgery, Department of Surgery, Bowman
Posterior cervical fusion in children JOE M. MCWHORTER, M.D., EBEN ALEXANDER, JR., M.D., COURTLAND H. DAVIS, JR., M.D., AND DAVID L. KELLY, JR., M.D. Section on Neurosurgery, Department of Surgery, Bowman
Cervical Spine Injury: A Clinical Decision Rule to Identify High-Risk Patients for Helical CT Screening
 Julian A. Hanson 1 C. Craig Blackmore 1,2 Frederick A. Mann 1 Anthony J. Wilson 1 Received July 2, 1999; accepted after revision August 31, 1999. 1 Department of Radiology, Harborview Medical Center, University
Julian A. Hanson 1 C. Craig Blackmore 1,2 Frederick A. Mann 1 Anthony J. Wilson 1 Received July 2, 1999; accepted after revision August 31, 1999. 1 Department of Radiology, Harborview Medical Center, University
Injury to the cervical spine (CS) occurs frequently after
 CLINICAL MANAGEMENT UPDATE Practice Management Guidelines for Identification of Cervical Spine Injuries Following Trauma: Update From the Eastern Association for the Surgery of Trauma Practice Management
CLINICAL MANAGEMENT UPDATE Practice Management Guidelines for Identification of Cervical Spine Injuries Following Trauma: Update From the Eastern Association for the Surgery of Trauma Practice Management
Standardize comprehensive care of the patient with severe traumatic brain injury
 Trauma Center Practice Management Guideline Iowa Methodist Medical Center Des Moines Management of Patients with Severe Traumatic Brain Injury (GCS < 9) ADULT Practice Management Guideline Contact: Trauma
Trauma Center Practice Management Guideline Iowa Methodist Medical Center Des Moines Management of Patients with Severe Traumatic Brain Injury (GCS < 9) ADULT Practice Management Guideline Contact: Trauma
Trauma CT Scanning Protocol
 Northern Trauma Network Trauma CT Scanning Protocol Background Whole body CT (WBCT) has assumed a pivotal position in trauma management. UK trauma is typically described as blunt and blind i.e. blunt trauma
Northern Trauma Network Trauma CT Scanning Protocol Background Whole body CT (WBCT) has assumed a pivotal position in trauma management. UK trauma is typically described as blunt and blind i.e. blunt trauma
Wounds and Injuries of the Spinal Column and Cord
 Wounds and Injuries of the Spinal Column and Cord Chapter 20 Wounds and Injuries of the Spinal Column and Cord Introduction Combat injuries of the spinal column, with or without associated spinal cord
Wounds and Injuries of the Spinal Column and Cord Chapter 20 Wounds and Injuries of the Spinal Column and Cord Introduction Combat injuries of the spinal column, with or without associated spinal cord
Cervical Spine Clearance Protocols
 Cervical Spine Clearance Protocols Spinal Interest Group 2018 3 rd March, 2018 Dr Helen Ackland, PhD Senior Clinical Trauma Research Fellow, National Trauma Research Institute, The Alfred Senior Lecturer,
Cervical Spine Clearance Protocols Spinal Interest Group 2018 3 rd March, 2018 Dr Helen Ackland, PhD Senior Clinical Trauma Research Fellow, National Trauma Research Institute, The Alfred Senior Lecturer,
Cervical spine. Assessment following trauma. Clinical assessment. Background. Objective. Discussion. Keywords. Helen Ackland Peter Cameron
 Child Injuries development Helen Ackland Peter Cameron Cervical spine Assessment following trauma Background Although cervical spine trauma is more common following high velocity mechanisms of injury resulting
Child Injuries development Helen Ackland Peter Cameron Cervical spine Assessment following trauma Background Although cervical spine trauma is more common following high velocity mechanisms of injury resulting
Chapter 24 Spinal Trauma Introduction to Spinal Injuries (1 of 2) Annually 15,000 permanent spinal cord injuries Commonly men years old
 1 2 3 4 5 6 7 Chapter 24 Spinal Trauma Introduction to Spinal Injuries (1 of 2) Annually 15,000 permanent spinal cord injuries Commonly men 16-30 years old Mechanism of Injury: Vehicle crashes: 48% : 21%
1 2 3 4 5 6 7 Chapter 24 Spinal Trauma Introduction to Spinal Injuries (1 of 2) Annually 15,000 permanent spinal cord injuries Commonly men 16-30 years old Mechanism of Injury: Vehicle crashes: 48% : 21%
Contributors. Thanks to Peter Miller, MD; LCDR Kevin Preston, MD; and Keith Newbrough, MD for their generous contribution of images:
 Contributors Thanks to Peter Miller, MD; LCDR Kevin Preston, MD; and Keith Newbrough, MD for their generous contribution of images: Peter Miller, MD, Indiana University School of Medicine Chapter 1: Figure
Contributors Thanks to Peter Miller, MD; LCDR Kevin Preston, MD; and Keith Newbrough, MD for their generous contribution of images: Peter Miller, MD, Indiana University School of Medicine Chapter 1: Figure
Dr. Richard Smith 26/04/16
 BENDIGO HEALTH EMERGENCY DEPARTMENT Spinal Trauma Clinical Practice Guidelines Dr. Richard Smith 26/04/16 1 Contents PURPOSE... 3 PREAMBLE... 3 POLICY... 4 INITIAL CLINICAL MANAGEMENT... 5 Basic exam components...
BENDIGO HEALTH EMERGENCY DEPARTMENT Spinal Trauma Clinical Practice Guidelines Dr. Richard Smith 26/04/16 1 Contents PURPOSE... 3 PREAMBLE... 3 POLICY... 4 INITIAL CLINICAL MANAGEMENT... 5 Basic exam components...
Spinal Trauma at the Pediatric Age
 Spinal Trauma at the Pediatric Age Burçak B LG NER Nejat AKALAN ABSTRACT Spinal trauma is relatively rare in pediatric patients. The anatomy and biomechanics of the growing spine produce failure patterns
Spinal Trauma at the Pediatric Age Burçak B LG NER Nejat AKALAN ABSTRACT Spinal trauma is relatively rare in pediatric patients. The anatomy and biomechanics of the growing spine produce failure patterns
Misdiagnosis in cervical spondylosis myelopathy.
 Journal of the International Society of Head and Neck Trauma (ISHANT) Case report Misdiagnosis in cervical spondylosis myelopathy. Dr. Reinel A. Junco Martin. Neurosurgeon. Assistant professor Miguel Enriquez
Journal of the International Society of Head and Neck Trauma (ISHANT) Case report Misdiagnosis in cervical spondylosis myelopathy. Dr. Reinel A. Junco Martin. Neurosurgeon. Assistant professor Miguel Enriquez
Medical evidence-based guidelines, when
 TOPIC Introduction to the Guidelines for the Management of Acute Cervical Spine and Spinal Cord Injuries Mark N. Hadley, MD* Beverly C. Walters, MD, MSc, FRCSC *Co-Lead Author, Guidelines Author Group;
TOPIC Introduction to the Guidelines for the Management of Acute Cervical Spine and Spinal Cord Injuries Mark N. Hadley, MD* Beverly C. Walters, MD, MSc, FRCSC *Co-Lead Author, Guidelines Author Group;
Immobilizing the spine New national approach
 NORWEGIAN NATIONAL ADVISORY UNIT ON TRAUMA Immobilizing the spine New national approach Torben Wisborg, MD, PhD Director Norwegian National Advisory Unit on Trauma Professor, University of Tromsø Consultant
NORWEGIAN NATIONAL ADVISORY UNIT ON TRAUMA Immobilizing the spine New national approach Torben Wisborg, MD, PhD Director Norwegian National Advisory Unit on Trauma Professor, University of Tromsø Consultant
Spine MRI and Spine CT Test Request Tip Sheet
 Spine MRI and Spine CT With/Without Contrast CT, MRI The study considered best for a specific clinical scenario should be ordered. The second study should be done ONLY if the first study does not provide
Spine MRI and Spine CT With/Without Contrast CT, MRI The study considered best for a specific clinical scenario should be ordered. The second study should be done ONLY if the first study does not provide
Cervical Spine Clearance in Obtunded Blunt Trauma Patients: A Prospective Study
 ORIGINAL ARTICLE Cervical Spine Clearance in Obtunded Blunt Trauma Patients: A Prospective Study Deirdre Hennessy, MSc, Sandy Widder, MD, FRCSC, David Zygun, MD, MSc, FRCPC, R. John Hurlbert, MD, FRSCS,
ORIGINAL ARTICLE Cervical Spine Clearance in Obtunded Blunt Trauma Patients: A Prospective Study Deirdre Hennessy, MSc, Sandy Widder, MD, FRCSC, David Zygun, MD, MSc, FRCPC, R. John Hurlbert, MD, FRSCS,
Resuscitation lateral cervical spine X-ray (LSCX): A useful mandatory screening tool in acute trauma?
 Resuscitation lateral cervical spine X-ray (LSCX): A useful mandatory screening tool in acute trauma? Poster No.: C-2397 Congress: ECR 2010 Type: Topic: Authors: Keywords: DOI: Scientific Exhibit Musculoskeletal
Resuscitation lateral cervical spine X-ray (LSCX): A useful mandatory screening tool in acute trauma? Poster No.: C-2397 Congress: ECR 2010 Type: Topic: Authors: Keywords: DOI: Scientific Exhibit Musculoskeletal
2. Blunt abdominal Trauma
 Abdominal Trauma 1. Evaluation and management depends on: a. Mechanism (Blunt versus Penetrating) b. Injury complex in addition to abdomen c. Haemodynamic stability assessment: i. Classically patient s
Abdominal Trauma 1. Evaluation and management depends on: a. Mechanism (Blunt versus Penetrating) b. Injury complex in addition to abdomen c. Haemodynamic stability assessment: i. Classically patient s
