A Case Series of Ocular Disease as the Primary Manifestation in Sarcoidosis
|
|
|
- Duane Adams
- 5 years ago
- Views:
Transcription
1 560 CASE REPORTS A Case Series of Ocular Disease as the Primary Manifestation in Sarcoidosis M Sivakumar,*M Med (Ophth), FRCS (Edin), S P Chee,**M Med (Ophth), FRCS (Edin), FRCOphth Abstract Sarcoidosis is an idiopathic, systemic, non-caseating, granulomatous disease with protean clinical manifestations. This disease is highly prevalent in the southern states of United States of America, especially among African-Americans, but uncommon among Asians. Though sarcoidosis concerns physicians of virtually all specialties, it is particularly important to ophthalmologists since a significant number of patients will seek initial medical examination because of ocular disease. Out of the 262 cases of uveitis examined at the Singapore National Eye Centre over a period of two years, 9 cases were diagnosed as sarcoidosis. We report here 4 patients with active sarcoidosis who presented to us with ocular symptoms as the first and primary manifestation of the disease. All 4 patients developed symptoms and signs of systemic sarcoidosis at a later date. The ocular manifestations included simultaneous bilateral chronic granulomatous iridocyclitis, intermediate uveitis, posterior uveitis characterised by vasculitis with candle wax drippings, and optic nerve head granuloma. Key words: Intermediate uveitis, Iridocyclitis, Optic nerve head granuloma, Posterior uveitis, Vasculitis Ann Acad Med Singapore 1998; 27:560-6 Introduction Sarcoidosis is an idiopathic, systemic, non-caseating, granulomatous disease with protean clinical manifestations. Although the first description of sarcoidosis was attributed to Hutchinson, 1 its ocular features received little attention until 1936 when Heerfordt s syndrome of uveitis, salivary gland enlargement and cranial nerve palsies was recognised as a sign of sarcoidosis. 2 Subsequently, sarcoidosis was recognised as one that commonly affects the eyes and ocular adnexae. The frequency of this disease is high in the southern states of USA, with almost three-fourths of the patients being African-Americans. 3 Sarcoidosis is considered relatively rare among the other races in the rest of the world. Case Reports We retrospectively examined 262 cases of uveitis seen in our centre between 1 February 1994 to 31 January 1996 obtained from our uveitis clinic database. Nine cases were diagnosed to have uveitis secondary to sarcoidosis. We report here 4 cases of sarcoidosis in whom ocular disease was the primary manifestation of the disease. Case 1 A 78-year-old Chinese female presented to us in 1994 with symptoms of gradual decrease in visual acuity in both eyes for a duration of 4 months. On examination, she had a visual acuity of 6/24 in the right eye and 6/36 in the left eye. The slit-lamp examination showed 10 to 15 medium sized keratic precipitates with an anterior chamber inflammation characterised by cells 2+ and flare 2+ bilaterally. There were Koeppe and Busacca nodules in the irides bilaterally. There was intense vitritis 3+ with snow balls. The right fundus also showed several choroidal scars in the posterior pole sparing the macular area. A diagnosis of bilateral chronic granulomatous panuveitis was made and she was investigated. A systemic review comprising of full blood count (FBC), erythrocyte sedimentation rate (ESR), chest X-ray, VDRL, and fluorescent treponemal antibody absorption test (FTA-ABS) were performed. All these test results were reported as normal. The Mantoux test showed no response. Fundus fluorescein angiography showed no active choroiditis or vasculitis. She was treated initially symptomatically with topical steroids and mydriatics. She defaulted follow-up for 7 months. During her subsequent follow up, the vitritis had increased in intensity and her visual acuity decreased to 6/24 in her right eye and counting fingers at 1 metre in her left eye and was reinvestigated. A subcutaneous nodule was observed over her right cheek. This time, her ESR was 16 mm/hour. Her FBC, liver function tests (LFTs) and total * Registrar ** Consultant Singapore National Eye Centre, Singapore Address for Reprints: Dr Chee Soon Phaik, Singapore National Eye Centre, 11 Third Hospital Avenue, Singapore Dr Meenakshi Sivakumar, the main author of this paper, was a registrar at the Singapore National Eye Centre. She passed away suddenly in December 1997 whilst visiting India. Her death is indeed a great loss to us.
2 561 serum calcium levels were all normal. She was started on systemic steroids, (tab. prednisolone 60 mg a day and tapered gradually) along with topical steroids and mydriatics for both eyes. The subcutaneous nodule over her right cheek (Fig. 1) decreased in size within a week of initiating systemic steroid therapy. An excision biopsy of the same was done. The histopathology report (Fig. 2) of the biopsied tissue showed coalescing collections of epithelioid histiocytes, abundant lymphocytes, and multinucleated giant cells suggestive of sarcoidosis or tuberculoid leprosy. A diagnosis of sarcoidosis was made based on the histopathology report. The dose of systemic steroid therapy was tapered. She developed a cataract as a complication of chronic uveitis, systemic and topical steroid therapies. She subsequently underwent an extracapsular cataract extraction with intraocular lens implantation in her left eye with perioperative steroid therapy. She was treated with tab. prednisolone 40 mg once a day for two weeks preoperatively and the dose was tapered postoperatively. Her current visual acuity is 6/18. Case 2 A 41-year-old Indian male presented to our hospital with a right-sided headache and decreased vision of 3 days duration. On examination his visual acuity was 6/ 6 in the right eye and 6/18 in the left eye. He had a left relative afferant pupillary defect (RAPD). The examination of his left fundus showed a swollen optic nerve head. His red/green colour vision, tested with Ishihara s chart was full. He was diagnosed as a case of left optic neuritis and was treated with IV methyl prednisolone 1 gm for 3 days, followed by oral prednisolone 45 mg/day and tapered over two weeks. His FBC, ESR and chest X-ray were within normal limits. The collagen vascular markers antinuclear factor (ANF) and rheumatoid factor (RF) were negative. His anti DsDNA was positive 36.8/ml (normal <18.0). The magnetic resonance imaging (MRI) of the brain and orbits revealed an enlargement and enhancement of the left optic nerve involving the proximal half of the nerve suggestive of an inflammatory origin. There was no space-occupying lesion. Ultrasound scan of the optic nerve showed elevation of the optic disc (Fig. 3). He was referred to an immunologist for systemic work up. The FBCs, serum antibody IgG, IgA and IgM levels were repeated and were within normal limits. AntiDsDNA was repeated and was found to be negative. A repeat chest X-ray revealed the presence of paratracheal lymph nodes. Three weeks after the initial presentation, his visual acuity improved to 6/12. The examination of his left eye showed a moderate RAPD, fine keratic precipitates, anterior chamber cells 2 +, flare 2 +, as well as retrolental cells. The examination of his fundus showed massive irregular swelling of the optic disc (Fig. 4), several segments of focal retinal vasculitis with perivascular sheathing, vitritis with snow balls. Red/green colour vision, tested with Ishihara s chart was decreased in the left eye (1/17 plates, test plate only). He was diagnosed as a case of sarcoidosis with optic nerve infiltration and was further investigated. Serum calcium levels and LFTs were normal. Mantoux test showed no response at 72 hours. He was given a pulse of oral prednisolone 90 mg a day for 7 days which was gradually tapered over the following weeks. His visual acuity gradually improved to 6/6 over 4 weeks. The disc granuloma decreased gradually in size and all signs of vasculitis and panuveitis subsided. The patient has been followed up for almost 2 years. He has fully recovered and regained his colour vision. Case 3 A 43-year-old Malay female presented to us with complaints of poor vision on and off for 6 months duration and a sudden loss of vision for a day in her left eye. On examination, her right eye had a visual acuity of 6/6 and her left eye had a visual acuity of hand movements. The patient s left eye examination showed mild Fig. 1. Right cheek showing a subcutaneous nodule (arrow). Fig. 2. Non-caseating epitheloid granuloma with giant cells seen on biopsy of the cheek nodule (haematoxylin-eosin staining x40). July 1998, Vol. 27 No. 4
3 562 Fig. 3. Swelling of the left optic nerve head as shown by B scan. Fig. 4. Left optic disc swelling due to infiltration of the nerve head by sarcoid granuloma. Fig. 5. Left eye with chronic granulomatous anterior uveitis and posterior synechiae. Fig. 6. Chest X-ray revealing bilateral hilar lymphadenopathy. Fig. 7. Cervical lymph node biopsy specimen showing multiple epitheloid granulomas with multinucleated giant cells (arrow) (haematoxylin-eosin staining x400). flare and occasional cells in the anterior chamber. Iris pigment deposits were noted on the anterior lens surface. There was no view of the fundus due to a vitreous haemorrhage. An ultrasound of the left eye was done which showed blood in the vitreous, posterior hyaloid detachment, and an irregular elevation over the optic nerve head. A presumptive diagnosis of posterior vitreous detachment with vitreous haemorrhage of the left eye was made. No treatment was instituted. Two months later, when the vitreous haemorrhage had cleared, there was evidence of vitreous veils with vitritis and retinal oedema. Initial systemic work-up done included: FBC, VDRL and chest X-ray. All tests were reported as normal. The ESR was 40 mm at the end of one hour. Her visual acuity improved to 6/9 in her left eye, but she continued to have a chronic anterior uveitis (Fig. 5), requiring topical steroid medication. She also developed a chronic anterior uveitis in her right eye requiring topical steroid eye drops. A year later she presented with bilateral vitritis, snow banking, neovascularisation of the discs, and sheathing of the retinal vessels. This time she was diagnosed as bilateral intermediate uveitis and was reinvestigated. Her FBC and serum calcium levels were within normal limits. The ESR was 16 mm at the end of 1 hour. The Mantoux test showed no response at the end of 72 hours. The X-ray of the chest showed bilateral hilar lymphadenopathy (Fig. 6) and she was referred to a respiratory physician. The bronchoscopic biopsy done showed evidence of non-ceaseating granulomatous inflammation suggestive of sarcoidosis. She was started on oral steroid therapy as well as topical
4 563 steroids. Currently her visual acuity is 6/12 in her right eye and 6/15 in her left eye and she has been tapered off systemic steroids and is under a regular follow up. Case 4 A 71-year-old Malay woman presented to us in 1993, with complaints of decreased vision and occasional redness for a duration of 4 months. She had diabetes mellitus for 10 years. On examination, she had a visual acuity of 6/12 in her right eye and 6/18 in her left eye. The slit lamp examination showed fine keratic precipitates on the cornea, occasional cells in the anterior chamber, and few areas of posterior synechiae bilaterally. The posterior segment was quiet and there was no evidence of diabetic retinopathy. She was started on topical steroids. A year later she developed granulomatous keratic precipitates as well as Koeppe and Busacca nodules on the iris with severe posterior synechiae. She was diagnosed to have bilateral chronic granulomatous anterior uveitis, and was investigated. Her FBC, VDRL, ESR, FTA-ABS and chest X-ray were within normal limits. The Mantoux test was non-reactive at 72 hours. One year later, she developed diplopia and was admitted to the neurology ward for investigation of a left complete third cranial nerve palsy. The clinical examination showed a left complete oculomotor nerve palsy, multiple bilateral cervical lymphadenopathy that were non-tender and rubbery in consistency, right axillary lymphadenopathy, multiple inguinal lymph nodes, with enlargement of liver and spleen. The computerised axial tomography (CAT) scan of the thorax showed multiple enlarged lymph nodes in the anterior and middle mediastinum. The CAT scan of the abdomen and pelvis revealed hepatosplenomegaly and enlargement of paraaortic lymph nodes. The CAT scan of the head was normal. A biopsy of a cervical lymph node was done. The histopathological examination showed multiple discrete compact epithelioid granules with a few multinucleated giant cells and a hyaline stroma suggestive of non-caeseating granulomatous lymphadenitis (Fig. 7). Her serum calcium level was 2.94 mmol/l, and ESR was 17 mm at the end of one hour. A diagnosis of systemic sarcoidosis was made on the basis of multiple lymphadenopathy, non-caeseating granuloma on biopsy, mononeuritis in the form of oculomotor cranial nerve palsy, raised serum calcium levels and hepatosplenomegaly. She was started on systemic steroids, tab. prednisolone 30 mg a day following which there was resolution of the lymphadenopathy, hepatoslenomegaly and III cranial nerve palsy. Currently she has chronic granulomatous anterior uveitis, with a visual acuity of 6/12 in each eye. Discussion Several studies have documented the common occurrence of ocular involvement in sarcoidosis. Estimates of the prevalence of ophthalmic involvement in sarcoidosis have ranged as high as 50% 4 but are generally closer to 25%. 5,6 In a study of manifestations of sarcoidosis worldwide, Siltzbach and associates 5 noted an overall 22% prevalence of ophthalmic involvement. Obenauf and associates 3 noted a 38% prevalence of ophthalmic involvement. James and associates 7 found 27.8% of patients to have ophthalmic manifestations in their large survey of 442 cases. These differences are related to the patient population studied, definitions of ophthalmic involvement and the nature of the evaluations conducted. Indeed, the highest prevalence rate was noted by Crick et al, 4 who classified keratoconjunctivitis sicca as evidence of lacrimal gland involvement in sarcoidosis. Since Ostenberg s first study on ophthalmic manifestations of sarcoidosis, it has been known that sarcoid may produce lesions in most tissues of the globe and its adnexa. The types of ocular abnormalities encountered are classified into three categories: (1) anterior segment disease, (2) posterior segment disease, and (3) orbital and other disease. In the acute stage, the ocular inflammation is generally unilateral, and as the disease becomes chronic, bilateral involvement usually develops. Chronic granulomatous uveitis, exemplified clinically by mutton-fat keratic precipitates, iris nodules, and synechiae, is the most common ocular manifestation of sarcoidosis as noted in our cases (1, 3 and 4). Acute iridocyclitis, typified by ciliary injection, aqueous cells and flare, and sometimes fine keratic precipitates, but without evidence of chronic inflammation, does occur in a small percentage of patients as seen in case 2. Intermediate uveitis can also be a presenting feature in sarcoidosis, with features of snowballs, string of pearls in the vitreous, vitritis with associated snowbanks as documented in our cases (1, 2 and 3). Posterior segment involvement in sarcoidosis is well documented. These can present as retinal periphlebitis, which can be focal with skip lesions, candlewax drippings, chroidal granulomata as documented in case 2. The disease can manifest with branch retinal vein occlusion, or retinal neovascularisation of the optic disc as seen in case 3, which resulted in vitreous haemorrhage. A variety of lesions of the optic nerve and disc have been reported: papillitis, retrobulbar optic neuritis, optic disc oedema secondary to increased intracranial pressure, optic atrophy and elevated masses extending intraocularly from the optic disc. In our series, case 2, presented with optic disc swelling due to sarcoid infiltration of the optic nerve. Orbital granulomas, lacrimal gland infiltrations, and cranial nerve palsies have also been described. Sarcoidosis can also present as classical panuveitis involving the anterior and posterior segments of the eye July 1998, Vol. 27 No. 4
5 564 as in case 1. The ocular disease can be protean with features of anterior uveitis, intermediate uveitis, panuveitis, or with optic nerve involvement. Table I summarises the ocular lesions noted in our 4 patients. Hence a diagnostic possibility of sarcoidosis should be there in the back of the ophthalmologist s mind while dealing with any patient of chronic uveitis. Sarcoidosis concerns physicians of virtually all specialties. It is particularly important to the ophthalmologist since a significant number of patients will seek initial medical examination because of ocular disease. Considering clinically detectable lesions, Obenauf and associates 3 in their study of 532 cases reported hilar lymphadenopathy and pulmonary abnormalities to be more common than ophthalmic manifestations. Clearly, all patients with suspected sarcoidosis deserve a thorough ophthalmologic examination. Conversely, patients with ocular findings suggestive of sarcoidosis should be examined for systemic disease. The commonly observed systemic features are hilar lymphadenopathy and pulmonary infiltrations as seen in cases 2 and 3. Multiple lymphadenopathy, oculomotor cranial nerve palsy, and hepatospenomegaly were noted in case 4. Cutaneous manifestations in sarcoidosis can be divided into those that are specific and those that are non-specific. 8 Specific lesions are those that on biopsy reveal non-caeseating granulomas. In case 1 a skin nodule developed which on excision biopsy showed non-caeseating granuloma with epitheloid cells. Non-specific lesions refer to cutaneous changes that on biopsy fail to reveal granuloma formation, but which are associated with sarcoidosis. Erythema nodosum is a principal example of a non-specific cutaneous lesion. The systemic features observed in our patients are summarised in Table II. All 4 patients reported here showed no response to Mantoux test, indicating a depression in cellular immunity that is seen in sarcoidosis (Table III). All our patients responded well to systemic or ocular steroid treatments. Diagnosis of Sarcoidosis Traditionally, diagnosis of sarcoidosis requires a positive Kveim s test, an elevated serum angiotensin converting enzyme (ACE) levels 9 and elevated serum lysozyme levels. Unfortunately, since the disease is so rare in this part of the world, these useful tests are not made readily available to us. So we adopt the following steps to aid us in the diagnosis of this enigmatic and perplexing disease. 1) In sarcoid suspect based on ocular features, the intraocular lesions we define as suggestive of sarcoidosis are granulomatous iritis with mutton-fat keratic precipitates or iris nodules, trabecular nodules, tent-like peripheral anterior synechiae, snowball or string-of-pearls vitreous opacities, retinal perivasculitis mainly involving the venules, perivascular cuffing, focal sheathing, candle-wax drippings, spotty retinochoroidal exudates and neovascularisation of the optic discs. 2) The initial systemic investigations recommended are blood cell count, ESR, chest roentgenography, LFTs, tuberculin skin test (Mantoux test) and serum ACE if available. Erythrocyte sedimentation rate is a useful tool as it is elevated in most cases but it is non-specific TABLE I: SUMMARY OF OCULAR FEATURES IN OUR FOUR CASES Panuveitis Optic nerve Intermediate Chronic infiltration uveitis granulomatous anterior uveitis Case 1 + _ Case Case 3 + _ Case 4 _ + + present absent TABLE III: SUMMARY OF THE POSITIVE INVESTIGATIONS IN OUR FOUR PATIENTS ESR Serum Chest Mantoux Non-caseating calcium X-ray test granuloma observed from: Case 1 _ Flat Skin nodule Case 2 + Flat _ Case 3 + _ + Flat Bronchial biopsy Case Flat Cervical node biopsy + positive negative TABLE II: SUMMARY OF THE SYSTEMIC FEATURES DIAGNOSED IN OUR FOUR PATIENTS Skin nodule Hilar Pulmonary Multiple Hepatosplenomegaly lymphadenopathy infiltration lymphadenopathy Case 1 + Case 2 _ + _ Case 3 + Case 4 _ present absent
6 565 as a diagnostic criteria. In chest X-rays one should look for bilateral hilar lymphadenopathy or pulmonary infiltrations. Pulmonary parenchymal lesions may be classified as (a) miliary size densities, (b) micronodular lesions, (c) large confluent mass lesions that may progress to cavitation, (d) interstitial fibrosis, or (e) alveolar sarcoid resembling pulmonary oedema. 10 A complete array of tests for liver functions needs to be done. An abnormal LFT indicates subclinical infiltration of the liver and could give additional support for the diagnosis. Mantoux test, if it shows no response at the end of 72 hours, is clinically significant and indicates a suppression of cellular immunity. This is particularly relevant to our local population as every one has received BCG vaccination. Epitheloid cells derived from macrophages are the most likely source of increased serum ACE activity in sarcoidosis. 11 Consequently, the serum ACE level appears to reflect the total body mass of ACE-producing granulomas and hence, disease activity. Serum ACE values are elevated in 60% to 90% of adult patients with sarcoidosis and they correlate well with disease activity. 8 Elevated serum ACE measurements in patients with granulomatous uveitis support a presumptive diagnosis of sarcoidosis If the initial investigations done are positive, then the patient should be further investigated. A complete systemic work up by a physician is recommended to look for pulmonary involvement, skin lesions, hepatosplenomegaly, lymhadenopathy and possibly any evidence of neurosarcoidosis. Serum calcium levels and total calcium levels are the next recommended tests. A normal value is between 2.1 and 2.6 mmol/ L. An elevated value is considered clinically significant and could add support to a diagnosis of sarcoidosis. Gallium citrate scans of the chest can be done, as they are more sensitive than routine chest roentgenograms for showing pulmonary involvement in sarcoid. Views of the head should be included in Gallium citrate scans to ascertain the status of the lacrimal gland whenever the diagnosis of sarcoidosis is being considered. 3) A definitive diagnosis can be achieved by biopsy of suspected tissues. If systemic examination reveals enlarged lymph nodes or suspicious skin lesions, then biopsy of the same is indicated. Histological feature observed in sarcoidosis is a non-caseating granuloma characterised by a central collection of monocytes-macrophages in various states of activation and differentiation. Among these activated monocytes and macrophages, monocytes that have differentiated into epitheloid cells (about 20µ in diameter), and Langhan s giant cells (as large as 300µ in diameter with as many as 30 nuclei) are believed to result from the fusion of two or more cells. This central collection of cells is surrounded by lymphocytes and a few plasma cells. Blind conjunctival biopsies yield diagnostic results in 10% to 28% of cases of suspected sarcoidosis. 6,9 Most authorities recommend conjunctival biopsies in all cases of suspected sarcoidosis because they are performed easily and virtually without risk. 6,9 4) More invasive procedures like bronchoalveolar lavage, transbronchial lung biopsy, or liver biopsy can be done, if there is a strong clinical suspicion and biopsy specimens elsewhere are non-diagnostic. The absence of absolute diagnostic criteria should not deter one from pursuing a logical diagnostic course after a detailed ophthalmic or systemic physical examination has suggested the possibility of sarcoidosis. As the mysteries of this enigmatic and perplexing disease are unravelled, more specific diagnostic criteria will undoubtedly be obtained. Conclusion The aim of this article is to highlight that sarcoidosis does exist in this region and the eye involvement can be the presenting symptom. So far, in our centre, 9 patients have been diagnosed with sarcoidosis on the basis of ocular features. Seven out of these 9 patients have ocular symptoms as the primary manifestation of the disease. Three of these 9 patients have had a histological confirmation of the diagnosis. Thus the ophthalmologist may be the first physician to see the patient. Therefore it is essential that the ophthalmologist be aware of the available diagnostic options and understands the manifestations of the disease. Sometimes the systemic involvement can occur many years after the ocular presentation and one needs to follow up the patient and take relevant history for the various systemic manifestations from time to time. REFERENCES 1. Hutchinson J. Illustrations of Clinical Surgery. London: J and A Churchill Ltd, Bruins Slot W J. Ziekte van Besnier Boeck en Febris uveoparotidea (Heerfordt). Ned Tijdschr Geneeskd 1936; 80: Obenauf C D, Shaw H E, Sydnor C F, Klintworth G K. Sarcoidosis and its ophthalmic manifestations. Am J Ophthalmol 1978; 86: Crick R P, Hoyle C, Smellie H. The eye in sarcoidosis. Br J Ophthalmol 1961; 45: Siltzbach L E, James D G, Neville E, Turia F J, Battesti J P, Sharma O M P, et al. Course and prognosis of sarcoidosis around the world. Am J Med 1985; 57: Karcioglu Z A, Brear R. Conjunctival biopsy in sarcoidosis. Am J Ophthalmol 1985; 99: James D G, Anderson R, Langley D, Ainslie D. Ocular sarcoidosis. Br J Ophthalmol 1964; 48: Kerdel F A, Moschella S L. Sarcoidosis an updated review. J Am Acad Dermatol 1984; 11:1-19. July 1998, Vol. 27 No. 4
7 Weinreb R N, Tessler H. Laboratory diagnosis of ophthalmic sarcoidosis. Surv Ophthalmol 1984; 28: Holden K R, Heller R M. Childhood sarcoidosis progressive systemic illness with micronodular pulmonary involvement. Am J Dis Child 1975; 129: Silverstein E, Pertschuck L P, Friedland J. Immunofluorescent localisation of angiotensin-converting enzyme in epithelioid and giant cells of sarcoidosis granulomas. Proc Natl Acad Sci USA 1979; 76: Romer F K, Schmidt P, Geday H. Angiotensin-converting enzyme in uveitis and sarcoidosis. Acta Ophthalmol 1980; 58: Weinreb, Barth R, Kimura S J. Limited gallium scans and angiotensinconverting enzyme in granulomatous uveitis. Ophthalmology 1980; 87: Weinreb R N, Kimura S J. Uveitis associated with sarcoidosis and angiotensin- converting enzyme. Trans Am Ophthalmol Soc 1979; LXXVII: Weinreb R N, Kimura S J. Uveitis associated with sarcoidosis and angiotensin-converting enzyme. Am J Ophthalmol 1980; 89: Weinreb R N, O Donnell J J, Sandman R, Char D H, Kimura S T. Angiotensin- converting enzyme in sarcoid uveitis. Invest Ophthalmol Vis Sci 1979; 18:
Sarcoidosis and Uveitis
 Sarcoidosis and Uveitis Nicholas Jones Royal Eye Hospital Manchester, UK Sarcoidosis a multisystem chronic inflammation causing multifocal non-caseating granulomas BUT Diagnosis often made indirectly (without
Sarcoidosis and Uveitis Nicholas Jones Royal Eye Hospital Manchester, UK Sarcoidosis a multisystem chronic inflammation causing multifocal non-caseating granulomas BUT Diagnosis often made indirectly (without
Rare Presentation of Ocular Toxoplasmosis
 Case Report Rare Presentation of Ocular Toxoplasmosis Rakhshandeh Alipanahi MD From Department of Ophthalmology, Nikookari Eye Hospital, Tabriz University of Medical Sciences, Tabriz, Iran. Correspondence:
Case Report Rare Presentation of Ocular Toxoplasmosis Rakhshandeh Alipanahi MD From Department of Ophthalmology, Nikookari Eye Hospital, Tabriz University of Medical Sciences, Tabriz, Iran. Correspondence:
Management of uveitis
 Management of uveitis DR. ANUPAMA KARANTH Anti-inflammatory agents -itis = inflammation Treatment : stop inflammation Use anti-inflammatory drugs Most potent of such agents : Corticosteroids Corticosteroids
Management of uveitis DR. ANUPAMA KARANTH Anti-inflammatory agents -itis = inflammation Treatment : stop inflammation Use anti-inflammatory drugs Most potent of such agents : Corticosteroids Corticosteroids
Moncef Khairallah, MD
 Moncef Khairallah, MD Department of Ophthalmology, Fattouma Bourguiba University Hospital Faculty of Medicine, University of Monastir Monastir, Tunisia INTRODUCTION IU: anatomic form of uveitis involving
Moncef Khairallah, MD Department of Ophthalmology, Fattouma Bourguiba University Hospital Faculty of Medicine, University of Monastir Monastir, Tunisia INTRODUCTION IU: anatomic form of uveitis involving
Various presentations of herpes simplex retinochoroiditis A case series
 Various presentations of herpes simplex retinochoroidits 47 Various presentations of herpes simplex retinochoroiditis A case series M. T. K. Perera 1, T. S. Keragala 1, M. Gamage 2 The Journal of the College
Various presentations of herpes simplex retinochoroidits 47 Various presentations of herpes simplex retinochoroiditis A case series M. T. K. Perera 1, T. S. Keragala 1, M. Gamage 2 The Journal of the College
UVEITIS IN SARCOIDOSIS. Dr. NURCHALIZA H. SIREGAR. Bagian Ilmu Penyakit Mata Fakultas Kedokteran Universitas Sumatera Utara
 UVEITIS IN SARCOIDOSIS Dr. NURCHALIZA H. SIREGAR Bagian Ilmu Penyakit Mata Fakultas Kedokteran Universitas Sumatera Utara UVEITIS IN SARCOIDOSIS Sarcoidosis, first recognised as a dermatological rarity
UVEITIS IN SARCOIDOSIS Dr. NURCHALIZA H. SIREGAR Bagian Ilmu Penyakit Mata Fakultas Kedokteran Universitas Sumatera Utara UVEITIS IN SARCOIDOSIS Sarcoidosis, first recognised as a dermatological rarity
Diffuse infiltrating retinoblastoma
 Brit. 1. Ophthal. (I 971) 55, 6oo Diffuse infiltrating retinoblastoma GWYN MORGAN Department of Pathology, Institute of Ophthalmology, University of London The term "diffuse infiltrating retinoblastoma"
Brit. 1. Ophthal. (I 971) 55, 6oo Diffuse infiltrating retinoblastoma GWYN MORGAN Department of Pathology, Institute of Ophthalmology, University of London The term "diffuse infiltrating retinoblastoma"
Cases CFEH. CFEH Facebook Case #4
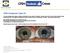 CFEH Cases CFEH Facebook Case #4 A 42 year old female has noticed a floater in her left eye for many years but no flashes. She also reports hazy vision in this eye that has been present all her life. She
CFEH Cases CFEH Facebook Case #4 A 42 year old female has noticed a floater in her left eye for many years but no flashes. She also reports hazy vision in this eye that has been present all her life. She
Neuro-Ocular Grand Rounds
 Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
UNDERSTAND MORE ABOUT UVEITIS UVEITIS
 UNDERSTAND MORE ABOUT UVEITIS UVEITIS Uveitis What is uveitis? Uveitis is inflammation of the uvea, the middle layer of your eye. The eye is shaped much like a tennis ball, with three different layers
UNDERSTAND MORE ABOUT UVEITIS UVEITIS Uveitis What is uveitis? Uveitis is inflammation of the uvea, the middle layer of your eye. The eye is shaped much like a tennis ball, with three different layers
Uveitis. Pt Info Brochure. Q: What is Uvea?
 Pt Info Brochure Uveitis Q: What is Uvea? A: Uvea is the middle layer of the eye. It is the most vascular structure of the eye. It provides nutrition to the other parts of the eye. The uvea is made up
Pt Info Brochure Uveitis Q: What is Uvea? A: Uvea is the middle layer of the eye. It is the most vascular structure of the eye. It provides nutrition to the other parts of the eye. The uvea is made up
Choroidal Neovascularization in Sympathetic Ophthalmia
 Choroidal Neovascularization in Sympathetic Ophthalmia Lucia Sobrin, Miguel Cordero Coma, C. Stephen Foster Case Report A 49-year-old man presented after a ruptured globe repair of his left eye status
Choroidal Neovascularization in Sympathetic Ophthalmia Lucia Sobrin, Miguel Cordero Coma, C. Stephen Foster Case Report A 49-year-old man presented after a ruptured globe repair of his left eye status
Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (CSC)
 HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
Case Report Atypical Presentation of Idiopathic Bilateral Optic Perineuritis in a Young Patient
 Case Reports in Ophthalmological Medicine Volume 2016, Article ID 6741925, 4 pages http://dx.doi.org/10.1155/2016/6741925 Case Report Atypical Presentation of Idiopathic Bilateral Optic Perineuritis in
Case Reports in Ophthalmological Medicine Volume 2016, Article ID 6741925, 4 pages http://dx.doi.org/10.1155/2016/6741925 Case Report Atypical Presentation of Idiopathic Bilateral Optic Perineuritis in
Kikuchi-Fujimoto Disease with Bilateral Uveitis
 Kikuchi-Fujimoto Disease with Bilateral Uveitis Hope R. Garner 1, Hilary E. Fazzone 1, Daniel E. Meltzer 1* 1. Department of Radiology, St. Luke's-Roosevelt Hospital Center, New York, NY, USA * Correspondence:
Kikuchi-Fujimoto Disease with Bilateral Uveitis Hope R. Garner 1, Hilary E. Fazzone 1, Daniel E. Meltzer 1* 1. Department of Radiology, St. Luke's-Roosevelt Hospital Center, New York, NY, USA * Correspondence:
COMMUNICATIONS OCULAR SARCOIDOSIS* it is the most troublesome and incapacitating. Its early recognition and treatment
 Brit. J. Ophthal. (1964) 48, 461. COMMUNICATIONS OCULAR SARCOIDOSIS* BY D. GERAINT JAMES Royal Northern Hospital and Royal Eye Medical Ophthalmology Unit, Lambeth Hospital R. ANDERSON AND D. LANGLEY Royal
Brit. J. Ophthal. (1964) 48, 461. COMMUNICATIONS OCULAR SARCOIDOSIS* BY D. GERAINT JAMES Royal Northern Hospital and Royal Eye Medical Ophthalmology Unit, Lambeth Hospital R. ANDERSON AND D. LANGLEY Royal
Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland
 Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
UVEITIS. Dr. Yılmaz ÖZYAZGAN
 UVEITIS Dr. Yılmaz ÖZYAZGAN UVEITIS DEFINITION BY STRICT DEFINITION, UVEITIS IS AN INFLAMMATION OF UVEAL TRACT. BUT IN PRACTICAL, IT IS GENERALLY NOT RESTRICTED TO THE UVEA AND INVOLVES OTHER ADJACENT
UVEITIS Dr. Yılmaz ÖZYAZGAN UVEITIS DEFINITION BY STRICT DEFINITION, UVEITIS IS AN INFLAMMATION OF UVEAL TRACT. BUT IN PRACTICAL, IT IS GENERALLY NOT RESTRICTED TO THE UVEA AND INVOLVES OTHER ADJACENT
Optical coherence tomography findings in a child with posterior scleritis
 European Journal of Ophthalmology / Vol. 18 no. 6, 2008 / pp. 1007-1010 SHORT OMMUNITIONS & SE REPORTS Optical coherence tomography findings in a child with posterior scleritis H. ERDÖL, M. KOL,. TÜRK
European Journal of Ophthalmology / Vol. 18 no. 6, 2008 / pp. 1007-1010 SHORT OMMUNITIONS & SE REPORTS Optical coherence tomography findings in a child with posterior scleritis H. ERDÖL, M. KOL,. TÜRK
Pediatric Ocular Sonography
 Pediatric Ocular Sonography Cicero J Torres A Silva, MD Associate Professor of Radiology 2016 SPR Pediatric Ultrasound Course Yale University School of Medicine None Disclosures Objectives of Presentation
Pediatric Ocular Sonography Cicero J Torres A Silva, MD Associate Professor of Radiology 2016 SPR Pediatric Ultrasound Course Yale University School of Medicine None Disclosures Objectives of Presentation
Malawi. Ocular leprosy in. Clinical and therapeutic survey of 8,325 leprosy. patients
 Brit. 5. Ophthal. (I 970) 54, I 07 Ocular leprosy in Malawi Clinical and therapeutic survey of 8,325 leprosy patients U. TICHO AND I. BEN SIRA Eye Department, Hadassah Medical Centre, Jerusalem, Israel
Brit. 5. Ophthal. (I 970) 54, I 07 Ocular leprosy in Malawi Clinical and therapeutic survey of 8,325 leprosy patients U. TICHO AND I. BEN SIRA Eye Department, Hadassah Medical Centre, Jerusalem, Israel
It has previously been shown that pine
 The effects of cortisone on pine pollen-induced uveitis in guinea pigs Stan L. Coleman and Samuel Canaan Injection of pine pollen into the vitreous of guinea pigs previously sensitized with Freund's adjuvant
The effects of cortisone on pine pollen-induced uveitis in guinea pigs Stan L. Coleman and Samuel Canaan Injection of pine pollen into the vitreous of guinea pigs previously sensitized with Freund's adjuvant
Bilateral nodular sarcoid choroiditis with vitreous haemorrhage
 British Journal of Ophthalmology, 1984, 68, 660-666 Bilateral nodular sarcoid choroiditis with vitreous haemorrhage LAURENCE S. STONE AND MARTIN EHRENBERG From the Departments of Ophthalmology, Eye Research
British Journal of Ophthalmology, 1984, 68, 660-666 Bilateral nodular sarcoid choroiditis with vitreous haemorrhage LAURENCE S. STONE AND MARTIN EHRENBERG From the Departments of Ophthalmology, Eye Research
SEGMENTAL LESIONS OF THE RETINAL ARTERIES*
 Brit. J. Ophthal. (1960) 44, 562. SEGMENTAL LESIONS OF THE RETINAL ARTERIES* BY R. K. BLACH London FEW cases with segmental lesions of the retinal arteries have been described. Suganuma (1927) reported
Brit. J. Ophthal. (1960) 44, 562. SEGMENTAL LESIONS OF THE RETINAL ARTERIES* BY R. K. BLACH London FEW cases with segmental lesions of the retinal arteries have been described. Suganuma (1927) reported
Complicated Cataract to Intraocular Tumors, Beware of the unexpected
 Complicated Cataract to Intraocular Tumors, Beware of the unexpected Ihab Saad Othman, MD, FRCS Professor of Ophthalmology Cairo University In this part of the world: We Master Phakoemulsification 1 Intraoperative/Second
Complicated Cataract to Intraocular Tumors, Beware of the unexpected Ihab Saad Othman, MD, FRCS Professor of Ophthalmology Cairo University In this part of the world: We Master Phakoemulsification 1 Intraoperative/Second
Role of high-resolution computerized tomography chest in identifying tubercular etiology in patients diagnosed as Eales disease
 Kharel (Sitaula) et al. Journal of Ophthalmic Inflammation and Infection (2017) 7:4 DOI 10.1186/s12348-016-0120-1 Journal of Ophthalmic Inflammation and Infection ORIGINAL RESEARCH Open Access Role of
Kharel (Sitaula) et al. Journal of Ophthalmic Inflammation and Infection (2017) 7:4 DOI 10.1186/s12348-016-0120-1 Journal of Ophthalmic Inflammation and Infection ORIGINAL RESEARCH Open Access Role of
doi: /j.jns
 doi: 10.1016/j.jns.2014.05.055 Title: Sixth nerve palsy associated with obstruction in Dorello s canal, accompanied by nodular type muscular sarcoidosis Author: Ayako Shioya 1), Hiroshi Takuma 1), Masanari
doi: 10.1016/j.jns.2014.05.055 Title: Sixth nerve palsy associated with obstruction in Dorello s canal, accompanied by nodular type muscular sarcoidosis Author: Ayako Shioya 1), Hiroshi Takuma 1), Masanari
Anterior Segment Disease and the Systemic Link Mile Brujic, OD, FAAO
 Anterior Segment Disease and the Systemic Link Mile Brujic, OD, FAAO brujic@prodigy.net Summary As optometry s role in health care increases, so does our responsibility to appropriately diagnose and appropriately
Anterior Segment Disease and the Systemic Link Mile Brujic, OD, FAAO brujic@prodigy.net Summary As optometry s role in health care increases, so does our responsibility to appropriately diagnose and appropriately
LEUKAEMIA*t INFILTRATION OF THE IRIS IN CHRONIC LYMPHATIC. pattemn * Received for pubiication November io, i967.
 Brit. J. Ophthal. (1968) 52, 781 INFILTRATION OF THE IRIS IN CHRONIC LYMPHATIC LEUKAEMIA*t BY BRIAN MARTIN The General Infirmary, Leeds OCULAR involvement is common in the leukaemias though the anterior
Brit. J. Ophthal. (1968) 52, 781 INFILTRATION OF THE IRIS IN CHRONIC LYMPHATIC LEUKAEMIA*t BY BRIAN MARTIN The General Infirmary, Leeds OCULAR involvement is common in the leukaemias though the anterior
DIAGNOSIS AND MANAGEMENT OF ANTERIOR UVEITIS POA SPRING CONFERENCE BERNARD H. BLAUSTEIN, O.D., F.A.A.O.
 DIAGNOSIS AND MANAGEMENT OF ANTERIOR UVEITIS POA SPRING CONFERENCE - 2009 Classification of Anterior Uveitis BERNARD H. BLAUSTEIN, O.D., F.A.A.O. A. Anatomic location 1. Iritis Cells and flare mostly in
DIAGNOSIS AND MANAGEMENT OF ANTERIOR UVEITIS POA SPRING CONFERENCE - 2009 Classification of Anterior Uveitis BERNARD H. BLAUSTEIN, O.D., F.A.A.O. A. Anatomic location 1. Iritis Cells and flare mostly in
Sarcoidosis: the clinical problem
 Postgraduate Medical Journal (1988) 64, 531-535 Sarcoidosis: the clinical problem Edmund Neville St Mary's Hospital, Portsmouth P03 6AD, UK. Summary: This paper reviews the clinical manifestations of acute
Postgraduate Medical Journal (1988) 64, 531-535 Sarcoidosis: the clinical problem Edmund Neville St Mary's Hospital, Portsmouth P03 6AD, UK. Summary: This paper reviews the clinical manifestations of acute
Bilateral multiple choroidal granulomas and systemic vasculitis as presenting features of tuberculosis in an immunocompetent patient
 Kumar et al. Journal of Ophthalmic Inflammation and Infection (2016) 6:40 DOI 10.1186/s12348-016-0109-9 Journal of Ophthalmic Inflammation and Infection BRIEF REPORT Open Access Bilateral multiple choroidal
Kumar et al. Journal of Ophthalmic Inflammation and Infection (2016) 6:40 DOI 10.1186/s12348-016-0109-9 Journal of Ophthalmic Inflammation and Infection BRIEF REPORT Open Access Bilateral multiple choroidal
Clinically Significant Macular Edema (CSME)
 Clinically Significant Macular Edema (CSME) 1 Clinically Significant Macular Edema (CSME) Sadrina T. Shaw OMT I Student July 26, 2014 Advisor: Dr. Uwaydat Clinically Significant Macular Edema (CSME) 2
Clinically Significant Macular Edema (CSME) 1 Clinically Significant Macular Edema (CSME) Sadrina T. Shaw OMT I Student July 26, 2014 Advisor: Dr. Uwaydat Clinically Significant Macular Edema (CSME) 2
CASE PRESENTATION. DR.Sravani 1 st yr PG Dept of Ophthalmology
 CASE PRESENTATION DR.Sravani 1 st yr PG Dept of Ophthalmology Name : X X X X X Age : 50yrs Sex : male Occupation : Farmer Residence : Mothkur CHIEF COMPLAINTS : - Diminision of vision in Right Eye since
CASE PRESENTATION DR.Sravani 1 st yr PG Dept of Ophthalmology Name : X X X X X Age : 50yrs Sex : male Occupation : Farmer Residence : Mothkur CHIEF COMPLAINTS : - Diminision of vision in Right Eye since
Temporal arteritis. Occurrence of ocular complications 7 years after diagnosis. University of Edinburgh, and Royal Infirmary of Edinburgh
 Brit. J. Ophthal. (I 972) 56, 584 Temporal arteritis Occurrence of ocular complications 7 years after diagnosis JAMES F. CULLEN Department of Ophthalmology, University of Edinburgh, and Royal Infirmary
Brit. J. Ophthal. (I 972) 56, 584 Temporal arteritis Occurrence of ocular complications 7 years after diagnosis JAMES F. CULLEN Department of Ophthalmology, University of Edinburgh, and Royal Infirmary
Role Of Various Factors In The Treatment Of Optic Neuritis----A Study Abstract Aim: Materials & Methods Discussion: Conclusion: Key words
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 9 Ver. X (September). 2016), PP 51-57 www.iosrjournals.org Role Of Various Factors In The Treatment
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 9 Ver. X (September). 2016), PP 51-57 www.iosrjournals.org Role Of Various Factors In The Treatment
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA
 OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
HLA-B27-related anterior Uveitis
 HLA-B27-related anterior Uveitis Nicholas Jones Manchester Uveitis Clinic The Royal Eye Hospital Manchester Anterior means anterior only IUSG classification: Anterior uveitis = Iris & pars plicata AU
HLA-B27-related anterior Uveitis Nicholas Jones Manchester Uveitis Clinic The Royal Eye Hospital Manchester Anterior means anterior only IUSG classification: Anterior uveitis = Iris & pars plicata AU
Neuro-Ophthalmic Masqueraders
 Neuro-Ophthalmic Masqueraders Leonid Skorin, Jr., OD, DO, MS, FAAO, FAOCO Mayo Clinic Health System in Albert Lea Denise Goodwin, OD, FAAO Pacific University College of Optometry Please silence all mobile
Neuro-Ophthalmic Masqueraders Leonid Skorin, Jr., OD, DO, MS, FAAO, FAOCO Mayo Clinic Health System in Albert Lea Denise Goodwin, OD, FAAO Pacific University College of Optometry Please silence all mobile
Haemorrhagic glaucoma
 Brit. j. Ophthal. (I97I) 55, 444 Haemorrhagic glaucoma Comparative study in diabetic and nondiabetic patients P. H. MADSEN From the Departments of Ophthalmology and Internal Medicine, the University Hospital,
Brit. j. Ophthal. (I97I) 55, 444 Haemorrhagic glaucoma Comparative study in diabetic and nondiabetic patients P. H. MADSEN From the Departments of Ophthalmology and Internal Medicine, the University Hospital,
Case History. The SEVEN HABITS of Highly Effective Anterior Uveitis Management. SLEx findings: SLEx corneal findings: y.o.
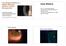 The SEVEN HABITS of Highly Effective Anterior Uveitis Management Case History! 68 y.o. Caucasian female of photophobia and blurred vision! As well as a headache over right eye for 2 days! Complains Paul
The SEVEN HABITS of Highly Effective Anterior Uveitis Management Case History! 68 y.o. Caucasian female of photophobia and blurred vision! As well as a headache over right eye for 2 days! Complains Paul
Mycobacterial Ocular Inflammation. Akbar Shakoor, M.D. John A. Moran Eye Center, University of Utah
 Mycobacterial Ocular Inflammation Akbar Shakoor, M.D. John A. Moran Eye Center, University of Utah Financial Disclosure I have no financial interests or relationships to disclose. Applied anatomy What
Mycobacterial Ocular Inflammation Akbar Shakoor, M.D. John A. Moran Eye Center, University of Utah Financial Disclosure I have no financial interests or relationships to disclose. Applied anatomy What
Differential diagnosis of posterior uveitis
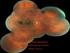 Differential diagnosis of posterior uveitis Diagnostic approach 45-year old male. Floaters and decreased vision since 1 week Fever, lymphadenopathy, myalgias, night sweats, two months ago Oral ulcer sporadically
Differential diagnosis of posterior uveitis Diagnostic approach 45-year old male. Floaters and decreased vision since 1 week Fever, lymphadenopathy, myalgias, night sweats, two months ago Oral ulcer sporadically
Indian Journal of Basic & Applied Medical Research; June 2013: Issue-7, Vol.-2, P
 Original article Clinial Study of different types of Uveitis in Western Maharashtra *Yellambkar ST, *Chavan WM,**Tayade MC *Dept. of Ophthalmology & **Department of Physiology, Rural Medical College, Pravara
Original article Clinial Study of different types of Uveitis in Western Maharashtra *Yellambkar ST, *Chavan WM,**Tayade MC *Dept. of Ophthalmology & **Department of Physiology, Rural Medical College, Pravara
Measure #191: Cataracts: 20/40 or Better Visual Acuity within 90 Days Following Cataract Surgery
 Measure #191: Cataracts: 20/40 or Better Visual Acuity within 90 Days Following Cataract Surgery 2012 PHYSICIAN QUALITY REPORTING OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY DESCRIPTION: Percentage
Measure #191: Cataracts: 20/40 or Better Visual Acuity within 90 Days Following Cataract Surgery 2012 PHYSICIAN QUALITY REPORTING OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY DESCRIPTION: Percentage
Dr Jo-Anne Pon. Dr Sean Every. 8:30-9:25 WS #70: Eye Essentials for GPs 9:35-10:30 WS #80: Eye Essentials for GPs (Repeated)
 Dr Sean Every Ophthalmologist Southern Eye Specialists Christchurch Dr Jo-Anne Pon Ophthalmologist Southern Eye Specialists, Christchurch Hospital, Christchurch 8:30-9:25 WS #70: Eye Essentials for GPs
Dr Sean Every Ophthalmologist Southern Eye Specialists Christchurch Dr Jo-Anne Pon Ophthalmologist Southern Eye Specialists, Christchurch Hospital, Christchurch 8:30-9:25 WS #70: Eye Essentials for GPs
A Case of Carotid-Cavernous Fistula
 A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome)
 Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
Re-emerging infections: Syphilis & Tuberculosis
 Re-emerging infections: Syphilis & Tuberculosis Nicholas Jones Manchester Royal Eye Hospital Syphilis and TB - historical plagues? Syphilis incidence over 40yrs Manchester: Manchester: The Syphilis Capital
Re-emerging infections: Syphilis & Tuberculosis Nicholas Jones Manchester Royal Eye Hospital Syphilis and TB - historical plagues? Syphilis incidence over 40yrs Manchester: Manchester: The Syphilis Capital
UVEITIS IN GENERAL. Information for patients UVEITIS CLINIC WHAT IS UVEITIS? MAIN CATEGORIES OF UVEITIS
 Information for patients UVEITIS CLINIC UVEITIS IN GENERAL WHAT IS UVEITIS? The uvea is a name given to the pigmented layer of tissue inside the eye. When all or part of the uvea becomes inflamed, the
Information for patients UVEITIS CLINIC UVEITIS IN GENERAL WHAT IS UVEITIS? The uvea is a name given to the pigmented layer of tissue inside the eye. When all or part of the uvea becomes inflamed, the
Case History. Slit lamp exam: Clinical Pearls in the Management of Iritis. 2- injection: Irregular SPK and staining AC: grade 3 cell & flare
 Clinical Pearls in the Management of Iritis Paul Karpecki, OD, FAAO Corneal Services and Ocular Disease Research Koffler Vision Group-Lexington, KY 68 y.o. Caucasian female Complains of photophobia and
Clinical Pearls in the Management of Iritis Paul Karpecki, OD, FAAO Corneal Services and Ocular Disease Research Koffler Vision Group-Lexington, KY 68 y.o. Caucasian female Complains of photophobia and
Primary Angle Closure Glaucoma
 www.eyesurgeonlondon.co.uk Primary Angle Closure Glaucoma What is Glaucoma? Glaucoma is a condition in which there is damage to the optic nerve. This nerve carries visual signals from the eye to the brain.
www.eyesurgeonlondon.co.uk Primary Angle Closure Glaucoma What is Glaucoma? Glaucoma is a condition in which there is damage to the optic nerve. This nerve carries visual signals from the eye to the brain.
NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS
 NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS Revision Date: 6/30/06 Distribution Date: 7/6/06 The Department of Ophthalmology at the NYU Medical Center
NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS Revision Date: 6/30/06 Distribution Date: 7/6/06 The Department of Ophthalmology at the NYU Medical Center
EYE TRAUMA: INCIDENCE
 Introduction EYE TRAUMA: INCIDENCE 2.5 million eye injuries per year in U.S. 40,000 60,000 of eye injuries lead to visual loss Introduction Final visual outcome of many ocular emergencies depends on prompt,
Introduction EYE TRAUMA: INCIDENCE 2.5 million eye injuries per year in U.S. 40,000 60,000 of eye injuries lead to visual loss Introduction Final visual outcome of many ocular emergencies depends on prompt,
Placoid pigment epitheliopathy with
 Brit. J. Ophthal. ( I 972) 56, 875 Placoid pigment epitheliopathy with retinal vasculitis and papillitis T. H. KIRKHAM, *T. J. FFYTCHE, AND M. D. SANDERS From the Department of Neuro-Ophthalmology, the
Brit. J. Ophthal. ( I 972) 56, 875 Placoid pigment epitheliopathy with retinal vasculitis and papillitis T. H. KIRKHAM, *T. J. FFYTCHE, AND M. D. SANDERS From the Department of Neuro-Ophthalmology, the
Role of Initial Preoperative Medical Management in Controlling Post-Operative Anterior Uveitis in Patients of Phacomorphic Glaucoma
 Original Article Role of Initial Preoperative Medical Management in Controlling Post-Operative Anterior Uveitis in Patients of Phacomorphic Glaucoma Irfan Qayyum Malik, M. Moin, A. Rehman, Mumtaz Hussain
Original Article Role of Initial Preoperative Medical Management in Controlling Post-Operative Anterior Uveitis in Patients of Phacomorphic Glaucoma Irfan Qayyum Malik, M. Moin, A. Rehman, Mumtaz Hussain
2/16/17. 3 main underlying causes are:
 Definition Etiology Signs/Symptoms Nathan Lighthizer, O.D., F.A.A.O. Assistant Professor Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic Northeastern State University Oklahoma College
Definition Etiology Signs/Symptoms Nathan Lighthizer, O.D., F.A.A.O. Assistant Professor Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic Northeastern State University Oklahoma College
Sarcoidosis. Sarcoidosis Care at National Jewish Health. Causes
 Sarcoidosis Sarcoidosis is a chronic disease that can affect any organ in the body, but most commonly affects the lungs. Very small (microscopic) clusters of inflammation or white cells, called granulomas,
Sarcoidosis Sarcoidosis is a chronic disease that can affect any organ in the body, but most commonly affects the lungs. Very small (microscopic) clusters of inflammation or white cells, called granulomas,
Macular Hole Associated with Vogt-Koyanagi-Harada Disease at the Acute Uveitic Stage
 Published online: September 15, 2015 2015 The Author(s) Published by S. Karger AG, Basel 1663 2699/15/0063 0328$39.50/0 This article is licensed under the Creative Commons Attribution-NonCommercial 4.0
Published online: September 15, 2015 2015 The Author(s) Published by S. Karger AG, Basel 1663 2699/15/0063 0328$39.50/0 This article is licensed under the Creative Commons Attribution-NonCommercial 4.0
Update on management of Anterior Uveitis
 Update on management of Anterior Uveitis Parthopratim Dutta Majumder Senior Consultant, Department of Uvea & Intraocular Inflammation Medical Research Foundation, Sankara Nethralaya ABCD of Treating a
Update on management of Anterior Uveitis Parthopratim Dutta Majumder Senior Consultant, Department of Uvea & Intraocular Inflammation Medical Research Foundation, Sankara Nethralaya ABCD of Treating a
OUR EYES & HOW WE SEE
 OUR EYES & HOW WE SEE UNDERSTAND MORE ABOUT OUR EYES & HOW WE SEE Our Eyes & How We See The eye is our visual gateway to the world. Within it, an array of delicate components labour away to give us the
OUR EYES & HOW WE SEE UNDERSTAND MORE ABOUT OUR EYES & HOW WE SEE Our Eyes & How We See The eye is our visual gateway to the world. Within it, an array of delicate components labour away to give us the
Corneal blood staining after hyphaema
 Brit. J_. Ophthal. (I 972) 56, 589 after hyphaema J. D. BRODRICK Sheffield has been described as a rare complication of contusion injury in which a hyphaema of relatively long duration and a raised intraocular
Brit. J_. Ophthal. (I 972) 56, 589 after hyphaema J. D. BRODRICK Sheffield has been described as a rare complication of contusion injury in which a hyphaema of relatively long duration and a raised intraocular
REFRESHER: ANTERIOR UVEITIS
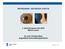 REFRESHER: ANTERIOR UVEITIS 2. SAoO Kongress 28.2.2018 Messe Luzern Dr. med. Christian Böni Augenklinik Universitätsspital Zürich Christian Böni Seite 1 Anterior Uveitis: Clinical Issues Diagnostics: yes
REFRESHER: ANTERIOR UVEITIS 2. SAoO Kongress 28.2.2018 Messe Luzern Dr. med. Christian Böni Augenklinik Universitätsspital Zürich Christian Böni Seite 1 Anterior Uveitis: Clinical Issues Diagnostics: yes
Frosted branch angiitis with undiagnosed Hodgkin lymphoma
 European Journal of Ophthalmology / Vol. 19 no. 2, 2009 / pp. 310-313 SHORT COMMUNICTIONS & CSE REPORTS Frosted branch angiitis with undiagnosed Hodgkin lymphoma MINH-TRI HU 1, PIERRE LISE 1, LURENCE DE
European Journal of Ophthalmology / Vol. 19 no. 2, 2009 / pp. 310-313 SHORT COMMUNICTIONS & CSE REPORTS Frosted branch angiitis with undiagnosed Hodgkin lymphoma MINH-TRI HU 1, PIERRE LISE 1, LURENCE DE
Mild NPDR. Moderate NPDR. Severe NPDR
 Diabetic retinopathy Diabetic retinopathy is the most common cause of blindness in adults aged 35-65 years-old. Hyperglycaemia is thought to cause increased retinal blood flow and abnormal metabolism in
Diabetic retinopathy Diabetic retinopathy is the most common cause of blindness in adults aged 35-65 years-old. Hyperglycaemia is thought to cause increased retinal blood flow and abnormal metabolism in
Metastatic tapioca iris melanoma
 British Journal of Ophthalmology, 1979, 63, 744-749 Metastatic tapioca iris melanoma KAMAL A. ZAKKA, ROBERT Y. FOOS, AND HECTOR SULIT From the Departments of Ophthalmology and Pathology, Jules Stein Eye
British Journal of Ophthalmology, 1979, 63, 744-749 Metastatic tapioca iris melanoma KAMAL A. ZAKKA, ROBERT Y. FOOS, AND HECTOR SULIT From the Departments of Ophthalmology and Pathology, Jules Stein Eye
Table of Contents 1 Orbit 3 2 Eyelids 7
 Table of Contents Preface, x List of abbreviations xi Glossary xii Section I Atlas 1 1 Orbit 3 Clinical signs associated with orbital neoplasia 3 Clinical signs associated with orbital cellulitis 3 Enophthalmos
Table of Contents Preface, x List of abbreviations xi Glossary xii Section I Atlas 1 1 Orbit 3 Clinical signs associated with orbital neoplasia 3 Clinical signs associated with orbital cellulitis 3 Enophthalmos
Case Report Pulmonary Sarcoidosis following Etanercept Treatment
 Case Reports in Rheumatology Volume 2012, Article ID 724013, 4 pages doi:10.1155/2012/724013 Case Report Pulmonary Sarcoidosis following Etanercept Treatment Kuljeet Bhamra and Richard Stevens Department
Case Reports in Rheumatology Volume 2012, Article ID 724013, 4 pages doi:10.1155/2012/724013 Case Report Pulmonary Sarcoidosis following Etanercept Treatment Kuljeet Bhamra and Richard Stevens Department
The Human Eye. Cornea Iris. Pupil. Lens. Retina
 The Retina Thin layer of light-sensitive tissue at the back of the eye (the film of the camera). Light rays are focused on the retina then transmitted to the brain. The macula is the very small area in
The Retina Thin layer of light-sensitive tissue at the back of the eye (the film of the camera). Light rays are focused on the retina then transmitted to the brain. The macula is the very small area in
3 main underlying causes are:
 Nathan Lighthizer, O.D., F.A.A.O. Assistant Professor Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic Northeastern State University Oklahoma College of Optometry Tahlequah, OK lighthiz@nsuok.edu
Nathan Lighthizer, O.D., F.A.A.O. Assistant Professor Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic Northeastern State University Oklahoma College of Optometry Tahlequah, OK lighthiz@nsuok.edu
Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and
 British Journal of Ophthalmology, 1977, 61, 278-284 Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and neovascular glaucoma LEILA LAATIKAINEN From Moorfields Eye Hospital,
British Journal of Ophthalmology, 1977, 61, 278-284 Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and neovascular glaucoma LEILA LAATIKAINEN From Moorfields Eye Hospital,
Glaucoma & Inflammation. Jorge L. Fernandez Bahamonde, MD.
 Glaucoma & Inflammation. Jorge L. Fernandez Bahamonde, MD. Definition. Inflammatory ocular conditions compromise outflow of aqueous humor. Keratitis Episcleritis. Scleritis. Uveitis Glaucoma & Keratitis.
Glaucoma & Inflammation. Jorge L. Fernandez Bahamonde, MD. Definition. Inflammatory ocular conditions compromise outflow of aqueous humor. Keratitis Episcleritis. Scleritis. Uveitis Glaucoma & Keratitis.
!! Definition. !! Etiology. !! Signs/Symptoms. !! Classification/Diagnosis. !! Systemic Associations. !! Lab Testing. !! Treatment. !!
 Nathan Lighthizer, O.D., F.A.A.O. Assistant Professor Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic Northeastern State University Oklahoma College of Optometry Tahlequah, OK lighthiz@nsuok.edu!!
Nathan Lighthizer, O.D., F.A.A.O. Assistant Professor Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic Northeastern State University Oklahoma College of Optometry Tahlequah, OK lighthiz@nsuok.edu!!
Kimura s Disease of the Orbit Successfully Treated with Radiotherapy Alone: A Case Report
 Published online: March 13, 2014 1663 2699/14/0051 0087$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial 3.0 Unported license (CC BY-NC)
Published online: March 13, 2014 1663 2699/14/0051 0087$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial 3.0 Unported license (CC BY-NC)
Note: This is an outcome measure and can be calculated solely using registry data.
 Measure #191 (NQF 0565): Cataracts: 20/40 or Better Visual Acuity within 90 Days Following Cataract Surgery -- National Quality Strategy Domain: Effective Clinical Care DESCRIPTION: Percentage of patients
Measure #191 (NQF 0565): Cataracts: 20/40 or Better Visual Acuity within 90 Days Following Cataract Surgery -- National Quality Strategy Domain: Effective Clinical Care DESCRIPTION: Percentage of patients
Directed conjunctival biopsy and impact of histologic sectioning methodology on the diagnosis of ocular sarcoidosis
 Bui et al. Journal of Ophthalmic Inflammation and Infection 2014, 4:8 ORIGINAL RESEARCH Directed conjunctival biopsy and impact of histologic sectioning methodology on the diagnosis of ocular sarcoidosis
Bui et al. Journal of Ophthalmic Inflammation and Infection 2014, 4:8 ORIGINAL RESEARCH Directed conjunctival biopsy and impact of histologic sectioning methodology on the diagnosis of ocular sarcoidosis
Sarcoid uveitis in a patient with multiple neurological lesions: a case report and review of the literature
 Ohno et al. Journal of Medical Case Reports (2018) 12:307 https://doi.org/10.1186/s13256-018-1842-5 CASE REPORT Open Access Sarcoid uveitis in a patient with multiple neurological lesions: a case report
Ohno et al. Journal of Medical Case Reports (2018) 12:307 https://doi.org/10.1186/s13256-018-1842-5 CASE REPORT Open Access Sarcoid uveitis in a patient with multiple neurological lesions: a case report
Ocular Pathology. I. Congenital and/or developmental. A. Trisomy 21. Hypertelorism (widely spaced eyes) Keratoconus (cone shaped cornea)
 I. Congenital and/or developmental Robbins Pathologic Basis of Disease, 6 th Ed. A. Trisomy 21 Hypertelorism (widely spaced eyes) Keratoconus (cone shaped cornea) Focal hypoplasia of iris Cataracts frequently
I. Congenital and/or developmental Robbins Pathologic Basis of Disease, 6 th Ed. A. Trisomy 21 Hypertelorism (widely spaced eyes) Keratoconus (cone shaped cornea) Focal hypoplasia of iris Cataracts frequently
Head prof. MUDr. E. Vlková, CSc.
 MUDr. Karkanová Michala, Oční klinika LF MU a FN Brno Head prof. MUDr. E. Vlková, CSc. 3 parts: iris (iris) ciliary body (corpus ciliare) choroid (choroidea) Function: regulating the entry of light into
MUDr. Karkanová Michala, Oční klinika LF MU a FN Brno Head prof. MUDr. E. Vlková, CSc. 3 parts: iris (iris) ciliary body (corpus ciliare) choroid (choroidea) Function: regulating the entry of light into
Chest radiograph of an. asymptomatic man. Case report. Case history
 Eleftheria Chaini 1, Niki Giannakou 2, Dimitra Haini 3, Anna Maria Athanassiadou 4, Angelos Tsipis 4, Nikolaos D. Hainis 5 elhaini@otenet.gr 1 Pulmonary Dept, Corfu General Hospital, Kontokali, Greece.
Eleftheria Chaini 1, Niki Giannakou 2, Dimitra Haini 3, Anna Maria Athanassiadou 4, Angelos Tsipis 4, Nikolaos D. Hainis 5 elhaini@otenet.gr 1 Pulmonary Dept, Corfu General Hospital, Kontokali, Greece.
Is Posner Schlossman Syndrome Benign?
 Is Posner Schlossman Syndrome Benign? Aliza Jap, FRCS (G), 1 Meenakshi Sivakumar, FRCS (Ed), M Med (Ophth), 2, Soon-Phaik Chee, FRCS (Ed), FRCOphth 2 Purpose: To determine the clinical course of patients
Is Posner Schlossman Syndrome Benign? Aliza Jap, FRCS (G), 1 Meenakshi Sivakumar, FRCS (Ed), M Med (Ophth), 2, Soon-Phaik Chee, FRCS (Ed), FRCOphth 2 Purpose: To determine the clinical course of patients
For details on measurement and recording of visual acuity, refer to Annex 1. VISION INTERPRETING RESULTS ABSTRACT
 management update on functional decline in older adults 2012 Unit No. 5 VISION Dr Au Eong Kah Guan, Ms Yulianti, Ms Fifiana ABSTRACT Among Singaporean adults of Chinese origin aged 40 to 79 years old,
management update on functional decline in older adults 2012 Unit No. 5 VISION Dr Au Eong Kah Guan, Ms Yulianti, Ms Fifiana ABSTRACT Among Singaporean adults of Chinese origin aged 40 to 79 years old,
Sarcoidosis with Skin Manifestations - Two Case Reports and Review of Literature
 Sarcoidosis with Skin Manifestations - Two Case Reports and Review of Literature Pages with reference to book, From 162 To 164 Shamaila Siddiqi, Aleern Qureshi ( Departments of Dermatology, The Aga Khan
Sarcoidosis with Skin Manifestations - Two Case Reports and Review of Literature Pages with reference to book, From 162 To 164 Shamaila Siddiqi, Aleern Qureshi ( Departments of Dermatology, The Aga Khan
Necrotizing retinitis of multifactorial etiology
 Romanian Journal of Ophthalmology, Volume 61, Issue 1, January-March 2017. pp:49-53 CASE REPORT Necrotizing retinitis of multifactorial etiology Pirvulescu Ruxandra Angela* **, Popa Cherecheanu Alina*
Romanian Journal of Ophthalmology, Volume 61, Issue 1, January-March 2017. pp:49-53 CASE REPORT Necrotizing retinitis of multifactorial etiology Pirvulescu Ruxandra Angela* **, Popa Cherecheanu Alina*
CATARACT SURGERY IN UVEITIS. Professor Harminder Singh Dua
 Research Institute of Ophthalmology, Cairo 11 th International Conference, 3-4 February, 2017 CATARACT SURGERY IN UVEITIS Professor Harminder Singh Dua MBBS, DO, DO(Lond), MS, MNAMS, FRCS, FRCOphth., FEBO,
Research Institute of Ophthalmology, Cairo 11 th International Conference, 3-4 February, 2017 CATARACT SURGERY IN UVEITIS Professor Harminder Singh Dua MBBS, DO, DO(Lond), MS, MNAMS, FRCS, FRCOphth., FEBO,
JOURNAL OF OPHTHALMOLOGY AND RELATED SCIENCES
 JOURNAL OF OPHTHALMOLOGY AND RELATED SCIENCES BILATERAL ACUTE TRANSILLUMINATION OF THE IRIS Kavitha Avadhani 1, MD, MS, Jay Kalliath 1, MS, FRCS 1 Department of Ophthalmology, NMC Speciality Hospital,
JOURNAL OF OPHTHALMOLOGY AND RELATED SCIENCES BILATERAL ACUTE TRANSILLUMINATION OF THE IRIS Kavitha Avadhani 1, MD, MS, Jay Kalliath 1, MS, FRCS 1 Department of Ophthalmology, NMC Speciality Hospital,
J of Evolution of Med and Dent Sci/ eissn , pissn / Vol. 4/ Issue 55/ July 09, 2015 Page 9665
 RARE PRESENTATION OF BILATERAL CHOROIDAL METASTASIS FROM PRIMARY MUCO-EPIDERMOID CARCINOMA OF THE PAROTID GLAND: A G. Premalatha 1, Ramya Seetamraju 2 HOW TO CITE THIS ARTICLE: G. Premalatha, Ramya Seetamraju.
RARE PRESENTATION OF BILATERAL CHOROIDAL METASTASIS FROM PRIMARY MUCO-EPIDERMOID CARCINOMA OF THE PAROTID GLAND: A G. Premalatha 1, Ramya Seetamraju 2 HOW TO CITE THIS ARTICLE: G. Premalatha, Ramya Seetamraju.
Nodular Muscular Sarcoidosis Extending to All Limb Muscles
 47 1997 CD4/8 MRI T1 T2 74.6 IU/l 46.0 µg/ml MRI [ ] MRI Nodular Muscular Sarcoidosis Extending to All Limb Muscles Takahiro Nishitake, Eishi Miyazaki, Masaru Ando, Tetsujiro Fukami, Osamu Matsuno, Takuya
47 1997 CD4/8 MRI T1 T2 74.6 IU/l 46.0 µg/ml MRI [ ] MRI Nodular Muscular Sarcoidosis Extending to All Limb Muscles Takahiro Nishitake, Eishi Miyazaki, Masaru Ando, Tetsujiro Fukami, Osamu Matsuno, Takuya
Pan-uveitis - A rare ocular manifestation of dengue
 Case report DOI: http://dx.doi.org/10.18320/jimd/201603.0147 JOURNAL OF INTERNATIONAL MEDICINE AND DENTISTRY To search..to know...to share p-issn: 2454-8847 e-issn: 2350-045X Pan-uveitis - A rare ocular
Case report DOI: http://dx.doi.org/10.18320/jimd/201603.0147 JOURNAL OF INTERNATIONAL MEDICINE AND DENTISTRY To search..to know...to share p-issn: 2454-8847 e-issn: 2350-045X Pan-uveitis - A rare ocular
Cutaneous Sarcoidosis Misdiagnosed as Leprosy. Report of Two Cases and Review of Literature
 Indian J Lepr 2016, 88 : 177-183 Hind Kusht Nivaran Sangh, New Delhi http://www.ijl.org.in Case Report Cutaneous Sarcoidosis Misdiagnosed as Leprosy. Report of Two Cases and Review of Literature 1 2 3
Indian J Lepr 2016, 88 : 177-183 Hind Kusht Nivaran Sangh, New Delhi http://www.ijl.org.in Case Report Cutaneous Sarcoidosis Misdiagnosed as Leprosy. Report of Two Cases and Review of Literature 1 2 3
Scleritis LEN V KOH OD
 Scleritis LEN V KOH OD 2014 PUCO 1 Introduction A painful, destructive, and potentially blinding disorder Highly symptomatic High association with systemic disease Immunosuppresssive agents 2014 PUCO 2
Scleritis LEN V KOH OD 2014 PUCO 1 Introduction A painful, destructive, and potentially blinding disorder Highly symptomatic High association with systemic disease Immunosuppresssive agents 2014 PUCO 2
Case Report: Indocyanine Green Dye Leakage from Retinal Artery in Branch Retinal Vein Occlusion
 Case Report: Indocyanine Green Dye Leakage from Retinal Artery in Branch Retinal Vein Occlusion Hiroki Fujita, Kyoko Ohno-Matsui, Soh Futagami and Takashi Tokoro Department of Visual Science, Tokyo Medical
Case Report: Indocyanine Green Dye Leakage from Retinal Artery in Branch Retinal Vein Occlusion Hiroki Fujita, Kyoko Ohno-Matsui, Soh Futagami and Takashi Tokoro Department of Visual Science, Tokyo Medical
Outline. Brief history and principles of ophthalmic ultrasound. Types of ocular ultrasound. Examination techniques. Types of Ultrasound
 Ultrasound and Intraocular Tumors 2015 Ophthalmic Photographers' Society Mid-Year Program Cagri G. Besirli MD, PhD Kellogg Eye Center University of Michigan Outline Brief history and principles of ophthalmic
Ultrasound and Intraocular Tumors 2015 Ophthalmic Photographers' Society Mid-Year Program Cagri G. Besirli MD, PhD Kellogg Eye Center University of Michigan Outline Brief history and principles of ophthalmic
OCULAR lesions occur in approximately 50 per cent of patients having
 MARVIN F. GREEN, M.D.,* AND ROSCOE J. KENNEDY, M.D. Department of Ophthalmology OCULAR lesions occur in approximately 50 per cent of patients having sarcoidosis. It is the purpose of this paper to review
MARVIN F. GREEN, M.D.,* AND ROSCOE J. KENNEDY, M.D. Department of Ophthalmology OCULAR lesions occur in approximately 50 per cent of patients having sarcoidosis. It is the purpose of this paper to review
manifestations are uncommon. Initial descriptions of the disease (Rosai and Dorfman, 1969) specifically
 Postgraduate Medical Journal (July 1980) 56, 521-525 Diffuse cutaneous involvement and sinus histiocytosis with massive lymphadenopathy A. A. WOODCOCK B.Sc., M.B., Ch.B., M.R.C.P. Summary Severe skin involvement
Postgraduate Medical Journal (July 1980) 56, 521-525 Diffuse cutaneous involvement and sinus histiocytosis with massive lymphadenopathy A. A. WOODCOCK B.Sc., M.B., Ch.B., M.R.C.P. Summary Severe skin involvement
OCCASIONAL COMMUNICATIONS
 UVEITIS: DIAGNOSIS AND MANAGEMENT T. Akerele and S. Lightman, Department of Clinical Ophthalmology, Institute of Ophthalmology, London and Moorfields Eye Hospital, London Uveitis is a generic term which
UVEITIS: DIAGNOSIS AND MANAGEMENT T. Akerele and S. Lightman, Department of Clinical Ophthalmology, Institute of Ophthalmology, London and Moorfields Eye Hospital, London Uveitis is a generic term which
Year 2 MBChB Clinical Skills Session Ophthalmoscopy. Reviewed & ratified by: Mr M Batterbury Consultant Ophthalmologist
 Year 2 MBChB Clinical Skills Session Ophthalmoscopy Reviewed & ratified by: o Mr M Batterbury Consultant Ophthalmologist Learning objectives o To understand the anatomy and physiology of the external and
Year 2 MBChB Clinical Skills Session Ophthalmoscopy Reviewed & ratified by: o Mr M Batterbury Consultant Ophthalmologist Learning objectives o To understand the anatomy and physiology of the external and
An Introduction to Radiology for TB Nurses
 An Introduction to Radiology for TB Nurses Garold O. Minns, MD September 14, 2017 TB Nurse Case Management September 12 14, 2017 EXCELLENCE EXPERTISE INNOVATION Garold O. Minns, MD has the following disclosures
An Introduction to Radiology for TB Nurses Garold O. Minns, MD September 14, 2017 TB Nurse Case Management September 12 14, 2017 EXCELLENCE EXPERTISE INNOVATION Garold O. Minns, MD has the following disclosures
Intraocular Tuberculosis
 Eye (1990) 4, 486-492 Intraocular Tuberculosis P. H. ROSEN*, D. 1. SPALTON and E. M. GRAHAM London Summary 1Welve patients with a diagnosis of intraocular tuberculosis are described. Nine patients presented
Eye (1990) 4, 486-492 Intraocular Tuberculosis P. H. ROSEN*, D. 1. SPALTON and E. M. GRAHAM London Summary 1Welve patients with a diagnosis of intraocular tuberculosis are described. Nine patients presented
