Renal Osteodystrophy. Chapter 6. I. Introduction. Classification of Bone Disease. Eric W. Young
|
|
|
- Barry Jerome Terry
- 6 years ago
- Views:
Transcription
1 Chapter 6 Renal Osteodystrophy Eric W. Young I. Introduction Renal osteodystrophy refers to bone disease that occurs in patients with kidney disease. Bone disease occurs across the full spectrum of kidney disease, ranging from early renal insufficiency to established chronic kidney disease and end-stage renal disease (ESRD). The severity of bone disease tends to be associated with the severity and duration of kidney disease. As a practical matter, the most clinically important bone disease occurs among patients with ESRD. Renal osteodystrophy presents with a characteristic spectrum of clinical, biochemical, and histologic abnormalities. Patients and physicians have access to a growing array of preventive and active treatments. II. Classification of Bone Disease Renal bone disease is usually classified according to the histologic appearance. Although definitive diagnosis in an individual patient requires a bone biopsy, much information about bone disease can be inferred from clinical and laboratory findings. Accordingly, most practitioners do not perform bone biopsies on a routine basis. Even in the absence of routine bone biopsies, knowledge of the histologic classification provides a useful framework for diagnosis and treatment. Osteitis fibrosa cystica is a high-turnover bone disease that is most prominently associated with hyperparathyroidism. Adynamic bone disease is a low bone turnover that is predominantly associated with low parathyroid hormone (PTH) activity. Osteomalacia is a low-turnover condition that is strongly associated with aluminum toxicity. Mixed uremic bone disease is characterized by the simultaneous appearance of multiple histologic patterns. In addition,
2 132 Eric W. Young patients with kidney disease may develop several other syndromes that may affect bone such as β 2 microglobulin disease (renal amyloidosis). Each histologic pattern is associated with characteristic clinical and biochemical features. A presumptive diagnosis is often possible, even without a bone biopsy. Different treatment approaches are indicated for each histologic pattern. It is likely that metabolic acidosis contributes to all forms of renal bone disease because of loss of bone calcium in the physiologic process of buffering the extracellular concentration of hydrogen. 1 III. Clinical Manifestations Overt bone symptoms are absent in most patients with kidney disease. However, clinical findings can be discerned in a significant number of patients. The prevalence and severity of clinical manifestations increase with duration of ESRD. Some patients experience bone pain, which may be vague and elusive. Renal osteodystrophy contributes to growth retardation in children with kidney disease, although other important factors are involved, including protein malnutrition. Patients with kidney disease have a demonstrated increased incidence of fractures, presumably related to altered bone architecture and strength. 2,3 A variety of clinical manifestations occur that are largely related to abnormal mineral metabolism rather than bone disease per se. Soft tissue manifestation may include spontaneous tendon rupture and soft tissue precipitation of calcium phosphate deposits. Calcium phosphate precipitation in skin triggers pruritus that may be severe and incapacitating in some patients. Conjunctival mineral deposition leads to local irritation, injection, and characteristic band keratopathy. Ocular findings provide a useful window to systemic mineral deposition. Although most studies of altered mineral metabolism in patients with kidney disease have focused on bone disease, there has been increasing recognition of an important relationship with mortality and cardiovascular disease. Patient mortality is strongly associated with the serum concentrations of calcium, phosphorus, and the calcium-phosphorus product. 4,5 Cardiovascular mortality is even more strongly associated with these mineral metabolism markers. 5 In addition, several studies have found that the prevalence of vascular calcification is associated with serum calcium and phosphorus levels. 6 These observations have contributed to the hypothesis that altered mineral metabolism in renal failure promotes vascular injury and premature atherosclerosis with all the attendant cardiovascular complications. Complications can affect all major vascular beds including the coronary, cerebral, and peripheral circulations. The hypothesis is supported by a growing body of clinical evidence. As such, addressing abnormal mineral metabolism associated with renal failure
3 6. Renal Osteodystrophy 133 is increasingly seen as prevention and treatment of cardiovascular as well as bone complications. IV. Osteitis Fibrosa Cystica Osteitis fibrosa cystica is the best understood bone disease associated with kidney failure. Once the most common form of bone disease, its prevalence has declined with the emergence of effective treatments. 7 Osteitis fibrosa cystica is strongly linked with hyperparathyroidism. Patients with renal disease develop hyperparathyroidism secondary to calcitriol deficiency, hypocalcemia, and hyperphosphatemia. Each of these factors stimulates production and secretion of PTH from the parathyroid glands. Calcitriol deficiency develops because of decreased activity of the 1αhydroxylase enzyme in the proximal tubule of the kidney. Renal 1α-hydroxylase is required to convert the vitamin D metabolite, 25-hydroxyvitamin D, into 1,25-dihydroxyvitamin D (calcitriol). Renal 1α-hydroxylase activity is reduced in part because of parenchymal cellular injury associated with the underlying process that produced kidney disease (e.g., diabetes, glomerulonephritis). In addition, hyperphosphatemia (see later) independently suppresses renal calcitriol production. The biologic actions of calcitriol include promotion of active intestinal calcium absorption and suppression of PTH secretion from the parathyroid glands. Calcitriol deficiency results in diminished calcium absorption and hypersecretion of PTH. In addition, kidney failure is associated with relative insensitivity to calcitriol at the level of the parathyroid calcitriol receptor. 8 The combination of decreased calcitriol production and calcitriol receptor insensitivity means that the normal suppressive action of calcitriol on PTH secretion is lost. Hypocalcemia occurs largely as a consequence of calcitriol deficiency. As noted previously, calcitriol normally stimulates active intestinal absorption of calcium. Low levels of serum calcium normally stimulate renal production of calcitriol in a classic physiologic feedback mechanism. However, calcitriol production is suppressed in patients with kidney disease. In addition, a small decrease in serum calcium concentration can be attributed to hyperphosphatemia. As the serum concentration of phosphate increases, precipitation and soft tissue deposition of calcium phosphate occurs, leading to a small decrement in the serum calcium concentration. The serum calcium concentration directly influences PTH secretion through the parathyroid gland calcium receptor. Calcium suppresses PTH secretion; PTH secretion increases as the serum calcium falls. Hyperphosphatemia is directly related to the loss of glomerular filtration, which is the hallmark of kidney disease. Phosphate is contained in many normal
4 134 Eric W. Young food items such as protein sources and dairy products. Dietary phosphate is absorbed in the intestine through both passive and active processes. Absorbed phosphate is normally eliminated by the kidney under the control of PTH in a process that ordinarily maintains a normal serum phosphate concentration. However, the blood phosphate concentration increases as glomerular filtration rate (GFR) declines in patients with kidney disease. Hyperphosphatemia contributes to hyperparathyroidism in two ways. First, phosphate directly suppresses calcitriol production. Second, hyperphosphatemia directly stimulates PTH secretion. 9,10 In fact, animal studies have shown that hyperparathyroidism of kidney disease can be prevented through dietary restriction of phosphorus and avoidance of hyperhosphatemia. 10 Over the short run, hyperparathyroidism is an appropriate adaptive mechanism to the mineral abnormalities that occur with kidney failure. 11 High PTH promotes renal excretion of phosphorus and production of calcitriol, which in turn increases intestinal calcium absorption. To a point, the secondary hyperparathyroidism of renal failure will resist the factors responsible for PTH secretion. However, the underlying abnormalities persist in patients with chronic kidney disease and the underlying problems (decreased calcitriol production, hypocalcimia, hyperphosphatemia) cannot be reversed. Hyperparathyroidism persists with its attendant long-term complications. High PTH has also been implicated as a major uremic toxin that contributes to a number of clinical manifestations of kidney disease such as anemia, neuromuscular symptoms, sexual dysfunction, and bone disease. Osteitis fibrosa cystica is the bone disease associated with hyperparathyroidism, regardless of the etiology of the excess PTH. Similar bone abnormalities are seen in patients with primary hyperparathyroidism due to a parathyroid adenoma (or hyperplasia) but no underlying kidney disease. Long-term exposure of bone to high levels of PTH results in increased bone turnover. Histologic examination reveals increased numbers of osteoblasts and osteoclasts. The rate of new bone formation is determined by administration of tetracycline at two distinct times before bone biopsy. Special stains are then used to visualize the incorporation of tetracycline into the bone front, giving an indication of bone formation. In osteitis fibrosa cystica, two distinct and well separated tetracycline lines are seen indicative of an increased rate of bone formation under PTH stimulation. Wide osteoid seams are seen indicating that bone is turning over faster than it can be mineralized. Foci of marrow fibrosis are characteristically seen. The resultant bone architecture is distinctly abnormal and intrinsically weaker and less durable than normal bone. As a result, patients with osteitis fibrosa cystica may develop bone pain and fractures. In general, osteitis fibrosa cystica is associated with high levels of intact PTH (often greater than 450 pg/ml). Newer generation PTH assays have been developed but are not yet sufficiently well characterized to alter the existing
5 6. Renal Osteodystrophy 135 clinical guidelines. 12 The blood concentration of alkaline phosphatase (both nonspecific and bone-specific) is elevated, reflecting the increased rate of bone cell activity, remodeling, metabolism, and turnover. Hypocalcemia and hyperphosphatemia are also characteristic, as described previously. However, prior values over an extended period of time are more important than isolated readings, which can be modified by diet and treatment much faster than the bone disease. Also, patients occasionally develop hypercalcemia as a result of very longstanding hyperparathyroidism and parathyroid gland hyperplasia (a condition sometimes referred to as tertiary hyperparathyroidism ). These biochemical features are characteristic of osteitis fibrosa cystica but not diagnositic. Definitive diagnosis requires a bone biopsy. However, specialized equipment and personnel are required for proper processing and interpretation of bone tissue. Many clinicians feel they are able to satisfactorily manage most patients without a bone biopsy. Prevention and treatment of osteitis fibrosa cystica are focused on the hyperparathyroidism. A low-phosphate diet should be prescribed. Phosphate binders should be used regularly to control hyperphosphatemia. Frequent and close follow-up is required. Direct suppression of PTH can be achieved with vitamin D analogues and calcimimetic compounds that emulate the action of calcium on the parathyroid calcium receptor. Available vitamin D compounds include calcitriol, paricalcitol, and doxercalciferol in both oral and intravenous forms. Large variations in vitamin D therapy exist among dialysis facilities and countries. 5 Differential patient survival has been found based on the type and route of vitamin D therapy, 13,14 although this finding has not been tested in clinical trials. Cinacalcet is an oral calcimimetic compound that effectively suppresses PTH. Cinacalcet can be used alone or in combination with a vitamin D compound. 15 Applied early, these approaches should prevent osteitis fibrosa cystica. In advanced cases, parathyroidectomy may be indicated to reduce PTH levels. For patients with active bone disease, these treatments can lower PTH and promote more physiologic bone remodeling with correction of abnormal bone architecture and, presumably, reduction in fracture risk. V. Adynamic Bone Disease Adynamic bone disease has emerged in recent years as the most common histologic form of renal osteodystrophy. 7 The growth in adynamic bone disease no doubt relates to improvements in treatment that have decreased the incidence of osteitis fibrosa cystica and osteomalacia. Adynamic bone disease is poorly understood at present. However, one common theme is relative suppression of PTH which, in turn, leads to decreased bone turnover. Low PTH levels are
6 136 Eric W. Young often attributable to the suppressive effects of vitamin D therapy, calciumcontaining phosphate binders, and perhaps relatively high concentrations of dialysate calcium. Approximately 50% of hemodialysis patients have an intact PTH concentration below the current K/DOQI lower bound guideline of 150 pg/ml. 5 Low bone turnover, like the high bone turnover seen in osteitis fibrosa cystica, leads to disruption of the normal bone architecture. The result is weakened bone that is potentially susceptible to fracture. An elevated risk of hip fractures was found in patients with low PTH concentrations and a presumed disposition to adymamic bone disease. 3 Adynamic bone disease is characterized by low bone turnover and mineralization rate, as determined by tetracycline labeling. Osteoclast and osteoblast activity is low. Specialized stains reveal thin osteoid seams and low osteoid mass. As noted, the major biochemical feature of adynamic bone disease is a low PTH concentration. Current guidelines call for an intact PTH concentration of 150 to 300 pg/ml 16 although there is controversy about the preferred range and assay type. Future guidelines may move toward higher PTH concentrations and new assay methods. 17 At present, treatment consists of attempting to desuppress PTH through withdrawal of vitamin D therapy, conversion to calcium-free phosphate binders, and use of lower dialysate calcium concentrations. Even with these measures, PTH remains inexplicably low in some patients. 5 VI. Osteomalacia Osteomalcia in patients with kidney disease is almost always attributable to aluminum intoxication. The usual cause of osteomalacia in patients without kidney failure is vitamin D deficiency. However, vitamin D deficiency in patients with renal disease is much more likely to be associated with osteitis fibrosa cystica as described earlier. These different patterns of bone disease associated with vitamin D deficiency probably reflect the complicated multifactorial and interactive nature of metabolic bone disease. Aluminum intoxication arises from contaminated dialysate fluid and oral aluminum-containing antacids administered for the purpose of binding dietary phosphate. Both sources introduced small amounts of aluminum into patients, either directly through the blood route (dialysate contamination) or indirectly through intestinal absorption (aluminum antacids). However, significant toxicity developed in many patients after years of low-level exposure in patients who lack normal renal routes of aluminum excretion. Removal of aluminum through dialysis is relatively inefficient.
7 6. Renal Osteodystrophy 137 Dialysate contamination occurs when dialysate fluid is prepared from water sources that have not been adequately purified. Many municipal water sources contain relatively high concentrations of aluminum. Water preparation procedures have been tightened since the recognition of the serious adverse impact of aluminum and other impurities. Aluminum antacids were used as phosphate binders for many years under the assumption of negligible and clinically insignificant intestinal absorption of aluminum. However, as noted, low-level exposure over many years in the absence of a route of excretion led to aluminum accumulation and toxicity. Aluminum gels have largely been replaced by alternative compounds. Initially, calcium salts were used. Several non-calcium compounds have recently been introduced as phosphate binding agents including sevelamer hydrochloride and lanthanum carbonate. These compounds do not increase the calcium load and may offer clinical advantages Widespread aluminum deposition has been reported in dialysis patients exposed to aluminum through dialysate and aluminum-containing antacids. Aluminum toxicity is a multisystem syndrome. Deposition in the central nervous system produced rapid and debilitating dementia ( dialysis dementia ). Bone marrow deposition resulted in microcytic anemia that failed to respond to iron or erythropoietin therapy. Aluminum deposition in emerging bone fronts during normal bone remodeling process led to the osteomalacia form of renal osteodystrophy. Thankfully, all the aluminum toxicity syndromes are now uncommon as a result of concerted efforts to minimize aluminum exposure. Osteomalcia due to aluminum is characterized by low bone turnover and mineralization. Tetracycline labeling generally reveals a single, poorly stained bone front instead of two distinct bands seen with normal bone remodeling. Osteoblast and osteoclast activity is low, presumably owing to direct cellular toxicity of aluminum. Wide unmineralized osteoid seams are found. Special stains reveal the presence of aluminum. Aluminum also deposits in parathyroid tissue and suppresses PTH production, resulting in characteristically low intact PTH blood levels. Blood alkaline phosphatase activity is generally not elevated, given the relative lack of bone turnover and metabolic activity. Patients generally exhibit characteristic hyperphosphatemia and hypocalcemia. However, hypercalcemia may emerge in later phases. Aluminum toxicity should be suspected in patients with a consistent clinical presentation and a plausible history of exposure over an extended period of time. An elevated blood aluminum level is supportive. A large increment in serum aluminum concentration after desferoximine (DFO) challenge strongly points to aluminum toxicity. Bone biopsy provides a definitive diagnosis but may not be necessary in all cases.
8 138 Eric W. Young Treatment consists of a prolonged course of aluminum chelation with DFO. DFO treatment improves the bone disease and anemia but is less effective for dementia. The best treatment is prevention through use of purified water for the dialysate and avoidance of aluminum-containing phosphate binders. VII. Mixed Bone Disease Mixed bone disease describes the combination of osteitis fibrosa cystica and defective bone mineralization. This insufficiently understood entity illustrates the complexity and poor understanding of renal osteodystrophy. References 1. Mehrotra R, Kopple JD, Wolfson M. Metabolic acidosis in maintenance dialysis patients: clinical considerations. Kidney Int Suppl 2003;S Kaji H, Suzuki M, Yano S, Sugimoto T, Chihara K, Hattori S, Sekita K. Risk factors for hip fracture in hemodialysis patients. Am J Nephrol 2002;22: Coco M, Rush H. Increased incidence of hip fractures in dialysis patients with low serum parathyroid hormone. Am J Kidney Dis 2000;36: Block GA, Hulbert-Shearon TE, Levin NW, Port FK. Association of serum phosphorus and calcium phosphate product with mortality risk in chronic hemodialysis patients: a national study. Am J Kidney Dis 1998;31: Young EW, Albert JM, Satayathum S, Goodkin DA, Pisoni RL, Akiba T, Akizawa T, Kurokawa K, Bommer J, Piera L, Port FK. Predictors and consequences of altered mineral metabolism: the Dialysis Outcomes and Practice Patterns Study. Kidney Int Under review, Goodman WG, London G, Amann K, Block GA, Giachelli C, Hruska KA, Ketteler M, Levin A, Massy Z, McCarron DA, Raggi P, Shanahan CM, Yorioka N. Vascular calcification in chronic kidney disease. Am J Kidney Dis 2004;43: Martin KJ, Olgaard K, Coburn JW, Coen GM, Fukagawa M, Langman C, Malluche HH, McCarthy JT, Massry SG, Mehls O, Salusky IB, Silver JM, Smogorzewski MT, Slatopolsky EM, McCann L. Diagnosis, assessment, and treatment of bone turnover abnormalities in renal osteodystrophy. Am J Kidney Dis 2004;43: Fukuda N, Tanaka H, Tominaga Y, Fukagawa M, Kurokawa K, Seino Y. Decreased 1,25- dihydroxyvitamin D3 receptor density is associated with a more severe form of parathyroid hyperplasia in chronic uremic patients. J Clin Invest 1993;92: Slatopolsky E, Finch J, Denda M, Ritter C, Zhong M, Dusso A, MacDonald PN, Brown AJ. Phosphorus restriction prevents parathyroid gland growth. High phosphorus directly stimulates PTH secretion in vitro. J Clin Invest 1996;97: Naveh-Many T, Rahamimov R, Livni N, Silver J. Parathyroid cell proliferation in normal and chronic renal failure rats. The effects of calcium, phosphate, and vitamin D. J Clin Invest 1995;96: Llach F. Secondary hyperparathyroidism in renal failure: the trade-off hypothesis revisited. Am J Kidney Dis 1995;25:
9 6. Renal Osteodystrophy Goodman WG. New assays for parathyroid hormone (PTH) and the relevance of PTH fragments in renal failure. Kidney Int Suppl 2003;S Teng M, Wolf M, Lowrie E, Ofsthun N, Lazarus JM, Thadhani R. Survival of patients undergoing hemodialysis with paricalcitol or calcitriol therapy. N Engl J Med 2003;349: Teng M, Wolf M, Ofsthun MN, Lazarus JM, Hernan MA, Camargo CA, Jr., Thadhani R. Activated injectable vitamin D and hemodialysis survival: a historical cohort study. J Am Soc Nephrol 2005;16: Block GA, Martin KJ, de Francisco AL, Turner SA, Avram MM, Suranyi MG, Hercz G, Cunningham J, Abu-Alfa AK, Messa P, Coyne DW, Locatelli F, Cohen RM, Evenepoel P, Moe SM, Fournier A, Braun J, McCary LC, Zani VJ, Olson KA, Drueke TB, Goodman WG. Cinacalcet for secondary hyperparathyroidism in patients receiving hemodialysis. N Engl J Med 2004;350: K/DOQI clinical practice guidelines for bone metabolism and disease in chronic kidney disease. Am J Kidney Dis 2003;42:S Martin KJ, Akhtar I, Gonzalez EA. Parathyroid hormone: new assays, new receptors. Semin Nephrol 2004;24: Chertow GM, Burke SK, Dillon MA, Slatopolsky E. Long-term effects of sevelamer hydrochloride on the calcium x phosphate product and lipid profile of haemodialysis patients. Nephrol Dial Transplant 1999;14: Chertow GM, Burke SK, Raggi P. Sevelamer attenuates the progression of coronary and aortic calcification in hemodialysis patients. Kidney Int 2002;62: D Haese PC, Spasovski GB, Sikole A, Hutchison A, Freemont TJ, Sulkova S, Swanepoel C, Pejanovic S, Djukanovic L, Balducci A, Coen G, Sulowicz W, Ferreira A, Torres A, Curic S, Popovic M, Dimkovic N, De Broe ME. A multicenter study on the effects of lanthanum carbonate (Fosrenol) and calcium carbonate on renal bone disease in dialysis patients. Kidney Int (Suppl) 2003;S Al-Baaj F, Speake M, Hutchison AJ. Control of serum phosphate by oral lanthanum carbonate in patients undergoing haemodialysis and continuous ambulatory peritoneal dialysis in a short-term, placebo-controlled study. Nephrol Dial Transplant 2005;20:
CKD: Bone Mineral Metabolism. Peter Birks, Nephrology Fellow
 CKD: Bone Mineral Metabolism Peter Birks, Nephrology Fellow CKD - KDIGO Definition and Classification of CKD CKD: abnormalities of kidney structure/function for > 3 months with health implications 1 marker
CKD: Bone Mineral Metabolism Peter Birks, Nephrology Fellow CKD - KDIGO Definition and Classification of CKD CKD: abnormalities of kidney structure/function for > 3 months with health implications 1 marker
Secondary Hyperparathyroidism: Where are we now?
 Secondary Hyperparathyroidism: Where are we now? Dylan M. Barth, Pharm.D. PGY-1 Pharmacy Resident Mayo Clinic 2017 MFMER slide-1 Objectives Identify risk factors for the development of complications caused
Secondary Hyperparathyroidism: Where are we now? Dylan M. Barth, Pharm.D. PGY-1 Pharmacy Resident Mayo Clinic 2017 MFMER slide-1 Objectives Identify risk factors for the development of complications caused
Therapeutic golas in the treatment of CKD-MBD
 Therapeutic golas in the treatment of CKD-MBD Hemodialysis clinic Clinical University Center Sarajevo Bantao, 04-08.10.2017, Sarajevo Abbvie Satellite symposium 06.10.2017 Chronic Kidney Disease Mineral
Therapeutic golas in the treatment of CKD-MBD Hemodialysis clinic Clinical University Center Sarajevo Bantao, 04-08.10.2017, Sarajevo Abbvie Satellite symposium 06.10.2017 Chronic Kidney Disease Mineral
Kobe University Repository : Kernel
 Title Author(s) Citation Issue date 2009-09 Resource Type Resource Version DOI URL Kobe University Repository : Kernel Marked increase in bone formation markers after cinacalcet treatment by mechanisms
Title Author(s) Citation Issue date 2009-09 Resource Type Resource Version DOI URL Kobe University Repository : Kernel Marked increase in bone formation markers after cinacalcet treatment by mechanisms
Metabolic Bone Disease (Past, Present and Future Challenges in the Management)
 Metabolic Bone Disease 871 151 Metabolic Bone Disease (Past, Present and Future Challenges in the Management) SNA RIZVI INTRODUCTION The past 40 years have seen some important historical events leading
Metabolic Bone Disease 871 151 Metabolic Bone Disease (Past, Present and Future Challenges in the Management) SNA RIZVI INTRODUCTION The past 40 years have seen some important historical events leading
HYDROCHLORIDE FOR THE TREATMENT OF SECONDARY HYPERPARATHYROIDISM IN PATIENTS WITH END-STAGE RENAL DISEASE ON MAINTENANCE DIALYSIS THERAPY
 UK RENAL PHARMACY GROUP SUBMISSION TO THE NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE on CINACALCET HYDROCHLORIDE FOR THE TREATMENT OF SECONDARY HYPERPARATHYROIDISM IN PATIENTS WITH END-STAGE RENAL DISEASE
UK RENAL PHARMACY GROUP SUBMISSION TO THE NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE on CINACALCET HYDROCHLORIDE FOR THE TREATMENT OF SECONDARY HYPERPARATHYROIDISM IN PATIENTS WITH END-STAGE RENAL DISEASE
CKD-MBD CKD mineral bone disorder
 CKD Renal bone disease Dr Mike Stone University Hospital Llandough Affects 5 10 % of population Increasingly common Ageing, diabetes, undetected hypertension Associated with: Cardiovascular disease Premature
CKD Renal bone disease Dr Mike Stone University Hospital Llandough Affects 5 10 % of population Increasingly common Ageing, diabetes, undetected hypertension Associated with: Cardiovascular disease Premature
Ramzi Vareldzis, MD Avanelle Jack, MD Dept of Internal Medicine Section of Nephrology and Hypertension LSU Health New Orleans September 13, 2016
 Ramzi Vareldzis, MD Avanelle Jack, MD Dept of Internal Medicine Section of Nephrology and Hypertension LSU Health New Orleans September 13, 2016 1 MBD + CKD in Elderly patients Our focus for today: CKD
Ramzi Vareldzis, MD Avanelle Jack, MD Dept of Internal Medicine Section of Nephrology and Hypertension LSU Health New Orleans September 13, 2016 1 MBD + CKD in Elderly patients Our focus for today: CKD
Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital
 Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital E-mail: snigwekar@mgh.harvard.edu March 13, 2017 Disclosures statement: Consultant: Allena, Becker
Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital E-mail: snigwekar@mgh.harvard.edu March 13, 2017 Disclosures statement: Consultant: Allena, Becker
The impact of improved phosphorus control: use of sevelamer hydrochloride in patients with chronic renal failure
 Nephrol Dial Transplant (2002) 17: 340 345 The impact of improved phosphorus control: use of sevelamer hydrochloride in patients with chronic renal failure Naseem Amin Genzyme Corporation, Cambridge, MA,
Nephrol Dial Transplant (2002) 17: 340 345 The impact of improved phosphorus control: use of sevelamer hydrochloride in patients with chronic renal failure Naseem Amin Genzyme Corporation, Cambridge, MA,
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Prevalence and Pattern of Mineral Bone Disorder in Chronic Kidney Disease Patients Using Serum
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Prevalence and Pattern of Mineral Bone Disorder in Chronic Kidney Disease Patients Using Serum
( ) , (Donabedian, 1980) We would not choose any treatment with poor outcomes
 ..., 2013 Amgen. 1 ? ( ), (Donabedian, 1980) We would not choose any treatment with poor outcomes 1. :, 2. ( ): 3. :.,,, 4. :, [Biomarkers Definitions Working Group, 2001]., (William M. Bennet, Nefrol
..., 2013 Amgen. 1 ? ( ), (Donabedian, 1980) We would not choose any treatment with poor outcomes 1. :, 2. ( ): 3. :.,,, 4. :, [Biomarkers Definitions Working Group, 2001]., (William M. Bennet, Nefrol
Incorporating K/DOQI Using a Novel Algorithm Approach: Regina Qu Appelle s Experience
 Incorporating K/DOQI Using a Novel Algorithm Approach: Regina Qu Appelle s Experience Michael Chan, Renal Dietitian Regina Qu Appelle Health Region BC Nephrology Days There is a strong association among
Incorporating K/DOQI Using a Novel Algorithm Approach: Regina Qu Appelle s Experience Michael Chan, Renal Dietitian Regina Qu Appelle Health Region BC Nephrology Days There is a strong association among
THE FIELD OF mineral metabolism and
 SPECIAL REPORT Controversies in Bone and Mineral Metabolism in Chronic Kidney Disease A Bridge to Improving Healthcare Outcomes and Quality of Life Sharon M. Moe, MD, FACP, and Tilman B. Drüeke, MD, FRCP
SPECIAL REPORT Controversies in Bone and Mineral Metabolism in Chronic Kidney Disease A Bridge to Improving Healthcare Outcomes and Quality of Life Sharon M. Moe, MD, FACP, and Tilman B. Drüeke, MD, FRCP
CKD-Mineral Bone Disorder (MBD) Pathogenesis of Metabolic Bone Disease. Grants: NIH, Abbott, Amgen, OPKO, Shire
 Pathogenesis of Metabolic Bone Disease Stuart M. Sprague, D.O. Chief, Division of Nephrology and Hypertension Professor of Medicine NorthShore University HealthSystem University of Chicago Pritzker School
Pathogenesis of Metabolic Bone Disease Stuart M. Sprague, D.O. Chief, Division of Nephrology and Hypertension Professor of Medicine NorthShore University HealthSystem University of Chicago Pritzker School
Persistent post transplant hyperparathyroidism. Shiva Seyrafian IUMS-97/10/18-8/1/2019
 Persistent post transplant hyperparathyroidism Shiva Seyrafian IUMS-97/10/18-8/1/2019 normal weight =18-160 mg In HPT= 500-1000 mg 2 Epidemiology Mild 2 nd hyperparathyroidism (HPT) resolve after renal
Persistent post transplant hyperparathyroidism Shiva Seyrafian IUMS-97/10/18-8/1/2019 normal weight =18-160 mg In HPT= 500-1000 mg 2 Epidemiology Mild 2 nd hyperparathyroidism (HPT) resolve after renal
A calcimimetic agent acutely suppresses parathyroid hormone levels in patients with chronic renal failure Rapid Communication
 Kidney International, Vol. 53 (1998), pp. 223 227 A calcimimetic agent acutely suppresses parathyroid hormone levels in patients with chronic renal failure Rapid Communication JOHN E. ANTONSEN, DONALD
Kidney International, Vol. 53 (1998), pp. 223 227 A calcimimetic agent acutely suppresses parathyroid hormone levels in patients with chronic renal failure Rapid Communication JOHN E. ANTONSEN, DONALD
Cinacalcet treatment in advanced CKD - is it justified?
 Cinacalcet treatment in advanced CKD - is it justified? Goce Spasovski ERBP Advisory Board member University of Skopje, R. Macedonia TSN Congress October 21, 2017, Antalya Session Objectives From ROD to
Cinacalcet treatment in advanced CKD - is it justified? Goce Spasovski ERBP Advisory Board member University of Skopje, R. Macedonia TSN Congress October 21, 2017, Antalya Session Objectives From ROD to
Calcium x phosphate product
 Date written: August 2005 Final submission: October 2005 Author: Carmel Hawley Calcium x phosphate product GUIDELINES No recommendations possible based on Level I or II evidence SUGGESTIONS FOR CLINICAL
Date written: August 2005 Final submission: October 2005 Author: Carmel Hawley Calcium x phosphate product GUIDELINES No recommendations possible based on Level I or II evidence SUGGESTIONS FOR CLINICAL
Treatment Options for Chronic Kidney
 Treatment Options for Chronic Kidney Disease: Metabolic Introduction Bone Disease to Renagel Goce Spasovski, R. Macedonia The 17th Budapest Nephrology School, August 29, 2010 Session Objectives Definition
Treatment Options for Chronic Kidney Disease: Metabolic Introduction Bone Disease to Renagel Goce Spasovski, R. Macedonia The 17th Budapest Nephrology School, August 29, 2010 Session Objectives Definition
Vascular calcification in stage 5 Chronic Kidney Disease patients on dialysis
 Vascular calcification in stage 5 Chronic Kidney Disease patients on dialysis Seoung Woo Lee Div. Of Nephrology and Hypertension, Dept. of Internal Medicine, Inha Unv. College of Medicine, Inchon, Korea
Vascular calcification in stage 5 Chronic Kidney Disease patients on dialysis Seoung Woo Lee Div. Of Nephrology and Hypertension, Dept. of Internal Medicine, Inha Unv. College of Medicine, Inchon, Korea
The role of calcimimetics in chronic kidney disease
 http://www.kidney-international.org & 2006 International Society of Nephrology The role of calcimimetics in chronic kidney disease A Gal-Moscovici 1,2 and SM Sprague 1 1 Division of Nephrology and Hypertension,
http://www.kidney-international.org & 2006 International Society of Nephrology The role of calcimimetics in chronic kidney disease A Gal-Moscovici 1,2 and SM Sprague 1 1 Division of Nephrology and Hypertension,
Renal Association Clinical Practice Guideline in Mineral and Bone Disorders in CKD
 Nephron Clin Pract 2011;118(suppl 1):c145 c152 DOI: 10.1159/000328066 Received: May 24, 2010 Accepted: December 6, 2010 Published online: May 6, 2011 Renal Association Clinical Practice Guideline in Mineral
Nephron Clin Pract 2011;118(suppl 1):c145 c152 DOI: 10.1159/000328066 Received: May 24, 2010 Accepted: December 6, 2010 Published online: May 6, 2011 Renal Association Clinical Practice Guideline in Mineral
Effect of lanthanum carbonate and calcium acetate in the treatment of hyperphosphatemia in patients of chronic kidney disease
 Research Article Effect of lanthanum and calcium acetate in the treatment of hyperphosphatemia in patients of chronic kidney disease P. Thomas Scaria, Reneega Gangadhar 1, Ramdas Pisharody 2 ABSTRACT Departments
Research Article Effect of lanthanum and calcium acetate in the treatment of hyperphosphatemia in patients of chronic kidney disease P. Thomas Scaria, Reneega Gangadhar 1, Ramdas Pisharody 2 ABSTRACT Departments
Hyperphosphatemia is associated with a
 TREATMENT OPTIONS IN THE MANAGEMENT OF PHOSPHATE RETENTION * George A. Porter, MD, FACP, and Hartmut H. Malluche, MD, FACP ABSTRACT Hyperphosphatemia is an independent risk factor for mortality and cardiovascular
TREATMENT OPTIONS IN THE MANAGEMENT OF PHOSPHATE RETENTION * George A. Porter, MD, FACP, and Hartmut H. Malluche, MD, FACP ABSTRACT Hyperphosphatemia is an independent risk factor for mortality and cardiovascular
Guidelines and new evidence on CKD - MBD treatment
 Guidelines and new evidence on CKD - MBD treatment Goce Spasovski ERBP Advisory Board member University of Skopje, R. Macedonia ERA-EDTA CME course IV Congress of Nephrology of B&H, April 25, 2015, Sarajevo,
Guidelines and new evidence on CKD - MBD treatment Goce Spasovski ERBP Advisory Board member University of Skopje, R. Macedonia ERA-EDTA CME course IV Congress of Nephrology of B&H, April 25, 2015, Sarajevo,
A new era in phosphate binder therapy: What are the options?
 http://www.kidney-international.org & 2006 International Society of Nephrology A new era in phosphate binder therapy: What are the options? IB Salusky 1 1 Department of Pediatrics, David Geffen School
http://www.kidney-international.org & 2006 International Society of Nephrology A new era in phosphate binder therapy: What are the options? IB Salusky 1 1 Department of Pediatrics, David Geffen School
Simultaneous Control of PTH and Ca P Is Sustained over Three Years of Treatment with Cinacalcet HCl
 Simultaneous Control of PTH and Ca P Is Sustained over Three Years of Treatment with Cinacalcet HCl Stuart M. Sprague,* Pieter Evenepoel, Mario P. Curzi, Maria Teresa González, Fred E. Husserl, Nelson
Simultaneous Control of PTH and Ca P Is Sustained over Three Years of Treatment with Cinacalcet HCl Stuart M. Sprague,* Pieter Evenepoel, Mario P. Curzi, Maria Teresa González, Fred E. Husserl, Nelson
Amol K Choulwar et al. / Journal of Pharmacy Research 2012,5(1), Available online through
 Research Article ISSN: 0974-6943 Amol K Choulwar et al. / Journal of Pharmacy Research 2012,5(1), Available online through www.jpronline.info Comparison of efficacy and safety of Cinacalcet versus Calcitriol
Research Article ISSN: 0974-6943 Amol K Choulwar et al. / Journal of Pharmacy Research 2012,5(1), Available online through www.jpronline.info Comparison of efficacy and safety of Cinacalcet versus Calcitriol
Reversal of adynamic bone disease by lowering of dialysate calcium
 http://www.kidney-international.org & 26 International Society of Nephrology original article Reversal of adynamic bone disease by lowering of dialysate calcium A Haris 1, DJ Sherrard 2 and G Hercz 3 1
http://www.kidney-international.org & 26 International Society of Nephrology original article Reversal of adynamic bone disease by lowering of dialysate calcium A Haris 1, DJ Sherrard 2 and G Hercz 3 1
Normal kidneys filter large amounts of organic
 ORIGINAL ARTICLE - NEPHROLOGY Effect Of Lanthanum Carbonate vs Calcium Acetate As A Phosphate Binder In Stage 3-4 CKD- Treat To Goal Study K.S. Sajeev Kumar (1), M K Mohandas (1), Ramdas Pisharody (1),
ORIGINAL ARTICLE - NEPHROLOGY Effect Of Lanthanum Carbonate vs Calcium Acetate As A Phosphate Binder In Stage 3-4 CKD- Treat To Goal Study K.S. Sajeev Kumar (1), M K Mohandas (1), Ramdas Pisharody (1),
Effect of percutaneous calcitriol injection therapy on secondary hyperparathyroidism in uraemic patients
 Nephrol Dial Transplant (2003) 18 [Suppl 3]: iii42 iii46 DOI: 10.1093/ndt/gfg1011 Effect of percutaneous calcitriol injection therapy on secondary hyperparathyroidism in uraemic patients Kazuhiro Shiizaki
Nephrol Dial Transplant (2003) 18 [Suppl 3]: iii42 iii46 DOI: 10.1093/ndt/gfg1011 Effect of percutaneous calcitriol injection therapy on secondary hyperparathyroidism in uraemic patients Kazuhiro Shiizaki
Hyperparathyroidism: Operative Considerations. Financial Disclosures: None. Hyperparathyroidism. Hyperparathyroidism 11/10/2012
 Hyperparathyroidism: Operative Considerations Financial Disclosures: None Steven J Wang, MD FACS Associate Professor Dept of Otolaryngology-Head and Neck Surgery University of California, San Francisco
Hyperparathyroidism: Operative Considerations Financial Disclosures: None Steven J Wang, MD FACS Associate Professor Dept of Otolaryngology-Head and Neck Surgery University of California, San Francisco
Complications of Chronic Kidney Disease: Anemia, Mineral Metabolism, and Cardiovascular Disease
 Med Clin N Am 89 (2005) 549 561 Complications of Chronic Kidney Disease: Anemia, Mineral Metabolism, and Cardiovascular Disease Shona Pendse, MD, Ajay K. Singh, MB, MRCP(UK)* Renal Division, Brigham and
Med Clin N Am 89 (2005) 549 561 Complications of Chronic Kidney Disease: Anemia, Mineral Metabolism, and Cardiovascular Disease Shona Pendse, MD, Ajay K. Singh, MB, MRCP(UK)* Renal Division, Brigham and
Introduction/objective: Adinamic bone disease (ABD) is a common finding in peritoneal. dialysis (PD) and is associated with a
 Original Article Low-calcium peritoneal dialysis solution is effective in bringing PTH levels to the range recommended by current guidelines in patients with PTH levels < 150 pg/dl Authors Thyago Proença
Original Article Low-calcium peritoneal dialysis solution is effective in bringing PTH levels to the range recommended by current guidelines in patients with PTH levels < 150 pg/dl Authors Thyago Proença
Contents. Authors Name: Christopher Wong: Consultant Nephrologist Anne Waddington: Renal Pharmacist Eimear Fegan : Renal Dietitian
 Cheshire and Merseyside Renal Units Guidelines on the Management of Chronic Kidney Disease - Mineral Bone Disorder (adapted from Greater Manchester) Authors Name: Christopher Wong: Consultant Nephrologist
Cheshire and Merseyside Renal Units Guidelines on the Management of Chronic Kidney Disease - Mineral Bone Disorder (adapted from Greater Manchester) Authors Name: Christopher Wong: Consultant Nephrologist
Sevelamer hydrochloride: a calcium- and metal-free phosphate binder
 DRUG PROFILE Sevelamer hydrochloride: a calcium- and metal-free phosphate binder Anthony J Bleyer & James Balwit Author for correspondence Wake Forest University School of Medicine, Section on Nephrology,
DRUG PROFILE Sevelamer hydrochloride: a calcium- and metal-free phosphate binder Anthony J Bleyer & James Balwit Author for correspondence Wake Forest University School of Medicine, Section on Nephrology,
Improved Assessment of Aortic Calcification in Japanese Patients Undergoing Maintenance Hemodialysis
 ORIGINAL ARTICLE Improved Assessment of Aortic Calcification in Japanese Patients Undergoing Maintenance Hemodialysis Masaki Ohya 1, Haruhisa Otani 2,KeigoKimura 3, Yasushi Saika 4, Ryoichi Fujii 4, Susumu
ORIGINAL ARTICLE Improved Assessment of Aortic Calcification in Japanese Patients Undergoing Maintenance Hemodialysis Masaki Ohya 1, Haruhisa Otani 2,KeigoKimura 3, Yasushi Saika 4, Ryoichi Fujii 4, Susumu
Malnutrition and Role of Nutrition in BMD:CKD
 Malnutrition and Role of Nutrition in BMD:CKD PNDS Continuing Nutrition Education Seminar Saturday, 30 th November 2013 Fayza Khan MSC (Foods and Nutrition) R.D President,PNDS Outline Objective Malnutrition
Malnutrition and Role of Nutrition in BMD:CKD PNDS Continuing Nutrition Education Seminar Saturday, 30 th November 2013 Fayza Khan MSC (Foods and Nutrition) R.D President,PNDS Outline Objective Malnutrition
The CARI Guidelines Caring for Australasians with Renal Impairment. Serum phosphate GUIDELINES
 Date written: August 2005 Final submission: October 2005 Author: Carmel Hawley Serum phosphate GUIDELINES No recommendations possible based on Level I or II evidence SUGGESTIONS FOR CLINICAL CARE (Suggestions
Date written: August 2005 Final submission: October 2005 Author: Carmel Hawley Serum phosphate GUIDELINES No recommendations possible based on Level I or II evidence SUGGESTIONS FOR CLINICAL CARE (Suggestions
2017 KDIGO Guidelines Update
 2017 KDIGO Guidelines Update Clinic for Hemodialysis Clinical Center University of Sarajevo 13 th Congress of the Balkan cities Association of Nephrology, Dialysis, and Artificial Organs Transplantation
2017 KDIGO Guidelines Update Clinic for Hemodialysis Clinical Center University of Sarajevo 13 th Congress of the Balkan cities Association of Nephrology, Dialysis, and Artificial Organs Transplantation
Original epidemiologic studies 1 have suggested that approximately
 Factors for Increased Morbidity and Mortality in Uremia: Hyperphosphatemia Nathan W. Levin, Frank A. Gotch, and Martin K. Kuhlmann Hyperphosphatemia is a metabolic abnormality present in the majority of
Factors for Increased Morbidity and Mortality in Uremia: Hyperphosphatemia Nathan W. Levin, Frank A. Gotch, and Martin K. Kuhlmann Hyperphosphatemia is a metabolic abnormality present in the majority of
Metabolic Bone Disease Related to Chronic Kidney Disease
 Metabolic Bone Disease Related to Chronic Kidney Disease Deborah Sellmeyer, MD Director, Johns Hopkins Metabolic Bone Center Dept of Medicine, Division of Endocrinology Disclosure DSMB member for denosumab
Metabolic Bone Disease Related to Chronic Kidney Disease Deborah Sellmeyer, MD Director, Johns Hopkins Metabolic Bone Center Dept of Medicine, Division of Endocrinology Disclosure DSMB member for denosumab
Management of CKD. Goce Spasovski, R. Macedonia
 Management of CKD complications Introduction Bone disease to Renagel Goce Spasovski, R. Macedonia Istanbul, June 4, 2011 Session Objectives - Mineral and Bone Disorders (MBD) Bone disease a part of CKD
Management of CKD complications Introduction Bone disease to Renagel Goce Spasovski, R. Macedonia Istanbul, June 4, 2011 Session Objectives - Mineral and Bone Disorders (MBD) Bone disease a part of CKD
Biochemical and pathologic abnormalities are a common
 CJASN epress. Published on March 4, 2009 as doi: 10.2215/CJN.03790808 Cinacalcet Lowers Serum Alkaline Phosphatase in Maintenance Hemodialysis Vasily Belozeroff,* William G. Goodman, Lulu Ren, and Kamyar
CJASN epress. Published on March 4, 2009 as doi: 10.2215/CJN.03790808 Cinacalcet Lowers Serum Alkaline Phosphatase in Maintenance Hemodialysis Vasily Belozeroff,* William G. Goodman, Lulu Ren, and Kamyar
chapter 1 & 2009 KDIGO
 http://www.kidney-international.org chapter 1 & 2009 DIGO Chapter 1: Introduction and definition of CD MBD and the development of the guideline statements idney International (2009) 76 (Suppl 113), S3
http://www.kidney-international.org chapter 1 & 2009 DIGO Chapter 1: Introduction and definition of CD MBD and the development of the guideline statements idney International (2009) 76 (Suppl 113), S3
Parathyroid Hormone, Calcium and Phosphorus Levels in Hemodialysis Patients at Al-Shifa Hospital, Gaza-Palestine
 IUG Journal of Natural and Engineering Studies Vol.22,No.1, pp 97-110 2014, ISSN 1726-6807, http://www.iugaza.edu.ps/ar/periodical/ Parathyroid Hormone, Calcium and Phosphorus Levels in Hemodialysis Patients
IUG Journal of Natural and Engineering Studies Vol.22,No.1, pp 97-110 2014, ISSN 1726-6807, http://www.iugaza.edu.ps/ar/periodical/ Parathyroid Hormone, Calcium and Phosphorus Levels in Hemodialysis Patients
Comparison of Serum Parathyroid Hormone (PTH) Levels in Hemodialysis and Peritoneal Dialysis Patients. Int.J.Curr.Res.Aca.Rev.2016; 4(11):
 Comparison of Serum Parathyroid Hormone (PTH) Levels in Hemodialysis and Peritoneal Dialysis Patients Seyed Seifollah Beladi Mousavi 1, Arman Shahriari 2 and Fatemeh Roumi 3 * 1 Department of Nephrology,
Comparison of Serum Parathyroid Hormone (PTH) Levels in Hemodialysis and Peritoneal Dialysis Patients Seyed Seifollah Beladi Mousavi 1, Arman Shahriari 2 and Fatemeh Roumi 3 * 1 Department of Nephrology,
The Calcium Conundrum: When, What and How to Give Calcium in Pediatric CKD/ESRD
 The Calcium Conundrum: When, What and How to Give Calcium in Pediatric CKD/ESRD Jess Tower MS RD LD 3/18/19 Children s Mercy Hospital jdtower@cmh.edu 816 460 1067 Disclosures Nothing to disclose 1 How
The Calcium Conundrum: When, What and How to Give Calcium in Pediatric CKD/ESRD Jess Tower MS RD LD 3/18/19 Children s Mercy Hospital jdtower@cmh.edu 816 460 1067 Disclosures Nothing to disclose 1 How
Sensipar. Sensipar (cinacalcet) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.46 Subject: Sensipar Page: 1 of 5 Last Review Date: June 22, 2018 Sensipar Description Sensipar (cinacalcet)
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.46 Subject: Sensipar Page: 1 of 5 Last Review Date: June 22, 2018 Sensipar Description Sensipar (cinacalcet)
Renal osteodystrophy with special emphasis on secondary hyperparathyroidism
 RENAL OSTEODYSTROPHY WITH SPECIAL EMPHASIS ON SECONDARY HYPERPARATHYROIDISM Artigo Original Rev Port Nefrol Hipert 2005; 19 (Suppl 1): 9-18 Renal osteodystrophy with special emphasis on secondary hyperparathyroidism
RENAL OSTEODYSTROPHY WITH SPECIAL EMPHASIS ON SECONDARY HYPERPARATHYROIDISM Artigo Original Rev Port Nefrol Hipert 2005; 19 (Suppl 1): 9-18 Renal osteodystrophy with special emphasis on secondary hyperparathyroidism
Benefits and Harms of Phosphate Binders in CKD: A Systematic Review of Randomized Controlled Trials
 Benefits and Harms of Phosphate Binders in CKD: A Systematic Review of Randomized Controlled Trials Sankar D. Navaneethan, MD, MPH, Suetonia C. Palmer, MBChB, Jonathan C. Craig, MBChB, PhD, Grahame J.
Benefits and Harms of Phosphate Binders in CKD: A Systematic Review of Randomized Controlled Trials Sankar D. Navaneethan, MD, MPH, Suetonia C. Palmer, MBChB, Jonathan C. Craig, MBChB, PhD, Grahame J.
Renal Osteodystrophy in Pediatric Patients on Peritoneal Dialysis
 Advances in Peritoneal Dialysis, Vol. 20, 2004 Francisco J. Cano, Marcela Valenzuela, Pedro Zambrano, Marta A. Azocar, Eduardo Wolff, Maria A. Delucchi, Eugenio E. Rodriguez Renal Osteodystrophy in Pediatric
Advances in Peritoneal Dialysis, Vol. 20, 2004 Francisco J. Cano, Marcela Valenzuela, Pedro Zambrano, Marta A. Azocar, Eduardo Wolff, Maria A. Delucchi, Eugenio E. Rodriguez Renal Osteodystrophy in Pediatric
Paricalcitol versus calcitriol treatment for hyperparathyroidism in pediatric hemodialysis patients
 Pediatr Nephrol (2006) 21:1434 1439 DOI 10.1007/s00467-006-0204-5 ORIGINAL ARTICLE Paricalcitol versus calcitriol treatment for hyperparathyroidism in pediatric hemodialysis patients Wacharee Seeherunvong
Pediatr Nephrol (2006) 21:1434 1439 DOI 10.1007/s00467-006-0204-5 ORIGINAL ARTICLE Paricalcitol versus calcitriol treatment for hyperparathyroidism in pediatric hemodialysis patients Wacharee Seeherunvong
The Parsabiv Beginner s Book
 The Parsabiv Beginner s Book A quick guide to help you learn about your treatment with Parsabiv and what to expect Indication Parsabiv (etelcalcetide) is indicated for the treatment of secondary hyperparathyroidism
The Parsabiv Beginner s Book A quick guide to help you learn about your treatment with Parsabiv and what to expect Indication Parsabiv (etelcalcetide) is indicated for the treatment of secondary hyperparathyroidism
The CARI Guidelines Caring for Australasians with Renal Impairment. Biochemical Targets. Calcium GUIDELINES
 Date written: August 2005 Final submission: October 2005 Author: Carmel Hawley Biochemical Targets CARMEL HAWLEY (Woolloongabba, Queensland) GRAHAME ELDER (Westmead, New South Wales) Calcium GUIDELINES
Date written: August 2005 Final submission: October 2005 Author: Carmel Hawley Biochemical Targets CARMEL HAWLEY (Woolloongabba, Queensland) GRAHAME ELDER (Westmead, New South Wales) Calcium GUIDELINES
CLINICAL PRACTICE GUIDELINE CKD-MINERAL AND BONE DISORDERS (CKD-MBD) Final Version (01/03/2015)
 CLINICAL PRACTICE GUIDELINE CKD-MINERAL AND BONE DISORDERS (CKD-MBD) Final Version (01/03/2015) Dr Simon Steddon, Consultant Nephrologist, Guy s and St Thomas NHS Foundation Trust, London Dr Edward Sharples,
CLINICAL PRACTICE GUIDELINE CKD-MINERAL AND BONE DISORDERS (CKD-MBD) Final Version (01/03/2015) Dr Simon Steddon, Consultant Nephrologist, Guy s and St Thomas NHS Foundation Trust, London Dr Edward Sharples,
Case 4 Generalised bone pain
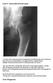 Case 4 Generalised bone pain C A 34- year- old woman presented complaining of multifocal pain in her chest and legs. The pain was intermittent, was aggravated by weight bearing. Initially was alleviated
Case 4 Generalised bone pain C A 34- year- old woman presented complaining of multifocal pain in her chest and legs. The pain was intermittent, was aggravated by weight bearing. Initially was alleviated
Secondary hyperparathyroidism in dialysis patients
 Secondary hyperparathyroidism in dialysis patients ( a critical approach of pharmacological treatments) Dominique JOLY Néphrologie Hôpital NECKER, Paris DFG Finn WF. J Am Soc Nephrol. 24;15:271A. Ca ++
Secondary hyperparathyroidism in dialysis patients ( a critical approach of pharmacological treatments) Dominique JOLY Néphrologie Hôpital NECKER, Paris DFG Finn WF. J Am Soc Nephrol. 24;15:271A. Ca ++
Awaisheh. Mousa Al-Abbadi. Abdullah Alaraj. 1 Page
 f #3 Awaisheh Abdullah Alaraj Mousa Al-Abbadi 1 Page *This sheet was written from Section 1 s lecture, in the first 10 mins the Dr. repeated all the previous material relating to osteoporosis from the
f #3 Awaisheh Abdullah Alaraj Mousa Al-Abbadi 1 Page *This sheet was written from Section 1 s lecture, in the first 10 mins the Dr. repeated all the previous material relating to osteoporosis from the
The Parathyroid Glands
 The Parathyroid Glands Bởi: OpenStaxCollege The parathyroid glands are tiny, round structures usually found embedded in the posterior surface of the thyroid gland ([link]). A thick connective tissue capsule
The Parathyroid Glands Bởi: OpenStaxCollege The parathyroid glands are tiny, round structures usually found embedded in the posterior surface of the thyroid gland ([link]). A thick connective tissue capsule
Month/Year of Review: September 2012 Date of Last Review: September 2010
 Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
NDT Advance Access published February 3, 2007
 NDT Advance Access published February 3, 2007 Nephrol Dial Transplant (2007) 1 of 6 doi:10.1093/ndt/gfl840 Original Article Implementation of K/DOQI Clinical Practice Guidelines for Bone Metabolism and
NDT Advance Access published February 3, 2007 Nephrol Dial Transplant (2007) 1 of 6 doi:10.1093/ndt/gfl840 Original Article Implementation of K/DOQI Clinical Practice Guidelines for Bone Metabolism and
International Journal of PharmTech Research CODEN (USA): IJPRIF, ISSN: Vol.7, No.4, pp ,
 International Journal of PharmTech Research CODEN (USA): IJPRIF, ISSN: 0974-4304 Vol.7, No.4, pp 560-565, 2014-2015 Comparison of Calcium, Phosphate and Intact Parathyroid Hormone Levels Pre- and Post-Parathyroidectomy
International Journal of PharmTech Research CODEN (USA): IJPRIF, ISSN: 0974-4304 Vol.7, No.4, pp 560-565, 2014-2015 Comparison of Calcium, Phosphate and Intact Parathyroid Hormone Levels Pre- and Post-Parathyroidectomy
Bone Disorders in CKD
 Osteoporosis in Dialysis Patients Challenges in Management David M. Klachko MD FACP Professor Emeritus of Medicine University of Missouri-Columbia Bone Disorders in CKD PTH-mediated high-turnover (osteitis
Osteoporosis in Dialysis Patients Challenges in Management David M. Klachko MD FACP Professor Emeritus of Medicine University of Missouri-Columbia Bone Disorders in CKD PTH-mediated high-turnover (osteitis
Treatment Options for Chronic Kidney. Goce Spasovski, R. Macedonia
 Treatment Options for Chronic Kidney Disease: Metabolic Introduction Bone Disease to Renagel Goce Spasovski, R. Macedonia Budapest, August 29, 2011 Session Objectives Definition of the problem of CKD-MBD
Treatment Options for Chronic Kidney Disease: Metabolic Introduction Bone Disease to Renagel Goce Spasovski, R. Macedonia Budapest, August 29, 2011 Session Objectives Definition of the problem of CKD-MBD
Mineral and bone disorder (MBD) affects the majority
 Consistent Control of Mineral and Bone Disorder in Incident Hemodialysis Patients Mark D. Danese,* Vasily Belozeroff, Karen Smirnakis, and Kenneth J. Rothman *Outcomes Insights, Inc., Newbury Park, California;
Consistent Control of Mineral and Bone Disorder in Incident Hemodialysis Patients Mark D. Danese,* Vasily Belozeroff, Karen Smirnakis, and Kenneth J. Rothman *Outcomes Insights, Inc., Newbury Park, California;
Achievement of recommended treatment targets for bone and mineral metabolism in haemodialysis patients using paricalcitol: An observational study
 Achievement of recommended treatment targets for bone and mineral metabolism in haemodialysis patients using paricalcitol: An observational study Fernstrom, Anders; Giaever, Jan; Granroth, Barbara; Hylander,
Achievement of recommended treatment targets for bone and mineral metabolism in haemodialysis patients using paricalcitol: An observational study Fernstrom, Anders; Giaever, Jan; Granroth, Barbara; Hylander,
Pathogenesis and Treatment of Renal Osteodystrophy
 Proceedings Blood Purif 2003;21:318 326 DOI: 10.1159/000072552 Eduardo Slatopolsky a Esther Gonzalez b Kevin Martin b a Renal Division, Washington University School of Medicine, St. Louis, Mo., and b Division
Proceedings Blood Purif 2003;21:318 326 DOI: 10.1159/000072552 Eduardo Slatopolsky a Esther Gonzalez b Kevin Martin b a Renal Division, Washington University School of Medicine, St. Louis, Mo., and b Division
Marie-Claude Monier-Faugere, Hanna Mawad, and Hartmut H. Malluche
 Opposite Effects of Calcitriol and Paricalcitol on the Parathyroid Hormone-(1-84)/Large Carboxy-Terminal- Parathyroid Hormone Fragments Ratio in Patients with Stage 5 Chronic Kidney Disease Marie-Claude
Opposite Effects of Calcitriol and Paricalcitol on the Parathyroid Hormone-(1-84)/Large Carboxy-Terminal- Parathyroid Hormone Fragments Ratio in Patients with Stage 5 Chronic Kidney Disease Marie-Claude
Clinical Guideline Bone chemistry management in adult renal patients on dialysis
 Clinical Guideline Bone chemistry management in adult renal patients on dialysis This guidance covers how to: Maintain serum phosphate 0.8 to 1.7mmol/L 1 Maintain serum corrected calcium 2.1 to 2.5mmol/L
Clinical Guideline Bone chemistry management in adult renal patients on dialysis This guidance covers how to: Maintain serum phosphate 0.8 to 1.7mmol/L 1 Maintain serum corrected calcium 2.1 to 2.5mmol/L
Secondary hyperparathyroidism an Update on Pathophysiology and Treatment
 Secondary hyperparathyroidism an Update on Pathophysiology and Treatment Klaus Olgaard Copenhagen Budapest Nephrology School August 2007 HPT IN CRF Renal mass Ca 2+ 1,25(OH) 2 D 3 CaR Hyperparathyroidism
Secondary hyperparathyroidism an Update on Pathophysiology and Treatment Klaus Olgaard Copenhagen Budapest Nephrology School August 2007 HPT IN CRF Renal mass Ca 2+ 1,25(OH) 2 D 3 CaR Hyperparathyroidism
Figures and tables in this presentation were adopted from various printed and electronic resorces and serve strictly for educational purposes.
 Academic lectures 3rd year of Medical faculty Figures and tables in this presentation were adopted from various printed and electronic resorces and serve strictly for educational purposes. ENDOCRINOLOGY
Academic lectures 3rd year of Medical faculty Figures and tables in this presentation were adopted from various printed and electronic resorces and serve strictly for educational purposes. ENDOCRINOLOGY
Nuove terapie in ambito Nefrologico: Etelcalcetide (AMG-416)
 Nuove terapie in ambito Nefrologico: Etelcalcetide (AMG-416) Antonio Bellasi, MD, PhD U.O.C. Nefrologia & Dialisi ASST-Lariana, Ospedale S. Anna, Como, Italy Improvement of mineral and bone metabolism
Nuove terapie in ambito Nefrologico: Etelcalcetide (AMG-416) Antonio Bellasi, MD, PhD U.O.C. Nefrologia & Dialisi ASST-Lariana, Ospedale S. Anna, Como, Italy Improvement of mineral and bone metabolism
The Skeletal Response to Aging: There s No Bones About It!
 The Skeletal Response to Aging: There s No Bones About It! April 7, 2001 Joseph E. Zerwekh, Ph.D. Interrelationship of Intestinal, Skeletal, and Renal Systems to the Overall Maintenance of Normal Calcium
The Skeletal Response to Aging: There s No Bones About It! April 7, 2001 Joseph E. Zerwekh, Ph.D. Interrelationship of Intestinal, Skeletal, and Renal Systems to the Overall Maintenance of Normal Calcium
Drugs for the treatment of secondary hyperparathyroidism and hyperphosphataemia
 NSW Therapeutic Advisory Group Level 5, 376 Victoria Street PO Box 766 Darlinghurst NSW 2010 Phone: 61 2 8382 2852 Fax: 61 2 8382 3529 Email: nswtag@stvincents.com.au www.nswtag.org.au Drugs for the treatment
NSW Therapeutic Advisory Group Level 5, 376 Victoria Street PO Box 766 Darlinghurst NSW 2010 Phone: 61 2 8382 2852 Fax: 61 2 8382 3529 Email: nswtag@stvincents.com.au www.nswtag.org.au Drugs for the treatment
Total Parathyroidectomy with Forearm Autotransplantation as the Treatment of Choice for Secondary Hyperparathyroidism
 The Journal of International Medical Research 2011; 39: 978 987 Total Parathyroidectomy with Forearm Autotransplantation as the Treatment of Choice for Secondary Hyperparathyroidism J NARANDA 1,2, R EKART
The Journal of International Medical Research 2011; 39: 978 987 Total Parathyroidectomy with Forearm Autotransplantation as the Treatment of Choice for Secondary Hyperparathyroidism J NARANDA 1,2, R EKART
Case Report Use of Percutaneous Ethanol Injection Therapy for Recurrent Secondary Hyperparathyroidism after Subtotal Parathyroidectomy
 SAGE-Hindawi Access to Research International Nephrology Volume 211, Article ID 246734, 6 pages doi:1.461/211/246734 Case Report Use of Percutaneous Ethanol Injection Therapy for Recurrent Secondary Hyperparathyroidism
SAGE-Hindawi Access to Research International Nephrology Volume 211, Article ID 246734, 6 pages doi:1.461/211/246734 Case Report Use of Percutaneous Ethanol Injection Therapy for Recurrent Secondary Hyperparathyroidism
Effectiveness and tolerability of sevelamer in the treatment of hyperphosphatemia in hemodialysis patients
 Open Access Journal of Journal of Parathyroid Disease 2017,5(1),17 24 http://www.jparathyroid.com Original Effectiveness and tolerability of sevelamer in the treatment of hyperphosphatemia in hemodialysis
Open Access Journal of Journal of Parathyroid Disease 2017,5(1),17 24 http://www.jparathyroid.com Original Effectiveness and tolerability of sevelamer in the treatment of hyperphosphatemia in hemodialysis
PRIMARY HYPERPARATHYROIDISM
 PRIMARY HYPERPARATHYROIDISM HYPERPARATHYROIDISM Inappropriate excess secretion of Parathyroid Hormone in Primary Hyperparathyroidism Appropriate Hypersecretion in Secondary Hyperparathyroidism PTH and
PRIMARY HYPERPARATHYROIDISM HYPERPARATHYROIDISM Inappropriate excess secretion of Parathyroid Hormone in Primary Hyperparathyroidism Appropriate Hypersecretion in Secondary Hyperparathyroidism PTH and
Lanthanum: A Safe Phosphate Binder
 Blackwell Publishing Inc Lanthanum: A Safe Phosphate Binder Veerle P. Persy, Geert J. Behets, An R. Bervoets, Marc E. De Broe, and Patrick C. D Haese University of Antwerp, Antwerp, Belgium ABSTRACT Accumulation
Blackwell Publishing Inc Lanthanum: A Safe Phosphate Binder Veerle P. Persy, Geert J. Behets, An R. Bervoets, Marc E. De Broe, and Patrick C. D Haese University of Antwerp, Antwerp, Belgium ABSTRACT Accumulation
UPDATE ON RENAL OSTEODYSTROPHY: PATHOGENESIS AND CLINICAL MANAGEMENT
 UPDATE ON RENAL OSTEODYSTROPHY: PATHOGENESIS AND CLINICAL MANAGEMENT KhashayarSakhaee,M.D. University of Texas Southwestern Medical Center at Dallas Internal Medicine Grand Rounds May 22, 1997 Name: Rank:
UPDATE ON RENAL OSTEODYSTROPHY: PATHOGENESIS AND CLINICAL MANAGEMENT KhashayarSakhaee,M.D. University of Texas Southwestern Medical Center at Dallas Internal Medicine Grand Rounds May 22, 1997 Name: Rank:
Since its inception in the 1970s, dialysis has allowed for
 http://www.revistanefrologia.com 2013 Revista Nefrología. Official Publication of the Spanish Nephrology Society editorial comment See original article on page 46 Are the K/DOQI objectives for bone mineral
http://www.revistanefrologia.com 2013 Revista Nefrología. Official Publication of the Spanish Nephrology Society editorial comment See original article on page 46 Are the K/DOQI objectives for bone mineral
Chapter 5: Evaluation and treatment of kidney transplant bone disease Kidney International (2009) 76 (Suppl 113), S100 S110; doi: /ki.2009.
 http://www.kidney-international.org & 2009 KDIGO Chapter 5: Evaluation and treatment of kidney transplant bone disease ; doi:10.1038/ki.2009.193 Grade for strength of recommendation a Strength Wording
http://www.kidney-international.org & 2009 KDIGO Chapter 5: Evaluation and treatment of kidney transplant bone disease ; doi:10.1038/ki.2009.193 Grade for strength of recommendation a Strength Wording
hypercalcemia of malignancy hyperparathyroidism PHPT the most common cause of hypercalcemia in the outpatient setting the second most common cause
 hyperparathyroidism A 68-year-old woman with documented osteoporosis has blood tests showing elevated serum calcium and parathyroid hormone (PTH) levels: 11.2 mg/dl (8.8 10.1 mg/dl) and 88 pg/ml (10-60),
hyperparathyroidism A 68-year-old woman with documented osteoporosis has blood tests showing elevated serum calcium and parathyroid hormone (PTH) levels: 11.2 mg/dl (8.8 10.1 mg/dl) and 88 pg/ml (10-60),
OPEN. Masahiro Yoshikawa 1,2, Osamu Takase 1,2, Taro Tsujimura
 www.nature.com/scientificreports Received: 26 September 2017 Accepted: 19 March 2018 Published: xx xx xxxx OPEN Long-term effects of low calcium dialysates on the serum calcium levels during maintenance
www.nature.com/scientificreports Received: 26 September 2017 Accepted: 19 March 2018 Published: xx xx xxxx OPEN Long-term effects of low calcium dialysates on the serum calcium levels during maintenance
Exer Ex cise Pa P tien tien with End End stag sta e g renal Disease
 Exercise in Patients with End stage Exercise in Patients with End stage renal Disease Chronic renal failure : gradual and progressive loss of the ability of the kidneys to function Structural kidney damage
Exercise in Patients with End stage Exercise in Patients with End stage renal Disease Chronic renal failure : gradual and progressive loss of the ability of the kidneys to function Structural kidney damage
Slowing the Progression of Vascular Calcification in Hemodialysis
 Slowing the Progression of Vascular Calcification in Hemodialysis J Am Soc Nephrol 14: S310 S314, 2003 GLENN M. CHERTOW Division of Nephrology, Department of Medicine, University of California San Francisco,
Slowing the Progression of Vascular Calcification in Hemodialysis J Am Soc Nephrol 14: S310 S314, 2003 GLENN M. CHERTOW Division of Nephrology, Department of Medicine, University of California San Francisco,
Ca, Phos and Vitamin D Metabolism in Pre-Dialysis Patients
 Ca, Phos and Vitamin D Metabolism in Pre-Dialysis Patients A. WADGYMAR, MD Credit Valley Hospital, Mississauga, Ontario, Canada. June 1, 2007 1 Case: 22 y/o referred to Renal Clinic Case: A.M. 29 y/o Man
Ca, Phos and Vitamin D Metabolism in Pre-Dialysis Patients A. WADGYMAR, MD Credit Valley Hospital, Mississauga, Ontario, Canada. June 1, 2007 1 Case: 22 y/o referred to Renal Clinic Case: A.M. 29 y/o Man
Glycaemic control and serum intact parathyroid hormone levels in diabetic patients on haemodialysis therapy
 Nephrol Dial Transplant (2008) 23: 315 320 doi: 10.1093/ndt/gfm639 Advance Access publication 23 October 2007 Original Article Glycaemic control and serum intact parathyroid hormone levels in diabetic
Nephrol Dial Transplant (2008) 23: 315 320 doi: 10.1093/ndt/gfm639 Advance Access publication 23 October 2007 Original Article Glycaemic control and serum intact parathyroid hormone levels in diabetic
White Rose Research Online URL for this paper: Version: Accepted Version
 This is a repository copy of Effect on mortality of elective parathyroid surgery in one hundred and three patients with chronic kidney disease : our experience. White Rose Research Online URL for this
This is a repository copy of Effect on mortality of elective parathyroid surgery in one hundred and three patients with chronic kidney disease : our experience. White Rose Research Online URL for this
The hart and bone in concert
 The hart and bone in concert Piotr Rozentryt III Department of Cardiology, Silesian Centre for Heart Disease, Silesian Medical University, Zabrze, Poland Disclosure Research grant, speaker`s fee, travel
The hart and bone in concert Piotr Rozentryt III Department of Cardiology, Silesian Centre for Heart Disease, Silesian Medical University, Zabrze, Poland Disclosure Research grant, speaker`s fee, travel
CKD FOR INTERNISTS. Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College
 CKD FOR INTERNISTS Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College INTRODUCTION In 2002, the National Kidney Foundation s Kidney Disease Outcomes Quality Initiative(KDOQI)
CKD FOR INTERNISTS Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College INTRODUCTION In 2002, the National Kidney Foundation s Kidney Disease Outcomes Quality Initiative(KDOQI)
02/27/2018. Objectives. To Replace or Not to Replace: Nutritional Vitamin D in Dialysis.
 To Replace or Not to Replace: Nutritional Vitamin D in Dialysis. Michael Shoemaker-Moyle, M.D. Assistant Professor of Clinical Medicine Objectives Review Vitamin D Physiology Review Current Replacement
To Replace or Not to Replace: Nutritional Vitamin D in Dialysis. Michael Shoemaker-Moyle, M.D. Assistant Professor of Clinical Medicine Objectives Review Vitamin D Physiology Review Current Replacement
Racial differences in bone turnover rate and hyperparathyroidism in hemodialysis patients
 Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine 1994 Racial differences in bone turnover rate and hyperparathyroidism
Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine 1994 Racial differences in bone turnover rate and hyperparathyroidism
Survival of Patients Undergoing Hemodialysis with Paricalcitol or Calcitriol Therapy
 The new england journal of medicine original article Survival of Patients Undergoing Hemodialysis with Paricalcitol or Calcitriol Therapy Ming Teng, M.D., Myles Wolf, M.D., M.M.Sc., Edmund Lowrie, M.D.,
The new england journal of medicine original article Survival of Patients Undergoing Hemodialysis with Paricalcitol or Calcitriol Therapy Ming Teng, M.D., Myles Wolf, M.D., M.M.Sc., Edmund Lowrie, M.D.,
K/DOQI-recommended intact PTH levels do not prevent low-turnover bone disease in hemodialysis patients
 http://www.kidney-international.org & 2008 International Society of Nephrology original article see commentary on page 674 K/DOQI-recommended intact PTH levels do not prevent low-turnover bone disease
http://www.kidney-international.org & 2008 International Society of Nephrology original article see commentary on page 674 K/DOQI-recommended intact PTH levels do not prevent low-turnover bone disease
Should cinacalcet be used in patients who are not on dialysis?
 Should cinacalcet be used in patients who are not on dialysis? Jorge B Cannata-Andía and José Luis Fernández-Martín Affiliations: Bone and Mineral Research Unit. Hospital Universitario Central de Asturias.
Should cinacalcet be used in patients who are not on dialysis? Jorge B Cannata-Andía and José Luis Fernández-Martín Affiliations: Bone and Mineral Research Unit. Hospital Universitario Central de Asturias.
Phosphate binders and metabolic acidosis in patients undergoing maintenance hemodialysis sevelamer hydrochloride, calcium carbonate, and bixalomer
 Hemodialysis International 2015; 19:5459 Phosphate binders and metabolic acidosis in patients undergoing maintenance hemodialysis sevelamer hydrochloride, calcium carbonate, and bixalomer Toru SANAI, 1
Hemodialysis International 2015; 19:5459 Phosphate binders and metabolic acidosis in patients undergoing maintenance hemodialysis sevelamer hydrochloride, calcium carbonate, and bixalomer Toru SANAI, 1
... . : ... PTH.
 IRMA Email msarookhani@qumsacir * CRD GFR D [1,25OH 2 D 3 ] SHPT GFR» «KDOQI SHPT Ca * P P P Selectra Overt HPT = = Ca * P P > GM II DSL i IRMA ± ± ± Ca * P % % % % % % % % % % % % % % % % pgml = = > ±
IRMA Email msarookhani@qumsacir * CRD GFR D [1,25OH 2 D 3 ] SHPT GFR» «KDOQI SHPT Ca * P P P Selectra Overt HPT = = Ca * P P > GM II DSL i IRMA ± ± ± Ca * P % % % % % % % % % % % % % % % % pgml = = > ±
