Immunology lecture. Immunity: Two Intrinsic Defense Systems. First line of defense skin and mucosa prevent entry of microorganisms
|
|
|
- Verity Mathews
- 6 years ago
- Views:
Transcription
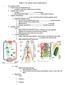
1 Immunology lecture D.HAMMOUDI.MD Immunity: Two Intrinsic Defense Systems Innate (nonspecific) system responds quickly and consists of:[3 line of defense] First line of defense skin and mucosa prevent entry of microorganisms Second line of defense antimicrobial proteins, p phagocytes, and other cells Inhibit spread of invaders throughout the body Inflammation is its most important mechanism 1
2 Immunity: Two Intrinsic Defense Systems Adaptive (specific) defense system Third line of defense mounts attack against particular foreign substances Takes longer to react than the innate system Works in conjunction with the innate system Innate and Adaptive Defenses Figure
3 Surface Barriers Skin, mucous membranes, and their secretions make up the first line of defense Keratin in the skin: Presents a physical barrier to most microorganisms Is resistant to weak acids and bases, bacterial enzymes, and toxins Mucosae provide similar mechanical barriers Epithelial Chemical Barriers Epithelial membranes produce protective chemicals that destroy microorganisms Skin acidity (ph of 3 to 5) inhibits bacterial growth Sebum contains chemicals toxic to bacteria Stomach mucosae secrete concentrated HCl and proteindigesting enzymes Saliva and lacrimal l fluid contain lysozyme Mucus traps microorganisms that enter the digestive and respiratory systems 3
4 Respiratory Tract Mucosae Mucus-coated hairs in the nose trap inhaled particles Mucosa of the upper respiratory tract is ciliated Cilia sweep dust- and bacteria-laden mucus away from lower respiratory passages Internal Defenses: Cells and Chemicals The body uses nonspecific cellular and chemical ca devices to protect itself Phagocytes and natural killer (NK) cells Antimicrobial proteins in blood and tissue fluid Inflammatory response enlists macrophages, mast cells, WBCs, and chemicals Harmful substances are identified by surface carbohydrates unique to infectious organisms 4
5 Phagocytes Macrophages are the chief phagocytic cells Free macrophages wander throughout a region in search of cellular debris Kupffer cells (liver) and microglia (brain) are fixed macrophages Figure 21.2a Phagocytes Neutrophils become phagocytic when encountering infectious material Eosinophils are weakly phagocytic against parasitic worms Mast cells bind and ingest a wide range of bacteria 5
6 Mast cells can be stimulated to degranulate by direct injury (e.g. physical or chemical), cross-linking of Immunoglobulin E (IgE) receptors, or by activated complement proteins A mast cell (or mastocyte) is a resident cell of several types of tissues and contains many granules rich in histamine and heparin. Although best known for their role in allergy and anaphylaxis, mast cells play an important protective role as well,being intimately involved in wound healing and defense against pathogens Prominent near the boundaries between the outside world and the internal milieu, such as the skin, mucosa of the lungs and digestive tract, as well as in the mouth, conjunctiva and nose 6
7 7
8 Mechanism of Phagocytosis 1/ Microbes adhere to the phagocyte 2/Pseudopods engulf the particle (antigen) into a phagosome 3/Phagosomes fuse with a lysosome to form a phagolysosome 4/Invaders in the phagolysosome are digested by proteolytic enzymes 5/Indigestible and residual material is removed by exocytosis 8
9 1 Microbe adheres to phagocyte. 2 Phagocyte forms pseudopods that eventually engulf the particle. Lysosome Acid hydrolase enzymes Phagocytic vesicle containing antigen (phagosome). 3 Phagocytic vesicle is fused with a lysosome. Phagolysosome 4 Microbe in fused vesicle is killed and digested by lysosomal enzymes within the phagolysosome, leaving a residual body. Residual body 5 Indigestible and residual material is removed by exocytosis. (b) Figure 21.2b 9
10 10
11 Natural Killer (NK) Cells Can lyse and kill cancer cells and virusinfected cells Are a small, distinct group of large granular lymphocytes React nonspecifically and eliminate cancerous and virus-infected cells Kill their target cells by releasing perforins and other cytolytic chemicals Secrete potent chemicals that enhance the inflammatory response 11
12 Inflammation: Tissue Response to Injury The inflammatory response is triggered whenever body tissues are injured Prevents the spread of damaging agents to nearby tissues Disposes of cell debris and pathogens Sets the stage for repair processes The four cardinal signs of acute inflammation are redness, heat, swelling, and pain Inflammation Response Begins with a flood of inflammatory chemicals released into the extracellular fluid Inflammatory mediators: Kinins, prostaglandins (PGs), complement, and cytokines Released by injured tissue, phagocytes, lymphocytes, and mast cells Cause local small blood vessels to dilate, resulting in hyperemia 12
13 Toll-like Receptors (TLRs) Macrophages and cells lining the gastrointestinal and respiratory tracts bear TLRs TLRs recognize specific classes of infecting microbes Activated TLRs trigger the release of cytokines that promote inflammation Inflammatory Response: Vascular Permeability Chemicals liberated by the inflammatory response increase the permeability of local capillaries Exudate fluid containing proteins, clotting factors, and antibodies Exudate seeps into tissue spaces causing local edema (swelling), which contributes to the sensation of pain 13
14 Inflammatory Response: Edema The surge of protein-rich fluids into tissue spaces (edema): Helps dilute harmful substances Brings in large quantities of oxygen and nutrients needed for repair Allows entry of clotting proteins, which h prevents the spread of bacteria Inflammatory Response: Phagocytic Mobilization Four main phases: Leukocytosis neutrophils are released from the bone marrow in response to leukocytosisinducing factors released by injured cells Margination neutrophils cling to the walls of capillaries in the injured area Diapedesis neutrophils squeeze through capillary walls and begin phagocytosis Chemotaxis inflammatory chemicals attract neutrophils to the injury site 14
15 Innate defenses Internal defenses Inflammatory chemicals diffusing from the inflamed site act as chemotactic agents 4 Positive chemotaxis 1 Neutrophils enter blood from bone marrow 2 Margination 3 Diapedesis Capillary wall Endothelium Basement membrane Figure
16 16
17 17
18 Figure
19 19
20 Antimicrobial Proteins Enhance the innate defenses by: Attacking microorganisms directly Hindering microorganisms ability to reproduce The most important antimicrobial proteins are: Interferon Complement proteins Interferon (IFN) Genes that synthesize IFN are activated when a host cell is invaded by a virus Interferon molecules leave the infected cell and enter neighboring cells Interferon stimulates the neighboring cells to activate genes for PKR (an antiviral protein) PKR nonspecifically blocks viral reproduction in the neighboring cell 20
21 Interferon (IFN) Figure 21.5 Interferon Family Family of related proteins each with slightly different physiological effects Lymphocytes secrete gamma (γ) interferon, but most other WBCs secrete alpha (α) interferon Fibroblasts secrete beta (β) interferon Interferons also activate macrophages and mobilize NKs FDA-approved alpha IFN is used: As an antiviral drug against hepatitis C virus To treat genital warts caused by the herpes virus 21
22 Complement 20 or so proteins that circulate in the blood in an inactive form Proteins include C1 through C9, factors B, D, and P, and regulatory proteins Provides a major mechanism for destroying foreign substances in the body Complement Amplifies all aspects of the inflammatory response Kills bacteria and certain other cell types (our cells are immune to complement) Enhances the effectiveness of both nonspecific and specific defenses 22
23 Complement Pathways Complement can be activated by two pathways: classical and alternative Classical pathway is linked to the immune system Depends on the binding of antibodies to invading organisms Subsequent binding of C1 to the antigen-antibody complexes (complement fixation) Alternative pathway is triggered by interaction among factors B, D, and P, and polysaccharide molecules present on microorganisms Complement Pathways Each pathway involves a cascade in which complement proteins are activated in a sequence where each step catalyzes the next Both pathways converge on C3, which cleaves into C3a and C3b 23
24 Complement Pathways C3b initiates formation of a membrane attack complex (MAC) MAC causes cell lysis by interfering with a cell s ability to eject Ca 2+ C3b also causes opsonization, and C3a causes inflammation Complement Pathways Figure
25 25
26 C-reactive Protein (CRP) CRP is produced by the liver in response to inflammatory molecules CRP is a clinical marker used to assess: The presence of an acute infection An inflammatory condition and its response to treatment Functions of C-reactive Protein Binds to PC receptor of pathogens and exposed self-antigens Plays a surveillance role in targeting damaged cells for disposal Activates complement 26
27 Fever Abnormally high body temperature in response to invading microorganisms The body s thermostat is reset upwards in response to pyrogens, chemicals secreted by leukocytes and macrophages exposed to bacteria and other foreign substances Fever High fevers are dangerous because they can denature enzymes Moderate fever can be beneficial, i as it causes: The liver and spleen to sequester iron and zinc (needed by microorganisms) An increase in the metabolic rate, which speeds up tissue repair 27
28 Adaptive (Specific) Defenses The adaptive immune system is a functional system that: Recognizes specific foreign substances Acts to immobilize, neutralize, or destroy foreign substances Amplifies inflammatory response and activates t complement Adaptive Immune Defenses The adaptive immune system is antigen-specific, systemic, and has memory It has two separate but overlapping arms: Humoral, or antibody-mediated immunity Cellular, or cell-mediated immunity 28
29 Antigens Substances that can mobilize the immune system and provoke an immune response The ultimate targets of all immune responses are mostly large, complex molecules not normally found in the body (nonself) Complete Antigens Important functional properties: Immunogenicity ability to stimulate proliferation of specific lymphocytes and antibody production Reactivity ability to react with products of activated lymphocytes and the antibodies released in response to them Complete antigens include foreign protein, nucleic acid, some lipids, and large polysaccharides 29
30 Haptens (Incomplete Antigens) Small molecules, such as peptides, nucleotides, and many hormones, that are not immunogenic but are reactive when attached to protein carriers If they link up with the body s proteins, the adaptive immune system may recognize them as foreign and mount a harmful attack (allergy) Haptens are found in poison ivy, dander, some detergents, and cosmetics Antigenic Determinants Only certain parts of an entire antigen are immunogenic Antibodies and activated lymphocytes bind to these antigenic determinants Most naturally occurring antigens have numerous antigenic determinants that: Mobilize several different lymphocyte populations Form different kinds of antibodies against it Large, chemically simple molecules (e.g., plastics) have little or no immunogenicity 30
31 Antigenic Determinants Figure 21.7 Self-Antigens: MHC Proteins Our cells are dotted with protein molecules (selfantigens) that are not antigenic to us but are strongly antigenic to others One type, MHC proteins, mark a cell as self The two classes of MHC proteins are: Class I MHC proteins found on virtually all body cells Class II MHC proteins found on certain cells in the immune response 31
32 MHC Proteins Are coded for by genes of the major histocompatibility complex (MHC) and are unique to an individual Each MHC molecule has a deep groove that displays a peptide, which is a normal cellular product of protein recycling In infected cells, MHC proteins bind to fragments of foreign antigens, which play a crucial role in mobilizing the immune system Cells of the Adaptive Immune System Two types of lymphocytes B lymphocytes oversee humoral immunity T lymphocytes non-antibody-producing cells that constitute the cell-mediated arm of immunity Antigen-presenting cells (APCs): Do not respond to specific antigens Play essential auxiliary roles in immunity 32
33 Lymphocytes Immature lymphocytes released from bone marrow are essentially identical Whether a lymphocyte matures into a B cell or a T cell depends on where in the body it becomes immunocompetent B cells mature in the bone marrow T cells mature in the thymus T Cell Selection in the Thymus Figure
34 T Cells T cells mature in the thymus under negative and positive selection pressures Negative selection eliminates T cells that are strongly anti-self Positive selection selects T cells with a weak response to self-antigens, which thus become both immunocompetent and self-tolerant B Cells B cells become immunocompetent and selftolerant in bone marrow Some self-reactive B cells are inactivated (anergy) while others are killed Other B cells undergo receptor editing in which there is a rearrangement of their receptors 34
35 Immunocompetent B or T cells Display a unique type of receptor that responds to a distinct antigen Become immunocompetent before they encounter antigens they may later attack Are exported to secondary lymphoid tissue where encounters with antigens occur Mature into fully functional antigen-activated cells upon binding with their recognized antigen It is genes, not antigens, that determine which foreign substances our immune system will recognize and resist Circulation in blood Thymus 2 Immunocompetent, but still naive, lymphocyte migrates via blood 1 Red bone marrow Immature lymphocytes Lymph nodes, spleen, and other lymphoid tissues 3 3 Activated Immunocompetent B and T cells recirculate in blood and lymph 1 Bone marrow 2 Key: = Site of lymphocyte origin = Site of development of immunocompetence as B or T cells; primary lymphoid organs = Site of antigen challenge, activation, and final diff erentiation of B and T cells 1 Lymphocytes destined to become T cells migrate to the thymus and develop immunocompetence there. B cells develop immunocompetence in red bone marrow. 2 After leaving the thymus or bone marrow as naïve immunocompetent cells, lymphocytes seed the lymph nodes, spleen, and other lymphoid tissues where the antigen challenge occurs. 3 Antigen-activated immunocompetent lymphocytes circulate continuously in the bloodstream and lymph and throughout the lymphoid organs of the body. Figure
36 Circulation in blood 1 Red bone marrow Immature lymphocytes Key: = Site of lymphocyte origin = Site of development of immunocompetence as B or T cells; primary lymphoid organs = Site of antigen challenge, activation, and final diff erentiation of B and T cells Thymus 1 Lymphocytes destined to become T cells migrate to the thymus and develop immunocompetence there. Figure 21.8 Circulation in blood 1 Red bone marrow Immature lymphocytes 1 Key: = Site of lymphocyte origin = Site of development of immunocompetence as B or T cells; primary lymphoid organs = Site of antigen challenge, activation, and final diff erentiation of B and T cells Thymus Bone marrow 1 Lymphocytes destined to become T cells migrate to the thymus and develop immunocompetence there. B cells develop immunocompetence in red bone marrow. Figure
37 Circulation in blood 1 Red bone marrow Immature lymphocytes 1 Key: = Site of lymphocyte origin = Site of development of immunocompetence as B or T cells; primary lymphoid organs = Site of antigen challenge, activation, and final diff erentiation of B and T cells Thymus 2 Immunocompetent, but still naive, lymphocyte migrates via blood Lymph nodes, spleen, and other lymphoid tissues Bone marrow 2 1 Lymphocytes destined to become T cells migrate to the thymus and develop immunocompetence there. B cells develop immunocompetence in red bone marrow. 2 After leaving the thymus or bone marrow as naïve immunocompetent cells, lymphocytes seed the lymph nodes, spleen, and other lymphoid tissues where the antigen challenge occurs. Figure 21.8 Circulation in blood Thymus 2 Immunocompetent, but still naive, lymphocyte migrates via blood 1 Red bone marrow Immature lymphocytes Lymph nodes, spleen, and other lymphoid tissues 3 3 Activated Immunocompetent B and T cells recirculate in blood and lymph 1 Bone marrow 2 Key: = Site of lymphocyte origin = Site of development of immunocompetence as B or T cells; primary lymphoid organs = Site of antigen challenge, activation, and final diff erentiation of B and T cells 1 Lymphocytes destined to become T cells migrate to the thymus and develop immunocompetence there. B cells develop immunocompetence in red bone marrow. 2 After leaving the thymus or bone marrow as naïve immunocompetent cells, lymphocytes seed the lymph nodes, spleen, and other lymphoid tissues where the antigen challenge occurs. 3 Antigen-activated immunocompetent lymphocytes circulate continuously in the bloodstream and lymph and throughout the lymphoid organs of the body. Figure
38 Antigen-Presenting Cells (APCs) Major rolls in immunity i are: To engulf foreign particles To present fragments of antigens on their own surfaces, to be recognized by T cells Major APCs are dendritic cells (DCs), macrophages, and activated B cells The major initiators of adaptive immunity are DCs, which migrate to the lymph nodes and secondary lymphoid organs, and present antigens to T and B cells Macrophages and Dendritic Cells Secrete soluble proteins that activate T cells Activated T cells in turn release chemicals that: Rev up the maturation and mobilization of DCs Prod macrophages to become activated macrophages, which are insatiable phagocytes that t secrete bactericidal id chemicals 38
39 Adaptive Immunity: Summary Two-fisted defensive system that uses lymphocytes, APCs, and specific molecules to identify and destroy nonself particles Its response depends upon the ability of its cells to: Recognize foreign substances (antigens) by binding to them Communicate with one another so that the whole system mounts a response specific to those antigens Humoral Immunity Response Antigen challenge first encounter between an antigen and a naive immunocompetent cell Takes place in the spleen or other lymphoid organ If the lymphocyte is a B cell: The challenging antigen provokes a humoral immune response Antibodies are produced against the challenger 39
40 Clonal Selection Stimulated B cell growth forms clones bearing the same antigen-specific receptors A naive, immunocompetent B cell is activated when antigens bind to its surface receptors and cross-link adjacent receptors Antigen binding is followed by receptormediated endocytosis of the cross-linked antigen-receptor complexes These activating events, plus T cell interactions, trigger clonal selection Primary Response (initial encounter with antigen) B lymphoblasts Proliferation to form a clone Antigen Antigen binding to a receptor on a specific B lymphocyte (B lymphocytes with non-complementary receptors remain inactive) Plasma cells Secreted antibody molecules Secondary Response (can be years later) Clone of cells identical to ancestral cells Memory B cell Subsequent challenge by same antigen Plasma cells Secreted antibody molecules Memory B cells Figure
41 Fate of the Clones Most clone cells become antibody-secreting plasma cells Plasma cells secrete specific antibody at the rate of 2000 molecules per second Fate of the Clones Secreted antibodies: Bind to free antigens Mark the antigens for destruction by specific or nonspecific mechanisms Clones that do not become plasma cells become memory cells that can mount an immediate response to subsequent exposures of the same antigen 41
42 Immunological Memory Primary immune response cellular differentiation and proliferation, which occurs on the first exposure to a specific antigen Lag period: 3 to 6 days after antigen challenge Peak levels of plasma antibody are achieved in 10 days Antibody levels then decline Immunological Memory Secondary immune response re-exposure to the same antigen Sensitized memory cells respond within hours Antibody levels peak in 2 to 3 days at much higher levels than in the primary response Antibodies bind with greater affinity, it and their levels in the blood can remain high for weeks to months 42
43 Primary and Secondary Humoral Responses Figure Active Humoral Immunity B cells encounter antigens and produce antibodies against them Naturally acquired response to a bacterial or viral infection Artificially acquired response to a vaccine of dead or attenuated ated pathogens Vaccines spare us the symptoms of disease, and their weakened antigens provide antigenic determinants that are immunogenic and reactive 43
44 Passive Humoral Immunity Differs from active immunity in the antibody source and the degree of protection B cells are not challenged by antigens Immunological memory does not occur Protection ends when antigens naturally degrade in the body Naturally acquired from the mother to her fetus via the placenta Artificially acquired from the injection of serum, such as gamma globulin Types of Acquired Immunity Figure
45 Antibodies Also called immunoglobulins Constitute the gamma globulin portion of blood proteins Are soluble proteins secreted by activated B cells and plasma cells in response to an antigen Are capable of binding specifically with that antigen There are five classes of antibodies: IgD, IgM, IgG, IgA, and IgE Classes of Antibodies IgD monomer attached to the surface of B cells, important in B cell activation IgM released by plasma cells during the primary immune response IgG the most abundant and diverse antibody in primary and secondary response; crosses the placenta and confers passive immunity 45
46 Classes of Antibodies IgA dimer that helps prevent attachment of pathogens to epithelial cell surfaces IgE monomer that binds to mast cells and basophils, causing histamine release when activated Basic Antibody Structure C i t f f l i l tid h i Consists of four looping polypeptide chains linked together with disulfide bonds Two identical heavy (H) chains and two identical light (L) chains The four chains bound together form an antibody monomer Each chain has a variable (V) region at one end and a constant (C) region at the other Variable regions of the heavy and light chains combine to form the antigen-binding site 46
47 Basic Antibody Structure Figure 21.13a Antibody Structure Antibodies responding to different antigens have different V regions but the C region is the same for all antibodies in a given class 47
48 Antibody Structure C regions form the stem of the Y-shaped antibody and: Determine the class of the antibody Serve common functions in all antibodies Dictate the cells and chemicals that the antibody can bind to Determine how the antibody class will function in elimination of antigens Mechanisms of Antibody Diversity Plasma cells make over a billion types of antibodies However, each cell only contains 100,000 genes that code for these polypeptides To code for this many antibodies, somatic recombination takes place: Gene segments are shuffled and combined in different ways by each B cell as it becomes immunocompetent Information of the newly assembled genes is expressed as B cell receptors and as antibodies 48
49 Antibody Diversity Random mixing of gene segments makes unique antibody genes that: Code for H and L chains Account for part of the variability in antibodies V gene segments, called hypervariable regions, mutate and dincrease antibody variation i Plasma cells can switch H chains, making two or more classes with the same V region Antibody Targets Antibodies themselves do not destroy antigen; they inactivate and tag it for destruction All antibodies form an antigen-antibody (immune) complex Defensive mechanisms used by antibodies are neutralization, agglutination, precipitation, and complement fixation 49
50 Complement Fixation and Activation Complement fixation: Main mechanism used against cellular antigens Antibodies bound to cells change shape and expose complement binding sites This triggers complement fixation and cell lysis Complement Fixation and Activation Complement activation: Enhances the inflammatory response Uses a positive feedback cycle to promote phagocytosis Enlists more and more defensive elements 50
51 Other Mechanisms of Antibody Action Neutralization antibodies bind to and block specific sites on viruses or exotoxins, thus preventing these antigens from binding to receptors on tissue cells Other Mechanisms of Antibody Action Agglutination antibodies bind the same determinant on more than one antigen Makes antigen-antibody complexes that are crosslinked into large lattices Cell-bound antigens are cross-linked, causing clumping (agglutination) Precipitation soluble molecules are crosslinked into large insoluble complexes 51
52 Mechanisms of Antibody Action Figure Monoclonal Antibodies Commercially prepared antibodies are used: To provide passive immunity In research, clinical testing, and cancer treatment Monoclonal antibodies are pure antibody preparations Specific for a single antigenic determinant Produced from descendents of a single cell 52
53 Monoclonal Antibodies Hybridomas cell hybrids made from a fusion of a tumor cell and a B cell Have desirable properties of both parent cells indefinite proliferation as well as the ability to produce a single type of antibody Cell-Mediated Immune Response Since antibodies are useless against intracellular antigens, cell-mediated immunity is needed Two major populations of T cells mediate cellular immunity: CD4 cells (T4 cells) are primarily helper T cells (T H ) CD8 cells (T8 cells) are cytotoxic T cells (T C ) that destroy cells harboring foreign antigens 53
54 Cell-Mediated Immune Response Other types of T cells are: Suppressor T cells (T S ) Memory T cells Major Types of T Cells Figure
55 Importance of Humoral Response Soluble antibodies The simplest ammunition of the immune response Interact in extracellular environments such as body secretions, tissue fluid, blood, and lymph Importance of Cellular Response T cells recognize and respond only to processed fragments of antigen displayed on the surface of body cells T cells are best suited for cell-to-cell interactions, and target: Cells infected with viruses, bacteria, a, or intracellular parasites Abnormal or cancerous cells Cells of infused or transplanted foreign tissue 55
56 Antigen Recognition and MHC Restriction Immunocompetent T cells are activated when the V regions of their surface receptors bind to a recognized antigen T cells must simultaneously l recognize: Nonself (the antigen) Self (a MHC protein of a body cell) MHC Proteins Both types of MHC proteins are important to T cell activation Class I MHC proteins Always recognized by CD8 T cells Display peptides from endogenous antigens 56
57 Class I MHC Proteins Endogenous antigens are: Degraded by proteases and enter the endoplasmic reticulum Transported via TAP (transporter associated with antigen processing) Loaded d onto class I MHC molecules l Displayed on the cell surface in association with a class I MHC molecule Extracellular fluid Plasma membrane Class I MHC Proteins of a tissue cell Class I MHC Antigenic peptide 4 Endoplasmic reticulum (ER) Cytoplasm of virus-invaded cell (a) Loaded MHC protein migrates to the plasma membrane, where it displays the antigenic peptide Class I MHC TAP 2 Endogenous antigen peptides enter ER via TAP 3 Endogenous antigen peptide loaded onto class I MHC Endogenous antigen (viral protein) 1 Endogenous antigen degraded by protease Figure 21.16a 57
58 Class II MHC Proteins Class II MHC proteins are found only on mature B cells, some T cells, and antigenpresenting cells A phagosome containing pathogens (with exogenous antigens) merges with a lysosome Invariant protein prevents class II MHC proteins from binding to peptides in the endoplasmic reticulum Class II MHC Proteins Class II MHC proteins migrate into the phagosomes where the antigen is degraded and the invariant chain is removed for peptide loading Loaded Class II MHC molecules then migrate to the cell membrane and display antigenic i peptide for recognition by CD4 cells 58
59 Extracellular fluid 1 Extracellular antigen Antigenic peptide (bacterium) phagocytized Plasma Class II MHC Proteins membrane of an APC 2 Lysosome merges with phagosome, forming a phagolysosome; antigen degraded (b) Cytoplasm of APC 4 Loaded MHC protein migrates to the plasma membrane 3 After synthesis at the ER, the class II MHC protein migrates in a vesicle, which fuses with the phagolysosome; invariant chain removed, antigen loaded Invariant chain prevents class II MHC binding to peptides in the ER Endoplasmic reticulum (ER) Figure 21.16b Antigen Recognition Provides the key for the immune system to recognize the presence of intracellular microorganisms MHC proteins are ignored by T cells if they are complexed with self protein fragments 59
60 Antigen Recognition If MHC proteins are complexed with endogenous or exogenous antigenic peptides, they: Indicate the presence of intracellular infectious microorganisms At Act as antigen hld holders Form the self part of the self-antiself complexes recognized by T cells T Cell Activation: Step One Antigen Binding T cell antigen receptors (TCRs): Bind to an antigen-mhc protein complex Have variable and constant regions consisting of two chains (alpha and beta) 60
61 T Cell Activation: Step One Antigen Binding MHC restriction T H and T C bind to different classes of MHC proteins T H cells bind to antigen linked to class II MHC proteins Mobile APCs (Langerhans cells) quickly alert the body to the presence of antigen by migrating to the lymph nodes and presenting antigen T C cells are activated by antigen fragments T Cell Activation: Step One Antigen complexed with class I MHC proteins Binding APCs produce co-stimulatory molecules that are required for T C activation TCR that acts to recognize the self-antiself complex is linked to multiple intracellular signaling pathways Other T cell surface proteins are involved in antigen binding (e.g., CD4 and CD8 help maintain coupling during antigen recognition) 61
62 T Cell Activation: Step One Antigen Binding Figure Before a T cell can undergo clonal expansion, it T Cell Activation: Step Two Costimulation signals This recognition may require binding to other must recognize one or more co-stimulatory surface receptors on an APC Macrophages produce surface B7 proteins when nonspecific defenses are mobilized B7 binding with the CD 28 receptor on the surface of T cells is a crucial co-stimulatory signal Other co-stimulatory signals include cytokines and interleukin 1 and 2 62
63 T Cell Activation: Step Two Costimulation Depending on receptor type, co-stimulators can cause T cells to complete their activation or abort activation Without co-stimulation, T cells: Become tolerant to that antigen Are unable to divide Do not secrete cytokines T Cell Activation: Step Two Costimulation T cells that are activated: Enlarge, proliferate, and form clones Differentiate and perform functions according to their T cell class 63
64 T Cell Activation: Step Two Costimulation Primary T cell response peaks within a week after signal exposure T cells then undergo apoptosis between days 7 and 30 Effector activity wanes as the amount of antigen declines The disposal of activated effector cells is a protective mechanism for the body Memory T cells remain and mediate secondary responses to the same antigen Cytokines Mediators involved in cellular immunity, including hormonelike glycoproteins released by activated T cells and macrophages Some are co-stimulators of T cells and T cell proliferation Interleukin 1 (IL-1) released by macrophages co- stimulates bound T cells to: Release interleukin 2 (IL-2) Synthesize more IL-2 receptors 64
65 Cytokines IL-2 is a key growth factor, which sets up a positive feedback cycle that encourages activated T cells to divide It is used therapeutically to enhance the body s defenses against cancer Other cytokines amplify and regulate immune and nonspecific responses Cytokines Examples include: Perforin and lymphotoxin cell toxins Gamma interferon enhances the killing power of macrophages Inflammatory factors 65
66 Helper T Cells (T H ) Regulatory cells that play a central role in the immune response Once primed by APC presentation of antigen, they: Chemically or directly stimulate proliferation of other T cells Stimulate B cells that have already become bound to antigen Without T H, there is no immune response Helper T Cells (TH) Figure 21.18a 66
67 T H cells interact directly with B cells that have Helper antigen fragments T Cell on their surfaces bound to MHC II receptors T H cells stimulate B cells to divide id more rapidly and begin antibody formation B cells may be activated without T H cells by binding to T cell independent antigens Most antigens, however, require T H costimulation to activate B cells Cytokines released by T H amplify nonspecific defenses Helper T Cells Figure 21.18b 67
68 Cytotoxic T Cell (T c ) T C cells, or killer T cells, are the only T cells that can directly attack and kill other cells They circulate throughout the body in search of body cells that display the antigen to which they have been sensitized Their targets include: Virus-infected i cells Cells with intracellular bacteria or parasites Cancer cells Foreign cells from blood transfusions or transplants Cytotoxic T Cells Bind to self-antiself complexes on all body cells Infected or abnormal cells can be destroyed as long as appropriate antigen and co-stimulatory stimuli (e.g., IL-2) are present Natural killer cells activate their killing machinery when they bind to MICA receptor MICA receptor MHC-related cell surface protein in cancer cells, virus-infected cells, and cells of transplanted organs 68
69 2/26/2009 In some cases, TC cells: Bind to the target release perforin into its Mechanisms ofcelltcand Action membrane x IIn the th presence off C Ca2+ perforin f i causes cell ll llysis i b by creating transmembrane pores Other TC cells induce cell death by: Secreting lymphotoxin, which fragments the target cell s DNA Secreting gamma interferon, which stimulates phagocytosis by macrophages Mechanisms of Tc Action Figure 21.19a 69
70 Other T Cells Suppressor T cells (T S ) regulatory cells that release cytokines, which suppress the activity of both T cells and B cells Gamma delta T cells (T gd ) 10% of all T cells found in the intestines that are triggered by binding to MICA receptors Figure
71 Organ Transplants The four major types of grafts are: Autografts graft transplanted from one site on the body to another in the same person Isografts grafts between identical twins Allografts transplants between individuals that are not identical twins, but belong to same species Xenografts grafts taken from another animal species Prevention of Rejection Prevention of tissue rejection is accomplished by using immunosuppressive drugs However, these drugs depress patient s immune system so it cannot fight off foreign agents 71
72 Immunodeficiencies Congenital and acquired conditions in which the function or production of immune cells, phagocytes, or complement is abnormal SCID severe combined immunodeficiency (SCID) syndromes; genetic defects that produce: A marked deficit in B and T cells Abnormalities in interleukin receptors Defective adenosine deaminase (ADA) enzyme Metabolites lethal to T cells accumulate SCID is fatal if untreated; treatment is with bone marrow transplants Acquired Immunodeficiencies Hodgkin s disease cancer of the lymph nodes leads to immunodeficiency by depressing lymph node cells Acquired immune deficiency syndrome (AIDS) cripples the immune system by interfering with the activity of helper T (CD4) cells Characterized by severe weight loss, night sweats, and swollen lymph nodes Opportunistic infections occur, including pneumocystis pneumonia and Kaposi s sarcoma 72
73 AIDS Caused by human immunodeficiency virus (HIV) transmitted via body fluids blood, semen, and vaginal secretions HIV enters the body via: Blood transfusions Contaminated needles Intimate sexual contact, including oral sex HIV: Destroys T H cells Depresses cell-mediated immunity AIDS HIV multiplies in lymph nodes throughout the asymptomatic period Symptoms appear in a few months to 10 years Attachment HIV s coat protein (gp120) attaches to the CD4 receptor A nearby protein (gp41) fuses the virus to the target cell 73
74 AIDS HIV enters the cell and uses reverse transcriptase to produce DNA from viral RNA This DNA (provirus) directs the host cell to make viral RNA (and proteins), enabling the virus to reproduce and infect other cells AIDS HIV reverse transcriptase is not accurate and produces frequent transcription errors This high mutation rate causes resistance to drugs Treatments include: Reverse transcriptase inhibitors (AZT) Protease inhibitors (saquinavir and ritonavir) New drugs currently being developed that block HIV s entry to helper T cells 74
75 Autoimmune Diseases Loss of the immune system s ability to distinguish self from nonself The body produces autoantibodies and sensitized T C cells that destroy its own tissues Examples include multiple sclerosis, myasthenia gravis, Graves disease, Type I (juvenile) diabetes mellitus, systemic lupus erythematosus (SLE), glomerulonephritis, and rheumatoid arthritis Mechanisms of Autoimmune Diseases Ineffective lymphocyte programming selfreactive T and B cells that should have been eliminated in the thymus and bone marrow escape into the circulation New self-antigens appear, generated by: Gene mutations that cause new proteins to appear Changes in self-antigens by hapten attachment or as a result of infectious damage 75
76 Mechanisms of Autoimmune Diseases If the determinants on foreign antigens resemble self-antigens: Antibodies made against foreign antigens crossreact with self-antigens Hypersensitivity Immune responses that cause tissue damage Different types of hypersensitivity reactions are distinguished by: Their time course Whether antibodies or T cells are the principle immune elements involved Antibody-mediated allergies are immediate and subacute hypersensitivities The most important cell-mediated allergic condition is delayed hypersensitivity 76
77 Immediate Hypersensitivity Acute (type I) hypersensitivities begin in seconds after contact with allergen Anaphylaxis initial allergen contact is asymptomatic but sensitizes the person Subsequent exposures to allergen cause: Release of histamine and inflammatory chemicals Systemic or local responses Immediate Hypersensitivity The mechanism involves IL-4 secreted by T cells IL-4 stimulates B cells to produce IgE IgE binds to mast cells and basophils causing them to degranulate, resulting in a flood of histamine release and inducing the inflammatory response 77
78 Subsequent (secondary) responses 4 More of same antigen invades body. 5 Antigen combines with IgE attached to mast cells (and basophils), which triggers degranulation and release of histamine (and other chemicals). Antigen Mast cell granules release contents after antigen binds with IgE antibodies Histamine 6 Histamine causes blood vessels to dilate and become leaky, which promotes edema; stimulates secretion of large amounts of mucus; and causes smooth muscles to contract (if respiratory system is site of antigen entry, asthma may ensue). Outpouring of fluid from capillaries Release of mucus Constriction of small respiratory passages (bronchioles) Figure Sensitization stage 1 Antigen (allergen) invades body. 2 Plasma cells produce large amounts of class IgE antibodies against allergen. 3 IgE antibodies attach to mast cells in body tissues (and to circulating basophils). Mast cell with fixed IgE antibodies IgE Granules containing histamine Subsequent (secondary) responses 4 More of same antigen invades body. 5Antigen combines with IgE attached to mast cells (and basophils), which triggers degranulation and release of histamine (and other chemicals). Antigen Mast cell granules release contents after antigen binds with IgE antibodies Histamine 6 Histamine causes blood vessels to dilate and become leaky, which promotes edema; stimulates secretion of large amounts of mucus; and causes smooth muscles to contract (if respiratory system is site of antigen entry, asthma may ensue). Outpouring of fluid from capillaries Release of mucus Constriction of small respiratory passages (bronchioles) Figure
79 Anaphylaxis Reactions include runny nose, itching reddened skin, and watery eyes If allergen is inhaled, asthmatic symptoms appear constriction of bronchioles and restricted airflow If allergen is ingested, cramping, vomiting, or diarrhea occur Antihistamines counteract these effects Anaphylactic Shock Response to allergen that directly enters the blood (e.g., insect bite, injection) Basophils and mast cells are enlisted throughout the body Systemic histamine releases may result in: Constriction of bronchioles Sudden vasodilation and fluid loss from the bloodstream Hypotensive shock and death Treatment epinephrine is the drug of choice 79
80 Subacute Hypersensitivities Caused by IgM and IgG, and transferred via blood plasma or serum Onset is slow (1 3 hours) after antigen exposure Duration is long lasting (10 15 hours) Cytotoxic (type II) reactions Antibodies bind to antigens on specific body cells, stimulating phagocytosis and complementmediated lysis of the cellular antigens Example: mismatched blood transfusion reaction Subacute Hypersensitivities Immune complex (type III) hypersensitivity Antigens are widely distributed through the body or blood Insoluble antigen-antibody complexes form Complexes cannot be cleared from a particular area of the body Intense inflammation, local cell lysis, and death may result Example: systemic lupus erythematosus (SLE) 80
81 Delayed Hypersensitivities (Type IV) Onset is slow (1 3 days) Mediated by mechanisms involving delayed hypersensitivity T cells and cytotoxic T cells Cytokines from activated T C are the mediators of the inflammatory response Antihistamines are ineffective and corticosteroid drugs are used to provide relief Delayed Hypersensitivities (Type IV) Example: allergic contact dermatitis (e.g., poison ivy) Involved in protective reactions against viruses, bacteria, fungi, protozoa, cancer, and rejection of foreign grafts or transplants 81
82 Developmental Aspects Immune system stem cells develop in the liver and spleen by the ninth week Later, bone marrow becomes the primary source of stem cells Lymphocyte development continues in the bone marrow and thymus system begins to wane Developmental Aspects T H 2 lymphocytes predominate in the newborn, and the T H 1 system is educated as the person encounters antigens The immune system is impaired by stress and depression With age, the immune system begins to wane 82
83 Immune Diseases or Conditions Wiskott-Aldrich Syndrome Guillain-Barre Syndrome ADA SCID Autoimmune lymphoprolifer ative syndrome celiac disease aplastic anemia psoriasis HIGM rabies systemic lupus erythemtosus elephantiasis leprosy arthritis anaphylaxis arteritis Crohn's disease allergic asthma Lyme Disease malaria mononucleosis MCL IFN-γ receptor deficiency conjunctivitis Trypanosomiasis scleroderma Graves Disease 83
The Immune System: Innate and Adaptive Body Defenses Outline PART 1: INNATE DEFENSES 21.1 Surface barriers act as the first line of defense to keep
 The Immune System: Innate and Adaptive Body Defenses Outline PART 1: INNATE DEFENSES 21.1 Surface barriers act as the first line of defense to keep invaders out of the body (pp. 772 773; Fig. 21.1; Table
The Immune System: Innate and Adaptive Body Defenses Outline PART 1: INNATE DEFENSES 21.1 Surface barriers act as the first line of defense to keep invaders out of the body (pp. 772 773; Fig. 21.1; Table
The Lymphatic System and Body Defenses
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Lymphatic System and Body Defenses 12PART B Adaptive Defense System: Third Line of Defense Immune
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Lymphatic System and Body Defenses 12PART B Adaptive Defense System: Third Line of Defense Immune
Disease causing organisms Resistance Immunity
 Part 1 Disease causing organisms Resistance Immunity Bacteria Most common pathogens Anthrax Cholera Staphylococcus epidermidis bacteria Bacterial diseases Tuberculosis Cholera Bubonic Plague Tetanus Effects
Part 1 Disease causing organisms Resistance Immunity Bacteria Most common pathogens Anthrax Cholera Staphylococcus epidermidis bacteria Bacterial diseases Tuberculosis Cholera Bubonic Plague Tetanus Effects
Body Defense Mechanisms
 BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 13 Body Defense Mechanisms Lecture Presentation Anne Gasc Hawaii Pacific University and University of
BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 13 Body Defense Mechanisms Lecture Presentation Anne Gasc Hawaii Pacific University and University of
Chapter 21: Innate and Adaptive Body Defenses
 Chapter 21: Innate and Adaptive Body Defenses I. 2 main types of body defenses A. Innate (nonspecific) defense: not to a specific microorganism or substance B. Adaptive (specific) defense: immunity to
Chapter 21: Innate and Adaptive Body Defenses I. 2 main types of body defenses A. Innate (nonspecific) defense: not to a specific microorganism or substance B. Adaptive (specific) defense: immunity to
Blood and Immune system Acquired Immunity
 Blood and Immune system Acquired Immunity Immunity Acquired (Adaptive) Immunity Defensive mechanisms include : 1) Innate immunity (Natural or Non specific) 2) Acquired immunity (Adaptive or Specific) Cell-mediated
Blood and Immune system Acquired Immunity Immunity Acquired (Adaptive) Immunity Defensive mechanisms include : 1) Innate immunity (Natural or Non specific) 2) Acquired immunity (Adaptive or Specific) Cell-mediated
Chapter 21 The Immune System: Innate and Adaptive Body Defenses
 Chapter 21 The Immune System: Innate and Adaptive Body Defenses 1/25/2016 1 Annie Leibovitz/Contact Press Images The Immune System Immune system provides resistance to disease Made up of two intrinsic
Chapter 21 The Immune System: Innate and Adaptive Body Defenses 1/25/2016 1 Annie Leibovitz/Contact Press Images The Immune System Immune system provides resistance to disease Made up of two intrinsic
All animals have innate immunity, a defense active immediately upon infection Vertebrates also have adaptive immunity
 1 2 3 4 5 6 7 8 9 The Immune System All animals have innate immunity, a defense active immediately upon infection Vertebrates also have adaptive immunity Figure 43.2 In innate immunity, recognition and
1 2 3 4 5 6 7 8 9 The Immune System All animals have innate immunity, a defense active immediately upon infection Vertebrates also have adaptive immunity Figure 43.2 In innate immunity, recognition and
Overview of the Lymphoid System
 Overview of the Lymphoid System The Lymphoid System Protects us against disease Lymphoid system cells respond to Environmental pathogens Toxins Abnormal body cells, such as cancers Overview of the Lymphoid
Overview of the Lymphoid System The Lymphoid System Protects us against disease Lymphoid system cells respond to Environmental pathogens Toxins Abnormal body cells, such as cancers Overview of the Lymphoid
NOTES: CH 43, part 2 Immunity; Immune Disruptions ( )
 NOTES: CH 43, part 2 Immunity; Immune Disruptions (43.3-43.4) Activated B & T Lymphocytes produce: CELL-MEDIATED IMMUNE RESPONSE: involves specialized T cells destroying infected host cells HUMORAL IMMUNE
NOTES: CH 43, part 2 Immunity; Immune Disruptions (43.3-43.4) Activated B & T Lymphocytes produce: CELL-MEDIATED IMMUNE RESPONSE: involves specialized T cells destroying infected host cells HUMORAL IMMUNE
Internal Defense Notes
 Internal environment of animals provides attractive area for growth of bacteria, viruses, fungi Harm via: 1. destruction of cells 2. production of toxic chemicals To protect against foreign invaders, humans
Internal environment of animals provides attractive area for growth of bacteria, viruses, fungi Harm via: 1. destruction of cells 2. production of toxic chemicals To protect against foreign invaders, humans
Third line of Defense
 Chapter 15 Specific Immunity and Immunization Topics -3 rd of Defense - B cells - T cells - Specific Immunities Third line of Defense Specific immunity is a complex interaction of immune cells (leukocytes)
Chapter 15 Specific Immunity and Immunization Topics -3 rd of Defense - B cells - T cells - Specific Immunities Third line of Defense Specific immunity is a complex interaction of immune cells (leukocytes)
Adaptive Immunity: Specific Defenses of the Host
 17 Adaptive Immunity: Specific Defenses of the Host SLOs Differentiate between innate and adaptive immunity, and humoral and cellular immunity. Define antigen, epitope, and hapten. Explain the function
17 Adaptive Immunity: Specific Defenses of the Host SLOs Differentiate between innate and adaptive immunity, and humoral and cellular immunity. Define antigen, epitope, and hapten. Explain the function
Immune System AP SBI4UP
 Immune System AP SBI4UP TYPES OF IMMUNITY INNATE IMMUNITY ACQUIRED IMMUNITY EXTERNAL DEFENCES INTERNAL DEFENCES HUMORAL RESPONSE Skin Phagocytic Cells CELL- MEDIATED RESPONSE Mucus layer Antimicrobial
Immune System AP SBI4UP TYPES OF IMMUNITY INNATE IMMUNITY ACQUIRED IMMUNITY EXTERNAL DEFENCES INTERNAL DEFENCES HUMORAL RESPONSE Skin Phagocytic Cells CELL- MEDIATED RESPONSE Mucus layer Antimicrobial
The Immune System. These are classified as the Innate and Adaptive Immune Responses. Innate Immunity
 The Immune System Biological mechanisms that defend an organism must be 1. triggered by a stimulus upon injury or pathogen attack 2. able to counteract the injury or invasion 3. able to recognise foreign
The Immune System Biological mechanisms that defend an organism must be 1. triggered by a stimulus upon injury or pathogen attack 2. able to counteract the injury or invasion 3. able to recognise foreign
Chapter 13 Lymphatic and Immune Systems
 The Chapter 13 Lymphatic and Immune Systems 1 The Lymphatic Vessels Lymphoid Organs Three functions contribute to homeostasis 1. Return excess tissue fluid to the bloodstream 2. Help defend the body against
The Chapter 13 Lymphatic and Immune Systems 1 The Lymphatic Vessels Lymphoid Organs Three functions contribute to homeostasis 1. Return excess tissue fluid to the bloodstream 2. Help defend the body against
Unit 12: The Lymphatic System and Body Defenses
 Unit 12: The Lymphatic System and Body Defenses I. The Lymphatic System A. Consists of two semi-independent parts 1. Lymphatic vessels 2. Lymphoid tissues and organs B. Lymphatic system functions 1. Transports
Unit 12: The Lymphatic System and Body Defenses I. The Lymphatic System A. Consists of two semi-independent parts 1. Lymphatic vessels 2. Lymphoid tissues and organs B. Lymphatic system functions 1. Transports
Immune system. Aims. Immune system. Lymphatic organs. Inflammation. Natural immune system. Adaptive immune system
 Aims Immune system Lymphatic organs Inflammation Natural immune system Adaptive immune system Major histocompatibility complex (MHC) Disorders of the immune system 1 2 Immune system Lymphoid organs Immune
Aims Immune system Lymphatic organs Inflammation Natural immune system Adaptive immune system Major histocompatibility complex (MHC) Disorders of the immune system 1 2 Immune system Lymphoid organs Immune
Chapter 23 Immunity Exam Study Questions
 Chapter 23 Immunity Exam Study Questions 1. Define 1) Immunity 2) Neutrophils 3) Macrophage 4) Epitopes 5) Interferon 6) Complement system 7) Histamine 8) Mast cells 9) Antigen 10) Antigens receptors 11)
Chapter 23 Immunity Exam Study Questions 1. Define 1) Immunity 2) Neutrophils 3) Macrophage 4) Epitopes 5) Interferon 6) Complement system 7) Histamine 8) Mast cells 9) Antigen 10) Antigens receptors 11)
Topics in Parasitology BLY Vertebrate Immune System
 Topics in Parasitology BLY 533-2008 Vertebrate Immune System V. Vertebrate Immune System A. Non-specific defenses against pathogens 1. Skin - physical barrier a. Tough armor protein KERATIN b. Surface
Topics in Parasitology BLY 533-2008 Vertebrate Immune System V. Vertebrate Immune System A. Non-specific defenses against pathogens 1. Skin - physical barrier a. Tough armor protein KERATIN b. Surface
General Biology. A summary of innate and acquired immunity. 11. The Immune System. Repetition. The Lymphatic System. Course No: BNG2003 Credits: 3.
 A summary of innate and acquired immunity General iology INNATE IMMUNITY Rapid responses to a broad range of microbes Course No: NG00 Credits:.00 External defenses Invading microbes (pathogens). The Immune
A summary of innate and acquired immunity General iology INNATE IMMUNITY Rapid responses to a broad range of microbes Course No: NG00 Credits:.00 External defenses Invading microbes (pathogens). The Immune
Unit 12 - The Lymphatic System and 1
 Unit 12 - The Lymphatic System and 1 I. Unit 12: The Lymphatic System and Body Defenses A. The Lymphatic System 1. Consists of two semi-independent parts a) Lymphatic vessels b) Lymphoid tissues and organs
Unit 12 - The Lymphatic System and 1 I. Unit 12: The Lymphatic System and Body Defenses A. The Lymphatic System 1. Consists of two semi-independent parts a) Lymphatic vessels b) Lymphoid tissues and organs
Chapter 24 The Immune System
 Chapter 24 The Immune System The Immune System Layered defense system The skin and chemical barriers The innate and adaptive immune systems Immunity The body s ability to recognize and destroy specific
Chapter 24 The Immune System The Immune System Layered defense system The skin and chemical barriers The innate and adaptive immune systems Immunity The body s ability to recognize and destroy specific
I. Lines of Defense Pathogen: Table 1: Types of Immune Mechanisms. Table 2: Innate Immunity: First Lines of Defense
 I. Lines of Defense Pathogen: Table 1: Types of Immune Mechanisms Table 2: Innate Immunity: First Lines of Defense Innate Immunity involves nonspecific physical & chemical barriers that are adapted for
I. Lines of Defense Pathogen: Table 1: Types of Immune Mechanisms Table 2: Innate Immunity: First Lines of Defense Innate Immunity involves nonspecific physical & chemical barriers that are adapted for
Third line of Defense. Topic 8 Specific Immunity (adaptive) (18) 3 rd Line = Prophylaxis via Immunization!
 Topic 8 Specific Immunity (adaptive) (18) Topics - 3 rd Line of Defense - B cells - T cells - Specific Immunities 1 3 rd Line = Prophylaxis via Immunization! (a) A painting of Edward Jenner depicts a cow
Topic 8 Specific Immunity (adaptive) (18) Topics - 3 rd Line of Defense - B cells - T cells - Specific Immunities 1 3 rd Line = Prophylaxis via Immunization! (a) A painting of Edward Jenner depicts a cow
Diseases-causing agents, pathogens, can produce infections within the body.
 BIO 212: ANATOMY & PHYSIOLOGY II 1 CHAPTER 16 Lecture: Dr. Lawrence G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. LYMPHATIC and IMMUNE Systems Body Defenses Against
BIO 212: ANATOMY & PHYSIOLOGY II 1 CHAPTER 16 Lecture: Dr. Lawrence G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. LYMPHATIC and IMMUNE Systems Body Defenses Against
Chapter 43. Immune System. phagocytosis. lymphocytes. AP Biology
 Chapter 43. Immune System phagocytosis lymphocytes 1 Why an immune system? Attack from outside lots of organisms want you for lunch! animals must defend themselves against unwelcome invaders viruses protists
Chapter 43. Immune System phagocytosis lymphocytes 1 Why an immune system? Attack from outside lots of organisms want you for lunch! animals must defend themselves against unwelcome invaders viruses protists
Physiology Unit 3. ADAPTIVE IMMUNITY The Specific Immune Response
 Physiology Unit 3 ADAPTIVE IMMUNITY The Specific Immune Response In Physiology Today The Adaptive Arm of the Immune System Specific Immune Response Internal defense against a specific pathogen Acquired
Physiology Unit 3 ADAPTIVE IMMUNITY The Specific Immune Response In Physiology Today The Adaptive Arm of the Immune System Specific Immune Response Internal defense against a specific pathogen Acquired
Medical Virology Immunology. Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University
 Medical Virology Immunology Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University Human blood cells Phases of immune responses Microbe Naïve
Medical Virology Immunology Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University Human blood cells Phases of immune responses Microbe Naïve
CELL BIOLOGY - CLUTCH CH THE IMMUNE SYSTEM.
 !! www.clutchprep.com CONCEPT: OVERVIEW OF HOST DEFENSES The human body contains three lines of against infectious agents (pathogens) 1. Mechanical and chemical boundaries (part of the innate immune system)
!! www.clutchprep.com CONCEPT: OVERVIEW OF HOST DEFENSES The human body contains three lines of against infectious agents (pathogens) 1. Mechanical and chemical boundaries (part of the innate immune system)
The Immune System All animals have innate immunity, a defense active immediately
 The Immune System All animals have innate immunity, a defense active immediately upon infection Vertebrates also have adaptive immunity Figure 43.2 INNATE IMMUNITY (all animals) Recognition of traits shared
The Immune System All animals have innate immunity, a defense active immediately upon infection Vertebrates also have adaptive immunity Figure 43.2 INNATE IMMUNITY (all animals) Recognition of traits shared
immunity produced by an encounter with an antigen; provides immunologic memory. active immunity clumping of (foreign) cells; induced by crosslinking
 active immunity agglutination allografts immunity produced by an encounter with an antigen; provides immunologic memory. clumping of (foreign) cells; induced by crosslinking of antigenantibody complexes.
active immunity agglutination allografts immunity produced by an encounter with an antigen; provides immunologic memory. clumping of (foreign) cells; induced by crosslinking of antigenantibody complexes.
Immune System Notes Innate immunity Acquired immunity lymphocytes, humoral response Skin lysozyme, mucus membrane
 Immune System Notes I. The immune system consists of innate and acquired immunity. A. An animal must defend itself against unwelcome intruders the many potentially dangerous viruses, bacteria, and other
Immune System Notes I. The immune system consists of innate and acquired immunity. A. An animal must defend itself against unwelcome intruders the many potentially dangerous viruses, bacteria, and other
4/28/2016. Host Defenses. Unit 8 Microorganisms & The Immune System. Types of Innate Defenses. Defensive Cells Leukocytes
 Host Defenses Unit 8 Microorganisms & The Immune System CH 16-18 Host defenses that produce resistance can be either innate or adaptive: Innate: those that protect against any type of invading agent Adaptive:
Host Defenses Unit 8 Microorganisms & The Immune System CH 16-18 Host defenses that produce resistance can be either innate or adaptive: Innate: those that protect against any type of invading agent Adaptive:
(b) fluid returns to venous end of capillary due to hydrostatic pressure and osmotic pressure
 (Slide 1) Lecture Notes: Lymphatic System and Immunity (Body Defenses) I. (Slide 2) Introduction A) General 1) Lymphatic System performs 2 basic functions: 2) Organs of the Lymphatic System (a) lymphatic
(Slide 1) Lecture Notes: Lymphatic System and Immunity (Body Defenses) I. (Slide 2) Introduction A) General 1) Lymphatic System performs 2 basic functions: 2) Organs of the Lymphatic System (a) lymphatic
What are bacteria? Microbes are microscopic(bacteria, viruses, prions, & some fungi etc.) How do the sizes of our cells, bacteria and viruses compare?
 7.1 Microbes, pathogens and you Chp. 7 Lymphatic System & Immunity The interaction between microbes and humans? Microbes are very abundant in the environment and as well as in and on our bodies GOOD: We
7.1 Microbes, pathogens and you Chp. 7 Lymphatic System & Immunity The interaction between microbes and humans? Microbes are very abundant in the environment and as well as in and on our bodies GOOD: We
11/25/2017. THE IMMUNE SYSTEM Chapter 43 IMMUNITY INNATE IMMUNITY EXAMPLE IN INSECTS BARRIER DEFENSES INNATE IMMUNITY OF VERTEBRATES
 THE IMMUNE SYSTEM Chapter 43 IMMUNITY INNATE IMMUNITY EXAMPLE IN INSECTS Exoskeleton made of chitin forms the first barrier to pathogens Digestive system is protected by a chitin-based barrier and lysozyme,
THE IMMUNE SYSTEM Chapter 43 IMMUNITY INNATE IMMUNITY EXAMPLE IN INSECTS Exoskeleton made of chitin forms the first barrier to pathogens Digestive system is protected by a chitin-based barrier and lysozyme,
INNATE IMMUNITY Non-Specific Immune Response. Physiology Unit 3
 INNATE IMMUNITY Non-Specific Immune Response Physiology Unit 3 Protection Against Infection The body has several defenses to protect itself from getting an infection Skin Mucus membranes Serous membranes
INNATE IMMUNITY Non-Specific Immune Response Physiology Unit 3 Protection Against Infection The body has several defenses to protect itself from getting an infection Skin Mucus membranes Serous membranes
I. Defense Mechanisms Chapter 15
 10/24/11 I. Defense Mechanisms Chapter 15 Immune System Lecture PowerPoint Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Defense Mechanisms Protect against
10/24/11 I. Defense Mechanisms Chapter 15 Immune System Lecture PowerPoint Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Defense Mechanisms Protect against
Campbell's Biology: Concepts and Connections, 7e (Reece et al.) Chapter 24 The Immune System Multiple-Choice Questions
 Campbell's Biology: Concepts and Connections, 7e (Reece et al.) Chapter 24 The Immune System 24.1 Multiple-Choice Questions 1) The body's innate defenses against infection include A) several nonspecific
Campbell's Biology: Concepts and Connections, 7e (Reece et al.) Chapter 24 The Immune System 24.1 Multiple-Choice Questions 1) The body's innate defenses against infection include A) several nonspecific
The Immune System. by Dr. Carmen Rexach Physiology Mt San Antonio College
 The Immune System by Dr. Carmen Rexach Physiology Mt San Antonio College What is the immune system? defense system found in vertebrates Two categories Nonspecific specific provides protection from pathogens
The Immune System by Dr. Carmen Rexach Physiology Mt San Antonio College What is the immune system? defense system found in vertebrates Two categories Nonspecific specific provides protection from pathogens
Defense mechanism against pathogens
 Defense mechanism against pathogens Immune System What is immune system? Cells and organs within an animal s body that contribute to immune defenses against pathogens ( ) Bacteria -Major entry points ;open
Defense mechanism against pathogens Immune System What is immune system? Cells and organs within an animal s body that contribute to immune defenses against pathogens ( ) Bacteria -Major entry points ;open
3/28/2012. Immune System. Activation of Innate Immunity. Innate (non-specific) Immunity
 Chapter 5 Outline Defense Mechansims Functions of B Lymphocytes Functions of T Lymphocytes Active and Passive Immunity Tumor Immunology Diseases Caused By Immune System Immune System Anatomy - Lymphoid
Chapter 5 Outline Defense Mechansims Functions of B Lymphocytes Functions of T Lymphocytes Active and Passive Immunity Tumor Immunology Diseases Caused By Immune System Immune System Anatomy - Lymphoid
Chapter 22: The Lymphatic System and Immunity
 Bio40C schedule Lecture Immune system Lab Quiz 2 this week; bring a scantron! Study guide on my website (see lab assignments) Extra credit Critical thinking questions at end of chapters 5 pts/chapter Due
Bio40C schedule Lecture Immune system Lab Quiz 2 this week; bring a scantron! Study guide on my website (see lab assignments) Extra credit Critical thinking questions at end of chapters 5 pts/chapter Due
1. Lymphatic vessels recover about of the fluid filtered by capillaries. A. ~1% C. ~25% E. ~85% B. ~10% D. ~50%
 BIOL2030 Huaman A&P II -- Exam 3 -- XXXX -- Form A Name: 1. Lymphatic vessels recover about of the fluid filtered by capillaries. A. ~1% C. ~25% E. ~85% B. ~10% D. ~50% 2. Special lymphatic vessels called
BIOL2030 Huaman A&P II -- Exam 3 -- XXXX -- Form A Name: 1. Lymphatic vessels recover about of the fluid filtered by capillaries. A. ~1% C. ~25% E. ~85% B. ~10% D. ~50% 2. Special lymphatic vessels called
Immune System. Biol 105 Chapter 13
 Immune System Biol 105 Chapter 13 Outline Immune System I. Function of the Immune system II. Barrier Defenses III. Nonspecific Defenses A. Immune system cells B. Inflammatory response C. Complementary
Immune System Biol 105 Chapter 13 Outline Immune System I. Function of the Immune system II. Barrier Defenses III. Nonspecific Defenses A. Immune system cells B. Inflammatory response C. Complementary
Overview. Barriers help animals defend against many dangerous pathogens they encounter.
 Immunity Overview Barriers help animals defend against many dangerous pathogens they encounter. The immune system recognizes foreign bodies and responds with the production of immune cells and proteins.
Immunity Overview Barriers help animals defend against many dangerous pathogens they encounter. The immune system recognizes foreign bodies and responds with the production of immune cells and proteins.
Chapters 20, 21. Lymphatic and Immune System. Overview. Specific Defenses 22/10/12. Part II. Specific Immunity BIOL242
 Chapters 20, 21. Lymphatic and Immune System Part II. Specific Immunity BIOL242 Overview Properties of specific immunity Antigen presentation and the MHC complexes T cell activation B cell activation Antibodies
Chapters 20, 21. Lymphatic and Immune System Part II. Specific Immunity BIOL242 Overview Properties of specific immunity Antigen presentation and the MHC complexes T cell activation B cell activation Antibodies
Chapter 12- The Lymphatic System and Body Defenses
 Chapter 12- The Lymphatic System and Body Defenses I. The Lymphatic System a. Consists of two semi-independent parts i. Lymphatic vessels and Lymphoid tissues and organs b. Lymphatic system functions i.
Chapter 12- The Lymphatic System and Body Defenses I. The Lymphatic System a. Consists of two semi-independent parts i. Lymphatic vessels and Lymphoid tissues and organs b. Lymphatic system functions i.
Chapter 38- Immune System
 Chapter 38- Immune System First Line of Defense: Barriers Nonspecific defenses, such as the skin and mucous membranes, are barriers to potential pathogens. In addition to being a physical barrier to pathogens,
Chapter 38- Immune System First Line of Defense: Barriers Nonspecific defenses, such as the skin and mucous membranes, are barriers to potential pathogens. In addition to being a physical barrier to pathogens,
Chapter 24 The Immune System
 Chapter 24 The Immune System PowerPoint Lectures for Biology: Concepts & Connections, Sixth Edition Campbell, Reece, Taylor, Simon, and Dickey Lecture by Edward J. Zalisko Introduction: The Kissing Disease?!?
Chapter 24 The Immune System PowerPoint Lectures for Biology: Concepts & Connections, Sixth Edition Campbell, Reece, Taylor, Simon, and Dickey Lecture by Edward J. Zalisko Introduction: The Kissing Disease?!?
Warm-up. Parts of the Immune system. Disease transmission. Disease transmission. Why an immune system? Chapter 43 3/9/2012.
 Warm-up Objective: Explain how antigens react with specific lymphocytes to induce immune response and immunological memory. Warm-up: Which of the following would normally contain blood with the least amount
Warm-up Objective: Explain how antigens react with specific lymphocytes to induce immune response and immunological memory. Warm-up: Which of the following would normally contain blood with the least amount
Immune System. Biol 105 Lecture 16 Chapter 13
 Immune System Biol 105 Lecture 16 Chapter 13 Outline Immune System I. Function of the Immune system II. Barrier Defenses III. Nonspecific Defenses A. Immune system cells B. Inflammatory response C. Complementary
Immune System Biol 105 Lecture 16 Chapter 13 Outline Immune System I. Function of the Immune system II. Barrier Defenses III. Nonspecific Defenses A. Immune system cells B. Inflammatory response C. Complementary
2014 Pearson Education, Inc. Exposure to pathogens naturally activates the immune system. Takes days to be effective Pearson Education, Inc.
 The innate immune interact with the adaptive immune system 1. Damage to skin causes bleeding = bradykinin activated, resulting in inflammation 2. Dendritic phagocytose pathogens Adaptive immunity 4. Dendritic
The innate immune interact with the adaptive immune system 1. Damage to skin causes bleeding = bradykinin activated, resulting in inflammation 2. Dendritic phagocytose pathogens Adaptive immunity 4. Dendritic
AP Biology. Why an immune system? Chapter 43. Immune System. Lines of defense. 1st: External defense. 2nd: Internal, broad range patrol
 Chapter 43. Immune System lymphocytes attacking cancer cell lymph phagocytic leukocyte Why an immune system? Attack from outside lots of organisms want you for lunch! animals must defend themselves against
Chapter 43. Immune System lymphocytes attacking cancer cell lymph phagocytic leukocyte Why an immune system? Attack from outside lots of organisms want you for lunch! animals must defend themselves against
Immunity. Chapter 38
 Immunity Chapter 38 Impacts, Issues Frankie s Last Wish Infection with a common, sexually transmitted virus (HPV) causes most cervical cancers including the one that killed Frankie McCullogh 38.1 Integrated
Immunity Chapter 38 Impacts, Issues Frankie s Last Wish Infection with a common, sexually transmitted virus (HPV) causes most cervical cancers including the one that killed Frankie McCullogh 38.1 Integrated
The Lymphatic System Dr. Gary Mumaugh
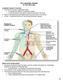 The Lymphatic System Dr. Gary Mumaugh Lymphatic System: Overview Consists of two semi-independent parts o A meandering network of lymphatic vessels o Lymphoid tissues and organs scattered throughout the
The Lymphatic System Dr. Gary Mumaugh Lymphatic System: Overview Consists of two semi-independent parts o A meandering network of lymphatic vessels o Lymphoid tissues and organs scattered throughout the
Unit 5 The Human Immune Response to Infection
 Unit 5 The Human Immune Response to Infection Unit 5-page 1 FOM Chapter 21 Resistance and the Immune System: Innate Immunity Preview: In Chapter 21, we will learn about the branch of the immune system
Unit 5 The Human Immune Response to Infection Unit 5-page 1 FOM Chapter 21 Resistance and the Immune System: Innate Immunity Preview: In Chapter 21, we will learn about the branch of the immune system
The Immune System is the Third Line of Defense Against Infection. Components of Human Immune System
 Chapter 17: Specific Host Defenses: The Immune Response The Immune Response Immunity: Free from burden. Ability of an organism to recognize and defend itself against specific pathogens or antigens. Immune
Chapter 17: Specific Host Defenses: The Immune Response The Immune Response Immunity: Free from burden. Ability of an organism to recognize and defend itself against specific pathogens or antigens. Immune
Outline. Animals: Immunity. Defenses Against Disease. Key Concepts:
 Animals: Immunity Defenses Against Disease Outline 1. Key concepts 2. Physical barriers: Skin, Mucus and HCL in stomach 3. Non-specific 4. Specific responses Immune System a. Components of Immune system
Animals: Immunity Defenses Against Disease Outline 1. Key concepts 2. Physical barriers: Skin, Mucus and HCL in stomach 3. Non-specific 4. Specific responses Immune System a. Components of Immune system
~ons~ecific Bod~ Defenses and Immunity
 ~ons~ecific Bod~ Defenses and Immunity The human body continually attempts to maintain homeostasis by counteracting harmful or disease-producing organisms called pathoqens or the toxins they produce. The
~ons~ecific Bod~ Defenses and Immunity The human body continually attempts to maintain homeostasis by counteracting harmful or disease-producing organisms called pathoqens or the toxins they produce. The
Essentials of Anatomy and Physiology, 9e (Marieb) Chapter 12 The Lymphatic System and Body Defenses. Short Answer. Figure 12.1
 Essentials of Anatomy and Physiology, 9e (Marieb) Chapter 12 The Lymphatic System and Body Defenses Short Answer Figure 12.1 Using Figure 12.1, identify the following: 1) A lymph capillary is indicated
Essentials of Anatomy and Physiology, 9e (Marieb) Chapter 12 The Lymphatic System and Body Defenses Short Answer Figure 12.1 Using Figure 12.1, identify the following: 1) A lymph capillary is indicated
CHAPTER-VII IMMUNOLOGY R.KAVITHA, M.PHARM, LECTURER, DEPARTMENT OF PHARMACEUTICS, SRM COLLEGE OF PHARMACY, SRM UNIVERSITY, KATTANKULATHUR.
 CHAPTER-VII IMMUNOLOGY R.KAVITHA, M.PHARM, LECTURER, DEPARTMENT OF PHARMACEUTICS, SRM COLLEGE OF PHARMACY, SRM UNIVERSITY, KATTANKULATHUR. The Immune Response Immunity: Free from burden. Ability of an
CHAPTER-VII IMMUNOLOGY R.KAVITHA, M.PHARM, LECTURER, DEPARTMENT OF PHARMACEUTICS, SRM COLLEGE OF PHARMACY, SRM UNIVERSITY, KATTANKULATHUR. The Immune Response Immunity: Free from burden. Ability of an
Immune System. Presented by Kazzandra Anton, Rhea Chung, Lea Sado, and Raymond Tanaka
 Immune System Presented by Kazzandra Anton, Rhea Chung, Lea Sado, and Raymond Tanaka Content Standards 35.1 In innate immunity, recognition and response rely on traits common to groups of pathogens 35.2
Immune System Presented by Kazzandra Anton, Rhea Chung, Lea Sado, and Raymond Tanaka Content Standards 35.1 In innate immunity, recognition and response rely on traits common to groups of pathogens 35.2
Immune System. Biology 105 Lecture 16 Chapter 13
 Immune System Biology 105 Lecture 16 Chapter 13 Outline: Immune System I. Functions of the immune system II. Barrier defenses III. Non-specific defenses A. Immune system cells B. Inflammatory response
Immune System Biology 105 Lecture 16 Chapter 13 Outline: Immune System I. Functions of the immune system II. Barrier defenses III. Non-specific defenses A. Immune system cells B. Inflammatory response
THE IMMUNE SYSTEM. There are specific defense mechanisms and nonspecific defense mechanisms also known as innate immune response.
 Chapter 43 THE IMMUNE SYSTEM Disease-causing microorganisms are called pathogens. They include bacteria, viruses, protozoans and fungi. Immunology is the study of specific defense mechanisms. Two major
Chapter 43 THE IMMUNE SYSTEM Disease-causing microorganisms are called pathogens. They include bacteria, viruses, protozoans and fungi. Immunology is the study of specific defense mechanisms. Two major
Chapter 17B: Adaptive Immunity Part II
 Chapter 17B: Adaptive Immunity Part II 1. Cell-Mediated Immune Response 2. Humoral Immune Response 3. Antibodies 1. The Cell-Mediated Immune Response Basic Steps of Cell-Mediated IR 1 2a CD4 + MHC cl.
Chapter 17B: Adaptive Immunity Part II 1. Cell-Mediated Immune Response 2. Humoral Immune Response 3. Antibodies 1. The Cell-Mediated Immune Response Basic Steps of Cell-Mediated IR 1 2a CD4 + MHC cl.
Lymphatic System. Where s your immunity idol?
 Lymphatic System Where s your immunity idol? Functions of the Lymphatic System Fluid Balance Drains excess fluid from tissues Lymph contains solutes from plasma Fat Absorption Lymphatic system absorbs
Lymphatic System Where s your immunity idol? Functions of the Lymphatic System Fluid Balance Drains excess fluid from tissues Lymph contains solutes from plasma Fat Absorption Lymphatic system absorbs
Immunology. Lecture- 8
 Immunology Lecture- 8 Immunological Disorders Immunodeficiency Autoimmune Disease Hypersensitivities Immunodeficiency 1. Immunodeficiency --> abnormal production or function of immune cells, phagocytes,
Immunology Lecture- 8 Immunological Disorders Immunodeficiency Autoimmune Disease Hypersensitivities Immunodeficiency 1. Immunodeficiency --> abnormal production or function of immune cells, phagocytes,
MONTGOMERY COUNTY COMMUNITY COLLEGE Department of Science LECTURE OUTLINE CHAPTERS 16, 17, 18 AND 19
 MONTGOMERY COUNTY COMMUNITY COLLEGE Department of Science LECTURE OUTLINE CHAPTERS 16, 17, 18 AND 19 CHAPTER 16: NONSPECIFIC DEFENSES OF THE HOST I. THE FIRST LINE OF DEFENSE A. Mechanical Barriers (Physical
MONTGOMERY COUNTY COMMUNITY COLLEGE Department of Science LECTURE OUTLINE CHAPTERS 16, 17, 18 AND 19 CHAPTER 16: NONSPECIFIC DEFENSES OF THE HOST I. THE FIRST LINE OF DEFENSE A. Mechanical Barriers (Physical
IMMUNITY AND DISEASE II
 IMMUNITY AND DISEASE II A. Evolution of the immune system. 1. Figure 1--57.25, p. 1167 from Raven and Johnson Biology 6 th ed. shows how the immune system evolved. Figure 1. How the immune system evolved.
IMMUNITY AND DISEASE II A. Evolution of the immune system. 1. Figure 1--57.25, p. 1167 from Raven and Johnson Biology 6 th ed. shows how the immune system evolved. Figure 1. How the immune system evolved.
Innate Immunity. Bởi: OpenStaxCollege
 Innate Immunity Bởi: OpenStaxCollege The vertebrate, including human, immune system is a complex multilayered system for defending against external and internal threats to the integrity of the body. The
Innate Immunity Bởi: OpenStaxCollege The vertebrate, including human, immune system is a complex multilayered system for defending against external and internal threats to the integrity of the body. The
Chapter 17. The Lymphatic System and Immunity. Copyright 2010, John Wiley & Sons, Inc.
 Chapter 17 The Lymphatic System and Immunity Immunity Innate Immunity Fast, non-specific and no memory Barriers, ph extremes, Phagocytes & NK cells, fever, inflammation, complement, interferon Adaptive
Chapter 17 The Lymphatic System and Immunity Immunity Innate Immunity Fast, non-specific and no memory Barriers, ph extremes, Phagocytes & NK cells, fever, inflammation, complement, interferon Adaptive
Chapter 07 Lecture Outline
 Chapter 07 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright 2016 McGraw-Hill Education. Permission required for reproduction
Chapter 07 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright 2016 McGraw-Hill Education. Permission required for reproduction
The Lymphatic System. Innate Immunity
 The Lymphatic System Innate Immunity 1 Types of Immunity Innate (non-specific) immunity Adaptive (specific) immunity The human body has several different ways that it defends itself against infection by
The Lymphatic System Innate Immunity 1 Types of Immunity Innate (non-specific) immunity Adaptive (specific) immunity The human body has several different ways that it defends itself against infection by
WHY IS THIS IMPORTANT?
 CHAPTER 16 THE ADAPTIVE IMMUNE RESPONSE WHY IS THIS IMPORTANT? The adaptive immune system protects us from many infections The adaptive immune system has memory so we are not infected by the same pathogen
CHAPTER 16 THE ADAPTIVE IMMUNE RESPONSE WHY IS THIS IMPORTANT? The adaptive immune system protects us from many infections The adaptive immune system has memory so we are not infected by the same pathogen
Chapter 13 Lecture Outline
 Chapter 13 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction
Chapter 13 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction
Innate vs Adaptive Response
 General Immunology Innate vs Adaptive Response Innate- non-specific (4 types of barriers) anatomic- ato mechanical ca (skin), ph, mucous, normal flora Physiologic- temperature, ph, chemicals (lysozyme,
General Immunology Innate vs Adaptive Response Innate- non-specific (4 types of barriers) anatomic- ato mechanical ca (skin), ph, mucous, normal flora Physiologic- temperature, ph, chemicals (lysozyme,
ANATOMY OF THE IMMUNE SYSTEM
 Immunity Learning objectives Explain what triggers an immune response and where in the body the immune response occurs. Understand how the immune system handles exogenous and endogenous antigen differently.
Immunity Learning objectives Explain what triggers an immune response and where in the body the immune response occurs. Understand how the immune system handles exogenous and endogenous antigen differently.
Adaptive Immunity. PowerPoint Lecture Presentations prepared by Mindy Miller-Kittrell, North Carolina State University C H A P T E R
 PowerPoint Lecture Presentations prepared by Mindy Miller-Kittrell, North Carolina State University C H A P T E R 16 Adaptive Immunity The Body s Third Line of Defense Adaptive Immunity Adaptive immunity
PowerPoint Lecture Presentations prepared by Mindy Miller-Kittrell, North Carolina State University C H A P T E R 16 Adaptive Immunity The Body s Third Line of Defense Adaptive Immunity Adaptive immunity
NOTES: CH 43, part 1 The Immune System - Nonspecific & Specific Defenses ( )
 NOTES: CH 43, part 1 The Immune System - Nonspecific & Specific Defenses (43.1-43.2) The lymphatic system is closely associated with the cardiovascular system. LYMPHATIC PATHWAYS Lymphatic capillaries
NOTES: CH 43, part 1 The Immune System - Nonspecific & Specific Defenses (43.1-43.2) The lymphatic system is closely associated with the cardiovascular system. LYMPHATIC PATHWAYS Lymphatic capillaries
Innate Immunity: Nonspecific Defenses of the Host
 PowerPoint Lecture Presentations prepared by Bradley W. Christian, McLennan Community College C H A P T E R 16 Innate Immunity: Nonspecific Defenses of the Host Host Response to Disease Resistance- ability
PowerPoint Lecture Presentations prepared by Bradley W. Christian, McLennan Community College C H A P T E R 16 Innate Immunity: Nonspecific Defenses of the Host Host Response to Disease Resistance- ability
Endeavour College of Natural Health endeavour.edu.au
 Endeavour College of Natural Health endeavour.edu.au BIOH122 Human Biological Science 2 Session 9 Immune System 2 Bioscience Department Endeavour College of Natural Health endeavour.edu.au o Adaptive (Specific)
Endeavour College of Natural Health endeavour.edu.au BIOH122 Human Biological Science 2 Session 9 Immune System 2 Bioscience Department Endeavour College of Natural Health endeavour.edu.au o Adaptive (Specific)
There are 2 major lines of defense: Non-specific (Innate Immunity) and. Specific. (Adaptive Immunity) Photo of macrophage cell
 There are 2 major lines of defense: Non-specific (Innate Immunity) and Specific (Adaptive Immunity) Photo of macrophage cell Development of the Immune System ery pl neu mφ nk CD8 + CTL CD4 + thy TH1 mye
There are 2 major lines of defense: Non-specific (Innate Immunity) and Specific (Adaptive Immunity) Photo of macrophage cell Development of the Immune System ery pl neu mφ nk CD8 + CTL CD4 + thy TH1 mye
Chapter 12: The Lymphatic System
 Chapter 12: The Lymphatic System Immune System Composed of many nonspecific and specific defenses Lymphatic System also plays an important role in establishing immunity Lymphatic System Major components
Chapter 12: The Lymphatic System Immune System Composed of many nonspecific and specific defenses Lymphatic System also plays an important role in establishing immunity Lymphatic System Major components
1. Overview of Innate Immunity
 Chapter 15: Innate Immunity 1. Overview of Innate Immunity 2. Inflammation & Phagocytosis 3. Antimicrobial Substances 1. Overview of Innate Immunity Chapter Reading pp. 449-456 The Body s Defenses The
Chapter 15: Innate Immunity 1. Overview of Innate Immunity 2. Inflammation & Phagocytosis 3. Antimicrobial Substances 1. Overview of Innate Immunity Chapter Reading pp. 449-456 The Body s Defenses The
Adaptive Immunity. PowerPoint Lecture Presentations prepared by Mindy Miller-Kittrell, North Carolina State University C H A P T E R
 CSLO7. Describe functions of host defenses and the immune system in combating infectious diseases and explain how immunizations protect against specific diseases. PowerPoint Lecture Presentations prepared
CSLO7. Describe functions of host defenses and the immune system in combating infectious diseases and explain how immunizations protect against specific diseases. PowerPoint Lecture Presentations prepared
Immunity. Acquired immunity differs from innate immunity in specificity & memory from 1 st exposure
 Immunity (1) Non specific (innate) immunity (2) Specific (acquired) immunity Characters: (1) Non specific: does not need special recognition of the foreign cell. (2) Innate: does not need previous exposure.
Immunity (1) Non specific (innate) immunity (2) Specific (acquired) immunity Characters: (1) Non specific: does not need special recognition of the foreign cell. (2) Innate: does not need previous exposure.
Principles of Adaptive Immunity
 Principles of Adaptive Immunity Chapter 3 Parham Hans de Haard 17 th of May 2010 Agenda Recognition molecules of adaptive immune system Features adaptive immune system Immunoglobulins and T-cell receptors
Principles of Adaptive Immunity Chapter 3 Parham Hans de Haard 17 th of May 2010 Agenda Recognition molecules of adaptive immune system Features adaptive immune system Immunoglobulins and T-cell receptors
phagocytic leukocyte Immune System lymphocytes attacking cancer cell lymph system
 phagocytic leukocyte Immune System lymphocytes attacking cancer cell lymph system 2006-2007 1) recognizing the presence of an infection; 2) containing the infection and working to eliminate it; 3) regulating
phagocytic leukocyte Immune System lymphocytes attacking cancer cell lymph system 2006-2007 1) recognizing the presence of an infection; 2) containing the infection and working to eliminate it; 3) regulating
4b. Innate (nonspecific) Immunity
 4b. Innate (nonspecific) Immunity Chapter 16: Innate (nonspecific) Immunity! Some terms:! Susceptibility: Lack of immunity to a disease.! Immunity: Ability to ward off disease.! Innate immunity: Defenses
4b. Innate (nonspecific) Immunity Chapter 16: Innate (nonspecific) Immunity! Some terms:! Susceptibility: Lack of immunity to a disease.! Immunity: Ability to ward off disease.! Innate immunity: Defenses
For questions 1-5, match the following with their correct descriptions. (24-39) A. Class I B. Class II C. Class III D. TH1 E. TH2
 Questions Made by SI ATTENDEES!! :) Page 1 of 6 Student-Made Practice Exam Activity All questions, answers, and slide numbers are based off of Monday s SI activity, where students/attendees created possible
Questions Made by SI ATTENDEES!! :) Page 1 of 6 Student-Made Practice Exam Activity All questions, answers, and slide numbers are based off of Monday s SI activity, where students/attendees created possible
Resisting infection. Cellular Defenses: Leukocytes. Chapter 16: Innate host defenses Phagocytosis Lymph Inflammation Complement
 Resisting infection Chapter 16: Innate host defenses Lymph Inflammation Complement Bio 139 Dr. Amy Rogers Innate defenses (ch. 16) Physical & chemical barriers; cellular defenses; inflammation, fever;
Resisting infection Chapter 16: Innate host defenses Lymph Inflammation Complement Bio 139 Dr. Amy Rogers Innate defenses (ch. 16) Physical & chemical barriers; cellular defenses; inflammation, fever;
Immunity and Infection. Chapter 17
 Immunity and Infection Chapter 17 The Chain of Infection Transmitted through a chain of infection (six links) Pathogen: Disease causing microorganism Reservoir: Natural environment of the pathogen Portal
Immunity and Infection Chapter 17 The Chain of Infection Transmitted through a chain of infection (six links) Pathogen: Disease causing microorganism Reservoir: Natural environment of the pathogen Portal
White Blood Cells (WBCs)
 YOUR ACTIVE IMMUNE DEFENSES 1 ADAPTIVE IMMUNE RESPONSE 2! Innate Immunity - invariant (generalized) - early, limited specificity - the first line of defense 1. Barriers - skin, tears 2. Phagocytes - neutrophils,
YOUR ACTIVE IMMUNE DEFENSES 1 ADAPTIVE IMMUNE RESPONSE 2! Innate Immunity - invariant (generalized) - early, limited specificity - the first line of defense 1. Barriers - skin, tears 2. Phagocytes - neutrophils,
Chapter 16 Innate Immunity: Nonspecific Defenses of the Host
 Module 10 Chapter 16 Innate Immunity: Nonspecific Defenses of the Host The concept of immunity Immunity: ability to protect against from microbes and their o Aka, Susceptibility: vulnerability or lack
Module 10 Chapter 16 Innate Immunity: Nonspecific Defenses of the Host The concept of immunity Immunity: ability to protect against from microbes and their o Aka, Susceptibility: vulnerability or lack
Defense & the Immune System. Immune System Agenda 4/28/2010. Overview. The bigger picture Non specific defenses Specific defenses (Immunity)
 Defense &The Immune System Overview Immune System Agenda The bigger picture Non specific defenses Specific defenses (Immunity) Defense & the Immune System Big Picture Defense Any means of preventing or
Defense &The Immune System Overview Immune System Agenda The bigger picture Non specific defenses Specific defenses (Immunity) Defense & the Immune System Big Picture Defense Any means of preventing or
Lymphatic System. The targets of the immune defenses are infectious organisms such as,, parasites, fungi, and some protists.
 Lymphatic System I. Non-specific Defenses The immune system is a body wide network of cells and organs that have evolved to defend the body against attacks by invaders. The targets of the immune defenses
Lymphatic System I. Non-specific Defenses The immune system is a body wide network of cells and organs that have evolved to defend the body against attacks by invaders. The targets of the immune defenses
April 01, Immune system.notebook
 I. First Line of Defense: Skin and Mucus Membranes Non Specific A. Skin Surface 1. dry, dead, thick, secretions 2. sweat and sebaceous glands: antibiotics, lactic acid, RNase B. Mucus (moist and sometimes
I. First Line of Defense: Skin and Mucus Membranes Non Specific A. Skin Surface 1. dry, dead, thick, secretions 2. sweat and sebaceous glands: antibiotics, lactic acid, RNase B. Mucus (moist and sometimes
Chapter 15 Adaptive, Specific Immunity and Immunization
 Chapter 15 Adaptive, Specific Immunity and Immunization Adaptive Immunity: The third line of defense Third line of defense acquired and specific. Dual System of B and T lymphocytes- Immunocompetence Antigen
Chapter 15 Adaptive, Specific Immunity and Immunization Adaptive Immunity: The third line of defense Third line of defense acquired and specific. Dual System of B and T lymphocytes- Immunocompetence Antigen
