Treatment of Sleep Apnea with Prosthetic Mandibular Advancement (PMA)
|
|
|
- Emily Bathsheba Davis
- 5 years ago
- Views:
Transcription
1 ~ Sleep, 15(6): American Sleep Disorders Association and Sleep Research Society Treatment of Sleep Apnea with Prosthetic Mandibular Advancement (PMA) Yoichi Nakazawa, Tetsuro Sakamoto, Rika Yasutake, Ken Yamaga, Tatayu Kotorii, Yasushi Miyahara, Yuh Ariyoshi and Tadarilitsu Kameyama Departments of Neuropsychiatry and Oral Surgery, School of Medicine, Kurume University, Kurume, Japan Summary: Nine males with sleep apnea DOES syndrome and three males with sleep apnea DIMS syndrome were treated with prosthetic mandibular advancement (PMA). The method uses a prosthesis, which is designed to advance the mandible 3-5 mm to prevent upper airway occlusion during sleep. The apnea index in the obstructive-type apnea and the percentage of time spent in obstructive apnea decreased significantly with PMA. Although the apnea index showed merely a tendency to decrease in central apnea (p < 0.1), the percentage of time spent in central apnea decreased significantly with PMA. A marked improvement in sleep structures was observed with PMA; a significant increase was seen in total sleep time, percent slow wave sleep (SWS) and percent rapid eye movement (REM) sleep, and the time spent in intra-sleep awakening decreased remarkably. PMA had excellent effects on snoring, and daytime hypersomnolence was reduced in almost all patients. Moreover, a survey on the therapeutic effects of PMA on sleep apnea syndrome and problems associated with wearing PMA was performed with a questionnaire for the sample of nine DOES patients and an additional 22 patients who were treated over a long time. The therapeutic effects could be maintained without any problems in about 213 of these patients. The therapeutic mechanisms of PMA in its reduction of both obstructive and central apnea are discussed. Key Words: Obstructive apnea-central apnea-prosthetic mandibular advancement-sleep changes. Sleep apnea, particularly the obstructive type, frequently results in many complications, including cardiovascular disorders, daytime drowsiness and nocturnal insomnia (I). Although the first step in the treatment of obstructive sleep apnea is the removal of any obvious causes of upper airway obstruction, such causes are not detected in many cases. Accordingly, surgical (2) [tracheostomy, uvulopalatopharyngoplasty (UPPP)], mechanical [continuous positive airway pressure (CPAP) (3-5), diaphragm pacing (6), tongue-retaining device (TRD) (7)] and medical [respiratory stimulants (8), central stimulants (9), progesterone (10), acetazolamide (11)] treatments have been employed in these cases. However, many of these treatment modalities are cumbersome and frequently have associated problems for patients, while they show therapeutic effects on sleep apnea. In 1984, Meier-Ewert et al. (12) reported that use of a prosthesis designed to nonsurgically pull the mandible 3-5 mm forward markedly reduced the occur- Accepted for publication July Address correspondence and reprint requests to Dr. Y oichi Nakazawa, Department of Neuropsychiatry, School of Medicine, Kurume University, 67 Asahi-machi, 830 Kurume, Japan. 499 rence of obstructive sleep apnea by opening the oropharyngeal airway. They termed this therapy "prosthetic mandibular advancement (PMA)" (12-14). Similar treatment modalities have been independently developed for sleep apnea by some researchers (15-19) and have been shown to reduce obstructive sleep apnea. In this study, we tried to treat some patients with sleep apnea syndrome by PMA and found it to be therapeutically effective not only on obstructive apnea but also on central apnea. Although it has been reported that CPAP and TRD decreased both types of sleep apnea, the reduction of central apnea with PMA has not been reported so far. Accordingly, the fact that PMA reduced not only obstructive apnea but also central apnea in the present study may support the hypothesis of a developmental mechanism for central apnea proposed by Lowe et al. (18,20) and Issa and Sullivan (4). SUBJECTS AND METHODS The subjects included nine male outpatients with sleep apnea DOES syndrome (SASDOES) and three male outpatients with sleep apnea DIMS syndrome
2 500 Y. NAKAZA W A ET AL. FIG. 1. Side view of prosthesis. (SASDIMS). The age of the patients ranged from 22 to 58 years (mean = 46.7 ± 13.0). No obvious cause for the sleep apnea could be detected by various examinations at the Department of Otorhinolaryngology, Kurume University Hospital, Japan, in the nose, throat or lower jaw of any of the patients, except for one patient in whom moderate hypertrophy of both the adenoid and palatine tonsils was identified. The prosthesis (Fig. I) was made at the Department Table 1. Frequency of SA Apnea index Time spent in SA/TST(%) Mean duration of SA (seconds) " = not significant. Table 2. of Oral Surgery, Kurume University Hospital. The procedures for making the prosthesis are as follows. First, plaster figures of the maxilla and mandible are molded. Protective plates are then made by pressing 2-mm-thick plastic discs onto both plaster figures. After the protective plates are fitted to both the maxilla and mandible, the mandible is advanced 3-5 mm and is fixed in that position. Following fixation, the prosthesis is promptly made with acrylic dental resin in the patient's mouth. With the 3-5-mm anterior advancement, the mandible is positioned about 4 mm inferior to its position during normal closure. After the patient had become accustomed to the prosthesis, polysomnographic (PSG) recording was conducted using the prosthesis, and the data were compared to those obtained without the prosthesis for each patient. PSG and sleep record analysis were performed according to the manual by Rechtschaffen and Kales (21). The recordings of ventilation and respiratory movements were performed by thermistors attached under a nostril and by an abdominal wall strain gauge, respectively. Each episode of lapse of ventilation lasting longer than 10 seconds was regarded as an episode of sleep apnea. Hypopnea was differentiated from apnea and was not estimated in the study, although it was observed in some patients. Statistical analysis was performed using the Student's t test and Mann-Whitney U test. Changes in sleep apnea parameters with prosthetic mandibular advancement (PAM) Pre-PMA ± ± ± ± 5.2 Post-PMA 138.0± ± ± ±4.4(n= II) Effects a/prosthetic mandibular advancement (PMA) on each type 0/ sleep apnea Pre-PMA Post PMA Frequency of OSk' ± ± 94.1 Frequency of CSA 89.4 ± ± 38.9 Frequency of MSA 79.7 ± ± 52.1 OSA index 22.6 ± ± 12.5 CSA index 14.2 ± ± 5.5 MSA index 13.7 ± ± 8.8 Time spent in OSA/TST (%) 16.2 ± ± 9.4 Time spent in CSA/TST (%) 9.2 ± ± 3.2 Time spent in MSA/TST (%) 12.5 ± I\ ± 8.7 Duration of OSA (seconds) 24.9 ± 5.8 (n = 12) 22.6 ± 3.9 (n = II) Duration of CSA (seconds) 20.4 ± 5.4 (n = II) 18.1 ± 2.8 (n = 10) Duration of MSA (seconds) 32.8 ± 4.0 (n = II) 29.4±7.7(n=ll) a Abbreviations: OSA = obstructive apnea; CSA = central apnea; MSA = mixed apnea; = not significant. p <0.01 <0.01 <0.01 " p <0.05 <0.05 <0.05 Sleep. Vol. /5. No.6, 1992
3 ' TREATMENT OF SLEEP APNEA WITH PMA 501 * * ** ** _ pre PMA _ post PMA * : p < 0.05 * * : p < 0.01 TST % sws % REM FIG. 2.. Comparison of sleep structures obtained before and after PMA treatment. TST -total sleep time; TISA-time of intra-sleep awakenmg. RESULTS The effects of PMA on sleep apnea The mean sleep apnea values before and during treatment with PMA are presented in Table 1. A significant reduction was found in the mean frequency of total apnea (p < 0.01), mean total apnea index (p < 0.01) and mean percentage of time spent in apnea (time spent in apnea/total sleep time) (p < 0.01), but not in the mean duration of all apneic episodes. The effects of PM A on each type of sleep apnea were investigated and the results are presented in Table 2. Although the reduction in the frequency of all apnea did not reach a significant level (p < 0.1), a significant decrease was found in the obstructive apnea index (p < 0.05). The apnea indices of central and mixed types did show a tendency to decrease (p < 0.1). The percentage of time spent in each obstructive and central apnea was significantly reduced with PMA (p < 0.05), but the percentage of time in mixed apnea did not decrease. No significant changes were observed in the mean durations of each apnea type with PMA. The changes in sleep structures with PMA The results are indicated in Fig. 2. The mean total sleep time increased from ± 78.2 minutes to ± 74.6 minutes with PMA (p < 0.05). Likewise, the mean % slow wave sleep (SWS) (p < 0.05) and % rapid eye movement (REM) sleep (p < 0.01) increased with PMA. Conversely, the time of intra-sleep awakening was significantly reduced with PMA (p < 0.01). Changes in subjective symptoms and snoring with PMA The results are indicated in Table 3. Daytime sleepiness was improved by PMA in all but two patients. TISA Insufficient nocturnal sleep was observed in two patients before treatment with PMA, and the sleeplessness disappeared with PMA and hypnotics. On the other hand, snoring was markedly improved with PMA in all patients, according to an estimation by the patients' family members. Subjective estimates in regard to the long-term wearing of PMA For this purpose, a questionnaire consisting of four questions was sent by mail to the nine patients and an additional 15 patients who were treated with PMA. They were requested to fill them out by answering the following questions: 1) Have you been using PMA up to now and how long have you been using it? 2) Do you think PMA is effective for snoring, periodic breathing and daytime hypersomnolence? 3) Did you feel any problems associated with wearing PMA? 4) Why did you stop using PMA if you were not wearing PMA? The questionnaire was collected from 21 patients, and the data are presented in Table 4. Table 3. Improved and unimproved symptoms with prosthetic mandibular advancement PMA Case Age Improved I 52 Insomnia 2 28 EDS," snoring 3 58 EDS, snoring 4 36 EDS, snoring 5 58 Snoring 6 57 EDS, snoring, insomnia 7 22 EDS, snoring 8 30 EDS, snoring 9 56 Insomnia b Snoring Insomnia," snoring EDS, snoring " EDS = excessive daytime somnolence. b Hypnotics intake. Not improved EDS EDS Sleep. Vol. 15. No
4 502 Y. NAKAZA W A ET AL. Table 4. Subjective estimates of long-term use of prosthetic mandibular advancement (PMA) 1. Have you been wearing PMA up to now, and how long have you been using it? Yes, every night Yes, frequently No 10 (48%) 4(19%) 7 (33%) Periods of wearing (months) Is PMA effective for snoring, periodic breathing and daytime' somnolence? Disap- No No peared Reduced change answer Snoring 0 11 (79%) 3(21%) 0 Periodic breathing 1 (7%) 11 (79%) 1 (7%) 1 (7%) Daytime somnolence 3(21%) 7 (50%) 4 (29%) 3. Did you feel any problems associated with wearing PMA? 14 patients who had been wearing PMA every night or frequently Gnathodynia 0 Occlusive disorder 3 (21%) Dullness of jaw 1 (7%) No problems 10 (71%) 7 patients who stopped wearing PMA Effective but cumbersome Gnathodynia Unable to wear No problems but ineffective " Because of an artificial tooth. 3 (43%) 2 (29%) 1 (14%)" 1 (14%) Ten patients (48% of 21 patients) had been using PMA every night for more than 4 months, and four patients (19% of2l patients) had been frequently wear ing it for more than 5 months. The effects of PMA estimated by patients or their family members on snor ing, periodic breathing and daytime hypersomnolence were analyzed for the 14 patients. Eleven patients re ported a reduction in snoring. Periodic breathing had disappeared in one patient and decreased in 11 pa tients. Daytime hypersomnolence had disappeared in three patients and decreased in seven. Problems as sociated with the long-term appliance of PMA were reported in six of the 14 patients. No one complained of gnathodynia, but one patient reported dullness of the temporomandibular joint. Of seven patients who had stopped wearing PMA, two abandoned it because of gnathodynia and three more stopped because the appliance was considered cumbersome, even though it decreased the symptoms of sleep apnea. DISCUSSION It is well known that sleep apnea syndrome often results in physical complications such as polycythemia and pulmonary and cardiovascular disorders. In more serious cases, cor pulmonale or right ventricular heart Sleep, Vol. IS, No.6, 1992 failure can be induced (1). In addition, patients with sleep apnea syndrome frequently complain of excessive daytime drowsiness and/or insufficient nocturnal sleep, which sometimes disturbs their social lives. For these reasons, an effective treatment for the syndrome is needed. All current treatments have some advantages but also have varying disadvantages, including respiratory infection following tracheostomy, necessity of using a complicated apparatus (CPAP, diaphragm pacing), expense of apparatus (CPAP), cumbersomeness ofthe apparatus (CPAP, tongue retaining device) and side effects (medication). In Japan, acetazolamide has been widely used since it was approved for use in the treatment of sleep apnea in However, some problems with its long-term administration, including lithogenesis (22) and progressive decrease in the therapeutic effect (11), remain. Because most patients require lifetime medication, drug safety is an important consideration and should not be ignored. PMA was introduced as a treatment for obstructive sleep apnea by Meier-Ewert et al. (12-14), who attempted to prevent upper airway occlusion by using a prosthesis to hold the mandible in a forward position. Similar treatment modalities have been independently developed by SolI and George (15), George (16), Bohnham et al. (17), Lowe et al. (18) and Schmidt-Nowara et al. (19). Their technique is based on the fact that sleep apnea frequently occurs in men with retrognathia or micrognathia, conditions that facilitate upper airway occlusion by backward movement of the tongue during sleep. As expected, they found that PMA provided excellent therapeutic effects on obstructive sleep apnea without unfavorable side effects. There was marked improvement in oxygen saturation, and snoring and daytime somnolence disappeared immediately. In the present study as well, we confirmed a significant decrease in obstructive apnea with PMA. These results indicate that PMA contributes to airway patency. Although the reduction of central apnea with PMA has not been reported so far, it is noteworthy that the percentage of time spent in central apnea was also significantly reduced by PMA, although the overall central apnea index showed only a tendency to decrease (p < 0.1). Issa and Sullivan (4,5) demonstrated that high pressure of CPAP prevented not only obstructive apnea but also central and mixed apnea and resulted in quiet breathing in all patients. On the other hand, Cartwright and Samelson (7) designed a device that holds the tongue slightly forward when negative pressure to one of its compartments is applied. This device, called a tongue-retaining device (TRD), is designed to advance the superior surface of the tongue away from the posterior pharyngeal wall. It has subsequently been found that not only obstructive but also central apnea is de- I i
5 TREATMENT OF SLEEP APNEA WITH PMA 503 creased considerably during use of the TRD. These results are consistent with those of the present study and suggest that both obstructive and central apnea share a common pathogenesis because modalities that maintain open upper airway are effective in both types of apnea. Although the causes of central apnea remain obscure, a mechanism that may induce central apnea has been experimentally demonstrated in humans and animals (23-28). Reflexes originating from the upper airway have been shown to alter the respiratory pattern in association with depth of anesthesia or sleep (27). If airway mucosa is stimulated by various stimuli during wakefulness or light anesthesia, a cough reflex is induced. However, an apneic reflex (central apnea) is induced by the same stimuli during sleep or deep anesthesia. Because upper airway occlusion occurs when the anterior wall of the oropharynx adheres to the posterior wall, central apnea results from obstructive apnea because receptors responsible for the reflex are stimulated. Actually, Issa and Sullivan (5) accounted for the reduction in all types of apnea by CPAP as follows: CPAP initially improves obstructive apnea by providing a pneumatic splint for the upper airway; this then induces secondary improvement and suppression of central apnea induced by reflective inhibition of respiration through activation of tracheal receptors during upper airway obstruction. Although the mechanisms by which PMA improves central apnea may be explained in the same way, the specific therapeutic mechanisms by which PMA suppresses obstructive apnea should be noted. PMA lowers the mandible about 4 mm, in addition to advancing the antherior pharyngeal wall. Lowe et al. (20) have demonstrated that, in man, voluntary or passive opening of the mandible produces definite enhancement of genioglossal EMG through activation of receptors located in the mandibular joint. Because the contraction of the genioglossal muscle opens the airway, this may also help to suppress/prevent airway obstruction. Subjective estimates regarding the long-term wearing of PM A suggest that the therapeutic effects of PM A on sleep apnea can be maintained in about 213 of patients without such problems as gnathodynia. Finally, we emphasize that PMA is simple and extremely easy for patients to use. Moreover, it is an important consideration that the cost ofthe prosthesis is very low ($5-6), and the prosthesis is light (15 g) and portable. Although the number of patients tested is limited in the present study, we think that PMA may be considered the treatment modality of choice for sleep apnea syndrome, except in serious cases. Acknowledgement: The authors sincerely thank Prof. Meier-Ewert for his helpful advice. REFERENCES I. Guilleminault C. Clinical features and evaluation of obstructive sleep apnea. In: Kryger MH, Roth T, Dement WC, eds. Principles and practice of sleep medicine. Tokyo: WB Saunders Co., 1989: Guilleminault C, Riley RW, Powell NB. Surgical treatment of obstructive sleep apnea. In: Kryger MH, Roth T, Dement WC, eds. Principles and practice of sleep medicine. Tokyo: WB Saunders Co., 1989: Sullivan CE, Berthon-Jones M, Issa FG. Remission of severe obesity-hypo ventilation syndrome after short-term treatment during sleep with nasal continuous positive airway pressure. A m Rev Respi Dis 1983;128: Issa FG, Sullivan CEo The immediate effects of nasal continuous positive airway pressure treatment on sleep pattern in patients with obstructive sleep apnea syndrome. Electroenceph Clin NeurophysioI1986;63: Issa FG, Sullivan CEo Reversal of central sleep apnea using nasal CPAP. Chest 1986;90: Farmer WC, Glen WWL, Gee JBL. Alveolar hypo ventilation syndrome: studies of ventilatory control in patients selected for diaphragm pacing. Am J Med 1978;64: Cartwright RD, Samelson CF. The effects of a nonsurgical treatment for obstructive sleep apnea. The tongue-retaining device. JAM A 1982;248: Davi MJ, Sankaran K, Simons FER, Seshia MM, Rigatto H. Physiologic changes induced by theophylline in the treatment of apnea in preterm infants. J Pediatr 1978;92: Kumashiro H, Sato M, Hirata J, Baba 0, Otsuki S. "Sleep apnea" and sleep regulating mechanism-a case effectively treated with monochlorimipramine. Folia Psychiat Neural Jap 1971; 25: Block AJ, Wynne JW, Boysen PG, Lindsey H, Martin C, Cantor B. Menopause, medroxyprogesterone and breathing during sleep. Am J Med 1981;70: White DP, Zwillich CW, Pickett CK, Douglas NJ, Findley LJ, Weil JV. Central sleep apnea: improvement with acetazolamide therapy. Arch Intern Med 1982;142: Meier-Ewert K, Schafer H, Kloss W. Treatment of sleep apnea by a mandibular protracting device. Berichtsband 7th Eurap Congr Sleep Res Munchen 1984: Kloss W, Meier-Ewert K, Schafer H. Zur Therapie des obstructiven Schlaf-Apnoe-Syndromes. Fortschr Neurol Psychiat 1986; 54: Meier-Ewert K, Brosing B. Treatment of sleep apnea by prosthetic mandibular advancement. In: Peter JH, Podszus T, von Wichert P, eds. Sleep related disorders and internal disease. Berlin: Springer-Verlag, 1987: Soli BA, George PT. Treatment of obstructive sleep apnea with a nocturnal airway-patency appliance. N Eng J Med 1985;313: George PT. A modified functional appliance for treatment of obstructive sleep apnea. J Clin Orthod 1987;21 : Bonham PE, Currier F, Orr WC, Othman J, Nanda RS. The effects of a modified functional appliance on obstructive sleep apnea. Am Orthod Dentofac Orthop 1988;94: Lowe AA, Fleetham J, Ryan F, Mathews B. Effects of a mandibular repositioning appliance used in the treatment of obstructive sleep apnea on tongue muscle activity. Prog Clin Bioi Res 1990;345: Schmidt-Nowara WW, Meade TE, Hays MB. Treatment of snoring and obstructive sleep apnea with a dental orthosis. Chest 1991;99: Lowe AA, Gurza SC, Sessle BJ. Regulation of genioglossus and masseter muscle activity in man. Arch Oral Bioi 1977;22: Rechtschaffen A, Kales A. A manual of standardized terminology, techniques, and scoring system for sleep stage of human subjects. Bethesda, MD, U.S. Department of Health, Education, and Welfare Public Health Service, Ahlstrand C, Tiselius H-C. Urine composition and stone for- Sleep, Vol. 15, No.6, 1992
6 504 Y. NAKAZA W A ET AL. mation during treatment with acetazolamide. Scand J Urol NephroI1987;2l: Mathew OP, Abu-Osba YK, Thach BT. Genioglossus muscle: responses to upper airway pressure changes: afferent pathways. J Appl Physiol Respirat Environ Exercise PhysioI1982;52: Hwang J-C, St. John WM, Bartlett D, Jr. Receptors responding to changes in upper airway pressure. Respir Physiol 1984;55: Mathew OP, Farber JP. Effect of upper airway negative pressure: on respiratory timing. Respir Physiol 1983;54: Sullivan CE, Murphy E, Kozar LF, Phillipson EA. Waking and ventilatory responses to laryngeal stimulation in sleeping dogs. J Appl Physiol Respirat Environ Exercise PhysioI1978;45: Nishino T, Hiraga K, Mizuguchi T, Honda Y. Respiratory reflex responses to stimulation of tracheal mucosa in enflurane-anesthetized humans. J Appl PhysioI1988;65: Sullivan CE, Kozar LF, Murphy E, Phillipson EA. Primary role of respiratory afferents in sustaining breathing rhythm. J Appl Physiol Respirat Environ Exercise Physio/ 1978;45: Sleep. Vol. 15. No
The Effect of a Mandibular Advancement Device on Apneas and Sleep in Patients With Obstructive Sleep Apnea*
 The Effect of a Mandibular Advancement Device on Apneas and Sleep in Patients With Obstructive Sleep Apnea* Marie Marklund, DDS; Karl A. Franklin, MD, PhD, FCCP; Carin Sahlin, RTA; and Rune Lundgren, MD,
The Effect of a Mandibular Advancement Device on Apneas and Sleep in Patients With Obstructive Sleep Apnea* Marie Marklund, DDS; Karl A. Franklin, MD, PhD, FCCP; Carin Sahlin, RTA; and Rune Lundgren, MD,
Effect of two types of mandibular advancement splints on snoring and obstructive sleep apnoea
 European Journal of Orthodontics 20 (1998) 293 297 1998 European Orthodontic Society Effect of two types of mandibular advancement splints on snoring and obstructive sleep apnoea J. Lamont*, D. R. Baldwin**,
European Journal of Orthodontics 20 (1998) 293 297 1998 European Orthodontic Society Effect of two types of mandibular advancement splints on snoring and obstructive sleep apnoea J. Lamont*, D. R. Baldwin**,
Snoring And Sleep Apnea in the U.S. Definitions Apnea: Cessation of ventilation for > 10 seconds. Defining Severity of OSA
 Snoring and Obstructive Sleep Apnea: Oral Appliance Therapy Management Midwest Society of Orthodontists October 16-17, 2009 Anthony J DiAngelis DMD, MPH Chief, Department of Dentistry, HCMC Professor,
Snoring and Obstructive Sleep Apnea: Oral Appliance Therapy Management Midwest Society of Orthodontists October 16-17, 2009 Anthony J DiAngelis DMD, MPH Chief, Department of Dentistry, HCMC Professor,
clinical investigations Evaluation of Variable Mandibular Advancement Appliance for Treatment of Snoring and Sleep Apnea*
 clinical investigations Evaluation of Variable Mandibular Advancement Appliance for Treatment of Snoring and Sleep Apnea* Jeffrey Pancer, DDS; Salem Al-Faifi, MD; Mohamed Al-Faifi, MD; and Victor Hoffstein,
clinical investigations Evaluation of Variable Mandibular Advancement Appliance for Treatment of Snoring and Sleep Apnea* Jeffrey Pancer, DDS; Salem Al-Faifi, MD; Mohamed Al-Faifi, MD; and Victor Hoffstein,
Sleep Disordered Breathing
 Sleep Disordered Breathing SDB SDB Is an Umbrella Term for Many Disorders characterized by a lack of drive to breathe Results n repetitive pauses in breathing with no effort Occurs for a minimum of 10
Sleep Disordered Breathing SDB SDB Is an Umbrella Term for Many Disorders characterized by a lack of drive to breathe Results n repetitive pauses in breathing with no effort Occurs for a minimum of 10
Alexandria Workshop on
 Alexandria Workshop on 1 Snoring & OSA Surgery Course Director: Yassin Bahgat MD Claudio Vicini MD Course Board: Filippo Montevecchi MD Pietro Canzi MD Snoring & Obstructive ti Sleep Apnea The basic information
Alexandria Workshop on 1 Snoring & OSA Surgery Course Director: Yassin Bahgat MD Claudio Vicini MD Course Board: Filippo Montevecchi MD Pietro Canzi MD Snoring & Obstructive ti Sleep Apnea The basic information
Alaska Sleep Education Center
 Alaska Sleep Education Center The 3 Types of Sleep Apnea Explained: Obstructive, Central, & Mixed Posted by Kevin Phillips on Jan 28, 2015 6:53:00 PM Sleep apnea is a very common sleep disorder, affecting
Alaska Sleep Education Center The 3 Types of Sleep Apnea Explained: Obstructive, Central, & Mixed Posted by Kevin Phillips on Jan 28, 2015 6:53:00 PM Sleep apnea is a very common sleep disorder, affecting
PEDIATRIC SLEEP GUIDELINES Version 1.0; Effective
 MedSolutions, Inc. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Requests for patients with atypical symptoms or clinical presentations
MedSolutions, Inc. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Requests for patients with atypical symptoms or clinical presentations
Influence of Sleep Posture on Response to Oral Appliance Therapy for Sleep Apnea Syndrome
 SLEEP-RELATED BREATHING DISORDERS Influence of Sleep Posture on Response to Oral Appliance Therapy for Sleep Apnea Syndrome Kazuya Yoshida DDS, PhD Department of Oral and Maxillofacial Surgery, Graduate
SLEEP-RELATED BREATHING DISORDERS Influence of Sleep Posture on Response to Oral Appliance Therapy for Sleep Apnea Syndrome Kazuya Yoshida DDS, PhD Department of Oral and Maxillofacial Surgery, Graduate
IEHP considers the treatment of obstructive sleep apnea (OSA) medically necessary according to the criteria outlined below:
 : Positive Airway Pressure, Oral Appliances, and Surgical Interventions Policy: Obstructive sleep apnea (OSA) is characterized by an interruption of breathing during sleep most commonly due to extra or
: Positive Airway Pressure, Oral Appliances, and Surgical Interventions Policy: Obstructive sleep apnea (OSA) is characterized by an interruption of breathing during sleep most commonly due to extra or
Management of OSA. saurabh maji
 Management of OSA saurabh maji INTRODUCTION Obstructive sleep apnea is a major public health problem Prevalence of OSAS in INDIA is 2.4% to 4.96% in men and 1% to 2 % in women In the rest of the world
Management of OSA saurabh maji INTRODUCTION Obstructive sleep apnea is a major public health problem Prevalence of OSAS in INDIA is 2.4% to 4.96% in men and 1% to 2 % in women In the rest of the world
in China Shanghai Office Beijing Office (+86) (+86)
 SLEEP Apnea in China Guide 2018-2019 Shanghai Office (+86) 21 2426 6400 Beijing Office (+86) 010 6464 0611 www.pacificprime.cn Follow us on WeChat t A comprehensive overview of sleep apnea Perhaps you
SLEEP Apnea in China Guide 2018-2019 Shanghai Office (+86) 21 2426 6400 Beijing Office (+86) 010 6464 0611 www.pacificprime.cn Follow us on WeChat t A comprehensive overview of sleep apnea Perhaps you
Increasing the Functional Residual Capacity May Reverse Obstructive Sleep Apnea
 Sleep 11(4):349-353, Raven Press, Ltd., New York 1988 Association of Professional Sleep Societies ncreasing the Functional Residual Capacity May Reverse Obstructive Sleep Apnea F. Series, Y. Cormier, N.
Sleep 11(4):349-353, Raven Press, Ltd., New York 1988 Association of Professional Sleep Societies ncreasing the Functional Residual Capacity May Reverse Obstructive Sleep Apnea F. Series, Y. Cormier, N.
University, India.) Corresponding author: Dr. Shubham Agarwal1
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 3 Ver.15 March. (2018), PP 59-63 www.iosrjournals.org Effect of Severity of OSA on Oxygen Saturation:
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 3 Ver.15 March. (2018), PP 59-63 www.iosrjournals.org Effect of Severity of OSA on Oxygen Saturation:
BTS sleep Course. Module 10 Therapies I: Mechanical Intervention Devices (Prepared by Debby Nicoll and Debbie Smith)
 BTS sleep Course Module 10 Therapies I: Mechanical Intervention Devices (Prepared by Debby Nicoll and Debbie Smith) S1: Overview of OSA Definition History Prevalence Pathophysiology Causes Consequences
BTS sleep Course Module 10 Therapies I: Mechanical Intervention Devices (Prepared by Debby Nicoll and Debbie Smith) S1: Overview of OSA Definition History Prevalence Pathophysiology Causes Consequences
Prefabricated Oral Appliances for Obstructive Sleep Apnea
 Medical Policy Manual Allied Health, Policy No. 36 Prefabricated Oral Appliances for Obstructive Sleep Apnea Next Review: May 2019 Last Review: April 2018 Effective: May 1, 2018 IMPORTANT REMINDER Medical
Medical Policy Manual Allied Health, Policy No. 36 Prefabricated Oral Appliances for Obstructive Sleep Apnea Next Review: May 2019 Last Review: April 2018 Effective: May 1, 2018 IMPORTANT REMINDER Medical
Snoring. Forty-five percent of normal adults snore at least occasionally and 25
 Snoring Insight into sleeping disorders and sleep apnea Forty-five percent of normal adults snore at least occasionally and 25 percent are habitual snorers. Problem snoring is more frequent in males and
Snoring Insight into sleeping disorders and sleep apnea Forty-five percent of normal adults snore at least occasionally and 25 percent are habitual snorers. Problem snoring is more frequent in males and
Pediatric Sleep-Disordered Breathing
 Pediatric Sleep-Disordered Breathing OSA in infants and young children is generally characterized by partial, persistent obstruction of the upper airway Continuum Benign primary snoring Upper-airway resistance
Pediatric Sleep-Disordered Breathing OSA in infants and young children is generally characterized by partial, persistent obstruction of the upper airway Continuum Benign primary snoring Upper-airway resistance
Upper Airway Obstruction
 Upper Airway Obstruction Adriaan Pentz Division of Otorhinolaryngology University of Stellenbosch and Tygerberg Hospital Stridor/Stertor Auditory manifestations of disordered respiratory function ie noisy
Upper Airway Obstruction Adriaan Pentz Division of Otorhinolaryngology University of Stellenbosch and Tygerberg Hospital Stridor/Stertor Auditory manifestations of disordered respiratory function ie noisy
OBSTRUCTIVE SLEEP APNEA and WORK Treatment Update
 OBSTRUCTIVE SLEEP APNEA and WORK Treatment Update David Claman, MD Professor of Medicine Director, UCSF Sleep Disorders Center 415-885-7886 Disclosures: None Chronic Sleep Deprivation (0 v 4 v 6 v 8 hrs)
OBSTRUCTIVE SLEEP APNEA and WORK Treatment Update David Claman, MD Professor of Medicine Director, UCSF Sleep Disorders Center 415-885-7886 Disclosures: None Chronic Sleep Deprivation (0 v 4 v 6 v 8 hrs)
Brian Palmer, D.D.S, Kansas City, Missouri, USA. April, 2001
 Brian Palmer, D.D.S, Kansas City, Missouri, USA A1 April, 2001 Disclaimer The information in this presentation is for basic information only and is not to be construed as a diagnosis or treatment for any
Brian Palmer, D.D.S, Kansas City, Missouri, USA A1 April, 2001 Disclaimer The information in this presentation is for basic information only and is not to be construed as a diagnosis or treatment for any
National Sleep Disorders Research Plan
 Research Plan Home Foreword Preface Introduction Executive Summary Contents Contact Us National Sleep Disorders Research Plan Return to Table of Contents SECTION 5 - SLEEP DISORDERS SLEEP-DISORDERED BREATHING
Research Plan Home Foreword Preface Introduction Executive Summary Contents Contact Us National Sleep Disorders Research Plan Return to Table of Contents SECTION 5 - SLEEP DISORDERS SLEEP-DISORDERED BREATHING
Upper airway resistance syndrome (UARS) Information for patients
 Upper airway resistance syndrome (UARS) Information for patients This leaflet answers common questions about upper airway resistance syndrome. If you would like further information, or have any concerns,
Upper airway resistance syndrome (UARS) Information for patients This leaflet answers common questions about upper airway resistance syndrome. If you would like further information, or have any concerns,
RESEARCH PACKET DENTAL SLEEP MEDICINE
 RESEARCH PACKET DENTAL SLEEP MEDICINE American Academy of Dental Sleep Medicine Dental Sleep Medicine Research Packet Page 1 Table of Contents Research: Oral Appliance Therapy vs. Continuous Positive Airway
RESEARCH PACKET DENTAL SLEEP MEDICINE American Academy of Dental Sleep Medicine Dental Sleep Medicine Research Packet Page 1 Table of Contents Research: Oral Appliance Therapy vs. Continuous Positive Airway
Sleep Apnea: Diagnosis & Treatment
 Disclosure Sleep Apnea: Diagnosis & Treatment Lawrence J. Epstein, MD Sleep HealthCenters Harvard Medical School Chief Medical Officer for Sleep HealthCenters Sleep medicine specialty practice group Consultant
Disclosure Sleep Apnea: Diagnosis & Treatment Lawrence J. Epstein, MD Sleep HealthCenters Harvard Medical School Chief Medical Officer for Sleep HealthCenters Sleep medicine specialty practice group Consultant
SLEEP APNOEA DR TAN KAH LEONG ALVIN CO-DIRECTOR SLEEP LABORATORY SITE CHIEF SDDC (SLEEP) DEPARTMENT OF OTORHINOLARYNGOLOGY, HEAD & NECK SURGERY
 SLEEP APNOEA DR TAN KAH LEONG ALVIN CO-DIRECTOR SLEEP LABORATORY SITE CHIEF SDDC (SLEEP) DEPARTMENT OF OTORHINOLARYNGOLOGY, HEAD & NECK SURGERY
SLEEP APNOEA DR TAN KAH LEONG ALVIN CO-DIRECTOR SLEEP LABORATORY SITE CHIEF SDDC (SLEEP) DEPARTMENT OF OTORHINOLARYNGOLOGY, HEAD & NECK SURGERY
The Mandibular Advancement Device and Patient Selection in the Treatment of Obstructive Sleep Apnea
 ORIGINAL ARTICLE The Mandibular Advancement Device and Patient Selection in the Treatment of Obstructive Sleep Apnea Chul Hee Lee, MD; Ji-Hun Mo, MD; Ik-Joon Choi, MD; Hyun Jong Lee, MD; Beom Seok Seo,
ORIGINAL ARTICLE The Mandibular Advancement Device and Patient Selection in the Treatment of Obstructive Sleep Apnea Chul Hee Lee, MD; Ji-Hun Mo, MD; Ik-Joon Choi, MD; Hyun Jong Lee, MD; Beom Seok Seo,
Sleep and the Heart Reversing the Effects of Sleep Apnea to Better Manage Heart Disease
 1 Sleep and the Heart Reversing the Effects of Sleep Apnea to Better Manage Heart Disease Rami Khayat, MD Professor of Internal Medicine Director, OSU Sleep Heart Program Medical Director, Department of
1 Sleep and the Heart Reversing the Effects of Sleep Apnea to Better Manage Heart Disease Rami Khayat, MD Professor of Internal Medicine Director, OSU Sleep Heart Program Medical Director, Department of
Treatment of Obstructive Sleep Apnea (OSA)
 MP9239 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes as shown below None Prevea360 Health Plan Medical Policy: 1.0 A continuous positive airway
MP9239 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes as shown below None Prevea360 Health Plan Medical Policy: 1.0 A continuous positive airway
Using the Pathophysiology of Obstructive Sleep Apnea (OSA) to Teach Cardiopulmonary Integration
 Using the Pathophysiology of Obstructive Sleep Apnea (OSA) to Teach Cardiopulmonary Integration Michael G. Levitzky, Ph.D. Department of Physiology Louisiana State University Health Sciences Center 1901
Using the Pathophysiology of Obstructive Sleep Apnea (OSA) to Teach Cardiopulmonary Integration Michael G. Levitzky, Ph.D. Department of Physiology Louisiana State University Health Sciences Center 1901
subjects Arousal responses to added inspiratory resistance during REM and non-rem sleep in normal M Gugger, S B6gershausen, L Schaffler
 Thorax 1993;48:125-129 Division of Pneumology M Gugger S Bogershausen Department of Neurology, University of Berne, Inselspital, CH-31 Berne, Switzerland L Schaffler Reprint requests to: Dr M Gugger Received
Thorax 1993;48:125-129 Division of Pneumology M Gugger S Bogershausen Department of Neurology, University of Berne, Inselspital, CH-31 Berne, Switzerland L Schaffler Reprint requests to: Dr M Gugger Received
Sleep Apnea. Herbert A Berger, MD Pulmonary Division Department of Internal Medicine University of Iowa
 Sleep Apnea Herbert A Berger, MD Pulmonary Division Department of Internal Medicine University of Iowa Disclosures No Relevant Financial Interests to Report Objectives Learn the history and physical examination
Sleep Apnea Herbert A Berger, MD Pulmonary Division Department of Internal Medicine University of Iowa Disclosures No Relevant Financial Interests to Report Objectives Learn the history and physical examination
Annals and Essences of Dentistry
 ROLE OF ORAL APPLIANCE IN CLINICAL MANAGEMENT OF OBSTRUCTIVE SLEEP APNEA IN CHILDREN * Balaji K, ** Tarasingh P * Associate Professor ** Asst. Professor Dept of Pedodontics and Preventive Dentistry, SVS
ROLE OF ORAL APPLIANCE IN CLINICAL MANAGEMENT OF OBSTRUCTIVE SLEEP APNEA IN CHILDREN * Balaji K, ** Tarasingh P * Associate Professor ** Asst. Professor Dept of Pedodontics and Preventive Dentistry, SVS
Childhood Obstructive Sleep Apnea
 Childhood Obstructive Sleep Apnea 1 PROF. RAJESHWAR DAYAL MD, FAMS,FIAP,DNB, DCH (LONDON) NATIONAL CONVENOR,IAP SLEEP PROGRAM NATIONAL VICE PRESIDENT IAP 2011 HEAD DEPARTMENT OF PAEDIATRICS S. N. MEDICAL
Childhood Obstructive Sleep Apnea 1 PROF. RAJESHWAR DAYAL MD, FAMS,FIAP,DNB, DCH (LONDON) NATIONAL CONVENOR,IAP SLEEP PROGRAM NATIONAL VICE PRESIDENT IAP 2011 HEAD DEPARTMENT OF PAEDIATRICS S. N. MEDICAL
Mandibular repositioning appliance (MRA) therapy for snoring
 Scientific investigations Effect of a Titration Polysomnogram on Treatment Success with a Mandibular Repositioning Appliance Fernanda R. Almeida, D.D.S. 1 ; Jonathan A. Parker, D.D.S. 2 ; James S. Hodges,
Scientific investigations Effect of a Titration Polysomnogram on Treatment Success with a Mandibular Repositioning Appliance Fernanda R. Almeida, D.D.S. 1 ; Jonathan A. Parker, D.D.S. 2 ; James S. Hodges,
Obstructive Sleep Apnea- Hypopnea Syndrome and Snoring: Surgical Options
 Obstructive Sleep Apnea- Hypopnea Syndrome and Snoring: Surgical Options Joshua L. Kessler, MD, FACS Boston ENT Associates Clinical Instructor, Otology and Laryngology Harvard Medical School Why Consider
Obstructive Sleep Apnea- Hypopnea Syndrome and Snoring: Surgical Options Joshua L. Kessler, MD, FACS Boston ENT Associates Clinical Instructor, Otology and Laryngology Harvard Medical School Why Consider
Sleep and the Heart. Physiologic Changes in Cardiovascular Parameters during Sleep
 Sleep and the Heart Rami N. Khayat, MD Professor of Internal Medicine Medical Director, Department of Respiratory Therapy Division of Pulmonary, Critical Care and Sleep Medicine The Ohio State University
Sleep and the Heart Rami N. Khayat, MD Professor of Internal Medicine Medical Director, Department of Respiratory Therapy Division of Pulmonary, Critical Care and Sleep Medicine The Ohio State University
Sleep and the Heart. Rami N. Khayat, MD
 Sleep and the Heart Rami N. Khayat, MD Professor of Internal Medicine Medical Director, Department of Respiratory Therapy Division of Pulmonary, Critical Care and Sleep Medicine The Ohio State University
Sleep and the Heart Rami N. Khayat, MD Professor of Internal Medicine Medical Director, Department of Respiratory Therapy Division of Pulmonary, Critical Care and Sleep Medicine The Ohio State University
Update on Sleep Apnea Diagnosis and Treatment
 Update on Sleep Apnea Diagnosis and Treatment Damien Stevens MD Pulmonary/Critical Care/Sleep Medicine Medical Director KU Medical Center Sleep Laboratory Objectives Discuss physiology of sleep and obstructive
Update on Sleep Apnea Diagnosis and Treatment Damien Stevens MD Pulmonary/Critical Care/Sleep Medicine Medical Director KU Medical Center Sleep Laboratory Objectives Discuss physiology of sleep and obstructive
Outline. Major variables contributing to airway patency/collapse. OSA- Definition
 Outline Alicia Gruber Kalamas, MD Associate Clinical Professor of Anesthesia & Perioperative Care University of California, San Francisco September 2011 Definition Pathophysiology Patient Risk Factors
Outline Alicia Gruber Kalamas, MD Associate Clinical Professor of Anesthesia & Perioperative Care University of California, San Francisco September 2011 Definition Pathophysiology Patient Risk Factors
Polysomnography (PSG) (Sleep Studies), Sleep Center
 Policy Number: 1036 Policy History Approve Date: 07/09/2015 Effective Date: 07/09/2015 Preauthorization All Plans Benefit plans vary in coverage and some plans may not provide coverage for certain service(s)
Policy Number: 1036 Policy History Approve Date: 07/09/2015 Effective Date: 07/09/2015 Preauthorization All Plans Benefit plans vary in coverage and some plans may not provide coverage for certain service(s)
SLEEP STUDIES IN THE VERY, VERY YOUNG
 SLEEP STUDIES IN THE VERY, VERY YOUNG Julie DeWitte, RCP, RPSGT, RST Assistant Department Administrator Kaiser Permanente Fontana Sleep Center AAST Director-at-Large Board Member NEONATES THROUGH INFANCY
SLEEP STUDIES IN THE VERY, VERY YOUNG Julie DeWitte, RCP, RPSGT, RST Assistant Department Administrator Kaiser Permanente Fontana Sleep Center AAST Director-at-Large Board Member NEONATES THROUGH INFANCY
Surgical Options for the Successful Treatment of Obstructive Sleep Apnea
 Surgical Options for the Successful Treatment of Obstructive Sleep Apnea Benjamin J. Teitelbaum, MD, FACS Otolaryngology Head and Neck Surgery Saint Agnes Medical Center Fresno, California Terms Apnea
Surgical Options for the Successful Treatment of Obstructive Sleep Apnea Benjamin J. Teitelbaum, MD, FACS Otolaryngology Head and Neck Surgery Saint Agnes Medical Center Fresno, California Terms Apnea
Oral appliances for the management of snoring and obstructive sleep apnoea
 S58 Thorax 1998;53(Suppl 2):S58 S64 Oral appliances for the management of snoring and obstructive sleep apnoea LS Bennett, RJO Davies, JR Stradling Oxford Sleep Unit, The Churchill Hospital, Osler Chest
S58 Thorax 1998;53(Suppl 2):S58 S64 Oral appliances for the management of snoring and obstructive sleep apnoea LS Bennett, RJO Davies, JR Stradling Oxford Sleep Unit, The Churchill Hospital, Osler Chest
Index. sleep.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Accidents. See Motor vehicle accidents. Acetazolamide, in OSA therapy, 531 Acetylcholinesterase inhibitors, in OSA therapy, 532 533 Acromegaly,
Note: Page numbers of article titles are in boldface type. A Accidents. See Motor vehicle accidents. Acetazolamide, in OSA therapy, 531 Acetylcholinesterase inhibitors, in OSA therapy, 532 533 Acromegaly,
Precision Sleep Medicine
 Precision Sleep Medicine Picking Winners Improves Outcomes and Avoids Side-Effects North American Dental Sleep Medicine Conference February 17-18, 2017 Clearwater Beach, FL John E. Remmers, MD Conflict
Precision Sleep Medicine Picking Winners Improves Outcomes and Avoids Side-Effects North American Dental Sleep Medicine Conference February 17-18, 2017 Clearwater Beach, FL John E. Remmers, MD Conflict
Emerging Nursing Roles in Collaborative Management of Sleep Disordered Breathing and Obstructive Sleep Apnoea
 Emerging Nursing Roles in Collaborative Management of Sleep Disordered Breathing and Obstructive Sleep Apnoea Sigma Theta Tau International 28th International Nursing Research Congress 27-31 July 2017
Emerging Nursing Roles in Collaborative Management of Sleep Disordered Breathing and Obstructive Sleep Apnoea Sigma Theta Tau International 28th International Nursing Research Congress 27-31 July 2017
Policy Specific Section: October 1, 2010 January 21, 2013
 Medical Policy Bi-level Positive Airway Pressure (BPAP/NPPV) Type: Medical Necessity/Not Medical Necessity Policy Specific Section: Durable Medical Equipment Original Policy Date: Effective Date: October
Medical Policy Bi-level Positive Airway Pressure (BPAP/NPPV) Type: Medical Necessity/Not Medical Necessity Policy Specific Section: Durable Medical Equipment Original Policy Date: Effective Date: October
Pediatric Considerations in the Sleep Lab
 AAST Technologist Fundamentals Date: May 7, 2017 Focus Conference Location: Orlando, Florida Workshop Pediatric Considerations in the Sleep Lab By Joel Porquez, BS, RST/RPSGT, CCSH X X X X X X Conflict
AAST Technologist Fundamentals Date: May 7, 2017 Focus Conference Location: Orlando, Florida Workshop Pediatric Considerations in the Sleep Lab By Joel Porquez, BS, RST/RPSGT, CCSH X X X X X X Conflict
EXPLORE NEW POSSIBILITIES
 EXPLORE NEW POSSIBILITIES TREATING SNORING AND SLEEP APNOEA HAS CHANGED FOREVER Introducing the Oventus O 2 Vent, a custom made, comfortable oral appliance with a unique airway design for the treatment
EXPLORE NEW POSSIBILITIES TREATING SNORING AND SLEEP APNOEA HAS CHANGED FOREVER Introducing the Oventus O 2 Vent, a custom made, comfortable oral appliance with a unique airway design for the treatment
Role of Oral Devices in Managing Sleep-disordered Breathing Patients
 Role of Oral Devices in Managing Sleep-disordered Breathing Patients Sleep-disordered breathing (SDB) includes mouth breathing, snoring, upper airway resistance syndrome (UARS), and obstructive sleep apnea
Role of Oral Devices in Managing Sleep-disordered Breathing Patients Sleep-disordered breathing (SDB) includes mouth breathing, snoring, upper airway resistance syndrome (UARS), and obstructive sleep apnea
Index SLEEP MEDICINE CLINICS. Note: Page numbers of article titles are in boldface type.
 549 SLEEP MEDICINE CLINICS Sleep Med Clin 1 (2007) 549 553 Note: Page numbers of article titles are in boldface type. A Abdominal motion, in assessment of sleep-related breathing disorders, 452 454 Adherence,
549 SLEEP MEDICINE CLINICS Sleep Med Clin 1 (2007) 549 553 Note: Page numbers of article titles are in boldface type. A Abdominal motion, in assessment of sleep-related breathing disorders, 452 454 Adherence,
Central Sleep Apnea. v Characteristics
 Central Sleep Apnea v Characteristics Respiratory pauses > 10 sec Due to failure of brain s respiratory center to send signal to respiratory muscles Tends to occur in infants (neurological immaturity)
Central Sleep Apnea v Characteristics Respiratory pauses > 10 sec Due to failure of brain s respiratory center to send signal to respiratory muscles Tends to occur in infants (neurological immaturity)
Dr Alireza Yarahmadi and Dr Arvind Perathur Mercy Medical Center - Winter Retreat Des Moines February 2012
 Dr Alireza Yarahmadi and Dr Arvind Perathur Mercy Medical Center - Winter Retreat Des Moines February 2012 Why screen of OSA prior to surgery? What factors increase the risk? When due to anticipate problems?
Dr Alireza Yarahmadi and Dr Arvind Perathur Mercy Medical Center - Winter Retreat Des Moines February 2012 Why screen of OSA prior to surgery? What factors increase the risk? When due to anticipate problems?
Kaniethapriya A.S, Ganesh Prasad S.
 Original Article A Comparative Study of Effects of Oropharyngeal Exercises and Continuous Positive Airway Pressure (CPAP) on Parameters of Sleep on Moderate Obstructive Sleep Apnea Syndrome (OSAS) Patients
Original Article A Comparative Study of Effects of Oropharyngeal Exercises and Continuous Positive Airway Pressure (CPAP) on Parameters of Sleep on Moderate Obstructive Sleep Apnea Syndrome (OSAS) Patients
A New, Clinically Proven Sleep Apnea Therapy for people unable to use CPAP.
 A New, Clinically Proven Sleep Apnea Therapy for people unable to use CPAP. Take Heart. If You Have OSA, You re Not Alone. Like you, more than 18 million Americans are estimated to have Obstructive Sleep
A New, Clinically Proven Sleep Apnea Therapy for people unable to use CPAP. Take Heart. If You Have OSA, You re Not Alone. Like you, more than 18 million Americans are estimated to have Obstructive Sleep
PEDIATRIC OBSTRUCTIVE SLEEP APNEA (OSA)
 PEDIATRIC OBSTRUCTIVE SLEEP APNEA (OSA) DEFINITION OSA Inspiratory airflow is either partly (hypopnea) or completely (apnea) occluded during sleep. The combination of sleep-disordered breathing with daytime
PEDIATRIC OBSTRUCTIVE SLEEP APNEA (OSA) DEFINITION OSA Inspiratory airflow is either partly (hypopnea) or completely (apnea) occluded during sleep. The combination of sleep-disordered breathing with daytime
Medicare C/D Medical Coverage Policy
 Medicare C/D Medical Coverage Policy Surgical Treatment of Obstructive Sleep Apnea Origination: June 26, 2000 Review Date: January 18, 2017 Next Review January, 2019 DESCRIPTION OF PROCEDURE OR SERVICE
Medicare C/D Medical Coverage Policy Surgical Treatment of Obstructive Sleep Apnea Origination: June 26, 2000 Review Date: January 18, 2017 Next Review January, 2019 DESCRIPTION OF PROCEDURE OR SERVICE
Sleep Diordered Breathing (Part 1)
 Sleep Diordered Breathing (Part 1) History (for more topics & presentations, visit ) Obstructive sleep apnea - first described by Charles Dickens in 1836 in Papers of the Pickwick Club, Dickens depicted
Sleep Diordered Breathing (Part 1) History (for more topics & presentations, visit ) Obstructive sleep apnea - first described by Charles Dickens in 1836 in Papers of the Pickwick Club, Dickens depicted
SLEEP DISORDERED BREATHING The Clinical Conditions
 SLEEP DISORDERED BREATHING The Clinical Conditions Robert G. Hooper, M.D. In the previous portion of this paper, the definitions of the respiratory events that are the hallmarks of problems with breathing
SLEEP DISORDERED BREATHING The Clinical Conditions Robert G. Hooper, M.D. In the previous portion of this paper, the definitions of the respiratory events that are the hallmarks of problems with breathing
SLEEP APNEA IN THE ELDERLY SLEEP THAT KNITS UP THE RAVELED SLEEVE OF CARE
 SLEEP APNEA IN THE ELDERLY SLEEP THAT KNITS UP THE RAVELED SLEEVE OF CARE OBJECTIVES 1. TO DESCRIBE THE NORMAL AGE RELATED CHANGES TO SLEEP 2. TO DESCRIBE THE SPECTRUM OF SLEEP-DISORDERED BREATHING. 3.
SLEEP APNEA IN THE ELDERLY SLEEP THAT KNITS UP THE RAVELED SLEEVE OF CARE OBJECTIVES 1. TO DESCRIBE THE NORMAL AGE RELATED CHANGES TO SLEEP 2. TO DESCRIBE THE SPECTRUM OF SLEEP-DISORDERED BREATHING. 3.
Pre-Operative Services Teaching Rounds 11 March 2011
 Pre-Operative Services Teaching Rounds 11 March 2011 Deborah Richman MBChB FFA(SA) Director Pre-Operative Services Department of Anesthesia Stony Brook University Medical Center, NY drichman@notes.cc.sunysb.edu
Pre-Operative Services Teaching Rounds 11 March 2011 Deborah Richman MBChB FFA(SA) Director Pre-Operative Services Department of Anesthesia Stony Brook University Medical Center, NY drichman@notes.cc.sunysb.edu
Bruxism: Revisiting an Old Problem with New Questions and Unique Solutions
 Jeff Rouse, DDS Txacad@aol.com 555 E. Basse #200 www.coredentistry.com San Antonio, TX 78209 210-828-3334 Bruxism: Revisiting an Old Problem with New Questions and Unique Solutions CORE Concept Wear and
Jeff Rouse, DDS Txacad@aol.com 555 E. Basse #200 www.coredentistry.com San Antonio, TX 78209 210-828-3334 Bruxism: Revisiting an Old Problem with New Questions and Unique Solutions CORE Concept Wear and
Persistent Obstructive Sleep Apnea After Tonsillectomy. Learning Objectives. Mary Frances Musso, DO Pediatric Otolaryngology
 Persistent Obstructive Sleep Apnea After Tonsillectomy Mary Frances Musso, DO Pediatric Otolaryngology Learning Objectives Recognize indications for tonsillectomy List patients at risk for persistent OSA
Persistent Obstructive Sleep Apnea After Tonsillectomy Mary Frances Musso, DO Pediatric Otolaryngology Learning Objectives Recognize indications for tonsillectomy List patients at risk for persistent OSA
Effect of Three Different Mandibular Advancement Devices and Two Different Bite Techniques on the Resultant Sleep Metrics
 Effect of Three Different Mandibular Advancement Devices and Two Different Bite Techniques on the Resultant Sleep Metrics Shamshudin (Sam) Kherani, DDS, FAGD, MICCMO Background It has been documented in
Effect of Three Different Mandibular Advancement Devices and Two Different Bite Techniques on the Resultant Sleep Metrics Shamshudin (Sam) Kherani, DDS, FAGD, MICCMO Background It has been documented in
OSA in children. About this information. What is obstructive sleep apnoea (OSA)?
 About this information This information explains all about sleep-related breathing problems in children, focusing on the condition obstructive sleep apnoea (OSA). It tells you what the risk factors are
About this information This information explains all about sleep-related breathing problems in children, focusing on the condition obstructive sleep apnoea (OSA). It tells you what the risk factors are
Dental Sleep Medicine Basics
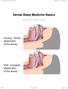 Dental Sleep Medicine Basics Written By: Patrick Tessier 2018 www.tap.wiki/ Page 1 of 8 INTRODUCTION Here are some basic aspect of Dental Sleep Medicine. This viewpoint is from an industry participant,
Dental Sleep Medicine Basics Written By: Patrick Tessier 2018 www.tap.wiki/ Page 1 of 8 INTRODUCTION Here are some basic aspect of Dental Sleep Medicine. This viewpoint is from an industry participant,
Technology Brief THE TREATMENT OF OBSTRUCTIVE SLEEP APNEA: AN OVERVIEW INTRODUCTION ISSUE 8.0 DECEMBER 1995
 Technology Brief ISSUE 8.0 DECEMBER 1995 THE TREATMENT OF OBSTRUCTIVE SLEEP APNEA: AN OVERVIEW INTRODUCTION Obstructive sleep apnea (OSA) is a disorder characterized by the intermittent cessation or decrement
Technology Brief ISSUE 8.0 DECEMBER 1995 THE TREATMENT OF OBSTRUCTIVE SLEEP APNEA: AN OVERVIEW INTRODUCTION Obstructive sleep apnea (OSA) is a disorder characterized by the intermittent cessation or decrement
Evaluation, Management and Long-Term Care of OSA in Adults
 Evaluation, Management and Long-Term Care of OSA in Adults AUGUST 2015 Providing diagnostic tools and therapies that are evidence-based is a key part of a successful sleep practice. This resource outlines
Evaluation, Management and Long-Term Care of OSA in Adults AUGUST 2015 Providing diagnostic tools and therapies that are evidence-based is a key part of a successful sleep practice. This resource outlines
Comparing Upper Airway Stimulation to Expansion Sphincter Pharyngoplasty: A Single University Experience
 771395AORXXX10.1177/0003489418771395Annals of Otology, Rhinology & LaryngologyHuntley et al research-article2018 Original Article Comparing Upper Airway Stimulation to Expansion Sphincter Pharyngoplasty:
771395AORXXX10.1177/0003489418771395Annals of Otology, Rhinology & LaryngologyHuntley et al research-article2018 Original Article Comparing Upper Airway Stimulation to Expansion Sphincter Pharyngoplasty:
Anyone of any shape or size may snore, but there are certain features which significantly increase the chance of snoring.
 Snoring Snoring is a common sleep related problem affecting more than 20% of the population at some stage in their lives. Snoring occurs when various parts of the throat, including the soft palate, tonsils
Snoring Snoring is a common sleep related problem affecting more than 20% of the population at some stage in their lives. Snoring occurs when various parts of the throat, including the soft palate, tonsils
Dr. Karan Madan Senior Resident
 SLEEP DISORDERED BREATHING DIAGNOSIS & MANAGEMENT Dr. Karan Madan Senior Resident Department of Pulmonary medicine Sleep disordered breathing (SDB) Definition- Sleep-disordered breathing (SDB) is present
SLEEP DISORDERED BREATHING DIAGNOSIS & MANAGEMENT Dr. Karan Madan Senior Resident Department of Pulmonary medicine Sleep disordered breathing (SDB) Definition- Sleep-disordered breathing (SDB) is present
Protriptyline in the treatment of sleep apnoea
 WA CONWAY, F ZORICK, P PICCIONE, T ROTH Thorax 1982;37:49-53 From the Department of Medicine, Pulmonary Medicine Division and Sleep Disorders Center, Henry Ford Hospital, Detroit, Michigan, USA ABSTRACT
WA CONWAY, F ZORICK, P PICCIONE, T ROTH Thorax 1982;37:49-53 From the Department of Medicine, Pulmonary Medicine Division and Sleep Disorders Center, Henry Ford Hospital, Detroit, Michigan, USA ABSTRACT
The treatment of obstructive sleep apnea syndrome
 Maxillofacial Surgery and Nasal CPAP* A Comparison of Treatment for Obstructive Sleep Apnea Syndrome Robert W Riley, D.D.S., M.D.; Nelson B. PoweU, M.D.; and Christian Guilleminault, M.D. Nasal continuous
Maxillofacial Surgery and Nasal CPAP* A Comparison of Treatment for Obstructive Sleep Apnea Syndrome Robert W Riley, D.D.S., M.D.; Nelson B. PoweU, M.D.; and Christian Guilleminault, M.D. Nasal continuous
Learning Objectives. And it s getting worse. The Big Picture. Dr. Roger Roubal
 Learning Objectives How to screen for sleep apnea; questions to ask your patients Industry treatment guidelines; when to consider an oral appliance vs. a CPAP What goals/thresholds to set for successful
Learning Objectives How to screen for sleep apnea; questions to ask your patients Industry treatment guidelines; when to consider an oral appliance vs. a CPAP What goals/thresholds to set for successful
Abdussalam Alahmari ENT Resident R2 KAUH 15/12/2015
 Abdussalam Alahmari ENT Resident R2 KAUH 15/12/2015 Physiology of sleep Snoring mechanism, causes, sites, symptoms, and management. Sleep apnea definitions, pathophysiology, risk factors, evaluation of
Abdussalam Alahmari ENT Resident R2 KAUH 15/12/2015 Physiology of sleep Snoring mechanism, causes, sites, symptoms, and management. Sleep apnea definitions, pathophysiology, risk factors, evaluation of
Role of Protriptyline and Acetazolamide in the Sleep Apnea/Hypopnea Syndrome
 Sleep 11(5):463-472, Raven Press, Ltd., New York 1988 Association of Professional Sleep Societies Role of Protriptyline and Acetazolamide in the Sleep Apnea/Hypopnea Syndrome K. F. Whyte, G. A. Gould,
Sleep 11(5):463-472, Raven Press, Ltd., New York 1988 Association of Professional Sleep Societies Role of Protriptyline and Acetazolamide in the Sleep Apnea/Hypopnea Syndrome K. F. Whyte, G. A. Gould,
During the therapeutic titration of nasal continuous
 Cardiogenic Oscillations on the Airflow Signal During Continuous Positive Airway Pressure as a Marker of Central Apnea* Indu Ayappa, PhD; Robert G. Norman, MS, RRT; and David M. Rapoport, MD, FCCP Therapeutic
Cardiogenic Oscillations on the Airflow Signal During Continuous Positive Airway Pressure as a Marker of Central Apnea* Indu Ayappa, PhD; Robert G. Norman, MS, RRT; and David M. Rapoport, MD, FCCP Therapeutic
Positive Airway Pressure and Oral Devices for the Treatment of Obstructive Sleep Apnea
 Positive Airway Pressure and Oral Devices for the Treatment of Obstructive Sleep Apnea Policy Number: Original Effective Date: MM.01.009 11/01/2009 Line(s) of Business: Current Effective Date: HMO; PPO
Positive Airway Pressure and Oral Devices for the Treatment of Obstructive Sleep Apnea Policy Number: Original Effective Date: MM.01.009 11/01/2009 Line(s) of Business: Current Effective Date: HMO; PPO
DOWNLOAD OR READ : TREATMENT FOR SNORING PROBLEMS PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : TREATMENT FOR SNORING PROBLEMS PDF EBOOK EPUB MOBI Page 1 Page 2 treatment for snoring problems treatment for snoring problems pdf treatment for snoring problems problem, presenting
DOWNLOAD OR READ : TREATMENT FOR SNORING PROBLEMS PDF EBOOK EPUB MOBI Page 1 Page 2 treatment for snoring problems treatment for snoring problems pdf treatment for snoring problems problem, presenting
Respiratory Management of Facioscapulohumeral Muscular Dystrophy. Nicholas S. Hill, MD Tufts Medical Center Boston, MA
 Respiratory Management of Facioscapulohumeral Muscular Dystrophy Nicholas S. Hill, MD Tufts Medical Center Boston, MA Respiratory Involvement in FSHD Very variable time of onset rate of progression Muscles
Respiratory Management of Facioscapulohumeral Muscular Dystrophy Nicholas S. Hill, MD Tufts Medical Center Boston, MA Respiratory Involvement in FSHD Very variable time of onset rate of progression Muscles
Excessive Daytime Sleepiness Associated with Insufficient Sleep
 Sleep, 6(4):319-325 1983 Raven Press, New York Excessive Daytime Sleepiness Associated with Insufficient Sleep T. Roehrs, F. Zorick, J. Sicklesteel, R. Wittig, and T. Roth Sleep Disorders and Research
Sleep, 6(4):319-325 1983 Raven Press, New York Excessive Daytime Sleepiness Associated with Insufficient Sleep T. Roehrs, F. Zorick, J. Sicklesteel, R. Wittig, and T. Roth Sleep Disorders and Research
Oral Appliances and their Clinical Applications
 Oral Appliances and their Clinical Applications Peter Cistulli MBBS, PhD, MBA, FRACP Professor of Respiratory Medicine & Head of Discipline of Sleep Medicine University of Sydney Director, Centre for Sleep
Oral Appliances and their Clinical Applications Peter Cistulli MBBS, PhD, MBA, FRACP Professor of Respiratory Medicine & Head of Discipline of Sleep Medicine University of Sydney Director, Centre for Sleep
WINDSOR DENTAL CARE 2224 WALKER ROAD SUITE 20 WINDSOR, ON N8W 5L7 PHONE FAX
 The quality of your sleep can impact you emotionally, physically and your overall general health. Poor sleep can cause chronic fatigue, daytime drowsiness, irritability and loss of focus. It affects your
The quality of your sleep can impact you emotionally, physically and your overall general health. Poor sleep can cause chronic fatigue, daytime drowsiness, irritability and loss of focus. It affects your
Obstructive sleep apnea: A dentist update
 Review article Obstructive sleep apnea: A dentist update Mithun K*, Ashith M V, Valerie Anithra Pereira, Deesha Kumari Email:dr.mithunknaik@gmail.com Abstract Sleep breathing disorder includes snoring,
Review article Obstructive sleep apnea: A dentist update Mithun K*, Ashith M V, Valerie Anithra Pereira, Deesha Kumari Email:dr.mithunknaik@gmail.com Abstract Sleep breathing disorder includes snoring,
Temperature controlled radiofrequency ablation for OSA
 Temperature controlled radiofrequency ablation for OSA Ridhwan Y. Baba, M.B.B.S. *1, V.V.S. Ramesh Metta, M.B.B.S. 1, Arjun Mohan, M.B.B.S. 2, M. Jeffery Mador, M.D. 2 1 Department of Internal Medicine,
Temperature controlled radiofrequency ablation for OSA Ridhwan Y. Baba, M.B.B.S. *1, V.V.S. Ramesh Metta, M.B.B.S. 1, Arjun Mohan, M.B.B.S. 2, M. Jeffery Mador, M.D. 2 1 Department of Internal Medicine,
Obstructive Sleep Apnea and COPD overlap syndrome. Financial Disclosures. Outline 11/1/2016
 Obstructive Sleep Apnea and COPD overlap syndrome Chitra Lal, MD, FCCP, FAASM Associate Professor of Medicine, Pulmonary, Critical Care, and Sleep, Medical University of South Carolina Financial Disclosures
Obstructive Sleep Apnea and COPD overlap syndrome Chitra Lal, MD, FCCP, FAASM Associate Professor of Medicine, Pulmonary, Critical Care, and Sleep, Medical University of South Carolina Financial Disclosures
Effect of Metabolic Acidosis Upon Sleep Apnea*
 Effect of Metabolic Upon Sleep Apnea* john T. Sharp, M.D., F.C.C.P.; WalterS. Druz, Ph.D.; Vivian D'Souza, M.D.; and Edward Diamond, M.D. The effects of metabolic acidosis upon the pattern of apnea during
Effect of Metabolic Upon Sleep Apnea* john T. Sharp, M.D., F.C.C.P.; WalterS. Druz, Ph.D.; Vivian D'Souza, M.D.; and Edward Diamond, M.D. The effects of metabolic acidosis upon the pattern of apnea during
Positive Airway Pressure and Oral Devices for the Treatment of Obstructive Sleep Apnea
 Positive Airway Pressure and Oral Devices for the Treatment of Obstructive Sleep Apnea Policy Number: Original Effective Date: MM.01.009 11/01/2009 Line(s) of Business: Current Effective Date: HMO; PPO;
Positive Airway Pressure and Oral Devices for the Treatment of Obstructive Sleep Apnea Policy Number: Original Effective Date: MM.01.009 11/01/2009 Line(s) of Business: Current Effective Date: HMO; PPO;
Basics of Polysomnography. Chitra Lal, MD, FCCP, FAASM Assistant professor of Medicine, Pulmonary, Critical Care and Sleep, MUSC, Charleston, SC
 Basics of Polysomnography Chitra Lal, MD, FCCP, FAASM Assistant professor of Medicine, Pulmonary, Critical Care and Sleep, MUSC, Charleston, SC Basics of Polysomnography Continuous and simultaneous recording
Basics of Polysomnography Chitra Lal, MD, FCCP, FAASM Assistant professor of Medicine, Pulmonary, Critical Care and Sleep, MUSC, Charleston, SC Basics of Polysomnography Continuous and simultaneous recording
Tired of being tired?
 Tired of being tired? Narval CC MRD ResMed.com/Narval Sleepiness and snoring are possible symptoms of sleep apnea. Did you know that one in every four adults has some form of sleep disordered-breathing
Tired of being tired? Narval CC MRD ResMed.com/Narval Sleepiness and snoring are possible symptoms of sleep apnea. Did you know that one in every four adults has some form of sleep disordered-breathing
NASAL CONTINUOUS POSITIVE AIRWAY PRESSURE FOR OBSTRUCTIVE SLEEP APNEA IN CHILDREN. Dr. Nguyễn Quỳnh Anh Department of Respiration 1
 1 NASAL CONTINUOUS POSITIVE AIRWAY PRESSURE FOR OBSTRUCTIVE SLEEP APNEA IN CHILDREN Dr. Nguyễn Quỳnh Anh Department of Respiration 1 CONTENTS 2 1. Preface 2. Definition 3. Etiology 4. Symptoms 5. Complications
1 NASAL CONTINUOUS POSITIVE AIRWAY PRESSURE FOR OBSTRUCTIVE SLEEP APNEA IN CHILDREN Dr. Nguyễn Quỳnh Anh Department of Respiration 1 CONTENTS 2 1. Preface 2. Definition 3. Etiology 4. Symptoms 5. Complications
(To be filled by the treating physician)
 CERTIFICATE OF MEDICAL NECESSITY TO BE ISSUED TO CGHS BENEFICIAREIS BEING PRESCRIBED BILEVEL CONTINUOUS POSITIVE AIRWAY PRESSURE (BI-LEVEL CPAP) / BI-LEVEL VENTILATORY SUPPORT SYSTEM Certification Type
CERTIFICATE OF MEDICAL NECESSITY TO BE ISSUED TO CGHS BENEFICIAREIS BEING PRESCRIBED BILEVEL CONTINUOUS POSITIVE AIRWAY PRESSURE (BI-LEVEL CPAP) / BI-LEVEL VENTILATORY SUPPORT SYSTEM Certification Type
전자선단층촬영기를이용한코골이환자의역동적상기도측정
 KISEP Rhinology Korean J Otolaryngol 3;46:-5 전자선단층촬영기를이용한코골이환자의역동적상기도측정 예미경 신승헌 김창균 이상흔 이종민 3 최재갑 4 Dynamic Upper Airway Study in Snoring Subjects Using Electron Beam Tomography Mi Kyung Ye, MD, Seung
KISEP Rhinology Korean J Otolaryngol 3;46:-5 전자선단층촬영기를이용한코골이환자의역동적상기도측정 예미경 신승헌 김창균 이상흔 이종민 3 최재갑 4 Dynamic Upper Airway Study in Snoring Subjects Using Electron Beam Tomography Mi Kyung Ye, MD, Seung
THE EFFECTS OF MEDROXYPROGESTERONE ACETATE AND ACETAZOLAMIDE ON THE NOCTURNAL OXYGEN SATURATION IN COPD PATIENTS
 THE EFFECTS OF MEDROXYPROGESTERONE ACETATE AND ACETAZOLAMIDE ON THE NOCTURNAL OXYGEN SATURATION IN COPD PATIENTS Wagenaar, M., Vos, P., Heijdra, Y., Herwaarden, C. van, Folgering, H. Departement of Pulmonary
THE EFFECTS OF MEDROXYPROGESTERONE ACETATE AND ACETAZOLAMIDE ON THE NOCTURNAL OXYGEN SATURATION IN COPD PATIENTS Wagenaar, M., Vos, P., Heijdra, Y., Herwaarden, C. van, Folgering, H. Departement of Pulmonary
PEDIATRIC PAP TITRATION PROTOCOL
 PURPOSE In order to provide the highest quality care for our patients, our sleep disorders facility adheres to the AASM Standards of Accreditation. The accompanying policy and procedure on pediatric titrations
PURPOSE In order to provide the highest quality care for our patients, our sleep disorders facility adheres to the AASM Standards of Accreditation. The accompanying policy and procedure on pediatric titrations
UPDATES IN SLEEP APNEA:
 UPDATES IN SLEEP APNEA: CPAP,CPAP COMPLIANCE, & ALTERNATIVES MICHELLE ZETOONY, DO, FCCP, FACOI BOARD CERTIFIED PULMONARY, CRITICAL CARE, SLEEP & INTERNAL MEDICINE CLEARWATER, FL DISCLOSURE I have no conflicts
UPDATES IN SLEEP APNEA: CPAP,CPAP COMPLIANCE, & ALTERNATIVES MICHELLE ZETOONY, DO, FCCP, FACOI BOARD CERTIFIED PULMONARY, CRITICAL CARE, SLEEP & INTERNAL MEDICINE CLEARWATER, FL DISCLOSURE I have no conflicts
Obstructive Sleep Apnea Syndrome
 SMGr up Obstructive Sleep Apnea Syndrome Alper Dilci, Handan Koyuncu and Vural Fidan* Otorhinolaryngology Department, Yunus Emre Government Hospital, Turkey *Corresponding author: Vural Fidan, Otorhinolaryngology
SMGr up Obstructive Sleep Apnea Syndrome Alper Dilci, Handan Koyuncu and Vural Fidan* Otorhinolaryngology Department, Yunus Emre Government Hospital, Turkey *Corresponding author: Vural Fidan, Otorhinolaryngology
GOT SLEEP? YOUR COMPLETE GUIDE TO UNDERSTANDING SLEEP APNEA
 Count me. I dare you. GOT SLEEP? YOUR COMPLETE GUIDE TO UNDERSTANDING SLEEP APNEA PRESENTED BY INTRODUCTION So what s the point of this ebook anyway? At The Maxillofacial Surgery Center, we want to inform
Count me. I dare you. GOT SLEEP? YOUR COMPLETE GUIDE TO UNDERSTANDING SLEEP APNEA PRESENTED BY INTRODUCTION So what s the point of this ebook anyway? At The Maxillofacial Surgery Center, we want to inform
