Department of Surgery, Eulji University College of Medicine, Seoul, Republic of Korea 2
|
|
|
- Frederick Bradley
- 5 years ago
- Views:
Transcription
1 Journal of Oncology Volume 2012, Article ID , 9 pages doi: /2012/ Clinical Study Robotic versus Endoscopic Thyroidectomy for Thyroid Cancers: A Multi-Institutional Analysis of Early Postoperative Outcomes and Surgical Learning Curves Jandee Lee, 1 Jong Ho Yun, 2 Un Jong Choi, 3 Sang-Wook Kang, 4 Jong Ju Jeong, 4 and Woong Youn Chung 4 1 Department of Surgery, Eulji University College of Medicine, Seoul, Republic of Korea 2 Department of Surgery, Asan Medical Center, Seoul, Republic of Korea 3 Department of Surgery, Wonkwang University School of Medicine, Iksan, Republic of Korea 4 Department of Surgery, Yonsei University College of Medicine, 134 Shinchon-dong, Seodaemun-ku, Seoul , Republic of Korea Correspondence should be addressed to Woong Youn Chung, ljd0906@naver.com Received 10 July 2012; Accepted 13 October 2012 Academic Editor: Thomas J. Fahey Copyright 2012 Jandee Lee et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Robotic thyroidectomy is an emerging technique with postoperative outcomes that are at least comparable to those of conventional endoscopic thyroidectomy, with some end-points appearing superior. Our multicenter series represents the largest comparison of robotic and endoscopic thyroidectomy to date, with results suggesting a comparable robot technology we used that could overcome some of the technical limitations associated with conventional endoscopic procedures, with reduced operation times and increased lymph node retrieval. Moreover, we found that the learning curve for robotic thyroidectomy was shorter than that for endoscopic thyroidectomy. 1. Introduction Endoscopic surgical techniques for thyroid cancer surgery can benefit patients by eliminating the anterior neck incision utilized in the traditional open approach. In addition to superior cosmetic results, endoscopic thyroidectomy can reduce postoperative pain and discomfort, shorten hospital stay, and enhance postoperative recovery [1 4]. Despite these advantages, however, endoscopic thyroidectomy has technical limitations, including the use of straight, rigid endoscopic instruments without articulation and a 2Dimensional (2D) view. The recent introduction of the da Vinci robot surgical system may be a major improvement in extracervical approaches for thyroid surgery and may be more ergonomic for surgeons than the endoscopic approach [5 7]. Among the advantages of the da Vinci robot are improved visualization via a 3D view, magnification, a tremor-filtering system, and instrument flexibility. To date, however, few studies have compared the postoperative outcomes in patients undergoing robotic and endoscopic thyroid surgery [8 11]. At present, endoscopic techniques are regarded as too time consuming and technically demanding to be adopted on a large-scale. The learning curve for endoscopic thyroidectomy performed by skilled endocrine surgeons has been estimated to be approximately 60 patients [12]. Use of a robot in thyroid surgery may shorten the learning curve, by providing a broader view of the surgical field and easier access to deep and narrow spaces through the use of multiarticulated instruments. We have previously reported the results of a multicenter study of learning curves for robotic thyroidectomy, based on a scientific analysis of a range of perioperative parameters [13]. However, there have been few comparisons of learning curves for robotic and endoscopic thyroidectomies. At present, the benefits of robotic thyroidectomy relative to endoscopic thyroidectomy, as determined by oncologic and functional outcomes, have not been fully clarified.
2 2 Journal of Oncology Moreover, there have been no multicenter studies comparing learning curves for these two methods. We therefore compared the operative outcomes and surgical learning curves of robotic and endoscopic thyroidectomy in patients with differentiated thyroid carcinoma (DTC). 2. Materials and Methods 2.1. Study Patients. This comparative, multicenter study evaluated patients who underwent robotic or endoscopic thyroidectomy at three large-volume centers with considerable experience in thyroid cancer surgery. Clinical and pathological data were collected retrospectively at each institution and entered into a dedicated database for analysis. Between November 2001 and June 2010, 2,612 patients with DTC underwent thyroidectomies at three centers, with all operations performed by four surgeons. Of these patients, 1796 underwent robotic thyroidectomy and 843 underwent conventional endoscopic thyroidectomy. At the time of surgery there was no intention to compare the two procedures. This study was approved by the institutional review boards (IRBs). At all institutions, perioperative workup included physical examination, high-resolution ultrasonography (US), and neck computed tomography (CT) and/or neck magnetic resonance imaging (MRI); preoperative staging US and neck CT (or MRI) was utilized to evaluate the degree of tumor invasion, including tumor size, extrathyroidal invasion, tumor infiltration of adjacent structures, and nodal involvement. Sonographic findings, such as loss of an echogenic thyroid capsule at the contact site of the primary tumor or contact with an adjacent thyroid capsule along more than 25% of the boundary of a tumor, were considered indicative of extrathyroidal extension [14]. In accordance with American Thyroid association (ATA) guidelines, a less than total thyroidectomy was performed in patients <45 years old, with a single lesion <1cm in size, no definitive evidence of extrathyroidal invasion or lymph node metastasis, no personal history of radiation therapy to the head or neck, and no first-degree family history of DTC [15]. A total thyroidectomy was performed in patients with multiple or bilateral lesions, or if definite extrathyroidal invasion was discovered during surgery. All patients underwent prophylactic ipsilateral pretracheal, prelaryngeal, and paraesophageal central compartment neck dissection (CCND) Postoperative Outcomes. Clinical parameters analyzed included patient characteristics, operative variables, extent of surgery, pathologic findings, and short-term operative outcomes. Pathologic examinations included assessments of disease tumor-node-metastasis (TNM) stage, number of lymph nodes harvested, and number of metastatic lymph nodes. We also assessed perioperative complications, including hematoma, seroma, vocal cord palsy, hypocalcemia, trachea injury, esophageal injury, chyle leakage, and brachial plexus neuropraxia. All patients were followed up in the same manner at the three centers, including clinical examinations within 1 week of discharge and a 3-to-6-month follow up that included a physical examination, neck US, assay of tumor markers (serum thyroglobulin concentration), and/or a 131 radioactive iodine ( 131 RAI) scan Learning Curves. To evaluate the learning curve for robotic versus endoscopic thyroidectomy, we used a protocol similar to those previously described for the evaluation of learning curves for thyroid surgery [5, 9]. That is, we assessed groups of about 100 (96 130) patients who underwent robotic and endoscopic less than total thyroidectomy performed by four surgeons at the time they started performing these operations independently. Each patient was assigned a case number without regard to tumor size or lymph node metastasis. Operation time was defined as the time from first incision to the completion of skin closure and included docking and undocking of the robot. Surgical learning curves were analyzed using a moving average method. The surgical techniques we use for endoscopic and robotic thyroidectomy have been described in detail elsewhere [8, 17 19] Statistics. Data were analyzed using SPSS 12.0 for Windows (SPSS Inc., Chicago, IL, USA). All data are expressed as means ± standard deviations (SDs), proportions, or absolute numbers. Continuous data were compared using Student s t- tests, and categorical data were analyzed using chi-squared or Fisher s exact tests. A P value < 0.05 was considered statistically significant. A moving average method was used to analyze operation time and learning curves. Creating an average that moves with the addition of new data results in smoothing of the process being analyzed, thus reducing the effects of fluctuations. We used a moving average of 20 to reduce variations and accentuate trends [20]. 3. Results 3.1. Demographic and Clinical Data. Table 1 shows the demographic data and extent of surgery for the 2,612 patients included in this study. Mean age and gender distribution were equivalent for the robotic and endoscopic groups, but types of operation differed significantly. Less than total thyroidectomy was performed in 693 patients (82.2%) in the endoscopic group and in 1,063 (60.1%) in the robotic group, whereas total thyroidectomy was performed in 150 patients (17.8%) in the endoscopic group and in 706 (39.9%) in the robotic group (P = 0.004). Modified radical neck dissection (MRND) was also performed more frequently in the robotic than in the endoscopic group (3.4% versus 1.7%, P<0.001) Pathologic Findings and Perioperative Outcomes. Pathologic results are shown in Table 2. There were no significant between differences groups in type of tumor, tumor size, multifocality, and bilaterality. However, the mean number of harvested lymph nodes was significantly higher in the robotic than in the endoscopic group (4.5 ± 2.6 versus2.9 ± 1.7, P < 0.001). More advanced T stage (P = 0.011), N stage
3 Journal of Oncology 3 Table 1: Demographics and extent of surgery in patients with thyroid carcinoma treated by robotic thyroidectomy versus endoscopic thyroidectomy. Robot group (n = 1769) Endoscopy group (n = 843) P value Age, mean (years), range 39.4 ± 9.1 (13 70) 37.5 ± 9.4 (6 50) NS Gender Female 1637 (92.5%) 824 (97.7%) Male 132 (7.5%) 19 (2.3%) NS Extent of surgery Less than total 1063 (60.1%) 693 (82.2%) Unilateral total 595 (33.6%) 307 (36.4%) Unilateral total + partial 177 (10.0%) 208 (24.7%) Unilateral total + subtotal 291 (16.4%) 178 (21.1%) Total 706 (39.9%) 150 (17.8%) Extent of neck node dissection No dissection 23 (1.3%) 59 (7.0%) <0.001 CCND 1675 (94.7%) 770 (91.3%) NS Selective node dissection 11 (0.6%) 0 (0%) NS MRND 60 (3.4%) 14 (1.7%) <0.001 NS : nonspecific finding, CCND : central compartment neck dissection, MRND : modified radical neck dissection. Table 2: Comparison of pathologic findings between patients treated with robotic thyroidectomy and endoscopic thyroidectomy. Robot group (n = 1769) Endoscopy group (n = 843) P value Pathology NS Papillary carcinoma 1758 (99.3%) 837 (99.3%) Follicular carcinoma 5 (0.3%) 6 (0.7%) Medullary carcinoma 5 (0.3%) Hurthle cell carcinoma 1 (0.1%) Tumor size, mean (cm) 0.5 ± ± 0.5 NS Multifocality NS Yes 469 (26.5) 110 (13.0%) No 1300 (73.5) 733 (87.0%) Bilaterality NS Yes 208 (11.8%) 72 (8.5%) No 1561 (88.2%) 771 (91.5%) Mean retrieved central LN (n) 4.5 ± ± 1.7 <0.001 Mean metastatic central LN (n) 1.2 ± ± 0.7 NS TNM stage T1 905 (51.2%) 513 (60.9%) T2 16 (0.9%) 15 (1.8%) T3 841 (47.5%) 314 (37.2%) T4a 7 (0.4%) 1 (0.1%) N (64.0%) 605 (71.7%) N1a 570 (32.2%) 224 (26.6%) N1b 68 (3.8%) 14 (1.7%) Stage Stage I 1480 (83.7%) 750 (89.0%) Stage II 275 (15.5%) 92 (10.9%) Stage IVa 14 (0.8%) 1 (0.1%) LN: lymph node. TNM: tumor-node-metastasis.
4 4 Journal of Oncology 250 Moving average (surgeon 1) 250 Moving average (surgeon 2) Operation time (minutes) Operation time (minutes) RT: cases MA (ET) MA (RT) ET: cases RT: cases MA (ET) MA (RT) ET: cases (a) (b) 250 Moving average (surgeon 3) 250 Moving average (surgeon 4) Operation time (minutes) Operation time (minutes) RT: cases MA (ET) MA (RT) ET: cases RT: cases MA (ET) MA (RT) ET: cases (c) (d) Figure 1: (a d) Individual learning curves for robotic thyroidectomy (RT) and endoscopic thyroidectomy (ET); The graph plots the time taken to perform each procedure as a function of the number of patients. The moving average method was used to determine changes in operation times for each surgeon. The time required for each surgeon to perform RT decreased after patients, whereas the time required by each to perform ET decreased after patients. (P = 0.001), and TNM stage (P = 0.002) tumors occurred more frequently in the robotic group. All 8 patients with T4a lesions showed local invasion of recurrent laryngeal nerve detected during operation, which could be not be noticed in preoperative imaging study, and underwent Maryland or endoscopic dissector shaving procedure. Total operation time for subtotal thyroidectomy was similar in the two groups, but was significantly shorter in the robotic than in the endoscopic group for total thyroidectomy (P <0.001). Postoperative hospital stay did not differ significantly (Table 3). Among the perioperative complications observed, transient hypocalcemia and transient hoarseness were the most frequent causes of postoperative morbidity, but there were no between differences groups in incidence. Transient hoarseness resolved in all patients within 6 months, as confirmed by postoperative laryngoscopy, and transient hypocalcemia resolved within 3 months. Transient traction injury from brachial plexus neuropraxia was observed in 3 patients in the robotic and 1 in the endoscopic group. This impairment resulted in pain
5 Journal of Oncology 5 Table 3: Comparison of perioperative outcomes between patients treated with robotic thyroidectomy and endoscopic thyroidectomy. Robot group (n = 1769) Endoscopy group (n = 843) P value Total operation time (min), range Total thyroidectomy ± ± 66.7 <0.001 Subtotal thyroidectomy ± ± 41.3 NS Postoperative hospital stay (days) 3.3 ± ± 1.1 NS Postoperative complications (n) Transient hypocalcemia 276/706 (39.1%) 55/150 (36.7%) Permanent hypocalcemia 0 (0%) 2 (0.2%) Transient hoarseness 68 (3.8%) 41 (4.9%) Permanent hoarseness 8 (0.5%) 1 (0.1%) Flap hematoma 10 (0.6%) 8 (0.9%) Observation 8 (0.5%) 5 (0.6%) Reoperation 2 (0.1%) 3 (0.4%) NS Seroma 40 (2.3%) 19 (0.3%) Tracheal injury 3 (0.2%) 4 (0.5%) Esophageal injury 0 (0%) 0 (0%) Transient chyle leakage 6 (0.3%) 3 (0.4%) Transient traction injury 3 (0.2%) 1 (0.1%) d/t brachial plexus neuropraxia and movement disorder of the shoulder and upper arm, but resolved spontaneously within 3 months. Of the 856 patients who underwent bilateral total thyroidectomy, 481 underwent 131 RAI ablation (range, mci) and a 131 RAI scan 5 7 days after 131 RAI ablation. The remaining 375 patients did not undergo 131 RAI ablation as they were deemed low risk (356 patients) or chose not to undergo such treatment (19 patients). No patient showed abnormal uptake on 131 I whole body scans. At the time of 131 RAI ablation (TSH stimulated), mean serum thyroglobulin levels were checked, serum thyroglobulin in 362 (75.2%) was <1 ng/ml and in the remaining 119 (24.8%) was >1ng/mL (3.1 ± 1.8, range ng/ml). Serum thyroglobulin levels were measured in 1,851 patients at 6 12 months postoperatively (TSH suppressed), with most being maintained at the lowest level (<1ng/mL). Mean thyroglobulin concentrations did not differ significantly in the robotic and endoscopic groups (0.72 ± 1.84 ng/ml versus 0.61 ± 1.99 ng/ml). Follow-up neck US and neck CT showed recurrence in six patients, 3 in each group, with 3 recurrences in a lateral neck node and 3 in the contralateral thyroid gland Learning Curves for Robotic and Endoscopic Thyroidectomies. When we compared the data on about 100 individual patients who underwent robotic and endoscopic less than total thyroidectomy by all involved surgeons, we observed no significant differences in patient-selection criteria. For both procedures, the operation times gradually decreased with accumulating experience. For all 4 surgeons, operation times reached a plateau after robotic and endoscopic less than total thyroidectomies (Figure 1). 4. Discussion Robotic thyroidectomy is an emerging technique with early outcomes that are at least comparable to those of conventional endoscopic thyroidectomy, with some end points appearing superior. Our series represents the largest comparison of robotic and endoscopic thyroidectomy to date, with results suggesting comparable operation times, perioperative outcomes, and complications. In addition, early-term oncologic outcomes demonstrated that robotic thyroidectomy resulted in acceptably complete resection and radical dissection, with an extremely low rate of recurrent disease at follow up. Moreover, to our knowledge, this study is the first multicenter trial to compare the learning curves of robotic and endoscopic thyroidectomy Comparison of Perioperative Outcomes with Robotic and Endoscopic Thyroidectomy. The goal of thyroidectomy plus neck dissection in patients with thyroid cancer is the complete surgical removal of the entire thyroid gland, along with radical cervical lymphadenectomy when necessary. Other goals include rapid convalescence and complete preservation of the recurrent and superior laryngeal nerves and the parathyroid gland. Only a few previous large series have compared perioperative outcomes in patients undergoing robotic and endoscopic thyroidectomy [8 11](Table 4). Our previous experience suggests that robotic thyroidectomy may be associated with decreased operation times and increased harvest of cervical LNs, outcomes related to the operative dexterity of the flexible robotic instruments, and a 3D surgical view [5 9]. In contrast, endoscopic thyroid dissection and lymph node retrieval may be more difficult and time consuming because of the straight angles
6 6 Journal of Oncology Table 4: Endoscopic versus robotic thyroidectomy studies. Case series comparing perioperative outcomes. Author, year Study design No. (patients) Approach Comparative parameters Lee et al. (2011) [9] Lang and Chow (2011) [11] Lee et al. (2011) [8] Kim et al. (2011) [10] Prospective, controlled, Single surgeon Retrospective, controlled, Single surgeon Retrospective, controlled, Single center Retrospective, Single center RT (163) versus ET (96) RT (7) ET (39) GT RT (580) ET (570) RT (69) ET (95) OT (138) Perioperative outcomes, GT surgical learning curve GT Perioperative outcomes Perioperative outcomes Perioperative BABA outcomes Perioperative results Operation time (ET > RT) Learning curve (ET > RT) Advanced cancer (RT > ET) Operation time (RT > ET) Operation time (ET > RT) Advanced cancer (RT > ET) Operation time (RT > ET > OT # ) Complication rate Oncologic safety (surgical completeness such as harvested lymph node) No difference Retrieved LN (RT > ET) No difference No data Transienthypoparathyroidism (RT > ET) No difference Retrieved LN (RT > ET) Surgical completeness (RT = OT > ET) Retrieved LN (RT = OT = ET) RT : robotic thyroidectomy, GT : gasless transaxillary approach, ET : endoscopic thyroidectomy, BABA : bilateral axillo-breast approach, OT # :openthyroidectomy. Other notable findings First comparative study between RT and ET. Showed superiorityofrtintermsof operation time, lymph node retrieval, and learning curve Described initial experience of RT in Hong Kong RT was found to be superior to ET in terms of operation time, and LN retrieval. First comparative study of RT versus OT by analyzing postoperative outcomes
7 Journal of Oncology 7 Table 5: Published data for surgical learning curves for robotic thyroidectomy. Author, year Study design Kang et al. (2009) [5] Lee et al. (2011) [9] Lee et al. (2011) [13] Kandil et al. (2012) [16] Retrospective (single surgeon) Retrospective (single surgeon) 163 GT Prospective (multicenter study) Prospective (single surgeon) No. (patients) Approach Pathology Operation Operation time Complications Methods for (Major) analysis 338 GT Benign (6) PTC (332) 644 GT PTC (151) FTCγ (1) Benign (11) PTC (616) FTC (13) Benign (15) 100 GT No data TT & CCND # (104) LTT & CCND (234) TT (48), LTT (115) CCND (149) TT & CCND (353) LTT & CCND (291) TT (22) LTT (69) CT (9) Total: ± 43.5 Console: 59.1±25.7 Total: ± 50.7 Console: 50.9 ± 11.4 Total: ± 78.2 ( 50 γγ ) ± 33.0 (>50) Console: 50.9 ± 11.4 Total: ± 63.8 ( 45 ) ± 71.5 (>45) Console: 51.3 ± 31.1 ( 45) 45 ± 36.4 (>45) 5/338 (1.5%) Moving average 2/163 (1.2%) Moving average 2/644 (0.3%) 1/100 (1.0%) Comparative analysis between beginners and experience surgeons Comparative analysis between early experience and late experience Surgical learning curve for robotic thyroidectomy RT ## (Console time): cases RT: cases, ET :50 60 cases RT (LTT): 40 cases RT (TT): 50 cases RT: 45 cases Complications (Major) : major complications mean permanent damages such as recurrent laryngeal nerve injury, permanent hypocalcemia, hematoma of muscle flap need to reoperation, hemorrhage of a major vessel need to reoperation, trachea injury, Honor s syndrome, major chyle leakage, and brachial plexus neuropraxia (not including minor complications such as transient hypocalcemia, transient hoarseness, wound seroma, wound infection, and hematoma of muscle flap only need to conservative management), GT : gasless transaxillary approach, PTC : papillary thyroid carcinoma, TT : total thyroidectomy, CCND # : central compartment node dissection, RT ## : robotic thyroidectomy, LTT : less than total thyroidectomy, ET : endoscopic thyroidectomy, FTC γ : follicular thyroid carcinoma, 50 γγ : experience for robotic thyroidectomy were less than 50 cases, CT : completion thyroidectomy, 45 : experience for robotic thyroidectomy was less than 45 cases.
8 8 Journal of Oncology of the endoscopic instruments and a 2D operative field [1 4]. Another superiority of robotic thyroidectomy over conventional endoscopic thyroidectomy is that surgeons use three arms during operation. In conventional endoscopy, the surgeon can steer only two arms during dissection, and this makes it difficult to create appropriate conditions for dissection. However, in robot technique, the surgeon can handle the Prograsp forceps during using the Maryland dissector, optimal dissection planes can be obtained by applying traction and countertraction to thyroid gland, and could position the thyroid gland to allow fine, dexterous dissection after swapping arms by controlling robotic arms himself [5 8]. A recent retrospective comparison of 580 patients who underwent robotic thyroidectomy and 570 who underwent conventional endoscopic thyroidectomy at a single center found that the operation time was shorter and the mean number of central LNs retrieved greater in the robotic than in the endoscopic group [8]. These findings were also observed in a recent comparison of robotic and endoscopic thyroidectomy performed by a single surgeon [9], providing further evidence that the robotic technique provides better results that conventional endoscopy in thyroid cancer patients [8 11]. Table 4 summarizes the published findings in studies comparing robotic and endoscopic thyroidectomy. Our findings were similar, in that mean operation times were 13.6% shorter (P < 0.001) and the numbers of LNs retrieved significantly greater (P <0.001) for robotic than for endoscopic total thyroidectomy. Objective comparisons are limited, however, by the lack of long-term surgical outcomes and by nonuniformity in defining, assessing, and reporting postoperative outcomes. Larger prospective studies, with uniform definitions of parameters, methodologies of data collection, and times of assessment are needed to compare operative outcomes of the two procedures Learning Curves for Robotic and Endoscopic Thyroidectomy. The operation time required by a single surgeon to perform robotic thyroidectomy using a gasless transaxillary approach was found to reach a plateau after operations [5]. In addition, the learning curve for inexperienced surgeons to perform robotic thyroidectomy was operations, whereas that for endoscopic thyroidectomy using a gasless transaxillary approach was operations [9]. An extensive review of the outcomes of learning curves for robotic thyroidectomy in the Republic of Korea categorized patients into two groups, those treated by surgeons with and without experience in robotic thyroid surgery [13]. The learning curves for robotic thyroidectomy were 50 for total and 40 for less than total thyroidectomies. Moreover, once through the learning curve period, operation times and perioperative parameters for previously inexperienced surgeons were similar to those of the experienced surgeons, indicating that the former had acquired the necessary technical skills to perform robotic thyroidectomy successfully [13]. Despite different methodologies and variables in different studies, the results of these investigations of surgical learning curves for robotic thyroidectomy showed similar operation time-related results [5, 9, 13, 16] (Table 5). Similar to these studies, we found that the learning curve was significantly shorter for the robotic than for the endoscopic technique. For all 4 enrolled surgeons at 3 centers, the learning curves were found to be patients for robotic and for endoscopic less than total thyroidectomy. In this study, we could not perform the comparative evaluation for learning curves between robotic and endoscopic total thyroidectomy, because the number of endoscopic total thyroidectomy cases was too low to analyze the learning curve for this procedure. This study had potential shortcomings. First, although all 4 surgeons in our study used the same technique, all procedures could not be completed with the same quality of manipulations. Second, patients were not randomized, as it was neither ethically nor geographically possible to move patients from one center to another. This was likely a result of selection bias of our patients and our overall experience with endoscopic and robotic surgery. Third, the short history of robotic thyroidectomy makes assertions on the oncologic safety and the surgical learning curve premature. In addition, the surgeon had experience in performing several endoscopic thyroidectomies prior to any robotic thyroidectomies, and this is likely to have influenced comparisons of operation times and learning curves. Therefore, further study is required to confirm these findings and to assess the surgical learning curve for surgeons who have no experience of endoscopic surgery. Moreover, a prospective and randomized study with longer follow-up period should be conducted to evaluate the role of robotic surgery in thyroid disease. In conclusion, we have shown that the robot technology we used could overcome some of the technical limitations associated with conventional endoscopic procedures, with reduced operation times and increased lymph node retrieval. Moreover, we found that the learning curve for robotic thyroidectomy was shorter than that for endoscopic thyroidectomy. Prospective randomized studies are required to evaluate the actual learning curves of inexperienced endoscopic surgeons for robotic thyroidectomy and lymph node dissection. Conflict of Interests All authors including Drs. J. Lee, J. H. Yun, U. J. Choi, S.-W. Kang, J. J. Jeong, and W. Y. Chung have no conflict of interests or financial ties to disclose. References [1] Y. Ikeda, H. Takami, Y. Sasaki, J. Takayama, M. Niimi, and S. Kan, Clinical benefits in endoscopic thyroidectomy by the axillary approach, Journal of the American College of Surgeons, vol. 196, no. 2, pp , [2] Y. Ikeda, H. Takami, Y. Sasaki, J. I. Takayama, and H. Kurihara, Are there significant benefits of minimally invasive endoscopic thyroidectomy? World Journal of Surgery, vol. 28, no. 11, pp , [3] Y. S. Chung, J. H. Choe, K. H. Kang et al., Endoscopic thyroidectomy for thyroid malignancies: comparison with
9 Journal of Oncology 9 conventional open thyroidectomy, World Journal of Surgery, vol. 31, no. 12, pp , [4]Y.W.Koh,J.H.Park,J.W.Kim,S.W.Lee,andE.C.Choi, Endoscopic hemithyroidectomy with prophylactic ipsilateral central neck dissection via an unilateral axillo-breast approach without gas insufflation for unilateral micropapillary thyroid carcinoma: preliminary report, Surgical Endoscopy and Other Interventional Techniques, vol. 24, no. 1, pp , [5] S. W. Kang, S. C. Lee, S. H. Lee et al., Robotic thyroid surgery using a gasless, transaxillary approach and the da Vinci S system: the operative outcomes of 338 consecutive patients, Surgery, vol. 146, no. 6, pp , [6] J. Lee, J. H. Yun, K. H. Nam, U. J. Choi, W. Y. Chung, and E. Y. Soh, Perioperative clinical outcomes after robotic thyroidectomy for thyroid carcinoma: a multicenter study, Surgical Endoscopy and Other Interventional Techniques, vol. 25, no. 3, pp , [7] J. Lee, S. W. Kang, J. J. Jung et al., Multicenter study of robotic thyroidectomy: short-term postoperative outcomes and surgeon ergonomic considerations, Annals of Surgical Oncology, vol. 18, no. 9, pp , [8]S.Lee,H.R.Ryu,J.H.Parketal., Excellenceinrobotic thyroid surgery: a comparative study of robot-assisted versus conventional endoscopic thyroidectomy in papillary thyroid microcarcinoma patients, Annals of Surgery, vol. 253, no. 6, pp , [9]J.Lee,J.H.Lee,K.Y.Nah,E.Y.Soh,andW.Y.Chung, Comparison of endoscopic and robotic thyroidectomy, Annals of Surgical Oncology, vol. 18, no. 5, pp , [10] W. W. Kim, J. S. Kim, S. M. Hur et al., Is robotic surgery superior to endoscopic and open surgeries in thyroid cancer? World Journal of Surgery, vol. 35, no. 4, pp , [11] B. H. H. Lang and M. P. Chow, A comparison of surgical outcomes between endoscopic and robotically assisted thyroidectomy: the authors initial experience, Surgical Endoscopy and Other Interventional Techniques, vol. 25, no. 5, pp , [12] S. Liu, M. Qiu, D. Z. Jiang et al., The learning curve for endoscopic thyroidectomy: a single surgeon s experience, Surgical Endoscopy and Other Interventional Techniques, vol. 23, no. 8, pp , [13] J. Lee, J. H. Yun, K. H. Nam, E. Y. Soh, and W. Y. Chung, The learning curve for robotic thyroidectomy: a multicenter study, Annals of Surgical Oncology, vol. 18, no. 1, pp , [14] J. S. Choi, J. Kim, J. Y. Kwak, M. J. Kim, H. S. Chang, and E. K. Kim, Preoperative staging of papillary thyroid carcinoma: comparison of ultrasound imaging and CT, American Journal of Roentgenology, vol. 193, no. 3, pp , [15] D. S. Cooper, G. M. Doherty, B. R. Haugen et al., Revised American thyroid association management guidelines for patients with thyroid nodules and differentiated thyroid cancer, Thyroid, vol. 19, no. 11, pp , [16] E. H. Kandil, S. I. Noureldine, L. Yao, and D. P. Slakey, Robotic transaxillary thyroidectomy: an examination of the first one hundred cases, Journal of the American College of Surgeons, vol. 214, no. 4, pp , [17]J.H.Yoon,C.H.Park,andW.Y.Chung, Gaslessendoscopic thyroidectomy via an axillary approach: experience of 30 cases, Surgical Laparoscopy, Endoscopy and Percutaneous Techniques, vol. 16, no. 4, pp , [18] J. J. Jong, S. W. Kang, J. S. Yun et al., Comparative study of endoscopic thyroidectomy versus conventional open thyroidectomy in papillary thyroid microcarcinoma (PTMC) patients, JournalofSurgicalOncology, vol. 100, no. 6, pp , [19] S. W. Kang, J. J. Jeong, J. S. Yun et al., Gasless endoscopic thyroidectomy using trans-axillary approach; surgical outcome of 581 patients, Endocrine Journal, vol. 56, no. 3, pp , [20] P. Diggle, Time Series: A Biostatistical Introduction, Oxford University Press, London, UK.
10 MEDIATORS of INFLAMMATION The Scientific World Journal Gastroenterology Research and Practice Journal of Diabetes Research International Journal of Journal of Endocrinology Immunology Research Disease Markers Submit your manuscripts at BioMed Research International PPAR Research Journal of Obesity Journal of Ophthalmology Evidence-Based Complementary and Alternative Medicine Stem Cells International Journal of Oncology Parkinson s Disease Computational and Mathematical Methods in Medicine AIDS Behavioural Neurology Research and Treatment Oxidative Medicine and Cellular Longevity
Jandee Lee, In Soon Kwon, Eun Hee Bae, and Woong Youn Chung
 ORIGINAL ARTICLE Endocrine Care Comparative Analysis of Oncological Outcomes and Quality of Life After Robotic versus Conventional Open Thyroidectomy With Modified Radical Neck Dissection in Patients With
ORIGINAL ARTICLE Endocrine Care Comparative Analysis of Oncological Outcomes and Quality of Life After Robotic versus Conventional Open Thyroidectomy With Modified Radical Neck Dissection in Patients With
Yonsei Experience of 5000 Gasless Transaxillary Robotic Thyroidectomies
 World J Surg (2018) 42:393 401 DOI 10.1007/s00268-017-4209-y ORIGINAL SCIENTIFIC REPORT Yonsei Experience of 5000 Gasless Transaxillary Robotic Thyroidectomies Min Jhi Kim 1 Kee-Hyun Nam 1 Seul Gi Lee
World J Surg (2018) 42:393 401 DOI 10.1007/s00268-017-4209-y ORIGINAL SCIENTIFIC REPORT Yonsei Experience of 5000 Gasless Transaxillary Robotic Thyroidectomies Min Jhi Kim 1 Kee-Hyun Nam 1 Seul Gi Lee
4/22/2010. Hakan Korkmaz, MD Assoc. Prof. of Otolaryngology Ankara Dıșkapı Training Hospital-Turkey.
 Management of Differentiated Thyroid Cancer: Head Neck Surgeon Perspective Hakan Korkmaz, MD Assoc. Prof. of Otolaryngology Ankara Dıșkapı Training Hospital-Turkey Thyroid gland Small endocrine gland:
Management of Differentiated Thyroid Cancer: Head Neck Surgeon Perspective Hakan Korkmaz, MD Assoc. Prof. of Otolaryngology Ankara Dıșkapı Training Hospital-Turkey Thyroid gland Small endocrine gland:
Can Robotic Thyroidectomy Be Performed Safely in Thyroid Carcinoma Patients?
 Review Article Endocrinol Metab 214;29:226-232 http://dx.doi.org/1.383/enm.214.29.3.226 pissn 293-596X eissn 293-5978 Can Robotic Thyroidectomy Be Performed Safely in Thyroid Carcinoma Patients? Young
Review Article Endocrinol Metab 214;29:226-232 http://dx.doi.org/1.383/enm.214.29.3.226 pissn 293-596X eissn 293-5978 Can Robotic Thyroidectomy Be Performed Safely in Thyroid Carcinoma Patients? Young
New technologies in Endocrine Surgery
 New technologies in Endocrine Surgery 1. Nerve monitoring 2. New technologies in Endocrine Surgery Jessica E. Gosnell MD Post graduate course in General Surgery March 28, 2012 1 2 Recurrent laryngeal nerve
New technologies in Endocrine Surgery 1. Nerve monitoring 2. New technologies in Endocrine Surgery Jessica E. Gosnell MD Post graduate course in General Surgery March 28, 2012 1 2 Recurrent laryngeal nerve
Reoperative central neck surgery
 Reoperative central neck surgery R. Pandev, I. Tersiev, M. Belitova, A. Kouizi, D. Damyanov University Clinic of Surgery, Section Endocrine Surgery University Hospital Queen Johanna ISUL Medical University
Reoperative central neck surgery R. Pandev, I. Tersiev, M. Belitova, A. Kouizi, D. Damyanov University Clinic of Surgery, Section Endocrine Surgery University Hospital Queen Johanna ISUL Medical University
Endoscopic Thyroidectomy Via the Cervico-axillary Approach for Thyroid Cancer: Initial Experience in a Single Institute
 ORIGINAL ARTICLE ISSN 1598-1703 (Print) ISSN 2287-6782 (Online) Korean J Endocr Surg 2017;17:19-24 https://doi.org/10.16956/kaes.2017.17.1.19 The Korean Journal of Endocrine Surgery Endoscopic Thyroidectomy
ORIGINAL ARTICLE ISSN 1598-1703 (Print) ISSN 2287-6782 (Online) Korean J Endocr Surg 2017;17:19-24 https://doi.org/10.16956/kaes.2017.17.1.19 The Korean Journal of Endocrine Surgery Endoscopic Thyroidectomy
Disclosures Nodal Management in Differentiated Thyroid Carcinoma
 Disclosures Nodal Management in Differentiated Thyroid Carcinoma Nothing to disclose Jonathan George, MD, MPH Assistant Professor UCSF Head and Neck Oncologic & Endocrine Surgery Objectives Overview Describe
Disclosures Nodal Management in Differentiated Thyroid Carcinoma Nothing to disclose Jonathan George, MD, MPH Assistant Professor UCSF Head and Neck Oncologic & Endocrine Surgery Objectives Overview Describe
Persistent & Recurrent Differentiated Thyroid Cancer
 Persistent & Recurrent Differentiated Thyroid Cancer Electron Kebebew University of California, San Francisco Department of Surgery Objectives Risk factors for persistent & recurrent disease Causes of
Persistent & Recurrent Differentiated Thyroid Cancer Electron Kebebew University of California, San Francisco Department of Surgery Objectives Risk factors for persistent & recurrent disease Causes of
THYROID CANCER IN CHILDREN. Humberto Lugo-Vicente MD FACS FAAP Professor Pediatric Surgery UPR School of Medicine
 THYROID CANCER IN CHILDREN Humberto Lugo-Vicente MD FACS FAAP Professor Pediatric Surgery UPR School of Medicine Thyroid nodules Rare Female predominance 4-fold as likely to be malignant Hx Radiation exposure?
THYROID CANCER IN CHILDREN Humberto Lugo-Vicente MD FACS FAAP Professor Pediatric Surgery UPR School of Medicine Thyroid nodules Rare Female predominance 4-fold as likely to be malignant Hx Radiation exposure?
Mandana Moosavi 1 and Stuart Kreisman Background
 Case Reports in Endocrinology Volume 2016, Article ID 6471081, 4 pages http://dx.doi.org/10.1155/2016/6471081 Case Report A Case Report of Dramatically Increased Thyroglobulin after Lymph Node Biopsy in
Case Reports in Endocrinology Volume 2016, Article ID 6471081, 4 pages http://dx.doi.org/10.1155/2016/6471081 Case Report A Case Report of Dramatically Increased Thyroglobulin after Lymph Node Biopsy in
A comparison of surgical outcomes between endoscopic and robotically assisted thyroidectomy: the authors initial experience
 Surg Endosc (2011) 25:1617 1623 DOI 10.1007/s00464-010-1450-y A comparison of surgical outcomes between endoscopic and robotically assisted thyroidectomy: the authors initial experience Brian Hung-Hin
Surg Endosc (2011) 25:1617 1623 DOI 10.1007/s00464-010-1450-y A comparison of surgical outcomes between endoscopic and robotically assisted thyroidectomy: the authors initial experience Brian Hung-Hin
Ultrasound for Pre-operative Evaluation of Well Differentiated Thyroid Cancer
 Ultrasound for Pre-operative Evaluation of Well Differentiated Thyroid Cancer Its Not Just About the Nodes AACE Advances in Medical and Surgical Management of Thyroid Cancer - 2017 Robert A. Levine, MD,
Ultrasound for Pre-operative Evaluation of Well Differentiated Thyroid Cancer Its Not Just About the Nodes AACE Advances in Medical and Surgical Management of Thyroid Cancer - 2017 Robert A. Levine, MD,
Gasless Endoscopic Thyroidectomy Using Trans-axillary Approach; Surgical Outcome of 581 Patients
 Endocrine Journal 2009, 56 (3), 361-369 Gasless Endoscopic Thyroidectomy Using Trans-axillary Approach; Surgical Outcome of 581 Patients Sa n g-wo o k Kang, Jo n g Ju Jeong, Ji-Su p Yun*, Ta e Yo n Sung,
Endocrine Journal 2009, 56 (3), 361-369 Gasless Endoscopic Thyroidectomy Using Trans-axillary Approach; Surgical Outcome of 581 Patients Sa n g-wo o k Kang, Jo n g Ju Jeong, Ji-Su p Yun*, Ta e Yo n Sung,
Current Issues in Thyroid Cancer Surgery in 2017
 Current Issues in Thyroid Cancer Surgery in 2017 Dr. David Goldstein MD Msc FRCSC FACS Associate Professor, Department Otolaryngology Head & Neck Surgery, U of T Department of Surgical Oncology, Princess
Current Issues in Thyroid Cancer Surgery in 2017 Dr. David Goldstein MD Msc FRCSC FACS Associate Professor, Department Otolaryngology Head & Neck Surgery, U of T Department of Surgical Oncology, Princess
The current status of robotic transaxillary thyroidectomy in the United States: an experience from two centers
 Original Article The current status of robotic transaxillary thyroidectomy in the United States: an experience from two centers Nisar Zaidi 1, Despoina Daskalaki 2, Pablo Quadri 2, Alexis Okoh 3, Pier
Original Article The current status of robotic transaxillary thyroidectomy in the United States: an experience from two centers Nisar Zaidi 1, Despoina Daskalaki 2, Pablo Quadri 2, Alexis Okoh 3, Pier
A variation in recurrence patterns of papillary thyroid cancer with disease progression: A long-term follow-up study
 ORIGINAL ARTICLE A variation in recurrence patterns of papillary thyroid cancer with disease progression: A long-term follow-up study Joon-Hyop Lee, MD, Yoo Seung Chung, MD, PhD,* Young Don Lee, MD, PhD
ORIGINAL ARTICLE A variation in recurrence patterns of papillary thyroid cancer with disease progression: A long-term follow-up study Joon-Hyop Lee, MD, Yoo Seung Chung, MD, PhD,* Young Don Lee, MD, PhD
Research Article A Study on Central Lymph Node Metastasis in 543 cn0 Papillary Thyroid Carcinoma Patients
 International Endocrinology Volume 2016, Article ID 1878194, 5 pages http://dx.doi.org/10.1155/2016/1878194 Research Article A Study on Central Lymph Node Metastasis in 543 cn0 Papillary Thyroid Carcinoma
International Endocrinology Volume 2016, Article ID 1878194, 5 pages http://dx.doi.org/10.1155/2016/1878194 Research Article A Study on Central Lymph Node Metastasis in 543 cn0 Papillary Thyroid Carcinoma
Clinical Study Utility of Surgeon-Performed Ultrasound Assessment of the Lateral Neck for Metastatic Papillary Thyroid Cancer
 Oncology Volume 2012, Article ID 973124, 4 pages doi:10.1155/2012/973124 Clinical Study Utility of Surgeon-Performed Ultrasound Assessment of the Lateral Neck for Metastatic Papillary Thyroid Cancer CortneyY.Lee,SamuelK.Snyder,TerryC.Lairmore,SeanC.Dupont,andDanielC.Jupiter
Oncology Volume 2012, Article ID 973124, 4 pages doi:10.1155/2012/973124 Clinical Study Utility of Surgeon-Performed Ultrasound Assessment of the Lateral Neck for Metastatic Papillary Thyroid Cancer CortneyY.Lee,SamuelK.Snyder,TerryC.Lairmore,SeanC.Dupont,andDanielC.Jupiter
How good are we at finding nodules? Thyroid Nodules Thyroid Cancer Epidemiology Initial management Long-term follow up Disease-free status
 New Perspectives in Thyroid Cancer Jennifer Sipos, MD Assistant Professor of Medicine Division of Endocrinology The Ohio State University Outline Thyroid Nodules Thyroid Cancer Epidemiology Initial management
New Perspectives in Thyroid Cancer Jennifer Sipos, MD Assistant Professor of Medicine Division of Endocrinology The Ohio State University Outline Thyroid Nodules Thyroid Cancer Epidemiology Initial management
Thyroid Nodule. Disclosure. Learning Objectives P A P A P A 3/18/2014. Nothing to disclose.
 Thyroid Nodule Evaluating the patient with a thyroid nodule and some management options. Miguel V. Valdez PA C Disclosure Nothing to disclose. Learning Objectives Examination of thyroid gland Options for
Thyroid Nodule Evaluating the patient with a thyroid nodule and some management options. Miguel V. Valdez PA C Disclosure Nothing to disclose. Learning Objectives Examination of thyroid gland Options for
Research Article The Cost of Prolonged Hospitalization due to Postthyroidectomy Hypocalcemia: A Case-Control Study
 Advances in Endocrinology, Article ID 954194, 4 pages http://dx.doi.org/10.1155/2014/954194 Research Article The Cost of Prolonged Hospitalization due to Postthyroidectomy Hypocalcemia: A Case-Control
Advances in Endocrinology, Article ID 954194, 4 pages http://dx.doi.org/10.1155/2014/954194 Research Article The Cost of Prolonged Hospitalization due to Postthyroidectomy Hypocalcemia: A Case-Control
Prediction of ipsilateral and contralateral central lymph node metastasis in unilateral papillary thyroid carcinoma: a retrospective study
 Original Article Prediction of ipsilateral and contralateral central lymph node metastasis in unilateral papillary thyroid carcinoma: a retrospective study Qiang Chen, Xiu-He Zou, Tao Wei, Qiu-Shi Huang,
Original Article Prediction of ipsilateral and contralateral central lymph node metastasis in unilateral papillary thyroid carcinoma: a retrospective study Qiang Chen, Xiu-He Zou, Tao Wei, Qiu-Shi Huang,
Dr J K Jekel Dept. Surgery University of Pretoria
 Dr J K Jekel Dept. Surgery University of Pretoria No Maybe ( T`s and C`s apply ) 1. Total thyroidectomy 2. Neck dissection only if nodes are involved 3. Ablative dose or doses of Radioactive Iodine 4.
Dr J K Jekel Dept. Surgery University of Pretoria No Maybe ( T`s and C`s apply ) 1. Total thyroidectomy 2. Neck dissection only if nodes are involved 3. Ablative dose or doses of Radioactive Iodine 4.
Long-term Follow-up for Patients with Papillary Thyroid Carcinoma Treated as Benign Nodules
 Long-term Follow-up for Patients with Papillary Thyroid Carcinoma Treated as Benign Nodules YASUHIRO ITO, TAKUYA HIGASHIYAMA, YUUKI TAKAMURA, AKIHIRO MIYA, KAORU KOBAYASHI, FUMIO MATSUZUKA, KANJI KUMA
Long-term Follow-up for Patients with Papillary Thyroid Carcinoma Treated as Benign Nodules YASUHIRO ITO, TAKUYA HIGASHIYAMA, YUUKI TAKAMURA, AKIHIRO MIYA, KAORU KOBAYASHI, FUMIO MATSUZUKA, KANJI KUMA
Changing trends in the management of well-differentiated thyroid carcinoma in Korea
 2016, 63 (6), 515-521 Original Changing trends in the management of well-differentiated thyroid carcinoma in Korea Yong Sang Lee, Hang-Seok Chang and Cheong Soo Park Thyroid Cancer Center, Department of
2016, 63 (6), 515-521 Original Changing trends in the management of well-differentiated thyroid carcinoma in Korea Yong Sang Lee, Hang-Seok Chang and Cheong Soo Park Thyroid Cancer Center, Department of
Gerard M. Doherty, MD
 Surgical Management of Differentiated Thyroid Cancer: Update on 2015 ATA Guidelines Gerard M. Doherty, MD Chair of Surgery Utley Professor of Surgery and Medicine Boston University Surgeon-in-Chief Boston
Surgical Management of Differentiated Thyroid Cancer: Update on 2015 ATA Guidelines Gerard M. Doherty, MD Chair of Surgery Utley Professor of Surgery and Medicine Boston University Surgeon-in-Chief Boston
Research Article Papillary Thyroid Cancer, Macrofollicular Variant: The Follow-Up and Analysis of Prognosis of 5 Patients
 yroid Research, Article ID 818134, 4 pages http://dx.doi.org/10.1155/2014/818134 Research Article Papillary Thyroid Cancer, Macrofollicular Variant: The Follow-Up and Analysis of Prognosis of 5 Patients
yroid Research, Article ID 818134, 4 pages http://dx.doi.org/10.1155/2014/818134 Research Article Papillary Thyroid Cancer, Macrofollicular Variant: The Follow-Up and Analysis of Prognosis of 5 Patients
Thyroid INTRODUCTION ANATOMY SUMMARY OF CHANGES
 AJC 7/14/06 1:19 PM Page 67 Thyroid C73.9 Thyroid gland SUMMARY OF CHANGES Tumor staging (T) has been revised and the categories redefined. T4 is now divided into T4a and T4b. Nodal staging (N) has been
AJC 7/14/06 1:19 PM Page 67 Thyroid C73.9 Thyroid gland SUMMARY OF CHANGES Tumor staging (T) has been revised and the categories redefined. T4 is now divided into T4a and T4b. Nodal staging (N) has been
10/24/2008. Surgery for Well-differentiated Thyroid Carcinoma- The Primary
 Surgery for Well-differentiated Thyroid Carcinoma- The Primary Head and Neck Endocrine Surgery Department of Otolaryngology-Head and Neck Surgery, UCSF October 24-25, 2008 Robert A. Sofferman, MD Professor
Surgery for Well-differentiated Thyroid Carcinoma- The Primary Head and Neck Endocrine Surgery Department of Otolaryngology-Head and Neck Surgery, UCSF October 24-25, 2008 Robert A. Sofferman, MD Professor
Coexistence of parathyroid adenoma and papillary thyroid carcinoma. Yong Sang Lee, Kee-Hyun Nam, Woong Youn Chung, Hang-Seok Chang, Cheong Soo Park
 J Korean Surg Soc 2011;81:316-320 http://dx.doi.org/10.4174/jkss.2011.81.5.316 ORIGINAL ARTICLE JKSS Journal of the Korean Surgical Society pissn 2233-7903 ㆍ eissn 2093-0488 Coexistence of parathyroid
J Korean Surg Soc 2011;81:316-320 http://dx.doi.org/10.4174/jkss.2011.81.5.316 ORIGINAL ARTICLE JKSS Journal of the Korean Surgical Society pissn 2233-7903 ㆍ eissn 2093-0488 Coexistence of parathyroid
Management of Recurrent Thyroid Cancer
 Management of Recurrent Thyroid Cancer Eric Genden, MD, MHA Isidore Professor and Chairman Department of Otolaryngology- Head and Neck Surgery Senior Associate Dean for Clinical Affairs The Icahn School
Management of Recurrent Thyroid Cancer Eric Genden, MD, MHA Isidore Professor and Chairman Department of Otolaryngology- Head and Neck Surgery Senior Associate Dean for Clinical Affairs The Icahn School
Osman Ilkay Ozdamar, 1 Gul Ozbilen Acar, 1 Cigdem Kafkasli, 1 M. Tayyar Kalcioglu, 1 Tulay Zenginkinet, 2 and H. Gonca Tamer 3. 1.
 Case Reports in Otolaryngology Volume 2015, Article ID 79658, 4 pages http://dx.doi.org/10.1155/2015/79658 Case Report Papillary Thyroid Microcarcinoma with a Large Cystic Dilated Lymph Node Metastasis
Case Reports in Otolaryngology Volume 2015, Article ID 79658, 4 pages http://dx.doi.org/10.1155/2015/79658 Case Report Papillary Thyroid Microcarcinoma with a Large Cystic Dilated Lymph Node Metastasis
Differentiated Thyroid Carcinoma
 Differentiated Thyroid Carcinoma The GOOD cancer? Jennifer Sipos, MD Associate Professor of Medicine Director, Benign Thyroid Program Division of Endocrinology, Diabetes and Metabolism The Ohio State University
Differentiated Thyroid Carcinoma The GOOD cancer? Jennifer Sipos, MD Associate Professor of Medicine Director, Benign Thyroid Program Division of Endocrinology, Diabetes and Metabolism The Ohio State University
Surgical Treatment for Papillary Thyroid Carcinoma in Japan: Differences from Other Countries
 REVIEW ARTICLE J Korean Thyroid Assoc Vol. 4, No. 2, November 2011 Surgical Treatment for Papillary Thyroid Carcinoma in Japan: Differences from Other Countries Yasuhiro Ito, MD and Akira Miyauchi, MD
REVIEW ARTICLE J Korean Thyroid Assoc Vol. 4, No. 2, November 2011 Surgical Treatment for Papillary Thyroid Carcinoma in Japan: Differences from Other Countries Yasuhiro Ito, MD and Akira Miyauchi, MD
Pre-operative Ultrasound of Lymph Nodes in Thyroid Cancer
 Pre-operative Ultrasound of Lymph Nodes in Thyroid Cancer AACE - Advances in Medical and Surgical Management of Thyroid Cancer - 2018 Robert A. Levine, MD, FACE, ECNU Thyroid Center of New Hampshire Geisel
Pre-operative Ultrasound of Lymph Nodes in Thyroid Cancer AACE - Advances in Medical and Surgical Management of Thyroid Cancer - 2018 Robert A. Levine, MD, FACE, ECNU Thyroid Center of New Hampshire Geisel
The clinical prognosis of patients with cn0 papillary thyroid microcarcinoma by central neck dissection
 Zhang et al. World Journal of Surgical Oncology (2015) 13:138 DOI 10.1186/s12957-015-0553-2 WORLD JOURNAL OF SURGICAL ONCOLOGY RESEARCH Open Access The clinical prognosis of patients with cn0 papillary
Zhang et al. World Journal of Surgical Oncology (2015) 13:138 DOI 10.1186/s12957-015-0553-2 WORLD JOURNAL OF SURGICAL ONCOLOGY RESEARCH Open Access The clinical prognosis of patients with cn0 papillary
Central Lymph Node Dissection In Patients With Papillary Thyroid Cancer: A Population Level Analysis Of Cases
 Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine January 2013 Central Lymph Node Dissection In Patients With Papillary
Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine January 2013 Central Lymph Node Dissection In Patients With Papillary
Long Term Follow-Up for Differentiated Thyroid Cancer: The Mayo Experience
 Long Term Follow-Up for Differentiated Thyroid Cancer: The Mayo Experience Geoffrey B. Thompson, MD Professor of Surgery College of Medicine, Mayo Clinic Differentiated Thyroid Cancer Objectives Overview
Long Term Follow-Up for Differentiated Thyroid Cancer: The Mayo Experience Geoffrey B. Thompson, MD Professor of Surgery College of Medicine, Mayo Clinic Differentiated Thyroid Cancer Objectives Overview
Review Article Thyroidectomy and Lymph Node Dissection in Papillary Thyroid Carcinoma
 SAGE-Hindawi Access to Research Thyroid Research Volume 2011, Article ID 634170, 6 pages doi:10.4061/2011/634170 Review Article Thyroidectomy and Lymph Node Dissection in Papillary Thyroid Carcinoma Yasuhiro
SAGE-Hindawi Access to Research Thyroid Research Volume 2011, Article ID 634170, 6 pages doi:10.4061/2011/634170 Review Article Thyroidectomy and Lymph Node Dissection in Papillary Thyroid Carcinoma Yasuhiro
Thyroid Surgery: Lobectomy, total thyroidectomy, LN biopsies or only watchful waiting?
 Thyroid Surgery: Lobectomy, total thyroidectomy, LN biopsies or only watchful waiting? Jacob Moalem, MD, FACS Associate Professor Endocrine Surgery and Endocrinology URMC Agenda 1. When is lobectomy alone
Thyroid Surgery: Lobectomy, total thyroidectomy, LN biopsies or only watchful waiting? Jacob Moalem, MD, FACS Associate Professor Endocrine Surgery and Endocrinology URMC Agenda 1. When is lobectomy alone
PEDIATRIC Ariel Katz MD
 PEDIATRIC Ariel Katz MD Dept. Otolaryngology Head &Neck Surgery Wolfson Medical Center Holon, Israel OBJECTIVES Overview/Background Epidemiology/Etiology Intro to Guidelines Workup Treatment Follow-Up
PEDIATRIC Ariel Katz MD Dept. Otolaryngology Head &Neck Surgery Wolfson Medical Center Holon, Israel OBJECTIVES Overview/Background Epidemiology/Etiology Intro to Guidelines Workup Treatment Follow-Up
Thyroid nodules - medical and surgical management. Endocrinology and Endocrine Surgery Manchester Royal Infirmary
 Thyroid nodules - medical and surgical management JRE Davis NR Parrott Endocrinology and Endocrine Surgery Manchester Royal Infirmary Thyroid nodules - prevalence Thyroid nodules common, increase with
Thyroid nodules - medical and surgical management JRE Davis NR Parrott Endocrinology and Endocrine Surgery Manchester Royal Infirmary Thyroid nodules - prevalence Thyroid nodules common, increase with
Evaluation of thyroid isthmusectomy as a potential treatment for papillary thyroid carcinoma limited to the isthmus: A clinical study of 73 patients
 ORIGINAL ARTICLE Evaluation of thyroid isthmusectomy as a potential treatment for papillary thyroid carcinoma limited to the isthmus: A clinical study of 73 patients Jianbiao Wang, MM, 1 Haili Sun, BM,
ORIGINAL ARTICLE Evaluation of thyroid isthmusectomy as a potential treatment for papillary thyroid carcinoma limited to the isthmus: A clinical study of 73 patients Jianbiao Wang, MM, 1 Haili Sun, BM,
Treatment of Cervical Lymph Node Metastases Differentiated Thyroid Cancer
 Treatment of Cervical Lymph Node Metastases Differentiated Thyroid Cancer Well Differentiated Thyroid Cancer Natural History and Prognosis EORTC AGES AMES MACIS QuickTime and a TIFF (LZW) decompressor
Treatment of Cervical Lymph Node Metastases Differentiated Thyroid Cancer Well Differentiated Thyroid Cancer Natural History and Prognosis EORTC AGES AMES MACIS QuickTime and a TIFF (LZW) decompressor
Research Article Predictions of the Length of Lumbar Puncture Needles
 Computational and Mathematical Methods in Medicine, Article ID 732694, 5 pages http://dx.doi.org/10.1155/2014/732694 Research Article Predictions of the Length of Lumbar Puncture Needles Hon-Ping Ma, 1,2
Computational and Mathematical Methods in Medicine, Article ID 732694, 5 pages http://dx.doi.org/10.1155/2014/732694 Research Article Predictions of the Length of Lumbar Puncture Needles Hon-Ping Ma, 1,2
Preoperative Evaluation
 Preoperative Evaluation Lateral compartment lymph nodes are easier to detect and are amenable to FNA Central compartment lymph nodes are much more difficult to detect and FNA (Tg washout testing is compromised)
Preoperative Evaluation Lateral compartment lymph nodes are easier to detect and are amenable to FNA Central compartment lymph nodes are much more difficult to detect and FNA (Tg washout testing is compromised)
Brian Hung-Hin Lang, MS, FRACS 1,2 and Kai-Pun Wong, MBBS, FRCS 1. Department of Surgery, Queen Mary Hospital, Hong Kong SAR, China
 Ann Surg Oncol (2013) 20:646 652 DOI 10.1245/s10434-012-2613-y ORIGINAL ARTICLE ENDOCRINE TUMORS A Comparison of Surgical Morbidity and Scar Appearance Between Gasless, Transaxillary Endoscopic Thyroidectomy
Ann Surg Oncol (2013) 20:646 652 DOI 10.1245/s10434-012-2613-y ORIGINAL ARTICLE ENDOCRINE TUMORS A Comparison of Surgical Morbidity and Scar Appearance Between Gasless, Transaxillary Endoscopic Thyroidectomy
Correspondence should be addressed to Stan H. M. Van Uum;
 Oncology Volume 2016, Article ID 6496750, 6 pages http://dx.doi.org/10.1155/2016/6496750 Research Article Recombinant Human Thyroid Stimulating Hormone versus Thyroid Hormone Withdrawal for Radioactive
Oncology Volume 2016, Article ID 6496750, 6 pages http://dx.doi.org/10.1155/2016/6496750 Research Article Recombinant Human Thyroid Stimulating Hormone versus Thyroid Hormone Withdrawal for Radioactive
Clinical Study Comparison of Conventional Open Thyroidectomy and Endoscopic Thyroidectomy via Breast Approach for Papillary Thyroid Carcinoma
 International Endocrinology Volume 2015, Article ID 239610, 5 pages http://dx.doi.org/10.1155/2015/239610 Clinical Study Comparison of Conventional Open Thyroidectomy and Endoscopic Thyroidectomy via Breast
International Endocrinology Volume 2015, Article ID 239610, 5 pages http://dx.doi.org/10.1155/2015/239610 Clinical Study Comparison of Conventional Open Thyroidectomy and Endoscopic Thyroidectomy via Breast
Papillary Thyroid Microcarcinoma Presenting as Horner s Syndrome: A Novel Clinical Presentation
 Case Report American Journal of Cancer Case Reports http://ivyunion.org/index.php/ajccr/ Page 1 of 6 Papillary Thyroid Microcarcinoma Presenting as Horner s Syndrome: A Novel Clinical Presentation Ammara
Case Report American Journal of Cancer Case Reports http://ivyunion.org/index.php/ajccr/ Page 1 of 6 Papillary Thyroid Microcarcinoma Presenting as Horner s Syndrome: A Novel Clinical Presentation Ammara
Frequency and pattern of central lymph node metastasis in papillary carcinoma of the thyroid isthmus
 ORIGINAL ARTICLE Frequency and pattern of central lymph node metastasis in papillary carcinoma of the thyroid isthmus Chang Myeon Song, MD, 1 Dong Won Lee, MD, 1 Yong Bae Ji, MD, PhD, 1 Jin Hyeok Jeong,
ORIGINAL ARTICLE Frequency and pattern of central lymph node metastasis in papillary carcinoma of the thyroid isthmus Chang Myeon Song, MD, 1 Dong Won Lee, MD, 1 Yong Bae Ji, MD, PhD, 1 Jin Hyeok Jeong,
Is Hepatic Resection Needed in the Patients with Peritoneal Side T2 Gallbladder Cancer?
 Is Hepatic Resection Needed in the Patients with Peritoneal Side T2 Gallbladder Cancer? Lee H, Park JY, Youn S, Kwon W, Heo JS, Choi SH, Choi DW Department of Surgery, Samsung Medical Center Sungkyunkwan
Is Hepatic Resection Needed in the Patients with Peritoneal Side T2 Gallbladder Cancer? Lee H, Park JY, Youn S, Kwon W, Heo JS, Choi SH, Choi DW Department of Surgery, Samsung Medical Center Sungkyunkwan
Management guideline for patients with differentiated thyroid cancer. Teeraporn Ratanaanekchai ENT, KKU 17 October 2007
 Management guideline for patients with differentiated thyroid Teeraporn Ratanaanekchai ENT, KKU 17 October 2007 Incidence (Srinagarind Hospital, 2005, both sex) Site (all) cases % 1. Liver 1178 27 2. Lung
Management guideline for patients with differentiated thyroid Teeraporn Ratanaanekchai ENT, KKU 17 October 2007 Incidence (Srinagarind Hospital, 2005, both sex) Site (all) cases % 1. Liver 1178 27 2. Lung
Minimally invasive thyroidectomy: a ten years experience
 Original Article Minimally invasive thyroidectomy: a ten years experience Paolo Del Rio, Lorenzo Viani, Chiara Montana Montana, Federico Cozzani, Mario Sianesi Unit of general Surgery and Organ Transplantation,
Original Article Minimally invasive thyroidectomy: a ten years experience Paolo Del Rio, Lorenzo Viani, Chiara Montana Montana, Federico Cozzani, Mario Sianesi Unit of general Surgery and Organ Transplantation,
Differentiated Thyroid Cancer: Initial Management
 Page 1 ATA HOME GIVE ONLINE ABOUT THE ATA JOIN THE ATA MEMBER SIGN-IN INFORMATION FOR PATIENTS FIND A THYROID SPECIALIST Home Management Guidelines for Patients with Thyroid Nodules and Differentiated
Page 1 ATA HOME GIVE ONLINE ABOUT THE ATA JOIN THE ATA MEMBER SIGN-IN INFORMATION FOR PATIENTS FIND A THYROID SPECIALIST Home Management Guidelines for Patients with Thyroid Nodules and Differentiated
The International Federation of Head and Neck Oncologic Societies. Current Concepts in Head and Neck Surgery and Oncology
 The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology www.ifhnos.net The International Federation of Head and Neck Oncologic Societies
The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology www.ifhnos.net The International Federation of Head and Neck Oncologic Societies
American Head and Neck Society - Journal Club Volume 22, July 2018
 - Table of Contents click the page number to go to the summary and full article link. Location and Causation of Residual Lymph Node Metastasis After Surgical Treatment of Regionally Advanced Differentiated
- Table of Contents click the page number to go to the summary and full article link. Location and Causation of Residual Lymph Node Metastasis After Surgical Treatment of Regionally Advanced Differentiated
Thyroid Cancer: When to Treat? MEGAN R. HAYMART, MD
 Thyroid Cancer: When to Treat? MEGAN R. HAYMART, MD ASSOCIATE PROFESSOR OF MEDICINE UNIVERSITY OF MICHIGAN MICHIGAN AACE 2018 ANNUAL MEETING Thyroid Cancer: When Not to Treat? FOCUS WILL BE ON LOW-RISK
Thyroid Cancer: When to Treat? MEGAN R. HAYMART, MD ASSOCIATE PROFESSOR OF MEDICINE UNIVERSITY OF MICHIGAN MICHIGAN AACE 2018 ANNUAL MEETING Thyroid Cancer: When Not to Treat? FOCUS WILL BE ON LOW-RISK
An Unexpected Cause of Hypoglycemia
 An Unexpected Cause of Hypoglycemia Stacey A. Milan, MD FACS Surgical Oncology Nothing to disclose Disclosures Objectives Identify indications for workup of hypoglycemia Define work up for hypoglycemic
An Unexpected Cause of Hypoglycemia Stacey A. Milan, MD FACS Surgical Oncology Nothing to disclose Disclosures Objectives Identify indications for workup of hypoglycemia Define work up for hypoglycemic
Adjuvant therapy for thyroid cancer
 Carcinoma of the thyroid Adjuvant therapy for thyroid cancer John Hay Department of Radiation Oncology Vancouver Cancer Centre Department of Surgery UBC 1% of all new malignancies 0.5% in men 1.5% in women
Carcinoma of the thyroid Adjuvant therapy for thyroid cancer John Hay Department of Radiation Oncology Vancouver Cancer Centre Department of Surgery UBC 1% of all new malignancies 0.5% in men 1.5% in women
Thyroid nodules 3/22/2011. Most thyroid nodules are benign. Thyroid nodules: differential diagnosis
 Most thyroid nodules are benign Thyroid nodules Postgraduate Course in General Surgery thyroid nodules occur in 77% of the world s population palpable thyroid nodules occur in about 5% of women and 1%
Most thyroid nodules are benign Thyroid nodules Postgraduate Course in General Surgery thyroid nodules occur in 77% of the world s population palpable thyroid nodules occur in about 5% of women and 1%
Correspondence should be addressed to Taha Numan Yıkılmaz;
 Advances in Medicine Volume 2016, Article ID 8639041, 5 pages http://dx.doi.org/10.1155/2016/8639041 Research Article External Validation of the Cancer of the Prostate Risk Assessment Postsurgical Score
Advances in Medicine Volume 2016, Article ID 8639041, 5 pages http://dx.doi.org/10.1155/2016/8639041 Research Article External Validation of the Cancer of the Prostate Risk Assessment Postsurgical Score
The International Federation of Head and Neck Oncologic Societies. Current Concepts in Head and Neck Surgery and Oncology
 The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology www.ifhnos.net The International Federation of Head and Neck Oncologic Societies
The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology www.ifhnos.net The International Federation of Head and Neck Oncologic Societies
Title. CitationInternational Cancer Conference Journal, 4(1): Issue Date Doc URL. Rights. Type. File Information
 Title Lymph node metastasis in the suprasternal space from Homma, Akihiro; Hatakeyama, Hiromitsu; Mizumachi, Ta Author(s) Tomohiro; Fukuda, Satoshi CitationInternational Cancer Conference Journal, 4(1):
Title Lymph node metastasis in the suprasternal space from Homma, Akihiro; Hatakeyama, Hiromitsu; Mizumachi, Ta Author(s) Tomohiro; Fukuda, Satoshi CitationInternational Cancer Conference Journal, 4(1):
Risk Adapted Follow-Up
 Risk Adapted Follow-Up Individualizing Follow- Up Strategies R Michael Tuttle, MD Clinical Director, Endocrinology Service Memorial Sloan Kettering Cancer Center Professor of Medicine Weill Medical College
Risk Adapted Follow-Up Individualizing Follow- Up Strategies R Michael Tuttle, MD Clinical Director, Endocrinology Service Memorial Sloan Kettering Cancer Center Professor of Medicine Weill Medical College
- RET/PTC rearrangement: 20% papillary thyroid cancer - RET: medullary thyroid cancer
 Thyroid Cancer UpToDate: Introduction: Risk Factors: Biology: Symptoms: Diagnosis: 1. Lenvina is the first line therapy with powerful durable response and superior PFS in pts with RAI-refractory disease.
Thyroid Cancer UpToDate: Introduction: Risk Factors: Biology: Symptoms: Diagnosis: 1. Lenvina is the first line therapy with powerful durable response and superior PFS in pts with RAI-refractory disease.
42 yr old male with h/o Graves disease and prior I 131 treatment presents with hyperthyroidism and undetectable TSH. 2 hr uptake 20%, 24 hr uptake 50%
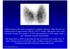 Pinhole images of the neck are acquired in multiple projections, 24hrs after the oral administration of approximately 200 µci of I123. Usually, 24hr uptake value if also calculated (normal 24 hr uptake
Pinhole images of the neck are acquired in multiple projections, 24hrs after the oral administration of approximately 200 µci of I123. Usually, 24hr uptake value if also calculated (normal 24 hr uptake
Case Report Five-Year Survival after Surgery for Invasive Micropapillary Carcinoma of the Stomach
 Case Reports in Surgery Volume 2013, Article ID 560712, 4 pages http://dx.doi.org/10.1155/2013/560712 Case Report Five-Year Survival after Surgery for Invasive Micropapillary Carcinoma of the Stomach Shigeo
Case Reports in Surgery Volume 2013, Article ID 560712, 4 pages http://dx.doi.org/10.1155/2013/560712 Case Report Five-Year Survival after Surgery for Invasive Micropapillary Carcinoma of the Stomach Shigeo
The role of prophylactic central compartment lymph node dissection in differentiated thyroid carcinoma
 Original Research Article The role of prophylactic central compartment lymph node dissection in differentiated thyroid carcinoma Nived Rao 1, M. Muralidhar 2*, M. Srinivasulu 3 1Senior Resident in Surgical
Original Research Article The role of prophylactic central compartment lymph node dissection in differentiated thyroid carcinoma Nived Rao 1, M. Muralidhar 2*, M. Srinivasulu 3 1Senior Resident in Surgical
Robotic Thyroidectomy: Pros and Cons of Various Surgical Approaches
 REVIEW ARTICLE ISSN 1598-1703 (Print) ISSN 2287-6782 (Online) Korean J Endocr Surg 2015;15:73-78 http://dx.doi.org/10.16956/kaes.2015.15.4.73 The Korean Journal of Endocrine Surgery Robotic Thyroidectomy:
REVIEW ARTICLE ISSN 1598-1703 (Print) ISSN 2287-6782 (Online) Korean J Endocr Surg 2015;15:73-78 http://dx.doi.org/10.16956/kaes.2015.15.4.73 The Korean Journal of Endocrine Surgery Robotic Thyroidectomy:
CAP Cancer Protocol and ecc Summary of Changes for August 2014 Thyroid Agile Release
 CAP Cancer Protocol and ecc Summary of Changes for August 2014 Thyroid Agile Release 2 REVISION HISTORY Date Author / Editor Comments 5/19/2014 Jaleh Mirza Created the document 8/12/2014 Samantha Spencer/Jaleh
CAP Cancer Protocol and ecc Summary of Changes for August 2014 Thyroid Agile Release 2 REVISION HISTORY Date Author / Editor Comments 5/19/2014 Jaleh Mirza Created the document 8/12/2014 Samantha Spencer/Jaleh
Biomedical Research 2017; 28 (21): ISSN X
 Biomedical Research 2017; 28 (21): 9497-9501 ISSN 0970-938X www.biomedres.info Analysis of relevant risk factor and recurrence prediction model construction of thyroid cancer after surgery. Shuai Lin 1#,
Biomedical Research 2017; 28 (21): 9497-9501 ISSN 0970-938X www.biomedres.info Analysis of relevant risk factor and recurrence prediction model construction of thyroid cancer after surgery. Shuai Lin 1#,
Thyroid nodules. Most thyroid nodules are benign
 Thyroid nodules Postgraduate Course in General Surgery Jessica E. Gosnell MD Assistant Professor March 22, 2011 Most thyroid nodules are benign thyroid nodules occur in 77% of the world s population palpable
Thyroid nodules Postgraduate Course in General Surgery Jessica E. Gosnell MD Assistant Professor March 22, 2011 Most thyroid nodules are benign thyroid nodules occur in 77% of the world s population palpable
Case Report PET/CT Imaging in Oncology: Exceptions That Prove the Rule
 Case Reports in Oncological Medicine Volume 2013, Article ID 865032, 4 pages http://dx.doi.org/10.1155/2013/865032 Case Report PET/CT Imaging in Oncology: Exceptions That Prove the Rule M. Casali, 1 A.
Case Reports in Oncological Medicine Volume 2013, Article ID 865032, 4 pages http://dx.doi.org/10.1155/2013/865032 Case Report PET/CT Imaging in Oncology: Exceptions That Prove the Rule M. Casali, 1 A.
Oral Presentation V. Surgical Outcome of Atypia of Undetermined Significance and Follicular Lesion of Undetermined Significance in Thyroid Nodule
 Oral Presentation V The Prevalence, Clinicopathologic Features, and Surgical Outcomes according to the Extent of Thyroidectomy in Differentiated Thyroid Cancer > 1 and < 4 cm 1 Jung Bum Choi, 2 SeulGi
Oral Presentation V The Prevalence, Clinicopathologic Features, and Surgical Outcomes according to the Extent of Thyroidectomy in Differentiated Thyroid Cancer > 1 and < 4 cm 1 Jung Bum Choi, 2 SeulGi
Fuqiang Li, Yijun Wu, Liang Chen, Liang Hu, Xiaosun Liu. Original Article
 Original Article Page 1 of 11 Evaluation of clinical risk factors for predicting insidious right central and posterior right recurrent laryngeal nerve lymph node metastasis in papillary thyroid microcarcinoma
Original Article Page 1 of 11 Evaluation of clinical risk factors for predicting insidious right central and posterior right recurrent laryngeal nerve lymph node metastasis in papillary thyroid microcarcinoma
Clinical Study Prognosis of Multifocal Papillary Thyroid Carcinoma
 International Endocrinology, Article ID 89382, 6 pages http://dx.doi.org/1.11/213/89382 Clinical Study Prognosis of Multifocal Papillary Thyroid Carcinoma Sheng-Fong Kuo, 1 Shu-Fu Lin, 1 Tzu-Chieh Chao,
International Endocrinology, Article ID 89382, 6 pages http://dx.doi.org/1.11/213/89382 Clinical Study Prognosis of Multifocal Papillary Thyroid Carcinoma Sheng-Fong Kuo, 1 Shu-Fu Lin, 1 Tzu-Chieh Chao,
Case Report Renal Cell Carcinoma Metastatic to Thyroid Gland, Presenting Like Anaplastic Carcinoma of Thyroid
 Case Reports in Urology Volume 2013, Article ID 651081, 4 pages http://dx.doi.org/10.1155/2013/651081 Case Report Renal Cell Carcinoma Metastatic to Thyroid Gland, Presenting Like Anaplastic Carcinoma
Case Reports in Urology Volume 2013, Article ID 651081, 4 pages http://dx.doi.org/10.1155/2013/651081 Case Report Renal Cell Carcinoma Metastatic to Thyroid Gland, Presenting Like Anaplastic Carcinoma
2 Unusual approaches to thyroidectomy
 UCSF School of Medicine Department of Surgery Section of Endocrine Surgery Disclosures Intuitive Surgical Unusual approaches to Research grant support Grand Rounds Consultant Prescient Surgical Shareholder,
UCSF School of Medicine Department of Surgery Section of Endocrine Surgery Disclosures Intuitive Surgical Unusual approaches to Research grant support Grand Rounds Consultant Prescient Surgical Shareholder,
Prophylactic Central Compartment Neck Dissection(CCND) for Papillary Thyroid Cancer: Con
 Prophylactic Central Compartment Neck Dissection(CCND) for Papillary Thyroid Cancer: Con Christopher R. McHenry, M.D. Vice Chairman Department of Surgery MetroHealth Medical Center Professor of Surgery
Prophylactic Central Compartment Neck Dissection(CCND) for Papillary Thyroid Cancer: Con Christopher R. McHenry, M.D. Vice Chairman Department of Surgery MetroHealth Medical Center Professor of Surgery
Case Report Overlap of Acute Cholecystitis with Gallstones and Squamous Cell Carcinoma of the Gallbladder in an Elderly Patient
 Case Reports in Surgery Volume 2015, Article ID 767196, 4 pages http://dx.doi.org/10.1155/2015/767196 Case Report Overlap of Acute Cholecystitis with Gallstones and Squamous Cell Carcinoma of the Gallbladder
Case Reports in Surgery Volume 2015, Article ID 767196, 4 pages http://dx.doi.org/10.1155/2015/767196 Case Report Overlap of Acute Cholecystitis with Gallstones and Squamous Cell Carcinoma of the Gallbladder
2015 American Thyroid Association Thyroid Nodule and Cancer Guidelines
 2015 American Thyroid Association Thyroid Nodule and Cancer Guidelines Angela M. Leung, MD, MSc, ECNU November 5, 2016 Outline Workup of nontoxic thyroid nodule(s) Ultrasound FNAB Management of FNAB results
2015 American Thyroid Association Thyroid Nodule and Cancer Guidelines Angela M. Leung, MD, MSc, ECNU November 5, 2016 Outline Workup of nontoxic thyroid nodule(s) Ultrasound FNAB Management of FNAB results
Case Report Asymptomatic Pulmonary Vein Stenosis: Hemodynamic Adaptation and Successful Ablation
 Case Reports in Cardiology Volume 2016, Article ID 4979182, 4 pages http://dx.doi.org/10.1155/2016/4979182 Case Report Asymptomatic Pulmonary Vein Stenosis: Hemodynamic Adaptation and Successful Ablation
Case Reports in Cardiology Volume 2016, Article ID 4979182, 4 pages http://dx.doi.org/10.1155/2016/4979182 Case Report Asymptomatic Pulmonary Vein Stenosis: Hemodynamic Adaptation and Successful Ablation
Operative bed recurrence of thyroid cancer: utility of a preoperative needle localization technique
 Original Article Operative bed recurrence of thyroid cancer: utility of a preoperative needle localization technique Oliver S. Eng 1, Scott B. Grant 2, Jason Weissler 3, Mitchell Simon 4, Sudipta Roychowdhury
Original Article Operative bed recurrence of thyroid cancer: utility of a preoperative needle localization technique Oliver S. Eng 1, Scott B. Grant 2, Jason Weissler 3, Mitchell Simon 4, Sudipta Roychowdhury
Solitary Contralateral Adrenal Metastases after Nephrectomy for Renal Cell Carcinoma
 Original Report ISSN 1537-744X; DOI 10.1100/tsw.2004.39 Solitary Contralateral Adrenal after Nephrectomy for Renal Cell Carcinoma Nikolaos Antoniou, M.D. and Demetrios Karanastasis, M.D. General Hospital
Original Report ISSN 1537-744X; DOI 10.1100/tsw.2004.39 Solitary Contralateral Adrenal after Nephrectomy for Renal Cell Carcinoma Nikolaos Antoniou, M.D. and Demetrios Karanastasis, M.D. General Hospital
5/18/2013. Most thyroid nodules are benign. Thyroid nodules: new techniques in evaluation
 Most thyroid nodules are benign Thyroid nodules: new techniques in evaluation Incidence Etiology Risk factors Diagnosis Gene classification system Treatment Postgraduate Course in General Surgery Jessica
Most thyroid nodules are benign Thyroid nodules: new techniques in evaluation Incidence Etiology Risk factors Diagnosis Gene classification system Treatment Postgraduate Course in General Surgery Jessica
Surgery for Recurrent Thyroid cancer: Considerations and limitations
 Surgery for Recurrent Thyroid cancer: Considerations and limitations 2016 Thyroid Master Class February 13, 2016 Ara A. Chalian MD, FACS Surgical Patient Safety Officer University Of Pennsylvania Health
Surgery for Recurrent Thyroid cancer: Considerations and limitations 2016 Thyroid Master Class February 13, 2016 Ara A. Chalian MD, FACS Surgical Patient Safety Officer University Of Pennsylvania Health
Goals & Objectives. Pros, Cons, and Options. Minimally-Invasive Thyroid Surgery: Pros, Cons, and Options 11/9/2012
 Minimally-Invasive Thyroid Surgery: Pros, Cons, and Options Minimally-Invasive Thyroid Surgery: Pros, Cons, and Options Merry Sebelik, MD, FACS Nothing to Disclose Merry E. Sebelik, MD, FACS University
Minimally-Invasive Thyroid Surgery: Pros, Cons, and Options Minimally-Invasive Thyroid Surgery: Pros, Cons, and Options Merry Sebelik, MD, FACS Nothing to Disclose Merry E. Sebelik, MD, FACS University
Case Report Metastatic Malignant Melanoma of Parotid Gland with a Regressed Primary Tumor
 Case Reports in Otolaryngology Volume 2016, Article ID 5393404, 4 pages http://dx.doi.org/10.1155/2016/5393404 Case Report Metastatic Malignant Melanoma of Parotid Gland with a Regressed Primary Tumor
Case Reports in Otolaryngology Volume 2016, Article ID 5393404, 4 pages http://dx.doi.org/10.1155/2016/5393404 Case Report Metastatic Malignant Melanoma of Parotid Gland with a Regressed Primary Tumor
Head & Neck Clinical Sub Group. Network Agreed Imaging Guidelines for UAT and Thyroid Cancer. Measure Nos: 11-1C-105i & 11-1C-106i
 Greater Manchester, Lancashire & South Cumbria Strategic Clinical Network & Senate Head & Neck Clinical Sub Group Network Agreed Imaging Guidelines for UAT and Thyroid Cancer Measure Nos: 11-1C-105i &
Greater Manchester, Lancashire & South Cumbria Strategic Clinical Network & Senate Head & Neck Clinical Sub Group Network Agreed Imaging Guidelines for UAT and Thyroid Cancer Measure Nos: 11-1C-105i &
3/29/2012. Thyroid cancer- what s new. Thyroid Cancer. Thyroid cancer is now the most rapidly increasing cancer in women
 Thyroid cancer- what s new Thyroid Cancer Changing epidemiology Molecular markers Lymph node dissection Technical advances rhtsh Genetic testing and prophylactic surgery Vandetanib What s new? Jessica
Thyroid cancer- what s new Thyroid Cancer Changing epidemiology Molecular markers Lymph node dissection Technical advances rhtsh Genetic testing and prophylactic surgery Vandetanib What s new? Jessica
Dynamic Risk Stratification:
 Dynamic Risk Stratification: Using Risk Estimates to Guide Initial Management R Michael Tuttle, MD Clinical Director, Endocrinology Service Memorial Sloan Kettering Cancer Center Professor of Medicine
Dynamic Risk Stratification: Using Risk Estimates to Guide Initial Management R Michael Tuttle, MD Clinical Director, Endocrinology Service Memorial Sloan Kettering Cancer Center Professor of Medicine
Case Report A Case of Primary Submandibular Gland Oncocytic Carcinoma
 Case Reports in Otolaryngology Volume 2013, Article ID 384238, 4 pages http://dx.doi.org/10.1155/2013/384238 Case Report A Case of Primary Submandibular Gland Oncocytic Carcinoma Kunihiko Tokashiki, Kiyoaki
Case Reports in Otolaryngology Volume 2013, Article ID 384238, 4 pages http://dx.doi.org/10.1155/2013/384238 Case Report A Case of Primary Submandibular Gland Oncocytic Carcinoma Kunihiko Tokashiki, Kiyoaki
Video-assisted thyroidectomy for papillary thyroid carcinoma
 Surg Endosc (2003) 17: 1604 1608 DOI: 10.1007/s00464-002-9220-0 Ó Springer-Verlag York Inc. 2003 Video-assisted thyroidectomy for papillary thyroid carcinoma R. Bellantone, 1 C. P. Lombardi, 1 M. Raffaelli,
Surg Endosc (2003) 17: 1604 1608 DOI: 10.1007/s00464-002-9220-0 Ó Springer-Verlag York Inc. 2003 Video-assisted thyroidectomy for papillary thyroid carcinoma R. Bellantone, 1 C. P. Lombardi, 1 M. Raffaelli,
Medicine. Optimal Cut-Off Values of Lymph Node Ratio Predicting Recurrence in Papillary Thyroid Cancer
 Medicine OBSERVATIONAL STUDY Optimal Cut-Off Values of Lymph Node Ratio Predicting Recurrence in Papillary Thyroid Cancer Seul Gi Lee, MD, Joon Ho, MD, Jung Bum Choi, MD, Tae Hyung Kim, MD, Min Jhi Kim,
Medicine OBSERVATIONAL STUDY Optimal Cut-Off Values of Lymph Node Ratio Predicting Recurrence in Papillary Thyroid Cancer Seul Gi Lee, MD, Joon Ho, MD, Jung Bum Choi, MD, Tae Hyung Kim, MD, Min Jhi Kim,
Research Article Therapeutic Outcomes of Patients with Multifocal Papillary Thyroid Microcarcinomas and Larger Tumors
 Hindawi International Endocrinology Volume 2017, Article ID 4208178, 8 pages https://doi.org/10.1155/2017/4208178 Research Article Therapeutic Outcomes of Patients with Multifocal Papillary Thyroid Microcarcinomas
Hindawi International Endocrinology Volume 2017, Article ID 4208178, 8 pages https://doi.org/10.1155/2017/4208178 Research Article Therapeutic Outcomes of Patients with Multifocal Papillary Thyroid Microcarcinomas
Index. Surg Oncol Clin N Am 16 (2007) Note: Page numbers of article titles are in boldface type.
 Surg Oncol Clin N Am 16 (2007) 465 469 Index Note: Page numbers of article titles are in boldface type. A Adjuvant therapy, preoperative for gastric cancer, staging and, 339 B Breast cancer, metabolic
Surg Oncol Clin N Am 16 (2007) 465 469 Index Note: Page numbers of article titles are in boldface type. A Adjuvant therapy, preoperative for gastric cancer, staging and, 339 B Breast cancer, metabolic
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons
 General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: ENDOCRINE 5-May-2013 DEVELOPED BY: Jonathan Serpell
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: ENDOCRINE 5-May-2013 DEVELOPED BY: Jonathan Serpell
Prognostic value of the 8 th tumor-node-metastasis classification for follicular carcinoma and poorly differentiated carcinoma of the thyroid in Japan
 2018, 65 (6), 621-627 ORIGINAL Prognostic value of the 8 th tumor-node-metastasis classification for follicular carcinoma and poorly differentiated carcinoma of the thyroid in Japan Yasuhiro Ito 1), Akira
2018, 65 (6), 621-627 ORIGINAL Prognostic value of the 8 th tumor-node-metastasis classification for follicular carcinoma and poorly differentiated carcinoma of the thyroid in Japan Yasuhiro Ito 1), Akira
