Assoc. Prof. Bilgen Başgut 2014
|
|
|
- Gervais Parks
- 5 years ago
- Views:
Transcription
1 Assoc. Prof. Bilgen Başgut 2014
2 CNS: Brain Spinal cord Central Nervous System PNS: Autonomic Sympathetic parasympath etic Somatic Peripheral Nervous System
3 Function of the CNS Receive and process information (spinal cord is usually the conduit) Initiate and maintain appropriate response physical emotional
4 The synapse Transmission of information from one neurone to another
5 Chemical v/s Electrical Synapses Electrical Synapses Rapid bidirectional transmission Gap junctions Ion current Electrotonic transmission Cytoplasmic continuity Chemical Synapses Slow unidirectional transmission Presynaptic vesicles, active zones, postsynaptic receptors Chemical neurotransmitters Complex amplifying excitatory/ inhibitory signals Synaptic cleft
6 Synaptic Transmission An AP reaches the axon terminal of the presynaptic cell and causes V-gated Ca2+ channels to open. Ca2+ rushes in, binds to regulatory proteins & initiates NT exocytosis. NTs diffuse across the synaptic cleft and then bind to receptors on the postsynaptic membrane and initiate some sort of response on the postsynaptic cell.
7 Chemical messengers Neurotransmitter (fast and slow synaptic transmission) Neuromodulator (diffuse, slower action)
8 Types of neurotransmitter Small molecules amino acids (glutamate, GABA) biogenic amines (ACh, NA, DA, 5-HT) Neuropeptides (cholecystokinin, Substance P, enkephalins) Diffusable gases nitric oxide Lipid mediators (e.g. endocannabinoids) Neurotrophins (e.g. nerve growth factor) Steroids
9
10 CNS DRUGS CLASSIFICATION Chemical structure Benzodiazepines, Butyrophenones Pharmacological MAO inhibitors, SSRI,. Clinical use Antidepressants, Antipsychotic agents
11 WHO Classification 1. Anxiolytic sedatives (hypnotics, sedatives, minor tranquillizers) Drugs that cause sleep and reduce anxiety Examples Barbiturates, benzodiazepines and ethanol
12 2. Antipsychotic drugs (neuroleptics, major tranquillizers, anti-schizophrenia Drugs that are effective in relieving symptoms of schizophrenic illness Examples Phenothiazines and butyrophenones
13 3. Antidepressant drugs (thymoleptics) Drugs that alleviate the symptoms of depressive illness Examples TCA, MAOI, SSRI
14 4. Psychomotor stimulants (Psychostimulants) Drugs that can cause wakefulness and euphoria Examples Amphetamines, Cocaine, and caffeine
15 5. Hallucinogenic drugs (psychodysleptics, psychotomimetics) Drugs that cause disturbance of perception and of behavior in ways that cannot be simply characterized as sedative or stimulant effects Examples Lysergic acid diethylamide (LSD), mescaline and phencyclidine
16 Others Analgesics (opiate) Anesthetics (Ketamine)
17 GENERAL AND LOCAL ANESTHETICS
18 OVERVIEW General anesthesia is a reversible state of central nervous system (CNS) depression. For patients undergoing surgical and other medical procedures, anesthesia provides the following important benefits: Sedation and reduction of anxiety Loss of consciousness Skeletal muscle relaxation Suppression of undesirable reflexes Analgesia
19 STAGES AND DEPTH OF ANESTHESIA General anesthesia can be divided into three stages: A. Induction, It is defined as the period of time from the onset of administration of the potent anesthetic to the development of effective surgical anesthesia in the patient. Induction of anesthesia depends on how fast effective concentrations of the anesthetic drug reach the brain. B. Maintenance ; provides a sustained surgical anesthesia. C. Recovery is the time from discontinuation of administration of anesthesia until consciousness and protective physiologic reflexes are regained. Recovery is essentially the reverse of induction and depends on how fast the anesthetic drug diffuses from the brain.
20 A.Induction General anesthesia in adults is normally induced with an IV anesthetic like propofol, which produces unconsciousness within seconds after injection. At that time, additional inhalation and/or IV drugs comprising the selected anesthetic combination may be given to produce the desired depth of surgical (Stage III) anesthesia. For children without IV access, inhalation induction is used with nonpungent agents, such as halothane or sevoflurane, to induce general anesthesia.
21 B.Maintenance of anesthesia Maintenance is the period during which the patient is surgically anesthetized. Anesthesia is commonly maintained by the administration of volatile anesthetics, which offer good control over the depth of anesthesia.
22 C.Recovery Postoperatively, the anesthetic admixture is withdrawn, and the patient is monitored for the return of consciousness. For most anesthetic agents, recovery is the reverse of induction. That is, redistribution from the site of action (rather than metabolism of the anesthetic) underlies recovery.
23 Depth of Anesthesia Depth of anesthesia is the degree to which the CNS is depressed and is a useful parameter for individualizing anesthesia. It has traditionally been divided into four sequential stages. Each stage is characterized by increased CNS depression, which is caused by accumulation of the anesthetic drug in the brain. With commonly used modern anesthetics, the stages are difficult to characterize clearly because of the rapid onset of surgical anesthesia.
24
25 An ideal anesthetic drug must; provide a smooth and rapid loss of consciousness allow for a prompt recovery after its administration is discontinued possess a wide margin of safety and be devoid of adverse effects. Because no single drug has all desirable properties mentioned, several groups of drugs are used in combination to produce optimal anesthesia.
26 PREANESTHETIC MEDICATIONS Antacids Anticholinergics Antiemetics Antihistamines Benzodiazepines Opioids Preanesthetic medications serve to calm the patient, relieve pain, and protect against undesirable effects of subsequently administered anesthetics or the surgical procedure itself.
27 Concomitant use of drugs; Commonly, surgical patients receive one or more of the following preanesthetic medications: H2 blockers to reduce gastric acidity (such as famotidine or ranitidine) Benzodiazepines to allay anxiety and facilitate amnesia (such as midazolam or diazepam) Opioids for analgesia (such as fentanyl) Antihistamines for prevention of allergic reactions; (such as diphenhydramine) Antiemetics to prevent nausea and the possible aspiration of stomach contents (such as ondansetron) Anticholinergics to prevent bradycardia and secretion of fluids into the respiratory tract (such as glycopyrrolate).
28 PARALYTICS / NEUROMUSCULAR BLOCKERS Neuromuscular blockers are used to abolish reflexes to facilitate tracheal intubation, and to provide muscle relaxation as needed for certain types of surgery. Their mechanism of action is blockade of the nicotinic acetylcholine receptors in the neuromuscular junction. These agents, which include cisatracurium, pancuronium, rocuronium, succinylcholine, and vecuronium,
29 Balanced anesthesia is a technique employed to compensate for the lack of an ideal anesthetic. Drugs are combined to make sure that : induction is smooth and rapid, analgesia and muscle relaxation are sufficient The agent used most commonly for these purposes: 1. short- acting barbiturates (for induction of anesthesia) 2. neuromuscular blocking agents (for muscle relaxation) 3. opioids and nitrous oxide (for analgesia) when administered concurrently, balanced anesthesia also lowers the dose of anesthetic required to maintain the desired level of surgical anesthesia. However, such coadministration can also enhance undesirable anesthetic effects (for example, hypoventilation), and may produce negative effects that are not observed when each drug is given individually.
30
31 Potent general anesthetics can be divided into two groups GENERAL ANESTHETICS: INHALED Desflurane SUPRANE Halothane FLUOTHANE Isoflurane FORANE Nitrous oxide NITROUS OXIDE Sevoflurane ULTANE GENERAL ANESTHETICS: INTRAVENOUS Barbiturates (eg. Thiopental, Methohexital) Benzodiazepines (eg. Midozolam, Diazepam) Propofol DIPRIVAN Ketamine KETALAR Opioid analgesics (eg. Morphine, Fentanyl, Sufentanil, Alfentanil, Remifentanil) Dexmedetomidine PRECEDEX Etomidate AMIDATE
32 INHALATION ANESTHETICS Inhalation anesthetics are used primarily for the maintenance of anesthesia after administration of an IV agent. One advantage of inhalation anesthetics is that the depth of anesthesia can be rapidly altered by changing the inhaled concentration of the drug.
33 Common features of inhalation anesthetics Modern inhalation anesthetics include the gas nitrous oxide as well as a number of volatile, halogenated hydrocarbons. As a group, these agents decrease cerebrovascular resistance, resulting in increased perfusion of the brain. The movement of these agents from the lungs to the different body compartments depends upon their solubility in blood and tissues as well as on blood flow. These factors play a role not only in induction, but also in recovery.
34 Potency The potency of inhaled anesthetics is defined quantitatively as the minimum alveolar concentration (MAC). Put another way, MAC of drug in the alveolar air produces inmobility in 50% of patients exposed to a painful stimulus. MAC is usually expressed as the percentage of gas in a mixture required to achieve the effect. MAC is small for potent anesthetics, such as sevoflurane, and large for less potent agents, such as nitrous oxide (N2O). Note that nitrous oxide alone cannot produce complete anesthesia, because an admixture with sufficient oxygen cannot approach its MAC value.
35
36 Potency (Continue) The more lipid soluble an anesthetic, the lower the concentration of anesthetic needed to produce anesthesia and, thus, the higher the potency of the anesthetic.
37
38
39 Mechanism of action The general anesthetics increase the sensitivity of the γ-aminobutyric acid (GABAA) receptors to the neurotransmitter, GABA, at clinically effective concentrations of the drug. This causes a prolongation of the inhibitory chloride ion current after a pulse of GABA release. Other receptors are also affected by volatile anesthetics. For example, the activity of the inhibitory glycine receptors in the spinal motor neurons is increased. In addition, the inhalation anesthetics block the excitatory postsynaptic current of the nicotinic receptors and the action of the excitatory neurotransmitter glutamic acid on N-methyl-D-apartate channel receptor. (Ketamine, nitrous oxide)
40 Halothane Halothane is a potent anesthetic but a relatively weak analgesic. Thus, halothane is usually coadministered with nitrous oxide, opioids, or local anesthetics. It is a potent bronchodilator and relaxes both skeletal and uterine muscle. Halothane is oxidatively metabolized in the body to tissue-toxic hydrocarbons (for example, trifluoroethanol) and bromide ion. These substances may be responsible for the toxic reaction (anorexia, nausea, and vomiting, and hepatitis) developing in some patients (especially females) after halothane anesthesia. To avoid this condition, halothane anesthesia is not repeated at intervals of less than 2 to 3 weeks. Halothane is not hepatotoxic in pediatric patients. Therefore, it is suitable in children for inhalation induction ( sevoflurane is now the agent of choice for this )
41 Halothane (continue) Like other halogenated hydrocarbons, halothane is vagomimetic and causes atropine-sensitive bradycardia. It has the undesirable property of causing cardiac arrhythmias. [Note: These are especially serious if hypercapnia (increased arterial carbon dioxide partial pressure) develops due to reduced alveolar ventilation or an increase in the plasma concentration of catecholamines.] Halothane, like the other halogenated anesthetics, produces concentrationdependent hypotension. Should it is necessary, it is recommended that a direct-acting vasoconstrictor (such as phenylephrine) can be given. It has the potential to induce Malignant hyperthermia in combination with the neuromuscular blocking agent succinylcholine
42 Isoflurane It is a very stable molecule that undergoes little metabolism and is not, therefore, toxic to the liver or kidney. It does not induce cardiac arrhythmias and does not sensitize the heart to the action of catecholamines. Like the other halogenated gases, it produces dose-dependent hypotension due to peripheral vasodilation. It has a pungent odor and stimulates respiratory reflexes (for example, breath-holding, salivation, coughing, and laryngospasm) and is, therefore, not used for inhalation induction. With higher blood solubility than desflurane and sevoflurane, isoflurane is typically used now only when cost is a factor.
43 Desflurane Desflurane provides very rapid onset and recovery due to its low blood solubility (the lowest of all the volatile anesthetics), causing it a popular anesthetic for outpatient surgery Because it has a low volatility, must be delivered using a special heated vaporizer. Like isoflurane, it decreases vascular resistance and perfuses all major tissues very well. Because it is irritating to the airway and can cause laryngospasm, coughing, and excessive secretions, desflurane is not used for inhalation inductions. Because it is relatively expensive, it is often not used for maintenance during extended anesthesia. Its degradation is minimal, and, therefore, tissue toxicity is rare.
44 Sevoflurane It has rapid onset and recovery due to low blood solubility. Sevoflurane has low pungency, allowing rapid induction without irritating the airway, thus making it suitable for inhalation induction in pediatric patients. It is replacing halothane for this purpose. Sevoflurane is metabolized by the liver, and compounds formed in the anesthesia circuit may be nephrotoxic if fresh gas flow is too low.
45 Nitrous oxide Nitrous oxide ( laughing gas ), is non-irritating and a potent analgesic but a weak general anesthetic. Nitrous oxide is frequently employed at concentrations of percent in combination with oxygen for analgesia, particularly in dental surgery. However, nitrous oxide at 80 percent (without adjunct agents) cannot produce surgical anesthesia. Therefore, it is commonly combined with other, more potent agents to attain pain-free anesthesia. Nitrous oxide is poorly soluble in blood and other tissues, allowing it to move very rapidly in and out of the body.
46 Nitrous oxide (continue) This anesthetic does not depress respiration, and it does not produce muscle relaxation. Under the usual circumstances of coadministration with other anesthetics, it also has moderate to no effect on the cardiovascular system or on increasing cerebral blood flow It is the least hepatotoxic of the inhalation anesthetics. Therefore, it is probably the safest of these anesthetics
47
48 INTRAVENOUS ANESTHETICS IV anesthetics cause the rapid induction of anesthesia. Anesthesia may then be maintained with an appropriate inhalation agent. IV anesthetics may be used as the sole agents for short procedures or administered as infusions to help maintain anesthesia during longer procedures. In lower doses, they may be used to provide sedation.
49 Induction After entering the blood stream, they pass along a concentration gradient from the blood into the brain. The rate of this transfer is dependent on: the arterial concentration of the unbound free drug, the lipid solubility of the drug, and the degree of ionization. Unbound, lipid-soluble, non-ionized molecules cross the blood-brain barrier most quickly. Once the drug has penetrated the CNS tissue, it exerts its effects. Like the inhalation anesthetics, the exact mode of action of the IV anesthetic drugs is unknown.
50 Propofol Propofol is an IV sedative/hypnotic used in the induction or maintenance of anesthesia. Propofol is widely used and has replaced thiopental as the first choice for anesthesia induction and sedation, because it produces a euphoric feeling in the patient and does not cause postanesthetic nausea and vomiting. The induction of anesthesia is smooth and occurs within about seconds of administration. Plasma levels decline rapidly as a result of redistribution, followed by a more prolonged period of hepatic metabolism and renal clearance. The initial redistribution half-life is between 2 and 4 minutes. The pharmacokinetics of propofol are not altered by moderate hepatic or renal failure.
51 Propofol (continue) Supplementation with narcotics for analgesia is required. Propofol decreases blood pressure without depressing the myocardium. It also reduces intracranial pressure, mainly due to systemic vasodilation. Propofol is commonly infused in lower doses to provide sedation for outpatient procedures. The incidence of postoperative nausea and vomiting is very low
52 Fospropofol Fospropofol is a new, water-soluble drug approved only for sedation. Fospropofol is metabolized to propofol in the body, and the pharmacological effects of fospropofol are attributed to propofol (thus, fospropofol is a prodrug of propofol). Because fospropofol is water soluble, the problems associated with lipidformulated propofol (such as pain at the IV injection site and increased chance for bacterial contamination) are expected to be less frequent.
53 Barbiturates Thiopental is a potent anesthetic but a weak analgesic. It is an ultrashort-acting barbiturate with high lipid solubility. When agents such as thiopental and methohexital are administered intravenously, they quickly enter the CNS and depress function, often in less than 1 minute. In contrast to the volatile anesthetics, thiopental is desirable drug for patient with head trauma and brain tumors However, diffusion out of the brain can also occur very rapidly because of redistribution of the drug to other body tissues, including skeletal muscle and, ultimately, adipose tissue.
54 Barbiturates (continue) The short duration of anesthetic action is due to the decrease of barbiturate concentration in the brain to a level below that necessary to produce anesthesia. The barbiturates are not significantly analgesic and, therefore, require some type of supplementary analgesic administration during anesthesia to avoid objectionable changes in blood pressure and autonomic function. Thiopental has minor effects on the cardiovascular system, but it may contribute to severe hypotension in patients with hypovolemia or shock. All barbiturates can cause apnea, coughing, chest wall spasm, laryngospasm, and bronchospasm. [Note: The latter is of particular concern for asthmatic patients.] Barbiturates are contraindicated in patients with acute intermittent porphyria.
55 Benzodiazepines The benzodiazepines are used in conjunction with anesthetics to sedate the patient. The most commonly used is midazolam. Diazepam and lorazepam are alternatives. All three facilitate amnesia while causing sedation, enhancing the inhibitory effects of various neurotransmitters, particularly GABA. Minimal cardiovascular depressant effects are seen, but all are potential respiratory depressants (especially when administered intravenously). They are metabolized by the liver with variable elimination half-lives, and erythromycin may prolong their effects. Benzodiazepines can induce a temporary form of anterograde amnesia in which the patient retains memory of past events, but new information is not transferred into long-term memory. Therefore, important treatment information should be repeated to the patient after the effects of the drug have worn off.
56 Opioids Because of their analgesic property, opioids are commonly used with anesthetics, such as in combination with nitrous oxide or volatile halogenated anesthetics. The most commonly used opioids are fentanyl and its congeners, sufentanil and remifentanil, because they induce analgesia more rapidly than morphine does. They may be administered either intravenously, epidurally, or intrathecally (into the cerebrospinal fluid). Opioids are not good amnesics, and they can all cause hypotension, respiratory depression, and muscle rigidity as well as postanesthetic nausea and vomiting. Opioid effects can be antagonized by naloxone.
57 Etomidate Etomidate is used to induce anesthesia. Induction is rapid, and the drug is short acting. It is a hypnotic agent but lacks analgesic activity. Its water solubility is poor, so etomidate is formulated in a propylene glycol solution. It causes minimal cardiovascular and respriratory depression (major advantage compared with other IV anesthetics) It is usually only used for patients with coronary artery disease or cardiovascular dysfunction such as shock. Etomidate is hydrolyzed in the liver. Its adverse effects include a decrease in plasma cortisol and aldosterone levels, which can persist for up to 8 hours. Therefore, Etomidate should not be infused for an extended time, because prolonged suppression of these hormones can be hazardous. Venous pain can occur on injection, and involuntary skeletal muscle movements are not uncommon. The latter are managed by administration of benzodiazepines and opioids.
58 Ketamine Ketamine a short-acting, nonbarbiturate anesthetic, induces a dissociated state in which the patient is unconscious (but may appear to be awake) and does not feel pain. This dissociative anesthesia provides sedation, amnesia, and immobility. Ketamine interacts with the N-methyl-D-aspartate receptor. It also stimulates the central sympathetic outflow, which, in turn, causes stimulation of the heart with increased blood pressure and CO. This property is especially beneficial in patients with either hypovolemic or cardiogenic shock as well as in patients with asthma. Therefore, ketamine is used when circulatory depression is undesirable. Ketamine is used mainly in children and elderly adults for short procedures. However, it is not widely used, because it increases cerebral blood flow and induces postoperative hallucinations ( nightmares ), particularly in adults.
59 Dexmedetomidine Dexmedetomidine is a sedative medication used by intensive care units and anesthesiologists. It is relatively unique in its ability to provide sedation without causing respiratory depression. Like clonidine, its mechanism of action is agonism of α2 receptors in certain parts of the brain. Dexmedetomidine has sedative, analgesic, sympatholytic, and anxiolytic effects that blunt many of the cardiovascular responses in the perioperative period. It reduces the volatile anesthetic, sedative and analgesic requirements of the patient without causing significant respiratory depression.
60
61 LOCAL ANESTHETICS Local anesthetics abolish sensation and, in higher concentrations, motor activity in a limited area of the body. They are applied or injected to block nerve conduction of sensory impulses from the periphery to the CNS. Local anesthesia is induced when propagation of action potentials is prevented, so that sensation cannot be transmitted from the source of stimulation to the brain. Local anesthetics work by blocking sodium ion channels to prevent the transient increase in permeability of the nerve membrane to sodium that is required for an action potential to occur. Delivery techniques include topical administration, infi ltration, ring blocks, peripheral nerve blocks, and neuraxial (spinal, epidural, or caudal) blocks. The small, unmyelinated nerve fi bers that conduct impulses for pain, temperature, and autonomic activity are most sensitive to the action of local anesthetics.
62 The most widely used of the local anesthetic compounds are : Amides Lidocaine Bupivacaine Mepivacaine Ropivacaine Prilocain Esters Procaine Chlor0procaine Tetracaine.
63 Metabolisms of local anesthetics Biotransformation of amides occurs primarily in the liver. Reduced hepatic function predisposes the patient to toxic effects. Esters are biotransformed by plasma cholinesterase (pseudocholinesterase). Patients with pseudocholinesterase.
64 Actions Local anesthetics cause vasodilation, when these drugs are administered alone. By adding the vasoconstrictor epinephrine to the local anesthetic, the rate of local anesthetic diffusion and absorption is decreased. Some of these local anesthetics agents confer additional benefits such as the antiarrhythmic effect of lidocaine when administered intravenously.
65 Clinical use of local anesthetics They may be administered topically and injection Topical anesthesia by applying directly to the skin or mucous membrane. Administration by injection Infiltration anesthesia Nerve block anesthesia Epidural anesthesia Spinal anesthesia
66
General anesthesia. No single drug capable of achieving these effects both safely and effectively.
 General anesthesia General anesthesia is essential to surgical practice, because it renders patients analgesic, amnesia, and unconscious reflexes, while causing muscle relaxation and suppression of undesirable
General anesthesia General anesthesia is essential to surgical practice, because it renders patients analgesic, amnesia, and unconscious reflexes, while causing muscle relaxation and suppression of undesirable
Chapter 25. General Anesthetics
 Chapter 25 1. Introduction General anesthetics: 1. Analgesia 2. Amnesia 3. Loss of consciousness 4. Inhibition of sensory and autonomic reflexes 5. Skeletal muscle relaxation An ideal anesthetic: 1. A
Chapter 25 1. Introduction General anesthetics: 1. Analgesia 2. Amnesia 3. Loss of consciousness 4. Inhibition of sensory and autonomic reflexes 5. Skeletal muscle relaxation An ideal anesthetic: 1. A
General Anesthesia. Mohamed A. Yaseen
 General Anesthesia Mohamed A. Yaseen M.S,c Surgery Before Anesthesia General Anesthesia ( GA ) Drug induced absence of perception of all sensation allowing surgery or other painful procedure to be carried
General Anesthesia Mohamed A. Yaseen M.S,c Surgery Before Anesthesia General Anesthesia ( GA ) Drug induced absence of perception of all sensation allowing surgery or other painful procedure to be carried
General Anesthesia. My goal in general anesthesia is to stop all of these in the picture above (motor reflexes, pain and autonomic reflexes).
 General Anesthesia General anesthesia is essential to surgical practice, because it renders patients analgesic, amnesia and unconscious reflexes, while causing muscle relaxation and suppression of undesirable
General Anesthesia General anesthesia is essential to surgical practice, because it renders patients analgesic, amnesia and unconscious reflexes, while causing muscle relaxation and suppression of undesirable
General anesthetics. Dr. Shamil AL-Noaimy Lecturer of Pharmacology Dept. of Pharmacology College of Medicine
 General anesthetics Dr. Shamil AL-Noaimy Lecturer of Pharmacology Dept. of Pharmacology College of Medicine Rationale General anesthesia is essential to surgical practice, because it renders patients analgesic,
General anesthetics Dr. Shamil AL-Noaimy Lecturer of Pharmacology Dept. of Pharmacology College of Medicine Rationale General anesthesia is essential to surgical practice, because it renders patients analgesic,
May 2013 Anesthetics SLOs Page 1 of 5
 May 2013 Anesthetics SLOs Page 1 of 5 1. A client is having a scalp laceration sutured and is to be given Lidocaine that contains Epinephrine. The nurse knows that this combination is desgined to: A. Cause
May 2013 Anesthetics SLOs Page 1 of 5 1. A client is having a scalp laceration sutured and is to be given Lidocaine that contains Epinephrine. The nurse knows that this combination is desgined to: A. Cause
General Anesthetics Pharmacology
 General Anesthetics Pharmacology Hiwa K. Saaed, PhD Department of Pharmacology & Toxicology College of Pharmacy, University of Sulaimani 2018-19 CLASSIFICATION General anesthetics Intravenous Inhalational
General Anesthetics Pharmacology Hiwa K. Saaed, PhD Department of Pharmacology & Toxicology College of Pharmacy, University of Sulaimani 2018-19 CLASSIFICATION General anesthetics Intravenous Inhalational
CHAPTER 11. General and Local Anesthetics. Anesthetics. Anesthesia. Eliza Rivera-Mitu, RN, MSN NDEG 26 A
 CHAPTER 11 General and Local Anesthetics Eliza Rivera-Mitu, RN, MSN NDEG 26 A Anesthetics Agents that depress the central nervous system (CNS) Depression of consciousness Loss of responsiveness to sensory
CHAPTER 11 General and Local Anesthetics Eliza Rivera-Mitu, RN, MSN NDEG 26 A Anesthetics Agents that depress the central nervous system (CNS) Depression of consciousness Loss of responsiveness to sensory
Chapter 19. Media Directory. Topical (Surface) Anesthesia. Spinal Anesthesia. Nerve-Block Anesthesia. Infiltration (Field-Block) Anesthesia
 Chapter 19 Drugs for Local and General Anesthesia Slide 18 Media Directory Lidocaine Animation Upper Saddle River, New Jersey 07458 All rights reserved. Topical (Surface) Anesthesia Creams, sprays, suppositories
Chapter 19 Drugs for Local and General Anesthesia Slide 18 Media Directory Lidocaine Animation Upper Saddle River, New Jersey 07458 All rights reserved. Topical (Surface) Anesthesia Creams, sprays, suppositories
Laith Mohammed Abbas Al-Huseini. M.B.Ch.B., M.Sc, M.Res, Ph.D. Department of Pharmacology and Therapeutics
 Laith Mohammed Abbas Al-Huseini M.B.Ch.B., M.Sc, M.Res, Ph.D Department of Pharmacology and Therapeutics I. Pre-anesthesia evaluation and preparation II. Pre-anesthesia medication III. Anesthesia steps:
Laith Mohammed Abbas Al-Huseini M.B.Ch.B., M.Sc, M.Res, Ph.D Department of Pharmacology and Therapeutics I. Pre-anesthesia evaluation and preparation II. Pre-anesthesia medication III. Anesthesia steps:
Neuromuscular Junction
 Muscle Relaxants Neuromuscular Junction Cholinergic antagonists Neuromuscular-blocking agents (mostly nicotinic antagonists): interfere with transmission of efferent impulses to skeletal muscles. These
Muscle Relaxants Neuromuscular Junction Cholinergic antagonists Neuromuscular-blocking agents (mostly nicotinic antagonists): interfere with transmission of efferent impulses to skeletal muscles. These
Drugs for Local and General Anesthesia. Copyright 2017, 2014, 2011 Pearson Education, Inc. All Rights Reserved
 Drugs for Local and General Anesthesia Anesthesia Local affecting a limited part of the body General resulting in loss of consciousness Local Anesthetics Five techniques for applying local anesthesia Topical
Drugs for Local and General Anesthesia Anesthesia Local affecting a limited part of the body General resulting in loss of consciousness Local Anesthetics Five techniques for applying local anesthesia Topical
Fundamentals of the Nervous System and Nervous Tissue: Part C
 PowerPoint Lecture Slides prepared by Janice Meeking, Mount Royal College C H A P T E R 11 Fundamentals of the Nervous System and Nervous Tissue: Part C Warm Up What is a neurotransmitter? What is the
PowerPoint Lecture Slides prepared by Janice Meeking, Mount Royal College C H A P T E R 11 Fundamentals of the Nervous System and Nervous Tissue: Part C Warm Up What is a neurotransmitter? What is the
NERVOUS SYSTEM NERVOUS SYSTEM. Somatic nervous system. Brain Spinal Cord Autonomic nervous system. Sympathetic nervous system
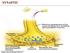 SYNAPTIC NERVOUS SYSTEM NERVOUS SYSTEM CENTRAL NERVOUS SYSTEM PERIPHERAL NERVOUS SYSTEM Brain Spinal Cord Autonomic nervous system Somatic nervous system Sympathetic nervous system Parasympathetic nervous
SYNAPTIC NERVOUS SYSTEM NERVOUS SYSTEM CENTRAL NERVOUS SYSTEM PERIPHERAL NERVOUS SYSTEM Brain Spinal Cord Autonomic nervous system Somatic nervous system Sympathetic nervous system Parasympathetic nervous
General and Local Anesthetics TURNING POINT PHARM THURSDAY IMC606 Neuroscience Module
 General and Local Anesthetics TURNING POINT PHARM THURSDAY IMC606 Neuroscience Module Peter Bradford, PhD pgb@buffalo.edu, JSMBS 3204 13-December-2018 Disclosures NO SIGNIFICANT FINANCIAL, GENERAL, OR
General and Local Anesthetics TURNING POINT PHARM THURSDAY IMC606 Neuroscience Module Peter Bradford, PhD pgb@buffalo.edu, JSMBS 3204 13-December-2018 Disclosures NO SIGNIFICANT FINANCIAL, GENERAL, OR
ANESTHESIA EXAM (four week rotation)
 SPARROW HEALTH SYSTEM ANESTHESIA SERVICES ANESTHESIA EXAM (four week rotation) Circle the best answer 1. During spontaneous breathing, volatile anesthetics A. Increase tidal volume and decrease respiratory
SPARROW HEALTH SYSTEM ANESTHESIA SERVICES ANESTHESIA EXAM (four week rotation) Circle the best answer 1. During spontaneous breathing, volatile anesthetics A. Increase tidal volume and decrease respiratory
What are the 6 types of neuroglia and their functions?!
 Warm Up! Take out your 11C Notes What are the 6 types of neuroglia and their functions?! Astrocytes Microglia Ependymal Cells Satellite Cells Schwann Cells Oligodendrocytes Support, brace, & nutrient transfer
Warm Up! Take out your 11C Notes What are the 6 types of neuroglia and their functions?! Astrocytes Microglia Ependymal Cells Satellite Cells Schwann Cells Oligodendrocytes Support, brace, & nutrient transfer
Overview. Normally, the process is completely reversible.
 Overview Local anesthetics produce a transient and reversible loss of sensation (analgesia) in a circumscribed region of the body without loss of consciousness. Normally, the process is completely reversible.
Overview Local anesthetics produce a transient and reversible loss of sensation (analgesia) in a circumscribed region of the body without loss of consciousness. Normally, the process is completely reversible.
Neurotransmitters. Chemical transmission of a nerve signal by neurotransmitters at a synapse
 Neurotransmitters A chemical released by one neuron that affects another neuron or an effector organ (e.g., muscle, gland, blood vessel). Neurotransmitters are small molecules that serve as messengers
Neurotransmitters A chemical released by one neuron that affects another neuron or an effector organ (e.g., muscle, gland, blood vessel). Neurotransmitters are small molecules that serve as messengers
ANESTHESIA DRUG REVIEW
 ANESTHESIA REVIEW CAPA S 39 TH ANNUAL CONFERENCE PALM SPRINGS OCTOBER 10, 2015 ROBERT F. KOPEL, MD, FACP, FCCP HOAG HOSPITAL CARDIAC ANESTHESIOLOGIST ASSISTANT CLINICAL PROFESSOR UCLA SCHOOL OF MEDICINE
ANESTHESIA REVIEW CAPA S 39 TH ANNUAL CONFERENCE PALM SPRINGS OCTOBER 10, 2015 ROBERT F. KOPEL, MD, FACP, FCCP HOAG HOSPITAL CARDIAC ANESTHESIOLOGIST ASSISTANT CLINICAL PROFESSOR UCLA SCHOOL OF MEDICINE
Inhalational Anesthesia. Munir Gharaibeh, MD, PhD, MHPE School of Medicine The University of Jordan February, 2018
 Inhalational Anesthesia School of Medicine The University of Jordan February, 2018 mgharaib@ju.edu.jo Inhalational Anesthesia n Gases or volatile liquids n Administration and Elimination is by the lungs
Inhalational Anesthesia School of Medicine The University of Jordan February, 2018 mgharaib@ju.edu.jo Inhalational Anesthesia n Gases or volatile liquids n Administration and Elimination is by the lungs
NEUROMUSCULAR BLOCKING AGENTS
 NEUROMUSCULAR BLOCKING AGENTS Edward JN Ishac, Ph.D. Associate Professor, Pharmacology and Toxicology Smith 742, 828-2127, Email: eishac@vcu.edu Learning Objectives: 1. Understand the physiology of the
NEUROMUSCULAR BLOCKING AGENTS Edward JN Ishac, Ph.D. Associate Professor, Pharmacology and Toxicology Smith 742, 828-2127, Email: eishac@vcu.edu Learning Objectives: 1. Understand the physiology of the
POST-INTUBATION ANALGESIA AND SEDATION. August 2012 J Pelletier
 POST-INTUBATION ANALGESIA AND SEDATION August 2012 J Pelletier Intubated patients experience pain and anxiety Mechanical ventilation, endotracheal tube Blood draws, positioning, suctioning Surgical procedures,
POST-INTUBATION ANALGESIA AND SEDATION August 2012 J Pelletier Intubated patients experience pain and anxiety Mechanical ventilation, endotracheal tube Blood draws, positioning, suctioning Surgical procedures,
Core Safety Profile. Pharmaceutical form(s)/strength: 5mg/ml and 25 mg/ml, Solution for injection, IM/IV FI/H/PSUR/0010/002 Date of FAR:
 Core Safety Profile Active substance: Esketamine Pharmaceutical form(s)/strength: 5mg/ml and 25 mg/ml, Solution for injection, IM/IV P-RMS: FI/H/PSUR/0010/002 Date of FAR: 29.05.2012 4.3 Contraindications
Core Safety Profile Active substance: Esketamine Pharmaceutical form(s)/strength: 5mg/ml and 25 mg/ml, Solution for injection, IM/IV P-RMS: FI/H/PSUR/0010/002 Date of FAR: 29.05.2012 4.3 Contraindications
DRUGS THAT ACT IN THE CNS
 DRUGS THAT ACT IN THE CNS Anxiolytic and Hypnotic Drugs Dr Karamallah S. Mahmood PhD Clinical Pharmacology 1 OTHER ANXIOLYTIC AGENTS/ A. Antidepressants Many antidepressants are effective in the treatment
DRUGS THAT ACT IN THE CNS Anxiolytic and Hypnotic Drugs Dr Karamallah S. Mahmood PhD Clinical Pharmacology 1 OTHER ANXIOLYTIC AGENTS/ A. Antidepressants Many antidepressants are effective in the treatment
Biology 3201 Nervous System #6: Effects of Drugs at Synapses
 Biology 3201 Nervous System #6: Effects of Drugs at Synapses Toxins prevent the release of acetylcholine ex. Clostridium botulinum (botulism: muscle paralysis)/ Clostridium tetani (tetanus: a disease characterized
Biology 3201 Nervous System #6: Effects of Drugs at Synapses Toxins prevent the release of acetylcholine ex. Clostridium botulinum (botulism: muscle paralysis)/ Clostridium tetani (tetanus: a disease characterized
Anesthesia: Analgesia: Loss of bodily SENSATION with or without loss of consciousness. Absence of the sense of PAIN without loss of consciousness
 1 2 Anesthesia: Loss of bodily SENSATION with or without loss of consciousness Analgesia: Absence of the sense of PAIN without loss of consciousness 3 1772: Joseph Priestly discovered Nitrous Oxide NO
1 2 Anesthesia: Loss of bodily SENSATION with or without loss of consciousness Analgesia: Absence of the sense of PAIN without loss of consciousness 3 1772: Joseph Priestly discovered Nitrous Oxide NO
The Nervous System. Chapter 4. Neuron 3/9/ Components of the Nervous System
 Chapter 4 The Nervous System 1. Components of the Nervous System a. Nerve cells (neurons) Analyze and transmit information Over 100 billion neurons in system Four defined regions Cell body Dendrites Axon
Chapter 4 The Nervous System 1. Components of the Nervous System a. Nerve cells (neurons) Analyze and transmit information Over 100 billion neurons in system Four defined regions Cell body Dendrites Axon
Local Anesthetics. Xiaoping Du Room E417 MSB Department of Pharmacology Phone (312) ;
 Local Anesthetics Xiaoping Du Room E417 MSB Department of Pharmacology Phone (312)355 0237; Email: xdu@uic.edu Summary: Local anesthetics are drugs used to prevent or relieve pain in the specific regions
Local Anesthetics Xiaoping Du Room E417 MSB Department of Pharmacology Phone (312)355 0237; Email: xdu@uic.edu Summary: Local anesthetics are drugs used to prevent or relieve pain in the specific regions
ISPUB.COM. Review Of Currently Used Inhalation Anesthetics: Part II. O Wenker SIDE EFFECTS OF INHALED ANESTHETICS CARDIOVASCULAR SYSTEM
 ISPUB.COM The Internet Journal of Anesthesiology Volume 3 Number 3 O Wenker Citation O Wenker.. The Internet Journal of Anesthesiology. 1998 Volume 3 Number 3. Abstract SIDE EFFECTS OF INHALED ANESTHETICS
ISPUB.COM The Internet Journal of Anesthesiology Volume 3 Number 3 O Wenker Citation O Wenker.. The Internet Journal of Anesthesiology. 1998 Volume 3 Number 3. Abstract SIDE EFFECTS OF INHALED ANESTHETICS
Integrated Cardiopulmonary Pharmacology Third Edition
 Integrated Cardiopulmonary Pharmacology Third Edition Chapter 3 Pharmacology of the Autonomic Nervous System Multimedia Directory Slide 19 Slide 37 Slide 38 Slide 39 Slide 40 Slide 41 Slide 42 Slide 43
Integrated Cardiopulmonary Pharmacology Third Edition Chapter 3 Pharmacology of the Autonomic Nervous System Multimedia Directory Slide 19 Slide 37 Slide 38 Slide 39 Slide 40 Slide 41 Slide 42 Slide 43
PCTH General Anaesthetics Nov 5 th 2013 (9:30-10:50) Location Woodward 6
 PCTH 325 - General Anaesthetics Nov 5 th 2013 (9:30-10:50) Location Woodward 6 M Walker (rsdaa@mail.ubc.ca) Anesthesiology, Pharmacology & Therapeutics, Faculty of Medicine, UBC Slides adapted from, and
PCTH 325 - General Anaesthetics Nov 5 th 2013 (9:30-10:50) Location Woodward 6 M Walker (rsdaa@mail.ubc.ca) Anesthesiology, Pharmacology & Therapeutics, Faculty of Medicine, UBC Slides adapted from, and
Nervous System Notes
 Nervous System Notes The nervous system consists of a network of nerve cells or neurons. I. A nervous system is an important part of a cell s (or an organism s) ability to respond to the environment. A.
Nervous System Notes The nervous system consists of a network of nerve cells or neurons. I. A nervous system is an important part of a cell s (or an organism s) ability to respond to the environment. A.
Anxiolytic, Sedative and Hypnotic Drugs. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Anxiolytic, Sedative and Hypnotic Drugs Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Anxiolytics: reduce anxiety Sedatives: decrease activity, calming
Anxiolytic, Sedative and Hypnotic Drugs Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Anxiolytics: reduce anxiety Sedatives: decrease activity, calming
Inhalation anesthesia. Somchai Wongpunkamol,MD Anes., CMU
 Inhalation anesthesia Somchai Wongpunkamol,MD nes., CMU Inhalation anesthetics is agent that possess anaesthetic qualities that are administered by breathing through an anaesthesia mask or ET tube connected
Inhalation anesthesia Somchai Wongpunkamol,MD nes., CMU Inhalation anesthetics is agent that possess anaesthetic qualities that are administered by breathing through an anaesthesia mask or ET tube connected
Slide 1. Slide 2. Slide 3. Local Anesthetics. Local Anesthetics. Lesson 9.1. History and Purpose of Anesthetics. Chapter 9
 Slide 1 Local Anesthetics Chapter 9 1 Slide 2 Lesson 9.1 History and Purpose of Anesthetics 1. Discuss the history and reasons for the use of local anesthetics in dentistry, including: List the properties
Slide 1 Local Anesthetics Chapter 9 1 Slide 2 Lesson 9.1 History and Purpose of Anesthetics 1. Discuss the history and reasons for the use of local anesthetics in dentistry, including: List the properties
Neuromuscular Blockers
 Neuromuscular Blockers Joanne Leung joanneleung22@hotmail.com Oct 14, 2014 Objectives After this lecture, you should be able to: Describe the physiology of the neuromuscular junction Differentiate the
Neuromuscular Blockers Joanne Leung joanneleung22@hotmail.com Oct 14, 2014 Objectives After this lecture, you should be able to: Describe the physiology of the neuromuscular junction Differentiate the
PCTH 400 Systematic Pharmacology
 Objectives At the end of this session, you will be able to: 1. Define the components of general anesthesia; PCTH 400 Systematic Pharmacology Inhaled s and Amnestic Agents Dr. Peter Choi (peter.choi@ubc.ca)
Objectives At the end of this session, you will be able to: 1. Define the components of general anesthesia; PCTH 400 Systematic Pharmacology Inhaled s and Amnestic Agents Dr. Peter Choi (peter.choi@ubc.ca)
Chapter 18. Skeletal Muscle Relaxants (Neuromuscular Blocking Agents)
 Chapter 18 Skeletal Muscle Relaxants (Neuromuscular Blocking Agents) Uses of Neuromuscular Blocking Facilitate intubation Surgery Agents Enhance ventilator synchrony Reduce intracranial pressure (ICP)
Chapter 18 Skeletal Muscle Relaxants (Neuromuscular Blocking Agents) Uses of Neuromuscular Blocking Facilitate intubation Surgery Agents Enhance ventilator synchrony Reduce intracranial pressure (ICP)
Pain: 1-2µg/kg q30-60min prn. effects in 10 minutes. Contraindications: Morphine is preferred in. Duration of Action: minutes. renal failure.
 Procedural Sedation / Analgesia / Anaesthesia Chart - Page 1 Diazepam (Valium) Anxiolytic / Sedative Etomidate (Amidate) Hypnotic / Anesthetic Fentanyl Citrate (Sublimaze) Narcotic Analgesic Dose Pediatric:
Procedural Sedation / Analgesia / Anaesthesia Chart - Page 1 Diazepam (Valium) Anxiolytic / Sedative Etomidate (Amidate) Hypnotic / Anesthetic Fentanyl Citrate (Sublimaze) Narcotic Analgesic Dose Pediatric:
Edyta Gołąbiewska PhD
 Edyta Gołąbiewska PhD The depth of anesthesia has been divided into four sequential stages: Stage 1: Analgesia (induction) Stage 2: Excitement Stage 3: Surgical anesthesia Stage 4: Medullary paralysis
Edyta Gołąbiewska PhD The depth of anesthesia has been divided into four sequential stages: Stage 1: Analgesia (induction) Stage 2: Excitement Stage 3: Surgical anesthesia Stage 4: Medullary paralysis
Review of Neurochemistry What are neurotransmitters?
 Review of Neurochemistry What are neurotransmitters? In molecular terms, neurotransmitters are molecules that ( ) and of neurons by, for example, increasing or decreasing enzymatic activity or altering
Review of Neurochemistry What are neurotransmitters? In molecular terms, neurotransmitters are molecules that ( ) and of neurons by, for example, increasing or decreasing enzymatic activity or altering
Local anaesthetic agents
 Local anaesthetic agents 1 Lecture Objectives: Awn khawaldeh 1.Definition 2. Classification of Local Anaesthetic Agents 2.1. Comparison between the two Classes. 3. Mode of action 4. composition of Local
Local anaesthetic agents 1 Lecture Objectives: Awn khawaldeh 1.Definition 2. Classification of Local Anaesthetic Agents 2.1. Comparison between the two Classes. 3. Mode of action 4. composition of Local
INHALATION AGENTS 2013/05/28 1
 INHALATION AGENTS 2013/05/28 1 2013/05/28 Isn t it romantic? 2 Administration 3 Physics Critical temperature Vapour vs. Gas Vapour pressure Blood Gas Partition Coefficient BGPC MAC 2013/05/28 4 Critical
INHALATION AGENTS 2013/05/28 1 2013/05/28 Isn t it romantic? 2 Administration 3 Physics Critical temperature Vapour vs. Gas Vapour pressure Blood Gas Partition Coefficient BGPC MAC 2013/05/28 4 Critical
ISPUB.COM. Review Of Currently Used Inhalation Anesthetics: Part I. O Wenker INTRODUCTION HISTORY
 ISPUB.COM The Internet Journal of Anesthesiology Volume 3 Number 2 O Wenker Citation O Wenker.. The Internet Journal of Anesthesiology. 1998 Volume 3 Number 2. Abstract INTRODUCTION Inhalation anesthetics
ISPUB.COM The Internet Journal of Anesthesiology Volume 3 Number 2 O Wenker Citation O Wenker.. The Internet Journal of Anesthesiology. 1998 Volume 3 Number 2. Abstract INTRODUCTION Inhalation anesthetics
Chapter 45: Synapses Transmission of Nerve Impulses Between Neurons. Chad Smurthwaite & Jordan Shellmire
 Chapter 45: Synapses Transmission of Nerve Impulses Between Neurons Chad Smurthwaite & Jordan Shellmire The Chemical Synapse The most common type of synapse used for signal transmission in the central
Chapter 45: Synapses Transmission of Nerve Impulses Between Neurons Chad Smurthwaite & Jordan Shellmire The Chemical Synapse The most common type of synapse used for signal transmission in the central
Mohammad Tarek. Wahab Al-tekreeti Tamer Barakat. Faisal Mohammad
 15 Mohammad Tarek Wahab Al-tekreeti Tamer Barakat Faisal Mohammad Things to remember Types of synapse: Neuron types and neurotransmitters When it happens between an axon and dendrites it is called axodendritic
15 Mohammad Tarek Wahab Al-tekreeti Tamer Barakat Faisal Mohammad Things to remember Types of synapse: Neuron types and neurotransmitters When it happens between an axon and dendrites it is called axodendritic
problems with, 29, 98 psychiatric patients, 96 rheumatic conditions, 97
 180 ACE inhibitors, 26 acetaminophen, see paracetamol acupressure, anti-emetic effect, 143 acute drugs, 64 5 adenoidectomy, 161 adrenaline, 64 α-2-chloroprocaine, 74, 81 age impact on patient selection,
180 ACE inhibitors, 26 acetaminophen, see paracetamol acupressure, anti-emetic effect, 143 acute drugs, 64 5 adenoidectomy, 161 adrenaline, 64 α-2-chloroprocaine, 74, 81 age impact on patient selection,
Action Potentials and Synaptic Transmission. BIO 219 Napa Valley College Dr. Adam Ross
 Action Potentials and Synaptic Transmission BIO 219 Napa Valley College Dr. Adam Ross Review of action potentials Nodes of Ranvier Nucleus Dendrites Cell body In saltatory conduction, the nerve impulses
Action Potentials and Synaptic Transmission BIO 219 Napa Valley College Dr. Adam Ross Review of action potentials Nodes of Ranvier Nucleus Dendrites Cell body In saltatory conduction, the nerve impulses
Chapter 17. Nervous System Nervous systems receive sensory input, interpret it, and send out appropriate commands. !
 Chapter 17 Sensory receptor Sensory input Integration Nervous System Motor output Brain and spinal cord Effector cells Peripheral nervous system (PNS) Central nervous system (CNS) 28.1 Nervous systems
Chapter 17 Sensory receptor Sensory input Integration Nervous System Motor output Brain and spinal cord Effector cells Peripheral nervous system (PNS) Central nervous system (CNS) 28.1 Nervous systems
BIOLOGY 12 TRANSMISSION OF IMPULSES ACROSS SYNAPSES
 Name: Pages: 326-327, 341-343 Date: BIOLOGY 12 TRANSMISSION OF IMPULSES ACROSS SYNAPSES How does a nerve impulse make a connection from an axon to the next nerve cell? The impulse must travel from the
Name: Pages: 326-327, 341-343 Date: BIOLOGY 12 TRANSMISSION OF IMPULSES ACROSS SYNAPSES How does a nerve impulse make a connection from an axon to the next nerve cell? The impulse must travel from the
SEDATION PHARMACOLOGY STUDY GUIDE RMS-PLLC 1
 SEDATION PHARMACOLOGY STUDY GUIDE RMS-PLLC 1 Responsiveness Continuum of Depth of Sedation Minimal Sedation/ Anxiolysis Normal response to verbal stimulation Moderate Sedation/ Analgesia Conscious Sedation
SEDATION PHARMACOLOGY STUDY GUIDE RMS-PLLC 1 Responsiveness Continuum of Depth of Sedation Minimal Sedation/ Anxiolysis Normal response to verbal stimulation Moderate Sedation/ Analgesia Conscious Sedation
Function of the Nervous System
 Nervous System Function of the Nervous System Receive sensory information, interpret it, and send out appropriate commands to form a response Composed of neurons (functional unit of the nervous system)
Nervous System Function of the Nervous System Receive sensory information, interpret it, and send out appropriate commands to form a response Composed of neurons (functional unit of the nervous system)
Sedation For Cardiac Procedures A Review of
 Sedation For Cardiac Procedures A Review of Sedative Agents Dr Simon Chan Consultant Anaesthesiologist Department of Anaesthesia and Intensive Care Prince of Wales Hospital Hong Kong 21 February 2009 Aims
Sedation For Cardiac Procedures A Review of Sedative Agents Dr Simon Chan Consultant Anaesthesiologist Department of Anaesthesia and Intensive Care Prince of Wales Hospital Hong Kong 21 February 2009 Aims
Skeletal Muscle Relaxants. Munir Gharaibeh, MD, PhD, MHPE Faculty of Medicine, The University of Jordan March, 2014
 Skeletal Muscle Relaxants Munir Gharaibeh, MD, PhD, MHPE Faculty of Medicine, The University of Jordan March, 2014 The nicotinic Acetycholine receptor Present at the neuromuscular junction, peripheral
Skeletal Muscle Relaxants Munir Gharaibeh, MD, PhD, MHPE Faculty of Medicine, The University of Jordan March, 2014 The nicotinic Acetycholine receptor Present at the neuromuscular junction, peripheral
LESSON ASSIGNMENT. LESSON OBJECTIVES 3-1. Given a group of definitions, select the definition of the term muscle relaxant.
 LESSON ASSIGNMENT LESSON 3 Skeletal Muscle Relaxants. TEXT ASSIGNMENT Paragraphs 3-1 through 3-7. LESSON OBJECTIVES 3-1. Given a group of definitions, select the definition of the term muscle relaxant.
LESSON ASSIGNMENT LESSON 3 Skeletal Muscle Relaxants. TEXT ASSIGNMENT Paragraphs 3-1 through 3-7. LESSON OBJECTIVES 3-1. Given a group of definitions, select the definition of the term muscle relaxant.
Anesthetics Locals and Generals.
 Anesthetics Locals and Generals http://wings.buffalo.edu/aru/preprohibition.htm 1 Overview Local anesthetics Esters Amides General anesthetics Parenteral Barbiturates Non-barbiturates Inhalation Volatile
Anesthetics Locals and Generals http://wings.buffalo.edu/aru/preprohibition.htm 1 Overview Local anesthetics Esters Amides General anesthetics Parenteral Barbiturates Non-barbiturates Inhalation Volatile
PAIN. Physiology of pain relating to pain management
 PAIN Physiology of pain relating to pain management What is pain? An unpleasant sensory and emotional experience associated with actual or potential tissue damage. (Melzac and Wall) The generation of pain
PAIN Physiology of pain relating to pain management What is pain? An unpleasant sensory and emotional experience associated with actual or potential tissue damage. (Melzac and Wall) The generation of pain
Anesthetic Techniques in Endoscopic Sinus and Skull Base Surgery
 Anesthetic Techniques in Endoscopic Sinus and Skull Base Surgery Martha Cordoba Amorocho, MD Iuliu Fat, MD Supplement to Cordoba Amorocho M, Fat I. Anesthetic techniques in endoscopic sinus and skull base
Anesthetic Techniques in Endoscopic Sinus and Skull Base Surgery Martha Cordoba Amorocho, MD Iuliu Fat, MD Supplement to Cordoba Amorocho M, Fat I. Anesthetic techniques in endoscopic sinus and skull base
Benztropine and trihexyphenidyl: Centrally acting antimuscarinic agents used for treatment of Parkinson disease & extrapyramidal symptoms.
 Scopolamine: Tertiary amine plant alkaloid. Produces peripheral effects similar to those of atropine. Unlike atropine, scopolamine has greater action on the CNS (observed at therapeutic doses). It has
Scopolamine: Tertiary amine plant alkaloid. Produces peripheral effects similar to those of atropine. Unlike atropine, scopolamine has greater action on the CNS (observed at therapeutic doses). It has
ANESTHETIZING DISEASED PATIENTS: URINARY; NEUROLOGICAL; TRAUMATIZED
 ANESTHETIZING DISEASED PATIENTS: URINARY; NEUROLOGICAL; TRAUMATIZED Lyon Lee DVM PhD DACVA Patients with Urinary Tract Diseases General considerations Three main factors to consider in anesthetizing urinary
ANESTHETIZING DISEASED PATIENTS: URINARY; NEUROLOGICAL; TRAUMATIZED Lyon Lee DVM PhD DACVA Patients with Urinary Tract Diseases General considerations Three main factors to consider in anesthetizing urinary
NEURONS COMMUNICATE WITH OTHER CELLS AT SYNAPSES 34.3
 NEURONS COMMUNICATE WITH OTHER CELLS AT SYNAPSES 34.3 NEURONS COMMUNICATE WITH OTHER CELLS AT SYNAPSES Neurons communicate with other neurons or target cells at synapses. Chemical synapse: a very narrow
NEURONS COMMUNICATE WITH OTHER CELLS AT SYNAPSES 34.3 NEURONS COMMUNICATE WITH OTHER CELLS AT SYNAPSES Neurons communicate with other neurons or target cells at synapses. Chemical synapse: a very narrow
Tranquilizers & Sedative-Hypnotics
 Tranquilizers & Sedative-Hypnotics 1 Tranquilizer or anxiolytic: Drugs used therapeutically to treat agitation or anxiety Sedative-Hypnotic: drugs used to sedate and aid in sleep Original sedatives (before
Tranquilizers & Sedative-Hypnotics 1 Tranquilizer or anxiolytic: Drugs used therapeutically to treat agitation or anxiety Sedative-Hypnotic: drugs used to sedate and aid in sleep Original sedatives (before
Chapter 12 Nervous Tissue. Copyright 2009 John Wiley & Sons, Inc. 1
 Chapter 12 Nervous Tissue Copyright 2009 John Wiley & Sons, Inc. 1 Terms to Know CNS PNS Afferent division Efferent division Somatic nervous system Autonomic nervous system Sympathetic nervous system Parasympathetic
Chapter 12 Nervous Tissue Copyright 2009 John Wiley & Sons, Inc. 1 Terms to Know CNS PNS Afferent division Efferent division Somatic nervous system Autonomic nervous system Sympathetic nervous system Parasympathetic
Chapter 13. Learning Objectives. Learning Objectives 9/11/2012. Poisonings, Overdoses, and Intoxications
 Chapter 13 Poisonings, Overdoses, and Intoxications Learning Objectives Discuss use of activated charcoal in treatment of poisonings List treatment options for acetaminophen overdose List clinical manifestations
Chapter 13 Poisonings, Overdoses, and Intoxications Learning Objectives Discuss use of activated charcoal in treatment of poisonings List treatment options for acetaminophen overdose List clinical manifestations
Neuro Basics SLO Practice (online) Page 1 of 5
 Neuro Basics SLO Practice (online) Page 1 of 5 1) Biogenic amines include ACh, NE, EPI and? a) Melatonin b) Dopamine c) Serotonin d) Histamine e) All of the neurotransmitters listed are biogenic amines.
Neuro Basics SLO Practice (online) Page 1 of 5 1) Biogenic amines include ACh, NE, EPI and? a) Melatonin b) Dopamine c) Serotonin d) Histamine e) All of the neurotransmitters listed are biogenic amines.
General anesthetics (GAs) History
 General anesthetics (GAs) History General anesthesia was introduced into clinical practice in the 19 th century with the use of volatile liquids such as diethyl ether and chloroform. Cardiac and hepatic
General anesthetics (GAs) History General anesthesia was introduced into clinical practice in the 19 th century with the use of volatile liquids such as diethyl ether and chloroform. Cardiac and hepatic
Toxicity Pathways Mediated by Ion Channels
 Toxicity Pathways Mediated by Ion Channels Philip J. Bushnell Neurotoxicology Division National Health and Environmental Effects Research Laboratory Office of Research and Development, US EPA Research
Toxicity Pathways Mediated by Ion Channels Philip J. Bushnell Neurotoxicology Division National Health and Environmental Effects Research Laboratory Office of Research and Development, US EPA Research
Anesthesia and Mitochondrial Cytopathies Bruce H. Cohen, MD, John Shoffner, MD, Glenn DeBoer, MD United Mitochondrial Disease Foundation, 1998
 Introduction Anesthesia and Mitochondrial Cytopathies Bruce H. Cohen, MD, John Shoffner, MD, Glenn DeBoer, MD United Mitochondrial Disease Foundation, 1998 This article will outline some basic aspects
Introduction Anesthesia and Mitochondrial Cytopathies Bruce H. Cohen, MD, John Shoffner, MD, Glenn DeBoer, MD United Mitochondrial Disease Foundation, 1998 This article will outline some basic aspects
Pharmacokinetics. Inhalational Agents. Uptake and Distribution
 Pharmacokinetics Inhalational Agents The pharmacokinetics of inhalational agents is divided into four phases Absorption Distribution (to the CNS Metabolism (minimal Excretion (minimal The ultimate goal
Pharmacokinetics Inhalational Agents The pharmacokinetics of inhalational agents is divided into four phases Absorption Distribution (to the CNS Metabolism (minimal Excretion (minimal The ultimate goal
Pharmacology: Inhalation Anesthetics
 Pharmacology: Inhalation Anesthetics This is an edited and abridged version of: Pharmacology: Inhalation Anesthetics by Jch Ko, DVM, MS, DACVA Oklahoma State University - Veterinary Medicine, February
Pharmacology: Inhalation Anesthetics This is an edited and abridged version of: Pharmacology: Inhalation Anesthetics by Jch Ko, DVM, MS, DACVA Oklahoma State University - Veterinary Medicine, February
Portions from Chapter 6 CHAPTER 7. The Nervous System: Neurons and Synapses. Chapter 7 Outline. and Supporting Cells
 CHAPTER 7 The Nervous System: Neurons and Synapses Chapter 7 Outline Neurons and Supporting Cells Activity in Axons The Synapse Acetylcholine as a Neurotransmitter Monoamines as Neurotransmitters Other
CHAPTER 7 The Nervous System: Neurons and Synapses Chapter 7 Outline Neurons and Supporting Cells Activity in Axons The Synapse Acetylcholine as a Neurotransmitter Monoamines as Neurotransmitters Other
SEEING KETAMINE IN A NEW LIGHT
 SEEING KETAMINE IN A NEW LIGHT BobbieJean Sweitzer, M.D., FACP Professor of Anesthesiology Director of Perioperative Medicine Northwestern University Bobbie.Sweitzer@northwestern.edu LEARNING OBJECTIVES
SEEING KETAMINE IN A NEW LIGHT BobbieJean Sweitzer, M.D., FACP Professor of Anesthesiology Director of Perioperative Medicine Northwestern University Bobbie.Sweitzer@northwestern.edu LEARNING OBJECTIVES
BIOL Week 6. Nervous System. Transmission at Synapses
 Collin County Community College BIOL 2401 Week 6 Nervous System 1 Transmission at Synapses Synapses are the site of communication between 2 or more neurons. It mediates the transfer of information and
Collin County Community College BIOL 2401 Week 6 Nervous System 1 Transmission at Synapses Synapses are the site of communication between 2 or more neurons. It mediates the transfer of information and
General Anesthetics. General Anesthesia Characteristics. Balanced Anesthesia. Types of General Anesthetics. Four Stages of Anesthesia
 History of Anesthesia General Anesthetics Pharmacology 604 K a t h e r i n e L. N i c h o l s o n, D. V. M., P h. D. Dept. Pharmacology/Toxicology k l n i c h o l @h s c. vcu. edu General Anesthesia Characteristics
History of Anesthesia General Anesthetics Pharmacology 604 K a t h e r i n e L. N i c h o l s o n, D. V. M., P h. D. Dept. Pharmacology/Toxicology k l n i c h o l @h s c. vcu. edu General Anesthesia Characteristics
Neuropharmacology NOTES
 Neuropharmacology NOTES Contents Topic Page # Lecture 1- Intro to Neurochemical Transmission & Neuromodulation 2 Lecture 2- Serotonin & Noradrenaline 7 Lecture 3- Acetylcholine & Dopamine 14 Lecture 4-
Neuropharmacology NOTES Contents Topic Page # Lecture 1- Intro to Neurochemical Transmission & Neuromodulation 2 Lecture 2- Serotonin & Noradrenaline 7 Lecture 3- Acetylcholine & Dopamine 14 Lecture 4-
Outline. Neuron Structure. Week 4 - Nervous System. The Nervous System: Neurons and Synapses
 Outline Week 4 - The Nervous System: Neurons and Synapses Neurons Neuron structures Types of neurons Electrical activity of neurons Depolarization, repolarization, hyperpolarization Synapses Release of
Outline Week 4 - The Nervous System: Neurons and Synapses Neurons Neuron structures Types of neurons Electrical activity of neurons Depolarization, repolarization, hyperpolarization Synapses Release of
Goals for sedation during mechanical ventilation
 New Uses of Old Medications Gina Riggi, PharmD, BCCCP, BCPS Clinical Pharmacist Trauma ICU Jackson Memorial Hospital Disclosure I do not have anything to disclose Objectives Describe the use of ketamine
New Uses of Old Medications Gina Riggi, PharmD, BCCCP, BCPS Clinical Pharmacist Trauma ICU Jackson Memorial Hospital Disclosure I do not have anything to disclose Objectives Describe the use of ketamine
Neural Tissue. Chapter 12 Part B
 Neural Tissue Chapter 12 Part B CNS Tumors - Neurons stop dividing at age 4 but glial cells retain the capacity to divide. - Primary CNS tumors in adults- division of abnormal neuroglia rather than from
Neural Tissue Chapter 12 Part B CNS Tumors - Neurons stop dividing at age 4 but glial cells retain the capacity to divide. - Primary CNS tumors in adults- division of abnormal neuroglia rather than from
Pharmacodynamics. Drugs usually elicit more than one effect. What the drug does to the body. How do drugs work? What do they do?
 Pharmacology 203 Windward Community College Pharmacodynamics What the drug does to the body How do drugs work? What do they do? In this fact sheet, we will look at the fundamental mechanisms of drug action.
Pharmacology 203 Windward Community College Pharmacodynamics What the drug does to the body How do drugs work? What do they do? In this fact sheet, we will look at the fundamental mechanisms of drug action.
Anesthesia For The Elderly. Yasser Sakawi, M.D. Associate Professor Anesthesiology Department
 Anesthesia For The Elderly Yasser Sakawi, M.D. Associate Professor Anesthesiology Department Topics of Discussion General concepts and definitions Aging and general organ function Cardiopulmonary function
Anesthesia For The Elderly Yasser Sakawi, M.D. Associate Professor Anesthesiology Department Topics of Discussion General concepts and definitions Aging and general organ function Cardiopulmonary function
Agonists: morphine, fentanyl Agonists-Antagonists: nalbuphine Antagonists: naloxone
 Opioid Definition All drugs, natural or synthetic, that bind to opiate receptors Agonists: morphine, fentanyl Agonists-Antagonists: nalbuphine Antagonists: naloxone Opioid agonists increase pain threshold
Opioid Definition All drugs, natural or synthetic, that bind to opiate receptors Agonists: morphine, fentanyl Agonists-Antagonists: nalbuphine Antagonists: naloxone Opioid agonists increase pain threshold
Warm-Up. Label the parts of the neuron below.
 Warm-Up Label the parts of the neuron below. A B C D E F G Warm-Up 1. One neuron transmits a nerve impulse at 40 m/s. Another conducts at the rate of 1 m/s. Which neuron has a myelinated axon? 2. List
Warm-Up Label the parts of the neuron below. A B C D E F G Warm-Up 1. One neuron transmits a nerve impulse at 40 m/s. Another conducts at the rate of 1 m/s. Which neuron has a myelinated axon? 2. List
1. Name the two major divisions of the nervous system and list the organs within each. Central Nervous System Peripheral Nervous System
 CHAPTER 10: NERVOUS SYSTEM I OBJECTIVES 1. Name the two major divisions of the nervous system and list the organs within each. Central Nervous System Peripheral Nervous System Brain Spinal Cord Cranial
CHAPTER 10: NERVOUS SYSTEM I OBJECTIVES 1. Name the two major divisions of the nervous system and list the organs within each. Central Nervous System Peripheral Nervous System Brain Spinal Cord Cranial
NERVOUS SYSTEM C H A P T E R 2 8
 NERVOUS SYSTEM C H A P T E R 2 8 CAN AN INJURED SPINAL CORD BE FIXED? Injuries to the spinal cord disrupt communication between the central nervous system (brain and spinal cord) and the rest of the body
NERVOUS SYSTEM C H A P T E R 2 8 CAN AN INJURED SPINAL CORD BE FIXED? Injuries to the spinal cord disrupt communication between the central nervous system (brain and spinal cord) and the rest of the body
Pharmacological methods of behaviour management
 Pharmacological methods of behaviour management Pharmacological methods CONCIOUS SEDATION?? Sedation is the use of a mild sedative (calming drug) to manage special needs or anxiety while a child receives
Pharmacological methods of behaviour management Pharmacological methods CONCIOUS SEDATION?? Sedation is the use of a mild sedative (calming drug) to manage special needs or anxiety while a child receives
Nervous System. Master controlling and communicating system of the body. Secrete chemicals called neurotransmitters
 Nervous System Master controlling and communicating system of the body Interacts with the endocrine system to control and coordinate the body s responses to changes in its environment, as well as growth,
Nervous System Master controlling and communicating system of the body Interacts with the endocrine system to control and coordinate the body s responses to changes in its environment, as well as growth,
Chapter 11 Introduction to the Nervous System and Nervous Tissue Chapter Outline
 Chapter 11 Introduction to the Nervous System and Nervous Tissue Chapter Outline Module 11.1 Overview of the Nervous System (Figures 11.1-11.3) A. The nervous system controls our perception and experience
Chapter 11 Introduction to the Nervous System and Nervous Tissue Chapter Outline Module 11.1 Overview of the Nervous System (Figures 11.1-11.3) A. The nervous system controls our perception and experience
- Neurotransmitters Of The Brain -
 - Neurotransmitters Of The Brain - INTRODUCTION Synapsis: a specialized connection between two neurons that permits the transmission of signals in a one-way fashion (presynaptic postsynaptic). Types of
- Neurotransmitters Of The Brain - INTRODUCTION Synapsis: a specialized connection between two neurons that permits the transmission of signals in a one-way fashion (presynaptic postsynaptic). Types of
Chapter 2. The Cellular and Molecular Basis of Cognition Cognitive Neuroscience: The Biology of the Mind, 2 nd Ed.,
 Chapter 2. The Cellular and Molecular Basis of Cognition Cognitive Neuroscience: The Biology of the Mind, 2 nd Ed., M. S. Gazzaniga, R. B. Ivry, and G. R. Mangun, Norton, 2002. Summarized by B.-W. Ku,
Chapter 2. The Cellular and Molecular Basis of Cognition Cognitive Neuroscience: The Biology of the Mind, 2 nd Ed., M. S. Gazzaniga, R. B. Ivry, and G. R. Mangun, Norton, 2002. Summarized by B.-W. Ku,
Anesthesia and Neuromuscular Blockade: A Guide for Hospital Pharmacists. Upon completion of this activity, participants will be better able to:
 Anesthesia and Neuromuscular Blockade: A Guide for Hospital Pharmacists EDUCATIONAL OBJECTIVES Upon completion of this activity, participants will be better able to: 1. Understand the use of neuromuscular
Anesthesia and Neuromuscular Blockade: A Guide for Hospital Pharmacists EDUCATIONAL OBJECTIVES Upon completion of this activity, participants will be better able to: 1. Understand the use of neuromuscular
The Nervous System -The master controlling and communicating system of the body
 The Nervous System -The master controlling and communicating system of the body Functions: -Sensory input -Integration -Motor output Organization of the Nervous System Central nervous system (CNS) -Brain
The Nervous System -The master controlling and communicating system of the body Functions: -Sensory input -Integration -Motor output Organization of the Nervous System Central nervous system (CNS) -Brain
(PP XI) Dr. Samir Matloob
 DRUGS ACTING ON THE CHOLINERGIC SYSTEM AND THE NEUROMUSCULAR BLOCKING DRUGS IV (NICOTINIC ANTAGONISTS) (PP XI) Dr. Samir Matloob Dept. of Pharmacology Baghdad College of Medicine Drugs acting on the cholinergic
DRUGS ACTING ON THE CHOLINERGIC SYSTEM AND THE NEUROMUSCULAR BLOCKING DRUGS IV (NICOTINIC ANTAGONISTS) (PP XI) Dr. Samir Matloob Dept. of Pharmacology Baghdad College of Medicine Drugs acting on the cholinergic
The Nervous System Mark Stanford, Ph.D.
 The Nervous System Functional Neuroanatomy and How Neurons Communicate Mark Stanford, Ph.D. Santa Clara Valley Health & Hospital System Addiction Medicine and Therapy Services The Nervous System In response
The Nervous System Functional Neuroanatomy and How Neurons Communicate Mark Stanford, Ph.D. Santa Clara Valley Health & Hospital System Addiction Medicine and Therapy Services The Nervous System In response
QUIZ/TEST REVIEW NOTES SECTION 7 NEUROPHYSIOLOGY [THE SYNAPSE AND PHARMACOLOGY]
![QUIZ/TEST REVIEW NOTES SECTION 7 NEUROPHYSIOLOGY [THE SYNAPSE AND PHARMACOLOGY] QUIZ/TEST REVIEW NOTES SECTION 7 NEUROPHYSIOLOGY [THE SYNAPSE AND PHARMACOLOGY]](/thumbs/86/94924826.jpg) QUIZ/TEST REVIEW NOTES SECTION 7 NEUROPHYSIOLOGY [THE SYNAPSE AND PHARMACOLOGY] Learning Objectives: Explain how neurons communicate stimulus intensity Explain how action potentials are conducted along
QUIZ/TEST REVIEW NOTES SECTION 7 NEUROPHYSIOLOGY [THE SYNAPSE AND PHARMACOLOGY] Learning Objectives: Explain how neurons communicate stimulus intensity Explain how action potentials are conducted along
Ideal Sedative Agent. Benzodiazepines 11/12/2013. Pharmacology of Benzodiazepines Used for Conscious Sedation in Dentistry.
 Pharmacology of Benzodiazepines Used for Conscious Sedation in Dentistry Peter Walker Ideal Sedative Agent Anxiolysis Analgesic No effect on CVS No effect on respiratory system Not metabolised Easy and
Pharmacology of Benzodiazepines Used for Conscious Sedation in Dentistry Peter Walker Ideal Sedative Agent Anxiolysis Analgesic No effect on CVS No effect on respiratory system Not metabolised Easy and
Summarized by B.-W. Ku, E. S. Lee, and B.-T. Zhang Biointelligence Laboratory, Seoul National University.
 Chapter 2. The Cellular l and Molecular Basis of Cognition Cognitive Neuroscience: The Biology of the Mind, 3 rd Ed., M. S. Gazzaniga, R. B. Ivry, and G. R. Mangun, Norton, 2008. Summarized by B.-W. Ku,
Chapter 2. The Cellular l and Molecular Basis of Cognition Cognitive Neuroscience: The Biology of the Mind, 3 rd Ed., M. S. Gazzaniga, R. B. Ivry, and G. R. Mangun, Norton, 2008. Summarized by B.-W. Ku,
Ideal Sedative Agent. Pharmacokinetics. Benzodiazepines. Pharmacodynamics 11/11/2013
 Ideal Sedative Agent Pharmacology of Benzodiazepines Used for Conscious Sedation in Dentistry Peter Walker Anxiolysis Analgesic No effect on CVS No effect on respiratory system Not metabolised Easy and
Ideal Sedative Agent Pharmacology of Benzodiazepines Used for Conscious Sedation in Dentistry Peter Walker Anxiolysis Analgesic No effect on CVS No effect on respiratory system Not metabolised Easy and
NEURAL TISSUE (NEUROPHYSIOLOGY) PART I (A): NEURONS & NEUROGLIA
 PART I (A): NEURONS & NEUROGLIA Neural Tissue Contains 2 kinds of cells: neurons: cells that send and receive signals neuroglia (glial cells): cells that support and protect neurons Neuron Types Sensory
PART I (A): NEURONS & NEUROGLIA Neural Tissue Contains 2 kinds of cells: neurons: cells that send and receive signals neuroglia (glial cells): cells that support and protect neurons Neuron Types Sensory
INTRODUCTION TO CNS PHARMACOLOGY
 INTRODUCTION TO CNS PHARMACOLOGY Central nervous system is nothing but a network of neuronal cells interacting each other with many inhibitory and excitatory neurotransmitters which regulate all the body
INTRODUCTION TO CNS PHARMACOLOGY Central nervous system is nothing but a network of neuronal cells interacting each other with many inhibitory and excitatory neurotransmitters which regulate all the body
