Transition from acute to chronic pain
|
|
|
- Preston Curtis
- 5 years ago
- Views:
Transcription
1 A Feizerfan FRCA G Sheh BHB MBChB FAFRM(RACP) FFPMANZCA Matrix reference 3E00 Key points Physiology of pain involves activation and complex interactions of autonomic, peripheral and central nervous systems, endocrine and immune systems. Persistent nociceptive stimulation may cause various changes in pain physiology leading to pain Cellular changes in the periphery and central nervous system result in peripheral and central Cerebral disorganization, pathophysiological changes in neurones are associated with a hyper-excitable neuronal state. Transition of acute to chronic pain may be minimized by early recognition of risk factors and early biopsychosocial pain management. A Feizerfan FRCA Pain Fellow in Combined Chronic Pain Fellowship Program at Concord Repatriation General Hospital and Royal Prince Alfred Hospital Sydney Australia G Sheh BHB MBChB FAFRM(RACP) FFPMANZCA Consultant Physician Pain Medicine and Rehabilitation Concord Repatriation General Hospital Hospital Road, Concord NSW 2139 Sydney Australia Tel: þ61 (2) Fax: þ61 (2) glen.sheh@sydney.edu.au (for correspondence) 98 Pain is commonly classified into acute and chronic. Acute pain implies a painful condition with a rapid onset or of a short course whereas chronic pain is referred to as a painful condition persisting beyond the normal time of healing. Transition of acute pain to chronic pain is an observed entity associated with enormous burden on the healthcare system. Minimization of this transition has been a challenge for decades. Numerous studies have investigated different factors that increase susceptibility in transition of acute to chronic pain. This article focuses on the basic science and pathophysiological changes during pain processing and clinical modalities aiming to minimize the risk of transition from acute to chronic pain. Pain physiology during acute tissue injury Acute tissue insults such as heat, cold, chemical or mechanical injury, cause disturbance in homeostasis, and stimulate the pain receptors, called nociceptors. Homeostasis can be restored by activation and complex interaction among autonomic, endocrine, immune, and nervous systems. 1 After an injury, a wide range of inflammatory mediators are released locally either from damaged tissue or by activated mast cells and neutrophils. These mediators are adenosine-5-triphosphate (ATP), bradykinin, prostaglandin E2, sodium (Na þ ), hydrogen (H þ ), potassium (K þ ), histamine, and serotonin. The released substances interact with their corresponding receptors located on the peripheral nociceptive neurones leading to depolarization of cell membrane and impulse generation within Ad and Cfibres. After tissue injury, cyclo-oxygenase-2 enzyme is activated and macrophages release proinflammatory substances such as interleukin-1b, interleukin-6, nerve growth factor, and tumour necrosis factor-alpha (TNF-a). Peripheral inflammation at the site of tissue injury activates C-fibres, which release substance P, calcitonin gene-related peptide (CGRP), neurokinin A and nitric oxide (NO) in a retrograde fashion called neurogenic inflammation. This amplifies the whole process resulting in an inflammatory soup. The end result is further activation of silent C fibres with a reduction of pain threshold and increased excitability. 1 Systemic inflammation is also activated along with the process of tissue injury. This activates the sympathetic system, releasing noradrenaline. Noradrenaline by itself further activates peripheral nociceptors. In summary, an acute nociceptive stimulation induces complex biochemical peripheral changes. These changes include: Up-regulation of substance P, phosphorylation of various enzymes (e.g. protein kinase A and C), activation of transient receptor potential vanilloid (TRPV) receptor and purinergic receptor, increased responsiveness of the nociceptors, and activation of silent nociceptors. All these changes potentiate nociception; leading to a state of peripheral hypersensitivity and hyperalgesia. 2 These changes are usually reversible once the tissue healing is completed. Generated action potential is transmitted from the injury site to the spinal cord via primary afferent sensory fibres with their cell bodies located at the dorsal root ganglion (DRG). The sensory fibres (except those arising from the face) form synapses in the dorsal horn of the spinal cord. The fibres arising from the face synapse at the nucleus caudalis. Primary afferent C and Ad fibres enter the spinal cord through the dorsal horn and synapse with the secondary afferent neurones at Rexed laminae I and II. Ab fibres that carry touch and pressure sensation, synapse at the laminae III VI. 3 In the laminae I V, there are three groups of second-order neurones. The first group is involved in proprioception. The second group includes nociceptive specific cells that synapse at laminae I and II. The third group of doi: /bjaceaccp/mku044 Advance Access publication 30 September, 2014 Continuing Education in Anaesthesia, Critical Care & Pain Volume 15 Number & The Author [2014]. Published by Oxford University Press on behalf of the British Journal of Anaesthesia. All rights reserved. For Permissions, please journals.permissions@oup.com
2 second-order neurones comprises wide dynamic range (WDR) neurones that synapse at lamina V. WDR neurones are usually in a dormant state until sensitization occurs. 3 Transmission of a nociceptive impulse from the primary afferent to the secondary afferent is facilitated by the secretion of excitatory substances such as glutamate, substance P, CGRP, and neurotrophic factors. Glutamate, the chief excitatory neurotransmitter in the central nervous system, is able to bind onto three different receptors located on the post-synaptic end. These are alpha-amino-3-hydroxy-5-methyl-4- isoxazoleproprionic acid (AMPA), N-methyl-D-aspartate (NMDA) and G-protein coupled metabotropic receptors. Among these, AMPA is the main receptor activated during acute nociception. 34 The NMDA receptor is not activated under acute noxious circumstances and it will be discussed further later. The second important excitatory substance is substance P working closely with glutamate generating nociceptive transmission. It is a neuropeptide functioning as a neurotransmitter or neuromodulator. Physically it is closely related to neurokinin A; hence substance P binds onto neurokinin receptors, which are abundant in spinoparabrachial pathway at lamina I. Apart from nociceptive transmission, the release of substance P has a positive influence on activation of glial cells. 5 The importance of glial cells will be explained later. While excitatory mechanisms facilitate the transmission of nociception to the brain, inhibitory mechanisms within the spinal cord dampen and impede the transmission. These inhibitory mechanisms consist of: inhibitory gamma-aminobutyric acid ergic and glycinergic interneurones, descending inhibitory pathways from the brain, production of endogenous opioids, and higher order brain functions responsible for distraction and cognitive function. The balance between excitatory and inhibitory functions determines the overall transmission of noxious stimuli to the brain. Ascending and descending pathways to the brain and pain matrix Ascending pathways or secondary afferent neurones from dorsal horn terminate at the thalamus and cerebral cortex. Spinothalamic tract is an important ascending pathway originating from lamina I, II, and V. Via the thalamus, it ends at the somatosensory cortex with an important role for sensory discrimination. Other important ascending pathways are the spinoparabrachial and spinomesencephalic tracts. They synapse at lamina I and project to the brainstem and medulla, and transmit the nociception. 2 Pain matrix is the brain network responding to nociceptive processing. It incorporates multiple cortical areas collaboratively activated by nociception and is divided into two parts. The first part is the nociceptive cortical matrix, consisting of posterior insula, medial parietal operculum and mid-cingulate cortex. These areas are responsible for the earliest response to a nociceptive input from spinothalamic tract. 6 Fine distinction, inter-individual variability of pain experience and consciousness are clinical interpretations managed by the second part of the pain matrix called the secondorder perceptual matrix. This area determines and reflects different individual responses when exposed to a similar nociception. The second-order matrix contains: (i) the mid/anterior insula, anterior cingulated cortex and prefrontal cortex, (ii) the periaqueductal gray matter (PAG) and rostroventromedial medulla (RVM), and (iii) reticular formation. 26 Descending pathways arise from PAG, RVM, and adjacent reticular formation secreting either noradrenaline or serotonin. Noradrenaline stimulates a2-adrenoceptors inhibiting release of neurotransmitters from primary afferent neurones. 37 The aim is to minimize the nociceptive transmission. Pathophysiological changes during the transition of acute to chronic pain Termination of acute nociception and full tissue recovery would result in restoration of normal homeostasis and end the pain process. However, continuous or repetitive nociceptive stimulation leads to a series of pathophysiological changes in pain processing. Complex changes are observed at all levels from the periphery to the brain resulting in persistent pain. Repetitive nociceptive stimulation may result in a prolonged inflammatory process through activation of lymphocytes and release of TNF-a and interleukins such as IL1, IL6, and IL1b. Chronic inflammation leads to a series of changes in the periphery such as: reduction of pain threshold in the primary afferent neurones, phosphorylation of protein kinases A and C, activation of TRPV1 receptors, up-regulation of voltage-gated sodium channels and TRPV1 receptors in DRG, and increased production of substance P and CGRP in the periphery and the spinal cord This mechanism is known as peripheral sensitization secondary to a prolonged inflammatory state (Fig. 1). Continuous nociception stimulation leads to a number of changes in gene and protein expression in both DRG and dorsal horn neurones. The most prominent change is an increase in the mrna coding for the production of various receptors and ion channels such as Na and TRPV1 receptors. 2 Changes in receptor kinetics lead to the hyperexcitable state of chronic pain. Another important receptor type in the spinal cord is the NMDA. This receptor remains inactive during acute noxious stimulation because of the tightly bound Mg plug. Continuous nociceptive stimulation causes prolonged slow depolarization of the neurones in the dorsal horn. This leads to massive influx of calcium which removes the Mg plug from NMDA receptors allowing glutamate to Continuing Education in Anaesthesia, Critical Care & Pain j Volume 15 Number
3 Fig 1 Pain physiology in periphery: neurogenic inflammation, reduced nociceptive threshold and up-regulation of receptors, and ion channels cause peripheral bind onto NMDA receptors. Activation of NMDA receptors leads to the wind-up phenomenon (Fig. 2). Once wind-up has developed, it induces and potentiates a WDR neuronal response to each stimulus. Subsequent sensory stimulation via Ab fibre (touch) ends up with exaggerated WDR neuronal output. Clinically, this manifests as allodynia. The end result of the wind-up process is neuroplasticity, which is a change in neuronal structure with potential enhancement of signal transduction. Prolonged nociceptive transmission to the spinal cord causes release of neuronal chemokines (fractalkine and monocytic chemotactic protein-1), neurotransmitters (substance P, CGRP, glutamate, and ATP) and neuromodulators ( prostaglandins and NO); and produces endogenous danger signals (heat shock proteins and the nuclear protein HMGB1). All these substances activate glial cells in the central nervous system. Glial cells are non-neuronal cells and are important in homeostasis and protection of neurones by means of myelin formation. Once glial cells are activated, they release various substances (IL-1, IL-6, TNF, chemokines, prostaglandins, excitatory amino acids, reactive oxygen species, and NO) into the central nervous system. The cumulative interactions result in enhanced neuronal excitability, up-regulation of AMPA and NMDA receptors, activation of tetrodotoxin-resistant sodium channels, and down-regulation of GABA receptors. These changes tip the balance towards an exaggerated excitable sensitized condition. 45 All these changes cause central sensitization, which are a state of reduced thresholds to stimulations associated with escalated neuronal activity response in the dorsal horn. 3 In the brain Pain matrix has been identified by radiological evidence. Imagings such as functional magnetic resonance imaging and positron emission tomography scans have identified five important pain centres and various changes in the pain matrix when sensitization occurs. The identified regions (and their associated clinical roles) are as follows: Thalamus where spinothalamic tract terminates (somatosensory discrimination), mid/anterior insula, anterior cingulated cortex and prefrontal cortex (affective and motivational components of pain), PAG and RVM (fight-or-flight responses and stress-induced analgesia), reticular formation (regulating descending pathways), and spinoparabrachial pathway to the hypothalamus and amygdala (autonomic and sensory coordination). Pathophysiological changes in the pain matrix reflect strong correlation between chronic pain and mental status. Mental issues vary 100 Continuing Education in Anaesthesia, Critical Care & Pain j Volume 15 Number
4 Fig 2 Pain physiology in spinal cord. Increased production of various substances in the DRG, activation of NMDA receptors, and glial cells cause central from maladaptive pain coping ability to anxiety and depression. Substance misuse and addiction are not uncommon. Psychological stressors tend to accentuate pain intensity and compromise an individual s ability to cope with pain. Therefore, biopsychosocial evaluation is a critical component of chronic pain management. 36 Approach to minimize the transition from acute to chronic pain-clinical application of basic science Physiological changes during the transition of acute to chronic pain are observed at various levels, from the peripheral to the central nervous system. Theoretically, if the pathophysiological changes during this transition could be prevented or reversed, we would be able to prevent or minimize the development of chronic pain in practice. Numerous studies have attempted to formulize analgesic approach to prevent this transition, but so far, there has been very limited promising evidence. Apart from ethical and humanitarian reasons, early management of patients with acute pain is paramount in minimizing the risk of chronic pain development. Early recognition of patients with a high risk of developing chronic pain is imperative in reducing chronic pain development (Table 1). 411 Upon risk stratification, appropriate preventative analgesia aiming at various levels of pain pathways would reduce the potential risk of developing chronic pain. Table 1 Risk factors for developing chronic pain (post-surgical) Patient factors Psychology vulnerability Preoperative anxiety Female gender (higher reported pain score) Younger age (adult) Worker s compensation Genetic factors Depression Unpleasant past experience with pain Social environment Medical factors Preoperative moderate-to-severe pain lasting more than 1 month Repeat surgery Radiotherapy to the area Nerve damage Chemotherapy Types of surgery (amputation, breast surgery, thoracotomy, herniorrhaphy, coronary artery bypass, and Caesarean section) Operations longer than 3 h Surgical technique, experience of surgeon, Prolonged postoperative pain/inflammation Duration of postoperative pain treatment The extent of tissue damage determines the severity of nociceptive stimulation, length of tissue healing process, and magnitude of inflammation. These factors affect the risk of chronic pain development. Careful tissue handling, avoidance of nerve damage and minimal invasive surgical techniques during surgery minimize tissue damage and potentially reduce the risk of chronic pain. Reduction of an inflammatory process may reduce the risk of sensitization in both the periphery and central nervous system. Continuing Education in Anaesthesia, Critical Care & Pain j Volume 15 Number
5 COX-2 inhibitors and NSAIDs have been proved to reduce inflammation. COX-2 inhibitors also prevent the breakdown of endocannabinoids, neuromodulatory substances, which reduces the release of neurostimulators (e.g. glutamate). 11 A long-term use of these two classes of medications leads to unwanted medical complications; which are not discussed in this article. Local anaesthetic infiltration of the surgical field is another effective technique to reduce the intensity of immediate postoperative pain. During the transition of acute to chronic pain, the activation of NMDA receptors and wind-up phenomenon are important changes in the spinal cord. Blocking the NMDA receptors with antagonist such as ketamine, nitrous oxide, and methadone would be effective in reducing the pain intensity and wind-up. 11 In the presence of intractable pain, particularly ketamine can be used as an adjunct of multimodal pharmacological treatment. However, because of its side-effect profile and highly addictive potential the treatment course should be limited to a short period. Adjuvants such as a-2-d ligands binding to voltage dependent calcium channels (gabapentin and pregabalin) are anti-neuropathic agents with the probable preventative effect. 411 The principle of utilizing multimodal analgesic approach is to provide synergistic pain control. This technique targets receptors at different levels of the pain pathway aiming to reduce neuronal excitability. Local and regional anaesthesia is another technique aiming to block the afferent transmission of pain signals reducing pain sensitivity. In theory, reduction of acute pain should reduce central neuroplasticity and minimize the risk of development of chronic pain, yet available evidence is limited. 11 In the brain matrix There is a strong link between individual preoperative expectation, psychological status, and postoperative pain intensity. 11 Functional MRI studies have demonstrated changes in the centres of the brain matrix of patients with chronic pain. These centres are mainly responsible for mood, affect, and behaviour. It seems reasonable to predict patients with significant psychosocial stressors being more prone to chronic pain development. Therefore, a biopsychosocial approach should be utilized in treating patients with a high risk of developing chronic pain. Conclusion Pain physiology involves complex immune, sensory, hormonal and inflammatory processes in the periphery, spinal cord, and brain. Repetitive nociceptive stimulation induces pathophysiological changes in the pain pathways leading to peripheral or central sensitization; hence, resulting in chronic pain in susceptible patients. Although evidence is limited, identifying risk factors and early multimodal approach and biopsychosocial assessment are reasonable steps to reduce the risk of developing chronic pain. Application of the basic science of pain pathways to clinical practice would improve the clinician s ability to deal with those patients at risk of chronic pain development. This may lead to more enthusiastic and exciting studies offering more robust evidence in preventing chronic pain. Advances and development of drugs preventing activation of glial cells, pharmacological agents aiming at the Na channel subtypes specific to nociceptors, and purinergic and TRPV receptor antagonists are ongoing with potential near-future innovations in the prevention of this transition. Declaration of interest None declared. References 1. Chapman CR, Tuckett RP, Song CW. Pain and stress in a systems perspective: reciprocal neural, endocrine, and immune interactions. J Pain 2008; 9: Physiology and psychology of acute pain. In: MacIntyre PE, Scott DA, Schug SA, Visser EJ, Walker SM. Acute Pain Management: Scientific Evidence. Australian and New Zealand College of Anaesthetists and Faculty of Pain Medicine, 3rdEdn. Canberra: Australian Government National Health and Medical Research Council, 2010; D Mello R, Dickenson AH. Spinal cord mechanisms of pain. Br J Anaesth 2008; 101: Voscopoulos C, Lema M. When does acute pain become chronic? Br J Anaesth 2010; 105 (S1): Watkins LR, Hutchinson MR, Rice KC, Maier SF. The toll of opioid-induced glial activation: improving the clinical efficacy of opioids by targeting glia. Trends Pharmacol Sci 2009; 30: Garcia-Larrea L, Peyron R. Pain matrices and neuropathic pain matrices: a review. Pain 2013; 154: S Heinricher MM, Tavares I, Leith JL, Lumb BM. Descending control of nociception: specificity, recruitment and plasticity. Brain Res Rev 2009; 60: Patapoutian A, Tate S, Woolf CJ. Transient receptor potential channels: targeting pain at the source. Nat Rev Drug Discov 2009; 8: Cummins TR, Sheets PL, Waxman SG. The roles of sodium channels in nociception: implications for mechanisms of pain. Pain 2007; 131: Hunt SP, Mantyh PW. The molecular dynamics of pain control. Nat Rev Neurosci 2001; 2: Kehlet H, Jensen TS, Woolf CJ. Persistent postsurgical pain: risk factors and prevention. Lancet 2006; 367: Continuing Education in Anaesthesia, Critical Care & Pain j Volume 15 Number
Pharmacology of Pain Transmission and Modulation
 Pharmacology of Pain Transmission and Modulation 2 Jürg Schliessbach and Konrad Maurer Nociceptive Nerve Fibers Pain is transmitted to the central nervous system via thinly myelinated Aδ and unmyelinated
Pharmacology of Pain Transmission and Modulation 2 Jürg Schliessbach and Konrad Maurer Nociceptive Nerve Fibers Pain is transmitted to the central nervous system via thinly myelinated Aδ and unmyelinated
Pathophysiology of Pain. Ramon Go MD Assistant Professor Anesthesiology and Pain medicine NYP-CUMC
 Pathophysiology of Pain Ramon Go MD Assistant Professor Anesthesiology and Pain medicine NYP-CUMC Learning Objectives Anatomic pathway of nociception Discuss the multiple target sites of pharmacological
Pathophysiology of Pain Ramon Go MD Assistant Professor Anesthesiology and Pain medicine NYP-CUMC Learning Objectives Anatomic pathway of nociception Discuss the multiple target sites of pharmacological
Receptors and Neurotransmitters: It Sounds Greek to Me. Agenda. What We Know About Pain 9/7/2012
 Receptors and Neurotransmitters: It Sounds Greek to Me Cathy Carlson, PhD, RN Northern Illinois University Agenda We will be going through this lecture on basic pain physiology using analogies, mnemonics,
Receptors and Neurotransmitters: It Sounds Greek to Me Cathy Carlson, PhD, RN Northern Illinois University Agenda We will be going through this lecture on basic pain physiology using analogies, mnemonics,
Pain Pathways. Dr Sameer Gupta Consultant in Anaesthesia and Pain Management, NGH
 Pain Pathways Dr Sameer Gupta Consultant in Anaesthesia and Pain Management, NGH Objective To give you a simplistic and basic concepts of pain pathways to help understand the complex issue of pain Pain
Pain Pathways Dr Sameer Gupta Consultant in Anaesthesia and Pain Management, NGH Objective To give you a simplistic and basic concepts of pain pathways to help understand the complex issue of pain Pain
Pathophysiology of Pain
 Pathophysiology of Pain Wound Inflammatory response Chemical mediators Activity in Pain Path PAIN http://neuroscience.uth.tmc.edu/s2/chapter08.html Chris Cohan, Ph.D. Dept. of Pathology/Anat Sci University
Pathophysiology of Pain Wound Inflammatory response Chemical mediators Activity in Pain Path PAIN http://neuroscience.uth.tmc.edu/s2/chapter08.html Chris Cohan, Ph.D. Dept. of Pathology/Anat Sci University
The anatomy and physiology of pain
 The anatomy and physiology of pain Charlotte E Steeds Abstract Pain is an unpleasant experience that results from both physical and psychological responses to injury. A complex set of pathways transmits
The anatomy and physiology of pain Charlotte E Steeds Abstract Pain is an unpleasant experience that results from both physical and psychological responses to injury. A complex set of pathways transmits
Pain Mechanisms. Prof Michael G Irwin MD, FRCA, FANZCA FHKAM Head Department of Anaesthesiology University of Hong Kong. The Somatosensory System
 ain Mechanisms rof Michael G Irwin MD, FRCA, FANZCA FHKAM Head Department of Anaesthesiology University of Hong Kong The Somatosensory System Frontal cortex Descending pathway eriaqueductal gray matter
ain Mechanisms rof Michael G Irwin MD, FRCA, FANZCA FHKAM Head Department of Anaesthesiology University of Hong Kong The Somatosensory System Frontal cortex Descending pathway eriaqueductal gray matter
Somatosensory Physiology (Pain And Temperature) Richard M. Costanzo, Ph.D.
 Somatosensory Physiology (Pain And Temperature) Richard M. Costanzo, Ph.D. OBJECTIVES After studying the material of this lecture the student should be familiar with: 1. The relationship between nociception
Somatosensory Physiology (Pain And Temperature) Richard M. Costanzo, Ph.D. OBJECTIVES After studying the material of this lecture the student should be familiar with: 1. The relationship between nociception
211MDS Pain theories
 211MDS Pain theories Definition In 1986, the International Association for the Study of Pain (IASP) defined pain as a sensory and emotional experience associated with real or potential injuries, or described
211MDS Pain theories Definition In 1986, the International Association for the Study of Pain (IASP) defined pain as a sensory and emotional experience associated with real or potential injuries, or described
PAIN MANAGEMENT in the CANINE PATIENT
 PAIN MANAGEMENT in the CANINE PATIENT Laurie Edge-Hughes, BScPT, MAnimSt (Animal Physio), CAFCI, CCRT Part 1: Laurie Edge-Hughes, BScPT, MAnimSt (Animal Physio), CAFCI, CCRT 1 Pain is the most common reason
PAIN MANAGEMENT in the CANINE PATIENT Laurie Edge-Hughes, BScPT, MAnimSt (Animal Physio), CAFCI, CCRT Part 1: Laurie Edge-Hughes, BScPT, MAnimSt (Animal Physio), CAFCI, CCRT 1 Pain is the most common reason
The perception of pain is a complex process,
 SPECIAL TOPIC Pathophysiology of Pain: A Practical Primer Adeline Fong, MRCP, MRCA, FANZCA Stephan A. Schug, MD, FANZCA, FFPMANZCA Perth, Australia Summary: The experience of pain is a subjective one and
SPECIAL TOPIC Pathophysiology of Pain: A Practical Primer Adeline Fong, MRCP, MRCA, FANZCA Stephan A. Schug, MD, FANZCA, FFPMANZCA Perth, Australia Summary: The experience of pain is a subjective one and
Name: Period: Chapter 2 Reading Guide The Biology of Mind
 Name: Period: Chapter 2 Reading Guide The Biology of Mind The Nervous System (pp. 55-58) 1. What are nerves? 2. Complete the diagram below with definitions of each part of the nervous system. Nervous System
Name: Period: Chapter 2 Reading Guide The Biology of Mind The Nervous System (pp. 55-58) 1. What are nerves? 2. Complete the diagram below with definitions of each part of the nervous system. Nervous System
Spinal Cord Injury Pain. Michael Massey, DO CentraCare Health St Cloud, MN 11/07/2018
 Spinal Cord Injury Pain Michael Massey, DO CentraCare Health St Cloud, MN 11/07/2018 Objectives At the conclusion of this session, participants should be able to: 1. Understand the difference between nociceptive
Spinal Cord Injury Pain Michael Massey, DO CentraCare Health St Cloud, MN 11/07/2018 Objectives At the conclusion of this session, participants should be able to: 1. Understand the difference between nociceptive
1 The Physiology of Pain
 1 The Physiology of Pain Rohit Juneja and Siân Jaggar Introduction Definitions Key Messages Pain is still underdiagnosed and undertreated. Pain is a subjective experience and may even be present in the
1 The Physiology of Pain Rohit Juneja and Siân Jaggar Introduction Definitions Key Messages Pain is still underdiagnosed and undertreated. Pain is a subjective experience and may even be present in the
When Acute Pain Becomes Chronic. Michael R. Clark, MD, MPH, MBA
 When Acute Pain Becomes Chronic Michael R. Clark, MD, MPH, MBA Disclosures Nothing to Disclose Learning Objectives Describe the phenomenon of the transition from acute to chronic pain Review risk factors
When Acute Pain Becomes Chronic Michael R. Clark, MD, MPH, MBA Disclosures Nothing to Disclose Learning Objectives Describe the phenomenon of the transition from acute to chronic pain Review risk factors
Pain and impulse conduction
 1 Pain and impulse conduction L.H.D.J. Booij According to the World Health Organisation pain is defined as an unpleasant sensation that occurs from imminent tissue damage. From a physiological perspective,
1 Pain and impulse conduction L.H.D.J. Booij According to the World Health Organisation pain is defined as an unpleasant sensation that occurs from imminent tissue damage. From a physiological perspective,
Chronic pain: We should not underestimate the contribution of neural plasticity. *Gwyn N Lewis 1, David A Rice 1,2
 Chronic pain: We should not underestimate the contribution of neural plasticity *Gwyn N Lewis 1, David A Rice 1,2 1 Health and Rehabilitation Research Institute, AUT University, Auckland, New Zealand 2
Chronic pain: We should not underestimate the contribution of neural plasticity *Gwyn N Lewis 1, David A Rice 1,2 1 Health and Rehabilitation Research Institute, AUT University, Auckland, New Zealand 2
Chapter 16. Sense of Pain
 Chapter 16 Sense of Pain Pain Discomfort caused by tissue injury or noxious stimulation, and typically leading to evasive action important /// helps to protect us lost of pain in diabetes mellitus = diabetic
Chapter 16 Sense of Pain Pain Discomfort caused by tissue injury or noxious stimulation, and typically leading to evasive action important /// helps to protect us lost of pain in diabetes mellitus = diabetic
Introduction to some interesting research questions: Molecular biology of the primary afferent nociceptor
 Introduction to some interesting research questions: Molecular biology of the primary afferent nociceptor NOCICEPTORS ARE NOT IDENTICAL PEPTIDE SubP/CGRP Trk A NON-PEPTIDE IB4 P2X 3 c-ret Snider and McMahon
Introduction to some interesting research questions: Molecular biology of the primary afferent nociceptor NOCICEPTORS ARE NOT IDENTICAL PEPTIDE SubP/CGRP Trk A NON-PEPTIDE IB4 P2X 3 c-ret Snider and McMahon
San Francisco Chronicle, June 2001
 PAIN San Francisco Chronicle, June 2001 CONGENITAL INSENSITIVITY TO PAIN PAIN IS A SUBJECTIVE EXPERIENCE: It is not a stimulus MAJOR FEATURES OF THE PAIN EXPERIENCE: Sensory discriminative Affective (emotional)
PAIN San Francisco Chronicle, June 2001 CONGENITAL INSENSITIVITY TO PAIN PAIN IS A SUBJECTIVE EXPERIENCE: It is not a stimulus MAJOR FEATURES OF THE PAIN EXPERIENCE: Sensory discriminative Affective (emotional)
Pain. Pain. Pain: One definition. Pain: One definition. Pain: One definition. Pain: One definition. Psyc 2906: Sensation--Introduction 9/27/2006
 Pain Pain Pain: One Definition Classic Paths A new Theory Pain and Drugs According to the international Association for the Study (Merskey & Bogduk, 1994), Pain is an unpleasant sensory and emotional experience
Pain Pain Pain: One Definition Classic Paths A new Theory Pain and Drugs According to the international Association for the Study (Merskey & Bogduk, 1994), Pain is an unpleasant sensory and emotional experience
What it Takes to be a Pain
 What it Takes to be a Pain Pain Pathways and the Neurophysiology of pain Dennis S. Pacl, MD, FACP, FAChPM Austin Palliative Care/ Hospice Austin A Definition of Pain complex constellation of unpleasant
What it Takes to be a Pain Pain Pathways and the Neurophysiology of pain Dennis S. Pacl, MD, FACP, FAChPM Austin Palliative Care/ Hospice Austin A Definition of Pain complex constellation of unpleasant
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007
 Proceedings of the World Small Animal Sydney, Australia 2007 Hosted by: Next WSAVA Congress REDUCING THE PAIN FACTOR AN UPDATE ON PERI-OPERATIVE ANALGESIA Sandra Forysth, BVSc DipACVA Institute of Veterinary,
Proceedings of the World Small Animal Sydney, Australia 2007 Hosted by: Next WSAVA Congress REDUCING THE PAIN FACTOR AN UPDATE ON PERI-OPERATIVE ANALGESIA Sandra Forysth, BVSc DipACVA Institute of Veterinary,
Seizure: the clinical manifestation of an abnormal and excessive excitation and synchronization of a population of cortical
 Are There Sharing Mechanisms of Epilepsy, Migraine and Neuropathic Pain? Chin-Wei Huang, MD, PhD Department of Neurology, NCKUH Basic mechanisms underlying seizures and epilepsy Seizure: the clinical manifestation
Are There Sharing Mechanisms of Epilepsy, Migraine and Neuropathic Pain? Chin-Wei Huang, MD, PhD Department of Neurology, NCKUH Basic mechanisms underlying seizures and epilepsy Seizure: the clinical manifestation
Lecture 22: A little Neurobiology
 BIO 5099: Molecular Biology for Computer Scientists (et al) Lecture 22: A little Neurobiology http://compbio.uchsc.edu/hunter/bio5099 Larry.Hunter@uchsc.edu Nervous system development Part of the ectoderm
BIO 5099: Molecular Biology for Computer Scientists (et al) Lecture 22: A little Neurobiology http://compbio.uchsc.edu/hunter/bio5099 Larry.Hunter@uchsc.edu Nervous system development Part of the ectoderm
biological psychology, p. 40 The study of the nervous system, especially the brain. neuroscience, p. 40
 biological psychology, p. 40 The specialized branch of psychology that studies the relationship between behavior and bodily processes and system; also called biopsychology or psychobiology. neuroscience,
biological psychology, p. 40 The specialized branch of psychology that studies the relationship between behavior and bodily processes and system; also called biopsychology or psychobiology. neuroscience,
Sensory coding and somatosensory system
 Sensory coding and somatosensory system Sensation and perception Perception is the internal construction of sensation. Perception depends on the individual experience. Three common steps in all senses
Sensory coding and somatosensory system Sensation and perception Perception is the internal construction of sensation. Perception depends on the individual experience. Three common steps in all senses
Cancer-induced bone pain
 Cancer-induced bone pain Common Prevalent in particular cancers: breast (73%), prostate (68%), thyroid (42%), lung (36%), renal (35%), colon (5%) Correlates with an increased morbidity Reduced performance
Cancer-induced bone pain Common Prevalent in particular cancers: breast (73%), prostate (68%), thyroid (42%), lung (36%), renal (35%), colon (5%) Correlates with an increased morbidity Reduced performance
CHAPTER 4 PAIN AND ITS MANAGEMENT
 CHAPTER 4 PAIN AND ITS MANAGEMENT Pain Definition: An unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage. Types of Pain
CHAPTER 4 PAIN AND ITS MANAGEMENT Pain Definition: An unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage. Types of Pain
PAIN IS A SUBJECTIVE EXPERIENCE: It is not a stimulus. MAJOR FEATURES OF THE PAIN EXPERIENCE: Sensory discriminative Affective (emotional) Cognitive
 PAIN PAIN IS A SUBJECTIVE EXPERIENCE: It is not a stimulus MAJOR FEATURES OF THE PAIN EXPERIENCE: Sensory discriminative Affective (emotional) Cognitive MEASUREMENT OF PAIN: A BIG PROBLEM Worst pain ever
PAIN PAIN IS A SUBJECTIVE EXPERIENCE: It is not a stimulus MAJOR FEATURES OF THE PAIN EXPERIENCE: Sensory discriminative Affective (emotional) Cognitive MEASUREMENT OF PAIN: A BIG PROBLEM Worst pain ever
Medical Neuroscience Tutorial
 Pain Pathways Medical Neuroscience Tutorial Pain Pathways MAP TO NEUROSCIENCE CORE CONCEPTS 1 NCC1. The brain is the body's most complex organ. NCC3. Genetically determined circuits are the foundation
Pain Pathways Medical Neuroscience Tutorial Pain Pathways MAP TO NEUROSCIENCE CORE CONCEPTS 1 NCC1. The brain is the body's most complex organ. NCC3. Genetically determined circuits are the foundation
Somatic Sensation (MCB160 Lecture by Mu-ming Poo, Friday March 9, 2007)
 Somatic Sensation (MCB160 Lecture by Mu-ming Poo, Friday March 9, 2007) Introduction Adrian s work on sensory coding Spinal cord and dorsal root ganglia Four somatic sense modalities Touch Mechanoreceptors
Somatic Sensation (MCB160 Lecture by Mu-ming Poo, Friday March 9, 2007) Introduction Adrian s work on sensory coding Spinal cord and dorsal root ganglia Four somatic sense modalities Touch Mechanoreceptors
Preemptive Analgesia: Does it Prevent Chronic Pain?
 Preemptive Analgesia: Does it Prevent Chronic Pain? Prof. Dr. Maged El-Ansary Al Azhar Univ. Al Azhar university, Cairo, Egypt 1. President of Egyptian Society for Regional Anesthesia & Pain Medicine 2.President
Preemptive Analgesia: Does it Prevent Chronic Pain? Prof. Dr. Maged El-Ansary Al Azhar Univ. Al Azhar university, Cairo, Egypt 1. President of Egyptian Society for Regional Anesthesia & Pain Medicine 2.President
Basic Neuroscience. Sally Curtis
 The Physiology of Pain Basic Neuroscience Sally Curtis sac3@soton.ac.uk The behaviour of humans is a result of the actions of nerves. Nerves form the basis of Thoughts, sensations and actions both reflex
The Physiology of Pain Basic Neuroscience Sally Curtis sac3@soton.ac.uk The behaviour of humans is a result of the actions of nerves. Nerves form the basis of Thoughts, sensations and actions both reflex
Primary Functions. Monitor changes. Integrate input. Initiate a response. External / internal. Process, interpret, make decisions, store information
 NERVOUS SYSTEM Monitor changes External / internal Integrate input Primary Functions Process, interpret, make decisions, store information Initiate a response E.g., movement, hormone release, stimulate/inhibit
NERVOUS SYSTEM Monitor changes External / internal Integrate input Primary Functions Process, interpret, make decisions, store information Initiate a response E.g., movement, hormone release, stimulate/inhibit
What is Pain? An unpleasant sensory and emotional experience associated with actual or potential tissue damage. Pain is always subjective
 Pain & Acupuncture What is Pain? An unpleasant sensory and emotional experience associated with actual or potential tissue damage. NOCICEPTION( the neural processes of encoding and processing noxious stimuli.)
Pain & Acupuncture What is Pain? An unpleasant sensory and emotional experience associated with actual or potential tissue damage. NOCICEPTION( the neural processes of encoding and processing noxious stimuli.)
Nervous System and Brain Review. Bio 3201
 Nervous System and Brain Review Bio 3201 Dont worry about: glial cells Oligodendrocytes Satelite cells etc Nervous System - Vital to maintaining homeostasis in organisms - Comprised of : brain, spinal
Nervous System and Brain Review Bio 3201 Dont worry about: glial cells Oligodendrocytes Satelite cells etc Nervous System - Vital to maintaining homeostasis in organisms - Comprised of : brain, spinal
Posterior White Column-Medial Lemniscal Pathway
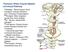 Posterior White Column-Medial Lemniscal Pathway Modality: Discriminative Touch Sensation (include Vibration) and Conscious Proprioception Receptor: Most receptors except free nerve endings Ist Neuron:
Posterior White Column-Medial Lemniscal Pathway Modality: Discriminative Touch Sensation (include Vibration) and Conscious Proprioception Receptor: Most receptors except free nerve endings Ist Neuron:
The Brain & Homeostasis. The Brain & Technology. CAT, PET, and MRI Scans
 The Brain & Homeostasis Today, scientists have a lot of information about what happens in the different parts of the brain; however they are still trying to understand how the brain functions. We know
The Brain & Homeostasis Today, scientists have a lot of information about what happens in the different parts of the brain; however they are still trying to understand how the brain functions. We know
AKA a painful lecture by Colleen Blanchfield, MD Full Circle Neuropsychiatric Wellness Center
 A lecture on PAIN AKA a painful lecture by Colleen Blanchfield, MD Full Circle Neuropsychiatric Wellness Center 1 Overview of the lecture Anatomy of the Pain Tract How a painful stimulus travels from the
A lecture on PAIN AKA a painful lecture by Colleen Blanchfield, MD Full Circle Neuropsychiatric Wellness Center 1 Overview of the lecture Anatomy of the Pain Tract How a painful stimulus travels from the
Pain teaching. Muhammad Laklouk
 Pain teaching Muhammad Laklouk Definition Pain An unpleasant sensory and emotional experience associated with actual or potential tissue damage or described in terms of such damage. Sensory (discriminatiory)
Pain teaching Muhammad Laklouk Definition Pain An unpleasant sensory and emotional experience associated with actual or potential tissue damage or described in terms of such damage. Sensory (discriminatiory)
The Nervous System. Biological School. Neuroanatomy. How does a Neuron fire? Acetylcholine (ACH) TYPES OF NEUROTRANSMITTERS
 Biological School The Nervous System It is all about the body!!!! It starts with an individual nerve cell called a NEURON. Synapse Neuroanatomy Neurotransmitters (chemicals held in terminal buttons that
Biological School The Nervous System It is all about the body!!!! It starts with an individual nerve cell called a NEURON. Synapse Neuroanatomy Neurotransmitters (chemicals held in terminal buttons that
Unit 3: The Biological Bases of Behaviour
 Unit 3: The Biological Bases of Behaviour Section 1: Communication in the Nervous System Section 2: Organization in the Nervous System Section 3: Researching the Brain Section 4: The Brain Section 5: Cerebral
Unit 3: The Biological Bases of Behaviour Section 1: Communication in the Nervous System Section 2: Organization in the Nervous System Section 3: Researching the Brain Section 4: The Brain Section 5: Cerebral
Neurobiology of Pain Adjuvant analgesia
 Neurobiology of Pain Adjuvant analgesia Jason Brooks Consultant Anaesthesia and Pain Management BCH March 2017 The Brief A broad overview of the abnormal and normal anatomy and physiology of pain pathways
Neurobiology of Pain Adjuvant analgesia Jason Brooks Consultant Anaesthesia and Pain Management BCH March 2017 The Brief A broad overview of the abnormal and normal anatomy and physiology of pain pathways
Psychophysical laws. Legge di Fechner: I=K*log(S/S 0 )
 Psychophysical laws Legge di Weber: ΔS=K*S Legge di Fechner: I=K*log(S/S 0 ) Sensory receptors Vision Smell Taste Touch Thermal senses Pain Hearing Balance Proprioception Sensory receptors Table 21-1 Classification
Psychophysical laws Legge di Weber: ΔS=K*S Legge di Fechner: I=K*log(S/S 0 ) Sensory receptors Vision Smell Taste Touch Thermal senses Pain Hearing Balance Proprioception Sensory receptors Table 21-1 Classification
Complex Acute Surgical Pain Management. Thomas Baribeault MSN, CRNA
 Complex Acute Surgical Pain Management Thomas Baribeault MSN, CRNA Introduction Anatomy and pathophysiology of acute surgical pain Pharmacology Chronic pain patient Opioid tolerant patient Introduction
Complex Acute Surgical Pain Management Thomas Baribeault MSN, CRNA Introduction Anatomy and pathophysiology of acute surgical pain Pharmacology Chronic pain patient Opioid tolerant patient Introduction
ANAT2010. Concepts of Neuroanatomy (II) S2 2018
 ANAT2010 Concepts of Neuroanatomy (II) S2 2018 Table of Contents Lecture 13: Pain and perception... 3 Lecture 14: Sensory systems and visual pathways... 11 Lecture 15: Techniques in Neuroanatomy I in vivo
ANAT2010 Concepts of Neuroanatomy (II) S2 2018 Table of Contents Lecture 13: Pain and perception... 3 Lecture 14: Sensory systems and visual pathways... 11 Lecture 15: Techniques in Neuroanatomy I in vivo
What is pain?: An unpleasant sensation. What is an unpleasant sensation?: Pain. - Aristotle.
 What is pain?: An unpleasant sensation. What is an unpleasant sensation?: Pain. - Aristotle. Nociception The detection of tissue damage or impending tissue damage, but There can be tissue damage without
What is pain?: An unpleasant sensation. What is an unpleasant sensation?: Pain. - Aristotle. Nociception The detection of tissue damage or impending tissue damage, but There can be tissue damage without
S E C T I O N I M E C H A N I S M S A N D E P I D E M I O L O G Y
 SECTION I MECHANISMS AND EPIDEMIOLOGY 1 Nociception: basic principles rie suzuki, shafaq sikandar, and anthony h. dickenson University College London Introduction Pain has been a major concern in the clinic
SECTION I MECHANISMS AND EPIDEMIOLOGY 1 Nociception: basic principles rie suzuki, shafaq sikandar, and anthony h. dickenson University College London Introduction Pain has been a major concern in the clinic
Neural Basis of Motor Control
 Neural Basis of Motor Control Central Nervous System Skeletal muscles are controlled by the CNS which consists of the brain and spinal cord. Determines which muscles will contract When How fast To what
Neural Basis of Motor Control Central Nervous System Skeletal muscles are controlled by the CNS which consists of the brain and spinal cord. Determines which muscles will contract When How fast To what
Neural Communication. Central Nervous System Peripheral Nervous System. Communication in the Nervous System. 4 Common Components of a Neuron
 Neural Communication Overview of CNS / PNS Electrical Signaling Chemical Signaling Central Nervous System Peripheral Nervous System Somatic = sensory & motor Autonomic = arousal state Parasympathetic =
Neural Communication Overview of CNS / PNS Electrical Signaling Chemical Signaling Central Nervous System Peripheral Nervous System Somatic = sensory & motor Autonomic = arousal state Parasympathetic =
UNIVERSITY OF JORDAN FACULTY OF MEDICINE DEPARTMENT OF PHYSIOLOGY & BIOCHEMISTRY NEUROPHYSIOLOGY (MEDICAL), SPRING 2014
 UNIVERSITY OF JORDAN FACULTY OF MEDICINE DEPARTMENT OF PHYSIOLOGY & BIOCHEMISTRY NEUROPHYSIOLOGY (MEDICAL), SPRING 2014 Textbook of Medical Physiology by: Guyton & Hall, 12 th edition 2011 Eman Al-Khateeb,
UNIVERSITY OF JORDAN FACULTY OF MEDICINE DEPARTMENT OF PHYSIOLOGY & BIOCHEMISTRY NEUROPHYSIOLOGY (MEDICAL), SPRING 2014 Textbook of Medical Physiology by: Guyton & Hall, 12 th edition 2011 Eman Al-Khateeb,
Prof Wayne Derman MBChB,BSc (Med)(Hons) PhD, FFIMS. Pain Management in the Elite Athlete: The 2017 IOC Consensus Statement
 Prof Wayne Derman MBChB,BSc (Med)(Hons) PhD, FFIMS Pain Management in the Elite Athlete: The 2017 IOC Consensus Statement 2 as 20 Experts published and leaders in their respective field 12 month lead in
Prof Wayne Derman MBChB,BSc (Med)(Hons) PhD, FFIMS Pain Management in the Elite Athlete: The 2017 IOC Consensus Statement 2 as 20 Experts published and leaders in their respective field 12 month lead in
Chapter 17. Nervous System Nervous systems receive sensory input, interpret it, and send out appropriate commands. !
 Chapter 17 Sensory receptor Sensory input Integration Nervous System Motor output Brain and spinal cord Effector cells Peripheral nervous system (PNS) Central nervous system (CNS) 28.1 Nervous systems
Chapter 17 Sensory receptor Sensory input Integration Nervous System Motor output Brain and spinal cord Effector cells Peripheral nervous system (PNS) Central nervous system (CNS) 28.1 Nervous systems
SOMATOSENSORY SYSTEMS AND PAIN
 SOMATOSENSORY SYSTEMS AND PAIN A 21 year old man presented with a stab wound of the right side of the neck (Panel A). Neurological examination revealed right hemiplegia and complete right-sided loss of
SOMATOSENSORY SYSTEMS AND PAIN A 21 year old man presented with a stab wound of the right side of the neck (Panel A). Neurological examination revealed right hemiplegia and complete right-sided loss of
Function of the Nervous System
 Nervous System Function of the Nervous System Receive sensory information, interpret it, and send out appropriate commands to form a response Composed of neurons (functional unit of the nervous system)
Nervous System Function of the Nervous System Receive sensory information, interpret it, and send out appropriate commands to form a response Composed of neurons (functional unit of the nervous system)
Neural Integration I: Sensory Pathways and the Somatic Nervous System
 15 Neural Integration I: Sensory Pathways and the Somatic Nervous System PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris An Introduction to Sensory Pathways and
15 Neural Integration I: Sensory Pathways and the Somatic Nervous System PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris An Introduction to Sensory Pathways and
Lesson 14. The Nervous System. Introduction to Life Processes - SCI 102 1
 Lesson 14 The Nervous System Introduction to Life Processes - SCI 102 1 Structures and Functions of Nerve Cells The nervous system has two principal cell types: Neurons (nerve cells) Glia The functions
Lesson 14 The Nervous System Introduction to Life Processes - SCI 102 1 Structures and Functions of Nerve Cells The nervous system has two principal cell types: Neurons (nerve cells) Glia The functions
The Nervous System. Nervous System Functions 1. gather sensory input 2. integration- process and interpret sensory input 3. cause motor output
 The Nervous System Nervous System Functions 1. gather sensory input 2. integration- process and interpret sensory input 3. cause motor output The Nervous System 2 Parts of the Nervous System 1. central
The Nervous System Nervous System Functions 1. gather sensory input 2. integration- process and interpret sensory input 3. cause motor output The Nervous System 2 Parts of the Nervous System 1. central
Biology 12 Human Biology - The Nervous System Name. Main reference: Biology Concepts and Connects Sixth edition Chapter 28
 Biology 12 Human Biology - The Nervous System Name Main reference: Biology Concepts and Connects Sixth edition Chapter 28 Vocabulary acetylcholine (ACh), acetylcholinesterase (AChE), action potential,
Biology 12 Human Biology - The Nervous System Name Main reference: Biology Concepts and Connects Sixth edition Chapter 28 Vocabulary acetylcholine (ACh), acetylcholinesterase (AChE), action potential,
Axon Nerve impulse. Axoplasm Receptor. Axomembrane Stimuli. Schwann cell Effector. Myelin Cell body
 Nervous System Review 1. Explain a reflex arc. 2. Know the structure, function and location of a sensory neuron, interneuron, and motor neuron 3. What is (a) Neuron Axon Nerve impulse Axoplasm Receptor
Nervous System Review 1. Explain a reflex arc. 2. Know the structure, function and location of a sensory neuron, interneuron, and motor neuron 3. What is (a) Neuron Axon Nerve impulse Axoplasm Receptor
Nervous System, Neuroanatomy, Neurotransmitters
 Nervous System, Neuroanatomy, Neurotransmitters Neurons Structure of neurons Soma Dendrites Spines Axon Myelin Nodes of Ranvier Neurons Structure of neurons Axon collaterals 1 Neurons Structure of neurons
Nervous System, Neuroanatomy, Neurotransmitters Neurons Structure of neurons Soma Dendrites Spines Axon Myelin Nodes of Ranvier Neurons Structure of neurons Axon collaterals 1 Neurons Structure of neurons
Pain classifications slow and fast
 Pain classifications slow and fast Fast Pain Slow Pain Sharp, pricking (Aδ) fiber Short latency Well localized Short duration Dull, burning (C) fiber Slower onset Diffuse Long duration Less emotional Emotional,
Pain classifications slow and fast Fast Pain Slow Pain Sharp, pricking (Aδ) fiber Short latency Well localized Short duration Dull, burning (C) fiber Slower onset Diffuse Long duration Less emotional Emotional,
*Anteriolateral spinothalamic tract (STT) : a sensory pathway that is positioned anteriorly and laterally in the spinal cord.
 *somatic sensations : PAIN *Anteriolateral spinothalamic tract (STT) : a sensory pathway that is positioned anteriorly and laterally in the spinal cord. *This pathway carries a variety of sensory modalities:
*somatic sensations : PAIN *Anteriolateral spinothalamic tract (STT) : a sensory pathway that is positioned anteriorly and laterally in the spinal cord. *This pathway carries a variety of sensory modalities:
CHAPTER 10 THE SOMATOSENSORY SYSTEM
 CHAPTER 10 THE SOMATOSENSORY SYSTEM 10.1. SOMATOSENSORY MODALITIES "Somatosensory" is really a catch-all term to designate senses other than vision, hearing, balance, taste and smell. Receptors that could
CHAPTER 10 THE SOMATOSENSORY SYSTEM 10.1. SOMATOSENSORY MODALITIES "Somatosensory" is really a catch-all term to designate senses other than vision, hearing, balance, taste and smell. Receptors that could
Brain and behaviour (Wk 6 + 7)
 Brain and behaviour (Wk 6 + 7) What is a neuron? What is the cell body? What is the axon? The basic building block of the nervous system, the individual nerve cell that receives, processes and transmits
Brain and behaviour (Wk 6 + 7) What is a neuron? What is the cell body? What is the axon? The basic building block of the nervous system, the individual nerve cell that receives, processes and transmits
MOLECULAR AND CELLULAR NEUROSCIENCE
 MOLECULAR AND CELLULAR NEUROSCIENCE BMP-218 November 4, 2014 DIVISIONS OF THE NERVOUS SYSTEM The nervous system is composed of two primary divisions: 1. CNS - Central Nervous System (Brain + Spinal Cord)
MOLECULAR AND CELLULAR NEUROSCIENCE BMP-218 November 4, 2014 DIVISIONS OF THE NERVOUS SYSTEM The nervous system is composed of two primary divisions: 1. CNS - Central Nervous System (Brain + Spinal Cord)
Neuropathic Pain in Palliative Care
 Neuropathic Pain in Palliative Care Neuropathic Pain in Advanced Cancer Affects 40% of patients Multiple concurrent pains are common Often complex pathophysiology with mixed components Nocioceptive Neuropathic
Neuropathic Pain in Palliative Care Neuropathic Pain in Advanced Cancer Affects 40% of patients Multiple concurrent pains are common Often complex pathophysiology with mixed components Nocioceptive Neuropathic
Pathophysiological Classification of Pain
 PATHOPHYSIOLOGY Overview Pathophysiological Classification of Pain Central sensitization/ dysfunctional pain Nociceptive pain - Somatic - Visceral Multiple pain mechanisms may coexist (mixed pain) Neuropathic
PATHOPHYSIOLOGY Overview Pathophysiological Classification of Pain Central sensitization/ dysfunctional pain Nociceptive pain - Somatic - Visceral Multiple pain mechanisms may coexist (mixed pain) Neuropathic
PAIN. Physiology of pain relating to pain management
 PAIN Physiology of pain relating to pain management What is pain? An unpleasant sensory and emotional experience associated with actual or potential tissue damage. (Melzac and Wall) The generation of pain
PAIN Physiology of pain relating to pain management What is pain? An unpleasant sensory and emotional experience associated with actual or potential tissue damage. (Melzac and Wall) The generation of pain
Sincerely, Ms. Paoloni and Mrs. Whitney
 Dear Students, Welcome to AP Psychology! We will begin our course of study focusing on the nervous system with a particular emphasis on how the brain and neurotransmitters influence our behaviors. In preparation
Dear Students, Welcome to AP Psychology! We will begin our course of study focusing on the nervous system with a particular emphasis on how the brain and neurotransmitters influence our behaviors. In preparation
Pre-op Interventions to Mitigate Post-op Acute and Chronic Pain
 Pre-op Interventions to Mitigate Post-op Acute and Chronic Pain H A R S H A S H A N T H A N N A. M D, M S C A S S O C I A T E P R O F E S S O R D E P A R T M E N T O F A N E S T H E S I A C H R O N I C
Pre-op Interventions to Mitigate Post-op Acute and Chronic Pain H A R S H A S H A N T H A N N A. M D, M S C A S S O C I A T E P R O F E S S O R D E P A R T M E N T O F A N E S T H E S I A C H R O N I C
Tony Dickenson, Neuroscience, Physiology and Pharmacology University College London PAIN - WHAT DOES IT DO TO US, AND WHAT CAN WE DO ABOUT IT?
 Tony Dickenson, Neuroscience, Physiology and Pharmacology University College London PAIN - WHAT DOES IT DO TO US, AND WHAT CAN WE DO ABOUT IT? Cortex - where and how much pain Limbic areas - unpleasantness
Tony Dickenson, Neuroscience, Physiology and Pharmacology University College London PAIN - WHAT DOES IT DO TO US, AND WHAT CAN WE DO ABOUT IT? Cortex - where and how much pain Limbic areas - unpleasantness
Study Guide Answer Key Nervous System
 Biology 12 Human Biology Textbook: BC Biology 12 Study Guide Answer Key Nervous System 1. Draw a neuron, label 3 parts and give the function of those parts. Dendrite: carry signals to the cell body Cell
Biology 12 Human Biology Textbook: BC Biology 12 Study Guide Answer Key Nervous System 1. Draw a neuron, label 3 parts and give the function of those parts. Dendrite: carry signals to the cell body Cell
Special Issue on Pain and Itch
 Special Issue on Pain and Itch Title: Recent Progress in Understanding the Mechanisms of Pain and Itch Guest Editor of the Special Issue: Ru-Rong Ji, PhD Chronic pain is a major health problem world-wide.
Special Issue on Pain and Itch Title: Recent Progress in Understanding the Mechanisms of Pain and Itch Guest Editor of the Special Issue: Ru-Rong Ji, PhD Chronic pain is a major health problem world-wide.
Chapter 14: The Cutaneous Senses
 Chapter 14: The Cutaneous Senses Somatosensory System There are three parts Cutaneous senses - perception of touch and pain from stimulation of the skin Proprioception - ability to sense position of the
Chapter 14: The Cutaneous Senses Somatosensory System There are three parts Cutaneous senses - perception of touch and pain from stimulation of the skin Proprioception - ability to sense position of the
Chapter 11 Introduction to the Nervous System and Nervous Tissue Chapter Outline
 Chapter 11 Introduction to the Nervous System and Nervous Tissue Chapter Outline Module 11.1 Overview of the Nervous System (Figures 11.1-11.3) A. The nervous system controls our perception and experience
Chapter 11 Introduction to the Nervous System and Nervous Tissue Chapter Outline Module 11.1 Overview of the Nervous System (Figures 11.1-11.3) A. The nervous system controls our perception and experience
Brian Kahan, D.O. FAAPMR, DABPM, DAOCRM, FIPP Center for Pain Medicine and Physiatric Rehabilitation 2002 Medical Parkway Suite 150 Annapolis, MD
 Brian Kahan, D.O. FAAPMR, DABPM, DAOCRM, FIPP Center for Pain Medicine and Physiatric Rehabilitation 2002 Medical Parkway Suite 150 Annapolis, MD 1630 Main Street Suite 215 Chester, MD 410-571-9000 www.4-no-pain.com
Brian Kahan, D.O. FAAPMR, DABPM, DAOCRM, FIPP Center for Pain Medicine and Physiatric Rehabilitation 2002 Medical Parkway Suite 150 Annapolis, MD 1630 Main Street Suite 215 Chester, MD 410-571-9000 www.4-no-pain.com
Acetylcholine (ACh) Action potential. Agonists. Drugs that enhance the actions of neurotransmitters.
 Acetylcholine (ACh) The neurotransmitter responsible for motor control at the junction between nerves and muscles; also involved in mental processes such as learning, memory, sleeping, and dreaming. (See
Acetylcholine (ACh) The neurotransmitter responsible for motor control at the junction between nerves and muscles; also involved in mental processes such as learning, memory, sleeping, and dreaming. (See
Somatic Sensory System I. Background
 Somatic Sensory System I. Background A. Differences between somatic senses and other senses 1. Receptors are distributed throughout the body as opposed to being concentrated at small, specialized locations
Somatic Sensory System I. Background A. Differences between somatic senses and other senses 1. Receptors are distributed throughout the body as opposed to being concentrated at small, specialized locations
Multimodal analgesic therapy has gained widespread
 TOPICAL REVIEW Analgesia for Anesthetized Patients Kip A. Lemke, DVM, MSc, Dipl. ACVA, and Catherine M. Creighton, DVM Many perioperative pain management protocols for cats and dogs are overly complex,
TOPICAL REVIEW Analgesia for Anesthetized Patients Kip A. Lemke, DVM, MSc, Dipl. ACVA, and Catherine M. Creighton, DVM Many perioperative pain management protocols for cats and dogs are overly complex,
3) Most of the organelles in a neuron are located in the A) dendritic region. B) axon hillock. C) axon. D) cell body. E) axon terminals.
 Chapter 48 Neurons, Synapses, and Signaling Multiple-Choice Questions 1) A simple nervous system A) must include chemical senses, mechanoreception, and vision. B) includes a minimum of 12 ganglia. C) has
Chapter 48 Neurons, Synapses, and Signaling Multiple-Choice Questions 1) A simple nervous system A) must include chemical senses, mechanoreception, and vision. B) includes a minimum of 12 ganglia. C) has
BIOLOGY 12 NERVOUS SYSTEM PRACTICE
 1 Name: BIOLOGY 12 NERVOUS SYSTEM PRACTICE Date: 1) Identify structures X, Y and Z and give one function of each. 2) Which processes are involved in the movement of molecule Y from point X to point Z?
1 Name: BIOLOGY 12 NERVOUS SYSTEM PRACTICE Date: 1) Identify structures X, Y and Z and give one function of each. 2) Which processes are involved in the movement of molecule Y from point X to point Z?
Human Nervous System. The nervous system has three functions
 Chapter 37 Human Nervous System The nervous system has three functions 1) Receive sensory input from both external and internal stimuli 2) Perform integration. (Coordinating all of the various inputs of
Chapter 37 Human Nervous System The nervous system has three functions 1) Receive sensory input from both external and internal stimuli 2) Perform integration. (Coordinating all of the various inputs of
All questions below pertain to mandatory material: all slides, and mandatory homework (if any).
 ECOL 182 Spring 2008 Dr. Ferriere s lectures Lecture 6: Nervous system and brain Quiz Book reference: LIFE-The Science of Biology, 8 th Edition. http://bcs.whfreeman.com/thelifewire8e/ All questions below
ECOL 182 Spring 2008 Dr. Ferriere s lectures Lecture 6: Nervous system and brain Quiz Book reference: LIFE-The Science of Biology, 8 th Edition. http://bcs.whfreeman.com/thelifewire8e/ All questions below
Neural Basis of Motor Control. Chapter 4
 Neural Basis of Motor Control Chapter 4 Neurological Perspective A basic understanding of the physiology underlying the control of voluntary movement establishes a more comprehensive appreciation and awareness
Neural Basis of Motor Control Chapter 4 Neurological Perspective A basic understanding of the physiology underlying the control of voluntary movement establishes a more comprehensive appreciation and awareness
POST-OP MULTIMODAL PAIN MANAGEMENT. Maripat Welz-Bosna Reading Hospital Medical Center Department of Medicine Hospitalist Services/Pain Management
 POST-OP MULTIMODAL PAIN MANAGEMENT Maripat Welz-Bosna Reading Hospital Medical Center Department of Medicine Hospitalist Services/Pain Management Objectives Understand the basic neurobiology of the pain
POST-OP MULTIMODAL PAIN MANAGEMENT Maripat Welz-Bosna Reading Hospital Medical Center Department of Medicine Hospitalist Services/Pain Management Objectives Understand the basic neurobiology of the pain
Chapter 3. Biological Processes
 Biological Processes Psychology, Fifth Edition, James S. Nairne What s It For? Biological Solutions Communicating internally Initiating and coordinating behavior Regulating growth and other internal functions
Biological Processes Psychology, Fifth Edition, James S. Nairne What s It For? Biological Solutions Communicating internally Initiating and coordinating behavior Regulating growth and other internal functions
NERVOUS SYSTEM C H A P T E R 2 8
 NERVOUS SYSTEM C H A P T E R 2 8 CAN AN INJURED SPINAL CORD BE FIXED? Injuries to the spinal cord disrupt communication between the central nervous system (brain and spinal cord) and the rest of the body
NERVOUS SYSTEM C H A P T E R 2 8 CAN AN INJURED SPINAL CORD BE FIXED? Injuries to the spinal cord disrupt communication between the central nervous system (brain and spinal cord) and the rest of the body
Ch. 45 Continues (Have You Read Ch. 45 yet?) u Central Nervous System Synapses - Synaptic functions of neurons - Information transmission via nerve
 Ch. 45 Continues (Have You Read Ch. 45 yet?) u Central Nervous System Synapses - Synaptic functions of neurons - Information transmission via nerve impulses - Impulse may be blocked in its transmission
Ch. 45 Continues (Have You Read Ch. 45 yet?) u Central Nervous System Synapses - Synaptic functions of neurons - Information transmission via nerve impulses - Impulse may be blocked in its transmission
PSYC& 100: Biological Psychology (Lilienfeld Chap 3) 1
 PSYC& 100: Biological Psychology (Lilienfeld Chap 3) 1 1 What is a neuron? 2 Name and describe the functions of the three main parts of the neuron. 3 What do glial cells do? 4 Describe the three basic
PSYC& 100: Biological Psychology (Lilienfeld Chap 3) 1 1 What is a neuron? 2 Name and describe the functions of the three main parts of the neuron. 3 What do glial cells do? 4 Describe the three basic
Modules 4 & 6. The Biology of Mind
 Modules 4 & 6 The Biology of Mind 1 Neuron - 100 Billion - Communication System Glial cells Cell body (nucleus) Dendrites Axon Axon Terminals (terminal buttons) Synaptic cleft 3 4 Communication Within
Modules 4 & 6 The Biology of Mind 1 Neuron - 100 Billion - Communication System Glial cells Cell body (nucleus) Dendrites Axon Axon Terminals (terminal buttons) Synaptic cleft 3 4 Communication Within
ANAT2010. Concepts of Neuroanatomy (II) S2 2018
 ANAT2010 Concepts of Neuroanatomy (II) S2 2018 Table of Contents Lecture 13: Pain and perception... 3 Lecture 14: Sensory systems and visual pathways... 11 Lecture 15: Techniques in Neuroanatomy I in vivo
ANAT2010 Concepts of Neuroanatomy (II) S2 2018 Table of Contents Lecture 13: Pain and perception... 3 Lecture 14: Sensory systems and visual pathways... 11 Lecture 15: Techniques in Neuroanatomy I in vivo
When does acute pain become chronic?
 British Journal of Anaesthesia 105 (S1): i69 i85 (2010) doi:10.1093/bja/aeq323 PAIN When does acute pain become chronic? C. Voscopoulos and M. Lema* Department of Anesthesiology, Critical Care, and Pain
British Journal of Anaesthesia 105 (S1): i69 i85 (2010) doi:10.1093/bja/aeq323 PAIN When does acute pain become chronic? C. Voscopoulos and M. Lema* Department of Anesthesiology, Critical Care, and Pain
5-Nervous system II: Physiology of Neurons
 5-Nervous system II: Physiology of Neurons AXON ION GRADIENTS ACTION POTENTIAL (axon conduction) GRADED POTENTIAL (cell-cell communication at synapse) SYNAPSE STRUCTURE & FUNCTION NEURAL INTEGRATION CNS
5-Nervous system II: Physiology of Neurons AXON ION GRADIENTS ACTION POTENTIAL (axon conduction) GRADED POTENTIAL (cell-cell communication at synapse) SYNAPSE STRUCTURE & FUNCTION NEURAL INTEGRATION CNS
Biology 3201 Quiz on Nervous System. Total 33 points
 Biology 3201 Quiz on Nervous System Total 33 points Name: Circle the best response to the following: (33 points) 1. What do we call the long fibre that carries impulses away from the nerve cell body? A.
Biology 3201 Quiz on Nervous System Total 33 points Name: Circle the best response to the following: (33 points) 1. What do we call the long fibre that carries impulses away from the nerve cell body? A.
Motor Control, Pain, Somatic Dysfunction, Core Stability. Richard G. Schuster, DO Shawn Kerger, DO, FAOASM 19 September 2016 OMED 2016 Anaheim, CA
 Motor Control, Pain, Somatic Dysfunction, Core Stability Richard G. Schuster, DO Shawn Kerger, DO, FAOASM 19 September 2016 OMED 2016 Anaheim, CA How do we move? Decision to move (Executive or Cognitive
Motor Control, Pain, Somatic Dysfunction, Core Stability Richard G. Schuster, DO Shawn Kerger, DO, FAOASM 19 September 2016 OMED 2016 Anaheim, CA How do we move? Decision to move (Executive or Cognitive
Organization of the nervous system. [See Fig. 48.1]
![Organization of the nervous system. [See Fig. 48.1] Organization of the nervous system. [See Fig. 48.1]](/thumbs/90/103926552.jpg) Nervous System [Note: This is the text version of this lecture file. To make the lecture notes downloadable over a slow connection (e.g. modem) the figures have been replaced with figure numbers as found
Nervous System [Note: This is the text version of this lecture file. To make the lecture notes downloadable over a slow connection (e.g. modem) the figures have been replaced with figure numbers as found
Nervous System C H A P T E R 2
 Nervous System C H A P T E R 2 Input Output Neuron 3 Nerve cell Allows information to travel throughout the body to various destinations Receptive Segment Cell Body Dendrites: receive message Myelin sheath
Nervous System C H A P T E R 2 Input Output Neuron 3 Nerve cell Allows information to travel throughout the body to various destinations Receptive Segment Cell Body Dendrites: receive message Myelin sheath
Joint Session with ACOFP, AOASM and AAO: Motor Control, Pain, Somatic Dysfunction, Core Stability. Shawn R. Kerger, DO, FAOSM Richard G.
 Joint Session with ACOFP, AOASM and AAO: Motor Control, Pain, Somatic Dysfunction, Core Stability Shawn R. Kerger, DO, FAOSM Richard G. Schuster, DO Motor Control, Pain, Somatic Dysfunction, Core Stability
Joint Session with ACOFP, AOASM and AAO: Motor Control, Pain, Somatic Dysfunction, Core Stability Shawn R. Kerger, DO, FAOSM Richard G. Schuster, DO Motor Control, Pain, Somatic Dysfunction, Core Stability
