Lead for Gastroenterology Lee Dodge Alcohol Liaison 03/03/2015. Clive Gibson Safeguarding Adults Lead Nurse 03/03/2015
|
|
|
- Arlene Cooper
- 6 years ago
- Views:
Transcription
1 Acute Alcohol Withdrawal Management for Adult Inpatients Type: Clinical Guideline Register No: 1409 Status: Public on ratification Developed in response to: Best Practice Contributes to CQC Outcome number: 4 Consulted With Post/Committee/Group Date Lauren Jones & Maria Richards Pharmacists 11/0/01 Adele Wisby Head of Nursing 1/01/01 Dr Rakesh Shah Consultant Gastroenterologist & Clinical 0/01/01 Lead for Gastroenterology Lee Dodge Alcohol Liaison 0/0/01 Clive Gibson Safeguarding Adults Lead Nurse 0/0/01 Doug Smale Local Security Management Specialist 0/0/01 Ryan Curtis Health & Safety Manager 0/0/01 Professionally Approved By Dr Alan Jackson Clinical Director Medicine 19/01/01 Version Number 1.1 Issuing Directorate Acute Medicine Ratified by: Document Ratification Group Ratified on: th March 01 Executive Management Board Sign Off April 01 Date Implementation Date 0th March 01 Next Review Date March 018 Author/Contact for Information Dr Chirag Oza, Consultant Gastroenterologist & Hepatologist Policy to be followed by (target staff) All Clinical Staff Distribution Method Intranet & Website Related Trust Policies (to be read in conjunction with) Document Review History Version Number Brief Reason for Change or Update Authored/Reviewed by Active Date 1.0 First version Dr Chirag Oza 0 March Update to 10.1 Maria Richards November 01 1
2 Index 1. Purpose. Scope. Staff Training 4. Definitions. Management first 4 hours. Management after the first 4 hours 7. Difficult to Control Patients 8. Discharge Planning 9. Breech Reporting 10. Audit & Monitoring 11. Useful Contacts 1. References Appendix 1 Clinical Alcohol Withdrawal Assessment (CIWA-Ar) Chart Appendix Dose Calculation
3 1. Purpose 1.1 This purpose of this clinical guideline is to: standardise the prescription of detoxification for alcohol withdrawal in all adult patients admitted with, or experiencing, alcohol withdrawal to minimise morbidity and mortality and maximise patient comfort through:.0 Scope Recognition of all alcohol misuser hospital attendees. Identification of sub-groups with, or at risk of, potentially life-threatening complications. Prompt initiation of appropriate medical management.1 This policy is to be used by all doctors, nurses, pharmacists and Allied Health Professionals.. This policy covers adult inpatients experiencing acute alcohol withdrawal (18 years and above) in Broomfield Hospital. It excludes outpatients.. This policy should be considered in all adult patients at risk of acute alcohol withdrawal, as identified by AUDIT-C in the Nursing Assessment, or identified during medical/surgical clerking at the time of admission (acute or planned). However, the decision for detoxification should be made by a senior doctor who has experience in managing these patients..4 Detoxification from alcohol in inpatients is usually indicated in the following cases: Definitely indicated if weekly alcohol consumption exceeds 100 units/week Probably required for patients drinking 0 to 100 units/week Not usually needed when intake is less than 0 units a week but may be required. Patients with complex alcohol withdrawal (e.g. DTs (delirium tremens), seizures, hallucinations, etc.), should be admitted for inpatient management of alcohol withdrawal as per the guidelines set out in this policy..0 Staff Training.1 All medical and nursing staff are to ensure that their knowledge, competencies and skills are up to date.. During induction, staff will receive instruction on current policies and guidelines and how to access them.. Staff will receive training on how to use this policy on the wards. This will be undertaken as face to face training by the Alcohol Liaison Nurse. This will be mandatory for all doctors and nurses working on wards where patients are admitted for more than 4 hours.
4 4.0 Definitions 4.1 Alcohol withdrawal This refers to a group of symptoms that may occur from suddenly stopping the use of alcohol after chronic or prolonged ingestion Symptoms and signs include (amongst others): Anxiety, agitation, irritability, depression, mood swings, insomnia, tremor of the hands, tongue, eyelids, fever (with or without infection), hypertension, tachycardia, sweating, nausea, vomiting, diarrhoea, headache, pallor, dilated pupils, amongst others. 4. Delirium Tremens 4..1 Delirium tremens (DTs) is the most severe form of alcohol l withdrawal manifested by altered mental status (global confusion) and sympathetic overdrive (autonomic hyperactivity), which can progress to cardiovascular collapse. 4.. DTs occur in about % of patients during withdrawal, usually - days after alcohol cessation or reduced alcohol intake. 4.. DTs are fatal in 1-0% of inappropriately managed patients, whilst prophylactic and proactive sedation reduces mortality to 1-% 4..4 Symptoms and signs include agitation, fever, hallucinations, confusion and seizures 4. Wernicke s Encephalopathy 4..1 This refers to the presence of neurological symptoms caused by biochemical lesions of the central nervous system, after exhaustion of B vitamin reserves, in particular thiamine. 4.. It classically presents with the triad of confusion, ataxia and ophthalmoplegia, but only 10% of patients present with all three features. 4.. It may develop rapidly or over a number of days. Inappropriately managed, it is the primary (or a contributory) cause of death in up to 0% of patients and results in permanent brain damage (Korsakoff s psychosis) in 8% of survivors. 4.4 Alcohol Units One unit equates to 10ml or 8g of pure ethanol The alcohol by volume (ABV) of a drink equates to the number of units contained in one litre of that drink, e.g. a 1 litre bottle of 40% spirit will contain 40 units of alcohol..0 Management first 4 hours.1 Patients who have capacity must consent (verbally) to the alcohol detoxification regime. If they are not consenting, urgent senior clinician review is necessary to ascertain appropriateness of admission. For those patients who do not have capacity to consent, an MCA will need to be filled out, and consideration for DoLS (deprivation of liberty) made if indicated.. For the first 4 hours of the admission (initial assessment and treatment) the admitting doctor (FY1/FY/CT/SpR/Consultant) should prescribe the following: Adults < yrs with no co-existing risk factors*: chlordiazepoxide -0mg PO - 4 hourly PRN as per CIWA-Ar chart (maximum 0mg in 4 hours) 4
5 Elderly (age > yrs) or in presence of co-existing risk factors*: chlordiazepoxide 10 mg -4 hourly PRN (maximum 0mg in 4 hours) *co-existing risk factors are liver impairment, frailty, renal impairment, concomitant opioids Pabrinex I+II, pairs (= 4 vials) IV TDS for days Thiamine 100mg PO BD for 0 days, after completion of IV Pabrinex Vitamin B Co. Strong tabs PO OD for 0 days, after completion of IV Pabrinex Diazepam 10-0mg (elderly 10mg) IV/PR PRN for seizures (patients are at risk of withdrawal seizures. Nurses are to assess the patient for the first 4 hours using a flexible regime via CIWA- Ar Withdrawal Scale (See Appendix 1.1 CIWA-Ar Assessment Tool), and administer chlordiazepoxide as follows: CIWA-Ar score Adults <yrs with no co-existing risk factors* Treatment Adults yrs and/or with co-existing risk factors* 0-9 (mild withdrawal) (moderate withdrawal) >1 (severe withdrawal) ASSESS CIWA-Ar EVERY -4 HOURS No treatment necessary Administer chlordiazepoxide mg STAT (then give mg every -4 hours PRN. Maximum daily dose of 0mg in 4 hours) Administer chlordiazepoxide 0mg STAT (then give 0mg every -4 hours PRN. Maximum daily dose of 0mg in 4 hours) ASSESS CIWA-Ar HOURLY No treatment necessary Administer chlordiazepoxide 10mg STAT (then give 10mg every -4 hours PRN. Maximum daily dose of 0mg in 4 hours) Administer chlordiazepoxide mg STAT (then give mg every -4 hours PRN. Maximum daily dose of 0mg in 4 hours) *co-existing risk factors are liver impairment, frailty, renal impairment, concomitant opioids.4 Patient should be assessed more frequently if scores remain high despite treatment, or if patient clinically appears to still be withdrawing. If patient is pregnant, ensure Obstetric team have been notified of admission.0 Management after the first 4 hours.1 After the first 4 hours, stop the chlordiazepoxide prescribed on a PRN basis.. Calculate total chlordiazepoxide administered during the first 4 hours and start a regular reducing regime accordingly.. Reduce the total dose needed in 4 hours by 0%, then divide this dose into 4 equal doses and prescribe as a fixed QDS dose for the detoxification regime..4 Continue to reduce the total daily dose by 0% daily over the following -7 days, and then stop the chlordiazepoxide (this is as an inpatient).
6 . Assess patient as per CIWA-Ar withdrawal scale every 4 hours. Review patients daily. A sign that the patient is receiving the right dose is that the CIWA scores should be reducing over time.. Patients should not normally be prescribed PRN chlordiazepoxide after the initial 4 hours. A patient who is still showing withdrawal symptoms and may need further PRN should be assessed and their detoxification regime reviewed. A patient who seems oversedated after first 4 hours should also have the reducing regime reviewed by review team. 7.0 Difficult to Control Patients 7.1 These patients should be urgently reviewed by Medical Staff. Consider switching to IV diazepam may be administered as a bolus at a rate of mg/min through a peripheral (large vein) or central route. A dose of -10mg every 0-0mins may be given until symptoms subside or the patient is sedated (max 0mg in 4hours). These patients should be managed either on MHDU or ITU. 7. In elderly patients use half the recommended diazepam dose. Beware of airway and respiratory complications. 7. For patients with liver failure, IV lorazepam 1-mg over mins (max hourly) may be used instead of diazepam (allowing for drug availability). 7.4 Consider using haloperidol PO/IM mg TDS as an alternative option 7. Consider extending the PRN dosing beyond 4hours in patients with delirium tremens 7. Consider using a longer withdrawal regimen if unable to stabilise after 4 hours 7.7 Discuss with the senior medical team and consider consulting with Psychiatric Liaison. 7.8 Strict cardiac & airways monitoring is essential. If this cannot be achieved then avoid IV sedation 7.9 Patients who are agitated or violent secondary to delirium tremens may require the presence of hospital security to ensure their own, other patient s, visitors and staff safety. In an emergency situation security are to be contacted using the bleep system. If long term security is required this is to be arranged with the Trust Security Manager, with advice as to what may be required from the LSMS (Local Security Management Specialist). 8.0 Discharge Planning 8.1 The detoxification regimen should be completed before the patient is discharged. 8. Make it clear on the prescription chart that chlordiazepoxide stops after the last day of the detoxification regime 8. At Consultant s discretion, patients can be given up to a maximum of 0mg chlordiazepoxide in discharge medication. Please specify it is not to be continued after this. 8.4 Patients who discharge themselves against medical advice should not be supplied with chlordiazepoxide to take away, and they should sign the Trust self discharge form. 8. All patients undergoing detoxification should be discharged on thiamine 100mg twice daily and Vitamin B Co Strong tabs daily for 0 days.
7 8. It is important that the GP is informed on the discharge letter not to add chlordiazepoxide to patients repeat medications. 9.0 Breech Reporting 9.1 Those patients who come to harm (withdrawal seizure, DTs, etc.) during their admission will require a Datix completed Audit & Monitoring 10.1 Pharmacy will monitor all acute prescriptions for chlordiazepoxide, and any concerns will be reported to the physician responsible for the patient. 10. Annual audit will be undertaken to monitor patient length of stay and any adverse events. This will be undertaken by the Gastroenterology department, and presented at one of the weekly Gastroenterology teaching sessions. 10. All reported (datixed) risk events will be reviewed at least annually and the Consultant Gastroenterologist & Hepatologist will report any findings/trends to the Clinical Director Useful Contacts Lee Dodge, Alcohol Liaison Nurse: Ext 4804, Mobile lee.dodge@meht.nhs.uk CHANGES (Community Drug & Alcohol Team) Tel: CHOICES Chelmsford (OpenRoad) Tel: Essex Young People s Drug and Alcohol Services (EYPDAS) Tel: References Taylor, D; Paton, C; Kerwin R (007). The Maudsley Prescribing Guidelines 9th Edition BNF. September 01 NICE guidelines: Alcohol-use disorders: physical complications (June 010) NICE guidelines: Nutrition support in adults (November 01) Parker AJ, Marshall EJ, Ball DM; Diagnosis and management of alcohol use disorders. BMJ. 008 Mar 1; (74): Health and Social Care Information Centre: Appendix 1 7
8 Clinical Alcohol Withdrawal Assessment (CIWA-Ar) Chart This chart is to be used in conjunction with the assessment questions overleaf Frequency of s: Hourly 4 Hourly Surname (or affix label): Ward: Forename(s): Date of Birth: Hospital Number: Consultant: NHS Number: Date Time Assess and rate each of the following: Nausea/Vomiting (0-7) Tremors (0-7) Paroxysmal Sweats (0-7) Anxiety (0-7) Agitation (0-7) Tactile Disturbances (0-7) Auditory Disturbances (0-7) Visual Disturbances (0-7) Headache (0-7) Orientation (0-7) Total CIWA-Ar Score Dose given (mg) Please sign drug chart If CIWA-Ar = Give mg Chlordiazepoxide If CIWA-Ar = 1 Give 0mg Chlordiazepoxide Nurse Signature Using the descriptions and questions overleaf, rate each withdrawal symptom, then add the scores together Nausea and Vomiting: Ask Do you feel sick to your stomach? Have you vomited? Tactile (touch) Disturbances: Ask Have you any itching, pins and needles sensations, any burning, any numbness, or do you feel bugs crawling 8
9 0 no nausea with no vomiting 1 mild nausea with no vomiting 4 intermittent nausea with dry heaves 7 constant nausea, frequent dry heaves and vomiting Tremor: Arms extended and fingers spread wide apart. 0 no tremor 1 not visible, but can be felt fingertip to fingertip 4 moderate, with patients arms extended 7 severe, even with arms not extended Paroxysmal Sweats: 0 no sweat visible 1 barely perceptible sweating, palms moist 4 beads of sweat obvious on forehead 7 drenching sweats Anxiety: Ask Do you feel nervous? 0 no anxiety, at ease 1 mildly anxious 4 moderately anxious or guarded, so anxiety is suggested 7 equivalent to acute panic states as seen in severe delirium or acute schizophrenic states Agitation: 0 normal activity 1 somewhat more than normal activity 4 moderately fidgety and restless 7 paces back and forth during interview, or thrashes about on or under your skin? 0 none 1 very mild itching, pins and needles, burning or numbness mild itching, pins and needles, burning or numbness moderate itching, pins and needles, burning or numbness 4 moderately severe hallucinations severe hallucinations extremely severe hallucinations 7 continuous hallucinations Auditory (hearing) Disturbances: Ask Are you more aware of sounds around you? Are they harsh? Do they frighten you? Are you hearing anything that is disturbing you? Are you hearing things you know are not there? 0 not present 1 very mild harshness or ability to frighten mild harshness or ability to frighten moderate harshness or ability to frighten 4 moderately severe hallucinations severe hallucinations extremely severe hallucinations 7 continuous hallucinations Visual (sight) Disturbances: Ask Does the light appear to be too bright? Is it s colour different? Does it hurt your eyes? Are you seeing anything that s disturbing you? Are you seeing anything that you know is not there? 0 not present 1 very mild sensitivity mild sensitivity moderate sensitivity 4 moderately severe hallucinations severe hallucinations extremely severe hallucinations 7 continuous hallucinations Headache, Fullness in Head: Ask Does your head feel different? Does it feel like there is a band around your head? Do not rate for dizziness or lightheadedness. Otherwise, rate severity. 0 not present 1 very mild mild moderate 4 moderately severe severe very severe 7 extremely severe Orientation and Clouding of Sensorium: Ask "What day is this? Where are you? Who am I?" 0 orientated and can do serial additions 1 cannot do serial additions or is uncertain about date disorientated for date by no more than calendar days disorientated for date by more than calendar days 4 disorientated for place or person Appendix 9
10 DOSE CALCULATION Simple Dose Equivalence: Diazepam 10 mg = chlordiazepoxide mg = lorazepam 1mg Chlordiazepoxide dose calculation after 4 hours: After the first 4 hours, stop the chlordiazepoxide prescribed on a PRN basis. Calculate total chlordiazepoxide administered during the first 4 hours and start a regular reducing regime accordingly. Reduce the total dose needed in 4 hours by 0%, then divide this dose into 4 equal doses and prescribe as a fixed QDS dose for the detoxification regime Continue to reduce the total daily dose by 0% daily over the following -7 days, and then stop the chlordiazepoxide (this is as an inpatient). Chlordiazepoxide should not been administered at the same time as other benzodiazepines (e.g. diazepam and lorazepam), but if other benzodiazepines have been given, the equivalent separate doses should be added to calculate the 4 hour total dose EXAMPLE DOSE CALCULATOR Record dose and time of any benzodiazepine (eg. chlordiazepoxide) given in 4 hour period Continue to reduce the total daily dose by 0% daily over the following -7 days, and then stop the chlordiazepoxide DATE AND TIME CIWA SCORE BENZODIAZEPINE GIVEN DOSE ADMINISTERED (mg) Total dose of Benzodiazepines at 4 hours NB: Convert other benzodiazepines to equivalent dose of chlordiazepoxide [Total dose reduced by 0%] [Total dose reduced by 0%} divided by 4 = QDS dose for next day 10
Alcohol withdrawal. Clinical features
 Alcohol withdrawal Clinical features Severity increase with amount consumed; uncommon with < drinks per day. Predictable pattern: patients with previous withdrawal seizures are at high risk for recurrence.
Alcohol withdrawal Clinical features Severity increase with amount consumed; uncommon with < drinks per day. Predictable pattern: patients with previous withdrawal seizures are at high risk for recurrence.
ALCOHOL WITHDRAWAL GUIDELINES
 ALCOHOL WITHDRAWAL GUIDELINES Policy author Accountable Executive Lead Approving body Policy reference Dr M Lewis, Gastroenterologist; Professor J A Vale, Clinical Toxicologist; Dr D A Robertson, Alcohol
ALCOHOL WITHDRAWAL GUIDELINES Policy author Accountable Executive Lead Approving body Policy reference Dr M Lewis, Gastroenterologist; Professor J A Vale, Clinical Toxicologist; Dr D A Robertson, Alcohol
Stabilization Algorithm
 VA/DoD Clinical Practice Guideline for the Management of Substance Use Disorders Stabilization Algorithm Stabilization Pocket Card 1 Patient and Time Information Clinical Institute Withdrawal Assessment
VA/DoD Clinical Practice Guideline for the Management of Substance Use Disorders Stabilization Algorithm Stabilization Pocket Card 1 Patient and Time Information Clinical Institute Withdrawal Assessment
Alcohol Detoxification (Inpatient) Prescribing Guidelines
 Alcohol Detoxification (Inpatient) Prescribing Guidelines Author: Sponsor/Executive: Responsible committee: Consultation & Approval: (Committee/Groups which signed off the procedure, including date) This
Alcohol Detoxification (Inpatient) Prescribing Guidelines Author: Sponsor/Executive: Responsible committee: Consultation & Approval: (Committee/Groups which signed off the procedure, including date) This
Guidelines for the In-Patient Management of Alcohol Withdrawal at Frimley Park Hospital NHS Foundation Trust
 Guidelines for the In-Patient Management of Alcohol Withdrawal at Frimley Park Hospital NHS Foundation Trust Authors: Dr Aftab Ala, Consultant Gastroenterologist & Hepatologist Dr Tasneem Pirani, ST4 in
Guidelines for the In-Patient Management of Alcohol Withdrawal at Frimley Park Hospital NHS Foundation Trust Authors: Dr Aftab Ala, Consultant Gastroenterologist & Hepatologist Dr Tasneem Pirani, ST4 in
APPENDIX 7 CLINICAL INSTITUTE NARCOTIC ASSESSMENT (CINA) SCALE FOR WITHDRAWAL SYMPTOMS
 APPENDIX 7 CLINICAL INSTITUTE NARCOTIC ASSESSMENT (CINA) SCALE FOR WITHDRAWAL SYMPTOMS The Clinical Institute Narcotic Assessment (CINA) Scale measures 11 signs and symptoms commonly seen in patients during
APPENDIX 7 CLINICAL INSTITUTE NARCOTIC ASSESSMENT (CINA) SCALE FOR WITHDRAWAL SYMPTOMS The Clinical Institute Narcotic Assessment (CINA) Scale measures 11 signs and symptoms commonly seen in patients during
Assessment Main title and management of alcohol dependence and withdrawal in the acute hospital: concise guidance
 CONCISE GUIDANCE Clinical Medicine 01, Vol 1, No : 71 Assessment Main title and management of alcohol dependence and withdrawal in the acute hospital: concise guidance Author head name Stephen Stewart
CONCISE GUIDANCE Clinical Medicine 01, Vol 1, No : 71 Assessment Main title and management of alcohol dependence and withdrawal in the acute hospital: concise guidance Author head name Stephen Stewart
Consulted With: Post/Committee/Group: Date: John Crome Drug and Alcohol Liaison Emergency Care
 THE MANAGEMENT OF OPIOID WITHDRAWAL IN ADULT PATIENTS Type: Clinical Guideline Register No: 18007 Status: Public on ratification Developed in response to: Contributes to CQC Outcome number: 12 Best practice
THE MANAGEMENT OF OPIOID WITHDRAWAL IN ADULT PATIENTS Type: Clinical Guideline Register No: 18007 Status: Public on ratification Developed in response to: Contributes to CQC Outcome number: 12 Best practice
Pharmacological Therapy Policy Practice Guidance Note Management of Acute Alcohol Withdrawal in Adults (Over 18) - V01. Planned review: December 2017
 Pharmacological Therapy Policy Practice Guidance Note Management of Acute Alcohol Withdrawal in Adults (Over 18) - V01 V01 issued: Issue 1- Dec 14 Issue 2 April 17 Planned review: December 2017 PPT-PGN
Pharmacological Therapy Policy Practice Guidance Note Management of Acute Alcohol Withdrawal in Adults (Over 18) - V01 V01 issued: Issue 1- Dec 14 Issue 2 April 17 Planned review: December 2017 PPT-PGN
Pharmacological Therapy Policy Practice Guidance Note Management of Acute Alcohol Withdrawal in Adults (Over 18) - V02. Planned review: Dec 2020
 Pharmacological Therapy Policy Practice Guidance Note Management of Acute Alcohol Withdrawal in Adults (Over 18) - V02 Issue No: Issue 1- Dec 17 Planned review: Dec 2020 PPT-PGN 22 Part of NTW(C)38 Pharmacological
Pharmacological Therapy Policy Practice Guidance Note Management of Acute Alcohol Withdrawal in Adults (Over 18) - V02 Issue No: Issue 1- Dec 17 Planned review: Dec 2020 PPT-PGN 22 Part of NTW(C)38 Pharmacological
Alcohol Withdrawal Guidelines
 SH CP 197 Alcohol Withdrawal Guidelines Summary: Keywords: Target Audience: Identification, assessment and management of alcohol dependence and harmful alcohol use in people presenting for assessment or
SH CP 197 Alcohol Withdrawal Guidelines Summary: Keywords: Target Audience: Identification, assessment and management of alcohol dependence and harmful alcohol use in people presenting for assessment or
Alcohol withdrawal including the Symptom triggered CIWA score Management
 Alcohol withdrawal including the Symptom triggered CIWA score Management Classification: Policy Lead Author: Ruth Brown Alcohol specialist Nurse Additional author(s): Hailey Pennington Authors Division:
Alcohol withdrawal including the Symptom triggered CIWA score Management Classification: Policy Lead Author: Ruth Brown Alcohol specialist Nurse Additional author(s): Hailey Pennington Authors Division:
Title Alcohol Withdrawal Management Guidelines
 Document Control Title Alcohol Withdrawal Management Guidelines Author Directorate Date Version Issued 0.1 Dec 2009 0.2 Mar 2010 0.3 Nov 2010 Status Draft 0.4 Sep 2015 1.0 Jan 2016 2.0 Nov Final 2018 Main
Document Control Title Alcohol Withdrawal Management Guidelines Author Directorate Date Version Issued 0.1 Dec 2009 0.2 Mar 2010 0.3 Nov 2010 Status Draft 0.4 Sep 2015 1.0 Jan 2016 2.0 Nov Final 2018 Main
Northern Ireland Alcohol Use Disorders Care Pathway. management in the acute hospital setting
 Northern Ireland Alcohol Use Disorders Care Pathway management in the acute hospital setting Main Content 1. Introduction 2 2. Alcohol Withdrawal Syndrome 3 2.1. Delirium tremens 3 2.2. Seizures 4 2.3.
Northern Ireland Alcohol Use Disorders Care Pathway management in the acute hospital setting Main Content 1. Introduction 2 2. Alcohol Withdrawal Syndrome 3 2.1. Delirium tremens 3 2.2. Seizures 4 2.3.
Acute Alcohol Withdrawal Protocol
 Acute Alcohol Withdrawal Protocol Controlled document This document is uncontrolled when downloaded or printed Reference number Version 1 Author WHHT: C268 Dr Mohamed Shariff Date ratified August 2014
Acute Alcohol Withdrawal Protocol Controlled document This document is uncontrolled when downloaded or printed Reference number Version 1 Author WHHT: C268 Dr Mohamed Shariff Date ratified August 2014
Clinical Guideline / Formulary Document Pharmacy Department Medicines Management Services
 Clinical Guideline / Formulary Document Pharmacy Department Medicines Management Services SUBSTANCE DEPENDENCY For full details of the of the medication discussed in this formulary including side effects,
Clinical Guideline / Formulary Document Pharmacy Department Medicines Management Services SUBSTANCE DEPENDENCY For full details of the of the medication discussed in this formulary including side effects,
SECTION 10: MANAGEMENT OF ALCOHOL, OPIOID AND BENZODIAZEPINE DEPENDENCE. Formulary and Prescribing Guidelines
 SECTION 10: MANAGEMENT OF ALCOHOL, OPIOID AND BENZODIAZEPINE DEPENDENCE Formulary and Prescribing Guidelines 10.1 Introduction This document covers the safe prescribing and management for service users
SECTION 10: MANAGEMENT OF ALCOHOL, OPIOID AND BENZODIAZEPINE DEPENDENCE Formulary and Prescribing Guidelines 10.1 Introduction This document covers the safe prescribing and management for service users
Education Pack for the Alcohol Liaison Nurse Service
 Education Pack for the Alcohol Liaison Nurse Service Welcome to the Alcohol Liaison Nurse Service, this pack is designed to help you get the most out of your time here with us today and set some objectives
Education Pack for the Alcohol Liaison Nurse Service Welcome to the Alcohol Liaison Nurse Service, this pack is designed to help you get the most out of your time here with us today and set some objectives
Northern Ireland Alcohol Use Disorders Care Pathway. management in the acute hospital setting
 Northern Ireland Alcohol Use Disorders Care Pathway management in the acute hospital setting Main Content 1. Introduction 2 2. Alcohol Withdrawal Syndrome 3 2.1. Delirium tremens 3 2.2. Seizures 4 2.3.
Northern Ireland Alcohol Use Disorders Care Pathway management in the acute hospital setting Main Content 1. Introduction 2 2. Alcohol Withdrawal Syndrome 3 2.1. Delirium tremens 3 2.2. Seizures 4 2.3.
GUIDELINES FOR ALCOHOL DETOXIFICATION AT HMP BEDFORD
 GUIDELINES FOR ALCOHOL DETOXIFICATION AT HMP BEDFORD Policy Details NHFT document reference MMG027/HMP Version 1 Date Ratified May 2017 Ratified by HMP Bedford Drugs and Therapeutics Committee Implementation
GUIDELINES FOR ALCOHOL DETOXIFICATION AT HMP BEDFORD Policy Details NHFT document reference MMG027/HMP Version 1 Date Ratified May 2017 Ratified by HMP Bedford Drugs and Therapeutics Committee Implementation
MANAGEMENT AND DETOXIFICATION FOR GAMMA- HYDROXYBUTYRATE (GHB) AND GAMMA-BUTARYL LACTONE (GBL) GUIDELINES SEPTEMBER 2017
 MANAGEMENT AND DETOXIFICATION FOR GAMMA- HYDROXYBUTYRATE (GHB) AND GAMMA-BUTARYL LACTONE (GBL) GUIDELINES SEPTEMBER 2017 Policy title Management and Detoxification for GHB and GBL Policy PHA61 reference
MANAGEMENT AND DETOXIFICATION FOR GAMMA- HYDROXYBUTYRATE (GHB) AND GAMMA-BUTARYL LACTONE (GBL) GUIDELINES SEPTEMBER 2017 Policy title Management and Detoxification for GHB and GBL Policy PHA61 reference
University Hospitals of Leicester NHS Trust
 University Hospitals of Leicester NHS Trust ACUTE ALCOHOL WITHDRAWAL MANAGEMENT Guidelines for Management of Acute Medical Emergencies Approved By: Policy and Guideline Committee Date Approved: 21 November
University Hospitals of Leicester NHS Trust ACUTE ALCOHOL WITHDRAWAL MANAGEMENT Guidelines for Management of Acute Medical Emergencies Approved By: Policy and Guideline Committee Date Approved: 21 November
Contributes to CQC Outcome number: 9&12 Consulted With Post/Committee/Group Date. Pharmacist. Alison Felton Head of Pharmacy/Deputy Chief.
 Prescribing paracetamol in adult inpatients at MEHT Type: Clinical Guideline Register No: 18005 Status: Public on ratification Developed in response to: In line with Basildon Contributes to CQC Outcome
Prescribing paracetamol in adult inpatients at MEHT Type: Clinical Guideline Register No: 18005 Status: Public on ratification Developed in response to: In line with Basildon Contributes to CQC Outcome
Lorraine Wilson, 74 years of age, is admitted. Alcohol Withdrawal. During Hospitalization. Early recognition and consistent intervention are critical.
 1.9 h o u r s Continuing Education Withdrawal During Hospitalization Early recognition and consistent intervention are critical. Overview: For a chronic drinker, sudden alcohol withdrawal because of an
1.9 h o u r s Continuing Education Withdrawal During Hospitalization Early recognition and consistent intervention are critical. Overview: For a chronic drinker, sudden alcohol withdrawal because of an
Policy on Pharmacological Therapies Practice Guidance Note Reducing Dosing Errors with Opioid Medicines V04
 Policy on Pharmacological Therapies Practice Guidance Note Reducing Dosing Errors with Opioid Medicines V04 Date issued Issue 1 Nov 2018 Planned review Nov 2021 PPT-PGN 18 part of NTW(C)38 Pharmaceutical
Policy on Pharmacological Therapies Practice Guidance Note Reducing Dosing Errors with Opioid Medicines V04 Date issued Issue 1 Nov 2018 Planned review Nov 2021 PPT-PGN 18 part of NTW(C)38 Pharmaceutical
CMBHS Clinical Management of Behavioral Health Services
 Client: CMBHS Clinical Management of Behavioral Health Services Detoxification Assessment Assessment Information (te: All are Required fields) Assessment Number Assessment Date Assessment Type Contact
Client: CMBHS Clinical Management of Behavioral Health Services Detoxification Assessment Assessment Information (te: All are Required fields) Assessment Number Assessment Date Assessment Type Contact
Contents. May 2016 KYN Long Training 2
 Contents Impact of alcohol on health and the NHS. Department of Health guidance and associated risk of drinking above these levels. How to calculate units of alcohol. Direct health implications to the
Contents Impact of alcohol on health and the NHS. Department of Health guidance and associated risk of drinking above these levels. How to calculate units of alcohol. Direct health implications to the
Critical Care Pharmacological Management of Delirium
 Critical Care Pharmacological Management of Delirium Policy Title: in the Critical Care Unit Executive Summary: This policy provides guidance Pharmacological Management of delirium in the Critical Care
Critical Care Pharmacological Management of Delirium Policy Title: in the Critical Care Unit Executive Summary: This policy provides guidance Pharmacological Management of delirium in the Critical Care
INPATIENT ALCOHOL WITHDRAWAL PRESCRIBING GUIDELINES MAY 2018
 INPATIENT ALCOHOL WITHDRAWAL PRESCRIBING GUIDELINES MAY 2018 Policy title Inpatient alcohol withdrawal Prescribing Guidelines Policy PHA28B reference Policy category Clinical Relevant to Trust-wide any
INPATIENT ALCOHOL WITHDRAWAL PRESCRIBING GUIDELINES MAY 2018 Policy title Inpatient alcohol withdrawal Prescribing Guidelines Policy PHA28B reference Policy category Clinical Relevant to Trust-wide any
ALCOHOL ASSESSMENT AND DETOXIFICATION POLICY FOR INPATIENTS
 ALCOHOL ASSESSMENT AND DETOXIFICATION POLICY FOR INPATIENTS Version: 4 Date issued: August 2017 Review date: August 2020 Applies to: All staff working within Trust Inpatient settings This document is available
ALCOHOL ASSESSMENT AND DETOXIFICATION POLICY FOR INPATIENTS Version: 4 Date issued: August 2017 Review date: August 2020 Applies to: All staff working within Trust Inpatient settings This document is available
Administration of High Dose Intra- Muscular Vitamin Supplements for Patients Undergoing Alcohol Detoxification. Standard Operating Procedure
 Administration of High Dose Intra- Muscular Vitamin Supplements for Patients Undergoing Alcohol Detoxification Standard Operating Procedure DOCUMENT CONTROL: Version: 3 Ratified by: Quality Assurance Sub
Administration of High Dose Intra- Muscular Vitamin Supplements for Patients Undergoing Alcohol Detoxification Standard Operating Procedure DOCUMENT CONTROL: Version: 3 Ratified by: Quality Assurance Sub
Withdrawal.
 Withdrawal Shamim Nejad, MD Director, Adult Burns & Trauma Psychiatry Division of Psychiatry and Medicine Medical Director, Addiction Consultation Team MGH Center for Addiction Medicine Massachusetts General
Withdrawal Shamim Nejad, MD Director, Adult Burns & Trauma Psychiatry Division of Psychiatry and Medicine Medical Director, Addiction Consultation Team MGH Center for Addiction Medicine Massachusetts General
MEDICALLY ASSISTED COMMUNITY ALCOHOL WITHDRAWAL GUIDELINES SEPTEMBER 2015
 MEDICALLY ASSISTED COMMUNITY ALCOHOL WITHDRAWAL GUIDELINES SEPTEMBER 2015 This policy supersedes all previous policies for medically assisted community alcohol withdrawal Policy title Guidelines for medically
MEDICALLY ASSISTED COMMUNITY ALCOHOL WITHDRAWAL GUIDELINES SEPTEMBER 2015 This policy supersedes all previous policies for medically assisted community alcohol withdrawal Policy title Guidelines for medically
Current Clinical Patterns in the Management of Alcohol Withdrawal Syndrome (AWS)
 1 Current Clinical Patterns in the Management of Alcohol Withdrawal Syndrome (AWS) The goal of the survey is to evaluate current practices for the inpatient management of AWS in adult hospitals located
1 Current Clinical Patterns in the Management of Alcohol Withdrawal Syndrome (AWS) The goal of the survey is to evaluate current practices for the inpatient management of AWS in adult hospitals located
Alcohol Issues in the Acute General Hospital Setting
 Alcohol Issues in the Acute General Hospital Setting (Guidelines and Management) This procedural document supersedes: PAT/T 25 version 3 - Guidelines for the Management of Alcohol Issues in the Acute General
Alcohol Issues in the Acute General Hospital Setting (Guidelines and Management) This procedural document supersedes: PAT/T 25 version 3 - Guidelines for the Management of Alcohol Issues in the Acute General
Alcohol Issues in the Acute General Hospital Setting
 Alcohol Issues in the Acute General Hospital Setting (Guidelines and Management) This procedural document supersedes: PAT/T 25 version 2 - Guidelines for the Management of Alcohol Issues in the Acute General
Alcohol Issues in the Acute General Hospital Setting (Guidelines and Management) This procedural document supersedes: PAT/T 25 version 2 - Guidelines for the Management of Alcohol Issues in the Acute General
NHS Fife Guidance for the Identification, Assessment and Management of Harmful Drinking and Alcohol Dependence
 NHS Fife Guidance for the Identification, Assessment and Management of Harmful Drinking and Alcohol Dependence Staff working in services provided and funded by the NHS who care for people who potentially
NHS Fife Guidance for the Identification, Assessment and Management of Harmful Drinking and Alcohol Dependence Staff working in services provided and funded by the NHS who care for people who potentially
Managing presenting alcohol users an Introduction to SPECTRUM (CRI) By Dr Gideon Felton MRCPsych Consultant Psychiatrist and Clinical Lead
 Managing presenting alcohol users an Introduction to SPECTRUM (CRI) By Dr Gideon Felton MRCPsych Consultant Psychiatrist and Clinical Lead PLAN OF PRESENTATION Assessment of alcohol dependence Psychiatric
Managing presenting alcohol users an Introduction to SPECTRUM (CRI) By Dr Gideon Felton MRCPsych Consultant Psychiatrist and Clinical Lead PLAN OF PRESENTATION Assessment of alcohol dependence Psychiatric
Prescribing for substance misuse: alcohol detoxification. Clinical background
 Prescribing for substance misuse: alcohol detoxification POMH-UK Quality Improvement Programme. Topic 14a: baseline Clinical background 1 2014 The Royal College of Psychiatrists. For further information
Prescribing for substance misuse: alcohol detoxification POMH-UK Quality Improvement Programme. Topic 14a: baseline Clinical background 1 2014 The Royal College of Psychiatrists. For further information
Provincial Clinical Knowledge Topic Alcohol Withdrawal, Adult Inpatient V 1.0
 Provincial Clinical Knowledge Topic Alcohol Withdrawal, Adult Inpatient V 1.0 Copyright: 2018, Alberta Health Services. This work is licensed under the Creative Commons Attribution-NonCommercial-NoDerivatives
Provincial Clinical Knowledge Topic Alcohol Withdrawal, Adult Inpatient V 1.0 Copyright: 2018, Alberta Health Services. This work is licensed under the Creative Commons Attribution-NonCommercial-NoDerivatives
DRAFT FOR CONSULTATION
 1) What is the accuracy of a tool and/or clinical judgement for the a) assessment b) monitoring of patients at risk of acute alcohol withdrawal? 2) Does the assessment and monitoring of patients with acute
1) What is the accuracy of a tool and/or clinical judgement for the a) assessment b) monitoring of patients at risk of acute alcohol withdrawal? 2) Does the assessment and monitoring of patients with acute
Benzodiazepines and Hypnotics
 Benzodiazepines and Hypnotics Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if Trust wide): Review date (when this version goes out of date):
Benzodiazepines and Hypnotics Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if Trust wide): Review date (when this version goes out of date):
ALCOHOL RELATED BRAIN DAMAGE (ARBD)
 FACT SHEET 01 ALCOHOL RELATED BRAIN DAMAGE (ARBD) This fact sheet will help you get a better understanding of Alcohol Related Brain Damage, how it can present, what causes it and how someone with ARBD
FACT SHEET 01 ALCOHOL RELATED BRAIN DAMAGE (ARBD) This fact sheet will help you get a better understanding of Alcohol Related Brain Damage, how it can present, what causes it and how someone with ARBD
Olanzapine Long-Acting Injection (Zypadhera ) - Guidelines for Prescribing and Administration (Version 3 May 2015)
 1. Key Points Olanzapine Long-Acting Injection (Zypadhera ) - Guidelines for Prescribing and Administration (Version 3 May 2015) 1.1 Olanzapine long acting injection (LAI) is indicated for the maintenance
1. Key Points Olanzapine Long-Acting Injection (Zypadhera ) - Guidelines for Prescribing and Administration (Version 3 May 2015) 1.1 Olanzapine long acting injection (LAI) is indicated for the maintenance
Critical Care Pharmacological Management of Delirium
 Critical Care Pharmacological Management of Delirium Policy Title: in the Critical Care Unit Executive Summary: This policy provides guidance Pharmacological Management of delirium in the Critical Care
Critical Care Pharmacological Management of Delirium Policy Title: in the Critical Care Unit Executive Summary: This policy provides guidance Pharmacological Management of delirium in the Critical Care
Multiple Choice Questions
 Multiple Choice Questions 25yo M presents without psychiatric or medical history, with complaint of tremor to the ER. He denies drinking alcohol but his friend at bedside takes you to the side and reports
Multiple Choice Questions 25yo M presents without psychiatric or medical history, with complaint of tremor to the ER. He denies drinking alcohol but his friend at bedside takes you to the side and reports
Provider Update: Alcohol Withdrawal Order Set Edits
 Provider Update: Alcohol Withdrawal Order Set Edits Situation: A revised Alcohol Withdrawal Order Set and new CIWA-Ar scoring tool will go LIVE February 12, 2018. Background: The latest guidelines for
Provider Update: Alcohol Withdrawal Order Set Edits Situation: A revised Alcohol Withdrawal Order Set and new CIWA-Ar scoring tool will go LIVE February 12, 2018. Background: The latest guidelines for
Methodist Hospital Alcohol Withdrawal Suggested Guidelines
 Methodist Hospital Alcohol Withdrawal Suggested Guidelines S. Prizada Sattar, MD Teri L Gabel, Pharm.D.,BCPP Sidney Kauzlarich, MD Subhash Bhatia, MD Mitzi Bollinger, RN S. Prizada Sattar, MD 6-20-3 Rationale
Methodist Hospital Alcohol Withdrawal Suggested Guidelines S. Prizada Sattar, MD Teri L Gabel, Pharm.D.,BCPP Sidney Kauzlarich, MD Subhash Bhatia, MD Mitzi Bollinger, RN S. Prizada Sattar, MD 6-20-3 Rationale
Pain and Itch Assessment and Management for the Burns Patient (Adults) Type: Clinical guideline Register No: Status: Public
 Pain and Itch Assessment and Management for the Burns Patient (Adults) Type: Clinical guideline Register No: 15025 Status: Public Developed in response to: Best Practice Contributes to CQC Regulation 9,11
Pain and Itch Assessment and Management for the Burns Patient (Adults) Type: Clinical guideline Register No: 15025 Status: Public Developed in response to: Best Practice Contributes to CQC Regulation 9,11
Supporting Last Days of Life Symptom Control Medication Guidance: Algorithm. Agitation & Anxiety
 Agitation & Anxiety (Exclude or treat REVERSIBLE causes*) Patient is anxious / frightened, but lucid Patient is confused, agitated and / or hallucinating MIDAZOLAM 2.5-5mg s/c (Max total 24 hour dose of
Agitation & Anxiety (Exclude or treat REVERSIBLE causes*) Patient is anxious / frightened, but lucid Patient is confused, agitated and / or hallucinating MIDAZOLAM 2.5-5mg s/c (Max total 24 hour dose of
Predictors of Severity of Alcohol Withdrawal in Hospitalized Patients
 Elmer Original Article ress Predictors of Severity of Alcohol Withdrawal in Hospitalized Patients Radhames Ramos a, Thierry Mallet b, Anthony DiVittis c b, d, e, Ronny Cohen Abstract Background: Alcohol
Elmer Original Article ress Predictors of Severity of Alcohol Withdrawal in Hospitalized Patients Radhames Ramos a, Thierry Mallet b, Anthony DiVittis c b, d, e, Ronny Cohen Abstract Background: Alcohol
Version Number: 5. Patient Group Direction drawn up by: Chief Pharmacist - Strategy. Group direction authorised by:
 PATIENT GROUP DIRECTION (PGD) FOR THE INPATIENT ADMINISTRATION OF ORAL LORAZEPAM TO WORKING AGE AND OLDER PEOPLE (includes persons in a Place of Safety suite) Version Number: 5 Patient Group Direction
PATIENT GROUP DIRECTION (PGD) FOR THE INPATIENT ADMINISTRATION OF ORAL LORAZEPAM TO WORKING AGE AND OLDER PEOPLE (includes persons in a Place of Safety suite) Version Number: 5 Patient Group Direction
Management of Alcohol Dependence
 STANDARD TREATMENT GUIDELINES Management of Alcohol Dependence Quick Reference Guide February 2016 Ministry of Health & Family Welfare Government of India 1 Table of Contents Objectives-... 3 Diagnosis...
STANDARD TREATMENT GUIDELINES Management of Alcohol Dependence Quick Reference Guide February 2016 Ministry of Health & Family Welfare Government of India 1 Table of Contents Objectives-... 3 Diagnosis...
PABRINEX PRESCRIBING PROTOCOL JULY This policy supersedes all previous policies for medically assisted community alcohol withdrawal
 PABRINEX PRESCRIBING PROTOCOL JULY 2015 This policy supersedes all previous policies for medically assisted community alcohol withdrawal Policy title Policy PHA55 reference Policy category Clinical Relevant
PABRINEX PRESCRIBING PROTOCOL JULY 2015 This policy supersedes all previous policies for medically assisted community alcohol withdrawal Policy title Policy PHA55 reference Policy category Clinical Relevant
NHS Grampian Protocol For The Prescribing And Administration Of Oral Opioids Following Trauma Or Surgery
 Acute Sector NHS Grampian Protocol For The Prescribing And Administration Of Oral Opioids Following Trauma Or Surgery Co-ordinators: Dr Karen Cranfield, Consultant Anaesthetist, Lead Acute Pain Sector
Acute Sector NHS Grampian Protocol For The Prescribing And Administration Of Oral Opioids Following Trauma Or Surgery Co-ordinators: Dr Karen Cranfield, Consultant Anaesthetist, Lead Acute Pain Sector
Substance Misuse Nurse service Belfast Trust
 Substance Misuse Nurse service Belfast Trust Alcohol is the most widely available socially acceptable drug in Northern Ireland It can be an addictive substance It is a depressant- slows down the central
Substance Misuse Nurse service Belfast Trust Alcohol is the most widely available socially acceptable drug in Northern Ireland It can be an addictive substance It is a depressant- slows down the central
Prescribing Framework for Naltrexone in Alcohol Relapse Prevention
 Prescribing Framework for Naltrexone in Alcohol Relapse Prevention Patients Name:.. NHS Number: Patients Address:... (Use addressograph sticker) GP s Name:... Communication We agree to treat this patient
Prescribing Framework for Naltrexone in Alcohol Relapse Prevention Patients Name:.. NHS Number: Patients Address:... (Use addressograph sticker) GP s Name:... Communication We agree to treat this patient
NCEPOD - Measuring the Units; A review of patients who died with alcohol-related liver disease
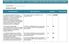 NCEPOD - Measuring the Units; A review of patients who died with alcohol-related liver disease Hospital Number Admission to hospital 5. Trusts should ensure that medical patients are reviewed by a consultant
NCEPOD - Measuring the Units; A review of patients who died with alcohol-related liver disease Hospital Number Admission to hospital 5. Trusts should ensure that medical patients are reviewed by a consultant
Guidance for community alcohol detoxification in clients with complex needs
 Document level: Clinical Service Unit (CSU) Code: DA3 Issue number: 1 Guidance for community alcohol detoxification in clients with complex needs Lead executive Medical Director Author and contact number
Document level: Clinical Service Unit (CSU) Code: DA3 Issue number: 1 Guidance for community alcohol detoxification in clients with complex needs Lead executive Medical Director Author and contact number
SiGMA/ MMHSCT GUIDELINES FOR ANTIPSYCHOTIC DRUG TREATMENT OF SCHIZOPHRENIA. [compatible with NICE guidance]
![SiGMA/ MMHSCT GUIDELINES FOR ANTIPSYCHOTIC DRUG TREATMENT OF SCHIZOPHRENIA. [compatible with NICE guidance] SiGMA/ MMHSCT GUIDELINES FOR ANTIPSYCHOTIC DRUG TREATMENT OF SCHIZOPHRENIA. [compatible with NICE guidance]](/thumbs/80/80440271.jpg) SiGMA/ MMHSCT GUIDELINES FOR ANTIPSYCHOTIC DRUG TREATMENT OF SCHIZOPHRENIA [compatible with NICE guidance] Medicines Management Committee August 2002 For review August 2003 Rationale The SiGMA algorithm
SiGMA/ MMHSCT GUIDELINES FOR ANTIPSYCHOTIC DRUG TREATMENT OF SCHIZOPHRENIA [compatible with NICE guidance] Medicines Management Committee August 2002 For review August 2003 Rationale The SiGMA algorithm
Prescribing for substance misuse: alcohol detoxification
 Prescribing for substance misuse: alcohol POMH-UK Quality Improvement Programme. Topic 14b (re-audit) Prepared by the Prescribing Observatory for Mental Health-UK for Non-participating Trusts Published
Prescribing for substance misuse: alcohol POMH-UK Quality Improvement Programme. Topic 14b (re-audit) Prepared by the Prescribing Observatory for Mental Health-UK for Non-participating Trusts Published
Prescribing Framework for Naltrexone in Relapse Prevention (Opioid Dependence)
 Hull & East Riding Prescribing Committee Prescribing Framework for Naltrexone in Relapse Prevention (Opioid Dependence) Patients Name: Unit Number: Patients Address:.. G.P s Name:.. Communication We agree
Hull & East Riding Prescribing Committee Prescribing Framework for Naltrexone in Relapse Prevention (Opioid Dependence) Patients Name: Unit Number: Patients Address:.. G.P s Name:.. Communication We agree
Guidance For The Detoxification Of Alcohol Dependent Patients In Community Or Outpatient Settings
 Guidance For The Detoxification Of Alcohol Dependent Patients In Community Or Outpatient Settings Co-ordinators: Fiona Raeburn, Specialist Pharmacist in Substance Misuse Reviewer: Dr Seonaid Anderson,
Guidance For The Detoxification Of Alcohol Dependent Patients In Community Or Outpatient Settings Co-ordinators: Fiona Raeburn, Specialist Pharmacist in Substance Misuse Reviewer: Dr Seonaid Anderson,
Medication Safety. Patient Safety. Setting Direction Julie Simmons, Medication Safety Pharmacist January 2016
 Medication Safety Patient Safety Setting Direction Julie Simmons, Medication Safety Pharmacist January 2016 1 The patient journey Admission Ward Transfer Ward stay Discharge Medication storage and supply
Medication Safety Patient Safety Setting Direction Julie Simmons, Medication Safety Pharmacist January 2016 1 The patient journey Admission Ward Transfer Ward stay Discharge Medication storage and supply
A new model for prescribing varenicline
 Pharmacist Independent Prescribers in partnership with A new model for prescribing varenicline Dear Stop Smoking Advisor You will be aware of the stop smoking drug varenicline that goes under the brand
Pharmacist Independent Prescribers in partnership with A new model for prescribing varenicline Dear Stop Smoking Advisor You will be aware of the stop smoking drug varenicline that goes under the brand
Peterborough Nalmefene Pathway Responsibilities for Specialist Services & GP
 Peterborough Nalmefene Pathway Responsibilities for Specialist Services & GP INTRODUCTION/BACKGROUND In November 2014 NICE (National Institute of Clinical Excellence) published the Technology Appraisal
Peterborough Nalmefene Pathway Responsibilities for Specialist Services & GP INTRODUCTION/BACKGROUND In November 2014 NICE (National Institute of Clinical Excellence) published the Technology Appraisal
A Guide to Alcoholism and Problem Drinking
 A Guide to Alcoholism and Problem Drinking Alcoholism is a word which many people use to mean alcohol dependence (alcohol addiction). Some people are problem drinkers without being dependent on alcohol.
A Guide to Alcoholism and Problem Drinking Alcoholism is a word which many people use to mean alcohol dependence (alcohol addiction). Some people are problem drinkers without being dependent on alcohol.
NHS Grampian Protocol For The Prescribing And Administration Of Oral Opioids Following Trauma Or Surgery in Adults. Consultation Group: See Page 5
 NHS...... Grampian Acute Sector NHS Grampian Protocol For The Prescribing And Administration Of Oral Opioids Following Trauma Or Surgery in Adults Co-ordinators: Consultant Anaesthetist, Lead Acute Pain
NHS...... Grampian Acute Sector NHS Grampian Protocol For The Prescribing And Administration Of Oral Opioids Following Trauma Or Surgery in Adults Co-ordinators: Consultant Anaesthetist, Lead Acute Pain
Job Title Name Signature Date. Director of Nursing Angela Wallace Signed Angela Wallace 30/6/2014
 PATIENT GROUP DIRECTIONS FOR SUPPLY OF VARENICLINE (CHAMPIX ) BY AUTHORISED COMMUNITY PHARMACISTS WORKING IN FORTH VALLEY Protocol Number 445 Version 1 Date protocol prepared: June 2014 Date protocol due
PATIENT GROUP DIRECTIONS FOR SUPPLY OF VARENICLINE (CHAMPIX ) BY AUTHORISED COMMUNITY PHARMACISTS WORKING IN FORTH VALLEY Protocol Number 445 Version 1 Date protocol prepared: June 2014 Date protocol due
PATIENT GROUP DIRECTION (PGD) FOR THE ADMINISTRATION OF ORAL DIAZEPAM TO WORKING AGE AND OLDER PEOPLE IN THE COMMUNITY
 PATIENT GROUP DIRECTION (PGD) FOR THE ADMINISTRATION OF ORAL DIAZEPAM TO WORKING AGE AND OLDER PEOPLE IN THE COMMUNITY Version Number: 5 Patient Group Direction drawn up by: Name Ray Lyon Dr Al Amaladoss
PATIENT GROUP DIRECTION (PGD) FOR THE ADMINISTRATION OF ORAL DIAZEPAM TO WORKING AGE AND OLDER PEOPLE IN THE COMMUNITY Version Number: 5 Patient Group Direction drawn up by: Name Ray Lyon Dr Al Amaladoss
POLICY DOCUMENT. CG/pain management in opioid dependency/03/15. Associate Director of Pharmacy
 POLICY DOCUMENT Document Title Reference Number PRESCRIBING FOR PAIN MANAGEMENT IN OPIOID DEPENDENT CLIENTS CG/pain management in opioid dependency/03/15 Policy Type Clinical Guideline Electronic File/Location
POLICY DOCUMENT Document Title Reference Number PRESCRIBING FOR PAIN MANAGEMENT IN OPIOID DEPENDENT CLIENTS CG/pain management in opioid dependency/03/15 Policy Type Clinical Guideline Electronic File/Location
SCENARIOS IN SUBSTANCE MISUSE. By Dr Gideon Felton Consultant Psychiatrist and Clinical Lead
 SCENARIOS IN SUBSTANCE MISUSE By Dr Gideon Felton Consultant Psychiatrist and Clinical Lead ALCOHOL SCENARIOS DON T PRESCRIBE LIBRIUM AS YOU ARE CONTRIBUTING TO A SECOND ADDICTION WITHOUT TREATING THE
SCENARIOS IN SUBSTANCE MISUSE By Dr Gideon Felton Consultant Psychiatrist and Clinical Lead ALCOHOL SCENARIOS DON T PRESCRIBE LIBRIUM AS YOU ARE CONTRIBUTING TO A SECOND ADDICTION WITHOUT TREATING THE
Behavioral Health Service Request Form Detox and Substance Abuse Rehab
 Medicaid Call for Pre-Certification of Admissions: 1-855-620-1861 Kentucky Medicaid Fax: 1-877-338-3686 Standard Request Requests for prior authorization (with supporting clinical information and documentation)
Medicaid Call for Pre-Certification of Admissions: 1-855-620-1861 Kentucky Medicaid Fax: 1-877-338-3686 Standard Request Requests for prior authorization (with supporting clinical information and documentation)
Emergency Control of the Acutely Disturbed Adult Patient GUIDELINES ON EMERGENCY CONTROL OF THE ACUTELY DISTURBED ADULT PATIENT... 2 ACTION...
 Delirium Toolkit Emergency Control of the Acutely Disturbed Adult Patient Table of Contents GUIDELINES ON EMERGENCY CONTROL OF THE ACUTELY DISTURBED ADULT PATIENT... 2 ACTION... 2 AFTERCARE... 3 NOTES...
Delirium Toolkit Emergency Control of the Acutely Disturbed Adult Patient Table of Contents GUIDELINES ON EMERGENCY CONTROL OF THE ACUTELY DISTURBED ADULT PATIENT... 2 ACTION... 2 AFTERCARE... 3 NOTES...
MANAGEMENT OF PATIENTS WITH PARKINSON S DISEASE WHO ARE NIL BY MOUTH OR WITH A COMPROMISED SWALLOW
 MANAGEMENT OF PATIENTS WITH PARKINSON S DISEASE WHO ARE NIL BY MOUTH OR WITH A COMPROMISED SWALLOW Author: Gordon W Duncan Status: Approved Authorised by: Clinical Policy Group Version: 1.0 Review date:
MANAGEMENT OF PATIENTS WITH PARKINSON S DISEASE WHO ARE NIL BY MOUTH OR WITH A COMPROMISED SWALLOW Author: Gordon W Duncan Status: Approved Authorised by: Clinical Policy Group Version: 1.0 Review date:
Ketorolac injection. Supportive care
 Supportive care Ketorolac injection Supportive care: specialist medicines This leaflet provides information on a medicine called ketorolac which is used to treat pain that is difficult to control. It is
Supportive care Ketorolac injection Supportive care: specialist medicines This leaflet provides information on a medicine called ketorolac which is used to treat pain that is difficult to control. It is
Clinical Guideline for the management of inpatients with Parkinson s disease
 Clinical Guideline for the management of inpatients with Parkinson s disease Introduction: Parkinson s disease (PD) is the second most common neurodegenerative disorder, characterised by bradykinesia,
Clinical Guideline for the management of inpatients with Parkinson s disease Introduction: Parkinson s disease (PD) is the second most common neurodegenerative disorder, characterised by bradykinesia,
Initiation of Clozapine Treatment Community Patients
 Initiation of Clozapine Treatment Community Patients Who Should Read This Policy Target Audience All clinical staff working in the community N/A N/A Initiation of Clozapine Treatment for Patients in the
Initiation of Clozapine Treatment Community Patients Who Should Read This Policy Target Audience All clinical staff working in the community N/A N/A Initiation of Clozapine Treatment for Patients in the
Guideline for use of Intramuscular Medication for Acutely Disturbed Behaviour in Mental Health and Associated Services
 NHS GGC Mental Health Service Guideline for use of Intramuscular Medication for Acutely Disturbed Behaviour in Mental Health and Associated Services Important Note: The Intranet version of this document
NHS GGC Mental Health Service Guideline for use of Intramuscular Medication for Acutely Disturbed Behaviour in Mental Health and Associated Services Important Note: The Intranet version of this document
ROLE OF HEALTH CARE PROVIDERS IN THE MANAGEMENT OF ALCOHOL AND DRUG USE RELATED PROBLEMS
 ROLE OF HEALTH CARE PROVIDERS IN THE MANAGEMENT OF ALCOHOL AND DRUG USE RELATED PROBLEMS Dr. Anita Rao? ASK SCREEN Refer HELP T T Ranganathan Clinical Research Foundation TTK Hospital IV Main Road, Indira
ROLE OF HEALTH CARE PROVIDERS IN THE MANAGEMENT OF ALCOHOL AND DRUG USE RELATED PROBLEMS Dr. Anita Rao? ASK SCREEN Refer HELP T T Ranganathan Clinical Research Foundation TTK Hospital IV Main Road, Indira
Sedation Hold/Interruption and Weaning Protocol ( Wake-up and Breathe )
 PROTOCOL Sedation Hold/Interruption and Weaning Protocol ( Wake-up and Breathe ) Page 1 of 6 Scope: Population: Outcome: Critical care clinicians and providers. All ICU patients intubated or mechanically
PROTOCOL Sedation Hold/Interruption and Weaning Protocol ( Wake-up and Breathe ) Page 1 of 6 Scope: Population: Outcome: Critical care clinicians and providers. All ICU patients intubated or mechanically
The causes of misuse:
 The Drug Misuse The causes of misuse: Availability of drugs. A vulnerable personality. Adverse social environment. Regular drug taking play a role. Determining misuse and dependence, it is unclear whether
The Drug Misuse The causes of misuse: Availability of drugs. A vulnerable personality. Adverse social environment. Regular drug taking play a role. Determining misuse and dependence, it is unclear whether
Patient Profile. Patient s details Initials: IF Age: 40 Gender: Male. Weight: 139.7kg Height: 510 metres BMI: >47
 Patient Profile Patient background and medication list Reason for selecting profile Interesting depression case whereby there were several opportunities for intervention as a pharmacist to ensure drug-related
Patient Profile Patient background and medication list Reason for selecting profile Interesting depression case whereby there were several opportunities for intervention as a pharmacist to ensure drug-related
Complicated Withdrawal
 Complicated Withdrawal Shamim Nejad, MD Medical Director, Division of Psychosocial Oncology Swedish Cancer Institute Swedish Medical Center Seattle, Washington Shamim.Nejad@Swedish.org Disclosures: Shamim
Complicated Withdrawal Shamim Nejad, MD Medical Director, Division of Psychosocial Oncology Swedish Cancer Institute Swedish Medical Center Seattle, Washington Shamim.Nejad@Swedish.org Disclosures: Shamim
Policy Register No: Status: Public. Contributes to Care Quality Commission Outcome 4
 Operational Policy for Transfer of ST Elevation MI (STEMI) patients to Essex Cardiothoracic Centre (ECTC) for Primary Percutaneous Coronary Intervention Policy Register No: 09122 Status: Public Developed
Operational Policy for Transfer of ST Elevation MI (STEMI) patients to Essex Cardiothoracic Centre (ECTC) for Primary Percutaneous Coronary Intervention Policy Register No: 09122 Status: Public Developed
Opioid rotation or switching may be considered if a patient obtains pain relief with one opioid and is suffering severe adverse effects.
 Dose equivalence and switching between opioids Key Messages Switching from one opioid to another should only be recommended or supervised by a healthcare practitioner with adequate competence and sufficient
Dose equivalence and switching between opioids Key Messages Switching from one opioid to another should only be recommended or supervised by a healthcare practitioner with adequate competence and sufficient
For patients and their carers this means smoother symptom control, better support in a crisis, and avoidance of admission if that is their choice.
 Bedfordshire Palliative Care Palliative Care Medicines Guidance This folder has been produced to support professionals providing palliative care in any setting. Its aim is to make best practice in palliative
Bedfordshire Palliative Care Palliative Care Medicines Guidance This folder has been produced to support professionals providing palliative care in any setting. Its aim is to make best practice in palliative
Guideline for the Identification and Management of Delirium (Including use of the THINK DELIRIUM Support Tool)
 Guideline for the Identification and Management of Delirium (Including use of the THINK DELIRIUM Support Tool) B27/2009 1. Introduction 1.1 Delirium is a common problem which occurs in about 15-20 out
Guideline for the Identification and Management of Delirium (Including use of the THINK DELIRIUM Support Tool) B27/2009 1. Introduction 1.1 Delirium is a common problem which occurs in about 15-20 out
PROOF. Intravenous Adult Community Therapy Team (IV-ACT Team) Intravenous antibiotics in the community
 Division of Medicine and Community Services Intravenous Adult Community Therapy Team (IV-ACT Team) Intravenous antibiotics in the community Patient information leaflet for patients receiving (IV) therapy
Division of Medicine and Community Services Intravenous Adult Community Therapy Team (IV-ACT Team) Intravenous antibiotics in the community Patient information leaflet for patients receiving (IV) therapy
Acute painful crisis in patients with sickle cell disease: Clinical Guidelines (HN-506a)
 Acute painful crisis in patients with sickle cell disease: Clinical Guidelines (HN-506a) Introduction The majority of acute painful crises in patients with sickle cell disease will be managed independently
Acute painful crisis in patients with sickle cell disease: Clinical Guidelines (HN-506a) Introduction The majority of acute painful crises in patients with sickle cell disease will be managed independently
Delirium. Patient Information Leaflet
 Delirium Patient Information Leaflet Betty, a lady who had been admitted to hospital with a broken hip, had been fully independent in her own home. A few days after surgery to repair her hip she became
Delirium Patient Information Leaflet Betty, a lady who had been admitted to hospital with a broken hip, had been fully independent in her own home. A few days after surgery to repair her hip she became
Management of Severe Agitation
 Management of Severe Agitation Key Points 1. The management of the severely agitated or violent patient embraces psychological, physical and pharmacological approaches. 2. Psychological methods focus on
Management of Severe Agitation Key Points 1. The management of the severely agitated or violent patient embraces psychological, physical and pharmacological approaches. 2. Psychological methods focus on
POLICY DOCUMENT. Pharmacy MMG/MPG. Approved By and Date Medicines Management roup March March 2016
 POLICY DOCUMENT Document Title High dose and combination antipsychotic guidance Reference Number n/a Policy Type Prescribing and Treatment Guideline Electronic File/Location Clinical Resources/Pharmacy/Prescribing
POLICY DOCUMENT Document Title High dose and combination antipsychotic guidance Reference Number n/a Policy Type Prescribing and Treatment Guideline Electronic File/Location Clinical Resources/Pharmacy/Prescribing
In our patients the cause of seizures can be broadly divided into structural and systemic causes.
 Guidelines for the management of Seizures Amalgamation and update of previous policies 7 (Seizure guidelines, ND, 2015) and 9 (Status epilepticus, KJ, 2011) Seizures can occur in up to 15% of the Palliative
Guidelines for the management of Seizures Amalgamation and update of previous policies 7 (Seizure guidelines, ND, 2015) and 9 (Status epilepticus, KJ, 2011) Seizures can occur in up to 15% of the Palliative
PAEDIATRIC DOSAGE GUIDELINES For management of post-operative acute pain
 Index No: MMG43 PAEDIATRIC DOSAGE GUIDELINES For management of post-operative acute pain Version: 3.1 (Includes anti-emetics and naloxone) Date ratified: July 2013 Ratified by: (Name of Committee) Name
Index No: MMG43 PAEDIATRIC DOSAGE GUIDELINES For management of post-operative acute pain Version: 3.1 (Includes anti-emetics and naloxone) Date ratified: July 2013 Ratified by: (Name of Committee) Name
Drug & Alcohol Detox:
 Drug & Alcohol Detox: Beginning Stages of Addiction Treatment If you ve tried to detox on your own and failed, you are not alone. The good news is that research shows those who commit to a rehabilitation
Drug & Alcohol Detox: Beginning Stages of Addiction Treatment If you ve tried to detox on your own and failed, you are not alone. The good news is that research shows those who commit to a rehabilitation
Managing presenting problems with benzodiazepines. By Dr Gideon Felton MRCPsych Consultant Psychiatrist and Clinical Lead
 Managing presenting problems with benzodiazepines By Dr Gideon Felton MRCPsych Consultant Psychiatrist and Clinical Lead OUTLINE OF PRESENTATION Why Benzodiazepines (BDZ s) are used Mechanism of Action
Managing presenting problems with benzodiazepines By Dr Gideon Felton MRCPsych Consultant Psychiatrist and Clinical Lead OUTLINE OF PRESENTATION Why Benzodiazepines (BDZ s) are used Mechanism of Action
Alcoholism. Social environment, stress, mental health, family history, age, ethnic group, and gender all influence the risk for the condition.
 SAY NO TO ALCOHOL Alcoholism Alcoholism is a chronic and often progressive disease that includes problems controlling your drinking, being preoccupied with alcohol, continuing to use alcohol even when
SAY NO TO ALCOHOL Alcoholism Alcoholism is a chronic and often progressive disease that includes problems controlling your drinking, being preoccupied with alcohol, continuing to use alcohol even when
MEDICATION GUIDE WELLBUTRIN (WELL byu-trin) (bupropion hydrochloride) Tablets
 MEDICATION GUIDE WELLBUTRIN (WELL byu-trin) (bupropion hydrochloride) Tablets Read this Medication Guide carefully before you start using WELLBUTRIN and each time you get a refill. There may be new information.
MEDICATION GUIDE WELLBUTRIN (WELL byu-trin) (bupropion hydrochloride) Tablets Read this Medication Guide carefully before you start using WELLBUTRIN and each time you get a refill. There may be new information.
