The perception of pain is a complex process,
|
|
|
- Ethelbert Charles
- 6 years ago
- Views:
Transcription
1 SPECIAL TOPIC Pathophysiology of Pain: A Practical Primer Adeline Fong, MRCP, MRCA, FANZCA Stephan A. Schug, MD, FANZCA, FFPMANZCA Perth, Australia Summary: The experience of pain is a subjective one and more than a simple sensation. Pain is commonly defined as an unpleasant sensory and emotional experience due to actual or potential tissue damage or described in such terms. Pain may be broadly classified into physiological and pathological pain. Nociceptive and inflammatory pains are physiological pain states, as they are protective and adaptive, whereas pathological pain is nonprotective and maladaptive. Nociception is the result of suprathreshold stimulation of peripheral nociceptors. Inflammatory pain follows release of various chemical mediators after tissue injury including surgery leading to peripheral sensitization. Nociceptive input is then transmitted to the spinal cord via primary afferents. Modulation of the nociceptive input occurs in the dorsal horn of the spinal cord, influenced by descending inhibitory systems. Central sensitization is a neuromodulatory change that results in the development of secondary hyperalgesia. The modulated nociceptive input then travels up the ascending tracts, mainly via the spinothalamic tract to the thalamus and subsequently to the higher centers of the brain. Pathological pain such as neuropathic pain and central nervous system dysfunctional pain are the result of neuroplasticity of the peripheral and central nervous system. Abnormal ectopic firing of neurons in the absence of a stimulus, increased neuronal hypersensitivity, changes within ion channels, and even alteration in gene expression and changes in the cortical representation are involved in the pathogenesis of these pain states. The development of persistent postsurgical pain is an example for this complex process. (Plast. Reconstr. Surg. 134: 8S, 2014.) The perception of pain is a complex process, as pain is not just a sensation, but has a significant emotional dimension, which is influenced by one s beliefs, expectations, culture, and past experience. According to the International Association for the Study of Pain, pain is defined as an unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage. 1 Acute pain occurs for a short period of time after injury, has a warning function, and promotes healing and therefore is physiologically useful. In contrast, chronic pain persists beyond the period of healing of an injury. It is increasingly recognized that acute and chronic pain may represent a continuum rather than 2 separate entities. Global statistics show that approximately 1 in 5 adults (20%) suffers from From the Department of Pain Management, Sir Charles Gairdner Hospital; and Pharmacology, Pharmacy and Anaesthesiology Unit, School of Medicine and Pharmacology, The University of Western Australia. Received for publication March 26, 2014; accepted May 12, Copyright 2014 by the American Society of Plastic Surgeons DOI: /PRS pain, which may be acute, chronic, intermittent, or a combination, and 1 in 10 adults (10%) is newly diagnosed with chronic pain each year. 2 Pain is a subjective experience, which is selfreported. In the acute pain setting, pain is assessed by taking a focused pain history and using various pain measurement tools, such as the numerical rating scale, visual analogue scale, and verbal rating scale. Observer assessment of pain includes observing the patient for facial expression and level of activity, as well as vital signs such as blood pressure, heart rate, and respiratory rate. Patients with chronic pain are assessed under the concept of a biopsychosocial model to include evaluation of physiological, psychological, and socio-environmental factors that influence the pain experience. Assessment of pain is limited in subgroups of patients who have difficulty communicating, such as in pediatrics (age < 2 years) with dementia Disclosure: Neither author has received funding for the writing of this review. They have no conflicts of interest to declare with regard to the contents of the review. 8S
2 Volume 134, Number 4S-2 Pathophysiology of Pain and intellectual impairment, or due to language barriers. A common and useful classification of pain separates physiological pain (nociceptive and/or inflammatory pain) and pathological pain [neuropathic and central nervous system (CNS) dysfunctional pain] (Table 1). 3 Understanding the neurobiology of pain, the changes that occur at the cellular, molecular, and genetic level are essential. It allows targeted management of pain using a combination of pharmacological, interventional, and nonpharmacological approaches. PHYSIOLOGICAL PAIN: NOCICEPTIVE AND INFLAMMATORY Nociceptive pain is caused by actual or threatened damage to nonneural tissue and is due to activation of pain receptors (nociceptors) by intense noxious stimuli. 1 Nociceptive pain has an important protective role because it evokes a painful sensation that draws immediate attention. The withdrawal reflex protects the organism from further injury. Inflammatory pain involves activation of the immune system as a result of tissue injury. It also has an adaptive and protective role. When tissue injury occurs following trauma (including surgery), infection, or ischemia, there is an increase in pain sensitivity due to peripheral sensitization. This results in behavioral changes, such as reduced movement and minimal physical contact, which promotes healing of the injured body part. Peripheral Nociceptors Painful stimuli, such as intense heat, cold, mechanical force, or chemical irritants, are detected by nociceptors, free nerve endings widely distributed in the body (skin, musculoskeletal system, viscera). 4 Nociceptors have a high threshold and their activation leads to generation of action potentials transmitted from the peripheral to CNS. The organization of the pain pathway is similar to that for other sensory modalities, including a receptor, primary afferent neuron, second-order neuron, and third-order neuron (Fig. 1). The dorsal root ganglia contain the cell bodies of the primary afferents that innervate the body with the exception of those innervating the head and neck, which are in the trigeminal ganglia. Two distinct types of nociceptors are described. 4 Thermomechanoreceptors responding to pinprick and sudden heat transmit via small myelinated fast conducting Aδ fibers. Polymodal receptors responding to thermal and chemical stimuli, such as hydrogen ions, potassium ions, bradykinin, serotonin, adenosine triphosphate, and prostaglandins, transmit via small unmyelinated slow conducting C fibers. Heat, for example, is detected by transient receptor potential channels; the most studied is the vanilloid-type transient receptor potential 1, which is sensitive to heat (>42 C), capsaicin, and hydrogen ions. 4 Other receptors postulated to signal noxious mechanical stimuli include acid-sensing ion channels and potassium channels. Nerve growth factor binds to the tyrosine kinase receptor TrKa and induces pain states, particularly due to inflammation. There are 2 types of voltage-gated sodium channels, which mediate conduction along primary sensory afferents to the CNS. 5 They are differentiated depending on their sensitivity to tetrodotoxin, the poison of the puffer fish. The rapidly inactivating fast sodium channels blocked by tetrodotoxin are present in all sensory neurons; Table 1. Classification of Pain 3 Physiological Pain Biologically useful: adaptive and protective Inflammatory pain Nociceptive pain Physiological protective system To minimize and avoid damage from intense noxious stimuli (eg, heat, cold, mechanical force, and chemical irritants) High threshold pain Pain results in immediate attention and withdrawal reflex Heightened sensitivity after tissue injury or infection Immune system is activated involving macrophages, mast cells, neutrophils, and granulocytes (inflammatory soup) Low threshold pain Tenderness discourages physical contact and movement, thus reducing further risk of injury and promoting healing Pathological Pain Maladaptive Neuropathic pain due to a lesion or disease of the somatosensory nervous system (eg, painful peripheral neuropathy, poststroke, and multiple sclerosis) CNS dysfunctional pain in conditions where there is no such damage or inflammation (eg, fibromyalgia, irritable bowel syndrome, and interstitial cystitis) Common features: Low-threshold pain Spontaneous pain Imbalance between excitatory/ inhibitory mechanisms Central sensitization 9S
3 Plastic and Reconstructive Surgery October Supplement 2014 Fig. 1. Basic structure of the pain pathway. these are the principal sites of action for local anesthetics. The tetrodotoxin-resistant sodium channels are present selectively on nociceptive fibers and are offering thereby interesting new targets for pain medications. 6 Nerve injury may lead to changes in the expression of these sodium channels explaining spontaneous depolarization in neuropathic pain states. The SCN9A gene is encoding one of these, the Na(v)1.7 channel; a loss of function mutation results in congenital insensitivity to pain, whereas a gain of function mutation leads to a severe painful state, erythromelalgia. 7 Pain Transmission in the Spinal Cord Small myelinated Aδ fibers, which respond to an initial stimulus, are faster conducting and terminate in lamina I and V of the dorsal horn. The main neurotransmitter here is the excitatory amino acid glutamate. Aδ fibers synapse directly with second-order neurons, which make up the ascending tracts. Small unmyelinated slow conducting C fibers, which transmit more a persistent ache, terminate in lamina II of the dorsal horn. The neurotransmitters involved in C fiber transmission include not only glutamate but also neuropeptides, such as substance P, calcitonin gene-related peptide, cholecystokinin, and brain-derived neurotrophic factor. C fibers often synapse indirectly with second-order neurons via interneurons. Aβ fibers conduct low-intensity mechanical stimuli like touch; they terminate in laminae III VI of the dorsal horn and may also be involved in transmission of chronic pain. 8 Various receptors are involved in the synaptic transmission in the dorsal horn. Most important are the α-amino-3-hydroxy-5-methyl- 4-isoxazolepropionic acid and N-methyl-d-aspartate (NMDA) receptors binding glutamate and 10S
4 Volume 134, Number 4S-2 Pathophysiology of Pain the neurokinin-1 receptors binding substance P. Noxious stimuli are initially mediated by glutamate acting on the α-amino-3-hydroxy-5-methyl-4- isoxazolepropionic acid receptor. With increasing intensity of stimuli, the NMDA receptor becomes activated, too, and other neuropeptides like substance P are released which bind to neurokinin-1 receptors; these processes lead to hyperexcitability of the second-order neuron. Ascending Pathways Nociception is conveyed from the dorsal horn to the brain via ascending tracts in the white matter of the spinal cord. 9 The second-order neurons cross over at the spinal cord before ascending to integrative centers in the thalamus. The 2 most important ascending tracts are the spinothalamic and the spinoreticular tracts. The lateral spinothalamic tract ascends directly to the ventral posterior lateral nucleus of the thalamus, serving the sensory discriminative aspect of pain perception. The medial spinothalamic tract sends collaterals to the periaqueductal grey matter, hypothalamus, and reticular system in the midbrain before reaching the medial thalamus; it is thought to be involved in mediating the autonomic and emotional component of pain. The spinoreticular tract arises from laminae VII and VIII of the dorsal horn, terminating in the reticular formation of the medulla and pons; it is believed to mediate the aversive component of pain. From the ventral posterior lateral and medial nuclei, third-order neurons project to higher cortical (somatosensory cortex) and to midbrain centers (limbic system). There are also important projections to the limbic system (hippocampus and amygdala) associated with memory, emotion, and behavior. MODULATION OF PAIN Gate Control Theory of Pain The revolutionary gate control theory of pain was proposed by Melzack and Wall 10 in Their gate in the spinal cord is located in the substantia gelatinosa (lamina II on Rexed s laminae) of the dorsal horn, and the opening and closure of the gate is influenced by several neural pathways. The gate is opened by small ascending C fibers and closed by descending and large ascending Aβ fibers. Pain occurs when the impulse flow exceeds a certain threshold that exceeds the inhibition elicited, thus opens the gate and activates the pain pathways. This theory led to concepts that pain could be controlled by modulation, by reducing excitation and increasing inhibition. 11 An example is use of transcutaneous electrical nerve stimulation for analgesia where stimulating Aβ fibers attenuates nociceptive impulses. However, although the theory revolutionized the thinking about pain, details are flawed, such as the oversimplification of the neural architecture of the spinal cord, the idea of how large afferent fiber stimulation produces modulation of C fibers, and the hypothesized modulatory system, which we are now aware includes descending small fiber projections from the brainstem. 12 Descending Inhibitory Pathways The spinal cord also carries descending pathways that modulate the transmission of pain signals at the dorsal horn. 13 Both inhibitory and facilitatory signals come mainly from areas in the brainstem, namely the periaqueductal grey matter, rostroventral medulla, and pontine tegmentum. The neurotransmitters involved are primarily noradrenaline and serotonin. Noradrenaline acts via postsynaptic α2-receptors, but the action of serotonin is less specific. Endogenous opioids, such as endorphins, dynorphins, and enkephalins, are also involved in descending inhibition at spinal and supraspinal level. Peripheral and Central Sensitization Peripheral sensitization is due to the local action of inflammatory mediators, such as prostaglandins, histamine, bradykinin, potassium and hydrogen ions, 5-hydroxytryptamine, adenosine triphosphate, and nitric oxide, released from damaged and immune cells. The effect of the inflammatory mediators on the peripheral terminals of high threshold nociceptors of sensory neurons leads to activation of intracellular signaling pathways. This triggers phosphorylation of ion channels and nociceptors on the terminal membrane, decreasing the threshold and increasing neuronal excitability. The hypersensitivity is known as primary hyperalgesia, as it reduces the intensity of the peripheral stimulus required to activate nociceptors at the site of inflammation. Primary hyperalgesia is reversible, as healing occurs, the amount of active mediator subsides and so does the local hyperexcitability. 14 In central sensitization, there is an increase in the excitability of the dorsal horn of the spinal cord leading to pain amplification. 15 Intense noxious peripheral stimuli such as surgery evoke large amounts of action potentials. Consequently, there is increased synaptic activity in the dorsal 11S
5 Plastic and Reconstructive Surgery October Supplement 2014 horn neurons compounded by humoral signals released from inflamed tissue. Activation of intracellular kinases produces alterations in proteins in dorsal horn neurons, and this increases the trafficking of ion channels and receptors to the membrane and change of their function by phosphorylation. Finally, there is even altered gene transcription in the sensory neurons and in the spinal cord. Central sensitization results in an abnormal response to a normal sensory input, and there is spread of sensitivity well beyond the peripheral site of injury, known as secondary hyperalgesia. 14 PATHOLOGICAL PAIN Pathological pain is called so as it has no biological function, is nonprotective and maladaptive, and is due to damage and/or abnormal functioning of the nervous system. Pathological pain has been recently subdivided into neuropathic pain following damage to or disease of the nervous system and CNS dysfunctional pain when there is no such damages but dysfunction of the CNS. Both conditions are largely the result of increased excitatory and decreased inhibitory activity in the CNS (Table 1). Examples of peripheral neuropathic pain include painful peripheral neuropathy, trigeminal neuralgia, and postherpetic neuralgia, whereas central neuropathic pain includes poststroke and spinal cord injury pain. Examples of dysfunctional pain include fibromyalgia, tension headache, and many visceral pain states such as irritable bowel syndrome. A detailed discussion is beyond the scope of this review. 15 Neuropathic Pain Neuropathic pain is defined as pain caused by a lesion or disease of the somatosensory nervous system. 16 The etiology includes trauma, ischemia, infection, or metabolic disturbances. This type of pain is qualitatively different from other types of pain; the diagnosis is often clinical based on characteristic pain symptoms (positive signs such as hyperalgesia and allodynia) (Table 2), which coexist with signs of altered sensory function (negative signs such as hypoesthesia or sensory deficits). 17 Characteristic descriptors of neuropathic pain include burning, electric shocks, shooting, numbness, itching, pins and needles. Neuropathic pain may be spontaneous or triggered by a stimulus. The pathophysiology of neuropathic pain is complex and involves peripheral and central mechanisms. Neuroplastic Changes and Pain Modulation in Neuropathic Pain When there is a lesion to the primary sensory neurons, they and their immediate noninjured neighbors start to fire action potentials spontaneously (ectopic discharge), following increased expression and altered trafficking of sodium channels. 17 This ectopic activity contributes to spontaneous pain and by inducing central sensitization will augment pain sensitivity and cause allodynia. In addition, there are changes in expression of synaptic transmitters and receptors and gene alteration that modify transmission and responsiveness. For example, upregulation of the α2δ subunit of voltage-gated calcium channels causes increased neurotransmission in abnormally active sensory neurons. 18 The α2δ subunit is the binding site for its modulators gabapentin and pregabalin, used to treat neuropathic pain and central sensitization. There are also neuroimmune changes that occur following peripheral nerve injury. If an axon is severed, its distal end degenerates and is engulfed by inflammatory cells. Tumor necrosis factor-α, a pain-producing signal molecule, then acts on these axons to increase ectopic activity. Finally, glial cells are activated in the spinal cord and interact with dorsal horn neurons to produce pain hypersensitivity. The important role of glial cells such as microglia and astrocytes in neuropathic pain has only recently been identified. The release of proinflammatory neuromodulators such as cytokines and chemokines from these glial cells plays a previously underestimated role in neuropathic pain and may provide new options for treatment. If reconnection of the injured axon with its target does not occur after a peripheral nerve injury, small nociceptor sensory neurons with unmyelinated axons start to die after many weeks. Sensory inflow to the CNS is permanently disrupted. The synaptic circuitry in the spinal cord is also modified and death by apoptosis of neurons in the dorsal horn occurs, and this seems to be related to excessive glutamate release. The neurons that die include inhibitory interneurons; hence, there is an irreversible reduction in local segmental inhibitory transmission in the dorsal horn. The changes are not limited to the spinal cord; they extend to alterations in the cortex and cortical grey matter. Some patients may demonstrate neuropathic pain that is dependent on the activity of the sympathetic nervous system. 19 Following a peripheral nerve 12S
6 Volume 134, Number 4S-2 Pathophysiology of Pain Table 2. Typical Features of Neuropathic Pain1,8,17 Hyperalgesia Allodynia Dysaesthesia Hyperpathia Hypoalgesia Increased response to a painful stimulus Pain due to a stimulus that does not normally cause pain Unpleasant abnormal sensation, whether spontaneous or evoked Painful syndrome characterized by an abnormally painful reaction to a stimulus, especially a repetitive stimulus, as well as an increased threshold Diminished response to a normally painful stimulus injury, axons develop increased α-adrenoreceptors and therefore have an exaggerated response to circulating catecholamines. Structural changes to the nerve also occur with sympathetic axons sprouting into the dorsal root ganglion surrounding the cell bodies of sensory neurons. These changes lead to sympathetically maintained pain, often as unilateral limb pain with associated features of vasomotor and sudomotor changes. Central mechanisms involved in the generation of neuropathic pain occur primarily in the dorsal horn and are thought to result in neuroplastic changes in the CNS.15 Windup occurs when there is repetitive C fiber inputs that act mainly on NMDA receptors. Windup is short lived (lasting seconds to minutes). Further central sensitization changes differ from windup in that the changes remain long after the C fiber input has ceased. Other described central mechanisms of neuropathic pain include central disinhibition, where there is loss of modulatory control mechanisms due to downregulation of inhibitory neurotransmitters, recruitment, Fig. 2. Risk factors for persistent postsurgical pain.14,20,21 13S
7 Plastic and Reconstructive Surgery October Supplement 2014 gene expression, role of glial cells, and anatomical reorganization of the spinal cord. Finally, changes in the representation of the affected area in the somatosensory cortex occur. Persistent Postsurgical Pain A specific example of neuropathic pain relevant to surgeons is persistent postsurgical pain (PPSP). Chronic pain is common after surgery. The reported incidences of PPSP vary widely, for example, mastectomy 20 50%, amputation 50 85%, hysterectomy 5 30%, cardiac surgery 30 55%, hernia repair 5 35%, and thoracotomy 5 65% 14,20 ; severe disabling pain (greater than 5 on a 10-point scale) occurs in 2 10% of cases. It has been suggested that PPSP should be defined as pain that persists for 2 months after surgery that is unexplained by other causes. 20 The mechanism for development of PPSP is complex; it is often neuropathic pain and maladaptive neuronal plasticity has occurred. 14 PPSP can be crippling resulting in disability and reduced quality of life and is a significant economic burden. Important risk factors include intraoperative nerve injury, preoperative pain, poorly controlled postoperative pain, and psychosocial factors. Figure 2 depicts factors contributing to PPSP. CONCLUSIONS The pain matrix is complex. Having gathered information on receptors, ion channels, and neurotransmitters over the last years, we now have a better understanding on nociceptive and inflammatory pain transmission and pathological pain states. This allows future development of potential new targets for analgesic therapy. Stephan A. Schug, MD, FANZCA, FFPMANZCA Pharmacology, Pharmacy and Anaesthesiology Unit School of Medicine and Pharmacology The University of Western Australia UWA Anaesthesiology Level 2, MRF Building, Royal Perth Hospital GPO Box X2213 Perth 6847, Australia stephan.schug@uwa.edu.au REFERENCES 1. IASP. IASP Taxonomy. Available at: org/education/content.aspx?itemnumber=1698&navitem Number=576. Accessed 27 March Goldberg DS, McGee SJ. Pain as a global public health priority. BMC Public Health 2011;11: Woolf CJ. What is this thing called pain? J Clin Invest. 2010;120: Woolf CJ, Ma Q. Nociceptors noxious stimulus detectors. Neuron 2007;55: Dib-Hajj SD, Binshtok AM, Cummins TR, et al. Voltage-gated sodium channels in pain states: role in pathophysiology and targets for treatment. Brain Res Rev. 2009;60: Silos-Santiago I. The role of tetrodotoxin-resistant sodium channels in pain states: are they the next target for analgesic drugs? Curr Opin Investig Drugs. 2008;9: Dib-Hajj SD, Yang Y, Waxman SG. Genetics and molecular pathophysiology of Na(v)1.7-related pain syndromes. Adv Genet. 2008;63: Schug SA, Daly H, Stannard KJD. Pathophysiology of pain. In: Thompson M, Fitridge R, eds. Mechanisms of Vascular Disease: A Reference Book for Vascular Specialists. Adelaide, Australia: University of Adelaide, Barr Smith Press; 2011: Garland EL. Pain processing in the human nervous system: a selective review of nociceptive and biobehavioral pathways. Prim Care 2012;39: Melzack R, Wall PD. Pain mechanisms: a new theory. Science 1965;150: Dickenson AH. Gate control theory of pain stands the test of time. Br J Anaesth. 2002;88: Moayedi M, Davis KD. Theories of pain: from specificity to gate control. J Neurophysiol. 2013;109: Heinricher MM, Tavares I, Leith JL, et al. Descending control of nociception: specificity, recruitment and plasticity. Brain Res Rev. 2009;60: Kehlet H, Jensen TS, Woolf CJ. Persistent postsurgical pain: risk factors and prevention. Lancet 2006;367: Woolf CJ. Central sensitization: implications for the diagnosis and treatment of pain. Pain 2011;152(3 Suppl):S Jensen TS, Baron R, Haanpää M, et al. A new definition of neuropathic pain. Pain 2011;152: Baron R, Binder A, Wasner G. Neuropathic pain: diagnosis, pathophysiological mechanisms, and treatment. Lancet Neurol. 2010;9: Taylor CP. Mechanisms of analgesia by gabapentin and pregabalin calcium channel alpha2-delta [Cavalpha2-delta] ligands. Pain 2009;142: Jänig W, Häbler HJ. Sympathetic nervous system: contribution to chronic pain. Prog Brain Res. 2000;129: Niraj G, Rowbotham DJ. Persistent postoperative pain: where are we now? Br J Anaesth. 2011;107: Macintyre PE, Schug SA, Scott D, et al. Acute Pain Management: Scientific Evidence. 3rd ed. Melbourne: ANZCA and FPM; S
The anatomy and physiology of pain
 The anatomy and physiology of pain Charlotte E Steeds Abstract Pain is an unpleasant experience that results from both physical and psychological responses to injury. A complex set of pathways transmits
The anatomy and physiology of pain Charlotte E Steeds Abstract Pain is an unpleasant experience that results from both physical and psychological responses to injury. A complex set of pathways transmits
211MDS Pain theories
 211MDS Pain theories Definition In 1986, the International Association for the Study of Pain (IASP) defined pain as a sensory and emotional experience associated with real or potential injuries, or described
211MDS Pain theories Definition In 1986, the International Association for the Study of Pain (IASP) defined pain as a sensory and emotional experience associated with real or potential injuries, or described
Chapter 16. Sense of Pain
 Chapter 16 Sense of Pain Pain Discomfort caused by tissue injury or noxious stimulation, and typically leading to evasive action important /// helps to protect us lost of pain in diabetes mellitus = diabetic
Chapter 16 Sense of Pain Pain Discomfort caused by tissue injury or noxious stimulation, and typically leading to evasive action important /// helps to protect us lost of pain in diabetes mellitus = diabetic
Receptors and Neurotransmitters: It Sounds Greek to Me. Agenda. What We Know About Pain 9/7/2012
 Receptors and Neurotransmitters: It Sounds Greek to Me Cathy Carlson, PhD, RN Northern Illinois University Agenda We will be going through this lecture on basic pain physiology using analogies, mnemonics,
Receptors and Neurotransmitters: It Sounds Greek to Me Cathy Carlson, PhD, RN Northern Illinois University Agenda We will be going through this lecture on basic pain physiology using analogies, mnemonics,
Pain Pathways. Dr Sameer Gupta Consultant in Anaesthesia and Pain Management, NGH
 Pain Pathways Dr Sameer Gupta Consultant in Anaesthesia and Pain Management, NGH Objective To give you a simplistic and basic concepts of pain pathways to help understand the complex issue of pain Pain
Pain Pathways Dr Sameer Gupta Consultant in Anaesthesia and Pain Management, NGH Objective To give you a simplistic and basic concepts of pain pathways to help understand the complex issue of pain Pain
Pharmacology of Pain Transmission and Modulation
 Pharmacology of Pain Transmission and Modulation 2 Jürg Schliessbach and Konrad Maurer Nociceptive Nerve Fibers Pain is transmitted to the central nervous system via thinly myelinated Aδ and unmyelinated
Pharmacology of Pain Transmission and Modulation 2 Jürg Schliessbach and Konrad Maurer Nociceptive Nerve Fibers Pain is transmitted to the central nervous system via thinly myelinated Aδ and unmyelinated
Pain. Pain. Pain: One definition. Pain: One definition. Pain: One definition. Pain: One definition. Psyc 2906: Sensation--Introduction 9/27/2006
 Pain Pain Pain: One Definition Classic Paths A new Theory Pain and Drugs According to the international Association for the Study (Merskey & Bogduk, 1994), Pain is an unpleasant sensory and emotional experience
Pain Pain Pain: One Definition Classic Paths A new Theory Pain and Drugs According to the international Association for the Study (Merskey & Bogduk, 1994), Pain is an unpleasant sensory and emotional experience
Somatosensory Physiology (Pain And Temperature) Richard M. Costanzo, Ph.D.
 Somatosensory Physiology (Pain And Temperature) Richard M. Costanzo, Ph.D. OBJECTIVES After studying the material of this lecture the student should be familiar with: 1. The relationship between nociception
Somatosensory Physiology (Pain And Temperature) Richard M. Costanzo, Ph.D. OBJECTIVES After studying the material of this lecture the student should be familiar with: 1. The relationship between nociception
Pathophysiology of Pain. Ramon Go MD Assistant Professor Anesthesiology and Pain medicine NYP-CUMC
 Pathophysiology of Pain Ramon Go MD Assistant Professor Anesthesiology and Pain medicine NYP-CUMC Learning Objectives Anatomic pathway of nociception Discuss the multiple target sites of pharmacological
Pathophysiology of Pain Ramon Go MD Assistant Professor Anesthesiology and Pain medicine NYP-CUMC Learning Objectives Anatomic pathway of nociception Discuss the multiple target sites of pharmacological
San Francisco Chronicle, June 2001
 PAIN San Francisco Chronicle, June 2001 CONGENITAL INSENSITIVITY TO PAIN PAIN IS A SUBJECTIVE EXPERIENCE: It is not a stimulus MAJOR FEATURES OF THE PAIN EXPERIENCE: Sensory discriminative Affective (emotional)
PAIN San Francisco Chronicle, June 2001 CONGENITAL INSENSITIVITY TO PAIN PAIN IS A SUBJECTIVE EXPERIENCE: It is not a stimulus MAJOR FEATURES OF THE PAIN EXPERIENCE: Sensory discriminative Affective (emotional)
Pathophysiology of Pain
 Pathophysiology of Pain Wound Inflammatory response Chemical mediators Activity in Pain Path PAIN http://neuroscience.uth.tmc.edu/s2/chapter08.html Chris Cohan, Ph.D. Dept. of Pathology/Anat Sci University
Pathophysiology of Pain Wound Inflammatory response Chemical mediators Activity in Pain Path PAIN http://neuroscience.uth.tmc.edu/s2/chapter08.html Chris Cohan, Ph.D. Dept. of Pathology/Anat Sci University
PAIN MANAGEMENT in the CANINE PATIENT
 PAIN MANAGEMENT in the CANINE PATIENT Laurie Edge-Hughes, BScPT, MAnimSt (Animal Physio), CAFCI, CCRT Part 1: Laurie Edge-Hughes, BScPT, MAnimSt (Animal Physio), CAFCI, CCRT 1 Pain is the most common reason
PAIN MANAGEMENT in the CANINE PATIENT Laurie Edge-Hughes, BScPT, MAnimSt (Animal Physio), CAFCI, CCRT Part 1: Laurie Edge-Hughes, BScPT, MAnimSt (Animal Physio), CAFCI, CCRT 1 Pain is the most common reason
ANAT2010. Concepts of Neuroanatomy (II) S2 2018
 ANAT2010 Concepts of Neuroanatomy (II) S2 2018 Table of Contents Lecture 13: Pain and perception... 3 Lecture 14: Sensory systems and visual pathways... 11 Lecture 15: Techniques in Neuroanatomy I in vivo
ANAT2010 Concepts of Neuroanatomy (II) S2 2018 Table of Contents Lecture 13: Pain and perception... 3 Lecture 14: Sensory systems and visual pathways... 11 Lecture 15: Techniques in Neuroanatomy I in vivo
Pain Mechanisms. Prof Michael G Irwin MD, FRCA, FANZCA FHKAM Head Department of Anaesthesiology University of Hong Kong. The Somatosensory System
 ain Mechanisms rof Michael G Irwin MD, FRCA, FANZCA FHKAM Head Department of Anaesthesiology University of Hong Kong The Somatosensory System Frontal cortex Descending pathway eriaqueductal gray matter
ain Mechanisms rof Michael G Irwin MD, FRCA, FANZCA FHKAM Head Department of Anaesthesiology University of Hong Kong The Somatosensory System Frontal cortex Descending pathway eriaqueductal gray matter
Spinal Cord Injury Pain. Michael Massey, DO CentraCare Health St Cloud, MN 11/07/2018
 Spinal Cord Injury Pain Michael Massey, DO CentraCare Health St Cloud, MN 11/07/2018 Objectives At the conclusion of this session, participants should be able to: 1. Understand the difference between nociceptive
Spinal Cord Injury Pain Michael Massey, DO CentraCare Health St Cloud, MN 11/07/2018 Objectives At the conclusion of this session, participants should be able to: 1. Understand the difference between nociceptive
ANAT2010. Concepts of Neuroanatomy (II) S2 2018
 ANAT2010 Concepts of Neuroanatomy (II) S2 2018 Table of Contents Lecture 13: Pain and perception... 3 Lecture 14: Sensory systems and visual pathways... 11 Lecture 15: Techniques in Neuroanatomy I in vivo
ANAT2010 Concepts of Neuroanatomy (II) S2 2018 Table of Contents Lecture 13: Pain and perception... 3 Lecture 14: Sensory systems and visual pathways... 11 Lecture 15: Techniques in Neuroanatomy I in vivo
What is Pain? An unpleasant sensory and emotional experience associated with actual or potential tissue damage. Pain is always subjective
 Pain & Acupuncture What is Pain? An unpleasant sensory and emotional experience associated with actual or potential tissue damage. NOCICEPTION( the neural processes of encoding and processing noxious stimuli.)
Pain & Acupuncture What is Pain? An unpleasant sensory and emotional experience associated with actual or potential tissue damage. NOCICEPTION( the neural processes of encoding and processing noxious stimuli.)
Seizure: the clinical manifestation of an abnormal and excessive excitation and synchronization of a population of cortical
 Are There Sharing Mechanisms of Epilepsy, Migraine and Neuropathic Pain? Chin-Wei Huang, MD, PhD Department of Neurology, NCKUH Basic mechanisms underlying seizures and epilepsy Seizure: the clinical manifestation
Are There Sharing Mechanisms of Epilepsy, Migraine and Neuropathic Pain? Chin-Wei Huang, MD, PhD Department of Neurology, NCKUH Basic mechanisms underlying seizures and epilepsy Seizure: the clinical manifestation
PAIN IS A SUBJECTIVE EXPERIENCE: It is not a stimulus. MAJOR FEATURES OF THE PAIN EXPERIENCE: Sensory discriminative Affective (emotional) Cognitive
 PAIN PAIN IS A SUBJECTIVE EXPERIENCE: It is not a stimulus MAJOR FEATURES OF THE PAIN EXPERIENCE: Sensory discriminative Affective (emotional) Cognitive MEASUREMENT OF PAIN: A BIG PROBLEM Worst pain ever
PAIN PAIN IS A SUBJECTIVE EXPERIENCE: It is not a stimulus MAJOR FEATURES OF THE PAIN EXPERIENCE: Sensory discriminative Affective (emotional) Cognitive MEASUREMENT OF PAIN: A BIG PROBLEM Worst pain ever
Pain and impulse conduction
 1 Pain and impulse conduction L.H.D.J. Booij According to the World Health Organisation pain is defined as an unpleasant sensation that occurs from imminent tissue damage. From a physiological perspective,
1 Pain and impulse conduction L.H.D.J. Booij According to the World Health Organisation pain is defined as an unpleasant sensation that occurs from imminent tissue damage. From a physiological perspective,
Transition from acute to chronic pain
 A Feizerfan FRCA G Sheh BHB MBChB FAFRM(RACP) FFPMANZCA Matrix reference 3E00 Key points Physiology of pain involves activation and complex interactions of autonomic, peripheral and central nervous systems,
A Feizerfan FRCA G Sheh BHB MBChB FAFRM(RACP) FFPMANZCA Matrix reference 3E00 Key points Physiology of pain involves activation and complex interactions of autonomic, peripheral and central nervous systems,
Sensory coding and somatosensory system
 Sensory coding and somatosensory system Sensation and perception Perception is the internal construction of sensation. Perception depends on the individual experience. Three common steps in all senses
Sensory coding and somatosensory system Sensation and perception Perception is the internal construction of sensation. Perception depends on the individual experience. Three common steps in all senses
Pain and Temperature Objectives
 Pain and Temperature Objectives 1. Describe the types of sensory receptors that transmit pain and temperature. 2. Understand how axon diameter relates to transmission of pain and temp information. 3. Describe
Pain and Temperature Objectives 1. Describe the types of sensory receptors that transmit pain and temperature. 2. Understand how axon diameter relates to transmission of pain and temp information. 3. Describe
UNIVERSITY OF JORDAN FACULTY OF MEDICINE DEPARTMENT OF PHYSIOLOGY & BIOCHEMISTRY NEUROPHYSIOLOGY (MEDICAL), SPRING 2014
 UNIVERSITY OF JORDAN FACULTY OF MEDICINE DEPARTMENT OF PHYSIOLOGY & BIOCHEMISTRY NEUROPHYSIOLOGY (MEDICAL), SPRING 2014 Textbook of Medical Physiology by: Guyton & Hall, 12 th edition 2011 Eman Al-Khateeb,
UNIVERSITY OF JORDAN FACULTY OF MEDICINE DEPARTMENT OF PHYSIOLOGY & BIOCHEMISTRY NEUROPHYSIOLOGY (MEDICAL), SPRING 2014 Textbook of Medical Physiology by: Guyton & Hall, 12 th edition 2011 Eman Al-Khateeb,
CHAPTER 10 THE SOMATOSENSORY SYSTEM
 CHAPTER 10 THE SOMATOSENSORY SYSTEM 10.1. SOMATOSENSORY MODALITIES "Somatosensory" is really a catch-all term to designate senses other than vision, hearing, balance, taste and smell. Receptors that could
CHAPTER 10 THE SOMATOSENSORY SYSTEM 10.1. SOMATOSENSORY MODALITIES "Somatosensory" is really a catch-all term to designate senses other than vision, hearing, balance, taste and smell. Receptors that could
*Anteriolateral spinothalamic tract (STT) : a sensory pathway that is positioned anteriorly and laterally in the spinal cord.
 *somatic sensations : PAIN *Anteriolateral spinothalamic tract (STT) : a sensory pathway that is positioned anteriorly and laterally in the spinal cord. *This pathway carries a variety of sensory modalities:
*somatic sensations : PAIN *Anteriolateral spinothalamic tract (STT) : a sensory pathway that is positioned anteriorly and laterally in the spinal cord. *This pathway carries a variety of sensory modalities:
CHAPTER 4 PAIN AND ITS MANAGEMENT
 CHAPTER 4 PAIN AND ITS MANAGEMENT Pain Definition: An unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage. Types of Pain
CHAPTER 4 PAIN AND ITS MANAGEMENT Pain Definition: An unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage. Types of Pain
What it Takes to be a Pain
 What it Takes to be a Pain Pain Pathways and the Neurophysiology of pain Dennis S. Pacl, MD, FACP, FAChPM Austin Palliative Care/ Hospice Austin A Definition of Pain complex constellation of unpleasant
What it Takes to be a Pain Pain Pathways and the Neurophysiology of pain Dennis S. Pacl, MD, FACP, FAChPM Austin Palliative Care/ Hospice Austin A Definition of Pain complex constellation of unpleasant
Medical Neuroscience Tutorial
 Pain Pathways Medical Neuroscience Tutorial Pain Pathways MAP TO NEUROSCIENCE CORE CONCEPTS 1 NCC1. The brain is the body's most complex organ. NCC3. Genetically determined circuits are the foundation
Pain Pathways Medical Neuroscience Tutorial Pain Pathways MAP TO NEUROSCIENCE CORE CONCEPTS 1 NCC1. The brain is the body's most complex organ. NCC3. Genetically determined circuits are the foundation
PAIN MODULATION. numerical value. adjectives. DR SYED SHAHID HABIB Professor & Consultant Dept. of Physiology College of Medicine & KKUH
 PAIN MODULATION numerical value adjectives DR SYED SHAHID HABIB Professor & Consultant Dept. of Physiology College of Medicine & KKUH OBJECTIVES At the end of this lecture you should be able to describe:
PAIN MODULATION numerical value adjectives DR SYED SHAHID HABIB Professor & Consultant Dept. of Physiology College of Medicine & KKUH OBJECTIVES At the end of this lecture you should be able to describe:
1 The Physiology of Pain
 1 The Physiology of Pain Rohit Juneja and Siân Jaggar Introduction Definitions Key Messages Pain is still underdiagnosed and undertreated. Pain is a subjective experience and may even be present in the
1 The Physiology of Pain Rohit Juneja and Siân Jaggar Introduction Definitions Key Messages Pain is still underdiagnosed and undertreated. Pain is a subjective experience and may even be present in the
Somatic Sensation (MCB160 Lecture by Mu-ming Poo, Friday March 9, 2007)
 Somatic Sensation (MCB160 Lecture by Mu-ming Poo, Friday March 9, 2007) Introduction Adrian s work on sensory coding Spinal cord and dorsal root ganglia Four somatic sense modalities Touch Mechanoreceptors
Somatic Sensation (MCB160 Lecture by Mu-ming Poo, Friday March 9, 2007) Introduction Adrian s work on sensory coding Spinal cord and dorsal root ganglia Four somatic sense modalities Touch Mechanoreceptors
Chapter 11 Introduction to the Nervous System and Nervous Tissue Chapter Outline
 Chapter 11 Introduction to the Nervous System and Nervous Tissue Chapter Outline Module 11.1 Overview of the Nervous System (Figures 11.1-11.3) A. The nervous system controls our perception and experience
Chapter 11 Introduction to the Nervous System and Nervous Tissue Chapter Outline Module 11.1 Overview of the Nervous System (Figures 11.1-11.3) A. The nervous system controls our perception and experience
SOMATOSENSORY SYSTEMS AND PAIN
 SOMATOSENSORY SYSTEMS AND PAIN A 21 year old man presented with a stab wound of the right side of the neck (Panel A). Neurological examination revealed right hemiplegia and complete right-sided loss of
SOMATOSENSORY SYSTEMS AND PAIN A 21 year old man presented with a stab wound of the right side of the neck (Panel A). Neurological examination revealed right hemiplegia and complete right-sided loss of
Pathophysiological Classification of Pain
 PATHOPHYSIOLOGY Overview Pathophysiological Classification of Pain Central sensitization/ dysfunctional pain Nociceptive pain - Somatic - Visceral Multiple pain mechanisms may coexist (mixed pain) Neuropathic
PATHOPHYSIOLOGY Overview Pathophysiological Classification of Pain Central sensitization/ dysfunctional pain Nociceptive pain - Somatic - Visceral Multiple pain mechanisms may coexist (mixed pain) Neuropathic
Motor Control, Pain, Somatic Dysfunction, Core Stability. Richard G. Schuster, DO Shawn Kerger, DO, FAOASM 19 September 2016 OMED 2016 Anaheim, CA
 Motor Control, Pain, Somatic Dysfunction, Core Stability Richard G. Schuster, DO Shawn Kerger, DO, FAOASM 19 September 2016 OMED 2016 Anaheim, CA How do we move? Decision to move (Executive or Cognitive
Motor Control, Pain, Somatic Dysfunction, Core Stability Richard G. Schuster, DO Shawn Kerger, DO, FAOASM 19 September 2016 OMED 2016 Anaheim, CA How do we move? Decision to move (Executive or Cognitive
Neuropathic Pain in Palliative Care
 Neuropathic Pain in Palliative Care Neuropathic Pain in Advanced Cancer Affects 40% of patients Multiple concurrent pains are common Often complex pathophysiology with mixed components Nocioceptive Neuropathic
Neuropathic Pain in Palliative Care Neuropathic Pain in Advanced Cancer Affects 40% of patients Multiple concurrent pains are common Often complex pathophysiology with mixed components Nocioceptive Neuropathic
Pain classifications slow and fast
 Pain classifications slow and fast Fast Pain Slow Pain Sharp, pricking (Aδ) fiber Short latency Well localized Short duration Dull, burning (C) fiber Slower onset Diffuse Long duration Less emotional Emotional,
Pain classifications slow and fast Fast Pain Slow Pain Sharp, pricking (Aδ) fiber Short latency Well localized Short duration Dull, burning (C) fiber Slower onset Diffuse Long duration Less emotional Emotional,
Chapter 9. Nervous System
 Chapter 9 Nervous System Central Nervous System (CNS) vs. Peripheral Nervous System(PNS) CNS Brain Spinal cord PNS Peripheral nerves connecting CNS to the body Cranial nerves Spinal nerves Neurons transmit
Chapter 9 Nervous System Central Nervous System (CNS) vs. Peripheral Nervous System(PNS) CNS Brain Spinal cord PNS Peripheral nerves connecting CNS to the body Cranial nerves Spinal nerves Neurons transmit
Posterior White Column-Medial Lemniscal Pathway
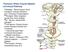 Posterior White Column-Medial Lemniscal Pathway Modality: Discriminative Touch Sensation (include Vibration) and Conscious Proprioception Receptor: Most receptors except free nerve endings Ist Neuron:
Posterior White Column-Medial Lemniscal Pathway Modality: Discriminative Touch Sensation (include Vibration) and Conscious Proprioception Receptor: Most receptors except free nerve endings Ist Neuron:
The biochemical origin of pain: The origin of all pain is inflammation and the inflammatory response: Inflammatory profile of pain syndromes
 The biochemical origin of pain: The origin of all pain is inflammation and the inflammatory response: Inflammatory profile of pain syndromes 1 Medical Hypothesis 2007, Vol. 69, pp. 1169 1178 Sota Omoigui
The biochemical origin of pain: The origin of all pain is inflammation and the inflammatory response: Inflammatory profile of pain syndromes 1 Medical Hypothesis 2007, Vol. 69, pp. 1169 1178 Sota Omoigui
Basic Neuroscience. Sally Curtis
 The Physiology of Pain Basic Neuroscience Sally Curtis sac3@soton.ac.uk The behaviour of humans is a result of the actions of nerves. Nerves form the basis of Thoughts, sensations and actions both reflex
The Physiology of Pain Basic Neuroscience Sally Curtis sac3@soton.ac.uk The behaviour of humans is a result of the actions of nerves. Nerves form the basis of Thoughts, sensations and actions both reflex
Chapter Nervous Systems
 The Nervous System Chapter Nervous Systems Which animals have nervous systems? (Which do not) What are the basic components of a NS? What kind of fish performs brain operations? What differentiates one
The Nervous System Chapter Nervous Systems Which animals have nervous systems? (Which do not) What are the basic components of a NS? What kind of fish performs brain operations? What differentiates one
Brian Kahan, D.O. FAAPMR, DABPM, DAOCRM, FIPP Center for Pain Medicine and Physiatric Rehabilitation 2002 Medical Parkway Suite 150 Annapolis, MD
 Brian Kahan, D.O. FAAPMR, DABPM, DAOCRM, FIPP Center for Pain Medicine and Physiatric Rehabilitation 2002 Medical Parkway Suite 150 Annapolis, MD 1630 Main Street Suite 215 Chester, MD 410-571-9000 www.4-no-pain.com
Brian Kahan, D.O. FAAPMR, DABPM, DAOCRM, FIPP Center for Pain Medicine and Physiatric Rehabilitation 2002 Medical Parkway Suite 150 Annapolis, MD 1630 Main Street Suite 215 Chester, MD 410-571-9000 www.4-no-pain.com
Mechanism of Pain Production
 Mechanism of Pain Production Pain conducting nerve fibers are small myelinated (A-delta) or unmyelinated nerve fibers (C-fibers). Cell bodies are in the dorsal root ganglia (DRG) or sensory ganglia of
Mechanism of Pain Production Pain conducting nerve fibers are small myelinated (A-delta) or unmyelinated nerve fibers (C-fibers). Cell bodies are in the dorsal root ganglia (DRG) or sensory ganglia of
Joint Session with ACOFP, AOASM and AAO: Motor Control, Pain, Somatic Dysfunction, Core Stability. Shawn R. Kerger, DO, FAOSM Richard G.
 Joint Session with ACOFP, AOASM and AAO: Motor Control, Pain, Somatic Dysfunction, Core Stability Shawn R. Kerger, DO, FAOSM Richard G. Schuster, DO Motor Control, Pain, Somatic Dysfunction, Core Stability
Joint Session with ACOFP, AOASM and AAO: Motor Control, Pain, Somatic Dysfunction, Core Stability Shawn R. Kerger, DO, FAOSM Richard G. Schuster, DO Motor Control, Pain, Somatic Dysfunction, Core Stability
Lecture 22: A little Neurobiology
 BIO 5099: Molecular Biology for Computer Scientists (et al) Lecture 22: A little Neurobiology http://compbio.uchsc.edu/hunter/bio5099 Larry.Hunter@uchsc.edu Nervous system development Part of the ectoderm
BIO 5099: Molecular Biology for Computer Scientists (et al) Lecture 22: A little Neurobiology http://compbio.uchsc.edu/hunter/bio5099 Larry.Hunter@uchsc.edu Nervous system development Part of the ectoderm
By the end of this lecture the students will be able to:
 UNIT VII: PAIN Objectives: By the end of this lecture the students will be able to: Review the concept of somatosensory pathway. Describe the function of Nociceptors in response to pain information. Describe
UNIT VII: PAIN Objectives: By the end of this lecture the students will be able to: Review the concept of somatosensory pathway. Describe the function of Nociceptors in response to pain information. Describe
Chronic pain: We should not underestimate the contribution of neural plasticity. *Gwyn N Lewis 1, David A Rice 1,2
 Chronic pain: We should not underestimate the contribution of neural plasticity *Gwyn N Lewis 1, David A Rice 1,2 1 Health and Rehabilitation Research Institute, AUT University, Auckland, New Zealand 2
Chronic pain: We should not underestimate the contribution of neural plasticity *Gwyn N Lewis 1, David A Rice 1,2 1 Health and Rehabilitation Research Institute, AUT University, Auckland, New Zealand 2
Prof Wayne Derman MBChB,BSc (Med)(Hons) PhD, FFIMS. Pain Management in the Elite Athlete: The 2017 IOC Consensus Statement
 Prof Wayne Derman MBChB,BSc (Med)(Hons) PhD, FFIMS Pain Management in the Elite Athlete: The 2017 IOC Consensus Statement 2 as 20 Experts published and leaders in their respective field 12 month lead in
Prof Wayne Derman MBChB,BSc (Med)(Hons) PhD, FFIMS Pain Management in the Elite Athlete: The 2017 IOC Consensus Statement 2 as 20 Experts published and leaders in their respective field 12 month lead in
AKA a painful lecture by Colleen Blanchfield, MD Full Circle Neuropsychiatric Wellness Center
 A lecture on PAIN AKA a painful lecture by Colleen Blanchfield, MD Full Circle Neuropsychiatric Wellness Center 1 Overview of the lecture Anatomy of the Pain Tract How a painful stimulus travels from the
A lecture on PAIN AKA a painful lecture by Colleen Blanchfield, MD Full Circle Neuropsychiatric Wellness Center 1 Overview of the lecture Anatomy of the Pain Tract How a painful stimulus travels from the
Anatomical Substrates of Somatic Sensation
 Anatomical Substrates of Somatic Sensation John H. Martin, Ph.D. Center for Neurobiology & Behavior Columbia University CPS The 2 principal somatic sensory systems: 1) Dorsal column-medial lemniscal system
Anatomical Substrates of Somatic Sensation John H. Martin, Ph.D. Center for Neurobiology & Behavior Columbia University CPS The 2 principal somatic sensory systems: 1) Dorsal column-medial lemniscal system
Fundamentals of the Nervous System and Nervous Tissue: Part C
 PowerPoint Lecture Slides prepared by Janice Meeking, Mount Royal College C H A P T E R 11 Fundamentals of the Nervous System and Nervous Tissue: Part C Warm Up What is a neurotransmitter? What is the
PowerPoint Lecture Slides prepared by Janice Meeking, Mount Royal College C H A P T E R 11 Fundamentals of the Nervous System and Nervous Tissue: Part C Warm Up What is a neurotransmitter? What is the
Primary Functions. Monitor changes. Integrate input. Initiate a response. External / internal. Process, interpret, make decisions, store information
 NERVOUS SYSTEM Monitor changes External / internal Integrate input Primary Functions Process, interpret, make decisions, store information Initiate a response E.g., movement, hormone release, stimulate/inhibit
NERVOUS SYSTEM Monitor changes External / internal Integrate input Primary Functions Process, interpret, make decisions, store information Initiate a response E.g., movement, hormone release, stimulate/inhibit
Pain teaching. Muhammad Laklouk
 Pain teaching Muhammad Laklouk Definition Pain An unpleasant sensory and emotional experience associated with actual or potential tissue damage or described in terms of such damage. Sensory (discriminatiory)
Pain teaching Muhammad Laklouk Definition Pain An unpleasant sensory and emotional experience associated with actual or potential tissue damage or described in terms of such damage. Sensory (discriminatiory)
Lesson 33. Objectives: References: Chapter 16: Reading for Next Lesson: Chapter 16:
 Lesson 33 Lesson Outline: Nervous System Structure and Function Neuronal Tissue Supporting Cells Neurons Nerves Functional Classification of Neuronal Tissue Organization of the Nervous System Peripheral
Lesson 33 Lesson Outline: Nervous System Structure and Function Neuronal Tissue Supporting Cells Neurons Nerves Functional Classification of Neuronal Tissue Organization of the Nervous System Peripheral
Department of Neurology/Division of Anatomical Sciences
 Spinal Cord I Lecture Outline and Objectives CNS/Head and Neck Sequence TOPIC: FACULTY: THE SPINAL CORD AND SPINAL NERVES, Part I Department of Neurology/Division of Anatomical Sciences LECTURE: Monday,
Spinal Cord I Lecture Outline and Objectives CNS/Head and Neck Sequence TOPIC: FACULTY: THE SPINAL CORD AND SPINAL NERVES, Part I Department of Neurology/Division of Anatomical Sciences LECTURE: Monday,
Chapter 4 Neuronal Physiology
 Chapter 4 Neuronal Physiology V edit. Pg. 99-131 VI edit. Pg. 85-113 VII edit. Pg. 87-113 Input Zone Dendrites and Cell body Nucleus Trigger Zone Axon hillock Conducting Zone Axon (may be from 1mm to more
Chapter 4 Neuronal Physiology V edit. Pg. 99-131 VI edit. Pg. 85-113 VII edit. Pg. 87-113 Input Zone Dendrites and Cell body Nucleus Trigger Zone Axon hillock Conducting Zone Axon (may be from 1mm to more
Introduction to some interesting research questions: Molecular biology of the primary afferent nociceptor
 Introduction to some interesting research questions: Molecular biology of the primary afferent nociceptor NOCICEPTORS ARE NOT IDENTICAL PEPTIDE SubP/CGRP Trk A NON-PEPTIDE IB4 P2X 3 c-ret Snider and McMahon
Introduction to some interesting research questions: Molecular biology of the primary afferent nociceptor NOCICEPTORS ARE NOT IDENTICAL PEPTIDE SubP/CGRP Trk A NON-PEPTIDE IB4 P2X 3 c-ret Snider and McMahon
What are the 6 types of neuroglia and their functions?!
 Warm Up! Take out your 11C Notes What are the 6 types of neuroglia and their functions?! Astrocytes Microglia Ependymal Cells Satellite Cells Schwann Cells Oligodendrocytes Support, brace, & nutrient transfer
Warm Up! Take out your 11C Notes What are the 6 types of neuroglia and their functions?! Astrocytes Microglia Ependymal Cells Satellite Cells Schwann Cells Oligodendrocytes Support, brace, & nutrient transfer
10.1: Introduction. Cell types in neural tissue: Neurons Neuroglial cells (also known as neuroglia, glia, and glial cells) Dendrites.
 10.1: Introduction Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Cell types in neural tissue: Neurons Neuroglial cells (also known as neuroglia, glia, and glial
10.1: Introduction Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Cell types in neural tissue: Neurons Neuroglial cells (also known as neuroglia, glia, and glial
The Nervous System. Nervous System Functions 1. gather sensory input 2. integration- process and interpret sensory input 3. cause motor output
 The Nervous System Nervous System Functions 1. gather sensory input 2. integration- process and interpret sensory input 3. cause motor output The Nervous System 2 Parts of the Nervous System 1. central
The Nervous System Nervous System Functions 1. gather sensory input 2. integration- process and interpret sensory input 3. cause motor output The Nervous System 2 Parts of the Nervous System 1. central
Nervous System. 2. Receives information from the environment from CNS to organs and glands. 1. Relays messages, processes info, analyzes data
 Nervous System 1. Relays messages, processes info, analyzes data 2. Receives information from the environment from CNS to organs and glands 3. Transmits impulses from CNS to muscles and glands 4. Transmits
Nervous System 1. Relays messages, processes info, analyzes data 2. Receives information from the environment from CNS to organs and glands 3. Transmits impulses from CNS to muscles and glands 4. Transmits
Lesson 14. The Nervous System. Introduction to Life Processes - SCI 102 1
 Lesson 14 The Nervous System Introduction to Life Processes - SCI 102 1 Structures and Functions of Nerve Cells The nervous system has two principal cell types: Neurons (nerve cells) Glia The functions
Lesson 14 The Nervous System Introduction to Life Processes - SCI 102 1 Structures and Functions of Nerve Cells The nervous system has two principal cell types: Neurons (nerve cells) Glia The functions
Chapter 17 Nervous System
 Chapter 17 Nervous System 1 The Nervous System Two Anatomical Divisions Central Nervous System (CNS) Brain and Spinal Cord Peripheral Nervous System (PNS) Two Types of Cells Neurons Transmit nerve impulses
Chapter 17 Nervous System 1 The Nervous System Two Anatomical Divisions Central Nervous System (CNS) Brain and Spinal Cord Peripheral Nervous System (PNS) Two Types of Cells Neurons Transmit nerve impulses
Chapter 17. Nervous System Nervous systems receive sensory input, interpret it, and send out appropriate commands. !
 Chapter 17 Sensory receptor Sensory input Integration Nervous System Motor output Brain and spinal cord Effector cells Peripheral nervous system (PNS) Central nervous system (CNS) 28.1 Nervous systems
Chapter 17 Sensory receptor Sensory input Integration Nervous System Motor output Brain and spinal cord Effector cells Peripheral nervous system (PNS) Central nervous system (CNS) 28.1 Nervous systems
Unit VIII Problem 1 Physiology: Sensory Pathway
 Unit VIII Problem 1 Physiology: Sensory Pathway - Process of sensation: Sensory receptors: they are specialized cells considered as biologic signal transducers which can detect stimuli and convert them
Unit VIII Problem 1 Physiology: Sensory Pathway - Process of sensation: Sensory receptors: they are specialized cells considered as biologic signal transducers which can detect stimuli and convert them
Cancer-induced bone pain
 Cancer-induced bone pain Common Prevalent in particular cancers: breast (73%), prostate (68%), thyroid (42%), lung (36%), renal (35%), colon (5%) Correlates with an increased morbidity Reduced performance
Cancer-induced bone pain Common Prevalent in particular cancers: breast (73%), prostate (68%), thyroid (42%), lung (36%), renal (35%), colon (5%) Correlates with an increased morbidity Reduced performance
SOMATOSENSORY SYSTEMS: Pain and Temperature Kimberle Jacobs, Ph.D.
 SOMATOSENSORY SYSTEMS: Pain and Temperature Kimberle Jacobs, Ph.D. Sensory systems are afferent, meaning that they are carrying information from the periphery TOWARD the central nervous system. The somatosensory
SOMATOSENSORY SYSTEMS: Pain and Temperature Kimberle Jacobs, Ph.D. Sensory systems are afferent, meaning that they are carrying information from the periphery TOWARD the central nervous system. The somatosensory
The Nervous System: Neural Tissue Pearson Education, Inc.
 13 The Nervous System: Neural Tissue Introduction Nervous System Characteristics Controls and adjust the activity of the body Provides swift but brief responses The nervous system includes: Central Nervous
13 The Nervous System: Neural Tissue Introduction Nervous System Characteristics Controls and adjust the activity of the body Provides swift but brief responses The nervous system includes: Central Nervous
What is pain?: An unpleasant sensation. What is an unpleasant sensation?: Pain. - Aristotle.
 What is pain?: An unpleasant sensation. What is an unpleasant sensation?: Pain. - Aristotle. Nociception The detection of tissue damage or impending tissue damage, but There can be tissue damage without
What is pain?: An unpleasant sensation. What is an unpleasant sensation?: Pain. - Aristotle. Nociception The detection of tissue damage or impending tissue damage, but There can be tissue damage without
CHAPTER 4 PAIN AND ITS MANAGEMENT
 CHAPTER 4 PAIN AND ITS MANAGEMENT Pain Definition: An unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage. Types of Pain
CHAPTER 4 PAIN AND ITS MANAGEMENT Pain Definition: An unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage. Types of Pain
Neural Integration I: Sensory Pathways and the Somatic Nervous System
 15 Neural Integration I: Sensory Pathways and the Somatic Nervous System PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris An Introduction to Sensory Pathways and
15 Neural Integration I: Sensory Pathways and the Somatic Nervous System PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris An Introduction to Sensory Pathways and
Biomechanics of Pain: Dynamics of the Neuromatrix
 Biomechanics of Pain: Dynamics of the Neuromatrix Partap S. Khalsa, D.C., Ph.D. Department of Biomedical Engineering The Neuromatrix From: Melzack R (1999) Pain Suppl 6:S121-6. NIOSH STAR Symposium May
Biomechanics of Pain: Dynamics of the Neuromatrix Partap S. Khalsa, D.C., Ph.D. Department of Biomedical Engineering The Neuromatrix From: Melzack R (1999) Pain Suppl 6:S121-6. NIOSH STAR Symposium May
Neural Basis of Motor Control
 Neural Basis of Motor Control Central Nervous System Skeletal muscles are controlled by the CNS which consists of the brain and spinal cord. Determines which muscles will contract When How fast To what
Neural Basis of Motor Control Central Nervous System Skeletal muscles are controlled by the CNS which consists of the brain and spinal cord. Determines which muscles will contract When How fast To what
SOMATIC SENSATION PART I: ALS ANTEROLATERAL SYSTEM (or SPINOTHALAMIC SYSTEM) FOR PAIN AND TEMPERATURE
 Dental Neuroanatomy Thursday, February 3, 2011 Suzanne S. Stensaas, PhD SOMATIC SENSATION PART I: ALS ANTEROLATERAL SYSTEM (or SPINOTHALAMIC SYSTEM) FOR PAIN AND TEMPERATURE Reading: Waxman 26 th ed, :
Dental Neuroanatomy Thursday, February 3, 2011 Suzanne S. Stensaas, PhD SOMATIC SENSATION PART I: ALS ANTEROLATERAL SYSTEM (or SPINOTHALAMIC SYSTEM) FOR PAIN AND TEMPERATURE Reading: Waxman 26 th ed, :
Neuropathic pain, pain matrix dysfunction, and pain syndromes
 Neuropathic pain, pain matrix dysfunction, and pain syndromes MSTN121 - Neurophysiology Session 3 Department of Myotherapy Session objectives Describe the mechanism of nociceptive chronic pain. Define
Neuropathic pain, pain matrix dysfunction, and pain syndromes MSTN121 - Neurophysiology Session 3 Department of Myotherapy Session objectives Describe the mechanism of nociceptive chronic pain. Define
CHAPTER 48: NERVOUS SYSTEMS
 CHAPTER 48: NERVOUS SYSTEMS Name I. AN OVERVIEW OF NERVOUS SYSTEMS A. Nervous systems perform the three overlapping functions of sensory input, integration, and motor output B. Networks of neurons with
CHAPTER 48: NERVOUS SYSTEMS Name I. AN OVERVIEW OF NERVOUS SYSTEMS A. Nervous systems perform the three overlapping functions of sensory input, integration, and motor output B. Networks of neurons with
All questions below pertain to mandatory material: all slides, and mandatory homework (if any).
 ECOL 182 Spring 2008 Dr. Ferriere s lectures Lecture 6: Nervous system and brain Quiz Book reference: LIFE-The Science of Biology, 8 th Edition. http://bcs.whfreeman.com/thelifewire8e/ All questions below
ECOL 182 Spring 2008 Dr. Ferriere s lectures Lecture 6: Nervous system and brain Quiz Book reference: LIFE-The Science of Biology, 8 th Edition. http://bcs.whfreeman.com/thelifewire8e/ All questions below
Warm-Up. Label the parts of the neuron below.
 Warm-Up Label the parts of the neuron below. A B C D E F G Warm-Up 1. One neuron transmits a nerve impulse at 40 m/s. Another conducts at the rate of 1 m/s. Which neuron has a myelinated axon? 2. List
Warm-Up Label the parts of the neuron below. A B C D E F G Warm-Up 1. One neuron transmits a nerve impulse at 40 m/s. Another conducts at the rate of 1 m/s. Which neuron has a myelinated axon? 2. List
Somatosensory System. Steven McLoon Department of Neuroscience University of Minnesota
 Somatosensory System Steven McLoon Department of Neuroscience University of Minnesota 1 Course News Dr. Riedl s review session this week: Tuesday (Oct 10) 4-5pm in MCB 3-146B 2 Sensory Systems Sensory
Somatosensory System Steven McLoon Department of Neuroscience University of Minnesota 1 Course News Dr. Riedl s review session this week: Tuesday (Oct 10) 4-5pm in MCB 3-146B 2 Sensory Systems Sensory
Chapter 2. The Cellular and Molecular Basis of Cognition Cognitive Neuroscience: The Biology of the Mind, 2 nd Ed.,
 Chapter 2. The Cellular and Molecular Basis of Cognition Cognitive Neuroscience: The Biology of the Mind, 2 nd Ed., M. S. Gazzaniga, R. B. Ivry, and G. R. Mangun, Norton, 2002. Summarized by B.-W. Ku,
Chapter 2. The Cellular and Molecular Basis of Cognition Cognitive Neuroscience: The Biology of the Mind, 2 nd Ed., M. S. Gazzaniga, R. B. Ivry, and G. R. Mangun, Norton, 2002. Summarized by B.-W. Ku,
Neurons, Synapses and Signaling. Chapter 48
 Neurons, Synapses and Signaling Chapter 48 Warm Up Exercise What types of cells can receive a nerve signal? Nervous Organization Neurons- nerve cells. Brain- organized into clusters of neurons, called
Neurons, Synapses and Signaling Chapter 48 Warm Up Exercise What types of cells can receive a nerve signal? Nervous Organization Neurons- nerve cells. Brain- organized into clusters of neurons, called
Name Biology 125 Midterm #2 ( ) Total Pages: 9
 Name - 1 - Biology 125 Midterm #2 (11-15-07) Part 1: (30 pts) Part 2: (40 pts) Part 3: (6 pts) Part 4: (12 pts) Part 5: (12 pts) Total Pages: 9 Total Score: (100 pts) 1 Name - 2 - Part 1: True or False.
Name - 1 - Biology 125 Midterm #2 (11-15-07) Part 1: (30 pts) Part 2: (40 pts) Part 3: (6 pts) Part 4: (12 pts) Part 5: (12 pts) Total Pages: 9 Total Score: (100 pts) 1 Name - 2 - Part 1: True or False.
Psychophysical laws. Legge di Fechner: I=K*log(S/S 0 )
 Psychophysical laws Legge di Weber: ΔS=K*S Legge di Fechner: I=K*log(S/S 0 ) Sensory receptors Vision Smell Taste Touch Thermal senses Pain Hearing Balance Proprioception Sensory receptors Table 21-1 Classification
Psychophysical laws Legge di Weber: ΔS=K*S Legge di Fechner: I=K*log(S/S 0 ) Sensory receptors Vision Smell Taste Touch Thermal senses Pain Hearing Balance Proprioception Sensory receptors Table 21-1 Classification
biological psychology, p. 40 The study of the nervous system, especially the brain. neuroscience, p. 40
 biological psychology, p. 40 The specialized branch of psychology that studies the relationship between behavior and bodily processes and system; also called biopsychology or psychobiology. neuroscience,
biological psychology, p. 40 The specialized branch of psychology that studies the relationship between behavior and bodily processes and system; also called biopsychology or psychobiology. neuroscience,
LECTURE STRUCTURE ASC171 NERVOUS SYSTEM PART 1: BACKGROUND 26/07/2015. Module 5
 LECTURE STRUCTURE PART 1: Background / Introduction PART 2: Structure of the NS, how it operates PART 3: CNS PART 4: PNS Why did the action potential cross the synaptic junction? To get to the other side
LECTURE STRUCTURE PART 1: Background / Introduction PART 2: Structure of the NS, how it operates PART 3: CNS PART 4: PNS Why did the action potential cross the synaptic junction? To get to the other side
S E C T I O N I M E C H A N I S M S A N D E P I D E M I O L O G Y
 SECTION I MECHANISMS AND EPIDEMIOLOGY 1 Nociception: basic principles rie suzuki, shafaq sikandar, and anthony h. dickenson University College London Introduction Pain has been a major concern in the clinic
SECTION I MECHANISMS AND EPIDEMIOLOGY 1 Nociception: basic principles rie suzuki, shafaq sikandar, and anthony h. dickenson University College London Introduction Pain has been a major concern in the clinic
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007
 Proceedings of the World Small Animal Sydney, Australia 2007 Hosted by: Next WSAVA Congress REDUCING THE PAIN FACTOR AN UPDATE ON PERI-OPERATIVE ANALGESIA Sandra Forysth, BVSc DipACVA Institute of Veterinary,
Proceedings of the World Small Animal Sydney, Australia 2007 Hosted by: Next WSAVA Congress REDUCING THE PAIN FACTOR AN UPDATE ON PERI-OPERATIVE ANALGESIA Sandra Forysth, BVSc DipACVA Institute of Veterinary,
Neurons Chapter 7 2/19/2016. Learning Objectives. Cells of the Nervous System. Cells of the Nervous System. Cells of the Nervous System
 Learning Objectives Neurons Chapter 7 Identify and describe the functions of the two main divisions of the nervous system. Differentiate between a neuron and neuroglial cells in terms of structure and
Learning Objectives Neurons Chapter 7 Identify and describe the functions of the two main divisions of the nervous system. Differentiate between a neuron and neuroglial cells in terms of structure and
NEURAL TISSUE (NEUROPHYSIOLOGY) PART I (A): NEURONS & NEUROGLIA
 PART I (A): NEURONS & NEUROGLIA Neural Tissue Contains 2 kinds of cells: neurons: cells that send and receive signals neuroglia (glial cells): cells that support and protect neurons Neuron Types Sensory
PART I (A): NEURONS & NEUROGLIA Neural Tissue Contains 2 kinds of cells: neurons: cells that send and receive signals neuroglia (glial cells): cells that support and protect neurons Neuron Types Sensory
Chapter 11: Functional Organization of Nervous Tissue
 Chapter 11: Functional Organization of Nervous Tissue I. Functions of the Nervous System A. List and describe the five major nervous system functions: 1. 2. 3. 4. 5. II. Divisions of the Nervous System
Chapter 11: Functional Organization of Nervous Tissue I. Functions of the Nervous System A. List and describe the five major nervous system functions: 1. 2. 3. 4. 5. II. Divisions of the Nervous System
When Acute Pain Becomes Chronic. Michael R. Clark, MD, MPH, MBA
 When Acute Pain Becomes Chronic Michael R. Clark, MD, MPH, MBA Disclosures Nothing to Disclose Learning Objectives Describe the phenomenon of the transition from acute to chronic pain Review risk factors
When Acute Pain Becomes Chronic Michael R. Clark, MD, MPH, MBA Disclosures Nothing to Disclose Learning Objectives Describe the phenomenon of the transition from acute to chronic pain Review risk factors
Chapter 6. Gathering information; the sensory systems
 Chapter 6 Gathering information; the sensory systems Gathering information the sensory systems The parts of the nervous system that receive and process information are termed sensory systems. There are
Chapter 6 Gathering information; the sensory systems Gathering information the sensory systems The parts of the nervous system that receive and process information are termed sensory systems. There are
Dendrites Receive impulse from the axon of other neurons through synaptic connection. Conduct impulse towards the cell body Axon
 Dendrites Receive impulse from the axon of other neurons through synaptic connection. Conduct impulse towards the cell body Axon Page 22 of 237 Conduct impulses away from cell body Impulses arise from
Dendrites Receive impulse from the axon of other neurons through synaptic connection. Conduct impulse towards the cell body Axon Page 22 of 237 Conduct impulses away from cell body Impulses arise from
Chapter 2. The Cellular and Molecular Basis of Cognition
 Chapter 2. The Cellular and Molecular Basis of Cognition Cognitive Neuroscience: The Biology of the Mind, 2 nd Ed., M. S. Gazzaniga,, R. B. Ivry,, and G. R. Mangun,, Norton, 2002. Summarized by B.-W. Ku,
Chapter 2. The Cellular and Molecular Basis of Cognition Cognitive Neuroscience: The Biology of the Mind, 2 nd Ed., M. S. Gazzaniga,, R. B. Ivry,, and G. R. Mangun,, Norton, 2002. Summarized by B.-W. Ku,
Nervous System. Master controlling and communicating system of the body. Secrete chemicals called neurotransmitters
 Nervous System Master controlling and communicating system of the body Interacts with the endocrine system to control and coordinate the body s responses to changes in its environment, as well as growth,
Nervous System Master controlling and communicating system of the body Interacts with the endocrine system to control and coordinate the body s responses to changes in its environment, as well as growth,
Unit 3: The Biological Bases of Behaviour
 Unit 3: The Biological Bases of Behaviour Section 1: Communication in the Nervous System Section 2: Organization in the Nervous System Section 3: Researching the Brain Section 4: The Brain Section 5: Cerebral
Unit 3: The Biological Bases of Behaviour Section 1: Communication in the Nervous System Section 2: Organization in the Nervous System Section 3: Researching the Brain Section 4: The Brain Section 5: Cerebral
MOLECULAR AND CELLULAR NEUROSCIENCE
 MOLECULAR AND CELLULAR NEUROSCIENCE BMP-218 November 4, 2014 DIVISIONS OF THE NERVOUS SYSTEM The nervous system is composed of two primary divisions: 1. CNS - Central Nervous System (Brain + Spinal Cord)
MOLECULAR AND CELLULAR NEUROSCIENCE BMP-218 November 4, 2014 DIVISIONS OF THE NERVOUS SYSTEM The nervous system is composed of two primary divisions: 1. CNS - Central Nervous System (Brain + Spinal Cord)
Neural Tissue. Chapter 12 Part B
 Neural Tissue Chapter 12 Part B CNS Tumors - Neurons stop dividing at age 4 but glial cells retain the capacity to divide. - Primary CNS tumors in adults- division of abnormal neuroglia rather than from
Neural Tissue Chapter 12 Part B CNS Tumors - Neurons stop dividing at age 4 but glial cells retain the capacity to divide. - Primary CNS tumors in adults- division of abnormal neuroglia rather than from
