COLLABORATION WITH OT IN TREATMENT OF DYSPHAGIA IN SEVERE DEMENTIA
|
|
|
- Darleen Wilkins
- 5 years ago
- Views:
Transcription
1 COLLABORATION WITH OT IN TREATMENT OF DYSPHAGIA IN SEVERE DEMENTIA Bob LeJeune; M.A., CCC SLP Progressive Step Rehab Sharon Kurfuerst; Ed.D.; OTR/L Christiana Health Services
2 Dementia Defined The American Psychiatric Association defines dementia as: A deterioration of intellectual capacities that has a significant negative impact on social and personal functioning A group of symptoms that may accompany certain diseases of physical conditions, but not a disease in and of itself
3 Dementia Defined (cont d) Dementia is a deterioration in intellectual capacity with impairments in at least 3 of the following spheres of mental activity: Language Visuospatial Skills Cognition Memory Personality
4 Types of Dementia Alzheimer s Disease Most common form of dementia Caused by a loss of brain cells Not reversible; not curable Disease process can be slowed Definitive diagnosis via autopsy
5 Types of Dementia (cont d) Vascular dementias, including multi infarct dementia Second most common form of dementia Caused by poor circulation of blood to the brain, often by repeated TIAs Progression can be slowed by controlling hypertension, diabetes, and overall vascular health
6 Types of Dementia (cont d) Lewy body dementia Caused by abnormal deposits of protein in nerve cells Symptoms often mimic Parkinson s Disease Thinking, attention, and concentration more impacted than memory and language Not reversible; not curable Same medicines used to slow Alzheimer s also have been shown to be effective here
7 Types of Dementia (cont d) Other Alcohol related dementia Pick s Disease (frontotemporal dementia) Senile dementia AIDS related dementia
8 Cognitive Disability With most dementias, progression of disease and/or predictable patterns of cognitive loss can be identified Cognitive disability requires making adjustments in daily activities and life roles Functional assessment helps to clarify the adjustments needed and the level of care that must be provided
9 Staging Dementia Staging dementia Helps facilitate documentation of the level of dementia that correlates to predictable characteristics of cognition, communication, mood, behavior, and ADL ability Provides a common language for all clinicians to use in caring for the person Assists in tracking the disease progression
10 Staging Dementia (cont d) Multiple tools exist (e.g., Global Deterioration Scale, Allen Cognitive Levels) Staging tools help provide a description of functional capabilities Global Deterioration Scale (GDS) most common interdisciplinary tool Breaks dementia into 7 stages that describe the degenerative process over 8 to 10 years
11 Global Deterioration Scale (GDS) Stage 1 No cognitive decline Stage 2 Very mild cognitive decline Stage 3 Mild cognitive decline Stage 4 Moderate cognitive decline
12 GDS (cont d) Stage 5 Moderately severe cognitive decline Stage 6 Severe cognitive decline Stage 7 Very severe cognitive decline ***today s focus will be on Stages 5 7
13 Stage 5 Characteristics Cannot survive without assistance Frequent disorientation to time and place Can follow some directions but cannot retain out of context Lives in the immediate situation Upset if you are not part of his/her reality Impatient, paranoid, suspicious Depression
14 Stage 5 (cont d) Needs assistance with multi step ADL (toileting, dressing) Performs best with activities that are error proof Can have difficulty with common objects Is unable to notice mistakes or solve problems Tunnel vision to 14 in front Uses different grasps for different objects
15 Stage 6 Characteristics Largely unaware of current events Abilities mimic that of 2 to 5 year old Resists unfamiliar and searches out familiar Wanders, has no boundaries, possessive of objects (theirs and those of others) Has a hard time sitting for meals Unable to recognize everyday objects
16 Stage 6 (cont d) Needs assistance both cognitive and physically with self care, except possibly self feeding May disrobe poor tolerance of dentures, hearing aids, glasses, socks, etc. Needs assistance to interpret issues of pain, anxiety, illness, hunger, thirst Postural difficulties (leaning, shuffling, sliding out of chair)
17 Stage 7 Characteristics Loss of basic psychomotor skills Cannot verbalize or manage physical needs Dependent on others for survival May respond to high contrast stimulus Dependent in ADL, including self feeding Emergence of significant dysphagia issues Significant postural and motor control issues At risk for skin breakdown, contractures, nutritional compromise, loss of swallowing function
18 Neurodevelopmental Treatment (NDT) Application for Feeding and Swallowing in Dementia
19 What is NDT? NDT is a problem solving approach to the examination and treatment of the impairments and functional limitations of individuals with neuropathology, primarily children with CP and adults with stroke or traumatic brain injury (TBI) These individuals have dysfunction in posture and movement that lead to limitations in functional activity NDT focuses on the analysis and treatment of sensorimotor impairments and functional limitations that physical therapists (PT), occupational therapists (OT), and speech and language pathologists (SLP) can address» NDTA (2009)
20 What is NDT? (cont d) Approach has a theoretical basis that is scientifically supported by the Neuronal Group Selection Theory (Edelman1987) Looks at the human body and how neurons are organized and compete to make connections as an individual experiences movement and selects and strengthens responses Relies on the development and enhancement of neurological maps or patterns of behavioral function Incorporates motor control and motor learning theories
21 Concepts of NDT The concept of neurodevelopmental treatment is based on the recognition of the importance of two factors: The interference of normal maturation of the brain by the lesion, leading to retardation or arrest of motor development The presence of abnormal patterns of posture and movement, due to a release of abnormal postural reflex activity
22 Concepts of NDT (cont d) Goal is the inhibition of the patterns of abnormal reflex activity and the facilitation of normal motor patterns Emphasis is placed on inhibiting abnormal patterns of posture and movement and on facilitating the greatest possible variety of innate normal basic motor patterns, such as head and trunk righting, arm hand support, and equilibrium reactions
23 Key Take Away to Remember The NDT approach involves viewing the individual as a whole person considering the entire body structure and function
24 Application to Dementia So what does this approach have to do with dementia? Normal course of development gets undone in reverse as the course of dementia progresses Functional biomechanical alignment, postural stability, and innate movement patterns can still be elicited or optimized even in the late stages of dementia
25 Application to Dementia (cont d) Sequentially, feeding and swallowing (i.e., sucking, swallowing, coordination of breath control) are the first ADL skills to be developed in the normal neuromotor developmental sequence Thus, they are also the last to be lost during the course of disease progression, including that of dementia
26 DYSPHAGIA AND SEVERE DEMENTIA: THE SCOPE OF THE PROBLEM
27 Individuals with Alzheimer s Disease weigh less than those with multi infarct dementia and less than non demented controls (Singh, 1988). Over half the residents in nursing homes are totally dependent in feeding (Siebens, et al, 1986). The cost of managing eating dependency accounts for 25% of the total cost of care in nursing homes
28 The severity of dementia will increase the chances of aspiration pneumonia (Wada, et al, 2001). Individuals with dementia are more at risk for dehydration due to inability to seek liquids, diminished thirst, a decrease in body mass (reducing water content of body), and decline in the ability to filtrated water due to renal failure (Garcia, 2001).
29 Poor oral care is not uncommon in the elderly and contributes not only to swallowing deficits but to weight loss, eating problems, dehydration, and behavioral problems. The ratio of hydration for thin versus nectar is 3 to 4 (4 ounces of thin equals 3 ounces of nectar) Thickening liquids adds approximately $.01 to the cost of every ounce of liquids
30 30% of all PEG tubes inserted in the US will be in individuals with dementia (Cervo, et al, 2006) As many as 10% of the total population in nursing homes in the US are being fed by PEG tubes (Cervo, et al, 2006)
31 WHY DO INDIVIDUALS WITH DEMENTIA HAVE DIFFICULTY EATING? Memory difficulties result in the individual thinking they have just eaten or when the next meal will be. Perceptual, spatial difficulties and motor impairment result in deficits in handling utensils and food. Language difficulties will decrease ability to express food preferences and/or problems with understanding mealtime instructions.
32 IMPACT OF COGNTIVE DEFICITS ON EATING/SWALLOWING Forgetting when their last meal occurred so they feel as if they are not hungry Difficulty in sitting for a meal Difficulty in recognizing food Impairment in expressing or knowing food preferences
33 Problems understanding mealtime instructions Socially inappropriate mealtime behavior Paranoia/delusions about food Difficulty in seating for a meal Slow eating Hallucinations regarding food
34 TYPES OF DYSPHAGIA ASSOCIATED WITH DEMENTIA Alzheimer s disease Vascular (multi infarct) dementia Lewy body dementia Pick s disease (frontotemporal dementia)
35 ALZHEIMER S DISEASE Reduced lingual peristalsis resulting in diffuse bolus formation and delayed bolus transit Difficulty with mouth opening Muscle spasms including oral musculature Difficulty with trunk and neck control resulting in poor posture Delayed initiation of the swallow reflex
36 VASCULAR (MULTI IMFARCT) DEMETIA Hemiparesis including oral musculature resulting in poor labial seal and reduced bolus control Reduced ability for hand to mouth activities
37 LEWY BODY DEMENTIA Deficits with attention to meal may lead to a lack of desire to eat Visual spatial deficits making self feeding difficult Recurrent hallucinations may lead to refusal for assistance in feeding Parkinson s motor features
38 PICK S DISEASE Lose social skills for eating and may result in eating quickly, cramming food increasing risks of aspiration Development of a likening to sweet foods
39 SOME EVALUATION SUGGESTIONS: Read the chart thoroughly noting diet level and restrictions (NAS, cardiac, etc) Review weight record and when available average consumption for each meal Look at typical positioning at meals and location that most meals are consumed Talk to the caregivers about behavioral issues they have with the individual at meals Look at positioning in bed and seated
40 Trial different levels of food/liquids without any facilitation techniques/strategies Consider doing the evaluation in two parts: early and late in the day When possible observe the caretaker feeding the resident When possible assess respiratory function through pulse oximetry or other measures
41 DIAGNOSIS OF DYSPHAGIA No Impairment: the individual is able to safely swallow all consistencies of liquids and solids without delay and without any signs of difficulty Mild Impairment: the individual has difficulty chewing the hardest consistency, slight increase in lingual peristalsis or slight delay in onset of the swallow reflex
42 Moderate Impairment: difficulty in chewing several consistencies, bolus control with liquids, coughing noted resulting in the individual reducing their consumption Severe Impairment: very little bolus formation and management, significant delay in onset of the swallow resulting in significant reduction in their ability to consume food sufficient for their nutritional needs
43 Profound Impairment: unaware of the need to eat or that food is present, symptoms of aspiration noted at each meal resulting in significant risk for malnutrition/dehydration and/or pneumonia
44 DETERMINING NEED FOR FURTHER DIAGNOSTIC PROCEDURES There is suspicion that pharyngeal stasis is occurring resulting in fever, reduced respiratory function, or other potentially lifethreatening issues There is questionable esophageal symptoms that negatively impacting the individuals ability to safely consume food
45 The symptoms of dysphagia are so diffuse that objective data is necessary to determine the presence of dysphagia and make safe recommendations for diet level and the need for intervention
46 TYPES OF DYSPHAGIA Oral Stage Dysphagia Pharyngeal Stage Dysphagia Esophageal Dysphagia Mixed Dysphagia
47 ORAL STAGE DYSPHAGIA Labial leaking resulting in anterior leakage reducing nutritional intake Reduced lingual peristalsis limiting the ability to form and manipulate the bolus posterior Pocketing or storage of food potentially providing debris that can trickle into the airway resulting in aspiration
48 PHARYGEAL STAGE DYSPHAGIA Delayed onset of the swallow reflex resulting in an open airway as the bolus is propelled posterior into the pharyngeal area Stasis in the area of the valleculae that could result in trickle aspiration Reduced closure of the airway causing solid food or liquid particles to travel into the lungs
49 ESOPHAGEAL DYSPHAGIA Reduced esophageal peristalsis resulting in food falling too slowing causing food or liquids to travel superiorly potential traveling into the airway Esophageal reflux where food is either at the inferior end of the esophagus or the stomach and is returned into the superior end of the esophagus
50 MIXED DYSPHAGIA A combination of symptoms (oral, pharyngeal, and/or esophageal)
51 DIET LEVEL CONSIDERATIONS Provide a diet level that is safe Provide a diet level that can be effectively AND efficiently provided by caretakers Provide a diet that will support the need for nutrition and hydration
52 There is minimal concern that the individual can safely hold a cup, glass, or utensil without injury or excessive spillage unless you are certain they will have assistance with all liquids including water at bedside
53 LIQUID LEVELS Thin Nectar Honey Pudding
54 THIN LIQUIDS There is no concern that the individual can consume the consistency with any type of liquid (water, juice, coffee, milk, etc) There is adequate labial seal There is little or no evidence of oral retention There is no evidence of pharyngeal symptoms (coughing, wet vocal quality, etc)
55 NECTAR LIQUIDS There is at least mild reduction in labial sealing causing anterior spillage There is a reduction in bolus transit whereby the slight increase in consistency will compensate for the deficit There is at least fair residue after the swallow with thin level liquids There is more than occasional pharyngeal symptoms with thin liquids
56 HONEY LIQUIDS There is significant anterior spillage to the extent that the majority of the liquids spills out of the oral cavity There is reduced lingual peristalsis so that the individual is unable to propel the bolus posterior or compensate for the deficit There is more than occasional difficulty with thin or nectar level liquids
57 PUDDING LIQUIDS There is such labial leakage that any other level of liquid would result in almost no liquids remaining in the oral cavity to be swallowing There is no lingual movement to facilitate posterior bolus propulsion
58 REGULAR FOOD There is little or no concern that the individual can consume any food presented with little or no alteration The level of food is safe whether the individual is able to self feed or be fed by a caretaker The individual is able to be consume adequate calories to meet their nutritional needs
59 MECHANICAL SOFT The individual has decreased ability to cut food into segments small enough to be safely ingested The individual has decreased mastication skills The individual has mild to moderate residue of solid food after the swallow The individual is unable to be positioned so that regular consistency is viewed as safe
60 PUREED LEVEL The individual has little or no labial seal so that the majority of a higher level consistency would not be ingested There is severe decrease in mastication skills so that the individual is unable to form a bolus or propel it timely posterior There are signs/symptoms of pharyngeal stasis
61 TO TREAT OR NOT TO TREAT There is the presence of dysphagia symptoms with their current diet There is a concern that the individual s ability to consume food will not meet their nutritional needs unless the food/liquid is altered Caregivers need education to safely present the food to the individual or provide the food to individuals who must be fed
62 There has been a change in their condition or medication that warrants intervention The individual s typical position for meals places them at risk for dysphagia The individual is responsive to commands (if they self feed) or allow you to feed them
63 TREATMENT CONSIDERATIONS:
64 Food intake is a social activity and should remain as such until it is not feasible or in the best interest of the patient you are treating or other individuals All treatment should focus on the rebuilding of normal neural pathways and as such a diet downgrade at the beginning of treatment may be indicated
65 Treatment should be a tactile experience; as such, you do not necessarily have to clean food debris outside the oral cavity unless the dignity of the patient is compromised or for reasons of safety Treatment should include a meal in bed and a meal while seated
66 Effective treatment may need to occur at a variety of times or with sessions that are split into smaller sections of time Treatment may include meals as well as snacks Treatment ALWAYS should include education specific to the patient AND to general good feeding techniques
67 Determine where it is best that both you and the patient sit during treatment Chewing and swallowing sounds will facilitate the multi sensory approach to the meal Conversations about food enhance the therapeutic process and the multi sensory approach to therapy
68 Conversations about food enhance the therapeutic process and the multi sensory approach to therapy It is easier to dehydrate than to starve so ALWAYS have liquids as a part of your treatment and end every treatment with liquids
69 TREATMENT STRATEGIES Oral stage Pharyngeal Stage Esophageal Stage
70 REDUCED LABIAL SEAL Use a straw rather than a spoon to present the bolus (best with pureed level foods or honey thick liquids) Touch or tap the lips with the spoon after the bolus is presented If the patient does not become agitated attempt to close the lower lip with either the spoon or with your hands
71 DECREASE LINGUAL MOBILITY (ANTERIOR POSTEROR) Add pressure to the tongue when presenting the bolus Use a straw to present the bolus outside the mouth and have the patient secure with their tongue and alternate locations When safe place the bolus in various places in the oral cavity When safe, place the bolus posterior in the oral cavity
72 REDUCED LINGUAL PERISTALSIS Alternate solids with liquids Consider liquifying solids Use the straw outside the mouth on each side to provide the bolus Consider downgrading the most difficult consistency (e.g. puree meats)
73 POCKETING/RESIDUE AFTER THE SWALLOW Provide liquids after each bite of solid and at least 120 cc at the end of the meal Keep the patient upright after the meal Reduce the size of the food bolus Chop food before presenting bolus
74 DELAYED INITIATION OF THE SWALLOW REFLEX If the patient does not become agitated physically tilt their head forward Consider downgrading diet Present bolus but do not provide until swallow is triggered
75 REGURGITATION Have the patient upright 30 minutes before the meal, upright during the meal and 30 to 45 minutes after the meal Feed the patient slowly with small bites and small sips Consult the dietician to determine if some foods need to be removed from the diet Consult nursing for potential medications to reduce reflux
76 Adaptive Equipment for Eating Adaptive Equipment for Eating Nonskid pads High rimmed plate Special cups Universal cuff fitted with utensil Adaptive handle utensil (weighted or built up) Swivel Utensil Mobile Arm Supports
77 Adaptive Cups
78 Adaptive Cups
79 Rocker Knife
80 Long Handled Utensils
81 \] Built up, Weighted, and Angled Utensils
82 Universal Cuff with Wrist Support and Angled Spoon
83 Swivel Spork
84 Universal Cuffs with Utensil
85 Coated Spoon
86 Final Considerations Eating is as much a cognitive, social, and emotional activity as it is a physiologic one For persons with dementia, the cognitive, social, and emotional aspects of eating cannot be ignored Preservation of feeding and swallowing abilities, or minimizing their decline, is possible in persons with dementia
87 WHEN TO DISCHARGE There is no change in their ability with skilled intervention There has been a sentinel event in their medical condition that does not allow any benefit from skilled intervention
88 SOME THOUGHTS ON NON ORAL FEEDING (PEG TUBE)
89 PEG tube insertion may reduce lower esophageal sphincter pressure thereby increasing the risk of aspiration and do not eliminate oral secretion aspiration There is also the risk of aspiration of stomach contents (Li, 2002) Weight loss and pressure ulcer development are associated with long term PEG tube feeding (Henderson, 1992)
90 May increase suffering and discomfort thereby decreasing quality of life PEG tube insertion does not eliminate the disease process that initially caused their dysphagia and/or the lack of appetite Mechanical problems such as tube leakage, tube blockage, and tube malfunction can place the individual at risk for infection, skin excoriation, and increased pain at the site
91 WHEN TO CONSIDER ENDING PO INTAKE Successive instances of aspiration pneumonia usually within a short period of time MBS indicates clear aspiration with no evidence of compensatory strategies or modified consistencies reducing the risk Signs/symptoms of aspiration occur daily over a period of time
92 IN SUMMARY Caring for the individual with dysphagia and severe dementia is most effective when other disciplines including caregivers are involved in the treatment process Always teach best practice for safety by example The treatment plan should center on a diet that is safe but provides adequate nutrition and hydration
93 QUESTIONS?????
Dysphagia Management in TCP. Susan Smith and Vanessa Barkla Speech Pathologists, Ballarat Health Services May 2012
 Dysphagia Management in TCP Susan Smith and Vanessa Barkla Speech Pathologists, Ballarat Health Services May 2012 The role of the Speech Pathologist To assess swallowing status To provide management and
Dysphagia Management in TCP Susan Smith and Vanessa Barkla Speech Pathologists, Ballarat Health Services May 2012 The role of the Speech Pathologist To assess swallowing status To provide management and
Dysphagia Identification and Management
 Dysphagia Identification and Management Presented By Speech-Language Pathologist Developmental Disabilities Administration DC Department on Disability Services Training Objectives After this training session
Dysphagia Identification and Management Presented By Speech-Language Pathologist Developmental Disabilities Administration DC Department on Disability Services Training Objectives After this training session
SWALLOWING DIFFICULTIES IN HD
 Nutrition, eating and swallowing needs, challenges and solutions Workshop SWALLOWING DIFFICULTIES IN HD Angela Nuzzi Speech and Language Pathologist (SLP) EHDN Language Coordinator - Italy The role of
Nutrition, eating and swallowing needs, challenges and solutions Workshop SWALLOWING DIFFICULTIES IN HD Angela Nuzzi Speech and Language Pathologist (SLP) EHDN Language Coordinator - Italy The role of
Swallowing Screen Why? How? and So What? พญ.พวงแก ว ธ ต สก ลช ย ภาคว ชาเวชศาสตร ฟ นฟ คณะแพทยศาสตร ศ ร ราชพยาบาล
 Swallowing Screen Why? How? and So What? พญ.พวงแก ว ธ ต สก ลช ย ภาคว ชาเวชศาสตร ฟ นฟ คณะแพทยศาสตร ศ ร ราชพยาบาล Dysphagia in Stroke The incidence of dysphagia after stroke ranging from 23-50% 1 Location
Swallowing Screen Why? How? and So What? พญ.พวงแก ว ธ ต สก ลช ย ภาคว ชาเวชศาสตร ฟ นฟ คณะแพทยศาสตร ศ ร ราชพยาบาล Dysphagia in Stroke The incidence of dysphagia after stroke ranging from 23-50% 1 Location
The Role of the Speech Language Pathologist & Spinal Cord Injury
 The Role of the Speech Language Pathologist & Spinal Cord Injury Facts According to the National Spinal Cord Injury Statistical Center (NSCISC) there are approxiamtely 12,000 new spinal cord injuries (SCI)
The Role of the Speech Language Pathologist & Spinal Cord Injury Facts According to the National Spinal Cord Injury Statistical Center (NSCISC) there are approxiamtely 12,000 new spinal cord injuries (SCI)
EATING SAFELY AND TALKING ABOUT IT KIERA N BERGGREN, MA/CCC-SLP, MS 2018 FSHD CONNECT CONFERENCE
 EATING SAFELY AND TALKING ABOUT IT KIERA N BERGGREN, MA/CCC-SLP, MS 2018 FSHD CONNECT CONFERENCE DISCLOSURES I have no personal financial relationships with commercial interests relevant to this presentation
EATING SAFELY AND TALKING ABOUT IT KIERA N BERGGREN, MA/CCC-SLP, MS 2018 FSHD CONNECT CONFERENCE DISCLOSURES I have no personal financial relationships with commercial interests relevant to this presentation
Chapter 27 & 28. Key Terms. Digestive System. Fig. 27-1, p. 443 Also known as the Gastrointestinal System (GI system)
 Chapter 27 & 28 Nutrition & Fluids Key Terms Aspiration Dehydration Edema Dysphagia Gastrostomy tube Intravenous therapy (IV) Digestive System Fig. 27-1, p. 443 Also known as the Gastrointestinal System
Chapter 27 & 28 Nutrition & Fluids Key Terms Aspiration Dehydration Edema Dysphagia Gastrostomy tube Intravenous therapy (IV) Digestive System Fig. 27-1, p. 443 Also known as the Gastrointestinal System
RECOMMENDATIONS & UPDATES IN THE MANAGEMENT OF POST- STROKE DYSPHAGIA
 RECOMMENDATIONS & UPDATES IN THE MANAGEMENT OF POST- STROKE DYSPHAGIA Feeding in the Acute Stroke Period: - Early initiation of feeding is beneficial w/c decreases the risk of infections, improve survival
RECOMMENDATIONS & UPDATES IN THE MANAGEMENT OF POST- STROKE DYSPHAGIA Feeding in the Acute Stroke Period: - Early initiation of feeding is beneficial w/c decreases the risk of infections, improve survival
HOMES AND SENIORS SERVICES. APPROVAL DATE: August 1985 REVISION DATE: January 2015 REVIEW DATE: May 2018
 POLICY: Page 1 of 10 Residents who experience signs and symptoms associated with dysphagia will have their nutrition and hydration needs met in a safe, coordinated manner as managed by the interdisciplinary
POLICY: Page 1 of 10 Residents who experience signs and symptoms associated with dysphagia will have their nutrition and hydration needs met in a safe, coordinated manner as managed by the interdisciplinary
Chapter 19. Nutrition and Fluids. All items and derived items 2015, 2011 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved.
 Chapter 19 Nutrition and Fluids Nutrition Nutrition--processes involved in the ingestion, digestion, absorption & use of foods & fluids by the body. The person s diet affects physical & mental wellbeing
Chapter 19 Nutrition and Fluids Nutrition Nutrition--processes involved in the ingestion, digestion, absorption & use of foods & fluids by the body. The person s diet affects physical & mental wellbeing
Palliative Care Swallowing Management HEATHER STORIE M.S.,CCC-SLP, BCS-S SPEECH LANGUAGE PATHOLOGY, BOARD CERTIFIED SWALLOWING SPECIALIST
 Palliative Care Swallowing Management HEATHER STORIE M.S.,CCC-SLP, BCS-S SPEECH LANGUAGE PATHOLOGY, BOARD CERTIFIED SWALLOWING SPECIALIST Objectives Gain a general understanding of normal swallowing Gain
Palliative Care Swallowing Management HEATHER STORIE M.S.,CCC-SLP, BCS-S SPEECH LANGUAGE PATHOLOGY, BOARD CERTIFIED SWALLOWING SPECIALIST Objectives Gain a general understanding of normal swallowing Gain
Reluctance or refusal to feed or eat. Understanding Feeding Aversion in a City Full of Foodies. Presentation Outline. Learning Objectives
 Understanding Feeding Aversion in a City Full of Foodies Amy Houtrow, MD, MPH Pediatric Physical Medicine & Rehabilitation UCSF Department of Pediatrics June 2, 2007 Learning Objectives Learners will be
Understanding Feeding Aversion in a City Full of Foodies Amy Houtrow, MD, MPH Pediatric Physical Medicine & Rehabilitation UCSF Department of Pediatrics June 2, 2007 Learning Objectives Learners will be
Safe swallowing strategies
 Learning Guide Safe swallowing strategies 27468 Apply safe swallowing strategies in a health or wellbeing setting Level 3 5 credits Name: Workplace: Issue 2.0 Copyright 2017 Careerforce All rights reserved.
Learning Guide Safe swallowing strategies 27468 Apply safe swallowing strategies in a health or wellbeing setting Level 3 5 credits Name: Workplace: Issue 2.0 Copyright 2017 Careerforce All rights reserved.
Assessing the Eating Needs of Personal Care Services (PCS) Beneficiaries Effective 12/1/2016
 Assessing the Eating Needs of Personal Care Services (PCS) Beneficiaries Effective 12/1/2016 The Freedom to Succeed November 22,2016 Content Introduction Signs and Symptoms Caring for Individuals with
Assessing the Eating Needs of Personal Care Services (PCS) Beneficiaries Effective 12/1/2016 The Freedom to Succeed November 22,2016 Content Introduction Signs and Symptoms Caring for Individuals with
Review of dysphagia in poststroke
 Review of dysphagia in poststroke patients Danielle Thompson, Speech and Language Therapist Northwick Park Hospital With acknowledgement to Mary McFarlane, Principal Speech and Language Therapist, Acute
Review of dysphagia in poststroke patients Danielle Thompson, Speech and Language Therapist Northwick Park Hospital With acknowledgement to Mary McFarlane, Principal Speech and Language Therapist, Acute
When Eating Becomes A Challenge Dysphagia
 When Eating Becomes A Challenge Dysphagia 1. DYSPHAGIA, WHAT IS IT? 2. IMPLICATIONS 3. ASSESSMENT 4. COMPENSATORY SWALLOWING AND EXERCISES 5. DIET TEXTURE ADJUSTMENTS Swallowing Dysfunction = Dysphagia
When Eating Becomes A Challenge Dysphagia 1. DYSPHAGIA, WHAT IS IT? 2. IMPLICATIONS 3. ASSESSMENT 4. COMPENSATORY SWALLOWING AND EXERCISES 5. DIET TEXTURE ADJUSTMENTS Swallowing Dysfunction = Dysphagia
Workbook. Apply safe swallowing strategies as a health assistant in an aged care, health or disability context. US Level 4 Credits 4. Name...
 Workbook Apply safe swallowing strategies as a health assistant in an aged care, health or disability context US 27468 Level 4 Credits 4 Name... US 27468 Level 4 Credits 4 All rights reserved. Careerforce
Workbook Apply safe swallowing strategies as a health assistant in an aged care, health or disability context US 27468 Level 4 Credits 4 Name... US 27468 Level 4 Credits 4 All rights reserved. Careerforce
Pediatric Modified Barium Swallow Studies. Presented by Jody Bousquet, MA, CCC- SLP Susan Shonbrun, MS, CCC- SLP November 7, 2015
 Pediatric Modified Barium Swallow Studies Presented by Jody Bousquet, MA, CCC- SLP Susan Shonbrun, MS, CCC- SLP November 7, 2015 Definition * Modified Barium Swallow Study * Assesses swallow functions
Pediatric Modified Barium Swallow Studies Presented by Jody Bousquet, MA, CCC- SLP Susan Shonbrun, MS, CCC- SLP November 7, 2015 Definition * Modified Barium Swallow Study * Assesses swallow functions
WEBINAR SERIES: AGING IN INDIVIDUALS WITH INTELLECTUAL AND DEVELOPMENTAL DISABILITIES
 WEBINAR SERIES: AGING IN INDIVIDUALS WITH INTELLECTUAL AND DEVELOPMENTAL DISABILITIES 1 CMS Medicare-Medicaid Coordination Office (MMCO) Established by Section 2602 of the Affordable Care Act Purpose:
WEBINAR SERIES: AGING IN INDIVIDUALS WITH INTELLECTUAL AND DEVELOPMENTAL DISABILITIES 1 CMS Medicare-Medicaid Coordination Office (MMCO) Established by Section 2602 of the Affordable Care Act Purpose:
Feeding and Oral Hygiene: How to Address the Challenges
 Feeding and Oral Hygiene: How to Address the Challenges Paige W. Roberts, OTR/L Occupational Therapist Pediatric Feeding Disorders Program Marcus Autism Center Disclaimer: This content is for personal
Feeding and Oral Hygiene: How to Address the Challenges Paige W. Roberts, OTR/L Occupational Therapist Pediatric Feeding Disorders Program Marcus Autism Center Disclaimer: This content is for personal
Clinical Swallowing Exam
 Clinical Evaluation Template 1 Clinical Exam Name: ID/Medical record number: Date of exam: Referred by: Reason for referral: Medical diagnosis: Date of onset of diagnosis: Other relevant medical history/diagnoses/surgery
Clinical Evaluation Template 1 Clinical Exam Name: ID/Medical record number: Date of exam: Referred by: Reason for referral: Medical diagnosis: Date of onset of diagnosis: Other relevant medical history/diagnoses/surgery
Chef Rick Schmitt, CDM, CFPP Assistant Dining Director/Executive Chef Westminster Towers Rock Hill, SC
 Chef Rick Schmitt, CDM, CFPP Assistant Dining Director/Executive Chef Westminster Towers Rock Hill, SC Water/Hydration Food/Nutrition Shelter/Security Love/Acceptance/Belonging Definition A chronic or
Chef Rick Schmitt, CDM, CFPP Assistant Dining Director/Executive Chef Westminster Towers Rock Hill, SC Water/Hydration Food/Nutrition Shelter/Security Love/Acceptance/Belonging Definition A chronic or
The Clinical Swallow Evaluation: What it can and cannot tell us. Introduction
 The Clinical Swallow Evaluation: What it can and cannot tell us Debra M. Suiter, Ph.D., CCC-SLP, BCS-S Director, Voice & Swallow Clinic Associate Professor, Division of Communication Sciences & Disorders
The Clinical Swallow Evaluation: What it can and cannot tell us Debra M. Suiter, Ph.D., CCC-SLP, BCS-S Director, Voice & Swallow Clinic Associate Professor, Division of Communication Sciences & Disorders
Meat. Chicken, steak, fish, beans, pork and veal products are members of the meat group.
 HOW NUTRITION AND FLUID NEEDS CHANGE WITH AGE Food and nutritional needs change as a person gets older and older. The need for a lot of calories decreases when a person gets older. These needs were highest
HOW NUTRITION AND FLUID NEEDS CHANGE WITH AGE Food and nutritional needs change as a person gets older and older. The need for a lot of calories decreases when a person gets older. These needs were highest
Role of Dining Services and Dietary Needs of the Resident, 2014
 Role of Dining Services and Dietary Needs of the Resident, 2014 It is the dining services role to provide quality meals and service to all residents that is as home-like as possible. This will be done
Role of Dining Services and Dietary Needs of the Resident, 2014 It is the dining services role to provide quality meals and service to all residents that is as home-like as possible. This will be done
Feeding Assistant Training Session #2
 Feeding Assistant Training Session #2 Dr. Heidi J. Silver, PhD, RDN Mrs. Abbie Hudson, BS, RDN Vanderbilt Center for Quality Aging & Qsource Vanderbilt Center for Human Nutrition Why is Nutrition Important?
Feeding Assistant Training Session #2 Dr. Heidi J. Silver, PhD, RDN Mrs. Abbie Hudson, BS, RDN Vanderbilt Center for Quality Aging & Qsource Vanderbilt Center for Human Nutrition Why is Nutrition Important?
Swallowing Disorders and Their Management in Patients with Multiple Sclerosis
 National Multiple Sclerosis Society 733 Third Avenue New York, NY 10017-3288 Clinical Bulletin Information for Health Professionals Swallowing Disorders and Their Management in Patients with Multiple Sclerosis
National Multiple Sclerosis Society 733 Third Avenue New York, NY 10017-3288 Clinical Bulletin Information for Health Professionals Swallowing Disorders and Their Management in Patients with Multiple Sclerosis
Swallowing problems. Patient information. Name: Date: Speech and Language Therapist: Reviewed: May 2016 Next review: June 2017 Version 1
 Patient information Swallowing problems Name: Date: Speech and Language Therapist: Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk Reviewed:
Patient information Swallowing problems Name: Date: Speech and Language Therapist: Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk Reviewed:
Dignified Dining: A guide to enhance dining experience for residents with dementia
 YOUR DATES HERE YOUR LOGO HERE Dignified Dining: A guide to enhance dining experience for residents with dementia Jessica Shyu, M.S., R.D. Senior Director of Nutrition & Wellness Morrison Senior Living
YOUR DATES HERE YOUR LOGO HERE Dignified Dining: A guide to enhance dining experience for residents with dementia Jessica Shyu, M.S., R.D. Senior Director of Nutrition & Wellness Morrison Senior Living
Feeding and Swallowing Problems in the Child with Special Needs
 Feeding and Swallowing Problems in the Child with Special Needs Joan Surfus, OTR/L, SWC Amy Lynch, MS, OTR/L Misericordia University This presentation is made possible, in part, by the support of the American
Feeding and Swallowing Problems in the Child with Special Needs Joan Surfus, OTR/L, SWC Amy Lynch, MS, OTR/L Misericordia University This presentation is made possible, in part, by the support of the American
Swallowing after a Total Laryngectomy
 Swallowing after a Total Laryngectomy Diane Longnecker, M.S.,CCC-SLP, BCS-S Baylor Institute for Rehabilitation at Baylor University Medical Center Dallas, TX Disclosure Statement No relevant financial
Swallowing after a Total Laryngectomy Diane Longnecker, M.S.,CCC-SLP, BCS-S Baylor Institute for Rehabilitation at Baylor University Medical Center Dallas, TX Disclosure Statement No relevant financial
Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing
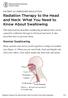 PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
SWALLOWING: HOW CAN WE HELP
 SWALLOWING: HOW CAN WE HELP Carol Romero-Clark, M.S., CCC-SLP University of New Mexico Hospital Speech Pathology Department November 10, 2017 What happens when you swallow? Mouth (Oral Phase) Your tongue
SWALLOWING: HOW CAN WE HELP Carol Romero-Clark, M.S., CCC-SLP University of New Mexico Hospital Speech Pathology Department November 10, 2017 What happens when you swallow? Mouth (Oral Phase) Your tongue
Slide 1. Slide 2 Disclosure. Slide 3 Objectives. Functional Mobility and Activities of Daily Living: Assessing and Treating Patients in Rehabilitation
 Slide 1 Functional Mobility and Activities of Daily Living: Assessing and Treating Patients in Rehabilitation Terry Carolan, MSPT, NCS Slide 2 Disclosure Terry Carolan has no industry disclosures to make
Slide 1 Functional Mobility and Activities of Daily Living: Assessing and Treating Patients in Rehabilitation Terry Carolan, MSPT, NCS Slide 2 Disclosure Terry Carolan has no industry disclosures to make
NUTRITION CARE ALERTS
 APPENDIX 10 A NUTRITION CARE ALERTS and for Caregivers in Nursing Facilities or at Home Proper nutrition care is vital to the health and well-being of nursing facility residents and seniors living in their
APPENDIX 10 A NUTRITION CARE ALERTS and for Caregivers in Nursing Facilities or at Home Proper nutrition care is vital to the health and well-being of nursing facility residents and seniors living in their
Every 67seconds, someone will develop Alzheimer's.
 We all need a purpose and responsibilities to live a healthy life. Dementia Care 101 Corrin Campbell BS, COTA/L & Michael Urban, MS, OTR/L, MBA Every 67seconds, someone will develop Alzheimer's. http://www.alz.org
We all need a purpose and responsibilities to live a healthy life. Dementia Care 101 Corrin Campbell BS, COTA/L & Michael Urban, MS, OTR/L, MBA Every 67seconds, someone will develop Alzheimer's. http://www.alz.org
Prepare Meals Before Eating
 Eating Technique Eating Techniques After bariatric surgery you must learn how to Eat smaller portions of food Eat slower Eating slowly is extremely important after bariatric surgery to prevent Nausea Vomiting
Eating Technique Eating Techniques After bariatric surgery you must learn how to Eat smaller portions of food Eat slower Eating slowly is extremely important after bariatric surgery to prevent Nausea Vomiting
Dysphagia and Swallowing. Jan Adams, DNP, MPA, RN and Karen Kern
 Dysphagia and Swallowing Jan Adams, DNP, MPA, RN and Karen Kern Scope of the Problem and Incidence 15 million people in the US have some form of Dysphagia. Every year, 1 million people are diagnosed with
Dysphagia and Swallowing Jan Adams, DNP, MPA, RN and Karen Kern Scope of the Problem and Incidence 15 million people in the US have some form of Dysphagia. Every year, 1 million people are diagnosed with
Chapter 20. Assisting With Nutrition and Fluids
 Chapter 20 Assisting With Nutrition and Fluids Food and water: Are physical needs Basics of Nutrition Are necessary for life A poor diet and poor eating habits: Increase the risk for diseases and infection
Chapter 20 Assisting With Nutrition and Fluids Food and water: Are physical needs Basics of Nutrition Are necessary for life A poor diet and poor eating habits: Increase the risk for diseases and infection
New Evidence-Based Support of a 3 Ounce Water Swallow Challenge Protocol
 New Evidence-Based Support of a 3 Ounce Water Swallow Challenge Protocol Steven B. Leder, Ph.D. Yale University School of Medicine New Haven, Connecticut Debra M. Suiter, Ph.D. VA Medical Center-Memphis
New Evidence-Based Support of a 3 Ounce Water Swallow Challenge Protocol Steven B. Leder, Ph.D. Yale University School of Medicine New Haven, Connecticut Debra M. Suiter, Ph.D. VA Medical Center-Memphis
Chapter 23. Nutrition Needs. Copyright 2019 by Elsevier, Inc. All rights reserved.
 Chapter 23 Nutrition Needs Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 23.1 Define the key terms and key abbreviations in this chapter. Explain the purpose and use of the MyPlate symbol.
Chapter 23 Nutrition Needs Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 23.1 Define the key terms and key abbreviations in this chapter. Explain the purpose and use of the MyPlate symbol.
Communication and Swallowing with PSP/CBD. Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist
 Communication and Swallowing with PSP/CBD Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist A Speech Therapist? Why? Swallowing (Dysphagia) Speech (Dysarthria, Dysphonia) Language (Aphasia) An Experienced
Communication and Swallowing with PSP/CBD Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist A Speech Therapist? Why? Swallowing (Dysphagia) Speech (Dysarthria, Dysphonia) Language (Aphasia) An Experienced
Relevant Listings for Evaluating Traumatic Brain Injury at Step 3 of the Sequential Evaluation
 Relevant Listings for Evaluating Traumatic Brain Injury at Step 3 of the Sequential Evaluation I. Neurological Disorders Revised Medical Criteria for Evaluating Neurological Disorders went into effect
Relevant Listings for Evaluating Traumatic Brain Injury at Step 3 of the Sequential Evaluation I. Neurological Disorders Revised Medical Criteria for Evaluating Neurological Disorders went into effect
What is Dysphagia? An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION What is Dysphagia? An information guide What is Dysphagia? If someone has dysphagia, this means they have difficulty in swallowing. Dysphagia
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION What is Dysphagia? An information guide What is Dysphagia? If someone has dysphagia, this means they have difficulty in swallowing. Dysphagia
NDTA BASIC ADULT COURSE KEY TO COURSE CONTENT
 Topic: Atypical Patterns of Movement Learning outcome(s) that pertain to occupational therapists 1. Identify the influence of atypical patterns of movement on: Postural alignment Transitional movements
Topic: Atypical Patterns of Movement Learning outcome(s) that pertain to occupational therapists 1. Identify the influence of atypical patterns of movement on: Postural alignment Transitional movements
Decline in Mental Capacity
 Decline in Mental Capacity Elder Law: Issues, Answers and Opportunities ALI-ABA, February 23-24, 2006 Robert B. Fleming 1 FLEMING & CURTI, P.L.C. 330 N. Granada Ave. Tucson, Arizona 85701 www.elder-law.com
Decline in Mental Capacity Elder Law: Issues, Answers and Opportunities ALI-ABA, February 23-24, 2006 Robert B. Fleming 1 FLEMING & CURTI, P.L.C. 330 N. Granada Ave. Tucson, Arizona 85701 www.elder-law.com
Creating Better Lives for People with Dementia
 Creating Better Lives for People with Dementia PRESENTED BY: Kim Warchol, OTR/L Founder and President of Dementia Care Specialists LeadingAge/LALA Conference Objectives 1. Identify prevalence and characteristics
Creating Better Lives for People with Dementia PRESENTED BY: Kim Warchol, OTR/L Founder and President of Dementia Care Specialists LeadingAge/LALA Conference Objectives 1. Identify prevalence and characteristics
No more tears at tea time: An occupational therapy approach to feeding difficulties
 Child Early Intervention Medical Centre Occupational Therapy Department Presents No more tears at tea time: An occupational therapy approach to feeding difficulties Presented by: Jennifer Logan Occupational
Child Early Intervention Medical Centre Occupational Therapy Department Presents No more tears at tea time: An occupational therapy approach to feeding difficulties Presented by: Jennifer Logan Occupational
If you have dementia, you may have some or all of the following symptoms.
 About Dementia Dementia may be caused by a number of illnesses that affect the brain. Dementia typically leads to memory loss, inability to do everyday things, difficulty in communication, confusion, frustration,
About Dementia Dementia may be caused by a number of illnesses that affect the brain. Dementia typically leads to memory loss, inability to do everyday things, difficulty in communication, confusion, frustration,
10/17/2017. Causes of Dementia Alzheimer's Disease Vascular Dementia Diffuse Lewy Body Disease Alcoholic Dementia Fronto-Temporal Dementia Others
 1 Dementia Dementia comes from the Latin word demens, meaning out of mind. It is the permanent loss of multiple intellectual functions. It is progressive deterioration of mental powers accompanied by changes
1 Dementia Dementia comes from the Latin word demens, meaning out of mind. It is the permanent loss of multiple intellectual functions. It is progressive deterioration of mental powers accompanied by changes
04/12/2019. Learning Objectives. An Approach to End of Life Conversations in Dementia Care for Speech-Language Pathologists
 1 An Approach to End of Life Conversations in Dementia Care for Speech-Language Emily Hornback, MS, CCC-SLP, BCS-S Communication Sciences & Disorders Learning Objectives 1. Increase knowledge of cognitive
1 An Approach to End of Life Conversations in Dementia Care for Speech-Language Emily Hornback, MS, CCC-SLP, BCS-S Communication Sciences & Disorders Learning Objectives 1. Increase knowledge of cognitive
Sensory. Physical. Cognitive. Language 4/12/2016 LEARNING OBJECTIVES AT ASSESSMENT: SKILLS EVALUATION OVERVIEW
 ASSISTIVE TECHNOLOGY ASSESSMENT: SEATING AND POSITIONING FOR ACCESS Anne Cronin 2016 LEARNING OBJECTIVES Describe the principles related to assessment and intervention in assistive technology (AT) service
ASSISTIVE TECHNOLOGY ASSESSMENT: SEATING AND POSITIONING FOR ACCESS Anne Cronin 2016 LEARNING OBJECTIVES Describe the principles related to assessment and intervention in assistive technology (AT) service
SECTION 1: as each other, or as me. THE BRAIN AND DEMENTIA. C. Boden *
 I read all the available books by other [people with] Alzheimer s disease but they never had quite the same problems as each other, or as me. I t s not like other diseases, where there is a standard set
I read all the available books by other [people with] Alzheimer s disease but they never had quite the same problems as each other, or as me. I t s not like other diseases, where there is a standard set
MS Learn Online Feature Presentation Swallowing Difficulties in Multiple Sclerosis Featuring Patricia Bednarik, MS, CCC-SLP, MSCS
 Page 1 MS Learn Online Feature Presentation Swallowing Difficulties in Multiple Sclerosis Featuring, MS, CCC-SLP, MSCS >>Kate Milliken: Welcome to MS Learn Online. I am Kate Milliken. Swallowing is something
Page 1 MS Learn Online Feature Presentation Swallowing Difficulties in Multiple Sclerosis Featuring, MS, CCC-SLP, MSCS >>Kate Milliken: Welcome to MS Learn Online. I am Kate Milliken. Swallowing is something
Choking and Aspiration Supplemental Reading Materials
 Choking and Aspiration Supplemental Reading Materials (Word Count: 1338 6.5 Minutes) The Supplementary Reading Materials for this training program consists of the following documents: Dining Assistive
Choking and Aspiration Supplemental Reading Materials (Word Count: 1338 6.5 Minutes) The Supplementary Reading Materials for this training program consists of the following documents: Dining Assistive
CLINICIANS CORNER So Is NDT Just Everything, Then? The Answers to Three Questions Pinpoint the NDT Approach
 From NDTA Network on the Net, 2006 CLINICIANS CORNER So Is NDT Just Everything, Then? The Answers to Three Questions Pinpoint the NDT Approach By Marcia Stamer, PT As an NDTA instructor, I learn a lot
From NDTA Network on the Net, 2006 CLINICIANS CORNER So Is NDT Just Everything, Then? The Answers to Three Questions Pinpoint the NDT Approach By Marcia Stamer, PT As an NDTA instructor, I learn a lot
Dysphagia after Stroke. Wendy Busby Stroke Service Dunedin Hospital
 Dysphagia after Stroke Wendy Busby Stroke Service Dunedin Hospital Incidence IN NEW ZEALAND 9,5000 new stroke per year Rate is decreasing More people surviving Major cause of disability in adults Prevalence
Dysphagia after Stroke Wendy Busby Stroke Service Dunedin Hospital Incidence IN NEW ZEALAND 9,5000 new stroke per year Rate is decreasing More people surviving Major cause of disability in adults Prevalence
COMMUNICATION. Communication and Swallowing post Tracheostomy. Role of SLT. Impact of Tracheostomy. Normal Speech. Facilitating Communication
 Communication and Swallowing post Tracheostomy. Role of SLT 1. 2. 3. Management of communication needs. Management of swallowing issues. Working with the multidisciplinary team to facilitate weaning. Impact
Communication and Swallowing post Tracheostomy. Role of SLT 1. 2. 3. Management of communication needs. Management of swallowing issues. Working with the multidisciplinary team to facilitate weaning. Impact
OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices OPTICS
 OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices Educational Booklet for Families Version April 26 th 2016 Page 1 of 12 This information booklet was originally
OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices Educational Booklet for Families Version April 26 th 2016 Page 1 of 12 This information booklet was originally
Section K Swallowing/ Nutritional Status
 Instructor Guide Section K Swallowing/ Nutritional Status Objectives State the intent of Section K Swallowing and Nutritional Status. Describe how to conduct an assessment of a resident s nutritional status.
Instructor Guide Section K Swallowing/ Nutritional Status Objectives State the intent of Section K Swallowing and Nutritional Status. Describe how to conduct an assessment of a resident s nutritional status.
15/11/2011. Swallowing
 Swallowing Swallowing starts from placement of the food in the mouth and continues until food enters the stomach. Dysphagia: any difficulty in moving food from mouth to stomach. Pharynx is shared for both
Swallowing Swallowing starts from placement of the food in the mouth and continues until food enters the stomach. Dysphagia: any difficulty in moving food from mouth to stomach. Pharynx is shared for both
Ancillary care team (nursing, therapists, etc):
 1 A. Preliminary Information Reason for referral: Chronological age (Adjusted age): Primary caregiver: Informant for evaluation: Primary language: Interpreter Family concerns Barriers to learning: B. Background
1 A. Preliminary Information Reason for referral: Chronological age (Adjusted age): Primary caregiver: Informant for evaluation: Primary language: Interpreter Family concerns Barriers to learning: B. Background
There are several reasons why a person with dementia may have a poor appetite and seem uninterested in eating.
 PBO 930022142 NPO 049-191 EATING If you are caring for someone with dementia you will want to ensure that they enjoy their food and that they eat a healthy, balanced diet. But for some people, as dementia
PBO 930022142 NPO 049-191 EATING If you are caring for someone with dementia you will want to ensure that they enjoy their food and that they eat a healthy, balanced diet. But for some people, as dementia
2013 Charleston Swallowing Conference
 Providing Quality Affordable Continuing Education and Treatment Materials for over 30 years. 2013 Charleston Swallowing Conference Session 9 Bedside Assessment: What Does It Tell You? 10:00 11:30 am Saturday,
Providing Quality Affordable Continuing Education and Treatment Materials for over 30 years. 2013 Charleston Swallowing Conference Session 9 Bedside Assessment: What Does It Tell You? 10:00 11:30 am Saturday,
Stroke. Objectives: After you take this class, you will be able to:
 Stroke Objectives: After you take this class, you will be able to: 1. Describe the signs of a stroke and how a stroke happens. 2. Discuss stroke risk factors. 3. Detail the care and rehabilitation of a
Stroke Objectives: After you take this class, you will be able to: 1. Describe the signs of a stroke and how a stroke happens. 2. Discuss stroke risk factors. 3. Detail the care and rehabilitation of a
VIDEOFLUOROSCOPIC SWALLOWING EXAM
 VIDEOFLUOROSCOPIC SWALLOWING EXAM INDENTIFYING INFORMATION May include the following: Name, ID/medical record number, date of birth, date of exam, referred by, reason for referral HISTORY/SUBJECTIVE INFORMATION
VIDEOFLUOROSCOPIC SWALLOWING EXAM INDENTIFYING INFORMATION May include the following: Name, ID/medical record number, date of birth, date of exam, referred by, reason for referral HISTORY/SUBJECTIVE INFORMATION
Alzheimer Disease and Related Dementias
 Alzheimer Disease and Related Dementias Defining Generic Key Terms and Concepts Mild cognitive impairment: (MCI) is a state of progressive memory loss after the age of 50 that is beyond what would be expected
Alzheimer Disease and Related Dementias Defining Generic Key Terms and Concepts Mild cognitive impairment: (MCI) is a state of progressive memory loss after the age of 50 that is beyond what would be expected
Sherri Shubin Cohen, MD, MPH Medical Director, Pediatric Feeding and Swallowing Center Program Director, Nutrition Fellowship The Children s Hospital
 Sherri Shubin Cohen, MD, MPH Medical Director, Pediatric Feeding and Swallowing Center Program Director, Nutrition Fellowship The Children s Hospital of Philadelphia Associate Professor of Clinical Pediatrics
Sherri Shubin Cohen, MD, MPH Medical Director, Pediatric Feeding and Swallowing Center Program Director, Nutrition Fellowship The Children s Hospital of Philadelphia Associate Professor of Clinical Pediatrics
The Person: Dementia Basics
 The Person: Dementia Basics Objectives 1. Discuss how expected age related changes in the brain might affect an individual's cognition and functioning 2. Discuss how changes in the brain due to Alzheimer
The Person: Dementia Basics Objectives 1. Discuss how expected age related changes in the brain might affect an individual's cognition and functioning 2. Discuss how changes in the brain due to Alzheimer
Restorative Rehabilitation Dining Programs
 Restorative Rehabilitation Dining Programs SUCCESSFUL DEVELOPMENT & IMPLEMENTATION LAURA ROBERTS, MS, CCC-SLP; BRS-S Course Objectives! Summarize goals of a typical rehab dining program.! Identify indicators
Restorative Rehabilitation Dining Programs SUCCESSFUL DEVELOPMENT & IMPLEMENTATION LAURA ROBERTS, MS, CCC-SLP; BRS-S Course Objectives! Summarize goals of a typical rehab dining program.! Identify indicators
Picky eating vs. Problem Feeding. Mary Louise Kennedy, OTR/L April 29, 2015
 Picky eating vs. Problem Feeding Mary Louise Kennedy, OTR/L April 29, 2015 Everyone likes to eat, right? We need to eat to stay alive. Eating should be fun and enjoyable. There are many cultural differences.
Picky eating vs. Problem Feeding Mary Louise Kennedy, OTR/L April 29, 2015 Everyone likes to eat, right? We need to eat to stay alive. Eating should be fun and enjoyable. There are many cultural differences.
DSM-5 MAJOR AND MILD NEUROCOGNITIVE DISORDERS (PAGE 602)
 SUPPLEMENT 2 RELEVANT EXTRACTS FROM DSM-5 The following summarizes the neurocognitive disorders in DSM-5. For the complete DSM-5 see Diagnostic and Statistical Manualof Mental Disorders, 5th edn. 2013,
SUPPLEMENT 2 RELEVANT EXTRACTS FROM DSM-5 The following summarizes the neurocognitive disorders in DSM-5. For the complete DSM-5 see Diagnostic and Statistical Manualof Mental Disorders, 5th edn. 2013,
DEMENTIA Dementia is NOT a normal part of aging Symptoms of dementia can be caused by different diseases Some symptoms of dementia may include:
 DEMENTIA Dementia is NOT a normal part of aging Symptoms of dementia can be caused by different diseases Some symptoms of dementia may include: 1. Memory loss The individual may repeat questions or statements,
DEMENTIA Dementia is NOT a normal part of aging Symptoms of dementia can be caused by different diseases Some symptoms of dementia may include: 1. Memory loss The individual may repeat questions or statements,
Dysphagia. A Problem Swallowing Foods or Liquids
 Dysphagia A Problem Swallowing Foods or Liquids What Is Dysphagia? If you have a problem swallowing foods or liquids, you may have dysphagia. It has a number of causes. Your doctor can find out what is
Dysphagia A Problem Swallowing Foods or Liquids What Is Dysphagia? If you have a problem swallowing foods or liquids, you may have dysphagia. It has a number of causes. Your doctor can find out what is
OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices OPTICS
 OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices Educational Booklet for Families Version June 16 2014 Page 1 of 11 This information booklet was originally
OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices Educational Booklet for Families Version June 16 2014 Page 1 of 11 This information booklet was originally
Nutricia. Nutrition and Dysphagia
 Nutricia Nutrition and Dysphagia 1 Introduction What is Dysphagia? The inability to swallow normally or freely. Disorder in the swallowing process that does not allow safe passing of food from the mouth
Nutricia Nutrition and Dysphagia 1 Introduction What is Dysphagia? The inability to swallow normally or freely. Disorder in the swallowing process that does not allow safe passing of food from the mouth
Preventing delirium while in the hospital
 Preventing delirium while in the hospital What is delirium? When an older person becomes ill and goes into the hospital, there is an increased risk of developing delirium and other problems. Delirium is
Preventing delirium while in the hospital What is delirium? When an older person becomes ill and goes into the hospital, there is an increased risk of developing delirium and other problems. Delirium is
In-Service Education. workbook 3. by Hartman Publishing, Inc. second edition
 In-Service Education workbook 3 second edition by Hartman Publishing, Inc. Alzheimer s Disease Dignity Diabetes Restraints and Restraint Alternatives Abuse and Neglect Death and Dying Managing Stress Perf
In-Service Education workbook 3 second edition by Hartman Publishing, Inc. Alzheimer s Disease Dignity Diabetes Restraints and Restraint Alternatives Abuse and Neglect Death and Dying Managing Stress Perf
Meals make sense An audit checklist to consider how far a Care Home is implementing quality care re the mealtime experience.
 Meals make sense An audit checklist to consider how far a Care Home is implementing quality care re the mealtime experience. Place a tick in one of the 3 boxes Yes, No, Partly in relation to your Care
Meals make sense An audit checklist to consider how far a Care Home is implementing quality care re the mealtime experience. Place a tick in one of the 3 boxes Yes, No, Partly in relation to your Care
Swallowing Awareness Day
 awareness for youth and adults INSIDE: Facts about eating and drinking checklist General information 9, 2011 Facts for youth and adults on swallowing issues Dysphagia is the medical term for any difficulty
awareness for youth and adults INSIDE: Facts about eating and drinking checklist General information 9, 2011 Facts for youth and adults on swallowing issues Dysphagia is the medical term for any difficulty
Karen Schoeneman Consul6ng 1
 + New Dining Standards of Practice How Do We Get There? Karen Schoeneman + How Did They Happen? 2 n CMS and Pioneer Network co-sponsored a symposium on the food and dining requirements, and culture change
+ New Dining Standards of Practice How Do We Get There? Karen Schoeneman + How Did They Happen? 2 n CMS and Pioneer Network co-sponsored a symposium on the food and dining requirements, and culture change
Breathing, voice and speech
 1) Goal Set a goal for the patient (if possible together with the patient) that can be reached within the nearest future one or two weeks. The goal should be concrete and measurable. 2a) Activity If possible
1) Goal Set a goal for the patient (if possible together with the patient) that can be reached within the nearest future one or two weeks. The goal should be concrete and measurable. 2a) Activity If possible
Seniors Helping Seniors September 7 & 12, 2016 Amy Abrams, MSW/MPH Education & Outreach Manager Alzheimer s San Diego
 Dementia Skills for In-Home Care Providers Seniors Helping Seniors September 7 & 12, 2016 Amy Abrams, MSW/MPH Education & Outreach Manager Alzheimer s San Diego Objectives Familiarity with the most common
Dementia Skills for In-Home Care Providers Seniors Helping Seniors September 7 & 12, 2016 Amy Abrams, MSW/MPH Education & Outreach Manager Alzheimer s San Diego Objectives Familiarity with the most common
NCFE Level 2 Certificate in The Principles of Dementia Care
 The Principles of Dementia Care S A M P LE NCFE Level 2 Certificate in The Principles of Dementia Care Part A 1 These learning resources and assessment questions have been approved and endorsed by ncfe
The Principles of Dementia Care S A M P LE NCFE Level 2 Certificate in The Principles of Dementia Care Part A 1 These learning resources and assessment questions have been approved and endorsed by ncfe
Speech and Language Therapy. Kerrie McCarthy Senior Speech and Language Therapist
 Speech and Language Therapy Kerrie McCarthy Senior Speech and Language Therapist Contents 1. Voice disorders 2. Swallow disorders 3. Videofluroscopy 4. Adult Acquired Communication Disorders 5. How to
Speech and Language Therapy Kerrie McCarthy Senior Speech and Language Therapist Contents 1. Voice disorders 2. Swallow disorders 3. Videofluroscopy 4. Adult Acquired Communication Disorders 5. How to
Moments of Joy: It s What YOU Choose to Do as a Caregiver. Teepa Snow
 Moments of Joy: It s What YOU Choose to Do as a Caregiver Teepa Snow Laughing VS Surviving My goal for you Understanding of what s happening with the person with dementia Support so you can survive Insight
Moments of Joy: It s What YOU Choose to Do as a Caregiver Teepa Snow Laughing VS Surviving My goal for you Understanding of what s happening with the person with dementia Support so you can survive Insight
FUNCTIONAL MOBILITY & ACTIVITIES OF DAILY LIVING. Courtney Silviotti, MS, OTR/L
 FUNCTIONAL MOBILITY & ACTIVITIES OF DAILY LIVING Courtney Silviotti, MS, OTR/L OBJECTIVES: FUNCTIONAL MOBILITY & ACTIVITIES OF DAILY LIVING Define Compare Review Examine Functional Mobility Activities
FUNCTIONAL MOBILITY & ACTIVITIES OF DAILY LIVING Courtney Silviotti, MS, OTR/L OBJECTIVES: FUNCTIONAL MOBILITY & ACTIVITIES OF DAILY LIVING Define Compare Review Examine Functional Mobility Activities
Dementia. Assessing Brain Damage. Mental Status Examination
 Dementia Assessing Brain Damage Mental status examination Information about current behavior and thought including orientation to reality, memory, and ability to follow instructions Neuropsychological
Dementia Assessing Brain Damage Mental status examination Information about current behavior and thought including orientation to reality, memory, and ability to follow instructions Neuropsychological
Rehab to Home. Stroke Recovery EDUCATION BOOKLET FOR: Care & Safety Tips. Frequently Asked Questions. Working Toward Independence. Adaptive Equipment
 Stroke Recovery Rehab to Home Care & Safety Tips Frequently Asked Questions Working Toward Independence Adaptive Equipment Summary of Progress Different Types of Therapy Personal Goals EDUCATION BOOKLET
Stroke Recovery Rehab to Home Care & Safety Tips Frequently Asked Questions Working Toward Independence Adaptive Equipment Summary of Progress Different Types of Therapy Personal Goals EDUCATION BOOKLET
How Speech and Swallowing are Affected with ALS
 Patient Education How Speech and Swallowing are Affected with ALS This handout describes how ALS affects speech and swallowing. For speech issues it covers tips for listeners and speakers and what can
Patient Education How Speech and Swallowing are Affected with ALS This handout describes how ALS affects speech and swallowing. For speech issues it covers tips for listeners and speakers and what can
Daniels SK & Huckabee ML (2008). Dysphagia Following Stroke. Muscles of Deglutition. Lateral & Mesial Premotor Area 6. Primary Sensory
 An Overview of Dysphagia in the Stroke Population Stephanie K. Daniels, PhD Michael E. DeBakey VA Medical Center PM & R, Baylor College of Medicine Communication Sciences and Disorders, University of Houston
An Overview of Dysphagia in the Stroke Population Stephanie K. Daniels, PhD Michael E. DeBakey VA Medical Center PM & R, Baylor College of Medicine Communication Sciences and Disorders, University of Houston
Medication for the Terminal Patient Who Can t Swallow. Annette T. Carron, DO Director Geriatrics & Palliative Care Botsford Hospital
 Medication for the Terminal Patient Who Can t Swallow Annette T. Carron, DO Director Geriatrics & Palliative Care Botsford Hospital Disclosure I have no financial relationships to disclose Route and medication
Medication for the Terminal Patient Who Can t Swallow Annette T. Carron, DO Director Geriatrics & Palliative Care Botsford Hospital Disclosure I have no financial relationships to disclose Route and medication
Managing Behaviors: Start with Yourself!
 Slide 1 Managing Behaviors: Start with Yourself! Teepa Snow, Positive Approach, LLC to be reused only with permission. Slide 2 Time Out Signal copyright - Positive Approach, LLC 2012 Slide 3 REALIZE It
Slide 1 Managing Behaviors: Start with Yourself! Teepa Snow, Positive Approach, LLC to be reused only with permission. Slide 2 Time Out Signal copyright - Positive Approach, LLC 2012 Slide 3 REALIZE It
Aging. Objectives 13/02/2013
 Deirdre Gillespie RN MN AHEADD (Assessment, Health, Education and Developmental Disabilities) dgillespie1@cogeco.ca 613-985-6154 Objectives Discussion about aging Aging and Developmental Disabilities Supporting
Deirdre Gillespie RN MN AHEADD (Assessment, Health, Education and Developmental Disabilities) dgillespie1@cogeco.ca 613-985-6154 Objectives Discussion about aging Aging and Developmental Disabilities Supporting
Video Fluoroscopic Swallowing Exam (VFSE)
 Scan for mobile link. Video Fluoroscopic Swallowing Exam (VFSE) A video fluoroscopic swallowing exam (VFSE) uses a form of real-time x-ray called fluoroscopy to evaluate a patient s ability to swallow
Scan for mobile link. Video Fluoroscopic Swallowing Exam (VFSE) A video fluoroscopic swallowing exam (VFSE) uses a form of real-time x-ray called fluoroscopy to evaluate a patient s ability to swallow
Respiration & Trunk control The Great Connection. Brief Review of Normal Development of the Rib Cage
 Respiration & Trunk control The Great Connection. are part of a complex combination of interactive systems. Muscles of respiration are part of the musculature of dynamic postural control. First 3 Years
Respiration & Trunk control The Great Connection. are part of a complex combination of interactive systems. Muscles of respiration are part of the musculature of dynamic postural control. First 3 Years
CARING FOR PATIENTS WITH DEMENTIA:
 CARING FOR PATIENTS WITH DEMENTIA: LESSON PLAN Lesson overview Time: One hour This lesson teaches useful ways to work with patients who suffer from dementia. Learning goals At the end of this session,
CARING FOR PATIENTS WITH DEMENTIA: LESSON PLAN Lesson overview Time: One hour This lesson teaches useful ways to work with patients who suffer from dementia. Learning goals At the end of this session,
PRACTICAL SOLUTIONS TO REHAB DEMENTIA CARE PART 1 PROMOTING EACH PERSON S BEST ABILITY TO FUNCTION
 The Dementia Problem PRACTICAL SOLUTIONS TO REHAB DEMENTIA CARE PART 1 PROMOTING EACH PERSON S BEST ABILITY TO FUNCTION Efficient, practical & compassionate service is more important than ever before Aging
The Dementia Problem PRACTICAL SOLUTIONS TO REHAB DEMENTIA CARE PART 1 PROMOTING EACH PERSON S BEST ABILITY TO FUNCTION Efficient, practical & compassionate service is more important than ever before Aging
Addressing Difficult Behaviors in Dementia
 Addressing Difficult Behaviors in Dementia GEORGE SCHOEPHOERSTER, MD GERIATRICIAN GENEVIVE/CENTRACARE CLINIC Objectives By the end of the session, you will be able to: 1) Explain the role of pain management
Addressing Difficult Behaviors in Dementia GEORGE SCHOEPHOERSTER, MD GERIATRICIAN GENEVIVE/CENTRACARE CLINIC Objectives By the end of the session, you will be able to: 1) Explain the role of pain management
I will explain the most important concepts of functional treatment while treating our 4 patients: Tom Clint Alice Dick
 Every step we ve covered so far, from Evaluation to Clinical Reasoning to Establishing Goals and Preparation for Function has laid the groundwork for the final step: Treatment Using Functional Activities.
Every step we ve covered so far, from Evaluation to Clinical Reasoning to Establishing Goals and Preparation for Function has laid the groundwork for the final step: Treatment Using Functional Activities.
