Neuropsychiatric features of corticobasal degeneration
|
|
|
- Doreen Brooks
- 6 years ago
- Views:
Transcription
1 J Neurol Neurosurg Psychiatry 1998;65: Neuropharmacology Unit, Defense and Veteran Head Injury Program, Jackson Foundation and the Medical Neurology Branch I Litvan National Institutes of Neurological Disorders and Stroke, National Institutes of Health, Bethesda, Maryland, USA I Litvan Department of Neurology J L Cummings M Mega Department of Psychiatry and Biobehavioral Science, UCLA School of Medicine, Los Angeles, CA, USA J L Cummings Correspondence to: Dr Irene Litvan, NINDS, NIH, Federal Building, Room 714, Bethesda, MD , USA. Telephone ; fax Received 2 February 1998 and in revised form 27 April 1998 Accepted 7 May 1998 Neuropsychiatric features of corticobasal degeneration Irene Litvan, JeVrey L Cummings, Michael Mega Abstract Objective To characterise the neuropsychiatric symptoms of patients with corticobasal degeneration (CBD). Methods The neuropsychiatric inventory (NPI), a tool with established validity and reliability, was administered to 15 patients with CBD (mean (SEM), age 67.9 (2) years); 34 patients with progressive supranuclear palsy (PSP) (66.6 (1.2) years); and 25 controls (70 (0.8) years), matched for age and education. Both patient groups had similar duration of symptoms and mini mental state examination scores. Semantic fluency and motor impairment were also assessed. Results Patients with CBD exhibited depression (73%), apathy (40%), irritability (20%), and agitation (20%) but less often had anxiety, disinhibition, delusions, or aberrant motor behaviour (for example, pacing). The depression and irritability of patients with CBD were more frequent and severe than those of patients with PSP. Conversely, patients with PSP exhibited significantly more apathy than patients with CBD. The presence of high depression and irritability and low apathy scale scores correctly diverentiated the patients with CBD 88% of the time. The irritability of patients with CBD was significantly associated with disinhibition (r=0.85) and apathy (r=0.72). In CBD, apathy was associated with disinhibition (r=0.67); disinhibition was associated with aberrant motor behaviour (r=0.68) and apathy (r=0.67); and aberrant motor behaviour with delusions (r=1.0). On the other hand, depression was not associated with any other behaviour, suggesting that it has a diverent pathophysiological mechanism. Symptom duration was associated with total motor scores (r=0.69). However, total motor score was not associated with any behaviour or cognitive scores. Conclusions The findings indicate that frontosubcortical pathways mediating cognition, emotion, and motor function in CBD are not avected in parallel. Patients with CBD and PSP have overlapping neuropsychiatric manifestations, but they express distinctive symptom profiles. Evaluating the behavioural abnormalities of parkinsonian patients may help clarify the role of the basal ganglia in behaviour. (J Neurol Neurosurg Psychiatry 1998;65: ) Keywords: corticobasal degeneration; progressive supranuclear palsy; neurobehaviour Corticobasal degeneration (CBD) is a neurodegenerative disorder characterised clinically by steadily progressive motor (for example, dystonia, asymmetric parkinsonism not benefitting from levodopa therapy, myoclonus, balance disturbances, and pyramidal signs) and cognitive (for example, ideomotor apraxia, alien hand syndrome, aphasia, visual and sensory neglect) disturbances presenting after the age of Neuropathologically, it features circumscribed parietal or frontoparietal atrophy, severe cortical neuronal loss, and intense astrogliosis, spongiosis, swollen and achromatic neurons (ballooned cells), neuropil threads, and occasionally, neurofibrillary tangles. In addition, basophilic argyrophilic and tau protein positive inclusions are found in the neurons of the substantia nigra and basal ganglia (subthalamic nucleus, striatum, and pallidum), and also may be present along the dentatorubrothalamic tracts. Feany and Dickson 3 recently described the astrocytic plaque as being pathognomonic of this disorder. Clinical and neuropathological variations have been described which overlap with progressive supranuclear palsy (PSP) and Pick s disease Several studies have characterised the motor and cognitive features of CBD, but the patients neuropsychiatric symptoms have rarely been described. Neuropsychiatric symptoms are important predictors of burden of the caregiver and the potential for admitting patients to institutions Thus identification and treatment of the associated behavioural abnormalities may be relevant for improving the quality of life of patients with CBD and their caregivers. In addition, increasing insight into the neurobiological basis of neuropsychiatric disorders facilitates understanding how behaviourally relevant circuits are involved in CBD. We administered the neuropsychiatric inventory (NPI), a tool with established validity and reliability, to assess the behavioural abnormalities of patients with CBD. 21 The NPI evaluates both the frequency and severity of 10 behaviours that are commonly reported in patients with cognitive disturbances: delusions, hallucinations, agitation, depression, anxiety, euphoria, apathy, disinhibition, irritability, and aberrant motor behaviour (for example, pacing). To better characterise the behavioural aspects of patients with CBD and to search for distinctive behavioural characteristics, we compared their performance on the NPI to that of a group of patients with PSP of similar age, education, and cognitive impairment and to age matched normal controls.
2 718 Litvan, Cummings, Mega Table 1 Characteristics Demographics of study group Corticobasal degeneration (n=15) Progressive supranuclear palsy (n=34) Healthy controls (n=25) Age (y) 67.9 (2) 66.6 (1.2) 70 (0.8) Sex 8M/7F 23M/11F 14M/11F Education (y) 14.3 (0.8) 14.4 (0.5) 13.2 (0.4) Duration (months) 46.5 (5.7) 52 (4.5) Mini mental state examination score 26.1 (1.2) 26 (0.8)* 28.6 (0.3) Total Mattis dementia rating scale score (4.2) (2.4) Total UPDRS motor scores 26.2 (2)* 21.2 (1.3) Data are presented as mean (SEM). UPDRS=unified Parkinson s disease rating scale score; UPDRS maximum score was 54, and included only motor evaluation of axial and most avected limb (bradykinesia, rigidity, tremor, or dystonia). *Patients with progressive supranuclear palsy had a significantly lower (worse) mini mental state examination score than controls (ANOVA, p<0.05), patients with corticobasal degeneration had a higher (worse) total motor score than those with progressive supranuclear palsy (p<0.05). The score of normal controls, not tested in this study with the Mattis dementia rating scale score, is >136. This analysis included 12 patients with corticobasal degeneration and 28 with progressive supranuclear palsy. Subjects and methods Fifteen patients with CBD and 34 with PSP, presenting to the National Institutes of Neurological Disorders and Stroke (NINDS) as outpatients, participated in the study (table 1). The patients with CBD were diagnosed according to the modified criteria of Lang et al. 4 which included a progressive course of an asymmetric parkinsonism not benefiting from levodopa therapy; the presence of either a dystonic limb or focal myoclonus; the presence of either ideomotor apraxia, alien limb syndrome, or cortical sensory loss; and absence of resting tremor, autonomic disturbance, or laboratory evidence of other disorders. The diagnosis of one of the 15 patients with CBD was later confirmed by necropsy. The PSP study subjects met the NINDS-Society for PSP, Inc (NINDS- PSP) clinical research criteria and 22 have previously been reported on. 22 Twenty five normal controls of the same age and educational levels were recruited at the University of California, Los Angeles (table 1). 21 Exclusion criteria for all subjects and patients comprised history of alcohol or substance misuse, head trauma with loss of consciousness, and psychiatric disorder preceding the onset of current disease. All participating subjects gave institutional consent. Caregivers and participating subjects were interviewed with the NPI, but as previously described, 21 the NPI is based on caregivers information. Briefly, screening questions for each behaviour were posed first, and if a positive response was obtained for one of the 10 neuropsychiatric domains, then this aspect was further explored with scripted questions. The behaviours were rated using a scale for the frequency (1 being occasionally, 2 often, 3 frequently, and 4 very frequently) and for the severity (1 being mild, 2 moderate, and 3 marked). The composite score for each behavioural domain is the product of the frequency and severity subscore for that particular behaviour (maximum 12). The total score of the NPI is the sum of the subscales scores. In addition, we administered the mini mental state examination (MSSE) 23 to all subjects, and the Mattis dementia rating scale 24 to 12 of the 15 patients with CBD and to 28 of 34 with PSP. There were no significant diverences between patients that were administered the Mattis dementia rating scale and those that were not, (age, education, MMSE scores, symptom duration, and motor scores). Verbal fluency (semantic fluency: number of names of items from a supermarket and phonemic fluency: number of words starting with the letter F, produced in one minute), and motor impairment (modified unified Parkinson s disease rating scale total motor score (UPDRS) 25 ) were assessed in the patients. We computed the motor function axially and in the most affected limb. Both patient groups had similar symptom duration, MMSE, and Mattis dementia rating scale scores, but the patients with CBD had a higher UPDRS total motor score (table 1). Statistical analyses included bootstrap analysis, analysis of variance (ANOVA), logistic regression, and discriminant function analyses. A histogram of NPI data disclosed that composite scores do not generate a normal distribution. Multiplying the frequency (1 4) by the severity (1 3) subscores will not produce a 5, 7, or 11 composite score. The use of nonparametric analysis (for example, the Mann- Whitney U test) partially accommodates such skewed data but results in a loss of power. Because NPI data generate a non-normal distribution, precluding traditional parametric analysis, a bootstrap analysis 26 was employed. The program Resampling Stats was used to evaluate significant diverences among patient groups mean composite scores for each of the 10 NPI behaviours. Bootstrap analysis combines the raw composite scores for any given behaviour of the entire dataset and randomly samples a number of these scores equal to the number making up the groups comprising the data set. A mean diverence composite score is then calculated from the randomly comprised samples. This is then repeated 1000 times on the dataset, producing a distribution of possible mean diverence composite scores. The mean diverences found can then be compared to this distribution of the possible mean diverence composite scores between two clinical groups for each behaviour on the NPI. The probability of finding the observed mean diverence based on the mean diverence generated by resampling is then recorded. This process was repeated 10 times for each of the 10 NPI behaviours to arrive at an average probability value for each comparison. If the observed diverence was greater than 95% of the diverences expected from random resampling in the bootstrap method, it was judged to be significant at the 0.05 level. To explore the relations among the diverent behaviours, symptom duration, and motor and overall cognitive functions, Spearman correlation coeycients were calculated for the composite scores of these, in a matrix for all patients with CBD (table 2). This exploratory analysis was not meant to establish strict significance, and thus a type 1 error was deemed preferable to missing a possible correlation (type 2 error). For this reason, no Bonferroni adjustment was made; however, an adjusted α level of 0.01 was required for significance.
3 Neuropsychiatric features of corticobasal degeneration 719 Table 2 Correlations of neuropsychiatric inventory (NPI) composite scores, motor, and global cognitive scores in corticobasal degeneration Depression Apathy Irritability Agitation Anxiety Disinhibition Delusions Results Patients with CBD exhibited depression (73%), apathy (40%), irritability (20%) and agitation (20%), but rarely (<14%) anxiety, disinhibition, delusions, or aberrant motor behaviour (table 3). No patient with CBD manifested euphoria or hallucinations. The depression and irritability of patients with CBD were significantly more frequent and severe than those of patients with PSP and normal controls. However, those with PSP exhibited significantly more apathy. The other behaviours were similar in the two patient groups (table 3). Logistic regression analysis indicated a significantly higher frequency of depression (χ 2 =13, p<0.001, odds ratio=1299) and irritability (χ 2 =15.4, p<0.001; odds ratio=27 065) and lower apathy (χ 2 =22; p<0.0001; odds ratio=0.0001) in patients with CBD compared with patients with PSP (overall model, 39.4; p<0.0001). A discriminant function analysis performed on the patient data set (CBD and PSP) disclosed that any patient with high depression and irritability scale scores and low apathy composite scores would be placed correctly in the CBD group 88% of the time in this patient sample (sensitivity 67%, specificity 97%, overall accuracy 88%). The irritability of patients with CBD was significantly associated with disinhibition and apathy (table 2). Their apathy was associated with disinhibition and anxiety; their disinhibition was associated with aberrant motor behaviour and delusions; their delusions were Aberrant motor behaviour Total NPI Duration Motor score MMSE MDRS Depression Apathy 0.05 Irritability ** Agitation Anxiety Disinhibition * 0.85*** Delusions ** 0.68** Aberrant motor behaviour ** 0.68** 1.0*** Total NPI score * Duration Motor score ** MMSE MDRS ** Verbal fluency Adjusted α= 0.01 was required for significance. p<0.03; *p<0.01; **p<0.005; ***p< Table 3 Mean (SEM, %) neuropsychiatric inventory (NPI) composite scores (maximum 12) of individual symptoms of patients with corticobasal degeneration and progressive supranuclear palsy, and healthy controls Behaviour (NPI composite scores) Corticobasal degeneration (n=15) Progressive supranuclear palsy (n=34) Healthy controls (n=25) Depression 3.4 (0.9, 73)* 0.5 (0.3, 18) 0.24 (0.3, 4) Apathy 1.8 (0.9, 40) 6 (0.7, 82)* 0 Irritability 1.13 (0.7, 20) 0.15 (0.09, 9) 0.08 (0.08, 4) Agitation 0.27 (0.2, 20) 0.06 (0.06, 3) 0 Anxiety 1.1 (0.7, 13) 0.24 (0.1, 12) 0 Disinhibition 1.1 (0.7, 13) 1.8 (0.6, 35) 0.16 (0.2, 4) Delusions 0.2 (0.2, 7) 0 0 Aberrant motor behaviour 0.07 (0.06, 7) 0.47 (0.4, 6) 0 Euphoria Hallucinations Total NPI score 9 (3.2, 87) 9.2 (1.2, 88) 0.5 (0.4, 1) *p<0.05, patients with progressive supranuclear palsy v patients with corticobasal degeneration; p<0.05 either patient group v controls; p<0.05, both patient groups v controls. associated with aberrant motor behaviour; and their anxiety was associated with delusions and aberrant motor behaviour. Although motor disturbances were not associated with any behaviour, they were associated with total MMSE, suggesting that some patients with CBD with the poorest motor function (higher scores) had better cognitive performance (higher total MMSE scores). A factor analysis was performed to investigate whether the strength of some correlations (for example, disinhibition, anxiety, apathy, irritability, aberrant motor behaviour) may suggest that these behaviours belong to a single syndrome rather than being independent behavioural domains. The analysis showed that these behaviours could be grouped into two factors: (1) irritability, disinhibition, and apathy and (2) anxiety and aberrant motor behaviour (p<0.0001). When we also included agitation and depression in the analysis, these behaviours were grouped into two factors: (1) agitation, apathy, disinhibition, irritability, and aberrant motor behaviour and (2) depression (p<0.0001). Anxiety was included with both but more with factor 1. Patients with CBD with left motor symptoms (n=7) had higher disinhibition (2 (SEM 1)), apathy (2.8 (SEM 2)) and irritability (2 (SEM 1)), and lower depression scores (2.4 (SEM 1)) than those with right motor symptoms (n=8; disinhibition, 0; apathy, 0.7 (SEM 0.6); irritability, 0.14 (SEM 0.1); depression, 4.6 (SEM 1.4), but none of these diverences were significant. Discussion This is the first study to systematically investigate the neuropsychiatric disturbances of patients with CBD. We found that most (87%) patients with CBD manifested neuropsychiatric symptoms, mostly depression (73%), apathy (40%), irritability (20%), and agitation (20%), and less commonly, anxiety, disinhibition, aberrant motor behaviours, or delusions. No patients evidenced euphoria or hallucinations as reported by caregivers on the NPI. Patients with CBD showed significantly more depression than both patients with PSP and controls; conversely, patients with PSP were more apathetic. Behaviouraly, patients with CBD were more likely (higher odds ratios) than those with PSP
4 720 Litvan, Cummings, Mega to exhibit depression and irritability in the absence of, or with low levels of, apathy. In fact, these features correctly identified the patients with CBD 88% of the time. However, patients with CBD also exhibited apathy which was unrelated to their depression. Apathy was manifested by inattention to usual interests, activities, or plans of family members, and by being less spontaneous and active than usual. Apathy of patients with CBD was associated with irritability, disinhibition, and anxiety suggesting possible common pathogenetic mechanisms. Irritability of patients with CBD was manifested by flashes of anger, impatience, being argumentative and diycult to get along with, unrelated to the frustration of their illness, and diverent from the patient s usual behaviour. Disinhibition was characterised by acting impulsively without considering the consequences and by being tactless or making crude remarks. Although, it could be argued that the combination of these features is counterintuitive, a factor analysis suggested that irritability, disinhibition, and apathy may belong to a single syndrome rather than being independent behavioural domains. This factor contains items indicative of frontal lobe dysfunction. In support of our findings, a recent study confirmed by necropsy showed that 58% of the patients with CBD studied had developed apathy, irritability, or disinhibition, often associated with frontal lobe release signs. 16 In the current study, depression was the most frequent neuropsychiatric symptom exhibited by patients with CBD. These results diver from those of our necropsy study in which only a few (7%) patients with CBD presented with depression at onset, although at least one third developed it during progression of disease. 16 Neuropsychiatric symptoms are usually not thoroughly ascertained, and necropsy studies probably underestimate their presence. We did not determine if our patients depression was reactive to their deficits, but the fact that it may antedate motor symptomatology (and was the first symptom in one of the 15 patients) indicates that at least in some patients with CBD, depression has a neurobiological basis. Depression in CBD was unrelated to any other behaviour, suggesting that its pathophysiological mechanism divered. Depression often occurs in other basal ganglia disorders such as Parkinson s disease and Huntington s disease, in which it may predate other symptoms Depressed patients with Parkinson s disease have more severe neuronal loss in the dorsal raphe than non-depressed patients 33 ; and in an 18 F-fluoro-2-deoxyglucose ( 18 F-FDG) PET study, there was significant hypometabolism in the caudate and orbital inferior frontal lobes. 34 In addition, the depression scores of the patients with Parkinson s disease inversely correlated with the decreased metabolic activity (lower metabolism correlated with greater depression). 34 Similarly, in an 18 F-FDG PET study, depressed patients with Huntington s disease showed orbitofrontal and thalamic hypometabolism. 35 Studies with 18 F-FDG PET in CBD disclose diminished metabolic activities in the frontal, temporal, sensorimotor, and parietal association cortices as well as in the caudate nucleus, lenticular nucleus, and thalamus. Studies with PET of regional oxygen uptake show significantly depressed values in the superior and posterior temporal, inferior parietal, and occipital cortices. In addition, there were significant abnormalities in the superior frontal, midfrontal, inferior frontal, frontal polar, and orbitofrontal areas of the prefrontal cortex. 38 Striatal fluorodopa uptake measured with PET discloses diminished fluorodopa uptake in both the caudate and putamen. These metabolic abnormalities tend to be asymmetric with greater involvement contralateral to the most avected side of the body. The regions avected are similar to those described as abnormal in patients with other neurologically based depression syndromes, although no specific metabolic studies of patients with CBD with and without depression have been reported. Pathological changes in CBD include involvement of several nuclei of frontosubcortical circuits posited to mediate cognitive and emotional functions. AVected areas include the prefrontal cortex, globus pallidus, subthalamic nucleus, substantia nigra, locus coeruleus, raphe nuclei, and midbrain tegmentum. 39 Biochemical deficits in CBD include a marked loss of noradrenaline and serotonin as well as a severe nigrostriatal dopamine deficiency. 40 Similar transmitter deficiencies characterise other basal ganglia disorders with depression such as Parkinson s disease. By contrast, in PSP the locus coeruleus and raphe nuclei are relatively preserved, and noradrenaline and serotonin concentrations are usually not avected. Additionally, in PSP, by contrast to what occurs in CBD and Parkinson s disease, involvement of the frontosubcortical circuits is bilateral and symmetric. Whether unilateral or asymmetric involvement of the orbitofrontal circuit is needed to manifest biological depression, and bilateral involvement of the medial frontal circuits is necessary for the presence of apathy, need further evaluation. Dysfunction of subcortical projections to premotor-motor and supplementary motor subcortical circuits explains the motor abnormalities exhibited by patients with CBD. Although in our study, patients symptom duration was associated with disinhibition (r=0.53) and motor scores (r=0.53), motor disturbances were unrelated to any behaviour or specific cognitive disturbance (for example, frontal dysfunction). Moreover, patients with CBD with worse motor dysfunction (higher scores) had less cognitive impairment (higher total MMSE scores), suggesting that the various frontosubcortical pathways in CBD are not avected in parallel, at relatively early stages of the disease. Because this finding was made in a cross sectional, not a longitudinal study, our results do not disagree with the previous studies, 16 which reported that cognitive symptoms progressed during the course of the disease. In support of our findings, we found that in cases confirmed by necropsy 16 (unpublished material), at early disease stages, motor dysfunction was inversely associated with cognitive impair-
5 Neuropsychiatric features of corticobasal degeneration 721 ment (unilateral rigidity was inversely correlated with impaired cognition during the first 3 years (r= 0.57, p<0.05); and unilateral dystonia was inversely related to cognitive disturbances at onset (r= 0.63, p<0.01)). Moreover, in the same data set, 16 bilateral motor disturbances were positively associated with cognitive disturbances (bilateral bradykinesia was associated with impaired cognition during the first 3 years (r=0.58, p<0.05)). These results suggest that at onset, patients may manifest either motor or cognitive disturbances which reflect the presence of neuronal degeneration in either motor or cognitive circuits. However, when motor symptoms are bilateral, usually with progression of the disease, patients show more obvious cognitive impairment. Because we evaluated patients at relatively early stages of their disease and used the score of the worse limb for the motor assessment, we found that at disease onset, degeneration of the diverent frontosubcortical circuits does not occur in parallel. It is not surprising that at early stages of the disease, the restricted cognitive disturbances patients exhibited hardly avected their performance on tests which evaluate overall mental status such as the MMSE. This study has several limitations. It was based on small sample size, thus limiting the generalisation of our findings. In addition, our psychiatric diagnoses were based mainly on a neuropsychiatric rating scale and not on clinical diagnoses. Future studies would benefit from including a larger sample and complete clinical and neuropsychiatric evaluations. Neuropsychiatric assessment may be helpful to better understand CBD and to better manage patients with this disorder. Future studies need to investigate whether depression in patients with CBD may benefit from treatment with antidepressant agents. We are grateful to the patients and their relatives for their kind cooperation in our research project and to Mrs Devee Schoenberg for her skillful editorial assistance. This study was supported by an NIA Alzheimer Disease Center grant (AG 10123) and the Sidell-Kogan Foundation. The work was presented in part at the 122nd Annual Meeting of the American Neurological Association, San Diego, California, 28 September to 1 October Rinne JO, Lee MS, Thompson PD, et al. Corticobasal degeneration. A clinical study of 36 cases. Brain 1994;117: Litvan I, Agid Y, Goetz C, et al. Accuracy of the clinical diagnosis of corticobasal degeneration: a clinicopathological study. Neurology 1997;48: Feany MB, Dickson DW. Widespread cytoskeletal pathology characterizes corticobasal degeneration. Am J Pathol 1995;146: Lang AE, Bergeron C, Pollanen MS, et al. Parietal Pick s disease mimicking cortical-basal ganglionic degeneration. Neurology 1994;44: Jendroska K, Rossor MN, Mathias CJ, et al. Morphological overlap between corticobasal degeneration and Pick s disease: a clinicopathological report. Mov Disord 1995;10: Bergeron C, Pollanen MS, Weyer L, et al. Unusual clinical presentations of cortical-basal ganglionic degeneration. Ann Neurol 1996;40: Feany MB, Mattiace LA, Dickson DW. Neuropathologic overlap of progressive supranuclear palsy, Pick s disease, and corticobasal degeneration. J Neuropathol Exp Neurol 1996;55: Bergeron C, Pollanen MS, Weyer L, et al. Cortical degeneration in progressive supranuclear palsy. A comparison with cortical-basal ganglionic degeneration. J Neuropathol Exp Neurology 1997;56: Schneider JA, Watts RL, Gearing M, et al. Corticobasal degeneration: neuropathologic and clinical heterogeneity. Neurology 1997;48: Brunt ER, van Weerden TW, Pruim J, et al. Unique myoclonic pattern in corticobasal degeneration. Mov Disord 1995;10: Thompson PD, Day BL, Rothwell JC, et al. The myoclonus in corticobasal degeneration. Evidence for two forms of cortical reflex myoclonus. Brain 1994;117: Leiguarda R, Lees AJ, Merello M, et al. The nature of apraxia in corticobasal degeneration. J Neurol Neurosurg Psychiatry 1994;57: Pillon B, Blin J, Vidailhet M, et al. The neuropsychological pattern of corticobasal degeneration: comparison with progressive supranuclear palsy and Alzheimer s disease. Neurology 1995;45: Vidailhet M, Rivaud S, Gouider-Khouja N, et al.eyemovements in parkinsonian syndromes. Ann Neurol 1994;35: Rey GJ, Tomer R, Levin BE, et al. Psychiatric symptoms, atypical dementia, and left visual field inattention in corticobasal ganglionic degeneration. Mov Disord 1995;10: Wenning GK, Litvan I, Jankovic J, et al. Natural history and survival of 14 corticobasal degeneration cases: a clinicopathologic study. J Neurol Neurosurg Psychiatry 1998, 64: Steele C, Rovner B, Chase GA, et al. Psychiatric symptoms and nursing home placement of patients with Alzheimer s disease. Am J Psychiatry 1990;147: Morriss RK, Rovner BW, Folstein MF, et al. Delusions in newly admitted residents of nursing homes. Am J Psychiatry 1990;147: Goetz CG, Stebbins GT. Risk factors for nursing home placement in advanced Parkinson s disease. Neurology 1993;43: Goetz CG, Stebbins GT. Mortality and hallucinations in nursing home patients with advanced Parkinson s disease. Neurology 1995;45: Cummings JL, Mega M, Gray K,et al. The Neuropsychiatric Inventory: comprehensive assessment of psychopathology in dementia. Neurology 1994;44: Litvan I, Mega MS, Cummings JL, et al. Neuropsychiatric aspects of progressive supranuclear palsy. Neurology 1997; 47: Folstein MF, Folstein SE, McHugh PR. Mini-mental state: a practical method for grading the mental state of patients for the clinician. J Psychiatr Res 1975;12: Mattis S. Mental status examination for organic mental syndrome in the elderly patient. In: Bellak L, Karasu TB, eds. Geriatric psychiatry. New York: Grune and Stratton, Fahn S, Elton RL, and members of the UPDRS Committee. Unified Parkinson s disease rating scale. Florham Park, NJ: Macmillan Healthcare Information, 1987: Efron B, Tibshirani R. Statistical data analysis in the computer age. Science 1991;253: Santamaria J, Tolosa E, Valles A. Parkinson s disease with depression: a possible subgroup of idiopathic parkinsonism. Neurology 1986;36: Cummings JL. Depression and Parkinson s disease: a review. Am J Psychiatry 1992;149: Cummings JL, Diaz C, Levy M, et al. Neuropsychiatric syndromes in neurodegenerative diseases: frequency and significance. Seminars in Clinical Neuropsychiatry 1996;1: Starkstein SE, Preziosi TJ, Bolduc PL, et al. Depression in Parkinson s disease. J Nerv Ment Dis 1990;178: Starkstein SE, Mayberg HS, Leiguarda R, et al. A prospective longitudinal study of depression, cognitive decline, and physical impairments in patients with Parkinson s disease. J Neurol Neurosurg Psychiatry 1992;55: Tandberg E, Larsen JP, Aarsland D, et al. The occurrence of depression in Parkinson s disease. A community-based study. Arch Neurol 1996;53: Paulus W, Jellinger K. The neuropathologic basis of diverent clinical subgroups of Parkinson s disease. J Neuropathol Exp Neurol 1991;50: Mayberg HS, Starkstein SE, Sadzot B, et al. Selective hypometabolism in the inferior frontal lobe in depressed patients with Parkinson s disease. Ann Neurol 1990;28: Mayberg HS, Starkstein SE, Peyser CE, et al. Paralimbic frontal lobe hypometabolism in depression associated with Huntington s disease. Neurology 1992;42: Blin J, Vidaihlet MJ, Pillon B, et al. Corticobasal degeneration: decreased and asymmetrical glucose consumption as studied with PET. Mov Disord 1992;7: Nagashama Y, Fukuyama H, Turjanski N, et al. Cerebral glucose metabolism in corticobasal degeneration: comparison with progressive supranuclear palsy and normal controls. Mov Disord 1997;12: Sawle GV, Brooks DJ, Marsden CD, et al. Corticobasal degeneration. A unique pattern of regional cortical oxygen hypometabolism and striatal fluorodopa uptake demonstrated by positron emission tomography. Brain 1991;114: Gibb WR, Luthert PJ, Marsden CD. Corticobasal degeneration. Brain 1989;112: Kish SJ, Gilbert JJ, Chang LJ, et al. Brain neurotransmitter abnormalities in neuronal intranuclear inclusion body disorder. Ann Neurol 1985;17:405 7.
Range of neuropsychiatric disturbances in patients with Parkinson s disease
 492 Section of Geriatric Psychiatry, Rogaland Psychiatric Hospital D Aarsland N G Lim C Janvin Department of Neurology, Central Hospital of Rogaland, Stavanger, Norway J P Larsen K Karlsen E Tandberg Departments
492 Section of Geriatric Psychiatry, Rogaland Psychiatric Hospital D Aarsland N G Lim C Janvin Department of Neurology, Central Hospital of Rogaland, Stavanger, Norway J P Larsen K Karlsen E Tandberg Departments
FDG-PET e parkinsonismi
 Parkinsonismi FDG-PET e parkinsonismi Valentina Berti Dipartimento di Scienze Biomediche, Sperimentali e Cliniche Sez. Medicina Nucleare Università degli Studi di Firenze History 140 PubMed: FDG AND parkinsonism
Parkinsonismi FDG-PET e parkinsonismi Valentina Berti Dipartimento di Scienze Biomediche, Sperimentali e Cliniche Sez. Medicina Nucleare Università degli Studi di Firenze History 140 PubMed: FDG AND parkinsonism
Neuropsychiatric Symptoms of Patients With Progressive Supranuclear Palsy and Parkinson s Disease
 Neuropsychiatric Symptoms of Patients With Progressive Supranuclear Palsy and Parkinson s Disease Dag Aarsland, M.D., Ph.D. Irene Litvan, M.D. Jan P. Larsen, M.D., Ph.D. Neuropsychiatric symptoms are common
Neuropsychiatric Symptoms of Patients With Progressive Supranuclear Palsy and Parkinson s Disease Dag Aarsland, M.D., Ph.D. Irene Litvan, M.D. Jan P. Larsen, M.D., Ph.D. Neuropsychiatric symptoms are common
Behavioral and psychological symptoms of dementia characteristic of mild Alzheimer patients
 Blackwell Science, LtdOxford, UKPCNPsychiatry and Clinical Neurosciences1323-13162005 Blackwell Publishing Pty Ltd593274279Original ArticleDementia and mild AlzheimersJ. Shimabukuro et al. Psychiatry and
Blackwell Science, LtdOxford, UKPCNPsychiatry and Clinical Neurosciences1323-13162005 Blackwell Publishing Pty Ltd593274279Original ArticleDementia and mild AlzheimersJ. Shimabukuro et al. Psychiatry and
FTD basics! Etienne de Villers-Sidani, MD!
 FTD basics! Etienne de Villers-Sidani, MD! Frontotemporal lobar degeneration (FTLD) comprises 3 clinical syndromes! Frontotemporal dementia (behavioral variant FTD)! Semantic dementia (temporal variant
FTD basics! Etienne de Villers-Sidani, MD! Frontotemporal lobar degeneration (FTLD) comprises 3 clinical syndromes! Frontotemporal dementia (behavioral variant FTD)! Semantic dementia (temporal variant
Update on functional brain imaging in Movement Disorders
 Update on functional brain imaging in Movement Disorders Mario Masellis, MSc, MD, FRCPC, PhD Assistant Professor & Clinician-Scientist Sunnybrook Health Sciences Centre University of Toronto 53 rd CNSF
Update on functional brain imaging in Movement Disorders Mario Masellis, MSc, MD, FRCPC, PhD Assistant Professor & Clinician-Scientist Sunnybrook Health Sciences Centre University of Toronto 53 rd CNSF
DIFFERENTIAL DIAGNOSIS SARAH MARRINAN
 Parkinson s Academy Registrar Masterclass Sheffield DIFFERENTIAL DIAGNOSIS SARAH MARRINAN 17 th September 2014 Objectives Importance of age in diagnosis Diagnostic challenges Brain Bank criteria Differential
Parkinson s Academy Registrar Masterclass Sheffield DIFFERENTIAL DIAGNOSIS SARAH MARRINAN 17 th September 2014 Objectives Importance of age in diagnosis Diagnostic challenges Brain Bank criteria Differential
Role of Neuropsychiatric Assessment in Diagnosis and Research
 Role of Neuropsychiatric Assessment 163 11 Role of Neuropsychiatric Assessment in Diagnosis and Research Dag Aarsland, Uwe Ehrt, and Clive Ballard INTRODUCTION Although the basal ganglia have traditionally
Role of Neuropsychiatric Assessment 163 11 Role of Neuropsychiatric Assessment in Diagnosis and Research Dag Aarsland, Uwe Ehrt, and Clive Ballard INTRODUCTION Although the basal ganglia have traditionally
Clinical Features and Treatment of Parkinson s Disease
 Clinical Features and Treatment of Parkinson s Disease Richard Camicioli, MD, FRCPC Cognitive and Movement Disorders Department of Medicine University of Alberta 1 Objectives To review the diagnosis and
Clinical Features and Treatment of Parkinson s Disease Richard Camicioli, MD, FRCPC Cognitive and Movement Disorders Department of Medicine University of Alberta 1 Objectives To review the diagnosis and
Dementia Update. October 1, 2013 Dylan Wint, M.D. Cleveland Clinic Lou Ruvo Center for Brain Health Las Vegas, Nevada
 Dementia Update October 1, 2013 Dylan Wint, M.D. Cleveland Clinic Lou Ruvo Center for Brain Health Las Vegas, Nevada Outline New concepts in Alzheimer disease Biomarkers and in vivo diagnosis Future trends
Dementia Update October 1, 2013 Dylan Wint, M.D. Cleveland Clinic Lou Ruvo Center for Brain Health Las Vegas, Nevada Outline New concepts in Alzheimer disease Biomarkers and in vivo diagnosis Future trends
Anosognosia, or loss of insight into one s cognitive
 REGULAR ARTICLES Anosognosia Is a Significant Predictor of Apathy in Alzheimer s Disease Sergio E. Starkstein, M.D., Ph.D. Simone Brockman, M.A. David Bruce, M.D. Gustavo Petracca, M.D. Anosognosia and
REGULAR ARTICLES Anosognosia Is a Significant Predictor of Apathy in Alzheimer s Disease Sergio E. Starkstein, M.D., Ph.D. Simone Brockman, M.A. David Bruce, M.D. Gustavo Petracca, M.D. Anosognosia and
White matter hyperintensities correlate with neuropsychiatric manifestations of Alzheimer s disease and frontotemporal lobar degeneration
 White matter hyperintensities correlate with neuropsychiatric manifestations of Alzheimer s disease and frontotemporal lobar degeneration Annual Scientific Meeting Canadian Geriatric Society Philippe Desmarais,
White matter hyperintensities correlate with neuropsychiatric manifestations of Alzheimer s disease and frontotemporal lobar degeneration Annual Scientific Meeting Canadian Geriatric Society Philippe Desmarais,
COGNITIVE SCIENCE 107A. Motor Systems: Basal Ganglia. Jaime A. Pineda, Ph.D.
 COGNITIVE SCIENCE 107A Motor Systems: Basal Ganglia Jaime A. Pineda, Ph.D. Two major descending s Pyramidal vs. extrapyramidal Motor cortex Pyramidal system Pathway for voluntary movement Most fibers originate
COGNITIVE SCIENCE 107A Motor Systems: Basal Ganglia Jaime A. Pineda, Ph.D. Two major descending s Pyramidal vs. extrapyramidal Motor cortex Pyramidal system Pathway for voluntary movement Most fibers originate
Non Alzheimer Dementias
 Non Alzheimer Dementias Randolph B Schiffer Department of Neuropsychiatry and Behavioral Science Texas Tech University Health Sciences Center 9/11/2007 Statement of Financial Disclosure Randolph B Schiffer,,
Non Alzheimer Dementias Randolph B Schiffer Department of Neuropsychiatry and Behavioral Science Texas Tech University Health Sciences Center 9/11/2007 Statement of Financial Disclosure Randolph B Schiffer,,
T he prevalence of Parkinson s disease (PD) is nearly 1% in
 708 PAPER Donepezil for cognitive impairment in Parkinson s disease: a randomised controlled study D Aarsland, K Laake, J P Larsen, C Janvin... See end of article for authors affiliations... Correspondence
708 PAPER Donepezil for cognitive impairment in Parkinson s disease: a randomised controlled study D Aarsland, K Laake, J P Larsen, C Janvin... See end of article for authors affiliations... Correspondence
Objectives. RAIN Difficult Diagnosis 2014: A 75 year old woman with falls. Case History: First visit. Case History: First Visit
 Objectives RAIN Difficult Diagnosis 2014: A 75 year old woman with falls Alexandra Nelson MD, PhD UCSF Memory and Aging Center/Gladstone Institute of Neurological Disease Recognize important clinical features
Objectives RAIN Difficult Diagnosis 2014: A 75 year old woman with falls Alexandra Nelson MD, PhD UCSF Memory and Aging Center/Gladstone Institute of Neurological Disease Recognize important clinical features
Neuropsychiatric Manifestations in Vascular Cognitive Impairment Patients with and without Dementia
 86 Neuropsychiatric Manifestations in Vascular Cognitive Impairment Patients with and without Dementia Pai-Yi Chiu 1,3, Chung-Hsiang Liu 2, and Chon-Haw Tsai 2 Abstract- Background: Neuropsychiatric profile
86 Neuropsychiatric Manifestations in Vascular Cognitive Impairment Patients with and without Dementia Pai-Yi Chiu 1,3, Chung-Hsiang Liu 2, and Chon-Haw Tsai 2 Abstract- Background: Neuropsychiatric profile
Pathogenesis of Degenerative Diseases and Dementias. D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria)
 Pathogenesis of Degenerative Diseases and Dementias D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) Dementias Defined: as the development of memory impairment and other cognitive deficits
Pathogenesis of Degenerative Diseases and Dementias D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) Dementias Defined: as the development of memory impairment and other cognitive deficits
A. General features of the basal ganglia, one of our 3 major motor control centers:
 Reading: Waxman pp. 141-146 are not very helpful! Computer Resources: HyperBrain, Chapter 12 Dental Neuroanatomy Suzanne S. Stensaas, Ph.D. April 22, 2010 THE BASAL GANGLIA Objectives: 1. What are the
Reading: Waxman pp. 141-146 are not very helpful! Computer Resources: HyperBrain, Chapter 12 Dental Neuroanatomy Suzanne S. Stensaas, Ph.D. April 22, 2010 THE BASAL GANGLIA Objectives: 1. What are the
Imaging biomarkers for Parkinson s disease
 3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Teaching Course 6 MDS-ES/EAN: Neuroimaging in movement disorders - Level 2 Imaging biomarkers for Parkinson
3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Teaching Course 6 MDS-ES/EAN: Neuroimaging in movement disorders - Level 2 Imaging biomarkers for Parkinson
CHAPTER 5 NEUROPSYCHOLOGICAL PROFILE OF ALZHEIMER S DISEASE
 CHAPTER 5 NEUROPSYCHOLOGICAL PROFILE OF ALZHEIMER S DISEASE 5.1 GENERAL BACKGROUND Neuropsychological assessment plays a crucial role in the assessment of cognitive decline in older age. In India, there
CHAPTER 5 NEUROPSYCHOLOGICAL PROFILE OF ALZHEIMER S DISEASE 5.1 GENERAL BACKGROUND Neuropsychological assessment plays a crucial role in the assessment of cognitive decline in older age. In India, there
Transcranial sonography in movement disorders
 Transcranial sonography in movement disorders Uwe Walter 1st Residential Training of the European Society of Neurosonology and Cerebral Hemodynamics September 7-12, 2008 Bertinoro, Italy Department of
Transcranial sonography in movement disorders Uwe Walter 1st Residential Training of the European Society of Neurosonology and Cerebral Hemodynamics September 7-12, 2008 Bertinoro, Italy Department of
Nature, prevalence and clinical significance. Barcelona, Spain
 Nature, prevalence and clinical significance Jaime Kulisevsky Barcelona, Spain 1 Non motor (neuropsychiatric) symptoms are an integral part of Parkinson s s disease (PD) Affective disorders And are associated
Nature, prevalence and clinical significance Jaime Kulisevsky Barcelona, Spain 1 Non motor (neuropsychiatric) symptoms are an integral part of Parkinson s s disease (PD) Affective disorders And are associated
ORIGINAL CONTRIBUTION. Neuropsychiatric Assessment of Patients With Hyperkinetic and Hypokinetic Movement Disorders
 ORIGINAL CONTRIBUTION Neuropsychiatric Assessment of Patients With Hyperkinetic and Hypokinetic Movement Disorders Irene Litvan, MD; Jane S. Paulsen, PhD; Michael S. Mega, MD; Jeffrey L. Cummings, MD Background:
ORIGINAL CONTRIBUTION Neuropsychiatric Assessment of Patients With Hyperkinetic and Hypokinetic Movement Disorders Irene Litvan, MD; Jane S. Paulsen, PhD; Michael S. Mega, MD; Jeffrey L. Cummings, MD Background:
Neuropathology of Neurodegenerative Disorders Prof. Jillian Kril
 Neurodegenerative disorders to be discussed Alzheimer s disease Lewy body diseases Frontotemporal dementia and other tauopathies Huntington s disease Motor Neuron Disease 2 Neuropathology of neurodegeneration
Neurodegenerative disorders to be discussed Alzheimer s disease Lewy body diseases Frontotemporal dementia and other tauopathies Huntington s disease Motor Neuron Disease 2 Neuropathology of neurodegeneration
III./3.1. Movement disorders with akinetic rigid symptoms
 III./3.1. Movement disorders with akinetic rigid symptoms III./3.1.1. Parkinson s disease Parkinson s disease (PD) is the second most common neurodegenerative disorder worldwide after Alzheimer s disease.
III./3.1. Movement disorders with akinetic rigid symptoms III./3.1.1. Parkinson s disease Parkinson s disease (PD) is the second most common neurodegenerative disorder worldwide after Alzheimer s disease.
What contributes to quality of life in patients with Parkinson s disease?
 308 Department of Neurology, Institute of Neurology, Queen Square, London WC1N 3BG, UK A Schrag M Jahanshahi N Quinn Correspondence to: Professor NP Quinn n.quinn@ion.ucl.ac.uk Received 2 Sepyember 1999
308 Department of Neurology, Institute of Neurology, Queen Square, London WC1N 3BG, UK A Schrag M Jahanshahi N Quinn Correspondence to: Professor NP Quinn n.quinn@ion.ucl.ac.uk Received 2 Sepyember 1999
A. General features of the basal ganglia, one of our 3 major motor control centers:
 Reading: Waxman pp. 141-146 are not very helpful! Computer Resources: HyperBrain, Chapter 12 Dental Neuroanatomy Suzanne S. Stensaas, Ph.D. March 1, 2012 THE BASAL GANGLIA Objectives: 1. What are the main
Reading: Waxman pp. 141-146 are not very helpful! Computer Resources: HyperBrain, Chapter 12 Dental Neuroanatomy Suzanne S. Stensaas, Ph.D. March 1, 2012 THE BASAL GANGLIA Objectives: 1. What are the main
Original Articles. Calne, resting tremor. Mortimer, Pirozzolo, Hansch, & Webster, postural disturbance III
 2004 97-106 Original Articles 1 2 3 1 1 2 3 47 22 III I II muscular rigidity postural disturbance resting tremor bradykinesia Calne, 2001 Mortimer, Pirozzolo, Hansch, & Webster, 1982 Tel: 02-23627076 E-mail:
2004 97-106 Original Articles 1 2 3 1 1 2 3 47 22 III I II muscular rigidity postural disturbance resting tremor bradykinesia Calne, 2001 Mortimer, Pirozzolo, Hansch, & Webster, 1982 Tel: 02-23627076 E-mail:
I do not have any disclosures
 Alzheimer s Disease: Update on Research, Treatment & Care Clinicopathological Classifications of FTD and Related Disorders Keith A. Josephs, MST, MD, MS Associate Professor & Consultant of Neurology Mayo
Alzheimer s Disease: Update on Research, Treatment & Care Clinicopathological Classifications of FTD and Related Disorders Keith A. Josephs, MST, MD, MS Associate Professor & Consultant of Neurology Mayo
ORIGINAL CONTRIBUTION. The Spectrum of Behavioral Responses to Cholinesterase Inhibitor Therapy in Alzheimer Disease
 ORIGINAL CONTRIBUTION The Spectrum of Behavioral Responses to Cholinesterase Inhibitor Therapy in Alzheimer Disease Michael S. Mega, MD, PhD; Donna M. Masterman, MD; Susan M. O Connor, RNC; Terry R. Barclay,
ORIGINAL CONTRIBUTION The Spectrum of Behavioral Responses to Cholinesterase Inhibitor Therapy in Alzheimer Disease Michael S. Mega, MD, PhD; Donna M. Masterman, MD; Susan M. O Connor, RNC; Terry R. Barclay,
Fatigue in patients with Parkinson s disease
 103 Fatigue in patients with Parkinson s disease Kazuo Abe, Mayako Takanashi and Takehiko Yanagihara Department of Neurology, Osaka University Graduate School of Medicine, Japan Purpose: Fatigue is a complaint
103 Fatigue in patients with Parkinson s disease Kazuo Abe, Mayako Takanashi and Takehiko Yanagihara Department of Neurology, Osaka University Graduate School of Medicine, Japan Purpose: Fatigue is a complaint
ORIGINAL CONTRIBUTION. Progression of Dysarthria and Dysphagia in Postmortem-Confirmed Parkinsonian Disorders
 ORIGINAL CONTRIBUTION Progression of Dysarthria and Dysphagia in Postmortem-Confirmed Parkinsonian Disorders Jörg Müller, MD; Gregor K. Wenning, MD, PhD; Marc Verny, MD; Ann McKee, MD; K. Ray Chaudhuri,
ORIGINAL CONTRIBUTION Progression of Dysarthria and Dysphagia in Postmortem-Confirmed Parkinsonian Disorders Jörg Müller, MD; Gregor K. Wenning, MD, PhD; Marc Verny, MD; Ann McKee, MD; K. Ray Chaudhuri,
Connections of basal ganglia
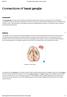 Connections of basal ganglia Introduction The basal ganglia, or basal nuclei, are areas of subcortical grey matter that play a prominent role in modulating movement, as well as cognitive and emotional
Connections of basal ganglia Introduction The basal ganglia, or basal nuclei, are areas of subcortical grey matter that play a prominent role in modulating movement, as well as cognitive and emotional
Screening and Management of Behavioral and Psychiatric Symptoms Associated with Dementia
 Screening and Management of Behavioral and Psychiatric Symptoms Associated with Dementia Measure Description Percentage of patients with dementia for whom there was a documented screening* for behavioral
Screening and Management of Behavioral and Psychiatric Symptoms Associated with Dementia Measure Description Percentage of patients with dementia for whom there was a documented screening* for behavioral
VL VA BASAL GANGLIA. FUNCTIONAl COMPONENTS. Function Component Deficits Start/initiation Basal Ganglia Spontan movements
 BASAL GANGLIA Chris Cohan, Ph.D. Dept. of Pathology/Anat Sci University at Buffalo I) Overview How do Basal Ganglia affect movement Basal ganglia enhance cortical motor activity and facilitate movement.
BASAL GANGLIA Chris Cohan, Ph.D. Dept. of Pathology/Anat Sci University at Buffalo I) Overview How do Basal Ganglia affect movement Basal ganglia enhance cortical motor activity and facilitate movement.
Use of the Neuropsychiatric Inventory to Characterize the Course of Neuropsychiatric Symptoms in Progressive Supranuclear Palsy
 ARTICLES Use of the Neuropsychiatric Inventory to Characterize the Course of Neuropsychiatric Symptoms in Progressive Supranuclear Palsy Milica Jecmenica-Lukic, M.D., Tatjana Pekmezovic, M.D., Ph.D., Igor
ARTICLES Use of the Neuropsychiatric Inventory to Characterize the Course of Neuropsychiatric Symptoms in Progressive Supranuclear Palsy Milica Jecmenica-Lukic, M.D., Tatjana Pekmezovic, M.D., Ph.D., Igor
A wide range of neuropsychiatric disturbances commonly
 36 PAPER Neuropsychiatric symptoms in patients with Parkinson s disease and dementia: frequency, profile and associated care giver stress D Aarsland, K Brønnick, U Ehrt, P P De Deyn, S Tekin, M Emre, J
36 PAPER Neuropsychiatric symptoms in patients with Parkinson s disease and dementia: frequency, profile and associated care giver stress D Aarsland, K Brønnick, U Ehrt, P P De Deyn, S Tekin, M Emre, J
Dementia and Healthy Ageing : is the pathology any different?
 Dementia and Healthy Ageing : is the pathology any different? Professor David Mann, Professor of Neuropathology, University of Manchester, Hope Hospital, Salford DEMENTIA Loss of connectivity within association
Dementia and Healthy Ageing : is the pathology any different? Professor David Mann, Professor of Neuropathology, University of Manchester, Hope Hospital, Salford DEMENTIA Loss of connectivity within association
Biomedical Technology Research Center 2011 Workshop San Francisco, CA
 Diffusion Tensor Imaging: Parkinson s Disease and Atypical Parkinsonism David E. Vaillancourt court1@uic.edu Associate Professor at UIC Departments t of Kinesiology i and Nutrition, Bioengineering, and
Diffusion Tensor Imaging: Parkinson s Disease and Atypical Parkinsonism David E. Vaillancourt court1@uic.edu Associate Professor at UIC Departments t of Kinesiology i and Nutrition, Bioengineering, and
Clinimetrics, clinical profile and prognosis in early Parkinson s disease Post, B.
 UvA-DARE (Digital Academic Repository) Clinimetrics, clinical profile and prognosis in early Parkinson s disease Post, B. Link to publication Citation for published version (APA): Post, B. (2009). Clinimetrics,
UvA-DARE (Digital Academic Repository) Clinimetrics, clinical profile and prognosis in early Parkinson s disease Post, B. Link to publication Citation for published version (APA): Post, B. (2009). Clinimetrics,
What if it s not Alzheimer s? Update on Lewy body dementia and frontotemporal dementia
 What if it s not Alzheimer s? Update on Lewy body dementia and frontotemporal dementia Dementia: broad term for any acquired brain condition impairing mental function such that ADLs are impaired. Includes:
What if it s not Alzheimer s? Update on Lewy body dementia and frontotemporal dementia Dementia: broad term for any acquired brain condition impairing mental function such that ADLs are impaired. Includes:
The Frontal Lobes. Anatomy of the Frontal Lobes. Anatomy of the Frontal Lobes 3/2/2011. Portrait: Losing Frontal-Lobe Functions. Readings: KW Ch.
 The Frontal Lobes Readings: KW Ch. 16 Portrait: Losing Frontal-Lobe Functions E.L. Highly organized college professor Became disorganized, showed little emotion, and began to miss deadlines Scores on intelligence
The Frontal Lobes Readings: KW Ch. 16 Portrait: Losing Frontal-Lobe Functions E.L. Highly organized college professor Became disorganized, showed little emotion, and began to miss deadlines Scores on intelligence
FRONTOTEMPORAL DEGENERATION: OVERVIEW, TRENDS AND DEVELOPMENTS
 FRONTOTEMPORAL DEGENERATION: OVERVIEW, TRENDS AND DEVELOPMENTS Norman L. Foster, M.D. Director, Center for Alzheimer s Care, Imaging and Research Chief, Division of Cognitive Neurology, Department of Neurology
FRONTOTEMPORAL DEGENERATION: OVERVIEW, TRENDS AND DEVELOPMENTS Norman L. Foster, M.D. Director, Center for Alzheimer s Care, Imaging and Research Chief, Division of Cognitive Neurology, Department of Neurology
Differential Diagnosis of Hypokinetic Movement Disorders
 Differential Diagnosis of Hypokinetic Movement Disorders Dr Donald Grosset Consultant Neurologist - Honorary Professor Institute of Neurological Sciences - Glasgow University Hypokinetic Parkinson's Disease
Differential Diagnosis of Hypokinetic Movement Disorders Dr Donald Grosset Consultant Neurologist - Honorary Professor Institute of Neurological Sciences - Glasgow University Hypokinetic Parkinson's Disease
212 Index C-SB-13,
 Index A Acetylcholinesterase inhibitor, treatment, 15 Age-associated memory impairment (AAMI), 5 Alzheimer s disease (AD), 40, 95 96 apolipoprotein E genotype and risk for, 58 cellular neurodegeneration
Index A Acetylcholinesterase inhibitor, treatment, 15 Age-associated memory impairment (AAMI), 5 Alzheimer s disease (AD), 40, 95 96 apolipoprotein E genotype and risk for, 58 cellular neurodegeneration
Cognitive and Behavioural Changes After Deep Brain Stimulation of the Subthalamic Nucleus in Parkinson s Disease
 17 Cognitive and Behavioural Changes After Deep Brain Stimulation of the Subthalamic Nucleus in Parkinson s Disease Antonio Daniele, Pietro Spinelli and Chiara Piccininni Istituto di Neurologia, Università
17 Cognitive and Behavioural Changes After Deep Brain Stimulation of the Subthalamic Nucleus in Parkinson s Disease Antonio Daniele, Pietro Spinelli and Chiara Piccininni Istituto di Neurologia, Università
Hallucinations and conscious access to visual inputs in Parkinson s disease
 Supplemental informations Hallucinations and conscious access to visual inputs in Parkinson s disease Stéphanie Lefebvre, PhD^1,2, Guillaume Baille, MD^4, Renaud Jardri MD, PhD 1,2 Lucie Plomhause, PhD
Supplemental informations Hallucinations and conscious access to visual inputs in Parkinson s disease Stéphanie Lefebvre, PhD^1,2, Guillaume Baille, MD^4, Renaud Jardri MD, PhD 1,2 Lucie Plomhause, PhD
Correlation between motor and cognitive functions in the progressive course of Parkinson s disease
 doi:10.1111/ncn3.53 ORIGINAL ARTICLE Correlation between motor and cognitive functions in the progressive course of Parkinson s disease Hidetomo Murakami,* Yoshiyuki Owan,* Yukiko Mori,* Kazuhisa Fujita,*
doi:10.1111/ncn3.53 ORIGINAL ARTICLE Correlation between motor and cognitive functions in the progressive course of Parkinson s disease Hidetomo Murakami,* Yoshiyuki Owan,* Yukiko Mori,* Kazuhisa Fujita,*
Lewy body disease (LBD) is the second most common
 REGULAR ARTICLES Lewy Body Disease: Can We Diagnose It? Michelle Papka, Ph.D. Ana Rubio, M.D., Ph.D. Randolph B. Schiffer, M.D. Christopher Cox, Ph.D. The authors assessed the accuracy of published clinical
REGULAR ARTICLES Lewy Body Disease: Can We Diagnose It? Michelle Papka, Ph.D. Ana Rubio, M.D., Ph.D. Randolph B. Schiffer, M.D. Christopher Cox, Ph.D. The authors assessed the accuracy of published clinical
Diagnosis before NIA AA The impact of FDG PET in. Diagnosis after NIA AA Neuropathology and PET image 2015/10/16
 The impact of FDG PET in degenerative dementia diagnosis Jung Lung, Hsu MD, Ph.D (Utrecht) Section of dementia and cognitive impairment Department of Neurology Chang Gung Memorial Hospital, Linkou, Taipei
The impact of FDG PET in degenerative dementia diagnosis Jung Lung, Hsu MD, Ph.D (Utrecht) Section of dementia and cognitive impairment Department of Neurology Chang Gung Memorial Hospital, Linkou, Taipei
Basal ganglia motor circuit
 Parkinson s Disease Basal ganglia motor circuit 1 Direct pathway (gas pedal) 2 Indirect pathway (brake) To release or augment the tonic inhibition of GPi on thalamus Direct pathway There is a tonic inhibition
Parkinson s Disease Basal ganglia motor circuit 1 Direct pathway (gas pedal) 2 Indirect pathway (brake) To release or augment the tonic inhibition of GPi on thalamus Direct pathway There is a tonic inhibition
Parkinsonism in corticobasal syndrome may not be primarily due to presynaptic dopaminergic deficiency
 Neurology Asia 2015; 20(1) : 23 27 Parkinsonism in corticobasal syndrome may not be primarily due to presynaptic dopaminergic deficiency 1 Ji Young Yun MD, 2 Jong-Min Kim MD, PhD, 3 Han-Joon Kim MD PhD,
Neurology Asia 2015; 20(1) : 23 27 Parkinsonism in corticobasal syndrome may not be primarily due to presynaptic dopaminergic deficiency 1 Ji Young Yun MD, 2 Jong-Min Kim MD, PhD, 3 Han-Joon Kim MD PhD,
Extrapyramidal Motor System. Basal Ganglia or Striatum. Basal Ganglia or Striatum 3/3/2010
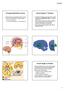 Extrapyramidal Motor System Basal Ganglia or Striatum Descending extrapyramidal paths receive input from other parts of motor system: From the cerebellum From the basal ganglia or corpus striatum Caudate
Extrapyramidal Motor System Basal Ganglia or Striatum Descending extrapyramidal paths receive input from other parts of motor system: From the cerebellum From the basal ganglia or corpus striatum Caudate
ORIGINAL CONTRIBUTION. Transcranial Brain Sonography Findings in Discriminating Between Parkinsonism and Idiopathic Parkinson Disease
 ORIGINAL CONTRIBUTION Transcranial Brain Sonography Findings in Discriminating Between Parkinsonism and Idiopathic Parkinson Disease Uwe Walter, MD; Dirk Dressler, MD; omas Probst, MD; Alexander Wolters,
ORIGINAL CONTRIBUTION Transcranial Brain Sonography Findings in Discriminating Between Parkinsonism and Idiopathic Parkinson Disease Uwe Walter, MD; Dirk Dressler, MD; omas Probst, MD; Alexander Wolters,
Parkinsonian Disorders with Dementia
 Parkinsonian Disorders with Dementia George Tadros Consultant in Old Age Liaison Psychiatry, RAID, Heartlands Hospital Professor of Dementia and Liaison Psychiatry, Aston Medical School Aston University
Parkinsonian Disorders with Dementia George Tadros Consultant in Old Age Liaison Psychiatry, RAID, Heartlands Hospital Professor of Dementia and Liaison Psychiatry, Aston Medical School Aston University
The motor regulator. 1) Basal ganglia/nucleus
 The motor regulator 1) Basal ganglia/nucleus Neural structures involved in the control of movement Basal Ganglia - Components of the basal ganglia - Function of the basal ganglia - Connection and circuits
The motor regulator 1) Basal ganglia/nucleus Neural structures involved in the control of movement Basal Ganglia - Components of the basal ganglia - Function of the basal ganglia - Connection and circuits
The Person: Dementia Basics
 The Person: Dementia Basics Objectives 1. Discuss how expected age related changes in the brain might affect an individual's cognition and functioning 2. Discuss how changes in the brain due to Alzheimer
The Person: Dementia Basics Objectives 1. Discuss how expected age related changes in the brain might affect an individual's cognition and functioning 2. Discuss how changes in the brain due to Alzheimer
Cognitive and motor assessment in autopsy-proven corticobasal degeneration
 Cognitive and motor assessment in autopsy-proven corticobasal degeneration R. Murray, BS; M. Neumann, MD; M.S. Forman, MD, PhD; J. Farmer, MSc; L. Massimo, LPN; A. Rice, BS; B.L. Miller, MD; J.K. Johnson,
Cognitive and motor assessment in autopsy-proven corticobasal degeneration R. Murray, BS; M. Neumann, MD; M.S. Forman, MD, PhD; J. Farmer, MSc; L. Massimo, LPN; A. Rice, BS; B.L. Miller, MD; J.K. Johnson,
A pathy refers to a set of behavioural, emotional, and
 579 PAPER The Lille apathy rating scale (LARS), a new instrument for detecting and quantifying apathy: validation in Parkinson s disease P Sockeel, K Dujardin, D Devos, C Denève, A Destée, L Defebvre...
579 PAPER The Lille apathy rating scale (LARS), a new instrument for detecting and quantifying apathy: validation in Parkinson s disease P Sockeel, K Dujardin, D Devos, C Denève, A Destée, L Defebvre...
7/3/2013 ABNORMAL PSYCHOLOGY SEVENTH EDITION CHAPTER FOURTEEN CHAPTER OUTLINE. Dementia, Delirium, and Amnestic Disorders. Oltmanns and Emery
 ABNORMAL PSYCHOLOGY SEVENTH EDITION Oltmanns and Emery PowerPoint Presentations Prepared by: Ashlea R. Smith, Ph.D. This multimedia and its contents are protected under copyright law. The following are
ABNORMAL PSYCHOLOGY SEVENTH EDITION Oltmanns and Emery PowerPoint Presentations Prepared by: Ashlea R. Smith, Ph.D. This multimedia and its contents are protected under copyright law. The following are
Final Scientific Progress Report
 CUREPSP Final Scientific Progress Report Tau in Peripheral Tissues of PSP and CBD. Brittany Dugger, PhD; University of California San Francisco Specific Aim: Using immunohistochemical methods on autopsy
CUREPSP Final Scientific Progress Report Tau in Peripheral Tissues of PSP and CBD. Brittany Dugger, PhD; University of California San Francisco Specific Aim: Using immunohistochemical methods on autopsy
Health related quality of life in Parkinson s disease: a prospective longitudinal study
 584 Department of Neurology, Central Hospital of Rogaland, Postbox 8100, N-4003 Stavanger, Norway K H Karlsen E Tandberg J P Larsen Department of Psychiatry D Årsland Correspondence to: Professor Jan P
584 Department of Neurology, Central Hospital of Rogaland, Postbox 8100, N-4003 Stavanger, Norway K H Karlsen E Tandberg J P Larsen Department of Psychiatry D Årsland Correspondence to: Professor Jan P
Lecture 42: Final Review. Martin Wessendorf, Ph.D.
 Lecture 42: Final Review Martin Wessendorf, Ph.D. Lecture 33 cortex Heilbronner 5 lobes of the cortex Lateral view (left side) Mid-saggital view (right side) Cellular organization of cortex White matter
Lecture 42: Final Review Martin Wessendorf, Ph.D. Lecture 33 cortex Heilbronner 5 lobes of the cortex Lateral view (left side) Mid-saggital view (right side) Cellular organization of cortex White matter
DEMENTIA 101: WHAT IS HAPPENING IN THE BRAIN? Philip L. Rambo, PhD
 DEMENTIA 101: WHAT IS HAPPENING IN THE BRAIN? Philip L. Rambo, PhD OBJECTIVES Terminology/Dementia Basics Most Common Types Defining features Neuro-anatomical/pathological underpinnings Neuro-cognitive
DEMENTIA 101: WHAT IS HAPPENING IN THE BRAIN? Philip L. Rambo, PhD OBJECTIVES Terminology/Dementia Basics Most Common Types Defining features Neuro-anatomical/pathological underpinnings Neuro-cognitive
Alzheimer's Disease An update on diagnostic criteria & Neuropsychiatric symptoms. l The diagnosis of AD l Neuropsychiatric symptoms l Place of the ICT
 Alzheimer's Disease An update on diagnostic criteria & Neuropsychiatric symptoms State of the art lecture March 4-2012 Philippe H Robert, Philippe Nice - France Robert The diagnosis of AD Neuropsychiatric
Alzheimer's Disease An update on diagnostic criteria & Neuropsychiatric symptoms State of the art lecture March 4-2012 Philippe H Robert, Philippe Nice - France Robert The diagnosis of AD Neuropsychiatric
N europsychiatric symptoms can induce marked disability
 PAPER Neuropsychiatric profiles in patients with Alzheimer s disease and vascular dementia J-L Fuh, S-J Wang, J L Cummings... See end of article for authors affiliations... Correspondence to: Dr J-L Fuh,
PAPER Neuropsychiatric profiles in patients with Alzheimer s disease and vascular dementia J-L Fuh, S-J Wang, J L Cummings... See end of article for authors affiliations... Correspondence to: Dr J-L Fuh,
Anatomy of the basal ganglia. Dana Cohen Gonda Brain Research Center, room 410
 Anatomy of the basal ganglia Dana Cohen Gonda Brain Research Center, room 410 danacoh@gmail.com The basal ganglia The nuclei form a small minority of the brain s neuronal population. Little is known about
Anatomy of the basal ganglia Dana Cohen Gonda Brain Research Center, room 410 danacoh@gmail.com The basal ganglia The nuclei form a small minority of the brain s neuronal population. Little is known about
WHAT IS DEMENTIA? An acquired syndrome of decline in memory and other cognitive functions sufficient to affect daily life in an alert patient
 DEMENTIA WHAT IS DEMENTIA? An acquired syndrome of decline in memory and other cognitive functions sufficient to affect daily life in an alert patient Progressive and disabling Not an inherent aspect of
DEMENTIA WHAT IS DEMENTIA? An acquired syndrome of decline in memory and other cognitive functions sufficient to affect daily life in an alert patient Progressive and disabling Not an inherent aspect of
responsiveness HMPAO SPECT in Parkinson's disease before and after levodopa: correlation with dopaminergic (SSmTc HMPAO) as a tracer in 21 patients
 18 1ournal of Neurology, Neurosurgery, and Psychiatry 1994;57:18-185 Department of Neurology H S Markus A J Lees Institute of Nuclear Medicine, University College and Middlesex School of Medicine, London,
18 1ournal of Neurology, Neurosurgery, and Psychiatry 1994;57:18-185 Department of Neurology H S Markus A J Lees Institute of Nuclear Medicine, University College and Middlesex School of Medicine, London,
HDSA Annual Convention June 2013 Behavior Issues: Irritability and Depression Peg Nopoulos, M.D.
 HDSA Annual Convention June 2013 Behavior Issues: Irritability and Depression Peg Nopoulos, M.D. Professor of Psychiatry, Neurology, and Pediatrics University of Iowa, Iowa City, Iowa The information provided
HDSA Annual Convention June 2013 Behavior Issues: Irritability and Depression Peg Nopoulos, M.D. Professor of Psychiatry, Neurology, and Pediatrics University of Iowa, Iowa City, Iowa The information provided
BEHAVIOURAL AND PSYCHOLOGICAL SYMPTOMS IN DEMENTIA
 BEHAVIOURAL AND PSYCHOLOGICAL SYMPTOMS IN DEMENTIA Unmet needs What might be your behavioural response to this experience? Content Definition What are BPSD? Prevalence How common are they? Aetiological
BEHAVIOURAL AND PSYCHOLOGICAL SYMPTOMS IN DEMENTIA Unmet needs What might be your behavioural response to this experience? Content Definition What are BPSD? Prevalence How common are they? Aetiological
Dr. Farah Nabil Abbas. MBChB, MSc, PhD
 Dr. Farah Nabil Abbas MBChB, MSc, PhD The Basal Ganglia *Functions in association with motor cortex and corticospinal pathways. *Regarded as accessory motor system besides cerebellum. *Receive most of
Dr. Farah Nabil Abbas MBChB, MSc, PhD The Basal Ganglia *Functions in association with motor cortex and corticospinal pathways. *Regarded as accessory motor system besides cerebellum. *Receive most of
Fluorodopa uptake and glucose metabolism in early stages of corticobasal degeneration
 J Neurol (1999) 246: 1151 1158 Steinkopff Verlag 1999 ORIGINAL COMMUNICATION Steven Laureys Eric Salmon Gaetan Garraux Philippe Peigneux Christian Lemaire Christian Degueldre George Franck Fluorodopa uptake
J Neurol (1999) 246: 1151 1158 Steinkopff Verlag 1999 ORIGINAL COMMUNICATION Steven Laureys Eric Salmon Gaetan Garraux Philippe Peigneux Christian Lemaire Christian Degueldre George Franck Fluorodopa uptake
Neurodegenerative Disease. April 12, Cunningham. Department of Neurosciences
 Neurodegenerative Disease April 12, 2017 Cunningham Department of Neurosciences NEURODEGENERATIVE DISEASE Any of a group of hereditary and sporadic conditions characterized by progressive dysfunction,
Neurodegenerative Disease April 12, 2017 Cunningham Department of Neurosciences NEURODEGENERATIVE DISEASE Any of a group of hereditary and sporadic conditions characterized by progressive dysfunction,
Basal Ganglia. Today s lecture is about Basal Ganglia and it covers:
 Basal Ganglia Motor system is complex interaction between Lower motor neurons (spinal cord and brainstem circuits) and Upper motor neurons (pyramidal and extrapyramidal tracts) plus two main regulators
Basal Ganglia Motor system is complex interaction between Lower motor neurons (spinal cord and brainstem circuits) and Upper motor neurons (pyramidal and extrapyramidal tracts) plus two main regulators
Brain imaging for the diagnosis of people with suspected dementia
 Why do we undertake brain imaging in dementia? Brain imaging for the diagnosis of people with suspected dementia Not just because guidelines tell us to! Exclude other causes for dementia Help confirm diagnosis
Why do we undertake brain imaging in dementia? Brain imaging for the diagnosis of people with suspected dementia Not just because guidelines tell us to! Exclude other causes for dementia Help confirm diagnosis
Fluorodeoxyglucose Positron Emission Tomography in Richardson s Syndrome and Progressive Supranuclear Palsy-Parkinsonism
 BRIEF REPORT Fluorodeoxyglucose Positron Emission Tomography in Richardson s Syndrome and Progressive Supranuclear Palsy-Parkinsonism Karin Srulijes, MD, 1,2 Matthias Reimold, MD, 3 Rajka M. Liscic, MD,
BRIEF REPORT Fluorodeoxyglucose Positron Emission Tomography in Richardson s Syndrome and Progressive Supranuclear Palsy-Parkinsonism Karin Srulijes, MD, 1,2 Matthias Reimold, MD, 3 Rajka M. Liscic, MD,
Neuropsychological pattern of striatonigral
 174 17ournal of Neurology, Neurosurgery, and Psychiatry 1 995;58: 174-179 INSERM U 289 and Federation de Neurologie, Hopital de la Salpetriere, 47 Boulevard de l'hopital, 75651 Paris cedex 13, France B
174 17ournal of Neurology, Neurosurgery, and Psychiatry 1 995;58: 174-179 INSERM U 289 and Federation de Neurologie, Hopital de la Salpetriere, 47 Boulevard de l'hopital, 75651 Paris cedex 13, France B
Parkinson e decadimento cognitivo. Stelvio Sestini
 Parkinson e decadimento cognitivo Stelvio Sestini Patients with PD can develop a spectrum of cognitive symptoms Heterogeneity of cognitive deficits The cognitive symptoms can evolve to dementia (Mov Disorder
Parkinson e decadimento cognitivo Stelvio Sestini Patients with PD can develop a spectrum of cognitive symptoms Heterogeneity of cognitive deficits The cognitive symptoms can evolve to dementia (Mov Disorder
Kurz MW, MD 1, 2, Larsen JP, MD, PhD 2, 3, Kvaloy JT, PhD 4, 5, Aarsland D, MD, PhD 2. Norway. Norway. Norway
 Paper V 1 Associations between family history of Parkinson s disease and dementia and risk of dementia in Parkinson s disease. A community-based, longitudinal study. Kurz MW, MD 1, 2, Larsen JP, MD, PhD
Paper V 1 Associations between family history of Parkinson s disease and dementia and risk of dementia in Parkinson s disease. A community-based, longitudinal study. Kurz MW, MD 1, 2, Larsen JP, MD, PhD
Basal ganglia Sujata Sofat, class of 2009
 Basal ganglia Sujata Sofat, class of 2009 Basal ganglia Objectives Describe the function of the Basal Ganglia in movement Define the BG components and their locations Describe the motor loop of the BG
Basal ganglia Sujata Sofat, class of 2009 Basal ganglia Objectives Describe the function of the Basal Ganglia in movement Define the BG components and their locations Describe the motor loop of the BG
COGNITIVE IMPAIRMENT IN PARKINSON S DISEASE
 1 GENERAL INTRODUCTION GENERAL INTRODUCTION PARKINSON S DISEASE Parkinson s disease (PD) is a neurodegenerative movement disorder, named after James Parkinson who described some of its characteristic
1 GENERAL INTRODUCTION GENERAL INTRODUCTION PARKINSON S DISEASE Parkinson s disease (PD) is a neurodegenerative movement disorder, named after James Parkinson who described some of its characteristic
For more information about how to cite these materials visit
 Author(s): Peter Hitchcock, PH.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Non-commercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Author(s): Peter Hitchcock, PH.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Non-commercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Clinicopathologic and genetic aspects of hippocampal sclerosis. Dennis W. Dickson, MD Mayo Clinic, Jacksonville, Florida USA
 Clinicopathologic and genetic aspects of hippocampal sclerosis Dennis W. Dickson, MD Mayo Clinic, Jacksonville, Florida USA The hippocampus in health & disease A major structure of the medial temporal
Clinicopathologic and genetic aspects of hippocampal sclerosis Dennis W. Dickson, MD Mayo Clinic, Jacksonville, Florida USA The hippocampus in health & disease A major structure of the medial temporal
Damage on one side.. (Notes) Just remember: Unilateral damage to basal ganglia causes contralateral symptoms.
 Lecture 20 - Basal Ganglia Basal Ganglia (Nolte 5 th Ed pp 464) Damage to the basal ganglia produces involuntary movements. Although the basal ganglia do not influence LMN directly (to cause this involuntary
Lecture 20 - Basal Ganglia Basal Ganglia (Nolte 5 th Ed pp 464) Damage to the basal ganglia produces involuntary movements. Although the basal ganglia do not influence LMN directly (to cause this involuntary
Making Things Happen 2: Motor Disorders
 Making Things Happen 2: Motor Disorders How Your Brain Works Prof. Jan Schnupp wschnupp@cityu.edu.hk HowYourBrainWorks.net On the Menu in This Lecture In the previous lecture we saw how motor cortex and
Making Things Happen 2: Motor Disorders How Your Brain Works Prof. Jan Schnupp wschnupp@cityu.edu.hk HowYourBrainWorks.net On the Menu in This Lecture In the previous lecture we saw how motor cortex and
Confronting the Clinical Challenges of Frontotemporal Dementia
 Confronting the Clinical Challenges of Frontotemporal Dementia A look at FTD s symptoms, pathophysiology, subtypes, as well as the latest from imaging studies. By Zac Haughn, Senior Associate Editor Ask
Confronting the Clinical Challenges of Frontotemporal Dementia A look at FTD s symptoms, pathophysiology, subtypes, as well as the latest from imaging studies. By Zac Haughn, Senior Associate Editor Ask
Views and Reviews. [ 123 I]FP-CIT (DaTscan) SPECT Brain Imaging in Patients with Suspected Parkinsonian Syndromes ABSTRACT
![Views and Reviews. [ 123 I]FP-CIT (DaTscan) SPECT Brain Imaging in Patients with Suspected Parkinsonian Syndromes ABSTRACT Views and Reviews. [ 123 I]FP-CIT (DaTscan) SPECT Brain Imaging in Patients with Suspected Parkinsonian Syndromes ABSTRACT](/thumbs/76/73233066.jpg) Views and Reviews [ 123 I]FP-CIT (DaTscan) SPECT Brain Imaging in Patients with Suspected Parkinsonian Syndromes Robert A. Hauser, MD, Donald G. Grosset, MD From the Departments of Neurology, Molecular
Views and Reviews [ 123 I]FP-CIT (DaTscan) SPECT Brain Imaging in Patients with Suspected Parkinsonian Syndromes Robert A. Hauser, MD, Donald G. Grosset, MD From the Departments of Neurology, Molecular
Evaluation of Parkinson s Patients and Primary Care Providers
 Evaluation of Parkinson s Patients and Primary Care Providers 2018 Movement Disorders Half Day Symposium Elise Anderson MD Medical Co-Director, PBSI Movement Disorders 6/28/2018 1 Disclosures GE Speaker,
Evaluation of Parkinson s Patients and Primary Care Providers 2018 Movement Disorders Half Day Symposium Elise Anderson MD Medical Co-Director, PBSI Movement Disorders 6/28/2018 1 Disclosures GE Speaker,
ALZHEIMER S DISEASE. Mary-Letitia Timiras M.D. Overlook Hospital Summit, New Jersey
 ALZHEIMER S DISEASE Mary-Letitia Timiras M.D. Overlook Hospital Summit, New Jersey Topics Covered Demography Clinical manifestations Pathophysiology Diagnosis Treatment Future trends Prevalence and Impact
ALZHEIMER S DISEASE Mary-Letitia Timiras M.D. Overlook Hospital Summit, New Jersey Topics Covered Demography Clinical manifestations Pathophysiology Diagnosis Treatment Future trends Prevalence and Impact
Mild Cognitive Impairment (MCI)
 October 19, 2018 Mild Cognitive Impairment (MCI) Yonas E. Geda, MD, MSc Professor of Neurology and Psychiatry Consultant, Departments of Psychiatry & Psychology, and Neurology Mayo Clinic College of Medicine
October 19, 2018 Mild Cognitive Impairment (MCI) Yonas E. Geda, MD, MSc Professor of Neurology and Psychiatry Consultant, Departments of Psychiatry & Psychology, and Neurology Mayo Clinic College of Medicine
Parkinson Disease. Lorraine Kalia, MD, PhD, FRCPC. Presented by: Ontario s Geriatric Steering Committee
 Parkinson Disease Lorraine Kalia, MD, PhD, FRCPC Key Learnings Parkinson Disease (L. Kalia) Key Learnings Parkinson disease is the most common but not the only cause of parkinsonism Parkinson disease is
Parkinson Disease Lorraine Kalia, MD, PhD, FRCPC Key Learnings Parkinson Disease (L. Kalia) Key Learnings Parkinson disease is the most common but not the only cause of parkinsonism Parkinson disease is
DEMENTIA WITH LEWY bodies (DLB) is the
 Psychiatry and Clinical Neurosciences 2017; 71: 409 416 doi:10.1111/pcn.12511 Regular Article Association of premorbid personality with behavioral and psychological symptoms in dementia with Lewy bodies:
Psychiatry and Clinical Neurosciences 2017; 71: 409 416 doi:10.1111/pcn.12511 Regular Article Association of premorbid personality with behavioral and psychological symptoms in dementia with Lewy bodies:
Dementia. Assessing Brain Damage. Mental Status Examination
 Dementia Assessing Brain Damage Mental status examination Information about current behavior and thought including orientation to reality, memory, and ability to follow instructions Neuropsychological
Dementia Assessing Brain Damage Mental status examination Information about current behavior and thought including orientation to reality, memory, and ability to follow instructions Neuropsychological
La neurosonologia. Ecografia cerebrale e nuove applicazioni nelle malattie neurodegenerative. Nelle patologie degenerative e vascolari cerebrali
 La neurosonologia Nelle patologie degenerative e vascolari cerebrali Andrea Pilotto Ecografia cerebrale e nuove applicazioni nelle malattie neurodegenerative Prof. Daniela Berg Department of Neurodegeneration
La neurosonologia Nelle patologie degenerative e vascolari cerebrali Andrea Pilotto Ecografia cerebrale e nuove applicazioni nelle malattie neurodegenerative Prof. Daniela Berg Department of Neurodegeneration
Depression and Anxiety in Parkinson s Disease. Bill Collins Symposium for Parkinson s Disease 2018 Robert Underwood, Ph.D. Licensed Psychologist
 Depression and Anxiety in Parkinson s Disease Bill Collins Symposium for Parkinson s Disease 2018 Robert Underwood, Ph.D. Licensed Psychologist Today s Discussion Review of Parkinson s Disease and Nonmotor
Depression and Anxiety in Parkinson s Disease Bill Collins Symposium for Parkinson s Disease 2018 Robert Underwood, Ph.D. Licensed Psychologist Today s Discussion Review of Parkinson s Disease and Nonmotor
Parkinson s Disease in the Elderly A Physicians perspective. Dr John Coyle
 Parkinson s Disease in the Elderly A Physicians perspective Dr John Coyle Overview Introduction Epidemiology and aetiology Pathogenesis Diagnosis and clinical features Treatment Psychological issues/ non
Parkinson s Disease in the Elderly A Physicians perspective Dr John Coyle Overview Introduction Epidemiology and aetiology Pathogenesis Diagnosis and clinical features Treatment Psychological issues/ non
NIH Public Access Author Manuscript Mov Disord. Author manuscript; available in PMC 2009 May 18.
 NIH Public Access Author Manuscript Published in final edited form as: Mov Disord. 2008 August 15; 23(11): 1602 1605. doi:10.1002/mds.22161. Emergence of Parkinsons Disease in Essential Tremor: A Study
NIH Public Access Author Manuscript Published in final edited form as: Mov Disord. 2008 August 15; 23(11): 1602 1605. doi:10.1002/mds.22161. Emergence of Parkinsons Disease in Essential Tremor: A Study
