Diabetes Care 36: , 2013
|
|
|
- Charlene Armstrong
- 6 years ago
- Views:
Transcription
1 Clinical Care/Education/Nutrition/Psychosocial Research O R I G I N A L A R T I C L E Short Sleep Duration Measured by Wrist Actimetry Is Associated With Deteriorated Glycemic Control in Type 1 Diabetes ANNE-LAURE BOREL, MD, PHD 1,2 JEAN-LOUIS PÉPIN, MD, PHD 1,3 LAURE NASSE, MSC 2 4 JEAN-PHILIPPE BAGUET, MD, PHD SOPHIE NETTER, MD 2 PIERRE-YVES BENHAMOU, MD, PHD 2 OBJECTIVEdSleep restriction has been associated with deteriorated insulin sensitivity. The effects of short sleep duration have been explored little in patients with type 1 diabetes. This study addresses the question of whether sleep curtailment affects HbA 1c levels in patients with type 1 diabetes. RESEARCH DESIGN AND METHODSdSeventy-nine adult patients with type 1 diabetes (median age 40 years [IQR 23 49]; 47% men) were recruited to wear a wrist actimetry sensor during 3 consecutive days to assess mean sleep duration during normal daily life. A subsample of 37 patients also performed 24-h ambulatory blood pressure monitoring (ABPM). Medical history, sleep questionnaires, and diabetes-related quality of life (DQOL) were assessed. RESULTSdPatients having shorter sleep durationdless than 6.5 h (n = 21)dhad higher levels of HbA 1c (P = 0.01) than patients with longer sleep duration, above 6.5 h (n = 58). In a multivariable regression model including shorter versus longer sleep duration, diabetes duration, DQOL score, and daily activity, sleep duration was the only variable independently associated with HbA 1c (R 2 = 10%). In patients who performed 24-h ABPM, patients with a nondipping pattern of blood pressure exhibited shorter sleep duration than patients with a dipping pattern of blood CONCLUSIONSdShorter sleep duration is associated with higher HbA 1c levels in patients with type 1 diabetes, as well as with a nondipping pattern of blood pressure, anticipating a longterm deleterious impact on the risk of microvascular complications. Further studies should test whether extending the duration of sleep may improve both HbA 1c and blood pressure in type 1 diabetes. V oluntary sleep curtailment is spreading among our societies, particularly in children and adolescents (1). Such chronic sleep deprivation is also frequent among patients suffering from type 1 diabetes as well as their families (2). Several prospective cohorts in the general population demonstrate a link between short sleep duration and incident obesity (3), type 2 diabetes (4 6), and hypertension (7,8). The main weakness of these studies, which Diabetes Care 36: , 2013 were conducted with large samples, is that sleep duration was not objectively assessed but only estimated subjectively by sleep questionnaires. Mechanisms underlying such associations seem to involve downregulation of the satiety hormone leptin and up-regulation of the appetite-stimulating hormone ghrelin, increasing hunger and food intake (9). Sleep restriction has been associated with deterioration of insulin sensitivity (10). ccccccccccccccccccccccccccccccccccccccccccccccccc From the 1 Hypoxia Pathophysiology (HP2) Laboratory, INSERM U1042, Joseph Fourier University, Grenoble, France; the 2 Endocrinology Department, University Hospital, Grenoble, France; the 3 CHU de Grenoble, Pole Locomotion, Rééducation & Physiologie, Clinique Physiologie, Sommeil et Exercice, Grenoble, France; and the 4 Cardiology Department, University Hospital, Grenoble, France. Corresponding author: Anne-Laure Borel, alborel@chu-grenoble.fr. Received 6 October 2012 and accepted 1 April DOI: /dc Clinical trial reg. no. NCT , clinicaltrials.gov by the American Diabetes Association. Readers may use this article as long as the work is properly cited, the use is educational and not for profit, and the work is not altered. See licenses/by-nc-nd/3.0/ for details. The effects of short sleep duration have been poorly explored in patients with type 1 diabetes. Short sleep duration has been associated with a nondipping pattern of blood pressure in patients with type 1 diabetes (11), which means that nocturnal blood pressure did not demonstrate the normal 10% decrease compared with daytime values. No study has yet addressed the question of the potential deleterious effect of sleep curtailment on HbA 1c in type 1 diabetes. Priou et al. (12) recently have shown that sleep apnea syndrome (obstructive sleep apnea [OSA]) was associated with increased levels of HbA 1c in subjects with OSA but without any diabetes, suggesting that sleep respiratory disorders could alter plasma glucose levels; however, this work did not evaluate the potential association of total sleep time with HbA 1c. Strict control of HbA 1c and blood pressure levels, including the normal dip of nocturnal blood pressure, have been clearly associated with lower incidence of microvascular complications in type 1 diabetes (13 15). Thus, this study looked for the effects of sleep duration on glycemic control and nocturnal blood pressure patterns in patients with type 1 diabetes. RESEARCH DESIGN AND METHODSdAdults with type 1 diabetes (81 men and women) (16) were recruited prospectively and at random from an outpatient clinic during the period ranging from December 2009 until April Participants were asked to wear a wrist actigraphy sensor for 3 consecutive days to objectively measure sleep duration in real-life conditions. One patient dropped out. One patient had invalid wrist actimetry values. Thus, 79 patients were included in the analyses. The exclusion criterion was unstable type 1 diabetes, that is, severe hypoglycemic events or acidoketosis during the previous 30 days. A subsample of 37 patients also performed a 24-h ambulatory blood pressure monitoring (ABPM) on a separate day, within 1 month after the actimetric 2902 DIABETES CARE, VOLUME 36, OCTOBER 2013 care.diabetesjournals.org
2 measurement. All patients provided informed consent and the study was approved by institutional ethics committee (Sud-Est V, France). The protocol was registered on clinicaltrial.gov (NCT ). Wrist actimetry The Actiwatch AW7 (Cambridge Neurotechnology Ltd., Cambridge, U.K.) is an actigraph that measures activity by means of a piezoelectric accelerometer that records the combination of intensity, amount, and duration of movement, and the corresponding voltage produced is converted and stored as an activity count. Activity counts were summed over 1-min intervals, called epochs. The software (Actiwatch activity and sleep analysis 7.31, Cambridge Neurotechnology Ltd.) was set to detect activity with medium sensitivity, that is, 40 counts per epoch. Determination of sleep and wakefulness by the software relies on an algorithm that looks at each data point and calculates a total score based on the activity counts from each epoch and those surrounding it. The event marker button on top of the Actiwatch had to be pressed when the participants went to bed and when they got up. The sleep analysis software determines the start of sleep by searching for a period of at least 10 min of consecutively recorded immobile data after bed time. To determine the end of sleep, the software analyzed the end of immobility corresponding to the time when patients got up. In addition, a selfreported sleep diary was completed by participants to determine bedtime, subjective sleep latency, wake-up and get-up times, sleep duration, as well as number of awakenings during the night, as recommended (17). The Actiwatch- AW7 was worn to the wrist during 3 consecutive days. This small device does not affect the subject s movements during normal activity. The ability of the device to measure sleep duration accurately and objectively has been reported previously (18). In addition to sleep duration, sleep latency, sleep fragmentation, and sleep efficiency as well as daily activity were analyzed automatically by the actimetry software. These measurements have been validated to be similar to those measured by polysomnography, the gold standard (19,20). Sleep questionnaires Pittsburgh Sleep Quality Index. The Pittsburgh Sleep Quality Index (PSQI) examined seven components (sleep quality, sleep latency, sleep duration, habitual sleep efficiency, sleep disturbances, use of sleep medications, and daytime dysfunction). A global score was fulfilled by all participants. With a total of 19 questions, participants rated the components on a scaleof0to3,withapossibletotalrange from 0 to 21 and with higher scores indicating worse sleep quality (.5 = poor sleepers) (21). Berlin questionnaire. The Berlin questionnaire evaluated the risk of having a sleep apnea syndrome (22). It consists of 10 questions on risk factors for OSA, subdivided into three symptom categories: 1) snoring behavior and apnea (six points); 2) wake-time sleepiness or fatigue (three points); and 3) the presence of obesity or hypertension (two points). The patient marks only one response per question and the ultimate interpretation of the answers suggests whether he or she has high risk of OSA (positive) or not (negative). If two or more categories are positive (categories 1 and 2: two or more points; category 3: one or more points), a person is considered at high risk of having OSA. Those who denied having persistent symptoms or who qualified for only one symptom category were placed in the lower-risk group. International restless leg syndrome severity score. For patients self-reporting a restless leg syndrome, its severity was assessed with the international restless leg syndrome (IRLS) severity score. The IRLS severity score rating scale comprises 10 questions that assess symptom severity and frequency on a 40-point scale (0 = no symptoms; 40 = very severe symptoms) (23). Diabetes quality of life. Quality of life was determined using the Diabetes Quality of Life (DQOL) questionnaire, as implemented during the Diabetes Control and Complications Trial and validated in French (24). The DQOL questionnaire was analyzed in five different subscales: satisfaction with life, impact of diabetes, social/vocational worry, diabetes-related worry, and health perception. It is a multiple-choice tool, with higher scores indicating higher quality of life. Biological measurements HbA 1c was measured by high-pressure liquid chromatography (normal values 4 6%) (Varian II; Bio-Rad, Hercules, CA). All HbA 1c values also were presented in millimoles per mole according to the NGSP s HbA 1c converter (available at Borel and Associates Microalbuminuria was measured by immunoturbidimetry (Nephelometer Analyser II; Berhing, Marburg, Germany). The level of microalbuminuria (milligrams per liter) was assessed using a urine sample collected at least 6 weeks after any urinary tract infections or acute hyperglycemic events and after exclusion of all other causes of albuminuria. 24-h ABPM The Enregistreur MAPA Q (Spacelabs Healthcare, Issaquah, WA) wasusedtorecord24-habpmwithan adapted-sized cuff. Blood pressure measurements were performed every 15 min. Blood pressure was considered nocturnal between 10:00 P.M. and 6:00 A.M. Menand women were considered to be nondippers if they had a day/night systolic blood pressure decrease of less than 10%. We included in the nondipper group four patients who were reverse dippers, that is, those whose daytime blood pressure was below the nocturnal blood They were no extreme dippers (nocturnal blood pressure dip.20%) among our population. Statistical analysis Results are expressed as mean (SD) for normally distributed variables and as median (interquartile range) for nonnormally distributed variables. Categorical variables were presented as number (percentage). The normal distribution of residuals was verified by stem and leaf plots and by Shapiro-Wilk tests. Parameters with skewed distributions (daily insulin dose, diabetes duration, sleep latency) were transformed by log or square root. Age, BMI, and microalbuminuria remained nonnormally distributed. Patients presenting with sleep duration less than 6.5 h (first quartile) were compared with patients with sleep duration longer than 6.5 h by ANOVA for normally distributed variables and by the Wilcoxon test for nonnormally distributed variables. Categorical variables were compared by x 2 test or Fischer test. Similar comparison tests were used to compare dippers with nondippers in the subsample of participants who performed a 24-h ABPM. Univariate Pearson correlations were made to identify factors associated with levels of HbA 1c. All variables tending to be associated with HbA 1c (P, 0.2), that is, short versus long sleep duration, diabetes duration, DQOL score, and daily level of care.diabetesjournals.org DIABETES CARE, VOLUME 36, OCTOBER
3 Sleep duration and HbA 1c in type 1 diabetes activity, were included in a multivariable linear regression model to assess the relative contribution of each factor to HbA 1c levels. The significance level was set at P, All analyses were performed using the SAS statistical package version 9.2 (SAS Institute, Cary, NC). RESULTSdCharacteristics of the whole sample of patients and differences between patients presenting with a shorter versus longer sleep duration are reported in Table 1. Thirty-eight patients (49%) were fulltime workers; none were shift workers. Seventeen patients (22%) were students, 11 (14%) were retired, and 12 (15%) did not work (1 missing data for work activity). The distribution of working status was not different between those who slept for shorter (,6.5 h) and longer (.6.5 h) durations (P = 0.411). Patients with shorter sleep duration presented with a higher prevalence of known sleep apnea syndrome (19 vs. 5%; P = 0.040) and restless leg syndrome (30 vs. 9%; P = 0.056) in their medical history than patients with longer sleep duration. The severity of restless leg syndrome was also higher in patients with shorter sleep duration. Beside known sleep apnea syndrome (8% of the patients), 27% of all patients presented with a positive score to the Berlin questionnaire, suggesting a high risk of undiagnosed sleep apnea syndrome. This risk tended to be higher in patients with shorter than with longer sleep duration (P = 0.060). Among patients with hypertension (n = 26), the use of b-blockers, angiotensinconverting enzyme inhibitors, angiotensin II type 1 receptor blockers, calcium channel blockers, thiazide, or antihypertensive therapy with central effect was not different between the two groups. Finally, HbA 1c was higher in patients with shorter sleep duration than in patients with longer sleep duration (8.5 [1.2] vs. 7.7 [1.0]% or 70 [13] vs. 60 [10] mmol/mol; P =0.001) (Fig. 1). Regression analyses Univariate Pearson correlations were computed to determine which variables were associated with the level of HbA 1c. Only the sleep duration dichotomized (threshold 6.5 h) between shorter versus longer sleep duration was significantly associated with HbA 1c. Shorter sleep duration increased the mean level of HbA 1c by 0.87% (10 mmol/mol). Diabetes duration, DQOL score, and daily level of activity tended to be associated with HbA 1c levels (P, 0.2). Therefore, these variables were included in a multivariable model along with sleep duration dichotomized between shorter versus longer sleep duration to assess the relative contribution of each variable to the level of HbA 1c. Sleep duration was the only variable independently associated with the level of HbA 1c,andthe model explained 10% of the HbA 1c variance. In this adjusted model, a 0.64% (7 mmol/mol) increase in HbA 1c level was associated with shorter sleep duration. 24-h ABPM. In the subsample of patients who performed a 24h-ABPM (n = 37), 12 patients presented with a dipping blood pressure pattern, 21 were nondippers, and 4 were reverse dippers. The four patients with a reverse dipping pattern were associated with nondipper patients for the analyses. The nondipping status of nocturnal blood pressure was found in 11 of 13 patients (85%) with shorter sleep duration and in 14 of 24 patients (58%) with longer sleep duration (P = 0.149,Fischer test). Of note, in this subsample of patients, those with shorter sleep duration also had higher levels of HbA 1c than those with longer sleep duration (8.9 [1.2] vs. 7.8 [0.8]% or 74 [14] vs. 61 [9] mmol/ mol, respectively; P = 0.002). Compared with dipping patients, nondipping patients were more often men and had shorter sleep duration, higher sleep latency, and lower sleep efficiency than dipping patients (Fig. 2). Diabetes duration, daily insulin dose, HbA 1c levels, and the presence of diabetes complications did not differ among dippers and nondippers (Table 2). CONCLUSIONSdThis study assessed the potential role of sleep duration on glycemic control in patients with type 1 diabetes. Sleep curtailment to less than 6.5 h was independently associated with a higher level of HbA 1c.Sleepdurationwas assessed objectively by wrist actigraphy when the majority of studies in the field used only sleep questionnaires. In addition, patients presenting with a nondipping pattern of nocturnal blood pressure also had shorter sleep duration as well as longer sleep latency and lower sleep efficiency than patients with a normal dipping pattern of nocturnal blood No study to date has specifically explored the effects of chronic sleep deprivation on glycemic control in patients with type 1 diabetes. However, several observations suggest that sleep deprivation may impact plasma glucose/insulin homeostasis. First, epidemiological studies (25 27) (see Spiegel et al. [28] for a review) suggest that short sleep duration is associated with an increased incidence of type 2 diabetes. Second, in patients without diabetes, experimental sleep deprivation was shown to alter plasma glucose/insulin homeostasis. Indeed, Spiegel et al. (29) performed a study of 6 nights of sleep deprivation (,4 h of sleep) in 11 healthy young men, followed by 6 nights of sleep recovery. An intravenous glucose tolerance test was performed at the end of each period. Sleep deprivation was associated with 40% decrease in glucose clearance and a 30% decrease in acute insulin response compared with results in the same subjects after sleep recovery. As a possible explanation for the deterioration in plasma glucose/insulin homeostasis during sleep restriction, these subjects also showed higher sympathetic activity and higher late-afternoon and evening cortisol levels after sleep restriction than after sleep recovery. These alterations were reproduced in a second study by Spiegel et al. (30) in which sleep deprivation also was associated with increased levels of the orexigenic hormone ghrelin and with reduced levels of leptin. Thus, sleep deprivation seems to affect plasma glucose/insulin homeostasis through several mechanisms: 1) sympathetic overactivity, 2) changes in food intake related hormones that are likely to increase appetite, and 3) increases in hormones that up-regulate glucose. These mechanisms are likely to alter plasma glucose/insulin homeostasis in patients with type 1 diabetes, and therefore their glycemic control. Sympathetic overactivity may also participate to poor blood pressure control. In a cohort including patients with type 1 diabetes and their first- and second-degree relatives, Estrada et al. (2) showed that 40.9% of these subjects slept insufficiently according to the U.S. age-specific recommendations for sleep duration. However, this study did not provide an additional analysis of patients with type 1 diabetes separate from their relatives without any diabetes. Our group has conducted a pilot study suggesting that patients with type 1 diabetes might have an elevated prevalence of sleep apnea syndrome (31). Accordingly, the risk of having undiagnosed sleep apnea syndrome was high (27%) in the current study. This risk tended to be higher in shorter than in longer sleepers, meaning that unknown sleep apnea syndrome may have participated in the 2904 DIABETES CARE, VOLUME 36, OCTOBER 2013 care.diabetesjournals.org
4 Borel and Associates Table 1dCharacteristics of patients Characteristics Total (n = 79) Shorter sleepers (,6.5 h) (n =21) Longer sleepers (.6.5 h) (n =58) P value Age (years) 40 (23 49) 43 (35 48) 38 (21 50) Sex, n (%) Male 37 (47) 10 (48) 27 (47) Female 42 (53) 11 (52) 31 (53) BMI (kg/m 2 ) 23.3 ( ) 23.4 ( ) 23.3 ( ) Type 1 diabetes disease profile Duration of disease (years) 16 (8 30) 21 (10 29) 13 (7 30) HbA 1c (%) 7.9 (1.1) 8.5 (1.2) 7.7 (1.0) HbA 1c (mmol/mol) 63 (12) 70 (13) 60 (10) Daily insulin dose (UI/24 h) 44 (31 62) 39 (32 58) 45 (30 62) Type of insulin regimen, n (%) Sequential insulin injections 38 (48) 10 (48) 28 (48) External insulin pump 41 (52) 11 (52) 30 (52) Retinopathy, n (%) 28 (36) 7 (35) 21 (36) Moderate 15 (56) 4 (19) 11 (19) Severe 5(6) 1(5) 4(7) Proliferative 7 (9) 2 (10) 5 (9) Nephropathy, n (%) 16 (20) 6 (29) 10 (17) Microalbuminuria 13 (16) 4 (19) 9 (16) Macroalbuminuria 1 (1) 0 (0) 1 (2) Renal deficiency 2 (3) 2 (10) 0 (0) Microalbuminuria (mg/l) 11 (9 21) 11 (11 29) 11 (8.5 16) DQOL score 78 (13) 73 (14) 80 (13) Comorbidities Hypertension, n (%) 26 (33) 10 (48) 16 (28) Dyslipidemia, n (%) 16 (20) 7 (33) 9 (16) Cardiovascular disease, n (%) 6 (8) 3 (14) 3 (5) Smoking status Current 9 (12) 4 (19) 5 (10) Former 9 (12) 1 (5) 8 (15) Nonsmoker 55 (75) 16 (76) 39 (75) Missing data Known sleep apnea, n (%) 6 (8) 4 (19) 2 (3) Insomnia, n (%) 6 (8) 2 (10) 4 (7) Restless legs syndrome, n (%) 10 (15) 6 (30) 4 (9) Actimetry Bedtime (h) 23.6 (1.2) 0.2 (1.5) 23.4 (1.0) Wake-up time (h) 7.4 (1.1) 6.8 (1.1) 7.7 (1.0) Sleep duration (min) 423 (61) 353 (43) 449 (44),0.001 Sleep latency (min) 5 (11 17) 11 (4 18) 10 (5 16) Sleep efficiency (%) 86.8 (4.7) 86.3 (5.2) 87.0 (4.6) Fragmentation index 26.2 (9.0) 26.3 (10.3) 26.2 (8.6) Daily activity 179 (99) 204 (95) 170 (100) Sleep questionnaires Pittsburgh score 4 (6 8) 6 (3 10) 6 (4 8) Positive Berlin questionnaire, n (%) 21 (27) 9 (43) 12 (21) IRLS score 0 (0 3) 4 (0 8) 0 (0 1) For continuous variables, normally distributed data are presented as mean (SD) and nonnormally distributed data as median (interquartile range). Data for categorical variables are presented as n (%). Comparisons between short vs. normal sleepers have been made by one-way ANOVA for normally distributed continuous variables, by the Wilcoxon test for nonnormally distributed continuous variables, and by x 2 or Fisher tests for categorical variables. Bold P values are statistically significant. reduced sleep duration of these patients. By contrast, the frequency of insomnia was not different between shorter and longer sleepers. Insomnia is defined by the difficulty to initiate and/or maintain sleep but is not necessarily associated with a reduction in objectively measured sleep time. Interestingly, Vgontzas et al. (32) have shown that the risk of incident diabetes among insomniac patients was increased only in patients with an objective sleep duration of less than 5 h per night. Van Dijk et al. (33) used questionnaires to assess subjective sleep characteristics of patients with type 1 diabetes compared with control care.diabetesjournals.org DIABETES CARE, VOLUME 36, OCTOBER
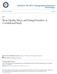
5 Sleep duration and HbA 1c in type 1 diabetes Figure 1dDistribution of HbA 1c levels in patients with shorter (,6.5 h) vs. longer (.6.5 h) sleep duration. Comparisons between short vs. normal sleepers were determined using oneway ANOVA and were statistically significant (P = 0.001). subjects without diabetes. They found that subjective sleep quality was impaired in patients with type 1 diabetes in relation to the sleep disturbance and daytime dysfunction items of the PSQI. They also presented higher levels of anxiety and depression in the Hospital Anxiety and Depression Scale than control subjects. However, sleep duration, number of short sleepers, and number of long sleepers were not different in patients with type 1 diabetes compared with control subjects. The mean sleep duration in the study by Van Dijk et al. was 7.2 h/night in patients and controls, which is comparable to the mean sleep duration found in the whole sample of patients in our study. Thus, symptoms associated with diabetes, such as thirst, nocturia, extreme glucose excursions, and mood alterations, may interfere with sleep quality and may contribute to sleep fragmentation but do not seem to alter sleep duration. In the present study, patients with shorter or longer sleep durations did not present any difference in sleep quality as assessed by the PSQI. However, patients with shorter sleep duration had delayed bedtime and earlier wake-up time compared with longer sleepers. This trend was observed at a population level using themunichchronotypequestionnaire,a simple, Internet-based questionnaire (34). Indeed, sleep duration has been reduced over the past decade by delaying bedtime, whereas get-up time on workdays has not changed. The sleep debt is often compensated for by oversleeping on free days, which induces a social jetlag, which is a chronic change in circadian rhythm every several days (35). These new paradigms may participate in glucose variability in type 1 diabetes. Further studies inquiring about the reason(s) for shorter sleep duration (e.g., voluntary sleep curtailment, constraints linked to professional status) or other factors and their specific effecton glucose control in patient with diabetes are warranted. Nocturnal blood pressure has a normal decline of more than 10% compared with daytime blood pressure, corresponding to the so-called dipping status. In type 1 diabetes, nondipping status is more prevalent (36) and is associated with increased risks for sustained hypertension, retinopathy, and nephropathy (15,36,37). Our group has previously shown that shorter sleep duration, assessed by a one-night polysomnography in a sleep laboratory, was associated with a nondipping pattern of blood pressure in patients with type 1 diabetes (11). In this previous study, patients spent the night in a sleep laboratory while polysomnography, 24-h ABPM, and continuous glucose monitoring were performed Figure 2dSleep characteristics of patients with a dipping vs. nondipping pattern of nocturnal blood A: Sleep duration. B: Sleep latency. C: Fragmentation index. D: Sleep efficiency derived from actimetric measurement. Results are mean (SD). For each patient, the data were the mean of the 3 consecutive days of measurements. *P, DIABETES CARE, VOLUME 36, OCTOBER 2013 care.diabetesjournals.org
6 Borel and Associates Table 2dCharacteristics of patients with dipping vs. nondipping blood pressure patterns Characteristics simultaneously. The current study assessed sleep duration using wrist actimetry at home and over 3 consecutive days to be closer to the routine sleep habits of patients. Results were concordant since patients with a nondipping blood pressure pattern had shorter sleep duration but longer sleep latency and lower sleep efficiency than patients with a dipping blood pressure pattern. Thus the present results show that short sleep duration is associated with deteriorated glycemic control and nocturnal blood pressure pattern in patients with type 1 diabetes. Both conditions are associated with an increased risk of developing microvascular complications (15,37,38). Thus, short sleep duration Total (n = 37) Nondippers (n =25) Dippers (n =12) P value Age (years) 44 (13) 42 (12) 49 (13) Sex, n (%) Male 18 (49) 15 (60) 3 (25) Female 19 (51) 10 (40) 9 (75) BMI (kg/m 2 ) 25.9 (4.7) 25.1 (4.0) 27.5 (5.7) Antihypertensive drugs, n (%) b-blockers 2 (6) 1 (4) 1 (8) Angiotensin conversion enzyme inhibitors 10 (29) 7 (30) 3 (25) Angiotensin II type 1 receptor blockers 9 (26) 5 (22) 4 (33) Calcium channel blocker 8 (23) 5 (22) 3 (25) Thiazide 4(11) 3(12) 1(8) Actimetry Sleep duration (min) 414 (67) 398 (65) 446 (64) Sleep.6.5 h, n (%) 24 (65) 14 (58) 10 (42) Sleep latency (min) 5 (11 18) 12 (8 24) 6 (4 10) Sleep efficiency (%) 86.4 (5.1) 84.6 (4.9) 89.8 (3.6) Fragmentation index 28.5 (9.9) 30.2 (9.5) 25.1 (10.2) Daily activity 226 (83) 225 (88) 228 (76) Sleep questionnaires Pittsburgh score 7 (4) 7 (5) 7 (2) Positive Berlin questionnaire, n (%) 14 (40) 8 (35) 6 (50) IRLS score 0 (0 3) 0 (0 5) 1 (0 1) h Ambulatory BP (mmhg) Systolic BP Mean 129 (12) 129 (14) 129 (8) Daytime 132 (12) 131 (13) 136 (8) Nighttime 120 ( ) 121 ( ) 117 ( ) Diastolic BP Mean 76 (7) 77 (8) 75 (6) Daytime 80 (7) 79 (8) 80 (6) Nighttime 69 (66 73) 70 (67 73) 66 (66 71) For continuous variables, normally distributed data are presented as mean (SD) and nonnormally distributed data as median (interquartile range). Data for categorical variables are presented as n (%). Comparisons between dippers vs. nondippers have been made by one-way ANOVA on normalized data for continuous variables and by x 2 or Fisher tests for categorical variables. Bold P values are statistically significant. BP, blood could affect the development of retinopathy and nephropathy by deteriorating synergistic glycemic levels and blood pressure in patients with type 1 diabetes. Further studies should address the efficiency of educational interventions aimed at enhancing sleep duration on glycemic levels and nocturnal blood AcknowledgmentsdThis study was supported by a grant from the Direction de la Recherche Clinique, University Hospital, Grenoble, France. No potential conflicts of interest relevant to this article were reported. A.-L.B. analyzed data and wrote the manuscript. J.-L.P. contributed to the discussion and reviewed/edited the manuscript. L.N. researched data and reviewed/edited the manuscript. J.-P.B. and S.N. researched data. P.-Y.B. researched data, contributed to the discussion, and reviewed/edited the manuscript. P.-Y.B. is the guarantor of this work and, as such, had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. References 1. Research IoMUCoSMa. Sleep Disorders and Sleep Deprivation: An Unmet Public Health Problem. Washington (DC). US, National Academies Press, Estrada CL, Danielson KK, Drum ML, Lipton RB. Insufficient sleep in young patients with diabetes and their families. Biol Res Nurs 2012;14: Chaput JP, Després JP, Bouchard C, Tremblay A. The association between sleep duration and weight gain in adults: a 6-year prospective study from the Quebec Family Study. Sleep 2008;31: Gangwisch JE, Heymsfield SB, Boden- Albala B, et al. Sleep duration as a risk factor for diabetes incidence in a large U.S. sample. Sleep 2007;30: Beihl DA, Liese AD, Haffner SM. Sleep duration as a risk factor for incident type 2 diabetes in a multiethnic cohort. Ann Epidemiol 2009;19: Chaput JP, Després JP, Bouchard C, Astrup A, Tremblay A. Sleep duration as a risk factor for the development of type 2 diabetes or impaired glucose tolerance: analyses of the Quebec Family Study. Sleep Med 2009;10: Cappuccio FP, Stranges S, Kandala NB, etal. Gender-specific associations of short sleep duration with prevalent and incident hypertension: the Whitehall II Study. Hypertension 2007;50: Knutson KL, Van Cauter E, Rathouz PJ, et al. Association between sleep and blood pressure in midlife: the CARDIA sleep study. Arch Intern Med 2009;169: Spiegel K, Tasali E, Penev P, Van Cauter E. Brief communication: Sleep curtailment in healthy young men is associated with decreased leptin levels, elevated ghrelin levels, and increased hunger and appetite. Ann Intern Med 2004;141: Morselli L, Leproult R, Balbo M, Spiegel K. Role of sleep duration in the regulation of glucose metabolism and appetite. Best Pract Res Clin Endocrinol Metab 2010;24: Borel AL, Benhamou PY, Baguet JP, et al. Short sleep duration is associated with a blood pressure nondipping pattern in type 1 diabetes: the DIAPASOM study. Diabetes Care 2009;32: Priou P, Le Vaillant M, Meslier N, et al; IRSR Sleep Cohort Group. Independent association between obstructive sleep care.diabetesjournals.org DIABETES CARE, VOLUME 36, OCTOBER
7 Sleep duration and HbA 1c in type 1 diabetes apnea severity and glycated hemoglobin in adults without diabetes. Diabetes Care 2012;35: Writing Team for the Diabetes Control and Complications Trial/Epidemiology of Diabetes Interventions and Complications Research Group. Sustained effect of intensive treatment of type 1 diabetes mellitus on development and progression of diabetic nephropathy: the Epidemiology of Diabetes Interventions and Complications (EDIC) study. JAMA 2003;290: Romero-Aroca P, Mendez-Marin I, Baget- Bernaldiz M, Fernéndez-Ballart J, Santos- Blanco E. Review of the relationship between renal and retinal microangiopathy in diabetes mellitus patients. Curr Diabetes Rev 2010;6: Benhamou PY, Halimi S, De Gaudemaris R, et al. Early disturbances of ambulatory blood pressure load in normotensive type I diabetic patients with microalbuminuria. Diabetes Care 1992;15: Expert Committee on the Diagnosis and Classification of Diabetes Mellitus. Report of the expert committee on the diagnosis and classification of diabetes mellitus. Diabetes Care 2003;26(Suppl 1):S5 S Littner M, Kushida CA, Anderson WM, et al; Standards of Practice Committee of the American Academy of Sleep Medicine. Practice parameters for the role of actigraphy in the study of sleep and circadian rhythms: an update for Sleep 2003; 26: Tryon WW. Issues of validity in actigraphic sleep assessment. Sleep 2004;27: Wang D, Wong KK, Dungan GC, 2nd, Buchanan PR, Yee BJ, Grunstein RR. The validity of wrist actimetry assessment of sleep with and without sleep apnea. J Clin Sleep Med 2008;4: Sadeh A. The role and validity of actigraphy in sleep medicine: an update. Sleep Med Rev 2011;15: Buysse DJ, Reynolds CF, 3rd, Monk TH, Berman SR, Kupfer DJ. The Pittsburgh Sleep Quality Index: a new instrument for psychiatric practice and research. Psychiatry Res 1989;28: Netzer NC, Stoohs RA, Netzer CM, Clark K, Strohl KP. Using the Berlin Questionnaire to identify patients at risk for the sleep apnea syndrome. Ann Intern Med 1999;131: Walters AS, LeBrocq C, Dhar A, et al; International Restless Legs Syndrome Study Group. Validation of the International Restless Legs Syndrome Study Group rating scale for restless legs syndrome. Sleep Med 2003;4: Renard E, Schaepelynck-Bélicar P; EVADIAC Group. Implantable insulin pumps. A position statement about their clinical use. Diabetes Metab 2007;33: Ayas NT, White DP, Al-Delaimy WK, et al. A prospective study of self-reported sleep duration and incident diabetes in women. Diabetes Care 2003;26: Mallon L, Broman JE, Hetta J. High incidence of diabetes in men with sleep complaints or short sleep duration: a 12-year follow-up study of a middle-aged population. Diabetes Care 2005;28: Yaggi HK, Araujo AB, McKinlay JB. Sleep duration as a risk factor for the development of type 2 diabetes. Diabetes Care 2006;29: Spiegel K, Tasali E, Leproult R, Van Cauter E. Effects of poor and short sleep on glucose metabolism and obesity risk. Nat Rev Endocrinol 2009;5: Spiegel K, Leproult R, Van Cauter E. Impact of sleep debt on metabolic and endocrine function. Lancet 1999;354: Spiegel K, Knutson K, Leproult R, Tasali E, Van Cauter E. Sleep loss: a novel risk factor for insulin resistance and Type 2 diabetes. J Appl Physiol 2005;99: Borel AL, Benhamou PY, Baguet JP, et al. High prevalence of obstructive sleep apnoea syndrome in a Type 1 diabetic adult population: a pilot study. Diabet Med 2010;27: Vgontzas AN, Liao D, Bixler EO, Chrousos GP, Vela-Bueno A. Insomnia with objective short sleep duration is associated with a high risk for hypertension. Sleep 2009;32: van Dijk M, Donga E, van Dijk JG, et al. Disturbed subjective sleep characteristics in adult patients with long-standing type 1 diabetes mellitus. Diabetologia 2011;54: Roenneberg T, Wirz-Justice A, Merrow M. Life between clocks: daily temporal patterns of human chronotypes. J Biol Rhythms 2003;18: Roenneberg T, Allebrandt KV, Merrow M, Vetter C. Social jetlag and obesity. Curr Biol 2012;22: Dost A, Klinkert C, Kapellen T, et al; DPV Science Initiative. Arterial hypertension determined by ambulatory blood pressure profiles: contribution to microalbuminuria risk in a multicenter investigation in 2,105 children and adolescents with type 1 diabetes. Diabetes Care 2008;31: Stella P, Tabak AG, Zgibor JC, Orchard TJ. Late diabetes complications and nondipping phenomenon in patients with Type 1 diabetes. Diabetes Res Clin Pract 2006;71: Nordwall M, Arnqvist HJ, Bojestig M, Ludvigsson J. Good glycemic control remains crucial in prevention of late diabetic complicationsdthe Linköping Diabetes Complications Study. Pediatr Diabetes 2009;10: DIABETES CARE, VOLUME 36, OCTOBER 2013 care.diabetesjournals.org
Cross-Sectional Associations Between Measures of Sleep and Markers of Glucose Metabolism Among Subjects With and Without Diabetes
 Epidemiology/Health Services Research O R I G I N A L A R T I C L E Cross-Sectional Associations Between Measures of Sleep and Markers of Glucose Metabolism Among Subjects With and Without Diabetes The
Epidemiology/Health Services Research O R I G I N A L A R T I C L E Cross-Sectional Associations Between Measures of Sleep and Markers of Glucose Metabolism Among Subjects With and Without Diabetes The
Sleep Apnea Symptoms in Diabetics and their First Degree Relatives
 www.ijpm.ir Sleep Apnea Symptoms in Diabetics and their First Degree Relatives Babak Amra, Farideh Sheikh Bahaee 1, Masoud Amini 1, Mohammad Golshan 2, Ingo Fietze 3, Thomas Penzel 3 Department of Internal
www.ijpm.ir Sleep Apnea Symptoms in Diabetics and their First Degree Relatives Babak Amra, Farideh Sheikh Bahaee 1, Masoud Amini 1, Mohammad Golshan 2, Ingo Fietze 3, Thomas Penzel 3 Department of Internal
Pooja Bansil, MPH; Elena V. Kuklina, MD, PhD; Robert K. Merritt, MA; Paula W. Yoon, ScD, MPH
 ORIGINAL PAPER Associations Between Sleep Disorders, Sleep Duration, Quality of Sleep, and Hypertension: Results From the National Health and Nutrition Examination Survey, 2005 to 2008 Pooja Bansil, MPH;
ORIGINAL PAPER Associations Between Sleep Disorders, Sleep Duration, Quality of Sleep, and Hypertension: Results From the National Health and Nutrition Examination Survey, 2005 to 2008 Pooja Bansil, MPH;
Sweet Dreams: The Relationship between Sleep Health and Your Weight
 Sweet Dreams: The Relationship between Sleep Health and Your Weight Jason C. Ong, PhD Associate Professor Department of Neurology Center for Circadian and Sleep Medicine Northwestern University Feinberg
Sweet Dreams: The Relationship between Sleep Health and Your Weight Jason C. Ong, PhD Associate Professor Department of Neurology Center for Circadian and Sleep Medicine Northwestern University Feinberg
Sleep Disturbances in Midlife Women: Kathryn A. Lee. Are there Ethnic or Class Differences, or Is it All Just Hormonal?
 Sleep Disturbances in Midlife Women: Are there Ethnic or Class Differences, or Is it All Just Hormonal? Kathryn A. Lee School of Nursing, UCSF Research supported by NIH grants #NR02247, NR03969, and Supplement
Sleep Disturbances in Midlife Women: Are there Ethnic or Class Differences, or Is it All Just Hormonal? Kathryn A. Lee School of Nursing, UCSF Research supported by NIH grants #NR02247, NR03969, and Supplement
Comparison of arbitrary definitions of circadian time periods with those determined by wrist actigraphy in analysis of ABPM data
 Journal of Human Hypertension (1999) 13, 449 453 1999 Stockton Press. All rights reserved 0950-9240/99 $12.00 http://www.stockton-press.co.uk/jhh ORIGINAL ARTICLE Comparison of arbitrary definitions of
Journal of Human Hypertension (1999) 13, 449 453 1999 Stockton Press. All rights reserved 0950-9240/99 $12.00 http://www.stockton-press.co.uk/jhh ORIGINAL ARTICLE Comparison of arbitrary definitions of
Waiting Time Distributions of Actigraphy Measured Sleep
 The Open Sleep Journal, 2008, 1, 1-5 1 Waiting Time Distributions of Actigraphy Measured Sleep J.E. Slaven*,1, A. Mnatsakanova 1, S. Li 1,2, J.M. Violanti 3, C.M. Burchfiel 1, B.J. Vila 4 and M.E. Andrew
The Open Sleep Journal, 2008, 1, 1-5 1 Waiting Time Distributions of Actigraphy Measured Sleep J.E. Slaven*,1, A. Mnatsakanova 1, S. Li 1,2, J.M. Violanti 3, C.M. Burchfiel 1, B.J. Vila 4 and M.E. Andrew
Sleep and Weight Control
 A Wake-up Call Charles H. Samuels, MD, CCFP, DABSM As presented at the Sleep and Respiration Rounds held at the Lung Association Sleep Centre at Foothills Medical Centre, Calgary, Alberta (May 2005) Jill
A Wake-up Call Charles H. Samuels, MD, CCFP, DABSM As presented at the Sleep and Respiration Rounds held at the Lung Association Sleep Centre at Foothills Medical Centre, Calgary, Alberta (May 2005) Jill
Overview of epidemiology of sleep and obesity risk
 Overview of epidemiology of sleep and obesity risk Sanjay R. Patel MD, MS Director, Center for Sleep and Cardiovascular Outcomes Research Visiting Professor of Medicine University of Pittsburgh What is
Overview of epidemiology of sleep and obesity risk Sanjay R. Patel MD, MS Director, Center for Sleep and Cardiovascular Outcomes Research Visiting Professor of Medicine University of Pittsburgh What is
Diabetes & Obstructive Sleep Apnoea risk. Jaynie Pateraki MSc RGN
 Diabetes & Obstructive Sleep Apnoea risk Jaynie Pateraki MSc RGN Non-REM - REM - Both - Unrelated - Common disorders of Sleep Sleep Walking Night terrors Periodic leg movements Sleep automatism Nightmares
Diabetes & Obstructive Sleep Apnoea risk Jaynie Pateraki MSc RGN Non-REM - REM - Both - Unrelated - Common disorders of Sleep Sleep Walking Night terrors Periodic leg movements Sleep automatism Nightmares
Metabolic, Endocrine, and Immune Consequences of Sleep Deprivation
 The Open Respiratory Medicine Journal, 2011, 5, 31-43 31 Metabolic, Endocrine, and Immune Consequences of Sleep Deprivation Laila AlDabal 1 and Ahmed S. BaHammam *,2 Open Access 1 Department of Pulmonary
The Open Respiratory Medicine Journal, 2011, 5, 31-43 31 Metabolic, Endocrine, and Immune Consequences of Sleep Deprivation Laila AlDabal 1 and Ahmed S. BaHammam *,2 Open Access 1 Department of Pulmonary
AGING, BLOOD PRESSURE & CARDIOVASCULAR DISEASE EVENT RISK. Michael Smolensky, Ph.D. The University of Texas Austin & Houston
 AGING, BLOOD PRESSURE & CARDIOVASCULAR DISEASE EVENT RISK Michael Smolensky, Ph.D. The University of Texas Austin & Houston Disclosures Partner: Circadian Ambulatory Diagnostics Consultant: Spot On Sciences
AGING, BLOOD PRESSURE & CARDIOVASCULAR DISEASE EVENT RISK Michael Smolensky, Ph.D. The University of Texas Austin & Houston Disclosures Partner: Circadian Ambulatory Diagnostics Consultant: Spot On Sciences
Diabetes and Hypertension
 Diabetes and Hypertension M.Nakhjvani,M.D Tehran University of Medical Sciences 20-8-96 Hypertension Common DM comorbidity Prevalence depends on diabetes type, age, BMI, ethnicity Major risk factor for
Diabetes and Hypertension M.Nakhjvani,M.D Tehran University of Medical Sciences 20-8-96 Hypertension Common DM comorbidity Prevalence depends on diabetes type, age, BMI, ethnicity Major risk factor for
ORIGINAL ARTICLE AMBULATORY BLOOD PRESSURE IN OBESITY. Introduction. Patients and Methods
 Vol. 2, Issue 1, pages 31-36 ORIGINAL ARTICLE AMBULATORY BLOOD PRESSURE IN OBESITY By Alejandro de la Sierra, MD Luis M. Ruilope, MD Hypertension Units, Hospital Clinico, Barcelona & Hospital 12 de Octubre,
Vol. 2, Issue 1, pages 31-36 ORIGINAL ARTICLE AMBULATORY BLOOD PRESSURE IN OBESITY By Alejandro de la Sierra, MD Luis M. Ruilope, MD Hypertension Units, Hospital Clinico, Barcelona & Hospital 12 de Octubre,
ΥΠΝΟΣ ΚΑΙ ΠΑΧΥΣΑΡΚΙΑ: ΜΙΑ ΑΜΦΙΔΡΟΜΗ ΣΧΕΣΗ?
 ΥΠΝΟΣ ΚΑΙ ΠΑΧΥΣΑΡΚΙΑ: ΜΙΑ ΑΜΦΙΔΡΟΜΗ ΣΧΕΣΗ? ΜΑΡΙΑ ΜΠΑΣΤΑ, ΕΠΙΚΟΥΡΗ ΚΑΘ. ΨΥΧΙΑΤΡΙΚΗΣ ΤΜΗΜΑ ΙΑΤΡΙΚΗΣ, ΠΑΝ/ΜΙΟ ΚΡΗΤΗΣ POST DOC FELLOSHIP SLEEP RESEARCH AND TREATMENT CENTRER, HERSHEY, PA EUROPEAN SOMNOLOGIST
ΥΠΝΟΣ ΚΑΙ ΠΑΧΥΣΑΡΚΙΑ: ΜΙΑ ΑΜΦΙΔΡΟΜΗ ΣΧΕΣΗ? ΜΑΡΙΑ ΜΠΑΣΤΑ, ΕΠΙΚΟΥΡΗ ΚΑΘ. ΨΥΧΙΑΤΡΙΚΗΣ ΤΜΗΜΑ ΙΑΤΡΙΚΗΣ, ΠΑΝ/ΜΙΟ ΚΡΗΤΗΣ POST DOC FELLOSHIP SLEEP RESEARCH AND TREATMENT CENTRER, HERSHEY, PA EUROPEAN SOMNOLOGIST
ORIGINAL INVESTIGATION. Association Between Sleep and Blood Pressure in Midlife
 ORIGINAL INVESTIGATION Association Between Sleep and Blood ressure in Midlife The CARDIA Sleep Study Kristen L. Knutson, hd; Eve Van Cauter, hd; aul J. Rathouz, hd; Lijing L. Yan, hd; Stephen B. Hulley,
ORIGINAL INVESTIGATION Association Between Sleep and Blood ressure in Midlife The CARDIA Sleep Study Kristen L. Knutson, hd; Eve Van Cauter, hd; aul J. Rathouz, hd; Lijing L. Yan, hd; Stephen B. Hulley,
Clinical Trial Synopsis TL , NCT#
 Clinical Trial Synopsis, NCT#00492011 Title of Study: A Randomized, Double-Blind, Placebo-Controlled, Parallel-Group Study to Evaluate the Ability of Ramelteon 1 mg, 4 mg, and 8 mg to Alleviate the Insomnia
Clinical Trial Synopsis, NCT#00492011 Title of Study: A Randomized, Double-Blind, Placebo-Controlled, Parallel-Group Study to Evaluate the Ability of Ramelteon 1 mg, 4 mg, and 8 mg to Alleviate the Insomnia
The Relationships between Sleep-Wake Cycle and Academic Performance in Medical Students
 Biological Rhythm Research 0165-0424/01/3202-263$16.00 2001, Vol. 32, No. 2, pp. 263 270 Swets & Zeitlinger The Relationships between Sleep-Wake Cycle and Academic Performance in Medical Students Ana Ligia
Biological Rhythm Research 0165-0424/01/3202-263$16.00 2001, Vol. 32, No. 2, pp. 263 270 Swets & Zeitlinger The Relationships between Sleep-Wake Cycle and Academic Performance in Medical Students Ana Ligia
Study «CLIMSOM & Sleep Quality»
 Study «CLIMSOM & Sleep Quality» 211 Actigraphic Measures 1. Contextof the Study 1 out of 5 suffer from insomnia. The environment is one of the most influential factors on sleep (noise, temperature and
Study «CLIMSOM & Sleep Quality» 211 Actigraphic Measures 1. Contextof the Study 1 out of 5 suffer from insomnia. The environment is one of the most influential factors on sleep (noise, temperature and
ANTIHYPERTENSIVE DRUG THERAPY IN CONSIDERATION OF CIRCADIAN BLOOD PRESSURE VARIATION*
 Progress in Clinical Medicine 1 ANTIHYPERTENSIVE DRUG THERAPY IN CONSIDERATION OF CIRCADIAN BLOOD PRESSURE VARIATION* Keishi ABE** Asian Med. J. 44(2): 83 90, 2001 Abstract: J-MUBA was a large-scale clinical
Progress in Clinical Medicine 1 ANTIHYPERTENSIVE DRUG THERAPY IN CONSIDERATION OF CIRCADIAN BLOOD PRESSURE VARIATION* Keishi ABE** Asian Med. J. 44(2): 83 90, 2001 Abstract: J-MUBA was a large-scale clinical
Primary hypertension in adults
 Primary hypertension in adults NICE provided the content for this booklet which is independent of any company or product advertised Hypertension Welcome NICE published an updated guideline on the diagnosis
Primary hypertension in adults NICE provided the content for this booklet which is independent of any company or product advertised Hypertension Welcome NICE published an updated guideline on the diagnosis
Blood pressure (BP) in healthy people follows a circadian
 The Effect of Measuring Ambulatory Blood Pressure on Nighttime Sleep and Daytime Activity Implications for Dipping Rajiv Agarwal and Robert P. Light Indiana University School of Medicine and Richard L.
The Effect of Measuring Ambulatory Blood Pressure on Nighttime Sleep and Daytime Activity Implications for Dipping Rajiv Agarwal and Robert P. Light Indiana University School of Medicine and Richard L.
Blood Pressure Monitoring in Chronic Kidney Disease
 Blood Pressure Monitoring in Chronic Kidney Disease Aldo J. Peixoto, MD FASN FASH Associate Professor of Medicine (Nephrology), YSM Associate Chief of Medicine, VACT Director of Hypertension, VACT American
Blood Pressure Monitoring in Chronic Kidney Disease Aldo J. Peixoto, MD FASN FASH Associate Professor of Medicine (Nephrology), YSM Associate Chief of Medicine, VACT Director of Hypertension, VACT American
Sleep Quality, Stress, and Eating Disorders: A Correlational Study
 Intuition: The BYU Undergraduate Journal in Psychology Volume 11 Issue 2 Article 3 2015 Sleep Quality, Stress, and Eating Disorders: A Correlational Study Follow this and additional works at: https://scholarsarchive.byu.edu/intuition
Intuition: The BYU Undergraduate Journal in Psychology Volume 11 Issue 2 Article 3 2015 Sleep Quality, Stress, and Eating Disorders: A Correlational Study Follow this and additional works at: https://scholarsarchive.byu.edu/intuition
Heart Failure and Sleep Disordered Breathing (SDB) Unhappy Bedfellows
 Question Heart Failure and Sleep Disordered Breathing (SDB) Unhappy Bedfellows 1 ResMed 2012 07 2 ResMed 2012 07 Open Airway 3 ResMed 2012 07 Flow Limitation Snore 4 ResMed 2012 07 Apnoea 5 ResMed 2012
Question Heart Failure and Sleep Disordered Breathing (SDB) Unhappy Bedfellows 1 ResMed 2012 07 2 ResMed 2012 07 Open Airway 3 ResMed 2012 07 Flow Limitation Snore 4 ResMed 2012 07 Apnoea 5 ResMed 2012
Sleepiness, Napping and Health Risk in the Elderly
 Sleepiness, Napping and Health Risk in the Elderly ANNE B. NEWMAN, MD, MPH PROFESSOR OF EPIDEMIOLOGY AND MEDICINE UNIVERSITY OF PITTSBURGH 8th Annual Bedside to Bench Conference Sleep, Circadian Rhythms,
Sleepiness, Napping and Health Risk in the Elderly ANNE B. NEWMAN, MD, MPH PROFESSOR OF EPIDEMIOLOGY AND MEDICINE UNIVERSITY OF PITTSBURGH 8th Annual Bedside to Bench Conference Sleep, Circadian Rhythms,
ORIGINAL INVESTIGATION. C-Reactive Protein Concentration and Incident Hypertension in Young Adults
 ORIGINAL INVESTIGATION C-Reactive Protein Concentration and Incident Hypertension in Young Adults The CARDIA Study Susan G. Lakoski, MD, MS; David M. Herrington, MD, MHS; David M. Siscovick, MD, MPH; Stephen
ORIGINAL INVESTIGATION C-Reactive Protein Concentration and Incident Hypertension in Young Adults The CARDIA Study Susan G. Lakoski, MD, MS; David M. Herrington, MD, MHS; David M. Siscovick, MD, MPH; Stephen
Excessive Daytime Sleepiness Associated with Insufficient Sleep
 Sleep, 6(4):319-325 1983 Raven Press, New York Excessive Daytime Sleepiness Associated with Insufficient Sleep T. Roehrs, F. Zorick, J. Sicklesteel, R. Wittig, and T. Roth Sleep Disorders and Research
Sleep, 6(4):319-325 1983 Raven Press, New York Excessive Daytime Sleepiness Associated with Insufficient Sleep T. Roehrs, F. Zorick, J. Sicklesteel, R. Wittig, and T. Roth Sleep Disorders and Research
Diabetes Care 32: , 2009
 Epidemiology/Health Services Research O R I G I N A L A R T I C L E Insomnia With Objective Short Sleep Duration Is Associated With Type 2 Diabetes A population-based study ALEXANDROS N. VGONTZAS, MD 1
Epidemiology/Health Services Research O R I G I N A L A R T I C L E Insomnia With Objective Short Sleep Duration Is Associated With Type 2 Diabetes A population-based study ALEXANDROS N. VGONTZAS, MD 1
Polysomnography (PSG) (Sleep Studies), Sleep Center
 Policy Number: 1036 Policy History Approve Date: 07/09/2015 Effective Date: 07/09/2015 Preauthorization All Plans Benefit plans vary in coverage and some plans may not provide coverage for certain service(s)
Policy Number: 1036 Policy History Approve Date: 07/09/2015 Effective Date: 07/09/2015 Preauthorization All Plans Benefit plans vary in coverage and some plans may not provide coverage for certain service(s)
(Insufficient) Sleep and CNS Inflammation
 (Insufficient) Sleep and CNS Inflammation Mark R. Opp, PhD Vice Chair for Basic Research UW Medicine Education and Research Endowed Chair in Anesthesiology Editor-in-Chief, Neurobiology of Sleep and Circadian
(Insufficient) Sleep and CNS Inflammation Mark R. Opp, PhD Vice Chair for Basic Research UW Medicine Education and Research Endowed Chair in Anesthesiology Editor-in-Chief, Neurobiology of Sleep and Circadian
The association between sleep duration, body mass index and metabolic measures in the Hordaland Health Study
 J. Sleep Res. (2007) 16, 66 76 The association between sleep duration, body mass index and metabolic measures in the Hordaland Health Study BJØRN BJORVATN 1,5, INA MARIE SAGEN 1, NICOLAS ØYANE 1, SIRI
J. Sleep Res. (2007) 16, 66 76 The association between sleep duration, body mass index and metabolic measures in the Hordaland Health Study BJØRN BJORVATN 1,5, INA MARIE SAGEN 1, NICOLAS ØYANE 1, SIRI
Original Article Is long sleep duratıon a new risk factor for obesity?
 Int J Clin Exp Med 2016;9(8):16741-16746 www.ijcem.com /ISSN:1940-5901/IJCEM0022504 Original Article? Yavuz Furuncuoğlu 1, Samim Emet 2, Murat Kose 2, Ayşe Çıkım Sertkaya 3, Şükrü Aras 4 1 Bahcesehir School
Int J Clin Exp Med 2016;9(8):16741-16746 www.ijcem.com /ISSN:1940-5901/IJCEM0022504 Original Article? Yavuz Furuncuoğlu 1, Samim Emet 2, Murat Kose 2, Ayşe Çıkım Sertkaya 3, Şükrü Aras 4 1 Bahcesehir School
Article printed from
 What Are Sleep Disorders? Sleep disorders are conditions that affect how much and how well you sleep. The causes range from poor habits that keep you awake to medical problems that disrupt your sleep cycle.
What Are Sleep Disorders? Sleep disorders are conditions that affect how much and how well you sleep. The causes range from poor habits that keep you awake to medical problems that disrupt your sleep cycle.
Sleep in the Patient with Diabetes
 Sleep in the Patient with Diabetes ANDREA RINN, DO SEPTEMBER, 2017 Learning Objectives 1. Recognize the correlation between sleep apnea and diabetes 2. Review potential relationships between sleep and
Sleep in the Patient with Diabetes ANDREA RINN, DO SEPTEMBER, 2017 Learning Objectives 1. Recognize the correlation between sleep apnea and diabetes 2. Review potential relationships between sleep and
Study on sleep quality and associated psychosocial factors among elderly in a rural population of Kerala, India
 International Journal of Community Medicine and Public Health George S et al. Int J Community Med Public Health. 2018 Feb;5(2):526-531 http://www.ijcmph.com pissn 2394-6032 eissn 2394-6040 Original Research
International Journal of Community Medicine and Public Health George S et al. Int J Community Med Public Health. 2018 Feb;5(2):526-531 http://www.ijcmph.com pissn 2394-6032 eissn 2394-6040 Original Research
Index. sleep.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Actigraphy, 475, 485, 496 Adolescents, sleep disorders in, 576 578 Adults, sleep disorders in, 578 580 Advanced sleep phase disorder, 482 Age,
Note: Page numbers of article titles are in boldface type. A Actigraphy, 475, 485, 496 Adolescents, sleep disorders in, 576 578 Adults, sleep disorders in, 578 580 Advanced sleep phase disorder, 482 Age,
Interactions between sleep, circadian function, and glucose metabolism: implications for risk and severity of diabetes
 Ann. N.Y. Acad. Sci. ISSN 0077-8923 ANNALS OF THE NEW YORK ACADEMY OF SCIENCES Issue: The Year in Diabetes and Obesity Interactions between sleep, circadian function, and glucose metabolism: implications
Ann. N.Y. Acad. Sci. ISSN 0077-8923 ANNALS OF THE NEW YORK ACADEMY OF SCIENCES Issue: The Year in Diabetes and Obesity Interactions between sleep, circadian function, and glucose metabolism: implications
Hypertension, which is a widely prevalent and treatable
 Chronic Kidney Disease and Nocturia Nocturia, Nocturnal Activity, and Nondipping Rajiv Agarwal, Robert P. Light, Jennifer E. Bills, Lindsey A. Hummel Abstract Patients with chronic kidney disease have
Chronic Kidney Disease and Nocturia Nocturia, Nocturnal Activity, and Nondipping Rajiv Agarwal, Robert P. Light, Jennifer E. Bills, Lindsey A. Hummel Abstract Patients with chronic kidney disease have
ORIGINAL INVESTIGATION. Overweight and Obese Patients in a Primary Care Population Report Less Sleep Than Patients With a Normal Body Mass Index
 ORIGINAL INVESTIGATION Overweight and Obese Patients in a Primary Care Population Report Less Sleep Than Patients With a Normal Body Mass Index Robert D. Vorona, MD; Maria P. Winn, MSN, FNP; Teresa W.
ORIGINAL INVESTIGATION Overweight and Obese Patients in a Primary Care Population Report Less Sleep Than Patients With a Normal Body Mass Index Robert D. Vorona, MD; Maria P. Winn, MSN, FNP; Teresa W.
The Association of Daytime and Nighttime Ambulatory Blood Pressure with Carotid IMT When Controlling for Daytime Physical Activity.
 The Association of Daytime and Nighttime Ambulatory Blood Pressure with Carotid IMT When Controlling for Daytime Physical Activity by Jeanette Garcia BS, University of Pittsburgh, 2004 MS, University of
The Association of Daytime and Nighttime Ambulatory Blood Pressure with Carotid IMT When Controlling for Daytime Physical Activity by Jeanette Garcia BS, University of Pittsburgh, 2004 MS, University of
There has been a substantial increase in the number of studies. The Validity of Wrist Actimetry Assessment of Sleep With and Without Sleep Apnea
 Scientific investigations The Validity of Wrist Actimetry Assessment of Sleep With and Without Sleep Apnea David Wang, Ph.D. 1,2 ; Keith K. Wong, MB. BS. 1,2 ; George C. Dungan II, RPSGT 1 ; Peter R. Buchanan,
Scientific investigations The Validity of Wrist Actimetry Assessment of Sleep With and Without Sleep Apnea David Wang, Ph.D. 1,2 ; Keith K. Wong, MB. BS. 1,2 ; George C. Dungan II, RPSGT 1 ; Peter R. Buchanan,
Dr Diana R Holdright. MD, FRCP, FESC, FACC, MBBS, DA, BSc. Consultant Cardiologist HYPERTENSION.
 Dr Diana R Holdright MD, FRCP, FESC, FACC, MBBS, DA, BSc. Consultant Cardiologist HYPERTENSION www.drholdright.co.uk Blood pressure is the pressure exerted on the walls of the arteries when the heart pumps;
Dr Diana R Holdright MD, FRCP, FESC, FACC, MBBS, DA, BSc. Consultant Cardiologist HYPERTENSION www.drholdright.co.uk Blood pressure is the pressure exerted on the walls of the arteries when the heart pumps;
Index SLEEP MEDICINE CLINICS. Note: Page numbers of article titles are in boldface type. Cerebrospinal fluid analysis, for Kleine-Levin syndrome,
 165 SLEEP MEDICINE CLINICS Index Sleep Med Clin 1 (2006) 165 170 Note: Page numbers of article titles are in boldface type. A Academic performance, effects of sleepiness in children on, 112 Accidents,
165 SLEEP MEDICINE CLINICS Index Sleep Med Clin 1 (2006) 165 170 Note: Page numbers of article titles are in boldface type. A Academic performance, effects of sleepiness in children on, 112 Accidents,
Sleep and Executive Performance
 Sleep and Executive Performance 2017 United Fresh Produce Executive Development Program Ana C. Krieger, MD, MPH, FAASM, FCCP Medical Director, Center for Sleep Medicine Associate Professor, Weill Cornell
Sleep and Executive Performance 2017 United Fresh Produce Executive Development Program Ana C. Krieger, MD, MPH, FAASM, FCCP Medical Director, Center for Sleep Medicine Associate Professor, Weill Cornell
Sleep Insomnia Severity Index (SISI) Pittsburgh Sleep Quality Inventory. POMS Vigor subscale
 Physical GLOBAL HEALTH PROMIS completed already Sleep PROMIS-Sleep Sleep Insomnia Severity Index () Pittsburgh Sleep Quality Inventory 8 items 7 items 18 items Vigor Vigor subscale 6 items 1 Sleep- PROMIS
Physical GLOBAL HEALTH PROMIS completed already Sleep PROMIS-Sleep Sleep Insomnia Severity Index () Pittsburgh Sleep Quality Inventory 8 items 7 items 18 items Vigor Vigor subscale 6 items 1 Sleep- PROMIS
Christopher D. Turnbull 1,2, Daniel J. Bratton 3, Sonya E. Craig 1, Malcolm Kohler 3, John R. Stradling 1,2. Original Article
 Original Article In patients with minimally symptomatic OSA can baseline characteristics and early patterns of CPAP usage predict those who are likely to be longer-term users of CPAP Christopher D. Turnbull
Original Article In patients with minimally symptomatic OSA can baseline characteristics and early patterns of CPAP usage predict those who are likely to be longer-term users of CPAP Christopher D. Turnbull
Obesity, Diabetes and Obstructive Sleep Apnea Syndrome (OSAS ) Jaakko Tuomilehto. Prof. MD, MA, PhD, FRCP (Edin)
 Obesity, Diabetes and Obstructive Sleep Apnea Syndrome (OSAS ) Jaakko Tuomilehto Prof. MD, MA, PhD, FRCP (Edin) Department of Chronic Disease Prevention, National Institute for Health and Welfare, Helsinki,
Obesity, Diabetes and Obstructive Sleep Apnea Syndrome (OSAS ) Jaakko Tuomilehto Prof. MD, MA, PhD, FRCP (Edin) Department of Chronic Disease Prevention, National Institute for Health and Welfare, Helsinki,
Relationship between Sleep and Obesity among Children in the Guelph Family Health Study. By: Sabrina Douglas
 Relationship between Sleep and Obesity among Children in the Guelph Family Health Study By: Sabrina Douglas A Thesis presented to The University of Guelph In partial fulfillment of requirements for the
Relationship between Sleep and Obesity among Children in the Guelph Family Health Study By: Sabrina Douglas A Thesis presented to The University of Guelph In partial fulfillment of requirements for the
Time of day for exercise on blood pressure reduction in dipping and nondipping hypertension
 (2005) 19, 597 605 & 2005 Nature Publishing Group All rights reserved 0950-9240/05 $30.00 www.nature.com/jhh ORIGINAL ARTICLE on blood pressure reduction in dipping and nondipping hypertension S Park,
(2005) 19, 597 605 & 2005 Nature Publishing Group All rights reserved 0950-9240/05 $30.00 www.nature.com/jhh ORIGINAL ARTICLE on blood pressure reduction in dipping and nondipping hypertension S Park,
Sleep and Obesity. Review INTRODUCTION
 Journal of Obesity & Metabolic Syndrome 2018;27:4-24 https://doi.org/10.7570/jomes.2018.27.1.4 Review pissn 2508-6235 eissn 2508-7576 Sleep and Obesity Chenzhao Ding 1, Lee Ling Lim 1,2, Li Xu 1, Alice
Journal of Obesity & Metabolic Syndrome 2018;27:4-24 https://doi.org/10.7570/jomes.2018.27.1.4 Review pissn 2508-6235 eissn 2508-7576 Sleep and Obesity Chenzhao Ding 1, Lee Ling Lim 1,2, Li Xu 1, Alice
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/33966 holds various files of this Leiden University dissertation. Author: Dijk, Marieke van Title: Type 1 diabetes and sleep : implications for glucoregulation
Cover Page The handle http://hdl.handle.net/1887/33966 holds various files of this Leiden University dissertation. Author: Dijk, Marieke van Title: Type 1 diabetes and sleep : implications for glucoregulation
SLEEP AND YOUR WEIGHT. Michelle Zetoony, DO, FCCP, FACOI.
 SLEEP AND YOUR WEIGHT Michelle Zetoony, DO, FCCP, FACOI http://dosleep.doctorsoffice.net OBJECTIVES What is sleep? As a culture, where does sleep fit in rank? Sleep and obesity Tips for better sleep WHAT
SLEEP AND YOUR WEIGHT Michelle Zetoony, DO, FCCP, FACOI http://dosleep.doctorsoffice.net OBJECTIVES What is sleep? As a culture, where does sleep fit in rank? Sleep and obesity Tips for better sleep WHAT
Chapter-V. Summary, Conclusions and Recommendations
 Summary, Conclusions and Recommendations INTRODUCTION The work included in this thesis entitled, Circadian heart rate and blood pressure variability in apparently healthy subjects using ABPM has been divided
Summary, Conclusions and Recommendations INTRODUCTION The work included in this thesis entitled, Circadian heart rate and blood pressure variability in apparently healthy subjects using ABPM has been divided
Utilizing Actigraphy Data and Multi-Dimensional Sleep Domains
 Utilizing Actigraphy Data and Multi-Dimensional Sleep Domains Katie L. Stone, Ph.D. For: WHI Investigator Meeting May 3-4, 2018 Chicago, Illinois Objectives Brief overview of sleep actigraphy data collection
Utilizing Actigraphy Data and Multi-Dimensional Sleep Domains Katie L. Stone, Ph.D. For: WHI Investigator Meeting May 3-4, 2018 Chicago, Illinois Objectives Brief overview of sleep actigraphy data collection
Teenagers: Sleep Patterns and School Performance
 The National Healthy Sleep Awareness Project involves a partnership between the American Academy of Sleep Medicine, Center for Disease Control and Sleep Research Society. The long term goal of the project
The National Healthy Sleep Awareness Project involves a partnership between the American Academy of Sleep Medicine, Center for Disease Control and Sleep Research Society. The long term goal of the project
Over the past 40 years, there have been dramatic increases SCIENTIFIC INVESTIGATIONS METHODS
 http://dx.doi.org/10.5664/jcsm.3448 Sleep Duration, Quality, or Stability and Obesity in an Urban Family Medicine Center Everett E. Logue, Ph.D. 1 ; Edward D. Scott, M.D., M.P.H. 1 ; Patrick A. Palmieri,
http://dx.doi.org/10.5664/jcsm.3448 Sleep Duration, Quality, or Stability and Obesity in an Urban Family Medicine Center Everett E. Logue, Ph.D. 1 ; Edward D. Scott, M.D., M.P.H. 1 ; Patrick A. Palmieri,
Disclosure statement: We have no financial relationships with a commercial interest/interests producing healthcare related products and/or services
 Disclosure statement: We have no financial relationships with a commercial interest/interests producing healthcare related products and/or services Glucose Intolerance and its Association with Sleep Disordered
Disclosure statement: We have no financial relationships with a commercial interest/interests producing healthcare related products and/or services Glucose Intolerance and its Association with Sleep Disordered
Quality of sleep in patients with chronic kidney disease
 Nephrol Dial Transplant (2004) 19: 95 99 DOI: 10.1093/ndt/gfg423 Original Article Quality of sleep in patients with chronic kidney disease Eduard A. Iliescu, Karen E. Yeates and David C. Holland Department
Nephrol Dial Transplant (2004) 19: 95 99 DOI: 10.1093/ndt/gfg423 Original Article Quality of sleep in patients with chronic kidney disease Eduard A. Iliescu, Karen E. Yeates and David C. Holland Department
6/3/2015. Insomnia An Integrative Approach. Objectives. Why An Integrative Approach? Integrative Model. Definition. Short-term Insomnia
 Insomnia An Integrative Approach Jeffrey S. Jump, M.D. Medical Director CHI Memorial Integrative Medicine Associates Objectives Understand the importance of sleep to health Identify patients with insomnia
Insomnia An Integrative Approach Jeffrey S. Jump, M.D. Medical Director CHI Memorial Integrative Medicine Associates Objectives Understand the importance of sleep to health Identify patients with insomnia
Brief Report: Sleep in Parents of Children with Autism Spectrum Disorders
 Brief Report: Sleep in Parents of Children with Autism Spectrum Disorders Lisa J. Meltzer, PHD Department of Pediatrics and Division of Pulmonary Medicine, University of Pennsylvania and The Children s
Brief Report: Sleep in Parents of Children with Autism Spectrum Disorders Lisa J. Meltzer, PHD Department of Pediatrics and Division of Pulmonary Medicine, University of Pennsylvania and The Children s
Obstructive sleep apnoea How to identify?
 Obstructive sleep apnoea How to identify? Walter McNicholas MD Newman Professor in Medicine, St. Vincent s University Hospital, University College Dublin, Ireland. Potential conflict of interest None Obstructive
Obstructive sleep apnoea How to identify? Walter McNicholas MD Newman Professor in Medicine, St. Vincent s University Hospital, University College Dublin, Ireland. Potential conflict of interest None Obstructive
Modern Management of Sleep Disorders
 Modern Management of Sleep Disorders Douglas C. Bauer, MD University of California, San Francisco No Disclosures Case 68 yr. old WF with >15 yr. of poor sleep Difficulty with both initiation and maintenance
Modern Management of Sleep Disorders Douglas C. Bauer, MD University of California, San Francisco No Disclosures Case 68 yr. old WF with >15 yr. of poor sleep Difficulty with both initiation and maintenance
DECLARATION OF CONFLICT OF INTEREST
 DECLARATION OF CONFLICT OF INTEREST Obstructive sleep apnoea How to identify? Walter McNicholas MD Newman Professor in Medicine, St. Vincent s University Hospital, University College Dublin, Ireland. Potential
DECLARATION OF CONFLICT OF INTEREST Obstructive sleep apnoea How to identify? Walter McNicholas MD Newman Professor in Medicine, St. Vincent s University Hospital, University College Dublin, Ireland. Potential
WHY SLEEP MATTERS: SLEEP HEALTH AND HYGIENE. KYRA P CLARK, MD, FACP Medical Director, Sleep Diagnostics Morehouse School of Medicine October 15, 2016
 WHY SLEEP MATTERS: SLEEP HEALTH AND HYGIENE KYRA P CLARK, MD, FACP Medical Director, Sleep Diagnostics Morehouse School of Medicine October 15, 2016 OBJECTIVES Discuss the prevalence sleep deprivation
WHY SLEEP MATTERS: SLEEP HEALTH AND HYGIENE KYRA P CLARK, MD, FACP Medical Director, Sleep Diagnostics Morehouse School of Medicine October 15, 2016 OBJECTIVES Discuss the prevalence sleep deprivation
Pilot study examining the effects of aircraft noise on sleep in communities near Philadelphia International Airport
 12th ICBEN Congress on Noise as a Public Health Problem Pilot study examining the effects of aircraft noise on sleep in communities near Philadelphia International Airport Mathias Basner 1, Maryam Witte
12th ICBEN Congress on Noise as a Public Health Problem Pilot study examining the effects of aircraft noise on sleep in communities near Philadelphia International Airport Mathias Basner 1, Maryam Witte
Parkinson s Disease Associated Sleep Disturbance Ehsan M. Hadi, MD, MPH. Dignity Health Neurological Institute
 Parkinson s Disease Associated Sleep Disturbance Ehsan M. Hadi, MD, MPH. Dignity Health Neurological Institute Parkinson s Disease 2 nd most common neurodegenerative disorder Peak age at onset is 60 years
Parkinson s Disease Associated Sleep Disturbance Ehsan M. Hadi, MD, MPH. Dignity Health Neurological Institute Parkinson s Disease 2 nd most common neurodegenerative disorder Peak age at onset is 60 years
Chapter-IV. Blood pressure and heart rate variability as function of ovarian cycle in young women
 Blood pressure and heart rate variability as function of ovarian cycle in young women INTRODUCTION In human females, the menstrual cycle begins with the onset of menstrual flow on day 1. The menstrual
Blood pressure and heart rate variability as function of ovarian cycle in young women INTRODUCTION In human females, the menstrual cycle begins with the onset of menstrual flow on day 1. The menstrual
NIH Public Access Author Manuscript Psychiatry Clin Neurosci. Author manuscript; available in PMC 2010 November 1.
 NIH Public Access Author Manuscript Published in final edited form as: Psychiatry Clin Neurosci. 2003 October ; 57(5): 542 544. An Open Pilot Study of Gabapentin vs. Trazodone to Treat Insomnia in Alcoholic
NIH Public Access Author Manuscript Published in final edited form as: Psychiatry Clin Neurosci. 2003 October ; 57(5): 542 544. An Open Pilot Study of Gabapentin vs. Trazodone to Treat Insomnia in Alcoholic
November 24, External Advisory Board Members:
 November 24, 2010 To: Fred W. Turek, Ph.D. Charles E. & Emma H. Morrison Professor of Biology Director, Center for Sleep and Circadian Biology Northwestern University RE: External Advisory Board Report
November 24, 2010 To: Fred W. Turek, Ph.D. Charles E. & Emma H. Morrison Professor of Biology Director, Center for Sleep and Circadian Biology Northwestern University RE: External Advisory Board Report
Note: Diagnosis and Management of Obstructive Sleep Apnea Syndrome is addressed separately in medical policy
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
5.2 Key priorities for implementation
 5.2 Key priorities for implementation From the full set of recommendations, the GDG selected ten key priorities for implementation. The criteria used for selecting these recommendations are listed in detail
5.2 Key priorities for implementation From the full set of recommendations, the GDG selected ten key priorities for implementation. The criteria used for selecting these recommendations are listed in detail
PREVENTION OF NOCTURNAL HYPOGLYCEMIA USING PREDICTIVE LOW GLUCOSE SUSPEND (PLGS)
 PREVENTION OF NOCTURNAL HYPOGLYCEMIA USING PREDICTIVE LOW GLUCOSE SUSPEND (PLGS) Pathways for Future Treatment and Management of Diabetes H. Peter Chase, MD Carousel of Hope Symposium Beverly Hilton, Beverly
PREVENTION OF NOCTURNAL HYPOGLYCEMIA USING PREDICTIVE LOW GLUCOSE SUSPEND (PLGS) Pathways for Future Treatment and Management of Diabetes H. Peter Chase, MD Carousel of Hope Symposium Beverly Hilton, Beverly
Review of self-reported instruments that measure sleep dysfunction in patients suffering from temporomandibular disorders and/or orofacial pain
 Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2015 Review of self-reported instruments that measure sleep dysfunction in
Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2015 Review of self-reported instruments that measure sleep dysfunction in
Individual Planning: A Treatment Plan Overview for Individuals Sleep Disorder Problems.
 COURSES ARTICLE - THERAPYTOOLS.US Individual Planning: A Treatment Plan Overview for Individuals Sleep Disorder Problems. Individual Planning: A Treatment Plan Overview for Individuals Sleep Disorder Problems.
COURSES ARTICLE - THERAPYTOOLS.US Individual Planning: A Treatment Plan Overview for Individuals Sleep Disorder Problems. Individual Planning: A Treatment Plan Overview for Individuals Sleep Disorder Problems.
Sleep Apnea: Vascular and Metabolic Complications
 Sleep Apnea: Vascular and Metabolic Complications Vahid Mohsenin, M.D. Professor of Medicine Yale University School of Medicine Director, Yale Center for Sleep Medicine Definitions Apnea: Cessation of
Sleep Apnea: Vascular and Metabolic Complications Vahid Mohsenin, M.D. Professor of Medicine Yale University School of Medicine Director, Yale Center for Sleep Medicine Definitions Apnea: Cessation of
Sleep Optimization and Diabetes Control: A Review of the Literature
 Diabetes Ther (2015) 6:425 468 DOI 10.1007/s13300-015-0141-z REVIEW Sleep Optimization and Diabetes Control: A Review of the Literature Teresa Arora. Shahrad Taheri To view enhanced content go to www.diabetestherapy-open.com
Diabetes Ther (2015) 6:425 468 DOI 10.1007/s13300-015-0141-z REVIEW Sleep Optimization and Diabetes Control: A Review of the Literature Teresa Arora. Shahrad Taheri To view enhanced content go to www.diabetestherapy-open.com
Sleep Concordance in Couples is Associated with Relationship Characteristics
 pii: sp-00514-14 http://dx.doi.org/10.5665/sleep.4744 SLEEP CONCORDANCE IN COUPLES Sleep Concordance in Couples is Associated with Relationship Characteristics Heather E. Gunn, PhD 1 ; Daniel J. Buysse,
pii: sp-00514-14 http://dx.doi.org/10.5665/sleep.4744 SLEEP CONCORDANCE IN COUPLES Sleep Concordance in Couples is Associated with Relationship Characteristics Heather E. Gunn, PhD 1 ; Daniel J. Buysse,
Coding for Sleep Disorders Jennifer Rose V. Molano, MD
 Practice Coding for Sleep Disorders Jennifer Rose V. Molano, MD Accurate coding is an important function of neurologic practice. This section of is part of an ongoing series that presents helpful coding
Practice Coding for Sleep Disorders Jennifer Rose V. Molano, MD Accurate coding is an important function of neurologic practice. This section of is part of an ongoing series that presents helpful coding
egfr > 50 (n = 13,916)
 Saxagliptin and Cardiovascular Risk in Patients with Type 2 Diabetes Mellitus and Moderate or Severe Renal Impairment: Observations from the SAVOR-TIMI 53 Trial Supplementary Table 1. Characteristics according
Saxagliptin and Cardiovascular Risk in Patients with Type 2 Diabetes Mellitus and Moderate or Severe Renal Impairment: Observations from the SAVOR-TIMI 53 Trial Supplementary Table 1. Characteristics according
Sleep Disturbance as a Geriatric Syndrome
 Sleep Disturbance as a Geriatric Syndrome Cathy Alessi, MD Geriatric Research, Education and Clinical Center; VA Greater Los Angeles David Geffen School of Medicine at UCLA Disclosures Current funding:
Sleep Disturbance as a Geriatric Syndrome Cathy Alessi, MD Geriatric Research, Education and Clinical Center; VA Greater Los Angeles David Geffen School of Medicine at UCLA Disclosures Current funding:
New Hypertension Guideline Recommendations for Adults July 7, :45-9:30am
 Advances in Cardiovascular Disease 30 th Annual Convention and Reunion UERM-CMAA, Inc. Annual Convention and Scientific Meeting July 5-8, 2018 New Hypertension Guideline Recommendations for Adults July
Advances in Cardiovascular Disease 30 th Annual Convention and Reunion UERM-CMAA, Inc. Annual Convention and Scientific Meeting July 5-8, 2018 New Hypertension Guideline Recommendations for Adults July
Ambulatory BP Monitoring: Getting the Diagnosis of Hypertension Right. Anthony J. Viera, MD, MPH, FAHA Professor and Chair
 Ambulatory BP Monitoring: Getting the Diagnosis of Hypertension Right Anthony J. Viera, MD, MPH, FAHA Professor and Chair Objectives Review limitations of office BP in making a correct diagnosis of hypertension
Ambulatory BP Monitoring: Getting the Diagnosis of Hypertension Right Anthony J. Viera, MD, MPH, FAHA Professor and Chair Objectives Review limitations of office BP in making a correct diagnosis of hypertension
General Outline. General Outline. Pathogenesis of Metabolic Dysfunction in Sleep Apnea: The Role of Sleep Fragmentation and Intermittent Hypoxemia
 Pathogenesis of Metabolic in Sleep Apnea: The Role of Sleep Fragmentation and Intermittent Hypoxemia Naresh M. Punjabi, MD, PhD Associate Professor of Medicine and Epidemiology Johns Hopkins University,
Pathogenesis of Metabolic in Sleep Apnea: The Role of Sleep Fragmentation and Intermittent Hypoxemia Naresh M. Punjabi, MD, PhD Associate Professor of Medicine and Epidemiology Johns Hopkins University,
Study No.: Title: Rationale: Phase: Study Period: Study Design: Centres: Indication: Treatment: Objectives: Primary Outcome/Efficacy Variable:
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
Sleep Quality and Restless Legs Syndrome among Health-care Workers: Shift Workers and Non-shift Workers
 Original Research Sleep Quality and Restless Legs Syndrome among Health-care Workers: Shift Workers and Non-shift Workers Zahra Banafsheh Alemohammad 1*, Seyed Mohammad Esmaeil Taghavi 1, Akbar Sharifian
Original Research Sleep Quality and Restless Legs Syndrome among Health-care Workers: Shift Workers and Non-shift Workers Zahra Banafsheh Alemohammad 1*, Seyed Mohammad Esmaeil Taghavi 1, Akbar Sharifian
Short Sleep Duration and Poor Sleep Quality Increase the Risk of Diabetes in Japanese Workers With No Family History of Diabetes
 Epidemiology/Health Services Research O R I G I N A L A R T I C L E Short Sleep Duration and Poor Sleep Quality Increase the Risk of Diabetes in Japanese Workers With No Family History of Diabetes TOSHIKO
Epidemiology/Health Services Research O R I G I N A L A R T I C L E Short Sleep Duration and Poor Sleep Quality Increase the Risk of Diabetes in Japanese Workers With No Family History of Diabetes TOSHIKO
0 Agenda. Agenda. 0 Chronic care principles 0 Patient centered care 0 The Big Five Co-Morbid Conditions
 0 Agenda Agenda 0 Chronic care principles 0 Patient centered care 0 The Big Five Co-Morbid Conditions 0 Bi-directionality of sleep and co-morbid conditions 2 Objectives 1. Apply principles of chronic care
0 Agenda Agenda 0 Chronic care principles 0 Patient centered care 0 The Big Five Co-Morbid Conditions 0 Bi-directionality of sleep and co-morbid conditions 2 Objectives 1. Apply principles of chronic care
Sleep and Ageing. Siobhan Banks PhD. Body and Brain at Work, Centre for Sleep Research University of South Australia
 Sleep and Ageing Siobhan Banks PhD Body and Brain at Work, Centre for Sleep Research University of South Australia Health and Active Ageing, 22 nd September 2015 Sleep and Aging How does sleep change as
Sleep and Ageing Siobhan Banks PhD Body and Brain at Work, Centre for Sleep Research University of South Australia Health and Active Ageing, 22 nd September 2015 Sleep and Aging How does sleep change as
Healthy Sleep Tips Along the Way!
 Women and Sleep What You Will Learn The Benefits and Importance of Sleep States and Stages of the Sleep Cycle Unique Physiology of Women s Sleep Common Disorders in Women that Affect Sleep Women s Role
Women and Sleep What You Will Learn The Benefits and Importance of Sleep States and Stages of the Sleep Cycle Unique Physiology of Women s Sleep Common Disorders in Women that Affect Sleep Women s Role
Underdiagnosis of Sleep Apnea Syndrome in U.S. Communities
 ORIGINAL ARTICLE Underdiagnosis of Sleep Apnea Syndrome in U.S. Communities Vishesh Kapur, M.D., 1 Kingman P. Strohl, M.D., 2 Susan Redline, M.D., M.P.H., 3 Conrad Iber, M.D., 4 George O Connor, M.D.,
ORIGINAL ARTICLE Underdiagnosis of Sleep Apnea Syndrome in U.S. Communities Vishesh Kapur, M.D., 1 Kingman P. Strohl, M.D., 2 Susan Redline, M.D., M.P.H., 3 Conrad Iber, M.D., 4 George O Connor, M.D.,
9/2/2016. Faculty. Sleep and Cardiometabolic Risk: What You Need to Know. Disclosures. Learning Objectives. Outline of Presentation
 9//16 Faculty Sleep and Cardiometabolic Risk: What You Need to Know Kristen L. Knutson, PhD Assistant Professor Department of edicine University of Chicago Chicago, Illinois Disclosures Learning Objectives
9//16 Faculty Sleep and Cardiometabolic Risk: What You Need to Know Kristen L. Knutson, PhD Assistant Professor Department of edicine University of Chicago Chicago, Illinois Disclosures Learning Objectives
Beyond Sleep Hygiene: Behavioral Approaches to Insomnia
 Beyond Sleep Hygiene: Behavioral Approaches to Insomnia Rocky Garrison, PhD, CBSM Damon Michael Williams, RN, PMHNP-BC In House Counseling Laughing Heart LLC 10201 SE Main St. 12 SE 14 th Ave. Suite 10
Beyond Sleep Hygiene: Behavioral Approaches to Insomnia Rocky Garrison, PhD, CBSM Damon Michael Williams, RN, PMHNP-BC In House Counseling Laughing Heart LLC 10201 SE Main St. 12 SE 14 th Ave. Suite 10
Correlation Between Sleep Quality and Blood Pressure Changes in Iranian Children
 J Compr Ped. 2015 February; 6(1): e24805. Published online 2015 February 21. DOI: 10.17795/compreped-24805 Research Article Correlation Between Sleep Quality and Blood Pressure Changes in Iranian Children
J Compr Ped. 2015 February; 6(1): e24805. Published online 2015 February 21. DOI: 10.17795/compreped-24805 Research Article Correlation Between Sleep Quality and Blood Pressure Changes in Iranian Children
Medical Policy. MP Actigraphy. Related Policies None
 Medical Policy MP 2.01.73 BCBSA Ref. Policy: 2.01.73 Last Review: 09/28/2017 Effective Date: 09/28/2017 Section: Medicine End Date: 06/26/2018 Related Policies None DISCLAIMER Our medical policies are
Medical Policy MP 2.01.73 BCBSA Ref. Policy: 2.01.73 Last Review: 09/28/2017 Effective Date: 09/28/2017 Section: Medicine End Date: 06/26/2018 Related Policies None DISCLAIMER Our medical policies are
Actigraphy. Policy Number: Last Review: 7/2018 Origination: 7/2008 Next Review: 1/2019
 Actigraphy Policy Number: 2.01.73 Last Review: 7/2018 Origination: 7/2008 Next Review: 1/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage for actigraphy. This is
Actigraphy Policy Number: 2.01.73 Last Review: 7/2018 Origination: 7/2008 Next Review: 1/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage for actigraphy. This is
0 Agenda. Agenda. 0 Chronic care principles 0 Patient centered care 0 The Big Five Co-Morbid Conditions
 0 Agenda Agenda 0 Chronic care principles 0 Patient centered care 0 The Big Five Co-Morbid Conditions 0 Bi-directionality of sleep and co-morbid conditions 2 Objectives 1. Apply principles of chronic care
0 Agenda Agenda 0 Chronic care principles 0 Patient centered care 0 The Big Five Co-Morbid Conditions 0 Bi-directionality of sleep and co-morbid conditions 2 Objectives 1. Apply principles of chronic care
What s In the New Hypertension Guidelines?
 American College of Physicians Ohio/Air Force Chapters 2018 Scientific Meeting Columbus, OH October 5, 2018 What s In the New Hypertension Guidelines? Max C. Reif, MD, FACP Objectives: At the end of the
American College of Physicians Ohio/Air Force Chapters 2018 Scientific Meeting Columbus, OH October 5, 2018 What s In the New Hypertension Guidelines? Max C. Reif, MD, FACP Objectives: At the end of the
Disclosures. Speaker: Teva, UCB, Purdue Advisory Board: Welltrinsic Sleep Network Consultant: Vapotherm, Inc. National Interpretor: Novasom
 So PAP Doesn t Work Rochelle Goldberg, MD, FAASM, FCCP Diplomat, American Board of Sleep Medicine Director Sleep Medicine Services Main Line Health Systems Lankenau Medical Center and Paoli Hospital Disclosures
So PAP Doesn t Work Rochelle Goldberg, MD, FAASM, FCCP Diplomat, American Board of Sleep Medicine Director Sleep Medicine Services Main Line Health Systems Lankenau Medical Center and Paoli Hospital Disclosures
NOCTURIA WHAT S KEEPING YOU UP AT NIGHT? Frances Stewart RN,NCA
 WHAT S KEEPING YOU UP AT NIGHT? Frances Stewart RN,NCA Objectives Be more knowledgeable in the diagnosis and treatment of nocturia Differentiate between urological causes of nocturia Select appropriate
WHAT S KEEPING YOU UP AT NIGHT? Frances Stewart RN,NCA Objectives Be more knowledgeable in the diagnosis and treatment of nocturia Differentiate between urological causes of nocturia Select appropriate
