BY BILL PRUITT, RRT, AE-C, CPFT, MBA, AND MICHAEL JACOBS, RN, CCRN, CEN, MSN
|
|
|
- Dale Harmon
- 5 years ago
- Views:
Transcription
1
2 C E 2.5 ANCC/AACN CONTACT HOURS Clearing away pulmonary secretions Excess or retained pulmonary secretions impair ventilation, invite infection, and may threaten survival. Find out who s at greatest risk and how to keep airways clear. BY BILL PRUITT, RRT, AE-C, CPFT, MBA, AND MICHAEL JACOBS, RN, CCRN, CEN, MSN JON KRAUSE EXCESS OR RETAINED pulmonary secretions cause a host of problems for the patient by increasing the work of breathing and setting the stage for infection. Frequent coughing as he tries to clear secretions drains his oxygen and energy reserves and makes muscles sore; coughing may also spread infection, cause vomiting, or trigger an asthma attack. Allowed to accumulate, excess pulmonary secretions impair gas exchange, which can lead to hypoxemia, pneumonia, respiratory failure, and death. Keeping your patient hydrated is a basic step to keeping airway secretions fluid and easier to clear. If he s on mechanical ventilation, he may need humidity added to the ventilator circuit to prevent the airway from drying out. If he s receiving supplemental oxygen and thick secretions are a problem, adding humidity (if the device allows) may be appropriate. Some patients are at greater risk for problems with pulmonary secretions than others. In this article, we ll describe who they are, how to spot problems early, and what to do to prevent complications. For details on the lungs normal lines of defense, see A nose (and more) for trouble. Who needs help? Anticipate problems if your patient has a disease that increases airway secretions. One or more of these mechanisms is at work. Increased mucus production by the goblet cells in the tracheobronchial tree inundates small airways with excess mucus. The mucociliary transport system, which works like an escalator to move airway secretions up the tracheobronchial tree where they can be expectorated, may be damaged or impaired. Airway inflammation and constriction can slow or prevent the upward movement of airway secretions, leaving excessive amounts below the level of airway inflammation or constriction. Let s take a closer look at how these mechanisms come into play with diseases likely to cause problems. Asthma is a chronic inflammatory disorder of the airways with intermittent acute exacerbations. It s characterized by the release of inflammatory mediators causing reversible spasms of the bronchial tubes, excessive mucus secretion, Nursing2005, July 37
3 failure of the mucociliary transport system, and airway inflammation and constriction. During an acute exacerbation, the patient complains of chest tightness and shortness of breath. Your assessment may reveal wheezing, tachypnea, tachycardia, and use of accessory muscles of respiration. As the asthma attack resolves and the airways open, the patient may develop a productive cough triggered by secretions that were retained during airway bronchospasm. Note that arterial blood gas (ABG) results may reflect respiratory alkalosis early in an asthma attack, proceed to a normal ph, then move into respiratory acidosis late in the attack because of elevated PaCO 2 levels. This transition occurs if airway bronchoconstriction is severe and unrelieved. Patients who have this progression into acidosis are at high risk for acute respiratory failure and death. Chronic bronchitis, a form of chronic obstructive pulmonary disease (COPD), is characterized by an increased number of goblet cells secreting excessive amounts of mucus. The airway walls become chronically inflamed, reducing airway diameters. These conditions raise the risk of mucus plugging. Your assessment may reveal crackles, wheezes, and gurgles on chest auscultation. Chronic bronchitis is diagnosed when the patient has a productive cough for at least 3 months in 2 consecutive years that can t be attributed to other causes. As the disease progresses, ABG analysis will reveal hypoxemia and respiratory acidosis with decreased PaO 2 and increased PaCO 2. Bronchiectasis is a respiratory disorder characterized by chronic bronchial dilation and inflammation. The mucociliary transport system is impaired, and mucus production increases. As excessive airway secretions pool, the epithelial layer lining the airways erodes, predisposing the patient to bacterial pulmonary infections. Muscular and elastic components supporting the airways also are destroyed, rendering the dilation and inflammation permanent. Possible causes of this disorder include foreign body aspiration, benign airway tumors, cystic fibrosis (CF), ciliary malfunction, or allergic bronchopulmonary aspergillosis. Your assessment may reveal inspiratory and expiratory crackles that clear with a cough. Results of ABG analysis are similar to those for chronic bronchitis. Cystic fibrosis is a genetic disorder characterized by overproduction of thick mucus affecting the respiratory, digestive, and reproductive systems. Excessive pulmonary mucus causes a lifetime of pulmonary inflammation, impaired breathing, and lung infections. To maintain lung function and avoid potentially fatal infections, patients must undergo a rigorous daily regimen to remove pulmonary secretions. In the past, few patients with CF lived beyond the teenage years. But treatment advances have extended the median survival age to 32 (as of 2000). Some patients even live into their 50s or 60s, so CF is no longer just a pediatric disorder. When you assess a patient with an advanced case of CF, or one who s having problems with secretions, you may find progressive dyspnea and crackles. Results of an ABG analysis will reveal hypoxemia and respiratory acidosis with decreased PaO 2 and increased PaCO 2. The patient may become increasingly fatigued and may have decreased activity tolerance. Pneumonia results in pooling of secretions and debris in the alveoli and lower airways, leading to hypoxemia and atelectasis. Bacterial or viral pneumonia develops when someone breathes in a pathogen or aspirates foreign matter (such as gastric contents) that breeds infection. The body responds by initiating the inflammatory process. Exudate and normal airway secretions begin to pool. As these pulmonary fluids collect they become viscous, depressing the mucociliary transport system. Typical respiratory signs and symptoms of pneumonia include cough (with or without mucus), chest pain, rapid breathing, crackles, wheezing, and shortness of breath. Nonrespiratory signs and symptoms include fever, sweating, headache, and weakness. Patients at particular risk for developing pneumonia include those with chronic illnesses such as diabetes; those with artificial airways; older adults; chronically ill, immunosuppressed, or immobile patients; and those who abuse alcohol. Neuromuscular diseases such as myasthenia gravis and Guillain- Barré syndrome cause respiratory muscle weakness, paralysis, or nerve conduction problems that can reduce cough effectiveness and lead to retained secretions. Trauma to the central nervous system can also disrupt the ability to cough or impair the cough reflex. Other contributing factors linked to retained or excessive secretions include smoking, which greatly increases production of airway secretions and damages the mucociliary transport system; air pollution or occupational exposure to irritants, which cause the same problems as tobacco smoke; and analgesia and sedation, which depress the cough reflex. Assessing your patient A thorough nursing assessment is the key to identifying subtle changes in your patient s status, including increased airway secretions that obstruct airflow. Follow trends in the patient s SpO 2 and 38 Nursing2005, Volume 35, Number 7
4 ABG values that could indicate impending respiratory difficulties. Follow these pointers for physical assessment: Inspection. Look for signs of increased work of breathing (because of resistance to airflow), increased respiratory rate, intercostal retractions, and increased use of accessory muscles to breathe. Palpation. Decreased fremitus (palpable vibrations transmitted through the bronchopulmonary tree to the chest wall when the patient speaks) indicate mucus plugging of a bronchus. Test for fremitus by using the ball or ulnar surface of your hand to palpate the chest while the patient repeatedly says 99. When he breathes deeply, you may also feel chest vibrations related to retained secretions; usually this is accompanied by audible rattling. Percussion. This technique is of limited use in trying to detect retained secretions because percussion penetrates only 2 to 3 inches (5 to 7.5 cm) in the chest. Still, a mucus plug that causes an atelectatic lung may produce a dull percussion note over the airless area. Auscultation. Adventitious (added) breath sounds are a hallmark of retained secretions, but you may need the patient s cooperation to properly assess breath sounds. A shallow- to mediumsized breath may not produce adventitious breath sounds, so ask him to breathe deeply through an open mouth. Retained secretions often cause crackles and wheezes that are more common on exhalation, but may also be present on inspiration. A nose (and more) for trouble The same airways that bring oxygen into the lungs also bring in dust, microbes, toxic particles, and smoke that can wreak havoc with normal lung function and the patient s health. Fortunately, the pulmonary system has several ways to keep itself clean. Filtering. Nasal hairs stop large particles as air moves into the nares. The mucus layer of the nasal epithelium traps more, smaller particles. Progressively smaller particles usually filter out in the lower airways and alveoli. Mucus. The nose, trachea, and much of the lower airway is lined with mucus-producing goblet cells and ciliated columnar epithelial cells whose cilia act like microscopic brooms. The cilia actually move the mucus blanket (with the trapped particles) toward the pharynx, a mechanism known as the mucociliary escalator. Goblet and ciliated cells gradually disappear as the airways get smaller and aren t present in the alveoli. The airways also are surrounded by smooth muscle that constricts to keep harmful particles from getting deep into the lungs. Coughing. The cough reflex helps remove secretions and particles that have landed in the lung. Rapid expiratory flows and positive pressure actually shear the mucus free from the airway walls and carry it out. The larynx, trachea, and mainstem bronchi have receptors that react to irritants and trigger the cough reflex. Cilia Ciliated columnar epithelial cells Clearing the pipes The first method you should try to clear secretions is also the simplest: Ask the patient to cough. If he s just had abdominal or thoracic surgery, make sure he has adequate analgesia first and show him how to use a BIRCK COX
5 pillow to splint his incision. Have tissues available to remove any secretions that he coughs up. Have him sit in high Fowler s position (or stand, if he can); an upright position lets him take in a deeper breath and generate a more forceful, effective cough. Tell him to wrap his arms around the pillow in a hugging motion, take a deep breath, hold it for a few seconds while squeezing the pillow tight against his body, then give two controlled coughs. Patients with COPD may have problems with premature airway closure when attempting a forceful cough. Teach these patients to use a huff cough, which starts from a middle to low inspiration (not a full inspiration), and to make two or three expiratory efforts with an open glottis. Assisted cough is indicated for a patient with a weak or paralyzed diaphragm. Place your hands on the patient s abdomen, then have him inhale deeply and cough. As he coughs, perform an abdominal thrust in the same way you would to clear an obstructed airway. (Remember your basic life support training.) For a patient who can t inhale, have a colleague give him a deep breath using a resuscitator bag connected to a mask (for a spontaneously breathing patient) or the artificial airway (for a mechanically ventilated patient). Incentive spirometry can help prevent atelectasis by filling the underventilated areas of the lung, reopening alveoli. Incentive spirometry and deep breathing and coughing improve ventilation and improve exercise tolerance in respiratory muscles. As a result, the patient may be able to generate a more forceful cough, helping to move secretions. Mucoactive agents to clear secretions include acetylcysteine, used to treat patients with chronic bronchitis, and dornase alfa, used to treat patients with CF. Another option is guaifenesin, which thins secretions and is a common ingredient in over-the-counter cold medications. Suctioning can help clear secretions, especially in patients with artificial airways. For patients who aren t intubated, use the nasotracheal route for suctioning the lower airways. If a patient has a reflex cough that clears secretions from the lower airway but can t remove secretions from his mouth, use a tonsil suction device such as a Yankauer suction device. Clearing retained secretions from the mouth helps reduce aspiration and infection risks. Careful attention to mouth care reduces microbial growth in the mouth and lowers the potential for hospitalacquired pneumonia. (For information on closed suctioning, see Clear the Air with Closed Suctioning on page 44.) To perform deep suction, use a sterile catheter to reach the lower airway (below the glottis). This stimulates a strong cough in many patients, which also helps clear secretions. Even if the patient has no cough reflex, though, deep suction will often clear secretions. Chest physiotherapy uses a combination of patient positioning (postural drainage) and chest percussion or vibration to dislodge and move secretions from smaller to larger airways. Patients with a lot of secretions (more than 25 ml/day of sputum), such as those with CF or bronchiectasis, are most likely to need chest physiotherapy. Once the patient is positioned appropriately, use your hands or a mechanical device to percuss or vibrate a specific area of the lung. Chest physiotherapy is usually performed two to four times a day; each procedure may last 10 to 30 minutes, depending on how many positions are being used for postural drainage. Positive expiratory pressure (PEP) consists of taking in a deep breath and exhaling through a device that resists airflow, creating positive pressure in the lung. This therapy helps refill underventilated areas of the lung, prevents premature airway closure, and prolongs expiration, making more air available to help dislodge and move secretions during coughing. Recently, PEP therapy has been combined with high-frequency compression/oscillation to mechanically move secretions in patients who aren t intubated. This combination therapy, given three to four times a day for 10 to 20 minutes each treatment, makes secretions less viscous and easier to move. The patient uses a portable, singlepatient-use device such as the Flutter valve or the Acapella. As he blows through the pipelike device, the expiratory flow causes a steel ball (or flipper and magnet) to move rapidly, generating 10 to 25 cm H 2 O of PEP and high-frequency oscillation. This dislodges secretions and lets them move into the larger airways. The Flutter device must be used when the patient is upright. The Acapella isn t gravity dependent, and aerosol treatments can be administered through it simultaneously with PEP treatment. High-frequency chest wall oscillation relies on a device to exert external forces on the chest to reduce mucus viscosity and mobilize secretions. This therapy also may enhance the activity and effectiveness of the cilia, which increases secretion mobility. The patient wears an inflated, nonstretchable vest attached to an air pulse delivery system that delivers oscillating pressures. (For more details, see Close to the Vest: A Novel Way to Keep Airways Clear in the December issue of Nursing2003.) He can take his aerosol treatments concurrently with this oscillation 40 Nursing2005, Volume 35, Number 7
6 therapy. Therapy typically includes two treatments a day, each lasting 20 minutes. Intrapulmonary percussive ventilation (IPV) is another highfrequency device used to move secretions, but this one creates pressure in the airways rather than through the chest wall. Delivered through a mask, this therapy is indicated for patients breathing spontaneously. During spontaneous breathing, the IPV device delivers positive airway pressure along with highfrequency microbursts of air. These microbursts are delivered on inspiration only or during the full inspiratory-expiratory cycle and create an oscillating effect in the airways. The device also delivers either a medication or 0.9% sodium chloride solution by aerosol. Treatments typically are given three to four times a day for 15 to 20 minutes each. Continuous lateral rotation therapy can help prevent pooled secretions in critically ill patients. The patient is placed in a specialized bed that rotates from side to side, moving up to about 45 degrees in lateral rotation. Gravity helps move secretions more centrally, making them easier for the patient to cough up (or for you to remove by suctioning). To perform bronchoscopy, a physician uses a flexible fiber-optic endoscope to view the airways; at the same time, he can use the device to remove secretions that can t be removed any other way. He may perform lavage with a sterile 0.9% sodium chloride solution to help clear secretions, or he may instill a mucolytic to break them down. The patient is sedated and given analgesia so he s comfortable during the procedure. Because it s invasive and stressful to the patient, as well as labor-intensive and costly, bronchoscopy is performed only as needed to manage secretions, with a day or more between treatments. Free and clear By knowing who s at risk for retained or excess pulmonary secretions and how to manage them, you can help your patient get the correct treatment and keep his airways open. SELECTED REFERENCES Fink J. Positive pressure techniques for airway clearance. Respiratory Care. 47(7): , July Fink J, Mahlmeister M. High-frequency oscillation of the airway and chest wall. Respiratory Care. 47(7): , July Rubin B, et al. Mucus-controlling drug therapy. In Rau Jr. J, Respiratory Care Pharmacology. St. Louis, Mo., Mosby, Inc., Wilkins R, et al. (eds). Egan s Fundamental of Respiratory Care, 8th edition. St. Louis, Mo., Mosby, Inc., Bill Pruitt is an instructor in the department of cardiorespiratory sciences at the University of South Alabama in Mobile and a p.r.n. respiratory therapist at Springhill Medical Center in Mobile. Michael Jacobs is a clinical assistant professor in the adult health department at the University of South Alabama s College of Nursing and a p.r.n. nursing supervisor and emergency department staff nurse at Ocean Springs (Miss.) Hospital. The authors have disclosed that they have no significant relationship with or financial interest in any commercial companies that pertain to this educational activity. SELECTED WEB SITE RT: The Journal for Respiratory Care Practitioners: Secretion Removal in the ICU articleid=r0502f03 Last accessed on June 1, C E Earn CE credit online: Go to and receive a certificate within minutes. INSTRUCTIONS Clearing away pulmonary secretions TEST INSTRUCTIONS To take the test online, go to our secure Web site at On the print form, record your answers in the test answer section of the CE enrollment form on page 42. Each question has only one correct answer. You may make copies of these forms. Complete the registration information and course evaluation. Mail the completed form and registration fee of $16.95 to: Lippincott Williams & Wilkins, CE Group, 2710 Yorktowne Blvd., Brick, NJ We will mail your certificate in 4 to 6 weeks. For faster service, include a fax number and we will fax your certificate within 2 business days of receiving your enrollment form. You will receive your CE certificate of earned contact hours and an answer key to review your results. There is no minimum passing grade. Registration deadline is July 31, DISCOUNTS and CUSTOMER SERVICE Send two or more tests in any nursing journal published by LWW together and deduct $0.95 from the price of each test. We also offer CE accounts for hospitals and other health care facilities on nursingcenter.com. Call for details. PROVIDER ACCREDITATION: This Continuing Nursing Education (CNE) activity for 2.5 contact hours is provided by Lippincott Williams & Wilkins (LWW), which is accredited as a provider of continuing education in nursing by the American Nurses Credentialing Center s Commission on Accreditation and by the American Association of Critical-Care Nurses (AACN , CERP Category A). This activity is also provider approved by the California Board of Registered Nursing, Provider Number CEP for 2.5 contact hours. LWW is also an approved provider of CNE in Alabama, Florida, and Iowa, and holds the following provider numbers: AL #ABNP0114, FL #FBN2454, IA #75. All of its home study activities are classified for Texas nursing continuing education requirements as Type 1. Your certificate is valid in all states. This means that your certificate of earned contact hours is valid no matter where you live. Nursing2005, July 41
7 C E 2.5 ANCC/AACN CONTACT HOURS Clearing away pulmonary secretions GENERAL PURPOSE To provide nurses with information to accurately assess and safely care for patients with excessive pulmonary secretions. LEARNING OBJECTIVES After reading the preceding article and taking this test, you should be able to: 1. Identify patients at risk for excess or retained pulmonary secretions. 2. Describe assessment findings related to excess or retained pulmonary secretions. 3. Describe nursing interventions to help keep airways clear. 1. To help maintain a clear airway, you should a. encourage prolonged coughing. b. keep the patient hydrated. c. limit environmental humidity. d. administer oxygen at a high flow rate. 2. Which condition results in excessive pulmonary secretions and airway constriction? a. bronchiectasis b. Guillain-Barré syndrome c. CF d. asthma 3. Which early assessment findings are most likely in a patient who has an acute exacerbation of asthma? a. fever and nasal congestion b. wheezing and bradypnea c. shortness of breath and tachycardia d. sneezing and hemoptysis 4. Which change in ABGs is found early in an asthma attack? a. increased ph level b. increased PaO 2 level c. decreased bicarbonate level d. increased PaCO 2 level 5. Which respiratory disorder is characterized by chronic bronchial dilation and inflammation? a. bronchiectasis c. chronic bronchitis b. asthma d. viral pneumonia 6. Chronic bronchitis is characterized by a. reversible spasms of the bronchial tubes. b. an increased number of goblet cells secreting excessive mucus. c. pooling of debris and secretions in the alveoli. d. nerve conduction problems. 7. ABG analysis in a patient with advanced CF commonly reveals a. metabolic acidosis. b. respiratory alkalosis. c. metabolic alkalosis. d. respiratory acidosis. 8. Which neuromuscular disease can cause respiratory muscle weakness and decreased cough effectiveness? a. CF b. bronchiectasis c. myasthenia gravis d. bacterial pneumonia 9. Which assessment finding best suggests increased work of breathing? a. frequent coughing b. purulent nasal discharge c. deep inspirations d. intercostal retractions 10. To assess a patient for fremitus a. inspect for diaphragmatic movement. b. palpate the chest wall while the patient repeatedly says 99. c. percuss the chest wall lightly. d. auscultate all lung lobes. ENROLLMENT FORM Nursing2005, July, Clearing away pulmonary secretions 11. When assessing for adventitious breath sounds, ask the patient to a. exhale completely and stop breathing in expiration. b. breathe in and out through the nose. c. breathe deeply through an open mouth. d. take quick, shallow breaths. 12. Teach patients with COPD who have problems with premature airway closure to use which type of cough? a. assisted c. closed glottis b. huff d. pursed lip 13. Performing an abdominal thrust as your patient inhales deeply and coughs is the best technique for a patient with a. chronic bronchitis. b. asthma. c. bronchiectasis. d. diaphragmatic paralysis. 14. Incentive spirometry can help reopen alveoli and prevent a. bronchospasm. b. atelectasis. c. asthma. d. bronchiectasis. 15. Which mucoactive agent is indicated to improve pulmonary function in patients with CF? a. acetylcysteine b. codeine c. dornase alfa d. guaifenesin A. Registration Information: Last name First name MI Address City State ZIP Telephone Fax Registration Deadline: July 31, 2007 Contact hours: 2.5 Pharmacology hours: 0.0 Fee: $16.95 LPN RN CNS NP CRNA CNM other Job title Specialty Type of facility Are you certified? Yes No Certified by State of license (1) License # State of license (2) License # Social Security # From time to time, we make our mailing list available to outside organizations to announce special offers. Please check here if you do not wish us to release your name and address. B. Test Answers: Darken one circle for your answer to each question C. Course Evaluation* 1. Did this CE activity's learning objectives relate to its general purpose? Yes No 2. Was the journal home study format an effective way to present the material? Yes No 3. Was the content relevant to your nursing practice? Yes No 4. How long did it take you to complete this CE activity? hours minutes 5. Suggestion for future topics D. Two Easy Ways to Pay: Check or money order enclosed (Payable to Lippincott Williams & Wilkins) Charge my Mastercard Visa American Express Card # Exp. date Signature *In accordance with the Iowa Board of Nursing administrative rules governing grievances, a copy of your evaluation of the CE offering may be submitted directly to the Iowa Board of Nursing.
RESPIRATORY REHABILITATION
 RESPIRATORY REHABILITATION By: Dr. Fatima Makee AL-Hakak University of kerbala College of nursing CHEST PHYSIOTHERAPY Chest physiotherapy (CPT) includes: 1.Postural drainage. 2.Chest percussion and vibration.
RESPIRATORY REHABILITATION By: Dr. Fatima Makee AL-Hakak University of kerbala College of nursing CHEST PHYSIOTHERAPY Chest physiotherapy (CPT) includes: 1.Postural drainage. 2.Chest percussion and vibration.
The Respiratory System
 130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
sounds are distant with inspiratory crackles. He sits on the edge of his chair, leaning forward, with both hands on his
 I NTE R P R ETI N G A R T E R I A L B L O O D G A S E S : EASY AS A B C Take this step-by-step approach to demystify the parameters of oxygenation, ventilation, acid-base balance. BY WILLIAM C. PRUITT,
I NTE R P R ETI N G A R T E R I A L B L O O D G A S E S : EASY AS A B C Take this step-by-step approach to demystify the parameters of oxygenation, ventilation, acid-base balance. BY WILLIAM C. PRUITT,
The objectives of this presentation are to
 1 The objectives of this presentation are to 1. Review the mechanics of airway clearance 2. Understand the difference between secretion mobilization and secretion clearance 3. Identify conditions that
1 The objectives of this presentation are to 1. Review the mechanics of airway clearance 2. Understand the difference between secretion mobilization and secretion clearance 3. Identify conditions that
Unconscious exchange of air between lungs and the external environment Breathing
 Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
Anatomy & Physiology 2 Canale. Respiratory System: Exchange of Gases
 Anatomy & Physiology 2 Canale Respiratory System: Exchange of Gases Why is it so hard to hold your breath for Discuss! : ) a long time? Every year carbon monoxide poisoning kills 500 people and sends another
Anatomy & Physiology 2 Canale Respiratory System: Exchange of Gases Why is it so hard to hold your breath for Discuss! : ) a long time? Every year carbon monoxide poisoning kills 500 people and sends another
Chapter 10 Respiration
 1 Chapter 10 Respiration Introduction/Importance of the Respiratory System All eukaryotic organisms need oxygen to perform cellular respiration (production of ATP), either aerobically or anaerobically.
1 Chapter 10 Respiration Introduction/Importance of the Respiratory System All eukaryotic organisms need oxygen to perform cellular respiration (production of ATP), either aerobically or anaerobically.
Function of the Respiratory System. Exchange CO2 (on expiration) for O2 (on inspiration)
 Function of the Respiratory System Exchange CO2 (on expiration) for O2 (on inspiration) Upper Respiratory Tract Includes: Nose Mouth Pharynx Larynx Function: Warms and humidifies the inspired air Filters
Function of the Respiratory System Exchange CO2 (on expiration) for O2 (on inspiration) Upper Respiratory Tract Includes: Nose Mouth Pharynx Larynx Function: Warms and humidifies the inspired air Filters
CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM
 CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM Pages 244-247 DO NOW What structures, do you think, are active participating in the breathing process? 2 WHAT ARE WE DOING IN TODAY S CLASS Finishing Digestion
CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM Pages 244-247 DO NOW What structures, do you think, are active participating in the breathing process? 2 WHAT ARE WE DOING IN TODAY S CLASS Finishing Digestion
5/5/2013. The Respiratory System. Chapter 16 Notes. The Respiratory System. Nasal Cavity. Sinuses
 The Respiratory System Chapter 16 Notes The Respiratory System Objectives List the general functions of the respiratory system. Identify the organs of the respiratory system. Describe the functions of
The Respiratory System Chapter 16 Notes The Respiratory System Objectives List the general functions of the respiratory system. Identify the organs of the respiratory system. Describe the functions of
Day-to-day management of Tracheostomies & Laryngectomies
 Humidification It is mandatory that a method of artificial humidification is utilised when a tracheostomy tube is in situ, for people requiring oxygen therapy dry oxygen should never be given to someone
Humidification It is mandatory that a method of artificial humidification is utilised when a tracheostomy tube is in situ, for people requiring oxygen therapy dry oxygen should never be given to someone
The Respiratory System. Dr. Ali Ebneshahidi
 The Respiratory System Dr. Ali Ebneshahidi Functions of The Respiratory System To allow gases from the environment to enter the bronchial tree through inspiration by expanding the thoracic volume. To allow
The Respiratory System Dr. Ali Ebneshahidi Functions of The Respiratory System To allow gases from the environment to enter the bronchial tree through inspiration by expanding the thoracic volume. To allow
Your Lungs and COPD. Patient Education Pulmonary Rehabilitation. A guide to how your lungs work and how COPD affects your lungs
 Patient Education Your Lungs and COPD A guide to how your lungs work and how COPD affects your lungs Your lungs are organs that process every breath you take. They provide oxygen (O 2 ) to the blood and
Patient Education Your Lungs and COPD A guide to how your lungs work and how COPD affects your lungs Your lungs are organs that process every breath you take. They provide oxygen (O 2 ) to the blood and
Pulmo-Park Pom-Pom Shooter: Measuring the Effect of Restricted Breathing on Peak Expiratory Flow (PEF) Student Information Page Activity 5D
 Pom-Pom Shooter: Measuring the Effect of Restricted Breathing on Peak Expiratory Flow (PEF) Student Information Page Activity 5D Students with asthma or other respiratory problems should not perform the
Pom-Pom Shooter: Measuring the Effect of Restricted Breathing on Peak Expiratory Flow (PEF) Student Information Page Activity 5D Students with asthma or other respiratory problems should not perform the
Chronic obstructive lung disease. Dr/Rehab F.Gwada
 Chronic obstructive lung disease Dr/Rehab F.Gwada Obstructive lung diseases Problem is in the expiratory phase Lung disease Restrictive lung disease Restriction may be with, or within the chest wall Problem
Chronic obstructive lung disease Dr/Rehab F.Gwada Obstructive lung diseases Problem is in the expiratory phase Lung disease Restrictive lung disease Restriction may be with, or within the chest wall Problem
Respiratory Diseases and Disorders
 Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
acapella vibratory PEP Therapy System Maximizing Therapy Effectiveness, Empowering Patient Compliance
 acapella vibratory PEP Therapy System Maximizing Therapy Effectiveness, Empowering Patient Compliance Investigating Questions Each acapella vibratory PEP therapy system uniquely provides PEP therapy by
acapella vibratory PEP Therapy System Maximizing Therapy Effectiveness, Empowering Patient Compliance Investigating Questions Each acapella vibratory PEP therapy system uniquely provides PEP therapy by
Aerosol Therapy. Aerosol Therapy. RSPT 1410 Humidity & Aerosol Therapy Part 4
 1 RSPT 1410 Humidity & Part 4 Wilkins Chapter 36; p. 801-806 2 Stability: the tendency for aerosol particles to remain in Size: the the particle, the greater the tendency toward stability the the particle,
1 RSPT 1410 Humidity & Part 4 Wilkins Chapter 36; p. 801-806 2 Stability: the tendency for aerosol particles to remain in Size: the the particle, the greater the tendency toward stability the the particle,
THE RESPIRATORY SYSTEM. Pages and
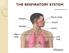 THE RESPIRATORY SYSTEM Pages 103-105 and 146-150 1 When the respiratory system is mentioned, people generally think of breathing, but breathing is only one of the activities of the respiratory system.
THE RESPIRATORY SYSTEM Pages 103-105 and 146-150 1 When the respiratory system is mentioned, people generally think of breathing, but breathing is only one of the activities of the respiratory system.
Disclaimer. Objectives. I can t cough it up! Airway Clearance Therapy. Heather Murgatroyd, RRT, RPSGT Field Clinical Specialist
 I can t cough it up! Airway Clearance Therapy Heather Murgatroyd, RRT, RPSGT Field Clinical Specialist 1 Disclaimer Name of presenter: Heather Murgatroyd, BA, RRT, RPSGT Name of employer: RespirTech I
I can t cough it up! Airway Clearance Therapy Heather Murgatroyd, RRT, RPSGT Field Clinical Specialist 1 Disclaimer Name of presenter: Heather Murgatroyd, BA, RRT, RPSGT Name of employer: RespirTech I
The RESPIRATORY System. Unit 3 Transportation Systems
 The RESPIRATORY System Unit 3 Transportation Systems Functions of the Respiratory System Warm, moisten, and filter incoming air Resonating chambers for speech and sound production Oxygen and Carbon Dioxide
The RESPIRATORY System Unit 3 Transportation Systems Functions of the Respiratory System Warm, moisten, and filter incoming air Resonating chambers for speech and sound production Oxygen and Carbon Dioxide
1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be
 1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be difficult to determine. Even for physician in hospital
1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be difficult to determine. Even for physician in hospital
Respiratory System. December 20, 2011
 Respiratory System December 20, 2011 Nasal Cavity: Contains cilia (hair cells) to prevent particles from entering the respiratory tract Mucus does the same, in addition to warming and moistening the air
Respiratory System December 20, 2011 Nasal Cavity: Contains cilia (hair cells) to prevent particles from entering the respiratory tract Mucus does the same, in addition to warming and moistening the air
Bronchitis. Anatomy of the Lungs The lungs allow us to fill our blood with oxygen. The oxygen we breathe is absorbed into our blood in the lungs.
 Bronchitis Introduction Bronchitis is an inflammation of the bronchial tubes, the airways that carry air to the lungs. It causes shortness of breath, wheezing and chest tightness as well as a cough that
Bronchitis Introduction Bronchitis is an inflammation of the bronchial tubes, the airways that carry air to the lungs. It causes shortness of breath, wheezing and chest tightness as well as a cough that
Chapter 10 The Respiratory System
 Chapter 10 The Respiratory System Biology 2201 Why do we breathe? Cells carry out the reactions of cellular respiration in order to produce ATP. ATP is used by the cells for energy. All organisms need
Chapter 10 The Respiratory System Biology 2201 Why do we breathe? Cells carry out the reactions of cellular respiration in order to produce ATP. ATP is used by the cells for energy. All organisms need
Pulmonary Pathophysiology
 Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Chronic Obstructive Pulmonary Disease (COPD) Copyright 2014 by Mosby, an imprint of Elsevier Inc.
 Chronic Obstructive Pulmonary Disease () 8.18.18 Copyright 2014 by Mosby, an imprint of Elsevier Inc. Description Airflow limitation not fully reversible progressive Abnormal inflammatory response of lungs
Chronic Obstructive Pulmonary Disease () 8.18.18 Copyright 2014 by Mosby, an imprint of Elsevier Inc. Description Airflow limitation not fully reversible progressive Abnormal inflammatory response of lungs
LUNGS. Requirements of a Respiratory System
 Respiratory System Requirements of a Respiratory System Gas exchange is the physical method that organisms use to obtain oxygen from their surroundings and remove carbon dioxide. Oxygen is needed for aerobic
Respiratory System Requirements of a Respiratory System Gas exchange is the physical method that organisms use to obtain oxygen from their surroundings and remove carbon dioxide. Oxygen is needed for aerobic
Anatomy Review. Anatomy Review. Respiratory Emergencies CHAPTER 16
 CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review 1 Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons
CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review 1 Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons
Chronic obstructive pulmonary disease
 Chronic obstructive pulmonary disease By: Dr. Fatima Makee AL-Hakak () University of kerbala College of nursing Out lines What is the? Overview Causes of Symptoms of What's the difference between and asthma?
Chronic obstructive pulmonary disease By: Dr. Fatima Makee AL-Hakak () University of kerbala College of nursing Out lines What is the? Overview Causes of Symptoms of What's the difference between and asthma?
Respiratory Emergencies
 CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons for
CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons for
Lecture Notes. Chapter 3: Asthma
 Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
Levine Children s Hospital. at Carolinas Medical Center. Respiratory Care Department
 Page 1 of 7 at Carolinas Medical Center 02.04 Pediatric Patient-Centered Respiratory Care Protocol Application of Chest Physical Therapy Created: 1/98 Reviewed: 4/03, 1/05, 6/08 Revised: Purpose: To describe
Page 1 of 7 at Carolinas Medical Center 02.04 Pediatric Patient-Centered Respiratory Care Protocol Application of Chest Physical Therapy Created: 1/98 Reviewed: 4/03, 1/05, 6/08 Revised: Purpose: To describe
The Human Respiration System
 The Human Respiration System Nasal Passage Overall function is to filter, warm and moisten air as it enters the body. The nasal passages are the primary site of air movement we tend to be nose breathers.
The Human Respiration System Nasal Passage Overall function is to filter, warm and moisten air as it enters the body. The nasal passages are the primary site of air movement we tend to be nose breathers.
PomPom SHOOTER. Activity Background: Common Obstructive Lung Disorders:
 CAUTION: Students with asthma or other respiratory problems should NOT perform the breathing exercises in this activity because they involve repeated maximal inhalations and exhalations and use of a breathing
CAUTION: Students with asthma or other respiratory problems should NOT perform the breathing exercises in this activity because they involve repeated maximal inhalations and exhalations and use of a breathing
an inflammation of the bronchial tubes
 BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
Chapter 11 The Respiratory System
 Biology 12 Name: Respiratory System Per: Date: Chapter 11 The Respiratory System Complete using BC Biology 12, page 342-371 11.1 The Respiratory System pages 346-350 1. Distinguish between A. ventilation:
Biology 12 Name: Respiratory System Per: Date: Chapter 11 The Respiratory System Complete using BC Biology 12, page 342-371 11.1 The Respiratory System pages 346-350 1. Distinguish between A. ventilation:
Section 2.1 Daily checks Humidification
 Bite- sized training from the GTC Section 2.1 Daily checks Humidification This is one of a series of bite- sized chunks of educational material developed by the Global Tracheostomy Collaborative. The GTC
Bite- sized training from the GTC Section 2.1 Daily checks Humidification This is one of a series of bite- sized chunks of educational material developed by the Global Tracheostomy Collaborative. The GTC
Respiratory Emergencies. Chapter 11
 Respiratory Emergencies Chapter 11 Respiratory System Anatomy and Function of the Lung Characteristics of Adequate Breathing Normal rate and depth Regular breathing pattern Good breath sounds on both sides
Respiratory Emergencies Chapter 11 Respiratory System Anatomy and Function of the Lung Characteristics of Adequate Breathing Normal rate and depth Regular breathing pattern Good breath sounds on both sides
Tuesday, December 13, 16. Respiratory System
 Respiratory System Trivia Time... What is the fastest sneeze speed? What is the surface area of the lungs? (hint... think of how large the small intestine was) How many breaths does the average person
Respiratory System Trivia Time... What is the fastest sneeze speed? What is the surface area of the lungs? (hint... think of how large the small intestine was) How many breaths does the average person
HASPI Medical Anatomy & Physiology 14b Lab Activity
 HASPI Medical Anatomy & Physiology 14b Lab Activity Name(s): Period: Date: Respiratory Distress Respiratory distress is a broad medical term that applies to any type of breathing difficulty and the associated
HASPI Medical Anatomy & Physiology 14b Lab Activity Name(s): Period: Date: Respiratory Distress Respiratory distress is a broad medical term that applies to any type of breathing difficulty and the associated
About the Respiratory System. Respiratory System. Human Respiratory System. Cellular Respiration. Nostrils. Label diagram
 Respiratory System Human Respiratory System A system to deliver oxygen (O2) to body cells & get rid of carbon dioxide (CO2) as a waste through cellular respiration. Two systems involved: Respiratory &
Respiratory System Human Respiratory System A system to deliver oxygen (O2) to body cells & get rid of carbon dioxide (CO2) as a waste through cellular respiration. Two systems involved: Respiratory &
CPAP. Pre-Hospital Treatment Using The Respironics Whisperflow CPAP Device. Charlottesville Albemarle Rescue Squad - CPAP
 CPAP Pre-Hospital Treatment Using The Respironics Whisperflow CPAP Device CPAP What Is It? C ontinuous P ositive A irway P ressure Anatomy Review Anatomy Review Anatomy Review Alveoli Anatomy Review Chest
CPAP Pre-Hospital Treatment Using The Respironics Whisperflow CPAP Device CPAP What Is It? C ontinuous P ositive A irway P ressure Anatomy Review Anatomy Review Anatomy Review Alveoli Anatomy Review Chest
Respiratory Disease. Dr Amal Damrah consultant Neonatologist and Paediatrician
 Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
The Respiratory System Structures of the Respiratory System Structures of the Respiratory System Structures of the Respiratory System Nose Sinuses
 CH 14 D.E. Human Biology The Respiratory System The Respiratory System OUTLINE: Mechanism of Breathing Transport of Gases between the Lungs and the Cells Respiratory Centers in the Brain Function Provides
CH 14 D.E. Human Biology The Respiratory System The Respiratory System OUTLINE: Mechanism of Breathing Transport of Gases between the Lungs and the Cells Respiratory Centers in the Brain Function Provides
Respiratory System. Respiratory System Overview. Component 3/Unit 11. Health IT Workforce Curriculum Version 2.0/Spring 2011
 Component 3-Terminology in Healthcare and Public Health Settings Unit 11-Respiratory System This material was developed by The University of Alabama at Birmingham, funded by the Department of Health and
Component 3-Terminology in Healthcare and Public Health Settings Unit 11-Respiratory System This material was developed by The University of Alabama at Birmingham, funded by the Department of Health and
Paramedic Rounds. Pre-Hospital Continuous Positive Airway Pressure (CPAP)
 Paramedic Rounds Pre-Hospital Continuous Positive Airway Pressure (CPAP) Morgan Hillier MD Class of 2011 Dr. Mike Peddle Assistant Medical Director SWORBHP Objectives Outline evidence for pre-hospital
Paramedic Rounds Pre-Hospital Continuous Positive Airway Pressure (CPAP) Morgan Hillier MD Class of 2011 Dr. Mike Peddle Assistant Medical Director SWORBHP Objectives Outline evidence for pre-hospital
RESPIRATORY PHYSIOLOGY Pre-Lab Guide
 RESPIRATORY PHYSIOLOGY Pre-Lab Guide NOTE: A very useful Study Guide! This Pre-lab guide takes you through the important concepts that where discussed in the lab videos. There will be some conceptual questions
RESPIRATORY PHYSIOLOGY Pre-Lab Guide NOTE: A very useful Study Guide! This Pre-lab guide takes you through the important concepts that where discussed in the lab videos. There will be some conceptual questions
Epiglottitis. Bronchitis. Bronchiolitis. Pneumonia. Croup syndrome. Miss. kamlah 2
 Miss. kamlah 1 Epiglottitis. Bronchitis. Bronchiolitis. Pneumonia. Croup syndrome. Miss. kamlah 2 Acute Epiglottitis Is an infection of the epiglottis, the long narrow structure that closes off the glottis
Miss. kamlah 1 Epiglottitis. Bronchitis. Bronchiolitis. Pneumonia. Croup syndrome. Miss. kamlah 2 Acute Epiglottitis Is an infection of the epiglottis, the long narrow structure that closes off the glottis
Chapter 10 Lecture Outline
 Chapter 10 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright 2016 McGraw-Hill Education. Permission required for reproduction
Chapter 10 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright 2016 McGraw-Hill Education. Permission required for reproduction
A Place For Airway Clearance Therapy In Today s Healthcare Environment
 A Place For Airway Clearance Therapy In Today s Healthcare Environment Michigan Society for Respiratory Care 2015 Fall Conference K. James Ehlen, MD October 6, 2015 Objectives Describe patients who will
A Place For Airway Clearance Therapy In Today s Healthcare Environment Michigan Society for Respiratory Care 2015 Fall Conference K. James Ehlen, MD October 6, 2015 Objectives Describe patients who will
11.3 RESPIRATORY SYSTEM DISORDERS
 11.3 RESPIRATORY SYSTEM DISORDERS TONSILLITIS Infection of the tonsils Bacterial or viral Symptoms: red and swollen tonsils, sore throat, fever, swollen glands Treatment: surgically removed Tonsils: in
11.3 RESPIRATORY SYSTEM DISORDERS TONSILLITIS Infection of the tonsils Bacterial or viral Symptoms: red and swollen tonsils, sore throat, fever, swollen glands Treatment: surgically removed Tonsils: in
Competency Title: Continuous Positive Airway Pressure
 Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Respiratory System. Introduction. Atmosphere. Some Properties of Gases. Human Respiratory System. Introduction
 Introduction Respiratory System Energy that we consume in our food is temporarily stored in the bonds of ATP (adenosine triphosphate) before being used by the cell. Cells use ATP for movement and to drive
Introduction Respiratory System Energy that we consume in our food is temporarily stored in the bonds of ATP (adenosine triphosphate) before being used by the cell. Cells use ATP for movement and to drive
Neuromuscular diseases (NMDs) include both hereditary and acquired diseases of the peripheral neuromuscular system. They are diseases of the
 Neuromuscular diseases (NMDs) include both hereditary and acquired diseases of the peripheral neuromuscular system. They are diseases of the peripheral nerves (neuropathies and anterior horn cell diseases),
Neuromuscular diseases (NMDs) include both hereditary and acquired diseases of the peripheral neuromuscular system. They are diseases of the peripheral nerves (neuropathies and anterior horn cell diseases),
Respiratory system. Applied Anatomy &Physiology
 Respiratory system Applied Anatomy &Physiology Anatomy The respiratory system consists of 1)The Upper airway : Nose, mouth and larynx 2)The Lower airways Trachea and the two lungs. Within the lungs,
Respiratory system Applied Anatomy &Physiology Anatomy The respiratory system consists of 1)The Upper airway : Nose, mouth and larynx 2)The Lower airways Trachea and the two lungs. Within the lungs,
Positive Expiratory pressure (PEP), Acapella and Flutter
 Positive Expiratory pressure (PEP), Acapella and Flutter Full Title of Guideline: Author (include email and role): Division & Speciality: Version: 3 Ratified by: Scope (Target audience, state if Trust
Positive Expiratory pressure (PEP), Acapella and Flutter Full Title of Guideline: Author (include email and role): Division & Speciality: Version: 3 Ratified by: Scope (Target audience, state if Trust
Using an Inhaler and Nebulizer
 Using an Inhaler and Nebulizer Introduction An inhaler is a handheld device that is used to deliver medication directly to your airways. A nebulizer is an electric or battery powered machine that turns
Using an Inhaler and Nebulizer Introduction An inhaler is a handheld device that is used to deliver medication directly to your airways. A nebulizer is an electric or battery powered machine that turns
Oxygenation. Chapter 45. Re'eda Almashagba 1
 Oxygenation Chapter 45 Re'eda Almashagba 1 Respiratory Physiology Structure and function Breathing: inspiration, expiration Lung volumes and capacities Pulmonary circulation Respiratory gas exchange: oxygen,
Oxygenation Chapter 45 Re'eda Almashagba 1 Respiratory Physiology Structure and function Breathing: inspiration, expiration Lung volumes and capacities Pulmonary circulation Respiratory gas exchange: oxygen,
B Unit III Notes 6, 7 and 8
 The Respiratory System Why do we breathe? B. 2201 Unit III Notes 6, 7 and 8 Respiratory System We know that our cells respire to produce ATP (energy). All organisms need energy to live, so that s why we
The Respiratory System Why do we breathe? B. 2201 Unit III Notes 6, 7 and 8 Respiratory System We know that our cells respire to produce ATP (energy). All organisms need energy to live, so that s why we
Chapter 13. Respiratory Emergencies
 Chapter 13 Respiratory Emergencies Introduction Patients often complain about dyspnea. Shortness of breath Symptom of many different conditions Cause can be difficult to determine. Even for physician in
Chapter 13 Respiratory Emergencies Introduction Patients often complain about dyspnea. Shortness of breath Symptom of many different conditions Cause can be difficult to determine. Even for physician in
Function: to supply blood with, and to rid the body of
 1 2 3 4 5 Bio 1102 Lec. 7 (guided): Chapter 10 The Respiratory System Respiratory System Function: to supply blood with, and to rid the body of Oxygen: needed by cells to break down food in cellular respiration
1 2 3 4 5 Bio 1102 Lec. 7 (guided): Chapter 10 The Respiratory System Respiratory System Function: to supply blood with, and to rid the body of Oxygen: needed by cells to break down food in cellular respiration
Airway and Ventilation. Emergency Medical Response
 Airway and Ventilation Lesson 14: Airway and Ventilation You Are the Emergency Medical Responder Your medical emergency response team has been called to the fitness center by building security on a report
Airway and Ventilation Lesson 14: Airway and Ventilation You Are the Emergency Medical Responder Your medical emergency response team has been called to the fitness center by building security on a report
The Respiratory System
 BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 14 The Respiratory System Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 14 The Respiratory System Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
Focus on Cystic Fibrosis. Cystic Fibrosis. Cystic Fibrosis
 Focus on (Relates to Chapter 29, Nursing Management: Obstructive Pulmonary Diseases, in the textbook) Copyright 2011, 2007 by Mosby, Inc., an affiliate of Elsevier Inc. Autosomal recessive, multisystem
Focus on (Relates to Chapter 29, Nursing Management: Obstructive Pulmonary Diseases, in the textbook) Copyright 2011, 2007 by Mosby, Inc., an affiliate of Elsevier Inc. Autosomal recessive, multisystem
Cardiovascular and Respiratory Disorders
 Cardiovascular and Respiratory Disorders Blood Pressure Normal blood pressure is 120/80 mmhg (millimeters of mercury) Hypertension is when the resting blood pressure is too high Systolic BP is 140 mmhg
Cardiovascular and Respiratory Disorders Blood Pressure Normal blood pressure is 120/80 mmhg (millimeters of mercury) Hypertension is when the resting blood pressure is too high Systolic BP is 140 mmhg
Chapter 13 Respiration & Excretion
 Chapter 13 Respiration & Excretion Breathing Did you know? Lungs are very spongy and elastic because of the millions of air sacs Lungs exchange about 10,000 L of air a day. Lungs would float like corks
Chapter 13 Respiration & Excretion Breathing Did you know? Lungs are very spongy and elastic because of the millions of air sacs Lungs exchange about 10,000 L of air a day. Lungs would float like corks
Anatomy and Physiology
 Anatomy and Physiology Respiratory Diagnostic Procedures 2004 Delmar Learning, a Division of Thomson Learning, Inc. Bell Work Complete cost of smoking exercise. We will go over this together! (Don t worry)!
Anatomy and Physiology Respiratory Diagnostic Procedures 2004 Delmar Learning, a Division of Thomson Learning, Inc. Bell Work Complete cost of smoking exercise. We will go over this together! (Don t worry)!
What is the next best step?
 Noninvasive Ventilation William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center What is the next best step? 65 year old female
Noninvasive Ventilation William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center What is the next best step? 65 year old female
Bronchiectasis. Information for patients Therapy Services - Surgical
 Bronchiectasis Information for patients Therapy Services - Surgical The aim of this booklet is to offer you practical suggestions for making the most of your lungs and coping with bronchiectasis. Contents
Bronchiectasis Information for patients Therapy Services - Surgical The aim of this booklet is to offer you practical suggestions for making the most of your lungs and coping with bronchiectasis. Contents
LESSON ASSIGNMENT. Physical Assessment of the Respiratory System. After completing this lesson, you should be able to:
 LESSON ASSIGNMENT LESSON 2 Physical Assessment of the Respiratory System. LESSON ASSIGNMENT Paragraphs 2-1 through 2-8. LESSON OBJECTIVES After completing this lesson, you should be able to: 2-1. Perform
LESSON ASSIGNMENT LESSON 2 Physical Assessment of the Respiratory System. LESSON ASSIGNMENT Paragraphs 2-1 through 2-8. LESSON OBJECTIVES After completing this lesson, you should be able to: 2-1. Perform
Cough Associated with Bronchitis
 Cough Associated with Bronchitis Bronchitis (bron-ki-tis) is a condition in which the bronchial tubes, the tubes that carry air to your lungs, become inflamed. People who have bronchitis often have a cough
Cough Associated with Bronchitis Bronchitis (bron-ki-tis) is a condition in which the bronchial tubes, the tubes that carry air to your lungs, become inflamed. People who have bronchitis often have a cough
Protocol for performing chest clearance techniques by nursing staff
 Protocol for performing chest clearance techniques by nursing staff Rationale The main indications for performing chest clearance techniques (CCT) are to assist in the removal of thick, tenacious secretions
Protocol for performing chest clearance techniques by nursing staff Rationale The main indications for performing chest clearance techniques (CCT) are to assist in the removal of thick, tenacious secretions
GOALS AND INSTRUCTIONAL OBJECTIVES
 October 4-7, 2004 Respiratory GOALS: GOALS AND INSTRUCTIONAL OBJECTIVES By the end of the week, the first quarter student will have an in-depth understanding of the diagnoses listed under Primary Diagnoses
October 4-7, 2004 Respiratory GOALS: GOALS AND INSTRUCTIONAL OBJECTIVES By the end of the week, the first quarter student will have an in-depth understanding of the diagnoses listed under Primary Diagnoses
10/17/2016 OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT COURSE OBJECTIVES COMMON CAUSES OF RESPIRATORY FAILURE
 OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT J U L I E Z I M M E R M A N, R N, M S N C L I N I C A L N U R S E S P E C I A L I S T E L O I S A C U T L E R, R R T, B S R C C L I N I C A L / E D U C
OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT J U L I E Z I M M E R M A N, R N, M S N C L I N I C A L N U R S E S P E C I A L I S T E L O I S A C U T L E R, R R T, B S R C C L I N I C A L / E D U C
Breathing Exercises in Airway diseases
 is a lung condition with abnormal permanent airway dilatation. It is a recurrent cough and colds. Not usually progressive or life threatening complication. Should it be progressive then will need aggressive
is a lung condition with abnormal permanent airway dilatation. It is a recurrent cough and colds. Not usually progressive or life threatening complication. Should it be progressive then will need aggressive
Glossary of Asthma Terms
 HealthyKidsExpress@bjc.org Asthma Words to Know Developed in partnership with Health Literacy Missouri Airways (Bronchi, Bronchial Tubes): The tubes in the lungs that let air in and out of the body. Airway
HealthyKidsExpress@bjc.org Asthma Words to Know Developed in partnership with Health Literacy Missouri Airways (Bronchi, Bronchial Tubes): The tubes in the lungs that let air in and out of the body. Airway
The primary function of the respiratory system is to supply the blood with oxygen in order for the blood to deliver oxygen to all parts of the body.
 Respiratory System The primary function of the respiratory system is to supply the blood with oxygen in order for the blood to deliver oxygen to all parts of the body. The respiratory system does this
Respiratory System The primary function of the respiratory system is to supply the blood with oxygen in order for the blood to deliver oxygen to all parts of the body. The respiratory system does this
RESPIRATORY COMPLICATIONS AFTER SCI
 SHEPHERD.ORG RESPIRATORY COMPLICATIONS AFTER SCI NORMA I RIVERA, RRT, RCP RESPIRATORY EDUCATOR SHEPHERD CENTER 2020 Peachtree Road, NW, Atlanta, GA 30309-1465 404-352-2020 DISCLOSURE STATEMENT I have no
SHEPHERD.ORG RESPIRATORY COMPLICATIONS AFTER SCI NORMA I RIVERA, RRT, RCP RESPIRATORY EDUCATOR SHEPHERD CENTER 2020 Peachtree Road, NW, Atlanta, GA 30309-1465 404-352-2020 DISCLOSURE STATEMENT I have no
Respiratory Physiology
 Respiratory Physiology Dr. Aida Korish Associate Prof. Physiology KSU The main goal of respiration is to 1-Provide oxygen to tissues 2- Remove CO2 from the body. Respiratory system consists of: Passages
Respiratory Physiology Dr. Aida Korish Associate Prof. Physiology KSU The main goal of respiration is to 1-Provide oxygen to tissues 2- Remove CO2 from the body. Respiratory system consists of: Passages
Reference Guide for Group Education
 A p l a n o f a c t i o n f o r l i f e Reference Guide for Group Education Session 1 Introduction to Living Well with COPD Education Program Participants Expectations Towards the Program Health in COPD
A p l a n o f a c t i o n f o r l i f e Reference Guide for Group Education Session 1 Introduction to Living Well with COPD Education Program Participants Expectations Towards the Program Health in COPD
Table of Contents. What is COPD? 1. Slowing the Progression of COPD 2. Treatment for COPD 3. Proper Inhaler Technique 5. Breathing Exercises 6
 1 Table of Contents What is COPD? 1 Slowing the Progression of COPD 2 Treatment for COPD 3 Proper Inhaler Technique 5 Breathing Exercises 6 Exercise 7 Nutrition 7 Avoiding Infection 8 Managing Daily Life
1 Table of Contents What is COPD? 1 Slowing the Progression of COPD 2 Treatment for COPD 3 Proper Inhaler Technique 5 Breathing Exercises 6 Exercise 7 Nutrition 7 Avoiding Infection 8 Managing Daily Life
Asthma. - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness.
 Obstructive diseases Asthma - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness. - Characterized by Intermittent and reversible (the
Obstructive diseases Asthma - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness. - Characterized by Intermittent and reversible (the
Respiratory System. Student Learning Objectives:
 Respiratory System Student Learning Objectives: Identify the primary structures of the respiratory system. Identify the major air volumes associated with ventilation. Structures to be studied: Respiratory
Respiratory System Student Learning Objectives: Identify the primary structures of the respiratory system. Identify the major air volumes associated with ventilation. Structures to be studied: Respiratory
The Respiratory System
 The Respiratory System By Mr. Danilo Villar Rogayan Jr. Instructor I, Department of Natural Sciences RMTU San Marcelino Introduction Function Move air in an out of lungs (ventilation) Delivers oxygen (O
The Respiratory System By Mr. Danilo Villar Rogayan Jr. Instructor I, Department of Natural Sciences RMTU San Marcelino Introduction Function Move air in an out of lungs (ventilation) Delivers oxygen (O
Chapter 39 Oxygenation. Copyright 2011 Wolters Kluwer Health Lippincott Williams & Wilkins
 Chapter 39 Oxygenation Factors Essential to Normal Functioning of the Respiratory System Integrity of the airway system to transport air to and from lungs Properly functioning alveolar system in lungs
Chapter 39 Oxygenation Factors Essential to Normal Functioning of the Respiratory System Integrity of the airway system to transport air to and from lungs Properly functioning alveolar system in lungs
Objectives. Pulmonary Assessment 12/13/2017
 Pulmonary Assessment Reid Blackwelder, MD, FAAFP Professor and Chair, Family Medicine Quillen Colege of Medicine, ETSU Objectives Understand anatomy and physiology of pulmonary assessment techniques Remember
Pulmonary Assessment Reid Blackwelder, MD, FAAFP Professor and Chair, Family Medicine Quillen Colege of Medicine, ETSU Objectives Understand anatomy and physiology of pulmonary assessment techniques Remember
NHS Training for Physiotherapy Support Workers. Workbook 14 The respiratory system
 NHS Training for Physiotherapy Support Workers Workbook 14 The respiratory system Contents Workbook 14 The respiratory system 1 14.1 Aim 3 14.2 Learning outcomes 3 14.3 The respiratory system 4 14.4 Breathing
NHS Training for Physiotherapy Support Workers Workbook 14 The respiratory system Contents Workbook 14 The respiratory system 1 14.1 Aim 3 14.2 Learning outcomes 3 14.3 The respiratory system 4 14.4 Breathing
Active Cycle of Breathing Technique
 Active Cycle of Breathing Technique Full Title of Guideline: Author (include email and role): Division & Speciality: Version: 3 Ratified by: Scope (Target audience, state if Trust wide): Review date (when
Active Cycle of Breathing Technique Full Title of Guideline: Author (include email and role): Division & Speciality: Version: 3 Ratified by: Scope (Target audience, state if Trust wide): Review date (when
Looking after your lungs
 choking awareness! Looking after your lungs Useful information and top tips Colds and chest infections can be common, especially in the autumn and winter months. It is therefore very important that you
choking awareness! Looking after your lungs Useful information and top tips Colds and chest infections can be common, especially in the autumn and winter months. It is therefore very important that you
The Respiratory System
 Elaine N. Marieb Katja Hoehn Human Anatomy & Physiology SEVENTH EDITION C H A P T E R PowerPoint Lecture Slides prepared by Vince Austin, Bluegrass Technical and Community College 22P A R T B The Respiratory
Elaine N. Marieb Katja Hoehn Human Anatomy & Physiology SEVENTH EDITION C H A P T E R PowerPoint Lecture Slides prepared by Vince Austin, Bluegrass Technical and Community College 22P A R T B The Respiratory
Respiratory Emergencies. Lesson Goal. Lesson Objectives 9/10/2012
 Respiratory Emergencies Lesson Goal Assess and provide timely treatment & transport to patients experiencing respiratory emergencies Lesson Objectives List parts of respiratory system and how they work
Respiratory Emergencies Lesson Goal Assess and provide timely treatment & transport to patients experiencing respiratory emergencies Lesson Objectives List parts of respiratory system and how they work
TOWN OF FAIRFIELD HEALTH DEPARTMENT PUBLIC HEALTH NURSING
 TOWN OF FAIRFIELD HEALTH DEPARTMENT PUBLIC HEALTH NURSING PROGRAM: School Health APPROVED BY: Board of Health POLICY: Nebulizer Therapy DATE: 5-10-93 PROCEDURE: a) Nebulizer Therapy With Non-oxygenated
TOWN OF FAIRFIELD HEALTH DEPARTMENT PUBLIC HEALTH NURSING PROGRAM: School Health APPROVED BY: Board of Health POLICY: Nebulizer Therapy DATE: 5-10-93 PROCEDURE: a) Nebulizer Therapy With Non-oxygenated
Pneumonia. Trachea , The Patient Education Institute, Inc. id Last reviewed: 11/11/2017 1
 Pneumonia Introduction Pneumonia is an inflammation and infection of the lungs. Pneumonia causes millions of deaths every year. It can affect anybody, but is more dangerous to older adults, babies and
Pneumonia Introduction Pneumonia is an inflammation and infection of the lungs. Pneumonia causes millions of deaths every year. It can affect anybody, but is more dangerous to older adults, babies and
Overview of COPD INTRODUCTION
 Overview of COPD INTRODUCTION Chronic obstructive pulmonary disease (COPD) is a common lung disease that affects millions of people, and it is the fourth leading cause of death in the United States. It
Overview of COPD INTRODUCTION Chronic obstructive pulmonary disease (COPD) is a common lung disease that affects millions of people, and it is the fourth leading cause of death in the United States. It
Basic mechanisms disturbing lung function and gas exchange
 Basic mechanisms disturbing lung function and gas exchange Blagoi Marinov, MD, PhD Pathophysiology Department, Medical University of Plovdiv Respiratory system 1 Control of breathing Structure of the lungs
Basic mechanisms disturbing lung function and gas exchange Blagoi Marinov, MD, PhD Pathophysiology Department, Medical University of Plovdiv Respiratory system 1 Control of breathing Structure of the lungs
COUGH Dr. A m A it i e t sh A g A garwa w l Le L ctu t rer Departm t ent t o f f M e M dic i in i e
 COUGH Dr. Amitesh Aggarwal Lecturer Department of Medicine Cough is an explosive expiration that provides a normal protective mechanism for clearing the tracheobronchial tree of secretions and foreign
COUGH Dr. Amitesh Aggarwal Lecturer Department of Medicine Cough is an explosive expiration that provides a normal protective mechanism for clearing the tracheobronchial tree of secretions and foreign
Hyperinflation Therapy and the Tools to Accomplish It!! Bill Barnes, RN, RRT Good Shepherd Rehabilitation Network
 Hyperinflation Therapy and the Tools to Accomplish It!! Bill Barnes, RN, RRT Good Shepherd Rehabilitation Network HYPERINFLATION THERAPY Challenges in Post Acute Care Deconditioning Malnutrition Hydration
Hyperinflation Therapy and the Tools to Accomplish It!! Bill Barnes, RN, RRT Good Shepherd Rehabilitation Network HYPERINFLATION THERAPY Challenges in Post Acute Care Deconditioning Malnutrition Hydration
Bronchospasm & SOB. Kim Kilmurray Senior Clinical Teaching Fellow
 Bronchospasm & SOB Kim Kilmurray Senior Clinical Teaching Fellow LEARNING OBJECTIVES Perform a comprehensive respiratory examination & link clinical signs to underlying pathology Identify the spectrum
Bronchospasm & SOB Kim Kilmurray Senior Clinical Teaching Fellow LEARNING OBJECTIVES Perform a comprehensive respiratory examination & link clinical signs to underlying pathology Identify the spectrum
CARDIOVASCULAR AND RESPIRATORY SYSTEMS
 CARDIOVASCULAR AND RESPIRATORY SYSTEMS KEY TERMS: Cardiovascular System, cardio, vascular, blood vessels, valves, arteries, capillaries, veins, systemic circulation, pulmonary circulation Your Cardiovascular
CARDIOVASCULAR AND RESPIRATORY SYSTEMS KEY TERMS: Cardiovascular System, cardio, vascular, blood vessels, valves, arteries, capillaries, veins, systemic circulation, pulmonary circulation Your Cardiovascular
