BEHAVIORAL SYMPTOMS manifest
|
|
|
- Brenda Carpenter
- 5 years ago
- Views:
Transcription
1 ORIGINAL CONTRIBUTION Left Frontotemporal Hypoperfusion Is Associated With Aggression in Patients With Dementia Nobutsugu Hirono, MD; Michael S. Mega, MD, PhD; Ivo D. Dinov, PhD; Fred Mishkin, MD; Jeffrey L. Cummings, MD Background: Aggressive behavior is common in patients with dementia. Temporolimbic and prefrontal cortical lesions can produce pathological aggression; however, involvement of these structures has not been established in aggressive patients with dementia. Objective: To study the relation between regional brain perfusion and aggressive behavior in patients with dementia. Methods: We compared the pattern of regional cerebral perfusion determined with technetium Tc 99m labeled hexamethylpropelene amineoxime single photon emission computed tomography in 2 groups of 10 patients with dementia with and without aggression, that were comparable for demographic factors, severity of cognitive impairments, and other behavioral symptoms as measured by the Neuropsychiatric Inventory. Results: Patients with aggression revealed significant (P.001) hypoperfusion in the left anterior temporal cortex; additional bilateral dorsofrontal and right parietal cortex were also found to be significantly hypoperfused. Conclusion: These results indicated an association between aggression and decreased perfusion in the left anterior temporal cortex. Arch Neurol. 2000;57: From the Division of Clinical Neurosciences, Hyogo Institute for Aging Brain and Cognitive Disorders, Himeji, Japan (Dr Hirono); Departments of Neurology (Drs Hirono, Mega, and Cummings) and Nuclear Medicine (Dr Mishkin), Harbor/UCLA Medical Center, Torrence; and the Laboratory of Neuroimaging (Drs Mega and Dinov) and Alzheimer s Disease Research Center (Drs Hirono, Mega, and Cummings), UCLA School of Medicine, Los Angeles, Calif. BEHAVIORAL SYMPTOMS manifest in patients with dementia and have a major influence on quality of life and social affiliations for patients and caregivers. Among these behavioral problems, aggressive outbursts are frequent and may pose the greatest caregiver distress. 1,2 Agitation or aggression are reported in 12% to 65% of patients with Alzheimer disease (AD) or other dementias. 1,3-12 Aggressive behavior causes serious burden and depression in caregivers, 1,2,6,13 and increases the likelihood of hospitalization, early institutionalization, and abuse of patients. 3,14-16 In the nursing home, aggressive behavior is associated with a need for increased staff supervision, 17 and the use of physical restraints. Moreover, aggressive behaviors may have severe adverse consequences, including injury, which may lead to the death of patients or others. 18 Therefore, evaluation and management of aggressive behaviors are of considerable importance in the care of patients with dementia. Although functional factors, such as pathological rearing, psychological trauma, and social stress, are important in the occurrence of aggression, regional brain lesions can produce pathological aggression in animals and humans. Among these regions, the temporolimbic and prefrontal cortices have been most frequently implicated. 19,20 Aggressive verbalization and rage occur with stimulation of the amygdala and hippocampus in animals. 21 Although destruction of the amygdala in monkeys and humans usually results in placidity, Rosvold et al 22 reported that amygdalectomy in submissive monkeys increased aggression, suggesting that amygdalar dysfunction modifies aggressive behavior in a variety of ways. Recently, Zagrodzka et al 23 reported that unilateral damage to the central nucleus of the amygdala alone increased the expression of aggressive behavior in the cat. Patients with temporal lobe epilepsy may have increased aggression during interictal periods in addition to ictal and postictal aggressive outbursts. 24,25 Furthermore, violent patients with focal lesions are most likely to have focal temporal abnormalities on electroencephalography and structural abnormalities in temporal lobes. 29 Functional neuroimaging studies using positron emission tomography 861
2 PATIENTS AND METHODS PATIENTS From a pool of 198 patients with dementia initially seen at the University of California Los Angeles (UCLA) Alzheimer s Disease Center, 20 outpatients who met all clinical criteria described below, comparable across demographic and behavioral domains and divided equally into those with and without agitation/aggression, were studied. All patients had acquired persistent decline involving at least 3 of the following domains: language, memory, visuospatial skills, cognition (ie, calculation, abstraction, judgment, and others), and emotion or personality. 42 All patients with AD met National Institute of Neurological and Communicative Disorders and Stroke Alzheimer s Disease and Related Disorders Association criteria for probable or possible AD. 43 All patients with vascular dementia met National Institute of Neurological Disorders and Stroke Alzheimer s Disease and Related Disorders Association International Workshop criteria for probable or possible vascular dementia 44 ; patients with large cortical strokes were excluded from the study. All patients with dementia who had Lewy bodies met the Consortium for Dementia with Lewy Bodies criteria for probable dementia with Lewy bodies. 45 Diagnostic evaluation for all patients included complete medical history, physical and neurological examination, magnetic resonance imaging or computed tomographic imaging, technetium Tc 99m labeled hexamethylpropylene amineoxime SPECT imaging of the brain, and electroencephalography, and routine blood tests (including thyrotropin level, vitamin B 12 level, and serological test for syphilis), and had caregivers who were willing to be interviewed. Exclusion criteria for all patients were delirium, history of alcohol or other substance abuse, history of head trauma with loss of consciousness, and history of psychiatric disorder preceding the onset of symptoms of dementia. Patients were physically well without pain or other identifiable precipitants of behavioral disturbances. Cognitive assessment included the Mini-Mental State Examination, 46 the Consortium to Establish a Registry for Alzheimer s Disease word memory test, the modified 15- item Boston Naming Test, 48 the Consortium to Establish a Registry for Alzheimer s Disease visuospatial task (copying a circle, diamond, overlapping rectangles, and cube), and a verbal fluency task (animal name generation in 1 minute). The 20 patients chosen were representative of the 198 patient pool having a similar sex, age, Mini-Mental State Examination score, and educational level of the larger group; the pool was assembled from all patients seen in the UCLA Alzheimer s Disease Center who had cognitive, behavioral, laboratory, structural, and functional (SPECT) imaging. BEHAVIORAL ASSESSMENT Caregivers were interviewed with the NPI following procedures previously described 49 in which screening questions for each behavior were posed first. The caregiver was asked if the behavior represented a change from that exhibited by the patient prior to the onset of the dementia and was present during the past month. If a positive response was obtained from the screening questions, then the behavioral domain was explored with scripted questions focusing on specific features of the behavioral disturbance. The caregiver then rated the behaviors; scores from 1 to 4 (with 4 being the most frequent) were obtained for the frequency and 1 to 3 (with 3 being the most severe) for the severity of each behavior (a composite score for each domain was the product of the frequency and severity subscores; maximum attainable score=12). The NPI has been shown to be valid and reliable 49 ; raters receive specific training in NPI administration and are retrained periodically to prevent drift. The 10 domains assessed by the NPI are delusions, hallucinations, agitation/aggression, depression, anxiety, euphoria, apathy, disinhibition, irritability, and abnormal motor output. The cognitive assessment was done concurrently with the NPI. SINGLE PHOTON EMISSION COMPUTED TOMOGRAPHY For all patients, an intravenous line was placed and a 15- minute period was allowed to pass for patients to regain a quiet comfortable state before the intravenous administration of 1110 MBq of technetium Tc 99m labeled hexamethylpropylene amineoxime (Ceretec; Amersham, Arlington Heights, Ill). Room lights were dimmed and quiet was observed to minimize patient visual and auditory stimuli during the brain uptake phase for another 15 minutes following or single photon emission computed tomography (SPECT) in aggressive individuals show hypometabolism or hypoperfusion in temporal lobes, particularly on the left side. 28,30-33 Dysfunction of the prefrontal cortex also has been implicated in aggressive behavior. Increased aggressive feelings are reported by patients with focal orbitofrontal lesions. 34 Neuropsychological and electroencepholographic 26 studies support a relationship between frontal lobe dysfunction and aggression, and functional neuroimaging studies indicate an association between aggression and hypometabolism in the prefrontal cortices, especially the orbitofrontal cortex. 28,30-32,38-40 The underlying mechanism for aggression in patients with dementia is unclear and involvement of the orbitofrontal and temporolimbic cortex has not been established. Studies evaluating focal brain lesions related to aggression in dementia are lacking. Sultzer et al 41 reported, in a study of 21 patients with AD, that the agitation/disinhibition factor score of the Neurobehavioral Rating Scale correlated with glucose metabolism in the frontal and temporal lobes, but they did not evaluate aggression separately. In this study, we compared the pattern of regional cerebral perfusion between 2 groups of 10 patients with dementia with and without agitation/aggression as measured by the Neuropsychiatry Inventory (NPI). The NPI emphasizes noncompliance, refusal to cooperate with the caregiver, obstinance, resistance, cursing, kicking, and being hard to handle within the agitation/aggression section. Groups were comparable on all demographic factors, severity of cognitive impairments, and all other be- 862
3 agnosed as having vascular dementia. Of the 10 nonaggressive patients with dementia 8 were diagnosed as having AD, 1 was diagnosed as having dementia with Lewy bodies, and 1 was diagnosed as having normal pressure hydrocephalus. Agitation/aggression was the only behavior assessed by the NPI that was statistically significantly (P.001) different between the 2 groups. The Figure and Table 3 show the Talairach and Tournoux atlas 57 location of the peak significance for regions with significantly lower perfusion in the 10 patients with dementia who had high aggression scores compared with the 10 nonaggressive patients. Patients with aggression revealed statistically significant (P.001) hypoperfusion in the left anterior temporal cortex (Brodmann areas 20, 21, and 38); the difference in the orbitofrontal cortices was not significant. Besides the regions we hyinjection of the radiolabeled substance. Approximately 1 hour after injection, during which time washout of the tracer from the brain had occurred, SPECT images of the brain were obtained using the a SPECT scanner (Picker Prism 3000XP SPECT scanner; Picker International Inc, Cleveland, Ohio) with low-energy, ultrahigh-resolution fan beam collimators. Images were reconstructed by filtered backprojection using lowpass filter, order 8, with a spatial frequency cutoff of 0.23 to 0.25 cycles per pixel. Transverse, sagittal, and coronal planes as pixel slices were generated. Pixel sizes were nominally mm. Resolution of the system was approximately 6-mm full-width half maximum. IMAGE PROCESSING Spatial alignment of all 20 SPECT data sets was accomplished via 12-parameter affine registration. 50 All data sets were first aligned to one randomly selected target to obtain an average SPECT which in turn was registered to the International Consortium of Human Brain Mapping probabilistic atlas. 51 To minimize resampling of data, the 2 above warping fields were concatenated and applied to each SPECT data set. The relative perfusion scans of each patient then underwent linear intensity normalization, on a voxel-by-voxel basis, to the global mean intensity value of all 10 patients within each group, thus equalizing the mean intensities across intragroup data sets. This normalization step did not alter the variance of data. Once all normalized data sets were in the common International Consortium of Human Brain Mapping probablistic atlas space, a voxel-by-voxel subtraction was conducted between the aggressive and nonaggressive groups. Subvolume thresholding (SVT) was used to create a statistical map of these subtraction results as previously described. 52 Briefly, SVT uses the probabilistic anatomical partitioning of the International Consortium of Human Brain Mapping atlas (partitions include the frontal, parietal, temporal, insular, and occipital cortex, along with the putamen, caudate, thalamus, and cerebellum) to model the different regions as separate stationary random fields thereby accommodating nonuniform global brain activity. In addition, the probability clouds of the International Consortium of Human Brain Mapping atlas allow us to control for spatial errors, imposed by registration and anatomical variability, by weighting the contribution of voxel intensities based on their location within an anatomical cloud. Thus, voxels within the center of a region have the highest probability of belonging to that region while voxels at the edge of a region have a lower chance of being accurately identified owing to registration error and normal anatomical variability. The SVT approach departs from other functional imaging techniques. In the first step of significance evaluation, an estimate of the pooled variance for the average voxel intensity, which is dependent on the topology of the anatomical subvolume of interest, is used to assess the globally significant variability of data within each region separately, permitting a functional-anatomical test of the subtraction paradigm. This novel approach is particularly suited for the assessment of functional imaging studies in dementia since parietal and temporal regions may have significantly different means and variances, across subjects, than frontal or subcortical regions given the local pathological distribution of dementing disease. 53,54 Ignoring these potential differences by modeling the entire data set as a stationary random field, done by many other functional assessments, will obliterate disease-specific variability. After the first SVT step identifies globally significant regions, the second step maps the location of voxels, with a difference z score above 2.5, in those regions. This is a standard procedure in most functional statistical mapping techniques with 2 exceptions: (1) voxel location tests are run only over those regions identified by the global search in step 1 and (2) variance estimates are pooled over subjects and across voxels. Once the locations of voxels within a region of interest have been assigned a z-score value, a significance level must be determined for voxels above a z- score threshold. The SVT local search within globally significant regions derived from the between-group subtraction is corrected for multiple voxelwise testing to control for type I errors in assessing significance. For each of the selected voxels outside of our a priori hypothesized regions, a Bonferroni correction is conducted by dividing the significance level associated with the z score by the number of voxels constituting a single search (this voxel number is equal to the size of the full-width half maximum of the scanner 6 mm). For voxels within our a priori hypothesized regions, we employed a bootstrap analysis 55,56 to determine the significance of the selected voxels. havioral symptoms captured by the NPI, including delusions, hallucinations, disinhibition, irritability, apathy, anxiety, and depression. We hypothesized that patients with dementia with significant agitation/aggression would have significantly lower anterior temporal and lateral orbitofrontal perfusion on SPECT analysis compared with patients without agitation/aggression. RESULTS Table 1 and Table 2 show the demographic features, psychotropic medications, Mini-Mental State Examination (all other cognitive indices assessed by our battery were comparable between groups), and behavioral profiles of the 2 groups. Of the 10 aggressive patients with dementia 8 were diagnosed as having AD, and 2 were di- 863
4 Table 1. Demographic and Medication Regimen for the Aggressive and Nonaggressive Groups With Dementia Characteristics pothesized would be affected in aggressive patients with dementia, patients with aggression also revealed significant (P.001) hypoperfusion in the right and left superior frontal cortices (Brodmann area 9) and the right superior parietal area (Brodmann area 7) with betweengroup differences after Bonferroni correction. Possible confounding effects of medication on cerebral perfusion were controlled for by composing the groups to have an equal percentage of patients with neuroleptic and antidepressant use in both groups. COMMENT Aggressive Group Nonaggressive Group Sex, M/F 4/6 4/6 Age, mean (SD), y (6.39) (6.82) Educational level, mean (SD), y (3.32) (3.43) Mini-Mental State Examination, (4.55) (4.92) mean (SD), score No. of patients with Alzheimer 8 8 disease No. of patients with vascular 2 0 dementia No. of patients with Lewy 0 1 bodies No. of patients with other 0 1 dementias Medication, % of patients Neuroleptic Antidepressant Table 2. Composite Scores on the Neuropsychiatric Inventory (NPI) for the Aggressive and Nonaggressive Groups* Domains Aggressive Group Nonaggressive Group NPI total score (5.84) (6.48) Agitation 3.70 (1.68) 0.20 (0.40) Hallucinations 0.20 (0.60) 0.00 (0.00) Depression 3.90 (1.51) 4.50 (2.58) Delusions 1.90 (2.51) 1.00 (1.41) Anxiety 1.80 (2.40) 2.10 (2.30) Euphoria 1.00 (1.55) 0.20 (0.40) Apathy 4.10 (3.65) 3.00 (2.90) Disinhibition 2.30 (3.03) 0.80 (1.83) Irritability 2.80 (1.83) 1.60 (2.01) Aberrant motor 1.50 (1.43) 1.40 (2.84) *All values are expressed as mean (SD). P.001 Several studies have suggested that aggressive behavior is associated with demographic factors including male gender 9,58,59 and increasing cognitive loss 3,17,59 in patients with dementia. Therefore, we minimized the confounding effects of these variables: age, sex, education level, psychotropic medications, Mini-Mental State Examination scores, and cognitive performance, all of which were similar between the patients groups with and without aggressive behavior. Moreover, because aggression has been associated with other neuropsychiatric manifestations including delusions, hallucinations, irritability, and depression, 8,11,58,60,61 we also ensured that the neuropsychiatric symptoms in the 2 groups were comparable. This approach aids identification of the brain regions that, when dysfunctional, may be specific to aggressive behavior. Generalizability of this study is limited by the small sample size. The study demonstrated a clear association between aggressive behavior and hypoperfusion in the left anterior temporal cortex but failed to demonstrate the expected involvement of the orbitofrontal cortices in patients with dementia. This failure might be caused by the lack of statistical power due to the small sample size. The anterior temporal cortex has reciprocal connections with the amygdaloid complex. The amygdala has abundant connections with association cortices of multiple cortical sensory systems; visceral brain areas including brainstem and hypothalamus; basal ganglia; and other limbic structures such as parahippocampal gyrus, insula, and cingulate cortices. 62,63 Anterior temporal structures have been posited to play an important role in associating sensory experiences with emotion. Dysfunction of these areas has been implicated in causing abnormal emotional associations to external sensory stimuli, and in provoking inappropriate aggressive acts to trivial or misinterpreted stimuli. 19,20,60 In addition to involvement of the left anterior temporal cortex, we found significant regional hypoperfusion in the right and left dorsolateral frontal and right superior parietal regions. Within the prefrontal regions, the disturbances of orbitofrontal cortices have been linked most often to aggression; however, several studies have shown the involvement of the dorsolateral frontal region in aggression. 28,30,32,38-40 Dorsolateral frontal regions are considered important to critical thinking and planning, 37 and reduced metabolic activity in these regions may lead to misinterpretation of environmental and social situations, which might be related to aggressive behavior. Raine et al 32 described significantly decreased glucose metabolism in both superior parietal regions in murderers as compared with normal controls. These findings also are compatible with the fact that aggressive behaviors are more frequent in patients with frontotemporal dementia, who usually have dysfunction of dorsolateral frontal regions as well as of anterior temporal structures, as compared with patients with AD. 64 The superior parietal lobes are critical for sensorimotor integration providing subjective knowledge of both the world and one s own body. 65 Dysfunction of the superior parietal lobes may cause the sensory information processing deficits and abnormal assessments of both the world and one s own body resulting in abnormal emotional responses. This study bears importantly on the understanding of agitation in dementias. Agitation encompasses many behaviors including aggressive behavior assessed by the NPI. The pathogenesis of agitation in dementia is controversial with some investigators considering it a primary symptom of brain dysfunction and others viewing it as a symptom of psychopathology. In this study, 864
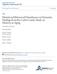
5 Z R L 1.5 Z L R Statistical map derived from normalized single photon emission computed tomography studies. The map reflects the a priori hypothesized temporal pole on the left (upper column) and those regions not hypothesized (lower column), that continued to show significant group differences even after Bonferroni correction, as being significantly more hypoperfused in the agitation/aggression group compared with 10 patients without agitation/aggression. Each row shows the coronal, sagittal, or axial views of the region whose Talairach and Tournoux atlas 57 coordinates and z scores are given in Table 3. Table 3. Talairach and Tournoux Atlas 57 Location of Brain Region s Peak Significance for the Statistical Map* patients had comparable levels of nonaggressive behaviors, differing only on the aggression/agitation scores of the NPI. Regional brain dysfunction was identified as the correlate of these behavioral differences. These observations support the hypothesis that this type of agitation can occur as a primary behavioral disturbance with unique anatomical underpinnings. CONCLUSIONS Axis Location Side z Score x y z Temporopolar cortex (BA 38) L Prefrontal (BA 9) L Prefrontal (BA 9) R Parietal (BA 7a) R *Talairach and Tournoux atlas 57 location of brain region s peak significance for the statistical map shown in Figure 1. These locations were derived from normalized brain perfusion, as measured by technetium Tc 99m labeled hexylmethylpropelene amineoxime single photon emission computed tomography. BA indicates Brodmann area. Hypothesized region (bootstrap P =.0003). Not hypothesized region (Bonferroni corrected). We prospectively studied aggressive behaviors in patients with dementia and the relevant regional cerebral hypoperfusion by using SPECT and an established method of neuropsychiatric assessment in dementia. We demonstrated an association between aggression and decreased perfusion in the left anterior temporal cortex. Our results support previous reports of anterior temporal involvement in aggressive behaviors, irrespective of disease origin. This finding might predict the development of aggression and the effectiveness of therapeutic interventions used for the patients with dysfunction in this region. Accepted for publication December 22, This investigation was supported by Career Development Award K08AG from the National Institute on Aging, National Institutes of Health, Bethesda, Md (Dr Mega); Alzheimer s Disease Research Center grant P50 AG16570 from the National Institute on Aging (Dr Cummings); an Alzheimer s Disease Research Center of California grant, Los Angeles (Dr Cummings); and the Sidell-Kagan Foundation, Los Angeles (Drs Mega and Cummings). Corresponding author: Nobutsugu Hirono, MD, Division of Clinical Neuroscience, Hyogo Institute for Aging Brain and Cognitive Disorders, 520 Saisho-ko, Himeji , Japan ( hirono@hiabcd.go.jp). REFERENCES 1. Nagaratnam N, Lewis-Jones M, Scott D, Palazzi L. Behavioral and psychiatric manifestations in dementia patients in a community: caregiver burden and outcome. Alzheimer Dis Assoc Disord. 1998;12: Rabins PV, Mace NL, Lucas MJ. The impact of dementia on the family. JAMA. 1982;248:
6 3. Ryden MB. Aggressive behavior in persons with dementia who live in the community. Alzheimer Dis Assoc Disord. 1988;2: Mendez MF, Martin RJ, Smyth KA, Whitehouse PJ. Psychiatric symptoms associated with Alzheimer s disease. J Neuropsychiatry Clin Neurosci. 1990;2: Burns A, Folstein S, Brandt J, Folstein M. Clinical assessment of irritability, aggression, and apathy in Huntington and Alzheimer disease. J Nerv Ment Dis. 1990; 178: Patel V, Hope T. Aggressive behavior in elderly people with dementia: a review. Int J Geriatr Psychiatry. 1993;8: Mega MS, Cummings JL, Fiorello T, Gornbein J. The spectrum of behavioral changes in Alzheimer s disease. Neurology. 1996;46: Aarsland D, Cummings JL, Yenner G, Miller B. Relationship of aggressive behavior to other neuropsychiatric symptoms in patients with Alzheimer s disease. Am J Psychiatry. 1996;153: Eastley R, Wilcock GK. Prevalence and correlates of aggressive behaviours occurring in patients with Alzheimer s disease. Int J Geriatr Psychiatry. 1997;12: Levy ML, Miller BL, Cummings JL, Fairbanks LA, Craig A. Alzheimer disease and frontotemporal dementias: behavioral distinctions. Arch Neurol. 1996;53: Chemerinski E, Petracca G, Teson A, Sabe L, Leiguarda R, Starkstein SE. Prevalence and correlates of aggressive behavior in Alzheimer s disease. J Neuropsychiatry Clin Neurosci. 1998;10: Binetti G, Mega MS, Magni E, et al. Behavioral disorders in Alzheimer disease: a transcultural perspective. Arch Neurol. 1998;55: Victoroff J, Mack WJ, Nielson KA. Psychiatric complications of dementia: impact on caregivers. Dementia Geriatr Cogn Disord. 1998;9: Chenowith B, Spencer B. Dementia: the experience of family caregivers. Gerontologist. 1986;26: Steele C, Rovner B, Chase GA, Folstein M. Psychiatric symptoms and nursing home placement of patients with Alzheimer s disease. Am J Psychiatry. 1990; 147: O Donnell BF, Drachman DA, Barnes HJ, Peterson KE, Swearer JM, Lew RA. Incontinence and troublesome behaviors predict institutionalization in dementia. J Geriatr Psychiatry Neurol. 1992;5: Aronson MK, Post DC, Guastadisegni P. Dementia, agitation, and care in the nursing home. J Am Geriatr Soc. 1993;41: Trimble GX. Attacks at nursing homes. CMAJ. 1988;138: Weiger WA, Bear DM. An approach to the neurology of aggression. J Psychiatr Res. 1988;22: Bear D. Neurological perspectives on aggressive behavior. J Neuropsychiatry Clin Neurosci. 1991;3:S3-S Trimble MR, Mendez MF, Cummings JL. Neuropsychiatric symptoms from the temporolimbic lobes. In: Salloway S, Malloy P, Cummings JL, eds. The Neuropsychiatry of Limbic and Subcortical Disorders. Washington DC: American Psychiatric Press; 1997: Rosvold HE, Mirsky AF, Pribram KH. Influence of amygdalectomy on social behavior in monkeys. J Comp Physiol A. 1954;47: Zagrodzka J, Hedberg CE, Mann GL, Morrison AR. Contrasting expressions of aggressive behavior released by lesions of the central nucleus of the amygdala during wakefulness and rapid eye movement sleep without atonia in cats. Behav Neurosci. 1998;112: Devinsky O, Bear D. Varieties of aggressive behavior in temporal lobe epilepsy. Am J Psychiatry. 1984;141: Elliott FA. Violence: the neurologic contribution: an overview. Arch Neurol. 1992; 49: Williams D. Neural factors related to habitual aggression: consideration of differences between those habitual aggressives and others who have committed crimes of violence. Brain. 1969;92: Bach-y-Rita G, Lion JR, Climent CE, Ervin FR. Episodic dyscontrol: a study of 130 violent patients. Am J Psychiatry. 1971;127: Volkow ND, Tancredi L. Neural substrates of violent behaviour. A preliminary study with positron emission tomography. Br J Psychiatry. 1987;151: Wong MT, Lumsden J, Fenton GW, et al. Electroencephalography, computed tomography and violence ratings of male patients in a maximum-security mental hospital. Acta Psychiatr Scand. 1994;90: Volkow ND, Tancredi LR, Grant C, et al. Brain glucose metabolism in violent psychiatric patients: a preliminary study. Psychiatry Res. 1995;61: Amen DG, Stubblefield M, Carmicheal B, Thisted R. Brain SPECT findings and aggressiveness. Ann Clin Psychiatry. 1996;8: Raine A, Buchsbaum M, LaCasse L. Brain abnormalities in murderers indicated by positron emission tomography. Biol Psychiatry. 1997;42: Seidenwurm D, Pounds TR, Globus A, Valk PE. Abnormal temporal lobe metabolism in violent subjects: correlation of imaging and neuropsychiatric findings. Am J Neuroradiol. 1997;18: Blumer D, Benson DF. Personality changes with frontal and temporal lobe lesions. In: Benson DF, Blumer D, eds. Psychiatric Aspects of Neurologic Disease. New York, NY: Grune & Stratton Inc; 1975: Yeudall LT, Fromm-Auch D. Neuropsychological impairments in various psycholopathological populations. In: Gruzelier J, Flor-Henry P, eds. Hemisphere Asymmetries of Function in Psychopathology. New York, NY: Elsevier/North- Holland Biomedical Press; 1979: Bryant ET, Scott ML, Golden CJ, Tori CD. Neuropsychological deficits, learning disability, and violent behavior. J Consult Clin Psychol. 1984;52: Raine A, Scerbo A. Biological theories of violence. In: Milner JS, ed. Neuropsychology of Aggression. Norwell, Mass: Kluwer Academic Publishers; 1991: Goyer PF, Andreason PJ, Semple WE, et al. Positron-emission tomography and personality disorders. Neuropsychopharmacology. 1994;10: Raine A, Phil D, Stoddard J, Bihrle S, Buchsbaum M. Prefrontal glucose deficits in murderers lacking psychosocial deprivation. Neuropsychiatry Neuropsychol Behav Neurol. 1998;11: Raine A, Buchsbaum MS, Stanley J, Lottenberg S, Abel L, Stoddard J. Selective reductions in prefrontal glucose metabolism in murderers. Biol Psychiatry. 1994; 36: Sultzer DL, Mahler ME, Mandelkern MA, et al. The relationship between psychiatric symptoms and regional cortical metabolism in Alzheimer s disease. J Neuropsychiatry Clin Neurosci. 1995;7: Cummings JL, Benson DF, LoVerme S. Reversible dementia: illustrative cases, definition, and review. JAMA. 1980;243: McKhann G, Drachman D, Folstein M, Katzman R, Price D, Stadlan EM. Clinical diagnosis of Alzheimer s disease: report of the NINCDS-ADRDA Work Group under the auspices of the Department of Health and Human Services Task Force on Alzheimer s Disease. Neurology. 1984;34: Roman GC, Tatemichi TK, Erkinjuntti T, et al. Vascular dementia: diagnostic criteria for research studies report of the NINDS-AIREN International Workshop. Neurology. 1993;43: McKeith IG, Galasko D, Kosaka K, et al. Clinical and pathological diagnosis of dementia with Lewy bodies (DLB): report of the CDLB International Workshop. Neurology. 1996;46: Folstein MF, Folstein SE, McHugh PR. Mini-mental state : a practical method for grading the mental state of patients for the clinician. J Psychiatry Res. 1975; 12: Consortium to Establish a Registry for Alzheimer s Disease Guide to the Clinical Assessment of Alzheimer s Disease and Other Dementias. (For information, contact: Albert Heyman, MD, Box 3203, Duke University Medical Center, Durham, NC ). 48. Kaplan E, Goodglass H, Weintraub S. The Boston Naming Test. Philadelphia, Pa: Lea & Febiger; Cummings JL, Mega MS, Gray K, Rosenberg-Thompson S, Carusi DA, Gornbein J. The neuropsychiatric inventory: comprehensive assessment of psychopathology in dementia. Neurology. 1994;44: Woods RP, Grafton ST, Watson JDG, Sicotte NL, Mazziotta JC. Automated image registration, II: intersubject validation of linear and nonlinear models. J Comput Assist Tomogr. 1998;22: Evans AC, Collins DL, Holmes CJ. Automated 3-D regional MRI segmentation and statistical probabilistic anatomical maps. In: Toga AW, Mazziotta JC, eds. Human Brain Mapping: The Methods. Orlando, Fla: Academic Press Inc, 1996: Dinov ID, Mega MS, Thompson PM, et al. Analyzing functional brain images in a probabilistic atlas: a validation of sub-volume thresholding. J Comput Assist Tomogr. 2000;24: Price JL, Davis PB, Morris JC, White DL. The distribution of tangles, plaques and related immunohistochemical markers in healthy aging and Alzheimer s disease. Neurobiol Aging. 1991;12: Braak H, Braak E. Neuropathological staging of Alzheimer-related changes. Acta Neuropathol. 1991;82: Efron B, Tibshirani R. Statistical data analysis in the computer age. Science. 1991; 253: Mega MS, O Connor SM, Lee L, Dinov ID, Cummings JL, Toga AW. Orbital frontal and anterior cingulate pretreatment perfusion defects on 99m Tc-HMPAO- SPECT are associated with behavioral response to cholinesterase inhibitor therapy in Alzheimer s disease [abstract]. Neurology. 1998;50:A Talairach J, Tournoux P. Principe et technique des etudes anatomiques. In: Rayport M, ed. Co-Planar Stereotaxic Atlas of the Human Brain 3-Dimensional Proportional System: An Approach to Cerebral Imaging. New York, NY: Thieme Medical Publishers Inc, 1988: Lyketsos CG, Steele C, Galik E, et al. Physical aggression in dementia patients and its relationship to depression. Am J Psychiatry. 1999;156: Copper JK, Mungas D, Weiler PG. Relation of cognitive status and abnormal behaviors in Alzheimer s disease. J Am Geriatr Soc. 1990;38: Flynn FG, Cummings JL, Gornbein J. Delusions in dementia syndromes: investigation of behavioral and neuropsychological correlates. J Neuropsychiatry Clin Neurosci. 1991;3: Deutsch LH, Bylsma FW, Rovner BW, Steele C, Folstein MF. Psychosis and physical aggression in probable Alzheimer s disease. Am J Psychiatry. 1991;148: Mega MS, Cummings JL, Salloway S, Malloy P. The limbic system: an anatomic, phylogenetic, and clinical perspective. J Neuropsychiatry Clin Neurosci. 1997;9: Van Hoesen GW. Ventromedial temporal lobe anatomy, with comments on Alzheimer s disease and temporal injury. In: Salloway S, Malloy P, Cummings JL, eds. The Neuropsychiatry of Limbic and Subcortical Disorders. Washington, DC: American Psychiatric Press, 1997: Miller BL, Darby A, Benson DF, Cummings JL, Miller MH. Aggressive, socially disruptive and antisocial behaviour associated with fronto-temporal dementia. Br J Psychiatry. 1997;170: Wolpert DM, Goodbody SJ, Husain M. Maintaining internal representations: the role of the human superior parietal lobe. Nat Neurosci. 1998;1:
ORIGINAL CONTRIBUTION. The Spectrum of Behavioral Responses to Cholinesterase Inhibitor Therapy in Alzheimer Disease
 ORIGINAL CONTRIBUTION The Spectrum of Behavioral Responses to Cholinesterase Inhibitor Therapy in Alzheimer Disease Michael S. Mega, MD, PhD; Donna M. Masterman, MD; Susan M. O Connor, RNC; Terry R. Barclay,
ORIGINAL CONTRIBUTION The Spectrum of Behavioral Responses to Cholinesterase Inhibitor Therapy in Alzheimer Disease Michael S. Mega, MD, PhD; Donna M. Masterman, MD; Susan M. O Connor, RNC; Terry R. Barclay,
Anosognosia, or loss of insight into one s cognitive
 REGULAR ARTICLES Anosognosia Is a Significant Predictor of Apathy in Alzheimer s Disease Sergio E. Starkstein, M.D., Ph.D. Simone Brockman, M.A. David Bruce, M.D. Gustavo Petracca, M.D. Anosognosia and
REGULAR ARTICLES Anosognosia Is a Significant Predictor of Apathy in Alzheimer s Disease Sergio E. Starkstein, M.D., Ph.D. Simone Brockman, M.A. David Bruce, M.D. Gustavo Petracca, M.D. Anosognosia and
Behavioral and psychological symptoms of dementia characteristic of mild Alzheimer patients
 Blackwell Science, LtdOxford, UKPCNPsychiatry and Clinical Neurosciences1323-13162005 Blackwell Publishing Pty Ltd593274279Original ArticleDementia and mild AlzheimersJ. Shimabukuro et al. Psychiatry and
Blackwell Science, LtdOxford, UKPCNPsychiatry and Clinical Neurosciences1323-13162005 Blackwell Publishing Pty Ltd593274279Original ArticleDementia and mild AlzheimersJ. Shimabukuro et al. Psychiatry and
Cerebral correlates of psychotic symptoms in Alzheimer s disease
 J Neurol Neurosurg Psychiatry 2000;69:167 171 167 Department of Neurology UCLA School of Medicine, UCLA School of Medicine, Los Angeles, California, USA L Lee I D Dinov AWToga J L Cummings Laboratory of
J Neurol Neurosurg Psychiatry 2000;69:167 171 167 Department of Neurology UCLA School of Medicine, UCLA School of Medicine, Los Angeles, California, USA L Lee I D Dinov AWToga J L Cummings Laboratory of
Screening and Management of Behavioral and Psychiatric Symptoms Associated with Dementia
 Screening and Management of Behavioral and Psychiatric Symptoms Associated with Dementia Measure Description Percentage of patients with dementia for whom there was a documented screening* for behavioral
Screening and Management of Behavioral and Psychiatric Symptoms Associated with Dementia Measure Description Percentage of patients with dementia for whom there was a documented screening* for behavioral
N europsychiatric symptoms can induce marked disability
 PAPER Neuropsychiatric profiles in patients with Alzheimer s disease and vascular dementia J-L Fuh, S-J Wang, J L Cummings... See end of article for authors affiliations... Correspondence to: Dr J-L Fuh,
PAPER Neuropsychiatric profiles in patients with Alzheimer s disease and vascular dementia J-L Fuh, S-J Wang, J L Cummings... See end of article for authors affiliations... Correspondence to: Dr J-L Fuh,
The course of neuropsychiatric symptoms in dementia. Part II: relationships among behavioural sub-syndromes and the influence of clinical variables
 INTERNATIONAL JOURNAL OF GERIATRIC PSYCHIATRY Int J Geriatr Psychiatry 2005; 20: 531 536. Published online in Wiley InterScience (www.interscience.wiley.com). DOI: 10.1002/gps.1317 The course of neuropsychiatric
INTERNATIONAL JOURNAL OF GERIATRIC PSYCHIATRY Int J Geriatr Psychiatry 2005; 20: 531 536. Published online in Wiley InterScience (www.interscience.wiley.com). DOI: 10.1002/gps.1317 The course of neuropsychiatric
Positron Emission Tomography Metabolic Correlates of Apathy in Alzheimer Disease
 ORIGINAL CONTRIBUTION Positron Emission Tomography Metabolic Correlates of Apathy in Alzheimer Disease Gad A. Marshall, MD; Lorena Monserratt, MA; Dylan Harwood, PhD; Mark Mandelkern, MD, PhD; Jeffrey
ORIGINAL CONTRIBUTION Positron Emission Tomography Metabolic Correlates of Apathy in Alzheimer Disease Gad A. Marshall, MD; Lorena Monserratt, MA; Dylan Harwood, PhD; Mark Mandelkern, MD, PhD; Jeffrey
Introduction, use of imaging and current guidelines. John O Brien Professor of Old Age Psychiatry University of Cambridge
 Introduction, use of imaging and current guidelines John O Brien Professor of Old Age Psychiatry University of Cambridge Why do we undertake brain imaging in AD and other dementias? Exclude other causes
Introduction, use of imaging and current guidelines John O Brien Professor of Old Age Psychiatry University of Cambridge Why do we undertake brain imaging in AD and other dementias? Exclude other causes
Behavioral and Psychologic Symptoms in Different Types of Dementia
 ORIGINAL ARTICLE Behavioral and Psychologic Symptoms in Different Types of Dementia Ming-Jang Chiu,* Ta-Fu Chen, Ping-Keung Yip, Mau-Sun Hua, 1 Li-Yu Tang 2 Background/Purpose: Behavioral and psychologic
ORIGINAL ARTICLE Behavioral and Psychologic Symptoms in Different Types of Dementia Ming-Jang Chiu,* Ta-Fu Chen, Ping-Keung Yip, Mau-Sun Hua, 1 Li-Yu Tang 2 Background/Purpose: Behavioral and psychologic
DEMENTIA WITH LEWY bodies (DLB) is the
 Psychiatry and Clinical Neurosciences 2017; 71: 409 416 doi:10.1111/pcn.12511 Regular Article Association of premorbid personality with behavioral and psychological symptoms in dementia with Lewy bodies:
Psychiatry and Clinical Neurosciences 2017; 71: 409 416 doi:10.1111/pcn.12511 Regular Article Association of premorbid personality with behavioral and psychological symptoms in dementia with Lewy bodies:
Neuropsychiatric Manifestations in Vascular Cognitive Impairment Patients with and without Dementia
 86 Neuropsychiatric Manifestations in Vascular Cognitive Impairment Patients with and without Dementia Pai-Yi Chiu 1,3, Chung-Hsiang Liu 2, and Chon-Haw Tsai 2 Abstract- Background: Neuropsychiatric profile
86 Neuropsychiatric Manifestations in Vascular Cognitive Impairment Patients with and without Dementia Pai-Yi Chiu 1,3, Chung-Hsiang Liu 2, and Chon-Haw Tsai 2 Abstract- Background: Neuropsychiatric profile
ORIGINAL CONTRIBUTION
 ORIGINAL CONTRIBUTION Medial Temporal Hypoperfusion and Aggression in Alzheimer Disease Krista L. Lanctôt, PhD; Nathan Herrmann, MD, FRCPC; Neelesh K. Nadkarni, MD; Farrell S. Leibovitch, MSc; Curtis B.
ORIGINAL CONTRIBUTION Medial Temporal Hypoperfusion and Aggression in Alzheimer Disease Krista L. Lanctôt, PhD; Nathan Herrmann, MD, FRCPC; Neelesh K. Nadkarni, MD; Farrell S. Leibovitch, MSc; Curtis B.
NEUROPSYCHOMETRIC TESTS
 NEUROPSYCHOMETRIC TESTS CAMCOG It is the Cognitive section of Cambridge Examination for Mental Disorders of the Elderly (CAMDEX) The measure assesses orientation, language, memory, praxis, attention, abstract
NEUROPSYCHOMETRIC TESTS CAMCOG It is the Cognitive section of Cambridge Examination for Mental Disorders of the Elderly (CAMDEX) The measure assesses orientation, language, memory, praxis, attention, abstract
Psychiatric and Behavioral Symptoms in Alzheimer s and Other Dementias. Aaron H. Kaufman, MD
 Psychiatric and Behavioral Symptoms in Alzheimer s and Other Dementias Aaron H. Kaufman, MD Psychiatric and Behavioral Symptoms in Alzheimer s and Other Dementias Aaron H. Kaufman, M.D. Health Sciences
Psychiatric and Behavioral Symptoms in Alzheimer s and Other Dementias Aaron H. Kaufman, MD Psychiatric and Behavioral Symptoms in Alzheimer s and Other Dementias Aaron H. Kaufman, M.D. Health Sciences
Range of neuropsychiatric disturbances in patients with Parkinson s disease
 492 Section of Geriatric Psychiatry, Rogaland Psychiatric Hospital D Aarsland N G Lim C Janvin Department of Neurology, Central Hospital of Rogaland, Stavanger, Norway J P Larsen K Karlsen E Tandberg Departments
492 Section of Geriatric Psychiatry, Rogaland Psychiatric Hospital D Aarsland N G Lim C Janvin Department of Neurology, Central Hospital of Rogaland, Stavanger, Norway J P Larsen K Karlsen E Tandberg Departments
Supplementary Online Content
 Supplementary Online Content Devenney E, Bartley L, Hoon C, et al. Progression in behavioral variant frontotemporal dementia: a longitudinal study. JAMA Neurol. Published online October 26, 2015. doi:10.1001/jamaneurol.2015.2061.
Supplementary Online Content Devenney E, Bartley L, Hoon C, et al. Progression in behavioral variant frontotemporal dementia: a longitudinal study. JAMA Neurol. Published online October 26, 2015. doi:10.1001/jamaneurol.2015.2061.
PREVALENCE AND CORRELATES OF ANXIETY IN ALZHEIMER S DISEASE
 166 Chemerinski et al. DEPRESSION AND ANXIETY 7:166 170 (1998) PREVALENCE AND CORRELATES OF ANXIETY IN ALZHEIMER S DISEASE Erán Chemerinski, M.D., 1 * Gustavo Petracca, M.D., 1 Facundo Manes, M.D., 2 Ramón
166 Chemerinski et al. DEPRESSION AND ANXIETY 7:166 170 (1998) PREVALENCE AND CORRELATES OF ANXIETY IN ALZHEIMER S DISEASE Erán Chemerinski, M.D., 1 * Gustavo Petracca, M.D., 1 Facundo Manes, M.D., 2 Ramón
ALZHEIMER DISEASE (AD) AFfects
 ORIGINAL CONTRIBUTION Executive Dysfunction in Alzheimer Disease Margaret M. Swanberg, DO; Rochelle E. Tractenberg, PhD, MPH; Richard Mohs, PhD; Leon J. Thal, MD; Jeffrey L. Cummings, MD Background: Executive
ORIGINAL CONTRIBUTION Executive Dysfunction in Alzheimer Disease Margaret M. Swanberg, DO; Rochelle E. Tractenberg, PhD, MPH; Richard Mohs, PhD; Leon J. Thal, MD; Jeffrey L. Cummings, MD Background: Executive
Hallucinations and conscious access to visual inputs in Parkinson s disease
 Supplemental informations Hallucinations and conscious access to visual inputs in Parkinson s disease Stéphanie Lefebvre, PhD^1,2, Guillaume Baille, MD^4, Renaud Jardri MD, PhD 1,2 Lucie Plomhause, PhD
Supplemental informations Hallucinations and conscious access to visual inputs in Parkinson s disease Stéphanie Lefebvre, PhD^1,2, Guillaume Baille, MD^4, Renaud Jardri MD, PhD 1,2 Lucie Plomhause, PhD
Brain imaging for the diagnosis of people with suspected dementia
 Why do we undertake brain imaging in dementia? Brain imaging for the diagnosis of people with suspected dementia Not just because guidelines tell us to! Exclude other causes for dementia Help confirm diagnosis
Why do we undertake brain imaging in dementia? Brain imaging for the diagnosis of people with suspected dementia Not just because guidelines tell us to! Exclude other causes for dementia Help confirm diagnosis
Neuroimaging for Diagnosis of Psychiatric Disorders
 Psychiatric Disorder Neuroimaging for Diagnosis of Psychiatric Disorders JMAJ 45(12): 538 544, 2002 Yoshio HIRAYASU Associate Professor, Department of Neuropsychiatry Kyorin University School of Medicine
Psychiatric Disorder Neuroimaging for Diagnosis of Psychiatric Disorders JMAJ 45(12): 538 544, 2002 Yoshio HIRAYASU Associate Professor, Department of Neuropsychiatry Kyorin University School of Medicine
Procedia - Social and Behavioral Sciences 159 ( 2014 ) WCPCG 2014
 Available online at www.sciencedirect.com ScienceDirect Procedia - Social and Behavioral Sciences 159 ( 2014 ) 743 748 WCPCG 2014 Differences in Visuospatial Cognition Performance and Regional Brain Activation
Available online at www.sciencedirect.com ScienceDirect Procedia - Social and Behavioral Sciences 159 ( 2014 ) 743 748 WCPCG 2014 Differences in Visuospatial Cognition Performance and Regional Brain Activation
Reliability of the Brazilian Portuguese version of the Neuropsychiatric Inventory (NPI) for patients with Alzheimer s disease and their caregivers
 International Psychogeriatrics (2008), 20:2, 383 393 C 2007 International Psychogeriatric Association doi:10.1017/s1041610207006254 Printed in the United Kingdom Reliability of the Brazilian Portuguese
International Psychogeriatrics (2008), 20:2, 383 393 C 2007 International Psychogeriatric Association doi:10.1017/s1041610207006254 Printed in the United Kingdom Reliability of the Brazilian Portuguese
O Connor 1. Appendix e-1
 O Connor 1 Appendix e-1 Neuropsychiatric assessment The Cambridge Behavioural Inventory Revised (CBI-R) 1, 2 is a proxy behavioural questionnaire that has been extensively used in studies involving FTD
O Connor 1 Appendix e-1 Neuropsychiatric assessment The Cambridge Behavioural Inventory Revised (CBI-R) 1, 2 is a proxy behavioural questionnaire that has been extensively used in studies involving FTD
Clinical Diagnosis. Step 1: Dementia or not? Diagnostic criteria for dementia (DSM-IV)
 Step 1: Dementia or not? Diagnostic criteria for dementia (DSM-IV) A. The development of multiple cognitive deficits manifested by both 1 and 2 1 1. Memory impairment 2. One (or more) of the following
Step 1: Dementia or not? Diagnostic criteria for dementia (DSM-IV) A. The development of multiple cognitive deficits manifested by both 1 and 2 1 1. Memory impairment 2. One (or more) of the following
Psychiatric Morbidity in Dementia Patients in a Neurology-Based Memory Clinic
 Original Articles 179 Psychiatric Morbidity in Dementia Patients in a Neurology-Based Memory Clinic Ching-Sen Shih 1, Sui-Hing Yan 2, Ying-Hoo Ho 1, Yuh-Te Lin 1, Jie-Yuan Li 1, and Yuk-Keung Lo 1 Abstract-
Original Articles 179 Psychiatric Morbidity in Dementia Patients in a Neurology-Based Memory Clinic Ching-Sen Shih 1, Sui-Hing Yan 2, Ying-Hoo Ho 1, Yuh-Te Lin 1, Jie-Yuan Li 1, and Yuk-Keung Lo 1 Abstract-
Differences in brain structure and function between the sexes has been a topic of
 Introduction Differences in brain structure and function between the sexes has been a topic of scientific inquiry for over 100 years. In particular, this topic has had significant interest in the past
Introduction Differences in brain structure and function between the sexes has been a topic of scientific inquiry for over 100 years. In particular, this topic has had significant interest in the past
Satoh M. 1, Ishikawa H. 1, Meguro K. 1,2, Kasuya M. 1, Ishii H. 3, and Yamaguchi S. 2
 CYRIC Annual Report 2009 VIII 15. Occipital Glucose Metabolic Decrease by Donepezil Treatment Correlated with the Improvement of Visual Hallucinations in Dementia with Lewy Bodies: the Osaki-Tajiri Project
CYRIC Annual Report 2009 VIII 15. Occipital Glucose Metabolic Decrease by Donepezil Treatment Correlated with the Improvement of Visual Hallucinations in Dementia with Lewy Bodies: the Osaki-Tajiri Project
Yin-Hui Siow MD, FRCPC Director of Nuclear Medicine Southlake Regional Health Centre
 Yin-Hui Siow MD, FRCPC Director of Nuclear Medicine Southlake Regional Health Centre Today Introduction to CT Introduction to MRI Introduction to nuclear medicine Imaging the dementias The Brain ~ 1.5
Yin-Hui Siow MD, FRCPC Director of Nuclear Medicine Southlake Regional Health Centre Today Introduction to CT Introduction to MRI Introduction to nuclear medicine Imaging the dementias The Brain ~ 1.5
Estimating the Validity of the Korean Version of Expanded Clinical Dementia Rating (CDR) Scale
 Estimating the Validity of the Korean Version of Expanded Clinical Dementia Rating (CDR) Scale Seong Hye Choi, M.D.*, Duk L. Na, M.D., Byung Hwa Lee, M.A., Dong-Seog Hahm, M.D., Jee Hyang Jeong, M.D.,
Estimating the Validity of the Korean Version of Expanded Clinical Dementia Rating (CDR) Scale Seong Hye Choi, M.D.*, Duk L. Na, M.D., Byung Hwa Lee, M.A., Dong-Seog Hahm, M.D., Jee Hyang Jeong, M.D.,
The Frontal Lobes. Anatomy of the Frontal Lobes. Anatomy of the Frontal Lobes 3/2/2011. Portrait: Losing Frontal-Lobe Functions. Readings: KW Ch.
 The Frontal Lobes Readings: KW Ch. 16 Portrait: Losing Frontal-Lobe Functions E.L. Highly organized college professor Became disorganized, showed little emotion, and began to miss deadlines Scores on intelligence
The Frontal Lobes Readings: KW Ch. 16 Portrait: Losing Frontal-Lobe Functions E.L. Highly organized college professor Became disorganized, showed little emotion, and began to miss deadlines Scores on intelligence
Dementia is a common neuropsychiatric disorder characterized by progressive impairment of
 Focused Issue of This Month Diagnosis and Treatment for Behavioral and Psychological Symptoms of Dementia Byoung Hoon Oh, MD Department of Psychiatry, Yonsei University College of Medicine E - mail : drobh@yuhs.ac
Focused Issue of This Month Diagnosis and Treatment for Behavioral and Psychological Symptoms of Dementia Byoung Hoon Oh, MD Department of Psychiatry, Yonsei University College of Medicine E - mail : drobh@yuhs.ac
WHAT IS DEMENTIA? An acquired syndrome of decline in memory and other cognitive functions sufficient to affect daily life in an alert patient
 DEMENTIA WHAT IS DEMENTIA? An acquired syndrome of decline in memory and other cognitive functions sufficient to affect daily life in an alert patient Progressive and disabling Not an inherent aspect of
DEMENTIA WHAT IS DEMENTIA? An acquired syndrome of decline in memory and other cognitive functions sufficient to affect daily life in an alert patient Progressive and disabling Not an inherent aspect of
Neuropsychiatric Inventory Nursing Home Version (NPI-NH)
 This is a Sample version of the Neuropsychiatric Inventory Nursing Home Version (NPI-NH) The full version of the Neuropsychiatric Inventory Nursing Home Version (NPI-NH) comes without sample watermark..
This is a Sample version of the Neuropsychiatric Inventory Nursing Home Version (NPI-NH) The full version of the Neuropsychiatric Inventory Nursing Home Version (NPI-NH) comes without sample watermark..
NEXT-Link DEMENTIA. A network of Danish memory clinics YOUR CLINICAL RESEARCH PARTNER WITHIN ALZHEIMER S DISEASE AND OTHER DEMENTIA DISEASES.
 NEXT-Link DEMENTIA A network of Danish memory clinics YOUR CLINICAL RESEARCH PARTNER WITHIN ALZHEIMER S DISEASE AND OTHER DEMENTIA DISEASES. NEXT-Link DEMENTIA NEXT-Link DEMENTIA is a network of Danish
NEXT-Link DEMENTIA A network of Danish memory clinics YOUR CLINICAL RESEARCH PARTNER WITHIN ALZHEIMER S DISEASE AND OTHER DEMENTIA DISEASES. NEXT-Link DEMENTIA NEXT-Link DEMENTIA is a network of Danish
Classic Evidence: Raine, Buchsbaum and LaCasse, 1997 Brain Abnormalities in Murderers indicated by PET (pg 16-19)
 Classic Evidence: Raine, Buchsbaum and LaCasse, 1997 Brain Abnormalities in Murderers indicated by PET (pg 16-19) Patrick has just been arrested for murder. He confesses to the crime of killing his next
Classic Evidence: Raine, Buchsbaum and LaCasse, 1997 Brain Abnormalities in Murderers indicated by PET (pg 16-19) Patrick has just been arrested for murder. He confesses to the crime of killing his next
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Abuse alcohol, aggression and, 52 53 substance, aggression and, 52 54 ACE. See Aid to Capacity Evaluation (ACE). AEDs. See Antiepileptic
Index Note: Page numbers of article titles are in boldface type. A Abuse alcohol, aggression and, 52 53 substance, aggression and, 52 54 ACE. See Aid to Capacity Evaluation (ACE). AEDs. See Antiepileptic
Behavioral and Psychological Symptoms of Dementia
 Behavioral and Psychological Symptoms of Dementia Akarachaid Pinidbunjerdkool MD*, Sansanee Saengwanitch MD*, Pasiri Sithinamsuwan MD* * Division of Neurology, Department of Medicine, Phramongkutklao Hospital
Behavioral and Psychological Symptoms of Dementia Akarachaid Pinidbunjerdkool MD*, Sansanee Saengwanitch MD*, Pasiri Sithinamsuwan MD* * Division of Neurology, Department of Medicine, Phramongkutklao Hospital
Myers Psychology for AP*
 Myers Psychology for AP* David G. Myers PowerPoint Presentation Slides by Kent Korek Germantown High School Worth Publishers, 2010 *AP is a trademark registered and/or owned by the College Board, which
Myers Psychology for AP* David G. Myers PowerPoint Presentation Slides by Kent Korek Germantown High School Worth Publishers, 2010 *AP is a trademark registered and/or owned by the College Board, which
Non Alzheimer Dementias
 Non Alzheimer Dementias Randolph B Schiffer Department of Neuropsychiatry and Behavioral Science Texas Tech University Health Sciences Center 9/11/2007 Statement of Financial Disclosure Randolph B Schiffer,,
Non Alzheimer Dementias Randolph B Schiffer Department of Neuropsychiatry and Behavioral Science Texas Tech University Health Sciences Center 9/11/2007 Statement of Financial Disclosure Randolph B Schiffer,,
Supplementary Information Methods Subjects The study was comprised of 84 chronic pain patients with either chronic back pain (CBP) or osteoarthritis
 Supplementary Information Methods Subjects The study was comprised of 84 chronic pain patients with either chronic back pain (CBP) or osteoarthritis (OA). All subjects provided informed consent to procedures
Supplementary Information Methods Subjects The study was comprised of 84 chronic pain patients with either chronic back pain (CBP) or osteoarthritis (OA). All subjects provided informed consent to procedures
Traumatic Brain Injury Screening in Correctional Populations. Abby Bernett. Marquette University
 TBI in Corrections 1 Traumatic Brain Injury Screening in Correctional Populations Abby Bernett Marquette University TBI in Corrections 2 Introduction The purpose of this paper is to describe the current
TBI in Corrections 1 Traumatic Brain Injury Screening in Correctional Populations Abby Bernett Marquette University TBI in Corrections 2 Introduction The purpose of this paper is to describe the current
Neuropsychiatric disturbances such as delusions,
 Differential Neuropsychiatric Responses to Tacrine in Alzheimer s Disease: Relationship to Dementia Severity Daniel Kaufer, M.D. Jeffrey L. Cummings, M.D. Dianne Christine, R.N. Neuropsychiatric symptom
Differential Neuropsychiatric Responses to Tacrine in Alzheimer s Disease: Relationship to Dementia Severity Daniel Kaufer, M.D. Jeffrey L. Cummings, M.D. Dianne Christine, R.N. Neuropsychiatric symptom
CHAPTER 5 NEUROPSYCHOLOGICAL PROFILE OF ALZHEIMER S DISEASE
 CHAPTER 5 NEUROPSYCHOLOGICAL PROFILE OF ALZHEIMER S DISEASE 5.1 GENERAL BACKGROUND Neuropsychological assessment plays a crucial role in the assessment of cognitive decline in older age. In India, there
CHAPTER 5 NEUROPSYCHOLOGICAL PROFILE OF ALZHEIMER S DISEASE 5.1 GENERAL BACKGROUND Neuropsychological assessment plays a crucial role in the assessment of cognitive decline in older age. In India, there
Management of the Acutely Agitated Long Term Care Patient
 Management of the Acutely Agitated Long Term Care Patient 80 60 Graying of the Population US Population Over Age 65 Millions of Persons 40 20 0 1900 1920 1940 1960 1980 1990 2010 2030 Year Defining Dementia
Management of the Acutely Agitated Long Term Care Patient 80 60 Graying of the Population US Population Over Age 65 Millions of Persons 40 20 0 1900 1920 1940 1960 1980 1990 2010 2030 Year Defining Dementia
BEHAVIOURAL AND PSYCHOLOGICAL SYMPTOMS IN DEMENTIA
 BEHAVIOURAL AND PSYCHOLOGICAL SYMPTOMS IN DEMENTIA Unmet needs What might be your behavioural response to this experience? Content Definition What are BPSD? Prevalence How common are they? Aetiological
BEHAVIOURAL AND PSYCHOLOGICAL SYMPTOMS IN DEMENTIA Unmet needs What might be your behavioural response to this experience? Content Definition What are BPSD? Prevalence How common are they? Aetiological
Differential Diagnosis of Alzheimer s Disease and Other Types of Dementia with Development of Neuroimaging Techniques (PET, SPECT, and MRI)
 www.jmscr.igmpublication.org Impact Factor 1.1147 ISSN (e)-2347-176x Differential Diagnosis of Alzheimer s Disease and Other Types of Dementia with Development of Neuroimaging Techniques (PET, SPECT, and
www.jmscr.igmpublication.org Impact Factor 1.1147 ISSN (e)-2347-176x Differential Diagnosis of Alzheimer s Disease and Other Types of Dementia with Development of Neuroimaging Techniques (PET, SPECT, and
CISC 3250 Systems Neuroscience
 CISC 3250 Systems Neuroscience Levels of organization Central Nervous System 1m 10 11 neurons Neural systems and neuroanatomy Systems 10cm Networks 1mm Neurons 100μm 10 8 neurons Professor Daniel Leeds
CISC 3250 Systems Neuroscience Levels of organization Central Nervous System 1m 10 11 neurons Neural systems and neuroanatomy Systems 10cm Networks 1mm Neurons 100μm 10 8 neurons Professor Daniel Leeds
Caring Sheet #11: Alzheimer s Disease:
 CARING SHEETS: Caring Sheet #11: Alzheimer s Disease: A Summary of Information and Intervention Suggestions with an Emphasis on Cognition By Shelly E. Weaverdyck, PhD Introduction This caring sheet focuses
CARING SHEETS: Caring Sheet #11: Alzheimer s Disease: A Summary of Information and Intervention Suggestions with an Emphasis on Cognition By Shelly E. Weaverdyck, PhD Introduction This caring sheet focuses
Mental and Behavioral Disturbances in Dementia: Findings from the Cache County Study on Memory in Aging
 Utah State University DigitalCommons@USU Psychology Faculty Publications Psychology 2000 Mental and Behavioral Disturbances in : Findings from the Cache County Study on Memory in Aging Constantine G. Lyketsos
Utah State University DigitalCommons@USU Psychology Faculty Publications Psychology 2000 Mental and Behavioral Disturbances in : Findings from the Cache County Study on Memory in Aging Constantine G. Lyketsos
fmri (functional MRI)
 Lesion fmri (functional MRI) Electroencephalogram (EEG) Brainstem CT (computed tomography) Scan Medulla PET (positron emission tomography) Scan Reticular Formation MRI (magnetic resonance imaging) Thalamus
Lesion fmri (functional MRI) Electroencephalogram (EEG) Brainstem CT (computed tomography) Scan Medulla PET (positron emission tomography) Scan Reticular Formation MRI (magnetic resonance imaging) Thalamus
Neuropsychiatric symptoms in 921 elderly subjects with dementia: a comparison between vascular and neurodegenerative types
 Acta Psychiatr Scand 2008: 117: 455 464 All rights reserved DOI: 10.1111/j.1600-0447.2008.01175.x Copyright Ó 2008 The Authors Journal Compilation Ó 2008 Blackwell Munksgaard ACTA PSYCHIATRICA SCANDINAVICA
Acta Psychiatr Scand 2008: 117: 455 464 All rights reserved DOI: 10.1111/j.1600-0447.2008.01175.x Copyright Ó 2008 The Authors Journal Compilation Ó 2008 Blackwell Munksgaard ACTA PSYCHIATRICA SCANDINAVICA
Research Article Behavioural and Psychological Symptoms in Poststroke Vascular Cognitive Impairment
 Behavioural Neurology, Article ID 430128, 5 pages http://dx.doi.org/10.1155/2014/430128 Research Article Behavioural and Psychological Symptoms in Poststroke Vascular Cognitive Impairment Meena Gupta,
Behavioural Neurology, Article ID 430128, 5 pages http://dx.doi.org/10.1155/2014/430128 Research Article Behavioural and Psychological Symptoms in Poststroke Vascular Cognitive Impairment Meena Gupta,
Supplementary Online Content
 Supplementary Online Content Redlich R, Opel N, Grotegerd D, et al. Prediction of individual response to electroconvulsive therapy via machine learning on structural magnetic resonance imaging data. JAMA
Supplementary Online Content Redlich R, Opel N, Grotegerd D, et al. Prediction of individual response to electroconvulsive therapy via machine learning on structural magnetic resonance imaging data. JAMA
IT IS WELL known that individuals with dementia. Classifying eating-related problems among institutionalized people with dementia.
 doi:10.1111/pcn.12375 Regular Article Classifying eating-related problems among institutionalized people with dementia Shunichiro Shinagawa, MD, PhD, 1 * Kazuki Honda, MD, PhD, 2 Tetsuo Kashibayashi, MD,
doi:10.1111/pcn.12375 Regular Article Classifying eating-related problems among institutionalized people with dementia Shunichiro Shinagawa, MD, PhD, 1 * Kazuki Honda, MD, PhD, 2 Tetsuo Kashibayashi, MD,
MITELMAN, SHIHABUDDIN, BRICKMAN, ET AL. basic necessities of life, including food, clothing, and shelter. Compared to patients with good-outcome schiz
 Article MRI Assessment of Gray and White Matter Distribution in Brodmann s Areas of the Cortex in Patients With Schizophrenia With Good and Poor Outcomes Serge A. Mitelman, M.D. Lina Shihabuddin, M.D.
Article MRI Assessment of Gray and White Matter Distribution in Brodmann s Areas of the Cortex in Patients With Schizophrenia With Good and Poor Outcomes Serge A. Mitelman, M.D. Lina Shihabuddin, M.D.
Clinical Characteristics of Behavioral and Psychological Symptoms in Patients with Drug-naïve Alzheimer s Disease
 Dementia and Neurocognitive Disorders 2012; 11: 87-94 ORIGINAL ARTICLE Clinical Characteristics of Behavioral and Psychological Symptoms in Patients with Drug-naïve Alzheimer s Disease Yong Tae Kwak, M.D.,
Dementia and Neurocognitive Disorders 2012; 11: 87-94 ORIGINAL ARTICLE Clinical Characteristics of Behavioral and Psychological Symptoms in Patients with Drug-naïve Alzheimer s Disease Yong Tae Kwak, M.D.,
Regional and Lobe Parcellation Rhesus Monkey Brain Atlas. Manual Tracing for Parcellation Template
 Regional and Lobe Parcellation Rhesus Monkey Brain Atlas Manual Tracing for Parcellation Template Overview of Tracing Guidelines A) Traces are performed in a systematic order they, allowing the more easily
Regional and Lobe Parcellation Rhesus Monkey Brain Atlas Manual Tracing for Parcellation Template Overview of Tracing Guidelines A) Traces are performed in a systematic order they, allowing the more easily
Supplementary Online Content
 Supplementary Online Content Atri A, Frölich L, Ballard C, et al. Effect of idalopirdine as adjunct to cholinesterase inhibitors on in cognition in patients with Alzheimer disease: three randomized clinical
Supplementary Online Content Atri A, Frölich L, Ballard C, et al. Effect of idalopirdine as adjunct to cholinesterase inhibitors on in cognition in patients with Alzheimer disease: three randomized clinical
Methods to examine brain activity associated with emotional states and traits
 Methods to examine brain activity associated with emotional states and traits Brain electrical activity methods description and explanation of method state effects trait effects Positron emission tomography
Methods to examine brain activity associated with emotional states and traits Brain electrical activity methods description and explanation of method state effects trait effects Positron emission tomography
The human brain. of cognition need to make sense gives the structure of the brain (duh). ! What is the basic physiology of this organ?
 The human brain The human brain! What is the basic physiology of this organ?! Understanding the parts of this organ provides a hypothesis space for its function perhaps different parts perform different
The human brain The human brain! What is the basic physiology of this organ?! Understanding the parts of this organ provides a hypothesis space for its function perhaps different parts perform different
Pick Paterson 1944
 383 33 1 1 28 4 383 391 2008 Key Words reduplicative paramnesia geographical mislocation double orientation identity right frontal lobe reduplicative paramnesia Pick 1901 1903 2 Ruff 1981 Staton 1982 Patterson
383 33 1 1 28 4 383 391 2008 Key Words reduplicative paramnesia geographical mislocation double orientation identity right frontal lobe reduplicative paramnesia Pick 1901 1903 2 Ruff 1981 Staton 1982 Patterson
A prospective study of dementia with Lewy bodies
 Age and Ageing 998; 27: 6-66 998, British Geriatrics Society A prospective study of dementia with Lewy bodies CLIVE G. BALLARD, JOHN O'BRIEN, KATH LOWERX GARETH A. AYRE, RICHARD HARRISON, ROBERT PERRY,
Age and Ageing 998; 27: 6-66 998, British Geriatrics Society A prospective study of dementia with Lewy bodies CLIVE G. BALLARD, JOHN O'BRIEN, KATH LOWERX GARETH A. AYRE, RICHARD HARRISON, ROBERT PERRY,
Investigating directed influences between activated brain areas in a motor-response task using fmri
 Magnetic Resonance Imaging 24 (2006) 181 185 Investigating directed influences between activated brain areas in a motor-response task using fmri Birgit Abler a, 4, Alard Roebroeck b, Rainer Goebel b, Anett
Magnetic Resonance Imaging 24 (2006) 181 185 Investigating directed influences between activated brain areas in a motor-response task using fmri Birgit Abler a, 4, Alard Roebroeck b, Rainer Goebel b, Anett
The Neuropsychology of
 The Neuropsychology of Stroke Tammy Kordes, Ph.D. Northshore Neurosciences Outline What is the Role of Neuropsychology Purpose of Neuropsychological Assessments Common Neuropsychological Disorders Assessment
The Neuropsychology of Stroke Tammy Kordes, Ph.D. Northshore Neurosciences Outline What is the Role of Neuropsychology Purpose of Neuropsychological Assessments Common Neuropsychological Disorders Assessment
Fatigue in patients with Parkinson s disease
 103 Fatigue in patients with Parkinson s disease Kazuo Abe, Mayako Takanashi and Takehiko Yanagihara Department of Neurology, Osaka University Graduate School of Medicine, Japan Purpose: Fatigue is a complaint
103 Fatigue in patients with Parkinson s disease Kazuo Abe, Mayako Takanashi and Takehiko Yanagihara Department of Neurology, Osaka University Graduate School of Medicine, Japan Purpose: Fatigue is a complaint
CEREBRAL BLOOD FLOW AND METABOLISM
 Supported by: HURO/0901/069/2.3.1 HU-RO-DOCS CEREBRAL BLOOD FLOW AND METABOLISM Part 3 Modern imaging methods SPECT, PET, nmri History of Nuclear Medicine Starts with the invention of the X-ray 1946: radioactive
Supported by: HURO/0901/069/2.3.1 HU-RO-DOCS CEREBRAL BLOOD FLOW AND METABOLISM Part 3 Modern imaging methods SPECT, PET, nmri History of Nuclear Medicine Starts with the invention of the X-ray 1946: radioactive
Dementia. Assessing Brain Damage. Mental Status Examination
 Dementia Assessing Brain Damage Mental status examination Information about current behavior and thought including orientation to reality, memory, and ability to follow instructions Neuropsychological
Dementia Assessing Brain Damage Mental status examination Information about current behavior and thought including orientation to reality, memory, and ability to follow instructions Neuropsychological
performance of verbal working memory tasks
 Proc. Natl. Acad. Sci. USA Vol. 90, pp. 878-882, February 1993 Neurobiology Functional activation of the human frontal cortex during the performance of verbal working memory tasks MICHAEL PETRIDES, BESSIE
Proc. Natl. Acad. Sci. USA Vol. 90, pp. 878-882, February 1993 Neurobiology Functional activation of the human frontal cortex during the performance of verbal working memory tasks MICHAEL PETRIDES, BESSIE
Four Tissue Segmentation in ADNI II
 Four Tissue Segmentation in ADNI II Charles DeCarli, MD, Pauline Maillard, PhD, Evan Fletcher, PhD Department of Neurology and Center for Neuroscience, University of California at Davis Summary Table of
Four Tissue Segmentation in ADNI II Charles DeCarli, MD, Pauline Maillard, PhD, Evan Fletcher, PhD Department of Neurology and Center for Neuroscience, University of California at Davis Summary Table of
Copyright 2002 American Academy of Neurology. Volume 58(8) 23 April 2002 pp
 Copyright 2002 American Academy of Neurology Volume 58(8) 23 April 2002 pp 1288-1290 Improved executive functioning following repetitive transcranial magnetic stimulation [Brief Communications] Moser,
Copyright 2002 American Academy of Neurology Volume 58(8) 23 April 2002 pp 1288-1290 Improved executive functioning following repetitive transcranial magnetic stimulation [Brief Communications] Moser,
Confusional state. Digit Span. Mini Mental State Examination MMSE. confusional state MRI
 10 304 29 3 confusional state MRI 29 3 304 311 2009 Key Words memory test attention brain region causative disease subcortical dementia 1 Confusional state Digit Span 1 1 5 4 Mini Mental State Examination
10 304 29 3 confusional state MRI 29 3 304 311 2009 Key Words memory test attention brain region causative disease subcortical dementia 1 Confusional state Digit Span 1 1 5 4 Mini Mental State Examination
CLINICAL TRIALS SECTION EDITOR: IRA SHOULSON, MD. Metabolic Patterns Associated With the Clinical Response to Galantamine Therapy
 CLINICAL TIALS SECTION EDITO: IA SHOULSON, MD Metabolic Patterns Associated With the Clinical esponse to Galantamine Therapy A Fludeoxyglucose F 18 Positron Emission Tomographic Study Michael S. Mega,
CLINICAL TIALS SECTION EDITO: IA SHOULSON, MD Metabolic Patterns Associated With the Clinical esponse to Galantamine Therapy A Fludeoxyglucose F 18 Positron Emission Tomographic Study Michael S. Mega,
Revised criteria for the clinical diagnosis of dementia with Lewy. Dementia with Lewy bodies. (Dementia with Lewy Bodies)
 Dementia with Lewy bodies First described: Okazaki H, 1961, Diffuse intracytoplasmic ganglionic inclusions (Lewy type) associated with progressive dementia and quadriparesis in flexion. J Neuropathol Exp
Dementia with Lewy bodies First described: Okazaki H, 1961, Diffuse intracytoplasmic ganglionic inclusions (Lewy type) associated with progressive dementia and quadriparesis in flexion. J Neuropathol Exp
Validation of apathy evaluation scale and assessment of severity of apathy in Alzheimer s diseasepcn_
 Psychiatry and Clinical Neurosciences 2012; 66: 227 234 doi:10.1111/j.1440-1819.2011.02315.x Regular Article Validation of apathy evaluation scale and assessment of severity of apathy in Alzheimer s diseasepcn_2315
Psychiatry and Clinical Neurosciences 2012; 66: 227 234 doi:10.1111/j.1440-1819.2011.02315.x Regular Article Validation of apathy evaluation scale and assessment of severity of apathy in Alzheimer s diseasepcn_2315
The place for treatments of associated neuropsychiatric and other symptoms
 The place for treatments of associated neuropsychiatric and other symptoms Luca Pani dg@aifa.gov.it London, 25 th November 2014 Workshop on Alzheimer s Disease European Medicines Agency London, UK Public
The place for treatments of associated neuropsychiatric and other symptoms Luca Pani dg@aifa.gov.it London, 25 th November 2014 Workshop on Alzheimer s Disease European Medicines Agency London, UK Public
A lzheimer s disease has many neuropsychiatric manifestations
 1396 PAPER Right prosubiculum amyloid plaque density correlates with anosognosia in Alzheimer s disease G A Marshall, D I Kaufer, O L Lopez, G R Rao, R L Hamilton, S T DeKosky... See end of article for
1396 PAPER Right prosubiculum amyloid plaque density correlates with anosognosia in Alzheimer s disease G A Marshall, D I Kaufer, O L Lopez, G R Rao, R L Hamilton, S T DeKosky... See end of article for
Downloaded from irje.tums.ac.ir at 9:18 IRDT on Saturday September 15th 2018
 .5159 :2 7 1390 : 88989123 4 3 2 1 1 : 2 3 4. :. :. 84 : Burden Iranian Version of Caregiver.. Neuropsychiatric Inventory ().. 85. 2/4 39/3 : ebrahemen@gmail.com : 89/10/4 : 89/8/26: :. : 40 (116 58).
.5159 :2 7 1390 : 88989123 4 3 2 1 1 : 2 3 4. :. :. 84 : Burden Iranian Version of Caregiver.. Neuropsychiatric Inventory ().. 85. 2/4 39/3 : ebrahemen@gmail.com : 89/10/4 : 89/8/26: :. : 40 (116 58).
High Resolution Ictal SPECT: Enhanced Epileptic Source Targeting?
 High Resolution Ictal SPECT: Enhanced Epileptic Source Targeting? Marvin A Rossi MD, PhD RUSH Epilepsy Center Research Lab http://www.synapticom.net Chicago, IL USA Medically-Refractory Epilepsy 500,000-800,000
High Resolution Ictal SPECT: Enhanced Epileptic Source Targeting? Marvin A Rossi MD, PhD RUSH Epilepsy Center Research Lab http://www.synapticom.net Chicago, IL USA Medically-Refractory Epilepsy 500,000-800,000
Diffusion Tensor Imaging in Psychiatry
 2003 KHBM DTI in Psychiatry Diffusion Tensor Imaging in Psychiatry KHBM 2003. 11. 21. 서울대학교 의과대학 정신과학교실 권준수 Neuropsychiatric conditions DTI has been studied in Alzheimer s disease Schizophrenia Alcoholism
2003 KHBM DTI in Psychiatry Diffusion Tensor Imaging in Psychiatry KHBM 2003. 11. 21. 서울대학교 의과대학 정신과학교실 권준수 Neuropsychiatric conditions DTI has been studied in Alzheimer s disease Schizophrenia Alcoholism
Comment on administration and scoring of the Neuropsychiatric Inventory in clinical trials
 Alzheimer s & Dementia 4 (2008) 390 394 Comment on administration and scoring of the Neuropsychiatric Inventory in clinical trials Donald J. Connor a, *, Marwan N. Sabbagh a, Jeffery L. Cummings b a Cleo
Alzheimer s & Dementia 4 (2008) 390 394 Comment on administration and scoring of the Neuropsychiatric Inventory in clinical trials Donald J. Connor a, *, Marwan N. Sabbagh a, Jeffery L. Cummings b a Cleo
Erin Cullnan Research Assistant, University of Illinois at Chicago
 Dr. Moises Gaviria Distinguished Professor of Psychiatry, University of Illinois at Chicago Director of Consultation Liaison Service, Advocate Christ Medical Center Director of the Older Adult Program,
Dr. Moises Gaviria Distinguished Professor of Psychiatry, University of Illinois at Chicago Director of Consultation Liaison Service, Advocate Christ Medical Center Director of the Older Adult Program,
Cerebral Cortex 1. Sarah Heilbronner
 Cerebral Cortex 1 Sarah Heilbronner heilb028@umn.edu Want to meet? Coffee hour 10-11am Tuesday 11/27 Surdyk s Overview and organization of the cerebral cortex What is the cerebral cortex? Where is each
Cerebral Cortex 1 Sarah Heilbronner heilb028@umn.edu Want to meet? Coffee hour 10-11am Tuesday 11/27 Surdyk s Overview and organization of the cerebral cortex What is the cerebral cortex? Where is each
Regional Cerebral Blood Flow Abnormalities Associated With Apathy and Depression in Alzheimer Disease
 ORIGINAL ARTICLE Regional Cerebral Blood Flow Abnormalities Associated With Apathy and Depression in Alzheimer Disease Ji Yeon Kang, MD,* Jae Sung Lee, PhD,*wz Hyejin Kang, PhD,* Hae-Woo Lee, MD,y Yu Kyeong
ORIGINAL ARTICLE Regional Cerebral Blood Flow Abnormalities Associated With Apathy and Depression in Alzheimer Disease Ji Yeon Kang, MD,* Jae Sung Lee, PhD,*wz Hyejin Kang, PhD,* Hae-Woo Lee, MD,y Yu Kyeong
Lewy body disease (LBD) is the second most common
 REGULAR ARTICLES Lewy Body Disease: Can We Diagnose It? Michelle Papka, Ph.D. Ana Rubio, M.D., Ph.D. Randolph B. Schiffer, M.D. Christopher Cox, Ph.D. The authors assessed the accuracy of published clinical
REGULAR ARTICLES Lewy Body Disease: Can We Diagnose It? Michelle Papka, Ph.D. Ana Rubio, M.D., Ph.D. Randolph B. Schiffer, M.D. Christopher Cox, Ph.D. The authors assessed the accuracy of published clinical
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 diagnosis and assessment bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
diagnosis and assessment bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
HDSA Annual Convention June 2013 Behavior Issues: Irritability and Depression Peg Nopoulos, M.D.
 HDSA Annual Convention June 2013 Behavior Issues: Irritability and Depression Peg Nopoulos, M.D. Professor of Psychiatry, Neurology, and Pediatrics University of Iowa, Iowa City, Iowa The information provided
HDSA Annual Convention June 2013 Behavior Issues: Irritability and Depression Peg Nopoulos, M.D. Professor of Psychiatry, Neurology, and Pediatrics University of Iowa, Iowa City, Iowa The information provided
ALZHEIMER S DISEASE. Mary-Letitia Timiras M.D. Overlook Hospital Summit, New Jersey
 ALZHEIMER S DISEASE Mary-Letitia Timiras M.D. Overlook Hospital Summit, New Jersey Topics Covered Demography Clinical manifestations Pathophysiology Diagnosis Treatment Future trends Prevalence and Impact
ALZHEIMER S DISEASE Mary-Letitia Timiras M.D. Overlook Hospital Summit, New Jersey Topics Covered Demography Clinical manifestations Pathophysiology Diagnosis Treatment Future trends Prevalence and Impact
Conversion Disorder in Young People. Consultant Child and Adolescent Psychiatrist Southampton Children s Hospital
 Conversion Disorder in Young People Dr Anthony Crabb Dr Anthony Crabb Consultant Child and Adolescent Psychiatrist Southampton Children s Hospital Conversion (noun) Pronunciation: /kənˈvəːʃ(ə)n/ The process
Conversion Disorder in Young People Dr Anthony Crabb Dr Anthony Crabb Consultant Child and Adolescent Psychiatrist Southampton Children s Hospital Conversion (noun) Pronunciation: /kənˈvəːʃ(ə)n/ The process
A new rapid landmark-based regional MRI segmentation method of the brain
 Journal of the Neurological Sciences 194 (2002) 35 40 www.elsevier.com/locate/jns A new rapid landmark-based regional MRI segmentation method of the brain A.L.W. Bokde a, S.J. Teipel a, *, Y. Zebuhr a,
Journal of the Neurological Sciences 194 (2002) 35 40 www.elsevier.com/locate/jns A new rapid landmark-based regional MRI segmentation method of the brain A.L.W. Bokde a, S.J. Teipel a, *, Y. Zebuhr a,
Pharmacological Treatment of Aggression in the Elderly
 Pharmacological Treatment of Aggression in the Elderly Howard Fenn, MD Adjunct Clinical Associate Professor Department of Psychiatry and Behavioral Sciences Stanford University Self-Assessment Question
Pharmacological Treatment of Aggression in the Elderly Howard Fenn, MD Adjunct Clinical Associate Professor Department of Psychiatry and Behavioral Sciences Stanford University Self-Assessment Question
. Neuropsychiatric Inventory (NPI) :
 Downloaded Downloaded from http://journals.tums.ac.ir/ from irje.tums.ac.ir at 9:18 on IRDT Monday, Saturday February September 27, 2012 15th 2018.5159 :2 7 1390 : 88989123 4 3 2 1 1 : 2 3 4. :. :. 84
Downloaded Downloaded from http://journals.tums.ac.ir/ from irje.tums.ac.ir at 9:18 on IRDT Monday, Saturday February September 27, 2012 15th 2018.5159 :2 7 1390 : 88989123 4 3 2 1 1 : 2 3 4. :. :. 84
Mild Cognitive Impairment (MCI)
 October 19, 2018 Mild Cognitive Impairment (MCI) Yonas E. Geda, MD, MSc Professor of Neurology and Psychiatry Consultant, Departments of Psychiatry & Psychology, and Neurology Mayo Clinic College of Medicine
October 19, 2018 Mild Cognitive Impairment (MCI) Yonas E. Geda, MD, MSc Professor of Neurology and Psychiatry Consultant, Departments of Psychiatry & Psychology, and Neurology Mayo Clinic College of Medicine
Introduction to Dementia: Complications
 Introduction to Dementia: Complications Created in March 2005 Duration: about 15 minutes Axel Juan, MD The Geriatrics Institute axel.juan@med.va.gov 305-575-3388 Credits Principal medical contributor:
Introduction to Dementia: Complications Created in March 2005 Duration: about 15 minutes Axel Juan, MD The Geriatrics Institute axel.juan@med.va.gov 305-575-3388 Credits Principal medical contributor:
Virtual Mentor American Medical Association Journal of Ethics August 2014, Volume 16, Number 8:
 Virtual Mentor American Medical Association Journal of Ethics August 2014, Volume 16, Number 8: 626-630. STATE OF THE ART AND SCIENCE Use of Art Making in Treating Older Patients with Dementia Laura T.
Virtual Mentor American Medical Association Journal of Ethics August 2014, Volume 16, Number 8: 626-630. STATE OF THE ART AND SCIENCE Use of Art Making in Treating Older Patients with Dementia Laura T.
Supplementary Online Content
 Supplementary Online Content Gregg NM, Kim AE, Gurol ME, et al. Incidental cerebral microbleeds and cerebral blood flow in elderly individuals. JAMA Neurol. Published online July 13, 2015. doi:10.1001/jamaneurol.2015.1359.
Supplementary Online Content Gregg NM, Kim AE, Gurol ME, et al. Incidental cerebral microbleeds and cerebral blood flow in elderly individuals. JAMA Neurol. Published online July 13, 2015. doi:10.1001/jamaneurol.2015.1359.
Behavior Problems: in Long Term Care and Assisted Living
 Behavior Problems: Dementia and Mental Illness in Long Term Care and Assisted Living Module I Dr. David A. Smith, M.D., FAAFP, CMD mmlearn.org is a program of Morningside Ministries Cell Phones and Pagers
Behavior Problems: Dementia and Mental Illness in Long Term Care and Assisted Living Module I Dr. David A. Smith, M.D., FAAFP, CMD mmlearn.org is a program of Morningside Ministries Cell Phones and Pagers
Case Report of the PET Scan Changes and Clinical Effects of Testosterone in the Treatment of a Stroke Patient
 Send Orders of Reprints at reprints@benthamscience.org The Open Andrology Journal, 2012, 4, 21-25 21 Open Access Case Report of the PET Scan Changes and Clinical Effects of Testosterone in the Treatment
Send Orders of Reprints at reprints@benthamscience.org The Open Andrology Journal, 2012, 4, 21-25 21 Open Access Case Report of the PET Scan Changes and Clinical Effects of Testosterone in the Treatment
Management of Agitation in Dementia. Kimberly Triplett Ferguson, MS4
 Management of Agitation in Dementia Kimberly Triplett Ferguson, MS4 Objectives 1. Review recommended evaluation of agitated patients with dementia. 2. Discuss evidence concerning nonpharmacologic management.
Management of Agitation in Dementia Kimberly Triplett Ferguson, MS4 Objectives 1. Review recommended evaluation of agitated patients with dementia. 2. Discuss evidence concerning nonpharmacologic management.
