Immediate or delayed repair of obstetric anal sphincter tears a randomised controlled trial*
|
|
|
- Merryl Simon
- 5 years ago
- Views:
Transcription
1 DOI: /j x General obstetrics Immediate or delayed repair of obstetric anal sphincter tears a randomised controlled trial* J Nordenstam, a,b A Mellgren, a,b D Altman, c ALópez, d C Johansson, a B Anzén, d Zhong-ze Li, e J Zetterström d a Division of Surgery, Department of Clinical Sciences, Karolinska Institutet, Danderyd Hospital, Stockholm, Sweden b Division of Colon and Rectal Surgery, Department of Surgery, University of Minnesota, Minneapolis, MN, USA c Department of Medical Epidemiology and Biostatistics, Karolinska Institutet, Stockholm, Sweden d Division of Obstetrics and Gynecology, Department of Clinical Sciences, Karolinska Institutet, Danderyd Hospital, Stockholm, Sweden e Biostatistics Core, University of Minnesota Cancer Center, Minneapolis, MN, USA Correspondence: Dr J Nordenstam, Division of Colon and Rectal Surgery, Department of Surgery, University of Minnesota, MMC 450, 420 Delaware Street SE, Minneapolis, MN 55455, USA. nord0464@umn.edu Accepted 20 February Objective To investigate if an 8- to 12-hour time delay of primary repair affects anal incontinence at 1-year follow up. Design Randomised controlled trial. Setting University hospital in Sweden. Population A total of 165 women diagnosed with a third- to fourth-degree perineal tear. Methods The participants were randomised to immediate or delayed (8- to 12-hour delay) end-to-end repair; 78 were allocated to immediate operation and 87 to a delayed repair. An incontinence and pelvic floor symptom was completed by the participants at baseline and at 6- and 12-month follow up. Main outcome measures Anal incontinence measured by the validated Pescatori incontinence score. Results A total of 161 (98%) and 155 (94%) women completed the two follow-up s. There was no significant difference in anal incontinence between the groups. There were no significant differences in pelvic floor symptoms between the groups. A multivariate proportional odds model revealed that increasing maternal age was significantly associated with both increased symptoms of faecal urgency and inability to discriminate flatus from faeces. Conclusion Delayed repair provided the same functional outcome at 1-year follow up. Delaying the repair should thus not be recommended routinely, but can be an alternative under special circumstances when appropriate surgical expertise is not readily available. Keywords Anal incontinence, obstetric anal sphincter tear, primary repair, randomised controlled trial. Please cite this paper as: Nordenstam J, Mellgren A, Altman D, López A, Johansson C, Anzén B, Li Z, Zetterström J. Immediate or delayed repair of obstetric anal sphincter tears a randomised controlled trial. BJOG 2008;115: Introduction *Presented in part at the Annual Meeting of the American Society of Colon and Rectal Surgeons, Philadelphia, The prevalence of faecal incontinence among women in the United States has been estimated to up to 12%. 1 3 Anal incontinence, which also includes incontinence for gas, is even more common. Childbirth is considered to be an important factor in the higher prevalence of anal incontinence in women. Occult or overt injuries to the anal sphincter complex can lead to immediate or delayed incontinence symptoms and the risk may be increased by the practice of obstetric interventions such as fundal pressure, instrumental delivery and episiotomy. 4 6 There is great variability in the reported prevalence of obstetric anal sphincter injuries in the literature and this implies that not all obstetric sphincter injuries are identified at the time of the delivery. 7,8 The optimal technique for primary repair of obstetric anal sphincter injury continues to be debated. End-to-end approximation repair of the anal sphincter injury is the most commonly used primary repair technique, while a few studies have advocated an overlapping repair technique. 9 A recent systematic review concluded that although the data were limited, early primary overlap repair appeared to be associated with a lower risk of faecal urgency and anal incontinence symptoms when compared with immediate primary end-to-end repair. 10 A partial sphincter ª 2008 The Authors Journal compilation ª RCOG 2008 BJOG An International Journal of Obstetrics and Gynaecology 857
2 Nordenstam et al. tear is, however, not compatible with an overlap repair, and several trials have concluded equivalence between the methods. 9,11,12 Child deliveries are evenly distributed over the hours and it is plausible that awaiting surgical expertise following detection of an obstetric anal sphincter injury may optimise the subjective outcome. However, it is also possible that the consequential time delay between the injury and the repair will affect the outcome of the repair. There are no previous studies addressing this issue. The aim of this study was to investigate if an 8- to 12-hour delay of the primary repair of obstetric anal sphincter injury affects the subjective outcome when compared with immediate primary repair with regard to anal incontinence. Methods The study was conducted over a 28-month period at Danderyd University Hospital, Stockholm, Sweden. The study was approved by the Research Ethics Committee at the Karolinska Institutet and midwives and obstetricians at the clinic received oral and written information on the objectives and planned execution of the study prior to study initiation. Subjects were given verbal and written information about the study while still at the hospital delivery ward, immediately following diagnosis of a third- or fourth-degree tear, and they were entered into the study by signing the informed consent form to participate. Inclusion criteria included vaginal delivery, proficiency in the Swedish language, obstetric anal sphincter injury according to the World Health Organization adopted ICD tenth revision. Exclusion criteria included excessive maternal bleeding from the vaginal rupture and medical conditions associated with a risk of abnormal obstetric bleeding. Women were randomised to immediate or delayed repair using opaque envelopes, each containing instructions for either immediate or delayed repair. The envelopes were shuffled and placed in a box in the delivery ward. Following childbirth, the responsible midwife inspected the vaginal laceration in accordance with hospital routines. First- and second-degree vaginal and perineal lacerations were classified and sutured by the midwife or an obstetrician. In cases where the responsible midwife suspected a third- or fourth-degree perineal injury, the attending obstetrician was consulted to confirm or refute this finding. In compliance with hospital routines, the physician s clinical assessment also included the classification proposed by Sultan and recommended by the Royal College of Obstetricians and Gynaecologists: less than 50% of the external anal sphincter thickness, more than 50% of the external anal sphincter thickness, total external anal sphincter rupture with torn internal anal sphincter and total external anal sphincter rupture with rupture of the rectal mucosa, registered in hospital charts. 13 If a third- or fourthdegree obstetric tear was confirmed and the woman agreed to participate in the study, the midwife selected the patient randomly by drawing the next sealed envelope from the randomisation box. In women randomised to immediate repair, standard procedures were followed and the obstetrician on call repaired the anal sphincter injury. Women randomised to a delayed repair waited at least 8 hours before a member of the study team repaired their injury. The study team consisted of three obstetricians and three colorectal surgeons. The experience of the participating study team physicians varied (Table 1). The three obstetricians also repaired injuries of women in the immediate group as they were on call. Infection prophylaxis consisting of intravenously administered cefuroxime (1.5 g) and metronidazole (1 g) was initiated before the surgery was started; all repairs were performed in the operating theatre. We used 3-0 Polysorb Ò (braided Lactomer) when repairing the anal mucosa, 0-0 Polysorb Ò for the sphincter and 2-0 Polysorb Ò for the perineal body. We used 4-0 Caprosyn Ò (monofilament polyglytone) for the perineal skin. Upon entering the study, each participant completed a selfreported baseline containing 22 questions on symptoms of anal incontinence and anorectal dysfunction. The women recorded the frequency of incontinence to gas, liquid and solid stool by responding to one of the alternatives of the following ordinal frequency scale: never, less than or once per week, more than once per week and daily. An incontinence score on a scale from 0 to 6 was calculated as described by Pescatori, where 0 corresponds to continence and 6 to daily incontinence of solid stool. 14 The scoring system has been used previously and has been shown to be reliable, sensitive to change and to correlate to clinical assessment of incontinence. 15,16 An identical self-reported was sent out and returned by ordinary mail at 6 and 12 months postpartum. A telephone call was made to subjects who did not respond within 3 weeks of the first mail-out, and a second letter was sent out after an additional 2 weeks if the subject still had not responded. Detailed medical data on maternal outcome were Table 1. Experience and degree of involvement of physicians Specialist experience (years) Operations immediate group (%) Operations delayed group (%), The table describes the experience level of the physicians involved in the study, and the percentage of operations in each of the two groups that were performed by physicians with a certain range of experience. 858 ª 2008 The Authors Journal compilation ª RCOG 2008 BJOG An International Journal of Obstetrics and Gynaecology
3 Immediate or delayed repair of sphincter tears retrieved from patient obstetric charts. The manuscript and data presentation are in accordance with the revised CONSORT statement for parallel group randomised trials. 17 Anal incontinence was chosen as the primary outcome variable and defined according to the incontinence score previously described. A power calculation was based on assumed proportions of anal incontinence at three time points in two different groups. The proportions were set at 0.1:0.1, 0.6:0.55 and 0.35:0.15, and then converted to the following Pescatori scores: 0.2:0.2, 1.75:1.5 and 1:0.4. The methodology proposed by Rochon 18 and the SAS macro GEESIZE was then used to perform the sample size calculation. A total of 150 women (75 in each group) were considered sufficient to detect the assumed difference between the two groups at 80% power and a = Group assignment was coded in the database and all statistical analyses were performed blinded until completed. For the descriptive statistics in Table 1, the Student s t test was used for continuous variables whereas Fisher s exact test was used for categorical variables. For pelvic floor symptoms that were ordinal variables and were measured repeatedly at baseline, 6 months and 12 months, we applied a proportional odds model to compare the probabilities of having increasing pelvic floor symptoms between groups and over time. 19 P values for multiple comparisons at different time points were adjusted by the Bonferroni method. Furthermore, for the symptoms of flatus incontinence, inability to discriminate faeces from flatus and faecal urgency, we adjusted for covariates such as age, number of childbirths, fundal pressure, instrument delivery, episiotomy and degree of surgery tear. For continuous variables that were measured repeatedly, such as the Pescatori incontinence score, we applied a linear mixed model with random subject effect to evaluate treatment group and time effects. 20 Time points were treated as discrete variables. We chose an unstructured covariance matrix. P values were adjusted by the Bonferroni method because we performed comparisons at different time points. We used the statistical software package SAS 9.1 (SAS Institute Inc., Cary, NC, USA) for all statistical analyses. The significance level was set at an alpha of Results During the study inclusion period, a total of 7272 women gave birth at Danderyd University Hospital, and 5561 of them delivered vaginally. A third- or fourth-degree obstetric anal sphincter injury was diagnosed in 416 women (7.5%) eligible for participation in the study. After receiving verbal and written information, 165 of the 416 (40%) patients gave their informed consent to participate and were subsequently randomised: 78 subjects to immediate and 87 subjects to delayed repair (Figure 1). Reasons for not participating in the study or not complying with the assigned group following randomisation are presented in the study flowchart (Figure 1). There were no significant differences in pretrial maternal characteristics, delivery characteristics or severity and distribution of anal sphincter injury between the groups (Table 2). Vaginal deliveries during time of study inclusion n=5561 No sphincter tears n=5145 Subjects excluded by clinician* n=56 Grade III-IV sphincter tears n=416 Subjects declining participation n=130 Randomised n=165 Subjects not participating for other reasons** n=65 Answered first n=78 Allocated to immediate repair n=78 Allocated to delayed repair n=87 Answered first n=87 Answered second n=78 Answered third n=71 Answered third n=84 Answered second n=83 Figure 1. CONSORT diagram of patient progress through the trial. Flowchart explains flow of subjects to the two treatment arms and shows the incidence of returned symptom at the three time points. *Exclusion criteria were met. **It is unknown why the subject not was included in the trial. ª 2008 The Authors Journal compilation ª RCOG 2008 BJOG An International Journal of Obstetrics and Gynaecology 859
4 Nordenstam et al. Table 2. Descriptive group statistics Immediate repair (n 5 78) Delayed repair (n 5 87) P value Maternal age * Gestational week Previous vaginal deliveries 0 64 (84.2) 69 (87.3) (14.5) 9 (11.4) 2 1 (1.3) 1 (1.2) Duration of second stage (minutes) Duration of third stage (minutes) Birthweight (g) Fundal pressure 22 (28.2) 33 (38.8) 0.18 Episiotomy 3 (3.9) 10 (11.9) 0.08 Instrumental delivery 21 (26.9) 31 (35.6) 0.24 Degree of anal sphincter injury,50% of EAS 24 (31.2) 12 (14.1) % of EAS 30 (38.9) 43 (50.6) Complete EAS rupture and IAS torn 23 (29.9) 30 (35.3) Wait for surgery ,0.001 (minutes) Time of surgery (minutes) EAS, external anal sphincter; IAS, internal anal sphincter. Values are given as mean SD or n (%). *P value from t test for continuous variable and from Fisher s exact test for categorical variables. At baseline, the degree and frequency of symptoms were similar in the two groups (Table 3). Twenty-six of 165 subjects (15.8%) reported anal incontinence, as defined by an incontinence score of two or higher. There were no significant differences between the study groups when comparing the probability of having increasing symptoms of flatus incontinence, liquid stool incontinence, solid stool incontinence, faecal urgency or the inability to distinguish flatus from faeces (Table 3). There were no significant differences in the adjusted Pescatori incontinence scores between the two study groups (Figure 2). The incontinence score increased between baseline and 6 months and this increase was statistically significant (P < ). This increase remained significant at 12 months (P < 0.001) although symptoms improved slightly between 6 and 12 months (Figure 2). The prevalence of anal incontinence symptoms, at 12 months, in relation to the extent of external anal sphincter injury is presented in Table 4. The Pescatori incontinence score was not significantly associated with the extent of sphincter injury (all three adjusted pairwise P = 1.0). No patient, in either group, had a breakdown of the wound or a wound abscess. When evaluating symptoms of flatus incontinence, inability to discriminate flatus from faeces and faecal urgency with adjustments for the covariates mentioned previously in the statistic analyses section, we did not find a significant difference in the probability of having an increase in any of the symptoms between groups. The increases in symptoms described in Table 3 remained after this multivariate analysis. Additionally, the symptom of faecal urgency now increased significantly between baseline and 6 months (P = 0.01). Age proved to be a predictor for flatus incontinence (P = 0.01), and the inability to discriminate flatus from faeces (P = 0.01) in this patient group. Discussion The most important finding of the present study was that a delayed primary repair of an obstetric anal sphincter injury was not associated with an adverse subjective outcome with regard to symptoms of anal incontinence. Known complications of primary repair after an obstetric anal sphincter tear include infections with abscess formation and wound breakdown, both primary to rectovaginal fistulas and anal incontinence The incidence of perineal wound dehiscence after a third- or fourth-degree obstetric sphincter tear has been reported to occur in up to 10% of cases. 24,25 In the present trial, there were no abscesses, wound breakdowns or rectovaginal fistulas in either of the groups. The fact that all included patients received prophylactic antibiotics may, in part, explain this finding. There are no randomised trials exploring the place of prophylactic antibiotics in the management of obstetric tears of the anal sphincters, 26 and the topic is omitted in the current recommendation from the American College of Obstetricians and Gynaecologists. 27 In this trial, all patients were repaired under optimal conditions in the operating theatre, and it seems probable that this controlled environment at surgery has had a favourable effect on the outcome as well. In the present study all patients, regardless of group randomisation, were operated using an approximation endto-end technique; the study was not designed to compare different operative techniques, but to evaluate whether a time delay between injury and repair is advantageous with regard to anal incontinence symptoms. The experience of physicians performing primary repairs varies, and some may feel inadequately trained to perform an optimal repair. 12,28,29 In cases when the responsible physician feels uncomfortable performing the procedure, our study suggests that delaying the operation until the adequate expertise is in place or up to 12 hours is safe and does not adversely affect anal continence status 1 year after delivery. However, our results do not suggest a benefit in delaying primary repair per se. 860 ª 2008 The Authors Journal compilation ª RCOG 2008 BJOG An International Journal of Obstetrics and Gynaecology
5 Immediate or delayed repair of sphincter tears Table 3. Pelvic floor symptoms at baseline, 6 and 12 months follow up by treatment group Baseline 6 months FU 12 months FU P value* P value Immediate Delayed Immediate Delayed Immediate Delayed Chance of symptoms deteriorating between baseline and 6 months Chance of symptoms deteriorating between baseline and 12 months Chance of symptoms being worse in one group than the other Flatus incontinence n 5 78 n 5 84 n 5 78 n 5 83 n 5 71 n 5 84,0.0001, Never 68 (87.2) 68 (81.0) 32 (41.1) 30 (36.1) 36 (50.7) 48 (57.1),1 per week 6 (7.7) 8 (9.5) 20 (25.6) 31 (37.4) 21 (29.6) 23 (27.4).1 per week 4 (5.1) 7 (8.3) 17 (21.8) 19 (22.9) 8 (11.3) 10 (11.9) Daily 1 (1.2) 9 (11.5) 3 (3.6) 6 (8.4) 3 (3.6) Liquid stool incontinence n 5 78 n 5 84 n 5 78 n 5 83 n 5 72 n Never 77 (98.7) 80 (95.2) 70 (89.7) 78 (94.0) 67 (93.1) 81 (96.4),1 per week 1 (1.3) 4 (4.8) 6 (7.7) 5 (6.0) 4 (5.5) 2 (2.4).1 per week 2 (2.6) 1 (1.4) 1 (1.2) Daily Solid stool incontinence n 5 78 n 5 84 n 5 78 n 5 83 n 5 72 n Never 78 (100) 83 (98.8) 73 (93.6) 79 (95.2) 71 (98.6) 84 (100),1 per week 1 (1.2) 4 (5.13) 3 (3.6).1 per week 1 (1.3) 1 (1.2) 1 (1.4) Daily Faecal urgency n 5 77 n 5 84 n 5 77 n 5 82 n 5 71 n Never 70 (90.9) 78 (92.9) 66 (85.7) 69 (84.2) 61 (85.9) 75 (89.3),1 per week 5 (6.5) 4 (4.8) 6 (7.8) 9 (11.0) 9 (12.7) 5 (5.9).1 per week 2 (2.6) 2 (2.4) 3 (3.9) 4 (4.9) 1 (1.4) 4 (4.8) Daily 2 (2.6) Inability to discriminate n 5 78 n 5 84 n 5 78 n 5 83 n 5 72 n flatus from faeces Never 77 (98.7) 81 (96.4) 71 (91.0) 75 (90.4) 65 (90.3) 75 (89.3),1 per week 1 (1.3) 2 (2.4) 5 (6.4) 6 (7.2) 6 (8.3) 8 (9.5).1 per week 1 (1.2) 2 (2.6) 2 (2.4) 1 (1.4) 1 (1.2) Daily FU, Follow up. (Patients answered the pelvic floor funciton questionaire at baseline, at 6- and at 12 months). Values are given as n (%). The frequency of pelvic floor function disturbances in the two study groups, as described by patients at baseline, 6 and 12 months are given. There is no significant interaction between treatment groups and time. P values of multiple comparisons at different time points are adjusted by the Bonferroni method. ª 2008 The Authors Journal compilation ª RCOG 2008 BJOG An International Journal of Obstetrics and Gynaecology 861
6 Nordenstam et al. Figure 2. Least square means of anal incontinence score according to Pescatori. The diagram shows the adjusted Pescatori score for anal incontinence over time. The dotted line represents the patients randomised to delayed repair whereas the continuous line represents the score for patients operated immediately. Several previous clinical trials have compared the end-toend technique with the overlapping technique, but it remains undecided if one technique is superior to the other. 9,11,12,30 The prevalence of faecal incontinence in this study is similar to these previous trials, emphasising that a meticulously performed operation by a physician of adequate competence likely results in acceptable results with both overlap and endto-end technique of primary repair. The incontinence symptoms worsened between baseline and both 6 and 12 months in both groups in this study. This is in concordance with previous studies. 6,31 Several previous studies, conducted over long time, have shown that symptoms of anal incontinence deteriorate over time. 32,33 However, in the present study, symptoms improved from 6 to 12 months. It is likely, but remains to be seen, that symptoms will deteriorate over additional time. We suggest that evaluation of incontinence symptoms should be delayed until at least 12 months after primary repair. In this study, 15.8% of women reported some degree of anal incontinence before the delivery that resulted in a sphincter tear. Hojberg et al. 34 reported a lower prevalence of 8.6% among women in a cross-sectional study. However, in their study, women at gestational week 16 were asked to answer their, whereas we asked women, while still in the delivery unit, to complete the symptoms. Additionally, only 7.4% of the women had more severe symptoms than incontinence to gas less than 1 per week, or a Pescatori score higher than 2. At 12 months, 39.4% of the women reported anal incontinence, but only 16.6% reported symptoms more severe than incontinence to gas less than 1 per week or a score higher than 2. Other authors have reported similar rates of gas incontinence, but higher rates of faecal incontinence 1 year after primary repair of an obstetric anal sphincter injury. 35,36 We believe that our comparatively low incidence of postpartum faecal incontinence may have several explanations: Vigilance in detecting anal sphincter injuries may be comparatively high at our institution and it is departmental policy that all primary repairs are performed under regional anaesthesia in the operating theatre. Other reports may include patients whose repair was conducted under less optimal conditions, which may affect the outcome. It is also possible that patients who decided to participate in the trial were healthier and more physically fit than the average population, resulting in a quicker return to normal physical activities, which in turn could have a positive effect on pelvic floor status. Previous reports have suggested that the extent of the anal sphincter tear may affect the prevalence of incontinence after primary repair. 37,38 The data presented in this study do not contradict these earlier reports, but no statistically significant difference between the three tear degrees could be shown. However, the effects of more extensive injury to the anal sphincter muscles may progress over time and a delayed onset of anal incontinence symptoms following childbirth is frequently reported. During the study inclusion period, nearly 8% of vaginal deliveries resulted in obstetric anal sphincter injury, an incidence comparable with a previous study from our institution. 6 Studies from other departments have, however, reported significantly lower incidences in the range of %. 39,40 The wide discrepancy in the reported incidence of obstetric anal sphincter injuries may have several explanations. 862 ª 2008 The Authors Journal compilation ª RCOG 2008 BJOG An International Journal of Obstetrics and Gynaecology
7 Immediate or delayed repair of sphincter tears Table 4. Prevalence of anal incontinence in relation to extent of external anal sphincter injury at 12 months follow-up IIIa (<50% injury to EAS) (n 5 36), n (%) IIIb (>50% injury to EAS) (n 5 73), n (%) IIIc (IAS also torn), (n 5 53), n (%) Flatus incontinence Never 22 (66.7) 36 (52.2) 25 (49.0),1/week 8 (24.2) 21 (30.4) 15 (29.4).1/week 3 (9.1) 7 (10.1) 8 (15.7) Daily 5 (7.3) 3 (5.9) Faecal urgency Never 30 (88.2) 58 (84.1) 46 (92.0),1/week 3 (8.8) 8 (11.6) 3 (6.0).1/week 1 (2.9) 3 (4.3) 1 (2.0) Daily Loose stool incontinence Never 32 (94.1) 66 (95.7) 48 (94.1),1/week 1 (2.9) 3 (4.3) 2 (3.9).1/week 1 (2.9) 1 (2.0) Daily Solid stool incontinence Never 33 (97.1) 69 (100) 51 (100),1/week.1/week 1 (2.9) Daily Discriminate flatus from faeces Never 33 (97.1) 60 (86.9) 45 (88.2),1/week 1 (2.9) 8 (11.6) 5 (9.8).1/week 1 (1.5) 1 (2.0) Daily Pescatori score 0.91 (1.36) 0.96 (1.21) 1.22 (1.32) EAS, external anal sphincter. IAS, internal anal sphincter. Total number of frequency for each outcome maybe smaller due to missing values. Degree of injury to EAS estimated at clinical examination. Classification of sphincter tears as proposed by Sultan. The high incidence of external and internal anal sphincter defects demonstrated by ultrasonography, suggest that the true incidence of obstetric anal sphincter tears may often be underreported. 8,41,42 Additionally, many institutions report their frequencies of sphincter injuries as a proportion of the total number of births. Consequently, an institution with high rates of caesarean sections will appear to have lower incidences of sphincter injuries than institutions that perform fewer caesarean sections. We report the percentage of vaginal deliveries that resulted in sphincter tears. Furthermore, the awareness and the recognition of obstetric anal sphincter injuries vary between institutions. Our department has been committed to the detection and treatment of obstetric sphincter complications for an extended period of time. Thus, the diagnostic vigilance of the delivery room team is high. It remains to be decided if maternal age at first time delivery may affect the incidence of third- and fourth-degree tears. Increasing maternal age was positively associated with increased symptoms of flatus incontinence, inability to discriminate flatus from faeces and an increased incontinence score. This finding is consistent with earlier reports. 43 These results suggest that older primiparous women may be more susceptible to developing symptoms following trauma to the anal sphincter complex. Considering the current trend in urban society with increasing maternal age at first delivery, the association between age at delivery and symptoms of anal incontinence need further research. Strengths of our study include the randomised design, the homogenous population characteristics, the minimal loss to follow up and the use of a validated instrument for the measurement of anal incontinence. The high response rate limits the risk for selection and ascertainment bias following randomisation, although one needs to consider the rather large number of subjects eligible for the trial that were not included. It is understandable that a newly delivered woman may hesitate to participate in a study requiring an obstetric tear to be left unsutured for 8 12 hours. We believe this to be the primary reason for eligible subjects to not participate in the trial. Additionally, the attitudes of individual midwives and obstetricians towards the study, as well as caregiver s ª 2008 The Authors Journal compilation ª RCOG 2008 BJOG An International Journal of Obstetrics and Gynaecology 863
8 Nordenstam et al. consideration of personality traits of individual patients, may have affected study inclusion. An additional weakness of this study is the fact that the three surgeons who were involved in the repair of the women in the delayed group did not participate in surgeries of women in the immediate group; it would have been preferred if the same physicians performed the repairs in both groups, but this was not practically possible. However, the three gynaecologists involved in the repairs of the women in the delayed group also performed repairs in the immediate group and the experience of the physicians, measured, as years in specialty, were similar between the groups (Table 1). Conclusion With the limitations of this study in mind, we conclude that there is no benefit or harm, with regards to anal continence, in delaying primary repair up to 12 hours after the delivery. Delaying the repair should thus not be recommended routinely, but can be an alternative in those cases when surgical expertise not is immediately available or when the responsible physician feels uncomfortable performing the repair without the assistance of a more experienced colleague. Contribution to authorship J.N. has carried the main responsibility for acquiring the data and drafting this manuscript. A.M. and J.Z. have collaborated in the conceptualization and the design of this study and also revised the manuscript. D.A. and Z.-z.L. have had the main responsibility for interpreting and analysing the data. Z.-z.L. is responsible for the statistics section and D.A. has contributed to the discussion. A.L., C.J. and B.A. have made contributions in data acquisition and manuscript revisions. All authors have approved the final manuscript. Details of Ethics Approval This study was approved by the Research Ethics Committee at the Karolinska Institutet in April 2001 (D-number ). Funding This research was supported by a grant from the Stockholm County Council. Acknowledgements We thank the staff at the department of Obstetrics and Gynaecology and Anaesthesiology, Danderyd Hospital for working with us to make this study possible. We also thank urotherapist Pia Pries, for managing the patient relations during this study. j References 1 Miner PB Jr. Economic and personal impact of fecal and urinary incontinence. Gastroenterology 2004;126 (Suppl 1):S Melville JL, FanM-Y, Newton K, FennerD.Fecalincontinence inuswomen: a population-based study. Am J Obstet Gynecol 2005;193: Bharucha AE, Zinsmeister AR, Locke GR, Seide BM, McKeon K, Schleck CD, et al. Prevalence and burden of fecal incontinence: a populationbased study in women. Gastroenterology 2005;129: Andrews V, Sultan AH, Thakar R, Jones PW. Risk factors for obstetric anal sphincter injury: a prospective study. Birth 2006;33: Buchhave P, Flatow L, Rydhstroem H, Thorbert G. Risk factors for rupture of the anal sphincter. Eur J Obstet Gynecol Reprod Biol 1999;87: Zetterstrom J, Lopez A, Anzen B, Norman M, Holmstrom B, Mellgren A. Anal sphincter tears at vaginal delivery: risk factors and clinical outcome of primary repair. Obstet Gynecol 1999;94: Groom KM, Paterson-Brown S. Can we improve on the diagnosis of third degree tears? Eur J Obstet Gynecol Reprod Biol 2002;101: Andrews V, Sultan AH, Thakar R, Jones PW. Occult anal sphincter injuries myth or reality? BJOG 2006;113: Fernando RJ, Sultan AH, Kettle C, Radley S, Jones P, O Brien PMS. Repair techniques for obstetric anal sphincter injuries: a randomized controlled trial. Obstet Gynecol 2006;107: Fernando R, Sultan AH, Kettle C, Thakar R, Radley S. Methods of repair for obstetric anal sphincter injury. Cochrane Database Syst Rev 2006; CD Garcia V, Rogers RG, Kim SS, Hall RJ, Kammerer-Doak DN. Primary repair of obstetric anal sphincter laceration: a randomized trial of two surgical techniques. Am J Obstet Gynecol 2005;192: Williams A, Adams EJ, Tincello DG, Alfirevic Z, Walkinshaw SA, Richmond DH. How to repair an anal sphincter injury after vaginal delivery: results of a randomised controlled trial [see comment]. BJOG 2006;113: Sultan AH. Editorial: obstetrical perineal injury and anal incontinence. Clin Risk 1999;5: Pescatori M, Anastasio G, Bottini C, Mentasti A. New grading and scoring for anal incontinence. Evaluation of 335 patients. Dis Colon Rectum 1992;35: Norderval S, Nsubuga D, Bjelke C, Frasunek J, Myklebust I, Vonen B. Anal incontinence after obstetric sphincter tears: incidence in a Norwegian county. Acta Obstet Gynecol Scand 2004;83: Vaizey CJ, Carapeti E, Cahill JA, Kamm MA. Prospective comparison of faecal incontinence grading systems. Gut 1999;44: Moher D, Schulz KF, Altman D, CONSORT Group (Consolidated Standards of Reporting Trials). The CONSORT statement: revised recommendations for improving the quality of reports of parallel-group randomized trials [see comment]. JAMA 2001;285: Rochon J. Application of GEE procedures for sample size calculations in repeated measures experiments. Stat Med 1998;17: McCullagh P. Regression models for ordinal data (with discussion). J R Stat Soc Ser A Stat Soc 1980;42: Verbeke G, Molenberghs G. Linear Mixed Models for Longitudinal Data, 1st edn. New York, USA: Springer Verlag, Pezim ME, Spencer RJ, Stanhope CR, Beart RW Jr, Ready RL, Ilstrup DM. Sphincter repair for fecal incontinence after obstetrical or iatrogenic injury. Dis Colon Rectum 1987;30: Rothenberger DA, Goldberg SM. The management of rectovaginal fistulae. Surg Clin North Am 1983;63: Corman ML. Anal sphincter reconstruction. Surg Clin North Am 1980; 60: Postpartum perineal morbidity after fourth-degree perineal repair. Am J Obstet Gynecol 1993;168: Venkatesh KS, Ramanujam PS, Larson DM, Haywood MA. Anorectal complications of vaginal delivery. Dis Colon Rectum 1989;32: ª 2008 The Authors Journal compilation ª RCOG 2008 BJOG An International Journal of Obstetrics and Gynaecology
9 Immediate or delayed repair of sphincter tears 26 Antibiotic prophylaxis for fourth-degree perineal tear during vaginal birth. Cochrane Database Syst Rev 2005:CD ACOG practice bulletin number 47, October 2003: prophylactic antibiotics in labor and delivery. Obstet Gynecol 2003;102: Fernando RJ, Sultan AH, Radley S, Jones PW, Johanson RB. Management of obstetric anal sphincter injury: a systematic review & national practice survey. BMC Health Serv Res 2002;2:9. 29 Sultan AH, Kamm MA, Hudson CN. Obstetric perineal trauma: an audit of training. J Obstet Gynecol 1995;15: Fitzpatrick M, Behan M, O Connell PR, O Herlihy C. A randomized clinical trial comparing primary overlap with approximation repair of third-degree obstetric tears. Am J Obstet Gynecol 2000;183: Fitzpatrick M, Fynes M, Cassidy M, Behan M, O Connell PR, O Herlihy C. Prospective study of the influence of parity and operative technique on the outcome of primary anal sphincter repair following obstetrical injury. Eur J Obstet Gynecol Reprod Biol 2000;89: Pollack J, Nordenstam J, Brismar S, Lopez A, Altman D, Zetterstrom J. Anal incontinence after vaginal delivery: a five-year prospective cohort study. Obstet Gynecol 2004;104: Fornell EU, Matthiesen L, Sjodahl R, Berg G. Obstetric anal sphincter injury ten years after: subjective and objective long term effects. BJOG 2005;112: Hojberg KE, Salvig JD, Winslow NA, Bek KM, Laurberg S, Secher NJ. Flatus and faecal incontinence: prevalence and risk factors at 16 weeks of gestation. BJOG 2000;107: Williams A. Third-degree perineal tears: risk factors and outcome after primary repair. J Obstet Gynecol 2003;23: Wagenius J, Laurin J. Clinical symptoms after anal sphincter rupture: a retrospective study. Acta Obstet Gynecol Scand 2003;82: Nichols CM, Lamb EH, Ramakrishnan V. Differences in outcomes after third- versus fourth-degree perineal laceration repair: a prospective study. Am J Obstet Gynecol 2005;193:530 4; discussion De Leeuw JW, Vierhout ME, Struijk PC, Hop WC, Wallenburg HC. Anal sphincter damage after vaginal delivery: functional outcome and risk factors for fecal incontinence. Acta Obstet Gynecol Scand 2001;80: Sultan AH, Kamm MA, Hudson CN, Bartram CI. Third degree obstetric anal sphincter tears: risk factors and outcome of primary repair. BMJ 1994;308: Walsh CJ, Mooney EF, Upton GJ, Motson RW. Incidence of third-degree perineal tears in labour and outcome after primary repair. Br J Surg 1996;83: Sultan AH, Kamm MA, Hudson CN, Thomas JM, Bartram CI. Analsphincter disruption during vaginal delivery. N Engl J Med 1993;329: Oberwalder M, Connor J, Wexner SD. Meta-analysis to determine the incidence of obstetric anal sphincter damage. Br J Surg 2003;90: Zetterstrom JP, Lopez A, Anzen B, Dolk A, Norman M, Mellgren A. Anal incontinence after vaginal delivery: a prospective study in primiparous women. Br J Obstet Gynaecol 1999;106: ª 2008 The Authors Journal compilation ª RCOG 2008 BJOG An International Journal of Obstetrics and Gynaecology 865
Anal Sphincter Injuries: Acute Management
 Anal Sphincter Injuries: Acute Management Dr Stephen Jeffery Urogynaecology Consultant Department of Obstetrics & Gynaecology Groote Schuur Hospital Colorectal Surgeons Gynaecologists Gynaecologists Colorectal
Anal Sphincter Injuries: Acute Management Dr Stephen Jeffery Urogynaecology Consultant Department of Obstetrics & Gynaecology Groote Schuur Hospital Colorectal Surgeons Gynaecologists Gynaecologists Colorectal
Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study
 ORIGINAL RESEARCH Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study Johan Pollack, MD, Johan Nordenstam, MD, Sophia Brismar, MD, Annika Lopez, MD, PhD, Daniel Altman, MD, and
ORIGINAL RESEARCH Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study Johan Pollack, MD, Johan Nordenstam, MD, Sophia Brismar, MD, Annika Lopez, MD, PhD, Daniel Altman, MD, and
Appendix B Protocol for management of obstetric anal sphincter injury THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS
 Appendix B Protocol for management of obstetric anal sphincter injury Document Type: THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS PURPOSE & SCOPE To provide a guideline that will assist in
Appendix B Protocol for management of obstetric anal sphincter injury Document Type: THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS PURPOSE & SCOPE To provide a guideline that will assist in
How to repair an anal sphincter injury after vaginal delivery: results of a randomised controlled trial
 DOI: 10.1111/j.1471-0528.2006.00806.x www.blackwellpublishing.com/bjog Intrapartum care How to repair an anal sphincter injury after vaginal delivery: results of a randomised controlled trial Abimbola
DOI: 10.1111/j.1471-0528.2006.00806.x www.blackwellpublishing.com/bjog Intrapartum care How to repair an anal sphincter injury after vaginal delivery: results of a randomised controlled trial Abimbola
Title: A modified surgical approach to women with obstetric anal sphincter tears
 Reviewer's report Title: A modified surgical approach to women with obstetric anal sphincter tears Version: 3 Date: 27 January 2010 Reviewer: Stig S Norderval Reviewer's report: Review on manuscript entitled:
Reviewer's report Title: A modified surgical approach to women with obstetric anal sphincter tears Version: 3 Date: 27 January 2010 Reviewer: Stig S Norderval Reviewer's report: Review on manuscript entitled:
Natural progression of anal incontinence after childbirth
 Int Urogynecol J (2009) 20:1029 1035 DOI 10.1007/s00192-009-0901-2 ORIGINAL ARTICLE Natural progression of anal incontinence after childbirth Johan Nordenstam & Daniel Altman & Sophia Brismar & Jan Zetterström
Int Urogynecol J (2009) 20:1029 1035 DOI 10.1007/s00192-009-0901-2 ORIGINAL ARTICLE Natural progression of anal incontinence after childbirth Johan Nordenstam & Daniel Altman & Sophia Brismar & Jan Zetterström
Obstetric Anal Sphincter Injury. An update on best practices. Objectives
 Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
Obstetric Anal Sphincter Injury- A guideline. Mr David Sim Ms Patricia McStay. Dr Martina Hogan Dept./Division Only: YES-IMWH Directorate Only: NO
 CLINICAL GUIDELINES ID TAG Title: Obstetric Anal Sphincter Injury- A guideline Author: Dr Foteini Verani Designation: Specialist Doctor Speciality / Division: Obstetrics-IMWH Directorate: Acute Services
CLINICAL GUIDELINES ID TAG Title: Obstetric Anal Sphincter Injury- A guideline Author: Dr Foteini Verani Designation: Specialist Doctor Speciality / Division: Obstetrics-IMWH Directorate: Acute Services
Royal College of Obstetricians and Gynaecologists
 Royal College of Obstetricians and Gynaecologists Consent Advice No. 9 June 2010 REPAIR OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS FOLLOWING CHILDBIRTH This is the first edition of this guidance. This
Royal College of Obstetricians and Gynaecologists Consent Advice No. 9 June 2010 REPAIR OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS FOLLOWING CHILDBIRTH This is the first edition of this guidance. This
Occult anal sphincter injuries myth or reality?
 DOI: 10.1111/j.1471-0528.2006.00799.x www.blackwellpublishing.com/bjog Intrapartum care Occult anal sphincter injuries myth or reality? Vasanth Andrews, a Abdul H Sultan, a Ranee Thakar, a Peter W Jones
DOI: 10.1111/j.1471-0528.2006.00799.x www.blackwellpublishing.com/bjog Intrapartum care Occult anal sphincter injuries myth or reality? Vasanth Andrews, a Abdul H Sultan, a Ranee Thakar, a Peter W Jones
Secondary Repair of Third Degree Perineal Tear Leading to Fecal Incontinence in 2 Cases
 CASE REPORT Secondary Repair of Third Degree Perineal Tear Leading to Fecal Incontinence in 2 Cases Vasant Kawade 1 and Abhijit Ambike 2 Professor and Head, Department of OBGY, B.K.L.Walawakarl Rural Medical
CASE REPORT Secondary Repair of Third Degree Perineal Tear Leading to Fecal Incontinence in 2 Cases Vasant Kawade 1 and Abhijit Ambike 2 Professor and Head, Department of OBGY, B.K.L.Walawakarl Rural Medical
OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION
 OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION COLM O HERLIHY, MD Professor and Chair University College Dublin Department of Obstetrics and Gynaecology National Maternity
OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION COLM O HERLIHY, MD Professor and Chair University College Dublin Department of Obstetrics and Gynaecology National Maternity
Risk factors and management of obstetric perineal injury
 Risk factors and management of obstetric perineal injury Ruwan J Fernando Abstract Perineal injury sustained during childbirth is a major aetiological factor in the development of perineal pain, sexual
Risk factors and management of obstetric perineal injury Ruwan J Fernando Abstract Perineal injury sustained during childbirth is a major aetiological factor in the development of perineal pain, sexual
EPISIOTOMY & PERINEAL TEARS Anatomy &Functionality May Dr. Annie Leong MBBS, FRANZCOG, CU
 EPISIOTOMY & PERINEAL TEARS Anatomy &Functionality May 2011 Dr. Annie Leong MBBS, FRANZCOG, CU Restore normal perineal anatomy Achieve good haemostasis Avoid infection and wound breakdown Avoid coital
EPISIOTOMY & PERINEAL TEARS Anatomy &Functionality May 2011 Dr. Annie Leong MBBS, FRANZCOG, CU Restore normal perineal anatomy Achieve good haemostasis Avoid infection and wound breakdown Avoid coital
Vincent Letouzey, MD, PhD
 How to protect the perineum and prevent obstetric perineal trauma Standards of OASIS diagnosis: Primary (clinical) and Secondary (ultrasound) Vincent Letouzey, MD, PhD Obst/Gyne Dept Nîmes University Hospital
How to protect the perineum and prevent obstetric perineal trauma Standards of OASIS diagnosis: Primary (clinical) and Secondary (ultrasound) Vincent Letouzey, MD, PhD Obst/Gyne Dept Nîmes University Hospital
Clinical Guideline for: The Management of Perineal Trauma following Childbirth
 For Use in: By: For: Division responsible for document: Key words: Name of document author: Job title of document author: Name of document author s Line Manager: Job title of author s Line Manager: Supported
For Use in: By: For: Division responsible for document: Key words: Name of document author: Job title of document author: Name of document author s Line Manager: Job title of author s Line Manager: Supported
Third & Fourth Degree Tears guideline (GL926)
 Third & Fourth Degree Tears guideline (GL926) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity Clinical Governance
Third & Fourth Degree Tears guideline (GL926) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity Clinical Governance
Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital
 Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital Capital city of Australia Population 350,000 but surrounding region of 500,000 Seat of government
Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital Capital city of Australia Population 350,000 but surrounding region of 500,000 Seat of government
The Perineal Clinic: - the management of women following OASI
 The Perineal Clinic: - the management of women following OASI Miss Gillian Fowler Consultant Urogynaecologist MBChB, MD, MRCOG Liverpool Women s Hospital. Margie Polden University Memorial of Liverpool
The Perineal Clinic: - the management of women following OASI Miss Gillian Fowler Consultant Urogynaecologist MBChB, MD, MRCOG Liverpool Women s Hospital. Margie Polden University Memorial of Liverpool
anal incontinence; endoanal ultrasonography; grading systems; obstetric sphincter tears; three-dimensional
 Ultrasound Obstet Gynecol 2012; 40: 207 214 Published online in Wiley Online Library (wileyonlinelibrary.com). DOI: 10.1002/uog.10154 Incontinence after primary repair of obstetric anal sphincter tears
Ultrasound Obstet Gynecol 2012; 40: 207 214 Published online in Wiley Online Library (wileyonlinelibrary.com). DOI: 10.1002/uog.10154 Incontinence after primary repair of obstetric anal sphincter tears
Anal incontinence after childbirth is more common than was previously believed. Anal incontinence after childbirth. Methods
 Anal incontinence after childbirth Research Recherche From *the Department of Obstetrics and Gynecology, University of Ottawa, Ottawa, Ont.; the Departments of Family Medicine and Social and Preventive
Anal incontinence after childbirth Research Recherche From *the Department of Obstetrics and Gynecology, University of Ottawa, Ottawa, Ont.; the Departments of Family Medicine and Social and Preventive
Effect of subsequent vaginal delivery on bowel symptoms and anorectal function in women who sustained a previous obstetric anal sphincter injury
 International Urogynecology Journal (2018) 29:1579 1588 https://doi.org/10.1007/s00192-018-3601-y ORIGINAL ARTICLE Effect of subsequent vaginal delivery on bowel symptoms and anorectal function in women
International Urogynecology Journal (2018) 29:1579 1588 https://doi.org/10.1007/s00192-018-3601-y ORIGINAL ARTICLE Effect of subsequent vaginal delivery on bowel symptoms and anorectal function in women
Postpartum Complications
 ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
AN INTERNATIONAL CONTINENCE SOCIETY (ICS) / INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR CHILDBIRTH TRAUMA
 AN INTERNATIONAL CONTINENCE SOCIETY (ICS) / INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR CHILDBIRTH TRAUMA NEED FOR A WORKING GROUP ON CHILDBIRTH TRAUMA A: Background
AN INTERNATIONAL CONTINENCE SOCIETY (ICS) / INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR CHILDBIRTH TRAUMA NEED FOR A WORKING GROUP ON CHILDBIRTH TRAUMA A: Background
Obstetric anal sphincter injury is the most common
 Repair Techniques for Obstetric Anal Sphincter Injuries A Randomized Controlled Trial Ruwan J. Fernando, MD, MRCOG, Abdul H. Sultan, MD, FRCOG, Christine Kettle, PhD, Simon Radley, MD, FRCS, Peter Jones,
Repair Techniques for Obstetric Anal Sphincter Injuries A Randomized Controlled Trial Ruwan J. Fernando, MD, MRCOG, Abdul H. Sultan, MD, FRCOG, Christine Kettle, PhD, Simon Radley, MD, FRCS, Peter Jones,
Faecal incontinence after childbirth
 Britisb Journal of Obstetrics and Gynaecology January 1997, Vol. 104, pp. 4650 Faecal incontinence after childbirth *Christine MacArthur Reader (Maternal and Child Epidemiology), *Debra E. Bick Research
Britisb Journal of Obstetrics and Gynaecology January 1997, Vol. 104, pp. 4650 Faecal incontinence after childbirth *Christine MacArthur Reader (Maternal and Child Epidemiology), *Debra E. Bick Research
Long-term ailments due to anal sphincter rupture caused by delivery - a hidden problem
 Eur. J. Obstet. Gynecol. Reprod. Biol., 27 (1988) 27-32 Elsevier 27 EJO 00556 Long-term ailments due to anal sphincter rupture caused by delivery - a hidden problem Knut Haadem, Sten Ohrlander and G6ran
Eur. J. Obstet. Gynecol. Reprod. Biol., 27 (1988) 27-32 Elsevier 27 EJO 00556 Long-term ailments due to anal sphincter rupture caused by delivery - a hidden problem Knut Haadem, Sten Ohrlander and G6ran
Repair of vaginal tears and episiotomy guidelines
 Repair of vaginal tears and episiotomy guidelines Purpose These guidelines assist practitioners in the repair of vaginal and perineal tears including the reasons for, and the techniques of performing an
Repair of vaginal tears and episiotomy guidelines Purpose These guidelines assist practitioners in the repair of vaginal and perineal tears including the reasons for, and the techniques of performing an
Guideline for Management and Repair of Perineal Trauma
 Guideline for Management and Repair of Perineal Trauma Author: Labour Ward Forum Specialty: Maternity Date Approved: September 2014 Approved by: W&CH Clinical Governance Committee Date for Review: August
Guideline for Management and Repair of Perineal Trauma Author: Labour Ward Forum Specialty: Maternity Date Approved: September 2014 Approved by: W&CH Clinical Governance Committee Date for Review: August
2/5/2016. Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach
 Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach Holly E Richter, PhD, MD, FACOG, FACS J Marion Sims Professor Obstetrics and Gynecology Professor
Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach Holly E Richter, PhD, MD, FACOG, FACS J Marion Sims Professor Obstetrics and Gynecology Professor
Hands-on Workshop. Cape Town, South Africa 3 August Chairpersons
 Hands-on Workshop www.perineum.net Cape Town, South Africa 3 August 2016 Chairpersons Mr Abdul H Sultan, MB.ChB (Natal), MD, FRCOG Consultant Obstetrician & Urogynaecologist Miss Ranee Thakar, MB.BS, MD,
Hands-on Workshop www.perineum.net Cape Town, South Africa 3 August 2016 Chairpersons Mr Abdul H Sultan, MB.ChB (Natal), MD, FRCOG Consultant Obstetrician & Urogynaecologist Miss Ranee Thakar, MB.BS, MD,
Urinary incontinence after obstetric anal sphincter injuries (OASIS) is there a relationship?
 DOI 10.1007/s00192-007-0431-8 ORIGINAL ARTICLE Urinary incontinence after obstetric anal sphincter injuries (OASIS) is there a relationship? Inka Scheer & Vasanth Andrews & Ranee Thakar & Abdul H. Sultan
DOI 10.1007/s00192-007-0431-8 ORIGINAL ARTICLE Urinary incontinence after obstetric anal sphincter injuries (OASIS) is there a relationship? Inka Scheer & Vasanth Andrews & Ranee Thakar & Abdul H. Sultan
period, cesarean delivery is thought to protect against anal incontinence, 3 albeit incompletely. In this study, we investigated anal incontinence
 Obstetrical anal sphincter laceration and anal incontinence 5-10 years after childbirth Emily C. Evers, MPH; Joan L. Blomquist, MD; Kelly C. McDermott, BS; Victoria L. Handa, MD, MHS OBJECTIVE: The purpose
Obstetrical anal sphincter laceration and anal incontinence 5-10 years after childbirth Emily C. Evers, MPH; Joan L. Blomquist, MD; Kelly C. McDermott, BS; Victoria L. Handa, MD, MHS OBJECTIVE: The purpose
A Case of Fecal Incontinence: Medical and Interventional Treatment Options
 A Case of Fecal Incontinence: Medical and Interventional Treatment Options HPI JP is a 69 year-old F with a 12-month history of FI. Her symptoms began after a colonoscopy She has been experiencing passive
A Case of Fecal Incontinence: Medical and Interventional Treatment Options HPI JP is a 69 year-old F with a 12-month history of FI. Her symptoms began after a colonoscopy She has been experiencing passive
Childbirth Trauma & Its Complications 23/ Mr Stergios K. Doumouchtsis
 Mr Stergios K. Doumouchtsis Consultant Obstetrician Gynaecologist & Urogynaecologist Childbirth Trauma & Its Complications Over eighty per cent of women sustain some degree of perineal trauma during childbirth.
Mr Stergios K. Doumouchtsis Consultant Obstetrician Gynaecologist & Urogynaecologist Childbirth Trauma & Its Complications Over eighty per cent of women sustain some degree of perineal trauma during childbirth.
Childbirth after pelvic floor surgery: analysis of Hospital Episode Statistics in England,
 DOI: 10.1111/1471-0528.12076 www.bjog.org Urogynaecology Childbirth after pelvic floor surgery: analysis of Hospital Episode Statistics in England, 2002 2008 A Pradhan, a DG Tincello, b R Kearney a a Department
DOI: 10.1111/1471-0528.12076 www.bjog.org Urogynaecology Childbirth after pelvic floor surgery: analysis of Hospital Episode Statistics in England, 2002 2008 A Pradhan, a DG Tincello, b R Kearney a a Department
Perineal Tears. Obstetrics & Gynaecology Women & Children s Group
 Perineal Tears Obstetrics & Gynaecology Women & Children s Group This leaflet has been designed to give you important information about your condition / procedure, and to answer some common queries that
Perineal Tears Obstetrics & Gynaecology Women & Children s Group This leaflet has been designed to give you important information about your condition / procedure, and to answer some common queries that
(UI Urine incontinence)! " # $% &'! ( ) * " " +, -. &/ !!" # $%& /'0 = ='' &!( )'*(" &%: "## $ "% % &' ( )* .!
 39/0/5: 39//8:! "#/7 / 6 4 3!!" # $%& /'0 -. (SI Stress incontinence) '' &!( )'*("&%!%!" #$ :!*8>4 &'!% = / ;
39/0/5: 39//8:! "#/7 / 6 4 3!!" # $%& /'0 -. (SI Stress incontinence) '' &!( )'*("&%!%!" #$ :!*8>4 &'!% = / ;
Fecal incontinence (FI) is a common symptom, not. Symptoms and Quality of Life in Community Women With Fecal Incontinence
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:1004 1009 Symptoms and Quality of Life in Community Women With Fecal Incontinence ADIL E. BHARUCHA,* ALAN R. ZINSMEISTER, G. RICHARD LOCKE,* CATHY SCHLECK,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:1004 1009 Symptoms and Quality of Life in Community Women With Fecal Incontinence ADIL E. BHARUCHA,* ALAN R. ZINSMEISTER, G. RICHARD LOCKE,* CATHY SCHLECK,
PERINEAL REPAIR: COMPARISON OF SUTURE MATERIALS AND SUTURING TECHNIQUES
 ORIGINAL ARTICLE PERINEAL REPAIR: COMPARISON OF SUTURE MATERIALS AND SUTURING TECHNIQUES FOUZIA PERVEEN, TEHMINA SHABBIR ABSTRACT Objective Study design Place & Duration of study To compare the outcome
ORIGINAL ARTICLE PERINEAL REPAIR: COMPARISON OF SUTURE MATERIALS AND SUTURING TECHNIQUES FOUZIA PERVEEN, TEHMINA SHABBIR ABSTRACT Objective Study design Place & Duration of study To compare the outcome
Midline episiotomy and anal incontinence: retrospective cohort study
 Obstetrics and Gynecology Epidemiology Center, Brigham and Women s Hospital, Harvard Medical School, 221 Longwood Avenue, Boston, MA 02115, Lisa B Signorello study coordinator Bernard L Harlow associate
Obstetrics and Gynecology Epidemiology Center, Brigham and Women s Hospital, Harvard Medical School, 221 Longwood Avenue, Boston, MA 02115, Lisa B Signorello study coordinator Bernard L Harlow associate
Childbirth and prolapse: long-term associations with the symptoms and objective measurement of pelvic organ prolapse
 DOI: 10.1111/1471-0528.12075 www.bjog.org Epidemiology Childbirth and prolapse: long-term associations with the symptoms and objective measurement of pelvic organ prolapse C Glazener, a A Elders, a C MacArthur,
DOI: 10.1111/1471-0528.12075 www.bjog.org Epidemiology Childbirth and prolapse: long-term associations with the symptoms and objective measurement of pelvic organ prolapse C Glazener, a A Elders, a C MacArthur,
K. Jundt 1, I. scheer 2, v. von Bodungen 1, F. Krumbachner 1, K. Friese 1, U. M. Peschers 3
 362 EU Ro PE an JoUR nal of MED I cal RE search Eur J Med Res (2010) 15: 362-366 I. Holzapfel Publishers 2010 WHat HaRM DoEs a second DElIvERy to the PElvIc FlooR? K. Jundt 1, I. scheer 2, v. von Bodungen
362 EU Ro PE an JoUR nal of MED I cal RE search Eur J Med Res (2010) 15: 362-366 I. Holzapfel Publishers 2010 WHat HaRM DoEs a second DElIvERy to the PElvIc FlooR? K. Jundt 1, I. scheer 2, v. von Bodungen
Impact of Delivery Types on Women s Postpartum Sexual Health
 Reproduction & Contraception (2003) 14 (4):237~242 Impact of Delivery Types on Women s Postpartum Sexual Health Huan-ying WANG 1, Xiao-yang XU 2, Zhen-wei YAO 1, Qin ZHOU 1 Key words: postpartum; sexual
Reproduction & Contraception (2003) 14 (4):237~242 Impact of Delivery Types on Women s Postpartum Sexual Health Huan-ying WANG 1, Xiao-yang XU 2, Zhen-wei YAO 1, Qin ZHOU 1 Key words: postpartum; sexual
A scoring system for the assessment of bowel and lower urinary tract symptoms in women
 BJOG: an International Journal of Obstetrics and Gynaecology April 2002, Vol. 109, pp. 424 430 A scoring system for the assessment of bowel and lower urinary tract symptoms in women L. Hiller a, H.D. Bradshaw
BJOG: an International Journal of Obstetrics and Gynaecology April 2002, Vol. 109, pp. 424 430 A scoring system for the assessment of bowel and lower urinary tract symptoms in women L. Hiller a, H.D. Bradshaw
Traumatic injury to the anal sphincter sustained in a thirdor
 Obstetric Anal Sphincter Injuries: A Survey of Clinical Practice Among Canadian Obstetricians Carolyn Best, BSc, MD, FRCSC, Harold P. Drutz, MD, FRCSC, May Alarab, MBChB, MRCOG, MRCPI, MSc Division of
Obstetric Anal Sphincter Injuries: A Survey of Clinical Practice Among Canadian Obstetricians Carolyn Best, BSc, MD, FRCSC, Harold P. Drutz, MD, FRCSC, May Alarab, MBChB, MRCOG, MRCPI, MSc Division of
In healthy young women, anal sphincter tear at
 Risk Factors for Anal Sphincter Tear During Vaginal Delivery Mary P. FitzGerald, MD, Anne M. Weber, MD, MS, Nancy Howden, MD, MS, Geoffrey W. Cundiff, MD, and Mort B. Brown, PhD, for the Pelvic Floor Disorders
Risk Factors for Anal Sphincter Tear During Vaginal Delivery Mary P. FitzGerald, MD, Anne M. Weber, MD, MS, Nancy Howden, MD, MS, Geoffrey W. Cundiff, MD, and Mort B. Brown, PhD, for the Pelvic Floor Disorders
2/25/2013. Speaker Disclosure. Learning Objectives. Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth
 Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth Jaime Sepulveda-Toro MD FACS FACOG Female Pelvic Medicine and Reconstructive Pelvic Surgery South Miami Hospital Speaker
Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth Jaime Sepulveda-Toro MD FACS FACOG Female Pelvic Medicine and Reconstructive Pelvic Surgery South Miami Hospital Speaker
A systematic review of etiological factors for postpartum fecal incontinence
 Acta Obstetricia et Gynecologica. 2010; 89: 302 314 ACTA REVIEW A systematic review of etiological factors for postpartum fecal incontinence ESTHER M.J. BOLS 1,2, ERIK J.M. HENDRIKS 1,2, BARY C.M. BERGHMANS
Acta Obstetricia et Gynecologica. 2010; 89: 302 314 ACTA REVIEW A systematic review of etiological factors for postpartum fecal incontinence ESTHER M.J. BOLS 1,2, ERIK J.M. HENDRIKS 1,2, BARY C.M. BERGHMANS
A retrospective postal survey of women s experiences of physiotherapy management following a third- or fourth-degree perineal tear
 Journal of the Association of Chartered Physiotherapists in Women s Health, Spring 2008, 102, 25 35 CLINICAL PAPER A retrospective postal survey of women s experiences of physiotherapy management following
Journal of the Association of Chartered Physiotherapists in Women s Health, Spring 2008, 102, 25 35 CLINICAL PAPER A retrospective postal survey of women s experiences of physiotherapy management following
Faecal incontinence persisting after childbirth: a 12 year longitudinal
 Author Posting. The Authors 2013. This is the authors version of the work. It is posted here for personal use, not for redistribution. The definitive version was published in British Journal of Obstetrics
Author Posting. The Authors 2013. This is the authors version of the work. It is posted here for personal use, not for redistribution. The definitive version was published in British Journal of Obstetrics
Rectal analgesia for the relief of perineal pain after childbirth: a randomised controlled trial of diclofenac suppositories
 BJOG: an International Journal of Obstetrics and Gynaecology October 2004, Vol. 111, pp. 1059 1064 DOI: 10.1111/j.1471-0528.2004.00156.x Rectal analgesia for the relief of perineal pain after childbirth:
BJOG: an International Journal of Obstetrics and Gynaecology October 2004, Vol. 111, pp. 1059 1064 DOI: 10.1111/j.1471-0528.2004.00156.x Rectal analgesia for the relief of perineal pain after childbirth:
World Journal of Colorectal Surgery
 World Journal of Colorectal Surgery Volume 3, Issue 3 2013 Article 5 Closed Versus Open Lateral Internal Sphincterotomy Technique in Treatment of Anal Fissure Seyed Reza Mousavi Jr Shohada Medical Center,
World Journal of Colorectal Surgery Volume 3, Issue 3 2013 Article 5 Closed Versus Open Lateral Internal Sphincterotomy Technique in Treatment of Anal Fissure Seyed Reza Mousavi Jr Shohada Medical Center,
Perineal and Anal Sphincter Trauma
 Perineal and Anal Sphincter Trauma Abdul H. Sultan, Ranee Thakar and Dee E. Fenner (Eds) Perineal and Anal Sphincter Trauma Diagnosis and Clinical Management Abdul H. Sultan, MB ChB, MD, FRCOG Consultant
Perineal and Anal Sphincter Trauma Abdul H. Sultan, Ranee Thakar and Dee E. Fenner (Eds) Perineal and Anal Sphincter Trauma Diagnosis and Clinical Management Abdul H. Sultan, MB ChB, MD, FRCOG Consultant
Proper analysis in clinical trials: how to report and adjust for missing outcome data
 DOI: 10.1111/1471-0528.12219 www.bjog.org Commentary Proper analysis in clinical trials: how to report and adjust for missing outcome data M Joshi, a, * A Royuela, b,c J Zamora b,c a Centre for Primary
DOI: 10.1111/1471-0528.12219 www.bjog.org Commentary Proper analysis in clinical trials: how to report and adjust for missing outcome data M Joshi, a, * A Royuela, b,c J Zamora b,c a Centre for Primary
Urinary and faecal incontinence following delayed primary repair of obstetric genital fistula
 BJOG: an International Journal of Obstetrics and Gynaecology July 2002, Vol. 109, pp. 828 832 Urinary and faecal incontinence following delayed primary repair of obstetric genital fistula Christine Murray,
BJOG: an International Journal of Obstetrics and Gynaecology July 2002, Vol. 109, pp. 828 832 Urinary and faecal incontinence following delayed primary repair of obstetric genital fistula Christine Murray,
The circumferential obstetric fistula: characteristics, management and outcomes
 DOI: 10.1111/j.1471-0528.2007.01329.x www.blackwellpublishing.com/bjog Short communication The circumferential obstetric fistula: characteristics, management and outcomes A Browning Barhirdar Hamlin Fistula
DOI: 10.1111/j.1471-0528.2007.01329.x www.blackwellpublishing.com/bjog Short communication The circumferential obstetric fistula: characteristics, management and outcomes A Browning Barhirdar Hamlin Fistula
Obstetric anal sphincter injuries: Incidence, risk factors, consequences and prevention
 Obstetric anal sphincter injuries: Incidence, risk factors, consequences and prevention Katariina Laine, MD PhD thesis 2013 Katariina Laine, MD Department of Obstetrics Oslo University Hospital, Ullevål
Obstetric anal sphincter injuries: Incidence, risk factors, consequences and prevention Katariina Laine, MD PhD thesis 2013 Katariina Laine, MD Department of Obstetrics Oslo University Hospital, Ullevål
Papers. Abstract. Introduction. Methods
 Conservative management of persistent postnatal urinary and faecal incontinence: randomised controlled trial Topic: 66;68;159;161 Cathryn M A Glazener, G Peter Herbison, P Don Wilson, Christine MacArthur,
Conservative management of persistent postnatal urinary and faecal incontinence: randomised controlled trial Topic: 66;68;159;161 Cathryn M A Glazener, G Peter Herbison, P Don Wilson, Christine MacArthur,
SUTURING AN EPISIOTOMY/GENITAL LACERATION
 WOMEN AND NEWBORN HEALTH SERVICE CLINICAL GUIDELINES SECTION B : GUIDELINES RELEVANT TO OBSTETRICS AND MIDWIFERY 5 INTRAPARTUM CARE 5.15 PERINEAL REPAIR Authorised by: OGCCU 5.15.1 SUTURING AN EPISIOTOMY/GENITAL
WOMEN AND NEWBORN HEALTH SERVICE CLINICAL GUIDELINES SECTION B : GUIDELINES RELEVANT TO OBSTETRICS AND MIDWIFERY 5 INTRAPARTUM CARE 5.15 PERINEAL REPAIR Authorised by: OGCCU 5.15.1 SUTURING AN EPISIOTOMY/GENITAL
UNDERSTANDING EPISIOTOMY C-SECTION AND RECTOCELE. Our suture portfolio meets all your procedural needs
 UNDERSTANDING EPISIOTOMY C-SECTION AND RECTOCELE Our suture portfolio meets all your procedural needs GYNECOLOGY Episiotomy A surgically planned incision on the perineum and the posterior vaginal wall,
UNDERSTANDING EPISIOTOMY C-SECTION AND RECTOCELE Our suture portfolio meets all your procedural needs GYNECOLOGY Episiotomy A surgically planned incision on the perineum and the posterior vaginal wall,
Care of your Perineum following 3 rd and 4 th degree tears
 Maternity Services Care of your Perineum following 3 rd and 4 th degree tears Introduction This leaflet aims to give you information about the repair and aftercare of the third or fourth degree tear you
Maternity Services Care of your Perineum following 3 rd and 4 th degree tears Introduction This leaflet aims to give you information about the repair and aftercare of the third or fourth degree tear you
THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS
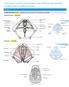 THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS MID2010 LEARNING OBJECTIVE 1 - REVIEW THE ANATOMY OF THE PELVIC FLOOR Superficial layers cavernosus Deep layer Coccygeus
THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS MID2010 LEARNING OBJECTIVE 1 - REVIEW THE ANATOMY OF THE PELVIC FLOOR Superficial layers cavernosus Deep layer Coccygeus
5 DIAGNOSIS. History taking
 5 DIAGNOSIS All of the photographs in Chapter 4 were taken in theatre before operation. This chapter deals with how one can recognize the type of fistula by history taking and examination. (Note that the
5 DIAGNOSIS All of the photographs in Chapter 4 were taken in theatre before operation. This chapter deals with how one can recognize the type of fistula by history taking and examination. (Note that the
Tertiary, regional and local pelvic floor service providers: the future. model? Andrew Williams
 Tertiary, regional and local pelvic floor service providers: the future Andrew Williams model? Pelvic Floor Unit Guy s and St Thomas NHS Foundation Trust Background 23% women suffer at least one pelvic
Tertiary, regional and local pelvic floor service providers: the future Andrew Williams model? Pelvic Floor Unit Guy s and St Thomas NHS Foundation Trust Background 23% women suffer at least one pelvic
Stapled transanal rectal resection for obstructed defaecation syndrome
 Stapled transanal rectal resection for obstructed Issued: June 2010 www.nice.org.uk/ipg351 NHS Evidence has accredited the process used by the NICE Interventional Procedures Programme to produce interventional
Stapled transanal rectal resection for obstructed Issued: June 2010 www.nice.org.uk/ipg351 NHS Evidence has accredited the process used by the NICE Interventional Procedures Programme to produce interventional
Obstetrical Anal Sphincter Injuries (OASIS): Prevention, Recognition, and Repair
 SOGC CLINICAL PRACTICE GUIDELINE No. 330, December 2015 Obstetrical Anal Sphincter Injuries (OASIS): Prevention, Recognition, and Repair This clinical practice guideline has been prepared by the Urogynaecology
SOGC CLINICAL PRACTICE GUIDELINE No. 330, December 2015 Obstetrical Anal Sphincter Injuries (OASIS): Prevention, Recognition, and Repair This clinical practice guideline has been prepared by the Urogynaecology
Do Unsutured Second-Degree Perineal Lacerations Affect Postpartum Functional Outcomes?
 Do Unsutured Second-Degree Perineal Lacerations Affect Postpartum Functional Outcomes? Lawrence M. Leeman, MD, Rebecca G. Rogers, MD, Betsy Greulich, CNM, and Leah L. Albers, DrPH Background: To compare
Do Unsutured Second-Degree Perineal Lacerations Affect Postpartum Functional Outcomes? Lawrence M. Leeman, MD, Rebecca G. Rogers, MD, Betsy Greulich, CNM, and Leah L. Albers, DrPH Background: To compare
Postoperative Care for Pelvic Fistulae. Peter Jeppson, MD October 3, 2017
 Postoperative Care for Pelvic Fistulae Peter Jeppson, MD October 3, 2017 No Disclosures Rational for Postoperative Care Intraoperative injury may be managed by: Identification Closure Continuous post-operative
Postoperative Care for Pelvic Fistulae Peter Jeppson, MD October 3, 2017 No Disclosures Rational for Postoperative Care Intraoperative injury may be managed by: Identification Closure Continuous post-operative
2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL)
 2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No. Service
2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No. Service
for a review under the Accident Compensation Act
 FairWay Resolution Limited Tā te Hinengaro Tōkeke Whakatau Review numbers: Application by for a review under the Accident Compensation Act Held at Date of hearing 2 November 2016, adjourned part-heard;
FairWay Resolution Limited Tā te Hinengaro Tōkeke Whakatau Review numbers: Application by for a review under the Accident Compensation Act Held at Date of hearing 2 November 2016, adjourned part-heard;
NONCLOSURE OF PERITONEUM; A COMPARITIVE TRIAL
 The Professional Medical Journal DOI: 10.29309/TPMJ/18.4404 NONCLOSURE OF PERITONEUM; A COMPARITIVE TRIAL ORIGINAL PROF-4404 1. MBBS, FCPS (Obs/Gyne) 2. MBBS, FCPS (Obs/Gyne) Consultant Gynecologist Razi
The Professional Medical Journal DOI: 10.29309/TPMJ/18.4404 NONCLOSURE OF PERITONEUM; A COMPARITIVE TRIAL ORIGINAL PROF-4404 1. MBBS, FCPS (Obs/Gyne) 2. MBBS, FCPS (Obs/Gyne) Consultant Gynecologist Razi
Episiotomy and obstetric outcomes among women living with type 3 female genital mutilation: a secondary analysis
 Rodriguez et al. Reproductive Health (2016) 13:131 DOI 10.1186/s12978-016-0242-9 RESEARCH Open Access Episiotomy and obstetric outcomes among women living with type 3 female genital mutilation: a secondary
Rodriguez et al. Reproductive Health (2016) 13:131 DOI 10.1186/s12978-016-0242-9 RESEARCH Open Access Episiotomy and obstetric outcomes among women living with type 3 female genital mutilation: a secondary
Consultation Guide: Specialised gynaecology surgery and complex urogynaecology conditions service specifications
 Consultation Guide: Specialised gynaecology surgery and complex urogynaecology conditions service specifications Consultation guide: Specialised gynaecology surgery and complex urogynaecology conditions
Consultation Guide: Specialised gynaecology surgery and complex urogynaecology conditions service specifications Consultation guide: Specialised gynaecology surgery and complex urogynaecology conditions
Repair of Perineal trauma, including 3 rd and 4 th degree tear
 MATERNITY GUIDELINES Repair of Perineal trauma, including 3 rd and 4 th degree tear Navigation Guidance document in the contents page the Press Ctrl on your keyboard and click on a heading to navigate
MATERNITY GUIDELINES Repair of Perineal trauma, including 3 rd and 4 th degree tear Navigation Guidance document in the contents page the Press Ctrl on your keyboard and click on a heading to navigate
The Pelvic Floor: Expecting (and Delivering!) Susan Barr, MD Assistant Professor Saint Louis University Division of Urogynecology
 The Pelvic Floor: What She Can Expect After Expecting (and Delivering!) Susan Barr, MD Assistant Professor Saint Louis University Division of Urogynecology Objectives Understand risk factors and treatment
The Pelvic Floor: What She Can Expect After Expecting (and Delivering!) Susan Barr, MD Assistant Professor Saint Louis University Division of Urogynecology Objectives Understand risk factors and treatment
Maternity Information Leaflet. Care of the Perineum (including Pelvic Floor Exercises) Version 2
 Maternity Information Leaflet Care of the Perineum (including Pelvic Floor Exercises) Version 2 Pelvic Floor Exercises The pelvic floor muscles are located between your legs, and run from your pubic bone
Maternity Information Leaflet Care of the Perineum (including Pelvic Floor Exercises) Version 2 Pelvic Floor Exercises The pelvic floor muscles are located between your legs, and run from your pubic bone
Current status in pelvic organ prolapse surgery: an evidence based review
 Current status in pelvic organ prolapse surgery: an evidence based review Christian Falconer, MD, PhD Department of Obstetrics and Gynecology Danderyd University Hospital Stockholm, Sweden Finnish Society
Current status in pelvic organ prolapse surgery: an evidence based review Christian Falconer, MD, PhD Department of Obstetrics and Gynecology Danderyd University Hospital Stockholm, Sweden Finnish Society
Bowel Disturbances Are the Most Important Risk Factors for Late Onset Fecal Incontinence: A Population-Based Case-Control Study in Women
 GASTROENTEROLOGY 2010;139:1559 1566 Bowel Disturbances Are the Most Important Risk Factors for Late Onset Fecal Incontinence: A Population-Based Case-Control Study in Women ADIL E. BHARUCHA,*, ALAN R.
GASTROENTEROLOGY 2010;139:1559 1566 Bowel Disturbances Are the Most Important Risk Factors for Late Onset Fecal Incontinence: A Population-Based Case-Control Study in Women ADIL E. BHARUCHA,*, ALAN R.
The Prevention of Early-onset Neonatal Group B Streptococcal Disease in UK Obstetric Units
 Royal College of Obstetricians and Gynaecologists and London School of Hygiene and Tropical Medicine The Prevention of Early-onset Neonatal Group B Streptococcal Disease in UK Obstetric Units An audit
Royal College of Obstetricians and Gynaecologists and London School of Hygiene and Tropical Medicine The Prevention of Early-onset Neonatal Group B Streptococcal Disease in UK Obstetric Units An audit
Pregnancy and childbirth: the effects on pelvic floor muscles
 Page 1 of 9 Pregnancy and childbirth: the effects on pelvic floor muscles 26 February, 2009 Stress incontinence can follow childbirth as pelvic floor muscles are damaged AUTHOR Julia Herbert, MSc, MCSP,
Page 1 of 9 Pregnancy and childbirth: the effects on pelvic floor muscles 26 February, 2009 Stress incontinence can follow childbirth as pelvic floor muscles are damaged AUTHOR Julia Herbert, MSc, MCSP,
Post-partum Anal Incontinence in SA: A myth or reality?
 Post-partum Anal Incontinence in SA: A myth or reality? TD Naidoo Consultant and Honorary Lecturer, Department of Obstetrics and Gynaecology, Grey s Hospital, Pietermaritzburg Metropolitan Hospitals Complex,
Post-partum Anal Incontinence in SA: A myth or reality? TD Naidoo Consultant and Honorary Lecturer, Department of Obstetrics and Gynaecology, Grey s Hospital, Pietermaritzburg Metropolitan Hospitals Complex,
A Population-Based Study of Pregnancy and Delivery Characteristics Among Women with Vulvodynia
 Pain Ther (2012) 1:2 DOI 10.1007/s40122-012-0002-7 ORIGINAL RESEARCH A Population-Based Study of Pregnancy and Delivery Characteristics Among Women with Vulvodynia Ruby H. N. Nguyen Elizabeth G. Stewart
Pain Ther (2012) 1:2 DOI 10.1007/s40122-012-0002-7 ORIGINAL RESEARCH A Population-Based Study of Pregnancy and Delivery Characteristics Among Women with Vulvodynia Ruby H. N. Nguyen Elizabeth G. Stewart
Injectable Bulking Agents for the Treatment of Fecal Incontinence. Policy Specific Section: September 27, 2013 January 1, 2015
 Medical Policy Injectable Bulking Agents for the Treatment of Fecal Incontinence Type: Investigational / Experimental Policy Specific Section: Surgery Original Policy Date: Effective Date: September 27,
Medical Policy Injectable Bulking Agents for the Treatment of Fecal Incontinence Type: Investigational / Experimental Policy Specific Section: Surgery Original Policy Date: Effective Date: September 27,
Epidural analgesia and backache: a randomized controlled comparison with intramuscular meperidine for analgesia during labour
 British Journal of Anaesthesia 89 (3): 466-72 (2002) analgesia and backache: a randomized controlled comparison with intramuscular meperidine for analgesia during labour B. A. Loughnan *, F. Carli 2, M.
British Journal of Anaesthesia 89 (3): 466-72 (2002) analgesia and backache: a randomized controlled comparison with intramuscular meperidine for analgesia during labour B. A. Loughnan *, F. Carli 2, M.
Dear Colleagues, EXTENSION OF PAUSE TO THE USE OF VAGINAL MESH
 29/03/2019 NHS Improvement and NHS England Wellington House 133-155 Waterloo Road London SE1 8UG 020 3747 0000 www.england.nhs.uk www.improvement.nhs.uk To: Regional Directors, Trust Medical Directors,
29/03/2019 NHS Improvement and NHS England Wellington House 133-155 Waterloo Road London SE1 8UG 020 3747 0000 www.england.nhs.uk www.improvement.nhs.uk To: Regional Directors, Trust Medical Directors,
Viscous Fluid Retention: A New Method for Evaluating Anorectal Function
 Viscous Fluid Retention: A New Method for Evaluating Anorectal Function Michael Srensen, M.D., Tine Tetzschner, M.D., le 0. Rasmussen, M.D., John Christiansen, M.D. From the Department of Surgery D, Glostrup
Viscous Fluid Retention: A New Method for Evaluating Anorectal Function Michael Srensen, M.D., Tine Tetzschner, M.D., le 0. Rasmussen, M.D., John Christiansen, M.D. From the Department of Surgery D, Glostrup
Mode of delivery and fecal incontinence at midlife: a study of 2,640 women in the Gazel cohort Fritel Xavier
 Mode of delivery and fecal incontinence at midlife: a study of 2,640 women in the Gazel cohort Fritel Xavier 1 *, Ringa Virginie 1, Varnoux Noëlle 1, Zins Marie 2 3, Bréart 1 Gérard 1 Recherches épidémiologiques
Mode of delivery and fecal incontinence at midlife: a study of 2,640 women in the Gazel cohort Fritel Xavier 1 *, Ringa Virginie 1, Varnoux Noëlle 1, Zins Marie 2 3, Bréart 1 Gérard 1 Recherches épidémiologiques
Introduction. A joint report by IUGA and the ICS 1 defines anal incontinence (AI) as the unintentional loss of faeces or flatus.
 TD Naidoo J Moodley Introduction A joint report by IUGA and the ICS 1 defines anal incontinence (AI) as the unintentional loss of faeces or flatus. Faecal incontinence is a complaint of involuntary loss
TD Naidoo J Moodley Introduction A joint report by IUGA and the ICS 1 defines anal incontinence (AI) as the unintentional loss of faeces or flatus. Faecal incontinence is a complaint of involuntary loss
2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL)
 E10d 2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No.
E10d 2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No.
INTERNATIONAL JOURNAL OF WOMEN'S HEALTH AND REPRODUCTION SCIENCES
 Original Article INTERNATIONAL JOURNAL OF WOMEN'S HEALTH AND REPRODUCTION SCIENCES http://www.ijwhr.net Urinary Incontinence During Pregnancy and Postpartum Incidence, Severity and Risk Factors in Alzahra
Original Article INTERNATIONAL JOURNAL OF WOMEN'S HEALTH AND REPRODUCTION SCIENCES http://www.ijwhr.net Urinary Incontinence During Pregnancy and Postpartum Incidence, Severity and Risk Factors in Alzahra
Maternal Mortality in Women with Sickle Cell Disease. Zainab Al-Jufairi, MHPE, FRCOG* Amarjit Sandhu, MD, FRCOG*
 Bahrain Medical Bulletin, Vol. 36, No. 4, December 2014 Maternal Mortality in Women with Sickle Cell Disease Zainab Al-Jufairi, MHPE, FRCOG* Amarjit Sandhu, MD, FRCOG* Background: Sickle cell disease (SCD)
Bahrain Medical Bulletin, Vol. 36, No. 4, December 2014 Maternal Mortality in Women with Sickle Cell Disease Zainab Al-Jufairi, MHPE, FRCOG* Amarjit Sandhu, MD, FRCOG* Background: Sickle cell disease (SCD)
Marietta Mahendeka, M.D. Obstetrician and Gynaecologist Bugando Medical Centre Tanzania. Tutor: Dr Luc de Bernis, WHO
 A COMPARATIVE STUDY OF THE MANAGEMENT OF VESICO AND/OR RECTO-VAGINAL FISTULAE AT BUGANDO MEDICAL CENTRE, MWANZA, TANZANIA, EAST AFRICA: A RETROSPECTIVE STUDY Marietta Mahendeka, M.D. Obstetrician and Gynaecologist
A COMPARATIVE STUDY OF THE MANAGEMENT OF VESICO AND/OR RECTO-VAGINAL FISTULAE AT BUGANDO MEDICAL CENTRE, MWANZA, TANZANIA, EAST AFRICA: A RETROSPECTIVE STUDY Marietta Mahendeka, M.D. Obstetrician and Gynaecologist
Cochrane Pregnancy and Childbirth Group Methodological Guidelines
 Cochrane Pregnancy and Childbirth Group Methodological Guidelines [Prepared by Simon Gates: July 2009, updated July 2012] These guidelines are intended to aid quality and consistency across the reviews
Cochrane Pregnancy and Childbirth Group Methodological Guidelines [Prepared by Simon Gates: July 2009, updated July 2012] These guidelines are intended to aid quality and consistency across the reviews
Approach to the Repair of Chronic Perineal Lacerations and Rectovaginal Fistula (RVF)
 Approach to the Repair of Chronic Perineal Lacerations and Rectovaginal Fistula (RVF) Blair B. Washington MD, MHA Urogynecology & Reconstructive Pelvic Surgery Virginia Mason Medical Center Disclosures
Approach to the Repair of Chronic Perineal Lacerations and Rectovaginal Fistula (RVF) Blair B. Washington MD, MHA Urogynecology & Reconstructive Pelvic Surgery Virginia Mason Medical Center Disclosures
Post - caesarean section pyrexia and its relation of rupture of membranes and prophylactic antibiotics
 MOJ Women s Health Research Article Open Access Post - caesarean section pyrexia and its relation of rupture of membranes and prophylactic antibiotics Abstract Objectives: To determine the incidence of
MOJ Women s Health Research Article Open Access Post - caesarean section pyrexia and its relation of rupture of membranes and prophylactic antibiotics Abstract Objectives: To determine the incidence of
The effect of pregnancy and mode of delivery on the prevalence of urinary and fecal incontinence
 American Journal of Obstetrics and Gynecology (2005) 193, 512 8 www.ajog.org The effect of pregnancy and mode of delivery on the prevalence of urinary and fecal incontinence Vikki McKinnie, MD, a Steven
American Journal of Obstetrics and Gynecology (2005) 193, 512 8 www.ajog.org The effect of pregnancy and mode of delivery on the prevalence of urinary and fecal incontinence Vikki McKinnie, MD, a Steven
Guide to Pelvic Floor Multicompartment Scanning
 Guide to Pelvic Floor Multicompartment Scanning These guidelines have been prepared by Giulio A. Santoro, MD, PhD, Head Pelvic Floor Unit, Section of Anal Physiology and Ultrasound, Coloproctology Service,
Guide to Pelvic Floor Multicompartment Scanning These guidelines have been prepared by Giulio A. Santoro, MD, PhD, Head Pelvic Floor Unit, Section of Anal Physiology and Ultrasound, Coloproctology Service,
Minimally Invasive Hysterectomies: A Survey of Current Practices. amongst members of the International Society for Gynaecologic Endoscopy
 Minimally Invasive Hysterectomies: A Survey of Current Practices amongst members of the International Society for Gynaecologic Endoscopy Abstract Study Objective This study aimed to explore the current
Minimally Invasive Hysterectomies: A Survey of Current Practices amongst members of the International Society for Gynaecologic Endoscopy Abstract Study Objective This study aimed to explore the current
