Clinical and electrophysiological evaluation of dysphagia in myasthenia gravis
|
|
|
- Henry French
- 5 years ago
- Views:
Transcription
1 848 Department of Clinical Neurophysiology C Ertekin Department of Neurology, Ege University Medical School Hospital, Bornova, I~zmir, Turkey N Yüceyar I~ Aydoǧdu Correspondence to: Professor Cumhur Ertekı n, 1357 SOK, No:1 Da:10 Nilhan Apt, Alsancak, I~zmı r, Turkey. Telephone ; fax Received 10 October 1997 and in final form 2 June 1998 Accepted 15 June 1998 Clinical and electrophysiological evaluation of dysphagia in myasthenia gravis Cumhur Ertekin, Nur Yüceyar, I~brahim Aydoǧdu J Neurol Neurosurg Psychiatry 1998;65: Abstract Objective To evaluate dysphagia at the oropharyngeal stage of swallowing and to determine the pathophysiological mechanisms of dysphagia in patients with myasthenia gravis. Methods Fifteen patients with myasthenia gravis with dysphagia and 10 patients without dysphagia were investigated by a combined electrophysiological and mechanical method described previously. Laryngeal movements were detected by a piezoelectric transducer and the related submental EMG (SM-EMG) and sometimes the EMG of cricopharyngeal muscle of the upper esophageal sphincter (CP- EMG) were recorded during dry or wet swallowing. The results of these electrophysiological variables were compared with those of normal age matched control subjects. Results In patients with myasthenia gravis with dysphagia, it was found that the time necessary for the larynx to remain in its superior position during swallowing and swallowing variability in successive swallows increased significantly compared with normal subjects and with patients with myasthenia gravis without dysphagia. The total duration of SM-EMG activity was also prolonged in both groups but more severely in the dysphagic patients. Electromyographic activity of the CP sphincter was found to be normal in the dysphagic patients investigated. All the patients with myasthenia gravis with dysphagia had pathological dysphagia limits (<20 ml water) whereas other patients except two, were within normal limits. Conclusions Because the electrophysiological variables related to oropharyngeal swallowing were prolonged even in patients with myasthenia gravis without dysphagia, it is concluded that the submental and laryngeal elevators are involved subclinically in myasthenia gravis and, because of compensating mechanisms, the patient may not be dysphagic. As the CP-EMG behaviour was found to be normal, a coordination disorder between normal CP sphincter muscle and the avected striated muscles of the laryngeal elevators may be one of the reasons for dysphagia in myasthenia gravis. This method also made it possible to investigate the myasthenic involvement in the laryngeal elevators that cannot be evaluated by other electrophysiological methods in myasthenia gravis. (J Neurol Neurosurg Psychiatry 1998;65: ) Keywords: myasthenia gravis; dysphagia; dysphagia limit; electrophysiology of swallowing; crycopharyngeal muscle; submental EMG In many patients with myasthenia gravis, fatiguability is usually first seen in the ocular muscles, but as soon as the bulbar muscles are involved, dysphagia occurs together with other bulbar muscle involvement. It has been reported 1 that 30% of 175 myasthenic patients had oral, pharyngeal, or laryngeal symptoms and 15% of them had dysphagia. However, in a larger patient population, diyculty in swallowing was reported to be the initial symptom in 6% of 1487 patients with myasthenia gravis and during the first month after the onset of disease, 15% of them had bulbar or oculobulbar involvement. 2 The prominence of dysphagia together with dysarthria and dysphonia may give rise to an erroneous diagnosis of primary bulbar involvement due to some other causes. If patients with bulbar myasthenia do not exhibit ptosis or diplopia which may be commonly associated with pharyngeal involvement, correct diagnosis can be diycult, and invasive laryngoscopical and fluoroscopical studies are sometimes made by ear, nose, and throat specialists or gastroenterologists in patients with pure bulbar symptoms or in patients with sole manifestations of dysphagia The mechanism and consequences of dysphagia in myasthenia gravis have been investigated by radiological methods Manometric studies have been also performed. 8 9 In this study, the pathophysiology of dysphagia was investigated by electrophysiological methods described previously Patients and methods Twenty five patients with myasthenia gravis were studied. Their clinical diagnoses were supported by EMG, repetitive nerve stimulation (decrement test), and single fibre EMG (jitter). Clinical responsiveness to anticholinesterase treatment was also important to support the diagnosis of the disorder. Acetylcholine receptor antibodies have not been measured. Mean age of patients was 44.2 (SD 13.7, range years). Fourteen were women. Clinical features of all patients are listed in table 1. The term dysphagia was applied when there were abnormal insistent symptoms (nasal regurgitation, the frequent feeling of
2 Dysphagia in myasthenia gravis 849 Table 1 Clinical features of patients with myasthenia gravis Patient Age/ sex Duration of MG(y) cleaning up of the mouth, the feeling of something being stuck behind the sternum) obtained from their questionaire and abnormal signs (cough during swallowing, accumulation of saliva in the mouth, wet voice after swallowing, palatal paresis) closely related with swallowing disorder. The patients with only uncertain symptoms but lacking any objective signs that could be related to swallowing were not considered to be dysphagic. Therefore, patients with myasthenia gravis were divided into two groups according to presentation of dysphagia at the time of investigation: (1) Dysphagia was either a prominent complaint (patients 1 5 in table 1) or had been present until anticholinesterase treatment before they were investigated in this study (patients 6 15 in table 1). These patients were found to be mildly dysphagic on clinical evaluation. (2) Patients in the second group did not have abnormal signs and symptoms related to dysphagia either at the time of investigation or Duration of dysphagia (months) Initial symptomatology Present symptomatology* 1 40/F 1 3 Ocular Ocular+bulbar 2 46/M 5/12 5 Bulbar Bulbar 3 36/M 2/12 2 Ocular+bulbar Ocular+bulbar 4 70/F 1 24 Generalised Generalised 5 34/F Ocular+bulbar Generalised 6 53/M 6/12 6 Ocular+bulbar Ocular+bulbar 7 55/M 1 6 Ocular+bulbar Ocular+bulbar 8 52/M 5 1 Ocular+bulbar generalised 9 76/M 3 2 Ocular Ocular+bulbar 10 32/F 4 3 Generalised Generalised 11 48/F Generalised Generalised 12 28/F 1 2 Bulbar Bulbar 13 53/M 9 12 Generalised Generalised 14 30/F 10 3 Ocular Generalised 15 34/F Bulbar Bulbar 16 50/M 3/12 None Ocular Ocular+bulbar 17 27/F 5 None Generalised Generalised 18 69/M 1.5 None ocular Generalised 19 32/F 3 None Generalised Generalised 20 25/F 1 None Ocular Generalised 21 49/F 1 None Ocular Ocular+bulbar 22 42/F 12 None Ocular+bulbar Ocular+bulbar 23 39/M 2 None Generalised Generalised 24 47/M 8 None Ocular Generalised 25 39/M 7/12 None Generalised Generalised *Clinical features of patients with myasthenia gravis; either dysphagic or not at the time of the investigation; none=without dysphagia. Table 2 The results of the questionnaire and clinical findings of patients with myasthesia gravis with dysphagia (A) (B) % (n=15) Complaints: Cough during swallowing 100 Feeling of being stuck behind the sternum 90 Nasal regurgitation 86 Feeling of the clean up of mouth 72 DiYculties in bolus formation and control 63 Abnormal posture during swallowing 54 Clinical findings: Dysphagia 100 Dysphonia 86 Facial weakness 80 Cough during a swallow 66 Saliva accumulation in mouth 60 Weak in voluntary cough 60 Palatal paresis 53 Loss of weight 46 Tongue weakness 40 Slow laryngeal elevation 40 Reduced gag reflex 26 Weakness in chewing muscles 20 Lung infection 6 earlier, but other cranial muscles were involved to varying extents (patients in table 1). Six patients with myasthenia gravis were followed up longitudinally for clinical and electrophysiological evaluations between 1 and 3 months. Table 2 shows the results of the dysphagia questionnaire and the clinical findings closely related to dysphagia in the 15 patients with myasthenia gravis and dysphagia. Informed consent was obtained from each patient. The investigation was approved by the ethics committee of our University Hospital. The mean values of swallowing variables obtained from patients with myasthenia gravis were compared with the mean values of 17 (four women, 13 men) normal control subjects (mean age 50.2 (SD 4.2, range: years)). Individual values obtained from each patient were also compared with the upper limit of the mean value (mean+2 SD) of 75 (34 women, 41 men) normal controls from our laboratory, matched with age. 12 The electrophysiological methods for evaluating oropharyngeal swallowing have been described previously Briefly, a mechanical sensor, which consists of a simple piezoelectric wafer with a rubber bulge ayxed at its centre, was placed between the cricoid and thyroid cartilages at the midline. Thus upward and downward laryngeal movements associated with swallowing could be detected. The sensor output was connected to one channel of the EMG apparatus and band pass filtered (between 0.01 Hz and 20 Hz). The sensor gave two deflections of generally opposing polarity during each swallow. The first deflection of the laryngeal sensor represents the upward movement of the larynx and the second deflection, its downward movement. The upward and downward deflections of the laryngeal sensor were sometimes diphasic or triphasic for technical reasons. Their shortest time with high amplitude at the beginning of deflexion from the baseline was important and accepted as the
3 850 Ertekin, Yüceyar, Aydoǧdu point of onset. The leading or the trailing edge of the first deflection was used to trigger the delay line circuitry of the recording apparatus so that all signals were time locked to the same instant. The onsets of two deflections in the laryngeal sensor signal recordings are denoted as 0 and 2. The 0 2 time interval is a time variable showing the duration of laryngeal superior movement plus relocation during swallowing. 10 The EMG activity was recorded on a Medelec Model MS-20 EMG apparatus using bipolar silver chloride EEG electrodes taped under the chin over the mylohyoid-geniohyoid anterior digastric muscle complex. The EMG signal was also band pass filtered (between 100 Hz and 10 Hz), amplified, rectified, and then integrated. The surface muscle activity was named submental EMG activity (SM-EMG). As these muscles are the laryngeal elevators, their activities were considered to give information about the onset and duration of swallowing denoted as the A-C interval. The preanalysis time was set at 800 ms and the total sweep time was set at 2 seconds. At least five successive sensor and EMG signals were recorded for each type of swallowing, dry or wet (3 ml tap water). The signals were examined as single traces and as a superimposition and averaging of several. Cricopharyngeal (CP) muscle of the upper oesophageal sphincter was recorded electromyographically in six patients with myasthenia gravis. The EMG was recorded using disposable concentric needle electrodes. The needle electrode was inserted through the skin at the level of the cricoid cartilage, about 1.5 cm lateral to its palpable lateral border in the posteromedial direction. High frequency, tonic EMG activity appeared on the oscilloscope screen as the electrode penetrated the muscle. CP muscle activity was also rectified, integrated, and averaged during all types of swallowing. Besides recording dry and wet swallowing patterns of SM-EMG and the sensor signals reflecting laryngeal movements, piecemeal deglutition and dysphagia limits were also measured electrophysiologically. This test is based on determining piecemeal deglutition which is a physiological phenomenon that occurs when a bolus of large volume is divided into two or more parts which are then swallowed successively. 5 All patients were instructed to swallow doses of water gradually increasing in quantity from 1 ml to 20 ml, and any recurrence of the EMG and laryngeal sensor signals related to swallowing within 8 seconds was accepted as a sign of dysphagia limit. 11 Mean (SD) values were calculated for all quantities measured and Student s t test was performed to assess the diverences in swallowing variables between the groups. Results CLINICAL FINDINGS RELATED TO DYSPHAGIA In 15 patients with myasthenia gravis and dysphagia, the degree of dysphagia was variable from patient to patient. For instance, it was severe enough for a nasogastric catheter to be used in three patients (1 3). These patients also had diplopia from the onset of the disease, except one (patient 2) in whom pure dysphagia was the first and the only manifestation of myasthenia gravis. Fifteen patients had symptoms and signs closely related to dysphagia and pharyngolaryngeal muscle involvement as shown in table 2. In all patients with dysphagia, Figure 1 Dysphagia limits of (A) a normal subject and (B) a patient with myasthenia gravis with dysphagia. Note that all volumes, increasing in quantity up to 30 ml water, were swallowed as one bolus in the normal subject whereas the patient with myasthenia gravis began to divide the bolus even at 3 ml water, defining his dysphagia limit. The bolus was divided more as the volume was increased (arrows above the CP-EMG indicate pause during swallowing). Laryngeal sensor signals (top traces in each pair) and integrated EMG activities of the cricopharyngeal muscle of the upper oesophageal sphincter (CP-EMG) (lower traces in each pair in patient with myasthenia gravis) and submental EMG (SM-EMG) (lower traces in each pair in normal subject).
4 Dysphagia in myasthenia gravis 851 Figure 2 (A) Dysphagia limit of a patient with myasthenia gravis under anticholinestrease treatment was within the normal limits. (B) After the withdrawal of treatment, the dysphagia limit became pathologically low (10 ml) with clinical signs of dysphagia. anticholinesterase and corticosteroid treatment always produced appreciable recovery from dysphagia. Six of them could be re-examined by electrophysiological methods after evective treatment of myasthenia gravis. ELECTROPHYSIOLOGICAL FINDINGS RELATED TO SWALLOWING (A) Dysphagia limit The existence of dysphagia in patients with myasthenia gravis could be indicated objectively by this electrophysiological evaluation, showing its usefulness as an electrodiagnostic test. Figure 1 shows dysphagia limits obtained from a patient with dysphagia and from a normal control subject. The normal control subject could swallow up to 30 ml water without dividing the material; but the patient with myasthenia gravis began to divide the bolus while swallowing 3 ml water and he divided it into even more portions as volume was increased. This pattern was never found in normal subjects unless they were required to swallow a volume >20 ml. Therefore the limit of dysphagia was found as <20 ml. 11 This method was so sensitive that the dysphagia limit was pathologically low even 18 hours after cessation of anticholinesterase medication in a non-dysphagic patient under anticholinesterase treatment (fig 2). This electrodiagnostic test was performed on patients with myasthenia gravis with dysphagia and the dysphagia limit was found to be <20 ml in all. Advanced dysphagic cases with myasthenia gravis had a dysphagia limit of 1 ml and sometimes they coughed, suggesting subglottal aspiration. Swallowing recovered both clinically and electrophysiologically after treatment and the dysphagia limit showed complete recovery. In two of 10 patients without dysphagia, the bolus limit was found to be 20 ml, with an occasional divided bolus. The other patients with myasthenia gravis without dysphagia had normal dysphagia limits. (B) Laryngeal movements and SM-EMG Figure 3 shows a comparison between a normal subject and a patient with myasthenia gravis with dysphagia. One of the important variables was the 0 2 time interval, and it was indeed prolonged in patients with myasthenia gravis. The second variable is usually measured from the second deflection peak representing the downward movement of the larynx in superimposed records in which the time between the earliest and latest peak values are quantitatively measured and called swallowing jitter. Swallowing jitter can be regarded as the variability in the swallowing apparatus under a given swallowing condition. It can be an important measure of the safety of swallowing during swallowing bolus with vari ous volumes. It has been found that the swallowing jitter is extremely high in patients with myasthenia gravis with dysphagia compared with normal subjects. Table 3 gives a summary of the statistical results of two groups of patients with myasthenia gravis compared with age matched normal control subjects. The 0 2 interval shows that the upper relocation time of the larynx during dry and wet swallowing was significantly prolonged in patients with myasthenia gravis with dysphagia (table 3). It was also prolonged in comparison with the group of patients with myasthenia gravis without dysphagia (p<0.05). Swallowing jitter in patients with myasthenia gravis with dysphagia lasted longer than that in normal controls and the second group of patients with myasthenia gravis (p<0.05). The features of SM-EMG were also pathological in myasthenia gravis. The total duration
5 852 Ertekin, Yüceyar, Aydoǧdu Table 3 ( ) of SM-EMG (denoted as the A-C interval) was significantly prolonged in dry and wet swallowing in both groups of patients with myasthenia gravis compared with normal controls as shown in figure 3. Prolongation of SM-EMG was more severe in patients with dysphagia than in those without dysphagia (p<0.01). The amplitude of the SM-EMG was significantly lower in the dysphagic groups but there was no significant reduction in amplitude in the second group of patients with myasthenia gravis without dysphagia compared with normal control subjects. Individual values obtained from each patient were also compared with the upper limit of normal values (mean+2 SD). At least one or Figure 3 A patient with myasthenia gravis and dysphagia (lower two traces) compared with a normal subject (upper two traces) during dry swallowing. Note that the 0 2 time interval; showing the time for laryngeal upward relocation, swallowing jitter, and the duration of the EMG activity of submental muscle (A-C interval) were prolonged when compared with the normal subject. The arrows above the laryngeal sensor records denotes the swallowing jitter. Summary of the statistical results of patients with myasthenia gravis compared with normal subjects* Myasthenia gravis (total) ( n=25) Myasthenia gravis (with dysphagia) (n=15) Myasthenia gravis(without dysphagia) (n=10) 3 ml water Dry swallowing 3 ml water Dry swallowing 3 ml water Dry swallowing 3 ml water Normal subjects (n=17) Dry swallowing 0 2 Interval (laryngeal 713 (178) 672 (193) 785 (175) 677 (168) 620 (139) NS 537 (170) NS 571 (85) 534 (108) relocation time) p<0.01 p<0.01 p<0.001 p<0.01 Swallowing variability 120 (81) 159 (111) 147 (86) 197 (110) 85 (60) NS 88 (71) NS 82 (39) 105 (46) (jitter) p<0.05 p<0.05 p<0.05 p<0.01 A-C interval (SM-EMG 1136 (257) 1273 (360) 1237 (288) 1420 (363) 1004 (130) 1052 (227) 863 (89) 896 (153) duration) p<0.001 p<0.001 p<0.001 p<0.001 p<0.01 p<0.05 SM-EMG amp 51 (34) NS 56 (37) p< (28) p< (28) p< (41) NS 68 (46) NS 62 (27) 82 (28) A-0 interval 328 (161) NS 382 (227) NS 323 (160) NS 36 7 (202) NS 334 (170) NS 404 (273) NS 286 (125) 312 (178) * Statistical comparisons between the patient groups have not been included in this table (see text). Swallowing variables except SM-EMG amp (µv) are in ms and the values are shown as mean (SD). A-O interval denotes the time interval at the onset of SM-EMG (A) and the onset of the laryngeal upward movements (0). This value is closely related to the time until triggering of the swallowing reflex.
6 Dysphagia in myasthenia gravis (295) Before treatment After treatment (219) (187) (77) (65) (23) 0 A-C interval O-2 interval Swallowing jitter Figure 4 The evect of treatment on the values of A-C interval (SM-EMG activity during swallowing), 0 2 sensor interval (time for laryngeal upward relocation), and swallowing jitter (variability of 0 2 time interval) of six patients with myasthenia gravis. The values are shown as mean (SD). Time (ms) more electrophysiological abnormalities were encountered in patients with dysphagia. On the other hand, one or more electrophysiological abnormalities were found in six out of 10 patients with myasthenia gravis without dysphagia. Electrophysiological evaluation disclosed that SM-EMG and laryngeal sensor findings are also useful indicators of involvement of laryngeal elevator muscles in patients with myasthenia gravis with and without dysphagia. After the treatment, all values of SM-EMG and laryngeal movement except amplitude values (0 2 interval, swallowing jitter, and SM-EMG duration) were reduced or shortened toward the normal limits in six patients with myasthenia gravis and dysphagia together with the clinical improvement (fig 4). The reduction in these quantities was found to be significant (p<0.001 for A-C interval, p<0.01 for swallowing jitter, and p<0.05 for 0 2 interval). (C) Cricopharyngeal sphincter EMG CP sphincter EMG was recorded in six patients with myasthenia gravis with dysphagia. The electrophysiological behaviour of CP-EMG during dry or wet swallowing was the same as in normal subjects. The CP-EMG behaviour can be seen with the SM-EMG in figure 5. During a swallow the tonic activity of CP muscle was switched ov for about 400 ms (CP-EMG pause); during this time the SM muscle complex was activated just before the onset of the CP-EMG pause. The normal before and after burst of activity around the Figure 5 Integrated SM-EMG activity and CP-EMG activity during swallowing of 3 ml water in a patient with myasthenia gravis. Lower pairs are the averaged traces. Upper pairs demonstrate the superposition of all traces. Points A and C denote the onset and the end of submental EMG activity. Pause is the silence of the tonic activity of CP-EMG during swallowing.
7 854 Ertekin, Yüceyar, Aydoǧdu Figure 6 Patient with myasthenia gravis with dysphagia (lower two traces) was compared with the normal subject with regard to the relation between the laryngeal movement and the relaxation of the CP sphincter. Note the prolongation in the laryngeal sensor signal and the increase in swallowing jitter despite the normal CP-EMG pause while swallowing 3 ml of bolus. The CP sphincter is prematurely closed in the patient with myasthenia gravis (oblique arrow). Arrows just below the laryngeal sensor signal in the lower pairs indicate the swallowing jitter with longer values in patients with myasthenia gravis with dysphagia compared with the swallowing jitter (above the laryngeal sensor signal in the upper pairs) of a normal subject. pause could be easily seen in CP muscle with normal values Thus no abnormalities were encountered in the CP muscle sphincter in six patients with myasthenia gravis plus dysphagia. On the other hand; coordination of laryngeal movement and the opening or relaxation of the CP sphincter may be disturbed probably due to the involvement of the suprahyoid and laryngeal elevator muscles and an intact CP sphincter. This is shown in figure 6, where the prolongation of the laryngeal upward movement (0 2 interval) and the increase in swallowing jitter are evident whereas the CP sphincter EMG has its normal pause without compensating the weakness of muscles which elevate the larynx. CP sphincter muscle showed a relatively early closure and probably this diverential involvement caused accumulation of pieces of material in the spaces of the pharynx after a swallow and played a part in laryngeal aspiration. Discussion Dysphagia is a common symptom in myasthenia gravis and has been documented in 6% of 1487 patients with myasthenia gravis as an initial symptom. 2 If it is the initial symptom and a prominent complaint, ear, nose, and throat specialists or gastroenterologists rather than neurologists may be consulted first. However, such patients are not very common. On the other hand, the incidence of dysphagia is probably underestimated. Based on our findings in this study, we have suggested two reasons for this. Firstly, dysphagia is so mild and insidious that the patient cannot be aware of his or her symptoms. Frequent involvement of ocular muscles apart from the pharyngeal and laryngeal muscles may dominate the complaints of patients with myasthenia gravis, so that dysphagia may be unnoticed by the patient. We have experienced this finding in our patients. Despite the common involvement of ocular
8 Dysphagia in myasthenia gravis 855 and pharyngeal muscles, the complaint of diplopia was more obvious and dysphagia has been missed by both the patients and the physicians. On the other hand, the myasthenic involvement in pharyngeal and laryngeal muscle groups has been rapidly cured with early and evective anticholinesterase treatment. The second reason for missing a swallowing disorder in myasthenia gravis is that the tongue, pharyngeal muscle of the oral floor, and other laryngeal elevators cannot be properly investigated by conventional electrodiagnostic methods. Myasthenic involvement was determined in the laryngeal elevators by means of the electrophysiological methods described. SM muscles have two actions in swallowing; one is the protection of the larynx by elevation, the second is the transportation of the bolus by a secondary support to the tongue to pump We have found that the SM muscles were activated for an abnormally long period during swallowing and the duration of SM-EMG was much longer in patients with myasthenia gravis with and without dysphagia. The prolongation of laryngeal upward movement and its relocation during swallowing (0 2 time interval) were also strictly related with long duration of SM-EMG. The prolonged activity of the weak SM muscles to keep the larynx at an anterosuperior relocation position during swallowing, must be the cause of longer duration of these variables. As these abnormalities are quite frequent in patients with myasthenia gravis without dysphagia, it can be proposed that SM muscles and other laryngeal elevators are also involved in myasthenia gravis without dysphagia but this can be shown objectively only by electrophysiological variables. Pure electrophysiological involvement of these muscles can be explained on the assumption the muscles are probably weak but are normal clinically. This is similar to the fact that in myasthenia gravis, although skeletal muscle power may be normal clinically it may be abnormal electrodiagnostically Subclinical weakness of the muscles investigated and weakness of other muscles such as the tongue and pharyngeal constrictor muscles, which are primarily related to swallowing, may not always result in dysphagia. Because either voluntary compensation (when the patient is aware of his or her swallowing impairment), or involuntary compensation mechanisms which occur through adjustments in the swallowing apparatus itself 21 may take place in the presence of weakness of oropharyngeal muscles. Thus patients with myasthenia gravis with a subclinical swallowing impairment may subconsciously alter the consistency of ingested food and the speed of eating and drinking and there may not be overt symptoms of dysphagia. 22 The prolongation of SM-EMG duration and 0 2 laryngeal sensor interval might be a type of compensating mechanism to prevent aspiration by keeping the larynx closed and elevated during swallowing. The increase in jitter and the lowering of the dysphagia limits in patients are another type of compensation for swallowing in the case of weakness of oral and pharyngeal muscles. Swallowing jitter can be adjusted from one swallow to another according to peripheral conditions. This may also be related to the change in the number of muscle fibres in transmission block from one swallow to another even if the same bolus volume is swallowed. This would result in further fluctuations as detected by the second deflections of the laryngeal sensor. After the anticholinesterase treatment, the increase in swallowing jitter has declined towards normal limits accompanied by clinical improvement. If the bolus is large enough, it is not sufficient to increase the times of swallowing events such as the 0 2 interval or SM-EMG duration; instead it becomes necessary to divide the bolus into portions and swallow them successively in piecemeal deglutition. Thus in the case of myasthenia gravis with dysphagia this mechanism works and the dysphagia limit is lowered below a 20 ml water bolus, which is the upper limit in normal subjects. 11 The lowering of the dysphagia limit therefore represents a more advanced stage of dysphagia (the clinically apparent stage). Indeed, whereas all of our patients with myasthenia gravis with dysphagia had abnormal dysphagia limit values, only two patients without dysphagia had a dysphagia limit at a 20 ml water bolus. EMG activity of the CP sphincter was normal in all patients investigated. The EMG behaviour of this sphincter muscle during swallowing has not been found diverent from that in normal subjects The videofluoroscopic and cinefluoroscopic studies have also disclosed that the CP sphincter is almost always normal in myasthenia gravis However, Huang et al 9 showed a significant decrease in sphincter pressure in a manometric study but they found that the relaxation and coordination of this sphincter were within normal limits. Similar to our findings, fluoroscopic studies disclosed that the tongue, laryngeal elevators, and pharyngeal constrictors are mostly involved in myasthenia gravis with dysphagia The selective involvement of the swallowing apparatus in myasthenia gravis can be explained by the fact that CP muscle is more dependent on a central swallowing programme and the central pattern generator in the bulbus, 27 and its action is semiautomatic and involuntary despite its striated nature. 28 Although the CP muscle of the upper esophageal sphincter is intact, this finding will be irrelevant as the myasthenic process advances to involve the tongue and the pharyngeal constrictor muscles, which pump and sweep the bolus, and the submental and other laryngeal elevator muscles which protect the larynx during swallowing. A coordination disorder between these suprahyoid laryngeal elevator muscles which are involved in myasthenia gravis and the intact cricopharyngeal muscle of the upper esophageal sphincter may be one of the causes of dysphagia and aspiration in MG. We are grateful to Professors G Çelebi and N Çelebisoy for their invaluable help. This study was supported by a grant from the Turkish Scientific and Technological Research Council (TU- BI~TAK) (Project No SBAG-1739).
9 856 Ertekin, Yüceyar, Aydoǧdu 1 Carpenter RC, Mc Donald TJ, Howard EM. The otolaryngologic presentation of myasthenia gravis. Laryngoscope 1979;89: Grob D, Arsura EL, Brunner NG, et al. The course of myasthenia gravis and therapies avecting outcome. Ann N Y Acad Sci 1987;505: Donner MW, Silbiger ML. Cinefluorographic analysis of pharyngeal swallowing in neuromuscular disorders. Am J Med Sci 1966; 25: Khan OA, Campbell WW. Myasthenia gravis presenting as dysphagia: clinical considerations. Am J Gastroenterol 1994; 89: Logeman JA. Evaluation and treatment of swallowing disorders. Austin, TX: Pro-ed, 1983:76. 6 Felson BJ, Klatte EC. Pharyngeal and upper esophageal dysphagia. JAMA 1976;235: Kilman WJ, Goyal RK. Disorder of pharyngeal and upper esophageal sphincter motor function. Arch Intern Med 1976;136: Kluin KJ, Bromberg MB, Feldman EL, et al. Dysphagia in elderly men with myasthenia gravis. J Neurol Sci 1996;138: Huang MH, King KL, Chien KY. Esophageal manometric studies in patients with myasthenia gravis. J Thorac Cardiovasc Surg 1988;95: Ertekin C, Pehlivan M, Aydogdu I, et al. An electrophysiological investigation of deglutition in man. Muscle Nerve 1995;18: Ertekin C, Aydogdu I, Yüceyar N. Piecemeal deglutition and dysphagia limit in normal subjects and in patients with swallowing disorders. J Neurol Neurosurg Psychiatry 1996; 61: Ertekin C. Clinical diagnosis and electrodiagnosis of swallowing disorders. In: Swenson MR, ed. Disorders of speech and swallowing. AAEM, 19th annual continuing education courses. Minnesota: Johnson, 1996; Ertekin C, Aydogdu I, Yüceyar N, et al. EVects of bolus volumes on the oropharyngeal swallowing an electrophysiological study in man. Am J Gastroenterol 1997;92: Pehlivan M, Yüceyar N, Ertekin C, et al. An electronic device measuring the frequency of spontaneous swallowing: digital phagometer. Dysphagia 1996;11: Cook IJ. Normal and disordered swallowing: new insights. Baillere s Clinical Gastroenterology 1991;5: Dodds WJ, Stewart ET, Logeman JA. Physiology and radiology of the normal oral and pharyngeal phases of swallowing. AJR Am J Roentgenol 1990;154: Mc Connell FM Scerenko D, Jackson RT, et al. Timing of major events of pharyngeal swallowing. Arch Otolaryngol Head Neck Surgery 1988;114: Sanders DB, Howard JF. Single-fiber electromyography in myasthenia gravis. Muscle Nerve 1986;9: Sanders DB, Howard JF, Johns TR. Single-fiber electromyography in myasthenia gravis. Neurology 1979;29: Stalberg E, Sanders DB. Electrophysiological tests of neuromuscular transmission. In: Stalberg E, Young RR, eds. Clinical neurophysiology. London: Butterworths, 1981: Buchholz DW, Bosma JF, Donner MW. Adaptation, compensation and decompensation of the pharyngeal swallowing. Gastrointest Radiol 1985;10: Jones B, Ravich WJ, Donner MV, et al. Pharyngoesophageal interrelationships: observations and working concepts. Gastrointest Radiol 1985;10: Elidan J, Schochina M, Gonen B, et al. Manometry and electromyography of the pharyngeal muscles in patients with dysphagia. Arch Otolaryngol Head Neck Surg 1990;116: Shipp T, Deatsch WW, Robertson K. Pharyngoesophageal muscle activity during swallowing in man. Laryngoscope 1970;80: Van Overbeek JJ, Wit HP, Paping RH, et al. Simultaneous manometry and electromyography in the pharyngoesophageal segment. Laryngoscope 1985;95: Silbiger ML, Pikielney R, Donner MW. Neuromuscular disorders avecting the pharynx-cineradiographic analysis. Invest Radiol 1967;2: Miller AJ. Deglutition. Physiol Rev 1982;62: Bonington A, Mahon M, Whitmore I. A histological and histochemical study of the cricopharyngeus muscle in man. J Anat 1988;156: J Neurol Neurosurg Psychiatry: first published as /jnnp on 1 December Downloaded from on 6 September 2018 by guest. Protected by copyright.
Electrophysiological Evaluation of Oropharyngeal Dysphagia in Parkinson s Disease
 REVIEW ARTICLE http://dx.doi.org/10.14802/jmd.14008 / J Mov Disord 2014;7(2):31-56 pissn 2005-940X / eissn 2093-4939 Electrophysiological Evaluation of Oropharyngeal Dysphagia in Parkinson s Disease Cumhur
REVIEW ARTICLE http://dx.doi.org/10.14802/jmd.14008 / J Mov Disord 2014;7(2):31-56 pissn 2005-940X / eissn 2093-4939 Electrophysiological Evaluation of Oropharyngeal Dysphagia in Parkinson s Disease Cumhur
Electrophysiological evaluation of oropharyngeal swallowing in myotonic dystrophy
 J Neurol Neurosurg Psychiatry 2001;70:363 371 363 Department of Clinical Neurophysiology, Ege University Medical School Hospital, Bornova, I~zmir, Turkey C Ertekin I~ Aydoğdu Department of Neurology C
J Neurol Neurosurg Psychiatry 2001;70:363 371 363 Department of Clinical Neurophysiology, Ege University Medical School Hospital, Bornova, I~zmir, Turkey C Ertekin I~ Aydoğdu Department of Neurology C
15/11/2011. Swallowing
 Swallowing Swallowing starts from placement of the food in the mouth and continues until food enters the stomach. Dysphagia: any difficulty in moving food from mouth to stomach. Pharynx is shared for both
Swallowing Swallowing starts from placement of the food in the mouth and continues until food enters the stomach. Dysphagia: any difficulty in moving food from mouth to stomach. Pharynx is shared for both
disorders Piecemeal deglutition and dysphagia limit in normal subjects and in patients with swallowing far, this has not been determined.
 J7ournal ofneurology, Neurosurgery, and Psychiatry 1996;61:491-496 Department of Clinical Neurophysiology and Neurology, Ege University Medical School Hospital, Bornova, Izmir, 51, Tiirkiye C Ertekin,
J7ournal ofneurology, Neurosurgery, and Psychiatry 1996;61:491-496 Department of Clinical Neurophysiology and Neurology, Ege University Medical School Hospital, Bornova, Izmir, 51, Tiirkiye C Ertekin,
Speech and Swallowing in KD: Soup to Nuts. Neil C. Porter, M.D. Assistant Professor of Neurology University of Maryland
 Speech and Swallowing in KD: Soup to Nuts Neil C. Porter, M.D. Assistant Professor of Neurology University of Maryland Disclosures I will not be speaking on off-label use of medications I have no relevant
Speech and Swallowing in KD: Soup to Nuts Neil C. Porter, M.D. Assistant Professor of Neurology University of Maryland Disclosures I will not be speaking on off-label use of medications I have no relevant
Swallowing Disorders and Their Management in Patients with Multiple Sclerosis
 National Multiple Sclerosis Society 733 Third Avenue New York, NY 10017-3288 Clinical Bulletin Information for Health Professionals Swallowing Disorders and Their Management in Patients with Multiple Sclerosis
National Multiple Sclerosis Society 733 Third Avenue New York, NY 10017-3288 Clinical Bulletin Information for Health Professionals Swallowing Disorders and Their Management in Patients with Multiple Sclerosis
Swallowing Screen Why? How? and So What? พญ.พวงแก ว ธ ต สก ลช ย ภาคว ชาเวชศาสตร ฟ นฟ คณะแพทยศาสตร ศ ร ราชพยาบาล
 Swallowing Screen Why? How? and So What? พญ.พวงแก ว ธ ต สก ลช ย ภาคว ชาเวชศาสตร ฟ นฟ คณะแพทยศาสตร ศ ร ราชพยาบาล Dysphagia in Stroke The incidence of dysphagia after stroke ranging from 23-50% 1 Location
Swallowing Screen Why? How? and So What? พญ.พวงแก ว ธ ต สก ลช ย ภาคว ชาเวชศาสตร ฟ นฟ คณะแพทยศาสตร ศ ร ราชพยาบาล Dysphagia in Stroke The incidence of dysphagia after stroke ranging from 23-50% 1 Location
Understanding your child s videofluoroscopic swallow study report
 Understanding your child s videofluoroscopic swallow study report This leaflet is given to you during your child s appointment in order to explain some of the words used by the speech and language therapist
Understanding your child s videofluoroscopic swallow study report This leaflet is given to you during your child s appointment in order to explain some of the words used by the speech and language therapist
TREATMENT OF DYSPHAGIA IN PATIENTS AFTER STROKE IN ESTONIA
 TREATMENT OF DYSPHAGIA IN PATIENTS AFTER STROKE IN ESTONIA ANNE URIKO SPORTS MEDICINE AND REHABILITATION CLINIG OF TARTU UNIVERSITY HOSPITAL 17.09.2010 DYSPHAGIA DIFFICULTY MOVING FOOD FROM MOUTH TO STOMACH
TREATMENT OF DYSPHAGIA IN PATIENTS AFTER STROKE IN ESTONIA ANNE URIKO SPORTS MEDICINE AND REHABILITATION CLINIG OF TARTU UNIVERSITY HOSPITAL 17.09.2010 DYSPHAGIA DIFFICULTY MOVING FOOD FROM MOUTH TO STOMACH
Dysphagia and Swallowing. Jan Adams, DNP, MPA, RN and Karen Kern
 Dysphagia and Swallowing Jan Adams, DNP, MPA, RN and Karen Kern Scope of the Problem and Incidence 15 million people in the US have some form of Dysphagia. Every year, 1 million people are diagnosed with
Dysphagia and Swallowing Jan Adams, DNP, MPA, RN and Karen Kern Scope of the Problem and Incidence 15 million people in the US have some form of Dysphagia. Every year, 1 million people are diagnosed with
Abstract. Abnormal peristaltic waves like aperistalsis of the esophageal body, high amplitude and broader waves,
 Original Article Esophageal Motility Disorders in Diabetics Waquaruddin Ahmed, Ejaz Ahmed Vohra Department of Medicine, Dr. Ziauddin Medical University, Karachi. Abstract Objective: To see the presence
Original Article Esophageal Motility Disorders in Diabetics Waquaruddin Ahmed, Ejaz Ahmed Vohra Department of Medicine, Dr. Ziauddin Medical University, Karachi. Abstract Objective: To see the presence
Cover Page. The handle holds various files of this Leiden University dissertation
 Cover Page The handle http://hdl.handle.net/1887/32744 holds various files of this Leiden University dissertation Author: Heemskerk, Anne-Wil Title: Dysphagia in Huntington s disease Issue Date: 2015-04-15
Cover Page The handle http://hdl.handle.net/1887/32744 holds various files of this Leiden University dissertation Author: Heemskerk, Anne-Wil Title: Dysphagia in Huntington s disease Issue Date: 2015-04-15
Swallowing Course (RHS )
 Swallowing Course (RHS ) Dr/Mohamed Farahat Ibrahim, M.D., Ph.D. Professor, Consultant Phoniatrician (Communication and Swallowing Disorders) Chairman, Communication and Swallowing Disorders Unit (CSDU)
Swallowing Course (RHS ) Dr/Mohamed Farahat Ibrahim, M.D., Ph.D. Professor, Consultant Phoniatrician (Communication and Swallowing Disorders) Chairman, Communication and Swallowing Disorders Unit (CSDU)
Is the Stimulation Frequency of the Repetitive Nerve Stimulation Test that You Choose Appropriate?
 186 Is the Stimulation Frequency of the Repetitive Nerve Stimulation Test that You Choose Appropriate? Yuan-Ting Sun and Thy-Sheng Lin Abstract- The repetitive nerve stimulation test (RNST) has been a
186 Is the Stimulation Frequency of the Repetitive Nerve Stimulation Test that You Choose Appropriate? Yuan-Ting Sun and Thy-Sheng Lin Abstract- The repetitive nerve stimulation test (RNST) has been a
Speech and Language Therapy. Kerrie McCarthy Senior Speech and Language Therapist
 Speech and Language Therapy Kerrie McCarthy Senior Speech and Language Therapist Contents 1. Voice disorders 2. Swallow disorders 3. Videofluroscopy 4. Adult Acquired Communication Disorders 5. How to
Speech and Language Therapy Kerrie McCarthy Senior Speech and Language Therapist Contents 1. Voice disorders 2. Swallow disorders 3. Videofluroscopy 4. Adult Acquired Communication Disorders 5. How to
Endoscopic carbon dioxide laser cricopharyngeal myotomy for relief of oropharyngeal dysphagia
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endoscopic carbon dioxide laser cricopharyngeal myotomy for relief of oropharyngeal dysphagia Difficulty
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endoscopic carbon dioxide laser cricopharyngeal myotomy for relief of oropharyngeal dysphagia Difficulty
The Clinical Swallow Evaluation: What it can and cannot tell us. Introduction
 The Clinical Swallow Evaluation: What it can and cannot tell us Debra M. Suiter, Ph.D., CCC-SLP, BCS-S Director, Voice & Swallow Clinic Associate Professor, Division of Communication Sciences & Disorders
The Clinical Swallow Evaluation: What it can and cannot tell us Debra M. Suiter, Ph.D., CCC-SLP, BCS-S Director, Voice & Swallow Clinic Associate Professor, Division of Communication Sciences & Disorders
Main Aspects of the Management of Neurogenic Dysphagia
 Main Aspects of the Management of Neurogenic Dysphagia Mario Prosiegel/München German Society of Neurology (DGN) prosiegel@t-online.de DYSPHAGIA October 8-10, 2015 Pavia, Italy Overview Diagnosis Causal
Main Aspects of the Management of Neurogenic Dysphagia Mario Prosiegel/München German Society of Neurology (DGN) prosiegel@t-online.de DYSPHAGIA October 8-10, 2015 Pavia, Italy Overview Diagnosis Causal
THE INTERIOR OF THE PHARYNX. By Dr. Muhammad Imran Qureshi
 THE INTERIOR OF THE PHARYNX By Dr. Muhammad Imran Qureshi The Cavity The cavity of the pharynx is divided into: 1. The Nasal part (called Nasopharynx) 2. The Oral part (called the Oropharynx), 3. And the
THE INTERIOR OF THE PHARYNX By Dr. Muhammad Imran Qureshi The Cavity The cavity of the pharynx is divided into: 1. The Nasal part (called Nasopharynx) 2. The Oral part (called the Oropharynx), 3. And the
Role of Laryngeal Movement and Effect of Aging on Swallowing Pressure in the Pharynx and Upper Esophageal Sphincter
 The Laryngoscope Lippincott Williams & Wilkins, Inc., Philadelphia 2000 The American Laryngological, Rhinological and Otological Society, Inc. Role of Laryngeal Movement and Effect of Aging on Swallowing
The Laryngoscope Lippincott Williams & Wilkins, Inc., Philadelphia 2000 The American Laryngological, Rhinological and Otological Society, Inc. Role of Laryngeal Movement and Effect of Aging on Swallowing
Applied physiology. 7- Apr- 15 Swallowing Course/ Anatomy and Physiology
 Applied physiology Temporal measures: Oral Transit Time (OTT) Pharyngeal Delay Time (PDT) Pharyngeal Transit Time (PTT) Oropharyngeal Swallowing Efficiency Score (OPSE score) 7- Apr- 15 Swallowing Course/
Applied physiology Temporal measures: Oral Transit Time (OTT) Pharyngeal Delay Time (PDT) Pharyngeal Transit Time (PTT) Oropharyngeal Swallowing Efficiency Score (OPSE score) 7- Apr- 15 Swallowing Course/
Cover Page. The handle holds various files of this Leiden University dissertation
 Cover Page The handle http://hdl.handle.net/1887/32744 holds various files of this Leiden University dissertation Author: Heemskerk, Anne-Wil Title: Dysphagia in Huntington s disease Issue Date: 2015-04-15
Cover Page The handle http://hdl.handle.net/1887/32744 holds various files of this Leiden University dissertation Author: Heemskerk, Anne-Wil Title: Dysphagia in Huntington s disease Issue Date: 2015-04-15
«Einschluckstörungen»
 18. Fortbildungskurs der SGG Brunnen 20.04.2018 «Einschluckstörungen» Troubles de la déglutition Swallowing disorders Dr Valérie Schweizer Unité de Phoniatrie Service ORL et chirurgie cervicofaciale CHUV
18. Fortbildungskurs der SGG Brunnen 20.04.2018 «Einschluckstörungen» Troubles de la déglutition Swallowing disorders Dr Valérie Schweizer Unité de Phoniatrie Service ORL et chirurgie cervicofaciale CHUV
SWALLOWING DIFFICULTIES IN HD
 Nutrition, eating and swallowing needs, challenges and solutions Workshop SWALLOWING DIFFICULTIES IN HD Angela Nuzzi Speech and Language Pathologist (SLP) EHDN Language Coordinator - Italy The role of
Nutrition, eating and swallowing needs, challenges and solutions Workshop SWALLOWING DIFFICULTIES IN HD Angela Nuzzi Speech and Language Pathologist (SLP) EHDN Language Coordinator - Italy The role of
Development of a Portable Non-Invasive Swallowing and Respiration Assessment Device
 Sensors 2015, 15, 12428-12453; doi:10.3390/s150612428 Article OPEN ACCESS sensors ISSN 1424-8220 www.mdpi.com/journal/sensors Development of a Portable Non-Invasive Swallowing and Respiration Assessment
Sensors 2015, 15, 12428-12453; doi:10.3390/s150612428 Article OPEN ACCESS sensors ISSN 1424-8220 www.mdpi.com/journal/sensors Development of a Portable Non-Invasive Swallowing and Respiration Assessment
Title. manometry system. Author(s) Takahashi, Haruo. Auris Nasus Larynx, 37(5), pp Issue Date
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Evaluation of swallowing pressure i sclerosis before and after cricopha manometry system. Takasaki, Kenji; Umeki, Hiroshi; En Takahashi, Haruo
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Evaluation of swallowing pressure i sclerosis before and after cricopha manometry system. Takasaki, Kenji; Umeki, Hiroshi; En Takahashi, Haruo
Effect of posture on swallowing.
 Effect of posture on swallowing. Ahmad H. Alghadir, Hamayun Zafar, Einas S. Al-Eisa, Zaheen A. Iqbal Rehabilitation Research Chair, College of Applied Medical Sciences, King Saud University, Riyadh, KSA.
Effect of posture on swallowing. Ahmad H. Alghadir, Hamayun Zafar, Einas S. Al-Eisa, Zaheen A. Iqbal Rehabilitation Research Chair, College of Applied Medical Sciences, King Saud University, Riyadh, KSA.
Respiratory Patterns Associated with Swallowing: Part 1. The Normal Adult Pattern and Changes with Age
 Respiratory Patterns Associated with Swallowing: Part 1. The Normal Adult Pattern and Changes with Age W. G. SELLEY, F. C. FLACK, R. E. ELLIS, W. A. BROOKS Summary Simple, non-invasive equipment was designed
Respiratory Patterns Associated with Swallowing: Part 1. The Normal Adult Pattern and Changes with Age W. G. SELLEY, F. C. FLACK, R. E. ELLIS, W. A. BROOKS Summary Simple, non-invasive equipment was designed
Asma Karameh. -Shatha Al-Jaberi محمد خطاطبة -
 -2 Asma Karameh -Shatha Al-Jaberi محمد خطاطبة - 1 P a g e Gastrointestinal motilities Chewing: once you introduce the first bolus to the mouth you started what we call chewing reflex appears by muscle
-2 Asma Karameh -Shatha Al-Jaberi محمد خطاطبة - 1 P a g e Gastrointestinal motilities Chewing: once you introduce the first bolus to the mouth you started what we call chewing reflex appears by muscle
Myasthenia Gravis. Mike Gilchrist 10/30/06
 Myasthenia Gravis Mike Gilchrist 10/30/06 Overview Background Pathogenesis Clinical Manifestations Diagnosis Treatment Associated Conditions Background Severe muscle disease Most common disorder of neuromuscular
Myasthenia Gravis Mike Gilchrist 10/30/06 Overview Background Pathogenesis Clinical Manifestations Diagnosis Treatment Associated Conditions Background Severe muscle disease Most common disorder of neuromuscular
EATING SAFELY AND TALKING ABOUT IT KIERA N BERGGREN, MA/CCC-SLP, MS 2018 FSHD CONNECT CONFERENCE
 EATING SAFELY AND TALKING ABOUT IT KIERA N BERGGREN, MA/CCC-SLP, MS 2018 FSHD CONNECT CONFERENCE DISCLOSURES I have no personal financial relationships with commercial interests relevant to this presentation
EATING SAFELY AND TALKING ABOUT IT KIERA N BERGGREN, MA/CCC-SLP, MS 2018 FSHD CONNECT CONFERENCE DISCLOSURES I have no personal financial relationships with commercial interests relevant to this presentation
Myasthenia gravis. David Hilton-Jones Oxford Neuromuscular Centre
 Myasthenia gravis David Hilton-Jones Oxford Neuromuscular Centre SWIM, Taunton, 2018 Myasthenia gravis Autoimmune disease Nature of Role of thymus Myasthenia gravis Autoimmune disease Nature of Role of
Myasthenia gravis David Hilton-Jones Oxford Neuromuscular Centre SWIM, Taunton, 2018 Myasthenia gravis Autoimmune disease Nature of Role of thymus Myasthenia gravis Autoimmune disease Nature of Role of
Respiratory Swallow Coordination in Healthy Individuals
 Cloud Publications International Journal of Advanced Speech and Hearing Research 2012, Volume 1, Issue 1, pp. 1-9, Article ID Med-03 Research Article Open Access Respiratory Swallow Coordination in Healthy
Cloud Publications International Journal of Advanced Speech and Hearing Research 2012, Volume 1, Issue 1, pp. 1-9, Article ID Med-03 Research Article Open Access Respiratory Swallow Coordination in Healthy
SCC - Parkinson Rehabilitation Program
 SCC - Parkinson Rehabilitation Program Introduction At the Spine Care Centre we don t treat Parkinson s Disease, we treat PEOPLE with Parkinson s Disease. Our goal is to assure that, in addition to improving
SCC - Parkinson Rehabilitation Program Introduction At the Spine Care Centre we don t treat Parkinson s Disease, we treat PEOPLE with Parkinson s Disease. Our goal is to assure that, in addition to improving
The Pharynx. Dr. Nabil Khouri MD. MSc, Ph.D
 The Pharynx Dr. Nabil Khouri MD. MSc, Ph.D Introduction The pharynx is the Musculo-fascial halfcylinder that links the oral and nasal cavities in the head to the larynx and esophagus in the neck Common
The Pharynx Dr. Nabil Khouri MD. MSc, Ph.D Introduction The pharynx is the Musculo-fascial halfcylinder that links the oral and nasal cavities in the head to the larynx and esophagus in the neck Common
Oro-pharyngeal and Esophageal Motility and Dysmotility John E. Pandolfino, MD, MSci
 Oro-pharyngeal and Esophageal Department of Medicine Feinberg School of Medicine Northwestern University 1 Oro-pharyngeal and Esophageal Motility Function: Oropharynx Transfer food Prevent aspiration Breathing
Oro-pharyngeal and Esophageal Department of Medicine Feinberg School of Medicine Northwestern University 1 Oro-pharyngeal and Esophageal Motility Function: Oropharynx Transfer food Prevent aspiration Breathing
Swallowing Strategies
 Department of Head and Neck Surgery Section of Speech Pathology & Audiology M.D. Anderson Cancer Center (713) 792-6525 Swallowing Strategies 1) POSTURAL CHANGES: a) Chin Tuck: (1) Delayed onset pharyngeal
Department of Head and Neck Surgery Section of Speech Pathology & Audiology M.D. Anderson Cancer Center (713) 792-6525 Swallowing Strategies 1) POSTURAL CHANGES: a) Chin Tuck: (1) Delayed onset pharyngeal
ORIGINAL ARTICLE. Pill Swallowing by Adults With Dysphagia. Giselle Carnaby-Mann, B App Sci, PGrad Dip (HSc), MPH, PhD; Michael Crary, PhD
 ORIGINAL ARTICLE Pill Swallowing by Adults With Dysphagia Giselle Carnaby-Mann, B App Sci, PGrad Dip (HSc), MPH, PhD; Michael Crary, PhD Objective: To evaluate differences in swallowing physiology and
ORIGINAL ARTICLE Pill Swallowing by Adults With Dysphagia Giselle Carnaby-Mann, B App Sci, PGrad Dip (HSc), MPH, PhD; Michael Crary, PhD Objective: To evaluate differences in swallowing physiology and
SUPER-SUPRAGLOTTIC SWALLOW IN IRRADIATED HEAD AND NECK CANCER PATIENTS
 SUPER-SUPRAGLOTTIC SWALLOW IN IRRADIATED HEAD AND NECK CANCER PATIENTS Jeri A. Logemann, PhD, 1 Barbara Roa Pauloski, PhD, 1 Alfred W. Rademaker, PhD, 2 Laura A. Colangelo, MS 2 1 Department of Communication
SUPER-SUPRAGLOTTIC SWALLOW IN IRRADIATED HEAD AND NECK CANCER PATIENTS Jeri A. Logemann, PhD, 1 Barbara Roa Pauloski, PhD, 1 Alfred W. Rademaker, PhD, 2 Laura A. Colangelo, MS 2 1 Department of Communication
POST POLIO SYNDROME (PPS) AND ITS EFFECTS ON SWALLOWING BY: LINDSAY JORDAN
 POST POLIO SYNDROME (PPS) AND ITS EFFECTS ON SWALLOWING BY: LINDSAY JORDAN WHAT IS POST POLIO SYNDROME (PPS)? Post-polio syndrome (PPS) is a condition that affects polio survivors years after recovery
POST POLIO SYNDROME (PPS) AND ITS EFFECTS ON SWALLOWING BY: LINDSAY JORDAN WHAT IS POST POLIO SYNDROME (PPS)? Post-polio syndrome (PPS) is a condition that affects polio survivors years after recovery
Feeding and Oral Hygiene: How to Address the Challenges
 Feeding and Oral Hygiene: How to Address the Challenges Paige W. Roberts, OTR/L Occupational Therapist Pediatric Feeding Disorders Program Marcus Autism Center Disclaimer: This content is for personal
Feeding and Oral Hygiene: How to Address the Challenges Paige W. Roberts, OTR/L Occupational Therapist Pediatric Feeding Disorders Program Marcus Autism Center Disclaimer: This content is for personal
Application of futility analysis to refine jitter recordings in myasthenia gravis
 Application of futility analysis to refine jitter recordings in myasthenia gravis The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters
Application of futility analysis to refine jitter recordings in myasthenia gravis The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters
The clinical gold standard in diagnostic dysphagia
 Clinical Measurement of Pharyngeal Surface Electromyography: Exploratory Research Sebastian H. Doeltgen, MSLT, Andrea Hofmayer, MA, Freya Gumbley, BSLT, Ulrike Witte, MSLT, Catherine Moran, PhD, Grant
Clinical Measurement of Pharyngeal Surface Electromyography: Exploratory Research Sebastian H. Doeltgen, MSLT, Andrea Hofmayer, MA, Freya Gumbley, BSLT, Ulrike Witte, MSLT, Catherine Moran, PhD, Grant
Myasthenia Gravis What is Myasthenia Gravis? Who is at risk of developing MG? Is MG hereditary? What are the symptoms of MG? What causes MG?
 Myasthenia Gravis What is Myasthenia Gravis? Myasthenia Gravis (MG) is a chronic, autoimmune disease that causes muscle weakness and excessive muscle fatigue. It is uncommon, affecting about 15 in every
Myasthenia Gravis What is Myasthenia Gravis? Myasthenia Gravis (MG) is a chronic, autoimmune disease that causes muscle weakness and excessive muscle fatigue. It is uncommon, affecting about 15 in every
Gender Differences in Normal Swallow Ahlam A. Nabieh, Ahmed M. Emam, Eman M. Mostafa and Rasha M. Hashem
 EJNSO Gender Differences in Normal Swallow Ahlam A. Nabieh, Ahmed M. Emam, Eman M. Mostafa and Rasha M. Hashem Phoniatrics unit, ENT department, Sohag University Abstract Introduction: Swallowing is a
EJNSO Gender Differences in Normal Swallow Ahlam A. Nabieh, Ahmed M. Emam, Eman M. Mostafa and Rasha M. Hashem Phoniatrics unit, ENT department, Sohag University Abstract Introduction: Swallowing is a
Identification number: TÁMOP /1/A
 Manifestation of Novel Social Challenges of the European Union in the Teaching Material of Medical Biotechnology Master s Programmes at the University of Pécs and at the University of Debrecen Identification
Manifestation of Novel Social Challenges of the European Union in the Teaching Material of Medical Biotechnology Master s Programmes at the University of Pécs and at the University of Debrecen Identification
Communication and Swallowing with PSP/CBD. Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist
 Communication and Swallowing with PSP/CBD Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist A Speech Therapist? Why? Swallowing (Dysphagia) Speech (Dysarthria, Dysphonia) Language (Aphasia) An Experienced
Communication and Swallowing with PSP/CBD Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist A Speech Therapist? Why? Swallowing (Dysphagia) Speech (Dysarthria, Dysphonia) Language (Aphasia) An Experienced
Increased motor unit fibre density in the external
 Journal of Neurology, Neurosurgery, and Psychiatry, 1980, 43, 343-347 Increased motor unit fibre density in the external anal sphincter muscle in ano-rectal incontinence: a single fibre EMG study M E NEILL
Journal of Neurology, Neurosurgery, and Psychiatry, 1980, 43, 343-347 Increased motor unit fibre density in the external anal sphincter muscle in ano-rectal incontinence: a single fibre EMG study M E NEILL
I 296. Electrophysiological investigations of cephalic tetanus. fbr C.)
 Journal of Neurology, Neurosurgery, and Psychiatry, 1973, 36, 296-301 Electrophysiological investigations of cephalic tetanus RICARDO GARCIA-MULLIN AND ROBERT B. DAROFF From the Department of Neurology,
Journal of Neurology, Neurosurgery, and Psychiatry, 1973, 36, 296-301 Electrophysiological investigations of cephalic tetanus RICARDO GARCIA-MULLIN AND ROBERT B. DAROFF From the Department of Neurology,
CONCETTI GENERALI SULLE DISFAGIE DI ORIGINE ESOFAGEA
 LA DISFAGIA ESOFAGEA Pavia, 12.1.217 CONCETTI GENERALI SULLE DISFAGIE DI ORIGINE ESOFAGEA Michele Di Stefano Clinica Medica 1 Fondazione IRCCS Policlinico S.Matteo Università di Pavia Pavia PHARYNGOESOPHAGEAL
LA DISFAGIA ESOFAGEA Pavia, 12.1.217 CONCETTI GENERALI SULLE DISFAGIE DI ORIGINE ESOFAGEA Michele Di Stefano Clinica Medica 1 Fondazione IRCCS Policlinico S.Matteo Università di Pavia Pavia PHARYNGOESOPHAGEAL
Myasthenia gravis. Page 1 of 7
 Myasthenia gravis What is myasthenia gravis? Myasthenia gravis (sometimes abbreviated to MG) is a chronic, autoimmune condition that causes muscle weakness and excessive muscle fatigue. It is rare, affecting
Myasthenia gravis What is myasthenia gravis? Myasthenia gravis (sometimes abbreviated to MG) is a chronic, autoimmune condition that causes muscle weakness and excessive muscle fatigue. It is rare, affecting
When Eating Becomes A Challenge Dysphagia
 When Eating Becomes A Challenge Dysphagia 1. DYSPHAGIA, WHAT IS IT? 2. IMPLICATIONS 3. ASSESSMENT 4. COMPENSATORY SWALLOWING AND EXERCISES 5. DIET TEXTURE ADJUSTMENTS Swallowing Dysfunction = Dysphagia
When Eating Becomes A Challenge Dysphagia 1. DYSPHAGIA, WHAT IS IT? 2. IMPLICATIONS 3. ASSESSMENT 4. COMPENSATORY SWALLOWING AND EXERCISES 5. DIET TEXTURE ADJUSTMENTS Swallowing Dysfunction = Dysphagia
Medicine, University of Lund, Sweden
 336 J. Phy8iol. (1961), 156, pp. 336-343 With 6 text-ftgures Printed in Great Britain AN ELECTROPHYSIOLOGIC STUDY OF THE NEURO- MUSCULAR JUNCTION IN MYASTHENIA GRAVIS BY 0. DAHLBACK, D. ELMQVIST, T. R.
336 J. Phy8iol. (1961), 156, pp. 336-343 With 6 text-ftgures Printed in Great Britain AN ELECTROPHYSIOLOGIC STUDY OF THE NEURO- MUSCULAR JUNCTION IN MYASTHENIA GRAVIS BY 0. DAHLBACK, D. ELMQVIST, T. R.
study. The subject was chosen as typical of a group of six soprano voices methods. METHOD
 254 J. Physiol. (I937) 9I, 254-258 6I2.784 THE MECHANISM OF PITCH CHANGE IN THE VOICE BY R. CURRY Phonetics Laboratory, King's College, Neweastle-on-Tyne (Received 9 August 1937) THE object of the work
254 J. Physiol. (I937) 9I, 254-258 6I2.784 THE MECHANISM OF PITCH CHANGE IN THE VOICE BY R. CURRY Phonetics Laboratory, King's College, Neweastle-on-Tyne (Received 9 August 1937) THE object of the work
Swallowing after a Total Laryngectomy
 Swallowing after a Total Laryngectomy Diane Longnecker, M.S.,CCC-SLP, BCS-S Baylor Institute for Rehabilitation at Baylor University Medical Center Dallas, TX Disclosure Statement No relevant financial
Swallowing after a Total Laryngectomy Diane Longnecker, M.S.,CCC-SLP, BCS-S Baylor Institute for Rehabilitation at Baylor University Medical Center Dallas, TX Disclosure Statement No relevant financial
Surgical aspects of dysphagia
 Dysphagia Why is dysphagia important? Surgery Surgical aspects of dysphagia Adrian P. Ireland aireland@eircom.net Academic RCSI Department of Surgery, Beaumont Hospital Why important Definitons Swallowing
Dysphagia Why is dysphagia important? Surgery Surgical aspects of dysphagia Adrian P. Ireland aireland@eircom.net Academic RCSI Department of Surgery, Beaumont Hospital Why important Definitons Swallowing
Larynx - cartilaginous structure holding the vocal folds which protrude into airstream
 1! Larynx - cartilaginous structure holding the vocal folds which protrude into airstream 2! Flow increase - like thumb over garden hose Pressure drop - narrower space forces pressure drop due to speed
1! Larynx - cartilaginous structure holding the vocal folds which protrude into airstream 2! Flow increase - like thumb over garden hose Pressure drop - narrower space forces pressure drop due to speed
NURSE-UP RESPIRATORY SYSTEM
 NURSE-UP RESPIRATORY SYSTEM FUNCTIONS OF THE RESPIRATORY SYSTEM Pulmonary Ventilation - Breathing Gas exchanger External Respiration between lungs and bloodstream Internal Respiration between bloodstream
NURSE-UP RESPIRATORY SYSTEM FUNCTIONS OF THE RESPIRATORY SYSTEM Pulmonary Ventilation - Breathing Gas exchanger External Respiration between lungs and bloodstream Internal Respiration between bloodstream
2013 Charleston Swallowing Conference
 Providing Quality Affordable Continuing Education and Treatment Materials for over 30 years. 2013 Charleston Swallowing Conference Session 9 Bedside Assessment: What Does It Tell You? 10:00 11:30 am Saturday,
Providing Quality Affordable Continuing Education and Treatment Materials for over 30 years. 2013 Charleston Swallowing Conference Session 9 Bedside Assessment: What Does It Tell You? 10:00 11:30 am Saturday,
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 7/2/2011 Radiology Quiz of the Week # 27 Page 1 CLINICAL PRESENTATION AND RADIOLOGY QUIZ
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 7/2/2011 Radiology Quiz of the Week # 27 Page 1 CLINICAL PRESENTATION AND RADIOLOGY QUIZ
MYASTHENIA GRAVIS. Mr. D.Raju, M.pharm, Lecturer
 MYASTHENIA GRAVIS Mr. D.Raju, M.pharm, Lecturer OUTLINE Background Anatomy Pathophysiology Clinical Presentation Treatment BACKGROUND Acquired autoimmune disorder Clinically characterized by: Weakness
MYASTHENIA GRAVIS Mr. D.Raju, M.pharm, Lecturer OUTLINE Background Anatomy Pathophysiology Clinical Presentation Treatment BACKGROUND Acquired autoimmune disorder Clinically characterized by: Weakness
CONCETTI GENERALI SULLE DISFAGIE DI ORIGINE ESOFAGEA
 MECCANISMI FISIOLOGICI AUTOMATICO-RIFLESSI DELL ESOFAGO CONCETTI GENERALI SULLE DISFAGIE DI ORIGINE ESOFAGEA Michele Di Stefano Clinica Medica 1 Fondazione IRCCS Policlinico S.Matteo Università di Pavia
MECCANISMI FISIOLOGICI AUTOMATICO-RIFLESSI DELL ESOFAGO CONCETTI GENERALI SULLE DISFAGIE DI ORIGINE ESOFAGEA Michele Di Stefano Clinica Medica 1 Fondazione IRCCS Policlinico S.Matteo Università di Pavia
The PHARYNX. Dr. Nabil Khouri MD Ph.D
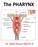 The PHARYNX Dr. Nabil Khouri MD Ph.D PHARYNX Fibromuscular tube lined with mucous membrane extends from base of skull to lower border of cricoid cartilage (C-6). 12-14 cm long At the lower border of cricoid
The PHARYNX Dr. Nabil Khouri MD Ph.D PHARYNX Fibromuscular tube lined with mucous membrane extends from base of skull to lower border of cricoid cartilage (C-6). 12-14 cm long At the lower border of cricoid
THREE STEPS TO SUCCESS
 THREE STEPS TO SUCCESS ICE TE EV REC OM PA THE LON GR U N ED IN ND ME NTE D MEDIC AL D THE SOLUTION AGAINST snoring sleep apnea CMD pain swallowing disorders etc. patented medical product easy causal effective
THREE STEPS TO SUCCESS ICE TE EV REC OM PA THE LON GR U N ED IN ND ME NTE D MEDIC AL D THE SOLUTION AGAINST snoring sleep apnea CMD pain swallowing disorders etc. patented medical product easy causal effective
Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing
 PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing
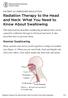 PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
Author's response to reviews
 Author's response to reviews Title: Dysphagia in Patients After Dental Extraction: Surface Electromyography Study Authors: Michael Vaiman (vaimed@yahoo.com) Oded Nahlieli (nahlieli@yahoo.com) Eli Eliav
Author's response to reviews Title: Dysphagia in Patients After Dental Extraction: Surface Electromyography Study Authors: Michael Vaiman (vaimed@yahoo.com) Oded Nahlieli (nahlieli@yahoo.com) Eli Eliav
Feeding and Swallowing Problems in the Child with Special Needs
 Feeding and Swallowing Problems in the Child with Special Needs Joan Surfus, OTR/L, SWC Amy Lynch, MS, OTR/L Misericordia University This presentation is made possible, in part, by the support of the American
Feeding and Swallowing Problems in the Child with Special Needs Joan Surfus, OTR/L, SWC Amy Lynch, MS, OTR/L Misericordia University This presentation is made possible, in part, by the support of the American
04 Development of the Face and Neck. Development of the Face Development of the neck
 04 Development of the Face and Neck Development of the Face Development of the neck Development of the face Overview of facial development The fourth week ~ the twelfth week of prenatal development Between
04 Development of the Face and Neck Development of the Face Development of the neck Development of the face Overview of facial development The fourth week ~ the twelfth week of prenatal development Between
New Directions in the Diagnostic Assessment of Swallowing Disorders in Children
 New Directions in the Diagnostic Assessment of Swallowing Disorders in Children Larissa Kate Noll BAppSc (Speech Pathology) School of Medicine Faculty of Health Sciences Flinders University South Australia
New Directions in the Diagnostic Assessment of Swallowing Disorders in Children Larissa Kate Noll BAppSc (Speech Pathology) School of Medicine Faculty of Health Sciences Flinders University South Australia
Electrodiagnosis of Neuromuscular Junction Disorders
 NMT overview Electrodiagnosis of Neuromuscular Junction Disorders Motor NAP arrives at nerve terminal Voltage-gated calcium channels open Ca +2 moves into presynaptic nerve terminal SNARE proteins elicit
NMT overview Electrodiagnosis of Neuromuscular Junction Disorders Motor NAP arrives at nerve terminal Voltage-gated calcium channels open Ca +2 moves into presynaptic nerve terminal SNARE proteins elicit
Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists
 Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists What is NCS/EMG? NCS examines the conduction properties of sensory and motor peripheral nerves. For both
Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists What is NCS/EMG? NCS examines the conduction properties of sensory and motor peripheral nerves. For both
SWALLOW PHYSIOLOGY IN PATIENTS WITH TRACH CUFF INFLATED OR DEFLATED: A RETROSPECTIVE STUDY
 SWALLOW PHYSIOLOGY IN PATIENTS WITH TRACH CUFF INFLATED OR DEFLATED: A RETROSPECTIVE STUDY Ruiying Ding, PhD, 1 Jeri A. Logemann, PhD 2 1 University of Wisconsin-Whitewater, Department of Communicative
SWALLOW PHYSIOLOGY IN PATIENTS WITH TRACH CUFF INFLATED OR DEFLATED: A RETROSPECTIVE STUDY Ruiying Ding, PhD, 1 Jeri A. Logemann, PhD 2 1 University of Wisconsin-Whitewater, Department of Communicative
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/20412 holds various files of this Leiden University dissertation. Author: Niks, E.H. Title: Myasthenia gravis with antibodies to muscle-specific kinase
Cover Page The handle http://hdl.handle.net/1887/20412 holds various files of this Leiden University dissertation. Author: Niks, E.H. Title: Myasthenia gravis with antibodies to muscle-specific kinase
64 Chiharu Ashida and Tomoshige Koga of blood gases as well as afferent gag reflex activities are sent to secondary NTS neurons in the medulla oblonga
 Kawasaki Journal of Medical Welfare Vol. 11, No. 2, 2006 63 68 Original Paper Effects of Arterial Oxygen Saturation on Gag Reflex in Humans Chiharu ASHIDA Λ and Tomoshige KOGA ΛΛ (Accepted November 4,
Kawasaki Journal of Medical Welfare Vol. 11, No. 2, 2006 63 68 Original Paper Effects of Arterial Oxygen Saturation on Gag Reflex in Humans Chiharu ASHIDA Λ and Tomoshige KOGA ΛΛ (Accepted November 4,
Swallowing disorder, aspiration: now what?
 Swallowing disorder, aspiration: now what? Poster No.: C-0691 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Kavka, M. Kysilko, M. Rocek; Prague/CZ Keywords: Swallowing disorders, Dynamic swallowing
Swallowing disorder, aspiration: now what? Poster No.: C-0691 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Kavka, M. Kysilko, M. Rocek; Prague/CZ Keywords: Swallowing disorders, Dynamic swallowing
RECOMMENDATIONS & UPDATES IN THE MANAGEMENT OF POST- STROKE DYSPHAGIA
 RECOMMENDATIONS & UPDATES IN THE MANAGEMENT OF POST- STROKE DYSPHAGIA Feeding in the Acute Stroke Period: - Early initiation of feeding is beneficial w/c decreases the risk of infections, improve survival
RECOMMENDATIONS & UPDATES IN THE MANAGEMENT OF POST- STROKE DYSPHAGIA Feeding in the Acute Stroke Period: - Early initiation of feeding is beneficial w/c decreases the risk of infections, improve survival
Larynx. Rudimentary. Behind the posterior surface : -stylopharyngeus - salpingopharyngeus -platopharyngeus
 Larynx The larynx is an organ that provides a protective sphincter at the inlet of the air passages and is responsible for voice production. It extends from C3-C6: *Posterior: the pharynx *Lateral: the
Larynx The larynx is an organ that provides a protective sphincter at the inlet of the air passages and is responsible for voice production. It extends from C3-C6: *Posterior: the pharynx *Lateral: the
Daniels SK & Huckabee ML (2008). Dysphagia Following Stroke. Muscles of Deglutition. Lateral & Mesial Premotor Area 6. Primary Sensory
 An Overview of Dysphagia in the Stroke Population Stephanie K. Daniels, PhD Michael E. DeBakey VA Medical Center PM & R, Baylor College of Medicine Communication Sciences and Disorders, University of Houston
An Overview of Dysphagia in the Stroke Population Stephanie K. Daniels, PhD Michael E. DeBakey VA Medical Center PM & R, Baylor College of Medicine Communication Sciences and Disorders, University of Houston
Nutricia. Nutrition and Dysphagia
 Nutricia Nutrition and Dysphagia 1 Introduction What is Dysphagia? The inability to swallow normally or freely. Disorder in the swallowing process that does not allow safe passing of food from the mouth
Nutricia Nutrition and Dysphagia 1 Introduction What is Dysphagia? The inability to swallow normally or freely. Disorder in the swallowing process that does not allow safe passing of food from the mouth
11/18/13 ECG SIGNAL ACQUISITION HARDWARE DESIGN. Origin of Bioelectric Signals
 ECG SIGNAL ACQUISITION HARDWARE DESIGN Origin of Bioelectric Signals 1 Cell membrane, channel proteins Electrical and chemical gradients at the semi-permeable cell membrane As a result, we get a membrane
ECG SIGNAL ACQUISITION HARDWARE DESIGN Origin of Bioelectric Signals 1 Cell membrane, channel proteins Electrical and chemical gradients at the semi-permeable cell membrane As a result, we get a membrane
Assessment Instruments for Your Patients with Myasthenia Gravis (MG)
 Assessment Instruments for Your Patients with Myasthenia Gravis (MG) Table of Contents Reported by patient Myasthenia Gravis Activities of Daily Living (MG-ADL): ~10 minutes 8-item outcome measure that
Assessment Instruments for Your Patients with Myasthenia Gravis (MG) Table of Contents Reported by patient Myasthenia Gravis Activities of Daily Living (MG-ADL): ~10 minutes 8-item outcome measure that
Human Physiology Lab (Biol 236L) Fall, 2015
 1 Human Physiology Lab (Biol 236L) Fall, 2015 Name: Nursing Case Study: Muscle Weakness Chief Complaint: A 26-year-old woman with muscle weakness in the face. Patient Presentation: A 26-year-old woman
1 Human Physiology Lab (Biol 236L) Fall, 2015 Name: Nursing Case Study: Muscle Weakness Chief Complaint: A 26-year-old woman with muscle weakness in the face. Patient Presentation: A 26-year-old woman
Digestive System Processes
 Unit 7 Digestive System Processes ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY Processes of the Digestive System Ingestion- getting food into the mouth Propulsion- moving foods through the digestive system
Unit 7 Digestive System Processes ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY Processes of the Digestive System Ingestion- getting food into the mouth Propulsion- moving foods through the digestive system
Clinical Swallowing Exam
 Clinical Evaluation Template 1 Clinical Exam Name: ID/Medical record number: Date of exam: Referred by: Reason for referral: Medical diagnosis: Date of onset of diagnosis: Other relevant medical history/diagnoses/surgery
Clinical Evaluation Template 1 Clinical Exam Name: ID/Medical record number: Date of exam: Referred by: Reason for referral: Medical diagnosis: Date of onset of diagnosis: Other relevant medical history/diagnoses/surgery
INTRAOPERATIVE NEUROPHYSIOLOGICAL MONITORING FOR MICROVASCULAR DECOMPRESSION SURGERY IN PATIENTS WITH HEMIFACIAL SPASM
 INTRAOPERATIVE NEUROPHYSIOLOGICAL MONITORING FOR MICROVASCULAR DECOMPRESSION SURGERY IN PATIENTS WITH HEMIFACIAL SPASM WILLIAM D. MUSTAIN, PH.D., CNIM, BCS-IOM DEPARTMENT OF OTOLARYNGOLOGY AND COMMUNICATIVE
INTRAOPERATIVE NEUROPHYSIOLOGICAL MONITORING FOR MICROVASCULAR DECOMPRESSION SURGERY IN PATIENTS WITH HEMIFACIAL SPASM WILLIAM D. MUSTAIN, PH.D., CNIM, BCS-IOM DEPARTMENT OF OTOLARYNGOLOGY AND COMMUNICATIVE
CLINICAL PRESENTATION
 MYASTHENIA GRAVIS INTRODUCTION Most common primary disorder of neuromuscular transmission Usually due to acquired immunological abnormality Also due to genetic abnormalities at neuromuscular junction.
MYASTHENIA GRAVIS INTRODUCTION Most common primary disorder of neuromuscular transmission Usually due to acquired immunological abnormality Also due to genetic abnormalities at neuromuscular junction.
Please refer back to the slides as these are extra notes only. Slide 2 -The Larynx is a Box of cartilage.
 [ANATOMY #3] 1 بسم رلاهللا Please refer back to the slides as these are extra notes only. Slide 2 -The Larynx is a Box of cartilage. -The lower border of c6 is the lower border of cricoid cartilage. -The
[ANATOMY #3] 1 بسم رلاهللا Please refer back to the slides as these are extra notes only. Slide 2 -The Larynx is a Box of cartilage. -The lower border of c6 is the lower border of cricoid cartilage. -The
Responses to electrical stimulation of denervated human muscle fibres recorded with single fibre EMG
 Journal of Neurology, Neurosurgery, and Psychiatry 1983;46:305-309 Responses to electrical stimulation of denervated human muscle fibres recorded with single fibre EMG JOZE TRONTELJ, ERIK STALBERG From
Journal of Neurology, Neurosurgery, and Psychiatry 1983;46:305-309 Responses to electrical stimulation of denervated human muscle fibres recorded with single fibre EMG JOZE TRONTELJ, ERIK STALBERG From
Clearance mechanisms of the aperistaltic esophagus. The pump-gun hypothesis.
 Gut Online First, published on December 14, 2005 as 10.1136/gut.2005.085423 Clearance mechanisms of the aperistaltic esophagus. The pump-gun hypothesis. Radu Tutuian 1, Daniel Pohl 1, Donald O Castell
Gut Online First, published on December 14, 2005 as 10.1136/gut.2005.085423 Clearance mechanisms of the aperistaltic esophagus. The pump-gun hypothesis. Radu Tutuian 1, Daniel Pohl 1, Donald O Castell
THE EFFECTS OF TWO REHABILITATION EXERCISES ON SUBMENTAL HYOLARYNGEAL MUSCULAR ACTIVITY. Teresa D. Hughes
 Running head: EFFECTS OF EXERCISES ON SUBMENTAL MUSCLE ACTIVITY THE EFFECTS OF TWO REHABILITATION EXERCISES ON SUBMENTAL HYOLARYNGEAL MUSCULAR ACTIVITY by Teresa D. Hughes Bachelor of Science, 2013 Texas
Running head: EFFECTS OF EXERCISES ON SUBMENTAL MUSCLE ACTIVITY THE EFFECTS OF TWO REHABILITATION EXERCISES ON SUBMENTAL HYOLARYNGEAL MUSCULAR ACTIVITY by Teresa D. Hughes Bachelor of Science, 2013 Texas
Neuromuscular Junction Testing ELBA Y. GERENA MALDONADO, MD ACTING ASSISTANT PROFESSOR UNIVERSITY OF WASHINGTON MEDICAL CENTER
 Neuromuscular Junction Testing ELBA Y. GERENA MALDONADO, MD ACTING ASSISTANT PROFESSOR UNIVERSITY OF WASHINGTON MEDICAL CENTER Objectives Neurophysiology Electrodiagnostic Evaluation Clinical Application
Neuromuscular Junction Testing ELBA Y. GERENA MALDONADO, MD ACTING ASSISTANT PROFESSOR UNIVERSITY OF WASHINGTON MEDICAL CENTER Objectives Neurophysiology Electrodiagnostic Evaluation Clinical Application
Cervical radiculopathy: diagnostic aspects and non-surgical treatment Kuijper, B.
 UvA-DARE (Digital Academic Repository) Cervical radiculopathy: diagnostic aspects and non-surgical treatment Kuijper, B. Link to publication Citation for published version (APA): Kuijper, B. (2011). Cervical
UvA-DARE (Digital Academic Repository) Cervical radiculopathy: diagnostic aspects and non-surgical treatment Kuijper, B. Link to publication Citation for published version (APA): Kuijper, B. (2011). Cervical
Index. Note: Page numbers of article titles are in boldface type.
 Neurol Clin N Am 20 (2002) 605 617 Index Note: Page numbers of article titles are in boldface type. A ALS. See Amyotrophic lateral sclerosis (ALS) Amyotrophic lateral sclerosis (ALS) active denervation
Neurol Clin N Am 20 (2002) 605 617 Index Note: Page numbers of article titles are in boldface type. A ALS. See Amyotrophic lateral sclerosis (ALS) Amyotrophic lateral sclerosis (ALS) active denervation
COMMUNICATION AND SWALLOWING DISORDERS IN PARKINSON S DISEASE Challenges, Treatments, and Resources
 COMMUNICATION AND SWALLOWING DISORDERS IN PARKINSON S DISEASE Challenges, Treatments, and Resources Rosemary B. Loftin, M.S. CCC/SLP Supervisor of Speech Pathology Services Mayo Clinic Hospital Arizona
COMMUNICATION AND SWALLOWING DISORDERS IN PARKINSON S DISEASE Challenges, Treatments, and Resources Rosemary B. Loftin, M.S. CCC/SLP Supervisor of Speech Pathology Services Mayo Clinic Hospital Arizona
Falk Symposium, , , Portorož. Physiology of Swallowing and Anti-Gastroesophageal. Reflux-Mechanisms. Mechanisms: C.
 Falk Symposium, 15.-16.6.07, 16.6.07, Portorož Physiology of Swallowing and Anti-Gastroesophageal Reflux-Mechanisms Mechanisms: Anything new from a radiologist s view? C.Kulinna-Cosentini Cosentini Medical
Falk Symposium, 15.-16.6.07, 16.6.07, Portorož Physiology of Swallowing and Anti-Gastroesophageal Reflux-Mechanisms Mechanisms: Anything new from a radiologist s view? C.Kulinna-Cosentini Cosentini Medical
MOVEMENT RULES. Dr. Tripat Deep Singh (MBBS, MD, RPSGT, RST) International Sleep Specialist (World Sleep Federation program)
 MOVEMENT RULES Dr. Tripat Deep Singh (MBBS, MD, RPSGT, RST) International Sleep Specialist (World Sleep Federation program) 1. Scoring Periodic Limb Movement in Sleep (PLMS) A. The following rules define
MOVEMENT RULES Dr. Tripat Deep Singh (MBBS, MD, RPSGT, RST) International Sleep Specialist (World Sleep Federation program) 1. Scoring Periodic Limb Movement in Sleep (PLMS) A. The following rules define
The Frequency of Gastroesophageal Reflux Disease in Nutcracker Esophagus and the Effect of Acid-Reduction Therapy on the Motor Abnormality
 Bahrain Medical Bulletin, Vol.22, No.4, December 2000 The Frequency of Gastroesophageal Reflux Disease in Nutcracker Esophagus and the Effect of Acid-Reduction Therapy on the Motor Abnormality Saleh Mohsen
Bahrain Medical Bulletin, Vol.22, No.4, December 2000 The Frequency of Gastroesophageal Reflux Disease in Nutcracker Esophagus and the Effect of Acid-Reduction Therapy on the Motor Abnormality Saleh Mohsen
Evaluating Swallowing Dysfunction Using a 100-ml Water Swallowing Test
 Dysphagia 19:43 47 (2004) DOI: 10.1007/s00455-003-0030-x Evaluating Swallowing Dysfunction Using a 100-ml Water Swallowing Test Meng-Chun Wu, MD, 1 Yeun-Chung Chang, MD, 2 Tyng-Guey Wang, MD, 1 and Li-Chan
Dysphagia 19:43 47 (2004) DOI: 10.1007/s00455-003-0030-x Evaluating Swallowing Dysfunction Using a 100-ml Water Swallowing Test Meng-Chun Wu, MD, 1 Yeun-Chung Chang, MD, 2 Tyng-Guey Wang, MD, 1 and Li-Chan
