A case of refractory Hashimoto s encephalopathy demonstrating improvement with plasmapheresis
|
|
|
- Marjory Austin
- 5 years ago
- Views:
Transcription
1 CASE REPORT A case of refractory Hashimoto s encephalopathy demonstrating improvement with plasmapheresis Sarah E. Nelson 1, Yasir N. Jassam 1, Lynne P. Taylor 2 1. Neurology, Tufts Medical Center, Boston, United States. 2. Hematology-Oncology, Tufts Medical Center, Boston, United States. Correspondence: Sarah Nelson. Address: 20 2nd Street, Unit H321, Cambridge, MA 02141, United States. snelson@tuftsmedicalcenter.org Received: February 27, 2014 Accepted: April 2, 2014 Online Published: April 10, 2014 DOI: /crim.v1n2p83 URL: Abstract Hashimoto s encephalopathy (HE) can present with multiple neurologic manifestations and various neuroimaging findings. While its progressive form is often well-recognized, patients with a waxing and waning course may provide diagnostic difficulty. Treatment with corticosteroids has been well-documented, but the benefit of immune-related therapies such as plasmapheresis has not been solidified. Here we describe a patient with waxing and waning signs and symptoms as well as significant fluctuations in neuroimaging findings that initially caused uncertainty regarding her diagnosis. After several largely negative tests including two brain biopsies, she was found to have high levels of anti-thyroid antibodies. Though sometimes found in disorders such as Hashimoto s thyroiditis and Graves disease, these laboratory values in the setting of unremarkable thyroid function tests and her symptoms and their initial responsiveness to corticosteroids helped solidify her diagnosis as HE. However, due to refractory symptoms and signs, this patient required plasmapheresis. We demonstrate clinical, serological, and radiological improvement with this yet unconfirmed therapy, thus raising questions about the appropriateness of the term steroid-responsive encephalopathy. Keywords Hashimoto disease, Autoimmune thyroiditis, Neuroimaging, Cognition disorders, Aphasia 1 Introduction Hashimoto s thyroiditis was first described by Hakaru Hashimoto in 1912 but it was Lord Brain who initially noted the association between thyroiditis and an unusual encephalopathy in 1966 that he called Hashimoto s encephalopathy [1-2]. It is unclear if the anti-thyroid antibodies that characterize this disorder are an autoimmune epiphenomenon or are pathogenic [1]. Many prefer the term steroid responsive encephalopathy associated with autoimmune thyroiditis because of this condition s responsiveness to corticosteroids greater than 90% of patients in some reviews [3, 4]. HE can present with several neurological manifestations and disease courses that can cause initial diagnostic confusion. Neuroimaging is often normal. We present a 74-year-old female with no personal or family history of autoimmune disease who presented with waxing and waning neurological symptoms and striking imaging findings for nearly a year before ultimately being diagnosed with HE. Her very thorough evaluation included multiple laboratory tests and studies in addition to two brain biopsies. In addition, we also demonstrate efficacy of plasmapheresis in our patient. Published by Sciedu Press 83
2 2 Case presentation A 74-year-old Russian female with a history of hypertension, coronary artery disease, diabetes mellitus, and treated hypothyroidism and a family history remarkable only for cardiovascular disorders presented in April 2012 with several months of confusion and aphasia. MRI brain demonstrated cortical T2 hyperintense lesions in multiple vascular territories. On further workup, MRA head and neck was unremarkable and transesophageal echocardiogram demonstrated an ejection fraction of 55% with no thrombus or interatrial shunt. With the conclusion that the patient had likely suffered from a cardioembolic stroke, she was placed on dabigatran. The patient was doing well when 10 days prior to her admission in May 2012 she became increasingly confused, stopped speaking English, and had difficulty understanding language. Though recurrent stroke was considered, a broad differential was initially entertained, including metabolic and infectious etiologies. However, initial negative serum studies included basic metabolic profile, liver function tests, renal function tests, coagulation values, thyroid stimulating hormone (TSH), thyrotropin binding inhibitory immunoglobulin, and vitamin B12 level. Complete blood count and urine and blood cultures were also unremarkable. For concern of a connective tissue disorder or malignancy as an etiology, C-reactive protein and erythrocyte sedimentation rate were tested and were unremarkable. In addition, CT chest, abdomen, and pelvis with and without contrast was unremarkable. Human immunodeficiency (HIV) 1 and 2 antibody and rapid plasma reagin were also tested given that HIV and syphilis can sometimes cause altered mental status, but these values were also unremarkable. Given the appearance of her previous MRI findings, Lyme antibody and angiotensin converting enzyme were sent but were normal. Furthermore, given the above unremarkable work-up, the patient underwent a lumbar puncture. However, negative cerebrospinal fluid (CSF) studies included oligoclonal bands, IgG index, myelin basic protein, herpes simplex virus 1 and 2, and protein. CSF protein was slightly elevated at 58 mg/dl (normal mg/dl), but CSF glucose and white blood cell count were unremarkable. An electroencephalogram (EEG) performed for concern of seizures showed only moderate cerebral dysfunction with possible right temporal/posterior cortical irritability. With the above studies largely unrevealing, HE was considered and anti-thyroid antibodies were then sent. These results showed thyroperoxidase (TPO) microsomal antibody 73 U/mL (normal U/mL) and thyroglobulin antibody U/mL (normal U/mL). Notably, in addition to an unremarkable TSH (3.21 µiu/ml (normal µiu/ml)), other thyroid function tests were total T3 62 ng/dl (normal ng/dl), free T ng/dl (normal ng/dl), and total T4 8.7 µg/dl (normal ug/dl). Her elevated anti-thyroid antibodies in the setting of her clinical presentation and normal thyroid function tests suggested that the patient was euthyroid. MRI brain showed multifocal areas of abnormal T2/FLAIR hyperintense signal involving the cortex and subcortical white matter in bilateral frontal, temporal, occipital, and parietal lobes some of which were increased or decreased in size or new with no enhancement noted (see Figure 1). To further clarify her diagnosis, she underwent a right temporal brain biopsy that showed marked reactive gliosis and rare lymphocytes with no evidence of encephalitis, lymphoma, or prion diseases. Despite this nonspecific biopsy result, the patient was treated empirically with corticosteroids for a presumed diagnosis of HE or central nervous system (CNS) lymphoma, thought possibly to have been missed on the biopsy. One month later, while still on corticosteroids, the patient was greatly improved. She was better able to converse in both English and Russian though was occasionally nonfluent and was independent in her activities of daily living. A follow-up MRI brain in July 2012 continued to show multifocal areas of abnormal T2/FLAIR hyperintensity involving the cortex and subcortical white matter with some lesions smaller and others new or increased in size. In an outpatient visit that month, her family noted that the patient s cognitive status was improving, including her attention, but was not yet at baseline. She was able to perform the cognitive tasks she had previously completed, asked good questions, and better engaged in Russian. Repeat thyroglobulin antibody at that time was U/mL. Due to her improving neurological examination she was weaned off corticosteroids. 84 ISSN E-ISSN
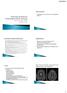
3 Figure 1. Axial FLAIR MRI brain over time. (Top row) Different axial slices from May 2012 demonstrating multifocal T2/FLAIR hyperintensities involving the cortex and subcortical white matter. (Second row) Similar axial slices as above from March 2013 demonstrating improvement in the multifocal T2/FLAIR hyperintensities. (Third row) Similar axial slices as above from June 2013 showing increased leukoencephalopathy. (Bottom row) Similar axial slices as above from August 2013 showing improved leukoencephalopathy. In late November 2012, however, the patient experienced increased confusion, and a repeat thyroglobulin antibody level in early December 2012 was > U/mL. A repeat brain biopsy completed in an attempt to confirm a diagnosis of presumed HE was performed in the left temporal region and was again nonspecific in demonstrating moderate to marked gliosis and no evidence for a lymphoproliferative disorder. Published by Sciedu Press 85
4 Despite the nondiagnostic second brain biopsy, she was diagnosed with HE due to her neurological symptoms, elevated anti-thyroid antibodies, response to corticosteroids, and relatively unremarkable supporting studies. She was restarted and improved on corticosteroids. MRI brain from March 2013 demonstrated marked improvement in the T2/FLAIR hyperintensities (see Figure 1). Unfortunately, however, the patient s symptoms continued to fluctuate. In May 2013 while still on corticosteroids, she presented with worsening aphasia and executive dysfunction including attentional deficits. Thyroglobulin antibody was U/mL, and MRI brain showed new lesions. Her corticosteroid dose was increased, and azathioprine was started for chronic immunosuppressive therapy. Nonetheless, deteriorating language and memory problems were noted in June MRI brain demonstrated increased foci of T2/FLAIR hyperintensities (see Figure 1). Due to the refractory nature of her symptoms despite treatment with corticosteroids and azathioprine, she was started on plasmapheresis. Thus far she has undergone plasmapheresis approximately every 2-3 days between June 28-July 8, 2013, October 8-21, 2013, and January 23-31, Since undergoing two courses of plasmapheresis to date, the patient has improved clinically: she has not experienced confusion, her language is without paraphrasic errors, and she maintains household activities. Interestingly, her anti-thyroid antibody levels decreased after at least two of her courses of plasmapheresis (antibody levels were not measured after her October 2013 plasmapheresis) (see Table 1). In addition, her neuroimaging findings have also improved since starting plasmaphereis (see Figure 1). She is currently maintained on corticosteroids, azathioprine, and plasmapheresis. Table 1. Clinical Correlation with Anti-Thyroid Antibody Levels Date TPO Microsomal Antibody ( U/ml) Thyroglobulin Antibody ( U/mL) Clinical Course May Initial presentation July 2012 NM Improved December 2012 NM > Worsened March 2013 NM NM Improved May Worsened June Worsened August NM Improved October NM Stable January 22, NM Worsened January 31, NM Improved Note: Abbreviations: TPO = thyroid peroxidase, NM = not measured. Normal values are provided in parentheses 3 Discussion While Hakaru Hashimoto first described Hashimoto s thyroiditis in 1912, the disorder now known as HE also known as Hashimoto s encephalitis, steroid-responsive encephalopathy associated with autoimmune thyroiditis, and nonvasculitic autoimmune inflammatory meningoencephalitis was first noted in 1966 by Lord Brain, who described what is considered the first case of this disorder [1, 2]. As demonstrated in our patient, multiple neurologic abnormalities can occur in patients with HE, including encephalopathy, stroke-like episodes, psychosis, visual hallucinations, aphasia, ataxia, seizures, myoclonus, and tremor. Supportive laboratory tests include thyroid-related antibodies such as anti-thyrotropin, anti-tpo, anti-thyroglobulin, and 86 ISSN E-ISSN
5 anti-alpha-enolase. An association with thyroid disorders is sometimes found but neurologic symptoms do not appear to depend on thyroid status [3, 4]. Though anti-alpha-enolase was not tested in our patient, her anti-thyroid antibodies were noted to be significantly elevated. As discussed above, diagnoses such as Hashimoto s thyroiditis and Graves disease can be considered in patients with elevated anti-thyroid antibodies but this was considered unlikely in our patient given her normal thyroid function tests and clinical exam. In the CSF the most frequent finding is elevated protein, as found in our patient, though anti-thyroid antibodies have also been noted (these were not tested in our patient) [1, 3]. EEG abnormalities are seen in a majority of patients, most commonly diffuse slowing but also triphasic waves, periodic sharp waves, and frontal rhythmic slowing [1, 4, 5]. There are no neuropathology findings specific to HE though an encephalitic or vasculitic process has been debated in the literature [1, 3, 4, 6, 7]. A relationship to CNS demyelination has also been shown [4, 8, 9]. Our patient s brain biopsies and EEG were overall considered nonspecific. The diagnosis of HE requires the presence of anti-thyroid antibodies, a progressive or relapsing-remitting course, and the exclusion of other etiologies [4, 10]. In 1999, Peschen-Rosin et al proposed the first set of diagnostic criteria: episodes of relapsing myoclonus, focal neurological deficits, seizures, or psychiatric disorders in addition to at least three of the following: heterogeneous but unrevealing MRI brain, abnormal EEG, high anti-thyroid antibody levels, elevated protein and/or oligoclonal bands in the CSF, and good response to steroids [11]. MRI brain findings are variable and can be normal or include focal or confluent white matter abnormalities, atrophy, and other cortex irregularities [1]. MRI abnormalities may improve with steroid treatment and can correlate with anti-thyroid antibody levels; in our patient it appears that her neuroimaging findings roughly improved along with her anti-thyroid antibody levels (see Table 1 and Figure 1) [1]. MRI findings can also change over time within the same patient [1, 4]. A review of 85 HE patients showed that 42 of 82 patients (52%) who had undergone neuroimaging had normal findings [3]. In a review of 121 patients, 71 patients were noted to have normal neuroimaging (it is unclear how many of these 121 patients underwent imaging, however) [4]. Those with abnormal scans most commonly exhibited cortical atrophy and nonspecific subcortical focal white matter abnormalities [3, 4]. Thus while neuroimaging in HE is often normal, our patient demonstrated the more typical HE imaging findings. Even so, imaging in our case fluctuated dramatically over time. Anti-thyroid antibodies is one of the signature features of HE, though as mentioned above there is uncertainty as to whether they are pathogenic or merely an autoimmune epiphenomenon [1]. While they do not necessarily parallel the clinical status of HE patients, exceptions have been noted [3, 4, 12]. Our patient is remarkable in that symptom improvement and worsening has roughly correlated with anti-thyroid antibody levels decreasing and increasing, respectively (see Table 1). The mean age of patients with HE was approximately mid-40-years-old in two reviews. Though our case could be considered unusual given that she initially presented at 74-years-old, a large age range in which this disorder can manifest has been found (9- to 78-years-old in one review, 8- to 86-years-old in another review) [3, 4]. Corticosteroids have been the mainstay of therapy for HE, and greater than 90% of patients improved on this therapy in two large reviews of HE patients [3, 4]. However, other treatments that can be beneficial in immune-mediated disorders, such as plasmapheresis and intravenous immunoglobulin (IVIG), have been used. In particular, the data on plasmapheresis is suggestive of a possible benefit but is not conclusive. Immuosuppressant medications have also been tried including azathioprine and cyclophosphamide [1, 3, 4]. Our patient initially benefited from steroids, and the effects of azathioprine likely remain to be seen. Significantly, however, our patient demonstrated clinical, serological, and radiological improvement with plasmapheresis. Our patient experienced a relapsing-remitting form of HE that was also difficult to treat. Various clinical courses can be seen in HE including progressive, relapsing-remitting, and stroke-like episodes though the progressive form may be the Published by Sciedu Press 87
6 most recognizable [1, 4]. In one review of 121 HE patients, 55 (45%) patients had relapsing courses and 10 (8%) were treatment-refractory, including some who did not respond to more than one therapy like our patient [4]. In another study including 85 HE patients, 51 (60%) patients suffered a relapsing-remitting course and 8 were refractory to treatments including glucocorticoids, glucocorticoids plus levothyroxine, levothyroxine, and IVIG [3]. We present a case of relapsing-remitting and treatment-refractory HE who, because of her varied neurological manifestations and neuroimaging findings over time, was initially challenging to diagnose. Ultimately, her positive anti-thyroid antibodies, symptomatic response to corticosteroids, and exclusion of other etiologies left little doubt of her diagnosis of HE. Our case is also unusual because significant fluctuations in her neuroimaging findings occurred over time. Correlation between clinical status and anti-thyroid antibody levels in HE is not always seen but was generally true in our patient. Finally, our demonstration of plasmapheresis efficacy adds to the small body of literature regarding the use of this therapy in HE patients. Physicians should consider the diagnosis of HE in patients presenting with relapsing-remitting symptoms and imaging that may be initially suggestive of other diagnoses. References [1] Schiess N, Pardo C. Hashimoto s encephalopathy. Ann NY Acad Sci. 2008; 1142: [2] Brain L, Jellinek EH, Ball K. Hashimoto s disease and encephalopathy. Lancet. 1966; 2(7462): [3] Chong JY, Rowland LP, Utiger RD. Hashimoto encephalopathy: syndrome or myth? Arch Neurol. 2003; 60: [4] Ferracci F, Carnevale A. The neurological disorder associated with thyroid autoimmunity. J Neurol. 2006; 253: [5] Henchey R, Cibula J, Helveston W, et al. Electroencephalographic findings in Hashimoto s encephalopathy. Neurology. 1995; 45: [6] Doherty CP, Schlossmacher M, Torres N, et al. Hashimoto s encephalopathy mimicking Creutzfeldt-Jakob disease: brain biopsy findings. J Neurol Neurosurg Psychiatry. 2002; 73: [7] Paulus W, Nolte KW. Neuropathology of Hashimoto s encephalopathy. J Neurol Neurosurg Psychiatry. 2003; 74: [8] Chaudhuri A, Behan PO. Hashimoto s encephalopathy: a relapsing form of acute disseminated encephalomyelitis. J Neurol Sci. 2005; 235: [9] Mahad DJ, Staugaitis S, Ruggieri P, et al. Steroid-responsive encephalopathy associated with autoimmune thyroiditis and primary CNS demyelination. J Neurol Sci. 2005; 228: [10] Mijajlovic M, Mikovic M, Dackovic J, et al. Clinical manifestations, diagnostic criteria and therapy of Hashimoto s encephalopathy: report of two cases. J Neurol Sci. 2010; 288: [11] Peschen-Rosin R, Schabet M, Dichgans J. Manifestation of Hashimoto s encephalopathy years before onset of thyroid disease. Eur Neurol. 1999; 41: [12] Yuceyar N, Karadeniz M, Erdogan M, et al. Thyrotoxic autoimmune encephalopathy in a female patient: only partial response to typical immunosuppressant treatment and remission after thyroidectomy. Clin Neurol Neurosurg. 2007; 109: ISSN E-ISSN
Case Report Paroxysmal Amnesia Attacks due to Hashimoto s Encephalopathy
 Case Reports in Medicine Volume 2016, Article ID 1267192, 4 pages http://dx.doi.org/10.1155/2016/1267192 Case Report Paroxysmal Amnesia Attacks due to Hashimoto s Encephalopathy Pelin Nar Senol, Aylin
Case Reports in Medicine Volume 2016, Article ID 1267192, 4 pages http://dx.doi.org/10.1155/2016/1267192 Case Report Paroxysmal Amnesia Attacks due to Hashimoto s Encephalopathy Pelin Nar Senol, Aylin
COPYRIGHT 2012 THE TRANSVERSE MYELITIS ASSOCIATION. ALL RIGHTS RESERVED
 The Transverse Myelitis Association...advocating for those with acute disseminated encephalomyelitis, neuromyelitis optica, optic neuritis and transverse myelitis ACUTE DISSEMINATED ENCEPHALOMYELITIS (ADEM)
The Transverse Myelitis Association...advocating for those with acute disseminated encephalomyelitis, neuromyelitis optica, optic neuritis and transverse myelitis ACUTE DISSEMINATED ENCEPHALOMYELITIS (ADEM)
Hashimoto s encephalopathy cases: Chinese experience
 Tang et al. BMC Neurology 2012, 12:60 RESEARCH ARTICLE Open Access Hashimoto s encephalopathy cases: Chinese experience Yi Tang 1, Yi Xing 1, Michael T Lin 2, Jin Zhang 1 and Jianping Jia 1* Abstract Background:
Tang et al. BMC Neurology 2012, 12:60 RESEARCH ARTICLE Open Access Hashimoto s encephalopathy cases: Chinese experience Yi Tang 1, Yi Xing 1, Michael T Lin 2, Jin Zhang 1 and Jianping Jia 1* Abstract Background:
Delirium in ICU due to Hashimoto s Encephalopathy: A Case Report
 International Journal of Advances in Health Sciences (IJHS) ISSN 2349-7033 Vol2, Issue6, 2015, pp731-735 http://www.ijhsonline.com Case Report Vijay Kumar Agarwal and B. Saroj Kumar Prusty Yashoda Hospitals,
International Journal of Advances in Health Sciences (IJHS) ISSN 2349-7033 Vol2, Issue6, 2015, pp731-735 http://www.ijhsonline.com Case Report Vijay Kumar Agarwal and B. Saroj Kumar Prusty Yashoda Hospitals,
Original Article Neuro-Psychiatric Manifestations of Hashimoto Thyroiditis Pak Armed Forces Med J 2018; 68 (2):
 Open Access Original Article Neuro-Psychiatric Manifestations of Hashimoto Thyroiditis Pak Armed Forces Med J 2018; 68 (2): 369-73 NEURO-PSYCHIATRIC MANIFESTATIONS OF HASHIMOTO THYROIDITIS; A CASE SERIES
Open Access Original Article Neuro-Psychiatric Manifestations of Hashimoto Thyroiditis Pak Armed Forces Med J 2018; 68 (2): 369-73 NEURO-PSYCHIATRIC MANIFESTATIONS OF HASHIMOTO THYROIDITIS; A CASE SERIES
Radiology Case Reports. Hashimoto's encephalopathy. Joana Ramalho, MD, and Mauricio Castillo, MD
 Radiology Case Reports Volume 6, Issue 1, 2011 Hashimoto's encephalopathy Joana Ramalho, MD, and Mauricio Castillo, MD We report a case of Hashimoto s encephalopathy with atypical and partially reversible
Radiology Case Reports Volume 6, Issue 1, 2011 Hashimoto's encephalopathy Joana Ramalho, MD, and Mauricio Castillo, MD We report a case of Hashimoto s encephalopathy with atypical and partially reversible
Neurosyphilis SYPHILIS OF THE CENTRAL NERVOUS SYSTEM AS A CAUSE OF COGNITIVE IMPAIRMENT AT YOUNGER AGE, DIAGNOSTIC DIFFICULTIES
 29 SYPHILIS OF THE CENTRAL NERVOUS SYSTEM AS A CAUSE OF COGNITIVE IMPAIRMENT AT YOUNGER AGE, DIAGNOSTIC DIFFICULTIES Nesteruk M 1 *, Nesteruk T 2, Mandecka M 3, Dorobek M 1 1. Neurology Clinic, MSW Hospital,
29 SYPHILIS OF THE CENTRAL NERVOUS SYSTEM AS A CAUSE OF COGNITIVE IMPAIRMENT AT YOUNGER AGE, DIAGNOSTIC DIFFICULTIES Nesteruk M 1 *, Nesteruk T 2, Mandecka M 3, Dorobek M 1 1. Neurology Clinic, MSW Hospital,
Human Herpes Virus-6 Limbic Encephalitis
 Case Studies [1] March 19, 2013 Case history: A 32-year-old Caucasian female with newly diagnosed acute myeloid leukemia (AML) was treated with induction chemotherapy and attained complete remission. She
Case Studies [1] March 19, 2013 Case history: A 32-year-old Caucasian female with newly diagnosed acute myeloid leukemia (AML) was treated with induction chemotherapy and attained complete remission. She
Electroencephalography. Role of EEG in NCSE. Continuous EEG in ICU 25/05/59. EEG pattern in status epilepticus
 EEG: ICU monitoring & 2 interesting cases Electroencephalography Techniques Paper EEG digital video electroencephalography Dr. Pasiri Sithinamsuwan PMK Hospital Routine EEG long term monitoring Continuous
EEG: ICU monitoring & 2 interesting cases Electroencephalography Techniques Paper EEG digital video electroencephalography Dr. Pasiri Sithinamsuwan PMK Hospital Routine EEG long term monitoring Continuous
Role of MRI in acute disseminated encephalomyelitis
 Original Research Article Role of MRI in acute disseminated encephalomyelitis Shashvat Modiya 1*, Jayesh Shah 2, C. Raychaudhuri 3 1 1 st year resident, 2 Associate Professor, 3 HOD and Professor Department
Original Research Article Role of MRI in acute disseminated encephalomyelitis Shashvat Modiya 1*, Jayesh Shah 2, C. Raychaudhuri 3 1 1 st year resident, 2 Associate Professor, 3 HOD and Professor Department
Neurology Department, The First Hospital of China Medical University, Nanjing North Street 155, Shenyang, Liaoning Province, China
 Psychiatric Symptoms as Bases for Differential Diagnosis of Pre-mortem Sporadic Creutzfeldt-Jakob Disease and Anti-N-Methyl D-aspartate Receptor Encephalitis Yujia Luo 1, Xi Cheng 1, Yang Jiao 2, Huibin
Psychiatric Symptoms as Bases for Differential Diagnosis of Pre-mortem Sporadic Creutzfeldt-Jakob Disease and Anti-N-Methyl D-aspartate Receptor Encephalitis Yujia Luo 1, Xi Cheng 1, Yang Jiao 2, Huibin
دمانس های اتوایمون دکتر رضائی طلب نورولوژیست آذر 95
 دمانس های اتوایمون دکتر رضائی طلب نورولوژیست آذر 95 Definition: Dementia According the DSM-5, dementia is defined as significant acquired cognitive impairment in one or more cognitive domains (eg, learning
دمانس های اتوایمون دکتر رضائی طلب نورولوژیست آذر 95 Definition: Dementia According the DSM-5, dementia is defined as significant acquired cognitive impairment in one or more cognitive domains (eg, learning
A Neurologist s Approach to Altered Mental Status
 A Neurologist s Approach to Altered Mental Status S. Andrew Josephson, MD Department of Neurology University of California San Francisco October 23, 2008 The speaker has no disclosures Case 1 A 71 year-old
A Neurologist s Approach to Altered Mental Status S. Andrew Josephson, MD Department of Neurology University of California San Francisco October 23, 2008 The speaker has no disclosures Case 1 A 71 year-old
MILD HYPERTHYROIDISM CAUSES A PSEUDO-ALZHEIMER S PATTERN OF CEREBRAL METABOLISM WHICH IS REVERSIBLE WITH CEREBRAL PERFUSION STIMULANTS
 MILD HYPERTHYROIDISM CAUSES A PSEUDO-ALZHEIMER S PATTERN OF CEREBRAL METABOLISM WHICH IS REVERSIBLE WITH CEREBRAL PERFUSION STIMULANTS Harold Thomas Pretorius, MD, PhD, and Nichole Richards Abstract Objective:
MILD HYPERTHYROIDISM CAUSES A PSEUDO-ALZHEIMER S PATTERN OF CEREBRAL METABOLISM WHICH IS REVERSIBLE WITH CEREBRAL PERFUSION STIMULANTS Harold Thomas Pretorius, MD, PhD, and Nichole Richards Abstract Objective:
Diagnosis and management of non-alzheimer dementias. Melissa Yu, M.D. Department of Neurology
 Diagnosis and management of non-alzheimer dementias Melissa Yu, M.D. Department of Neurology AGENDA Introduction When to think of alternate diagnoses Other forms of dementia Other reasons for confusion
Diagnosis and management of non-alzheimer dementias Melissa Yu, M.D. Department of Neurology AGENDA Introduction When to think of alternate diagnoses Other forms of dementia Other reasons for confusion
Cerebral Toxoplasmosis in HIV-Infected Patients. Ahmed Saad,MD,FACP
 Cerebral Toxoplasmosis in HIV-Infected Patients Ahmed Saad,MD,FACP Introduction Toxoplasmosis: Caused by the intracellular protozoan, Toxoplasma gondii. Immunocompetent persons with primary infection
Cerebral Toxoplasmosis in HIV-Infected Patients Ahmed Saad,MD,FACP Introduction Toxoplasmosis: Caused by the intracellular protozoan, Toxoplasma gondii. Immunocompetent persons with primary infection
May He Rest in Peace
 May He Rest in Peace Neurologic Complications of AIDS Medical Knowledge Fiesta 2012 Paul K. King MD pkingmd@yahoo.com Objectives definition of HIV/AIDS what are the neurologic complications of AIDS how
May He Rest in Peace Neurologic Complications of AIDS Medical Knowledge Fiesta 2012 Paul K. King MD pkingmd@yahoo.com Objectives definition of HIV/AIDS what are the neurologic complications of AIDS how
Decoding Your Thyroid Tests and Results
 Decoding Your Thyroid Tests and Results Wondering about your thyroid test results? Learn about each test and what low, optimal, and high results may mean so you can work with your doctor to choose appropriate
Decoding Your Thyroid Tests and Results Wondering about your thyroid test results? Learn about each test and what low, optimal, and high results may mean so you can work with your doctor to choose appropriate
EEG IN FOCAL ENCEPHALOPATHIES: CEREBROVASCULAR DISEASE, NEOPLASMS, AND INFECTIONS
 246 Figure 8.7: FIRDA. The patient has a history of nonspecific cognitive decline and multiple small WM changes on imaging. oligodendrocytic tumors of the cerebral hemispheres (11,12). Electroencephalogram
246 Figure 8.7: FIRDA. The patient has a history of nonspecific cognitive decline and multiple small WM changes on imaging. oligodendrocytic tumors of the cerebral hemispheres (11,12). Electroencephalogram
A challenging neurological complication in a young HIV-infected woman
 A challenging neurological complication in a young HIV-infected woman Ianache Irina-Cristiana Vi tor Ba es Clini al Hospital for Infectious and Tropical Diseases Bucharest - HIV/AIDS department Assessment
A challenging neurological complication in a young HIV-infected woman Ianache Irina-Cristiana Vi tor Ba es Clini al Hospital for Infectious and Tropical Diseases Bucharest - HIV/AIDS department Assessment
10/27/2013. Funding from the Autoimmune Encephalitis Alliance. Heather Van Mater, MD MS October 27, 2013
 Funding from the Alliance Heather Van Mater, MD October 27, 2013 1 2 Aviv, et al. MR imaging and angiography of primary CNS of childhood. AJNR Am J Neuroradiol. 2006; 27: 192-199 Aviv, et al. of primary
Funding from the Alliance Heather Van Mater, MD October 27, 2013 1 2 Aviv, et al. MR imaging and angiography of primary CNS of childhood. AJNR Am J Neuroradiol. 2006; 27: 192-199 Aviv, et al. of primary
Case Report. Herpes simplex virus encephalitis presenting as frontal lobe hemorrhage
 1 Case Report Herpes simplex virus encephalitis presenting as frontal lobe hemorrhage Authors: Shila, MD, *Jessica Erfan, MPAS, PA-C, Ray Bogitch, MD, Jefferson T. Miley, MD Department of Neurology, Dell
1 Case Report Herpes simplex virus encephalitis presenting as frontal lobe hemorrhage Authors: Shila, MD, *Jessica Erfan, MPAS, PA-C, Ray Bogitch, MD, Jefferson T. Miley, MD Department of Neurology, Dell
Autoimmune encephalopathieslatest. Prof Belinda Lennox Department of Psychiatry, University of Oxford
 Autoimmune encephalopathieslatest advances Prof Belinda Lennox Department of Psychiatry, University of Oxford Belinda.lennox@psych.ox.ac.uk RCP Advanced Medicine 20 th June 2016 Declarations of Interest
Autoimmune encephalopathieslatest advances Prof Belinda Lennox Department of Psychiatry, University of Oxford Belinda.lennox@psych.ox.ac.uk RCP Advanced Medicine 20 th June 2016 Declarations of Interest
Central Nervous System Immune Reconstitution Disease: Pathology
 Central Nervous System Immune Reconstitution Disease: Pathology F.Gray, H.Adle-Biassette, F.Héran, G. Pialoux, A.Moulignier, APHP Hôpital Lariboisière Université Paris VII Introduction of HAART, which
Central Nervous System Immune Reconstitution Disease: Pathology F.Gray, H.Adle-Biassette, F.Héran, G. Pialoux, A.Moulignier, APHP Hôpital Lariboisière Université Paris VII Introduction of HAART, which
Objective. Clinical characteristic. Case 1: M/70 8/11/2014. Autoimmune epilepsy: A new cause of seizure & status epilepticus
 Objective Autoimmune epilepsy: A new cause of seizure & status epilepticus Metha Apiwattanakul MD. Neuroimmunology Unit Prasat Neurological Institute How to identify autoimmune epilepsy, are there any
Objective Autoimmune epilepsy: A new cause of seizure & status epilepticus Metha Apiwattanakul MD. Neuroimmunology Unit Prasat Neurological Institute How to identify autoimmune epilepsy, are there any
Helpful Information for evaluation of new neurological symptoms in patients receiving TYSABRI
 Helpful Information for evaluation of new neurological symptoms in patients receiving TYSABRI This information is provided as an educational resource for healthcare providers and should be considered current
Helpful Information for evaluation of new neurological symptoms in patients receiving TYSABRI This information is provided as an educational resource for healthcare providers and should be considered current
Reactivation of herpesvirus under fingolimod: A case of severe herpes simplex encephalitis
 Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2015 Reactivation of herpesvirus under fingolimod: A case of severe herpes
Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2015 Reactivation of herpesvirus under fingolimod: A case of severe herpes
The Neurology of HIV Infection. Carolyn Barley Britton, MD, MS Associate Professor of Clinical Neurology Columbia University
 The Neurology of HIV Infection Carolyn Barley Britton, MD, MS Associate Professor of Clinical Neurology Columbia University HIV/AIDS Epidemiology World-wide pandemic, 40 million affected U.S.- Disproportionate
The Neurology of HIV Infection Carolyn Barley Britton, MD, MS Associate Professor of Clinical Neurology Columbia University HIV/AIDS Epidemiology World-wide pandemic, 40 million affected U.S.- Disproportionate
AUTOIMMUNE ENCEPHALITIS
 AUTOIMMUNE ENCEPHALITIS Shruti Agnihotri, MD Assistant Professor Department of Neurology, UAB August 12, 2017 DISCLOSURES No financial disclosure Evolving evidence Page 2 OBJECTIVES Review the types of
AUTOIMMUNE ENCEPHALITIS Shruti Agnihotri, MD Assistant Professor Department of Neurology, UAB August 12, 2017 DISCLOSURES No financial disclosure Evolving evidence Page 2 OBJECTIVES Review the types of
Marchiafava Bignami Disease (MBD) and Diffusion Tensor Image (DTI) Tractography. Priscilla Chukwueke, MD, MPH
 Marchiafava Bignami Disease (MBD) and Diffusion Tensor Image (DTI) Tractography Priscilla Chukwueke, MD, MPH INTRODUCTION Definition: A rare CNS disease characterized by demyelination of the Corpus Callosum.
Marchiafava Bignami Disease (MBD) and Diffusion Tensor Image (DTI) Tractography Priscilla Chukwueke, MD, MPH INTRODUCTION Definition: A rare CNS disease characterized by demyelination of the Corpus Callosum.
Case Report High Grade Glioma Mimicking Voltage Gated Potassium Channel Complex Associated Antibody Limbic Encephalitis
 Case Reports in Neurological Medicine, Article ID 458790, 4 pages http://dx.doi.org/10.1155/2014/458790 Case Report High Grade Glioma Mimicking Voltage Gated Potassium Channel Complex Associated Antibody
Case Reports in Neurological Medicine, Article ID 458790, 4 pages http://dx.doi.org/10.1155/2014/458790 Case Report High Grade Glioma Mimicking Voltage Gated Potassium Channel Complex Associated Antibody
Difficult Diagnosis: Case History. 7 months prior, she happened to have undergone a C-spine MRI after a car accident
 Relevant Disclosures: None Difficult Diagnosis: Recent Advances in Neurology 2013 Jeffrey M. Gelfand, MD Assistant Professor UCSF Neuroinflammation and MS Center UCSF Department of Neurology Case History
Relevant Disclosures: None Difficult Diagnosis: Recent Advances in Neurology 2013 Jeffrey M. Gelfand, MD Assistant Professor UCSF Neuroinflammation and MS Center UCSF Department of Neurology Case History
Case 9 10/29/2018. CJD (Creutzfeldt -Jakob Disease) CJD (Creutzfeldt -Jakob Disease) CJD (Creutzfeldt -Jakob Disease)
 CJD (Creutzfeldt -Jakob Disease) Rare fatal neurodegen dz caused by infectious protein Prion (lacks nucleic acid)- causes spongiform changes of the brain and neuronal death. 4 types: scjd- 85% of cases
CJD (Creutzfeldt -Jakob Disease) Rare fatal neurodegen dz caused by infectious protein Prion (lacks nucleic acid)- causes spongiform changes of the brain and neuronal death. 4 types: scjd- 85% of cases
Research Article [ 18 F]-Fluoro-Deoxy-Glucose Positron Emission Tomography Scan Should Be Obtained Early in Cases of Autoimmune Encephalitis
![Research Article [ 18 F]-Fluoro-Deoxy-Glucose Positron Emission Tomography Scan Should Be Obtained Early in Cases of Autoimmune Encephalitis Research Article [ 18 F]-Fluoro-Deoxy-Glucose Positron Emission Tomography Scan Should Be Obtained Early in Cases of Autoimmune Encephalitis](/thumbs/72/67118353.jpg) Autoimmune Diseases Volume 2016, Article ID 9450452, 6 pages http://dx.doi.org/10.1155/2016/9450452 Research Article [ 18 F]-Fluoro-Deoxy-Glucose Positron Emission Tomography Scan Should Be Obtained Early
Autoimmune Diseases Volume 2016, Article ID 9450452, 6 pages http://dx.doi.org/10.1155/2016/9450452 Research Article [ 18 F]-Fluoro-Deoxy-Glucose Positron Emission Tomography Scan Should Be Obtained Early
Scope. EEG patterns in Encephalopathy. Diffuse encephalopathy. EEG in adult patients with. EEG in diffuse encephalopathy
 Scope EEG patterns in Encephalopathy Dr.Pasiri Sithinamsuwan Division of Neurology Department of Medicine Phramongkutklao Hospital Diffuse encephalopathy EEG in specific encephalopathies Encephalitides
Scope EEG patterns in Encephalopathy Dr.Pasiri Sithinamsuwan Division of Neurology Department of Medicine Phramongkutklao Hospital Diffuse encephalopathy EEG in specific encephalopathies Encephalitides
Hippocampal Sclerosis in LGI1 and CSPR2 Positive Limbic Encephalopathy: Case Report
 Hippocampal Sclerosis in LGI1 and CSPR2 Positive Limbic Encephalopathy: Ammar Taha Abdulaziz 1, Le Zhang 1, Dong Zhou 2, JinMei Li 3, Abstract Background: Limbic encephalopathy (LE) is a sub-acute neuropsychiatric
Hippocampal Sclerosis in LGI1 and CSPR2 Positive Limbic Encephalopathy: Ammar Taha Abdulaziz 1, Le Zhang 1, Dong Zhou 2, JinMei Li 3, Abstract Background: Limbic encephalopathy (LE) is a sub-acute neuropsychiatric
MRI in Differential Diagnosis. CMSC, June 2, Jill Conway, MD, MA, MSCE
 MRI in Differential Diagnosis CMSC, June 2, 2016 Jill Conway, MD, MA, MSCE Director, Carolinas MS Center Clerkship Director, UNCSOM-Charlotte Campus Charlotte, NC Disclosures Speaking, consulting, and/or
MRI in Differential Diagnosis CMSC, June 2, 2016 Jill Conway, MD, MA, MSCE Director, Carolinas MS Center Clerkship Director, UNCSOM-Charlotte Campus Charlotte, NC Disclosures Speaking, consulting, and/or
Applying Chimeric Antigen Receptor T cells (CAR-T) to hematologic malignancies
 Applying Chimeric Antigen Receptor T cells (CAR-T) to hematologic malignancies Anne W. Beaven, MD Associate Professor Duke University Medical Center Duke Debates April 21, 2017 Chimeric Antigen Receptor
Applying Chimeric Antigen Receptor T cells (CAR-T) to hematologic malignancies Anne W. Beaven, MD Associate Professor Duke University Medical Center Duke Debates April 21, 2017 Chimeric Antigen Receptor
Demyelinating Diseases of the Brain
 Department of Radiology University of California San Diego Demyelinating Diseases of the Brain John R. Hesselink, M.D. T1-Weighted Images Normal White Matter Contents Axons with envelope of myelin Neuroglia
Department of Radiology University of California San Diego Demyelinating Diseases of the Brain John R. Hesselink, M.D. T1-Weighted Images Normal White Matter Contents Axons with envelope of myelin Neuroglia
Sawada J, Orimoto R, Misu T, Katayama T, Aizawa H, Asanome A, Takahashi K, Saito T, Anei R, Kamada K, Miyokawa N, Takahashi T, Fujihara K, Hasebe N.
 Mult Scler (2014.9) 20(10):1413-1416. A case of pathology-proven neuromyelitis optica spectrum disorder with Sjögren syndrome manifesting aphasia and apraxia due to a localized cerebral white matter lesion.
Mult Scler (2014.9) 20(10):1413-1416. A case of pathology-proven neuromyelitis optica spectrum disorder with Sjögren syndrome manifesting aphasia and apraxia due to a localized cerebral white matter lesion.
Dementia Update. October 1, 2013 Dylan Wint, M.D. Cleveland Clinic Lou Ruvo Center for Brain Health Las Vegas, Nevada
 Dementia Update October 1, 2013 Dylan Wint, M.D. Cleveland Clinic Lou Ruvo Center for Brain Health Las Vegas, Nevada Outline New concepts in Alzheimer disease Biomarkers and in vivo diagnosis Future trends
Dementia Update October 1, 2013 Dylan Wint, M.D. Cleveland Clinic Lou Ruvo Center for Brain Health Las Vegas, Nevada Outline New concepts in Alzheimer disease Biomarkers and in vivo diagnosis Future trends
Grand-round meeting for Dementia - A patient with rapidly progressing dementia. Dr. Ho Ka Shing Tuen Mun Hospital
 Grand-round meeting for Dementia - A patient with rapidly progressing dementia Dr. Ho Ka Shing Tuen Mun Hospital Mr. Wong, 60 years old Security guard Ex-smoker for over 20 years, non-drinker Premorbid
Grand-round meeting for Dementia - A patient with rapidly progressing dementia Dr. Ho Ka Shing Tuen Mun Hospital Mr. Wong, 60 years old Security guard Ex-smoker for over 20 years, non-drinker Premorbid
Prion diseases or transmissible spongiform encephalopathies (TSEs)
 Prion diseases or transmissible spongiform encephalopathies (TSEs) rare progressive neurodegenerative disorders that affect both humans and animals. They are distinguished by long incubation periods, characteristic
Prion diseases or transmissible spongiform encephalopathies (TSEs) rare progressive neurodegenerative disorders that affect both humans and animals. They are distinguished by long incubation periods, characteristic
Lancet Neurology 2016 Apr; 15(4): The estimated incidence is 5-10 patients per inhabitants per year.
 Lancet Neurology 2016 Apr; 15(4):391-404 Position Paper 1 A clinical approach to diagnosis of autoimmune encephalitis Graus F, Titulaer MJ, Balu R, Benseler S, Bien CG, Cellucci T, Cortese I, Dale RC,
Lancet Neurology 2016 Apr; 15(4):391-404 Position Paper 1 A clinical approach to diagnosis of autoimmune encephalitis Graus F, Titulaer MJ, Balu R, Benseler S, Bien CG, Cellucci T, Cortese I, Dale RC,
Supplementary Online Content
 Supplementary Online Content Quek AM, Britton JW, McKeon A, et al. Autoimmune epilepsy: clinical characteristics and response to immunotherapy. Arch Neurol. Published online March 26, 2012. doi:10.1001/archneurol.2011.2985.
Supplementary Online Content Quek AM, Britton JW, McKeon A, et al. Autoimmune epilepsy: clinical characteristics and response to immunotherapy. Arch Neurol. Published online March 26, 2012. doi:10.1001/archneurol.2011.2985.
Contents 1 Immunology for the Non-immunologist 2 Neurology for the Non-neurologist 3 Neuroimmunology for the Non-neuroimmunologist
 1 Immunology for the Non-immunologist... 1 1 The Beginnings of Immunology... 1 2 The Components of the Healthy Immune Response... 2 2.1 White Blood Cells... 4 2.2 Molecules... 8 References... 13 2 Neurology
1 Immunology for the Non-immunologist... 1 1 The Beginnings of Immunology... 1 2 The Components of the Healthy Immune Response... 2 2.1 White Blood Cells... 4 2.2 Molecules... 8 References... 13 2 Neurology
Delirium & Dementia. Nicholas J. Silvestri, MD
 Delirium & Dementia Nicholas J. Silvestri, MD Outline Delirium vs. Dementia Neural pathways relating to consciousness Encephalopathy Stupor Coma Dementia Delirium vs. Dementia Delirium Abrupt onset Lasts
Delirium & Dementia Nicholas J. Silvestri, MD Outline Delirium vs. Dementia Neural pathways relating to consciousness Encephalopathy Stupor Coma Dementia Delirium vs. Dementia Delirium Abrupt onset Lasts
Situaciones estresantes en el lupus
 Situaciones estresantes en el lupus Munther A Khamashta MD FRCP PhD Director: Lupus Research Unit Barcelona, Noviembre 2008 What is Lupus? Lupus is a neurological disease and sometimes affects other organs
Situaciones estresantes en el lupus Munther A Khamashta MD FRCP PhD Director: Lupus Research Unit Barcelona, Noviembre 2008 What is Lupus? Lupus is a neurological disease and sometimes affects other organs
Neuropsychiatric SLE (NPSLE) Dr. MTL NYO FCP(SA), Cert Rheum (Phys) Division of Rheumatology Department of Internal Medicine DGMAH / SMU
 Neuropsychiatric SLE (NPSLE) Dr. MTL NYO FCP(SA), Cert Rheum (Phys) Division of Rheumatology Department of Internal Medicine DGMAH / SMU NPSLE represents a diagnostic and therapeutic challenge Wide range
Neuropsychiatric SLE (NPSLE) Dr. MTL NYO FCP(SA), Cert Rheum (Phys) Division of Rheumatology Department of Internal Medicine DGMAH / SMU NPSLE represents a diagnostic and therapeutic challenge Wide range
Accepted Manuscript. Comparison of costs and outcomes of patients presenting with a rare brainstem syndrome. Devin E. Prior, Vijay Renga
 Accepted Manuscript Comparison of costs and outcomes of patients presenting with a rare brainstem syndrome Devin E. Prior, Vijay Renga PII: S2405-6502(18)30036-4 DOI: https://doi.org/10.1016/j.ensci.2018.11.004
Accepted Manuscript Comparison of costs and outcomes of patients presenting with a rare brainstem syndrome Devin E. Prior, Vijay Renga PII: S2405-6502(18)30036-4 DOI: https://doi.org/10.1016/j.ensci.2018.11.004
Case Report Immunotherapy Responsive Autoimmune Subacute Encephalitis: AReportofTwoCases
 Case Reports in Medicine Volume 2010, Article ID 837371, 4 pages doi:10.1155/2010/837371 Case Report Immunotherapy Responsive Autoimmune Subacute Encephalitis: AReportofTwoCases Manoj Mittal, Nancy Hammond,
Case Reports in Medicine Volume 2010, Article ID 837371, 4 pages doi:10.1155/2010/837371 Case Report Immunotherapy Responsive Autoimmune Subacute Encephalitis: AReportofTwoCases Manoj Mittal, Nancy Hammond,
Five Most Common Problems in Surgical Neuropathology
 Five Most Common Problems in Surgical Neuropathology If the brain were so simple that we could understand it, we would be so simple that we couldn t Emerson Pugh What is your greatest difficulty in neuropathology?
Five Most Common Problems in Surgical Neuropathology If the brain were so simple that we could understand it, we would be so simple that we couldn t Emerson Pugh What is your greatest difficulty in neuropathology?
Case Report LGI1-antibody encephalitis with subsequent rapid progression of diffuse cerebral atrophy: a case report
 Int J Clin Exp Med 2016;9(3):7041-7045 www.ijcem.com /ISSN:1940-5901/IJCEM0020965 Case Report LGI1-antibody encephalitis with subsequent rapid progression of diffuse cerebral atrophy: a case report Fang
Int J Clin Exp Med 2016;9(3):7041-7045 www.ijcem.com /ISSN:1940-5901/IJCEM0020965 Case Report LGI1-antibody encephalitis with subsequent rapid progression of diffuse cerebral atrophy: a case report Fang
Introduction to Dementia: Diagnosis & Evaluation. Created in March 2005 Duration: about 15 minutes
 Introduction to Dementia: Diagnosis & Evaluation Created in March 2005 Duration: about 15 minutes Axel Juan, MD The Geriatrics Institute axel.juan@med.va.gov 305-575-3388 Credits Principal medical contributor:
Introduction to Dementia: Diagnosis & Evaluation Created in March 2005 Duration: about 15 minutes Axel Juan, MD The Geriatrics Institute axel.juan@med.va.gov 305-575-3388 Credits Principal medical contributor:
ENCEPHALOPATHY RECOGNIZING METABOLIC AND ANOXIC CHANGES
 ENCEPHALOPATHY RECOGNIZING METABOLIC AND ANOXIC CHANGES ENCEPHALOPATHY Encephalopathy is a general term that means brain disease, damage, or malfunction. The major symptom of encephalopathy is an altered
ENCEPHALOPATHY RECOGNIZING METABOLIC AND ANOXIC CHANGES ENCEPHALOPATHY Encephalopathy is a general term that means brain disease, damage, or malfunction. The major symptom of encephalopathy is an altered
Subacute Sclerosing Panencephalitis in a Child with HIV Co-Infection
 CM&R Rapid Release. Published online ahead of print October 24, 2016 as doi:10.3121/cmr.2016.1331 Case Report Subacute Sclerosing Panencephalitis in a Child with HIV Co-Infection Pradeep Kumar Maurya,
CM&R Rapid Release. Published online ahead of print October 24, 2016 as doi:10.3121/cmr.2016.1331 Case Report Subacute Sclerosing Panencephalitis in a Child with HIV Co-Infection Pradeep Kumar Maurya,
Meet the Professor CASE 2
 Meet the Professor CASE 2 Case One ID: 60 year old man Chief Complaint: Altered sensorium and abdominal distension for 2 days Summary History of Present Illness Over the past 3 months word finding difficulties
Meet the Professor CASE 2 Case One ID: 60 year old man Chief Complaint: Altered sensorium and abdominal distension for 2 days Summary History of Present Illness Over the past 3 months word finding difficulties
Periodic and Rhythmic Patterns. Suzette M LaRoche, MD Mission Health Epilepsy Center Asheville, North Carolina
 Periodic and Rhythmic Patterns Suzette M LaRoche, MD Mission Health Epilepsy Center Asheville, North Carolina Continuum of EEG Activity Neuronal Injury LRDA GPDs SIRPIDs LPDs + NCS Burst-Suppression LPDs
Periodic and Rhythmic Patterns Suzette M LaRoche, MD Mission Health Epilepsy Center Asheville, North Carolina Continuum of EEG Activity Neuronal Injury LRDA GPDs SIRPIDs LPDs + NCS Burst-Suppression LPDs
Themes Non-Traumatic Intracranial Emergencies
 Themes Non-Traumatic Intracranial Emergencies Diffuse Lesion: Infection vs Infarction Focal Lesion: Infection vs Tumor Kevin Abrams, M.D. Chief of Radiology Medical Director of Neuroradiology & MRI Baptist
Themes Non-Traumatic Intracranial Emergencies Diffuse Lesion: Infection vs Infarction Focal Lesion: Infection vs Tumor Kevin Abrams, M.D. Chief of Radiology Medical Director of Neuroradiology & MRI Baptist
Interactive Cases: Demyelinating Diseases and Mimics. Disclosures. Case 1 25 yo F with nystagmus; look for tumor 4/14/2017
 Interactive Cases: Demyelinating Diseases and Mimics Disclosures None Brad Wright, MD 27 March 2017 Case 1 25 yo F with nystagmus; look for tumor What do you suspect? A. Demyelinating disease B. Malignancy
Interactive Cases: Demyelinating Diseases and Mimics Disclosures None Brad Wright, MD 27 March 2017 Case 1 25 yo F with nystagmus; look for tumor What do you suspect? A. Demyelinating disease B. Malignancy
Michael A. Lane, Vijay Renga, Andrew R. Pachner, and Jeffrey A. Cohen. Correspondence should be addressed to Michael A. Lane;
 Case Reports in Neurological Medicine Volume 2015, Article ID 892047, 4 pages http://dx.doi.org/10.1155/2015/892047 Case Report Late Occurrence of PML in a Patient Treated for Lymphoma with Immunomodulatory
Case Reports in Neurological Medicine Volume 2015, Article ID 892047, 4 pages http://dx.doi.org/10.1155/2015/892047 Case Report Late Occurrence of PML in a Patient Treated for Lymphoma with Immunomodulatory
PRACTICAL NEUROLOGY. Reversible. dementias Blackwell Science Ltd
 138 PRACTICAL NEUROLOGY Reversible dementias JUNE 2002 139 Gunhild Waldemar Memory Disorders Research Unit, Department of Neurology, Rigshospitalet, Copenhagen University Hospital, 9 Blegdamsvej, DK-2100
138 PRACTICAL NEUROLOGY Reversible dementias JUNE 2002 139 Gunhild Waldemar Memory Disorders Research Unit, Department of Neurology, Rigshospitalet, Copenhagen University Hospital, 9 Blegdamsvej, DK-2100
Dementia. Stephen S. Flitman, MD Medical Director 21st Century Neurology
 Dementia Stephen S. Flitman, MD Medical Director 21st Century Neurology www.neurozone.org Dementia is a syndrome Progressive memory loss, plus Progressive loss of one or more cognitive functions: Language
Dementia Stephen S. Flitman, MD Medical Director 21st Century Neurology www.neurozone.org Dementia is a syndrome Progressive memory loss, plus Progressive loss of one or more cognitive functions: Language
First clinical attack of inflammatory or demyelinating disease in the CNS. Alteration in consciousness ranging from somnolence or coma
 ADEM Clinical features First clinical attack of inflammatory or demyelinating disease in the CNS Acute or subacute onset Affects multifocal areas of the CNS Polysymptomatic presentation Must include encephalopathy:
ADEM Clinical features First clinical attack of inflammatory or demyelinating disease in the CNS Acute or subacute onset Affects multifocal areas of the CNS Polysymptomatic presentation Must include encephalopathy:
Paraneoplastic limbic encephalitis in a patient with rectal adenocarcinoma: A rare entity
 Hooda et al. 6 CASE REPORT PEER REVIEWED OPEN ACCESS Paraneoplastic limbic encephalitis in a patient with rectal adenocarcinoma: A rare entity Kusum Hooda, Nishant Gupta, Charu Chanana, Pranav Sharma,
Hooda et al. 6 CASE REPORT PEER REVIEWED OPEN ACCESS Paraneoplastic limbic encephalitis in a patient with rectal adenocarcinoma: A rare entity Kusum Hooda, Nishant Gupta, Charu Chanana, Pranav Sharma,
Imaging in a confused patient: Infections and Inflammation
 American Society of Neuroimaging Imaging in a confused patient: Infections and Inflammation January 21, 2017 Los Angeles, California Joshua P. Klein, MD, PhD, FANA, FAAN, FASN Chief, Division of Hospital
American Society of Neuroimaging Imaging in a confused patient: Infections and Inflammation January 21, 2017 Los Angeles, California Joshua P. Klein, MD, PhD, FANA, FAAN, FASN Chief, Division of Hospital
Clinical Genetics & Dementia
 Clinical Genetics & Dementia Dr Nayana Lahiri Consultant in Clinical Genetics & Honorary Senior Lecturer Nayana.lahiri@nhs.net Aims of the Session To appreciate the potential utility of family history
Clinical Genetics & Dementia Dr Nayana Lahiri Consultant in Clinical Genetics & Honorary Senior Lecturer Nayana.lahiri@nhs.net Aims of the Session To appreciate the potential utility of family history
The Role of MRI in Multiple Sclerosis
 September 2006 The Role of MRI in Multiple Sclerosis David Cochran, Harvard Medical School Year IV Meet our patient WM 49yoF presents to Multiple Sclerosis Clinic for follow-up regarding worsening symptoms
September 2006 The Role of MRI in Multiple Sclerosis David Cochran, Harvard Medical School Year IV Meet our patient WM 49yoF presents to Multiple Sclerosis Clinic for follow-up regarding worsening symptoms
Reassessment: Neuroimaging in the Emergency Patient Presenting with Seizure
 Reassessment: Neuroimaging in the Emergency Patient Presenting with Seizure This evidence-based report provides clinicians with information to identify which seizure patients in the emergency department
Reassessment: Neuroimaging in the Emergency Patient Presenting with Seizure This evidence-based report provides clinicians with information to identify which seizure patients in the emergency department
Differential diagnose of cerebral infections. Peter Uldall Rigshospitalet
 Differential diagnose of cerebral infections Peter Uldall Rigshospitalet Encephalitis Definition: Inflammation of the brain parachyma Markers: Inflammatory cells of CNS MRI Aetiology: 1) Infectious agents
Differential diagnose of cerebral infections Peter Uldall Rigshospitalet Encephalitis Definition: Inflammation of the brain parachyma Markers: Inflammatory cells of CNS MRI Aetiology: 1) Infectious agents
Neuroradiology of AIDS
 Neuroradiology of AIDS Frank Minja,, HMS IV Gillian Lieberman MD September 2002 AIDS 90% of HIV patients have CNS involvement 1 10% of AIDS patients present first with neurological symptoms 2 73-80% of
Neuroradiology of AIDS Frank Minja,, HMS IV Gillian Lieberman MD September 2002 AIDS 90% of HIV patients have CNS involvement 1 10% of AIDS patients present first with neurological symptoms 2 73-80% of
NEW ONSET SYMPTOMS OF CONVERSION AFTER INCARCERATION. Anise Noggle, MD CPMC-PGY3 NCPS March 25, 2017
 NEW ONSET SYMPTOMS OF CONVERSION AFTER INCARCERATION Anise Noggle, MD CPMC-PGY3 NCPS March 25, 2017 Case Presentation ID: 25 YO male with 3 weeks of b/l LE weakness, dysarthria, memory loss, paresthesias.
NEW ONSET SYMPTOMS OF CONVERSION AFTER INCARCERATION Anise Noggle, MD CPMC-PGY3 NCPS March 25, 2017 Case Presentation ID: 25 YO male with 3 weeks of b/l LE weakness, dysarthria, memory loss, paresthesias.
Autoimmune Encephalitis
 Evaluation Approach for Suspected Autoimmune Encephalitis M.R ASHRAFI PROFESSOR OF PEDIATRIC NEUROLOGY CHILDREN S MEDICAL CENTER PEDIATRIC CENTER OF EXCELLENCE TEHRAN UNIVERSITY OF MEDICAL SCIENCES TEHRAN
Evaluation Approach for Suspected Autoimmune Encephalitis M.R ASHRAFI PROFESSOR OF PEDIATRIC NEUROLOGY CHILDREN S MEDICAL CENTER PEDIATRIC CENTER OF EXCELLENCE TEHRAN UNIVERSITY OF MEDICAL SCIENCES TEHRAN
MULTI-SYSTEM SARCOIDOSIS CAUSING PANHYPOPITUITARISM: RAPID IMPROVEMENT WITH CORTICOSTEROID THERAPY Rashid Mahboob, MD; Ali A.
 ENDOCRINE PRACTICE Rapid Electronic Article in Press Rapid Electronic Articles in Press are preprinted manuscripts that have been reviewed and accepted for publication, but have yet to be edited, typeset
ENDOCRINE PRACTICE Rapid Electronic Article in Press Rapid Electronic Articles in Press are preprinted manuscripts that have been reviewed and accepted for publication, but have yet to be edited, typeset
SWI including phase and magnitude images
 On-line Table: MRI imaging recommendation and summary of key features Sequence Pathologies Visible Key Features T1 volumetric high-resolution whole-brain reformatted in axial, coronal, and sagittal planes
On-line Table: MRI imaging recommendation and summary of key features Sequence Pathologies Visible Key Features T1 volumetric high-resolution whole-brain reformatted in axial, coronal, and sagittal planes
Dementia With A Twist
 Dementia With A Twist Christina Tieu Geriatric Update for the Primary Care Provider November 17 th, 2016 2016 MFMER slide-1 79 y/o woman originally from Greece CC: paranoia, abulia and mutism Accompanied
Dementia With A Twist Christina Tieu Geriatric Update for the Primary Care Provider November 17 th, 2016 2016 MFMER slide-1 79 y/o woman originally from Greece CC: paranoia, abulia and mutism Accompanied
IMAGING OF INTRACRANIAL INFECTIONS
 IMAGING OF INTRACRANIAL INFECTIONS Dr Carolina Kachramanoglou LYSHOLM DEPARTMENT OF NEURORADIOLOGY NATIONAL HOSPITAL FOR NEUROLOGY AND NEUROSURGERY Plan Introduce MR sequences that are useful in the diagnosis
IMAGING OF INTRACRANIAL INFECTIONS Dr Carolina Kachramanoglou LYSHOLM DEPARTMENT OF NEURORADIOLOGY NATIONAL HOSPITAL FOR NEUROLOGY AND NEUROSURGERY Plan Introduce MR sequences that are useful in the diagnosis
The Transverse Myelitis Association Page 39
 The Transverse Myelitis Association Page 39 Neurosarcoidosis: Clinical, Pathological and Therapeutic Issues Carlos Pardo, M.D. Directory, Transverse Myelitis Center Department of Neurology Johns Hopkins
The Transverse Myelitis Association Page 39 Neurosarcoidosis: Clinical, Pathological and Therapeutic Issues Carlos Pardo, M.D. Directory, Transverse Myelitis Center Department of Neurology Johns Hopkins
Accepted Manuscript. Cerebral fat embolism syndrome in sickle cell disease without evidence of shunt
 Accepted Manuscript Cerebral fat embolism syndrome in sickle cell disease without evidence of shunt Cody L. Nathan, Whitley W. Aamodt, Tanuja Yalamarti, Calli Dogon, Paul Kinniry PII: S2405-6502(18)30044-3
Accepted Manuscript Cerebral fat embolism syndrome in sickle cell disease without evidence of shunt Cody L. Nathan, Whitley W. Aamodt, Tanuja Yalamarti, Calli Dogon, Paul Kinniry PII: S2405-6502(18)30044-3
1st interactive course in MS advanced managment
 6-7 December - Toronto, Canada 1st interactive course in MS advanced managment IMPROVING THE PATIENT S LIFE THROUGH MEDICAL EDUCATION www.excemed.org Liesly Lee Sunnybrook Health Sciences Centre. Department
6-7 December - Toronto, Canada 1st interactive course in MS advanced managment IMPROVING THE PATIENT S LIFE THROUGH MEDICAL EDUCATION www.excemed.org Liesly Lee Sunnybrook Health Sciences Centre. Department
Case Report Chronic Lymphocytic Inflammation with Pontine Perivascular Enhancement Responsive to Steroids, with Cranial and Caudal Extension
 Hindawi Case Reports in Neurological Medicine Volume 2017, Article ID 2593096, 4 pages https://doi.org/10.1155/2017/2593096 Case Report Chronic Lymphocytic Inflammation with Pontine Perivascular Enhancement
Hindawi Case Reports in Neurological Medicine Volume 2017, Article ID 2593096, 4 pages https://doi.org/10.1155/2017/2593096 Case Report Chronic Lymphocytic Inflammation with Pontine Perivascular Enhancement
Cognitive disorders. Dr S. Mashaphu Department of Psychiatry
 Cognitive disorders Dr S. Mashaphu Department of Psychiatry Delirium Syndrome characterised by: Disturbance of consciousness Impaired attention Change in cognition Develops over hours-days Fluctuates during
Cognitive disorders Dr S. Mashaphu Department of Psychiatry Delirium Syndrome characterised by: Disturbance of consciousness Impaired attention Change in cognition Develops over hours-days Fluctuates during
Case #1. Inter-ictal EEG. Difficult Diagnosis Pediatrics. 15 mos girl with medically refractory infantile spasms 2/13/2010
 Difficult Diagnosis Pediatrics Joseph E. Sullivan M.D. Assistant Professor of Clinical Neurology & Pediatrics Director, UCSF Pediatric Epilepsy Center University of California San Francisco Case #1 15
Difficult Diagnosis Pediatrics Joseph E. Sullivan M.D. Assistant Professor of Clinical Neurology & Pediatrics Director, UCSF Pediatric Epilepsy Center University of California San Francisco Case #1 15
Appendix B: Provincial Case Definitions for Reportable Diseases
 Ministry of Health and Long-Term Care Infectious Diseases Protocol Appendix B: Provincial Case Definitions for Reportable Diseases Disease: Creutzfeldt-Jakob Disease, all types Revised Creutzfeldt-Jakob
Ministry of Health and Long-Term Care Infectious Diseases Protocol Appendix B: Provincial Case Definitions for Reportable Diseases Disease: Creutzfeldt-Jakob Disease, all types Revised Creutzfeldt-Jakob
IVIG (intravenous immunoglobulin) Bivigam, Carimune NF, Flebogamma, Gammagard, Gammagard S/D, Gammaked, Gammaplex, Gamunex-C, Octagam, Privigen
 Pre - PA Allowance None Prior-Approval Requirements Diagnoses Patient must have ONE of the following documented indications: 1. Primary Immunodeficiency Disease (PID) with ONE of the a. Hypogammaglobulinemia,
Pre - PA Allowance None Prior-Approval Requirements Diagnoses Patient must have ONE of the following documented indications: 1. Primary Immunodeficiency Disease (PID) with ONE of the a. Hypogammaglobulinemia,
MANAGEMENT OF SUSPECTED VIRAL ENCEPHALITIS IN CHILDREN
 MANAGEMENT OF SUSPECTED VIRAL ENCEPHALITIS IN CHILDREN OVERVIEW 1980s: dramatically improved by aciclovir HSV encephalitis in adults Delays treatment(> 48h after hospital admission): associated with a
MANAGEMENT OF SUSPECTED VIRAL ENCEPHALITIS IN CHILDREN OVERVIEW 1980s: dramatically improved by aciclovir HSV encephalitis in adults Delays treatment(> 48h after hospital admission): associated with a
1 Maiser. 5-Fluorouracil (5-FU) Induced Acute Toxic Leukoencephalopathy. Samuel Maiser, MD. Department of Neurology, University of Minnesota
 1 Maiser 5-Fluorouracil (5-FU) Induced Acute Toxic Leukoencephalopathy Samuel Maiser, MD Department of Neurology, University of Minnesota Case This is a 57-year-old right-handed male with a history of
1 Maiser 5-Fluorouracil (5-FU) Induced Acute Toxic Leukoencephalopathy Samuel Maiser, MD Department of Neurology, University of Minnesota Case This is a 57-year-old right-handed male with a history of
e) None of the above e) None of the above
 Neurology 1) For the management of an acute delirium acquired in the hospital, which one of the following options would be least appropriate? a) Treating the underlying cause b) Promptly increasing antibiotic
Neurology 1) For the management of an acute delirium acquired in the hospital, which one of the following options would be least appropriate? a) Treating the underlying cause b) Promptly increasing antibiotic
A Child with Cross Eye. Nia Kurniati
 A Child with Cross Eye Nia Kurniati Background When dealing with new case with potential social problem, complication related to ARV treatment may pose difficulties Restricted resource to address potential
A Child with Cross Eye Nia Kurniati Background When dealing with new case with potential social problem, complication related to ARV treatment may pose difficulties Restricted resource to address potential
CNS Infections in the Pediatric Age Group
 CNS Infections in the Pediatric Age Group Introduction CNS infections are frequently life-threatening In the Philippines, bacterial meningitis is one of the top leading causes of mortality in children
CNS Infections in the Pediatric Age Group Introduction CNS infections are frequently life-threatening In the Philippines, bacterial meningitis is one of the top leading causes of mortality in children
Clinical commentary. Epileptic Disord 2014; 16 (4): limbic epilepsy. Received June 19, 2014; Accepted September 03, 2014
 Clinical commentary Epileptic Disord 2014; 16 (4): 494-9 Effectiveness of multimodality treatment for autoimmune limbic epilepsy Divyanshu Dubey, John Konikkara, Pradeep N. Modur, Mark Agostini, Puneet
Clinical commentary Epileptic Disord 2014; 16 (4): 494-9 Effectiveness of multimodality treatment for autoimmune limbic epilepsy Divyanshu Dubey, John Konikkara, Pradeep N. Modur, Mark Agostini, Puneet
CIDP + MMN - how to diagnose and treat. Dr Hadi Manji
 CIDP + MMN - how to diagnose and treat Dr Hadi Manji Outline Introduction CIDP Diagnosis Clinical features MRI Nerve conduction tests Lumbar puncture Nerve biopsy Treatment IV Ig Steroids Plasma Exchnage
CIDP + MMN - how to diagnose and treat Dr Hadi Manji Outline Introduction CIDP Diagnosis Clinical features MRI Nerve conduction tests Lumbar puncture Nerve biopsy Treatment IV Ig Steroids Plasma Exchnage
When the drugs don t work- a case of HSV encephalitis.
 When the drugs don t work- a case of HSV encephalitis. Nicky Price Consultant Virologist Public Health Wales 67 year old Caucasian Female Presenting complaint 2 day history of: Confusion Shivering Headache
When the drugs don t work- a case of HSV encephalitis. Nicky Price Consultant Virologist Public Health Wales 67 year old Caucasian Female Presenting complaint 2 day history of: Confusion Shivering Headache
Sporadic CJD in a patient with relapsing-remitting multiple sclerosis on an immunomodulatory treatment
 Acta Neurol. Belg., 2011, 111, 232-236 Sporadic CJD in a patient with relapsing-remitting multiple sclerosis on an immunomodulatory treatment Tereza Gabelić 1,2, Mario Habek 1,2, inga Zerr 3, Joanna Gawinecka
Acta Neurol. Belg., 2011, 111, 232-236 Sporadic CJD in a patient with relapsing-remitting multiple sclerosis on an immunomodulatory treatment Tereza Gabelić 1,2, Mario Habek 1,2, inga Zerr 3, Joanna Gawinecka
Heterogeneity of Demyelinating Disease: Definitions and Overlap Overview
 Heterogeneity of Demyelinating Disease: Definitions and Overlap Overview Brian Weinshenker, MD, FRCP(C) Disclosures Royalties related to patent for discovery of NMO-IgG licensed to RSR Ltd; Oxford University
Heterogeneity of Demyelinating Disease: Definitions and Overlap Overview Brian Weinshenker, MD, FRCP(C) Disclosures Royalties related to patent for discovery of NMO-IgG licensed to RSR Ltd; Oxford University
MRI Findings from a Case of Fulminating Adult-onset Measles Encephalitis
 CASE REPORT MRI Findings from a Case of Fulminating Adult-onset Measles Encephalitis Kazutaka Jin 1, Shigeru Sato 2, Ryuji Saito 2, Ayumu Ohnuma 2, Hiroshi Nomura 2 and Yasuto Itoyama 3 Abstract We report
CASE REPORT MRI Findings from a Case of Fulminating Adult-onset Measles Encephalitis Kazutaka Jin 1, Shigeru Sato 2, Ryuji Saito 2, Ayumu Ohnuma 2, Hiroshi Nomura 2 and Yasuto Itoyama 3 Abstract We report
Meningeal carcinomatosis presenting with leukoencephalopathylike imaging findings
 Accepted Manuscript Meningeal carcinomatosis presenting with leukoencephalopathylike imaging findings Hiroshi Tsuji, Shioya Ayako, Norio Takayashiki, Toshiyuki Irie, Satoshi Itoi, Taisuke Kodama, Yuki
Accepted Manuscript Meningeal carcinomatosis presenting with leukoencephalopathylike imaging findings Hiroshi Tsuji, Shioya Ayako, Norio Takayashiki, Toshiyuki Irie, Satoshi Itoi, Taisuke Kodama, Yuki
Tumefactive multiple sclerosis lesions: Diagnostic challenge for the radiologist
 Tumefactive multiple sclerosis lesions: Diagnostic challenge for the radiologist Poster No.: C-0679 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Gargallo Vaamonde, M. Iridoy Zulet, I. Rubio
Tumefactive multiple sclerosis lesions: Diagnostic challenge for the radiologist Poster No.: C-0679 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Gargallo Vaamonde, M. Iridoy Zulet, I. Rubio
Example Clinician Educational Material for Providers of Immune Effector Cellular Therapy
 Example Clinician Educational Material for Providers of Immune Effector Cellular Therapy Disclaimer: This example is just one of many potential examples of clinician education material that can be provided
Example Clinician Educational Material for Providers of Immune Effector Cellular Therapy Disclaimer: This example is just one of many potential examples of clinician education material that can be provided
Non-convulsive status epilepticus of frontal origin as the first manifestation of Hashimoto s encephalopathy
 Original article with video sequences Epileptic Disord 2011; 13 (3): 253-8 Non-convulsive status epilepticus of frontal origin as the first manifestation of Hashimoto s encephalopathy Giulia Monti, Matteo
Original article with video sequences Epileptic Disord 2011; 13 (3): 253-8 Non-convulsive status epilepticus of frontal origin as the first manifestation of Hashimoto s encephalopathy Giulia Monti, Matteo
