STUDENT EXPOSURE TO BLOOD OR OTHER POTENTIALLY INFECTIOUS MATERIALS
|
|
|
- Eugene Burke
- 6 years ago
- Views:
Transcription
1 STUDENT EXPOSURE TO BLOOD OR OTHER POTENTIALLY INFECTIOUS MATERIALS (See Bloodborne Pathogen Worksheet and Post Exposure Prophylaxis consent immediately following this policy ) 1. Student must report immediately any occupational exposure to blood or body fluids to their faculty member (See bottom of page for definitions of exposure and body fluids). 2. Obtain any necessary assistance to clean/flush wound, mucous membranes, or eyes, or otherwise provide necessary palliative measures to the contaminated area at the time of exposure. 3. After completing the Bloodborne Pathogen Exposure Worksheet,the faculty member immediately calls the Johns Hopkins Hospital Exposure Hotline at STIX ( ) to discuss immediate evaluation and a treatment plan. 4. The faculty member will assist the student with transportation to the Johns Hopkins Hospital if directed by the Hotline. 5. After this initial consultation with the Hotline, the student is instructed to schedule an appointment for follow-up at the Occupational Injury Clinic at Johns Hopkins Hospital (Blalock 139, phone # ). Clinic hours are 7:30 am 4 pm Monday through Friday. 6. Please contact the Associate Dean for Enrollment Management and Student Affairs, at or by beeper at for assistance. 7. The faculty member initiates follow-up to determine the source patient s HIV, HBV, or HCV status and to evaluate whether the source and/or exposure are considered high risk 8. Faculty faxes a copy of the Bloodborne Exposure Worksheet to the Occupational Injury Clinic at with attention to Conrad Utanes, RN, Clinic Manager. 9. In all cases, a hospital or clinic incident report must be completed. The student should complete the employee incident report, have the supervisor sign it and bring it to the Occupational Injury Clinic when he/she comes for evaluation. 10. The clinical faculty sends a copy of both the Exposure Worksheet and the Incident report to the course coordinator. 11. The course coordinator initials the report after determining that all appropriate follow-up has been arranged, and sends the report to the Director of the Baccalaureate program with a copy to the Associate Dean for Student Affairs. Definitions 1. Exposure a. a percutaneous injury (e.g. needlestick or cut with a sharp object) involving blood, tissue or other body fluids (see definitions below) or b. contact of a mucous membrane or non-intact skin (e.g., the skin is chapped, abraded, or afflicted with dermatitis) with blood, tissue or other body fluids or c. contact of blood, tissue or other body fluids with intact skin when the duration of contact is prolonged (i.e., several minutes or more) or involves an extensive area, or d. direct contact (i.e., without or with ineffective barrier protection) to concentrated HIV in a research or production facility
2 2. Body Fluids Associated with HIV a. blood, semen, vaginal secretions, or other body fluids contaminated with visible blood that have been implicated in the transmission of HIV infection ( including saliva with visible blood but excluding tears, sweat, non-bloody urine or feces, and human breast milk in occupational settings) b. cerebrospinal, synovial, pleural, peritoneal, pericardial or amniotic fluids, which have an undetermined risk for transmitting HIV 3. Body Fluids Associated with HBV or HCV a. see HIV Body Fluids above b. saliva, sputum, or vomitus 4. HIV PEP post exposure prophylaxis which usually includes a 28-day regimen of AZT (associated with a 79% decrease in HIV transmission), 3TC, and a protease inhibitor if indicated. 5. HBV PEP may include HBIG (hepatitis B immune globulin) for short term, immediate protection when titer is unknown and risk is high; and HBV vaccine (if unvaccinated or negative titer) 6. HCV PEP no current recommendations do not give IG (old recommendation) 7. HIV High Risk Sources a. infected patient with initial acute infection b. infected patient with terminal illness c. infected patient with high viral load d. injection drug user e. hemophiliac (receipt of blood or blood products before 1985) f. homosexual/bisexual g. unprotected sexual contact with multiple partners h. sexual partner of any of the above 8. HBV and HCV High Risk Sources a. see above plus hemodialysis patients b. transfusion recipients (prior to 1985 or receipt of multiple recent transfusions) 9. High Risk Factors for Transmission of Any Bloodborne Pathogen a. Device is visibly contaminated with blood b. Procedure where device was placed directly in a vein or an artery c. Deep injury d. Injury with a hollow bore needle e. Exposure involving a large volume of blood Key questions about bloodborne exposures Exposure-Related Questions 1. Was wound treated immediately? How? (recommend washing wounds with soap & water, flushing mucous membranes with sterile water, or sending to ED if necessary) (con t next page)
3 2. Did an exposure occur? (see above definitions) When? (if > 72 hrs ago, HIV PEP is not necessary, but f/u is still needed; optimal HIV PEP is within 1-2 hrs How? (include activity, part of body, type of device, amount of fluid, severity or depth of exposure) Source-Related Questions 1. Is source (patient or other source) known? (if no information on source, HIV PEP is not necessary, but f/u is still needed). If known, what is patient s name and history or social security number? 2. Is patient HBV positive (surface antigen, e-antigen, surface or core antibody)? Date and test results? 3. Is patient HCV positive (antibody)? Date and test results? 4. Is patient HIV positive (western blot)? Date and test results? 5. If untested (or testing is > 4 weeks old), is patient available for testing? Name and phone number(s) of order writing person(s)? Was written consent for HIV obtained from patient? 6. Is patient high risk for HBV, HCV or HIV (see definitions)? Student-Related Questions 1. Has student had the HBV vaccine? Dates (3) of vaccine? Does student have a positive HBV titer? Date of titer? 2. When was student s last tetanus vaccine? 3. Is student willing to consider testing for HBV, HCV, and/or HIV? Give student copy of Exposure Booklet. If source patient is asked to consent, the exposed Health Care Worker must consent to have HIV testing (MD law). 4. Does student want to hear about PEP options? (Student should consider pregnancy status, history of renal or hepatic disease, current medications, other immunosuppressive medical conditions, toxicity of PEP medications, risk of transmission, lethality of diseases, etc.) May 2013
4 The Johns Hopkins University School of Nursing Bloodborne Pathogen Worksheet *To be completed by clinical faculty immediately after an exposure is reported. Student Name Date of Incident Time of Incident Clinical Site Location 1. Description of Incident: include (a) activity at time of exposure (e.g., needlestick while removing vacutainer needle from barrel after blood draw); (b) part of body exposed (e.g., left thumb); (c) type of device (e.g., contaminated vacutainer needle); and (d) severity or depth of injury (e.g. residual blood on needle tip, broke surface of skin, minimal bleeding). 2. Treatment of Exposed Area: include (a) actions taken (e.g., washed wound with soap and water or see attached ED sheet) and (b) timing of actions (e.g., washed within 3 minutes of exposure) 3. Source/Patient: include (a) patient Name and (b) history number or social security number (e.g., John Doe, HX # ) or record unknown source. 4. Risk Status of Source/Patient: refer to the attached definitions section and list any high risk conditions (e.g., injection drug user, unprotected sex with multiple partners) as acknowledged by the patient or providers; or record none known or denies all high risk conditions ; use patient/provider quotes. 5. Patient Test Results/Tests Ordered: include (a) Names of all blood tests performed in the past and tests ordered at the time of exposure (e.g., HBV antigen, anti-hcv or Western blot); (b) dates; (c) results e.g., positive, negative, or pending; and (d) locations (e.g., lab/hospital name or record never tested or not ordered. Do not allow HIV test to be sent to the state laboratory. We want a turnaround time of < 5 days. a. HBV b. HCV c. HIV* *If HIV positive, include patient medications (including past failed meds). Current CD4 count & viral load
5 6. Order-Writing Person: include (a) Name; (b) title, and (c) phone number(s) of person(s) authorized to write orders for patient (e.g., Jane Doe, CRNP; ) 7. Student HBV Status: include (a) approximate dates (all 3) of HBV vaccine and (b) date and results of any HBV titer or record no HBV vaccine or no HBV titer. 8. Last Student Tetanus: include approximate date or number of years since last tetanus 9. Exposure Information: indicate (a) whether student received and/or reviewed Exposure booklet; and (b) any counseling given or other information/comments 10. Student Decision: indicate whether student decided to contact 5-STIX for PEP counseling use student quotes: Print Name of Faculty Completing Worksheet Date Worksheet Completed Then, as indicated: 1. Call the Hotline at STIX ( ) to review worksheet and for student to receive PEP counseling. 2. If directed by the Hotline, arrange immediate transportation to the Occupational Injury Clinic (Blalock 139 Johns Hopkins Hospital) or other site as directed by OIC. 3. Fax worksheet (all sides) ASAP to the Occupational Injury Clinic at ; Attention: Conrad Utanes, RN, Clinic Manager. Mark form confidential. Instruct student to schedule a follow-up visit by calling (410) Deliver the original form to the Course Coordinator who will review it and forward to the Associate Dean for Academic Affairs and the Associate Dean for Student Affairs. 5. Questions? Call Associate Dean for Enrollment Management and Student Affairs at (410) or on beeper at (410)
6 The Johns Hopkins University School of Nursing POST EXPOSURE PROPHYLAXIS (PEP) CONSENT I hereby consent to receive PEP for an HIV exposure. I have read or had read to me the information regarding the use of anti-retroviral drugs as given to me by health care professional in JHH Occupational Health. I have been given the opportunity to ask questions with a Health Care Professional and understand that there are possible risks involved in taking anti-retroviral drugs. I have read the drug information regarding the medication. I understand these drugs are not FDA approved to prevent infection after an exposure on the job and that the use of anti-retroviral drugs in this way is considered experimental. In spite of this and a lack of scientific understanding and research, I have freely decided to take the anti-retroviral drugs. Healthcare Worker Consenting Employee JHU SON Student Signature Date (Print Full Name) DECLINATION STATEMENT I have read or had read to me the information about PEPE and have had an opportunity to discuss the use of the anti-retroviral drugs with a Health Care Professional and I decline PEP at this time. Healthcare Worker Consenting Employee JHU SON Student Signature Date (Print Full Name) POST EXPOSURE FOLLOW UP This is to certify that I have been given follow up dates to have the appropriate blood testing and/or treatments. I understand it is my responsibility to return to clinic on the due dates that have been given to me. Healthcare Worker Consenting Employee JHU SON Student Signature Date (Print Full Name) (con't on next page )
7 INFORMATION FOR FEMALE HEALTHCARE WORKERS/JHU SON STUDENT OF CHILDBEARING AGE Post Exposure Prophylaxis (PEP) includes the administration of COMBIVIR (this is a combination of AZR and 3TC). AZT is considered to have few side effects in the last 6 months of pregnancy and in pregnant women already infected with HIV, AZT can prevent maternal fetal transmission. A study by the National Cancer Institute (NCI) demonstrated an increase in incidence of liver, lung and genitor-urinary tumors in the offspring of mice receiving high doses of AZT (near maximum tolerated dose) during days of gestation. A second study at Glaxo-Wellcome, Inc., demonstrate no increase in incidence of tumors in offspring of mice receiving a variety of regimens of AZT in doses and schedules intended to simulate clinic drug regimens. "Pregnancy should not preclude the use of optimal PEP regimens, and PEP should not be denied to a HCW solely on the basis of pregnancy". However, as discussed previously, an occupationally exposed pregnant HCW must be provided with full information about what is known and not known regarding the potential benefits and risk associated with use of the antiretroviral drugs to her and her fetus for her to make an informed decision regarding the use of PEP. The choice of anti-retroviral drugs to use for PEP in pregnant HCW's is complicated by the potential need to alter doing because of physiologic changes associated with pregnancy and the potential for short or long term effects on the fetus and newborn. Thus, considerations that should be discussed after the HCW has read the information booklet regarding the potential risk for HIV transmission based on the type of exposure: the stage of pregnancy ( the first trimester being the period of maximal organogenesis and risk for teratogenesis)" and what is known about the pharmacokinetics, safety and tolerability of the drug or combination of drugs in pregnancy" (MWR 1998:47(No.RR-7):21. NIH review and recommendation is that Combivir can be given to pregnant women with HIV infection because the risk; benefit ratio is acceptable. With a low probability event such as exposure of a healthcare worker (the risk of occupational transmission of HIV is 0,3% or about 1 infection for every 330 exposures), the risks usually outweigh the benefits. WAIVER I have read and discussed the above information on Combivir regarding the risks inherent in taking Post Exposure Prophylaxis in women of childbearing age. If I have been prescribed another anti-retroviral medication, I have read the drug insert/handout that was given to me by Pharmacy. I have been advised and understand the risks to an unborn child, however, I refuse to take the recommended pregnancy test, or I already know that I am pregnant and I want to be started on PEPE immediately. On my behalf and on behalf of my unborn child, I hereby release The Johns Hopkins Health System, The Johns Hopkins Hospital, the Johns Hopkins University, their officers, agents and employees from any and all claims associated with my electing to take Post Exposure Prophylaxis. Witness Signature of JHU SON Student Date
To provide the guidelines for the management of healthcare workers who have had an occupational exposure to blood and/or body fluids.
 TITLE/DESCRIPTION: MANAGEMENT OF OCCUPATIONAL EXPOSURE TO HBV, HCV, and HIV INDEX NUMBER: EFFECTIVE DATE: APPLIES TO: ISSUING AUTHORITY: 01/01/2009 01/01/2013 All GCC Countries GULF COOPERATION COUNCIL
TITLE/DESCRIPTION: MANAGEMENT OF OCCUPATIONAL EXPOSURE TO HBV, HCV, and HIV INDEX NUMBER: EFFECTIVE DATE: APPLIES TO: ISSUING AUTHORITY: 01/01/2009 01/01/2013 All GCC Countries GULF COOPERATION COUNCIL
EXPOSURE (HIV/HEPATITIS) BLOOD & BODY FLUIDS
 Page(s): 1 of 11 PURPOSE To set a standardized procedure to ensure that employees are evaluated in a consistent and timely manner.. POLICY A. The treatment of Team Member exposure to bloodborne pathogens
Page(s): 1 of 11 PURPOSE To set a standardized procedure to ensure that employees are evaluated in a consistent and timely manner.. POLICY A. The treatment of Team Member exposure to bloodborne pathogens
Clinical Education Initiative OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS. Antonio E. Urbina, MD
 Clinical Education Initiative Support@ceitraining.org OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS Antonio E. Urbina, MD 5/22/2013 Occupational Post-Exposure Prophylaxis [Video Transcript] 00:00:15 - [Tony]
Clinical Education Initiative Support@ceitraining.org OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS Antonio E. Urbina, MD 5/22/2013 Occupational Post-Exposure Prophylaxis [Video Transcript] 00:00:15 - [Tony]
INITIAL EVALUATION AND MANAGEMENT FOLLOWING EXPOSURE TO BLOOD OR BODY FLUIDS
 Page 1 of 11 Original Date of Issue: June 1991 Reviewed 2/96 5/97 11/98 11/99 5/01 5/02 12/05 Revised 9/95 5/97 5/00 7/02 3/06 6/08 6/10 The following are the procedures to be followed when a person sustains
Page 1 of 11 Original Date of Issue: June 1991 Reviewed 2/96 5/97 11/98 11/99 5/01 5/02 12/05 Revised 9/95 5/97 5/00 7/02 3/06 6/08 6/10 The following are the procedures to be followed when a person sustains
MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet. Instructions for Employees/Students:
 MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet MUSC has established these protocols in accordance with the OSHA Bloodborne Pathogen Standard and Center for Disease Control recommendations
MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet MUSC has established these protocols in accordance with the OSHA Bloodborne Pathogen Standard and Center for Disease Control recommendations
El Paso - Ambulatory Clinic Policy and Procedure
 Regulation Reference: Title: NEEDLESTICK INJURIES/EXPOSURES TO BODY FLUIDS, CARE & FOLLOW UP Policy Number: EP 7.3 Effective Date: 6/2010 Policy Statement: A system is established and maintained to assure
Regulation Reference: Title: NEEDLESTICK INJURIES/EXPOSURES TO BODY FLUIDS, CARE & FOLLOW UP Policy Number: EP 7.3 Effective Date: 6/2010 Policy Statement: A system is established and maintained to assure
Blood/Body Fluid Exposure Option
 Introduction: Transmission of bloodborne pathogens [e.g., Hepatitis B virus (HBV), Hepatitis C virus (HBC), Human Immunodeficiency Virus (HIV)] from patients to healthcare workers (HCW) is an important
Introduction: Transmission of bloodborne pathogens [e.g., Hepatitis B virus (HBV), Hepatitis C virus (HBC), Human Immunodeficiency Virus (HIV)] from patients to healthcare workers (HCW) is an important
Bloodborne Pathogens Exposure Procedure
 Bloodborne Pathogens Exposure Procedure Background: Bloodborne pathogens are infectious microorganisms present in blood that can cause disease in humans. These pathogens include, but are not limited to,
Bloodborne Pathogens Exposure Procedure Background: Bloodborne pathogens are infectious microorganisms present in blood that can cause disease in humans. These pathogens include, but are not limited to,
Exposures at Non-MUSC Clinical Sites
 BLOOD BORNE PATHOGEN EXPOSURE CHECKLIST Exposures at Non-MUSC Clinical Sites (Students on clinical rotations at Roper Hospital, Trident Hospital, Affiliated Local Clinical Sites, Out of Town Clinical Sites,
BLOOD BORNE PATHOGEN EXPOSURE CHECKLIST Exposures at Non-MUSC Clinical Sites (Students on clinical rotations at Roper Hospital, Trident Hospital, Affiliated Local Clinical Sites, Out of Town Clinical Sites,
Needlestick and Splash Exposure Flow Chart Page 1 Clinical Practice Guidelines
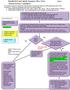 Needlestick and Splash Exposure Flow Chart Page 1 If ANY student experiences a needlestick or splash exposure ANY time of day/night, they need to page #11709 which will be forwarded to: (**in the event
Needlestick and Splash Exposure Flow Chart Page 1 If ANY student experiences a needlestick or splash exposure ANY time of day/night, they need to page #11709 which will be forwarded to: (**in the event
Bloodbourne Pathogens (BBP) Occupational Post-Exposure Chemophrophylaxis
 Bloodbourne Pathogens (BBP) Audience: All personnel in the. Purpose: The purpose of this document is to establish UTMB policy for the initiation of prophylaxis after occupational exposure to the human
Bloodbourne Pathogens (BBP) Audience: All personnel in the. Purpose: The purpose of this document is to establish UTMB policy for the initiation of prophylaxis after occupational exposure to the human
Safety Regulations and Procedures Occupational Health Bloodborne Pathogens Exposure Control Plan S80.10, updated, May Contains information for:
 APPENDIX A Safety Regulations and Procedures Occupational Health Bloodborne Pathogens Exposure Control Plan S80.10, updated, May 2018 BLOODBORNE PATHOGEN EXPOSURE INCIDENT PACKET Contains information for:
APPENDIX A Safety Regulations and Procedures Occupational Health Bloodborne Pathogens Exposure Control Plan S80.10, updated, May 2018 BLOODBORNE PATHOGEN EXPOSURE INCIDENT PACKET Contains information for:
Management of Workplace Exposure to Blood-borne Pathogens
 Management of Workplace Exposure to Blood-borne Pathogens 11/22/2017 Management of Workplace Exposure to Blood-borne Pathogens BY SOLYMOLE KURUVILLA, PHD, RN, ACNP-BC DIRECTOR, OCCUPATIONAL HEALTH SERVICES
Management of Workplace Exposure to Blood-borne Pathogens 11/22/2017 Management of Workplace Exposure to Blood-borne Pathogens BY SOLYMOLE KURUVILLA, PHD, RN, ACNP-BC DIRECTOR, OCCUPATIONAL HEALTH SERVICES
One of your office personnel
 Doug Campos-Outcalt, MD, MPA Department of Family and Community Medicine, University of Arizona College of Medicine, Phoenix HIV postexposure prophylaxis: Who should get it? CORRESPONDENCE Doug Campos-Outcalt,
Doug Campos-Outcalt, MD, MPA Department of Family and Community Medicine, University of Arizona College of Medicine, Phoenix HIV postexposure prophylaxis: Who should get it? CORRESPONDENCE Doug Campos-Outcalt,
Definitions. Appendix A
 Definitions Appendix A 1. Blood means human blood, human blood components, and products made from human blood. 2. Bloodborne Pathogens means pathogenic microorganisms that are present in human blood and
Definitions Appendix A 1. Blood means human blood, human blood components, and products made from human blood. 2. Bloodborne Pathogens means pathogenic microorganisms that are present in human blood and
Revised April WGH ER #5 Hospital Rd. Whitehorse Phone: (867) Outside of Whitehorse: Local Community Health Centre/Clinic/ER
 Where to access care Who to consult and when Please consult whenever questions arise on how to proceed with postexposure management and when exposure is beyond the scope of guidelines. Blood and Body Fluid
Where to access care Who to consult and when Please consult whenever questions arise on how to proceed with postexposure management and when exposure is beyond the scope of guidelines. Blood and Body Fluid
Exposure. What Healthcare Personnel Need to Know
 Information from the Centers for Disease Control and Prevention National Center for Infectious Diseases Divison of Healthcare Quality Promotion and Division of Viral Hepatitis For additional brochures
Information from the Centers for Disease Control and Prevention National Center for Infectious Diseases Divison of Healthcare Quality Promotion and Division of Viral Hepatitis For additional brochures
Bloodborne Pathogen Exposure STUDENT. Blood Borne Pathogen Exposure. Student. Rev:
 Blood Borne Pathogen Exposure Student INSTRUCTIONS 1. Student: Get name, DOB and, if available, health record number of source patient Obtain form and assist your supervisor with providing information
Blood Borne Pathogen Exposure Student INSTRUCTIONS 1. Student: Get name, DOB and, if available, health record number of source patient Obtain form and assist your supervisor with providing information
POLICY ON BLOOD AND BODY FLUID EXPOSURE (NEEDLE STICK)
 POLICY ON BLOOD AND BODY FLUID EXPOSURE (NEEDLE STICK) Dated: January 1, 2018 Supersedes: Blood and Body Fluid Exposure (Needle stick) dated July 1, 2015 I. POLICY It is the policy of New York Medical
POLICY ON BLOOD AND BODY FLUID EXPOSURE (NEEDLE STICK) Dated: January 1, 2018 Supersedes: Blood and Body Fluid Exposure (Needle stick) dated July 1, 2015 I. POLICY It is the policy of New York Medical
HIV and PEP. LTC Rose Ressner WRNMMC ID staff Oct 2014 UNCLASSIFIED
 HIV and PEP LTC Rose Ressner WRNMMC ID staff Oct 2014 UNCLASSIFIED Disclaimer The views expressed in this presentation are those of the speaker and do not reflect the official policy of the Department
HIV and PEP LTC Rose Ressner WRNMMC ID staff Oct 2014 UNCLASSIFIED Disclaimer The views expressed in this presentation are those of the speaker and do not reflect the official policy of the Department
Effective Date: 6/10/2013 Review Date: 6/10/2016
 Policy Title: Sterilization and Disinfection of Patient-Care Items Policy Number: 11 6.2.2. Examples of useful items to maintain in the office sterilization log are as following: o Date and time of cycle
Policy Title: Sterilization and Disinfection of Patient-Care Items Policy Number: 11 6.2.2. Examples of useful items to maintain in the office sterilization log are as following: o Date and time of cycle
Blood-Borne Pathogens and Post-Exposure Prophylaxis
 Blood-Borne Pathogens and Post-Exposure Prophylaxis Christopher Behrens MD Northwest Association of Occupational and Environmental Medicine October 2017 with thanks to Shireesha Dhanireddy MD Disclosures
Blood-Borne Pathogens and Post-Exposure Prophylaxis Christopher Behrens MD Northwest Association of Occupational and Environmental Medicine October 2017 with thanks to Shireesha Dhanireddy MD Disclosures
Contamination Incidents Frequently Asked Questions
 Contamination Incidents Frequently Asked Questions WWR- 004 Index 1. What is a contamination injury? 2. What should I do immediately if I have sustained a contamination injury? 3. What should I do immediately
Contamination Incidents Frequently Asked Questions WWR- 004 Index 1. What is a contamination injury? 2. What should I do immediately if I have sustained a contamination injury? 3. What should I do immediately
CONTINUING CARE ADMINISTRATIVE MANUAL POLICY
 CONTINUING CARE ADMINISTRATIVE MANUAL POLICY NUMBER III-10 DATE Draft June 8, 2010 PAGE 1 OF 3 APPROVED BY: SITE: CATEGORY TITLE: Vice President & Senior Operating Officer, Rehab & Continuing Care Edmonton
CONTINUING CARE ADMINISTRATIVE MANUAL POLICY NUMBER III-10 DATE Draft June 8, 2010 PAGE 1 OF 3 APPROVED BY: SITE: CATEGORY TITLE: Vice President & Senior Operating Officer, Rehab & Continuing Care Edmonton
Post Blood & Body Fluid Exposure Checklist
 Post Blood & Body Fluid Exposure Checklist Employee Name: : First Aid completed (If exposure was to eye, irrigate for 20 minutes at the nearest eye wash station. If exposure was to skin, wash affected
Post Blood & Body Fluid Exposure Checklist Employee Name: : First Aid completed (If exposure was to eye, irrigate for 20 minutes at the nearest eye wash station. If exposure was to skin, wash affected
3/23/2016. Managing Bloodborne Pathogen Exposures. Managing Bloodborne Pathogen Exposures
 This webinar begins at 11 a.m., Eastern. You will not hear anything over your telephone line until the program starts. If the system did not prompt you to enter your phone number and receive a call back,
This webinar begins at 11 a.m., Eastern. You will not hear anything over your telephone line until the program starts. If the system did not prompt you to enter your phone number and receive a call back,
Bloodborne Pathogens Across the Continuum of Care Sue Sebazco, Arlington, Texas A Webber Training Teleclass
 Bloodborne Pathogens Across the Continuum of Care Objectives Sue Sebazco, RN, BS, CIC Infection Control/Employee Health Director Arlington, TX Pittsburg Mercy Health System skrystofiak@mercy.pmhs.org Define
Bloodborne Pathogens Across the Continuum of Care Objectives Sue Sebazco, RN, BS, CIC Infection Control/Employee Health Director Arlington, TX Pittsburg Mercy Health System skrystofiak@mercy.pmhs.org Define
B. Tasks and Procedures where employees, students or contractors can be exposed to bloodborne pathogens:
 Page 1 of 6 BLOODBORNE PATHOGEN PROGRAM INTRODUCTION The intended purpose of this document is to comply with OSHA s Occupational Exposures to Bloodborne Pathogens in Title 29 Code of Federal Regulations
Page 1 of 6 BLOODBORNE PATHOGEN PROGRAM INTRODUCTION The intended purpose of this document is to comply with OSHA s Occupational Exposures to Bloodborne Pathogens in Title 29 Code of Federal Regulations
Bloodborne Pathogens. Exposure Control Plan
 Bloodborne Pathogens Exposure Control Plan Maryland Institute College of Art Revision Date(s): January 2007/January 2008 Maryland Institute College of Art (MICA) Subject: Occupational/Non-occupational
Bloodborne Pathogens Exposure Control Plan Maryland Institute College of Art Revision Date(s): January 2007/January 2008 Maryland Institute College of Art (MICA) Subject: Occupational/Non-occupational
PEDIATRIC EMERGENCY DEPARTMENT CLINICAL GUIDELINE: NON- OCCUPATIONAL EXPOSURE TO BLOOD-BORNE PATHOGENS (HIV, Hepatitis B, AND Hepatitis C)
 General Definition: Blood-borne pathogens are infectious agents that can be transmitted through contact with blood or certain other body fluids. The primary pathogens are HIV, Hepatitis B, and C. Before
General Definition: Blood-borne pathogens are infectious agents that can be transmitted through contact with blood or certain other body fluids. The primary pathogens are HIV, Hepatitis B, and C. Before
BAY-ARENAC BEHAVIORAL HEALTH AUTHORITY POLICIES AND PROCEDURES MANUAL
 Page: 1 of 8 Policy Bay-Arenac Behavioral Health Authority (BABHA) is committed to high standards of employee and consumer safety practices. This standard will include the prevention, surveillance, identification
Page: 1 of 8 Policy Bay-Arenac Behavioral Health Authority (BABHA) is committed to high standards of employee and consumer safety practices. This standard will include the prevention, surveillance, identification
University of Louisville Campus Health Services 401 East Chestnut Street Suite110 P: F:
 University of Louisville Campus Health Services 401 East Chestnut Street Suite110 P: 502-852-2708 F: 502-852-0660 hlthoff@louisville.edu Training Objectives Understand the OSHA Bloodborne Pathogens Regulation
University of Louisville Campus Health Services 401 East Chestnut Street Suite110 P: 502-852-2708 F: 502-852-0660 hlthoff@louisville.edu Training Objectives Understand the OSHA Bloodborne Pathogens Regulation
NEOMED ACADEMIC POLICY
 (A) PURPOSE The purpose of this Policy is to delineate the management of incidents of exposure to blood-borne pathogens that occur to students while they are in the educational setting. (B) SCOPE This
(A) PURPOSE The purpose of this Policy is to delineate the management of incidents of exposure to blood-borne pathogens that occur to students while they are in the educational setting. (B) SCOPE This
43. Guidelines on Needle stick Injury
 43. Guidelines on Needle stick Injury The following information is abstracted from the South African Department of Health guidelines entitled: Management of Occupational Exposure to the Human Immunodeficiency
43. Guidelines on Needle stick Injury The following information is abstracted from the South African Department of Health guidelines entitled: Management of Occupational Exposure to the Human Immunodeficiency
Blood Borne Pathogen Exposure Employee
 Blood Borne Pathogen Exposure Employee INSTRUCTIONS 1. Employee: Get name, DOB and, if available, health record number of source patient Obtain form and assist your supervisor with providing information
Blood Borne Pathogen Exposure Employee INSTRUCTIONS 1. Employee: Get name, DOB and, if available, health record number of source patient Obtain form and assist your supervisor with providing information
Bloodborne Pathogens and Exposure Control
 Bloodborne Pathogens and Exposure Control 2016 Information in the Exposure Control Plan The Bloodborne Pathogen Exposure Control Plan was developed to communicate information to you about: - Your risk
Bloodborne Pathogens and Exposure Control 2016 Information in the Exposure Control Plan The Bloodborne Pathogen Exposure Control Plan was developed to communicate information to you about: - Your risk
Bloodborne Pathogens. Montclair Kimberley Academy 1
 Bloodborne Pathogens Montclair Kimberley Academy 1 Introduction! Approximately 5.6 million workers in health care and other facilities are at risk of exposure to bloodborne pathogens such as human immunodeficiency
Bloodborne Pathogens Montclair Kimberley Academy 1 Introduction! Approximately 5.6 million workers in health care and other facilities are at risk of exposure to bloodborne pathogens such as human immunodeficiency
Bloodborne Pathogens. By Deborah Massarella RN, MSN
 Bloodborne Pathogens By Deborah Massarella RN, MSN 2010, 2014 Objectives At conclusion of in-service learners will: 1. Identify two types of personal protective equipment. 2. Identify two prevention measures
Bloodborne Pathogens By Deborah Massarella RN, MSN 2010, 2014 Objectives At conclusion of in-service learners will: 1. Identify two types of personal protective equipment. 2. Identify two prevention measures
Exposure. Blood. Department of Health & Human Services
 Exposure to Blood What Health-Care Workers Need to Know Department of Health & Human Services OCCUPATIONAL EXPOSURES TO BLOOD Introduction Health-care workers are at risk for occupational exposure to bloodborne
Exposure to Blood What Health-Care Workers Need to Know Department of Health & Human Services OCCUPATIONAL EXPOSURES TO BLOOD Introduction Health-care workers are at risk for occupational exposure to bloodborne
Colgate University. Bloodborne Pathogens Exposure Control Plan
 Colgate University Bloodborne Pathogens Exposure Control Plan COLGATE UNIVERSITY BLOODBORNE PATHOGENS EXPOSURE CONTROL PLAN I. STATEMENT OF POLICY It is the policy of Colgate University (CU) to limit or
Colgate University Bloodborne Pathogens Exposure Control Plan COLGATE UNIVERSITY BLOODBORNE PATHOGENS EXPOSURE CONTROL PLAN I. STATEMENT OF POLICY It is the policy of Colgate University (CU) to limit or
Infection Control Standard Precautions. CDC Recommendations: Application of Standard Precautions for All Patients
 Infection Control Standard Precautions Standard Precautions Hand Hygiene CDC Recommendations: Application of Standard Precautions for All Patients Component Personal Protective Equipment (PPE) Gloves Mask,
Infection Control Standard Precautions Standard Precautions Hand Hygiene CDC Recommendations: Application of Standard Precautions for All Patients Component Personal Protective Equipment (PPE) Gloves Mask,
2017 BLOODBORNE PATHOGENS
 2017 BLOODBORNE PATHOGENS OSHA TERMS UPDATES HEPATITIS B HEPATITIS C HIV REPORTING AN EXPOSURE To have a basic understanding of bloodborne pathogens and the role of Greenwood School District 50 and OSHA.
2017 BLOODBORNE PATHOGENS OSHA TERMS UPDATES HEPATITIS B HEPATITIS C HIV REPORTING AN EXPOSURE To have a basic understanding of bloodborne pathogens and the role of Greenwood School District 50 and OSHA.
Greenwood School District 50 OSHA UPDATE BLOODBORNE PATHOGENS
 Greenwood School District 50 OSHA UPDATE 2012 BLOODBORNE PATHOGENS TOPICS OSHA TERMS UPDATES HEPATITIS B HEPATITIS C HIV REPORTING AN EXPOSURE OBJECTIVES To have a basic understanding of bloodborne pathogens
Greenwood School District 50 OSHA UPDATE 2012 BLOODBORNE PATHOGENS TOPICS OSHA TERMS UPDATES HEPATITIS B HEPATITIS C HIV REPORTING AN EXPOSURE OBJECTIVES To have a basic understanding of bloodborne pathogens
SIV/SHIV Exposure Medical Response Guidance for the University of Wisconsin-Madison
 SIV/SHIV SIV/SHIV Exposure Medical Response Guidance for the University of Wisconsin-Madison 1.0 Instructions: Information in this guidance is meant to inform both laboratory staff and health professionals
SIV/SHIV SIV/SHIV Exposure Medical Response Guidance for the University of Wisconsin-Madison 1.0 Instructions: Information in this guidance is meant to inform both laboratory staff and health professionals
Bloodborne Pathogens: Recognition and Treatment 2011
 Bloodborne Pathogens: Recognition and Treatment 2011 Occupational Health Services at The Summit Rita M. Lopez, APRN-BC, MSN 751-4189 rlopez@krmc.org OBJECTIVES DEFINE Bloodborne Pathogen Exposure WHO must
Bloodborne Pathogens: Recognition and Treatment 2011 Occupational Health Services at The Summit Rita M. Lopez, APRN-BC, MSN 751-4189 rlopez@krmc.org OBJECTIVES DEFINE Bloodborne Pathogen Exposure WHO must
Needlestick Policy and Actions to be taken after Exposure to Blood and Body Fluids (including HIV Post- Exposure Prophylaxis).
 LTHT Infection Control Policies Needlestick Policy and Actions to be taken after Exposure to Blood and Body Fluids (including HIV Post- Exposure Prophylaxis). This policy covers the immediate actions to
LTHT Infection Control Policies Needlestick Policy and Actions to be taken after Exposure to Blood and Body Fluids (including HIV Post- Exposure Prophylaxis). This policy covers the immediate actions to
Occupational Exposures to Bloodborne Pathogen (BBP) Training
 Occupational Exposures to Bloodborne Pathogen (BBP) Training OSHA 29 CFR 1910.1030 Protects workers exposed to blood or other potentially infectious diseases Who are at Risk? Workers in many different
Occupational Exposures to Bloodborne Pathogen (BBP) Training OSHA 29 CFR 1910.1030 Protects workers exposed to blood or other potentially infectious diseases Who are at Risk? Workers in many different
Bloodborne Pathogens. Post-Exposure Incident Packet. An Informational Guide
 Bloodborne Pathogens Post-Exposure Incident Packet An Informational Guide Faribault Public Schools Bloodborne Pathogens Post-Exposure Incident Packet This packet has been developed as an informational
Bloodborne Pathogens Post-Exposure Incident Packet An Informational Guide Faribault Public Schools Bloodborne Pathogens Post-Exposure Incident Packet This packet has been developed as an informational
Blood Borne Pathogens. Becky Walch, R.N. Micheel Valdez, L.V.N.
 Blood Borne Pathogens Becky Walch, R.N. Micheel Valdez, L.V.N. Examples of Blood Borne Pathogens Hepatitis B Hepatitis C Other Hepatitis HIV Hepatitis Hepatitis means inflammation of the liver. Hepatitis
Blood Borne Pathogens Becky Walch, R.N. Micheel Valdez, L.V.N. Examples of Blood Borne Pathogens Hepatitis B Hepatitis C Other Hepatitis HIV Hepatitis Hepatitis means inflammation of the liver. Hepatitis
BLOODBORNE DISEASES. Prevention of transmission for school staff. for staff not directly responsible for providing care or cleaning up blood
 BLOODBORNE DISEASES Prevention of transmission for school staff for staff not directly responsible for providing care or cleaning up blood MASSACHUSETTS DIVISION OF OCCUPATIONAL SAFETY Robert Prezioso,
BLOODBORNE DISEASES Prevention of transmission for school staff for staff not directly responsible for providing care or cleaning up blood MASSACHUSETTS DIVISION OF OCCUPATIONAL SAFETY Robert Prezioso,
NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS
 NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS Hepatitis B, Hepatitis C and HIV may be contracted through exposure to any body fluid, particularly blood. IMMEDIATE ACTION
NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS Hepatitis B, Hepatitis C and HIV may be contracted through exposure to any body fluid, particularly blood. IMMEDIATE ACTION
Hepatitis B Control. Table of Contents
 Control Table of Contents 1.0 INTRODUCTION... 1 2.0 GOALS... 1 3.0 DEFINITIONS... 1 4.0 CASE MANAGEMENT... 3 5.0 HEPATITIS B POST- EXPOSURE MANAGEMENT... 4 TABLE 1: HEPATITIS B POST EXPOSURE PROPHYLAXIS...
Control Table of Contents 1.0 INTRODUCTION... 1 2.0 GOALS... 1 3.0 DEFINITIONS... 1 4.0 CASE MANAGEMENT... 3 5.0 HEPATITIS B POST- EXPOSURE MANAGEMENT... 4 TABLE 1: HEPATITIS B POST EXPOSURE PROPHYLAXIS...
Introduction to Blood Borne Pathogens
 Introduction to Blood Borne Pathogens What are blood pathogens? Any infectious microorganism in the human blood that can cause disease is a Blood borne pathogen. Three of these pathogens include hepatitis
Introduction to Blood Borne Pathogens What are blood pathogens? Any infectious microorganism in the human blood that can cause disease is a Blood borne pathogen. Three of these pathogens include hepatitis
Blood borne Pathogen Exposure Policy for Students
 Blood borne Pathogen Exposure Policy for Students A University of Rhode Island (URI) student or intern who sustains an exposure from a needle stick, instrument stick, or mucous membranes to non-intact
Blood borne Pathogen Exposure Policy for Students A University of Rhode Island (URI) student or intern who sustains an exposure from a needle stick, instrument stick, or mucous membranes to non-intact
Bloodborne Pathogens. Kathleen Stefek, RN, MSN
 Bloodborne Pathogens Kathleen Stefek, RN, MSN What are Bloodborne Pathogens? Infectious agents carried in the blood and other body fluids that are capable of infecting a host (people like you and me) with
Bloodborne Pathogens Kathleen Stefek, RN, MSN What are Bloodborne Pathogens? Infectious agents carried in the blood and other body fluids that are capable of infecting a host (people like you and me) with
Blood-borne Pathogens Exposure Policy
 Blood-borne Pathogens Exposure Policy Contents Blood Borne Pathogen(s) Exposure (BBPE) -Post-Exposure Prophylaxis... 1 STUDENT CHECKLIST... 3 PROGRAM CHECKLIST... 4 PROVIDER CHECKLIST... 5 POST-EXPOSURE
Blood-borne Pathogens Exposure Policy Contents Blood Borne Pathogen(s) Exposure (BBPE) -Post-Exposure Prophylaxis... 1 STUDENT CHECKLIST... 3 PROGRAM CHECKLIST... 4 PROVIDER CHECKLIST... 5 POST-EXPOSURE
Training for Employees of Taylor Special Care Services, Inc.
 Training for Employees of Taylor Special Care Services, Inc. TSCS Taylor Special Care Services housing staffing counseling on-going support Simon Pop, MBA Chief Operating Officer 2015 2016 Guidelines:
Training for Employees of Taylor Special Care Services, Inc. TSCS Taylor Special Care Services housing staffing counseling on-going support Simon Pop, MBA Chief Operating Officer 2015 2016 Guidelines:
Dare County Schools. Bloodborne Pathogens Exposure Control Plan
 Dare County Schools Bloodborne Pathogens Exposure Control Plan 2017 Dare County Schools Bloodborne Pathogens Exposure Control Page 1 of 12 Dare County Schools Bloodborne Pathogen Program Purpose An infection
Dare County Schools Bloodborne Pathogens Exposure Control Plan 2017 Dare County Schools Bloodborne Pathogens Exposure Control Page 1 of 12 Dare County Schools Bloodborne Pathogen Program Purpose An infection
Post Exposure Prophylaxis (PEP)
 Post Exposure Prophylaxis (PEP) Occupational exposure Occupational exposure refers to exposure to potential blood-borne infections (HIV, HBV and HCV) that may occur in healthcare settings during performance
Post Exposure Prophylaxis (PEP) Occupational exposure Occupational exposure refers to exposure to potential blood-borne infections (HIV, HBV and HCV) that may occur in healthcare settings during performance
Bloodborne Pathogens Training. IEA, Inc.
 Bloodborne Pathogens Training IEA, Inc. Review the potential hazard of exposure to blood and other potentially infectious materials (OPIMs). Review safe work practices to prevent occupational exposure
Bloodborne Pathogens Training IEA, Inc. Review the potential hazard of exposure to blood and other potentially infectious materials (OPIMs). Review safe work practices to prevent occupational exposure
Module 1: HIV epidemiology, transmission and prevention
 Session 2 Module goals Module 1 Participants will be able to: -offer an insight into the epidemiological situation in the country and worldwide -present the HIV transmission modes and the broad approaches
Session 2 Module goals Module 1 Participants will be able to: -offer an insight into the epidemiological situation in the country and worldwide -present the HIV transmission modes and the broad approaches
HIV Occupational Transmission and Exposure. Marsh Gelbart 2010
 HIV Occupational Transmission and Exposure Marsh Gelbart 2010 Rationale for Post Exposure Prophylaxis (PEP) It was estimated that the risk for HIV transmission after percutaneous exposures involving larger
HIV Occupational Transmission and Exposure Marsh Gelbart 2010 Rationale for Post Exposure Prophylaxis (PEP) It was estimated that the risk for HIV transmission after percutaneous exposures involving larger
PROCEDURE TITLE: BLOOD BORNE PATHOGENS EXPOSURE CONTROL PLAN PROCEDURE NO.: 5.21:1
 PROCEDURE TITLE: BLOOD BORNE PATHOGENS EXPOSURE CONTROL PLAN PROCEDURE NO.: 5.21:1 RELATED POLICY: 5.21REV PAGE NO.: 1 OF 9 RESPONSIBLE ADMINISTRATOR(S): VPF&A/EHS EFECTIVE DATE: 07/11/14 NEXT REVIEW DATE:
PROCEDURE TITLE: BLOOD BORNE PATHOGENS EXPOSURE CONTROL PLAN PROCEDURE NO.: 5.21:1 RELATED POLICY: 5.21REV PAGE NO.: 1 OF 9 RESPONSIBLE ADMINISTRATOR(S): VPF&A/EHS EFECTIVE DATE: 07/11/14 NEXT REVIEW DATE:
Bloodborne pathogens and Standard Precautions
 Bloodborne pathogens and Standard Precautions Teaching plan To use this lesson for self-study, the learner should read the material, do the activity, and take the test. For group study, the leader may
Bloodborne pathogens and Standard Precautions Teaching plan To use this lesson for self-study, the learner should read the material, do the activity, and take the test. For group study, the leader may
Drew University Bloodborne Pathogens Exposure Control Plan and Procedures
 PURPOSE To provide a written plan for preventing and/or minimizing exposure to bloodborne pathogens for those Drew University personnel who may be involved in the handling of human blood, blood products,
PURPOSE To provide a written plan for preventing and/or minimizing exposure to bloodborne pathogens for those Drew University personnel who may be involved in the handling of human blood, blood products,
May Safety Subject. Bloodborne Pathogens
 May Safety Subject Bloodborne Pathogens Everyone is at risk to contact bloodborne pathogens. Some more than others. Universal precautions means treating all objects as potentially contaminated Personal
May Safety Subject Bloodborne Pathogens Everyone is at risk to contact bloodborne pathogens. Some more than others. Universal precautions means treating all objects as potentially contaminated Personal
Guidelines for Post- Exposure Prophylaxis for HAV, HBV, HCV & HIV
 Guidelines for Post- Exposure Prophylaxis for HAV, HBV, HCV & HIV By Dr. Sinan Butrus F.I.C.M.S Clinical Standards & Guidelines Kurdistan Board For Medical Specialties An exposure that might place health
Guidelines for Post- Exposure Prophylaxis for HAV, HBV, HCV & HIV By Dr. Sinan Butrus F.I.C.M.S Clinical Standards & Guidelines Kurdistan Board For Medical Specialties An exposure that might place health
Pre and Post Exposure Prophylaxis. Laila AL Dabal MD FRCP MSc Infectious Diseases Unit Dubai Health Authority 15 March 2018
 Pre and Post Exposure Prophylaxis Laila AL Dabal MD FRCP MSc Infectious Diseases Unit Dubai Health Authority 15 March 2018 Indications for Pre and Post Exposure Prophylaxis: occupational and non-occupational
Pre and Post Exposure Prophylaxis Laila AL Dabal MD FRCP MSc Infectious Diseases Unit Dubai Health Authority 15 March 2018 Indications for Pre and Post Exposure Prophylaxis: occupational and non-occupational
Management of Needlestick and Mucous Membrane Exposures To Blood/Body Fluids
 Management of Needlestick and Mucous Membrane Exposures To Blood/Body Fluids August 2004 Table Of Contents Protocol - Management of Needlestick and Mucous Membrane Exposures to Blood/Body Fluids Assessment
Management of Needlestick and Mucous Membrane Exposures To Blood/Body Fluids August 2004 Table Of Contents Protocol - Management of Needlestick and Mucous Membrane Exposures to Blood/Body Fluids Assessment
Non-Occupational Post-Exposure HIV Prophylaxis npep
 Non-Occupational Post-Exposure HIV Prophylaxis npep Peter Meacher MD (Chief Medical Officer) Anthony Vavasis MD (Director of Medicine) Callen-Lorde Community Health Center Objectives - at the end of the
Non-Occupational Post-Exposure HIV Prophylaxis npep Peter Meacher MD (Chief Medical Officer) Anthony Vavasis MD (Director of Medicine) Callen-Lorde Community Health Center Objectives - at the end of the
Bloodborne Pathogen Module. Chelmsford Public Schools September, 2016
 Bloodborne Pathogen Module Chelmsford Public Schools September, 2016 Why is this important? v OSHA BB Pathogen Standard anyone whose job requires exposure to BB pathogens is required to complete training
Bloodborne Pathogen Module Chelmsford Public Schools September, 2016 Why is this important? v OSHA BB Pathogen Standard anyone whose job requires exposure to BB pathogens is required to complete training
Management of Exposure to Needlestick Injuries & Body Fluids
 Management of Exposure to Needlestick Injuries & Body Fluids Clinical S.O.P. No.:28 Compiled by: Approved by: Review date: November 2016 DOCUMENT HISTORY Version Detail of purpose / change Author / edited
Management of Exposure to Needlestick Injuries & Body Fluids Clinical S.O.P. No.:28 Compiled by: Approved by: Review date: November 2016 DOCUMENT HISTORY Version Detail of purpose / change Author / edited
Safety Committee Prototypical Safety Program Manual
 1 Bloodborne Pathogens Exposure Control Plan Policy The Department Bloodborne Pathogens Exposure Control Plan is designed to comply with the requirements of the OSHA Bloodborne Pathogens Standard, 29 CFR
1 Bloodborne Pathogens Exposure Control Plan Policy The Department Bloodborne Pathogens Exposure Control Plan is designed to comply with the requirements of the OSHA Bloodborne Pathogens Standard, 29 CFR
The Bloodborne Pathogen Standard. An Overview
 The Bloodborne Pathogen Standard An Overview The Standard l In 1990, OSHA (Occupational Safety and Health Administration), developed the Bloodborne Pathogen Standard to protect workers by limiting occupational
The Bloodborne Pathogen Standard An Overview The Standard l In 1990, OSHA (Occupational Safety and Health Administration), developed the Bloodborne Pathogen Standard to protect workers by limiting occupational
Bloodborne Pathogens Training (OHS_BIO500) Course Material
 Introduction (OHS_BIO500) Course Material Welcome to the Bloodborne Pathogens (BBP) Training Course (OHS_BIO500). UAB Campus Employees whose job duties put them at increased risk for exposure to bloodborne
Introduction (OHS_BIO500) Course Material Welcome to the Bloodborne Pathogens (BBP) Training Course (OHS_BIO500). UAB Campus Employees whose job duties put them at increased risk for exposure to bloodborne
Blood Borne Pathogens
 Bloomer School District Blood Borne Pathogens Developed by: Tammy Kornesczuk, RN Act Rather Than Re-act School Staff tend to be nurturing and care-taking people Don t rush to help without putting on gloves
Bloomer School District Blood Borne Pathogens Developed by: Tammy Kornesczuk, RN Act Rather Than Re-act School Staff tend to be nurturing and care-taking people Don t rush to help without putting on gloves
WVU Occupational Medicine Program for evaluation and treatment of persons exposed to Lentivirus Vectors
 Hazard Description: Lentivirus vector systems are derived from HIV and similar viruses because of being very effective at inserting genetic material into the genome of target cells. While most researchers
Hazard Description: Lentivirus vector systems are derived from HIV and similar viruses because of being very effective at inserting genetic material into the genome of target cells. While most researchers
01.02 Blood Borne Pathogens (BBP) Occupational Post Exposure Management
 01.02 Blood Borne Pathogens (BBP) Occupational Post Exposure Purpose Audience Policy Definitions Establish protocol for management of occupational exposures to blood or potentially infectious materials.
01.02 Blood Borne Pathogens (BBP) Occupational Post Exposure Purpose Audience Policy Definitions Establish protocol for management of occupational exposures to blood or potentially infectious materials.
NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS
 NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS Hepatitis B, Hepatitis C and HIV may be contracted through exposure to any body fluid, particularly blood. IMMEDIATE ACTION
NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS Hepatitis B, Hepatitis C and HIV may be contracted through exposure to any body fluid, particularly blood. IMMEDIATE ACTION
HIV prophylaxis for health care providers. Dr. A. K. M. Humayon Kabir Assistant Professor Department of Medicine Dhaka Medical College Hospital
 HIV prophylaxis for health care providers. Dr. A. K. M. Humayon Kabir Assistant Professor Department of Medicine Dhaka Medical College Hospital HIV continues to be a major global public health issue, Approximately
HIV prophylaxis for health care providers. Dr. A. K. M. Humayon Kabir Assistant Professor Department of Medicine Dhaka Medical College Hospital HIV continues to be a major global public health issue, Approximately
01.02 Blood Borne Pathogens (BBP) Occupational Post Exposure Prophylaxis
 01.02 Blood Borne Pathogens (BBP) Occupational Post Exposure Purpose Audience Establish protocol for management of occupational exposures to blood or potentially infectious materials. All employees of
01.02 Blood Borne Pathogens (BBP) Occupational Post Exposure Purpose Audience Establish protocol for management of occupational exposures to blood or potentially infectious materials. All employees of
You will now begin the Bloodborne Pathogen Refresher Training.
 You will now begin the Bloodborne Pathogen Refresher Training. The following program will review your occupational risks and the steps that you and your Client must take to reduce your risks of exposure.
You will now begin the Bloodborne Pathogen Refresher Training. The following program will review your occupational risks and the steps that you and your Client must take to reduce your risks of exposure.
Guidance for management of exposure events where there is a risk of transmission of blood borne viruses
 Guidance for management of exposure events where there is a risk of transmission of blood borne viruses (HIV, Hepatitis B and Hepatitis C) in the community SUMMARY Where a child is thought to have had
Guidance for management of exposure events where there is a risk of transmission of blood borne viruses (HIV, Hepatitis B and Hepatitis C) in the community SUMMARY Where a child is thought to have had
Infection/Disease Control HEPATITIS CONTROL PROGRAM
 OPERATING PROCEDURE NO. 153-29 Florida State Hospital Chattahoochee, Florida July 8, 2009 Infection/Disease Control HEPATITIS CONTROL PROGRAM 1. Purpose: To establish consistent surveillance, reporting,
OPERATING PROCEDURE NO. 153-29 Florida State Hospital Chattahoochee, Florida July 8, 2009 Infection/Disease Control HEPATITIS CONTROL PROGRAM 1. Purpose: To establish consistent surveillance, reporting,
May Safety Subject. Bloodborne Pathogens
 May Safety Subject Bloodborne Pathogens Everyone is at risk to contact bloodborne pathogens. Some more than others. Universal precautions means treating all objects as potentially contaminated Personal
May Safety Subject Bloodborne Pathogens Everyone is at risk to contact bloodborne pathogens. Some more than others. Universal precautions means treating all objects as potentially contaminated Personal
Blood Borne Pathogens (BBP)
 Blood Borne Pathogens (BBP) Healthcare facilities are high-risk areas for exposure to bloodborne pathogens, so protect yourself and remind others to do the same. There are three bloodborne pathogens of
Blood Borne Pathogens (BBP) Healthcare facilities are high-risk areas for exposure to bloodborne pathogens, so protect yourself and remind others to do the same. There are three bloodborne pathogens of
I. PROCEEDINGS AFTER EXPOSURE TO BLOOD OR OTHER POTENTIALLY INFECTIOUS MATERIALS (OPIM) WHICH MIGHT TRANSFER AN INFECTION WITH HAEMATOGENOUS VIRUSES
 Annex no. 1 to the enactment No. 13/XIV R/2010 of the Rector of the Medical University in Wrocław dated April 12, 2010 Proceedings after occupational exposure to HIV, HBV and HCV 1 LEGAL GROUNDS: 1. The
Annex no. 1 to the enactment No. 13/XIV R/2010 of the Rector of the Medical University in Wrocław dated April 12, 2010 Proceedings after occupational exposure to HIV, HBV and HCV 1 LEGAL GROUNDS: 1. The
Bloodborne Pathogens Training For School Personnel
 Bloodborne Pathogens Training For School Personnel OSHA Defined: Occupational Safety and Health Administration Published a standard to reduce or eliminate health risk, resulting in: Annual training of
Bloodborne Pathogens Training For School Personnel OSHA Defined: Occupational Safety and Health Administration Published a standard to reduce or eliminate health risk, resulting in: Annual training of
Bloodborne Pathogens and Universal Precautions
 Bloodborne Pathogens and Universal Precautions Parkway School District 2012-2013 Revised 9/19/2012 What Are Bloodborne Pathogens(BBPs) Bloodborne pathogens (BBPs) are disease causing microorganisms carried
Bloodborne Pathogens and Universal Precautions Parkway School District 2012-2013 Revised 9/19/2012 What Are Bloodborne Pathogens(BBPs) Bloodborne pathogens (BBPs) are disease causing microorganisms carried
A. Background for Trainer: B. What OSHA Requires: Bloodborne Pathogens. Lesson Plan 6080a
 Lesson Plan 6080a This training session outline is designed to follow the accompanying booklet, OSHA s Bloodborne Pathogens Standard. The booklet reviews what employees who are potentially exposed to the
Lesson Plan 6080a This training session outline is designed to follow the accompanying booklet, OSHA s Bloodborne Pathogens Standard. The booklet reviews what employees who are potentially exposed to the
EMPLOYEE HEALTH TABLE OF CONTENTS
 EMPLOYEE HEALTH TABLE OF CONTENTS PHYSICAL ASSESSMENT.2 REPORTING EMPLOYEE INFECTIONS...3 SUMMARY OF IMPORTANT RECOMMENDATIONS AND WORK RESTRICTIONS FOR PERSONNEL WITH INFECTIOUS DISEASES.4 HEPATITIS B
EMPLOYEE HEALTH TABLE OF CONTENTS PHYSICAL ASSESSMENT.2 REPORTING EMPLOYEE INFECTIONS...3 SUMMARY OF IMPORTANT RECOMMENDATIONS AND WORK RESTRICTIONS FOR PERSONNEL WITH INFECTIOUS DISEASES.4 HEPATITIS B
Infection Prevention and Control - General Orientation
 Infection Prevention and Control - General Orientation Hand Hygiene-CDC Isolation Precautions - CDC Medical Waste - OSHA Environmental Cleaning - CDC Safe Injection Practices - CDC Bloodborne Pathogens
Infection Prevention and Control - General Orientation Hand Hygiene-CDC Isolation Precautions - CDC Medical Waste - OSHA Environmental Cleaning - CDC Safe Injection Practices - CDC Bloodborne Pathogens
Immunization Policy. "UIC/COD-sponsored graduate education program" is one for which UIC/COD maintains academic responsibility.
 I. PURPOSE Immunization Policy TITLE: CLINICAL HEALTHCARE PROVIDERS - IMMUNIZATIONS AND HEALTH REQUIREMENTS To prevent or reduce the risk of transmission of vaccine-preventable and other communicable diseases
I. PURPOSE Immunization Policy TITLE: CLINICAL HEALTHCARE PROVIDERS - IMMUNIZATIONS AND HEALTH REQUIREMENTS To prevent or reduce the risk of transmission of vaccine-preventable and other communicable diseases
Bloodborne Pathogens and Regulated Medical Waste
 Bloodborne Pathogens and Regulated Medical Waste OSHA Ensure employees can safely perform their normal duties without undue health risks Bloodborne Pathogen (BBP) Standard developed to protect employees
Bloodborne Pathogens and Regulated Medical Waste OSHA Ensure employees can safely perform their normal duties without undue health risks Bloodborne Pathogen (BBP) Standard developed to protect employees
IMPORTANT HEALTH INFORMATION
 IMPORTANT HEALTH INFORMATION SU-6523MI Page 1 of 8 Table of Contents Page What is an HIV test?..........................................1 Will the HIV test tell me if I have AIDS?............................1
IMPORTANT HEALTH INFORMATION SU-6523MI Page 1 of 8 Table of Contents Page What is an HIV test?..........................................1 Will the HIV test tell me if I have AIDS?............................1
East Carolina University Student Health Service
 Page 1 of 5 Policy: BLOOD AND OTHER POTENTIALLY INFECTIOUS MATERIAL EXPOSURE POLICY FOR STUDENTS, WITH CLINICAL EXPOSURES s (SHS) will adapt and modify the policies and procedures of ECU Prospective Health
Page 1 of 5 Policy: BLOOD AND OTHER POTENTIALLY INFECTIOUS MATERIAL EXPOSURE POLICY FOR STUDENTS, WITH CLINICAL EXPOSURES s (SHS) will adapt and modify the policies and procedures of ECU Prospective Health
Code: GBGAA-R Amended: 08/09/10 Amended: 08/06/18 HERMON SCHOOL DEPARTMENT BLOODBORNE PATHOGENS EXPOSURE CONTROL PLAN
 Code: GBGAA-R Amended: 08/09/10 Amended: 08/06/18 HERMON SCHOOL DEPARTMENT BLOODBORNE PATHOGENS EXPOSURE CONTROL PLAN April 2018 Table of Contents Exposure Determination... 3 Hepatitis B Vaccine... 4 Universal
Code: GBGAA-R Amended: 08/09/10 Amended: 08/06/18 HERMON SCHOOL DEPARTMENT BLOODBORNE PATHOGENS EXPOSURE CONTROL PLAN April 2018 Table of Contents Exposure Determination... 3 Hepatitis B Vaccine... 4 Universal
Emergency Department Blood/Body Fluid Exposure Instructions
 Emergency Department Blood/Body Fluid Exposure Instructions For employees sent to the Emergency Department after hours to be evaluated for needle stick / body fluid exposure 1. Floor or unit Charge RN
Emergency Department Blood/Body Fluid Exposure Instructions For employees sent to the Emergency Department after hours to be evaluated for needle stick / body fluid exposure 1. Floor or unit Charge RN
