Acute stroke management has changed over the past 10
|
|
|
- Martin Ramsey
- 5 years ago
- Views:
Transcription
1 Emergency Calls in Acute Stroke René Handschu, MD; Reinhard Poppe; Joachim Rauß; Bernhard Neundörfer, MD, PhD; Frank Erbguth, MD, PhD Background and Purpose In the last 10 years, stroke has become a medical emergency. Subsequently, early recognition of stroke symptoms and rapid activation of the medical system are essential. We sought to investigate what witnesses or victims of an acute stroke syndrome recognize and report in the actual situation. Methods We analyzed the recordings of all patients admitted to our stroke unit via the Emergency Medical System (EMS) dispatch center in Nuremberg within 1 year. With a structured evaluation form, the calls were screened for symptoms reported and for any diagnosis or other facts mentioned spontaneously or in response to a question by the dispatcher. We also evaluated data about EMS response and patient condition on admission. Results Of 482 patients treated in our stroke unit, 141 calls were evaluated. Main symptoms reported included speech problems (25.5%), motor deficits (21.9%), and disturbances of consciousness (14.8%). In many cases, a fall (21.2%) was presented as the main problem. Sensory deficits (7.8%) and vertigo (5.6%) were rarely mentioned. In 28 calls (19.8%), stroke was mentioned as a possible cause of the acute health problems. The dispatcher suspected a stroke in 51.7% of all cases. Conclusions This is one of the first studies to investigate emergency calls in acute stroke. We found that motor deficits and speech problems were the most dramatic symptoms that led to activation of the EMS. Other symptoms were less frequently reported, or atypical descriptions were given. Educational efforts are needed to improve recognition of atypical stroke symptoms by stroke victims and EMS professionals. (Stroke. 2003;34: ) Key Words: diagnosis education emergency medical services signs and symptoms stroke, acute Acute stroke management has changed over the past 10 years with the development of new therapeutic strategies toward rapid evaluation and treatment. Some therapies such as thrombolysis can be administered only within certain time windows. Still, the vast majority of acute stroke patients do not receive effective treatment in time primarily because of prolonged time between onset of first symptoms and first attempts at seeking medical attention. 1,2 Thus, immediate recognition of stroke symptoms and activation of the medical system is a crucial factor in improving outcome for acute stroke patients. Accordingly, rapid recognition of stroke warning signs is also the first part of the stroke chain of survival in the American Stroke Association s Operation Stroke. 3 Limited knowledge of signs, symptoms, and risk factors for stroke was noted as a factor associated with delay in activation of the medical system. 4 6 To face this dilemma, educational programs have been initiated, 4,7 and various studies have investigated knowledge of stroke symptoms in the general population 7 9 and in risk groups 9,10 through the use of structured questionnaires or telephone interviews. Data from this work may not exactly reflect what is actually happening if somebody really activates the emergency medical system (EMS) in case of a possible stroke. The knowledge people gain from educational programs or recall in answering interview questions may be somewhat different from what they actually recognize in the unexpected situation of somebody next to them sustaining a stroke or transient ischemic attack (TIA). Subjects involved and calling for help could differ from those targeted and reached by public awareness projects. On the other hand, people may realize that there is something wrong and call for medical help even if they have no idea that the problem is a sign of stroke or what stroke means at all. Little is known about how people really act if a stroke or TIA happens to someone in their surroundings because we normally cannot watch and analyze such situations. Posthoc interviews might draw a distorted image because remembering an exciting and frightening situation will not produce a true description. Therefore, we conducted a prospective study in cooperation with the EMS and analyzed emergency calls of patients treated in our stroke unit to investigate what witnesses or victims of an acute stroke syndrome recognize and report in the actual situation. Materials and Methods In Germany, organization of the EMS is under the control of the federal states. To organize its EMS, the state of Bavaria is divided Received September 13, 2002; final revision received October 24, 2002; accepted November 1, From the Department of Neurology, Friedrich-Alexander-Universitaet Erlangen-Nürnberg, Erlangen (R.H., B.N.); Bavarian Red Cross, Nürnberg EMS Dispatch Center, Nürnberg (R.P., J.R.); and Department of Neurology, City General Hospital, Nürnberg (F.E.), Germany. Reprint requests to Dr René Handschu, Department of Neurology, Friedrich-Alexander Universitaet, Stroke Unit, Schwabachanlage 6, D Erlangen, Germany. rene.handschu@neuro.med.uni-erlangen.de 2003 American Heart Association, Inc. Stroke is available at DOI: /01.STR F 1005
2 1006 Stroke April 2003 Figure 1. Symptoms (sym) reported in 141 emergency calls. into 26 districts. Within each district, 1 dispatch center is responsible for all EMS activities. Seeking urgent medical help, people call the telephone number and are connected directly to the dispatch center closest to them. Once the call is registered and completed, the dispatcher activates the closest appropriate ambulance unit. Ambulance units are operated by organizations like the Bavarian Red Cross, the Workers Samaritan Foundation, and St John s Ambulance and are staffed with at least 1 fully trained paramedic and 1 or 2 emergency medical technicians (EMTs). In contrast to many other countries, in Germany an emergency physician is on call 24 hours a day to be sent out to the scene and meet the paramedics in cases of severe and potentially life-threatening events. According to state law, all telephone calls coming in to the dispatch center and the radio communication between dispatcher and ambulance units in the district are tape recorded for documentation and liability reasons. Erlangen University Hospital is located in the Nuremberg EMS district but also receives patients from neighboring districts. There are 2 EMS ambulance stations based in the city of Erlangen and at least 1 in every large neighboring community. One ambulance unit, based at the University Medical Center, transports the EMS physician and 2 paramedics. In neighboring cities, EMS physicians leave the local hospital or their offices in separate cars and meet the paramedic ambulance unit at the scene (rendezvous system). Every patient admitted to the Stroke Unit of the University Hospital in Erlangen (Department of Neurology) after calling the EMS dispatch center in Nuremberg through within 1 year was included in this study. The patient and the person calling the EMS were asked for informed consent for evaluation of the call. After informed consent was given, analysis of the tape recordings at the dispatch center was begun. Calls were screened with a structured evaluation form for symptoms reported, any diagnosis or medical syndrome named by the caller, information about onset and duration of symptoms, and other facts mentioned spontaneously or in response to questions by the dispatcher. Descriptions of symptoms were transcribed from the tapes without any change by the EMS center and later categorized by the investigators. We also evaluated reactions and decisions by the EMS dispatcher. Data about the resultant EMS response and especially symptoms and history documented were extracted from EMS records. On admission to the stroke unit, all patients received a standardized examination, including a detailed history, physical and detailed neurological examination, and scores for the Glasgow Coma Scale (GCS) and National Institutes of Health Stroke Scale (NIHSS). Emergency calls with any healthcare professional reporting to the dispatcher were not analyzed. The study was approved by the headquarters of the Bavarian Red Cross, which operates the Nuremberg EMS dispatch center, and by the university. Results Of 482 patients treated in our stroke unit during the study period, 196 (40.7%) came in after activation of EMS. Because 57 cases were brought in from other EMS districts or we could not identify the person calling or obtain informed consent, 141 calls concerning 137 different patients (139 cases) were finally evaluated. Mean age of patients was 65.4 years (range, 21 to 91 years); 56.4% were male. Mean duration of all calls was 1 minute 23 seconds (range, 38 seconds to 4 minutes 12 seconds). Median latency from onset of symptoms to call was 38 minutes (2 to 960 minutes). In 26.2% of all calls, only 1 symptom was reported; in 36.8%, 2 symptoms were identified; in the remaining cases, 3 symptoms were presented. We found that 41.1% of all callers were the patient s spouse; in 23.4% of the calls, other relatives placed the call; in 19.8%, neighbors, colleagues, or friends called; in 8.5%, a person not related to the patient placed the call; and in 7.1% of all calls, the patients themselves made the call. Mean age of callers was 53.4 years; 58.2% of them were female. Symptoms most frequently reported included speech problems (25.5%), limb weakness (21.9%), and disturbances of consciousness (14.8%). In many cases, a fall (21.2%) was presented as the main problem. Problems with sensation (7.8%) and vertigo (5.6%) were rarely mentioned. Any information about onset or duration of symptoms was given by 14.1% of all callers and was documented in 28.7% of all EMS records. Most symptoms were reported spontaneously by the person calling. After dispatcher inquiry, only speech problems and alterations in consciousness were elicited as additional symptoms in a relevant number of calls. Figure 1 shows the frequency of symptoms spontaneously reported by callers and after query by the dispatcher. Figure 2 gives some examples of typical statements made in calls. Exact percentages of symptoms reported in calls are given in Table 1, together with symptoms documented in EMS records and findings on admission to the stroke unit. Many symptoms were more frequent on scene than reported in calls
3 Handschu et al Emergency Calls in Acute Stroke 1007 Figure 2. Original citations from some emergency calls. and even more frequent on admission. NIHSS score was 4.34 points on average (range, 0 to 22) and GCS score was 14.2 points (range, 9 to 15) on admission to the stroke unit. In 28 calls (19.8%), stroke was mentioned as a possible cause of the acute health problems. In 9.9% of all cases, other medical conditions besides stroke (eg, myocardial infarction) were mentioned. The dispatcher assumed and coded for stroke in 51.7% of all analyzed cases. Other diagnoses coded included cardiac diseases (15.6%), syncope (4.9%), and unconsciousness (3.5%). In records of EMS physicians, a cerebrovascular disorder was coded in 83.7% of all documented cases (n 74). Final diagnosis at discharge from the Department of Neurology was ischemic stroke in 63.3%; 13.0% were coded as intracerebral hemorrhage; and 15.8% had had a TIA. We found that 7.9% (n 11) had a nonstroke diagnosis. Symptoms reported in cases with a nonstroke diagnosis were suggestive mainly of a possible stroke (see Table 2) and similar to those reported in cases with a final diagnosis of cerebrovascular disease. In the resulting EMS response, the priority of activations was high (lights and sirens) in 79.3% of all 140 EMS runs. In 52.8%, an EMS physician was at the scene with the paramedics; in 22.8%, only a paramedic unit was sent to the scene; and in 17.8%, only an EMT unit was sent. The TABLE 1. Symptoms Noted at Various Stages of Stroke Care helicopter, which is staffed with a physician and paramedic, was activated in 6 cases (4.3%). Median time from call to arrival on scene was 12 minutes (range, 5 to 57 minutes) and from arrival on scene to first hospital arrival was 51 minutes (range, 23 to 70 minutes). In 21 cases, the first hospital arrival of the patient was outside the Department of Neurology at the University of Erlangen. Those patients were brought to a different hospital or to the Department of Internal Medicine at the University Hospital. Median delay from time on scene to arrival at our stroke unit was 72 minutes (range, 23 to 403 minutes). See Figure 3 for a view of the time flow. Discussion This is one of the first studies to investigate emergency calls in cases of acute stroke. To gain sufficient information about clinical presentation on admission and to obtain informed consent from patients and their relatives, we decided to investigate calls about patients seen in our stroke unit. This cohort may be biased because there are stroke cases in the covered region that are not included in this study, especially in outlying regions where some of the patients were seen exclusively in general hospitals. In Erlangen, where almost two thirds of all cases happened, most stroke patients are seen by the Department of Neurology, whether primarily (85.3%) 11 or after transfer if a diagnosis of stroke was made. An additional bias may exist in that cases analyzed in this study are only those with primary activation of the EMS system. In these cases, the event was already recognized as an emergency, in contrast to situations in which individuals seek help by calling or visiting their primary care physician s office or by calling friends or family members. Unfortunately, in a study setting like ours, it is impossible to analyze what the latter group recognized and thought when seeking medical attention because calls and conversations such as those in physician s offices are not documented on a regular basis. Symptoms reported by callers included various descriptions of different neurological or nonneurological disturbances. See Figure 2 for examples. Present Reported in Emergency Calls, % (n 141) Documented on Scene, % (n 140) Found on Admission, % (n 139) Limb weakness/paresis Fall/atypical motor description Facial paresis Speech problems Impaired consciousness Confusion Sensory deficit Vertigo Headache Nonspecific symptoms Onset of symptoms Stroke mentioned
4 1008 Stroke April 2003 TABLE 2. Symptoms Reported in Nonstroke Cases Final Diagnosis n Dispatcher Coding Symptoms Reported in Calls Epileptic seizure 4 Stroke (3), seizure (1) Limb weakness, reduced consciousness, confusion, stroke mentioned in 2 calls Psychosomatic disorder 3 Stroke (2), cardiac disease (1) Sensory deficit, limb weakness, dizziness/vertigo Vestibulopathy 2 Stroke (1), cardiac disease (1) Dizziness/vertigo, nausea Transient global amnesia 1 Seizure Disorientation Pneumonia/dehydration 1 Unspecified medical disease Speech problem, dyspnea n 11. Transcribed into categories of neurological deficits, speech problems and motor deficits were the categories most frequently reported. Motor deficits such as a sudden weakness and especially speech problems such as incoherent answers or the inability to talk are dramatic symptoms. They interfere with daily life and are therefore rapidly recognized. Even more so, these symptoms may imply that something serious is happening, leading to activation of the EMS. Motor problems were often reported by their consequences, resulting in a person sinking or falling down, noted as fall in Table 1 and Figure 1. Falls were the symptom category most frequently reported spontaneously. When limb weakness and fall are taken together, descriptions of motor deficits were the most frequently reported neurological symptoms in our calls. Other symptoms such as sensory deficits or dizziness or vertigo were less frequently reported. In more than one fourth of cases, other nonstroke symptoms like chest pain, dyspnea, or paleness were reported with or without stroke symptoms. Most symptoms and descriptions were reported spontaneously. Only a small additional number was obtained after questioning by the dispatcher mainly in the symptom categories of speech problems and consciousness. Standard questionnaires at the dispatch center include mainly vital signs such as heartbeat, breathing, and consciousness. Stroke symptoms are currently not included. Routine questioning for such symptoms not only would increase number of symptoms reported to more than 1 or 2 but could clarify the background of symptoms, eg, that a fall goes with a paresis. Compared with findings on initial examination in our stroke unit, most symptom categories were more frequent on admission than reported on calls and even more frequent on admission than documented in EMS records. Especially for symptoms such as sensory deficits or facial paresis for which the frequency was 5 times higher on admission than reported in calls, this shift may indicate that symptoms are underrecognized by the person calling for help. On the other hand, impaired consciousness and confusion have higher frequencies in calls and even higher frequency in EMS reports than on admission. It is possible that all these confused or stuporous patients improved. However, we found that some of them had symptoms of aphasia not documented before hospital admission. It appears that aphasia is sometimes misinterpreted as altered consciousness by the public and even trained staff, including physicians, in the prehospital setting. A direct comparison of the frequency of symptoms in emergency calls, in EMS records, and on admission seems problematic. One reason is that they are fixed at different time points and that there is a mean latency of 1 hour 40 minutes between call and admission to the stroke unit. Within this time, symptoms may improve or disappear, or new symptoms may arise. Given the fact that some of our patients had a TIA and sometimes arrived without any symptoms, it may be speculated that the higher rates of symptoms documented on admission will be due not only to worsening strokes but also to symptoms not recognized or documented. A second cause limiting comparison of symptom frequency is the different quality of their sources. Callers just report symptoms that they are most aware of, many times only 1 or 2 symptoms. On the other hand, symptoms on admission are findings from a structured neurological examination for acute stroke patients, including administration of NIHSS. On-scene documentation is normally done by the physician, if involved, or the paramedics using standardized documentation forms on a different level. These forms do not provide special reminders for stroke symptoms. Physician documentation forms provide tick boxes for the GCS and for muscle strength of legs and arms, whereas paramedic forms only ask for consciousness as a special neurological condition. All other information about stroke symptoms is given by free notes, which are added optionally. So, what is documented as symptoms by EMS staff, whether paramedics or physicians, could be a mixture of symptoms, findings, and history. The impression emerging from our data that stroke symptoms are, if not unrecognized completely, sometimes Figure 3. Time flow from first symptoms to hospital arrival (median values).
5 Handschu et al Emergency Calls in Acute Stroke 1009 not documented very well by EMS staff is due partially to the methods and forms of documentation. In only 19.8% of all calls was any word indicating stroke or TIA mentioned. So, only every fifth person involved in a stroke emergency was aware of a possible stroke. A recent study from the United States reported a much higher rate of callers mentioning stroke. 12 The sample size of that study was smaller, and in contrast to our findings, family members of patients were the minority of callers. Additionally, that work was conducted in an urban population, whereas our study area was partially rural. However, the infrequent use of the word stroke is a hint for insufficient knowledge about stroke symptoms in the population of our study area, and the people calling for help in the previous work 12 were probably younger and better educated. Dispatchers coded for stroke after the call in more than half of our cases, a rate similar to the identification rate of EMS dispatchers in the Cincinnati area. 13 Furthermore, the vast majority of cases received a high-priority response often as a potentially life-threatening event requiring the presence of an emergency physician on scene. Contrary to previous findings, 12 in our study, a stroke seems to be taken as a serious event by the dispatchers, who are usually fully trained paramedics with several years of experience in the field. To summarize, there is a striking need for educational efforts to improve recognition of especially nondramatic and atypical stroke symptoms in the general population but also in family members of patients at high risk for stroke. More public information on stroke pathology and risk factors is necessary. In addition, EMS dispatchers knowledge about typical and atypical stroke symptoms should be increased, and stroke symptoms must be included in routine questionnaires for EMS dispatchers. Paramedics and EMS physicians in the field should receive training in evaluating stroke patients, and documentation of signs and symptoms present on the scene should be emphasized. Acknowledgments This work is dedicated to the memory of Peter Rück, a close friend and colleague, paramedic, and emergency physician, who died far too early 5 years ago. We want to thank all EMS dispatchers, paramedics, and physicians in the Nuremberg district, as well as our patients and their relatives, or whoever took the phone to get a stroke patient to treatment, for taking part in this study. We also want to thank Dr Heike Schmolck for her support and advice in preparing this manuscript. References 1. Barber PA, Zhang J, Demchuk AM, Hill MD, Buchan AM. Why are stroke patients excluded from TPA therapy? An analysis of patient eligibility. Neurology. 2001;56: Chiu D, Krieger D, Villar-Cordova C, Kasner SE, Morgenstern LB, Bratina PL, Yatsu FM, Grotta JC. Intravenous tissue plasminogen activator for acute ischemic stroke: feasibility, safety and efficacy in the first year of clinical practice. Stroke. 1998;29: Operation stroke. Available at: http// presenter.jhtml?identifier Accessed August 23, Alberts MJ, Perry A, Dawson DV, Bertels C. Effects of public and professional education on reducing the delay in presentation and referral of stroke patients. Stroke. 1992;23: Williams LS, Bruno A, Rouch D, Marriot DJ. Stroke patients knowledge of stroke: influence on time to presentation. Stroke. 1997;28: Fogelholm R, Murros K, Rissanen A, Ilmavirta M. Factors delaying hospital admission after acute stroke. Stroke. 1996;27: Stern BE, Berman ME, Thomas JJ, Klassen AC. Community education for stroke awareness: an efficacy study. Stroke. 1999;30: Pancioli AM, Broderick J, Kothari R, Brott T, Tuchfarber A, Miller R, Khoury J, Jauch E. Public perception of stroke warning signs and knowledge of potential risk factors. JAMA. 1998;279: Yoon SS, Byles J. Perceptions of stroke in the general public and patients with stroke: a qualitative study. BMJ. 2002;324: Kothari R, Sauerbeck L, Jauch E, Broderick J, Brott T, Khoury J, Tiepu L. Patients awareness of stroke signs, symptoms. and risk factors. Stroke. 1997;28: Kolominsky-Rabas PL, Sarti C, Heuschmann PU, Graf C, Siemonsen S, Neundoerfer B, Katalinic A, Lang E, Gassmann KG, von Stockert TR. A prospective community-based study of stroke in Germany: the Erlangen Stroke Project (ESPro): incidence and case fatality at 1, 3, and 12 months. Stroke. 1998;29: Porteous GH, Corry MD, Smith WS. Emergency medical services dispatcher identification of stroke and transient ischemic attack. Prehosp Emerg Care. 1999;3: Kothari R, Barsan W, Brott T, Broderick J, Ashbrock S. Frequency and accuracy of prehospital diagnosis of acute stroke. Stroke. 1995;26:
Stroke remains the third leading cause of death and the
 Stroke Symptoms and the Decision to Call for an Ambulance Ian Mosley, MBus; Marcus Nicol, PhD; Geoffrey Donnan, MD; Ian Patrick, ASM; Helen Dewey, PhD Background and Purpose Few acute stroke patients are
Stroke Symptoms and the Decision to Call for an Ambulance Ian Mosley, MBus; Marcus Nicol, PhD; Geoffrey Donnan, MD; Ian Patrick, ASM; Helen Dewey, PhD Background and Purpose Few acute stroke patients are
Patient characteristics. Intervention Comparison Length of followup. Outcome measures. Number of patients. Evidence level.
 5.0 Rapid recognition of symptoms and diagnosis 5.1. Pre-hospital health professional checklists for the prompt recognition of symptoms of TIA and stroke Evidence Tables ASM1: What is the accuracy of a
5.0 Rapid recognition of symptoms and diagnosis 5.1. Pre-hospital health professional checklists for the prompt recognition of symptoms of TIA and stroke Evidence Tables ASM1: What is the accuracy of a
STROKE is a major cause of disability and
 218 STROKE DELAYS Morris et al. STROKE CARE DELAYS EDUCATION AND PRACTICE Time Delays in Accessing Stroke Care in the Emergency Department DEXTER L. MORRIS, PHD, MD, WAYNE D. ROSAMOND, PHD, ALBERT R. HINN,
218 STROKE DELAYS Morris et al. STROKE CARE DELAYS EDUCATION AND PRACTICE Time Delays in Accessing Stroke Care in the Emergency Department DEXTER L. MORRIS, PHD, MD, WAYNE D. ROSAMOND, PHD, ALBERT R. HINN,
Stroke: Journal of the American Heart Association
 1 of 12 8/13/2018, 10:33 AM Skip to Content Stroke: Journal of the American Heart Association Issue: Volume 31(1), January 2000, p 71 Copyright: 2000 American Heart Association, Inc. Publication Type:
1 of 12 8/13/2018, 10:33 AM Skip to Content Stroke: Journal of the American Heart Association Issue: Volume 31(1), January 2000, p 71 Copyright: 2000 American Heart Association, Inc. Publication Type:
Pre-Hospital Stroke Care: Bringing It To The Street. by Bob Atkins, NREMT-Paramedic AEMD EMS Director Bedford Regional Medical Center
 Pre-Hospital Stroke Care: Bringing It To The Street by Bob Atkins, NREMT-Paramedic AEMD EMS Director Bedford Regional Medical Center Overview/Objectives Explain the reasons or rational behind the importance
Pre-Hospital Stroke Care: Bringing It To The Street by Bob Atkins, NREMT-Paramedic AEMD EMS Director Bedford Regional Medical Center Overview/Objectives Explain the reasons or rational behind the importance
: STROKE. other pertinent information such as recent trauma, illicit drug use, pertinent medical history or use of oral contraceptives.
 INTRODUCTION A cerebral vascular accident (CVA) or stroke is a lack of blood supply to the brain as a result of either ischemia or hemorrhage. 80% of CVAs are a result of ischemia (embolic or thrombotic)
INTRODUCTION A cerebral vascular accident (CVA) or stroke is a lack of blood supply to the brain as a result of either ischemia or hemorrhage. 80% of CVAs are a result of ischemia (embolic or thrombotic)
Stroke is the second leading cause of death and the most
 Acute Stroke Management in the Local General Hospital René Handschu, MD; Andreas Garling, MD; Peter Ulrich Heuschmann, MD; Peter L. Kolominsky-Rabas, MD; Frank Erbguth, MD, PhD; Bernhard Neundörfer, MD,
Acute Stroke Management in the Local General Hospital René Handschu, MD; Andreas Garling, MD; Peter Ulrich Heuschmann, MD; Peter L. Kolominsky-Rabas, MD; Frank Erbguth, MD, PhD; Bernhard Neundörfer, MD,
3.2 Emergency Medical Services Canadian Best Practice Recommendations for Stroke Care, 4th Edition Update
 Last Updated: May 21st, 2013 Canadian Best Practice Recommendations for Stroke Care, 4th Edition 2012-2013 Update Table of Contents Evidence Tables... 3 EMS Management of Acute Stroke... 3 Summary of the
Last Updated: May 21st, 2013 Canadian Best Practice Recommendations for Stroke Care, 4th Edition 2012-2013 Update Table of Contents Evidence Tables... 3 EMS Management of Acute Stroke... 3 Summary of the
Table 2.0 Canadian Stroke Best Practices Table of Standardized Acute Stroke Out-of- Hospital Diagnostic Screening Tools
 Table 2.0 Canadian Stroke Best Practices Table of Standardized Acute Stroke Out-of- Hospital Diagnostic Screening Tools Assessment Tool Cincinnati Pre-Hospital Stroke Scale (CPSS) Number and description
Table 2.0 Canadian Stroke Best Practices Table of Standardized Acute Stroke Out-of- Hospital Diagnostic Screening Tools Assessment Tool Cincinnati Pre-Hospital Stroke Scale (CPSS) Number and description
What Do You Think of My Posterior?
 What Do You Think of My Posterior? Posterior Stroke and Stroke Mimics Peter Panagos, MD, FACEP, FAHA Associate Professor Emergency Medicine and Neurology Washington University School of Medicine Disclosures
What Do You Think of My Posterior? Posterior Stroke and Stroke Mimics Peter Panagos, MD, FACEP, FAHA Associate Professor Emergency Medicine and Neurology Washington University School of Medicine Disclosures
Objectives. Stroke Facts 2/27/2015. EMS in Stroke Care: A Critical Partnership
 EMS in Stroke Care: A Critical Partnership Spokane County EMS Objectives Identify the types and time limitations for acute ischemic stroke treatment options Identify the importance of early identification
EMS in Stroke Care: A Critical Partnership Spokane County EMS Objectives Identify the types and time limitations for acute ischemic stroke treatment options Identify the importance of early identification
GUIDELINES FOR THE EARLY MANAGEMENT OF PATIENTS WITH ACUTE ISCHEMIC STROKE
 2018 UPDATE QUICK SHEET 2018 American Heart Association GUIDELINES FOR THE EARLY MANAGEMENT OF PATIENTS WITH ACUTE ISCHEMIC STROKE A Summary for Healthcare Professionals from the American Heart Association/American
2018 UPDATE QUICK SHEET 2018 American Heart Association GUIDELINES FOR THE EARLY MANAGEMENT OF PATIENTS WITH ACUTE ISCHEMIC STROKE A Summary for Healthcare Professionals from the American Heart Association/American
Factors Delaying Hospital Arrival after Acute Stroke in Southern Taiwan. Teng-Yeow Tan, MD; Ku-Chou Chang, MD; Chia-Wei Liou, MD
 Original Article 458 Factors Delaying Hospital Arrival after Acute Stroke in Southern Taiwan Teng-Yeow Tan, MD; Ku-Chou Chang, MD; Chia-Wei Liou, MD Background: Acute stroke management emphasizes prompt
Original Article 458 Factors Delaying Hospital Arrival after Acute Stroke in Southern Taiwan Teng-Yeow Tan, MD; Ku-Chou Chang, MD; Chia-Wei Liou, MD Background: Acute stroke management emphasizes prompt
Does Use of the Recognition Of Stroke In the Emergency Room Stroke Assessment Tool Enhance Stroke Recognition by Ambulance Clinicians?
 Does Use of the Recognition Of Stroke In the Emergency Room Stroke Assessment Tool Enhance Stroke Recognition by Ambulance Clinicians? Rachael T. Fothergill, PhD; Julia Williams, PhD; Melanie J. Edwards,
Does Use of the Recognition Of Stroke In the Emergency Room Stroke Assessment Tool Enhance Stroke Recognition by Ambulance Clinicians? Rachael T. Fothergill, PhD; Julia Williams, PhD; Melanie J. Edwards,
STROKE INTRODUCTION OBJECTIVES. When the student has finished this module, he/she will be able to:
 STROKE INTRODUCTION Stroke is the medical term for a specific type of neurological event that causes damage to the brain. There are two types of stroke, but both types of stroke cause the same type of
STROKE INTRODUCTION Stroke is the medical term for a specific type of neurological event that causes damage to the brain. There are two types of stroke, but both types of stroke cause the same type of
Supplementary Online Content
 Supplementary Online Content Wolters FJ, Li L, Gutnikov SA, Mehta Z, Rothwell PM. Medical attention seeking after transient ischemic attack and minor stroke in relation to the UK Face, Arm, Speech, Time
Supplementary Online Content Wolters FJ, Li L, Gutnikov SA, Mehta Z, Rothwell PM. Medical attention seeking after transient ischemic attack and minor stroke in relation to the UK Face, Arm, Speech, Time
Making every second count Challenges in acute stroke management Prehospital management of acute ischaemic stroke: how can we do better?
 Making every second count Challenges in acute stroke management Prehospital management of acute ischaemic stroke: how can we do better? Patrick Goldstein, MD, Lille, France NIH-recommended emergency department
Making every second count Challenges in acute stroke management Prehospital management of acute ischaemic stroke: how can we do better? Patrick Goldstein, MD, Lille, France NIH-recommended emergency department
BY: Ramon Medina EMT-LP/RN
 BY: Ramon Medina EMT-LP/RN Discuss types of strokes Discuss the physical and neurological assessment of stroke patients Discuss pertinent historical findings Discuss pre-hospital and emergency management
BY: Ramon Medina EMT-LP/RN Discuss types of strokes Discuss the physical and neurological assessment of stroke patients Discuss pertinent historical findings Discuss pre-hospital and emergency management
ND STROKE Coordinators Case Studies. STEMI and Stroke Conference, Fargo, ND, August 5, 2014
 ND STROKE Coordinators Case Studies STEMI and Stroke Conference, Fargo, ND, August 5, 2014 STROKE Coordinator Case Study Essentia Health, Fargo Essentia Health Stroke Alert Process Within 24 hours of Last
ND STROKE Coordinators Case Studies STEMI and Stroke Conference, Fargo, ND, August 5, 2014 STROKE Coordinator Case Study Essentia Health, Fargo Essentia Health Stroke Alert Process Within 24 hours of Last
Factors Influencing Pre-Hospital Delay after Ischemic Stroke and Transient Ischemic Attack
 ORIGINAL ARTICLE Factors Influencing Pre-Hospital Delay after Ischemic Stroke and Transient Ischemic Attack Yuko Tanaka 1, Makoto Nakajima 1, Teruyuki Hirano 2 and Makoto Uchino 2 Abstract Background and
ORIGINAL ARTICLE Factors Influencing Pre-Hospital Delay after Ischemic Stroke and Transient Ischemic Attack Yuko Tanaka 1, Makoto Nakajima 1, Teruyuki Hirano 2 and Makoto Uchino 2 Abstract Background and
Stroke: clinical presentations, symptoms and signs
 Stroke: clinical presentations, symptoms and signs Professor Peter Sandercock University of Edinburgh EAN teaching course Burkina Faso 8 th November 2017 Clinical diagnosis is important to Ensure stroke
Stroke: clinical presentations, symptoms and signs Professor Peter Sandercock University of Edinburgh EAN teaching course Burkina Faso 8 th November 2017 Clinical diagnosis is important to Ensure stroke
Chapter 18. Objectives. Objectives 01/09/2013. Altered Mental Status, Stroke, and Headache
 Chapter 18 Altered Mental Status, Stroke, and Headache Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives
Chapter 18 Altered Mental Status, Stroke, and Headache Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives
Stroke Transfer Checklist
 Stroke Transfer Checklist When preparing to transfer an acute stroke patient to the UF Health Shands Comprehensive Stroke Center, please make every attempt to include the following information: Results
Stroke Transfer Checklist When preparing to transfer an acute stroke patient to the UF Health Shands Comprehensive Stroke Center, please make every attempt to include the following information: Results
In the last decade, various therapeutic strategies were
 Telemedicine in Emergency Evaluation of Acute Stroke Interrater Agreement in Remote Video Examination With a Novel Multimedia System René Handschu, MD; Rebekka Littmann, MD; Udo Reulbach, MD; Charly Gaul,
Telemedicine in Emergency Evaluation of Acute Stroke Interrater Agreement in Remote Video Examination With a Novel Multimedia System René Handschu, MD; Rebekka Littmann, MD; Udo Reulbach, MD; Charly Gaul,
Understanding Stroke
 MINTO PREVENTION & REHABILITATION CENTRE CENTRE DE PREVENTION ET DE READAPTATION MINTO Understanding Stroke About This Kit Stroke is the fourth leading cause of death in Canada after heart disease and
MINTO PREVENTION & REHABILITATION CENTRE CENTRE DE PREVENTION ET DE READAPTATION MINTO Understanding Stroke About This Kit Stroke is the fourth leading cause of death in Canada after heart disease and
Stroke Belt Consortium
 Field Triage And Diversion of Acute Stroke Charles Sand, MD Stroke Belt Consortium 10/26/12 WCF EMS Acute Stroke Advisory Committee Formed 2001 5 Original members Now > 100 members interdisciplinary expertise
Field Triage And Diversion of Acute Stroke Charles Sand, MD Stroke Belt Consortium 10/26/12 WCF EMS Acute Stroke Advisory Committee Formed 2001 5 Original members Now > 100 members interdisciplinary expertise
Acute Ischaemic Stroke Pathways Drip and Ship
 Acute Ischaemic Stroke Pathways Drip and Ship Professor Gary Ford Chief Executive Officer, Oxford Academic Health Science Network Consultant Stroke Physician, Oxford University Hospitals Visiting Professor
Acute Ischaemic Stroke Pathways Drip and Ship Professor Gary Ford Chief Executive Officer, Oxford Academic Health Science Network Consultant Stroke Physician, Oxford University Hospitals Visiting Professor
Mohamed Al-Khaled, MD,* Christine Matthis, MD, and J urgen Eggers, MD*
 Predictors of In-hospital Mortality and the Risk of Symptomatic Intracerebral Hemorrhage after Thrombolytic Therapy with Recombinant Tissue Plasminogen Activator in Acute Ischemic Stroke Mohamed Al-Khaled,
Predictors of In-hospital Mortality and the Risk of Symptomatic Intracerebral Hemorrhage after Thrombolytic Therapy with Recombinant Tissue Plasminogen Activator in Acute Ischemic Stroke Mohamed Al-Khaled,
WHAT IS A STROKE? What causes a stroke? What disabilities can result from a stroke?
 Know Stroke Stroke is the third leading cause of death in the United States and a leading cause of serious, long-term disability in adults. About 600,000 new strokes are reported in the U.S. each year.
Know Stroke Stroke is the third leading cause of death in the United States and a leading cause of serious, long-term disability in adults. About 600,000 new strokes are reported in the U.S. each year.
It s Not All One Sided. James Smith, MD (Smitty)
 It s Not All One Sided James Smith, MD (Smitty) Disclosures Chair, NE State EMS Board Medical Director, Emergency Services, GPH Medical Director, GPH LifeNet, NPFD, Maxwell, Tryon, Chase County, NP Rec
It s Not All One Sided James Smith, MD (Smitty) Disclosures Chair, NE State EMS Board Medical Director, Emergency Services, GPH Medical Director, GPH LifeNet, NPFD, Maxwell, Tryon, Chase County, NP Rec
Heart of England Foundation Trust ACUTE STROKE PATHWAY EMERGENCY DEPARTMENT ATTACHMENTS
 STROKE Name: PID: DOB: Consultant: Heart of England Foundation Trust ACUTE STROKE PATHWAY EMERGENCY DEPARTMENT ATTACHMENTS November 2010 TIME IS BRAIN SUSPECTED STROKE Onset Within 6 Hours? (FAST TEST
STROKE Name: PID: DOB: Consultant: Heart of England Foundation Trust ACUTE STROKE PATHWAY EMERGENCY DEPARTMENT ATTACHMENTS November 2010 TIME IS BRAIN SUSPECTED STROKE Onset Within 6 Hours? (FAST TEST
Primary Stroke Center Quality & Performance Measures
 Primary Stroke Center Quality & Performance Measures This section of the manual contains information related to the quality performance of Primary Stroke Centers. Brain Attack Coalition Definitions Recognition
Primary Stroke Center Quality & Performance Measures This section of the manual contains information related to the quality performance of Primary Stroke Centers. Brain Attack Coalition Definitions Recognition
Better identification of patients who may benefit from therapy
 Jon Jui MD, MPH Large Vessel Occlusion Low rates of re-canalization after tpa Only 25 % of large vessel strokes re-canalization after tpa Newer invasive techniques Solitaire vs Merci Better identification
Jon Jui MD, MPH Large Vessel Occlusion Low rates of re-canalization after tpa Only 25 % of large vessel strokes re-canalization after tpa Newer invasive techniques Solitaire vs Merci Better identification
Stroke Workshop. Pre-Workshop Handout. With Walter Himmel, Meeta Patel & Anton Helman
 2018 Stroke Workshop Pre-Workshop Handout With Walter Himmel, Meeta Patel & Anton Helman Instructions for Getting the Most Out of The EMU Stroke Workshop Handout This workshop has been designed around
2018 Stroke Workshop Pre-Workshop Handout With Walter Himmel, Meeta Patel & Anton Helman Instructions for Getting the Most Out of The EMU Stroke Workshop Handout This workshop has been designed around
Presentation Time to Hospital and Recognition of Stroke in Patients with Ischemic Stroke
 Presentation Time to Hospital and Recognition of Stroke in Patients with Ischemic Stroke Ji Hoe Heo, M.D., Hwa Young Cheon, M.D., Chung Mo Nam, Ph.D.*, Dong Chan Kim, R.N., Gyung Whan Kim, M.D., Byung
Presentation Time to Hospital and Recognition of Stroke in Patients with Ischemic Stroke Ji Hoe Heo, M.D., Hwa Young Cheon, M.D., Chung Mo Nam, Ph.D.*, Dong Chan Kim, R.N., Gyung Whan Kim, M.D., Byung
Slide 1. Slide 2. Slide 3 EMS STROKE CARE AND CSTAT OREGON STROKE NETWORK CONFERENCE 2018 SHAWN WOOD, CLINICAL MANAGER DISCLOSURES MY PATH TO EMS
 Slide 1 EMS STROKE CARE AND CSTAT OREGON STROKE NETWORK CONFERENCE 2018 SHAWN WOOD, CLINICAL MANAGER METRO WEST AMBULANCE Slide 2 DISCLOSURES No Financial Conflicts. I work as the Clinical Manager for
Slide 1 EMS STROKE CARE AND CSTAT OREGON STROKE NETWORK CONFERENCE 2018 SHAWN WOOD, CLINICAL MANAGER METRO WEST AMBULANCE Slide 2 DISCLOSURES No Financial Conflicts. I work as the Clinical Manager for
Awareness of stroke among stroke patients in a tertiary-care level hospital in northwest India
 Research Article Awareness of stroke among stroke patients in a tertiary-care level hospital in northwest India Sulena Sulena, Banshi Lal Kumawat, Anjani Kumar Sharma Department of Neurology, SMS Medical
Research Article Awareness of stroke among stroke patients in a tertiary-care level hospital in northwest India Sulena Sulena, Banshi Lal Kumawat, Anjani Kumar Sharma Department of Neurology, SMS Medical
The Blackouts Checklist i
 The Blackouts Checklist i The Blackouts Checklist key aim is to help you and your doctor reach the correct diagnosis for any unexplained loss of consciousness (blackout). The Checklist gives you information
The Blackouts Checklist i The Blackouts Checklist key aim is to help you and your doctor reach the correct diagnosis for any unexplained loss of consciousness (blackout). The Checklist gives you information
Concurrent Admission Reviews Milliman and Second Level Physician Review Criteria
 Concurrent Admission Reviews Milliman and Second Level Physician Review Criteria Patient Status: Understanding Inpatient and Outpatient Observation Focusing on Chest Pain, TIAs, Syncope and Dizziness Which
Concurrent Admission Reviews Milliman and Second Level Physician Review Criteria Patient Status: Understanding Inpatient and Outpatient Observation Focusing on Chest Pain, TIAs, Syncope and Dizziness Which
Stroke & the Emergency Department. Dr. Barry Moynihan, March 2 nd, 2012
 Stroke & the Emergency Department Dr. Barry Moynihan, March 2 nd, 2012 Outline Primer Stroke anatomy & clinical syndromes Diagnosing stroke Anterior / Posterior Thrombolysis Haemorrhage The London model
Stroke & the Emergency Department Dr. Barry Moynihan, March 2 nd, 2012 Outline Primer Stroke anatomy & clinical syndromes Diagnosing stroke Anterior / Posterior Thrombolysis Haemorrhage The London model
Non-epileptic attacks
 Non-epileptic attacks A short guide for patients and families Information for patients Neurology Psychotherapy Service What are non-epileptic attacks? Non-epileptic attacks are episodes in which people
Non-epileptic attacks A short guide for patients and families Information for patients Neurology Psychotherapy Service What are non-epileptic attacks? Non-epileptic attacks are episodes in which people
Medical Emergencies. Emergency Medical Response
 Medical Emergencies Lesson 23: Medical Emergencies You Are the Emergency Medical Responder You are the emergency medical responder (EMR) responding to a scene on a downtown street involving a male who
Medical Emergencies Lesson 23: Medical Emergencies You Are the Emergency Medical Responder You are the emergency medical responder (EMR) responding to a scene on a downtown street involving a male who
PHANTOM-S study Prehospital acute neurologic therapy and optimization of medical care in stroke Matthias Wendt on behalf of the PHANTOM-S study group
 PHANTOM-S study Prehospital acute neurologic therapy and optimization of medical care in stroke Matthias Wendt on behalf of the PHANTOM-S study group Recent guidelines 1. Intravenous rtpa (0.9 mg/kg, maximum
PHANTOM-S study Prehospital acute neurologic therapy and optimization of medical care in stroke Matthias Wendt on behalf of the PHANTOM-S study group Recent guidelines 1. Intravenous rtpa (0.9 mg/kg, maximum
Thrombolytic Therapy in Clinical Practice The Norwegian Experience
 Thrombolytic Therapy in Clinical Practice The Norwegian Experience Thomassen Lars Thomassen, Ulrike Waje-Andreassen, Halvor Næss ABSTRACT Background: Awaiting the European approval of thrombolysis, we
Thrombolytic Therapy in Clinical Practice The Norwegian Experience Thomassen Lars Thomassen, Ulrike Waje-Andreassen, Halvor Næss ABSTRACT Background: Awaiting the European approval of thrombolysis, we
Canadian Best Practice Recommendations for Stroke Care. (Updated 2008) Section # 3 Section # 3 Hyperacute Stroke Management
 Canadian Best Practice Recommendations for Stroke Care (Updated 2008) Section # 3 Section # 3 Hyperacute Stroke Management Reorganization of Recommendations 2008 2006 RECOMMENDATIONS: 2008 RECOMMENDATIONS:
Canadian Best Practice Recommendations for Stroke Care (Updated 2008) Section # 3 Section # 3 Hyperacute Stroke Management Reorganization of Recommendations 2008 2006 RECOMMENDATIONS: 2008 RECOMMENDATIONS:
HPI Signs and Symptoms Considerations
 SECTION: Adult General Medical Emergencies PROTOCOL TITLE: Medical Stroke/TIA REVISED: 07/2017 Protocol OVERVIEW: Stroke is a major cause of disability and a leading cause of death in the U.S. There are
SECTION: Adult General Medical Emergencies PROTOCOL TITLE: Medical Stroke/TIA REVISED: 07/2017 Protocol OVERVIEW: Stroke is a major cause of disability and a leading cause of death in the U.S. There are
11/2/2016. The Acute Phase of Cerebrovascular Accident. L. Michael Peterson, DO Medical Director HealthNet Aeromedical Services Charleston, WV
 The Acute Phase of Cerebrovascular Accident L. Michael Peterson, DO Medical Director HealthNet Aeromedical Services Charleston, WV 1 Faculty Disclosure Information 1. SPEAKER: L. Michael Peterson, D.O.
The Acute Phase of Cerebrovascular Accident L. Michael Peterson, DO Medical Director HealthNet Aeromedical Services Charleston, WV 1 Faculty Disclosure Information 1. SPEAKER: L. Michael Peterson, D.O.
Stroke 101. Maine Cardiovascular Health Summit. Eileen Hawkins, RN, MSN, CNRN Pen Bay Stroke Program Coordinator November 7, 2013
 Stroke 101 Maine Cardiovascular Health Summit Eileen Hawkins, RN, MSN, CNRN Pen Bay Stroke Program Coordinator November 7, 2013 Stroke Statistics Definition of stroke Risk factors Warning signs Treatment
Stroke 101 Maine Cardiovascular Health Summit Eileen Hawkins, RN, MSN, CNRN Pen Bay Stroke Program Coordinator November 7, 2013 Stroke Statistics Definition of stroke Risk factors Warning signs Treatment
911 Dispatch initiated! Stroke Assessment-!! Decreasing time to treatment at Stroke Centers
 911 Dispatch initiated! Stroke Assessment-!! Decreasing time to treatment at Stroke Centers David Miramontes MD FACEP NREMT Emily Kidd MD FACEP Office of the Medical Director Stroke Embolic Strokes are
911 Dispatch initiated! Stroke Assessment-!! Decreasing time to treatment at Stroke Centers David Miramontes MD FACEP NREMT Emily Kidd MD FACEP Office of the Medical Director Stroke Embolic Strokes are
911 Dispatch initiated Stroke Assessment- How to decrease time to treatment at Stroke Centers
 911 Dispatch initiated Stroke Assessment- How to decrease time to treatment at Stroke Centers David Miramontes MD FACEP NREMT Office of the Medical Director Conflicts of Interest Full Time Employee University
911 Dispatch initiated Stroke Assessment- How to decrease time to treatment at Stroke Centers David Miramontes MD FACEP NREMT Office of the Medical Director Conflicts of Interest Full Time Employee University
Hanna K. Al-Makhamreh, M.D., FACC Interventional Cardiologist
 Hanna K. Al-Makhamreh, M.D., FACC Interventional Cardiologist Introduction. Basic Life Support (BLS). Advanced Cardiac Life Support (ACLS). Cardiovascular diseases (CVDs) are the number one cause of death
Hanna K. Al-Makhamreh, M.D., FACC Interventional Cardiologist Introduction. Basic Life Support (BLS). Advanced Cardiac Life Support (ACLS). Cardiovascular diseases (CVDs) are the number one cause of death
Chapter 15. Neurologic Emergencies
 Chapter 15 Neurologic Emergencies Introduction (1 of 4) Stroke is the third leading cause of death in the United States. After heart disease and cancer It is common in geriatric patients. More men than
Chapter 15 Neurologic Emergencies Introduction (1 of 4) Stroke is the third leading cause of death in the United States. After heart disease and cancer It is common in geriatric patients. More men than
Despite availability of reperfusion therapy for treatment
 erceptual, Social, and Behavioral Factors Associated With Delays in Seeking Medical Care in atients With Symptoms of Acute Stroke Lori Mandelzweig, hd; Uri Goldbourt, hd; Valentina Boyko, MSc; David Tanne,
erceptual, Social, and Behavioral Factors Associated With Delays in Seeking Medical Care in atients With Symptoms of Acute Stroke Lori Mandelzweig, hd; Uri Goldbourt, hd; Valentina Boyko, MSc; David Tanne,
Stroke School for Internists Part 1
 Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
HOW TO HANDLE BASIC MEDICAL EMERGENCIES
 HOW TO HANDLE BASIC MEDICAL EMERGENCIES INTRODUCTION At some point in your career as a Certified Nursing Assistant (CNA) you may be the first person on the scene at a medical emergency. You may witness
HOW TO HANDLE BASIC MEDICAL EMERGENCIES INTRODUCTION At some point in your career as a Certified Nursing Assistant (CNA) you may be the first person on the scene at a medical emergency. You may witness
Statewide Acute Stroke Triage The Washington Story
 Statewide Acute Stroke Triage The Washington Story David Tirschwell, MD, MSc Medical Director of Comprehensive Stroke Care Professor, Department of Neurology UW Medicine Comprehensive Stroke Center at
Statewide Acute Stroke Triage The Washington Story David Tirschwell, MD, MSc Medical Director of Comprehensive Stroke Care Professor, Department of Neurology UW Medicine Comprehensive Stroke Center at
Diagnostic Accuracy of Stroke Referrals From Primary Care, Emergency Room Physicians, and Ambulance Staff Using the Face Arm Speech Test
 Diagnostic Accuracy of Stroke Referrals From Primary Care, Emergency Room Physicians, and Ambulance Staff Using the Face Arm Speech Test Joseph Harbison, MRCP; Omar Hossain, MRCP; Damian Jenkinson, FRCP;
Diagnostic Accuracy of Stroke Referrals From Primary Care, Emergency Room Physicians, and Ambulance Staff Using the Face Arm Speech Test Joseph Harbison, MRCP; Omar Hossain, MRCP; Damian Jenkinson, FRCP;
The Fainting Checklist
 Take Fainting to Heart There is no such thing as a simple faint The Fainting Checklist BMA Patient Information Awards www.stars-international.org Registered Charity No. 1084898 Registered Non-Profit 501(c)(3)
Take Fainting to Heart There is no such thing as a simple faint The Fainting Checklist BMA Patient Information Awards www.stars-international.org Registered Charity No. 1084898 Registered Non-Profit 501(c)(3)
Rural Minnesota STEMI Systems of Care
 CARDIOVASCULAR HEALTH UNIT Rural Minnesota STEMI Systems of Care Almost 250,000 Americans experience ST-elevation Myocardial Infarction (STEMI), the deadliest form of heart attack, each year. Of approximately
CARDIOVASCULAR HEALTH UNIT Rural Minnesota STEMI Systems of Care Almost 250,000 Americans experience ST-elevation Myocardial Infarction (STEMI), the deadliest form of heart attack, each year. Of approximately
Strokes , The Patient Education Institute, Inc. hp Last reviewed: 11/11/2017 1
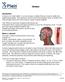 Strokes Introduction A stroke or a brain attack is a very serious condition that can result in death and significant disability. This disease is ranked as the third leading cause of death in the United
Strokes Introduction A stroke or a brain attack is a very serious condition that can result in death and significant disability. This disease is ranked as the third leading cause of death in the United
OHSU HEALTH CARE SYSTEM PRACTICE GUIDELINES
 OHSU HEALTH CARE SYSTEM NEUROSCIENCES (includes ischemic stroke, TIA, intracerebral hemorrhage and non-subarachnoid hemorrhage) Last Reviewed Date: September 2013 POLICY STATEMENT: OHSU hospitals and clinics
OHSU HEALTH CARE SYSTEM NEUROSCIENCES (includes ischemic stroke, TIA, intracerebral hemorrhage and non-subarachnoid hemorrhage) Last Reviewed Date: September 2013 POLICY STATEMENT: OHSU hospitals and clinics
Stroke Mimics. Atlantic Canada Stroke Conference. Dr Warren Fieldus FRCP
 Stroke Mimics Atlantic Canada Stroke Conference Dr Warren Fieldus FRCP No Conflicts of Interest the plan stroke or no stroke QEII Acute Stroke Protocol things to do before the CT common stroke mimics (25
Stroke Mimics Atlantic Canada Stroke Conference Dr Warren Fieldus FRCP No Conflicts of Interest the plan stroke or no stroke QEII Acute Stroke Protocol things to do before the CT common stroke mimics (25
EMS & Stroke NECC. Peter Moyer MD,MPH Medical Director Boston EMS, Fire and Police 9/13/06
 EMS & Stroke NECC Peter Moyer MD,MPH Medical Director Boston EMS, Fire and Police 9/13/06 No financial interests to disclose EMS key and underappreciated role in stroke Stroke recognition by stroke victim
EMS & Stroke NECC Peter Moyer MD,MPH Medical Director Boston EMS, Fire and Police 9/13/06 No financial interests to disclose EMS key and underappreciated role in stroke Stroke recognition by stroke victim
RECOGNISE AND REMOVE
 RECOGNISE AND REMOVE Remember the 4 R s of concussion management: RECOGNISE REMOVE RECOVER RETURN Identifying concussion is not always easy, and players may not exhibit the signs or symptoms immediately
RECOGNISE AND REMOVE Remember the 4 R s of concussion management: RECOGNISE REMOVE RECOVER RETURN Identifying concussion is not always easy, and players may not exhibit the signs or symptoms immediately
COUNTY OF SAN LUIS OBISPO HEALTH AGENCY. Jeff Hamm Health Agency Director Penny Borenstein, MD, MPH Health Officer/Public Health Director
 COUNTY OF SAN LUIS OBISPO HEALTH AGENCY PUBLIC HEALTH DEPARTMENT Jeff Hamm Health Agency Director Penny Borenstein, MD, MPH Health Officer/Public Health Director County of SLO Emergency Medical Services
COUNTY OF SAN LUIS OBISPO HEALTH AGENCY PUBLIC HEALTH DEPARTMENT Jeff Hamm Health Agency Director Penny Borenstein, MD, MPH Health Officer/Public Health Director County of SLO Emergency Medical Services
EPIDEMIOLOGY AND TREATMENT OF CARDIOVASCULAR EMERGENCIES IN URBAN VS. REMOTE AREAS
 EPIDEMIOLOGY AND TREATMENT OF CARDIOVASCULAR EMERGENCIES IN URBAN VS. REMOTE AREAS Andrea Semplicini Medicina Interna 1 Ospedale SS. Giovanni e Paolo - Venezia Azienda ULSS 12 Veneziana Dipartimento Medicina
EPIDEMIOLOGY AND TREATMENT OF CARDIOVASCULAR EMERGENCIES IN URBAN VS. REMOTE AREAS Andrea Semplicini Medicina Interna 1 Ospedale SS. Giovanni e Paolo - Venezia Azienda ULSS 12 Veneziana Dipartimento Medicina
CBT/OTEP 442 Stroke. Seattle-King County EMS. Print version of EMS Online Course
 Seattle-King County EMS Seattle-King County Emergency Medical Services Division Public Health - Seattle/King County 401 5th Avenue, Suite 1200 Seattle, WA 98104 (206) 296-4693 January 2009 (rev. 4/1/09)
Seattle-King County EMS Seattle-King County Emergency Medical Services Division Public Health - Seattle/King County 401 5th Avenue, Suite 1200 Seattle, WA 98104 (206) 296-4693 January 2009 (rev. 4/1/09)
ABNORMAL STROKE EXAM FINDINGS:
 Stroke Assessment Scenario Case Information PATIENT INFORMATION: 68-year-old male patient complaining of left sided weakness and an unsteady gait. Reported last normal time 3 minutes prior to EMS arrival
Stroke Assessment Scenario Case Information PATIENT INFORMATION: 68-year-old male patient complaining of left sided weakness and an unsteady gait. Reported last normal time 3 minutes prior to EMS arrival
List of Exhibits Adult Stroke
 List of Exhibits Adult Stroke List of Exhibits Adult Stroke i. Ontario Stroke Audit Hospital and Patient Characteristics Exhibit i. Hospital characteristics from the Ontario Stroke Audit, 200/ Exhibit
List of Exhibits Adult Stroke List of Exhibits Adult Stroke i. Ontario Stroke Audit Hospital and Patient Characteristics Exhibit i. Hospital characteristics from the Ontario Stroke Audit, 200/ Exhibit
Two Decades of Evidenced-based Outcomes Research: The Erlangen Stroke Registry
 Two Decades of Evidenced-based Outcomes Research: The Erlangen Stroke Registry 06.06.2017 Prof. Dr. Peter Kolominsky-Rabas, MD, PhD, MBA Interdisciplinary Center for Health Technology Assessment (HTA)
Two Decades of Evidenced-based Outcomes Research: The Erlangen Stroke Registry 06.06.2017 Prof. Dr. Peter Kolominsky-Rabas, MD, PhD, MBA Interdisciplinary Center for Health Technology Assessment (HTA)
Mini Research Paper: Traumatic Brain Injury. Allison M McGee. Salt Lake Community College
 Running Head: Mini Research Paper: Traumatic Brain Injury Mini Research Paper: Traumatic Brain Injury Allison M McGee Salt Lake Community College Abstract A Traumatic Brain Injury (also known as a TBI)
Running Head: Mini Research Paper: Traumatic Brain Injury Mini Research Paper: Traumatic Brain Injury Allison M McGee Salt Lake Community College Abstract A Traumatic Brain Injury (also known as a TBI)
3. Screening Subject Identification Screening Overview
 3. Screening 3.1 Subject Identification Each site will be responsible for identifying and recruiting participants into the study. It is known that screening methods vary across sites. It is, however, important
3. Screening 3.1 Subject Identification Each site will be responsible for identifying and recruiting participants into the study. It is known that screening methods vary across sites. It is, however, important
Updated tpa Guidelines: Expanding the opportunity for good outcomes. Benjamin Morrow, MSN RN UPMC Stroke Institute
 Updated tpa Guidelines: Expanding the opportunity for good outcomes Benjamin Morrow, MSN RN UPMC Stroke Institute 1 Outline History Current State Review Exclusions: Minor stroke symptoms Severe strokes
Updated tpa Guidelines: Expanding the opportunity for good outcomes Benjamin Morrow, MSN RN UPMC Stroke Institute 1 Outline History Current State Review Exclusions: Minor stroke symptoms Severe strokes
Time to Hospital Evaluation in Patients of Acute Stroke for Alteplase Therapy
 1 Original Article Time to Hospital Evaluation in Patients of Acute Stroke for Alteplase Therapy Asad Mahmood,* Muhammad Ashraf Sharif,** Umar Zafar Ali,* Muhammad Naeem Khan* From *Military Hospital (MH),
1 Original Article Time to Hospital Evaluation in Patients of Acute Stroke for Alteplase Therapy Asad Mahmood,* Muhammad Ashraf Sharif,** Umar Zafar Ali,* Muhammad Naeem Khan* From *Military Hospital (MH),
Urgent and Emergency Care Clinical Audit Toolkit
 Urgent and Emergency Care Clinical Audit Toolkit The Care UK Out of Hours service in the East of England uses various tools to ensure quality This includes the use of Clinical Audit This audit toolkit
Urgent and Emergency Care Clinical Audit Toolkit The Care UK Out of Hours service in the East of England uses various tools to ensure quality This includes the use of Clinical Audit This audit toolkit
Thrombolytic therapy can improve neurological outcomes
 Prehospital Notification by Emergency Medical Services Reduces Delays in Stroke Evaluation Findings From the North Carolina Stroke Care Collaborative Mehul D. Patel, MSPH; Kathryn M. Rose, PhD; Emily C.
Prehospital Notification by Emergency Medical Services Reduces Delays in Stroke Evaluation Findings From the North Carolina Stroke Care Collaborative Mehul D. Patel, MSPH; Kathryn M. Rose, PhD; Emily C.
REGIONAL STROKE TRIAGE PLAN
 REGIONAL STROKE TRIAGE PLAN Rappahannock EMS Council 435 Hunter Street Fredericksburg, VA 22401 Phone: (540) 373-0249 Fax: (540) 373-0249 E-mail: rems@vaems.org www.remscouncil.org Board of Directors Approved:
REGIONAL STROKE TRIAGE PLAN Rappahannock EMS Council 435 Hunter Street Fredericksburg, VA 22401 Phone: (540) 373-0249 Fax: (540) 373-0249 E-mail: rems@vaems.org www.remscouncil.org Board of Directors Approved:
Informant Interview Form Instructions (IFI) Version C 05/05/2014
 Informant Interview Form Instructions (IFI) Version C 05/05/2014 I. GENERAL INSTRUCTIONS The purpose of the informant interview is to obtain information about possible CHD events in order to classify cause
Informant Interview Form Instructions (IFI) Version C 05/05/2014 I. GENERAL INSTRUCTIONS The purpose of the informant interview is to obtain information about possible CHD events in order to classify cause
Seizures. What is a seizure? How does it occur?
 Seizures What is a seizure? A seizure is a symptom, not a disease. It happens when nerve cells in the brain function abnormally and there is a sudden abnormal electrical signal in the brain. The seizure
Seizures What is a seizure? A seizure is a symptom, not a disease. It happens when nerve cells in the brain function abnormally and there is a sudden abnormal electrical signal in the brain. The seizure
Understanding Inpatient and Outpatient Observation Status Determination. Focusing on Chest Pain, TIAs, Syncope and Dizziness
 Understanding Inpatient and Outpatient Observation Status Determination Focusing on Chest Pain, TIAs, Syncope and Dizziness Medicare Compliance Inpatient Admissions & Outpatient Observation Monitoring
Understanding Inpatient and Outpatient Observation Status Determination Focusing on Chest Pain, TIAs, Syncope and Dizziness Medicare Compliance Inpatient Admissions & Outpatient Observation Monitoring
Stroke: The First Critical Hour. Alina Candal, RN, PCC, MICN Kevin Andruss, MD, FACEP
 Stroke: The First Critical Hour Alina Candal, RN, PCC, MICN Kevin Andruss, MD, FACEP Disclosures We have no actual or potential conflicts of interest in relation to this presentation. Objectives Discuss
Stroke: The First Critical Hour Alina Candal, RN, PCC, MICN Kevin Andruss, MD, FACEP Disclosures We have no actual or potential conflicts of interest in relation to this presentation. Objectives Discuss
THE FRAMINGHAM STUDY Protocol for data set vr_soe_2009_m_0522 CRITERIA FOR EVENTS. 1. Cardiovascular Disease
 THE FRAMINGHAM STUDY Protocol for data set vr_soe_2009_m_0522 CRITERIA FOR EVENTS 1. Cardiovascular Disease Cardiovascular disease is considered to have developed if there was a definite manifestation
THE FRAMINGHAM STUDY Protocol for data set vr_soe_2009_m_0522 CRITERIA FOR EVENTS 1. Cardiovascular Disease Cardiovascular disease is considered to have developed if there was a definite manifestation
Emergency Care 3/9/15. Multimedia Directory. Topics. Emergency Care for Behavioral and. Psychiatric Emergencies CHAPTER
 Emergency Care THIRTEENTH EDITION CHAPTER 23 Behavioral and Psychiatric Emergencies and Suicide Multimedia Directory Slide 42 Applications of Mechanical Restraints Video Topics Behavioral and Psychiatric
Emergency Care THIRTEENTH EDITION CHAPTER 23 Behavioral and Psychiatric Emergencies and Suicide Multimedia Directory Slide 42 Applications of Mechanical Restraints Video Topics Behavioral and Psychiatric
HeartRescue Global Policy Brief STEMI: ST-segment elevation myocardial infarction. HeartRescue Global MEDTRONIC FOUNDATION
 HeartRescue Global Policy Brief STEMI: ST-segment elevation myocardial infarction HeartRescue Global MEDTRONIC FOUNDATION STEMI, or ST Segment Elevation Myocardial Infarction, is one form of cardiovascular
HeartRescue Global Policy Brief STEMI: ST-segment elevation myocardial infarction HeartRescue Global MEDTRONIC FOUNDATION STEMI, or ST Segment Elevation Myocardial Infarction, is one form of cardiovascular
Chapter 15 Neurological Emergencies Stroke (1 of 2) Stroke (2 of 2) Seizures Altered Mental Status (AMS) Brain Structure and Function
 1 Chapter 15 Neurological Emergencies 2 Stroke (1 of 2) Stroke is the leading cause of death in the United States. After heart disease and cancer It is common in geriatric patients. More than women have
1 Chapter 15 Neurological Emergencies 2 Stroke (1 of 2) Stroke is the leading cause of death in the United States. After heart disease and cancer It is common in geriatric patients. More than women have
Helicopter Transport of Stroke Patients and Its Influence on Thrombolysis Rates Data From the Austrian Stroke Unit Registry
 Helicopter Transport of Stroke Patients and Its Influence on Thrombolysis Rates Data From the Austrian Stroke Unit Registry Veronika Reiner-Deitemyer, MD; Yvonne Teuschl, PhD; Karl Matz, MD; Martina Reiter,
Helicopter Transport of Stroke Patients and Its Influence on Thrombolysis Rates Data From the Austrian Stroke Unit Registry Veronika Reiner-Deitemyer, MD; Yvonne Teuschl, PhD; Karl Matz, MD; Martina Reiter,
Chapter 15 Neurological Emergencies Stroke (1 of 2) Stroke (2 of 2) Seizures Altered Mental Status (AMS)
 1 2 3 4 5 Chapter 15 Neurological Emergencies Stroke (1 of 2) Stroke is the leading cause of death in the United States. After heart disease and cancer It is common in geriatric patients. More than women
1 2 3 4 5 Chapter 15 Neurological Emergencies Stroke (1 of 2) Stroke is the leading cause of death in the United States. After heart disease and cancer It is common in geriatric patients. More than women
P1: OTA/XYZ P2: ABC c01 BLBK231-Ginsberg December 23, :43 Printer Name: Yet to Come. Part 1. The Neurological Approach COPYRIGHTED MATERIAL
 Part 1 The Neurological Approach COPYRIGHTED MATERIAL 1 2 Chapter 1 Neurological history-taking The diagnosis and management of diseases of the nervous system have been revolutionized in recent years by
Part 1 The Neurological Approach COPYRIGHTED MATERIAL 1 2 Chapter 1 Neurological history-taking The diagnosis and management of diseases of the nervous system have been revolutionized in recent years by
What Is A Concussion?
 What Is A Concussion? A concussion is a brain injury, and all brain injuries are serious. Concussions can range from mild to severe, and they can change the way your brain normally functions. Symptoms
What Is A Concussion? A concussion is a brain injury, and all brain injuries are serious. Concussions can range from mild to severe, and they can change the way your brain normally functions. Symptoms
Alan Barber. Professor of Clinical Neurology University of Auckland
 Alan Barber Professor of Clinical Neurology University of Auckland Presented with L numbness & slurred speech 2 episodes; 10 mins & 2 hrs Hypertension Type II DM Examination P 80/min reg, BP 160/95, normal
Alan Barber Professor of Clinical Neurology University of Auckland Presented with L numbness & slurred speech 2 episodes; 10 mins & 2 hrs Hypertension Type II DM Examination P 80/min reg, BP 160/95, normal
Vascular Disorders. Nervous System Disorders (Part B-1) Module 8 -Chapter 14. Cerebrovascular disease S/S 1/9/2013
 Nervous System Disorders (Part B-1) Module 8 -Chapter 14 Overview ACUTE NEUROLOGIC DISORDERS Vascular Disorders Infections/Inflammation/Toxins Metabolic, Endocrinologic, Nutritional, Toxic Neoplastic Traumatic
Nervous System Disorders (Part B-1) Module 8 -Chapter 14 Overview ACUTE NEUROLOGIC DISORDERS Vascular Disorders Infections/Inflammation/Toxins Metabolic, Endocrinologic, Nutritional, Toxic Neoplastic Traumatic
Monthly Safety Meeting. 25 September 2014 Please sign roster
 Monthly Safety Meeting 25 September 2014 Please sign roster Before we begin Please sign the safety meeting roster Used to log safety currency in eservices Safety currency necessary for participation in
Monthly Safety Meeting 25 September 2014 Please sign roster Before we begin Please sign the safety meeting roster Used to log safety currency in eservices Safety currency necessary for participation in
2017 AYL Emergency Action Plan
 2017 AYL Emergency Action Plan The purpose of this document is to provide instructions to athletic trainers, coaches, and parents in the event of a medical emergency regarding Arizona Youth Lacrosse (AYL)
2017 AYL Emergency Action Plan The purpose of this document is to provide instructions to athletic trainers, coaches, and parents in the event of a medical emergency regarding Arizona Youth Lacrosse (AYL)
Team Work in Treatment of Acute Ischemic Stroke
 Diagnosis and Treatment in Acute Ischemic stroke July, 15 th 2016. Bach Mai Hospital Team Work in Treatment of Acute Ischemic Stroke Prof. Pham Minh Thong 1 Time is brain Ischemic stroke: big global burden
Diagnosis and Treatment in Acute Ischemic stroke July, 15 th 2016. Bach Mai Hospital Team Work in Treatment of Acute Ischemic Stroke Prof. Pham Minh Thong 1 Time is brain Ischemic stroke: big global burden
Critical Review Form Therapy
 Critical Review Form Therapy A transient ischaemic attack clinic with round-the-clock access (SOS-TIA): feasibility and effects, Lancet-Neurology 2007; 6: 953-960 Objectives: To evaluate the effect of
Critical Review Form Therapy A transient ischaemic attack clinic with round-the-clock access (SOS-TIA): feasibility and effects, Lancet-Neurology 2007; 6: 953-960 Objectives: To evaluate the effect of
QUESTION EXAMPLES ECG
 ACEM Fellowship VAQ Examination QUESTION EXAMPLES ECG ECG 1: A 16 year old boy with a congenital heart problem presents to your ED with syncopal episodes. An ECG is taken. Describe and interpret his ECG
ACEM Fellowship VAQ Examination QUESTION EXAMPLES ECG ECG 1: A 16 year old boy with a congenital heart problem presents to your ED with syncopal episodes. An ECG is taken. Describe and interpret his ECG
TENNESSEE STROKE REGISTRY QUARTERLY REPORT
 TENNESSEE STROKE REGISTRY QUARTERLY REPORT Volume 1, Issue 3 September 2018 This report is published quarterly using data from the Tennessee Stroke Registry. Inside this report Data on diagnosis, gender
TENNESSEE STROKE REGISTRY QUARTERLY REPORT Volume 1, Issue 3 September 2018 This report is published quarterly using data from the Tennessee Stroke Registry. Inside this report Data on diagnosis, gender
STROKE TRAINING FOR EMS PROFESSIONALS
 1 STROKE TRAINING FOR EMS PROFESSIONALS COURSE OBJECTIVES About Stroke Stroke Policy Recommendations Stroke Protocols and Stroke Hospital Care Stroke Assessment Tools Pre-Notification Stroke Treatment
1 STROKE TRAINING FOR EMS PROFESSIONALS COURSE OBJECTIVES About Stroke Stroke Policy Recommendations Stroke Protocols and Stroke Hospital Care Stroke Assessment Tools Pre-Notification Stroke Treatment
TIA Transient Ischaemic Attack?
 TIA Transient Ischaemic Attack? OR Transient loss of function (TLOF) Tal Anjum Consultant Stroke Physician, Morriston Hospital Training & education lead, WASP (Welsh Association of Stroke Physicians) Qs.
TIA Transient Ischaemic Attack? OR Transient loss of function (TLOF) Tal Anjum Consultant Stroke Physician, Morriston Hospital Training & education lead, WASP (Welsh Association of Stroke Physicians) Qs.
