Slide 1. Slide 2. Slide 3. Acute Pancreatitis: An Evidence-Based Clinical Approach in Case. Important Clinical Questions
|
|
|
- Leon Barton
- 5 years ago
- Views:
Transcription
1 Slide 1 Acute Pancreatitis: An Evidence-Based Clinical Approach in 2014 David G. Forcione, MD Associate Director Interventional Endoscopy Slide 2 Case A 68 yo M p/w acute onset of sharp epigastric pain, which has been unrelenting for 6 hours. +nausea/vomiting PMHx: HTN, CAD, GERD, remote PUD Initial VS: HR 114, BP 140/90 mm Hg, RR 24, T 37.6 C, O2 Sat 92% (RA) Labs: Amylase 1270 U/L (ULN 100), Lipase 3430 U/L (ULN 60) HCT 47%, WBC 18K, Ca mg/dl, ALT 295, AST 221, AP 217, TB 0.9 mg/dl, Glucose 240 mg/dl, BUN 47, Cr 1.3 Slide 3 Important Clinical Questions Is this acute pancreatitis? What is the cause? What imaging studies are important at this time? Does this patient need an ICU? How should I manage this patient? Fluids? Antibiotics? Nutrition? ERCP? Surgery?
2 Slide Updated guidelines on classification and management Am J Gastro 2013 Gut 2012 Slide 5 Epidemiology of Acute Pancreatitis One of the most common GI tract disorders $2.6 billion (2009) Ann Epidem 2007 Slide 6 Diagnostic Criteria >2 criteria should be met: Characteristic abdominal pain Amylase and/or lipase >3x upper limit normal Characteristic cross sectional imaging findings
3 Slide 7 What is pancreatitis type pain? Characteristic Findings NOT Location Epigastric/LUQ Crampy Onset Acute Colicky Quality Deep,penetrating/ Periumbilical knife-like, burning, Lower gas pocket abdominal sensation Caveats Immunosuppressed Acuity Severe, constant Altered MS Radiation Band-like upper abdomen Chronic pain Chronic pancreatitis Mid/Upper back Associated Features Anorexia, Nausea, Vomiting Slide 8 Serologic Testing Onset Levels Duration Source Caveats Amylase (<100 U/L) <4 hrs Height of elevation does not correlate with severity/prognosis Daily tracking: limited value 3-5 days Pancreatic Salivary 1) May be WNL in AP due to EtOH or hypertrig 2) Non-pancreatic conditions 3) Renal failure Lipase (<60 U/L) <3 hrs Height of elevation does not correlate with severity/prognosis Daily tracking: limited value 7-10 days Panc, Intestinal Salivary, Hepatic 1) Diabetics: higher baseline 2) Non-pancreatic conditions 3) Renal failure Slide 9 Approach to Serologic Testing Lipase is more specific than amylase >3x ULN: 98% specificity for AP Amylase/lipase levels.<3xuln WITH abdominal sxs WITHOUT abdominal sxs Pancreatitis Pancreatitis Gastroenteritis Renal failure Peptic ulcer disease Salivary (fractionation) Cholecystitis HIV SBO Metabolic acidosis (DKA) Mesenteric ischemia Macroamylase/lipase Appendicitis Drugs Celiac disease IBD Gynecologic
4 Slide 10 Role of Early Imaging TUS for all piotential cases of biliary pancreatitis Cross sectional imaging may be clinically indicated Diagnostic uncertainty Dx AP with clinical deterioration hrs after presentation Routine use of CT in ED for diagnosis of AP is unwarranted Dx is made by Hx/PE/Serologies Most pts have uncomplicated courses CT and MR appear comparable Necrosis may not be evident for 2-3 days >90% sensitivity/specificity Pros CT : availability, faster, cheaper Pros MR: CBD stones, non-contrast (renal failure/allergy) Challenging scenarios Pancreatic neoplasms Slide 11 Case 68 yo M p/w acute onset of sharp epigastric pain, which has been unrelenting for 6 hours. +nausea/vomiting PMHx: HTN, CAD, GERD, TUS: remote PUD Gallstones w/o cholecystitis Initial VS: HR 114, BP 140/90 CBD 6 mm (otherwise nl) mm Hg, RR 24, T 37.6 C, O2 Sat 92% (RA) CT: pancreatitis without necrosis Labs: Amylase 1270 U/L (ULN 100), Lipase 3430 U/L (ULN 60) HCT 47%, WBC 18K, ALT 295, AST 221, AP 217, TB 0.9 mg/dl Slide 12 Establish an etiology Important! Can be established in most cases Diagnosis-specific treatments Target reversible causes Prevention of future attacks Overusage of idiopathic and chronic pancreatitis labels
5 Slide 13 Etiology of Acute Pancreatitis: 2014 Other Alcohol Biliary Alcohol Biliary Slide 14 Most common etiologies: Biliary Biliary (50%) Pathogenesis Mechanical obstruction Reflux of bile into pancreas duct Spectrum Gallstones Sludge (TPN) Microlithiasis 3-7% pts with gallstones- >AP Men: greatest risk of bil AP (size<5 mm) Women: highest incidence (higher prevalence of stones) Slide 15
6 Slide 16 Biliary Pancreatitis - Findings Subacute/acute onset of pain 4-6 hrs post prandial (fatty meal) ALT elevation >150 U/L (3x ULN) PPV of 95% for the diagnosis of gallstone pancreatitis (sens 45%) TUS in all pts with AP Natural Hx: Most often resolves on its own (stone passes) Subset pts benefit from ERCP (cholangitis/obstruction) CCY recommended in all candidates (to prevent recurrent attacks) Slide 17 Most common etiologies: Alcohol Alcohol (30%) Pathogenesis Direct oxidative stress on pancreas Increases pancreatic enzyme synthesis Disrupts intracellular membranes- >autodigestion Activates stellate cells of the pancreas->fibrosis <5% heavy drinkers >5 yrs of heavy use (>50 gm/day ~ 3-4/drinks/day) Isolated alcoholic binges rarely, if ever, cause pancreatitis) Other sensitizers: Genetics, Tobacco, Anatomy Slide 18 Most important causes?: the other 20%: Structural Pancreas divisum Choledochocele Sphincter of Oddi dysfunction Neoplasm (5-14%) Ampullary mass Cystic neoplasms (IPMN) Ductal AdenoCA Mets to pancreas Inflammatory Celiac disease Autoimmune Pancreatitis Vascular Vasculitis (PAN, SLE) Atheroembolism Cholesterol embolism Intra-op shock (CABG) Traumatic Post-ERCP Trauma (blunt) Metabolic Hypertriglyceridemia: >1000 mg/dl Hypercalcemia Exogenous Drugs: uncommon (6-MP, DDI, pentamadine, diuretics, flagyl, ACEI, tamoxifen) Infection: mumps, HIV, Legionella, Ascaris Smoking Genetic (CFTR/SPINK/PRSS1) <25 yo, recurrent AP, FHx
7 Slide 19 How to diagnose the other 20% High degree of clinical suspicion don t assume! All pts Lipids, Ca++ Careful family history Medication review (uncommon!) Travel history Imaging if >1 attack (<40 yrs old): pancreas divisum Evaluation for neoplasm with imaging (CT/MRI/EUS) Pts >40 yrs old first episode of AP Additional sxs: wt loss, new DM, FHx Smoldering or relapsing course Do not assume cysts seen with acute pancreatitis are pseudocysts; THINK CYSTIC NEOPLASM Controversial Sphincter of Oddi dysfunction Post cholecystectomy microlithiasis Slide 20 Spectrum of Acute Pancreatitis Frequency 80% Subtypes Cross sectional Imaging Course Interstitial None Infected Homogenous Sterile enhnacement Necrosis (nonenhancement, >30%) Edema/stranding Collections Resolves within 1 week Necrotizing 20% Location Peripancreatic + Pancreatic Peripancreatic Pancreatic (rare) Morphology Variable Slide 21 Initial Assessment and Risk Stratification Most patients do well (80%) Development of systemic inflammatory response syndrome (SIRS) and organ failure (OF) are associated with morbidity and mortality SIRS presence within first 24 hrs predicts organ failure SIRS 1) Temperature <36 C or >38 C >2 = SIRS 2) Respirations >20/min or PaCO2 <32 mmhg 3) Heart rate >90/min 4) WBC <4,000/mm(3) or WBC >12,000/mm(3)
8 Slide 22 Defining Organ Failure in 2014: Marshall Scoring System (PaO2/FiO2) (Cr) >2 = organ failure Slide 23 Classification of AP Atlanta Classification (1992) Revised Classification (2012) Slide 24 Patterns of Diseases Based on SIRS and OF 80% PTS AP Resolution 15% PTS AP SIRS OF Stabilization AP SIRS OF Stabilization Death
9 Slide 25 Mortality Rates of AP All comers: 2-3% Mild AP (interstitial): 1% Necrotizing pancreatitis: 17% Sterile: 12% Infected: 30% Multi-organ failure: 47% Experience counts <10% mortality for necrotizing pancreatitis in expert centers Slide 26 Case 68 yo M p/w acute onset of TUS: sharp epigastric pain, which Gallstones w/o cholecystitis has been unrelenting for 6 CBD 6 mm (otherwise nl) hours. +nausea/vomiting PMHx: HTN, CAD, GERD, CT: pancreatitis without necrosis remote PUD Initial VS: HR 114, BP 140/90 SIRS: YES mm Hg, RR 24, T 37.6 C, Organ Failure: NO O2 Sat 92% (RA) Labs: Amylase 1270 U/L (ULN 100), Lipase 3430 U/L (ULN 60) HCT 47%, WBC 18K, ALT 295, AST 221, AP 217, TB 0.9 mg/dl Slide 27 Can we predict severity? 2014: remain unable to accurately predict which pts with AP will develop severe disease Many scoring systems developed/available.few are practical and can be used early Clinical Scoring Systems Ranson (1976) APACHE II (14 inputs) BISAP Serologic CRP, HCT, BUN Radiologic Balthazar CT score
10 Slide 28 Can we predict severity? 2014: remain unable to accurately predict which pts with AP will develop severe disease Many scoring systems developed/available.few are practical and can be used early Clinical Scoring Systems Ranson (1976) APACHE II (14 inputs) BISAP Serologic CRP, HCT, BUN Radiologic Balthazar CT score Slide 29 Clinical Scoring system: BISAP (2008) BUN>25 mg/dl Impaired mental status (GCS <15) SIRS 1) Temperature <36 C or >38 C 2) Respirations >20/min or PaCO2 <32 mmhg 3) Heart rate >90/min 4) WBC <4,000/mm(3) or WBC >12,000/mm(3) or more than 10% bands found on blood smear. Age >60 Pleural effusion Slide 30 Case 68 yo M p/w acute onset of TUS: sharp epigastric pain, which Gallstones w/o cholecystitis has been unrelenting for 6 CBD 6 mm (otherwise nl) hours. +nausea/vomiting PMHx: HTN, CAD, GERD, CT: pancreatitis without necrosis remote PUD Initial VS: HR 114, BP 140/90 SIRS: YES mm Hg, RR 24, T 37.6 C, Organ Failure: NO O2 Sat 92% (RA) Labs: Amylase 1270 U/L (ULN 100), Lipase 3430 U/L (ULN BISAP= 3 (age, SIRS, BUN>25) 60) 5% mortality HCT 47%, WBC 18K, ALT 295, AST 221, AP 217, TB 0.9 mg/dl
11 Slide 31 Serologic tests as predictors of severity: CRP CRP The most widely studied inflammatory marker in AP >150 mg/l at 48 hrs PPV 67%, NPV 86% for severe pancreatitis Slide 32 Serologic tests as predictors of severity: BUN BUN Elevation at presentation (>22 mg/dl) Failure to decline in 24 hrs Marker of volume status/third spacing Slide 33 Serologic tests as predictors of severity: HCT Hematocrit Hemoconcentration (HCT>44%) at admission Reflects degree of third spacing Failure to reverse hemoconcentration is a/w worse outcomes Pts with HCT <44% and with decline in first 24hrs a/w benign clinical course
12 Slide 34 Need to look at the whole picture The Doctor Luke Fildes, 1891 Slide 35 Cross Sectional Imaging: Early Use Has Limited Value Necrosis takes time to develop 3 studies on early imaging Pts with a clinical dx of AP 50% CT scan, 15% MRI No alternative dx found Low frequency of necrosis (<5%) 2.5x CT/MRI over no change in severity of AP Use: dx uncertainty, pts not improving by day 4, or suspected local complication (lumenal obstruction, pseudoaneurysm) Slide 36 Defining Pancreatitis by Imaging: Sharing A Common Terminology
13 Slide 37 Acute Pancreatitis- Interstitial Edematous Acute Peripancreatic Fluid Collections Pseudocysts Slide 38 Acute Necrotizing Pancreatitis Acute Necrotic Collection Walled Off Pancreatic Necrosis WOPN Slide 39 Management Update 2014 Initial Treatment Strategies Role of ERCP Role/Timing of CCY Nutritional Considerations Management of Necrosis Antibiotics? Debridement Indications? Timing? Methods?
14 Slide 40 Multidisciplinary Approach is Essential GI Nursing Radiology Pancreatitis Internist Nutritionist Intensivist Surgery Slide 41 Initial Treatment Strategies (0-36 hrs): The Critical Window No medication has been shown to be effective for AP Early Aggressive Hydration (EAH) is essential! Offsets the cascade Inflammation Cell death Microvascular Permeability Hypovolemia Vomiting Reduce PO Tachypnea Diaphoresis Third spacing Slide 42 How to employ EAH? Needs to be individualized.based on age/comorbidities (Cr, EF%)
15 Slide 43 Employing an EAH plan Bolus: 20 ml/kg (1-2L) Infusion: 3 ml/kg/hr ( ml/hr) Lactated Ringers vs NS LR associated with lower CRP levels LR associated with less SIRS WHY?? Better electrolyte balance More ph balanced NS-> Non gap met acidosis->trypsinogen activation Guide fluid at 12 and 24 hrs based on BUN, HCT, clinical status (resp status, UO) Slide 44 Beware of over-hydration! After 24 hrs, need to be mindful of volume status Volume overload/pulmonary edema Abdominal compartment syndrome Sepsis?Lower survival Slide 45 Initial Treatment Strategies Part II Best Supportive Measures DVT prophylaxis Incenctive spirometry PPI prophylaxis Electrolyte stabilization Nutrition Control/Prevention of extrapancreatic infection
16 Slide 46 Role of early ERCP 1) Acute biliary pancreatitis: Most times ->stone passes Spontaneously-> no role for ERCP Clinical trials (6 meta-anlalysis) reduced M+M when ERCP impemented within 24h: Clinical or radiologic evidence of biliary obstruction (Tb>5, dilated ducts) and/or Ascending cholangitis Use MRCP/EUS to guide grey cases 2) Acute traumatic pancreatitis Stenting of ductal disruption (pancreatic duct) Slide 47 Slide 48 Update on Post-ERCP pancreatitis (PEP) Remains the most common complication decreasing frequency Frequency (5-40%) Most mild Severe: 1/500 Mechanisms: early enzyme activation Thermal Hydrostatic pressure
17 Slide 49 Prophylactic Measures Against PEP #1: Do not do the ERCP! #2: Guidewire cannulation #3: Periprocedural IVF #4: Pancreatic duct stenting #5: Rectal NSAIDs PEP reduced by 60% with rectal indomethacin Slide 50 Role of Cholecystectomy Lap CCY vs Wait and See (Lancet 2002): 120 pts randomized High rate of recurrent events (18% within 90 days) Mild biliary AP: CCY during index hospitalization Severe biliary AP: wait until pancreatitis resolves due to higher risk of infection Pts too frail for CCY? Consider ERCP/biliary sphincterotomy->eliminate risk of biliary AP Empric CCY for recurrent idiopathic AP,? Microlithiasis. Not indicated >50% recurrence of AP Slide 51 Nutritional Considerations Rethinking NPO Historically: NPO -> clears over days 1 st 24 hrs: NPO Multiple studies demonstrate providing oral feeding early in AP (pts without ileus) a/w: Reduced LOS Reduced infectious complications Reduced M+M Low residue, low fat soft diet = clear liquids
18 Slide 52 Nutritional Support: Intolerant of PO Avoid TPN = complications (infection/thrombosis), expensive Enteral feeding options a/w better outcomes, less expensive, safer Nasogastric: easier Nasojejunal: more physiologic NIH sponsored study NG vs NJT Slide 53 Case 68 yo M acute biliary pancreatitis (ALT, U/S) and evidence of SIRS (HR/RR/WBC) on admission without organ failure BISAP 3 HCT 44%, BUN 47 mg/dl GI Consulted NPO on admission EAH instituted (LR) Anti-emetics, PCA, PPI, no antibiotics HCT 44%->36% at 24 hrs BUN 47 mg/dl->39 mg d/l at 24 hrs Improving LFTs, no cholangitis: ERCP not recommended No evidence of OF Started on clears in 24 hrs then ADAT Lap CCY on HD 4 D/C home HD 5 Slide 54 Management of Necrosis Antibiotics? Debridement Indications? Timing? Method?
19 Slide 55 Role of Antibiotics in AP Infectious complications = major source of M+M Extrapancreatic (pneumonia, line, UTI, CDiff, cholangitis) Pancreatic (infected necrosis) A/w higher mortality rate (30%) than sterile necrosis Since 1993, 11 abx trials (quinolone, carbapenems) No advantage of empiric abx for necrotizing pancreatitis NNT = 1429 One trial (1995) suggest selective gut decontamination with oral antifungal/antibacterial -> reduced M+M Probiotics = increased M+M Slide 56 When should antibiotics be used? Extrapancreatic infections Suspected infected pancreatic necrosis Cinical deterioration No improvement after 7-10 days Persistent fever without source Gas on CT Options CT guided FNA (issues!) Empiric treatment: carbapenems, quinolones No evidence to support routine addition of antifungals Slide 57 Managing Necrosis.Debride or Not? Historically ANY Necrosis = early debridement Outcomes: High M+M 2014: Infected necrosis + unstable = urgent open surgical debridement 2014: Delay debridement for >30 days if stable Allows for necrosis to become organized May be able to avoid entirely asx necrosis does not require treatment
20 Slide 58 Methods of debridement Stable pts with symptomatic mature (>30 days) or walled off pancreatic necrosis/wopn Surgical debridement Open Laparoscopic VARDs Percutaneous (IR): limited Endoscopic Interventional Endoscopist Step up approach Factors: Size Location Vasculature Pancreatic Necrosis Local expertise/experience Surgery Interventional Radiology Slide 59 Endoscopic Necrosectomy Optimal for pts with WOPN in close apposition to stomach or duodenum Optimally done in tertiary care centers with expertise and back-up Assess contents with MRI (how much fluid vs solid) EUS guidance Create a tract (15-18mm) between stomach/duodenum and WOPN Enter space with scope and debride Leave stents from stomach into cyst space 24 hr lavage with saline/abx Repeat manuel debridement every 2-7 days depending upon amount/purulence Slide 60
21 Slide 61 Slide 62 Slide 63
22 Slide 64 Slide 65 Slide 66
23 Slide 67 Slide 68 Slide 69
24 Slide 70 Slide 71 Slide 72
25 Slide 73 Slide 74 Slide 75 Data for Endoscopic Management of WOPN 2011 (GI Endoscopy) 104 pts/6 centers Mean time to procedure: 63 days Successful resolution: 91% LOS: 12 days Complications: 14% Bleeding Death (6%) 2012 (JAMA) 22 pts/4 centers RCT Endoscopic vs VARDS Better outcomes with endoscopic
26 Slide Slide 77 Serosa to Serosa Apposition 77 Slide 78 78
27 Slide Slide Slide 81 Take Home Messages 1. AP is a clinical diagnosis 2. Establish a specific etiology for AP 3. BUN/HCT are useful markers of severity. 4. Early aggressive hydration is essential Avoid hemoconcentration! 5. No role for empiric antibiotics. Use selectively 6. Urgent ERCP for obstruction/cholangitis 7. Post ERCP pancreatitis prophylaxis = standard of care 8. Earlier impementation of enteral nutrition; avoid TPN 9. Necrosectomy is best done in >4 weeks in stable, sxs pts 10. Minimally invasive approaches are effective for WOPN
28 Slide 82 THANK YOU!!
ACG Clinical Guideline: Management of Acute Pancreatitis
 ACG Clinical Guideline: Management of Acute Pancreatitis Scott Tenner, MD, MPH, FACG 1, John Baillie, MB, ChB, FRCP, FACG 2, John DeWitt, MD, FACG 3 and Santhi Swaroop Vege, MD, FACG 4 1 State University
ACG Clinical Guideline: Management of Acute Pancreatitis Scott Tenner, MD, MPH, FACG 1, John Baillie, MB, ChB, FRCP, FACG 2, John DeWitt, MD, FACG 3 and Santhi Swaroop Vege, MD, FACG 4 1 State University
Pancreatic Benign April 27, 2016
 Department of Surgery Pancreatic Benign April 27, 2016 James Choi Dr. Hernandez Objectives Medical Expert: 1. Anatomy and congenital anomalies of the pancreas and pancreatic duct (divisum, annular pancreas
Department of Surgery Pancreatic Benign April 27, 2016 James Choi Dr. Hernandez Objectives Medical Expert: 1. Anatomy and congenital anomalies of the pancreas and pancreatic duct (divisum, annular pancreas
Management of Acute Pancreatitis and its Complications Aspirus Grand Rounds June 6, 2017 Eric A. Johnson MD
 Management of Acute Pancreatitis and its Complications Aspirus Grand Rounds June 6, 2017 Eric A. Johnson MD Disclosure: None In accordance with the Standards of the Wisconsin Medical Society, all those
Management of Acute Pancreatitis and its Complications Aspirus Grand Rounds June 6, 2017 Eric A. Johnson MD Disclosure: None In accordance with the Standards of the Wisconsin Medical Society, all those
Severe necrotizing pancreatitis. ICU Fellowship Training Radboudumc
 Severe necrotizing pancreatitis ICU Fellowship Training Radboudumc Acute pancreatitis Patients with acute pancreatitis van Dijk SM. Gut 2017;66:2024-2032 Diagnosis Revised Atlanta classification Abdominal
Severe necrotizing pancreatitis ICU Fellowship Training Radboudumc Acute pancreatitis Patients with acute pancreatitis van Dijk SM. Gut 2017;66:2024-2032 Diagnosis Revised Atlanta classification Abdominal
The Bile Duct (and Pancreas) and the Physician
 The Bile Duct (and Pancreas) and the Physician Javaid Iqbal Consultant in Gastroenterology and Pancreato-biliary Medicine University Hospital South Manchester Not so common?! Two weeks 38 ERCP s 20 15
The Bile Duct (and Pancreas) and the Physician Javaid Iqbal Consultant in Gastroenterology and Pancreato-biliary Medicine University Hospital South Manchester Not so common?! Two weeks 38 ERCP s 20 15
Management of Acute Pancreatitis
 Management of Acute Pancreatitis A Clinical Practice Guideline developed by the University of Toronto s Best Practice in Surgery JA Greenberg, M Bawazeer, J Hsu, J Marshall, JO Friedrich, A Nathens, N
Management of Acute Pancreatitis A Clinical Practice Guideline developed by the University of Toronto s Best Practice in Surgery JA Greenberg, M Bawazeer, J Hsu, J Marshall, JO Friedrich, A Nathens, N
PANCREATIC PSEUDOCYSTS. Madhuri Rao MD PGY-5 Kings County Hospital Center
 PANCREATIC PSEUDOCYSTS Madhuri Rao MD PGY-5 Kings County Hospital Center 34 yo M Case Presentation PMH: Chronic pancreatitis (ETOH related) PSH: Nil Meds: Nil NKDA www.downstatesurgery.org Symptoms o Chronic
PANCREATIC PSEUDOCYSTS Madhuri Rao MD PGY-5 Kings County Hospital Center 34 yo M Case Presentation PMH: Chronic pancreatitis (ETOH related) PSH: Nil Meds: Nil NKDA www.downstatesurgery.org Symptoms o Chronic
Endoscopic Management of Acute Pancreatitis. Theo Doukides, MD Gastroenterology and Therapeutic Endoscopy February 13, 2018
 Endoscopic Management of Acute Pancreatitis Theo Doukides, MD Gastroenterology and Therapeutic Endoscopy February 13, 2018 Objectives Assessment of acute pancreatitis Early management Who needs an ERCP
Endoscopic Management of Acute Pancreatitis Theo Doukides, MD Gastroenterology and Therapeutic Endoscopy February 13, 2018 Objectives Assessment of acute pancreatitis Early management Who needs an ERCP
Disclosures. Extra-hepatic Biliary Disease and the Pancreas. Objectives. Pancreatitis 10/3/2018. No relevant financial disclosures to report
 Extra-hepatic Biliary Disease and the Pancreas Disclosures No relevant financial disclosures to report Jeffrey Coughenour MD FACS Clinical Associate Professor of Surgery and Emergency Medicine Division
Extra-hepatic Biliary Disease and the Pancreas Disclosures No relevant financial disclosures to report Jeffrey Coughenour MD FACS Clinical Associate Professor of Surgery and Emergency Medicine Division
Acute Pancreatitis:
 American College of Gastroenterology 2014 Acute Pancreatitis Scott Tenner, MD, MPH, FACG Clinical Professor of Medicine State University of New York Health Sciences Center Director, Brooklyn Gastroenterology
American College of Gastroenterology 2014 Acute Pancreatitis Scott Tenner, MD, MPH, FACG Clinical Professor of Medicine State University of New York Health Sciences Center Director, Brooklyn Gastroenterology
U Nordic Forum - Trauma & Emergency Radiology. Lecture Objectives. MDCT in Acute Pancreatitis. Acute Pancreatitis: Etiologies
 Nordic Forum - Trauma & Emergency Radiology Lecture Objectives MDCT in Acute Pancreatitis Borut Marincek Institute of Diagnostic Radiology niversity Hospital Zurich, Switzerland To describe the role of
Nordic Forum - Trauma & Emergency Radiology Lecture Objectives MDCT in Acute Pancreatitis Borut Marincek Institute of Diagnostic Radiology niversity Hospital Zurich, Switzerland To describe the role of
Management of Gallbladder Disease
 Management of Gallbladder Disease Steven B. Johnson, MD, FACS, FCCM Professor and Chairman, Department of Surgery Program Director, Phoenix Integrated Surgical Residency University of Arizona College of
Management of Gallbladder Disease Steven B. Johnson, MD, FACS, FCCM Professor and Chairman, Department of Surgery Program Director, Phoenix Integrated Surgical Residency University of Arizona College of
Acute Pancreatitis. Encourage You to Read!
 Acute Pancreatitis Laith H. Jamil, MD, FACG Associate Director of Interventional Endoscopy Cedars Sinai Medical Center Los Angeles, CA Encourage You to Read! Copyright 2015 American College of Gastroenterology
Acute Pancreatitis Laith H. Jamil, MD, FACG Associate Director of Interventional Endoscopy Cedars Sinai Medical Center Los Angeles, CA Encourage You to Read! Copyright 2015 American College of Gastroenterology
Management of Gallbladder Disease. Cory Buschmann, MD PGY-5 11/28/2017
 Management of Gallbladder Disease Cory Buschmann, MD PGY-5 11/28/2017 Financial disclosures None Content Scope of gallbladder diseases Evaluation H&P Labs Imaging Cholecystectomy vs cholecystostomy Ancillary
Management of Gallbladder Disease Cory Buschmann, MD PGY-5 11/28/2017 Financial disclosures None Content Scope of gallbladder diseases Evaluation H&P Labs Imaging Cholecystectomy vs cholecystostomy Ancillary
Siddharth Gosavi, Vydehi Institute of Medical Sciences & Research Centre, India Under the guidance of Gillian Lieberman, MD
 Under the guidance of Gillian Lieberman, MD March 2016 RADIOLOGICAL HALLMARKS OF NECROTIZING PANCREATITIS Siddharth Gosavi, Vydehi Institute of Medical Sciences & Research Centre, India Under the guidance
Under the guidance of Gillian Lieberman, MD March 2016 RADIOLOGICAL HALLMARKS OF NECROTIZING PANCREATITIS Siddharth Gosavi, Vydehi Institute of Medical Sciences & Research Centre, India Under the guidance
Exocrine functions: secretion of digestive enzymes (eg. lipase, amylase,
 Chapter 91 Pancreas Episode Overview: 1. List 10 differential diagnoses for acute pancreatitis 2. List 10 causes of pancreatitis. Which are most common in adults? Which one is most common in pediatrics?
Chapter 91 Pancreas Episode Overview: 1. List 10 differential diagnoses for acute pancreatitis 2. List 10 causes of pancreatitis. Which are most common in adults? Which one is most common in pediatrics?
Disclosures. Overview. Case 1. Common Bile Duct Sizes 10/14/2016. General GI + Advanced Endoscopy: NAFLD/Stones/Pancreatitis
 Disclosures General GI + Advanced Endoscopy: NAFLD/Stones/Pancreatitis 123 Blank Blank, LLC Aldo Maspons, MD Assistant Professor Director of Endoscopy Department of Pediatrics Texas Tech University Health
Disclosures General GI + Advanced Endoscopy: NAFLD/Stones/Pancreatitis 123 Blank Blank, LLC Aldo Maspons, MD Assistant Professor Director of Endoscopy Department of Pediatrics Texas Tech University Health
CLINICAL MANIFESTATIONS AND DIAGNOSIS OF ACUTE PANCREATITIS. Raed Abu Sham a, M.D
 CLINICAL MANIFESTATIONS AND DIAGNOSIS OF ACUTE PANCREATITIS Raed Abu Sham a, M.D ACUTE PANCREATITIS Acute inflammatory process of the pancreas that resolves both clinically and histologically. It is usually
CLINICAL MANIFESTATIONS AND DIAGNOSIS OF ACUTE PANCREATITIS Raed Abu Sham a, M.D ACUTE PANCREATITIS Acute inflammatory process of the pancreas that resolves both clinically and histologically. It is usually
Figure 2: Post-cholecystectomy biliary-like pain
 Figure 2: Post-cholecystectomy biliary-like pain 1 patient with recurrent episodes of pain (not daily), in the epigastrium/right upper quadrant, lasting >30 mins, building to a steady level, interrupting
Figure 2: Post-cholecystectomy biliary-like pain 1 patient with recurrent episodes of pain (not daily), in the epigastrium/right upper quadrant, lasting >30 mins, building to a steady level, interrupting
Resident Teaching Conference 10/16/09 Rondi Kauffmann Resident presenter William Nealon Faculty presenter
 Resident Teaching Conference 10/16/09 Rondi Kauffmann Resident presenter William Nealon Faculty presenter KC 59 year old male Referred to Surgery clinic for incidentally discovered 5cm x 3cm pancreatic
Resident Teaching Conference 10/16/09 Rondi Kauffmann Resident presenter William Nealon Faculty presenter KC 59 year old male Referred to Surgery clinic for incidentally discovered 5cm x 3cm pancreatic
American College of Gastroenterology Guideline: Management of Acute Pancreatitis
 PRACTICE GUIDELINES nature publishing group 1 American College of Gastroenterology Guideline: Management of Acute Pancreatitis Scott Tenner, MD, MPH, FACG1, John Baillie, MB, ChB, FRCP, FACG 2, Joh n D
PRACTICE GUIDELINES nature publishing group 1 American College of Gastroenterology Guideline: Management of Acute Pancreatitis Scott Tenner, MD, MPH, FACG1, John Baillie, MB, ChB, FRCP, FACG 2, Joh n D
LOKUN! I got stomach ache!
 LOKUN! I got stomach ache! Mr L is a 67year old Chinese gentleman who is a non smoker, social drinker. He has a medical history significant for Hypertension, Hyperlipidemia, Type 2 Diabetes Mellitus, Chronic
LOKUN! I got stomach ache! Mr L is a 67year old Chinese gentleman who is a non smoker, social drinker. He has a medical history significant for Hypertension, Hyperlipidemia, Type 2 Diabetes Mellitus, Chronic
ESPEN Congress Brussels 2005
 ESPEN Congress Brussels 2005 Therapeutic endoscopy of pancreatic diseases. How endoscopy may improve nutrition? Myriam Delhaye Therapeutic endoscopy of pancreatic diseases. How endoscopy may improve nutrition?
ESPEN Congress Brussels 2005 Therapeutic endoscopy of pancreatic diseases. How endoscopy may improve nutrition? Myriam Delhaye Therapeutic endoscopy of pancreatic diseases. How endoscopy may improve nutrition?
General Surgery Service
 General Surgery Service Patient Care Goals and Objectives Stomach/Duodenum and Bariatric assessed for a) Obesity surgery b) Treatment of i) Adenocarcinoma of the stomach ii) GIST iii) Carcinoid 2) Optimize
General Surgery Service Patient Care Goals and Objectives Stomach/Duodenum and Bariatric assessed for a) Obesity surgery b) Treatment of i) Adenocarcinoma of the stomach ii) GIST iii) Carcinoid 2) Optimize
stents she/he is providing appropriate or inappropriate care?
 Pancreatic Stents Are They Now State of the Art Care? To Help Limit Post ERCP Pancreatitis Glen A. Lehman, M.D. Professor of Medicine and Radiology Division of Gastroenterology/Hepatology Indiana University
Pancreatic Stents Are They Now State of the Art Care? To Help Limit Post ERCP Pancreatitis Glen A. Lehman, M.D. Professor of Medicine and Radiology Division of Gastroenterology/Hepatology Indiana University
PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE. PRESENTED BY: Susan DePasquale, CGRN, MSN
 PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE PRESENTED BY: Susan DePasquale, CGRN, MSN Pancreatic Fluid Collection (PFC) A result of pancreatic duct (PD) and side branch disruption,
PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE PRESENTED BY: Susan DePasquale, CGRN, MSN Pancreatic Fluid Collection (PFC) A result of pancreatic duct (PD) and side branch disruption,
Multi modality Imaging in Acute Pancreatitis. Marsha Lynch, HMS III Gillian Lieberman, MD BIDMC Core Clerkship in Radiology March 2009
 Multi modality Imaging in Acute Pancreatitis Marsha Lynch, HMS III Gillian Lieberman, MD BIDMC Core Clerkship in Radiology March 2009 Our Patient R: Introduction 52M with 10d history of nausea, vomiting
Multi modality Imaging in Acute Pancreatitis Marsha Lynch, HMS III Gillian Lieberman, MD BIDMC Core Clerkship in Radiology March 2009 Our Patient R: Introduction 52M with 10d history of nausea, vomiting
ERCP / PTC Surgical Laparoscopic vs open Timing and order of approach
 Choledocholithiasis Which Approach and When? Lygia Stewart, MD University of California, San Francisco 2010 Naffziger Post-Graduate Course Clinical Manifestations of Choledocholithiasis Asymptomatic (no
Choledocholithiasis Which Approach and When? Lygia Stewart, MD University of California, San Francisco 2010 Naffziger Post-Graduate Course Clinical Manifestations of Choledocholithiasis Asymptomatic (no
7/11/2017. We re gonna help a lot of people today. Biliary/Pancreatic Endoscopy. AGS July 1-2, Kenneth M. Sigman, MD
 Biliary/Pancreatic Endoscopy AGS July 1-2, 2017 Kenneth M. Sigman, MD We re gonna help a lot of people today 1 2 3 4 Cannulation It all starts with cannulation Double Wire Cannulation Difficult cannulations
Biliary/Pancreatic Endoscopy AGS July 1-2, 2017 Kenneth M. Sigman, MD We re gonna help a lot of people today 1 2 3 4 Cannulation It all starts with cannulation Double Wire Cannulation Difficult cannulations
General'Surgery'Service'
 General'Surgery'Service' Patient Care Goals and Objectives 1)! Stomach/Duodenum and Bariatric 2)! Interpret the results of clinical evaluations (history, physical examination) performed on patients being
General'Surgery'Service' Patient Care Goals and Objectives 1)! Stomach/Duodenum and Bariatric 2)! Interpret the results of clinical evaluations (history, physical examination) performed on patients being
ERCP complications and challenges in their diagnosis and management.
 ERCP complications and challenges in their diagnosis and management. Sandie R Thomson Chair of the Division of Gastroenterology, University of Cape Town ERCP Do I have a good Indication? . Algorithm for
ERCP complications and challenges in their diagnosis and management. Sandie R Thomson Chair of the Division of Gastroenterology, University of Cape Town ERCP Do I have a good Indication? . Algorithm for
Pathophysiology ACUTE PANCREATITIS
 Pancreatitis Pathophysiology ACUTE PANCREATITIS BILIARY OBSTRUCTION Duct obstruction in the bile duct, pancreatic duct, or both. Increasing pressure Unregulated activation of digestive enzymes. Inflammation
Pancreatitis Pathophysiology ACUTE PANCREATITIS BILIARY OBSTRUCTION Duct obstruction in the bile duct, pancreatic duct, or both. Increasing pressure Unregulated activation of digestive enzymes. Inflammation
ESPEN Congress The Hague 2017
 ESPEN Congress The Hague 2017 Meeting nutritional needs of acute care patients Feeding acute pancreatitis patients J. Luttikhold (NL) FEEDING ACUTE PANCREATITIS PATIENTS Joanna Luttikhold, MD PhD Registrar
ESPEN Congress The Hague 2017 Meeting nutritional needs of acute care patients Feeding acute pancreatitis patients J. Luttikhold (NL) FEEDING ACUTE PANCREATITIS PATIENTS Joanna Luttikhold, MD PhD Registrar
Joint Trust Management of Acute Severe Pancreatitis in Adults
 A clinical guideline recommended for use For Use in: By: For: Division responsible for document: All clinical areas (as a reference for screening) ITU/HDU (for definitive care) All medical staff likely
A clinical guideline recommended for use For Use in: By: For: Division responsible for document: All clinical areas (as a reference for screening) ITU/HDU (for definitive care) All medical staff likely
Emergency Surgery Course Graz, March ACUTE PANCREATITIS. Carlos Mesquita Coimbra
 ACUTE PANCREATITIS Carlos Mesquita Coimbra ESSENTIALS (1) AP occurs when digestive enzymes become activated while still in the pancreas, causing inflammation repeated bouts of AP can lead to chronic pancreatitis
ACUTE PANCREATITIS Carlos Mesquita Coimbra ESSENTIALS (1) AP occurs when digestive enzymes become activated while still in the pancreas, causing inflammation repeated bouts of AP can lead to chronic pancreatitis
Pancreatic Lesions. Valerie Jefford Pediatric Surgery Rounds June 6, 2003
 Pancreatic Lesions Valerie Jefford Pediatric Surgery Rounds June 6, 2003 Embryology 4 th week 2 buds of endodermal origin from caudal foregut Dorsal and ventral bud Ventral migrates dorsally with CBD (below/behind
Pancreatic Lesions Valerie Jefford Pediatric Surgery Rounds June 6, 2003 Embryology 4 th week 2 buds of endodermal origin from caudal foregut Dorsal and ventral bud Ventral migrates dorsally with CBD (below/behind
Nothing to declare. Probable causes for the change
 acute pancreatitis March 25, 2017 C. S PITCHUMONI. MD,MACP,MACG,MPH.FRCP (c) Adjunct Professor of Medicine New York Medical College Professor of Medicine Rutgers university Nothing to declare Lesser sac?
acute pancreatitis March 25, 2017 C. S PITCHUMONI. MD,MACP,MACG,MPH.FRCP (c) Adjunct Professor of Medicine New York Medical College Professor of Medicine Rutgers university Nothing to declare Lesser sac?
ERCP and EUS: What s New and What Should We Do?
 ERCP and EUS: What s New and What Should We Do? Rajesh N. Keswani, MD Associate Professor of Medicine Division of Gastroenterology Northwestern University Feinberg School of Medicine EUS/ERCP in 2015 THE
ERCP and EUS: What s New and What Should We Do? Rajesh N. Keswani, MD Associate Professor of Medicine Division of Gastroenterology Northwestern University Feinberg School of Medicine EUS/ERCP in 2015 THE
GASTROENTEROLOGY ESSENTIALS
 GASTROENTEROLOGY ESSENTIALS Practical Gastroenterology 8/25/2018 Jahnavi Koppala, MBBS Abdullah Abdussalam, MD A 48-year-old male was evaluated for noncardiac chest pain. Treatment with PPI twice daily
GASTROENTEROLOGY ESSENTIALS Practical Gastroenterology 8/25/2018 Jahnavi Koppala, MBBS Abdullah Abdussalam, MD A 48-year-old male was evaluated for noncardiac chest pain. Treatment with PPI twice daily
Early management of complicated gallstones and acute pancreatitis
 Early management of complicated gallstones and acute pancreatitis A/Prof Richard Cade George Kalogeropoulos ( Fellow) HPB/Upper GI Unit Eastern Health, Melbourne biliary colic/acute cholecystitis common
Early management of complicated gallstones and acute pancreatitis A/Prof Richard Cade George Kalogeropoulos ( Fellow) HPB/Upper GI Unit Eastern Health, Melbourne biliary colic/acute cholecystitis common
The Pancreas. Basic Anatomy. Endocrine pancreas. Exocrine pancreas. Pancreas vasculature. Islets of Langerhans. Acinar cells Ductal System
 SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
Case 1- B.N. 66 yr old F with PMHx of breast cancer s/ p mastectomy, HTN, DM presented with dysphagia to solids and liquids.
 Case 1- B.N 66 yr old F with PMHx of breast cancer s/ p mastectomy, HTN, DM presented with dysphagia to solids and liquids. Reports retching to clear esophagus. Case 1- B.N EGD: Stricture in the distal
Case 1- B.N 66 yr old F with PMHx of breast cancer s/ p mastectomy, HTN, DM presented with dysphagia to solids and liquids. Reports retching to clear esophagus. Case 1- B.N EGD: Stricture in the distal
GENERAL SURGERY FOR SMART PEOPLE JOE NOLD MD, FACS WICHITA SURGICAL SPECIALISTS
 GENERAL SURGERY FOR SMART PEOPLE JOE NOLD MD, FACS WICHITA SURGICAL SPECIALISTS CONFLICTS/DECLARATIONS I have no financial conflicts or declarations I AM always willing to see a consult for you TEXT TOPICS
GENERAL SURGERY FOR SMART PEOPLE JOE NOLD MD, FACS WICHITA SURGICAL SPECIALISTS CONFLICTS/DECLARATIONS I have no financial conflicts or declarations I AM always willing to see a consult for you TEXT TOPICS
Sphincter of Oddi Dysfunction: What s the Verdict in 2014?
 SGNA March 2014 Sphincter of Oddi Dysfunction: What s the Verdict in 2014? Evan L. Fogel, M.D. Professor of Clinical Medicine ERCP Fellowship Director Division of Gastroenterology/Hepatology Indiana University
SGNA March 2014 Sphincter of Oddi Dysfunction: What s the Verdict in 2014? Evan L. Fogel, M.D. Professor of Clinical Medicine ERCP Fellowship Director Division of Gastroenterology/Hepatology Indiana University
The role of ERCP in chronic pancreatitis
 The role of ERCP in chronic pancreatitis Marianna Arvanitakis Erasme University Hospital, ULB, Brussels, Belgium 10 th Nottingham Endoscopy Masterclass SPEAKER DECLARATIONS This presenter has the following
The role of ERCP in chronic pancreatitis Marianna Arvanitakis Erasme University Hospital, ULB, Brussels, Belgium 10 th Nottingham Endoscopy Masterclass SPEAKER DECLARATIONS This presenter has the following
6/17/2016. ERCP in June 26, Kenneth M. Sigman, M.D. Birmingham Gastroenterology Associates
 ERCP in 2016 June 26, 2016 Kenneth M. Sigman, M.D. Birmingham Gastroenterology Associates 1 2 3 Diagnostic/Therapeutic ERCP Biliary Obstruction Benign stricture Malignant Stones Ductal injuries Cholangitis
ERCP in 2016 June 26, 2016 Kenneth M. Sigman, M.D. Birmingham Gastroenterology Associates 1 2 3 Diagnostic/Therapeutic ERCP Biliary Obstruction Benign stricture Malignant Stones Ductal injuries Cholangitis
Acute Pancreatitis. Falk Symposium 161 Dresden
 Acute Pancreatitis Falk Symposium 161 Dresden 12.10.2007 Incidence of Acute Pancreatitis (Malmö) Lindkvist B, et al Clin Gastroenterol Hepatol 2004;2:831-837 Gallstones Alcohol AGA Medical Position Statement
Acute Pancreatitis Falk Symposium 161 Dresden 12.10.2007 Incidence of Acute Pancreatitis (Malmö) Lindkvist B, et al Clin Gastroenterol Hepatol 2004;2:831-837 Gallstones Alcohol AGA Medical Position Statement
Abdominal Pain. Luke Donnelly, MD Emergency Medicine
 Abdominal Pain Luke Donnelly, MD Emergency Medicine Objectives Approach to abdominal pain Evaluation Critical diagnoses and treatments Abdominal Pain Most Common ER Complaint Broad Differential Can often
Abdominal Pain Luke Donnelly, MD Emergency Medicine Objectives Approach to abdominal pain Evaluation Critical diagnoses and treatments Abdominal Pain Most Common ER Complaint Broad Differential Can often
Chronic Pancreatitis: When to Scope? Gregory A. Cote, MD, MS Assistant Professor of Medicine Indiana University School of Medicine
 Chronic Pancreatitis: When to Scope? Gregory A. Cote, MD, MS Assistant Professor of Medicine Indiana University School of Medicine Endoscopy & Chronic Pancreatitis Diagnosis EUS ERCP Exocrine Function
Chronic Pancreatitis: When to Scope? Gregory A. Cote, MD, MS Assistant Professor of Medicine Indiana University School of Medicine Endoscopy & Chronic Pancreatitis Diagnosis EUS ERCP Exocrine Function
DISCLAIMER. No Conflict of Interest
 DISCLAIMER No Conflict of Interest EXCLAIMER No Interest in Conflict GALLSTONES FAQs and FACTS John Dunn, FRACS Laparoscopy Auckland YOU GOTTA KNOW THIS STUFF HOW DO THEY FORM? Gallbladder Lithogenic
DISCLAIMER No Conflict of Interest EXCLAIMER No Interest in Conflict GALLSTONES FAQs and FACTS John Dunn, FRACS Laparoscopy Auckland YOU GOTTA KNOW THIS STUFF HOW DO THEY FORM? Gallbladder Lithogenic
Endoscopic Ultrasonography Clinical Impact. Giancarlo Caletti. Gastroenterologia Università di Bologna. Caletti
 Clinical Impact Giancarlo Gastroenterologia Università di Bologna AUSL di Imola,, Castel S. Pietro Terme (BO) 1982 Indications Diagnosis of Submucosal Tumors (SMT) Staging of Neoplasms Evaluation of Pancreato-Biliary
Clinical Impact Giancarlo Gastroenterologia Università di Bologna AUSL di Imola,, Castel S. Pietro Terme (BO) 1982 Indications Diagnosis of Submucosal Tumors (SMT) Staging of Neoplasms Evaluation of Pancreato-Biliary
Lahey Clinic Internal Medicine Residency Program: Curriculum for Gastroenterology
 Lahey Clinic Internal Medicine Residency Program: Curriculum for Gastroenterology Faculty representative: David L. Burns, MD, CNSP Resident representative: Tom Castiglione, MD Revision date: March 6, 2006
Lahey Clinic Internal Medicine Residency Program: Curriculum for Gastroenterology Faculty representative: David L. Burns, MD, CNSP Resident representative: Tom Castiglione, MD Revision date: March 6, 2006
Surgical Management of Acute Pancreatitis
 Surgical Management of Acute Pancreatitis Steven J. Hughes, MD, FACS Cracchiolo Family Professor of Surgery and Chief, General Surgery Overview Biliary pancreatitis a cost effective algorithm Key concepts
Surgical Management of Acute Pancreatitis Steven J. Hughes, MD, FACS Cracchiolo Family Professor of Surgery and Chief, General Surgery Overview Biliary pancreatitis a cost effective algorithm Key concepts
Does Sphincter of Oddi Dysfunction Even Exist Anymore?
 Does Sphincter of Oddi Dysfunction Even Exist Anymore? Grace H. Elta, MD, FACG Professor of Medicine University of Michigan Sphincter of Oddi Dysfunction Best studied clinical association: Biliary pain
Does Sphincter of Oddi Dysfunction Even Exist Anymore? Grace H. Elta, MD, FACG Professor of Medicine University of Michigan Sphincter of Oddi Dysfunction Best studied clinical association: Biliary pain
Randomized Controlled Trials in Pancreatic Diseases. James Buxbaum MD University of Southern California Los Angeles County Hospital
 Randomized Controlled Trials in Pancreatic Diseases James Buxbaum MD University of Southern California Los Angeles County Hospital Randomized Trials in Pancreatic Diseases Focus acute pancreatitis Challenges
Randomized Controlled Trials in Pancreatic Diseases James Buxbaum MD University of Southern California Los Angeles County Hospital Randomized Trials in Pancreatic Diseases Focus acute pancreatitis Challenges
Caring for the Patient with Acute Pancreatitis. Disclosure. Objectives
 Caring for the Patient with Acute Pancreatitis Bruce D. Askey, MS, ANP-BC Associate Lecturer Fitzgerald Health Education North Andover, MA Adult Nurse Practitioner Dept. of Hepatology/Gastroenterology
Caring for the Patient with Acute Pancreatitis Bruce D. Askey, MS, ANP-BC Associate Lecturer Fitzgerald Health Education North Andover, MA Adult Nurse Practitioner Dept. of Hepatology/Gastroenterology
Pancreas composed of 2 parts: 1- exocrine gland 2- endocrine gland
 pancreas Pancreas composed of 2 parts: 1- exocrine gland 2- endocrine gland Acute pancreatitis Inflammation of the pancreas associated with acinar cell injury Clinical features: 1-abdominal pain cardinal
pancreas Pancreas composed of 2 parts: 1- exocrine gland 2- endocrine gland Acute pancreatitis Inflammation of the pancreas associated with acinar cell injury Clinical features: 1-abdominal pain cardinal
Sphincter of Oddi Dysfunction: Where do we stand in 2015?
 IU GI Motility Conference August 5, 2015 Sphincter of Oddi Dysfunction: Where do we stand in 2015? Evan L. Fogel, M.D. Professor of Medicine ERCP Fellowship Director Division of Gastroenterology/Hepatology
IU GI Motility Conference August 5, 2015 Sphincter of Oddi Dysfunction: Where do we stand in 2015? Evan L. Fogel, M.D. Professor of Medicine ERCP Fellowship Director Division of Gastroenterology/Hepatology
9/21/15. Joshua Pruitt, MD, FAAEM Medical Director, LifeGuard Air Ambulance Iowa PA Society Fall CME Conference September 29, 2015
 Unless they prove otherwise. ~Every ED attending ever Joshua Pruitt, MD, FAAEM Medical Director, LifeGuard Air Ambulance Iowa PA Society Fall CME Conference September 29, 2015 AAA with rupture Mesenteric
Unless they prove otherwise. ~Every ED attending ever Joshua Pruitt, MD, FAAEM Medical Director, LifeGuard Air Ambulance Iowa PA Society Fall CME Conference September 29, 2015 AAA with rupture Mesenteric
Morning Report. Allison Haden, MD October 1, 2002
 Morning Report Allison Haden, MD October 1, 2002 68 yo WM with N/V and abdominal pain Became ill about 2 weeks ago, per pt. intermittent nausea: worse w/eating vomiting within 30min of eating, nonbilious,
Morning Report Allison Haden, MD October 1, 2002 68 yo WM with N/V and abdominal pain Became ill about 2 weeks ago, per pt. intermittent nausea: worse w/eating vomiting within 30min of eating, nonbilious,
Abdo Pain rules & regulations. Mark Hartnell 2010
 Abdo Pain rules & regulations Mark Hartnell 2010 Aims Simple rules which might help in patients with abdominal pain Talk about some myths and realities Discuss some practical how to s in day to day treatment
Abdo Pain rules & regulations Mark Hartnell 2010 Aims Simple rules which might help in patients with abdominal pain Talk about some myths and realities Discuss some practical how to s in day to day treatment
Case Discussion Splenic Abscess
 Case Discussion Splenic Abscess Personal Data Gender: male Birth Date: 1928/Mar/06th Allergy: Mefenamic Smoking: 0.5 PPD for 55 years Alcohol: negative (?) 4 Months Ago Abdominal pain: epigastric area
Case Discussion Splenic Abscess Personal Data Gender: male Birth Date: 1928/Mar/06th Allergy: Mefenamic Smoking: 0.5 PPD for 55 years Alcohol: negative (?) 4 Months Ago Abdominal pain: epigastric area
Case 1. Intro to Gallbladder & Pancreas Pathology. Case 1 DIAGNOSIS??? Acute Cholecystitis. Acute Cholecystitis. Helen Remotti M.D.
 Cholecystitis acute chronic Gallbladder tumors Adenomyoma (benign) Adenocarcinoma Pancreatitis acute chronic Pancreatic tumors Intro to Gallbladder & Pancreas Pathology Helen Remotti M.D. Case 1 70 year
Cholecystitis acute chronic Gallbladder tumors Adenomyoma (benign) Adenocarcinoma Pancreatitis acute chronic Pancreatic tumors Intro to Gallbladder & Pancreas Pathology Helen Remotti M.D. Case 1 70 year
Background. RUQ Ultrasound Normal, Recommend Clinical Correlation. Sohail R. Shah, MD, MSHA, FACS, FAAP Texas Children s Hosptial
 RUQ Ultrasound Normal, Recommend Clinical Correlation Sohail R. Shah, MD, MSHA, FACS, FAAP Texas Children s Hosptial Background Incidence of pediatric gallbladder disease continues to rise U.S. Pediatric
RUQ Ultrasound Normal, Recommend Clinical Correlation Sohail R. Shah, MD, MSHA, FACS, FAAP Texas Children s Hosptial Background Incidence of pediatric gallbladder disease continues to rise U.S. Pediatric
Acute pancreatitis Case reports. Clinical problems. Use of antibiotics? (P 1 & 2) Surgical treatment of AP? (P 3 & 4)
 Case reports Clinical problems Use of antibiotics? (P 1 & 2) Surgical treatment of AP? (P 3 & 4) Case reports Case 1 Case 1 Patient KD History M, 63 y Obesity BMI 30.3 kg/m 2 Gallbladder stones No concomitant
Case reports Clinical problems Use of antibiotics? (P 1 & 2) Surgical treatment of AP? (P 3 & 4) Case reports Case 1 Case 1 Patient KD History M, 63 y Obesity BMI 30.3 kg/m 2 Gallbladder stones No concomitant
JUST ANOTHER CASE OF BELLY PAIN A CASE PRESENTATION. Michael Shamoon Albert Einstein College of Medicine September 10, 2013
 A CASE PRESENTATION Michael Shamoon Albert Einstein College of Medicine September 10, 2013 Mr. L 24y/o african-american man CC: abdominal pain, nausea & vomiting since 9am VS: T 98.3, HR 85, RR 18, BP
A CASE PRESENTATION Michael Shamoon Albert Einstein College of Medicine September 10, 2013 Mr. L 24y/o african-american man CC: abdominal pain, nausea & vomiting since 9am VS: T 98.3, HR 85, RR 18, BP
Acute Abdomen. Nirav Patel MD, FACS Banner University Medical Center - Phoenix
 Acute Abdomen Nirav Patel MD, FACS Banner University Medical Center - Phoenix ? Diffuse periumbilical with localization to RLQ + Nausea, anorexia, fevers - Diarrhea, emesis Exacerbated by movement, bumps
Acute Abdomen Nirav Patel MD, FACS Banner University Medical Center - Phoenix ? Diffuse periumbilical with localization to RLQ + Nausea, anorexia, fevers - Diarrhea, emesis Exacerbated by movement, bumps
Does it matter what we drain?
 Endoscopic Management of Pancreatic Fluid Collections Shyam Varadarajulu, MD Medical Director Center for Interventional Endoscopy Florida Hospital, Orlando Does it matter what we drain? Makes all the difference!
Endoscopic Management of Pancreatic Fluid Collections Shyam Varadarajulu, MD Medical Director Center for Interventional Endoscopy Florida Hospital, Orlando Does it matter what we drain? Makes all the difference!
16 April 2010 Resident Teaching Conference. Pancreatitis. W. H. Nealon, M.D., F.A.C.S. J.J. Smith, M.D., D.W.D.
 16 April 2010 Resident Teaching Conference Pancreatitis W. H. Nealon, M.D., F.A.C.S. J.J. Smith, M.D., D.W.D. Santorini Wirsung anatomy.med.umich.edu/.../ duodenum_ans.html Bud and ductology Ventral pancreatic
16 April 2010 Resident Teaching Conference Pancreatitis W. H. Nealon, M.D., F.A.C.S. J.J. Smith, M.D., D.W.D. Santorini Wirsung anatomy.med.umich.edu/.../ duodenum_ans.html Bud and ductology Ventral pancreatic
GASTRO-INTESTINAL TRACT INFECTIONS - ANTIMICROBIAL MANAGEMENT
 GASTRO-INTESTINAL TRACT INFECTIONS - ANTIMICROBIAL MANAGEMENT Name & Title Of Author: Dr Linda Jewes, Consultant Microbiologist Date Amended: December 2016 Approved by Committee/Group: Drugs & Therapeutics
GASTRO-INTESTINAL TRACT INFECTIONS - ANTIMICROBIAL MANAGEMENT Name & Title Of Author: Dr Linda Jewes, Consultant Microbiologist Date Amended: December 2016 Approved by Committee/Group: Drugs & Therapeutics
Biliary MRI w Eovist
 Biliary MRI w Eovist Is there any added value? Elmar M. Merkle, MD Director of MR Imaging Duke University Medical Center elmar.merkle@duke.edu Declaration of Conflict of Interest or Relationship Research
Biliary MRI w Eovist Is there any added value? Elmar M. Merkle, MD Director of MR Imaging Duke University Medical Center elmar.merkle@duke.edu Declaration of Conflict of Interest or Relationship Research
Pancreatic Disease. Chapter. Overview. Diagnosis of the Disease. Francisco Igor B. Macedo and Danny Sleeman. Laboratory Testing
 Chapter 128 Pancreatic Disease Francisco Igor B. Macedo and Danny Sleeman Overview Acute pancreatitis has an annual incidence of 5 to 40 per 100,000 with an overall mortality of 1.5 per 100,000 (1). The
Chapter 128 Pancreatic Disease Francisco Igor B. Macedo and Danny Sleeman Overview Acute pancreatitis has an annual incidence of 5 to 40 per 100,000 with an overall mortality of 1.5 per 100,000 (1). The
Case Scenario 1. Discharge Summary
 Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Prof. (DR.) MD. ISMAIL PATWARY. MBBS, FCPS, MD, FACP, FRCP(Glasgow, Edin) Professor, Dept. of Medicine, Sylhet women s Medical College, Sylhet
 Prof. (DR.) MD. ISMAIL PATWARY MBBS, FCPS, MD, FACP, FRCP(Glasgow, Edin) Professor, Dept. of Medicine, Sylhet women s Medical College, Sylhet CHRONIC PANCREATITIS Defined as a progressive inflammatory
Prof. (DR.) MD. ISMAIL PATWARY MBBS, FCPS, MD, FACP, FRCP(Glasgow, Edin) Professor, Dept. of Medicine, Sylhet women s Medical College, Sylhet CHRONIC PANCREATITIS Defined as a progressive inflammatory
What to do and not do before seeking surgical consultation for a patient with suspected pancreatic cancer
 What to do and not do before seeking surgical consultation for a patient with suspected pancreatic cancer 9 Th Annual Symposium on Gastrointestinal Cancers, St. Louis University School of Medicine Carlos
What to do and not do before seeking surgical consultation for a patient with suspected pancreatic cancer 9 Th Annual Symposium on Gastrointestinal Cancers, St. Louis University School of Medicine Carlos
Chronic Pancreatitis. Ara Sahakian, M.D. Assistant Professor of Medicine USC core lecture
 Chronic Pancreatitis Ara Sahakian, M.D. Assistant Professor of Medicine USC core lecture What is Chronic Pancreatitis Progressive inflammatory disease Pancreatic parenchyma replaced w/fibrous tissue Destruction
Chronic Pancreatitis Ara Sahakian, M.D. Assistant Professor of Medicine USC core lecture What is Chronic Pancreatitis Progressive inflammatory disease Pancreatic parenchyma replaced w/fibrous tissue Destruction
Acute Pancreatitis: New Developments and Strategies for the Hospitalist
 REVIEWS Acute Pancreatitis: New Developments and Strategies for the Hospitalist John F. Dick, III, MD 1 *, Timothy B. Gardner, MD, MS 2, Edward J. Merrens, MD, MS 1 1 Geisel School of Medicine, Section
REVIEWS Acute Pancreatitis: New Developments and Strategies for the Hospitalist John F. Dick, III, MD 1 *, Timothy B. Gardner, MD, MS 2, Edward J. Merrens, MD, MS 1 1 Geisel School of Medicine, Section
A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY
 A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center Welcome The St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center is a leader
A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center Welcome The St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center is a leader
Sphincter of Oddi dysfunction: SOD after EPISOD, Now what do we do?
 Sphincter of Oddi dysfunction: SOD after EPISOD, Now what do we do? Priya A. Jamidar, M.D., FASGE Professor of Medicine, Director of Endoscopy Yale School Y A L E S CH OO L O F MEDIC IN E February in Connecticut
Sphincter of Oddi dysfunction: SOD after EPISOD, Now what do we do? Priya A. Jamidar, M.D., FASGE Professor of Medicine, Director of Endoscopy Yale School Y A L E S CH OO L O F MEDIC IN E February in Connecticut
CLINICAL CASE OF THE MONTH. A 35 Year Old Woman with Abdominal Pain
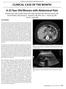 CASE REPORT JOURNAL OF THE LOUISIANA STATE MEDICAL SOCIETY CLINICAL CASE OF THE MONTH A 35 Year Old Woman with Abdominal Pain Melissa Spera, MD, Camille Thelin, MD, Abby Gandolfi, MD, Nicholas Clayton,
CASE REPORT JOURNAL OF THE LOUISIANA STATE MEDICAL SOCIETY CLINICAL CASE OF THE MONTH A 35 Year Old Woman with Abdominal Pain Melissa Spera, MD, Camille Thelin, MD, Abby Gandolfi, MD, Nicholas Clayton,
The role of endoscopy in the diagnosis and treatment of cystic pancreatic neoplasms
 The role of endoscopy in the diagnosis and treatment of cystic pancreatic neoplasms CYSTIC LESIONS AND FLUID COLLECTIONS OF THE PANCREAS Their pathology ranges from pseudocysts and pancreatic necrosis
The role of endoscopy in the diagnosis and treatment of cystic pancreatic neoplasms CYSTIC LESIONS AND FLUID COLLECTIONS OF THE PANCREAS Their pathology ranges from pseudocysts and pancreatic necrosis
Role of Imaging Methods in Diagnosis of Acute Pancreatitis. Válek V. Radiologická klinika, FN Brno a LF MU v Brně
 Role of Imaging Methods in Diagnosis of Acute Pancreatitis Válek V. Radiologická klinika, FN Brno a LF MU v Brně New Classification: Acute Pancreatitis 2007 revision of Atlanta classification and definitions
Role of Imaging Methods in Diagnosis of Acute Pancreatitis Válek V. Radiologická klinika, FN Brno a LF MU v Brně New Classification: Acute Pancreatitis 2007 revision of Atlanta classification and definitions
ACG Postgraduate Course. Multidisciplinary Approach to Acute Pancreatitis Medical Management of Acute Pancreatitis
 ACG Postgraduate Course Multidisciplinary Approach to Acute Pancreatitis Medical Management of Acute Pancreatitis Timothy B. Gardner, MD MS FACG Assistant Professor of Medicine Geisel School of Medicine
ACG Postgraduate Course Multidisciplinary Approach to Acute Pancreatitis Medical Management of Acute Pancreatitis Timothy B. Gardner, MD MS FACG Assistant Professor of Medicine Geisel School of Medicine
Acute Pancreatitis. Case: NG. Idiopathic Pancreatitis is Common. Investigation and Management of Idiopathic Acute Recurrent Pancreatitis (IARP)
 BRIGHAM AND WOMENS HOSPITAL Investigation and Management of (IARP) Acute Pancreatitis j Darwin L. Conwell MD, MS Associate Professor of Medicine Harvard Medical School Boston, MA Case: NG 54 year old female
BRIGHAM AND WOMENS HOSPITAL Investigation and Management of (IARP) Acute Pancreatitis j Darwin L. Conwell MD, MS Associate Professor of Medicine Harvard Medical School Boston, MA Case: NG 54 year old female
Vesalius SCALpel : Biliary (see also: biliary/pancreatic folios) Physiology
 Vesalius SCALpel : Biliary (see also: biliary/pancreatic folios) Physiology 95% of bile acids reabsorbed; colic and chenodeoxycolic primary bile acids cholecystokinin (CCK) major stimulus of gallbladder
Vesalius SCALpel : Biliary (see also: biliary/pancreatic folios) Physiology 95% of bile acids reabsorbed; colic and chenodeoxycolic primary bile acids cholecystokinin (CCK) major stimulus of gallbladder
A Prospective Study of Bedside Index for Severity in Acute Pancreatitis Score in Acute Pancreatitis
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2018/210 A Prospective Study of Bedside Index for Severity in Acute Pancreatitis Score in Acute Pancreatitis S Kasturi Bai
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2018/210 A Prospective Study of Bedside Index for Severity in Acute Pancreatitis Score in Acute Pancreatitis S Kasturi Bai
Best of UEG week 2017 (Pancreas-biliary)
 Best of UEG week 2017 (Pancreas-biliary) Marianna Arvanitakis Erasme University Hospital, ULB, Brussels, Belgium 10 th Nottingham Endoscopy Masterclass SPEAKER DECLARATIONS This presenter has the following
Best of UEG week 2017 (Pancreas-biliary) Marianna Arvanitakis Erasme University Hospital, ULB, Brussels, Belgium 10 th Nottingham Endoscopy Masterclass SPEAKER DECLARATIONS This presenter has the following
IMAGING OF ACUTE AND CHRONIC PANCREATITIS, INCLUDING EXOCRINE FUNCTION
 IMAGING OF ACUTE AND CHRONIC PANCREATITIS, INCLUDING EXOCRINE FUNCTION Andrew T. Trout, MD @AndrewTroutMD Disclosures Grant support National Pancreas Foundation In-kind support - ChiRhoClin modified from:
IMAGING OF ACUTE AND CHRONIC PANCREATITIS, INCLUDING EXOCRINE FUNCTION Andrew T. Trout, MD @AndrewTroutMD Disclosures Grant support National Pancreas Foundation In-kind support - ChiRhoClin modified from:
Management of Pancreatic Fistulae
 Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
SOD (Sphincter of Oddi Dysfunction)
 SOD (Sphincter of Oddi Dysfunction) SOD refers to the mechanical malfunctioning of the Sphincter of Oddi, which is the valve muscle that regulates the flow of bile and pancreatic juice into the duodenum.
SOD (Sphincter of Oddi Dysfunction) SOD refers to the mechanical malfunctioning of the Sphincter of Oddi, which is the valve muscle that regulates the flow of bile and pancreatic juice into the duodenum.
Diseases of pancreas - Chronic pancreatitis
 Corso di laurea in Medicina e Chirurgia Anno accademico 2015-2016 V Anno di corso- Primo Semestre Corso Integrato : Patologia Sistemica C- Gastroenterologia Prof. Stefano Fiorucci Diseases of pancreas
Corso di laurea in Medicina e Chirurgia Anno accademico 2015-2016 V Anno di corso- Primo Semestre Corso Integrato : Patologia Sistemica C- Gastroenterologia Prof. Stefano Fiorucci Diseases of pancreas
Evaluation of Children with Blunt Abdominal Trauma. James F. Holmes, MD, MPH UC Davis School of Medicine
 Evaluation of Children with Blunt Abdominal Trauma James F. Holmes, MD, MPH UC Davis School of Medicine Objectives Epidemiology of intra-abdominal injury (IAI) Physical examination findings with IAI Laboratory
Evaluation of Children with Blunt Abdominal Trauma James F. Holmes, MD, MPH UC Davis School of Medicine Objectives Epidemiology of intra-abdominal injury (IAI) Physical examination findings with IAI Laboratory
Case Report (1) Sphincter of Oddi Dysfunction. Case Report (3) Case Report (2) Case Report (4) Case Report (5)
 Dr David Westaby Imperial NHS Trust Imperial College Medical School London Case Report (1)! TD 33yr old male! Feb May 2010: Recurrent episodes of abdominal pain! June 2010 Episode severe abdominal pain
Dr David Westaby Imperial NHS Trust Imperial College Medical School London Case Report (1)! TD 33yr old male! Feb May 2010: Recurrent episodes of abdominal pain! June 2010 Episode severe abdominal pain
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds
 Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
A patient with an unusual congenital anomaly of the pancreaticobiliary tree
 A patient with an unusual congenital anomaly of the pancreaticobiliary tree Thomas Hocker, HMS IV BIDMC Core Radiology Case Presentation September 17, 2007 Review of Normal Pancreaticobiliary Tract Anatomy
A patient with an unusual congenital anomaly of the pancreaticobiliary tree Thomas Hocker, HMS IV BIDMC Core Radiology Case Presentation September 17, 2007 Review of Normal Pancreaticobiliary Tract Anatomy
Pictorial review of Benign Biliary tract abnormality on MRCP/MRI Liver with Endoscopic (including splyglass) and Endoscopic Ultrasound correlation
 Pictorial review of Benign Biliary tract abnormality on MRCP/MRI Liver with Endoscopic (including splyglass) and Endoscopic Ultrasound correlation Poster No.: C-2617 Congress: ECR 2015 Type: Educational
Pictorial review of Benign Biliary tract abnormality on MRCP/MRI Liver with Endoscopic (including splyglass) and Endoscopic Ultrasound correlation Poster No.: C-2617 Congress: ECR 2015 Type: Educational
Pancreatitis. Acute Pancreatitis
 Pancreatitis Pancreatitis is an inflammation of the pancreas. The pancreas is a large gland behind the stomach and close to the duodenum. The duodenum is the upper part of the small intestine. The pancreas
Pancreatitis Pancreatitis is an inflammation of the pancreas. The pancreas is a large gland behind the stomach and close to the duodenum. The duodenum is the upper part of the small intestine. The pancreas
Adv Pathophysiology Unit 9: GI Page 1 of 10
 Adv Pathophysiology Unit 9: GI Page 1 of 10 Learning objectives for this file: 1. Recognize positive physical and lab findings that point to the diagnosis 2. Appreciate the appearance of the affected organ
Adv Pathophysiology Unit 9: GI Page 1 of 10 Learning objectives for this file: 1. Recognize positive physical and lab findings that point to the diagnosis 2. Appreciate the appearance of the affected organ
Antibiotic Therapy for Prophylaxis of Infection in Severe Pancreatitis is Overrated. Jessica Yu, R2 10/26/09
 Antibiotic Therapy for Prophylaxis of Infection in Severe Pancreatitis is Overrated Jessica Yu, R2 10/26/09 Of 12 with pancreatitis 15% will get necrosis Of these, 40-70% progress to infection week 2-3
Antibiotic Therapy for Prophylaxis of Infection in Severe Pancreatitis is Overrated Jessica Yu, R2 10/26/09 Of 12 with pancreatitis 15% will get necrosis Of these, 40-70% progress to infection week 2-3
Gastroenterology. Certification Examination Blueprint. Purpose of the exam
 Gastroenterology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified gastroenterologist
Gastroenterology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified gastroenterologist
