Published OnlineFirst October 14, 2009; DOI: / CCR
|
|
|
- Linette Blair
- 5 years ago
- Views:
Transcription
1 Published OnlineFirst October 14, 2009; DOI: / CCR Imaging, Diagnosis, Prognosis Lymphocytic Reaction to Colorectal Cancer Is Associated with Longer Survival, Independent of Lymph Node Count, Microsatellite Instability, and CpG Island Methylator Phenotype Shuji Ogino, 1,3,6 Katsuhiko Nosho, 3 Natsumi Irahara, 3 Jeffrey A. Meyerhardt, 3 Yoshifumi Baba, 3 Kaori Shima, 3 Jonathan N. Glickman, 1 Cristina R. Ferrone, 4 Mari Mino-Kenudson, 5 Noriko Tanaka, 7 Glenn Dranoff, 3 Edward L. Giovannucci, 2,6,8 and Charles S. Fuchs 2,3 Abstract Purpose: Host immune response to tumor may be an important prognostic factor for colon cancer patients. However, little is known on prognostic significance of histopathologic lymphoid reaction to tumor, independent of the number of lymph nodes examined and tumoral molecular alterations, including microsatellite instability (MSI) and the CpG island methylator phenotype (CIMP), both of which are associated with lymphocytic reaction and clinical outcome. Experimental Design: Using 843 colorectal cancer patients in two independent prospective cohorts, we examined patient prognosis in relation to four components of lymphocytic reaction (i.e., Crohn's-like reaction, peritumoral reaction, intratumoral periglandular reaction, and tumor-infiltrating lymphocytes) and overall lymphocytic score (0-12). CIMP was determined using eight markers including CACNA1G, CDKN2A (p16), CRABP1, IGF2, MLH1, NEUROG1, RUNX3, and SOCS1. Cox proportional hazard models computed hazard ratio for mortality, adjusted for covariates including tumor stage, body mass index, lymph node count, KRAS, BRAF, p53, cyclooxygenase-2 (PTGS2), MSI, CIMP, and LINE-1 methylation. Results: Increasing overall lymphocytic reaction score including tumor-infiltrating lymphocytes was associated with a significant improvement in colorectal cancer specific and overall survival (log-rank P < 0.003). These findings remained significant (adjusted hazard ratio estimates, ; P trend < 0.009) in multivariate models that adjusted for covariates, including body mass index, MSI, CIMP, LINE-1 hypomethylation, and cyclooxygenase-2. The beneficial effect of tumoral lymphocytic reaction was consistent across strata of clinical, pathologic, and molecular characteristics. Conclusions: Lymphocytic reactions to tumor were associated with improved prognosis among colorectal cancer patients, independent of lymph node count and other clinical, pathologic, and molecular characteristics. (Clin Cancer Res 2009;15(20): ) Authors' Affiliations: 1 Department of Pathology and 2 Channing Laboratory, Department of Medicine, Brigham and Women's Hospital and Harvard Medical School; 3 Department of Medical Oncology, Dana-Farber Cancer Institute and Harvard Medical School; 4 Surgery and 5 Pathology, Massachusetts General Hospital and Harvard Medical School; and 6 Epidemiology, 7 Biostatistics, and 8 Nutrition, Harvard School of Public Health, Boston, Massachusetts Received 6/4/09; revised 6/26/09; accepted 7/15/09; published OnlineFirst 10/13/09. Grant support: U.S. NIH grants P01 CA87969 (S. Hankinson), P01 CA55075 (W. Willett), P50 CA (C.S. Fuchs), and K07 CA (S. Ogino); the Bennett Family Fund; the Entertainment Industry Foundation National Colorectal Cancer Research Alliance; and a fellowship grant from the Japan Society for Promotion of Science (K. Nosho). The content is solely the responsibility of the authors and does not necessarily represent the official views of National Cancer Institute or NIH. Funding agencies did not have any role in the design of the study; the collection, analysis, or interpretation of the data; the decision to submit the manuscript for publication; or the writing of the manuscript. The corresponding author had full access to all of the data and takes full responsibility for the veracity of the data and analysis. The costs of publication of this article were defrayed in part by the payment of page charges. This article must therefore be hereby marked advertisement in accordance with 18 U.S.C. Section 1734 solely to indicate this fact. Note: Supplementary data for this article are available at Clinical Cancer Research Online ( Requests for reprints: Shuji Ogino, Center for Molecular Oncologic Pathology, Dana-Farber Cancer Institute, Brigham and Women's Hospital, Harvard Medical School, Room JF-215C, 44 Binney Street, Boston, MA Phone: ; Fax: ; shuji_ogino@dfci. harvard.edu. F 2009 American Association for Cancer doi: / ccr Clin Cancer Res 2009;15(20) October 15,
2 Published OnlineFirst October 14, 2009; DOI: / CCR Lymphocytic Reaction and Prognosis in Colorectal Cancer Translational Relevance Host immune response to tumor is an important prognostic factor in colorectal cancer. However, little is known on prognostic significance of lymphocytic reaction to tumor, independent of the number of lymph nodes and tumoral molecular alterations (including microsatellite instability and the CpG island methylator phenotype). We have used the database of 843 colorectal cancers in two independent cohort studies, with available clinical information, adequate follow-up, and important molecular events in colon cancers. To our knowledge, this is the first large study to show the influence of lymphocytic reaction on clinical outcome independent of lymph node count and molecular features including BRAF mutation, microsatellite instability, CpG island methylator phenotype, and long interspersed nucleotide element-1 hypomethylation, all of which are potential confounders. Lymphocytic reaction can be readily evaluated in routine pathology practice. Moreover, stimulating host immune response is a promising therapeutic strategy. Thus, our findings are relevant to practice in oncology. Greater lymphocytic reaction to colorectal cancer observed by pathologic examination has been associated with longer patient survival (1 6). However, the true nature of this association and the exact mechanisms underlying it remain uncertain. Lymphocytic reaction may be an indicator of host immune response to tumor cells, leading to improved survival. Specific subsets of infiltrating lymphocytes (e.g., CD57 +,CD8 +, CD45RO +,or FOXP3 + cells) have been associated with improved clinical outcome in colorectal cancer (7 12). In addition, immune reaction to tumor may cause enlargement of lymph nodes, which may contribute to an increase in the number of recovered lymph nodes and thereby more accurate staging of colorectal cancer. In fact, lymphocytic reaction to colorectal cancer has been associated with an increase in the recovered node count (13), which has, in turn, consistently been associated with improved patient survival in colorectal cancer (13 18). Alternatively, lymphocytic reaction to tumor may reflect specific tumoral molecular alterations associated with indolent tumor behavior. Indeed, studies have shown that lymphocytic reaction to colorectal cancer is associated with microsatellite instability (MSI-high; refs ) and the CpG island methylator phenotype (CIMP; ref. 22). Studies have suggested that truncated peptides, which are produced by MSI and frameshift mutations, may be immunogenic and contribute to host immune response (23, 24). Because lymphocytic reaction, lymph node count, MSI, and CIMP have all been associated with prognosis (13 18, 25, 26), all of these variables can confound each other in survival analysis. To assess a prognostic role of lymphocytic reaction independent of lymph node count and tumoral molecular features, it is necessary to examine the lymph node count and tumoral molecular features. We therefore examined the prognostic significance of lymphocytic reaction to tumor in 843 stage I to IV colorectal cancer patients identified in two independent prospective cohort studies. Because we concurrently assessed the number of recovered lymph nodes as well as related molecular variables such as MSI, CIMP, BRAF mutation, and long interspersed nucleotide element-1 (LINE-1) hypomethylation, we could evaluate the effect of lymphocytic reaction to tumor, independent of these potential confounders. Materials and Methods Study population. We used the databases of two independent prospective cohort studies: the Nurses' Health Study (N = 121,701 women followed since 1976) and the Health Professionals Follow-up Study (N = 51,529 men followed since 1986; ref. 27). Every 2 years, participants were sent follow-up questionnaires to identify newly diagnosed cancer in themselves and their first-degree relatives. When a participant reported colorectal cancer, study physicians reviewed medical records as well as recorded tumor-node-metastasis stage, tumor location, and the number of positive and negative lymph nodes. We collected paraffinembedded tissue blocks from hospitals where patients underwent tumor resections (27). We excluded cases preoperatively treated with radiation and/or chemotherapy. Based on the availability of tissue specimens for pathologic analyses, we included a total of 843 stage I to IV colorectal cancer cases diagnosed up to 2002 (Table 1). Patients were observed until death or June 30, 2006, whichever came first. Ascertainment of deaths included reporting by the family or postal authorities. In addition, the names of persistent nonresponders were searched in the National Death Index. We identified >98% of deaths in the cohorts by these methods. The cause of death was assigned by physicians unaware of tumoral pathologic or molecular data. Written informed consent was obtained from all study subjects. This study was approved by the Human Subjects Committees at Brigham and Women's Hospital and the Harvard School of Public Health. Histopathologic evaluations. Tissue sections from all colorectal cancer cases were examined by a pathologist (S.O.) unaware of other data. Of the 843 tumors, 3 tumor tissue blocks were available in 284 cases, 2 in 297 cases, and 1 in the remaining 262 cases. Tumor grade was categorized as high or low ( 50% versus >50% glandular area). Four components of lymphocytic reactions [Crohn's-like lymphoid reaction, peritumoral lymphocytic reaction, intratumoral periglandular reaction, and tumor-infiltrating lymphocytes (TIL)] were examined (Fig. 1). Crohn's-like reaction was defined as transmural lymphoid reaction. Peritumoral lymphocytic reaction was defined as discrete lymphoid reactions surrounding tumor. Intratumoral periglandular reaction was defined as lymphocytic reaction in tumor stroma within tumor mass. TIL was defined as lymphocytes on top of cancer cells. For any given tumor, each of the four lymphocytic reaction components was scored as 0 (absent), 1+ (mild), 2+ (moderate), or 3+ (marked). The overall lymphocytic reaction score (0-12) was the sum of scores for the above four reaction components. Due to a skewed distribution of the lymphocytic scores (Supplementary Table S1), the majority of cases were in the group of scores 0 to 2. Most of them had a score of 2. Thus, the reference group (i.e., low score) was set as those with scores 0 to 2, which provided the robust reference group. We divided non low-score cases into two groups because of a wide range of scores from 3 to 12. We set the cutoff between middle and high groups as 6 versus 7 because it was in the middle of the total score of 12. A random selection of 398 cases were reexamined by a second pathologist (J.N.G.) unaware of other data, and the correlation on the lymphocytic scores between the two pathologists was good (Spearman correlation r =0.65,P < ; κ = 0.55 for score <3 versus 3, P < ). Kappa coefficients between the lymphocytic scores by the two pathologists for additional cutoffs were as follows: 0.49 for <2 versus 2; 0.53 for <4 versus 4; 0.46 for <5 versus 5; 0.50 for <6 versus 6; 0.49 for <7 versus 7; 0.55 for <8 versus 8; 0.57 for <9 versus 9; and 0.47 for <10 versus Clin Cancer Res 2009;15(20) October 15, 2009
3 Imaging, Diagnosis, Prognosis Published OnlineFirst October 14, 2009; DOI: / CCR Table 1. Clinical, pathologic, and molecular features according to lymphocytic reactions to colorectal cancer Clinical or molecular feature All cases, n (%) Overall lymphocytic reaction score,* n (%) P Total, n Sex Male (HPFS) 361 (43) 240 (44) 90 (39) 31 (48) 0.32 Female (NHS) 482 (57) 309 (56) 140 (61) 33 (52) Mean age (y) ± SD 66.3 ± ± ± ± Body mass index (kg/m 2 ) < (84) 425 (83) 185 (85) 53 (87) (16) 90 (17) 33 (15) 8 (13) Family history of colorectal cancer in first-degree relative(s) (-) 637 (76) 411 (75) 178 (77) 48 (75) 0.75 (+) 206 (24) 138 (25) 52 (23) 16 (25) Year of diagnosis Prior to (18) 105 (19) 37 (16) 6 (9.4) (71) 381 (69) 164 (71) 53 (83) (12) 63 (11) 29 (13) 5 (7.8) Tumor location Proximal (cecum to transverse) 381 (45) 206 (38) 131 (57) 44 (69) < Distal colon (splenic flexure to sigmoid) 267 (32) 185 (34) 65 (28) 17 (27) Rectum 195 (23) 158 (29) 34 (15) 3 (4.7) AJCC tumor stage I 187 (22) 129 (24) 44 (19) 14 (22) II 242 (29) 139 (25) 76 (33) 27 (42) III 242 (29) 150 (27) 74 (32) 18 (28) IV 118 (14) 95 (17) 21 (9.1) 2 (3.1) Unknown 54 (6.4) 36 (6.6) 15 (6.5) 3 (4.7) No. of lymph nodes examined (12) 62 (14) 14 (7.3) 4 (7.1) (15) 76 (17) 24 (13) 5 (8.9) (36) 162 (37) 67 (35) 16 (29) (37) 138 (32) 87 (45) 31 (55) No. of negative lymph nodes (19) 99 (23) 27 (14) 5 (8.9) < (18) 92 (21) 25 (13) 8 (14) (33) 138 (32) 70 (36) 15 (27) (30) 109 (25) 70 (36) 28 (50) Tumor grade Low 755 (90) 515 (95) 200 (87) 40 (63) < High 82 (9.8) 28 (5.2) 30 (13) 24 (37) MSI MSI-low/MSS 702 (85) 503 (94) 169 (74) 30 (47) < MSI-high 124 (15) 31 (5.8) 59 (26) 34 (53) CIMP CIMP-low/0 685 (84) 488 (93) 165 (73) 32 (50) < CIMP-high 127 (16) 34 (6.5) 61 (27) 32 (50) Mean LINE-1 methylation (%) ± SD 61.2 ± ± ± ± BRAF mutation (-) 699 (86) 479 (91) 178 (81) 42 (68) < (+) 112 (14) 49 (9.3) 43 (19) 20 (32) KRAS mutation (-) 528 (63) 346 (64) 135 (59) 47 (73) 0.11 (+) 304 (37) 195 (36) 92 (41) 17 (27) p53 expression (-) 471 (57) 271 (50) 150 (66) 50 (78) < (+) 358 (43) 267 (50) 77 (34) 14 (22) COX-2 expression (-) 136 (16) 74 (14) 50 (22) 12 (19) (+) 701 (84) 470 (86) 179 (78) 52 (81) NOTE: Percentages in parentheses indicate the proportion of tumors with a specific clinical, pathologic, or molecular feature in all patients or patients with a specific category of lymphocytic reactions. Abbreviations: HPFS, Health Professionals Follow-up Study; MSS, microsatellite stable; NHS, Nurses' Health Study; AJCC, American Joint Committee on Cancer. *Overall lymphocytic reaction score is the sum of scores for Crohn's-like reaction (0-3), peritumoral reaction (0-3), intratumoral periglandular reaction (0-3), and TIL (0-3). Clin Cancer Res 2009;15(20) October 15,
4 Published OnlineFirst October 14, 2009; DOI: / CCR Lymphocytic Reaction and Prognosis in Colorectal Cancer Fig. 1. Lymphocytic reaction to colorectal cancer and survival of stage I to IV colorectal cancer patients. A, Crohn's-like reaction (open arrowheads) and peritumoral reaction (arrows; original magnification, 20). B, peritumoral reaction (arrows) and intratumoral periglandular reaction (open block arrows; original magnification, 40). C, intratumoral periglandular reaction (open block arrows) and TIL (solid arrowheads; original magnification, 400). D, TIL (solid arrowheads; original magnification, 400). E, Kaplan-Meier curves for colon cancer specific survival (top) and overall survival (bottom) with the numbers of at-risk individuals, according to the overall lymphocytic reaction score (L score). F, smoothing spline plots of HR for colorectal cancer specific mortality (left) and overall mortality (right) according to lymphocytic reaction score (with score 0 as a reference). Hatched lines, 95% confidence interval. Pyrosequencing of KRAS and BRAF and MSI analysis. DNA from paraffin-embedded tissue was extracted, and PCR and pyrosequencing targeted for KRAS codons 12 and 13 (28) and BRAF codon 600 (29) were done. MSI status was determined using microsatellite markers, D2S123, D5S346, D17S250, BAT25, BAT26, BAT40, D18S55, D18S56, D18S67, and D18S487 (i.e., 10-marker panel; ref. 30). MSI-high was defined as the presence of instability in 30% of the markers, and MSI-low/microsatellite stability (MSS) as no or <30% unstable markers. Real-time PCR for CpG island methylation and pyrosequencing to measure LINE-1 methylation. Sodium bisulfite treatment on tumor DNA and subsequent real-time PCR (MethyLight) assays were validated and done as previously described (31). We quantified promoter 6415 Clin Cancer Res 2009;15(20) October 15, 2009
5 Imaging, Diagnosis, Prognosis Published OnlineFirst October 14, 2009; DOI: / CCR methylation in eight CIMP-specific genes (CACNA1G, CDKN2A, CRABP1, IGF2, MLH1, NEUROG1, RUNX3, and SOCS1; refs ). CIMP-high was defined as 6 of 8 methylated promoters using the eight-marker CIMP panel, and CIMP-low/0 as 0 to 5 methylated promoters, according to the previously established criteria (33). To accurately quantify relatively high LINE-1 methylation levels, we used pyrosequencing as previously described (35, 36). Immunohistochemistry for p53 and cyclooxygenase-2. Tissue microarrays were constructed (37). p53 (38) and cyclooxygenase-2 (COX-2) immunohistochemistry was done as previously described (27, 30). Appropriate positive and negative controls were included in each run of immunohistochemistry. All immunohistochemically stained slides were interpreted by a pathologist (S.O.) unaware of other data. A random sample of 118 and 108 tumors were reexamined for p53 and COX-2, respectively, by a second observer (p53 by K.N., and COX-2 by R. Dehari, Kanagawa Cancer Center) unaware of other data, and the concordance between the two observers was substantial (κ = 0.75, P < , for p53; and κ = 0.62, P < , for COX-2). Statistical analysis. All analyses used SAS version 9.1 (SAS Institute) and all P values were two-sided. The χ 2 test was used to assess an association between categorical variables. The ANOVA was done to compare mean age and mean LINE-1 methylation level across the three lymphocytic categories. The κ coefficients were calculated to assess agreements between the two observers for lymphocytic reaction scores and immunohistochemical data. In the analysis of colorectal cancer specific survival, death as a result of colorectal cancer was the primary end point, and deaths as a result of other causes were censored. The Kaplan-Meier method was used to describe the distribution of survival time, and the log-rank test was done. We used stage-matched (stratified) Cox proportional hazard models to calculate hazard ratio (HR) of death according to lymphocytic reaction, adjusted for age at diagnosis (continuous), sex, year of diagnosis (continuous), body mass index ( 30 versus <30 kg/m 2 ), family history of colorectal cancer in any first-degree relative (present versus absent), tumor location (proximal versus distal colon versus rectum), tumor grade (high versus low), negative lymph node count (ordinal categories; 0-3, 4-6, 7-12, and 13), MSI (high versus low/mss), CIMP (high versus low/0), LINE-1 methylation (continuous), KRAS, BRAF, p53, and COX-2. Tumor stage (I, IIA, IIB, IIIA, IIIB, IIIC, IV, unknown) was used as a matching (stratifying) variable (using the strata option in the SAS proc phreg command) to minimize residual confounding; this fine tumor staging also included information on the number of positive lymph nodes. When we included all of the four lymphocytic reaction components (Crohn's-like reaction, peritumoral reaction, periglandular reaction, and TIL) in multivariate Cox models, these four variables were collinear with each other. Spearman correlation coefficients among these four variables are shown in Supplementary Table S2. Thus, we analyzed each of the four components separately in Cox models. In the summary analysis, we used overall lymphocytic reaction score (0-12; the sum of scores for the four components). We classified tumors into three categories [overall reaction score 0-2 (low) versus 3-6 (middle) versus 7-12 (high)]. We examined the possibility of a nonlinear relation between the lymphocytic reaction score and survival, nonparametrically with restricted cubic splines. In addition, we added squared term of lymphocytic score and/or cubic term of lymphocytic score in a multivariate model, and we did not observe any significant improvement in model fitting (all P > 0.5 by likelihood ratio tests). Nonetheless, our data presentations were mainly based on categorized groups according to the lymphocytic score because categorized data were easily understandable. In the Cox regression analyses, the proportionality of hazards assumption was satisfied by evaluating time-dependent variables, which were the cross-product of the ordinal lymphocytic score variable and survival time (P = for colorectal cancer specific survival; P = 0.18 for overall survival). For cases with missing information on the negative lymph node count, we assign a separate ( missing ) indicator variable. For cases with missing information in other categorical covariates [including body mass index (5.8% missing), tumor grade (0.7%), MSI (2.0%), CIMP (3.7%), KRAS (1.3%), BRAF (3.8%), p53 (1.7%), and COX-2 (0.7%)], we included those cases in a majority category to minimize the number of variables in multivariate Cox models. We confirmed that excluding cases with missing information in any of the covariates did not substantially alter the results (data not shown). An interaction was assessed by including the cross product of the ordinal lymphocytic score variable and another variable of interest in a multivariate Cox model, and P values for interaction were conservatively interpreted, considering multiple hypothesis testing. Results Lymphocytic reaction to colorectal cancer. We examined lymphocytic reaction by light microscopy in 843 stage I to IV colorectal cancers identified in the two prospective cohort studies. We scored Crohn's-like reaction, peritumoral reaction, intratumoral periglandular reaction, and TIL as 0 (absent), 1+ (mild), 2+ (moderate), or 3+ (strong). Then, we calculated overall lymphocytic reaction score (0-12) as the sum of scores for the four components. As shown in Table 1, tumors with middle (score 3-6) to high (score 7-12) lymphocytic scores were associated with older age, proximal location, larger negative node count, stages I to III, high tumor grade, MSI-high, CIMP-high, LINE-1 hypermethylation, BRAF mutation, and negative p53 (all P < 0.003). Overall lymphocytic reaction score and colorectal cancer survival. We examined patient survival according to the overall lymphocytic reaction score. There were a total of 373 deaths including 225 colorectal cancer specific deaths. Five-year colorectal cancer specific survival was 73% among patients with a score of 0 to 2, 83% among patients with a score of 3 to 6, and 89% among patients with a score of 7 to 12 (log-rank P < ), and 5-year overall survival was 67% among patients with a score of 0 to 2, 77% for a score of 3 to 6, and 88% for a score of 7 to 12 (logrank P = 0.002; Fig. 1E). We examined the possibility of a nonlinear relation between the lymphocytic reaction score and survival, nonparametrically with restricted cubic splines (Fig. 1F). This flexible method allowed us to examine the relation with survival without any categorization of the lymphocytic reaction score. Increasing lymphocytic reaction score was associated with a progressive decrease in mortality. In multivariate Cox regression analyses, overall lymphocytic reaction score was associated with a significant improvement in colorectal cancer specific and overall survival (P trend = and P trend = 0.002, respectively; Table 2). The attenuation of effect of lymphocytic reaction score on colorectal cancer specific survival in the multivariate analysis was principally due to adjustment for tumor stage. A high lymphocytic reaction score was inversely associated with stage IV (Table 1). No other major confounders were identified. Each lymphocytic reaction component and colorectal cancer survival. We examined patient survival according to each of the four lymphocytic reaction components (Fig. 2). All components of the lymphocytic reactions were associated with improved colorectal cancer specific survival (long-rank P <0.014). We examined the prognostic significance of each component in stage-adjusted and multivariate Cox models (Table 3). Crohn'slike reaction, peritumoral reaction, and periglandular reaction seemed to be associated with long cancer-specific survival in multivariate analysis (P trend < 0.053; Table 3). Clin Cancer Res 2009;15(20) October 15,
6 Published OnlineFirst October 14, 2009; DOI: / CCR Lymphocytic Reaction and Prognosis in Colorectal Cancer Table 2. Lymphocytic reaction score and survival of patients with stage I to IV colorectal cancer Overall Total, lymphocytic n (%) reaction score* Colorectal cancer specific survival Univariate Deaths/ personyears Stagematched Multivariate Univariate Overall survival Deaths/ personyears Stagematched Multivariate 0-2 (low) 549 (65) 175/4,323 1 (reference) 1 (reference) 1 (reference) 268/4,323 1 (reference) 1 (reference) 1 (reference) 3-6 (middle) 230 (27) 43/1, ( ) 0.64 ( ) 0.61 ( ) 88/1, ( ) 0.80 ( ) 0.71 ( ) 7-12 (high) 64 (7.6) 7/ ( ) 0.60 ( ) 0.53 ( ) 17/ ( ) 0.74 ( ) 0.49 ( ) P for trend < NOTE: The multivariate, stage-matched Cox regression model included age, year of diagnosis, sex, family history of colorectal cancer, tumor location, tumor grade, negative lymph node count, KRAS, BRAF, p53, LINE-1 methylation, MSI, and CIMP. Abbreviation: 95% CI, 95% confidence interval. *Overall lymphocytic reaction score is the sum of scores for Crohn's-like reaction (0-3), peritumoral reaction (0-3), intratumoral periglandular reaction (0-3), and TIL (0-3). Stratified analysis of lymphocytic reaction score and survival. We further examined whether the prognostic influence of the lymphocytic reaction score was modified by any of the other patient and tumoral features (Supplementary figure). The prognostic effect of the lymphocytic reaction score was not significantly modified by any of the variables examined (all P interaction > 0.30). Notably, the effect of the lymphocytic reaction score did not significantly differ across tumor stages (P interaction = 0.32) or between the two independent cohort studies (P interaction = 0.73). Fig. 2. Kaplan-Meier survival curves for colon cancer specific survival (left) and overall survival (right) according to each of the four components of lymphocytic reactions to stage I to IV colorectal cancer: Crohn's-like reaction (A), peritumoral reaction (B), intratumoral periglandular reaction (C), and TIL (D) Clin Cancer Res 2009;15(20) October 15, 2009
7 Imaging, Diagnosis, Prognosis Published OnlineFirst October 14, 2009; DOI: / CCR Discussion We examined the prognostic significance of lymphocytic reaction to tumor in a population of stage I to IV colorectal cancer patients who were concurrently assessed for other clinical and molecular predictors of patient outcome. We observed a significant relation between lymphocytic reaction and patient survival, independent of patient characteristics and other related molecular variables including the number of lymph nodes, p53, KRAS, BRAF, MSI, CIMP, and LINE-1 hypomethylation. Although each of the four components of lymphocytic reactions (Crohn's-like reaction, peritumoral reaction, intratumoral periglandular reaction, and TIL) seemed to predict longer survival of patients, the association with survival was most robust when overall lymphocytic score was used. Our results may support the role of the host immune reaction to tumor as an independent prognostic factor among colorectal cancer patients. The four components of lymphocytic reactions can be assessed on routine histopathologic examination of resected colorectal cancer, and an evaluation of these features can be implemented in clinical practice. Our study also supports the use of immune cells as potential cancer treatment. The stimulation of immune response has a number of theoretical advantages over other forms of cancer therapy (1). Immune cells can direct to antigen-expressing tumor cells wherever they are located in the body and can proliferate until all tumor cells are eradicated. Immunologic memory can be generated for surveillance against any tumor recurrence (1). Finally, targeting host immune cells may avoid the emergence of resistance mutations that are commonly observed during targeted treatment against molecules within cancer cells. Examining prognostic and predictive factors is important in cancer research (39 45). Lymphocytic reaction to colorectal cancer has been associated with longer survival in colorectal cancer (2 6, 8). However, the mechanism underlying the survival advantage associated with lymphocytic reaction to tumor remains uncertain. Lymphocytic reaction may be an indicator of host immune response to tumor cells, leading to improved survival (7, 46). In addition, immune response may cause enlargement of lymph nodes, which may contribute to an increase in the recovered lymph node count and thereby more accurate staging of colorectal cancer. In fact, lymphocytic reaction to colorectal cancer has been associated with an increased lymph node count (13), and lymph node count has consistently been associated with improved survival of colorectal cancer patients (13 18). Alternatively, lymphocytic reaction to tumor may reflect specific tumoral molecular alterations associated with indolent tumor behavior. Tumoral lymphocytic reaction has been associated with MSI-high (19, 47), which, in turn, is associated with longer patient survival (25). Recent studies have further shown that MSI-high in colorectal cancer is associated with CIMP, BRAF mutation (33, 48), and high LINE-1 methylation level (35), and all of these factors (MSI, CIMP, BRAF mutation and LINE-1 methylation) have been independently related with prognosis of colon cancer patients (26, 36, 49). Therefore, numerous pathologic and molecular features (lymph node count, MSI, CIMP, BRAF mutation, and LINE-1 methylation) could account for the beneficial effect of lymphocytic reaction to tumor. However, none of the previous studies of lymphocytic reaction and patient survival has comprehensively examined the aforementioned molecular features in colorectal cancer beyond MSI. In our analysis, the benefit associated with higher tumoral Table 3. Lymphocytic reaction component and survival in stage I to IV colorectal cancer Lymphocytic reaction Total, n Colorectal cancer specific survival Overall survival Deaths/ personyears Stagematched Multivariate Deaths/ personyears Stagematched Multivariate Crohn's-like reaction* /4,778 1 (reference) 1 (reference) 292/4,778 1 (reference) 1 (reference) /1, ( ) 0.77 ( ) 61/1, ( ) 0.80 ( ) / ( ) 0.53 ( ) 20/ ( ) 0.51 ( ) P for trend Peritumoral reaction* /292 1 (reference) 1 (reference) 29/292 1 (reference) 1 (reference) /5, ( ) 0.72 ( ) 317/5, ( ) 0.76 ( ) / ( ) 0.38 ( ) 27/ ( ) 0.48 ( ) P for trend Intratumoral periglandular reaction* /231 1 (reference) 1 (reference) 25/231 1 (reference) 1 (reference) /5, ( ) 0.65 ( ) 320/5, ( ) 0.67 ( ) / ( ) 0.37 ( ) 28/ ( ) 0.42 ( ) P for trend TIL* /5,054 1 (reference) 1 (reference) 290/5,054 1 (reference) 1 (reference) / ( ) 0.81 ( ) 51/ ( ) 0.77 ( ) / ( ) 0.72 ( ) 32/ ( ) 0.73 ( ) P for trend NOTE: The multivariate, stage-matched Cox regression model included age, year of diagnosis, sex, family history of colorectal cancer, tumor location, tumor grade, negative lymph node count, KRAS, BRAF, p53, LINE-1 methylation, MSI, CIMP, and each of the lymphocytic reaction components listed in the table. *The score represents reaction as follows: 0 (absent); 1+ (mild); 2+ (moderate); 3+ (strong). Clin Cancer Res 2009;15(20) October 15,
8 Published OnlineFirst October 14, 2009; DOI: / CCR Lymphocytic Reaction and Prognosis in Colorectal Cancer lymphocytic reaction remained significant after adjusting for these various pathologic and molecular features. One unresolved question is whether subtyping of infiltrating lymphocytes provides any additional information beyond histopathologic evaluation of lymphocytic reaction patterns. Previous studies have shown that the presence, degree, or localization of infiltrates by a specific subtype of lymphocytes (e.g., CD57 +,CD8 +, CD45RO +,orfoxp3 + lymphocytes) is associated with patient outcome in colorectal cancer (7 12). In addition, high tumoral expression of chemokine CXCL16 hasbeenassociatedwithtilandgoodprognosis(50).however, none of these studies (7 12, 50) has comprehensively evaluated the distinct histopathologic patterns of lymphocytic infiltrates described in the current study. Moreover, none of the previous studies has examined the potential confounding effect of the number of lymph nodes examined and molecular features of colorectal cancer beyond MSI (i.e., CIMP, BRAF mutation, and LINE-1 methylation). Thus, confounding effect by these variables (lymph node count and tumoral molecular features) cannot be excluded in the previous studies (7 12, 50). Additional studies are necessary to clarify whether lymphocyte subtyping adds any additional or independent prognostic information beyond histopathologic evaluation of lymphocytic reaction patterns. We calculated the lymphocytic reaction score using the four components (i.e., Crohn's-like reaction, peritumoral reaction, intratumoral periglandular reaction, and TIL). TIL seemed to be less significantly associated with patient survival than the other three components. Although using an overall score of the three components yielded similar results (data not shown), the significance and the magnitude of the effect were attenuated. Thus, in this study, we provide the data based on the four components. Nonetheless, utilization of the three components without TIL may represent a potentially reasonable alternative approach. We confirmed the positive relation between lymphocytic reaction and lymph node count, which has been previously reported (13). The recovered lymph node count has consistently been associated with longer survival of colorectal cancer patients (13 18). Our data provide evidence supporting that the recovered node count is influenced by host immune reaction to tumor. Nonetheless, the best effort should be made to recover and examine as many lymph nodes as possible for accurate staging. Additional studies are necessary to assess whether the beneficial prognostic effect of the lymph node count is independent of lymphocytic reaction to tumor. There are limitations in this study. For example, data on cancer treatment were limited. Nonetheless, it is unlikely that chemotherapy use substantially differed according to lymphocytic reactions to tumor because such data were not typically used for treatment decision making. In addition, beyond cause of mortality, data on cancer recurrences were not available in these cohorts. Nonetheless, given that the median survival for metastatic colon cancer was approximately 10 to 12 months during much of the time period of this study, colorectal cancer specific survival should be a reasonable surrogate for cancer-specific outcomes. There are advantages in using the database of the two independent prospective cohort studies, the Nurses' Health Study and the Health Professionals Follow-up Study, to examine prognostic significance of lymphocytic reaction and its interactions with tumoral and host factors. Anthropometric measurements, family history, other clinical information, pathologic and tumor staging data, and tumoral molecular features were prospectively collected blinded to patient outcome. Cohort participants who developed cancer were treated at hospitals throughout the United States, and thus more representative of colorectal cancers in the general U.S. population than patients in a single to several hospitals. There were no demographic difference between cases with tumor tissue analyzed and those without tumor tissue analyzed (27). Lymphocytic reaction to colorectal cancer was examined by the single study pathologist, and a subset of cases were reexamined by a second pathologist for the agreement study. Finally, our rich tumor database enabled us to simultaneously assess pathologic and tumoral molecular features and control for confounding by a number of tumoral molecular alterations. None of the previous studies on lymphocytic reactions and patient outcome has examined as many molecular variables as we did in this study. In summary, our large cohort study suggests that lymphocytic reaction to tumor is associated with longer survival of colorectal cancer patients, independent of other clinical, pathologic, and tumoral molecular characteristics. Our data suggest a possible role of host immune response as an independent prognostic factor in colorectal cancer patients. Future studies are needed to confirm these results as well as to elucidate exact mechanisms by which lymphocytic reaction to tumor affects clinical outcome in colorectal cancer. Disclosure of Potential Conflicts of Interest J.N. Glickman is currently an employee of Caris Diagnostics, Inc., which offers service related to pathologic diagnosis. No other conflicts of interest exist. Acknowledgments We thank the Nurses' Health Study and the Health Professionals Followup Study cohort participants who have generously agreed to provide us with biological specimens and information through responses to questionnaires; hospitals and pathology departments throughout the United States for providing us with tumor tissue materials; and Frank Speizer, Walter Willett, Susan Hankinson, Meir Stampfer, and many other staff members who have implemented and maintained the prospective cohort studies. References 1. Disis ML, Bernhard H, Jaffee EM. Use of tumour-responsive T cells as cancer treatment. Lancet 2009;373: Ohtani H. Focus on TILs: prognostic significance of tumor infiltrating lymphocytes in human colorectal cancer. Cancer Immun 2007;7:4. 3. Pages F, Galon J, Fridman WH. The essential role of the in situ immune reaction in human colorectal cancer. J Leukoc Biol 2008;84: Ropponen KM, Eskelinen MJ, Lipponen PK, Alhava E, Kosma VM. Prognostic value of tumourinfiltrating lymphocytes (TILs) in colorectal cancer. J Pathol 1997;182: Morris M, Platell C, Iacopetta B. Tumor-infiltrating lymphocytes and perforation in colon cancer predict positive response to 5-fluorouracil chemotherapy. Clin Cancer Res 2008;14: Graham DM, Appelman HD. Crohn's-like lymphoid reaction and colorectal carcinoma: a potential histologic prognosticator. Mod Pathol 1990;3: Pages F, Berger A, Camus M, et al. Effector memory T cells, early metastasis, and survival in colorectal cancer. N Engl J Med 2005;353: Coca S, Perez-Piqueras J, Martinez D, et al. The prognostic significance of intratumoral natural 6419 Clin Cancer Res 2009;15(20) October 15, 2009
9 Imaging, Diagnosis, Prognosis Published OnlineFirst October 14, 2009; DOI: / CCR killer cells in patients with colorectal carcinoma. Cancer 1997;79: Chiba T, Ohtani H, Mizoi T, et al. Intraepithelial CD8 + T-cell-count becomes a prognostic factor after a longer follow-up period in human colorectal carcinoma: possible association with suppression of micrometastasis. Br J Cancer 2004; 91: Galon J, Costes A, Sanchez-Cabo F, et al. Type, density, and location of immune cells within human colorectal tumors predict clinical outcome. Science 2006;313: Zlobec I, Terracciano LM, Lugli A. Local recurrence in mismatch repair-proficient colon cancer predicted by an infiltrative tumor border and lack of CD8 + tumor-infiltrating lymphocytes. Clin Cancer Res 2008;14: Salama P, Phillips M, Grieu F, et al. Tumorinfiltrating FOXP3 + T regulatory cells show strong prognostic significance in colorectal cancer. J Clin Oncol 2009;27: George S, Primrose J, Talbot R, et al. Will Rogers revisited: prospective observational study of survival of 3592 patients with colorectal cancer according to number of nodes examined by pathologists. Br J Cancer 2006;95: Goldstein NS. Lymph node recoveries from 2427 pt3 colorectal resection specimens spanning 45 years: recommendations for a minimum number of recovered lymph nodes based on predictive probabilities. Am J Surg Pathol 2002; 26: Le Voyer TE, Sigurdson ER, Hanlon AL, et al. Colon cancer survival is associated with increasing number of lymph nodes analyzed: a secondary survey of intergroup trial INT J Clin Oncol 2003;21: Baxter NN, Virnig DJ, Rothenberger DA, Morris AM, Jessurun J, Virnig BA. Lymph node evaluation in colorectal cancer patients: a population-based study. J Natl Cancer Inst 2005;97: Bui L, Rempel E, Reeson D, Simunovic M. Lymph node counts, rates of positive lymph nodes, and patient survival for colon cancer surgery in Ontario, Canada: a population-based study. J Surg Oncol 2006;93: Chang GJ, Rodriguez-Bigas MA, Skibber JM, Moyer VA. Lymph node evaluation and survival after curative resection of colon cancer: systematic review. J Natl Cancer Inst 2007;99: Alexander J, Watanabe T, Wu TT, Rashid A, Li S, Hamilton SR. Histopathological identification of colon cancer with microsatellite instability. Am J Pathol 2001;158: Shia J, Ellis NA, Paty PB, et al. Value of histopathology in predicting microsatellite instability in hereditary nonpolyposis colorectal cancer and sporadic colorectal cancer. Am J Surg Pathol 2003;27: Jenkins MA, Hayashi S, O'Shea AM, et al. Pathology features in Bethesda guidelines predict colorectal cancer microsatellite instability: a population-based study. Gastroenterology 2007;133: Ogino S, Odze RD, kawasaki T, et al. Correlation of pathologic features with CpG island methylator phenotype (CIMP) by quantitative DNA methylation analysis in colorectal carcinoma. Am J Surg Pathol 2006;30: Schwitalle Y, Kloor M, Eiermann S, et al. Immune response against frameshift-induced neopeptides in HNPCC patients and healthy HNPCC mutation carriers. Gastroenterology 2008;134: Tougeron D, Fauquembergue E, Rouquette A, et al. Tumor-infiltrating lymphocytes in colorectal cancers with microsatellite instability are correlated with the number and spectrum of frameshift mutations. Mod Pathol 2009;22: Popat S, Hubner R, Houlston RS. Systematic review of microsatellite instability and colorectal cancer prognosis. J Clin Oncol 2005;23: Ogino S, Nosho K, Kirkner GJ, et al. CpG island methylator phenotype, microsatellite instability, BRAF mutation and clinical outcome in colon cancer. Gut 2009;58: Chan AT, Ogino S, Fuchs CS. Aspirin and the risk of colorectal cancer in relation to the expression of COX-2. N Engl J Med 2007;356: Ogino S, Kawasaki T, Brahmandam M, et al. Sensitive sequencing method for KRAS mutation detection by pyrosequencing. J Mol Diagn 2005;7: Ogino S, Kawasaki T, Kirkner GJ, Loda M, Fuchs CS. CpG island methylator phenotypelow (CIMP-low) in colorectal cancer: possible associations with male sex and KRAS mutations. J Mol Diagn 2006;8: Ogino S, Brahmandam M, Cantor M, et al. Distinct molecular features of colorectal carcinoma with signet ring cell component and colorectal carcinoma with mucinous component. Mod Pathol 2006;19: Ogino S, kawasaki T, Brahmandam M, et al. Precision and performance characteristics of bisulfite conversion and real-time PCR (Methy- Light) for quantitative DNA methylation analysis. J Mol Diagn 2006;8: Ogino S, Cantor M, Kawasaki T, et al. CpG island methylator phenotype (CIMP) of colorectal cancer is best characterised by quantitative DNA methylation analysis and prospective cohort studies. Gut 2006;55: Ogino S, Kawasaki T, Kirkner GJ, Kraft P, Loda M, Fuchs CS. Evaluation of markers for CpG island methylator phenotype (CIMP) in colorectal cancer by a large population-based sample. J Mol Diagn 2007;9: Weisenberger DJ, Siegmund KD, Campan M, et al. CpG island methylator phenotype underlies sporadic microsatellite instability and is tightly associated with BRAF mutation in colorectal cancer. Nat Genet 2006;38: OginoS,KawasakiT,NoshoK,etal.LINE-1 hypomethylation is inversely associated with microsatellite instability and CpG methylator phenotype in colorectal cancer. Int J Cancer 2008;122: Ogino S, Nosho K, Kirkner GJ, et al. A cohort study of tumoral LINE-1 hypomethylation and prognosis in colon cancer. J Natl Cancer Inst 2008;100: Ogino S, Brahmandam M, kawasaki T, Kirkner GJ, Loda M, Fuchs CS. Combined analysis of COX-2 and p53 expressions reveals synergistic inverse correlations with microsatellite instability and CpG island methylator phenotype in colorectal cancer. Neoplasia 2006;8: Ogino S, kawasaki T, Kirkner GJ, Yamaji T, Loda M, Fuchs CS. Loss of nuclear p27 (CDKN1B/KIP1) in colorectal cancer is correlated with microsatellite instability and CIMP. Mod Pathol 2007; 20: Cheng YW, Pincas H, Bacolod MD, et al. CpG island methylator phenotype associates with low-degree chromosomal abnormalities in colorectal cancer. Clin Cancer Res 2008;14: French AJ, Sargent DJ, Burgart LJ, et al. Prognostic significance of defective mismatch repair and BRAF V600E in patients with colon cancer. Clin Cancer Res 2008;14: Ginty F, Adak S, Can A, et al. The relative distribution of membranous and cytoplasmic met is a prognostic indicator in stage I and II colon cancer. Clin Cancer Res 2008;14: Jorissen RN, Lipton L, Gibbs P, et al. DNA copy-number alterations underlie gene expression differences between microsatellite stable and unstable colorectal cancers. Clin Cancer Res 2008;14: Suehiro Y, Wong CW, Chirieac LR, et al. Epigenetic-genetic interactions in the APC/WNT, RAS/ RAF, and P53 pathways in colorectal carcinoma. Clin Cancer Res 2008;14: Weichert W, Roske A, Niesporek S, et al. Class I histone deacetylase expression has independent prognostic impact in human colorectal cancer: specific role of class I histone deacetylases in vitro and in vivo. Clin Cancer Res 2008;14: Zlobec I, Baker K, Terracciano LM, Lugli A. RHAMM, p21 combined phenotype identifies microsatellite instability-high colorectal cancers with a highly adverse prognosis. Clin Cancer Res 2008;14: Johnson PM, Porter GA, Ricciardi R, Baxter NN. Increasing negative lymph node count is independently associated with improved longterm survival in stage IIIBand IIIC colon cancer. J Clin Oncol 2006;24: Jass JR, Do K-A, Simms LA, et al. Morphology of sporadic colorectal cancer with DNA replication errors. Gut 1998;42: Samowitz W, Albertsen H, Herrick J, et al. Evaluation of a large, population-based sample supports a CpG island methylator phenotype in colon cancer. Gastroenterology 2005;129: Samowitz WS, Sweeney C, Herrick J, et al. Poor survival associated with the BRAF V600E mutation in microsatellite-stable colon cancers. Cancer Res 2005;65: Hojo S, Koizumi K, Tsuneyama K, et al. High-level expression of chemokine CXCL16 by tumor cells correlates with a good prognosis and increased tumor-infiltrating lymphocytes in colorectal cancer. Cancer Res 2007; 67: Clin Cancer Res 2009;15(20) October 15,
10 Published OnlineFirst October 14, 2009; DOI: / CCR Lymphocytic Reaction to Colorectal Cancer Is Associated with Longer Survival, Independent of Lymph Node Count, Microsatellite Instability, and CpG Island Methylator Phenotype Shuji Ogino, Katsuhiko Nosho, Natsumi Irahara, et al. Clin Cancer Res 2009;15: Published OnlineFirst October 14, Updated version Supplementary Material Access the most recent version of this article at: doi: / ccr Access the most recent supplemental material at: Cited articles Citing articles This article cites 50 articles, 19 of which you can access for free at: This article has been cited by 33 HighWire-hosted articles. Access the articles at: alerts Sign up to receive free -alerts related to this article or journal. Reprints and Subscriptions Permissions To order reprints of this article or to subscribe to the journal, contact the AACR Publications Department at To request permission to re-use all or part of this article, use this link Click on "Request Permissions" which will take you to the Copyright Clearance Center's (CCC) Rightslink site.
Clinical and Pathological Significance of Epigenomic Changes in Colorectal Cancer
 Clinical and Pathological Significance of Epigenomic Changes in Colorectal Cancer Shuji Ogino, M.D., Ph.D. Associate Professor of Pathology Harvard Medical School Brigham and Women s Hospital Dana-Farber
Clinical and Pathological Significance of Epigenomic Changes in Colorectal Cancer Shuji Ogino, M.D., Ph.D. Associate Professor of Pathology Harvard Medical School Brigham and Women s Hospital Dana-Farber
The Role of the CpG Island Methylator Phenotype on Survival Outcome in Colon Cancer
 Gut and Liver, Vol. 9, No. 2, March 215, pp. 22-27 ORiginal Article The Role of the CpG Island Methylator Phenotype on Survival Outcome in Colon Cancer Ki Joo Kang*, Byung-Hoon Min, Kyung Ju Ryu, Kyoung-Mee
Gut and Liver, Vol. 9, No. 2, March 215, pp. 22-27 ORiginal Article The Role of the CpG Island Methylator Phenotype on Survival Outcome in Colon Cancer Ki Joo Kang*, Byung-Hoon Min, Kyung Ju Ryu, Kyoung-Mee
Colorectal Cancer Expression of Peroxisome Proliferator-Activated Receptor (PPARG, PPARgamma) Is Associated With Good Prognosis
 GASTROENTEROLOGY 2009;136:1242 1250 Colorectal Cancer Expression of Peroxisome Proliferator-Activated Receptor (PPARG, PPARgamma) Is Associated With Good Prognosis SHUJI OGINO,*,, KAORI SHIMA,* YOSHIFUMI
GASTROENTEROLOGY 2009;136:1242 1250 Colorectal Cancer Expression of Peroxisome Proliferator-Activated Receptor (PPARG, PPARgamma) Is Associated With Good Prognosis SHUJI OGINO,*,, KAORI SHIMA,* YOSHIFUMI
Evaluation of Markers for CpG Island Methylator Phenotype (CIMP) in Colorectal Cancer by a Large Population-Based Sample
 JMD CME Program Journal of Molecular Diagnostics, Vol. 9, No. 3, July 2007 Copyright American Society for Investigative Pathology and the Association for Molecular Pathology DOI: 10.2353/jmoldx.2007.060170
JMD CME Program Journal of Molecular Diagnostics, Vol. 9, No. 3, July 2007 Copyright American Society for Investigative Pathology and the Association for Molecular Pathology DOI: 10.2353/jmoldx.2007.060170
High risk stage II colon cancer
 High risk stage II colon cancer Joel Gingerich, MD, FRCPC Assistant Professor Medical Oncologist University of Manitoba CancerCare Manitoba Disclaimer No conflict of interests 16 October 2010 Overview
High risk stage II colon cancer Joel Gingerich, MD, FRCPC Assistant Professor Medical Oncologist University of Manitoba CancerCare Manitoba Disclaimer No conflict of interests 16 October 2010 Overview
Department of Pathology, Brigham and Women s Hospital, Harvard Medical School, Boston, MA, USA
 & 2008 USCAP, Inc All rights reserved 0893-3952/08 $30.00 www.modernpathology.org CpG island methylator phenotype-low (CIMP-low) colorectal cancer shows not only few methylated CIMP-high-specific CpG islands,
& 2008 USCAP, Inc All rights reserved 0893-3952/08 $30.00 www.modernpathology.org CpG island methylator phenotype-low (CIMP-low) colorectal cancer shows not only few methylated CIMP-high-specific CpG islands,
CpG Island Methylator Phenotype-Low (CIMP-Low) in Colorectal Cancer: Possible Associations with Male Sex and KRAS Mutations
 Journal of Molecular Diagnostics, Vol. 8, No. 5, November 2006 Copyright American Society for Investigative Pathology and the Association for Molecular Pathology DOI: 10.2353/jmoldx.2006.060082 CpG Island
Journal of Molecular Diagnostics, Vol. 8, No. 5, November 2006 Copyright American Society for Investigative Pathology and the Association for Molecular Pathology DOI: 10.2353/jmoldx.2006.060082 CpG Island
Epigenetic profiling of synchronous colorectal neoplasias by quantitative DNA methylation analysis
 & 2006 USCAP, Inc All rights reserved 0893-3952/06 $30.00 www.modernpathology.org Epigenetic profiling of synchronous colorectal neoplasias by quantitative DNA methylation analysis Shuji Ogino 1,2,3, Mohan
& 2006 USCAP, Inc All rights reserved 0893-3952/06 $30.00 www.modernpathology.org Epigenetic profiling of synchronous colorectal neoplasias by quantitative DNA methylation analysis Shuji Ogino 1,2,3, Mohan
COLORECTAL PATHWAY GROUP, MANCHESTER CANCER. Guidelines for the assessment of mismatch. Colorectal Cancer
 COLORECTAL PATHWAY GROUP, MANCHESTER CANCER Guidelines for the assessment of mismatch repair (MMR) status in Colorectal Cancer March 2017 1 Background Mismatch repair (MMR) deficiency is seen in approximately
COLORECTAL PATHWAY GROUP, MANCHESTER CANCER Guidelines for the assessment of mismatch repair (MMR) status in Colorectal Cancer March 2017 1 Background Mismatch repair (MMR) deficiency is seen in approximately
Colorectal cancer Chapelle, J Clin Oncol, 2010
 Colorectal cancer Chapelle, J Clin Oncol, 2010 Early-Stage Colorectal cancer: Microsatellite instability, multigene assay & emerging molecular strategy Asit Paul, MD, PhD 11/24/15 Mr. X: A 50 yo asymptomatic
Colorectal cancer Chapelle, J Clin Oncol, 2010 Early-Stage Colorectal cancer: Microsatellite instability, multigene assay & emerging molecular strategy Asit Paul, MD, PhD 11/24/15 Mr. X: A 50 yo asymptomatic
COLORECTAL PATHWAY GROUP, MANCHESTER CANCER. Guidelines for the assessment of mismatch. Colorectal Cancer
 COLORECTAL PATHWAY GROUP, MANCHESTER CANCER Guidelines for the assessment of mismatch repair (MMR) status in Colorectal Cancer January 2015 1 Background Mismatch repair (MMR) deficiency is seen in approximately
COLORECTAL PATHWAY GROUP, MANCHESTER CANCER Guidelines for the assessment of mismatch repair (MMR) status in Colorectal Cancer January 2015 1 Background Mismatch repair (MMR) deficiency is seen in approximately
WHAT SHOULD WE DO WITH TUMOUR BUDDING IN EARLY COLORECTAL CANCER?
 CANCER STAGING TNM and prognosis in CRC WHAT SHOULD WE DO WITH TUMOUR BUDDING IN EARLY COLORECTAL CANCER? Alessandro Lugli, MD Institute of Pathology University of Bern Switzerland Maastricht, June 19
CANCER STAGING TNM and prognosis in CRC WHAT SHOULD WE DO WITH TUMOUR BUDDING IN EARLY COLORECTAL CANCER? Alessandro Lugli, MD Institute of Pathology University of Bern Switzerland Maastricht, June 19
Lymph node ratio as a prognostic factor in stage III colon cancer
 Lymph node ratio as a prognostic factor in stage III colon cancer Emad Sadaka, Alaa Maria and Mohamed El-Shebiney. Clinical Oncology department, Faculty of Medicine, Tanta University, Egypt alaamaria1@hotmail.com
Lymph node ratio as a prognostic factor in stage III colon cancer Emad Sadaka, Alaa Maria and Mohamed El-Shebiney. Clinical Oncology department, Faculty of Medicine, Tanta University, Egypt alaamaria1@hotmail.com
Aspirin Use, Tumor PIK3CA Mutation, and Colorectal-Cancer Survival
 T h e n e w e ngl a nd j o u r na l o f m e dic i n e original article Aspirin Use, Tumor PIK3CA Mutation, and Colorectal-Cancer Survival Xiaoyun Liao, M.D., Ph.D., Paul Lochhead, M.B., Ch.B., Reiko Nishihara,
T h e n e w e ngl a nd j o u r na l o f m e dic i n e original article Aspirin Use, Tumor PIK3CA Mutation, and Colorectal-Cancer Survival Xiaoyun Liao, M.D., Ph.D., Paul Lochhead, M.B., Ch.B., Reiko Nishihara,
T ranscriptional inactivation by cytosine methylation at
 1000 GASTROINTESTINAL CANCER CpG island methylator phenotype () of colorectal cancer is best characterised by quantitative DNA methylation analysis and prospective cohort studies S Ogino, M Cantor, T Kawasaki,
1000 GASTROINTESTINAL CANCER CpG island methylator phenotype () of colorectal cancer is best characterised by quantitative DNA methylation analysis and prospective cohort studies S Ogino, M Cantor, T Kawasaki,
Colorectal Carcinoma Reporting in 2009
 Colorectal Carcinoma Reporting in 2009 Overview Colorectal carcinoma- new and confusing AJCC TNM issues Wendy L. Frankel, M.D. Vice-Chair and Director of AP Department of Pathology The Ohio State University
Colorectal Carcinoma Reporting in 2009 Overview Colorectal carcinoma- new and confusing AJCC TNM issues Wendy L. Frankel, M.D. Vice-Chair and Director of AP Department of Pathology The Ohio State University
Whether regional lymph nodes evaluation should be equally required for both right and left colon cancer
 /, Vol. 7, No. 37 Whether regional lymph nodes evaluation should be equally required for both right and left colon cancer Xu Guan 1,*, Wei Chen 2,*, Zheng Liu 3,*, Zheng Jiang 3, Hanqing Hu 1, Zhixun Zhao
/, Vol. 7, No. 37 Whether regional lymph nodes evaluation should be equally required for both right and left colon cancer Xu Guan 1,*, Wei Chen 2,*, Zheng Liu 3,*, Zheng Jiang 3, Hanqing Hu 1, Zhixun Zhao
Cancer Programs Practice Profile Reports (CP 3 R) Rapid Quality Reporting System (RQRS)
 O COLON MEASURE SPECIFICATIONS Cancer Programs Practice Profile Reports (CP 3 R) Rapid Quality Reporting System (RQRS) Introduction The Commission on Cancer s (CoC) National Cancer Data Base (NCDB) staff
O COLON MEASURE SPECIFICATIONS Cancer Programs Practice Profile Reports (CP 3 R) Rapid Quality Reporting System (RQRS) Introduction The Commission on Cancer s (CoC) National Cancer Data Base (NCDB) staff
Supplementary Table 1. PIK3CA mutation in colorectal cancer
 Liao X et al. PIK3CA Mutation in Colorectal Cancer. Page 1 Supplementary Table 1. PIK3CA mutation in colorectal cancer Exon Domain Nucleotide change* Amino acid change* cases 9 Helical c.1621t>a p.e541t
Liao X et al. PIK3CA Mutation in Colorectal Cancer. Page 1 Supplementary Table 1. PIK3CA mutation in colorectal cancer Exon Domain Nucleotide change* Amino acid change* cases 9 Helical c.1621t>a p.e541t
Guidelines for the assessment of mismatch repair (MMR) status in Colorectal Cancer
 Guidelines for the assessment of mismatch repair (MMR) status in Colorectal Cancer Start date: May 2015 Review date: April 2018 1 Background Mismatch repair (MMR) deficiency is seen in approximately 15%
Guidelines for the assessment of mismatch repair (MMR) status in Colorectal Cancer Start date: May 2015 Review date: April 2018 1 Background Mismatch repair (MMR) deficiency is seen in approximately 15%
Clinicopathologic Characteristics of Left-Sided Colon Cancers with High Microsatellite Instability
 The Korean Journal of Pathology 29; 43: 428-34 DOI: 1.4132/KoreanJPathol.29.43.5.428 Clinicopathologic Characteristics of Left-Sided Colon Cancers with High Microsatellite Instability Sang Kyum Kim Junjeong
The Korean Journal of Pathology 29; 43: 428-34 DOI: 1.4132/KoreanJPathol.29.43.5.428 Clinicopathologic Characteristics of Left-Sided Colon Cancers with High Microsatellite Instability Sang Kyum Kim Junjeong
ORIGINAL ARTICLE. and treatment of patients
 ONLINE FIRST ORIGINAL ARTICLE Predictors of Lymph Node Count in Colorectal Cancer Resections Data From US Nationwide Prospective Cohort Studies Teppei Morikawa, MD, PhD; Noriko Tanaka, PhD; Aya Kuchiba,
ONLINE FIRST ORIGINAL ARTICLE Predictors of Lymph Node Count in Colorectal Cancer Resections Data From US Nationwide Prospective Cohort Studies Teppei Morikawa, MD, PhD; Noriko Tanaka, PhD; Aya Kuchiba,
Early colorectal cancer Quality and rules for a good pathology report Histoprognostic factors
 Early colorectal cancer Quality and rules for a good pathology report Histoprognostic factors Frédéric Bibeau, MD, PhD Pathology department Biopathology unit Institut du Cancer de Montpellier France Quality
Early colorectal cancer Quality and rules for a good pathology report Histoprognostic factors Frédéric Bibeau, MD, PhD Pathology department Biopathology unit Institut du Cancer de Montpellier France Quality
Serrated Polyps and a Classification of Colorectal Cancer
 Serrated Polyps and a Classification of Colorectal Cancer Ian Chandler June 2011 Structure Serrated polyps and cancer Molecular biology The Jass classification The familiar but oversimplified Vogelsteingram
Serrated Polyps and a Classification of Colorectal Cancer Ian Chandler June 2011 Structure Serrated polyps and cancer Molecular biology The Jass classification The familiar but oversimplified Vogelsteingram
Clinicopathologic Factors Identify Sporadic Mismatch Repair Defective Colon Cancers
 Anatomic Pathology / MORPHOLOGY IN MMR-DEFECTIVE COLON CANCER Clinicopathologic Factors Identify Sporadic Mismatch Repair Defective Colon Cancers Britta Halvarsson, MD, PhD, 1 Harald Anderson, PhD, 2 Katarina
Anatomic Pathology / MORPHOLOGY IN MMR-DEFECTIVE COLON CANCER Clinicopathologic Factors Identify Sporadic Mismatch Repair Defective Colon Cancers Britta Halvarsson, MD, PhD, 1 Harald Anderson, PhD, 2 Katarina
BRAF Testing In The Elderly: Same As in Younger Patients?
 EGFR, K-RAS, K BRAF Testing In The Elderly: Same As in Younger Patients? Nadine Jackson McCleary MD MPH Gastrointestinal Oncology Dana-Farber/Harvard Cancer Care Boston, MA, USA Outline Colorectal cancer
EGFR, K-RAS, K BRAF Testing In The Elderly: Same As in Younger Patients? Nadine Jackson McCleary MD MPH Gastrointestinal Oncology Dana-Farber/Harvard Cancer Care Boston, MA, USA Outline Colorectal cancer
General Session 7: Controversies in Screening and Surveillance in Colorectal Cancer
 General Session 7: Controversies in Screening and Surveillance in Colorectal Cancer Complexities of Pathological Assessment: Serrated Polyps/Adenomas Carolyn Compton, MD, PhD Professor of Life Sciences,
General Session 7: Controversies in Screening and Surveillance in Colorectal Cancer Complexities of Pathological Assessment: Serrated Polyps/Adenomas Carolyn Compton, MD, PhD Professor of Life Sciences,
DNMT3B Expression Might Contribute to CpG Island Methylator Phenotype in Colorectal Cancer
 Human Cancer Biology DNMT3B Expression Might Contribute to CpG Island Methylator Phenotype in Colorectal Cancer Katsuhiko Nosho, 1 Kaori Shima, 1 Natsumi Irahara, 1 Shoko Kure, 1 Yoshifumi Baba, 1 Gregory
Human Cancer Biology DNMT3B Expression Might Contribute to CpG Island Methylator Phenotype in Colorectal Cancer Katsuhiko Nosho, 1 Kaori Shima, 1 Natsumi Irahara, 1 Shoko Kure, 1 Yoshifumi Baba, 1 Gregory
What Pathology can tell us in the approach of localized colorectal cancer
 What Pathology can tell us in the approach of localized colorectal cancer A/Prof Tony Lim Kiat Hon Department of Anatomical Pathology Singapore General Hospital ESMO 2017 Singapore Nov 1 2 Do we still
What Pathology can tell us in the approach of localized colorectal cancer A/Prof Tony Lim Kiat Hon Department of Anatomical Pathology Singapore General Hospital ESMO 2017 Singapore Nov 1 2 Do we still
Anatomic Molecular Pathology: An Emerging Field
 Anatomic Molecular Pathology: An Emerging Field Antonia R. Sepulveda M.D., Ph.D. University of Pennsylvania asepu@mail.med.upenn.edu 2008 ASIP Annual Meeting Anatomic pathology (U.S.) is a medical specialty
Anatomic Molecular Pathology: An Emerging Field Antonia R. Sepulveda M.D., Ph.D. University of Pennsylvania asepu@mail.med.upenn.edu 2008 ASIP Annual Meeting Anatomic pathology (U.S.) is a medical specialty
CpG islands are DNA segments of at least 0.5 kb in size,
 Four Molecular Subtypes of Colorectal Cancer and Their Precursor Lesions Gyeong Hoon Kang, MD N Context. In addition to chromosomal instability and microsatellite instability (MSI), a third pathway, epigenetic
Four Molecular Subtypes of Colorectal Cancer and Their Precursor Lesions Gyeong Hoon Kang, MD N Context. In addition to chromosomal instability and microsatellite instability (MSI), a third pathway, epigenetic
Disclosures. Outline. What IS tumor budding?? Tumor Budding in Colorectal Carcinoma: What, Why, and How. I have nothing to disclose
 Tumor Budding in Colorectal Carcinoma: What, Why, and How Disclosures I have nothing to disclose Soo-Jin Cho, MD, PhD Assistant Professor UCSF Dept of Pathology Current Issues in Anatomic Pathology 2017
Tumor Budding in Colorectal Carcinoma: What, Why, and How Disclosures I have nothing to disclose Soo-Jin Cho, MD, PhD Assistant Professor UCSF Dept of Pathology Current Issues in Anatomic Pathology 2017
Development of Carcinoma Pathways
 The Construction of Genetic Pathway to Colorectal Cancer Moriah Wright, MD Clinical Fellow in Colorectal Surgery Creighton University School of Medicine Management of Colon and Diseases February 23, 2019
The Construction of Genetic Pathway to Colorectal Cancer Moriah Wright, MD Clinical Fellow in Colorectal Surgery Creighton University School of Medicine Management of Colon and Diseases February 23, 2019
Peritoneal Involvement in Stage II Colon Cancer
 Anatomic Pathology / PERITONEAL INVOLVEMENT IN STAGE II COLON CANCER Peritoneal Involvement in Stage II Colon Cancer A.M. Lennon, MB, MRCPI, H.E. Mulcahy, MD, MRCPI, J.M.P. Hyland, MCh, FRCS, FRCSI, C.
Anatomic Pathology / PERITONEAL INVOLVEMENT IN STAGE II COLON CANCER Peritoneal Involvement in Stage II Colon Cancer A.M. Lennon, MB, MRCPI, H.E. Mulcahy, MD, MRCPI, J.M.P. Hyland, MCh, FRCS, FRCSI, C.
Lynch Syndrome Screening for Endometrial Cancer: Basic Concepts 1/16/2017
 1 Hi, my name is Sarah Kerr. I m a pathologist at Mayo Clinic, where I participate in our high volume Lynch syndrome tumor testing practice. Today I hope to cover some of the basics needed to understand
1 Hi, my name is Sarah Kerr. I m a pathologist at Mayo Clinic, where I participate in our high volume Lynch syndrome tumor testing practice. Today I hope to cover some of the basics needed to understand
A Review from the Genetic Counselor s Perspective
 : A Review from the Genetic Counselor s Perspective Erin Sutcliffe, MS, CGC Certified Genetic Counselor Cancer Risk Evaluation Program INTRODUCTION Errors in base pair matching that occur during DNA replication,
: A Review from the Genetic Counselor s Perspective Erin Sutcliffe, MS, CGC Certified Genetic Counselor Cancer Risk Evaluation Program INTRODUCTION Errors in base pair matching that occur during DNA replication,
Only Estrogen receptor positive is not enough to predict the prognosis of breast cancer
 Young Investigator Award, Global Breast Cancer Conference 2018 Only Estrogen receptor positive is not enough to predict the prognosis of breast cancer ㅑ Running head: Revisiting estrogen positive tumors
Young Investigator Award, Global Breast Cancer Conference 2018 Only Estrogen receptor positive is not enough to predict the prognosis of breast cancer ㅑ Running head: Revisiting estrogen positive tumors
Molecular Pathological Epidemiology (MPE): Novel Integrative Pathology Science (9/24/ min)
 Molecular Pathological Epidemiology (MPE): Novel Integrative Pathology Science (9/24/12. 50 min) Shuji Ogino, MD, PhD, MS (Epidemiology) Associate Professor of Pathology Harvard Medical School Dana-Farber
Molecular Pathological Epidemiology (MPE): Novel Integrative Pathology Science (9/24/12. 50 min) Shuji Ogino, MD, PhD, MS (Epidemiology) Associate Professor of Pathology Harvard Medical School Dana-Farber
LOINC. Clinical information. RCPA code. Record if different to report header Operating surgeon name and contact details. Absent.
 Complete as narrative or use the structured format below 55752-0 17.02.28593 Clinical information 22027-7 17.02.30001 Record if different to report header Operating surgeon name and contact details 52101004
Complete as narrative or use the structured format below 55752-0 17.02.28593 Clinical information 22027-7 17.02.30001 Record if different to report header Operating surgeon name and contact details 52101004
Prospective Study of Family History and Colorectal Cancer
 DOI:10.1093/jnci/djs482 Advance Access publication November 21, 2012 The Author 2012. Published by Oxford University Press. All rights reserved. For Permissions, please e-mail: journals.permissions@oup.com.
DOI:10.1093/jnci/djs482 Advance Access publication November 21, 2012 The Author 2012. Published by Oxford University Press. All rights reserved. For Permissions, please e-mail: journals.permissions@oup.com.
Colorectal Cancer Structured Pathology Reporting Proforma DD MM YYYY
 Colorectal Cancer Structured Pathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.03). Family name Given name(s) Date of birth DD MM YYYY S1.02 Clinical details
Colorectal Cancer Structured Pathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.03). Family name Given name(s) Date of birth DD MM YYYY S1.02 Clinical details
Mismatch repair status, inflammation and outcome in patients with primary operable colorectal cancer
 Mismatch repair status, inflammation and outcome in patients with primary operable colorectal cancer Park JH, Powell AG, Roxburgh CSD, Richards CH, Horgan PG, McMillan DC, Edwards J James Park Clinical
Mismatch repair status, inflammation and outcome in patients with primary operable colorectal cancer Park JH, Powell AG, Roxburgh CSD, Richards CH, Horgan PG, McMillan DC, Edwards J James Park Clinical
Measure Description. Denominator Statement
 CMS ID/CMS QCDR ID: CAP 18 Title: Mismatch Repair (MMR) or Microsatellite Instability (MSI) Biomarker Testing to Inform Clinical Management and Treatment Decisions in Patients with Primary or Metastatic
CMS ID/CMS QCDR ID: CAP 18 Title: Mismatch Repair (MMR) or Microsatellite Instability (MSI) Biomarker Testing to Inform Clinical Management and Treatment Decisions in Patients with Primary or Metastatic
Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers
 日大医誌 75 (1): 10 15 (2016) 10 Original Article Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers Naotaka Uchida 1), Yasuki Matsui 1), Takeshi Notsu 1) and Manabu
日大医誌 75 (1): 10 15 (2016) 10 Original Article Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers Naotaka Uchida 1), Yasuki Matsui 1), Takeshi Notsu 1) and Manabu
Microsatellite instability and other molecular markers: how useful are they?
 Microsatellite instability and other molecular markers: how useful are they? Pr Frédéric Bibeau, MD, PhD Head, Pathology department CHU de Caen, Normandy University, France ESMO preceptorship, Barcelona,
Microsatellite instability and other molecular markers: how useful are they? Pr Frédéric Bibeau, MD, PhD Head, Pathology department CHU de Caen, Normandy University, France ESMO preceptorship, Barcelona,
Immunotherapy in Colorectal cancer
 Immunotherapy in Colorectal cancer Ahmed Zakari, MD Associate Professor University of Central Florida, College of Medicine Medical Director, Gastro Intestinal Cancer Program Florida Hospital Cancer Institute
Immunotherapy in Colorectal cancer Ahmed Zakari, MD Associate Professor University of Central Florida, College of Medicine Medical Director, Gastro Intestinal Cancer Program Florida Hospital Cancer Institute
Disclosures. Clinical and molecular features to guide adjuvant therapy. Personalized Medicine - Decision Tools -
 Disclosures Clinical and molecular features to guide adjuvant therapy Daniel Sargent Professor of Biostatistics & Oncology Mayo Clinic Consulting activities Amgen Pfizer Roche/Genentech Sanofi-Aventis
Disclosures Clinical and molecular features to guide adjuvant therapy Daniel Sargent Professor of Biostatistics & Oncology Mayo Clinic Consulting activities Amgen Pfizer Roche/Genentech Sanofi-Aventis
Colorectal carcinoma (CRC) was traditionally thought of
 Testing for Defective DNA Mismatch Repair in Colorectal Carcinoma A Practical Guide Lawrence J. Burgart, MD Context. Significant bench and clinical data have been generated during the last decade regarding
Testing for Defective DNA Mismatch Repair in Colorectal Carcinoma A Practical Guide Lawrence J. Burgart, MD Context. Significant bench and clinical data have been generated during the last decade regarding
Novel Methods of Lymph Node Evaluation for Predicting the Prognosis of Colorectal Cancer Patients with Inadequate Lymph Node Harvest
 pissn 1598-2998, eissn 25-9256 Cancer Res Treat. 216;48(1):216-224 Original Article http://dx.doi.org/1.4143/crt.214.312 Open Access Novel Methods of Lymph Node Evaluation for Predicting the Prognosis
pissn 1598-2998, eissn 25-9256 Cancer Res Treat. 216;48(1):216-224 Original Article http://dx.doi.org/1.4143/crt.214.312 Open Access Novel Methods of Lymph Node Evaluation for Predicting the Prognosis
Prognostic significance of K-Ras mutation rate in metastatic colorectal cancer patients. Bruno Vincenzi Università Campus Bio-Medico di Roma
 Prognostic significance of K-Ras mutation rate in metastatic colorectal cancer patients Bruno Vincenzi Università Campus Bio-Medico di Roma Colorectal cancer 3 rd most common cancer worldwide Approximately
Prognostic significance of K-Ras mutation rate in metastatic colorectal cancer patients Bruno Vincenzi Università Campus Bio-Medico di Roma Colorectal cancer 3 rd most common cancer worldwide Approximately
Correlation of B-Catenin Localization with Cyclooxygenase-2 Expression and CpG Island Methylator Phenotype (CIMP) in Colorectal Cancer 1
 RESEARCH ARTICLE Neoplasia. Vol. 9, No. 7, July 2007, pp. 569 577 569 www.neoplasia.com Correlation of B-Catenin Localization with Cyclooxygenase-2 Expression and CpG Island Methylator Phenotype (CIMP)
RESEARCH ARTICLE Neoplasia. Vol. 9, No. 7, July 2007, pp. 569 577 569 www.neoplasia.com Correlation of B-Catenin Localization with Cyclooxygenase-2 Expression and CpG Island Methylator Phenotype (CIMP)
Androgen deprivation therapy for treatment of localized prostate cancer and risk of
 Androgen deprivation therapy for treatment of localized prostate cancer and risk of second primary malignancies Lauren P. Wallner, Renyi Wang, Steven J. Jacobsen, Reina Haque Department of Research and
Androgen deprivation therapy for treatment of localized prostate cancer and risk of second primary malignancies Lauren P. Wallner, Renyi Wang, Steven J. Jacobsen, Reina Haque Department of Research and
The pathological phenotype of colon cancer with microsatellite instability
 Dan Med J 63/2 February 2016 danish medical JOURNAL 1 The pathological phenotype of colon cancer with microsatellite instability Helene Schou Andersen 1, 2, Claus Anders Bertelsen 1, Rikke Henriksen 1,
Dan Med J 63/2 February 2016 danish medical JOURNAL 1 The pathological phenotype of colon cancer with microsatellite instability Helene Schou Andersen 1, 2, Claus Anders Bertelsen 1, Rikke Henriksen 1,
Surgical Management of Metastatic Colon Cancer: analysis of the Surveillance, Epidemiology and End Results (SEER) database
 Surgical Management of Metastatic Colon Cancer: analysis of the Surveillance, Epidemiology and End Results (SEER) database Hadi Khan, MD 1, Adam J. Olszewski, MD 2 and Ponnandai S. Somasundar, MD 1 1 Department
Surgical Management of Metastatic Colon Cancer: analysis of the Surveillance, Epidemiology and End Results (SEER) database Hadi Khan, MD 1, Adam J. Olszewski, MD 2 and Ponnandai S. Somasundar, MD 1 1 Department
Please Silence Your Cell Phones. Thank You
 Please Silence Your Cell Phones Thank You TUMOR BUDDING IN PRE OPERATIVE BIOPSIES AND RESECTIONS Alessandro Lugli, MD Institute of Pathology and Translational Research Unit (TRU) University of Bern Bern,
Please Silence Your Cell Phones Thank You TUMOR BUDDING IN PRE OPERATIVE BIOPSIES AND RESECTIONS Alessandro Lugli, MD Institute of Pathology and Translational Research Unit (TRU) University of Bern Bern,
Patient age and cutaneous malignant melanoma: Elderly patients are likely to have more aggressive histological features and poorer survival
 MOLECULAR AND CLINICAL ONCOLOGY 7: 1083-1088, 2017 Patient age and cutaneous malignant melanoma: Elderly patients are likely to have more aggressive histological features and poorer survival FARUK TAS
MOLECULAR AND CLINICAL ONCOLOGY 7: 1083-1088, 2017 Patient age and cutaneous malignant melanoma: Elderly patients are likely to have more aggressive histological features and poorer survival FARUK TAS
THE FUTURE OF IMMUNOTHERAPY IN COLORECTAL CANCER. Prof. Dr. Hans Prenen, MD, PhD Oncology Department University Hospital Antwerp, Belgium
 THE FUTURE OF IMMUNOTHERAPY IN COLORECTAL CANCER Prof. Dr. Hans Prenen, MD, PhD Oncology Department University Hospital Antwerp, Belgium DISCLAIMER Please note: The views expressed within this presentation
THE FUTURE OF IMMUNOTHERAPY IN COLORECTAL CANCER Prof. Dr. Hans Prenen, MD, PhD Oncology Department University Hospital Antwerp, Belgium DISCLAIMER Please note: The views expressed within this presentation
CpG Island Methylator Phenotype in Primary Gastric Carcinoma
 Showa Univ J Med Sci 25 2, 127 132, June 2013 Original CpG Island Methylator Phenotype in Primary Gastric Carcinoma Masayuki TOJO 1, Kazuo KONISHI 1, Yuichiro YANO 1, Atsushi KATAGIRI 1, Hisako NOZAWA
Showa Univ J Med Sci 25 2, 127 132, June 2013 Original CpG Island Methylator Phenotype in Primary Gastric Carcinoma Masayuki TOJO 1, Kazuo KONISHI 1, Yuichiro YANO 1, Atsushi KATAGIRI 1, Hisako NOZAWA
National Surgical Adjuvant Breast and Bowel Project (NSABP) Foundation Annual Progress Report: 2009 Formula Grant
 National Surgical Adjuvant Breast and Bowel Project (NSABP) Foundation Annual Progress Report: 2009 Formula Grant Reporting Period July 1, 2012 June 30, 2013 Formula Grant Overview The National Surgical
National Surgical Adjuvant Breast and Bowel Project (NSABP) Foundation Annual Progress Report: 2009 Formula Grant Reporting Period July 1, 2012 June 30, 2013 Formula Grant Overview The National Surgical
A DISSERTATION SUBMITTED TO THE FACULTY OF THE GRADUATE SCHOOL OF THE UNIVERSITY OF MINNESOTA BY. Helen Mari Parsons
 A Culture of Quality? Lymph Node Evaluation for Colon Cancer Care A DISSERTATION SUBMITTED TO THE FACULTY OF THE GRADUATE SCHOOL OF THE UNIVERSITY OF MINNESOTA BY Helen Mari Parsons IN PARTIAL FULFILLMENT
A Culture of Quality? Lymph Node Evaluation for Colon Cancer Care A DISSERTATION SUBMITTED TO THE FACULTY OF THE GRADUATE SCHOOL OF THE UNIVERSITY OF MINNESOTA BY Helen Mari Parsons IN PARTIAL FULFILLMENT
BMJ Open. A Nationwide Danish Cohort Study challenging the Categorization into Right Sided and Left Sided Colon Cancer
 A Nationwide Danish Cohort Study challenging the Categorization into Right Sided and Left Sided Colon Cancer Journal: BMJ Open Manuscript ID: bmjopen-0-000 Article Type: Research Date Submitted by the
A Nationwide Danish Cohort Study challenging the Categorization into Right Sided and Left Sided Colon Cancer Journal: BMJ Open Manuscript ID: bmjopen-0-000 Article Type: Research Date Submitted by the
Histo-prognostic factors what histopathology has to offer for clinical decision making
 Histo-prognostic factors what histopathology has to offer for clinical decision making Daniela E. Aust Institute for Pathology, University Hospital Dresden, Germany Center for Molecular Tumor Diagnostics
Histo-prognostic factors what histopathology has to offer for clinical decision making Daniela E. Aust Institute for Pathology, University Hospital Dresden, Germany Center for Molecular Tumor Diagnostics
Variables Impacting Lymph Node Recovery in Colectomy Resection Specimens Removed for Colorectal Adenocarcinoma
 Send Orders for Reprints to reprints@benthamscience.net The Open Pathology Journal, 2013, 7, 1-6 1 Open Access Variables Impacting Lymph Node Recovery in Colectomy Resection Specimens Removed for Colorectal
Send Orders for Reprints to reprints@benthamscience.net The Open Pathology Journal, 2013, 7, 1-6 1 Open Access Variables Impacting Lymph Node Recovery in Colectomy Resection Specimens Removed for Colorectal
Ramya Thota 1, Xiang Fang 2, Shanmuga Subbiah 3. Introduction
 Original Article Clinicopathological features and survival outcomes of primary signet ring cell and mucinous adenocarcinoma of colon: retrospective analysis of VACCR database Ramya Thota 1, Xiang Fang
Original Article Clinicopathological features and survival outcomes of primary signet ring cell and mucinous adenocarcinoma of colon: retrospective analysis of VACCR database Ramya Thota 1, Xiang Fang
IGFBP3 Promoter Methylation in Colorectal Cancer: Relationship with Microsatellite Instability, CpG Island Methylator Phenotype, and p53 1
 RESEARCH ARTICLE Neoplasia. Vol. 9, No. 12, December 2007, pp. 1091 1098 1091 www.neoplasia.com IGFBP3 Promoter Methylation in Colorectal Cancer: Relationship with Microsatellite Instability, CpG Island
RESEARCH ARTICLE Neoplasia. Vol. 9, No. 12, December 2007, pp. 1091 1098 1091 www.neoplasia.com IGFBP3 Promoter Methylation in Colorectal Cancer: Relationship with Microsatellite Instability, CpG Island
Introduction ORIGINAL RESEARCH
 Cancer Medicine ORIGINAL RESEARCH Open Access The effect of radiation therapy in the treatment of adult soft tissue sarcomas of the extremities: a long- term community- based cancer center experience Jeffrey
Cancer Medicine ORIGINAL RESEARCH Open Access The effect of radiation therapy in the treatment of adult soft tissue sarcomas of the extremities: a long- term community- based cancer center experience Jeffrey
Colorectal cancer (CRC) is a common disease that
 GASTROENTEROLOGY 2011;140:1174 1181 5-Fluorouracil Adjuvant Chemotherapy Does Not Increase Survival in Patients With CpG Island Methylator Phenotype Colorectal Cancer RODRIGO JOVER,*, THUY PHUONG NGUYEN,
GASTROENTEROLOGY 2011;140:1174 1181 5-Fluorouracil Adjuvant Chemotherapy Does Not Increase Survival in Patients With CpG Island Methylator Phenotype Colorectal Cancer RODRIGO JOVER,*, THUY PHUONG NGUYEN,
CAP Laboratory Improvement Programs. Summary of Microsatellite Instability Test Results From Laboratories Participating in Proficiency Surveys
 CAP Laboratory Improvement Programs Summary of Microsatellite Instability Test Results From Laboratories Participating in Proficiency Surveys Proficiency Survey Results From 2005 to 2012 Theresa A. Boyle,
CAP Laboratory Improvement Programs Summary of Microsatellite Instability Test Results From Laboratories Participating in Proficiency Surveys Proficiency Survey Results From 2005 to 2012 Theresa A. Boyle,
PD-L1 and Immunotherapy of GI cancers: What do you need to know
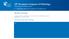 None. PD-L1 and Immunotherapy of GI cancers: What do you need to know Rondell P. Graham September 3, 2017 2017 MFMER slide-2 Disclosure No conflicts of interest to disclose 2017 MFMER slide-3 Objectives
None. PD-L1 and Immunotherapy of GI cancers: What do you need to know Rondell P. Graham September 3, 2017 2017 MFMER slide-2 Disclosure No conflicts of interest to disclose 2017 MFMER slide-3 Objectives
ASSESSMENT OF MLH1 PROMOTER METHYLATION IN ENDOMETRIAL CANCER USING PYROSEQUENCING TECHNOLOGY OBJECTIVES
 ASSESSMENT OF MLH1 PROMOTER METHYLATION IN ENDOMETRIAL CANCER USING PYROSEQUENCING TECHNOLOGY Authors: Duilio Della Libera, Alessandra D Urso, Federica Modesti, Georgeta Florea, Marta Gobbato Hospital:
ASSESSMENT OF MLH1 PROMOTER METHYLATION IN ENDOMETRIAL CANCER USING PYROSEQUENCING TECHNOLOGY Authors: Duilio Della Libera, Alessandra D Urso, Federica Modesti, Georgeta Florea, Marta Gobbato Hospital:
Difference in the recurrence rate between right- and left-sided colon cancer: a 17-year experience at a single institution
 Surg Today (2014) 44:1685 1691 DOI 10.1007/s00595-013-0748-5 ORIGINAL ARTICLE Difference in the recurrence rate between right- and left-sided colon cancer: a 17-year experience at a single institution
Surg Today (2014) 44:1685 1691 DOI 10.1007/s00595-013-0748-5 ORIGINAL ARTICLE Difference in the recurrence rate between right- and left-sided colon cancer: a 17-year experience at a single institution
Cover Page. The handle holds various files of this Leiden University dissertation
 Cover Page The handle http://hdl.handle.net/1887/55957 holds various files of this Leiden University dissertation Author: Dekker T.J.A. Title: Optimizing breast cancer survival models based on conventional
Cover Page The handle http://hdl.handle.net/1887/55957 holds various files of this Leiden University dissertation Author: Dekker T.J.A. Title: Optimizing breast cancer survival models based on conventional
Universal Screening for Lynch Syndrome
 Universal Screening for Lynch Syndrome St. Vincent/Ameripath protocol proposal Lynch syndrome (HNPCC) 1/35 individuals with colorectal cancer has Lynch syndrome Over half individuals are >50 at time of
Universal Screening for Lynch Syndrome St. Vincent/Ameripath protocol proposal Lynch syndrome (HNPCC) 1/35 individuals with colorectal cancer has Lynch syndrome Over half individuals are >50 at time of
CME/SAM. Poorly Differentiated Colorectal Cancers. Correlation of Microsatellite Instability With Clinicopathologic Features and Survival
 Poorly Differentiated Colorectal Cancers Correlation of Microsatellite Instability With Clinicopathologic Features and Survival Haitao Xiao, MD, 1,2 Yong Sik Yoon, MD, 1,3 Seung-Mo Hong, MD, 4 Seon Ae
Poorly Differentiated Colorectal Cancers Correlation of Microsatellite Instability With Clinicopathologic Features and Survival Haitao Xiao, MD, 1,2 Yong Sik Yoon, MD, 1,3 Seung-Mo Hong, MD, 4 Seon Ae
Introduction. Why Do MSI/MMR Analysis?
 Clinical Significance Of MSI, KRAS, & EGFR Pathway In Colorectal Carcinoma UCSF & Stanford Current Issues In Anatomic Pathology Introduction Microsatellite instability and mismatch repair protein deficiency
Clinical Significance Of MSI, KRAS, & EGFR Pathway In Colorectal Carcinoma UCSF & Stanford Current Issues In Anatomic Pathology Introduction Microsatellite instability and mismatch repair protein deficiency
Case Presentation Diana Lim, MBBS, FRCPA, FRCPath Senior Consultant Department of Pathology, National University Health System, Singapore Assistant Pr
 Case Presentation Diana Lim, MBBS, FRCPA, FRCPath Senior Consultant Department of Pathology, National University Health System, Singapore Assistant Professor Yong Loo Lin School of Medicine, National University
Case Presentation Diana Lim, MBBS, FRCPA, FRCPath Senior Consultant Department of Pathology, National University Health System, Singapore Assistant Professor Yong Loo Lin School of Medicine, National University
Clinical Significance of Lymph Node Ratio in Stage III Colorectal Cancer
 Original Article Journal of the Korean Society of http://dx.doi.org/10.3393/jksc.2011.27.5.260 pissn 2093-7822 eissn 2093-7830 Clinical Significance of Lymph Node Ratio in Stage III Colorectal Cancer Yo
Original Article Journal of the Korean Society of http://dx.doi.org/10.3393/jksc.2011.27.5.260 pissn 2093-7822 eissn 2093-7830 Clinical Significance of Lymph Node Ratio in Stage III Colorectal Cancer Yo
Differential lymph node retrieval in rectal cancer: associated factors and effect on survival
 Original Article Differential lymph node retrieval in rectal cancer: associated factors and effect on survival Cedrek McFadden 1, Brian McKinley 1, Brian Greenwell 2, Kaylee Knuckolls 1, Patrick Culumovic
Original Article Differential lymph node retrieval in rectal cancer: associated factors and effect on survival Cedrek McFadden 1, Brian McKinley 1, Brian Greenwell 2, Kaylee Knuckolls 1, Patrick Culumovic
Androgen Receptor Expression in Renal Cell Carcinoma: A New Actionable Target?
 Androgen Receptor Expression in Renal Cell Carcinoma: A New Actionable Target? New Frontiers in Urologic Oncology Juan Chipollini, MD Clinical Fellow Department of Genitourinary Oncology Moffitt Cancer
Androgen Receptor Expression in Renal Cell Carcinoma: A New Actionable Target? New Frontiers in Urologic Oncology Juan Chipollini, MD Clinical Fellow Department of Genitourinary Oncology Moffitt Cancer
* * * * Supplementary Figure 1. DS Lv CK HSA CK HSA. CK Col-3. CK Col-3. See overleaf for figure legend. Cancer cells
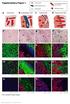 Supplementary Figure 1 Cancer cells Desmoplastic stroma Hepatocytes Pre-existing sinusoidal blood vessel New blood vessel a Normal liver b Desmoplastic HGP c Pushing HGP d Replacement HGP e f g h i DS
Supplementary Figure 1 Cancer cells Desmoplastic stroma Hepatocytes Pre-existing sinusoidal blood vessel New blood vessel a Normal liver b Desmoplastic HGP c Pushing HGP d Replacement HGP e f g h i DS
Colon cancer: practical molecular diagnostics. Wade S. Samowitz, M.D. University of Utah and ARUP
 Colon cancer: practical molecular diagnostics Wade S. Samowitz, M.D. University of Utah and ARUP Disclosure Dr. Samowitz may receive royalties in the future related to the Ventana BRAF V600E antibody.
Colon cancer: practical molecular diagnostics Wade S. Samowitz, M.D. University of Utah and ARUP Disclosure Dr. Samowitz may receive royalties in the future related to the Ventana BRAF V600E antibody.
B Base excision repair, in MUTYH-associated polyposis and colorectal cancer, BRAF testing, for hereditary colorectal cancer, 696
 Index Note: Page numbers of article titles are in boldface type. A Adenomatous polyposis, familial. See Familial adenomatous polyposis. Anal anastomosis, ileal-pouch, proctocolectomy with, in FAP, 591
Index Note: Page numbers of article titles are in boldface type. A Adenomatous polyposis, familial. See Familial adenomatous polyposis. Anal anastomosis, ileal-pouch, proctocolectomy with, in FAP, 591
A916: rectum: adenocarcinoma
 General facts of colorectal cancer The colon has cecum, ascending, transverse, descending and sigmoid colon sections. Cancer can start in any of the r sections or in the rectum. The wall of each of these
General facts of colorectal cancer The colon has cecum, ascending, transverse, descending and sigmoid colon sections. Cancer can start in any of the r sections or in the rectum. The wall of each of these
RNA preparation from extracted paraffin cores:
 Supplementary methods, Nielsen et al., A comparison of PAM50 intrinsic subtyping with immunohistochemistry and clinical prognostic factors in tamoxifen-treated estrogen receptor positive breast cancer.
Supplementary methods, Nielsen et al., A comparison of PAM50 intrinsic subtyping with immunohistochemistry and clinical prognostic factors in tamoxifen-treated estrogen receptor positive breast cancer.
Molecular Diagnosis for Colorectal Cancer Patients
 Molecular Diagnosis for Colorectal Cancer Patients Antonia R. Sepulveda MD, PhD, FCAP October, 20, 2010 www.cap.org Welcome to the PHC Webinar Series This talk on The Molecular Diagnosis for Colorectal
Molecular Diagnosis for Colorectal Cancer Patients Antonia R. Sepulveda MD, PhD, FCAP October, 20, 2010 www.cap.org Welcome to the PHC Webinar Series This talk on The Molecular Diagnosis for Colorectal
Current Status of Biomarkers (including DNA Tumor Markers and Immunohistochemistry in the Laboratory Diagnosis of Tumors)
 Current Status of Biomarkers (including DNA Tumor Markers and Immunohistochemistry in the Laboratory Diagnosis of Tumors) Kael Mikesell, DO McKay-Dee Hospital May 14, 2015 Outline Update to DNA Testing
Current Status of Biomarkers (including DNA Tumor Markers and Immunohistochemistry in the Laboratory Diagnosis of Tumors) Kael Mikesell, DO McKay-Dee Hospital May 14, 2015 Outline Update to DNA Testing
ORIGINAL ARTICLE. Colon Cancer and Low Lymph Node Count. James W. Jakub, MD; Greg Russell, MS; Cindy L. Tillman, CTR; Craig Lariscy, MD
 ORIGINAL ARTICLE Colon Cancer and Low Lymph Node Count Who Is to Blame? James W. Jakub, MD; Greg Russell, MS; Cindy L. Tillman, CTR; Craig Lariscy, MD Objective: To identify the factors that contribute
ORIGINAL ARTICLE Colon Cancer and Low Lymph Node Count Who Is to Blame? James W. Jakub, MD; Greg Russell, MS; Cindy L. Tillman, CTR; Craig Lariscy, MD Objective: To identify the factors that contribute
The incidence of pulmonary adenocarcinoma is
 THE PROGNOSTIC VALUE OF NATURAL KILLER CELL INFILTRATION IN RESECTED PULMONARY ADENOCARCINOMA Iwao Takanami, MD Ken Takeuchi, MD Masatoshi Giga, MD Objective: Natural cytotoxicity caused by mediated natural
THE PROGNOSTIC VALUE OF NATURAL KILLER CELL INFILTRATION IN RESECTED PULMONARY ADENOCARCINOMA Iwao Takanami, MD Ken Takeuchi, MD Masatoshi Giga, MD Objective: Natural cytotoxicity caused by mediated natural
Gastrointestinal and Hernia Ward, Ningbo No.2 Hospital, Xibei Street 41, Ningbo, Zhejiang, China. * Equal contributors.
 Int J Clin Exp Med 2017;10(5):8165-8173 www.ijcem.com /ISSN:1940-5901/IJCEM0045461 Original Article Impact of primary tumor location on the overall survival of patients with stage IV colorectal cancer:
Int J Clin Exp Med 2017;10(5):8165-8173 www.ijcem.com /ISSN:1940-5901/IJCEM0045461 Original Article Impact of primary tumor location on the overall survival of patients with stage IV colorectal cancer:
Modified primary tumour/vessel tumour/nodal tumour classification for patients with invasive ductal carcinoma of the breast
 British Journal of Cancer (2011) 105, 698 708 All rights reserved 0007 0920/11 www.bjcancer.com Modified primary tumour/vessel tumour/nodal tumour classification for patients with invasive ductal carcinoma
British Journal of Cancer (2011) 105, 698 708 All rights reserved 0007 0920/11 www.bjcancer.com Modified primary tumour/vessel tumour/nodal tumour classification for patients with invasive ductal carcinoma
Comparison of the Mismatch Repair System between Primary and Metastatic Colorectal Cancers Using Immunohistochemistry
 Journal of Pathology and Translational Medicine 2017; 51: 129-136 ORIGINAL ARTICLE Comparison of the Mismatch Repair System between Primary and Metastatic Colorectal Cancers Using Immunohistochemistry
Journal of Pathology and Translational Medicine 2017; 51: 129-136 ORIGINAL ARTICLE Comparison of the Mismatch Repair System between Primary and Metastatic Colorectal Cancers Using Immunohistochemistry
Survival Prediction Models for Estimating the Benefit of Post-Operative Radiation Therapy for Gallbladder Cancer and Lung Cancer
 Survival Prediction Models for Estimating the Benefit of Post-Operative Radiation Therapy for Gallbladder Cancer and Lung Cancer Jayashree Kalpathy-Cramer PhD 1, William Hersh, MD 1, Jong Song Kim, PhD
Survival Prediction Models for Estimating the Benefit of Post-Operative Radiation Therapy for Gallbladder Cancer and Lung Cancer Jayashree Kalpathy-Cramer PhD 1, William Hersh, MD 1, Jong Song Kim, PhD
Colon Cancer Prediction based on Artificial Neural Network
 Global Journal of Computer Science and Technology Interdisciplinary Volume 13 Issue 3 Version 1.0 Year 2013 Type: Double Blind Peer Reviewed International Research Journal Publisher: Global Journals Inc.
Global Journal of Computer Science and Technology Interdisciplinary Volume 13 Issue 3 Version 1.0 Year 2013 Type: Double Blind Peer Reviewed International Research Journal Publisher: Global Journals Inc.
Molecular Subtyping of Endometrial Cancer: A ProMisE ing Change
 Molecular Subtyping of Endometrial Cancer: A ProMisE ing Change Charles Matthew Quick, M.D. Associate Professor of Pathology Director of Gynecologic Pathology University of Arkansas for Medical Sciences
Molecular Subtyping of Endometrial Cancer: A ProMisE ing Change Charles Matthew Quick, M.D. Associate Professor of Pathology Director of Gynecologic Pathology University of Arkansas for Medical Sciences
Immunotherapy for dmmr metastatic colorectal cancer. Prof.dr. Kees Punt Dept. Medical Oncology AUMC
 Immunotherapy for dmmr metastatic colorectal cancer Prof.dr. Kees Punt Dept. Medical Oncology AUMC Active specific immunotherapy (ASI) in stage II-III colon cancer Vaccination with autologous tumor + BCG
Immunotherapy for dmmr metastatic colorectal cancer Prof.dr. Kees Punt Dept. Medical Oncology AUMC Active specific immunotherapy (ASI) in stage II-III colon cancer Vaccination with autologous tumor + BCG
IJC International Journal of Cancer
 IJC International Journal of Cancer The clinical impact of tumour-infiltrating lymphocytes in colorectal cancer differs by anatomical subsite: A cohort study Jonna Berntsson 1, Maria C Svensson 1, Karin
IJC International Journal of Cancer The clinical impact of tumour-infiltrating lymphocytes in colorectal cancer differs by anatomical subsite: A cohort study Jonna Berntsson 1, Maria C Svensson 1, Karin
Serrated Colorectal Polyps New Challenges to Old Dogma. Kenneth Batts, M.D. Abbott Northwestern Hospital Minneapolis, MN
 Serrated Colorectal Polyps New Challenges to Old Dogma Kenneth Batts, M.D. Abbott Northwestern Hospital Minneapolis, MN A Sneak Preview.... This was in the good old days: Adenomas HPPs Mixed Polyps A Sneak
Serrated Colorectal Polyps New Challenges to Old Dogma Kenneth Batts, M.D. Abbott Northwestern Hospital Minneapolis, MN A Sneak Preview.... This was in the good old days: Adenomas HPPs Mixed Polyps A Sneak
The effect of delayed adjuvant chemotherapy on relapse of triplenegative
 Original Article The effect of delayed adjuvant chemotherapy on relapse of triplenegative breast cancer Shuang Li 1#, Ding Ma 2#, Hao-Hong Shi 3#, Ke-Da Yu 2, Qiang Zhang 1 1 Department of Breast Surgery,
Original Article The effect of delayed adjuvant chemotherapy on relapse of triplenegative breast cancer Shuang Li 1#, Ding Ma 2#, Hao-Hong Shi 3#, Ke-Da Yu 2, Qiang Zhang 1 1 Department of Breast Surgery,
Signet-Ring Cell Carcinoma of the Colon: A Case Report and Review of the Literature
 Published online: November 4, 2015 2015 The Author(s) Published by S. Karger AG, Basel 1662 6575/15/0083 0466$39.50/0 This article is licensed under the Creative Commons Attribution-NonCommercial 4.0 International
Published online: November 4, 2015 2015 The Author(s) Published by S. Karger AG, Basel 1662 6575/15/0083 0466$39.50/0 This article is licensed under the Creative Commons Attribution-NonCommercial 4.0 International
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/22278 holds various files of this Leiden University dissertation. Author: Cunha Carvalho de Miranda, Noel Filipe da Title: Mismatch repair and MUTYH deficient
Cover Page The handle http://hdl.handle.net/1887/22278 holds various files of this Leiden University dissertation. Author: Cunha Carvalho de Miranda, Noel Filipe da Title: Mismatch repair and MUTYH deficient
