ALCOHOL WITHDRAWAL GUIDELINES
|
|
|
- Mary Morton
- 5 years ago
- Views:
Transcription
1 ALCOHOL WITHDRAWAL GUIDELINES Policy author Accountable Executive Lead Approving body Policy reference Dr M Lewis, Gastroenterologist; Professor J A Vale, Clinical Toxicologist; Dr D A Robertson, Alcohol Lead. Clinical Director Emergency Care Governance Group for Medicine; Drugs & Therapeutics Committee SWBH/Gastro/09 ESSENTIAL READING FOR THE FOLLOWING STAFF GROUPS: 1 All Medical staff All Clinical staff STAFF GROUPS WHICH SHOULD BE AWARE OF THE POLICY FOR REFERENCE PURPOSES: 1 All Medical/Clinical staff POLICY APPROVAL DATE: June 01 POLICY IMPLEMENTATION DATE: June 01 DATE POLICY TO BE REVIEWED: June 018 Alcohol withdrawal guidelines Page 1 of 7
2 Version No Date Approved DOCUMENT CONTROL AND HISTORY Date of implementation Next Review Date Reason for change (e.g. full rewrite, amendment to reflect new legislation, updated flowchart, etc.) 4 January 009 January 009 January 011 December 011 December 011 December 014 June 01 June 01 June 018 To reflect new alcohol services, and reconfiguration of AMUs. Alcohol withdrawal guidelines Page of 7
3 1. INTRODUCTION Alcohol withdrawal syndrome is a common medical problem and follows the abrupt discontinuation of, or at least the rapid decrease in intake of, alcohol, the use of which has been heavy and prolonged. The syndrome usually begins within -8 hours of alcohol cessation or reduction, though alcohol withdrawal delirium does not usually develop for days after stopping drinking and usually lasts for at least 48 7 hours. For this reason a detailed alcohol history should be taken from all patients admitted to hospital. The alcohol withdrawal syndrome may develop in patients admitted to hospital for an unrelated illness (e.g. for an operation) or patients may present in a confused state or following an alcohol related seizure to the Emergency Department. In both these circumstances, which are medical emergencies, the diagnosis may be delayed, usually because it is not considered.. GENERAL POINTS The capacity of patients with alcohol intoxication or alcohol withdrawal should be assessed according to the Mental Capacity Act 00 (policy for assessing mental capacity (Pt Care/0). Patients who have capacity to make their own decisions may elect to discharge themselves. For further advice about assessing capacity, junior staff should first approach the senior members of their team and, if necessary, thereafter help can be obtained from the on-call psychiatrist. Contact security to help manage aggressive behaviour.. ASSESSMENT/TRIAGE Rapid triage is required to determine the severity of symptoms of alcohol withdrawal which should be assessed using the CIWA score (see attached form). Optimal management is determined by the patient s CIWA score, their commitment to alcohol cessation and their response to therapy (see Therapy Schedule). 4. EARLY SIGNS OF WITHDRAWAL (CIWA <8) Assuming that there are no other reasons for remaining in hospital, patients who show only early signs of withdrawal (CIWA <8) can be discharged and recommended to continue drinking alcohol. If such patients are keen to be considered for alcohol detoxification, they should be referred either for urgent out-patient review at City Hospital (typically within 1- weeks), prior to planned alcohol detoxification on the West Midlands Poisons Unit by telephoning (Fax: ), or for consideration of outpatient help withdrawing from alcohol, they can be referred to outpatient alcohol services (Swanswell at Sandwell; Reach Out Recovery at City).. WHERE SHOULD PATIENTS WITH ALCOHOL WITHDRAWAL SYNDROME BE MANAGED? If the patient s predominant clinical problem is alcohol withdrawal and the patient has a CIWA score >8, the patient should be discussed promptly by a member of the medical team with the Clinical Toxicologist on-call for the West Midlands Poisons Unit at City Hospital before treatment is commenced (Contact Switchboard for rota). If a patient is admitted with a diagnosis of alcohol withdrawal syndrome and is not referred on admission to the Clinical Toxicologist on call for the West Midlands Poisons Alcohol withdrawal guidelines Page of 7
4 Unit, subsequent transfer to the Poisons Unit will be a matter of consultant to consultant discussion. If a patient presents at Sandwell they should be discussed with the on-call Clinical Toxicologist as above (Contact Switchboard for rota). If the patient is unfit to be transferred to City Hospital advice should still be sought from the Clinical Toxicologist on-call for the West Midlands Poisons Unit. Consideration should be given to transferring the patient to Priory after referral to the Gastroenterology Team. In the rare instance where a patient at Sandwell with severe alcohol withdrawal is very difficult to manage, transfer to HDU should be considered, but this should only happen after discussion with the Sandwell consultant in charge of the patient s care.. THIAMINE SUPPLEMENTATION Alcohol dependent individuals are often thiamine deficient. Thiamine prevents Wernicke s encephalopathy and Korsakoff s psychosis and should therefore be administered to such patients on admission. If Korsakoff s psychosis or Wernicke s encephalopathy is suspected or considered likely to occur, parenteral administration of B vitamins is appropriate e.g. Pabrinex high potency injection intravenously over 10 minutes. In other cases, oral thiamine 100 mg b.d. should be given. Thiamine and vitamin B complex should be continued on discharge. 7. TREATMENT OF HALLUCINATIONS Patients presenting with alcohol withdrawal should be initially treated using diazepam. In patients who have had appropriate doses of diazepam in whom hallucinations remain a predominant feature of their alcohol withdrawal syndrome, an antipsychotic agent such as haloperidol. mg IM (maximum 1 mg daily) may be a useful adjunct. 8. ALCOHOL RELATED SEIZURES For patients presenting with a single fit resulting from alcohol withdrawal, inpatient detoxification is usually only indicated if they have other significant features of withdrawal (CIWA >8), when they should be referred immediately to the Clinical Toxicologist on-call for the West Midlands Poisons Unit at City Hospital (Contact Switchboard for rota). Routine CT head scans in such patients are unnecessary. It is important to consider early discharge of patients with alcohol related seizures if, on recovery from the seizure the CIWA score is <8, to prevent the development of more severe withdrawal. If the patient expresses a commitment to giving up alcohol and has a CIWA <8, the patient can be referred for outpatient review by Professor Vale or Dr Bradberry at City Hospital (typically within 1- weeks), by telephoning (Fax: ). 9. PLANNED ALCOHOL DETOXIFICATION WEST MIDLANDS POISONS UNIT Following out-patient assessment by Professor Vale and Dr Bradberry, patients committed to sobriety will be admitted to the West Midlands Poisons Unit for planned detoxification which takes some 7 hours in uncomplicated cases. The aims of detoxification are to: Provide safe withdrawal from alcohol to enable the patient to become alcohol free; Provide withdrawal that is humane, thus protecting the patient s dignity; Prepare the patient for an alcohol free existence. Alcohol withdrawal guidelines Page 4 of 7
5 Medical and nursing staff on the West Midlands Poisons Unit have substantial experience of managing alcohol withdrawal using a symptom-triggered regimen which is fully in accord with the NICE Guidelines (010). For patients unable/unwilling to come to City Hospital planned in-patient detoxification may be arranged with Dr Singhal, consultant gastroenterologist, on Priory. COMMUNITY ALCOHOL SERVICES Patients with no co-morbidities can be taken through alcohol detoxification in the community. Swanswell and Reach Out Recovery can provide this approach to appropriate individuals. Please contact them on discharge. 10. DISCHARGE Patients managed on the West Midlands Poisons Unit will be offered follow-up at the clinics of Professor Vale and Dr Bradberry. If the patient has not been managed on the West Midlands Poisons Unit, consider referral to Professor Vale or Dr Bradberry particularly if the patient is committed to giving up alcohol. For those not so committed, consider referral to the hospital-based representatives of the Community alcohol teams. Contact via switchboard. Consultant Clinical Toxicologists: Professor Vale, Dr Bradberry (Secretary: ) Monday AM Clinic Alcohol providers: City contact: Phone: Reach Out Recovery: ; Birmingham.secure@cri.cjsm.net Sandwell contact: SPOC: support@swanswell.org.cjsm.net Alcohol withdrawal guidelines Page of 7
6 Appendix 1 West Midlands Poisons Unit: Alcohol Withdrawal Assessment Form [Clinical Institute Withdrawal Assessment for Alcohol, revised (CIWA-Ar)] Name DOB Hospital Number a) Nausea and vomiting 0 No nausea or vomiting 1 4 Intermittent nausea with dry heaves 7 Constant nausea, frequent dry heaves and vomiting b) Paroxysmal sweats 0 No sweats visible 1 Barely perceptible sweating, palms moist 4 Beads of sweat obvious on forehead 7 Drenching sweats c) Anxiety 0 No anxiety, at ease 1 4 Moderately anxious, guarded 7 Acute panic state, consistent with severe delirium or acute schizophrenia d) Agitation 0 Normal activity 1 Somewhat more than normal activity 4 Moderately fidgety and restless 7 Paces back and forth during most of the interview or constantly thrashes about e) Tremor 0 No tremor 1 Not visible, but can be felt at fingertips 4 Moderate when patient's hands extended 7 Severe, even with arms not extended f) Headache 0 Not present 1 Very mild Mild Moderate 4 Moderately severe Severe Very severe 7 Extremely severe g) Auditory disturbances 0 Not present 1 Very mild harshness or ability to frighten Mild harshness or ability to frighten Moderate harshness or ability to frighten 4 Moderately severe hallucinations Severe hallucination Extremely severe hallucinations 7 Continuous hallucinations h) Visual disturbances 0 Not present 1 Very mild photosensitivity Mild photosensitivity Moderate photosensitivity 4 Moderately severe visual hallucinations Severe visual hallucinations Extremely severe visual hallucinations 7 Continuous visual hallucinations i) Tactile disturbances 0 None 1 Very mild paraesthesias Mild paraesthesias Moderate paraesthesias 4 Moderately severe hallucinations Severe hallucinations Extremely severe hallucinations 7 Continuous hallucinations j) Orientation 0 Oriented and can do serial additions 1 Cannot do serial additions Disoriented for date by no more than calendar days Disoriented for date by more than calendar days 4 Disoriented for place and/or patient Date Time Score Total a b c d e f g h i j Heart Rate / BP Diazepam dose (route) Total score is a simple sum of each item score (maximum score is 7) <8 Mild withdrawal 8-1 Moderate withdrawal >1 Severe withdrawal Alcohol withdrawal guidelines Page of 7
7 Appendix Management of Alcohol Withdrawal Syndrome Perform CIWA-Ar Score. Refer urgently to Clinical Toxicologist on call (Contact Switchboard for rota) if CIWA >8 <8 8 1 >1 Consider discharge, but make out-patient referral to alcohol services. If there are other reasons for the patient to remain in hospital, repeat CIWA score in h. + h If CIWA <8 repeat CIWA score every h. Give diazepam 0-40 mg stat orally. Repeat CIWA score in 0 min while awaiting transfer of patient to AMU. Discuss with Clinical Toxicologist on call (via Switchboard) if concerns. + 0 min CIWA still 8 1, give diazepam another 0-40 mg stat orally. Repeat CIWA in 0min. + 0 min If a bed is still not available on the Poisons Unit (AMU-), and CIWA remains 8 1, discuss with Clinical Toxicologist. Give further diazepam as advised. Refer urgently to Clinical Toxicologist on call (Contact Switchboard for rota). While transfer to the Poisons Unit (AMU-) is being arranged, give diazepam 0 40 mg IV**. +1 min If CIWA >1, give diazepam 0 40 mg IV** every 1 minutes until CIWA is < 1 and transfer to the Poisons Unit (AMU-) or HDU as soon as bed available. Regular Medical Review is mandatory for all patients with a CIWA >8. **Intravenous diazepam should be given only if the SO can be monitored before and after administration and flumazenil is available. Ensure Clinical Toxicologist is aware of decision to give IV diazepam. If immediate concerns, seek ITU support. Alcohol withdrawal guidelines Page 7 of 7
Alcohol withdrawal. Clinical features
 Alcohol withdrawal Clinical features Severity increase with amount consumed; uncommon with < drinks per day. Predictable pattern: patients with previous withdrawal seizures are at high risk for recurrence.
Alcohol withdrawal Clinical features Severity increase with amount consumed; uncommon with < drinks per day. Predictable pattern: patients with previous withdrawal seizures are at high risk for recurrence.
Stabilization Algorithm
 VA/DoD Clinical Practice Guideline for the Management of Substance Use Disorders Stabilization Algorithm Stabilization Pocket Card 1 Patient and Time Information Clinical Institute Withdrawal Assessment
VA/DoD Clinical Practice Guideline for the Management of Substance Use Disorders Stabilization Algorithm Stabilization Pocket Card 1 Patient and Time Information Clinical Institute Withdrawal Assessment
Lead for Gastroenterology Lee Dodge Alcohol Liaison 03/03/2015. Clive Gibson Safeguarding Adults Lead Nurse 03/03/2015
 Acute Alcohol Withdrawal Management for Adult Inpatients Type: Clinical Guideline Register No: 1409 Status: Public on ratification Developed in response to: Best Practice Contributes to CQC Outcome number:
Acute Alcohol Withdrawal Management for Adult Inpatients Type: Clinical Guideline Register No: 1409 Status: Public on ratification Developed in response to: Best Practice Contributes to CQC Outcome number:
APPENDIX 7 CLINICAL INSTITUTE NARCOTIC ASSESSMENT (CINA) SCALE FOR WITHDRAWAL SYMPTOMS
 APPENDIX 7 CLINICAL INSTITUTE NARCOTIC ASSESSMENT (CINA) SCALE FOR WITHDRAWAL SYMPTOMS The Clinical Institute Narcotic Assessment (CINA) Scale measures 11 signs and symptoms commonly seen in patients during
APPENDIX 7 CLINICAL INSTITUTE NARCOTIC ASSESSMENT (CINA) SCALE FOR WITHDRAWAL SYMPTOMS The Clinical Institute Narcotic Assessment (CINA) Scale measures 11 signs and symptoms commonly seen in patients during
Assessment Main title and management of alcohol dependence and withdrawal in the acute hospital: concise guidance
 CONCISE GUIDANCE Clinical Medicine 01, Vol 1, No : 71 Assessment Main title and management of alcohol dependence and withdrawal in the acute hospital: concise guidance Author head name Stephen Stewart
CONCISE GUIDANCE Clinical Medicine 01, Vol 1, No : 71 Assessment Main title and management of alcohol dependence and withdrawal in the acute hospital: concise guidance Author head name Stephen Stewart
Guidelines for the In-Patient Management of Alcohol Withdrawal at Frimley Park Hospital NHS Foundation Trust
 Guidelines for the In-Patient Management of Alcohol Withdrawal at Frimley Park Hospital NHS Foundation Trust Authors: Dr Aftab Ala, Consultant Gastroenterologist & Hepatologist Dr Tasneem Pirani, ST4 in
Guidelines for the In-Patient Management of Alcohol Withdrawal at Frimley Park Hospital NHS Foundation Trust Authors: Dr Aftab Ala, Consultant Gastroenterologist & Hepatologist Dr Tasneem Pirani, ST4 in
Alcohol Detoxification (Inpatient) Prescribing Guidelines
 Alcohol Detoxification (Inpatient) Prescribing Guidelines Author: Sponsor/Executive: Responsible committee: Consultation & Approval: (Committee/Groups which signed off the procedure, including date) This
Alcohol Detoxification (Inpatient) Prescribing Guidelines Author: Sponsor/Executive: Responsible committee: Consultation & Approval: (Committee/Groups which signed off the procedure, including date) This
Title Alcohol Withdrawal Management Guidelines
 Document Control Title Alcohol Withdrawal Management Guidelines Author Directorate Date Version Issued 0.1 Dec 2009 0.2 Mar 2010 0.3 Nov 2010 Status Draft 0.4 Sep 2015 1.0 Jan 2016 2.0 Nov Final 2018 Main
Document Control Title Alcohol Withdrawal Management Guidelines Author Directorate Date Version Issued 0.1 Dec 2009 0.2 Mar 2010 0.3 Nov 2010 Status Draft 0.4 Sep 2015 1.0 Jan 2016 2.0 Nov Final 2018 Main
Pharmacological Therapy Policy Practice Guidance Note Management of Acute Alcohol Withdrawal in Adults (Over 18) - V01. Planned review: December 2017
 Pharmacological Therapy Policy Practice Guidance Note Management of Acute Alcohol Withdrawal in Adults (Over 18) - V01 V01 issued: Issue 1- Dec 14 Issue 2 April 17 Planned review: December 2017 PPT-PGN
Pharmacological Therapy Policy Practice Guidance Note Management of Acute Alcohol Withdrawal in Adults (Over 18) - V01 V01 issued: Issue 1- Dec 14 Issue 2 April 17 Planned review: December 2017 PPT-PGN
Alcohol withdrawal including the Symptom triggered CIWA score Management
 Alcohol withdrawal including the Symptom triggered CIWA score Management Classification: Policy Lead Author: Ruth Brown Alcohol specialist Nurse Additional author(s): Hailey Pennington Authors Division:
Alcohol withdrawal including the Symptom triggered CIWA score Management Classification: Policy Lead Author: Ruth Brown Alcohol specialist Nurse Additional author(s): Hailey Pennington Authors Division:
Alcohol Withdrawal Guidelines
 SH CP 197 Alcohol Withdrawal Guidelines Summary: Keywords: Target Audience: Identification, assessment and management of alcohol dependence and harmful alcohol use in people presenting for assessment or
SH CP 197 Alcohol Withdrawal Guidelines Summary: Keywords: Target Audience: Identification, assessment and management of alcohol dependence and harmful alcohol use in people presenting for assessment or
Lorraine Wilson, 74 years of age, is admitted. Alcohol Withdrawal. During Hospitalization. Early recognition and consistent intervention are critical.
 1.9 h o u r s Continuing Education Withdrawal During Hospitalization Early recognition and consistent intervention are critical. Overview: For a chronic drinker, sudden alcohol withdrawal because of an
1.9 h o u r s Continuing Education Withdrawal During Hospitalization Early recognition and consistent intervention are critical. Overview: For a chronic drinker, sudden alcohol withdrawal because of an
Withdrawal.
 Withdrawal Shamim Nejad, MD Director, Adult Burns & Trauma Psychiatry Division of Psychiatry and Medicine Medical Director, Addiction Consultation Team MGH Center for Addiction Medicine Massachusetts General
Withdrawal Shamim Nejad, MD Director, Adult Burns & Trauma Psychiatry Division of Psychiatry and Medicine Medical Director, Addiction Consultation Team MGH Center for Addiction Medicine Massachusetts General
Pharmacological Therapy Policy Practice Guidance Note Management of Acute Alcohol Withdrawal in Adults (Over 18) - V02. Planned review: Dec 2020
 Pharmacological Therapy Policy Practice Guidance Note Management of Acute Alcohol Withdrawal in Adults (Over 18) - V02 Issue No: Issue 1- Dec 17 Planned review: Dec 2020 PPT-PGN 22 Part of NTW(C)38 Pharmacological
Pharmacological Therapy Policy Practice Guidance Note Management of Acute Alcohol Withdrawal in Adults (Over 18) - V02 Issue No: Issue 1- Dec 17 Planned review: Dec 2020 PPT-PGN 22 Part of NTW(C)38 Pharmacological
Clinical Guideline / Formulary Document Pharmacy Department Medicines Management Services
 Clinical Guideline / Formulary Document Pharmacy Department Medicines Management Services SUBSTANCE DEPENDENCY For full details of the of the medication discussed in this formulary including side effects,
Clinical Guideline / Formulary Document Pharmacy Department Medicines Management Services SUBSTANCE DEPENDENCY For full details of the of the medication discussed in this formulary including side effects,
Northern Ireland Alcohol Use Disorders Care Pathway. management in the acute hospital setting
 Northern Ireland Alcohol Use Disorders Care Pathway management in the acute hospital setting Main Content 1. Introduction 2 2. Alcohol Withdrawal Syndrome 3 2.1. Delirium tremens 3 2.2. Seizures 4 2.3.
Northern Ireland Alcohol Use Disorders Care Pathway management in the acute hospital setting Main Content 1. Introduction 2 2. Alcohol Withdrawal Syndrome 3 2.1. Delirium tremens 3 2.2. Seizures 4 2.3.
GUIDELINES FOR ALCOHOL DETOXIFICATION AT HMP BEDFORD
 GUIDELINES FOR ALCOHOL DETOXIFICATION AT HMP BEDFORD Policy Details NHFT document reference MMG027/HMP Version 1 Date Ratified May 2017 Ratified by HMP Bedford Drugs and Therapeutics Committee Implementation
GUIDELINES FOR ALCOHOL DETOXIFICATION AT HMP BEDFORD Policy Details NHFT document reference MMG027/HMP Version 1 Date Ratified May 2017 Ratified by HMP Bedford Drugs and Therapeutics Committee Implementation
Methodist Hospital Alcohol Withdrawal Suggested Guidelines
 Methodist Hospital Alcohol Withdrawal Suggested Guidelines S. Prizada Sattar, MD Teri L Gabel, Pharm.D.,BCPP Sidney Kauzlarich, MD Subhash Bhatia, MD Mitzi Bollinger, RN S. Prizada Sattar, MD 6-20-3 Rationale
Methodist Hospital Alcohol Withdrawal Suggested Guidelines S. Prizada Sattar, MD Teri L Gabel, Pharm.D.,BCPP Sidney Kauzlarich, MD Subhash Bhatia, MD Mitzi Bollinger, RN S. Prizada Sattar, MD 6-20-3 Rationale
Managing presenting alcohol users an Introduction to SPECTRUM (CRI) By Dr Gideon Felton MRCPsych Consultant Psychiatrist and Clinical Lead
 Managing presenting alcohol users an Introduction to SPECTRUM (CRI) By Dr Gideon Felton MRCPsych Consultant Psychiatrist and Clinical Lead PLAN OF PRESENTATION Assessment of alcohol dependence Psychiatric
Managing presenting alcohol users an Introduction to SPECTRUM (CRI) By Dr Gideon Felton MRCPsych Consultant Psychiatrist and Clinical Lead PLAN OF PRESENTATION Assessment of alcohol dependence Psychiatric
Delirium. Quick reference guide. Issue date: July Diagnosis, prevention and management
 Issue date: July 2010 Delirium Diagnosis, prevention and management Developed by the National Clinical Guideline Centre for Acute and Chronic Conditions About this booklet This is a quick reference guide
Issue date: July 2010 Delirium Diagnosis, prevention and management Developed by the National Clinical Guideline Centre for Acute and Chronic Conditions About this booklet This is a quick reference guide
MANAGEMENT AND DETOXIFICATION FOR GAMMA- HYDROXYBUTYRATE (GHB) AND GAMMA-BUTARYL LACTONE (GBL) GUIDELINES SEPTEMBER 2017
 MANAGEMENT AND DETOXIFICATION FOR GAMMA- HYDROXYBUTYRATE (GHB) AND GAMMA-BUTARYL LACTONE (GBL) GUIDELINES SEPTEMBER 2017 Policy title Management and Detoxification for GHB and GBL Policy PHA61 reference
MANAGEMENT AND DETOXIFICATION FOR GAMMA- HYDROXYBUTYRATE (GHB) AND GAMMA-BUTARYL LACTONE (GBL) GUIDELINES SEPTEMBER 2017 Policy title Management and Detoxification for GHB and GBL Policy PHA61 reference
Northern Ireland Alcohol Use Disorders Care Pathway. management in the acute hospital setting
 Northern Ireland Alcohol Use Disorders Care Pathway management in the acute hospital setting Main Content 1. Introduction 2 2. Alcohol Withdrawal Syndrome 3 2.1. Delirium tremens 3 2.2. Seizures 4 2.3.
Northern Ireland Alcohol Use Disorders Care Pathway management in the acute hospital setting Main Content 1. Introduction 2 2. Alcohol Withdrawal Syndrome 3 2.1. Delirium tremens 3 2.2. Seizures 4 2.3.
University Hospitals of Leicester NHS Trust
 University Hospitals of Leicester NHS Trust ACUTE ALCOHOL WITHDRAWAL MANAGEMENT Guidelines for Management of Acute Medical Emergencies Approved By: Policy and Guideline Committee Date Approved: 21 November
University Hospitals of Leicester NHS Trust ACUTE ALCOHOL WITHDRAWAL MANAGEMENT Guidelines for Management of Acute Medical Emergencies Approved By: Policy and Guideline Committee Date Approved: 21 November
Administration of High Dose Intra- Muscular Vitamin Supplements for Patients Undergoing Alcohol Detoxification. Standard Operating Procedure
 Administration of High Dose Intra- Muscular Vitamin Supplements for Patients Undergoing Alcohol Detoxification Standard Operating Procedure DOCUMENT CONTROL: Version: 3 Ratified by: Quality Assurance Sub
Administration of High Dose Intra- Muscular Vitamin Supplements for Patients Undergoing Alcohol Detoxification Standard Operating Procedure DOCUMENT CONTROL: Version: 3 Ratified by: Quality Assurance Sub
Education Pack for the Alcohol Liaison Nurse Service
 Education Pack for the Alcohol Liaison Nurse Service Welcome to the Alcohol Liaison Nurse Service, this pack is designed to help you get the most out of your time here with us today and set some objectives
Education Pack for the Alcohol Liaison Nurse Service Welcome to the Alcohol Liaison Nurse Service, this pack is designed to help you get the most out of your time here with us today and set some objectives
CMBHS Clinical Management of Behavioral Health Services
 Client: CMBHS Clinical Management of Behavioral Health Services Detoxification Assessment Assessment Information (te: All are Required fields) Assessment Number Assessment Date Assessment Type Contact
Client: CMBHS Clinical Management of Behavioral Health Services Detoxification Assessment Assessment Information (te: All are Required fields) Assessment Number Assessment Date Assessment Type Contact
Behavioral Health Service Request Form Detox and Substance Abuse Rehab
 Medicaid Call for Pre-Certification of Admissions: 1-855-620-1861 Kentucky Medicaid Fax: 1-877-338-3686 Standard Request Requests for prior authorization (with supporting clinical information and documentation)
Medicaid Call for Pre-Certification of Admissions: 1-855-620-1861 Kentucky Medicaid Fax: 1-877-338-3686 Standard Request Requests for prior authorization (with supporting clinical information and documentation)
Acute Alcohol Withdrawal Protocol
 Acute Alcohol Withdrawal Protocol Controlled document This document is uncontrolled when downloaded or printed Reference number Version 1 Author WHHT: C268 Dr Mohamed Shariff Date ratified August 2014
Acute Alcohol Withdrawal Protocol Controlled document This document is uncontrolled when downloaded or printed Reference number Version 1 Author WHHT: C268 Dr Mohamed Shariff Date ratified August 2014
Behavioral Health Service Request Form Detox and Substance Abuse Rehab
 Arkansas 855-538-0454 Connecticut 855-538-0454 Florida 855-538-0454 Georgia 800-424-5412 Illinois 800-504-2766 Kentucky 855-620-1861 Louisiana 855-538-0454 Arkansas 855-710-0159 Connecticut 888-365-3233
Arkansas 855-538-0454 Connecticut 855-538-0454 Florida 855-538-0454 Georgia 800-424-5412 Illinois 800-504-2766 Kentucky 855-620-1861 Louisiana 855-538-0454 Arkansas 855-710-0159 Connecticut 888-365-3233
MEDICALLY ASSISTED COMMUNITY ALCOHOL WITHDRAWAL GUIDELINES SEPTEMBER 2015
 MEDICALLY ASSISTED COMMUNITY ALCOHOL WITHDRAWAL GUIDELINES SEPTEMBER 2015 This policy supersedes all previous policies for medically assisted community alcohol withdrawal Policy title Guidelines for medically
MEDICALLY ASSISTED COMMUNITY ALCOHOL WITHDRAWAL GUIDELINES SEPTEMBER 2015 This policy supersedes all previous policies for medically assisted community alcohol withdrawal Policy title Guidelines for medically
Management of Alcohol Dependence
 STANDARD TREATMENT GUIDELINES Management of Alcohol Dependence Quick Reference Guide February 2016 Ministry of Health & Family Welfare Government of India 1 Table of Contents Objectives-... 3 Diagnosis...
STANDARD TREATMENT GUIDELINES Management of Alcohol Dependence Quick Reference Guide February 2016 Ministry of Health & Family Welfare Government of India 1 Table of Contents Objectives-... 3 Diagnosis...
Behavioral Health Service Request Form Detox and Substance Abuse Rehab
 Please Submit to the Dedicated Fax Line Below Medicaid Call for Pre-Certification of Admissions: 888-453-2534 New Jersey Medicaid Fax: 855-703-8082 Lev el of Care: Place of Serv ice: Detox Substance Abuse
Please Submit to the Dedicated Fax Line Below Medicaid Call for Pre-Certification of Admissions: 888-453-2534 New Jersey Medicaid Fax: 855-703-8082 Lev el of Care: Place of Serv ice: Detox Substance Abuse
NCEPOD - Measuring the Units; A review of patients who died with alcohol-related liver disease
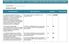 NCEPOD - Measuring the Units; A review of patients who died with alcohol-related liver disease Hospital Number Admission to hospital 5. Trusts should ensure that medical patients are reviewed by a consultant
NCEPOD - Measuring the Units; A review of patients who died with alcohol-related liver disease Hospital Number Admission to hospital 5. Trusts should ensure that medical patients are reviewed by a consultant
NHS Fife Guidance for the Identification, Assessment and Management of Harmful Drinking and Alcohol Dependence
 NHS Fife Guidance for the Identification, Assessment and Management of Harmful Drinking and Alcohol Dependence Staff working in services provided and funded by the NHS who care for people who potentially
NHS Fife Guidance for the Identification, Assessment and Management of Harmful Drinking and Alcohol Dependence Staff working in services provided and funded by the NHS who care for people who potentially
Treatment of Alcohol and Opiate Withdrawal
 Objectives Treatment of Alcohol and Opiate Withdrawal Renee Striker, Pharm.D., BCPS, BCPP Pharmacy Clinical Specialist Huron Hospital East Cleveland, Ohio Outline the diagnostic criteria for substance
Objectives Treatment of Alcohol and Opiate Withdrawal Renee Striker, Pharm.D., BCPS, BCPP Pharmacy Clinical Specialist Huron Hospital East Cleveland, Ohio Outline the diagnostic criteria for substance
ALCOHOL ASSESSMENT AND DETOXIFICATION POLICY FOR INPATIENTS
 ALCOHOL ASSESSMENT AND DETOXIFICATION POLICY FOR INPATIENTS Version: 4 Date issued: August 2017 Review date: August 2020 Applies to: All staff working within Trust Inpatient settings This document is available
ALCOHOL ASSESSMENT AND DETOXIFICATION POLICY FOR INPATIENTS Version: 4 Date issued: August 2017 Review date: August 2020 Applies to: All staff working within Trust Inpatient settings This document is available
Emergency Control of the Acutely Disturbed Adult Patient GUIDELINES ON EMERGENCY CONTROL OF THE ACUTELY DISTURBED ADULT PATIENT... 2 ACTION...
 Delirium Toolkit Emergency Control of the Acutely Disturbed Adult Patient Table of Contents GUIDELINES ON EMERGENCY CONTROL OF THE ACUTELY DISTURBED ADULT PATIENT... 2 ACTION... 2 AFTERCARE... 3 NOTES...
Delirium Toolkit Emergency Control of the Acutely Disturbed Adult Patient Table of Contents GUIDELINES ON EMERGENCY CONTROL OF THE ACUTELY DISTURBED ADULT PATIENT... 2 ACTION... 2 AFTERCARE... 3 NOTES...
SECTION 10: MANAGEMENT OF ALCOHOL, OPIOID AND BENZODIAZEPINE DEPENDENCE. Formulary and Prescribing Guidelines
 SECTION 10: MANAGEMENT OF ALCOHOL, OPIOID AND BENZODIAZEPINE DEPENDENCE Formulary and Prescribing Guidelines 10.1 Introduction This document covers the safe prescribing and management for service users
SECTION 10: MANAGEMENT OF ALCOHOL, OPIOID AND BENZODIAZEPINE DEPENDENCE Formulary and Prescribing Guidelines 10.1 Introduction This document covers the safe prescribing and management for service users
INPATIENT ALCOHOL WITHDRAWAL PRESCRIBING GUIDELINES MAY 2018
 INPATIENT ALCOHOL WITHDRAWAL PRESCRIBING GUIDELINES MAY 2018 Policy title Inpatient alcohol withdrawal Prescribing Guidelines Policy PHA28B reference Policy category Clinical Relevant to Trust-wide any
INPATIENT ALCOHOL WITHDRAWAL PRESCRIBING GUIDELINES MAY 2018 Policy title Inpatient alcohol withdrawal Prescribing Guidelines Policy PHA28B reference Policy category Clinical Relevant to Trust-wide any
Multiple Choice Questions
 Multiple Choice Questions 25yo M presents without psychiatric or medical history, with complaint of tremor to the ER. He denies drinking alcohol but his friend at bedside takes you to the side and reports
Multiple Choice Questions 25yo M presents without psychiatric or medical history, with complaint of tremor to the ER. He denies drinking alcohol but his friend at bedside takes you to the side and reports
Acute painful crisis in patients with sickle cell disease: Clinical Guidelines (HN-506a)
 Acute painful crisis in patients with sickle cell disease: Clinical Guidelines (HN-506a) Introduction The majority of acute painful crises in patients with sickle cell disease will be managed independently
Acute painful crisis in patients with sickle cell disease: Clinical Guidelines (HN-506a) Introduction The majority of acute painful crises in patients with sickle cell disease will be managed independently
Behavioral Health Service Request Form Detox and Substance Abuse Rehab
 Please Submit to the Dedicated Fax Line Below Medicaid Call for Pre-Certification of Admissions: 888-588-9842 South Carolina Medicaid Fax: 888-339-8293 Lev el of Care: Place of Serv ice: Detox Substance
Please Submit to the Dedicated Fax Line Below Medicaid Call for Pre-Certification of Admissions: 888-588-9842 South Carolina Medicaid Fax: 888-339-8293 Lev el of Care: Place of Serv ice: Detox Substance
FOR RESIDENTIAL FACILITIES
 AGED CASP 1a - APMHS REFERRAL ACASP 1a AGED PERSONS MENTAL HEALTH SERVICE REFERRAL FOR RESIDENTIAL FACILITIES Surname:. Rapid UR:. Given names:... D.O.B.:. Sex: Address: Phone:.. Medicare Number:. Date
AGED CASP 1a - APMHS REFERRAL ACASP 1a AGED PERSONS MENTAL HEALTH SERVICE REFERRAL FOR RESIDENTIAL FACILITIES Surname:. Rapid UR:. Given names:... D.O.B.:. Sex: Address: Phone:.. Medicare Number:. Date
Current Clinical Patterns in the Management of Alcohol Withdrawal Syndrome (AWS)
 1 Current Clinical Patterns in the Management of Alcohol Withdrawal Syndrome (AWS) The goal of the survey is to evaluate current practices for the inpatient management of AWS in adult hospitals located
1 Current Clinical Patterns in the Management of Alcohol Withdrawal Syndrome (AWS) The goal of the survey is to evaluate current practices for the inpatient management of AWS in adult hospitals located
Prescribing for substance misuse: alcohol detoxification. Clinical background
 Prescribing for substance misuse: alcohol detoxification POMH-UK Quality Improvement Programme. Topic 14a: baseline Clinical background 1 2014 The Royal College of Psychiatrists. For further information
Prescribing for substance misuse: alcohol detoxification POMH-UK Quality Improvement Programme. Topic 14a: baseline Clinical background 1 2014 The Royal College of Psychiatrists. For further information
Delirium. Approach. Symptom Update Masterclass:
 Symptom Update Masterclass: Delirium Jason Boland Senior Clinical Lecturer and Honorary Consultant in Palliative Medicine Wolfson Centre for Palliative Care Research Hull York Medical School University
Symptom Update Masterclass: Delirium Jason Boland Senior Clinical Lecturer and Honorary Consultant in Palliative Medicine Wolfson Centre for Palliative Care Research Hull York Medical School University
DRAFT FOR CONSULTATION
 1) What is the accuracy of a tool and/or clinical judgement for the a) assessment b) monitoring of patients at risk of acute alcohol withdrawal? 2) Does the assessment and monitoring of patients with acute
1) What is the accuracy of a tool and/or clinical judgement for the a) assessment b) monitoring of patients at risk of acute alcohol withdrawal? 2) Does the assessment and monitoring of patients with acute
Provider Update: Alcohol Withdrawal Order Set Edits
 Provider Update: Alcohol Withdrawal Order Set Edits Situation: A revised Alcohol Withdrawal Order Set and new CIWA-Ar scoring tool will go LIVE February 12, 2018. Background: The latest guidelines for
Provider Update: Alcohol Withdrawal Order Set Edits Situation: A revised Alcohol Withdrawal Order Set and new CIWA-Ar scoring tool will go LIVE February 12, 2018. Background: The latest guidelines for
2010 National Audit of Dementia (Care in General Hospitals) North West London Hospitals NHS Trust
 Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: rth West London Hospitals NHS Trust The 2010 national audit
Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: rth West London Hospitals NHS Trust The 2010 national audit
Chapter 7. Screening and Assessment
 Chapter 7 Screening and Assessment Screening And Assessment Starting the dialogue and begin relationship Each are sizing each other up Information gathering Listening to their story Asking the questions
Chapter 7 Screening and Assessment Screening And Assessment Starting the dialogue and begin relationship Each are sizing each other up Information gathering Listening to their story Asking the questions
Complicated Withdrawal
 Complicated Withdrawal Shamim Nejad, MD Medical Director, Division of Psychosocial Oncology Swedish Cancer Institute Swedish Medical Center Seattle, Washington Shamim.Nejad@Swedish.org Disclosures: Shamim
Complicated Withdrawal Shamim Nejad, MD Medical Director, Division of Psychosocial Oncology Swedish Cancer Institute Swedish Medical Center Seattle, Washington Shamim.Nejad@Swedish.org Disclosures: Shamim
Westminster Memory Services Pathways Toolkit (updated October 2016)
 Westminster Memory Services Pathways Toolkit (updated October 2016) Contents Aims... 2 Memory loss experienced by service users... 2 Signs of memory loss... 2 Alcohol dependency and memory loss... 3 Other
Westminster Memory Services Pathways Toolkit (updated October 2016) Contents Aims... 2 Memory loss experienced by service users... 2 Signs of memory loss... 2 Alcohol dependency and memory loss... 3 Other
ROLE OF HEALTH CARE PROVIDERS IN THE MANAGEMENT OF ALCOHOL AND DRUG USE RELATED PROBLEMS
 ROLE OF HEALTH CARE PROVIDERS IN THE MANAGEMENT OF ALCOHOL AND DRUG USE RELATED PROBLEMS Dr. Anita Rao? ASK SCREEN Refer HELP T T Ranganathan Clinical Research Foundation TTK Hospital IV Main Road, Indira
ROLE OF HEALTH CARE PROVIDERS IN THE MANAGEMENT OF ALCOHOL AND DRUG USE RELATED PROBLEMS Dr. Anita Rao? ASK SCREEN Refer HELP T T Ranganathan Clinical Research Foundation TTK Hospital IV Main Road, Indira
Guidelines for the Management of Behavioural and Psychological Symptoms of Dementia (BPSD) Summary document for Primary Care
 Guidelines for the Management of Behavioural and Psychological Symptoms of Dementia (BPSD) Summary document for Primary Care Guidelines for the Management of Behavioural and Psychological Symptoms of Dementia
Guidelines for the Management of Behavioural and Psychological Symptoms of Dementia (BPSD) Summary document for Primary Care Guidelines for the Management of Behavioural and Psychological Symptoms of Dementia
Psychotropic Medication
 FOM 802-1 1 of 10 OVERVIEW The use of psychotropic medication as part of a child s comprehensive mental health treatment plan may be beneficial and should include consideration of all alternative interventions.
FOM 802-1 1 of 10 OVERVIEW The use of psychotropic medication as part of a child s comprehensive mental health treatment plan may be beneficial and should include consideration of all alternative interventions.
Guideline for use of Intramuscular Medication for Acutely Disturbed Behaviour in Mental Health and Associated Services
 NHS GGC Mental Health Service Guideline for use of Intramuscular Medication for Acutely Disturbed Behaviour in Mental Health and Associated Services Important Note: The Intranet version of this document
NHS GGC Mental Health Service Guideline for use of Intramuscular Medication for Acutely Disturbed Behaviour in Mental Health and Associated Services Important Note: The Intranet version of this document
Provincial Clinical Knowledge Topic Alcohol Withdrawal, Adult Inpatient V 1.0
 Provincial Clinical Knowledge Topic Alcohol Withdrawal, Adult Inpatient V 1.0 Copyright: 2018, Alberta Health Services. This work is licensed under the Creative Commons Attribution-NonCommercial-NoDerivatives
Provincial Clinical Knowledge Topic Alcohol Withdrawal, Adult Inpatient V 1.0 Copyright: 2018, Alberta Health Services. This work is licensed under the Creative Commons Attribution-NonCommercial-NoDerivatives
2010 National Audit of Dementia (Care in General Hospitals) Chelsea and Westminster Hospital NHS Foundation Trust
 Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: NHS Foundation Trust The 2010 national audit of dementia
Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: NHS Foundation Trust The 2010 national audit of dementia
Olanzapine Long-Acting Injection (Zypadhera ) - Guidelines for Prescribing and Administration (Version 3 May 2015)
 1. Key Points Olanzapine Long-Acting Injection (Zypadhera ) - Guidelines for Prescribing and Administration (Version 3 May 2015) 1.1 Olanzapine long acting injection (LAI) is indicated for the maintenance
1. Key Points Olanzapine Long-Acting Injection (Zypadhera ) - Guidelines for Prescribing and Administration (Version 3 May 2015) 1.1 Olanzapine long acting injection (LAI) is indicated for the maintenance
Admit date: 1-WM 2-WM 3.2-WM 3.7-WM 4-WM DSM-V diagnoses: Please list all diagnoses (psychiatric, chemical dependency and medical)
 https://providers.amerigroup.com Substance Use Disorder Withdrawal Management Prior Authorization and Continued Care Request (Use for American Society of Addiction Medicine [ASAM] withdrawal management
https://providers.amerigroup.com Substance Use Disorder Withdrawal Management Prior Authorization and Continued Care Request (Use for American Society of Addiction Medicine [ASAM] withdrawal management
Substance Misuse Nurse service Belfast Trust
 Substance Misuse Nurse service Belfast Trust Alcohol is the most widely available socially acceptable drug in Northern Ireland It can be an addictive substance It is a depressant- slows down the central
Substance Misuse Nurse service Belfast Trust Alcohol is the most widely available socially acceptable drug in Northern Ireland It can be an addictive substance It is a depressant- slows down the central
Guidance for community alcohol detoxification in clients with complex needs
 Document level: Clinical Service Unit (CSU) Code: DA3 Issue number: 1 Guidance for community alcohol detoxification in clients with complex needs Lead executive Medical Director Author and contact number
Document level: Clinical Service Unit (CSU) Code: DA3 Issue number: 1 Guidance for community alcohol detoxification in clients with complex needs Lead executive Medical Director Author and contact number
Alcoholism. Social environment, stress, mental health, family history, age, ethnic group, and gender all influence the risk for the condition.
 SAY NO TO ALCOHOL Alcoholism Alcoholism is a chronic and often progressive disease that includes problems controlling your drinking, being preoccupied with alcohol, continuing to use alcohol even when
SAY NO TO ALCOHOL Alcoholism Alcoholism is a chronic and often progressive disease that includes problems controlling your drinking, being preoccupied with alcohol, continuing to use alcohol even when
CP80 Version: V01. Acute Oncology Management Service Date approved: 8 th May 2015 Date ratified: 1 st June 2015 Review date: 1 st June 2017
 STANDARD OPERATING PROCEDURE (SOP) AND PATHWAY FOR THE MANAGEMENT OF PATIENTS WITH METASTATIC SPINAL CORD COMPRESSION (MSCC) WITHIN THE CHRISTIE (Refer to the Manchester Cancer Network MSCC Pathway flowchart)
STANDARD OPERATING PROCEDURE (SOP) AND PATHWAY FOR THE MANAGEMENT OF PATIENTS WITH METASTATIC SPINAL CORD COMPRESSION (MSCC) WITHIN THE CHRISTIE (Refer to the Manchester Cancer Network MSCC Pathway flowchart)
Predictors of Severity of Alcohol Withdrawal in Hospitalized Patients
 Elmer Original Article ress Predictors of Severity of Alcohol Withdrawal in Hospitalized Patients Radhames Ramos a, Thierry Mallet b, Anthony DiVittis c b, d, e, Ronny Cohen Abstract Background: Alcohol
Elmer Original Article ress Predictors of Severity of Alcohol Withdrawal in Hospitalized Patients Radhames Ramos a, Thierry Mallet b, Anthony DiVittis c b, d, e, Ronny Cohen Abstract Background: Alcohol
Alcohol Issues in the Acute General Hospital Setting
 Alcohol Issues in the Acute General Hospital Setting (Guidelines and Management) This procedural document supersedes: PAT/T 25 version 3 - Guidelines for the Management of Alcohol Issues in the Acute General
Alcohol Issues in the Acute General Hospital Setting (Guidelines and Management) This procedural document supersedes: PAT/T 25 version 3 - Guidelines for the Management of Alcohol Issues in the Acute General
Management of Severe Agitation
 Management of Severe Agitation Key Points 1. The management of the severely agitated or violent patient embraces psychological, physical and pharmacological approaches. 2. Psychological methods focus on
Management of Severe Agitation Key Points 1. The management of the severely agitated or violent patient embraces psychological, physical and pharmacological approaches. 2. Psychological methods focus on
Guidance For The Detoxification Of Alcohol Dependent Patients In Community Or Outpatient Settings
 Guidance For The Detoxification Of Alcohol Dependent Patients In Community Or Outpatient Settings Co-ordinators: Fiona Raeburn, Specialist Pharmacist in Substance Misuse Reviewer: Dr Seonaid Anderson,
Guidance For The Detoxification Of Alcohol Dependent Patients In Community Or Outpatient Settings Co-ordinators: Fiona Raeburn, Specialist Pharmacist in Substance Misuse Reviewer: Dr Seonaid Anderson,
WAHT-T&O-006 It is the responsibility of every individual to check that this is the latest version/copy of this document.
 OPERATIONAL GUIDELINES FOR OCCUPATIONAL THERAPY ASSESSMENT AND TREATMENT OF ADULTS WITH TRAUMATIC HEAD INJURY ADMITTED/TRANSFERRED OR ATTENDING A&E AT WORCESTERSHIRE ROYAL HOSPITAL This guidance does t
OPERATIONAL GUIDELINES FOR OCCUPATIONAL THERAPY ASSESSMENT AND TREATMENT OF ADULTS WITH TRAUMATIC HEAD INJURY ADMITTED/TRANSFERRED OR ATTENDING A&E AT WORCESTERSHIRE ROYAL HOSPITAL This guidance does t
A NEW RATING SCALE FOR THE ASSESSMENT OF THE ALCOHOL-WITHDRAWAL SYNDROME (AWS SCALE)
 Alcohol & Alcoholism Vol. 32, No. 6, pp. 753-760, 1997 A NEW RATING SCALE FOR THE ASSESSMENT OF THE ALCOHOL-WITHDRAWAL SYNDROME (AWS SCALE) TILMAN WETTERLING*, ROLF-DETER KANTTZ, BETTINA BESTERS, DOROTHEA
Alcohol & Alcoholism Vol. 32, No. 6, pp. 753-760, 1997 A NEW RATING SCALE FOR THE ASSESSMENT OF THE ALCOHOL-WITHDRAWAL SYNDROME (AWS SCALE) TILMAN WETTERLING*, ROLF-DETER KANTTZ, BETTINA BESTERS, DOROTHEA
Complicated Withdrawal
 Complicated Withdrawal Shamim Nejad, MD Director, Adult Burns & Trauma Psychiatry Division of Psychiatry and Medicine Medical Director, Addiction Consultation Team MGH Center for Addiction Medicine Massachusetts
Complicated Withdrawal Shamim Nejad, MD Director, Adult Burns & Trauma Psychiatry Division of Psychiatry and Medicine Medical Director, Addiction Consultation Team MGH Center for Addiction Medicine Massachusetts
Calvary Riverina Drug and Alcohol Centre
 Calvary Riverina Drug and Alcohol Centre Changing lives Changing behaviours Working towards recovery Choosing a better life Continuing the Mission of the Sisters of the Little Company of Mary Who we are?
Calvary Riverina Drug and Alcohol Centre Changing lives Changing behaviours Working towards recovery Choosing a better life Continuing the Mission of the Sisters of the Little Company of Mary Who we are?
Delirium. Information for patients, relatives and carers. Nursing and Patient Experience. Royal Surrey County Hospital. Patient information leaflet
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Delirium Information for patients, relatives and carers Nursing and Patient Experience What is delirium? Delirium is a word
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Delirium Information for patients, relatives and carers Nursing and Patient Experience What is delirium? Delirium is a word
Critical Care Pharmacological Management of Delirium
 Critical Care Pharmacological Management of Delirium Policy Title: in the Critical Care Unit Executive Summary: This policy provides guidance Pharmacological Management of delirium in the Critical Care
Critical Care Pharmacological Management of Delirium Policy Title: in the Critical Care Unit Executive Summary: This policy provides guidance Pharmacological Management of delirium in the Critical Care
Ahsan U. Rashid, M.D., F.A.C.P.
 Ahsan U. Rashid, M.D., F.A.C.P. OPIOID MAINTENANCE AND CONSENT Instructions: Review this document before signing. This document will help both the patient and caregivers in establishing a medical program
Ahsan U. Rashid, M.D., F.A.C.P. OPIOID MAINTENANCE AND CONSENT Instructions: Review this document before signing. This document will help both the patient and caregivers in establishing a medical program
SiGMA/ MMHSCT GUIDELINES FOR ANTIPSYCHOTIC DRUG TREATMENT OF SCHIZOPHRENIA. [compatible with NICE guidance]
![SiGMA/ MMHSCT GUIDELINES FOR ANTIPSYCHOTIC DRUG TREATMENT OF SCHIZOPHRENIA. [compatible with NICE guidance] SiGMA/ MMHSCT GUIDELINES FOR ANTIPSYCHOTIC DRUG TREATMENT OF SCHIZOPHRENIA. [compatible with NICE guidance]](/thumbs/80/80440271.jpg) SiGMA/ MMHSCT GUIDELINES FOR ANTIPSYCHOTIC DRUG TREATMENT OF SCHIZOPHRENIA [compatible with NICE guidance] Medicines Management Committee August 2002 For review August 2003 Rationale The SiGMA algorithm
SiGMA/ MMHSCT GUIDELINES FOR ANTIPSYCHOTIC DRUG TREATMENT OF SCHIZOPHRENIA [compatible with NICE guidance] Medicines Management Committee August 2002 For review August 2003 Rationale The SiGMA algorithm
2010 National Audit of Dementia (Care in General Hospitals) Guy's and St Thomas' NHS Foundation Trust
 Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: Guy's and St Thomas' NHS Foundation Trust The 2010 national
Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: Guy's and St Thomas' NHS Foundation Trust The 2010 national
Peterborough Nalmefene Pathway Responsibilities for Specialist Services & GP
 Peterborough Nalmefene Pathway Responsibilities for Specialist Services & GP INTRODUCTION/BACKGROUND In November 2014 NICE (National Institute of Clinical Excellence) published the Technology Appraisal
Peterborough Nalmefene Pathway Responsibilities for Specialist Services & GP INTRODUCTION/BACKGROUND In November 2014 NICE (National Institute of Clinical Excellence) published the Technology Appraisal
PATIENT GROUP DIRECTION (PGD) FOR THE ADMINISTRATION OF ORAL DIAZEPAM TO WORKING AGE AND OLDER PEOPLE IN THE COMMUNITY
 PATIENT GROUP DIRECTION (PGD) FOR THE ADMINISTRATION OF ORAL DIAZEPAM TO WORKING AGE AND OLDER PEOPLE IN THE COMMUNITY Version Number: 5 Patient Group Direction drawn up by: Name Ray Lyon Dr Al Amaladoss
PATIENT GROUP DIRECTION (PGD) FOR THE ADMINISTRATION OF ORAL DIAZEPAM TO WORKING AGE AND OLDER PEOPLE IN THE COMMUNITY Version Number: 5 Patient Group Direction drawn up by: Name Ray Lyon Dr Al Amaladoss
Version Number: 5. Patient Group Direction drawn up by: Chief Pharmacist - Strategy. Group direction authorised by:
 PATIENT GROUP DIRECTION (PGD) FOR THE INPATIENT ADMINISTRATION OF ORAL LORAZEPAM TO WORKING AGE AND OLDER PEOPLE (includes persons in a Place of Safety suite) Version Number: 5 Patient Group Direction
PATIENT GROUP DIRECTION (PGD) FOR THE INPATIENT ADMINISTRATION OF ORAL LORAZEPAM TO WORKING AGE AND OLDER PEOPLE (includes persons in a Place of Safety suite) Version Number: 5 Patient Group Direction
Home intravenous and intramuscular antibiotics
 Home intravenous and intramuscular antibiotics Children s Community Nursing Service 0161 206 2370 All Rights Reserved 2018. Document for issue as handout. This booklet has been given to you because your
Home intravenous and intramuscular antibiotics Children s Community Nursing Service 0161 206 2370 All Rights Reserved 2018. Document for issue as handout. This booklet has been given to you because your
DUAL DIAGNOSIS POLICY JANUARY This policy supersedes all previous policies for Dual Diagnosis
 DUAL DIAGNOSIS POLICY JANUARY 2017 This policy supersedes all previous policies for Dual Diagnosis DUAL DIAGNOSIS POLICY_CL37_JANUARY 2017 Policy title Policy reference Policy category Dual Diagnosis CL37
DUAL DIAGNOSIS POLICY JANUARY 2017 This policy supersedes all previous policies for Dual Diagnosis DUAL DIAGNOSIS POLICY_CL37_JANUARY 2017 Policy title Policy reference Policy category Dual Diagnosis CL37
Complicated Withdrawal
 Complicated Withdrawal Shamim Nejad, MD Medical Director, Psycho-Oncology Services Swedish Cancer Institute Swedish Medical Center Seattle, Washington Shamim.Nejad@Swedish.org Disclosures: Shamim Nejad,
Complicated Withdrawal Shamim Nejad, MD Medical Director, Psycho-Oncology Services Swedish Cancer Institute Swedish Medical Center Seattle, Washington Shamim.Nejad@Swedish.org Disclosures: Shamim Nejad,
Medical Necessity Criteria 2017
 Medical Necessity Criteria 2017 The New Directions Medical Necessity Criteria have been revised. The new version will be effective January 1, 2017. See https://www.ndbh.com/providers/behavioralhealthplanproviders.aspx.
Medical Necessity Criteria 2017 The New Directions Medical Necessity Criteria have been revised. The new version will be effective January 1, 2017. See https://www.ndbh.com/providers/behavioralhealthplanproviders.aspx.
A Care Pathway exists for the management of neutropenic fever. Copies of the care pathway document are available in EAU, A&E, Deanesly and CHU.
 Subject: Neutropenic Fever Guideline for Junior Doctors Date of Implementation: January 2010 Date of Review: January 2012 Director Responsible for Implementation and Review: Policy location: Consultant
Subject: Neutropenic Fever Guideline for Junior Doctors Date of Implementation: January 2010 Date of Review: January 2012 Director Responsible for Implementation and Review: Policy location: Consultant
AACN PCCN Review. Behavioral
 AACN PCCN Review Behavioral Presenter: Carol A. Rauen, RN, MS, CCNS, CCRN, PCCN, CEN Independent Clinical Nurse Specialist & Education Consultant rauen.carol104@gmail.com 0 Behavioral I. INTRODUCTION PCCN
AACN PCCN Review Behavioral Presenter: Carol A. Rauen, RN, MS, CCNS, CCRN, PCCN, CEN Independent Clinical Nurse Specialist & Education Consultant rauen.carol104@gmail.com 0 Behavioral I. INTRODUCTION PCCN
2010 National Audit of Dementia (Care in General Hospitals)
 Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: Barking, Havering and Redbridge Hospitals NHS Trust The 2010
Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: Barking, Havering and Redbridge Hospitals NHS Trust The 2010
Guideline for the Identification and Management of Delirium (Including use of the THINK DELIRIUM Support Tool)
 Guideline for the Identification and Management of Delirium (Including use of the THINK DELIRIUM Support Tool) B27/2009 1. Introduction 1.1 Delirium is a common problem which occurs in about 15-20 out
Guideline for the Identification and Management of Delirium (Including use of the THINK DELIRIUM Support Tool) B27/2009 1. Introduction 1.1 Delirium is a common problem which occurs in about 15-20 out
GREATER MANCHESTER INTERFACE PRESCRIBING GROUP
 GREATER MANCHESTER INTERFACE PRESCRIBING GROUP On behalf of the GREATER MANCHESTER MEDICINES MANAGEMENT GROUP SHARED CARE GUIDELINE FOR THE PRESCRIBING OF SELECTIVE SEROTONIN REUPTAKE INHIBITORS (SSRIs)
GREATER MANCHESTER INTERFACE PRESCRIBING GROUP On behalf of the GREATER MANCHESTER MEDICINES MANAGEMENT GROUP SHARED CARE GUIDELINE FOR THE PRESCRIBING OF SELECTIVE SEROTONIN REUPTAKE INHIBITORS (SSRIs)
Ambulatory Emergency Care Pathways. Painless Obstructive Jaundice
 Ambulatory Emergency Care Pathways Painless Obstructive Jaundice Effective Date: December 2011 Content Summary Ref Title Description 1 Condition Details Identifies pathway details and clinical sign-off
Ambulatory Emergency Care Pathways Painless Obstructive Jaundice Effective Date: December 2011 Content Summary Ref Title Description 1 Condition Details Identifies pathway details and clinical sign-off
Addictions in General Practice 16 th November 2017
 Addictions in General Practice 16 th November 2017 Dr Anshul Swami in Addictions Consultant Psychiatrist Priory Hospital North London, Southgate Consultant telephone: 020 8920 5616 Consultant email: SueGranger@priorygroup.com
Addictions in General Practice 16 th November 2017 Dr Anshul Swami in Addictions Consultant Psychiatrist Priory Hospital North London, Southgate Consultant telephone: 020 8920 5616 Consultant email: SueGranger@priorygroup.com
Bock Associates 221 West 2 nd Street, Suite 607 Little Rock, AR 72201
 Bock Associates 221 West 2 nd Street, Suite 607 Little Rock, AR 72201 State Project Director- Bliss Beeman, RN Clinical Associate- Shelley Smith, RN Administrative Assistant- Viki DeClerk bockarkansas@gmail.com
Bock Associates 221 West 2 nd Street, Suite 607 Little Rock, AR 72201 State Project Director- Bliss Beeman, RN Clinical Associate- Shelley Smith, RN Administrative Assistant- Viki DeClerk bockarkansas@gmail.com
MMG003 GUIDELINES FOR THE USE OF HYPNOTICS FOR THE TREATMENT OF INSOMNIA
 MMG003 GUIDELINES FOR THE USE OF HYPNOTICS FOR THE TREATMENT OF INSOMNIA Page 1 of 11 Table of Contents Why we need this Guideline... 3 What the Policy is trying to do... 3 Which stakeholders have been
MMG003 GUIDELINES FOR THE USE OF HYPNOTICS FOR THE TREATMENT OF INSOMNIA Page 1 of 11 Table of Contents Why we need this Guideline... 3 What the Policy is trying to do... 3 Which stakeholders have been
Psychosis with coexisting substance misuse
 Psychosis with coexisting substance misuse Clinical case scenarios for primary, secondary and third sector services Implementing NICE guidance March 2011 OTC α blocker information sheet for GP s (2010)
Psychosis with coexisting substance misuse Clinical case scenarios for primary, secondary and third sector services Implementing NICE guidance March 2011 OTC α blocker information sheet for GP s (2010)
ALCOHOL RELATED BRAIN DAMAGE (ARBD)
 FACT SHEET 01 ALCOHOL RELATED BRAIN DAMAGE (ARBD) This fact sheet will help you get a better understanding of Alcohol Related Brain Damage, how it can present, what causes it and how someone with ARBD
FACT SHEET 01 ALCOHOL RELATED BRAIN DAMAGE (ARBD) This fact sheet will help you get a better understanding of Alcohol Related Brain Damage, how it can present, what causes it and how someone with ARBD
AGED SPECIFIC ASSESSMENT TOOLS. Anna Ciotta Senior Clinical Neuropsychologist Peninsula Mental Health Services
 AGED SPECIFIC ASSESSMENT TOOLS Anna Ciotta Senior Clinical Neuropsychologist Peninsula Mental Health Services Issues in assessing the Elderly Association between biological, psychological, social and cultural
AGED SPECIFIC ASSESSMENT TOOLS Anna Ciotta Senior Clinical Neuropsychologist Peninsula Mental Health Services Issues in assessing the Elderly Association between biological, psychological, social and cultural
4.Do a Mini Mental State Examination on your study buddy.
 MCQ PYCHIATRIC DIORDER UAN TUCKER 1.High yield indicators of an organic illness include all of these except? a) disorientation b) rapid onset c) no pre morbid decline d) a score of 23 on Folsteins Mini
MCQ PYCHIATRIC DIORDER UAN TUCKER 1.High yield indicators of an organic illness include all of these except? a) disorientation b) rapid onset c) no pre morbid decline d) a score of 23 on Folsteins Mini
Risk assessment of moderate to severe alcohol withdrawal Predictors for seizures and delirium tremens
 Risk assessment of moderate to severe alcohol withdrawal Predictors for seizures and delirium tremens Results of a retrospective Cohort Study Florian Eyer, MD Toxicological Department Klinikum rechts der
Risk assessment of moderate to severe alcohol withdrawal Predictors for seizures and delirium tremens Results of a retrospective Cohort Study Florian Eyer, MD Toxicological Department Klinikum rechts der
Schizophrenia. This factsheet provides a basic description of schizophrenia, its symptoms and the treatments and support options available.
 This factsheet provides a basic description of schizophrenia, its symptoms and the treatments and support options available. What is schizophrenia? Schizophrenia is a severe mental health condition. However,
This factsheet provides a basic description of schizophrenia, its symptoms and the treatments and support options available. What is schizophrenia? Schizophrenia is a severe mental health condition. However,
