What's in a Review? Key Factors to Include and Exclude
|
|
|
- Beryl Horton
- 5 years ago
- Views:
Transcription
1 What's in a Review? Key Factors to Include and Exclude Deanne Wilk, BSN, RN, CCDS, CCS, CMS Manager, Clinical Documentation Improvement Penn State Health Hershey This is the Full Title of a Session Hershey, PA 1
2 Learning Objectives At the completion of this educational activity, the learner will be able to: Define the CDI review Demonstrate construction of CDI review elements Contrast the balance of the review and production goals Differentiate various quality focus reviews Distinguish advanced CDI review factors 2
3 CDI Review Purpose and Definition 3
4 CDI Review Purpose and Definition The CDI review is that information captured to communicate CDI principles and other pertinent factors relevant to the individual institution. 4
5 Review Purpose Quality Compliance Revenue Documentation quality Documentation compliance Coding specificity Quality initiatives Present on admission (POA) Coding accuracy Patient care and outcomes Coding appropriateness Value based purchasing Public reporting Medical necessity Denials 5
6 Goals of the Review Documentation Clear, concise, complete Organizational and regulatory bylaw compliance UHDDS and Official Coding Guidelines followed Clinical support Clinical indicators Medical necessity Diagnostics and medications Patient care Patient severity Complications POA Quality 6
7 Review Prioritization Sample 7
8 Initial Subsequent Medicare Top DRGs with opportunity Unit/complex cases Surgical cases post surgery or transfers in Poor documentation providers Blues Queries outstanding Medicare No MCC/CC x 2 Low APR Surgical cases post surgery or transfers in Blues Top DRGs with opportunity Complex cases and mortalities to achieve MCC/CCs (x 2+) and 4/4 SOI/ROM Surgical cases for complications/psis Poor provider documentation Commercial Medicaid Commercial *Prioritization should always be facility specific Medicaid Self Pay Self Pay 8
9 What s In a Review? 9
10 When Performing a Review, Ask Yourself Why is the patient here? What do I need to prove or disprove about this patient? Diagnoses Normal and abnormal What is important to capture in my review so that I remember on the subsequent review? What is important for me to capture if someone else reviews this patient after me? CDI or coding What do I need to follow up? Self talk What coding needs further specification? 10
11 Chart Review Workflow ED Progress notes Nursing notes H & P Diagnostics Query Consults OR Follow up and focus 11
12 Emergency Department Vitals initial: May need for SIRS, sepsis, infections, respiratory failure, POA status support, medical necessity. Compare to subsequent vitals. Chief complaint (CC): Must relate to principal diagnosis. What did the patient or family say? Confusion? Behavioral disturbance? Not eating or drinking? Fall? (Where, how, doing what?) Relevant physical findings: Diagnosis support (pressure injuries, respiratory failure, malnutrition). Relevant PMH: Chronic conditions. Diagnoses to capture. What medications were they on coming in, and is there a diagnosis to match? Are there antibiotics, and what are they still treating? Recent surgery or surgery that removed an organ or limb? (HCC captures) DNR or palliative care status? (mortality risk factors) POA (devices, ostomy site): Complications, recent surgery, conditions still being treated (PNA, cancer, UTI). Patient Safety Indicators (PSIs)? Confusion/AMS/skin ulcers: Present? Diagnosis to match? Query or follow up needed? Dx/impression: Medical necessity. Diagnoses to capture. Does it relate to admission diagnosis? 12
13 History and Physical CC: Does it compare or contrast to ED diagnosis? Must relate to principal diagnosis. Diagnoses to capture. Vitals or significant changes from ED record: What is new or different? What is further supported or not mentioned or no longer supported clinically? Query required? Follow up in first progress notes? Relevant PMH: Chronic conditions not documented in ED. Alzheimer's or Parkinson's or encephalopathy? What did nursing or ED say about their behavior? HCC risk factors. Relevant physical findings: Complete physical exam reviewed for normal and abnormal. Ostomy site presence and appearance. Skin dry? Skin moist but patient dehydrated. Pressure injury but no mention on skin assessment. Sepsis diagnosed but patient in No Acute Distress (NAD) and no findings of chills, rigors, or clamminess. Respiratory failure but no SOB, work of breathing, elevated respiratory rate, accessory muscle use. Wheelchair/bed bound, disability, lack of mobility, DNR status = mortality risk factors. Significant findings: Diagnoses to capture. Normal and abnormal. Diagnostics to prove or disprove a diagnosis. Clinical support for your diagnoses? Dx/impression: Diagnoses to capture. What has changed from the ED diagnoses and are they clinically supported? Query required? Follow up required? What is the plan? What diagnostics do you need to follow up on? 13
14 Progress Notes, Consults, and Nursing Notes Diagnoses: Diagnosis capture. New diagnoses clinically supported? Diagnostic findings with a relevant diagnosis? Does it prove or disprove a diagnosis? Significant skin assessment: Nursing compared to provider. Pressure injuries and staging. Status changes: What is different today? What is new or different from what the consult vs attending is documenting? Query needed for discrepancy of documentation? Significant findings: What is normal or abnormal? Why? Is it clinically supported? Is it diagnosed? Is there a query needed? Impression/plan: Diagnosis capture. Clinical support query necessary? What is supporting the diagnosis (diagnostics)? Relevant nutrition notes with abnormal BMI: Do they clinically support nutrition diagnosis? Educate them to write patient meets indicators for. 14
15 Operative Note or Bedside Procedures OP report: Coding specificity required to get the right DRG. Don t review surgery cases until after the operation. Compare the brief op note with the dictated report for discrepancies. Postop dx: How is it different than the preop dx? Significant findings: Complications, blood loss, extra procedures. Complications: Is it documented as a complication? Does it need to be referred to patient safety or reviewed as a PSI? 15
16 Diagnostics and Medications Pertinent diagnostics: Review your diagnostics together to save time as it provides a timeline comparison. Normal and abnormal. Lab, radiology, EKG, echo. Does it prove or disprove a diagnosis? Query required on abnormal findings with no diagnosis? Relevant abnormal trends such as: WBC = Infection or immunosuppression, cancer Na, K, Mg = hyper/hypo conditions INR, PT, PTT = bleeding, coagulopathy (mortality risk factors) H/H = anemia, cancers Amylase/lipase = pancreatitis Protein/albumin/pre albumin = malnutrition (labs sometimes used by auditors) LFTs = liver disease Significant/incidental findings: Findings diagnosed and documented in the record. Is the report copied/pasted or corroborated by the provider in documentation? Radiology reports (renal calculus, gallbladder sludge, liver mass, lung mass) severity factors. Labs with abnormals not diagnosed. EKG with arrhythmias and blocks. Echo with regurgitation, insufficiency and ejection fraction %. Abnormal BMI: Always capture BMI. BMI code only relevant with a nutritional diagnosis to match. Query needed? Significant medication diagnoses: Diagnosis to match medication? Is there a new medication introduced? Why? Changed in antibiotics? Why? (Complex vs simple PNA?) Sepsis? Surgical infection? (PSI?) Do the medications clinically support the diagnoses documented? 16
17 Summary Follow up CDI comments: Summation of what needs further review: Diagnoses, diagnostics, reports, consults. Queries. Note last progress note reviewed. Pertinent notes to self and others: Self talk. What you want to tell yourself or others for current or subsequent reviews. What are your thoughts? What conditions are still uncertain or need follow up, clinically supported or possibly queried? Possible queries: May query but not enough clinical indicators to support a query. Strive for 2 or more clinical indicators to query. Focus review/follow up: Focus reviews performed and noted (risk factors, PSIs, etc. and if record forwarded to physician advisor): Specific reviews for your institution such as: Quality: mortality, readmissions, PSIs, HACs, infections, devices and lines, never events, pressure injuries HCC risk factors APR DRG conditions: SOI/ROM High denial DRGs: principal dx unrelated, malnutrition, one MCC/CC, sepsis, pneumonia PEPPER report outliers Length of stay: LOS excessive for severity Queries: Queries performed to clarify documentation and/or coding: Document your queries to remind yourself and others what needs to be followed up on. 17
18 How Do YOU Document Your Review? Use common abbreviations and symbols in your review. Condense wording vs fluffy and full sentences CT head 5/1 cerebral edema Query K 3.1 Although CDI reviews are a personal expression and preference, you will save time and frustration if you are consistent in how and what you write in your reviews. Decide together as a team what is important to capture, how to write, and what you will write! 18
19 Talk to Yourself! Don t forget to talk to yourself in the review. Saves time when summarizing, querying, and following up Also helps subsequent reviewers know what you were thinking Differentiate provider documentation from your self talk and your summary of findings. Provider in quotes: CT shows cerebral edema CDI summary in regular text: Patient CT 5/1 with cerebral edema CDI self talk in parentheses: (query on TBI from 5/1 CT findings of cerebral edema) Common self talk: Query Follow up (malnutrition, EKG, echo, surgery, electrolytes, H/H) 19
20 Quality Over Quantity: How to Balance Review Quality and Production Rates 20
21 Quality Over Quantity It is important to set up new staff correctly with a focus on QUALITY review over QUANTITY Quantity will increase with time, but quality must be ingrained from the start Utilize a review template Teaches new staff what to capture Keeps reviews consistent for the team Quality standards can be measured Easy to memorize and will decrease review time 21
22 Review Template ED: Vitals initial: Chief complaint (CC): Relevant physical findings: Relevant PMH: POA (devices, ostomy site): Confusion/AMS/skin ulcers: Dx/impression: H&P: CC: Vitals or significant changes from ED record: Relevant PMH: Relevant physical findings: Significant findings (diagnoses, diagnostics, labs): Dx/impression: PN, consults, nursing notes: Diagnoses: Significant skin assessment: Status changes: Significant findings: Impression/plan: Relevant nutrition notes with abnormal BMI: OP report: Postop DX: Significant findings: Complications: Diagnostics and medications: Pertinent diagnostics (labs, radiology, cardiology): Relevant abnormal trends: Significant/incidental findings: Abnormal BMI: Significant medication diagnoses: Incidental/significant findings: Follow up/cdi comments: Summation of what needs further review: Pertinent notes to self and others: Possible queries: Focus review/follow up: Focus reviews performed and noted (risk factors, PSIs, etc. and if record forwarded to physician advisor): Queries: Queries performed to clarify documentation and/or coding: 22
23 Production and the Review Initial review Avg mins depending on service, severity and LOS. Prioritize (payer, service, etc.). Don t review cases without an ED/H&P or first progress note. Don t review surgical cases until after surgery. Key in on your template requirements vs reading every word and getting bogged down with the case itself. Mondays and Tuesdays are usually Initial reviews only with no subsequent reviews. Hold for later in week or perform Wednesday Friday while adding in initial reviews. Remember, the goal is to have impact vs going through the motions to push your production numbers higher. Subsequent review Avg mins depending on service and severity. Read your review notes and pick up from last progress note. Key in on new diagnostics, diagnoses, and findings. FOLLOW UP the query to get the case resolved: Call, text, page, , face to face, escalate in order to get it answered quickly and off your list. Again, the goal is to have impact. Determine if there is an impact potential. If not, stop reviewing it and go review another initial case! Don t let production quotas destroy your review process, impact, and provider education. High production does not always equal high impact and revenue; it may lower quality by burning out CDI staff. 23
24 Advancing the CDI Review 24
25 Advancing Your Reviews With Value Based CDI CMI MCC/CC (re evaluate case < one MCC/CC) DRG High financial impact DRGs Top DRGs with opportunity for improvement (OFI) SOI/ROM Evaluate score (4/4) Query impacts Service lines with high impact requiring queries Quality PSI HAC Mortality risk factors Readmissions LOS Bundles Focus reviews Coding and documentation Accuracy, specificity, severity, consistency, clinical support Denials prevention Track denials Financial impacts, volume, type Clinical indicators UHDDS guidelines, coding guidelines, facilitydefined clinical indicators Education/liaison Poor provider documentation Opportunities for improvement Interdisciplinary coordination and collaboration Risk adjustment HCCs/chronic conditions ICD 10 CM Guidelines.pdf 25
26 Reviews for Education Use your review information to educate providers. Put education examples in your review to pull later for rounding and education purposes. Pertinent patient history: Type 2 DM, poorly controlled Wheelchair bound at baseline ED summary: Left buttocks ulcer WOCN: Left buttocks pressure ulcer, stage 3 Sacral pressure ulcer, stage 3 connecting right buttocks ulcer to left buttocks pressure ulcer Progress note: Sacral ulcer Right buttocks ulcer Query response: Pressure ulcers on right buttocks (stage 3), left buttocks (stage 2), and sacrum (stage 2) 26
27 Thank you. Questions? In order to receive your continuing education certificate(s) for this program, you must complete the online evaluation. The link can be found in the continuing education section at the front of the program guide. 27
28 ED: CC/injury: Cause/action of injury: Significant findings: PMH: Physical findings (Foley, confusion/ams, ulcers): Diagnoses: Impression: Vital signs: Meds (Dx for med?): Lab/radiology: Readmission: POA: H&P: CC: PMH: Physical findings (Foley, confusion/ams, ulcers): Significant findings: Diagnoses: Plan: Vital signs/bmi: Meds/labs: PN: Diagnoses: Status changes: Significant findings: Impression: Plan: Radiology/lab/EKG: Findings: Impression:
29 NN/therapy notes (behavior, stroke residuals, dysphagia): CN (palliative care order/consult, clinical nutrition, WOCN): Impression: Plan: OP report: Postop Dx: Significant Dx: Relevant findings: Complications: Focus review/follow up: Risk factors: PSI: Quality: Pertinent notes to self and others: What needs further review: Queries: Subsequent review: OR/diagnostic studies: PN: CN: Postop complications: Queries: Follow up:
Who's Driving the DRG Bus: Selecting the Appropriate Principal Diagnosis
 7th Annual Association for Clinical Documentation Improvement Specialists Conference Who's Driving the DRG Bus: Selecting the Appropriate Principal Diagnosis MedPartners CDI: Karen Newhouser, RN, BSN,
7th Annual Association for Clinical Documentation Improvement Specialists Conference Who's Driving the DRG Bus: Selecting the Appropriate Principal Diagnosis MedPartners CDI: Karen Newhouser, RN, BSN,
At the completion of this educational activity, the learner will be able to:
 How CDI and Coding Can Travel Together in the Outpatient Realm Deanne Wilk, BSN, RN, CCDS, CCS Manager, Clinical Documentation Improvement Milton S. Hershey Medical Center Hershey, PA Melissa Maguire,
How CDI and Coding Can Travel Together in the Outpatient Realm Deanne Wilk, BSN, RN, CCDS, CCS Manager, Clinical Documentation Improvement Milton S. Hershey Medical Center Hershey, PA Melissa Maguire,
2015 HCPro, a division of BLR. All rights reserved. These materials may not be duplicated without express written permission.
 A Matter of Life or Death: CDI Impact on Mortality Risk Adjustment Allison Clerval, RN, BSN, CCDS Kathleen Shindle, RN, BSN, CCDS Clinical Documentation Supervisors Thomas Jefferson University Hospital
A Matter of Life or Death: CDI Impact on Mortality Risk Adjustment Allison Clerval, RN, BSN, CCDS Kathleen Shindle, RN, BSN, CCDS Clinical Documentation Supervisors Thomas Jefferson University Hospital
Learning Objectives. Clinical Validation. Ultimate Test for Queries:
 1 Ultimate Test for Queries Cesar M. Limjoco, MD Kelli A. Estes, RN, CCDS Learning Objectives At the completion of this educational activity, the learner will be able to: Understand the true mission of
1 Ultimate Test for Queries Cesar M. Limjoco, MD Kelli A. Estes, RN, CCDS Learning Objectives At the completion of this educational activity, the learner will be able to: Understand the true mission of
Expanding Clinical Validation Into Outpatient CDI. At the completion of this educational activity, the learner will be able to:
 Expanding Clinical Validation Into Outpatient CDI Tara Bell, RN, MSN, CCDS, CCM Manager, CDI & UR Services United Audit Systems, Inc. Cincinnati, OH 1 Learning Objectives At the completion of this educational
Expanding Clinical Validation Into Outpatient CDI Tara Bell, RN, MSN, CCDS, CCM Manager, CDI & UR Services United Audit Systems, Inc. Cincinnati, OH 1 Learning Objectives At the completion of this educational
4/1/2014 ICD-10 CM/PCS. Benefits to ICD-10. Fewer queries and/or requests for additional clarification. Fewer denials based on medical necessity
 Clinical Documentation and ICD-10 Presented by: Altegra Health 1 ICD-10 CM/PCS ICD-10 will be the official HIPAA-transaction set to communicate all patient conditions and all inpatient treatments, beginning
Clinical Documentation and ICD-10 Presented by: Altegra Health 1 ICD-10 CM/PCS ICD-10 will be the official HIPAA-transaction set to communicate all patient conditions and all inpatient treatments, beginning
How to Get a Customized Wheelchair through Florida Medicaid. Created by the Florida Developmental Disabilities Council, Inc.
 How to Get a Customized Wheelchair through Florida Medicaid Created by the Florida Developmental Disabilities Council, Inc. How to Get a Customized Wheelchair through Florida Medicaid What is a customized
How to Get a Customized Wheelchair through Florida Medicaid Created by the Florida Developmental Disabilities Council, Inc. How to Get a Customized Wheelchair through Florida Medicaid What is a customized
Register today! Visit or call 877/
 The bestselling CDI Boot Camp is now available online! Clinical Documentation Improvement Boot CampSM CDI-specific education covering: Medical record review and physician queries MS-DRGs and IPPS reimbursement
The bestselling CDI Boot Camp is now available online! Clinical Documentation Improvement Boot CampSM CDI-specific education covering: Medical record review and physician queries MS-DRGs and IPPS reimbursement
Making Inpatient Audits FAIR Again
 2016 GHIMA Annual Meeting & Exhibit "Charting the Course...A World of Opportunities." Making Inpatient Audits FAIR Again By: Sabrina A. Clark, RHIA HRA Strategies, LLC 770 317 3697 OUTLINE Inpatient Coding
2016 GHIMA Annual Meeting & Exhibit "Charting the Course...A World of Opportunities." Making Inpatient Audits FAIR Again By: Sabrina A. Clark, RHIA HRA Strategies, LLC 770 317 3697 OUTLINE Inpatient Coding
Mortality Risk Adjustment and HCCs: Is This the New 'Sweet Spot' for Physician Buy In?
 Mortality Risk Adjustment and HCCs: Is This the New 'Sweet Spot' for Physician Buy In? Kyra Brown, RHIA, CCS, CCDS Clinical Documentation Manager/Educator Erlanger Chattanooga, TN 1 Learning Objectives
Mortality Risk Adjustment and HCCs: Is This the New 'Sweet Spot' for Physician Buy In? Kyra Brown, RHIA, CCS, CCDS Clinical Documentation Manager/Educator Erlanger Chattanooga, TN 1 Learning Objectives
Querying Your Physicians for Inpatient MS-DRG & POA Are You in Compliance?
 Querying Your Physicians for Inpatient MS-DRG & POA Are You in Compliance? Betty B. Bibbins, MD, FACOG, CHC, C-CDI Specialist, CPEHR, CPHIT President & Chief Medical Officer DocuComp LLC BibbinsMD@DocuCompLLC.com
Querying Your Physicians for Inpatient MS-DRG & POA Are You in Compliance? Betty B. Bibbins, MD, FACOG, CHC, C-CDI Specialist, CPEHR, CPHIT President & Chief Medical Officer DocuComp LLC BibbinsMD@DocuCompLLC.com
Denial Avoidance: Five Proven Strategies for Reducing Your Denials
 Denial Avoidance: Five Proven Strategies for Reducing Your Denials Kimberly Carr and Jon LaFleur, March 30, 2017 What would you recommend to NOT annoy physicians and keep their continued cooperation and
Denial Avoidance: Five Proven Strategies for Reducing Your Denials Kimberly Carr and Jon LaFleur, March 30, 2017 What would you recommend to NOT annoy physicians and keep their continued cooperation and
How to Get a Customized Wheelchair through Florida Medicaid
 How to Get a Customized Wheelchair through Florida Medicaid To advocate and promote meaningful participation in all aspects of life for Floridians with developmental disabilities What is a customized wheelchair?
How to Get a Customized Wheelchair through Florida Medicaid To advocate and promote meaningful participation in all aspects of life for Floridians with developmental disabilities What is a customized wheelchair?
How R are you coding severe sepsis? Why the R-code matters
 How R are you coding severe sepsis? Why the R-code matters WHITE PAPER Summary: This article briefly reviews aspects of differing definitions of severe sepsis, and provides commentary on perceived areas
How R are you coding severe sepsis? Why the R-code matters WHITE PAPER Summary: This article briefly reviews aspects of differing definitions of severe sepsis, and provides commentary on perceived areas
Documenting in the World of ICD-10 Capturing all your CCs and MCCs Crystal Coen, RN, MSN, FNP-BC NPSS Asheville, NC
 Documenting in the World of ICD-10 Capturing all your CCs and MCCs Crystal Coen, RN, MSN, FNP-BC 2017 NPSS Asheville, NC Objectives Understand the importance of documenting to the highest specificity Understand
Documenting in the World of ICD-10 Capturing all your CCs and MCCs Crystal Coen, RN, MSN, FNP-BC 2017 NPSS Asheville, NC Objectives Understand the importance of documenting to the highest specificity Understand
Rapid Response Teams. January 17, Safe Table Webinar
 Rapid Response Teams January 17, 2017 Safe Table Webinar Christin Gordanier, MSN, RN, Inpatient Nursing Director at Virginia Mason Medical Center in Seattle, Washington. Alice Ferguson, BSN, RN, Project
Rapid Response Teams January 17, 2017 Safe Table Webinar Christin Gordanier, MSN, RN, Inpatient Nursing Director at Virginia Mason Medical Center in Seattle, Washington. Alice Ferguson, BSN, RN, Project
Writing with purpose. Make IT real and simple. On the Medicine Wards for Medical Students, Interns, and Residents
 Writing with purpose Make IT real and simple On the Medicine Wards 2017-2018 for Medical Students, Interns, and Residents Omar S. Darwish, MS, DO Health Science Assistant Professor Coordinator of the M&M
Writing with purpose Make IT real and simple On the Medicine Wards 2017-2018 for Medical Students, Interns, and Residents Omar S. Darwish, MS, DO Health Science Assistant Professor Coordinator of the M&M
Aligning Quality Outcomes Data with Financial Performance
 Aligning Quality Outcomes Data with Financial Performance Driving Case Mix and Revenue Improvement Susan E. Belley, M.Ed., RHIA Cleveland Clinic Garri L. Garrison, RN, CPC, CMC, CPUR 3M Health Information
Aligning Quality Outcomes Data with Financial Performance Driving Case Mix and Revenue Improvement Susan E. Belley, M.Ed., RHIA Cleveland Clinic Garri L. Garrison, RN, CPC, CMC, CPUR 3M Health Information
9/15/2017. Joyce Turner RN Director of Clinical Program Development
 Joyce Turner RN Director of Clinical Program Development A toxic response to an infection that spirals out of control attacking the body s own organs and tissues. The infection can be bacterial, viral
Joyce Turner RN Director of Clinical Program Development A toxic response to an infection that spirals out of control attacking the body s own organs and tissues. The infection can be bacterial, viral
Navigating the Challenges of Hospice Coding. Coding has never been so important for the hospice industry.
 Navigating the Challenges of Hospice Coding Coding has never been so important for the hospice industry. Presentation team: Dawn B. Cheek RN, BSN Clinical Consulting Manager, McBee Associates, Inc. Elizabeth
Navigating the Challenges of Hospice Coding Coding has never been so important for the hospice industry. Presentation team: Dawn B. Cheek RN, BSN Clinical Consulting Manager, McBee Associates, Inc. Elizabeth
Diagnosis Coding is About to be Much More Important. Matthew Menendez
 Diagnosis Coding is About to be Much More Important Matthew Menendez Agenda What is CMS doing with MACRA? What is an HCC code and why should I care? Brief MIPS overview How does risk adjustment impact
Diagnosis Coding is About to be Much More Important Matthew Menendez Agenda What is CMS doing with MACRA? What is an HCC code and why should I care? Brief MIPS overview How does risk adjustment impact
MOVE IN THE RIGHT DIRECTION: Malnutrition Diagnosis, Documentation & Physical Assessment!
 4/3/2014 PRESENTERS MOVE IN THE RIGHT DIRECTION: Malnutrition Diagnosis, Documentation & Physical Assessment! Michelle Hoppman, RD, LRD, CDE Allison Ferguson, RD, CNSC Director, Nutrition Division Executive
4/3/2014 PRESENTERS MOVE IN THE RIGHT DIRECTION: Malnutrition Diagnosis, Documentation & Physical Assessment! Michelle Hoppman, RD, LRD, CDE Allison Ferguson, RD, CNSC Director, Nutrition Division Executive
National Medicare RAC Summit March 5, 2009 Provider Lessons From Demonstration States
 National Medicare RAC Summit March 5, 2009 Provider Lessons From Demonstration States Lynn H. Grieves Chief Compliance Officer MemorialCare Medical Centers lgrieves@memorialcare.org MemorialCare Health
National Medicare RAC Summit March 5, 2009 Provider Lessons From Demonstration States Lynn H. Grieves Chief Compliance Officer MemorialCare Medical Centers lgrieves@memorialcare.org MemorialCare Health
Focus On Signs and Symptoms
 Focus On Signs and Symptoms Decreasing Primary Care Access Help Your Patients with Their Insurance Benefits Risk Management and Reimbursement Align Don t Forget to Document Abnormal Vitals and Labs Document
Focus On Signs and Symptoms Decreasing Primary Care Access Help Your Patients with Their Insurance Benefits Risk Management and Reimbursement Align Don t Forget to Document Abnormal Vitals and Labs Document
MOVE IN THE RIGHT DIRECTION: Malnutrition Diagnosis, Documentation & Physical Assessment!
 MOVE IN THE RIGHT DIRECTION: Malnutrition Diagnosis, Documentation & Physical Assessment! Michelle Hoppman, RD, LRD, CDE Director, Nutrition Division Executive Success Coach DM&A michelle@destination10.com
MOVE IN THE RIGHT DIRECTION: Malnutrition Diagnosis, Documentation & Physical Assessment! Michelle Hoppman, RD, LRD, CDE Director, Nutrition Division Executive Success Coach DM&A michelle@destination10.com
Sepsis Denials. Presented by James Donaher, RHIA, CDIP, CCS, CCS-P
 Sepsis Denials Presented by James Donaher, RHIA, CDIP, CCS, CCS-P Sepsis-1 2 From the first Sepsis Definition Conference in 1991 Defined sepsis as systemic response syndrome (SIRS) due to infection SIRS
Sepsis Denials Presented by James Donaher, RHIA, CDIP, CCS, CCS-P Sepsis-1 2 From the first Sepsis Definition Conference in 1991 Defined sepsis as systemic response syndrome (SIRS) due to infection SIRS
Partial Hospitalization Program Program for Evaluating Payment Patterns Electronic Report. User s Guide Sixth Edition. Prepared by
 Partial Hospitalization Program Program for Evaluating Payment Patterns Electronic Report User s Guide Sixth Edition Prepared by Partial Hospitalization Program Program for Evaluating Payment Patterns
Partial Hospitalization Program Program for Evaluating Payment Patterns Electronic Report User s Guide Sixth Edition Prepared by Partial Hospitalization Program Program for Evaluating Payment Patterns
STROKE INTRODUCTION OBJECTIVES. When the student has finished this module, he/she will be able to:
 STROKE INTRODUCTION Stroke is the medical term for a specific type of neurological event that causes damage to the brain. There are two types of stroke, but both types of stroke cause the same type of
STROKE INTRODUCTION Stroke is the medical term for a specific type of neurological event that causes damage to the brain. There are two types of stroke, but both types of stroke cause the same type of
Highlights of the NEW 2017 Codes ICD-10- CM
 Highlights of the NEW 2017 Codes ICD-10- CM Maine HIMA September 22, 2016 ICD-10-CM o 1943 New Codes o 422 Revised Codes o 305 Deleted Codes Overall Picture o Which revisions apply most to your facility?
Highlights of the NEW 2017 Codes ICD-10- CM Maine HIMA September 22, 2016 ICD-10-CM o 1943 New Codes o 422 Revised Codes o 305 Deleted Codes Overall Picture o Which revisions apply most to your facility?
Legislation POLST. Palliative and Hospice Care: End of Life Decisions. Palliative and Hospice Care End of Life Decisions John F. Bertagnolli, Jr, DO
 Palliative and Hospice Care End of Life Decisions John F. Bertagnolli, Jr, DO Legislation On 12/21/11 Gov. Christie signed legislation that enables patients to indicate their preferences regarding life
Palliative and Hospice Care End of Life Decisions John F. Bertagnolli, Jr, DO Legislation On 12/21/11 Gov. Christie signed legislation that enables patients to indicate their preferences regarding life
Objectives. Medicare Spending per Beneficiary: Analyzing MSPB Data to Identify Primary Drivers
 Medicare Spending per Beneficiary: Analyzing MSPB Data to Identify Primary Drivers August 22, 2017 Objectives Understand the basics of the hospital specific MSPB data files and reports Review the factors
Medicare Spending per Beneficiary: Analyzing MSPB Data to Identify Primary Drivers August 22, 2017 Objectives Understand the basics of the hospital specific MSPB data files and reports Review the factors
This is the Full Title of a Session
 Inpatient Psychiatric Hospitals: Let's Talk About Quality Care and Reimbursement Potential Linda Jackson, RHIT Director, Health Information Management Arkansas State Hospital This is the Full Title of
Inpatient Psychiatric Hospitals: Let's Talk About Quality Care and Reimbursement Potential Linda Jackson, RHIT Director, Health Information Management Arkansas State Hospital This is the Full Title of
Anemia. Revenue Cycle Solutions Consulting & Management Services. The ICD-10 Success Series Webconference December 3, 2014
 Revenue Cycle Solutions Consulting & Management Services Anemia The ICD-10 Success Series Webconference December 3, 2014 Managing Your Audio Use Telephone Use Mic and Speakers If you select the use telephone
Revenue Cycle Solutions Consulting & Management Services Anemia The ICD-10 Success Series Webconference December 3, 2014 Managing Your Audio Use Telephone Use Mic and Speakers If you select the use telephone
A Guide for Effective Communication in Healthcare Patients
 A Guide for Effective Communication in Healthcare Patients It is important for your health and well-being that you communicate clearly with your doctors and staff. Asking questions can avoid mistakes and
A Guide for Effective Communication in Healthcare Patients It is important for your health and well-being that you communicate clearly with your doctors and staff. Asking questions can avoid mistakes and
OPERATIONALIZING HIERARCHICAL CONDITION CATEGORIES (HCC SCORING)
 OPERATIONALIZING HIERARCHICAL CONDITION CATEGORIES (HCC SCORING) OBJECTIVES 1 DEFINE HIERARCHICAL CONDITION CATEGORIES We will cover how Hierarchical Condition Categories (HCC) are determined and the Risk
OPERATIONALIZING HIERARCHICAL CONDITION CATEGORIES (HCC SCORING) OBJECTIVES 1 DEFINE HIERARCHICAL CONDITION CATEGORIES We will cover how Hierarchical Condition Categories (HCC) are determined and the Risk
NYSDOH Sepsis Q&A Session from February 2018 Data Abstraction Meetings Table of Content
 NYSDOH Sepsis Q&A Session from February 2018 Data Abstraction Meetings Table of Content Adherence variables Q: within 3 hours of the start datetime. How can we document that monotherapy was started before
NYSDOH Sepsis Q&A Session from February 2018 Data Abstraction Meetings Table of Content Adherence variables Q: within 3 hours of the start datetime. How can we document that monotherapy was started before
Leveraging the Value of Midas+ DataVision Toolpacks. Brenda Pettyjohn RN, CPHQ Midas+ DataVision Clinical Consultant
 Leveraging the Value of Midas+ DataVision Toolpacks Brenda Pettyjohn RN, CPHQ Midas+ DataVision Clinical Consultant Objectives Identify at least 1-2 uses for each of the Toolpacks Identify populations
Leveraging the Value of Midas+ DataVision Toolpacks Brenda Pettyjohn RN, CPHQ Midas+ DataVision Clinical Consultant Objectives Identify at least 1-2 uses for each of the Toolpacks Identify populations
Physical Therapy Diagnosis and Documentation Tips
 1 This tool is designed to assist the Physical Therapist in consultation with the physician, in the selection of an appropriate according to Medicare coverage guidelines. The documentation tips will add
1 This tool is designed to assist the Physical Therapist in consultation with the physician, in the selection of an appropriate according to Medicare coverage guidelines. The documentation tips will add
SEP-1 CHALLENGING CASES WITH DR. TOWNSEND
 UW MEDICINE PATIENTS ARE FIRST SEP-1 CHALLENGING CASES WITH DR. TOWNSEND AMADAE AREVALO RN, MSN, CCRN KATIE MEHRING RN, BSN, CCDS AMANDA SIGALA, RN, BSN, MPH, CPHQ JUNE 12, 2018 OBJECTIVES 1. Summarize
UW MEDICINE PATIENTS ARE FIRST SEP-1 CHALLENGING CASES WITH DR. TOWNSEND AMADAE AREVALO RN, MSN, CCRN KATIE MEHRING RN, BSN, CCDS AMANDA SIGALA, RN, BSN, MPH, CPHQ JUNE 12, 2018 OBJECTIVES 1. Summarize
Talking with your doctors about palliative care Dr. Mary Anne Huggins and Barbara Pidcock
 Talking with your doctors about palliative care Dr. Mary Anne Huggins and Barbara Pidcock You will have appointments with your family doctor, and with specialists. It will help you if you write your brief
Talking with your doctors about palliative care Dr. Mary Anne Huggins and Barbara Pidcock You will have appointments with your family doctor, and with specialists. It will help you if you write your brief
Sepsis: Mitigating Denials Amid Definition Disparity
 Sepsis: Mitigating Denials Amid Definition Disparity White Paper - April 2017 Sepsis Criteria at a Glance The Society of Critical Care Medicine (SCCM) met in 2016 to update the definition of sepsis. During
Sepsis: Mitigating Denials Amid Definition Disparity White Paper - April 2017 Sepsis Criteria at a Glance The Society of Critical Care Medicine (SCCM) met in 2016 to update the definition of sepsis. During
Hospital Transition Management. Barbara Wood, BSN, MBA
 Hospital Transition Management Barbara Wood, BSN, MBA Director, Embedded Care Management Programs OBJECTIVES Improve health care quality for our patients by streamlining care transitions Reduce avoidable
Hospital Transition Management Barbara Wood, BSN, MBA Director, Embedded Care Management Programs OBJECTIVES Improve health care quality for our patients by streamlining care transitions Reduce avoidable
2015 HCPro, a division of BLR. All rights reserved. These materials may not be duplicated without express written permission.
 Pediatric CDI: Lessons Learned From a Tertiary, Freestanding Children's Hospital Jodi P. Carter, MD, CDI Physician Champion Nancy C. Rush, RN, BSN, CCM, CDI Manager Mary Ellen Fee, RN, CCDS, CDI Specialist
Pediatric CDI: Lessons Learned From a Tertiary, Freestanding Children's Hospital Jodi P. Carter, MD, CDI Physician Champion Nancy C. Rush, RN, BSN, CCM, CDI Manager Mary Ellen Fee, RN, CCDS, CDI Specialist
Why is an outpatient transplant best for you?
 Outpatient Autologous Transplant Why is an outpatient transplant best for you? An outpatient transplant allows you to: stay in the comfort of your own home sleep in your own bed eat your usual foods be
Outpatient Autologous Transplant Why is an outpatient transplant best for you? An outpatient transplant allows you to: stay in the comfort of your own home sleep in your own bed eat your usual foods be
Living Well With MDS. Begin at the Beginning... And, that s why we re here! Management of Disease Symptoms. What is MDS? What is MDS?
 Begin at the Beginning... Living Well With MDS Barbara Weinstein, RN BSN CCRP 2009 internet based survey conducted by the AAMDSIF 358 patients surveyed 55% did not know their International Prognostic Scoring
Begin at the Beginning... Living Well With MDS Barbara Weinstein, RN BSN CCRP 2009 internet based survey conducted by the AAMDSIF 358 patients surveyed 55% did not know their International Prognostic Scoring
Appendix. Potentially Preventable Complications (PPCs) identify. complications that can occur during an admission. There are 64
 Calikoglu S, Murray R, Feeney D. Hospital pay-for-performance programs in Maryland produced strong results, including reduced hospital-acquired infections. Health Aff (Millwood). 2012;31(12). Appendix
Calikoglu S, Murray R, Feeney D. Hospital pay-for-performance programs in Maryland produced strong results, including reduced hospital-acquired infections. Health Aff (Millwood). 2012;31(12). Appendix
3/20/2017. CONNECTING THE LATEST GUIDANCE FY2017 FOR ICD-10 MATTERS Kyla D. Harrison, RN, BSN, HCS-D, COS-C Visiting Nurse Association of Kansas City
 CONNECTING THE LATEST GUIDANCE FY2017 FOR ICD-10 MATTERS Kyla D. Harrison, RN, BSN, HCS-D, COS-C Visiting Nurse Association of Kansas City Coding needs met in many different ways: 1. Fulltime Coders HCS-D
CONNECTING THE LATEST GUIDANCE FY2017 FOR ICD-10 MATTERS Kyla D. Harrison, RN, BSN, HCS-D, COS-C Visiting Nurse Association of Kansas City Coding needs met in many different ways: 1. Fulltime Coders HCS-D
Geriatric Medicine Clerkship Orientation. Aval-Na Ree Green (modified by Huai Cheng)
 Geriatric Medicine Clerkship Orientation Aval-Na Ree Green (modified by Huai Cheng) Welcome! Goals The geriatric clerkship is designed to prepare medical students to provide evidence-based, competent,
Geriatric Medicine Clerkship Orientation Aval-Na Ree Green (modified by Huai Cheng) Welcome! Goals The geriatric clerkship is designed to prepare medical students to provide evidence-based, competent,
Muscular Dystrophy UK s Adult North Star Network. Care recommendations for adults with Duchenne a consultation
 Muscular Dystrophy UK s Adult North Star Network Care recommendations for adults with Duchenne a consultation Background: The North Star Network was set up in 2003 to help drive improvements in services
Muscular Dystrophy UK s Adult North Star Network Care recommendations for adults with Duchenne a consultation Background: The North Star Network was set up in 2003 to help drive improvements in services
Guidelines for Incorporating & Strengthening Perspective-Taking & Self-Authorship into Division of Student Life Programs
 Guidelines for Incorporating & Strengthening Perspective-Taking & Self-Authorship into Division of Student Life Programs Your program or service has been identified as potentially high impact in helping
Guidelines for Incorporating & Strengthening Perspective-Taking & Self-Authorship into Division of Student Life Programs Your program or service has been identified as potentially high impact in helping
Q&A CDI Q A Q A WEEK. Technology. How long have you had electronic health records?
 & CDI WEEK Technology s part of the seventh annual Clinical Documentation Improvement Week, CDIS has conducted a series of interviews with CDI professionals on a variety of emerging industry topics. Caryn
& CDI WEEK Technology s part of the seventh annual Clinical Documentation Improvement Week, CDIS has conducted a series of interviews with CDI professionals on a variety of emerging industry topics. Caryn
Clinical Documentation Improvement Program Family Medicine Service April 4, 2011 Session 1
 Clinical Documentation Improvement Program 2011 Family Medicine Service April 4, 2011 Session 1 2010 Goal Update Physician Query Response Rate 97.8% Goal for 2010 $4.3 million Goal 96% Financial Impact
Clinical Documentation Improvement Program 2011 Family Medicine Service April 4, 2011 Session 1 2010 Goal Update Physician Query Response Rate 97.8% Goal for 2010 $4.3 million Goal 96% Financial Impact
10/17/2013. Billing and Coding in Long Term Care: Keeping the Wolves at Bay. Disclosure
 Billing and Coding in Long Term Care: Keeping the Wolves at Bay Maine Medical Directors Association Annual Conference October 11, 2013 Alva S Baker, MD, CMD-R Disclosure Dr. Baker has indicated that he
Billing and Coding in Long Term Care: Keeping the Wolves at Bay Maine Medical Directors Association Annual Conference October 11, 2013 Alva S Baker, MD, CMD-R Disclosure Dr. Baker has indicated that he
Diagnosis Coding Problematic Areas: Coding & Sequencing
 Diagnosis Coding Problematic Areas: Coding & Sequencing OBJECTIVES Guideline information Sepsis, Severe Sepsis, Septic Shock HIV Diabetes Under/Over-dosing Hypertension Ulcers Burns INCLUDES, USE ADDITIONAL
Diagnosis Coding Problematic Areas: Coding & Sequencing OBJECTIVES Guideline information Sepsis, Severe Sepsis, Septic Shock HIV Diabetes Under/Over-dosing Hypertension Ulcers Burns INCLUDES, USE ADDITIONAL
Life is pleasant. Death is peaceful. It s the transition that s troublesome. Isaac Asimov ( )
 Life is pleasant. Death is peaceful. It s the transition that s troublesome. Isaac Asimov (1920-1992) Objectives Palliative care versus hospice care. Admission guidelines to hospice services. Having the
Life is pleasant. Death is peaceful. It s the transition that s troublesome. Isaac Asimov (1920-1992) Objectives Palliative care versus hospice care. Admission guidelines to hospice services. Having the
Monthly Campaign Webinar. October 20, 2016
 Monthly Campaign Webinar October 20, 2016 TODAY S WEBINAR Together 2 Goal Updates Webinar Reminders Goal Post October Newsletter Highlights National Day of Action Embed Point-of-Care Tools Q&A Scott Hines,
Monthly Campaign Webinar October 20, 2016 TODAY S WEBINAR Together 2 Goal Updates Webinar Reminders Goal Post October Newsletter Highlights National Day of Action Embed Point-of-Care Tools Q&A Scott Hines,
CareFirst Hospice. Health care for the end of life. CareFirst
 Hospice Health care for the end of life 1 What is Hospice? Hospice is a philosophy- When a person in end stages of an illness can no longer receive, or wants to receive, life sustaining treatment, he or
Hospice Health care for the end of life 1 What is Hospice? Hospice is a philosophy- When a person in end stages of an illness can no longer receive, or wants to receive, life sustaining treatment, he or
TOTAL HIP AND KNEE REPLACEMENTS. FISCAL YEAR 2002 DATA July 1, 2001 through June 30, 2002 TECHNICAL NOTES
 TOTAL HIP AND KNEE REPLACEMENTS FISCAL YEAR 2002 DATA July 1, 2001 through June 30, 2002 TECHNICAL NOTES The Pennsylvania Health Care Cost Containment Council April 2005 Preface This document serves as
TOTAL HIP AND KNEE REPLACEMENTS FISCAL YEAR 2002 DATA July 1, 2001 through June 30, 2002 TECHNICAL NOTES The Pennsylvania Health Care Cost Containment Council April 2005 Preface This document serves as
Clinical Documentation Improvement: Reporting Opportunities
 Clinical Documentation Improvement: Reporting Opportunities Karee Burns, RN, BSN Midas+ Solutions Consultant Waheed Baqai, MPH, CPH Director Clinical Decision Support Loma Linda University Medical Center
Clinical Documentation Improvement: Reporting Opportunities Karee Burns, RN, BSN Midas+ Solutions Consultant Waheed Baqai, MPH, CPH Director Clinical Decision Support Loma Linda University Medical Center
ECMO Extracorporeal Membrane Oxygenation
 ECMO Extracorporeal Membrane Oxygenation patienteducation.osumc.edu ECMO Table of Contents ECMO: Extracorporeal Membrane Oxygenation... 3 ECMO Treatment... 5 Care Team... 7 Discontinuing ECMO... 8 Notes,
ECMO Extracorporeal Membrane Oxygenation patienteducation.osumc.edu ECMO Table of Contents ECMO: Extracorporeal Membrane Oxygenation... 3 ECMO Treatment... 5 Care Team... 7 Discontinuing ECMO... 8 Notes,
Key Performance Indicators to Direct Audit Plans
 Key Performance Indicators to Direct Audit Plans Lori Laubach, Principal MD Audit User Group June 15 17, 2014 1 The material appearing in this presentation is for informational purposes only and is not
Key Performance Indicators to Direct Audit Plans Lori Laubach, Principal MD Audit User Group June 15 17, 2014 1 The material appearing in this presentation is for informational purposes only and is not
This is a guide for volunteers in UTS HELPS Buddy Program. UTS.EDU.AU/CURRENT-STUDENTS/SUPPORT/HELPS/
 VOLUNTEER GUIDE This is a guide for volunteers in UTS HELPS Buddy Program. UTS.EDU.AU/CURRENT-STUDENTS/SUPPORT/HELPS/ CONTENTS 1 2 3 4 5 Introduction: Your role as a Buddy Getting started Helping with
VOLUNTEER GUIDE This is a guide for volunteers in UTS HELPS Buddy Program. UTS.EDU.AU/CURRENT-STUDENTS/SUPPORT/HELPS/ CONTENTS 1 2 3 4 5 Introduction: Your role as a Buddy Getting started Helping with
Arkansas Health Care Payment Improvement Initiative Congestive Heart Failure Algorithm Summary
 Arkansas Health Care Payment Improvement Initiative Congestive Heart Failure Algorithm Summary Congestive Heart Failure Algorithm Summary v1.2 (1/5) Triggers PAP assignment Exclusions Episode time window
Arkansas Health Care Payment Improvement Initiative Congestive Heart Failure Algorithm Summary Congestive Heart Failure Algorithm Summary v1.2 (1/5) Triggers PAP assignment Exclusions Episode time window
The emotional side of diabetes
 The emotional side of diabetes Diabetes can take a lot of effort to manage. So it s not surprising that many people who have it feel overwhelmed. If you have felt that way, you re not alone. Read on to
The emotional side of diabetes Diabetes can take a lot of effort to manage. So it s not surprising that many people who have it feel overwhelmed. If you have felt that way, you re not alone. Read on to
ACDIS Answers. Clinical Documentation Improvement FAQs
 ACDIS Answers Clinical Documentation Improvement FAQs ACDIS Answers: Clinical Documentation Improvement FAQs LAURIE L. PRESCOTT, MSN, RN, CCDS, CDIP, CRC SHARME BRODIE, RN, CCDS ALLEN FRADY, RN, BSN, CCDS,
ACDIS Answers Clinical Documentation Improvement FAQs ACDIS Answers: Clinical Documentation Improvement FAQs LAURIE L. PRESCOTT, MSN, RN, CCDS, CDIP, CRC SHARME BRODIE, RN, CCDS ALLEN FRADY, RN, BSN, CCDS,
Medicare hospice benefit. Katherine Dietrich, DO HMDC FACP CPE
 Medicare hospice benefit Katherine Dietrich, DO HMDC FACP CPE Disclosures Hospice Compassus Medical Director Billings MT Which of the following is correct about the Medicare Hospice Benefit? A. Once a
Medicare hospice benefit Katherine Dietrich, DO HMDC FACP CPE Disclosures Hospice Compassus Medical Director Billings MT Which of the following is correct about the Medicare Hospice Benefit? A. Once a
Welcome to the ACSM/Exercise is Medicine Professional Credential online workshop presented by Health & Exercise Connections, LLC
 Welcome to the ACSM/Exercise is Medicine Professional Credential online workshop presented by Health & Exercise Connections, LLC Objectives 1. Provide candidates with an overview of content related to
Welcome to the ACSM/Exercise is Medicine Professional Credential online workshop presented by Health & Exercise Connections, LLC Objectives 1. Provide candidates with an overview of content related to
Sepsis 3.0: The Impact on Quality Improvement Programs
 Sepsis 3.0: The Impact on Quality Improvement Programs Mitchell M. Levy MD, MCCM Professor of Medicine Chief, Division of Pulmonary, Sleep, and Critical Care Warren Alpert Medical School of Brown University
Sepsis 3.0: The Impact on Quality Improvement Programs Mitchell M. Levy MD, MCCM Professor of Medicine Chief, Division of Pulmonary, Sleep, and Critical Care Warren Alpert Medical School of Brown University
Who, Me? Starting THE Conversation
 Who, Me? Starting THE Conversation Nancy Flowers, LCSW Social Work Manager Rainbow Hospice and Palliative Care nflowers@rainbowhospice.org 847-685-9900 Objectives Clarify the importance of advance directives
Who, Me? Starting THE Conversation Nancy Flowers, LCSW Social Work Manager Rainbow Hospice and Palliative Care nflowers@rainbowhospice.org 847-685-9900 Objectives Clarify the importance of advance directives
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 8 Episodes
 TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 8 Episodes Acute Seizure, Syncope, Acute Gastroenteritis, Pediatric Pneumonia, Bronchiolitis, Colposcopy, Hysterectomy,
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 8 Episodes Acute Seizure, Syncope, Acute Gastroenteritis, Pediatric Pneumonia, Bronchiolitis, Colposcopy, Hysterectomy,
Using Health IT to Support Oral Health Integration: Dealing with Common Barriers. Jeff Hummel, MD, MPH Qualis Health November 5, 2015
 Using Health IT to Support Oral Health Integration: Dealing with Common Barriers Jeff Hummel, MD, MPH Qualis Health November 5, 2015 Goals for this Session Understand 3 aspects of oral health information
Using Health IT to Support Oral Health Integration: Dealing with Common Barriers Jeff Hummel, MD, MPH Qualis Health November 5, 2015 Goals for this Session Understand 3 aspects of oral health information
THE POTENTIAL IMPACT OF VITALSTIM THERAPY ON HEALTHCARE COSTS: A White PaperVitalStim Therapy has significant
 Dysphagia THE POTENTIAL IMPACT OF VITALSTIM THERAPY ON HEALTHCARE COSTS: A White PaperVitalStim Therapy has significant Contents potential to dramatically impact the health care costs arising from oropharyngeal
Dysphagia THE POTENTIAL IMPACT OF VITALSTIM THERAPY ON HEALTHCARE COSTS: A White PaperVitalStim Therapy has significant Contents potential to dramatically impact the health care costs arising from oropharyngeal
Advance Care Planning: What s the Physician s Role? Dr. Tim Jessick Palliative Medicine Aurora West Allis Medical Center October, 2015
 Advance Care Planning: What s the Physician s Role? Dr. Tim Jessick Palliative Medicine Aurora West Allis Medical Center October, 2015 Objectives Define usual medical care vs palliative care vs hospice
Advance Care Planning: What s the Physician s Role? Dr. Tim Jessick Palliative Medicine Aurora West Allis Medical Center October, 2015 Objectives Define usual medical care vs palliative care vs hospice
Polling Question #1. Risk Adjustment in the Inpatient Hospital Setting
 1 Risk Adjustment in the Inpatient Hospital Setting Mark N. Dominesey, RN, BSN, MBA, CCDS, CDIP, CHTS CP Manager of CDI Children s National Medical Center Washington, DC 2 Polling Question #1 Does your
1 Risk Adjustment in the Inpatient Hospital Setting Mark N. Dominesey, RN, BSN, MBA, CCDS, CDIP, CHTS CP Manager of CDI Children s National Medical Center Washington, DC 2 Polling Question #1 Does your
Expectations for Ostomy Patients Discharged to a SNF
 Expectations for Ostomy Patients Discharged to a SNF Following your surgery and hospital stay you will enter a Skilled Nursing Facility (SNF) to continue your recovery. This material has 3 parts: 1. Precautions
Expectations for Ostomy Patients Discharged to a SNF Following your surgery and hospital stay you will enter a Skilled Nursing Facility (SNF) to continue your recovery. This material has 3 parts: 1. Precautions
DIVISION OF HOSPITAL MEDICINE PERIOPERATIVE MEDICINE
 DIVISION OF HOSPITAL MEDICINE PERIOPERATIVE MEDICINE Hip Fracture Management: Role of Internists SESSION OUTLINE INTRODUCTION Hip fractures are a major cause of hospitalization, morbidity and mortality,
DIVISION OF HOSPITAL MEDICINE PERIOPERATIVE MEDICINE Hip Fracture Management: Role of Internists SESSION OUTLINE INTRODUCTION Hip fractures are a major cause of hospitalization, morbidity and mortality,
At the completion of this educational activity, the learner will be able to understand:
 Claims vs. Submission: Understanding the Difference Sonia Trepina, MPA Director, Risk Adjustment & Ambulatory CDI Services Enjoin Asheville, NC Brett Senor, MD, CRC, CCDS Physician Associate, CDI Quality
Claims vs. Submission: Understanding the Difference Sonia Trepina, MPA Director, Risk Adjustment & Ambulatory CDI Services Enjoin Asheville, NC Brett Senor, MD, CRC, CCDS Physician Associate, CDI Quality
About this consent form
 Protocol Title: Development of the smoking cessation app Smiling instead of Smoking Principal Investigator: Bettina B. Hoeppner, Ph.D. Site Principal Investigator: n/a Description of Subject Population:
Protocol Title: Development of the smoking cessation app Smiling instead of Smoking Principal Investigator: Bettina B. Hoeppner, Ph.D. Site Principal Investigator: n/a Description of Subject Population:
6/30/2015. Lunch and Learn. Objectives. Who owns Quality and Patient Safety? We all do It s a Balance of Responsibility
 Lunch and Learn Patient Safety Indicators June 11, 2014 Objectives List at least 3 entities that drive patient quality and safety initiatives Define AHRQ Patient Safety Indicators Describe the 10 diagnoses
Lunch and Learn Patient Safety Indicators June 11, 2014 Objectives List at least 3 entities that drive patient quality and safety initiatives Define AHRQ Patient Safety Indicators Describe the 10 diagnoses
Malnutrition: An independent Risk Factor for Postoperative Complications
 Malnutrition: An independent Risk Factor for Postoperative Complications Bryan P. Hooks, D.O. University of Pittsburgh-Horizon June 24, 2017 Orthopedic Surgeon-Adult Reconstruction Disclosures: None Objectives:
Malnutrition: An independent Risk Factor for Postoperative Complications Bryan P. Hooks, D.O. University of Pittsburgh-Horizon June 24, 2017 Orthopedic Surgeon-Adult Reconstruction Disclosures: None Objectives:
Sepsis clinical evolution: Understand essential challenges to developing effective queries
 Understand essential challenges to developing effective queries ADVICE FROM THE ACDIS REGULATORY COMMITTEE Summary: This paper provides a timeline of the various sepsis definitions and their implications
Understand essential challenges to developing effective queries ADVICE FROM THE ACDIS REGULATORY COMMITTEE Summary: This paper provides a timeline of the various sepsis definitions and their implications
Advice for patients, families and carers
 Advice for patients, families and carers On 14 July 2015, reports came out which showed that strong medicines called antipsychotics and other medicines to treat mental illness were being used to treat
Advice for patients, families and carers On 14 July 2015, reports came out which showed that strong medicines called antipsychotics and other medicines to treat mental illness were being used to treat
Effectively Managing Sepsis Denials
 Effectively Managing Sepsis Denials Krysten Brooks, RN, BSN, MBA Senior Inpatient Consultant 3M Health Information Systems This is the Full Title of a Session Atlanta, GA 1 Learning Objectives At the completion
Effectively Managing Sepsis Denials Krysten Brooks, RN, BSN, MBA Senior Inpatient Consultant 3M Health Information Systems This is the Full Title of a Session Atlanta, GA 1 Learning Objectives At the completion
2016 AMC Quality and Accountability Performance Scorecard Vidant Medical Center. Overall Rank. Overall Score 63.4% Efficiency 7.
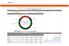 2016 AMC Quality and Accountability Performance Scorecard Vidant Medical Center Star Rating Mortality 12.66% of 25% Domain Performance Overall Rank 27 Overall Score 63.4% Equity 5.00% of 5% Efficiency
2016 AMC Quality and Accountability Performance Scorecard Vidant Medical Center Star Rating Mortality 12.66% of 25% Domain Performance Overall Rank 27 Overall Score 63.4% Equity 5.00% of 5% Efficiency
Risk Adjustment and Hierarchical Condition Category Coding
 Risk Adjustment 101 Agenda Risk Adjustment Model Hierarchical Condition Categories (HCC) Patient Example Documentation MEAT Documentation Guidance Chronic Conditions Risk Score Calculations Steps for Physician
Risk Adjustment 101 Agenda Risk Adjustment Model Hierarchical Condition Categories (HCC) Patient Example Documentation MEAT Documentation Guidance Chronic Conditions Risk Score Calculations Steps for Physician
CARF Continuous Quality & Survey Readiness: Leadership Meeting Agenda
 March 18, 2016 CARF Continuous Quality & Survey Readiness: Leadership Meeting Agenda The following information may or may not be appropriate to your clinical setting. Please review the information and
March 18, 2016 CARF Continuous Quality & Survey Readiness: Leadership Meeting Agenda The following information may or may not be appropriate to your clinical setting. Please review the information and
New York City Development of the Geriatric Collaborative
 New York City - 2014 Development of the Geriatric Collaborative The Clinical Problem More than 50% persons age 65 years will have some surgical procedure in the remainder of his or her lifetime Outcome
New York City - 2014 Development of the Geriatric Collaborative The Clinical Problem More than 50% persons age 65 years will have some surgical procedure in the remainder of his or her lifetime Outcome
Screening and Clinical Assessment for Dysphagia: How to Decide.
 Screening and Clinical Assessment for Dysphagia: How to Decide. How to Decide. ASHA Convention 2014 James L. Coyle, Ph.D., CCC-SLP, BCS-S Associate Professor, Communication Science & Disorders, University
Screening and Clinical Assessment for Dysphagia: How to Decide. How to Decide. ASHA Convention 2014 James L. Coyle, Ph.D., CCC-SLP, BCS-S Associate Professor, Communication Science & Disorders, University
Charting Smarter, not Longer: Basic Concepts in Outpatient Coding
 Charting Smarter, not Longer: Basic Concepts in Outpatient Coding Workshop WA01 SGIM 29 th Annual Meeting April 27, 2006 Sponsored by the SGIM Clinical Practice Task Force (CPTF) Faculty: Jeannine Engel,
Charting Smarter, not Longer: Basic Concepts in Outpatient Coding Workshop WA01 SGIM 29 th Annual Meeting April 27, 2006 Sponsored by the SGIM Clinical Practice Task Force (CPTF) Faculty: Jeannine Engel,
Determining MS-DRGs. Kimberly Cunningham CPC, CIC, CCS. Copyright/Disclaimer text
 Determining MS-DRGs Kimberly Cunningham CPC, CIC, CCS Copyright/Disclaimer text No part of this presentation may be reproduced or transmitted in any form or by any means (graphically, electronically, or
Determining MS-DRGs Kimberly Cunningham CPC, CIC, CCS Copyright/Disclaimer text No part of this presentation may be reproduced or transmitted in any form or by any means (graphically, electronically, or
Real Data, Real Time, Real Results
 Real Data, Real Time, Real Results Angela McCann, RN, MPH Quality Improvement Specialist Northeast Health Care Quality Foundation Adverse Drug Events / Readmissions Workshop March 15, 2013 Concord, NH
Real Data, Real Time, Real Results Angela McCann, RN, MPH Quality Improvement Specialist Northeast Health Care Quality Foundation Adverse Drug Events / Readmissions Workshop March 15, 2013 Concord, NH
(Signature) British Sign Language
 (Signature) British Sign Language BSL Level 1 Week 1 Aim: to introduce learners to BSL, course, tutor and learners On arrival please write your first name on the flip chart large enough for people to read
(Signature) British Sign Language BSL Level 1 Week 1 Aim: to introduce learners to BSL, course, tutor and learners On arrival please write your first name on the flip chart large enough for people to read
Stroke Coordinator: ROI. Author: Debbie Roper, RN, MSN (d.r. Stroke) Vice President of Roper Resources, Inc.
 Stroke Coordinator: ROI Author: Debbie Roper, RN, MSN (d.r. Stroke) Vice President of Roper Resources, Inc. debbie@roper-resources.com 214-864-8993 Disclosure Debbie Roper is a speaker for: Genentech Activase
Stroke Coordinator: ROI Author: Debbie Roper, RN, MSN (d.r. Stroke) Vice President of Roper Resources, Inc. debbie@roper-resources.com 214-864-8993 Disclosure Debbie Roper is a speaker for: Genentech Activase
Effect of Ortho-Geriatric Co-Management on Hip Fractures
 Effect of Ortho-Geriatric Co-Management on Hip Fractures Kenji Shigemoto Takeshi Sawaguchi Daigo Sakagoshi Kenichi Goshima Yu Hatsuchi Dept. Orthop. Surg. Toyama Municipal Hospital, Toyama, Japan Purpose
Effect of Ortho-Geriatric Co-Management on Hip Fractures Kenji Shigemoto Takeshi Sawaguchi Daigo Sakagoshi Kenichi Goshima Yu Hatsuchi Dept. Orthop. Surg. Toyama Municipal Hospital, Toyama, Japan Purpose
Objectives 2/11/2016 HOSPICE 101
 HOSPICE 101 Overview Hospice History and Statistics What is Hospice? Who qualifies for services? Levels of Service The Admission Process Why Not to Wait Objectives Understand how to determine hospice eligibility
HOSPICE 101 Overview Hospice History and Statistics What is Hospice? Who qualifies for services? Levels of Service The Admission Process Why Not to Wait Objectives Understand how to determine hospice eligibility
Not all NLP is Created Equal:
 Not all NLP is Created Equal: CAC Technology Underpinnings that Drive Accuracy, Experience and Overall Revenue Performance Page 1 Performance Perspectives Health care financial leaders and health information
Not all NLP is Created Equal: CAC Technology Underpinnings that Drive Accuracy, Experience and Overall Revenue Performance Page 1 Performance Perspectives Health care financial leaders and health information
NEW DEFINITION FORMAT AND DIFFICULT VARIABLE DEFINITIONS
 NEW DEFINITION FORMAT AND DIFFICULT VARIABLE DEFINITIONS Bruce L. Hall, MD, PhD, MBA, FACS Clinical Support Physician Lead Paula Farrell, RN, BSN ACS NSQIP Clinical Support Specialist Case Studies &
NEW DEFINITION FORMAT AND DIFFICULT VARIABLE DEFINITIONS Bruce L. Hall, MD, PhD, MBA, FACS Clinical Support Physician Lead Paula Farrell, RN, BSN ACS NSQIP Clinical Support Specialist Case Studies &
Lauren DiBiase, MS, CIC Associate Director Public Health Epidemiologist Hospital Epidemiology UNC Hospitals
 Lauren DiBiase, MS, CIC Associate Director Public Health Epidemiologist Hospital Epidemiology UNC Hospitals Statistics Numbers that describe the health of the population The science used to interpret these
Lauren DiBiase, MS, CIC Associate Director Public Health Epidemiologist Hospital Epidemiology UNC Hospitals Statistics Numbers that describe the health of the population The science used to interpret these
RN Behavioral Health Care Manager in Primary Care Settings
 RN Behavioral Health Care Manager in Primary Care Settings Integrated Care and the Expanding Role of Nurses Seattle Airport Marriott, SeaTac, WA Tuesday, January 9, 2018 The Healthier Washington Practice
RN Behavioral Health Care Manager in Primary Care Settings Integrated Care and the Expanding Role of Nurses Seattle Airport Marriott, SeaTac, WA Tuesday, January 9, 2018 The Healthier Washington Practice
From A to Z-Codes Matter
 From A to Z-Codes Matter Susan Wallace, MEd, RHIA, CCS, CDIP, CCDS, FAHIMA While ALL ICD-10-CM codes are important, the Z-codes in ICD-10-CM are frequently considered step-children, supplemental codes
From A to Z-Codes Matter Susan Wallace, MEd, RHIA, CCS, CDIP, CCDS, FAHIMA While ALL ICD-10-CM codes are important, the Z-codes in ICD-10-CM are frequently considered step-children, supplemental codes
