journals/eano/index.html Homepage: Online Database Featuring Author, Key Word and Full-Text Search
|
|
|
- Emmeline Wheeler
- 5 years ago
- Views:
Transcription
1 Volume 3 (2013) // Issue 2 // e-issn Neurology Neurosurgery Medical Oncology Radiotherapy Paediatric Neurooncology Neuropathology Neuroradiology Neuroimaging Nursing Patient Issues Journey of Intraoperative Magnetic Resonance Imaging into Daily Use: A Review Scherer M, Jungk C, Unterberg AW European Association of NeuroOncology Magazine 2013; 3 (2) Homepage: journals/eano/index.html Online Database Featuring Author, Key Word and Full-Text Search Member of the THE EUROPEAN ASSOCIATION OF NEUROONCOLOGY Indexed in EMBASE
2 Journey of Intraoperative Magnetic Resonance Imaging into Daily Use: A Review Moritz Scherer, Christine Jungk, Andreas Unterberg Abstract: The introduction of intraoperative MRI (imri) for resection guidance was a milestone of technical innovation in neurosurgery more than a decade ago. Based on the general opinion that more radical and preferably complete tumour resection leads to significantly longer survival of glioma patients, advantages of this method have become increasingly evident ever since. imri appears to be the most effective way to safely extend tumour resections and precisely delineate tumour boundaries in both highand low-grade tumours. This review covers recent literature illustrating the contribution of imri to more radical tumour resections and underscores why bringing this method into daily routine of glioma surgery was only a logical consequence. EANO Mag 2013; 3 (2): Key words: glioma surgery, extent of resection, patient survival, intraoperative magnetic resonance imaging, volumetric analysis Introduction Alongside adjuvant radio- and chemotherapy, surgery remains a mainstay in the treatment of patients with intracranial gliomas. Similar to recent advances in the field of neuro-oncology, resection techniques of intracranial gliomas have undergone many changes in the past decades. New technological developments range from microneurosurgery and multimodal neuro-navigation to routine implementation of highfield MRI scanners for intraoperative resection control in latest history. All these advances provide assistance to the operating surgeon, ensuring removal of as much tumour tissue as possible without causing any additional neurologic squalor. The contribution of intraoperative MRI imaging (imri) to maximized tumour resection, patient safety, and outcome has been subject of many studies since the first appearance of this method in the late 1990s. Following a controversial debate, maximum extended safe tumour resection has been proven to harbour significant survival benefits for glioma patients. The role of imri is to guide such maximum extended safe tumour resection and its unprecedented precision in delineating tumour borders has become evident in recent research. Regardless of its clinical benefits, high costs and manpower requirements still pose heavy limitations to widespread availability of imri which makes this method subject to economical and ethical considerations. This review outlines the significance of maximum extended safe tumour resection in present-day multidisciplinary glioma treatment, explains how imri can provide substantial decision guidance to the operating surgeon, and demonstrates how such a sophisticated method can be implemented into the daily routine of neurosurgical procedures. Received on January 15, 2013; accepted on January 16, 2013; Pre-Publishing Online on February 12, 2013 From the Department of Neurosurgery, Heidelberg University Hospital, Germany Correspondence to: Moritz Scherer, MD, Department of Neurosurgery, Heidelberg University Hospital, Im Neuenheimer Feld 400, Heidelberg, Germany; . moritz.scherer@med.uni-heidelberg.de Benefit of Extended Tumour Resections for Patient Prognosis Diagnosed with an intracranial mass lesion, patients need confirmation of histological diagnosis in order to receive adequate and specific therapy. Treatment guidelines for intracranial tumours explicitly recommend that tissue specimens be obtained before commencement of radio- or chemotherapy. In case of intracranial gliomas, the least surgery can offer is to provide the histological diagnosis required for further adjuvant therapies. Beyond that, maximum extensive safe surgery is increasingly accepted as an independent, positive, prognostic factor [1]. In recent years, routine acquisition of early post-resection MRI scans within hrs after surgery has provided the opportunity to evaluate the correlation between the extent of resection (EOR) and different outcome measures. Among the many studies dedicated to this matter, heterogeneity of data and patient samples is huge. Up-to-date, large, randomized, controlled trials evaluating the value of maximized resection vs partial resections are lacking and ethically debatable. Many conclusions are drawn from subgroup analyses based on patient data acquired in another context. Additionally, retrospectively designed and single-centre reports are unfortunately subject to a biased patient sample regarding age, overall performance, imaging modalities, or adjuvant therapy regimens. Nevertheless, there is a growing body of evidence supporting the pursuit of maximized safe resection in the treatment of intracranial gliomas. In case of high-grade gliomas (HGG), besides yielding a histological diagnosis surgery is also performed to relieve symptoms caused by the rapidly growing tumour mass and brain oedema. Due to the inevitable tumour invasion into healthy brain parenchyma, it is obviously never possible to remove all tumour cells but rather important to achieve substantial relief from tumour burden in terms of gross total resection (GTR, ie no residual contrast enhancement [CE] on post-resection scan). As opposed to subtotal or partial resection of the tumour (STR or PR, nodular or solid CE residual, respectively), GTR has been shown in various studies to have significant impact on patient survival. Besides known prognostic factors EUR ASSOC NEUROONCOL MAG 2013; 3 (2) For personal use only. Not to be reproduced without permission of Krause & Pachernegg GmbH. 61
3 Table 1. Increase of EOR in all cases where resection was continued after an intraoperative MRI scan. Author, Year [Ref] Cases (n) WHO grade imri EOR (%) Final EOR (%) ± (%) p Nimsky et al, 2004 [20] 17 I IV 88.6 ± ± < 0.01 Schneider et al, 2005 [21] 31 IV NC Hatiboglu et al, 2009 [19] 21 I IV 76 (35 97) 96 (48 100) +20 < Kuhnt et al, 2011 [22] 76 I IV ± ± < 0.01 Scherer et al, I IV 90.1 ± ± NC (unpublished data) NC: not calculated Table 2. Rates of successfully reached, predefined resection goals after a first imri scan, a postoperative scan, and the incidence of ongoing resections. Author, Cases WHO Predefined Success Success OP Ongoing p Year [Ref] (n) grade goal after 1 st on post- resection imri (%) MRI (%) (%) Knauth et al, 1999 [24] 38 III IV GTR Nimsky et al, 2004 [20] 47 I IV GTR/IR < for IR Hatiboglu et al, 2009 [19] 44 I IV GTR/IR NC Kuhnt et al, 2011 [22] 293 I IV GTR/IR NC Senft et al, 2011 [18] 24 (IV) GTR NC Scherer et al, I IV GTR/IR NC (unpublished data) GTR: gross total resection; IR: incomplete resection; HGG: high-grade glioma; NC: not calculated such as age and Karnofsky performance status (KPS), GTR has been shown to be another independent positive prognostic factor in HGG [1 8]. To our knowledge, evidence of the highest available quality can be derived from a German multicentre, randomized, controlled trial by Stummer et al that compares 5-aminolevulinic acid (5-ALA) fluorescenceguided with conventional white-light HGG resections [9]. In a balanced re-stratification for resection extent, all patients who underwent GTR experienced prolongation of overall survival compared to incompletely resected patients (16.7 vs 11.8 months, respectively; p < ) [1, 7]. In addition, another high-volume series of McGirt et al evaluated 1250 patients harbouring a high-grade glioma and found a survival benefit up to 5 months when comparing GTR to PR (13 vs 8 months, respectively) [8]. These results were adjusted for factors with known association to survival such as age, KPS, or adjuvant therapies. Sanai et al present a thorough analysis of the current literature with a focus on precise calculation of EOR and clear statistical measures. They report a statistically significant beneficial effect from maximized EOR in 16/28 HGG studies [6]. Although prognosis in HGG remains poor, these recent results should be valued as encouraging. We see the impact of extended safe resection upon overall survival in glioblastoma alongside with the beneficial effects of concomitant radio-chemotherapy as reported by Stupp et al in 2005, formerly offering a median 2.5-month longer survival compared to previous standard treatment [10]. Even though this study did not include mandatory postoperative imaging and EOR was partly assessed by means of inaccurate estimation of the operating surgeon, in a post-hoc data analysis by Gorlia et al EOR was shown to have a significant impact on patient survival. Building on this and remembering that 5- ALA data was acquired before the implementation of concomitant adjuvant radiochemotherapy, supplemental effects should be expected when both approaches are combined. Maximized safe resection followed by an individualized, targeted therapy is expected to further prolong overall survival for patients with HGG in the future [11]. Low-grade glioma (LGG) patients often show mild to nil clinical symptoms but eventual malignant tumour progression will aggravate symptoms and reduce life expectancy. As most of WHO I and II tumours are not easily amenable for radioor chemotherapy due to their slow cell proliferation compared to their high-grade counterparts, watch-and-wait regimens are still applied after biopsy until a definite therapy is initiated [12]. To date, this approach should be questioned when surgery alternately can safely remove the tumour, diminishing the risk of malignant transformation or occurrence of neurologic symptoms or seizures. Besides, even small and deeply located lesions can be safely approached with today s techniques so that factors complicating surgery such as growth, malignant transformation, and tumour infiltration can be anticipated instead. The literature provides support for radical surgery in supratentorial LGG amenable for safe resection as the treatment of choice [13, 14]. Even though formal quality of evidence is weak, a systematic review of Sanai et al quotes 9/10 selected LGG studies as being in favour of extensive resection of LGG lesions. In uni- and multivariate analyses, EOR was revealed to be a significant positive prognosticator in 7 of these studies [6]. Even in case of tumour recurrence, Ahmadi et al could show a clearly beneficial effect of more radical surgery in terms of time to malignant progression and overall survival [15]. 62 EUR ASSOC NEUROONCOL MAG 2013; 3 (2)
4 imri for Intraoperative Resection Control Accurate delineation of tumour and normal brain parenchyma remains one of the major challenges in glioma surgery. In recent years, many technical advancements have been developed to assist the surgeon in locating and precisely confining brain tumours. Alongside with multimodal neuronavigation, intraoperative ultrasound, and 5-ALA in glioblastomas, intraoperative MRI acquisition is used in a growing number of centres for tumour resection control. Initial evaluation following the introduction of this method quickly showed beneficial effects of imri in glioma surgery. Reports of increased EOR and improved patient prognosis have accumulated over recent years and other advantages such as compensation for brainshift phenomena through intraoperative update of neuronavigation have been pointed out [16]. Moreover, surgeons have been exposed to commonly overestimate their own resection extent, which strengthens the call for routine intraoperative resection guidance based on the given correlation between resection radicality and patient prognosis [17]. In HGG, imri resection control is often compared to fluorescence-guided resection with 5-ALA, which has been shown to lead to more frequent GTR compared to white-light surgery. To corroborate the contribution of imri to a more radical EOR, a bundle of retrospective studies and cohort analyses have been published. Following the design of the 5-ALA study, Senft et al recently conducted a randomized controlled trial to further elucidate the use of imri. In their cohort of 49 HGG cases scheduled for total tumour resection, randomization assigned patients either to receive low-field imriguided or conventional microneurosurgical extirpation of the tumour. In the imri resection group, this surgical goal was achieved in 96 % of cases compared to only 68 % in the conventional group (23 vs 17 of 49 patients, respectively) [18]. Adding up to other likeminded results, this study for the first time validated the gain of imri resection control in a randomized controlled fashion. For HGG resections, imri-guided surgery leads to a higher frequency of GTR at least comparable to results achieved using 5-ALA fluorescence. In LGG, only intraoperative ultrasound (ius) can help as an alternate imaging modality during surgery. High-field imri scanners are of special value in LGG surgery since they offer high anatomical resolution along with full-scale diagnostic capability. Sharp T2 and FLAIR sequences, MR-spectroscopy, and diffusion-weighted imaging (DWI) contribute greatly to a precise delineation of residual non-enhancing intracranial lesions. So far, there are only few retrospective studies available evaluating LGG outcomes after imri-guided resection. A group from the Brigham and Women s Hospital in Boston compared long-term results derived from their imri-guided LGG resections to results from a national registry. Their central finding was a significant reduction of 1-, 2-, and 5-year age- and histology-adjusted death rates compared to the national registry when imri was used for resection guidance (1.9 % [95-% CI: %], 3.6 % [95-% CI: %], and 17.6 % [95-% CI: %], respectively). Stratifying for total and subtotal LGG tumour removal, a 1.4 times higher risk of recurrence (95-% CI: ) and a 4.9 times higher risk of death (95-% CI: ) was apparent when lesions were only removed subtotally [14]. These tendencies suggest a correlation between imri-guided extent of resection and longer patient survival also in low-grade tumours. But again formal evidence is weak, with the non-homogeneity of data and study groups impeding final conclusions until results are confirmed in larger, randomized, matched or other controlled populations. Regarding EOR, volumetric analysis did also quantify the increased amount of tumour that could be removed by means of imri in some studies (Table 1). EOR could be increased from a median 76 % to 96 % in one series, and residual tumour fractions could be reduced from 21.4 ± 13.8 to 6.9 ± 10.3 % in another series across all WHO grades [19, 20]. Accordingly, Kuhnt et al and Schneider et al showed an increase in EOR from % and 69.3 % at the point where MRI was performed intraoperatively to a final EOR of approximately 85 % on postoperative MRI scans [21, 23]. A preliminary analysis of our own prospective volumetric imri data has yielded similar results. In 101 analyzed patients operated under imri guidance in 2011, EOR was increased from 90.1 % ± 15.6 % on intraoperative images to a final EOR of 99.8 % ± 0.8 % (Scherer et al, unpublished data, 2012). In all of these studies, up to 20 % of the overall tumour resection was not performed until after an imri scan confirmed tumour remnants. To deduct an increased extent of resection solely from the intraoperative use of imri would be much of a hasty reaction. Since surgeons were aware of the feasibility of imri right from the beginning of surgery, this possibility biased the decision of when to do the first intraoperative scan and led to a more defensive resection strategy in those studies. Accordingly, the absolute values of EOR increase after imri partly represent the surgeon s uncertainty in tumour delineation or the difficulty of surgery rather than the direct contribution of imri to more radical tumour surgery. Rates of continued surgery after intraoperative resection control by means of imri are another interesting aspect when assessing the value of this intraoperative imaging modality. Among the imri studies presented here (Table 2), 21 out of 44 patients (47 %) [19] and 17 out of 47 patients (36 %) [20], respectively, underwent further tumour resection after imri resection control. Another report by Kuhnt et al states a 26-% incidence of additional resections after the first intraoperative scan. Referring to our own data analyzing the routine use of imri guidance for all glioma resections at our department, we observed high frequencies of ongoing resections beyond all WHO grades. In total, 71 of 101 (70.3 %) cases received additional tumour resection after imri with even higher rates for WHO II and III tumours (Scherer et al, unpublished data, 2012). In their randomized controlled cohort of WHO IV tumours, Senft et al reported additional tumour resection in 1/3 of cases of imri application, leading to successful accomplishment of GTR in all of these patients. In their conclusion, imri was accountable for rhe 30-% increase in complete resections and it was evident that without its use neither group would have differed significantly from the other [18, 23]. EUR ASSOC NEUROONCOL MAG 2013; 3 (2) 63
5 Table 3. Postoperative neurological deficits (visual, motor, language) after imri-guided surgery, permanent deficits at > 4 months after surgery. Author, Year [Ref] Postoperative Permanent Deficits deficits (%) Further No further resections resections after imri (%) after imri (%) Schneider et al, [21] Hatiboglu et al, [19] Kuhnt et al, [22] Senft et al, [18] Table 4. Outcome of patients operated under imri guidance with respect to the EOR. Data presented as difference in median survival times. Author, Year [Ref] Survival Resection ± (months) p Wirtz et al, OS GTR vs IR [25] Schneider et al, OS GTR vs IR [21] Kuhnt et al, OS GTR vs IR [22] Senft et al, PFS GTR vs IR [18] GTR: gross total resection; IR: incomplete resection; OS: overall survival; PFS: progression-free survival While these questions concern rather technical aspects of imri-guided surgery, it is important to focus on the true goal of surgery, which is to achieve maximized safe tumour resection in order to prolong patient survival. Among all imri studies that have documented their cases with respect to the preoperatively defined resection goal it becomes evident that this surgical goal can be attained in a vast majority of cases where imri was used (Table 2). While the predefined goal was already reached in % of cases when a first imri was performed, continued resections after imri led to eventual success in up to 100 % of cases. This implicates that independently from other available modalities for resection control imri is a convincingly precise and efficient way to push resection boundaries and achieve the goal of surgery in an overwhelming majority of tumour resections across all WHO grades. Most importantly, imri-guided extended resection radicality was not achieved at the cost of any increased morbidity. Neither did the randomized study of Senft et al show a significant accumulation of deficits when comparing the imri with the white-light group (3 vs 2 permanent deficits; 13 % vs 8 %, respectively), nor did Kuhnt et al observe any aggravation of motor or speech deficits when comparing their cohort of additionally resected tumours with those resections terminated after an imri resection control (7.7 % vs 12.5 % accumulated morbidity at discharge, respectively; Table 3). As mentioned earlier, prolonged survival after extended glioma surgery has been reported many times in general. Some studies have also directly addressed the contribution of imri-guided extended tumour resection upon patient overall survival [18, 21, 22, 25 27]. Among the HGG series, Kuhnt et al present a series including 135 glioblastoma patients operated using 1.5 T high-field imri guidance. EOR > 98 % and age < 65 were independent positive prognosticators leading to a 5-month longer overall survival when more radical surgery could be achieved (14 months [95-% CI: ] vs 9 months [95-% CI: ]) for EOR > 98 % and < 98 %, respectively (p < ) [22]. Results from other cohorts point in the same direction with a longer overall or progression-free survival after complete vs incomplete tumour resection (Table 4). Comparable to 5-ALA data, beneficial effects of extended surgical radicality have thus been observed independently of the technique used for resection guidance in HGG. In their review, Kubben et al attempted not only to examine the benefit on survival but also to evaluate clinical performance and quality of life before and after imri-guided surgery. Focusing on precise EOR calculation, detailed reports of quality of life, and long-term documentation of patient survival, 12 non-randomized cohort studies out of 682 published studies from 1999 until 2010 were selected. Even though all included studies showed increased overall EORs, reliable data on the quality of life or prolonged survival was sparse. Only 3/12 studies included patient follow-up, each showing significantly longer median survival times. Another 3/12 studies evaluated clinical performance but failed to show a correlation to extended tumour resections. Data concerning quality of life after surgery was not provided by any study [28]. Performance scores are often documented before surgery in order to identify the calculated status as an outcome predictor; postoperative performance status, however, often remains elusive. Although a slight reduction in KPS within 2 weeks after surgery has been reported by Mehdorn et al, yet the value of this finding is unclear due to unbalanced and selected cohorts in this study [27]. So, apart from focal motor or speech deficits, the question of how patients are doing shortly after extended glioma surgery and during their assumedly longer survival has remained mostly unanswered. Although not truly online, like intraoperative ultrasound (ius) and 5-ALA, intraoperatively acquired MR imaging can reliably help the surgeon to delineate tumour tissue from healthy brain parenchyma. Especially in areas that are hard to explore with US or fluorescent light, imri might be superior in detecting residual tumour. Likewise, in LGG or anaplastic gliomas, where 5-ALA shows no or only weaker detection rates, imri has full distinction power leading to a greater EOR across all tumour entities without adding any specific neurologic morbidity. Spatial precision of tumour delineation of imri combined with multimodal neuronavigation is unprecedented. This offers the chance not only to enhance complete tumour resections but also to guide partial resections with borders close to eloquent areas, limiting resection extent precisely to only harmless tumour parts. Compared to any other intraoperative imaging modality imri enables the sur- 64 EUR ASSOC NEUROONCOL MAG 2013; 3 (2)
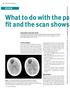
6 Figure year-old male with seizures diagnosed with a WHO II astrocytoma by stereotactic biopsy. Complete tumour resection was scheduled. (A) Preoperative definition of target tumour volume of cm3 on T2 FLAIR images. (B) On the first imri, a 1.92-cm 3 residual tumour is detected at the ventral aspect of the resection cavity on sharp FLAIR images. (C) Postoperative MRI shows no signs of tumour remnants. imri guidance led to a fully successful procedure with no added neurologic morbidity. geon to achieve the seemingly contradictory goal of extending radicality while improving safety. In summary, the literature shows clear benefits from improved imri-guided resection radicality such as lower risk of recurrence, longer progression-free survival, lower 1 5-year death rates (LGG), and longer overall survival (HGG). However, formal evidence for this knowledge is still lacking. Due to inconsistency of data acquisition and presentation, mixed patient populations, and other technical limitations such as different measurements of EOR or MRI field strengths it has so far been virtually impossible to elaborate a clear meta-analysis of existing studies dealing with this topic. As further randomized controlled trials evaluating the extent of resection and its effect on survival are ethically debatable from our current state of knowledge, well-designed, prospective, observa- tional studies might be the only way to underscore the importance and benefit from more radical surgery for the treatment of intracranial gliomas in the future. Precise and prospectively addressed definitions of surgical goals (GTR, no residual contrast enhancement, vs PR, residual contrast enhancement), routine postoperative imaging hrs after surgery and volumetric documentation of resection extent should be the least common ground for future data collections. This welldefined baseline data will help to merge knowledge in the field and to present high-volume multicentre series providing age- and histology-adjusted estimates of survival rates with respect to the achieved EOR. Beyond technical aspects, future studies also have to focus on clinical performance and quality of life along with survival benefits in order to give sustainable answers to the questions evolving around the use of imri in glioma surgery. EUR ASSOC NEUROONCOL MAG 2013; 3 (2) 65
7 Feasibility of Routine imri: Implementation into Daily Surgery Since acquisition and maintenance costs are still a substantial drag to a greater prevalence of imri units in hospitals today, it is important to take into account all therapeutic indications and their benefits for patients to justify their establishment. High-field imri machines offer the full range of diagnostic sequences and high anatomical resolution. Accordingly, imri imaging can also assist in stereotactic biopsies, placement of catheters, or deep-brain stimulating electrodes and, lastly, transsphenoidal resections of pituitary tumours. From an economical point of view, frequent utilization of an imri promotes a faster return of initial investments while cutting maintenance costs at the same time. Hence, frequent and effective use of an imri unit will serve both medicine and management. Routine implementation of an imri into daily surgical routine can only be accomplished under certain conditions. Patient safety has to be given top priority, which can easily be jeopardized by a strong magnetic field within an operating room (OR). Among different imri-suite set-ups, instead of placing the imri scanner in the OR itself, in our opinion a 2- room solution has obvious advantages for routine daily use. Our set-up in Heidelberg, where the patient is transported into the imri next door, allows us to perform regular surgery without any relevant limitations with regard to positioning or surgical instruments. Moreover, this set-up allows us to use the imri unit from 2 ORs, fostering efficient multiple daily use for various indications. Besides, separating the magnet from the OR is a relevant safety aspect, especially when the OR is used for cases where imri will not be used. Regardless of the imri set-up, dedicated standards of imri procedures and vigorous staff training are inevitable. On the one hand, standardized work-flows warrant patient safety while on the other hand, a straightforward imri procedure with reduced transfer times also contributes to efficient use of OR and labour time. In Heidelberg, routine use of imri began when a new 1.5 T magnet was installed in June Since then, more than 670 surgical procedures have been performed using imri guidance. In our institution, all intracranial gliomas eligible for GTR are scheduled to undergo surgery with imri guidance. Whenever applicable, partial tumour resections are planned to be operated with imri resection control in order to safely increase radicality in these patients as well. In 2011, we initiated a prospective collection of our imriguided glioma resections in a volumetric database. Intended extent of tumour resection, imri residual tumour volumes, and postoperative tumour volumes are documented along with other patient parameters. An illustrative case demonstrating our routine procedures and volumetric documentation is shown in Figure 1 and some of our preliminary data, as mentioned above, is presented in Tables 1 and 2. Implementing imri into routine glioma surgery certainly causes challenges and will most likely affect the strategic approach to a tumour as well as the manner of surgery itself. As a consequence of routine imri use in glioma surgery one might expect the frequency of post-imri resections to increase over time, together with residual tumour volumes seen in a first intraoperative scan. This would resemble a more defensive surgical strategy in the first place. A preliminary analysis of our data seems to confirm this hypothesis with continued tumour resections performed after imri scans in almost 2 /3 of all patients. It might also be interesting to follow learning curves of young neurosurgeons over their time of training since imri provides immediate feedback on the resection progress. By means of this prospective single-institution database of unselected glioma cases, we hope to be able to address unanswered questions and confirm beneficial effects of imri surgery for glioma patients in the future. A newly formed German imri study group will further pursue this approach and try to derive a similar multi-centre database in order to merge data and produce solid evidence fostering the use and prevalence of imri in neurosurgery. Conflict of Interest The authors state that no conflict of interest exists. References: 1. Stummer W, van den Bent MJ, Westphal M. Cytoreductive surgery of glioblastoma as the key to successful adjuvant therapies: new arguments in an old discussion. Acta Neurochir 2011; 153: Ewelt C, Floeth FW, Felsberg J, et al. Finding the anaplastic focus in diffuse gliomas: the value of Gd-DTPA enhanced MRI, FET- PET, and intraoperative, ALA-derived tissue fluorescence. Clin Neurol Neurosurg 2011; 113: Keles GE, Anderson B, Berger MS. The effect of extent of resection on time to tumor progression and survival in patients with glioblastoma multiforme of the cerebral hemisphere. Surg Neurol 1999; 52: Lacroix M, Abi-Said D, Fourney DR, et al. A multivariate analysis of 416 patients with glioblastoma multiforme: prognosis, extent of resection, and survival. J Neurosurg 2001; 95: Laws ER, Parney IF, Huang W, et al. Survival following surgery and prognostic factors for recently diagnosed malignant glioma: data from the Glioma Outcomes Project. J Neurosurg 2003; 99: Sanai N, Berger MS. Glioma extent of resection and its impact on patient outcome. Neurosurgery 2008; 62: Stummer W, Tonn JC, Mehdorn HM, et al. Counterbalancing risks and gains from extended resections in malignant glioma surgery: a supplemental analysis from the randomized 5-aminolevulinic acid glioma resection study. Clinical article. J Neurosurg 2011; 114: McGirt MJ, Chaichana KL, Gathinji M, et al. Independent association of extent of resection with survival in patients with malignant brain astrocytoma. J Neurosurg 2009; 110: Stummer W, Pichlmeier U, Meinel T, et al. Fluorescence-guided surgery with 5-aminolevulinic acid for resection of malignant glioma: a randomised controlled multicentre phase III trial. Lancet Oncol 2006; 7: Stupp R, Mason WP, van den Bent MJ, et al. Radiotherapy plus concomitant and adjuvant temozolomide for glioblastoma. N Engl J Med 2005; 352: Gorlia T, van den Bent MJ, Hegi ME, et al. Nomograms for predicting survival of patients with newly diagnosed glioblastoma: prognostic factor analysis of EORTC and NCIC trial /CE.3. Lancet Oncol 2008; 9: Jakola AS, Myrmel KS, Kloster R, et al. Comparison of a strategy favoring early surgical resection vs a strategy favoring watchful waiting in low-grade gliomas. JAMA 2012; 308: Keles GE, Lamborn KR, Berger MS. Lowgrade hemispheric gliomas in adults: a critical review of extent of resection as a factor influencing outcome. J Neurosurg 2001; 95: Claus EB, Horlacher A, Hsu L, et al. Survival rates in patients with low-grade glioma after intraoperative magnetic resonance image guidance. Cancer 2005; 103: Ahmadi R, Dictus C, Hartmann C, et al. Long-term outcome and survival of surgically treated supratentorial low-grade glioma in adult patients. Acta Neurochir (Wien) 2009; 151: Wirtz CR, Bonsanto MM, Knauth M, et al. Intraoperative magnetic resonance imaging to update interactive navigation in neurosurgery: method and preliminary experience. Comput Aided Surg 1997; 2: Albert FK, Forsting M, Sartor K, et al. Early postoperative magnetic resonance imaging after resection of malignant glioma: objective evaluation of residual tumor and its influence on regrowth and prognosis. Neurosurgery 1994; 34: Senft C, Bink A, Franz K, et al. Intraoperative MRI guidance and extent of resection in glioma surgery: a randomised, controlled trial. Lancet Oncol 2011; 12: Hatiboglu MA, Weinberg JS, Suki D, et al. Impact of intraoperative high-field magnetic resonance imaging guidance on glioma surgery: a prospective volumetric analysis. Neurosurgery 2009; 64: Nimsky C, Fujita A, Ganslandt O, et al. Volumetric assessment of glioma removal 66 EUR ASSOC NEUROONCOL MAG 2013; 3 (2)
8 by intraoperative high-field magnetic resonance imaging. Neurosurgery 2004; 55: Schneider JP, Trantakis C, Rubach M, et al. Intraoperative MRI to guide the resection of primary supratentorial glioblastoma multiforme a quantitative radiological analysis. Neuroradiology 2005; 47: Kuhnt D, Becker A, Ganslandt O, et al. Correlation of the extent of tumor volume resection and patient survival in surgery of glioblastoma multiforme with high-field intraoperative MRI guidance. Neuro Oncol 2011; 13: Kuhnt D, Ganslandt O, Schlaffer SM, et al. Quantification of glioma removal by intraoperative high-field magnetic resonance imaging an update. Neurosurgery 2011; 69: Knauth M, Wirtz CR, Tronnier VM, et al. Intraoperative MR imaging increases the extent of tumor resection in patients with high-grade gliomas. AJNR Am J Neuroradiol 1999; 20: Wirtz CR, Knauth M, Staubert A, et al. Clinical evaluation and follow-up results for intraoperative magnetic resonance imaging in neurosurgery. Neurosurgery 2000; 46: Hirschberg H, Samset E, Hol PK, et al. Impact of intraoperative MRI on the surgical results for high-grade gliomas. Minim Invasive Neurosurg 2005; 48: Mehdorn HM, Schwartz F, Dawirs S, et al. High-field imri in glioblastoma surgery: improvement of resection radicality and survival for the patient? Acta Neurochir Suppl 2011; 109: Kubben PL, Ter Meulen KJ, Schijns OE, et al. Intraoperative MRI-guided resection of glioblastoma multiforme: a systematic review. Lancet Oncol 2011; 12: EUR ASSOC NEUROONCOL MAG 2013; 3 (2) 67
See the corresponding editorial in this issue, pp 1 2. J Neurosurg 115:3 8, An extent of resection threshold for newly diagnosed glioblastomas
 See the corresponding editorial in this issue, pp 1 2. J Neurosurg 115:3 8, 2011 An extent of resection threshold for newly diagnosed glioblastomas Clinical article Nader Sanai, M.D., 1 Mei-Yin Polley,
See the corresponding editorial in this issue, pp 1 2. J Neurosurg 115:3 8, 2011 An extent of resection threshold for newly diagnosed glioblastomas Clinical article Nader Sanai, M.D., 1 Mei-Yin Polley,
Scottish Medicines Consortium
 Scottish Medicines Consortium temozolomide 5, 20, 100 and 250mg capsules (Temodal ) Schering Plough UK Ltd No. (244/06) New indication: for the treatment of newly diagnosed glioblastoma multiforme concomitantly
Scottish Medicines Consortium temozolomide 5, 20, 100 and 250mg capsules (Temodal ) Schering Plough UK Ltd No. (244/06) New indication: for the treatment of newly diagnosed glioblastoma multiforme concomitantly
Low grade glioma: a journey towards a cure
 Editorial Page 1 of 5 Low grade glioma: a journey towards a cure Ali K. Choucair SIU School of Medicine, Springfield, IL, USA Correspondence to: Ali K. Choucair, MD. Professor of Neurology, Director of
Editorial Page 1 of 5 Low grade glioma: a journey towards a cure Ali K. Choucair SIU School of Medicine, Springfield, IL, USA Correspondence to: Ali K. Choucair, MD. Professor of Neurology, Director of
성균관대학교삼성창원병원신경외과학교실신경종양학 김영준. KNS-MT-03 (April 15, 2015)
 성균관대학교삼성창원병원신경외과학교실신경종양학 김영준 INTRODUCTIONS Low grade gliomas (LGG) - heterogeneous group of tumors with astrocytic, oligodendroglial, ependymal, or mixed cellular histology - In adults diffuse, infiltrating
성균관대학교삼성창원병원신경외과학교실신경종양학 김영준 INTRODUCTIONS Low grade gliomas (LGG) - heterogeneous group of tumors with astrocytic, oligodendroglial, ependymal, or mixed cellular histology - In adults diffuse, infiltrating
CURRICULUM VITAE Prof. Dr. med. Walter Stummer
 CURRICULUM VITAE Prof. Dr. med. Walter Stummer Date of birth: April 19, 1964, in Düsseldorf, Germany Medical education: 1984-91: Medical School, Ludwig-Maximilians-University, Munich 1988-90: Doctoral
CURRICULUM VITAE Prof. Dr. med. Walter Stummer Date of birth: April 19, 1964, in Düsseldorf, Germany Medical education: 1984-91: Medical School, Ludwig-Maximilians-University, Munich 1988-90: Doctoral
Concepts for a personalized neurosurgical oncology. XXIV Annual Conference Pietro Paoletti 27. November 2015
 Concepts for a personalized neurosurgical oncology Jörg-Christian Tonn Dept. of Neurosurgery Ludwig-Maximilian University München Großhadern Germany XXIV Annual Conference Pietro Paoletti 27. November
Concepts for a personalized neurosurgical oncology Jörg-Christian Tonn Dept. of Neurosurgery Ludwig-Maximilian University München Großhadern Germany XXIV Annual Conference Pietro Paoletti 27. November
Concomitant (without adjuvant) temozolomide and radiation to treat glioblastoma: A retrospective study
 Concomitant (without adjuvant) temozolomide and radiation to treat glioblastoma: A retrospective study T Sridhar 1, A Gore 1, I Boiangiu 1, D Machin 2, R P Symonds 3 1. Department of Oncology, Leicester
Concomitant (without adjuvant) temozolomide and radiation to treat glioblastoma: A retrospective study T Sridhar 1, A Gore 1, I Boiangiu 1, D Machin 2, R P Symonds 3 1. Department of Oncology, Leicester
Intraoperative MR Imaging Increases the Extent of Tumor Resection in Patients with High-Grade Gliomas
 AJNR Am J Neuroradiol 20:1642 1646, October 1999 Intraoperative MR Imaging Increases the Extent of Tumor Resection in Patients with High-Grade Gliomas Michael Knauth, Christian R. Wirtz, Volker M. Tronnier,
AJNR Am J Neuroradiol 20:1642 1646, October 1999 Intraoperative MR Imaging Increases the Extent of Tumor Resection in Patients with High-Grade Gliomas Michael Knauth, Christian R. Wirtz, Volker M. Tronnier,
Radioterapia no Tratamento dos Gliomas de Baixo Grau
 Radioterapia no Tratamento dos Gliomas de Baixo Grau Dr. Luis Souhami University Montreal - Canada Low Grade Gliomas Relatively rare Heterogeneous, slow growing tumors WHO Classification Grade I Pilocytic
Radioterapia no Tratamento dos Gliomas de Baixo Grau Dr. Luis Souhami University Montreal - Canada Low Grade Gliomas Relatively rare Heterogeneous, slow growing tumors WHO Classification Grade I Pilocytic
Imaging for suspected glioma
 Imaging for suspected glioma 1.1.1 Offer standard structural MRI (defined as T2 weighted, FLAIR, DWI series and T1 pre- and post-contrast volume) as the initial diagnostic test for suspected glioma, unless
Imaging for suspected glioma 1.1.1 Offer standard structural MRI (defined as T2 weighted, FLAIR, DWI series and T1 pre- and post-contrast volume) as the initial diagnostic test for suspected glioma, unless
Systemic Treatment. Third International Neuro-Oncology Course. 23 May 2014
 Low-Grade Astrocytoma of the CNS: Systemic Treatment Third International Neuro-Oncology Course São Paulo, Brazil 23 May 2014 John de Groot, MD Associate Professor, Neuro-Oncology UT MD Anderson Cancer
Low-Grade Astrocytoma of the CNS: Systemic Treatment Third International Neuro-Oncology Course São Paulo, Brazil 23 May 2014 John de Groot, MD Associate Professor, Neuro-Oncology UT MD Anderson Cancer
Intraoperative perception and estimates on extent of resection during awake glioma surgery: overcoming the learning curve
 CLINICAL ARTICLE J Neurosurg 128:1410 1418, 2018 Intraoperative perception and estimates on extent of resection during awake glioma surgery: overcoming the learning curve Darryl Lau, MD, 1 Shawn L. Hervey-Jumper,
CLINICAL ARTICLE J Neurosurg 128:1410 1418, 2018 Intraoperative perception and estimates on extent of resection during awake glioma surgery: overcoming the learning curve Darryl Lau, MD, 1 Shawn L. Hervey-Jumper,
ORIGINAL PAPERS. The Impact of Surgery on the Efficacy of Adjuvant Therapy in Glioblastoma Multiforme
 ORIGINAL PAPERS Adv Clin Exp Med 2015, 24, 2, 279 287 DOI: 10.17219/acem/40456 Copyright by Wroclaw Medical University ISSN 1899 5276 Anna Brzozowska 1, 2, A D, Anna Toruń 3, G, Maria Mazurkiewicz1, 2,
ORIGINAL PAPERS Adv Clin Exp Med 2015, 24, 2, 279 287 DOI: 10.17219/acem/40456 Copyright by Wroclaw Medical University ISSN 1899 5276 Anna Brzozowska 1, 2, A D, Anna Toruń 3, G, Maria Mazurkiewicz1, 2,
Carmustine implants and Temozolomide for the treatment of newly diagnosed high grade glioma
 National Institute for Health and Clinical Excellence Health Technology Appraisal Carmustine implants and Temozolomide for the treatment of newly diagnosed high grade glioma Personal statement Conventional
National Institute for Health and Clinical Excellence Health Technology Appraisal Carmustine implants and Temozolomide for the treatment of newly diagnosed high grade glioma Personal statement Conventional
LOW GRADE ASTROCYTOMAS
 LOW GRADE ASTROCYTOMAS This article was provided to us by David Schiff, MD, Associate Professor of Neurology, Neurosurgery, and Medicine at University of Virginia, Charlottesville. We appreciate his generous
LOW GRADE ASTROCYTOMAS This article was provided to us by David Schiff, MD, Associate Professor of Neurology, Neurosurgery, and Medicine at University of Virginia, Charlottesville. We appreciate his generous
Small and Big Operations: New Tools of the Trade for Brain Tumors. Disclosure. Incidence of Childhood Cancer
 Small and Big Operations: New Tools of the Trade for Brain Tumors Nalin Gupta MD PhD Chief, Division of Pediatric Neurosurgery Departments of Neurosurgery and Pediatrics University of California San Francisco
Small and Big Operations: New Tools of the Trade for Brain Tumors Nalin Gupta MD PhD Chief, Division of Pediatric Neurosurgery Departments of Neurosurgery and Pediatrics University of California San Francisco
Survival of High Grade Glioma Patients Treated by Three Radiation Schedules with Chemotherapy: A Retrospective Comparative Study
 Original Article Research in Oncology June 2017; Vol. 13, No. 1: 18-22. DOI: 10.21608/resoncol.2017.552.1022 Survival of High Grade Glioma Patients Treated by Three Radiation Schedules with Chemotherapy:
Original Article Research in Oncology June 2017; Vol. 13, No. 1: 18-22. DOI: 10.21608/resoncol.2017.552.1022 Survival of High Grade Glioma Patients Treated by Three Radiation Schedules with Chemotherapy:
HHS Public Access Author manuscript World Neurosurg. Author manuscript; available in PMC 2016 August 01.
 Intra-Operative Magnetic Resonance Imaging In Intracranial Glioma Resection: A Single Center Retrospective Blinded Volumetric Study Olutayo Ibukunolu Olubiyi, MD, MPH, Aysegul Ozdemir, MD, Fatih Incekara,
Intra-Operative Magnetic Resonance Imaging In Intracranial Glioma Resection: A Single Center Retrospective Blinded Volumetric Study Olutayo Ibukunolu Olubiyi, MD, MPH, Aysegul Ozdemir, MD, Fatih Incekara,
SURGICAL MANAGEMENT OF BRAIN TUMORS
 SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
The role of intraoperative magnetic resonance imaging in glioma surgery
 1 di 10 05/04/2013 18.14 Surg Neurol Int. 2012; 3(Suppl 4): S320 S327. Published online 2012 October 31. doi: 10.4103/2152-7806.103029 PMCID: PMC3514913 The role of intraoperative magnetic resonance imaging
1 di 10 05/04/2013 18.14 Surg Neurol Int. 2012; 3(Suppl 4): S320 S327. Published online 2012 October 31. doi: 10.4103/2152-7806.103029 PMCID: PMC3514913 The role of intraoperative magnetic resonance imaging
Collection of Recorded Radiotherapy Seminars
 IAEA Human Health Campus Collection of Recorded Radiotherapy Seminars http://humanhealth.iaea.org The Role of Radiosurgery in the Treatment of Gliomas Luis Souhami, MD Professor Department of Radiation
IAEA Human Health Campus Collection of Recorded Radiotherapy Seminars http://humanhealth.iaea.org The Role of Radiosurgery in the Treatment of Gliomas Luis Souhami, MD Professor Department of Radiation
THE EFFECTIVE OF BRAIN CANCER AND XAY BETWEEN THEORY AND IMPLEMENTATION. Mustafa Rashid Issa
 THE EFFECTIVE OF BRAIN CANCER AND XAY BETWEEN THEORY AND IMPLEMENTATION Mustafa Rashid Issa ABSTRACT: Illustrate malignant tumors that form either in the brain or in the nerves originating in the brain.
THE EFFECTIVE OF BRAIN CANCER AND XAY BETWEEN THEORY AND IMPLEMENTATION Mustafa Rashid Issa ABSTRACT: Illustrate malignant tumors that form either in the brain or in the nerves originating in the brain.
This study was designed to evaluate an online prognosis
 Neuro-Oncology 15(8):1074 1078, 2013. doi:10.1093/neuonc/not033 Advance Access publication March 29, 2013 NEURO-ONCOLOGY Can the prognosis of individual patients with glioblastoma be predicted using an
Neuro-Oncology 15(8):1074 1078, 2013. doi:10.1093/neuonc/not033 Advance Access publication March 29, 2013 NEURO-ONCOLOGY Can the prognosis of individual patients with glioblastoma be predicted using an
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM LOW GRADE GLIOMAS CNS Site Group Low Grade Gliomas Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2. PREVENTION 3 3. SCREENING
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM LOW GRADE GLIOMAS CNS Site Group Low Grade Gliomas Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2. PREVENTION 3 3. SCREENING
Visualization strategies for major white matter tracts identified by diffusion tensor imaging for intraoperative use
 International Congress Series 1281 (2005) 793 797 www.ics-elsevier.com Visualization strategies for major white matter tracts identified by diffusion tensor imaging for intraoperative use Ch. Nimsky a,b,
International Congress Series 1281 (2005) 793 797 www.ics-elsevier.com Visualization strategies for major white matter tracts identified by diffusion tensor imaging for intraoperative use Ch. Nimsky a,b,
Prior to 1993, the only data available in the medical
 Neuro-Oncology Prospective clinical trials of intracranial low-grade glioma in adults and children Edward G. Shaw 1 and Jeffrey H. Wisoff Department of Radiation Oncology, Wake Forest University School
Neuro-Oncology Prospective clinical trials of intracranial low-grade glioma in adults and children Edward G. Shaw 1 and Jeffrey H. Wisoff Department of Radiation Oncology, Wake Forest University School
UPDATES ON CHEMOTHERAPY FOR LOW GRADE GLIOMAS
 UPDATES ON CHEMOTHERAPY FOR LOW GRADE GLIOMAS Antonio M. Omuro Department of Neurology Memorial Sloan-Kettering Cancer Center II International Neuro-Oncology Congress Sao Paulo, 08/17/12 CHALLENGES IN
UPDATES ON CHEMOTHERAPY FOR LOW GRADE GLIOMAS Antonio M. Omuro Department of Neurology Memorial Sloan-Kettering Cancer Center II International Neuro-Oncology Congress Sao Paulo, 08/17/12 CHALLENGES IN
Newcastle Neuro-oncology Team Audit of Outcome of Glioblastoma Multiforme Chemoradiotherapy Treatment
 Newcastle Neuro-oncology Team Audit of Outcome of Glioblastoma Multiforme Chemoradiotherapy Treatment Jennifer Wright Neurosurgery SSC Audit Team Jennifer Wright, Rachel Tresman, Cyril Dubois, Surash Surash,
Newcastle Neuro-oncology Team Audit of Outcome of Glioblastoma Multiforme Chemoradiotherapy Treatment Jennifer Wright Neurosurgery SSC Audit Team Jennifer Wright, Rachel Tresman, Cyril Dubois, Surash Surash,
Clinical Trials for Adult Brain Tumors - the Imaging Perspective
 Clinical Trials for Adult Brain Tumors - the Imaging Perspective Whitney B. Pope, M.D., Ph.D. Department of Radiology David Geffen School of Medicine at UCLA August 22, 2015 1 Disclosure of Financial Relationships
Clinical Trials for Adult Brain Tumors - the Imaging Perspective Whitney B. Pope, M.D., Ph.D. Department of Radiology David Geffen School of Medicine at UCLA August 22, 2015 1 Disclosure of Financial Relationships
Cilengitide (Impetreve) for glioblastoma multiforme. February 2012
 Cilengitide (Impetreve) for glioblastoma multiforme February 2012 This technology summary is based on information available at the time of research and a limited literature search. It is not intended to
Cilengitide (Impetreve) for glioblastoma multiforme February 2012 This technology summary is based on information available at the time of research and a limited literature search. It is not intended to
HHS Public Access Author manuscript World Neurosurg. Author manuscript; available in PMC 2016 June 01.
 Extra-operatve MRI (eomri) for Brain Tumor Surgery Initial Results at a Single Institution Muhammad M. Abd-El-Barr, MD, PhD a, Seth M. Santos, PA-C a, Linda S. Aglio, MD, MS b, Geoffrey S. Young, MD c,
Extra-operatve MRI (eomri) for Brain Tumor Surgery Initial Results at a Single Institution Muhammad M. Abd-El-Barr, MD, PhD a, Seth M. Santos, PA-C a, Linda S. Aglio, MD, MS b, Geoffrey S. Young, MD c,
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM ANAPLASTIC GLIOMAS CNS Site Group Anaplastic Gliomas Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM ANAPLASTIC GLIOMAS CNS Site Group Anaplastic Gliomas Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION
Surgery guided by 5-aminolevulinic fluorescence in glioblastoma: volumetric analysis of extent of resection in singlecenter
 Surgery guided by 5-aminolevulinic fluorescence in glioblastoma: volumetric analysis of extent of resection in singlecenter experience Ricardo Díez Valle; Sonia Tejada Solis; Miguel Ángel Idoate Gastearena;
Surgery guided by 5-aminolevulinic fluorescence in glioblastoma: volumetric analysis of extent of resection in singlecenter experience Ricardo Díez Valle; Sonia Tejada Solis; Miguel Ángel Idoate Gastearena;
Neurosurgical Management of Brain Tumours. Nicholas Little Neurosurgeon RNSH
 Neurosurgical Management of Brain Tumours Nicholas Little Neurosurgeon RNSH General Most common tumours are metastatic 10x more common than primary Incidence of primary neoplasms is 20 per 100000 per year
Neurosurgical Management of Brain Tumours Nicholas Little Neurosurgeon RNSH General Most common tumours are metastatic 10x more common than primary Incidence of primary neoplasms is 20 per 100000 per year
Technology appraisal guidance Published: 27 June 2007 nice.org.uk/guidance/ta121
 Carmustine implants and temozolomide for the treatment of newly diagnosed high-grade glioma Technology appraisal guidance Published: 27 June 2007 nice.org.uk/guidance/ta121 NICE 2018. All rights reserved.
Carmustine implants and temozolomide for the treatment of newly diagnosed high-grade glioma Technology appraisal guidance Published: 27 June 2007 nice.org.uk/guidance/ta121 NICE 2018. All rights reserved.
Appraisal of carmustine. implants and temozolomide. for newly diagnosed high. Brain and Spine Foundation
 Appraisal of carmustine implants and temozolomide for newly diagnosed high grade glioma Brain and Spine Foundation June 2005 Submission to the National Institute for Health and Clinical Excellence Brain
Appraisal of carmustine implants and temozolomide for newly diagnosed high grade glioma Brain and Spine Foundation June 2005 Submission to the National Institute for Health and Clinical Excellence Brain
Clinical Management Protocol Chemotherapy [Glioblastoma Multiforme (CNS)] Protocol for Planning and Treatment
![Clinical Management Protocol Chemotherapy [Glioblastoma Multiforme (CNS)] Protocol for Planning and Treatment Clinical Management Protocol Chemotherapy [Glioblastoma Multiforme (CNS)] Protocol for Planning and Treatment](/thumbs/87/96032554.jpg) Protocol for Planning and Treatment The process to be followed when a course of chemotherapy is required to treat: GLIOBLASTOMA MULTIFORME (CNS) Patient information given at each stage following agreed
Protocol for Planning and Treatment The process to be followed when a course of chemotherapy is required to treat: GLIOBLASTOMA MULTIFORME (CNS) Patient information given at each stage following agreed
National Institute for Health and Clinical Excellence. Single Technology Appraisal (STA)
 National Institute for Health and Clinical Excellence Appendix C Comment 1: the draft scope Single Technology Appraisal (STA) Carmustine implants for the treatment of recurrent glioblastoma multiforme
National Institute for Health and Clinical Excellence Appendix C Comment 1: the draft scope Single Technology Appraisal (STA) Carmustine implants for the treatment of recurrent glioblastoma multiforme
Diffuse infiltrative LGGs of the cerebral hemispheres
 J Neurosurg 117:1039 1052, 2012 Low-grade glioma surgery in eloquent areas: volumetric analysis of extent of resection and its impact on overall survival. A single-institution experience in 190 patients
J Neurosurg 117:1039 1052, 2012 Low-grade glioma surgery in eloquent areas: volumetric analysis of extent of resection and its impact on overall survival. A single-institution experience in 190 patients
PROCARBAZINE, lomustine, and vincristine (PCV) is
 RAPID PUBLICATION Procarbazine, Lomustine, and Vincristine () Chemotherapy for Anaplastic Astrocytoma: A Retrospective Review of Radiation Therapy Oncology Group Protocols Comparing Survival With Carmustine
RAPID PUBLICATION Procarbazine, Lomustine, and Vincristine () Chemotherapy for Anaplastic Astrocytoma: A Retrospective Review of Radiation Therapy Oncology Group Protocols Comparing Survival With Carmustine
Primary brain tumours and cerebral metastases workshop
 Primary brain tumours and cerebral workshop 22.4.16 Summary of workshop group discussions on the content of the scope Scope section Title: Primary brain tumours and cerebral Who the guideline is for People
Primary brain tumours and cerebral workshop 22.4.16 Summary of workshop group discussions on the content of the scope Scope section Title: Primary brain tumours and cerebral Who the guideline is for People
University of Zurich. Temozolomide and MGMT forever? Zurich Open Repository and Archive. Weller, M. Year: 2010
 University of Zurich Zurich Open Repository and Archive Winterthurerstr. 190 CH-8057 Zurich Year: 2010 Temozolomide and MGMT forever? Weller, M Weller, M (2010). Temozolomide and MGMT forever? Neuro-Oncology,
University of Zurich Zurich Open Repository and Archive Winterthurerstr. 190 CH-8057 Zurich Year: 2010 Temozolomide and MGMT forever? Weller, M Weller, M (2010). Temozolomide and MGMT forever? Neuro-Oncology,
To achieve excellence in surgical neuro-oncology, the
 CHAPTER 2 Defining and Achieving Excellence in Surgical Neuro-Oncology Mitchel S. Berger, MD To achieve excellence in surgical neuro-oncology, the neurosurgeon must achieve 3 particular things. The first
CHAPTER 2 Defining and Achieving Excellence in Surgical Neuro-Oncology Mitchel S. Berger, MD To achieve excellence in surgical neuro-oncology, the neurosurgeon must achieve 3 particular things. The first
University of Alberta. Evaluation of Concomitant Temozolomide Treatment in Glioblastoma Multiforme Patients in Two Canadian Tertiary Care Centers
 University of Alberta Evaluation of Concomitant Temozolomide Treatment in Glioblastoma Multiforme Patients in Two Canadian Tertiary Care Centers by Ibrahim Alnaami A thesis submitted to the Faculty of
University of Alberta Evaluation of Concomitant Temozolomide Treatment in Glioblastoma Multiforme Patients in Two Canadian Tertiary Care Centers by Ibrahim Alnaami A thesis submitted to the Faculty of
21/03/2017. Disclosure. Practice Changing Articles in Neuro Oncology for 2016/17. Gliomas. Objectives. Gliomas. No conflicts to declare
 Practice Changing Articles in Neuro Oncology for 2016/17 Disclosure No conflicts to declare Frances Cusano, BScPharm, ACPR April 21, 2017 Objectives Gliomas To describe the patient selection, methodology
Practice Changing Articles in Neuro Oncology for 2016/17 Disclosure No conflicts to declare Frances Cusano, BScPharm, ACPR April 21, 2017 Objectives Gliomas To describe the patient selection, methodology
Postoperative Deterioration in Health Related Quality of Life as Predictor for Survival in Patients with Glioblastoma: A Prospective Study
 Postoperative Deterioration in Health Related Quality of Life as Predictor for Survival in Patients with Glioblastoma: A Prospective Study Asgeir S. Jakola 1,2,3 *, Sasha Gulati 1,4, Clemens Weber 1, Geirmund
Postoperative Deterioration in Health Related Quality of Life as Predictor for Survival in Patients with Glioblastoma: A Prospective Study Asgeir S. Jakola 1,2,3 *, Sasha Gulati 1,4, Clemens Weber 1, Geirmund
Citation Pediatrics international (2015), 57.
 Title Long-term efficacy of bevacizumab a pediatric glioblastoma. Umeda, Katsutsugu; Shibata, Hirofum Author(s) Hiramatsu, Hidefumi; Arakawa, Yoshi Nishiuchi, Ritsuo; Adachi, Souichi; Ken-Ichiro Citation
Title Long-term efficacy of bevacizumab a pediatric glioblastoma. Umeda, Katsutsugu; Shibata, Hirofum Author(s) Hiramatsu, Hidefumi; Arakawa, Yoshi Nishiuchi, Ritsuo; Adachi, Souichi; Ken-Ichiro Citation
Early postoperative tumor progression predicts clinical outcome in glioblastoma implication for clinical trials
 J Neurooncol (2017) 132:249 254 DOI 10.1007/s11060-016-2362-z CLINICAL STUDY Early postoperative tumor progression predicts clinical outcome in glioblastoma implication for clinical trials Andreas Merkel
J Neurooncol (2017) 132:249 254 DOI 10.1007/s11060-016-2362-z CLINICAL STUDY Early postoperative tumor progression predicts clinical outcome in glioblastoma implication for clinical trials Andreas Merkel
Improved Survival after Gross Total Resection of Malignant Gliomas in Pediatric Patients from the HIT-GBM Studies
 Improved Survival after Gross Total Resection of Malignant Gliomas in Pediatric Patients from the HIT-GBM Studies CHRISTOF M. KRAMM 1, SABINE WAGNER 2, STEFAN VAN GOOL 3, HANSJÖRG SCHMID 4, RONALD STRÄTER
Improved Survival after Gross Total Resection of Malignant Gliomas in Pediatric Patients from the HIT-GBM Studies CHRISTOF M. KRAMM 1, SABINE WAGNER 2, STEFAN VAN GOOL 3, HANSJÖRG SCHMID 4, RONALD STRÄTER
TABLES. Table 1: Imaging. Congress of Neurological Surgeons Author (Year) Description of Study Classification Process / Evidence Class
 TABLES Table 1: Imaging Kremer et al (2002) 2 Study Design: Prospective followed case series. Patient Population: Fifty adult patients with NFPA Study Description: Patients underwent MRI before surgery,
TABLES Table 1: Imaging Kremer et al (2002) 2 Study Design: Prospective followed case series. Patient Population: Fifty adult patients with NFPA Study Description: Patients underwent MRI before surgery,
Supratentorial Glioblastoma Multiforme: The Role of Surgical Resection Versus Biopsy Among Older Patients
 Ann Surg Oncol DOI 10.1245/s10434-010-1242-6 ORIGINAL ARTICLE NEURO-ONCOLOGY Supratentorial Glioblastoma Multiforme: The Role of Surgical Resection Versus Biopsy Among Older Patients Kaisorn L. Chaichana,
Ann Surg Oncol DOI 10.1245/s10434-010-1242-6 ORIGINAL ARTICLE NEURO-ONCOLOGY Supratentorial Glioblastoma Multiforme: The Role of Surgical Resection Versus Biopsy Among Older Patients Kaisorn L. Chaichana,
NICE guideline Published: 11 July 2018 nice.org.uk/guidance/ng99
 Brain tumours (primary) and brain metastases in adults NICE guideline Published: 11 July 2018 nice.org.uk/guidance/ng99 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Brain tumours (primary) and brain metastases in adults NICE guideline Published: 11 July 2018 nice.org.uk/guidance/ng99 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Zurich Open Repository and Archive. Long-term survival of glioblastoma patients treated with radiotherapy and lomustine plus temozolomide
 University of Zurich Zurich Open Repository and Archive Winterthurerstr. 190 CH-8057 Zurich http://www.zora.uzh.ch Year: 2009 Long-term survival of glioblastoma patients treated with radiotherapy and lomustine
University of Zurich Zurich Open Repository and Archive Winterthurerstr. 190 CH-8057 Zurich http://www.zora.uzh.ch Year: 2009 Long-term survival of glioblastoma patients treated with radiotherapy and lomustine
Clinical Policy: Electric Tumor Treating Fields (Optune) Reference Number: PA.CP.MP.145
 Clinical Policy: Electric Tumor Treating Fields (Optune) Reference Number: PA.CP.MP.145 Effective Date: 01/18 Last Review Date: 04/18 Coding Implications Revision Log Description Electric tumor treating
Clinical Policy: Electric Tumor Treating Fields (Optune) Reference Number: PA.CP.MP.145 Effective Date: 01/18 Last Review Date: 04/18 Coding Implications Revision Log Description Electric tumor treating
Incidence of Early Pseudo-progression in a Cohort of Malignant Glioma Patients Treated With Chemoirradiation With Temozolomide
 405 Incidence of Early Pseudo-progression in a Cohort of Malignant Glioma Patients Treated With Chemoirradiation With Temozolomide Walter Taal, MD 1 Dieta Brandsma, MD, PhD 1 Hein G. de Bruin, MD, PhD
405 Incidence of Early Pseudo-progression in a Cohort of Malignant Glioma Patients Treated With Chemoirradiation With Temozolomide Walter Taal, MD 1 Dieta Brandsma, MD, PhD 1 Hein G. de Bruin, MD, PhD
AMERICAN BRAIN TUMOR ASSOCIATION. Oligodendroglioma and Oligoastrocytoma
 AMERICAN BRAIN TUMOR ASSOCIATION Oligodendroglioma and Oligoastrocytoma ACKNOWLEDGEMENTS ABOUT THE AMERICAN BRAIN TUMOR ASSOCIATION Founded in 1973, the American Brain Tumor Association (ABTA) was the
AMERICAN BRAIN TUMOR ASSOCIATION Oligodendroglioma and Oligoastrocytoma ACKNOWLEDGEMENTS ABOUT THE AMERICAN BRAIN TUMOR ASSOCIATION Founded in 1973, the American Brain Tumor Association (ABTA) was the
Oncological Management of Brain Tumours. Anna Maria Shiarli SpR in Clinical Oncology 15 th July 2013
 Oncological Management of Brain Tumours Anna Maria Shiarli SpR in Clinical Oncology 15 th July 2013 Outline General considerations of Primary Brain Tumours: epidemiology, pathology, presentation. Diagnosis
Oncological Management of Brain Tumours Anna Maria Shiarli SpR in Clinical Oncology 15 th July 2013 Outline General considerations of Primary Brain Tumours: epidemiology, pathology, presentation. Diagnosis
General Identification. Name: 江 X X Age: 29 y/o Gender: Male Height:172cm, Weight: 65kg Date of admission:95/09/27
 General Identification Name: 江 X X Age: 29 y/o Gender: Male Height:172cm, Weight: 65kg Date of admission:95/09/27 Chief Complaint Sudden onset of seizure for several minutes Present illness This 29-year
General Identification Name: 江 X X Age: 29 y/o Gender: Male Height:172cm, Weight: 65kg Date of admission:95/09/27 Chief Complaint Sudden onset of seizure for several minutes Present illness This 29-year
Management of single brain metastasis: a practice guideline
 PRACTICE GUIDELINE SERIES Management of single brain metastasis: a practice guideline A. Mintz MD,* J. Perry MD, K. Spithoff BHSc, A. Chambers MA, and N. Laperriere MD on behalf of the Neuro-oncology Disease
PRACTICE GUIDELINE SERIES Management of single brain metastasis: a practice guideline A. Mintz MD,* J. Perry MD, K. Spithoff BHSc, A. Chambers MA, and N. Laperriere MD on behalf of the Neuro-oncology Disease
PRESURGICAL PLANNING. Strongly consider neuropsychological evaluation before functional imaging study Strongly consider functional imaging study
 NOTE: Consider Clinical Trials as treatment options for eligible patients. Page 1 of 6 RADIOLOGICAL PRESENTATION PRESURGICAL PLANNING TREATMENT Imaging study suggestive of glioma 1 Left hemisphere speech/motor
NOTE: Consider Clinical Trials as treatment options for eligible patients. Page 1 of 6 RADIOLOGICAL PRESENTATION PRESURGICAL PLANNING TREATMENT Imaging study suggestive of glioma 1 Left hemisphere speech/motor
Introduction. Keywords Low-grade astrocytoma Volumetric analysis Extent of resection IDH1 Intraoperative MRI Survival
 J Neurooncol (2016) 129:319 328 DOI 10.1007/s11060-016-2177-y CLINIcAL STUDY Prognostic value of the extent of resection in supratentorial WHO grade II astrocytomas stratified for IDH1 mutation status:
J Neurooncol (2016) 129:319 328 DOI 10.1007/s11060-016-2177-y CLINIcAL STUDY Prognostic value of the extent of resection in supratentorial WHO grade II astrocytomas stratified for IDH1 mutation status:
Bevacizumab rescue therapy extends the survival in patients with recurrent malignant glioma
 Original Article Bevacizumab rescue therapy extends the survival in patients with recurrent malignant glioma Lin-Bo Cai, Juan Li, Ming-Yao Lai, Chang-Guo Shan, Zong-De Lian, Wei-Ping Hong, Jun-Jie Zhen,
Original Article Bevacizumab rescue therapy extends the survival in patients with recurrent malignant glioma Lin-Bo Cai, Juan Li, Ming-Yao Lai, Chang-Guo Shan, Zong-De Lian, Wei-Ping Hong, Jun-Jie Zhen,
Oligodendrogliomas & Oligoastrocytomas
 Oligodendrogliomas & Oligoastrocytomas ABOUT THE AMERICAN BRAIN TUMOR ASSOCIATION Founded in 1973, the American Brain Tumor Association (ABTA) was the first national nonprofit organization dedicated solely
Oligodendrogliomas & Oligoastrocytomas ABOUT THE AMERICAN BRAIN TUMOR ASSOCIATION Founded in 1973, the American Brain Tumor Association (ABTA) was the first national nonprofit organization dedicated solely
After primary tumor treatment, 30% of patients with malignant
 ESTS METASTASECTOMY SUPPLEMENT Alberto Oliaro, MD, Pier L. Filosso, MD, Maria C. Bruna, MD, Claudio Mossetti, MD, and Enrico Ruffini, MD Abstract: After primary tumor treatment, 30% of patients with malignant
ESTS METASTASECTOMY SUPPLEMENT Alberto Oliaro, MD, Pier L. Filosso, MD, Maria C. Bruna, MD, Claudio Mossetti, MD, and Enrico Ruffini, MD Abstract: After primary tumor treatment, 30% of patients with malignant
Epidemiology and outcome research of glioma patients in Southern Switzerland: A population based analysis
 Epidemiology and outcome research of glioma patients in Southern Switzerland: A population based analysis G. Pesce 1, A. Bordoni, F. Montanaro, R. Renella 3, A. Richetti 1, D. Boscherini 3, S. Mauri 4,
Epidemiology and outcome research of glioma patients in Southern Switzerland: A population based analysis G. Pesce 1, A. Bordoni, F. Montanaro, R. Renella 3, A. Richetti 1, D. Boscherini 3, S. Mauri 4,
Modeling the effects of resection, radiation and chemotherapy in glioblastoma
 J Neurooncol (09) 91:287 293 DOI 10.1007/s11060-008-9710-6 CLINICAL STUDY - PATIENT STUDY Modeling the effects of resection, radiation and chemotherapy in glioblastoma Jianjun Paul Tian Æ Avner Friedman
J Neurooncol (09) 91:287 293 DOI 10.1007/s11060-008-9710-6 CLINICAL STUDY - PATIENT STUDY Modeling the effects of resection, radiation and chemotherapy in glioblastoma Jianjun Paul Tian Æ Avner Friedman
Objectives. Presenter Disclosure Information 11/29/2016
 Current State of Neurosurgical Treatment of Cerebral Glioma and Clinical Trials Testing Future Advances John D. Heiss, M.D. Chair, Surgical Neurology Branch, NINDS, National Institutes of Health Presenter
Current State of Neurosurgical Treatment of Cerebral Glioma and Clinical Trials Testing Future Advances John D. Heiss, M.D. Chair, Surgical Neurology Branch, NINDS, National Institutes of Health Presenter
Multimodal Imaging in Extratemporal Epilepsy Surgery
 Open Access Case Report DOI: 10.7759/cureus.2338 Multimodal Imaging in Extratemporal Epilepsy Surgery Christian Vollmar 1, Aurelia Peraud 2, Soheyl Noachtar 1 1. Epilepsy Center, Dept. of Neurology, University
Open Access Case Report DOI: 10.7759/cureus.2338 Multimodal Imaging in Extratemporal Epilepsy Surgery Christian Vollmar 1, Aurelia Peraud 2, Soheyl Noachtar 1 1. Epilepsy Center, Dept. of Neurology, University
Ultrasound-guided versus traditional surgical resection of supratentorial gliomas in a limited-resources neurosurgical setting
 Ibrahim et al. Egyptian Journal of Neurosurgery (2018) 33:24 https://doi.org/10.1186/s41984-018-0024-5 Egyptian Journal of Neurosurgery RESEARCH Ultrasound-guided versus traditional surgical resection
Ibrahim et al. Egyptian Journal of Neurosurgery (2018) 33:24 https://doi.org/10.1186/s41984-018-0024-5 Egyptian Journal of Neurosurgery RESEARCH Ultrasound-guided versus traditional surgical resection
Spinal cord compression as a first presentation of cancer: A case report
 J Pain Manage 2013;6(4):319-322 ISSN: 1939-5914 Nova Science Publishers, Inc. Spinal cord compression as a first presentation of cancer: A case report Nicholas Lao, BMSc(C), Michael Poon, MD(C), Marko
J Pain Manage 2013;6(4):319-322 ISSN: 1939-5914 Nova Science Publishers, Inc. Spinal cord compression as a first presentation of cancer: A case report Nicholas Lao, BMSc(C), Michael Poon, MD(C), Marko
Ependymoma Programme Synopsis
 Ependymoma Programme Synopsis TITLE SPONSOR PROTOCOL NUMBER EUDRACT NUMBER NATIONAL INVESTIGATOR- COORDINATOR SIOP Ependymoma program II: An International Clinical Program for the diagnosis and treatment
Ependymoma Programme Synopsis TITLE SPONSOR PROTOCOL NUMBER EUDRACT NUMBER NATIONAL INVESTIGATOR- COORDINATOR SIOP Ependymoma program II: An International Clinical Program for the diagnosis and treatment
3-D conformal radiotherapy with concomitant and adjuvant temozolomide for patients with glioblastoma multiforme and evaluation of prognostic factors
 research article 213 3-D conformal radiotherapy with concomitant and adjuvant temozolomide for patients with glioblastoma multiforme and evaluation of prognostic factors Yilmaz Tezcan and Mehmet Koc Department
research article 213 3-D conformal radiotherapy with concomitant and adjuvant temozolomide for patients with glioblastoma multiforme and evaluation of prognostic factors Yilmaz Tezcan and Mehmet Koc Department
THE DIFFUSE LOW-GRADE GLIOmas
 ORIGINAL CONTRIBUTION ONLINE FIRST Comparison of a Strategy Favoring Early Surgical Resection vs a Strategy Favoring Watchful Waiting in Low-Grade Gliomas Asgeir S. Jakola, MD Kristin S. Myrmel, MD Roar
ORIGINAL CONTRIBUTION ONLINE FIRST Comparison of a Strategy Favoring Early Surgical Resection vs a Strategy Favoring Watchful Waiting in Low-Grade Gliomas Asgeir S. Jakola, MD Kristin S. Myrmel, MD Roar
Lynn S. Ashby 1*, Kris A. Smith 2 and Baldassarre Stea 3
 Ashby et al. World Journal of Surgical Oncology (2016) 14:225 DOI 10.1186/s12957-016-0975-5 REVIEW Gliadel wafer implantation combined with standard radiotherapy and concurrent followed by adjuvant temozolomide
Ashby et al. World Journal of Surgical Oncology (2016) 14:225 DOI 10.1186/s12957-016-0975-5 REVIEW Gliadel wafer implantation combined with standard radiotherapy and concurrent followed by adjuvant temozolomide
Tristate Lung Meeting 2014 Pro-Con Debate: Surgery has no role in the management of certain subsets of N2 disease
 Tristate Lung Meeting 2014 Pro-Con Debate: Surgery has no role in the management of certain subsets of N2 disease Jennifer E. Tseng, MD UFHealth Cancer Center-Orlando Health Sep 12, 2014 Background Approximately
Tristate Lung Meeting 2014 Pro-Con Debate: Surgery has no role in the management of certain subsets of N2 disease Jennifer E. Tseng, MD UFHealth Cancer Center-Orlando Health Sep 12, 2014 Background Approximately
Role of intraoperative ultrasound in achieving complete resection of intra-axial solid brain tumours
 1343 ORIGINAL ARTICLE Role of intraoperative ultrasound in achieving complete resection of intra-axial solid brain tumours Abdul Razaque Mari, 1 Irfanullah Shah, 2 Muhammed Imran, 3 Junaid Ashraf 4 Abstract
1343 ORIGINAL ARTICLE Role of intraoperative ultrasound in achieving complete resection of intra-axial solid brain tumours Abdul Razaque Mari, 1 Irfanullah Shah, 2 Muhammed Imran, 3 Junaid Ashraf 4 Abstract
Regional Neuro-Oncology Service Information Evening
 Regional Neuro-Oncology Service Information Evening Dr Tom Flannery Information Evening hosted by Brainwaves NI, in partnership with the Northern Ireland Regional Neuro-Oncology Multi Disciplinary Team.
Regional Neuro-Oncology Service Information Evening Dr Tom Flannery Information Evening hosted by Brainwaves NI, in partnership with the Northern Ireland Regional Neuro-Oncology Multi Disciplinary Team.
Extending resection and preserving function: modern concepts of glioma surgery
 Published 4 February 2015, doi:10.4414/smw.2015.14082 Cite this as: Extending resection and preserving function: modern concepts of glioma surgery Philippe Schucht, Jürgen Beck, Kathleen Seidel, Andreas
Published 4 February 2015, doi:10.4414/smw.2015.14082 Cite this as: Extending resection and preserving function: modern concepts of glioma surgery Philippe Schucht, Jürgen Beck, Kathleen Seidel, Andreas
Treatment and outcomes for glioblastoma in elderly compared with non-elderly patients: a population-based study
 ORIGINAL ARTICLE Treatment and outcomes for glioblastoma in elderly compared with non-elderly patients: a population-based study E.R. Morgan md,* A. Norman md, K. Laing md, and M.D. Seal md ABSTRACT Purpose
ORIGINAL ARTICLE Treatment and outcomes for glioblastoma in elderly compared with non-elderly patients: a population-based study E.R. Morgan md,* A. Norman md, K. Laing md, and M.D. Seal md ABSTRACT Purpose
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MENINGIOMA CNS Site Group Meningioma Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION 3 2. PREVENTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MENINGIOMA CNS Site Group Meningioma Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION 3 2. PREVENTION
Brain tumours (primary) and brain metastases in adults
 Brain tumours (primary) and brain metastases in adults NICE guideline Draft for consultation, January 0 This guideline covers diagnosing, monitoring and managing any type of primary brain tumour or brain
Brain tumours (primary) and brain metastases in adults NICE guideline Draft for consultation, January 0 This guideline covers diagnosing, monitoring and managing any type of primary brain tumour or brain
What to do with the pa fit and the scan shows
 84 PRACTICAL NEUROLOGY REVIEW What to do with the pa fit and the scan shows Jeremy Rees* and Ludvic Zrinzo *Consultant Neurologist and Specialist Registrar Neurosurgery, National Hospital for Neurology
84 PRACTICAL NEUROLOGY REVIEW What to do with the pa fit and the scan shows Jeremy Rees* and Ludvic Zrinzo *Consultant Neurologist and Specialist Registrar Neurosurgery, National Hospital for Neurology
HSV1716 Dose levels and Cohort size Dose level No of Patients HSV1716 Dosage 1* 3 to 6 1 ml of 1 x 10 5 infectious units HSV1716 per ml 2
 Abstract and Schema: Description and Rationale: Pediatric high grade gliomas have a progressive initial course and high risk of relapse/ progression; making the 5-year overall survival rate 15-35% with
Abstract and Schema: Description and Rationale: Pediatric high grade gliomas have a progressive initial course and high risk of relapse/ progression; making the 5-year overall survival rate 15-35% with
NON-SURGICAL STRATEGY FOR ADULT EPENDYMOMA
 NON-SURGICAL STRATEGY FOR ADULT EPENDYMOMA Roberta Rudà Department of Neuro-Oncology University and City of Health and Science Hospital of Turin, Italy EORTC EANO ESMO Conference 2015 Istanbul, March 27-28
NON-SURGICAL STRATEGY FOR ADULT EPENDYMOMA Roberta Rudà Department of Neuro-Oncology University and City of Health and Science Hospital of Turin, Italy EORTC EANO ESMO Conference 2015 Istanbul, March 27-28
Evaluation of Lung Cancer Response: Current Practice and Advances
 Evaluation of Lung Cancer Response: Current Practice and Advances Jeremy J. Erasmus I have no financial relationships, arrangements or affiliations and this presentation will not include discussion of
Evaluation of Lung Cancer Response: Current Practice and Advances Jeremy J. Erasmus I have no financial relationships, arrangements or affiliations and this presentation will not include discussion of
Zurich Open Repository and Archive. Long-term survival of glioblastoma patients treated with radiotherapy and lomustine plus temozolomide
 University of Zurich Zurich Open Repository and Archive Winterthurerstr. 19 CH-857 Zurich http://www.zora.uzh.ch Year: 29 Long-term survival of glioblastoma patients treated with radiotherapy and lomustine
University of Zurich Zurich Open Repository and Archive Winterthurerstr. 19 CH-857 Zurich http://www.zora.uzh.ch Year: 29 Long-term survival of glioblastoma patients treated with radiotherapy and lomustine
Navigating Treatment Pathways in Relapsed/Refractory Hodgkin Lymphoma
 Welcome to Managing Hodgkin Lymphoma. I am Dr. John Sweetenham from Huntsman Cancer Institute at the University of Utah. In today s presentation, I will be discussing navigating treatment pathways in relapsed
Welcome to Managing Hodgkin Lymphoma. I am Dr. John Sweetenham from Huntsman Cancer Institute at the University of Utah. In today s presentation, I will be discussing navigating treatment pathways in relapsed
Pediatric Brain Tumors: Updates in Treatment and Care
 Pediatric Brain Tumors: Updates in Treatment and Care Writer Classroom Rishi R. Lulla, MD MS Objectives Introduce the common pediatric brain tumors Discuss current treatment strategies for pediatric brain
Pediatric Brain Tumors: Updates in Treatment and Care Writer Classroom Rishi R. Lulla, MD MS Objectives Introduce the common pediatric brain tumors Discuss current treatment strategies for pediatric brain
Optimal Management of Isolated HER2+ve Brain Metastases
 Optimal Management of Isolated HER2+ve Brain Metastases Eliot Sims November 2013 Background Her2+ve patients 15% of all breast cancer Even with adjuvant trastuzumab 10-15% relapse Trastuzumab does not
Optimal Management of Isolated HER2+ve Brain Metastases Eliot Sims November 2013 Background Her2+ve patients 15% of all breast cancer Even with adjuvant trastuzumab 10-15% relapse Trastuzumab does not
Laser Interstitial Thermal Therapy (LITT) in Neuro-Oncology. Tim Lucas, MD, PhD Neurosurgery
 Laser Interstitial Thermal Therapy (LITT) in Neuro-Oncology Tim Lucas, MD, PhD Neurosurgery Timothy.Lucas@uphs.upenn.edu 2016 Laser Interstitial Thermal Therapy (LITT) in Neuro-Oncology Tim Lucas, MD,
Laser Interstitial Thermal Therapy (LITT) in Neuro-Oncology Tim Lucas, MD, PhD Neurosurgery Timothy.Lucas@uphs.upenn.edu 2016 Laser Interstitial Thermal Therapy (LITT) in Neuro-Oncology Tim Lucas, MD,
Institute of Oncology & Radiobiology. Havana, Cuba. INOR
 Institute of Oncology & Radiobiology. Havana, Cuba. INOR 1 Transition from 2-D 2 D to 3-D 3 D conformal radiotherapy in high grade gliomas: : our experience in Cuba Chon. I, MD - Chi. D, MD - Alert.J,
Institute of Oncology & Radiobiology. Havana, Cuba. INOR 1 Transition from 2-D 2 D to 3-D 3 D conformal radiotherapy in high grade gliomas: : our experience in Cuba Chon. I, MD - Chi. D, MD - Alert.J,
Volume 14, Issue 4, Oncology special
 Volume 14, Issue 4, 2012 - Oncology special The growing role of interventional oncology within multidisciplinary cancer care Interventional radiology (IR) is already well established within the field of
Volume 14, Issue 4, 2012 - Oncology special The growing role of interventional oncology within multidisciplinary cancer care Interventional radiology (IR) is already well established within the field of
Selecting the Optimal Treatment for Brain Metastases
 Selecting the Optimal Treatment for Brain Metastases Clinical Practice Today CME Co-provided by Learning Objectives Upon completion, participants should be able to: Understand the benefits, limitations,
Selecting the Optimal Treatment for Brain Metastases Clinical Practice Today CME Co-provided by Learning Objectives Upon completion, participants should be able to: Understand the benefits, limitations,
Temozolomide in the treatment of recurrent malignant glioma in Chinese patients!"#$%&'()*+,-./0,1234
 Key words: Astrocytoma; Brain neoplasms; Disease-free survival; Glioblastoma; Neoplasm recurrence!!"!"!"#$ DTM Chan WS Poon YL Chan HK Ng Hong Kong Med J 2005;11:452-6 The Chinese University of Hong Kong,
Key words: Astrocytoma; Brain neoplasms; Disease-free survival; Glioblastoma; Neoplasm recurrence!!"!"!"#$ DTM Chan WS Poon YL Chan HK Ng Hong Kong Med J 2005;11:452-6 The Chinese University of Hong Kong,
FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR PILOCYTIC ASTROCYTOMA
 1 EVIDENCE SUMMARY REPORT FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR PILOCYTIC ASTROCYTOMA QUESTIONS TO BE ADDRESSED: SUMMARY 1. What is the evidence for the clinical
1 EVIDENCE SUMMARY REPORT FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR PILOCYTIC ASTROCYTOMA QUESTIONS TO BE ADDRESSED: SUMMARY 1. What is the evidence for the clinical
Positively Impacting Patient Outcomes With imri Suite
 In Practice Positively Impacting Patient Outcomes With imri Suite In Practice Something pretty amazing is happening in the middle of America s Dairyland. Neurosurgery tumor resection and deep brain stimulation
In Practice Positively Impacting Patient Outcomes With imri Suite In Practice Something pretty amazing is happening in the middle of America s Dairyland. Neurosurgery tumor resection and deep brain stimulation
Surgical resection versus watchful waiting in low-grade gliomas
 Annals of Oncology 28: 1942 1948, 217 doi:1.193/annonc/mdx23 Published online 5 May 217 ORIGINAL ARTICLE Surgical resection versus watchful waiting in low-grade gliomas A. S. Jakola 1,2,3 *, A. J. Skjulsvik
Annals of Oncology 28: 1942 1948, 217 doi:1.193/annonc/mdx23 Published online 5 May 217 ORIGINAL ARTICLE Surgical resection versus watchful waiting in low-grade gliomas A. S. Jakola 1,2,3 *, A. J. Skjulsvik
Response to postoperative radiotherapy as a prognostic factor for patients with low-grade gliomas
 ONCOLOGY LETTERS 4: 455-460, 2012 Response to postoperative radiotherapy as a prognostic factor for patients with low-grade gliomas MICHAL SPYCH 1,2, LESZEK GOTTWALD 3, EMILIA JESIEŃ LEWANDOWICZ 1,2, SŁAWOMIR
ONCOLOGY LETTERS 4: 455-460, 2012 Response to postoperative radiotherapy as a prognostic factor for patients with low-grade gliomas MICHAL SPYCH 1,2, LESZEK GOTTWALD 3, EMILIA JESIEŃ LEWANDOWICZ 1,2, SŁAWOMIR
Survival Analysis of Glioblastoma Multiforme
 DOI:10.22034/APJCP.2018.19.9.2613 RESEARCH ARTICLE Editorial Process: Submission:04/24/2018 Acceptance:08/19/2018 Supapan Witthayanuwat, Montien Pesee*, Chunsri Supaadirek, Narudom Supakalin, Komsan Thamronganantasakul,
DOI:10.22034/APJCP.2018.19.9.2613 RESEARCH ARTICLE Editorial Process: Submission:04/24/2018 Acceptance:08/19/2018 Supapan Witthayanuwat, Montien Pesee*, Chunsri Supaadirek, Narudom Supakalin, Komsan Thamronganantasakul,
Early Post-Operative MRI: Correlation with Progression-Free Survival and Overall Survival Time in Malignant Gliomas
 J. Exp. Clin. Cancer Res., 25, 2, 2006 Early Post-Operative MRI: Correlation with Progression-Free Survival and Overall Survival Time in Malignant Gliomas A. Vidiri 1, C. M. Carapella 2, A. Pace 3, A.
J. Exp. Clin. Cancer Res., 25, 2, 2006 Early Post-Operative MRI: Correlation with Progression-Free Survival and Overall Survival Time in Malignant Gliomas A. Vidiri 1, C. M. Carapella 2, A. Pace 3, A.
