New methods for the management of esophageal varices
|
|
|
- Clare Garrison
- 6 years ago
- Views:
Transcription
1 PO Box 2345, Beijing , China World J Gastroenterol 2007 March 21; 13(11): World Journal of Gastroenterology ISSN wjg@wjgnet.com 2007 The WJG Press. All rights reserved. New methods for the management of esophageal varices EDITORIAL Hiroshi Yoshida, Yasuhiro Mamada, Nobuhiko Taniai, Takashi Tajiri Hiroshi Yoshida, Yasuhiro Mamada, Nobuhiko Taniai, Takashi Tajiri, Department of Surgery, Nippon Medical School, Tokyo , Japan Correspondence to: Hiroshi Yoshida, MD, Department of Surgery, Nippon Medical School, Sendagi, Bunkyo-ku, Tokyo , Japan. hiroshiy@nms.ac.jp Telephone: Fax: Received: Accepted: Abstract Bleeding from esophageal varices (EVs) is a catastrophic complication of chronic liver disease. Many years ago, surgical procedures such as esophageal transection or distal splenorenal shunting were the only treatments for EVs. In the 1970s, interventional radiology procedures such as transportal obliteration, left gastric artery embolization, and partial splenic artery embolization were introduced, improving the survival of patients with bleeding EVs. In the 1980s, endoscopic treatment, endoscopic injection sclerotherapy (EIS), and endoscopic variceal ligation (EVL), further contributed to improved survival. We combined IVR with endoscopic treatment or EIS with EVL. Most patients with EVs treated endoscopically required followup treatment for recurrent varices. Proper management of recurrent EVs can significantly improve patients quality of life. Recently, we have performed EVL at 2-mo (bimonthly) intervals for the management of EVs. Longer intervals between treatment sessions resulted in a higher rate of total eradication and lower rates of recurrence and additional treatment The WJG Press. All rights reserved. Key words: Esophageal varices; Surgery; Interventional radiology; Embolization; Endoscopic treatment; Bi-monthly Yoshida H, Mamada Y, Taniai N, Tajiri T. New methods for the management of esophageal varices. World J Gastroenterol 2007; 13(11): INTRODUCTION Bleeding from esophageal varices (EVs) or gastric varices (GVs) is a catastrophic complication of chronic liver disease. There are various treatments for EVs. Many years ago, operation was the only treatment option available. In the 1970s, techniques for interventional radiology were developed, improving the survival of patients with bleeding EVs. In the 1980s, endoscopic treatment further contributed to improved survival. In this paper, we review the evolution of treatments for EVs. DIAGNOSIS OF ESOPHAGEAL VARICES The Esophagogastric Varices Grading System of the Japan Society for Portal Hypertension [1] evaluates EVs on the basis of color [white (Cw) or blue (Cb)], form [small and straight (F1), nodular (F2), or large or coiled (F3)], and red color signs (RC0-3). Pathomorphology of esophageal varices Bleeding from an EV most commonly occurs in the critical area 3 cm proximal to the esophagocardiac junction. Fine longitudinal veins in the lamina propria originate at the esophagocardiac junction and transverse the lamina propria toward this critical area. EVs consist of multiple dilated veins. Veins that rupture are usually located in the lamina propria [2]. The mucosal layer covering an EV is somewhat thinner than that covering a GV. The lamina muscularis mucosa of the esophagus is loose, and venous pressure in the submucosa is transmitted through communicating branches to veins in the lamina propria. In contrast, the lamina muscularis mucosa of the gastric mucosa is tough and tightly integrated with the lamina propria [3]. Red color signs are elevated red areas that are important for predicting the risk of variceal bleeding. Histologically, red color signs are associated with a thinning epithelial layer. Incidence and risk factors for bleeding from esophageal varices The incidence of variceal bleeding in patients with previously untreated EVs ranges from 16% to 75.6% [4,5]. In an earlier study examining the natural course of GVs, our group treated bleeding from GVs in 4 of 52 patients over a mean follow-up of 41 mo. Hemorrhage was successfully controlled in all 4 of these patients. Cumulative bleeding rates at 1, 3, and 5 years were 3.8%, 9.4%, and 9.4%, respectively [6]. The overall incidence of bleeding is thus higher for EVs than for GVs. In another study, our group examined 70 cirrhotic patients with first episodes of bleeding from EVs or GVs; no patient had received prior treatment [7]. Red color signs were more common in EVs than in GVs. Mucosal
2 1642 ISSN CN /R World J Gastroenterol March 21, 2007 Volume 13 Number 11 erosions and ulcers at bleeding varices were more common in GVs than in EVs. Gastric erosions and ulcers were also more common in GVs than in EVs. Red color signs were frequently encountered in EVs, but were not found in fundal varices. All cardiac varices showing red color signs communicated with EVs, which also showed red color signs. The lack of red color signs in fundal varices might have been caused by the thick overlying mucosa. Gastric ulcers that develop on GVs invade the protective layer of the gastric mucosa. Invasion of the mucosal barrier overlying GVs increases the risk of massive bleeding, especially when fundal varices are involved. Such invasions might be an important precondition for variceal hemorrhage. Endoscopic risk factors for bleeding from EVs include the presence of raised red markings, cherry-red spots, blue coloration, and large size [8]. The North Italian Endoscopic Club for the Study and Treatment of Esophageal Varices [9] reported that red color signs on EVs are predictive of bleeding. TREATMETN OF ESOPHAGEAL VARICES Treatment modalities for EVs include surgery, interventional radiology, and endoscopic treatment. Surgery A number of surgical procedures have been developed to manage EVs. These can be broadly classified as shunting procedures and nonshunting procedures. Shunting procedures: The goal of shunting is to reduce the incidence of variceal bleeding by lowering the pressure in the portal system with a portal-systemic shunt. A standard portocaval shunt effectively reduces the incidence of variceal bleeding; however, impaired metabolism of hepatic protein after the procedure frequently causes hepatic encephalopathy due to hyperammonemia [10-12]. In 1967, Warren developed the distal splenorenal shunt (DSRS) to preserve portal blood flow through the liver, while lowering variceal pressure [13]. This approach was developed in the hope of preventing bleeding as well as hyperammonemia. Despite these initial expectations, DSRS has been found to effectively prevent rebleeding, but not eliminate the risk of hyperammonemia. To solve this problem, our group designed a DSRS with splenopancreatic disconnection and gastric transection, modifications to prevent the loss of shunt selectivity. Our modified DSRS has been confirmed to reduce the incidence of postoperative hyperammonemia [14]. Non-shunting procedures: As an alternative to shunting, Hassab [15] and Sugiura [16] developed methods for gastroesophageal decongestion and splenectomy for the treatment of varices. The Hassab operation devascularizes the distal esophagus and proximal stomach. Splenectomy, selective vagotomy, and pyloroplasty can be performed concomitantly with the procedure. Sugiura [16] developed a procedure for esophageal transection in patients with EVs and GVs. While both the Hassab and Sugiura procedures solve the problem of hepatic encephalopathy, varices are likely to recur earlier than they do after DSRS [17]. Interventional radiology In the 1970s, interventional radiology (IVR) techniques were developed for the treatment of EVs. Transportal obliteration, left gastric artery embolization, and partial splenic artery embolization are the principal IVR techniques used to treat EVs. Before performing IVR, portal hemodynamics should be determined. Angiography can determine the hemodynamics of varices during embolization. Transportal obliteration: Two methods have been used to obliterate the feeding veins of EVs: percutaneous transhepatic obliteration and trans-ileocolic vein obliteration. These methods are performed similarly. A catheter is inserted directly into the portal vein, and the portal circulation is visualized by portography. A balloon catheter is inserted selectively into the inflow site of the feeding veins of the varices. The balloon is inflated, and a test dose of contrast medium is injected to determine the optimal volume of sclerosant. Five percent ethanolamine oleate with iopamidol (EOI), 500 ml/l glucose, or both are injected to obliterate the feeding vein(s). Steel coils are then used to complete obliteration [18]. The procedure is highly effective, although the complete disappearance rate of EVs is not so high after transportal obliteration alone. Partial splenic artery embolization: Partial splenic artery embolization (PSE) has been performed to treat hypersplenism, EVs, GVs, portal hypertensive gastropathy, pancreatic carcinoma, and portosystemic encephalopathy [18-29]. The femoral artery approach is used for superselective catheterization of the splenic artery. The tip of a catheter is placed as distally as possible in either the hilus of the spleen or in an intrasplenic artery. Embolization is achieved by injecting 2-mm gelatin-sponge cubes suspended in a saline solution containing antibiotics [23,30]. Similar to transportal obliteration, complete disappearance of EVs is difficult to achieve by PSE alone. PSE is thus a supplemental treatment for EVs. Endoscopic treatment Two endoscopic techniques are used to treat EVs: endoscopic injection sclerotherapy (EIS) and endoscopic variceal ligation (EVL) [31-37]. Whenever possible, endoscopic treatment was performed at 2-wk intervals by three expert endoscopists, using a television endoscopy system with computer-stored endoscopic images. After premedication with an intramuscular injection of scopolamine butylbromide (20 mg), atropine sulfate (0.25 mg), pentazocine (15 mg), hydroxyzine (25 mg), and diazepam (5 mg) were injected intravenously. A one-channel endoscope was then inserted. A flexible endoscopic sheath (Sumitomo Bakelite, Tokyo, Japan) was used to permit reinsertion of the endoscope and to prevent aspiration. Endoscopic injection sclerotherapy: EIS can be accomplished by either intravariceal EIS or extravariceal EIS [32-34,38]. (1) Intravariceal EIS. An anal-side balloon was inserted into the stomach, and a 22-gauge needle was inserted into the target EV 2 to 3 cm proximal to the gastroesophageal junction. The sclerosant (50 ml/l EOI) was infused into
3 Yoshida H et al. New methods for the management of esophageal varices 1643 the EV, and flow was monitored by X-ray fluoroscopy to confirm filling of the feeder vessel or the pericardiac venous plexus. Suction was maintained at the puncture point while the needle was in the EV. The same procedure was repeated for other variceal columns in the lower esophagus. Additional injections could not be performed, and the injection site was compressed by inflating the analside balloon with air. In the treatment of EVs, intravariceal EIS obliterates both interconnecting perforating veins and feeding veins of EVs. Nearby, however, some dilated winding cardiac veins transverse the submucosa and directly join the EVs. This allows most cardiac varices to be treated concomitantly with EVs when correcting the latter by intravariceal EIS. Intravariceal EIS is useful for obliterating feeding veins of recurrent EVs after operation [34]. However, EIS is associated with high incidences of local and systemic complications [39]. (2) Extravariceal EIS. Extravariceal EIS was performed with 10 ml/l polidocanol to treat remaining varices by paravariceal injection [40]. The end point of primary treatment was the failure to detect any residual varices between the ulcers created by extravariceal EIS during the first hospitalization. Extravariceal EIS achieves local eradication, but does not completely disrupt the interconnecting perforating and feeder vessels [41]. Endoscopic variceal ligation: There are various EVL devices for the treatment of EVs. We use a pneumoactivated EVL device (Sumitomo Bakelite) to treat EVs. EVL is increasingly used because of its safety and simplicity and because no sclerosant is required. EVL achieves local eradication, but does not completely disrupt the interconnecting perforating and feeder vessels [41]. We have devised a new intensive EVL method to more consistently eradicate EVs [31]. In comparison, the average total number of rubber bands used per patient was 9.6 in the standard EVL group and 19.9 in the intensive EVL group. EVs were completely obliterated in all patients in the intensive EVL group, but not in all patients in the standard EVL group [31]. Nevertheless, early recurrences of EVs after EVL have been reported [32]. Combination of endoscopic treatment and interventional radiology Our group previously reported that endoscopic treatment combined with IVR techniques significantly reduced longterm rates of rebleeding and retreatment in patients with EVs [18,24,26,27]. Combination of endoscopic variceal ligation and partial splenic artery embolization: Cumulative recurrence rates at 1 and 2 years were lower in the EVL + PSE group than in the intensive EVL group (P = 0.042), suggesting that EVL + PSE therapy is effective for the management of EVs [24]. Endoscopic treatment versus endoscopic treatment combined with interventional radiology: Cumulative retreatment rates in patients with Child s class C disease were lower after endoscopic treatment + IVR than after endoscopic treatment alone (P = 0.025). A combination of endoscopic therapy and IVR is effective therapy for EVs, especially in patients with poor liver function [18]. Combination of endoscopic injection sclerotherapy and endoscopic variceal ligation: Several investigators have examined the efficacy of EVL combined with EIS for the treatment of EVs [42-44]. Saeed et al [42] and Laine et al [43] compared a single session of treatment with EVL plus low-volume EIS with a single session of EVL alone and concluded that EVL alone is superior to combination therapy. EVL was performed first, followed by intravariceal EIS immediately proximal to the ligature. The main limitation of this method is that only half of the feeding vessels are treated because the sclerosants are injected into the EV proximal to the ligature; distal vessels therefore do not undergo sclerosis. EVL followed by EIS intrinsically differs from EIS followed by EVL. Moreover, the combination of intravariceal EIS and EVL differs from that of extravariceal EIS and EVL. EVL and extravariceal EIS both eradicate varices locally, with no effect on interconnecting perforating or feeding vessels [41]. Takase et al [45] concluded that feeder vessels must be obliterated to prevent recurrence. Beginning in November 1994, we developed a new technique combining EVL with EIS, called endoscopic scleroligation (ESL). In this technique, intravariceal EIS is performed before ligation. The puncture needle was removed after sclerosant infusion, and EVL was done simultaneously, including the placement of bands at the injection site. The same procedure was repeated for other EVs around the lower esophagus. Additional sclerosants were not injected. Intensive EVL was performed for EVs in the lower to middle esophagus [32]. Intravariceal endoscopic injection sclerotherapy followed by endoscopic variceal ligation (ESL) versus intensive endoscopic variceal ligation: Both methods were equally effective with respect to complete eradication of EVs. Among patients in whom complete eradication was achieved, cumulative recurrence rates at 1 and 3 years were lower in the ESL group than in the intensive EVL group (P < 0.01). ESL was thus superior to intensive EVL in preventing variceal recurrence [32]. Intravariceal endoscopic injection sclerotherapy followed by endoscopic variceal ligation (ESL) versus EVL followed by extravariceal EIS: Cumulative recurrence rates at 1 and 3 years in the ESL group were much lower than those in the EVL + extravariceal EIS group (P < ) [33]. Because intravariceal EIS was performed before ligation in ESL, all interconnecting perforating veins and feeder vessels were obliterated. This study supports the conclusion that the incidence of variceal recurrence is lower after ESL than after EVL + extravariceal EIS, although both methods were equally effective initially in terms of completely eradicating EVs. Endoscopic variceal ligation followed by extravariceal endoscopic injection sclerotherapy versus intensive endoscopic variceal ligation: Fewer treatment sessions were needed (P < 0.005), and more O-rings were required (P < ) in the EVL group than in the EVL + extravariceal EIS group. Cumulative recurrence rates at 1 and 3 years were higher in the EVL group
4 1644 ISSN CN /R World J Gastroenterol March 21, 2007 Volume 13 Number 11 than in the EVL + extravariceal EIS group (P < 0.05). Endoscopic examination at first recurrence showed that varices were more severe in form (P < 0.001), but less frequently associated with red color signs (P < ) and intramucosal venous dilatation (P < ) in the EVL group than in the EVL + extravariceal EIS group. Fewer rehospitalizations were required for additional treatment (P < ), and more patients received only endoscopic treatment for recurrent varices (P < 0.05) in the EVL group than in the EVL + extravariceal EIS group. These findings indicate that multiple EVL sessions are an effective treatment strategy for EVs [38]. New methods for the management of EVs: EVL at 2-mo intervals EVL and extravariceal EIS are not always effective, and early recurrences have been reported [32]. Furthermore, most patients with endoscopically treated EVs require followup therapy for recurrent varices. Proper management of recurrent EVs can significantly improve patients quality of life. In our previous study, the number of EVL sessions during the first hospitalization was 2.5 ± 0.5 [38]. Most EVs were ligated and deprived of blood after the first session. The remaining EVs were ligated in the second and subsequent sessions of EVL. Our findings suggested that the first EVL session had the most important role in blocking blood flow and stimulating shunt formation. After EVL alone, 1.8 subsequent hospitalizations were required for additional treatment of recurrent varices [38]. We judged that multiple blockages (at least three) of blood flow to EVs effectively stimulated shunt formation. We therefore defined three sessions to be one course in subsequent studies. The second treatment session after recanalization of variceal blood flow had a greater impact on the stimulation of shunt formation than did prior treatment sessions. This finding suggested that a prolonged interval between EVL sessions may improve treatment outcomes for EVs. However, we found that the bleeding rate of incompletely eradicated EVs was high and that bleeding from completely eradicated EVs occurred after only 6 mo [32]. We therefore based the following study on the premise that three treatment sessions performed at 2-mo intervals (i.e., the third session begins 4 mo after the first session) would effectively prevent bleeding from EVs. Endoscopic variceal ligation bi-weekly versus bimonthly: We conventionally performed EVL treatment once every 2 wk (bi-weekly). We compared the short- and long-term results of EVL performed in three sessions with a total of 16 O-rings at two different intervals, i.e., biweekly (conventional interval) versus bi-monthly. A total of 63 patients with EVs were randomly assigned to receive one of these EVL treatments. Outcomes were assessed by an experienced physician who was blinded to the patients treatment assignments. The overall rates of variceal recurrence and additional treatment were both higher after EVL bi-weekly than after EVL bi-monthly (P < 0.001). We concluded that EVL once every 2 mo (bi-monthly) resulted in better outcomes than EVL once every 2 wk (bi-weekly) in patients with EVs. Treatment sessions separated by a longer interval had a higher rate of total eradication and lower rates of recurrence and additional treatment [36]. REFERENCES 1 The Japan Society for Portal Hypertension. The general rules for study of portal hypertension. 2nd ed. Tokyo: Kanehara Co., 2004: Arakawa M, Kage M. Haemorrhage in the upper digestive tract due to portal hypertension: clinicopathological examinations of the foci of haemorrhage. J Gastroenterol Hepatol 1989; 4 Suppl 1: Ide K, Nagasaki Y, Tomimatsu H, Nakashima T, Arakawa M, Kojiro M. Pathomorphologic and angio-architectural studies of oesophagogastric varices. J Gastroenterol Hepatol 1989; 4 Suppl 1: Paquet KJ, Kalk JF, Klein CP, Gad HA. Prophylactic sclerotherapy for esophageal varices in high-risk cirrhotic patients selected by endoscopic and hemodynamic criteria: a randomized, single-center controlled trial. Endoscopy 1994; 26: Triger DR, Smart HL, Hosking SW, Johnson AG. Prophylactic sclerotherapy for esophageal varices: long-term results of a single-center trial. Hepatology 1991; 13: Tajiri T, Onda M, Yoshida H, Mamada Y, Taniai N, Yamashita K. The natural history of gastric varices. Hepatogastroenterology 2002; 49: Yoshida H, Onda M, Tajiri T, Mamada Y, Taniai N. Endoscopic findings of bleeding esophagogastric varices. Hepatogastroenterology 2002; 49: Beppu K, Inokuchi K, Koyanagi N, Nakayama S, Sakata H, Kitano S, Kobayashi M. Prediction of variceal hemorrhage by esophageal endoscopy. Gastrointest Endosc 1981; 27: Prediction of the first variceal hemorrhage in patients with cirrhosis of the liver and esophageal varices. A prospective multicenter study. The North Italian Endoscopic Club for the Study and Treatment of Esophageal Varices. N Engl J Med 1988; 319: Millikan WJ Jr, Warren WD, Henderson JM, Smith RB 3rd, Salam AA, Galambos JT, Kutner MH, Keen JH. The Emory prospective randomized trial: selective versus nonselective shunt to control variceal bleeding. Ten year follow-up. Ann Surg 1985; 201: Rikkers LF, Jin G. Variceal hemorrhage: surgical therapy. Gastroenterol Clin North Am 1993; 22: Rikkers LF, Sorrell WT, Jin G. Which portosystemic shunt is best? Gastroenterol Clin North Am 1992; 21: Warren WD, Zeppa R, Fomon JJ. Selective trans-splenic decompression of gastroesophageal varices by distal splenorenal shunt. Ann Surg 1967; 166: Tajiri T, Onda M, Yoshida H, Mamada Y, Taniai N, Umehara M, Toba M, Yamashita K. Long-term results of modified distal splenorenal shunts for the treatment of esophageal varices. Hepatogastroenterology 2000; 47: Hassab MA. Gastroesophageal decongestion and splenectomy in the treatment of esophageal varices in bilharzial cirrhosis: further studies with a report on 355 operations. Surgery 1967; 61: Sugiura M, Futagawa S. A new technique for treating esophageal varices. J Thorac Cardiovasc Surg 1973; 66: Tajiri T, Onda M, Yoshida H, Mamada Y, Taniai N, Yamashita K. Comparison of the long-term results of distal splenorenal shunt and esophageal transection for the treatment of esophageal varices. Hepatogastroenterology 2000; 47: Taniai N, Onda M, Tajiri T, Yoshida H, Mamada Y. Combined endoscopic and radiologic intervention to treat esophageal varices. Hepatogastroenterology 2002; 49: Shimizu T, Onda M, Tajiri T, Yoshida H, Mamada Y, Taniai N, Aramaki T, Kumazaki T. Bleeding portal-hypertensive gastropathy managed successfully by partial splenic embolization. Hepatogastroenterology 2002; 49:
5 Yoshida H et al. New methods for the management of esophageal varices Tajiri T, Onda M, Taniai N, Yoshida H, Mamada Y. A comparison of combination endoscopic therapy and interventional radiology with esophageal transection for the treatment of esophageal varices. Hepatogastroenterology 2002; 49: Yoshida H, Onda M, Tajiri T, Akimaru K, Uchida E, Arima Y, Mamada Y, Taniai N, Yamamoto K, Kaneko M, Kumazaki T. New techniques: splenic artery embolization followed by intraarterial infusion chemotherapy for the treatment of pancreatic cancer. Hepatogastroenterology 1999; 46: Yoshida H, Onda M, Tajiri T, Uchida E, Arima Y, Mamada Y, Yamamoto K, Kaneko M, Terada Y, Kumazaki T. Experience with intraarterial infusion of styrene maleic acid neocarzinostatin (SMANCS)-lipiodol in pancreatic cancer. Hepatogastroenterology 1999; 46: Yoshida H, Mamada Y, Taniai N, Yamamoto K, Kaneko M, Kawano Y, Mizuguchi Y, Kumazaki T, Tajiri T. Long-term results of partial splenic artery embolization as supplemental treatment for portal-systemic encephalopathy. Am J Gastroenterol 2005; 100: Taniai N, Onda M, Tajiri T, Toba M, Yoshida H. Endoscopic variceal ligation (EVL) combined with partial splenic embolization (PSE). Hepatogastroenterology 1999; 46: Taniai N, Onda M, Tajiri T, Yoshida H, Mamada Y. Interventional radiology and endoscopic therapy for recurrent esophageal varices. Hepatogastroenterology 2001; 48: Yoshioka M, Onda M, Tajiri T, Akimaru K, Yoshida H, Mamada Y, Taniai N, Mineta S, Hirakata A, Kumazaki T. Control of isolated gastric varices by combination therapy using embolization and endoscopic scleroligation therapy. Hepatogastroenterology 2002; 49: Taniai N, Yoshida H, Mamada Y, Tajiri T. The treatment of gastric fundal varices--endoscopic therapy versus interventional radiology. Hepatogastroenterology 2005; 52: Takahashi T, Arima Y, Yokomuro S, Yoshida H, Mamada Y, Taniai N, Kawano Y, Mizuguchi Y, Shimizu T, Akimaru K, Tajiri T. Splenic artery embolization before laparoscopic splenectomy in children. Surg Endosc 2005; 19: Shimizu T, Tajiri T, Yoshida H, Yokomuro S, Mamada Y, Taniai N, Kawano Y, Takahashi T, Arima Y, Aramaki T, Kumazaki T. Hand-assisted laparoscopic hepatectomy after partial splenic embolization. Surg Endosc 2003; 17: Tajiri T, Onda M, Yoshida H, Mamada Y, Taniai N, Kumazaki T. Long-term hematological and biochemical effects of partial splenic embolization in hepatic cirrhosis. Hepatogastroenterology 2002; 49: Masumori K, Onda M, Tajiri T, Kim DY, Toba M, Umehara M, Yoshida H, Mamada Y, Nishikubo H, Taniai N, Kojima T, Matsuzaki S, Yamashita K. Modified endoscopic variceal ligation. Dig Endosc 1995; 7: Umehara M, Onda M, Tajiri T, Toba M, Yoshida H, Yamashita K. Sclerotherapy plus ligation versus ligation for the treatment of esophageal varices: a prospective randomized study. Gastrointest Endosc 1999; 50: Tajiri T, Onda M, Yoshida H, Mamada Y, Taniai N, Umehara M, Toba M, Yamashita K. Endoscopic scleroligation is a superior new technique for preventing recurrence of esophageal varices. J Nippon Med Sch 2002; 69: Yoshida H, Onda M, Tajiri T, Toba M, Umehara M, Mamada Y, Taniai N, Yamashita K. Endoscopic injection sclerotherapy for the treatment of recurrent esophageal varices after esophageal transection. Dig Endosc 2002; 14: Yoshida H, Onda M, Tajiri T, Mamada Y, Taniai N. New techniques: combined endoscopic injection sclerotherapy and ligation for acute bleeding from gastric varices. Hepatogastroenterology 2002; 49: Yoshida H, Mamada Y, Taniai N, Yamamoto K, Kawano Y, Mizuguchi Y, Shimizu T, Takahashi T, Tajiri T. A randomized control trial of bi-monthly versus bi-weekly endoscopic variceal ligation of esophageal varices. Am J Gastroenterol 2005; 100: Sarin SK, Govil A, Jain AK, Guptan RC, Issar SK, Jain M, Murthy NS. Prospective randomized trial of endoscopic sclerotherapy versus variceal band ligation for esophageal varices: influence on gastropathy, gastric varices and variceal recurrence. J Hepatol 1997; 26: Yoshida H, Tajiri T, Mamada Y, Taniai N, Hirakata A, Kawano Y, Mizuguchi Y, Shimizu T, Takahashi T. Comparison of characteristics of recurrent esophageal varices after endoscopic ligation versus endoscopic ligation plus sclerotherapy. Hepatogastroenterology 2004; 51: Schuman BM, Beckman JW, Tedesco FJ, Griffin JW Jr, Assad RT. Complications of endoscopic injection sclerotherapy: a review. Am J Gastroenterol 1987; 82: Obara K, Sakamoto H, Kasukawa R. Prediction of the recurrence of esophageal varices based on portal vein pressure and oxygen tension in portal and peripheral blood. Gastroenterol Jpn 1991; 26: Hou MC, Lin HC, Kuo BI, Chen CH, Lee FY, Lee SD. Comparison of endoscopic variceal injection sclerotherapy and ligation for the treatment of esophageal variceal hemorrhage: a prospective randomized trial. Hepatology 1995; 21: Saeed ZA, Stiegmann GV, Ramirez FC, Reveille RM, Goff JS, Hepps KS, Cole RA. Endoscopic variceal ligation is superior to combined ligation and sclerotherapy for esophageal varices: a multicenter prospective randomized trial. Hepatology 1997; 25: Laine L, Stein C, Sharma V. Randomized comparison of ligation versus ligation plus sclerotherapy in patients with bleeding esophageal varices. Gastroenterology 1996; 110: Lo GH, Lai KH, Cheng JS, Lin CK, Huang JS, Hsu PI, Huang HC, Chiang HT. The additive effect of sclerotherapy to patients receiving repeated endoscopic variceal ligation: a prospective, randomized trial. Hepatology 1998; 28: Takase Y, Shibuya S, Chikamori F, Orii K, Iwasaki Y. Recurrence factors studied by percutaneous transhepatic portography before and after endoscopic sclerotherapy for esophageal varices. Hepatology 1990; 11: S- Editor Zhu LH L- Editor Zhu LH E- Editor Ma WH
Evidence-Base Management of Esophageal and Gastric Varices
 Evidence-Base Management of Esophageal and Gastric Varices Rino Alvani Gani Hepatobiliary Division Department of Internal Medicine Faculty of Medicine Universitas Indonesia Cipto Mangunkusumo National
Evidence-Base Management of Esophageal and Gastric Varices Rino Alvani Gani Hepatobiliary Division Department of Internal Medicine Faculty of Medicine Universitas Indonesia Cipto Mangunkusumo National
Michele Bettinelli RN CCRN Lahey Health and Medical Center
 Michele Bettinelli RN CCRN Lahey Health and Medical Center Differentiate the types of varices Identify glue preparations utilized when treating gastric varices Review the process of glue administration
Michele Bettinelli RN CCRN Lahey Health and Medical Center Differentiate the types of varices Identify glue preparations utilized when treating gastric varices Review the process of glue administration
Surgical Rescue of Surgical Failures
 HPB Surgery, 1999, Vol. 11, pp. 151-155 Reprints available directly from the publisher Photocopying permitted by license only (C) 1999 OPA (Overseas Publishers Association) N.V. Published by license under
HPB Surgery, 1999, Vol. 11, pp. 151-155 Reprints available directly from the publisher Photocopying permitted by license only (C) 1999 OPA (Overseas Publishers Association) N.V. Published by license under
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acute variceal bleeding management of, 251 262 balloon tamponade of esophagus in, 257 258 endoscopic therapies in, 255 257. See also Endoscopy,
Index Note: Page numbers of article titles are in boldface type. A Acute variceal bleeding management of, 251 262 balloon tamponade of esophagus in, 257 258 endoscopic therapies in, 255 257. See also Endoscopy,
Gastroesophageal Variceal Bleeding Successfully Controlled by Partial Splenic Embolization
 CASE REPORT Gastroesophageal Variceal Bleeding Successfully Controlled by Partial Splenic Embolization Takayuki Kogure, Jun Inoue, Eiji Kakazu, Masashi Ninomiya and Tooru Shimosegawa Abstract A 53-year-old
CASE REPORT Gastroesophageal Variceal Bleeding Successfully Controlled by Partial Splenic Embolization Takayuki Kogure, Jun Inoue, Eiji Kakazu, Masashi Ninomiya and Tooru Shimosegawa Abstract A 53-year-old
SUMMARY AND CONCLUSION
 - 100 - SUMMARY AND CONCLUSION The problem of portal hypertension and its alarming complications is still attracting the attentions of surgeons and physicians all over the world. Portal hypertension usually
- 100 - SUMMARY AND CONCLUSION The problem of portal hypertension and its alarming complications is still attracting the attentions of surgeons and physicians all over the world. Portal hypertension usually
Studies on the Results of the Nonshunting Procedures for Portal Hypertension*)
 Hiroshima Journal of Medical Sciences Vol. 32, No. 3, 241,...,246, September, 1983 HIJM 32-38 241 Studies on the Results of the Nonshunting Procedures for Portal Hypertension*) Motomu KODAMA, Tsuneo TAN
Hiroshima Journal of Medical Sciences Vol. 32, No. 3, 241,...,246, September, 1983 HIJM 32-38 241 Studies on the Results of the Nonshunting Procedures for Portal Hypertension*) Motomu KODAMA, Tsuneo TAN
Endoscopic management of esophagogastric varices in Japan
 Review Article Page 1 of 6 Endoscopic management of esophagogastric varices in Japan Hisamitsu Miyaaki, Tatsuki Ichikawa, Naota Taura, Satoshi Miuma, Hajime Isomoto, Kazuhiko Nakao Department of Gastroenterology
Review Article Page 1 of 6 Endoscopic management of esophagogastric varices in Japan Hisamitsu Miyaaki, Tatsuki Ichikawa, Naota Taura, Satoshi Miuma, Hajime Isomoto, Kazuhiko Nakao Department of Gastroenterology
Portogram shows opacification of gastroesophageal varices.
 Portogram shows opacification of gastroesophageal varices. http://clinicalgate.com/radiologic-hepatobiliary-interventions/ courtesyhttp://emedicine.medscape.com/article/372708-overview DR.Thulfiqar Baiae
Portogram shows opacification of gastroesophageal varices. http://clinicalgate.com/radiologic-hepatobiliary-interventions/ courtesyhttp://emedicine.medscape.com/article/372708-overview DR.Thulfiqar Baiae
BRTO: Updates to Techniques
 Session XIV: BRTO, PARTO and Portal Hypertension GEST2016 BRTO: Updates to Techniques Hiro Kiyosue Oita University Hospital, Japan Hiro Kiyosue, MD Royalty: Cook, Medkit Consulting Fee: Stryker Japan,
Session XIV: BRTO, PARTO and Portal Hypertension GEST2016 BRTO: Updates to Techniques Hiro Kiyosue Oita University Hospital, Japan Hiro Kiyosue, MD Royalty: Cook, Medkit Consulting Fee: Stryker Japan,
PORTAL HYPERTENSION. Tianjin Medical University LIU JIAN
 PORTAL HYPERTENSION Tianjin Medical University LIU JIAN DEFINITION Portal hypertension is present if portal venous pressure exceeds 10mmHg (1.3kPa). Normal portal venous pressure is 5 10mmHg (0.7 1.3kPa),
PORTAL HYPERTENSION Tianjin Medical University LIU JIAN DEFINITION Portal hypertension is present if portal venous pressure exceeds 10mmHg (1.3kPa). Normal portal venous pressure is 5 10mmHg (0.7 1.3kPa),
VARICEAL BLEEDING. Ram Subramanian MD Hepatology & Critical Care Medical Director of Liver Transplant Emory University, Atlanta.
 VARICEAL BLEEDING Ram Subramanian MD Hepatology & Critical Care Medical Director of Liver Transplant Emory University, Atlanta Disclosures: None OUTLINE Pathophysiology of portal hypertension Splanchnic
VARICEAL BLEEDING Ram Subramanian MD Hepatology & Critical Care Medical Director of Liver Transplant Emory University, Atlanta Disclosures: None OUTLINE Pathophysiology of portal hypertension Splanchnic
Cyanoacrylate Glue versus Band Ligation for Acute Gastric Variceal Hemorrhage - A randomized controlled trial at Services Hospital, Lahore
 ORIGINAL ARTICLE Cyanoacrylate Glue versus Band Ligation for Acute Gastric Variceal Hemorrhage - A randomized controlled trial at Services Hospital, Lahore ISMAIL HASSAN 1, ASMA SIDDIQUE 2, MUHAMMAD IBRAR
ORIGINAL ARTICLE Cyanoacrylate Glue versus Band Ligation for Acute Gastric Variceal Hemorrhage - A randomized controlled trial at Services Hospital, Lahore ISMAIL HASSAN 1, ASMA SIDDIQUE 2, MUHAMMAD IBRAR
Manejo Actual del Sangrado por Varices Gástricas
 Manejo Actual del Sangrado por Varices Gástricas Juan Carlos Garcia-Pagán Barcelona Hepatic Hemodynamic Laboratory. Liver Unit. IMDIM. Hospital Clinic. IDIBAPS. Ciberehd. XXIV Congreso de la Asociación
Manejo Actual del Sangrado por Varices Gástricas Juan Carlos Garcia-Pagán Barcelona Hepatic Hemodynamic Laboratory. Liver Unit. IMDIM. Hospital Clinic. IDIBAPS. Ciberehd. XXIV Congreso de la Asociación
Practical Approach to Endoscopic Management for Bleeding Gastric Varices
 Review Article http://dx.doi.org/10.3348/kjr.2012.13.s1.s40 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2012;13(S1):S40-S44 Practical Approach to Endoscopic Management for Bleeding Gastric Varices
Review Article http://dx.doi.org/10.3348/kjr.2012.13.s1.s40 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2012;13(S1):S40-S44 Practical Approach to Endoscopic Management for Bleeding Gastric Varices
Ruptured duodenal varices arising from the main portal vein successfully treated with endoscopic injection sclerotherapy: a case report
 The Korean Journal of Hepatology 2011;17:152-156 DOI: 10.3350/kjhep.2011.17.2.152 Case Report Ruptured duodenal varices arising from the main portal vein successfully treated with endoscopic injection
The Korean Journal of Hepatology 2011;17:152-156 DOI: 10.3350/kjhep.2011.17.2.152 Case Report Ruptured duodenal varices arising from the main portal vein successfully treated with endoscopic injection
Role of paraoesophageal collaterals and perforating veins on outcome of endoscopic sclerotherapy for oesophageal varices: an endosonographic study
 Gut 1996; 38: 759-764 Role of paraoesophageal collaterals and perforating veins on outcome of endoscopic sclerotherapy for oesophageal varices: an endosonographic study 759 R K Dhiman, G Choudhuri, V A
Gut 1996; 38: 759-764 Role of paraoesophageal collaterals and perforating veins on outcome of endoscopic sclerotherapy for oesophageal varices: an endosonographic study 759 R K Dhiman, G Choudhuri, V A
BY DEVASCULARIZATION AND PROXIMAL
 HPB Surgery, 1994, Vol. 7, pp. 201-209 Reprints available directly from the publisher Photocopying permitted by license only (C) 1994 Harwood Academic Publishers GmbH Printed in the United States of America
HPB Surgery, 1994, Vol. 7, pp. 201-209 Reprints available directly from the publisher Photocopying permitted by license only (C) 1994 Harwood Academic Publishers GmbH Printed in the United States of America
Esophageal Varices Beta-Blockers or Band Ligation. Cesar Yaghi MD Hotel-Dieu de France University Hospital Universite Saint Joseph
 Esophageal Varices Beta-Blockers or Band Ligation Cesar Yaghi MD Hotel-Dieu de France University Hospital Universite Saint Joseph Esophageal Varices Beta-Blockers or Band Ligation? Risk of esophageal variceal
Esophageal Varices Beta-Blockers or Band Ligation Cesar Yaghi MD Hotel-Dieu de France University Hospital Universite Saint Joseph Esophageal Varices Beta-Blockers or Band Ligation? Risk of esophageal variceal
Table 1 Cases studied
 Fig. 1 Intra-operative measurements using the ultrasonic Doppler duplex sys temin a patient with idiopathic portal hypertension. The shunt blood flow was measured at the splenic hilus just after the shunt
Fig. 1 Intra-operative measurements using the ultrasonic Doppler duplex sys temin a patient with idiopathic portal hypertension. The shunt blood flow was measured at the splenic hilus just after the shunt
carcinoma at a single Japanese Inst Citation Hepato-Gastroenterology, 56(91-92),
 NAOSITE: Nagasaki University's Ac Title Author(s) Treatment of concomitant gastric va carcinoma at a single Japanese Inst Nanashima, Atsushi; Sumida, Yorihis Kenichirou; Tomoshige, Kouichi; Tak Fukuoka,
NAOSITE: Nagasaki University's Ac Title Author(s) Treatment of concomitant gastric va carcinoma at a single Japanese Inst Nanashima, Atsushi; Sumida, Yorihis Kenichirou; Tomoshige, Kouichi; Tak Fukuoka,
Endoscopic treatment of gastroesophageal varices in young infants with cyanoacrylate glue: a pilot study
 ORIGINAL ARTICLE Endoscopic treatment of gastroesophageal varices in young infants with cyanoacrylate glue: a pilot study Christine Rivet, MD, Carlos Robles-Medranda, MD, Jérôme Dumortier, MD, PhD, Catherine
ORIGINAL ARTICLE Endoscopic treatment of gastroesophageal varices in young infants with cyanoacrylate glue: a pilot study Christine Rivet, MD, Carlos Robles-Medranda, MD, Jérôme Dumortier, MD, PhD, Catherine
Primary Prophylaxis against Variceal Hemorrhage Pharmacotherapy vs Endoscopic Band Ligation
 Primary Prophylaxis against Variceal Hemorrhage Pharmacotherapy vs Endoscopic Band Ligation Siwaporn Chainuvati, MD Faculty of Medicine Siriraj Hospital Outline Natural history of esophageal varices Which
Primary Prophylaxis against Variceal Hemorrhage Pharmacotherapy vs Endoscopic Band Ligation Siwaporn Chainuvati, MD Faculty of Medicine Siriraj Hospital Outline Natural history of esophageal varices Which
ACG & AASLD Joint Clinical Guideline: Prevention and Management of Gastroesophageal Varices and Variceal Hemorrhage in Cirrhosis
 ACG & AASLD Joint Clinical Guideline: Prevention and Management of Gastroesophageal Varices and Variceal Hemorrhage in Cirrhosis Guadalupe Garcia-Tsao, M.D., 1 Arun J. Sanyal, M.D., 2 Norman D. Grace,
ACG & AASLD Joint Clinical Guideline: Prevention and Management of Gastroesophageal Varices and Variceal Hemorrhage in Cirrhosis Guadalupe Garcia-Tsao, M.D., 1 Arun J. Sanyal, M.D., 2 Norman D. Grace,
Endoscopic sclerotherapy: A risk factor for splanchnic venous thrombosis
 Endoscopic sclerotherapy: A risk factor for splanchnic venous thrombosis Steven D. Leach, MD, George H. Meier, MD, and Richard J. Gusberg, MD, New Haven, Conn. Endoscopic sclerotherapy has been widely
Endoscopic sclerotherapy: A risk factor for splanchnic venous thrombosis Steven D. Leach, MD, George H. Meier, MD, and Richard J. Gusberg, MD, New Haven, Conn. Endoscopic sclerotherapy has been widely
Endoscopic Management of Vascular Lesions of the GI tract
 Endoscopic Management of Vascular Lesions of the GI tract Lake Louise, June 2014 Sergio Zepeda Gómez MD Assistant Professor Division of Gastroenterology University of Alberta, Edmonton Best Practice &
Endoscopic Management of Vascular Lesions of the GI tract Lake Louise, June 2014 Sergio Zepeda Gómez MD Assistant Professor Division of Gastroenterology University of Alberta, Edmonton Best Practice &
Variceal bleeding. Mainz,
 Variceal bleeding Mainz, 21.09.2008 Risk of complications 5 years 10 years Ascites 10 % 25 % HCC 10 % 25 % Bleeding < 5 % 5-10 % Enceph. < 5 % < 5 % Typical situation : Mortality 10 % to 40 % Sequence
Variceal bleeding Mainz, 21.09.2008 Risk of complications 5 years 10 years Ascites 10 % 25 % HCC 10 % 25 % Bleeding < 5 % 5-10 % Enceph. < 5 % < 5 % Typical situation : Mortality 10 % to 40 % Sequence
Review Article Role of Self-Expandable Metal Stents in Acute Variceal Bleeding
 Hindawi Publishing Corporation International Journal of Hepatology Volume 2012, Article ID 418369, 6 pages doi:10.1155/2012/418369 Review Article Role of Self-Expandable Metal Stents in Acute Variceal
Hindawi Publishing Corporation International Journal of Hepatology Volume 2012, Article ID 418369, 6 pages doi:10.1155/2012/418369 Review Article Role of Self-Expandable Metal Stents in Acute Variceal
THE WARREN SHUNT: EFFECT OF ALCOHOLISM ON PORTAL PERFUSION. Gastroenterology; 100, Irving Street, NW Washington DC
 70 HPB INTERNATIONAL 11. Niederhuber, J.E. (1985) Arterial chemotherapy for metastatic colorectal cancer in the liver. Conference Advantages in Regional Cancer Therapy. Giessen, West Germany 12. Weiss,
70 HPB INTERNATIONAL 11. Niederhuber, J.E. (1985) Arterial chemotherapy for metastatic colorectal cancer in the liver. Conference Advantages in Regional Cancer Therapy. Giessen, West Germany 12. Weiss,
Research Article Validation of an Endoscopic Fibre-Optic Pressure Sensor for Noninvasive Measurement of Variceal Pressure
 Hindawi Publishing Corporation BioMed Research International Volume 2016, Article ID 1893474, 7 pages http://dx.doi.org/10.1155/2016/1893474 Research Article Validation of an Endoscopic Fibre-Optic Pressure
Hindawi Publishing Corporation BioMed Research International Volume 2016, Article ID 1893474, 7 pages http://dx.doi.org/10.1155/2016/1893474 Research Article Validation of an Endoscopic Fibre-Optic Pressure
Endoscopic Resection of a Rectal. Carcinoid Tumor with an Esophageal. Variceal Ligation Device. Report of a Case and Literature Review
 2006 7 28-32 Endoscopic Resection of a Rectal Carcinoid Tumor with an Esophageal Variceal Ligation Device Report of a Case and Literature Review Wei-Feng Feng, An-Liang Chou, Jen-En Tzeng, and Kuo-Chih
2006 7 28-32 Endoscopic Resection of a Rectal Carcinoid Tumor with an Esophageal Variceal Ligation Device Report of a Case and Literature Review Wei-Feng Feng, An-Liang Chou, Jen-En Tzeng, and Kuo-Chih
NYU School of Medicine Department of Radiology Rotation-Specific House Staff Evaluation
 Vascular & Interventional Radiology Rotation 1 Core competency in vascular and interventional radiology during the first resident rotation consists of clinical objectives, technical objectives and image
Vascular & Interventional Radiology Rotation 1 Core competency in vascular and interventional radiology during the first resident rotation consists of clinical objectives, technical objectives and image
بسم الله الرحمن الرحيم أوتيتم من العلم إال قليال وما
 بسم الله الرحمن الرحيم أوتيتم من العلم إال قليال وما 1 2 Goals of the Lecture: What is the portal vein? How common is PVT? What conditions are associated with PVT? How does patient with PVT present? How
بسم الله الرحمن الرحيم أوتيتم من العلم إال قليال وما 1 2 Goals of the Lecture: What is the portal vein? How common is PVT? What conditions are associated with PVT? How does patient with PVT present? How
Virtual Mentor American Medical Association Journal of Ethics December 2008, Volume 10, Number 12:
 Virtual Mentor American Medical Association Journal of Ethics December 2008, Volume 10, Number 12: 805-809. CLINICAL PEARL Indications for Use of TIPS in Treating Portal Hypertension Elizabeth C. Verna,
Virtual Mentor American Medical Association Journal of Ethics December 2008, Volume 10, Number 12: 805-809. CLINICAL PEARL Indications for Use of TIPS in Treating Portal Hypertension Elizabeth C. Verna,
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A ACLF. See Acute-on-chronic liver failure (ACLF) Acute kidney injury (AKI) in ACLF patients, 967 Acute liver failure (ALF), 957 964 causes
Index Note: Page numbers of article titles are in boldface type. A ACLF. See Acute-on-chronic liver failure (ACLF) Acute kidney injury (AKI) in ACLF patients, 967 Acute liver failure (ALF), 957 964 causes
Useful Endoscopic Ultrasonography Parameters and a Predictive Model for the Recurrence of Esophageal Varices and Bleeding after Variceal Ligation
 Gut and Liver, Vol. 11, No. 6, November 2017, pp. 843-851 ORiginal Article Useful Endoscopic Ultrasonography Parameters and a Predictive Model for the Recurrence of Esophageal Varices and Bleeding after
Gut and Liver, Vol. 11, No. 6, November 2017, pp. 843-851 ORiginal Article Useful Endoscopic Ultrasonography Parameters and a Predictive Model for the Recurrence of Esophageal Varices and Bleeding after
Current status of hepatic surgery in Korea
 Korean J Hepatol. 2009 Dec; 15(Suppl 6):S60 - S64. DOI: 10.3350/kjhep.2009.15.S6.S60 Current status of hepatic surgery in Korea Kyung Sik Kim Department of Surgery, Severance Hospital, Yonsei University
Korean J Hepatol. 2009 Dec; 15(Suppl 6):S60 - S64. DOI: 10.3350/kjhep.2009.15.S6.S60 Current status of hepatic surgery in Korea Kyung Sik Kim Department of Surgery, Severance Hospital, Yonsei University
Clinical application of kelp micro gelation (KMG) in partial splenic embolization
 European Review for Medical and Pharmacological Sciences 2018; 22: 1776-1781 Clinical application of kelp micro gelation (KMG) in partial splenic embolization D.-J. HUANG 1,2, J.-Z. HUANG 3, Y. YANG 2,
European Review for Medical and Pharmacological Sciences 2018; 22: 1776-1781 Clinical application of kelp micro gelation (KMG) in partial splenic embolization D.-J. HUANG 1,2, J.-Z. HUANG 3, Y. YANG 2,
Left-sided portal hypertension with a patent splenic vein: An impossible or a not-so-uncommon scenario?
 Khan et al. 108 CASE REPORT PEER REVIEWED OPEN ACCESS Left-sided portal hypertension with a patent splenic vein: An impossible or a not-so-uncommon scenario? Iftikhar Khan, Ghassan Ramahi, Saif Zaabi,
Khan et al. 108 CASE REPORT PEER REVIEWED OPEN ACCESS Left-sided portal hypertension with a patent splenic vein: An impossible or a not-so-uncommon scenario? Iftikhar Khan, Ghassan Ramahi, Saif Zaabi,
On-Call Upper GI Bleeding. Upper Gastrointestinal Bleeding
 On-Call Upper GI Bleeding John R Saltzman MD, FACG Director of Endoscopy Brigham and Women s Hospital Associate Professor of Medicine Harvard Medical School Upper Gastrointestinal Bleeding 300,000000 hospitalizations/year
On-Call Upper GI Bleeding John R Saltzman MD, FACG Director of Endoscopy Brigham and Women s Hospital Associate Professor of Medicine Harvard Medical School Upper Gastrointestinal Bleeding 300,000000 hospitalizations/year
Tranjugular Intrahepatic Portosystemic Shunt
 Tranjugular Intrahepatic Portosystemic Shunt Christopher Selhorst July 25, 2005 BIDMC Radiology Overview Portal Hypertension Indications, Contraindications The Procedure Case Review Complications Outcomes
Tranjugular Intrahepatic Portosystemic Shunt Christopher Selhorst July 25, 2005 BIDMC Radiology Overview Portal Hypertension Indications, Contraindications The Procedure Case Review Complications Outcomes
Carvedilol or Propranolol in the Management of Portal Hypertension?
 Evidence Based Case Report Carvedilol or Propranolol in the Management of Portal Hypertension? Arranged by: dr. Saskia Aziza Nursyirwan RESIDENCY PROGRAM OF INTERNAL MEDICINE DEPARTMENT UNIVERSITY OF INDONESIA
Evidence Based Case Report Carvedilol or Propranolol in the Management of Portal Hypertension? Arranged by: dr. Saskia Aziza Nursyirwan RESIDENCY PROGRAM OF INTERNAL MEDICINE DEPARTMENT UNIVERSITY OF INDONESIA
Patient guide: pfm Nit-Occlud PDA coil occlusion system. Catheter occlusion of. Patent Ductus Arteriosus. with the
 Patient guide: Catheter occlusion of Patent Ductus Arteriosus with the pfm Nit-Occlud PDA coil occlusion system pfm Produkte für die Medizin - AG Wankelstr. 60 D - 50996 Cologne Phone: +49 (0) 2236 96
Patient guide: Catheter occlusion of Patent Ductus Arteriosus with the pfm Nit-Occlud PDA coil occlusion system pfm Produkte für die Medizin - AG Wankelstr. 60 D - 50996 Cologne Phone: +49 (0) 2236 96
A Prospective, Randomized Trial of Butyl Cyanoacrylate Injection Versus Band Ligation in the Management of Bleeding Gastric Varices
 A Prospective, Randomized Trial of Butyl Cyanoacrylate Injection Versus Band Ligation in the Management of Bleeding Gastric Varices GIN-HO LO, KWOK-HUNG LAI, JIN-SHIUNG CHENG, MEI-HSIU CHEN, AND HUNG-TING
A Prospective, Randomized Trial of Butyl Cyanoacrylate Injection Versus Band Ligation in the Management of Bleeding Gastric Varices GIN-HO LO, KWOK-HUNG LAI, JIN-SHIUNG CHENG, MEI-HSIU CHEN, AND HUNG-TING
Upper gastrointestinal bleeding in children. Nguyễn Diệu Vinh, MD Department of Gastroenterology
 Upper gastrointestinal bleeding in children Nguyễn Diệu Vinh, MD Department of Gastroenterology INTRODUCTION Upper gastrointestinal (UGI) bleeding : arising proximal to the ligament of Treitz in the distal
Upper gastrointestinal bleeding in children Nguyễn Diệu Vinh, MD Department of Gastroenterology INTRODUCTION Upper gastrointestinal (UGI) bleeding : arising proximal to the ligament of Treitz in the distal
BRTO /PARTO Indications and outcomes
 BRTO /PARTO Indications and outcomes Saher Sabri, MD Associate Professor of Radiology and Surgery Division of Interventional Radiology University of Virginia Health System Saher Sabri, M.D. Speakers Bureau:
BRTO /PARTO Indications and outcomes Saher Sabri, MD Associate Professor of Radiology and Surgery Division of Interventional Radiology University of Virginia Health System Saher Sabri, M.D. Speakers Bureau:
EUS-guided thrombin injection for management of gastric fundal varices
 EUS-guided thrombin injection for management of gastric fundal varices Authors John W. Frost, Srisha Hebbar Institution Royal Stoke University Hospital Gastroenterology, Stokeon-Trent, United Kingdom of
EUS-guided thrombin injection for management of gastric fundal varices Authors John W. Frost, Srisha Hebbar Institution Royal Stoke University Hospital Gastroenterology, Stokeon-Trent, United Kingdom of
Variceal bleeding is a major cause of morbidity in patients
 GASTROENTEROLOGY 2010;139:1238 1245 Equal Efficacy of Endoscopic Variceal Ligation and Propranolol in Preventing Variceal Bleeding in Patients With Noncirrhotic Portal Hypertension SHIV KUMAR SARIN,*,,
GASTROENTEROLOGY 2010;139:1238 1245 Equal Efficacy of Endoscopic Variceal Ligation and Propranolol in Preventing Variceal Bleeding in Patients With Noncirrhotic Portal Hypertension SHIV KUMAR SARIN,*,,
Transjugular Intrahepatic Portosystemic Shunt Reduction for Management of Recurrent Hepatic Encephalopathy
 CLINICAL IMAGES Ochsner Journal 17:311 316, 2017 Ó Academic Division of Ochsner Clinic Foundation Transjugular Intrahepatic Portosystemic Shunt Reduction for Management of Recurrent Hepatic Encephalopathy
CLINICAL IMAGES Ochsner Journal 17:311 316, 2017 Ó Academic Division of Ochsner Clinic Foundation Transjugular Intrahepatic Portosystemic Shunt Reduction for Management of Recurrent Hepatic Encephalopathy
Cholangiocarcinoma (Bile Duct Cancer)
 Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Clinical Study EUS-Assisted Evaluation of Rectal Varices before Banding
 Gastroenterology Research and Practice Volume 2013, Article ID 619187, 7 pages http://dx.doi.org/10.1155/2013/619187 Clinical Study EUS-Assisted Evaluation of Rectal Varices before Banding Malay Sharma,
Gastroenterology Research and Practice Volume 2013, Article ID 619187, 7 pages http://dx.doi.org/10.1155/2013/619187 Clinical Study EUS-Assisted Evaluation of Rectal Varices before Banding Malay Sharma,
V ariceal haemorrhage is a major cause of mortality and
 270 LIVER DISEASE The role of the transjugular intrahepatic portosystemic stent shunt (TIPSS) in the management of bleeding gastric : clinical and haemodynamic correlations D Tripathi, G Therapondos, E
270 LIVER DISEASE The role of the transjugular intrahepatic portosystemic stent shunt (TIPSS) in the management of bleeding gastric : clinical and haemodynamic correlations D Tripathi, G Therapondos, E
Image Analysis of Magnifying Endoscopy for Differentiation between Early Gastric Cancers and Gastric Erosions
 Showa Univ J Med Sci 29 3, 297 306, September 2017 Original Image Analysis of Magnifying Endoscopy for Differentiation between Early Gastric Cancers and Gastric Erosions Shotaro HANAMURA, Kuniyo GOMI,
Showa Univ J Med Sci 29 3, 297 306, September 2017 Original Image Analysis of Magnifying Endoscopy for Differentiation between Early Gastric Cancers and Gastric Erosions Shotaro HANAMURA, Kuniyo GOMI,
urhealth March 2018 Nu Mu Lambda...
 March 2018 1 Health & Wellness Committee Bro. Trenton Taylor Committee Chair Bro. William J. Bennett, M.D., Ph.D. Medical Editor Contents Portal Hypertension 3 12 Renal Artery Stenosis 13-16 Holiday Depression
March 2018 1 Health & Wellness Committee Bro. Trenton Taylor Committee Chair Bro. William J. Bennett, M.D., Ph.D. Medical Editor Contents Portal Hypertension 3 12 Renal Artery Stenosis 13-16 Holiday Depression
Long-Term Hemodynamic Effects of Portocaval
 HPB Surgery, 1996, Vol.9, pp.209-213 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V. Published in The
HPB Surgery, 1996, Vol.9, pp.209-213 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V. Published in The
Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus
 Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus Br J Surg 38 oct. 1950 Definition of Barrett's esophagus A change in the esophageal epithelium of any length that can be recognized
Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus Br J Surg 38 oct. 1950 Definition of Barrett's esophagus A change in the esophageal epithelium of any length that can be recognized
Perforated peptic ulcer
 Perforated peptic ulcer - Despite the widespread use of gastric anti-secretory agents and eradication therapy, the incidence of perforated peptic ulcer has changed little, age limits increase NSAIDs elderly
Perforated peptic ulcer - Despite the widespread use of gastric anti-secretory agents and eradication therapy, the incidence of perforated peptic ulcer has changed little, age limits increase NSAIDs elderly
LIVER CIRRHOSIS. The liver extracts nutrients from the blood and processes them for later use.
 LIVER CIRRHOSIS William Sanchez, M.D. & Jayant A. Talwalkar, M.D., M.P.H. Advanced Liver Disease Study Group Miles and Shirley Fiterman Center for Digestive Diseases Mayo College of Medicine Rochester,
LIVER CIRRHOSIS William Sanchez, M.D. & Jayant A. Talwalkar, M.D., M.P.H. Advanced Liver Disease Study Group Miles and Shirley Fiterman Center for Digestive Diseases Mayo College of Medicine Rochester,
SAM PROVIDER TOOLKIT
 THE AMERICAN BOARD OF PATHOLOGY Maintenance of Certification (MOC) Program SAM PROVIDER TOOLKIT Developing Self-Assessment Modules (SAMs) www.abpath.org The American Board of Pathology (ABP) approves educational
THE AMERICAN BOARD OF PATHOLOGY Maintenance of Certification (MOC) Program SAM PROVIDER TOOLKIT Developing Self-Assessment Modules (SAMs) www.abpath.org The American Board of Pathology (ABP) approves educational
Hepatocellular Carcinoma: Diagnosis and Management
 Hepatocellular Carcinoma: Diagnosis and Management Nizar A. Mukhtar, MD Co-director, SMC Liver Tumor Board April 30, 2016 1 Objectives Review screening/surveillance guidelines Discuss diagnostic algorithm
Hepatocellular Carcinoma: Diagnosis and Management Nizar A. Mukhtar, MD Co-director, SMC Liver Tumor Board April 30, 2016 1 Objectives Review screening/surveillance guidelines Discuss diagnostic algorithm
Diagnosis of tumor extension in biliary carcinoma has. Differential Diagnosis and Treatment of Biliary Strictures
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
Patrick S. Kamath, MD, and David M. Nagorney, MD
 gastrointestinal tract and abdomen PORTAL HYPERTENSION Patrick S. Kamath, MD, and David M. Nagorney, MD Portal hypertension is diagnosed when the hepatic veinpressure gradient (HVPG), which reflects hepatic
gastrointestinal tract and abdomen PORTAL HYPERTENSION Patrick S. Kamath, MD, and David M. Nagorney, MD Portal hypertension is diagnosed when the hepatic veinpressure gradient (HVPG), which reflects hepatic
COPYRIGHTED MATERIAL. 1 Approach to the patient with gross gastrointestinal bleeding. Grace H. Elta, Mimi Takami
 1 Approach to the patient with gross gastrointestinal bleeding Grace H. Elta, Mimi Takami Gastrointestinal (GI) bleeding is a common clinical problem that requires more than 300 000 hospitalizations annually
1 Approach to the patient with gross gastrointestinal bleeding Grace H. Elta, Mimi Takami Gastrointestinal (GI) bleeding is a common clinical problem that requires more than 300 000 hospitalizations annually
Balloon-Occluded Retrograde Transvenous Obliteration of Gastric Fundal Varices with Hemorrhage
 Mikiya Kitamoto 1,2 Michio Imamura 1 Koji Kamada 1 Hiroshi Aikata 1 Yoshiiku Kawakami 1 Akiko Matsumoto 1 Yoshika Kurihara 1 Hirotaka Kono 1 Hiroo Shirakawa 1 Toshio Nakanishi 1,3 Katsuhide Ito 4 Kazuaki
Mikiya Kitamoto 1,2 Michio Imamura 1 Koji Kamada 1 Hiroshi Aikata 1 Yoshiiku Kawakami 1 Akiko Matsumoto 1 Yoshika Kurihara 1 Hirotaka Kono 1 Hiroo Shirakawa 1 Toshio Nakanishi 1,3 Katsuhide Ito 4 Kazuaki
Perforation of a Duodenal Ulcer into a Non-Parasitic Liver Cyst: A Rare Case of a Penetrate Hole Blockaded with Conservative Medical Management
 CASE REPORT Perforation of a Duodenal Ulcer into a Non-Parasitic Liver Cyst: A Rare Case of a Penetrate Hole Blockaded with Conservative Medical Management Koichi Ono 1, Masaharu Takeda 1, Eiichi Makihata
CASE REPORT Perforation of a Duodenal Ulcer into a Non-Parasitic Liver Cyst: A Rare Case of a Penetrate Hole Blockaded with Conservative Medical Management Koichi Ono 1, Masaharu Takeda 1, Eiichi Makihata
Imaging in gastric cancer
 Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Information Technology Solutions
 2016 2014 CPT Esophagoscopy Changes - Gastroenterology CPT Changes Information Technology Solutions ASGE LOGO AND INFO Esophagogastroduodenoscopy CPT Codes 43235-43270 The American Society for Gastrointestinal
2016 2014 CPT Esophagoscopy Changes - Gastroenterology CPT Changes Information Technology Solutions ASGE LOGO AND INFO Esophagogastroduodenoscopy CPT Codes 43235-43270 The American Society for Gastrointestinal
Splenic artery ligature associated with endoscopic banding for schistosomal portal hypertension
 Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.3748/wjg.v20.i44.16734 World J Gastroenterol 2014 November 28; 20(44): 16734-16738 ISSN 1007-9327
Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.3748/wjg.v20.i44.16734 World J Gastroenterol 2014 November 28; 20(44): 16734-16738 ISSN 1007-9327
HIV. KEY WORDS: HIV, esophageal varices, endoscopic injection sclerotherapy (EIS), endoscopic variceal ligation (EVL)
 2013; 19: 25 32 HIV 1, 2 1 1 1 1 HIV 7 3 HCV, 2 HBV B C 2 HCC 2 F 2 RC 1 2.1 F 1 RC 0 30.4 4 HCV 9 HCC 13.5 3 HCC 1 1 AIDS B C HIV HIV HCV HIV KEY WORDS: HIV, esophageal varices, endoscopic injection sclerotherapy
2013; 19: 25 32 HIV 1, 2 1 1 1 1 HIV 7 3 HCV, 2 HBV B C 2 HCC 2 F 2 RC 1 2.1 F 1 RC 0 30.4 4 HCV 9 HCC 13.5 3 HCC 1 1 AIDS B C HIV HIV HCV HIV KEY WORDS: HIV, esophageal varices, endoscopic injection sclerotherapy
GI bleeding in chronic liver disease
 GI bleeding in chronic liver disease Stuart McPherson Consultant Hepatologist Liver Unit, Freeman Hospital, Newcastle upon Tyne and Institute of Cellular Medicine, Newcastle University. Case 54 year old
GI bleeding in chronic liver disease Stuart McPherson Consultant Hepatologist Liver Unit, Freeman Hospital, Newcastle upon Tyne and Institute of Cellular Medicine, Newcastle University. Case 54 year old
Update in abdominal Surgery in cirrhotic patients
 Update in abdominal Surgery in cirrhotic patients Safi Dokmak HBP department and liver transplantation Beaujon Hospital, Clichy, France Cairo, 5 April 2016 Cirrhosis Prevalence in France (1%)* Patients
Update in abdominal Surgery in cirrhotic patients Safi Dokmak HBP department and liver transplantation Beaujon Hospital, Clichy, France Cairo, 5 April 2016 Cirrhosis Prevalence in France (1%)* Patients
Percutaneous transsplenic catheterization of the portal venous system
 Acta Radiologica ISSN: 0284-1851 (Print) 1600-0455 (Online) Journal homepage: https://www.tandfonline.com/loi/iard20 Percutaneous transsplenic catheterization of the portal veus system H.-L. Liang, C.-F.
Acta Radiologica ISSN: 0284-1851 (Print) 1600-0455 (Online) Journal homepage: https://www.tandfonline.com/loi/iard20 Percutaneous transsplenic catheterization of the portal veus system H.-L. Liang, C.-F.
Clinical Study Transjugular Intrahepatic Portosystemic Shunt for the Treatment of Portal Hypertension in Noncirrhotic Patients with Portal Cavernoma
 Gastroenterology Research and Practice, Article ID 659726, 8 pages http://dx.doi.org/10.1155/2014/659726 Clinical Study Transjugular Intrahepatic Portosystemic Shunt for the Treatment of Portal Hypertension
Gastroenterology Research and Practice, Article ID 659726, 8 pages http://dx.doi.org/10.1155/2014/659726 Clinical Study Transjugular Intrahepatic Portosystemic Shunt for the Treatment of Portal Hypertension
The Role of Endoscopy in the Diagnosis and Management of Upper Gastrointestinal Bleeding.
 Original Article ISSN (O):2395-2822; ISSN (P):2395-2814 The Role of Endoscopy in the Diagnosis and Management of Upper Gastrointestinal Bleeding. Faroze A. Khan 1, M. H. Raza 2, Vikrant 1 1 Senior Resident,
Original Article ISSN (O):2395-2822; ISSN (P):2395-2814 The Role of Endoscopy in the Diagnosis and Management of Upper Gastrointestinal Bleeding. Faroze A. Khan 1, M. H. Raza 2, Vikrant 1 1 Senior Resident,
Sclerosing Agents: Tips & Tricks Session: Liquid Embolics
 Sclerosing Agents: Tips & Tricks Session: Liquid Embolics Jeffrey S. Pollak, M.D. Robert I. White, Jr., M.D. Professor of Interventional Radiology Yale University School of Medicine Department of Radiology
Sclerosing Agents: Tips & Tricks Session: Liquid Embolics Jeffrey S. Pollak, M.D. Robert I. White, Jr., M.D. Professor of Interventional Radiology Yale University School of Medicine Department of Radiology
Sandipan Ghose, Md. Azizul Hoque, Md. Khalilur Rahman, Mohd. Harun-or-Rashid
 Sandipan Ghose, Md. Azizul Hoque, Md. Khalilur Rahman, Mohd. Harun-or-Rashid Liver cirrhosis may be defined as a diffuse process characterized by fibrosis and conversion of normal liver architecture into
Sandipan Ghose, Md. Azizul Hoque, Md. Khalilur Rahman, Mohd. Harun-or-Rashid Liver cirrhosis may be defined as a diffuse process characterized by fibrosis and conversion of normal liver architecture into
4/24/2015. History of Reflux Surgery. Recent Innovations in the Surgical Treatment of Reflux
 Recent Innovations in the Surgical Treatment of Reflux Scott Carpenter, DO, FACOS, FACS Mercy Hospital Ardmore Ardmore, OK History of Reflux Surgery - 18 th century- first use of term heartburn - 1934-
Recent Innovations in the Surgical Treatment of Reflux Scott Carpenter, DO, FACOS, FACS Mercy Hospital Ardmore Ardmore, OK History of Reflux Surgery - 18 th century- first use of term heartburn - 1934-
Barbara Rus Gadžijev Peter Popovič Klinični inštitut za radiologijo UKC Ljubljana
 STROKOVNI SESTANEK ZDRUŽENJA HEMATOLOGOV SLOVENIJE IN ZDRUŽENJA ZA TRANSFUZIJSKO MEDICINO, Terme Zreče, 17.-18.4.2015 Barbara Rus Gadžijev Peter Popovič Klinični inštitut za radiologijo UKC Ljubljana goals,
STROKOVNI SESTANEK ZDRUŽENJA HEMATOLOGOV SLOVENIJE IN ZDRUŽENJA ZA TRANSFUZIJSKO MEDICINO, Terme Zreče, 17.-18.4.2015 Barbara Rus Gadžijev Peter Popovič Klinični inštitut za radiologijo UKC Ljubljana goals,
Gastric fundal varices with hemorrhage are
 alloon-occluded Retrograde Transvenous Obliteration of Gastric Varices review of the anatomy, technique, and outcomes. Y SHER S. SRI, MD; ULKU C. TUR, MD; WEL E.. SD, MD; UH WHN PRK, MD; ND JOHN F. NGLE,
alloon-occluded Retrograde Transvenous Obliteration of Gastric Varices review of the anatomy, technique, and outcomes. Y SHER S. SRI, MD; ULKU C. TUR, MD; WEL E.. SD, MD; UH WHN PRK, MD; ND JOHN F. NGLE,
Non-exposed endoscopic wall-inversion surgery for gastrointestinal stromal tumor
 Technical Note Non-exposed endoscopic wall-inversion surgery for gastrointestinal stromal tumor Takashi Mitsui 1, Hiroharu Yamashita 1, Susumu Aikou 1, Keiko Niimi 2, Mitsuhiro Fujishiro 2, Yasuyuki Seto
Technical Note Non-exposed endoscopic wall-inversion surgery for gastrointestinal stromal tumor Takashi Mitsui 1, Hiroharu Yamashita 1, Susumu Aikou 1, Keiko Niimi 2, Mitsuhiro Fujishiro 2, Yasuyuki Seto
Visceral aneurysm. Diagnosis and Interventions M.NEDEVSKA
 Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
pitfall Table 1 4 disorientation pitfall pitfall Table 1 Tel:
 11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
Esophageal seeding after endoscopic ultrasound-guided fine-needle aspiration of a mediastinal tumor
 Esophageal seeding after endoscopic ultrasound-guided fine-needle aspiration of a mediastinal tumor Authors Kensuke Yokoyama 1,JunUshio 1,NorikatsuNumao 1, Kiichi Tamada 1, Noriyoshi Fukushima 2, Alan
Esophageal seeding after endoscopic ultrasound-guided fine-needle aspiration of a mediastinal tumor Authors Kensuke Yokoyama 1,JunUshio 1,NorikatsuNumao 1, Kiichi Tamada 1, Noriyoshi Fukushima 2, Alan
CCTC Minnesota Procedure: Minnesota Tube, Assisting with Insertion and Care of Patient
 CCTC Minnesota Procedure: Minnesota Tube, Assisting with Insertion and Care of Patient Purpose: To control bleeding from esophageal or gastric varices that have not responded to medical therapy (ie. Sclerotherapy,
CCTC Minnesota Procedure: Minnesota Tube, Assisting with Insertion and Care of Patient Purpose: To control bleeding from esophageal or gastric varices that have not responded to medical therapy (ie. Sclerotherapy,
REPEATED INTRANODAL LYMPHANGIOGRAPHY FOR THE TREATMENT OF LYMPHATIC LEAKAGE
 59 Lymphology 48 (2015) 59-63 REPEATED INTRANODAL LYMPHANGIOGRAPHY FOR THE TREATMENT OF LYMPHATIC LEAKAGE S. Kariya, M. Nakatani, R. Yoshida, Y. Ueno, A. Komemushi, N. Tanigawa Department of Radiology,
59 Lymphology 48 (2015) 59-63 REPEATED INTRANODAL LYMPHANGIOGRAPHY FOR THE TREATMENT OF LYMPHATIC LEAKAGE S. Kariya, M. Nakatani, R. Yoshida, Y. Ueno, A. Komemushi, N. Tanigawa Department of Radiology,
Tools of the Gastroenterologist: Introduction to GI Endoscopy
 Tools of the Gastroenterologist: Introduction to GI Endoscopy Objectives Endoscopy Upper endoscopy Colonoscopy Endoscopic retrograde cholangiopancreatography (ERCP) Endoscopic ultrasound (EUS) Endoscopic
Tools of the Gastroenterologist: Introduction to GI Endoscopy Objectives Endoscopy Upper endoscopy Colonoscopy Endoscopic retrograde cholangiopancreatography (ERCP) Endoscopic ultrasound (EUS) Endoscopic
gastric varices, gastrorenal shunt, endoscopic sclerotherapy, Hassab's operation Key words: 1 cases 6 cases 5 cases
 Key words: gastric varices, gastrorenal shunt, endoscopic sclerotherapy, Hassab's operation 1 cases 6 cases 5 cases LC: Liver cirrhosis HCC: Hepatocellular carcinoma PHP : Prehepatic portal hypertension
Key words: gastric varices, gastrorenal shunt, endoscopic sclerotherapy, Hassab's operation 1 cases 6 cases 5 cases LC: Liver cirrhosis HCC: Hepatocellular carcinoma PHP : Prehepatic portal hypertension
Feasibility of endoscopic mucosa-submucosa clip closure method (with video)
 Feasibility of endoscopic mucosa-submucosa clip closure method (with video) Authors Toshihiro Nishizawa 1, Shigeo Banno 2, Satoshi Kinoshita 1,HidekiMori 2, Yoshihiro Nakazato 3,YuichiroHirai 2,Yoko Kubosawa
Feasibility of endoscopic mucosa-submucosa clip closure method (with video) Authors Toshihiro Nishizawa 1, Shigeo Banno 2, Satoshi Kinoshita 1,HidekiMori 2, Yoshihiro Nakazato 3,YuichiroHirai 2,Yoko Kubosawa
Portal hypertension is the main complication of cirrhosis
 GASTROENTEROLOGY 2001;120:726 748 Current Management of the Complications of Cirrhosis and Portal Hypertension: Variceal Hemorrhage, Ascites, and Spontaneous Bacterial Peritonitis GUADALUPE GARCIA TSAO
GASTROENTEROLOGY 2001;120:726 748 Current Management of the Complications of Cirrhosis and Portal Hypertension: Variceal Hemorrhage, Ascites, and Spontaneous Bacterial Peritonitis GUADALUPE GARCIA TSAO
Original Article INTRODUCTION. pissn eissn X
 pissn 2287-2728 eissn 2287-285X Original Article Clinical and Molecular Hepatology 2016;22:466-476 Emergency endoscopic variceal ligation in cirrhotic patients with blood clots in the stomach but no active
pissn 2287-2728 eissn 2287-285X Original Article Clinical and Molecular Hepatology 2016;22:466-476 Emergency endoscopic variceal ligation in cirrhotic patients with blood clots in the stomach but no active
Having a PEG tube inserted
 Having a PEG tube inserted This information leaflet is for patients who are having a PEG (Percutaneous Endoscopic Gastrostomy) tube inserted. It explains what is involved, what to expect and what significant
Having a PEG tube inserted This information leaflet is for patients who are having a PEG (Percutaneous Endoscopic Gastrostomy) tube inserted. It explains what is involved, what to expect and what significant
(a) (b) Plate 16.1 Esophageal tear after passage of the echoendoscope.
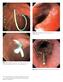 Plate 16.1 Esophageal tear after passage of the echoendoscope. Plate 11.1 Prophylactic pancreatic duct stents. 3-Fr, 4-cm long single-pigtail stent. 5-Fr, 3-cm long flanged stent. Plate 16.2 Esophageal
Plate 16.1 Esophageal tear after passage of the echoendoscope. Plate 11.1 Prophylactic pancreatic duct stents. 3-Fr, 4-cm long single-pigtail stent. 5-Fr, 3-cm long flanged stent. Plate 16.2 Esophageal
Review Article Self-Expandable Metal Stents in the Treatment of Acute Esophageal Variceal Bleeding
 Hindawi Publishing Corporation Gastroenterology Research and Practice Volume 2011, Article ID 910986, 6 pages doi:10.1155/2011/910986 Review Article Self-Expandable Metal Stents in the Treatment of Acute
Hindawi Publishing Corporation Gastroenterology Research and Practice Volume 2011, Article ID 910986, 6 pages doi:10.1155/2011/910986 Review Article Self-Expandable Metal Stents in the Treatment of Acute
Detection of Esophageal Varices in Liver Cirrhosis Using Non-invasive Parameters
 ORIGINAL ARTICLE Detection of Esophageal Varices in Liver Cirrhosis Using Non-invasive Parameters Johana Prihartini*, LA Lesmana**, Chudahman Manan***, Rino A Gani** ABSTRACT Aim: recent guidelines recommend
ORIGINAL ARTICLE Detection of Esophageal Varices in Liver Cirrhosis Using Non-invasive Parameters Johana Prihartini*, LA Lesmana**, Chudahman Manan***, Rino A Gani** ABSTRACT Aim: recent guidelines recommend
ACUTE CHOLANGITIS AS a result of an occluded
 Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
Department of Surgery, Aizu Central Hospital, Fukushima
 Case Reports Resection of Asynchronous Quadruple Advanced Colonic Carcinomas Followed by Reconstruction with Ileal Interposition between the Transverse Colon and Rectum Sho Mineta 1, Kimiyoshi Shimanuki
Case Reports Resection of Asynchronous Quadruple Advanced Colonic Carcinomas Followed by Reconstruction with Ileal Interposition between the Transverse Colon and Rectum Sho Mineta 1, Kimiyoshi Shimanuki
th Annual AISF Meeting 44 th th th, 2011 Rome, February 23 rd -26
 44 th 44 th Annual AISF Meeting Rome, February 23 rd -26 th th, 2011 Update on the Baveno Consensus Conference Roberto de Franchis Department of of Clinical Sciences, University of of Milan, Head, Gastroenterology
44 th 44 th Annual AISF Meeting Rome, February 23 rd -26 th th, 2011 Update on the Baveno Consensus Conference Roberto de Franchis Department of of Clinical Sciences, University of of Milan, Head, Gastroenterology
Endoscopic pancreatic necrosectomy in 2017
 Endoscopic pancreatic necrosectomy in 2017 Mouen Khashab, MD Associate Professor of Medicine Director of Therapeutic Endoscopy The Johns Hopkins Hospital Revised Atlanta Classification Entity Acute fluid
Endoscopic pancreatic necrosectomy in 2017 Mouen Khashab, MD Associate Professor of Medicine Director of Therapeutic Endoscopy The Johns Hopkins Hospital Revised Atlanta Classification Entity Acute fluid
The role of endoscopy in the management of variceal hemorrhage
 GUIDELINE The role of endoscopy in the management of variceal hemorrhage This is one of a series of statements discussing the use of GI endoscopy in common clinical situations. The Standards of Practice
GUIDELINE The role of endoscopy in the management of variceal hemorrhage This is one of a series of statements discussing the use of GI endoscopy in common clinical situations. The Standards of Practice
