EUS-guided pancreatic cyst ablation: a critical review (with video) Hyoung-Chul Oh, MD, 1 William R. Brugge, MD 2
|
|
|
- Natalie Shields
- 5 years ago
- Views:
Transcription
1 TECHNICAL REVIEW EUS-guided pancreatic cyst ablation: a critical review (with video) Hyoung-Chul Oh, MD, 1 William R. Brugge, MD 2 The widespread use of cross-sectional imaging has dramatically increased the number of incidental pancreatic cystic lesions. The prevalence is age related. Based on screening CT/magnetic resonance imaging, the prevalence is 2.5% in adults and as high as 8% in the elderly. 1,2 Although most pancreatic cysts are incidentally detected, pancreatic cysts represent a wide spectrum of histopathology, and neoplastic cysts are more prevalent than previously estimated. Some histologic types including mucinous cystic neoplasms (MCNs) and intraductal papillary mucinous neoplasms (IPMNs) have malignant potential. 3,4 Differentiation of pancreatic cysts with malignant potential from those with benign behavior is an essential step in formulating a management strategy. High-resolution imaging technologies including CT, magnetic resonance imaging, and EUS allow a morphologic description of a pancreatic cyst in detail. However, the accuracy of cross-sectional imaging in the typing of pancreatic cysts is limited. Cyst fluid analysis for tumor markers such as carcinoembryonic antigen is useful in differentiating mucinous from nonmucinous cysts. Based on histologic controls, good diagnostic accuracy has been reported (sensitivity of 73% and specificity of 84%). 5 However, a substantial portion (as high as 50%) of pancreatic cysts remains indeterminate, even after extensive evaluation including cyst fluid aspiration. 6 On the other hand, surgical resection of a pancreatic cystic neoplasm is associated with a perioperative morbidity of 20% to 40% and a mortality rate of 2% Therefore, making a clinical decision as to whether to operate or observe an incidentally detected pancreatic cyst that is indeterminate by conventional diagnostic modality Abbreviations: IPMN, intraductal papillary mucinous neoplasm; MCN, mucinous cystic neoplasm; SCA, serous cystadenoma. DISCLOSURE: The authors disclosed no financial relationships relevant to this publication. Dr Oh was supported by the 2012 ASGE Cook Medical Don Wilson Award. This video can be viewed directly from the GIE website or by using the QR code and your mobile device. Download a free QR code scanner by searching QR Scanner in your mobile device s app store. Copyright 2013 by the American Society for Gastrointestinal Endoscopy /$ is challenging. A personalized management strategy is often deployed, applying a risk-benefit analysis to each patient. 3 This clinical dilemma has raised the need to develop a safe, effective, and minimally invasive approach for the treatment of pancreatic cysts. EUS-guided FNA of cyst fluid has been widely used for the differential diagnosis of pancreatic cysts. Based on the accumulated experience with EUSguided FNA, pancreatic tissue ablation by EUS-guided injection of ethanol or other ablative agents can be performed safely, with few procedure-related adverse events Percutaneous injection with ethanol has been widely used for the ablation of cystic lesions of the kidney, liver, 19,20 and thyroid gland without serious adverse events. EUS-guided injection of a variety of antitumor agents into pancreatic cancer has been reported to be feasible and safe By using similar principles, ablation of neoplastic cyst epithelium has been attempted with a chemotherapeutic agent. 27 EUS-guided pancreatic cyst ablation has been investigated in a variety of clinical trials. In this technical review, procedural basics and special considerations of cyst ablation and its clinical outcomes including safety and treatment response are summarized by reviewing the published literature. Briefly, the terms used for cyst ablation in this review may be defined as follows: ablation relates to the destruction of the cyst epithelium; injection refers to the act of forceful placement of an ablative agent into a cyst; and lavage is the act of repeated injections and aspiration. EUS-GUIDED CYST ABLATION TECHNIQUE An imaging evaluation of a pancreatic cystic lesion can determine the internal structure with regard to the number of septations, the wall thickness, and the presence of a mural nodule or mass. EUS imaging can be performed with a radial scanning echoendoscope or a curvilineararray echoendoscope. Both instruments provide highresolution imaging, but linear endosonography has the option of FNA. With a curvilinear-array echoendoscope, the cyst may be punctured via a transgastric or transduodenal route with the use of a 22-gauge needle. Cyst fluid aspiration is relatively simple and has a low rate of adverse events. The collection of cyst fluid provides important diagnostic material, as well as space for the ablative agent in the cyst cavity. After subtotal evacuation of the cyst, 526 GASTROINTESTINAL ENDOSCOPY Volume 77, No. 4 :
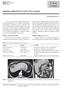
2 Oh & Brugge EUS-guided pancreatic cyst ablation Figure 1. Stepwise EUS-guided pancreatic cyst ablation therapy. Step 1: FNA (left) within a septated cyst (heavy black line). Step 2: 5-minute ethanol (middle) lavage of the cyst, followed by aspiration of the ethanol. Step 3: injection of paclitaxel (right) into the cyst, resulting in expansion of the cyst to its original diameter. injection is performed with a volume of fluid equal to that initially aspirated, and the cyst is lavaged for 3 to 5 minutes, alternately filling and emptying the cavity. Ethanol is the simplest agent for cyst ablation because it is easily obtained and injected. The injected ethanol is evacuated at the end of lavage, leaving just enough fluid to outline the cyst cavity. A second ablative agent (eg, a chemotherapeutic agent such as paclitaxel) may be injected and left in the cyst cavity; the total injection volume should not exceed the volume of aspirated fluid. During the procedure, the needle tip is carefully maintained within the cyst to avoid parenchymal injury or a leak in the cyst wall. At the completion of the injection or lavage, the needle is removed from the cyst cavity (Fig. 1) (Video 1, available online at Ablative agents Ethanol is an inexpensive, widely available, low-viscosity agent that is easy to inject through a small-gauge needle. Ethanol injected into hepatic cysts induces cell membrane lysis, protein denaturation, and vascular occlusion within 10 minutes but penetrates the fibrous capsule slowly. 28,29 The minimally effective ethanol concentration for tissue ablation in hepatic cysts is 40%. 30 The mean maximum postprocedure blood ethanol concentration is approximately 130 mg/ml at 3 to 4 hours after ethanol instillation, and clinical signs of ethanol intoxication have been noted in two thirds of cases but resolved without treatment. 21 Paclitaxel, a widely used chemotherapeutic agent, inhibits cell processes that are dependent on microtubules. It is hydrophobic and viscous in nature and hence can exert a durable effect on the epithelium within the cyst cavity with a low risk of leakage. 31 In an animal study with intravesical instillation of paclitaxel (500 g in20mlof water), the tissue concentration in the bladder wall was two- to threefold greater than the plasma concentration obtained after intravenous infusion of 250 mg/m Because of the high viscosity of its cosolvent, Cremophor (castor oil), the paclitaxel solution needs to be diluted 1:1 in 0.9% normal saline solution (a final dose concentration of 3 mg/ml paclitaxel) for injection. However, another formula of paclitaxel with a less viscous delivery vehicle (polymeric micelle) can be used without dilution (a dose concentration of 6 mg/ml). 6 Special consideration for EUS-guided cyst ablation The morphologic characteristics of a cyst will guide the approaches to cyst injection and ablation therapy. Cyst injection therapy has the greatest chance of successful ablation in unilocular or oligolocular cysts with fewer than 2 to 3 locules. In the presence of 3 or more locules, a single needle pass may not provide a sufficient drug delivery to all locules within a cyst. It is important to determine the optimal angle at which the needle can be introduced into the maximal number of targeted locules. When all punctured locules cannot be visualized on an endosonographic image, needle passage across a septation may be indicated. The simultaneous collapse of locules across the septum during cyst fluid evacuation and the spread of echogenic bubbles across the septation during injection of ablative agents are indicative of a good distribution of the ablative agent into the locules. A missed locule may result in regrowth of a cyst and treatment failure. Additional needle passes through different angles may increase not only the effectiveness of cyst ablation but also the risk of Volume 77, No. 4 : 2013 GASTROINTESTINAL ENDOSCOPY 527
3 EUS-guided pancreatic cyst ablation Oh & Brugge Table 1. Summary of previous reports of EUS-guided cyst ablations Authors No. of patients Ablative agent Follow-up period Complete resolution Gan et al %-80% ethanol 6-12 mo 35% (8/23) Oh et al %/99% ethanol with paclitaxel Median 9 mo (range 6-23 mo) 79% (11/14) Oh et al 37 * 10 99% ethanol with paclitaxel Median 8.5 mo (range 6-18 mo) 60% (6/10) DeWitt et al % ethanol 3-4 mo after second lavage 33% (12/36) Oh et al % ethanol with paclitaxel Median 20 mo (range 12-44) 62% (29/27) DiMaio et al % ethanol 13 mo after first lavage 38% (5/13) *Included only patients with a septated cyst. Included study population of 2 preliminary reports. 29,30 Included patients with multiple ablations. adverse events. A second needle puncture may be considered when it can be performed without increasing the risk of adverse events. In a case report, an 8-cm septated cyst was punctured twice at different angles, and cyst injection was performed with each needle pass. On follow-up CT, the cyst size decreased markedly, and septa observed on the initial CT scan were no longer visible. Two needle passes increased an ablation effect by improving the contact between the cyst locules and the ablative agent. 33 Nearly complete evacuation of cyst fluid before injection therapy increases the surface area directly exposed to the ablative agent and improves the efficacy of ablation. However, cyst fluid rich in mucinous content may not be effectively aspirated because of high viscosity. Even though cyst fluid may not be completely evacuated during initial aspiration, ethanol lavage may reduce the viscosity of mucin-containing fluid and lead to improved evacuation of cyst fluid as well as ablation of the epithelial lining. Therefore, ethanol lavage is usually performed before the injection of a second ablative agent. The presence of a communication between the cyst and main pancreatic duct may result in flow of the injected ablative agent through the communicating duct into the main pancreatic duct. This outflow may not only diminish the ablative effect but may also increase the risk of unexpected ductal change or pancreatitis. Although a mucous plug might obstruct the communicating duct in branchduct IPMN and lavage may not increase the frequency of pancreatitis, 34,35 repeated injection and aspiration during lavage may open an outflow tract. Dilution of the injected agent with pancreatic duct fluid will interfere with the effects of the injectant. Practically, injection and lavage rarely result in flow of the ablative agent into the main pancreatic duct. However, if a cyst is not restored to its original size during ethanol injection, vigorous lavage with repeated injection and aspiration should be avoided because of the probable communication with the main pancreatic duct. On the other hand, endoscopic retrograde pancreatography may be useful for determining the presence of communication between the main pancreatic duct and cyst, but it should be considered in select cases because of the possible risk of pancreatitis. RESULTS OF CLINICAL TRIAL To date, 3 clinical trials of cyst injection therapy, 6,34,36 3 preliminary cases series, 27,35,37 1 long-term follow-up report, 38 and 1 case report 33 have been reported. These reports were summarized in Table 1. In the initial pilot study, patients underwent ethanol lavage with a concentration escalation from 5% to 80% ethanol and were followed for 6 to 12 months. Eight of 23 patients (35%) with complete follow-up had complete resolution. All septated cysts persisted despite ethanol ablation therapy. There was no significant difference in cyst resolution according to the ethanol concentration (5%-40% vs 50%-80%). Five patients underwent surgical resection. All 5 patients had a diagnosis of MCN, and a variable degree of epithelial ablation (up to complete) was observed on surgical pathology. To increase the ablative effect, in new trials, a chemotherapeutic agent (paclitaxel) has been combined with ethanol ablation therapy. 27 It was hypothesized that the epithelial distortion by ethanol could allow the diffusion of paclitaxel in the injured epithelium. In a pilot feasibility study with ethanol and paclitaxel, 14 patients were followed for more than 6 months after injection therapy, and complete resolution was achieved in 11 patients. Paclitaxel used in the study was highly hydrophobic and viscous in nature, complicating the injection technique. Although this study was a preliminary case series, the cyst resolution rate (79%) was greater than the previously observed rate with ethanol alone (33%), suggesting a synergistic effect between ethanol and paclitaxel. One of the important factors that may influence the treatment response is the presence of septations within the cyst. In a case series of 10 patients with septated cysts, 37 complete resolution was achieved in 6 patients after eth- 528 GASTROINTESTINAL ENDOSCOPY Volume 77, No. 4 :
4 Oh & Brugge EUS-guided pancreatic cyst ablation anol lavage and paclitaxel injection. Two patients with a persistent cyst demonstrated an initial decrease in diameter at 6 months, but an increase in size at 12 months. The histopathology of the resected specimen and review of EUS images revealed that regrowth of the cyst resulted from the remnant mucinous epithelium arising from the incompletely lavaged locules. Careful patient selection and tailored intervention based on the internal structure of the cyst is required to improve ablation efficacy and minimize the missed locules, especially when a cyst is septated. Although an ablation effect was demonstrated in the resected cysts of subjects in the pilot study, further evidence of cyst ablation was demonstrated by a randomized, double-blind trial of 42 patients comparing ethanol with saline solution lavage. 36 Ethanol lavage resulted in a significant decrease in cyst size at 3 months after initial ablation compared with saline solution alone. Thirty-three of 42 patients enrolled for the initial randomization underwent a second unblinded ethanol lavage. There was no significant difference in cyst size of subjects exposed to 1 or 2 injections of ethanol. Complete resolution as shown by CT scan was achieved in 33%. Four patients underwent surgery and received a diagnosis of having an IPMN (n 3) or MCN (n 1). Epithelial ablation ranging from 0% (saline solution alone) to 50% to 100% (1 or 2 ethanol lavages) was observed in the histopathology of the resected cysts. The durability of cyst ablation is an important issue because cyst resolution achieved for a short-term period may not ensure the long-term ablative effect and ultimately the prevention of malignant transformation. In a clinical trial of 47 patients who underwent ethanol lavage and paclitaxel injection, 6 29 patients (62%) showed complete resolution of the cyst over a median follow-up of 22 months (range months) (Fig. 2). Four patients underwent surgery and had a diagnosis of MCN (n 2), serous cystadenoma (SCA) (n 1), or a neuroendocrine tumor (n 1). The histopathologic extent of epithelial ablation ranged from 0% to 100%, and a spectrum of histopathologic changes including epithelial denudation with fibrosis and an atrophied epithelium was observed (Fig. 3). A small cyst volume was predictive of complete resolution of the cyst by CT scanning. Two MCN cysts that were nearly resolved at 6-month follow-up demonstrated regrowth at 12 months. The return of the cyst may represent remnant epithelial regrowth. The resolution rate in this study (69%), greater than that in the previous study with ethanol alone, might be a result of the combination injection of ethanol and paclitaxel. In another follow-up report, 38 9 patients who had complete resolution as shown on a CT scan after 1 or 2 ethanol lavages were followed over a median of 26 months (range months). Cyst recurrence on CT scan was not observed in any patient. Imaging evidence of cyst resolution includes complete disappearance of cyst, small low-density focus on CT or EUS, or residual calcification. Imaging-based resolution Figure 2. A, B, A 36-mm unilocular cyst in the body of the pancreas. C, Dense calcification replaced the original cyst on follow-up CT scan at 30 months after cyst ablation. Volume 77, No. 4 : 2013 GASTROINTESTINAL ENDOSCOPY 529
5 EUS-guided pancreatic cyst ablation Oh & Brugge Figure 3. Spectrum of histopathologic changes after cyst ablation: atrophied epithelium (A), transitional area (B), persistent mucinous epithelium (C). may not correlate, however, with histologic ablation. Close monitoring should be continued even after complete resolution, but surveillance policy may be modified based on risk analysis. To improve the ablative effect of cyst injection therapy, procedural techniques including a second needle pass at a different angle and booster ablation have been tried. In 1 case series of 13 patients with branch-duct IPMN, 35 multiple sessions of cyst lavage were performed. Although cyst diameter and surface area showed no significant decrease after 1 ethanol lavage session, these parameters decreased after 2 ethanol lavage sessions. Complete resolution was achieved in 38% (5/13) only after 2 lavage sessions. 35 The presence and number of septations were not predictive of the response to injection therapy. When 2 needle injections with different needle angles were used, an 8-cm cyst was shown to be nearly eliminated on CT scanning. 33 Multiple cyst injection therapy may induce additional effects on the remnant epithelium or locules, but multiple injections have not consistently resulted in a better resolution rate. The relative effectiveness is probably related to the degree of contact between the ablative agent and the cyst epithelium. SAFETY OF CYST ABLATION The safety of an investigational treatment modality is a major concern when it is first applied clinically. Procedurerelated adverse events described in the 3 representative clinical trials are summarized in Table 2. Most adverse events were mild and self-limited. Abdominal pain just after cyst ablation was the most common acute complication. Contrary to initial concerns, the frequency of ablation-related pancreatitis was low (2%, 3/152). The risk of pancreatitis was increased if there was inadvertent injection of an ablative agent into the pancreatic parenchyma. Surprisingly, in cases of injection of branch-duct IPMN with main duct communication, pancreatitis was rare. Thick mucin in the communicating duct may prevent 530 GASTROINTESTINAL ENDOSCOPY Volume 77, No. 4 :
6 Oh & Brugge EUS-guided pancreatic cyst ablation Table 2. Cyst ablation related adverse events Adverse events, n* (%) Gan et al 34 (N 25) DeWitt et al 36 (N 75) Oh et al 6 (N 52) Overall (N 152)* Abdominal pain (7.9) Acute pancreatitis (2.0) Fever (0.7) Pericystic spillage (0.7) Splenic vein obliteration (0.7) *Total number of patients who underwent 1 session of EUS-guided cyst ablation. the leakage of the ablative agent into the main pancreatic duct. 35 Venous obliteration and thrombosis in the venous system adjacent to the cyst have been reported in 2 patients who underwent ethanol lavage and paclitaxel injection. 39 Extensive inflammation within and around the cyst induced by the injection itself or pericystic leak of the ablative agent may result in local extension of inflammation into the adjacent vessels. These adverse events may become serious because portal hypertension and collateral formation may develop. In addition, substantial difficulty may be encountered in subsequent surgical resection for the persistent cyst. For prevention of procedure-related adverse events, it is important to maintain the needle in the visual plane and within the cyst cavity during the entire procedure. The optimal volume of ablative agent needs to be cautiously titrated and an aggressive lavage procedure should be avoided, especially when a cyst is in close proximity to the portosplenic venous system. The ablative agent related systemic adverse events of intravenous administration have not been observed in patients undergoing local injection. Hypersensitivity reaction to paclitaxel, a worrisome and unexpected complication, has not occurred, even without premedication of a steroid and histamine antagonist. CONTROVERSIES IN PANCREATIC CYST ABLATION There are some concerns about ablation of benign cysts that meet the criteria for observation. Second, others have raised concerns of a false sense of success after cyst elimination seen on imaging. The possibility of residual viable epithelium undermines the hope of complete eradication. 40 An imaging surveillance policy for asymptomatic nonsurgical candidates has become widely accepted by surgeons and gastroenterologists. However, lifelong monitoring is burdensome economically and psychologically for the elderly. Cyst ablation of a benign cyst may be an attractive option if a cyst can be readily and successfully ablated by using a minimally invasive method. With successful elimination of a cyst shown by cross-sectional imaging, the subsequent imaging intervals could be prolonged, if not eliminated. Early treatment of premalignant diseases with lessinvasive modalities has resulted in paradigm shifts in the management of gastric and colon adenomas, as well as Barrett s esophagus. Although the role of EUS-guided pancreatic cyst ablation is still under evaluation and its potential benefits are theoretical, eradication of a premalignant cyst may also have a role in the prevention of malignant change. PROPOSED INDICATIONS EUS-guided pancreatic cyst ablation is still an investigational modality and should be judiciously used in select patients based on strict inclusion criteria that may predict high treatment efficacy while minimizing procedurerelated risks. Most patients in published clinical trials underwent cyst ablation at the time of diagnostic FNA. This practice resulted in the inclusion of a wide variety of cysts and types of epithelium. In the future, it would be ideal for the patient to have an established diagnosis before injection therapy. The ideal cyst candidate for ablation should have (1) a benign appearance without any malignant feature, (2) a diameter between 2 and 4 cm, (3) a unilocular or oligolocular morphology, and (4) no communication with the main pancreatic duct. The ideal size of the cyst for injection therapy is based on 2 competing factors, the risk of malignancy and the success rate, and both are related to the cyst diameter. It is generally accepted that a cyst larger than 3 to 4 cm in diameter may have an increased malignant potential. A cyst diameter less than 3.5 cm was predictive of cyst resolution after ablation therapy. On the other hand, a minimum cyst diameter of 2 cm may ensure the safety and feasibility of ablation therapy. Volume 77, No. 4 : 2013 GASTROINTESTINAL ENDOSCOPY 531
7 EUS-guided pancreatic cyst ablation Oh & Brugge Ideally, patient selection should be based on the specific type of cyst. MCN is the ideal target for EUSguided cyst ablation because it has malignant potential and is often unilocular. Cyst ablation should be considered only when the viscous mucinous cyst fluid can be effectively aspirated. There are some concerns about the treatment of a benign cyst such as SCA. Because SCAs may exhibit significant growth, they may ultimately lead to cyst-related symptom. 41,42 Cyst ablation may be considered for macrocystic SCAs that demonstrate a size increase during follow-up. Branch-duct IPMNs may also be good candidates because they may be unilocular, demonstrate malignant potential, and are highly prevalent in elderly patients. In terms of specific clinical indications, cyst ablation may be considered for the following clinical scenarios: (1) a 2- to 4-cm benign branch-duct IPMN or MCN located in the head or body of the pancreas, (2) a 2- to 4-cm benign branch-duct IPMN or MCN located in the tail of the pancreas in a high-risk surgical patient, (3) a 2- to 4-cm branch-duct IPMN or MCN with high-risk features (nodule or enlarging size) in a high-risk surgical patient. FUTURE PERSPECTIVES EUS-guided cyst ablation is a promising modality that may become an alternative to surgical resection, but should not be performed clinically at this time. Instead, cyst ablation therapy should be performed by using an institutional review board based protocol. For this paradigm shift, some limitations associated with cyst ablation need to be overcome. Procedural modifications may improve the treatment efficacy: (1) a second needle pass in septated cysts, (2) a booster ablation for a large cyst that demonstrates a plateau in response after initial ablation, and (3) maintenance ethanol concentration in the cyst during ethanol lavage. 43 Discovery and development of novel ablative agents that may exert durable activity by using slow-releasing formulations may provide improved ablation rates. 14 Long-term studies over 5 to 10 years after cyst ablation will provide the critical long-term outcomes including prevention of cancer development in premalignant cysts and procedure-related risk profile. The roles of emerging therapeutic modalities including radiofrequency ablation and photodynamic therapy need to be evaluated in future research. In radiofrequency ablation, the heating of the cyst fluid could deliver thermal injury not only directly to the exposed epithelium but also transmission through septations, resulting in complete ablation of septated cysts. In photodynamic therapy, the sensitization of the cyst epithelium by systemic injection of photosensitizer may limit its efficacy. Therefore, the development of locally injectable photosensitizer may enhance its clinical application in cyst ablation. REFERENCES 1. Laffan TA, Horton KM, Klein AP, et al. Prevalence of unsuspected pancreatic cysts on MDCT. AJR Am J Roentgenol 2008;191: de Jong K, Nio CY, Hermans JJ, et al. High prevalence of pancreatic cysts detected by screening magnetic resonance imaging examinations. Clin Gastroenterol Hepatol 2010;8: Brugge WR, Lauwers GY, Sahani D, et al. Cystic neoplasms of the pancreas. N Engl J Med 2004;351: Oh HC, Kim MH, Hwang CY, et al. Cystic lesions of the pancreas: challenging issues in clinical practice. Am J Gastroenterol 2008;103:229-39; quiz 8, Brugge WR. Evaluation of pancreatic cystic lesions with EUS. Gastrointest Endosc 2004;59: Oh HC, Seo DW, Song TJ, et al. Endoscopic ultrasonography-guided ethanol lavage with paclitaxel injection treats patients with pancreatic cysts. Gastroenterology 2011;140: Allen PJ, D Angelica M, Gonen M, et al. A selective approach to the resection of cystic lesions of the pancreas: results from 539 consecutive patients. Ann Surg 2006;244: Goh BK, Tan YM, Cheow PC, et al. Cystic lesions of the pancreas: an appraisal of an aggressive resectional policy adopted at a single institution during 15 years. Am J Surg 2006;192: Galanis C, Zamani A, Cameron JL, et al. Resected serous cystic neoplasms of the pancreas: a review of 158 patients with recommendations for treatment. J Gastrointest Surg 2007;11: Ferrone CR, Correa-Gallego C, Warshaw AL, et al. Current trends in pancreatic cystic neoplasms. Arch Surg 2009;144: Gaujoux S, Brennan MF, Gonen M, et al. Cystic lesions of the pancreas: changes in the presentation and management of 1,424 patients at a single institution over a 15-year time period. J Am Coll Surg 2011;212: ; discussion Aslanian H, Salem RR, Marginean C, et al. EUS-guided ethanol injection of normal porcine pancreas: a pilot study. Gastrointest Endosc 2005;62: Matthes K, Mino-Kenudson M, Sahani DV, et al. Concentrationdependent ablation of pancreatic tissue by EUS-guided ethanol injection. Gastrointest Endosc 2007;65: Matthes K, Mino-Kenudson M, Sahani DV, et al. EUS-guided injection of paclitaxel (OncoGel) provides therapeutic drug concentrations in the porcine pancreas (with video). Gastrointest Endosc 2007;65: Jurgensen C, Schuppan D, Neser F, et al. EUS-guided alcohol ablation of an insulinoma. Gastrointest Endosc 2006;63: Bean WJ. Renal cysts: treatment with alcohol. Radiology 1981;138: Hanna RM, Dahniya MH. Aspiration and sclerotherapy of symptomatic simple renal cysts: value of two injections of a sclerosing agent. AJR Am J Roentgenol 1996;167: Mohsen T, Gomha MA. Treatment of symptomatic simple renal cysts by percutaneous aspiration and ethanol sclerotherapy. BJU Int 2005;96: Larssen TB, Viste A, Jensen DK, et al. Single-session alcohol sclerotherapy in benign symptomatic hepatic cysts. Acta Radiol 1997;38: Yang CF, Liang HL, Pan HB, et al. Single-session prolonged alcoholretention sclerotherapy for large hepatic cysts. AJR Am J Roentgenol 2006;187: Monzani F, Lippi F, Goletti O, et al. Percutaneous aspiration and ethanol sclerotherapy for thyroid cysts. J Clin Endocrinol Metab 1994;78: Bennedbaek FN, Hegedus L. Treatment of recurrent thyroid cysts with ethanol: a randomized double-blind controlled trial. J Clin Endocrinol Metab 2003;88: Del Prete S, Caraglia M, Russo D, et al. Percutaneous ethanol injection efficacy in the treatment of large symptomatic thyroid cystic nodules: ten-year follow-up of a large series. Thyroid 2002;12: Chang KJ, Nguyen PT, Thompson JA, et al. Phase I clinical trial of allogeneic mixed lymphocyte culture (cytoimplant) delivered by endoscopic 532 GASTROINTESTINAL ENDOSCOPY Volume 77, No. 4 :
8 Oh & Brugge EUS-guided pancreatic cyst ablation ultrasound-guided fine-needle injection in patients with advanced pancreatic carcinoma. Cancer 2000;88: Hecht JR, Bedford R, Abbruzzese JL, et al. A phase I/II trial of intratumoral endoscopic ultrasound injection of ONYX-015 with intravenous gemcitabine in unresectable pancreatic carcinoma. Clin Cancer Res 2003;9: Chang KJ, Lee JG, Holcombe RF, et al. Endoscopic ultrasound delivery of an antitumor agent to treat a case of pancreatic cancer. Nat Clin Pract Gastroenterol Hepatol 2008;5: Oh HC, Seo DW, Lee TY, et al. New treatment for cystic tumors of the pancreas: EUS-guided ethanol lavage with paclitaxel injection. Gastrointest Endosc 2008;67: Bean WJ, Rodan BA. Hepatic cysts: treatment with alcohol. AJR Am J Roentgenol 1985;144: Gelczer RK, Charboneau JW, Hussain S, et al. Complications of percutaneous ethanol ablation. J Ultrasound Med 1998;17: Okano A, Hajiro K, Takakuwa H, et al. Alcohol sclerotherapy of hepatic cysts: its effect in relation to ethanol concentration. Hepatol Res 2000; 17: Rowinsky EK, Donehower RC. Paclitaxel (taxol). N Engl J Med 1995;332: Song D, Wientjes MG, Au JL. Bladder tissue pharmacokinetics of intravesical taxol. Cancer Chemother Pharmacol 1997;40: Oh HC, Seo DW, Song TJ. Resolution of a septated pancreatic cyst by booster endoscopic ultrasonography-guided ablation. J Dig Dis 2011; 12: Gan SI, Thompson CC, Lauwers GY, et al. Ethanol lavage of pancreatic cystic lesions: initial pilot study. Gastrointest Endosc 2005;61: DiMaio CJ, DeWitt JM, Brugge WR. Ablation of pancreatic cystic lesions: the use of multiple endoscopic ultrasound-guided ethanol lavage sessions. Pancreas 2011;40: DeWitt J, McGreevy K, Schmidt CM, et al. EUS-guided ethanol versus saline solution lavage for pancreatic cysts: a randomized, double-blind study. Gastrointest Endosc 2009;70: Oh HC, Seo DW, Kim SC, et al. Septated cystic tumors of the pancreas: is it possible to treat them by endoscopic ultrasonography-guided intervention? Scand J Gastroenterol 2009;44: DeWitt J, DiMaio CJ, Brugge WR. Long-term follow-up of pancreatic cysts that resolve radiologically after EUS-guided ethanol ablation. Gastrointest Endosc 2010;72: Oh HC, Seo DW, Kim SC. Portal Vein thrombosis after EUS-guided pancreatic cyst ablation. Dig Dis Sci 2012;57: Fernandez-Del Castillo C. EUS treatment of pancreatic cysts: let s keep the alcohol (and the chemotherapy) locked in the cupboard. Gastroenterology 2011;140: Tseng JF, Warshaw AL, Sahani DV, et al. Serous cystadenoma of the pancreas: tumor growth rates and recommendations for treatment. Ann Surg 2005;242:413-9; discussion Khashab MA, Shin EJ, Amateau S, et al. Tumor size and location correlate with behavior of pancreatic serous cystic neoplasms. Am J Gastroenterol 2011;106: Xu XX, Du Y, Yang HF, et al. CT-guided sclerotherapy with ethanol concentration monitoring for treatment of renal cysts. AJR Am J Roentgenol 2011;196:W Received September 15, Accepted October 29, Current affiliations: Division of Gastroenterology, Chung-Ang University College of Medicine, Seoul, Korea (1), Gastrointestinal Unit, Massachusetts General Hospital, Harvard Medical School, Boston, Massachusetts, USA (2). Reprint requests: William R. Brugge, MD, Gastrointestinal Unit, Massachusetts General Hospital, Blake 452c, 55 Fruit Street, Boston, MA Volume 77, No. 4 : 2013 GASTROINTESTINAL ENDOSCOPY 533
The role of endoscopy in the diagnosis and treatment of cystic pancreatic neoplasms
 The role of endoscopy in the diagnosis and treatment of cystic pancreatic neoplasms CYSTIC LESIONS AND FLUID COLLECTIONS OF THE PANCREAS Their pathology ranges from pseudocysts and pancreatic necrosis
The role of endoscopy in the diagnosis and treatment of cystic pancreatic neoplasms CYSTIC LESIONS AND FLUID COLLECTIONS OF THE PANCREAS Their pathology ranges from pseudocysts and pancreatic necrosis
Evaluation of AGA and Fukuoka Guidelines for EUS and surgical resection of incidental pancreatic cysts
 Evaluation of AGA and Fukuoka Guidelines for EUS and surgical resection of incidental pancreatic cysts Authors Alexander Lee 1, Vivek Kadiyala 2,LindaS.Lee 3 Institutions 1 Texas Digestive Disease Consultants,
Evaluation of AGA and Fukuoka Guidelines for EUS and surgical resection of incidental pancreatic cysts Authors Alexander Lee 1, Vivek Kadiyala 2,LindaS.Lee 3 Institutions 1 Texas Digestive Disease Consultants,
ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts
 ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts Grace H. Elta, MD, FACG 1, Brintha K. Enestvedt, MD, MBA 2, Bryan G. Sauer, MD, MSc, FACG (GRADE Methodologist) 3 and Anne Marie Lennon,
ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts Grace H. Elta, MD, FACG 1, Brintha K. Enestvedt, MD, MBA 2, Bryan G. Sauer, MD, MSc, FACG (GRADE Methodologist) 3 and Anne Marie Lennon,
Types of IPMN. Pancreas Cysts: An Incidental Finding or Harbinger of Malignancy. Cysts: Early Neoplasia. Mucinous Cystic Lesions. EUS-guided FNA EUS
 Pancreas Cysts: An Incidental Finding or Harbinger of Malignancy EUS-guided FNA William R. Brugge,, MD, FACG Professor of Medicine Harvard Medical School Director, GI Endoscopy Unit Massachusetts General
Pancreas Cysts: An Incidental Finding or Harbinger of Malignancy EUS-guided FNA William R. Brugge,, MD, FACG Professor of Medicine Harvard Medical School Director, GI Endoscopy Unit Massachusetts General
Cystic Pancreatic Lesions: Approach to Diagnosis
 Cystic Pancreatic Lesions: Approach to Diagnosis Poster No.: R-0130 Congress: RANZCR-AOCR 2012 Type: Educational Exhibit Authors: A. AGARWAL, R. M. Mendelson; Perth/AU Keywords: Cysts, Biopsy, Endoscopy,
Cystic Pancreatic Lesions: Approach to Diagnosis Poster No.: R-0130 Congress: RANZCR-AOCR 2012 Type: Educational Exhibit Authors: A. AGARWAL, R. M. Mendelson; Perth/AU Keywords: Cysts, Biopsy, Endoscopy,
An Approach to Pancreatic Cysts. Introduction
 An Approach to Pancreatic Cysts Nalini M. Guda, MD Aurora St. Luke s Medical Center, Milwaukee Clinical Adjunct Professor of Medicine, University of Wisconsin School of Medicine and Public Health Introduction
An Approach to Pancreatic Cysts Nalini M. Guda, MD Aurora St. Luke s Medical Center, Milwaukee Clinical Adjunct Professor of Medicine, University of Wisconsin School of Medicine and Public Health Introduction
Pancreatic Cysts. Darius C. Desai, MD FACS St. Luke s University Health Network
 Pancreatic Cysts Darius C. Desai, MD FACS St. Luke s University Health Network None Disclosures Incidence Widespread use of cross sectional imaging Seen in over 2% of patients having abdominal imaging
Pancreatic Cysts Darius C. Desai, MD FACS St. Luke s University Health Network None Disclosures Incidence Widespread use of cross sectional imaging Seen in over 2% of patients having abdominal imaging
Is alcohol required for effective pancreatic cyst ablation? The prospective randomized CHARM trial pilot study
 E63 Is alcohol required for effective pancreatic cyst ablation? The prospective randomized CHARM trial pilot study Authors Matthew T. Moyer 1, Charles E. Dye 1, Setareh Sharzehi 1, Brooke Ancrile 1, Abraham
E63 Is alcohol required for effective pancreatic cyst ablation? The prospective randomized CHARM trial pilot study Authors Matthew T. Moyer 1, Charles E. Dye 1, Setareh Sharzehi 1, Brooke Ancrile 1, Abraham
doi: /den.12628
 Digestive Endoscopy 2016; 28: 599 606 doi: 10.1111/den.12628 Original Article Endoscopic ultrasound-guided ablation of branch-duct intraductal papillary mucinous neoplasms: Feasibility and safety tests
Digestive Endoscopy 2016; 28: 599 606 doi: 10.1111/den.12628 Original Article Endoscopic ultrasound-guided ablation of branch-duct intraductal papillary mucinous neoplasms: Feasibility and safety tests
Original article. Introduction!
 382 Original article Peritoneal seeding in intraductal papillary mucinous neoplasm of the pancreas patients who underwent endoscopic ultrasound-guided fine-needle aspiration: The PIPE Study Authors Won
382 Original article Peritoneal seeding in intraductal papillary mucinous neoplasm of the pancreas patients who underwent endoscopic ultrasound-guided fine-needle aspiration: The PIPE Study Authors Won
Patient History. A 58 year old man presents with a 16 mm cyst in the pancreatic tail. The cyst is unilocular with a thick wall and no mural nodule.
 Case 1 Martha Bishop Pitman, MD Director of Cytopathology Massachusetts General Hospital Associate Professor of Pathology Harvard Medical School Boston, MA Patient History A 58 year old man presents with
Case 1 Martha Bishop Pitman, MD Director of Cytopathology Massachusetts General Hospital Associate Professor of Pathology Harvard Medical School Boston, MA Patient History A 58 year old man presents with
Matthew McCollough, M.D. April 9, 2009 University of Louisville
 Matthew McCollough, M.D. April 9, 2009 University of Louisville List the differential diagnosis for pancreatic cysts Review the epidemiology Illustrate the types of cysts through case discussions Discuss
Matthew McCollough, M.D. April 9, 2009 University of Louisville List the differential diagnosis for pancreatic cysts Review the epidemiology Illustrate the types of cysts through case discussions Discuss
Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases
 Jichi Medical University Journal Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases Noritoshi Mizuta, Hiroshi Noda, Nao Kakizawa, Nobuyuki Toyama,
Jichi Medical University Journal Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases Noritoshi Mizuta, Hiroshi Noda, Nao Kakizawa, Nobuyuki Toyama,
The Pancreas. Basic Anatomy. Endocrine pancreas. Exocrine pancreas. Pancreas vasculature. Islets of Langerhans. Acinar cells Ductal System
 SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
X-ray Corner. Imaging of The Pancreas. Pantongrag-Brown L
 X-ray Corner 125 Imaging of The Pancreas Modern imaging modalities commonly used in pancreas include ultrasound (US), CT, and MRI. Pancreas is a retroperitoneal organ which makes it difficult to visualize
X-ray Corner 125 Imaging of The Pancreas Modern imaging modalities commonly used in pancreas include ultrasound (US), CT, and MRI. Pancreas is a retroperitoneal organ which makes it difficult to visualize
Intraductal papillary mucinous neoplasm (IPMN) is a distinct
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:815 819 Evaluation of the Guidelines for Management of Pancreatic Branch-Duct Intraductal Papillary Mucinous Neoplasm RAYMOND S. TANG,* BENJAMIN WEINBERG,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:815 819 Evaluation of the Guidelines for Management of Pancreatic Branch-Duct Intraductal Papillary Mucinous Neoplasm RAYMOND S. TANG,* BENJAMIN WEINBERG,
Outline. Intraductal Papillary Mucinous Neoplasm (IPMN) Guideline Review 4/6/2017. Case Example Background Classification Histology Guidelines
 Intraductal Papillary Mucinous Neoplasm (IPMN) Guideline Review The Nurse Practitioner Association New York State Capital Region Teaching Day Matthew Warndorf MD Case Example Background Classification
Intraductal Papillary Mucinous Neoplasm (IPMN) Guideline Review The Nurse Practitioner Association New York State Capital Region Teaching Day Matthew Warndorf MD Case Example Background Classification
Management A Guideline Based Approach to the Incidental Pancreatic Cysts. Common Cystic Pancreatic Neoplasms.
 Management 2016 A Guideline Based Approach to the Incidental Pancreatic Cysts ISMRM 2016 Masoom Haider, MD, FRCP(C) Professor of Radiology, University of Toronto Clinician Scientist, Ontario Institute
Management 2016 A Guideline Based Approach to the Incidental Pancreatic Cysts ISMRM 2016 Masoom Haider, MD, FRCP(C) Professor of Radiology, University of Toronto Clinician Scientist, Ontario Institute
Citation American Journal of Surgery, 196(5)
 NAOSITE: Nagasaki University's Ac Title Author(s) Multifocal branch-duct pancreatic i neoplasms Tajima, Yoshitsugu; Kuroki, Tamotsu Amane; Adachi, Tomohiko; Mishima, T Kanematsu, Takashi Citation American
NAOSITE: Nagasaki University's Ac Title Author(s) Multifocal branch-duct pancreatic i neoplasms Tajima, Yoshitsugu; Kuroki, Tamotsu Amane; Adachi, Tomohiko; Mishima, T Kanematsu, Takashi Citation American
Review Article Endoscopic Ultrasound-Guided Radiofrequency Ablation of the Pancreatic Tumors: A Promising Tool in Management of Pancreatic Tumors
 Hindawi Publishing Corporation Canadian Journal of Gastroenterology and Hepatology Volume 2016, Article ID 4189358, 5 pages http://dx.doi.org/10.1155/2016/4189358 Review Article Endoscopic Ultrasound-Guided
Hindawi Publishing Corporation Canadian Journal of Gastroenterology and Hepatology Volume 2016, Article ID 4189358, 5 pages http://dx.doi.org/10.1155/2016/4189358 Review Article Endoscopic Ultrasound-Guided
Role of Endoscopic Ultrasonography in the Diagnosis and Treatment of Cystic Tumors of the Pancreas
 ROUND TABLE Role of Endoscopic Ultrasonography in the Diagnosis and Treatment of Cystic Tumors of the Pancreas Manoop S Bhutani Center for Endoscopic Ultrasound - Center for Endoscopic Research, Training
ROUND TABLE Role of Endoscopic Ultrasonography in the Diagnosis and Treatment of Cystic Tumors of the Pancreas Manoop S Bhutani Center for Endoscopic Ultrasound - Center for Endoscopic Research, Training
Serous Cystic Neoplasm: Do We Have to Wait Till It Causes Trouble?
 Korean Journal of HBP Surgery Case Report Vol. 15, No. 2, May 2011 Serous Cystic Neoplasm: Do We Have to Wait Till It Causes Trouble? Serous cystic neoplasm (SCN) of the pancreas is considered a benign
Korean Journal of HBP Surgery Case Report Vol. 15, No. 2, May 2011 Serous Cystic Neoplasm: Do We Have to Wait Till It Causes Trouble? Serous cystic neoplasm (SCN) of the pancreas is considered a benign
Neoplasias Quisticas del Páncreas
 SEAP -Aproximación Práctica a la Patología Gastrointestinal- Madrid, 26 de mayo, 2006 Neoplasias Quisticas del Páncreas Gregory Y. Lauwers, M.D. Director, Service Massachusetts General Hospital Harvard
SEAP -Aproximación Práctica a la Patología Gastrointestinal- Madrid, 26 de mayo, 2006 Neoplasias Quisticas del Páncreas Gregory Y. Lauwers, M.D. Director, Service Massachusetts General Hospital Harvard
Nonsurgical Management of Asymptomatic Incidental Pancreatic Cysts
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:813 817 Nonsurgical Management of Asymptomatic Incidental Pancreatic Cysts MAOR LAHAV, YAKOV MAOR, BENJAMIN AVIDAN, BEN NOVIS, and SIMON BAR MEIR Department
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:813 817 Nonsurgical Management of Asymptomatic Incidental Pancreatic Cysts MAOR LAHAV, YAKOV MAOR, BENJAMIN AVIDAN, BEN NOVIS, and SIMON BAR MEIR Department
Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma
 Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma Authors: R. Revert Espí, Y. Fernandez Nuñez, I. Carbonell, D. P. Gómez valencia,
Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma Authors: R. Revert Espí, Y. Fernandez Nuñez, I. Carbonell, D. P. Gómez valencia,
Research Article The Changing Spectrum of Surgically Treated Cystic Neoplasms of the Pancreas
 HPB Surgery Volume 2015, Article ID 791704, 7 pages http://dx.doi.org/10.1155/2015/791704 Research Article The Changing Spectrum of Surgically Treated Cystic Neoplasms of the Pancreas Jennifer K. Plichta,
HPB Surgery Volume 2015, Article ID 791704, 7 pages http://dx.doi.org/10.1155/2015/791704 Research Article The Changing Spectrum of Surgically Treated Cystic Neoplasms of the Pancreas Jennifer K. Plichta,
Case 1. Case 1: EUS Report 5/1/2017. Interesting Cases of Pancreatic Masses
 Interesting Cases of Pancreatic Masses Martha Bishop Pitman, MD Professor of Pathology Harvard Medical School Director of Cytopathology Massachusetts General Hospital Boston, MA MASSACHUSETTS GENERAL PHYSICIANS
Interesting Cases of Pancreatic Masses Martha Bishop Pitman, MD Professor of Pathology Harvard Medical School Director of Cytopathology Massachusetts General Hospital Boston, MA MASSACHUSETTS GENERAL PHYSICIANS
Unusual Pancreatic Neoplasms RTC 2/11/2011
 Unusual Pancreatic Neoplasms RTC 2/11/2011 Objectives Intraductal Papillary Mucinous Neoplasm (IPMN) Mucinous Cystic Neoplasm (MCN) Islet Cell Tumors Insulinoma Glucagonoma VIPoma Somatostatinoma Gastrinoma
Unusual Pancreatic Neoplasms RTC 2/11/2011 Objectives Intraductal Papillary Mucinous Neoplasm (IPMN) Mucinous Cystic Neoplasm (MCN) Islet Cell Tumors Insulinoma Glucagonoma VIPoma Somatostatinoma Gastrinoma
Pancreatic Cyst. Introduction. EUS Findings of Pancreatic Cysts. Symposium
 Symposium Symposium II - Pancreatobiliary System : Endoscopic Approach for the Early Detection of Pancreatobiliary Malignancy in Ji Kon Ryu Department of Internal Medicine, Seoul National University College
Symposium Symposium II - Pancreatobiliary System : Endoscopic Approach for the Early Detection of Pancreatobiliary Malignancy in Ji Kon Ryu Department of Internal Medicine, Seoul National University College
The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
Cystic Lesions of the Pancreas: Changes in the Presentation and Management of 1,424 Patients at a Single Institution over a 15-Year Time Period
 Cystic Lesions of the Pancreas: Changes in the Presentation and Management of 1,424 Patients at a Single Institution over a 15-Year Time Period Sébastien Gaujoux, MD, PhD, Murray F Brennan, MD, FACS, Mithat
Cystic Lesions of the Pancreas: Changes in the Presentation and Management of 1,424 Patients at a Single Institution over a 15-Year Time Period Sébastien Gaujoux, MD, PhD, Murray F Brennan, MD, FACS, Mithat
Hepatobiliary and Pancreatic Malignancies
 Hepatobiliary and Pancreatic Malignancies Gareth Eeson MD MSc FRCSC Surgical Oncologist and General Surgeon Kelowna General Hospital Interior Health Consultant, Surgical Oncology BC Cancer Agency Centre
Hepatobiliary and Pancreatic Malignancies Gareth Eeson MD MSc FRCSC Surgical Oncologist and General Surgeon Kelowna General Hospital Interior Health Consultant, Surgical Oncology BC Cancer Agency Centre
A Selective Approach to Resection of Cystic Lesions of the Pancreas: Results From 539 Consecutive Patients
 LETTER TO THE EDITOR A Selective Approach to Resection of Cystic Lesions of the Pancreas: Results From 539 Consecutive Patients To the Editor: I would like to congratulate Dr. Allen and colleagues for
LETTER TO THE EDITOR A Selective Approach to Resection of Cystic Lesions of the Pancreas: Results From 539 Consecutive Patients To the Editor: I would like to congratulate Dr. Allen and colleagues for
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds
 Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
40th European Congress of Cytology Liverpool, UK, 2-5 th October 2016
 40th European Congress of Cytology Liverpool, UK, 2-5 th October 2016 EUS FNA of abdominal organs: An approach to reporting and triage for ancillary testing Date and time: Sunday 2 nd October 2016 15.00-16.30
40th European Congress of Cytology Liverpool, UK, 2-5 th October 2016 EUS FNA of abdominal organs: An approach to reporting and triage for ancillary testing Date and time: Sunday 2 nd October 2016 15.00-16.30
Endoscopic ultrasound-guided ablation of pancreatic cystic neoplasms: ready for prime time?
 REVIEW ARTICLE Annals of Gastroenterology (2019) 32, 1-7 Endoscopic ultrasound-guided ablation of pancreatic cystic neoplasms: ready for prime time? Andrew Ofosu a, Daryl Ramai b, Douglas G. Adler c The
REVIEW ARTICLE Annals of Gastroenterology (2019) 32, 1-7 Endoscopic ultrasound-guided ablation of pancreatic cystic neoplasms: ready for prime time? Andrew Ofosu a, Daryl Ramai b, Douglas G. Adler c The
The Role of Molecular Analysis in the Diagnosis and Surveillance of Pancreatic Cystic Neoplasms
 JOP. J Pancreas (Online) 20 Mar 20; (2):-9. RESEARCH ARTICLE The Role of Molecular Analysis in the Diagnosis and Surveillance of Pancreatic Cystic Neoplasms Megan Winner, Amrita Sethi 2, John M Poneros
JOP. J Pancreas (Online) 20 Mar 20; (2):-9. RESEARCH ARTICLE The Role of Molecular Analysis in the Diagnosis and Surveillance of Pancreatic Cystic Neoplasms Megan Winner, Amrita Sethi 2, John M Poneros
Report of a case of pancreatic hemangioma: A difficult preoperative diagnosis
 www.edoriumjournals.com CASE REPORT PEER REVIEWED OPEN ACCESS Report of a case of pancreatic hemangioma: A difficult preoperative diagnosis AL Hashmi Al Warith, Lagrange Xavier, Fara Régis, Camerlo Antoine
www.edoriumjournals.com CASE REPORT PEER REVIEWED OPEN ACCESS Report of a case of pancreatic hemangioma: A difficult preoperative diagnosis AL Hashmi Al Warith, Lagrange Xavier, Fara Régis, Camerlo Antoine
High Prevalence of Pancreatic Cysts Detected by Screening Magnetic Resonance Imaging Examinations
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:806 811 High Prevalence of Pancreatic Cysts Detected by Screening Magnetic Resonance Imaging Examinations KOEN DE JONG,* C. YUNG NIO, JOHN J. HERMANS, MARCEL
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:806 811 High Prevalence of Pancreatic Cysts Detected by Screening Magnetic Resonance Imaging Examinations KOEN DE JONG,* C. YUNG NIO, JOHN J. HERMANS, MARCEL
Evaluation and Management of Cystic Lesions of the Pancreas: When to Resect, When to Follow and When to Forget
 Evaluation and Management of Cystic Lesions of the Pancreas: When to Resect, When to Follow and When to Forget Randall Brand, MD Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition
Evaluation and Management of Cystic Lesions of the Pancreas: When to Resect, When to Follow and When to Forget Randall Brand, MD Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition
Select problems in cystic pancreatic lesions
 Disclosure Select problems in cystic pancreatic lesions Five Prime Therapeutics shareholder Adicet Bio shareholder Bristol-Meyer Squibb advisory board grace.kim@ucsf.edu Pancreatic cystic lesions Intraductal
Disclosure Select problems in cystic pancreatic lesions Five Prime Therapeutics shareholder Adicet Bio shareholder Bristol-Meyer Squibb advisory board grace.kim@ucsf.edu Pancreatic cystic lesions Intraductal
Paolo Giorgio Arcidiacono MD FASGE
 LOCAL ABLATIVE TREATMENT OF PANCREATIC SOLID LESIONS. WHERE ARE WE NOW? Paolo Giorgio Arcidiacono MD FASGE Pancreato-Biliary Endoscopy & Endosonography Division Pancreas Translational & Clinical Research
LOCAL ABLATIVE TREATMENT OF PANCREATIC SOLID LESIONS. WHERE ARE WE NOW? Paolo Giorgio Arcidiacono MD FASGE Pancreato-Biliary Endoscopy & Endosonography Division Pancreas Translational & Clinical Research
Endoscopic Ultrasonography Clinical Impact. Giancarlo Caletti. Gastroenterologia Università di Bologna. Caletti
 Clinical Impact Giancarlo Gastroenterologia Università di Bologna AUSL di Imola,, Castel S. Pietro Terme (BO) 1982 Indications Diagnosis of Submucosal Tumors (SMT) Staging of Neoplasms Evaluation of Pancreato-Biliary
Clinical Impact Giancarlo Gastroenterologia Università di Bologna AUSL di Imola,, Castel S. Pietro Terme (BO) 1982 Indications Diagnosis of Submucosal Tumors (SMT) Staging of Neoplasms Evaluation of Pancreato-Biliary
Introduction E389. Background and study aims Guidelines for management
 Impact of endoscopic ultrasound on diagnosis and management of presumed mucinous neoplasms when done for pancreatic cyst morphology change on non-invasive surveillance imaging Authors Kamraan Madhani 1,
Impact of endoscopic ultrasound on diagnosis and management of presumed mucinous neoplasms when done for pancreatic cyst morphology change on non-invasive surveillance imaging Authors Kamraan Madhani 1,
Accuracy of CT in predicting malignant potential of cystic pancreatic neoplasms
 HPB, 2008; 10: 483490 ORIGINAL ARTICLE Accuracy of CT in predicting malignant potential of cystic pancreatic neoplasms WILLIAM E. FISHER a, SALLY E. HODGES a, VIVEK YAGNIK b, FANNIE E. MORÓN b, MENG-FEN
HPB, 2008; 10: 483490 ORIGINAL ARTICLE Accuracy of CT in predicting malignant potential of cystic pancreatic neoplasms WILLIAM E. FISHER a, SALLY E. HODGES a, VIVEK YAGNIK b, FANNIE E. MORÓN b, MENG-FEN
Cystic lesions of the pancreas
 REVIEW ARTICLE Annals of Gastroenterology (2016) 29, 155-161 Cystic lesions of the pancreas Ioannis Karoumpalis a, Dimitrios K. Christodoulou b General Hospital of Athens G. Gennimatas, Athens; University
REVIEW ARTICLE Annals of Gastroenterology (2016) 29, 155-161 Cystic lesions of the pancreas Ioannis Karoumpalis a, Dimitrios K. Christodoulou b General Hospital of Athens G. Gennimatas, Athens; University
Endoscopic Ultrasound Guided Trucut Biopsy of the Cyst Wall for Diagnosing Cystic Pancreatic Tumors
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:974 979 Endoscopic Ultrasound Guided Trucut Biopsy of the Cyst Wall for Diagnosing Cystic Pancreatic Tumors MICHAEL J. LEVY,* THOMAS C. SMYRK, RAGHURAM P.
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:974 979 Endoscopic Ultrasound Guided Trucut Biopsy of the Cyst Wall for Diagnosing Cystic Pancreatic Tumors MICHAEL J. LEVY,* THOMAS C. SMYRK, RAGHURAM P.
CASE 01 LA Path Slide Seminar 13 March, 08. Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center
 CASE 01 LA Path Slide Seminar 13 March, 08 Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center Clinical History 60 year old male presented with obstructive jaundice
CASE 01 LA Path Slide Seminar 13 March, 08 Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center Clinical History 60 year old male presented with obstructive jaundice
Fine-Needle Aspiration Biopsy of Solid Pancreatic Masses: Comparison of CT and Endoscopic Sonography Guidance
 Comparison of Guidance Techniques for Pancreatic Mass Biopsy Abdominal Imaging Original Research A C D E M N E U T R Y L I A M C A I G O F I N G Sukru Mehmet Erturk 1 Koenraad J. Mortelé 1 Kemal Tuncali
Comparison of Guidance Techniques for Pancreatic Mass Biopsy Abdominal Imaging Original Research A C D E M N E U T R Y L I A M C A I G O F I N G Sukru Mehmet Erturk 1 Koenraad J. Mortelé 1 Kemal Tuncali
Diagnosis and Management of Cystic Pancreatic Lesions
 Gastrointestinal Imaging Best Practices/Review Sahani et al. Cystic Pancreatic Lesions Gastrointestinal Imaging Best Practices/Review Dushyant V. Sahani 1 Avinash Kambadakone 1 Michael Macari 2 Noaki Takahashi
Gastrointestinal Imaging Best Practices/Review Sahani et al. Cystic Pancreatic Lesions Gastrointestinal Imaging Best Practices/Review Dushyant V. Sahani 1 Avinash Kambadakone 1 Michael Macari 2 Noaki Takahashi
Esophageal seeding after endoscopic ultrasound-guided fine-needle aspiration of a mediastinal tumor
 Esophageal seeding after endoscopic ultrasound-guided fine-needle aspiration of a mediastinal tumor Authors Kensuke Yokoyama 1,JunUshio 1,NorikatsuNumao 1, Kiichi Tamada 1, Noriyoshi Fukushima 2, Alan
Esophageal seeding after endoscopic ultrasound-guided fine-needle aspiration of a mediastinal tumor Authors Kensuke Yokoyama 1,JunUshio 1,NorikatsuNumao 1, Kiichi Tamada 1, Noriyoshi Fukushima 2, Alan
Pancreatic Cystic Neoplasms: Guidelines and beyond
 Pancreatic Cystic Neoplasms: Guidelines and beyond Kenneth J. Chang, MD, FACG, FASGE Executive Director, Comprehensive Digestive Disease Center Professor and Chief, Gastroenterology Vincent & Anna Kong
Pancreatic Cystic Neoplasms: Guidelines and beyond Kenneth J. Chang, MD, FACG, FASGE Executive Director, Comprehensive Digestive Disease Center Professor and Chief, Gastroenterology Vincent & Anna Kong
Intraductal Papillary Mucinous Neoplasms: We Still Have a Way to Go! Francesco M. Serafini, MD, FACS
 Intraductal Papillary Mucinous Neoplasms: We Still Have a Way to Go! Francesco M. Serafini, MD, FACS Brooklyn VAMC September 21 st GI Grand Rounds - What is it? - Clinical entity that has emerged from
Intraductal Papillary Mucinous Neoplasms: We Still Have a Way to Go! Francesco M. Serafini, MD, FACS Brooklyn VAMC September 21 st GI Grand Rounds - What is it? - Clinical entity that has emerged from
Diagnostic performance of endoscopic ultrasound-guided fine-needle aspiration in pancreatic lesions
 European Review for Medical and Pharmacological Sciences 2018; 22: 1397-1401 Diagnostic performance of endoscopic in pancreatic lesions Q.-M. WU 1, Y.-N. GUO 1, Y.-Q. XU 1 Digestive Department of Beijing
European Review for Medical and Pharmacological Sciences 2018; 22: 1397-1401 Diagnostic performance of endoscopic in pancreatic lesions Q.-M. WU 1, Y.-N. GUO 1, Y.-Q. XU 1 Digestive Department of Beijing
A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY
 A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center Welcome The St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center is a leader
A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center Welcome The St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center is a leader
Surgical management and results for cystic neoplasms of pancreas
 Korean J Hepatobiliary Pancreat Surg 2013;17:118-125 Original Article Surgical management and results for cystic neoplasms of pancreas Kyung Won Han 1, Ryun Ha 1, Kun Kuk Kim 1, Jung Nam Lee 1, Yeon Suk
Korean J Hepatobiliary Pancreat Surg 2013;17:118-125 Original Article Surgical management and results for cystic neoplasms of pancreas Kyung Won Han 1, Ryun Ha 1, Kun Kuk Kim 1, Jung Nam Lee 1, Yeon Suk
Benign nodular thyroid disease is common, and 15% 25% of
 CLINICAL REPORT HEAD & NECK Combination Therapy Consisting of Ethanol and Radiofrequency Ablation for Predominantly Cystic Thyroid Nodules H.M. Yoon, J.H. Baek, J.H. Lee, E.J. Ha, J.K. Kim, J.H. Yoon,
CLINICAL REPORT HEAD & NECK Combination Therapy Consisting of Ethanol and Radiofrequency Ablation for Predominantly Cystic Thyroid Nodules H.M. Yoon, J.H. Baek, J.H. Lee, E.J. Ha, J.K. Kim, J.H. Yoon,
Contrast-Enhanced Ultrasonograpic Findings in Pancreatic Tumors
 Int. J. Med. Sci. 2008, 5 203 Short Research Communication International Journal of Medical Sciences ISSN 1449-1907 www.medsci.org 2008 5(4):203-208 Ivyspring International Publisher. All rights reserved
Int. J. Med. Sci. 2008, 5 203 Short Research Communication International Journal of Medical Sciences ISSN 1449-1907 www.medsci.org 2008 5(4):203-208 Ivyspring International Publisher. All rights reserved
CT 101 :Pancreas and Spleen
 CT 101 :Pancreas and Spleen Shikha Khullar,, MD, MPH Division of Radiology University of South Alabama The Pancreas Normal Pancreas 3 Phase Pancreatic CT Non contrast Arterial phase : 30-35 35 second
CT 101 :Pancreas and Spleen Shikha Khullar,, MD, MPH Division of Radiology University of South Alabama The Pancreas Normal Pancreas 3 Phase Pancreatic CT Non contrast Arterial phase : 30-35 35 second
Appendix 5. EFSUMB Newsletter. Gastroenterological Ultrasound
 EFSUMB Newsletter 87 Examinations should encompass the full range of pathological conditions listed below A log book listing the types of examinations undertaken should be kept Training should usually
EFSUMB Newsletter 87 Examinations should encompass the full range of pathological conditions listed below A log book listing the types of examinations undertaken should be kept Training should usually
Cystic lesions of the pancreas are composed of a broad
 2C: Pancreaticobiliary Problems cystic lesions in the pancreas William R. Brugge, MD, FACG Cystic lesions of the pancreas are composed of a broad range of neoplastic cysts and inflammatory pseudocysts.
2C: Pancreaticobiliary Problems cystic lesions in the pancreas William R. Brugge, MD, FACG Cystic lesions of the pancreas are composed of a broad range of neoplastic cysts and inflammatory pseudocysts.
CASE REPORT. Abstract. Introduction. Case Report
 CASE REPORT Branch Duct Intraductal Papillary Mucinous Neoplasms of the Pancreas Involving Type 1 Localized Autoimmune Pancreatitis with Normal Serum IgG4 Levels Successfully Diagnosed by Endoscopic Ultrasound-guided
CASE REPORT Branch Duct Intraductal Papillary Mucinous Neoplasms of the Pancreas Involving Type 1 Localized Autoimmune Pancreatitis with Normal Serum IgG4 Levels Successfully Diagnosed by Endoscopic Ultrasound-guided
Appendix 9: Endoscopic Ultrasound in Gastroenterology
 Appendix 9: Endoscopic Ultrasound in Gastroenterology This curriculum is intended for clinicians who perform endoscopic ultrasonography (EUS) in gastroenterology. It includes standards for theoretical
Appendix 9: Endoscopic Ultrasound in Gastroenterology This curriculum is intended for clinicians who perform endoscopic ultrasonography (EUS) in gastroenterology. It includes standards for theoretical
Video Microscopy Tutorial 19
 Video Microscopy Tutorial 19 EUS FNA of Pancreatic Cysts Martha Pitman, MD There are no disclosures necessary. EUS-FNA of Pancreatic Cysts Martha Bishop Pitman, M.D. Massachusetts General Hospital Harvard
Video Microscopy Tutorial 19 EUS FNA of Pancreatic Cysts Martha Pitman, MD There are no disclosures necessary. EUS-FNA of Pancreatic Cysts Martha Bishop Pitman, M.D. Massachusetts General Hospital Harvard
Endoscopic ultrasound-guided through-the-needle microforceps biopsy in the evaluation of pancreatic cystic lesions: a multicenter study
 Endoscopic ultrasound-guided through-the-needle microforceps biopsy in the evaluation of pancreatic cystic lesions: a multicenter study Authors Dennis Yang 1, Jason B. Samarasena 2,LaithH.Jamil 3, Kenneth
Endoscopic ultrasound-guided through-the-needle microforceps biopsy in the evaluation of pancreatic cystic lesions: a multicenter study Authors Dennis Yang 1, Jason B. Samarasena 2,LaithH.Jamil 3, Kenneth
Mural nodules are predictors of malignancy in mucusproducing. Histologic and Imaging Features of Mural Nodules in Mucinous Pancreatic Cysts.
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:192 198 Histologic and Imaging Features of Mural Nodules in Mucinous Pancreatic Cysts NING ZHONG,*, LIZHI ZHANG, NAOKI TAKAHASHI, VLADISLAV SHALMIYEV,*
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:192 198 Histologic and Imaging Features of Mural Nodules in Mucinous Pancreatic Cysts NING ZHONG,*, LIZHI ZHANG, NAOKI TAKAHASHI, VLADISLAV SHALMIYEV,*
Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review
 Review Article Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review Min-Jie Yang, Su Li, Yong-Guang Liu, Na Jiao, Jing-Shan Gong Department of Radiology, Shenzhen
Review Article Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review Min-Jie Yang, Su Li, Yong-Guang Liu, Na Jiao, Jing-Shan Gong Department of Radiology, Shenzhen
Endoscopic Ultrasonography Assessment for Ampullary and Bile Duct Malignancy
 Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
ORIGINAL ARTICLE. The Impact of Laparoscopy and Laparoscopic Ultrasound on the Management of Pancreatic
 ORIGINAL ARTICLE The Impact of Laparoscopy and Laparoscopic Ultrasound on the Management of Pancreatic Cystic Lesions Pinhas P. Schachter, MD; Yona Avni, MD; Gabriela Gvirtz, MD; Ada Rosen, MD; Abraham
ORIGINAL ARTICLE The Impact of Laparoscopy and Laparoscopic Ultrasound on the Management of Pancreatic Cystic Lesions Pinhas P. Schachter, MD; Yona Avni, MD; Gabriela Gvirtz, MD; Ada Rosen, MD; Abraham
Endoscopic ultrasonography in suspected pancreatic malignancy and indecisive CT
 O r i g i n a l a r t i c l e Endoscopic ultrasonography in suspected pancreatic malignancy and indecisive CT O.L.M. Meijer 1, R.K. Weersma 1, E.J. van der Jagt 2, H.M. van Dullemen 1 * Departments of
O r i g i n a l a r t i c l e Endoscopic ultrasonography in suspected pancreatic malignancy and indecisive CT O.L.M. Meijer 1, R.K. Weersma 1, E.J. van der Jagt 2, H.M. van Dullemen 1 * Departments of
PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies. Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels
 PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels 1. Diagnosis. 2. Multidisciplinary approach. 3. Therapeutic planning. 4. How? 5. Follow-up
PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels 1. Diagnosis. 2. Multidisciplinary approach. 3. Therapeutic planning. 4. How? 5. Follow-up
Giant pancreatic mucinous cystadenoma with malignant transformation
 Case Report Brunei Int Med J. 2014; 10 (3): 177-182 Giant pancreatic mucinous cystadenoma with malignant transformation Jerica CHAI 1, Vui Heng CHONG 2, Ian BICKLE 1 1 Department of Radiology and 2 Department
Case Report Brunei Int Med J. 2014; 10 (3): 177-182 Giant pancreatic mucinous cystadenoma with malignant transformation Jerica CHAI 1, Vui Heng CHONG 2, Ian BICKLE 1 1 Department of Radiology and 2 Department
Review Article Epidemiology, Diagnosis, and Management of Cystic Lesions of the Pancreas
 Gastroenterology Research and Practice Volume 2012, Article ID 147465, 8 pages doi:10.1155/2012/147465 Review Article Epidemiology, Diagnosis, and Management of Cystic Lesions of the Pancreas Koen de Jong,
Gastroenterology Research and Practice Volume 2012, Article ID 147465, 8 pages doi:10.1155/2012/147465 Review Article Epidemiology, Diagnosis, and Management of Cystic Lesions of the Pancreas Koen de Jong,
Mucin-Producing Neoplasms of the Pancreas: An Analysis of Distinguishing Clinical and Epidemiologic Characteristics
 Mucin-Producing Neoplasms of the Pancreas: An Analysis of Distinguishing Clinical and Epidemiologic Characteristics The Harvard community has made this article openly available. Please share how this access
Mucin-Producing Neoplasms of the Pancreas: An Analysis of Distinguishing Clinical and Epidemiologic Characteristics The Harvard community has made this article openly available. Please share how this access
Intraductal Papillary Mucinous Neoplasms: The Bologna Experience
 ORIGINAL ARTICLE INTRADUCTAL PAPILLARY MUCINOUS NEOPLASM Intraductal Papillary Mucinous Neoplasms: The Bologna Experience Riccardo Casadei 1, Carlo Alberto Pacilio 1, Claudio Ricci 1, Giovanni Taffurelli
ORIGINAL ARTICLE INTRADUCTAL PAPILLARY MUCINOUS NEOPLASM Intraductal Papillary Mucinous Neoplasms: The Bologna Experience Riccardo Casadei 1, Carlo Alberto Pacilio 1, Claudio Ricci 1, Giovanni Taffurelli
Endoscopic Management of Barrett s Esophagus
 Endoscopic Management of Barrett s Esophagus Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Barrett s Esophagus Consequence of chronic GERD Mean
Endoscopic Management of Barrett s Esophagus Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Barrett s Esophagus Consequence of chronic GERD Mean
ORIGINAL ARTICLE. Abstract. Introduction
 ORIGINAL ARTICLE Annals of Gastroenterology (2015) 28, 1-8 Pancreatic cysts suspected to be branch duct intraductal papillary mucinous neoplasm without concerning features have low risk for development
ORIGINAL ARTICLE Annals of Gastroenterology (2015) 28, 1-8 Pancreatic cysts suspected to be branch duct intraductal papillary mucinous neoplasm without concerning features have low risk for development
Serous Cystadenomas Follow a Benign and Asymptomatic Course and Do Not Present a Significant Size Change During Follow-Up
 REVISTA DE INVESTIGACIÓN CLÍNICA Contents available at PubMed www.clinicalandtranslationalinvestigation.com Rev Inves Clin. 2015;67:344-9 PERMANYER BRIEF COMMUNICATIONS Serous Cystadenomas Follow a Benign
REVISTA DE INVESTIGACIÓN CLÍNICA Contents available at PubMed www.clinicalandtranslationalinvestigation.com Rev Inves Clin. 2015;67:344-9 PERMANYER BRIEF COMMUNICATIONS Serous Cystadenomas Follow a Benign
Role of Imaging Methods in Diagnosis of Acute Pancreatitis. Válek V. Radiologická klinika, FN Brno a LF MU v Brně
 Role of Imaging Methods in Diagnosis of Acute Pancreatitis Válek V. Radiologická klinika, FN Brno a LF MU v Brně New Classification: Acute Pancreatitis 2007 revision of Atlanta classification and definitions
Role of Imaging Methods in Diagnosis of Acute Pancreatitis Válek V. Radiologická klinika, FN Brno a LF MU v Brně New Classification: Acute Pancreatitis 2007 revision of Atlanta classification and definitions
Patient with incidental pancreatic cyst
 Clinical problem Diego Aponte M, MD 1 1 Internal Medicine Gastroenterology Specialist. Gastroenterology Academic Coordinator for Graduate Level. Fundación Sanitas. Bogotá, Colombia.... Received: 07-09-10
Clinical problem Diego Aponte M, MD 1 1 Internal Medicine Gastroenterology Specialist. Gastroenterology Academic Coordinator for Graduate Level. Fundación Sanitas. Bogotá, Colombia.... Received: 07-09-10
Cystic pancreatic lesions A proposal for a network approach. Chris Briggs Consultant HPB Surgeon Peninsula HPB Unit Derriford Hospital, Plymouth
 Cystic pancreatic lesions A proposal for a network approach Chris Briggs Consultant HPB Surgeon Peninsula HPB Unit Derriford Hospital, Plymouth Aims Brief overview of cystic pancreatic lesions International
Cystic pancreatic lesions A proposal for a network approach Chris Briggs Consultant HPB Surgeon Peninsula HPB Unit Derriford Hospital, Plymouth Aims Brief overview of cystic pancreatic lesions International
Killing Tumors with Scans Not Scalpels: Kidney Cancer Ablation. Basics. What is Percutaneous Ablation? Where are your kidneys?
 Killing Tumors with Scans Not Scalpels: Kidney Cancer Ablation Ronald J. Zagoria, M.D. UCSF Professor and Vice Chair Abdominal Imaging Section Chief Basics Where are your kidneys? What is ablation? Facts
Killing Tumors with Scans Not Scalpels: Kidney Cancer Ablation Ronald J. Zagoria, M.D. UCSF Professor and Vice Chair Abdominal Imaging Section Chief Basics Where are your kidneys? What is ablation? Facts
EUS guided liver biopsy
 EUS guided liver biopsy Abdul El Chafic, MD Ochsner Medical Center Department of Gastroenterology Section of Advanced endoscopy Disclosure/ Disclaimer I have a financial interest/arrangement of affiliation
EUS guided liver biopsy Abdul El Chafic, MD Ochsner Medical Center Department of Gastroenterology Section of Advanced endoscopy Disclosure/ Disclaimer I have a financial interest/arrangement of affiliation
Public Statement: Medical Policy Statement:
 Medical Policy Title: Radiofrequency Ablation ARBenefits Approval: 10/26/2011 of Tumors Effective Date: 01/01/2012 Document: ARB0300 Revision Date: Code(s): 20982 Ablation, bone tumor(s), radiofrequency,
Medical Policy Title: Radiofrequency Ablation ARBenefits Approval: 10/26/2011 of Tumors Effective Date: 01/01/2012 Document: ARB0300 Revision Date: Code(s): 20982 Ablation, bone tumor(s), radiofrequency,
Performance of novel tissue harmonic echo imaging using endoscopic ultrasound for pancreatic diseases
 E Performance of novel tissue harmonic echo imaging using endoscopic ultrasound for pancreatic diseases Authors Kazuyuki Matsumoto, *, Akio Katanuma, *, Hiroyuki Maguchi, Kuniyuki Takahashi, Manabu Osanai,
E Performance of novel tissue harmonic echo imaging using endoscopic ultrasound for pancreatic diseases Authors Kazuyuki Matsumoto, *, Akio Katanuma, *, Hiroyuki Maguchi, Kuniyuki Takahashi, Manabu Osanai,
X-Ray Corner. Imaging Approach to Cystic Liver Lesions. Pantongrag-Brown L. Solitary cystic liver lesions. Hepatic simple cyst (Figure 1)
 THAI J 136 Imaging Approach to Cystic Liver Lesions GASTROENTEROL 2013 X-Ray Corner Imaging Approach to Cystic Liver Lesions Pantongrag-Brown L Cystic liver lesions are common findings in daily practice
THAI J 136 Imaging Approach to Cystic Liver Lesions GASTROENTEROL 2013 X-Ray Corner Imaging Approach to Cystic Liver Lesions Pantongrag-Brown L Cystic liver lesions are common findings in daily practice
Gastrointestinal Intervention
 Gastrointest Interv 2013; 2:17 23 Contents lists available at SciVerse ScienceDirect Gastrointestinal Intervention journal homepage: www.gi-intervention.org Review Article EUS-guided interventional management
Gastrointest Interv 2013; 2:17 23 Contents lists available at SciVerse ScienceDirect Gastrointestinal Intervention journal homepage: www.gi-intervention.org Review Article EUS-guided interventional management
PersPeCTIves. Controversies in the management of pancreatic ipmn. Masao Tanaka
 PersPeCTIves OpiniOn Controversies in the management of pancreatic ipmn Masao Tanaka Abstract Although considerable progress has been made in our understanding of intraductal papillary mucinous neoplasm
PersPeCTIves OpiniOn Controversies in the management of pancreatic ipmn Masao Tanaka Abstract Although considerable progress has been made in our understanding of intraductal papillary mucinous neoplasm
Liver Cancer (Hepatocellular Carcinoma or HCC) Overview
 Liver Cancer (Hepatocellular Carcinoma or HCC) Overview Recent advances in liver cancer care seek to address the rising incidence of liver cancer, which has steadily increased over the past three decades.
Liver Cancer (Hepatocellular Carcinoma or HCC) Overview Recent advances in liver cancer care seek to address the rising incidence of liver cancer, which has steadily increased over the past three decades.
performed to help sway the clinician in what the appropriate diagnosis is, which can substantially alter the treatment of management.
 Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Imaging in gastric cancer
 Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Cystic Disease of the Liver Work Up and Management. Louis Ferrari MD, PGY 3 6/9/16 SUNY Downstate Medical Center
 Cystic Disease of the Liver Work Up and Management Louis Ferrari MD, PGY 3 6/9/16 SUNY Downstate Medical Center The Case 73F presents to clinic after diagnostic laparoscopy at OSH. Known liver mass for
Cystic Disease of the Liver Work Up and Management Louis Ferrari MD, PGY 3 6/9/16 SUNY Downstate Medical Center The Case 73F presents to clinic after diagnostic laparoscopy at OSH. Known liver mass for
Surgical outcomes of multifocal branch duct intraductal papillary mucinous neoplasms of pancreas
 Korean J Hepatobiliary Pancreat Surg 2014;18:152-158 http://dx.doi.org/10.14701/kjhbps.2014.18.4.152 Original Article Surgical outcomes of multifocal branch duct intraductal papillary mucinous neoplasms
Korean J Hepatobiliary Pancreat Surg 2014;18:152-158 http://dx.doi.org/10.14701/kjhbps.2014.18.4.152 Original Article Surgical outcomes of multifocal branch duct intraductal papillary mucinous neoplasms
Solid Pancreatic Tumors with Unilocular Cyst-Like Appearance on CT: Differentiation from Unilocular Cystic Tumors Using CT
 Original Article Gastrointestinal Imaging http://dx.doi.org/10.3348/kjr.2014.15.6.704 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2014;15(6):704-711 Solid Pancreatic Tumors with Unilocular Cyst-Like
Original Article Gastrointestinal Imaging http://dx.doi.org/10.3348/kjr.2014.15.6.704 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2014;15(6):704-711 Solid Pancreatic Tumors with Unilocular Cyst-Like
Gemstone Spectral Imaging quantifies lesion characteristics for a confident diagnosis
 GE Healthcare Gemstone Spectral Imaging quantifies lesion characteristics for a confident diagnosis CT clinical case study lesion characterization Desiree Morgan, MD Vice Chair of Clinical Research Professor
GE Healthcare Gemstone Spectral Imaging quantifies lesion characteristics for a confident diagnosis CT clinical case study lesion characterization Desiree Morgan, MD Vice Chair of Clinical Research Professor
ORIGINAL ARTICLE. Fate of the Pancreatic Remnant After Resection for an Intraductal Papillary Mucinous Neoplasm
 ONLINE FIRST ORIGINAL ARTICLE Fate of the Pancreatic Remnant After Resection for an Intraductal Papillary Mucinous Neoplasm A Longitudinal Level II Cohort Study Toshiyuki Moriya, MD, PhD; L. William Traverso,
ONLINE FIRST ORIGINAL ARTICLE Fate of the Pancreatic Remnant After Resection for an Intraductal Papillary Mucinous Neoplasm A Longitudinal Level II Cohort Study Toshiyuki Moriya, MD, PhD; L. William Traverso,
Wiriyaporn Ridtitid, John M.DeWitt, C. Max Schmidt, Alexandra Roch, Jennifer Schaffter Stuart, Stuart Sherman, Mohammad A.
 Management of Branch duct Intraductal Papillary Mucinous Neoplasms: A Large Single Center Study to Assess Predictors of Malignancy and Long Term Outcomes Wiriyaporn Ridtitid, John M.DeWitt, C. Max Schmidt,
Management of Branch duct Intraductal Papillary Mucinous Neoplasms: A Large Single Center Study to Assess Predictors of Malignancy and Long Term Outcomes Wiriyaporn Ridtitid, John M.DeWitt, C. Max Schmidt,
Anatomy of the biliary tract
 Harvard-MIT Division of Health Sciences and Technology HST.121: Gastroenterology, Fall 2005 Instructors: Dr. Jonathan Glickman Anatomy of the biliary tract Figure removed due to copyright reasons. Biliary
Harvard-MIT Division of Health Sciences and Technology HST.121: Gastroenterology, Fall 2005 Instructors: Dr. Jonathan Glickman Anatomy of the biliary tract Figure removed due to copyright reasons. Biliary
Autoimmune Pancreatitis: A Great Imitator
 Massachusetts General Hospital Harvard Medical School Autoimmune Pancreatitis: A Great Imitator Dushyant V Sahani MD dsahani@partners.org Autoimmune Pancreatitis: Learning Objectives Clinical manifestations
Massachusetts General Hospital Harvard Medical School Autoimmune Pancreatitis: A Great Imitator Dushyant V Sahani MD dsahani@partners.org Autoimmune Pancreatitis: Learning Objectives Clinical manifestations
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
