NEPHROLOGY BOARD REVIEW MANUAL. Table of Contents
|
|
|
- Theresa Matthews
- 6 years ago
- Views:
Transcription
1 NEPHROLOGY BOARD REVIEW MANUAL PUBLISHING STAFF PRESIDENT, GROUP PUBLISHER Bruce M. White EDITORIAL DIRECTOR Debra Dreger EDITOR Robert Litchkofski ASSISTANT EDITOR Laurie Garrison EDITORIAL ASSISTANTS Rita E. Gould A.C. Arkles SPECIAL PROGRAMS DIRECTOR Barbara T. White PRODUCTION DIRECTOR Suzanne S. Banish PRODUCTION ASSOCIATES Tish Berchtold Klus Christie Grams Mary Beth Cunney ADVERTISING/PROJECT MANAGER Patricia Payne Castle NOTE FROM THE PUBLISHER: This publication has been developed without involvement of or review by the American Board of Internal Medicine. Endorsed by the Association for Hospital Medical Education The Association for Hospital Medical Education endorses HOSPITAL PHYSICIAN for the purpose of presenting the latest developments in medical education as they affect residency programs and clinical hospital practice. Uremic Bone Disease Series Editor and Contributing Author: Stanley Goldfarb, MD, FACP Professor of Medicine Interim Chairman Department of Medicine University of Pennsylvania School of Medicine Philadelphia, PA Table of Contents Introduction Forms of Renal Osteodystrophy Pathogenesis of Hyperparathyroid Bone Disease Management of Secondary Hyperparathyroidism Resistant Hyperparathyroidism and Parathyroidectomy Dialysis-Related Amyloidosis References Cover Illustration by Scott Holladay Copyright 2001, Turner White Communications, Inc., 125 Strafford Avenue, Suite 220, Wayne, PA , All rights reserved. No part of this publication may be reproduced, stored in a retrieval system, or transmitted in any form or by any means, mechanical, electronic, photocopying, recording, or otherwise, without the prior written permission of Turner White Communications, Inc. The editors are solely responsible for selecting content. Although the editors take great care to ensure accuracy, Turner White Communications, Inc., will not be liable for any errors of omission or inaccuracies in this publication. Opinions expressed are those of the authors and do not necessarily reflect those of Turner White Communications, Inc. Nephrology Volume 4, Part 1 1
2 NEPHROLOGY BOARD REVIEW MANUAL Uremic Bone Disease Series Editor and Contributing Author: Stanley Goldfarb, MD, FACP Professor of Medicine Interim Chairman Department of Medicine University of Pennsylvania School of Medicine Philadelphia, PA INTRODUCTION Uremic bone disease continues to present a diagnostic and therapeutic challenge to clinicians who care for patients with end-stage renal disease (ESRD). Tremendous advances have been made in many aspects of uremic bone disease, including assessing the status of hyperparathyroidism, measuring components of vitamin D, evaluating bone and joint disease by various imaging modalities, and understanding the pathogenesis of and therapy for soft-tissue calcifications. However, a distressingly large number of patients continue to develop hyperparathyroidism after prolonged hemodialysis treatment, and control of hyperphosphatemia and its attendant soft-tissue calcification remains a major clinical problem. In this review, we will examine the pathophysiologic factors that underlie the development of renal osteodystrophy and dialysis-related amyloidosis, consider the major therapeutic interventions, and develop an approach to the treatment of these often perplexing and challenging clinical disorders. CASE PATIENT PRESENTATION History A 44-year-old patient with a history of focal glomerulosclerosis presents for his biannual general health evaluation. He has been treated with hemodialysis for the past 9 years and generally has been compliant with his thrice-weekly hemodialysis treatments. He underwent cadaveric renal transplantation 4 years ago but rapidly rejected the kidney. He works part-time as an accountant. On questioning, the patient reports that he has noticed some generalized pain in his arms and legs. The pain is unrelated to any particular activity. He denies any focal complaints. The rest of the history is noncontributory. Medications include a calcium channel blocker for hypertension, epoetin 10,000 U twice weekly, and 3 tablets of calcium acetate with each meal. Physical Examination The patient appears well nourished and well developed. There is a well-functioning arteriovenous fistula in his left arm. He is afebrile and has a blood pressure of 140/90 mm Hg and pulse of 80 bpm. Extremities are otherwise normal. The rest of the examination is unremarkable. Laboratory Studies Laboratory testing reveals the following: hemoglobin, 11.8 g/dl; blood urea nitrogen, 78 mg/dl; creatinine, 8.1 mg/dl; calcium, 8.7 mg/dl; phosphorus, 6.2 mg/dl; and albumin, 3.5 g/dl. Immunoassay reveals an intact immunoreactive parathyroid hormone (ipth) level of 700 pg/ml. 2 Hospital Physician Board Review Manual
3 Table. Classification of Renal Osteodystrophy Disorder Description Pathogenesis Frequency (%)* Osteitis fibrosa cystica Peritrabecular fibrosis, increased remodeling (resorption and formation) Secondary hyperparathyroidism, secondary role of cytokines and growth factor 50 Osteomalacia Increased osteoid, defective mineralization Aluminum deposition plus unknown factors 7 Mixed disease Features of both osteitis fibrosa and osteomalacia Secondary hyperparathyroidism and aluminum deposition, plus unknown factors 13 Mild disease Slightly increased remodeling Early or treated secondary hyperparathyroidism 3 Adynamic renal bone disease Hypocellular bone surfaces, no remodeling Aluminum deposition, parathyroid hormone suppression, and other factors (eg, deficiency of bone growth factors or increased suppressors of bone modeling) 27 *The frequency at the start of therapy for end-stage renal disease is shown. Although the data are based on a small series, the distribution of disorders is similar to that generally seen in current clinical practice. Data are from Hutchison AJ, Whitehouse RW, Boulton HF, et al. Correlation of bone histology with parathyroid hormone, vitamin D 3 and radiology in end-stage renal disease. Kidney Int 1993;44: Adapted with permission from Hruska KA, Teitelbaum S. Renal osteodystrophy. N Engl J Med 1995;333:170. Copyright 1995 Massachusetts Medical Society. All rights reserved. FORMS OF RENAL OSTEODYSTROPHY What forms of metabolic bone disease occur in patients with renal failure? What is the likely cause of this patient s bone pain? Renal failure inevitably leads to metabolic bone disease. The term renal osteodystrophy describes the variety of metabolic bone disorders that occur as a complication of renal failure (Table). The 2 dominant forms of renal osteodystrophy are osteitis fibrosa cystica and osteomalacia, with many patients showing mixed osteodystrophy in which aspects of both disorders are present. Symptoms due to these disorders, such as fractures and bone pain with osteomalacia or bone pain in osteitis fibrosa, generally do not occur until the patient is already on maintenance dialysis. 1 However, with more sensitive tests such as bone biopsy, a significant proportion of individuals with renal failure can be shown to experience significant morbidity early in the course of renal failure due to abnormalities of bone and mineral metabolism. In fact, half the individuals with a 50% reduction in glomerular filtration rate (GFR) have abnormal bone histology, 2 and almost all individuals have it at the start of dialysis. 3 Renal osteodystrophy is the result of prolonged and severe metabolic derangement in calcium, phosphorus, vitamin D, and parathyroid hormone (PTH) activity. Bone can respond to these changes in only a limited fashion. However, these responses all lead to significant impairment in global bone structure. OSTEITIS FIBROSA CYSTICA Osteitis fibrosa cystica is characterized by increased bone turnover due to secondary hyperparathyroidism. Secondary hyperparathyroidism is virtually universally present to some degree in patients with chronic renal failure and usually takes the form of diffuse hyperplasia of the parathyroid glands. In early renal failure, alterations in vitamin D metabolism, characterized by decreased levels of 1,25(OH) 2 D 3 (calcitriol) and moderately decreased levels of ionized calcium, may allow greater synthesis and secretion of PTH. In later stages of renal disease or in patients on hemodialysis, these abnormalities may be more severe and the symptoms correspondingly more intense. Symptoms may include progressive and debilitating bone disease, pruritus that does not respond to medical or dialytic therapy, progressive extraskeletal calcification (ie, calciphylaxis) that is usually associated with hyperphosphatemia refractory to oral phosphate binders, and otherwise unexplained symptomatic myopathy. Nephrology Volume 4, Part 1 3
4 OSTEOMALACIA Osteomalacia is characterized by low rates of bone formation and dissolution (bone turnover) with an increased volume of unmineralized bone (osteoid) and an accumulation of unmineralized osteoid. Aluminum deposition in bone is thought to be the cause of this condition in most, but not all, patients with osteomalacia. Osteomalacia is often seen in bone biopsies taken in patients with ESRD, 1 although its prevalence is decreasing with widespread elimination of aluminum-containing phosphate binder therapy. 4 The type of osteomalacia associated with ESRD differs from that caused by vitamin D deficiency. Aluminum accumulation in bone causes defective mineralization and increased matrix synthesis by existing osteoblasts while inhibiting osteoclast-associated bone resorption. The fact that low bone turnover osteomalacia has not completely disappeared following the dramatic reduction in the use of aluminum-based phosphate binders suggests that other factors, perhaps related to some aspect of vitamin D metabolism, might play a role in the development of this condition. 5 Patients with osteomalacia often have bone pain, fractures, and marked musculoskeletal disability. ADYNAMIC BONE DISEASE In the past 25 years, a third, seemingly new, and increasingly common form of renal osteodystrophy known as adynamic bone disease has been defined. Adynamic bone disease remains a poorly understood entity. This disease is most common in patients with ESRD who do not have secondary hyperparathyroidism (eg, after parathyroidectomy), who have been aggressively treated with calcium and vitamin D, or who have diabetes mellitus or aluminum intoxication. There is a strong association between continuous ambulatory peritoneal dialysis and adynamic bone disease that may be related to the greater transfer of calcium from the dialysate to the patient and subsequent suppression of PTH secretion. 1 Although adynamic bone disease initially was thought not to cause symptoms, subsequent follow-up has shown that the fracture rate and mortality rate are increased in patients with this disease compared with patients with other forms of osteodystrophy. 1 Patients with adynamic bone disease have a tendency to become hypercalcemic when receiving calcitriol. This probably reflects a decrease in the ability of the skeleton to take up calcium after gastrointestinal absorption is stimulated by the vitamin. BONE DISEASE IN CASE PATIENT In the case patient, the very high PTH level strongly suggests that the bone pain is a manifestation of intense hyperparathyroid effect on bone. A test that would be useful to confirm the diagnosis is measurement of bonespecific alkaline phosphatase levels, which may provide useful information in conjunction with PTH measurements. Elevated bone-specific alkaline phosphatase (20 ng/ml) in plasma, alone or in combination with increased plasma PTH (above 200 pg/ml), appears to be highly sensitive and specific for high turnover bone disease. 6 Radiographic examination of bone can also provide important information regarding the presence of hyperparathyroidism (vide infra). However, radiographic findings are less sensitive than PTH levels and will not establish the type of bone disease. PATHOGENESIS OF HYPERPARATHYROID BONE DISEASE What are the mechanisms by which abnormalities of vitamin D, calcium, and phosphate lead to hyperparathyroidism in patients with ESRD? ALTERATIONS IN VITAMIN D METABOLISM The vitamin D hormone calcitriol (1,25(OH) 2 D 3 ), the most active metabolite of vitamin D, controls parathyroid gland growth and suppresses the synthesis and secretion of PTH. Calcitriol is produced in the renal cortex through the actions of the enzyme 25(OH) 2 D-1-hydroxylase on the precursor molecule 25(OH)D, which is made in the liver; thus, a reduction in the level of calcitriol is one of the earliest manifestations of renal damage. Calcitriol production is normally stimulated by a direct action of PTH whenever there is a fall in the serum calcium level. When such a decrease occurs, the actions of calcitriol lead to an increase of gastrointestinal calcium absorption and an increase in the effect of PTH to cause mobilization of calcium from bone stores. As the serum calcium rises, PTH levels are normally suppressed through several pathways, including the activation of the calciumsensing receptor on the surface of parathyroid cells and through a direct action of calcitriol to suppress the parathyroid cells and PTH secretion. This latter effect occurs through calcitriol s ability to potently decrease the transcription of the PTH gene. This action was first demonstrated in in vitro parathyroid cell cultures, where calcitriol led to a marked decrease in PTH messenger ribonucleic acid (mrna) levels and a consequent decrease in PTH secretion. 7 The physiologic relevance of these findings was established by in vivo studies in rats and subsequently in a variety of human studies. 8 Calcitriol might further regulate the PTH gene at the 4 Hospital Physician Board Review Manual
5 level of the calcitriol receptor. This protein acts as a nuclear receptor of the steroid receptor family, binds to the PTH gene regulatory elements, and suppresses PTH gene transcription. 9 In chronic renal disease, the damaged kidney s lack of capacity to synthesize adequate amounts of the active form of vitamin D clearly contributes to the rise in PTH levels. However, there may be other factors that result in resistance to the action of calcitriol, including circulating or cellular factors that interfere with the binding of vitamin D to its receptor or defects in receptor synthesis. Calcitriol therapy has been successfully utilized to reverse hyperparathyroidism. 10 The utility of intravenous calcitriol in suppressing PTH levels in patients with ESRD and secondary hyperparathyroidism is well established. However, because of its potent action to stimulate intestinal calcium absorption and bone calcium mobilization, calcitriol treatment can induce hypercalcemia, often precluding the use of therapeutic doses. HYPERPHOSPHATEMIA Hyperphosphatemia is also a persistent problem among patients with chronic renal failure and is important in the pathogenesis of hyperparathyroidism. As kidneys fail, their capacity to excrete phosphate is impaired and serum phosphate levels begin to rise. Increased phosphate levels have a number of consequences, including a decrease in ionized calcium and an increase in serum PTH levels (described below). Studies in experimental renal failure in dogs have shown that a restriction of dietary phosphorus in proportion to the decrease in GFR can prevent the development of secondary hyperparathyroidism. 11 In addition to decreasing the levels of ionized calcium, high serum phosphorus decreases the production of calcitriol. As GFR falls below 25 ml/min, most patients develop hyperphosphatemia; in this setting hypocalcemia appears to be directly related to the markedly increased levels of serum phosphorus. The mechanism by which hyperphosphatemia reduces the concentration of ionized calcium is not known. It may decrease the release of calcium from bone and/or affect the activity of the renal enzyme 1-hydroxylase, which converts 25(OH)D to 1,25(OH) 2 D 3. 12,13 Recent studies have suggested that phosphate ion per se could influence PTH secretion. This hypothesis springs from observations that elevated phosphate levels may directly alter release of PTH in in vitro cell culture systems or in experimental animals, without a measurable change in calcium levels. 14 Unfortunately, it may be very difficult to perfectly maintain the level of ionized calcium in both in vitro and in vivo systems when there is a concomitant change in the phosphate level, because the 2 are bound and highly interactive. Therefore, the direct effect of phosphate independent of calcium or of calcitriol remains somewhat speculative. HYPOCALCEMIA Serum calcium levels are typically low in patients with chronic renal failure. The etiology of low calcium levels is complex but includes reductions in gastrointestinal calcium absorption due to reduced activity of calcitriol, resistance to the effects of calcitriol to promote calcium uptake in the gastrointestinal tract and calcium mobilization from bone, hyperphosphatemia, and reduced dietary calcium intake as overall nutrition declines in the uremic state. 15 The parathyroid gland is exquisitely sensitive to small changes in serum calcium. Variations in serum calcium are recognized by the calcium-sensing receptor, a 7-transmembrane receptor with a large extracellular amino-terminal region. 16 Small changes in extracellular calcium lead to large changes in PTH secretion, although the response of the receptor may be less robust in uremia. The relative insensitivity in uremia could be due to down-regulation of synthesis of the calciumsensing receptor protein in the parathyroid gland in ESRD. 17 A fall in serum calcium leads not only to an increase in PTH secretion but also to increases in PTH mrna levels and parathyroid cell proliferation. The effect is post-transcriptional in vivo and involves protein RNA interactions at the 3'-untranslated region of the PTH mrna. This protein-rna binding leads to stabilization or inhibition of degradation of the mrna and thereby results in an opportunity for greater synthesis of PTH protein. 18 Hypocalcemia acts through several other pathways to increase PTH secretion over the short term as well as the long term. It stimulates PTH secretion through changes in the calcium-sensing receptor linked to the cyclic adenosine monophosphate (camp) signaling system in parathyroid cells, and increases PTH mrna levels over hours and days, thus enhancing cellular synthesis of PTH. Most importantly for the development of glandular enlargement and severe hyperparathyroidism, hypocalcemia increases parathyroid cell number after a stimulus of many weeks. 19 In general, the parathyroid gland is poised to secrete increased amounts of PTH in the face of a decline in serum calcium level, but a rise in serum calcium has only a minimal effect in suppressing baseline PTH synthesis and secretion. 20 In summary, in early renal failure, decreased levels of calcitriol and moderate decreases in ionized calcium result in greater synthesis and secretion of PTH. As the disease progresses, there may be a decrease in the number of vitamin D receptors within the parathyroid gland and the Nephrology Volume 4, Part 1 5
6 A B C D E Figure. Specimens of normal trabecular bone and trabecular bone showing the histologic types of renal osteodystrophy. Noncalcified iliac-biopsy specimens from patients with end-stage renal disease were fixed in Millonig s fluid and stained with a modified Masson stain (original magnification, 40). (A) Normal trabecular bone. (B) Osteitis fibrosa with prominent peritrabecular fibrosis (F), which is the hallmark of this disease. (C) Osteomalacia with increased unmineralized bone matrix (osteoid, red). Decreased rates of remodeling are suggested by the decreased activity and number of osteoclasts. The osteoid accumulates and is poorly resorbed. (D) Mixed disease, characterized by areas of fibrosis (F) and increased remodeling activity adjacent to areas of increased osteoid deposition, with poor mineralization and remodeling. (E) Adynamic bone disease, characterized by an absence of remodeling activity. The number of bone cells (osteoblasts and osteoclasts) is decreased, and there is minimal evidence of osteoid production. Adapted with permission from Hruska KA, Teitelbaum SL. Renal osteodystrophy. N Engl J Med 1995;333:167. Copyright 1995 Massachusetts Medical Society. All rights reserved. 6 Hospital Physician Board Review Manual
7 gastrointestinal tract, and a decrease in the density of calcium receptors in the parathyroid glands. Also, there may be an ill-defined antagonism to the actions of PTH to mobilize bone calcium in ESRD. All these effects render the parathyroid glands more resistant to calcitriol and limit calcium availability, thereby stimulating the parathyroid gland. Hyperphosphatemia may induce hyperfunction of the parathyroid glands, although whether this effect of phosphorus is independent from calcium and calcitriol remains somewhat inconclusive. Hypocalcemia, perhaps by a post-transcriptional mechanism at the level of PTH mrna, increases PTH synthesis and secretion. Chronic stimulation of the gland may induce cellular hyperplasia and thereby lead to very high PTH levels and even to transformation of the glandular hyperplasia into an independently functioning form of nonsuppressible or tertiary hyperparathyroidism. What are the likely pathologic characteristics of hyperparathyroid bone disease in this patient? HYPERPARATHYROID BONE DISEASE Chronic and often marked PTH excess produces a number of pathologic changes in bone that ultimately translate into bone that is more prone to fracture or to be painful (Figure). Normal bone shows a lamellar distribution of osteoid, a complex of extracellular matrix material that is primed to become calcified and to form the organic substrate for bone. Osteoid is present on a small amount of the bone surface (< 25%), and about 40% of the osteoid is covered with mature osteoblasts, cells that produce the extracellular matrix material. Bone resorption occurs at only 7% of the bone surface, and osteoclasts (ie, the multinucleated cells that stimulate bone resorption) are present on less than 2% of the bone surface. Hyperparathyroid bone shows dramatic differences from normal bone. There is a great deal of fibrous tissue in the bone marrow, the osteoid has a woven appearance, and there are increased numbers and activity of osteoblasts, expansion of osteoid surfaces, and numerous osteoclasts and resorptive surfaces. In very advanced cases, fibrosis replaces bone marrow entirely, reflecting the irregular activity of osteoblasts in which the regular activity of individual cells is decreased. MANAGEMENT OF SECONDARY HYPERPARATHYROIDISM What therapies are used to control hyperparathyroidism in patients with ESRD? CONTROL OF HYPERPHOSPHATEMIA The main problem in general, and perhaps the major problem in the management of divalent ion metabolism and the control of secondary hyperparathyroidism, is insufficient control of hyperphosphatemia. 21 Serum phosphate is notoriously difficult to control due to the extremely complex kinetics of elimination of phosphate during dialysis treatments. Phosphate diffusion from the intracellular to extracellular compartment is low relative to the rate of removal of phosphate during high-efficiency dialysis sessions. This leads to a relatively small mass of phosphate removed at each dialysis treatment and to a positive phosphate balance. In Japanese patients with an average weight of 52 kg and an average duration of hemodialysis of 4.2 ± 0.5 hours, 22 predialytic serum phosphate is 5.8 mg/dl. In other countries, the values tend to be even higher. Obviously, if patents receive insufficient amounts of hemodialysis, the problem of hyperphosphatemia may be exaggerated. Hyperphosphatemia not only lowers the serum calcium but may also lead to soft-tissue calcifications. The combination of marked hyperphosphatemia and a normal, low normal, or elevated plasma calcium concentration results in an elevated calcium-phosphate product. This theoretical term is derived by multiplying the plasma phosphate level in mg/dl by the total plasma calcium level in mg/dl. While no specific data have established a particularly dangerous value, it is generally accepted that if the product exceeds 70, there is an increased likelihood that precipitates of calcium phosphate will appear in arteries, joints, and other soft tissues, including the heart and heart valves; this process is known as metastatic calcification. The standard approach to the control of serum phosphate in ESRD patients is to employ phosphate binders such as calcium carbonate, calcium acetate, and aluminum-based compounds. These agents act to restrict gastrointestinal absorption of phosphate and therefore should be taken at the time of meals. Unfortunately, the use of these agents is limited by side effects such as hypercalcemia, skeletal and neurologic toxicities associated with the use of aluminum-containing agents, and difficulty with compliance since therapy usually involves taking many pills. Large doses of calcium carbonate or acetate with meals are commonly used to control phosphate absorption, and this therapy currently represents a standard of care. However, the use of these agents in patients receiving calcitriol increases the risk of hypercalcemia. 23 Thus, control of serum phosphate remains a challenge. This has prompted the development of novel phosphate-binding Nephrology Volume 4, Part 1 7
8 compounds, such as polyallylamine hydrochloride, that are effective but expensive. USE OF VITAMIN D Because prophylactic use of calcitriol is the most effective means of suppressing PTH levels to the near normal range, the hormone should be added to the treatment program of all patients with ESRD, particularly those patients with plasma ipth values above 300 pg/ml. It is common practice to give calcitriol intravenously after every dialysis treatment if the PTH level is elevated, the serum phosphate level is less than 6 mg/dl, and the calcium level is less than 10.5 mg/dl. Individual calcitriol doses typically range from 0.5 to 4 µg, with the average tolerated dose being about 2.5 µg. 24 Initially, it was thought that calcitrol should be given in a pattern of intravenous pulses in order to overcome any resistance to the actions of the hormone in renal failure that could result from reduced PTH cell receptors for vitamin D or some other form of interference. The direct cellular effect of calcitriol to suppress the transcription of the PTH gene was the basis for this therapy. Subsequent studies have shown that oral administration is as effective as intravenous administration, 25 although in patients with limited financial resources, the use of expensive oral agents may not be feasible. Intravenous therapy generally qualifies for various forms of reimbursement. Recent studies have pointed out some of the deficiencies in the use of calcitriol as the principal means of suppressing the hyperparathyroidism of ESRD. First, even with the aggressive use of calcitriol, most registries of ESRD patients receiving hemodialysis suggest that 15% of patients will eventually need to undergo surgical parathyroidectomy. Second, hypercalcemia continues to occur in patients treated with calcitriol, and the induction of softtissue calcification may be an important cause of later morbidity and mortality. Recently developed analogs of calcitriol hold the promise of more selectively depressing PTH levels with a minimal tendency to produce hypercalcemia. New vitamin D metabolites have been synthesized and studied in patients with ESRD. Some of these have shown a reduced tendency to raise phosphate and/or calcium while maintaining good control of the parathyroid glands: 22-oxacalcitriol, 26 paricalcitol (19 nor-1,25-dihydroxyvitamin D 2 ), and doxercalciferol (1α-hydroxyvitamin D 2 ) have all shown high efficacy when compared with placebo. 27 The results of randomized studies comparing the new vitamin D metabolites with calcitriol are either not yet available or show uncertain benefits in relation to hypercalcemia, hyperphosphatemia, and hyperparathyroidism. Moreover, the reason these agents are less likely to produce hypercalcemia compared to calcitriol likely resides in different pharmacokinetic characteristics rather than a different mechanism of action. 28 TREATMENT OF CASE PATIENT Measurement of bone-specific alkaline phosphatase is done to confirm the diagnosis of osteitis fibrosa and reveals a level of 35 ng/ml. The patient is treated with the phosphate binder calcium acetate and calcitriol 4 µg given intravenously after each dialysis treatment. After a 3-month course of this therapy, the patient s bone pain persists. Laboratory analysis reveals the following: serum calcium, 11.1 mg/dl; serum phosphate, 5.8 mg/dl; and plasma ipth, 980 pg/ml. Radiographs of hands and clavicles show subperiosteal resorption at the radial surface of the metacarpals and the distal head of the clavicles. RESISTANT HYPERPARATHYROIDISM AND PARATHYROIDECTOMY What is the significance of these laboratory and radiologic studies? What characteristics of the parathyroid glands suggest that parathyroid surgery will be necessary? RESISTANT HYPERPARATHYROIDISM This patient s clinical and radiologic picture is most consistent with resistant hyperparathyroidism. The radiologic picture of hyperparathyroidism is characterized by subperiosteal erosions, which can occur at any site in the skeleton but are most often present in the hands along the radial margins of the middle phalanges of the second and third fingers. In the most severe cases, one may see so-called brown tumors in which cavities develop in bone. These cavities consist of excessive osteoclast-induced bone resorption, fibrous tissue, and, ultimately, necrosis and liquefaction. Such cavities appear as cysts in bone, can occur anywhere in the skeleton, and may expand bone. The appellation osteitis fibrosa cystica described by von Recklinghausen is thus derived. The finding of hyperparathyroidism resistant to calcitriol, despite the presence of hypercalcemia, suggests that parathyroidectomy will be required in this patient. Parathyroidectomy is indicated in any symptomatic patient who has nonsuppressible serum PTH levels. GLAND HYPERPLASIA Size is an important aspect of the parathyroid glands of those patients requiring surgery. A normal parathyroid 8 Hospital Physician Board Review Manual
9 gland weighs 30 to 40 mg, while a hyperplastic gland in secondary hyperparathyroidism may weigh as much as 2 to 3 g. Large parathyroid glands in patients with ESRD in whom hyperparathyroidism is suspected on clinical grounds usually show asymmetrical enlargement and nodularity when examined pathologically. There are 2 types of parathyroid hyperplasia: diffuse hyperplasia and nodular hyperplasia (usually a fibrous capsule surrounds nodules). Nodular hyperplasia is the more advanced type of hyperplasia and is seen more often in large glands. The characteristics of cells in nodular and diffuse hyperplasia are strikingly different. 29 It appears that parathyroid hyperplasia actually progresses from diffuse cellular hyperplasia to the nodular form. Some cells with more pronounced reduction of vitamin D receptor and calcium-sensing receptor in areas of diffuse hyperplasia begin to proliferate more vigorously, leading to formation of individual nodules and finally to nodular hyperplasia. In the most advanced type of parathyroid hyperplasia in ESRD, 1 of the nodules may grow to occupy the whole gland, forming a single hyperfunctioning nodule. 26 What are the options for intervening and reducing the mass of parathyroid tissue? PARATHYROID SURGERY The therapy of choice for hyperparathyroidism refractory to calcitriol and phosphate restriction is parathyroidectomy, although this operation can be tedious and difficult. In patients with primary hyperparathyroidism, bilateral neck exploration by an experienced parathyroid surgeon is curative in more than 95% of cases. 30 Therefore, routine preoperative parathyroid imaging is considered neither generally necessary nor cost-effective before a first parathyroidectomy. 31 The most popular surgical procedures used to treat renal hyperparathyroidism are subtotal parathyroidectomy and total parathyroidectomy with intramuscular implantation of parathyroid tissue. With both techniques, a small amount of abnormal parathyroid tissue is left in the patient. Because the stimuli to secretion of PTH may persist after the operation, the remaining glandular tissue may be continually stimulated and hyperparathyroidism may recur. Total parathyroidectomy without grafting has been advocated to avoid these recurrences. 32 However, the complete absence of PTH may lead to defects in bone such as adynamic bone disease. 33 Recently, minimally invasive endoscopic surgical procedures have been proposed for the removal of excess parathyroid tissue. However, it will be difficult to demonstrate clear advantages of such procedures over the current standard open parathyroid exploration. 34 Recent studies from Japan suggest that minimally invasive approaches using percutaneous injection following ultrasonic localization of glands may be a more effective and less morbid approach. In this new approach, selective percutaneous ethanol injection therapy (PEIT) of the parathyroid gland is performed. 35 In selective PEIT, all glands with nodular hyperplasia are selectively destroyed by ethanol and the remaining glands with diffuse hyperplasia are controlled by medical therapy, including the standard calcitriol infusions and phosphate restriction. The indications for PEIT are similar to those for parathyroidectomy: osteitis fibrosa bone disease with associated high PTH levels, marked parathyroid hyperplasia, and resistance to medical therapy. Patients with 1 or 2 enlarged glands with nodular hyperplasia are good candidates for this therapy. Doppler color imaging is required to assure destruction of the tissue, to recognize the recurrence of cell growth, and to assess the need for additional ethanol injection. In contrast to surgical parathyroidectomy, the risk of hypoparathyroidism is minimal. PATIENT FOLLOW-UP The patient successfully undergoes parathyroidectomy and autotransplantation of the glands. Diffuse hyperplasia with a single large nodule is seen. He is treated with calcitriol 2 µg after each dialysis treatment and remains on calcium acetate as a phosphate binder. During a general health evaluation 3 years after surgery, the patient complains of shoulder pain that has persisted for the past 3 months. What other skeletal-related complications of longterm chronic dialysis therapy may develop in this patient despite correction of hyperparathyroidism? DIALYSIS-RELATED AMYLOIDOSIS CLINICAL FEATURES Carpal tunnel syndrome, chronic joint pain, and destructive arthropathy are seen in many patients who have been treated with hemodialysis for a period of 8 to 10 years. 36 This condition has been given several names, including dialysis-related amyloidosis, dialysis-associated arthropathy, dialysis-associated spondyloarthropathy, and carpal tunnel syndromes. 37 The chronic arthralgias are usually bilateral and often initially involve the shoulders. Other joints may be involved as well, particularly the knees, wrists, and small joints of the hands. Chronic joint edema, recurrent hemarthrosis, and chronic Nephrology Volume 4, Part 1 9
10 tenosynovitis of the hands are common features of the disease. Destruction of large peripheral joints and of the spine may occur. Massive amyloid deposits are almost always observed at the site of the destructive lesions and are therefore considered pathogenetic. 38 However, dialysisrelated amyloidosis is also a systemic disease as the amyloid deposition sites may be the same as those found in other forms of amyloidosis (ie, the subcutaneous tissues and skin, and less frequently the rectal mucosa, liver, spleen, and blood vessels). 39 Key radiologic features of β 2 -microglobulin amyloidosis are subchondral bone cysts or articular erosions that result from replacement of subchondral bone by amyloid deposits. Their frequency increases with patient survival, and they may be found in 50% to 60% of patients treated with dialysis for more than 10 years. 40 Since the lesions typically are cystic and occur at the ends of long bones, they may be mistaken for brown tumors and lead to a diagnosis of hyperparathyroid bone disease. The cystic lesions tend to enlarge with time and may be associated with pathologic fractures of the carpal bones, fingers, femoral and humeral heads, acetabulum, tibial plateau, and distal radius, further confusing the diagnosis. PATHOGENESIS Dialysis-related amyloidosis has a complex pathogenesis. The amyloid deposits contain β 2 -microglobulin proteins, and the condition depends on disordered metabolism of this protein. In patients with reduced renal function, the pathogenetic mechanisms include reduced elimination and enhanced production of β 2 -microglobulin amyloid fibrils. Similar to glucose s capacity to form adducts with proteins and thereby alter the degradation of proteins such as collagen, 41 nonenzymatic modifications of β 2 -microglobulin probably play a role, including β 2 -microglobulin protein modification with advanced glycation end-products. These modified β 2 -microglobulin products induce a local inflammatory response and β 2 -microglobulin amyloid formation. There is some evidence that the type of hemodialysis membrane used in long-term treatment may contribute to the pathogenesis of β 2 -microglobulin amyloidosis. The prevalence of amyloid cysts is higher in patients treated with standard cuprophane membrane than in those treated with more biocompatible membranes such as polyacrylonitrile AN 69 or polysulfone. 42 The structure, surface area, permeability, and biocompatibility may all contribute the change of plasma β 2 -microglobulin during dialysis. The use of standard cuprophane and cellulose acetate membranes does not allow one to remove significant amounts of β 2 -microglobulin, while the use of highly permeable membranes (ie, polysulfone or polyacrylonitrile) leads to greater clearance of the molecule during dialysis 43 and subsequent lower plasma levels of the molecule. 44 DIAGNOSIS AND TREATMENT The diagnosis of dialysis-related amyloidosis is based on the presence of typical clinical features and synovial biopsy or bone biopsy demonstrating the presence of amyloid fibrils. The plasma β 2 -microglobulin level can be measured and, in fact, is increased in dialyzed patients at a level ranging from 30 to 50 mg/l (normal value, 0.8 to 3.0 mg/l); however, it is a nonspecific finding because the level can be elevated without the presence of amyloid in bone or other tissues. In a study of 26 patients receiving hemodialysis treatment (mean time, 12.2 years) for chronic renal failure who developed dialysis-related amyloidosis, histological confirmation of amyloid visceral involvement was demonstrated by abdominal fat aspiration and rectal biopsy in 58% of the patients. 45 Twodimensional ultrasonography may also be useful in diagnosing dialysis-related amyloidosis of the shoulder by demonstrating increased rotator cuff thickness or a thickened synovial sheath of the biceps tendon. 46 Specific treatment of the complications of dialysisrelated amyloidosis and early surgical correction of carpal tunnel syndrome are often indicated. Surgical repair of the shoulder with removal of synovium infiltrated by amyloid is often very effective, although the lesions and the symptoms tend to recur. 47 Joint replacement can relieve pain and restore lost mobility and should be considered. Given the important role of the dialysis membrane as discussed above, membranes with greater biocompatibility and permeability should be used. Dialysis duration and frequency should be modified to increase the likelihood of removal of the etiologic β 2 -microglobulin. 48 Successful renal transplantation reduces plasma β 2 -microglobulin levels to normal and may produce prompt resolution of the amyloid deposits. In one long-term study, all patients receiving renal transplant had nearly complete clinical recovery. 49 REFERENCES 1. Hruska KA, Teitelbaum SL. Renal osteodystrophy. N Engl J Med 1995;333: Hutchison AJ, Whitehouse RW, Boulton HF, et al. Correlation of bone histology with parathyroid hormone, vitamin D 3 and radiology in end-stage renal disease. Kidney Int 1993;44: Smith A, Faugere M, Abreo K. Aluminium associated bone disease in renal failure. A study on prevalence, 10 Hospital Physician Board Review Manual
11 histopathology, etiology and diagnosis in 197 patients. Am J Nephrol 1986;6: Moriniere P, Cohen-Solal A, Belbrik S, et al. Disappearance of aluminic bone disease in a long term asymptomatic dialysis population restricting Al(OH) 3 intake: emergence of an idiopathic adynamic bone disease not related to aluminum. Nephron 1989;53: Eastwood JB, Stamp TC, De Wardener HE, et al. The effect of 25-hydroxyvitamin D 3 in osteomalacia of chronic renal failure. Clin Sci Mol Med 1977;52: Urena P, Hruby M, Ferreira A, et al. Plasma total versus bone alkaline phosphatase as markers of bone turnover in hemodialysis patients. J Am Soc Nephrol 1996;7: Cantley LK, Russell J, Lettieri D, Sherwood LM. 1,25- Dihydroxyvitamin D 3 suppresses parathyroid hormone secretion from bovine parathyroid cells in tissue culture. Endocrinology 1985;117: Slatopolsky E, Delmez JA. Pathogenesis of secondary hyperparathyroidism. Am J Kid Dis 1994;23: Silver J, Naveh-Many T, Mayer H, et al. Regulation by vitamin D metabolites of parathyroid hormone gene transcription in vivo in the rat. J Clin Invest 1986;78: Andress DL, Keith MD, Norris C, et al. Intravenous calcitriol in the treatment of refractory osteitis fibrosa of chronic renal failure. N Engl J Med 1989;321: Slatopolsky E, Caglar S, Gradowska L, et al. On the prevention of secondary hyperparathyroidism in experimental chronic renal disease using proportional reduction of dietary phosphorus intake. Kidney Int 1972;2: Reiss E, Canterbury MJ, Bercovitz MA, Kaplan EL. The role of phosphate in the secretion of parathyroid hormone in man. J Clin Invest 1970;49: Lucas PA, Brown RC, Woodhead JS, Coles G. 1,25 dihydroxycholecalciferol and parathyroid hormone in advanced renal failure: effects of simultaneous protein and phosphorus restriction. Clin Nephrol 1986;25: Hernandez A, Concepcion MT, Rodriguez M, et al. High phosphorus diet increases prepropth mrna independent of calcium and calcitriol in normal rats. Kidney Int 1996;50: Hutchison AJ. Predialysis management of divalent ion metabolism. Kidney Int Suppl 1999;73:S Brown EM, Pollak M, Seidman CE, et al. Calcium-ionsensing cell-surface receptors. N Engl J Med 1995;333: Kifor O, Moore FD Jr, Wang P, et al. Reduced immunostaining for the extracellular Ca2+-sensing receptor in primary and uremic secondary hyperparathyroidism. J Clin Endocrinol Metab 1996;81: Moallem E, Silver J, Kilav R, Naveh-Many T. RNA protein binding and post-transcriptional regulation of PTH gene expression by calcium and phosphate. J Biol Chem 1998;273: Naveh-Many T, Silver J. Regulation of parathyroid hormone gene expression by hypocalcemia, hypercalcemia, and vitamin D in the rat. J Clin Invest 1990;86: Silver J, Yalcindag C, Sela-Brown A, et al. Regulation of the parathyroid hormone gene by vitamin D, calcium and phosphate. Kidney Int 1999;73:S Ritz E, Schömig M, Bommer J. Osteodystrophy in the millennium. Kidney Int 1999;73:S Shinzato T, Nakai S, Akiba T, et al. Current status of renal replacement therapy in Japan. Results of the annual survey of the Japanese Society for Dialysis Therapy. Nephrol Dial Transplant 1997;12: Ritz E, Passlick-Deetjen J, Lippert J. What is the appropriate dialysate calcium concentration for the dialysis patient? Nephrol Dial Transplant 1996;11 Suppl 3: Levine BS, Song M. Pharmacokinetics and efficacy of pulse oral versus intravenous calcitriol in hemodialysis patients. J Am Soc Nephrol 1996;7: Quarles LD, Yohay DA, Carroll BA, et al. Prospective trial of pulse oral versus intravenous calcitriol treatment of hyperparathyroidism in ESRD. Kidney Int 1994;45: Monier-Faugere MC, Geng Z, Friedler RM, et al. 22-oxacalcitriol suppresses secondary hyperparathyroidism without inducing low bone turnover in dogs with renal failure. Kidney Int 1999;55: Frazao JM, Chesney RW, Coburn JW. Intermittent oral 1alpha-hydroxyvitamin D 2 is effective and safe for the suppression of secondary hyperparathyroidism in hemodialysis patients. 1alphaD 2 Study Group. Nephrol Dial Transplant 1998;13 Suppl 3: Brown AJ, Finch J, Grieff M, et al. The mechanism for the disparate actions of calcitriol and 22-oxacalcitriol in the intestine. Endocrinology 1993;133: Fukagawa M, Tominaga Y, Kitaoka M, et al. Medical and surgical aspects of parathyroidectomy. Kidney Int 1999; 73:S Pattou F, Huglo D, Proye C. Radionuclide scanning in parathyroid diseases. Br J Surg 1998;85: National Institutes of Health conference. Diagnosis and management of asymptomatic primary hyperparathyroidism: consensus development conference statement. Ann Intern Med 1991;114: Ureña P, Kubrusly M, Mannstadt M, et al. Total or subtotal parathyroidectomy in uremic patients? Clin Nephrol 1994;41: Kinnaert P, Salmon I, Decoster-Gervy C, et al. Long-term results of subcutaneous parathyroid grafts in uremic patients. Arch Surg 2000;135: Gauger PG, Reeve TS, Delbridge LW. Endoscopically assisted, minimally invasive parathyroidectomy. Br J Surg 1999;86: Kitaoka M, Fukagawa M, Ogata E, Kurokawa K. Reduction Nephrology Volume 4, Part 1 11
12 of functioning parathyroid cell mass by ethanol injection in chronic dialysis patients. Kidney Int 1994;46: van Ypersele de Strihou C, Jadoul M, Malghem L, et al. Effect of dialysis membrane and patient s age on signs of dialysis-related amyloidosis. Kidney Int 1991;39: Drueke TB. Extraskeletal problems and amyloid. Kidney Int Suppl 1999;73:S Bardin T, Zingraff J, Shirahama T, et al. Hemodialysisassociated amyloidosis and beta-2 microglobulin. Clinical and immunohistochemical study. Am J Med 1987;83: Zhou H, Pfeifer U, Linke R. Generalized amyloidosis from beta 2-microglobulin, with caecal perforation after long-term haemodialysis. Virchows Arch A Pathol Anat Histopathol 1991;419: Munoz-Gomez J, Bergada-Barado E, Gomez-Perez R, et al. Amyloid arthropathy in patients undergoing periodical haemodialysis for chronic renal failure: a new complication. Ann Rheum Dis 1985;44: Yang CW, Vlassara H, Peten EP, et al. Advanced glycation end products up-regulate gene expression found in diabetic glomerular disease. Proc Natl Acad Sci USA 1994; 91: Miura Y, Ishiyama T, Inomata A, et al. Radiolucent bone cysts and the type of dialysis membrane used in patients undergoing long-term hemodialysis. Nephron 1992;60: Floge J, Granolleras C, Bingel M, et al. Beta 2-microglobulin kinetics during haemodialysis and haemofiltration. Nephrol Dial Transplant 1987;1: Locatelli F, Mastrangelo F, Redaelli B, et al. Effects of different membranes and dialysis technologies on patient treatment tolerance and nutritional parameters. The Italian Cooperative Dialysis Study Group. Kidney Int 1996;50: Campistol JM, Sole M, Munoz-Gomez J, et al. Systemic involvement of dialysis-amyloidosis. Am J Nephrol 1990; 10: Cardinal E, Buckwalter KA, Braunstein EM, et al. Amyloidosis of the shoulder in patients on chronic hemodialysis: sonographic findings. AJR Am J Roentgenol 1996; 166: Takenaka R, Fukatsu A, Matsuo S, et al. Surgical treatment of hemodialysis-related shoulder arthropathy. Clin Nephrol 1992;38: Tan SY, Pepys MB, Hawkins PN. Treatment of amyloidosis. Am J Kidney Dis 1995;26: Tan SY, Irish A, Winearls CG, et al. Long term effect of renal transplantation on dialysis-related amyloid deposits and symptomatology. Kidney Int 1996;50: Copyright 2001 by Turner White Communications Inc., Wayne, PA. All rights reserved. 12 Hospital Physician Board Review Manual
Kobe University Repository : Kernel
 Title Author(s) Citation Issue date 2009-09 Resource Type Resource Version DOI URL Kobe University Repository : Kernel Marked increase in bone formation markers after cinacalcet treatment by mechanisms
Title Author(s) Citation Issue date 2009-09 Resource Type Resource Version DOI URL Kobe University Repository : Kernel Marked increase in bone formation markers after cinacalcet treatment by mechanisms
Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital
 Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital E-mail: snigwekar@mgh.harvard.edu March 13, 2017 Disclosures statement: Consultant: Allena, Becker
Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital E-mail: snigwekar@mgh.harvard.edu March 13, 2017 Disclosures statement: Consultant: Allena, Becker
Secondary Hyperparathyroidism: Where are we now?
 Secondary Hyperparathyroidism: Where are we now? Dylan M. Barth, Pharm.D. PGY-1 Pharmacy Resident Mayo Clinic 2017 MFMER slide-1 Objectives Identify risk factors for the development of complications caused
Secondary Hyperparathyroidism: Where are we now? Dylan M. Barth, Pharm.D. PGY-1 Pharmacy Resident Mayo Clinic 2017 MFMER slide-1 Objectives Identify risk factors for the development of complications caused
hypercalcemia of malignancy hyperparathyroidism PHPT the most common cause of hypercalcemia in the outpatient setting the second most common cause
 hyperparathyroidism A 68-year-old woman with documented osteoporosis has blood tests showing elevated serum calcium and parathyroid hormone (PTH) levels: 11.2 mg/dl (8.8 10.1 mg/dl) and 88 pg/ml (10-60),
hyperparathyroidism A 68-year-old woman with documented osteoporosis has blood tests showing elevated serum calcium and parathyroid hormone (PTH) levels: 11.2 mg/dl (8.8 10.1 mg/dl) and 88 pg/ml (10-60),
Persistent post transplant hyperparathyroidism. Shiva Seyrafian IUMS-97/10/18-8/1/2019
 Persistent post transplant hyperparathyroidism Shiva Seyrafian IUMS-97/10/18-8/1/2019 normal weight =18-160 mg In HPT= 500-1000 mg 2 Epidemiology Mild 2 nd hyperparathyroidism (HPT) resolve after renal
Persistent post transplant hyperparathyroidism Shiva Seyrafian IUMS-97/10/18-8/1/2019 normal weight =18-160 mg In HPT= 500-1000 mg 2 Epidemiology Mild 2 nd hyperparathyroidism (HPT) resolve after renal
Therapeutic golas in the treatment of CKD-MBD
 Therapeutic golas in the treatment of CKD-MBD Hemodialysis clinic Clinical University Center Sarajevo Bantao, 04-08.10.2017, Sarajevo Abbvie Satellite symposium 06.10.2017 Chronic Kidney Disease Mineral
Therapeutic golas in the treatment of CKD-MBD Hemodialysis clinic Clinical University Center Sarajevo Bantao, 04-08.10.2017, Sarajevo Abbvie Satellite symposium 06.10.2017 Chronic Kidney Disease Mineral
A calcimimetic agent acutely suppresses parathyroid hormone levels in patients with chronic renal failure Rapid Communication
 Kidney International, Vol. 53 (1998), pp. 223 227 A calcimimetic agent acutely suppresses parathyroid hormone levels in patients with chronic renal failure Rapid Communication JOHN E. ANTONSEN, DONALD
Kidney International, Vol. 53 (1998), pp. 223 227 A calcimimetic agent acutely suppresses parathyroid hormone levels in patients with chronic renal failure Rapid Communication JOHN E. ANTONSEN, DONALD
CKD: Bone Mineral Metabolism. Peter Birks, Nephrology Fellow
 CKD: Bone Mineral Metabolism Peter Birks, Nephrology Fellow CKD - KDIGO Definition and Classification of CKD CKD: abnormalities of kidney structure/function for > 3 months with health implications 1 marker
CKD: Bone Mineral Metabolism Peter Birks, Nephrology Fellow CKD - KDIGO Definition and Classification of CKD CKD: abnormalities of kidney structure/function for > 3 months with health implications 1 marker
Awaisheh. Mousa Al-Abbadi. Abdullah Alaraj. 1 Page
 f #3 Awaisheh Abdullah Alaraj Mousa Al-Abbadi 1 Page *This sheet was written from Section 1 s lecture, in the first 10 mins the Dr. repeated all the previous material relating to osteoporosis from the
f #3 Awaisheh Abdullah Alaraj Mousa Al-Abbadi 1 Page *This sheet was written from Section 1 s lecture, in the first 10 mins the Dr. repeated all the previous material relating to osteoporosis from the
Complications observed in end-stage renal disease may be due to
 Complications of Dialysis: Selected Topics Robert W. Hamilton Complications observed in end-stage renal disease may be due to the side effects of treatment or to the alterations of pathophysiology that
Complications of Dialysis: Selected Topics Robert W. Hamilton Complications observed in end-stage renal disease may be due to the side effects of treatment or to the alterations of pathophysiology that
Hyperparathyroidism: Operative Considerations. Financial Disclosures: None. Hyperparathyroidism. Hyperparathyroidism 11/10/2012
 Hyperparathyroidism: Operative Considerations Financial Disclosures: None Steven J Wang, MD FACS Associate Professor Dept of Otolaryngology-Head and Neck Surgery University of California, San Francisco
Hyperparathyroidism: Operative Considerations Financial Disclosures: None Steven J Wang, MD FACS Associate Professor Dept of Otolaryngology-Head and Neck Surgery University of California, San Francisco
Case 4 Generalised bone pain
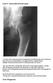 Case 4 Generalised bone pain C A 34- year- old woman presented complaining of multifocal pain in her chest and legs. The pain was intermittent, was aggravated by weight bearing. Initially was alleviated
Case 4 Generalised bone pain C A 34- year- old woman presented complaining of multifocal pain in her chest and legs. The pain was intermittent, was aggravated by weight bearing. Initially was alleviated
Incorporating K/DOQI Using a Novel Algorithm Approach: Regina Qu Appelle s Experience
 Incorporating K/DOQI Using a Novel Algorithm Approach: Regina Qu Appelle s Experience Michael Chan, Renal Dietitian Regina Qu Appelle Health Region BC Nephrology Days There is a strong association among
Incorporating K/DOQI Using a Novel Algorithm Approach: Regina Qu Appelle s Experience Michael Chan, Renal Dietitian Regina Qu Appelle Health Region BC Nephrology Days There is a strong association among
chapter 1 & 2009 KDIGO
 http://www.kidney-international.org chapter 1 & 2009 DIGO Chapter 1: Introduction and definition of CD MBD and the development of the guideline statements idney International (2009) 76 (Suppl 113), S3
http://www.kidney-international.org chapter 1 & 2009 DIGO Chapter 1: Introduction and definition of CD MBD and the development of the guideline statements idney International (2009) 76 (Suppl 113), S3
Metabolic Bone Disease (Past, Present and Future Challenges in the Management)
 Metabolic Bone Disease 871 151 Metabolic Bone Disease (Past, Present and Future Challenges in the Management) SNA RIZVI INTRODUCTION The past 40 years have seen some important historical events leading
Metabolic Bone Disease 871 151 Metabolic Bone Disease (Past, Present and Future Challenges in the Management) SNA RIZVI INTRODUCTION The past 40 years have seen some important historical events leading
Renal Osteodystrophy. Chapter 6. I. Introduction. Classification of Bone Disease. Eric W. Young
 Chapter 6 Renal Osteodystrophy Eric W. Young I. Introduction Renal osteodystrophy refers to bone disease that occurs in patients with kidney disease. Bone disease occurs across the full spectrum of kidney
Chapter 6 Renal Osteodystrophy Eric W. Young I. Introduction Renal osteodystrophy refers to bone disease that occurs in patients with kidney disease. Bone disease occurs across the full spectrum of kidney
CKD-MBD CKD mineral bone disorder
 CKD Renal bone disease Dr Mike Stone University Hospital Llandough Affects 5 10 % of population Increasingly common Ageing, diabetes, undetected hypertension Associated with: Cardiovascular disease Premature
CKD Renal bone disease Dr Mike Stone University Hospital Llandough Affects 5 10 % of population Increasingly common Ageing, diabetes, undetected hypertension Associated with: Cardiovascular disease Premature
CKD-Mineral Bone Disorder (MBD) Pathogenesis of Metabolic Bone Disease. Grants: NIH, Abbott, Amgen, OPKO, Shire
 Pathogenesis of Metabolic Bone Disease Stuart M. Sprague, D.O. Chief, Division of Nephrology and Hypertension Professor of Medicine NorthShore University HealthSystem University of Chicago Pritzker School
Pathogenesis of Metabolic Bone Disease Stuart M. Sprague, D.O. Chief, Division of Nephrology and Hypertension Professor of Medicine NorthShore University HealthSystem University of Chicago Pritzker School
HYDROCHLORIDE FOR THE TREATMENT OF SECONDARY HYPERPARATHYROIDISM IN PATIENTS WITH END-STAGE RENAL DISEASE ON MAINTENANCE DIALYSIS THERAPY
 UK RENAL PHARMACY GROUP SUBMISSION TO THE NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE on CINACALCET HYDROCHLORIDE FOR THE TREATMENT OF SECONDARY HYPERPARATHYROIDISM IN PATIENTS WITH END-STAGE RENAL DISEASE
UK RENAL PHARMACY GROUP SUBMISSION TO THE NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE on CINACALCET HYDROCHLORIDE FOR THE TREATMENT OF SECONDARY HYPERPARATHYROIDISM IN PATIENTS WITH END-STAGE RENAL DISEASE
Glycaemic control and serum intact parathyroid hormone levels in diabetic patients on haemodialysis therapy
 Nephrol Dial Transplant (2008) 23: 315 320 doi: 10.1093/ndt/gfm639 Advance Access publication 23 October 2007 Original Article Glycaemic control and serum intact parathyroid hormone levels in diabetic
Nephrol Dial Transplant (2008) 23: 315 320 doi: 10.1093/ndt/gfm639 Advance Access publication 23 October 2007 Original Article Glycaemic control and serum intact parathyroid hormone levels in diabetic
Effect of percutaneous calcitriol injection therapy on secondary hyperparathyroidism in uraemic patients
 Nephrol Dial Transplant (2003) 18 [Suppl 3]: iii42 iii46 DOI: 10.1093/ndt/gfg1011 Effect of percutaneous calcitriol injection therapy on secondary hyperparathyroidism in uraemic patients Kazuhiro Shiizaki
Nephrol Dial Transplant (2003) 18 [Suppl 3]: iii42 iii46 DOI: 10.1093/ndt/gfg1011 Effect of percutaneous calcitriol injection therapy on secondary hyperparathyroidism in uraemic patients Kazuhiro Shiizaki
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Prevalence and Pattern of Mineral Bone Disorder in Chronic Kidney Disease Patients Using Serum
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Prevalence and Pattern of Mineral Bone Disorder in Chronic Kidney Disease Patients Using Serum
II. RELATION TO BONE DISEASE INTRODUCTION. M.M. POPOVTZER, W.E. HUFFER, W.P. GElS, W.S. HAMMOND, T.E. STARZL
 II. RELATION TO BONE DISEASE M.M. POPOVTZER, W.E. HUFFER, W.P. GElS, W.S. HAMMOND, T.E. STARZL INTRODUCTION It has been generally assumed that azotemic osteodystrophy resolves after kidney transplantation
II. RELATION TO BONE DISEASE M.M. POPOVTZER, W.E. HUFFER, W.P. GElS, W.S. HAMMOND, T.E. STARZL INTRODUCTION It has been generally assumed that azotemic osteodystrophy resolves after kidney transplantation
PRIMARY HYPERPARATHYROIDISM
 PRIMARY HYPERPARATHYROIDISM HYPERPARATHYROIDISM Inappropriate excess secretion of Parathyroid Hormone in Primary Hyperparathyroidism Appropriate Hypersecretion in Secondary Hyperparathyroidism PTH and
PRIMARY HYPERPARATHYROIDISM HYPERPARATHYROIDISM Inappropriate excess secretion of Parathyroid Hormone in Primary Hyperparathyroidism Appropriate Hypersecretion in Secondary Hyperparathyroidism PTH and
Ramzi Vareldzis, MD Avanelle Jack, MD Dept of Internal Medicine Section of Nephrology and Hypertension LSU Health New Orleans September 13, 2016
 Ramzi Vareldzis, MD Avanelle Jack, MD Dept of Internal Medicine Section of Nephrology and Hypertension LSU Health New Orleans September 13, 2016 1 MBD + CKD in Elderly patients Our focus for today: CKD
Ramzi Vareldzis, MD Avanelle Jack, MD Dept of Internal Medicine Section of Nephrology and Hypertension LSU Health New Orleans September 13, 2016 1 MBD + CKD in Elderly patients Our focus for today: CKD
Hypocalcemia 6/8/12. Normal value. Physiologic functions. Nephron a functional unit of kidney. Influencing factors in Calcium and Phosphate Balance
 Normal value Hypocalcemia Serum calcium Total mg/dl Ionized mg/dl Cord blood 9.0 ~ 11.5 5.0 ~ 6.o New born (1 st 24 hrs) 9.0 ~ 10.6 4.3 ~ 5.1 24~ 48 hrs 7.0 ~12.0 4.0 ~4.7 Child 8.8 ~10.8 4.8 ~4.92 There
Normal value Hypocalcemia Serum calcium Total mg/dl Ionized mg/dl Cord blood 9.0 ~ 11.5 5.0 ~ 6.o New born (1 st 24 hrs) 9.0 ~ 10.6 4.3 ~ 5.1 24~ 48 hrs 7.0 ~12.0 4.0 ~4.7 Child 8.8 ~10.8 4.8 ~4.92 There
Jemds.com. Original Article STUDY OF RENAL OSTEODYSTROPHY IN CHRONIC RENAL FAILURE
 STUDY OF RENAL OSTEODYSTROPHY IN CHRONIC RENAL FAILURE Nalina Thimmappa 1, Giriraja Kanakapura Vrushabaih 2, Pula Laxmi Bindumathi 3, Pooja Pillai 4, Bhaskar Balasundaram 5 1Associate Professor, Department
STUDY OF RENAL OSTEODYSTROPHY IN CHRONIC RENAL FAILURE Nalina Thimmappa 1, Giriraja Kanakapura Vrushabaih 2, Pula Laxmi Bindumathi 3, Pooja Pillai 4, Bhaskar Balasundaram 5 1Associate Professor, Department
The role of calcimimetics in chronic kidney disease
 http://www.kidney-international.org & 2006 International Society of Nephrology The role of calcimimetics in chronic kidney disease A Gal-Moscovici 1,2 and SM Sprague 1 1 Division of Nephrology and Hypertension,
http://www.kidney-international.org & 2006 International Society of Nephrology The role of calcimimetics in chronic kidney disease A Gal-Moscovici 1,2 and SM Sprague 1 1 Division of Nephrology and Hypertension,
Metabolic Bone Disease Related to Chronic Kidney Disease
 Metabolic Bone Disease Related to Chronic Kidney Disease Deborah Sellmeyer, MD Director, Johns Hopkins Metabolic Bone Center Dept of Medicine, Division of Endocrinology Disclosure DSMB member for denosumab
Metabolic Bone Disease Related to Chronic Kidney Disease Deborah Sellmeyer, MD Director, Johns Hopkins Metabolic Bone Center Dept of Medicine, Division of Endocrinology Disclosure DSMB member for denosumab
Chapter 5: Evaluation and treatment of kidney transplant bone disease Kidney International (2009) 76 (Suppl 113), S100 S110; doi: /ki.2009.
 http://www.kidney-international.org & 2009 KDIGO Chapter 5: Evaluation and treatment of kidney transplant bone disease ; doi:10.1038/ki.2009.193 Grade for strength of recommendation a Strength Wording
http://www.kidney-international.org & 2009 KDIGO Chapter 5: Evaluation and treatment of kidney transplant bone disease ; doi:10.1038/ki.2009.193 Grade for strength of recommendation a Strength Wording
Effects of Diabetes Mellitus, Age, and Duration of Dialysis on Parathormone in Chronic Hemodialysis Patients. Hamid Nasri 1, Soleiman Kheiri 2
 Saudi J Kidney Dis Transplant 2008;19(4):608-613 2008 Saudi Center for Organ Transplantation Saudi Journal of Kidney Diseases and Transplantation Original Article Effects of Diabetes Mellitus, Age, and
Saudi J Kidney Dis Transplant 2008;19(4):608-613 2008 Saudi Center for Organ Transplantation Saudi Journal of Kidney Diseases and Transplantation Original Article Effects of Diabetes Mellitus, Age, and
The Effect of High-Flux Hemodialysis on Dialysis-Associated Amyloidosis
 Renal Failure, 1:31-34, 2005 Copyright 2005 Taylor & Francis Inc. ISSN: 0886-022X print / 1525-6049 online DOI: 10.1081/JDI-200042868 Taylor & Francis Taylor 6. Francis Croup CLINICAL STUDY The Effect
Renal Failure, 1:31-34, 2005 Copyright 2005 Taylor & Francis Inc. ISSN: 0886-022X print / 1525-6049 online DOI: 10.1081/JDI-200042868 Taylor & Francis Taylor 6. Francis Croup CLINICAL STUDY The Effect
PRIMARY HYPERPARATHYROIDISM PRIMARY HYPERPARATHYROIDISM. Hyperparathyroidism Etiology. Common Complex Insidious Chronic Global Only cure is surgery
 ENDOCRINE DISORDER PRIMARY HYPERPARATHYROIDISM Roseann P. Velez, DNP, FNP Francis J. Velez, MD, FACS Common Complex Insidious Chronic Global Only cure is surgery HYPERPARATHYROIDISM PARATHRYOID GLANDS
ENDOCRINE DISORDER PRIMARY HYPERPARATHYROIDISM Roseann P. Velez, DNP, FNP Francis J. Velez, MD, FACS Common Complex Insidious Chronic Global Only cure is surgery HYPERPARATHYROIDISM PARATHRYOID GLANDS
New vitamin D analogs
 Kidney International, Vol. 63, Supplement 85 (2003), pp. S83 S87 New vitamin D analogs EDUARDO SLATOPOLSKY, JANE FINCH, and ALEX BROWN Renal Division, Department of Internal Medicine, Washington University
Kidney International, Vol. 63, Supplement 85 (2003), pp. S83 S87 New vitamin D analogs EDUARDO SLATOPOLSKY, JANE FINCH, and ALEX BROWN Renal Division, Department of Internal Medicine, Washington University
Normal kidneys filter large amounts of organic
 ORIGINAL ARTICLE - NEPHROLOGY Effect Of Lanthanum Carbonate vs Calcium Acetate As A Phosphate Binder In Stage 3-4 CKD- Treat To Goal Study K.S. Sajeev Kumar (1), M K Mohandas (1), Ramdas Pisharody (1),
ORIGINAL ARTICLE - NEPHROLOGY Effect Of Lanthanum Carbonate vs Calcium Acetate As A Phosphate Binder In Stage 3-4 CKD- Treat To Goal Study K.S. Sajeev Kumar (1), M K Mohandas (1), Ramdas Pisharody (1),
Different effects of calcitriol and parathytoidectomy on the PTH-calcium curve in dialysis patients with severe hyperparathyroidism
 Nephrol Dial Transplant (996) : 8-87 Original Article Nephrology Dialysis Transplantation Different effects of calcitriol and parathytoidectomy on the PTH-calcium curve in dialysis patients with severe
Nephrol Dial Transplant (996) : 8-87 Original Article Nephrology Dialysis Transplantation Different effects of calcitriol and parathytoidectomy on the PTH-calcium curve in dialysis patients with severe
Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary
 Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 1 Agent Indication Dosing and Administration Natpara (parathyroid hormone) subcutaneous
Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 1 Agent Indication Dosing and Administration Natpara (parathyroid hormone) subcutaneous
Hyperphosphatemia is associated with a
 TREATMENT OPTIONS IN THE MANAGEMENT OF PHOSPHATE RETENTION * George A. Porter, MD, FACP, and Hartmut H. Malluche, MD, FACP ABSTRACT Hyperphosphatemia is an independent risk factor for mortality and cardiovascular
TREATMENT OPTIONS IN THE MANAGEMENT OF PHOSPHATE RETENTION * George A. Porter, MD, FACP, and Hartmut H. Malluche, MD, FACP ABSTRACT Hyperphosphatemia is an independent risk factor for mortality and cardiovascular
Bone and Mineral. Comprehensive Menu for the Management of Bone and Mineral Related Diseases
 Bone and Mineral Comprehensive Menu for the Management of Bone and Mineral Related Diseases Innovation to Assist in Clinical Diagnosis and Treatment DiaSorin offers a specialty line of Bone and Mineral
Bone and Mineral Comprehensive Menu for the Management of Bone and Mineral Related Diseases Innovation to Assist in Clinical Diagnosis and Treatment DiaSorin offers a specialty line of Bone and Mineral
Case Report Use of Percutaneous Ethanol Injection Therapy for Recurrent Secondary Hyperparathyroidism after Subtotal Parathyroidectomy
 SAGE-Hindawi Access to Research International Nephrology Volume 211, Article ID 246734, 6 pages doi:1.461/211/246734 Case Report Use of Percutaneous Ethanol Injection Therapy for Recurrent Secondary Hyperparathyroidism
SAGE-Hindawi Access to Research International Nephrology Volume 211, Article ID 246734, 6 pages doi:1.461/211/246734 Case Report Use of Percutaneous Ethanol Injection Therapy for Recurrent Secondary Hyperparathyroidism
Ultrasound examination in diagnosis of morphological variants of parathyroid hyperplasia in patients with secondary hyperparathyroidism
 Ultrasound examination in diagnosis of morphological variants of parathyroid hyperplasia in patients with secondary hyperparathyroidism Poster No.: C-0304 Congress: ECR 2015 Type: Authors: Keywords: DOI:
Ultrasound examination in diagnosis of morphological variants of parathyroid hyperplasia in patients with secondary hyperparathyroidism Poster No.: C-0304 Congress: ECR 2015 Type: Authors: Keywords: DOI:
Frequency of Metabolic Bone Disease in Haemodialysis Patients
 Frequency of Metabolic Bone Disease in Haemodialysis Patients Pages with reference to book, From 83 To 86 Rizwan Hussain, Arshad Ahmed, Abdul Salam Soomro, Saeed Hassan Chishty, Syed Ali Jaffar Naqvi (
Frequency of Metabolic Bone Disease in Haemodialysis Patients Pages with reference to book, From 83 To 86 Rizwan Hussain, Arshad Ahmed, Abdul Salam Soomro, Saeed Hassan Chishty, Syed Ali Jaffar Naqvi (
Comparison of Serum Parathyroid Hormone (PTH) Levels in Hemodialysis and Peritoneal Dialysis Patients. Int.J.Curr.Res.Aca.Rev.2016; 4(11):
 Comparison of Serum Parathyroid Hormone (PTH) Levels in Hemodialysis and Peritoneal Dialysis Patients Seyed Seifollah Beladi Mousavi 1, Arman Shahriari 2 and Fatemeh Roumi 3 * 1 Department of Nephrology,
Comparison of Serum Parathyroid Hormone (PTH) Levels in Hemodialysis and Peritoneal Dialysis Patients Seyed Seifollah Beladi Mousavi 1, Arman Shahriari 2 and Fatemeh Roumi 3 * 1 Department of Nephrology,
Calcium x phosphate product
 Date written: August 2005 Final submission: October 2005 Author: Carmel Hawley Calcium x phosphate product GUIDELINES No recommendations possible based on Level I or II evidence SUGGESTIONS FOR CLINICAL
Date written: August 2005 Final submission: October 2005 Author: Carmel Hawley Calcium x phosphate product GUIDELINES No recommendations possible based on Level I or II evidence SUGGESTIONS FOR CLINICAL
Sensipar (cinacalcet)
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
UPDATE ON RENAL OSTEODYSTROPHY: PATHOGENESIS AND CLINICAL MANAGEMENT
 UPDATE ON RENAL OSTEODYSTROPHY: PATHOGENESIS AND CLINICAL MANAGEMENT KhashayarSakhaee,M.D. University of Texas Southwestern Medical Center at Dallas Internal Medicine Grand Rounds May 22, 1997 Name: Rank:
UPDATE ON RENAL OSTEODYSTROPHY: PATHOGENESIS AND CLINICAL MANAGEMENT KhashayarSakhaee,M.D. University of Texas Southwestern Medical Center at Dallas Internal Medicine Grand Rounds May 22, 1997 Name: Rank:
Indian Journal of Nephrology Indian J Nephrol 2001;11:
 160 ARTICLE Microglobulin in chronic renal failure and effect of different dialyzer membrane on its clearance T Jeloka, MD Mathur*, R Kaur*, R Kohli, NP Singh, SNA Rizvi Department of Medicine and Microbiology*
160 ARTICLE Microglobulin in chronic renal failure and effect of different dialyzer membrane on its clearance T Jeloka, MD Mathur*, R Kaur*, R Kohli, NP Singh, SNA Rizvi Department of Medicine and Microbiology*
Case study Group 2 presentation
 Case study Group 2 presentation Patient profile HN 3095-57 Female 60 years old Hometown : Sa Kaeo province Occupation : farmer No drug and food allergy Chief complain Left neck mass 10 years PTA that gradually
Case study Group 2 presentation Patient profile HN 3095-57 Female 60 years old Hometown : Sa Kaeo province Occupation : farmer No drug and food allergy Chief complain Left neck mass 10 years PTA that gradually
Secondary hyperparathyroidism an Update on Pathophysiology and Treatment
 Secondary hyperparathyroidism an Update on Pathophysiology and Treatment Klaus Olgaard Copenhagen Budapest Nephrology School August 2007 HPT IN CRF Renal mass Ca 2+ 1,25(OH) 2 D 3 CaR Hyperparathyroidism
Secondary hyperparathyroidism an Update on Pathophysiology and Treatment Klaus Olgaard Copenhagen Budapest Nephrology School August 2007 HPT IN CRF Renal mass Ca 2+ 1,25(OH) 2 D 3 CaR Hyperparathyroidism
Malnutrition and Role of Nutrition in BMD:CKD
 Malnutrition and Role of Nutrition in BMD:CKD PNDS Continuing Nutrition Education Seminar Saturday, 30 th November 2013 Fayza Khan MSC (Foods and Nutrition) R.D President,PNDS Outline Objective Malnutrition
Malnutrition and Role of Nutrition in BMD:CKD PNDS Continuing Nutrition Education Seminar Saturday, 30 th November 2013 Fayza Khan MSC (Foods and Nutrition) R.D President,PNDS Outline Objective Malnutrition
Title:Relationship between parathyroid mass and parathyroid hormone level in hemodialysis patients with secondary hyperparathyroidism
 Author's response to reviews Title:Relationship between parathyroid mass and parathyroid hormone level in hemodialysis patients with secondary hyperparathyroidism Authors: Li Fang (fangli@njmu.edu.cn)
Author's response to reviews Title:Relationship between parathyroid mass and parathyroid hormone level in hemodialysis patients with secondary hyperparathyroidism Authors: Li Fang (fangli@njmu.edu.cn)
Bone Disorders in CKD
 Osteoporosis in Dialysis Patients Challenges in Management David M. Klachko MD FACP Professor Emeritus of Medicine University of Missouri-Columbia Bone Disorders in CKD PTH-mediated high-turnover (osteitis
Osteoporosis in Dialysis Patients Challenges in Management David M. Klachko MD FACP Professor Emeritus of Medicine University of Missouri-Columbia Bone Disorders in CKD PTH-mediated high-turnover (osteitis
Calcium metabolism and the Parathyroid Glands. Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands
 Calcium metabolism and the Parathyroid Glands Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands Calcium is an essential element for contraction of voluntary/smooth
Calcium metabolism and the Parathyroid Glands Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands Calcium is an essential element for contraction of voluntary/smooth
Month/Year of Review: September 2012 Date of Last Review: September 2010
 Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Endocrine Regulation of Calcium and Phosphate Metabolism
 Endocrine Regulation of Calcium and Phosphate Metabolism Huiping Wang ( 王会平 ), PhD Department of Physiology Rm C516, Block C, Research Building, School of Medicine Tel: 88208252 Email: wanghuiping@zju.edu.cn
Endocrine Regulation of Calcium and Phosphate Metabolism Huiping Wang ( 王会平 ), PhD Department of Physiology Rm C516, Block C, Research Building, School of Medicine Tel: 88208252 Email: wanghuiping@zju.edu.cn
PREVALENCE AND PATTERNS OF HYPERPARATHYROIDISM AND MINERAL BONE DISEASE IN PATIENTS WITH CHRONIC KIDNEY DISEASE AT KENYATTA NATIONAL HOSPITAL
 PREVALENCE AND PATTERNS OF HYPERPARATHYROIDISM AND MINERAL BONE DISEASE IN PATIENTS WITH CHRONIC KIDNEY DISEASE AT KENYATTA NATIONAL HOSPITAL DR. ANNE MUGERA The Problem Chronic Kidney disease is a worldwide
PREVALENCE AND PATTERNS OF HYPERPARATHYROIDISM AND MINERAL BONE DISEASE IN PATIENTS WITH CHRONIC KIDNEY DISEASE AT KENYATTA NATIONAL HOSPITAL DR. ANNE MUGERA The Problem Chronic Kidney disease is a worldwide
Vascular calcification in stage 5 Chronic Kidney Disease patients on dialysis
 Vascular calcification in stage 5 Chronic Kidney Disease patients on dialysis Seoung Woo Lee Div. Of Nephrology and Hypertension, Dept. of Internal Medicine, Inha Unv. College of Medicine, Inchon, Korea
Vascular calcification in stage 5 Chronic Kidney Disease patients on dialysis Seoung Woo Lee Div. Of Nephrology and Hypertension, Dept. of Internal Medicine, Inha Unv. College of Medicine, Inchon, Korea
Functions of the Skeletal System. Chapter 6: Osseous Tissue and Bone Structure. Classification of Bones. Bone Shapes
 Chapter 6: Osseous Tissue and Bone Structure Functions of the Skeletal System 1. Support 2. Storage of minerals (calcium) 3. Storage of lipids (yellow marrow) 4. Blood cell production (red marrow) 5. Protection
Chapter 6: Osseous Tissue and Bone Structure Functions of the Skeletal System 1. Support 2. Storage of minerals (calcium) 3. Storage of lipids (yellow marrow) 4. Blood cell production (red marrow) 5. Protection
Basic and clinical aspects of parathyroid hyperplasia in chronic kidney disease
 http://www.kidney-international.org & 2006 International Society of Nephrology Basic and clinical aspects of parathyroid hyperplasia in chronic kidney disease M Fukagawa 1, S Nakanishi 1 and JJ Kazama
http://www.kidney-international.org & 2006 International Society of Nephrology Basic and clinical aspects of parathyroid hyperplasia in chronic kidney disease M Fukagawa 1, S Nakanishi 1 and JJ Kazama
OMICS Journals are welcoming Submissions
 OMICS Journals are welcoming Submissions OMICS International welcomes submissions that are original and technically so as to serve both the developing world and developed countries in the best possible
OMICS Journals are welcoming Submissions OMICS International welcomes submissions that are original and technically so as to serve both the developing world and developed countries in the best possible
Sensipar. Sensipar (cinacalcet) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.46 Subject: Sensipar Page: 1 of 5 Last Review Date: June 22, 2018 Sensipar Description Sensipar (cinacalcet)
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.46 Subject: Sensipar Page: 1 of 5 Last Review Date: June 22, 2018 Sensipar Description Sensipar (cinacalcet)
The Skeletal Response to Aging: There s No Bones About It!
 The Skeletal Response to Aging: There s No Bones About It! April 7, 2001 Joseph E. Zerwekh, Ph.D. Interrelationship of Intestinal, Skeletal, and Renal Systems to the Overall Maintenance of Normal Calcium
The Skeletal Response to Aging: There s No Bones About It! April 7, 2001 Joseph E. Zerwekh, Ph.D. Interrelationship of Intestinal, Skeletal, and Renal Systems to the Overall Maintenance of Normal Calcium
Yueming Sun Æ Huihua Cai Æ Jianfeng Bai Æ Hanlin Zhao Æ Yi Miao
 World J Surg (2009) 33:1674 1679 DOI 10.1007/s00268-009-0086-3 Endoscopic Total Parathyroidectomy and Partial Parathyroid Tissue Autotransplantation for Patients with Secondary Hyperparathyroidism: A New
World J Surg (2009) 33:1674 1679 DOI 10.1007/s00268-009-0086-3 Endoscopic Total Parathyroidectomy and Partial Parathyroid Tissue Autotransplantation for Patients with Secondary Hyperparathyroidism: A New
Non-protein nitrogenous substances (NPN)
 Non-protein nitrogenous substances (NPN) A simple, inexpensive screening test a routine urinalysis is often the first test conducted if kidney problems are suspected. A small, randomly collected urine
Non-protein nitrogenous substances (NPN) A simple, inexpensive screening test a routine urinalysis is often the first test conducted if kidney problems are suspected. A small, randomly collected urine
NATIONAL QUALITY FORUM Renal EM Submitted Measures
 NATIONAL QUALITY FORUM Renal EM Submitted Measures Measure ID/ Title Measure Description Measure Steward Topic Area #1662 Percentage of patients aged 18 years and older with a diagnosis of CKD ACE/ARB
NATIONAL QUALITY FORUM Renal EM Submitted Measures Measure ID/ Title Measure Description Measure Steward Topic Area #1662 Percentage of patients aged 18 years and older with a diagnosis of CKD ACE/ARB
The Calcium Conundrum: When, What and How to Give Calcium in Pediatric CKD/ESRD
 The Calcium Conundrum: When, What and How to Give Calcium in Pediatric CKD/ESRD Jess Tower MS RD LD 3/18/19 Children s Mercy Hospital jdtower@cmh.edu 816 460 1067 Disclosures Nothing to disclose 1 How
The Calcium Conundrum: When, What and How to Give Calcium in Pediatric CKD/ESRD Jess Tower MS RD LD 3/18/19 Children s Mercy Hospital jdtower@cmh.edu 816 460 1067 Disclosures Nothing to disclose 1 How
Radiologic features of a pyrophosphate-like arthropathy associated with long-term dialysis
 Skeletal Radiol (1987) 16:437-441 Skeletal Radiology Radiologic features of a pyrophosphate-like arthropathy associated with long-term dialysis Ethan M. Braunstein, M.D. 1, Kathleen Menerey, M.D. 2, William
Skeletal Radiol (1987) 16:437-441 Skeletal Radiology Radiologic features of a pyrophosphate-like arthropathy associated with long-term dialysis Ethan M. Braunstein, M.D. 1, Kathleen Menerey, M.D. 2, William
Vitamin D: Is it a superhero??
 Vitamin D: Is it a superhero?? Dr. Ashraf Abdel Basset Bakr Prof. of Pediatrics 1 2 History of vitamin D discovery Sources of vitamin D and its metabolism 13 Actions of vitamin D 4 Vitamin D deficiency
Vitamin D: Is it a superhero?? Dr. Ashraf Abdel Basset Bakr Prof. of Pediatrics 1 2 History of vitamin D discovery Sources of vitamin D and its metabolism 13 Actions of vitamin D 4 Vitamin D deficiency
HYPERPARATHYROIDIS M FAISAL GHANI SIDDIQUI MBBS; FCPS; PGDIP-BIOMEDICAL ETHICS; MCPS-HPE
 HYPERPARATHYROIDIS M FAISAL GHANI SIDDIQUI MBBS; FCPS; PGDIP-BIOMEDICAL ETHICS; MCPS-HPE PROFESSOR OF SURGERY J I N N A H S I N D H M E D I C A L U N I V E R S I T Y PREAMBLE Anatomy & physiology of the
HYPERPARATHYROIDIS M FAISAL GHANI SIDDIQUI MBBS; FCPS; PGDIP-BIOMEDICAL ETHICS; MCPS-HPE PROFESSOR OF SURGERY J I N N A H S I N D H M E D I C A L U N I V E R S I T Y PREAMBLE Anatomy & physiology of the
2.0 Synopsis. Paricalcitol Capsules M Clinical Study Report R&D/15/0380. (For National Authority Use Only)
 2.0 Synopsis AbbVie Inc. Name of Study Drug: ABT-358/Zemplar (paricalcitol) Capsules Name of Active Ingredient: paricalcitol Individual Study Table Referring to Part of Dossier: Volume: Page: (For National
2.0 Synopsis AbbVie Inc. Name of Study Drug: ABT-358/Zemplar (paricalcitol) Capsules Name of Active Ingredient: paricalcitol Individual Study Table Referring to Part of Dossier: Volume: Page: (For National
Factors Affecting Calcium Metabolism in Disorders of the Kidney*
 ANNALS OF CLINICAL AND LABORATORY SCIENCE, Vol. 11, No. 4 Copyright 1981, Institute for Clinical Science, Inc. Factors Affecting Calcium Metabolism in Disorders of the Kidney* MURRAY J. FAVUS, M.D. Departm
ANNALS OF CLINICAL AND LABORATORY SCIENCE, Vol. 11, No. 4 Copyright 1981, Institute for Clinical Science, Inc. Factors Affecting Calcium Metabolism in Disorders of the Kidney* MURRAY J. FAVUS, M.D. Departm
Pseudohypoparathyroidism Showing Positive Phosphaturic and Negative Cyclic AMP Excretion Response to Parathyroid Hormone
 Pseudohypoparathyroidism Showing Positive Phosphaturic and Negative Cyclic AMP Excretion Response to Parathyroid Hormone KIICHIRO HIGASHI, KENICHI HONDA*, MITSUO MORITA*, TERUHISA UMEDA*, TATSUYA SHIMADA,
Pseudohypoparathyroidism Showing Positive Phosphaturic and Negative Cyclic AMP Excretion Response to Parathyroid Hormone KIICHIRO HIGASHI, KENICHI HONDA*, MITSUO MORITA*, TERUHISA UMEDA*, TATSUYA SHIMADA,
Case Report A Reference Finding Rarely Seen in Primary Hyperparathyroidism: Brown Tumor
 Case Reports in Medicine Volume 2012, Article ID 432676, 4 pages doi:10.1155/2012/432676 Case Report A Reference Finding Rarely Seen in Primary Hyperparathyroidism: Brown Tumor F. Mantar, 1 S. Gunduz,
Case Reports in Medicine Volume 2012, Article ID 432676, 4 pages doi:10.1155/2012/432676 Case Report A Reference Finding Rarely Seen in Primary Hyperparathyroidism: Brown Tumor F. Mantar, 1 S. Gunduz,
Parathyroid Imaging. A Guide to Parathyroid Surgery
 Parathyroid Imaging A Guide to Parathyroid Surgery Primary Hyperparathyroidism (PHPT) 3 rd most common endocrine disorder after diabetes and hyperthyroidism Prevalence in women 2% Often discovered in asymptomatic
Parathyroid Imaging A Guide to Parathyroid Surgery Primary Hyperparathyroidism (PHPT) 3 rd most common endocrine disorder after diabetes and hyperthyroidism Prevalence in women 2% Often discovered in asymptomatic
Southern Derbyshire Shared Care Pathology Guidelines. Primary Hyperparathyroidism
 Southern Derbyshire Shared Care Pathology Guidelines Primary Hyperparathyroidism Please use this Guideline in Conjunction with the Hypercalcaemia Guideline Definition Driven by hyperfunction of one or
Southern Derbyshire Shared Care Pathology Guidelines Primary Hyperparathyroidism Please use this Guideline in Conjunction with the Hypercalcaemia Guideline Definition Driven by hyperfunction of one or
Renal bone disease 1990: An unmet challenge for the nephrologist
 Kidney International, Vol. 38 (1990), pp. 193 2 11 Renal bone disease 1990: An unmet challenge for the nephrologist EDITORIAL REVIEW The replacement of excretory kidney function by dialysis or by renal
Kidney International, Vol. 38 (1990), pp. 193 2 11 Renal bone disease 1990: An unmet challenge for the nephrologist EDITORIAL REVIEW The replacement of excretory kidney function by dialysis or by renal
Cinacalcet treatment in advanced CKD - is it justified?
 Cinacalcet treatment in advanced CKD - is it justified? Goce Spasovski ERBP Advisory Board member University of Skopje, R. Macedonia TSN Congress October 21, 2017, Antalya Session Objectives From ROD to
Cinacalcet treatment in advanced CKD - is it justified? Goce Spasovski ERBP Advisory Board member University of Skopje, R. Macedonia TSN Congress October 21, 2017, Antalya Session Objectives From ROD to
PART FOUR. Metabolism and Nutrition
 PART FOUR Metabolism and Nutrition Advances in Peritoneal Dialysis, Vol. 21, 2005 Maria Mesquita, 1 Eric Wittersheim, 2 Anne Demulder, 2 Max Dratwa, 1 Pierre Bergmann 3 Bone Cytokines and Renal Osteodystrophy
PART FOUR Metabolism and Nutrition Advances in Peritoneal Dialysis, Vol. 21, 2005 Maria Mesquita, 1 Eric Wittersheim, 2 Anne Demulder, 2 Max Dratwa, 1 Pierre Bergmann 3 Bone Cytokines and Renal Osteodystrophy
Radiographic Appearance Of Primary Hyperparathyroidism With Atypical Parathyroid Adenoma
 ISPUB.COM The Internet Journal of Internal Medicine Volume 6 Number 2 Radiographic Appearance Of Primary Hyperparathyroidism With Atypical Parathyroid Adenoma P George, N Philip, B Pawar Citation P George,
ISPUB.COM The Internet Journal of Internal Medicine Volume 6 Number 2 Radiographic Appearance Of Primary Hyperparathyroidism With Atypical Parathyroid Adenoma P George, N Philip, B Pawar Citation P George,
Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary
 Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 2 Available Product Indication Dosing and Administration Natpara (parathyroid hormone)
Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 2 Available Product Indication Dosing and Administration Natpara (parathyroid hormone)
Secondary hyperparathyroidism in chronic kidney disease recent paradigm shift in clinical management
 Secondary hyperparathyroidism in chronic kidney disease recent paradigm shift in clinical management Complete this course and earn 1 CME POINT Dr. HO Chung Ping MBBS (HK), MRCP, FRCP (Glas, Edin), FHKCP,
Secondary hyperparathyroidism in chronic kidney disease recent paradigm shift in clinical management Complete this course and earn 1 CME POINT Dr. HO Chung Ping MBBS (HK), MRCP, FRCP (Glas, Edin), FHKCP,
Pathogenesis and Treatment of Renal Osteodystrophy
 Proceedings Blood Purif 2003;21:318 326 DOI: 10.1159/000072552 Eduardo Slatopolsky a Esther Gonzalez b Kevin Martin b a Renal Division, Washington University School of Medicine, St. Louis, Mo., and b Division
Proceedings Blood Purif 2003;21:318 326 DOI: 10.1159/000072552 Eduardo Slatopolsky a Esther Gonzalez b Kevin Martin b a Renal Division, Washington University School of Medicine, St. Louis, Mo., and b Division
Level 1 Strong We recommendyshould A High Moderate Level 2 Weak We suggestymight C Low Very low. K Hyperphosphatemia has been associated with poor
 chapter 4.1 http://www.kidney-international.org & 2009 KDIGO Chapter 4.1: Treatment of CKD MBD targeted at lowering high serum phosphorus and maintaining serum calcium ; doi:10.1038/ki.2009.192 Grade for
chapter 4.1 http://www.kidney-international.org & 2009 KDIGO Chapter 4.1: Treatment of CKD MBD targeted at lowering high serum phosphorus and maintaining serum calcium ; doi:10.1038/ki.2009.192 Grade for
development of erosive osteoarthritis?
 Annals of the Rheumatic Diseases, 1989; 48, 183-187 Scientific papers Is chronic renal failure a risk factor for the development of erosive osteoarthritis? I J S DUNCAN,' N P HURST,' A DISNEY,2 R SEBBEN,3
Annals of the Rheumatic Diseases, 1989; 48, 183-187 Scientific papers Is chronic renal failure a risk factor for the development of erosive osteoarthritis? I J S DUNCAN,' N P HURST,' A DISNEY,2 R SEBBEN,3
The Role of the Laboratory in Metabolic Bone Disease
 The Role of the Laboratory in Metabolic Bone Disease Howard Morris PhD, FAACB, FFSc(RCPA) President, IFCC Professor of Medical Sciences, University of South Australia, Clinical Scientist, SA Pathology
The Role of the Laboratory in Metabolic Bone Disease Howard Morris PhD, FAACB, FFSc(RCPA) President, IFCC Professor of Medical Sciences, University of South Australia, Clinical Scientist, SA Pathology
* It is proportionate to body size and the reference value is usually expressed after correction for body surface area as 120 ± 25 ml/min/1.
 Ahmad Al-zoubi Glomerular filtration rate : is the sum of the ultrafiltration rates from plasma into the Bowman s space in each nephron and is a measure of renal excretory function *co : 6L *renal blood
Ahmad Al-zoubi Glomerular filtration rate : is the sum of the ultrafiltration rates from plasma into the Bowman s space in each nephron and is a measure of renal excretory function *co : 6L *renal blood
Medical and surgical aspects of parathyroidectomy
 Kidney International, Vol. 56, Suppl. 73 (1999), pp. S-65 S-69 Medical and surgical aspects of parathyroidectomy MASAFUMI FUKAGAWA, YOSHIHIRO TOMINAGA, MASAFUMI KITAOKA, TAKATOSHI KAKUTA, and KIYOSHI KUROKAWA
Kidney International, Vol. 56, Suppl. 73 (1999), pp. S-65 S-69 Medical and surgical aspects of parathyroidectomy MASAFUMI FUKAGAWA, YOSHIHIRO TOMINAGA, MASAFUMI KITAOKA, TAKATOSHI KAKUTA, and KIYOSHI KUROKAWA
The impact of improved phosphorus control: use of sevelamer hydrochloride in patients with chronic renal failure
 Nephrol Dial Transplant (2002) 17: 340 345 The impact of improved phosphorus control: use of sevelamer hydrochloride in patients with chronic renal failure Naseem Amin Genzyme Corporation, Cambridge, MA,
Nephrol Dial Transplant (2002) 17: 340 345 The impact of improved phosphorus control: use of sevelamer hydrochloride in patients with chronic renal failure Naseem Amin Genzyme Corporation, Cambridge, MA,
02/27/2018. Objectives. To Replace or Not to Replace: Nutritional Vitamin D in Dialysis.
 To Replace or Not to Replace: Nutritional Vitamin D in Dialysis. Michael Shoemaker-Moyle, M.D. Assistant Professor of Clinical Medicine Objectives Review Vitamin D Physiology Review Current Replacement
To Replace or Not to Replace: Nutritional Vitamin D in Dialysis. Michael Shoemaker-Moyle, M.D. Assistant Professor of Clinical Medicine Objectives Review Vitamin D Physiology Review Current Replacement
Pathologic Fracture of the Femur in Brown Tumor Induced in Parathyroid Carcinoma: A Case Report
 CASE REPORT Hip Pelvis 28(3): 173-177, 2016 http://dx.doi.org/10.5371/hp.2016.28.3.173 Print ISSN 2287-3260 Online ISSN 2287-3279 Pathologic Fracture of the Femur in Brown Tumor Induced in Parathyroid
CASE REPORT Hip Pelvis 28(3): 173-177, 2016 http://dx.doi.org/10.5371/hp.2016.28.3.173 Print ISSN 2287-3260 Online ISSN 2287-3279 Pathologic Fracture of the Femur in Brown Tumor Induced in Parathyroid
Amol K Choulwar et al. / Journal of Pharmacy Research 2012,5(1), Available online through
 Research Article ISSN: 0974-6943 Amol K Choulwar et al. / Journal of Pharmacy Research 2012,5(1), Available online through www.jpronline.info Comparison of efficacy and safety of Cinacalcet versus Calcitriol
Research Article ISSN: 0974-6943 Amol K Choulwar et al. / Journal of Pharmacy Research 2012,5(1), Available online through www.jpronline.info Comparison of efficacy and safety of Cinacalcet versus Calcitriol
( ) , (Donabedian, 1980) We would not choose any treatment with poor outcomes
 ..., 2013 Amgen. 1 ? ( ), (Donabedian, 1980) We would not choose any treatment with poor outcomes 1. :, 2. ( ): 3. :.,,, 4. :, [Biomarkers Definitions Working Group, 2001]., (William M. Bennet, Nefrol
..., 2013 Amgen. 1 ? ( ), (Donabedian, 1980) We would not choose any treatment with poor outcomes 1. :, 2. ( ): 3. :.,,, 4. :, [Biomarkers Definitions Working Group, 2001]., (William M. Bennet, Nefrol
Racial differences in bone turnover rate and hyperparathyroidism in hemodialysis patients
 Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine 1994 Racial differences in bone turnover rate and hyperparathyroidism
Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine 1994 Racial differences in bone turnover rate and hyperparathyroidism
Figures and tables in this presentation were adopted from various printed and electronic resorces and serve strictly for educational purposes.
 Academic lectures 3rd year of Medical faculty Figures and tables in this presentation were adopted from various printed and electronic resorces and serve strictly for educational purposes. ENDOCRINOLOGY
Academic lectures 3rd year of Medical faculty Figures and tables in this presentation were adopted from various printed and electronic resorces and serve strictly for educational purposes. ENDOCRINOLOGY
Approach to a patient with hypercalcemia
 Approach to a patient with hypercalcemia Ana-Maria Chindris, MD Division of Endocrinology Mayo Clinic Florida 2013 MFMER slide-1 Background Hypercalcemia is a problem frequently encountered in clinical
Approach to a patient with hypercalcemia Ana-Maria Chindris, MD Division of Endocrinology Mayo Clinic Florida 2013 MFMER slide-1 Background Hypercalcemia is a problem frequently encountered in clinical
CKD FOR INTERNISTS. Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College
 CKD FOR INTERNISTS Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College INTRODUCTION In 2002, the National Kidney Foundation s Kidney Disease Outcomes Quality Initiative(KDOQI)
CKD FOR INTERNISTS Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College INTRODUCTION In 2002, the National Kidney Foundation s Kidney Disease Outcomes Quality Initiative(KDOQI)
Effect of lanthanum carbonate and calcium acetate in the treatment of hyperphosphatemia in patients of chronic kidney disease
 Research Article Effect of lanthanum and calcium acetate in the treatment of hyperphosphatemia in patients of chronic kidney disease P. Thomas Scaria, Reneega Gangadhar 1, Ramdas Pisharody 2 ABSTRACT Departments
Research Article Effect of lanthanum and calcium acetate in the treatment of hyperphosphatemia in patients of chronic kidney disease P. Thomas Scaria, Reneega Gangadhar 1, Ramdas Pisharody 2 ABSTRACT Departments
Reversal of adynamic bone disease by lowering of dialysate calcium
 http://www.kidney-international.org & 26 International Society of Nephrology original article Reversal of adynamic bone disease by lowering of dialysate calcium A Haris 1, DJ Sherrard 2 and G Hercz 3 1
http://www.kidney-international.org & 26 International Society of Nephrology original article Reversal of adynamic bone disease by lowering of dialysate calcium A Haris 1, DJ Sherrard 2 and G Hercz 3 1
Introduction/objective: Adinamic bone disease (ABD) is a common finding in peritoneal. dialysis (PD) and is associated with a
 Original Article Low-calcium peritoneal dialysis solution is effective in bringing PTH levels to the range recommended by current guidelines in patients with PTH levels < 150 pg/dl Authors Thyago Proença
Original Article Low-calcium peritoneal dialysis solution is effective in bringing PTH levels to the range recommended by current guidelines in patients with PTH levels < 150 pg/dl Authors Thyago Proença
17. CALCIUM AND PHOSPHOROUS METABOLISM. Calcium. Role of calcium ROLE OF CALCIUM STORAGE. Calcium movement
 17. CALCIUM AND PHOSPHOROUS METABOLISM Many physiological processes are regulated directly or indirectly by calcium. Furthermore, the main physical structure of vertebrates and other species depend on
17. CALCIUM AND PHOSPHOROUS METABOLISM Many physiological processes are regulated directly or indirectly by calcium. Furthermore, the main physical structure of vertebrates and other species depend on
