Needlestick Policy and Actions to be taken after Exposure to Blood and Body Fluids (including HIV Post- Exposure Prophylaxis).
|
|
|
- Emil Fields
- 5 years ago
- Views:
Transcription
1 LTHT Infection Control Policies Needlestick Policy and Actions to be taken after Exposure to Blood and Body Fluids (including HIV Post- Exposure Prophylaxis). This policy covers the immediate actions to be taken following percutaneous or mucocutaneous exposure to blood and body fluids. Scope of policy This policy applies to: All patients at LTHT All staff working on LTHT property either on a permanent or temporary basis. Policy contents: Body fluids that may transmit blood borne viruses pg 2 What is meant by exposure pg 2 Immediate first aid following exposure to blood/body fluids pg 2 Hepatitis B, Hepatitis C and HIV pg 3 Action following exposure from source patient pg 4 Action following exposure from HCW to another individual pg 5 Who provides specialist advice pg 5 Appendix 1 risk assessment pg 7, 8 Appendix 2 action following exposure pg 9 Appendix 3 PEP information and advice pg 10 Appendix 4 Out of Hours Needlestick Checklist Form pg 11 Appendix 5 - Example Microbiology Forms pg 12 Key Points Each health care worker (HCW) needs to be aware of the actions they should take if exposure has occurred; both for their own benefit and if they are involved in the immediate management of exposed workers. If significant exposure has taken place and HIV post exposure prophylaxis (PEP) is indicated then ideally it should be commenced within one hour.(see appendix 3) 1
2 Body fluids that may transmit blood borne viruses Blood Saliva (associated with dentistry) Cerebro-spinal fluid Pericardial fluid Peritoneal fluid Pleural fluid Synovial fluid Unfixed human tissues and organs Exudate or tissue fluid from burns/wounds Any other body fluid if visibly blood stained. Vaginal fluid Semen Amniotic fluid Human breast milk What is meant by exposure? Percutaneous injuries e.g. from used needles, bites and other wounds from sharp items. Mucocutaneous exposure e.g. splashes into the mouth, eyes etc, or splashes onto broken skin e.g. existing cuts, eczema etc. Exposure to low risk body fluids e.g. urine, vomit, faeces, sputum and saliva (except when associated with dental work) is not normally considered a risk unless visibly stained with blood. Exposure of unbroken skin to blood and body fluids has not been associated with blood borne virus transmission. Injuries with unused needles or sharps should be washed and covered with a waterproof plaster. A record of the injury should be made on an IR 1 form but there is no requirement to inform Occupational Health Services or the Site Matron. Immediate first aid following exposure to blood/body fluids. Percutaneous injuries from used needles, bites, cuts from sharp objects etc, should be gently encouraged to bleed. Do NOT suck the wound. The wound should then be washed with soap and water, dried and covered with a waterproof plaster. Splashes onto non-intact skin (e.g. abrasions, cuts, and eczema) should be cleaned liberally with water. Splashes into the eyes, mouth or other mucous membranes should be irrigated with copious amounts of clean water. If contact lenses are worn, eye irrigation should take place before and after removing the lenses. The injury/incident should then be reported to the person in charge of the ward or area and a written record made on an IR 1 form. 2
3 Protection against Hepatitis B Virus The risk of infection with HBV in unimmunised individuals following a sharps or splash injury from a HBV positive source patient is in the region of 1 in 50, rising to 1 in 2.5 to 1 in 3 if the source patient is also e antigen positive (DoH 1998, Gerberdring 1995). The action needed in the immediate post exposure period to protect the health care worker against hepatitis B is dependent on the vaccination status of the health care worker and (where known) the hepatitis B surface antigen status of the source patient. This will be managed by the OHS. For details of what action is necessary out of hours see page 4 (action following exposure from a source patient). Please note, if hepatitis B immunoglobulin is required this is available from the Health Protection Agency (HPA) at Seacroft (tel or out of hours via Seacroft Lodge ). Protection against Hepatitis C Virus Currently there is no vaccination or post exposure prophylaxis against hepatitis C. The risk of infection to an individual following a needlestick injury from a HCV positive patient is 1 in 30 (DoH 1998). If the source patient is found or known to be hepatitis C positive, then the exposed individual will require follow up by Occupational Health Services (OHS). Treatment in the early stages of infection has been shown to be very successful.the source patient should be referred to an appropriate specialist where necessary. Protection issues against HIV Currently there is no vaccination, however post exposure prophylaxis is available. Studies have indicated that the average risk for HIV transmission after percutaneous exposure to HIV infected blood in health care settings is about 0.3% or 3 per 1000 injuries (Department of Health 2000). However some factors are associated with increased risk of HIV infection, these include :- Deep injury Visible blood on the device which caused the injury Injury with a needle that had been in the source patient s artery or vein Terminal HIV related illness in the source patient The initial risk assessment is based on the potential for viral transmission, i.e. the type of body fluid involved, the route and severity of exposure. For example, some occupational exposures after careful assessment may not be considered to be significant, that is they do not have potential for HIV transmission i.e. splashes onto intact skin. In such circumstances PEP is not indicated. Further information pertaining to PEP including access to and prescribing of can be found in appendix 3. 3
4 Action following exposure from a source patient After sustaining an injury, the individual concerned should perform immediate first aid as outlined on page 2. During the out of office hours period use and complete the checklist form found in appendix 4. A risk assessment of the source patient should be carried out as soon as the injury occurs. This should ideally be carried out by the clinician responsible for the patient, but may also be performed by competent other e.g. Ward/Nurse Manager when they are not available (eg out of hours). Consent for blood should be obtained by the person completing the risk assessment. Detailed advice pertaining to risk assessment can be found in appendix 1. Information pertaining to PEP if indicated can be found in appendix 3. If PEP is indicated out of hours, the recipient should report to A&E for further treatment. A sample of the source patient s blood should be obtained in a clotted sample tube and sent to Microbiology to test for Hepatitis B, Hepatitis C and HIV (see appendix 5 for example of completed microbiology form). The sample must be obtained with informed consent (either from the donor or, in the case of a minor, from their guardian), by the individual carrying out the risk assessment, and this should be documented in the patient s notes. Blood samples may not be obtained from clients who are unconscious, confused or deceased unless extenuating circumstances exist. Obtain specialist advice if required (see page 5). The recipient should provide a sample of blood in a clotted sample tube, to be sent to Microbiology (see appendix 5 for example of completed microbiology form). The HCW must be informed that the baseline blood sample will be stored for 2 years. The Hepatitis B vaccination history of the recipient should be obtained. If appropriate, the sample is tested for Hepatitis B antibodies. Blood samples may be sent from the clinical area or OHS. If the recipient has been vaccinated against Hepatitis B no further treatment is required immediately. If the recipient has no history of vaccination the first dose of vaccine should be given. In hours this will be managed by OHS, out of hours this will be prescribed and given in A&E. For further specialist advice contact the Virologist Injuries from an unknown source are usually classed as low risk. Action following exposure should include all steps except, obviously collection of donor bloods. All recipient exposures must be reported to OHS as soon as possible, either immediately or if the injury occurs out of hours, on the next working day. 4
5 (Injuries from a known HIV positive source or that have resulted in the prescription of PEP must be reported under RIDDOR by OHS). All injuries should be recorded on an IR1 form and reported to Occupational Health Services either at LGI (ext 23267) or SJUH (ext 65228). This should be done as soon as the injury occurs or, if out of office hours, on the next working day. Action following exposure from a HCW to another individual If exposure occurs from a HCW under-taking an exposure prone procedure to a patient (recipient), refer to annex G in HIV Post Exposure Prophylaxis: Guidance from the UK Chief Medical Officers' Expert Advisory Group on AIDS. UK Health Departments. Feb 2004, or contact Infection Control for advice. Who provides specialist advice? During office hours Occupational Health Services will co-ordinate immediate follow up of exposed HCWs and will contact specialists in genito-urinary medicine or infectious diseases if necessary. Outside of office hours the following can be contacted by the site matron/designated deputy or A+E for HIV specialist advice. For incidents occurring at Seacroft or St. James Hospitals contact the oncall Registrar or Consultant in Infectious Diseases via SJUH switchboard. For incidents occurring at LGI, Chapel Allerton, Wharfedale, and Cookridge Hospitals contact the on-call Registrar or Consultant in Genito- Urinary Medicine via LGI switchboard. Or Outside of office hours the following can be contacted by the site matron/designated deputy or A+E for Hepatitis B specialist advice. Contact the on call Virologist via switchboard Out of hours if PEP is indicated (PEP is indicated if the source patient is identified as high risk following completion of the risk assessment (appendix 1) which will be co-ordinated by the site matron), the A+E doctor will prescribe and dispense the necessary medicines immediately. If PEP is indicated the site matron/designated deputy must ensure the relevant HIV specialist is contacted so that urgent follow up can take place the next day. If there are any doubts or questions over whether PEP should be started the site matron should not hesitate to contact the appropriate HIV specialist. Out of hours if Hepatitis B vaccination is indicated (if the source patient is identified as high risk following completion of the risk assessment (appendix 1) and the site matron has established vaccination history), the A+E doctor is to 5
6 prescribe and dispense the necessary medicine. If there are any doubts or questions over whether the recipient requires Hepatitis B vaccination the site matron should not hesitate to contact the on call virologist References and further reading. Guidance for Clinical Health Care Workers: Protection Against Infection with Blood borne Viruses. Recommendations of the Expert Advisory Group on AIDS and the Advisory Group on Hepatitis. UK Health Departments HIV Post Exposure Prophylaxis : Guidance from the UK Chief Medical Officers' Expert Advisory Group on AIDS. UK Health Departments. Feb Gerberding JL Management of Occupational Exposures to Blood Borne Viruses. New England Journal of Medicine, Vol 332, No 7, Feb 16 th Policy Development Group Fiona Allen Janice Colbeck Anna Di Biasio Mark Farrah David Green Helen Jolly Janet Maynard Jane Minton Pam Mellor Eric Monteiro Mark Wilcox Policy Development Group Lead Gillian Hodgson Advisory members to the development group Graham Johnson Tony Hale Bill Bagnel Rachel Allsop Policy date: October 2001 Revised date: December 2004 Review date: December
Contamination Incidents Frequently Asked Questions
 Contamination Incidents Frequently Asked Questions WWR- 004 Index 1. What is a contamination injury? 2. What should I do immediately if I have sustained a contamination injury? 3. What should I do immediately
Contamination Incidents Frequently Asked Questions WWR- 004 Index 1. What is a contamination injury? 2. What should I do immediately if I have sustained a contamination injury? 3. What should I do immediately
Sunny Smiles Clinical Guidelines
 Sunny Smiles Clinical Guidelines Accidental Inoculation Injury - Guidance for healthcare professionals on dealing with needle-stick injuries to members Date Written: April 2010 Contents 1 Local Contacts...3
Sunny Smiles Clinical Guidelines Accidental Inoculation Injury - Guidance for healthcare professionals on dealing with needle-stick injuries to members Date Written: April 2010 Contents 1 Local Contacts...3
Guidance for management of exposure events where there is a risk of transmission of blood borne viruses
 Guidance for management of exposure events where there is a risk of transmission of blood borne viruses (HIV, Hepatitis B and Hepatitis C) in the community SUMMARY Where a child is thought to have had
Guidance for management of exposure events where there is a risk of transmission of blood borne viruses (HIV, Hepatitis B and Hepatitis C) in the community SUMMARY Where a child is thought to have had
Sharps injuries and exposure to blood and high risk body fluids SOP:
 Clinical Sharps injuries and exposure to blood and high risk body fluids SOP: Document Control Summary Status: Replacement. Replaces: Management of clinical sharps injuries and exposure to blood and high
Clinical Sharps injuries and exposure to blood and high risk body fluids SOP: Document Control Summary Status: Replacement. Replaces: Management of clinical sharps injuries and exposure to blood and high
Sharps and Blood/Body Fluid Contamination Injury Immediate Actions
 Infection Prevention and Control Assurance - Standard Operating Procedure 8 (IPC SOP 8) Sharps and Blood/Body Fluid Contamination Injury Immediate Actions Why we have a procedure? The Health and Social
Infection Prevention and Control Assurance - Standard Operating Procedure 8 (IPC SOP 8) Sharps and Blood/Body Fluid Contamination Injury Immediate Actions Why we have a procedure? The Health and Social
To provide the guidelines for the management of healthcare workers who have had an occupational exposure to blood and/or body fluids.
 TITLE/DESCRIPTION: MANAGEMENT OF OCCUPATIONAL EXPOSURE TO HBV, HCV, and HIV INDEX NUMBER: EFFECTIVE DATE: APPLIES TO: ISSUING AUTHORITY: 01/01/2009 01/01/2013 All GCC Countries GULF COOPERATION COUNCIL
TITLE/DESCRIPTION: MANAGEMENT OF OCCUPATIONAL EXPOSURE TO HBV, HCV, and HIV INDEX NUMBER: EFFECTIVE DATE: APPLIES TO: ISSUING AUTHORITY: 01/01/2009 01/01/2013 All GCC Countries GULF COOPERATION COUNCIL
Management of Exposure to Needlestick Injuries & Body Fluids
 Management of Exposure to Needlestick Injuries & Body Fluids Clinical S.O.P. No.:28 Compiled by: Approved by: Review date: November 2016 DOCUMENT HISTORY Version Detail of purpose / change Author / edited
Management of Exposure to Needlestick Injuries & Body Fluids Clinical S.O.P. No.:28 Compiled by: Approved by: Review date: November 2016 DOCUMENT HISTORY Version Detail of purpose / change Author / edited
Blood/Body Fluid Exposure Option
 Introduction: Transmission of bloodborne pathogens [e.g., Hepatitis B virus (HBV), Hepatitis C virus (HBC), Human Immunodeficiency Virus (HIV)] from patients to healthcare workers (HCW) is an important
Introduction: Transmission of bloodborne pathogens [e.g., Hepatitis B virus (HBV), Hepatitis C virus (HBC), Human Immunodeficiency Virus (HIV)] from patients to healthcare workers (HCW) is an important
EXPOSURE (HIV/HEPATITIS) BLOOD & BODY FLUIDS
 Page(s): 1 of 11 PURPOSE To set a standardized procedure to ensure that employees are evaluated in a consistent and timely manner.. POLICY A. The treatment of Team Member exposure to bloodborne pathogens
Page(s): 1 of 11 PURPOSE To set a standardized procedure to ensure that employees are evaluated in a consistent and timely manner.. POLICY A. The treatment of Team Member exposure to bloodborne pathogens
TRUST POLICY AND PROCEDURES FOR THE MANAGEMENT OF INOCULATION INCIDENTS
 TRUST POLICY AND PROCEDURES FOR THE MANAGEMENT OF INOCULATION INCIDENTS Reference Number CL-RM 2014 022 Version: 2.6 Status Final Authors: Dr D.Gnanarajah, Consultant Microbiologist Dr Apoola Consultant
TRUST POLICY AND PROCEDURES FOR THE MANAGEMENT OF INOCULATION INCIDENTS Reference Number CL-RM 2014 022 Version: 2.6 Status Final Authors: Dr D.Gnanarajah, Consultant Microbiologist Dr Apoola Consultant
Clinical Education Initiative OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS. Antonio E. Urbina, MD
 Clinical Education Initiative Support@ceitraining.org OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS Antonio E. Urbina, MD 5/22/2013 Occupational Post-Exposure Prophylaxis [Video Transcript] 00:00:15 - [Tony]
Clinical Education Initiative Support@ceitraining.org OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS Antonio E. Urbina, MD 5/22/2013 Occupational Post-Exposure Prophylaxis [Video Transcript] 00:00:15 - [Tony]
Management of Workplace Exposure to Blood-borne Pathogens
 Management of Workplace Exposure to Blood-borne Pathogens 11/22/2017 Management of Workplace Exposure to Blood-borne Pathogens BY SOLYMOLE KURUVILLA, PHD, RN, ACNP-BC DIRECTOR, OCCUPATIONAL HEALTH SERVICES
Management of Workplace Exposure to Blood-borne Pathogens 11/22/2017 Management of Workplace Exposure to Blood-borne Pathogens BY SOLYMOLE KURUVILLA, PHD, RN, ACNP-BC DIRECTOR, OCCUPATIONAL HEALTH SERVICES
Management of sharps injuries in the healthcare setting
 Link to this article online for CPD/CME credits Management of sharps injuries in the healthcare setting Anna Riddell, 1 Ioana Kennedy, 2 C Y William Tong 1 3 1 Department of Infection, Barts Health NHS
Link to this article online for CPD/CME credits Management of sharps injuries in the healthcare setting Anna Riddell, 1 Ioana Kennedy, 2 C Y William Tong 1 3 1 Department of Infection, Barts Health NHS
Exposures at Non-MUSC Clinical Sites
 BLOOD BORNE PATHOGEN EXPOSURE CHECKLIST Exposures at Non-MUSC Clinical Sites (Students on clinical rotations at Roper Hospital, Trident Hospital, Affiliated Local Clinical Sites, Out of Town Clinical Sites,
BLOOD BORNE PATHOGEN EXPOSURE CHECKLIST Exposures at Non-MUSC Clinical Sites (Students on clinical rotations at Roper Hospital, Trident Hospital, Affiliated Local Clinical Sites, Out of Town Clinical Sites,
POLICY ON BLOOD AND BODY FLUID EXPOSURE (NEEDLE STICK)
 POLICY ON BLOOD AND BODY FLUID EXPOSURE (NEEDLE STICK) Dated: January 1, 2018 Supersedes: Blood and Body Fluid Exposure (Needle stick) dated July 1, 2015 I. POLICY It is the policy of New York Medical
POLICY ON BLOOD AND BODY FLUID EXPOSURE (NEEDLE STICK) Dated: January 1, 2018 Supersedes: Blood and Body Fluid Exposure (Needle stick) dated July 1, 2015 I. POLICY It is the policy of New York Medical
Blood and Body Fluid Exposure
 Blood and Body Fluid Exposure Infection Prevention and Control Contents Policy... 1 Purpose... 1 Scope/Audience... 1 Definitions... 2 Associated documents... 2 1.1 Indications for BBFE reporting... 2 1.2
Blood and Body Fluid Exposure Infection Prevention and Control Contents Policy... 1 Purpose... 1 Scope/Audience... 1 Definitions... 2 Associated documents... 2 1.1 Indications for BBFE reporting... 2 1.2
Peninsula Dental Social Enterprise (PDSE)
 Peninsula Dental Social Enterprise (PDSE) Inoculation Incidents and Blood Borne Viruses Version 1.0 Date approved: October 2013 Approved by: The Board Review due: March 2016 Contents Section Topic Page
Peninsula Dental Social Enterprise (PDSE) Inoculation Incidents and Blood Borne Viruses Version 1.0 Date approved: October 2013 Approved by: The Board Review due: March 2016 Contents Section Topic Page
MANAGEMENT OF OCCUPATIONAL AND NON-OCCUPATIONAL EXPOSURES TO BLOODBORNE VIRUSES INCLUDING NEEDLESTICK INJURIES & SEXUAL EXPOSURES
 NHS GREATER GLASGOW CONTROL OF INFECTION COMMITTEE GUIDELINE MANAGEMENT OF OCCUPATIONAL AND NON-OCCUPATIONAL EXPOSURES TO BLOODBORNE VIRUSES INCLUDING NEEDLESTICK INJURIES & SEXUAL EXPOSURES Effective
NHS GREATER GLASGOW CONTROL OF INFECTION COMMITTEE GUIDELINE MANAGEMENT OF OCCUPATIONAL AND NON-OCCUPATIONAL EXPOSURES TO BLOODBORNE VIRUSES INCLUDING NEEDLESTICK INJURIES & SEXUAL EXPOSURES Effective
One of your office personnel
 Doug Campos-Outcalt, MD, MPA Department of Family and Community Medicine, University of Arizona College of Medicine, Phoenix HIV postexposure prophylaxis: Who should get it? CORRESPONDENCE Doug Campos-Outcalt,
Doug Campos-Outcalt, MD, MPA Department of Family and Community Medicine, University of Arizona College of Medicine, Phoenix HIV postexposure prophylaxis: Who should get it? CORRESPONDENCE Doug Campos-Outcalt,
INFECTION CONTROL PROCEDURE FOR NEEDLESTICK AND SIMILAR SHARPS INJURIES
 Reference Number: UHB 019 Version Number: 2 Date of Next Review: October 2018 Previous Trust/LHB Reference Number: UHB075 INFECTION CONTROL PROCEDURE FOR NEEDLESTICK AND SIMILAR SHARPS INJURIES INTRODUCTION
Reference Number: UHB 019 Version Number: 2 Date of Next Review: October 2018 Previous Trust/LHB Reference Number: UHB075 INFECTION CONTROL PROCEDURE FOR NEEDLESTICK AND SIMILAR SHARPS INJURIES INTRODUCTION
Infection Control Standard Precautions. CDC Recommendations: Application of Standard Precautions for All Patients
 Infection Control Standard Precautions Standard Precautions Hand Hygiene CDC Recommendations: Application of Standard Precautions for All Patients Component Personal Protective Equipment (PPE) Gloves Mask,
Infection Control Standard Precautions Standard Precautions Hand Hygiene CDC Recommendations: Application of Standard Precautions for All Patients Component Personal Protective Equipment (PPE) Gloves Mask,
3/23/2016. Managing Bloodborne Pathogen Exposures. Managing Bloodborne Pathogen Exposures
 This webinar begins at 11 a.m., Eastern. You will not hear anything over your telephone line until the program starts. If the system did not prompt you to enter your phone number and receive a call back,
This webinar begins at 11 a.m., Eastern. You will not hear anything over your telephone line until the program starts. If the system did not prompt you to enter your phone number and receive a call back,
MANAGEMENT OF EXPOSURE TO HEALTH CARE ASSOCIATED INFECTIONS (HCAI) AND INOCULATION INCIDENTS (INCLUDING SAFE MANAGEMENT OF SHARPS)
 MANAGEMENT OF EXPOSURE TO HEALTH CARE ASSOCIATED INFECTIONS (HCAI) AND INOCULATION INCIDENTS (INCLUDING SAFE MANAGEMENT OF SHARPS) INFECTION PREVENTION AND CONTROL POLICY NO. 4 Applies to: Staff employed
MANAGEMENT OF EXPOSURE TO HEALTH CARE ASSOCIATED INFECTIONS (HCAI) AND INOCULATION INCIDENTS (INCLUDING SAFE MANAGEMENT OF SHARPS) INFECTION PREVENTION AND CONTROL POLICY NO. 4 Applies to: Staff employed
43. Guidelines on Needle stick Injury
 43. Guidelines on Needle stick Injury The following information is abstracted from the South African Department of Health guidelines entitled: Management of Occupational Exposure to the Human Immunodeficiency
43. Guidelines on Needle stick Injury The following information is abstracted from the South African Department of Health guidelines entitled: Management of Occupational Exposure to the Human Immunodeficiency
Bloodborne Pathogens Across the Continuum of Care Sue Sebazco, Arlington, Texas A Webber Training Teleclass
 Bloodborne Pathogens Across the Continuum of Care Objectives Sue Sebazco, RN, BS, CIC Infection Control/Employee Health Director Arlington, TX Pittsburg Mercy Health System skrystofiak@mercy.pmhs.org Define
Bloodborne Pathogens Across the Continuum of Care Objectives Sue Sebazco, RN, BS, CIC Infection Control/Employee Health Director Arlington, TX Pittsburg Mercy Health System skrystofiak@mercy.pmhs.org Define
Effective Date: 6/10/2013 Review Date: 6/10/2016
 Policy Title: Sterilization and Disinfection of Patient-Care Items Policy Number: 11 6.2.2. Examples of useful items to maintain in the office sterilization log are as following: o Date and time of cycle
Policy Title: Sterilization and Disinfection of Patient-Care Items Policy Number: 11 6.2.2. Examples of useful items to maintain in the office sterilization log are as following: o Date and time of cycle
INITIAL EVALUATION AND MANAGEMENT FOLLOWING EXPOSURE TO BLOOD OR BODY FLUIDS
 Page 1 of 11 Original Date of Issue: June 1991 Reviewed 2/96 5/97 11/98 11/99 5/01 5/02 12/05 Revised 9/95 5/97 5/00 7/02 3/06 6/08 6/10 The following are the procedures to be followed when a person sustains
Page 1 of 11 Original Date of Issue: June 1991 Reviewed 2/96 5/97 11/98 11/99 5/01 5/02 12/05 Revised 9/95 5/97 5/00 7/02 3/06 6/08 6/10 The following are the procedures to be followed when a person sustains
Village By Village HIV/AIDS Policy
 The Old Sweet Shop Teme Street, Tenbury Wells, Worcs. WR15 8BB Phone: 07887 870090 Web: villagebyvillage.org.uk Email: neil@villagebyvillage.org.uk Registered Charity Number 1116952 18/9/07 Village By
The Old Sweet Shop Teme Street, Tenbury Wells, Worcs. WR15 8BB Phone: 07887 870090 Web: villagebyvillage.org.uk Email: neil@villagebyvillage.org.uk Registered Charity Number 1116952 18/9/07 Village By
SHARPS PROCEDURE PROCEDURE FOR THE SAFE USE & DISPOSAL OF SHARPS AND THE MANAGEMENT OF SHARPS INJURIES AND BLOOD EXPOSURE INCIDENTS.
 SHARPS PROCEDURE PROCEDURE FOR THE SAFE USE & DISPOSAL OF SHARPS AND THE MANAGEMENT OF SHARPS INJURIES AND BLOOD EXPOSURE INCIDENTS February 2012 Version 1.0 1 CONTENTS Section Page 1.0 Introduction 3
SHARPS PROCEDURE PROCEDURE FOR THE SAFE USE & DISPOSAL OF SHARPS AND THE MANAGEMENT OF SHARPS INJURIES AND BLOOD EXPOSURE INCIDENTS February 2012 Version 1.0 1 CONTENTS Section Page 1.0 Introduction 3
Bloodborne Pathogens Exposure Procedure
 Bloodborne Pathogens Exposure Procedure Background: Bloodborne pathogens are infectious microorganisms present in blood that can cause disease in humans. These pathogens include, but are not limited to,
Bloodborne Pathogens Exposure Procedure Background: Bloodborne pathogens are infectious microorganisms present in blood that can cause disease in humans. These pathogens include, but are not limited to,
Needlestick and Splash Exposure Flow Chart Page 1 Clinical Practice Guidelines
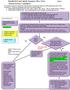 Needlestick and Splash Exposure Flow Chart Page 1 If ANY student experiences a needlestick or splash exposure ANY time of day/night, they need to page #11709 which will be forwarded to: (**in the event
Needlestick and Splash Exposure Flow Chart Page 1 If ANY student experiences a needlestick or splash exposure ANY time of day/night, they need to page #11709 which will be forwarded to: (**in the event
Safety Regulations and Procedures Occupational Health Bloodborne Pathogens Exposure Control Plan S80.10, updated, May Contains information for:
 APPENDIX A Safety Regulations and Procedures Occupational Health Bloodborne Pathogens Exposure Control Plan S80.10, updated, May 2018 BLOODBORNE PATHOGEN EXPOSURE INCIDENT PACKET Contains information for:
APPENDIX A Safety Regulations and Procedures Occupational Health Bloodborne Pathogens Exposure Control Plan S80.10, updated, May 2018 BLOODBORNE PATHOGEN EXPOSURE INCIDENT PACKET Contains information for:
Introduction to Blood Borne Pathogens
 Introduction to Blood Borne Pathogens What are blood pathogens? Any infectious microorganism in the human blood that can cause disease is a Blood borne pathogen. Three of these pathogens include hepatitis
Introduction to Blood Borne Pathogens What are blood pathogens? Any infectious microorganism in the human blood that can cause disease is a Blood borne pathogen. Three of these pathogens include hepatitis
NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS
 NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS Hepatitis B, Hepatitis C and HIV may be contracted through exposure to any body fluid, particularly blood. IMMEDIATE ACTION
NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS Hepatitis B, Hepatitis C and HIV may be contracted through exposure to any body fluid, particularly blood. IMMEDIATE ACTION
Colgate University. Bloodborne Pathogens Exposure Control Plan
 Colgate University Bloodborne Pathogens Exposure Control Plan COLGATE UNIVERSITY BLOODBORNE PATHOGENS EXPOSURE CONTROL PLAN I. STATEMENT OF POLICY It is the policy of Colgate University (CU) to limit or
Colgate University Bloodborne Pathogens Exposure Control Plan COLGATE UNIVERSITY BLOODBORNE PATHOGENS EXPOSURE CONTROL PLAN I. STATEMENT OF POLICY It is the policy of Colgate University (CU) to limit or
PROTECTION FROM OCCUPATIONAL ACQUIRED/TRANSMITTED COMMUNICABLE DISEASES Policy
 PROTECTION FROM OCCUPATIONAL ACQUIRED/TRANSMITTED COMMUNICABLE DISEASES Policy 1 Policy title Protection from Occupational Acquired /Transmitted Communicable Diseases Policy COR 60 reference Policy category
PROTECTION FROM OCCUPATIONAL ACQUIRED/TRANSMITTED COMMUNICABLE DISEASES Policy 1 Policy title Protection from Occupational Acquired /Transmitted Communicable Diseases Policy COR 60 reference Policy category
CONTINUING CARE ADMINISTRATIVE MANUAL POLICY
 CONTINUING CARE ADMINISTRATIVE MANUAL POLICY NUMBER III-10 DATE Draft June 8, 2010 PAGE 1 OF 3 APPROVED BY: SITE: CATEGORY TITLE: Vice President & Senior Operating Officer, Rehab & Continuing Care Edmonton
CONTINUING CARE ADMINISTRATIVE MANUAL POLICY NUMBER III-10 DATE Draft June 8, 2010 PAGE 1 OF 3 APPROVED BY: SITE: CATEGORY TITLE: Vice President & Senior Operating Officer, Rehab & Continuing Care Edmonton
MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet. Instructions for Employees/Students:
 MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet MUSC has established these protocols in accordance with the OSHA Bloodborne Pathogen Standard and Center for Disease Control recommendations
MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet MUSC has established these protocols in accordance with the OSHA Bloodborne Pathogen Standard and Center for Disease Control recommendations
Prevention and Management of Occupational Exposure to Blood Borne Viruses, Post Exposure Prophylaxis and Prevention of Sharps Injuries Policy
 Prevention and Management of Occupational Exposure to Blood Borne Viruses, Post Exposure Prophylaxis and Prevention of Sharps Injuries Policy Author(s) & Designation Lead Clinician if appropriate In consultation
Prevention and Management of Occupational Exposure to Blood Borne Viruses, Post Exposure Prophylaxis and Prevention of Sharps Injuries Policy Author(s) & Designation Lead Clinician if appropriate In consultation
Gwynedd Mercy University Bloodborne Pathogen Safety and Awareness Training
 Gwynedd Mercy University Bloodborne Pathogen Safety and Awareness Training Education is the KEY Here are Gwynedd Mercy University, we recognize the importance of providing a safe working environment for
Gwynedd Mercy University Bloodborne Pathogen Safety and Awareness Training Education is the KEY Here are Gwynedd Mercy University, we recognize the importance of providing a safe working environment for
Definitions. Appendix A
 Definitions Appendix A 1. Blood means human blood, human blood components, and products made from human blood. 2. Bloodborne Pathogens means pathogenic microorganisms that are present in human blood and
Definitions Appendix A 1. Blood means human blood, human blood components, and products made from human blood. 2. Bloodborne Pathogens means pathogenic microorganisms that are present in human blood and
NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS
 NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS Hepatitis B, Hepatitis C and HIV may be contracted through exposure to any body fluid, particularly blood. IMMEDIATE ACTION
NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS Hepatitis B, Hepatitis C and HIV may be contracted through exposure to any body fluid, particularly blood. IMMEDIATE ACTION
Sharps Management, Needle-Stick Injuries and Exposure to Blood Borne Viruses Procedure ICPr005
 Sharps Management, Needle-Stick Injuries and Exposure to Blood Borne Viruses Procedure ICPr005 Version Date Date of Next Reason for Change (eg. full rewrite, No. Ratified/ Implementation Review amendment
Sharps Management, Needle-Stick Injuries and Exposure to Blood Borne Viruses Procedure ICPr005 Version Date Date of Next Reason for Change (eg. full rewrite, No. Ratified/ Implementation Review amendment
Bloodborne Pathogens and Exposure Control
 Bloodborne Pathogens and Exposure Control 2016 Information in the Exposure Control Plan The Bloodborne Pathogen Exposure Control Plan was developed to communicate information to you about: - Your risk
Bloodborne Pathogens and Exposure Control 2016 Information in the Exposure Control Plan The Bloodborne Pathogen Exposure Control Plan was developed to communicate information to you about: - Your risk
Blood Borne Pathogens. Becky Walch, R.N. Micheel Valdez, L.V.N.
 Blood Borne Pathogens Becky Walch, R.N. Micheel Valdez, L.V.N. Examples of Blood Borne Pathogens Hepatitis B Hepatitis C Other Hepatitis HIV Hepatitis Hepatitis means inflammation of the liver. Hepatitis
Blood Borne Pathogens Becky Walch, R.N. Micheel Valdez, L.V.N. Examples of Blood Borne Pathogens Hepatitis B Hepatitis C Other Hepatitis HIV Hepatitis Hepatitis means inflammation of the liver. Hepatitis
Sharps Injuries Management
 Sharps Injuries Management and other blood or body fluid exposure incidents This procedural document supersedes: PAT/IC 14 v.5 Sharps Injuries Management and other blood or body fluid exposure incidents
Sharps Injuries Management and other blood or body fluid exposure incidents This procedural document supersedes: PAT/IC 14 v.5 Sharps Injuries Management and other blood or body fluid exposure incidents
I. PROCEEDINGS AFTER EXPOSURE TO BLOOD OR OTHER POTENTIALLY INFECTIOUS MATERIALS (OPIM) WHICH MIGHT TRANSFER AN INFECTION WITH HAEMATOGENOUS VIRUSES
 Annex no. 1 to the enactment No. 13/XIV R/2010 of the Rector of the Medical University in Wrocław dated April 12, 2010 Proceedings after occupational exposure to HIV, HBV and HCV 1 LEGAL GROUNDS: 1. The
Annex no. 1 to the enactment No. 13/XIV R/2010 of the Rector of the Medical University in Wrocław dated April 12, 2010 Proceedings after occupational exposure to HIV, HBV and HCV 1 LEGAL GROUNDS: 1. The
Bloodborne Pathogens. Exposure Control Plan
 Bloodborne Pathogens Exposure Control Plan Maryland Institute College of Art Revision Date(s): January 2007/January 2008 Maryland Institute College of Art (MICA) Subject: Occupational/Non-occupational
Bloodborne Pathogens Exposure Control Plan Maryland Institute College of Art Revision Date(s): January 2007/January 2008 Maryland Institute College of Art (MICA) Subject: Occupational/Non-occupational
B. Tasks and Procedures where employees, students or contractors can be exposed to bloodborne pathogens:
 Page 1 of 6 BLOODBORNE PATHOGEN PROGRAM INTRODUCTION The intended purpose of this document is to comply with OSHA s Occupational Exposures to Bloodborne Pathogens in Title 29 Code of Federal Regulations
Page 1 of 6 BLOODBORNE PATHOGEN PROGRAM INTRODUCTION The intended purpose of this document is to comply with OSHA s Occupational Exposures to Bloodborne Pathogens in Title 29 Code of Federal Regulations
Exposure. What Healthcare Personnel Need to Know
 Information from the Centers for Disease Control and Prevention National Center for Infectious Diseases Divison of Healthcare Quality Promotion and Division of Viral Hepatitis For additional brochures
Information from the Centers for Disease Control and Prevention National Center for Infectious Diseases Divison of Healthcare Quality Promotion and Division of Viral Hepatitis For additional brochures
Title Management of Inoculation Injuries Policy
 Document Control Title Author Directorate Nursing Date Version Issued 1.0 March 2007 1.1 April 2008 1.1 May 2008 2.0 May 2008 2.1 Sept 2008 2.2 October 2008 2.3 Nov 2008 Status Revision Revision Final
Document Control Title Author Directorate Nursing Date Version Issued 1.0 March 2007 1.1 April 2008 1.1 May 2008 2.0 May 2008 2.1 Sept 2008 2.2 October 2008 2.3 Nov 2008 Status Revision Revision Final
STUDENT EXPOSURE TO BLOOD OR OTHER POTENTIALLY INFECTIOUS MATERIALS
 STUDENT EXPOSURE TO BLOOD OR OTHER POTENTIALLY INFECTIOUS MATERIALS (See Bloodborne Pathogen Worksheet and Post Exposure Prophylaxis consent immediately following this policy ) 1. Student must report immediately
STUDENT EXPOSURE TO BLOOD OR OTHER POTENTIALLY INFECTIOUS MATERIALS (See Bloodborne Pathogen Worksheet and Post Exposure Prophylaxis consent immediately following this policy ) 1. Student must report immediately
Sharps Policy: Safe Handling and Disposal of Sharps
 Sharps Policy: Safe Handling and Disposal of Sharps Document Control Sheet Name of document: Sharps Policy: Safe Handling and Disposal of Sharps Version: 8 Status: Owner: In review Infection Prevention
Sharps Policy: Safe Handling and Disposal of Sharps Document Control Sheet Name of document: Sharps Policy: Safe Handling and Disposal of Sharps Version: 8 Status: Owner: In review Infection Prevention
Drew University Bloodborne Pathogens Exposure Control Plan and Procedures
 PURPOSE To provide a written plan for preventing and/or minimizing exposure to bloodborne pathogens for those Drew University personnel who may be involved in the handling of human blood, blood products,
PURPOSE To provide a written plan for preventing and/or minimizing exposure to bloodborne pathogens for those Drew University personnel who may be involved in the handling of human blood, blood products,
Blood Borne Pathogens (BBP)
 Blood Borne Pathogens (BBP) Healthcare facilities are high-risk areas for exposure to bloodborne pathogens, so protect yourself and remind others to do the same. There are three bloodborne pathogens of
Blood Borne Pathogens (BBP) Healthcare facilities are high-risk areas for exposure to bloodborne pathogens, so protect yourself and remind others to do the same. There are three bloodborne pathogens of
HEPATITIS B GUIDANCE FOR THE PROTECTION OF HEALTH CARE WORKERS AND PATIENTS. All clinical areas of the Trust. Prevent spread of Hepatitis B virus
 Trust Policy and Procedure PP(15)027 Document Ref No: HEPATITIS B GUIDANCE FOR THE PROTECTION OF HEALTH CARE WORKERS AND PATIENTS For use in: For use by: For use for: Document owner: Status: All clinical
Trust Policy and Procedure PP(15)027 Document Ref No: HEPATITIS B GUIDANCE FOR THE PROTECTION OF HEALTH CARE WORKERS AND PATIENTS For use in: For use by: For use for: Document owner: Status: All clinical
Bloodborne Pathogens. Montclair Kimberley Academy 1
 Bloodborne Pathogens Montclair Kimberley Academy 1 Introduction! Approximately 5.6 million workers in health care and other facilities are at risk of exposure to bloodborne pathogens such as human immunodeficiency
Bloodborne Pathogens Montclair Kimberley Academy 1 Introduction! Approximately 5.6 million workers in health care and other facilities are at risk of exposure to bloodborne pathogens such as human immunodeficiency
Universal Precautions
 Universal Precautions emphasizes the need for workers and students to consider all blood and body fluids as potentially infected with HIV, HBV, and / or other blood-borne pathogens, and to adhere rigorously
Universal Precautions emphasizes the need for workers and students to consider all blood and body fluids as potentially infected with HIV, HBV, and / or other blood-borne pathogens, and to adhere rigorously
EU Directive for Safer Sharps. Anna Pronyszyn Infection Prevention Nurse Conusultant
 EU Directive for Safer Sharps Anna Pronyszyn Infection Prevention Nurse Conusultant Regulation and Legislation Health and Social Care Act 2008 Occupier s Liability Act 1957 Health and Safety at Work Act
EU Directive for Safer Sharps Anna Pronyszyn Infection Prevention Nurse Conusultant Regulation and Legislation Health and Social Care Act 2008 Occupier s Liability Act 1957 Health and Safety at Work Act
A. Background for Trainer: B. What OSHA Requires: Bloodborne Pathogens. Lesson Plan 6080a
 Lesson Plan 6080a This training session outline is designed to follow the accompanying booklet, OSHA s Bloodborne Pathogens Standard. The booklet reviews what employees who are potentially exposed to the
Lesson Plan 6080a This training session outline is designed to follow the accompanying booklet, OSHA s Bloodborne Pathogens Standard. The booklet reviews what employees who are potentially exposed to the
Trust Guideline for the Management of Incidents which have the potential to transmit Blood Borne Viruses
 transmit Blood Borne Viruses A clinical guideline recommended for use For Use in: By: For: Division responsible for document: Key words: Name and job titles of document author: Name and job title of document
transmit Blood Borne Viruses A clinical guideline recommended for use For Use in: By: For: Division responsible for document: Key words: Name and job titles of document author: Name and job title of document
SIV/SHIV Exposure Medical Response Guidance for the University of Wisconsin-Madison
 SIV/SHIV SIV/SHIV Exposure Medical Response Guidance for the University of Wisconsin-Madison 1.0 Instructions: Information in this guidance is meant to inform both laboratory staff and health professionals
SIV/SHIV SIV/SHIV Exposure Medical Response Guidance for the University of Wisconsin-Madison 1.0 Instructions: Information in this guidance is meant to inform both laboratory staff and health professionals
Blood-Borne Pathogens and Post-Exposure Prophylaxis
 Blood-Borne Pathogens and Post-Exposure Prophylaxis Christopher Behrens MD Northwest Association of Occupational and Environmental Medicine October 2017 with thanks to Shireesha Dhanireddy MD Disclosures
Blood-Borne Pathogens and Post-Exposure Prophylaxis Christopher Behrens MD Northwest Association of Occupational and Environmental Medicine October 2017 with thanks to Shireesha Dhanireddy MD Disclosures
SHARPS MANAGEMENT AND INOCULATION INJURIES
 Community Infection Prevention and Control Guidance for Health and Social Care Sharps Management and Inoculation Injuries Version 1.01 May 15 Harrogate and District NHS Foundation Trust Sharps Management
Community Infection Prevention and Control Guidance for Health and Social Care Sharps Management and Inoculation Injuries Version 1.01 May 15 Harrogate and District NHS Foundation Trust Sharps Management
Bloodborne Pathogen Module. Chelmsford Public Schools September, 2016
 Bloodborne Pathogen Module Chelmsford Public Schools September, 2016 Why is this important? v OSHA BB Pathogen Standard anyone whose job requires exposure to BB pathogens is required to complete training
Bloodborne Pathogen Module Chelmsford Public Schools September, 2016 Why is this important? v OSHA BB Pathogen Standard anyone whose job requires exposure to BB pathogens is required to complete training
Revised April WGH ER #5 Hospital Rd. Whitehorse Phone: (867) Outside of Whitehorse: Local Community Health Centre/Clinic/ER
 Where to access care Who to consult and when Please consult whenever questions arise on how to proceed with postexposure management and when exposure is beyond the scope of guidelines. Blood and Body Fluid
Where to access care Who to consult and when Please consult whenever questions arise on how to proceed with postexposure management and when exposure is beyond the scope of guidelines. Blood and Body Fluid
Bloodborne Pathogens and Regulated Medical Waste
 Bloodborne Pathogens and Regulated Medical Waste OSHA Ensure employees can safely perform their normal duties without undue health risks Bloodborne Pathogen (BBP) Standard developed to protect employees
Bloodborne Pathogens and Regulated Medical Waste OSHA Ensure employees can safely perform their normal duties without undue health risks Bloodborne Pathogen (BBP) Standard developed to protect employees
QUALITY LIFE CONCEPTS Policy on Bloodborne Pathogens
 QUALITY LIFE CONCEPTS Policy on Bloodborne Pathogens A24 TUBERCULOSIS TESTING Quality Life Concepts is committed to protecting its employees and individuals who will be served by vigilance and regular
QUALITY LIFE CONCEPTS Policy on Bloodborne Pathogens A24 TUBERCULOSIS TESTING Quality Life Concepts is committed to protecting its employees and individuals who will be served by vigilance and regular
You will now begin the Bloodborne Pathogen Refresher Training.
 You will now begin the Bloodborne Pathogen Refresher Training. The following program will review your occupational risks and the steps that you and your Client must take to reduce your risks of exposure.
You will now begin the Bloodborne Pathogen Refresher Training. The following program will review your occupational risks and the steps that you and your Client must take to reduce your risks of exposure.
INFECTION CONTROL POLICY
 INFECTION CONTROL POLICY The OHC&AT Board of Directors has agreed this Policy and as such, it applies across the organisation 15 th December 2017. Jay Mercer Darren Coghlan Chair of OHCAT Board Chair of
INFECTION CONTROL POLICY The OHC&AT Board of Directors has agreed this Policy and as such, it applies across the organisation 15 th December 2017. Jay Mercer Darren Coghlan Chair of OHCAT Board Chair of
El Paso - Ambulatory Clinic Policy and Procedure
 Regulation Reference: Title: NEEDLESTICK INJURIES/EXPOSURES TO BODY FLUIDS, CARE & FOLLOW UP Policy Number: EP 7.3 Effective Date: 6/2010 Policy Statement: A system is established and maintained to assure
Regulation Reference: Title: NEEDLESTICK INJURIES/EXPOSURES TO BODY FLUIDS, CARE & FOLLOW UP Policy Number: EP 7.3 Effective Date: 6/2010 Policy Statement: A system is established and maintained to assure
University of Louisville Campus Health Services 401 East Chestnut Street Suite110 P: F:
 University of Louisville Campus Health Services 401 East Chestnut Street Suite110 P: 502-852-2708 F: 502-852-0660 hlthoff@louisville.edu Training Objectives Understand the OSHA Bloodborne Pathogens Regulation
University of Louisville Campus Health Services 401 East Chestnut Street Suite110 P: 502-852-2708 F: 502-852-0660 hlthoff@louisville.edu Training Objectives Understand the OSHA Bloodborne Pathogens Regulation
May Safety Subject. Bloodborne Pathogens
 May Safety Subject Bloodborne Pathogens Everyone is at risk to contact bloodborne pathogens. Some more than others. Universal precautions means treating all objects as potentially contaminated Personal
May Safety Subject Bloodborne Pathogens Everyone is at risk to contact bloodborne pathogens. Some more than others. Universal precautions means treating all objects as potentially contaminated Personal
2017 BLOODBORNE PATHOGENS
 2017 BLOODBORNE PATHOGENS OSHA TERMS UPDATES HEPATITIS B HEPATITIS C HIV REPORTING AN EXPOSURE To have a basic understanding of bloodborne pathogens and the role of Greenwood School District 50 and OSHA.
2017 BLOODBORNE PATHOGENS OSHA TERMS UPDATES HEPATITIS B HEPATITIS C HIV REPORTING AN EXPOSURE To have a basic understanding of bloodborne pathogens and the role of Greenwood School District 50 and OSHA.
SHARPS POLICY: SAFE HANDLING AND DISPOSAL OF SHARPS
 SHARPS POLICY: SAFE HANDLING AND DISPOSAL OF SHARPS Version 10. Feb 2017 First issued Oct 2008 Reviewed Feb 2017 Document Control Sheet Name of document: Sharps Policy: Safe Handling and Disposal of Sharps
SHARPS POLICY: SAFE HANDLING AND DISPOSAL OF SHARPS Version 10. Feb 2017 First issued Oct 2008 Reviewed Feb 2017 Document Control Sheet Name of document: Sharps Policy: Safe Handling and Disposal of Sharps
Safety Services Guidance. Guidance on working with blood and body fluids
 Guidance on working with blood and body fluids Key word(s): Blood, body fluids, sputum, blood borne viruses, BBV Target audience: Laboratory personnel Contents Introduction... 2 Assessing the risks...
Guidance on working with blood and body fluids Key word(s): Blood, body fluids, sputum, blood borne viruses, BBV Target audience: Laboratory personnel Contents Introduction... 2 Assessing the risks...
The Bloodborne Pathogen Standard. An Overview
 The Bloodborne Pathogen Standard An Overview The Standard l In 1990, OSHA (Occupational Safety and Health Administration), developed the Bloodborne Pathogen Standard to protect workers by limiting occupational
The Bloodborne Pathogen Standard An Overview The Standard l In 1990, OSHA (Occupational Safety and Health Administration), developed the Bloodborne Pathogen Standard to protect workers by limiting occupational
Greenwood School District 50 OSHA UPDATE BLOODBORNE PATHOGENS
 Greenwood School District 50 OSHA UPDATE 2012 BLOODBORNE PATHOGENS TOPICS OSHA TERMS UPDATES HEPATITIS B HEPATITIS C HIV REPORTING AN EXPOSURE OBJECTIVES To have a basic understanding of bloodborne pathogens
Greenwood School District 50 OSHA UPDATE 2012 BLOODBORNE PATHOGENS TOPICS OSHA TERMS UPDATES HEPATITIS B HEPATITIS C HIV REPORTING AN EXPOSURE OBJECTIVES To have a basic understanding of bloodborne pathogens
Question 1. Blood Borne Viruses: Some important basic facts 6. What does BBV stand for? A. Blood Based Virus. B. Blood Borne Viruses
 Question 1 What does BBV stand for? A. Blood Based Virus B. Blood Borne Viruses C. Basic Blood Viruses Blood Borne Viruses: Some important basic facts 6 Question 1 What does BBV stand for? A. Blood Based
Question 1 What does BBV stand for? A. Blood Based Virus B. Blood Borne Viruses C. Basic Blood Viruses Blood Borne Viruses: Some important basic facts 6 Question 1 What does BBV stand for? A. Blood Based
The Prevention of Infection with Blood Borne Viruses [BBV]
![The Prevention of Infection with Blood Borne Viruses [BBV] The Prevention of Infection with Blood Borne Viruses [BBV]](/thumbs/93/112976583.jpg) The Prevention of Infection with Blood Borne Viruses [BBV] Control of Infection Manual Section G Study Morning 25 th November 2014 Marissa Herron Occupational Health Support Nurse [BBV] Aim To raise awareness
The Prevention of Infection with Blood Borne Viruses [BBV] Control of Infection Manual Section G Study Morning 25 th November 2014 Marissa Herron Occupational Health Support Nurse [BBV] Aim To raise awareness
Occupational Exposures to Bloodborne Pathogen (BBP) Training
 Occupational Exposures to Bloodborne Pathogen (BBP) Training OSHA 29 CFR 1910.1030 Protects workers exposed to blood or other potentially infectious diseases Who are at Risk? Workers in many different
Occupational Exposures to Bloodborne Pathogen (BBP) Training OSHA 29 CFR 1910.1030 Protects workers exposed to blood or other potentially infectious diseases Who are at Risk? Workers in many different
INFECTION PREVENTION AND CONTROL POLICY
 Document title: Infection Prevention and Control Policy CCG document ref: Author / originator: Date of approval: Tanya Kidson 29 th Approving committee: Quality Committee Responsible director: Category:
Document title: Infection Prevention and Control Policy CCG document ref: Author / originator: Date of approval: Tanya Kidson 29 th Approving committee: Quality Committee Responsible director: Category:
Occupational Exposure to Blood Borne Viruses
 Occupational Exposure to Blood Borne Viruses Marissa Herron Occupational Health Support Nurse [BBV] 2014 Aim To raise awareness of the key information and procedures in NHS Lanarkshire's Control of Infection
Occupational Exposure to Blood Borne Viruses Marissa Herron Occupational Health Support Nurse [BBV] 2014 Aim To raise awareness of the key information and procedures in NHS Lanarkshire's Control of Infection
Bloodborne Pathogen Refresher Training
 Bloodborne Pathogen Refresher Training This program will review your occupational risks and the steps that you and the County must take to reduce your risks of exposure. Employees must report any occupational
Bloodborne Pathogen Refresher Training This program will review your occupational risks and the steps that you and the County must take to reduce your risks of exposure. Employees must report any occupational
Bloodborne Pathogens Training
 Bloodborne Pathogens Training OSHA S Bloodborne Pathogen Standard 29CFR 1910.1030 Employers must: Develop an Exposure Control Plan (ECP) that details their Bloodborne Pathogens (BBP) Program Provide employees
Bloodborne Pathogens Training OSHA S Bloodborne Pathogen Standard 29CFR 1910.1030 Employers must: Develop an Exposure Control Plan (ECP) that details their Bloodborne Pathogens (BBP) Program Provide employees
Blood and Body Fluid Spillage Procedure
 Blood and Body Fluid Spillage Procedure (IPC Manual) DOCUMENT CONTROL: Version: v1.1 Ratified by: Clinical Policies Review and Approval Group Date ratified: 8 January 2019 Name of originator/author: Senior
Blood and Body Fluid Spillage Procedure (IPC Manual) DOCUMENT CONTROL: Version: v1.1 Ratified by: Clinical Policies Review and Approval Group Date ratified: 8 January 2019 Name of originator/author: Senior
Bloodbourne Pathogens (BBP) Occupational Post-Exposure Chemophrophylaxis
 Bloodbourne Pathogens (BBP) Audience: All personnel in the. Purpose: The purpose of this document is to establish UTMB policy for the initiation of prophylaxis after occupational exposure to the human
Bloodbourne Pathogens (BBP) Audience: All personnel in the. Purpose: The purpose of this document is to establish UTMB policy for the initiation of prophylaxis after occupational exposure to the human
June 4, Page 1 of 5 POLICY STATEMENT
 POLICY STATEMENT This policy has been written to inform all staff, clients, relatives and other visitors to the homes of service users about the risks associated with MRSA, AIDS and HIV hazards in the
POLICY STATEMENT This policy has been written to inform all staff, clients, relatives and other visitors to the homes of service users about the risks associated with MRSA, AIDS and HIV hazards in the
Bloodborne Infectious Diseases
 Bloodborne Infectious Diseases Dr. Kaya Süer Near East University Faculty of Medicine Infectious Diseases and Clinical Microbiology Bloodborne Pathogens Bloodborne pathogens Pathogenic organisms present
Bloodborne Infectious Diseases Dr. Kaya Süer Near East University Faculty of Medicine Infectious Diseases and Clinical Microbiology Bloodborne Pathogens Bloodborne pathogens Pathogenic organisms present
Post Exposure Prophylaxis (PEP)
 Post Exposure Prophylaxis (PEP) Occupational exposure Occupational exposure refers to exposure to potential blood-borne infections (HIV, HBV and HCV) that may occur in healthcare settings during performance
Post Exposure Prophylaxis (PEP) Occupational exposure Occupational exposure refers to exposure to potential blood-borne infections (HIV, HBV and HCV) that may occur in healthcare settings during performance
Author and Designation Equality Impact Assessment Associated Documents. Supporting References
 Title Policy for the prevention and Management of Needlestick and Sharps Injuries (Inoculation Incidents) Description of document This policy promotes sharps safety with the aim to prevent needlestick
Title Policy for the prevention and Management of Needlestick and Sharps Injuries (Inoculation Incidents) Description of document This policy promotes sharps safety with the aim to prevent needlestick
HIV and PEP. LTC Rose Ressner WRNMMC ID staff Oct 2014 UNCLASSIFIED
 HIV and PEP LTC Rose Ressner WRNMMC ID staff Oct 2014 UNCLASSIFIED Disclaimer The views expressed in this presentation are those of the speaker and do not reflect the official policy of the Department
HIV and PEP LTC Rose Ressner WRNMMC ID staff Oct 2014 UNCLASSIFIED Disclaimer The views expressed in this presentation are those of the speaker and do not reflect the official policy of the Department
ALBUQUERQUE PUBLIC SCHOOLS
 ALBUQUERQUE PUBLIC SCHOOLS BLOODBORNE PATHOGENS EXPOSURE CONTROL PLAN Risk Management Department 1 ALBUQUERQUE PUBLIC SCHOOLS RISK MANAGEMENT DEPARTMENT BLOODBORNE PATHOGENS EXPOSURE CONTROL PLAN TABLE
ALBUQUERQUE PUBLIC SCHOOLS BLOODBORNE PATHOGENS EXPOSURE CONTROL PLAN Risk Management Department 1 ALBUQUERQUE PUBLIC SCHOOLS RISK MANAGEMENT DEPARTMENT BLOODBORNE PATHOGENS EXPOSURE CONTROL PLAN TABLE
Bloodborne Pathogens Training (OHS_BIO500) Course Material
 Introduction (OHS_BIO500) Course Material Welcome to the Bloodborne Pathogens (BBP) Training Course (OHS_BIO500). UAB Campus Employees whose job duties put them at increased risk for exposure to bloodborne
Introduction (OHS_BIO500) Course Material Welcome to the Bloodborne Pathogens (BBP) Training Course (OHS_BIO500). UAB Campus Employees whose job duties put them at increased risk for exposure to bloodborne
Post Blood & Body Fluid Exposure Checklist
 Post Blood & Body Fluid Exposure Checklist Employee Name: : First Aid completed (If exposure was to eye, irrigate for 20 minutes at the nearest eye wash station. If exposure was to skin, wash affected
Post Blood & Body Fluid Exposure Checklist Employee Name: : First Aid completed (If exposure was to eye, irrigate for 20 minutes at the nearest eye wash station. If exposure was to skin, wash affected
Dr Helena Nixon Specialist Occupational Physician University Hospital Birmingham
 A Study in Scarlet Dr Helena Nixon Specialist Occupational Physician University Hospital Birmingham World Map April 2006 World developing nations World life expectancy Why the interest in BBVs? Estimated
A Study in Scarlet Dr Helena Nixon Specialist Occupational Physician University Hospital Birmingham World Map April 2006 World developing nations World life expectancy Why the interest in BBVs? Estimated
Training for Employees of Taylor Special Care Services, Inc.
 Training for Employees of Taylor Special Care Services, Inc. TSCS Taylor Special Care Services housing staffing counseling on-going support Simon Pop, MBA Chief Operating Officer 2015 2016 Guidelines:
Training for Employees of Taylor Special Care Services, Inc. TSCS Taylor Special Care Services housing staffing counseling on-going support Simon Pop, MBA Chief Operating Officer 2015 2016 Guidelines:
Exposure. Blood. Department of Health & Human Services
 Exposure to Blood What Health-Care Workers Need to Know Department of Health & Human Services OCCUPATIONAL EXPOSURES TO BLOOD Introduction Health-care workers are at risk for occupational exposure to bloodborne
Exposure to Blood What Health-Care Workers Need to Know Department of Health & Human Services OCCUPATIONAL EXPOSURES TO BLOOD Introduction Health-care workers are at risk for occupational exposure to bloodborne
HEPATITIS B VIRUS: PROTECTING EMPLOYEES AND PATIENTS
 HUMAN RESOURCES (WITH OCCUPATIONAL HEALTH) HEPATITIS B VIRUS: PROTECTING EMPLOYEES AND PATIENTS DOCUMENT REF: PHRMHEPAB (Version No. 5.0) Name and designation of policy author(s) Approved by (committee,
HUMAN RESOURCES (WITH OCCUPATIONAL HEALTH) HEPATITIS B VIRUS: PROTECTING EMPLOYEES AND PATIENTS DOCUMENT REF: PHRMHEPAB (Version No. 5.0) Name and designation of policy author(s) Approved by (committee,
IMOGAM RABIES PASTEURIZED - HUMAN RABIES IMMUNOGLOBULIN. Active ingredient: Human proteins mg
 IMOGAM RABIES PASTEURIZED - HUMAN RABIES IMMUNOGLOBULIN COMPOSITION 1 ml of human rabies immunoglobulin contains: Active ingredient: Human proteins 100 180 mg containing (IgG class) human rabies immunoglobulins
IMOGAM RABIES PASTEURIZED - HUMAN RABIES IMMUNOGLOBULIN COMPOSITION 1 ml of human rabies immunoglobulin contains: Active ingredient: Human proteins 100 180 mg containing (IgG class) human rabies immunoglobulins
