ORIGINAL ARTICLE. Received August 28, 2008; accepted December 22, 2008.
|
|
|
- Piers Wilkerson
- 5 years ago
- Views:
Transcription
1 LIVER TRANSPLANTATION 15: , 2009 ORIGINAL ARTICLE Extended Right Liver Grafts Obtained by an Ex Situ Split Can Be Used Safely for Primary and Secondary Transplantation with Acceptable Biliary Morbidity Atsushi Takebe, 1,3 Harald Schrem, 1 Bastian Ringe, 1 Frank Lehner, 1 Christian Strassburg, 2 Juergen Klempnauer, 1 and Thomas Becker 1 Departments of 1 General, Visceral, and Transplantation Surgery and 2 Gastroenterology, Hepatology, and Endocrinology, Medizinische Hochschule Hannover, Hannover, Germany; and 3 Division of Hepato-Biliary- Pancreatic Surgery, Kobe University Graduate School of Medicine, Kobe, Japan Split liver transplantation (SLT) is clearly beneficial for pediatric recipients. However, the increased risk of biliary complications in adult recipients of SLT in comparison with whole liver transplantation (WLT) remains controversial. The objective of this study was to investigate the incidence and clinical outcome of biliary complications in an SLT group using split extended right grafts (ERGs) after ex situ splitting in comparison with WLT in adults. The retrospectively collected data for 80 consecutive liver transplants using ERGs after ex situ splitting between 1998 and 2007 were compared with the data for 80 liver transplants using whole liver grafts in a matched-pair analysis paired by the donor age, recipient age, indications, Model for End-Stage Liver Disease score, and high-urgency status. The cold ischemic time was significantly longer in the SLT group (P 0.006). As expected, bile leakage from the transected surface occurred only in the SLT group (15%) without any mortality or graft loss. The incidence of all other early or late biliary complications (eg, anastomotic leakage and stenosis) was not different between SLT and WLT. The 1- and 5-year patient and graft survival rates showed no statistical difference between SLT and WLT [83.2% and 82.0% versus 88.5% and 79.8% (P 0.92) and 70.8% and 67.5% versus 83.6% and 70.0% (P 0.16), respectively]. In conclusion, ERGs can be used safely without any increased mortality and with acceptable morbidity, and they should also be considered for retransplantation. The significantly longer cold ischemic time in the SLT group indicates the potential for improved results and should thus be considered in the design of allocation policies. Liver Transpl 15: , AASLD. Received August 28, 2008; accepted December 22, In 1988, the first description of successful split liver transplantation (SLT) using a left lateral graft (LLG) for a pediatric recipient and the remnant extended right graft (ERG) for an adult recipient was reported by our institution. 1 Since then, with increasing experience and improvement of the surgical technique, the significant potential of SLT became apparent, and this modality soon became common practice. 2-5 SLT demonstrated great merit for very small children who were otherwise very unlikely find a suitable donor of a full size liver graft. Living-related liver donation of LLGs for pediatric recipients was introduced later into the repertoire of liver transplant techniques 6 and is now a well-established method with the disadvantage of the inherent risks for the healthy living donor. Therefore, SLT still has a place in pediatric and adult liver transplantation. Abbreviations: AST, aspartate aminotransferase; BMI, body mass index; CIT, cold ischemic time; ERG, extended right graft; GRBW, graft/body weight ratio; HAT, hepatic arterial thrombosis; HU, high urgency; ICU, intensive care unit; LDLT, living donor liver transplantation; LLG, left lateral graft; MELD, Model for End-Stage Liver Disease; NS, not significant; PNF, primary nonfunction of the graft; SLT, split liver transplantation; WLG, whole liver graft; WLT, whole liver transplantation. Address reprint requests to Thomas Becker, M.D., Ph.D., Department of General, Abdominal, and Transplantation Surgery, Medizinische Hochschule Hannover, Carl-Neuberg-Straße 1, 30625, Hannover, Germany. Telephone: ; FAX: ; becker.thomas@mh-hannover.de DOI /lt Published online in Wiley InterScience ( American Association for the Study of Liver Diseases.
2 SAFE USE OF EX SITU EXTENDED RIGHT LIVER GRAFTS 731 Today, the splitting procedure can be done either in situ during the liver procurement procedure in the braindead donor or alternatively ex situ after whole liver harvesting, but both methods are considered to increase the risk for biliary complications. 7 Biliary complications belong to the most serious morbidities of all types of liver transplantation 8 and are closely related to the graft and preoperative recipient conditions. 9 An analysis of living donor liver transplantation (LDLT) 10 has shown that partial liver grafts have a higher incidence of biliary complications because of their transected surface and the operation procedure, which includes surgical dissection in the hepatic hilum. Even though the number of published cases is comparatively limited so far, high rates of biliary morbidity have also been reported for ERGs with an incidence of 10% to 34% Despite this clear disadvantage, the use of ERGs after an in situ or ex situ split is basically acceptable for most patients because of the ubiquitous shortage of donor organs. In clinical practice, in situ splitting to avoid longer cold ischemic times (CITs), with associated damage to the graft leading potentially to significant increases in morbidity and mortality, is often restrained by logistical and technical efforts and expertise as well as financial expenditures, all of which are necessary for its success. Although most publications on SLT using in situ split ERGs have demonstrated comparable patient and graft survival in comparison with whole liver transplantation (WLT), the value and safety of ex situ splitting in obtaining ERGs for liver transplantation remain controversial, even though in practice about half of all SLT procedures in Europe and the United States are done after an ex situ split. 2,16,17 Some centers hesitate to use ERGs obtained by an ex situ split either in general or for complicated or retransplant cases. In most published series, ERGs have been mainly or exclusively used for primary liver transplantation in adult recipients This study investigates the common complications and details the biliary complications and results after the transplantation of ERGs obtained by ex situ splitting in comparison with whole liver grafts. This study also includes high-urgency cases and retransplants, all of which were performed at our institute. Our aim is to evaluate the value of the use of ex situ split ERGs in comparison with whole liver grafts under different circumstances. PATIENTS AND METHODS This study evaluated 80 consecutive split liver transplants using ERGs after ex situ splitting within the last decade ( ). In this period, among a total of 1205 liver transplants, 80 ERGs and 94 LLGs, which were all obtained by ex situ splitting, were used. These 80 recipients of ERGs were selected for this study and matched to adult recipients who received WLGs in the same period of time. The following matching criteria were used: 1. Donor age ( 50 and 50). 2. Recipient age ( 50 and 50). 3. Indication. 4. Model for End-Stage Liver Disease (MELD) score. 5. High-urgency status according to the Eurotransplant status. Definition of Complications Vascular complications were defined as problems in the hepatic artery, portal vein, or hepatic vein requiring therapeutic invasive interventions. Renal dysfunction was defined as renal failure requiring transient hemodialysis. Respiratory insufficiency was defined as prolonged intubation ( 5 days) or reintubation. Neurological complications were diagnosed by a neurologist. Postoperative bleeding was identified as bleeding requiring 3 units of blood after transplantation or needed surgical management. Ascites was defined as uncontrollable ascites with drug therapy. A wound malignancy was defined as some type of wound complication that needed secondary surgical management. Acute rejection was diagnosed by pathological findings. An infection event was defined as any kind of infection that required antibiotics or an invasive procedure. Biliary complications were defined as bile leakage from the transected liver surface or bile leakage from the anastomosis site (including leakage from the cystic duct and stump of the left bile duct) or bile duct necrosis or stenosis. Donor and Recipient Selection Well-experienced transplant surgeons made decisions based on macroscopic observation and the anatomical situation on the basis of these criteria: 1. Donor age below 50 years. 2. Hemodynamic stability. 3. Preferable donor intensive care unit (ICU) stay of less than 5 days. 4. No status of hypernatremia with Na 170 mmol/l. Every patient with any condition who agreed to receive ERGs was considered to be a potential recipient of SLT. Surgical Technique The ex situ splitting procedure has been described in a previous report. 18 In summary, (1) preoperative cholangiography and angiography were not performed on the donor, (2) a surgical metal probe was used to demonstrate all vessels, (3) the sharp-knife technique 19 was used for the parenchymal transection, and (4) the bile duct was transected to allow minimum dissection in the hepatic hilum at the final step. The implantation techniques of ERGs and WLGs were identical. Furthermore, (1) neither the piggyback technique nor a venous-venous bypass was used; (2) no portocaval shunt was made; (3) the arterial tree of the celiac trunk and the common bile duct of the graft were used with the ERG for anastomosis; (4) in most cases, the vascular anastomosis was performed in an end-to-end fashion for the portal vein and the suprahepatic and infrahepatic vena cava, whereas arterial reconstruction was performed with the branch-patch technique (gastroduodenal artery gastroduodenal artery) 20 ; (5) for biliary recon-
3 732 TAKEBE ET AL. TABLE 1. Donor and Recipient Characteristics SLT (n 80) WLT (n 80) P Donor Age (years) 33.0 (7 60) 38.1 (14 64) NS Stay in ICU (days) 3.9 (1 14) 5.45 (1 44) Graft weight (g) 1141 ( ) 1753 ( ) GRBW (%) 1.78 ( ) 2.36 ( ) CIT (minutes) 747 ( ) 662 ( ) Recipient Age (years) 41.6 (15 65) 43.4 (18 64) NS MELD 16.2 (6 40) 17.2 (6 40) NS Number of HU 8 (10.0%) 8 (10.0%) NS Follow-up (months) 40.0 ( ) 40.0 (0 109) NS Abbreviations: CIT, cold ischemic time; GRBW, graft/body weight ratio; HU, high urgency; ICU, intensive care unit; MELD, Model for End-Stage Liver Disease; NS, not significant; SLT, split liver transplantation; WLT, whole liver transplantation. struction, the first choice was the duct-to-duct method by end-to-end anastomosis depending on the indications for transplantation; and (6) biliary drainage (Ttube) was used rarely and only for high-risk cases. A Roux-en-Y biliary reconstruction was used for cholestatic disease. Statistics In a matched-pair analysis, continuous variables were compared with the Mann-Whitney U test, and categorical variables were compared with Fisher s exact test. The survival rates were calculated according to the Kaplan- Meier method. Differences in the survival curves were compared with log-rank statistics. Statistical significance was defined as P JMP version 5.0 (SAS Institute, Cary, NC) was used for all statistical analysis. RESULTS Donor and Recipient Characteristics The characteristics of the donors and recipients are compared in Table 1. The median length of the donor ICU stay was 1.5 days shorter (P 0.045) and the median CIT was 85 minutes longer (P 0.006) in the SLT group. As expected, the graft weight (P 0.001) and graft/body weight ratio (P 0.001) were significantly higher in the WLT group in comparison with SLT. There was no significant difference between WLT and SLT in terms of the chosen matching criteria described previously. The median follow-up durations of SLT and WLT were equal (40 months). The most frequent indication for transplantation was cholestatic disease (36.3%). There were 10 cases of retransplantation (12.5%) in both groups. The causes of retransplantation were distributed identically between SLT and WLT, and half of them were high-urgency cases (Table 2). Comparison of Common Complications in the SLT and WLT Groups TABLE 2. Indications for Transplantation n % Fulminant liver failure Cholestatic disease Cirrhosis Malignant tumor Metabolic disease Cystic liver or benign tumor Retransplantation PNF (HU) 2 Vascular complication (HU) 3 Recurrence of hepatitis 2 Chronic rejection 3 Total Abbreviations: HU, high urgency; PNF, primary nonfunction of the graft. The incidences of complications in the SLT and WLT groups are compared in Table 3. Not only crucial complications [vascular complications, biliary complications, and primary nonfunction of the graft (PNF)] but also milder ones occurred at statistically comparable rates. There were no statistical differences in the average length of stay in the ICU in both groups. Biliary Complications To evaluate the detailed incidence of biliary complications in the SLT group, the type of biliary reconstruction and the specific biliary complications are shown in Table 4. Forty-eight patients (60.0%) in the SLT group and 50 patients in the WLT group (62.5%) received duct-toduct biliary reconstruction. A T-tube was used in 5 patients (6.3%) in the SLT group and in 1 patient (1.2%) in the WLT group. For 2 patients in the SLT group and 1 patient in the WLT group, the biliary reconstruction was not accomplished because of hemodynamic instability during the transplantation. However, a second operation intended for biliary reconstruction was canceled in all 3 cases because of the patient s death. In total, 32 biliary complications in 26 patients in the SLT group (32.5%) and 25 biliary complications in 19 pa-
4 SAFE USE OF EX SITU EXTENDED RIGHT LIVER GRAFTS 733 TABLE 3. Common Complications of Liver Transplantation SLT [n (%)] WLT [n (%)] P Primary nonfunction 6 (7.5) 2 (2.5) NS Vascular complications 12 (15.0) 6 (7.5) NS Biliary complications 26 (32.5) 19 (23.8) NS Cardiac complications 2 (2.5) 2 (2.5) NS Renal dysfunction 10 (10.0) 16 (20.0) NS Respiratory insufficient 10 (10.0) 13 (16.3) NS Neurological complications 2 (2.5) 3 (3.8) NS Postoperative bleeding 9 (11.3) 9 (11.3) NS Ascites 8 (10.0) 7 (8.8) NS Wound malignancy 6 (7.5) 7 (8.8) NS Acute rejection 15 (18.8) 12 (15.0) NS Infection event 15 (18.8) 7 (8.8) NS Date of ICU stay 16.0 (0 124) 14.1 (1 118) NS Abbreviations: ICU, intensive care unit; NS, not significant; SLT, split liver transplantation; WLT, whole liver transplantation. TABLE 4. Biliary Reconstruction and Details of Biliary Complications SLT [n (%)] WLT [n (%)] P Biliary reconstruction Duct to duct 48 (60.0) 50 (62.5) NS Roux-en-Y 32 (40.0) 29 (36.3) NS No reconstruction 2* (2.5) 1* (1.2) NS Biliary complications Total 26 (32.5) 19 (23.8) NS Early onset ( 90 days) 21 (26.3) 11 (13.8) 0.04 Leakage (transected surface) 12 (15.0) 0 (0.0) Leakage (anastomotic) 5 (6.3) 5 (6.3) NS Bile duct necrosis 5 (6.3) 2 (2.5) NS Anastomotic stenosis 2 (2.5) 6 (7.5) NS Related graft loss 2 (2.5) 2 (2.5) NS Late onset ( 90 days) 9 (11.3) 10 (12.5) NS Anastomotic stenosis 9 (11.3) 10 (12.5) NS Related graft loss 1 (1.3) 0 (0.0) NS Abbreviations: NS, not significant; SLT, split liver transplantation; WLT, whole liver transplantation. *Because of the patient s death, biliary reconstruction was not performed. Including leakage from the anastomotic site, cystic duct, and stump of the left bile duct. tients in the WLT group (23.8%) were observed during the study period. SLT demonstrated a higher risk of early-onset ( 90 days) biliary complications (26.3% versus 13.8%, P 0.04) in comparison with WLT. However, except for bile leakage from the transected surface, which is a particular complication of SLT, the number of patients with other early-onset biliary complications was the same in both groups (n 11, 13.8%). All of the late-onset ( 90 days) biliary complications in both groups were characterized by anastomotic stenosis. The incidence of anastomotic stenosis was not significantly different between the SLT and WLT groups. Overall, there were 5 graft losses (SLT 3, WLT 2) that were related to biliary complications. The difference in the incidence of these graft losses was not statistically significant between SLT and WLT. The possible clinical factors associated with early- and late-onset biliary complications after SLT were statistically analyzed. These factors included donor factors (age, length of the donor s ICU stay, graft/body weight ratio, and CIT), patient factors (age, body mass index, preoperative MELD score, urgency of operation, and indication), and other factors such as the type of biliary reconstruction and the postoperative maximum aspartate aminotransferase value. A univariate analysis did not indicate that any of these factors were a risk factor for the observed biliary complications. Bile Leakage from the Transected Surface After SLT After SLT, 12 patients were diagnosed with bile leakage from the transected surface, which is particularly inherent to SLT in comparison with WLT. In 8 of these 12 patients, this was a solitary biliary complication. This type of complication was easily controlled by percuta-
5 734 TAKEBE ET AL. TABLE 5. Univariate Analysis of Factors Associated with Leakage from the Transected Surface Leakage( ) Leakage( ) P Total number Donor age (yrs) 28.2 (17 54) 33.9 (7 60) NS Donor ICU stay (days) 4.75 (1 14) 3.83 (1 11) NS GRBW 1.79 ( ) 1.73 ( ) NS CIT (min) ( ) ( ) NS Recipient age (yrs) 36.1 (18 58) 42.6 (15 65) NS Recipient BMI (kg/m 2 ) 23.2 (17 32) 23.1 (15 35) NS MELD score 13.9 (6 27) 16.8 (6 40) NS HU 1 (8.3%) 7 (10.3%) NS Cholestatic disease 8 (66.7%) 21 (30.9%) Retransplantation 1 (8.33%) 9 (13.2%) NS Duct to duct 5 (41.7%) 43 (63.2%) NS Maximum AST (IU/L) 2062 ( ) 2314 ( ) NS Abbreviations: AST, aspartate aminotransferase; BMI, body mass index; CIT, cold ischemic time; GRBW, graft/body weight ratio; HU, high urgency; ICU, intensive care unit; MELD, Model for End-Stage Liver Disease; NS, not significant. neous drainage in 2 of 8 cases, whereas reoperation (abdominal drainage or repair of the point of leakage) was necessary in the other 6 patients (6/8, 75.0%). There was no graft loss in these 8 cases. Four patients were diagnosed with combined biliary complications. In 2 of those patients, bile leakage from the transected surface was combined with bile leakage from the anastomotic site. One patient received endoscopic biliary drainage, whereas the other underwent new biliary reconstruction. Two patients were retransplanted because of bile duct necrosis combined with bile leakage from the transected surface. One of these 2 patients died after retransplantation. Late-onset biliary complications were not associated with bile leakage from the transected surface (P 0.83). The association between leakage from the transected surface and the aforementioned clinical factors was analyzed statistically (Table 5). The incidence of leakage from the transected surface was found to be significantly higher only in patients with cholestatic disease (66.7% versus 30.9%, P 0.019) in comparison with patients who were transplanted for other indications. All other clinical factors had no significant association with this biliary complication. Patient and Graft Survival Kaplan-Meier estimations of graft and patient survival were compared by a log-rank analysis. The 1- and 5-year survival of SLT patients was 83.2% and 82.0%, respectively. The patient survival of WLT patients at the same time points was 88.5% and 79.8%, respectively (Fig. 1A). The differences between SLT and WLT in overall graft survival did not reach statistical significance (P 0.92). The 1- and 5-year graft survival rates showed no statistical difference between SLT and WLT (70.8% and 67.5% versus 83.6% and 70.0%, P 0.16; Fig. 1B). Twenty-five grafts were lost after SLT during the last decade (19 graft losses in the WLT group). Seventeen graft losses occurred within the first month after transplantation (10 in the WLT group). With significance for graft survival, the incidence of PNF and hepatic arterial thrombosis (HAT) was slightly increased in the SLT group (PNF, 7.5% versus 2.5%, P 0.13; HAT, 13.6% versus 6.3%, P 0.17) in comparison with the WLT group, but this difference did not reach statistical significance. DISCUSSION The major aim of SLT is to provide a graft of a suitable size for a small child without decreasing the number of available donor organs for adult recipients. Although the initial results for SLT were not satisfying, later, with the establishment of modern surgical techniques and further progress in the field of liver transplantation, several reports could demonstrate that SLT has potential equal to that of WLT not only for pediatric recipients but also for adult recipients. 2,13,15 Because of the ubiquitous shortage of donor organs, ERGs have become an essential option for almost every adult recipient, especially in high-volume transplantation centers with sufficient experience with this procedure. The current study clearly supports this opinion because the results have demonstrated that ERGs can be transplanted with comparable results in comparison with WLT with respect to patient and graft survival, and the significantly increased morbidity due to biliary complications appears to be acceptable. This is remarkable because in the current series, ERGs were also used for high-urgency and retransplant cases, whereas other published series used ERGs only for primary transplantation in stable patients It is well accepted that early and late biliary complications are still some of the most severe morbidities after liver transplantation, and their incidence has been reported to be between 10% and 30% after liver transplants from brain-dead donors In addition, it has been reported that the potential risk for biliary morbidities is associated with both the type of biliary recon-
6 SAFE USE OF EX SITU EXTENDED RIGHT LIVER GRAFTS 735 Figure 1. The overall survival of the SLT and WLT groups ( ). (A) The overall patient survival of the SLT and WLT groups. The 1- and 5-year survival rates (Kaplan-Meier) were 83.2% and 82.0% in the SLT group and 88.5% and 79.8% in the WLT group (P 0.92). (B) The overall graft survival in the SLT and WLT groups. The 1- and 5-year survival rates (Kaplan-Meier) were 70.8% and 67.5% in the SLT group and 83.6% and 70.0% in the WLT group (P 0.162). Abbreviations: SLT, split liver transplantation; WLT, whole liver transplantation. struction and the type of parenchymal transection. Therefore, in partial liver transplantation, reduced-size liver transplantation, SLT, and LDLT, a higher incidence of biliary complications is to be expected Especially in terms of bile leakage from the anastomotic site and late-onset stenosis, the published reports have also noted that the incidence of biliary complications is significantly higher in full right grafts after living-related donation in comparison with WLGs. 27,28 The preservation of the blood supply to the biliary tract at the donor and recipient ends is the major concern in biliary reconstruction because of its significance for a successful biliary anastomosis. An ischemic biliary tract will lead to a critical biliary complication known as an ischemic-type biliary lesion. 29,30 The dissection along the biliary tract should not be close to the wall of the biliary duct so that the fine arterial plexus covering the surface of the biliary tract remains intact and is not damaged. In addition, the right side of the hepatic hilum is normally not dissected. As a result of these technical principles, there is no difference between SLT and WLT in terms of biliary morbidity except for transected surface leakage. In this context, it is noteworthy that in the current study, fatal biliary morbidity in the SLT and WLT groups was similar in the short term and the long term. This result strongly supports the principal approach to using ERGs. In addition, biliary complications are related to the patient s condition, blood type incompatibility, CIT, HAT, and cytomegalovirus infection Among the parameters that we investigated, no factors associated with biliary complications were identified. In particular, it should be emphasized that severe preoperative conditions of the recipient (eg, high MELD score, high urgency, and retransplantation) were not associated with increased biliary complications in the SLT group. In this study, it became clear that bile leakage from the transected surface is the only additional biliary morbidity of SLT in comparison with WLT. Even with visualization of the biliary anatomy by cholangiograms prior to transection or by methylene blue injections into the biliary tree, it is difficult to avoid this complication completely. 36,37 In comparison with the lower incidence of this complication in full right grafts of LDLT, 28,38 the current results show that ERGs have a higher potential risk for biliary leakage from the transected surface. The variant biliary anatomy for segment I or IV may be difficult to recognize without preoperative examination of the biliary tree anatomy. This may be the major reason for the difference between full right grafts of LDLT and ERGs. A compromise to ERGs for adult recipients is more acceptable than a compromise to LLGs for pediatric recipients. Thereafter, the transection planes that ignore strict segmental liver anatomy at the cost of ERGs in order to preserve the relevant vessels of LLGs may be another cause of this difference. Few reports have been published on the risk factors for bile leakage from the transected surface. The decompression of the biliary tract with a T-tube may reduce bile leakage at both the anastomotic site and transected surface. 12 In our practice, on the basis of our experience, we do not use T-drains routinely. Some articles on in situ splitting data show comparable incidences of biliary complications for SLT and WLT. 14,15,39 In addition, for adult living donors who donate an LLG for pediatric transplantation, only very small incidences of bile leakage from the transacted surface have been reported. 40 This may indicate a potential advantage for in situ splitting. For the vast majority of shipped grafts, the donor harvesting operations are performed by transplant teams that are completely independent of and unrelated to the team that performs the recipient operation in Germany. This circumstance may be a confounding factor for the high percentage of ex situ splitting versus in situ splitting. Furthermore, in comparison with in situ splitting, the ex situ procedure of splitting requires much fewer financial and human resources in order to be successful. Because the ex situ
7 736 TAKEBE ET AL. splitting procedure is done in most cases in the transplant center that intends to use the LLGs, acceptance of ERGs by other centers requires a high degree of professional trust in order to overcome skepticism about the quality of the ERGs. The current study clearly shows that this trust must be justified. In several studies, a multivariate analysis of a huge number of liver transplants has demonstrated that split or reduced liver grafts are not significant risk factors for HAT and PNF. 41,42 However, in the current study, the incidence of HAT and PNF was slightly higher in the SLT group than in the WLT group without reaching statistical significance. This observation should not be neglected with respect to the slightly less favorable graft survival curve for SLT, especially in the early postoperative phase. Prolonged CIT is one of the critical risk factors for HAT and PNF. 43,44 The present results show that the SLT group has a significantly prolonged CIT in comparison with the WLT group. In addition, the CIT is extended both by the splitting time itself and, in many cases with shipped ERGs, by the transport time to the center that accepts the ERGs for transplantation. To redress the difference in CIT between SLT and WLT is one of the biggest assignments of ex situ splitting. There are no other reports about ERGs after ex situ splitting for adult recipients with a meaningful number of cases and without recipient selection. Therefore, it is difficult to precisely compare the current data with results published by other transplant centers. In terms of the short-term survival rate, the current data can be compared with the University of California at Los Angeles group (1-year patient/graft survival, 78%/69%), 4 even though in this report only the in situ technique was applied. A comparison of the current results with a report published by the Hamburg group (5-year patient/graft survival, 78.4%/77.3%) 15 and a report published by the Bergamo group (5-year patient/graft survival, 94%/94%) 13 shows room for improvement. The probable reasons for these differences are that at least 50% of their data were based on in situ split transplantation and that more difficult cases such as secondary transplantation were eliminated in both reports. The results of a multicenter analysis for right trisegmental grafts after ex situ splitting from Texas showed a shorter CIT (average CIT, 586 minutes) in ex situ split transplantation in comparison with the current results (average CIT, 747 minutes). 11 Therefore, every effort should be made to shorten the CIT, although that study reported much less favorable long-term patient survival (40%-50% after 5 years) in comparison with the current results. The number of patients with a very severe preoperative condition (MELD 30) was insufficient to reach statistical significance (SLT 8, WLT 8). Nevertheless, the comparable mortality in the 2 groups (SLT 3/8, WLT 3/8) suggests that ERGs have sufficient potential even in very severe situations. In addition, no contraindications have been identified for the use of an ERG for high-risk patients if the clinical circumstances are well balanced. The average MELD score in both groups was around 17. This number seemed to be slightly inconsistent with the average condition of the recipients. For this reason, before the conversion of the allocation rules of ERGs to agree with normal allocation rules with the MELD system in Germany, ERGs are predominately used for recipients with cholestatic disease who have a very small chance of getting a suitable organ graft despite the risk of cholangiocarcinoma and the repeated risk of cholangitis. This study has shown that cholestatic disease is a significant risk factor for bile leakage from the transected surface. Unfortunately, there is no satisfactory explanation for this observation at the moment. It is important to note in this context that there was no significantly higher incidence of late biliary complications in patients with cholestatic disease after the transplantation of ERGs in comparison with WLTs. In conclusion, the use of ERGs contributes significantly to enabling pediatric liver transplantation, and ERGs can be used safely without increased mortality and with acceptable morbidity and should also be considered for retransplantation. The significantly longer CIT in the SLT group indicates a relevant potential for improved results that should be considered in the design of allocation policies and for the distribution of local resources in order to allow simultaneous transplantation of both grafts after liver splitting at the same center. REFERENCES 1. Pichlmayr R, Ringe B, Gubernatis G, Hauss J, Bunzendahl H. Transplantation of a donor liver to 2 recipients (splitting transplantation) a new method in the further development of segmental liver transplantation [in German]. Langenbecks Arch Chir 1988;373: Renz JF, Emond JC, Yersiz H, Ascher NL, Busuttil RW. Split-liver transplantation in the United States: outcomes of a national survey. Ann Surg 2004;239: Mirza DF, Achilleos O, Pirenne J, Buckels JA, McMaster P, Mayer AD. Encouraging results of split-liver transplantation. Br J Surg 1998;85: Yersiz H, Renz JF, Farmer DG, Hisatake GM, McDiarmid SV, Busuttil RW. One hundred in situ split-liver transplantations: a single-center experience. Ann Surg 2003; 238: ; discussion Broering DC, Mueller L, Ganschow R, Kim JS, Achilles EG, Schafer H, et al. Is there still a need for living-related liver transplantation in children? Ann Surg 2001;234: ; discussion Strong RW, Lynch SV, Ong TH, Matsunami H, Koido Y, Balderson GA. Successful liver transplantation from a living donor to her son. N Engl J Med 1990;322: Busuttil RW, Goss JA. Split liver transplantation. Ann Surg 1999;229: Greif F, Bronsther OL, Van Thiel DH, Casavilla A, Iwatsuki S, Tzakis A, et al. The incidence, timing, and management of biliary tract complications after orthotopic liver transplantation. Ann Surg 1994;219: Pascher A, Neuhaus P. Bile duct complications after liver transplantation. Transpl Int 2005;18: Trotter JF, Wachs M, Everson GT, Kam I. Adult-to-adult transplantation of the right hepatic lobe from a living donor. N Engl J Med 2002;346: Washburn K, Halff G, Mieles L, Goldstein R, Goss JA. Split-liver transplantation: results of statewide usage of
8 SAFE USE OF EX SITU EXTENDED RIGHT LIVER GRAFTS 737 the right trisegmental graft. Am J Transplant 2005;5: Wojcicki M, Silva MA, Jethwa P, Gunson B, Bramhall SR, Mayer D, et al. Biliary complications following adult right lobe ex vivo split liver transplantation. Liver Transpl 2006; 12: Corno V, Colledan M, Dezza MC, Guizzetti M, Lucianetti A, Maldini G, et al. Extended right split liver graft for primary transplantation in children and adults. Transpl Int 2006; 19: Broering DC, Topp S, Schaefer U, Fischer L, Gundlach M, Sterneck M, et al. Split liver transplantation and risk to the adult recipient: analysis using matched pairs. J Am Coll Surg 2002;195: Wilms C, Walter J, Kaptein M, Mueller L, Lenk C, Sterneck M, et al. Long-term outcome of split liver transplantation using right extended grafts in adulthood: a matched pair analysis. Ann Surg 2006;244: ; discussion de Ville de Goyet J. Split liver transplantation in Europe 1988 to Transplantation 1995;59: Adam R, McMaster P, O Grady JG, Castaing D, Klempnauer JL, Jamieson N, et al. Evolution of liver transplantation in Europe: report of the European Liver Transplant Registry. Liver Transpl 2003;9: Yan JQ, Becker T, Peng CH, Li HW, Klempnauer J. Split liver transplantation: a reliable approach to expand donor pool. Hepatobiliary Pancreat Dis Int 2005;4: Azoulay D, Astarcioglu I, Bismuth H, Castaing D, Majno P, Adam R, et al. Split-liver transplantation. The Paul Brousse policy. Ann Surg 1996;224: ; discussion Busuttil RW, Colonna JO II, Hiatt JR, Brems JJ, el Khoury G, Goldstein LI, et al. The first 100 liver transplants at UCLA. Ann Surg 1987;206: Sutcliffe R, Maguire D, Mroz A, Portmann B, O Grady J, Bowles M, et al. Bile duct strictures after adult liver transplantation: a role for biliary reconstructive surgery? Liver Transpl 2004;10: Lerut J, Gordon RD, Iwatsuki S, Esquivel CO, Todo S, Tzakis A, et al. Biliary tract complications in human orthotopic liver transplantation. Transplantation 1987;43: Stratta RJ, Wood RP, Langnas AN, Hollins RR, Bruder KJ, Donovan JP, et al. Diagnosis and treatment of biliary tract complications after orthotopic liver transplantation. Surgery 1989;106: ; discussion Noujaim HM, Gunson B, Mayer DA, Mirza DF, Buckels JA, Candinas D, et al. Worth continuing doing ex situ liver graft splitting? A single-center analysis. Am J Transplant 2003;3: Reichert PR, Renz JF, Rosenthal P, Bacchetti P, Lim RC, Roberts JP, et al. Biliary complications of reduced-organ liver transplantation. Liver Transpl Surg 1998;4: Renz JF, Yersiz H, Farmer DG, Hisatake GM, Ghobrial RM, Busuttil RW. Changing faces of liver transplantation: partial-liver grafts for adults. J Hepatobiliary Pancreat Surg 2003;10: Olthoff KM, Merion RM, Ghobrial RM, Abecassis MM, Fair JH, Fisher RA, et al. Outcomes of 385 adult-to-adult living donor liver transplant recipients: a report from the A2ALL consortium. Ann Surg 2005;242: ; discussion Malago M, Testa G, Frilling A, Nadalin S, Valentin-Gamazo C, Paul A, et al. Right living donor liver transplantation: an option for adult patients: single institution experience with 74 patients. Ann Surg 2003;238: ; discussion Schlitt HJ, Meier PN, Nashan B, Oldhafer KJ, Boeker K, Flemming P, et al. Reconstructive surgery for ischemictype lesions at the bile duct bifurcation after liver transplantation. Ann Surg 1999;229: Sanchez-Urdazpal L, Gores GJ, Ward EM, Maus TP, Wahlstrom HE, Moore SB, et al. Ischemic-type biliary complications after orthotopic liver transplantation. Hepatology 1992;16: Tung BY, Kimmey MB. Biliary complications of orthotopic liver transplantation. Dig Dis 1999;17: Colonna JO II, Shaked A, Gomes AS, Colquhoun SD, Jurim O, McDiarmid SV, et al. Biliary strictures complicating liver transplantation. Incidence, pathogenesis, management, and outcome. Ann Surg 1992;216: ; discussion Sanchez-Urdazpal L, Batts KP, Gores GJ, Moore SB, Sterioff S, Wiesner RH, et al. Increased bile duct complications in liver transplantation across the ABO barrier. Ann Surg 1993;218: Abbasoglu O, Levy MF, Vodapally MS, Goldstein RM, Husberg BS, Gonwa TA, et al. Hepatic artery stenosis after liver transplantation incidence, presentation, treatment, and long term outcome. Transplantation 1997;63: Halme L, Hockerstedt K, Lautenschlager I. Cytomegalovirus infection and development of biliary complications after liver transplantation. Transplantation 2003;75: Balzan S, Farges O, Sommacale D, Dondero F, Plasse M, Belghiti J. Direct bile duct visualization during the preparation of split livers. Liver Transpl 2004;10: Goss JA, Yersiz H, Shackleton CR, Seu P, Smith CV, Markowitz JS, et al. In situ splitting of the cadaveric liver for transplantation. Transplantation 1997;64: Miller CM, Gondolesi GE, Florman S, Matsumoto C, Munoz L, Yoshizumi T, et al. One hundred nine living donor liver transplants in adults and children: a single-center experience. Ann Surg 2001;234: ; discussion Spada M, Cescon M, Aluffi A, Zambelli M, Guizzetti M, Lucianetti A, et al. Use of extended right grafts from in situ split livers in adult liver transplantation: a comparison with whole-liver transplants. Transplant Proc 2005;37: Broering DC, Wilms C, Bok P, Fischer L, Mueller L, Hillert C, et al. Evolution of donor morbidity in living related liver transplantation: a single-center analysis of 165 cases. Ann Surg 2004;240: ; discussions Busuttil RW, Farmer DG, Yersiz H, Hiatt JR, McDiarmid SV, Goldstein LI, et al. Analysis of long-term outcomes of 3200 liver transplantations over two decades: a singlecenter experience. Ann Surg 2005;241: ; discussion Kashyap R, Jain A, Reyes J, Demetris AJ, Elmagd KA, Dodson SF, et al. Causes of retransplantation after primary liver transplantation in 4000 consecutive patients: 2 to 19 years follow-up. Transplant Proc 2001;33: Silva MA, Jambulingam PS, Gunson BK, Mayer D, Buckels JA, Mirza DF, et al. Hepatic artery thrombosis following orthotopic liver transplantation: a 10-year experience from a single centre in the United Kingdom. Liver Transpl 2006;12: Stahl JE, Kreke JE, Malek FA, Schaefer AJ, Vacanti J. Consequences of cold-ischemia time on primary nonfunction and patient and graft survival in liver transplantation: a meta-analysis. PLoS ONE 2008;3:e2468.
Split Graft Liver Transplant for Paediatric Patients in Hong Kong
 HK J Paediatr (new series) 2009;14:181-185 Split Graft Liver Transplant for Paediatric Patients in Hong Kong PHY CHUNG, KKY WONG, PKH TAM, KL CHAN, KKC NG, SC CHAN, TWC HUI, BH YONG, ST FAN, CM LO Abstract
HK J Paediatr (new series) 2009;14:181-185 Split Graft Liver Transplant for Paediatric Patients in Hong Kong PHY CHUNG, KKY WONG, PKH TAM, KL CHAN, KKC NG, SC CHAN, TWC HUI, BH YONG, ST FAN, CM LO Abstract
Split liver transplantation and risk to the adult recipient: analysis using matched pairs
 Volume 195, Issue 5, Pages 648-657 (November 2002) Split liver transplantation and risk to the adult recipient: analysis using matched pairs Dieter C. Broering, Stefan Topp, Ulrich Schaefer, Lutz Fischer,
Volume 195, Issue 5, Pages 648-657 (November 2002) Split liver transplantation and risk to the adult recipient: analysis using matched pairs Dieter C. Broering, Stefan Topp, Ulrich Schaefer, Lutz Fischer,
Outcomes in partial liver transplantation: deceased donor split-liver vs. live donor liver transplantation
 DOI:10.1111/j.1477-2574.201360.x HPB ORIGINAL ARTICLE Outcomes in partial liver transplantation: deceased donor split-liver vs. live donor liver transplantation Reza F. Saidi, Nicolas Jabbour, YouFu Li,
DOI:10.1111/j.1477-2574.201360.x HPB ORIGINAL ARTICLE Outcomes in partial liver transplantation: deceased donor split-liver vs. live donor liver transplantation Reza F. Saidi, Nicolas Jabbour, YouFu Li,
Technique of Split-Liver Transplant for Two Adult Recipients
 F'UJIUWA H.EAL,THCAREi, INC. PRESENTS IMAGES mljk?zr 3TUiVU?MAZ7ON Technique of Split-Liver Transplant for Two Adult Recipients Abhinuv Humur, KhuLid Khwuju> Timothy D. SieLu$'John R. Luke, und WiLLium
F'UJIUWA H.EAL,THCAREi, INC. PRESENTS IMAGES mljk?zr 3TUiVU?MAZ7ON Technique of Split-Liver Transplant for Two Adult Recipients Abhinuv Humur, KhuLid Khwuju> Timothy D. SieLu$'John R. Luke, und WiLLium
Vasculobiliary Complications Following Adult Right Lobe Split Liver Transplantation From the Perspective of Reconstruction Techniques
 LIVER TRANSPLANTATION 21:63 71, 2015 ORIGINAL ARTICLE Vasculobiliary Complications Following Adult Right Lobe Split Liver Transplantation From the Perspective of Reconstruction Techniques Moustafa Mabrouk
LIVER TRANSPLANTATION 21:63 71, 2015 ORIGINAL ARTICLE Vasculobiliary Complications Following Adult Right Lobe Split Liver Transplantation From the Perspective of Reconstruction Techniques Moustafa Mabrouk
Outcomes in adult recipients of right-sided liver grafts in split-liver procedures
 DOI:10.1111/j.1477-2574.2009.00147.x HPB ORIGINAL ARTICLE Outcomes in adult recipients of right-sided liver grafts in split-liver procedures Luca Viganò 1 *, Alexis Laurent 1 *, Claude Tayar 1, Jean-Claude
DOI:10.1111/j.1477-2574.2009.00147.x HPB ORIGINAL ARTICLE Outcomes in adult recipients of right-sided liver grafts in split-liver procedures Luca Viganò 1 *, Alexis Laurent 1 *, Claude Tayar 1, Jean-Claude
Surgical Injuries of Postmortem Donor Livers: Incidence and Impact on Outcome After Adult Liver Transplantation
 LIVER TRANSPLANTATION 12:1365-1370, 2006 ORIGINAL ARTICLE Surgical Injuries of Postmortem Donor Livers: Incidence and Impact on Outcome After Adult Liver Transplantation Danielle M. Nijkamp, 1 Maarten
LIVER TRANSPLANTATION 12:1365-1370, 2006 ORIGINAL ARTICLE Surgical Injuries of Postmortem Donor Livers: Incidence and Impact on Outcome After Adult Liver Transplantation Danielle M. Nijkamp, 1 Maarten
Information for patients (and their families) waiting for liver transplantation
 Information for patients (and their families) waiting for liver transplantation Waiting list? What is liver transplant? Postoperative conditions? Ver.: 5/2017 1 What is a liver transplant? Liver transplantation
Information for patients (and their families) waiting for liver transplantation Waiting list? What is liver transplant? Postoperative conditions? Ver.: 5/2017 1 What is a liver transplant? Liver transplantation
Donor Hypernatremia Influences Outcomes Following Pediatric Liver Transplantation
 8 Original Article Donor Hypernatremia Influences Outcomes Following Pediatric Liver Transplantation Neema Kaseje 1 Samuel Lüthold 2 Gilles Mentha 3 Christian Toso 3 Dominique Belli 2 Valérie McLin 2 Barbara
8 Original Article Donor Hypernatremia Influences Outcomes Following Pediatric Liver Transplantation Neema Kaseje 1 Samuel Lüthold 2 Gilles Mentha 3 Christian Toso 3 Dominique Belli 2 Valérie McLin 2 Barbara
Predicted Lifetimes for Adult and Pediatric Split Liver Versus Adult Whole Liver Transplant Recipients
 American Journal of Transplantation 2004; 4: 1792 1797 Blackwell Munksgaard Copyright C Blackwell Munksgaard 2004 doi: 10.1111/j.1600-6143.2004.00594.x Predicted Lifetimes for Adult and Pediatric Split
American Journal of Transplantation 2004; 4: 1792 1797 Blackwell Munksgaard Copyright C Blackwell Munksgaard 2004 doi: 10.1111/j.1600-6143.2004.00594.x Predicted Lifetimes for Adult and Pediatric Split
Results of Choledochojejunostomy in the Treatment of Biliary Complications After Liver Transplantation in the Era of Nonsurgical Therapies
 Results of Choledochojejunostomy in the Treatment of Biliary Complications After Liver Transplantation in the Era of Nonsurgical Therapies Brian R. Davidson, Rakesh Rai, Ashim Nandy, Nilesh Doctor, Andrew
Results of Choledochojejunostomy in the Treatment of Biliary Complications After Liver Transplantation in the Era of Nonsurgical Therapies Brian R. Davidson, Rakesh Rai, Ashim Nandy, Nilesh Doctor, Andrew
The New England Journal of Medicine. Review Article 16,000 14,000 12,000. No. of Patients 10,000 8,000 6,000 4,000 2,000
 Review Article Medical Progress ADULT-TO-ADULT TRANSPLANTATION OF THE RIGHT HEPATIC LOBE FROM A LIVING DONOR JAMES F. TROTTER, M.D., MICHAEL WACHS, M.D., GREGORY T. EVERSON, M.D., AND IGAL KAM, M.D. TRANSPLANTATION
Review Article Medical Progress ADULT-TO-ADULT TRANSPLANTATION OF THE RIGHT HEPATIC LOBE FROM A LIVING DONOR JAMES F. TROTTER, M.D., MICHAEL WACHS, M.D., GREGORY T. EVERSON, M.D., AND IGAL KAM, M.D. TRANSPLANTATION
Outcomes of Full-Right-Full-Left Split Liver Transplantation in Adults in the USA: A Propensity-Score Matched Analysis
 Outcomes of Full-Right-Full-Left Split Liver Transplantation in Adults in the USA: A Propensity-Score Matched Analysis The Harvard community has made this article openly available. Please share how this
Outcomes of Full-Right-Full-Left Split Liver Transplantation in Adults in the USA: A Propensity-Score Matched Analysis The Harvard community has made this article openly available. Please share how this
Ischemic-type biliary lesions (ITBL) are reported to. Prevention of Ischemic-Type Biliary Lesions by Arterial Back-Table Pressure Perfusion
 Prevention of Ischemic-Type Biliary Lesions by Arterial Back-Table Pressure Perfusion Christian Moench, * Kerstin Moench, Ansgar W. Lohse, Jochen Thies, * and Gerd Otto * Ischemic-type biliary lesions
Prevention of Ischemic-Type Biliary Lesions by Arterial Back-Table Pressure Perfusion Christian Moench, * Kerstin Moench, Ansgar W. Lohse, Jochen Thies, * and Gerd Otto * Ischemic-type biliary lesions
With the spread of orthotopic liver transplantation
 Original Article / Transplantation Liver retransplantation for ischemic-type biliary lesions after orthotopic liver transplantation: a clinical report of 66 cases Zhi-Jun Zhu, Wei Rao, Ji-San Sun, Jin-Zhen
Original Article / Transplantation Liver retransplantation for ischemic-type biliary lesions after orthotopic liver transplantation: a clinical report of 66 cases Zhi-Jun Zhu, Wei Rao, Ji-San Sun, Jin-Zhen
Biliary Anatomy in Living-related Liver Transplantation
 The 5th IHPBA Congress - Istanbul Biliary Anatomy in Living-related Liver Transplantation biliary trees hilar plate Assessment for Vascular Anatomy 1. 3DCT portal vein hepatic vein hepatic artery 2. No
The 5th IHPBA Congress - Istanbul Biliary Anatomy in Living-related Liver Transplantation biliary trees hilar plate Assessment for Vascular Anatomy 1. 3DCT portal vein hepatic vein hepatic artery 2. No
pitfall Table 1 4 disorientation pitfall pitfall Table 1 Tel:
 11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
The pediatric end-stage liver disease (PELD) score
 Selection of Pediatric Candidates Under the PELD System Sue V. McDiarmid, 1 Robert M. Merion, 2 Dawn M. Dykstra, 2 and Ann M. Harper 3 Key Points 1. The PELD score accurately predicts the 3 month probability
Selection of Pediatric Candidates Under the PELD System Sue V. McDiarmid, 1 Robert M. Merion, 2 Dawn M. Dykstra, 2 and Ann M. Harper 3 Key Points 1. The PELD score accurately predicts the 3 month probability
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,700 108,500 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,700 108,500 1.7 M Open access books available International authors and editors Downloads Our
Liver Transplantation in Children: Techniques and What the Surgeon Wants to Know from Imaging
 Liver Transplantation in Children: Techniques and What the Surgeon Wants to Know from Imaging Jaimie D. Nathan, MD Associate Professor of Surgery and Pediatrics Associate Surgical Director, Liver Transplant
Liver Transplantation in Children: Techniques and What the Surgeon Wants to Know from Imaging Jaimie D. Nathan, MD Associate Professor of Surgery and Pediatrics Associate Surgical Director, Liver Transplant
Liver Transplantation
 1 Liver Transplantation Department of Surgery Yonsei University Wonju College of Medicine Kim Myoung Soo M.D. ysms91@wonju.yonsei.ac.kr http://gs.yonsei.ac.kr History Development of Liver transplantation
1 Liver Transplantation Department of Surgery Yonsei University Wonju College of Medicine Kim Myoung Soo M.D. ysms91@wonju.yonsei.ac.kr http://gs.yonsei.ac.kr History Development of Liver transplantation
ORIGINAL ARTICLE. Received April 30, 2007; accepted June
 LIVER TRANSPLANTATION 13:1405-1413, 2007 ORIGINAL ARTICLE Human Leukocyte Antigen and Adult Living- Donor Liver Transplantation Outcomes: An Analysis of the Organ Procurement and Transplantation Network
LIVER TRANSPLANTATION 13:1405-1413, 2007 ORIGINAL ARTICLE Human Leukocyte Antigen and Adult Living- Donor Liver Transplantation Outcomes: An Analysis of the Organ Procurement and Transplantation Network
Long-term Outcomes After Third Liver Transplant
 ArtıcLe Long-term Outcomes After Third Liver Transplant C. Burcin Taner, 1 Deniz Balci, 1 Darrin L. Willingham, 1 Andrew P. Keaveny, 1 Barry G. Rosser, 1 Juan M. Canabal, 1 Timothy S. J. Shine, 2 Denise
ArtıcLe Long-term Outcomes After Third Liver Transplant C. Burcin Taner, 1 Deniz Balci, 1 Darrin L. Willingham, 1 Andrew P. Keaveny, 1 Barry G. Rosser, 1 Juan M. Canabal, 1 Timothy S. J. Shine, 2 Denise
Liver retransplantation for adult recipients
 Korean J Hepatobiliary Pancreat Surg 2013;17:1-7 Review Article Liver retransplantation for adult recipients Shin Hwang, Chul-Soo Ahn, Ki-Hun Kim, Deok-Bog Moon, Tae-Yong Ha, Gi-Won Song, Dong-Hwan Jung,
Korean J Hepatobiliary Pancreat Surg 2013;17:1-7 Review Article Liver retransplantation for adult recipients Shin Hwang, Chul-Soo Ahn, Ki-Hun Kim, Deok-Bog Moon, Tae-Yong Ha, Gi-Won Song, Dong-Hwan Jung,
Adult-to-adult living donor liver transplantation Triumphs and challenges
 Falk Symposium No. 163 on Chronic Inflammation of Liver and Gut Adult-to-adult living donor liver transplantation Triumphs and challenges ST Fan, MS, MD, PhD, DSc Professor Sun CY Chair of Hepatobiliary
Falk Symposium No. 163 on Chronic Inflammation of Liver and Gut Adult-to-adult living donor liver transplantation Triumphs and challenges ST Fan, MS, MD, PhD, DSc Professor Sun CY Chair of Hepatobiliary
For the past two decades, the number of patients
 When Shouldn t We Retransplant? Michael A. Zimmerman and R. Mark Ghobrial Key Points 1. In the setting of early graft failure after primary transplantation, orthotopic liver retransplantation (re-olt)
When Shouldn t We Retransplant? Michael A. Zimmerman and R. Mark Ghobrial Key Points 1. In the setting of early graft failure after primary transplantation, orthotopic liver retransplantation (re-olt)
Pediatric Liver Transplantation Outcomes in Korea
 ORIGINAL ARTICLE Cell Therapy & Organ Transplantation http://dx.doi.org/6/jkms.8..4 J Korean Med Sci 0; 8: 4-47 Pediatric Liver Transplantation Outcomes in Korea Jong Man Kim,, * Kyung Mo Kim,, * Nam-Joon
ORIGINAL ARTICLE Cell Therapy & Organ Transplantation http://dx.doi.org/6/jkms.8..4 J Korean Med Sci 0; 8: 4-47 Pediatric Liver Transplantation Outcomes in Korea Jong Man Kim,, * Kyung Mo Kim,, * Nam-Joon
CHEN AND DE VILLA have recently reported their experience in performing splits in donors older than 50 years. 11 Their results were favourable; surviv
 SPLIT LIVER TRANSPLANTATION Asian Journal of Surgery Excerpta Medica Asia Ltd Split Liver Transplantation Chao-Long Chen and Vanessa H. de Villa, Liver Transplant Program, Department of Surgery, Chang
SPLIT LIVER TRANSPLANTATION Asian Journal of Surgery Excerpta Medica Asia Ltd Split Liver Transplantation Chao-Long Chen and Vanessa H. de Villa, Liver Transplant Program, Department of Surgery, Chang
Citation Transplantation Proceedings, 47(3),
 NAOSITE: Nagasaki University's Ac Title Author(s) Hybrid Procedure in Living Donor Li Soyama, Akihiko; Takatsuki, Mitsuhi Tomohiko; Kitasato, Amane; Kinoshit Baimakhanov, Zhassulan; Kuroki, Tam Citation
NAOSITE: Nagasaki University's Ac Title Author(s) Hybrid Procedure in Living Donor Li Soyama, Akihiko; Takatsuki, Mitsuhi Tomohiko; Kitasato, Amane; Kinoshit Baimakhanov, Zhassulan; Kuroki, Tam Citation
Classification and Prognosis of Intrahepatic Biliary Stricture After Liver Transplantation
 LIVER TRANSPLANTATION 13:1736-1742, 2007 ORIGINAL ARTICLE Classification and Prognosis of Intrahepatic Biliary Stricture After Liver Transplantation Hae Won Lee, 1 Kyung-Suk Suh, 1 Woo Young Shin, 1 Eung-Ho
LIVER TRANSPLANTATION 13:1736-1742, 2007 ORIGINAL ARTICLE Classification and Prognosis of Intrahepatic Biliary Stricture After Liver Transplantation Hae Won Lee, 1 Kyung-Suk Suh, 1 Woo Young Shin, 1 Eung-Ho
OPERATIVE TECHNIQUES AND HAZARDS
 OPERATIVE TECHNIQUES AND HAZARDS CHRIS O SULLIVAN MD FRCSI CONSULTANT HBP AND LIVER TRANSPLANT SURGEON FREEMAN HOSPITAL, N-UPON-TYNE CAVAL RECONSTRUCTION IN ORTHOTOPIC LIVER TRANSPLANTATION RESECTION OF
OPERATIVE TECHNIQUES AND HAZARDS CHRIS O SULLIVAN MD FRCSI CONSULTANT HBP AND LIVER TRANSPLANT SURGEON FREEMAN HOSPITAL, N-UPON-TYNE CAVAL RECONSTRUCTION IN ORTHOTOPIC LIVER TRANSPLANTATION RESECTION OF
Twenty Years of Follow-Up of Aortohepatic Conduits in Liver Transplantation
 LIVER TRANSPLANTATION 14:1486-1490, 2008 ORIGINAL ARTICLE Twenty Years of Follow-Up of Aortohepatic s in Liver Transplantation Dmitriy Nikitin, Linda W. Jennings, Tariq Khan, Edmund Q. Sanchez, Srinath
LIVER TRANSPLANTATION 14:1486-1490, 2008 ORIGINAL ARTICLE Twenty Years of Follow-Up of Aortohepatic s in Liver Transplantation Dmitriy Nikitin, Linda W. Jennings, Tariq Khan, Edmund Q. Sanchez, Srinath
Removing Patients from the Liver Transplant Wait List: A Survey of US Liver Transplant Programs
 LIVER TRANSPLANTATION 14:303-307, 2008 ORIGINAL ARTICLE Removing Patients from the Liver Transplant Wait List: A Survey of US Liver Transplant Programs Kevin P. Charpentier 1 and Arun Mavanur 2 1 Rhode
LIVER TRANSPLANTATION 14:303-307, 2008 ORIGINAL ARTICLE Removing Patients from the Liver Transplant Wait List: A Survey of US Liver Transplant Programs Kevin P. Charpentier 1 and Arun Mavanur 2 1 Rhode
Current State of Living Donor Liver Transplantation
 REVIEW Current State of Living Donor Liver Transplantation Paige M. Porret, Kim M. Olthoff The discrepancy between the number of patients waiting for a liver and the available number of deceased donors
REVIEW Current State of Living Donor Liver Transplantation Paige M. Porret, Kim M. Olthoff The discrepancy between the number of patients waiting for a liver and the available number of deceased donors
One of the most important problems for patients
 Selection of Donors and Recipients for Living Donor Liver Transplantation Key Points 1. Living donor liver transplantation (LDLT) is increasingly used for adults with end-stage liver disease. 2. Standards
Selection of Donors and Recipients for Living Donor Liver Transplantation Key Points 1. Living donor liver transplantation (LDLT) is increasingly used for adults with end-stage liver disease. 2. Standards
Significant allograft dysfunction after liver transplantation
 Bile Duct Strictures After Adult Liver Transplantation: A Role for Biliary Reconstructive Surgery? Robert Sutcliffe, 1 Donal Maguire, 1 Andrej Mróz, 2 Bernard Portmann, 1 John O Grady, 1 Matthew Bowles,
Bile Duct Strictures After Adult Liver Transplantation: A Role for Biliary Reconstructive Surgery? Robert Sutcliffe, 1 Donal Maguire, 1 Andrej Mróz, 2 Bernard Portmann, 1 John O Grady, 1 Matthew Bowles,
Predictors of cardiac allograft vasculopathy in pediatric heart transplant recipients
 Pediatr Transplantation 2013: 17: 436 440 2013 John Wiley & Sons A/S. Pediatric Transplantation DOI: 10.1111/petr.12095 Predictors of cardiac allograft vasculopathy in pediatric heart transplant recipients
Pediatr Transplantation 2013: 17: 436 440 2013 John Wiley & Sons A/S. Pediatric Transplantation DOI: 10.1111/petr.12095 Predictors of cardiac allograft vasculopathy in pediatric heart transplant recipients
POST TRANSPLANT OUTCOMES IN PSC
 POST TRANSPLANT OUTCOMES IN PSC Kidist K. Yimam, MD Medical Director, Autoimmune Liver Disease Program Division of Hepatology and Liver Transplantation California Pacific Medical Center (CPMC) PSC Partners
POST TRANSPLANT OUTCOMES IN PSC Kidist K. Yimam, MD Medical Director, Autoimmune Liver Disease Program Division of Hepatology and Liver Transplantation California Pacific Medical Center (CPMC) PSC Partners
Induction Immunosuppression With Rabbit Antithymocyte Globulin in Pediatric Liver Transplantation
 LIVER TRANSPLANTATION 12:1210-1214, 2006 ORIGINAL ARTICLE Induction Immunosuppression With Rabbit Antithymocyte Globulin in Pediatric Liver Transplantation Ashesh Shah, 1 Avinash Agarwal, 1 Richard Mangus,
LIVER TRANSPLANTATION 12:1210-1214, 2006 ORIGINAL ARTICLE Induction Immunosuppression With Rabbit Antithymocyte Globulin in Pediatric Liver Transplantation Ashesh Shah, 1 Avinash Agarwal, 1 Richard Mangus,
Surgical management of HCC. Evangelos Prassas Hepatobiliary and Pancreatic Surgery / Liver Transplantation Kings College Hospital / London
 Surgical management of HCC Evangelos Prassas Hepatobiliary and Pancreatic Surgery / Liver Transplantation Kings College Hospital / London Global distribution of HCC and staging systems WEST 1. Italy (Milan,
Surgical management of HCC Evangelos Prassas Hepatobiliary and Pancreatic Surgery / Liver Transplantation Kings College Hospital / London Global distribution of HCC and staging systems WEST 1. Italy (Milan,
Liver Splitting During Normothermic Organ Preservation
 LETTERS FROM THE FRONTLINE Liver Splitting During Normothermic Organ Preservation TO THE EDITOR: Although widely established as a means to increase the number of patients who can benefit from transplantation,
LETTERS FROM THE FRONTLINE Liver Splitting During Normothermic Organ Preservation TO THE EDITOR: Although widely established as a means to increase the number of patients who can benefit from transplantation,
Studies on bile duct Injury and the protective role of oxygenated machine perfusion in liver transplantation Karimian, Negin
 University of Groningen Studies on bile duct Injury and the protective role of oxygenated machine perfusion in liver transplantation Karimian, Negin IMPORTANT NOTE: You are advised to consult the publisher's
University of Groningen Studies on bile duct Injury and the protective role of oxygenated machine perfusion in liver transplantation Karimian, Negin IMPORTANT NOTE: You are advised to consult the publisher's
Liver transplantation for hepatocellular carcinoma with live donors or extended criteria donors: a propensity score-matched comparison
 ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 722-727 Liver transplantation for hepatocellular carcinoma with live donors or extended criteria donors: a propensity score-matched comparison Georgios
ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 722-727 Liver transplantation for hepatocellular carcinoma with live donors or extended criteria donors: a propensity score-matched comparison Georgios
Late Surgical Complications Following Liver Transplantation
 LIVER TRANSPLANTATION 15:S12-S18, 2009 AASLD/ILTS SYLLABUS Late Surgical Complications Following Liver Transplantation Paige M. Porrett, John Hsu, and Abraham Shaked Division of Transplantation, Department
LIVER TRANSPLANTATION 15:S12-S18, 2009 AASLD/ILTS SYLLABUS Late Surgical Complications Following Liver Transplantation Paige M. Porrett, John Hsu, and Abraham Shaked Division of Transplantation, Department
Living Donor Liver Transplantation for Hepatocellular Carcinoma: It Is All about Donors?
 Original Article Living Donor Liver Transplantation for Hepatocellular Carcinoma: It Is All about Donors? R. F. Saidi 1 *, Y. Li 2, S. A. Shah 2, N. Jabbour 2 1 Division of Organ Transplantation, Department
Original Article Living Donor Liver Transplantation for Hepatocellular Carcinoma: It Is All about Donors? R. F. Saidi 1 *, Y. Li 2, S. A. Shah 2, N. Jabbour 2 1 Division of Organ Transplantation, Department
Surgery for hilar cholangiocirconoma
 Department of Surgery University Hospital RWTH Aachen Surgery for hilar cholangiocirconoma Ulf Peter Neumann Agenda Operating on the most complex tumor in HBP Surgery Preoperative management Does the patient
Department of Surgery University Hospital RWTH Aachen Surgery for hilar cholangiocirconoma Ulf Peter Neumann Agenda Operating on the most complex tumor in HBP Surgery Preoperative management Does the patient
Liver transplantation is a gold standard of therapy. Estimation of Standard Liver Volume for Liver Transplantation in the Korean Population
 Estimation of Standard Liver Volume for Liver Transplantation in the Korean Population Hee Chul Yu, 1,2 Heecheon You, 3 Ho Lee, 4 Zhe-Wu Jin, 1 Jang Il Moon, 5 and Baik Hwan Cho 1,2 The standard liver
Estimation of Standard Liver Volume for Liver Transplantation in the Korean Population Hee Chul Yu, 1,2 Heecheon You, 3 Ho Lee, 4 Zhe-Wu Jin, 1 Jang Il Moon, 5 and Baik Hwan Cho 1,2 The standard liver
Peri-operative challenges and long-term outcomes in liver transplantation for polycystic liver disease
 DOI:10.1111/j.1477-2574.2012.00579.x HPB ORIGINAL ARTICLE Peri-operative challenges and long-term outcomes in liver transplantation for polycystic liver disease Roberto Gedaly, Paige Guidry, Daniel Davenport,
DOI:10.1111/j.1477-2574.2012.00579.x HPB ORIGINAL ARTICLE Peri-operative challenges and long-term outcomes in liver transplantation for polycystic liver disease Roberto Gedaly, Paige Guidry, Daniel Davenport,
Survival Outcomes Following Liver Transplantation (SOFT) Score: A Novel Method to Predict Patient Survival Following Liver Transplantation
 American Journal of Transplantation 2008; 8: 2537 2546 Wiley Periodicals Inc. C 2008 The Authors Journal compilation C 2008 The American Society of Transplantation and the American Society of Transplant
American Journal of Transplantation 2008; 8: 2537 2546 Wiley Periodicals Inc. C 2008 The Authors Journal compilation C 2008 The American Society of Transplantation and the American Society of Transplant
Biliary Complications in Liver Transplantation
 10 Biliary Complications in Liver Transplantation Ilka de Fatima Santana Ferreira Boin, Fernando Romani de Araujo, Elaine Cristina de Ataide, Anaisa Portes Ramos and Ciro Garcia Montes Unit of Liver Transplantation
10 Biliary Complications in Liver Transplantation Ilka de Fatima Santana Ferreira Boin, Fernando Romani de Araujo, Elaine Cristina de Ataide, Anaisa Portes Ramos and Ciro Garcia Montes Unit of Liver Transplantation
Original article: new surgical approaches to the Klatskin tumour
 Alimentary Pharmacology & Therapeutics Original article: new surgical approaches to the Klatskin tumour T. M. VAN GULIK*, S. DINANT*, O. R. C. BUSCH*, E. A. J. RAUWS, H. OBERTOP* & D. J. GOUMA Departments
Alimentary Pharmacology & Therapeutics Original article: new surgical approaches to the Klatskin tumour T. M. VAN GULIK*, S. DINANT*, O. R. C. BUSCH*, E. A. J. RAUWS, H. OBERTOP* & D. J. GOUMA Departments
Successful Application of Supraceliac Aortohepatic Conduit Using Saphenous Venous Graft in Right Lobe Living Donor Liver Transplantation
 LETTERS FROM THE FRONTLINE Successful Application of Supraceliac Aortohepatic Conduit Using Saphenous Venous Graft in Right Lobe Living Donor Liver Transplantation TO THE EDITOR: Hepatic artery (HA) reconstruction
LETTERS FROM THE FRONTLINE Successful Application of Supraceliac Aortohepatic Conduit Using Saphenous Venous Graft in Right Lobe Living Donor Liver Transplantation TO THE EDITOR: Hepatic artery (HA) reconstruction
Liver Transplantation for Alcoholic Liver Disease in the United States: 1988 to 1995
 Liver Transplantation for Alcoholic Liver Disease in the United States: 1988 to 1995 Steven H. Belle, Kimberly C. Beringer, and Katherine M. Detre T he Scientific Liver Transplant Registry (LTR) was established
Liver Transplantation for Alcoholic Liver Disease in the United States: 1988 to 1995 Steven H. Belle, Kimberly C. Beringer, and Katherine M. Detre T he Scientific Liver Transplant Registry (LTR) was established
Liver Transplantation for Biliary Atresia: 19-Year, Single-Center Experience
 Liver Transplantation for Biliary Atresia: 19-Year, Single-Center Experience L Thomas Chin 1, Anthony M D Alessandro 1, Stuart J Knechtle 1, Luis A Fernandez 1, Glen Leverson 1, Robert H Judd 2, Elizabeth
Liver Transplantation for Biliary Atresia: 19-Year, Single-Center Experience L Thomas Chin 1, Anthony M D Alessandro 1, Stuart J Knechtle 1, Luis A Fernandez 1, Glen Leverson 1, Robert H Judd 2, Elizabeth
A Matched Pair Analysis of Multicenter Longterm Follow-up After Split-Liver Transplantation With Extended Right Grafts
 ORIGINAL ARTICLE A Matched Pair Analysis of Multicenter Longterm Follow-up After Split-Liver Transplantation With Extended Right Grafts Mitchell W. Ross, 1 Matteo Cescon, 2 Roberta Angelico, 3 Enzo Andorno,
ORIGINAL ARTICLE A Matched Pair Analysis of Multicenter Longterm Follow-up After Split-Liver Transplantation With Extended Right Grafts Mitchell W. Ross, 1 Matteo Cescon, 2 Roberta Angelico, 3 Enzo Andorno,
In-situ v Normothermic Regional Perfusion for Abdominal Organs
 In-situ v Normothermic Regional Perfusion for Abdominal Organs ANGEL RUIZ M.D. DONATION AND TRANSPLNAT COORDINATION UNIT MEDICAL DIRECTION HOSPITAL CLÍNIC DE BARCELONA Introduction Donation after circulatory
In-situ v Normothermic Regional Perfusion for Abdominal Organs ANGEL RUIZ M.D. DONATION AND TRANSPLNAT COORDINATION UNIT MEDICAL DIRECTION HOSPITAL CLÍNIC DE BARCELONA Introduction Donation after circulatory
Variations in Surgical Anatomy of the Portal Vein in Living Donor Liver Transplantation
 Kasr El Aini Journal of Surgery VOL., 9, NO 3 January 2008 19 Variations in Surgical Anatomy of the Portal Vein in Living Donor Liver Transplantation A. Ayad ; W. Tobar; M.Hassan; A.Hosny; M.El Shazly;
Kasr El Aini Journal of Surgery VOL., 9, NO 3 January 2008 19 Variations in Surgical Anatomy of the Portal Vein in Living Donor Liver Transplantation A. Ayad ; W. Tobar; M.Hassan; A.Hosny; M.El Shazly;
Postoperative Hyperbilirubinemia and Graft Outcome in Living Donor Liver Transplantation
 LIVER TRANSPLANTATION 13:1538-1544, 2007 ORIGINAL ARTICLE Postoperative Hyperbilirubinemia and Graft Outcome in Living Donor Liver Transplantation Shigeru Marubashi, Keizo Dono, Hiroaki Nagano, Tadafumi
LIVER TRANSPLANTATION 13:1538-1544, 2007 ORIGINAL ARTICLE Postoperative Hyperbilirubinemia and Graft Outcome in Living Donor Liver Transplantation Shigeru Marubashi, Keizo Dono, Hiroaki Nagano, Tadafumi
Split Versus Whole Liver Transplantation
 Split Versus Whole Liver Transplantation OPTN/UNOS Ethics Committee Prepared by: Lee Bolton UNOS Policy Department Executive Summary... 1 What problem will this resource solve?... 1 Why should you support
Split Versus Whole Liver Transplantation OPTN/UNOS Ethics Committee Prepared by: Lee Bolton UNOS Policy Department Executive Summary... 1 What problem will this resource solve?... 1 Why should you support
Liver Transplantation Using Donation After Cardiac Death Donors: Long-Term Follow-Up from a Single Center
 American Journal of Transplantation 2009; 9: 773 781 Wiley Periodicals Inc. C 2009 The Authors Journal compilation C 2009 The American Society of Transplantation and the American Society of Transplant
American Journal of Transplantation 2009; 9: 773 781 Wiley Periodicals Inc. C 2009 The Authors Journal compilation C 2009 The American Society of Transplantation and the American Society of Transplant
I number of factors, including donor and recipient
 Contribution of True Cold and Rewarming - Ischemia Times to Factors Determining Outcome After Orthotopic liver Transplantation Teerha Piratvisuth, J. Michael Tredger, Karen A. Hayllar, and Roger Williams
Contribution of True Cold and Rewarming - Ischemia Times to Factors Determining Outcome After Orthotopic liver Transplantation Teerha Piratvisuth, J. Michael Tredger, Karen A. Hayllar, and Roger Williams
Perioperative Events in Living and Deceased Donor Liver Transplant Recipients: A Case Control Study
 8 The Open Transplantation Journal, 2011, 5, 8-14 Open Access Perioperative Events in Living and Deceased Donor Liver Transplant Recipients: A Case Control Study Bhargavi Gali *,1, David J. Plevak 1, David
8 The Open Transplantation Journal, 2011, 5, 8-14 Open Access Perioperative Events in Living and Deceased Donor Liver Transplant Recipients: A Case Control Study Bhargavi Gali *,1, David J. Plevak 1, David
What Is the Real Gain After Liver Transplantation?
 LIVER TRANSPLANTATION 15:S1-S5, 9 AASLD/ILTS SYLLABUS What Is the Real Gain After Liver Transplantation? James Neuberger Organ Donation and Transplantation, NHS Blood and Transplant, Bristol, United Kingdom;
LIVER TRANSPLANTATION 15:S1-S5, 9 AASLD/ILTS SYLLABUS What Is the Real Gain After Liver Transplantation? James Neuberger Organ Donation and Transplantation, NHS Blood and Transplant, Bristol, United Kingdom;
Readmission to the hospital after discharge is an important
 Defining Readmission Risk Factors for Liver Transplantation Recipients Neil Shankar, Paul Marotta, MD, William Wall, MD, Mamoun AlBasheer, MD, Roberto Hernandez-Alejandro, MD, and Natasha Chandok, MD,
Defining Readmission Risk Factors for Liver Transplantation Recipients Neil Shankar, Paul Marotta, MD, William Wall, MD, Mamoun AlBasheer, MD, Roberto Hernandez-Alejandro, MD, and Natasha Chandok, MD,
Extensive Use of Split Liver for Pediatric Liver Transplantation: A Single-Center Experience
 ORIGINAL ARTICLES Extensive Use of Split Liver for Pediatric Liver Transplantation: A Single-Center Experience Marco Spada, Bruno Gridelli, Michele Colledan, Andrea Segalin, Alessandro Lucianetti, Wanda
ORIGINAL ARTICLES Extensive Use of Split Liver for Pediatric Liver Transplantation: A Single-Center Experience Marco Spada, Bruno Gridelli, Michele Colledan, Andrea Segalin, Alessandro Lucianetti, Wanda
Liver Transplantation
 Liver Transplantation Dr Mathew Jacob - MRCS FRCS CCT (UK) Lead Consultant HPB/Transplant Surgeon Aster Integrated Liver Care Program AsterMedcity, kochi, kerala, India mathew@transplantationliver.com
Liver Transplantation Dr Mathew Jacob - MRCS FRCS CCT (UK) Lead Consultant HPB/Transplant Surgeon Aster Integrated Liver Care Program AsterMedcity, kochi, kerala, India mathew@transplantationliver.com
Liver Transplantation Following Donation After Cardiac Death: An Analysis Using Matched Pairs
 LIVER TRANSPLANTATION 15:1072-1082, 2009 ORIGINAL ARTICLE Liver Transplantation Following Donation After Cardiac Death: An Analysis Using Matched Pairs James K. Pine, Amer Aldouri, Alistair L. Young, Mervyn
LIVER TRANSPLANTATION 15:1072-1082, 2009 ORIGINAL ARTICLE Liver Transplantation Following Donation After Cardiac Death: An Analysis Using Matched Pairs James K. Pine, Amer Aldouri, Alistair L. Young, Mervyn
Anne Barkman. The University of Kansas School of Nursing
 Expanding Donor Criteria: Is it Safe? Anne Barkman The University of Kansas School of Nursing About the author: Anne Barkman is from Leawood, Kansas. She was an academic honor roll recipient for Fall 2010,
Expanding Donor Criteria: Is it Safe? Anne Barkman The University of Kansas School of Nursing About the author: Anne Barkman is from Leawood, Kansas. She was an academic honor roll recipient for Fall 2010,
Living donor liver transplantation: Eastern experiences
 Living donor liver transplantation: Eastern experiences K Tanaka 1, Y Ogura 1, T Kiuchi 1, Y Inomata 2, S Uemoto 3 and H Furukawa 4 "Deportment of Transplantation and Immunology, Kyoto University Hospital,
Living donor liver transplantation: Eastern experiences K Tanaka 1, Y Ogura 1, T Kiuchi 1, Y Inomata 2, S Uemoto 3 and H Furukawa 4 "Deportment of Transplantation and Immunology, Kyoto University Hospital,
Living related donor liver transplantation in Iranian children: a 12- year experience
 Gastroenterology and Hepatology From Bed to Bench. 2013 RIGLD, Research Institute for Gastroenterology and Liver Diseases ORIGINAL ARTICLE Living related donor liver transplantation in Iranian children:
Gastroenterology and Hepatology From Bed to Bench. 2013 RIGLD, Research Institute for Gastroenterology and Liver Diseases ORIGINAL ARTICLE Living related donor liver transplantation in Iranian children:
Fifteen Years and 382 Extended Right Grafts From In Situ Split Livers in a Multicenter Study: Are These Still Extended Criteria Liver Grafts?
 LIVER TRANSPLANTATION 21:500 511, 2015 ORIGINAL ARTICLE Fifteen Years and 382 Extended Right Grafts From In Situ Split Livers in a Multicenter Study: Are These Still Extended Criteria Liver Grafts? Umberto
LIVER TRANSPLANTATION 21:500 511, 2015 ORIGINAL ARTICLE Fifteen Years and 382 Extended Right Grafts From In Situ Split Livers in a Multicenter Study: Are These Still Extended Criteria Liver Grafts? Umberto
Surgical Management of CBD Injury Jin Seok Heo
 Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
LIVER TRANSPLANTATION FOR OVERLAP SYNDROMES OF AUTOIMMUNE LIVER DISEASES
 LIVER TRANSPLANTATION FOR OVERLAP SYNDROMES OF AUTOIMMUNE LIVER DISEASES No conflict of interest Objectives Introduction Methods Results Conclusions Objectives Introduction Methods Results Conclusions
LIVER TRANSPLANTATION FOR OVERLAP SYNDROMES OF AUTOIMMUNE LIVER DISEASES No conflict of interest Objectives Introduction Methods Results Conclusions Objectives Introduction Methods Results Conclusions
Liver transplantation is the only hope for patients with terminal. Indication and Prognosis of Liver Transplantation. Abstract
 Indication and Prognosis of Liver Transplantation Jae Won Joh, M.D. Department of General Surgery Sungkyunkwan University School of Medicine Samsung Medical Center E mail: jwjoh@smc.samsung.co.kr Abstract
Indication and Prognosis of Liver Transplantation Jae Won Joh, M.D. Department of General Surgery Sungkyunkwan University School of Medicine Samsung Medical Center E mail: jwjoh@smc.samsung.co.kr Abstract
Living-donor liver transplantation European experiences
 Nephrol Dial Transplant (2004) 19 [Suppl 4]: iv16 iv21 doi:10.1093/ndt/gfh1036 Living-donor liver transplantation European experiences Utz Settmacher, Tom Theruvath, Andreas Pascher and Peter Neuhaus Department
Nephrol Dial Transplant (2004) 19 [Suppl 4]: iv16 iv21 doi:10.1093/ndt/gfh1036 Living-donor liver transplantation European experiences Utz Settmacher, Tom Theruvath, Andreas Pascher and Peter Neuhaus Department
The first liver transplant in a human was performed
 Liver Transplantation With Monosegments. Technical Aspects and Outcome: A Meta-Analysis Marcelo Enne, 1 Lucio Pacheco-Moreira, 1 Elizabeth Balbi, 2 Alexandre Cerqueira, 1 Giuseppe Santalucia, 3 and José
Liver Transplantation With Monosegments. Technical Aspects and Outcome: A Meta-Analysis Marcelo Enne, 1 Lucio Pacheco-Moreira, 1 Elizabeth Balbi, 2 Alexandre Cerqueira, 1 Giuseppe Santalucia, 3 and José
Hepatic Artery Reconstruction in Living Donor Liver Transplant Experience at King Hussein Medical Center
 Hepatic Artery Reconstruction in Living Donor Liver Transplant Experience at King Hussein Medical Center Khaldoun J. Haddadin MD FRCS (Eng)*, Nasser Q. Ahmad MD MRCSI*, Abdelhamid M. Aladwan MD ** ABSTRACT
Hepatic Artery Reconstruction in Living Donor Liver Transplant Experience at King Hussein Medical Center Khaldoun J. Haddadin MD FRCS (Eng)*, Nasser Q. Ahmad MD MRCSI*, Abdelhamid M. Aladwan MD ** ABSTRACT
Erratum to: Int J Hematol (2014) 99: DOI /s
 Int J Hematol (216) 13:725 729 DOI 1.17/s12185-16-1987-1 ERRATUM Erratum to: Prolonged thrombocytopenia after living donor liver transplantation is a strong prognostic predictor irrespective of history
Int J Hematol (216) 13:725 729 DOI 1.17/s12185-16-1987-1 ERRATUM Erratum to: Prolonged thrombocytopenia after living donor liver transplantation is a strong prognostic predictor irrespective of history
Proceedings S.Z.P.G.M.I. Vol: 32(1): pp , 2018.
 Proceedings S.Z.P.G.M.I. Vol: 32(1): pp. 50-55, 2018. PSZMC-670-32-1-2018 Choose Well, Cut Well and Get Well Living Donor Liver Transplants Sumbul Naz 1, Amer Latif 2, Tariq Ali Bangash 2, Asim Rana 2
Proceedings S.Z.P.G.M.I. Vol: 32(1): pp. 50-55, 2018. PSZMC-670-32-1-2018 Choose Well, Cut Well and Get Well Living Donor Liver Transplants Sumbul Naz 1, Amer Latif 2, Tariq Ali Bangash 2, Asim Rana 2
Radiology Rounds A Newsletter for Referring Physicians Massachusetts General Hospital Department of Radiology
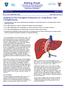 Radiology Rounds A Newsletter for Referring Physicians Massachusetts General Hospital Department of Radiology Imaging for Pre-Transplant Evaluation of Living Donor Liver Transplantation Imaging plays a
Radiology Rounds A Newsletter for Referring Physicians Massachusetts General Hospital Department of Radiology Imaging for Pre-Transplant Evaluation of Living Donor Liver Transplantation Imaging plays a
Biliary complications after right lobe living donor liver transplantation: a single-centre experience
 DOI:10.1111/j.1477-2574.2011.00401.x HPB ORIGINAL ARTICLE Biliary complications after right lobe living donor liver transplantation: a single-centre experience Onur Yaprak 1, Murat Dayangac 1, Murat Akyildiz
DOI:10.1111/j.1477-2574.2011.00401.x HPB ORIGINAL ARTICLE Biliary complications after right lobe living donor liver transplantation: a single-centre experience Onur Yaprak 1, Murat Dayangac 1, Murat Akyildiz
Optimal Bile Duct Division Using Real- Time Indocyanine Green Near-Infrared Fluorescence Cholangiography During Laparoscopic Donor Hepatectomy
 LETTERS FROM THE FRONTLINE Optimal Bile Duct Division Using Real- Time Indocyanine Green Near-Infrared Fluorescence Cholangiography During Laparoscopic Donor Hepatectomy TO THE EDITOR: Despite advances
LETTERS FROM THE FRONTLINE Optimal Bile Duct Division Using Real- Time Indocyanine Green Near-Infrared Fluorescence Cholangiography During Laparoscopic Donor Hepatectomy TO THE EDITOR: Despite advances
The Incidence, Timing, and Management of Biliary Tract Complications After Orthotopic Liver Transplantation
 A:"
A:"
Liver transplant for biliary atresia
 Jean de Ville de Goyet ISMETT Director of the Department for the Treatment and Study of Pediatric Abdominal Diseases and Abdominal Transplantation The first human liver transplant was performed on a pediatric
Jean de Ville de Goyet ISMETT Director of the Department for the Treatment and Study of Pediatric Abdominal Diseases and Abdominal Transplantation The first human liver transplant was performed on a pediatric
Vascular Imaging in the Pediatric Abdomen. Jonathan Swanson, MD
 Vascular Imaging in the Pediatric Abdomen Jonathan Swanson, MD Goals and Objectives To understand the imaging approach, appearance, and clinical manifestations of the common pediatric abdominal vascular
Vascular Imaging in the Pediatric Abdomen Jonathan Swanson, MD Goals and Objectives To understand the imaging approach, appearance, and clinical manifestations of the common pediatric abdominal vascular
TIAN AND OTHERS common hepatic artery. For LDLT, a microvascular technique was employed to anastomose the donor artery to either the right or left hep
 Original Article Treatment of Hepatic Artery Thrombosis After Orthotopic Liver Transplantation Ming Guo Tian, Wai Kuen Tso, 1 Chung Mau Lo, Chi Leung Liu and Sheung Tat Fan, Departments of Surgery and
Original Article Treatment of Hepatic Artery Thrombosis After Orthotopic Liver Transplantation Ming Guo Tian, Wai Kuen Tso, 1 Chung Mau Lo, Chi Leung Liu and Sheung Tat Fan, Departments of Surgery and
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Current status of hepatic surgery in Korea
 Korean J Hepatol. 2009 Dec; 15(Suppl 6):S60 - S64. DOI: 10.3350/kjhep.2009.15.S6.S60 Current status of hepatic surgery in Korea Kyung Sik Kim Department of Surgery, Severance Hospital, Yonsei University
Korean J Hepatol. 2009 Dec; 15(Suppl 6):S60 - S64. DOI: 10.3350/kjhep.2009.15.S6.S60 Current status of hepatic surgery in Korea Kyung Sik Kim Department of Surgery, Severance Hospital, Yonsei University
Outcome Analysis in Adult-to-Adult Living Donor Liver Transplantation Using the Left Lobe. Patients
 Outcome Analysis in Adult-to-Adult Living Donor Liver Transplantation Using the Left Lobe Yuji Soejima, Mitsuo Shimada, Taketoshi Suehiro, Shoji Hiroshige, Mizuki Ninomiya, Satoko Shiotani, Noboru Harada,
Outcome Analysis in Adult-to-Adult Living Donor Liver Transplantation Using the Left Lobe Yuji Soejima, Mitsuo Shimada, Taketoshi Suehiro, Shoji Hiroshige, Mizuki Ninomiya, Satoko Shiotani, Noboru Harada,
Seronegative (also known as non-a, non-b or non-a,
 Outcomes Following Liver Transplantation for Seronegative Acute Liver Failure: Experience During a 12-Year Period With More Than 100 Patients Alan J. Wigg, 1,2 Bridget K. Gunson, 1 and David J. Mutimer
Outcomes Following Liver Transplantation for Seronegative Acute Liver Failure: Experience During a 12-Year Period With More Than 100 Patients Alan J. Wigg, 1,2 Bridget K. Gunson, 1 and David J. Mutimer
BILIARY TRACT COMPLICATIONS IN HUMAN ORTHOTOPIC LIVER TRANSPLANTATION 1,2
 004-33/8/430-004$02.00/0 TRANSPLANTATION Copyright (c) 98 by The Williams & Wilkins Co. Vol. 43, No. Printed in U.S.A. BILIARY TRACT COMPLICATIONS IN HUMAN ORTHOTOPIC LIVER TRANSPLANTATION,2 JAN LERUT,
004-33/8/430-004$02.00/0 TRANSPLANTATION Copyright (c) 98 by The Williams & Wilkins Co. Vol. 43, No. Printed in U.S.A. BILIARY TRACT COMPLICATIONS IN HUMAN ORTHOTOPIC LIVER TRANSPLANTATION,2 JAN LERUT,
Live Donor Liver Transplantation: A Life Saving Option for End Stage Liver Disease
 Live Donor Liver Transplantation: A Life Saving Option for End Stage Liver Disease Abhi Humar, MD Clinical Director, Thomas E. Starzl Transplantation Institute 1 PITTSBURGH THE BIRTHPLACE OF LIVER TRANSPLANTATION
Live Donor Liver Transplantation: A Life Saving Option for End Stage Liver Disease Abhi Humar, MD Clinical Director, Thomas E. Starzl Transplantation Institute 1 PITTSBURGH THE BIRTHPLACE OF LIVER TRANSPLANTATION
Pancreas After Islet Transplantation: A First Report of the International Pancreas Transplant Registry
 American Journal of Transplantation 2016; 16: 688 693 Wiley Periodicals Inc. Brief Communication Copyright 2015 The American Society of Transplantation and the American Society of Transplant Surgeons doi:
American Journal of Transplantation 2016; 16: 688 693 Wiley Periodicals Inc. Brief Communication Copyright 2015 The American Society of Transplantation and the American Society of Transplant Surgeons doi:
Twenty Years of Liver Transplantation for Budd- Chiari Syndrome: A National Registry Analysis
 LIVER TRANSPLANTATION 13:1285-1294, 2007 ORIGINAL ARTICLE Twenty Years of Liver Transplantation for Budd- Chiari Syndrome: A National Registry Analysis Dorry L. Segev, 1 Geoffrey C. Nguyen, 2 Jayme E.
LIVER TRANSPLANTATION 13:1285-1294, 2007 ORIGINAL ARTICLE Twenty Years of Liver Transplantation for Budd- Chiari Syndrome: A National Registry Analysis Dorry L. Segev, 1 Geoffrey C. Nguyen, 2 Jayme E.
Adult living donor versus deceased donor liver transplantation., 2009; 8 (4): At our center the waiting list mortality from 1994 to 1997 a
 298 Fisher RA, et al., 2009; 8 (4): 298-307 ORIGINAL ARTICLE October-December, Vol. 8 No.4, 2009: 298-307 Adult living donor versus deceased donor liver transplantation: A 10-year prospective single center
298 Fisher RA, et al., 2009; 8 (4): 298-307 ORIGINAL ARTICLE October-December, Vol. 8 No.4, 2009: 298-307 Adult living donor versus deceased donor liver transplantation: A 10-year prospective single center
Management of HepatoCellular Carcinoma
 9th Symposium GIC St Louis - 2010 Management of HepatoCellular Carcinoma Overview Pierre A. Clavien, MD, PhD Department of Surgery University Hospital Zurich Zurich, Switzerland Hepatocellular carcinoma
9th Symposium GIC St Louis - 2010 Management of HepatoCellular Carcinoma Overview Pierre A. Clavien, MD, PhD Department of Surgery University Hospital Zurich Zurich, Switzerland Hepatocellular carcinoma
Quantitative Survival Model for Short-Term Survival After Adult-to-Adult Living Donor Liver Transplantation
 LIVER TRANSPLANTATION 12:904-911, 2006 ORIGINAL ARTICLE Quantitative Survival Model for Short-Term Survival After Adult-to-Adult Living Donor Liver Transplantation Ichiro Tsunematsu, 1 3 Yasuhiro Ogura,
LIVER TRANSPLANTATION 12:904-911, 2006 ORIGINAL ARTICLE Quantitative Survival Model for Short-Term Survival After Adult-to-Adult Living Donor Liver Transplantation Ichiro Tsunematsu, 1 3 Yasuhiro Ogura,
Outcomes in 139 Cases of Biliary Tract Reconstructions from a Transplant Surgery Center
 Outcomes in 139 Cases of Biliary Tract Reconstructions from a Transplant Surgery Center Salvatore Gruttadauria, Cataldo Doria, Davide Cintorino, Dhruv Singhal Roberto Verzaro, Carlo Scotti Foglieni, Ignazio
Outcomes in 139 Cases of Biliary Tract Reconstructions from a Transplant Surgery Center Salvatore Gruttadauria, Cataldo Doria, Davide Cintorino, Dhruv Singhal Roberto Verzaro, Carlo Scotti Foglieni, Ignazio
UEMS & EBS: DIVISION OF TRANSPLANT SURGERY
 CURRICULUM AND SYLLABUS TRANSPLANTATION Module 1: Multi-organ retrieval Ability to evaluate donor suitability Ability to retrieve abdominal organs for transplantation Evaluation of donor/ organs suitability
CURRICULUM AND SYLLABUS TRANSPLANTATION Module 1: Multi-organ retrieval Ability to evaluate donor suitability Ability to retrieve abdominal organs for transplantation Evaluation of donor/ organs suitability
Heart Transplantation for Patients with a Fontan Procedure
 Heart Transplantation for Patients with a Fontan Procedure Kirk R. Kanter MD Professor of Surgery Pediatric Cardiac Surgery Emory University School of Medicine Children s Healthcare of Atlanta Atlanta,
Heart Transplantation for Patients with a Fontan Procedure Kirk R. Kanter MD Professor of Surgery Pediatric Cardiac Surgery Emory University School of Medicine Children s Healthcare of Atlanta Atlanta,
