Clinical Importance of Purulence in Methicillin- Resistant Staphylococcus aureus Skin and Soft Tissue Infections
|
|
|
- Alberta Dorsey
- 6 years ago
- Views:
Transcription
1 Clinical Importance of Purulence in Methicillin- Resistant Staphylococcus aureus Skin and Soft Tissue Infections Susan E. Crawford, MD, Michael Z. David, MD, PhD, Daniel Glikman, MD, Kimberly J. King, MS, Susan Boyle-Vavra, PhD, and Robert S. Daum, MD Background: The so-called community-associated methicillin-resistant Staphylococcus aureus (MRSA) strains are more frequently susceptible to non ß-lactam antibiotics (including clindamycin) than health care-associated MRSA strains. We assessed whether predictive clinical characteristics of presumptive MRSA infections can be identified to guide choice of empiric antibiotic therapy. Methods: A clinical syndrome was assigned to each inpatient and outpatient at the University of Chicago Medical Center with an MRSA infection in 2004 to Antimicrobial susceptibilities and molecular characteristics of MRSA isolates were assessed. Patients were stratified by lesion characteristics. Results: Of MRSA isolates from 262 patients with purulent skin and soft tissue infections (SSTIs), 231 (88%) were susceptible to clindamycin, 253 (97%) contained staphylococcal chromosomal cassette mec (SCCmec) IV, and 245 (94%) contained Panton-Valentine leukocidin (pvl) genes, characteristics associated with community-associated MRSA strains. The presence of a purulent SSTI had a positive predictive value of 88% for a clindamycin-susceptible MRSA isolate. Among 87 isolates from a nonpurulent SSTI, 44% were susceptible to clindamycin and 34% contained pvl genes. In 179 invasive MRSA disease isolates, 33% were clindamycin-susceptible and 26% carried pvl genes. Conclusions: A purulent MRSA SSTI strongly predicted the presence of a clindamycin-susceptible MRSA isolate. Presence of the pvl genes was almost universal among MRSA isolates causing purulent SSTIs; this was less common in nonpurulent SSTIs and other clinical syndromes. (J Am Board Fam Med 2009;22: ) Methicillin-resistant Staphylococcus aureus (MRSA) isolates were first recognized in the 1960s 1,2 and This article was externally peer reviewed. Submitted 5 February 2009; revised 11 May 2009; accepted 19 May From the Department of Pediatrics, The University of Chicago, IL (SEC, MZD, DG, KJK, SB-V, RSD); and the Infectious Disease Unit and Pediatrics, Western Galilee Hospital, Nahariya, Israel (DG). Funding: Support has been provided by the Centers for Disease Control and Prevention (R01 CCR and R01 C ), the National Institute of Allergy and Infectious Diseases (R01 A A1), and the Grant Healthcare Foundation (RSD, SB-V). Support has also been provided by Centers for Disease Control and Prevention grant R01 C (RSD, MZD) and National Institute of Allergy and Infectious Diseases grant 1R01A A2 (SEC). Conflict of interest: Grant funding has been provided to RSD from the National Institute of Allergy and Infectious Diseases, the Centers for Disease Control and Prevention, as well as Grant Healthcare Foundation, Sage Products, Inc., Pfizer, Sanofi Pasteur, BD, and Clorox. RSD has served on paid advisory boards for Clorox, GlaxoSmithKline, Pfizer, and the MRSA National Faculty Meeting (sponsored by Astellas and Theravance). Corresponding author: Michael Z. David, MD, PhD, Section of Infectious Diseases, Department of Medicine, The University of Chicago, 5841 S. Maryland Avenue, MC 6054, Chicago, IL ( mdavid@medicine.bsd.uchicago.edu). were largely confined to patients with certain health care exposures. 3 During the past 10 years, novel MRSA isolates have been recognized among previously healthy members of the community who often lack these health care-associated (HA) MRSA risk factors. 4,5 Both clinical information and molecular isolate characteristics have been used to distinguish patients with HA MRSA and community-associated (CA) MRSA infections. 6 HA MRSA isolates are typically resistant to multiple antimicrobial drugs, including clindamycin, and, in the United States, belong to multilocus sequence type (MLST) 5 and contain the methicillin resistance element staphylococcal chromosomal cassette mec (SCCmec) type II. 7 In contrast, CA MRSA-type isolates are frequently susceptible to clindamycin (with some exceptions) 8,9 ; belong to MLST 8 or 1; contain SCCmec type IV or, rarely, type V; and bear the genes for the Panton Valentine leukocidin (pvl) Skin and soft tissue infections (SSTIs) account for approximately 80% of infections caused by doi: /jabfm Purulence in MRSA Infections 647
2 CA MRSA strains, 13 although severe, life-threatening disease syndromes have also been described. 5,14 16 HA MRSA-type isolates, in contrast, are seldom associated with purulent SSTIs but have instead been associated with catheterrelated bacteremia, postoperative wound infections, and infections with onset 48 hours or more after hospitalization. 17 Recent analyses of MRSA infections with onset in the community have revealed a complex epidemiology with both HA and CA MRSA strains circulating in the community Moreover, nosocomial MRSA infections and MRSA infections among patients with health care-related risk factors have been caused by various isolate types, including CA MRSA strains The epidemiologic case definition of CA MRSA used by the Centers for Disease Control and Prevention (CDC) employs the lack of HA risk factors as follows: culture from an outpatient or within 48 hours of hospital admission and no history of hemodialysis, surgery, residence in a long-term care facility, or hospitalization during the previous 12 months; no indwelling catheter or percutaneous device at the time of culture; and no previous isolation of MRSA. We have shown, however, that application of this definition to a patient with an MRSA infection substantially underestimates the prevalence of infection caused by CA MRSA strains. 20 Although the CDC criteria do accurately identify a portion of the CA MRSA isolate disease burden in the community, many patients with health care exposures (who would be classified as having HA MRSA) have disease caused by CA MRSA strains. This underestimate of disease caused by CA MRSA strains is important because the CA MRSA isolates are often susceptible to more classes of antimicrobial drugs than are HA MRSA strains. As the complex epidemiology of MRSA disease has evolved, we hypothesized that there might be identifiable clinical features that would distinguish disease caused by CA MRSA strains from disease caused by HA MRSA strains and that would allow clinicians to choose appropriate initial empiric therapy for putative MRSA infections. In particular, we hypothesized that the presence of a purulent SSTI might be a useful predictor of a CA MRSA strain with clindamycin susceptibility in the era of epidemic MRSA disease. Methods Setting Pediatric and adult patients served by the inpatient, outpatient and emergency department facilities at the University of Chicago Medical Center (UCMC) were asked to participate in this study, as described previously. 20 The institution has 577 inpatient beds and 26,200 annual admissions. More than 71,000 visits are made to the emergency department annually. UCMC serves an inner city population and draws tertiary referrals from the surrounding region. Microbiologic Studies The UCMC Clinical Microbiology Laboratory prospectively identified all MRSA isolates collected between July 1, 2004, and June 30, 2005, from patients in all clinical settings, as previously reported. 20 The antibiotic susceptibility profile of each isolate was determined by Vitek testing (biomérieux Vitek, Hazelwood, MO) for oxacillin, clindamycin, erythromycin, and gentamicin. Isolates that were resistant to erythromycin but susceptible to clindamycin by Vitek testing underwent a D test to detect inducible clindamycin resistance. All assays were performed in accordance with Clinical and Laboratory Standards Institute guidelines. 26 Molecular Studies For all MRSA isolates, polymerase chain reaction assays for meca, SCCmec type, lukf-pv, and luks-pv (which encode pvl) were conducted and MLST was determined, as described previously. 20,27,28 Patient Information A review of all consenting patients electronic medical records including hospital discharge summaries and radiographic, laboratory, pathology, operative, and outpatient clinic reports was conducted and a clinical syndrome was assigned to each MRSA patient s isolate using all available data by 2 physician investigators (SEC and DG), as described previously. 20 The clinical syndrome and molecular type were independently assigned without knowledge of the susceptibility or the molecular testing results on the isolate. This study was approved by the Institutional Review Board of the Biological Sciences Division of the University of Chicago. 648 JABFM November December 2009 Vol. 22 No. 6
3 Definitions In a previous report, 20 we stratified isolates according to the site from which the culture was obtained, including skin and soft tissue, respiratory, blood, bone and joint, and the urinary tract. For this investigation, each patient s isolate was assigned a more detailed syndrome classification. Among patients with isolates from SSTIs, a lesion requiring incision and drainage or a lesion with spontaneously draining purulent fluid (as described by the treating physician) was defined as an abscess. This group included treating cliniciandesignated diagnoses of abscesses as well as carbuncles, furuncles, boils, and cellulitis with purulent drainage. The diagnosis of pustule was assigned when an isolate was obtained from a pus-containing, 1 to 2 mm, superficial skin lesion. A chronic ulcer or an open pressure sore with nonpurulent drainage (if drainage was present) found in a patient with diabetes, peripheral vascular disease, or another underlying disease predisposing to these conditions was termed a wound. Patients with an isolate from the respiratory tract were assigned a diagnosis of ventilator-associated pneumonia, pneumonia with empyema, or other pneumonia. Any designation of MRSA pneumonia required the presence of respiratory symptoms such as cough, signs such as tachypnea and rales, consistent findings on a chest radiograph, and the prescription by the treating physician of an antibiotic effective against MRSA. Isolates colonizing the respiratory tract without attendant clinical illness and those obtained from the respiratory tract of patients with cystic fibrosis during routine surveillance were not included for analysis. Some patients had several foci of infection. An identified anatomic focus of infection was assigned priority in designating the syndrome. For example, a patient with bacteremia and osteomyelitis was categorized as having osteomyelitis. Bacteremia without a focus of infection was termed bacteremia without focus. An isolate that was shown to be susceptible to clindamycin by Vitek testing (biomérieux Vitek), resistant to erythromycin, and showed a positive D test was considered resistant to clindamycin. Statistical Analysis Categorical data were compared using the 2 or Fisher exact tests, as appropriate. All calculations were performed using Stata 9.0 (StataCorp, College Station, TX). P.05 was considered significant. Results The UCMC Clinical Microbiology Laboratories identified 1225 MRSA isolates during the study period. After excluding multiple isolates from the same patient, confirming the species as S. aureus and the presence of meca, as well as excluding respiratory colonization or skin surveillance culture isolates and the 35 patients who declined to participate, 548 MRSA isolates were designated for further analysis. Of these 548 MRSA isolates, 362 (66%) contained SCCmec type IV and 321 (89%) of these isolates were pvl positive. Three hundred sixteen (87%) of the isolates containing SCCmec type IV were susceptible to clindamycin. Among the 46 SCCmec type IV isolates resistant to clindamycin, 21 (46%) were detected by single-agent testing and 25 (54%) were detected by D test. Among SCCmec IV-bearing isolates, 319 (88%) were ST8, 20 (5%) were ST1, and 11 (3%) were ST5. One hundred seventy-nine (33%) contained SCCmec type II. None of the 179 were pvl positive and 9 (5%) were susceptible to clindamycin. Among the isolates resistant to clindamycin, 152 (85%) were resistant on single-agent testing and 18 (10%) showed a positive D test. By MLST, 154 (86%) SCCmec II-bearing isolates were ST5, 14 (8%) were ST231, and only 3 (2%) were ST8. Seven isolates had a SCCmec element that could not be classified as SCCmec types I through VI. None of them were pvl positive; all belonged to ST5 and were isolated from patients with one or more HA risk factors. One was susceptible to clindamycin. A site of isolation and specific syndrome was identified for each of the 548 MRSA isolates, as seen in Tables 1 and 2. The designation of abscess strongly predicted the presence of a clindamycin-susceptible, SCCmec type IV-containing, pvl positive isolate (Table 2). Two hundred eight (89%) of the 234 MRSA abscess isolates were susceptible to clindamycin; SCCmec type IV was found in 229 of these (98%) and pvl genes were found in 223 (95%). Of the 229 SCCmec type IV-containing isolates found in abscesses, only 6 (2.6%) lacked the pvl genes. Twenty-eight MRSA isolates were obtained from patients with a purulent SSTI that was not doi: /jabfm Purulence in MRSA Infections 649
4 Table 1. Characteristics of Methicillin-Resistant Staphylococcus aureus Isolates from Patients Without Skin and Soft Tissue Infections (n 199) Syndrome Strains Tested (n 199) Strains Susceptible to Clindamycin Strains Containing SCCmec IV Strains with the PVL Genes Respiratory tract* 63 (32) 13 (21) 16 (25) 13 (21) Pneumonia 26 5 (19) 6 (23) 5 (19) Empyema 4 2 (50) 2 (50) 2 (50) Ventilator-associated pneumonia 19 4 (21) 5 (26) 4 (21) Other respiratory isolates 14 2 (14) 3 (21) 2 (14) Bacteremia syndromes 60 (30) 14 (23) 19 (32) 11 (18) Bacteremia 18 4 (22) 6 (33) 5 (28) Line infection 38 8 (21) 10 (26) 4 (11) Endocarditis 4 2 (50) 2 (50) 2 (50) Bone and joint 33 (17) 16 (48) 17 (52) 13 (39) Osteomyelitis 18 7 (39) 9 (50) 7 (39) Septic arthritis 12 7 (58) 7 (58) 5 (42) Septic bursitis 3 2 (66) 1 (33) 1 (33) Urinary tract 23 (12) 5 (22) 4 (17) 3 (13) Other 20 (10) 9 (45) 9 (45) 5 (25) All data provided as n (%). *Isolates from the upper respiratory tract designated as colonization isolates were excluded; isolates from patients with cystic fibrosis were also excluded. Includes isolates obtained from patients with bronchitis, chronic laryngitis, sinusitis, tracheitis, and acute otitis media. Isolates with an untypeable SCCmec element were included. As defined by modified Duke criteria. Including intra-abdominal fluid, deep intraperitoneal abscess, gall bladder, pericardial fluid, conjunctiva or the external ear canal. PVL, Panton-Valentine leukocidin. designated as an abscess. The syndromes for these patients were designated as a pustule, paronychia, pyomyositis, or felon. Twenty-three (82%) of these nonabscess purulent MRSA SSTI isolates were susceptible to clindamycin; 24 (86%) contained SCCmec type IV and 22 (79%) were pvl positive. Table 2. Characteristics of Methicillin-Resistant Staphylococcus aureus Isolates from Patients with Skin and Soft Tissue Infections (n 349) Type of Infection Strains Tested (n 349) Strains Susceptible to Clindamycin Strains Containing SCCmec IV Strains with the PVL Genes Purulent SSTI 262 (75) 231 (88) 253 (97) 245 (94) Abscess (89) 229 (98) 223 (95) Pustules (88) 13 (81) 13 (81) Paronychia 4 3 (75) 4 (100) 3 (75) Pyomyositis 6 4 (67) 5 (83) 4 (67) Felon 2 2 (100) 2 (100) 2 (100) Nonpurulent SSTI 87 (25) 38 (44) 44 (51) 30 (34) Postoperative wound infection 42* 15 (36) 16 (38) 10 (24) Wound 17 8 (47) 9 (53) 5 (29) Wound and foreign body 18* 12 (67) 13 (72) 9 (50) Burns 8 2 (25) 5 (63) 5 (63) Impetigo 2 1 (50) 1 (50) 1 (50) All data provided as n (%). *Isolates with an untypeable SCCmec element were included. SSTI, skin and soft tissue infenction; PVL, Panton-Valentine leukocidin. 650 JABFM November December 2009 Vol. 22 No. 6
5 Table 3. Characteristics of Methicillin-resistant Staphylococcus aureus Isolates from Patients with Purulent and Nonpurulent Skin and Soft Tissue Infections Characteristic Purulent SSTI* (n 262) Nonpurulent SSTI* (n 87) P Contains SCCmec IV 253 (97) 44 (51).001 Contains SCCmec II 9 (3) 41 (47).001 Positive for PVL genes 245 (94) 30 (34).001 Susceptibility to: Clindamycin 231 (88) 38 (44).001 Ciprofloxacin 237 (90) 31 (36).001 Gentamicin 261 (99) 77 (89).001 Erythromycin 19 (7) 11 (13).1 Rifampin 260 (99) 83 (95).04 Trimethoprim-sulfamethoxazole 232 (100) 31 (97).1 *Data provided as n (%). Two hundred thirty-two isolates from purulent SSTIs and 32 from nonpurulent SSTIs were tested for susceptibility to trimethoprim-sulfamethoxazole. SSTI, skin and soft tissue infenction; PVL, Panton-Valentine leukocidin. When clinical data regarding abscess and nonabscess purulent SSTIs were pooled, 88% were caused by MRSA isolates that were susceptible to clindamycin, 97% contained SCCmec IV, and 94% were pvl positive. Eighty-nine percent of purulent SSTI isolates belonged to ST8, 5% belonged to ST1, and 4% belonged to ST5; 2% of isolates belonged to other MLST types. Overall, the positive predictive value of a purulent SSTI for clindamycin susceptibility was 88%. The high percent of clindamycin-susceptible strains in all purulent SSTI isolates did not differ significantly (P.37) among isolates obtained from children or adults. The 87 MRSA isolates from nonpurulent SSTIs were obtained from patients with infected wounds in the presence or absence of an associated foreign body (eg, nonpurulent drainage at a central venous catheter insertion site), a burn, impetigo, or a postoperative wound infection. The isolates from these patients contained SCCmec types II and IV with approximately equal frequency (47% and 51%, respectively); 38 (44%) were susceptible to clindamycin and 30 (34%) were pvl positive. ST5 was represented among 47% of nonpurulent SSTI isolates; ST8 was found in 41% of the isolates and 12% of isolates had other MLST types. Clindamycin susceptibility was not reliably predicted by clinical syndrome among patients with a nonpurulent SSTI (Table 3). It is noteworthy that 97% of the SCCmec IVcontaining isolates found in patients with purulent SSTIs contained the pvl genes compared with only 30 of 44 (68%) of the isolates that contained SCCmec IV obtained from patients with nonpurulent SSTIs (P.001). Among isolates associated with disease from the respiratory tract, bloodstream, bone or joint, or the urinary tract, we found that none of these non- SSTI syndromes were strongly associated with clindamycin susceptibility, pvl gene carriage, or SCCmec type IV (Table 1). A patient with isolation of MRSA from a normally sterile body site including blood, pleural fluid, joint/synovial fluid, or bone was considered to have invasive MRSA disease. 11 Of the 95 isolates from patients with invasive MRSA disease, 31 (33%) were susceptible to clindamycin, 37 (39%) contained SCCmec type IV, and 25 (26%) carried the pvl genes. Using the CDC case definition for CA MRSA, only 228 of 390 (58%) patients with pvl-positive isolates that contained SCCmec type IV would have been classified as CA MRSA, whereas 162 (42%) of the patients with pvl-positive isolates that contained SCCmec type IV would have been classified as HA MRSA cases. Of the patients with a purulent MRSA SSTI (n 262), 91 (35%) had a health care risk factor that would result in their isolate being classified as HA MRSA by the CDC definition. Of these 91 isolates, 74 (81%) were susceptible to clindamycin, 82 (90%) possessed the pvl genes, and 85 (93%) contained SCCmec type IV. doi: /jabfm Purulence in MRSA Infections 651
6 Table 4. Comparison of Purulent and Nonpurulent Skin and Soft Tissue Infections among Patients with One or More Health Care Risk Factors as Defined by the Centers for Disease Control and Prevention (n 169) Characteristic Purulent SSTI* (n 91) Nonpurulent SSTI* (n 78) P Contains SCCmec IV 85 (93) 36 (46).001 Contains SCCmec II 6 (7) 40 (51).001 Positive for PVL genes 82 (90) 23 (29).001 Susceptible to clindamycin 74 (81) 32 (41).001 *All data provided as n (%). SSTI, skin and soft tissue infenction; PVL, Panton-Valentine leukocidin. In contrast, among the 87 isolates from patients with a nonpurulent SSTI, 78 (90%) were identified as HA MRSA by CDC criteria. Of these, 32 (41%) were susceptible to clindamycin, 36 (46%) contained SCCmec type IV, and 23 (29%) carried the pvl genes. Thus, even among those patients with a CDC-defined health care risk factor, those with a purulent MRSA SSTI were significantly more likely to have a clindamycin-susceptible, pvl-positive, SCCmec type IV isolate than patients with nonpurulent SSTIs (P.001; Table 4). Discussion The presence of a purulent SSTI strongly predicted the presence of an MRSA isolate that was susceptible to clindamycin, contained SCCmec type IV, and possessed the pvl genes, regardless of the presence of CDC health care risk factors. In contrast, among the patients with nonpurulent SSTIs with respiratory, bone and joint, bloodstream, and urinary tract infections from which MRSA was isolated, strains containing both SCCmec types II and IV were responsible for infection. The absence of a CDC health care risk factor also identified a subset of patients whose MRSA isolate was susceptible to clindamycin and contained SCCmec IV and the pvl genes. 20 However, the CDC criteria for CA MRSA identified a smaller subset of patients for whom clindamycin therapy would be effective. Thirteen percent of strains that contained SCCmec type IV and 11% of MRSA isolated from purulent SSTIs were resistant to clindamycin. This rate of clindamycin resistance among CA MRSA strains is comparable with that reported by others, 29 but the rate varies geographically and temporally. 30 Clindamycin has been suggested as firstline therapy in the treatment of putative staphylococcal SSTIs in areas in which MRSA strains comprise 10% of S. aureus infections. 31 Clindamycin is often effective in the treatment of infections caused by MRSA strains possessing the inducible form of clindamycin resistance. However, a few failures have been reported, 32 and for this reason we considered isolates with a positive D test as resistant to clindamycin. Alternatives for the empiric treatment of CA MRSA SSTIs must be considered should the rate of clindamycin resistance increase; some consider trimethoprim-sulfamethoxazole (TMP/SMX) as first-line therapy for this reason and because of its better tolerability in some cases, 33 although few reported data attest to its efficacy. Indeed, we found TMP/SMX susceptibility to be near universal in isolates tested from both purulent and nonpurulent SSTIs. Therapy with TMP/SMX is not recommended when infection caused by group A Streptococcus is likely. Caution must be used when trying to interpret institution-specific rates of clindamycin resistance among MRSA isolates. Antibiograms often reflect susceptibility among pooled MRSA isolates and do not distinguish between isolates that contain SCCmec IV that are usually susceptible to clindamycin and those isolates that contain SCCmec II that are usually resistant to clindamycin. Institutions may find it helpful to stratify reporting of MRSA antibiograms by clinical syndromes. Such stratification would be helpful for practitioners when monitoring antibiotic susceptibility patterns and serve as a practical guide in the treatment options for MRSA infections. It has been suggested that pvl might be an important virulence factor in CA MRSA disease. However, animal infection studies have provided contradictory results. 34,35 Our data show near universality of pvl genes in isolates from purulent SSTIs and their substantially lower prevalence in all other MRSA clinical syndromes. Of note, we 652 JABFM November December 2009 Vol. 22 No. 6
7 also found that pvl genes were significantly more common among strains that contain SCCmec type IV found in purulent SSTIs than in those strains containing SCCmec IV found in nonpurulent SSTIs or non-ssti syndromes. This suggests that pvl may not solely be a marker for SCCmec type IV strains but that it also may be important in the pathogenesis of purulent lesions characteristic of certain CA MRSA infections. 35,36 Further studies are needed to delineate the role of pvl in the pathogenesis of MRSA infections. Our study has several limitations. We only studied infections caused by MRSA and did not include those caused by methicillin-sensitive S. aureus. Our study represents clinical and isolate data from one center and may not be representative of other areas. The burden of community and hospital disease caused by MRSA was high in our center (approximately 60% of S. aureus isolates), but it is also high in many other US medical centers. 30 Antibiotic resistance rates among CA MRSA isolates may have changed since this study period. In addition, clinical features of methicillin-sensitive S. aureus and MRSA infections have been found to be indistinguishable. 37 Therefore, a putative S. aureus infection can be presumed to be MRSA and treated as such until culture results are obtained, but this approach may vary geographically. We relied on physician documentation to assign a clinical syndrome category and assigned these syndromes retrospectively. For example, furuncles, carbuncles, and superficial primary cutaneous abscesses were grouped together as abscess because the detail provided by observer description made it difficult to stratify them further. Drainage from a postoperative wound infection or around a central venous catheter or another foreign body was often not described in sufficient detail. Therefore, if purulence was not described, we assigned the designation nonpurulent. It is not known if such drainage, if purulent, would also predict the presence of an isolate that was susceptible to clindamycin, that contained SCCmec IV, and that was pvl positive. Conclusion The diagnosis of a purulent, putative MRSA skin lesion predicts the presence of an MRSA isolate susceptible to clindamycin, bearing the SCCmec type IV element, and carrying pvl genes, regardless of the presence of HA risk factors. Epidemiologic studies of MRSA infections that excluded patients with health care risk factors have probably underestimated the burden of clindamycin-susceptible MRSA disease. 13 Recognition of a purulent SSTI will permit clinicians to select from a broader range of empiric antimicrobial drugs including clindamycin (when such therapy is deemed necessary), even among patients with CDC-defined, health carerelated risk factors. References 1. Barber M. Methicillin-resistant staphylococci. J Clin Pathol 1961;14: Barrett FF, McGehee RF, Finland M. Methicillinresistant Staphylococcus aureus at Boston City Hospital. N Eng J Med 1968;279: Doebbeling BN. The epidemiology of methicillinresistant Staphylococcus aureus colonisation and infection. J Chemother 1995;7(Suppl 3): Herold BC, Immergluck LC, Maranan MC, et al. Community-acquired methicillin-resistant Staphylococcus aureus in children with no identified predisposing risk. JAMA 1998;279: Centers for Disease Control and Prevention. Four pediatric deaths from community-acquired methicillin-resistant Staphylococcus aureus Minnesota and North Dakota, MMWR Morb Mortal Wkly Rep 1999;48: Naimi TS, LeDell KH, Como-Sabetti K, et al. Comparison of community- and health care-associated methicillin-resistant Staphylococcus aureus infection. JAMA 2003;290: Ito T, Katayama Y, Asada K, et al. Structural comparison of three types of staphylococcal cassette chromosome mec integrated in the chromosome in methicillin-resistant Staphylococcus aureus. Antimicrob Agents Chemother 2001;45: Diep BA, Chambers HF, Graber CJ, et al. Emergence of multidrug-resistant, community-associated, methicillin-resistant Staphylococcus aureus clone USA300 in men who have sex with men. Ann Intern Med 2008; 148: Han LL, McDougal LK, Gorwitz RJ, et al. High frequencies of clindamycin and tetracycline resistance in methicillin-resistant Staphylococcus aureus pulsed-field type USA300 isolates collected at a Boston ambulatory health center. J Clin Microbiol 2007; 45: Ma XX, Ito T, Tiensasitorn C, et al. Novel type of staphylococcal cassette chromosome mec identified in community-acquired methicillin-resistant Staphylococcus aureus strains. Antimicrob Agents Chemother 2002;46: Daum RS, Ito T, Hiramatsu K, et al. A novel methicillin-resistance cassette in community-acquired medoi: /jabfm Purulence in MRSA Infections 653
8 thicillin-resistant Staphylococcus aureus isolates of diverse genetic backgrounds. J Infect Dis 2002;186: Vandenesch F, Naimi T, Enright MC, et al. Community-acquired methicillin-resistant Staphylococcus aureus carrying Panton-Valentine leukocidin genes: worldwide emergence. Emerg Infect Dis 2003;9: Fridkin SK, Hageman JC, Morrison M, et al. Active Bacterial Core Surveillance Program of the Emerging Infections Program Network. Methicillin-resistant Staphylococcus aureus disease in three communities. N Engl J Med 2005;352: Adem PV, Montgomery CP, Husain AN, et al. Staphylococcus aureus sepsis and the Waterhouse- Friderichsen syndrome in children. N Engl J Med 2005;353: Francis JS, Doherty MC, Lopatin U, et al. Severe community-onset pneumonia in healthy adults caused by methicillin-resistant Staphylococcus aureus carrying the Panton-Valentine leukocidin genes. Clin Infect Dis 2005;40: Miller LG, Perdreau-Remington F, Rieg G, et al. Necrotizing fasciitis caused by community-associated methicillin-resistant Staphylococcus aureus in Los Angeles. N Engl J Med 2005;352: Diekema DJ, Pfaller MA, Schmitz FJ, et al. Survey of infections due to Staphylococcus species: frequency of occurrence and antimicrobial susceptibility of isolates collected in the United States, Canada, Latin America, Europe, and the Western Pacific region for the SEN- TRY Antimicrobial Surveillance Program, Clin Infect Dis 2001;32(Suppl):S Charlebois ED, Perdreau-Remington F, Kreiswirth B, et al. Origins of community strains of methicillinresistant Staphylococcus aureus. Clin Infect Dis 2004; 39: Klevens RM, Morrison MA, Nadle J, et al. Active Bacterial Core Surveillance MRSA Investigators. Invasive methicillin-resistant Staphylococcus aureus infections in the United States. JAMA 2007;298: David MZ, Glikman D, Crawford SE, et al. What is community-associated methicillin-resistant Staphylococcus aureus? J Infect Dis 2008;197: Maree CL, Daum RS, Boyle-Vavra S, Matayoshi K, Miller LG. Community-associated methicillin-resistant Staphylococcus aureus isolates causing healthcare-associated infections. Emerg Infect Dis 2007; 13: Gonzalez BE, Rueda AM, Shelburne SA 3rd, Musher DM, Hamill RJ, Hulten KG. Community-associated strains of methicillin-resistant Staphylococcus aureus as the cause of healthcare-associated infection. Infect Control Hosp Epidemiol 2006;27: Healy CM, Hulten KG, Palazzi DL, Campbell JR, Baker CJ. Emergence of new strains of methicillinresistant Staphylococcus aureus in a neonatal intensive care unit. Clin Infect Dis 2004;39: Saiman L, O Keefe M, Graham PL 3rd, et al. Hospital transmission of community-acquired methicillin-resistant Staphylococcus aureus among postpartum women. Clin Infect Dis 2003;37: Klevens RM, Morrison MA, Fridkin SK, et al. Community-associated methicillin-resistant Staphylococcus aureus and healthcare risk factors. Emerg Infect Dis 2006;12: National Committee for Clinical Laboratory Standards. Performance standards for antimicrobial disk susceptibility testing. 14th Informational Supplement. Villanova, PA: National Committee for Clinical Laboratory Standards; David MZ, Crawford SE, Boyle-Vavra S, Hostetler MA, Kim DC, Daum RS. Contrasting pediatric and adult methicillin-resistant Staphylococcus aureus isolates. Emerg Infect Dis 2006;12: Boyle-Vavra S, Ereshefsky B, Wang CC, Daum RS. Successful multiresistant community-associated methicillin-resistant Staphylococcus aureus lineage from Taipei, Taiwan, that carries either the novel Staphylcoccal chromosome cassette (SCCmec) type VT or SCCmec type IV. J Clin Micro 2005;43: Kaplan SL, Hulten KG, Gonzalez BE, et al. Threeyear surveillance of community-acquired Staphylococcus aureus infections in children. Clin Infect Dis 2005;40: Moran GJ, Krishnadasan A, Gorwitz RJ, et al. Methicillin-resistant S. aureus infections among patients in the emergency department. N Engl J Med 2006; 355: Daum RS. Skin and soft-tissue infections caused by methicillin-resistant Staphylococcus aureus. N Engl J Med 2007;357: Frank AL, Marcinak JF, Mangat PD, et al. Clindamycin treatment of methicillin-resistant Staphylococcus aureus infections in children. Pediatr Infect Dis J 2002;21: Szumowski JD, Cohen DE, Kanaya F, Mayer KH. Treatment and outcomes of infections by methicillin-resistant Staphylococcus aureus at an ambulatory clinic. Antimicrob Agents Chemother 2007;51: Voyich JM, Otto M, Mathema B, et al. Is Panton- Valentine leukocidin the major virulence determinant in community-associated methicillin-resistant Staphylococcus aureus disease? J Infect Dis 2006;194: Labandeira-Rey M, Couzon F, Boisset S, et al. Staphylococcus aureus Panton-Valentine leukocidin causes necrotizing pneumonia. Science 2007;23: Ward PD, Turner WH. Identification of staphylococcal Panton-Valentine leukocidin as a potent dermonecrotic toxin. Infect Immun 1980;28: Miller LG, Perdreau-Remington F, Bayer AS, et al. Clinical and epidemiologic characteristics cannot distinguish community-associated methicillin-resistant Staphylococcus aureus infection from methicillinsusceptible S. aureus infection: a prospective investigation. Clin Infect Dis 2007;44: JABFM November December 2009 Vol. 22 No. 6
La menace du Community-associated MRSA dans notre pays
 La menace du Community-associated MRSA dans notre pays Bibliothèque Royale de Belgique 17/12/2010 Dr Olivier Denis Laboratoire de référence des MRSA ULB, Hôpital Erasme Brussels MRSA transmission between
La menace du Community-associated MRSA dans notre pays Bibliothèque Royale de Belgique 17/12/2010 Dr Olivier Denis Laboratoire de référence des MRSA ULB, Hôpital Erasme Brussels MRSA transmission between
Available online at journal homepage:
 Journal of Microbiology, Immunology and Infection (2012) 45, 208e213 Available online at www.sciencedirect.com journal homepage: www.e-jmii.com ORIGINAL ARTICLE Risk factors and molecular analysis of Panton-Valentine
Journal of Microbiology, Immunology and Infection (2012) 45, 208e213 Available online at www.sciencedirect.com journal homepage: www.e-jmii.com ORIGINAL ARTICLE Risk factors and molecular analysis of Panton-Valentine
Clinical and Molecular Characteristics of Community- Acquired Methicillin-Resistant Staphylococcus Aureus Infections In Chinese Neonates
 Clinical and Molecular Characteristics of Community- Acquired Methicillin-Resistant Staphylococcus Aureus Infections In Chinese Neonates Xuzhuang Shen Beijing Children's Hospital, Capital Medical University,
Clinical and Molecular Characteristics of Community- Acquired Methicillin-Resistant Staphylococcus Aureus Infections In Chinese Neonates Xuzhuang Shen Beijing Children's Hospital, Capital Medical University,
Rochester Patient Safety C. difficile Prevention Collaborative: Long Term Care Antimicrobial Stewardship (funded by NYSDOH)
 Rochester Patient Safety C. difficile Prevention Collaborative: Long Term Care Antimicrobial Stewardship (funded by NYSDOH) Clinical Practice Guideline* for the Diagnosis and Management of Acute Bacterial
Rochester Patient Safety C. difficile Prevention Collaborative: Long Term Care Antimicrobial Stewardship (funded by NYSDOH) Clinical Practice Guideline* for the Diagnosis and Management of Acute Bacterial
Characterization of community and hospital Staphylococcus aureus isolates in Southampton, UK
 Journal of Medical Microbiology (2010), 59, 1084 1088 DOI 10.1099/jmm.0.018986-0 Characterization of community and hospital Staphylococcus aureus isolates in Southampton, UK S. M. Green, 1 P. Marsh, 1
Journal of Medical Microbiology (2010), 59, 1084 1088 DOI 10.1099/jmm.0.018986-0 Characterization of community and hospital Staphylococcus aureus isolates in Southampton, UK S. M. Green, 1 P. Marsh, 1
Methicillin-Resistant Staphylococcus aureus (MRSA) S urveillance Report 2008 Background Methods
 Methicillin-Resistant Staphylococcus aureus (MRSA) Surveillance Report 2008 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Department of Human Services
Methicillin-Resistant Staphylococcus aureus (MRSA) Surveillance Report 2008 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Department of Human Services
Panton Valentine leukocidin associated staphylococcal disease: a cross-sectional study at a London hospital, England
 ORIGINAL ARTICLE BACTERIOLOGY Panton Valentine leukocidin associated staphylococcal disease: a cross-sectional study at a London hospital, England L. J. Shallcross 1, K. Williams 2, S. Hopkins 2, R. W.
ORIGINAL ARTICLE BACTERIOLOGY Panton Valentine leukocidin associated staphylococcal disease: a cross-sectional study at a London hospital, England L. J. Shallcross 1, K. Williams 2, S. Hopkins 2, R. W.
The Curious Intersection of HIV and Staphylococcus aureus with a Focus on MRSA
 The Curious Intersection of HIV and Staphylococcus aureus with a Focus on MRSA Franklin D. Lowy, MD Columbia University College of Physicians & Surgeons New York, NY Topics to Be Covered Background Some
The Curious Intersection of HIV and Staphylococcus aureus with a Focus on MRSA Franklin D. Lowy, MD Columbia University College of Physicians & Surgeons New York, NY Topics to Be Covered Background Some
Wen-Tsung Lo, Ching-Shen Tang, Shyi-Jou Chen, Ching-Feng Huang, Min-Hua Tseng, and Chih-Chien Wang
 MAJOR ARTICLE Panton-Valentine Leukocidin Is Associated with Exacerbated Skin Manifestations and Inflammatory Response in Children with Community-Associated Staphylococcal Scarlet Fever Wen-Tsung Lo, Ching-Shen
MAJOR ARTICLE Panton-Valentine Leukocidin Is Associated with Exacerbated Skin Manifestations and Inflammatory Response in Children with Community-Associated Staphylococcal Scarlet Fever Wen-Tsung Lo, Ching-Shen
NIH Public Access Author Manuscript Infect Control Hosp Epidemiol. Author manuscript; available in PMC 2010 December 28.
 NIH Public Access Author Manuscript Published in final edited form as: Infect Control Hosp Epidemiol. 2010 July ; 31(7): 694 700. doi:10.1086/653206. Predictive Ability of Positive Clinical Culture Results
NIH Public Access Author Manuscript Published in final edited form as: Infect Control Hosp Epidemiol. 2010 July ; 31(7): 694 700. doi:10.1086/653206. Predictive Ability of Positive Clinical Culture Results
Genetic diversity of community-associated methicillin-resistant Staphylococcus aureus in southern Stockholm,
 ORIGINAL ARTICLE 10.1111/j.1469-0691.2007.01941.x Genetic diversity of community-associated methicillin-resistant Staphylococcus aureus in southern Stockholm, 2000 2005 H. Fang, G. Hedin, G. Li and C.
ORIGINAL ARTICLE 10.1111/j.1469-0691.2007.01941.x Genetic diversity of community-associated methicillin-resistant Staphylococcus aureus in southern Stockholm, 2000 2005 H. Fang, G. Hedin, G. Li and C.
The Challenge of Managing Staphylococcus aureus Bacteremia
 The Challenge of Managing Staphylococcus aureus Bacteremia M A R G A R E T G R A Y B S P F C S H P C L I N I C A L P R A C T I C E M A N A G E R N O R T H / I D P H A R M A C I S T A L B E R T A H E A
The Challenge of Managing Staphylococcus aureus Bacteremia M A R G A R E T G R A Y B S P F C S H P C L I N I C A L P R A C T I C E M A N A G E R N O R T H / I D P H A R M A C I S T A L B E R T A H E A
The economic burden of community-associated methicillin-resistant Staphylococcus aureus (CA-MRSA)
 ORIGINAL ARTICLE BACTERIOLOGY The economic burden of community-associated methicillin-resistant Staphylococcus aureus (CA-MRSA) B. Y. Lee 1, A. Singh 1, M. Z. David 2, S. M. Bartsch 1, R. B. Slayton 1,
ORIGINAL ARTICLE BACTERIOLOGY The economic burden of community-associated methicillin-resistant Staphylococcus aureus (CA-MRSA) B. Y. Lee 1, A. Singh 1, M. Z. David 2, S. M. Bartsch 1, R. B. Slayton 1,
Of 142 cases where sex was known, 56 percent were male; of 127cases where race was known, 90 percent were white, 4 percent were
 Group B Streptococcus Surveillance Report 2014 Oregon Active Bacterial Core Surveillance (ABCs) Center for Public Health Practice Updated: November 2015 Background The Active Bacterial Core surveillance
Group B Streptococcus Surveillance Report 2014 Oregon Active Bacterial Core Surveillance (ABCs) Center for Public Health Practice Updated: November 2015 Background The Active Bacterial Core surveillance
Nosocomial transmission of community-associated methicillin-resistant Staphylococcus aureus in Danish Hospitals
 J Antimicrob Chemother 2012; 67: 1775 1780 doi:10.1093/jac/dks125 Advance Access publication 20 April 2012 Nosocomial transmission of community-associated methicillin-resistant Staphylococcus aureus in
J Antimicrob Chemother 2012; 67: 1775 1780 doi:10.1093/jac/dks125 Advance Access publication 20 April 2012 Nosocomial transmission of community-associated methicillin-resistant Staphylococcus aureus in
Incidence per 100,
 Group B Streptococcus Surveillance Report 2005 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Department of Human Services Updated: January 2007 Background
Group B Streptococcus Surveillance Report 2005 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Department of Human Services Updated: January 2007 Background
Incidence per 100,000
 Streptococcus pneumoniae Surveillance Report 2005 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Department of Human Services Updated: March 2007 Background
Streptococcus pneumoniae Surveillance Report 2005 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Department of Human Services Updated: March 2007 Background
Endogenous Invasive Community- Methicillin-Resistant Staphylococcus aureus Endophthalmitis
 Endogenous Invasive Community- Acquired Methicillin-Resistant Staphylococcus aureus Endophthalmitis: Observations in Two Cases Jessica R. Newman, D.O., Lisa A. Clough, M.D., Stephen Waller, M.D., Fernando
Endogenous Invasive Community- Acquired Methicillin-Resistant Staphylococcus aureus Endophthalmitis: Observations in Two Cases Jessica R. Newman, D.O., Lisa A. Clough, M.D., Stephen Waller, M.D., Fernando
GUIDE TO INFECTION CONTROL IN THE HOSPITAL. Carbapenem-resistant Enterobacteriaceae
 GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 47: Carbapenem-resistant Enterobacteriaceae Authors E-B Kruse, MD H. Wisplinghoff, MD Chapter Editor Michelle Doll, MD, MPH) Topic Outline Key Issue Known
GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 47: Carbapenem-resistant Enterobacteriaceae Authors E-B Kruse, MD H. Wisplinghoff, MD Chapter Editor Michelle Doll, MD, MPH) Topic Outline Key Issue Known
Pseudomonas aeruginosa
 JOURNAL OF CLINICAL MICROBIOLOGY, July 1983, p. 16-164 95-1137/83/716-5$2./ Copyright C) 1983, American Society for Microbiology Vol. 18, No. 1 A Three-Year Study of Nosocomial Infections Associated with
JOURNAL OF CLINICAL MICROBIOLOGY, July 1983, p. 16-164 95-1137/83/716-5$2./ Copyright C) 1983, American Society for Microbiology Vol. 18, No. 1 A Three-Year Study of Nosocomial Infections Associated with
Source: Portland State University Population Research Center (
 Neisseria meningitidis Surveillance Report 2009 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Health Authority Updated: June 2011 Background The Active
Neisseria meningitidis Surveillance Report 2009 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Health Authority Updated: June 2011 Background The Active
Staphylococcus aureus Colonization and Infection in New York State Prisons
 MAJOR ARTICLE Staphylococcus aureus Colonization and Infection in New York State Prisons Franklin D. Lowy, 1,2 Allison E. Aiello, 5 Meera Bhat, 1 Vicki D. Johnson-Lawrence, 5 Mei-Ho Lee, 1 Earl Burrell,
MAJOR ARTICLE Staphylococcus aureus Colonization and Infection in New York State Prisons Franklin D. Lowy, 1,2 Allison E. Aiello, 5 Meera Bhat, 1 Vicki D. Johnson-Lawrence, 5 Mei-Ho Lee, 1 Earl Burrell,
Clinical Failure of Vancomycin Treatment of Staphylococcus aureus Infection in a Tertiary Care Hospital in Southern Brazil
 224 BJID 2003; 7 (June) Clinical Failure of Vancomycin Treatment of Staphylococcus aureus Infection in a Tertiary Care Hospital in Southern Brazil Larissa Lutz, Adão Machado, Nadia Kuplich and Afonso Luís
224 BJID 2003; 7 (June) Clinical Failure of Vancomycin Treatment of Staphylococcus aureus Infection in a Tertiary Care Hospital in Southern Brazil Larissa Lutz, Adão Machado, Nadia Kuplich and Afonso Luís
Infectious Disease Hot Topics: 2008
 Infectious Disease Hot Topics: 2008 Joseph Domachowske MD Professor of Pediatrics, Microbiology and Immunology Golisano Children s Hospital at SUNY Upstate Medical University Topic 1: COMMUNITY-ASSOCIATED
Infectious Disease Hot Topics: 2008 Joseph Domachowske MD Professor of Pediatrics, Microbiology and Immunology Golisano Children s Hospital at SUNY Upstate Medical University Topic 1: COMMUNITY-ASSOCIATED
Clinical Feature: Community-acquired. Pneumonia Caused by Panton-Valentine
 Mini Review imedpub Journals http://www.imedpub.com Journal of Intensive and Critical Care ISSN 2471-8505 DOI: 10.21767/2471-8505.100016 Clinical Feature: Community-acquired Pneumonia Caused by Panton-Valentine
Mini Review imedpub Journals http://www.imedpub.com Journal of Intensive and Critical Care ISSN 2471-8505 DOI: 10.21767/2471-8505.100016 Clinical Feature: Community-acquired Pneumonia Caused by Panton-Valentine
Whole genome sequencing & new strain typing methods in IPC. Lyn Gilbert ACIPC conference Hobart, November 2015
 Whole genome sequencing & new strain typing methods in IPC Lyn Gilbert ACIPC conference Hobart, November 2015 Why do strain typing? Evolution, population genetics, geographic distribution 2 Why strain
Whole genome sequencing & new strain typing methods in IPC Lyn Gilbert ACIPC conference Hobart, November 2015 Why do strain typing? Evolution, population genetics, geographic distribution 2 Why strain
Staph Infections. including MRSA
 Staph Infections including MRSA What is a Staph infection? STAPH Staphylococcus aureus, often referred to simply as staph, are bacteria commonly carried on the skin or in the nose of healthy people. SYMPTOMS
Staph Infections including MRSA What is a Staph infection? STAPH Staphylococcus aureus, often referred to simply as staph, are bacteria commonly carried on the skin or in the nose of healthy people. SYMPTOMS
Staph aureus: New nasties and how to tackle them!
 Staph aureus: New nasties and how to tackle them! Brenda Dale Health Protection Unit, Dartington Adam Brown Doncaster and Bassetlaw Hospitals NHS Foundation Trust Hosted by Maria Bennallick maria@webbertraining.com
Staph aureus: New nasties and how to tackle them! Brenda Dale Health Protection Unit, Dartington Adam Brown Doncaster and Bassetlaw Hospitals NHS Foundation Trust Hosted by Maria Bennallick maria@webbertraining.com
Received 24 August 2010/Returned for modification 7 November 2010/Accepted 7 February 2011
 JOURNAL OF CLINICAL MICROBIOLOGY, Apr. 2011, p. 1583 1587 Vol. 49, No. 4 0095-1137/11/$12.00 doi:10.1128/jcm.01719-10 Copyright 2011, American Society for Microbiology. All Rights Reserved. Clinical and
JOURNAL OF CLINICAL MICROBIOLOGY, Apr. 2011, p. 1583 1587 Vol. 49, No. 4 0095-1137/11/$12.00 doi:10.1128/jcm.01719-10 Copyright 2011, American Society for Microbiology. All Rights Reserved. Clinical and
GROUP A STREPTOCOCCUS (GAS) INVASIVE
 GROUP A STREPTOCOCCUS (GAS) INVASIVE Case definition CONFIRMED CASE Laboratory confirmation of infection with or without clinical evidence of invasive disease: isolation of group A streptococcus (Streptococcus
GROUP A STREPTOCOCCUS (GAS) INVASIVE Case definition CONFIRMED CASE Laboratory confirmation of infection with or without clinical evidence of invasive disease: isolation of group A streptococcus (Streptococcus
How Common is MRSA in Adult Septic Arthritis?
 INFECTIOUS DISEASE/BRIEF RESEARCH REPORT How Common is MRSA in Adult Septic Arthritis? Bradley W. Frazee, MD Christopher Fee, MD Larry Lambert, MPH From the Department of Emergency Medicine, Alameda County
INFECTIOUS DISEASE/BRIEF RESEARCH REPORT How Common is MRSA in Adult Septic Arthritis? Bradley W. Frazee, MD Christopher Fee, MD Larry Lambert, MPH From the Department of Emergency Medicine, Alameda County
A Case of Acute Pyogenic Sacroiliitis and Bacteremia Caused by Community-Acquired Methicillin- Resistant Staphylococcus aureus
 Case Report http://dx.doi.org/10.3947/ic.2013.45.4.441 Infect Chemother 2013;45(4):441-445 pissn 2093-2340 eissn 2092-6448 Infection & Chemotherapy A Case of Acute Pyogenic Sacroiliitis and Bacteremia
Case Report http://dx.doi.org/10.3947/ic.2013.45.4.441 Infect Chemother 2013;45(4):441-445 pissn 2093-2340 eissn 2092-6448 Infection & Chemotherapy A Case of Acute Pyogenic Sacroiliitis and Bacteremia
Enhanced EARS-Net Surveillance REPORT FOR 2012 DATA
 Enhanced EARS-Net Surveillance REPORT FOR DATA 1 In this report Main results for Proposed changes to the enhanced programme Abbreviations Used Here BSI Bloodstream Infections CVC Central Venous Catheter
Enhanced EARS-Net Surveillance REPORT FOR DATA 1 In this report Main results for Proposed changes to the enhanced programme Abbreviations Used Here BSI Bloodstream Infections CVC Central Venous Catheter
Four studies caught my eye this past
 For mass reproduction, content licensing and permissions contact Dowden Health Media. NEW DEVELOPMENTS THAT ARE CHANGING PATIENT CARE Patrick Duff, MD Professor, Division of Maternal Fetal Medicine, Department
For mass reproduction, content licensing and permissions contact Dowden Health Media. NEW DEVELOPMENTS THAT ARE CHANGING PATIENT CARE Patrick Duff, MD Professor, Division of Maternal Fetal Medicine, Department
NIH Public Access Author Manuscript Infect Control Hosp Epidemiol. Author manuscript; available in PMC 2014 September 02.
 NIH Public Access Author Manuscript Published in final edited form as: Infect Control Hosp Epidemiol. 2013 June ; 34(6): 581 587. doi:10.1086/670631. Predictors of Hospitals with Endemic Community-Associated
NIH Public Access Author Manuscript Published in final edited form as: Infect Control Hosp Epidemiol. 2013 June ; 34(6): 581 587. doi:10.1086/670631. Predictors of Hospitals with Endemic Community-Associated
Pyomyositis and Necrotizing Pneumonia in a Young Soldier Caused by Methicillin-Susceptible Staphylococcus aureus of Sequence Type 59 Lineage
 DOI 10.6314/JIMT.2016.27(1).07 2016 27 49-54 Pyomyositis and Necrotizing Pneumonia in a Young Soldier Caused by Methicillin-Susceptible Staphylococcus aureus of Sequence Type 59 Lineage Pei-Hsiung Kuo
DOI 10.6314/JIMT.2016.27(1).07 2016 27 49-54 Pyomyositis and Necrotizing Pneumonia in a Young Soldier Caused by Methicillin-Susceptible Staphylococcus aureus of Sequence Type 59 Lineage Pei-Hsiung Kuo
Antibiotic Management of Pediatric Osteomyelitis
 Reprinted from www.antimicrobe.org Sandra Arnold, M.D. Antibiotic Management of Pediatric Osteomyelitis Several points uncertainty exist regarding the antimicrobial management of acute hematogenous osteomyelitis,
Reprinted from www.antimicrobe.org Sandra Arnold, M.D. Antibiotic Management of Pediatric Osteomyelitis Several points uncertainty exist regarding the antimicrobial management of acute hematogenous osteomyelitis,
Gram Positive Coccus Staphylococci Dr. Hala Al Daghistani
 Medical bacteriology Gram Positive Coccus Staphylococci Dr. Hala Al Daghistani The Staphylococci are gram-positive spherical cells, nonmotile, usually arranged in grapelike irregular clusters. Some are
Medical bacteriology Gram Positive Coccus Staphylococci Dr. Hala Al Daghistani The Staphylococci are gram-positive spherical cells, nonmotile, usually arranged in grapelike irregular clusters. Some are
Necrotizing Fasciitis Caused by Community-Associated Methicillin-Resistant Staphylococcus aureus in Los Angeles
 original article Necrotizing Fasciitis Caused by Community-Associated Methicillin-Resistant Staphylococcus aureus in Los Angeles Loren G. Miller, M.D., M.P.H., Francoise Perdreau-Remington, Ph.D., Gunter
original article Necrotizing Fasciitis Caused by Community-Associated Methicillin-Resistant Staphylococcus aureus in Los Angeles Loren G. Miller, M.D., M.P.H., Francoise Perdreau-Remington, Ph.D., Gunter
Vancomycin: Class: Antibiotic.
 Vancomycin: Class: Antibiotic. Indications: Treatment of patients with infections caused by staphylococcal species and streptococcal Species. Available dosage form in the hospital: 1G VIAL, 500MG VIAL.
Vancomycin: Class: Antibiotic. Indications: Treatment of patients with infections caused by staphylococcal species and streptococcal Species. Available dosage form in the hospital: 1G VIAL, 500MG VIAL.
Skin and soft tissue (SSTI) sepsis (surgery, antimicrobial therapy and more)
 Skin and soft tissue (SSTI) sepsis (surgery, antimicrobial therapy and more) Christian Eckmann Antibiotic Stewardship Expert ECDC Chief of Staff Department of General, Visceral and Thoracic Surgery Klinikum
Skin and soft tissue (SSTI) sepsis (surgery, antimicrobial therapy and more) Christian Eckmann Antibiotic Stewardship Expert ECDC Chief of Staff Department of General, Visceral and Thoracic Surgery Klinikum
Staph Infection Fact Sheet
 What is Staphylococcus aureus (staph)? Staphylococcus aureus, often referred to simply as staph, are bacteria commonly carried on the skin or in the nose of healthy people. Approximately 25% to 30% of
What is Staphylococcus aureus (staph)? Staphylococcus aureus, often referred to simply as staph, are bacteria commonly carried on the skin or in the nose of healthy people. Approximately 25% to 30% of
Received 31 January 2007/Returned for modification 29 March 2007/Accepted 12 June 2007
 JOURNAL OF CLINICAL MICROBIOLOGY, Aug. 2007, p. 2554 2563 Vol. 45, No. 8 0095-1137/07/$08.00 0 doi:10.1128/jcm.00245-07 Copyright 2007, American Society for Microbiology. All Rights Reserved. The Emergence
JOURNAL OF CLINICAL MICROBIOLOGY, Aug. 2007, p. 2554 2563 Vol. 45, No. 8 0095-1137/07/$08.00 0 doi:10.1128/jcm.00245-07 Copyright 2007, American Society for Microbiology. All Rights Reserved. The Emergence
Brice Taylor Assistant Professor Division of Pulmonary and Critical Care Medicine
 Brice Taylor Assistant Professor Division of Pulmonary and Critical Care Medicine Discuss advances in predicting prognosis Understand dwhat we know (and don t know) about the Microbiology Recognize important
Brice Taylor Assistant Professor Division of Pulmonary and Critical Care Medicine Discuss advances in predicting prognosis Understand dwhat we know (and don t know) about the Microbiology Recognize important
Haemophilus influenzae Surveillance Report 2012 Oregon Active Bacterial Core Surveillance (ABCs) Center for Public Health Practice Updated: July 2014
 Haemophilus influenzae Surveillance Report 2012 Oregon Active Bacterial Core Surveillance (ABCs) Center for Public Health Practice Updated: July 2014 Background The Active Bacterial Core surveillance (ABCs)
Haemophilus influenzae Surveillance Report 2012 Oregon Active Bacterial Core Surveillance (ABCs) Center for Public Health Practice Updated: July 2014 Background The Active Bacterial Core surveillance (ABCs)
Objectives. Pneumonia. Pneumonia. Epidemiology. Prevalence 1/7/2012. Community-Acquired Pneumonia in infants and children
 Objectives Community-Acquired in infants and children Review of Clinical Practice Guidelines by the Pediatric Infectious Diseases Society and the Infectious Diseases Society of America - 2011 Sabah Charania,
Objectives Community-Acquired in infants and children Review of Clinical Practice Guidelines by the Pediatric Infectious Diseases Society and the Infectious Diseases Society of America - 2011 Sabah Charania,
Epidemiology of Infectious Complications of H1N1 Influenza Virus Infection
 Epidemiology of Infectious Complications of H1N1 Influenza Virus Infection Lyn Finelli, DrPH, MS Lead, Influenza Surveillance and Outbreak Response Epidemiology and Prevention Branch Influenza Division
Epidemiology of Infectious Complications of H1N1 Influenza Virus Infection Lyn Finelli, DrPH, MS Lead, Influenza Surveillance and Outbreak Response Epidemiology and Prevention Branch Influenza Division
MRSA The Facts. Staphylococcus aureus MRSA. Staphylococcus aureus, often referred to simply as "staph," What is Staphylococcus aureus?
 MRSA SOME FACTS This leaflet is written to provide information to anyone who may be going to use the health service in Glasgow and Clyde or who just wishes to know more about Meticillin resistant Staphylococcus
MRSA SOME FACTS This leaflet is written to provide information to anyone who may be going to use the health service in Glasgow and Clyde or who just wishes to know more about Meticillin resistant Staphylococcus
Risk Factors for Community- Associated Methicillin-Resistant Staphylococcus aureus Skin Infections among HIV-Positive Men Who Have Sex with Men
 BRIEF REPORT HIV/AIDS Risk Factors for Community- Associated Methicillin-Resistant Staphylococcus aureus Skin Infections among HIV-Positive Men Who Have Sex with Men Nolan E. Lee, 1,a,b Melanie M. Taylor,
BRIEF REPORT HIV/AIDS Risk Factors for Community- Associated Methicillin-Resistant Staphylococcus aureus Skin Infections among HIV-Positive Men Who Have Sex with Men Nolan E. Lee, 1,a,b Melanie M. Taylor,
Haemophilus influenzae, Invasive Disease rev Jan 2018
 Haemophilus influenzae, Invasive Disease rev Jan 2018 BASIC EPIDEMIOLOGY Infectious Agent Haemophilus influenzae (H. influenzae) is a small, Gram-negative bacillus, a bacterium capable of causing a range
Haemophilus influenzae, Invasive Disease rev Jan 2018 BASIC EPIDEMIOLOGY Infectious Agent Haemophilus influenzae (H. influenzae) is a small, Gram-negative bacillus, a bacterium capable of causing a range
Dr. Andrew Simor, University of Toronto A Webber Training Teleclass
 The Changing Face of : Evolving Epidemiology Andrew E. Simor, MD, FRCPC, FACP Sunnybrook Health Sciences Centre University of Toronto Disclosures I have received grants, and served as a consultant on Advisory
The Changing Face of : Evolving Epidemiology Andrew E. Simor, MD, FRCPC, FACP Sunnybrook Health Sciences Centre University of Toronto Disclosures I have received grants, and served as a consultant on Advisory
Epidemiology and Etiology of Community-Acquired Pneumonia 761 Lionel A. Mandell
 LOWER RESPIRATORY TRACT INFECTIONS Preface Thomas M. File, Jr xiii Community-Acquired Pneumonia: Pathophysiology and Host Factors with Focus on Possible New Approaches to Management of Lower Respiratory
LOWER RESPIRATORY TRACT INFECTIONS Preface Thomas M. File, Jr xiii Community-Acquired Pneumonia: Pathophysiology and Host Factors with Focus on Possible New Approaches to Management of Lower Respiratory
December 3, 2015 Severe Sepsis and Septic Shock Antibiotic Guide
 Severe Sepsis and Septic Shock Antibiotic Guide Surviving Sepsis: The choice of empirical antimicrobial therapy depends on complex issues related to the patient s history, including drug intolerances,
Severe Sepsis and Septic Shock Antibiotic Guide Surviving Sepsis: The choice of empirical antimicrobial therapy depends on complex issues related to the patient s history, including drug intolerances,
Epidemiological and Genetic Diversity of Staphylococcus aureus Causing Bloodstream Infection in Shanghai,
 Epidemiological and Genetic Diversity of Staphylococcus aureus Causing Bloodstream Infection in Shanghai, 2009-2011 Xu Chen 1., Wen-Kui Wang 2., Li-Zhong Han 1 *, Ying Liu 3, Hong Zhang 4, Jin Tang 5,
Epidemiological and Genetic Diversity of Staphylococcus aureus Causing Bloodstream Infection in Shanghai, 2009-2011 Xu Chen 1., Wen-Kui Wang 2., Li-Zhong Han 1 *, Ying Liu 3, Hong Zhang 4, Jin Tang 5,
Staphylococci. What s to be Covered. Clinical Scenario #1
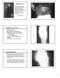 Staphylococci Micrococcus, which, when limited in its extent and activity, causes acute suppurative inflammation (phlegmon), produces, when more extensive and intense in its action on the human system,
Staphylococci Micrococcus, which, when limited in its extent and activity, causes acute suppurative inflammation (phlegmon), produces, when more extensive and intense in its action on the human system,
What s to be Covered. Microbiology of staphylococci Epidemiology of S. aureus infections Pathogenesis of S. aureus infections
 Staphylococci Micrococcus, which, when limited in its extent and activity, causes acute suppurative inflammation (phlegmon), produces, when more extensive and intense in its action on the human system,
Staphylococci Micrococcus, which, when limited in its extent and activity, causes acute suppurative inflammation (phlegmon), produces, when more extensive and intense in its action on the human system,
Pulmonary Manifestations in Children with Invasive Community-Acquired Staphylococcus aureus Infection
 MAJOR ARTICLE Pulmonary Manifestations in Children with Invasive Community-Acquired Staphylococcus aureus Infection Blanca E. Gonzalez, 1,3 Kristina G. Hulten, 1,3 Megan K. Dishop, 1,2,3 Linda B. Lamberth,
MAJOR ARTICLE Pulmonary Manifestations in Children with Invasive Community-Acquired Staphylococcus aureus Infection Blanca E. Gonzalez, 1,3 Kristina G. Hulten, 1,3 Megan K. Dishop, 1,2,3 Linda B. Lamberth,
Severe β-lactam allergy. Alternative (use for mild-moderate β-lactam allergy) therapy
 Recommended Empirical Antibiotic Regimens for MICU Patients Notes: The antibiotic regimens shown are general guidelines and should not replace clinical judgment. Always assess for antibiotic allergies.
Recommended Empirical Antibiotic Regimens for MICU Patients Notes: The antibiotic regimens shown are general guidelines and should not replace clinical judgment. Always assess for antibiotic allergies.
Prosthetic Valve Endocarditis Caused by ST8 SCCmecIVl Type Community-associated Methicillin-resistant Staphylococcus aureus: A Case Report
 doi: 10.2169/internalmedicine.1415-18 Intern Med Advance Publication http://internmed.jp CASE REPORT Prosthetic Valve Endocarditis Caused by ST8 SCCmecIVl Type Community-associated Methicillin-resistant
doi: 10.2169/internalmedicine.1415-18 Intern Med Advance Publication http://internmed.jp CASE REPORT Prosthetic Valve Endocarditis Caused by ST8 SCCmecIVl Type Community-associated Methicillin-resistant
Western Australian Methicillin-Resistant Staphylococcus aureus (MRSA) and Vancomycin Resistant Enterococcus (VRE) Epidemiology and Typing Report
 Australian Collaborating Centre for Enterococcus and Staphylococcus Species (ACCESS) Typing and Research Microbiology and Infectious Diseases Department PathWest Laboratory Medicine-WA, Royal Perth Hospital
Australian Collaborating Centre for Enterococcus and Staphylococcus Species (ACCESS) Typing and Research Microbiology and Infectious Diseases Department PathWest Laboratory Medicine-WA, Royal Perth Hospital
INFECTIOUS DISEASES IN THE LONG TERM CARE FACILITY
 INFECTIOUS DISEASES IN THE LONG TERM CARE FACILITY The following is a list of the most common infectious diseases that are to be found in the long term care facility. Precautions are recommended and the
INFECTIOUS DISEASES IN THE LONG TERM CARE FACILITY The following is a list of the most common infectious diseases that are to be found in the long term care facility. Precautions are recommended and the
Staphylococcus aureus Community-Acquired Pneumonia During the 2006 to 2007 Influenza Season
 INFECTIOUS DISEASE/ORIGINAL RESEARCH Staphylococcus aureus Community-Acquired Pneumonia During the 2006 to 2007 Influenza Season Alexander J. Kallen, MD, MPH Joan Brunkard, PhD Zachary Moore, MD, MPH Philip
INFECTIOUS DISEASE/ORIGINAL RESEARCH Staphylococcus aureus Community-Acquired Pneumonia During the 2006 to 2007 Influenza Season Alexander J. Kallen, MD, MPH Joan Brunkard, PhD Zachary Moore, MD, MPH Philip
Catheter-Associated Urinary Tract Infection (CAUTI) Event
 Catheter-Associated Urinary Tract Infection () Event Introduction: The urinary tract is the most common site of healthcare-associated infection, accounting for more than 30% of infections reported by acute
Catheter-Associated Urinary Tract Infection () Event Introduction: The urinary tract is the most common site of healthcare-associated infection, accounting for more than 30% of infections reported by acute
Methicillin Resistant Staphylococcus aureus (MRSA) in Persons with HIV: Increased Prevalence, Increased Mortality
 Methicillin Resistant Staphylococcus aureus (MRSA) in Persons with HIV: Increased Prevalence, Increased Mortality Jason E. Farley, PhD, MPH, NP Assistant Professor Johns Hopkins University School of Nursing
Methicillin Resistant Staphylococcus aureus (MRSA) in Persons with HIV: Increased Prevalence, Increased Mortality Jason E. Farley, PhD, MPH, NP Assistant Professor Johns Hopkins University School of Nursing
Enhanced EARS-Net Surveillance 2017 First Half
 1 Enhanced EARS-Net Surveillance 2017 First Half In this report Main results for 2017, first half Breakdown of factors by organism and resistance subtype Device-association Data quality assessment Key
1 Enhanced EARS-Net Surveillance 2017 First Half In this report Main results for 2017, first half Breakdown of factors by organism and resistance subtype Device-association Data quality assessment Key
Emergence of Klebsiella pneumoniae ST258 with KPC-2 in Hong Kong. Title. Ho, PL; Tse, CWS; Lai, EL; Lo, WU; Chow, KH
 Title Emergence of Klebsiella pneumoniae ST258 with KPC-2 in Hong Kong Author(s) Ho, PL; Tse, CWS; Lai, EL; Lo, WU; Chow, KH Citation International Journal Of Antimicrobial Agents, 2011, v. 37 n. 4, p.
Title Emergence of Klebsiella pneumoniae ST258 with KPC-2 in Hong Kong Author(s) Ho, PL; Tse, CWS; Lai, EL; Lo, WU; Chow, KH Citation International Journal Of Antimicrobial Agents, 2011, v. 37 n. 4, p.
Eve Boakes, 1 Helene Marbach, 1 Steven Lynham, 2 Malcolm Ward, 2 Jonathan D. Edgeworth 1 and Jonathan A. Otter 1,3
 Journal of Medical Microbiology (2016), 65, 1429 1433 DOI 10.1099/jmm.0.000379 Comparative analysis of phenol-soluble modulin production and Galleria mellonella killing by community-associated and healthcare-associated
Journal of Medical Microbiology (2016), 65, 1429 1433 DOI 10.1099/jmm.0.000379 Comparative analysis of phenol-soluble modulin production and Galleria mellonella killing by community-associated and healthcare-associated
Original Article Clinical Microbiology INTRODUCTION
 Original Article Clinical Microbiology Ann Lab Med 2019;39:158-166 https://doi.org/10.3343/alm.2019.39.2.158 ISSN 2234-3806 eissn 2234-3814 Impact of Community-Onset Methicillin-Resistant Staphylococcus
Original Article Clinical Microbiology Ann Lab Med 2019;39:158-166 https://doi.org/10.3343/alm.2019.39.2.158 ISSN 2234-3806 eissn 2234-3814 Impact of Community-Onset Methicillin-Resistant Staphylococcus
Infection Control Manual Residential Care Part 3 Infection Control Standards IC6: Additional Precautions
 IC6: 0110 Appendix I Selection Table Infection Control Manual esidential Care IC6: Additional Legend: outine Practice * reportable to Public Health C - Contact ** reportable by Lab D - Droplet A - Airborne
IC6: 0110 Appendix I Selection Table Infection Control Manual esidential Care IC6: Additional Legend: outine Practice * reportable to Public Health C - Contact ** reportable by Lab D - Droplet A - Airborne
2.3 Invasive Group A Streptococcal Disease
 2.3 Invasive Group A Streptococcal Disease Summary Total number of cases, 2015 = 107 Crude incidence rate, 2015 = 2.3 per 100,000 population Notifications In 2015, 107 cases of invasive group A streptococcal
2.3 Invasive Group A Streptococcal Disease Summary Total number of cases, 2015 = 107 Crude incidence rate, 2015 = 2.3 per 100,000 population Notifications In 2015, 107 cases of invasive group A streptococcal
2009 (Pandemic) H1N1 Influenza Virus
 2009 (Pandemic) H1N1 Influenza Virus September 15, 2009 Olympia, Washington Anthony A Marfin Washington State Department of Health Goals Understand current situation & pattern of transmission of 2009 H1N1
2009 (Pandemic) H1N1 Influenza Virus September 15, 2009 Olympia, Washington Anthony A Marfin Washington State Department of Health Goals Understand current situation & pattern of transmission of 2009 H1N1
Catheter-Associated Urinary Tract Infection (CAUTI) Event
 Device-associated Events Catheter-Associated Urinary Tract Infection () Event Introduction: The urinary tract is the most common site of healthcare-associated infection, accounting for more than 30% of
Device-associated Events Catheter-Associated Urinary Tract Infection () Event Introduction: The urinary tract is the most common site of healthcare-associated infection, accounting for more than 30% of
Pediatric Infections: Treatment of Resistant Pathogens. Focus : MRSA and DRSP Infections, Including Pneumonia. Blaise L. Congeni M.D.
 Pediatric Infections: Treatment of Resistant Pathogens Focus : MRSA and DRSP Infections, Including Pneumonia Blaise L. Congeni M.D. Patient 1-LP 8 yo with 8 days of fever and 6 days of cough. She had consistently
Pediatric Infections: Treatment of Resistant Pathogens Focus : MRSA and DRSP Infections, Including Pneumonia Blaise L. Congeni M.D. Patient 1-LP 8 yo with 8 days of fever and 6 days of cough. She had consistently
Paediatric OPAT provision the challenges and opportunities. Dr Sanjay Patel Consultant in Paediatric Infectious Diseases
 Paediatric OPAT provision the challenges and opportunities Dr Sanjay Patel Consultant in Paediatric Infectious Diseases Challenges:- Contents Economies of scale Where can p-opat be delivered? Risk averse
Paediatric OPAT provision the challenges and opportunities Dr Sanjay Patel Consultant in Paediatric Infectious Diseases Challenges:- Contents Economies of scale Where can p-opat be delivered? Risk averse
HEALTHCARE-ASSOCIATED PNEUMONIA: EPIDEMIOLOGY, MICROBIOLOGY & PATHOPHYSIOLOGY
 HEALTHCARE-ASSOCIATED PNEUMONIA: EPIDEMIOLOGY, MICROBIOLOGY & PATHOPHYSIOLOGY David Jay Weber, M.D., M.P.H. Professor of Medicine, Pediatrics, & Epidemiology Associate Chief Medical Officer, UNC Health
HEALTHCARE-ASSOCIATED PNEUMONIA: EPIDEMIOLOGY, MICROBIOLOGY & PATHOPHYSIOLOGY David Jay Weber, M.D., M.P.H. Professor of Medicine, Pediatrics, & Epidemiology Associate Chief Medical Officer, UNC Health
Genotyping of 353 Staphylococcus aureus bloodstream isolates. collected in at a Norwegian University Hospital and
 JCM Accepts, published online ahead of print on 11 July 2012 J. Clin. Microbiol. doi:10.1128/jcm.01352-12 Copyright 2012, American Society for Microbiology. All Rights Reserved. 1 2 3 Genotyping of 353
JCM Accepts, published online ahead of print on 11 July 2012 J. Clin. Microbiol. doi:10.1128/jcm.01352-12 Copyright 2012, American Society for Microbiology. All Rights Reserved. 1 2 3 Genotyping of 353
Reemergence of antibiotic-resistant Staphylococcus aureus in the genomics era
 Review series Reemergence of antibiotic-resistant Staphylococcus aureus in the genomics era Frank R. DeLeo 1 and Henry F. Chambers 2 1 Laboratory of Human Bacterial Pathogenesis, Rocky Mountain Laboratories,
Review series Reemergence of antibiotic-resistant Staphylococcus aureus in the genomics era Frank R. DeLeo 1 and Henry F. Chambers 2 1 Laboratory of Human Bacterial Pathogenesis, Rocky Mountain Laboratories,
Annual Surveillance Summary: Pseudomonas aeruginosa Infections in the Military Health System (MHS), 2017
 i Annual Surveillance Summary: Pseudomonas aeruginosa Infections in the Military Health System (MHS), 2017 Jessica R. Spencer and Uzo Chukwuma Approved for public release. Distribution is unlimited. The
i Annual Surveillance Summary: Pseudomonas aeruginosa Infections in the Military Health System (MHS), 2017 Jessica R. Spencer and Uzo Chukwuma Approved for public release. Distribution is unlimited. The
Objectives. Define classes of uncomplicated skin and soft tissue infection (SSTI) that drive empiric antimicrobial selection
 Objectives Define classes of uncomplicated skin and soft tissue infection (SSTI) that drive empiric antimicrobial selection Purulent SSTI Non-purulent SSTI Recognize conditions that suggest complications
Objectives Define classes of uncomplicated skin and soft tissue infection (SSTI) that drive empiric antimicrobial selection Purulent SSTI Non-purulent SSTI Recognize conditions that suggest complications
Dissemination of New Methicillin-Resistant Staphylococcus aureus Clones in the Community
 JOURNAL OF CLINICAL MICROBIOLOGY, Nov. 2002, p. 4289 4294 Vol. 40, No. 11 0095-1137/02/$04.00 0 DOI: 10.1128/JCM.40.11.4289 4294.2002 Copyright 2002, American Society for Microbiology. All Rights Reserved.
JOURNAL OF CLINICAL MICROBIOLOGY, Nov. 2002, p. 4289 4294 Vol. 40, No. 11 0095-1137/02/$04.00 0 DOI: 10.1128/JCM.40.11.4289 4294.2002 Copyright 2002, American Society for Microbiology. All Rights Reserved.
MRSA: Implications in Sports Medicine
 MRSA: Implications in Sports Medicine Staphylococcus aureus, often referred to as staph, are bacteria commonly carried on the skin or in the nose of healthy people Staphylococcus Aureus Occasionally, staph
MRSA: Implications in Sports Medicine Staphylococcus aureus, often referred to as staph, are bacteria commonly carried on the skin or in the nose of healthy people Staphylococcus Aureus Occasionally, staph
Infections Amenable to OPAT. (Nabin Shrestha + Ajay Mathur)
 3 Infections Amenable to OPAT (Nabin Shrestha + Ajay Mathur) Decisions regarding outpatient treatment of infections vary with the institution, the prescribing physician, the individual patient s condition
3 Infections Amenable to OPAT (Nabin Shrestha + Ajay Mathur) Decisions regarding outpatient treatment of infections vary with the institution, the prescribing physician, the individual patient s condition
Michael S. Niederman, M.D. Clinical Director Pulmonary and Critical Care Medicine New York Presbyterian Hospital Weill Cornell Medical Center
 CA-MRSA Pneumonia Michael S. Niederman, M.D. Clinical Director Pulmonary and Critical Care Medicine New York Presbyterian Hospital Weill Cornell Medical Center Professor of Clinical Medicine Weill Cornell
CA-MRSA Pneumonia Michael S. Niederman, M.D. Clinical Director Pulmonary and Critical Care Medicine New York Presbyterian Hospital Weill Cornell Medical Center Professor of Clinical Medicine Weill Cornell
WHICH ANTIFUNGAL AGENT IS THE CHOICE FOR SUSPECTED FUNGAL INFECTIONS?
 WHICH ANTIFUNGAL AGENT IS THE CHOICE FOR SUSPECTED FUNGAL INFECTIONS? Assoc. Prof. Dr. Serkan SENER Acibadem University Medical School Department of Emergency Medicine, Istanbul Acibadem Ankara Hospital,
WHICH ANTIFUNGAL AGENT IS THE CHOICE FOR SUSPECTED FUNGAL INFECTIONS? Assoc. Prof. Dr. Serkan SENER Acibadem University Medical School Department of Emergency Medicine, Istanbul Acibadem Ankara Hospital,
Outpatient parenteral antibiotic therapy with daptomycin: insights from a patient registry
 doi: 10.1111/j.1742-1241.2008.01824.x ORIGINAL PAPER Outpatient parenteral antibiotic therapy with daptomycin: insights from a patient registry W. J. Martone, K. C. Lindfield, D. E. Katz OnlineOpen: This
doi: 10.1111/j.1742-1241.2008.01824.x ORIGINAL PAPER Outpatient parenteral antibiotic therapy with daptomycin: insights from a patient registry W. J. Martone, K. C. Lindfield, D. E. Katz OnlineOpen: This
Received 24 September 2009/Returned for modification 8 November 2009/Accepted 19 December 2009
 JOURNAL OF CLINICAL MICROBIOLOGY, Mar. 2010, p. 720 727 Vol. 48, No. 3 0095-1137/10/$12.00 doi:10.1128/jcm.01890-09 Copyright 2010, American Society for Microbiology. All Rights Reserved. Emergence of
JOURNAL OF CLINICAL MICROBIOLOGY, Mar. 2010, p. 720 727 Vol. 48, No. 3 0095-1137/10/$12.00 doi:10.1128/jcm.01890-09 Copyright 2010, American Society for Microbiology. All Rights Reserved. Emergence of
MRSA: A TEAM APPROACH
 Eric Bosley, MD Laura Stadler, MD John MD J h Draus, D MRSA: A TEAM APPROACH PART I: OUTPATIENT ISSUES AND MANAGEMENT NOT REQUIRING I&D OR HOSPITALIZATION Eric L. Bosley, MD, FAAP Pediatric Associates,
Eric Bosley, MD Laura Stadler, MD John MD J h Draus, D MRSA: A TEAM APPROACH PART I: OUTPATIENT ISSUES AND MANAGEMENT NOT REQUIRING I&D OR HOSPITALIZATION Eric L. Bosley, MD, FAAP Pediatric Associates,
Invasive Bacterial Disease
 Invasive Bacterial Disease All Streptococcus pneumoniae Electronic Disease Surveillance System Division of Surveillance and Disease Control Infectious Disease Epidemiology Program : 304-558-5358 or 800-423-1271
Invasive Bacterial Disease All Streptococcus pneumoniae Electronic Disease Surveillance System Division of Surveillance and Disease Control Infectious Disease Epidemiology Program : 304-558-5358 or 800-423-1271
D DAVID PUBLISHING. 1. Introduction. Kathryn Koliha 1, Julie Falk 1, Rachana Patel 1 and Karen Kier 2
 Journal of Pharmacy and Pharmacology 5 (2017) 607-615 doi: 10.17265/2328-2150/2017.09.001 D DAVID PUBLISHING Comparative Evaluation of Pharmacist-Managed Vancomycin Dosing in a Community Hospital Following
Journal of Pharmacy and Pharmacology 5 (2017) 607-615 doi: 10.17265/2328-2150/2017.09.001 D DAVID PUBLISHING Comparative Evaluation of Pharmacist-Managed Vancomycin Dosing in a Community Hospital Following
Staphylococcus aureus bacteraemia Cases in Denmark 2017
 Staphylococcus aureus bacteraemia Cases in Denmark 2017 Statens Serum Institut Page 2 of 20 This report describes the laboratory and clinical characteristics of the 2,104 cases of Staphylococcus aureus
Staphylococcus aureus bacteraemia Cases in Denmark 2017 Statens Serum Institut Page 2 of 20 This report describes the laboratory and clinical characteristics of the 2,104 cases of Staphylococcus aureus
Ageing and the burden of diseases in the elderly. Karl-Heinz Krause Geneva University Hospitals and Medical Faculty
 Ageing and the burden of diseases in the elderly Karl-Heinz Krause Geneva University Hospitals and Medical Faculty - Norwegian Surveillance System for Communicable Diseases (MSIS) - Clinicians and laboratories
Ageing and the burden of diseases in the elderly Karl-Heinz Krause Geneva University Hospitals and Medical Faculty - Norwegian Surveillance System for Communicable Diseases (MSIS) - Clinicians and laboratories
Skin and Soft Tissue Infections (SSTI): More than a skin deep review. Vicky Parente, MD Sea Pines Conference July 12th, 2018
 Skin and Soft Tissue Infections (SSTI): More than a skin deep review Vicky Parente, MD Sea Pines Conference July 12th, 2018 Objectives To review the anatomy and classification of SSTIs To understand the
Skin and Soft Tissue Infections (SSTI): More than a skin deep review Vicky Parente, MD Sea Pines Conference July 12th, 2018 Objectives To review the anatomy and classification of SSTIs To understand the
Clinical significance of potential contaminants in blood cultures among patients in a medical center
 Potential J Microbiol contaminants Immunol Infect. in blood cultures 2007;40:438-444 Original Article Clinical significance of potential contaminants in blood cultures among patients in a medical center
Potential J Microbiol contaminants Immunol Infect. in blood cultures 2007;40:438-444 Original Article Clinical significance of potential contaminants in blood cultures among patients in a medical center
THE USE OF THE PENICILLINASE-RESISTANT
 Therapeutic problems THE USE OF THE PENICILLINASE-RESISTANT PENICILLIN IN THE PNEUMONIAS OF CHILDREN MARTHA D. Yow, MARY A. SOUTH AND CHARLES G. HESS From the Department of Pediatrics, Baylor University
Therapeutic problems THE USE OF THE PENICILLINASE-RESISTANT PENICILLIN IN THE PNEUMONIAS OF CHILDREN MARTHA D. Yow, MARY A. SOUTH AND CHARLES G. HESS From the Department of Pediatrics, Baylor University
THE INCIDENCE of infections caused by
 Vancomycin Prescribing Practices in Hospitalized Chronic Hemodialysis Patients Kevin Green, MD, Gerald Schulman, MD, David W. Haas, MD, William Schaffner, MD, and Erika M.C. D Agata, MD, MPH To determine
Vancomycin Prescribing Practices in Hospitalized Chronic Hemodialysis Patients Kevin Green, MD, Gerald Schulman, MD, David W. Haas, MD, William Schaffner, MD, and Erika M.C. D Agata, MD, MPH To determine
Nosocomial infections surveillance in RIPAS Hospital
 Original Article Brunei Int Med J. 212; 8 (6): 32-333 Nosocomial infections surveillance in RIPAS Hospital Muppidi SATYAVANI, 1, 2 Junita MOMIN, ² and Samuel Kai San YAPP 2, 3 ¹ Department of Microbiology,
Original Article Brunei Int Med J. 212; 8 (6): 32-333 Nosocomial infections surveillance in RIPAS Hospital Muppidi SATYAVANI, 1, 2 Junita MOMIN, ² and Samuel Kai San YAPP 2, 3 ¹ Department of Microbiology,
PATIENT DEMOGRAPHICS. Surname. Given name. Pacific Islander (non-maori) ADMISSION DETAILS
 Reviewer / hospital Date review started PATIENT DEMOGRAPHICS MRN DOB Sex Patient sticky label if available, else enter details here Surname Post-code Given name Australian Aborigine / TSI Middle Eastern
Reviewer / hospital Date review started PATIENT DEMOGRAPHICS MRN DOB Sex Patient sticky label if available, else enter details here Surname Post-code Given name Australian Aborigine / TSI Middle Eastern
Alberta Health Services Infection Prevention and Control - Initiatives and Services. Surveillance Protocol January 12, 2010 Rev.
 Alberta Health Services Infection Prevention and Control - Initiatives and Services Hospital Acquired Bloodstream Infections (HABSI) Hospital Wide- in Acute Care and Acute Rehabilitation Facilities Surveillance
Alberta Health Services Infection Prevention and Control - Initiatives and Services Hospital Acquired Bloodstream Infections (HABSI) Hospital Wide- in Acute Care and Acute Rehabilitation Facilities Surveillance
Central Line-Associated Infections (CLABSI) Settings Toolkit
 Central Line-Associated Infections (CLABSI) in Non-Intensive Care Unit (non-icu) Settings Toolkit Activity C: ELC Prevention Collaboratives Alex Kallen, MD, MPH and Priti Patel, MD, MPH Division of Healthcare
Central Line-Associated Infections (CLABSI) in Non-Intensive Care Unit (non-icu) Settings Toolkit Activity C: ELC Prevention Collaboratives Alex Kallen, MD, MPH and Priti Patel, MD, MPH Division of Healthcare
