Association of 24 h systolic blood pressure variability and cardiovascular disease in patients with obstructive sleep apnea
|
|
|
- Willis Gregory
- 6 years ago
- Views:
Transcription
1 Ke et al. BMC Cardiovascular Disorders (2017) 17:287 DOI /s y RESEARCH ARTICLE Open Access Association of 24 h systolic blood pressure variability and cardiovascular disease in patients with obstructive sleep apnea Xiao Ke 1, Yan Sun 2, Rongfeng Yang 1, Jiawen Liang 3, Shaoyun Wu 3, Chengheng Hu 3* and Xing Wang 3* Abstract Background: To evaluate association of 24 h systolic blood pressure (SBP) variability and obstructive sleep apnea (OSA) as defined by the apnea-hypopnea index 5/h; and association of 24 h SBP variability and prevalent cardiovascular disease (CVD) in OSA patients. Methods: Participants underwent polysomongraphy to evaluate the presence of OSA, and 24 h ambulatory blood pressure monitoring was applied to evaluate 24 h SBP variability as indexed by weighted 24 h standard deviation (SD) of SBP. Between-group differences were evaluated in participants with and without OSA. Participants with OSA were divided into high and low 24 h SBP variability groups and between-group differences were evaluated. Results: Mean age of 384 participants was 50 years old and 42.2% had OSA. Mean 24 h systolic/diastolic BP were 130/78 mmhg, with mean weighted 24 h SD of systolic/diastolic BP were 12.9/7.3 mmhg. Compared to those without OSA, OSA participants had higher clinic-, 24 h-, daytime- and nighttime-sbp, and weighted 24 h, daytime- and nighttime-sd of SBP. Age, prevalent CVD and OSA, usage of angiotensin converting enzyme inhibitor/ angiotensin receptor blocker, calcium channel blocker and diuretic were significantly associated with 24 h SBP variability. In OSA patients, compared to those with low variability, participants with high variability had higher weighted 24 h, daytime- and nighttime-sd of SBP. After adjusted for covariates including clinic-sbp and 24 h SBP, per 1-SD increment weighted 24 h SD of SBP was associated with 21% increased prevalent CVD. Conclusions: Patients with newly-diagnosed OSA have higher 24 h SBP variability compared to those without OSA; in OSA patients, increased 24 h SBP variability is associated with increased prevalence of CVD. Keywords: Obstructive sleep apnea, Blood pressure variability, Cardiovascular diseases Background Hypertension is a well-known risk factor for cardiovascular diseases (CVD) and all-cause mortality [1, 2]. Most previous clinical trials used systolic blood pressure (SBP) as the therapeutic target and showed that decreasing SBP was beneficial for improving cardiovascular outcomes [3, 4]. After the publication of the SPRINT trial [5], the optimal SBP target for patients with hypertension has once again underwent intensive debate. Notably, BP is featured by high variability whereby the therapeutic BP target is debatable [6]. Importantly, prior observational studies and meta-analysis indicate * Correspondence: huchengheng138@163.com; @163.com Equal contributors 3 Department of Cardiology, The First Affiliated Hospital of Sun Yat-sen University, 58 Zhongshan Road 2, Guangzhou , China Full list of author information is available at the end of the article that other than SBP level, SBP variability was also independently associated with cardiovascular outcomes [7 10]. Obstructive sleep apnea (OSA) is another major risk factor for CVD and cardiovascular mortality [11, 12]. In addition, prior prospective cohort studies demonstrate that patients with OSA have an increased incidence of hypertension compared to those without OSA [13, 14]. The underlying mechanisms are multifactorial including endothelial dysfunction, increased sympathetic output and arterial stiffness [15]. Notably, these pathological alterations are also associated with BP variability. Therefore, one may anticipate that OSA patients may have higher BP variability compared those without OSA; in addition, regarding the association of SBP variability and CVD, it may be possible that OSA patients with high The Author(s) Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
2 Ke et al. BMC Cardiovascular Disorders (2017) 17:287 Page 2 of 6 SBP variability may have higher prevalence of CVD compared to their OSA counterparts with low SBP variability. Nevertheless, up till now, few studies have investigated these aspects in patients with OSA. Therefore, using a cross-sectional design, we plans to evaluate whether OSA is independently associated with 24 h SBP variability; in addition, in patients with OSA, whether 24 h SBP variability is associated with prevalence of CVD. Methods Participants enrolment Written informed consents were obtained from studied participants before recruitment and current study was approved by the Research Ethic Committee of Shenzhen Sun Yat-sen Cardiovascular Hospital. All participants were treated in accordance to the Declaration of Helsinki. Included criteria were as follows: participants who have documented essential hypertension and agreed to have polysomnography (PSG) evaluation. Excluded criteria were as follows: those who have a diagnosis OSA before or already have been treated with continuous positive airway pressure (CPAP), have documented diabetes mellitus and chronic kidney disease, and have ischemic stroke, myocardial infarction, or congestive heart failure in the past 12 months. Data collection Demographic and clinical data including age, gender, smoking status, previous medical history and current medications usage were collected by using selfadministered questionnaire with the help of investigators; anthropometric data including body mass index (BMI, calculated by weight in kilograms divided by height in squared meters), systolic/diastolic BP (SBP/ DBP) and heart rate at rest were measured (HEM7200, Omron Healthcare, Tokyo, Japan) by investigators in accordance to the guideline recommendation [16]. In brief, BP was measured 3 times and the last two BP readings were averaged for the clinic-sbp/dbp. Overnight fasting venous blood was drawn for serum fasting plasma glucose (FPG), lipid profiles, high-sensitivity C-reactive protein (Hs-CRP) and creatinine (Cr) measurements. Cardiovascular disease included coronary heart disease (CHD) which was diagnosed based on clinical symptoms and coronary angiography or computer tomography with contrast, and ischemic stroke which was diagnosed based on clinical symptoms and signs and computer tomography or magnetic resonance imaging, and transient ischemic attack were excluded. Variability of BP evaluation Variability of 24 h SBP were assessed using 24 h ambulatory blood pressure monitoring (24 h ABPM, The Spacelabs 90,217, Spacelabs Inc., Redmond, Wash), which was conducted in accordance to the European Society Hypertension practice guideline for ABPM [17]. Daytime and nighttime intervals were determined using sleep time reported by patients, and at least 20 valid awake and 7 valid asleep measurements should be recorded. The weighted standard deviation (SD) of 24 h SBP was used as the variability of 24-SBP. OSA evaluation OSA evaluation was performed using PSG (Philips) and those with central sleep apnea were excluded. According to the AASM guideline [18], airflow total blockage for >10 s, or >50% reduction in respiratory airflow with >3% reduction in saturation of arterial oxygen (SaO 2 ) for >10 s is defined as apnea or hypopnea events, and the apnea-hypopnea index (AHI) is calculated by the total number of apnea and hypopnea events per sleep hour, with AHI 5 events/h was diagnosed as OSA [18]. Statistical analysis Continuous variables were expressed as mean ± SD and between-group differences were evaluated by the independent Student t test. Categorical variables were expressed as number and frequency of cases, and between-group differences were assessed by the Chi-square analysis or Fisher exact test. Association of weighted 24 h SD of SBP and parameters of interest were evaluated using the linear regression analysis. Logistic regression analysis was applied to evaluate the association of weighted 24 h SD of SBP and prevalent CVD. Statistical analysis was conducted by the SPSS 17.0 software (SPSS Inc., Chicago, USA). Results General characteristics From June of 2016 to June of 2017, a total of 393 participants were enrolled from outpatient clinic. Among them, 5 patients could not finish 24 h ABPM and 4 patients subsequently diagnosed as central sleep apnea were excluded, therefore, 384 participants were included into final analysis. No significant differences in clinical characteristics between the excluded patients and included participants were observed. Overall, the mean age was 50 years old and male participants accounted for 64.1%. The mean AHI was 8.3 events/h and 42.2% of participants were diagnosed as OSA. The mean clinic- SBP/DBP were 141/86 mmhg, and the mean 24 h SBP/ DBP were 130/78 mmhg, with mean weighted 24 h SD of SBP/DBP were 12.9/7.3 mmhg. Clinical characteristics comparisons between participants with and without OSA As shown in the Table 1, the mean age of OSA patients was 53 years old, male participants accounted for 65.4%,
3 Ke et al. BMC Cardiovascular Disorders (2017) 17:287 Page 3 of 6 Table 1 Characteristics comparison between participants with and without OSA Variables Without OSA (n = 222) OSA (n = 162) Age (years) 47 ± ± 15* Male, n (%) 140 (63.1) 106 (65.4) BMI (kg/m 2 ) 23.3 ± ± 6.8* Current smoking, n (%) 78 (35.1) 78 (48.1) # Clinic-SBP (mm Hg) 139 ± ± 18* Clinic-DBP (mm Hg) 85 ± 9 86 ± 10 Clinic-HR (bpm) 75 ± ± 12 FPG (mmol/l) 5.6 ± ± 0.6 TC (mmol/l) 5.0 ± ± 0.5 TG (mmol/l) 1.8 ± ± 0.8 HDL-C (mmol/l) 1.0 ± ± 0.4 LDL-C (mmol/l) 3.2 ± ± 0.6 Cr (umol/l) 74.9 ± ± 13.6 Hs-CRP (mg/dl) 7.2 ± ± 4.8* AHI (events/h) 3.4 ± ± 6.2 # CVD, n (%) 79 (35.6) 66 (40.7)* Anti-platelet agent, n (%) 98 (44.1) 68 (42.0) Statins, n (%) 79 (35.6) 59 (36.4) ACEI/ARB, n (%) 160 (72.1) 119 (73.5) CCB, n (%) 42 (18.9) 33 (20.4) Diuretic, n (%) 70 (31.5) 52 (32.1) Beta-blocker, n (%) 43 (19.4) 37 (22.8) Alpha-blocker, n (%) 12 (5.4) 10 (6.2) Anti-HTN medications number 1.7 ± ± 0.8* BMI = body mass index; SBP/DBP = systolic/diastolic blood pressure; HR = heart rate; bpm = beat per minute; FPG = fasting plasma glucose; TC = total cholesterol; TG = triglyceride; HDL-C = high density lipoprotein-cholesterol; LDL-C = low density lipoprotein-cholesterol; Cr = creatinine; Hs-CRP = high sensitivity C-reactive protein; SD = standard deviation; AHI = apnea hypopnea index; OSA = obstructive sleep apnea; CVD = cardiovascular disease; ACEI/ARB = angiotensin converting enzyme inhibitor/angiotensin receptor blocker; CCB = calcium channel blocker; *P < 0.05 and # P < 0.01 vs without OSA group 48.1% were current cigarette smokers, 40.7% had prevalent CVD and the mean number of anti-hypertensive medications was 2.5. Compared to those without OSA, participants with OSA were more elderly, had higher BMI, proportion of smokers and serum Hs-CRP level, and also had higher prevalence of CVD. The mean number of antihypertensive medications and clinic-sbp (143 ± 18 mmhg vs 139 ± 15 mmhg) were also significantly higher. 24 h BP parameters comparisons between participants with and without OSA As presented in the Table 2, compared to those without OSA, participants with OSA had significantly higher 24 h SBP (134 ± 14 mmhg vs 128 ± 12 mmhg) and weighted 24 h SD of SBP (14.2 ± 4.6 mmhg vs 10.3 ± 3.1 mmhg). In addition, the daytime and nighttime SBP, Table 2 24 h BP parameters comparisons between participants with and without OSA Variables Without OSA (n = 222) OSA (n = 162) 24 h SBP (mm Hg) 128 ± ± 14* 24 h DBP (mm Hg) 76 ± 9 79 ± h HR (beat per minute) 71 ± ± 9 Weighted 24 h SD of SBP (mm Hg) 10.3 ± ± 4.6* Weighted 24 h SD of DBP (mm Hg) 6.8 ± ± 2.0 Daytime-SBP (mm Hg) 133 ± ± 16* Daytime-DBP (mm Hg) 80 ± ± 12 Daytime-HR (beat per minute) 77 ± ± 14 Weighted daytime-sd of SBP (mm Hg) 12.5 ± ± 4.9* Weighted daytime-sd of DBP (mm Hg) 7.7 ± ± 2.5 Nighttime-SBP (mm Hg) 122 ± ± 12* Nighttime-DBP (mm Hg) 71 ± 7 74 ± 9 Nighttime-HR (beat per minute) 65 ± 8 66 ± 8 Weighted nighttime-sd of SBP (mm Hg) 9.1 ± ± 2.5* Weighted nighttime-sd of DBP (mm Hg) 6.1 ± ± 1.8 *P < 0.05 vs without OSA group; SD = standard deviation; SBP/DBP = systolic/ diastolic blood pressure; HR = heart rate; bpm = beat per minute weighted daytime- and nighttime-sd of SBP were also significantly higher in OSA group versus without OSA group. No statistical significances in parameters of DBP were observed. Association of weighted 24 h SD of SBP and parameters of interest Linear regression analysis was applied to evaluate whether the presence of OSA and other parameters of interest were independently associated with 24 h SBP variability. As presented in the Table 3, age, presence of CHD and Table 3 Association of weighted 24 h SD of SBP and parameters of interest Independent variables Coefficient SE P value Age (years) <0.05 Male (vs female) NS BMI (kg/m 2 ) NS Smoking (yes vs no) NS Hs-CRP (mg/dl) NS CVD (yes vs no) <0.05 ACEI/ARB (yes vs no) <0.05 CCB (yes vs no) <0.05 Diuretic (yes vs no) <0.05 Beta-blocker (yes vs no) NS Alpha-blocker (yes vs no) NS OSA (yes vs no) <0.05 Abbreviation is the same as the Table 1; NS = non-significant
4 Ke et al. BMC Cardiovascular Disorders (2017) 17:287 Page 4 of 6 OSA, and usage of angiotensin converting enzyme inhibitor/angiotensin receptor blocker (ACEI/ARB) were positively associated with weighted 24 h SD of SBP; and usage of calcium channel blocker (CCB) and diuretic were negatively associated with weighted 24 h SD of SBP. Comparisons between high and low variability of 24 h SBP groups in participants with OSA Participants with OSA were separated into two groups based on the median value of weighted 24 h SD of SBP, and as presented in the Table 4, compared to the low variability group, participants in the high variability group were more elderly, had higher mean 24 h-, daytime- and nighttime-sbp, and mean weighted 24 h, daytime- and nighttime-sd of SBP (P < 0.05 for all comparisons). The mean AHI (13.8 ± 7.6 vs 9.9 ± 4.5) was also significantly different. In addition, the prevalence of CVD and the proportion of participants using ACEI/ ARB were also significantly higher in the high versus low variability groups. Association between weighted 24 h SD of SBP and CVD in OSA patients Logistic regression analysis was applied to evaluate the association between weighted 24 h SD of SBP and composite CVD in OSA patients. As presented in the Table 5, in the unadjusted model, per 1-SD increment 24 h SD of SBP was associated with nearly 2-fold increased prevalence of CVD, and after gradually adjusted for potential covariates, per 1-SD increment in weighted 24 h SD of SBP remained associated with 21% increased prevalence of CVD even after adjusted for clinic-sbp and 24 h SBP. In addition, the association of weighted 24 h SD of SBP and prevalent CVD in non-osa patients was also evaluated and no statistical significance was observed after adjusted for 24 h SBP (odds ratio 1.05, and 95% confidence interval , P = 0.127). Discussion The principal findings of our current study include: first, patients with newly diagnosed OSA have higher 24 h SBP variability compared to those without OSA, and the potential determinants of 24 h SBP variability includes age, prevalent CVD and OSA, usage of ACEI/ARB, CCB and diuretic; second, in patients with OSA, higher 24 h SBP variability is associated with higher prevalence of CVD, even after adjusted for traditional risk factors including clinic-sbp and 24 h SBP. In recent years, numerous observational studies and meta-analysis have consistently showed that increased SBP variability was associated with cardiovascular events. For example, Ohkuma et al. [8] conducted a post-hoc analysis of the ADVANCE trial, and they found that in patients with diabetes mellitus, visit-to-visit Table 4 Comparisons between high and low variability of 24 h SBP groups in participants with OSA Variables Low variability (n = 81) High variability (n = 81) Age (years) 50 ± ± 16* Male, n (%) 52 (64.2) 54 (66.4) BMI (kg/m 2 ) 27.3 ± ± 6.9 Current smoking, n (%) 38 (46.9) 40 (49.4) Clinic-SBP (mm Hg) 142 ± ± 18 Clinic-DBP (mm Hg) 85 ± ± 10 Clinic-HR (bpm) 78 ± 9 79 ± 13 FPG (mmol/l) 5.5 ± ± 0.4 TC (mmol/l) 5.1 ± ± 0.4 TG (mmol/l) 1.8 ± ± 0.8 HDL-C (mmol/l) 1.1 ± ± 0.4 LDL-C (mmol/l) 3.4 ± ± 0.6 Cr (umol/l) 70.6 ± ± 13.9 Hs-CRP (mg/dl) 8.8 ± ± h SBP (mm Hg) 132 ± ± 15* 24 h DBP (mm Hg) 78 ± ± HR (beat per minute) 72 ± ± 13 Weighted 24 h SD of SBP (mm Hg) 12.6 ± ± 4.9* Weighted 24 h SD of DBP (mm Hg) 7.4 ± ± 2.2 Daytime-SBP (mm Hg) 137 ± ± 18* Daytime-DBP (mm Hg) 81 ± ± 14 Daytime-HR (beat per minute) 77 ± ± 15 Weighted daytime-sd of SBP (mm Hg) 14.7 ± ± 5.2* Weighted daytime-sd of DBP (mm Hg) 8.1 ± ± 2.3 Nighttime-SBP (mm Hg) 128 ± ± 14* Nighttime-DBP (mm Hg) 73 ± 6 77 ± 8 Nighttime-HR (beat per minute) 64 ± 7 68 ± 9 Weighted nighttime-sd of SBP (mm Hg) 10.8 ± ± 2.1* Weighted nighttime-sd of DBP (mm Hg) 6.5 ± ± 1.3 AHI (events/h) 9.9 ± ± 7.6* CVD, n (%) 31 (38.3) 35 (43.2)* Anti-platelet agent, n (%) 34 (42.0) 34 (42.0) Statins, n (%) 29 (35.8) 30 (37.0) ACEI/ARB, n (%) 58 (71.6) 61 (75.3)* CCB, n (%) 17 (21.0) 16 (19.8) Diuretic, n (%) 26 (32.1) 26 (32.1) Beta-blocker, n (%) 18 (22.2) 37 (23.5) Alpha-blocker, n (%) 5 (6.2) 5 (6.2) Anti-HTN medications number 2.3 ± ± 0.9 Abbreviation is the same as the Table 1; *P < 0.05 vs low variability group variability in SBP predicted cardiovascular events and mortality; in addition, addition of visit-to-visit variability in SBP improved predictive value of traditional CVD risk model. Okada et al. [9] reported that high visit-to-visit
5 Ke et al. BMC Cardiovascular Disorders (2017) 17:287 Page 5 of 6 Table 5 Association of weighted 24 h SD of SBP and prevalent CVD in OSA patients OR and 95% CI P value Unadjusted 1.97 ( ) <0.001 Model ( ) Model ( ) Model ( ) OR = odds ratio; CI = confidence interval; model 1 = adjusted for age and male gender; model 2 = model 1 + further adjusted for smoking, body mass index, fasting plasma glucose, total cholesterol, high-sensitivity C-reactive protein, apnea-hypopnea index and clinic-sbp; model 3 = model 1+ model 2 + further adjusted for 24 h SBP variability in BP was associated with cardiac diastolic dysfunction and carotid atherosclerosis. In a cohort study, Muntner et al. [7] observed that higher visit-tovisit BP variability predicted CVD and mortality. In a systemic review and meta-analysis [10], Diaz et al. reported that for each 5 mmhg increased SD of SBP was associated with 17%, 27%, 20% and 22% of higher risk of stroke, CHD, cardiovascular mortality and all-cause mortality. Consistent to previous reports, our current study also showed that higher SBP variability as assessed by 24 h ABPM was independently associated with prevalence of CVD even after adjusted for traditional risk factors including age, male gender, smoking, total cholesterol, clinic-sbp and 24 h SBP. However, compared to prior studies, our current study enrolled participants with newly-diagnosed OSA, in whom haven t been sufficiently evaluated before. In addition, prior studies used visit-to-visit variability in SBP, and our current study used 24 h SBP variability as assessed by 24 h ABPM which provided novel insights into the association of variability of 24 h SBP and prevalence of CVD in patients with OSA. Interestingly and importantly, as anticipated, we observed that patients with newly-diagnosed OSA, compared to those without OSA, had significantly higher 24 h- SBP variability. As we have already mentioned before that patients with OSA commonly have increased sympathetic nerve output, potential endothelial dysfunction and arterial stiffness which together render them at increased probability of short-term and long-term BP fluctuation. In addition, we also observed that in the linear regression analysis, age, presence of CVD and OSA and usage of ACEI/ARB were potential determinants of BP fluctuation. Notably, aging, presence of CVD and OSA are all independently associated with arterial stiffness and endothelial dysfunction, which in turn may cause BP fluctuation. Consistent to prior reports [19 22], we also observed that usage of ACEI/ARB seemed to increase BP variability while CCB and diuretic tended to decrease BP variability. The underlying mechanisms are still unclear yet. However, the data from our current study indicate that in OSA patients with hypertension, it is clinically relevant to monitor and compare BP variability with different classics of anti-hypertensive medications. There are several limitations of our current study. First of all, the inherent limitation in terms of cross-sectional design could not allow us to draw causal relationship; however, our current study provides novel insight into the association of 24 h SBP variability and prevalence of CVD in patients with OSA; second, in contrast to using visit-to-visit variability in clinic or home BP, we used 24 h ABPM to evaluate the 24 h SBP variability and therefore, the findings from our current study should not extrapolated to those using visit-to-visit variability in home or clinic BP. Last but not least, participants enrolled in our current study were all newly-diagnosed OSA and without diabetes mellitus or chronic kidney disease. Therefore, the findings should not be extrapolated to these populations groups. Conclusion In summary, patients with newly-diagnosed OSA have higher 24 h SBP variability compared to those without OSA, and age, prevalent CVD and OSA are the potential determinants of 24 h SBP variability, while anti-hypertensive medications may also influence 24 h SBP variability. In patients with OSA, those with high 24 h SBP variability appear to have higher prevalence of CVD compared to their OSA counterparts with low 24 h SBP variability. Future randomized controlled trials are warranted to evaluate whether improving OSA could contribute to improving 24 h SBP variability and cardiovascular outcomes. Abbreviation (24 h ABPM): 24 h ambulatory blood pressure monitoring; (ACEI/ARB): Angiotensin converting enzyme inhibitor/angiotensin receptor blocker; (AHI): Apnea-hypopnea index; (BMI): Body mass index; (CCB): Calcium channel blocker; (CHD): Coronary heart disease; (CPAP): Continuous positive airway pressure; (Cr): Creatinine; (CVD):Cardiovasculardisease;(DBP):Diastolicbloodpressure;(FPG):Fastingplasma glucose; (Hs-CRP): High-sensitivity C-reactive protein; (OSA): Obstructive sleep apnea; (PSG): Polysomnography; (SaO 2 ): Saturation of arterial oxygen; (SBP): Systolic blood pressure; (SD): Standard deviation Acknowledgments We thank Chen Zhang, PhD, for assisting us in performing statistical analysis of our paper. Funding The study was supported by grants from the Science and Technology project of Shenzhen city of China (JCYJ and JCYJ ); by grants from the Research Project(Doctoral Innovation Program) of Health Planning system of Shenzhen city(szbc ); by grants from the Science and Technology project of Guangzhou city of China (NO ); by the Sanming Project of Medicine in Shenzhen city of China; and by grants from the National Natural Science Foundation of China (NO and NO ). Availability of data and materials The data that support the findings of this study are available from corresponding authors but restrictions apply to the availability of these data, which were used under license for the current study, and so are not publicly
6 Ke et al. BMC Cardiovascular Disorders (2017) 17:287 Page 6 of 6 available. Data are however available from the authors upon reasonable request and with permission of corresponding authors. Authors contributions XW and CHH designed the study, reviewed and corrected the manuscript. XK and YS analyzed the data and wrote the manuscript. XK, YS, YRF, JWL and SYW helped in collecting the data. YRF, JWL and SYW helped in data interpretation. YRF, JWL and SYW helped in study design, getting the permission for data access, supervising data analysis, and correcting the manuscript. All authors read and approved the final manuscript. Ethics approval and consent to participate Written informed consents were obtained from studied participants before recruitment and current study was approved by the Research Ethic Committee of Shenzhen Sun Yat-sen Cardiovascular Hospital. All participants were treated in accordance to the Declaration of Helsinki. Competing interests The authors declare that they have no competing interests. Consent for publication All authors approved for the publication of current study. Publisher s Note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations. Author details 1 Department of Cardiology, Shenzhen Sun Yat-sen Cardiovascular Hospital, Dongmen North Road 1021, Shenzhen , China. 2 Department of Endocrinology, Xili People s Hospital of Nanshan District, Shenzhen , China. 3 Department of Cardiology, The First Affiliated Hospital of Sun Yat-sen University, 58 Zhongshan Road 2, Guangzhou , China. 11. Jean-Louis G, Zizi F, Brown D, Ogedegbe G, Borer J, McFarlane S. Obstructive sleep apnea and cardiovascular disease: evidence and underlying mechanisms. Minerva Pneumol. 2009;48(4): Jin J. Screening for obstructive sleep apnea in adults. JAMA. 2017;317(4): Konecny T, Kara T, Somers VK. Obstructive sleep apnea and hypertension: an update. Hypertension. 2014;63(2): Cai A, Wang L, Zhou Y. Hypertension and obstructive sleep apnea. Hypertens Res. 2016;39(6): Javaheri S, Barbe F, Campos-Rodriguez F, et al. Sleep apnea: types, mechanisms, and clinical cardiovascular consequences. J Am Coll Cardiol. 2017;69(7): Chobanian AV, Bakris GL, Black HR, et al. The seventh report of the joint National Committee on prevention, detection, evaluation, and treatment of high blood pressure: the JNC 7 report. JAMA. 2003;289(19): Parati G, Stergiou G, O'Brien E, et al. European Society of Hypertension practice guidelines for ambulatory blood pressure monitoring. J Hypertens. 2014;32(7): Sleep-related breathing disorders in adults: recommendations for syndrome definition and measurement techniques in clinical research. The Report of an American Academy of Sleep Medicine Task Force. Sleep (5): Webb AJ, Fischer U, Mehta Z, Rothwell PM. Effects of antihypertensive-drug class on interindividual variation in blood pressure and risk of stroke: a systematic review and meta-analysis. Lancet. 2010;375(9718): Muntner P, Levitan EB, Lynch AI, et al. Effect of chlorthalidone, amlodipine, and lisinopril on visit-to-visit variability of blood pressure: results from the antihypertensive and lipid-lowering treatment to prevent heart attack trial. J Clin Hypertens (Greenwich). 2014;16(5): Hussein WF, Chang TI. Visit-to-visit variability of systolic blood pressure and cardiovascular disease. Curr Hypertens Rep. 2015;17(3): Mancia G, Facchetti R, Parati G, Zanchetti A. Visit-to-visit blood pressure variability in the European Lacidipine study on atherosclerosis: methodological aspects and effects of antihypertensive treatment. J Hypertens. 2012;30(6): Received: 13 September 2017 Accepted: 28 November 2017 References 1. Mancia G, Fagard R, Narkiewicz K, et al ESH/ESC guidelines for the management of arterial hypertension: the task force for the management of arterial hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC). J Hypertens. 2013;31(7): James PA, Oparil S, Carter BL, et al evidence-based guideline for the management of high blood pressure in adults: report from the panel members appointed to the eighth joint National Committee (JNC 8). JAMA. 2014;311(5): Xie X, Atkins E, Lv J, et al. Effects of intensive blood pressure lowering on cardiovascular and renal outcomes: updated systematic review and metaanalysis. Lancet. 2016;387(10017): Brunström M, Carlberg B. Effect of antihypertensive treatment at different blood pressure levels in patients with diabetes mellitus: systematic review and meta-analyses. BMJ. 2016;352:i Wright JT, Williamson JD, Whelton PK, et al. A randomized trial of intensive versus standard blood-pressure control. N Engl J Med. 2015;373(22): Whelton PK, Pollock BDI. It time to employ a measure of visit-to-visit variability in clinical practice. Hypertension. 2017;70(2): Muntner P, Whittle J, Lynch AI, et al. Visit-to-visit variability of blood pressure and coronary heart disease, stroke, heart failure, and mortality: a cohort study. Ann Intern Med. 2015;163(5): Ohkuma T, Woodward M, Jun M, et al. Prognostic value of variability in systolic blood pressure related to vascular events and premature death in type 2 diabetes mellitus: the ADVANCE-ON study. Hypertension. 2017;70(2): Okada R, Okada A, Okada T, Nanasato M, Wakai K. Visit-to-visit blood pressure variability is a marker of cardiac diastolic function and carotid atherosclerosis. BMC Cardiovasc Disord. 2014;14: Diaz KM, Tanner RM, Falzon L, et al. Visit-to-visit variability of blood pressure and cardiovascular disease and all-cause mortality: a systematic review and meta-analysis. Hypertension. 2014;64(5): Submit your next manuscript to BioMed Central and we will help you at every step: We accept pre-submission inquiries Our selector tool helps you to find the most relevant journal We provide round the clock customer support Convenient online submission Thorough peer review Inclusion in PubMed and all major indexing services Maximum visibility for your research Submit your manuscript at
Which antihypertensives are more effective in reducing diastolic hypertension versus systolic hypertension? May 24, 2017
 Which antihypertensives are more effective in reducing diastolic hypertension versus systolic hypertension? May 24, 2017 The most important reason for treating hypertension in primary care is to prevent
Which antihypertensives are more effective in reducing diastolic hypertension versus systolic hypertension? May 24, 2017 The most important reason for treating hypertension in primary care is to prevent
JNC Evidence-Based Guidelines for the Management of High Blood Pressure in Adults
 JNC 8 2014 Evidence-Based Guidelines for the Management of High Blood Pressure in Adults Table of Contents Why Do We Treat Hypertension? Blood Pressure Treatment Goals Initial Therapy Strength of Recommendation
JNC 8 2014 Evidence-Based Guidelines for the Management of High Blood Pressure in Adults Table of Contents Why Do We Treat Hypertension? Blood Pressure Treatment Goals Initial Therapy Strength of Recommendation
Slide notes: References:
 1 2 3 Cut-off values for the definition of hypertension are systolic blood pressure (SBP) 135 and/or diastolic blood pressure (DBP) 85 mmhg for home blood pressure monitoring (HBPM) and daytime ambulatory
1 2 3 Cut-off values for the definition of hypertension are systolic blood pressure (SBP) 135 and/or diastolic blood pressure (DBP) 85 mmhg for home blood pressure monitoring (HBPM) and daytime ambulatory
Serum levels of galectin-1, galectin-3, and galectin-9 are associated with large artery atherosclerotic
 Supplementary Information The title of the manuscript Serum levels of galectin-1, galectin-3, and galectin-9 are associated with large artery atherosclerotic stroke Xin-Wei He 1, Wei-Ling Li 1, Cai Li
Supplementary Information The title of the manuscript Serum levels of galectin-1, galectin-3, and galectin-9 are associated with large artery atherosclerotic stroke Xin-Wei He 1, Wei-Ling Li 1, Cai Li
Risk Assessment of developing type 2 diabetes mellitus in patient on antihypertensive medication
 41 Research Article Risk Assessment of developing type 2 diabetes mellitus in patient on antihypertensive medication Amarjeet Singh*, Sudeep bhardwaj, Ashutosh aggarwal Department of Pharmacology, Seth
41 Research Article Risk Assessment of developing type 2 diabetes mellitus in patient on antihypertensive medication Amarjeet Singh*, Sudeep bhardwaj, Ashutosh aggarwal Department of Pharmacology, Seth
Update on Current Trends in Hypertension Management
 Friday General Session Update on Current Trends in Hypertension Management Shawna Nesbitt, MD Associate Dean, Minority Student Affairs Associate Professor, Department of Internal Medicine Office of Student
Friday General Session Update on Current Trends in Hypertension Management Shawna Nesbitt, MD Associate Dean, Minority Student Affairs Associate Professor, Department of Internal Medicine Office of Student
Hypertension Update Clinical Controversies Regarding Age and Race
 Hypertension Update Clinical Controversies Regarding Age and Race Allison Helmer, PharmD, BCACP Assistant Clinical Professor Auburn University Harrison School of Pharmacy July 22, 2017 DISCLOSURE/CONFLICT
Hypertension Update Clinical Controversies Regarding Age and Race Allison Helmer, PharmD, BCACP Assistant Clinical Professor Auburn University Harrison School of Pharmacy July 22, 2017 DISCLOSURE/CONFLICT
ALLHAT. Major Outcomes in High Risk Hypertensive Patients Randomized to Angiotensin-Converting Enzyme Inhibitor or Calcium Channel Blocker vs Diuretic
 1 U.S. Department of Health and Human Services National Institutes of Health Major Outcomes in High Risk Hypertensive Patients Randomized to Angiotensin-Converting Enzyme Inhibitor or Calcium Channel Blocker
1 U.S. Department of Health and Human Services National Institutes of Health Major Outcomes in High Risk Hypertensive Patients Randomized to Angiotensin-Converting Enzyme Inhibitor or Calcium Channel Blocker
Blood Pressure Targets: Where are We Now?
 Blood Pressure Targets: Where are We Now? Diana Cao, PharmD, BCPS-AQ Cardiology Assistant Professor Department of Clinical & Administrative Sciences California Northstate University College of Pharmacy
Blood Pressure Targets: Where are We Now? Diana Cao, PharmD, BCPS-AQ Cardiology Assistant Professor Department of Clinical & Administrative Sciences California Northstate University College of Pharmacy
Int. J. Pharm. Sci. Rev. Res., 36(1), January February 2016; Article No. 06, Pages: JNC 8 versus JNC 7 Understanding the Evidences
 Research Article JNC 8 versus JNC 7 Understanding the Evidences Anns Clara Joseph, Karthik MS, Sivasakthi R, Venkatanarayanan R, Sam Johnson Udaya Chander J* RVS College of Pharmaceutical Sciences, Coimbatore,
Research Article JNC 8 versus JNC 7 Understanding the Evidences Anns Clara Joseph, Karthik MS, Sivasakthi R, Venkatanarayanan R, Sam Johnson Udaya Chander J* RVS College of Pharmaceutical Sciences, Coimbatore,
ΑΡΥΙΚΗ ΠΡΟΔΓΓΙΗ ΤΠΔΡΣΑΙΚΟΤ ΑΘΔΝΟΤ. Μ.Β.Παπαβαζιλείοσ Καρδιολόγος FESC - Γιεσθύνηρια ιζμανόγλειον ΓΝΑ Clinical Hypertension Specialist ESH
 ΑΡΥΙΚΗ ΠΡΟΔΓΓΙΗ ΤΠΔΡΣΑΙΚΟΤ ΑΘΔΝΟΤ Μ.Β.Παπαβαζιλείοσ Καρδιολόγος FESC - Γιεσθύνηρια ιζμανόγλειον ΓΝΑ Clinical Hypertension Specialist ESH Hypertension Co-Morbidities HTN Commonly Clusters with Other Risk
ΑΡΥΙΚΗ ΠΡΟΔΓΓΙΗ ΤΠΔΡΣΑΙΚΟΤ ΑΘΔΝΟΤ Μ.Β.Παπαβαζιλείοσ Καρδιολόγος FESC - Γιεσθύνηρια ιζμανόγλειον ΓΝΑ Clinical Hypertension Specialist ESH Hypertension Co-Morbidities HTN Commonly Clusters with Other Risk
What s In the New Hypertension Guidelines?
 American College of Physicians Ohio/Air Force Chapters 2018 Scientific Meeting Columbus, OH October 5, 2018 What s In the New Hypertension Guidelines? Max C. Reif, MD, FACP Objectives: At the end of the
American College of Physicians Ohio/Air Force Chapters 2018 Scientific Meeting Columbus, OH October 5, 2018 What s In the New Hypertension Guidelines? Max C. Reif, MD, FACP Objectives: At the end of the
JNC 8 -Controversies. Sagren Naidoo Nephrologist CMJAH
 JNC 8 -Controversies Sagren Naidoo Nephrologist CMJAH Joint National Committee (JNC) Panel appointed by the National Heart, Lung, and Blood Institute (NHLBI) First guidelines (JNC-1) published in 1977
JNC 8 -Controversies Sagren Naidoo Nephrologist CMJAH Joint National Committee (JNC) Panel appointed by the National Heart, Lung, and Blood Institute (NHLBI) First guidelines (JNC-1) published in 1977
T. Suithichaiyakul Cardiomed Chula
 T. Suithichaiyakul Cardiomed Chula The cardiovascular (CV) continuum: role of risk factors Endothelial Dysfunction Atherosclerosis and left ventricular hypertrophy Myocardial infarction & stroke Endothelial
T. Suithichaiyakul Cardiomed Chula The cardiovascular (CV) continuum: role of risk factors Endothelial Dysfunction Atherosclerosis and left ventricular hypertrophy Myocardial infarction & stroke Endothelial
Clinical Updates in the Treatment of Hypertension JNC 7 vs. JNC 8. Lauren Thomas, PharmD PGY1 Pharmacy Practice Resident South Pointe Hospital
 Clinical Updates in the Treatment of Hypertension JNC 7 vs. JNC 8 Lauren Thomas, PharmD PGY1 Pharmacy Practice Resident South Pointe Hospital Objectives Review the Eighth Joint National Committee (JNC
Clinical Updates in the Treatment of Hypertension JNC 7 vs. JNC 8 Lauren Thomas, PharmD PGY1 Pharmacy Practice Resident South Pointe Hospital Objectives Review the Eighth Joint National Committee (JNC
Increased Lipoprotein-associated phospholipase A2 activity portends an increased risk of resistant hypertension
 Li et al. Lipids in Health and Disease (2016) 15:15 DOI 10.1186/s12944-016-0184-9 RESEARCH Increased Lipoprotein-associated phospholipase A2 activity portends an increased risk of resistant hypertension
Li et al. Lipids in Health and Disease (2016) 15:15 DOI 10.1186/s12944-016-0184-9 RESEARCH Increased Lipoprotein-associated phospholipase A2 activity portends an increased risk of resistant hypertension
Hypertension Update Background
 Hypertension Update Background Overview Aaron J. Friedberg, MD Assistant Professor, Clinical Division of General Internal Medicine The Ohio State University Wexner Medical Center Management Guideline Comparison
Hypertension Update Background Overview Aaron J. Friedberg, MD Assistant Professor, Clinical Division of General Internal Medicine The Ohio State University Wexner Medical Center Management Guideline Comparison
AGING, BLOOD PRESSURE & CARDIOVASCULAR DISEASE EVENT RISK. Michael Smolensky, Ph.D. The University of Texas Austin & Houston
 AGING, BLOOD PRESSURE & CARDIOVASCULAR DISEASE EVENT RISK Michael Smolensky, Ph.D. The University of Texas Austin & Houston Disclosures Partner: Circadian Ambulatory Diagnostics Consultant: Spot On Sciences
AGING, BLOOD PRESSURE & CARDIOVASCULAR DISEASE EVENT RISK Michael Smolensky, Ph.D. The University of Texas Austin & Houston Disclosures Partner: Circadian Ambulatory Diagnostics Consultant: Spot On Sciences
Antihypertensive Trial Design ALLHAT
 1 U.S. Department of Health and Human Services Major Outcomes in High Risk Hypertensive Patients Randomized to Angiotensin-Converting Enzyme Inhibitor or Calcium Channel Blocker vs Diuretic National Institutes
1 U.S. Department of Health and Human Services Major Outcomes in High Risk Hypertensive Patients Randomized to Angiotensin-Converting Enzyme Inhibitor or Calcium Channel Blocker vs Diuretic National Institutes
DISCLOSURE PHARMACIST OBJECTIVES 9/30/2014 JNC 8: A REVIEW OF THE LONG-AWAITED/MUCH-ANTICIPATED HYPERTENSION GUIDELINES. I have nothing to disclose.
 JNC 8: A REVIEW OF THE LONG-AWAITED/MUCH-ANTICIPATED HYPERTENSION GUIDELINES Tiffany Dickey, PharmD Assistant Professor, UAMS COP Clinical Pharmacy Specialist, Mercy Hospital Northwest AR DISCLOSURE I
JNC 8: A REVIEW OF THE LONG-AWAITED/MUCH-ANTICIPATED HYPERTENSION GUIDELINES Tiffany Dickey, PharmD Assistant Professor, UAMS COP Clinical Pharmacy Specialist, Mercy Hospital Northwest AR DISCLOSURE I
NIH Public Access Author Manuscript JAMA Intern Med. Author manuscript; available in PMC 2015 August 01.
 NIH Public Access Author Manuscript Published in final edited form as: JAMA Intern Med. 2014 August ; 174(8): 1397 1400. doi:10.1001/jamainternmed.2014.2492. Prevalence and Characteristics of Systolic
NIH Public Access Author Manuscript Published in final edited form as: JAMA Intern Med. 2014 August ; 174(8): 1397 1400. doi:10.1001/jamainternmed.2014.2492. Prevalence and Characteristics of Systolic
Hypertension Update. Aaron J. Friedberg, MD
 Hypertension Update Aaron J. Friedberg, MD Assistant Professor, Clinical Division of General Internal Medicine The Ohio State University Wexner Medical Center Background Diagnosis Management Overview Guideline
Hypertension Update Aaron J. Friedberg, MD Assistant Professor, Clinical Division of General Internal Medicine The Ohio State University Wexner Medical Center Background Diagnosis Management Overview Guideline
CARDIOVASCULAR RISK FACTORS & TARGET ORGAN DAMAGE IN GREEK HYPERTENSIVES
 CARDIOVASCULAR RISK FACTORS & TARGET ORGAN DAMAGE IN GREEK HYPERTENSIVES C. Liakos, 1 G. Vyssoulis, 1 E. Karpanou, 2 S-M. Kyvelou, 1 V. Tzamou, 1 A. Michaelides, 1 A. Triantafyllou, 1 P. Spanos, 1 C. Stefanadis
CARDIOVASCULAR RISK FACTORS & TARGET ORGAN DAMAGE IN GREEK HYPERTENSIVES C. Liakos, 1 G. Vyssoulis, 1 E. Karpanou, 2 S-M. Kyvelou, 1 V. Tzamou, 1 A. Michaelides, 1 A. Triantafyllou, 1 P. Spanos, 1 C. Stefanadis
 Touyz, R. M., and Dominiczak, A. F. (2016) Hypertension guidelines: is it time to reappraise blood pressure thresholds and targets? Hypertension, 67(4), pp. 688-689. There may be differences between this
Touyz, R. M., and Dominiczak, A. F. (2016) Hypertension guidelines: is it time to reappraise blood pressure thresholds and targets? Hypertension, 67(4), pp. 688-689. There may be differences between this
The Evolution To Treatment Of Hypertension With Advanced Formulation
 The Evolution To Treatment Of Hypertension With Advanced Formulation Dr. Donald Ang MBChB (UK) FRCP (Edin) MD (UK) CCST Cardiology (UK) FESC (Europe) Consultant Cardiologist Island Hospital Penang High
The Evolution To Treatment Of Hypertension With Advanced Formulation Dr. Donald Ang MBChB (UK) FRCP (Edin) MD (UK) CCST Cardiology (UK) FESC (Europe) Consultant Cardiologist Island Hospital Penang High
Evolving Concepts on Hypertension: Implications of Three Guidelines (JNC 8 Panel, ESH/ESC, NICE/BSH)
 Evolving Concepts on Hypertension: Implications of Three Guidelines (JNC 8 Panel, ESH/ESC, NICE/BSH) Sidney C. Smith, Jr. MD, FACC, FAHA, FESC Professor of Medicine/Cardiology University of North Carolina
Evolving Concepts on Hypertension: Implications of Three Guidelines (JNC 8 Panel, ESH/ESC, NICE/BSH) Sidney C. Smith, Jr. MD, FACC, FAHA, FESC Professor of Medicine/Cardiology University of North Carolina
Autonomic nervous system, inflammation and preclinical carotid atherosclerosis in depressed subjects with coronary risk factors
 Autonomic nervous system, inflammation and preclinical carotid atherosclerosis in depressed subjects with coronary risk factors Carmine Pizzi 1 ; Lamberto Manzoli 2, Stefano Mancini 3 ; Gigliola Bedetti
Autonomic nervous system, inflammation and preclinical carotid atherosclerosis in depressed subjects with coronary risk factors Carmine Pizzi 1 ; Lamberto Manzoli 2, Stefano Mancini 3 ; Gigliola Bedetti
4/4/17 HYPERTENSION TARGETS: WHAT DO WE DO NOW? SET THE STAGE BP IN CLINICAL TRIALS?
 HYPERTENSION TARGETS: WHAT DO WE DO NOW? MICHAEL LEFEVRE, MD, MSPH PROFESSOR AND VICE CHAIR DEPARTMENT OF FAMILY AND COMMUNITY MEDICINE UNIVERSITY OF MISSOURI 4/4/17 DISCLOSURE: MEMBER OF THE JNC 8 PANEL
HYPERTENSION TARGETS: WHAT DO WE DO NOW? MICHAEL LEFEVRE, MD, MSPH PROFESSOR AND VICE CHAIR DEPARTMENT OF FAMILY AND COMMUNITY MEDICINE UNIVERSITY OF MISSOURI 4/4/17 DISCLOSURE: MEMBER OF THE JNC 8 PANEL
Module 2. Global Cardiovascular Risk Assessment and Reduction in Women with Hypertension
 Module 2 Global Cardiovascular Risk Assessment and Reduction in Women with Hypertension 1 Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored,
Module 2 Global Cardiovascular Risk Assessment and Reduction in Women with Hypertension 1 Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored,
How do we diagnose hypertension today? Presentation Subtitle
 How do we diagnose hypertension today? Presentation Subtitle Renata Cífková Case 1 JM, a 64-year-old lady referred to our center because of undesirable effects of her antihypertensive medication Personal
How do we diagnose hypertension today? Presentation Subtitle Renata Cífková Case 1 JM, a 64-year-old lady referred to our center because of undesirable effects of her antihypertensive medication Personal
DISCLOSURES OUTLINE OUTLINE 9/29/2014 ANTI-HYPERTENSIVE MANAGEMENT OF CHRONIC KIDNEY DISEASE
 ANTI-HYPERTENSIVE MANAGEMENT OF CHRONIC KIDNEY DISEASE DISCLOSURES Editor-in-Chief- Nephrology- UpToDate- (Wolters Klewer) Richard J. Glassock, MD, MACP Geffen School of Medicine at UCLA 1 st Annual Internal
ANTI-HYPERTENSIVE MANAGEMENT OF CHRONIC KIDNEY DISEASE DISCLOSURES Editor-in-Chief- Nephrology- UpToDate- (Wolters Klewer) Richard J. Glassock, MD, MACP Geffen School of Medicine at UCLA 1 st Annual Internal
DEPARTMENT OF GENERAL MEDICINE WELCOMES
 DEPARTMENT OF GENERAL MEDICINE WELCOMES 1 Dr.Mohamed Omar Shariff, 2 nd Year Post Graduate, Department of General Medicine. DR.B.R.Ambedkar Medical College & Hospital. 2 INTRODUCTION Leading cause of global
DEPARTMENT OF GENERAL MEDICINE WELCOMES 1 Dr.Mohamed Omar Shariff, 2 nd Year Post Graduate, Department of General Medicine. DR.B.R.Ambedkar Medical College & Hospital. 2 INTRODUCTION Leading cause of global
Sleep Apnea: Vascular and Metabolic Complications
 Sleep Apnea: Vascular and Metabolic Complications Vahid Mohsenin, M.D. Professor of Medicine Yale University School of Medicine Director, Yale Center for Sleep Medicine Definitions Apnea: Cessation of
Sleep Apnea: Vascular and Metabolic Complications Vahid Mohsenin, M.D. Professor of Medicine Yale University School of Medicine Director, Yale Center for Sleep Medicine Definitions Apnea: Cessation of
High-dose monotherapy vs low-dose combination therapy of calcium channel blockers and angiotensin receptor blockers in mild to moderate hypertension
 (2005) 19, 491 496 & 2005 Nature Publishing Group All rights reserved 0950-9240/05 $30.00 www.nature.com/jhh ORIGINAL ARTICLE High-dose monotherapy vs low-dose combination therapy of calcium channel blockers
(2005) 19, 491 496 & 2005 Nature Publishing Group All rights reserved 0950-9240/05 $30.00 www.nature.com/jhh ORIGINAL ARTICLE High-dose monotherapy vs low-dose combination therapy of calcium channel blockers
Long-Term Care Updates
 Long-Term Care Updates August 2015 By Darren Hein, PharmD Hypertension is a clinical condition in which the force of blood pushing on the arteries is higher than normal. This increases the risk for heart
Long-Term Care Updates August 2015 By Darren Hein, PharmD Hypertension is a clinical condition in which the force of blood pushing on the arteries is higher than normal. This increases the risk for heart
Using the New Hypertension Guidelines
 Using the New Hypertension Guidelines Kamal Henderson, MD Department of Cardiology, Preventive Medicine, University of North Carolina School of Medicine Kotchen TA. Historical trends and milestones in
Using the New Hypertension Guidelines Kamal Henderson, MD Department of Cardiology, Preventive Medicine, University of North Carolina School of Medicine Kotchen TA. Historical trends and milestones in
Jared Moore, MD, FACP
 Hypertension 101 Jared Moore, MD, FACP Assistant Program Director, Internal Medicine Residency Clinical Assistant Professor of Internal Medicine Division of General Medicine The Ohio State University Wexner
Hypertension 101 Jared Moore, MD, FACP Assistant Program Director, Internal Medicine Residency Clinical Assistant Professor of Internal Medicine Division of General Medicine The Ohio State University Wexner
Todd S. Perlstein, MD FIFTH ANNUAL SYMPOSIUM
 Todd S. Perlstein, MD FIFTH ANNUAL SYMPOSIUM Faculty Disclosure I have no financial interest to disclose No off-label use of medications will be discussed FIFTH ANNUAL SYMPOSIUM Recognize changes between
Todd S. Perlstein, MD FIFTH ANNUAL SYMPOSIUM Faculty Disclosure I have no financial interest to disclose No off-label use of medications will be discussed FIFTH ANNUAL SYMPOSIUM Recognize changes between
Cedars Sinai Diabetes. Michael A. Weber
 Cedars Sinai Diabetes Michael A. Weber Speaker Disclosures I disclose that I am a Consultant for: Ablative Solutions, Boston Scientific, Boehringer Ingelheim, Eli Lilly, Forest, Medtronics, Novartis, ReCor
Cedars Sinai Diabetes Michael A. Weber Speaker Disclosures I disclose that I am a Consultant for: Ablative Solutions, Boston Scientific, Boehringer Ingelheim, Eli Lilly, Forest, Medtronics, Novartis, ReCor
Hypertension. Risk of cardiovascular disease beginning at 115/75 mmhg doubles with every 20/10mm Hg increase. (Grade B)
 Practice Guidelines and Principles: Guidelines and principles are intended to be flexible. They serve as reference points or recommendations, not rigid criteria. Guidelines and principles should be followed
Practice Guidelines and Principles: Guidelines and principles are intended to be flexible. They serve as reference points or recommendations, not rigid criteria. Guidelines and principles should be followed
Adherence to Antihypertensive Medication in the older hypertensive patients: the role of blood pressure measurement assistance
 Research Article Pharmaceutical Adherence to Antihypertensive Medication in the older hypertensive patients: the role of blood pressure measurement assistance Aim: To evaluate the compliance of patients
Research Article Pharmaceutical Adherence to Antihypertensive Medication in the older hypertensive patients: the role of blood pressure measurement assistance Aim: To evaluate the compliance of patients
hypertension Head of prevention and control of CVD disease office Ministry of heath
 hypertension t. Samavat MD,Cadiologist,MPH Head of prevention and control of CVD disease office Ministry of heath RECOMMENDATIONS FOR HYPERTENSION DIAGNOSIS, ASSESSMENT, AND TREATMENT Definition of hypertension
hypertension t. Samavat MD,Cadiologist,MPH Head of prevention and control of CVD disease office Ministry of heath RECOMMENDATIONS FOR HYPERTENSION DIAGNOSIS, ASSESSMENT, AND TREATMENT Definition of hypertension
SUPPLEMENTARY DATA. Supplementary Table 1. Baseline Patient Characteristics
 Supplementary Table 1. Baseline Patient Characteristics Normally distributed data are presented as mean (±SD), data that were not of a normal distribution are presented as median (ICR). The baseline characteristics
Supplementary Table 1. Baseline Patient Characteristics Normally distributed data are presented as mean (±SD), data that were not of a normal distribution are presented as median (ICR). The baseline characteristics
None. Disclosure: Relationships with Industry Conflicts of Interests. Learning Objectives: Participants will be able to:
 2014 Evidence-Based Guideline for the Management of High Blood Pressure in Adults: Report from the Panel Members Appointed to the Eighth Joint National Committee (JNC 8) James W. Shaw, MD Memorial Lecture
2014 Evidence-Based Guideline for the Management of High Blood Pressure in Adults: Report from the Panel Members Appointed to the Eighth Joint National Committee (JNC 8) James W. Shaw, MD Memorial Lecture
Diabetes Mellitus: A Cardiovascular Disease
 Diabetes Mellitus: A Cardiovascular Disease Nestoras Mathioudakis, M.D. Assistant Professor of Medicine Division of Endocrinology, Diabetes, & Metabolism September 30, 2013 1 The ABCs of cardiovascular
Diabetes Mellitus: A Cardiovascular Disease Nestoras Mathioudakis, M.D. Assistant Professor of Medicine Division of Endocrinology, Diabetes, & Metabolism September 30, 2013 1 The ABCs of cardiovascular
Yuqing Zhang, M.D., FESC Department of Cardiology, Fu Wai Hospital. CAMS & PUMC, Beijing, China
 What Can We Learn from the Observational Studies and Clinical Trials of Prehypertension? Yuqing Zhang, M.D., FESC Department of Cardiology, Fu Wai Hospital. CAMS & PUMC, Beijing, China At ARIC visit 4
What Can We Learn from the Observational Studies and Clinical Trials of Prehypertension? Yuqing Zhang, M.D., FESC Department of Cardiology, Fu Wai Hospital. CAMS & PUMC, Beijing, China At ARIC visit 4
Validation of the SEJOY BP-1307 upper arm blood pressure monitor for home. blood pressure monitoring according to the European Society of Hypertension
 Validation of the SEJOY BP-1307 upper arm blood pressure monitor for home blood pressure monitoring according to the European Society of Hypertension International Protocol revision 2010 Short title: Validation
Validation of the SEJOY BP-1307 upper arm blood pressure monitor for home blood pressure monitoring according to the European Society of Hypertension International Protocol revision 2010 Short title: Validation
Chapman University Digital Commons. Chapman University. Michael S. Kelly Chapman University,
 Chapman University Chapman University Digital Commons Pharmacy Faculty Articles and Research School of Pharmacy 12-30-2016 Assessment of Achieved Systolic Blood Pressure in Newly Treated Hypertensive Patients
Chapman University Chapman University Digital Commons Pharmacy Faculty Articles and Research School of Pharmacy 12-30-2016 Assessment of Achieved Systolic Blood Pressure in Newly Treated Hypertensive Patients
When should blood pressure be lowered? Should treatment be guided by blood pressure values or total cardiovascular risk?
 OF JOURNAL HYPERTENSION JH R RESEARCH Journal of HYPERTENSION RESEARCH www.hypertens.org/jhr Editorial J Hypertens Res (2016) 2(2):47 51 When should blood pressure be lowered? Should treatment be guided
OF JOURNAL HYPERTENSION JH R RESEARCH Journal of HYPERTENSION RESEARCH www.hypertens.org/jhr Editorial J Hypertens Res (2016) 2(2):47 51 When should blood pressure be lowered? Should treatment be guided
300 Biomed Environ Sci, 2018; 31(4):
 300 Biomed Environ Sci, 2018; 31(4): 300-305 Letter to the Editor Combined Influence of Insulin Resistance and Inflammatory Biomarkers on Type 2 Diabetes: A Population-based Prospective Cohort Study of
300 Biomed Environ Sci, 2018; 31(4): 300-305 Letter to the Editor Combined Influence of Insulin Resistance and Inflammatory Biomarkers on Type 2 Diabetes: A Population-based Prospective Cohort Study of
Combination therapy Giuseppe M.C. Rosano, MD, PhD, MSc, FESC, FHFA St George s Hospitals NHS Trust University of London
 Combination therapy Giuseppe M.C. Rosano, MD, PhD, MSc, FESC, FHFA St George s Hospitals NHS Trust University of London KCS Congress: Impact through collaboration CONTACT: Tel. +254 735 833 803 Email:
Combination therapy Giuseppe M.C. Rosano, MD, PhD, MSc, FESC, FHFA St George s Hospitals NHS Trust University of London KCS Congress: Impact through collaboration CONTACT: Tel. +254 735 833 803 Email:
Hypertension and obesity. Dr Wilson Sugut Moi teaching and referral hospital
 Hypertension and obesity Dr Wilson Sugut Moi teaching and referral hospital No conflict of interests to declare Obesity Definition: excessive weight that may impair health BMI Categories Underweight BMI
Hypertension and obesity Dr Wilson Sugut Moi teaching and referral hospital No conflict of interests to declare Obesity Definition: excessive weight that may impair health BMI Categories Underweight BMI
Statin therapy in patients with Mild to Moderate Coronary Stenosis by 64-slice Multidetector Coronary Computed Tomography
 Statin therapy in patients with Mild to Moderate Coronary Stenosis by 64-slice Multidetector Coronary Computed Tomography Hyo Eun Park 1, Eun-Ju Chun 2, Sang-Il Choi 2, Soyeon Ahn 2, Hyung-Kwan Kim 3,
Statin therapy in patients with Mild to Moderate Coronary Stenosis by 64-slice Multidetector Coronary Computed Tomography Hyo Eun Park 1, Eun-Ju Chun 2, Sang-Il Choi 2, Soyeon Ahn 2, Hyung-Kwan Kim 3,
Hypertension. Does it Matter What Medications We Use? Nishant K. Sekaran, M.D. M.Sc. Intermountain Heart Institute
 Hypertension Does it Matter What Medications We Use? Nishant K. Sekaran, M.D. M.Sc. Intermountain Heart Institute Hypertension 2017 Classification BP Category Systolic Diastolic Normal 120 and 80 Elevated
Hypertension Does it Matter What Medications We Use? Nishant K. Sekaran, M.D. M.Sc. Intermountain Heart Institute Hypertension 2017 Classification BP Category Systolic Diastolic Normal 120 and 80 Elevated
New Hypertension Guideline Recommendations for Adults July 7, :45-9:30am
 Advances in Cardiovascular Disease 30 th Annual Convention and Reunion UERM-CMAA, Inc. Annual Convention and Scientific Meeting July 5-8, 2018 New Hypertension Guideline Recommendations for Adults July
Advances in Cardiovascular Disease 30 th Annual Convention and Reunion UERM-CMAA, Inc. Annual Convention and Scientific Meeting July 5-8, 2018 New Hypertension Guideline Recommendations for Adults July
The Hypertension Clinic is a part of the Internal Medicine
 Original Article Hypertension Registry at the Bangkok Hospital Medical Center: The First 7 Months Experience OBJECTIVE: The Hypertension Registry at the Bangkok Hospital Medical Center was established
Original Article Hypertension Registry at the Bangkok Hospital Medical Center: The First 7 Months Experience OBJECTIVE: The Hypertension Registry at the Bangkok Hospital Medical Center was established
Supplementary Online Content. Abed HS, Wittert GA, Leong DP, et al. Effect of weight reduction and
 1 Supplementary Online Content 2 3 4 5 6 Abed HS, Wittert GA, Leong DP, et al. Effect of weight reduction and cardiometabolic risk factor management on sympton burden and severity in patients with atrial
1 Supplementary Online Content 2 3 4 5 6 Abed HS, Wittert GA, Leong DP, et al. Effect of weight reduction and cardiometabolic risk factor management on sympton burden and severity in patients with atrial
Using Cardiovascular Risk to Guide Antihypertensive Treatment Implications For The Pre-elderly and Elderly
 Using Cardiovascular Risk to Guide Antihypertensive Treatment Implications For The Pre-elderly and Elderly Paul Muntner, PhD MHS Professor and Vice Chair Department of Epidemiology University of Alabama
Using Cardiovascular Risk to Guide Antihypertensive Treatment Implications For The Pre-elderly and Elderly Paul Muntner, PhD MHS Professor and Vice Chair Department of Epidemiology University of Alabama
Characteristics and Future Cardiovascular Risk of Patients With Not-At- Goal Hypertension in General Practice in France: The AVANT AGE Study
 ORIGINAL PAPER Characteristics and Future Cardiovascular Risk of Patients With Not-At- Goal Hypertension in General Practice in France: The AVANT AGE Study Yi Zhang, MD, PhD; 1 Helene Lelong, MD; 2 Sandrine
ORIGINAL PAPER Characteristics and Future Cardiovascular Risk of Patients With Not-At- Goal Hypertension in General Practice in France: The AVANT AGE Study Yi Zhang, MD, PhD; 1 Helene Lelong, MD; 2 Sandrine
2017 High Blood Pressure Clinical Practice Guideline
 2017 High Blood Pressure Clinical Practice Guideline Applying the Latest Hypertension Guideline to Your Practice Carmine D Amico, D.O., F.A.C.C. 2017 ACC / AHA / AAPA / ABC / ACPM / AGS / APhA / ASH /
2017 High Blood Pressure Clinical Practice Guideline Applying the Latest Hypertension Guideline to Your Practice Carmine D Amico, D.O., F.A.C.C. 2017 ACC / AHA / AAPA / ABC / ACPM / AGS / APhA / ASH /
Prevention of Heart Failure: What s New with Hypertension
 Prevention of Heart Failure: What s New with Hypertension Ali AlMasood Prince Sultan Cardiac Center Riyadh 3ed Saudi Heart Failure conference, Jeddah, 13 December 2014 Background 20-30% of Saudi adults
Prevention of Heart Failure: What s New with Hypertension Ali AlMasood Prince Sultan Cardiac Center Riyadh 3ed Saudi Heart Failure conference, Jeddah, 13 December 2014 Background 20-30% of Saudi adults
HYPERTENSION GUIDELINES WHERE ARE WE IN 2014
 HYPERTENSION GUIDELINES WHERE ARE WE IN 2014 Donald J. DiPette MD FACP Special Assistant to the Provost for Health Affairs Distinguished Health Sciences Professor University of South Carolina University
HYPERTENSION GUIDELINES WHERE ARE WE IN 2014 Donald J. DiPette MD FACP Special Assistant to the Provost for Health Affairs Distinguished Health Sciences Professor University of South Carolina University
Aquifer Hypertension Guidelines Module
 Aquifer Hypertension Guidelines Module 2018 Aquifer Hypertension Guidelines Module 1 1. Introduction. In 2013 the National Heart Lung and Blood Institute (NHLBI) asked the American College of Cardiology
Aquifer Hypertension Guidelines Module 2018 Aquifer Hypertension Guidelines Module 1 1. Introduction. In 2013 the National Heart Lung and Blood Institute (NHLBI) asked the American College of Cardiology
Target Blood Pressure Attainment in Diabetic Hypertensive Patients: Need for more Diuretics? Waleed M. Sweileh, PhD
 Target Blood Pressure Attainment in Diabetic Hypertensive Patients: Need for more Diuretics? Waleed M. Sweileh, PhD Associate Professor, Clinical Pharmacology Corresponding author Waleed M. Sweileh, PhD
Target Blood Pressure Attainment in Diabetic Hypertensive Patients: Need for more Diuretics? Waleed M. Sweileh, PhD Associate Professor, Clinical Pharmacology Corresponding author Waleed M. Sweileh, PhD
A fixed-dose combination of bisoprolol and amlodipine in daily practice treatment of hypertension: Results of a noninvestigational
 Hostalek U et al. Medical Research Archives, vol. 5, issue 11, November 2017 issue Page 1 of 11 RESEARCH ARTICLE A fixed-dose combination of bisoprolol and amlodipine in daily practice treatment of hypertension:
Hostalek U et al. Medical Research Archives, vol. 5, issue 11, November 2017 issue Page 1 of 11 RESEARCH ARTICLE A fixed-dose combination of bisoprolol and amlodipine in daily practice treatment of hypertension:
In the Literature 1001 BP of 1.1 mm Hg). The trial was stopped early based on prespecified stopping rules because of a significant difference in cardi
 Is Choice of Antihypertensive Agent Important in Improving Cardiovascular Outcomes in High-Risk Hypertensive Patients? Commentary on Jamerson K, Weber MA, Bakris GL, et al; ACCOMPLISH Trial Investigators.
Is Choice of Antihypertensive Agent Important in Improving Cardiovascular Outcomes in High-Risk Hypertensive Patients? Commentary on Jamerson K, Weber MA, Bakris GL, et al; ACCOMPLISH Trial Investigators.
Randomized Design of ALLHAT BP Trial
 Outcomes in Hypertensive Black and Nonblack Patients Treated with Chlorthalidone, Amlodipine, and Lisinopril* *Wright JT, Dunn JK, Cutler JA et al. JAMA 2005:293:1595-1608. 42,418 High-risk hypertensive
Outcomes in Hypertensive Black and Nonblack Patients Treated with Chlorthalidone, Amlodipine, and Lisinopril* *Wright JT, Dunn JK, Cutler JA et al. JAMA 2005:293:1595-1608. 42,418 High-risk hypertensive
Management of Hypertension in special groups. DR-Mohammed Salah Assistant Lecturer of Cardiology Mansoura University
 Management of Hypertension in special groups BY DR-Mohammed Salah Assistant Lecturer of Cardiology Mansoura University AGENDA SPECIAL GROUPS SPECIFIC DRUDS FOR SPECIAL GROUPS TARGET BP FOR SPECIAL GROUPS:
Management of Hypertension in special groups BY DR-Mohammed Salah Assistant Lecturer of Cardiology Mansoura University AGENDA SPECIAL GROUPS SPECIFIC DRUDS FOR SPECIAL GROUPS TARGET BP FOR SPECIAL GROUPS:
The role of physical activity in the prevention and management of hypertension and obesity
 The 1 st World Congress on Controversies in Obesity, Diabetes and Hypertension (CODHy) Berlin, October 26-29 2005 The role of physical activity in the prevention and management of hypertension and obesity
The 1 st World Congress on Controversies in Obesity, Diabetes and Hypertension (CODHy) Berlin, October 26-29 2005 The role of physical activity in the prevention and management of hypertension and obesity
Approximately 73.6 million adults in the United States have
 n clinical n Hypertension Treatment and Control Within an Independent Nurse Practitioner Setting Wendy L. Wright, MS; Joan E. Romboli, MSN; Margaret A. DiTulio, MS, MBA; Jenifer Wogen, MS; and Daniel A.
n clinical n Hypertension Treatment and Control Within an Independent Nurse Practitioner Setting Wendy L. Wright, MS; Joan E. Romboli, MSN; Margaret A. DiTulio, MS, MBA; Jenifer Wogen, MS; and Daniel A.
New Lipid Guidelines. PREVENTION OF CARDIOVASCULAR DISEASE IN WOMEN: Implications of the New Guidelines for Hypertension and Lipids.
 PREVENTION OF CARDIOVASCULAR DISEASE IN WOMEN: Implications of the New Guidelines for Hypertension and Lipids Robert B. Baron MD MS Professor and Associate Dean UCSF School of Medicine Disclosure No relevant
PREVENTION OF CARDIOVASCULAR DISEASE IN WOMEN: Implications of the New Guidelines for Hypertension and Lipids Robert B. Baron MD MS Professor and Associate Dean UCSF School of Medicine Disclosure No relevant
Supplementary Online Content
 Supplementary Online Content Kavousi M, Leening MJG, Nanchen D, et al. Comparison of application of the ACC/AHA guidelines, Adult Treatment Panel III guidelines, and European Society of Cardiology guidelines
Supplementary Online Content Kavousi M, Leening MJG, Nanchen D, et al. Comparison of application of the ACC/AHA guidelines, Adult Treatment Panel III guidelines, and European Society of Cardiology guidelines
An Epidemiological Overview
 An Epidemiological Overview Cardiovascular disease (CVD) is the leading cause of death in the U.S. In 2005 CVD accounted for approximately 38 percent of all deaths CVD has been the number one killer in
An Epidemiological Overview Cardiovascular disease (CVD) is the leading cause of death in the U.S. In 2005 CVD accounted for approximately 38 percent of all deaths CVD has been the number one killer in
CVD Prevention, Who to Consider
 Continuing Professional Development 3rd annual McGill CME Cruise September 20 27, 2015 CVD Prevention, Who to Consider Dr. Guy Tremblay Excellence in Health Care and Lifelong Learning Global CV risk assessment..
Continuing Professional Development 3rd annual McGill CME Cruise September 20 27, 2015 CVD Prevention, Who to Consider Dr. Guy Tremblay Excellence in Health Care and Lifelong Learning Global CV risk assessment..
Is there a mechanism of interaction between hypertension and dyslipidaemia?
 Is there a mechanism of interaction between hypertension and dyslipidaemia? Neil R Poulter International Centre for Circulatory Health NHLI, Imperial College London Daegu, Korea April 2005 Observational
Is there a mechanism of interaction between hypertension and dyslipidaemia? Neil R Poulter International Centre for Circulatory Health NHLI, Imperial College London Daegu, Korea April 2005 Observational
The Latest Generation of Clinical
 The Latest Generation of Clinical Guidelines: HTN and HLD Dave Brackett Clinical Guideline Purpose Uniform approach Awareness of key details Diagnosis Treatment Monitoring Evidence based approach Inform
The Latest Generation of Clinical Guidelines: HTN and HLD Dave Brackett Clinical Guideline Purpose Uniform approach Awareness of key details Diagnosis Treatment Monitoring Evidence based approach Inform
Hypertension and Cardiovascular Disease
 Hypertension and Cardiovascular Disease Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any form or by any means graphic,
Hypertension and Cardiovascular Disease Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any form or by any means graphic,
New Recommendations for the Treatment of Hypertension: From Population Salt Reduction to Personalized Treatment Targets
 New Recommendations for the Treatment of Hypertension: From Population Salt Reduction to Personalized Treatment Targets Sidney C. Smith, Jr. MD, FACC, FAHA Professor of Medicine/Cardiology University of
New Recommendations for the Treatment of Hypertension: From Population Salt Reduction to Personalized Treatment Targets Sidney C. Smith, Jr. MD, FACC, FAHA Professor of Medicine/Cardiology University of
Objectives. JNC 7 Is Nice But What s Up With JNC 8? Why Do We Care? Hypertension Background: Prevalence
 JNC 7 Is Nice But What s Up With JNC 8? 37 th Annual CAPA Conference October 4 th 2013 Ignacio de Artola, Jr. M.D. Assistant Professor of Clinical Family Medicine Medical Director, Primary Care Physician
JNC 7 Is Nice But What s Up With JNC 8? 37 th Annual CAPA Conference October 4 th 2013 Ignacio de Artola, Jr. M.D. Assistant Professor of Clinical Family Medicine Medical Director, Primary Care Physician
Traitements associés chez l hypertendu: Statines, Aspirine
 Traitements associés chez l hypertendu: Statines, Aspirine Pr Jean-Jacques Mourad CHU Avicenne, Université Paris 13, Bobigny DU HTA, Mars 2012 jean-jacques.mourad@avc.aphp.fr Global Mortality 2000: Impact
Traitements associés chez l hypertendu: Statines, Aspirine Pr Jean-Jacques Mourad CHU Avicenne, Université Paris 13, Bobigny DU HTA, Mars 2012 jean-jacques.mourad@avc.aphp.fr Global Mortality 2000: Impact
Hypertension targets: sorting out the confusion. Brian Rayner, Division of Nephrology and Hypertension, University of Cape Town
 Hypertension targets: sorting out the confusion Brian Rayner, Division of Nephrology and Hypertension, University of Cape Town Historical Perspective The most famous casualty of this approach was the
Hypertension targets: sorting out the confusion Brian Rayner, Division of Nephrology and Hypertension, University of Cape Town Historical Perspective The most famous casualty of this approach was the
TIP. Documentation and coding guide. Disease definitions* Prevalence and statistics associated with HTN**
 Documentation and coding guide Disease definitions* HTN is diagnosed when the average of two or more (systolic of diastolic) blood pressure readings are found to be elevated on two or more office visits
Documentation and coding guide Disease definitions* HTN is diagnosed when the average of two or more (systolic of diastolic) blood pressure readings are found to be elevated on two or more office visits
Hypertension Update. Mayo Clinic 90 th Annual Clinical Reviews November 2 nd and 16 th, 2016
 Mayo Clinic 90 th Annual Clinical Reviews November 2 nd and 16 th, 2016 Hypertension Update Vincent J. Canzanello, M.D. Consultant, Division of Nephrology and Hypertension Professor or Medicine College
Mayo Clinic 90 th Annual Clinical Reviews November 2 nd and 16 th, 2016 Hypertension Update Vincent J. Canzanello, M.D. Consultant, Division of Nephrology and Hypertension Professor or Medicine College
Significance of Cardiac Rehabilitation on Visit-to-Visit Variability of Blood Pressure in Patients With Cardiovascular Disease in a 12-Month Follow-Up
 Elmer ress Original Article J Clin Med Res. 2017;9(4):345-352 Significance of Cardiac Rehabilitation on Visit-to-Visit Variability of Blood Pressure in Patients With Cardiovascular Disease in a 12-Month
Elmer ress Original Article J Clin Med Res. 2017;9(4):345-352 Significance of Cardiac Rehabilitation on Visit-to-Visit Variability of Blood Pressure in Patients With Cardiovascular Disease in a 12-Month
(n=6279). Continuous variables are reported as mean with 95% confidence interval and T1 T2 T3. Number of subjects
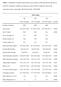 Table 1. Distribution of baseline characteristics across tertiles of OPG adjusted for age and sex (n=6279). Continuous variables are reported as mean with 95% confidence interval and categorical values
Table 1. Distribution of baseline characteristics across tertiles of OPG adjusted for age and sex (n=6279). Continuous variables are reported as mean with 95% confidence interval and categorical values
Cardiovascular Health Practice Guideline Outpatient Management of Coronary Artery Disease 2003
 Authorized By: Medical Management Guideline Committee Approval Date: 12/13/01 Revision Date: 12/11/03 Beta-Blockers Nitrates Calcium Channel Blockers MEDICATIONS Indicated in post-mi, unstable angina,
Authorized By: Medical Management Guideline Committee Approval Date: 12/13/01 Revision Date: 12/11/03 Beta-Blockers Nitrates Calcium Channel Blockers MEDICATIONS Indicated in post-mi, unstable angina,
EFFICACY & SAFETY OF ORAL TRIPLE DRUG COMBINATION OF TELMISARTAN, AMLODIPINE AND HYDROCHLOROTHIAZIDE IN THE MANAGEMENT OF NON-DIABETIC HYPERTENSION
 EFFICACY & SAFETY OF ORAL TRIPLE DRUG COMBINATION OF TELMISARTAN, AMLODIPINE AND HYDROCHLOROTHIAZIDE IN THE MANAGEMENT OF NON-DIABETIC HYPERTENSION Khemchandani D. 1 and * Arif A. Faruqui 2 1 Bairagarh,
EFFICACY & SAFETY OF ORAL TRIPLE DRUG COMBINATION OF TELMISARTAN, AMLODIPINE AND HYDROCHLOROTHIAZIDE IN THE MANAGEMENT OF NON-DIABETIC HYPERTENSION Khemchandani D. 1 and * Arif A. Faruqui 2 1 Bairagarh,
VA/DoD Clinical Practice Guideline for the Diagnosis and Management of Hypertension - Pocket Guide Update 2004 Revision July 2005
 VA/DoD Clinical Practice Guideline for the Diagnosis and Management of Hypertension - Pocket Guide Update 2004 Revision July 2005 1 Any adult in the health care system 2 Obtain blood pressure (BP) (Reliable,
VA/DoD Clinical Practice Guideline for the Diagnosis and Management of Hypertension - Pocket Guide Update 2004 Revision July 2005 1 Any adult in the health care system 2 Obtain blood pressure (BP) (Reliable,
CVD risk assessment using risk scores in primary and secondary prevention
 CVD risk assessment using risk scores in primary and secondary prevention Raul D. Santos MD, PhD Heart Institute-InCor University of Sao Paulo Brazil Disclosure Honoraria for consulting and speaker activities
CVD risk assessment using risk scores in primary and secondary prevention Raul D. Santos MD, PhD Heart Institute-InCor University of Sao Paulo Brazil Disclosure Honoraria for consulting and speaker activities
Use of Antihypertensive Medications in Patients with type -2 Diabetes in Ajman, UAE
 Use of Antihypertensive Medications in Patients with type -2 Diabetes in Ajman, UAE ORIGINAL ARTICLE Mohammed Arifulla 1, Lisha Jenny John 1, Jayadevan Sreedharan 2, Jayakumary Muttappallymyalil 3, Jenny
Use of Antihypertensive Medications in Patients with type -2 Diabetes in Ajman, UAE ORIGINAL ARTICLE Mohammed Arifulla 1, Lisha Jenny John 1, Jayadevan Sreedharan 2, Jayakumary Muttappallymyalil 3, Jenny
Egyptian Hypertension Guidelines
 Egyptian Hypertension Guidelines 2014 Egyptian Hypertension Guidelines Dalia R. ElRemissy, MD Lecturer of Cardiovascular Medicine Cairo University Why Egyptian Guidelines? Guidelines developed for rich
Egyptian Hypertension Guidelines 2014 Egyptian Hypertension Guidelines Dalia R. ElRemissy, MD Lecturer of Cardiovascular Medicine Cairo University Why Egyptian Guidelines? Guidelines developed for rich
2014 HYPERTENSION GUIDELINES
 2014 HYPERTENSION GUIDELINES Eileen M. Twomey, Pharm.D., BCPS 1 Learning Objectives Describe specific blood pressure thresholds at which antihypertensive therapy should be initiated and blood pressure
2014 HYPERTENSION GUIDELINES Eileen M. Twomey, Pharm.D., BCPS 1 Learning Objectives Describe specific blood pressure thresholds at which antihypertensive therapy should be initiated and blood pressure
Consensus Core Set: Cardiovascular Measures Version 1.0
 Consensus Core Set: Cardiovascular s NQF 0330 Hospital 30-day, all-cause, riskstandardized readmission rate (RSRR) following heart failure hospitalization 0229 Hospital 30-day, all-cause, riskstandardized
Consensus Core Set: Cardiovascular s NQF 0330 Hospital 30-day, all-cause, riskstandardized readmission rate (RSRR) following heart failure hospitalization 0229 Hospital 30-day, all-cause, riskstandardized
Difficult-to-Control & Resistant Hypertension. Anthony Viera, MD, MPH, FAHA Professor and Chair
 Difficult-to-Control & Resistant Hypertension Anthony Viera, MD, MPH, FAHA Professor and Chair Objectives Define resistant hypertension Discuss evaluation strategy for patient with HTN that appears difficult
Difficult-to-Control & Resistant Hypertension Anthony Viera, MD, MPH, FAHA Professor and Chair Objectives Define resistant hypertension Discuss evaluation strategy for patient with HTN that appears difficult
Supplementary Table 1. Baseline Characteristics by Quintiles of Systolic and Diastolic Blood Pressures
 Supplementary Data Supplementary Table 1. Baseline Characteristics by Quintiles of Systolic and Diastolic Blood Pressures Quintiles of Systolic Blood Pressure Quintiles of Diastolic Blood Pressure Q1 Q2
Supplementary Data Supplementary Table 1. Baseline Characteristics by Quintiles of Systolic and Diastolic Blood Pressures Quintiles of Systolic Blood Pressure Quintiles of Diastolic Blood Pressure Q1 Q2
The monthly ESH guide through publications
 NEWSLETTER APRIL 2016 The monthly ESH guide through publications Edited by: Prof Costas Tsioufis, ESH Secretary and Dr Alex Kasiakogias Effects of hypertension treatment on heart failure: insights from
NEWSLETTER APRIL 2016 The monthly ESH guide through publications Edited by: Prof Costas Tsioufis, ESH Secretary and Dr Alex Kasiakogias Effects of hypertension treatment on heart failure: insights from
Talking about blood pressure
 Talking about blood pressure Mrs Khan 56 BP 158/99 BMI 32 Total cholesterol 5.4 (HDL 0.8) HbA1c 43 She has been promising to do more exercise and eat more healthily for the last 2 years but her weight
Talking about blood pressure Mrs Khan 56 BP 158/99 BMI 32 Total cholesterol 5.4 (HDL 0.8) HbA1c 43 She has been promising to do more exercise and eat more healthily for the last 2 years but her weight
2/10/2014. Hypertension: Highlights of Hypertension Guidelines: Making the Most of Limited Evidence. Issues with contemporary guidelines
 Hypertension: 214 Highlights of Hypertension Guidelines: Making the Most of Limited Evidence Michael A, Weber, MD Editor-in-Chief, The Journal of Clinical Hypertension, Professor of Medicine, Division
Hypertension: 214 Highlights of Hypertension Guidelines: Making the Most of Limited Evidence Michael A, Weber, MD Editor-in-Chief, The Journal of Clinical Hypertension, Professor of Medicine, Division
Diabetes and Hypertension
 Diabetes and Hypertension William C. Cushman, MD, FAHA, FACP, FASH Chief, Preventive Medicine, Veterans Affairs Medical Center Professor, Preventive Medicine, Medicine, and Physiology University of Tennessee
Diabetes and Hypertension William C. Cushman, MD, FAHA, FACP, FASH Chief, Preventive Medicine, Veterans Affairs Medical Center Professor, Preventive Medicine, Medicine, and Physiology University of Tennessee
Cardiovascular Risk Factors: Distribution and Prevalence in a Rural Population of Bangladesh
 "Insight Heart" is also available at www.squarepharma.com.bd Cardiovascular Risk Factors: Distribution and Prevalence in a Rural Population of Bangladesh Coronary heart disease has been emerging as an
"Insight Heart" is also available at www.squarepharma.com.bd Cardiovascular Risk Factors: Distribution and Prevalence in a Rural Population of Bangladesh Coronary heart disease has been emerging as an
