Yonsei Experience of 5000 Gasless Transaxillary Robotic Thyroidectomies
|
|
|
- Willa Blankenship
- 5 years ago
- Views:
Transcription
1 World J Surg (2018) 42: DOI /s y ORIGINAL SCIENTIFIC REPORT Yonsei Experience of 5000 Gasless Transaxillary Robotic Thyroidectomies Min Jhi Kim 1 Kee-Hyun Nam 1 Seul Gi Lee 1 Jung Bum Choi 1 Tae Hyung Kim 1 Cho Rok Lee 1 Jandee Lee 1 Sang-Wook Kang 1 Jong Ju Jeong 1 Woong Youn Chung 1 Published online: 6 September 2017 Ó Société Internationale de Chirurgie 2017 Abstract Background Since the use of robot systems in thyroid surgery was introduced in 2007, we have advanced a novel method of robotic thyroidectomy (RT) using a gasless transaxillary approach (TAA). We report our experience with this technique and detail the surgical outcome of 5000 robotic thyroidectomies. Methods From October 2007 to May 2016, we successfully performed 5000 robotic thyroidectomies using a gasless TAA at the Department of Surgery, Yonsei University Health System. The medical records of the patients are reviewed retrospectively, and the details of clinicopathologic characteristics, operation times, perioperative complications, and oncologic outcomes are analyzed. Results The 5000 patients with thyroid tumor (4804 with cancer and 196 with benign tumor) underwent RT using a gasless TAA. Mean operation time was ± min. The most common histologic subtype of thyroid cancer was papillary (98%), and the mean tumor size was 8.0 ± 6.0 mm. Stage I was found in 85.4% patients regarding tumor nodes metastasis staging. The 196 benign tumors consisted of 104 adenomatous hyperplasias (53.0%), 43 follicular adenomas (21.9%), 30 Graves diseases (15.3%), and 19 others (9.7%). Postoperative complication occurred in 24.1% without any serious one, and overall morbidity tended to decrease over time. No disease-specific mortality was observed during the follow-up period. Locoregional recurrence was developed in 26 patients (0.5%). Conclusion The authors have tried to improve RT technique using gasless TAA and achieved acceptable surgical outcomes. The rapid evolution of surgical robot technology and our constant effort to advance RT technique using gasless TAA would make it possible to reduce the perioperative morbidity and gain the best possible operative and oncologic outcomes. Introduction The incidence of thyroid cancer has increased worldwide during the last decade, with thyroid surgery becoming one of the most common surgical procedures. Conventional & Woong Youn Chung woungyounc@yuhs.ac 1 Department of Surgery, Severance Hospital, Yonsei Cancer Center, Yonsei University College of Medicine, 50-1, Yonsei-ro, Seodaemun-gu, Seoul 03722, Korea open thyroid surgery leaves a scar on the anterior neck, which can be a cosmetic issue for some patients. Desire for the lack of visible scars has led to the introduction of endoscopic surgeries in the late nineteenth century. Endoscopic cervical approaches to the thyroid and parathyroid glands were initiated by Gagner [1] and Huscher et al. [2]. The endoscopic technique has subsequently been augmented with various approaches such as anterior chest, axillary, breast, and cervical approaches [3 5]. At our institution, Chung et al. [6] invented the new endoscopic thyroidectomy (ET) technique using a gasless transaxillary approach (TAA) in November 2001.
2 394 World J Surg (2018) 42: However, ET showed several limitations, including restricted vision, difficulty in instrument handling, and lack of tactile perception [7, 8]. The disadvantages of endoscopic surgery necessitated more technical advancements, and the concept of using a robot in surgery was introduced. Robotic surgery was developed to overcome the limitations of the ET technique and to enhance the capabilities of surgeons. Since the da Vinci surgical system (Intuitive Surgical, Sunnyvale, CA, USA) was approved by the US Food and Drug Administration in 2000 for certain laparoscopic procedures, its application has rapidly become more widespread [9]. However, since the conventional approach is safe and timehonored, robotic thyroidectomy (RT) remains controversial especially in the West including the USA, where the FDA has revoked approval on the use of robotic thyroidectomy and parathyroidectomy in 2011 [10]. Our institution utilized the robot system in thyroid surgery, and first introduced the RT technique using gasless TAA in October 2007 [7]. We have made constant effort to advance our RT technique since then. As robotic experience accumulated, we could change the surgical incision from double incision to single axillary incision, developing a less invasive RT technique using gasless TAA while maintaining surgical outcomes. Until May 2016, we have performed 5000 cases of RT using a gasless TAA. We herein report our experience and detail the surgical outcome of the total 5000 patients. Materials and methods Patients From October 2007 to May 2016, 5000 patients with thyroid tumor underwent RT using a gasless TAA at the Department of Surgery, Yonsei University Health System. Of these, 4804 patients (96%) had thyroid cancer and 196 (4%) had a benign tumor. All operations were performed with the da Vinci S, Si, or Xi surgical robotic system (Intuitive Surgical). Less than total thyroidectomy (LTT) was performed in 3 patients (62.5%), and bilateral total thyroidectomy (BTT) was conducted in 1543 (30.9%). LTT was defined as total resection on one lobe of the thyroid and partial or subtotal resection on the opposite lobe. Robotic modified radical neck dissection (MRND) was performed in 334 patients (6.7%) with lateral neck node metastases. All patients with thyroid cancer underwent prophylactic ipsilateral central compartment neck dissection. The eligibility criteria for RT were as follows: (1) follicular proliferation with tumor size B5cm, and (2) differentiated thyroid cancer without contraindications to RT. The exclusion criteria were (1) previous head-and-neck surgery or irradiation, (2) definite tumor invasion to an adjacent organ (recurrent laryngeal nerve [RLN], esophagus, or trachea), (3) multiple lateral neck node metastases or perinodal metastatic lymph node infiltration, and (4) distant metastasis. Patients with thyroid tumor were divided into four groups according to operation dates: first period (October 2007 November 2011, n = 1033), second period (December 2011 January 2012, n = 1367), third period (February 2012 March 2014, n = 1489), and fourth period (April 2014 May 2016, n = 904). Details of clinicopathologic characteristics, operation times, perioperative complications, and oncologic outcomes were reviewed retrospectively. This study was approved by the Institutional Review Board of Yonsei University Health System ( ). For benign tumors, surgical management was indicated as follows: (1) follicular/hürthle cell lesions of diameter \5 cm, (2) nodules with indefinite suspicious ultrasonographic findings, (3) nodules with fine needle aspiration biopsy (FNAB) findings suspicious for malignancy, and (4) Graves disease (GD). Among patients with GD, those who were intractable to medical treatment and had contraindications to radioactive iodine (RAI) therapy, those with severe exophthalmoses, and those seeking pregnancy within 1 year were included. Frozen sections were obtained from all suspicious lesions with inconclusive FNAB results. When a lesion was considered malignant, treatment was provided according to ATA guidelines [11]. Operative methods We have previously described the procedures for RT and robotic MRND [7, 12 14]. We started RT using a gasless TAA with two separate incisions: one in the axilla and one in the anterior chest. After performing [750 cases of RT, we modified our technique by using a single incision on the axilla, from September 2009 for RT and from March 2013 for robotic MRND. Outcome assessment All patients were administered with levothyroxine for thyroid-stimulating hormone (TSH) suppression immediately after surgery. To evaluate postoperative morbidity, the parathyroid function was assessed by measuring serum calcium and intact parathyroid hormone (ipth) concentrations preoperatively, and at 1 week and 3 months postoperatively. Hypoparathyroidism was defined as a reduction in serum ipth concentration below the normal limit, regardless of hypocalcemic symptoms [15]. Postoperative laryngoscopy was performed in patients with
3 World J Surg (2018) 42: transient hoarseness after surgery. Permanent hypoparathyroidism and RLN palsy were defined as nonrecovery within 6 months. Thyroid function tests (TSH, ft3, and ft4) and serum calcium levels were determined at 1, 3, and 6 months postoperatively. TSH-suppressed serum thyroglobulin (Tg) levels were measured, and ultrasonography (US) was performed at 3- or 6-month intervals. RAI ablation was performed based on stage and risk factors, according to ATA guidelines, at 4 12 weeks after surgery [11]. The patients underwent posttherapy whole-body scans and diagnostic whole-body scans 2 5 days after RAI ablation, and abnormal RAI uptakes were investigated [16]. To evaluate the long-term oncologic outcomes, suppressed serum Tg concentration was measured annually, and all patients underwent regular follow-up US. Patients with evidence of recurrence or distant metastasis were assessed with other imaging modalities, such as neck computed tomography (CT) and/or positron emission tomography-ct. Regional neck node recurrence was confirmed with US-guided FNAB. Overall survival was defined as the time from the date of initial surgery to the date of last follow-up or death. Recurrence-free survival (RFS) was defined as the time from the date of surgery to the date of detection of the first recurrence on imaging. Study endpoints The primary endpoint of the study was to review clinicopathologic characteristics and surgical outcomes of 5000 patients with thyroid tumor. The second endpoint was to demonstrate feasibility and safety of RT technique using gasless TAA by comparing the rate of perioperative morbidities according to the periods. Statistical analysis Categorical data were reported as rates and proportions, while the median and ranges were calculated for continuous data. To compare the rate of perioperative complications according to operation period, patients were regrouped into two groups: patients of the first, second, and third periods; and patients of the fourth period. Surgical complications and complication rates were assessed for each group, and among-group comparisons were expressed as numbers and proportions. Differences in categorical variables were compared by Chi square test and Fisher s exact test, as appropriate. A P value of \0.05 was considered statistically significant. Statistical analyses were performed using IBM SPSS Statistics for Windows, version 23.0 (IBM Corp., Armonk, NY). Results The clinical characteristics of 5000 patients (558 men and 4442 women; mean age, 38.3 ± 9.3 years) were reviewed. Primary operations were performed on 4963 patients (4767 with cancer and 196 with benign tumor). The mean total operation time was ± min (Table 1). No case was converted to conventional open surgery. Concerning the 196 benign tumors, the mean tumor size was 2.1 ± 1.4 cm. Adenomatous hyperplasia was the most common finding (104 patients). Forty-three lesions were diagnosed as follicular adenoma. GD was indicated for surgery in 30 cases (Table 2). Table 3 shows the histopathologic characteristics of 4804 patients with thyroid cancer. The mean tumor diameter was 0.8 ± 0.6 cm. Papillary thyroid carcinoma (PTC) was the most common histologic type (4751 patients [98.9%]). Multiple or bilateral lesions were observed in 1188 (24.7%) and 598 cases (12.4%), respectively. According to the tumor node metastasis stage classification, 2530 patients (52.9%) had T1 cancer lesions, followed by 2171 patients (45.4%) with T3 lesions. In 25 patients with T4a lesions, direct cancer invasion into adjacent organs was noted, as follows: 15 RLN, 6 trachea (perichondrium), 1 esophagus (longitudinal muscle layer), and 1 internal jugular vein (tunica adventitia) invasions. In 20 patients, the invaded organs were successfully preserved after shaving with robotic scissors; however, the RLN was sacrificed in four patients owing to complete tumor invasion of the nerve core. The remaining one patient had a widely invasive follicular carcinoma. Concerning N stage, central neck node metastases (N1a) and lateral neck metastases (N1b) were found in 1407 (29.3%) and 363 (7.6%) patients, respectively. No patient had distant metastasis (Table 3). For 334 patients with lateral neck metastasis, BTT with MRND was performed in 311 patients, and redo operations consisting of 8 completion total thyroidectomy with MRNDs and 15 MRNDs were conducted in 23 patients with tumor recurrence. The mean tumor size was 1.3 ± 0.7 cm. The mean numbers of retrieved central and lateral lymph nodes were 6.3 ± 5.1 and 34.1 ± 17.5, respectively (Table 4). To figure out changing trends in our RT experience, patients were organized into four groups according to their operation dates and then re-evaluated. The trends of RT with experience showed several changes in clinical performance status. Specifically, BTT with MRND cases increased and total operation times decreased (Table 5). In terms of postoperative complications, 884 patients (48.1% of BTT cases) experienced transient hypocalcemia, which resolved within 3 months. Twenty-five patients
4 396 World J Surg (2018) 42: Table 1 Clinical characteristics of patients Variables N = 5000 Age (years) 38.3 ± 9.3 Sex ratio (male:female) 558:4442 (ratio 1:8.0) Pathologic type, malignant:benign (n, %) 4804 (96%):196 (4%) Operation type, primary:redo (n, %) 4963 (99%):37 (1%) Operation time (min) ± (range ) Postoperative hospital stay (days) 3.3 ± 3.0 (range 2 7) Table 2 Pathologic characteristics of patients with benign tumors Variables n = 196 Mean tumor size (cm) 2.1 ± 1.4 Pathology (n) Adenomatous hyperplasia 104 Follicular adenoma 43 Hürthle cell adenoma 11 Lymphocytic thyroiditis 10 Graves disease 30 Others 5 a a Hyalinizing trabecular tumor: two cases, maltoma: one case, bronchogenic cyst: one case, and neurofibroma: one case (1.3% of BTT cases) were found to have permanent hypocalcemia. Transient hoarseness appeared in 126 patients (2.5%), which resolved within 3 months. Most cases of chyle leakage were successfully managed conservatively; however, three patients had massive chyle leakage requiring reoperation. There were 18 cases (0.4%) of RLN injury, 7 cases (0.1%) of tracheal wall injury, and 2 cases (0.04%) of vessel injuries (carotid artery or brachiocephalic vein). All RLN injuries were treated by using injection laryngoplasty with Rofilan. Tracheal wall and vessel injuries were managed through primary repair by using robotic instruments. Horner s syndrome occurred in four patients. Three patients underwent lateral neck dissection due to extensive lateral neck node metastases. The remaining one patient had isthmus cancer with extrathyroidal extension and central LN metastases. Extensive manipulation and dissection of tissues around the carotid sheath would have led to compression of the cervical plexus. The symptoms spontaneously resolved within 2 months. The technique-related complications that were seen exclusively in RT were axillary skin flap perforation in eight patients (0.2%) and transient brachial nerve paralysis in four patients (0.1%). Transient brachial nerve paralysis occurred owing to the hyperextension of the lesion side arm, and all patients spontaneously recovered within 2 months (Table 6). Moreover, accumulation of robotic experience resulted in a smaller overall morbidity rate in the fourth period. Comparative analyses revealed that patients of the fourth period experienced significantly less transient hypocalcemia, permanent hypocalcemia, and overall morbidity compared to previous periods (Table 7). Of 1863 thyroid cancer patients who had BTT, 1460 (80.0%) underwent adjuvant RAI therapy, and no abnormal uptake was seen in 1380 patients (94.5%) according to diagnostic whole-body scans. At 3 months after surgery, the serum TSH-suppressed Tg level was less than 1 ng/ml in 1038 patients (55.7%). During the follow-up, tumor recurrence was detected by imaging and confirmed in 26 patients (0.5%) (Table 8). Patients with tumor recurrence consisted of 15 patients who had hemithyroidectomy and 11 patients who had total thyroidectomy. Despite the fact that the latter group had all received RAI ablation, five patients had serum Tg C 1 ng/ ml after 5 years of surgery. Patients who had no RAI treatment showed higher percentages of persistent serum Tg elevation. However, no structural recurrence was found in these patients during follow-up. The most common sites of recurrence were the lateral neck nodes (14 patients). Recurrence in the contralateral thyroid and in the central neck node was found in nine and three patients, respectively. No recurrence was detected in distant organs. All patients with recurrence underwent reoperation (robotic surgery in 15 and conventional open method in 11). The median RFS of these patients was 39.5 ± 30.0 months. No disease-specific mortality was observed during the follow-up period. The median RFS of 4804 thyroid cancer patients was 52.5 ± 27.1 months. Discussion In the current study, the trends in our RT tended to include more advanced cases with less invasive method, shorter operation time, and less perioperative complications over time. These can be explained by the rapid evolution of robot technology. Moreover, accumulation of robotic
5 World J Surg (2018) 42: Table 3 Pathologic characteristics of patients with thyroid cancer Variables n = 4804 Tumor size (cm) 0.8 ± 0.6 (range ) Pathology, n(%) Papillary carcinoma 4751 (98.9%) (papillary microcarcinoma) (3617 [75.3%]) Follicular carcinoma 38 (0.79%) Papillary carcinoma? follicular carcinoma 4 (0.08%) Medullary carcinoma 9 (0.19%) Papillary carcinoma? medullary carcinoma 1 (0.02%) Hürthle cell carcinoma 1 (0.02%) Multiplicity, n (%) 1188 (24.7%) Bilaterality, n (%) 598 (12.4%) Retrieved lymph node, n Central neck node 4.9 ± 4.0 (range 0 40) Lateral node 27.8 ± 19.8 (range 1 146) T stage, n (%) T1/T2/T3/T (25.9)/57 (1.2)/2171 (45.4)/25 (0.5) N stage, n (%) N0/N1a/N1b 3034 (63.1)/1407 (29.3)/363 (7.6) TNM stage, n (%) I/II/III/IV 4102 (85.4)/7 (0.2)/622 (12.9)/73 (1.5) Table 4 Pathologic characteristics of patients with lateral neck metastasis Variables n = 334 Tumor size (cm) 1.3 ± 0.7 (range ) Extracapsular invasion, n (%) 258 (77.9%) Multiplicity, n (%) 143 (43.2%) Bilaterality, n (%) 100 (30.2%) Retrieved lymph node, n Central neck node 6.3 ± 5.1 (range 0 40) Lateral node 34.1 ± 17.5 (range 1 146) T stage, n (%) T1/T2/T3/T4 59 (17.8)/8 (2.4)/236 (71.2)/8 (2.4) TNM stage, n (%) I/IV 273 (82.4)/58 (17.5) experience and constant efforts to develop more effective techniques may have led to preferable outcomes. Robotic surgery is an innovative and new technique representing minimally invasive surgery in the current surgical trends. The outstanding advantages of robotic surgery are overcoming the technical limitations of endoscopic surgery and providing three-dimensional imaging, motion scaling, tremor elimination, and additional degrees of freedom [9, 17, 18]. The application of robot technology in thyroid surgery has provided a safe and feasible approach for preexisting ET. Several institutions subsequently substantiated the technical efficiency and positive potential of RT, and reported their successful experience with this technique [8, 19]. Considering the advantages of RT, many thyroid surgeons performed [6000 RTs with or without neck dissection in South Korea between 2007 and 2011 [13, 14, 20, 21]. At our institution, we have performed[650 ETs using a gasless TAA from Our RT technique using gasless TAA is based on the feasibility of ET in papillary microcarcinoma of the thyroid, which is defined as PTC with diameter B1 cm [6]; however, the first application of robotics to thyroid surgery was limited to well-differentiated thyroid carcinoma with tumor size B2 cm without definite extrathyroidal tumor invasion, or to follicular neoplasms with tumor size B5 cm[8]. We have continued to refine the surgical techniques in RT based on the principles and protocols described for the indication. As robotic experience accumulated, we were able to successfully manage unexpected advanced cases, such as those with definite adjacent muscle invasion or perinodal infiltration. The indications for RT have expanded, including more aggressive disease, with more technical advancements and increase in the skill of surgeons over time (Table 5). Superficial invasion to adjacent organs such as the trachea, RLN, and neck vessels became manageable by using the technique of shaving with robotic scissors. Currently, the only contraindication of RT at our institution
6 398 World J Surg (2018) 42: Table 5 Clinicopathologic characteristics of patients with thyroid cancer according to period (n = 4804) First period (n = 1036) Second period (n = 1370) Third period (n = 1492) Fourth period (n = 906) Operation type, n (%) LTT 644 (62.2) 787 (57.4) 906 (60.7) 624 (68.9) BTT 352 (34.0) 484 (35.3) 480 (32.2) 199 (21.9) Additional MRND 40 (3.8) 99 (7.2) 106 (7.1) 83 (9.2) Total operation time LTT ± ± ± ± 29.5 BTT ± ± ± ± 39.4 Additional MRND ± ± ± ± 92.8 Working space time LTT 31.4 ± ± ± ± 14.3 BTT 32.6 ± ± ± ± 18.1 Additional MRND 59.2 ± ± ± ± 36.2 Docking time LTT 5.6 ± ± ± ± 1.8 BTT 5.4 ± ± ± ± 1.5 Additional MRND 5.3 ± ± ± ± 3.9 Console time LTT 47.8 ± ± ± ± 17.6 BTT 68.1 ± ± ± ± 21.3 Additional MRND ± ± ± ± 54.8 Positive nodes Central nodes 0.9 ± ± ± ± 2.2 Lateral nodes 3.0 ± ± ± ± 4.8 T stage, n (%) T1 527 (50.9) 727 (53.1) 813 (54.5) 480 (53.0) T2 11 (1.0) 15 (1.1) 18 (1.2) 19 (2.1) T3 492 (47.5) 625 (45.6) 652 (43.7) 397 (43.8) T4 6 (0.6) 3 (0.2) 9 (0.6) 10 (1.1) N stage, n (%) N0 651 (62.8) 896 (65.4) 976 (65.4) 526 (58.1) N1a 344 (33.2) 375 (27.4) 407 (27.3) 293 (32.3) N1b 41 (4.0) 99 (7.2) 109 (7.3) 87 (9.6) TNM stage, n (%) I 873 (84.3) 1150 (84.0) 1290 (86.5) 776 (85.7) II 0 (0) 2 (0.1) 4 (0.2) 2 (0.2) III 154 (14.8) 193 (14.1) 177 (11.9) 111(12.2) IV 9 (0.9) 25 (1.8) 21 (1.4) 17 (1.9) LTT less than total thyroidectomy, BTT bilateral total thyroidectomy, MRND modified radical neck dissection is deep tumor infiltration to adjacent structures requiring extensive resection of the trachea or neck vessels. Our experience resulted in [300 cases of MRND with acceptable perioperative outcomes and excellent cosmesis [22]. Furthermore, the robotic technique enabled the management of GD and multinodular goiter, which were difficult to manage with an endoscopic method owing to the large volume of engorged fragile thyroid tissue. Surgeons with experience in RT can successfully extract large thyroid glands with excellent cosmesis, without increasing the complication rates [23]. Through the application of the robotic technique in thyroid surgery, our institution aimed to achieve comparable postoperative outcomes and enhance patient
7 World J Surg (2018) 42: Table 6 Perioperative complications of the 5000 total patients according to period Complication (n, %) First period (n = 1052) Second period (n = 1421) Third period (n = 1563) Fourth period (n = 964) Total (N = 5000) Transient hypocalcemia (n/btt, %) 161 (161/393, 41.0) 256 (256/579, 44.2) 372 (372/589, 63.2) 95 (95/276, 34.4) 884 (884/1837, 48.1) Permanent hypocalcemia (n/btt, %) 5 (5/393, 1.3) 10 (10/579, 1.7) 10 (10/589, 1.6) 0 (0/964, 0) 25 (25/1837, 1.3) Transient voice change 56 (5.3) 18 (1.3) 27 (1.7) 25 (2.6) 126 (2.5) Seroma 23 (2.2) 23 (1.6) 23 (1.5) 6 (0.6) 75 (1.5) Hematoma [reoperation] 6 [1] (0.6) 5 [1] (0.4) 5 [2] (0.3) 5 [1] (0.5) 21 [5] (0.4) Chyle leak [reoperation] 5 [1] (0.5) 11 [0] (0.8) 9 [0] (0.6) 4 [2] (0.4) 29 [3] (0.6) RLN injury 6 (0.6) 4 (0.3) 6 (0.4) 2 (0.2) 18 (0.4) Horner syndrome 1 (0.1) 0 (0) 2 (0.1) 1 (0.1) 4 (0.1) Trachea injury 4 (0.44) 1 (0.1) 2 (0.1) 0 (0) 7 (0.1) Vessel injury (carotid artery, brachiocephalic 0 (0) 1 (0.1) 1(0.1) 0 (0) 2 (0.04) vein) Flap injury (burn) 2 (0.2) 1 (0.1) 2 (0.1) 3 (0.3) 8 (0.2) Traction injury of lesion side arm 2 (0.2) 0 (0) 2 (0.1) 0 (0) 4 (0.1) SAN injury 0 (0) 0 (0) 0 (0) 1 (0.1) 1 (0.02) Overall morbidity 271 (25.8) 330 (23.2) 461(29.5) 142 (14.7) 1204 (24.1) BTT bilateral total thyroidectomy, RLN recurrent laryngeal nerve, SAN spinal accessory nerve Table 7 Comparative analyses of perioperative complications of the 5000 patients at different periods Complication (n, %) First? Second? Third Period (N = 4036) Fourth Period (N = 964) P value Transient hypocalcemia (n/btt, %) 789 (789/1561,50.5) 95 (95/276,34.4) \0.001 Permanent hypocalcemia (n/btt, %) 25 (25/1561,0.1) 0 (0/964,0) \0.001 Transient voice change 101 (2.5) 25 (2.6) Seroma 69 (1.7) 6 (0.6) Hematoma [reoperation] 16 [4] (0.3) 5 [1] (0.5) Chyle leak [reoperation] 25 [1] (0.6) 4 [2] (0.4) RLN injury 16 (0.3) 2 (0.2) [0.999 Horner syndrome 3 (0.1) 1 (0.1) [0.999 Trachea injury 6 (0.1) 1 (0.1) [0.999 Vessel injury (carotid artery, brachiocephalic vein) 2 (0.04) 0 (0) [0.999 Flap injury (burn) 4 (0.1) 3 (0.3) Traction injury of lesion side arm 4 (0.1) 0 (0) [0.999 SAN injury 0 (0) 1 (0.1) Overall Morbidity 1062 (26.3) 142 (14.7) \0.001 BTT bilateral total thyroidectomy, RLN recurrent laryngeal nerve, SAN spinal accessory nerve satisfaction after surgery. We conducted comparative studies between RT and open thyroidectomy or ET to evaluate the oncologic and functional outcomes, technical efficiency, and safety. We retrospectively reviewed the medical records of patients undergoing RT, and single- and multicenter trials were also conducted. Our constant efforts in developing surgical techniques and training programs have resulted in similar postoperative complications and surgical completeness, as well as comparable 5-year oncologic outcomes [16, 22, 24, 25]. According to our prospective functional study, less sensory change in the neck, less swallowing difficulty, and much
8 400 World J Surg (2018) 42: Table 8 Treatment outcomes of patients with thyroid cancer Study patients, n (%) LTT (n = 2941) TT (±MRND) (n = 1863) Postoperative RAI ablation 1460 (78.3%) Ablation success based on DxWBS 1380 (94.5%) Serum Tg \ 1.0 ng/ml after 3 months 1038 (55.7%) (without TSH:) Recurrence 15 (0.3%) 11 (0.2%) LTT less than total thyroidectomy, TT total thyroidectomy, MRND modified radical neck dissection, RAI radioactive iodine, DxWBS diagnostic whole-body scan, Tg thyroglobulin better cosmetic satisfaction were observed in patients who underwent RT [26]. RT is a complex and sophisticated surgical procedure and needs a longer total operation time than open or endoscopic surgery. The operation time gradually decreased with increasing surgeon skill and reached steady states after cases for RT and after cases for ET [27]. The advantages of RT may be due to the threedimensional magnified camera vision, use of multiarticulated instruments, and the fine coordination of robotic hands, resulting in more ergonomically favorable conditions [18]. Although large numbers of results have already been reported, the technical reproducibility of RT remains unproven. Most studies have been nonrandomized retrospective studies, which is the limitation in this field. Prospective studies in large numbers of patients are needed to accurately assess the effects of RT in terms of various postoperative outcomes. Despite the limitations, our institution has accomplished the first 5000 cases of RT using gasless TAA worldwide. Our results may provide a good starting point to guide future studies with a longer followup. RT is a revolutionary technology; however, the robotic equipment and the operative field have a learning curve. RT requires complete understanding of the robotic instruments, approach routes, and neck anatomy, which can lead to a dexterous and sophisticated technique in performing the procedure. Thus, sufficient training is essential, and careful observation of an expert s technique and animal or cadaveric studies are required. Surgeons should also consider the patient factors affecting outcomes in RT, including age, body habitus, disease aggressiveness, associated comorbidities, and safety. The stepwise extension of surgical methods and indications after proper training and sufficient experience will lead to the ideal application of robotic thyroid surgery. Over the last nine years, the authors tried to improve RT technique using gasless TAA and achieved acceptable surgical outcomes. We believe that the rapid evolution of surgical robot technology, in addition to our constant efforts to advance RT technique using gasless TAA, would help reduce perioperative morbidity and gain the best possible operative and oncologic outcomes. Compliance with ethical standards Conflict of interest There are no conflicts of interest or financial ties to disclose. References 1. Gagner M (1996) Endoscopic subtotal parathyroidectomy in patients with primary hyperparathyroidism. Br J Surg 83: Huscher CS, Chiodini S, Napolitano C et al (1997) Endoscopic right thyroid lobectomy. Surg Endosc 11: Shimizu K, Akira S, Jasmi AY et al (1999) Video-assisted neck surgery: endoscopic resection of thyroid tumors with a very minimal neck wound. J Am Coll Surg 188: Ikeda Y, Takami H, Sasaki Y et al (2000) Endoscopic neck surgery by the axillary approach. J Am Coll Surg 191: Ohgami M, Ishii S, Arisawa Y et al (2000) Scarless endoscopic thyroidectomy: breast approach for better cosmesis. Surg Laparosc Endosc Percutan Tech 10: Kang SW, Jeong JJ, Yun JS et al (2009) Gasless endoscopic thyroidectomy using trans-axillary approach; surgical outcome of 581 patients. Endocr J 56: Kang SW, Jeong JJ, Nam KH et al (2009) Robot-assisted endoscopic thyroidectomy for thyroid malignancies using a gasless transaxillary approach. J Am Coll Surg 209:e1 e7 8. Kang SW, Jeong JJ, Yun JS et al (2009) Robot-assisted endoscopic surgery for thyroid cancer: experience with the first 100 patients. Surg Endosc 23: Goh HK, Ng YH, Teo DT (2010) Minimally invasive surgery for head and neck cancer. Lancet Oncol 11: Lang BH, Wong CK, Tsang JS et al (2015) A systematic review and meta-analysis evaluating completeness and outcomes of robotic thyroidectomy. Laryngoscope 125: Cooper DS, Doherty GM, Haugen BR et al (2009) Revised American Thyroid Association management guidelines for patients with thyroid nodules and differentiated thyroid cancer. Thyroid 19: Ryu HR, Kang SW, Lee SH et al (2010) Feasibility and safety of a new robotic thyroidectomy through a gasless, transaxillary single-incision approach. J Am Coll Surg 211:e13 e Kang SW, Lee SH, Ryu HR et al (2010) Initial experience with robot-assisted modified radical neck dissection for the management of thyroid carcinoma with lateral neck node metastasis. Surgery 148:
9 World J Surg (2018) 42: Kang SW, Park JH, Jeong JS et al (2011) Prospects of robotic thyroidectomy using a gasless, transaxillary approach for the management of thyroid carcinoma. Surg Laparosc Endosc Percutan Tech 21: Rivere AE, Brooks AJ, Hayek GA et al (2014) Parathyroid hormone levels predict posttotal thyroidectomy hypoparathyroidism. Am Surg 80: Lee S, Lee CR, Lee SC et al (2014) Surgical completeness of robotic thyroidectomy: a prospective comparison with conventional open thyroidectomy in papillary thyroid carcinoma patients. Surg Endosc 28: Fuchs KH (2002) Minimally invasive surgery. Endoscopy 34: Lee J, Chung WY (2013) Robotic surgery for thyroid disease. Eur Thyroid J 2: Lee KE, Rao J, Youn YK (2009) Endoscopic thyroidectomy with the da Vinci robot system using the bilateral axillary breast approach (BABA) technique: our initial experience. Surg Laparosc Endosc Percutan Tech 19:e71 e Tae K, Song CM, Ji YB et al (2016) Oncologic outcomes of robotic thyroidectomy: 5-year experience with propensity score matching. Surg Endosc 30: Cho JN, Park WS, Min SY et al (2016) Surgical outcomes of robotic thyroidectomy vs. conventional open thyroidectomy for papillary thyroid carcinoma. World J Surg Oncol 14: Kim MJ, Lee J, Lee SG et al (2017) Transaxillary robotic modified radical neck dissection: a 5-year assessment of operative and oncologic outcomes. Surg Endosc 31: Park JH, Lee CR, Park S et al (2013) Initial experience with robotic gasless transaxillary thyroidectomy for the management of graves disease: comparison of conventional open versus robotic thyroidectomy. Surg Laparosc Endosc Percutan Tech 23:e173 e Kang SW, Lee SH, Park JH et al (2012) A comparative study of the surgical outcomes of robotic and conventional open modified radical neck dissection for papillary thyroid carcinoma with lateral neck node metastasis. Surg Endosc 26: Lee SG, Lee J, Kim MJ et al (2016) Long-term oncologic outcome of robotic versus open total thyroidectomy in PTC: a casematched retrospective study. Surg Endosc 30: Lee J, Kwon IS, Bae EH et al (2013) Comparative analysis of oncological outcomes and quality of life after robotic versus conventional open thyroidectomy with modified radical neck dissection in patients with papillary thyroid carcinoma and lateral neck node metastases. J Clin Endocrinol Metab 98: Lee J, Yun JH, Nam KH et al (2011) The learning curve for robotic thyroidectomy: a multicenter study. Ann Surg Oncol 18:
Department of Surgery, Eulji University College of Medicine, Seoul, Republic of Korea 2
 Journal of Oncology Volume 2012, Article ID 734541, 9 pages doi:10.1155/2012/734541 Clinical Study Robotic versus Endoscopic Thyroidectomy for Thyroid Cancers: A Multi-Institutional Analysis of Early Postoperative
Journal of Oncology Volume 2012, Article ID 734541, 9 pages doi:10.1155/2012/734541 Clinical Study Robotic versus Endoscopic Thyroidectomy for Thyroid Cancers: A Multi-Institutional Analysis of Early Postoperative
Jandee Lee, In Soon Kwon, Eun Hee Bae, and Woong Youn Chung
 ORIGINAL ARTICLE Endocrine Care Comparative Analysis of Oncological Outcomes and Quality of Life After Robotic versus Conventional Open Thyroidectomy With Modified Radical Neck Dissection in Patients With
ORIGINAL ARTICLE Endocrine Care Comparative Analysis of Oncological Outcomes and Quality of Life After Robotic versus Conventional Open Thyroidectomy With Modified Radical Neck Dissection in Patients With
Can Robotic Thyroidectomy Be Performed Safely in Thyroid Carcinoma Patients?
 Review Article Endocrinol Metab 214;29:226-232 http://dx.doi.org/1.383/enm.214.29.3.226 pissn 293-596X eissn 293-5978 Can Robotic Thyroidectomy Be Performed Safely in Thyroid Carcinoma Patients? Young
Review Article Endocrinol Metab 214;29:226-232 http://dx.doi.org/1.383/enm.214.29.3.226 pissn 293-596X eissn 293-5978 Can Robotic Thyroidectomy Be Performed Safely in Thyroid Carcinoma Patients? Young
Endoscopic Thyroidectomy Via the Cervico-axillary Approach for Thyroid Cancer: Initial Experience in a Single Institute
 ORIGINAL ARTICLE ISSN 1598-1703 (Print) ISSN 2287-6782 (Online) Korean J Endocr Surg 2017;17:19-24 https://doi.org/10.16956/kaes.2017.17.1.19 The Korean Journal of Endocrine Surgery Endoscopic Thyroidectomy
ORIGINAL ARTICLE ISSN 1598-1703 (Print) ISSN 2287-6782 (Online) Korean J Endocr Surg 2017;17:19-24 https://doi.org/10.16956/kaes.2017.17.1.19 The Korean Journal of Endocrine Surgery Endoscopic Thyroidectomy
Persistent & Recurrent Differentiated Thyroid Cancer
 Persistent & Recurrent Differentiated Thyroid Cancer Electron Kebebew University of California, San Francisco Department of Surgery Objectives Risk factors for persistent & recurrent disease Causes of
Persistent & Recurrent Differentiated Thyroid Cancer Electron Kebebew University of California, San Francisco Department of Surgery Objectives Risk factors for persistent & recurrent disease Causes of
A comparison of surgical outcomes between endoscopic and robotically assisted thyroidectomy: the authors initial experience
 Surg Endosc (2011) 25:1617 1623 DOI 10.1007/s00464-010-1450-y A comparison of surgical outcomes between endoscopic and robotically assisted thyroidectomy: the authors initial experience Brian Hung-Hin
Surg Endosc (2011) 25:1617 1623 DOI 10.1007/s00464-010-1450-y A comparison of surgical outcomes between endoscopic and robotically assisted thyroidectomy: the authors initial experience Brian Hung-Hin
4/22/2010. Hakan Korkmaz, MD Assoc. Prof. of Otolaryngology Ankara Dıșkapı Training Hospital-Turkey.
 Management of Differentiated Thyroid Cancer: Head Neck Surgeon Perspective Hakan Korkmaz, MD Assoc. Prof. of Otolaryngology Ankara Dıșkapı Training Hospital-Turkey Thyroid gland Small endocrine gland:
Management of Differentiated Thyroid Cancer: Head Neck Surgeon Perspective Hakan Korkmaz, MD Assoc. Prof. of Otolaryngology Ankara Dıșkapı Training Hospital-Turkey Thyroid gland Small endocrine gland:
THYROID CANCER IN CHILDREN. Humberto Lugo-Vicente MD FACS FAAP Professor Pediatric Surgery UPR School of Medicine
 THYROID CANCER IN CHILDREN Humberto Lugo-Vicente MD FACS FAAP Professor Pediatric Surgery UPR School of Medicine Thyroid nodules Rare Female predominance 4-fold as likely to be malignant Hx Radiation exposure?
THYROID CANCER IN CHILDREN Humberto Lugo-Vicente MD FACS FAAP Professor Pediatric Surgery UPR School of Medicine Thyroid nodules Rare Female predominance 4-fold as likely to be malignant Hx Radiation exposure?
Reoperative central neck surgery
 Reoperative central neck surgery R. Pandev, I. Tersiev, M. Belitova, A. Kouizi, D. Damyanov University Clinic of Surgery, Section Endocrine Surgery University Hospital Queen Johanna ISUL Medical University
Reoperative central neck surgery R. Pandev, I. Tersiev, M. Belitova, A. Kouizi, D. Damyanov University Clinic of Surgery, Section Endocrine Surgery University Hospital Queen Johanna ISUL Medical University
New technologies in Endocrine Surgery
 New technologies in Endocrine Surgery 1. Nerve monitoring 2. New technologies in Endocrine Surgery Jessica E. Gosnell MD Post graduate course in General Surgery March 28, 2012 1 2 Recurrent laryngeal nerve
New technologies in Endocrine Surgery 1. Nerve monitoring 2. New technologies in Endocrine Surgery Jessica E. Gosnell MD Post graduate course in General Surgery March 28, 2012 1 2 Recurrent laryngeal nerve
Coexistence of parathyroid adenoma and papillary thyroid carcinoma. Yong Sang Lee, Kee-Hyun Nam, Woong Youn Chung, Hang-Seok Chang, Cheong Soo Park
 J Korean Surg Soc 2011;81:316-320 http://dx.doi.org/10.4174/jkss.2011.81.5.316 ORIGINAL ARTICLE JKSS Journal of the Korean Surgical Society pissn 2233-7903 ㆍ eissn 2093-0488 Coexistence of parathyroid
J Korean Surg Soc 2011;81:316-320 http://dx.doi.org/10.4174/jkss.2011.81.5.316 ORIGINAL ARTICLE JKSS Journal of the Korean Surgical Society pissn 2233-7903 ㆍ eissn 2093-0488 Coexistence of parathyroid
Thyroid Nodule. Disclosure. Learning Objectives P A P A P A 3/18/2014. Nothing to disclose.
 Thyroid Nodule Evaluating the patient with a thyroid nodule and some management options. Miguel V. Valdez PA C Disclosure Nothing to disclose. Learning Objectives Examination of thyroid gland Options for
Thyroid Nodule Evaluating the patient with a thyroid nodule and some management options. Miguel V. Valdez PA C Disclosure Nothing to disclose. Learning Objectives Examination of thyroid gland Options for
A variation in recurrence patterns of papillary thyroid cancer with disease progression: A long-term follow-up study
 ORIGINAL ARTICLE A variation in recurrence patterns of papillary thyroid cancer with disease progression: A long-term follow-up study Joon-Hyop Lee, MD, Yoo Seung Chung, MD, PhD,* Young Don Lee, MD, PhD
ORIGINAL ARTICLE A variation in recurrence patterns of papillary thyroid cancer with disease progression: A long-term follow-up study Joon-Hyop Lee, MD, Yoo Seung Chung, MD, PhD,* Young Don Lee, MD, PhD
Minimally invasive thyroidectomy: a ten years experience
 Original Article Minimally invasive thyroidectomy: a ten years experience Paolo Del Rio, Lorenzo Viani, Chiara Montana Montana, Federico Cozzani, Mario Sianesi Unit of general Surgery and Organ Transplantation,
Original Article Minimally invasive thyroidectomy: a ten years experience Paolo Del Rio, Lorenzo Viani, Chiara Montana Montana, Federico Cozzani, Mario Sianesi Unit of general Surgery and Organ Transplantation,
Long-term Follow-up for Patients with Papillary Thyroid Carcinoma Treated as Benign Nodules
 Long-term Follow-up for Patients with Papillary Thyroid Carcinoma Treated as Benign Nodules YASUHIRO ITO, TAKUYA HIGASHIYAMA, YUUKI TAKAMURA, AKIHIRO MIYA, KAORU KOBAYASHI, FUMIO MATSUZUKA, KANJI KUMA
Long-term Follow-up for Patients with Papillary Thyroid Carcinoma Treated as Benign Nodules YASUHIRO ITO, TAKUYA HIGASHIYAMA, YUUKI TAKAMURA, AKIHIRO MIYA, KAORU KOBAYASHI, FUMIO MATSUZUKA, KANJI KUMA
How good are we at finding nodules? Thyroid Nodules Thyroid Cancer Epidemiology Initial management Long-term follow up Disease-free status
 New Perspectives in Thyroid Cancer Jennifer Sipos, MD Assistant Professor of Medicine Division of Endocrinology The Ohio State University Outline Thyroid Nodules Thyroid Cancer Epidemiology Initial management
New Perspectives in Thyroid Cancer Jennifer Sipos, MD Assistant Professor of Medicine Division of Endocrinology The Ohio State University Outline Thyroid Nodules Thyroid Cancer Epidemiology Initial management
Surgical Treatment for Papillary Thyroid Carcinoma in Japan: Differences from Other Countries
 REVIEW ARTICLE J Korean Thyroid Assoc Vol. 4, No. 2, November 2011 Surgical Treatment for Papillary Thyroid Carcinoma in Japan: Differences from Other Countries Yasuhiro Ito, MD and Akira Miyauchi, MD
REVIEW ARTICLE J Korean Thyroid Assoc Vol. 4, No. 2, November 2011 Surgical Treatment for Papillary Thyroid Carcinoma in Japan: Differences from Other Countries Yasuhiro Ito, MD and Akira Miyauchi, MD
Evaluation of thyroid isthmusectomy as a potential treatment for papillary thyroid carcinoma limited to the isthmus: A clinical study of 73 patients
 ORIGINAL ARTICLE Evaluation of thyroid isthmusectomy as a potential treatment for papillary thyroid carcinoma limited to the isthmus: A clinical study of 73 patients Jianbiao Wang, MM, 1 Haili Sun, BM,
ORIGINAL ARTICLE Evaluation of thyroid isthmusectomy as a potential treatment for papillary thyroid carcinoma limited to the isthmus: A clinical study of 73 patients Jianbiao Wang, MM, 1 Haili Sun, BM,
Gasless Endoscopic Thyroidectomy Using Trans-axillary Approach; Surgical Outcome of 581 Patients
 Endocrine Journal 2009, 56 (3), 361-369 Gasless Endoscopic Thyroidectomy Using Trans-axillary Approach; Surgical Outcome of 581 Patients Sa n g-wo o k Kang, Jo n g Ju Jeong, Ji-Su p Yun*, Ta e Yo n Sung,
Endocrine Journal 2009, 56 (3), 361-369 Gasless Endoscopic Thyroidectomy Using Trans-axillary Approach; Surgical Outcome of 581 Patients Sa n g-wo o k Kang, Jo n g Ju Jeong, Ji-Su p Yun*, Ta e Yo n Sung,
The current status of robotic transaxillary thyroidectomy in the United States: an experience from two centers
 Original Article The current status of robotic transaxillary thyroidectomy in the United States: an experience from two centers Nisar Zaidi 1, Despoina Daskalaki 2, Pablo Quadri 2, Alexis Okoh 3, Pier
Original Article The current status of robotic transaxillary thyroidectomy in the United States: an experience from two centers Nisar Zaidi 1, Despoina Daskalaki 2, Pablo Quadri 2, Alexis Okoh 3, Pier
Changing trends in the management of well-differentiated thyroid carcinoma in Korea
 2016, 63 (6), 515-521 Original Changing trends in the management of well-differentiated thyroid carcinoma in Korea Yong Sang Lee, Hang-Seok Chang and Cheong Soo Park Thyroid Cancer Center, Department of
2016, 63 (6), 515-521 Original Changing trends in the management of well-differentiated thyroid carcinoma in Korea Yong Sang Lee, Hang-Seok Chang and Cheong Soo Park Thyroid Cancer Center, Department of
Thyroid nodules 3/22/2011. Most thyroid nodules are benign. Thyroid nodules: differential diagnosis
 Most thyroid nodules are benign Thyroid nodules Postgraduate Course in General Surgery thyroid nodules occur in 77% of the world s population palpable thyroid nodules occur in about 5% of women and 1%
Most thyroid nodules are benign Thyroid nodules Postgraduate Course in General Surgery thyroid nodules occur in 77% of the world s population palpable thyroid nodules occur in about 5% of women and 1%
Ultrasound for Pre-operative Evaluation of Well Differentiated Thyroid Cancer
 Ultrasound for Pre-operative Evaluation of Well Differentiated Thyroid Cancer Its Not Just About the Nodes AACE Advances in Medical and Surgical Management of Thyroid Cancer - 2017 Robert A. Levine, MD,
Ultrasound for Pre-operative Evaluation of Well Differentiated Thyroid Cancer Its Not Just About the Nodes AACE Advances in Medical and Surgical Management of Thyroid Cancer - 2017 Robert A. Levine, MD,
Current Issues in Thyroid Cancer Surgery in 2017
 Current Issues in Thyroid Cancer Surgery in 2017 Dr. David Goldstein MD Msc FRCSC FACS Associate Professor, Department Otolaryngology Head & Neck Surgery, U of T Department of Surgical Oncology, Princess
Current Issues in Thyroid Cancer Surgery in 2017 Dr. David Goldstein MD Msc FRCSC FACS Associate Professor, Department Otolaryngology Head & Neck Surgery, U of T Department of Surgical Oncology, Princess
Brian Hung-Hin Lang, MS, FRACS 1,2 and Kai-Pun Wong, MBBS, FRCS 1. Department of Surgery, Queen Mary Hospital, Hong Kong SAR, China
 Ann Surg Oncol (2013) 20:646 652 DOI 10.1245/s10434-012-2613-y ORIGINAL ARTICLE ENDOCRINE TUMORS A Comparison of Surgical Morbidity and Scar Appearance Between Gasless, Transaxillary Endoscopic Thyroidectomy
Ann Surg Oncol (2013) 20:646 652 DOI 10.1245/s10434-012-2613-y ORIGINAL ARTICLE ENDOCRINE TUMORS A Comparison of Surgical Morbidity and Scar Appearance Between Gasless, Transaxillary Endoscopic Thyroidectomy
Prediction of ipsilateral and contralateral central lymph node metastasis in unilateral papillary thyroid carcinoma: a retrospective study
 Original Article Prediction of ipsilateral and contralateral central lymph node metastasis in unilateral papillary thyroid carcinoma: a retrospective study Qiang Chen, Xiu-He Zou, Tao Wei, Qiu-Shi Huang,
Original Article Prediction of ipsilateral and contralateral central lymph node metastasis in unilateral papillary thyroid carcinoma: a retrospective study Qiang Chen, Xiu-He Zou, Tao Wei, Qiu-Shi Huang,
Robotic retroauricular thyroidectomy: initial experience from India
 Review Article Robotic retroauricular thyroidectomy: initial experience from India Krishnakumar Thankappan 1, Surender Dabas 2, Mandar Deshpande 3 1 Department of Head and Neck surgery and Oncology, Amrita
Review Article Robotic retroauricular thyroidectomy: initial experience from India Krishnakumar Thankappan 1, Surender Dabas 2, Mandar Deshpande 3 1 Department of Head and Neck surgery and Oncology, Amrita
Management guideline for patients with differentiated thyroid cancer. Teeraporn Ratanaanekchai ENT, KKU 17 October 2007
 Management guideline for patients with differentiated thyroid Teeraporn Ratanaanekchai ENT, KKU 17 October 2007 Incidence (Srinagarind Hospital, 2005, both sex) Site (all) cases % 1. Liver 1178 27 2. Lung
Management guideline for patients with differentiated thyroid Teeraporn Ratanaanekchai ENT, KKU 17 October 2007 Incidence (Srinagarind Hospital, 2005, both sex) Site (all) cases % 1. Liver 1178 27 2. Lung
Gerard M. Doherty, MD
 Surgical Management of Differentiated Thyroid Cancer: Update on 2015 ATA Guidelines Gerard M. Doherty, MD Chair of Surgery Utley Professor of Surgery and Medicine Boston University Surgeon-in-Chief Boston
Surgical Management of Differentiated Thyroid Cancer: Update on 2015 ATA Guidelines Gerard M. Doherty, MD Chair of Surgery Utley Professor of Surgery and Medicine Boston University Surgeon-in-Chief Boston
- RET/PTC rearrangement: 20% papillary thyroid cancer - RET: medullary thyroid cancer
 Thyroid Cancer UpToDate: Introduction: Risk Factors: Biology: Symptoms: Diagnosis: 1. Lenvina is the first line therapy with powerful durable response and superior PFS in pts with RAI-refractory disease.
Thyroid Cancer UpToDate: Introduction: Risk Factors: Biology: Symptoms: Diagnosis: 1. Lenvina is the first line therapy with powerful durable response and superior PFS in pts with RAI-refractory disease.
Volume 2 Issue ISSN
 Volume 2 Issue 3 2012 ISSN 2250-0359 Correlation of fine needle aspiration and final histopathology in thyroid disease: a series of 702 patients managed in an endocrine surgical unit *Chandrasekaran Maharajan
Volume 2 Issue 3 2012 ISSN 2250-0359 Correlation of fine needle aspiration and final histopathology in thyroid disease: a series of 702 patients managed in an endocrine surgical unit *Chandrasekaran Maharajan
Thyroid Cancer: When to Treat? MEGAN R. HAYMART, MD
 Thyroid Cancer: When to Treat? MEGAN R. HAYMART, MD ASSOCIATE PROFESSOR OF MEDICINE UNIVERSITY OF MICHIGAN MICHIGAN AACE 2018 ANNUAL MEETING Thyroid Cancer: When Not to Treat? FOCUS WILL BE ON LOW-RISK
Thyroid Cancer: When to Treat? MEGAN R. HAYMART, MD ASSOCIATE PROFESSOR OF MEDICINE UNIVERSITY OF MICHIGAN MICHIGAN AACE 2018 ANNUAL MEETING Thyroid Cancer: When Not to Treat? FOCUS WILL BE ON LOW-RISK
Disclosures. Learning objectives. Case 1A. Autoimmune Thyroid Disease: Medical and Surgical Issues. I have nothing to disclose.
 Disclosures Autoimmune Thyroid Disease: Medical and Surgical Issues I have nothing to disclose. Chrysoula Dosiou, MD, MS Clinical Assistant Professor Division of Endocrinology Stanford University School
Disclosures Autoimmune Thyroid Disease: Medical and Surgical Issues I have nothing to disclose. Chrysoula Dosiou, MD, MS Clinical Assistant Professor Division of Endocrinology Stanford University School
Thyroid nodules - medical and surgical management. Endocrinology and Endocrine Surgery Manchester Royal Infirmary
 Thyroid nodules - medical and surgical management JRE Davis NR Parrott Endocrinology and Endocrine Surgery Manchester Royal Infirmary Thyroid nodules - prevalence Thyroid nodules common, increase with
Thyroid nodules - medical and surgical management JRE Davis NR Parrott Endocrinology and Endocrine Surgery Manchester Royal Infirmary Thyroid nodules - prevalence Thyroid nodules common, increase with
Frequency and pattern of central lymph node metastasis in papillary carcinoma of the thyroid isthmus
 ORIGINAL ARTICLE Frequency and pattern of central lymph node metastasis in papillary carcinoma of the thyroid isthmus Chang Myeon Song, MD, 1 Dong Won Lee, MD, 1 Yong Bae Ji, MD, PhD, 1 Jin Hyeok Jeong,
ORIGINAL ARTICLE Frequency and pattern of central lymph node metastasis in papillary carcinoma of the thyroid isthmus Chang Myeon Song, MD, 1 Dong Won Lee, MD, 1 Yong Bae Ji, MD, PhD, 1 Jin Hyeok Jeong,
Robotic Thyroidectomy: Pros and Cons of Various Surgical Approaches
 REVIEW ARTICLE ISSN 1598-1703 (Print) ISSN 2287-6782 (Online) Korean J Endocr Surg 2015;15:73-78 http://dx.doi.org/10.16956/kaes.2015.15.4.73 The Korean Journal of Endocrine Surgery Robotic Thyroidectomy:
REVIEW ARTICLE ISSN 1598-1703 (Print) ISSN 2287-6782 (Online) Korean J Endocr Surg 2015;15:73-78 http://dx.doi.org/10.16956/kaes.2015.15.4.73 The Korean Journal of Endocrine Surgery Robotic Thyroidectomy:
2015 American Thyroid Association Thyroid Nodule and Cancer Guidelines
 2015 American Thyroid Association Thyroid Nodule and Cancer Guidelines Angela M. Leung, MD, MSc, ECNU November 5, 2016 Outline Workup of nontoxic thyroid nodule(s) Ultrasound FNAB Management of FNAB results
2015 American Thyroid Association Thyroid Nodule and Cancer Guidelines Angela M. Leung, MD, MSc, ECNU November 5, 2016 Outline Workup of nontoxic thyroid nodule(s) Ultrasound FNAB Management of FNAB results
Disclosures Nodal Management in Differentiated Thyroid Carcinoma
 Disclosures Nodal Management in Differentiated Thyroid Carcinoma Nothing to disclose Jonathan George, MD, MPH Assistant Professor UCSF Head and Neck Oncologic & Endocrine Surgery Objectives Overview Describe
Disclosures Nodal Management in Differentiated Thyroid Carcinoma Nothing to disclose Jonathan George, MD, MPH Assistant Professor UCSF Head and Neck Oncologic & Endocrine Surgery Objectives Overview Describe
Differentiated Thyroid Cancer: Initial Management
 Page 1 ATA HOME GIVE ONLINE ABOUT THE ATA JOIN THE ATA MEMBER SIGN-IN INFORMATION FOR PATIENTS FIND A THYROID SPECIALIST Home Management Guidelines for Patients with Thyroid Nodules and Differentiated
Page 1 ATA HOME GIVE ONLINE ABOUT THE ATA JOIN THE ATA MEMBER SIGN-IN INFORMATION FOR PATIENTS FIND A THYROID SPECIALIST Home Management Guidelines for Patients with Thyroid Nodules and Differentiated
Thyroid Cancer. Diagnosis? Learn why da Vinci Surgery may be your best treatment option
 Thyroid Cancer Diagnosis? Learn why da Vinci Surgery may be your best treatment option The Treatment: Thyroid Surgery Your doctor will discuss treatment options with you in detail. Generally, treatments
Thyroid Cancer Diagnosis? Learn why da Vinci Surgery may be your best treatment option The Treatment: Thyroid Surgery Your doctor will discuss treatment options with you in detail. Generally, treatments
Pre-operative Ultrasound of Lymph Nodes in Thyroid Cancer
 Pre-operative Ultrasound of Lymph Nodes in Thyroid Cancer AACE - Advances in Medical and Surgical Management of Thyroid Cancer - 2018 Robert A. Levine, MD, FACE, ECNU Thyroid Center of New Hampshire Geisel
Pre-operative Ultrasound of Lymph Nodes in Thyroid Cancer AACE - Advances in Medical and Surgical Management of Thyroid Cancer - 2018 Robert A. Levine, MD, FACE, ECNU Thyroid Center of New Hampshire Geisel
Video-assisted thyroidectomy for papillary thyroid carcinoma
 Surg Endosc (2003) 17: 1604 1608 DOI: 10.1007/s00464-002-9220-0 Ó Springer-Verlag York Inc. 2003 Video-assisted thyroidectomy for papillary thyroid carcinoma R. Bellantone, 1 C. P. Lombardi, 1 M. Raffaelli,
Surg Endosc (2003) 17: 1604 1608 DOI: 10.1007/s00464-002-9220-0 Ó Springer-Verlag York Inc. 2003 Video-assisted thyroidectomy for papillary thyroid carcinoma R. Bellantone, 1 C. P. Lombardi, 1 M. Raffaelli,
Four Cases of Malignant Pleural Effusion in Patients with Papillary Thyroid Carcinoma
 Endocrinol Metab 26(4):330-334, December 2011 CASE REPORT Four Cases of Malignant Pleural Effusion in Patients with Papillary Thyroid Carcinoma Min Ji Jeon, Ji Hye Yim, Eui Young Kim, Won Gu Kim, Tae Yong
Endocrinol Metab 26(4):330-334, December 2011 CASE REPORT Four Cases of Malignant Pleural Effusion in Patients with Papillary Thyroid Carcinoma Min Ji Jeon, Ji Hye Yim, Eui Young Kim, Won Gu Kim, Tae Yong
Thyroid nodules. Most thyroid nodules are benign
 Thyroid nodules Postgraduate Course in General Surgery Jessica E. Gosnell MD Assistant Professor March 22, 2011 Most thyroid nodules are benign thyroid nodules occur in 77% of the world s population palpable
Thyroid nodules Postgraduate Course in General Surgery Jessica E. Gosnell MD Assistant Professor March 22, 2011 Most thyroid nodules are benign thyroid nodules occur in 77% of the world s population palpable
Anil D Rao Consultant Dept of Surgery Khoo Teck Puat Hospital
 Thyroid Surgery Without a Neck Scar Challenging The Traditional Approach Anil D Rao Consultant Dept of Surgery Khoo Teck Puat Hospital BACKGROUND Open approach is well established. Traditional Safe Applicable
Thyroid Surgery Without a Neck Scar Challenging The Traditional Approach Anil D Rao Consultant Dept of Surgery Khoo Teck Puat Hospital BACKGROUND Open approach is well established. Traditional Safe Applicable
Thyroid and Parathyroid Surgery
 Med 5 Surgery Refresher Course 2013 2014 Thyroid and Parathyroid Surgery Dr Shirley Liu Resident Specialist Honorary Clinical Assistant Professor Team 2 Surgery Prince of Wales Hospital Case scenario:
Med 5 Surgery Refresher Course 2013 2014 Thyroid and Parathyroid Surgery Dr Shirley Liu Resident Specialist Honorary Clinical Assistant Professor Team 2 Surgery Prince of Wales Hospital Case scenario:
10/24/2008. Surgery for Well-differentiated Thyroid Carcinoma- The Primary
 Surgery for Well-differentiated Thyroid Carcinoma- The Primary Head and Neck Endocrine Surgery Department of Otolaryngology-Head and Neck Surgery, UCSF October 24-25, 2008 Robert A. Sofferman, MD Professor
Surgery for Well-differentiated Thyroid Carcinoma- The Primary Head and Neck Endocrine Surgery Department of Otolaryngology-Head and Neck Surgery, UCSF October 24-25, 2008 Robert A. Sofferman, MD Professor
Thyroid INTRODUCTION ANATOMY SUMMARY OF CHANGES
 AJC 7/14/06 1:19 PM Page 67 Thyroid C73.9 Thyroid gland SUMMARY OF CHANGES Tumor staging (T) has been revised and the categories redefined. T4 is now divided into T4a and T4b. Nodal staging (N) has been
AJC 7/14/06 1:19 PM Page 67 Thyroid C73.9 Thyroid gland SUMMARY OF CHANGES Tumor staging (T) has been revised and the categories redefined. T4 is now divided into T4a and T4b. Nodal staging (N) has been
Prophylactic Central Compartment Neck Dissection(CCND) for Papillary Thyroid Cancer: Con
 Prophylactic Central Compartment Neck Dissection(CCND) for Papillary Thyroid Cancer: Con Christopher R. McHenry, M.D. Vice Chairman Department of Surgery MetroHealth Medical Center Professor of Surgery
Prophylactic Central Compartment Neck Dissection(CCND) for Papillary Thyroid Cancer: Con Christopher R. McHenry, M.D. Vice Chairman Department of Surgery MetroHealth Medical Center Professor of Surgery
Clinical Study Comparison of Conventional Open Thyroidectomy and Endoscopic Thyroidectomy via Breast Approach for Papillary Thyroid Carcinoma
 International Endocrinology Volume 2015, Article ID 239610, 5 pages http://dx.doi.org/10.1155/2015/239610 Clinical Study Comparison of Conventional Open Thyroidectomy and Endoscopic Thyroidectomy via Breast
International Endocrinology Volume 2015, Article ID 239610, 5 pages http://dx.doi.org/10.1155/2015/239610 Clinical Study Comparison of Conventional Open Thyroidectomy and Endoscopic Thyroidectomy via Breast
Operative bed recurrence of thyroid cancer: utility of a preoperative needle localization technique
 Original Article Operative bed recurrence of thyroid cancer: utility of a preoperative needle localization technique Oliver S. Eng 1, Scott B. Grant 2, Jason Weissler 3, Mitchell Simon 4, Sudipta Roychowdhury
Original Article Operative bed recurrence of thyroid cancer: utility of a preoperative needle localization technique Oliver S. Eng 1, Scott B. Grant 2, Jason Weissler 3, Mitchell Simon 4, Sudipta Roychowdhury
5/18/2013. Most thyroid nodules are benign. Thyroid nodules: new techniques in evaluation
 Most thyroid nodules are benign Thyroid nodules: new techniques in evaluation Incidence Etiology Risk factors Diagnosis Gene classification system Treatment Postgraduate Course in General Surgery Jessica
Most thyroid nodules are benign Thyroid nodules: new techniques in evaluation Incidence Etiology Risk factors Diagnosis Gene classification system Treatment Postgraduate Course in General Surgery Jessica
The clinical prognosis of patients with cn0 papillary thyroid microcarcinoma by central neck dissection
 Zhang et al. World Journal of Surgical Oncology (2015) 13:138 DOI 10.1186/s12957-015-0553-2 WORLD JOURNAL OF SURGICAL ONCOLOGY RESEARCH Open Access The clinical prognosis of patients with cn0 papillary
Zhang et al. World Journal of Surgical Oncology (2015) 13:138 DOI 10.1186/s12957-015-0553-2 WORLD JOURNAL OF SURGICAL ONCOLOGY RESEARCH Open Access The clinical prognosis of patients with cn0 papillary
Introduction. Materials and methods Y-N XU 1,2, J-D WANG 1,2
 1 di 5 11/04/2016 17:54 G Chir Vol. 31 - n. 5 - pp. 205-209 Maggio 2010 Y-N XU 1,2, J-D WANG 1,2 Introduction The World Health Organization (WHO) defined papillary thyroid microcarcinomas (PTMC) as tumors
1 di 5 11/04/2016 17:54 G Chir Vol. 31 - n. 5 - pp. 205-209 Maggio 2010 Y-N XU 1,2, J-D WANG 1,2 Introduction The World Health Organization (WHO) defined papillary thyroid microcarcinomas (PTMC) as tumors
The role of prophylactic central compartment lymph node dissection in differentiated thyroid carcinoma
 Original Research Article The role of prophylactic central compartment lymph node dissection in differentiated thyroid carcinoma Nived Rao 1, M. Muralidhar 2*, M. Srinivasulu 3 1Senior Resident in Surgical
Original Research Article The role of prophylactic central compartment lymph node dissection in differentiated thyroid carcinoma Nived Rao 1, M. Muralidhar 2*, M. Srinivasulu 3 1Senior Resident in Surgical
Index. radiologic.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A ACC. See Adrenal cortical carcinoma. Acromegaly and the pituitary gland, 551 Acute suppurative thyroiditis, 405, 406 Addison, Thomas and
Index Note: Page numbers of article titles are in boldface type. A ACC. See Adrenal cortical carcinoma. Acromegaly and the pituitary gland, 551 Acute suppurative thyroiditis, 405, 406 Addison, Thomas and
The International Federation of Head and Neck Oncologic Societies. Current Concepts in Head and Neck Surgery and Oncology
 The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology www.ifhnos.net The International Federation of Head and Neck Oncologic Societies
The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology www.ifhnos.net The International Federation of Head and Neck Oncologic Societies
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons
 General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: ENDOCRINE 5-May-2013 DEVELOPED BY: Jonathan Serpell
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: ENDOCRINE 5-May-2013 DEVELOPED BY: Jonathan Serpell
LYMPHATIC DRAINAGE IN THE HEAD & NECK
 LYMPHATIC DRAINAGE IN THE HEAD & NECK Like other parts of the body, the head and neck contains lymph nodes (commonly called glands). Which form part of the overall Lymphatic Drainage system of the body.
LYMPHATIC DRAINAGE IN THE HEAD & NECK Like other parts of the body, the head and neck contains lymph nodes (commonly called glands). Which form part of the overall Lymphatic Drainage system of the body.
PEDIATRIC Ariel Katz MD
 PEDIATRIC Ariel Katz MD Dept. Otolaryngology Head &Neck Surgery Wolfson Medical Center Holon, Israel OBJECTIVES Overview/Background Epidemiology/Etiology Intro to Guidelines Workup Treatment Follow-Up
PEDIATRIC Ariel Katz MD Dept. Otolaryngology Head &Neck Surgery Wolfson Medical Center Holon, Israel OBJECTIVES Overview/Background Epidemiology/Etiology Intro to Guidelines Workup Treatment Follow-Up
42 yr old male with h/o Graves disease and prior I 131 treatment presents with hyperthyroidism and undetectable TSH. 2 hr uptake 20%, 24 hr uptake 50%
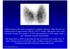 Pinhole images of the neck are acquired in multiple projections, 24hrs after the oral administration of approximately 200 µci of I123. Usually, 24hr uptake value if also calculated (normal 24 hr uptake
Pinhole images of the neck are acquired in multiple projections, 24hrs after the oral administration of approximately 200 µci of I123. Usually, 24hr uptake value if also calculated (normal 24 hr uptake
Differentiated Thyroid Carcinoma
 Differentiated Thyroid Carcinoma The GOOD cancer? Jennifer Sipos, MD Associate Professor of Medicine Director, Benign Thyroid Program Division of Endocrinology, Diabetes and Metabolism The Ohio State University
Differentiated Thyroid Carcinoma The GOOD cancer? Jennifer Sipos, MD Associate Professor of Medicine Director, Benign Thyroid Program Division of Endocrinology, Diabetes and Metabolism The Ohio State University
Thyroid Surgery: Lobectomy, total thyroidectomy, LN biopsies or only watchful waiting?
 Thyroid Surgery: Lobectomy, total thyroidectomy, LN biopsies or only watchful waiting? Jacob Moalem, MD, FACS Associate Professor Endocrine Surgery and Endocrinology URMC Agenda 1. When is lobectomy alone
Thyroid Surgery: Lobectomy, total thyroidectomy, LN biopsies or only watchful waiting? Jacob Moalem, MD, FACS Associate Professor Endocrine Surgery and Endocrinology URMC Agenda 1. When is lobectomy alone
Citation Auris, nasus, larynx (2011), 38(3):
 TitleManagement of metastasis to the thy Author(s) Ishikawa, Masaaki; Hirano, Shigeru; Citation Auris, nasus, larynx (2011), 38(3): Issue Date 2011-06 URL http://hdl.handle.net/2433/139807 Right 2010 Elsevier
TitleManagement of metastasis to the thy Author(s) Ishikawa, Masaaki; Hirano, Shigeru; Citation Auris, nasus, larynx (2011), 38(3): Issue Date 2011-06 URL http://hdl.handle.net/2433/139807 Right 2010 Elsevier
Management of Recurrent Thyroid Cancer
 Management of Recurrent Thyroid Cancer Eric Genden, MD, MHA Isidore Professor and Chairman Department of Otolaryngology- Head and Neck Surgery Senior Associate Dean for Clinical Affairs The Icahn School
Management of Recurrent Thyroid Cancer Eric Genden, MD, MHA Isidore Professor and Chairman Department of Otolaryngology- Head and Neck Surgery Senior Associate Dean for Clinical Affairs The Icahn School
Dynamic Risk Stratification:
 Dynamic Risk Stratification: Using Risk Estimates to Guide Initial Management R Michael Tuttle, MD Clinical Director, Endocrinology Service Memorial Sloan Kettering Cancer Center Professor of Medicine
Dynamic Risk Stratification: Using Risk Estimates to Guide Initial Management R Michael Tuttle, MD Clinical Director, Endocrinology Service Memorial Sloan Kettering Cancer Center Professor of Medicine
CAP Cancer Protocol and ecc Summary of Changes for August 2014 Thyroid Agile Release
 CAP Cancer Protocol and ecc Summary of Changes for August 2014 Thyroid Agile Release 2 REVISION HISTORY Date Author / Editor Comments 5/19/2014 Jaleh Mirza Created the document 8/12/2014 Samantha Spencer/Jaleh
CAP Cancer Protocol and ecc Summary of Changes for August 2014 Thyroid Agile Release 2 REVISION HISTORY Date Author / Editor Comments 5/19/2014 Jaleh Mirza Created the document 8/12/2014 Samantha Spencer/Jaleh
Avi Khafif, MD, Rami Ben-Yosef, MD, Avrum Abergel, MD, Ada Kesler, MD, Roee Landsberg, MD, Dan M. Fliss, MD
 ORIGINAL ARTICLE ELECTIVE PARATRACHEAL NECK DISSECTION FOR LATERAL METASTASES FROM PAPILLARY CARCINOMA OF THE THYROID: IS IT INDICATED? Avi Khafif, MD, Rami Ben-Yosef, MD, Avrum Abergel, MD, Ada Kesler,
ORIGINAL ARTICLE ELECTIVE PARATRACHEAL NECK DISSECTION FOR LATERAL METASTASES FROM PAPILLARY CARCINOMA OF THE THYROID: IS IT INDICATED? Avi Khafif, MD, Rami Ben-Yosef, MD, Avrum Abergel, MD, Ada Kesler,
Preoperative Evaluation
 Preoperative Evaluation Lateral compartment lymph nodes are easier to detect and are amenable to FNA Central compartment lymph nodes are much more difficult to detect and FNA (Tg washout testing is compromised)
Preoperative Evaluation Lateral compartment lymph nodes are easier to detect and are amenable to FNA Central compartment lymph nodes are much more difficult to detect and FNA (Tg washout testing is compromised)
Case Papillary thyroid carcinoma(ptc):local recurrence post thyroidectomy
 Case 16070 Papillary thyroid carcinoma(ptc):local recurrence post thyroidectomy Dr Alka Ashmita Singhal, Dr Deepak Sarin 1, Dr Monika Aggarwal, Dr Haimanti Sarin2 Medanta The Medicity Hospital, Medanta
Case 16070 Papillary thyroid carcinoma(ptc):local recurrence post thyroidectomy Dr Alka Ashmita Singhal, Dr Deepak Sarin 1, Dr Monika Aggarwal, Dr Haimanti Sarin2 Medanta The Medicity Hospital, Medanta
Oral Presentation V. Surgical Outcome of Atypia of Undetermined Significance and Follicular Lesion of Undetermined Significance in Thyroid Nodule
 Oral Presentation V The Prevalence, Clinicopathologic Features, and Surgical Outcomes according to the Extent of Thyroidectomy in Differentiated Thyroid Cancer > 1 and < 4 cm 1 Jung Bum Choi, 2 SeulGi
Oral Presentation V The Prevalence, Clinicopathologic Features, and Surgical Outcomes according to the Extent of Thyroidectomy in Differentiated Thyroid Cancer > 1 and < 4 cm 1 Jung Bum Choi, 2 SeulGi
 To the Patient and Family This booklet has been written for people who have received a diagnosis of thyroid cancer or who are being tested for this illness. If you have questions that are not answered
To the Patient and Family This booklet has been written for people who have received a diagnosis of thyroid cancer or who are being tested for this illness. If you have questions that are not answered
Dr J K Jekel Dept. Surgery University of Pretoria
 Dr J K Jekel Dept. Surgery University of Pretoria No Maybe ( T`s and C`s apply ) 1. Total thyroidectomy 2. Neck dissection only if nodes are involved 3. Ablative dose or doses of Radioactive Iodine 4.
Dr J K Jekel Dept. Surgery University of Pretoria No Maybe ( T`s and C`s apply ) 1. Total thyroidectomy 2. Neck dissection only if nodes are involved 3. Ablative dose or doses of Radioactive Iodine 4.
Risk Adapted Follow-Up
 Risk Adapted Follow-Up Individualizing Follow- Up Strategies R Michael Tuttle, MD Clinical Director, Endocrinology Service Memorial Sloan Kettering Cancer Center Professor of Medicine Weill Medical College
Risk Adapted Follow-Up Individualizing Follow- Up Strategies R Michael Tuttle, MD Clinical Director, Endocrinology Service Memorial Sloan Kettering Cancer Center Professor of Medicine Weill Medical College
Fuqiang Li, Yijun Wu, Liang Chen, Liang Hu, Xiaosun Liu. Original Article
 Original Article Page 1 of 11 Evaluation of clinical risk factors for predicting insidious right central and posterior right recurrent laryngeal nerve lymph node metastasis in papillary thyroid microcarcinoma
Original Article Page 1 of 11 Evaluation of clinical risk factors for predicting insidious right central and posterior right recurrent laryngeal nerve lymph node metastasis in papillary thyroid microcarcinoma
Treatment of Cervical Lymph Node Metastases Differentiated Thyroid Cancer
 Treatment of Cervical Lymph Node Metastases Differentiated Thyroid Cancer Well Differentiated Thyroid Cancer Natural History and Prognosis EORTC AGES AMES MACIS QuickTime and a TIFF (LZW) decompressor
Treatment of Cervical Lymph Node Metastases Differentiated Thyroid Cancer Well Differentiated Thyroid Cancer Natural History and Prognosis EORTC AGES AMES MACIS QuickTime and a TIFF (LZW) decompressor
Review Article Thyroidectomy and Lymph Node Dissection in Papillary Thyroid Carcinoma
 SAGE-Hindawi Access to Research Thyroid Research Volume 2011, Article ID 634170, 6 pages doi:10.4061/2011/634170 Review Article Thyroidectomy and Lymph Node Dissection in Papillary Thyroid Carcinoma Yasuhiro
SAGE-Hindawi Access to Research Thyroid Research Volume 2011, Article ID 634170, 6 pages doi:10.4061/2011/634170 Review Article Thyroidectomy and Lymph Node Dissection in Papillary Thyroid Carcinoma Yasuhiro
ORIGINAL ARTICLE. Incidental Parathyroidectomy During Thyroid Surgery Does Not Cause Transient Symptomatic Hypocalcemia
 ORIGINAL ARTICLE Incidental Parathyroidectomy During Thyroid Surgery Does Not Cause Transient Symptomatic Hypocalcemia Aaron R. Sasson, MD; James F. Pingpank, Jr, MD; R. Wesley Wetherington, MD; Alexandra
ORIGINAL ARTICLE Incidental Parathyroidectomy During Thyroid Surgery Does Not Cause Transient Symptomatic Hypocalcemia Aaron R. Sasson, MD; James F. Pingpank, Jr, MD; R. Wesley Wetherington, MD; Alexandra
Surgery for Recurrent Thyroid cancer: Considerations and limitations
 Surgery for Recurrent Thyroid cancer: Considerations and limitations 2016 Thyroid Master Class February 13, 2016 Ara A. Chalian MD, FACS Surgical Patient Safety Officer University Of Pennsylvania Health
Surgery for Recurrent Thyroid cancer: Considerations and limitations 2016 Thyroid Master Class February 13, 2016 Ara A. Chalian MD, FACS Surgical Patient Safety Officer University Of Pennsylvania Health
Papillary Thyroid Microcarcinoma Presenting as Horner s Syndrome: A Novel Clinical Presentation
 Case Report American Journal of Cancer Case Reports http://ivyunion.org/index.php/ajccr/ Page 1 of 6 Papillary Thyroid Microcarcinoma Presenting as Horner s Syndrome: A Novel Clinical Presentation Ammara
Case Report American Journal of Cancer Case Reports http://ivyunion.org/index.php/ajccr/ Page 1 of 6 Papillary Thyroid Microcarcinoma Presenting as Horner s Syndrome: A Novel Clinical Presentation Ammara
Distant and Lymph Node Metastases of Thyroid Nodules with No Pathological Evidence of Malignancy: A Limitation of Pathological Examination
 Endocrine Journal 2008, 55 (5), 889 894 Distant and Lymph Node Metastases of Thyroid Nodules with No Pathological Evidence of Malignancy: A Limitation of Pathological Examination YASUHIRO ITO, TOMONORI
Endocrine Journal 2008, 55 (5), 889 894 Distant and Lymph Node Metastases of Thyroid Nodules with No Pathological Evidence of Malignancy: A Limitation of Pathological Examination YASUHIRO ITO, TOMONORI
Comparison of indocyanine green fluorescence and parathyroid autofluorescence imaging in the identification of parathyroid glands during thyroidectomy
 Original Article Comparison of indocyanine green fluorescence and parathyroid autofluorescence imaging in the identification of parathyroid glands during thyroidectomy Bora Kahramangil, Eren Berber Department
Original Article Comparison of indocyanine green fluorescence and parathyroid autofluorescence imaging in the identification of parathyroid glands during thyroidectomy Bora Kahramangil, Eren Berber Department
원격전이가최초증상으로발현된분화갑상선암. Differentiated Thyroid Carcinoma Presenting Distant Metastses as a Initial Sign
 원격전이가최초증상으로발현된분화갑상선암 Differentiated Thyroid Carcinoma Presenting Distant Metastses as a Initial Sign Jandee Lee, M.D., Kee-Hyun Nam, M.D., Chi-Young Lim, M.D., Woong Youn Chung, M.D. and Cheong Soo Park,
원격전이가최초증상으로발현된분화갑상선암 Differentiated Thyroid Carcinoma Presenting Distant Metastses as a Initial Sign Jandee Lee, M.D., Kee-Hyun Nam, M.D., Chi-Young Lim, M.D., Woong Youn Chung, M.D. and Cheong Soo Park,
Thyroid Nodules. Dr. HAKIMI, SpAK Dr. MELDA DELIANA, SpAK Dr. SISKA MAYASARI LUBIS, SpA
 Thyroid Nodules ENDOCRINOLOGY DIVISION ENDOCRINOLOGY DIVISION Dr. HAKIMI, SpAK Dr. MELDA DELIANA, SpAK Dr. SISKA MAYASARI LUBIS, SpA Anatomical Considerations The Thyroid Nodule Congenital anomalies Thyroglossal
Thyroid Nodules ENDOCRINOLOGY DIVISION ENDOCRINOLOGY DIVISION Dr. HAKIMI, SpAK Dr. MELDA DELIANA, SpAK Dr. SISKA MAYASARI LUBIS, SpA Anatomical Considerations The Thyroid Nodule Congenital anomalies Thyroglossal
Robotic thyroidectomy versus endoscopic thyroidectomy: a meta-analysis
 Lin et al. World Journal of Surgical Oncology 2012, 10:239 WORLD JOURNAL OF SURGICAL ONCOLOGY REVIEW Open Access Robotic thyroidectomy versus endoscopic thyroidectomy: a meta-analysis Shuang Lin 1, Zhi-Heng
Lin et al. World Journal of Surgical Oncology 2012, 10:239 WORLD JOURNAL OF SURGICAL ONCOLOGY REVIEW Open Access Robotic thyroidectomy versus endoscopic thyroidectomy: a meta-analysis Shuang Lin 1, Zhi-Heng
Correlation analyses of thyroid-stimulating hormone and thyroid autoantibodies with differentiated thyroid cancer
 JBUON 2018; 23(5): 1467-1471 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Correlation analyses of thyroid-stimulating hormone and thyroid autoantibodies
JBUON 2018; 23(5): 1467-1471 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Correlation analyses of thyroid-stimulating hormone and thyroid autoantibodies
Gasless Transaxillary Robot-Assisted Neck Dissection: A Preclinical Feasibility Study in Four Cadavers
 Original Article http://dx.doi.org/10.3349/ymj.2012.53.1.193 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 53(1):193-197, 2012 Gasless Transaxillary Robot-Assisted Neck Dissection: A Preclinical Feasibility
Original Article http://dx.doi.org/10.3349/ymj.2012.53.1.193 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 53(1):193-197, 2012 Gasless Transaxillary Robot-Assisted Neck Dissection: A Preclinical Feasibility
Adjuvant therapy for thyroid cancer
 Carcinoma of the thyroid Adjuvant therapy for thyroid cancer John Hay Department of Radiation Oncology Vancouver Cancer Centre Department of Surgery UBC 1% of all new malignancies 0.5% in men 1.5% in women
Carcinoma of the thyroid Adjuvant therapy for thyroid cancer John Hay Department of Radiation Oncology Vancouver Cancer Centre Department of Surgery UBC 1% of all new malignancies 0.5% in men 1.5% in women
Perigastric Lymph Node Metastasis from Papillary Thyroid Carcinoma in a Patient with Early Gastric Cancer: The First Case Report
 J Gastric Cancer 2014;14(3):215-219 http://dx.doi.org/10.5230/jgc.2014.14.3.215 Perigastric Lymph Node Metastasis from Papillary Thyroid Carcinoma in a Patient with Early Gastric Cancer: The First Gui-Ae
J Gastric Cancer 2014;14(3):215-219 http://dx.doi.org/10.5230/jgc.2014.14.3.215 Perigastric Lymph Node Metastasis from Papillary Thyroid Carcinoma in a Patient with Early Gastric Cancer: The First Gui-Ae
WTC 2013 Panel Discussion: Minimal disease
 WTC 2013 Panel Discussion: Minimal disease Susan J. Mandel MD MPH Panelists Ken Ain Yasuhiro Ito Stephanie Lee Erich Sturgis Mark Urken Faculty/Presenter Disclosure Relationships with commercial interests
WTC 2013 Panel Discussion: Minimal disease Susan J. Mandel MD MPH Panelists Ken Ain Yasuhiro Ito Stephanie Lee Erich Sturgis Mark Urken Faculty/Presenter Disclosure Relationships with commercial interests
Title. CitationInternational Cancer Conference Journal, 4(1): Issue Date Doc URL. Rights. Type. File Information
 Title Lymph node metastasis in the suprasternal space from Homma, Akihiro; Hatakeyama, Hiromitsu; Mizumachi, Ta Author(s) Tomohiro; Fukuda, Satoshi CitationInternational Cancer Conference Journal, 4(1):
Title Lymph node metastasis in the suprasternal space from Homma, Akihiro; Hatakeyama, Hiromitsu; Mizumachi, Ta Author(s) Tomohiro; Fukuda, Satoshi CitationInternational Cancer Conference Journal, 4(1):
Preoperative information for thyroid surgery
 Review Article Preoperative information for thyroid surgery Vaninder K. Dhillon, Jonathon O. Russell, Mai G. Al Khadem, Ralph P. Tufano Division of Head and Neck Endocrine Surgery, Department of Otolaryngology-Head
Review Article Preoperative information for thyroid surgery Vaninder K. Dhillon, Jonathon O. Russell, Mai G. Al Khadem, Ralph P. Tufano Division of Head and Neck Endocrine Surgery, Department of Otolaryngology-Head
Management of Thyroid Nodules
 Management of Thyroid Nodules 38 y/o female with solid 1.5 cm right Thyroid nodule. TSH=0.68 Vincent J. Reid, MD., FACS Thyroid Cancer Incidence & Mortality 1974 to 2004 Overall Women Men Mortality 1 Cancer
Management of Thyroid Nodules 38 y/o female with solid 1.5 cm right Thyroid nodule. TSH=0.68 Vincent J. Reid, MD., FACS Thyroid Cancer Incidence & Mortality 1974 to 2004 Overall Women Men Mortality 1 Cancer
Papillary Thyroid Carcinoma with Retropharyngeal Node Metastasis Demonstrating Negative I-131 but Positive FDG Uptake on PET/CT
 CASE REPORT ISSN 1598-1703 (Print) ISSN 2287-6782 (Online) Korean J Endocr Surg 2016;16:18-23 http://dx.doi.org/10.16956/kaes.2016.16.1.18 The Korean Journal of Endocrine Surgery Papillary Thyroid Carcinoma
CASE REPORT ISSN 1598-1703 (Print) ISSN 2287-6782 (Online) Korean J Endocr Surg 2016;16:18-23 http://dx.doi.org/10.16956/kaes.2016.16.1.18 The Korean Journal of Endocrine Surgery Papillary Thyroid Carcinoma
Prognostic value of the 8 th tumor-node-metastasis classification for follicular carcinoma and poorly differentiated carcinoma of the thyroid in Japan
 2018, 65 (6), 621-627 ORIGINAL Prognostic value of the 8 th tumor-node-metastasis classification for follicular carcinoma and poorly differentiated carcinoma of the thyroid in Japan Yasuhiro Ito 1), Akira
2018, 65 (6), 621-627 ORIGINAL Prognostic value of the 8 th tumor-node-metastasis classification for follicular carcinoma and poorly differentiated carcinoma of the thyroid in Japan Yasuhiro Ito 1), Akira
What is Thyroid Cancer? Here are four types of thyroid cancer:
 What is Thyroid Cancer? Thyroid cancer is a group of malignant tumors that originate from the thyroid gland. The thyroid is a gland in the front of the neck. The thyroid gland absorbs iodine from the bloodstream
What is Thyroid Cancer? Thyroid cancer is a group of malignant tumors that originate from the thyroid gland. The thyroid is a gland in the front of the neck. The thyroid gland absorbs iodine from the bloodstream
B Berry, J. 25 see also suspensory ligament of Berry biopsy see fine-needle aspiration biopsy (FNAB); open wedge biopsy
 174 Index Index Page numbers in italics refer to illustrations A abscess 80, 137 adenoma 61 parathyroid 18, 18 19, 62, 84 differential diagnosis 84, 84, 85, 85 thyroid 63 follicular 62, 63, 64 macrofollicular
174 Index Index Page numbers in italics refer to illustrations A abscess 80, 137 adenoma 61 parathyroid 18, 18 19, 62, 84 differential diagnosis 84, 84, 85, 85 thyroid 63 follicular 62, 63, 64 macrofollicular
The International Federation of Head and Neck Oncologic Societies. Current Concepts in Head and Neck Surgery and Oncology
 The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology www.ifhnos.net The International Federation of Head and Neck Oncologic Societies
The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology www.ifhnos.net The International Federation of Head and Neck Oncologic Societies
Carcinoma of thyroid - clinical presentation and outcome
 Med. J. Malaysia Vol. 46 No. 3 September 1991 Carcinoma of thyroid - clinical presentation and outcome K. Sothy, MBBS M. Mafauzy, MBBS, MRCP, M.Med. Sci. W.B. Wan Mohamad, MD, MRCP B.E. Mustaffa, MBBS,
Med. J. Malaysia Vol. 46 No. 3 September 1991 Carcinoma of thyroid - clinical presentation and outcome K. Sothy, MBBS M. Mafauzy, MBBS, MRCP, M.Med. Sci. W.B. Wan Mohamad, MD, MRCP B.E. Mustaffa, MBBS,
Minimalistic Initial Therapy Options For Low Risk Papillary Thyroid Cancer
 Minimalistic Initial Therapy Options For Low Risk Papillary Thyroid Cancer An emphasis on proper patient selection R Michael Tuttle, MD Clinical Director, Endocrinology Service Memorial Sloan Kettering
Minimalistic Initial Therapy Options For Low Risk Papillary Thyroid Cancer An emphasis on proper patient selection R Michael Tuttle, MD Clinical Director, Endocrinology Service Memorial Sloan Kettering
