When is a tracheostomy indicated? an acute or chronic upper airway. of oral or gastric secretions in. (ET) tube and facilitate longterm
|
|
|
- Erika Gilbert
- 5 years ago
- Views:
Transcription
1 Learn all about managing a "trach" to protect your patient from complications. By Elizabeth Neville Regan, RN, MSN, and Lisa Dallachiesa, RN, BS m 2.0 ANCC CONTAG HOURS cartilage. Made surgically or percutaneously; A TRACHEOSTOMY IS an opening in the anterior wall of the trachea inferior to the cricoid it provides tracheal access for airway management via a temporary or permanent tracheostomy tube. Patients with tracheostomies aren't limited to critical care settings and can be found in all nursing units. No matter where you work, you need a basic understanding of the nursing care required for these patients. In this article, we'll provide a practical overview. When is a tracheostomy indicated? A tracheostomy can be used to bypass an acute or chronic upper airway obstruction, allow removal of tracheobronchial secretions, and prevent aspiration of oral or gastric secretions in unresponsive with chronic respiratory be performed patients. For patients failure, it may to replace an endotracheal (ET) tube and facilitate longterm mechanical ventilation.! Upper airway obstruction from conditions inflammation, such as tumors, can result fracture, foreign bodies, or laryngeal spasm. Patients with prolonged unresponsiveness secondary to such conditions as drug intoxication or traumatic brain injury may need a tracheostomy to maintain a patent airway In addition, patients needing an ET tube for 10 to 14 days or longer should be considered possible candidates for a tracheostomy? The most recent American College of Chest Physicians consensus statement recommending a specific time frame for conversion to tracheostomy was published in These guidelines recommended the translaryngeal route (ET tube) if the need for an artificial airway is How to care for a patient with a 34 I Nursingl009 I August wvwv.nursing2009.com
2 anticipated to be no longer than 10 days, and favored tracheostomy if an artificial airway is anticipated for longer than 21 days3 The literature suggests that the earlier the patient undergoes tracheostomy, the more likely he'll benefit.' Benefits of tracheostomy include avoiding further direct laryngeal injury from the ET tube, facilitating airway suctioning oral care, increasing patient mobility, improving patient comfort, allowing and speech, and facilitating oral feedmgs." Complications associated with tracheostomy are largely determined technique used. by the A peek at techniques The standard surgical tracheostomy (ST), also known as an open tracheostomy, is usually performed in the OR under general anesthesia. In percutaneous dilatational tracheostomy (PDT), the tracheal stoma is created through dilation of an incision rather than surgery. PDT may be performed under local anesthesia, moderate sedation/analgesia, or general anesthesia in the OR or at the bedside. Indications for PDT are the same as for ST, but PDT requires careful patient selection to assure a safe and successful outcome. (See Contraindications to PDT.) Advantages of PDT over ST include eliminating the need for general anesthesia and the OR, and lower costs." Because the PDT requires a smaller Contra indications to PDYs Absolute Uncorrected coagulopathy Infection over the site Extreme ventilatory and oxygenation demands Tracheal obstruction Relative Unfavorable neck anatomy Emergency airway management Use the ventilator, not a manual resuscitation bag, to provide hyperoxygenation before suctioning to reduce hemodynamic changes. skin incision, patients experience less tissue trauma and a lower risk of complications such as wound infection, wound scarring, and peristomal bleeding. And because the procedure can be performed at the bedside in the ICU, PDT reduces the risk associated with transferring critically ill patients to the OR. For a look at the types of tracheostomy tubes available and why they're used, see Tracheostomy tube design review. What can go wrong? Early complications associated with ST include bleeding, pneumothorax, embolism, recurrent laryngeal nerve damage, and posterior injury: Long-term air tracheal wall complications include airway obstruction from accumulation of secretions or protrusion of the cuff over the opening of the tube, infection, rupture artery, dysphagia, of the innominate tracheoesophageal fistula, tracheal dilation, and tracheal ischemia and necrosis. 1 The complication rate of PDT is low and similar to that of ST, especially the rates of major infection or bleeding." However, airway loss associated with tracheal tube displacement is significantly more likely to occur in PDT due to the narrow dilated tract and lack of formal stoma creation. Responding to inadvertent decannulation Tracheal tube decannulation (dislodgment) in the first few days after surgery is a medical emergency: Keep supplies for reinserting the tube at the bedside, including suctioning equipment, a new tracheostomy (dilator), tube with obturator and a curved hemostat. Oxygen and equipment for ET intubation also should be readily available. If decannulation emergency response reinsertion. occurs, call the team to attempt Use a bag-valve mask to ventilate your patient through the upper airway: Ventilate gently to prevent air from escaping through the stoma or carefully occlude the stoma with a gloved hand to maximize oxygenation. The patient will be panicked, so stay with him and assure him that help is on the way: When the emergency team arrives, a clinician will try to insert a new tracheostomy tube through the opening, using a hemostat and obturator. If she doesn't succeed and the patient's condition worsens, she may place an ET tube through his mouth to establish an airway: If the patient has a disruption between the upper and lower airways (for example, after tumor resection), making mask ventilation and endotracheal intubation through the upper airway impossible, ventilate him through the stoma. Monitor him to make sure he's adequately and oxygenated for surgery: To prevent accidental decannulation, ventilated before he's prepared tracheal make sure the tube is properly secured, minimize manipulation of the tube and traction on the tube from oxygen or ventilator and teach the patient to move cautiously until the tract is healed." tubing, 36 I Nursingl009 I August
3 Tracheostomy care basics Provide tracheostomy care every 4 to 8 hours.f Knowing how to properly care for a patient with a tracheostomy is vital because inappropriate or inadequate care may lead to complications and even death. Although details vary depending on the type of tracheostomy tube, tracheostomy care includes cleaning or changing the inner cannula, changing the dressing and tracheostomy tube holder, and suctioning if needed. Most tracheostomy tubes have disposable inner cannulas, which are replaced and secured using aseptic technique. Never clean and reuse a disposable cannula. Reusable inner cannulas require careful cleaning. Perform hand hygiene, don a face shield (or goggles and mask) and sterile gloves, and maintain aseptic technique during the procedure. Unlock and remove the inner cannula and place it in a solution of equal parts hydrogen peroxide and 0.9% sodium chloride unless the manufacturer directs otherwise. Remove encrusted secretions from the lumen with sterile pipe cleaners. After cleaning, rinse the cannula thoroughly with sterile 0.9% sodium chloride solution. Reinsert the inner cannula and securely lock it into place. While providing tracheostomy care, inspect the skin for signs of irritation or infection, such as erythema, pain, or discharge. Thoroughly assess the skin around the tracheostomy for evidence of skin breakdown related to the tracheostomy device, tube securement device, or mucus and secretions." Clean the area around the tracheostomy tube with a noncytotoxic cleanser using a sterile cotton-tipped applicator. Then rinse the skin with water and dry it gently with sterile gauze." If you see skin breakdown, consult a woundjostomy/continence nurse for an individualized patient plan of care. Tracheostomy tube design review 11 The healthcare market has exploded with tracheostomy tube designs in the last 10 years. Here's a quick look at how some of the various options compare. Metal tracheostomy tubes aren't commonly used today due to their expense, rigid construction, the lack of a cuff, and the lack of a 15 mm connector to attach a ventilator or bag-valve mask. Plastic tracheostomy tubes soften at body temperature, conforming to patient anatomy and centering the distal tip in the trachea. Uncuiied tracheostomy tubes are generally reserved for I ~. I infant~ an~ children because.they are less traumatic t? sur- ftf~ rounding tissue. They allow airway clearance but provide. '\} no protection from aspiration. Cuffed tracheostomy tubes allow for airway clearance, offer some protection from aspiration, and facilitate positive-pressure ventilation when the cuff is inflated. High-volume, low-pressure cuffs are most commonly used for adults. Dual-cannula tracheostomy tubes have a disposable or reusable inner cannula, which is cleaned or replaced regularly; the inner cannula can be removed if the tracheostomy tube becomes occluded. PDT tubes have a tapered distal tip and are designed for use with percutaneous tracheostomies. Minitracheostomy tubes are small bore, generally uncuffed, and used primarily for secretion clearance. They're inserted into the trachea through the cricothyroid membrane or the tracheal stoma after decannulation for administration of oxygen. They're used primarily for patients who have problems with airway clearance because they allow bronchial lavage and suctioning with a 10 Fr suction catheter. They're generally unsuitable for positive pressure ventilation.p Foam cuff tracheostomy tubes are self-inflating with a large diameter highresidual-volume cuff composed of polyurethane foam covered by a silicone sheath. The foam cuff addresses the issue of high lateral tracheal-wall pressures that lead to complications such as tracheal necrosis and stenosis. Before insertion, air in the cuff is removed by attaching a syringe to the pilot port. Once the tube is in place, the syringe is removed to allow the pilot port to open to atmospheric pressure (room air) and the cuff self-inflates. Once inflated, it conforms to the size and shape of the patient's trachea. Be sure to keep the pilot port open to prevent cuff deflation. Adjustable flange tracheostomy tubes have a spiral wire reinforced flexible design with a longer proximal length facilitating placement in patients with a large neck. The adjustable flange allows bedside adjustments to meet extralength tracheostomy needs. Because the locking mechanism on the flanges tends to deteriorate over time, these tubes are usually reserved for temporary use. Fenestrated tracheostomy tubes are similar in construction to the standard cuffed tube, with the addition of an opening in the posterior portion of the tube above the cuff. They have a removable inner cannula and a plastic plug. With the inner cannula removed, the cuff deflated, and the normal air passage occluded, the patient can inhale and exhale through the fenestrations and around the tube. This tube allows clinicians to assess the patient's ability to breathe through the normal oral/nasal route (preparing the patient for decannulation) and permits air to pass by the vocal cords (allowing phonation). August I Nursingl009 I 37
4 Absorbing secretions helps prevent maceration and skin breakdown. Place a prepackaged, sterile tracheostomy dressing under the tube flanges. Always use a manufactured split sponge rather than cutting a gauze pad. Never place anything with loose fibers around the stoma or tracheostomy they can cause irritation. tube because Inform the health care provider if sutures used to secure the tube after insertion are irritating the skin or preventing routine maintenance. Obtain an order for suture removal 7 days after tracheostomy tube insertion. If twill tape was used, change it to a Velcro-securing device as soon as possible because it's more comfortable less likely to abrade the skin." Maintaining humidification is another key nursing responsibility. Normally, the nasopharynx and humidifies inhaled air. Because the tracheostomy tube bypasses the upper airway, you need to provide adequate humidity keep the airway moist. In hospitalized patients, this can be accomplished by a heat and moisture exchanger on a mechanical ventilator or a 'l-piece or tracheostomy mask. In addition, your patient must be properly hydrated; example, with LV fluids. Monitor and record cuff pressures to for every shift and more often if the tube is changed or repositioned, if the volume of cuff air changes, or a leak occurs (see Maintaining safe, effective cuff pressures). Sudioning tips and precautions Because the patient can't cough effectively to clear secretions, be prepared to suction him as needed. Suctioning raises the risk of hypoxemia, bronchospasm, and other adverse reactions, so suction only when needed, not on a set schedule, and suction for the shortest time necessary to clear secretions. Indications for suctioning include coughing, secretions in the airway, respiratory distress, presence of rhonchi on auscultation, pressures increased peak airway on the ventilator, and decreasing Sao, or Pao 2 9 Besides hypoxemia and bronchospasm, complications associated with suctioning include atelectasis, dysrhythmias (including bradycardia), increased intracranial pressure, and airway trauma. Bradycardia is attributed to vagal nerve stimulation. Atelectasis may occur when the outer diameter the suction catheter is greater than one-half of the inner diameter tracheostomy of the tube, which can prevent airflow around the catheter. Choosing a catheter that's the right size can help prevent greater negative pressures in the airway and potentially falls in Pao Maintaining safe, effedive cuff pressures minimize Some tracheostomy The maximum acceptable tracheostomy tube cuff pressure is 25 mm Hg. Tracheal capillary perfusion pressure is normally 25 to 35 mm Hg; higher pressure exerted by the inflated cuff can produce tracheal ischemia and mucosal injury. Cuff pressure management is an important aspect of care to prevent complications associated with incorrect cuff pressures. The clinician who manages the tracheal cuff pressure will vary depending on the institution and the location of the patient. Low cuff pressure can lead to silent aspiration. Silent aspiration can be defined as foreign material entering the trach or lungs without an outward sign (coughing or respiratory difficulty). High cuff pressure could lead to tracheal erosion or fistula. A common reason for high cuff pressure is a tube that's too small in diameter, resulting in overfilling of the cuff to achieve a seal in the trachea. Another common cause of high cuff pressure is malposition of the tube. of tube manufacturers provide a chart to help you choose the most appropriate suction catheter for your patient, based on the internal diameter of the tracheostomy tube. Suctioning can be an uncomfortable and scary experience for the patient, so thoroughly explain the procedure to him before you start. Maintain aseptic technique while suctioning. To help prevent hypoxemia, hyperoxygenate him before and after suetioning. As you suction, look for signs of hypoxemia, such as hypertension, dysrhythmias, and a drop in Sp02 by pulse oximetry. If this occurs, stop suctioning and hyperoxygenate the patient. Limit the duration of each suction pass to 10 to 15 seconds or less, and make only 1 or 2 passes. 10 Limit suction pressure to 120 mm Hg or less to minimize airway trauma. If the patient is on mechanical ventilation, allow time for the increased oxygen percentage to come through the ventilator tubing and reach the patient. Use the ventilator, not a manual resuscitation bag, to provide hyperoxygenation before suctioning to reduce hemodynamic changes 10 Don't instill 0.9% sodium chloride before suctioning adults with an artificial airway. Although irrigating the tube before suctioning was once standard to help remove secretions, this practice is no longer recommended for routine care. Ensuring patients are adequately hydrated can facilitate removal of respiratory secretions.l'' Document the patient's response each time you suction, including his vital signs, cardiac rhythm, oxygen saturation, amount and consistency of secretions, breath sounds, and the frequency of needed suctioning. 38 I Nursing2009 I August Communication tips Losing the ability to communicate is incredibly stressful for a patient with a tracheostomy tube. Nonverbal interwww.nursing2009.com
5 ventions that can help facilitate communication include sign language, gestures, lip reading, pointing, facial expressions, or eye blinking. Use simple devices, such as pencil and paper, magic slates, magnetic boards with plastic letters, symbol boards, and flashcards to help the patient communicate. Teach him and his family communication methods appropriate for his condition. Consider a consultation with a speech therapist to aid in communication. utrition is an important aspect of tracheostomy care as well. The tracheostomy tube may impair swallowing and compromise the patients nutritional status. He may also have a loss of appetite due to his altered airway, which affects his sense of smell. Consult with a nutritionist to ensure his nutritional needs are being met. Breathe easy Knowing how a tracheostomy is performed, what equipment how to respond if complications can help you maintain is used, and arise your patient's respiratory function and keep him safe and comfortable. <> REFERENCES 1. Smeltzer S, Bare B, Hinkle ], Cheever K. Brunner & Suddarth~ Textbook of Medical- Surgical Nursing. 11 th ed. Philadelphia, PA: Lipincott Williams and Wilkins; 2008: Zollinger jr, RM, Zollinger Sr, RM. Zollinger~ Atlas oj Surgical Operations. 8th ed. ew York, NY: McGraw-Hill; Clum S, Rumbak M. Mortality and tracheostomy Crit Care Med. 2007;35(3): Angel LF, Irn S. Timing of tracheotomy and the comparison of surgical vs. percutaneous dilational tracheotomy Pulmon Crit Care Update. 2003;13(12). 5. Ernst A, Silvestri CA, johnstone D. lnterventional pulmonary procedures: guidelines from the American College of Chest Physicians. Chest. 2003;123(5): Bhatti N, Mirski M. Tatlipinar A. Koch WM. Goldenberg D. Reduction of complication rate in percutaneous dilation tracheostomies. laryngoscope. 2007;117(1): Dixon B. Tasota FJ. Inadvertent tracheal decannulation. Nursing. 2003;33(1): Dennis-Rouse MD. Davidson je. An evidencebased evaluation of tracheostomy care practices. Crit Care Nurs Q. 2008;31(2): Higgins KM. Punthakee X. Meta-analysis comparison of open versus percutaneous tracheostomy, Laryngoscope. 2007;117(3): Joanna Briggs Institute. Tracheal suctioning of adults with an artificial airway. Best Practice. 2000;4(4): Hess D. Tracheostomy tubes and related appliances. Respir Care. 2005;50(4): Urden L. Stacy K. Lough M. The/ans Critical Care Nursing Diagnosis and Management. 5th ed. S!. Louis. MO: Mosby; 2006: Elizabeth Neville Regan is a nursing educator coordinator and Lisa Dallachiesa is a nursing educator at Suburban Hospital in Bethesda, Md. The authors have disclosed that they have no financial relationships related to this article.
Policy x.xxx. Issued: Artificial Airways and Airway Care. ABC Home Medical Company Policy & Procedure Manual. A. Tracheostomy Tubes ( trach tubes)
 A. Tracheostomy Tubes ( trach tubes) A tracheotomy is a surgical procedure whereby an opening is cut into the trachea of the patient for the purpose of inserting a tube (trach tube). The trach tube allows
A. Tracheostomy Tubes ( trach tubes) A tracheotomy is a surgical procedure whereby an opening is cut into the trachea of the patient for the purpose of inserting a tube (trach tube). The trach tube allows
TRACHEOSTOMY CARE. Tracheostomy- Surgically created hole that extends from the neck skin into the windpipe or trachea.
 1 TRACHEOSTOMY CARE Definitions: Trachea-Windpipe Tracheostomy- Surgically created hole that extends from the neck skin into the windpipe or trachea. Outer Cannula- The outer part of a trach tube. Usually
1 TRACHEOSTOMY CARE Definitions: Trachea-Windpipe Tracheostomy- Surgically created hole that extends from the neck skin into the windpipe or trachea. Outer Cannula- The outer part of a trach tube. Usually
Welcome to the Specialized Medical Services respiratory training webinar series!
 Welcome to the Specialized Medical Services respiratory training webinar series! SMS is your LTC facility single source for oxygen, medical equipment, respiratory care services and supplies nationwide.
Welcome to the Specialized Medical Services respiratory training webinar series! SMS is your LTC facility single source for oxygen, medical equipment, respiratory care services and supplies nationwide.
Adult Patients Going Home with a Tracheostomy
 Physiotherapy Department Adult Patients Going Home with a Tracheostomy Darent Valley Hospital Darenth Wood Road Dartford Kent DA2 8DA www.dvh.nhs.uk In case of emergencies you will need to dial 999 If
Physiotherapy Department Adult Patients Going Home with a Tracheostomy Darent Valley Hospital Darenth Wood Road Dartford Kent DA2 8DA www.dvh.nhs.uk In case of emergencies you will need to dial 999 If
Clearing the air.. How to assist and rescue neck breathing patients. Presented by: Don Hall MCD, CCC/SLP Sarah Markel RRT, MHA
 Clearing the air.. How to assist and rescue neck breathing patients Presented by: Don Hall MCD, CCC/SLP Sarah Markel RRT, MHA Learning Objectives Define common terms identified with total (laryngectomy)
Clearing the air.. How to assist and rescue neck breathing patients Presented by: Don Hall MCD, CCC/SLP Sarah Markel RRT, MHA Learning Objectives Define common terms identified with total (laryngectomy)
TRACHEOSTOMY. Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion
 TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
Disclosures. Learning Objectives. Coeditor/author. Associate Science Editor, American Heart Association
 Tracheotomy Challenges for airway specialists Elizabeth H. Sinz, MD Professor of Anesthesiology & Neurosurgery Associate Dean for Clinical Simulation Disclosures Coeditor/author Associate Science Editor,
Tracheotomy Challenges for airway specialists Elizabeth H. Sinz, MD Professor of Anesthesiology & Neurosurgery Associate Dean for Clinical Simulation Disclosures Coeditor/author Associate Science Editor,
Rota-Trach Double Lumen Tracheostomy Tube VITALTEC
 Rota-Trach Double Lumen Tracheostomy Tube VITALTEC Contents INTRODUCTION HISTORY REVIEW ANATOMY & PHYSIOLOGY OPERATIVE PROCEDURE THE RANGE OF TRACHEOSTOMY TUBES ROTA-TRACH TRACHEOSTOMY TUBE INTRODUCTION
Rota-Trach Double Lumen Tracheostomy Tube VITALTEC Contents INTRODUCTION HISTORY REVIEW ANATOMY & PHYSIOLOGY OPERATIVE PROCEDURE THE RANGE OF TRACHEOSTOMY TUBES ROTA-TRACH TRACHEOSTOMY TUBE INTRODUCTION
Policies and Procedures. I.D. Number: 1154
 Policies and Procedures Title: TRACHEOSTOMY TUBE CHANGE - PEDIATRIC I.D. Number: 1154 Authorization: [X ] SHR Nursing Practice Committee Source: Nursing Date Effective: October 2008 Date Revised: March
Policies and Procedures Title: TRACHEOSTOMY TUBE CHANGE - PEDIATRIC I.D. Number: 1154 Authorization: [X ] SHR Nursing Practice Committee Source: Nursing Date Effective: October 2008 Date Revised: March
8/8/2013. Disclaimer. Tracheostomy Care in the Home. Polling Question 1. Upper Airway and Respiratory System
 Disclaimer Appendix 3 Declaration of Vested Interest Form Name of presenter: Heather Murgatroyd RRT RPSGT Name of employer: DeVilbiss Healthcare Tracheostomy Care in the Home Heather Murgatroyd, RRT, RPSGT
Disclaimer Appendix 3 Declaration of Vested Interest Form Name of presenter: Heather Murgatroyd RRT RPSGT Name of employer: DeVilbiss Healthcare Tracheostomy Care in the Home Heather Murgatroyd, RRT, RPSGT
CARING FOR THE TRACHEOSTOMISED PATIENT: WHAT TO LOOK OUT FOR
 CARING FOR THE TRACHEOSTOMISED PATIENT: WHAT TO LOOK OUT FOR DR MOHD NAZRI ALI Anaesthesiologist & Intensivist HRPZ II, Kota Bharu, Kelantan Tracheostomy The Enabling Disability Tracheostomy Are becoming
CARING FOR THE TRACHEOSTOMISED PATIENT: WHAT TO LOOK OUT FOR DR MOHD NAZRI ALI Anaesthesiologist & Intensivist HRPZ II, Kota Bharu, Kelantan Tracheostomy The Enabling Disability Tracheostomy Are becoming
Module 22 TRACHEOSTOMY CARE AND SUCTIONING. Unit 1 Basic Information Related to Tracheostomy
 580 Module 22 TRACHEOSTOMY CARE AND SUCTIONING Unit 1 Basic Information Related to Tracheostomy OBJECTIVES Upon completion of this unit, you should be able to: Define selected essential terms related to
580 Module 22 TRACHEOSTOMY CARE AND SUCTIONING Unit 1 Basic Information Related to Tracheostomy OBJECTIVES Upon completion of this unit, you should be able to: Define selected essential terms related to
All bedside percutaneously placed tracheostomies
 Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
Facility Name: Name: Date: Tracheostomy Care Evaluation Checklist
 Name: Date: Tracheostomy Care Evaluation Checklist Objective: Learner will be able to demonstrate tracheostomy care with a disposable inner cannula. Review facility protocol for caring for Airway Management:
Name: Date: Tracheostomy Care Evaluation Checklist Objective: Learner will be able to demonstrate tracheostomy care with a disposable inner cannula. Review facility protocol for caring for Airway Management:
Tracheostomy. Hope Building Neurosurgery
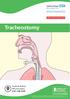 Tracheostomy Hope Building Neurosurgery 0161 206 5055 All Rights Reserved 2017. Document for issue as handout. Unique Identifier: CS36(17). Review date: November 2019 What is a tracheostomy? A tracheostomy
Tracheostomy Hope Building Neurosurgery 0161 206 5055 All Rights Reserved 2017. Document for issue as handout. Unique Identifier: CS36(17). Review date: November 2019 What is a tracheostomy? A tracheostomy
Waitin In The Wings. Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider
 Waitin In The Wings Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider 1 CombiTube Kit General Description The CombiTube is A double-lumen tube with
Waitin In The Wings Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider 1 CombiTube Kit General Description The CombiTube is A double-lumen tube with
Tracheostomy and laryngectomy airway emergencies: an overview for medical and nursing staff
 2013 Medical Journal Tracheostomy and laryngectomy airway emergencies: an overview for medical and nursing staff Steven Lobaz 1 and Paul Bush 2 1 ST6 and 2 Consultant Department of Anaesthesia and Intensive
2013 Medical Journal Tracheostomy and laryngectomy airway emergencies: an overview for medical and nursing staff Steven Lobaz 1 and Paul Bush 2 1 ST6 and 2 Consultant Department of Anaesthesia and Intensive
Competency 1: General principles and equipment required to safely manage a patient with a tracheostomy tube.
 Competency 1: General principles and equipment required to safely manage a patient with a tracheostomy tube. Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Competency 1: General principles and equipment required to safely manage a patient with a tracheostomy tube. Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
The essential principles of tracheostomy care
 The essential principles of tracheostomy care Deborah Dawson Consultant Nurse Critical Care Excellence in specialist and community healthcare Key publications https://www.stgeorges.nhs.uk/gps-andclinicians/clinical-resources/tracheostomyguidelines/
The essential principles of tracheostomy care Deborah Dawson Consultant Nurse Critical Care Excellence in specialist and community healthcare Key publications https://www.stgeorges.nhs.uk/gps-andclinicians/clinical-resources/tracheostomyguidelines/
This information was created and reviewed through a partnership with the UAMS Patient and Family Advisory Councils.
 Tracheostomy Care You have a: Cuffed Tracheostomy Cuffless Tracheostomy What is a tracheostomy? A tracheostomy (sometimes called a trach rhymes with cake ) is a small opening, or stoma, in your throat.
Tracheostomy Care You have a: Cuffed Tracheostomy Cuffless Tracheostomy What is a tracheostomy? A tracheostomy (sometimes called a trach rhymes with cake ) is a small opening, or stoma, in your throat.
I. Subject: Therapeutic Bronchoscopy and Bronchoscope Assisted Intubation
 I. Subject: Therapeutic Bronchoscopy and Bronchoscope Assisted Intubation II. Policy: Therapeutic flexible fiberoptic bronchoscopy procedures and bronchoscope assisted intubations will be performed by
I. Subject: Therapeutic Bronchoscopy and Bronchoscope Assisted Intubation II. Policy: Therapeutic flexible fiberoptic bronchoscopy procedures and bronchoscope assisted intubations will be performed by
PRODUCTS FOR THE DIFFICULT AIRWAY. Courtesy of Cook Critical Care
 PRODUCTS FOR THE DIFFICULT AIRWAY Courtesy of Cook Critical Care EMERGENCY CRICOTHYROTOMY Thyroid Cartilage Access Site Cricoid Cartilage Identify the cricothyroid membrane between the cricoid and thyroid
PRODUCTS FOR THE DIFFICULT AIRWAY Courtesy of Cook Critical Care EMERGENCY CRICOTHYROTOMY Thyroid Cartilage Access Site Cricoid Cartilage Identify the cricothyroid membrane between the cricoid and thyroid
Kapitex Healthcare. making things clearer for tracheostomy patients
 Kapitex Healthcare making things clearer for tracheostomy patients preface In publishing this booklet, Kapitex Healthcare Ltd hopes to provide information and understanding for both the patient and carer
Kapitex Healthcare making things clearer for tracheostomy patients preface In publishing this booklet, Kapitex Healthcare Ltd hopes to provide information and understanding for both the patient and carer
Bronchoscopy SICU Protocol
 Bronchoscopy SICU Protocol Updated January 2013 Outline Clinical indications Considerations Preparation Bronchoscopy technique Bronchoalveolar Lavage (BAL) Post-procedure Purpose Bronchoscopy is a procedure
Bronchoscopy SICU Protocol Updated January 2013 Outline Clinical indications Considerations Preparation Bronchoscopy technique Bronchoalveolar Lavage (BAL) Post-procedure Purpose Bronchoscopy is a procedure
Other methods for maintaining the airway (not definitive airway as still unprotected):
 Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Foundations of Critical Care Nursing Course. Tracheostomy Workbook
 Foundations of Critical Care Nursing Course Tracheostomy Workbook 1 Key Reference: Dawson D (2014) Essential principles:trachepstomy care in the adult patient, Nursing in Critical Care, Vol 19, 2 p.63-72.
Foundations of Critical Care Nursing Course Tracheostomy Workbook 1 Key Reference: Dawson D (2014) Essential principles:trachepstomy care in the adult patient, Nursing in Critical Care, Vol 19, 2 p.63-72.
Changing tracheostomy tubes
 Changing tracheostomy tubes Changing the tracheostomy tube should be a multidisciplinary decision. The first change should always be performed or supervised by a suitably trained member of the medical
Changing tracheostomy tubes Changing the tracheostomy tube should be a multidisciplinary decision. The first change should always be performed or supervised by a suitably trained member of the medical
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device
 I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
Neonatal Airway Disorders, Treatments, and Outcomes. Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center
 Neonatal Airway Disorders, Treatments, and Outcomes Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center Disclosure I have nothing to disclose Neonatal and Pediatric Tracheostomy Tracheostomy
Neonatal Airway Disorders, Treatments, and Outcomes Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center Disclosure I have nothing to disclose Neonatal and Pediatric Tracheostomy Tracheostomy
Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy
 Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who are
Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who are
Tracheostomy management Kate Regan MRCP FRCA Katharine Hunt FRCA
 Kate Regan MRCP FRCA Katharine Hunt FRCA The use of tracheostomy has increased over recent years. Traditionally, it was confined to the emergency management of upper airway obstruction; more recently,
Kate Regan MRCP FRCA Katharine Hunt FRCA The use of tracheostomy has increased over recent years. Traditionally, it was confined to the emergency management of upper airway obstruction; more recently,
1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to
 1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only. In
1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only. In
Chapter 40 Advanced Airway Management
 1 2 3 4 5 Chapter 40 Advanced Airway Management Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only.
1 2 3 4 5 Chapter 40 Advanced Airway Management Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only.
Airway Management in the ICU
 Airway Management in the ICU New developments in management of epistaxis. April 28, 2008 Methods of airway control Non surgical BIPAP CPAP Mask ventilation Laryngeal Mask Intubation Surgical Cricothyrotomy
Airway Management in the ICU New developments in management of epistaxis. April 28, 2008 Methods of airway control Non surgical BIPAP CPAP Mask ventilation Laryngeal Mask Intubation Surgical Cricothyrotomy
Translaryngeal tracheostomy
 Translaryngeal tracheostomy Issued: August 2013 NICE interventional procedure guidance 462 guidance.nice.org.uk/ipg462 NICE has accredited the process used by the NICE Interventional Procedures Programme
Translaryngeal tracheostomy Issued: August 2013 NICE interventional procedure guidance 462 guidance.nice.org.uk/ipg462 NICE has accredited the process used by the NICE Interventional Procedures Programme
Caring for Your TRACHEOSTOMY. Getting On with Your Life
 Caring for Your TRACHEOSTOMY Getting On with Your Life A New Pathway for Air Have you had a tracheostomy? Or, are you about to have one? If so, you may be wondering what the future holds for you. It s
Caring for Your TRACHEOSTOMY Getting On with Your Life A New Pathway for Air Have you had a tracheostomy? Or, are you about to have one? If so, you may be wondering what the future holds for you. It s
Small Volume Nebulizer Treatment (Hand-Held)
 Small Volume Aerosol Treatment Page 1 of 6 Purpose Policy Physician's Order Small Volume Nebulizer Treatment To standardize the delivery of inhalation aerosol drug therapy via small volume (hand-held)
Small Volume Aerosol Treatment Page 1 of 6 Purpose Policy Physician's Order Small Volume Nebulizer Treatment To standardize the delivery of inhalation aerosol drug therapy via small volume (hand-held)
Tracheostomy: Procedures, Timing and Tubes
 TRACHEOSTOMY: PROCEDURES, TIMING AND TUBES Gail M. Sudderth RRT Clinical Specialist Passy-Muir Inc. gsudderth@passy-muir.com (949) 833-8255 Objectives Explain how the timing of the tracheotomy and tube
TRACHEOSTOMY: PROCEDURES, TIMING AND TUBES Gail M. Sudderth RRT Clinical Specialist Passy-Muir Inc. gsudderth@passy-muir.com (949) 833-8255 Objectives Explain how the timing of the tracheotomy and tube
Anatomy and Physiology. The airways can be divided in to parts namely: The upper airway. The lower airway.
 Airway management Anatomy and Physiology The airways can be divided in to parts namely: The upper airway. The lower airway. Non-instrumental airway management Head Tilt and Chin Lift Jaw Thrust Advanced
Airway management Anatomy and Physiology The airways can be divided in to parts namely: The upper airway. The lower airway. Non-instrumental airway management Head Tilt and Chin Lift Jaw Thrust Advanced
Checklist for Going Home with a Tracheostomy Tube... page 4. Parts of a Tracheostomy Set... page 5. Tracheostomy Skin Care (Stoma Care)...
 Tracheostomy Care This booklet was developed by UPMC/Jefferson Regional Home Health, L.P. in collaboration with the respiratory care nurses and therapists across the. Table of contents Introduction...
Tracheostomy Care This booklet was developed by UPMC/Jefferson Regional Home Health, L.P. in collaboration with the respiratory care nurses and therapists across the. Table of contents Introduction...
Emergency)tracheostomy)management)/)Patent)upper)airway)
 Emergency)tracheostomy)management)/)Patent)upper)airway) Call,for,airway,expert,help,,Look,,listen,&,feel,at,the,mouth,and,tracheostomy) A)Mapleson)C)system)(e.g.) Waters)circuit ))may)help)assessment)if)available)
Emergency)tracheostomy)management)/)Patent)upper)airway) Call,for,airway,expert,help,,Look,,listen,&,feel,at,the,mouth,and,tracheostomy) A)Mapleson)C)system)(e.g.) Waters)circuit ))may)help)assessment)if)available)
PEMSS PROTOCOLS INVASIVE PROCEDURES
 PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
Interfacility Protocol Protocol Title:
 Interfacility Protocol Protocol Title: Mechanical Ventilator Monitoring & Management Original Adoption Date: 05/2009 Past Protocol Updates 05/2009, 12/2013 Date of Most Recent Update: March 23, 2015 Medical
Interfacility Protocol Protocol Title: Mechanical Ventilator Monitoring & Management Original Adoption Date: 05/2009 Past Protocol Updates 05/2009, 12/2013 Date of Most Recent Update: March 23, 2015 Medical
F: Respiratory Care. College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 59
 F: Respiratory Care College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 59 Competency: F-1 Airway Management F-1-1 F-1-2 F-1-3 F-1-4 F-1-5 Demonstrate knowledge and ability
F: Respiratory Care College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 59 Competency: F-1 Airway Management F-1-1 F-1-2 F-1-3 F-1-4 F-1-5 Demonstrate knowledge and ability
H: Respiratory Care. Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79
 H: Respiratory Care Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79 Competency: H-1 Airway Management H-1-1 H-1-2 H-1-3 H-1-4 H-1-5 Demonstrate knowledge
H: Respiratory Care Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79 Competency: H-1 Airway Management H-1-1 H-1-2 H-1-3 H-1-4 H-1-5 Demonstrate knowledge
10/17/2016 OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT COURSE OBJECTIVES COMMON CAUSES OF RESPIRATORY FAILURE
 OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT J U L I E Z I M M E R M A N, R N, M S N C L I N I C A L N U R S E S P E C I A L I S T E L O I S A C U T L E R, R R T, B S R C C L I N I C A L / E D U C
OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT J U L I E Z I M M E R M A N, R N, M S N C L I N I C A L N U R S E S P E C I A L I S T E L O I S A C U T L E R, R R T, B S R C C L I N I C A L / E D U C
Advanced Airway Management. University of Colorado Medical School Rural Track
 Advanced Airway Management University of Colorado Medical School Rural Track Advanced Airway Management Basic Airway Management Airway Suctioning Oxygen Delivery Methods Laryngeal Mask Airway ET Intubation
Advanced Airway Management University of Colorado Medical School Rural Track Advanced Airway Management Basic Airway Management Airway Suctioning Oxygen Delivery Methods Laryngeal Mask Airway ET Intubation
This interdisciplinary clinical support document provides guidelines for the safe establishment of an artificial airway.
 PURPOSE This interdisciplinary clinical support document provides guidelines for the safe establishment of an artificial airway. POLICY STATEMENTS Endotracheal intubation will be performed by the Most
PURPOSE This interdisciplinary clinical support document provides guidelines for the safe establishment of an artificial airway. POLICY STATEMENTS Endotracheal intubation will be performed by the Most
CLINICAL CONSIDERATIONS FOR THE BUNNELL LIFE PULSE HIGH-FREQUENCY JET VENTILATOR
 CLINICAL CONSIDERATIONS FOR THE BUNNELL LIFE PULSE HIGH-FREQUENCY JET VENTILATOR 801-467-0800 Phone 800-800-HFJV (4358) Hotline TABLE OF CONTENTS Respiratory Care Considerations..3 Physician Considerations
CLINICAL CONSIDERATIONS FOR THE BUNNELL LIFE PULSE HIGH-FREQUENCY JET VENTILATOR 801-467-0800 Phone 800-800-HFJV (4358) Hotline TABLE OF CONTENTS Respiratory Care Considerations..3 Physician Considerations
AIRWAY MANAGEMENT AND VENTILATION
 AIRWAY MANAGEMENT AND VENTILATION D1 AIRWAY MANAGEMENT AND VENTILATION Basic airway management and ventilation The laryngeal mask airway and Combitube Advanced techniques of airway management D2 Basic
AIRWAY MANAGEMENT AND VENTILATION D1 AIRWAY MANAGEMENT AND VENTILATION Basic airway management and ventilation The laryngeal mask airway and Combitube Advanced techniques of airway management D2 Basic
ENDOTRACHEAL INTUBATION POLICY
 POLICY Indications: Ineffective ventilation with mask and t-piece, or mask and bag technique Inability to maintain a patent airway Need or anticipation of need for prolonged ventilation Need for endotracheal
POLICY Indications: Ineffective ventilation with mask and t-piece, or mask and bag technique Inability to maintain a patent airway Need or anticipation of need for prolonged ventilation Need for endotracheal
SESSION 3 OXYGEN THERAPY
 SESSION 3 OXYGEN THERAPY Harith Eranga Yapa Department of Nursing Faculty of Health Sciences The Open University of Sri Lanka 1 Outline Methods of delivery Complications of oxygen therapy Artificial airways
SESSION 3 OXYGEN THERAPY Harith Eranga Yapa Department of Nursing Faculty of Health Sciences The Open University of Sri Lanka 1 Outline Methods of delivery Complications of oxygen therapy Artificial airways
CCTC Minnesota Procedure: Minnesota Tube, Assisting with Insertion and Care of Patient
 CCTC Minnesota Procedure: Minnesota Tube, Assisting with Insertion and Care of Patient Purpose: To control bleeding from esophageal or gastric varices that have not responded to medical therapy (ie. Sclerotherapy,
CCTC Minnesota Procedure: Minnesota Tube, Assisting with Insertion and Care of Patient Purpose: To control bleeding from esophageal or gastric varices that have not responded to medical therapy (ie. Sclerotherapy,
Tracheostomy. Information for patients and relatives
 Tracheostomy Information for patients and relatives page 2 What is a tracheostomy? A tracheostomy is a small hole (stoma) made at the front of the neck, which goes into the trachea (windpipe). A tube called
Tracheostomy Information for patients and relatives page 2 What is a tracheostomy? A tracheostomy is a small hole (stoma) made at the front of the neck, which goes into the trachea (windpipe). A tube called
TRACHEOSTOMY 186 INTENSIVE CARE
 186 INTENSIVE CARE Table 7.4 Indications for tracheostomy Upper-airway obstruction Prolonged mechanical ventilation To facilitate bronchopulmonary toilet To maintain and protect the airway use of oral
186 INTENSIVE CARE Table 7.4 Indications for tracheostomy Upper-airway obstruction Prolonged mechanical ventilation To facilitate bronchopulmonary toilet To maintain and protect the airway use of oral
Full Range of Tracheostomy Solutions
 Full Range of Tracheostomy Solutions Every Breath Counts Choices by Setting Throughout the hospital or home Smiths Medical tracheostomy tubes are designed for performance ER The Portex Cricothyroidotomy
Full Range of Tracheostomy Solutions Every Breath Counts Choices by Setting Throughout the hospital or home Smiths Medical tracheostomy tubes are designed for performance ER The Portex Cricothyroidotomy
TRUSTED SOLUTIONS FOR SIMPLIFIED PATIENT CARE. Shiley Tracheostomy Product Guide GettyImages
 TRUSTED SOLUTIONS FOR SIMPLIFIED PATIENT CARE. Shiley Tracheostomy Product Guide GettyImages 503532118 TABLE OF CONTENTS Shiley Flexible Adult Tracheostomy Tubes 3 Shiley Extended-Length Tracheostomy Tubes
TRUSTED SOLUTIONS FOR SIMPLIFIED PATIENT CARE. Shiley Tracheostomy Product Guide GettyImages 503532118 TABLE OF CONTENTS Shiley Flexible Adult Tracheostomy Tubes 3 Shiley Extended-Length Tracheostomy Tubes
Policies & Procedures. RNSP - RN Procedure. I.D. Number: 1097
 Policies & Procedures Title: ESOPHAGEAL TAMPONADE TUBE (MINNESOTA Tube) ASSISTING WITH INSERTION, CARE OF A PATIENT, ASSISTING WITH REMOVAL RNSP - RN Procedure I.D. Number: 1097 Authorization [x] Nursing
Policies & Procedures Title: ESOPHAGEAL TAMPONADE TUBE (MINNESOTA Tube) ASSISTING WITH INSERTION, CARE OF A PATIENT, ASSISTING WITH REMOVAL RNSP - RN Procedure I.D. Number: 1097 Authorization [x] Nursing
Endoscopy. Pulmonary Endoscopy
 Pulmonary 1 Direct visualization of TB tree Developed in 1890 s to remove foreign bodies - rigid metal tube Advances added light system, Sx Flexible fiberoptic scopes introduced in early 1960 s 2 Used
Pulmonary 1 Direct visualization of TB tree Developed in 1890 s to remove foreign bodies - rigid metal tube Advances added light system, Sx Flexible fiberoptic scopes introduced in early 1960 s 2 Used
Changing Your Trach Tube
 Patient & Family Guide 2017 Changing Your Trach Tube www.nshealth.ca Changing Your Trach Tube Your entire trach tube should be changed about once a month, or sooner if you notice an odour (smell) or get
Patient & Family Guide 2017 Changing Your Trach Tube www.nshealth.ca Changing Your Trach Tube Your entire trach tube should be changed about once a month, or sooner if you notice an odour (smell) or get
LESSON ASSIGNMENT. After completing this lesson, you should be able to:
 LESSON ASSIGNMENT LESSON 3 Cricothyroidotomy LESSON ASSIGNMENT Paragraphs 3-1 through 3-7. LESSON OBJECTIVES After completing this lesson, you should be able to: 3-1. Define cricothyroidotomy. 3-2. Identify
LESSON ASSIGNMENT LESSON 3 Cricothyroidotomy LESSON ASSIGNMENT Paragraphs 3-1 through 3-7. LESSON OBJECTIVES After completing this lesson, you should be able to: 3-1. Define cricothyroidotomy. 3-2. Identify
Translaryngeal Tracheostomy - TLT Fantoni Method
 Translaryngeal Tracheostomy - TLT Fantoni Method Fantoni A., Ripamonti D., Lesmo A. About the Authors Fantoni Antonio Chief Emeritus of Department of Anaesthesia and Intensive Care - San Carlo Borromeo
Translaryngeal Tracheostomy - TLT Fantoni Method Fantoni A., Ripamonti D., Lesmo A. About the Authors Fantoni Antonio Chief Emeritus of Department of Anaesthesia and Intensive Care - San Carlo Borromeo
Advanced Airway Management
 CHAPTER 37 Advanced Airway Management Airway Anatomy and Physiology Review Respiratory System: The Airway Respiratory System (Supine) Physiology: Factors of Adequate Breathing Functioning brainstem Open
CHAPTER 37 Advanced Airway Management Airway Anatomy and Physiology Review Respiratory System: The Airway Respiratory System (Supine) Physiology: Factors of Adequate Breathing Functioning brainstem Open
Continuous Aerosol Therapy
 PROCEDURE - : Page 1 of 5 Purpose Policy Physician's Order To standardize the administration of continuous aerosol therapy. Respiratory Care Services provides equipment and therapy according to physician
PROCEDURE - : Page 1 of 5 Purpose Policy Physician's Order To standardize the administration of continuous aerosol therapy. Respiratory Care Services provides equipment and therapy according to physician
Chapter 11. Children with Special Healthcare Needs. Objectives. Definition 9/11/2012. Define children with special healthcare needs.
 Chapter 11 Children with Special Healthcare Needs Objectives Define children with special healthcare needs. Define technology-assisted children. Discuss specific assessment and management considerations
Chapter 11 Children with Special Healthcare Needs Objectives Define children with special healthcare needs. Define technology-assisted children. Discuss specific assessment and management considerations
2. Need for serial arterial blood gas determinations. 2. Anticipation of the initiation of thrombolytic therapy
 I. Subject: Arterial Cannulation II. Policy: Arterial cannulation will be performed upon a physician's order by Cardiopulmonary and Respiratory Therapy personnel certified in the arterial catheterization
I. Subject: Arterial Cannulation II. Policy: Arterial cannulation will be performed upon a physician's order by Cardiopulmonary and Respiratory Therapy personnel certified in the arterial catheterization
Tracheostomy discharge information. Information for community nurses, patients and carers
 Tracheostomy discharge information Information for community nurses, patients and carers What is a tracheostomy? A tracheostomy is a surgical incision (cut) through the neck tissues into the trachea leaving
Tracheostomy discharge information Information for community nurses, patients and carers What is a tracheostomy? A tracheostomy is a surgical incision (cut) through the neck tissues into the trachea leaving
Equipment: NRP algorithm, MRSOPA table, medication chart, SpO 2 table Warm
 NRP Skills Stations Performance Skills Station OR Integrated Skills Station STATION: Assisting with and insertion of endotracheal tube (ETT) Equipment: NRP algorithm, MRSOPA table, medication chart, SpO
NRP Skills Stations Performance Skills Station OR Integrated Skills Station STATION: Assisting with and insertion of endotracheal tube (ETT) Equipment: NRP algorithm, MRSOPA table, medication chart, SpO
Day-to-day management of Tracheostomies & Laryngectomies
 Humidification It is mandatory that a method of artificial humidification is utilised when a tracheostomy tube is in situ, for people requiring oxygen therapy dry oxygen should never be given to someone
Humidification It is mandatory that a method of artificial humidification is utilised when a tracheostomy tube is in situ, for people requiring oxygen therapy dry oxygen should never be given to someone
ADVANCED AIRWAY MANAGEMENT
 The Advanced Airway Management protocol should be used on all patients requiring advanced airway management procedures. This protocol is divided into three sections the Crash Airway Algorithm, the Rapid
The Advanced Airway Management protocol should be used on all patients requiring advanced airway management procedures. This protocol is divided into three sections the Crash Airway Algorithm, the Rapid
Shiley Tracheostomy Products Quick Reference Guide
 Shiley Tracheostomy Products Quick Reference Guide SHILEY ACCESSORIES 8A DIC SIC DICFN 8B 8C 8A. Inner Cannula, Disposable (DIC) with integral 15mm snap-lock connector, individually sterile packaged, required
Shiley Tracheostomy Products Quick Reference Guide SHILEY ACCESSORIES 8A DIC SIC DICFN 8B 8C 8A. Inner Cannula, Disposable (DIC) with integral 15mm snap-lock connector, individually sterile packaged, required
Basic Airway Management
 Basic Airway Management Dr. Madhurita Singh, Assoc. Professor, Dept. of Critical Care, CMC Vellore. This is the first module in a series on management of airway and ventilation in critically ill patients.
Basic Airway Management Dr. Madhurita Singh, Assoc. Professor, Dept. of Critical Care, CMC Vellore. This is the first module in a series on management of airway and ventilation in critically ill patients.
*gurgle* *snore* *slaver* Tracheostomy Emergencies with Trachy Tracey Helen Lyall ACCP LUHT 03/06/2016
 *gurgle* *snore* *slaver* Tracheostomy Emergencies with Trachy Tracey Helen Lyall ACCP LUHT 03/06/2016 Learning objectives Describe the difference in anatomy between a tracheotomy and a laryngectomy Understand
*gurgle* *snore* *slaver* Tracheostomy Emergencies with Trachy Tracey Helen Lyall ACCP LUHT 03/06/2016 Learning objectives Describe the difference in anatomy between a tracheotomy and a laryngectomy Understand
Collaborative Regional Benchmarking Group (North of England, North Yorkshire & Humber and West Yorkshire)
 Collaborative Regional Benchmarking Group (North of England, North Yorkshire & Humber and West Yorkshire) Best Practice Guidance Endo Tracheal Tube Care These recommendations are based on the current evidence
Collaborative Regional Benchmarking Group (North of England, North Yorkshire & Humber and West Yorkshire) Best Practice Guidance Endo Tracheal Tube Care These recommendations are based on the current evidence
Management of Pediatric Tracheostomy
 Management of Pediatric Tracheostomy Deepak Mehta Associate Professor Of Otolaryngology Director Pediatric Aerodigestive Center Definitions Tracheotomy: The making of an incision in the trachea The name
Management of Pediatric Tracheostomy Deepak Mehta Associate Professor Of Otolaryngology Director Pediatric Aerodigestive Center Definitions Tracheotomy: The making of an incision in the trachea The name
Carole Wegner RN, MSN And Lori Leiser CRT
 Airway Clearance Carole Wegner RN, MSN And Lori Leiser CRT Topics Suctioning and suctioning equipment Medications to facilitate t airway clearance Bronchial hygiene modalities Preparing for suctioning
Airway Clearance Carole Wegner RN, MSN And Lori Leiser CRT Topics Suctioning and suctioning equipment Medications to facilitate t airway clearance Bronchial hygiene modalities Preparing for suctioning
Pediatric Patients. BCFPD Paramedic Education Program. EMS Education Paramedic Level
 Pediatric Patients BCFPD Program Basic Considerations Much of the initial patient assessment can be done during visual examination of the scene. Involve the caregiver or parent as much as possible. Allow
Pediatric Patients BCFPD Program Basic Considerations Much of the initial patient assessment can be done during visual examination of the scene. Involve the caregiver or parent as much as possible. Allow
Section 2.1 Daily checks Humidification
 Bite- sized training from the GTC Section 2.1 Daily checks Humidification This is one of a series of bite- sized chunks of educational material developed by the Global Tracheostomy Collaborative. The GTC
Bite- sized training from the GTC Section 2.1 Daily checks Humidification This is one of a series of bite- sized chunks of educational material developed by the Global Tracheostomy Collaborative. The GTC
Tracheostomy Sim Course
 Patients Name: Robert Smith Patients Age / DOB: 45 year old gentleman on medical ward Major Medical Problem Displaced tracheostomy tube Learning Goal Medical Early recognition of displaced tracheostomy
Patients Name: Robert Smith Patients Age / DOB: 45 year old gentleman on medical ward Major Medical Problem Displaced tracheostomy tube Learning Goal Medical Early recognition of displaced tracheostomy
Adult Intubation Skill Sheet
 Adult Intubation 2. Opens the airway manually and inserts an oral airway *** 3. Ventilates the patient with BVM attached to oxygen at 15 lpm *** 4. Directs assistant to oxygenate the patient 5. Selects
Adult Intubation 2. Opens the airway manually and inserts an oral airway *** 3. Ventilates the patient with BVM attached to oxygen at 15 lpm *** 4. Directs assistant to oxygenate the patient 5. Selects
PMV 2020 (CLEAR) INSTRUCTION BOOKLET. Touching Lives and Advancing Patient Care Through Education. David A. Muir Inventor of the PMV
 PASSY-MUIR LOW PROFILE TRACHEOSTOMY SWALLOWING AND SPEAKING VALVE PMV 2020 (CLEAR) INSTRUCTION BOOKLET David A. Muir Inventor of the PMV PASSY-MUIR LOW PROFILE TRACHEOSTOMY SWALLOWING AND SPEAKING VALVE
PASSY-MUIR LOW PROFILE TRACHEOSTOMY SWALLOWING AND SPEAKING VALVE PMV 2020 (CLEAR) INSTRUCTION BOOKLET David A. Muir Inventor of the PMV PASSY-MUIR LOW PROFILE TRACHEOSTOMY SWALLOWING AND SPEAKING VALVE
Tracheotomy Care Handbook. Bloomer, Jessica
 Tracheotomy Care Handbook Bloomer, Jessica 1 TABLE OF CONTENTS I II III V VI INTRODUCTION What is a tracheostomy? 2 TRACHEOTOMY CARE Types and Parts of Tracheotomy Tubes 3 Tracheotomy Suctioning 4 Tracheotomy
Tracheotomy Care Handbook Bloomer, Jessica 1 TABLE OF CONTENTS I II III V VI INTRODUCTION What is a tracheostomy? 2 TRACHEOTOMY CARE Types and Parts of Tracheotomy Tubes 3 Tracheotomy Suctioning 4 Tracheotomy
Airway Management. DFMRT Casualty Care Examination Course. Revision notes for. January Les Gordon
 Airway Management Revision notes for DFMRT Casualty Care Examination Course January 2013 Les Gordon Indicating special information in Revision Notes presentations New information since Casualty Care in
Airway Management Revision notes for DFMRT Casualty Care Examination Course January 2013 Les Gordon Indicating special information in Revision Notes presentations New information since Casualty Care in
Tracheostomy/ Laryngectomy PRODUCT CATALOG
 1 Tracheostomy/ Laryngectomy PRODUCT CATALOG 2 3 is a highly experienced manufacturer of medical devices for tracheostomized and laryngectomized patients. For many years we have been supplying our customers
1 Tracheostomy/ Laryngectomy PRODUCT CATALOG 2 3 is a highly experienced manufacturer of medical devices for tracheostomized and laryngectomized patients. For many years we have been supplying our customers
COMMUNICATION. Communication and Swallowing post Tracheostomy. Role of SLT. Impact of Tracheostomy. Normal Speech. Facilitating Communication
 Communication and Swallowing post Tracheostomy. Role of SLT 1. 2. 3. Management of communication needs. Management of swallowing issues. Working with the multidisciplinary team to facilitate weaning. Impact
Communication and Swallowing post Tracheostomy. Role of SLT 1. 2. 3. Management of communication needs. Management of swallowing issues. Working with the multidisciplinary team to facilitate weaning. Impact
DISCOVER NEW HORIZONS IN FLUID DRAINAGE. Bringing Safety and Convenience to Fluid Drainage Management
 DISCOVER NEW HORIZONS IN FLUID DRAINAGE Bringing Safety and Convenience to Fluid Drainage Management DRAIN ASEPT Pleural and Peritoneal Drainage Catheter System 600mL or 1,000mL Evacuated Drainage Bottle
DISCOVER NEW HORIZONS IN FLUID DRAINAGE Bringing Safety and Convenience to Fluid Drainage Management DRAIN ASEPT Pleural and Peritoneal Drainage Catheter System 600mL or 1,000mL Evacuated Drainage Bottle
HeartCode PALS. PALS Actions Overview > Legend. Contents
 HeartCode PALS PALS Actions Overview > Legend Action buttons (round buttons) Clicking a round button initiates an action. Clicking this button, for example, checks the child s carotid pulse. Menu buttons
HeartCode PALS PALS Actions Overview > Legend Action buttons (round buttons) Clicking a round button initiates an action. Clicking this button, for example, checks the child s carotid pulse. Menu buttons
How to use the Control-Cric to perform a surgical cricothyrotomy
 TRAININGGROUNDS How to use the Control-Cric to perform a surgical cricothyrotomy Product Description The Control-Cric is a System which verifies tracheal location during a surgical airway procedure, without
TRAININGGROUNDS How to use the Control-Cric to perform a surgical cricothyrotomy Product Description The Control-Cric is a System which verifies tracheal location during a surgical airway procedure, without
RSPT Tracheal Aspiration. Tracheal Aspiration. RSPT 1410 Tracheal Aspiration
 1 RSPT 1410 2 is the use of to facilitate the removal of secretions from the respiratory tract. Under normal circumstances, patients with normal coughing do not have difficulty in removing secretions.
1 RSPT 1410 2 is the use of to facilitate the removal of secretions from the respiratory tract. Under normal circumstances, patients with normal coughing do not have difficulty in removing secretions.
Information for patients preparing for a tracheostomy at Toronto General Hospital
 Tracheostomy Information for patients preparing for a tracheostomy at Toronto General Hospital This booklet will answer the following questions: What is a tracheostomy or trach? Why do I need a tracheostomy?
Tracheostomy Information for patients preparing for a tracheostomy at Toronto General Hospital This booklet will answer the following questions: What is a tracheostomy or trach? Why do I need a tracheostomy?
This information will help you care for your tracheostomy while you re in the hospital and at home.
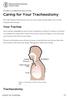 PATIENT & CAREGIVER EDUCATION Caring for Your Tracheostomy This information will help you care for your tracheostomy while you re in the hospital and at home. Your Trachea Your trachea (windpipe) is part
PATIENT & CAREGIVER EDUCATION Caring for Your Tracheostomy This information will help you care for your tracheostomy while you re in the hospital and at home. Your Trachea Your trachea (windpipe) is part
Emergency First Response (EFR) Skills Assessment Sheets V4 June 2017
 Emergency First Response () Skills Assessment Sheets V4 June 2017 Airway management & ventilation Airway management & ventilation Trauma jaw thrust 1 Hand positions 2 Perform jaw thrust / mouth open 3
Emergency First Response () Skills Assessment Sheets V4 June 2017 Airway management & ventilation Airway management & ventilation Trauma jaw thrust 1 Hand positions 2 Perform jaw thrust / mouth open 3
The Adult with A Tracheostomy
 The Adult with A Tracheostomy You have a tracheostomy (trach), a surgical incision (opening) made into the trachea or windpipe (figure 1). A small plastic tube called a trach, is placed into the opening
The Adult with A Tracheostomy You have a tracheostomy (trach), a surgical incision (opening) made into the trachea or windpipe (figure 1). A small plastic tube called a trach, is placed into the opening
Airway/Breathing. Chapter 5
 Airway/Breathing Chapter 5 Airway/Breathing Introduction Skillful, rapid assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur
Airway/Breathing Chapter 5 Airway/Breathing Introduction Skillful, rapid assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 8.1 Define key terms introduced in this chapter. Slides 12 15, 21, 24, 31-34, 39, 40, 54 8.2 Describe the anatomy and physiology of the upper and lower
Introduction to Emergency Medical Care 1 OBJECTIVES 8.1 Define key terms introduced in this chapter. Slides 12 15, 21, 24, 31-34, 39, 40, 54 8.2 Describe the anatomy and physiology of the upper and lower
I. Subject: Medication Delivery by Metered Dose Inhaler (MDI)
 I. Subject: Medication Delivery by Metered Dose Inhaler (MDI) II. Policy: Aerosol medication administration by metered dose inhaler will be performed upon a physician's order by Respiratory Therapy personnel.
I. Subject: Medication Delivery by Metered Dose Inhaler (MDI) II. Policy: Aerosol medication administration by metered dose inhaler will be performed upon a physician's order by Respiratory Therapy personnel.
General Medical Procedure. Emergency Airway Techniques (General Airway Protocol)
 General Medical Procedure Appropriate airway management is often the most important intervention a prehospital care provider makes, as ensuring adequate oxygenation and ventilation is crucial to the survival
General Medical Procedure Appropriate airway management is often the most important intervention a prehospital care provider makes, as ensuring adequate oxygenation and ventilation is crucial to the survival
Tracheostomy Guidelines for NHS Wales
 Tracheostomy Guidelines for NHS Wales Prepared by the All Wales Tracheostomy Advisory Group, chaired by Duncan Ingrams, Assistant Medical Director ABUHB. 1 Introduction April 2018 Formulating one set of
Tracheostomy Guidelines for NHS Wales Prepared by the All Wales Tracheostomy Advisory Group, chaired by Duncan Ingrams, Assistant Medical Director ABUHB. 1 Introduction April 2018 Formulating one set of
Tracheostomy and Ventilator Education Program Module 10: Communication Supplies
 Tracheostomy and Ventilator Education Program Module 10: Communication Supplies Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who
Tracheostomy and Ventilator Education Program Module 10: Communication Supplies Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who
Overview. Chapter 37. Advanced Airway Techniques. Sellick Maneuver 9/11/2012
 Chapter 37 Advanced Airway Techniques Slide 1 Sellick Maneuver Purpose Anatomic Location Technique Special Considerations Overview Advanced Airway Management of Adults Esophageal Tracheal Combitubes Tracheal
Chapter 37 Advanced Airway Techniques Slide 1 Sellick Maneuver Purpose Anatomic Location Technique Special Considerations Overview Advanced Airway Management of Adults Esophageal Tracheal Combitubes Tracheal
