Risk factors and management of obstetric perineal injury
|
|
|
- Jared Stafford
- 6 years ago
- Views:
Transcription
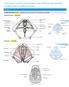
1 Risk factors and management of obstetric perineal injury Ruwan J Fernando Abstract Perineal injury sustained during childbirth is a major aetiological factor in the development of perineal pain, sexual dysfunction, prolapse and disturbance in bowel and bladder function. Preferential use of the vacuum extractor, restricting the use of episiotomy, repair of anal sphincter rupture by a trained doctor and selective caesarean section in these women can be beneficial in preventing complications. More focused training of midwives and doctors in perineal and anal sphincter anatomy and repair is needed to minimize the morbidity associated with inadequate repair and missed tears. Future research must address ways to predict and minimize severe perineal injury, and the management of subsequent pregnancies following anal sphincter injury. Keywords anal sphincter; childbirth; delivery; episiotomy; incontinence; perineum; third degree tears Introduction The morbidity associated with perineal injury related to childbirth is a major health problem that affects thousands of women. As many as 91% of women report at least one new persistent symptom 8 weeks after delivery. Over 60% of women suffer perineal injury (either perineal tear or episiotomy) following spontaneous vaginal delivery and approximately 1000 women per day require perineal repair following vaginal birth. Complications of perineal trauma following childbirth include haemorrhage, haematoma and abscess formation, perineal pain and discomfort, fistula formation, dyspareunia and anal incontinence. In addition, there has been an increase in litigation related to the complications of perineal trauma following childbirth. Increased awareness of maternal morbidity following vaginal birth has led some women to request elective caesarean delivery despite being without any medical indications for this. However, elective caesarean delivery is associated with a fourfold risk of maternal morbidity compared with vaginal birth. In view of these facts, the modern obstetrician needs focused training to identify and manage women who are at high risk of developing postpartum morbidity and thereby re-establish women s confidence in vaginal delivery. Ruwan J Fernando MS MD MRCOG Department of Urogynaecology, Ground Floor, Cambridge Wing, St Mary s Hospital, Praed Street, London W2 1NY, UK. Classification of perineal injury Traditionally, perineal trauma following childbirth has been classified as first-, second- or third-degree tears. However this classification is incomplete and has created considerable confusion. The following descriptive classification (Figure 1) suggested by Sultan has now been incorporated into the Royal College of Obstetricians and Gynaecologists and international guidelines. 1 First-degree tear involving the perineal or vaginal skin only 2 Second-degree tear perineal skin and muscles torn, but intact anal sphincter 3 Third-degree tear perineal skin, muscles and anal sphincter are torn a less than 50% of the external anal sphincter thickness is torn b more than 50% of the external anal sphincter thickness is torn, but internal anal sphincter intact c both external and internal anal sphincters are torn, but anal mucosa intact 4 Fourth-degree tear perineal skin, muscles, anal sphincter and anal mucosa torn 5 Buttonhole tear anal sphincter intact but anal mucosa torn Third- and fourth-degree tears that involve the anal sphincter complex are also termed obstetric anal sphincter injury. Anatomically, an episiotomy involves the same structures as a second-degree perineal tear. Causes of and risk factors for perineal injury Greater birthweight Birthweight of more than 4 kg is associated with maternal perineal injury, especially third- and fourth-degree tears. This may be attributed to the larger head circumference, prolonged labour and difficult delivery, particularly when this is instrumental. A large baby is also likely to disrupt the fascial supports of the pelvic floor and cause stretch injury to the pelvic and pudendal nerves. Even after safe delivery of the head, shoulder dystocia is associated with perineal and anal sphincter trauma. Malposition and malpresentation Malposition, particularly the persistent occipitoposterior position, leads to a larger presenting diameter and is associated with difficult delivery. Face and brow presentations are known risk factors for anal sphincter injury. Breech deliveries do not appear to increase the risk, but this may be attributed to stringent selection criteria and a low threshold for caesarean section during labour. Duration of labour and rate of delivery Precipitate labour is associated with cervical, perineal, labial and urethral injury due to the lack of time available for the maternal tissues to adjust to the forces of delivery and for controlled delivery with an episiotomy if necessary. Furthermore, delivery following precipitate labour is more likely to occur under less favourable circumstances such as during transit to hospital, in a standing position and often without experienced assistance. There is evidence to suggest that a prolonged active second stage of labour causes pudendal nerve damage. There is evidence that perineal damage may occur in the first stage of labour. Caesarean OBSTETRICS, GYNAECOLOGY AND REPRODUCTIVE MEDICINE 17: Elsevier Ltd. All rights reserved.
2 1st-degree injury Injury to the perineal skin only. Perineal muscles are intact. 2nd-degree injury Injury to the perineum involving perineal muscles but not the anal sphincter. 4th-degree injury Injury to the perineum involving the EAS and IAS and rectal mucosa 3rd-degree injury Injury to the perineum involving the external anal sphincter (EAS) and the internal anal sphincter (IAS) 3a <50% of EAS thickness torn 3b >50% of EAS thickness torn 3c IAS torn Figure 1 Classification of obstetric anal sphincter injury. section performed after the onset of labour, resulting in cervical dilatation of more than 8 cm, may be associated with pudendal nerve damage. It has been suggested that the passive second stage of labour should be accelerated with oxytocics particularly in women who have an epidural, rather than resorting to instrumental delivery, which can cause more trauma. Episiotomy Episiotomy is defined as surgical excision of the perineum to facilitate delivery. Although episiotomy is the commonest operation performed in obstetrics, there is little evidence to demonstrate any benefit with its routine use. Randomized studies have shown that median episiotomy is more likely to extend into the anal sphincter than mediolateral episiotomy (12% vs 2%). The Cochrane database shows that restriction of the use of episiotomy is associated with less posterior trauma. Although anterior perineal trauma was increased it had no effect on the development of urinary incontinence. It has been suggested that the ideal episiotomy rate should be no more than 20 30%. Instrumental delivery Instrumental delivery is an integral part of obstetrics, and though it reduces the caesarean section rate, maternal morbidity is higher than that following unassisted delivery. The injuries caused by instrumental delivery include both cervical laceration and anal sphincter injury. Although it is well recognized that forceps delivery has a higher maternal injury rate than vacuum extraction, it is important for the operator to be versatile with the use of both instruments. Certain circumstances preclude the use of the vacuum extractor; these include prematurity, face presentation, potential fetal bleeding tendency, delivery of the aftercoming head at breech presentation, lift out at caesarean section and equipment failure. Forceps delivery is likely to cause injury as the instrument occupies almost 10% more space in the pelvis. The shanks of the forceps stretch the perineum and can cause injury, particularly to the anal sphincter when pulling in the posterolateral direction to encourage flexion of the head. Unlike the vacuum extractor, which can become detached, the forceps does not have such a fail-safe mechanism and therefore excessive force can be applied, particularly under epidural anaesthesia. As mentioned above, the benefits of episiotomy during spontaneous delivery have been questioned, and while an episiotomy is not absolutely necessary with the vacuum extractor, it is invariably performed with the forceps. Interestingly, one study has reported that a reduction in the episiotomy rate from about 90% to 30% during instrumental delivery (n=2041) was associated with a reduction in the rate of fourth-degree tears and no significant change in the third-degree tear rate. Metal cups appear to be more suitable for occipitoposterior, transverse and difficult occipitoanterior position deliveries, while soft cups seem to be OBSTETRICS, GYNAECOLOGY AND REPRODUCTIVE MEDICINE 17: Elsevier Ltd. All rights reserved.
3 appropriate for straightforward deliveries as they are significantly more likely to fail to achieve vaginal delivery (OR 1.65, 95% CI ). Although they were associated with less scalp injury (OR 0.45, 95% CI ), there was no difference between the two groups in terms of maternal injury. A Cochrane review, which included the guidelines of 10 trials, concluded that use of the vacuum extractor for assisted vaginal delivery, compared with forceps delivery, was associated with significantly less maternal trauma (OR 0.41, 95% CI ) and with less general and regional anaesthesia. There were more deliveries with vacuum extraction (OR 1.69, 95% CI ) and fewer caesarean sections were performed in the vacuum extractor group, though the vacuum extractor was associated with an increase in neonatal cephalhaematomata and retinal haemorrhages. Serious neonatal injury was uncommon with either instrument. Use of the vacuum extractor rather than forceps thus appears to reduce maternal morbidity, though the reduction in cephalhaematoma and retinal haemorrhages seen with forceps may be a compensatory benefit. However, in a 5-year follow-up of a randomized controlled trial (RCT) comparing forceps with vacuum extraction, no significant differences were found in terms of visual problems or child development. Birthing position There is evidence that delivery in the standing delivery position may be associated with a higher incidence of perineal injury. However, a Cochrane review has shown that, with the possible exception of increased blood loss, delivery in the upright posture has no demonstrated deleterious effects on the mother or the fetus. Current evidence on the effectiveness of various delivery positions is inconclusive and it is therefore suggested that women should be encouraged to deliver in whichever position is most comfortable for them. Principles of the management of perineal injury The principles of management are as follows. Recognition and proper classification are important. Perineal injury should be examined under adequate analgesia and light. A combined vaginal and rectal examination is needed to exclude associated anal sphincter injury. Immediate repair of perineal injury rather than delayed repair is advisable, as immediate repair reduces the bleeding and pain associated with the injury, which may otherwise impair early breast-feeding and bonding. Immediate repair also prevents the development of oedema, which may affect subsequent recognition of the structures involved, and reduces the risk of infection. If there is any doubt about the extent of the injury, a second opinion must be sought. The presence of an experienced person during the assessment of perineal injury has increased the rate of detection of anal sphincter injury. The labia, clitoris and urethra should also be examined. Management of episiotomy and first- and second-degree perineal tears Non-suturing of first- and second-degree perineal tears has been described. There are only two, small RCTs in the literature, both of which showed no significant difference in short-term discomfort, but showed an association with poorer wound healing. Based on the current evidence, non-suturing is recommended only for first-degree perineal tears that are not actively bleeding and have regular and well-approximated wound edges. Episiotomies and second-degree tears are conventionally sutured in three stages. The traditional interrupted suturing technique involves: a continuous locking suture in the vagina commencing from the apex and finishing at the level of fourchette with a loop knot re-approximation of the deep and superficial perineal muscles with three or four interrupted sutures skin suturing with continuous subcutaneous or interrupted transcutaneous sutures. Another method for the repair of episiotomy and second-degree perineal tears is the continuous non-locking (Fleming s) technique, in which a continuous non-locking suture is used to approximate the vagina and the deep and superficial perineal muscles without tension. Skin edges are apposed with a subcutaneous suture. A recent large RCT involving 1542 women showed that the continuous non-locking technique is associated with a significant reduction in short- and long-term perineal pain and less frequent need for suture removal compared with the interrupted suturing technique. Suture materials used in the repair of episiotomy and first- and second-degree perineal tears range from catgut to synthetic absorbable sutures such as Dexon and Vicryl, though the use of catgut has been discontinued in Europe. A Cochrane review has shown that absorbable synthetic suture materials are associated with less perineal pain, use of analgesia, wound dehiscence and wound re-suturing than is catgut. A recently introduced absorbable suture material, Vicryl Rapide, dissolves earlier than Vicryl. A large RCT has shown that Vicryl Rapide is associated with significantly less superficial dyspareunia and a significant reduction in the need for suture removal up to 3 months after delivery. Following the repair of episiotomy or second-degree perineal injury, adequate analgesia such as diclofenac suppositories is recommended. If there are associated urethral, labial, clitoral or vaginal tears, or if the repair is difficult, insertion of an indwelling catheter for 24 hours is recommended to prevent acute urine retention. Proper documentation, including a diagrammatic description of the structures involved, is good medical practice. The patient must be informed about the extent of the trauma and the repair, pain relief, diet and pelvic floor exercises. Follow-up is not essential for uncomplicated episiotomy or first- or second-degree perineal injury. Principles and technique of primary sphincter repair of third- and fourth-degree tears Such repairs should be performed only by a doctor experienced in anal sphincter repair or by a trainee under supervision. They should be conducted in the operating theatre, with good lighting, appropriate equipment and aseptic conditions. The full extent of the injury should be evaluated by a careful vaginal and rectal examination, and it should be graded according to the classification above. Detailed notes should be made of the findings and OBSTETRICS, GYNAECOLOGY AND REPRODUCTIVE MEDICINE 17: Elsevier Ltd. All rights reserved.
4 the subsequent repair. A pictorial representation of the tears is useful when reviewing the notes in the event of complications, audit or litigation. General or regional (spinal, epidural, caudal) anaesthesia is an important prerequisite, particularly for overlap repair, as the inherent tone in the sphincter muscle can cause the torn muscle ends to retract within its sheath. Muscle relaxation is necessary to retrieve the ends, especially if overlapping of the muscles without tension is intended. In a fourth-degree tear, the torn anal epithelium is repaired with interrupted Vicryl (polyglactin) 3/0 sutures with the knots tied in the anal lumen. The sphincter muscles are repaired with 3/0 polydioxanone (PDS) dyed sutures. Compared with a braided suture, these monofilamentous sutures are less likely to precipitate infection, and the author has not encountered problems with suture migration and therefore recommends PDS. Internal sphincter repair The internal anal sphincter should be identified and any tear should be repaired separately from the external sphincter. The internal anal sphincter lies between the external sphincter and the anal epithelium. It is paler than the striated external sphincter and the muscle fibres run in a circular manner. The internal sphincter resembles the flesh of raw fish, as opposed to the red meat appearance of the external sphincter. The ends of the torn muscle are grasped with Allis forceps and an end-to-end repair is performed with interrupted or mattress 3/0 PDS sutures. A torn internal sphincter should be approximated with mattress or single interrupted sutures, as overlapping can be technically difficult. External sphincter repair Different techniques of repair of the external sphincter have been described. The most commonly used technique in the UK appears to be end-to-end repair with figure-of-eight sutures. As figureof-eight sutures are haemostatic, they may cause ischaemia of the muscle ends, and therefore mattress sutures are preferable if an end-to-end repair is being considered. Colorectal surgeons prefer the overlap technique for patients who present with faecal incontinence, though longer-term follow-up suggests that the symptoms may deteriorate with time. Based on this, Sultan et al. described an overlap technique for the external sphincter and separate approximation of the internal sphincter. The torn ends of the external anal sphincter are identified and grasped with Allis tissue forceps. To perform an overlap, the muscle may need to be mobilized by dissection with a pair of McIndoe scissors, separating it from the ischio-anal fat laterally. If the overlap technique is preferred, the external sphincter should be grasped with Allis forceps and pulled across to overlap in a double-breast manner. The torn ends of the external sphincter can then be overlapped as shown in Figure 1, using PDS 3/0 sutures. It is important that the full length of the external sphincter is identified to ensure complete approximation or overlap. Compared with the overlap technique, lack of complete apposition is more likely to occur with the end-to-end technique. Anal length has been shown to be the best predictor of faecal incontinence following secondary sphincter surgery. A shorter anal length has been reported following end to-end primary repair of the external anal sphincter, probably as a result of incomplete apposition. An advantage of the overlap repair is that the full length of the external sphincter must be visualized, and overlapping allows a greater surface area of contact between muscle. Unlike in endto-end repair, if further retraction of the overlapped muscle ends were to occur, it is highly likely that muscle continuity would be maintained. Although Sultan et al. achieved favourable results with the overlap technique, this could have been a reflection of operator expertise. There are four completed RCTS comparing the primary endto-end and overlap techniques for external anal sphincter repair following obstetric injuries. In the first, by Fitzpatrick et al., 112 patients were randomised to the end-to-end or overlap technique. All sphincters were repaired with Maxon, but the patients were followed-up for only 3 months. There were no significant differences in outcome in either arm of the study. In the second RCT, by Fernando et al., 64 patients were randomised to the overlap and end-to-end techniques, performed by only two trained clinicians. Faecal urgency at 12 months was reported in 32% of the end-to-end group and 3.2% of the overlap group (p = 0.02), and 24% of the end-to-end group reported faecal incontinence associated with urgency compared with none of the overlap group (p = 0.01). Compared with the other RCTs, which used larger groups of trained clinicians to perform repairs, this study showed an improvement in outcome with overlap repair but may not be applicable to all labour wards. In the third RCT, by Williams et al., 112 participants were randomized to four groups: to end-end or overlap repair of the torn anal sphincters, and braided polyglactin (coated Vicryl) 2/0 or PDS 3/0. In this study, there were no significant differences in anal continence rates or quality-of-life scores in the four groups after 12 months of follow-up. In the fourth RCT, by Garcia et al., 41 women with complete third- or fourth-degree perineal tears were randomized to overlap and end-to-end groups and followed-up for 3 months. There were 23 women in the end-to-end group and 18 in the overlap group, but only 15 and 11, respectively, returned for followup. No significant differences were found between the groups in terms of symptoms of faecal incontinence and transperineal ultrasound findings. However, the authors acknowledged that the randomization was inaccurate and that their study was underpowered. In a separate RCT of secondary repair, 24 patients were randomized to end-to-end or overlap repair. At a median followup of 26 months, there were no significant differences in anal continence. Other studies have evaluated secondary sphincter repair for anal incontinence in colorectal patients and showed a significant increase in continence rate with overlap repair. However, one study showed a deterioration of anal incontinence 5 years after secondary repair for obstetric anal sphincter injury. The evidence to date indicates that there is no significant difference in short-term outcome between the end-to-end and the overlap technique and therefore either technique can be used. In grade 3a tears, the overlapping technique is not possible without completely dividing the external anal sphincter. However, as most of the fibres are intact tears, complete division of the external anal sphincter is not justified and the OBSTETRICS, GYNAECOLOGY AND REPRODUCTIVE MEDICINE 17: Elsevier Ltd. All rights reserved.
5 torn fibres are best approximated with interrupted sutures. In grade 3b tears, if the overlapping technique is used it is advisable to divide the remaining few intact fibres to facilitate the repair. Great care should be taken when reconstructing the perineal muscles, to provide support to the sphincter repair. A short, deficient perineum makes the anal sphincter more vulnerable to trauma during subsequent vaginal deliveries. Muscles of the perineal body are reconstructed with interrupted Vicryl 2/0 sutures after closing the vaginal epithelium with a continuous Vicryl 3/0 suture. Lastly, the perineal skin is approximated with a Vicryl 3/0 subcuticular suture. A rectovaginal examination should be performed to confirm complete repair and ensure that all tampons or swabs have been removed. Antibiotics Intravenous antibiotics (cefuroxime 1.5 g and metronidazole 500 mg) should be commenced intraoperatively and continued orally for 1 week. Although there are no randomized trials to substantiate the benefit of this practice, infection could jeopardize the repair and lead to incontinence or fistula formation. Postoperative care Severe perineal discomfort, particularly following instrumental delivery, is a known cause of urine retention, and following regional anaesthesia it can be up to 12 hours before bladder sensation returns. A Foley catheter should be inserted for about 24 hours unless the midwifery staff can ensure that spontaneous voiding occurs at least every 3 hours. As passage of a large bolus of hard stool may disrupt the repair, a stool softener (lactulose 15 ml b.d.) and a bulking agent such as Fybogel (ispaghula husk, one sachet b.d.) is prescribed for at least 2 weeks postoperatively. It is important to ensure that bowel action has occurred before the patient is discharged. Follow-up and subsequent pregnancies following third- and fourth-degree tears The woman must understand the extent of the tear and how to seek help if symptoms of infection or incontinence develop. All women should be warned of the possible sequelae of anal sphincter disruption, and ideally should be assessed 6 12 weeks post-partum by anorectal physiology tests and anal ultrasonography (Figure 2). Asymptomatic women with low squeeze pressures and a defect of more than one quadrant are at increased risk of developing anal incontinence following another vaginal delivery and therefore counseling should include the option of caesarean section (Figure 3). If manometry and anal ultrasonography facilities are unavailable locally, symptomatic women should be referred to a specialist centre for these investigations. Women who are asymptomatic and have no clinical evidence of a deficient perineum or low anal sphincter tone can undergo vaginal delivery by an experienced midwife or doctor. As there is no evidence that elective prophylactic episiotomy prevents another tear, episiotomy should only be performed if clinically indicated; that is if the perineum is thick and inelastic and an episiotomy will prevent multiple radial tears. Figure 2 Endoanal scan demonstrating a persistent defect (between arrows) of the external anal sphincter (EAS) following end-to-end repair. The internal anal sphincter is intact (reproduced from: Fernando RJ, Sultan AH. Curr Obstet Gynaecol 2004; 14: ). Symptomatic women with severe injuries should be offered a secondary sphincter repair and subsequent pregnancies should be delivered by caesarean section. Women with mild symptoms should be managed with advice on the avoidance of gas-producing foods, regulation of bowel action, bulking agents, constipating agents such as loperamide and codeine phosphate, and biofeedback. This group of women are at risk of deterioration following a subsequent vaginal delivery and should therefore be offered caesarean section. The risk of a repeat third-degree tear is low, but no randomized studies have been performed to evaluate the benefit of routine Caesarean section. Medicolegal implications Although the creation of a third- or fourth-degree tear is seldom found to be an issue of culpability, missing a tear is considered to be negligent. It is essential that a rectal examination is performed before and after any perineal repair and that the findings are carefully documented in the notes. At least 20% of consultant obstetricians continue to classify a tear of the anal sphincter that has not breached the anal mucosa as a second-degree tear. As a consequence, the safe principles of repair mentioned above are not applied and repair and subsequent management are likely to be inadequate. Poor note-keeping, repair by an inexperienced doctor, deviation from recommended safe practice, failure to inform and counsel the woman, failure to inform the general practitioner, and inappropriate follow-up and advice regarding subsequent pregnancies are common issues raised at litigation. As more than two-thirds of doctors practicing obstetrics feel inadequately trained, it is important that focused and intensive training is made available. In this regard, Sultan and colleagues have introduced an ongoing course using video presentations, specially designed models and fresh animal anorectal specimens to demonstrate the anatomy and techniques of OBSTETRICS, GYNAECOLOGY AND REPRODUCTIVE MEDICINE 17: Elsevier Ltd. All rights reserved.
6 Hospital follow up Anal endosonography and manometry Asymptomatic Severe symptoms Large defect/low pressures Mild symptoms Avoid traumatic delivery Experienced person Prophylactic episiotomy of unproven benefit Traumatic delivery expected Big baby Occipito-posterior position Slow progress in labour Secondary sphincter repair Offer caesarean section Conservative management Dietary advice Constipating agents (codeine phosphate loperamide) Physiotherapy and biofeedback Figure 3 Flow diagram to demonstrate pathway in the management of acute obstetric anal sphincter injury. repair. The feedback from attendees is that this type of training should be an essential part of the modular training for specialist registrars. Further reading deleeuw JW, Struijk PC, Viererhout ME, Wallenburg HCS. Risk factors for third degree perineal ruptures during delivery. Br J Obstet Gynaecol 2001; 108: Fernando RJ, Sultan AH, Kettle C, Radley S, Jones PW, O Brien PMS. Repair techniques for obstetric anal sphincter injuries a randomized controlled trial. Obstet Gynecol 2006; 107: Fernando R, Sultan AH, Kettle C, Thakar R, Radley S. Methods of repair for obstetric anal sphincter injury. Cochrane Database Syst Rev 2006; 3: CD Fernando RJ, Sultan AH, Radley S, Jones PW, Johanson RB. Management of obstetric anal sphincter injury a systematic review and national practice survey. BMC Health Serv Res 2002; 2: 9. Fitzpatrick M, Behan M, O Connell R, O Herlihy C. A randomised clinical trial comparing primary overlap with approximation repair of third degree tears. Am J Obstet Gynecol 2000; 183: Garcia V, Rogers RG, Kim SS, Hall RJ, Kammerer-Doak DN. Primary repair of obstetric anal sphincter laceration: a randomized trial of two surgical techniques. Am J Obstet Gynecol 2005; 192: Kettle C, Hills RK, Jones P, Darby L, Gray R, Johanson R. Continuous versus interrupted perineal repair with standard or rapidly absorbed sutures after spontaneous vaginal birth: a randomised controlled trial. Lancet 2002; 359: Kettle C, Johanson RB. Absorbable synthetic versus catgut suture material for perineal repair (Cochrane review). In: The Cochrane library, issue 4. Oxford: Update Software; Sultan AH, Thakar R. Lower genital tract and anal sphincter trauma. Best Pract Res Clin Obstet Gynaecol 2002; 16: Thakar R, Sultan AH. Management of obstetric anal sphincter injury. Obstet Gynecol 2003; 5: Williams A, Adams EJ, Tincello DG, Alfirevic Z, Walkinshaw SA, Richmond DH. How to repair an anal sphincter injury after vaginal delivery: results of a randomised controlled trial. Br J Obstet Gynaecol 2006; 113: Practice points Clarify the classification of perineal tears and identify risk factors for injury Safe practice, education, training, management of subsequent pregnancies following anal sphincter injury and prevention of injuries should be emphasized investigations comprise anal ultrasonography, manometry, electromyography, urodynamics and MRI Research directions Timing of pelvic floor exercises Benefits of episiotomy in instrumental delivery Prevention of anal sphincter injury Role of immediate endoanal scanning in the detection of anal sphincter injury Randomized trials of the management of subsequent pregnancies following anal sphincter rupture OBSTETRICS, GYNAECOLOGY AND REPRODUCTIVE MEDICINE 17: Elsevier Ltd. All rights reserved.
Appendix B Protocol for management of obstetric anal sphincter injury THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS
 Appendix B Protocol for management of obstetric anal sphincter injury Document Type: THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS PURPOSE & SCOPE To provide a guideline that will assist in
Appendix B Protocol for management of obstetric anal sphincter injury Document Type: THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS PURPOSE & SCOPE To provide a guideline that will assist in
Anal Sphincter Injuries: Acute Management
 Anal Sphincter Injuries: Acute Management Dr Stephen Jeffery Urogynaecology Consultant Department of Obstetrics & Gynaecology Groote Schuur Hospital Colorectal Surgeons Gynaecologists Gynaecologists Colorectal
Anal Sphincter Injuries: Acute Management Dr Stephen Jeffery Urogynaecology Consultant Department of Obstetrics & Gynaecology Groote Schuur Hospital Colorectal Surgeons Gynaecologists Gynaecologists Colorectal
Obstetric Anal Sphincter Injury- A guideline. Mr David Sim Ms Patricia McStay. Dr Martina Hogan Dept./Division Only: YES-IMWH Directorate Only: NO
 CLINICAL GUIDELINES ID TAG Title: Obstetric Anal Sphincter Injury- A guideline Author: Dr Foteini Verani Designation: Specialist Doctor Speciality / Division: Obstetrics-IMWH Directorate: Acute Services
CLINICAL GUIDELINES ID TAG Title: Obstetric Anal Sphincter Injury- A guideline Author: Dr Foteini Verani Designation: Specialist Doctor Speciality / Division: Obstetrics-IMWH Directorate: Acute Services
Clinical Guideline for: The Management of Perineal Trauma following Childbirth
 For Use in: By: For: Division responsible for document: Key words: Name of document author: Job title of document author: Name of document author s Line Manager: Job title of author s Line Manager: Supported
For Use in: By: For: Division responsible for document: Key words: Name of document author: Job title of document author: Name of document author s Line Manager: Job title of author s Line Manager: Supported
Repair of vaginal tears and episiotomy guidelines
 Repair of vaginal tears and episiotomy guidelines Purpose These guidelines assist practitioners in the repair of vaginal and perineal tears including the reasons for, and the techniques of performing an
Repair of vaginal tears and episiotomy guidelines Purpose These guidelines assist practitioners in the repair of vaginal and perineal tears including the reasons for, and the techniques of performing an
EPISIOTOMY & PERINEAL TEARS Anatomy &Functionality May Dr. Annie Leong MBBS, FRANZCOG, CU
 EPISIOTOMY & PERINEAL TEARS Anatomy &Functionality May 2011 Dr. Annie Leong MBBS, FRANZCOG, CU Restore normal perineal anatomy Achieve good haemostasis Avoid infection and wound breakdown Avoid coital
EPISIOTOMY & PERINEAL TEARS Anatomy &Functionality May 2011 Dr. Annie Leong MBBS, FRANZCOG, CU Restore normal perineal anatomy Achieve good haemostasis Avoid infection and wound breakdown Avoid coital
Third & Fourth Degree Tears guideline (GL926)
 Third & Fourth Degree Tears guideline (GL926) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity Clinical Governance
Third & Fourth Degree Tears guideline (GL926) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity Clinical Governance
Obstetric Anal Sphincter Injury. An update on best practices. Objectives
 Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
Guideline for Management and Repair of Perineal Trauma
 Guideline for Management and Repair of Perineal Trauma Author: Labour Ward Forum Specialty: Maternity Date Approved: September 2014 Approved by: W&CH Clinical Governance Committee Date for Review: August
Guideline for Management and Repair of Perineal Trauma Author: Labour Ward Forum Specialty: Maternity Date Approved: September 2014 Approved by: W&CH Clinical Governance Committee Date for Review: August
Royal College of Obstetricians and Gynaecologists
 Royal College of Obstetricians and Gynaecologists Consent Advice No. 9 June 2010 REPAIR OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS FOLLOWING CHILDBIRTH This is the first edition of this guidance. This
Royal College of Obstetricians and Gynaecologists Consent Advice No. 9 June 2010 REPAIR OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS FOLLOWING CHILDBIRTH This is the first edition of this guidance. This
Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital
 Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital Capital city of Australia Population 350,000 but surrounding region of 500,000 Seat of government
Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital Capital city of Australia Population 350,000 but surrounding region of 500,000 Seat of government
Childbirth Trauma & Its Complications 23/ Mr Stergios K. Doumouchtsis
 Mr Stergios K. Doumouchtsis Consultant Obstetrician Gynaecologist & Urogynaecologist Childbirth Trauma & Its Complications Over eighty per cent of women sustain some degree of perineal trauma during childbirth.
Mr Stergios K. Doumouchtsis Consultant Obstetrician Gynaecologist & Urogynaecologist Childbirth Trauma & Its Complications Over eighty per cent of women sustain some degree of perineal trauma during childbirth.
The Perineal Clinic: - the management of women following OASI
 The Perineal Clinic: - the management of women following OASI Miss Gillian Fowler Consultant Urogynaecologist MBChB, MD, MRCOG Liverpool Women s Hospital. Margie Polden University Memorial of Liverpool
The Perineal Clinic: - the management of women following OASI Miss Gillian Fowler Consultant Urogynaecologist MBChB, MD, MRCOG Liverpool Women s Hospital. Margie Polden University Memorial of Liverpool
OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION
 OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION COLM O HERLIHY, MD Professor and Chair University College Dublin Department of Obstetrics and Gynaecology National Maternity
OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION COLM O HERLIHY, MD Professor and Chair University College Dublin Department of Obstetrics and Gynaecology National Maternity
THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS
 THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS MID2010 LEARNING OBJECTIVE 1 - REVIEW THE ANATOMY OF THE PELVIC FLOOR Superficial layers cavernosus Deep layer Coccygeus
THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS MID2010 LEARNING OBJECTIVE 1 - REVIEW THE ANATOMY OF THE PELVIC FLOOR Superficial layers cavernosus Deep layer Coccygeus
Hands-on Workshop. Cape Town, South Africa 3 August Chairpersons
 Hands-on Workshop www.perineum.net Cape Town, South Africa 3 August 2016 Chairpersons Mr Abdul H Sultan, MB.ChB (Natal), MD, FRCOG Consultant Obstetrician & Urogynaecologist Miss Ranee Thakar, MB.BS, MD,
Hands-on Workshop www.perineum.net Cape Town, South Africa 3 August 2016 Chairpersons Mr Abdul H Sultan, MB.ChB (Natal), MD, FRCOG Consultant Obstetrician & Urogynaecologist Miss Ranee Thakar, MB.BS, MD,
Secondary Repair of Third Degree Perineal Tear Leading to Fecal Incontinence in 2 Cases
 CASE REPORT Secondary Repair of Third Degree Perineal Tear Leading to Fecal Incontinence in 2 Cases Vasant Kawade 1 and Abhijit Ambike 2 Professor and Head, Department of OBGY, B.K.L.Walawakarl Rural Medical
CASE REPORT Secondary Repair of Third Degree Perineal Tear Leading to Fecal Incontinence in 2 Cases Vasant Kawade 1 and Abhijit Ambike 2 Professor and Head, Department of OBGY, B.K.L.Walawakarl Rural Medical
Postpartum Complications
 ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
Vincent Letouzey, MD, PhD
 How to protect the perineum and prevent obstetric perineal trauma Standards of OASIS diagnosis: Primary (clinical) and Secondary (ultrasound) Vincent Letouzey, MD, PhD Obst/Gyne Dept Nîmes University Hospital
How to protect the perineum and prevent obstetric perineal trauma Standards of OASIS diagnosis: Primary (clinical) and Secondary (ultrasound) Vincent Letouzey, MD, PhD Obst/Gyne Dept Nîmes University Hospital
SUTURING AN EPISIOTOMY/GENITAL LACERATION
 WOMEN AND NEWBORN HEALTH SERVICE CLINICAL GUIDELINES SECTION B : GUIDELINES RELEVANT TO OBSTETRICS AND MIDWIFERY 5 INTRAPARTUM CARE 5.15 PERINEAL REPAIR Authorised by: OGCCU 5.15.1 SUTURING AN EPISIOTOMY/GENITAL
WOMEN AND NEWBORN HEALTH SERVICE CLINICAL GUIDELINES SECTION B : GUIDELINES RELEVANT TO OBSTETRICS AND MIDWIFERY 5 INTRAPARTUM CARE 5.15 PERINEAL REPAIR Authorised by: OGCCU 5.15.1 SUTURING AN EPISIOTOMY/GENITAL
How to repair an anal sphincter injury after vaginal delivery: results of a randomised controlled trial
 DOI: 10.1111/j.1471-0528.2006.00806.x www.blackwellpublishing.com/bjog Intrapartum care How to repair an anal sphincter injury after vaginal delivery: results of a randomised controlled trial Abimbola
DOI: 10.1111/j.1471-0528.2006.00806.x www.blackwellpublishing.com/bjog Intrapartum care How to repair an anal sphincter injury after vaginal delivery: results of a randomised controlled trial Abimbola
Perineal Tears. Obstetrics & Gynaecology Women & Children s Group
 Perineal Tears Obstetrics & Gynaecology Women & Children s Group This leaflet has been designed to give you important information about your condition / procedure, and to answer some common queries that
Perineal Tears Obstetrics & Gynaecology Women & Children s Group This leaflet has been designed to give you important information about your condition / procedure, and to answer some common queries that
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives
 Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
Repair of Perineal trauma, including 3 rd and 4 th degree tear
 MATERNITY GUIDELINES Repair of Perineal trauma, including 3 rd and 4 th degree tear Navigation Guidance document in the contents page the Press Ctrl on your keyboard and click on a heading to navigate
MATERNITY GUIDELINES Repair of Perineal trauma, including 3 rd and 4 th degree tear Navigation Guidance document in the contents page the Press Ctrl on your keyboard and click on a heading to navigate
Obstetrical Anal Sphincter Injuries (OASIS): Prevention, Recognition, and Repair
 SOGC CLINICAL PRACTICE GUIDELINE No. 330, December 2015 Obstetrical Anal Sphincter Injuries (OASIS): Prevention, Recognition, and Repair This clinical practice guideline has been prepared by the Urogynaecology
SOGC CLINICAL PRACTICE GUIDELINE No. 330, December 2015 Obstetrical Anal Sphincter Injuries (OASIS): Prevention, Recognition, and Repair This clinical practice guideline has been prepared by the Urogynaecology
Obstetric anal sphincter injury is the most common
 Repair Techniques for Obstetric Anal Sphincter Injuries A Randomized Controlled Trial Ruwan J. Fernando, MD, MRCOG, Abdul H. Sultan, MD, FRCOG, Christine Kettle, PhD, Simon Radley, MD, FRCS, Peter Jones,
Repair Techniques for Obstetric Anal Sphincter Injuries A Randomized Controlled Trial Ruwan J. Fernando, MD, MRCOG, Abdul H. Sultan, MD, FRCOG, Christine Kettle, PhD, Simon Radley, MD, FRCS, Peter Jones,
Care of your Perineum following 3 rd and 4 th degree tears
 Maternity Services Care of your Perineum following 3 rd and 4 th degree tears Introduction This leaflet aims to give you information about the repair and aftercare of the third or fourth degree tear you
Maternity Services Care of your Perineum following 3 rd and 4 th degree tears Introduction This leaflet aims to give you information about the repair and aftercare of the third or fourth degree tear you
Postoperative Care for Pelvic Fistulae. Peter Jeppson, MD October 3, 2017
 Postoperative Care for Pelvic Fistulae Peter Jeppson, MD October 3, 2017 No Disclosures Rational for Postoperative Care Intraoperative injury may be managed by: Identification Closure Continuous post-operative
Postoperative Care for Pelvic Fistulae Peter Jeppson, MD October 3, 2017 No Disclosures Rational for Postoperative Care Intraoperative injury may be managed by: Identification Closure Continuous post-operative
Taking care of your perineum before, during and after birth
 Taking care of your perineum before, during and after birth A Parent Information Leaflet Where is is my my perineum and and what what happens happens during childbirth? during childbirth? Your perineum
Taking care of your perineum before, during and after birth A Parent Information Leaflet Where is is my my perineum and and what what happens happens during childbirth? during childbirth? Your perineum
Guidelines on the Management of Complications related to Female Genital Mutilation
 Guidelines on the Management of Complications related to Female Genital Mutilation Scoping Survey Instructions The following is a list of 33 potential questions which could guide the evidence retrieval
Guidelines on the Management of Complications related to Female Genital Mutilation Scoping Survey Instructions The following is a list of 33 potential questions which could guide the evidence retrieval
Title: A modified surgical approach to women with obstetric anal sphincter tears
 Reviewer's report Title: A modified surgical approach to women with obstetric anal sphincter tears Version: 3 Date: 27 January 2010 Reviewer: Stig S Norderval Reviewer's report: Review on manuscript entitled:
Reviewer's report Title: A modified surgical approach to women with obstetric anal sphincter tears Version: 3 Date: 27 January 2010 Reviewer: Stig S Norderval Reviewer's report: Review on manuscript entitled:
Long-term ailments due to anal sphincter rupture caused by delivery - a hidden problem
 Eur. J. Obstet. Gynecol. Reprod. Biol., 27 (1988) 27-32 Elsevier 27 EJO 00556 Long-term ailments due to anal sphincter rupture caused by delivery - a hidden problem Knut Haadem, Sten Ohrlander and G6ran
Eur. J. Obstet. Gynecol. Reprod. Biol., 27 (1988) 27-32 Elsevier 27 EJO 00556 Long-term ailments due to anal sphincter rupture caused by delivery - a hidden problem Knut Haadem, Sten Ohrlander and G6ran
Maternity Information Leaflet. Care of the Perineum (including Pelvic Floor Exercises) Version 2
 Maternity Information Leaflet Care of the Perineum (including Pelvic Floor Exercises) Version 2 Pelvic Floor Exercises The pelvic floor muscles are located between your legs, and run from your pubic bone
Maternity Information Leaflet Care of the Perineum (including Pelvic Floor Exercises) Version 2 Pelvic Floor Exercises The pelvic floor muscles are located between your legs, and run from your pubic bone
Occult anal sphincter injuries myth or reality?
 DOI: 10.1111/j.1471-0528.2006.00799.x www.blackwellpublishing.com/bjog Intrapartum care Occult anal sphincter injuries myth or reality? Vasanth Andrews, a Abdul H Sultan, a Ranee Thakar, a Peter W Jones
DOI: 10.1111/j.1471-0528.2006.00799.x www.blackwellpublishing.com/bjog Intrapartum care Occult anal sphincter injuries myth or reality? Vasanth Andrews, a Abdul H Sultan, a Ranee Thakar, a Peter W Jones
5 DIAGNOSIS. History taking
 5 DIAGNOSIS All of the photographs in Chapter 4 were taken in theatre before operation. This chapter deals with how one can recognize the type of fistula by history taking and examination. (Note that the
5 DIAGNOSIS All of the photographs in Chapter 4 were taken in theatre before operation. This chapter deals with how one can recognize the type of fistula by history taking and examination. (Note that the
Faecal incontinence after childbirth
 Britisb Journal of Obstetrics and Gynaecology January 1997, Vol. 104, pp. 4650 Faecal incontinence after childbirth *Christine MacArthur Reader (Maternal and Child Epidemiology), *Debra E. Bick Research
Britisb Journal of Obstetrics and Gynaecology January 1997, Vol. 104, pp. 4650 Faecal incontinence after childbirth *Christine MacArthur Reader (Maternal and Child Epidemiology), *Debra E. Bick Research
Stapled transanal rectal resection for obstructed defaecation syndrome
 Stapled transanal rectal resection for obstructed Issued: June 2010 www.nice.org.uk/ipg351 NHS Evidence has accredited the process used by the NICE Interventional Procedures Programme to produce interventional
Stapled transanal rectal resection for obstructed Issued: June 2010 www.nice.org.uk/ipg351 NHS Evidence has accredited the process used by the NICE Interventional Procedures Programme to produce interventional
Number of pages: This policy and procedure guideline applies to all obstetrics and gynecology medical and midwifery staff.
 Saudi Society of Obstetrics and Gynaecology Policy and Procedure Title/Description: REPAIR OF PERINEAL TRAUMA Effective Date: 1st July 2016 1. PURPOSE Department: Obstetrics and Gynecology (Labour & Birth)
Saudi Society of Obstetrics and Gynaecology Policy and Procedure Title/Description: REPAIR OF PERINEAL TRAUMA Effective Date: 1st July 2016 1. PURPOSE Department: Obstetrics and Gynecology (Labour & Birth)
PERINEAL REPAIR: COMPARISON OF SUTURE MATERIALS AND SUTURING TECHNIQUES
 ORIGINAL ARTICLE PERINEAL REPAIR: COMPARISON OF SUTURE MATERIALS AND SUTURING TECHNIQUES FOUZIA PERVEEN, TEHMINA SHABBIR ABSTRACT Objective Study design Place & Duration of study To compare the outcome
ORIGINAL ARTICLE PERINEAL REPAIR: COMPARISON OF SUTURE MATERIALS AND SUTURING TECHNIQUES FOUZIA PERVEEN, TEHMINA SHABBIR ABSTRACT Objective Study design Place & Duration of study To compare the outcome
for a review under the Accident Compensation Act
 FairWay Resolution Limited Tā te Hinengaro Tōkeke Whakatau Review numbers: Application by for a review under the Accident Compensation Act Held at Date of hearing 2 November 2016, adjourned part-heard;
FairWay Resolution Limited Tā te Hinengaro Tōkeke Whakatau Review numbers: Application by for a review under the Accident Compensation Act Held at Date of hearing 2 November 2016, adjourned part-heard;
Patient Advice for Third & Fourth Degree Tears
 Patient Advice for Third & Fourth Degree Tears Please read this leaflet carefully. It is important that you take note of any instructions or advice given. If you have any questions or problems that are
Patient Advice for Third & Fourth Degree Tears Please read this leaflet carefully. It is important that you take note of any instructions or advice given. If you have any questions or problems that are
Surgical repair of vaginal wall prolapse using mesh
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
UNDERSTANDING EPISIOTOMY C-SECTION AND RECTOCELE. Our suture portfolio meets all your procedural needs
 UNDERSTANDING EPISIOTOMY C-SECTION AND RECTOCELE Our suture portfolio meets all your procedural needs GYNECOLOGY Episiotomy A surgically planned incision on the perineum and the posterior vaginal wall,
UNDERSTANDING EPISIOTOMY C-SECTION AND RECTOCELE Our suture portfolio meets all your procedural needs GYNECOLOGY Episiotomy A surgically planned incision on the perineum and the posterior vaginal wall,
Physiotherapy advice following your third or fourth degree perineal tear
 Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
8 A SIMPLE FISTULA REPAIR, STEP BY STEP
 8 A SIMPLE FISTULA REPAIR, STEP BY STEP The first step is to suture the labia to the thighs and cover the anus with a swab (Figure 31). Figure 31 The labia are sutured to the thighs and the anus is covered
8 A SIMPLE FISTULA REPAIR, STEP BY STEP The first step is to suture the labia to the thighs and cover the anus with a swab (Figure 31). Figure 31 The labia are sutured to the thighs and the anus is covered
Pelvic Floor Ultrasound Imaging. Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague)
 Pelvic Floor Ultrasound Imaging Workshop IUGA 2015 Nice Faculty: Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague) The use of translabial ultrasound
Pelvic Floor Ultrasound Imaging Workshop IUGA 2015 Nice Faculty: Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague) The use of translabial ultrasound
PROTOCOL FOR BLADDER CARE MANAGEMENT DURING INTRAPARTUM AND POSTNATAL PERIOD
 PROTOCOL FOR BLADDER CARE MANAGEMENT DURING INTRAPARTUM AND POSTNATAL PERIOD Specialty: Obstetrics Date Approved: Revised September 2015 Approved by: Labour Ward Forum Date for Review: September 2018 Overview
PROTOCOL FOR BLADDER CARE MANAGEMENT DURING INTRAPARTUM AND POSTNATAL PERIOD Specialty: Obstetrics Date Approved: Revised September 2015 Approved by: Labour Ward Forum Date for Review: September 2018 Overview
Pregnancy and childbirth: the effects on pelvic floor muscles
 Page 1 of 9 Pregnancy and childbirth: the effects on pelvic floor muscles 26 February, 2009 Stress incontinence can follow childbirth as pelvic floor muscles are damaged AUTHOR Julia Herbert, MSc, MCSP,
Page 1 of 9 Pregnancy and childbirth: the effects on pelvic floor muscles 26 February, 2009 Stress incontinence can follow childbirth as pelvic floor muscles are damaged AUTHOR Julia Herbert, MSc, MCSP,
This information is intended as an overview only
 This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
Immediate or delayed repair of obstetric anal sphincter tears a randomised controlled trial*
 DOI: 10.1111/j.1471-0528.2008.01726.x www.blackwellpublishing.com/bjog General obstetrics Immediate or delayed repair of obstetric anal sphincter tears a randomised controlled trial* J Nordenstam, a,b
DOI: 10.1111/j.1471-0528.2008.01726.x www.blackwellpublishing.com/bjog General obstetrics Immediate or delayed repair of obstetric anal sphincter tears a randomised controlled trial* J Nordenstam, a,b
John Laughlin 4 th year Cardiff University Medical Student
 John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
Approach to the Repair of Chronic Perineal Lacerations and Rectovaginal Fistula (RVF)
 Approach to the Repair of Chronic Perineal Lacerations and Rectovaginal Fistula (RVF) Blair B. Washington MD, MHA Urogynecology & Reconstructive Pelvic Surgery Virginia Mason Medical Center Disclosures
Approach to the Repair of Chronic Perineal Lacerations and Rectovaginal Fistula (RVF) Blair B. Washington MD, MHA Urogynecology & Reconstructive Pelvic Surgery Virginia Mason Medical Center Disclosures
2/25/2013. Speaker Disclosure. Learning Objectives. Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth
 Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth Jaime Sepulveda-Toro MD FACS FACOG Female Pelvic Medicine and Reconstructive Pelvic Surgery South Miami Hospital Speaker
Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth Jaime Sepulveda-Toro MD FACS FACOG Female Pelvic Medicine and Reconstructive Pelvic Surgery South Miami Hospital Speaker
ARTIFICIAL MESH REPAIR FOR TREATMENT OF PELVIC ORGAN PROLAPSE
 Pelvic Floor Unit / Department of Gynaecology Ward 17, Singleton Hospital, Sketty, Swansea, SA2 8QA 01792 205666 Secretary Direct Line: 01792 285688. Fax: 01792 285874 ARTIFICIAL MESH REPAIR FOR TREATMENT
Pelvic Floor Unit / Department of Gynaecology Ward 17, Singleton Hospital, Sketty, Swansea, SA2 8QA 01792 205666 Secretary Direct Line: 01792 285688. Fax: 01792 285874 ARTIFICIAL MESH REPAIR FOR TREATMENT
LAPAROSCOPIC REPAIR OF PELVIC FLOOR
 LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
Interventional procedures guidance Published: 12 October 2016 nice.org.uk/guidance/ipg566
 Single-incision short sling mesh insertion for stress urinary incontinence in women Interventional procedures guidance Published: 12 October 2016 nice.org.uk/guidance/ipg566 Your responsibility This guidance
Single-incision short sling mesh insertion for stress urinary incontinence in women Interventional procedures guidance Published: 12 October 2016 nice.org.uk/guidance/ipg566 Your responsibility This guidance
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
AN INTERNATIONAL CONTINENCE SOCIETY (ICS) / INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR CHILDBIRTH TRAUMA
 AN INTERNATIONAL CONTINENCE SOCIETY (ICS) / INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR CHILDBIRTH TRAUMA NEED FOR A WORKING GROUP ON CHILDBIRTH TRAUMA A: Background
AN INTERNATIONAL CONTINENCE SOCIETY (ICS) / INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR CHILDBIRTH TRAUMA NEED FOR A WORKING GROUP ON CHILDBIRTH TRAUMA A: Background
2/5/2016. Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach
 Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach Holly E Richter, PhD, MD, FACOG, FACS J Marion Sims Professor Obstetrics and Gynecology Professor
Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach Holly E Richter, PhD, MD, FACOG, FACS J Marion Sims Professor Obstetrics and Gynecology Professor
Pelvic Floor Disorders. Amir Darakhshan MD FRCS (Gen Surg) Consultant Colorectal and General Surgeon
 Pelvic Floor Disorders Amir Darakhshan MD FRCS (Gen Surg) Consultant Colorectal and General Surgeon What is Pelvic Floor Disorder Surgical perspective symptoms of RED, FI or prolapse on the background
Pelvic Floor Disorders Amir Darakhshan MD FRCS (Gen Surg) Consultant Colorectal and General Surgeon What is Pelvic Floor Disorder Surgical perspective symptoms of RED, FI or prolapse on the background
Stop Coping. Start Living. Talk to your doctor about pelvic organ prolapse and sacrocolpopexy
 Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Surgical treatment of urinary stress incontinence with tension free vaginal tape
 Surgical treatment of urinary stress incontinence with tension free vaginal tape Gynaecology department 01935 384 385 yeovilhospital.nhs.uk Many surgical operations are available for the treatment of
Surgical treatment of urinary stress incontinence with tension free vaginal tape Gynaecology department 01935 384 385 yeovilhospital.nhs.uk Many surgical operations are available for the treatment of
RANZCOG Advanced Training Modules
 RANZCOG Advanced Training Modules Generalist Obstetrics ATM and Generalist Gynaecology ATM The Generalist ATMs in each of Obstetrics and Gynaecology provide a framework for trainees to consolidate and
RANZCOG Advanced Training Modules Generalist Obstetrics ATM and Generalist Gynaecology ATM The Generalist ATMs in each of Obstetrics and Gynaecology provide a framework for trainees to consolidate and
Bladder care postpartum including bladder care for women with epidural analgesia (GL792)
 Bladder care postpartum including bladder care for women with epidural analgesia (GL792) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children's Services Clinical Governance Committee
Bladder care postpartum including bladder care for women with epidural analgesia (GL792) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children's Services Clinical Governance Committee
A PATIENT GUIDE TO Understanding Stress Urinary Incontinence
 A PATIENT GUIDE TO Understanding Stress Urinary Incontinence Q: What is SUI? A: Stress urinary incontinence is defined as the involuntary leakage of urine. The problem afflicts approximately 18 million
A PATIENT GUIDE TO Understanding Stress Urinary Incontinence Q: What is SUI? A: Stress urinary incontinence is defined as the involuntary leakage of urine. The problem afflicts approximately 18 million
The Pelvic Floor: Expecting (and Delivering!) Susan Barr, MD Assistant Professor Saint Louis University Division of Urogynecology
 The Pelvic Floor: What She Can Expect After Expecting (and Delivering!) Susan Barr, MD Assistant Professor Saint Louis University Division of Urogynecology Objectives Understand risk factors and treatment
The Pelvic Floor: What She Can Expect After Expecting (and Delivering!) Susan Barr, MD Assistant Professor Saint Louis University Division of Urogynecology Objectives Understand risk factors and treatment
EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time
 EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time Menachem Alcalay,M.D, Urogynecology unit, Sheba Medical
EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time Menachem Alcalay,M.D, Urogynecology unit, Sheba Medical
2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL)
 E10d 2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No.
E10d 2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No.
Gynecology Dr. Sallama Lecture 3 Genital Prolapse
 Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Pelvic organ prolapse. Information for patients Continence Service
 Pelvic organ prolapse Information for patients Continence Service What is a pelvic organ prolapse? A pelvic organ prolapse occurs when the uterus (womb), vagina, bladder or bowel slips out of place, resulting
Pelvic organ prolapse Information for patients Continence Service What is a pelvic organ prolapse? A pelvic organ prolapse occurs when the uterus (womb), vagina, bladder or bowel slips out of place, resulting
Perineal Trauma Assessment, Repair and Safe Practice
 1. Purpose This document outlines the guideline and the procedure details for the assessment and repair of perineal trauma in postpartum women. Genital tract trauma can occur spontaneously during a vaginal
1. Purpose This document outlines the guideline and the procedure details for the assessment and repair of perineal trauma in postpartum women. Genital tract trauma can occur spontaneously during a vaginal
Ben Herbert Alex Wojtowicz
 Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL)
 2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No. Service
2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No. Service
Focus on Post-Partum Incontinence
 Focus on Post-Partum Incontinence A one day intensive course for Nurses, Midwives and Physiotherapists Old Main Building Law Faculty Stellenbosch 24 January 2013 9h00-17h00 Sponsored by the International
Focus on Post-Partum Incontinence A one day intensive course for Nurses, Midwives and Physiotherapists Old Main Building Law Faculty Stellenbosch 24 January 2013 9h00-17h00 Sponsored by the International
GI Physiology - Investigating and treating patients with pelvic floor dysfunction. Lynne Smith Department of GI Physiology NGH Sheffield
 GI Physiology - Investigating and treating patients with pelvic floor dysfunction Lynne Smith Department of GI Physiology NGH Sheffield Aims o o o To give an overview of lower GI investigations To demonstrate
GI Physiology - Investigating and treating patients with pelvic floor dysfunction Lynne Smith Department of GI Physiology NGH Sheffield Aims o o o To give an overview of lower GI investigations To demonstrate
anal incontinence; endoanal ultrasonography; grading systems; obstetric sphincter tears; three-dimensional
 Ultrasound Obstet Gynecol 2012; 40: 207 214 Published online in Wiley Online Library (wileyonlinelibrary.com). DOI: 10.1002/uog.10154 Incontinence after primary repair of obstetric anal sphincter tears
Ultrasound Obstet Gynecol 2012; 40: 207 214 Published online in Wiley Online Library (wileyonlinelibrary.com). DOI: 10.1002/uog.10154 Incontinence after primary repair of obstetric anal sphincter tears
Women s & Children s Directorate The TVT Operation - a guide for patients
 Women s & Children s Directorate The TVT Operation - a guide for patients This leaflet was written for women who are considering having a TVT operation. If you have any questions that aren't answered by
Women s & Children s Directorate The TVT Operation - a guide for patients This leaflet was written for women who are considering having a TVT operation. If you have any questions that aren't answered by
Post operative voiding dysfunction and the Value of Urodynamics. Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist
 Post operative voiding dysfunction and the Value of Urodynamics Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist Learning objectives: v Pathophysiology of post op voiding dysfunction.
Post operative voiding dysfunction and the Value of Urodynamics Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist Learning objectives: v Pathophysiology of post op voiding dysfunction.
Effect of subsequent vaginal delivery on bowel symptoms and anorectal function in women who sustained a previous obstetric anal sphincter injury
 International Urogynecology Journal (2018) 29:1579 1588 https://doi.org/10.1007/s00192-018-3601-y ORIGINAL ARTICLE Effect of subsequent vaginal delivery on bowel symptoms and anorectal function in women
International Urogynecology Journal (2018) 29:1579 1588 https://doi.org/10.1007/s00192-018-3601-y ORIGINAL ARTICLE Effect of subsequent vaginal delivery on bowel symptoms and anorectal function in women
Pelvic Support Problems
 AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
The Management of Female Urinary Incontinence. Part 1: Aetiology and Investigations
 The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
Pelvic organ prolapse
 Page 1 of 11 Pelvic organ prolapse Introduction The aim of this leaflet is to give you information about a pelvic organ prolapse, its causes and available treatments but does not replace advice given by
Page 1 of 11 Pelvic organ prolapse Introduction The aim of this leaflet is to give you information about a pelvic organ prolapse, its causes and available treatments but does not replace advice given by
Consultation Guide: Specialised gynaecology surgery and complex urogynaecology conditions service specifications
 Consultation Guide: Specialised gynaecology surgery and complex urogynaecology conditions service specifications Consultation guide: Specialised gynaecology surgery and complex urogynaecology conditions
Consultation Guide: Specialised gynaecology surgery and complex urogynaecology conditions service specifications Consultation guide: Specialised gynaecology surgery and complex urogynaecology conditions
JMSCR Volume 03 Issue 03 Page March 2015
 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Quality of Life among Patients after Vaginal Hysterectomy and Pelvic Floor Repair Operation ABSTRACT Authors S Lovereen 1, F A Suchi 2,
www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Quality of Life among Patients after Vaginal Hysterectomy and Pelvic Floor Repair Operation ABSTRACT Authors S Lovereen 1, F A Suchi 2,
1) What conditions is vaginal mesh used to commonly treat? Vaginal mesh is used to treat two different health issues in women:
 Vaginal Mesh Frequently Asked Questions 1) What conditions is vaginal mesh used to commonly treat? Vaginal mesh is used to treat two different health issues in women: a) stress urinary incontinence (SUI)
Vaginal Mesh Frequently Asked Questions 1) What conditions is vaginal mesh used to commonly treat? Vaginal mesh is used to treat two different health issues in women: a) stress urinary incontinence (SUI)
Physiotherapy advice following your vaginal birth
 Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Sacrocolpopexy. Department of Gynaecology. Patient Information
 Sacrocolpopexy Department of Gynaecology 2 Patient Information What What is is a a sacrocolpopexy? This is an operation carried out to correct prolapse of the vaginal vault in patients who had a hysterectomy.
Sacrocolpopexy Department of Gynaecology 2 Patient Information What What is is a a sacrocolpopexy? This is an operation carried out to correct prolapse of the vaginal vault in patients who had a hysterectomy.
Le fort s operation for prolapse uterus: A forgotten procedure
 2017; 1(2): 52-56 ISSN (P): 2522-6614 ISSN (E): 2522-6622 Gynaecology Journal www.gynaecologyjournal.com 2017; 1(2): 52-56 Received: 12-09-2017 Accepted: 13-10-2017 Dr. Jasmine Lall 3 rd Year Resident,
2017; 1(2): 52-56 ISSN (P): 2522-6614 ISSN (E): 2522-6622 Gynaecology Journal www.gynaecologyjournal.com 2017; 1(2): 52-56 Received: 12-09-2017 Accepted: 13-10-2017 Dr. Jasmine Lall 3 rd Year Resident,
Prolapse & Urogynaecology. Hester Mannion and Fabi Sica
 Prolapse & Urogynaecology Hester Mannion and Fabi Sica Take home messages Prolapse and associated incontinence is very common It has a devastating effect on the QoL of the patient and their partner Strategies
Prolapse & Urogynaecology Hester Mannion and Fabi Sica Take home messages Prolapse and associated incontinence is very common It has a devastating effect on the QoL of the patient and their partner Strategies
Posterior Vaginal Wall Prolapse Repair And Repair of Perineum
 Posterior Vaginal Wall Prolapse Repair And Repair of Perineum Patient Information Leaflet BSUG Patient Information Sheet Disclaimer This patient information sheet was put together by members of the BSUG
Posterior Vaginal Wall Prolapse Repair And Repair of Perineum Patient Information Leaflet BSUG Patient Information Sheet Disclaimer This patient information sheet was put together by members of the BSUG
Promoting Continence with Physiotherapy
 A Common problem for Men and women Promoting Continence with Physiotherapy This leaflet contains information about physiotherapy advice and treatment for anyone with bladder and bowel problems. This may
A Common problem for Men and women Promoting Continence with Physiotherapy This leaflet contains information about physiotherapy advice and treatment for anyone with bladder and bowel problems. This may
Faecal Incontinence Information Leaflet THE DIGESTIVE SYSTEM
 THE DIGESTIVE SYSTEM This factsheet is about faecal incontinence Faecal (or anal) incontinence is the loss of stool, liquid or gas from the bowel at an undesirable time. Males and females of any age may
THE DIGESTIVE SYSTEM This factsheet is about faecal incontinence Faecal (or anal) incontinence is the loss of stool, liquid or gas from the bowel at an undesirable time. Males and females of any age may
INTRAPARTUM AND POSTNATAL BLADDER CARE
 INTRAPARTUM AND POSTNATAL BLADDER CARE BACKGROUND Urinary retention is uncommon but carries significant morbidity and the risk is increased by a number of factors including epidural analgesia (Teo, et
INTRAPARTUM AND POSTNATAL BLADDER CARE BACKGROUND Urinary retention is uncommon but carries significant morbidity and the risk is increased by a number of factors including epidural analgesia (Teo, et
Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study
 ORIGINAL RESEARCH Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study Johan Pollack, MD, Johan Nordenstam, MD, Sophia Brismar, MD, Annika Lopez, MD, PhD, Daniel Altman, MD, and
ORIGINAL RESEARCH Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study Johan Pollack, MD, Johan Nordenstam, MD, Sophia Brismar, MD, Annika Lopez, MD, PhD, Daniel Altman, MD, and
Post-operative Analgesia for Caesarean Section
 Post-operative Analgesia for Caesarean Section Introduction Good quality analgesia after any surgery leads to earlier mobilisation, fewer pulmonary and cardiac complications, a reduced risk of DVT and
Post-operative Analgesia for Caesarean Section Introduction Good quality analgesia after any surgery leads to earlier mobilisation, fewer pulmonary and cardiac complications, a reduced risk of DVT and
Fecal Incontinence. What is fecal incontinence?
 Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Patient Information. Tension Free Vaginal/ Obturator Tape (TVT) Royal Devon and Exeter NHS Foundation Trust
 Tension Free Vaginal/Obturator Tape (TVT) Royal Devon and Exeter NHS Foundation Trust Patient Information Tension Free Vaginal/ Obturator Tape (TVT) Reference Number: CW 08 011 003 (version date: September
Tension Free Vaginal/Obturator Tape (TVT) Royal Devon and Exeter NHS Foundation Trust Patient Information Tension Free Vaginal/ Obturator Tape (TVT) Reference Number: CW 08 011 003 (version date: September
