The Ratio of Atypical Ductal Hyperplasia Foci to Core Numbers in Needle Biopsy: A Practical Index Predicting Breast Cancer in Subsequent Excision
|
|
|
- Trevor Richards
- 5 years ago
- Views:
Transcription
1 The Korean Journal of Pathology 2012; 46: ORIGINAL ARTICLE The Ratio of Atypical Ductal Hyperplasia Foci to Core Numbers in Needle Biopsy: A Practical Index Predicting Breast Cancer in Subsequent Excision Jeong-Ju Lee Hee Jin Lee Jun Kang Jeong-Hyeon Jo Gyungyub Gong Department of Pathology, Asan Medical Center, University of Ulsan College of Medicine, Seoul, Korea Received: June 22, 2011 Revised: September 8, 2011 Accepted: October 7, 2011 Corresponding Author Gyungyub Gong, M.D. Department of Pathology, Asan Medical Center, University of Ulsan College of Medicine, Pungnap 2-dong, Songpa-gu, Seoul , Korea Tel: Fax: gygong@amc.seoul.kr Background: Although core needle biopsy (CNB) is considered to be the standard technique for histological diagnosis of breast lesions, it is less reliable for diagnosing atypical ductal hyperplasia (ADH). We therefore assessed the characteristics of CNB-diagnosed ADH that are more likely to be associated with more advanced lesions on subsequent surgical excision. Methods: We retrospectively examined 239 consecutive CNBs, 127 of which were diagnosed as ADH following surgical excision, performed at Asan Medical Center between 1995 and Archival slides were analyzed for the number of cores per specimen, the number of ADH foci, and the ratio of ADH foci to number of cores (FC ratio). Results: We found that ADH foci in 3 or more cores (p= 0.003) and the presence of ADH in 3 or more foci (p= 0.002) were correlated with malignancy following excision lesion. Moreover, an FC> 1.1 was significantly associated with malignancy in the subsequent excision (p= 0.000). Conclusions: Including the number of ADH foci, the number of cores involved according to ADH, FC ratio, and histologic type in a pathology report of CNB may help in making clinical decisions about surgical excision. Key Words: Atypical ductal hyperplasia; Core needle biopsy; Predictive pathologic factor Image-guided core needle biopsy (CNB) has become the procedure of choice to investigate mammographically suspicious lesions of the breast and has been shown to be effective at ruling out the possibility of cancer. Overall, histologic findings of CNB are in agreement with surgical biopsy in more than 95% of patients. 1-3 However, significant discordance has been reported in the CNB diagnosis of atypical ductal hyperplasia (ADH), with the likelihood of ductal carcinoma in situ (DCIS) or invasive carcinoma on subsequent surgical excision ranging from 7% to 87%. 1,4-9 ADH is a proliferative breast lesion associated with an increased risk of breast cancer with some, but not all, features of low grade DCIS. 10 ADH is characterized by relatively small, monomorphic cells with generally rounded nuclei that are evenly spaced and have well-defined borders. The cells may grow in arcades, rigid bridges or bars of uniform thickness, as micropapillae that are usually broader at the tips than at the base (clubshaped), in solid patterns, or in fenestrated (cribriform) patterns with cells polarized around the extracellular lumens within the proliferation. 10 ADH lesions have also been defined as lesions <2 mm in size with all the cytologic and architectural features of low-grade DCIS. 11 Distinguishing between ADH and low grade DCIS can be difficult using the limited tissue samples obtained by CNB. In addition, ADH foci may be present at the periphery of areas of DCIS; thus, even an unequivocal diagnosis of ADH does not preclude the presence of more advanced lesions in adjacent breast tissue. Due to the risks of false negative biopsy results, it is currently recommended that surgery is not undertaken on lesions diagnosed as ADH by CNB. 12,13 The identification of patients with ADH diagnosed by CNB who can be spared surgical excision is an area of active investigation. Some of these studies have suggested that the extent and histologic pattern of ADH present in CNB specimens can be used to predict the likelihood of the presence of more advanced lesions (DCIS or invasive carcinoma). 5,9 Although previous studies have suggested that the number of ADH foci in core biopsy specimens could be a predictor of malignancy in surgically excised specimens, 5 the number of ADH foci may be propor- pissn The Korean Society of Pathologists/The Korean Society for Cytopathology 15 eissn
2 16 Lee J-J, et al. tional to the number of cores obtained per lesion. The number of biopsy cores can vary due to technical differences. To compensate for this variability, we have devised a new parameter, the ratio of ADH foci to number of cores (FC ratio), defined as the ratio of the number of ADH foci to the number of biopsy cores. In addition to the extent and histologic pattern of ADH in CNB specimens, Ki-67 concentrations in ADH may predict breast cancer. A study examining Ki-67 levels and 10-year and longer-term risk of breast cancer in a cohort of women with atypical hyperplasia reported that Ki-67 concentration is a timevarying biomarker of the risk of breast cancer. 14 However, the clinical significance of Ki-67 in ADH of CNB has not been determined. We have therefore assessed the characteristics of CNBdiagnosed ADH, including pathologic findings, FC ratio, and Ki-67 labeling index, that are more likely to be associated with more advanced lesions on subsequent surgical excision. MATERIALS AND METHODS We examined the surgical pathology files of Asan Medical Center, Seoul, Korea, for all patients with CNB-diagnosed ADH between January 1995 and August Of the 239 CNB-diagnosed patients, 62 were diagnosed with DCIS or invasive carcinoma in the same breast and were therefore excluded. Of the 177 patients diagnosed by CNB with ADH as the most significant lesion, 127 underwent follow-up surgical excision, and 50 did not. Of the latter, some refused further surgery, and others underwent excision at other institutions, with their slides unavailable for review; these patients were therefore excluded. Thus, our study population consisted of 127 patients. All underwent biopsies using a vacuum assisted device with an 11-gauge automated needle or nonvacuum assisted device with a 14-gauge automated needle. All core biopsies and subsequently excised tissue sections were fixed in 10% buffered formaldehyde, embedded in paraffin, and stained with hematoxylin and eosin (H&E). All H&E-stained slides of the CNB specimens were reviewed by two pathologists, blind to the results of subsequent excisional biopsy, to confirm the diagnosis of ADH using established criteria. 10,11 Following the verification of the presence of ADH in CNB specimens, the extent of involvement was determined by evaluation of the number of large ducts and/or terminal duct lobular units affected by ADH, as described previously. 5 When multiple foci of ADH were present, the size of the largest focus was determined. We also analyzed the predominant histologic pattern of ADH (cribriform, micropapillary, papillary or solid) (Fig. 1), the presence of calcifications, number of tissue cores obtained, and number of tissue cores showing ADH involvement. Clinical parameters, including patient age, affected side, and mammographic and ultrasonographic findings, were obtained from patients electronic medical records. All H&E-stained slides of the subsequent surgical excisions were reviewed by two additional pathologists, blind to the CNB results, to confirm the final diagnosis. Surgically excised specimens were evaluated for the presence of invasive carcinoma, DC- IS, lobular carcinoma in situ (LCIS), and residual ADH, using established criteria. 10 The presence of a prior biopsy site was confirmed in all cases. Samples from 79 patients were available for paraffin blocks. Sections were cut at 3 μm thicknesses, deparaffinized in xylene, and rehydrated with graded ethanol. Samples were assayed for Ki-67 expression using a monoclonal mouse anti-human Ki-67 antibody (Zymed, San Francisco, CA, USA) using standard immunohistochemical methods and a Ventana BenchMark XT immunostainer (Ventana Medical Systems, Tucson, AZ, USA). These slides were evaluated by a pathologist blind to the clinical data, who calculated the Ki-67 percentage (representing the proportion of the nuclear positivity for Ki-67) in each ADH lesion. The number of cores obtained, ADH foci, and cores showing ADH involvement, the size of the largest ADH focus, and the Ki-67 labeling index were compared using the Kruskal-Wallis 1-way analysis of variance by ranks. Other clinical and pathological characteristics were cross-tabulated with diagnostic yield in a C R contingency table. Pearson chi-squared test statistics were estimated for every contingency table to test the null hypothesis that the diagnostic yields and clinical characteristics were independent against the alternative that there was an association between them. A 2-sided p-value<0.05 was considered statistically significant. All statistical analyses were performed using SPSS ver.15 (SPSS Inc., Chicago, IL, USA). RESULTS The 127 women assessed ranged in age from 21 to 62 years (mean, years); their clinical and demographic data are summarized in Table 1. Mammographic and/or ultrasonographic evaluation showed that 25 lesions were microcalcifications, 70 were masses, 13 were combined masses with microcalcifications,
3 A Practical Index Predicting Breast Cancer in Subsequent Excision 17 A B C D Fig. 1. Histologic patterns of atypical ductal hyperplasia. (A) Cribriform. (B) Micropapillary. (C) Papillary. (D) Solid. Table 1. Clinical features of the 127 patients with atypical ductal hyperplasia Features Age (yr) Mean Range Side of lesion Left Right Positive family history First-degree relative Other relative None Radiologic findings Microcalcifications Mass Microcalcifications and mass Others No. of patients (%) (41) 75 (59) 6 (5) 2 (1) 119 (94) 25 (20) 70 (55) 13 (10) 19 (15) and 19 showed other findings. The number of cores obtained from each lesion ranged from 1 to 14 (median, 5), the aggregate length of cores obtained from each lesion ranged from 7 to 240 mm (mean, 51 mm) and the median number of cores showing ADH involvement was 2. The median number of ADH foci was 2, and the mean size of ADH foci was 1.0 mm. The predominant histologic pattern of ADH in CNB specimens was cribriform, observed in 88 patients (69.3%), followed by micropapillary in 19 (15.0%), papillary in 9 (7.1%), and solid in 11 (8.7%) patients. The presence of microcalcifications was confirmed histologically in 48 CNBs (37.8%). The Ki-67 labeling index ranged from 0% to 30% (mean, 4.3%). Histologic evaluation of the surgically excised specimens show ed that 42 (33.1%) were benign breast tissue without evidence of atypia, 54 (42.5%) were residual ADH, and 31 (24.4%) were malignant, including DCIS in 25 patients, LCIS in 3, DCIS with LCIS in 1, and invasive carcinoma in 2. Utilizing the Nottingham modification of Scarff-Bloom-Ri chardson histologic grading system, 13 cases (52%) of DCIS were nuclear grade 2, 11 cases (44%) of DCIS were nuclear grade 1, and one case (4%) of DCIS was nuclear grade 3. Two cases of
4 18 Lee J-J, et al. Table 2. Correlation of clinicopathologic characteristics of ADH in CNB specimens with diagnosis after surgical excision Variables Diagnosis after surgical excision Benign ADH Malignancy p-value Age (yr) a < Radiologic findings (No. of patients) a Microcalcifications Mass Microcalcifications and mass Others No. of cores obtained b c Aggregate length of cores b (mm) c No. of cores with ADH involvement b c No. of ADH foci b c ADH size b (mm) c ADH type a Cribriform Papillary Micropapillary Solid Microcalcifications a Present Absence Ki-67 labeling index b (%) c ADH, atypical ductal hyperplasia; CNB, core needle biopsy. a Chi-squared test; b Mean value; c Kruskal-Wallis test. LCIS were accompanied with ADH, but one case of LCIS was purely LCIS. Invasive carcinomas included invasive ductal carcinoma and papillary carcinoma which were nuclear grade 2 and histologic grade 2. The correlations between the extent and types of ADH lesions and other features of the CNB specimens with the results of the surgical excisional specimens are summarized in Table 2. There were no statistically significant differences related to the side of the lesion, family history of breast cancer and radiologically observed microcalcifications. The number of ADH foci, the number of cores showing ADH involvement and ADH size differed significantly among the groups according to their diagnosis based on surgically excised specimens. In contrast, patient age, number of cores obtained, aggregate length of cores, presence of microcalcification in CNB specimens and Ki-67 labeling index were not related to the diagnosis on excised specimens. When the predominant histologic pattern of ADH seen in the CNB specimens was correlated with the corresponding findings on subsequent surgical excision, there was an association between solid ADH and subsequent malignancy, as well as an association between cribriform ADH and subsequent benign lesions. Table 3. Correlation of the extent of ADH in CNB specimens with diagnosis on surgical excision Variables Diagnosis on surgical excision Benign Among the 67 patients with ADH limited to 1 or 2 foci in CNB specimens, 8 (12%) were diagnosed with malignancy, 31 (46%) with residual ADH, and 28 (42%) with lesions having benign histologic features without atypia (Table 3). Among the 60 patients with ADH affecting 3 or more foci in CNB specimens, 23 (38%) were diagnosed with malignancy, 23 (38%) with ADH, and 14 (24%) with benign lesions without atypia. The sensitivity and specificity of ADH involving 3 or more foci in predicting the presence of a malignancy were 74.2% and 61.5%, respectively. Similar results were observed when we considered the number of cores showing ADH involvement. The sensitivity and specificity of ADH involving 3 or more cores in predicting worse lesions (DCIS/LCIS or invasive carcinoma) were 58.1% and 69.8%, respectively. We divided the CNB specimens into two groups. The cut off value was an FC ratio of 1.1 based on the maximum area under the receiver operating characteristic curve. Of the 122 patients with CNB specimens having FC ratios<1.1, 42 (35%) were diagnosed with malignancy, 54 (44%) with residual ADH, and 26 (21%) with benign lesions without atypia (Table 3). In contrast, of the 5 patients with CNB specimens having FC ratios 1.1, all 5 (100%) were diagnosed with malignancy after surgical excision. The sensitivity and specificity of an FC ratio 1.1 in predicting the presence of a malignancy were 16.1% and 100%, respectively. DISCUSSION ADH/ALH Malignancy p-value a No. of ADH foci No. of cores showing ADH involvement FC ratio < ADH, atypical ductal hyperplasia; CNB, core needle biopsy; ALH, atypical lobular hyperplasia; FC ratio, ratio of ADH foci to number of cores. a Chi-squared test. We have assessed the clinicopathological and radiological findings of ADH diagnosed by CNB to determine the factors that can distinguish between ADH and cancer, including DCIS,
5 A Practical Index Predicting Breast Cancer in Subsequent Excision 19 LCIS, and invasive carcinoma. ADH is a type of histologically borderline lesion that is difficult to distinguish from low grade DICS on small tissue samples provided by CNB. Because of this difficulty, clinicopathologic and radiologic findings that can distinguish between ADH and DCIS are valuable in planning patient management. Several studies have examined various mammographic, clinical, and pathologic factors that may predict the presence of a more significant lesion following surgical excision after a CNB diagnosis of ADH. 7,15,16 For example, the combination of a mass with microcalcifications on ultrasonography has been associated with an underestimation of cancer, 17 although we found no association between microcalcifications, on ultrasonography or mammography, and subsequent cancer on excision. Although no universal agreement has been reached about the number of cores necessary to achieve an accurate histologic diagnosis, previous studies have demonstrated that underestimation of malignancy decreases as the average number of cores obtained per lesion increases. 2,18 For example, underestimation at CNB diminished as the mean number of cores per lesion increased from 6.3 to 9.5, with an even further reduction in the underestimation rate when more than 10 cores were acquired per lesion. 19,20 While acknowledging that a certain number of tissue cores are needed for categorization of the lesion, other studies found that the underestimation rate was not related to the number of cores obtained, suggesting that numbers alone may not accurately reflect how thoroughly the lesion is sampled by CNB In contrast to previous findings, 19,20 however, we did not observe a statistically significant correlation between the number of tissue cores removed and the results on final surgical excision. We found a significant correlation between the number of cores showing ADH involvement and the likelihood of malignant lesions after subsequent excision. The number of cores showing ADH involvement has been shown to be significantly higher in patients with a follow-up excisional diagnosis of DCIS compared with patients with a benign lesion or an ADH by excisional biopsy. 25 Although all patients with ADH limited to 1 or 2 foci did not have more malignant lesions on open biopsy, patients with ADH involving 4 or more foci had a higher probability of an underlying, more advanced lesion on excision, with 86.6% of the latter having DCIS or invasive carcinoma. 5 Moreover, we found that ADH involving 3 or more foci in CNB is an indicator of a more significant lesion after excision. Although a previous study reported no association between largest ADH size and subsequent malignancy, 25 we found that largest ADH size was correlated with subsequent malignancy after surgical excision of the lesion. Moreover, a strong association was observed between micropapillary ADH and subsequent DCIS, 5 whereas another study found no association between increased risk of carcinoma on excision and a micropapillary pattern of ADH. 26 We also observed an association between solid ADH and subsequent cancer on excision, whereby 7 of these 11 patients (64%) were diagnosed with malignancy. Histologic examination has shown calcifications in mammary ducts within areas of ADH, but without cell necrosis. 27 In DCIS, the calcifications develop in secretions and are dystrophic calcifications secondary to necrotic tumor cells. 28,29 Our findings were not in agreement with these earlier results. One study found an association between a high Ki-67 labeling index (>2%) in atypical hyperplasia and increased risk of breast cancer within 10 years after atypia. 30 The cumulative incidence of breast cancer at 10 years was also high in patients with a high Ki-67 labeling index. 24,30 In contrast, we found that the Ki-67 labeling index was not significantly correlated with the short-term risk of breast cancer. We also found that FC ratio, representing the number of ADH foci divided by the number of cores, is an indicator for surgical excision in patients with core biopsy samples of breast lesion with ADH. An FC ratio 1.1 is associated with a significantly higher probability of malignancy on subsequent excisions (p= 0.000). The FC ratio compensates for the variability in the number of biopsy cores, is highly specific and is useful for predicting malignancy on follow-up excision. In summary, our study in a series of 127 cases of ADH diagnosed by CNB indicates that microcalcifications on ultrasonography or mammography, determination of the extent (ADH foci, cores involved with ADH), FC ratio, and solid histologic type of ADH can be applied to predict the presence of malignancy found by surgical excision. Including the number of ADH foci, the number of cores involved according to ADH, FC ratio, and histologic type in a pathology report may help in making clinical decisions about surgical excision. Conflicts of Interest No potential conflict of interest relevant to this article was reported. REFERENCES 1. Dahlstrom JE, Sutton S, Jain S. Histological precision of stereotactic
6 20 Lee J-J, et al. core biopsy in diagnosis of malignant and premalignant breast lesions. Histopathology 1996; 28: Jackman RJ, Nowels KW, Shepard MJ, Finkelstein SI, Marzoni FA Jr. Stereotaxic large-core needle biopsy of 450 nonpalpable breast lesions with surgical correlation in lesions with cancer or atypical hyperplasia. Radiology 1994; 193: Parker SH, Lovin JD, Jobe WE, Burke BJ, Hopper KD, Yakes WF. Nonpalpable breast lesions: stereotactic automated large-core biopsies. Radiology 1991; 180: Bonnett M, Wallis T, Rossmann M, et al. Histopathologic analysis of atypical lesions in image-guided core breast biopsies. Mod Pathol 2003; 16: Ely KA, Carter BA, Jensen RA, Simpson JF, Page DL. Core biopsy of the breast with atypical ductal hyperplasia: a probabilistic approach to reporting. Am J Surg Pathol 2001; 25: Harvey JM, Sterrett GF, Frost FA. Atypical ductal hyperplasia and atypia of uncertain significance in core biopsies from mammographically detected lesions: correlation with excision diagnosis. Pathology 2002; 34: Jackman RJ, Birdwell RL, Ikeda DM. Atypical ductal hyperplasia: can some lesions be defined as probably benign after stereotactic 11-gauge vacuum-assisted biopsy, eliminating the recommendation for surgical excision? Radiology 2002; 224: Renshaw AA, Cartagena N, Schenkman RH, Derhagopian RP, Gould EW. Atypical ductal hyperplasia in breast core needle biopsies: correlation of size of the lesion, complete removal of the lesion, and the incidence of carcinoma in follow-up biopsies. Am J Clin Pathol 2001; 116: Sneige N, Lim SC, Whitman GJ, et al. Atypical ductal hyperplasia diagnosis by directional vacuum-assisted stereotactic biopsy of breast microcalcifications: considerations for surgical excision. Am J Clin Pathol 2003; 119: Page DL, Dupont WD, Rogers LW, Rados MS. Atypical hyperplastic lesions of the female breast: a long-term follow-up study. Cancer 1985; 55: Tavassoli FA, Norris HJ. A comparison of the results of long-term follow-up for atypical intraductal hyperplasia and intraductal hyperplasia of the breast. Cancer 1990; 65: Bassett L, Winchester DP, Caplan RB, et al. Stereotactic core-needle biopsy of the breast: a report of the Joint Task Force of the American College of Radiology, American College of Surgeons, and College of American Pathologists. CA Cancer J Clin 1997; 47: Jacobs TW, Connolly JL, Schnitt SJ. Nonmalignant lesions in breast core needle biopsies: to excise or not to excise? Am J Surg Pathol 2002; 26: Liu X, Elojeimy S, Turner LS, et al. Acid ceramidase inhibition: a novel target for cancer therapy. Front Biosci 2008; 13: Brown TA, Wall JW, Christensen ED, et al. Atypical hyperplasia in the era of stereotactic core needle biopsy. J Surg Oncol 1998; 67: Hoang JK, Hill P, Cawson JN. Can mammographic findings help discriminate between atypical ductal hyperplasia and ductal carcinoma in situ after needle core biopsy? Breast 2008; 17: Chae BJ, Lee A, Song BJ, Jung SS. Predictive factors for breast cancer in patients diagnosed atypical ductal hyperplasia at core needle biopsy. World J Surg Oncol 2009; 7: Zografos GC, Zagouri F, Sergentanis TN, et al. Minimizing underestimation rate of microcalcifications excised via vacuum-assisted breast biopsy: a blind study. Breast Cancer Res Treat 2008; 109: Jackman RJ, Burbank F, Parker SH, et al. Stereotactic breast biopsy of nonpalpable lesions: determinants of ductal carcinoma in situ underestimation rates. Radiology 2001; 218: Jackman RJ, Burbank F, Parker SH, et al. Atypical ductal hyperplasia diagnosed at stereotactic breast biopsy: improved reliability with 14-gauge, directional, vacuum-assisted biopsy. Radiology 1997; 204: Darling ML, Smith DN, Lester SC, et al. Atypical ductal hyperplasia and ductal carcinoma in situ as revealed by large-core needle breast biopsy: results of surgical excision. AJR Am J Roentgenol 2000; 175: Liberman L, Cohen MA, Dershaw DD, Abramson AF, Hann LE, Rosen PP. Atypical ductal hyperplasia diagnosed at stereotaxic core biopsy of breast lesions: an indication for surgical biopsy. AJR Am J Roentgenol 1995; 164: Philpotts LE, Lee CH, Horvath LJ, Lange RC, Carter D, Tocino I. Underestimation of breast cancer with II-gauge vacuum suction biopsy. AJR Am J Roentgenol 2000; 175: Winchester DJ, Bernstein JR, Jeske JM, et al. Upstaging of atypical ductal hyperplasia after vacuum-assisted 11-gauge stereotactic core needle biopsy. Arch Surg 2003; 138: Wagoner MJ, Laronga C, Acs G. Extent and histologic pattern of atypical ductal hyperplasia present on core needle biopsy specimens of the breast can predict ductal carcinoma in situ in subsequent excision. Am J Clin Pathol 2009; 131: Doren E, Hulvat M, Norton J, et al. Predicting cancer on excision of atypical ductal hyperplasia. Am J Surg 2008; 195: Helvie MA, Hessler C, Frank TS, Ikeda DM. Atypical hyperplasia of the breast: mammographic appearance and histologic correlation. Radiology 1991; 179: Holland R, Hendriks JH. Microcalcifications associated with ductal carcinoma in situ: mammographic-pathologic correlation. Semin
7 A Practical Index Predicting Breast Cancer in Subsequent Excision 21 Diagn Pathol 1994; 11: Slanetz PJ, Giardino AA, Oyama T, et al. Mammographic appearance of ductal carcinoma in situ does not reliably predict histologic subtype. Breast J 2001; 7: Santisteban M, Reynolds C, Barr Fritcher EG, et al. Ki67: a time-varying biomarker of risk of breast cancer in atypical hyperplasia. Breast Cancer Res Treat 2010; 121:
Michael J. Wagoner, MD, 1 Christine Laronga, MD, 2 and Geza Acs, MD, PhD 1-3. Abstract
 Anatomic Pathology / ADH in Breast Core Needle Biopsy Specimens Extent and Histologic Pattern of Atypical Ductal Hyperplasia Present on Core Needle Biopsy Specimens of the Breast Can Predict Ductal Carcinoma
Anatomic Pathology / ADH in Breast Core Needle Biopsy Specimens Extent and Histologic Pattern of Atypical Ductal Hyperplasia Present on Core Needle Biopsy Specimens of the Breast Can Predict Ductal Carcinoma
Atypical Ductal Hyperplasia and Ductal Carcinoma In Situ as Revealed by Large-Core Needle Breast Biopsy: Results of Surgical Excision
 Marla L. Rosenfield Darling 1 Darrell N. Smith 1 Susan C. Lester 2 Carolyn Kaelin 3 Donna-Lee G. Selland 1 Christine M. Denison 1 Pamela J. DiPiro 1 David I. Rose 1 Esther Rhei 3 Jack E. Meyer 1 Received
Marla L. Rosenfield Darling 1 Darrell N. Smith 1 Susan C. Lester 2 Carolyn Kaelin 3 Donna-Lee G. Selland 1 Christine M. Denison 1 Pamela J. DiPiro 1 David I. Rose 1 Esther Rhei 3 Jack E. Meyer 1 Received
Note: This copy is for your personal, non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, cont
 Note: This copy is for your personal, non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. Risk of Upgrade
Note: This copy is for your personal, non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. Risk of Upgrade
Underestimation of Atypical Ductal Hyperplasia at Sonographically Guided Core Biopsy of the Breast
 Women s Imaging Original Research Jang et al. Sonographic Breast Biopsy Women s Imaging Original Research WOMEN S IMAGING Underestimation of Atypical Ductal Hyperplasia at Sonographically Guided Core Biopsy
Women s Imaging Original Research Jang et al. Sonographic Breast Biopsy Women s Imaging Original Research WOMEN S IMAGING Underestimation of Atypical Ductal Hyperplasia at Sonographically Guided Core Biopsy
Women s Imaging Original Research
 Women s Imaging Original Research Villa et al. Biopsy of Atypical Ductal Hyperplasia Women s Imaging Original Research WOMEN S IMAGING Alessandro Villa 1 Alberto Tagliafico 2 Fabio Chiesa 1 Maurizio Chiaramondia
Women s Imaging Original Research Villa et al. Biopsy of Atypical Ductal Hyperplasia Women s Imaging Original Research WOMEN S IMAGING Alessandro Villa 1 Alberto Tagliafico 2 Fabio Chiesa 1 Maurizio Chiaramondia
Image-guided core needle biopsy has become a standard
 Pathologic Review of Atypical Hyperplasia Identified by Image-Guided Breast Needle Core Biopsy Correlation With Excision Specimen I-Tien Yeh, MD; Diana Dimitrov, MD; Pamela Otto, MD; Alexander R. Miller,
Pathologic Review of Atypical Hyperplasia Identified by Image-Guided Breast Needle Core Biopsy Correlation With Excision Specimen I-Tien Yeh, MD; Diana Dimitrov, MD; Pamela Otto, MD; Alexander R. Miller,
Diagnostic benefits of ultrasound-guided. CNB) versus mammograph-guided biopsy for suspicious microcalcifications. without definite breast mass
 Volume 118 No. 19 2018, 531-543 ISSN: 1311-8080 (printed version); ISSN: 1314-3395 (on-line version) url: http://www.ijpam.eu ijpam.eu Diagnostic benefits of ultrasound-guided biopsy versus mammography-guided
Volume 118 No. 19 2018, 531-543 ISSN: 1311-8080 (printed version); ISSN: 1314-3395 (on-line version) url: http://www.ijpam.eu ijpam.eu Diagnostic benefits of ultrasound-guided biopsy versus mammography-guided
Underestimation of cancer in case of diagnosis of atypical ductal hyperplasia (ADH) by vacuum assisted core needle biopsy
 reports of practical oncology and radiotherapy 1 7 (2 0 1 2) 129 133 Available online at www.sciencedirect.com journal homepage: http://www.elsevier.com/locate/rpor Original research article Underestimation
reports of practical oncology and radiotherapy 1 7 (2 0 1 2) 129 133 Available online at www.sciencedirect.com journal homepage: http://www.elsevier.com/locate/rpor Original research article Underestimation
Stereotactic 11-Gauge Vacuum- Assisted Breast Biopsy: A Validation Study
 Georg Pfarl 1 Thomas H. Helbich 1 Christopher C. Riedl 1 Teresa Wagner 2 Michael Gnant 3 Margaretha Rudas 4 Laura Liberman 5 Received March 11, 2002; accepted after revision May 17, 2002. 1 Department
Georg Pfarl 1 Thomas H. Helbich 1 Christopher C. Riedl 1 Teresa Wagner 2 Michael Gnant 3 Margaretha Rudas 4 Laura Liberman 5 Received March 11, 2002; accepted after revision May 17, 2002. 1 Department
Journal of Breast Cancer
 Journal of Breast Cancer ORIGINAL ARTICLE J Breast Cancer 2012 December; 15(4): 407-411 Validation of a Scoring System for Predicting Malignancy in Patients Diagnosed with Atypical Ductal Hyperplasia Using
Journal of Breast Cancer ORIGINAL ARTICLE J Breast Cancer 2012 December; 15(4): 407-411 Validation of a Scoring System for Predicting Malignancy in Patients Diagnosed with Atypical Ductal Hyperplasia Using
Atypical papillary lesions after core needle biopsy and subsequent breast carcinoma
 Asian Biomedicine Vol. 5 No. 2 April 2011; 243-248 DOI: 10.5372/1905-7415.0502.031 Original article Atypical papillary lesions after core needle biopsy and subsequent breast carcinoma Tuenchit Khamapirad
Asian Biomedicine Vol. 5 No. 2 April 2011; 243-248 DOI: 10.5372/1905-7415.0502.031 Original article Atypical papillary lesions after core needle biopsy and subsequent breast carcinoma Tuenchit Khamapirad
Atypical ductal hyperplasia diagnosed at ultrasound guided biopsy of breast mass
 Atypical ductal hyperplasia diagnosed at ultrasound guided biopsy of breast mass Poster No.: C-1483 Congress: ECR 2014 Type: Authors: Keywords: DOI: Scientific Exhibit J. Cho, J. Chung, E. S. Cha, J. E.
Atypical ductal hyperplasia diagnosed at ultrasound guided biopsy of breast mass Poster No.: C-1483 Congress: ECR 2014 Type: Authors: Keywords: DOI: Scientific Exhibit J. Cho, J. Chung, E. S. Cha, J. E.
CNB vs Surgical Excision
 Update on Core Needle Biopsy of Non-palpable Breast Lesions Nour Sneige, M.D. UT MD Anderson Cancer Center Houston, Tx Image-Guided CNB of Breast Lesions An alternative to surgical biospy CNB vs Surgical
Update on Core Needle Biopsy of Non-palpable Breast Lesions Nour Sneige, M.D. UT MD Anderson Cancer Center Houston, Tx Image-Guided CNB of Breast Lesions An alternative to surgical biospy CNB vs Surgical
Sonographically Guided Core Biopsy of the Breast: Comparison of 14-Gauge Automated Gun and 11-Gauge Directional Vacuum-Assisted Biopsy Methods
 Sonographically Guided Core Biopsy of the Breast: Comparison of 14-Gauge Automated Gun and 11-Gauge Directional Vacuum-Assisted Biopsy Methods Nariya Cho, MD 1 Woo Kyung Moon, MD 1 Joo Hee Cha, MD 1 Sun
Sonographically Guided Core Biopsy of the Breast: Comparison of 14-Gauge Automated Gun and 11-Gauge Directional Vacuum-Assisted Biopsy Methods Nariya Cho, MD 1 Woo Kyung Moon, MD 1 Joo Hee Cha, MD 1 Sun
Journal of Breast Cancer
 Journal of Breast Cancer ORIGINAL ARTICLE J Breast Cancer 2014 September; 17(3): 265-269 Absence of Residual Microcalcifications in Atypical Ductal Hyperplasia Diagnosed via Stereotactic Vacuum-Assisted
Journal of Breast Cancer ORIGINAL ARTICLE J Breast Cancer 2014 September; 17(3): 265-269 Absence of Residual Microcalcifications in Atypical Ductal Hyperplasia Diagnosed via Stereotactic Vacuum-Assisted
Epithelial Columnar Breast Lesions: Histopathology and Molecular Markers
 29th Annual International Conference Advances in the Application of Monoclonal Antibodies in Clinical Oncology and Symposium on Cancer Stem Cells 25 th -27t h June, 2012, Mykonos, Greece Epithelial Columnar
29th Annual International Conference Advances in the Application of Monoclonal Antibodies in Clinical Oncology and Symposium on Cancer Stem Cells 25 th -27t h June, 2012, Mykonos, Greece Epithelial Columnar
Multicenter Evaluation of the Breast Lesion Excision System, a Percutaneous, Vacuum-Assisted, Intact-Specimen Breast Biopsy Device
 945 Multicenter Evaluation of the Breast Lesion Excision System, a Percutaneous, Vacuum-Assisted, Intact-Specimen Breast Biopsy Device Angela Sie, MD 1 David C. Bryan, MD 2 Victor Gaines, MD 3 Larry K.
945 Multicenter Evaluation of the Breast Lesion Excision System, a Percutaneous, Vacuum-Assisted, Intact-Specimen Breast Biopsy Device Angela Sie, MD 1 David C. Bryan, MD 2 Victor Gaines, MD 3 Larry K.
Benign Breast Disease and Breast Cancer Risk
 Benign Breast Disease and Breast Cancer Risk Jean F. Simpson, M.D. Vanderbilt University Nashville, Tennessee December 1, 2011 Nashville Nashville Lebanon 1 Cedars of Lebanon State Park The American University
Benign Breast Disease and Breast Cancer Risk Jean F. Simpson, M.D. Vanderbilt University Nashville, Tennessee December 1, 2011 Nashville Nashville Lebanon 1 Cedars of Lebanon State Park The American University
Interpretation of Breast Pathology in the Era of Minimally Invasive Procedures
 Shahla Masood, M.D. Professor and Chair Department of Pathology and Laboratory Medicine University of Florida College of Medicine Jacksonville Medical Director, UF Health Breast Center Chief of Pathology
Shahla Masood, M.D. Professor and Chair Department of Pathology and Laboratory Medicine University of Florida College of Medicine Jacksonville Medical Director, UF Health Breast Center Chief of Pathology
Proliferative Breast Disease: implications of core biopsy diagnosis. Proliferative Breast Disease
 Proliferative Breast Disease: implications of core biopsy diagnosis Jean F. Simpson, M.D. Breast Pathology Consultants, Inc. Nashville, TN Proliferative Breast Disease Must be interpreted in clinical and
Proliferative Breast Disease: implications of core biopsy diagnosis Jean F. Simpson, M.D. Breast Pathology Consultants, Inc. Nashville, TN Proliferative Breast Disease Must be interpreted in clinical and
Sonographically-Guided 14-Gauge Core Needle Biopsy for Papillary Lesions of the Breast
 Sonographically-Guided 14-Gauge Core Needle Biopsy for Papillary Lesions of the Breast Eun Sook Ko, MD Nariya Cho, MD Joo Hee Cha, MD Jeong Seon Park, MD Sun Mi Kim, MD Woo Kyung Moon, MD Index terms:
Sonographically-Guided 14-Gauge Core Needle Biopsy for Papillary Lesions of the Breast Eun Sook Ko, MD Nariya Cho, MD Joo Hee Cha, MD Jeong Seon Park, MD Sun Mi Kim, MD Woo Kyung Moon, MD Index terms:
04/10/2018 HIGH RISK BREAST LESIONS. Pathology Perspectives of High Risk Breast Lesions ELEVATED RISK OF BREAST CANCER HISTORICAL PERSPECTIVES
 Pathology Perspectives of High Risk Breast Lesions Savitri Krishnamurthy MD Professor of Pathology Deputy Division Head Director of Clinical Trials, Research and Development The University of Texas MD
Pathology Perspectives of High Risk Breast Lesions Savitri Krishnamurthy MD Professor of Pathology Deputy Division Head Director of Clinical Trials, Research and Development The University of Texas MD
Atypical Ductal Hyperplasia of the Breast:
 Atypical Ductal Hyperplasia of the Breast: Radiologic and Histopathologic Correlation 1 Ji Young Lee, M.D., Bo Kyoung Seo, M.D. 2, Jung Hyck Kim, M.D., Yu Whan Oh, M.D., Kyu Ran Cho, M.D., Eun Jeong Choi,
Atypical Ductal Hyperplasia of the Breast: Radiologic and Histopathologic Correlation 1 Ji Young Lee, M.D., Bo Kyoung Seo, M.D. 2, Jung Hyck Kim, M.D., Yu Whan Oh, M.D., Kyu Ran Cho, M.D., Eun Jeong Choi,
PAPER. Upstaging of Atypical Ductal Hyperplasia After Vacuum-Assisted 11-Gauge Stereotactic Core Needle Biopsy
 PAPER Upstaging of Atypical Ductal Hyperplasia After Vacuum-Assisted 11-Gauge Stereotactic Core Needle Biopsy David J. Winchester, MD; Joel R. Bernstein, MD; Jan M. Jeske, MD; Mary H. Nicholson, MD; Elizabeth
PAPER Upstaging of Atypical Ductal Hyperplasia After Vacuum-Assisted 11-Gauge Stereotactic Core Needle Biopsy David J. Winchester, MD; Joel R. Bernstein, MD; Jan M. Jeske, MD; Mary H. Nicholson, MD; Elizabeth
Atypical Ductal Hyperplasia and Papillomas: A Comparison of Ultrasound Guided Breast Biopsy and Stereotactic Guided Breast Biopsy
 Atypical Ductal Hyperplasia and Papillomas: A Comparison of Ultrasound Guided Breast Biopsy and Stereotactic Guided Breast Biopsy Breast Cancer is the most common cancer diagnosed in women in the United
Atypical Ductal Hyperplasia and Papillomas: A Comparison of Ultrasound Guided Breast Biopsy and Stereotactic Guided Breast Biopsy Breast Cancer is the most common cancer diagnosed in women in the United
Flat Epithelial Atypia
 Flat Epithelial Atypia Richard Owings, M.D. University of Arkansas for Medical Sciences Department of Pathology Flat epithelial atypia can be a difficult lesion May be a subtle diagnosis Lots of changes
Flat Epithelial Atypia Richard Owings, M.D. University of Arkansas for Medical Sciences Department of Pathology Flat epithelial atypia can be a difficult lesion May be a subtle diagnosis Lots of changes
Proliferative Epithelial lesions of the Breast. Sami Shousha, MD, FRCPath Charing Cross Hospital & Imperial College, London
 Proliferative Epithelial lesions of the Breast Sami Shousha, MD, FRCPath Charing Cross Hospital & Imperial College, London Amman, November2013 Proliferative Epithelial Lesions of the Breast Usual type
Proliferative Epithelial lesions of the Breast Sami Shousha, MD, FRCPath Charing Cross Hospital & Imperial College, London Amman, November2013 Proliferative Epithelial Lesions of the Breast Usual type
Treatment options for the precancerous Atypical Breast lesions. Prof. YOUNG-JIN SUH The Catholic University of Korea
 Treatment options for the precancerous Atypical Breast lesions Prof. YOUNG-JIN SUH The Catholic University of Korea Not so benign lesions? Imaging abnormalities(10% recall) lead to diagnostic evaluation,
Treatment options for the precancerous Atypical Breast lesions Prof. YOUNG-JIN SUH The Catholic University of Korea Not so benign lesions? Imaging abnormalities(10% recall) lead to diagnostic evaluation,
Stereotactic Core-Needle Biopsy of Non-Mass Calcifications: Outcome and Accuracy at Long-Term Follow-Up
 Stereotactic Core-Needle Biopsy of Non-Mass Calcifications: Outcome and Accuracy at Long-Term Follow-Up Boo-Kyung Han, MD 1 Yeon Hyeon Choe, MD 1 Young-Hyeh Ko, MD 2 Seok-Jin Nam, MD 3 Jung-Han Kim, MD
Stereotactic Core-Needle Biopsy of Non-Mass Calcifications: Outcome and Accuracy at Long-Term Follow-Up Boo-Kyung Han, MD 1 Yeon Hyeon Choe, MD 1 Young-Hyeh Ko, MD 2 Seok-Jin Nam, MD 3 Jung-Han Kim, MD
Mammographic features and correlation with biopsy findings using 11-gauge stereotactic vacuum-assisted breast biopsy (SVABB)
 Original article Annals of Oncology 14: 450 454, 2003 DOI: 10.1093/annonc/mdh088 Mammographic features and correlation with biopsy findings using 11-gauge stereotactic vacuum-assisted breast biopsy (SVABB)
Original article Annals of Oncology 14: 450 454, 2003 DOI: 10.1093/annonc/mdh088 Mammographic features and correlation with biopsy findings using 11-gauge stereotactic vacuum-assisted breast biopsy (SVABB)
Significance of flat epithelial atypia on mammotome core needle biopsy: should it be excised? B
 Human Pathology (2007) 38, 35 41 www.elsevier.com/locate/humpath Original contribution Significance of flat epithelial atypia on mammotome core needle biopsy: should it be excised? B Lakshmi P. Kunju MD,
Human Pathology (2007) 38, 35 41 www.elsevier.com/locate/humpath Original contribution Significance of flat epithelial atypia on mammotome core needle biopsy: should it be excised? B Lakshmi P. Kunju MD,
Anatomic Pathology / Mucocele-like Lesions on Breast Core Biopsy. Mucocele-like Lesions Diagnosed on Breast Core Biopsy
 Anatomic Pathology / Mucocele-like Lesions on Breast Core Biopsy Mucocele-like Lesions Diagnosed on Breast Core Biopsy Assessment of Upgrade Rate and Need for Surgical Excision Brian Sutton, MD, 1 Simone
Anatomic Pathology / Mucocele-like Lesions on Breast Core Biopsy Mucocele-like Lesions Diagnosed on Breast Core Biopsy Assessment of Upgrade Rate and Need for Surgical Excision Brian Sutton, MD, 1 Simone
Pathology of Lobular & Ductal Preneoplasia. Syed A Hoda, MD Weill-Cornell, New York, NY
 Pathology of Lobular & Ductal Preneoplasia Syed A Hoda, MD Weill-Cornell, New York, NY Proliferative Epithelial Changes in Breast A wide range of proliferative epithelial changes occur in the breast There
Pathology of Lobular & Ductal Preneoplasia Syed A Hoda, MD Weill-Cornell, New York, NY Proliferative Epithelial Changes in Breast A wide range of proliferative epithelial changes occur in the breast There
Atypical proliferative lesions diagnosed on core biopsy - 6 year review
 Atypical proliferative lesions diagnosed on core biopsy - 6 year review Dr Angela Harris, Dr Julie Weigner & Dr Ricardo Vilain NSW Health Pathology Pathology North, Hunter Anatomical Pathology & Cytology
Atypical proliferative lesions diagnosed on core biopsy - 6 year review Dr Angela Harris, Dr Julie Weigner & Dr Ricardo Vilain NSW Health Pathology Pathology North, Hunter Anatomical Pathology & Cytology
Ductal Proliferations of the Breast: The Good, the Bad, and the Ugly
 Ductal Proliferations of the Breast: The Good, the Bad, and the Ugly Melinda F. Lerwill, MD CRITERIA FOR DISTINGUISHING LOW-GRADE DUCTAL CARCINOMA IN SITU FROM USUAL DUCTAL HYPERPLASIA CYTOLOGY Low-grade
Ductal Proliferations of the Breast: The Good, the Bad, and the Ugly Melinda F. Lerwill, MD CRITERIA FOR DISTINGUISHING LOW-GRADE DUCTAL CARCINOMA IN SITU FROM USUAL DUCTAL HYPERPLASIA CYTOLOGY Low-grade
Percutaneous Biopsy of the Breast
 Percutaneous Biopsy of the Breast Expires Tuesday, March 31, 2020 Radiology Brooke A. Caldwell, M.D. Objectives 1. Describe the pros and cons of surgical biopsy and the reasoning behind the development
Percutaneous Biopsy of the Breast Expires Tuesday, March 31, 2020 Radiology Brooke A. Caldwell, M.D. Objectives 1. Describe the pros and cons of surgical biopsy and the reasoning behind the development
Learning Curve for Stereotactic Breast Biopsy: How Many Cases Are Enough?
 Laura Liberman 1 Catherine L. Benton D. David Dershaw Andrea F. Abramson Linda R. LaTrenta Elizabeth A. Morris Received July 17, 2000; accepted after revision September 7, 2000. Supported by grant C015709
Laura Liberman 1 Catherine L. Benton D. David Dershaw Andrea F. Abramson Linda R. LaTrenta Elizabeth A. Morris Received July 17, 2000; accepted after revision September 7, 2000. Supported by grant C015709
Surgical Pathology Issues of Practical Importance
 Surgical Pathology Issues of Practical Importance Anne Moore, MD Medical Oncology Syed Hoda, MD Surgical Pathology The pathologist is central to the team approach needed to manage the patient with breast
Surgical Pathology Issues of Practical Importance Anne Moore, MD Medical Oncology Syed Hoda, MD Surgical Pathology The pathologist is central to the team approach needed to manage the patient with breast
Surgical Management of High- Risk Breast Lesions
 Surgical Management of High- Risk Breast Lesions Amy C. Degnim, MD a, Tari A. King, MD b, * KEYWORDS High-risk lesion Atypical hyperplasia Lobular carcinoma in situ Percutaneous breast biopsy Breast cancer
Surgical Management of High- Risk Breast Lesions Amy C. Degnim, MD a, Tari A. King, MD b, * KEYWORDS High-risk lesion Atypical hyperplasia Lobular carcinoma in situ Percutaneous breast biopsy Breast cancer
Original Report. Mucocele-Like Tumors of the Breast: Mammographic and Sonographic Appearances. Katrina Glazebrook 1 Carol Reynolds 2
 Katrina Glazebrook 1 Carol Reynolds 2 Received January 2, 2002; accepted after revision August 28, 2002. 1 Department of Radiology, Mayo Clinic, 200 First St. S.W., Rochester, MN 55905. Address correspondence
Katrina Glazebrook 1 Carol Reynolds 2 Received January 2, 2002; accepted after revision August 28, 2002. 1 Department of Radiology, Mayo Clinic, 200 First St. S.W., Rochester, MN 55905. Address correspondence
Original Article Breast Imaging
 Original Article Breast Imaging http://dx.doi.org/10.3348/kjr.2014.15.6.697 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2014;15(6):697-703 Percutaneous Ultrasound-Guided Vacuum-Assisted Removal versus
Original Article Breast Imaging http://dx.doi.org/10.3348/kjr.2014.15.6.697 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2014;15(6):697-703 Percutaneous Ultrasound-Guided Vacuum-Assisted Removal versus
The Hot Topic for today is a biopsy from a 58-year-old woman who had worrisome mammographic calcifications on screening.
 The Hot Topic for today is a biopsy from a 58-year-old woman who had worrisome mammographic calcifications on screening. 1 My name is Dan Visscher; I am a consultant in the Division of Anatomic Pathology
The Hot Topic for today is a biopsy from a 58-year-old woman who had worrisome mammographic calcifications on screening. 1 My name is Dan Visscher; I am a consultant in the Division of Anatomic Pathology
Imaging-Guided Core Needle Biopsy of Papillary Lesions of the Breast
 Eric L. Rosen 1 Rex C. Bentley 2 Jay A. Baker 1 Mary Scott Soo 1 Received January 30, 2002; accepted after revision April 12, 2002. 1 Department of Radiology, Breast Imaging Division, Duke University Medical
Eric L. Rosen 1 Rex C. Bentley 2 Jay A. Baker 1 Mary Scott Soo 1 Received January 30, 2002; accepted after revision April 12, 2002. 1 Department of Radiology, Breast Imaging Division, Duke University Medical
A E K Ibrahim, A C Bateman, J M Theaker, J L Low, B Addis, P Tidbury, C Rubin, M Briley, G T Royle
 J Clin Pathol 2001;54:121 125 121 Departments of Histopathology and Cytopathology,, Tremona Road,, SO16 6YO, UK A E K Ibrahim A C Bateman J M Theaker B Addis P Tidbury Medical Statistics and Computing,
J Clin Pathol 2001;54:121 125 121 Departments of Histopathology and Cytopathology,, Tremona Road,, SO16 6YO, UK A E K Ibrahim A C Bateman J M Theaker B Addis P Tidbury Medical Statistics and Computing,
Poster No.: C-0466 Congress: ECR 2010 Scientific Exhibit
 Up-right stereotactic vacuum-assisted biopsy (UP-VAB) of non palpable breast lesions: Results and correlations with radiological suspicion (BI-RADS classification) Poster No.: C-0466 Congress: ECR 2010
Up-right stereotactic vacuum-assisted biopsy (UP-VAB) of non palpable breast lesions: Results and correlations with radiological suspicion (BI-RADS classification) Poster No.: C-0466 Congress: ECR 2010
Diagnostic accuracy for different strategies of image-guided breast intervention in cases of nonpalpable breast lesions
 British Journal of Cancer (2004) 90, 595 600 All rights reserved 0007 0920/04 $25.00 www.bjcancer.com Diagnostic accuracy for different strategies of image-guided breast intervention in cases of nonpalpable
British Journal of Cancer (2004) 90, 595 600 All rights reserved 0007 0920/04 $25.00 www.bjcancer.com Diagnostic accuracy for different strategies of image-guided breast intervention in cases of nonpalpable
Disclosures 5/27/2012. Outline of Talk. Outline of Talk. When Is LCIS Clinically Significant? Classic LCIS. Classic LCIS
 When Is LCIS Clinically Significant? Disclosures I have nothing to disclose Yunn-Yi Chen, MD, PhD Professor Outline of Talk Outline of Talk Classic LCIS Classic LCIS Definition of lobular differentiation
When Is LCIS Clinically Significant? Disclosures I have nothing to disclose Yunn-Yi Chen, MD, PhD Professor Outline of Talk Outline of Talk Classic LCIS Classic LCIS Definition of lobular differentiation
Advocating Nonsurgical Management of Patients With Small, Incidental Radial Scars at the Time of Needle Core Biopsy. A Study of 77 Cases
 Advocating Nonsurgical Management of Patients With Small, Incidental Radial Scars at the Time of Needle Core Biopsy A Study of 77 Cases Cathleen Matrai, MD; Timothy M. D Alfonso, MD; Lindsay Pharmer, MD;
Advocating Nonsurgical Management of Patients With Small, Incidental Radial Scars at the Time of Needle Core Biopsy A Study of 77 Cases Cathleen Matrai, MD; Timothy M. D Alfonso, MD; Lindsay Pharmer, MD;
Fine-needle aspiration cytology (FNAC) and core needle biopsy
 146 CANCER CYTOPATHOLOGY A Comparison of Aspiration Cytology and Core Needle Biopsy in the Evaluation of Breast Lesions Pieter J. Westenend, M.D., Ph.D. 1 Ali R. Sever, M.D. 2 Hannie J. C. Beekman-de Volder
146 CANCER CYTOPATHOLOGY A Comparison of Aspiration Cytology and Core Needle Biopsy in the Evaluation of Breast Lesions Pieter J. Westenend, M.D., Ph.D. 1 Ali R. Sever, M.D. 2 Hannie J. C. Beekman-de Volder
Recurrence following Treatment of Ductal Carcinoma in Situ with Skin-Sparing Mastectomy and Immediate Breast Reconstruction
 Recurrence following Treatment of Ductal Carcinoma in Situ with Skin-Sparing Mastectomy and Immediate Breast Reconstruction Aldona J. Spiegel, M.D., and Charles E. Butler, M.D. Houston, Texas Skin-sparing
Recurrence following Treatment of Ductal Carcinoma in Situ with Skin-Sparing Mastectomy and Immediate Breast Reconstruction Aldona J. Spiegel, M.D., and Charles E. Butler, M.D. Houston, Texas Skin-sparing
Columnar Cell Lesions
 Columnar Cell Lesions Laura C. Collins, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA Question? Columnar cell lesions are: a) Annoying lesions
Columnar Cell Lesions Laura C. Collins, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA Question? Columnar cell lesions are: a) Annoying lesions
CLINICAL SIGNIFICANCE OF BENIGN EPITHELIAL CHANGES
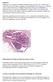 Papillomas. Papillomas are composed of multiple branching fibrovascular cores, each having a connective tissue axis lined by luminal and myoepithelial cells ( Fig. 23-11 ). Growth occurs within a dilated
Papillomas. Papillomas are composed of multiple branching fibrovascular cores, each having a connective tissue axis lined by luminal and myoepithelial cells ( Fig. 23-11 ). Growth occurs within a dilated
Cytyc Corporation - Case Presentation Archive - March 2002
 FirstCyte Ductal Lavage History: 68 Year Old Female Gail Index: Unknown Clinical History: Negative Mammogram in 1995 6 yrs. later presents with bloody nipple discharge Subsequent suspicious mammogram Suspicious
FirstCyte Ductal Lavage History: 68 Year Old Female Gail Index: Unknown Clinical History: Negative Mammogram in 1995 6 yrs. later presents with bloody nipple discharge Subsequent suspicious mammogram Suspicious
Stereotactic vacuum-assisted breast biopsy under lateral decubitus position
 ORIGINAL ARTICLE pissn 2288-6575 eissn 2288-6796 http://dx.doi.org/10.4174/astr.2016.90.1.16 Annals of Surgical Treatment and Research Stereotactic vacuum-assisted breast biopsy under lateral decubitus
ORIGINAL ARTICLE pissn 2288-6575 eissn 2288-6796 http://dx.doi.org/10.4174/astr.2016.90.1.16 Annals of Surgical Treatment and Research Stereotactic vacuum-assisted breast biopsy under lateral decubitus
Controversies and Problematic Issues in Core Needle Biopsies (To excise or not to excise)
 Controversies and Problematic Issues in Core Needle Biopsies (To excise or not to excise) Laura C. Collins, M.D. Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA Schematic Representation
Controversies and Problematic Issues in Core Needle Biopsies (To excise or not to excise) Laura C. Collins, M.D. Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA Schematic Representation
Columnar Cell Lesions. Columnar Cell Lesions and Flat Epithelial Atypia
 Columnar Cell Lesions and Stuart J. Schnitt, M.D. Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA, USA Columnar Cell Lesions Lesions characterized by columnar epithelial cells
Columnar Cell Lesions and Stuart J. Schnitt, M.D. Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA, USA Columnar Cell Lesions Lesions characterized by columnar epithelial cells
Department of Radiology, Research Institute of Radiological Science, Yonsei University, College of Medicine, Seodaemun-gu, Seoul, Republic of Korea
 The British Journal of Radiology, 85 (2012), e349 e356 Comparison of the underestimation rate in cases with ductal carcinoma in situ at ultrasound-guided core biopsy: 14-gauge automated core-needle biopsy
The British Journal of Radiology, 85 (2012), e349 e356 Comparison of the underestimation rate in cases with ductal carcinoma in situ at ultrasound-guided core biopsy: 14-gauge automated core-needle biopsy
Breast calcifications are important mammographic features in the
 Diagn Interv Radiol 2012; 18:354 359 Turkish Society of Radiology 2012 BREAST IMAGING ORIGINAL ARTICLE Causes of failure in removing calcium in microcalcification-only lesions using 11-gauge stereotactic
Diagn Interv Radiol 2012; 18:354 359 Turkish Society of Radiology 2012 BREAST IMAGING ORIGINAL ARTICLE Causes of failure in removing calcium in microcalcification-only lesions using 11-gauge stereotactic
Excisional biopsy or long term follow-up results in breast high-risk lesions diagnosed at core needle biopsy
 Excisional biopsy or long term follow-up results in breast high-risk lesions diagnosed at core needle biopsy Poster No.: C-2515 Congress: ECR 2015 Type: Authors: Scientific Exhibit Ö. S. Okcu 1, A. Oktay
Excisional biopsy or long term follow-up results in breast high-risk lesions diagnosed at core needle biopsy Poster No.: C-2515 Congress: ECR 2015 Type: Authors: Scientific Exhibit Ö. S. Okcu 1, A. Oktay
Palpable Breast Lesions Cytomorphological Analysis and Scoring System with Histopatholgical Correlation
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. III (October. 2016), PP 25-29 www.iosrjournals.org Palpable Breast Lesions Cytomorphological
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. III (October. 2016), PP 25-29 www.iosrjournals.org Palpable Breast Lesions Cytomorphological
Utility of Adequate Core Biopsy Samples from Ultrasound Biopsies Needed for Today s Breast Pathology
 Utility of Adequate Core Biopsy Samples from Ultrasound Biopsies Needed for Today s Breast Pathology Ugur Ozerdem, M.D. 1 Abstract Background: There is a paradigm shift in breast biopsy philosophy. In
Utility of Adequate Core Biopsy Samples from Ultrasound Biopsies Needed for Today s Breast Pathology Ugur Ozerdem, M.D. 1 Abstract Background: There is a paradigm shift in breast biopsy philosophy. In
Lobular Carcinoma In Situ Variants in Breast Cores
 Lobular Carcinoma In Situ Variants in Breast Cores Potential for Misdiagnosis, Upgrade Rates at Surgical Excision, and Practical Implications Megan E. Sullivan, MD; Seema A. Khan, MD; Yurdanur Sullu, MD;
Lobular Carcinoma In Situ Variants in Breast Cores Potential for Misdiagnosis, Upgrade Rates at Surgical Excision, and Practical Implications Megan E. Sullivan, MD; Seema A. Khan, MD; Yurdanur Sullu, MD;
Emad A Rakha, Bernard Chi-Shern Ho, Veena K Naik, Soumadri Sen, Lisa Hamilton, Zsolt Hodi, Ian Ellis, Andrew Hs Lee
 Outcome of breast lesions diagnosed as lesion of uncertain malignant potential (B3) or suspicious of malignancy (B4) on needle core biopsy including detailed review of epithelial atypia Emad A Rakha, Bernard
Outcome of breast lesions diagnosed as lesion of uncertain malignant potential (B3) or suspicious of malignancy (B4) on needle core biopsy including detailed review of epithelial atypia Emad A Rakha, Bernard
Breast Lesions of Uncertain Malignant Potential: A Challenge for Surgeons
 Breast Lesions of Uncertain Malignant Potential: A Challenge for Surgeons Deslauriers Nancy 1, Sidéris Lucas 1, Dufresne Michel-Pierre 2, Mitchell Andrew 3, Drolet Pierre 4, Dubé Pierre 1, Leclerc Yves
Breast Lesions of Uncertain Malignant Potential: A Challenge for Surgeons Deslauriers Nancy 1, Sidéris Lucas 1, Dufresne Michel-Pierre 2, Mitchell Andrew 3, Drolet Pierre 4, Dubé Pierre 1, Leclerc Yves
Columnar Cell Lesions and Flat Epithelial Atypia
 Columnar Cell Lesions and Flat Epithelial Atypia Laura C. Collins, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School, Boston, MA Terminology for Columnar Cell
Columnar Cell Lesions and Flat Epithelial Atypia Laura C. Collins, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School, Boston, MA Terminology for Columnar Cell
Breast Lesion Excision System-Intact (BLES): A Stereotactic Method of Biopsy of Suspicius Non-Palpable Mammographic Lesions.
 Breast Lesion Excision System-Intact (BLES): A Stereotactic Method of Biopsy of Suspicius Non-Palpable Mammographic Lesions. Poster No.: C-1595 Congress: ECR 2014 Type: Authors: Scientific Exhibit I. Georgiou
Breast Lesion Excision System-Intact (BLES): A Stereotactic Method of Biopsy of Suspicius Non-Palpable Mammographic Lesions. Poster No.: C-1595 Congress: ECR 2014 Type: Authors: Scientific Exhibit I. Georgiou
Evaluation of Breast Specimens Removed by Needle Localization Technique
 Evaluation of Breast Specimens Removed by Needle Localization Technique Specimen Handling: The breast specimen when received should be measured and grossly inspected for any orientation designated by the
Evaluation of Breast Specimens Removed by Needle Localization Technique Specimen Handling: The breast specimen when received should be measured and grossly inspected for any orientation designated by the
Percutaneous Core Needle Biopsy of Radial Scars of the Breast: When Is Excision Necessary?
 R. James Brenner 1, 2 Roger J. Jackman 3 Steve H. Parker 4 W. Phil Evans III 5 Liane Philpotts 6 Beth M. Deutch 7 Mary C. Lechner 8 Daniel Lehrer 9 Paul Sylvan 10 Rebecca Hunt 11 Steven J. Adler 12 Nancy
R. James Brenner 1, 2 Roger J. Jackman 3 Steve H. Parker 4 W. Phil Evans III 5 Liane Philpotts 6 Beth M. Deutch 7 Mary C. Lechner 8 Daniel Lehrer 9 Paul Sylvan 10 Rebecca Hunt 11 Steven J. Adler 12 Nancy
Consensus Guideline on Image-Guided Percutaneous Biopsy of Palpable and Nonpalpable Breast Lesions
 Consensus Guideline on Image-Guided Percutaneous Biopsy of Palpable and Nonpalpable Breast Lesions Purpose: To outline the use of minimally invasive biopsy techniques (MIBT) for palpable and nonpalpable
Consensus Guideline on Image-Guided Percutaneous Biopsy of Palpable and Nonpalpable Breast Lesions Purpose: To outline the use of minimally invasive biopsy techniques (MIBT) for palpable and nonpalpable
BI-RADS Categorization As a Predictor of Malignancy 1
 Susan G. Orel, MD Nicole Kay, BA Carol Reynolds, MD Daniel C. Sullivan, MD BI-RADS Categorization As a Predictor of Malignancy 1 Index terms: Breast, biopsy, 00.1261 Breast neoplasms, localization, 00.125,
Susan G. Orel, MD Nicole Kay, BA Carol Reynolds, MD Daniel C. Sullivan, MD BI-RADS Categorization As a Predictor of Malignancy 1 Index terms: Breast, biopsy, 00.1261 Breast neoplasms, localization, 00.125,
Disclosures. Premalignant Lesions of the Breast: What Clinicians Want and Why. NY Times: Prone to Error: Earliest Steps to Find Cancer.
 Disclosures Premalignant Lesions of the Breast: What Clinicians Want and Why I have nothing to disclose Rick Baehner, MD Assistant Professor, UCSF Pathology NY Times: Prone to Error: Earliest Steps to
Disclosures Premalignant Lesions of the Breast: What Clinicians Want and Why I have nothing to disclose Rick Baehner, MD Assistant Professor, UCSF Pathology NY Times: Prone to Error: Earliest Steps to
IBCM 2, April 2009, Sarajevo, Bosnia and Herzegovina
 Preoperative diagnosis and treatment planning in breast cancer The pathologist s perspective L. Mazzucchelli Istituto Cantonale di Patologia Locarno, Switzerland IBCM 2, 23-25 April 2009, Sarajevo, Bosnia
Preoperative diagnosis and treatment planning in breast cancer The pathologist s perspective L. Mazzucchelli Istituto Cantonale di Patologia Locarno, Switzerland IBCM 2, 23-25 April 2009, Sarajevo, Bosnia
Extent of Lumpectomy for Breast Cancer After Diagnosis by Stereotactic Core Versus Wire Localization Biopsy
 Annals of Surgical Oncology, 6(4):330 335 Published by Lippincott Williams & Wilkins 1999 The Society of Surgical Oncology, Inc. Extent of Lumpectomy for Breast Cancer After Diagnosis by Stereotactic Core
Annals of Surgical Oncology, 6(4):330 335 Published by Lippincott Williams & Wilkins 1999 The Society of Surgical Oncology, Inc. Extent of Lumpectomy for Breast Cancer After Diagnosis by Stereotactic Core
Papillary Lesions of the breast
 Papillary Lesions of the breast Emad Rakha Professor of Breast Pathology The University of Nottingham Papillary lesions of the breast are a heterogeneous group of disease, which are characterised by neoplastic
Papillary Lesions of the breast Emad Rakha Professor of Breast Pathology The University of Nottingham Papillary lesions of the breast are a heterogeneous group of disease, which are characterised by neoplastic
Index words: Breast US Breast neoplasm Breast cancer
 Index words: Breast US Breast neoplasm Breast cancer 125 47.. 53. (),, taller than wide. 50.. 126 Table 1. + 34 24-106 145,, + 139 167-1 2 + 65 37-75 132 47. duct extension. 127 taller than wide + 62 95-78
Index words: Breast US Breast neoplasm Breast cancer 125 47.. 53. (),, taller than wide. 50.. 126 Table 1. + 34 24-106 145,, + 139 167-1 2 + 65 37-75 132 47. duct extension. 127 taller than wide + 62 95-78
Diagnostic accuracy of ultrasonography-guided core needle biopsy for breast lesions
 Singapore Med J 01; 5(1) 40 Diagnostic accuracy of ultrasonography-guided core needle biopsy for breast lesions Wiratkapun Cl, MD, Treesit T1, MD, Wibulpolprasert E1, MD, Lertsithichai P, MD, MSc INTRODUCTION
Singapore Med J 01; 5(1) 40 Diagnostic accuracy of ultrasonography-guided core needle biopsy for breast lesions Wiratkapun Cl, MD, Treesit T1, MD, Wibulpolprasert E1, MD, Lertsithichai P, MD, MSc INTRODUCTION
Clinical Studies MATERIALS AND METHODS. Image-guided large-core needle biopsies of breast lesions
 British Journal of Cancer (005) 9, 31 35 All rights reserved 0007 090/05 $30.00 www.bjcancer.com Ultrasound-guided large-core needle biopsies of breast lesions: analysis of 96 cases to determine the number
British Journal of Cancer (005) 9, 31 35 All rights reserved 0007 090/05 $30.00 www.bjcancer.com Ultrasound-guided large-core needle biopsies of breast lesions: analysis of 96 cases to determine the number
6/3/2010. Outline of Talk. Lobular Breast Cancer: Definition of lobular differentiation. Common Problems in Diagnosing LCIS in Core Biopsies
 Outline of Talk Lobular Breast Cancer: Common Problems in Diagnosing LCIS in Core Biopsies Definition of lobular differentiation Variants of LCIS that: carry risk for unsampled invasive cancer mimic DCIS
Outline of Talk Lobular Breast Cancer: Common Problems in Diagnosing LCIS in Core Biopsies Definition of lobular differentiation Variants of LCIS that: carry risk for unsampled invasive cancer mimic DCIS
Incidence and Management of Complex Fibroadenomas
 Incidence and Management of Complex Fibroadenomas Women s Imaging Original Research 214.fm 11/29/07 WOMEN S IMAGING Miri Sklair-Levy 1 Tamar Sella 1 Tanir Alweiss 2 Ilia Craciun 1 Eugene Libson 1 Bella
Incidence and Management of Complex Fibroadenomas Women s Imaging Original Research 214.fm 11/29/07 WOMEN S IMAGING Miri Sklair-Levy 1 Tamar Sella 1 Tanir Alweiss 2 Ilia Craciun 1 Eugene Libson 1 Bella
Atypical And Suspicious Categories In Fine Needle Aspiration Cytology Of The Breast
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-853, p-issn: 2279-861.Volume 15, Issue 1 Ver. III (October. 216), PP 57-61 www.iosrjournals.org Atypical And Suspicious Categories in
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-853, p-issn: 2279-861.Volume 15, Issue 1 Ver. III (October. 216), PP 57-61 www.iosrjournals.org Atypical And Suspicious Categories in
The management of B3 lesions with emphasis on lobular neoplasia
 The management of B3 lesions with emphasis on lobular neoplasia Abeer Shaaban Queen Elizabeth Hospital Birmingham NHSBSP core biopsy categories B1 - Normal B2 - Benign B3 Uncertain malignant potential
The management of B3 lesions with emphasis on lobular neoplasia Abeer Shaaban Queen Elizabeth Hospital Birmingham NHSBSP core biopsy categories B1 - Normal B2 - Benign B3 Uncertain malignant potential
Incidence of ductal lesions
 Ductal Proliferative Lesions of the Breast: From FEA to ADH to DCIS Incidence of ductal lesions Pre-mammography: DCIS < 3% of breast cancers, large palpable masses, with invasion Mammography: DCIS 25%
Ductal Proliferative Lesions of the Breast: From FEA to ADH to DCIS Incidence of ductal lesions Pre-mammography: DCIS < 3% of breast cancers, large palpable masses, with invasion Mammography: DCIS 25%
Ductal carcinoma in situ, underestimation, ultrasound-guided core needle biopsy
 Ductal carcinoma in situ diagnosed after an ultrasoundguided 14-gauge core needle biopsy of breast masses: Can underestimation be predicted preoperatively? Poster No.: C-0442 Congress: ECR 2010 Type: Scientific
Ductal carcinoma in situ diagnosed after an ultrasoundguided 14-gauge core needle biopsy of breast masses: Can underestimation be predicted preoperatively? Poster No.: C-0442 Congress: ECR 2010 Type: Scientific
Women s Imaging Original Research
 Women s Imaging Original Research Linda et al. Biopsy of Radial Scars Without Atypia Women s Imaging Original Research WOMEN S IMAGING Anna Linda 1 Chiara Zuiani 1 Alessandro Furlan 1 Viviana Londero 1
Women s Imaging Original Research Linda et al. Biopsy of Radial Scars Without Atypia Women s Imaging Original Research WOMEN S IMAGING Anna Linda 1 Chiara Zuiani 1 Alessandro Furlan 1 Viviana Londero 1
BI-RADS CATEGORIZATION AND BREAST BIOPSY categorization in the selection of appropriate breast biopsy technique is also discussed. Patients and method
 Original Article Positive Predictive Value of BI-RADS Categorization in an Asian Population Yah-Yuen Tan, Siew-Bock Wee, Mona P.C. Tan and Bee-Kiang Chong, 1 Departments of General Surgery and 1Diagnostic
Original Article Positive Predictive Value of BI-RADS Categorization in an Asian Population Yah-Yuen Tan, Siew-Bock Wee, Mona P.C. Tan and Bee-Kiang Chong, 1 Departments of General Surgery and 1Diagnostic
Breast Pathology. Breast Development
 Breast Pathology Lecturer: Hanina Hibshoosh, M.D. Reading: Kumar, Cotran, Robbins, Basic Pathology, 6th Edition, pages 623-635 Breast Development 5th week - thickening of the epidermis - milk line 5th
Breast Pathology Lecturer: Hanina Hibshoosh, M.D. Reading: Kumar, Cotran, Robbins, Basic Pathology, 6th Edition, pages 623-635 Breast Development 5th week - thickening of the epidermis - milk line 5th
Breast Intraductal Papillomas Without Atypia in Radiologic- Pathologic Concordant Core-Needle Biopsies: Rate of Upgrade to Carcinoma at Excision
 Breast Intraductal Papillomas Without Atypia in Radiologic- Pathologic Concordant Core-Needle Biopsies: Rate of Upgrade to Carcinoma at Excision Fresia Pareja, MD, PhD 1 ; Adriana D. Corben, MD 1 ; Sandra
Breast Intraductal Papillomas Without Atypia in Radiologic- Pathologic Concordant Core-Needle Biopsies: Rate of Upgrade to Carcinoma at Excision Fresia Pareja, MD, PhD 1 ; Adriana D. Corben, MD 1 ; Sandra
Stereotactic large core needle biopsy for all nonpalpable breast lesions?
 Breast Cancer Research and Treatment 73: 177 182, 2002. 2002 Kluwer Academic Publishers. Printed in the Netherlands. Report Stereotactic large core needle biopsy for all nonpalpable breast lesions? L.E.
Breast Cancer Research and Treatment 73: 177 182, 2002. 2002 Kluwer Academic Publishers. Printed in the Netherlands. Report Stereotactic large core needle biopsy for all nonpalpable breast lesions? L.E.
Ductal Carcinoma in Situ. Laura C. Collins, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA
 Ductal Carcinoma in Situ Laura C. Collins, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA Definition of DCIS WHO 2012 A neoplastic proliferation
Ductal Carcinoma in Situ Laura C. Collins, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA Definition of DCIS WHO 2012 A neoplastic proliferation
Percutaneous Biopsy and Sentinel Lymphadenectomy: Minimally Invasive. he diagnosis and treatment of nonpalpable. Breast Cancer
 Laura Liberman 1 Hiram S. Cody III 2 Received January 30, 2001; accepted after revision April 3, 2001. Supported by a grant from the New York State Department of Health (C015709). 1 Department of Radiology,
Laura Liberman 1 Hiram S. Cody III 2 Received January 30, 2001; accepted after revision April 3, 2001. Supported by a grant from the New York State Department of Health (C015709). 1 Department of Radiology,
Cystic Hypersecretory Carcinoma of the Breast:
 J Korean Soc Radiol 2010;62:287-294 Cystic Hypersecretory Carcinoma of the Breast: Sonographic Features with a Histological Correlation 1 Sang Yu Nam, M.D., Boo-Kyung Han, M.D., Jung Hee Shin, M.D., Eun
J Korean Soc Radiol 2010;62:287-294 Cystic Hypersecretory Carcinoma of the Breast: Sonographic Features with a Histological Correlation 1 Sang Yu Nam, M.D., Boo-Kyung Han, M.D., Jung Hee Shin, M.D., Eun
Immunohistochemical studies (ER & Ki-67) in Proliferative breast lesions adjacent to malignancy
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 3 Ver. IV. (Mar. 2014), PP 84-89 Immunohistochemical studies (ER & Ki-67) in Proliferative
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 3 Ver. IV. (Mar. 2014), PP 84-89 Immunohistochemical studies (ER & Ki-67) in Proliferative
3/27/2017. Disclosure of Relevant Financial Relationships. Papilloma???
 Management of Papillary Lesions Diagnosed at Rad Path Concordant Core Biopsy (CNB) Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to
Management of Papillary Lesions Diagnosed at Rad Path Concordant Core Biopsy (CNB) Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to
STEREOTACTIC BREAST BIOPSY: CORRELATION WITH HISTOLOGY
 3-rd Baltic Congress of Radiology, October 8-9, 2010 Riga Rūta Briedienė, Rūta Grigienė, Raimundas Meškauskas Institute of Oncology Vilnius University, National Centre of Pathology STEREOTACTIC BREAST
3-rd Baltic Congress of Radiology, October 8-9, 2010 Riga Rūta Briedienė, Rūta Grigienė, Raimundas Meškauskas Institute of Oncology Vilnius University, National Centre of Pathology STEREOTACTIC BREAST
Case study 1. Rie Horii, M.D., Ph.D. Division of Pathology Cancer Institute Hospital, Japanese Foundation for Cancer Research
 NCCN/JCCNB Seminar in Japan April 15, 2012 Case study 1 Rie Horii, M.D., Ph.D. Division of Pathology Cancer Institute Hospital, Japanese Foundation for Cancer Research Present illness: A 50y.o.premenopausal
NCCN/JCCNB Seminar in Japan April 15, 2012 Case study 1 Rie Horii, M.D., Ph.D. Division of Pathology Cancer Institute Hospital, Japanese Foundation for Cancer Research Present illness: A 50y.o.premenopausal
Papillary Lesions of the Breast A Practical Approach to Diagnosis. (Arch Pathol Lab Med. 2016;140: ; doi: /arpa.
 Papillary Lesions of the Breast A Practical Approach to Diagnosis (Arch Pathol Lab Med. 2016;140:1052 1059; doi: 10.5858/arpa.2016-0219-RA) Papillary lesions of the breast Span the spectrum of benign,
Papillary Lesions of the Breast A Practical Approach to Diagnosis (Arch Pathol Lab Med. 2016;140:1052 1059; doi: 10.5858/arpa.2016-0219-RA) Papillary lesions of the breast Span the spectrum of benign,
Three-dimensional ultrasound-validated large-core needle biopsy: is it a reliable method for the histological assessment of breast lesions?
 Ultrasound Obstet Gynecol 2004; 23: 393 397 Published online 24 February 2004 in Wiley InterScience (www.interscience.wiley.com). DOI: 10.1002/uog.1001 Three-dimensional ultrasound-validated large-core
Ultrasound Obstet Gynecol 2004; 23: 393 397 Published online 24 February 2004 in Wiley InterScience (www.interscience.wiley.com). DOI: 10.1002/uog.1001 Three-dimensional ultrasound-validated large-core
Papillary Lesions of the Breast
 Papillary Lesions of the Breast Laura C. Collins, M.D. Associate Professor of Pathology Associate Director, Division of Anatomic Pathology Beth Israel Deaconess Medical Center and Harvard Medical School
Papillary Lesions of the Breast Laura C. Collins, M.D. Associate Professor of Pathology Associate Director, Division of Anatomic Pathology Beth Israel Deaconess Medical Center and Harvard Medical School
Good afternoon everyone. First of all many thanks to Dr. Bonaventura and Dr. Arn for inviting
 PATHOLOGY IN-SITU CARCINOMA, ROHIT BHARGAVA, MD 1 Good afternoon everyone. First of all many thanks to Dr. Bonaventura and Dr. Arn for inviting me here, it s great to be here and I m going to talk about
PATHOLOGY IN-SITU CARCINOMA, ROHIT BHARGAVA, MD 1 Good afternoon everyone. First of all many thanks to Dr. Bonaventura and Dr. Arn for inviting me here, it s great to be here and I m going to talk about
Management of Patients Diagnosed With Lobular Carcinoma in Situ at Needle Core Biopsy at a Community-Based Outpatient Facility
 Women s Imaging Original Research Destounis et al. Management of LCIS Diagnosed at Core Needle Biopsy Women s Imaging Original Research FOCUS ON: Stamatia V. Destounis 1 Philip F. Murphy Posy J. Seifert
Women s Imaging Original Research Destounis et al. Management of LCIS Diagnosed at Core Needle Biopsy Women s Imaging Original Research FOCUS ON: Stamatia V. Destounis 1 Philip F. Murphy Posy J. Seifert
