Treating refractory depression in Parkinson s disease: a meta-analysis of transcranial magnetic stimulation
|
|
|
- Dwain Mitchell
- 6 years ago
- Views:
Transcription
1 Lesenskyj et al. Translational Neurodegeneration (2018) 7:8 REVIEW Treating refractory depression in Parkinson s disease: a meta-analysis of transcranial magnetic stimulation Alexandra M. Lesenskyj 1, Megan P. Samples 2, Jill M. Farmer 2 and Christina R. Maxwell 2* Open Access Abstract Background: Parkinson s disease (PD) is often accompanied by clinically identified depression. Providing effective pharmacotherapies that concomitantly treat both motor and psychological symptoms can pose a challenge to physicians. For this reason, alternatives to standard anti-depressant treatments, such as repetitive transcranial magnetic stimulation (rtms), have been evaluated within the Parkinson s population. Methods: A literature search was conducted on the PubMed database for all studies that evaluated rtms as a treatment in patients with both depression and PD. A meta-analysis was performed on all studies that reported mean pre- and post-rtms depression inventory scores. Widely used depression inventories included both self-report and clinician-administered measures. Effect size for individual study groups and across all studies was calculated. Results: Six of 7 studies meeting inclusion criteria reported significantly improved depression scores, large effect sizes, and significant p-values. Total weighted average effect size was calculated at 1.32 across all study groups that applied rtms. Conclusions: Across all but one study, rtms appears to effectively reduce depression scores among self-reported and clinician administered inventories. The total weight average effect size showed that, when considering study sample sizes and degree of findings, this form of neurostimulation can relieve PD patients of their depressive symptoms. Further, rtms is a promising alternative to traditional anti-depressant therapies when treating refractory depression in patients with PD. Keywords: Parkinson s disease, Depression, Transcranial magnetic stimulation Background The prevalence of depression in Parkinson s disease (PD) is underestimated at 40 % [1]. The comorbidity between PD and depression requires a careful balance of multiple pharmacotherapies [2]. Shared pathophysiology between the two conditions poses a challenge with respect to treating both motor and non-motor symptoms effectively. Dopamine is a common target in the treatment of both depression and Parkinson s disease, often complicating effective management of symptoms [3]. Treatment is additionally complicated because this relationship occurs across a wide range of patients with varying responsiveness * Correspondence: Crm327@drexel.edu 2 Drexel Neurosciences Institute, 245 N 15th Street ms 423, Philadelphia, PA 19102, USA Full list of author information is available at the end of the article to typical anti-depressive medications [4]. For this reason, several alternative anti-depressant therapies have been explored for the treatment of depression in the PD population [5 8]. One novel treatment for depression in the general population is transcranial magnetic stimulation (TMS). This neurostimulative technique utilizes non-invasive coils that produce magnetic fields and currents that in turn affect neurons within specific cortical areas [9]. In particular, TMS to the left dorsolateral prefrontal cortex (DLPFC) and dorsomedial prefrontal cortex have been identified as viable treatment options [8, 10 12]. Clinical trials have examined both psychological and physiological changes that occur in correlation with TMS. These studies consider several depression inventories as well as electrochemical changes occurring in depressed patients subsequent to TMS. The Author(s) Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
2 Lesenskyj et al. Translational Neurodegeneration (2018) 7:8 Page 2 of 6 Several widely accepted depression surveys have been used to demonstrate change in depressive symptoms when evaluating TMS [7, 8, 13]. In a sham-controlled randomized trial, George and colleagues used the Hamilton Depression Rating Scale (HAM-D), a clinicianadministered tool, as a means to show that daily high frequency repetitive TMS (rtms) to the left DLPFC yields high rates of remission as compared to sham stimulation [7]. Another multi-site trial used the Montgomery-Asberg Depression Rating Scale (MADRS) as a primary measure to show that TMS was more effective than sham treatment; in this study, the MADRS as well as the 17 and 24 item HAM-D were significantly improved at 4 and 6 weeks [8]. A self-report measure, the Beck Depression Inventory (), has also been used to show remission in patients with depression who have been treated with this neurostimulation [13]. In addition to the psychological changes, physiological changes have been observed in patients with depression who were treated with TMS [14]. Functional connectivity of depressed patients may be made stable when certain phenotypes are treated with stimulation to the left DLPFC [15, 16]. Those patients who respond to high frequency stimulation show initially high functional connectivity in various brain regions that may indicate longstanding changes in connectivity associated with improved depression scores [17]. Success with TMS when treating depression raises the question of whether this method will be safe and effective in the Parkinson s disease (PD) population. TMS has been assessed in the treatment of motor symptoms in PD [18]. These studies attest to the safety of this method and moderate ability to improve tremors [19, 20]. Recent research has begun to evaluate TMS for non-motor symptoms in PD patients [21]. Several studies of varying quality and design suggest that TMS is a promising alternative therapy to typical anti-depressant medications used for patients with PD [22 27]. This meta-analysis seeks to quantitatively and qualitatively evaluate the findings of these studies. This review aims to determine the relative efficacy of TMS as a treatment for clinical depression in PD patients. Methods Search criteria A literature search was completed on the PubMed research database for key words transcranial magnetic stimulation (TMS), Parkinson s disease, and depression. Other search terms did not increase the number of studies found. No time restrictions were used in the search. Inclusion criteria Inclusion criteria required a study population of patients diagnosed with Parkinson s disease, concomitant clinically identified depression, and treatment via TMS. Research articles were only included if pre- and post-treatment measures of depression (i.e. 17 or 24 item HAM-D, MADRS, or ) were provided. Studies including median and interquartile range (IQR) were included in the qualitative review portion of this study; however, these studies were excluded from the meta-analysis calculations because they did not provide information regarding whether the data distribution was normal. Data analysis The Parkinson s disease and depression diagnostic criteria used in each study was noted. Mean and standard deviation were recorded for the various depression inventories prior to and following TMS treatment. All stimulation treatment parameters (timing, intensity, location, etc.) were recorded. Administration of concomitant medication with known anti-depressant qualities were also considered. Using Comprehensive Meta-Analysis software version 3 (BioStat Englewood, NJ), Hedges G and p-values were calculated for all studies that provided pre- and poststimulation means and standard deviations for the reported depression inventories. Hedge s G values provided information on the effect size of each individual group within the studies considered. An effect size of 0.20 was considered small, 0.50 considered medium, 0.80 considered large, and > 1.20 considered very large. The total weighted average effect size was then calculated for all of the study groups implementing rtms treatment. All study groups that applied rtms to the DLPFC were grouped to find overall effect size as well. Results A search on the PubMed research database, using the aforementioned terms, yielded 13 studies. Seven of these publications were identified as meeting the inclusion criteria for this review: 1 multi-center double-blinded sham-controlled parallel-group study, 2 randomized double-blind sham controlled studies, 1 sham-controlled trial, 2 prospective open-label studies, and 1 retrospective study (Table 1). Six of the studies reported significant improvement for at least 30 days following treatment; however, one study reported variable improvement in depression depending on stimulation area. Two studies solely reported median scores and IQR, thus containing insufficient data for the quantitative portion of this meta-analysis [25, 26]. All seven studies measured depression pre- and posttreatment via one or more of the following depression inventories: HAM-D, MADRS, or. Number of treatments, time period of treatments, stimulation location, and follow-up timing varied across studies. Table 2 and Table 3 show that, with one exception, all studies reported a large effect size and significant p-values [18].
3 Lesenskyj et al. Translational Neurodegeneration (2018) 7:8 Page 3 of 6 Table 1 Descriptive findings of 7 studies reporting on rtms as a treatment for depression in PD Reference Type Improvement Number Mean age (years) Sessions/stimulation Time Period (days) Primary rtms Site rtms Side Follow-up Depression Scales Brys (2016) [18] Multi-center No /1000 to 2000 at 10 Hz 14 DLPFC L 30 days HAM-D Dragasevic (2002) [22] Prospective Yes /100 at 0.5 Hz 10 DLPFC B 21 days 30 days HAM-D Epstein (2007) [23] Prospective Yes /1000 at 10 Hz 20 DLPFC L 6 weeks HAM-D Fregni (2004) [24] Sham-controlled Yes /40 at 15 Hz 14 DLPFC L 2 weeks 8 weeks HAM-D Makkos (2016) [25] Randomized sham-controlled Yes /600 at 5 Hz 10 M1 B 1 day 30 days MADRS Pal (2010) [26] Randomized sham-controlled Yes /600 at 5 Hz 10 DLPFC L 1 day 30 days MADRS Torres (2015) [27] Retrospective Yes /1000 at 10 Hz a 21 PFC B 30 day HAM-D DLPFC dorsolateral prefrontal cortex, M1 motor cortex, PFC prefrontal cortex, L left, B bilateral a 1000stim at 10 Hz for PFC; 900 stim at 1 Hz for M1
4 Lesenskyj et al. Translational Neurodegeneration (2018) 7:8 Page 4 of 6 Table 2 Effect size of studies reporting mean changes in HAM-D. Epstein et al. (2007) used the 17 and 21 item HAM-D inventory, noted under Treatment. Post-treatment population sizes (n) that changed are noted under corresponding studies groups by parentheses Reference Treatment Number Hedge s G p-value Brys (2016) [18] M1 Stim + DLPFC Stim 20 (19) Brys (2016) [18] M1 Stim + DLPFC Sham < Brys (2016) [18] M1 Sham + DLPFC Stim Brys (2016) [18] M1 Sham + DLPFC Sham < Dragasevic (2002) [22] DLPFC Stim Epstein (2007) [23] DLPFC Stim (17) 14 (8) Epstein (2007) [23] DLPFC Stim (21) 14 (8) Fregni (2004) [24] DLPFC Stim + Medication Sham < Fregni (2004) [24] DLPFC Sham + Medication < Torres (2015) [27] PFC Stim < Additionally, total weighted average effect size was calculated at 1.32 across all study groups that applied rtms. The weighted average effect size of study groups that applied the treatment to the DLPFC only was Discussion This meta-analysis sought to evaluate the efficacy of rtms to alleviate depression in patients with PD. Of 7 studies meeting the inclusion criteria, 5 contained sufficient data on depression (HAM-D and/or ) to perform quantitative evaluations. Because both inventories were used across the 5 studies, evaluation of rtms from both clinician and patient perspectives was possible. Apart from Brys and colleagues (2016), all studies reported rtms to be highly effective in improving depression (Hedge s G > 1.2). To bolster these findings, individual p-values show that this trend was not observed by chance (p < 0.05). When all study groups implementing rtms were combined, high efficacy was observed by both patients and clinicians. Combining study groups that specifically examined rtms to the DLPFC yielded an even higher treatment efficacy. Results of this meta-analysis confirm that rtms significantly lowers both the self-reported and the health care provider-determined HAM-D. Ultimately, these findings suggest that rtms may be an effective treatment for depression in patients with PD. Stimulation sites Three studies report significant findings when administering rtms to specifically the left DLPFC, the location most commonly targeted when treating depression in the non-parkinson s population [23, 24, 26]. An open study by Epstein and colleagues directly sought to examine the treatment s effects in an inpatient setting [23]. The study yielded improvement at post-treatment visits (3 days-post) as well as at 3 6 week follow-up. Our results echoed these findings, showing an extremely notable relationship with high significance between treatment and improved HAM-D and scores (Tables 2 and 3). In a sham-controlled trial, Fregni et al. compare treatment of depression with medication to treatment with magnetic stimulation [24]. The authors found that treatment with rtms is equally as effective as fluoxetine in treating depression and in most cases better tolerated. In both self-report and cliniciandetermined measures, very large effect sizes with high significance were found for the medication and stimulation groups, showing equally notable effects on depression (Tables 2 and 3). Similarly, Pal and colleagues use a randomized, double-blind, placebo-controlled study to evaluate rtms to the left DLPFC. In both short term and long term follow-up evaluations (MADRS and ), patients reported significant improvement in depressive symptoms. Interestingly, long term follow-ups (at 30 days) yield a larger significant improvement in depression scores than the immediate (1 day-post) followup. Although effect size could not be evaluated due to insufficient data, the authors provide evidence that patients with PD who experience mild to moderate depression may respond favorable to rtms. Table 3 Effect size of studies reporting mean changes in Reference Treatment Number Hedge s G p-value Dragasevic (2002) [22] DLPFC Stim Fregni (2004) [24] DLPFC Stim + Medication Sham < Fregni (2004) [24] DLPFC Sham + Medication < Torres (2015) [27] PFC Stim < 0.001
5 Lesenskyj et al. Translational Neurodegeneration (2018) 7:8 Page 5 of 6 Two studies reported on the effects of bilateral prefrontal cortex stimulation. In an open study, Dragasevic and colleagues studied bilateral rtms to the prefrontal cortex [22]. The authors found that the HAM-D and improved significantly upon immediate follow-up, as well as 21 and 30 days post-treatment. These results are strengthened by a significant and noteworthy effect size post-treatment (Tables 2 and 3). In a retrospective study, Torres and coworkers identify the effects of TMS on various symptoms experienced by patients with PD, including depression [27]. Significant improvement was seen in HAM-D and scores from before to after, and extended to follow-up evaluation. As seen with the previous studies, a high effect size and significance further illustrate these reports (Tables 2 and 3). Torres et al. once again demonstrate the efficacy of TMS as a treatment for Parkinson s patients with depression. Unlike the previously discussed studies, Makkos and colleagues solely tested for improvement in depression with stimulation to the motor cortex [25]. In a randomized, double-blind, placebo-controlled project, the authors applied bilateral rtms to the M1 cortical region of patients. According to the MADRS and the PDQ-39, depression severity and health related quality of life improved significantly for the treatment group. As with the study by Pal and colleagues, insufficient data prevent an effect size analysis. Alternative findings Among the studies considered in this review, the most common location of TMS stimulation was the left DLPFC; however, bilateral DLPFC and M1 stimulation was also reported (Table 1). In their multi-center trial, Brys and colleagues examined potential effects of rtms to the motor cortex (M1) and left DLPFC on both motor functioning and mood [18]. Among the 50 patients who completed all study visits, the authors found that stimulation to M1 yielded improved motor function; however, unexpectedly, stimulation to the left DLPFC yielded no significant changes in the depression 1 month after treatment. When stimulation of M1 and the left DLPFC were done together, no synergistic effect was observed. The authors purport that while stimulation did not appear to effectively treat patient mood, a longer duration of treatment may yield different results. Effect sizes and p-values calculated for each experimental group in this study mirrored the contradictory findings reported by Brys and colleagues (Tables 2 and 3). With regard to M1 stimulation alone, a very large effect size was calculated; this suggests that M1 rtms stimulation reduces depression (p < 0.05). Alternatively, little to no effect was observed following stimulation to the DLPFC alone, raising some doubt about the efficacy of rtms. However, when further evaluated, the result was found to have no significance (p = 0.495), challenging the reliability of the finding. When both M1 and DLPFC were stimulated together a moderate effect size was observed. Full sham treatment yielded high effect sizes. Together these results seem to indicate that three of the experimental groups appear to have some effect on reducing depression: M1 stimulation, simultaneous M1 and DLPFC stimulation, and full placebo stimulation. Total weighted average effect size Despite the contradictory findings by Brys and coworkers, calculation of total weighted average effect size helped to resolve any discrepancy between the study results. When all study groups that applied rtms stimulation were considered together and weighted based on sample size, effect size (1.32) overwhelmingly suggested a notable reduction in depression following rtms. Further, among all study groups applying rtms to the DLPFC specifically an even more notable effect was found (1.37). These weighted overall calculations serve to remedy any concern regarding the contradictory study. Despite these findings, it is important to recognize that only one of the studies in the quantitative analysis used a true sham treatment as a control and subsequently reported a strong placebo effect (Hedge s G > 1.2;p < 0.05) [18]. A major limitation for all treatments of depression is the high placebo effect. We acknowledge that the findings reported in this meta-analysis could be a result of placebo. Future studies, must incorporate reliable control groups in order to examine a potential placebo effect. Along these lines, experimental design and stimulation parameters varied greatly across all studies. New research must begin to establish standards for variables such as stimulation frequency and location. To this end, it is of note that stimulation parameters in Table 1 vary considerably between papers with the same target and standardization of these parameters may be difficult due to individual demographic variability. Provided that rtms treatment parameters can be standardized in this way, our findings bring light to a promising alternative anti-depressant therapy. As examined from both clinician and patient perspectives, this meta-analysis strongly suggests that rtms can relieve clinical depression in patients with Parkinson s disease. Conclusions This meta-analysis qualitatively and quantitatively evaluated the use of rtms for the treatment of refractory depression in patients with PD. Individual study groups and overall effect sizes yielded promising reductions in self-reported and clinician-administered inventories. These findings encourage further exploration of rtms as an alternative to traditional anti-depressant pharmacology in the Parkinson s population.
6 Lesenskyj et al. Translational Neurodegeneration (2018) 7:8 Page 6 of 6 Abbreviations : Beck Depression Inventory; DLPFC: Dorsolateral prefrontal cortex; HAM- D: Hamilton Depression Inventory; IQR: Interquartile range; MADRS: Montgomery-Asberg Depression Rating Scale; PD: Parkinson s disease; rtms: Repetitive transcranial magnetic stimulation Acknowledgements Funding Availability of data and materials All data generated or analyzed during this study are included in this published article. Authors contributions AL performed the literature search for this meta-analysis. AL and MS performed all statistical analyses. AL, CM, and JF contributed to the writing of this manuscript. All authors read and approved the final manuscript. Ethics approval and consent to participate Consent for publication Competing interests The authors declare that they have no competing interests. Author details 1 Rowan University School of Osteopathic Medicine, Stratford, NJ 08048, USA. 2 Drexel Neurosciences Institute, 245 N 15th Street ms 423, Philadelphia, PA 19102, USA. Received: 22 August 2017 Accepted: 6 March 2018 References 1. Rihmer Z, Gonda X, Dome P. Depression in Parkinson's disease. Ideggyogy Sz. 2014;67(7 8): Berg D, Lang AE, Postuma RB, Maetzler W, Deuschl G, Gasser T, Siderowf A, Schapira AH, Oertel W, Obeso JA, et al. Changing the research criteria for the diagnosis of Parkinson's disease: obstacles and opportunities. Lancet Neurol. 2013;12(5): Leentjens AF. Depression in Parkinson's disease: conceptual issues and clinical challenges. J Geriatr Psychiatry Neurol. 2004;17(3): Schapira AHV, Chaudhuri KR, Jenner P. Non-motor features of Parkinson disease. Nat Rev Neurosci. 2017;18(7): Perera T, George MS, Grammer G, Janicak PG, Pascual-Leone A, Wirecki TS. The clinical TMS Society consensus review and treatment recommendations for TMS therapy for major depressive disorder. Brain Stimul. 2016;9(3): Gaynes BN, Lloyd SW, Lux L, Gartlehner G, Hansen RA, Brode S, Jonas DE, Swinson Evans T, Viswanathan M, Lohr KN. Repetitive transcranial magnetic stimulation for treatment-resistant depression: a systematic review and meta-analysis. J Clin Psychiatry. 2014;75(5): quiz George MS, Lisanby SH, Avery D, McDonald WM, Durkalski V, Pavlicova M, Anderson B, Nahas Z, Bulow P, Zarkowski P, et al. Daily left prefrontal transcranial magnetic stimulation therapy for major depressive disorder: a sham-controlled randomized trial. Arch Gen Psychiatry. 2010;67(5): O'Reardon JP, Solvason HB, Janicak PG, Sampson S, Isenberg KE, Nahas Z, McDonald WM, Avery D, Fitzgerald PB, Loo C, et al. Efficacy and safety of transcranial magnetic stimulation in the acute treatment of major depression: a multisite randomized controlled trial. Biol Psychiatry. 2007;62(11): Cantone M, Bramanti A, Lanza G, Pennisi M, Bramanti P, Pennisi G, Bella R. Cortical plasticity in depression. ASN Neuro. 2017;9(3): Janicak PG, Dokucu ME. Transcranial magnetic stimulation for the treatment of major depression. Neuropsychiatr Dis Treat. 2015;11: Rostami R, Kazemi R, Nitsche MA, Gholipour F, Salehinejad MA. Clinical and demographic predictors of response to rtms treatment in unipolar and bipolar depressive disorders. Clin Neurophysiol. 2017;128(10): Drysdale AT, Grosenick L, Downar J, Dunlop K, Mansouri F, Meng Y, Fetcho RN, Zebley B, Oathes DJ, Etkin A, et al. Resting-state connectivity biomarkers define neurophysiological subtypes of depression. Nat Med. 2017;23(1): ConnollyKR,HelmerA,CristanchoMA,Cristancho P, O'Reardon JP. Effectiveness of transcranial magnetic stimulation in clinical practice post-fda approval in the United States: results observed with the first 100 consecutive cases of depression at an academic medical center. J Clin Psychiatry. 2012;73(4):e Dubin M. Imaging TMS: antidepressant mechanisms and treatment optimization. Int Rev Psychiatry. 2017;29(2): Fox MD, Liu H, Pascual-Leone A. Identification of reproducible individualized targets for treatment of depression with TMS based on intrinsic connectivity. NeuroImage. 2013;66: Baeken C, Marinazzo D, Wu GR, Van Schuerbeek P, De Mey J, Marchetti I, Vanderhasselt MA, Remue J, Luypaert R, De Raedt R. Accelerated HF-rTMS in treatment-resistant unipolar depression: insights from subgenual anterior cingulate functional connectivity. World J Biol Psychiatry. 2014;15(4): Salomons TV, Dunlop K, Kennedy SH, Flint A, Geraci J, Giacobbe P, Downar J. Resting-state cortico-thalamic-striatal connectivity predicts response to dorsomedial prefrontal rtms in major depressive disorder. Neuropsychopharmacology. 2014;39(2): Brys M, Fox MD, Agarwal S, Biagioni M, Dacpano G, Kumar P, Pirraglia E, Chen R, Wu A, Fernandez H, et al. Multifocal repetitive TMS for motor and mood symptoms of Parkinson disease: a randomized trial. Neurology. 2016; 87(18): Chou YH, Hickey PT, Sundman M, Song AW, Chen NK. Effects of repetitive transcranial magnetic stimulation on motor symptoms in Parkinson disease: a systematic review and meta-analysis. JAMA Neurol. 2015;72(4): Elahi B, Chen R. Effect of transcranial magnetic stimulation on Parkinson motor function systematic review of controlled clinical trials. Mov Disord. 2009;24(3): Helmich RC, Siebner HR, Bakker M, Münchau A, Bloem BR. Repetitive transcranial magnetic stimulation to improve mood and motor function in Parkinson's disease. J Neurol Sci. 2006;248(1 2): Dragasevic N, Potrebić A, Damjanović A, Stefanova E, Kostić VS. Therapeutic efficacy of bilateral prefrontal slow repetitive transcranial magnetic stimulation in depressed patients with Parkinson's disease: an open study. Mov Disord. 2002;17(3): Epstein CM, Evatt ML, Funk A, Girard-Siqueira L, Lupei N, Slaughter L, Athar S, Green J, McDonald W, DeLong MR. An open study of repetitive transcranial magnetic stimulation in treatment-resistant depression with Parkinson's disease. Clin Neurophysiol. 2007;118(10): Fregni F, Santos CM, Myczkowski ML, Rigolino R, Gallucci-Neto J, Barbosa ER, Valente KD, Pascual-Leone A, Marcolin MA. Repetitive transcranial magnetic stimulation is as effective as fluoxetine in the treatment of depression in patients with Parkinson's disease. J Neurol Neurosurg Psychiatry. 2004;75(8): Makkos A, Pál E, Aschermann Z, Janszky J, Balázs É, Takács K, Karádi K, Komoly S, Kovács N. High-frequency repetitive transcranial magnetic stimulation can improve depression in Parkinson's disease: a randomized, double-blind, placebo-controlled study. Neuropsychobiology. 2016;73(3): Pal E, Nagy F, Aschermann Z, Balazs E, Kovacs N. The impact of left prefrontal repetitive transcranial magnetic stimulation on depression in Parkinson's disease: a randomized, double-blind, placebo-controlled study. Mov Disord. 2010;25(14): Torres F, Villalon E, Poblete P, Moraga-Amaro R, Linsambarth S, Riquelme R, Zangen A, Stehberg J. Retrospective evaluation of deep transcranial magnetic stimulation as add-on treatment for Parkinson's disease. Front Neurol. 2015;6:210.
Transcranial Magnetic Stimulation for the Treatment of Depression
 Transcranial Magnetic Stimulation for the Treatment of Depression Paul E. Holtzheimer, MD Associate Professor Departments of Psychiatry and Surgery Geisel School of Medicine at Dartmouth Dartmouth-Hitchcock
Transcranial Magnetic Stimulation for the Treatment of Depression Paul E. Holtzheimer, MD Associate Professor Departments of Psychiatry and Surgery Geisel School of Medicine at Dartmouth Dartmouth-Hitchcock
HHS Public Access Author manuscript J Neuropsychiatry Clin Neurosci. Author manuscript; available in PMC 2017 September 11.
 HHS Public Access Author manuscript Published in final edited form as: J Neuropsychiatry Clin Neurosci. 2017 ; 29(2): 179 182. doi:10.1176/appi.neuropsych.16100181. Initial Response to Transcranial Magnetic
HHS Public Access Author manuscript Published in final edited form as: J Neuropsychiatry Clin Neurosci. 2017 ; 29(2): 179 182. doi:10.1176/appi.neuropsych.16100181. Initial Response to Transcranial Magnetic
Statement on Repetitive Transcranial Magnetic Stimulation for Depression. Position statement CERT03/17
 Statement on Repetitive Transcranial Magnetic Stimulation for Depression Position statement CERT03/17 Approved by the Royal College of Psychiatrists, Committee on ECT and Related Treatments: February 2017
Statement on Repetitive Transcranial Magnetic Stimulation for Depression Position statement CERT03/17 Approved by the Royal College of Psychiatrists, Committee on ECT and Related Treatments: February 2017
Transcranial Magnetic Stimulation
 Transcranial Magnetic Stimulation Date of Origin: 7/24/2018 Last Review Date: 7/24/2018 Effective Date: 08/01/18 Dates Reviewed: 7/24/2018 Developed By: Medical Necessity Criteria Committee I. Description
Transcranial Magnetic Stimulation Date of Origin: 7/24/2018 Last Review Date: 7/24/2018 Effective Date: 08/01/18 Dates Reviewed: 7/24/2018 Developed By: Medical Necessity Criteria Committee I. Description
TRANSCRANIAL MAGNETIC STIMULATION
 TRANSCRANIAL MAGNETIC STIMULATION Optum Behavioral Clinical Policy Policy Number: BH727BCPTMS_112017 Effective Date: November, 2017 Table of Contents Page BENEFIT CONSIDERATIONS... 1 COVERAGE RATIONALE...
TRANSCRANIAL MAGNETIC STIMULATION Optum Behavioral Clinical Policy Policy Number: BH727BCPTMS_112017 Effective Date: November, 2017 Table of Contents Page BENEFIT CONSIDERATIONS... 1 COVERAGE RATIONALE...
NeuroField, Inc., Bishop, California, USA Published online: 02 Mar 2012.
 Journal of Neurotherapy: Investigations in Neuromodulation, Neurofeedback and Applied Neuroscience The Effect of Neurofield Pulsed EMF on Parkinson's Disease Symptoms and QEEG Nicholas J. Dogris a a NeuroField,
Journal of Neurotherapy: Investigations in Neuromodulation, Neurofeedback and Applied Neuroscience The Effect of Neurofield Pulsed EMF on Parkinson's Disease Symptoms and QEEG Nicholas J. Dogris a a NeuroField,
Accepted Manuscript. Peter Fettes, Sarah Peters, Peter Giacobbe, Jonathan Downar
 Accepted Manuscript Neural correlates of successful orbitofrontal 1 Hz rtms following unsuccessful dorsolateral and dorsomedial prefrontal rtms in major depression: A case report Peter Fettes, Sarah Peters,
Accepted Manuscript Neural correlates of successful orbitofrontal 1 Hz rtms following unsuccessful dorsolateral and dorsomedial prefrontal rtms in major depression: A case report Peter Fettes, Sarah Peters,
Modulation of the Neural Circuitry Underlying Obsessive-Compulsive Disorder
 BRAIN STIMULATION LABORATORY Modulation of the Neural Circuitry Underlying Obsessive-Compulsive Disorder OCD Awareness Day NOLAN WILLIAMS, M.D. Instructor Department of Psychiatry Stanford University October
BRAIN STIMULATION LABORATORY Modulation of the Neural Circuitry Underlying Obsessive-Compulsive Disorder OCD Awareness Day NOLAN WILLIAMS, M.D. Instructor Department of Psychiatry Stanford University October
FDA CLEARS NEUROSTAR TMS THERAPY FOR THE TREATMENT OF DEPRESSION
 FOR IMMEDIATE RELEASE FDA CLEARS NEUROSTAR TMS THERAPY FOR THE TREATMENT OF DEPRESSION First and Only Non-systemic and Non-invasive Treatment Cleared for Patients Who Have Not Benefited From Prior Antidepressant
FOR IMMEDIATE RELEASE FDA CLEARS NEUROSTAR TMS THERAPY FOR THE TREATMENT OF DEPRESSION First and Only Non-systemic and Non-invasive Treatment Cleared for Patients Who Have Not Benefited From Prior Antidepressant
Efficacy and Safety of Transcranial Magnetic Stimulation in Patients with Depression
 Showa Univ J Med Sci 30 1, 97 106, March 2018 Original Efficacy and Safety of Transcranial Magnetic Stimulation in Patients with Depression Yu KAWAGUCHI 1 and Akira IWANAMI 2 Abstract : Transcranial magnetic
Showa Univ J Med Sci 30 1, 97 106, March 2018 Original Efficacy and Safety of Transcranial Magnetic Stimulation in Patients with Depression Yu KAWAGUCHI 1 and Akira IWANAMI 2 Abstract : Transcranial magnetic
Transcranial magnetic stimulation has become an increasingly
 Within-Session Mood Changes From TMS in Depressed Patients Tobias Dang, M.D. David H. Avery, M.D. Joan Russo, Ph.D. Transcranial magnetic stimulation has become an increasingly well studied tool in neuropsychiatry.
Within-Session Mood Changes From TMS in Depressed Patients Tobias Dang, M.D. David H. Avery, M.D. Joan Russo, Ph.D. Transcranial magnetic stimulation has become an increasingly well studied tool in neuropsychiatry.
Copyright 2002 American Academy of Neurology. Volume 58(8) 23 April 2002 pp
 Copyright 2002 American Academy of Neurology Volume 58(8) 23 April 2002 pp 1288-1290 Improved executive functioning following repetitive transcranial magnetic stimulation [Brief Communications] Moser,
Copyright 2002 American Academy of Neurology Volume 58(8) 23 April 2002 pp 1288-1290 Improved executive functioning following repetitive transcranial magnetic stimulation [Brief Communications] Moser,
Original Effective Date: 8/28/2013. Subject: Transcranial Magnetic Stimulation for the Treatment of Major Depression
 Subject: Transcranial Magnetic Stimulation for the Treatment of Major Depression Guidance Number: MCG-104 Revision Date(s): Original Effective Date: 8/28/2013 Medical Coverage Guidance Approval Date: 8/28/2013
Subject: Transcranial Magnetic Stimulation for the Treatment of Major Depression Guidance Number: MCG-104 Revision Date(s): Original Effective Date: 8/28/2013 Medical Coverage Guidance Approval Date: 8/28/2013
What is Repetitive Transcranial Magnetic Stimulation?
 rtms for Refractory Depression: Findings and Future Jonathan Downar, MD PhD Asst Professor, Dept of Psychiatry University of Toronto, Canada Co-Director, rtms Clinic Toronto Western Hospital University
rtms for Refractory Depression: Findings and Future Jonathan Downar, MD PhD Asst Professor, Dept of Psychiatry University of Toronto, Canada Co-Director, rtms Clinic Toronto Western Hospital University
Review. M. Gross 1, L. Nakamura 1, A. Pascual-Leone 2 F. Fregni 2 1 Department of Psychiatry, University of S¼o Paulo, S¼o
 Acta Psychiatr Scand 2007: 116: 165 173 All rights reserved DOI: 10.1111/j.1600-0447.2007.01049.x Copyright Ó 2007 The Authors Journal Compilation Ó 2007 Blackwell Munksgaard ACTA PSYCHIATRICA SCANDINAVICA
Acta Psychiatr Scand 2007: 116: 165 173 All rights reserved DOI: 10.1111/j.1600-0447.2007.01049.x Copyright Ó 2007 The Authors Journal Compilation Ó 2007 Blackwell Munksgaard ACTA PSYCHIATRICA SCANDINAVICA
Transcranial Magnetic Stimulation Therapy for Patients with Refractory Depression: Clinical-Effectiveness and Guidelines
 TITLE: Transcranial Magnetic Stimulation Therapy for Patients with Refractory Depression: Clinical-Effectiveness and Guidelines DATE: 14 April 2009 RESEARCH QUESTIONS: 1. What is the clinical-effectiveness
TITLE: Transcranial Magnetic Stimulation Therapy for Patients with Refractory Depression: Clinical-Effectiveness and Guidelines DATE: 14 April 2009 RESEARCH QUESTIONS: 1. What is the clinical-effectiveness
Subject: Transcranial Magnetic Stimulation
 01-93875-18 Original Effective Date: 06/15/02 Reviewed: 12/06/18 Revised: 12/15/18 Subject: Transcranial Magnetic Stimulation THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION, CERTIFICATION, EXPLANATION
01-93875-18 Original Effective Date: 06/15/02 Reviewed: 12/06/18 Revised: 12/15/18 Subject: Transcranial Magnetic Stimulation THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION, CERTIFICATION, EXPLANATION
Transcranial Magnetic Stimulation:
 Transcranial Magnetic Stimulation: What has experience told us? Jonathan Downar MD PhD FRCPC MRI-Guided rtms Clinic University Health Network www.rtmsclinic.ca Disclosures Research funding: Canadian Institutes
Transcranial Magnetic Stimulation: What has experience told us? Jonathan Downar MD PhD FRCPC MRI-Guided rtms Clinic University Health Network www.rtmsclinic.ca Disclosures Research funding: Canadian Institutes
 http://web.uct.ac.za/depts/psychology/postgraduate/hons2008projects/sarah.drowley.pdf ftp://ftp.psy.gla.ac.uk/pub/gregor/tmseeg4marine/ort%20clinneurophysiol%202009.pdf J Nerv Ment Dis. 2010 Sep;198(9):679-81.
http://web.uct.ac.za/depts/psychology/postgraduate/hons2008projects/sarah.drowley.pdf ftp://ftp.psy.gla.ac.uk/pub/gregor/tmseeg4marine/ort%20clinneurophysiol%202009.pdf J Nerv Ment Dis. 2010 Sep;198(9):679-81.
Neuromodulation Approaches to Treatment Resistant Depression
 1 Alternative Treatments: Neuromodulation Approaches to Treatment Resistant Depression Audrey R. Tyrka, MD, PhD Assistant Professor Brown University Department of Psychiatry Associate Chief, Mood Disorders
1 Alternative Treatments: Neuromodulation Approaches to Treatment Resistant Depression Audrey R. Tyrka, MD, PhD Assistant Professor Brown University Department of Psychiatry Associate Chief, Mood Disorders
Review Paper. Introduction
 Review Paper Unilateral and bilateral repetitive transcranial magnetic stimulation for treatment-resistant depression: a meta-analysis of randomized controlled trials over decades Shayan Sehatzadeh, MD,
Review Paper Unilateral and bilateral repetitive transcranial magnetic stimulation for treatment-resistant depression: a meta-analysis of randomized controlled trials over decades Shayan Sehatzadeh, MD,
Transcranial Magnetic Stimulation (TMS)
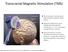 Transcranial Magnetic Stimulation (TMS) The treatment coil produces MRI-strength magnetic field pulses. Magnetic field pulses pass unimpeded through the cranium for 2-3 cm. and induce a small electric
Transcranial Magnetic Stimulation (TMS) The treatment coil produces MRI-strength magnetic field pulses. Magnetic field pulses pass unimpeded through the cranium for 2-3 cm. and induce a small electric
TRANSCRANIAL MAGNETIC STIMULATION: CLINICAL UPDATE FOR PSYCHIATRIC APPLICATIONS ANNA MAZUR, PH.D. OSU DEPT. OF PSYCHIATRY AND BEHAVIORAL SCIENCES
 TRANSCRANIAL MAGNETIC STIMULATION: CLINICAL UPDATE FOR PSYCHIATRIC APPLICATIONS ANNA MAZUR, PH.D. OSU DEPT. OF PSYCHIATRY AND BEHAVIORAL SCIENCES FINANCIAL DISCLOSURE I have financial relationships to
TRANSCRANIAL MAGNETIC STIMULATION: CLINICAL UPDATE FOR PSYCHIATRIC APPLICATIONS ANNA MAZUR, PH.D. OSU DEPT. OF PSYCHIATRY AND BEHAVIORAL SCIENCES FINANCIAL DISCLOSURE I have financial relationships to
HCT Medical Policy. Transcranial Magnetic Stimulation (TMS) for Major Depression Policy # 121 Current Effective Date: 05/24/2016.
 HCT Medical Policy Transcranial Magnetic Stimulation (TMS) for Major Depression Policy # 121 Current Effective Date: 05/24/2016 Medical Policies are developed by HealthyCT to assist in administering plan
HCT Medical Policy Transcranial Magnetic Stimulation (TMS) for Major Depression Policy # 121 Current Effective Date: 05/24/2016 Medical Policies are developed by HealthyCT to assist in administering plan
Repetitive Transcranial Magnetic Stimulation (rtms)
 Page 1 of 33 Medical Policies - Mental Health Repetitive Transcranial Magnetic Stimulation (rtms) Print Number: PSY301.015 Effective Date: 07-01-2014 Coverage: Initial rtms Treatment Repetitive transcranial
Page 1 of 33 Medical Policies - Mental Health Repetitive Transcranial Magnetic Stimulation (rtms) Print Number: PSY301.015 Effective Date: 07-01-2014 Coverage: Initial rtms Treatment Repetitive transcranial
PSYCHOPHARMACOLOGY BULLETIN: Vol. 42 No. 2 5
 DEMITRACK_MWM_549.QXP 7/14/9 1:46 PM Page 5 ORIGINAL RESEARCH Key Words: major depression, treatment resistance, transcranial magnetic stimulation, TMS, antidepressant, efficacy, safety, randomized clinical
DEMITRACK_MWM_549.QXP 7/14/9 1:46 PM Page 5 ORIGINAL RESEARCH Key Words: major depression, treatment resistance, transcranial magnetic stimulation, TMS, antidepressant, efficacy, safety, randomized clinical
Effective Date: July 27, 2016
 Medical Review Criteria Transcranial Magnetic Stimulation Effective Date: July 27, 2016 Subject: Transcranial Magnetic Stimulation Policy: An initial course of left prefrontal TMS 1 is covered for: Patients
Medical Review Criteria Transcranial Magnetic Stimulation Effective Date: July 27, 2016 Subject: Transcranial Magnetic Stimulation Policy: An initial course of left prefrontal TMS 1 is covered for: Patients
The Evidence Base for rtms Reimbursement
 The Evidence Base for rtms Reimbursement Bradley N. Gaynes, MD, MPH Professor of Psychiatry Associate Chair of Research Training and Education Institute of Medicine Workshop March 3, 2015 What do we know,
The Evidence Base for rtms Reimbursement Bradley N. Gaynes, MD, MPH Professor of Psychiatry Associate Chair of Research Training and Education Institute of Medicine Workshop March 3, 2015 What do we know,
Transcranial Magnetic Stimulation: Scientific Underpinnings and Practical Applications
 Transcranial Magnetic Stimulation: Scientific Underpinnings and Practical Applications Jon Draud, MS, MD Clinical Professor of Psychiatry University of Tennessee College of Medicine Memphis, Tennessee
Transcranial Magnetic Stimulation: Scientific Underpinnings and Practical Applications Jon Draud, MS, MD Clinical Professor of Psychiatry University of Tennessee College of Medicine Memphis, Tennessee
Transcranial Direct-Current Stimulation
 Introduction (tdcs) is a non-invasive form of brain stimulation similar to transcranial magnetic stimulation, but instead of using magnets, it uses a lowintensity, constant current applied through scalp
Introduction (tdcs) is a non-invasive form of brain stimulation similar to transcranial magnetic stimulation, but instead of using magnets, it uses a lowintensity, constant current applied through scalp
Therapeutic Uses of Noninvasive Brain Stimulation Current & Developing
 Therapeutic Uses of Noninvasive Brain Stimulation Current & Developing Alvaro Pascual-Leone, MD, PhD Berenson-Allen Center for Noninvasive Brain Stimulation Harvard Catalyst Beth Israel Deaconess Medical
Therapeutic Uses of Noninvasive Brain Stimulation Current & Developing Alvaro Pascual-Leone, MD, PhD Berenson-Allen Center for Noninvasive Brain Stimulation Harvard Catalyst Beth Israel Deaconess Medical
Short-term efficacy of repetitive transcranial magnetic stimulation (rtms) in depressionreanalysis of data from meta-analyses up to 2010
 Kedzior and Reitz BMC Psychology 2014, 2:39 RESEARCH ARTICLE Open Access Short-term efficacy of repetitive transcranial magnetic stimulation (rtms) in depressionreanalysis of data from meta-analyses up
Kedzior and Reitz BMC Psychology 2014, 2:39 RESEARCH ARTICLE Open Access Short-term efficacy of repetitive transcranial magnetic stimulation (rtms) in depressionreanalysis of data from meta-analyses up
Repetitive transcranial magnetic stimulation for depression
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Repetitive transcranial magnetic stimulation for depression Depression causes low mood or sadness that can
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Repetitive transcranial magnetic stimulation for depression Depression causes low mood or sadness that can
Transcranial direct current stimulation (tdcs)
 Clinical Memorandum Transcranial direct current stimulation (tdcs) August 2018 Authorising Committee/Department: Responsible Committee Responsible Department: Document Code: Board Section of Electroconvulsive
Clinical Memorandum Transcranial direct current stimulation (tdcs) August 2018 Authorising Committee/Department: Responsible Committee Responsible Department: Document Code: Board Section of Electroconvulsive
Therapeutic Neuromodulation: Overview of a Novel Treatment Platform
 Therapeutic Neuromodulation: Overview of a Novel Treatment Platform David G. Brock, MD; and Mark A. Demitrack, MD Shutterstock David G. Brock, MD, is Medical Director, Neuronetics, Inc. Mark A. Demitrack,
Therapeutic Neuromodulation: Overview of a Novel Treatment Platform David G. Brock, MD; and Mark A. Demitrack, MD Shutterstock David G. Brock, MD, is Medical Director, Neuronetics, Inc. Mark A. Demitrack,
( Transcranial Magnetic Stimulation, TMS) TMS, TMS TMS TMS TMS TMS TMS Q189
 102 2004 35 2 3 : 1 2 2 ( 1 DK29220 ; 2 100083) ( Transcranial Magnetic Stimulation TMS) TMS TMS TMS TMS TMS TMS TMS ; ; ; Q189 Transcranial Magnetic Stimulation ( TMS) : Physiology Psychology Brain Mapping
102 2004 35 2 3 : 1 2 2 ( 1 DK29220 ; 2 100083) ( Transcranial Magnetic Stimulation TMS) TMS TMS TMS TMS TMS TMS TMS ; ; ; Q189 Transcranial Magnetic Stimulation ( TMS) : Physiology Psychology Brain Mapping
Case 2:15-cv MWF-JPR Document Filed 03/20/17 Page 1 of 36 Page ID #:388 EXHIBIT 1
 Case 2:15-cv-07074-MWF-JPR Document 65-10 Filed 03/20/17 Page 1 of 36 Page ID #:388 EXHIBIT 1 Case 2:15-cv-07074-MWF-JPR Document 65-10 Filed 03/20/17 Page 2 of 36 Page ID #:389 Cigna Medical Coverage
Case 2:15-cv-07074-MWF-JPR Document 65-10 Filed 03/20/17 Page 1 of 36 Page ID #:388 EXHIBIT 1 Case 2:15-cv-07074-MWF-JPR Document 65-10 Filed 03/20/17 Page 2 of 36 Page ID #:389 Cigna Medical Coverage
TRANSCRANIAL MAGNETIC STIMULATION
 MEDICAL POLICY TRANSCRANIAL MAGNETIC STIMULATION Policy Number: 2013T0536F Effective Date: December 1, 2013 Table of Contents COVERAGE RATIONALE... BACKGROUND... CLINICAL EVIDENCE... U.S. FOOD AND DRUG
MEDICAL POLICY TRANSCRANIAL MAGNETIC STIMULATION Policy Number: 2013T0536F Effective Date: December 1, 2013 Table of Contents COVERAGE RATIONALE... BACKGROUND... CLINICAL EVIDENCE... U.S. FOOD AND DRUG
The Effect of Pramipexole on Depressive Symptoms in Parkinson's Disease.
 Kobe J. Med. Sci., Vol. 56, No. 5, pp. E214-E219, 2010 The Effect of Pramipexole on Depressive Symptoms in Parkinson's Disease. NAOKO YASUI 1, KENJI SEKIGUCHI 1, HIROTOSHI HAMAGUCHI 1, and FUMIO KANDA
Kobe J. Med. Sci., Vol. 56, No. 5, pp. E214-E219, 2010 The Effect of Pramipexole on Depressive Symptoms in Parkinson's Disease. NAOKO YASUI 1, KENJI SEKIGUCHI 1, HIROTOSHI HAMAGUCHI 1, and FUMIO KANDA
Transcranial magnetic stimulation in clinical practice
 BJPsych Advances (2016), vol. 22, 373 379 doi: 10.1192/apt.bp.115.015206 Transcranial magnetic stimulation in clinical practice Sheila Hardy, Lorraine Bastick, Alex O Neill-Kerr, Priyadharshini Sabesan,
BJPsych Advances (2016), vol. 22, 373 379 doi: 10.1192/apt.bp.115.015206 Transcranial magnetic stimulation in clinical practice Sheila Hardy, Lorraine Bastick, Alex O Neill-Kerr, Priyadharshini Sabesan,
Predictors of Response to Repetitive Transcranial Magnetic Stimulation in Depression: A Review of Recent Updates
 Review https://doi.org/10.9758/cpn.2019.17.1.25 pissn 1738-1088 / eissn 2093-4327 Clinical Psychopharmacology and Neuroscience 2019;17(1):25-33 Copyrightc 2019, Korean College of Neuropsychopharmacology
Review https://doi.org/10.9758/cpn.2019.17.1.25 pissn 1738-1088 / eissn 2093-4327 Clinical Psychopharmacology and Neuroscience 2019;17(1):25-33 Copyrightc 2019, Korean College of Neuropsychopharmacology
Frequently Asked Questions FAQS. NeuroStar TMS Therapies
 Frequently Asked Questions FAQS NeuroStar TMS Therapies Provided by Dr Terrence A. Boyadjis MD 790 E Market Street Suite 245 West Chester, PA 19382 610.738.9576 FAQS About TMS Therapies Page 1 NeuroStar
Frequently Asked Questions FAQS NeuroStar TMS Therapies Provided by Dr Terrence A. Boyadjis MD 790 E Market Street Suite 245 West Chester, PA 19382 610.738.9576 FAQS About TMS Therapies Page 1 NeuroStar
Introduction. Cheng-Long Xie 1,2 Jie Chen. Shi-Yi Lin 1 Xiao-Dong Xue
 DOI 10.1007/s10072-015-2345-4 REVIEW ARTICLE Repetitive transcranial magnetic stimulation (rtms) for the treatment of depression in Parkinson disease: a meta-analysis of randomized controlled clinical
DOI 10.1007/s10072-015-2345-4 REVIEW ARTICLE Repetitive transcranial magnetic stimulation (rtms) for the treatment of depression in Parkinson disease: a meta-analysis of randomized controlled clinical
obsessive-compulsive disorder; OCD
 9(1), 50 56, 2017 OCD OCD DBSECT tdcsrtms DBS ECT 6 tdcs rtms obsessive-compulsive disorder; OCD 2013 OCD 2012 deep brain stimulation; DBS electroconvulsive therapy; ECT transcranial direct current stimulation;
9(1), 50 56, 2017 OCD OCD DBSECT tdcsrtms DBS ECT 6 tdcs rtms obsessive-compulsive disorder; OCD 2013 OCD 2012 deep brain stimulation; DBS electroconvulsive therapy; ECT transcranial direct current stimulation;
High-frequency rtms for the Treatment of Chronic Fatigue Syndrome: A Case Series
 CASE REPORT High-frequency rtms for the Treatment of Chronic Fatigue Syndrome: A Case Series Wataru Kakuda 1,2, Ryo Momosaki 1, Naoki Yamada 1 and Masahiro Abo 1 Abstract Structural and functional abnormalities
CASE REPORT High-frequency rtms for the Treatment of Chronic Fatigue Syndrome: A Case Series Wataru Kakuda 1,2, Ryo Momosaki 1, Naoki Yamada 1 and Masahiro Abo 1 Abstract Structural and functional abnormalities
Is There Evidence for Effectiveness of Transcranial Magnetic Stimulation in the Treatment of Psychiatric Disorders?
 [EVIDENCE-BASED PHARMACOLOGY] by BIJU BASIL, MD, DPM; JAMAL MAHMUD, MD, DPM; MAJU MATHEWS, MD, MRCPsych, DIP PSYCH; CARLOS RODRIGUEZ, MD; and BABATUNDE ADETUNJI, MD, DPM Dr. Basil is a resident, Dr. Mahmud
[EVIDENCE-BASED PHARMACOLOGY] by BIJU BASIL, MD, DPM; JAMAL MAHMUD, MD, DPM; MAJU MATHEWS, MD, MRCPsych, DIP PSYCH; CARLOS RODRIGUEZ, MD; and BABATUNDE ADETUNJI, MD, DPM Dr. Basil is a resident, Dr. Mahmud
Non-therapeutic and investigational uses of non-invasive brain stimulation
 Non-therapeutic and investigational uses of non-invasive brain stimulation Robert Chen, MA, MBBChir, MSc, FRCPC Catherine Manson Chair in Movement Disorders Professor of Medicine (Neurology), University
Non-therapeutic and investigational uses of non-invasive brain stimulation Robert Chen, MA, MBBChir, MSc, FRCPC Catherine Manson Chair in Movement Disorders Professor of Medicine (Neurology), University
CIMR. What is the CIMR? May In this issue. Quarterly Newsletter. Volume 1, Issue 2
 What is Department of : What is the? The has recently been established at University Health Network to promote the understanding of depression and mood disorders; to develop innovative evidence-based therapeutic
What is Department of : What is the? The has recently been established at University Health Network to promote the understanding of depression and mood disorders; to develop innovative evidence-based therapeutic
Rapid Transcranial Magnetic Stimulation (rtms) and Normalisation of the
 1 Rapid Transcranial Magnetic Stimulation (rtms) and Normalisation of the Dexamethasone Suppression Test (DST). Short Title: Normalisation of DST with rtms Saxby Pridmore, M.D Department of Psychological
1 Rapid Transcranial Magnetic Stimulation (rtms) and Normalisation of the Dexamethasone Suppression Test (DST). Short Title: Normalisation of DST with rtms Saxby Pridmore, M.D Department of Psychological
Transcranial Magnetic Stimulation
 Transcranial Magnetic Stimulation Scientific evidence in major depression and schizophrenia C.W. Slotema Parnassia Bavo Group The Hague, the Netherlands Faraday s law (1831) Electrical current magnetic
Transcranial Magnetic Stimulation Scientific evidence in major depression and schizophrenia C.W. Slotema Parnassia Bavo Group The Hague, the Netherlands Faraday s law (1831) Electrical current magnetic
Naoyuki Takeuchi, MD, PhD 1, Takeo Tada, MD, PhD 2, Masahiko Toshima, MD 3, Yuichiro Matsuo, MD 1 and Katsunori Ikoma, MD, PhD 1 ORIGINAL REPORT
 J Rehabil Med 2009; 41: 1049 1054 ORIGINAL REPORT REPETITIVE TRANSCRANIAL MAGNETIC STIMULATION OVER BILATERAL HEMISPHERES ENHANCES MOTOR FUNCTION AND TRAINING EFFECT OF PARETIC HAND IN PATIENTS AFTER STROKE
J Rehabil Med 2009; 41: 1049 1054 ORIGINAL REPORT REPETITIVE TRANSCRANIAL MAGNETIC STIMULATION OVER BILATERAL HEMISPHERES ENHANCES MOTOR FUNCTION AND TRAINING EFFECT OF PARETIC HAND IN PATIENTS AFTER STROKE
Setting up atms Clinic. Daniel Press, M.D. Assistant Professor in Neurology, Harvard Medical School and Beth Israel Deaconess Medical Center
 Setting up atms Clinic Daniel Press, M.D. Assistant Professor in Neurology, Harvard Medical School and Beth Israel Deaconess Medical Center Contents Safety and training of personnel Equipment Certification
Setting up atms Clinic Daniel Press, M.D. Assistant Professor in Neurology, Harvard Medical School and Beth Israel Deaconess Medical Center Contents Safety and training of personnel Equipment Certification
Transcranial magnetic stimulation for the treatment of major depression
 Neuropsychiatric Disease and Treatment open access to scientific and medical research Open Access Full Text Article Review Transcranial magnetic stimulation for the treatment of major depression Philip
Neuropsychiatric Disease and Treatment open access to scientific and medical research Open Access Full Text Article Review Transcranial magnetic stimulation for the treatment of major depression Philip
NEW DIRECTIONS BEHAVIORAL HEALTH, L.L.C.
 NEW DIRECTIONS BEHAVIORAL HEALTH, L.L.C. Medical Policy Repetitive Transcranial Magnetic Stimulation for Treatment of Major Depression Original Effective date: 10/13/2014 Reviewed: 3/2015, 11/2015, 11/2016,
NEW DIRECTIONS BEHAVIORAL HEALTH, L.L.C. Medical Policy Repetitive Transcranial Magnetic Stimulation for Treatment of Major Depression Original Effective date: 10/13/2014 Reviewed: 3/2015, 11/2015, 11/2016,
DBS efficacia, complicanze in cronico e nuovi orizzonti terapeutici
 DBS efficacia, complicanze in cronico e nuovi orizzonti terapeutici TECNICHE DI NEUROMODULAZIONE Invasiva: odeep Brain Stimulation Non Invasiva: o Transcranial Magnetic Stimulation (TMS) o Transcranial
DBS efficacia, complicanze in cronico e nuovi orizzonti terapeutici TECNICHE DI NEUROMODULAZIONE Invasiva: odeep Brain Stimulation Non Invasiva: o Transcranial Magnetic Stimulation (TMS) o Transcranial
2018 Otsuka Pharmaceutical Development & Commercialization, Inc., Rockville, MD Lundbeck, LLC.
 Neuromodulation Techniques: State of the Science Philip G. Janicak, MD Adjunct Professor Department of Psychiatry and Behavioral Sciences, Northwestern University Feinberg School of Medicine Consultant
Neuromodulation Techniques: State of the Science Philip G. Janicak, MD Adjunct Professor Department of Psychiatry and Behavioral Sciences, Northwestern University Feinberg School of Medicine Consultant
Update on Repetitive Transcranial Magnetic Stimulation in Obsessive-Compulsive Disorder: Different Targets
 Curr Psychiatry Rep (2011) 13:289 294 DOI 10.1007/s11920-011-0205-3 Update on Repetitive Transcranial Magnetic Stimulation in Obsessive-Compulsive Disorder: Different Targets Rianne M. Blom & Martijn Figee
Curr Psychiatry Rep (2011) 13:289 294 DOI 10.1007/s11920-011-0205-3 Update on Repetitive Transcranial Magnetic Stimulation in Obsessive-Compulsive Disorder: Different Targets Rianne M. Blom & Martijn Figee
NOW I M A NEUROSTAR. Let Your Best Self Shine
 NOW I M A NEUROSTAR. Let Your Best Self Shine It s Time for a New You NeuroStar Advanced Therapy is an in-office treatment that requires no anesthesia or sedation. You are awake and alert during treatment
NOW I M A NEUROSTAR. Let Your Best Self Shine It s Time for a New You NeuroStar Advanced Therapy is an in-office treatment that requires no anesthesia or sedation. You are awake and alert during treatment
Administration of repetitive transcranial magnetic stimulation (rtms)
 Professional Practice Guideline 16 Administration of repetitive transcranial magnetic stimulation (rtms) November 2018 Authorising Body: Responsible Committee/Department: Responsible Department: Document
Professional Practice Guideline 16 Administration of repetitive transcranial magnetic stimulation (rtms) November 2018 Authorising Body: Responsible Committee/Department: Responsible Department: Document
LEASE DO NOT COPY. Setting up atms Clinic
 Setting up atms Clinic Daniel Press, M.D. Assistant Professor in Neurology, Harvard Medical School and Beth Israel Deaconess Medical Center Contents Safety and training of personnel Equipment Certification
Setting up atms Clinic Daniel Press, M.D. Assistant Professor in Neurology, Harvard Medical School and Beth Israel Deaconess Medical Center Contents Safety and training of personnel Equipment Certification
Supplementary Online Content
 Supplementary Online Content Redlich R, Opel N, Grotegerd D, et al. Prediction of individual response to electroconvulsive therapy via machine learning on structural magnetic resonance imaging data. JAMA
Supplementary Online Content Redlich R, Opel N, Grotegerd D, et al. Prediction of individual response to electroconvulsive therapy via machine learning on structural magnetic resonance imaging data. JAMA
Supplementary materials
 Supplementary materials Kedzior, K.K., Gellersen, H., Brachetti, A., Berlim, M.T., 2015. Deep transcranial magnetic stimulation (DTMS) in the treatment of major depression: an exploratory systematic review
Supplementary materials Kedzior, K.K., Gellersen, H., Brachetti, A., Berlim, M.T., 2015. Deep transcranial magnetic stimulation (DTMS) in the treatment of major depression: an exploratory systematic review
Brain Stimulation 6 (2013) 254e260. Contents lists available at SciVerse ScienceDirect. Brain Stimulation. journal homepage:
 Brain Stimulation 6 (2013) 254e260 Contents lists available at SciVerse ScienceDirect Brain Stimulation journal homepage: www.brainstimjrnl.com The Role of Electrode Location and Stimulation Polarity in
Brain Stimulation 6 (2013) 254e260 Contents lists available at SciVerse ScienceDirect Brain Stimulation journal homepage: www.brainstimjrnl.com The Role of Electrode Location and Stimulation Polarity in
Clinical Policy: Transcranial Magnetic Stimulation
 Clinical Policy: Reference Number: CP.MP.172 Last Review Date: 12/18 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and legal information. Description
Clinical Policy: Reference Number: CP.MP.172 Last Review Date: 12/18 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and legal information. Description
Pridmore S. Download of Psychiatry, Chapter 29. Last modified: September,
 Pridmore S. Download of Psychiatry, Chapter 29. Last modified: September, 2017. 1 CHAPTER 29 TRANSCRANIAL MAGNETIC STIMULATION (TMS) Introduction ECT demonstrates that, for certain psychiatric disorders,
Pridmore S. Download of Psychiatry, Chapter 29. Last modified: September, 2017. 1 CHAPTER 29 TRANSCRANIAL MAGNETIC STIMULATION (TMS) Introduction ECT demonstrates that, for certain psychiatric disorders,
Repetitive Transcranial Magnetic Stimulation as a for Treatment of Refractory Depression and other Psychiatric/Neurologic Disorders
 Repetitive Transcranial Magnetic Stimulation as a for Treatment of Refractory Depression and other Psychiatric/Neurologic Disorders Policy Number: Original Effective Date: MM.12.015 08/01/2014 Line(s)
Repetitive Transcranial Magnetic Stimulation as a for Treatment of Refractory Depression and other Psychiatric/Neurologic Disorders Policy Number: Original Effective Date: MM.12.015 08/01/2014 Line(s)
Neural model of emotional regulation structures - Circuits involving prefrontal cortex and subcortical limbic structures - MDE associated with
 Topics Brain and signalling changes in depression Ketamine activity in refractory depression Mechanism of Action New Data Dose finding Route of Administration Activity in Other Disorders Neural model of
Topics Brain and signalling changes in depression Ketamine activity in refractory depression Mechanism of Action New Data Dose finding Route of Administration Activity in Other Disorders Neural model of
funzioni motorie e cognitive (nella malattia di Parkinson) Laura Avanzino
 Department of Experimental Medicine, section of Human Physiology Centre for Parkinson s Disease and Movement Disorders - University of Genoa funzioni motorie e cognitive (nella malattia di Parkinson) Laura
Department of Experimental Medicine, section of Human Physiology Centre for Parkinson s Disease and Movement Disorders - University of Genoa funzioni motorie e cognitive (nella malattia di Parkinson) Laura
BRAIN STIMULATION AN ALTERNATIVE TO DRUG THERAPY IN MATERNAL DEPRESSION?
 BRAIN STIMULATION AN ALTERNATIVE TO DRUG THERAPY IN MATERNAL DEPRESSION? Kira Stein, MD Medical Director West Coast Life Center Sherman Oaks, California CA Maternal Mental Health Initiative - 2013 2013
BRAIN STIMULATION AN ALTERNATIVE TO DRUG THERAPY IN MATERNAL DEPRESSION? Kira Stein, MD Medical Director West Coast Life Center Sherman Oaks, California CA Maternal Mental Health Initiative - 2013 2013
Introduction to TMS Transcranial Magnetic Stimulation
 Introduction to TMS Transcranial Magnetic Stimulation Lisa Koski, PhD, Clin Psy TMS Neurorehabilitation Lab Royal Victoria Hospital 2009-12-14 BIC Seminar, MNI Overview History, basic principles, instrumentation
Introduction to TMS Transcranial Magnetic Stimulation Lisa Koski, PhD, Clin Psy TMS Neurorehabilitation Lab Royal Victoria Hospital 2009-12-14 BIC Seminar, MNI Overview History, basic principles, instrumentation
Magellan Care Guidelines
 2018 2019 Magellan Care Guidelines Introduction Effective July 1, 2018 June 30, 2019 Updated April 4, 2018 In California, Magellan does business as Human Affairs International of California, Inc. and/or
2018 2019 Magellan Care Guidelines Introduction Effective July 1, 2018 June 30, 2019 Updated April 4, 2018 In California, Magellan does business as Human Affairs International of California, Inc. and/or
Biological treatments: Electroconvulsive Therapy, Transcranial Magnetic Stimulation, Light therapy
 Biological treatments: Electroconvulsive Therapy, Transcranial Magnetic Stimulation, Light therapy Basic trainee talk 23 May 2007 ECT When is ECT used. Depression. Severe, melancholic. Resistant to treatment.
Biological treatments: Electroconvulsive Therapy, Transcranial Magnetic Stimulation, Light therapy Basic trainee talk 23 May 2007 ECT When is ECT used. Depression. Severe, melancholic. Resistant to treatment.
HHS Public Access Author manuscript JAMA Neurol. Author manuscript; available in PMC 2015 May 08.
 Effects of Repetitive Transcranial Magnetic Stimulation on Motor Symptoms in Parkinson Disease: A Systematic Review and Meta-analysis Ying-hui Chou, ScD, Patrick T. Hickey, DO, Mark Sundman, BS, Allen
Effects of Repetitive Transcranial Magnetic Stimulation on Motor Symptoms in Parkinson Disease: A Systematic Review and Meta-analysis Ying-hui Chou, ScD, Patrick T. Hickey, DO, Mark Sundman, BS, Allen
KEY SUMMARY. Mirapexin /Sifrol (pramipexole): What it is and how it works. What is Mirapexin /Sifrol (pramipexole)?
 KEY SUMMARY 1. Mirapexin /Sifrol (pramipexole*) is a selective non-ergot dopamine agonist approved as immediate release since 1997 for the treatment of the signs and symptoms of idiopathic Parkinson's
KEY SUMMARY 1. Mirapexin /Sifrol (pramipexole*) is a selective non-ergot dopamine agonist approved as immediate release since 1997 for the treatment of the signs and symptoms of idiopathic Parkinson's
Nonpharmacologic Interventions for Treatment-Resistant Depression. Public Meeting December 9, 2011
 Nonpharmacologic Interventions for Treatment-Resistant Depression Public Meeting December 9, 2011 New England CEPAC Goal: To improve the application of evidence to guide practice and policy in New England
Nonpharmacologic Interventions for Treatment-Resistant Depression Public Meeting December 9, 2011 New England CEPAC Goal: To improve the application of evidence to guide practice and policy in New England
Clinical Policy: Safinamide (Xadago) Reference Number: CP.CPA.308 Effective Date: Last Review Date: Line of Business: Commercial
 Clinical Policy: Safinamide (Xadago) Reference Number: CP.CPA.308 Effective Date: 05.16.17 Last Review Date: 08.17 Line of Business: Commercial Revision Log See Important Reminder at the end of this policy
Clinical Policy: Safinamide (Xadago) Reference Number: CP.CPA.308 Effective Date: 05.16.17 Last Review Date: 08.17 Line of Business: Commercial Revision Log See Important Reminder at the end of this policy
Patients with disorders of consciousness: how to treat them?
 Patients with disorders of consciousness: how to treat them? Aurore THIBAUT PhD Student Coma Science Group LUCA meeting February 25 th 2015 Pharmacological treatments Amantadine Giacino (2012) 184 TBI
Patients with disorders of consciousness: how to treat them? Aurore THIBAUT PhD Student Coma Science Group LUCA meeting February 25 th 2015 Pharmacological treatments Amantadine Giacino (2012) 184 TBI
Keywords: deep brain stimulation; subthalamic nucleus, subjective visual vertical, adverse reaction
 Re: Cost effectiveness of rasagiline and pramipexole as treatment strategies in early Parkinson's disease in the UK setting: an economic Markov model evaluation Norbert Kovacs 1*, Jozsef Janszky 1, Ferenc
Re: Cost effectiveness of rasagiline and pramipexole as treatment strategies in early Parkinson's disease in the UK setting: an economic Markov model evaluation Norbert Kovacs 1*, Jozsef Janszky 1, Ferenc
Transcranial Brain Stimulation for Treatment of Psychiatric Disorders
 Transcranial Brain Stimulation for Treatment of Psychiatric Disorders Advances in Biological Psychiatry Vol. 23 Series Editors D. Ebert, Freiburg K.P. Ebmeier, Oxford W.F. Gattaz, São Paulo W.P. Kaschka,
Transcranial Brain Stimulation for Treatment of Psychiatric Disorders Advances in Biological Psychiatry Vol. 23 Series Editors D. Ebert, Freiburg K.P. Ebmeier, Oxford W.F. Gattaz, São Paulo W.P. Kaschka,
A practical guide to the use of repetitive transcranial magnetic stimulation in the treatment of depression
 Brain Stimulation (2012) 5, 287 96 www.brainstimjrnl.com A practical guide to the use of repetitive transcranial magnetic stimulation in the treatment of depression Paul B. Fitzgerald, a Zafiris J. Daskalakis
Brain Stimulation (2012) 5, 287 96 www.brainstimjrnl.com A practical guide to the use of repetitive transcranial magnetic stimulation in the treatment of depression Paul B. Fitzgerald, a Zafiris J. Daskalakis
University of Groningen. Negative symptoms of schizophrenia de Lange, Jozarni
 University of Groningen Negative symptoms of schizophrenia de Lange, Jozarni IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check
University of Groningen Negative symptoms of schizophrenia de Lange, Jozarni IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check
Downloaded from:
 Arnup, SJ; Forbes, AB; Kahan, BC; Morgan, KE; McKenzie, JE (2016) The quality of reporting in cluster randomised crossover trials: proposal for reporting items and an assessment of reporting quality. Trials,
Arnup, SJ; Forbes, AB; Kahan, BC; Morgan, KE; McKenzie, JE (2016) The quality of reporting in cluster randomised crossover trials: proposal for reporting items and an assessment of reporting quality. Trials,
Anticholinergics. COMT* Inhibitors. Dopaminergic Agents. Dopamine Agonists. Combination Product
 Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301-1079 Phone 503-945-5220 Fax 503-947-1119 Class Update: Parkinson s Drugs Month/Year of Review:
Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301-1079 Phone 503-945-5220 Fax 503-947-1119 Class Update: Parkinson s Drugs Month/Year of Review:
CENTENE PHARMACY AND THERAPEUTICS NEW DRUG REVIEW 3Q17 July August
 BRAND NAME Xadago GENERIC NAME Safinamide MANUFACTURER Newron Pharmaceuticals SpA holds license; granted approval. US WorldMeds, LLC exclusive licensee and distributor in the U.S. DATE OF APPROVAL March
BRAND NAME Xadago GENERIC NAME Safinamide MANUFACTURER Newron Pharmaceuticals SpA holds license; granted approval. US WorldMeds, LLC exclusive licensee and distributor in the U.S. DATE OF APPROVAL March
INTRODUCTION. Vijay Pathak 1, Vinod Kumar Sinha 2, Samir Kumar Praharaj 3
 Original Article http://dx.doi.org/10.9758/cpn.2015.13.3.245 pissn 1738-1088 / eissn 2093-4327 Clinical Psychopharmacology and Neuroscience 2015;13(3):245-249 Copyrightc 2015, Korean College of Neuropsychopharmacology
Original Article http://dx.doi.org/10.9758/cpn.2015.13.3.245 pissn 1738-1088 / eissn 2093-4327 Clinical Psychopharmacology and Neuroscience 2015;13(3):245-249 Copyrightc 2015, Korean College of Neuropsychopharmacology
Remission From Depression Is Possible
 Remission From Depression Is Possible About Depression Over 350 million people worldwide suffer from depression 1 While medications may help manage symptoms of depression, many patients are not satisfied
Remission From Depression Is Possible About Depression Over 350 million people worldwide suffer from depression 1 While medications may help manage symptoms of depression, many patients are not satisfied
Clinical Applications of tdcs: past, present and future
 Clinical Applications of tdcs: past, present and future Felipe Fregni, MD, PhD, MPH, MMSc, MEd Spaulding Neuromodulation Center Spaulding Rehabilitation Hospital Massachusetts General Hospital Harvard
Clinical Applications of tdcs: past, present and future Felipe Fregni, MD, PhD, MPH, MMSc, MEd Spaulding Neuromodulation Center Spaulding Rehabilitation Hospital Massachusetts General Hospital Harvard
Transcranial Magnetic Stimulation as a Treatment of Depression and Other Psychiatric/Neurologic Disorders Corporate Medical Policy
 Transcranial Magnetic Stimulation as a Treatment of Depression and Other Psychiatric/Neurologic Disorders Corporate Medical Policy File Name: Transcranial Magnetic Stimulation as a Treatment of Depression
Transcranial Magnetic Stimulation as a Treatment of Depression and Other Psychiatric/Neurologic Disorders Corporate Medical Policy File Name: Transcranial Magnetic Stimulation as a Treatment of Depression
Transcranial Direct Current Stimulation (tdcs) A Promising Treatment for Depression?
 Transcranial Direct Current Stimulation (tdcs) A Promising Treatment for Depression? transcranial Direct Current Stimulation (tdcs) Alternating current (AC) 1-3 ma, 9V Direct Current (DC) Direct current:
Transcranial Direct Current Stimulation (tdcs) A Promising Treatment for Depression? transcranial Direct Current Stimulation (tdcs) Alternating current (AC) 1-3 ma, 9V Direct Current (DC) Direct current:
Transcranial Magnetic Stimulation and Cranial Electrical Stimulation (CES) as a Treatment of Depression and Other Psychiatric/Neurologic Disorders
 Transcranial Magnetic Stimulation and Cranial Electrical Stimulation (CES) as a Treatment of Depression and Other Psychiatric/Neurologic Disorders Policy Number: 2.01.50 Last Review: 10/2017 Origination:
Transcranial Magnetic Stimulation and Cranial Electrical Stimulation (CES) as a Treatment of Depression and Other Psychiatric/Neurologic Disorders Policy Number: 2.01.50 Last Review: 10/2017 Origination:
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Transcranial Magnetic Stimulation (TMS) Page 1 of 24 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: See also: Transcranial Magnetic Stimulation (TMS) Vagus Nerve
Transcranial Magnetic Stimulation (TMS) Page 1 of 24 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: See also: Transcranial Magnetic Stimulation (TMS) Vagus Nerve
ORIGINAL CONTRIBUTION
 ORIGINAL CONTRIBUTION Common Misdiagnosis of a Common Neurological Disorder How Are We Misdiagnosing Essential Tremor? Samay Jain, MD; Steven E. Lo, MD; Elan D. Louis, MD, MS Background: As a common neurological
ORIGINAL CONTRIBUTION Common Misdiagnosis of a Common Neurological Disorder How Are We Misdiagnosing Essential Tremor? Samay Jain, MD; Steven E. Lo, MD; Elan D. Louis, MD, MS Background: As a common neurological
Neuromodulation and Non- Pharmacological Approaches
 Multimodal approaches to pain management and potential synergies Neuromodulation and Non- Pharmacological Approaches Richard Wilson, MD Director, Division of Neurologic Rehabilitation MetroHealth Rehabilitation
Multimodal approaches to pain management and potential synergies Neuromodulation and Non- Pharmacological Approaches Richard Wilson, MD Director, Division of Neurologic Rehabilitation MetroHealth Rehabilitation
Deep transcranial magnetic stimulation add-on for treatment of negative symptoms and cognitive deficits of schizophrenia: a feasibility study
 International Journal of Neuropsychopharmacology (2011), 14, 991 996. f CINP 2011 doi:10.1017/s1461145711000642 Deep transcranial magnetic stimulation add-on for treatment of negative symptoms and cognitive
International Journal of Neuropsychopharmacology (2011), 14, 991 996. f CINP 2011 doi:10.1017/s1461145711000642 Deep transcranial magnetic stimulation add-on for treatment of negative symptoms and cognitive
Objectives. APNA 27th Annual Conference Session 1021: October 9, Brain Stimulation Techniques. Rosedale, Ecklesdafer, Kormos, Freedland, Knapp 1
 The Significant Promise of Therapeutic Neuromodulation: Implications for Psychiatric Mental (PMH) Health Nursing Mary Rosedale PhD, PMHNP BC Donna Ecklesdafer, MSN, RN Theresa Kormos, MSN, PMHCNS BC Michelle
The Significant Promise of Therapeutic Neuromodulation: Implications for Psychiatric Mental (PMH) Health Nursing Mary Rosedale PhD, PMHNP BC Donna Ecklesdafer, MSN, RN Theresa Kormos, MSN, PMHCNS BC Michelle
TREATMENT-SPECIFIC ABNORMAL SYNAPTIC PLASTICITY IN EARLY PARKINSON S DISEASE
 TREATMENT-SPECIFIC ABNORMAL SYNAPTIC PLASTICITY IN EARLY PARKINSON S DISEASE Angel Lago-Rodriguez 1, Binith Cheeran 2 and Miguel Fernández-Del-Olmo 3 1. Prism Lab, Behavioural Brain Sciences, School of
TREATMENT-SPECIFIC ABNORMAL SYNAPTIC PLASTICITY IN EARLY PARKINSON S DISEASE Angel Lago-Rodriguez 1, Binith Cheeran 2 and Miguel Fernández-Del-Olmo 3 1. Prism Lab, Behavioural Brain Sciences, School of
Interventions for Relapsing Depression: TMS, ECT, and Ketamine
 Interventions for Relapsing Depression: TMS, ECT, and Ketamine MDD top cause of disability; suicide only top-10 cause of death currently increasing. 10-15% lifetime prevalence A third of patients do not
Interventions for Relapsing Depression: TMS, ECT, and Ketamine MDD top cause of disability; suicide only top-10 cause of death currently increasing. 10-15% lifetime prevalence A third of patients do not
The effectiveness of transcranial direct current stimulation on ambulation in persons with Parkinson s Disease: A Systematic Review
 The effectiveness of transcranial direct current stimulation on ambulation in persons with Parkinson s Disease: A Systematic Review Caitlin Liberatore, SPT Melissa McEnroe, SPT Brian Esterle, SPT Lindsay
The effectiveness of transcranial direct current stimulation on ambulation in persons with Parkinson s Disease: A Systematic Review Caitlin Liberatore, SPT Melissa McEnroe, SPT Brian Esterle, SPT Lindsay
