Congenital lung malformations antenatal and postnatal evaluation and management
|
|
|
- Silvia Burke
- 6 years ago
- Views:
Transcription
1 European Journal of Cardio-thoracic Surgery 27 (2005) Review Congenital lung malformations antenatal and postnatal evaluation and management Ganesh Shanmugam, Kenneth MacArthur, James C. Pollock* Department of Paediatric Cardio Thoracic Surgery, Royal Hospital for Sick Children, Dalnair Street, Glasgow G3 8SJ, Scotland, UK Received 24 March 2004; received in revised form 1 October 2004; accepted 6 October 2004; Available online 24 November 2004 Summary We reviewed our institutional experience with pulmonary resection for congenital bronchopulmonary malformations and analysed the management and outcome of pregnancies with a prenatal diagnosis of congenital lung malformations. Between January 1993 and December 2003, 31 patients underwent evaluation and pulmonary resection for bronchopulmonary malformations. Common clinical presentations were respiratory distress (9), respiratory infections/pneumonias (22), and dyspnoea (9). Diagnostic modalities included chest radiography, CT scan (22), MRI scan (7), arteriography (1), and bronchoscopy (5). There were 13 congenital cystic adenomatoid malformations (CCAM), six pulmonary sequestrations, three bronchogenic cysts, and nine congenital lobar emphysemas (CLE). Fifteen patients who underwent resection were diagnosed by antenatal ultrasound. No foetus had hydrops or associated malformations. No pregnancy was terminated. There was no foetal demise. Regression of the sonographic appearance was observed in six cases. Amniotic puncture was required for hydramnios in three cases. Eight emergency resections were performed (CCAM 4; CLE 3; Bronchogenic cyst 1). Surgical procedures included 24 lobectomies, one right middle lobectomy with a wedge resection of the right lower lobe, one completion right lower lobectomy, four sequestrectomies, one mediastinal mass excision and one wedge resection for a bronchogenic cyst. There were no deaths. Postoperative complications included: persistent air leak (nz2; one requiring completion lobectomy) and pneumothorax (1). Persistent mild symptoms were present in five patients, at long-term follow-up. Congenital cystic adenomatoid malformation and congenital lobar emphysema were the commonest congenital anomalies. Congenital lung malformations are increasingly diagnosed antenatally, sometimes necessitating emergent surgical resection. The natural history is variable. All infants with a prenatal diagnosis require postnatal evaluation. Patients should be evaluated for associated disorders. The presence of mass effects is an indication for therapeutic decompression. The risk of pulmonary compression, infection and malignant degeneration makes resection imperative, even in asymptomatic patients. Lobectomy is the procedure of choice, is well tolerated, and leads to excellent outcomes. q 2004 Elsevier B.V. All rights reserved. Keywords: Congenital cystic adenomatoid malformation; Congenital lobar emphysema; Bronchogenic cyst; Lung resection; Sequestration 1. Introduction This study represents the 10-year experience of a single institution with the diagnosis and management congenital lung malformations. 2. Materials and methods Between January 1993 and December 2003, 31 patients (14 female; 17 male; mean age at surgery months; range 3 days to 12 years) underwent pulmonary resection for congenital pulmonary anomalies. There were 8 neonates, 14 infants and 9 children. Mean weight at surgery was 8.05 kg. Common clinical presentations were respiratory * Corresponding author. Tel.: C address: jim.pollock@yorkhill.scot.nhs.uk (J.C. Pollock). distress (8), respiratory infections/pneumonias (16), and dyspnoea (7). The spectrum of broncho-pulmonary malformations included 13 congenital cystic adenomatoid malformations, four extralobar and two intralobar pulmonary sequestrations, three bronchogenic/enteric cysts, and nine congenital lobar emphysemas Associated anomalies Associated cardiac anomalies included patent ductus arteriosus (1) and atrial setal defect (2). Non-cardiac anomalies occurred in four patients (Wilms tumour 1; Down s syndrome 1; duodenal and jejunal duplication cysts 1; polycystic kidney 1). Three patients had bronchial asthma and one patient had associated acute lymphatic leukemia. All patients had chest radiography. Diagnostic studies included CT scan (22), MRI (7), arteriography (1) and bronchoscopy (5) /$ - see front matter q 2004 Elsevier B.V. All rights reserved. doi: /j.ejcts
2 46 G. Shanmugam et al. / European Journal of Cardio-thoracic Surgery 27 (2005) Type of resection Eight emergency resections were performed (CCAM 4; CLE 3; Bronchogenic cyst 1). Surgical procedures included 24 lobectomies, one right middle lobectomy with a wedge resection of the right lower lobe, one completion right lower lobectomy, four sequestrectomies, one mediastinal mass excision and one wedge resection for a bronchogenic cyst. Surgical access was by right or left thoracotomy in most patients, and rethoracotomy in one. All resected specimens were submitted for histopathology Congenital cystic adenomatoid malformation (nz13) There were four neonates and six infants. Mean age at surgery was 18.2 months (range 7 days to 9 years). Nine patients had recurrent pneumonias. Nine antenatally diagnosed patients underwent resection within the first year of life. Four neonates (mean age 11 days) presenting with moderate (nz2), or severe respiratory distress necessitating preoperative ventilation (nz2), required an emergency lobectomy. The mean age of the five infants was 4.7 months. Surgical treatment for congenital cystic adenomatoid malformation consisted of right upper lobectomy (2), right middle lobectomy (2), right lower lobectomy (3), left upper lobectomy (3), and left lower lobectomy (2). One patient underwent a right middle lobectomy and a wedge resection of the right lower lobe for extensive CCAM, but developed a prolonged air leak postoperatively and required a completion right lower lobectomy. Histopathologically, eight specimens had Stocker Type 1 and five had Stocker Type 2 CCAM. No Type 3 lesions were seen. Three out of 13 patients had mild respiratory symptoms at follow up (lymphatic leukemia 1; recurrent respiratory infection 1, bronchial asthma 1). Fig. 1. Chest radiograph showing marked tracheal and mediastinal shift, in a patient who required emergency lobectomy. patients (one intralobar and two extra lobar) were asymptomatic, while three presented with recurrent respiratory infections. No patient had cardiovascular symptoms. All extra lobar sequestrations were located between the left lower lobe and the diaphragm. One intralobar sequestration (Fig. 2) was located in the left lower lobe while the other was located in the right lower lobe. Five patients (extralobar 4; intralobar 1) were diagnosed antenatally. Surgical treatment consisted of sequestrectomy (4), right lower lobectomy (1) and left lower lobectomy (1). One patient with an intralobar sequestration underwent right lower lobectomy, for a large lung abscess. The other patients with intralobar sequestration had dense adhesions at surgery. The anomalous arterial supply to the sequestrated lobes arose from the abdominal aorta in five cases (extralobar 4, intralobar 1), and from the thoracic aorta in the other. The venous drainage was to a systemic vein (extralobar 4), or a pulmonary vein (intralobar 2). All patients were asymptomatic at follow up Congenital lobar emphysema (nz9) There were three neonates and four infants. Mean age at surgery was 9.7 months (range 3 days to 3 years). Cases of lobar hyperinflation secondary to intraluminal or extrinsic obstruction were excluded. Three neonates had respiratory distress and marked mediastinal shift (Fig. 1), requiring an emergency lobectomy. One patient required ventilation preoperatively. Bronchoscopy was performed in four children to rule out intrinsic obstruction. A pulmonary angiogram was done in one patient to rule out extrinsic vascular compression. Surgical treatment consisted of right upper lobectomy (1), right middle lobectomy (4), and left upper lobectomy (4). None of these patients had pulmonary hypoplasia. Two out of nine patients (with bronchial asthma) had mild wheeze at longterm follow-up Sequestration (intralobar 2; extralobar 4) There were four infants and two children. Mean age at surgery was 48.6 months (range 4 months 12 years). Three Fig. 2. Intralobar sequestration of the left lower lobe.
3 G. Shanmugam et al. / European Journal of Cardio-thoracic Surgery 27 (2005) Bronchogenic (nz2) and enteric cysts (nz1) Three patients underwent resection for bronchogenic/enteric cysts. Mean age at surgery was 26.3 months (range 3 days to 51 months). One neonate aged 3 days (diagnosed antenatally to have CCAM) required excision of a mediastinal mass due to pressure effects from a large enteric cyst in the right paravertebral gutter. This neonate had associated duodenal and jejunal cysts. Surgery for bronchogenic cysts in the two children with recurrent infections consisted of right middle lobectomy (1) and wedge resection (1). Histopathologically, these cysts were lined by squamous epithelium. All patients were asymptomatic at follow up Antenatal diagnosis Fifteen of the 31 patients who underwent resection, had lung lesions diagnosed on antenatal ultrasound. This included nine congenital cystic adenomatoid malformations (all marocystic), five sequestrations and one enteric cyst, which was antenatally diagnosed as a congenital cystic adenomatoid malformation. In addition, antenatal ultrasound detected lesions in six fetuses, which regressed by the end of the pregnancy. Foetuses with an antenatal diagnosis were followed up with sonograms at regular intervals until delivery to monitor location, size, and associated mass effects. Following the initial diagnosis on antenatal ultrasound, the in utero course of these patients evolved as described. In ten patients, antenatal ultrasound at the end of pregnancy was considered to demonstrate resolution of the anomaly. Five infants with CCAM were shown to have a persistent lesion, which was not demonstrable on radiographs but could be depicted on postpartum multi-slice CT scans. The five sequestration patients were shown to have persistent lesions on both chest radiographs and CT scan. In six patients, serial antenatal sonograms towards the end of pregnancy demonstrated spontaneous resolution of the malformation, which was confirmed by postpartum ultrasound, radiographs and CT scans. Serial therapeutic amniocenteses were performed in three fetuses with polyhydramnios. Re-accumulation of fluid occurred in one foetus while the others improved. All patients in this group underwent emergent resection. In two fetuses, the malformation remained stable and neither progressed nor regressed. There were no associated mass effects with these lesions. One patient diagnosed to have CCAM on antenatal ultrasound, was shown to have an enteric cyst on postoperative histopathology. There was no evidence of progression of hydrops, mediastinal shift, or cyst enlargement in any of the foetuses on sequential scanning. No foetuses in this series had other structural anomalies detected on ultrasound. No pregnancy was terminated. There were no instances of foetal demise. Of the 15 patients diagnosed antenatally, five neonates underwent emergency resection (4 congenital cystic adenomatoid malformations; 1 enteric cyst). All four patients with congenital cystic adenomatoid malformation (including one patient with multilobar CCAM) who underwent an emergent resection had Stocker type 2 features on histopathology. This included the patient with multilobar CCAM. Ten out of 15 (66.67%) antenatally diagnosed malformations (including all five sequestration patients) required only elective resections later in life. Nine out of ten cases of antenatally diagnosed CCAM were confirmed postnatally as having a CCAM. The other neonate had an enteric cyst Statistics Data are presented as means and range. 3. Results There was no operative or late mortality. There were no neoplastic changes in any of the resected specimens. Two patients had a prolonged air leak, one of whom required a completion right lower lobectomy. One patient had a pneumothorax. Ten patients were extubated on the table. Mean duration of ventilation was 2.4 h (range 2 6 h). Mean intensive care and hospital stays were 1.04 and 6.5 days, respectively. Mean follow up was 48.7 months (range 1 month 10 years). Persistent mild symptoms were present in five patients (congenital cystic adenomatoid malformation 3 and congenital lobar emphysema 2). 4. Discussion Congenital pulmonary malformations are infrequent but fascinating disorders of lung development. They frequently present with respiratory distress necessitating prompt diagnosis and treatment Congenital cystic adenomatoid malformation Congenital cystic adenomatoid malformation (Fig. 3a c) results from a cessation of bronchial maturation and concomitant overgrowth of mesenchymal elements, which produce the adenomatoid appearance [1]. Stocker and associates outlined the classification of these lesions based on the size, shape, spacing of the cysts and histologic appearance Type 1 lesions have the best prognosis, while Type 3 lesions are usually associated with a dismal prognosis. CT scan is our imaging modality of choice for the detailed evaluation of CCAM. Conran and Stocker [2] demonstrated the coexistence of a sequestration in up to 50% of cases. None of our patients had an associated sequestration. Surgical resection results in good symptom relief and long-term outcome. Prognosis is, however, bad for those with bilobar and bilateral lesions, and those with pulmonary hypoplasia [3]. Only one patient in our series had bilobar CCAM. In our experience, cases with more extensive unilobar or bilobar congenital cystic adenomatoid malformation were the ones where serial therapeutic amniocentesis (nz3) was performed. These were also the neonates who presented with respiratory distress, needed urgent and more extensive resections (nz4) and showed Stocker type 2-lesions on
4 48 G. Shanmugam et al. / European Journal of Cardio-thoracic Surgery 27 (2005) Impaired pulmonary function is uncommon unless more than one lobe is resected. Infants and children tolerate lobectomy well with compensatory lung growth so that total lung volume and gas exchange capacity return toward normal during somatic maturation. Long-term symptoms tend to occur in those with associated lung disorders like asthma. Preoperative pulmonary function tests may be especially beneficial in such patients as well as those with multilobar or bilateral involvement where more extensive resections may be anticipated. Based on our experience, we would prefer to perform a lobectomy in those with extensive but unilobar involvement and those who undergo emergent resections. In those with mutilobar involvement, the extent and type of resection would be determined by the extent of lung involvement and the presence of associated disorders Congenital lobar emphysema Fig. 3. CT (a) and MRI (b and c) images of CCAM. histopathology. The others had a more stable intrauterine course, usually underwent elective resection and had better histopathological features. However, all of them had the macrocystic variant of CCAM on antenatal ultrasound, which tends to have a better prognosis. Rhabdomyosarcoma and bronchio alveolar carcinoma are reported complications of CCAM. Increased cell proliferation, decreased apoptosis [4], and malignant transformation of the glandular component [5], have been cited as carcinogenic mechanisms in CCAM. Lobectomy is, therefore, safe effective, precludes air leaks and infections and completely removes potentially malignant tissue that might exist among the cystic lesions. There is debate about the advisability of segmental resection versus lobectomy for CCAM. In infants with extensive CCAM, non-anatomic pulmonary resection has been promoted as a parenchymal sparing technique that permits preservation of normal pulmonary remnants, which then demonstrate the capacity for expansion, growth, and function. However, this can be complicated by prolonged air leaks and recurrent postoperative infections, necessitating repeat surgery and lobectomy, due to incomplete removal of abnormal lung tissue. This occurred in one of our patients. Some authors believe that the possibility of prolonged postoperative air leak should not discourage surgeons from attempting conservative resections whenever this proves feasible. However, the numbers have been small. Congenital lobar emphysema (CLE) is a marked pulmonary hyperinflation state, usually involving the left upper and right middle lobes. The most constant pathological finding is cartilage deficiency resulting in bronchomalacia, and causing collapse on expiration followed by air-block hyperinflation. Some cases are associated with intraluminal bronchial obstruction that, by definition is not acquired by aspiration of a foreign body or mucus plugging, but is caused by abnormal mucosal folds, bronchial stenosis or kinking. CLE manifested as severe respiratory distress in three patients, and with wheezing, cough or recurrent chest infections in the six older children. Chest radiograph and CT (Fig. 4), findings include hyperlucency (with scant pulmonary markings) of the involved lobe, herniation of the hyperinflated lobe to the opposite side with mediastinal shift and adjacent lobe collapse. The diaphragm on both sides may be displaced downward. CT shows stretched attenuated vessels in the emphysematous lobe. It is very important not to confuse CLE Fig. 4. Congenital lobar emphysema left upper lobe.
5 G. Shanmugam et al. / European Journal of Cardio-thoracic Surgery 27 (2005) with a pneumothorax; an intercostal tube further increases respiratory distress. Bronchoscopy is necessary particularly in older children, to exclude endobronchial masses, before assigning a diagnosis of CLE to these patients. Bronchoscopy was done in four cases to rule out mucus plug, granuloma, or foreign body. A pulmonary angiogram was done in one case where there was a suspicion of external/vascular compression of the bronchus or trachea. Neonates with CLE tolerate positive pressure ventilation poorly, and rapid thoracotomy may be necessary to relieve the compression of the remaining normal lung tissue. The surgeon should be, therefore, present at anaesthetic induction. At thoracotomy, the abnormal lobe usually herniates through the opened hemithorax white the remaining lung is atelectatic. Even following lobectomy, children continue to have mild wheezing especially during respiratory infections. The children in our series who had postoperative symptoms were also asthmatic Sequestration The frequency of intralobar to extralobar sequestration is about 3:1 [6]. In our series, however, the ratio was 1:2. An intralobar pulmonary sequestration is usually located in the posterior basilar region of the lower lobe, and presents as recurrent bouts of pneumonia or abscesses in the affected lobe. Extralobar sequestration is often found in the left posterior costophrenic angle. Symptoms are caused by left-to-right or left-to-left shunting causing high output failure, anatomic impingements, or associated anatomic defects. Ten percent remain asymptomatic and persist to adulthood [7]. Associated congenital abnormalities are common, occurring in up to 65% of cases. They include diaphragmatic hernias, pectus excavatum, foregut duplications, and congenital heart defects. The term bronchopulmonary foregut malformation was introduced in reference to pulmonary sequestrations with a communication with the oesophagus or stomach, which may be an obliterated fibrous cord or a patent tract. A barium study is beneficial in such cases. Preoperative delineation of the anomalous vasculature minimizes fatal outcomes from haemorrhage caused by accidental division of the systemic artery. The aberrant arteries may be extremely retractile and friable. They must be suture-ligated with care to prevent bleeding following retraction into the mediastinum or the abdomen. Retrograde aortography has been the traditional approach to diagnosing pulmonary sequestration especially in those cases with multiple arteries supplying the sequestration. Helical CT [8] and colour Doppler sonography can delineate the feeding vessels non-invasively [9]. Contrastenhanced magnetic resonance angiography has replaced the need for conventional angiography [10], by displaying the aberrant artery without flow or respiratory artefact. A reported limitation of MRI is that small anomalous vessels may not be detected. Several authors have proposed conservative treatment for the majority of patients and reserved surgical intervention only in case of complications. Numerous reports have described serious complications arising from sequestrations, such as fungal infection [11], tuberculosis [12], fatal haemoptysis [13], massive hemothorax [14], cardiovascular problems [15], benign tumors [16], and even malignant degeneration [17]. It has, therefore, been our policy to resect sequestrations to establish a diagnosis, and prevent serious complications. Sequestrectomy for ELS is fairly straightforward, as the malformation is well separated from the normal lung by its own pleural envelope. In intralobar sequestration, inflammatory changes from previous infections can produce dense, vascular adhesions, obliterate the intersegmental plane and make intraoperative identification of the aberrant blood supply difficult. Lobectomy, therefore, is the treatment of choice. Early resection prior to the development of chronic inflammation may permit a parenchymalsparing resection Bronchogenic cysts Bronchogenic cysts are primitive foregut remnants that originate from embryonic bud tissue before the bronchi were formed. They present as respiratory distress (mediastinal cysts) in neonates, or as pulmonary sepsis (space occupying and infected parenchymal cysts) in older infants. The most common presenting symptoms are cough, stridor or wheezing due to airway compression. Bronchogenic (Fig. 5a and b) and enteric (Fig. 5c) cysts occurred in three patients in our series. Two of the resected cysts were lined with squamous epithelium, presumably due to the recurrent infection. Rupture into pleural space, compression atelectasis, infection, neoplastic change, and cyst haemorrhage are potential complications, leading to more extensive resections and increased operative risk. Maier and associates classified bronchogenic cysts into five groups by location: paratracheal, and miscellaneous including pericardial, cervical, subcutaneous and abdominal sites. Up to 1/3 of bronchogenic cysts remain asymptomatic. Unless the patient is a poor surgical risk, the only reason for following a lesion long-term would be if serial films demonstrated progressive resolution indicating the possibility of an acquired infectious cyst that has the potential for complete resolution. Simple cysts can usually be resected without loss of any significant functional lung tissue unless long-term compression atelectasis or superimposed infections have caused adjacent parenchymal abnormalities. Barium studies can demonstrate abnormal communication of the respiratory tract with the esophagus or stomach Video assisted thoracoscopic surgery Video assisted thoracoscopy minimizes access trauma and postoperative pain and has been used to resect these lesions. Serious and life threatening blood loss may result from pulmonary hilar dissection. Other complications include conversion to thoracotomy due to adhesions to vital structures and intraoperative injuries.
6 50 G. Shanmugam et al. / European Journal of Cardio-thoracic Surgery 27 (2005) tissue with release of vasoactive factors. Expanding congenital intrathoracic lesions can cause pulmonary hypoplasia due to compression of the developing lung. The hypoplastic lung is inadequate for normal gas exchange owing to an insufficient number of airway and vascular branches and additional vasomuscular hypertrophy. This can result in pulmonary hypertension and persistent fetal circulation Prognostic features and counselling Prognostic features that require consideration for prenatal counseling include the size and type of mass, laterality, progression or regression of the mass, cardiac deviation, hydrops, polyhydramnios, pulmonary hypoplasia, type 3 lesions and associated anomalies. Large, bilateral and microcystic lesions tend to have a more adverse prognosis Natural history The natural history of these lung masses is variable. From a sonographic standpoint congenital malformations could (1) show progression in size and/or development of hydrops; (2) remain stable throughout pregnancy; and (3) decrease in size or disappear. The timing of this phenomenon of regression is variable but tends to be in the mid-third trimester, usually at weeks gestation Accuracy of prenatal detection Fig. 5. Chest radiograph (a) and CT (b) reveal a bronchogenic cyst. MRI image of a large enteric cyst in the right paravertebral gutter Antenatal diagnosis Prenatal sonographic now makes it possible to define the natural history of congenital lung malformations, determine the pathophysiologic features affecting clinical outcome, and formulate management based on prognosis CCAM classification Adzick [18] described two types of CCAM by gross anatomy, ultrasonographic findings, and prognosis microcystic lesions (cysts!5 mm; solid appearance) are often associated with foetal hydrops and have a poor prognosis. Macrocystic lesions (single or multiple cystso5 mm) have a more favourable prognosis Pathophysiology Pathophysiological effects on the fetus and the mother can be demonstrated on prenatal ultrasound [19]. Development of hydrops (skin edema, pleural effusion, ascites, and pericardial effusion) is associated with poor foetal outcome [20]. Vena caval, oesophageal and cardiac compression are responsible for fetal hydrops with ascites pleural and pericardial effusions, and skin and scalp edema. Fetal hydrops causes placentomegaly and endothelial injury occurs in the poorly perfused megaplacental The accuracy in classifying these lesions on prenatal ultrasound has increased significantly. However, although prenatal ultrasound is becoming increasingly sophisticated, diagnostic errors are possible. Sequestration can be difficult to confirm. The anomalous arterial supply can be difficult to visualize despite color doppler, owing to the small size of the vessel and its proximity to the heart and prevertebral vessels. The prenatal diagnosis of congenital lobar emphysema is only rarely reported in the literature and the sonographic features have not been well characterized. Problems of diagnostic accuracy and resolution may render counseling difficult. More recently antenatal magnetic resonance imaging has provided further information on the nature of these lesions and helped to differentiate them from extrathoracic abnormalities such as congenital diaphragmatic hernia, which is important in parental counseling Foetal intervention The goals of antenatal treatment are to prevent fetal demise and/or irreversible lung injury. Symptomatic treatment of polyhydramnios includes, repetitive amniocentesis, indomethacin therapy, and video-endoscopic or ultrasonoguided placement of a thoracoamniotic shunt [20]. The finding that fetuses with hydrops are at high risk for fetal or neonatal demise without intervention led to fetal lobectomy. Pioneering work by Harrison and Adzick suggested removal of lesions through a hysterotomy and thoracotomy, but prevention of premature contractions and premature labor remain in an important problem.
7 G. Shanmugam et al. / European Journal of Cardio-thoracic Surgery 27 (2005) Foetuses with CCAM but without hydrops have a good chance for survival with maternal transport, planned delivery, and immediate neonatal resuscitation and surgery. Whether fetal surgery in these cases would be beneficial is difficult to say given the possibility of spontaneous regression. Fetal surgery is currently reserved for only those fetuses with hydrops and a uniformly fatal outcome Postnatal evaluation Prenatal lesions on sonograms can resolve partially or completely on sonograms performed late in gestation. Suspected resolution of the ultrasound appearances in utero, however, does not necessarily imply complete resolution of the primary pathology. Normal radiographic findings do not preclude persistence on CT scan. Hence, all infants with an antenatal diagnosis of congenital lung malformations require postnatal evaluation based on chest radiographs and CT even if the lesions apparently disappear during pregnancy or if they are asymptomatic Postnatal surgery Selection of patients for surgery depends on postpartum respiratory distress, as well as on postnatal radiology. Symptomatic patients and those in respiratory distress undergo surgical resection. Neonatal pulmonary surgery is safe, provided no other life-threatening problems are involved Asymptomatic patients The management of asymptomatic patients is controversial. Some authors advocate close observation, whereas others favor elective resection in every case because of the risks of recurrent infection or malignant transformation. Early surgery reduces complication related morbidity and parental anxiety. Besides, alveolar multiplication continues in the first years of life. Compensatory lung growth after resection is, therefore, possible in infants, but not in adults. Patients with CCAM, bronchogenic cysts and intralobar sequestration frequently had multiple abscesses in the resected lobes, consequent to the recurrent respiratory infections. Early diagnosis and surgery precludes the formation of abscesses and adhesions, if segmental resection is to be considered in these patients. We, therefore, believe that the risks of pulmonary compression, infection and malignant degeneration make surgical exploration imperative, even in asymptomatic patients. 5. Conclusion Antenatally diagnosed lesions should be closely monitored since the natural history is variable. One in three neonates with antenatally diagnosed lesions require emergent resection. While antenatal diagnosis may not be completely accurate, the detection of mass effects is crucial and constitutes the indications for prenatal intervention. Postnatal evaluation is important even for asymptomatic neonates and those whose lesions show regression on late prenatal ultrasound. Patients should be evaluated for associated congenital anomalies. CT scan is our investigation of choice for the evaluation of postnatal lesions. Bronchoscopy is necessary especially in children with congenital lobar emphysema. In older children, the technical problems of anaesthesia, surgery, and postoperative care reduce. This has to be balanced against the ability of infants and very young children to replace lost lung parenchyma. The risk of pulmonary compression, infection and malignant degeneration makes surgical exploration imperative, even in asymptomatic patients. Lobectomy is our treatment of choice but segmental resection is an important option and should be considered when larger resections may not be tolerated. Surgical resection results in symptomatic relief and long-term outcome, except for the cases with pulmonary hypoplasia, and those with associated disorders. Emergency surgery in patients with severe respiratory distress is sometimes necessary to achieve an optimum outcome. References [1] Haller Jr JA, Golladay ES, Pickard LR, Tepas JJ, Shorter NA, Shermeta DW. Surgical management of lung bud anomalies: lobar emphysema, bronchogenic cyst, cystic adenomatoid malformation, and intralobar pulmonary sequestration. Ann Thorac Surg 1979;28: [2] Conran RM, Stocker JT. Extralobar sequestration with frequently associated congenital cystic adenomatoid malformation, Type 2: report of 50 cases. Ped Dev Pathol 1999;2: [3] Bailey PV, Tracy Jr T, Connors RH, DeMello D, Lewis JE, Weber TR. Congenital bronchopulmonary malformations. Diagnostic and therapeutic considerations. J Thorac Cardiovasc Surg 1990;99: [4] Cass DL, Quinn TM, Yang EY, Liechty KW, Crombleholme TM, Flake AW, Adzick NS. Increased cell proliferation and decreased apoptosis characterize congenital cystic adenomatoid malformation of the lung. J Pediatr Surg 1998;33: [5] Wang NS, Chen MF, Chen FF. The glandular component in congenital cystic adenomatoid malformation of the lung. Respirology 1999;4: [6] Sauvanet A, Regnard JF, Calanducci F, Rojas-Miranda A, Dartevelle A, Levasseur P. Pulmonary sequestration: surgical aspects based on 61 cases. Rev Pneumol Clin 1991;47: [7] Felker RE, Tonkin ILD. Imaging of pulmonary sequestration. Am J Roentgenol 1990;154: [8] Ko SF, Ng SH, Lee TY, Wan YL, Liang CD, Lin JW, Chen WJ, Hseih MJ. Noninvasive imaging of bronchopulmonary sequestration. Am J Roentgenol 2000;175: [9] Hernanz-Schulman JW, Stein SM, Neblett WW, Atkinson JB, Kirchner SG, Heller RM, Merrill WH, Fleischer AC. Pulmonary sequestration: diagnosis with color Doppler sonography and a new theory of associated hydrothorax. Radiology 1991;180: [10] Savic B, Birtel FJ, Tholen W, Funke HD, Knoche R. Lung separation: report of seven case review of 540 published cases. Thorax 1979;34: [11] Freixinet J, De Cos J, Rodriguez de Castro F, Julia G, Romero T. Colonisation with Aspergillus of an intralobar pulmonary sequestration. Thorax 1995;50:810 1.
8 52 G. Shanmugam et al. / European Journal of Cardio-thoracic Surgery 27 (2005) [12] Elia S, Alifano M, Gentile M, Somma P, D Armiento GP, Ferrante G. Infection with mycobacterium tuberculosis complicating a pulmonary sequestration. Ann Thorac Surg 1998;66: [13] Rubin EM, Garcia H, Horowitz MD, Guerra JJ. Fatal massive hemoptysis secondary to intralobar sequestration. Chest 1994;106: [14] Avishai V, Dolev E, Weissberg D, Zajdel Land Priel IE. Extralobar sequestration presenting as massive hemothorax. Chest 1996;109: [15] Fabre OH, Porte HL, Godart FR, Rey C, Wurtz AJ. Long-term cardiovascular consequences of undiagnosed intralobar pulmonary sequestration. Ann Thorac Surg 1998;65: [16] Paksoy N, Demircan A, Altiner M, Artvinli M. Localised fibrous mesothelioma arising in intralobar pulmonary sequestration. Thorax 1992;47: [17] Gatzinsky P, Olling S. A case of carcinoma in intralobar pulmonary sequestration. Thorac Cardiovasc Surg 1988;36: [18] Adzick NS, Harrison MR. Management of the fetus with a cystic adenomatoid malformation. J Pediatr Surg 1985;20(5): [19] Sakala EP, Perrott WS, Grube GL. Sonographic characteristics of antenatally diagnosed extralobar pulmonary sequestration and congenital cystic adenomatoid malformation. Obstet Gynecol Surv 1994;49: [20] Adzick NS, Harrison MR, Glick PL, Golbus MS, Anderson RL, Mahony BS, Callen PW, Hirsch JH, Luthy DA, Filly RA, DeLorimier AA. Fetal cystic adenomatoid malformation: prenatal diagnosis and natural history. J Pediatr Surg 1985;20:483 8.
Surgical indications: Non-malignant pulmonary diseases. Punnarerk Thongcharoen
 Surgical indications: Non-malignant pulmonary diseases Punnarerk Thongcharoen Non-malignant Malignant as a pathological term: Cancer Non-malignant = not cancer Malignant as an adjective: Disposed to cause
Surgical indications: Non-malignant pulmonary diseases Punnarerk Thongcharoen Non-malignant Malignant as a pathological term: Cancer Non-malignant = not cancer Malignant as an adjective: Disposed to cause
Lung sequestration and Scimitar syndrome
 Lung sequestration and Scimitar syndrome Imaging approaches M. Mearadji International Foundation for Pediatric Imaging Aid Rotterdam, The Netherlands Pulmonary sequestration Pulmonary sequestration (PS)
Lung sequestration and Scimitar syndrome Imaging approaches M. Mearadji International Foundation for Pediatric Imaging Aid Rotterdam, The Netherlands Pulmonary sequestration Pulmonary sequestration (PS)
Congenital Lung Malformations: Radiologic-Pathologic Correlation
 Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 51-60, Abr.-Jun., 2006 Congenital Lung Malformations: Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 51-60, Abr.-Jun., 2006 Congenital Lung Malformations: Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
Imaging of the Lung in Children
 Imaging of the Lung in Children Imaging methods X-Ray of the Lung (Anteroposterior, ) CT, HRCT MRI USG Congenital developmental defects of the lungs Agenesis, aplasia, hypoplasia Tension pulmonary anomalies
Imaging of the Lung in Children Imaging methods X-Ray of the Lung (Anteroposterior, ) CT, HRCT MRI USG Congenital developmental defects of the lungs Agenesis, aplasia, hypoplasia Tension pulmonary anomalies
Case Report Coexistent Congenital Diaphragmatic Hernia with Extrapulmonary Sequestration
 Canadian Respiratory Journal Volume 2016, Article ID 1460480, 4 pages http://dx.doi.org/10.1155/2016/1460480 Case Report Coexistent Congenital Diaphragmatic Hernia with Extrapulmonary Sequestration Nao
Canadian Respiratory Journal Volume 2016, Article ID 1460480, 4 pages http://dx.doi.org/10.1155/2016/1460480 Case Report Coexistent Congenital Diaphragmatic Hernia with Extrapulmonary Sequestration Nao
Case Report Pulmonary Sequestration with Renal Aplasia and Elevated SUV Level in PET/CT
 Case Reports in Pulmonology Volume 2012, Article ID 276012, 4 pages doi:10.1155/2012/276012 Case Report Pulmonary Sequestration with Renal Aplasia and Elevated SUV Level in PET/CT Serdar Şen, 1 Nilgün
Case Reports in Pulmonology Volume 2012, Article ID 276012, 4 pages doi:10.1155/2012/276012 Case Report Pulmonary Sequestration with Renal Aplasia and Elevated SUV Level in PET/CT Serdar Şen, 1 Nilgün
Case Based Fetal Lung Masses
 Case Based Fetal Lung Masses Advances in Fetal and Neonatal Imaging Course Orlando, Florida, January 28, 2017 Leann E. Linam, MD Associate Professor Radiology University of Arkansas for Medical Sciences/
Case Based Fetal Lung Masses Advances in Fetal and Neonatal Imaging Course Orlando, Florida, January 28, 2017 Leann E. Linam, MD Associate Professor Radiology University of Arkansas for Medical Sciences/
Thoracoscopic treatment of congenital malformation of the lung
 Jemis, 1 2013 Thoracoscopic treatment of congenital malformation of the lung Preliminary experience with preoperative 3D virtual rendering F. Destro M. Maffi T. Gargano G. Ruggeri L. Soler M. Lima Table
Jemis, 1 2013 Thoracoscopic treatment of congenital malformation of the lung Preliminary experience with preoperative 3D virtual rendering F. Destro M. Maffi T. Gargano G. Ruggeri L. Soler M. Lima Table
Pulmonary Sequestration
 July 26, 2004 Pulmonary Sequestration Jonathan Shaw, Harvard Medical School Year IV What do these two patients have in common? Patient 1: 50 y.o. non-smoking female with several months cough and hemoptysis;
July 26, 2004 Pulmonary Sequestration Jonathan Shaw, Harvard Medical School Year IV What do these two patients have in common? Patient 1: 50 y.o. non-smoking female with several months cough and hemoptysis;
Molla Teshome MD, Habtamu Belete MD Aurora Health Care Internal Medicine Residency Program
 Molla Teshome MD, Habtamu Belete MD Aurora Health Care Internal Medicine Residency Program History 32 year-old male who presented with a 4 days history of: Productive cough Right sided pleuritic chest
Molla Teshome MD, Habtamu Belete MD Aurora Health Care Internal Medicine Residency Program History 32 year-old male who presented with a 4 days history of: Productive cough Right sided pleuritic chest
SWISS SOCIETY OF NEONATOLOGY. Bilateral pulmonary sequestration in a neonate
 SWISS SOCIETY OF NEONATOLOGY Bilateral pulmonary sequestration in a neonate February 2008 2 Woerner A, Schwendener K, Casaulta C, Raio L, Wolf R, Zachariou Z, Nelle M, Division of Neonatology, (WA, SK,
SWISS SOCIETY OF NEONATOLOGY Bilateral pulmonary sequestration in a neonate February 2008 2 Woerner A, Schwendener K, Casaulta C, Raio L, Wolf R, Zachariou Z, Nelle M, Division of Neonatology, (WA, SK,
Heart and Lungs. LUNG Coronal section demonstrates relationship of pulmonary parenchyma to heart and chest wall.
 Heart and Lungs Normal Sonographic Anatomy THORAX Axial and coronal sections demonstrate integrity of thorax, fetal breathing movements, and overall size and shape. LUNG Coronal section demonstrates relationship
Heart and Lungs Normal Sonographic Anatomy THORAX Axial and coronal sections demonstrate integrity of thorax, fetal breathing movements, and overall size and shape. LUNG Coronal section demonstrates relationship
Congenital lung anomalies: can we postpone resection?
 Journal of Pediatric Surgery (2012) 47, 87 92 www.elsevier.com/locate/jpedsurg Congenital lung anomalies: can we postpone resection? Nadja Colon a, Cameron Schlegel a, John Pietsch a, Dai H. Chung a,b,
Journal of Pediatric Surgery (2012) 47, 87 92 www.elsevier.com/locate/jpedsurg Congenital lung anomalies: can we postpone resection? Nadja Colon a, Cameron Schlegel a, John Pietsch a, Dai H. Chung a,b,
It s Rare So Be Aware: Pleuropulmonary Blastoma Mimicking Congenital Pulmonary Airway Malformation
 e10 Case Report: Thoracic THIEME It s Rare So Be Aware: Pleuropulmonary Blastoma Mimicking Congenital Pulmonary Airway Malformation Fayza Haider 1 Khulood Al Saad 2 Fatima Al-Hashimi 3 Hakima Al-Hashimi
e10 Case Report: Thoracic THIEME It s Rare So Be Aware: Pleuropulmonary Blastoma Mimicking Congenital Pulmonary Airway Malformation Fayza Haider 1 Khulood Al Saad 2 Fatima Al-Hashimi 3 Hakima Al-Hashimi
Case report Esophageal lung: a rare case of communicating bronchopulmonary foregut malformation
 Case report Esophageal lung: a rare case of communicating bronchopulmonary foregut malformation 1 Dr.Varsha Rathi, 2 Dr. Saurabh Deshpande*, 3 Dr.Almas Nazim, 4 Dr.Shilpa Domkundwar 1 Professor, Department
Case report Esophageal lung: a rare case of communicating bronchopulmonary foregut malformation 1 Dr.Varsha Rathi, 2 Dr. Saurabh Deshpande*, 3 Dr.Almas Nazim, 4 Dr.Shilpa Domkundwar 1 Professor, Department
PULMONARY VENOLOBAR SYNDROME. Dr.C.Anandhi DNB Resident, Southern Railway Headquarters Hospital.
 PULMONARY VENOLOBAR SYNDROME Dr.C.Anandhi DNB Resident, Southern Railway Headquarters Hospital. Presenting complaint: 10 yrs old girl with recurrent episodes of lower respiratory tract infection from infancy.
PULMONARY VENOLOBAR SYNDROME Dr.C.Anandhi DNB Resident, Southern Railway Headquarters Hospital. Presenting complaint: 10 yrs old girl with recurrent episodes of lower respiratory tract infection from infancy.
ISUOG Basic Training. Assessing the Neck & Chest Gihad Chalouhi, Lebanon
 ISUOG Basic Training Assessing the Neck & Chest Gihad Chalouhi, Lebanon Learning objectives 9 & 10 At the end of the lecture you will be able to: recognise the differences between the normal & most common
ISUOG Basic Training Assessing the Neck & Chest Gihad Chalouhi, Lebanon Learning objectives 9 & 10 At the end of the lecture you will be able to: recognise the differences between the normal & most common
24. An infant with recurrent pneumonia underwent a frontal chest radiograph (Fig 24-A) followed by
 24. An infant with recurrent pneumonia underwent a frontal chest radiograph (Fig 24-A) followed by diagnosis? ndings, what is the most likely A. Pulmonary sequestration B. Congenital pulmonary airway malformation
24. An infant with recurrent pneumonia underwent a frontal chest radiograph (Fig 24-A) followed by diagnosis? ndings, what is the most likely A. Pulmonary sequestration B. Congenital pulmonary airway malformation
B-I-2 CARDIAC AND VASCULAR RADIOLOGY
 (YEARS 1 3) CURRICULUM FOR RADIOLOGY 13 B-I-2 CARDIAC AND VASCULAR RADIOLOGY KNOWLEDGE To describe the normal anatomy of the heart and vessels including the lymphatic system as demonstrated by radiographs,
(YEARS 1 3) CURRICULUM FOR RADIOLOGY 13 B-I-2 CARDIAC AND VASCULAR RADIOLOGY KNOWLEDGE To describe the normal anatomy of the heart and vessels including the lymphatic system as demonstrated by radiographs,
HOW TO IMAGE AND DESCRIBE CONGENITAL LUNG MALFORMATIONS
 HOW TO IMAGE AND DESCRIBE CONGENITAL LUNG MALFORMATIONS Paul Thacker, MD Assistant Professor Departments of Radiology and Pediatrics Medical University of South Carolina DISCLOSURES I have no relevant
HOW TO IMAGE AND DESCRIBE CONGENITAL LUNG MALFORMATIONS Paul Thacker, MD Assistant Professor Departments of Radiology and Pediatrics Medical University of South Carolina DISCLOSURES I have no relevant
Lung Cancer - Suspected
 Lung Cancer - Suspected Shared Decision Making Lung Cancer: http://www.enhertsccg.nhs.uk/ Patient presents with abnormal CXR Lung cancer - clinical presentation History and Examination Incidental finding
Lung Cancer - Suspected Shared Decision Making Lung Cancer: http://www.enhertsccg.nhs.uk/ Patient presents with abnormal CXR Lung cancer - clinical presentation History and Examination Incidental finding
A STUDY OF MORPHOLOGY AND VARIATIONS OF LUNGS IN ADULTS AND FOETUS
 International Journal of Advancements in Research & Technology, Volume 3, Issue 4, April-2014 150 A STUDY OF MORPHOLOGY AND VARIATIONS OF LUNGS IN ADULTS AND FOETUS ZAREENA.SK (assistant professor of anatomy)
International Journal of Advancements in Research & Technology, Volume 3, Issue 4, April-2014 150 A STUDY OF MORPHOLOGY AND VARIATIONS OF LUNGS IN ADULTS AND FOETUS ZAREENA.SK (assistant professor of anatomy)
-Tamara Wahbeh. -Razan Abu Rumman. Dr. Mohammed Al-Muhtaseb
 -2 -Tamara Wahbeh -Razan Abu Rumman Dr. Mohammed Al-Muhtaseb I tried to include everything the doctor mentioned in both the lecture and his slides in the simplest way possible, so hopefully there would
-2 -Tamara Wahbeh -Razan Abu Rumman Dr. Mohammed Al-Muhtaseb I tried to include everything the doctor mentioned in both the lecture and his slides in the simplest way possible, so hopefully there would
CONGENITAL LUNG LESION Round Table. Objectives. Congenital Lung Lesions: Anatomy and Physiology Leah Barefoot, DNP, CPNP-PC
 CONGENITAL LUNG LESION Round Table L. Barefoot, E. Paton, C. Schultz, R. Caskey, M. O Day Objectives Review the anatomy and pathophysiology of congenital lung lesions List the preoperative evaluation of
CONGENITAL LUNG LESION Round Table L. Barefoot, E. Paton, C. Schultz, R. Caskey, M. O Day Objectives Review the anatomy and pathophysiology of congenital lung lesions List the preoperative evaluation of
Undergraduate Teaching
 Prof. James F Meaney Undergraduate Teaching Chest X-Ray Understanding the normal anatomical by reference to cross sectional imaging Radiology? It s FUN! Cryptic puzzle Sudoku (Minecraft?) It s completely
Prof. James F Meaney Undergraduate Teaching Chest X-Ray Understanding the normal anatomical by reference to cross sectional imaging Radiology? It s FUN! Cryptic puzzle Sudoku (Minecraft?) It s completely
Discussing feline tracheal disease
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Discussing feline tracheal disease Author : ANDREW SPARKES Categories : Vets Date : March 24, 2008 ANDREW SPARKES aims to
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Discussing feline tracheal disease Author : ANDREW SPARKES Categories : Vets Date : March 24, 2008 ANDREW SPARKES aims to
PRESENCE OF LOWER ACCESSORY LOBES IN THE LUNGS
 Int. J. Pharm. Med. & Bio. Sc. 2013 Hemanth Kommuru et al., 2013 Research Paper ISSN 2278 5221 www.ijpmbs.com Vol. 2, No. 3, July 2013 2013 IJPMBS. All Rights Reserved PRESENCE OF LOWER ACCESSORY LOBES
Int. J. Pharm. Med. & Bio. Sc. 2013 Hemanth Kommuru et al., 2013 Research Paper ISSN 2278 5221 www.ijpmbs.com Vol. 2, No. 3, July 2013 2013 IJPMBS. All Rights Reserved PRESENCE OF LOWER ACCESSORY LOBES
Basic Data. Sex:Male 31 years old Occupation: 搬家工人
 Basic Data Sex:Male 31 years old Occupation: 搬家工人 Chief Complaint Intermittent chest pain with shortness of breath for 2-3 months. Present Illness 4 months ago, he started having occasional chest pain
Basic Data Sex:Male 31 years old Occupation: 搬家工人 Chief Complaint Intermittent chest pain with shortness of breath for 2-3 months. Present Illness 4 months ago, he started having occasional chest pain
CONGENITAL LUNG MALFORMATIONS, UPDATE AND TREATMENT
 CONGENITAL LUNG MALFORMATIONS, UPDATE AND TREATMENT STEVEN ROTHENBERG MD.(1) 1. Department of Pediatrics. The Rocky Mountain Hospital For Children. Hospital for Children, Denver, Colorado, USA. steverberg@aol.com
CONGENITAL LUNG MALFORMATIONS, UPDATE AND TREATMENT STEVEN ROTHENBERG MD.(1) 1. Department of Pediatrics. The Rocky Mountain Hospital For Children. Hospital for Children, Denver, Colorado, USA. steverberg@aol.com
4/16/2017. Learning Objectives. Interpretation of the Chest Radiograph. Components. Production of the Radiograph. Density & Appearance
 Interpretation of the Arthur Jones, EdD, RRT Learning Objectives Identify technical defects in chest radiographs Identify common radiographic abnormalities This Presentation is Approved for 1 CRCE Credit
Interpretation of the Arthur Jones, EdD, RRT Learning Objectives Identify technical defects in chest radiographs Identify common radiographic abnormalities This Presentation is Approved for 1 CRCE Credit
Index. Note: Page numbers of article titles are in boldface type
 Index Note: Page numbers of article titles are in boldface type A Acute coronary syndrome, perioperative oxygen in, 599 600 Acute lung injury (ALI). See Lung injury and Acute respiratory distress syndrome.
Index Note: Page numbers of article titles are in boldface type A Acute coronary syndrome, perioperative oxygen in, 599 600 Acute lung injury (ALI). See Lung injury and Acute respiratory distress syndrome.
Bronchogenic Carcinoma
 A 55-year-old construction worker has smoked 2 packs of ciggarettes daily for the past 25 years. He notes swelling in his upper extremity & face, along with dilated veins in this region. What is the most
A 55-year-old construction worker has smoked 2 packs of ciggarettes daily for the past 25 years. He notes swelling in his upper extremity & face, along with dilated veins in this region. What is the most
ORIGINAL ARTICLE. Complete video-assisted thoracoscopic surgery for pulmonary sequestration
 ORIGINAL ARTICLE Complete video-assisted thoracoscopic surgery for pulmonary sequestration Jian-Fei Shen, Xiao-Xue Zhang, Shu-Ben Li, Zhi-Hua Guo, Zhi-Qiang Xu, Xiao-Sun Shi, Jian-Xing He Department of
ORIGINAL ARTICLE Complete video-assisted thoracoscopic surgery for pulmonary sequestration Jian-Fei Shen, Xiao-Xue Zhang, Shu-Ben Li, Zhi-Hua Guo, Zhi-Qiang Xu, Xiao-Sun Shi, Jian-Xing He Department of
Lung- and airway emergencies
 Lung- and airway emergencies Charlotte de Lange,MD,PhD Pediatric Radiology unit, Oslo University Hospital, Norway 5th Nordic course - Emergency Radiology Oslo 18-21.5.2015 clange@ous-hf.no How come pediatric
Lung- and airway emergencies Charlotte de Lange,MD,PhD Pediatric Radiology unit, Oslo University Hospital, Norway 5th Nordic course - Emergency Radiology Oslo 18-21.5.2015 clange@ous-hf.no How come pediatric
Clinical spectrum of congenital cystic disease of the lung in children 1
 European Journal of Cardio-thoracic Surgery 15 (1999) 11 17 Clinical spectrum of congenital cystic disease of the lung in children 1 Shin-ichi Takeda*, Shinichiro Miyoshi, Masayoshi Inoue, Ken-ichi Omori,
European Journal of Cardio-thoracic Surgery 15 (1999) 11 17 Clinical spectrum of congenital cystic disease of the lung in children 1 Shin-ichi Takeda*, Shinichiro Miyoshi, Masayoshi Inoue, Ken-ichi Omori,
disease, bronchopulmonary dysplasia, pulmonary hypoplasia and congenital diaphragmatic hernia.
 Neonatal Chest Imaging - What the Nurse Should Know Expires Monday, April 30, 2018 Nursing Michael J. Diament, M.D. Objectives 1. Describe a good technique for positioning a neonate for the purpose of
Neonatal Chest Imaging - What the Nurse Should Know Expires Monday, April 30, 2018 Nursing Michael J. Diament, M.D. Objectives 1. Describe a good technique for positioning a neonate for the purpose of
Case Report Left Upper Lobectomy for Congenital Lobar Emphysema in a Low Weight Infant
 Case Reports in Surgery Volume 2016, Article ID 4182741, 4 pages http://dx.doi.org/10.1155/2016/4182741 Case Report Left Upper Lobectomy for Congenital Lobar Emphysema in a Low Weight Infant Meletios Kanakis,
Case Reports in Surgery Volume 2016, Article ID 4182741, 4 pages http://dx.doi.org/10.1155/2016/4182741 Case Report Left Upper Lobectomy for Congenital Lobar Emphysema in a Low Weight Infant Meletios Kanakis,
Subject Index. Bacterial infection, see Suppurative lung disease, Tuberculosis
 Subject Index Abscess, virtual 107 Adenoidal hypertrophy, features 123 Airway bleeding, technique 49, 50 Airway stenosis, see Stenosis, airway Anaesthesia biopsy 47 complications 27, 28 flexible 23 26
Subject Index Abscess, virtual 107 Adenoidal hypertrophy, features 123 Airway bleeding, technique 49, 50 Airway stenosis, see Stenosis, airway Anaesthesia biopsy 47 complications 27, 28 flexible 23 26
CASE REPORTS. Idiopathic Unilateral Hyperlucent Lung
 CASE REPORTS Idiopathic Unilateral Hyperlucent Lung The Swyer-James Syndrome J. Judson McNamara, M.D., Harold C. Urschel, M.D., J. H. Arndt, M.D., Herman Ulevitch, M.D., and W. B. Kingsley, M.D. I diopathic
CASE REPORTS Idiopathic Unilateral Hyperlucent Lung The Swyer-James Syndrome J. Judson McNamara, M.D., Harold C. Urschel, M.D., J. H. Arndt, M.D., Herman Ulevitch, M.D., and W. B. Kingsley, M.D. I diopathic
Extralobar lung sequestration associated with fatal
 Thorax (1971), 26, 125. Extralobar lung sequestration associated with fatal neonatal respiratory distress A. J. BLIEK and D. J. MULHOLLAND The Departments of Radiology and Pathology, Royal Alexandra Hospital,
Thorax (1971), 26, 125. Extralobar lung sequestration associated with fatal neonatal respiratory distress A. J. BLIEK and D. J. MULHOLLAND The Departments of Radiology and Pathology, Royal Alexandra Hospital,
There are four general types of congenital lung disorders:
 Pediatric Pulmonology Conditions Evaluated and Treated As a parent, watching a child suffer from a respiratory disorder can be frightening and worrisome. Our respiratory specialists provide compassionate
Pediatric Pulmonology Conditions Evaluated and Treated As a parent, watching a child suffer from a respiratory disorder can be frightening and worrisome. Our respiratory specialists provide compassionate
Shedding Light on Neonatal X-rays. Objectives. Indications for X-Rays 5/14/2018
 Shedding Light on Neonatal X-rays Barbara C. Mordue, MSN, NNP-BC Neonatal Nurse Practitioner LLUH Children s Hospital, NICU Objectives Utilize a systematic approach to neonatal x-ray interpretation Identify
Shedding Light on Neonatal X-rays Barbara C. Mordue, MSN, NNP-BC Neonatal Nurse Practitioner LLUH Children s Hospital, NICU Objectives Utilize a systematic approach to neonatal x-ray interpretation Identify
INDEPENDENT LUNG VENTILATION
 INDEPENDENT LUNG VENTILATION Giuseppe A. Marraro, MD Director Anaesthesia and Intensive Care Department Paediatric Intensive Care Unit Fatebenefratelli and Ophthalmiatric Hospital Milan, Italy gmarraro@picu.it
INDEPENDENT LUNG VENTILATION Giuseppe A. Marraro, MD Director Anaesthesia and Intensive Care Department Paediatric Intensive Care Unit Fatebenefratelli and Ophthalmiatric Hospital Milan, Italy gmarraro@picu.it
Management of antenatally diagnosed pulmonary sequestration associated with congenital cystic adenomatoid malformation
 Thorax 1999;54:701 706 701 Wessex Regional Center for Pediatric Surgery, Southampton General Hospital, Southampton SO16 6YD, UK M Samuel D M Burge Correspondence to: Dr M Samuel, Department of Pediatric
Thorax 1999;54:701 706 701 Wessex Regional Center for Pediatric Surgery, Southampton General Hospital, Southampton SO16 6YD, UK M Samuel D M Burge Correspondence to: Dr M Samuel, Department of Pediatric
Children are not small adults Children are Not Small Adults Anatomic considerations Pliable bony & cartilagenous structures - Significant thoracic inj
 PEDIATRIC CHEST TRAUMA Children are not small adults Role of imaging Spectrum of injury Children are not small adults Children are Not Small Adults Anatomic considerations Pliable bony & cartilagenous
PEDIATRIC CHEST TRAUMA Children are not small adults Role of imaging Spectrum of injury Children are not small adults Children are Not Small Adults Anatomic considerations Pliable bony & cartilagenous
Learning Radiology: Recognizing the Basics. Text with Student Consult Online Access Code
 Learning Radiology: Recognizing the Basics. Text with Student Consult Online Access Code Herring, W ISBN-13: 9780323074445 Table of Contents 1. Recognizing Anything The "colorful" world of radiology A
Learning Radiology: Recognizing the Basics. Text with Student Consult Online Access Code Herring, W ISBN-13: 9780323074445 Table of Contents 1. Recognizing Anything The "colorful" world of radiology A
Bronchopulmonary foregut malformation: A pictorial review.
 Bronchopulmonary foregut malformation: A pictorial review. Poster No.: C-1676 Congress: ECR 2013 Type: Educational Exhibit Authors: N. L. Eun, C. S. Yoon, M.-J. Lee, M.-J. Kim ; Rep. of KOREA/ 1 2 2 2
Bronchopulmonary foregut malformation: A pictorial review. Poster No.: C-1676 Congress: ECR 2013 Type: Educational Exhibit Authors: N. L. Eun, C. S. Yoon, M.-J. Lee, M.-J. Kim ; Rep. of KOREA/ 1 2 2 2
Prenatal and Neonatal MRI of Sacrococcygeal Teratoma With Surgical Correlation
 Prenatal and Neonatal MRI of Sacrococcygeal Teratoma With Surgical Correlation Ali Mahmood, M.D., and Nadia F. Mahmood, M.D. Citation: Mahmood A, Mahmood NF. Prenatal and Neonatal MRI of Sacrococcygeal
Prenatal and Neonatal MRI of Sacrococcygeal Teratoma With Surgical Correlation Ali Mahmood, M.D., and Nadia F. Mahmood, M.D. Citation: Mahmood A, Mahmood NF. Prenatal and Neonatal MRI of Sacrococcygeal
Congenital Pulmonary Airways Malformation: an update
 Congenital Pulmonary Airways Malformation: an update Poster No.: P-0111 Congress: ESTI 2014 Type: Educational Poster Authors: S. M. Mak, B. Annan, S. P. G. Padley, A. G. Nicholson; London/UK Keywords:
Congenital Pulmonary Airways Malformation: an update Poster No.: P-0111 Congress: ESTI 2014 Type: Educational Poster Authors: S. M. Mak, B. Annan, S. P. G. Padley, A. G. Nicholson; London/UK Keywords:
Evaluation of Clinical Outcomes in Neonates Undergoing Lung Resection for Congenital Lesions
 e4 Original Article THIEME Evaluation of Clinical Outcomes in Neonates Undergoing Lung Resection for Congenital Lesions Hemonta Kumar Dutta 1 Madhuchanda Bora 2 Diganta Saikia 2 1 Department of Pediatric
e4 Original Article THIEME Evaluation of Clinical Outcomes in Neonates Undergoing Lung Resection for Congenital Lesions Hemonta Kumar Dutta 1 Madhuchanda Bora 2 Diganta Saikia 2 1 Department of Pediatric
Surgical treatment of bullous lung disease
 Surgical treatment of bullous lung disease PD POTGIETER, SR BENATAR, RP HEWITSON, AD FERGUSON Thorax 1981 ;36:885-890 From the Respiratory Clinic, Groote Schuur Hospita', and Departments of Medicine, Anaesthetics,
Surgical treatment of bullous lung disease PD POTGIETER, SR BENATAR, RP HEWITSON, AD FERGUSON Thorax 1981 ;36:885-890 From the Respiratory Clinic, Groote Schuur Hospita', and Departments of Medicine, Anaesthetics,
Heart and Soul Evaluation of the Fetal Heart
 Heart and Soul Evaluation of the Fetal Heart Ivana M. Vettraino, M.D., M.B.A. Clinical Associate Professor, Michigan State University College of Human Medicine Objectives Review the embryology of the formation
Heart and Soul Evaluation of the Fetal Heart Ivana M. Vettraino, M.D., M.B.A. Clinical Associate Professor, Michigan State University College of Human Medicine Objectives Review the embryology of the formation
PRACTICAL GUIDE TO FETAL ECHOCARDIOGRAPHY IC Huggon and LD Allan
 PRACTICAL GUIDE TO FETAL ECHOCARDIOGRAPHY IC Huggon and LD Allan Fetal Cardiology Unit, Harris Birthright Research Centre for Fetal Medicine, King's College Hospital, London, UK IMPORTANCE OF PRENATAL
PRACTICAL GUIDE TO FETAL ECHOCARDIOGRAPHY IC Huggon and LD Allan Fetal Cardiology Unit, Harris Birthright Research Centre for Fetal Medicine, King's College Hospital, London, UK IMPORTANCE OF PRENATAL
Congenital Pulmonary Airways Malformation: an update
 Congenital Pulmonary Airways Malformation: an update Poster No.: P-0111 Congress: ESTI 2014 Type: Educational Poster Authors: S. M. Mak, B. Annan, S. P. G. Padley, A. G. Nicholson; London/UK Keywords:
Congenital Pulmonary Airways Malformation: an update Poster No.: P-0111 Congress: ESTI 2014 Type: Educational Poster Authors: S. M. Mak, B. Annan, S. P. G. Padley, A. G. Nicholson; London/UK Keywords:
Pulmonary Sequestration Causing Severe Cardiac Failure Requiring Lobectomy in an Extreme Preterm Infant
 Scholarship@Western Surgery Publications Surgery Department 10-2015 Pulmonary Sequestration Causing Severe Cardiac Failure Requiring Lobectomy in an Extreme Preterm Infant Rohit Nagar Andreana Bütter,
Scholarship@Western Surgery Publications Surgery Department 10-2015 Pulmonary Sequestration Causing Severe Cardiac Failure Requiring Lobectomy in an Extreme Preterm Infant Rohit Nagar Andreana Bütter,
Clinical presentation and characteristics of 25 adult cases of pulmonary sequestration
 Original Article Clinical presentation and characteristics of 25 adult cases of pulmonary sequestration Mateusz Polaczek 1,2, Inga Baranska 3, Malgorzata Szolkowska 4, Jacek Zych 1, Piotr Rudzinski 5,
Original Article Clinical presentation and characteristics of 25 adult cases of pulmonary sequestration Mateusz Polaczek 1,2, Inga Baranska 3, Malgorzata Szolkowska 4, Jacek Zych 1, Piotr Rudzinski 5,
Epidermiology Early pulmonary embolism
 Epidermiology Early pulmonary embolism Sitang Nirattisaikul Faculty of Medicine, Prince of Songkla University 3 rd most common cause of cardiovascular death in the United States, following ischemic heart
Epidermiology Early pulmonary embolism Sitang Nirattisaikul Faculty of Medicine, Prince of Songkla University 3 rd most common cause of cardiovascular death in the United States, following ischemic heart
Cardiopulmonary Syndromes: Conditions With Concomitant Cardiac and Pulmonary Abnormalities
 Cardiopulmonary Syndromes: Conditions With Concomitant Cardiac and Pulmonary Abnormalities Carlos S. Restrepo M.D. Professor of Radiology The University of Texas HSC at San Antonio Cardiopulmonary Syndromes
Cardiopulmonary Syndromes: Conditions With Concomitant Cardiac and Pulmonary Abnormalities Carlos S. Restrepo M.D. Professor of Radiology The University of Texas HSC at San Antonio Cardiopulmonary Syndromes
Congenital Diaphragmatic Hernia information for parents. David M Notrica MD FACS FAAP Pediatric Surgeons of Phoenix
 Congenital Diaphragmatic Hernia information for parents David M Notrica MD FACS FAAP Pediatric Surgeons of Phoenix CDH Congenital absence of a portion of the diaphragm allowing abdominal contents to migrate
Congenital Diaphragmatic Hernia information for parents David M Notrica MD FACS FAAP Pediatric Surgeons of Phoenix CDH Congenital absence of a portion of the diaphragm allowing abdominal contents to migrate
Perinatal Imaging in Congenital Thoracic Cystic Malformations.
 Perinatal Imaging in Congenital Thoracic Cystic Malformations. Poster No.: C-0898 Congress: ECR 2013 Type: Educational Exhibit Authors: R. Llorens, G. Montoliu, A. Moreno, F. Menor; Valencia/ES Keywords:
Perinatal Imaging in Congenital Thoracic Cystic Malformations. Poster No.: C-0898 Congress: ECR 2013 Type: Educational Exhibit Authors: R. Llorens, G. Montoliu, A. Moreno, F. Menor; Valencia/ES Keywords:
Thoracic Surgery; An Overview
 Thoracic Surgery What we see Thoracic Surgery; An Overview James P. Locher, Jr, MD Methodist Cardiovascular and Thoracic Surgery Lung cancer Mets Fungus and TB Lung abcess and empyema Pleural based disease
Thoracic Surgery What we see Thoracic Surgery; An Overview James P. Locher, Jr, MD Methodist Cardiovascular and Thoracic Surgery Lung cancer Mets Fungus and TB Lung abcess and empyema Pleural based disease
Introduction to Chest Radiography
 Introduction to Chest Radiography RSTH 366: DIAGNOSTIC TECHNIQUES Alan Alipoon BS, RCP, RRT Instructor Department of Cardiopulmonary Sciences 1 Introduction Discovered in 1895 by Wilhelm Roentgen Terminology
Introduction to Chest Radiography RSTH 366: DIAGNOSTIC TECHNIQUES Alan Alipoon BS, RCP, RRT Instructor Department of Cardiopulmonary Sciences 1 Introduction Discovered in 1895 by Wilhelm Roentgen Terminology
X-Rays. Prepared by Prof.Dr. Magda Hassab Allah Assist.lecturer Marwa Al Hady
 X-Rays Prepared by Prof.Dr. Magda Hassab Allah Assist.lecturer Marwa Al Hady CHEST X-RAYS Normal Chest X-ray Comments on chest X ray includes examination of 1- Bony cage (ribs,clavicles &vertebral column
X-Rays Prepared by Prof.Dr. Magda Hassab Allah Assist.lecturer Marwa Al Hady CHEST X-RAYS Normal Chest X-ray Comments on chest X ray includes examination of 1- Bony cage (ribs,clavicles &vertebral column
Pulmonary Pathophysiology
 Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Chest X rays and Case Studies. No disclosures. Outline 5/31/2018. Carlo Manalo, M.D. Department of Radiology Loma Linda University Children s Hospital
 Chest X rays and Case Studies Carlo Manalo, M.D. Department of Radiology Loma Linda University Children s Hospital No disclosures. Outline Importance of history Densities delineated on radiography An approach
Chest X rays and Case Studies Carlo Manalo, M.D. Department of Radiology Loma Linda University Children s Hospital No disclosures. Outline Importance of history Densities delineated on radiography An approach
SURGICAL TECHNIQUE. Radical treatment for left upper-lobe cancer via complete VATS. Jun Liu, Fei Cui, Shu-Ben Li. Introduction
 SURGICAL TECHNIQUE Radical treatment for left upper-lobe cancer via complete VATS Jun Liu, Fei Cui, Shu-Ben Li The First Affiliated Hospital of Guangzhou Medical College, Guangzhou, China ABSTRACT KEYWORDS
SURGICAL TECHNIQUE Radical treatment for left upper-lobe cancer via complete VATS Jun Liu, Fei Cui, Shu-Ben Li The First Affiliated Hospital of Guangzhou Medical College, Guangzhou, China ABSTRACT KEYWORDS
SWISS SOCIETY OF NEONATOLOGY. Cantrell s pentalogy: an unusual midline defect
 SWISS SOCIETY OF NEONATOLOGY Cantrell s pentalogy: an unusual midline defect October 2004 2 Cevey-Macherel MN, Meijboom EJ, Di Bernardo S, Truttmann AC, Division of Neonatology and Division of Pediatric
SWISS SOCIETY OF NEONATOLOGY Cantrell s pentalogy: an unusual midline defect October 2004 2 Cevey-Macherel MN, Meijboom EJ, Di Bernardo S, Truttmann AC, Division of Neonatology and Division of Pediatric
CONGENITAL LOBAR EMPHYSEMA
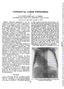 CONGENITAL LOBAR EMPHYSEMA BY R. H. WHITE-JONES and L. J. TEMPLE From Whiston County Hospital, Lancs., and Broadgreen Hospital, Liverpool Regional obstructive emphysema is not uncommon and is due in most
CONGENITAL LOBAR EMPHYSEMA BY R. H. WHITE-JONES and L. J. TEMPLE From Whiston County Hospital, Lancs., and Broadgreen Hospital, Liverpool Regional obstructive emphysema is not uncommon and is due in most
Situs inversus. Dr praveena pulmonology- final year post graduate
 Situs inversus Dr praveena pulmonology- final year post graduate Definiton History Types Cause Clinical features Diagnosis Treatment Definition The term situs inversus is a short form of the latin phrase
Situs inversus Dr praveena pulmonology- final year post graduate Definiton History Types Cause Clinical features Diagnosis Treatment Definition The term situs inversus is a short form of the latin phrase
HelmiLubis, RidwanMuchtarDaulay, WismanDalimunthe, Rini Savitri Daulay
 Congenital Malformation of the Lung and Airways HelmiLubis, RidwanMuchtarDaulay, WismanDalimunthe, Rini Savitri Daulay DivisiRespirologiDepartemenIlmuKesehatanAnak FakultasKedokteran Universitas Sumatera
Congenital Malformation of the Lung and Airways HelmiLubis, RidwanMuchtarDaulay, WismanDalimunthe, Rini Savitri Daulay DivisiRespirologiDepartemenIlmuKesehatanAnak FakultasKedokteran Universitas Sumatera
PAEDIATRIC RESPIRATORY MEDICINE- LOGBOOK 1
 PAEDIATRIC RESPIRATORY MEDICINE- LOGBOOK 1 Module A1 In-patient management of acute respiratory illness 1. Record of a total of 50 cases in 24 36 months to reflect competencies outlined in curriculum Bronchiolitis
PAEDIATRIC RESPIRATORY MEDICINE- LOGBOOK 1 Module A1 In-patient management of acute respiratory illness 1. Record of a total of 50 cases in 24 36 months to reflect competencies outlined in curriculum Bronchiolitis
Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012
 Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012 INTRODUCTION PNEUMOTHORAX HEMOPTYSIS RESPIRATORY FAILURE Cystic Fibrosis Autosomal Recessive Genetically
Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012 INTRODUCTION PNEUMOTHORAX HEMOPTYSIS RESPIRATORY FAILURE Cystic Fibrosis Autosomal Recessive Genetically
Right lung. -fissures:
 -Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
-Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
Surgery has been proven to be beneficial for selected patients
 Thoracoscopic Lung Volume Reduction Surgery Robert J. McKenna, Jr, MD Surgery has been proven to be beneficial for selected patients with severe emphysema. Compared with medical management, lung volume
Thoracoscopic Lung Volume Reduction Surgery Robert J. McKenna, Jr, MD Surgery has been proven to be beneficial for selected patients with severe emphysema. Compared with medical management, lung volume
Neonatal Airway Disorders, Treatments, and Outcomes. Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center
 Neonatal Airway Disorders, Treatments, and Outcomes Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center Disclosure I have nothing to disclose Neonatal and Pediatric Tracheostomy Tracheostomy
Neonatal Airway Disorders, Treatments, and Outcomes Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center Disclosure I have nothing to disclose Neonatal and Pediatric Tracheostomy Tracheostomy
SETTING Fudan University Shanghai Cancer Center. RESPONSIBLE PARTY Haiquan Chen MD.
 OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
In ESH we usually see blunt chest trauma but penetrating injuries also treated here (usually as single injuries, like stab wound)
 Chest Trauma Dr Csaba Dioszeghy MD PhD FRCEM FFICM FERC East Surrey Hospital Emergency Department Scope Thoracic injuries are common and can be life threatening In ESH we usually see blunt chest trauma
Chest Trauma Dr Csaba Dioszeghy MD PhD FRCEM FFICM FERC East Surrey Hospital Emergency Department Scope Thoracic injuries are common and can be life threatening In ESH we usually see blunt chest trauma
Spectrum of Pulmonary Sequestration M. Wayne Flye, M.D., Martin Conley, M.D., and Donald Silver, M.D.
 Spectrum of Pulmonary Sequestration M. Wayne Flye, M.D., Martin Conley, M.D., and Donald Silver, M.D. ABSTRACT Bronchopulmonary sequestration was diagnosed in 17 patients ranging in age from newborn to
Spectrum of Pulmonary Sequestration M. Wayne Flye, M.D., Martin Conley, M.D., and Donald Silver, M.D. ABSTRACT Bronchopulmonary sequestration was diagnosed in 17 patients ranging in age from newborn to
PULMONARY TUBERCULOSIS RADIOLOGY
 PULMONARY TUBERCULOSIS RADIOLOGY RADIOLOGICAL MODALITIES Medical radiophotography Radiography Fluoroscopy Linear (conventional) tomography Computed tomography Pulmonary angiography, bronchography Ultrasonography,
PULMONARY TUBERCULOSIS RADIOLOGY RADIOLOGICAL MODALITIES Medical radiophotography Radiography Fluoroscopy Linear (conventional) tomography Computed tomography Pulmonary angiography, bronchography Ultrasonography,
PDF hosted at the Radboud Repository of the Radboud University Nijmegen
 PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/23566
PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/23566
Non-Small Cell Lung Cancer: Disease Spectrum and Management in a Tertiary Care Hospital
 Non-Small Cell Lung Cancer: Disease Spectrum and Management in a Tertiary Care Hospital Muhammad Rizwan Khan,Sulaiman B. Hasan,Shahid A. Sami ( Department of Surgery, The Aga Khan University Hospital,
Non-Small Cell Lung Cancer: Disease Spectrum and Management in a Tertiary Care Hospital Muhammad Rizwan Khan,Sulaiman B. Hasan,Shahid A. Sami ( Department of Surgery, The Aga Khan University Hospital,
Chest and cardiovascular
 Module 1 Chest and cardiovascular A. Doss and M. J. Bull 1. Regarding the imaging modalities of the chest: High resolution computed tomography (HRCT) uses a slice thickness of 4 6 mm to identify mass lesions
Module 1 Chest and cardiovascular A. Doss and M. J. Bull 1. Regarding the imaging modalities of the chest: High resolution computed tomography (HRCT) uses a slice thickness of 4 6 mm to identify mass lesions
Life-Threatening Respiratory Distress from Mediastinal Masses in Infants
 Life-Threatening Respiratory Distress from Mediastinal Masses in Infants J. Alex Haller, Jr., M.D., Dennis W. Shermeta, M.D., James S. Donahoo, M.D., and John J. White, M.D. ABSTRACT From 1972 through
Life-Threatening Respiratory Distress from Mediastinal Masses in Infants J. Alex Haller, Jr., M.D., Dennis W. Shermeta, M.D., James S. Donahoo, M.D., and John J. White, M.D. ABSTRACT From 1972 through
Adam J. Hansen, MD UHC Thoracic Surgery
 Adam J. Hansen, MD UHC Thoracic Surgery Sometimes seen on Chest X-ray (CXR) Common incidental findings on computed tomography (CT) chest and abdomen done for other reasons Most lung cancers discovered
Adam J. Hansen, MD UHC Thoracic Surgery Sometimes seen on Chest X-ray (CXR) Common incidental findings on computed tomography (CT) chest and abdomen done for other reasons Most lung cancers discovered
UERMMMC Department of Radiology. Basic Chest Radiology
 UERMMMC Department of Radiology Basic Chest Radiology PHYSICS DENSITIES BONE SOFT TISSUES WATER FAT AIR TELEROENTGENOGRAM Criteria for an Ideal Chest Radiograph 1. Upright 2. Posteroanterior View 3. Full
UERMMMC Department of Radiology Basic Chest Radiology PHYSICS DENSITIES BONE SOFT TISSUES WATER FAT AIR TELEROENTGENOGRAM Criteria for an Ideal Chest Radiograph 1. Upright 2. Posteroanterior View 3. Full
Video-assisted thoracic surgery for pulmonary sequestration: a safe alternative procedure
 Original Article Video-assisted thoracic surgery for pulmonary sequestration: a safe alternative procedure Lu-Ming Wang, Jin-Lin Cao, Jian Hu Department of Thoracic Surgery, The First Affiliated Hospital,
Original Article Video-assisted thoracic surgery for pulmonary sequestration: a safe alternative procedure Lu-Ming Wang, Jin-Lin Cao, Jian Hu Department of Thoracic Surgery, The First Affiliated Hospital,
Systematic approach to Fetal Echocardiography. Objectives. Introduction 11/2/2015
 Systematic approach to Fetal Echocardiography. Pediatric Echocardiography Conference, JCMCH November 7, 2015 Rajani Anand Objectives Fetal cardiology pre-test Introduction Embryology and Physiology of
Systematic approach to Fetal Echocardiography. Pediatric Echocardiography Conference, JCMCH November 7, 2015 Rajani Anand Objectives Fetal cardiology pre-test Introduction Embryology and Physiology of
Surgical Management of Lung Bud Anomalies: Lobar Emphysema, Bronchogenic Cyst, Cystic Adenomatoid Malformation, and Intralobar Pulmonary Sequestration
 Surgical Management of Lung Bud Anomalies: Lobar Emphysema, Bronchogenic Cyst, Cystic Adenomatoid Malformation, and Intralobar Pulmonary Sequestration J. Alex Haller, Jr., M.D., E. S. Golladay, M.D., Laurens
Surgical Management of Lung Bud Anomalies: Lobar Emphysema, Bronchogenic Cyst, Cystic Adenomatoid Malformation, and Intralobar Pulmonary Sequestration J. Alex Haller, Jr., M.D., E. S. Golladay, M.D., Laurens
VASCULAR RINGS A CASE - BASED REVIEW
 VASCULAR RINGS A CASE - BASED REVIEW Beverley Newman, BSc. MB.Bch. FACR Professor of Radiology Stanford University and Lucile Packard Children s Hospital Q1,2,3 Frontal chest radiographs on three different
VASCULAR RINGS A CASE - BASED REVIEW Beverley Newman, BSc. MB.Bch. FACR Professor of Radiology Stanford University and Lucile Packard Children s Hospital Q1,2,3 Frontal chest radiographs on three different
OSAMA A. ABDULMAJID, ABDELMOMEN M. EBEID, MOHAMED M. MOTAWEH, and IBRAHIM S. KLEIBO
 Aspirated foreign bodies in the tracheobronchial tree: report of 250 cases Thorax (1976), 31, 635. OSAMA A. ABDULMAJID, ABDELMOMEN M. EBEID, MOHAMED M. MOTAWEH, and IBRAHIM S. KLEIBO Thoracic Surgical
Aspirated foreign bodies in the tracheobronchial tree: report of 250 cases Thorax (1976), 31, 635. OSAMA A. ABDULMAJID, ABDELMOMEN M. EBEID, MOHAMED M. MOTAWEH, and IBRAHIM S. KLEIBO Thoracic Surgical
ULTRASOUND OF THE FETAL HEART
 ULTRASOUND OF THE FETAL HEART Cameron A. Manbeian, MD Disclosure Statement Today s faculty: Cameron Manbeian, MD does not have any relevant financial relationships with commercial interests or affiliations
ULTRASOUND OF THE FETAL HEART Cameron A. Manbeian, MD Disclosure Statement Today s faculty: Cameron Manbeian, MD does not have any relevant financial relationships with commercial interests or affiliations
Giant Solitary Fibrous Tumor of the Pleura: An Analysis of Five Patients
 World J Surg (2010) 34:2553 2557 DOI 10.1007/s00268-010-0715-x Giant Solitary Fibrous Tumor of the Pleura: An Analysis of Five Patients Juntang Guo Xiangyang Chu Yu-e Sun Lianbin Zhang Naikang Zhou Published
World J Surg (2010) 34:2553 2557 DOI 10.1007/s00268-010-0715-x Giant Solitary Fibrous Tumor of the Pleura: An Analysis of Five Patients Juntang Guo Xiangyang Chu Yu-e Sun Lianbin Zhang Naikang Zhou Published
Swyer-James Syndrome: An Infrequent Cause Of Bronchiectasis?
 ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 12 Number 1 Swyer-James Syndrome: An Infrequent Cause Of Bronchiectasis? A Huaringa, S Malek, M Haro, L Tapia Citation A Huaringa, S Malek, M
ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 12 Number 1 Swyer-James Syndrome: An Infrequent Cause Of Bronchiectasis? A Huaringa, S Malek, M Haro, L Tapia Citation A Huaringa, S Malek, M
Bronchioles. Alveoli. Type I alveolar cells are very thin simple squamous epithelial cells and form most of the lining of an alveolus.
 276 Bronchioles Bronchioles continue on to form bronchi. The primary identifying feature is the loss of hyaline cartilage. The epithelium has become simple ciliated columnar, and there is a complete ring
276 Bronchioles Bronchioles continue on to form bronchi. The primary identifying feature is the loss of hyaline cartilage. The epithelium has become simple ciliated columnar, and there is a complete ring
Original Article. Double Aortic Arch in Infants and Children CH XIE, FQ GONG, GP JIANG, SL FU. Key words. Background
 HK J Paediatr (new series) 2018;23:233-238 Original Article Double Aortic Arch in Infants and Children CH XIE, FQ GONG, GP JIANG, SL FU Abstract Key words Background: This study aimed to report the diagnosis,
HK J Paediatr (new series) 2018;23:233-238 Original Article Double Aortic Arch in Infants and Children CH XIE, FQ GONG, GP JIANG, SL FU Abstract Key words Background: This study aimed to report the diagnosis,
Lecture 2: Clinical anatomy of thoracic cage and cavity II
 Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
OBJECTIVES. Solitary Solid Spiculated Nodule. What would you do next? Case Based Discussion: State of the Art Management of Lung Nodules.
 Organ Imaging : September 25 2015 OBJECTIVES Case Based Discussion: State of the Art Management of Lung Nodules Dr. Elsie T. Nguyen Dr. Kazuhiro Yasufuku 1. To review guidelines for follow up and management
Organ Imaging : September 25 2015 OBJECTIVES Case Based Discussion: State of the Art Management of Lung Nodules Dr. Elsie T. Nguyen Dr. Kazuhiro Yasufuku 1. To review guidelines for follow up and management
Tubes and lines in neonatal chest radiograph
 Tubes and lines in neonatal chest radiograph Poster No.: C-1008 Congress: ECR 2014 Type: Educational Exhibit Authors: R. TUMMA, N. AHMED, V. Prasad ; Hyderabad/IN, 1 2 1 1 2 HYDERABAD, ANDHRA PRADESH/IN
Tubes and lines in neonatal chest radiograph Poster No.: C-1008 Congress: ECR 2014 Type: Educational Exhibit Authors: R. TUMMA, N. AHMED, V. Prasad ; Hyderabad/IN, 1 2 1 1 2 HYDERABAD, ANDHRA PRADESH/IN
Exam 2 Respiratory Disorders
 Exam 2 Respiratory Disorders Common Cold Common Cold Pathology Common Cold Consequences Rhinosinusitis Rhinosinusitis Pathology Rhinosinusitis ostia can close due to Influenza (Flu) Influenza Pathology
Exam 2 Respiratory Disorders Common Cold Common Cold Pathology Common Cold Consequences Rhinosinusitis Rhinosinusitis Pathology Rhinosinusitis ostia can close due to Influenza (Flu) Influenza Pathology
