Target Audience: Emergency Medicine Residents (junior and senior level postgraduate learners), Medical Students
|
|
|
- Randall Stevens
- 5 years ago
- Views:
Transcription
1 Caustic Ingestion Authors: Bailey M. Roche, Jonathan B. Ford, MD Reviewers: Miriam T. Davis, MD; Jennifer Hannum, MD Target Audience: Emergency Medicine Residents (junior and senior level postgraduate learners), Medical Students Primary Learning Objectives: 1. Identify intentional versus unintentional caustic ingestions 2. Recognize signs of impending airway compromise and intubate early if necessary 3. Consult with Gastroenterology (GI) early for prognostic esophagogastroduodenoscopy (EGD) 4. Recognize and identify signs of perforation and consult surgery as needed 5. Order appropriate imaging and laboratory studies Secondary Learning Objectives: detailed technical/behavioral goals, didactic points 1. Describe the difference between acidic and alkaline chemicals 2. Describe role of activated charcoal (AC) in caustic ingestions 3. Identify limitations of physical exam findings as predictors of esophageal injury 4. Describe management differences for pediatric unintentional caustic ingestions vs intentional ingestions 5. Describe the role of antibiotics for caustic ingestion Critical actions checklist: 1. Perform early endotracheal intubation 2. Order chest X-ray (CXR) 3. Avoid attempts at GI decontamination 4. Obtain early GI consultation 5. Consider perforation when patient deteriorates 6. Consult Poison Center/Toxicologist 7. Administer antibiotics 8. Consult Surgery Environment: Emergency Department treatment area 1. Room Set Up ED noncritical care area a. Manikin Set Up Mid or high fidelity simulator, simulated sweat, simulated oropharyngeal swelling b. Props Standard ED equipment 2. Distractors ED noise, patient s ex-girlfriend in room and hysterical
2 For Examiner Only CASE SUMMARY SYNOPSIS OF HISTORY/ Scenario Background This takes place in a tertiary care center. The patient is a 17-year-old male with a history of depression and prior alcohol abuse who presents to the emergency department with his ex-girlfriend after ingesting Poolife Rapid Shock. The patient s ex-girlfriend says they recently broke up, and he called her after drinking about half of a 1L bottle of the pool cleaner in an attempt at self-harm. The patient is alert but not talking. PMH: depression, prior alcohol abuse PSHx: none Medications: fluoxetine Allergies: no known drug allergies SH: Prior alcohol abuse, social smoker, lives with parents and is in high-school SYNOPSIS OF PHYSICAL Patient is anxious. His vitals are significant for tachycardia and tachypnea. His mucous membranes are edematous, there are visible partial thickness burns of the lips, tongue, and posterior oropharynx; he has stridor and drooling Neurologic exam is non-focal. He is alert but not talking, follows commands Skin is diaphoretic. 2
3 For Examiner Only HISTORY You are called to see a new patient (17-year-old male) in the pediatric area of the emergency department. You see a diaphoretic male who is alert, but breathing rapidly and not talking. Onset of Symptoms: Background Info: Today 17-year-old male with a history of depression and prior alcohol abuse who presents to the emergency department with his ex-girlfriend after ingesting Poolife Rapid Shock. The patient s ex-girlfriend says they recently broke up, and he called her after drinking about half of a 1L bottle of Poolife Rapid Shock in an attempt at self-harm. History cannot be obtained from the patient because he is not talking. Additional History From Ex-Girlfriend: He has had some problems with alcohol in the past, but he has been sober for over a year. They broke up last week and he has been taking it really hard. She knows he has depression. Chief Complaint: Past Medical Hx: Past Surgical Hx: Habits: Family Med Hx: Mouth pain prior alcohol abuse, depression none Smoking: Occasional ETOH: prior abuse, sober for 1 year Drugs: none Diabetes, CVA Social Hx: Marital Status: Single Children: None Education: High School Employment: Unemployed ROS: Patient is unable to answer. 3
4 CASE CONTINUATION The ex-girlfriend is hysterical and continuously asks if he is going to be ok. Vital Signs: BP: 110/73 mmhg P: 122/minute R: 27/minute T: 37.1C (98.6F) POx: 98% (FiO 2 =0.21) Primary Survey Airway Lips swollen and burned, tongue swollen, posterior oropharyngeal edema and erythema, saliva pooling in the mouth Breathing Tachypnea, stridor, 100% POx Circulation Tachycardia (120s/minute), SBP 110s mmhg Disability Patient is alert but not talking, in some obvious distress Exposure No trauma, rash, drug patches. Patient is diaphoretic Required Actions within the First Two Minutes Establish safety net (IV, oxygen, cardiac monitor, two large bore IVs, draw blood for labs) A/B Provide supplemental oxygen C Cardiac monitor; NS IV bolus; ECG D Finger stick glucose = 121 mg/dl; diagnostics should be ordered by this time Branch Points IF PATIENT IS NOT INTUBATED, then his stridor worsens. IFHE REMAINS UNINTUBATED FOLLOWING THE ONSET OF STRIDOR, then his airway will obstruct, and he will enter respiratory arrest. 4
5 PHYSICAL EXAMINATION General Appearance: Pale, diaphoretic male. Unresponsive. Vital Signs: BP: 110/73 mmhg P: 122/minute R: 27/minute T: 37.1C (98.6F) POx: 98% (FiO 2 =0.21) Head: Normal Eyes: Pupils equal, round and reactive to light, pupils 3 mm bilaterally Ears: Tympanic membranes are normal. Mouth: Partial thickness burns to the upper and lower lips, edematous tongue and posterior oropharyngeal edema and erythema with saliva pooling in the mouth Neck: No tenderness or deformity on exam, full range of motion Skin: Moist skin/sweaty, no rashes, warm Chest: Increased respiratory rate without any accessory muscle use Lungs: Clear, equal bilaterally Heart: Tachycardic, S1 S2, no murmurs Back: Normal Abdomen: Soft, nontender, no signs of trauma, no rebound/guarding, normal bowel sounds Extremities: No signs of trauma, no edema, pulses are present Genital: Normal male genitalia Rectal: Normal tone, guaiac negative Neurological: Non-focal exam, no clonus Mental Status: Alert and following commands but not talking Required Actions within the Next Two Minutes Obtain CXR, assess for tube placement, signs of aspiration pneumonitis, signs of perforation Should send basic labs including CBC, BMP, lactate, ASA, APAP; obtain ECG Call Poison Center or Toxicologist Consult GI 5
6 Branch Points IF POISONCENTER/TOXICOLOGIST IS CALLED, then the Poison Center/Toxicologist should tell participants that Poolife Rapid Shock has chlorine and is converted to hydrochloric acid when it makes contact with water CASE CONTINUATION The patient s hemodynamics worsen: he becomes more tachycardic to the 120s- 130s/minute, and his BP drops to SBP 70s mmhg despite fluid resuscitation. His repeat exam is essentially unchanged aside from a somewhat distended abdomen that is tense His initial lactate is 6.2 Required Actions within the Next Several Minutes Start patient on vasopressors (can attempt more fluids, but his BP will be unresponsive) Consult Surgery emergently for suspected perforation (can obtain imaging first to confirm, but this is not required) Start broad-spectrum antibiotics Admit to ICU/Send to OR Branch Points IF PERFORATION IS NOT RECOGNIZED CLINICALLY OR BY IMAGING, then the patient continues to deteriorate despite maximally supportive care. LACTATE TRENDS UPWARDS, AND PATIENT SUFFERS A CARDIAC ARREST AND DIES Required Actions Over the Next Several Minutes Examinee should contact ICU physician for admission by this time Patient should be admitted to ICU 6
7 For Examiner Only 1. Perform early endotracheal intubation CRITICAL ACTIONS Perform early endotracheal intubation in the management of a patient with a caustic ingestion and the imminent potential for airway edema and compromise. Cueing Guideline: Nurse can ask if the doctor wants to do anything about the patient s stridor, if endotracheal intubation is deferred initially. 2. Order chest X-ray (CXR) Order CXR in the management of a patient with a caustic ingestion to help determine if perforation or aspiration has occurred. Cueing Guideline: The nurse asks if the doctor would like a CXR. 3. Avoid attempts at GI decontamination GI decontamination with activated charcoal (AC) or whole bowel irrigation (WBI) is ineffective and contraindicated in the context of a caustic ingestion. Cueing Guideline: The nurse may say, Are you sure it is appropriate to attempt AC administration or WBI in this patient? 4. Obtain early GI consultation Participants should obtain GI consultation early in the management of a patient with a caustic ingestion for possible advanced diagnostics(egd). Cueing Guideline: Nurse can ask if the doctor has called the GI consultant yet. 5. Consider perforation when patient deteriorates When the patient deteriorates in the context of a caustic ingestion, participants should consider perforation as a possible cause (and consult surgery, see below). Cueing Guideline: Nurse can ask if the doctor can explain why the patient has suddenly deteriorated. 6. Consult Poison Center/Toxicologist The Poison Center or Toxicology Service should be consulted for further management recommendations. Cueing Guideline: Nurse can ask if the doctor has called the Poison Center/Toxicologist yet. 7. Administer antibiotics When the patient deteriorates in the context of a caustic ingestion, participants should consider perforation as a possible cause and administer broad-spectrum antibiotics. Cueing Guideline: Nurse can ask if the doctor would like to do something if perforation is suspected (and this has been verbalized). 7
8 8. Consult Surgery When the patient deteriorates in the context of a caustic ingestion, participants should consider perforation as a possible cause and consult surgery. Cueing Guideline: Nurse can ask if the doctor has called the surgical consultant yet. 8
9 Critical Actions Checklist 1 Resident Name Case Description Skills measured Core competencies: PC Patient care, MK Medical knowledge, IC Interpersonal and communication skills P Professionalism, PB Practice-based learning and improvement SB Systems-based practice Very Unacceptable Unacceptable Acceptable Very Acceptable Data Acquisition (D) PC MK I Problem Solving (S) PC MK PB Patient Management (M) PC MK IC P PB SB Resource Utilization (R) PC PB SB Health Care Provided (H) PC SB Interpersonal Relations (I) IC P Comprehension of Pathophysiology (P) MK PB Clinical Competence (C) PC MK IC P PB SB Critical Actions Yes No Comments: Perform early endotracheal intubation Order CXR Avoid attempts at GI decontamination Obtain early GI consultation Consider perforation when patient deteriorates Consult Poison Center/Toxicologist Administer antibiotics Yes No Consult Surgery Dangerous actions 1 Modified ABEM Oral Certification Examination checklist and scoresheet 9
10 For Examiner Only STIMULUS INVENTORY #1 Complete blood count #2 Basic metabolic panel #3 Urinalysis #4 Liver function tests #5 Venous blood gas #6 Coagulation studies #7 Toxicology #8 Radiology (CXR, CT abdomen) #9 A: Initial Lactate B: Repeat Lactate #10 ECG 10
11 For Examiner Only LAB DATA & IMAGING RESULTS Stimulus #1 Stimulus #5 Complete Blood Count (CBC) Venous Blood Gas WBC 18,500/mm 3 ph 7.30 Hemoglobin 13.2 g/dl pco 2 27 mmhg Hematocrit 40% po 2 40 mmhg Platelets 219,000/mm 3 HCO 3 base deficit 16 meq/l 9 Differential O 2 Sat 55% PMNLs 70% Lymphocytes 26% Stimulus #6 Monocytes 2% Coagulation Studies Eosinophils 1% PT/INR 13.1 seconds / 1.1 PTT 18 seconds Stimulus #2 Basic Metabolic Panel (BMP) Stimulus #7 Sodium 145 meq/l Toxicology Potassium 3.6 meq/l Salicylate Undetectable Chloride 110 meq/l Acetaminophen Undetectable Bicarbonate 16 meq/l Ethanol Undetectable Glucose 129 mg/dl Urine drug screen BUN 17 mg/dl Amphetamines Negative Creatinine 1.1 mg/dl Benzodiazepines Negative Cocaine Negative Stimulus #3 Opiates Negative Urinalysis TCAs Negative Color Yellow THC Negative Specific gravity Glucose Negative Stimulus #8 Protein Negative Radiology Ketones Trace Upright CXR Pneumoperitoneum LE/Nitrites Negative CT abdomen Pneumoperitoneum Blood Negative WBC/RBC 0/hpf / 0/hpf Stimulus #9A and #9B Crystals/bacteria Negative Lactate Initial / Repeat 6.2 / 7.8 mmol/l Stimulus #4 Liver Function Tests Stimulus #10 AST 49 IU/L ECG Sinus tachycardia. No T wave or ST elevation; ALT 32 IU/L No right ventricular strain ALP 110 IU/L T. Bilirubin 1.2 mg/dl D. Bilirubin 0.2 mg/dl NOTE: A portable supine CXR will not Albumin 4.3 mg/dl reveal pneumoperitoneum ( free air ) 11
12 Stimulus #1 Complete Blood Count (CBC) WBC 18,500/mm 3 Hemoglobin 13.2 g/dl Hematocrit 40% Platelets 219,000/mm 3 Differential PMNLs 70% Lymphocytes 26% Monocytes 2% Eosinophils 1% 12
13 Stimulus #2 Basic Metabolic Panel (BMP) Sodium 145 meq/l Potassium 3.6 meq/l Chloride 110 meq/l Bicarbonate 16 meq/l Glucose 129 mg/dl BUN 17 mg/dl Creatinine 1.1 mg/dl 13
14 Stimulus #3 Urinalysis Color / ph Yellow Specific gravity Glucose Negative Protein Negative Ketones Trace LE/Nitrites Negative Blood Negative WBC/RBC 0/hpf / 0/hpf Crystals/bacteria Negative 14
15 Stimulus #4 Liver Function Tests AST 49 IU/L ALT 32 IU/L ALP 110 IU/L T. Bilirubin 1.2 mg/dl D. Bilirubin 0.2 mg/dl Albumin 4.3 mg/dl 15
16 Stimulus #5 Venous Blood Gas ph 7.30 pco 2 27 mmhg po 2 40 mmhg HCO 3 base deficit 16 meq/l 9 O 2 Sat 55% 16
17 Stimulus #6 Coagulation Studies PT/INR 13.1 seconds / 1.1 PTT 18 seconds 17
18 Stimulus #7 Toxicology Salicylate Acetaminophen Ethanol Urine drug screen Amphetamines Benzodiazepines Cocaine Opiates TCAs THC Undetectable Undetectable Undetectable Negative Negative Negative Negative Negative Negative 18
19 Stimulus #8 Radiology Upright CXR CT abdomen Pneumoperitoneum Pneumoperitoneum 19
20 Stimulus #9A Lactate Value 6.2 mmol/l 20
21 Stimulus #9B Repeat Lactate Value 7.8 mmol/l 21
22 Stimulus #10 22
23 Debriefing Materials Caustic Ingestion Sources of Exposure: Caustic chemicals are commonly found in home and work environments. Their uses include oven cleaners, clogged drain openers, concrete cleaners, automotive detailing, paint stripping, metal or glass etching, and swimming pool treatments to name a few. Clinically significant injuries occur from caustics that have a ph < 3 or > 11. However, the concentration, volume, and intent of the ingestion (i.e., accidental versus intentional) contribute to the potential for serious injury. Typical household bleach is not usually considered a caustic due to its low concentration, but higher concentrations are available. Typical acetic acid (i.e., vinegar) is not a caustic, but highly concentrated solutions are easily purchased and can lead to significant morbidity or death with only small ingestions. Pathophysiology: Caustic chemicals burn the oral and GI mucosa Strongly basic chemicals cause liquefactive necrosis leading to deep burns. Basic chemicals tend to cause more injury to the esophagus than to the stomach. Strongly acidic chemicals cause coagulative necrosis, may not penetrate as deep as basic chemicals, and may cause injury to both the esophagus and stomach. Severity of Ingestion: Depends on the ph, concentration, and volume of chemical ingested The physical exam is often not reliable in excluding severe injury particularly in adult and intentional ingestions Prognosis depends on severity of GI injury The Zargar modified endoscopic classification of burns is used to predict which patients may have early and late complications such as perforation and stricture formation. o Grade 0 normal examination o Grade 1 edema and hyperemia of the mucosa o Grade 2a friability, hemorrhages, erosions, blisters, whitish membranes, exudates and superficial ulcerations o Grade 2b grade 2a plus deep discrete or circumferential ulceration o Grade 3a multiple ulcerations and small scattered areas of necrosis o Grade 3b extensive areas of necrosis Grade 2a or better are associated with minimal early or late complications, whereas grade 2b or higher are associated with a high rate of stricture formation (71% in one series) and perforation. Organ System Effects: Gastrointestinal: o Nausea and abdominal pain. May be unable to swallow secretions. Vomiting may occur. Pulmonary: o Caustic chemicals may be aspirated during attempted ingestion and therefore cause direct lung injury. Coughing and breathlessness may occur. Cardiovascular: 23
24 o Tachycardia, hypotension, and sometimes chest pain. Dermatologic: o Erythema and edema of the face, lips, tongue and oral mucosa is possible but the physical exam does not often correlate with the EGD findings. Adults may conceal ingestion by using funnels or hoses to minimize injury to oropharynx. o Pediatric patients (<6 years of age) who unintentionally ingest chemicals often stop when they feel pain or encounter a bad taste. Burns may be limited to the lips and/or anterior tongue. Diagnostic Testing: Chemistry panel o Repeat as needed Chest X-ray o Assess for perforation or aspiration o Assess endotracheal tube placement Obtain hepatic, hematologic, and coagulation profiles for patients with clinical evidence of moderate-to-severe toxicity Chest x-ray is indicated if evidence of severe intoxication, pulmonary edema, or hypoxemia is present Treatment: Endotracheal intubation if needed Activated Charcoal is not indicated as it does not typically adsorb the caustic substances and it can interfere with EGD staging Antibiotics are typically not indicated, as they have not clearly been shown to be beneficial. However, in cases of perforation, broad-spectrum antibiotics are indicated. Studies do not show any benefit with steroids as an agent to reduce stricture formation. Consultations: Consult the regional poison center or a local medical toxicologist for additional information and patient care recommendations. Consult Gastroenterology for early EGD or surgery if suspected perforation. Disposition: Admit patients with major signs and symptoms to an ICU. Unintentional pediatric ingestions may be given a trial of oral intake if oral injury is limited to lips and anterior tongue and they are well appearing. Inability to tolerate secretions, oral intake, or posterior tongue or pharyngeal injury should prompt a GI consultation for EGD. Most adult patients with intentional ingestions should be considered for early EGD due to their ability to conceal ingestion by limiting oral injury, and the physical exam does not correlate with EGD findings of esophageal injury. Consult psychiatric service personnel for stabilized patients with intentional overdose. Take-Home Points: Caustic chemicals are common in home and work environments Ingestions may be accidental or intentional. Unintentional ingestions are more common in pediatric patients < 6 years of age 24
25 Chemicals with ph < 3 or > 11 may cause serious injury but concentration and volume ingested contribute to the potential to cause injury The physical exam does not correlate with EGD findings Consult the Poison Control Center or Toxicologist for guidance on properties of chemical ingested and appropriate management Treatment principles include stabilizing the ABCs, consulting appropriate services, and maintaining a high suspicion for perforation References: Zargar SA, Kochhar R, et al. The role of fiberoptic endoscopy in the management of corrosive ingestion and modified endoscopic classification of burns, Gastrointestinal Endoscopy, Volume 37, Issue 2, March 1991, Pages Goldfrank, Lewis R. Goldfrank's Toxicologic Emergencies. New York: McGraw-Hill Medical Pub. Division, Tenth Edition Print. 25
Target Audience: Emergency Medicine Residents (junior and senior level postgraduate learners), Medical Students
 Cocaine Overdose Authors: Andrew Stolbach Reviewer: Tammi Schaeffer Target Audience: Emergency Medicine Residents (junior and senior level postgraduate learners), Medical Students Primary Learning Objectives:
Cocaine Overdose Authors: Andrew Stolbach Reviewer: Tammi Schaeffer Target Audience: Emergency Medicine Residents (junior and senior level postgraduate learners), Medical Students Primary Learning Objectives:
Target Audience: Emergency Medicine Residents, Medical Students
 Target Audience: Emergency Medicine Residents, Medical Students Primary Learning Objectives: 1. Recognize signs, symptoms, and course of scorpion envenomation 2. Understand differential diagnosis for scorpion
Target Audience: Emergency Medicine Residents, Medical Students Primary Learning Objectives: 1. Recognize signs, symptoms, and course of scorpion envenomation 2. Understand differential diagnosis for scorpion
Target Audience: Emergency Medicine Residents (junior and senior level postgraduate learners), Medical Students
 Carbon Monoxide Poisoning Authors: Jeff Holmes, MD / Tammi Schaeffer, MD Reviewers: Adam Pomerlau, MD Target Audience: Emergency Medicine Residents (junior and senior level postgraduate learners), Medical
Carbon Monoxide Poisoning Authors: Jeff Holmes, MD / Tammi Schaeffer, MD Reviewers: Adam Pomerlau, MD Target Audience: Emergency Medicine Residents (junior and senior level postgraduate learners), Medical
Opioid Overdose (CASE OPTION: Concomitant Acetaminophen Toxicity) Authors: Andrew Stolbach
 Opioid Overdose (CASE OPTION: Concomitant Acetaminophen Toxicity) Authors: Andrew Stolbach Reviewer: Joseph Yanta Target Audience: Emergency Medicine Residents (junior and senior level postgraduate learners),
Opioid Overdose (CASE OPTION: Concomitant Acetaminophen Toxicity) Authors: Andrew Stolbach Reviewer: Joseph Yanta Target Audience: Emergency Medicine Residents (junior and senior level postgraduate learners),
Hydrofluoric Acid Toxicity Author: Z. Kazzi / E. A. Numur / S. Kini. Target Audience: Emergency Medicine Residents
 Hydrofluoric Acid Toxicity Author: Z. Kazzi / E. A. Numur / S. Kini Reviewer: S. M. Varney Target Audience: Emergency Medicine Residents Primary Learning Objectives: 1. Demonstrate a general approach to
Hydrofluoric Acid Toxicity Author: Z. Kazzi / E. A. Numur / S. Kini Reviewer: S. M. Varney Target Audience: Emergency Medicine Residents Primary Learning Objectives: 1. Demonstrate a general approach to
Target Audience: Emergency Medicine Residents (junior and senior level postgraduate learners), Medical Students
 Rattlesnake Bite Authors: Laura Morrison, MD / Ryan Chuang, MD Reviewers: Shawn M. Varney, MD Target Audience: Emergency Medicine Residents (junior and senior level postgraduate learners), Medical Students
Rattlesnake Bite Authors: Laura Morrison, MD / Ryan Chuang, MD Reviewers: Shawn M. Varney, MD Target Audience: Emergency Medicine Residents (junior and senior level postgraduate learners), Medical Students
pthaigastro.org Caustic injury The 5 th Pediatric GI Days Pediatric GI & Liver Emergency : Current Practical Management
 The 5 th Pediatric GI Days Pediatric GI & Liver Emergency : Current Practical Management Caustic injury Phisek Yimyaem Pediatric Department, Khon Kaen Regional Hospital 18 July 2013 Outlines Introduction
The 5 th Pediatric GI Days Pediatric GI & Liver Emergency : Current Practical Management Caustic injury Phisek Yimyaem Pediatric Department, Khon Kaen Regional Hospital 18 July 2013 Outlines Introduction
Repeated Supratherapeutic Acetaminophen Toxicity Author: Jeff Holmes, MD / Tammi Schaeffer, DO
 Repeated Supratherapeutic Acetaminophen Toxicity Author: Jeff Holmes, MD / Tammi Schaeffer, DO Reviewer: Adam Pomerlau, MD Target Audience: Emergency Medicine Residents, Medical Students Primary Learning
Repeated Supratherapeutic Acetaminophen Toxicity Author: Jeff Holmes, MD / Tammi Schaeffer, DO Reviewer: Adam Pomerlau, MD Target Audience: Emergency Medicine Residents, Medical Students Primary Learning
Diphenhydramine-Acetaminophen Overdose Author: Andrew Stolbach, MD. Target Audience: Emergency Medicine Residents, Medical Students
 Diphenhydramine-Acetaminophen Overdose Author: Andrew Stolbach, MD Reviewer: Tammi Schaeffer, DO Target Audience: Emergency Medicine Residents, Medical Students Primary Learning Objectives: 1. Recognize
Diphenhydramine-Acetaminophen Overdose Author: Andrew Stolbach, MD Reviewer: Tammi Schaeffer, DO Target Audience: Emergency Medicine Residents, Medical Students Primary Learning Objectives: 1. Recognize
Diphenhydramine Overdose Author: L. Keith French. Target Audience: Emergency Medicine Residents, Medical Students
 Diphenhydramine Overdose Author: L. Keith French Reviewer: Andrew Stolbach Target Audience: Emergency Medicine Residents, Medical Students Primary Learning Objectives: 1. Recognize signs and symptoms of
Diphenhydramine Overdose Author: L. Keith French Reviewer: Andrew Stolbach Target Audience: Emergency Medicine Residents, Medical Students Primary Learning Objectives: 1. Recognize signs and symptoms of
Acute Aspirin Overdose Author: Shawn M. Varney. Target Audience: Emergency Medicine Residents, Medical Students
 Acute Aspirin Overdose Author: Shawn M. Varney Reviewers: Joseph Yanta Target Audience: Emergency Medicine Residents, Medical Students Primary Learning Objectives: 1. Recognize signs and symptoms of aspirin
Acute Aspirin Overdose Author: Shawn M. Varney Reviewers: Joseph Yanta Target Audience: Emergency Medicine Residents, Medical Students Primary Learning Objectives: 1. Recognize signs and symptoms of aspirin
Chapter 153 Caustics. Episode Overview: Wisecracks. Key Points: Rosen s in Perspective
 Chapter 153 Caustics Episode Overview: 1) Compare acid and alkali caustic burns 2) Describe clinical features of significant airway and esophageal injury by caustics 3) What are indications for endoscopy
Chapter 153 Caustics Episode Overview: 1) Compare acid and alkali caustic burns 2) Describe clinical features of significant airway and esophageal injury by caustics 3) What are indications for endoscopy
Poison (Toxicant): any substance or agent capable of producing a deleterious response in a biological system or living organism.
 Poison (Toxicant): any substance or agent capable of producing a deleterious response in a biological system or living organism. Poisoning= overdose toxicity intoxication= toxicity due to foreign substance
Poison (Toxicant): any substance or agent capable of producing a deleterious response in a biological system or living organism. Poisoning= overdose toxicity intoxication= toxicity due to foreign substance
Target Audience: Emergency Medicine Residents (junior and senior level postgraduate learners), Medical Students
 Digoxin Toxicity Authors: Laura Morrison, MD / Ryan Chuang, MD Reviewers: Shawn M. Varney, MD Target Audience: Emergency Medicine Residents (junior and senior level postgraduate learners), Medical Students
Digoxin Toxicity Authors: Laura Morrison, MD / Ryan Chuang, MD Reviewers: Shawn M. Varney, MD Target Audience: Emergency Medicine Residents (junior and senior level postgraduate learners), Medical Students
Med 536 Communicating About Prognosis Workshop. Case 2
 Med 536 Communicating About Prognosis Workshop Case 2 ID / CC: 33 year-old man with intracranial hemorrhage History of the Presenting Illness 33 year-old man with a prior history of melanoma of the neck
Med 536 Communicating About Prognosis Workshop Case 2 ID / CC: 33 year-old man with intracranial hemorrhage History of the Presenting Illness 33 year-old man with a prior history of melanoma of the neck
Pediatric Ingestion Injuries: Assessment & Treatment
 Pediatric Ingestion Injuries: Assessment & Treatment Benjamin L. Eithun, MSN, CRNP, RN, CPNP-AC, CCRN, TCRN Andrea L. Williams, PhD, RN UW Health & AFCH Case #1 Presentation Dispatched to Sandstone Ridge
Pediatric Ingestion Injuries: Assessment & Treatment Benjamin L. Eithun, MSN, CRNP, RN, CPNP-AC, CCRN, TCRN Andrea L. Williams, PhD, RN UW Health & AFCH Case #1 Presentation Dispatched to Sandstone Ridge
Ethylene Glycol Ingestion Author: Joseph H. Yanta, MD. Target Audience: Emergency Medicine Residents, Medical Students
 Ethylene Glycol Ingestion Author: Joseph H. Yanta, MD Reviewer: Dan Rusyniak, MD Target Audience: Emergency Medicine Residents, Medical Students Primary Learning Objectives: 1. Recognize signs and symptoms
Ethylene Glycol Ingestion Author: Joseph H. Yanta, MD Reviewer: Dan Rusyniak, MD Target Audience: Emergency Medicine Residents, Medical Students Primary Learning Objectives: 1. Recognize signs and symptoms
Documentation Dissection
 History of Present Illness: Documentation Dissection The patient is a 50-year-old male c/o symptoms for past 4 months 1, severe 2 bloating and stomach cramps, some nausea, vomiting, diarrhea. In last 3
History of Present Illness: Documentation Dissection The patient is a 50-year-old male c/o symptoms for past 4 months 1, severe 2 bloating and stomach cramps, some nausea, vomiting, diarrhea. In last 3
Student Guide Module 4: Pediatric Trauma
 Student Guide Module 4: Pediatric Trauma Problem based learning exercise objectives Understand how to manage traumatic injuries in mass casualty events. Discuss the features and the approach to pediatric
Student Guide Module 4: Pediatric Trauma Problem based learning exercise objectives Understand how to manage traumatic injuries in mass casualty events. Discuss the features and the approach to pediatric
SMALL GROUP DISCUSSION
 MHD II, Session 1 Student Copy Page 1 SMALL GROUP DISCUSSION MHD II Session 1 Gastroinestinal Monday, January 9, 2017 STUDENT COPY MHD II, Session 1 Student Copy Page 2 CASE 1 CHIEF CONCERN: "I'm passing
MHD II, Session 1 Student Copy Page 1 SMALL GROUP DISCUSSION MHD II Session 1 Gastroinestinal Monday, January 9, 2017 STUDENT COPY MHD II, Session 1 Student Copy Page 2 CASE 1 CHIEF CONCERN: "I'm passing
Down the Tube: Caustic Ingestions. Significance & Management in the ED. Laura Chng PGY-3
 Down the Tube: Caustic Ingestions Significance & Management in the ED Laura Chng PGY-3 Caustic Ingestions Not common but you ll see them Controversial You drank WHAT? ED management can change outcome Who
Down the Tube: Caustic Ingestions Significance & Management in the ED Laura Chng PGY-3 Caustic Ingestions Not common but you ll see them Controversial You drank WHAT? ED management can change outcome Who
CASE-BASED SMALL GROUP DISCUSSION MHD II
 MHD II, Session 11, Student Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD II Session 11 April 11, 2016 STUDENT COPY MHD II, Session 11, Student Copy Page 2 CASE HISTORY 1 Chief complaint: Our baby
MHD II, Session 11, Student Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD II Session 11 April 11, 2016 STUDENT COPY MHD II, Session 11, Student Copy Page 2 CASE HISTORY 1 Chief complaint: Our baby
Suspected Foreign Body Ingestion
 Teresa Liang Suspected Foreign Body Ingestion 1. General Presentation Background: Of more than 100,000 cases of foreign body ingestion reported each year in the United States, 80% occur in children, with
Teresa Liang Suspected Foreign Body Ingestion 1. General Presentation Background: Of more than 100,000 cases of foreign body ingestion reported each year in the United States, 80% occur in children, with
Caustic Esophageal Injury. Aliu Sanni, MD SUNY Downstate Medical Center March 21, 2013
 Caustic Esophageal Injury Aliu Sanni, MD SUNY Downstate Medical Center March 21, 2013 Case presentation 3F with no PMH presented to outside facility after drinking unmarked bottle containing oven cleaner
Caustic Esophageal Injury Aliu Sanni, MD SUNY Downstate Medical Center March 21, 2013 Case presentation 3F with no PMH presented to outside facility after drinking unmarked bottle containing oven cleaner
CASE-BASED SMALL GROUP DISCUSSION
 MHD I, Session 11, Student Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD I SESSION 11 Renal Block Acid- Base Disorders November 7, 2016 MHD I, Session 11, Student Copy Page 2 Case #1 Cc: I have had
MHD I, Session 11, Student Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD I SESSION 11 Renal Block Acid- Base Disorders November 7, 2016 MHD I, Session 11, Student Copy Page 2 Case #1 Cc: I have had
Med 536 Communicating About Prognosis Workshop. Case 1
 Med 536 Communicating About Prognosis Workshop Case 1 ID / CC: 39 year-old woman status-post motor-vehicle collision History of the Presenting Illness Previously healthy 39 year-old woman was found in
Med 536 Communicating About Prognosis Workshop Case 1 ID / CC: 39 year-old woman status-post motor-vehicle collision History of the Presenting Illness Previously healthy 39 year-old woman was found in
Pediatric Asthma. Concepts (in order of emphasis) Jared, 10 years old
 Pediatric Asthma Jared, 10 years old Overview This scenario is a rich application of the priority setting required by the nurse to rescue a child with an acute asthmatic exacerbation. Concepts (in order
Pediatric Asthma Jared, 10 years old Overview This scenario is a rich application of the priority setting required by the nurse to rescue a child with an acute asthmatic exacerbation. Concepts (in order
Scenario #4A: Geriatric Trauma Resuscitation Version-5
 Scenario #4A: Geriatric Trauma Resuscitation Version-5 Goals & Objectives: 1. Discuss the principles of initial assessment of a geriatric trauma patient. 2. Recognize physiologic and anatomic changes that
Scenario #4A: Geriatric Trauma Resuscitation Version-5 Goals & Objectives: 1. Discuss the principles of initial assessment of a geriatric trauma patient. 2. Recognize physiologic and anatomic changes that
1/29/2014. Objectives. The unstable overdose patient. Unstable overdose case #1. Outline
 Objectives The unstable overdose patient Craig Smollin MD Associate Medical Director California Poison Control Center, SF Division Discuss clinical scenarios unique to the acutely poisoned patient and
Objectives The unstable overdose patient Craig Smollin MD Associate Medical Director California Poison Control Center, SF Division Discuss clinical scenarios unique to the acutely poisoned patient and
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University
 Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
MHD I SESSION X. Renal Disease
 MHD I, Session X, Student Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD I SESSION X Renal Disease Monday, November 11, 2013 MHD I, Session X, Student Copy Page 2 Case #1 Cc: I have had weeks of diarrhea
MHD I, Session X, Student Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD I SESSION X Renal Disease Monday, November 11, 2013 MHD I, Session X, Student Copy Page 2 Case #1 Cc: I have had weeks of diarrhea
Clinical Pathway: Management Of The Life-Threatening Overdose
 Clinical Pathway: Management Of The Life-Threatening Overdose Intravenous access Oxygen Pulse oximetry n-invasive blood pressure monitoring Accu-Check ECG monitoring and ECG Chest x-ray Respiratory depression?
Clinical Pathway: Management Of The Life-Threatening Overdose Intravenous access Oxygen Pulse oximetry n-invasive blood pressure monitoring Accu-Check ECG monitoring and ECG Chest x-ray Respiratory depression?
ROS: all remaining ROS negative
 Case # 1 CC: altered mental status HPI: 13 yo male presents with altered metal status. Child`s mother was called by the school nurse to pick her child up from school today due to child`s unusual behavior.
Case # 1 CC: altered mental status HPI: 13 yo male presents with altered metal status. Child`s mother was called by the school nurse to pick her child up from school today due to child`s unusual behavior.
Sample Case Study. The patient was a 77-year-old female who arrived to the emergency room on
 Sample Case Study The patient was a 77-year-old female who arrived to the emergency room on February 25 th with a chief complaint of shortness of breath and a deteriorating pulmonary status along with
Sample Case Study The patient was a 77-year-old female who arrived to the emergency room on February 25 th with a chief complaint of shortness of breath and a deteriorating pulmonary status along with
A walk through a STEMI
 A walk through a STEMI M.M. s Story Kim Robison Ashley Corcoran Situation M.M. is an 82 year old male brought in by private vehicle on 10/22/17 to the Emergency Department Pt. c/o left arm numbness, pain
A walk through a STEMI M.M. s Story Kim Robison Ashley Corcoran Situation M.M. is an 82 year old male brought in by private vehicle on 10/22/17 to the Emergency Department Pt. c/o left arm numbness, pain
* Final Report * ED Triage Entered On: 01/16/2014 8:45 EST Performed On: 01/16/2014 8:42 EST by
 Result date: Result status: 16 January 2014 8:42 EST Auth (Verified) * Final Report * ED Triage Entered On: 01/16/2014 8:45 EST Performed On: 01/16/2014 8:42 EST by Assessment I Chief Complaint : Diarrhea
Result date: Result status: 16 January 2014 8:42 EST Auth (Verified) * Final Report * ED Triage Entered On: 01/16/2014 8:45 EST Performed On: 01/16/2014 8:42 EST by Assessment I Chief Complaint : Diarrhea
Rural STEMI System of Care Success. Nicole Huber, PA-C Cumberland Healthcare Emergency Department
 Rural STEMI System of Care Success Nicole Huber, PA-C Cumberland Healthcare Emergency Department DISCLOSURES I HAVE NO ACTUAL OR POTENTIAL CONFLICT OF INTEREST IN RELATION TO THIS PRESENTATION Ideal Process
Rural STEMI System of Care Success Nicole Huber, PA-C Cumberland Healthcare Emergency Department DISCLOSURES I HAVE NO ACTUAL OR POTENTIAL CONFLICT OF INTEREST IN RELATION TO THIS PRESENTATION Ideal Process
Discharge Summary-Page 1
 Discharge Summary-Page 1 Admission diagnosis: 1. Gastritis. 2. Alcoholic cirrhosis, ascites, grade 1 esophageal varices. 3. Recent left knee arthroplasty. 4. Osteoporosis naqmq : 1. Three chest X-rays
Discharge Summary-Page 1 Admission diagnosis: 1. Gastritis. 2. Alcoholic cirrhosis, ascites, grade 1 esophageal varices. 3. Recent left knee arthroplasty. 4. Osteoporosis naqmq : 1. Three chest X-rays
Subject ID: I N D # # U A * Consent Date: Day Month Year
 IND Study # Eligibility Checklist Pg 1 of 15 Instructions: Check the appropriate box for each Inclusion and Exclusion Criterion below. Each criterion must be marked and all protocol criteria have to be
IND Study # Eligibility Checklist Pg 1 of 15 Instructions: Check the appropriate box for each Inclusion and Exclusion Criterion below. Each criterion must be marked and all protocol criteria have to be
DIAGNOSIS AND MANAGEMENT OF DIURETIC RESISTANCE. Jules B. Puschett, M.D.
 DIAGNOSIS AND MANAGEMENT OF DIURETIC RESISTANCE Jules B. Puschett, M.D. Diuretic Resistance A clinical circumstance in which patients do not respond to a combination of salt restriction and even large
DIAGNOSIS AND MANAGEMENT OF DIURETIC RESISTANCE Jules B. Puschett, M.D. Diuretic Resistance A clinical circumstance in which patients do not respond to a combination of salt restriction and even large
REASON FOR REFERRAL Referred for blisters and rash of mucous membranes and skin.
 Report 1 Listen to the audio to fill in the blanks. Name: DERMATOLOGY CONSULTATION REPORT REASON FOR REFERRAL Referred for blisters and rash of mucous membranes and skin. HISTORY OF PRESENT ILLNESS Rash
Report 1 Listen to the audio to fill in the blanks. Name: DERMATOLOGY CONSULTATION REPORT REASON FOR REFERRAL Referred for blisters and rash of mucous membranes and skin. HISTORY OF PRESENT ILLNESS Rash
History Data Panel. Case 030 Preg Trauma. Presenting Complaint Altered mental status s/p MVC. Person Giving Information EMS
 History Data Panel Presenting Complaint Altered mental status s/p MVC Person Giving Information EMS History of Present Illness 28 year old woman, 35 weeks pregnant per report of her husband the passenger.
History Data Panel Presenting Complaint Altered mental status s/p MVC Person Giving Information EMS History of Present Illness 28 year old woman, 35 weeks pregnant per report of her husband the passenger.
Example Clinician Educational Material for Providers of Immune Effector Cellular Therapy
 Example Clinician Educational Material for Providers of Immune Effector Cellular Therapy Disclaimer: This example is just one of many potential examples of clinician education material that can be provided
Example Clinician Educational Material for Providers of Immune Effector Cellular Therapy Disclaimer: This example is just one of many potential examples of clinician education material that can be provided
County General Hospital 546 That Street. Some Town, YY DISCHARGE SUMMARY
 County General Hospital 546 That Street. Some Town, YY 12347 111-222-9998 DISCHARGE SUMMARY PATIENT: Collette Rose UNIT#: 345678 ADMISSION DATE: June 5, 1995 ACCT#: 98734513 DISCHARGE DATE: June 13, 1995
County General Hospital 546 That Street. Some Town, YY 12347 111-222-9998 DISCHARGE SUMMARY PATIENT: Collette Rose UNIT#: 345678 ADMISSION DATE: June 5, 1995 ACCT#: 98734513 DISCHARGE DATE: June 13, 1995
Transfusion Reactions
 Transfusion Reactions From A to T Provincial Blood Coordinating Program Daphne Osborne MN PANC (C) RN We want you to know Definition Appropriate actions Classification Complete case studies Transfusion
Transfusion Reactions From A to T Provincial Blood Coordinating Program Daphne Osborne MN PANC (C) RN We want you to know Definition Appropriate actions Classification Complete case studies Transfusion
LOKUN! I got stomach ache!
 LOKUN! I got stomach ache! Mr L is a 67year old Chinese gentleman who is a non smoker, social drinker. He has a medical history significant for Hypertension, Hyperlipidemia, Type 2 Diabetes Mellitus, Chronic
LOKUN! I got stomach ache! Mr L is a 67year old Chinese gentleman who is a non smoker, social drinker. He has a medical history significant for Hypertension, Hyperlipidemia, Type 2 Diabetes Mellitus, Chronic
Organ Donor Management Recommended Guidelines ADULT CARDIAC DEATH (DCD)
 Date: Time: = Always applicable = Check if applicable ADMISSION INSTRUCTIONS Move to Comfort Care Note in chart. Contact initiated with BC Transplant Consent for Organ Donation obtained Code Status: Full
Date: Time: = Always applicable = Check if applicable ADMISSION INSTRUCTIONS Move to Comfort Care Note in chart. Contact initiated with BC Transplant Consent for Organ Donation obtained Code Status: Full
SMALL ANIMAL SOFT TISSUE CASE-BASED EXAMINATION
 SMALL ANIMAL SOFT TISSUE CASE-BASED EXAMINATION CASE-BASED EXAMINATION INSTRUCTIONS The case-based examination measures surgical principles in case management prior to, during, and after surgery. Information
SMALL ANIMAL SOFT TISSUE CASE-BASED EXAMINATION CASE-BASED EXAMINATION INSTRUCTIONS The case-based examination measures surgical principles in case management prior to, during, and after surgery. Information
SMALL GROUP DISCUSSION
 MHD II, Seesion II Student Copy - Page 1 SMALL GROUP DISCUSSION MHD II Session II JANUARY 15, 2014 Recent Review highlighting disease process in Case 2: Fasano A, Catassi, C. NEJM 2012; 367: 2419-26 STUDENT
MHD II, Seesion II Student Copy - Page 1 SMALL GROUP DISCUSSION MHD II Session II JANUARY 15, 2014 Recent Review highlighting disease process in Case 2: Fasano A, Catassi, C. NEJM 2012; 367: 2419-26 STUDENT
Pain can produce unstable hemodynamics
 Pain can produce unstable hemodynamics 30-year-old male came to emergency department for severe epigastric pain for 6 hours as well as nausea and vomiting. 1)BP: 130/70mmHg 2)HR:
Pain can produce unstable hemodynamics 30-year-old male came to emergency department for severe epigastric pain for 6 hours as well as nausea and vomiting. 1)BP: 130/70mmHg 2)HR:
Canadian Trauma Trials Collaborative. Occult Pneumothorax in Critical Care (OPTICC): Standardized Data Collection Sheet
 Canadian Trauma Trials Collaborative STUDY CENTRE: Institution: City / Province: / Occult Pneumothorax in Critical Care (OPTICC): Standardized Sheet PATIENT DEMOGRAPHICS: First Name: Health record number
Canadian Trauma Trials Collaborative STUDY CENTRE: Institution: City / Province: / Occult Pneumothorax in Critical Care (OPTICC): Standardized Sheet PATIENT DEMOGRAPHICS: First Name: Health record number
Biochemical indicators of caustic ingestion and/or accompanying esophageal injury in children
 The Turkish Journal of Pediatrics 2003; 45: 21-25 Original Biochemical indicators of caustic ingestion and/or accompanying esophageal injury in children Selçuk Otçu, Ýbrahim Karnak, Feridun Cahit Tanyel
The Turkish Journal of Pediatrics 2003; 45: 21-25 Original Biochemical indicators of caustic ingestion and/or accompanying esophageal injury in children Selçuk Otçu, Ýbrahim Karnak, Feridun Cahit Tanyel
Prehospital Resuscitation for the 21 st Century Simulation Case. VF/Asystole
 Prehospital Resuscitation for the 21 st Century Simulation Case VF/Asystole Case History 1 (hypovolemic cardiac arrest secondary to massive upper GI bleed) 56 year-old male patient who fainted in the presence
Prehospital Resuscitation for the 21 st Century Simulation Case VF/Asystole Case History 1 (hypovolemic cardiac arrest secondary to massive upper GI bleed) 56 year-old male patient who fainted in the presence
Pediatric Advanced Life Support
 Pediatric Advanced Life Support Pediatric Chain of Survival Berg M D et al. Circulation 2010;122:S862-S875 Prevention Early cardiopulmonary resuscitation (CPR) Prompt access to the emergency response system
Pediatric Advanced Life Support Pediatric Chain of Survival Berg M D et al. Circulation 2010;122:S862-S875 Prevention Early cardiopulmonary resuscitation (CPR) Prompt access to the emergency response system
The student guide to simulation
 CETL 2008 1 The following guide will introduce you to what the simulators can do But firstly a few words on communication Please verbally and non-verbally communicate with the simulator as if it were a
CETL 2008 1 The following guide will introduce you to what the simulators can do But firstly a few words on communication Please verbally and non-verbally communicate with the simulator as if it were a
Patient: Becky Smith DOB: 01/26/XXXX Age: 5 y/o Attending: Dr. D. Miles Allergies: NKA MR#: 203. Patient Chart #203 Becky Smith
 Patient Chart #203 Becky Smith 1 Property of CSCLV CSCLV Rev: 06/04/2018 Chief Complaint: Abdominal pain. Informant: Parents. HISTORY & PHYSICAL HPI: Ill looking patient, healthy until 2 days ago when
Patient Chart #203 Becky Smith 1 Property of CSCLV CSCLV Rev: 06/04/2018 Chief Complaint: Abdominal pain. Informant: Parents. HISTORY & PHYSICAL HPI: Ill looking patient, healthy until 2 days ago when
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv
 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
Diabetic Ketoacidosis: When Sugar Isn t Sweet!!!
 Diabetic Ketoacidosis: When Sugar Isn t Sweet!!! W Ricks Hanna Jr MD Assistant Professor of Pediatrics University of Tennessee Health Science Center LeBonheur Children s Hospital Introduction Diabetes
Diabetic Ketoacidosis: When Sugar Isn t Sweet!!! W Ricks Hanna Jr MD Assistant Professor of Pediatrics University of Tennessee Health Science Center LeBonheur Children s Hospital Introduction Diabetes
CASE-BASED SMALL GROUP DISCUSSION
 MHD II, Session XII, STUDENT Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION Session XII MHD II April 21, 2014 STUDENT COPY Helpful Resource: ACP Medicine online available through LUHS Library Infectious
MHD II, Session XII, STUDENT Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION Session XII MHD II April 21, 2014 STUDENT COPY Helpful Resource: ACP Medicine online available through LUHS Library Infectious
Case presentation. Dr Rammohan Reddy 1 st year PG, Dept of DVL, Kamineni Institute of Medical Sciences, Narketpally.
 Case presentation Dr Rammohan Reddy 1 st year PG, Dept of DVL, Kamineni Institute of Medical Sciences, Narketpally. Name : XXX Age : 33 years Sex : Female Occupation : Farmer IP no : 201608905 DOA : 15-02-2016
Case presentation Dr Rammohan Reddy 1 st year PG, Dept of DVL, Kamineni Institute of Medical Sciences, Narketpally. Name : XXX Age : 33 years Sex : Female Occupation : Farmer IP no : 201608905 DOA : 15-02-2016
Burn Priorities of Care: Triage/Treatment/Transfer. Via Christi Regional Burn Center Sarah Fischer, MSN, RN
 Burn Priorities of Care: Triage/Treatment/Transfer Via Christi Regional Burn Center Sarah Fischer, MSN, RN Disclosure I have nothing to disclose Objectives Identify American Burn Association referral criteria
Burn Priorities of Care: Triage/Treatment/Transfer Via Christi Regional Burn Center Sarah Fischer, MSN, RN Disclosure I have nothing to disclose Objectives Identify American Burn Association referral criteria
Pediatric Gastroenterology Referral Guidelines
 Suggested Pre-Referral Workup This is a general suggestion of possible testing to confirm a suspected diagnosis. Although referrals will be accepted without the suggested work up being complete, to ensure
Suggested Pre-Referral Workup This is a general suggestion of possible testing to confirm a suspected diagnosis. Although referrals will be accepted without the suggested work up being complete, to ensure
CASE-BASED SMALL GROUP DISCUSSION SESSION 6 MHD I. October 14, 2015
 Session 6, MHD I, STUDENT Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION SESSION 6 MHD I October 14, 2015 Helpful Resources McPhee, SJ, Hammer GD. Pathophysiology of Disease: An Introduction to Clinical
Session 6, MHD I, STUDENT Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION SESSION 6 MHD I October 14, 2015 Helpful Resources McPhee, SJ, Hammer GD. Pathophysiology of Disease: An Introduction to Clinical
PHYSIOLOGY AND MANAGEMENT OF THE SEPTIC PATIENT
 PHYSIOLOGY AND MANAGEMENT OF THE SEPTIC PATIENT Melanie Sanchez, RN, MSNE, OCN, CCRN Clinical Nurse III City of Hope National Medical Center HOW THE EXPERTS TREAT HEMATOLOGIC MALIGNANCIES LAS VEGAS, NV
PHYSIOLOGY AND MANAGEMENT OF THE SEPTIC PATIENT Melanie Sanchez, RN, MSNE, OCN, CCRN Clinical Nurse III City of Hope National Medical Center HOW THE EXPERTS TREAT HEMATOLOGIC MALIGNANCIES LAS VEGAS, NV
Standardized Nurse Activated Protocols (SNAPs)
 SNAPs by presenting complaint/problem help nurses initiate care before the patient is seen by a physician. SNAPs should be approved by ED team consensus If patient unstable in any way, immediately notify
SNAPs by presenting complaint/problem help nurses initiate care before the patient is seen by a physician. SNAPs should be approved by ED team consensus If patient unstable in any way, immediately notify
EMT OPTIONAL SKILL. Cell Phones and Pagers. Epinephrine Auto-injector. Course Outline 9/2017
 EMT OPTIONAL SKILL Epinephrine Auto-injector Cell Phones and Pagers Be courteous to your classmates! Please set your cell phones and/or pagers to silent or turn them off. Course Outline Introduction and
EMT OPTIONAL SKILL Epinephrine Auto-injector Cell Phones and Pagers Be courteous to your classmates! Please set your cell phones and/or pagers to silent or turn them off. Course Outline Introduction and
Upper Gastrointestinal (GI) Tract X-ray (Radiography)
 Upper Gastrointestinal (GI) Tract X-ray (Radiography) What is Upper Gastrointestinal (GI) Tract Radiography? What are some common uses of the procedure? How should I prepare? What does the equipment look
Upper Gastrointestinal (GI) Tract X-ray (Radiography) What is Upper Gastrointestinal (GI) Tract Radiography? What are some common uses of the procedure? How should I prepare? What does the equipment look
Organ Donor Management Recommended Guidelines ADULT Brain Death (NDD)
 Date: Time: = Always applicable = Check if applicable ADMISSION INSTRUCTIONS Neurological Determination of Death (NDD) has been performed by at least 2 licensed physicians Contact initiated with BC Transplant
Date: Time: = Always applicable = Check if applicable ADMISSION INSTRUCTIONS Neurological Determination of Death (NDD) has been performed by at least 2 licensed physicians Contact initiated with BC Transplant
Esophageal injuries. 新光急診張志華醫師 Facebook.com/jack119
 Esophageal injuries 新光急診張志華醫師 Facebook.com/jack119 Pre-test 1 What is the most common cause of esophageal injuries? A. Traffic accidents B. Gunshot wounds C. Iatrogenic Pre-test 2 Which contrast agent
Esophageal injuries 新光急診張志華醫師 Facebook.com/jack119 Pre-test 1 What is the most common cause of esophageal injuries? A. Traffic accidents B. Gunshot wounds C. Iatrogenic Pre-test 2 Which contrast agent
9/15/2017. Joyce Turner RN Director of Clinical Program Development
 Joyce Turner RN Director of Clinical Program Development A toxic response to an infection that spirals out of control attacking the body s own organs and tissues. The infection can be bacterial, viral
Joyce Turner RN Director of Clinical Program Development A toxic response to an infection that spirals out of control attacking the body s own organs and tissues. The infection can be bacterial, viral
BOARD REVIEW QUESTIONS
 September 2017 Volume 17 Issue 9 Challenging ABEM style questions for enhanced learning and deeper understanding of the EMRAP program www.emrap.org Editor-in-Chief: Mel Herbert, MD Executive Editor: Stuart
September 2017 Volume 17 Issue 9 Challenging ABEM style questions for enhanced learning and deeper understanding of the EMRAP program www.emrap.org Editor-in-Chief: Mel Herbert, MD Executive Editor: Stuart
Understanding Blood Tests
 PATIENT EDUCATION patienteducation.osumc.edu Your heart pumps the blood in your body through a system of blood vessels. Blood delivers oxygen and nutrients to all parts of the body. It also carries away
PATIENT EDUCATION patienteducation.osumc.edu Your heart pumps the blood in your body through a system of blood vessels. Blood delivers oxygen and nutrients to all parts of the body. It also carries away
Waitin In The Wings. Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider
 Waitin In The Wings Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider 1 CombiTube Kit General Description The CombiTube is A double-lumen tube with
Waitin In The Wings Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider 1 CombiTube Kit General Description The CombiTube is A double-lumen tube with
Case TWO. Vital Signs: Temperature 36.6degC BP 137/89 HR 110 SpO2 97% on Room Air
 Mr N is a 64year old Chinese gentleman who is a heavy drinker, still actively drinking, and chronic smoker of >40pack year history. He has a past medical history significant for Hypertension, Hyperlipidemia,
Mr N is a 64year old Chinese gentleman who is a heavy drinker, still actively drinking, and chronic smoker of >40pack year history. He has a past medical history significant for Hypertension, Hyperlipidemia,
Emergency Department Triage
 Emergency Department Triage Julia Fuzak, MD, Patrick Mahar, MD The Children s Hosital Denver, CO, USA 1/30/09 Hospital Pediatrico Juan Manuel Marquez Habana, Cuba Objectives What is does triage mean? Why
Emergency Department Triage Julia Fuzak, MD, Patrick Mahar, MD The Children s Hosital Denver, CO, USA 1/30/09 Hospital Pediatrico Juan Manuel Marquez Habana, Cuba Objectives What is does triage mean? Why
EM Cases Course 2017 Toxicology Module
 EM Cases Course 2017 Toxicology Module quick IV access and diazepam is administered. The seizure stops. The first set of vitals show: HR 30bpm, BP 70/40. His ECG is shown below. Margaret Thompson & JP
EM Cases Course 2017 Toxicology Module quick IV access and diazepam is administered. The seizure stops. The first set of vitals show: HR 30bpm, BP 70/40. His ECG is shown below. Margaret Thompson & JP
IMMEDIATE EMERGENCY BURN CARE » THERMAL BURNS » ELECTRICAL BURNS » CHEMICAL BURNS FIRST AID FOR THE THREE MAJOR CATEGORIES
 IMMEDIATE EMERGENCY BURN CARE 1. Treat according to BLS or ACLS Protocol 2. Use airway and C-Spine precautions. 3. Stop the burning process. FIRST AID FOR THE THREE MAJOR CATEGORIES» THERMAL BURNS + Stop
IMMEDIATE EMERGENCY BURN CARE 1. Treat according to BLS or ACLS Protocol 2. Use airway and C-Spine precautions. 3. Stop the burning process. FIRST AID FOR THE THREE MAJOR CATEGORIES» THERMAL BURNS + Stop
Staging Sepsis for the Emergency Department: Physician
 Staging Sepsis for the Emergency Department: Physician Sepsis Continuum 1 Sepsis Continuum SIRS = 2 or more clinical criteria, resulting in Systemic Inflammatory Response Syndrome Sepsis = SIRS + proven/suspected
Staging Sepsis for the Emergency Department: Physician Sepsis Continuum 1 Sepsis Continuum SIRS = 2 or more clinical criteria, resulting in Systemic Inflammatory Response Syndrome Sepsis = SIRS + proven/suspected
EmergencyKT: Management of Thermal Injury in Adult Patients
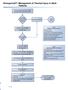 EmergencyKT: Management of Thermal Injury in Adult Patients Remove patient from source of injury, including burned clothing and jewelry Does patient appear to have minor burns? (See Box A) No Notify Burn
EmergencyKT: Management of Thermal Injury in Adult Patients Remove patient from source of injury, including burned clothing and jewelry Does patient appear to have minor burns? (See Box A) No Notify Burn
Video Fluoroscopic Swallowing Exam (VFSE)
 Scan for mobile link. Video Fluoroscopic Swallowing Exam (VFSE) A video fluoroscopic swallowing exam (VFSE) uses a form of real-time x-ray called fluoroscopy to evaluate a patient s ability to swallow
Scan for mobile link. Video Fluoroscopic Swallowing Exam (VFSE) A video fluoroscopic swallowing exam (VFSE) uses a form of real-time x-ray called fluoroscopy to evaluate a patient s ability to swallow
Clinician Blood Panel Results
 Page 1 of 7 Blood Panel - Markers Out of Range and Patterns (Pattern: proprietary formula using one or more Blood Markers) Blood Panel: Check for Markers that are out of Lab Range ***NOTE*** Only one supplement
Page 1 of 7 Blood Panel - Markers Out of Range and Patterns (Pattern: proprietary formula using one or more Blood Markers) Blood Panel: Check for Markers that are out of Lab Range ***NOTE*** Only one supplement
Calcium (Ca 2+ ) mg/dl
 Quick Guide to Laboratory Values Use this handy cheat-sheet to help you monitor laboratory values related to fluid and electrolyte status. Remember, normal values may vary according to techniques used
Quick Guide to Laboratory Values Use this handy cheat-sheet to help you monitor laboratory values related to fluid and electrolyte status. Remember, normal values may vary according to techniques used
Hypothermia Short Set-Critical Care HYPOTHERMIA SS- CRITICAL CARE
 Hypothermia Short Set-Critical Care HYPOTHERMIA SS- CRITICAL CARE Inclusion Criteria all must be present Cardiac arrest with return of spontaneous circulation (ROSC) ROSC within 60 mins of witnessed arrest;
Hypothermia Short Set-Critical Care HYPOTHERMIA SS- CRITICAL CARE Inclusion Criteria all must be present Cardiac arrest with return of spontaneous circulation (ROSC) ROSC within 60 mins of witnessed arrest;
Case Scenario 3: Shock and Sepsis
 Name: Molly Boyle 1. Define the term shock (Lewis textbook): Shock is a syndrome characterized by decreased perfusion and impaired metabolism. Shock can have a number of causes that result in damage to
Name: Molly Boyle 1. Define the term shock (Lewis textbook): Shock is a syndrome characterized by decreased perfusion and impaired metabolism. Shock can have a number of causes that result in damage to
SEPSIS: IT ALL BEGINS WITH INFECTION. Theresa Posani, MS, RN, ACNS-BC, CCRN M/S CNS/Sepsis Coordinator Texas Health Harris Methodist Ft.
 SEPSIS: IT ALL BEGINS WITH INFECTION Theresa Posani, MS, RN, ACNS-BC, CCRN M/S CNS/Sepsis Coordinator Texas Health Harris Methodist Ft. Worth 1 2 3 OBJECTIVES Review the new Sepsis 3 definitions of sepsis
SEPSIS: IT ALL BEGINS WITH INFECTION Theresa Posani, MS, RN, ACNS-BC, CCRN M/S CNS/Sepsis Coordinator Texas Health Harris Methodist Ft. Worth 1 2 3 OBJECTIVES Review the new Sepsis 3 definitions of sepsis
Real Cases: Bad Outcomes
 Real Cases: Bad Outcomes Fredrick M. Abrahamian, D.O., FACEP, FIDSA Clinical Professor of Medicine UCLA School of Medicine Director of Education Department of Emergency Medicine Olive View-UCLA Medical
Real Cases: Bad Outcomes Fredrick M. Abrahamian, D.O., FACEP, FIDSA Clinical Professor of Medicine UCLA School of Medicine Director of Education Department of Emergency Medicine Olive View-UCLA Medical
Pain Rating Scale GG. PAIN MANAGEMENT (NEW 10) 1. Initiate General Patient Care.
 GG. PAIN MANAGEMENT (NEW 10) 1. Initiate General Patient Care. 2. Presentation Pain may be present in many different conditions. Management of pain in the field can help to reduce suffering, make transport
GG. PAIN MANAGEMENT (NEW 10) 1. Initiate General Patient Care. 2. Presentation Pain may be present in many different conditions. Management of pain in the field can help to reduce suffering, make transport
INHALANT ABUSE AND RESPIRATORY FAILURE. Chalita Waenlor, MD
 INHALANT ABUSE AND RESPIRATORY FAILURE Chalita Waenlor, MD Inhalants Substances with significant acute and chronic toxicity. Wide variety of chemical structures with the majority being hydrocarbons (aliphatic,
INHALANT ABUSE AND RESPIRATORY FAILURE Chalita Waenlor, MD Inhalants Substances with significant acute and chronic toxicity. Wide variety of chemical structures with the majority being hydrocarbons (aliphatic,
SMALL ANIMAL SOFT TISSUE CASE- BASED EXAMINATION
 SMALL ANIMAL SOFT TISSUE CASE- BASED EXAMINATION CASE-BASED EXAMINATION INSTRUCTIONS The case-based examination measures surgical principles in case management prior to, during, and after surgery. Information
SMALL ANIMAL SOFT TISSUE CASE- BASED EXAMINATION CASE-BASED EXAMINATION INSTRUCTIONS The case-based examination measures surgical principles in case management prior to, during, and after surgery. Information
Competency Log Professional Responder Courses
 Competency Log Professional Responder Courses Check off each competency once successfully demonstrated. This log may be used as a support tool when teaching a Professional Responder course. Refer to the
Competency Log Professional Responder Courses Check off each competency once successfully demonstrated. This log may be used as a support tool when teaching a Professional Responder course. Refer to the
2. Have your symptoms affected your ability to carry out your daily activities? YES NO
 QUESTIONNAIRE Page 1 of 5 Date: Referring MD (Name, Address, Phone Number): Primary Care Physician (Name and Address, Phone Number): Reason for visit: 1. How long have you had symptoms? Describe your symptoms?
QUESTIONNAIRE Page 1 of 5 Date: Referring MD (Name, Address, Phone Number): Primary Care Physician (Name and Address, Phone Number): Reason for visit: 1. How long have you had symptoms? Describe your symptoms?
Use of Blood Lactate Measurements in the Critical Care Setting
 Use of Blood Lactate Measurements in the Critical Care Setting John G Toffaletti, PhD Director of Blood Gas and Clinical Pediatric Labs Professor of Pathology Duke University Medical Center Chief, VAMC
Use of Blood Lactate Measurements in the Critical Care Setting John G Toffaletti, PhD Director of Blood Gas and Clinical Pediatric Labs Professor of Pathology Duke University Medical Center Chief, VAMC
Candidate number BOOK THREE. NSW Fellowship Course - SAQ trial paper
 BOOK THREE QUESTION 19 (20 marks) DOUBLE QUESTION A 12 month old Asian boy is brought to the ED by his parents. Over the last 48 hours his mother noticed him becoming increasingly pale and lethargic and
BOOK THREE QUESTION 19 (20 marks) DOUBLE QUESTION A 12 month old Asian boy is brought to the ED by his parents. Over the last 48 hours his mother noticed him becoming increasingly pale and lethargic and
 55-year-old male with 2nd and 3rd degree burns to face, chest, and arms on 25% of the body Respirations: 34 Pulse: 120 Mental Status: moans to painful stimulus Mucous membranes charred Stridor 10 cm scalp
55-year-old male with 2nd and 3rd degree burns to face, chest, and arms on 25% of the body Respirations: 34 Pulse: 120 Mental Status: moans to painful stimulus Mucous membranes charred Stridor 10 cm scalp
Medical Case History and Examination (2) 31 years old Gender. Male Nationality. Bengali Religion. Muslim Marital Status
 Medical Case History and Examination (2) - Demographic Data: Patient s name Suman **** CPR 86025**** Age 31 years old Gender Male Nationality Bengali Religion Muslim Marital Status Unmarried Date of Admission
Medical Case History and Examination (2) - Demographic Data: Patient s name Suman **** CPR 86025**** Age 31 years old Gender Male Nationality Bengali Religion Muslim Marital Status Unmarried Date of Admission
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 14 Practical Anesthesia Key Points 2 14.1 General Anesthesia Have a clear plan before starting anesthesia Never use an unfamiliar anesthetic technique in an emergency
Surgical Care at the District Hospital 1 14 Practical Anesthesia Key Points 2 14.1 General Anesthesia Have a clear plan before starting anesthesia Never use an unfamiliar anesthetic technique in an emergency
Case Scenarios. Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC. Consultant, Critical Care Medicine Medanta, The Medicity
 Case Scenarios Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity Case 1 A 36 year male with cirrhosis and active GI bleeding is intubated to protect his airway,
Case Scenarios Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity Case 1 A 36 year male with cirrhosis and active GI bleeding is intubated to protect his airway,
Objectives. Case Presentation. Respiratory Emergencies
 Respiratory Emergencies Objectives Describe how to assess airway and breathing, including interpreting information from the PAT and ABCDEs. Differentiate between respiratory distress, respiratory failure,
Respiratory Emergencies Objectives Describe how to assess airway and breathing, including interpreting information from the PAT and ABCDEs. Differentiate between respiratory distress, respiratory failure,
Assessment of the Adolescent, Pre-Teen, and Teen Student for School Nurses
 Assessment of the Adolescent, Pre-Teen, and Teen Student for School Nurses KIMBERLY RICHARDS RN, BSN CLINICAL UNIT LEADER NOVANT HEALTH MATTHEWS MEDICAL CENTER MEDICAL SURGICAL/HOSPICE ONCOLOGY Agenda
Assessment of the Adolescent, Pre-Teen, and Teen Student for School Nurses KIMBERLY RICHARDS RN, BSN CLINICAL UNIT LEADER NOVANT HEALTH MATTHEWS MEDICAL CENTER MEDICAL SURGICAL/HOSPICE ONCOLOGY Agenda
Diabetic Emergencies. Chapter 15
 Diabetic Emergencies Chapter 15 Diabetes- is a disorder of glucose metabolism or difficulty metabolizing carbohydrates, fats and proteins Full name is diabetes mellitus which refers to the presence of
Diabetic Emergencies Chapter 15 Diabetes- is a disorder of glucose metabolism or difficulty metabolizing carbohydrates, fats and proteins Full name is diabetes mellitus which refers to the presence of
