County General Hospital 546 That Street. Some Town, YY DISCHARGE SUMMARY
|
|
|
- Kristin Houston
- 6 years ago
- Views:
Transcription
1 County General Hospital 546 That Street. Some Town, YY DISCHARGE SUMMARY PATIENT: Collette Rose UNIT#: ADMISSION DATE: June 5, 1995 ACCT#: DISCHARGE DATE: June 13, 1995 DOB: 12/04/78 ATTENDING PHYSICIAN: Jackson, Samantha ROOM/BED: F. 346-B Issac Johnson, DSA dictating for Dr. Samantha Jackson DISCHARGE DIAGNOSES: 1. Major Depression 2. Alcohol Abuse HISTORY OF PRESENT ILLNESS: This is an 18-year-old Caucasian female with a recent history of major depression and suicide attempt. She ingested nearly an entire bottle of acetaminophen. Her sister discovered her passed out in the bathtub and called 911. She was brought to the emergency department by ambulance. She was admitted for further evaluation, stabilization and medication management. ALLERGIES: No known drug allergies. HOSPITAL COURSE: Treatment began in the ambulance on the way to the hospital. Activated charcoal was administered. Upon admission, gastric lavage was conducted to clean out the contents of her stomach. Patient s BAC level was She was given fluids to rehydrate her system after respiratory stabilization. On the morning of June 13, the patient had calmed down in response to the medication and care provided the last 7 days. She denied AH/VH. She denied any suicidal or homicidal ideations. She was prescribed fluoxetine 20mg, once daily. Dr. Jackson noted that she would need to follow up with social services and XYZ Community Mental Health Center for ongoing treatment. CONDITION AT DISCHARGE: The patient was wanting to be discharged. She was alert and oriented x3. Vital signs were stable. Her last recorded blood pressure was 107/61, heart rate 75. Lungs were clear. Abdomen was soft, nontender, nondistended with positive bowel sounds. She was
2 discharged on June 13, 1995, with discharge instructions given and medications reconciled. LABORATORY DATA: On June 5, sodium 143, potassium 3.8, chloride 109, co2 of 28, anion gap 6.0, glucose 122, BUN 17, creatinine 1.1, total protein 6.5, albumin 3.4, globulin 3.1, calcium 8.8, phosphorus 3.7, total bilirubin 0.3, AST 14, ALT 15, alkaline phosphatase 88, magnesium 2.2, triglycerides 50, cholesterol 150, HDL cholesterol 45, and LDL 120. Hematology values on June 6, white blood count 11.6, hemoglobin and hematocrit 12.3 and 36.5 respectively, with platelet count of 282,000. DISCHARGE MEDICATIONS: 1. Fluoxetine 20 mg DISCHARGE INSTRUCTIONS: Follow up with Social Services as instructed r.e. housing. Follow-up with XYZ Community Mental Health Center for ongoing treatment. Dictated by Issac Johnson DSA DD: 06/14/ :25:34 DT: 06/14/ :15:25 CGHANYHSC; Job# Authenticated by Samantha Jackson MD on 06/15/ :45:21 PM
3 County General Hospital 546 That Street. Some Town, YY HISTORY AND PHYSICAL REPORT PATIENT: Collette Rose UNIT#: ADMISSION DATE: June 5, 1995 ACCT#: ADMITTING PHYSICIAN: Jackson, Samantha DOB: 12/04/78 ATTENDING PHYSICIAN: Jackson, Samantha ROOM/BED: F. 346-B DICTATING PHYSICIAN: Jackson, Samantha CHIEF COMPLAINT: The patient came in with major depression following a suicide attempt. HISTORY OF PRESENT ILLNESS: This is an 18-year-old Caucasian female with major depression. She complains of feelings of hopelessness. She has lost interest in every day activities that used to bring her joy, including caring for her son. She is sleeping hours a day and not caring for her hygiene. She complains of little energy. She reports that she has lost 15 lbs in the last month. She appears to be underweight for her height. PAST MEDICAL HISTORY: The patient has a prior suicide attempt as a juvenile. In 1991, when the patient was 13 years old she took an entire bottle of acetaminophen to stop the pain. SOCIAL HISTORY: She is single, she recently had a son, is currently unemployed and homeless. She does not smoke, denies drinking or using drugs but smelled of alcohol at admittance. FAMILY HISTORY: MEDICATIONS: REVIEW OF SYSTEMS: All other systems are reviewed, otherwise negative. ALLERGIES: PHYSICAL EXAMINATION: GENERAL: The patient is lying in the bed, quietly crying. Occasionally sleeps.
4 VITAL SIGNS: Significant for patient s temperature of 99.2, pulse of 88, respiratory rate of 18, blood pressure of 107/61, and pulse ox of 97%. HEENT: Pupils equal, round, reactive to light and accommodation. Extraocular muscles are intact. No icterus, no pallor noted. NECK: Supple, no jugular venous distention, no thyromegaly. CARDIOVASCULAR: Regular rate and rhythm, s1, s2 heard. No murmurs, gallops, or rubs. CHEST: Clear to auscultation. Abdomen: Soft, tender to the touch, nondistended. EXTREMETIES: No edema, No cyanosis. NUEROLOGIC: Alert and oriented x3 and follows all commands. LABORATORY DATA: The patient s CBC was within normal limits. The patient s CMP was also within normal limits. ASSESSMENT AND PLAN: Abdominal pain. The patient will be given calcium carbonate and acetaminophen. Anxiety and agitation. The patient will be given Fluoxetine 20 mg to stabilize. The patient will get social worker involved for further plan of care. We will start the patient on antidepressant medications. If this history and physical was performed prior to admission, but within the last 30 days, indicate by initialing one of the following: I have reassessed the patient and notes that there are no significant changes to the assessment. I have reassessed the patient and note the following significant changes occurred: DD: 06/05/ :25:30 DT: 06/05/ :14:09 CGHANYHSC; Job# Authenticated by Samantha Jackson MD on 06/07/ :49:45 AM Samantha Jackson Report ID: Electronically Signed by Samantha Jackson on 06/07/1995 at 0932
5 County General Hospital 546 That Street. Some Town, YY DISCHARGE SUMMARY PATIENT: Collette Rose UNIT#: ADMISSION DATE: January 5, 2012 ACCT#: DISCHARGE DATE: January 8, 2012 DOB: 12/04/78 ATTENDING PHYSICIAN: Jackson, Samantha ROOM/BED: F. 346-B Issac Johnson, DSA dictating for Dr. Samantha Jackson DISCHARGE DIAGNOSES: 1. Bipolar I Disorder, most recent episode, manic 2. Alcohol Abuse HISTORY OF PRESENT ILLNESS: This is a 33-year-old Caucasian female with a recent history of bipolar disorder, manic episode. She was picked up by a patrol call when business owners reported her harassing their patrons as she yelled at them to buy a copy of her book. She was talking rapidly, could not focus on questions and began hyperventilating. She was admitted for further evaluation, stabilization and medication management. PREVIOUS ADMISSIONS: 2011 March Inpatient Psychiatric 2010 April Inpatient Psychiatric 2007 August 1-3 Inpatient Psychiatric 2007 Jan 1-3 Inpatient Psychiatric 2006 June Inpatient Psychiatric 2005 Feb Inpatient Psychiatric 2004 Sept 1-4 Inpatient Psychiatric 2003 Dec Inpatient Psychiatric 2001 Nov 6-10 Inpatient Psychiatric 2000 Mar Inpatient Psychiatric 1997 Feb Inpatient Psychiatric 1995 June 5-3 Inpatient Psychiatric 1991 May 6-10 Inpatient Psychiatric ALLERGIES: No known drug allergies.
6 HOSPITAL COURSE: Patient was admitted to the psychiatric unit for stabilization on medication. She was placed under close observation and given a regular diet. Her breathing calmed once she was placed in a bed but she continued to tell the nurses about the book and the book tour that she was going to go on with her daughter. Her pressured speech and delusions of grandeur lasted for the first 48 hours. On the morning of January 8th, the patient had stabilized in response to the medication and care provided the last 3 days. She denied AH/VH. She denied any suicidal or homicidal ideations. She was prescribed Lamictal 300 mg and Seroquel 100 mg to help her sleep. She was prescribed metoprolol tartrate 100 mg for her hypertension. Dr. Jackson noted that she would need to follow up with social services and XYZ Community Mental Health Center for ongoing treatment. CONDITION AT DISCHARGE: The patient was wanting to be discharged. She was alert and oriented x3. Vital signs were stable. Her last recorded blood pressure was 140/90, heart rate 75. Lungs were clear. Abdomen was soft, nontender, nondistended with positive bowel sounds. She was discharged on January 8, 2012, with discharge instructions given and medications reconciled. LABORATORY DATA: On January 5, sodium 143, potassium 3.8, chloride 109, co2 of 28, anion gap 6.0, glucose 122, BUN 17, creatinine 1.1, total protein 6.5, albumin 3.4, globulin 3.1, calcium 8.8, phosphorus 3.7, total bilirubin 0.3, AST 14, ALT 15, alkaline phosphatase 88, magnesium 2.2, triglycerides 50, cholesterol 150, HDL cholesterol 45, and LDL 120. Hematology values on June 6, white blood count 11.6, hemoglobin and hematocrit 12.3 and 36.5 respectively, with platelet count of 282,000. DISCHARGE MEDICATIONS: 1. Lamictal 300 mg, po opd 2. Seroquel 100 mg, po qhs 3. Metoprolol tartrate 100 mg, po opd DISCHARGE INSTRUCTIONS: Follow up with Social Services as instructed r.e. benefits application and housing. Follow-up with XYZ Community Mental Health Center for ongoing treatment. Dictated by Issac Johnson DSA DD: 01/09/ :25:34 DT: 01/09/ :15:25 CGHANYHSC; Job# Authenticated by Samantha Jackson MD on 01/11/ :45:21 PM
7 County General Hospital 546 That Street. Some Town, YY HISTORY AND PHYSICAL REPORT PATIENT: Collette Rose UNIT#: ADMISSION DATE: January 5, 2012 ACCT#: ADMITTING PHYSICIAN: Jackson, Samantha DOB: 12/04/78 ATTENDING PHYSICIAN: Jackson, Samantha ROOM/BED: F. 346-B DICTATING PHYSICIAN: Jackson, Samantha CHIEF COMPLAINT: The patient was brought to the hospital because of a public disturbance. She is experiencing a manic episode. HISTORY OF PRESENT ILLNESS: This patient has a known history of bipolar disorder. She has a long history of mood swings for the past several years. She has been on Lithium and Lamictal and she has been noncompliant with medications. For the past few weeks she has had depressed mood, she was anhedonic, had decreased energy, decreased appetite and difficulty falling and maintaining sleeping. In the last few days she has been experiencing a manic episode. Officers report a change in her demeanor. She has been attending the County Probation Alternatives Program and is currently sober, but is not taking any medications. She has delusions of grandeur and pressured speech. She is not able to focus on a line of questions or one topic. She is preoccupied with sharing information about a supposed book that she has written and how she is going to use the proceeds to take her daughter on a book tour to Europe. She denies any auditory hallucinations during the interview. She denies any suicidal or homicidal ideation. PAST MEDICAL HISTORY: The patient has prior suicide attempts as a juvenile and young adult. She has been diagnosed with major depression and bipolar disorder. Her most recent episode is manic. Records indicate that she has diabetes and high blood pressure. SOCIAL HISTORY: The patient was born in Middleton, PA and spent most of her adult life in Any Town. The patient is currently experiencing homelessness. She is single and has 2 kids who are not currently in her custody. She has a sister who she maintains contact with. She has an 8 th grade education and is unable to maintain employment. She has a significant history of physical and sexual abuse. No military history. FAMILY HISTORY:
8 MEDICATIONS: REVIEW OF SYSTEMS: All other systems are reviewed, otherwise negative. ALLERGIES: PHYSICAL EXAMINATION: GENERAL: The patient is lying in the bed quietly talking to herself. VITAL SIGNS: Significant for patient s temperature of 99.2, pulse of 88, respiratory rate of 18, blood pressure of 150/91, and pulse ox of 97%. HEENT: Pupils equal, round, reactive to light and accommodation. Extraocular muscles are intact. No icterus, no pallor noted. NECK: Supple, no jugular venous distention, no thyromegaly. CARDIOVASCULAR: Regular rate and rhythm, s1, s2 heard. No murmurs, gallops, or rubs. CHEST: Clear to auscultation. Abdomen: Soft, tender to the touch, nondistended. EXTREMETIES: No edema, No cyanosis. NUEROLOGIC: Alert and oriented x3 and follows all commands. LABORATORY DATA: The patient s CBC was within normal limits. The patient s CMP was also within normal limits. Tox screens were negative for alcohol. ASSESSMENT AND PLAN: Mania. The patient will be given Lamictal 300mg to stabilize. The patient will get social worker involved for further plan of care. We will start the patient on Seroquel to aid her sleep. Hypertension. The patient was given metaprolol tartrate 100mg to control her blood pressure. If this history and physical was performed prior to admission, but within the last 30 days, indicate by initialing one of the following: I have reassessed the patient and notes that there are no significant changes to the assessment. I have reassessed the patient and note the following significant changes occurred: DD: 01/07/ :25:30 DT: 01/07/ :14:09 CGHANYHSC; Job# Authenticated by Samantha Jackson MD on 01/08/ :49:45 AM
9 Samantha Jackson Report ID: Electronically Signed by Samantha Jackson on 01/08/2012 at 0932
County General Hospital 546 That Street Some Town, YY DISCHARGE SUMMARY
 County General Hospital 546 That Street Some Town, YY 12345 111-222-9998 DISCHARGE SUMMARY PATIENT: Michael F. Byrnes UNIT#: 345678 ADMISSION DATE: June 5, 2006 ACCT#: 98734512 DISCHARGE DATE: June 6,
County General Hospital 546 That Street Some Town, YY 12345 111-222-9998 DISCHARGE SUMMARY PATIENT: Michael F. Byrnes UNIT#: 345678 ADMISSION DATE: June 5, 2006 ACCT#: 98734512 DISCHARGE DATE: June 6,
CASE-BASED SMALL GROUP DISCUSSION
 MHD I, Session 11, Student Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD I SESSION 11 Renal Block Acid- Base Disorders November 7, 2016 MHD I, Session 11, Student Copy Page 2 Case #1 Cc: I have had
MHD I, Session 11, Student Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD I SESSION 11 Renal Block Acid- Base Disorders November 7, 2016 MHD I, Session 11, Student Copy Page 2 Case #1 Cc: I have had
Documentation Dissection
 History of Present Illness: Documentation Dissection The patient is a 50-year-old male c/o symptoms for past 4 months 1, severe 2 bloating and stomach cramps, some nausea, vomiting, diarrhea. In last 3
History of Present Illness: Documentation Dissection The patient is a 50-year-old male c/o symptoms for past 4 months 1, severe 2 bloating and stomach cramps, some nausea, vomiting, diarrhea. In last 3
CASE-BASED SMALL GROUP DISCUSSION MHD II
 MHD II, Session 11, Student Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD II Session 11 April 11, 2016 STUDENT COPY MHD II, Session 11, Student Copy Page 2 CASE HISTORY 1 Chief complaint: Our baby
MHD II, Session 11, Student Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD II Session 11 April 11, 2016 STUDENT COPY MHD II, Session 11, Student Copy Page 2 CASE HISTORY 1 Chief complaint: Our baby
Patient Encounters in the Primary Care Setting
 Patient Encounters in the Primary Care Setting Carmine D Amico, D.O. Clinical Cases Overview Learning objectives Clinical case presentations Questions for audience participation 1 Clinical Cases Learning
Patient Encounters in the Primary Care Setting Carmine D Amico, D.O. Clinical Cases Overview Learning objectives Clinical case presentations Questions for audience participation 1 Clinical Cases Learning
County Probation Alternatives Program
 County Probation Alternatives Program Name: Collette Rose DOB: 12/04/1978 Client number: 10409 Date of Initial Contact: Dec 12, 2011 Date of Evaluation: Dec 12, 2011 Primary Counselor: Barbara Jackson,
County Probation Alternatives Program Name: Collette Rose DOB: 12/04/1978 Client number: 10409 Date of Initial Contact: Dec 12, 2011 Date of Evaluation: Dec 12, 2011 Primary Counselor: Barbara Jackson,
MHD I SESSION X. Renal Disease
 MHD I, Session X, Student Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD I SESSION X Renal Disease Monday, November 11, 2013 MHD I, Session X, Student Copy Page 2 Case #1 Cc: I have had weeks of diarrhea
MHD I, Session X, Student Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD I SESSION X Renal Disease Monday, November 11, 2013 MHD I, Session X, Student Copy Page 2 Case #1 Cc: I have had weeks of diarrhea
SMALL GROUP DISCUSSION
 MHD II, Session 1 Student Copy Page 1 SMALL GROUP DISCUSSION MHD II Session 1 Gastroinestinal Monday, January 9, 2017 STUDENT COPY MHD II, Session 1 Student Copy Page 2 CASE 1 CHIEF CONCERN: "I'm passing
MHD II, Session 1 Student Copy Page 1 SMALL GROUP DISCUSSION MHD II Session 1 Gastroinestinal Monday, January 9, 2017 STUDENT COPY MHD II, Session 1 Student Copy Page 2 CASE 1 CHIEF CONCERN: "I'm passing
Rural STEMI System of Care Success. Nicole Huber, PA-C Cumberland Healthcare Emergency Department
 Rural STEMI System of Care Success Nicole Huber, PA-C Cumberland Healthcare Emergency Department DISCLOSURES I HAVE NO ACTUAL OR POTENTIAL CONFLICT OF INTEREST IN RELATION TO THIS PRESENTATION Ideal Process
Rural STEMI System of Care Success Nicole Huber, PA-C Cumberland Healthcare Emergency Department DISCLOSURES I HAVE NO ACTUAL OR POTENTIAL CONFLICT OF INTEREST IN RELATION TO THIS PRESENTATION Ideal Process
SMALL GROUP DISCUSSION
 MHD II, Seesion II Student Copy - Page 1 SMALL GROUP DISCUSSION MHD II Session II JANUARY 15, 2014 Recent Review highlighting disease process in Case 2: Fasano A, Catassi, C. NEJM 2012; 367: 2419-26 STUDENT
MHD II, Seesion II Student Copy - Page 1 SMALL GROUP DISCUSSION MHD II Session II JANUARY 15, 2014 Recent Review highlighting disease process in Case 2: Fasano A, Catassi, C. NEJM 2012; 367: 2419-26 STUDENT
Note for Jane Doe on 02/10/ Chart 3642
 Note for Jane Doe on 02/10/2005 - Chart 3642 Consultation was requested by Dr. Smith Chief Complaint (1/1): This 31 year old Caucasian female presents today for evaluation of chest pain. Chest pains HPI:
Note for Jane Doe on 02/10/2005 - Chart 3642 Consultation was requested by Dr. Smith Chief Complaint (1/1): This 31 year old Caucasian female presents today for evaluation of chest pain. Chest pains HPI:
CSS Correctional Service System
 Mental Health Services Staff Referral Form 04/06/2012 Medical Evaluation (To Be Completed By The Medical Staff) Reason for Referral- Check and Explain All That Apply Actively Suicidal or Homicidal Self-Reported
Mental Health Services Staff Referral Form 04/06/2012 Medical Evaluation (To Be Completed By The Medical Staff) Reason for Referral- Check and Explain All That Apply Actively Suicidal or Homicidal Self-Reported
CARDIOVASCULAR CASE-BASED SMALL GROUP DISCUSSION
 MHD I Session VIII Student Copy Page 1 CARDIOVASCULAR CASE-BASED SMALL GROUP DISCUSSION MHD I SESSION VIII OCTOBER 22, 2014 STUDENT COPY MHD I Session VIII Student Copy Page 2 Case 1 Chief Complaint I
MHD I Session VIII Student Copy Page 1 CARDIOVASCULAR CASE-BASED SMALL GROUP DISCUSSION MHD I SESSION VIII OCTOBER 22, 2014 STUDENT COPY MHD I Session VIII Student Copy Page 2 Case 1 Chief Complaint I
Discharge Summary-Page 1
 Discharge Summary-Page 1 Admission diagnosis: 1. Gastritis. 2. Alcoholic cirrhosis, ascites, grade 1 esophageal varices. 3. Recent left knee arthroplasty. 4. Osteoporosis naqmq : 1. Three chest X-rays
Discharge Summary-Page 1 Admission diagnosis: 1. Gastritis. 2. Alcoholic cirrhosis, ascites, grade 1 esophageal varices. 3. Recent left knee arthroplasty. 4. Osteoporosis naqmq : 1. Three chest X-rays
Understanding Blood Tests
 PATIENT EDUCATION patienteducation.osumc.edu Your heart pumps the blood in your body through a system of blood vessels. Blood delivers oxygen and nutrients to all parts of the body. It also carries away
PATIENT EDUCATION patienteducation.osumc.edu Your heart pumps the blood in your body through a system of blood vessels. Blood delivers oxygen and nutrients to all parts of the body. It also carries away
Substance Abuse History: 5 to 6 drinks every 2 weeks. No recent use of alcohol, tobacco, or drugs.
 Date of Admission: [DATE] Date of Discharge: [DATE] History of Present Illness: This is a 39-year-old Caucasian married male with no previous psych history who is brought in by his wife on the urging of
Date of Admission: [DATE] Date of Discharge: [DATE] History of Present Illness: This is a 39-year-old Caucasian married male with no previous psych history who is brought in by his wife on the urging of
SESSION 5 - Cardiovascular
 Small Group Session I, MHD 5 - STUDENT Copy Page 1 MECHANISMS OF HUMAN DISEASE AND PHARMACOLOGY & THERAPEUTICS CASE-BASED SMALL GROUP DISCUSSION SESSION 5 - Cardiovascular MHD I Friday, September 29, 2017
Small Group Session I, MHD 5 - STUDENT Copy Page 1 MECHANISMS OF HUMAN DISEASE AND PHARMACOLOGY & THERAPEUTICS CASE-BASED SMALL GROUP DISCUSSION SESSION 5 - Cardiovascular MHD I Friday, September 29, 2017
PSYCHIATRIC CLINIC, LLC 123 Main Street Anywhere, US (O) (F) Nesmith, Kelly.
 Page 1 of 7 PSYCHIATRIC CLINIC, LLC 123 Main Street Anywhere, US 12345-6789 555-678-9100 (O) 555-678-9111 (F) DATE ADMITTED: 4/24/2017 DATE DISCHARGED: This discharge summary consists of 1. Initial Assessment
Page 1 of 7 PSYCHIATRIC CLINIC, LLC 123 Main Street Anywhere, US 12345-6789 555-678-9100 (O) 555-678-9111 (F) DATE ADMITTED: 4/24/2017 DATE DISCHARGED: This discharge summary consists of 1. Initial Assessment
MHD I Session VIII Renal Disease November 6, 2013 STUDENT COPY
 MHD I, Session VIII, Student Copy Page 1 MHD I Session VIII Renal Disease November 6, 2013 STUDENT COPY MHD I, Session VIII, Student Copy Page 2 Case #1 Chief Complaint: I have been feeling just lousy
MHD I, Session VIII, Student Copy Page 1 MHD I Session VIII Renal Disease November 6, 2013 STUDENT COPY MHD I, Session VIII, Student Copy Page 2 Case #1 Chief Complaint: I have been feeling just lousy
Patient: Becky Smith DOB: 01/26/XXXX Age: 5 y/o Attending: Dr. D. Miles Allergies: NKA MR#: 203. Patient Chart #203 Becky Smith
 Patient Chart #203 Becky Smith 1 Property of CSCLV CSCLV Rev: 06/04/2018 Chief Complaint: Abdominal pain. Informant: Parents. HISTORY & PHYSICAL HPI: Ill looking patient, healthy until 2 days ago when
Patient Chart #203 Becky Smith 1 Property of CSCLV CSCLV Rev: 06/04/2018 Chief Complaint: Abdominal pain. Informant: Parents. HISTORY & PHYSICAL HPI: Ill looking patient, healthy until 2 days ago when
Med 536 Communicating About Prognosis Workshop. Case 2
 Med 536 Communicating About Prognosis Workshop Case 2 ID / CC: 33 year-old man with intracranial hemorrhage History of the Presenting Illness 33 year-old man with a prior history of melanoma of the neck
Med 536 Communicating About Prognosis Workshop Case 2 ID / CC: 33 year-old man with intracranial hemorrhage History of the Presenting Illness 33 year-old man with a prior history of melanoma of the neck
75 year old woman with Hyponatremia. Sharon H. Chou, MD Endorama September 13, 2012
 75 year old woman with Hyponatremia Sharon H. Chou, MD Endorama September 13, 2012 History of Present Illness 75 yo woman who was previously healthy until the past month when she had recurrent admissions
75 year old woman with Hyponatremia Sharon H. Chou, MD Endorama September 13, 2012 History of Present Illness 75 yo woman who was previously healthy until the past month when she had recurrent admissions
SESSION 5 - Cariovascular
 Small Group Session I, MHD 5 - STUDENT Copy Page 1 MECHANISMS OF HUMAN DISEASE AND PHARMACOLOGY & THERAPEUTICS CASE-BASED SMALL GROUP DISCUSSION SESSION 5 - Cariovascular MHD I Friday, September 30, 2016
Small Group Session I, MHD 5 - STUDENT Copy Page 1 MECHANISMS OF HUMAN DISEASE AND PHARMACOLOGY & THERAPEUTICS CASE-BASED SMALL GROUP DISCUSSION SESSION 5 - Cariovascular MHD I Friday, September 30, 2016
Case Presentation. Dr. K. MonaLisa PG in Psy
 Case Presentation Dr. K. MonaLisa PG in Psy Name : XYZ Age : 35 years Sex : Female Religion : Hindu Marital status : Married Residence : Nalgonda Education : Intermediate Occupation : House-wife Socio-economic
Case Presentation Dr. K. MonaLisa PG in Psy Name : XYZ Age : 35 years Sex : Female Religion : Hindu Marital status : Married Residence : Nalgonda Education : Intermediate Occupation : House-wife Socio-economic
SMALL GROUP DISCUSSION
 MHD II, Session 2 Student Copy - Page 1 SMALL GROUP DISCUSSION MHD II Session 2 Gastroinestinal JANUARY 12, 2017 STUDENT COPY CASE 1 MHD II, Session 2 Student Copy - Page 2 CHIEF COMPLAINT: "My bowels
MHD II, Session 2 Student Copy - Page 1 SMALL GROUP DISCUSSION MHD II Session 2 Gastroinestinal JANUARY 12, 2017 STUDENT COPY CASE 1 MHD II, Session 2 Student Copy - Page 2 CHIEF COMPLAINT: "My bowels
An Uncommon Presentation of Large B-cell Lymphoma of the kidney A Case Report and Literature Review
 An Uncommon Presentation of Large B-cell Lymphoma of the kidney A Case Report and Literature Review CHRISTOPHER ADILETTA M.D., AJAZ SHAWL M.D. ST. JOSEPH S HEALTH, SYRACUSE, NY Our Patient Case We present
An Uncommon Presentation of Large B-cell Lymphoma of the kidney A Case Report and Literature Review CHRISTOPHER ADILETTA M.D., AJAZ SHAWL M.D. ST. JOSEPH S HEALTH, SYRACUSE, NY Our Patient Case We present
Chemistry Reference Ranges and Critical Values
 Alanine Aminotransferase (ALT, SGPT) 3-9 years 9-18 years 1-9 years 9-18 years 10-25 U/L 10-35 U/L 10-30 U/L 10-25 U/L 10-30 U/L 10-35 U/L 10-25 U/L 10-35 U/L 10-25 U/L 10-20 U/L 10-35 U/L Albumin 0-6
Alanine Aminotransferase (ALT, SGPT) 3-9 years 9-18 years 1-9 years 9-18 years 10-25 U/L 10-35 U/L 10-30 U/L 10-25 U/L 10-30 U/L 10-35 U/L 10-25 U/L 10-35 U/L 10-25 U/L 10-20 U/L 10-35 U/L Albumin 0-6
Chemistry Reference Ranges and Critical Values
 Alanine Aminotransferase (ALT, SGPT) 3-9 years 9-18 years 1-9 years 9-18 years 10-30 U/L 10-30 U/L 10-20 U/L Albumin 0-6 days 6 days - 37 months 37 months - 7 years 7-20 years 2.6-3.6 g/dl 3.4-4.2 g/dl
Alanine Aminotransferase (ALT, SGPT) 3-9 years 9-18 years 1-9 years 9-18 years 10-30 U/L 10-30 U/L 10-20 U/L Albumin 0-6 days 6 days - 37 months 37 months - 7 years 7-20 years 2.6-3.6 g/dl 3.4-4.2 g/dl
AMPS : A Quick, Effective Approach To The Primary Care Psychiatric Interview
 AMPS : A Quick, Effective Approach To The Primary Care Psychiatric Interview February 7, 2012 Robert McCarron, D.O. Assosicate Clinical Professor Internal Medicine / Psychiatry / Pain Medicine UC Davis,
AMPS : A Quick, Effective Approach To The Primary Care Psychiatric Interview February 7, 2012 Robert McCarron, D.O. Assosicate Clinical Professor Internal Medicine / Psychiatry / Pain Medicine UC Davis,
Using the DSM-5 in the Differential Diagnosis of Depression
 Using the DSM-5 in the Differential Diagnosis of Depression Wayne Bentham, MD Clinical Assistant Professor Department of Psychiatry and Behavioral Sciences University of Washington School of Medicine Depressive
Using the DSM-5 in the Differential Diagnosis of Depression Wayne Bentham, MD Clinical Assistant Professor Department of Psychiatry and Behavioral Sciences University of Washington School of Medicine Depressive
Date of Admission: [DATE]. Date of Discharge:
![Date of Admission: [DATE]. Date of Discharge: Date of Admission: [DATE]. Date of Discharge:](/thumbs/74/71277118.jpg) Date of Admission: [DATE]. Date of Discharge: History of Present Illness: Mr. [NAME] AKA [NAME] is a 31-year-old male who presents to the [PLACE] Trauma Surgery Service as a moderate trauma on [DATE] following
Date of Admission: [DATE]. Date of Discharge: History of Present Illness: Mr. [NAME] AKA [NAME] is a 31-year-old male who presents to the [PLACE] Trauma Surgery Service as a moderate trauma on [DATE] following
North Shore Youth Eating Disorders Program NEW CLIENT REFERRAL
 North Shore Youth Eating Disorders Program NEW CLIENT REFERRAL The North Shore Youth Eating Disorders Program (NSYEDP) is a multidisciplinary team consisting of a medical professional, dietitian, and counsellor.
North Shore Youth Eating Disorders Program NEW CLIENT REFERRAL The North Shore Youth Eating Disorders Program (NSYEDP) is a multidisciplinary team consisting of a medical professional, dietitian, and counsellor.
THE DREADED RUN- ON SENTENCE AND OTHER PUNCTUATION RULES THAT KEEP YOU UP AT NIGHT!!!!
 THE DREADED RUN- ON SENTENCE AND OTHER PUNCTUATION RULES THAT KEEP YOU UP AT NIGHT!!!! Is punctuation giving you NIGHTMARES??? Does it give you a headache? When you think of punctuation, do you want to
THE DREADED RUN- ON SENTENCE AND OTHER PUNCTUATION RULES THAT KEEP YOU UP AT NIGHT!!!! Is punctuation giving you NIGHTMARES??? Does it give you a headache? When you think of punctuation, do you want to
5AB Dysrhythmia Interpretation and Management 2016
 5AB Dysrhythmia Interpretation and Management 2016 How to complete your biennial ECG review: A website has been created that contains the basic review information. Use this as a reference during your review.
5AB Dysrhythmia Interpretation and Management 2016 How to complete your biennial ECG review: A website has been created that contains the basic review information. Use this as a reference during your review.
Patient Name Date of Birth Page 1 of 6
 2545 W. Hillcrest Dr. #205 Thousand Oaks, CA 91320 Admissions: 888.822.8938 Fax: 805.273.5246 Dear Medical Professional, This patient is seeking care to address eating disorder behaviors. For the patient
2545 W. Hillcrest Dr. #205 Thousand Oaks, CA 91320 Admissions: 888.822.8938 Fax: 805.273.5246 Dear Medical Professional, This patient is seeking care to address eating disorder behaviors. For the patient
CSS Correctional Service System
 Mental Health Services Staff Referral Form 09/20/2007 Medical Evaluation (To Be Completed By The Medical Staff) Reason for Referral- Check and Explain All That Apply Actively Suicidal or Homicidal Self-Reported
Mental Health Services Staff Referral Form 09/20/2007 Medical Evaluation (To Be Completed By The Medical Staff) Reason for Referral- Check and Explain All That Apply Actively Suicidal or Homicidal Self-Reported
PCCSS, LLP Pulmonary, Critical Care & Sleep Specialists
 NAME: AGE: DOB: DATE: REQUESTING PHYSICIAN: NOTE: Please help us find out about you by filling out the Patient side of this form on pages 1 3. If you don t know the answer to one of the questions, ask
NAME: AGE: DOB: DATE: REQUESTING PHYSICIAN: NOTE: Please help us find out about you by filling out the Patient side of this form on pages 1 3. If you don t know the answer to one of the questions, ask
CASE-BASED SMALL GROUP DISCUSSION
 MHD II, Session XII, STUDENT Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION Session XII MHD II April 21, 2014 STUDENT COPY Helpful Resource: ACP Medicine online available through LUHS Library Infectious
MHD II, Session XII, STUDENT Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION Session XII MHD II April 21, 2014 STUDENT COPY Helpful Resource: ACP Medicine online available through LUHS Library Infectious
A walk through a STEMI
 A walk through a STEMI M.M. s Story Kim Robison Ashley Corcoran Situation M.M. is an 82 year old male brought in by private vehicle on 10/22/17 to the Emergency Department Pt. c/o left arm numbness, pain
A walk through a STEMI M.M. s Story Kim Robison Ashley Corcoran Situation M.M. is an 82 year old male brought in by private vehicle on 10/22/17 to the Emergency Department Pt. c/o left arm numbness, pain
10 Essential Blood Tests PART 1
 Presents 10 Essential Blood Tests PART 1 The Blood Chemistry Webinars With DR. DICKEN WEATHERBY Creator of the Blood Chemistry Software Essential Blood Test #1: Basic Chem Screen and CBC http://bloodchemsoftware.com
Presents 10 Essential Blood Tests PART 1 The Blood Chemistry Webinars With DR. DICKEN WEATHERBY Creator of the Blood Chemistry Software Essential Blood Test #1: Basic Chem Screen and CBC http://bloodchemsoftware.com
ADULTS WITH COMPLEX BEHAVIORAL SUPPORT NEEDS. Betsey Benson, Ph.D. Vanessa Rodriguez, Ph.D., BCBA-D Nisonger Institute 2015
 ADULTS WITH COMPLEX BEHAVIORAL SUPPORT NEEDS Betsey Benson, Ph.D. Vanessa Rodriguez, Ph.D., BCBA-D Nisonger Institute 2015 Transitions School to Work or Other Guardianship Home Mental Health Physical Health
ADULTS WITH COMPLEX BEHAVIORAL SUPPORT NEEDS Betsey Benson, Ph.D. Vanessa Rodriguez, Ph.D., BCBA-D Nisonger Institute 2015 Transitions School to Work or Other Guardianship Home Mental Health Physical Health
Adams Memorial Hospital Decatur, Indiana EXPLANATION OF LABORATORY TESTS
 Adams Memorial Hospital Decatur, Indiana EXPLANATION OF LABORATORY TESTS Your health is important to us! The test descriptions listed below are for educational purposes only. Laboratory test interpretation
Adams Memorial Hospital Decatur, Indiana EXPLANATION OF LABORATORY TESTS Your health is important to us! The test descriptions listed below are for educational purposes only. Laboratory test interpretation
ADULT INTAKE/PSYCHOSOCIAL ASSESSMENT. Name: Date: Referred by:
 ADULT INTAKE/PSYCHOSOCIAL ASSESSMENT Name: Date: Referred by: Date of Birth: SSN: Identifying Information (age, marital status, ethnicity, and sex) 1. Reason for Referral: (Why are you here? Describe problems,
ADULT INTAKE/PSYCHOSOCIAL ASSESSMENT Name: Date: Referred by: Date of Birth: SSN: Identifying Information (age, marital status, ethnicity, and sex) 1. Reason for Referral: (Why are you here? Describe problems,
Case TWO. Vital Signs: Temperature 36.6degC BP 137/89 HR 110 SpO2 97% on Room Air
 Mr N is a 64year old Chinese gentleman who is a heavy drinker, still actively drinking, and chronic smoker of >40pack year history. He has a past medical history significant for Hypertension, Hyperlipidemia,
Mr N is a 64year old Chinese gentleman who is a heavy drinker, still actively drinking, and chronic smoker of >40pack year history. He has a past medical history significant for Hypertension, Hyperlipidemia,
CASE-BASED SMALL GROUP DISCUSSION MHD II SESSION VI
 MHD II, Session VI, Student Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD II SESSION VI Wednesday, MARCH 26, 2014 STUDENT COPY MHD II, Session VI, Student Copy Page 2 CASE 1 History: A 57-year-old
MHD II, Session VI, Student Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD II SESSION VI Wednesday, MARCH 26, 2014 STUDENT COPY MHD II, Session VI, Student Copy Page 2 CASE 1 History: A 57-year-old
Behavioral Emergencies. Lesson Goal. Lesson Objectives 9/10/2012
 Behavioral Emergencies Lesson Goal Recognize, assess, & treat patients with behavioral emergencies, including patients with psychiatric history & substance abuse Lesson Objectives Define these terms: Suicide
Behavioral Emergencies Lesson Goal Recognize, assess, & treat patients with behavioral emergencies, including patients with psychiatric history & substance abuse Lesson Objectives Define these terms: Suicide
Bisan Salhi, M.D. 69 Jesse Hill Jr. Dr. Atlanta, GA Phone:
 Bisan Salhi, M.D. 69 Jesse Hill Jr. Dr. Atlanta, GA 30303 Phone: 734-657-4539 30 June 2006 Dear Sir or Madam: 1. Thank you for the opportunity to evaluate Mr. Liviu Negut. Enclosed is my preliminary medical
Bisan Salhi, M.D. 69 Jesse Hill Jr. Dr. Atlanta, GA 30303 Phone: 734-657-4539 30 June 2006 Dear Sir or Madam: 1. Thank you for the opportunity to evaluate Mr. Liviu Negut. Enclosed is my preliminary medical
Hawthorne Veteran and Family Resource Center. Recuperative Care Program Referral Form. 250 N. Ash Street. Escondido, CA 92027
 Hawthorne Veteran and Family Resource Center Recuperative Care Program Referral Form 250 N. Ash Street Escondido, CA 92027 Referring party: Date of Referral: / / Contact number: ( ) - Last admission: /
Hawthorne Veteran and Family Resource Center Recuperative Care Program Referral Form 250 N. Ash Street Escondido, CA 92027 Referring party: Date of Referral: / / Contact number: ( ) - Last admission: /
PATIENT SLEEP QUESTIONNAIRE
 PATIENT SLEEP QUESTIONNAIRE Name: Date of Birth: Today s Date Primary Care Physician Telephone # Physician ordering test (Other than PCP): Physician s Tel. #: _ Age: Years Height: Feet Inches Weight: Lb
PATIENT SLEEP QUESTIONNAIRE Name: Date of Birth: Today s Date Primary Care Physician Telephone # Physician ordering test (Other than PCP): Physician s Tel. #: _ Age: Years Height: Feet Inches Weight: Lb
DIAGNOSIS AND MANAGEMENT OF DIURETIC RESISTANCE. Jules B. Puschett, M.D.
 DIAGNOSIS AND MANAGEMENT OF DIURETIC RESISTANCE Jules B. Puschett, M.D. Diuretic Resistance A clinical circumstance in which patients do not respond to a combination of salt restriction and even large
DIAGNOSIS AND MANAGEMENT OF DIURETIC RESISTANCE Jules B. Puschett, M.D. Diuretic Resistance A clinical circumstance in which patients do not respond to a combination of salt restriction and even large
ADULT History Form (To be filled out by the person seeking treatment)
 1 ADULT History Form (To be filled out by the person seeking treatment) Client s Name Date: SS# - - DOB: / / Age: Person completing this form: Client Other: (give name) Who referred you to Namsate Counseling?
1 ADULT History Form (To be filled out by the person seeking treatment) Client s Name Date: SS# - - DOB: / / Age: Person completing this form: Client Other: (give name) Who referred you to Namsate Counseling?
RITUXIMAB RHEUMATOLOGY VASCULITIS
 . PHYSICIAN (Patient Sticker) ORDER SET : CDH 208-237 Approved - Page 1 of 5 Patient: DOB: Gender: Patient Phone #: Height: Weight: Diagnosis: ICD-10 Code: Treatment Start Date: Provider Facility Name:
. PHYSICIAN (Patient Sticker) ORDER SET : CDH 208-237 Approved - Page 1 of 5 Patient: DOB: Gender: Patient Phone #: Height: Weight: Diagnosis: ICD-10 Code: Treatment Start Date: Provider Facility Name:
Get to know yourself better. Attend our health screening event.
 Gateway Technical College Get to know yourself better. Attend our health screening event. Putting your knowledge to action is Powerful. Get the information and guidance you need with the Wellness Screening
Gateway Technical College Get to know yourself better. Attend our health screening event. Putting your knowledge to action is Powerful. Get the information and guidance you need with the Wellness Screening
Psychosocial Factors in a TB Patient Adriana Vasquez, MD July 30, 2008
 Becoming a TB Nurse Expert San Antonio, Texas July 30-31, 2008 Psychosocial Factors in a TB Patient Adriana Vasquez, MD July 30, 2008 TUBERCULOSIS and MENTAL ILLNESS Adriana Vasquez, MD Staff physician
Becoming a TB Nurse Expert San Antonio, Texas July 30-31, 2008 Psychosocial Factors in a TB Patient Adriana Vasquez, MD July 30, 2008 TUBERCULOSIS and MENTAL ILLNESS Adriana Vasquez, MD Staff physician
Delta Check Calculation Guide
 Delta Check Calculation Guide National Technology 2017, All Rights Reserved By Senior Scientific Researcher, Asmaa Taher Table of Contents Definition... 2 Purpose... 2 Delta Check Research Studies... 2
Delta Check Calculation Guide National Technology 2017, All Rights Reserved By Senior Scientific Researcher, Asmaa Taher Table of Contents Definition... 2 Purpose... 2 Delta Check Research Studies... 2
HOME HEALTH RE-REGISTRATION/CONCURRENT REVIEW TEMPLATE
 HOME HEALTH RE-REGISTRATION/CONCURRENT REVIEW TEMPLATE Provider EDS/CMAP ID # (Medicaid 9-digit ID) ALL FIELDS WITH * ARE REQUIRED Name of clinician who filled out this form Contact number Facility/Provider
HOME HEALTH RE-REGISTRATION/CONCURRENT REVIEW TEMPLATE Provider EDS/CMAP ID # (Medicaid 9-digit ID) ALL FIELDS WITH * ARE REQUIRED Name of clinician who filled out this form Contact number Facility/Provider
To appreciate the unique problems of older surgical patients. To describe the differential and management
 To appreciate the unique problems of older surgical patients. t To describe the differential and management of acute abdomen in the older. To recognize and tend to hospital complications in olderpatients.
To appreciate the unique problems of older surgical patients. t To describe the differential and management of acute abdomen in the older. To recognize and tend to hospital complications in olderpatients.
* Final Report * ED Triage Entered On: 01/16/2014 8:45 EST Performed On: 01/16/2014 8:42 EST by
 Result date: Result status: 16 January 2014 8:42 EST Auth (Verified) * Final Report * ED Triage Entered On: 01/16/2014 8:45 EST Performed On: 01/16/2014 8:42 EST by Assessment I Chief Complaint : Diarrhea
Result date: Result status: 16 January 2014 8:42 EST Auth (Verified) * Final Report * ED Triage Entered On: 01/16/2014 8:45 EST Performed On: 01/16/2014 8:42 EST by Assessment I Chief Complaint : Diarrhea
What Does My Blood Test Mean
 What Does My Blood Test Mean CBC with Differential This means that your doctor wants to know the amounts and proportions among the various components of your blood, explained below. The term differential
What Does My Blood Test Mean CBC with Differential This means that your doctor wants to know the amounts and proportions among the various components of your blood, explained below. The term differential
BEHAVIORAL HEALTH INITIAL CLINICAL REVIEW FORM
 BEHAVIORAL HEALTH INITIAL CLINICAL REVIEW FORM (Please address each area. An incomplete form may result in a delay of your request.) Submit completed form to: Email: BHRequests@Molinahealthcare.com Fax:
BEHAVIORAL HEALTH INITIAL CLINICAL REVIEW FORM (Please address each area. An incomplete form may result in a delay of your request.) Submit completed form to: Email: BHRequests@Molinahealthcare.com Fax:
Itemized Billing and Procedure Description for the AspireAssist
 Itemized Billing and Procedure Description for the AspireAssist The following describes the recommended therapy course for the first year for a patient undergoing AspireAssist therapy. Although providers
Itemized Billing and Procedure Description for the AspireAssist The following describes the recommended therapy course for the first year for a patient undergoing AspireAssist therapy. Although providers
More than 1 million people die worldwide every year from suicide!!!
 Chapter 115 Suicide Episode Overview: 1) Name 10 risk factors for suicide 2) Name an additional 5 risk factors for adolescent suicide 3) Describe the SAD PERSONS scale 4) Describe 4 potential targeted
Chapter 115 Suicide Episode Overview: 1) Name 10 risk factors for suicide 2) Name an additional 5 risk factors for adolescent suicide 3) Describe the SAD PERSONS scale 4) Describe 4 potential targeted
BEHAVIORAL HEALTH CONCURRENT CLINICAL REVIEW FORM
 BEHAVIORAL HEALTH CONCURRENT CLINICAL REVIEW FORM (Please address each area. An incomplete form may result in a delay of your request.) Submit completed form to: Email: BHRequests@Molinahealthcare.com
BEHAVIORAL HEALTH CONCURRENT CLINICAL REVIEW FORM (Please address each area. An incomplete form may result in a delay of your request.) Submit completed form to: Email: BHRequests@Molinahealthcare.com
CASE-BASED SMALL GROUP DISCUSSION. MHD II Session VII. Friday, March 28, 2014 STUDENT COPY
 CASE-BASED SMALL GROUP DISCUSSION MHD II Session VII Friday, March 28, 2014 STUDENT COPY Helpful resources ACP Medicine available online through Loyola Health Science Library Endocrinology and Metabolism
CASE-BASED SMALL GROUP DISCUSSION MHD II Session VII Friday, March 28, 2014 STUDENT COPY Helpful resources ACP Medicine available online through Loyola Health Science Library Endocrinology and Metabolism
Acute Stroke with Alteplase Administration Order Set
 Review Due Date: 2017 October PATIENT CARE DERS Weight: Adverse Reactions or Intolerances Drug No Yes (list) Food No Yes (list) _ Latex No Yes Admission Admit to Neurology service: Dr. Critical Care Diagnosis:
Review Due Date: 2017 October PATIENT CARE DERS Weight: Adverse Reactions or Intolerances Drug No Yes (list) Food No Yes (list) _ Latex No Yes Admission Admit to Neurology service: Dr. Critical Care Diagnosis:
Legal 2000 and the Mental Health Crisis in Clark County. Lesley R. Dickson, M.D. Executive Director, Nevada Psychiatric Association
 Legal 2000 and the Mental Health Crisis in Clark County Lesley R. Dickson, M.D. Executive Director, Nevada Psychiatric Association Civil action: Civil Commitment Definition a legal action to recover money
Legal 2000 and the Mental Health Crisis in Clark County Lesley R. Dickson, M.D. Executive Director, Nevada Psychiatric Association Civil action: Civil Commitment Definition a legal action to recover money
Alcohol Opiates Other:
 Pages 1 and 2 must be completed in full for all referrals (incomplete forms will not be processed) Additional Required Information Form must be completed for all referrals Medication Clinic (Pg. 3), ECT
Pages 1 and 2 must be completed in full for all referrals (incomplete forms will not be processed) Additional Required Information Form must be completed for all referrals Medication Clinic (Pg. 3), ECT
Multiphasic Blood Analysis
 Understanding Your Multiphasic Blood Analysis Test Results Mon General thanks you for participating in the multiphasic blood analysis. This test can be an early warning of health problems, including coronary
Understanding Your Multiphasic Blood Analysis Test Results Mon General thanks you for participating in the multiphasic blood analysis. This test can be an early warning of health problems, including coronary
DIAN KUANG 馬 萬. Giovanni Maciocia
 DIAN KUANG 癫狂 馬 萬 Giovanni Maciocia 里 BIPOLAR DISORDER (MANIC-DEPRESSION) DIAN Qi and Phlegm stagnating Heart and Spleen deficiency with Phlegm Qi deficiency with Phlegm KUANG Phlegm-Fire harassing upwards
DIAN KUANG 癫狂 馬 萬 Giovanni Maciocia 里 BIPOLAR DISORDER (MANIC-DEPRESSION) DIAN Qi and Phlegm stagnating Heart and Spleen deficiency with Phlegm Qi deficiency with Phlegm KUANG Phlegm-Fire harassing upwards
DUKEMedicine. SMITH, JAMES MRN: D DOB: 2/6/1993, Sex: M Adm: 2/15/2016, D/C: 2/15/2016
 History Chief Complaint Patient presents with Motor Vehicle Crash HPI James Smith is a 23 y.o. male here today for evaluation of injuries sustained today in a MVA. He was a restrained driver of a car struck
History Chief Complaint Patient presents with Motor Vehicle Crash HPI James Smith is a 23 y.o. male here today for evaluation of injuries sustained today in a MVA. He was a restrained driver of a car struck
Behavioral Health Initial Clinical Review Form
 Behavioral Health Initial Clinical Review Form (Address all areas. An incomplete form may result in a delay of your request.) Submit completed form to: Online: Provider Portal Fax: 844-618-9572 Date Form
Behavioral Health Initial Clinical Review Form (Address all areas. An incomplete form may result in a delay of your request.) Submit completed form to: Online: Provider Portal Fax: 844-618-9572 Date Form
Client Name: Date of Birth: Address: City: Zip code: Hm #: ( ) -. Cell#: ( ) -. Wrk#: ( ) -. Otr#: ( ) -.
 New Client Intake Date: Client Name: Date of Birth: Address: City: Zip code: Hm #: ( ) -. Cell#: ( ) -. Wrk#: ( ) -. Otr#: ( ) -. Employer Email: Emergency Contact Name Relationship Phone number TREATMENT
New Client Intake Date: Client Name: Date of Birth: Address: City: Zip code: Hm #: ( ) -. Cell#: ( ) -. Wrk#: ( ) -. Otr#: ( ) -. Employer Email: Emergency Contact Name Relationship Phone number TREATMENT
Client: Date of Birth: Date of Report: MENTAL STATUS EXAMINATION REPORT 1. Identifying Information
 Client: Date of Birth: MENTAL STATUS EXAMINATION REPORT 1. Identifying Information Date of Report: 2. Reason for Assessment (Please indicate referral source, precipitating circumstances and chief complaints)
Client: Date of Birth: MENTAL STATUS EXAMINATION REPORT 1. Identifying Information Date of Report: 2. Reason for Assessment (Please indicate referral source, precipitating circumstances and chief complaints)
A 45 year old African American man presents to the IMC with a chief complaint of my
 AN EVIDENCE BASED APPROACH TO HYPERTENSION AND HYPERLIPIDENIA: A CASE STUDY A 45 year old African American man presents to the IMC with a chief complaint of my pressure is high. Apparently he recently
AN EVIDENCE BASED APPROACH TO HYPERTENSION AND HYPERLIPIDENIA: A CASE STUDY A 45 year old African American man presents to the IMC with a chief complaint of my pressure is high. Apparently he recently
THE PSYCHIATRIC MEDICAL HISTORY. Prof. Paz García-Portilla
 THE PSYCHIATRIC MEDICAL HISTORY Prof. Paz García-Portilla MEDICAL HISTORY (HX) Clinical data set gained by a physician by asking specific questions to the patient (or proxy), with the aim of obtaining
THE PSYCHIATRIC MEDICAL HISTORY Prof. Paz García-Portilla MEDICAL HISTORY (HX) Clinical data set gained by a physician by asking specific questions to the patient (or proxy), with the aim of obtaining
2/29/2016. By Lisa Amaya, Physician Assistant ATSU graduate 2006
 By Lisa Amaya, Physician Assistant ATSU graduate 2006 Identifying unusual presentations Evaluating the history of the patient Conducting a physical exam Recognize that these presentations may be subtle
By Lisa Amaya, Physician Assistant ATSU graduate 2006 Identifying unusual presentations Evaluating the history of the patient Conducting a physical exam Recognize that these presentations may be subtle
Major Depression Major Depression
 Contemporary Psychiatric-Mental Health Nursing Third Edition CHAPTER 17 Mood Disorders Major Depression Major Depression Characterized by a change in several aspects of a person s life and emotional state
Contemporary Psychiatric-Mental Health Nursing Third Edition CHAPTER 17 Mood Disorders Major Depression Major Depression Characterized by a change in several aspects of a person s life and emotional state
Get to know yourself better. Attend our health screening event.
 Get to know yourself better. Attend our health screening event. Putting your knowledge to action is Powerful. Get the information and guidance you need with the Wellness Screening Program. 1 SIMPLE ACTION
Get to know yourself better. Attend our health screening event. Putting your knowledge to action is Powerful. Get the information and guidance you need with the Wellness Screening Program. 1 SIMPLE ACTION
Name:, Sex:, Age: Ethnicity, Race. Date of Birth:, address: Address:, City: State:, County,, Zip: Telephone numbers: Home: ( ),Work: ( )
 Adult Patient Information Name:, Sex:, Age: Ethnicity, Race Date of Birth:, Email address: Address:, City: State:, County,, Zip: Telephone numbers: Home: ( ),Work: ( ) Cell: ( ) Referral by: Person to
Adult Patient Information Name:, Sex:, Age: Ethnicity, Race Date of Birth:, Email address: Address:, City: State:, County,, Zip: Telephone numbers: Home: ( ),Work: ( ) Cell: ( ) Referral by: Person to
Bipolar Disorder Clinical Practice Guideline Summary for Primary Care
 Bipolar Disorder Clinical Practice Guideline Summary for Primary Care DIAGNOSIS AND CLINICAL ASSESSMENT Bipolar Disorder is categorized by extreme mood cycling; manifested by periods of euphoria, grandiosity,
Bipolar Disorder Clinical Practice Guideline Summary for Primary Care DIAGNOSIS AND CLINICAL ASSESSMENT Bipolar Disorder is categorized by extreme mood cycling; manifested by periods of euphoria, grandiosity,
Specialized Mental Health Referral Specialized Mental Health, GRT2 Grand River Hospital Freeport Site 3570 King St East, Kitchener, Ontario N2A 2W1
 Specialized Mental Health Referral Specialized Mental Health, GRT2 Grand River Hospital Freeport Site 3570 King St East, Kitchener, Ontario N2A 2W1 Prior to faxing - please call the program secretary at
Specialized Mental Health Referral Specialized Mental Health, GRT2 Grand River Hospital Freeport Site 3570 King St East, Kitchener, Ontario N2A 2W1 Prior to faxing - please call the program secretary at
PSYCHIATRIC INTAKE AND TREATMENT PLAN-PART I TO BE FILLED BY PATIENT PLEASE PRINT
 DOB: / / / PSYCHIATRIC INTAKE AND TREATMENT PLAN-PART I TO BE FILLED BY PATIENT PLEASE PRINT Date Age Gender M F Current address: Married. Single Separated Divorced Widowed If patient is a child, he/she
DOB: / / / PSYCHIATRIC INTAKE AND TREATMENT PLAN-PART I TO BE FILLED BY PATIENT PLEASE PRINT Date Age Gender M F Current address: Married. Single Separated Divorced Widowed If patient is a child, he/she
BIPOLAR. DISORDER What you need to know BECAUSE...CARING COMES NATURALLY TO US
 BIPOLAR DISORDER What you need to know BECAUSE...CARING COMES NATURALLY TO US What is Bipolar Disorder Bipolar disorder is a mental illness that causes unusual swings in mood, energy and activity levels,
BIPOLAR DISORDER What you need to know BECAUSE...CARING COMES NATURALLY TO US What is Bipolar Disorder Bipolar disorder is a mental illness that causes unusual swings in mood, energy and activity levels,
Brief Notes on the Mental Health of Children and Adolescents
 Brief Notes on the Mental Health of Children and Adolescents The future of our country depends on the mental health and strength of our young people. However, many children have mental health problems
Brief Notes on the Mental Health of Children and Adolescents The future of our country depends on the mental health and strength of our young people. However, many children have mental health problems
Annual Wellness Visit Form 2016
 Annual Wellness Visit Form 6 Initial G48/Subsequent G49 (circle one) Subjective: Past Medical History (mark X to confirm and note duration for chronic conditions only) Conditions Yrs Conditions Yrs Others:
Annual Wellness Visit Form 6 Initial G48/Subsequent G49 (circle one) Subjective: Past Medical History (mark X to confirm and note duration for chronic conditions only) Conditions Yrs Conditions Yrs Others:
Mood Disorders. Moderate depression that will go away without therapy. Restlessness, inability to concentrate, and rapid speech. Dysthymic Disorder
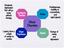 Moderate depression that will go away without therapy Dysthymic Disorder Mania Restlessness, inability to concentrate, and rapid speech Mood Disorders Lasting from a couple of weeks to months Major Depression
Moderate depression that will go away without therapy Dysthymic Disorder Mania Restlessness, inability to concentrate, and rapid speech Mood Disorders Lasting from a couple of weeks to months Major Depression
DSM5: How to Understand It and How to Help
 DSM5: How to Understand It and How to Help Introduction: The DSM5 is a foreign language! Three Questions: I. The first was, What the key assumptions made to determine the organization of the DSM5? A. Mental
DSM5: How to Understand It and How to Help Introduction: The DSM5 is a foreign language! Three Questions: I. The first was, What the key assumptions made to determine the organization of the DSM5? A. Mental
MEDICAL HISTORY. 23-Jan-2018 to 23-Jan VCA Miller-Robertson Animal Hospital 8807 Melrose Ave, Los Angeles, CA (310)
 8807 Melrose Ave, Los Angeles, CA 90069 (310) 657-7050 MEDICAL HISTORY 23-Jan-2018 to 23-Jan-2018 Client Linnea Engdahl (1810) C: Linnea: (310) 351-9547 Patient Abby (6487) Canine Mixed Breed 3y (22-Jan-2015)
8807 Melrose Ave, Los Angeles, CA 90069 (310) 657-7050 MEDICAL HISTORY 23-Jan-2018 to 23-Jan-2018 Client Linnea Engdahl (1810) C: Linnea: (310) 351-9547 Patient Abby (6487) Canine Mixed Breed 3y (22-Jan-2015)
Research Data Available
 Research Data Available Main Questionnaire General Topic Socio-economic status Occupational exposure Physical activity Mobile phone usage Sleeping patterns smoking Childhood conditions/illnesses/family
Research Data Available Main Questionnaire General Topic Socio-economic status Occupational exposure Physical activity Mobile phone usage Sleeping patterns smoking Childhood conditions/illnesses/family
Presented by Bevan Gibson Southern IL Professional Development Center -Part of the Illinois Community College Board Service Center Network
 Bipolar Disorder: What It Means to You and Your Classroom Presented by Bevan Gibson Southern IL Professional Development Center -Part of the Illinois Community College Board Service Center Network Introduction
Bipolar Disorder: What It Means to You and Your Classroom Presented by Bevan Gibson Southern IL Professional Development Center -Part of the Illinois Community College Board Service Center Network Introduction
CLIENT INFORMATION FORM. Name: Date: Address: Gender: City: State: Zip: Date of Birth: Social Security Number:
 Name: Address: Gender: City: State: Zip: Date of Birth: Social Security Number: Contact Telephone Numbers Please complete relevant information and indicate the number at which you wish to be contacted
Name: Address: Gender: City: State: Zip: Date of Birth: Social Security Number: Contact Telephone Numbers Please complete relevant information and indicate the number at which you wish to be contacted
LOKUN! I got stomach ache!
 LOKUN! I got stomach ache! Mr L is a 67year old Chinese gentleman who is a non smoker, social drinker. He has a medical history significant for Hypertension, Hyperlipidemia, Type 2 Diabetes Mellitus, Chronic
LOKUN! I got stomach ache! Mr L is a 67year old Chinese gentleman who is a non smoker, social drinker. He has a medical history significant for Hypertension, Hyperlipidemia, Type 2 Diabetes Mellitus, Chronic
Amy Eisenhauer Developed for Pulse Check 2016
 Amy Eisenhauer Developed for Pulse Check 2016 Understand alcoholism, co-morbid diseases, and treatment options Possible emergent presentations Discuss societal and EMS perceptions of alcohol related illness
Amy Eisenhauer Developed for Pulse Check 2016 Understand alcoholism, co-morbid diseases, and treatment options Possible emergent presentations Discuss societal and EMS perceptions of alcohol related illness
Mood Disorders. Dr. Vidumini De Silva
 Mood Disorders Dr. Vidumini De Silva Depression - Lowering of mood Mania - Heightening of mood Depressive Disorder Overview Introduction Clinical Features Aetiology Course and prognosis What s your management
Mood Disorders Dr. Vidumini De Silva Depression - Lowering of mood Mania - Heightening of mood Depressive Disorder Overview Introduction Clinical Features Aetiology Course and prognosis What s your management
Disability Risk Management in Today s Workforce: Chronic Pain and Opioid Addiction
 Disability Risk Management in Today s Workforce: Chronic Pain and Opioid Addiction Michael V. Genovese, M.D., J.D. Chief Medical Advisor, Acadia Healthcare Recovery Division The vast majority of painful
Disability Risk Management in Today s Workforce: Chronic Pain and Opioid Addiction Michael V. Genovese, M.D., J.D. Chief Medical Advisor, Acadia Healthcare Recovery Division The vast majority of painful
THE PSYCHIATRIC PATIENT JENNIFER NOCE REGIONAL CLINICAL EDUCATION MANAGER CCEMPT/FP-C/CCP-C
 THE PSYCHIATRIC PATIENT JENNIFER NOCE REGIONAL CLINICAL EDUCATION MANAGER CCEMPT/FP-C/CCP-C Objectives The student will be able to recognize behaviors that pose a risk Assess and manage basic principles
THE PSYCHIATRIC PATIENT JENNIFER NOCE REGIONAL CLINICAL EDUCATION MANAGER CCEMPT/FP-C/CCP-C Objectives The student will be able to recognize behaviors that pose a risk Assess and manage basic principles
REASON FOR REFERRAL Referred for blisters and rash of mucous membranes and skin.
 Report 1 Listen to the audio to fill in the blanks. Name: DERMATOLOGY CONSULTATION REPORT REASON FOR REFERRAL Referred for blisters and rash of mucous membranes and skin. HISTORY OF PRESENT ILLNESS Rash
Report 1 Listen to the audio to fill in the blanks. Name: DERMATOLOGY CONSULTATION REPORT REASON FOR REFERRAL Referred for blisters and rash of mucous membranes and skin. HISTORY OF PRESENT ILLNESS Rash
Specialized Mental Health - Seniors Inpatient Services
 Specialized Mental Health - Seniors Inpatient Services Specialized Mental Health Grand River Hospital - Freeport Site 3570 King St East Kitchener, Ontario N2A 2W1 Prior to faxing - please call the program
Specialized Mental Health - Seniors Inpatient Services Specialized Mental Health Grand River Hospital - Freeport Site 3570 King St East Kitchener, Ontario N2A 2W1 Prior to faxing - please call the program
MEDICATION GUIDE. Quetiapine (kwe-tye-a-peen) Tablets USP
 MEDICATION GUIDE Quetiapine (kwe-tye-a-peen) Tablets USP Read this Medication Guide before you start taking quetiapine tablets and each time you get a refill. There may be new information. This information
MEDICATION GUIDE Quetiapine (kwe-tye-a-peen) Tablets USP Read this Medication Guide before you start taking quetiapine tablets and each time you get a refill. There may be new information. This information
25/04/2017. To ensure that the Rx meets CPSS standards. To provide patient-centered, individualized care. To safely dispense the patient s medication
 To ensure that the Rx meets CPSS standards To provide patient-centered, individualized care To safely dispense the patient s medication To assess for clinical stability and progress in treatment Kirsty
To ensure that the Rx meets CPSS standards To provide patient-centered, individualized care To safely dispense the patient s medication To assess for clinical stability and progress in treatment Kirsty
