رناد زكريا Dr. ahmad Dr. ahmad. P a g e 1
|
|
|
- Egbert Parker
- 5 years ago
- Views:
Transcription
1 5 رناد زكريا Dr. ahmad Dr. ahmad P a g e 1
2 Before we start. -This sheet was written according to section 2 s record and reviewed according to section 1 s record by Ruba Hussien with all thanks and I referred to last year sheets. - In this sheet, the topic about anemia will end and we ll start talking about polycythemia. - For you who want to go through the book this sheet will cover the pages &425 & In the previous lecture, we were talking about hemolytic anemia of intrinsic factor and we discussed the heredity types: 1-Membranopathies spherocytosis. 2-Hemoglobinopathies thalassemia and sickle cell disease. 3- Enzymopathies G6PD deficiency (it's our topic in this sheet). And the Acquired type, which is Paroxysmal nocturnal hemoglobinuria (it's our topic in this sheet as well). Enzymopathies G6PD deficiency G6PD is an enzyme which produces NADPH; NADPH will in turn reduce glutathione which will find reactive oxygen species and get rid of them. - So if we have G6PD deficiency, this cycle (shown in the figure) will break, making RBCs more prone to oxidative stress. - Cells that are more prone to oxidative stress are the old senescent RBCs; in other words, young RBCs are not affected as severely as old RBCs. - Remember that the half-life of an RBC is 120 days and with daily production and turnover of cells, old and new RBCs are found in the blood. P a g e 2
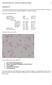
3 - G6PD deficiency is an X-linked disorder more common in males. - Many G6PD variants exist (over 400); those associated with disease are mainly two: 1- G6PD A- (common in African Americans). 2- G6PD Mediterranean (common in Middle East). - the Mediterranean is more severe than G6PD A-. *Hemolysis in G6PD deficiency is acute and episodic compared to hemolysis in spherocytosis where it is chronic. For example, if a patient who doesn t have chronic hemolysis and got exposed to an acute attack, he will suffer from hemolytic anemia; on the other hand, spherocytosis patients always have hemolysis even if it was presymptomatic or subclavian. **The acute attacks that cause acute episodic hemolysis in G6PD deficiency are: 1-Infections: most common cause. 2-Drugs: antimalarials, nitrofurantoin (old antibiotic for UTIs, especially in females). 3-Certain foods: fava beans; one of the least common causes. - Once the oxidative stress occurs, the old RBCs will undergo hemolysis. The acute episodic hemolysis will stop even when the patient takes the drug that causes the hemolysis or still has an infection. Why? Because the new RBCs have the ability to fight this oxidative stress more than the old ones, so once the old RBCs undergo hemolysis, the patient will come back to being normal. - After oxidation, the oxidized hemoglobin denatures and precipitates, forming intracellular inclusions called Heinz bodies. - Or the less severely damaged cells lose their deformability and suffer further injury when splenic phagocytes attempt to "pluck out" the Heinz bodies, creating so called bite cells. Remember: Heinz bodies are denatured hemoglobin molecules; when there is oxidative stress on the hemoglobin, the sulfhydryl groups within the amino acids will combine with each other causing precipitation (Heinz bodies). P a g e 3
4 This is the denatured globin Why are cells in the picture above cells (containing denatured globin) yellow compared to the normal color of RBCs? Because Heinz bodies are not seen by Wright Giemsa stain which we normally use (our routine stain that we use in every blood test; i.e. in staining peripheral blood and bone marrow); that s why we use a special stain known collectively as supravital stains, specifically crystal violet. ** Hemolysis in G6PD can be either intra- or extravascular depending on how much the oxidizing is or how strong the attack is. ** Since it s episodic and acute (rather than chronic) hemolysis, features related to chronic hemolysis (splenomegaly and gallbladder stones) are typically absent. Anemia s where splenomegaly and gallbladder stones are absent are: a. Aplastic anemia b. Sickle cell anemia c. G6PD deficiency Acquired: Paroxysmal nocturnal hemoglobinuria (PNH): - PNH is rare, is due to an acquired mutation (not an inherited disease), and is caused by a mutation on the protein found on RBCs that protect them from the complement system. P a g e 4
5 - Not all cells are affected; one clone in the body has this mutation. It's kind of similar to leukemia or any cancer; one clone of the disease is affected not the whole cells in the body, but here this condition is not neoplastic. **Mutations don t mean they are inherited. -To be inherited, the mutations must be germ cell mutations. - PNH results from acquired mutations in the phosphatidylinositol glycan complementation group A gene (PIGA), an enzyme that is essential for the synthesis of certain membrane-associated complement regulatory proteins -PIGA gene is present on the X chromosome. - A mutation in PIGA gene will result in decreased production of PIGA protein on the cellular membrane less CD55 and CD59 to counter complement proteins the cell will be more prone to complement fixation and hemolysis. - It is the only hemolytic anemia resulting from an acquired genetic mutation. Clinical manifestations 1- Low level chronic hemolytic anemia. 2- It's NOCTURNAL, why? Because the fixation of complement is enhanced by the slight decrease in blood ph that accompanies sleep, rendering cells more prone to hemolysis. 3- It has some association with aplastic anemia and thrombosis that s why the most encountered clinical scenario is when you suspect PNH in a young patient with anemia and thrombosis. 4- High incidence of bone marrow disorders like myelodysplastic syndrome and leukemia. ** The treatment of those patients will increase the risk of Neisseria infection, why? Because the treatment will fight the complement proteins, and complements specifically the last 5 proteins, which are called membrane attack complex (MAC) are really important in fighting Neisseria. If you inhibit these proteins, you will risk that the P a g e 5
6 patient might be affected by Neisseria. ** That was the last topic in anemia lectures. We will start with the new topic which is: Polycythemia Denotes an abnormally high red cell count, usually with a corresponding increase in the hemoglobin level. **In polycythemia, these two criteria usually go side by side, so whenever you hear polycythemia, it means high RBC count as well as elevated hemoglobin level. ** While in anemia, the decrease in hemoglobin level does not necessarily reflect low RBC Count. For example, in beta-thalassemia minor, there s a normal or increased RBC count (Erythrocytosis) associated with low hemoglobin level. ** Polycythemia may be absolute or relative. Relative Polycythemia - Occurs when there s a decrease in plasma volume with no change in the total RBC mass. * It results from dehydration, which occurs with diarrhea, vomiting or diuretic therapy. * Remember the case of the pregnant woman that has low blood count as a result of fluid retention that leads to an increase in RBC concentration, but she doesn t have anemia. The same concept is applied here. Absolute Polycythemia - In absolute polycythemia, the increase of RBC count is due to overproduction of RBCs in the bone marrow. * It s classified into primary and secondary absolute polycythemia. * It s described as primary when increased red blood cell mass results from autonomous proliferation of erythroid progenitors, independent of erythropoietin. While in secondary, this overproduction is induced by erythropoietin (no problem in the RBC). P a g e 6
7 In other words, -Primary polycythemia is associated with low erythropoietin levels -Secondary polycythemia is associated with elevated erythropoietin levels 1- Secondary absolute polycythemia: As we just mentioned, secondary absolute polycythemia results from excess stimulation of erythroid progenitors by erythropoietin. **But how does this occur and what is the relation between erythropoietin and oxygen? 1- Hypoxia is sensed by kidney cells. 2- Kidneys cells also have a transcription factor called HIF (hypoxia induced factor). 3- If hypoxia occurs, kidney cells will sense it and HIF factor will be stabilized; therefore, it will act as a transcriptional factor for many genes. One of them is the gene that codes for erythropoietin. 4- Finally, increased erythropoietin secretion by kidney cells would increase RBC production. ** Keep in mind, in high oxygen tension, HIF will be destroyed and thus inactivated. **Two types of hypoxia occur generalized hypoxia and localized hypoxia: a. Generalized hypoxia, like in smoking, High altitude and High affinity hemoglobins. Hemoglobin in these cases have high affinity to oxygen. P a g e 7
8 b. Localized hypoxia, like in renal artery stenosis and polycystic kidney disease ** Moreover, some tumors can secrete erythropoietin. Examples are Wilms tumor, Renal cell carcinoma, Cerebellar hemangioma, Hepatocellular carcinoma. 2- Primary absolute polycythemia: - Erythropoietin production will be low. The most common cause of primary absolute polycythemia is polycythemia vera. ** Polycythemia vera is characterized by increased marrow production of red cells, granulocytes, and platelets (panmyelosis), so when we take a bone marrow biopsy, we will see proliferation of all myeloid cells. - So, it s an acquired, clonal neoplasm of bone marrow stem cells (Chronic myeloproliferative neoplasm). ** PCV is Strongly associated with JAK2 mutation. Such mutation is present in more than 97% of PV cases: - It s strongly associated with PCV, but it s not specific as seen in 50% of cases of some other chronic myeloproliferative disorders, such as essential thrombocythemia and primary myelofibrosis. - The most common JAK2 mutation is a Valine-to-phenylalanine substitution at residue 617. ** At first, the patient will have mild splenomegaly which will then become more severe (as a result of the congestion of the spleen). Also, the bone marrow will become hypercellular. **Late in the disease course, bone marrow fibrosis and significant organomegaly is present, PCV carries a 2% risk for transforming to acute myeloid leukemia. - In myeloproliferative neoplasm, the spleen will be very large. ** Myeloproliferative neoplasms (we will talk about them in other lectures). They are four major neoplasms: P a g e 8
9 a. polycythemia vera b. primary myelofibrosis c. essential thrombocythemia d. chronic myelogenous leukemia Clinical Features: 1- Pruritis. 2- Headache; dizziness. 3- Hyperuricemia and gout. 4- Increased risk of both major bleeding and thrombotic episodes, why? Because of the high levels of RBCs that cause viscosity in the blood, bleeding would occur because of dysfunctional platelets, so what kills in PCV is the thrombosis not the neoplasm itself. Examples: a. Deep venous thrombosis. b. Stroke. c. Myocardial infarction. d. Bowel infarction. e. Budd-Chiari syndrome formation of a blood clot within the hepatic veins which may progress to cirrhosis. f. Epistaxis and bleeding gums. ** Major hemorrhage can occur in ~10% of the patients. ** Spent phase fibrosis and splenomegaly. **2% might transform to acute myeloid leukemia THROMBOSIS IS THE MAJOR RISK FOR MORTLAITY IN THESE PATIENTS. Treatment: Treatment is Phlebotomy and administration of JAK2 inhibitors: - If you have high count of RBCs, you have to donate them, as simple as that. -And recently, JAK2 inhibitors have been developed. P a g e 9
10 Criteria for PCV diagnosis according to WHO: Major criteria: 1. Haemoglobin >18.5 g/dl in men, 16.5 g/dl in women. Or other evidence of increased red cell volume. 2. Presence of JAK2 V617F or other functionally similar mutations such as JAK2 exon 12 mutation. Minor criteria: 1. Bone marrow biopsy showing hyper-cellularity for age with trilineage growth (panmyelosis) with prominent erythroid, granulocytic and megakaryocytic proliferation. 2. Serum erythropoietin level below the reference range for normal. 3. Endogenous erythroid colony formation in vitro. (Not commonly used). - To diagnose PCV, you have to observe two major and minor criteria, or the first major criterion with two minor criteria. - The second major criterion is not sufficient, because JAK2 mutation is not specific for PCV. The Doctor s Questions: 1- Relative polycythemia occurs in the setting of: A. Wilms tumor B. Dehydration C. Renal cell carcinoma D. Polycythemia vera. E. Hypoxia P a g e 10
11 2- All of the following are examples of secondary absolute polycythemia, except: A. Smokers B. Renal artery stenosis C. Polycystic kidney D. Polycythemia vera E. High altitude 3- The risk of acute myeloid leukemia in polycythemia vera is: A. 2% B. 10% C. 30% D. 50% E. 70% 4- One of the following is a major criterion for PV: A. High hemoglobin B. Hypercellular bone marrow C. Low erythropoietin level D. High erythropoietin level E. Endogenous erythroid colony formation in vitro Answers: 1: B, 2: D, 3: A, 4: A "If you are not willing to risk the usual, you will have to settle for the ordinary." Sorry for any mistake P a g e 11
12 P a g e 12
Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms
 Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms Myelodysplastic syndrome (MDS) A multipotent stem cell that can differentiate into any of the myeloid lineage cells (RBCs, granulocytes, megakaryocytes)
Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms Myelodysplastic syndrome (MDS) A multipotent stem cell that can differentiate into any of the myeloid lineage cells (RBCs, granulocytes, megakaryocytes)
The Internists Approach to Polycythemia and Implications of Uncontrolled Disease
 The Internists Approach to Polycythemia and Implications of Uncontrolled Disease Mary Jo K. Voelpel, DO, FACOI, MA, CS Associate Clinical Professor MSU-COM Disclosures NONE Overview 1. Objectives 2. Case
The Internists Approach to Polycythemia and Implications of Uncontrolled Disease Mary Jo K. Voelpel, DO, FACOI, MA, CS Associate Clinical Professor MSU-COM Disclosures NONE Overview 1. Objectives 2. Case
Myelodysplastic Syndromes Myeloproliferative Disorders
 Myelodysplastic Syndromes Myeloproliferative Disorders Myelodysplastic Syndromes characterized by maturation defects that are associated with ineffective hematopoiesis and a high risk of transformation
Myelodysplastic Syndromes Myeloproliferative Disorders Myelodysplastic Syndromes characterized by maturation defects that are associated with ineffective hematopoiesis and a high risk of transformation
Polycthemia Vera (Rubra)
 Polycthemia Vera (Rubra) Polycthemia Vera (Rubra) Increased red cells Clonal Myeloid lineages also increased 2-13 cases per million Mean age: 60 years Sites of Involvement Bone marrow Peripheral blood
Polycthemia Vera (Rubra) Polycthemia Vera (Rubra) Increased red cells Clonal Myeloid lineages also increased 2-13 cases per million Mean age: 60 years Sites of Involvement Bone marrow Peripheral blood
Dana Alsulaibi. - Ahmad Almuhtaseb. - Tariq Al - Adaily
 - 2 - Dana Alsulaibi - Ahmad Almuhtaseb - Tariq Al - Adaily This sheet will talk about 4 diseases that cause hemolytic anemia, best of luck! 1) Hereditary Spherocytosis Transferred through inheritance
- 2 - Dana Alsulaibi - Ahmad Almuhtaseb - Tariq Al - Adaily This sheet will talk about 4 diseases that cause hemolytic anemia, best of luck! 1) Hereditary Spherocytosis Transferred through inheritance
CLINICAL CASE PRESENTATION
 European Winter School of Internal Medicine 2015 Riga, Latvia, 26-30 January CLINICAL CASE PRESENTATION Vasiliy Chulkov South Ural State Medical University (Chelyabinsk, Russia) CHELYABINSK CLINICAL HISTORY
European Winter School of Internal Medicine 2015 Riga, Latvia, 26-30 January CLINICAL CASE PRESENTATION Vasiliy Chulkov South Ural State Medical University (Chelyabinsk, Russia) CHELYABINSK CLINICAL HISTORY
Chronic Myeloproliferative Disorders
 1 Chronic Myeloproliferative Disorders 15th 9 April2015 Polycythemia vera Essential thrombocythemia Idiopathic primary myelofibrosis 2 Learning objectives To appreciate types of polycythaemia (erythrocytosis)
1 Chronic Myeloproliferative Disorders 15th 9 April2015 Polycythemia vera Essential thrombocythemia Idiopathic primary myelofibrosis 2 Learning objectives To appreciate types of polycythaemia (erythrocytosis)
Polycythemia Vera and other Myeloproliferative Neoplasms. A.Mousavi
 Polycythemia Vera and other Myeloproliferative Neoplasms A.Mousavi Chronic MPNs Multipotent hematopoietic progenitor cell is origin. Overproduction of one or more formed element of blood cells without
Polycythemia Vera and other Myeloproliferative Neoplasms A.Mousavi Chronic MPNs Multipotent hematopoietic progenitor cell is origin. Overproduction of one or more formed element of blood cells without
4 Jumana Jihad Dr. Ahmad Mansour Dr. Ahmad Mansour
 4 Jumana Jihad Dr. Ahmad Mansour Dr. Ahmad Mansour Anemia Decreased blood production Increased blood loss Hemolytic Hemorrhage Extravascular Intravascular Hemolytic (Further classification( Extrinsic Intrinsic
4 Jumana Jihad Dr. Ahmad Mansour Dr. Ahmad Mansour Anemia Decreased blood production Increased blood loss Hemolytic Hemorrhage Extravascular Intravascular Hemolytic (Further classification( Extrinsic Intrinsic
Pathology. #11 Acute Leukemias. Farah Banyhany. Dr. Sohaib Al- Khatib 23/2/16
 35 Pathology #11 Acute Leukemias Farah Banyhany Dr. Sohaib Al- Khatib 23/2/16 1 Salam First of all, this tafreegh is NOT as long as you may think. If you just focus while studying this, everything will
35 Pathology #11 Acute Leukemias Farah Banyhany Dr. Sohaib Al- Khatib 23/2/16 1 Salam First of all, this tafreegh is NOT as long as you may think. If you just focus while studying this, everything will
Chronic Idiopathic Myelofibrosis (CIMF)
 Chronic Idiopathic Myelofibrosis (CIMF) CIMF Synonyms Agnogenic myeloid metaplasia Myelosclerosis with myeloid metaplasia Chronic granulocytic-megakaryocytic myelosis CIMF Megakaryocytic proliferation
Chronic Idiopathic Myelofibrosis (CIMF) CIMF Synonyms Agnogenic myeloid metaplasia Myelosclerosis with myeloid metaplasia Chronic granulocytic-megakaryocytic myelosis CIMF Megakaryocytic proliferation
WHO Update to Myeloproliferative Neoplasms
 WHO Update to Myeloproliferative Neoplasms Archana M Agarwal, MD, Associate Professor of Pathology University of Utah Department of Pathology/ARUP Laboratories Myeloproliferative Neoplasms The categories
WHO Update to Myeloproliferative Neoplasms Archana M Agarwal, MD, Associate Professor of Pathology University of Utah Department of Pathology/ARUP Laboratories Myeloproliferative Neoplasms The categories
74y old Female with chronic elevation of Platelet count. August 18, 2005 Faizi Ali, MD Hematopathology Fellow
 74y old Female with chronic elevation of Platelet count August 18, 2005 Faizi Ali, MD Hematopathology Fellow Clinical History Patient is a 74y old otherwise healthy Caucasian female with no major complaint
74y old Female with chronic elevation of Platelet count August 18, 2005 Faizi Ali, MD Hematopathology Fellow Clinical History Patient is a 74y old otherwise healthy Caucasian female with no major complaint
12 Dynamic Interactions between Hematopoietic Stem and Progenitor Cells and the Bone Marrow: Current Biology of Stem Cell Homing and Mobilization
 Table of Contents: PART I: Molecular and Cellular Basis of Hematology 1 Anatomy and Pathophysiology of the Gene 2 Genomic Approaches to Hematology 3 Regulation of Gene Expression, Transcription, Splicing,
Table of Contents: PART I: Molecular and Cellular Basis of Hematology 1 Anatomy and Pathophysiology of the Gene 2 Genomic Approaches to Hematology 3 Regulation of Gene Expression, Transcription, Splicing,
Bone Marrow Transplantation
 Bone Marrow Transplantation Introduction Bone marrow is the spongy tissue inside all of your bones, including your hip and thigh bones. The bone marrow is like a factory that makes different types of blood
Bone Marrow Transplantation Introduction Bone marrow is the spongy tissue inside all of your bones, including your hip and thigh bones. The bone marrow is like a factory that makes different types of blood
HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD. Part 4 MYELOID NEOPLASMS
 HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD Part 4 MYELOID NEOPLASMS Introduction: o Myeloid neoplasms are divided into three major categories: o Acute
HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD Part 4 MYELOID NEOPLASMS Introduction: o Myeloid neoplasms are divided into three major categories: o Acute
Welcome to Master Class for Oncologists. Session 3: 9:15 AM - 10:00 AM
 Welcome to Master Class for Oncologists Session 3: 9:15 AM - 10:00 AM Miami, FL December 18, 2009 Myeloproliferative Neoplasms: Bringing Order to Complexity and Achieving Optimal Outcomes Speaker: Andrew
Welcome to Master Class for Oncologists Session 3: 9:15 AM - 10:00 AM Miami, FL December 18, 2009 Myeloproliferative Neoplasms: Bringing Order to Complexity and Achieving Optimal Outcomes Speaker: Andrew
بسم هللا الرحمن الرحيم
 بسم هللا الرحمن الرحيم WBCs disorders *Slide 2: - we will focus on the disorders that are related to the # of WBCs - in children the # of lymphocyte is more than it in adults,sometimes more than neutrophils
بسم هللا الرحمن الرحيم WBCs disorders *Slide 2: - we will focus on the disorders that are related to the # of WBCs - in children the # of lymphocyte is more than it in adults,sometimes more than neutrophils
Opportunities for Optimal Testing in the Myeloproliferative Neoplasms. Curtis A. Hanson, MD
 Opportunities for Optimal Testing in the Myeloproliferative Neoplasms Curtis A. Hanson, MD 2013 MFMER slide-1 DISCLOSURES: Relevant Financial Relationship(s) None Off Label Usage None 2013 MFMER slide-2
Opportunities for Optimal Testing in the Myeloproliferative Neoplasms Curtis A. Hanson, MD 2013 MFMER slide-1 DISCLOSURES: Relevant Financial Relationship(s) None Off Label Usage None 2013 MFMER slide-2
Hemolytic anemias (2 of 2)
 Hemolytic anemias (2 of 2) Sickle Cell Anemia The most common familial hemolytic anemia in the world Sickle cell anemia is the prototypical (and most prevalent) hemoglobinopathy Mutation in the β-globin
Hemolytic anemias (2 of 2) Sickle Cell Anemia The most common familial hemolytic anemia in the world Sickle cell anemia is the prototypical (and most prevalent) hemoglobinopathy Mutation in the β-globin
Department of Clinical Haematology
 Diagnosis in Primary Care and referral pathway for patients with a raised haematocrit Why implement this pathway? A raised haemoglobin or haematocrit is a common finding and can be a reason for referral.
Diagnosis in Primary Care and referral pathway for patients with a raised haematocrit Why implement this pathway? A raised haemoglobin or haematocrit is a common finding and can be a reason for referral.
2013 Pathology Student
 About this guide If you re reading this introduction, it means you are probably either a) covering hematopathology in your pathology class right now, or b) studying for boards. Either way, you ve come
About this guide If you re reading this introduction, it means you are probably either a) covering hematopathology in your pathology class right now, or b) studying for boards. Either way, you ve come
Done by :Aseel Twaijer & Laith Sorour Hemolytic Anemias
 Hemolytic Anemias Hemolytic anemias share the following features: - A shortened red cell life < 120 days - Elevated erythropoietin levels (compensatory increase in erythropoiesis) - Accumulation of hemoglobin
Hemolytic Anemias Hemolytic anemias share the following features: - A shortened red cell life < 120 days - Elevated erythropoietin levels (compensatory increase in erythropoiesis) - Accumulation of hemoglobin
Theme: Making Further Advancements in the Treatment of Hematologic Diseases - Frontline therapies and future prospects -
 Theme: Making Further Advancements in the Treatment of Hematologic Diseases - Frontline therapies and future prospects - Professor Yutaka YATOMI, M.D., Ph.D., The Department of Clinical Laboratory Medicine,
Theme: Making Further Advancements in the Treatment of Hematologic Diseases - Frontline therapies and future prospects - Professor Yutaka YATOMI, M.D., Ph.D., The Department of Clinical Laboratory Medicine,
POLYCYTHEMIA VERA (PV)
 LIVING WITH POLYCYTHEMIA VERA (PV) Information, resources, and support for wherever you are on your journey with PV. For more information, visit PVvoices.com today. POLYCYTHEMIA VERA (polly-sigh-thee-me-ah-vair-ah)
LIVING WITH POLYCYTHEMIA VERA (PV) Information, resources, and support for wherever you are on your journey with PV. For more information, visit PVvoices.com today. POLYCYTHEMIA VERA (polly-sigh-thee-me-ah-vair-ah)
Paroxysmal Nocturnal Hemoglobinuria
 Paroxysmal Nocturnal Hemoglobinuria Barry Skikne MD, FACP, FCP(SA) Professor of Hematology Division of Hematologic Malignancies and Cellular Therapeutics Cardinal Clinical Manifestations PNH Clonal disease
Paroxysmal Nocturnal Hemoglobinuria Barry Skikne MD, FACP, FCP(SA) Professor of Hematology Division of Hematologic Malignancies and Cellular Therapeutics Cardinal Clinical Manifestations PNH Clonal disease
Heme 9 Myeloid neoplasms
 Heme 9 Myeloid neoplasms The minimum number of blasts to diagnose acute myeloid leukemia is 5% 10% 20% 50% 80% AML with the best prognosis is AML with recurrent cytogenetic abnormality AML with myelodysplasia
Heme 9 Myeloid neoplasms The minimum number of blasts to diagnose acute myeloid leukemia is 5% 10% 20% 50% 80% AML with the best prognosis is AML with recurrent cytogenetic abnormality AML with myelodysplasia
RBCs Disorders 2. Dr. Nabila Hamdi MD, PhD
 RBCs Disorders 2 Dr. Nabila Hamdi MD, PhD ILOs Discuss the classification of anemia into hypochromic-microcytic, normochromicnormocytic and macrocytic. Categorize laboratory test procedures used in the
RBCs Disorders 2 Dr. Nabila Hamdi MD, PhD ILOs Discuss the classification of anemia into hypochromic-microcytic, normochromicnormocytic and macrocytic. Categorize laboratory test procedures used in the
Disclosures. Myeloproliferative Neoplasms: A Case-Based Approach. Objectives. Myeloproliferative Neoplasms. Myeloproliferative Neoplasms
 Myeloproliferative Neoplasms: A Case-Based Approach Disclosures No conflicts of interests regarding the topic being presented Adam M. Miller, MD PGY-4 Resident Physician Department of Pathology and Laboratory
Myeloproliferative Neoplasms: A Case-Based Approach Disclosures No conflicts of interests regarding the topic being presented Adam M. Miller, MD PGY-4 Resident Physician Department of Pathology and Laboratory
Hemoglobin and anemia BCH 471
 Hemoglobin and anemia BCH 471 OBJECTIVES Quantitative determination of hemoglobin in a blood sample. Hemoglobin structure Hemoglobin (Hb) is a porphyrin iron (II) protein in RBCs that transport oxygen
Hemoglobin and anemia BCH 471 OBJECTIVES Quantitative determination of hemoglobin in a blood sample. Hemoglobin structure Hemoglobin (Hb) is a porphyrin iron (II) protein in RBCs that transport oxygen
The Power of Peripheral Blood Smears: Apparent Diagnostic Clues (Part 1) (Wednesday, October 19, 2011)
 The Power of Peripheral Blood Smears: Apparent Diagnostic Clues (Part 1) (Wednesday, October 19, 2011) By Gene Gulati, Ph.D., SH(ASCP) Conflict of Interest None Plan for the Course Review blood smears,
The Power of Peripheral Blood Smears: Apparent Diagnostic Clues (Part 1) (Wednesday, October 19, 2011) By Gene Gulati, Ph.D., SH(ASCP) Conflict of Interest None Plan for the Course Review blood smears,
Lec.2 Medical Physiology Blood Physiology Z.H.Kamil
 Destruction of Red Blood Cells When red blood cells are delivered from the bone marrow into the circulatory system, they normally circulate an average of 120 days before being destroyed. Even though mature
Destruction of Red Blood Cells When red blood cells are delivered from the bone marrow into the circulatory system, they normally circulate an average of 120 days before being destroyed. Even though mature
THE UNIVERSITY OF JORDAN FACULTY OF MEDICINE DEPARTMENT OF PATHOLOGY HEMOLYTIC ANEMIAS. Dr. Tariq Aladily
 THE UNIVERSITY OF JORDAN FACULTY OF MEDICINE DEPARTMENT OF PATHOLOGY HEMOLYTIC ANEMIAS Third year medical students First semester Faculty 2018/2019 of Medicine Hereditary Spherocytosis Intrinsic defects
THE UNIVERSITY OF JORDAN FACULTY OF MEDICINE DEPARTMENT OF PATHOLOGY HEMOLYTIC ANEMIAS Third year medical students First semester Faculty 2018/2019 of Medicine Hereditary Spherocytosis Intrinsic defects
Myeloid neoplasms. Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories:
 Myeloid neoplasms Note: Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories: 1. AML : Acute myeloid leukemia(stem cell with myeloid
Myeloid neoplasms Note: Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories: 1. AML : Acute myeloid leukemia(stem cell with myeloid
MYELOPROLIFARATIVE NEOPLASMS. Dr. Hasan Fahmawi, MRCP(UK), FRCP(Edin).
 MYELOPROLIFARATIVE NEOPLASMS Dr. Hasan Fahmawi, MRCP(UK), FRCP(Edin). These are a group of chronic conditions characterised by clonal proliferation of marrow precursor cells. PRV, essential thrombocyathaemia,
MYELOPROLIFARATIVE NEOPLASMS Dr. Hasan Fahmawi, MRCP(UK), FRCP(Edin). These are a group of chronic conditions characterised by clonal proliferation of marrow precursor cells. PRV, essential thrombocyathaemia,
Emerging diagnostic and risk stratification criteria
 PV STATE OF MIND Polycythemia vera: Emerging diagnostic and risk stratification criteria Rami S. Komrokji, MD Moffitt Cancer Center, Tampa, Florida Disclosure These slides were developed by Incyte Corporation
PV STATE OF MIND Polycythemia vera: Emerging diagnostic and risk stratification criteria Rami S. Komrokji, MD Moffitt Cancer Center, Tampa, Florida Disclosure These slides were developed by Incyte Corporation
THE UNIVERSITY OF JORDAN FACULTY OF MEDICINE DEPARTMENT OF PATHOLOGY
 THE UNIVERSITY OF JORDAN FACULTY OF MEDICINE DEPARTMENT OF PATHOLOGY INTRODUCTION TO ANEMIA Third year medical students First semester 2018/2019 Dr. RBC DISORDERS Lecturer: Dr. Tariq Al-Adaily Email: TNALADILY@ju.edu.jo
THE UNIVERSITY OF JORDAN FACULTY OF MEDICINE DEPARTMENT OF PATHOLOGY INTRODUCTION TO ANEMIA Third year medical students First semester 2018/2019 Dr. RBC DISORDERS Lecturer: Dr. Tariq Al-Adaily Email: TNALADILY@ju.edu.jo
Anemia (3).ms4.25.Oct.15 Hemolytic Anemia. Abdallah Abbadi
 Anemia (3).ms4.25.Oct.15 Hemolytic Anemia Abdallah Abbadi Case 3 24 yr old female presented with anemia syndrome and jaundice. She was found to have splenomegaly. Hb 8, wbc 12k, Plt 212k, retics 12%, LDH
Anemia (3).ms4.25.Oct.15 Hemolytic Anemia Abdallah Abbadi Case 3 24 yr old female presented with anemia syndrome and jaundice. She was found to have splenomegaly. Hb 8, wbc 12k, Plt 212k, retics 12%, LDH
QUESTIONS OF HEMATOLOGY AND THEIR ANSWERS
 QUESTIONS OF HEMATOLOGY AND THEIR ANSWERS WHAT IS TRUE AND WHAT IS FALSE? Questions 1 Iron deficiency anemia a) Is usually associated with a raised MCV. b) The MCH is usually low. c) Is most commonly due
QUESTIONS OF HEMATOLOGY AND THEIR ANSWERS WHAT IS TRUE AND WHAT IS FALSE? Questions 1 Iron deficiency anemia a) Is usually associated with a raised MCV. b) The MCH is usually low. c) Is most commonly due
Myeloproliferative Disorders in the Elderly: Clinical Presentation and Role of Bone Marrow Examination
 Myeloproliferative Disorders in the Elderly: Clinical Presentation and Role of Bone Marrow Examination Arati V. Rao, M.D. Division of Medical Oncology and Geriatrics Duke University Medical Center Durham
Myeloproliferative Disorders in the Elderly: Clinical Presentation and Role of Bone Marrow Examination Arati V. Rao, M.D. Division of Medical Oncology and Geriatrics Duke University Medical Center Durham
Glucose-6-Phosphate Dehydrogenase
 Glucose-6-Phosphate Dehydrogenase Is the major enzyme in the pentose phosphate pathway (also called the phosphogluconate pathway or the hexose monophosphate shunt) which is a metabolic pathway parallel
Glucose-6-Phosphate Dehydrogenase Is the major enzyme in the pentose phosphate pathway (also called the phosphogluconate pathway or the hexose monophosphate shunt) which is a metabolic pathway parallel
DONE BY : RaSHA RAKAN & Bushra Saleem
 DONE BY : RaSHA RAKAN & Bushra Saleem Hemolytic anemias (2 of 2) Sickle Cell Anemia The most common familial hemolytic anemia in the world Sickle cell anemia is the prototypical (and most prevalent) hemoglobinopathy
DONE BY : RaSHA RAKAN & Bushra Saleem Hemolytic anemias (2 of 2) Sickle Cell Anemia The most common familial hemolytic anemia in the world Sickle cell anemia is the prototypical (and most prevalent) hemoglobinopathy
SESSION 1 Reactive cytopenia and dysplasia
 SESSION 1 Reactive cytopenia and dysplasia Falko Fend, Tübingen & Alexandar Tzankov, Basel 1 Disclosure of speaker s interests (Potential) conflict of interest none Potentially relevant company relationships
SESSION 1 Reactive cytopenia and dysplasia Falko Fend, Tübingen & Alexandar Tzankov, Basel 1 Disclosure of speaker s interests (Potential) conflict of interest none Potentially relevant company relationships
MYELOPROLIFERATIVE NEOPLASMS
 9 : 2 MYELOPROLIFERATIVE NEOPLASMS Introduction William Dameshek in 1951 introduced the term Myeloproliferative disorders (MPD). This included polycythemia vera (PV), essential thrombocythemia (ET), primary
9 : 2 MYELOPROLIFERATIVE NEOPLASMS Introduction William Dameshek in 1951 introduced the term Myeloproliferative disorders (MPD). This included polycythemia vera (PV), essential thrombocythemia (ET), primary
Zeina Al-Assaf. Mustafa Khader. Nayef Karadsheh
 6 Zeina Al-Assaf Mustafa Khader Nayef Karadsheh 1 P a g e Metabolism in mature erythrocytes: During the maturation of RBCs most of its intracellular organelles are lost such as the nucleus and the mitochondria,
6 Zeina Al-Assaf Mustafa Khader Nayef Karadsheh 1 P a g e Metabolism in mature erythrocytes: During the maturation of RBCs most of its intracellular organelles are lost such as the nucleus and the mitochondria,
Myeloproliferative Neoplasms and Treatment Overview
 Myeloproliferative Neoplasms and Treatment Overview George Nesr Clinical Research Fellow in Haematology Haematology Department Imperial College Healthcare NHS Trust Overview Historical Background Pathogenesis
Myeloproliferative Neoplasms and Treatment Overview George Nesr Clinical Research Fellow in Haematology Haematology Department Imperial College Healthcare NHS Trust Overview Historical Background Pathogenesis
RBCs Disorders 2. Dr. Nabila Hamdi MD, PhD
 RBCs Disorders 2 Dr. Nabila Hamdi MD, PhD ILOs Discuss the classification of anemia into hypochromic-microcytic, normochromicnormocytic and macrocytic. Categorize laboratory test procedures used in the
RBCs Disorders 2 Dr. Nabila Hamdi MD, PhD ILOs Discuss the classification of anemia into hypochromic-microcytic, normochromicnormocytic and macrocytic. Categorize laboratory test procedures used in the
PNH Glossary of Terms
 AA Absolute neutrophil count Alendronate Allergen ALT Anemia Antibodies Anticoagulant Anticoagulation Antigen Antithymocyte globulin (ATG) Aplastic Aplastic anemia Band Bilirubin Blast cells Bone marrow
AA Absolute neutrophil count Alendronate Allergen ALT Anemia Antibodies Anticoagulant Anticoagulation Antigen Antithymocyte globulin (ATG) Aplastic Aplastic anemia Band Bilirubin Blast cells Bone marrow
MPL W515L K mutation
 MPL W515L K mutation BCR-ABL genotyping The exact chromosomal defect in Philadelphia chromosome is a translocation. Parts of two chromosomes, 9 and 22, switch places. The result is a fusion gene, created
MPL W515L K mutation BCR-ABL genotyping The exact chromosomal defect in Philadelphia chromosome is a translocation. Parts of two chromosomes, 9 and 22, switch places. The result is a fusion gene, created
Anemia. A case-based approach. David B. Sykes, MD, PhD Hematology, MGH Cancer Center June 8, 2017
 Anemia A case-based approach David B. Sykes, MD, PhD Hematology, MGH Cancer Center June 8, 2017 Recognizing trends Learning Objectives MCV, RDW, Ferritin, LDH, Reticulocytes Managing complex patients 1.
Anemia A case-based approach David B. Sykes, MD, PhD Hematology, MGH Cancer Center June 8, 2017 Recognizing trends Learning Objectives MCV, RDW, Ferritin, LDH, Reticulocytes Managing complex patients 1.
Approach to Hemolysis
 Objectives: Approach to Hemolysis To know the function of platelets and the relationship between the platelet count in peripheral blood and the extent of abnormal bleeding. To know about the diseases associated
Objectives: Approach to Hemolysis To know the function of platelets and the relationship between the platelet count in peripheral blood and the extent of abnormal bleeding. To know about the diseases associated
YEREVAN STATE MEDICAL UNIVERSITY DEPARTMENT OF HEMATOLOGY COURSE DESCRIPTION HEMATOLOGY
 1. Module/unit Code II. 1.2. 2. Module/unit Title Hematology 3. Subject Field Internal Diseases Group 4. Faculty/Department General Medicine, Department of Hematology 5. Programme(s) to which the Doctor
1. Module/unit Code II. 1.2. 2. Module/unit Title Hematology 3. Subject Field Internal Diseases Group 4. Faculty/Department General Medicine, Department of Hematology 5. Programme(s) to which the Doctor
Why do patients with polycythemia vera clot? Kinsey McCormick Hematology Fellows conference August 10, 2012
 Why do patients with polycythemia vera clot? Kinsey McCormick Hematology Fellows conference August 10, 2012 Outline Case presentation Overview of PV Disease course Mechanisms of thrombosis Case Presentation
Why do patients with polycythemia vera clot? Kinsey McCormick Hematology Fellows conference August 10, 2012 Outline Case presentation Overview of PV Disease course Mechanisms of thrombosis Case Presentation
Examination Tests from Pathological Physiology. Pavel Maruna et al. Reviewed by: Prof. MUDr. Emanuel Nečas, DrSc. Prof. MUDr. Jaroslav Veselý, CSc.
 Examination Tests from Pathological Physiology Pavel Maruna et al. Reviewed by: Prof. MUDr. Emanuel Nečas, DrSc. Prof. MUDr. Jaroslav Veselý, CSc. Authors: Prof. MUDr. Pavel Maruna, CSc. Doc. MUDr. Martin
Examination Tests from Pathological Physiology Pavel Maruna et al. Reviewed by: Prof. MUDr. Emanuel Nečas, DrSc. Prof. MUDr. Jaroslav Veselý, CSc. Authors: Prof. MUDr. Pavel Maruna, CSc. Doc. MUDr. Martin
COEXISTENCE OF β-thalassemia AND POLYCYTHEMIA VERA: A CHICKEN-AND-EGG DEBATE?
 COEXISTENCE OF β-thalassemia AND POLYCYTHEMIA VERA: A CHICKEN-AND-EGG DEBATE? M. DE SLOOVERE (1), L. HARLET (2), S. VAN STEENWEGHEN (3), E. MOREAU (1), D. DE SMET (1) (1) DEPARTMENT OF LABORATORY MEDICINE,
COEXISTENCE OF β-thalassemia AND POLYCYTHEMIA VERA: A CHICKEN-AND-EGG DEBATE? M. DE SLOOVERE (1), L. HARLET (2), S. VAN STEENWEGHEN (3), E. MOREAU (1), D. DE SMET (1) (1) DEPARTMENT OF LABORATORY MEDICINE,
Around million aged erythrocytes/hour are broken down.
 Anemia Degradation ofheme Around 100 200 million aged erythrocytes/hour are broken down. The degradation process starts in reticuloendothelial cells in the spleen, liver, and bone marrow. [1] The tetrapyrrole
Anemia Degradation ofheme Around 100 200 million aged erythrocytes/hour are broken down. The degradation process starts in reticuloendothelial cells in the spleen, liver, and bone marrow. [1] The tetrapyrrole
Anemia (3).ms Hemolytic Anemia. Abdallah Abbadi Feras Fararjeh
 Anemia (3).ms4.26.2.18 Hemolytic Anemia Abdallah Abbadi Feras Fararjeh Case 3 24 yr old female presented with anemia syndrome and jaundice. She was found to have splenomegaly. Hb 8, wbc 12k, Plt 212k,
Anemia (3).ms4.26.2.18 Hemolytic Anemia Abdallah Abbadi Feras Fararjeh Case 3 24 yr old female presented with anemia syndrome and jaundice. She was found to have splenomegaly. Hb 8, wbc 12k, Plt 212k,
Characterization of blood donors with high haemoglobin concentration
 STATE OF THE ART 2A-S05-02 ISBT Science Series (2013) 8, 114 118 ISBT Science Series 2013 International Society of Blood Transfusion Characterization of blood donors with high haemoglobin concentration
STATE OF THE ART 2A-S05-02 ISBT Science Series (2013) 8, 114 118 ISBT Science Series 2013 International Society of Blood Transfusion Characterization of blood donors with high haemoglobin concentration
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Acute lymphoblastic leukemia, in India, 439 440 pediatric, global approach to, 420 424 core resources in low- and middle-income countries, 423
Note: Page numbers of article titles are in boldface type. A Acute lymphoblastic leukemia, in India, 439 440 pediatric, global approach to, 420 424 core resources in low- and middle-income countries, 423
Extra Notes 3. Warm. In the core (center) of the body, where the temperature is 37 C.
 Extra Notes 3 *The numbers of the slides are according to the last year slides. Slide 33 Autoimmune hemolytic anemia : Abnormal circulating antibodies that target normal antigen on the RBC and cause lysis.
Extra Notes 3 *The numbers of the slides are according to the last year slides. Slide 33 Autoimmune hemolytic anemia : Abnormal circulating antibodies that target normal antigen on the RBC and cause lysis.
Year 2003 Paper two: Questions supplied by Tricia
 QUESTION 65 A 36-year-old man presents in a post-ictal state after an observed generalised seizure. Full blood investigation shows: haemoglobin 0 g/l [128-175] mean corpuscular volume (MCV) 106 fl [80-7]
QUESTION 65 A 36-year-old man presents in a post-ictal state after an observed generalised seizure. Full blood investigation shows: haemoglobin 0 g/l [128-175] mean corpuscular volume (MCV) 106 fl [80-7]
General Characterisctics
 Anemia General Characterisctics Definition: anemia is a decrease in red blood cells. Happens due to underproduction, increased destruction or loss of red cells. Diagnosis of anemia: Hgb < 135 (men) Hgb
Anemia General Characterisctics Definition: anemia is a decrease in red blood cells. Happens due to underproduction, increased destruction or loss of red cells. Diagnosis of anemia: Hgb < 135 (men) Hgb
Polycythemia Vera and Essential Thombocythemia A Single Institution Experience
 INDIAN JOURNAL OF MEDICAL & PAEDIATRIC ONCOLOGY Vol. 29 No 4, 2008 7 Original Article-I Polycythemia Vera and Essential Thombocythemia A Single Institution Experience CECIL ROSS, NAVYA, VANAMALA AND KARUNA
INDIAN JOURNAL OF MEDICAL & PAEDIATRIC ONCOLOGY Vol. 29 No 4, 2008 7 Original Article-I Polycythemia Vera and Essential Thombocythemia A Single Institution Experience CECIL ROSS, NAVYA, VANAMALA AND KARUNA
3 Ruba hussein Dr. ahmad Dr. ahmad
 3 Ruba hussein Dr. ahmad Dr. ahmad The arrangement of this sheet differs from that of the record. Anemia of peripheral removal in which we are losing hemoglobin and RBCs mass and the two major Causes are:
3 Ruba hussein Dr. ahmad Dr. ahmad The arrangement of this sheet differs from that of the record. Anemia of peripheral removal in which we are losing hemoglobin and RBCs mass and the two major Causes are:
Technical Bulletin No. 100
 CPAL Central Pennsylvania Alliance Laboratory Technical Bulletin No. 100 August 2, 2012 JAK2 AND MPL 515 MUTATIONAL ANALYSIS Contact: Dr. Jeffrey Wisotzkey, 717-851-1422 Technical Director, CPAL Jill A.
CPAL Central Pennsylvania Alliance Laboratory Technical Bulletin No. 100 August 2, 2012 JAK2 AND MPL 515 MUTATIONAL ANALYSIS Contact: Dr. Jeffrey Wisotzkey, 717-851-1422 Technical Director, CPAL Jill A.
20/01/1439. Prof. M. Rushdi. Prof. Mahmoud Rushdi Faculty of Veterinary Medicine Assiut University Egypt.
 By Prof. Mahmoud Rushdi Faculty of Veterinary Medicine Assiut University Egypt 1 CBC in Dog 2 1 Evaluation of the red blood cells (RBCs) Erythrocytes picture Determination of RBCs count (/mm 3 or T/l)
By Prof. Mahmoud Rushdi Faculty of Veterinary Medicine Assiut University Egypt 1 CBC in Dog 2 1 Evaluation of the red blood cells (RBCs) Erythrocytes picture Determination of RBCs count (/mm 3 or T/l)
A. Blood is considered connective tissue. RBC. A. Blood volume and composition 1. Volume varies - average adult has 5 liters
 A. Blood is considered connective tissue. RBC A. Blood volume and composition 1. Volume varies - average adult has 5 liters 2. 45% cells by volume called hematocrit (HCT) a. red blood cells (RBC) mostly
A. Blood is considered connective tissue. RBC A. Blood volume and composition 1. Volume varies - average adult has 5 liters 2. 45% cells by volume called hematocrit (HCT) a. red blood cells (RBC) mostly
Increased Number of Red Blood Cells (Polycythemia) Basics
 Increased Number of Red Blood Cells (Polycythemia) Basics OVERVIEW Blood consists of red blood cells (the most numerous cells normally), white blood cells, platelets, and plasma (the liquid portion of
Increased Number of Red Blood Cells (Polycythemia) Basics OVERVIEW Blood consists of red blood cells (the most numerous cells normally), white blood cells, platelets, and plasma (the liquid portion of
C. treatment with Desferal (deferoxamine mesylate USP, iron-chelating agent)
 HEMOLYTIC ANEMIAS Single choice tests 1. Select the clinical manifestation that is not characteristic for the hemolytic crisis: A. decrease of the red blood cell count B. reticulocytosis C. jaundice D.
HEMOLYTIC ANEMIAS Single choice tests 1. Select the clinical manifestation that is not characteristic for the hemolytic crisis: A. decrease of the red blood cell count B. reticulocytosis C. jaundice D.
SICKLE CELL DISEASE. Dr. MUBARAK ABDELRAHMAN MD PEDIATRICS AND CHILD HEALTH. Assistant Professor FACULTY OF MEDICINE -JAZAN
 SICKLE CELL DISEASE Dr. MUBARAK ABDELRAHMAN MD PEDIATRICS AND CHILD HEALTH Assistant Professor FACULTY OF MEDICINE -JAZAN Objective: The student should be able: To identify the presentation, diagnosis,
SICKLE CELL DISEASE Dr. MUBARAK ABDELRAHMAN MD PEDIATRICS AND CHILD HEALTH Assistant Professor FACULTY OF MEDICINE -JAZAN Objective: The student should be able: To identify the presentation, diagnosis,
MDS 101. What is bone marrow? Myelodysplastic Syndrome: Let s build a definition. Dysplastic? Syndrome? 5/22/2014. What does bone marrow do?
 101 May 17, 2014 Myelodysplastic Syndrome: Let s build a definition Myelo bone marrow Gail J. Roboz, M.D. Director, Leukemia Program Associate Professor of Medicine What is bone marrow? What does bone
101 May 17, 2014 Myelodysplastic Syndrome: Let s build a definition Myelo bone marrow Gail J. Roboz, M.D. Director, Leukemia Program Associate Professor of Medicine What is bone marrow? What does bone
Disclosure BCR/ABL1-Negative Classical Myeloproliferative Neoplasms
 Disclosure BCR/ABL1-Negative Classical Myeloproliferative Neoplasms Sonam Prakash declares affiliation with Incyte Corporation: Advisor for Hematopathology Publications Steering Committee Sonam Prakash,
Disclosure BCR/ABL1-Negative Classical Myeloproliferative Neoplasms Sonam Prakash declares affiliation with Incyte Corporation: Advisor for Hematopathology Publications Steering Committee Sonam Prakash,
WHICH OF THE FOLLOWING COMPRISE A
 HEMATOLOGY QUESTION REVIEW WHICH OF THE FOLLOWING COMPRISE A LOGICAL SEQUENCE OF VESSELS AS BLOOD EXITS THE HEART? a. capillaries; arteries; veins b. veins; capillaries; arteries c. arteries; capillaries;
HEMATOLOGY QUESTION REVIEW WHICH OF THE FOLLOWING COMPRISE A LOGICAL SEQUENCE OF VESSELS AS BLOOD EXITS THE HEART? a. capillaries; arteries; veins b. veins; capillaries; arteries c. arteries; capillaries;
SYLLABUS ON HEMATOLOGY FOR THE 4-YEAR STUDENTS, MEDICINE-2. Total hours number 70 hours, including course 20 hours, seminars 50 hours.
 SYLLABUS ON HEMATOLOGY FOR THE 4-YEAR STUDENTS, MEDICINE- Total hours number 70 hours, including course 0 hours, seminars 0 hours. Aim of the subject of Hematology: The study of etiology, pathogenesis,
SYLLABUS ON HEMATOLOGY FOR THE 4-YEAR STUDENTS, MEDICINE- Total hours number 70 hours, including course 0 hours, seminars 0 hours. Aim of the subject of Hematology: The study of etiology, pathogenesis,
10/27/2017 PAROXYSMAL NOCTURNAL HEMOGLOBINURIA DANIEL LANDAU, MD PNH TYPICAL CASE
 PAROXYSMAL NOCTURNAL HEMOGLOBINURIA Daniel Landau, MD Orlando Health: UF Health Cancer Center Hematologist/ Oncologist Orlando Health University of Florida Cancer Center Section Chief of Hematology/Oncology
PAROXYSMAL NOCTURNAL HEMOGLOBINURIA Daniel Landau, MD Orlando Health: UF Health Cancer Center Hematologist/ Oncologist Orlando Health University of Florida Cancer Center Section Chief of Hematology/Oncology
Dairion Gatot, Soegiarto Ganie, Savita Handayani. Divisi Hematologi & Onkologi Medik Departemen Ilmu Penyakit Dalam FK-USU/RS H.Adam Malik Medan 2009
 HAEMOLYTIC ANAEMIA Dairion Gatot, Soegiarto Ganie, Savita Handayani. Divisi Hematologi & Onkologi Medik Departemen Ilmu Penyakit Dalam FK-USU/RS H.Adam Malik Medan 2009 WHEN BY THEN Hb 9 g% transfusion
HAEMOLYTIC ANAEMIA Dairion Gatot, Soegiarto Ganie, Savita Handayani. Divisi Hematologi & Onkologi Medik Departemen Ilmu Penyakit Dalam FK-USU/RS H.Adam Malik Medan 2009 WHEN BY THEN Hb 9 g% transfusion
Hemoglobinopathies Diagnosis and management
 Hemoglobinopathies Diagnosis and management Morgan L. McLemore, M.D. Hematology/Leukemia Department of Hematology and Oncology Winship Cancer Institute at Emory University mlmclem@emory.edu Disclosures
Hemoglobinopathies Diagnosis and management Morgan L. McLemore, M.D. Hematology/Leukemia Department of Hematology and Oncology Winship Cancer Institute at Emory University mlmclem@emory.edu Disclosures
Disorders of Blood Cells & Blood Coagulation
 Disorders of Blood Cells & Blood Coagulation HIHIM 409 WBC count RBC count WBC differential Hemoglobin (HGB) Hematocrit (HCT) % of volume occupied by RBCs CBC Red cell indices Mean cell volume (MCV) average
Disorders of Blood Cells & Blood Coagulation HIHIM 409 WBC count RBC count WBC differential Hemoglobin (HGB) Hematocrit (HCT) % of volume occupied by RBCs CBC Red cell indices Mean cell volume (MCV) average
JAK2 V617F analysis. Indication: monitoring of therapy
 JAK2 V617F analysis BCR-ABL genotyping The exact chromosomal defect in Philadelphia chromosome is a translocation. Parts of two chromosomes, 9 and 22, switch places. The result is a fusion gene, created
JAK2 V617F analysis BCR-ABL genotyping The exact chromosomal defect in Philadelphia chromosome is a translocation. Parts of two chromosomes, 9 and 22, switch places. The result is a fusion gene, created
HEMOLYTIC ANEMIA Anemia of increased destruction Normochromic, normochromic anemia Shortened RBC survival Reticulocytosis - Response to increased RBC
 HEMOLYTIC ANEMIAS Edited by: GR. Bahoush, MD. HEMOLYTIC ANEMIA Anemia of increased destruction Normochromic, normochromic anemia Shortened RBC survival Reticulocytosis - Response to increased RBC destruction
HEMOLYTIC ANEMIAS Edited by: GR. Bahoush, MD. HEMOLYTIC ANEMIA Anemia of increased destruction Normochromic, normochromic anemia Shortened RBC survival Reticulocytosis - Response to increased RBC destruction
Average adult = 8-10 pints of blood. Functions:
 Average adult = 8-10 pints of blood Functions: Transports nutrients, oxygen, cellular waste products, and hormones Aids in distribution of heat Regulates acid-base balance Helps protect against infection
Average adult = 8-10 pints of blood Functions: Transports nutrients, oxygen, cellular waste products, and hormones Aids in distribution of heat Regulates acid-base balance Helps protect against infection
Hematology 101. Blanche P Alter, MD, MPH, FAAP Clinical Genetics Branch Division of Cancer Epidemiology and Genetics Bethesda, MD
 Hematology 101 Blanche P Alter, MD, MPH, FAAP Clinical Genetics Branch Division of Cancer Epidemiology and Genetics Bethesda, MD Hematocrits Plasma White cells Red cells Normal, Hemorrhage, IDA, Leukemia,
Hematology 101 Blanche P Alter, MD, MPH, FAAP Clinical Genetics Branch Division of Cancer Epidemiology and Genetics Bethesda, MD Hematocrits Plasma White cells Red cells Normal, Hemorrhage, IDA, Leukemia,
Case Workshop of Society for Hematopathology and European Association for Haematopathology
 Case 148 2007 Workshop of Society for Hematopathology and European Association for Haematopathology Robert P Hasserjian Department of Pathology Massachusetts General Hospital Boston, MA Clinical history
Case 148 2007 Workshop of Society for Hematopathology and European Association for Haematopathology Robert P Hasserjian Department of Pathology Massachusetts General Hospital Boston, MA Clinical history
Tim R. Randolph. PhD, MT(ASCP) Chair and Associate Professor Department of Biomedical Laboratory Science Saint Louis University
 Tim R. Randolph. PhD, MT(ASCP) Chair and Associate Professor Department of Biomedical Laboratory Science Saint Louis University Anemias Over 30 types Myeloproliferative Neoplasm Polycythemia Leukemia AML:M6
Tim R. Randolph. PhD, MT(ASCP) Chair and Associate Professor Department of Biomedical Laboratory Science Saint Louis University Anemias Over 30 types Myeloproliferative Neoplasm Polycythemia Leukemia AML:M6
Bone marrow histopathology in Ph - CMPDs. - the new WHO classification - Juergen Thiele Cologne, Germany
 Bone marrow histopathology in Ph - CMPDs - the new WHO classification - Juergen Thiele Cologne, Germany Current issues in MPNs concerning morphology 1.Prodromal stages of disease 2.Impact of histopathology
Bone marrow histopathology in Ph - CMPDs - the new WHO classification - Juergen Thiele Cologne, Germany Current issues in MPNs concerning morphology 1.Prodromal stages of disease 2.Impact of histopathology
Latest updates in Myeloproliferative Neoplasms. Elizabeth Hexner, MD, MSTR
 Latest updates in Myeloproliferative Neoplasms Elizabeth Hexner, MD, MSTR Disclosures Nothing to disclose Agenda/Goals Treatment goals in PV Indications for cytoreduction in patients polycythemia vera
Latest updates in Myeloproliferative Neoplasms Elizabeth Hexner, MD, MSTR Disclosures Nothing to disclose Agenda/Goals Treatment goals in PV Indications for cytoreduction in patients polycythemia vera
Composition of Blood
 Composition of Blood Erythrocytes Disorders of Erythrocytes Hematocrit Leukocytes Disorders of Leukocytes Platelets Hemostasis Disorders of Clotting Blood Types Blood Transfusion Unit 7 Blood Composition
Composition of Blood Erythrocytes Disorders of Erythrocytes Hematocrit Leukocytes Disorders of Leukocytes Platelets Hemostasis Disorders of Clotting Blood Types Blood Transfusion Unit 7 Blood Composition
The primary medical content categories of the blueprint are shown below, with the percentage assigned to each for a typical exam:
 Hematology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified hematologist
Hematology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified hematologist
HAEMOLYTIC ANAEMIA. Dr. Hasan Fahmawi, MRCP(London), FRCP(Edin) Consultant Physician
 HAEMOLYTIC ANAEMIA Dr. Hasan Fahmawi, MRCP(London), FRCP(Edin) Consultant Physician Haemolysis Definition shortening of the normal red blood lifespan of 120 days Increase in unconjugated bilirubin, increased
HAEMOLYTIC ANAEMIA Dr. Hasan Fahmawi, MRCP(London), FRCP(Edin) Consultant Physician Haemolysis Definition shortening of the normal red blood lifespan of 120 days Increase in unconjugated bilirubin, increased
Case Presentation No. 075
 Case Presentation No. 075 Session 4. Myelodysplastic Syndrome Cristina Montalvo, MD Baylor College of Medicine Houston, Texas 2007 Workshop of Society for Hematopathology and European Association for Haematopathology
Case Presentation No. 075 Session 4. Myelodysplastic Syndrome Cristina Montalvo, MD Baylor College of Medicine Houston, Texas 2007 Workshop of Society for Hematopathology and European Association for Haematopathology
HEMATOLOGY Maintenance of Certification (MOC) Examination Blueprint
 HEMATOLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Hematology MOC exam blueprint Based on feedback from physicians that MOC assessments should
HEMATOLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Hematology MOC exam blueprint Based on feedback from physicians that MOC assessments should
Hematopoietic Growth Factors Colony Stimulating Factors. Erythropoietin (Epoetin alfa). Granulocyte-macrophage colonystimulating factor (G-CSF).
 Hematopoietic Growth Factors Colony Stimulating Factors. Erythropoietin (Epoetin alfa). Granulocyte colony-stimulating factor(g-csf). Granulocyte-macrophage colonystimulating factor (G-CSF). Interleukin-11
Hematopoietic Growth Factors Colony Stimulating Factors. Erythropoietin (Epoetin alfa). Granulocyte colony-stimulating factor(g-csf). Granulocyte-macrophage colonystimulating factor (G-CSF). Interleukin-11
[COMPREHENSIVE GENETIC ASSAY PANEL ON
 2014 SN GENELAB AND RESEARCH CENTER DR. SALIL VANIAWALA, PH.D [COMPREHENSIVE GENETIC ASSAY PANEL ON MYELOPROLIFERATIVE NEOPLASMS] SN Genelab presents one of the most comprehensive genetic assay panel for
2014 SN GENELAB AND RESEARCH CENTER DR. SALIL VANIAWALA, PH.D [COMPREHENSIVE GENETIC ASSAY PANEL ON MYELOPROLIFERATIVE NEOPLASMS] SN Genelab presents one of the most comprehensive genetic assay panel for
UNDERSTANDING POLYCYTHEMIA VERA (PV) A guide for patients and caregivers
 UNDERSTANDING POLYCYTHEMIA VERA (PV) A guide for patients and caregivers Jakafi is used to treat adults with polycythemia vera who have already taken a medicine called hydroxyurea and it did not work well
UNDERSTANDING POLYCYTHEMIA VERA (PV) A guide for patients and caregivers Jakafi is used to treat adults with polycythemia vera who have already taken a medicine called hydroxyurea and it did not work well
PNH. PNH A study case 5/9/2012. PNH Current Thinking on the Disease, Diagnosis, and Treatment. Where have we been, where are we going?
 PNH Current Thinking on the Disease, Diagnosis, and Treatment Where have we been, where are we going? Carlos M. de Castro, MD Duke University Medical Center PNH Case What is PNH? What causes PNH? Relationship
PNH Current Thinking on the Disease, Diagnosis, and Treatment Where have we been, where are we going? Carlos M. de Castro, MD Duke University Medical Center PNH Case What is PNH? What causes PNH? Relationship
Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data
 Instructions for Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data (Form 2114) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the Myelodysplasia/Myeloproliferative
Instructions for Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data (Form 2114) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the Myelodysplasia/Myeloproliferative
Acute haemolysis and appearance of PNH-like clones in patients with vitamin B12 deficiency and iron deficiency after iron dextran administration
 Acute haemolysis and appearance of PNH-like clones in patients with vitamin B12 deficiency and iron deficiency after iron dextran administration Chun-Liang Lin 1, Chin-Chan Lin 1,Wen-Jyi Lo 2,Yu-Chien
Acute haemolysis and appearance of PNH-like clones in patients with vitamin B12 deficiency and iron deficiency after iron dextran administration Chun-Liang Lin 1, Chin-Chan Lin 1,Wen-Jyi Lo 2,Yu-Chien
Year 2004 Paper two: Questions supplied by Megan 1
 Year 2004 Paper two: Questions supplied by Megan 1 QUESTION 93 A 16yo adolescent male presents with lethargy and lower respiratory tract infection. Physical examination shows him to be febrile, icteric
Year 2004 Paper two: Questions supplied by Megan 1 QUESTION 93 A 16yo adolescent male presents with lethargy and lower respiratory tract infection. Physical examination shows him to be febrile, icteric
