Pyoderma gangrenosum in myelodysplasia and acute leukaemia
|
|
|
- Marybeth Audra Joseph
- 5 years ago
- Views:
Transcription
1 Postgraduate Medical Journal (1985) 61, Pyoderma gangrenosum in myelodysplasia and acute leukaemia Peter Jacobs', S. Palmer2 and E.C. Gordon-Smith2 'The University ofcape Town Leukaemia Centre and the Department ofhaematology, Groote Schuur Hospital, Observatory, 7925, Cape Town, South Africa and 'The Department ofhaematology, Royal Postgraduate Medical School, London, UK. Summary: Pyoderma gangrenosum is a rare occurrence in patients with haematological malignancy. This characteristic but nonspecific inflammatory process with skin destruction occurred in 4 patients with myelodysplasia, in one with acute leukaemic transformation of myelofibrosis, and in de novo acute myeloblastic leukaemia in another. Clinically, the cutaneous lesion in these patients differed from that associated with inflammatory bowel disease, arthritis, or the idiopathic type of pyoderma gangrenosum by having the vesiculo-bulious borders. Histopathological differences were also evident since more superficial layers of the skin were involved in the ulceration than typically encountered in patients with non-malignant systemic disease. Despite the less penetrating nature of this variant, treatment of the pyoderma gangrenosum is unsatisfactory and in the absence of effective therapy for the underlying disease, healing occurred only in the patient with acute leukaemia who achieved complete remission in response to chemotherapy. Introduction Pyoderma gangrenosum describes a nonspecific form of cutaneous ulceration that is progressive, begins as a tender erythematous nodule, then forms a pustule, followed by rapid central necrosis characterized by oedematous and dusky overhanging borders with a surrounding margin of erythema (Brunsting et al., 1930). The ulcers typically enlarge to exceed 10 cm in diameter, persist for weeks or months, and heal with scarring, often to recur over a period of years. Although in many instances there is no clear association with any underlying systemic disease, giving rise to the concept of idiopathic pyoderma gangrenosum, the classical clinical association is with ulcerative colitis, where an incidence between 1% and 3% has been reported (Sloan et al., 1950; Perry & Brunsting, 1957). Pyoderma gangrenosum may also be found with arthritis (Stolman et al., 1975; Holt, 1980), and in a number of less clearly defined disorders (Wolff & Stingl, 1983). Maldonada and his associates (1968) first reported the occurrence of this entity with leukaemia. Subsequently, an atypical variant was described in chronic granulocytic and myelomonocytic leukaemia, where Correspondence: Professor P. Jacobs, F.R.C.P. (Edin), F.R.C.Path. (UK), Department of Haematology - Research Centre, University of Cape Town Medical School, Anzio Road, Observatory 7925, Cape Town, South Africa. Accepted: 27 February 1985 the lesions were more superficial and their margins bullous (Perry & Winkelmann, 1972). Further experience (Tay, 1973; Fayolle et al., 1974; Goldin, 1974; Lewis et al., 1978) has emphasized clinical differences between the typical lesions of the idiopathic type, those associated with inflammatory bowel disease or arthritis, and the ulceration found together with haematological malignancy. In the former examples this destructive skin lesion extends into and involves the reticular layer of the dermis and the subcutis, but usually spares the subcutaneous tissue. In contrast, the skin pathology found with myelodysplasia or leukaemia is more superficial and has vesiculo-bullous borders. No specific causative agent has been isolated and while pathergy, which describes the phenomenon of trivial trauma provoking new lesions or aggravating existing ones (Wolff & Stingl, 1983), has been reported, there is generally spontaneous healing in parallel with resolution or control of the underlying disorder. In patients with the myelodysplastic syndrome, relentless progression of the induration and the ulcer occur, providing an ideal nidus for secondary infection, leadi-ng -to- septicaemia and death. In those patients where leukaemia responds to treatment, complete healing of the ulcer may occur. These points are emphasized by our experience with 4 patients having preleukaemia and 2 with acute leukaemia, all having pyoderma gangrenosum. )D The Fellowship of Postgraduate Medicine, 1985
2 690 P. JACOBS et al. Case histories Case 1 A 39 year old male developed severe anaemia in October 1977 when a bone marrow biopsy showed dyserythropoiesis and a mild increase in blast cells. Over the next 2 y he was maintained on intermittent red cell transfusions. Two weeks after a transfusion, in October 1979, the patient noticed pain in his left calf. The following day a bruise developed over the left ankle. Over the next 10 d this slowly enlarged to form a superficial haematoma. Surgical drainage was attempted but this was followed by the development of a large ulcer. He was transferred to Hammersmith Hospital in December At that time he had a large necrotic ulcer measuring 11 cm x 8 cm over the left medial malleolus. The edge of the ulcer showed the typical rolled edge and blue-grey colour of pyoderma gangrenosum. The patient was febrile and had a palpable spleen 4 cm below the costal margin. Haematology results showed haemoglobin 8.3 g/dl, white blood count 3.3 x 109/l, and platelets 15 x 109/l. Differential count showed 8% blast cells, 8% myelocytes, 4% metamyelocytes, 44% neutrophils, 27% lymphocytes and 9% monocytes. The neutrophils were abnormal, with marked hypogranularity and abnormal segmentation. The bone marrow was hypercellular with abnormal granulopoiesis, dyserythropoiesis and scanty mononuclear megakaryocytes. Blast cells constituted 8% of the differential count. Bone marrow chromosomes showed a consistent pseudodiploid abnormality. A diagnosis of myelodysplastic syndrome without leukaemic change was made. Initial treatment with prednisone at 60 mg/day resulted in a good response with decreased erythema and some healing. However, as the dose of prednisone was reduced relapse of the pyoderma occurred. A month after commencement of prednisone the dose had been reduced to 20 mg/day and at that time the patient developed swelling in his right scrotum. Initially, this was thought to be an epididymo-orchitis. However, there was no response to antibiotics and the lesion rapidly advanced to pyoderma gangrenosum. This eventually resulted in a scrotal-rectal fistula, the patient dying soon after from secondary infection. No specific pathogens were cultured from the early lesions. During his stay in hospital there was no evidence of development of an overt leukaemia. Case 2 A 58 year old man first presented in July 1979 with symptoms of aching limbs. He was noted to be anorexic, and subsequent blood test showed a pancytopenia. Over the next 9 months he required red cell transfusion every 4 weeks. Corticosteroids were given but this made no difference to his pancytopenia. In March 1980, on a dose of 15 mg prednisone a day he developed a painful haematoma on his left leg. This eventually broke down and developed into a large chronic ulcer. When seen at Hammersmith Hospital he had pyoderma gangrenosum on his shin, measuring 15 cm in diameter. He had no lymphadenopathy and his spleen was not palpable. Haematology results showed haemoglobin 14.4 g/dl, white blood count 0.9 x 109/l with 18% neutrophils, and platelets 22 x 109/l. The bone marrow aspirate and trephine biopsy were both hypocellular with marked depression of granulopoiesis and erythropoiesis. Blast cells constituted 20% of the differential count. The appearances were those of a refractory anaemia with increased blast cells. His subsequent course was one of gradual deterioration. He became progressively more pancytopenic and suffered recurrent infections. The pyoderma gangrenosum failed to heal but had not extended at the time of his death from septicaemia. The patient did not progress to overt leukaemia. Case 3 A 78 year old white man presented in February 1980 short of breath with haemorrhagic lesions over the scrotum. Examination revealed bruises over the arms and legs and 3 cm hepatosplenomegaly. Haemoglobin was 6.9 g/dl, MCV 105 fl, white blood count of 2.3 x 109/l with 22% neutrophils, 45% lymphocytes, 3% eosinophils, 5% monocytes, 20% hypogranular myelocytes and promyelocytes, with 5% myeloblasts. Platelets were 58 x 109/l and there were 5 nucleated red cells for every 100 white cells in the differential count. Bone marrow aspiration and trephine biopsy showed hypercellularity, megaloblastic haematopoiesis, and 10% atypical myeloblasts. In view of the patient's age and unwillingness to undergo any form of chemotherapy he was treated with blood transfusions. Quality of life remained excellent and peripheral blast count varied between 4% and 36%. Five months after diagnosis a hot tender swelling developed on the right thigh following very minor injury. This became a red indurated area of cellulitis that formed an abscess which spontaneously ruptured. Culture of the sero-sanguineous material was negative. The centre of this cutaneous lesion became a black necrotic eschar measuring 10 cm in diameter and the edges were rolled and purple in colour. Biopsy showed nonspecific inflammatory changes. Culture of curettings and skin biopsy grew a staphylococcus resistant to cloxacillin, two strains of bacteroides, and a scanty growth of Klebsiella and Clostridium welchii. Shortly after this a second lesion
3 developed on the left lower chest and biopsy again showed nonspecific inflammatory infiltrate only; cultures were negative. The clinical picture of both lesions was considered to be that of pyoderma gangrenosum and the patient treated on 1 mg/kg of prednisone orally each day, red cell transfusions as necessary to maintain haemoglobin between 10 and 12 g/dl, and no specific therapy for the preleukaemia. Despite regular dressings the lesions, which remained clean, failed to granulate and progressed gradually. Nine months after diagnosis the blast count gradually rose to over 70%, thrombocytopenia became more severe and the patient developed pneumonia and septicaemia, and died in November Case 4 A 60 year old man presented in November 1976 for a routine medical examination. Haemoglobin was 11.9 g/dl, MCV 95 fl, white blood count 1.3 x 109/l. Myelodysplastic features were present in the granulocytic series. Bone marrow was hypercellular with increase in ringed sideroblasts, monocytes were prominent, and hypogranularity was evident in the myeloid series. A diagnosis of preleukaemia was made and the patient observed without therapy. In February of 1978 he again sought medical attention because of boils. At this time haemoglobin was 8.3 g/dl, white cell count and morphology unchanged, but platelets were 53 x 109/l. In June, one of the boils had become indurated and formed a mass in his left calf, measuring 8 x 10 cm with a large surrounding erythematous area. A clinical diagnosis of cellulitis was made and the patient treated with antibiotics. There was a slow improvement in the erythema, but localization and spontaneous rupture with central breakdown and extensive tissue necrosis occurred within 4 weeks. By September of that year 3 further similar lesions had occurred and with the clinical condition relatively stable, the patient was managed on transfusions only. In March of the following year the patient presented again with a large perianal swelling and a mass in the left quadriceps. The perianal lesion resolved slowly but that in the thigh broke down, draining serosanguineous fluid which was repeatedly negative on blood culture. Within 2 months further lesions had developed and the patient admitted with septicaemic shock and died. Terminally, granulocytes were absent from the peripheral circulation. Bone marrow examination was unchanged from the initial study and showed no leukaemic transformation. Case 5 The patient, a 44 year old woman, first presented in PYODERMA GANGRENOSUM IN MALIGNANCY 691 August 1980 with spontaneous bruising and tiredness. Bone marrow aspiration was unsuccessful but the bone marrow trephine biopsy showed malignant myelofibrosis with marked increase in reticulin and collagen, megakaryocytic proliferation and increased blast cells. From August 1980 to March 1981 she was given intermittent blood transfusion and remained reasonably well. In March 1981 she was readmitted to hospital with symptoms of tiredness and bleeding. Haematology results at that time showed haemoglobin 5 g/dl, white blood count 0.4 x 109/l, and platelets 12 x 109/l. She was given systemic antibiotics for continuing fever and commenced on prednisone. While in hospital she developed severe pain in both legs. Within 24 h she developed two areas of erythema and bruising on her lower limbs. In April 1981 she was transferred to Hammersmith Hospital. On both legs there were single raised tender purple nodules covered by shiny smooth skin. The larger nodule showed early bullous formation and measured 5 cm x 4 cm and over the next 3 d ulcerated to show the typical features of a superficial bullous pyoderma gangrenosum. No specific pathogens were cultured from the lesion. Haematology on admission showed haemoglobin 10.3 g/dl, white blood count 1.3 x 109/l, and platelets 7 x 109/l. The differential count showed 65% blast cells, 5% segmented neutrophils, 25% lymphocytes, and 4% monocytes. The trephine biopsy showed replacement of normal elements with blast cells. Reticulin was moderately increased. The appearances were those of an acute leukaemic transformation of myelofibrosis. Dapsone was added to the prednisone with no beneficial effect, and both the pyoderma gangrenosum and the leukaemia progressed rapidly. The patient had been unwilling to have a trial of chemotherapy and died of septicaemia shortly afterwards. Case 6 A 19 year old woman attended the casualty section of Groote Schuur Hospital for a large necrotic ulcer on her right leg (Figure 1). She had no previous illness. On examination she was found to have a haemoglobin of 5 g/dl, given a blood transfusion, and, after dressing the wound, was discharged, to be followed as an outpatient. Three weeks later she re-presented with a fever of 38.5 C and was empirically treated with antibiotics. Dressings to the wound continued but this now measured 16 cm x 12 cm and was noted to have a gangrenous centre. Blood count showed haemoglobin of 6 g/dl, total white blood count of 1.5 x 109/1, with 7% neutrophils, 3% band forms, 1% eosinophils, 3% basophils, 70% lymphocytes, and 16% myeloblasts; platelet count was 60 x 1009/l. Bone marrow aspiration and trephine showed extensive replacement with
4 692 P. JACOBS et al.... : Figure 1 A large necrotic ulcer is seen on the right leg of the sixth patient. This was the presenting sign of her underlying leukaemia. myeloblasts and a diagnosis of acute leukaemia was made. The patient achieved complete remission in response to cytosine arabinoside, doxorubicin, and VP (Jacobs et al., 1984), and after two courses of consolidation treatment entered a maintenance programme. The skin lesion healed completely, although slowly, over a period of 8 weeks (Figure 2) from commencing chemotherapy but recurred in the same site 16 months later when the patient relapsed. Further chemotherapy was unsuccessful and she eventually died from overwhelming sepsis. Discussion The pathogenesis of pyoderma gangrenosum is uncertain and circumstantial evidence suggests -that it is a form of vasculitis (Allen & Reeves, 1977). In our patients, with the exception of the one having acute leukaemia who responded to chemotherapy, the lesions were extensive, often multiple, penetrated the deeper layers of the dermis, failed to heal, and were thought to be the site from which bacterial invasion eventually led to septicaemia and death of the 5 individuals. It is, however, noteworthy that in the sixth patient, although the lesion at first appeared to penetrate deeply into the dermis, slow but complete healing took place once remission had been induced with chemotherapy; eventually only an area of increased pigmentation remained. This latter experience would therefore be consistent with the suggestion that in haematological malignancy, despite initial and perhaps misleading appearances, more superficial ulceration may exist. It is not clear to what extent neutropenia or granulocyte dysfunction may decrease durin thex heln - 4 I' *. X% a s _ Fry ''.5 haste. Th upiigygorsra tion of tissue is well demonstrated and eventually only an area of pigmentation remained. leucocyte-mediated tissue destruction in these individuals. The occurrence of pyoderma gangrenosum is recognized with acute and chronic leukaemia; both lymphoblastic and myeloblastic (Perry & Winkelman, 1972; Lewis et at., 1978; Ortonne et at., 1979). However, its association with acute myeloproliferative disease (Toolis et at., 1978; Caughman et at., 1983) and the myelodysplastic or preleukaemic syndromes appears to have been less well described. The latter poses particularly difficult therapeutic challenges since the available evidence in rheumatoid arthritis and ulcerative colitis, as well as with our sixth patient, suggests that healing of the ulcer is only likely to occur once underlying disease has either been controlled or eradicated. In the latter group of patients treatment is not satisfactory and it remains to be seen whether the use of maturation-inducing agents such as low-dose cytosine arabinoside or administration of retinoids which, in laboratory culture systems may diminish proliferation and facilitate differentiation, will bring
5 References ALLEN, B.R. & REEVES, W.G. (1977). Skin disease. In Immunology in Medicine. A Comprehensive Guide to Clinical Immunology. Holborow, E.J. & Reeves, W.G., (Eds) pp Academic Press: London. BRUNSTING, L.A., GOECKERMAN, W.H. & O'LEARY, P.A. (1930). Pyoderma (echthyma) gangrenosum: clinical and experimental observation in five cases occurring in adults. Archives of Dermatology and Syphilology, 22, 655. CAUGHMAN, W., STERN, R. & HAYNES, H. (1983). Neutrophilic dermatosis ofmyeloproliferative disorders. Atypical forms of pyoderma gangrenosum and Sweet's syndrome associated with meloproliferative disorders. Journal of the American Academy of Dermatology, 9, 751. CRAWFORD, S.E., SHERMAN, R. & FAVARA, B. (1967). Pyoderma gangrenosum with response to cyclophosphamide therapy. Journal of Pediatrics, 71, 255. FAYOLLE, J., ENAY, G. & WOEHRIE, R. (1974). Pyoderma gangrenosum et leucose aigue myeloblastique: Cas personnel et revue de la literature. Lyon Medical, 232, 85. GOLDIN, D. (1974). Pyoderma gangrenosum with chronic myeloid leukaemia. Proceedings of the Royal Society of Medicine, 67, HOLT, P.J., DAVIES, M.G., SAUNDERS, K.C. & NUKI, G. (1980). Pyoderma gangrenosum: clinical and laboratory findings in 15 patients with special reference to polyarthritis. Medicine (Baltimore), 59, 114. JACOBS, P., DUBOVSKY, D.W. & WOOD, L. (1984). In adult acute nonlymphoblastic leukaemia extended maintenance PYODERMA GANGRENOSUM IN MALIGNANCY 693 about comparable in vivo changes which may then allow tissue repair. In more general terms, approaches to specific therapy have also been unrewarding. Systemic adrenocorticosteroids have produced rapid clinical improvement in many cases, particularly of inflammatory bowel disease and rheumatoid arthritis, where healing may reflect decreasing activity of the inflammatory process. Similarly, sulphone derivatives (Perry & Winkelman, 1972), antimetabolites (Crawford et al., 1967; Maldonada et al., 1968) or clofazimine (Thomsen & Rothenberg, 1979; Holt et al., 1980) may have an effect; here again, it is not clear whether benefit is related to the effect of the therapeutic agent on the ulcer or, as seems more probable, on the underlying disease, with spontaneous slow resolution of the skin lesion following thereafter. However, with clofazimine the enhanced intracellular killing of bacteria and increased phagocytosis of neutrophils shown in vitro and in vivo suggest an effect at cellular level, but the exact mechanism of action in this disease remains unknown. Swift healing of the lesions has also been reported (Lewis et al., 1978) in one leukaemic patient following commencement of cytosine arabinoside and daunorubicin therapy. The latter workers drew attention to one curious observation in their two patients where rapid resolution of previously extensive erythema, oedema, and intense local tenderness followed excision of necrotic tissue in one and response in a single lesion following an extensive biopsy whilst others continued to enlarge. It is concluded that pyoderma gangrenosum may occur with greater frequency than is generally appreciated in patients with acute and chronic leukaemia as well as in the myelodysplastic syndromes. Particularly in this latter group of individuals, an atypical form of the ulcers may exist with involvement of the more superficial layers of the skin and an unusual vesiculo-bullous border. Treatment remains unsatisfactory and is only likely to take place slowly and spontaneously with induction of complete remission in acute leukaemia; the possibility that a similar response may follow the use of maturation-inducing agents in the myelodysplastic syndrome remains speculative. Acknowledgements Supported by the University of Cape Town Leukaemia Centre and Staff Research Fund, the Medical Research Council and National Cancer Institute. We thank Jackie Davies for secretarial assistance and the Medical Superintendent of Groote Schuur Hospital for permission to publish. chemotherapy has no benefit. American Journal of Hematology, 16, 255. LEWIS, S.J., POH-FITZPATRICK, M.B. & WALTHER, R.R. (1978). Atypical pyoderma gangrenosum with leukemia. Journal of the American Medical Association, 239, 935. MALDONADA, N., TORRES, V., MENDEZ-CASHION, D., PEREZ-SANTIAGO, E. & DE COSTA, M.C. (1968). Pyoderma gangrenosum treated with 6-mercaptopurine and followed by acute leukaemia. Journal ofpediatrics, 72, 409. ORTONNE, J.P., THIVOLET, J., CHOUVET, B. & COIFFET, J. (1979). Pyoderma gangrensum, ovarian carcinoma treated with melphalan and acute myelomonocytic leukaemia: report of one case and literature review (Fren). Anales de Dermatologie et de Venereologie, 106, 251. PERRY, H.O. & BRUNSTING, L.A. (1957). Pyoderma gangrenosum: a clinical study of nineteen cases. Archives of Dermatology 75, 380. PERRY, H.O. & WINKELMANN, R.K. (1972). Bullous pyoderma gangrenosum and leukaemia. Archives of Dermatology, 106, 901. SLOAN, W.P., BARGEN, J.A. & GAGE, R.P. (1950). Life histories of patients with chronic ulcerative coliti.: A review of 2000 cases. Gastroenterology, 16, 25. STOLMAN, L.P., ROSENTHAL, D., YAWORSKY, R. & HORAN, F. (1975). Pyoderma gangrenosum and rheumatoid arthritis. Archives ofdermatology, 111, TAY, C.A. (1973). Pyoderma gangrenosum and leukemia.
6 694 P. JACOBS et al. Archives of Dermatology, 108, 580. THOMSEN, K. & ROTHENBORG, H.W. (1979). Clofazimine in the treatment of pyoderma gangrenosum. Archives of Dermatology, 115, 851. TOOLIS, F., PARKER, A.C. & BARNETSON, R. (1978). Pyoderma gangrenosum associated with acute myeloproliferative dissease (?erythroleukaemia). Postgraduate Medicine, 54, 830. WOLFF, K. & STINGL, G.(1983). Pyoderma gangrenosum. In Dermatology in General Medicine, pp Fitzpatrick, T.B., Arndt, K.A., Clark, W.H., van Scott, E.J. & Vaughan. J.H. (eds). McGraw-Hill: New York. Postgrad Med J: first published as /pgmj on 1 August Downloaded from on 2 October 2018 by guest. Protected by
CASE REPORT ATYPICAL BULLOUS PYODERMA GANGRENOSUM WITH EARLY LESIONS MIMICKING CHICKEN POX
 ATYPICAL BULLOUS PYODERMA GANGRENOSUM WITH EARLY LESIONS MIMICKING CHICKEN POX Ramesh M 1, Kavya Raju Nayak 2, M.G. Gopal 3, Sharath Kumar B.C 4, Nandini A.S 5 HOW TO CITE THIS ARTICLE: Ramesh M, Kavya
ATYPICAL BULLOUS PYODERMA GANGRENOSUM WITH EARLY LESIONS MIMICKING CHICKEN POX Ramesh M 1, Kavya Raju Nayak 2, M.G. Gopal 3, Sharath Kumar B.C 4, Nandini A.S 5 HOW TO CITE THIS ARTICLE: Ramesh M, Kavya
Clinical & Laboratory Assessment
 Clinical & Laboratory Assessment Dr Roger Pool NHLS & University of Pretoria Clinical Assessment (History) Anaemia ( haemoglobin) Dyspnoea (shortness of breath) Tiredness Angina Headache Clinical Assessment
Clinical & Laboratory Assessment Dr Roger Pool NHLS & University of Pretoria Clinical Assessment (History) Anaemia ( haemoglobin) Dyspnoea (shortness of breath) Tiredness Angina Headache Clinical Assessment
Hematology Unit Lab 2 Review Material
 Objectives Hematology Unit Lab 2 Review Material - 2018 Laboratory Instructors: 1. Assist students during lab session Students: 1. Review the introductory material 2. Study the case histories provided
Objectives Hematology Unit Lab 2 Review Material - 2018 Laboratory Instructors: 1. Assist students during lab session Students: 1. Review the introductory material 2. Study the case histories provided
Leukemias. Prof. Mutti Ullah Khan Head of Department Medical Unit-II Holy Family Hospital Rawalpindi Medical College
 Leukemias Prof. Mutti Ullah Khan Head of Department Medical Unit-II Holy Family Hospital Rawalpindi Medical College Introduction Leukaemias are malignant disorders of the haematopoietic stem cell compartment,
Leukemias Prof. Mutti Ullah Khan Head of Department Medical Unit-II Holy Family Hospital Rawalpindi Medical College Introduction Leukaemias are malignant disorders of the haematopoietic stem cell compartment,
Abscess. A abscess is a localized collection of pus in the skin and may occur on any skin surface and be formed in any part of body.
 Abscess A abscess is a localized collection of pus in the skin and may occur on any skin surface and be formed in any part of body. Ethyology Bacteria causing cutaneous abscesses are typically indigenous
Abscess A abscess is a localized collection of pus in the skin and may occur on any skin surface and be formed in any part of body. Ethyology Bacteria causing cutaneous abscesses are typically indigenous
MYELODYSPLASTIC SYNDROMES
 MYELODYSPLASTIC SYNDROMES Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra university hospital, Isfahan university of medical sciences Key Features ESSENTIALS OF DIAGNOSIS Cytopenias
MYELODYSPLASTIC SYNDROMES Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra university hospital, Isfahan university of medical sciences Key Features ESSENTIALS OF DIAGNOSIS Cytopenias
HAEMATOLOGICAL MALIGNANCY
 HAEMATOLOGICAL MALIGNANCY Reference Compulsory reading Haematology at Glance 2 nd ed. Atul Mehta & Victor Hoffbrand Chapters: 20 to 31 Pages: 46 to 69 Pathogenesis of Haematological Malignancy Figure (a)
HAEMATOLOGICAL MALIGNANCY Reference Compulsory reading Haematology at Glance 2 nd ed. Atul Mehta & Victor Hoffbrand Chapters: 20 to 31 Pages: 46 to 69 Pathogenesis of Haematological Malignancy Figure (a)
Extensive bone marrow infarction followed by myelofibrosis in a patient with Ph' positive chronic granulocytic leukaemia
 J Clin Pathol 1980; 33: 449-453 Extensive bone marrow infarction followed by myelofibrosis in a patient with Ph' positive chronic granulocytic leukaemia BARBARA BAIN From the Department of Haematology,
J Clin Pathol 1980; 33: 449-453 Extensive bone marrow infarction followed by myelofibrosis in a patient with Ph' positive chronic granulocytic leukaemia BARBARA BAIN From the Department of Haematology,
BLASTIC CRISIS AND MYELOFIBROSIS SIMULTANEOUS COMPLICATIONS IN A CASE OF CHRONIC MYELOCYTIC LEUKEMIA
 BLASTIC CRISIS AND MYELOFIBROSIS SIMULTANEOUS COMPLICATIONS IN A CASE OF CHRONIC MYELOCYTIC LEUKEMIA Abstract Pages with reference to book, From 151 To 153 Khalid Hassan ( Department of Pathology (Haematology)
BLASTIC CRISIS AND MYELOFIBROSIS SIMULTANEOUS COMPLICATIONS IN A CASE OF CHRONIC MYELOCYTIC LEUKEMIA Abstract Pages with reference to book, From 151 To 153 Khalid Hassan ( Department of Pathology (Haematology)
Atypical bullous pyoderma gangrenosum associated
 J Clin Pathol 1987;40:387-392 Atypical bullous pyoderma gangrenosum associated with myeloid malignancies C R M HAY,* A G MESSENGER,t D W K COTTON,$ S S BLEEHEN,t D A WINFIELD* From the University Departments
J Clin Pathol 1987;40:387-392 Atypical bullous pyoderma gangrenosum associated with myeloid malignancies C R M HAY,* A G MESSENGER,t D W K COTTON,$ S S BLEEHEN,t D A WINFIELD* From the University Departments
Group of malignant disorders of the hematopoietic tissues characteristically associated with increased numbers of white cells in the bone marrow and
 Group of malignant disorders of the hematopoietic tissues characteristically associated with increased numbers of white cells in the bone marrow and / or peripheral blood Classified based on cell type
Group of malignant disorders of the hematopoietic tissues characteristically associated with increased numbers of white cells in the bone marrow and / or peripheral blood Classified based on cell type
Rory McCulloch. Specialty Trainee Haematology Royal Devon & Exeter Hospital
 Rory McCulloch Specialty Trainee Haematology Royal Devon & Exeter Hospital Anaemia 1 Haematological disorders Anaemia 2 Non-haematological disorders Substrates: Iron, folate, vitamin B12 Red cell mass
Rory McCulloch Specialty Trainee Haematology Royal Devon & Exeter Hospital Anaemia 1 Haematological disorders Anaemia 2 Non-haematological disorders Substrates: Iron, folate, vitamin B12 Red cell mass
Pyoderma gangrenosum presenting with acute generalised haemorrhagic bullae
 H.K. Dermatol. Venereol. Bull. (2003) 11, 155-159 Case Report Pyoderma gangrenosum presenting with acute generalised haemorrhagic bullae YH Chan, WYM Tang, WY Lam A 31-year-old Chinese man presented with
H.K. Dermatol. Venereol. Bull. (2003) 11, 155-159 Case Report Pyoderma gangrenosum presenting with acute generalised haemorrhagic bullae YH Chan, WYM Tang, WY Lam A 31-year-old Chinese man presented with
HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT
 HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT Nirmala Ponnuthurai, Sabeera Begum, Lee Bang Rom Paediatric Dermatology Unit, Institute of Paediatric, Hospital Kuala Lumpur, Malaysia Abstract
HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT Nirmala Ponnuthurai, Sabeera Begum, Lee Bang Rom Paediatric Dermatology Unit, Institute of Paediatric, Hospital Kuala Lumpur, Malaysia Abstract
Introduction to Haematology. Prof Roger Pool Department of Haematology University of Pretoria
 Introduction to Haematology Prof Roger Pool Department of Haematology University of Pretoria Suggested reading Haematology at a Glance Atul Mehta & Victor Hoffbrand Second Edition Published by Blackwell
Introduction to Haematology Prof Roger Pool Department of Haematology University of Pretoria Suggested reading Haematology at a Glance Atul Mehta & Victor Hoffbrand Second Edition Published by Blackwell
Superficial Granulomatous Pyoderma of the Face: A Case Report and Review of the Literature
 Superficial Granulomatous Pyoderma of the Face: A Case Report and Review of the Literature Sarah M. Persing, MPH, a and Donald Laub Jr, MD, FACS a,b a University of Vermont College of Medicine, Burlington;
Superficial Granulomatous Pyoderma of the Face: A Case Report and Review of the Literature Sarah M. Persing, MPH, a and Donald Laub Jr, MD, FACS a,b a University of Vermont College of Medicine, Burlington;
Juvenile Myelomonocytic Leukemia (JMML)
 Juvenile Myelomonocytic Leukemia (JMML) JMML: Definition Monoclonal hematopoietic disorder of childhood characterized by proliferation of the granulocytic and monocytic lineages Erythroid and megakaryocytic
Juvenile Myelomonocytic Leukemia (JMML) JMML: Definition Monoclonal hematopoietic disorder of childhood characterized by proliferation of the granulocytic and monocytic lineages Erythroid and megakaryocytic
1 Introduction. 1.1 Cancer. Introduction
 Introduction 1 1.1 Cancer 1 Introduction Cancer is the most precarious disease characterized by uncontrolled proliferation of cells without any physiological demands of the organism. Cancer may be defined
Introduction 1 1.1 Cancer 1 Introduction Cancer is the most precarious disease characterized by uncontrolled proliferation of cells without any physiological demands of the organism. Cancer may be defined
Hematology 101. Blanche P Alter, MD, MPH, FAAP Clinical Genetics Branch Division of Cancer Epidemiology and Genetics Bethesda, MD
 Hematology 101 Blanche P Alter, MD, MPH, FAAP Clinical Genetics Branch Division of Cancer Epidemiology and Genetics Bethesda, MD Hematocrits Plasma White cells Red cells Normal, Hemorrhage, IDA, Leukemia,
Hematology 101 Blanche P Alter, MD, MPH, FAAP Clinical Genetics Branch Division of Cancer Epidemiology and Genetics Bethesda, MD Hematocrits Plasma White cells Red cells Normal, Hemorrhage, IDA, Leukemia,
Year 2002 Paper two: Questions supplied by Jo 1
 Year 2002 Paper two: Questions supplied by Jo 1 Question 70 A 25 year old previously well male student presents with recent exertional dyspnoea, epistaxis and bruising. There is no history of medication,
Year 2002 Paper two: Questions supplied by Jo 1 Question 70 A 25 year old previously well male student presents with recent exertional dyspnoea, epistaxis and bruising. There is no history of medication,
manifestations are uncommon. Initial descriptions of the disease (Rosai and Dorfman, 1969) specifically
 Postgraduate Medical Journal (July 1980) 56, 521-525 Diffuse cutaneous involvement and sinus histiocytosis with massive lymphadenopathy A. A. WOODCOCK B.Sc., M.B., Ch.B., M.R.C.P. Summary Severe skin involvement
Postgraduate Medical Journal (July 1980) 56, 521-525 Diffuse cutaneous involvement and sinus histiocytosis with massive lymphadenopathy A. A. WOODCOCK B.Sc., M.B., Ch.B., M.R.C.P. Summary Severe skin involvement
Diseases Of The Blood
 Diseases Of The Blood DR. Associate Professor Of Pathology Faculty Of Medicine Ain Shams University Red Blood Cells and Anemia RBC=4-6 million/mm 2 Hb=12-18 g/dl Oxygen Carrying Molecule Hemoglobin Tetramer:
Diseases Of The Blood DR. Associate Professor Of Pathology Faculty Of Medicine Ain Shams University Red Blood Cells and Anemia RBC=4-6 million/mm 2 Hb=12-18 g/dl Oxygen Carrying Molecule Hemoglobin Tetramer:
r). SUPPLEMENTARY/SECOND OPPORTUNITY EXAMINATION PAPER nnmlbih UNIVERSITY Sophia Blaauw INSTRUCTIONS FACULTY OF HEALTH AND APPLIED SCIENCES
 r). nnmlbih UNIVERSITY OF SCIEFICE nnd TECHNOLOGY FACULTY OF HEALTH AND APPLIED SCIENCES DEPARTMENT OF HEALTH SCIENCES QUALIFICATION: BACHELOR OF MEDICAL LABORATORY SCIENCES QUALIFICATION CODE: 08BMLS
r). nnmlbih UNIVERSITY OF SCIEFICE nnd TECHNOLOGY FACULTY OF HEALTH AND APPLIED SCIENCES DEPARTMENT OF HEALTH SCIENCES QUALIFICATION: BACHELOR OF MEDICAL LABORATORY SCIENCES QUALIFICATION CODE: 08BMLS
MYELOPROLIFARATIVE NEOPLASMS. Dr. Hasan Fahmawi, MRCP(UK), FRCP(Edin).
 MYELOPROLIFARATIVE NEOPLASMS Dr. Hasan Fahmawi, MRCP(UK), FRCP(Edin). These are a group of chronic conditions characterised by clonal proliferation of marrow precursor cells. PRV, essential thrombocyathaemia,
MYELOPROLIFARATIVE NEOPLASMS Dr. Hasan Fahmawi, MRCP(UK), FRCP(Edin). These are a group of chronic conditions characterised by clonal proliferation of marrow precursor cells. PRV, essential thrombocyathaemia,
MORPHOLOGY OF BONE MARROW ASPIRATES. Dr.Prasanna N Kumar Head Department of Pathology, Oman Medical College, Oman
 MORPHOLOGY OF BONE MARROW ASPIRATES Dr.Prasanna N Kumar Head Department of Pathology, Oman Medical College, Oman BONE MARROW ASPIRATION Sites Sternum Anterior or posterior iliac spines Aspiration from
MORPHOLOGY OF BONE MARROW ASPIRATES Dr.Prasanna N Kumar Head Department of Pathology, Oman Medical College, Oman BONE MARROW ASPIRATION Sites Sternum Anterior or posterior iliac spines Aspiration from
Case Presentation No. 075
 Case Presentation No. 075 Session 4. Myelodysplastic Syndrome Cristina Montalvo, MD Baylor College of Medicine Houston, Texas 2007 Workshop of Society for Hematopathology and European Association for Haematopathology
Case Presentation No. 075 Session 4. Myelodysplastic Syndrome Cristina Montalvo, MD Baylor College of Medicine Houston, Texas 2007 Workshop of Society for Hematopathology and European Association for Haematopathology
Letter 63: Childhood Leukemia: Blood Test Results Normalised After Four Months On Herbs
 Letter 63: Childhood Leukemia: Blood Test Results Normalised After Four Months On Herbs Kontribusi Dari Dr. Chris Teo Wednesday, 03 September 2008 Cancer Care August / September 2008 Danny (M355/not real
Letter 63: Childhood Leukemia: Blood Test Results Normalised After Four Months On Herbs Kontribusi Dari Dr. Chris Teo Wednesday, 03 September 2008 Cancer Care August / September 2008 Danny (M355/not real
Acute Lymphoblastic Leukaemia
 Acute Lymphoblastic Leukaemia Terri Boyer 17 th October 2006 Overview Disease information: Aetiology of ALL proposed theory, contributing factors Symptoms Complications Diagnostic approaches - morphology
Acute Lymphoblastic Leukaemia Terri Boyer 17 th October 2006 Overview Disease information: Aetiology of ALL proposed theory, contributing factors Symptoms Complications Diagnostic approaches - morphology
If unqualified, Complete remission is considered to be Haematological complete remission
 Scroll right to see the database codes for Disease status and Response Diagnosis it refers to Disease status or response to treatment AML ALL CML CLL MDS or MD/MPN or acute leukaemia secondary to previous
Scroll right to see the database codes for Disease status and Response Diagnosis it refers to Disease status or response to treatment AML ALL CML CLL MDS or MD/MPN or acute leukaemia secondary to previous
If unqualified, Complete remission is considered to be Haematological complete remission
 Scroll right to see the database codes for Disease status and Response Diagnosis it refers to Disease status or response to treatment AML ALL CML CLL MDS or MD/MPN or acute leukaemia secondary to previous
Scroll right to see the database codes for Disease status and Response Diagnosis it refers to Disease status or response to treatment AML ALL CML CLL MDS or MD/MPN or acute leukaemia secondary to previous
Myelodysplastic Syndromes Myeloproliferative Disorders
 Myelodysplastic Syndromes Myeloproliferative Disorders Myelodysplastic Syndromes characterized by maturation defects that are associated with ineffective hematopoiesis and a high risk of transformation
Myelodysplastic Syndromes Myeloproliferative Disorders Myelodysplastic Syndromes characterized by maturation defects that are associated with ineffective hematopoiesis and a high risk of transformation
Adult Acute leukemia. Matthew Seftel. August
 Adult Acute leukemia Matthew Seftel August 21 2007 mseftel@cancercare.mb.ca Principles 3 cases Diagnosis and classification of acute leukemia (AL) Therapy Emergencies Remission induction BMT Complications
Adult Acute leukemia Matthew Seftel August 21 2007 mseftel@cancercare.mb.ca Principles 3 cases Diagnosis and classification of acute leukemia (AL) Therapy Emergencies Remission induction BMT Complications
Disclosures. Myeloproliferative Neoplasms: A Case-Based Approach. Objectives. Myeloproliferative Neoplasms. Myeloproliferative Neoplasms
 Myeloproliferative Neoplasms: A Case-Based Approach Disclosures No conflicts of interests regarding the topic being presented Adam M. Miller, MD PGY-4 Resident Physician Department of Pathology and Laboratory
Myeloproliferative Neoplasms: A Case-Based Approach Disclosures No conflicts of interests regarding the topic being presented Adam M. Miller, MD PGY-4 Resident Physician Department of Pathology and Laboratory
Case Workshop of Society for Hematopathology and European Association for Haematopathology
 Case 148 2007 Workshop of Society for Hematopathology and European Association for Haematopathology Robert P Hasserjian Department of Pathology Massachusetts General Hospital Boston, MA Clinical history
Case 148 2007 Workshop of Society for Hematopathology and European Association for Haematopathology Robert P Hasserjian Department of Pathology Massachusetts General Hospital Boston, MA Clinical history
The function of the bone marrow. Living with Aplastic Anemia. A Case Study - I. Hypocellular bone marrow failure 5/14/2018
 The function of the bone marrow Larry D. Cripe, MD Indiana University Simon Cancer Center Bone Marrow Stem Cells Mature into Blood Cells Mature Blood Cells and Health Type Function Term Red Cells Carry
The function of the bone marrow Larry D. Cripe, MD Indiana University Simon Cancer Center Bone Marrow Stem Cells Mature into Blood Cells Mature Blood Cells and Health Type Function Term Red Cells Carry
Treat the whole patient, not just the hole in the patient! 3/21/2017 CAN YOU CONNECT THE DOTS?? PHILOSOPHY OBJECTIVES
 CAN YOU CONNECT THE DOTS?? Boone Hospital Wound Healing Center Kimberly Jamison, MD, FACP, FAPWCA, PCWC Kim Mitchell, RN, BSN OBJECTIVES Describe the basic concepts of chronic wound care to ensure an optimal
CAN YOU CONNECT THE DOTS?? Boone Hospital Wound Healing Center Kimberly Jamison, MD, FACP, FAPWCA, PCWC Kim Mitchell, RN, BSN OBJECTIVES Describe the basic concepts of chronic wound care to ensure an optimal
Myeloproliferative Disorders: Diagnostic Enigmas, Therapeutic Dilemmas. James J. Stark, MD, FACP
 Myeloproliferative Disorders: Diagnostic Enigmas, Therapeutic Dilemmas James J. Stark, MD, FACP Medical Director, Cancer Program and Palliative Care Maryview Medical Center Professor of Medicine, EVMS
Myeloproliferative Disorders: Diagnostic Enigmas, Therapeutic Dilemmas James J. Stark, MD, FACP Medical Director, Cancer Program and Palliative Care Maryview Medical Center Professor of Medicine, EVMS
A case of Sweet's syndrome with marked facial swelling and fluid collection
 Hong Kong J. Dermatol. Venereol. (2017) 25, 128-132 Case Report A case of Sweet's syndrome with marked facial swelling and fluid collection JE Seol, SH Park, DH Kim, JN Kang, H Kim A 43-year-old woman
Hong Kong J. Dermatol. Venereol. (2017) 25, 128-132 Case Report A case of Sweet's syndrome with marked facial swelling and fluid collection JE Seol, SH Park, DH Kim, JN Kang, H Kim A 43-year-old woman
Dual Wavelength Phototherapy System
 Dual Wavelength Phototherapy System The AKLARUS Blue and Red Combination System is an effective, drugfree alternative for treating acne & photodamaged skin. The non-invasive Aklarus treatment has been
Dual Wavelength Phototherapy System The AKLARUS Blue and Red Combination System is an effective, drugfree alternative for treating acne & photodamaged skin. The non-invasive Aklarus treatment has been
2 nd step do Bone Marrow Study If possible both the aspiration and
 Blood Malignancies-I Prof. Herman Hariman,SpPK a (KH). Ph.D.(U.K) Prof. Dr. Adikoesoema Aman, SpPK (KH) Dept. Clinpath, FK-USU First do the Full Blood Count Hb, WBCS, Platelets Morphology!! Such as blasts,
Blood Malignancies-I Prof. Herman Hariman,SpPK a (KH). Ph.D.(U.K) Prof. Dr. Adikoesoema Aman, SpPK (KH) Dept. Clinpath, FK-USU First do the Full Blood Count Hb, WBCS, Platelets Morphology!! Such as blasts,
Participants Identification No. % Evaluation. Mitotic figure Educational Erythrocyte precursor, abnormal 1 0.
 Cell Identification Mitotic figure 212 99.5 Educational Erythrocyte precursor, abnormal BMD-02 The arrowed cell is a mitotic figure. It was correctly identified by 99.5% of the participants. A cell containing
Cell Identification Mitotic figure 212 99.5 Educational Erythrocyte precursor, abnormal BMD-02 The arrowed cell is a mitotic figure. It was correctly identified by 99.5% of the participants. A cell containing
2007 Workshop of Society for Hematopathology & European Association for Hematopathology Indianapolis, IN, USA Case # 228
 2007 Workshop of Society for Hematopathology & European Association for Hematopathology Indianapolis, IN, USA Case # 228 Vishnu V. B Reddy, MD University of Alabama at Birmingham Birmingham, AL USA 11/03/07
2007 Workshop of Society for Hematopathology & European Association for Hematopathology Indianapolis, IN, USA Case # 228 Vishnu V. B Reddy, MD University of Alabama at Birmingham Birmingham, AL USA 11/03/07
Abnormal blood counts in children Dr Tina Biss Consultant Paediatric Haematologist Newcastle upon Tyne Hospitals NHS Foundation Trust
 Abnormal blood counts in children Dr Tina Biss Consultant Paediatric Haematologist Newcastle upon Tyne Hospitals NHS Foundation Trust Regional Paediatric Specialty Trainees teaching 4 th July 2017 Scope
Abnormal blood counts in children Dr Tina Biss Consultant Paediatric Haematologist Newcastle upon Tyne Hospitals NHS Foundation Trust Regional Paediatric Specialty Trainees teaching 4 th July 2017 Scope
The AML subtypes are based on how mature (developed) the cancer cells are at the time of diagnosis and how different they are from normal cells.
 What is Acute Myeloid Leukemia (AML)? Acute myeloid leukemia (AML) is a cancer of cells in the blood, bone marrow and lymph nodes. AML is also called acute nonlymphocytic leukemia, acute myeloblastic leukemia,
What is Acute Myeloid Leukemia (AML)? Acute myeloid leukemia (AML) is a cancer of cells in the blood, bone marrow and lymph nodes. AML is also called acute nonlymphocytic leukemia, acute myeloblastic leukemia,
CASE REPORT LEUKEMIA CUTIS- A CASE REPORT
 LEUKEMIA CUTIS- A CASE REPORT C. Nirmala 1, Mangal V. Kulkarni 2. 1. Associate Professor, Department Of Pathology, Bangalore Medical College &RI 2. Tutor, Department Of Pathology, Bangalore Medical College
LEUKEMIA CUTIS- A CASE REPORT C. Nirmala 1, Mangal V. Kulkarni 2. 1. Associate Professor, Department Of Pathology, Bangalore Medical College &RI 2. Tutor, Department Of Pathology, Bangalore Medical College
SWOG ONCOLOGY RESEARCH PROFESSIONAL (ORP) MANUAL LEUKEMIA FORMS CHAPTER 16A REVISED: DECEMBER 2017
 LEUKEMIA FORMS The guidelines and figures below are specific to Leukemia studies. The information in this manual does NOT represent a complete set of required forms for any leukemia study. Please refer
LEUKEMIA FORMS The guidelines and figures below are specific to Leukemia studies. The information in this manual does NOT represent a complete set of required forms for any leukemia study. Please refer
EDUCATIONAL COMMENTARY DIFFERENTIATING IMMATURE PERIPHERAL BLOOD CELLS
 Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE credits click on Continuing Education on the left side of the
Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE credits click on Continuing Education on the left side of the
Recognizing Pyoderma Gangrenosum in a Patient with History of Essential Thrombocytosis
 Open Journal of Clinical & Medical Case Reports Volume 2 (2016) Issue 17 ISSN 2379-1039 Recognizing Pyoderma Gangrenosum in a Patient with History of Essential Thrombocytosis * Amier Ahmad, Md ; Kevin
Open Journal of Clinical & Medical Case Reports Volume 2 (2016) Issue 17 ISSN 2379-1039 Recognizing Pyoderma Gangrenosum in a Patient with History of Essential Thrombocytosis * Amier Ahmad, Md ; Kevin
SH A CASE OF PERSISTANT NEUTROPHILIA: BCR-ABL
 SH2017-0124 A CASE OF PERSISTANT NEUTROPHILIA: BCR-ABL NEGATIVE John R Goodlad 1, Pedro Martin-Cabrera 2, Catherine Cargo 2 1. Department of Pathology, NHS Greater Glasgow & Clyde, QEUH, Glasgow 2. Haematological
SH2017-0124 A CASE OF PERSISTANT NEUTROPHILIA: BCR-ABL NEGATIVE John R Goodlad 1, Pedro Martin-Cabrera 2, Catherine Cargo 2 1. Department of Pathology, NHS Greater Glasgow & Clyde, QEUH, Glasgow 2. Haematological
بسم هللا الرحمن الرحيم
 بسم هللا الرحمن الرحيم WBCs disorders *Slide 2: - we will focus on the disorders that are related to the # of WBCs - in children the # of lymphocyte is more than it in adults,sometimes more than neutrophils
بسم هللا الرحمن الرحيم WBCs disorders *Slide 2: - we will focus on the disorders that are related to the # of WBCs - in children the # of lymphocyte is more than it in adults,sometimes more than neutrophils
Case Rep Dermatol 2016;8: DOI: / Published online: April 21, 2016
 Published online: April 21, 2016 2016 The Author(s) Published by S. Karger AG, Basel 1662 6567/16/0081 0097$39.50/0 This article is licensed under the Creative Commons Attribution-NonCommercial 4.0 International
Published online: April 21, 2016 2016 The Author(s) Published by S. Karger AG, Basel 1662 6567/16/0081 0097$39.50/0 This article is licensed under the Creative Commons Attribution-NonCommercial 4.0 International
What is MDS? Epidemiology, Diagnosis, Classification & Risk Stratification
 What is MDS? Epidemiology, Diagnosis, Classification & Risk Stratification Rami Komrokji, MD Clinical Director Malignant Hematology Moffitt Cancer Center Normal Blood and Bone Marrow What is MDS Myelodysplastic
What is MDS? Epidemiology, Diagnosis, Classification & Risk Stratification Rami Komrokji, MD Clinical Director Malignant Hematology Moffitt Cancer Center Normal Blood and Bone Marrow What is MDS Myelodysplastic
All Wales Lymphoma Panel Lymphoma Course April 2015 Wales Millennium Centre Cardiff
 All Wales Lymphoma Panel Lymphoma Course 23-24 April 2015 Wales Millennium Centre Cardiff Case Histories Online slides at: http://dental.uwcm.ac.uk:82/awlp%20course%202015/view.apml? Professor Sebastian
All Wales Lymphoma Panel Lymphoma Course 23-24 April 2015 Wales Millennium Centre Cardiff Case Histories Online slides at: http://dental.uwcm.ac.uk:82/awlp%20course%202015/view.apml? Professor Sebastian
Bilateral Chest X-Ray Shadowing and Bilateral leg lesions - A case of Pulmonary Kaposi Sarcoma
 Article ID: WMC005047 ISSN 2046-1690 Bilateral Chest X-Ray Shadowing and Bilateral leg lesions - A case of Pulmonary Kaposi Sarcoma Peer review status: No Corresponding Author: Dr. Mohammad Fawad Khattak,
Article ID: WMC005047 ISSN 2046-1690 Bilateral Chest X-Ray Shadowing and Bilateral leg lesions - A case of Pulmonary Kaposi Sarcoma Peer review status: No Corresponding Author: Dr. Mohammad Fawad Khattak,
Uncommon clinical presentations of leprosy: apropos of three cases
 Lepr Rev (2016) 87, 246 251 CASE REPORT Uncommon clinical presentations of leprosy: apropos of three cases RASHMI JINDAL* & NADIA SHIRAZI** *Department of Dermatology, Venereology & Leprosy, Himalayan
Lepr Rev (2016) 87, 246 251 CASE REPORT Uncommon clinical presentations of leprosy: apropos of three cases RASHMI JINDAL* & NADIA SHIRAZI** *Department of Dermatology, Venereology & Leprosy, Himalayan
CASE 106. Pancytopenia in the setting of marrow hypoplasia, a PNH clone, and a DNMT3A mutation
 CASE 106 Pancytopenia in the setting of marrow hypoplasia, a PNH clone, and a DNMT3A mutation Gabriel C. Caponetti, MD University of Pennsylvania, US Clinical history 69, F peripheral neuropathy, refractory
CASE 106 Pancytopenia in the setting of marrow hypoplasia, a PNH clone, and a DNMT3A mutation Gabriel C. Caponetti, MD University of Pennsylvania, US Clinical history 69, F peripheral neuropathy, refractory
REGISTRATION PATIENT DETAILS
 PATIENT DETAILS Person completing form: (please print) FOR REGIONAL REFERRAL CENTER USE ONLY Registration: Approved Date: / / Not approved RRC telephone contact with primary MD: Date: / / Reviewers Signature:
PATIENT DETAILS Person completing form: (please print) FOR REGIONAL REFERRAL CENTER USE ONLY Registration: Approved Date: / / Not approved RRC telephone contact with primary MD: Date: / / Reviewers Signature:
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS LYMPHOMA. April 16, 2008
 MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS LYMPHOMA April 16, 2008 FACULTY COPY GOAL: Learn the appearance of normal peripheral blood elements and lymph nodes. Recognize abnormal peripheral blood
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS LYMPHOMA April 16, 2008 FACULTY COPY GOAL: Learn the appearance of normal peripheral blood elements and lymph nodes. Recognize abnormal peripheral blood
WHAT IS YOUR DIAGNOSIS?
 WHAT IS YOUR DIAGNOSIS? A 1.5 year, male neuter, domestic shorthair cat was presented to the R(D)SVS Internal Medicine Service with a three month history of pica (ingestion of cat litter and licking concrete)
WHAT IS YOUR DIAGNOSIS? A 1.5 year, male neuter, domestic shorthair cat was presented to the R(D)SVS Internal Medicine Service with a three month history of pica (ingestion of cat litter and licking concrete)
Myeloid neoplasms. Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories:
 Myeloid neoplasms Note: Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories: 1. AML : Acute myeloid leukemia(stem cell with myeloid
Myeloid neoplasms Note: Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories: 1. AML : Acute myeloid leukemia(stem cell with myeloid
MS.4/ 1.Nov/2015. Acute Leukemia: AML. Abdallah Abbadi
 MS.4/ 1.Nov/2015. Acute Leukemia: AML Abdallah Abbadi Case 9: Acute Leukemia 29 yr old lady complains of fever and painful gums for 1 week. She developed easy bruising and hemorrhagic spots on her trunk
MS.4/ 1.Nov/2015. Acute Leukemia: AML Abdallah Abbadi Case 9: Acute Leukemia 29 yr old lady complains of fever and painful gums for 1 week. She developed easy bruising and hemorrhagic spots on her trunk
By Dr. Mohamed Saad Daoud
 By Dr. Mohamed Saad Daoud Part I Introduction Types of White Blood Cells Genesis of the White Blood Cells Life Span of the White Blood Cells Dr. Mohamed Saad Daoud 2 Leucocytes Introduction: Infectious
By Dr. Mohamed Saad Daoud Part I Introduction Types of White Blood Cells Genesis of the White Blood Cells Life Span of the White Blood Cells Dr. Mohamed Saad Daoud 2 Leucocytes Introduction: Infectious
WBCs Disorders 1. Dr. Nabila Hamdi MD, PhD
 WBCs Disorders 1 Dr. Nabila Hamdi MD, PhD ILOs Compare and contrast ALL, AML, CLL, CML in terms of age distribution, cytogenetics, morphology, immunophenotyping, laboratory diagnosis clinical features
WBCs Disorders 1 Dr. Nabila Hamdi MD, PhD ILOs Compare and contrast ALL, AML, CLL, CML in terms of age distribution, cytogenetics, morphology, immunophenotyping, laboratory diagnosis clinical features
Evaluation of bone marrow aspirate in paediatric patients with pancytopenia: a 2 years study
 International Journal of Research in Medical Sciences Baig MA. Int J Res Med Sci. 2015 Oct;3(10):2775-2779 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20150830
International Journal of Research in Medical Sciences Baig MA. Int J Res Med Sci. 2015 Oct;3(10):2775-2779 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20150830
CHALLENGING CASES PRESENTATION
 CHALLENGING CASES PRESENTATION Michael C. Wiemann, MD, FACP Program Co-Chair and Vice President Indy Hematology Education President, Clinical St. John Providence Physician Network Detroit, Michigan 36
CHALLENGING CASES PRESENTATION Michael C. Wiemann, MD, FACP Program Co-Chair and Vice President Indy Hematology Education President, Clinical St. John Providence Physician Network Detroit, Michigan 36
Participants Identification No. % Evaluation. Mitotic figure Educational Erythrocyte precursor, abnormal/
 Cell Identification BMD-09 Participants Identification No. % Evaluation Mitotic figure 233 96.7 Educational Erythrocyte precursor, abnormal/ 4 1.7 Educational dysplastic nuclear features Erythrocyte precursor
Cell Identification BMD-09 Participants Identification No. % Evaluation Mitotic figure 233 96.7 Educational Erythrocyte precursor, abnormal/ 4 1.7 Educational dysplastic nuclear features Erythrocyte precursor
Skin Integrity and Wound Care
 Skin Integrity and Wound Care By Dr. Amer Hasanien & Dr. Ali Saleh Skin Integrity and Wound Care Skin integrity: the presence of normal Skin & Uninterrupted skin layers by wounds. Factors affecting appearance
Skin Integrity and Wound Care By Dr. Amer Hasanien & Dr. Ali Saleh Skin Integrity and Wound Care Skin integrity: the presence of normal Skin & Uninterrupted skin layers by wounds. Factors affecting appearance
Pathology of Hematopoietic and Lymphoid tissue
 CONTENTS Pathology of Hematopoietic and Lymphoid tissue White blood cells and lymph nodes Quantitative disorder of white blood cells Reactive lymphadenopathies Infectious lymphadenitis Tumor metastasis
CONTENTS Pathology of Hematopoietic and Lymphoid tissue White blood cells and lymph nodes Quantitative disorder of white blood cells Reactive lymphadenopathies Infectious lymphadenitis Tumor metastasis
ADx Bone Marrow Report. Patient Information Referring Physician Specimen Information
 ADx Bone Marrow Report Patient Information Referring Physician Specimen Information Patient Name: Specimen: Bone Marrow Site: Left iliac Physician: Accession #: ID#: Reported: 08/19/2014 - CHRONIC MYELOGENOUS
ADx Bone Marrow Report Patient Information Referring Physician Specimen Information Patient Name: Specimen: Bone Marrow Site: Left iliac Physician: Accession #: ID#: Reported: 08/19/2014 - CHRONIC MYELOGENOUS
Myelodysplastic Syndromes: Everyday Challenges and Pitfalls
 Myelodysplastic Syndromes: Everyday Challenges and Pitfalls Kathryn Foucar, MD kfoucar@salud.unm.edu Henry Moon lecture May 2007 Outline Definition Conceptual overview; pathophysiologic mechanisms Incidence,
Myelodysplastic Syndromes: Everyday Challenges and Pitfalls Kathryn Foucar, MD kfoucar@salud.unm.edu Henry Moon lecture May 2007 Outline Definition Conceptual overview; pathophysiologic mechanisms Incidence,
Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms
 Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms Myelodysplastic syndrome (MDS) A multipotent stem cell that can differentiate into any of the myeloid lineage cells (RBCs, granulocytes, megakaryocytes)
Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms Myelodysplastic syndrome (MDS) A multipotent stem cell that can differentiate into any of the myeloid lineage cells (RBCs, granulocytes, megakaryocytes)
This was a multicenter study conducted at 11 sites in the United States and 11 sites in Europe.
 Protocol CAM211: A Phase II Study of Campath-1H (CAMPATH ) in Patients with B- Cell Chronic Lymphocytic Leukemia who have Received an Alkylating Agent and Failed Fludarabine Therapy These results are supplied
Protocol CAM211: A Phase II Study of Campath-1H (CAMPATH ) in Patients with B- Cell Chronic Lymphocytic Leukemia who have Received an Alkylating Agent and Failed Fludarabine Therapy These results are supplied
Candidates must answer ALL questions
 Time allowed: Three hours. Part 1 examination Haematology: First paper Tuesday 22 March 2016 Candidates must answer ALL questions Question 1: General Haematology A 16 year old non-european is referred
Time allowed: Three hours. Part 1 examination Haematology: First paper Tuesday 22 March 2016 Candidates must answer ALL questions Question 1: General Haematology A 16 year old non-european is referred
Heme 9 Myeloid neoplasms
 Heme 9 Myeloid neoplasms The minimum number of blasts to diagnose acute myeloid leukemia is 5% 10% 20% 50% 80% AML with the best prognosis is AML with recurrent cytogenetic abnormality AML with myelodysplasia
Heme 9 Myeloid neoplasms The minimum number of blasts to diagnose acute myeloid leukemia is 5% 10% 20% 50% 80% AML with the best prognosis is AML with recurrent cytogenetic abnormality AML with myelodysplasia
Myelodysplastic syndromes
 Haematology 601 Myelodysplastic syndromes The myelodysplastic syndromes are a group of disorders predominantly affecting elderly people, leading to ineffective haematopoiesis, and they have the potential
Haematology 601 Myelodysplastic syndromes The myelodysplastic syndromes are a group of disorders predominantly affecting elderly people, leading to ineffective haematopoiesis, and they have the potential
There are two main causes of a low platelet count
 Thrombocytopenia Thrombocytopenia is a condition in which a person's blood has an unusually low level of platelets Platelets, also called thrombocytes, are found in a person's blood along with red blood
Thrombocytopenia Thrombocytopenia is a condition in which a person's blood has an unusually low level of platelets Platelets, also called thrombocytes, are found in a person's blood along with red blood
CHAPTER:4 LEUKEMIA. BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY 8/12/2009
 LEUKEMIA CHAPTER:4 1 BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY Leukemia A group of malignant disorders affecting the blood and blood-forming tissues of
LEUKEMIA CHAPTER:4 1 BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY Leukemia A group of malignant disorders affecting the blood and blood-forming tissues of
Myelodysplastic Syndrome Case 158
 Myelodysplastic Syndrome Case 158 Dong Chen MD PhD Division of Hematopathology Mayo Clinic Clinical History 86 year old man Persistent borderline anemia and thrombocytopenia. His past medical history was
Myelodysplastic Syndrome Case 158 Dong Chen MD PhD Division of Hematopathology Mayo Clinic Clinical History 86 year old man Persistent borderline anemia and thrombocytopenia. His past medical history was
Department of Medicine, Govt. Dharmapuri Medical College, Tamil Nadu, India * Corresponding author
 Original Research Article To evaluate the clinical and etiological profile of patients presenting with pancytopenia in Government Dharmapuri Medical College Hospital, Dharmapuri P. S. Rani 1*, K. Sureshkumar
Original Research Article To evaluate the clinical and etiological profile of patients presenting with pancytopenia in Government Dharmapuri Medical College Hospital, Dharmapuri P. S. Rani 1*, K. Sureshkumar
MDS 101. What is bone marrow? Myelodysplastic Syndrome: Let s build a definition. Dysplastic? Syndrome? 5/22/2014. What does bone marrow do?
 101 May 17, 2014 Myelodysplastic Syndrome: Let s build a definition Myelo bone marrow Gail J. Roboz, M.D. Director, Leukemia Program Associate Professor of Medicine What is bone marrow? What does bone
101 May 17, 2014 Myelodysplastic Syndrome: Let s build a definition Myelo bone marrow Gail J. Roboz, M.D. Director, Leukemia Program Associate Professor of Medicine What is bone marrow? What does bone
Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data
 Instructions for Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data (Form 2114) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the Myelodysplasia/Myeloproliferative
Instructions for Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data (Form 2114) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the Myelodysplasia/Myeloproliferative
Notes for the 2 nd histology lab
 Notes for the 2 nd histology lab Note : Please refer to the slides and see the morphological characteristics of each cell, as the practical exam will be in the form of figures. SLIDE #2 Erythropoiesis
Notes for the 2 nd histology lab Note : Please refer to the slides and see the morphological characteristics of each cell, as the practical exam will be in the form of figures. SLIDE #2 Erythropoiesis
Glistening, Skin-Colored Nodule
 To Print: Click your browser's PRINT button. NOTE: To view the article with Web enhancements, go to: http://www.medscape.com/viewarticle/436334 Medscape Dermatology Clinic Glistening, Skin-Colored Nodule
To Print: Click your browser's PRINT button. NOTE: To view the article with Web enhancements, go to: http://www.medscape.com/viewarticle/436334 Medscape Dermatology Clinic Glistening, Skin-Colored Nodule
Pathology. #11 Acute Leukemias. Farah Banyhany. Dr. Sohaib Al- Khatib 23/2/16
 35 Pathology #11 Acute Leukemias Farah Banyhany Dr. Sohaib Al- Khatib 23/2/16 1 Salam First of all, this tafreegh is NOT as long as you may think. If you just focus while studying this, everything will
35 Pathology #11 Acute Leukemias Farah Banyhany Dr. Sohaib Al- Khatib 23/2/16 1 Salam First of all, this tafreegh is NOT as long as you may think. If you just focus while studying this, everything will
PULMONARY MEDICINE BOARD REVIEW. Financial Conflicts of Interest. Question #1: Question #1 (Cont.): None. Christopher H. Fanta, M.D.
 PULMONARY MEDICINE BOARD REVIEW Christopher H. Fanta, M.D. Pulmonary and Critical Care Division Brigham and Women s Hospital Partners Asthma Center Harvard Medical School Financial Conflicts of Interest
PULMONARY MEDICINE BOARD REVIEW Christopher H. Fanta, M.D. Pulmonary and Critical Care Division Brigham and Women s Hospital Partners Asthma Center Harvard Medical School Financial Conflicts of Interest
Leukocytosis - Some Learning Points
 Leukocytosis - Some Learning Points Koh Liang Piu Department of Hematology-Oncology National University Cancer Institute National University Health System Objectives of this talk: 1. To provide some useful
Leukocytosis - Some Learning Points Koh Liang Piu Department of Hematology-Oncology National University Cancer Institute National University Health System Objectives of this talk: 1. To provide some useful
HEMATOLOGIC MALIGNANCIES BIOLOGY
 HEMATOLOGIC MALIGNANCIES BIOLOGY Failure of terminal differentiation Failure of differentiated cells to undergo apoptosis Failure to control growth Neoplastic stem cell FAILURE OF TERMINAL DIFFERENTIATION
HEMATOLOGIC MALIGNANCIES BIOLOGY Failure of terminal differentiation Failure of differentiated cells to undergo apoptosis Failure to control growth Neoplastic stem cell FAILURE OF TERMINAL DIFFERENTIATION
VETERINARY HEMATOLOGY ATLAS OF COMMON DOMESTIC AND NON-DOMESTIC SPECIES COPYRIGHTED MATERIAL SECOND EDITION
 VETERINARY HEMATOLOGY ATLAS OF COMMON DOMESTIC AND NON-DOMESTIC SPECIES SECOND EDITION COPYRIGHTED MATERIAL CHAPTER ONE HEMATOPOIESIS GENERAL FEATURES All blood cells have a finite life span, but in normal
VETERINARY HEMATOLOGY ATLAS OF COMMON DOMESTIC AND NON-DOMESTIC SPECIES SECOND EDITION COPYRIGHTED MATERIAL CHAPTER ONE HEMATOPOIESIS GENERAL FEATURES All blood cells have a finite life span, but in normal
DERMATOLOGICAL EMERGENCIES. DR. Ian Hoyle MBBS DIP IMC RCS (Ed), DA (UK),FRACGP,FACRRM,DIP DERM(Wales) TASMANIAN SKIN AND BODY CENTRE
 DERMATOLOGICAL EMERGENCIES DR. Ian Hoyle MBBS DIP IMC RCS (Ed), DA (UK),FRACGP,FACRRM,DIP DERM(Wales) TASMANIAN SKIN AND BODY CENTRE Dermatological Emergencies INFECTIONS ERYTHRODERMA DRUG ERUPTIONS STEVENS-JOHNSON
DERMATOLOGICAL EMERGENCIES DR. Ian Hoyle MBBS DIP IMC RCS (Ed), DA (UK),FRACGP,FACRRM,DIP DERM(Wales) TASMANIAN SKIN AND BODY CENTRE Dermatological Emergencies INFECTIONS ERYTHRODERMA DRUG ERUPTIONS STEVENS-JOHNSON
Large granular lymphocytic leukaemia (LGLL)
 Bloodwise Patient Information Large granular lymphocytic leukaemia (LGLL) For anyone affected by blood cancer Large granular lymphocytic leukaemia (LGLL) This fact sheet will help you to understand LGLL,
Bloodwise Patient Information Large granular lymphocytic leukaemia (LGLL) For anyone affected by blood cancer Large granular lymphocytic leukaemia (LGLL) This fact sheet will help you to understand LGLL,
Pathology of Hematopoietic and Lymphoid tissue
 Pathology of Hematopoietic and Lymphoid tissue Peerayut Sitthichaiyakul, M.D. Department of Pathology and Forensic Medicine Faculty of Medicine, Naresuan University CONTENTS White blood cells and lymph
Pathology of Hematopoietic and Lymphoid tissue Peerayut Sitthichaiyakul, M.D. Department of Pathology and Forensic Medicine Faculty of Medicine, Naresuan University CONTENTS White blood cells and lymph
PRODIGY Quick Reference Guide
 PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
Myelodysplastic Syndromes (MDS) Diagnosis, Treatments & Support
 Myelodysplastic Syndromes (MDS) Diagnosis, Treatments & Support LLS Mission & Goals Our mission. Cure leukemia, lymphoma, Hodgkin s disease and myeloma, and improve the quality of life of patients and
Myelodysplastic Syndromes (MDS) Diagnosis, Treatments & Support LLS Mission & Goals Our mission. Cure leukemia, lymphoma, Hodgkin s disease and myeloma, and improve the quality of life of patients and
Hematopoiesis Simplified: Part 1 Erythropoiesis
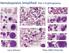 Hematopoiesis Simplified: Part 1 Erythropoiesis Larry Johnson Texas A&M University Hematopoiesis Simplified: Part 1 Erythropoiesis Objectives are to: Identify the developmental cells of erythropoiesis
Hematopoiesis Simplified: Part 1 Erythropoiesis Larry Johnson Texas A&M University Hematopoiesis Simplified: Part 1 Erythropoiesis Objectives are to: Identify the developmental cells of erythropoiesis
Hematopathology Case Study
 Hematopathology Case Study AMP Outreach Course 2009 AMP Annual Meeting John Greg Howe Ph.D. Department of Laboratory Medicine Yale University School of Medicine November 19, 2009 HISTORY Case History An
Hematopathology Case Study AMP Outreach Course 2009 AMP Annual Meeting John Greg Howe Ph.D. Department of Laboratory Medicine Yale University School of Medicine November 19, 2009 HISTORY Case History An
A case of rosacea fulminans in a pregnant woman
 Hong Kong J. Dermatol. Venereol. (2018) 26, 122-126 Views and Practice A case of rosacea fulminans in a pregnant woman JE Seol, SH Park, JU Kim, GJ Cho, SH Moon, H Kim Introduction Rosacea fulminans (RF)
Hong Kong J. Dermatol. Venereol. (2018) 26, 122-126 Views and Practice A case of rosacea fulminans in a pregnant woman JE Seol, SH Park, JU Kim, GJ Cho, SH Moon, H Kim Introduction Rosacea fulminans (RF)
Blood Cell Identification Graded
 BCP-21 Blood Cell Identification Graded Case History The patient is a 37-year-old female with a history of multiple sickle cell crises. She now presents with avascular necrosis of the left hip. Laboratory
BCP-21 Blood Cell Identification Graded Case History The patient is a 37-year-old female with a history of multiple sickle cell crises. She now presents with avascular necrosis of the left hip. Laboratory
Complete Blood Count in Primary Care
 QUIZ FEEDBACK Complete Blood Count in Primary Care bpac nz better medicine GP Review Panel: Dr Janine Bailey, Motueka Dr Susie Lawless, Dunedin Dr Randall Sturm, Auckland Dr Neil Whittaker, Nelson Specialist
QUIZ FEEDBACK Complete Blood Count in Primary Care bpac nz better medicine GP Review Panel: Dr Janine Bailey, Motueka Dr Susie Lawless, Dunedin Dr Randall Sturm, Auckland Dr Neil Whittaker, Nelson Specialist
Pyoderma gangrenosum rare manifestation of crohn s disease in 14 year old child: Case report
 Damor et al. 46 CASE REPORT OPEN ACCESS Pyoderma gangrenosum rare manifestation of crohn s disease in 14 year old child: Case report Ajay Damor, Varsha Shah, Lalit Nainiwal, Bhadra Trivedi, Rohit Agrawal,
Damor et al. 46 CASE REPORT OPEN ACCESS Pyoderma gangrenosum rare manifestation of crohn s disease in 14 year old child: Case report Ajay Damor, Varsha Shah, Lalit Nainiwal, Bhadra Trivedi, Rohit Agrawal,
Interesting Case Series. Skin Grafting in Pyoderma Gangrenosum
 Interesting Case Series Skin Grafting in Pyoderma Gangrenosum Marco Romanelli, MD, PhD, Agata Janowska, MD, Teresa Oranges, MD, and Valentina Dini, MD, PhD Department of Dermatology, University of Pisa,
Interesting Case Series Skin Grafting in Pyoderma Gangrenosum Marco Romanelli, MD, PhD, Agata Janowska, MD, Teresa Oranges, MD, and Valentina Dini, MD, PhD Department of Dermatology, University of Pisa,
