Moyamoya disease is a progressive cerebrovascular. Pial synangiosis in patients with moyamoya younger than 2 years of age.
|
|
|
- Johnathan Hoover
- 6 years ago
- Views:
Transcription
1 J Neurosurg Pediatrics 13: , 2014 AANS, 2014 Pial synangiosis in patients with moyamoya younger than 2 years of age Clinical article Eric M. Jackson, M.D., Ning Lin, M.D., Sunil Manjila, M.D., R. Michael Scott, M.D., and Edward R. Smith, M.D. Department of Neurosurgery, Children s Hospital Boston, Harvard Medical School, Boston, Massachusetts Object. Patients with moyamoya who are younger than 2 years of age represent a therapeutic challenge because of their frequent neurological instability and concomitant anesthetic risks. The authors report their experience with pial synangiosis revascularization in this population. Methods. The authors reviewed the clinical and radiographic records of all patients with moyamoya in a consecutive series of patients under 2 years of age, who underwent cerebral revascularization surgery using pial synangiosis at a single institution. Results. During a 12-year period ( ), 34 procedures (bilateral in 15 patients, unilateral in 4) were performed in 19 patients younger than 2 years (out of a total of 456 procedures in 240 patients). Eighteen of these patients presented with either stroke or transient ischemic attack. The average age of the 19 patients at first surgery was 1.4 years (range 6 months 1.9 years). Unanticipated staged operations occurred in 3 patients, due to persistent electroencephalographic changes during the initial surgery in 2 cases and due to brain swelling during the procedure requiring ventriculostomy in the other. There were 2 perioperative strokes; both patients had postoperative seizures but made clinical recoveries. The average follow-up was 7 years (range 1 14 years). Long term, at follow-up, 13 patients (68%) were clinically independent for their age, with 8 (42%) having no significant deficit. Late complications included subdural hygroma evacuation (1), additional revascularization procedures performed years later for frontal lobe ischemia (2), late infarction (1), and asymptomatic ischemic change on routine follow-up MRI studies (1). All patients who had both pre- and postoperative angiography demonstrated progression of disease. Conclusions. Despite the challenges inherent to this population, the majority of children with moyamoya under the age of 2 years have a good long-term prognosis. The data from this study support the use of pial synangiosis as a safe, effective, and durable method for treatment of moyamoya for most children in this potentially high-risk population. ( Key Words pial synangiosis moyamoya pediatric vascular disorders Abbreviations used in this paper: DSA = digital subtraction an giography; EDAS = encephaloduroarteriosynangiosis; EEG = electroencephalographic; IRB = institutional review board; mrs = modified Rankin Scale; STA = superficial temporal artery; TIA = transient ischemic attack. Moyamoya disease is a progressive cerebrovascular arteriopathy and a common cause of stroke in the pediatric population. 9,14 It is characterized by stenosis and occlusion of the distal internal carotid arteries and, less often, the proximal anterior cerebral and middle cerebral arteries. Associated with the stenosis is the development of collateral vessels from perforating arteries at the base of the brain, which gives the puff of smoke appearance. Surgical revascularization of the ischemic cerebral hemispheres, either with direct or indirect methods, significantly improves the long-term outcome for children with moyamoya. 3,5,6,10,13,15,16 Young children with moyamoya have been historically thought to be the most severely affected and most challenging to treat subgroup of all moyamoya patients. 5,8,12 The clinical course in these patients is frequently dynamic and rapidly progressing, leading to major strokes on presentation and poor eventual outcome. Furthermore, infants with moyamoya have severely compromised cerebrovascular reserve and are usually felt to have increased anesthetic risks. 17 Despite the fact that aggressive surgical management is usually warranted, moyamoya surgery This article contains some figures that are displayed in color on line but in black-and-white in the print edition. 420 J Neurosurg: Pediatrics / Volume 13 / April 2014
2 Moyamoya patients under 2 years of age in patients less than 2 years of age is performed infrequently, and there is limited literature that separates out this youngest age group of moyamoya patients. Here we present a single-center experience in treating moyamoya patients younger than 2 years with pial synangiosis. Methods Patient Selection A consecutive surgical series of patients with moyamoya arteriopathy who underwent pial synangiosis from 1994 through 2005 was reviewed to identify all patients who were younger than 2 years at the time of surgery. All patients who underwent surgery within this time period were included. In accordance with an institutional review board (IRB)-approved protocol, medical records were retrospectively reviewed to determine patient demographic information, age at presentation and initial surgery, symptoms at presentation, comorbid conditions, results of radiographic studies, perioperative and late complications, and long-term outcomes. The modified Rankin Scale (mrs) score at late follow-up and the Matsushima Scale score on postoperative digital subtraction angiography (DSA) were used to evaluate the outcome of this cohort. All these data are collected routinely as part of an IRBapproved protocol and longitudinal moyamoya database. Surgery and Perioperative Management The technique of pial synangiosis has been described previously. 1 Briefly, the superficial temporal artery (STA) is mapped with Doppler ultrasonography, and an STA graft is isolated and dissected free. A craniotomy is performed in the frontotemporal region, and the dura mater is opened into multiple flaps. The arachnoid membrane is dissected widely to expose the pial surface, and the STA graft is sewn to the pia mater with 10 0 monofilament nylon sutures. The dura mater is left open to prevent constriction of the arterial graft and to provide additional surface area for collateralization from meningeal vessels. Patients routinely are administered aspirin right up to the day of surgery and resume on postoperative Day 1. Patients who present with bilateral disease and require treatments to both hemispheres are usually operated bilaterally under a single anesthesia, assuming no operative or anesthetic complications or electroencephalographic (EEG) changes. Postoperative DSA is routinely performed 1 year after synangiosis surgery. Results Demographics A total of 240 patients were operated on for moyamoya during the study period. Nineteen (8%) of those patients were under 2 years of age at the time of their first operation and were included in the study. The demographic and clinical characteristics of the study cohort are summarized in Table 1. There were 11 female and 8 male patients in the group. Their average age at presentation was 1.1 years (range 2 months 1.7 years). Their average J Neurosurg: Pediatrics / Volume 13 / April 2014 age at the time of their first surgery was 1.4 years (range 6 months 1.9 years). A number of patients had associated diseases: 3 had neurofibromatosis Type 1, 2 had Noonan syndrome, and 1 had Alagille syndrome. Three patients had other vascular diseases 2 had cutaneous hemangiomas and 1 had a facial arteriovenous malformation. Moreover, there were familial associations in the study cohort 2 patients included were siblings and 1 patient had a mother with surgically treated moyamoya. Presentation Eighteen of the patients presented with evidence of cerebral ischemia (Table 2). Seventeen patients had clinical and imaging evidence of infarction. Four patients presented initially with seizures and were noted to have infarction on the imaging workup for the seizures. One patient had crescendo transient ischemic attacks (TIAs) with deep white matter changes on imaging. The remaining patient in the study group was worked up secondary to family history (2 siblings with moyamoya). She was noted to have significant asymptomatic disease and underwent prophylactic surgery. Operative Treatment All patients in the series underwent pial synangiosis as described above. 1 Thirty-four treated hemispheres were included in this analysis, out of a total of 456 surgically treated hemispheres in the entire series of 240 pedi- TABLE 1: Clinical and demographic characteristics of the study cohort* Characteristic Value no. of patients 19 age at presentation mean 1.1 yrs range 2 mos 1.7 yrs age at 1st op mean 1.4 yrs range 6 mos 1.9 yrs sex female 11 (57.9%) male 8 (42.1%) bilateral moyamoya yes 17 (88.9%) no 2 (11.1%) associated disease/condition NF1 3 Graves disease 2 Noonan syndrome 2 Alagille syndrome 1 facial AVM 1 hemangioma 2 * Values represent numbers of patients (%) unless otherwise indicated. AVM = arteriovenous malformation; NF1 = neurofibromatosis Type
3 E. M. Jackson et al. TABLE 2: Presenting symptoms in 19 patients with moyamoya disease younger than 2 years of age Presenting Symptom No. of Patients (%) TIA 18 (94.7) stroke 17 (89.5) seizure 4 (21.1) hemorrhage 0 (0.0) asymptomatic 1 (5.3) atric patients treated during this time period. Two operated hemispheres were excluded from the study. In one of these cases, the patient had a second hemisphere operated upon in a staged fashion after her second birthday. In the other. the patient had a myosynangiosis during the same anesthesia session on the opposite side due to the absence of a donor vessel following earlier treatment of a facial hemangioma. Twelve patients had bilateral procedures during a single session of anesthesia (including dural synangiosis in 1 patient without donor vessel). Three patients had staged bilateral procedures (one procedure was performed after 1 patient s second birthday). Four patients had unilateral procedures. Perioperative Complications Three patients underwent unanticipated staged procedures. Two patients had the second hemisphere treated in a staged procedure because of persistent EEG changes during the initial surgery. The third patient had significant brain swelling after the first operation requiring the placement of an external ventriculostomy drain (Table 3). Two patients developed perioperative infarcts, both of whom presented with seizures 12 hours postoperatively in one case and 36 hours postoperatively in the other. Both patients had immediate CT scans that demonstrated infarction. At the time of the operation, the first patient was noted to have an area of white, devascularized brain that was larger than the preoperative scans had suggested; the exact cause of the new event could not be determined. The second patient who suffered a stroke was undergoing the staged second-side procedure following an initial synangiosis that was complicated by EEG changes and brain swelling, suggesting that this patient had marked cerebrovascular instability under anesthesia. TABLE 3: Perioperative and delayed complications after pial synangiosis in 19 patients with moyamoya disease younger than 2 years of age Variable No. of Patients (%) perioperative complications persistent EEG change 2 brain swelling 1 seizures 2* infarction 2 delayed complications during follow-up hematoma evacuation 1 repeat synangiosis 2 infarction 1 asymptomatic MRI change 1 death 0 long-term outcome favorable (mrs 0 2) 13 (68.4%) unfavorable (mrs 3 6) 6 (31.6%) * In both cases, workup demonstrated infarction. Radiographic Outcome After Hospital Discharge Complete pre- and postoperative angiographic data with Suzuki grades 18 were available for 6 patients (11 hemispheres). All 6 patients (10 of 11 hemispheres) demonstrated progression of disease on postoperative DSA at 1 year after synangiosis surgery (Fig. 1). The 1 hemisphere that did not demonstrate progression had been graded 4 5 preoperatively. While we recommended postoperative DSA to all patients, some parents declined the procedure. As a result, data on 19 hemispheres in 10 patients were available to assess the development of collaterals following synangiosis surgery (Fig. 1). Eleven hemispheres were considered Matsushima A (57.9%); 6 were considered B (31.6%); and 2 were considered C (10.5%). 11 Clinical Outcome at Long-Term Follow-Up Outcomes (clinical and radiological) were reviewed with an average follow-up period of 7 years (range 1 14 years). Patients had an mrs score 15 calculated based on their most recent clinic note. Of the 19 patients, 8 had a score of either 0 or 1, 5 had a score of 2, 3 had a score of 3, 4 had a score of 4, and 0 had a score of 5 or 6 (Fig. 2). Thirteen patients (68.4%) were clinically independent for their age, with 8 (42.1%) having no significant deficit. Overall, 18 patients (94.7%) had improved or stable neurological status at follow-up compared with that prior to surgery. Delayed complications during follow-up are summarized in Table 3. No patient died during the followup period (mortality 0%). Of the 19 patients, 3 had additional neurosurgical procedures. One patient who had initially presented with significant bilateral infarcts and had undergone surgery on an urgent basis returned to the operating room 1 year later for drainage of subdural fluid collections, which were found to be under low pressure. Two other patients underwent repeat synangiosis for persistent TIA symptoms in the anterior cerebral artery territory. One patient had a right frontal pericranial synangiosis performed 4 years later. Of note, this hemisphere had been treated in a nonstandard fashion because of the absence of a donor vessel due to a facial hemangioma. The other patient returned to the operating room twice, for right frontal pericranial synangiosis 5 years after the original surgery and for right frontotemporal and parietotemporal dural synangiosis 8 years after the original surgery. One patient had a late infarct, presenting with right foot weakness 4 years postoperatively with evidence of 422 J Neurosurg: Pediatrics / Volume 13 / April 2014
4 Moyamoya patients under 2 years of age Fig. 1. Illustrative case involving an 18-month-old boy with bilateral moyamoya treated with bilateral pial synangiosis. The patient presented with seizures, and brain MRI demonstrated infarction (arrow) on T2-weighted sequence (A) and slow cortical flow ( ivy sign, arrowheads) on FLAIR sequence (B). Preoperative DSA showed moyamoya arteriopathy in both hemispheres, with Suzuki Grade III on the right (C) and Grade II on the left (D). (The arrows indicate changes typical of the respective grades.) Postoperative injections from the external carotid arteries showed significant collaterals developed around the pial synangiosis, with Matsushima Grade A revascularization in both hemispheres (E and F). infarction on CT. These symptoms improved with time. An additional patient was noted to have new asymptomatic ischemic T2 signal changes on follow-up MRI. Discussion In this patient series, we chose a 2-year age cutoff to define a moyamoya patient population that we and others have noted to frequently have a fulminant clinical course and a poor long-term prognosis. Other measures to define this high-risk population, such as patient weight or radiographic measures of brain development, such as myelination status, might be equally useful Young children with moyamoya usually present with a severe ischemic burden and advanced arteriopathy and are frequently noted to have a poor prognosis. 5,6,8,12 Matsushima et al. 12 studied mental and cognitive outcomes following encephaloduroarteriosynangiosis (EDAS) in pa tients with onset of disease before 5 years of age. They found that children who presented at less than 2 years of age had a poor mental prognosis, with 7 of 8 patients having an IQ less than 80 (less than 61 in all 7 cases). Kim et al. 8 demonstrated that patients younger than 3 years had a higher rate of infarction at presentation (87%) and lower J Neurosurg: Pediatrics / Volume 13 / April 2014 rate of favorable outcome (58%) than older pediatric populations. Moreover, 39% of patients (9 of 23) in this age group (0 3 years of age) had additional infarctions while awaiting surgery, suggesting a rapidly progressive clinical course. 8 Our data were consistent with these prior reports and showed that children with moyamoya under 2 years of age presented with advanced disease. Eighteen (94.7%) Fig. 2. Modified Rankin Scale scores during long-term follow-up for patients who presented with moyamoya at less than 2 years of age. The x-axis indicates mrs scores; the y-axis percentages of patients. 423
5 E. M. Jackson et al. of the patients in the study presented with symptoms and imaging findings consistent with significant ischemia. The single patient without significant ischemia had been screened secondary to significant family history. Moyamoya disease in very young children (under 2 years of age) poses a significant challenge to the treating neurosurgeon. The small vascular caliber of donor vessels usually renders direct bypass technically challenging, and in these patients, indirect revascularization techniques are frequently used. Patients in this age group have markedly limited cerebrovascular reserve; as a result, it is essential to avoid hypotension, hypovolemia, and hyperthermia during induction and throughout the operation. Postoperatively, pain control is of vital importance to prevent persistent crying and hyperventilation. Additionally, we strongly believe that antiplatelet therapy should be given before and after surgery, and that intravenous fluid administration should be generous (1.5 times maintenance) postoperatively until the patient is able to tolerate good oral intake. Although our study cohort is small, the results suggest that pial synangiosis can be safely performed in children with moyamoya less than 2 years of age, although 2 patients in our series suffered perioperative strokes (rate of 10.5% per patient, 5.6% per treated hemisphere) despite careful attention to the perioperative treatment measures outlined above. There was no infectious complication or perioperative mortality. These results compare favorably to prior reports in the literature on moyamoya patients in a similar age group. In a large retrospective series, S. K. Kim et al. 8 divided 204 patients treated with EDAS into 3 age categories and reported a 17% perioperative stroke rate (4 of 23 cases) in patients under 3 years of age. S. H. Kim et al. 7 analyzed 90 children treated for moyamoya and found that age less than 3 years at time of operation was a significant factor associated with perioperative stroke (occurring in 5 [27.8%] of 18 cases). Postoperative angiography demonstrated Matsushima A-B revascularization in 89.5% of treated hemispheres in our series, which was similar to reports from our institution 15 and others 2 on children with moyamoya of all age groups. In the long-term follow-up, despite young age and advanced disease at presentation, most patients (13 [68.4%] of 19) had favorable outcomes and were functionally independent. These results, compared with the natural history of 65% 82% stroke risk over 5 years, 4,9 suggest that pial synangiosis can be an effective and durable method of treating moyamoya patients under 2 years of age. These clinical findings also support the notion that aggressive surgical management is necessary and essential to improve the outcome for moyamoya children in the very young age group. There are several limitations to be considered in interpreting these results. The study was a retrospective case series and sample size was small. Postoperative angiography was declined by some patients families, which could introduce additional selection bias. Nevertheless, our findings confirm that young children with moyamoya less than 2 years of age present with significant disease burden and ischemia. Conclusions Pial synangiosis is a safe, effective, and durable treatment for moyamoya patients under 2 years of age with a relatively low perioperative complication rate. Following synangiosis surgery, the majority of these patients have a favorable outcome and functional independence. Disclosure The authors report no conflict of interest concerning the materials or methods used in this study or the findings specified in this paper. Author contributions to the study and manuscript preparation include the following. Conception and design: Smith, Jackson, Lin, Scott. Acquisition of data: Smith, Jackson, Lin, Scott. Analysis and interpretation of data: Smith, Jackson, Lin, Scott. Drafting the article: Smith, Jackson, Lin, Scott. Critically revising the article: all authors. Reviewed submitted version of manuscript: all authors. Approved the final version of the manuscript on behalf of all authors: Smith. Administrative/technical/material support: Smith. Study supervision: Smith, Scott. References 1. Adelson PD, Scott RM: Pial synangiosis for moyamoya syndrome in children. Pediatr Neurosurg 23:26 33, Golby AJ, Marks MP, Thompson RC, Steinberg GK: Direct and combined revascularization in pediatric moyamoya disease. Neurosurgery 45:50 60, Guzman R, Lee M, Achrol A, Bell-Stephens T, Kelly M, Do HM, et al: Clinical outcome after 450 revascularization procedures for moyamoya disease. Clinical article. J Neurosurg 111: , Hallemeier CL, Rich KM, Grubb RL Jr, Chicoine MR, Moran CJ, Cross DT III, et al: Clinical features and outcome in North American adults with moyamoya phenomenon. Stroke 37: , Imaizumi T, Hayashi K, Saito K, Osawa M, Fukuyama Y: Long-term outcomes of pediatric moyamoya disease monitored to adulthood. Pediatr Neurol 18: , Isono M, Ishii K, Kamida T, Inoue R, Fujiki M, Kobayashi H: Long-term outcomes of pediatric moyamoya disease treated by encephalo-duro-arterio-synangiosis. Pediatr Neurosurg 36:14 21, Kim SH, Choi JU, Yang KH, Kim TG, Kim DS: Risk factors for postoperative ischemic complications in patients with moyamoya disease. J Neurosurg 103 (5 Suppl): , Kim SK, Seol HJ, Cho BK, Hwang YS, Lee DS, Wang KC: Moyamoya disease among young patients: its aggressive clinical course and the role of active surgical treatment. Neurosurgery 54: , Kuroda S, Houkin K: Moyamoya disease: current concepts and future perspectives. Lancet Neurol 7: , Lin N, Baird L, Koss M, Kopecky KE, Gone E, Ullrich NJ, et al: Discovery of asymptomatic moyamoya arteriopathy in pediatric syndromic populations: radiographic and clinical progression. Neurosurg Focus 31(6):E6, Matsushima T, Inoue T, Suzuki SO, Fujii K, Fukui M, Hasuo K: Surgical treatment of moyamoya disease in pediatric patients comparison between the results of indirect and direct revascularization procedures. Neurosurgery 31: , Matsushima Y, Aoyagi M, Masaoka H, Suzuki R, Ohno K: Mental outcome following encephaloduroarteriosynangiosis in children with moyamoya disease with the onset earlier than 5 years of age. Childs Nerv Syst 6: , Roach ES, Golomb MR, Adams R, Biller J, Daniels S, Deve- 424 J Neurosurg: Pediatrics / Volume 13 / April 2014
6 Moyamoya patients under 2 years of age ber G, et al: Management of stroke in infants and children: a scientific statement from a Special Writing Group of the American Heart Association Stroke Council and the Council on Cardiovascular Disease in the Young. Stroke 39: , Scott RM, Smith ER: Moyamoya disease and moyamoya syndrome. N Engl J Med 360: , Scott RM, Smith JL, Robertson RL, Madsen JR, Soriano SG, Rockoff MA: Long-term outcome in children with moyamoya syndrome after cranial revascularization by pial synangiosis. J Neurosurg 100 (2 Suppl Pediatrics): , Smith ER, Scott RM: Surgical management of moyamoya syndrome. Skull Base 15:15 26, Soriano SG, Sethna NF, Scott RM: Anesthetic management of children with moyamoya syndrome. Anesth Analg 77: , Suzuki J, Takaku A: Cerebrovascular moyamoya disease. Disease showing abnormal net-like vessels in base of brain. Arch Neurol 20: , 1969 Manuscript submitted May 17, Accepted January 10, The data reported in this manuscript were presented at the International Stroke Conference in New Orleans, Louisiana, February 1 3, Current affiliation for Dr. Jackson: Johns Hopkins University, Baltimore, Maryland. Please include this information when citing this paper: published online February 14, 2014; DOI: / PEDS Address correspondence to: Edward R. Smith, M.D., Department of Neurosurgery, Hunnewell 2, 300 Longwood Ave., Boston, MA edward.smith@childrens.harvard.edu. J Neurosurg: Pediatrics / Volume 13 / April
INSTITUTE OF NEUROSURGERY & DEPARTMENT OF PICU
 CEREBRAL BYPASS An Innovative Treatment for Arteritis INSTITUTE OF NEUROSURGERY & DEPARTMENT OF PICU CASE 1 q 1 year old girl -recurrent seizure, right side limb weakness, excessive cry and irritability.
CEREBRAL BYPASS An Innovative Treatment for Arteritis INSTITUTE OF NEUROSURGERY & DEPARTMENT OF PICU CASE 1 q 1 year old girl -recurrent seizure, right side limb weakness, excessive cry and irritability.
In patients with moyamoya the clinical significance of. Preoperative transdural collateral vessels in moyamoya as radiographic biomarkers of disease
 CLINICAL ARTICLE J Neurosurg Pediatr 19:289 295, 2017 Preoperative transdural collateral vessels in moyamoya as radiographic biomarkers of disease Armide Storey, BS, 1 R. Michael Scott, MD, 1 Richard Robertson,
CLINICAL ARTICLE J Neurosurg Pediatr 19:289 295, 2017 Preoperative transdural collateral vessels in moyamoya as radiographic biomarkers of disease Armide Storey, BS, 1 R. Michael Scott, MD, 1 Richard Robertson,
Anesthetic Management of Child with Moyamoya Disease for Pial Synangiosis
 Anesthetic Management of Child with Moyamoya Disease for Pial Synangiosis Craig D. McClain, MD, MPH Boston Children s Hospital and Harvard Medical School Case Presentation 14 year old male with bilateral
Anesthetic Management of Child with Moyamoya Disease for Pial Synangiosis Craig D. McClain, MD, MPH Boston Children s Hospital and Harvard Medical School Case Presentation 14 year old male with bilateral
MOYA Moya disease is a rare idiopathic
 Research Papers Moya Moya Cases Treated with Encephaloduroarteriosynangiosis Parimal Tripathi, Varsha Tripathi, Ronak J. Naik and Jaimin M. Patel From Gujarat Cancer & Research Institute, Ahmedabad; Sterling
Research Papers Moya Moya Cases Treated with Encephaloduroarteriosynangiosis Parimal Tripathi, Varsha Tripathi, Ronak J. Naik and Jaimin M. Patel From Gujarat Cancer & Research Institute, Ahmedabad; Sterling
Anaesthesia recommendations for patients suffering from. Moyamoya disease
 orphananesthesia Anaesthesia recommendations for patients suffering from Disease name: Moyamoya disease ICD 10: I67.5 Moyamoya disease Synonyms: Moyamoya means something hazy, like a puff of cigarette
orphananesthesia Anaesthesia recommendations for patients suffering from Disease name: Moyamoya disease ICD 10: I67.5 Moyamoya disease Synonyms: Moyamoya means something hazy, like a puff of cigarette
Neurosurg Focus 5 (5):Article 4, 1998
 Neurosurg Focus 5 (5):Article 4, 1998 Multiple combined indirect procedure for the surgical treatment of children with moyamoya disease. A comparison with single indirect anastomosis with direct anastomosis
Neurosurg Focus 5 (5):Article 4, 1998 Multiple combined indirect procedure for the surgical treatment of children with moyamoya disease. A comparison with single indirect anastomosis with direct anastomosis
Title. CitationWorld Neurosurgery, 80(5): Issue Date Doc URL. Rights. Rights(URL)
 Title Effective Surgical Revascularization Improves Cerebr Moyamoya Disease Kawabori, Masahito; Kuroda, Satoshi; Nakayama, Naoki Author(s) Nagara CitationWorld Neurosurgery, 80(5): 612-619 Issue Date 2013-11
Title Effective Surgical Revascularization Improves Cerebr Moyamoya Disease Kawabori, Masahito; Kuroda, Satoshi; Nakayama, Naoki Author(s) Nagara CitationWorld Neurosurgery, 80(5): 612-619 Issue Date 2013-11
Title in Children. Issue Date Copyright 2011 S. Karger AG, Base.
 NAOSITE: Nagasaki University's Ac Title Author(s) Clinical Features and Long-Term Fol in Children. Hayashi, Kentaro; Horie, Nobutaka; Citation Pediatric Neurosurgery, 47(1), pp.1 Issue Date 2011-09 URL
NAOSITE: Nagasaki University's Ac Title Author(s) Clinical Features and Long-Term Fol in Children. Hayashi, Kentaro; Horie, Nobutaka; Citation Pediatric Neurosurgery, 47(1), pp.1 Issue Date 2011-09 URL
Overview Blood supply of the brain What is moyamoya disease? > 1
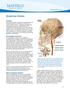 Moyamoya Disease Overview Moyamoya disease is caused by blocked arteries at the base of the brain. The name "moyamoya" means "puff of smoke" in Japanese and describes the appearance of tiny vessels that
Moyamoya Disease Overview Moyamoya disease is caused by blocked arteries at the base of the brain. The name "moyamoya" means "puff of smoke" in Japanese and describes the appearance of tiny vessels that
Young So, MD; Ho-Young Lee, MD; Seung-Ki Kim, MD; Jae Sung Lee, PhD; Kyu-Chang Wang, MD; Byung-Kyu Cho, MD; Eunjoo Kang, PhD; Dong Soo Lee, MD
 Prediction of the Clinical Outcome of Pediatric Moyamoya Disease With Postoperative Basal/Acetazolamide Stress Brain Perfusion SPECT After Revascularization Surgery Young So, MD; Ho-Young Lee, MD; Seung-Ki
Prediction of the Clinical Outcome of Pediatric Moyamoya Disease With Postoperative Basal/Acetazolamide Stress Brain Perfusion SPECT After Revascularization Surgery Young So, MD; Ho-Young Lee, MD; Seung-Ki
Moyamoya syndrome associated with cocaine abuse Case report
 Neurosurg Focus 5 (5):Article 7, 1998 Moyamoya syndrome associated with cocaine abuse Case report Marc S. Schwartz, M.D., and R. Michael Scott, M.D. Division of Neurosurgery, Albany Medical College, Albany,
Neurosurg Focus 5 (5):Article 7, 1998 Moyamoya syndrome associated with cocaine abuse Case report Marc S. Schwartz, M.D., and R. Michael Scott, M.D. Division of Neurosurgery, Albany Medical College, Albany,
Clinicoepidemiological Features of Asymptomatic Moyamoya Disease in Adult Patients
 Journal of Cerebrovascular and Endovascular Neurosurgery pissn 2234-8565, eissn 2287-3139, http://dx.doi.org/10.7461/jcen.2014.16.3.241 Original Article Clinicoepidemiological Features of Asymptomatic
Journal of Cerebrovascular and Endovascular Neurosurgery pissn 2234-8565, eissn 2287-3139, http://dx.doi.org/10.7461/jcen.2014.16.3.241 Original Article Clinicoepidemiological Features of Asymptomatic
Longitudinal anterior-to-posterior shift of collateral channels in patients with moyamoya disease: an implication for its hemorrhagic onset
 CLINICAL ARTICLE Longitudinal anterior-to-posterior shift of collateral channels in patients with moyamoya disease: an implication for its hemorrhagic onset Shusuke Yamamoto, MD, Satoshi Hori, MD, PhD,
CLINICAL ARTICLE Longitudinal anterior-to-posterior shift of collateral channels in patients with moyamoya disease: an implication for its hemorrhagic onset Shusuke Yamamoto, MD, Satoshi Hori, MD, PhD,
Supratentorial cerebral arteriovenous malformations : a clinical analysis
 Original article: Supratentorial cerebral arteriovenous malformations : a clinical analysis Dr. Rajneesh Gour 1, Dr. S. N. Ghosh 2, Dr. Sumit Deb 3 1Dept.Of Surgery,Chirayu Medical College & Research Centre,
Original article: Supratentorial cerebral arteriovenous malformations : a clinical analysis Dr. Rajneesh Gour 1, Dr. S. N. Ghosh 2, Dr. Sumit Deb 3 1Dept.Of Surgery,Chirayu Medical College & Research Centre,
History of revascularization
 History of revascularization Author (year) Kredel, 1942 Woringer& Kunlin, 1963 Donaghy& Yasargil, 1968 Loughheed 1971 Kikuchini & Karasawa1973 Karasawa, 1977 Story, 1978 Sundt, 1982 EC/IC bypass study
History of revascularization Author (year) Kredel, 1942 Woringer& Kunlin, 1963 Donaghy& Yasargil, 1968 Loughheed 1971 Kikuchini & Karasawa1973 Karasawa, 1977 Story, 1978 Sundt, 1982 EC/IC bypass study
Moyamoya. Moyamoya Disease Double Trouble. Epidemiology 1/16/2015
 Moyamoya Moyamoya Disease Double Trouble Jan Boerke, ACNP AACN Brunch January 24, 2015 Moyamoya - puff of smoke in Japanese Describes the look of the tangle of tiny vessels formed to compensate for the
Moyamoya Moyamoya Disease Double Trouble Jan Boerke, ACNP AACN Brunch January 24, 2015 Moyamoya - puff of smoke in Japanese Describes the look of the tangle of tiny vessels formed to compensate for the
Direct Bypass Techniques for the Treatment of Pediatric Moyamoya Disease
 Direct Bypass Techniques for the Treatment of Pediatric Moyamoya Disease Raphael Guzman, MD a, Gary K. Steinberg, MD, PhD b, * KEYWORDS Moyamoya disease Pediatric Direct bypass INDICATIONS Moyamoya disease
Direct Bypass Techniques for the Treatment of Pediatric Moyamoya Disease Raphael Guzman, MD a, Gary K. Steinberg, MD, PhD b, * KEYWORDS Moyamoya disease Pediatric Direct bypass INDICATIONS Moyamoya disease
Moyamoya disease (MMD), an idiopathic disease. Direct versus indirect revascularization in the treatment of moyamoya disease
 CLINICAL ARTICLE J Neurosurg 129:480 489, 2018 Direct versus indirect revascularization in the treatment of moyamoya disease *Seong-eun Park, BSc, Ju-seong Kim, MD, Eun Kyung Park, MD, Kyu-Won Shim, MD,
CLINICAL ARTICLE J Neurosurg 129:480 489, 2018 Direct versus indirect revascularization in the treatment of moyamoya disease *Seong-eun Park, BSc, Ju-seong Kim, MD, Eun Kyung Park, MD, Kyu-Won Shim, MD,
Moyamoya disease (MMD) is a rare steno-occlusive
 CLINICAL ARTICLE J Neurosurg 126:1573 1577, 2017 Low flow velocity in the middle cerebral artery predicting infarction after bypass surgery in adult moyamoya disease *Hoyeon Cho, MD, 1 Kyung Il Jo, MD,
CLINICAL ARTICLE J Neurosurg 126:1573 1577, 2017 Low flow velocity in the middle cerebral artery predicting infarction after bypass surgery in adult moyamoya disease *Hoyeon Cho, MD, 1 Kyung Il Jo, MD,
Unstable moyamoya disease: clinical features and impact on perioperative ischemic complications
 clinical article J Neurosurg 122:400 407, 2015 Unstable moyamoya disease: clinical features and impact on perioperative ischemic complications Takeshi Funaki, MD, 1 Jun C. Takahashi, MD, PhD, 1 Yasushi
clinical article J Neurosurg 122:400 407, 2015 Unstable moyamoya disease: clinical features and impact on perioperative ischemic complications Takeshi Funaki, MD, 1 Jun C. Takahashi, MD, PhD, 1 Yasushi
Neurosurgical Treatment of Moyamoya Disease: Bypass Surgery for the Brain
 Neurosurgical Treatment of Moyamoya Disease: Bypass Surgery for the Brain Christopher Payne Currently, no medical treatment exists to prevent the progression of moyamoya disease, and neurosurgical treatment
Neurosurgical Treatment of Moyamoya Disease: Bypass Surgery for the Brain Christopher Payne Currently, no medical treatment exists to prevent the progression of moyamoya disease, and neurosurgical treatment
Michael Horowitz, MD Pittsburgh, PA
 Michael Horowitz, MD Pittsburgh, PA Introduction Cervical Artery Dissection occurs by a rupture within the arterial wall leading to an intra-mural Hematoma. A possible consequence is an acute occlusion
Michael Horowitz, MD Pittsburgh, PA Introduction Cervical Artery Dissection occurs by a rupture within the arterial wall leading to an intra-mural Hematoma. A possible consequence is an acute occlusion
Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature
 Romanian Neurosurgery Volume XXXI Number 3 2017 July-September Article Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature Ashish Kumar Dwivedi, Pradeep Kumar,
Romanian Neurosurgery Volume XXXI Number 3 2017 July-September Article Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature Ashish Kumar Dwivedi, Pradeep Kumar,
A CASE OF RECURRENT ALTERNATING TRANSIENT HEMIPARESIS Dr. Shunmuga Arumugasamy.S DNB Resident Railway Hospital, Perambur.
 A CASE OF RECURRENT ALTERNATING TRANSIENT HEMIPARESIS Dr. Shunmuga Arumugasamy.S DNB Resident Railway Hospital, Perambur. 6 year old school going child. Apparently normal till 3 yrs when she developed
A CASE OF RECURRENT ALTERNATING TRANSIENT HEMIPARESIS Dr. Shunmuga Arumugasamy.S DNB Resident Railway Hospital, Perambur. 6 year old school going child. Apparently normal till 3 yrs when she developed
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
MMD is a rare cerebrovascular disease first described by
 ORIGINAL RESEARCH M.A. Mogensen P. Karzmark P.D. Zeifert J. Rosenberg M. Marks G.K. Steinberg L.J. Dorfman Neuroradiologic Correlates of Cognitive Impairment in Adult Moyamoya Disease BACKGROUND AND PURPOSE:
ORIGINAL RESEARCH M.A. Mogensen P. Karzmark P.D. Zeifert J. Rosenberg M. Marks G.K. Steinberg L.J. Dorfman Neuroradiologic Correlates of Cognitive Impairment in Adult Moyamoya Disease BACKGROUND AND PURPOSE:
CT perfusion in Moyamoya disease
 CT perfusion in Moyamoya disease Poster No.: C-1726 Congress: ECR 2015 Type: Scientific Exhibit Authors: K. C. Lam, C. P. Tsang, K. K. Wong, R. LEE ; HK, Hong Kong/HK Keywords: Hemodynamics / Flow dynamics,
CT perfusion in Moyamoya disease Poster No.: C-1726 Congress: ECR 2015 Type: Scientific Exhibit Authors: K. C. Lam, C. P. Tsang, K. K. Wong, R. LEE ; HK, Hong Kong/HK Keywords: Hemodynamics / Flow dynamics,
Neuroscience. Journal. Moyamoya disease a review and case illustration. P A L M E T T O H E A L T H Vol. 2 Issue 3 Summer 2016
 Neuroscience P A L M E T T O H E A L T H Vol. 2 Issue 3 Summer 2016 Journal Moyamoya disease a review and case illustration pg. 5 Choroid Plexus Papilloma in adults pg. 8 As physician co-leaders of Palmetto
Neuroscience P A L M E T T O H E A L T H Vol. 2 Issue 3 Summer 2016 Journal Moyamoya disease a review and case illustration pg. 5 Choroid Plexus Papilloma in adults pg. 8 As physician co-leaders of Palmetto
Moyamoya disease presenting as acute onset cortical blindness: a case report
 Romanian Neurosurgery Volume XXX Number 1 2016 January-March Article Moyamoya disease presenting as acute onset cortical blindness: a case report Dudi Maniram, Bansal Rajeev, Srivastava Trilochan, Sardana
Romanian Neurosurgery Volume XXX Number 1 2016 January-March Article Moyamoya disease presenting as acute onset cortical blindness: a case report Dudi Maniram, Bansal Rajeev, Srivastava Trilochan, Sardana
Emergency EC-IC bypass for symptomatic atherosclerotic ischemic stroke
 Emergency EC-IC bypass for symptomatic atherosclerotic ischemic stroke Tetsuyoshi Horiuchi, Junpei Nitta, Shigetoshi Ishizaka, Kohei Kanaya, Takao Yanagawa, and Kazuhiro Hongo. Department of Neurosurgery,
Emergency EC-IC bypass for symptomatic atherosclerotic ischemic stroke Tetsuyoshi Horiuchi, Junpei Nitta, Shigetoshi Ishizaka, Kohei Kanaya, Takao Yanagawa, and Kazuhiro Hongo. Department of Neurosurgery,
Recent Advances in Neurology Difficult Cases
 Patient X: History Part 1 Recent Advances in Neurology Difficult Cases Heather J. Fullerton, MD, MAS Professor of Neurology & Pediatrics Director, Pediatric Brain Center Previously healthy 14-year old
Patient X: History Part 1 Recent Advances in Neurology Difficult Cases Heather J. Fullerton, MD, MAS Professor of Neurology & Pediatrics Director, Pediatric Brain Center Previously healthy 14-year old
Title. Author(s) 黒田, 敏 ; 川堀, 真人 ; 宮本, 倫行 ; 笹森, 徹 ; 遠藤, 将吾 ; 中山, 若樹 ; 石川, 達哉. Citation 脳卒中の外科, 37(5): Issue Date Doc URL.
 Title 側頭葉から後頭葉にかけて高度の虚血を有するもやもや病に対する脳血行再建術 Author(s) 黒田, 敏 ; 川堀, 真人 ; 宮本, 倫行 ; 笹森, 徹 ; 遠藤, 将吾 ; 中山, 若樹 ; 石川, 達哉 Citation 脳卒中の外科, 37(5): 345-349 Issue Date 2009 Doc URL http://hdl.handle.net/2115/70929
Title 側頭葉から後頭葉にかけて高度の虚血を有するもやもや病に対する脳血行再建術 Author(s) 黒田, 敏 ; 川堀, 真人 ; 宮本, 倫行 ; 笹森, 徹 ; 遠藤, 将吾 ; 中山, 若樹 ; 石川, 達哉 Citation 脳卒中の外科, 37(5): 345-349 Issue Date 2009 Doc URL http://hdl.handle.net/2115/70929
 Impact of posterior cerebral artery Titleclinical and social outcome of pedi Dissertation_ 全文 ) Author(s) Funaki, Takeshi Citation Kyoto University ( 京都大学 ) Issue Date 2015-01-23 URL http://dx.doi.org/10.14989/doctor.r
Impact of posterior cerebral artery Titleclinical and social outcome of pedi Dissertation_ 全文 ) Author(s) Funaki, Takeshi Citation Kyoto University ( 京都大学 ) Issue Date 2015-01-23 URL http://dx.doi.org/10.14989/doctor.r
Moyamoya disease in the midwestern United States
 Neurosurg Focus 5 (5):Article 1, 1998 Moyamoya disease in the midwestern United States Nicholas M. Wetjen, B.S., P. Charles Garell, M.D., Nicholas V. Stence, and Christopher M. Loftus, M.D. Division of
Neurosurg Focus 5 (5):Article 1, 1998 Moyamoya disease in the midwestern United States Nicholas M. Wetjen, B.S., P. Charles Garell, M.D., Nicholas V. Stence, and Christopher M. Loftus, M.D. Division of
Moyamoya disease is an unusual form of chronic, occlusive
 Angiographic Dilatation and Branch Extension of the Anterior Choroidal and Posterior Communicating Arteries Are Predictors of Hemorrhage in Adult Moyamoya Patients Motohiro Morioka, MD; Jun-Ichiro Hamada,
Angiographic Dilatation and Branch Extension of the Anterior Choroidal and Posterior Communicating Arteries Are Predictors of Hemorrhage in Adult Moyamoya Patients Motohiro Morioka, MD; Jun-Ichiro Hamada,
Moyamoya disease (MMD), a cerebral vascular
 clinical article J Neurosurg 125:308 314, 2016 Surgical outcomes following encephaloduroarteriosynangiosis in adult moyamoya disease associated with Type 2 diabetes *Bin Ren, BS, 1,2 Zheng-Shan Zhang,
clinical article J Neurosurg 125:308 314, 2016 Surgical outcomes following encephaloduroarteriosynangiosis in adult moyamoya disease associated with Type 2 diabetes *Bin Ren, BS, 1,2 Zheng-Shan Zhang,
Moyamoya Disease in China Its Clinical Features and Outcomes
 Moyamoya Disease in China Its Clinical Features and Outcomes Lian Duan, MD, PhD; Xiang-Yang Bao, MM; Wei-Zhong Yang, BS; Wan-Chao Shi, MD; De-Sheng Li, MD; Zheng-Shan Zhang, MM; Rui Zong, MM; Cong Han,
Moyamoya Disease in China Its Clinical Features and Outcomes Lian Duan, MD, PhD; Xiang-Yang Bao, MM; Wei-Zhong Yang, BS; Wan-Chao Shi, MD; De-Sheng Li, MD; Zheng-Shan Zhang, MM; Rui Zong, MM; Cong Han,
Neurosurgical decision making in structural lesions causing stroke. Dr Rakesh Ranjan MS, MCh, Dip NB (Neurosurgery)
 Neurosurgical decision making in structural lesions causing stroke Dr Rakesh Ranjan MS, MCh, Dip NB (Neurosurgery) Subarachnoid Hemorrhage Every year, an estimated 30,000 people in the United States experience
Neurosurgical decision making in structural lesions causing stroke Dr Rakesh Ranjan MS, MCh, Dip NB (Neurosurgery) Subarachnoid Hemorrhage Every year, an estimated 30,000 people in the United States experience
Slide 1. Slide 2 Conflict of Interest Disclosure. Slide 3 Stroke Facts. The Treatment of Intracranial Stenosis. Disclosure
 Slide 1 The Treatment of Intracranial Stenosis Helmi Lutsep, MD Vice Chair and Dixon Term Professor, Department of Neurology, Oregon Health & Science University Chief of Neurology, VA Portland Health Care
Slide 1 The Treatment of Intracranial Stenosis Helmi Lutsep, MD Vice Chair and Dixon Term Professor, Department of Neurology, Oregon Health & Science University Chief of Neurology, VA Portland Health Care
Moyamoya Disease A Vasculopathy and an Uncommon Cause of Recurrent Cerebrovascular Accidents
 Moyamoya Disease A Vasculopathy and an Uncommon Cause of Recurrent Cerebrovascular Accidents Yasmin S. Hamirani, Md 1 *, Mohammad Valikhani, Md 2, Allison Sweney, Ms Iii 2, Hafsa Khan, Md 2, Mohammad Pathan,
Moyamoya Disease A Vasculopathy and an Uncommon Cause of Recurrent Cerebrovascular Accidents Yasmin S. Hamirani, Md 1 *, Mohammad Valikhani, Md 2, Allison Sweney, Ms Iii 2, Hafsa Khan, Md 2, Mohammad Pathan,
Ischemic stroke is a prevalent and devastating complication
 CLINICAL ARTICLE J Neurosurg Pediatr 20:232 238, 2017 Effectiveness of surgical revascularization for stroke prevention in pediatric patients with sickle cell disease and moyamoya syndrome Wuyang Yang,
CLINICAL ARTICLE J Neurosurg Pediatr 20:232 238, 2017 Effectiveness of surgical revascularization for stroke prevention in pediatric patients with sickle cell disease and moyamoya syndrome Wuyang Yang,
Neurosurgical Management of Stroke
 Overview Hemorrhagic Stroke Ischemic Stroke Aneurysmal Subarachnoid hemorrhage Neurosurgical Management of Stroke Jesse Liu, MD Instructor, Neurological Surgery Initial management In hospital management
Overview Hemorrhagic Stroke Ischemic Stroke Aneurysmal Subarachnoid hemorrhage Neurosurgical Management of Stroke Jesse Liu, MD Instructor, Neurological Surgery Initial management In hospital management
Thirteen-year Experience of 44 Patients with Adult Hemorrhagic Moyamoya Disease from a Single Institution: Clinical Analysis by Management Modality
 Journal of Cerebrovascular and Endovascular Neurosurgery ISSN 2234-8565, EISSN 2287-3139, http://dx.doi.org/10.7461/jcen.2013.15.3.191 Clinical Article Thirteen-year Experience of 44 Patients with Adult
Journal of Cerebrovascular and Endovascular Neurosurgery ISSN 2234-8565, EISSN 2287-3139, http://dx.doi.org/10.7461/jcen.2013.15.3.191 Clinical Article Thirteen-year Experience of 44 Patients with Adult
Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine
 Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine Institute The Oregon Clinic Disclosure I declare that neither
Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine Institute The Oregon Clinic Disclosure I declare that neither
Double STA-MCA Anatomosis for Bilateral Carotid Occlusion
 Double STA-MCA Anatomosis for Bilateral Carotid Occlusion -Case Report and Literature Review- Sandra vuignier 1, Kenji Kanamaru 2, Tomohiro Araki 2 1 Department of Neurosurgery, Nagoya University School
Double STA-MCA Anatomosis for Bilateral Carotid Occlusion -Case Report and Literature Review- Sandra vuignier 1, Kenji Kanamaru 2, Tomohiro Araki 2 1 Department of Neurosurgery, Nagoya University School
Perils of Mechanical Thrombectomy in Acute Asymptomatic Large Vessel Occlusion
 Perils of Mechanical Thrombectomy in Acute Asymptomatic Large Vessel Occlusion Aman B. Patel, MD Robert & Jean Ojemann Associate Professor Director, Cerebrovascular Surgery Director, Neuroendovascular
Perils of Mechanical Thrombectomy in Acute Asymptomatic Large Vessel Occlusion Aman B. Patel, MD Robert & Jean Ojemann Associate Professor Director, Cerebrovascular Surgery Director, Neuroendovascular
Preoperative risk factors for carotid endarterectomy: Defining the patient at high risk
 Preoperative risk factors for carotid endarterectomy: Defining the patient at high risk Amy B. Reed, MD, a Peter Gaccione, MA, b Michael Belkin, MD, b Magruder C. Donaldson, MD, b John A. Mannick, MD,
Preoperative risk factors for carotid endarterectomy: Defining the patient at high risk Amy B. Reed, MD, a Peter Gaccione, MA, b Michael Belkin, MD, b Magruder C. Donaldson, MD, b John A. Mannick, MD,
Moyamoya disease (MMD) is a progressive stenoocclusive
 J Neurosurg 121:432 440, 2014 AANS, 2014 The frequency of postoperative stroke in moyamoya disease following combined revascularization: a single-university series and systematic review Clinical article
J Neurosurg 121:432 440, 2014 AANS, 2014 The frequency of postoperative stroke in moyamoya disease following combined revascularization: a single-university series and systematic review Clinical article
Moyamoya disease in children
 Childs Nerv Syst (2010) 26:1297 1308 DOI 10.1007/s00381-010-1209-8 SPECIAL ANNUAL ISSUE Moyamoya disease in children David M. Ibrahimi & Rafael J. Tamargo & Edward S. Ahn Received: 8 June 2010 /Accepted:
Childs Nerv Syst (2010) 26:1297 1308 DOI 10.1007/s00381-010-1209-8 SPECIAL ANNUAL ISSUE Moyamoya disease in children David M. Ibrahimi & Rafael J. Tamargo & Edward S. Ahn Received: 8 June 2010 /Accepted:
SURGICAL MANAGEMENT OF MOYAMOYA DISEASE- RETROSPECTIVE ANALYSIS OF A SINGLE INSTITUTION SERIES
 SURGICAL MANAGEMENT OF MOYAMOYA DISEASE- RETROSPECTIVE ANALYSIS OF A SINGLE INSTITUTION SERIES Submitted for M.Ch Neurosurgery By Dr. Ranjit Devidas Rangnekar October 2016 Department of Neurosurgery Sree
SURGICAL MANAGEMENT OF MOYAMOYA DISEASE- RETROSPECTIVE ANALYSIS OF A SINGLE INSTITUTION SERIES Submitted for M.Ch Neurosurgery By Dr. Ranjit Devidas Rangnekar October 2016 Department of Neurosurgery Sree
Case Report INTRODUCTION
 Journal of Cerebrovascular and Endovascular Neurosurgery pissn 2234-8565, eissn 2287-3139, https//doi.org/10.7461/jcen.2018.20.2.127 Case Report Revision Superficial Temporal Artery-Middle Cerebral Artery
Journal of Cerebrovascular and Endovascular Neurosurgery pissn 2234-8565, eissn 2287-3139, https//doi.org/10.7461/jcen.2018.20.2.127 Case Report Revision Superficial Temporal Artery-Middle Cerebral Artery
Occlusive cerebrovascular disease. A Novel Chronic Cerebral Hypoperfusion Model with Cognitive Impairment and Low Mortality Rate in Rats
 FPⅧ-1 A Novel Chronic Cerebral Hypoperfusion Model with Cognitive Impairment and Low Mortality Rate in Rats Ahmed Said Mansour 1, Kuniyasu Niizuma 2, Sherif Rashad 2, Hidenori Endo 2, Toshiki Endo 3, Kenichi
FPⅧ-1 A Novel Chronic Cerebral Hypoperfusion Model with Cognitive Impairment and Low Mortality Rate in Rats Ahmed Said Mansour 1, Kuniyasu Niizuma 2, Sherif Rashad 2, Hidenori Endo 2, Toshiki Endo 3, Kenichi
CEA and cerebral protection Volodymyr labinskyy, MD
 CEA and cerebral protection Volodymyr labinskyy, MD VA Hospital 7/26/2012 63 year old male presents for the vascular evaluation s/p TIA in January 2012 PMH: HTN, long term active smoker, Hep C PSH: None
CEA and cerebral protection Volodymyr labinskyy, MD VA Hospital 7/26/2012 63 year old male presents for the vascular evaluation s/p TIA in January 2012 PMH: HTN, long term active smoker, Hep C PSH: None
Moyamoya disease (MMD) is a rare, chronic disorder
 LITERATURE REVIEW J Neurosurg 126:1523 1529, 2017 Direct versus indirect revascularization procedures for moyamoya disease: a comparative effectiveness study Luke Macyszyn, MD, MA, Mark Attiah, MD, MS,
LITERATURE REVIEW J Neurosurg 126:1523 1529, 2017 Direct versus indirect revascularization procedures for moyamoya disease: a comparative effectiveness study Luke Macyszyn, MD, MA, Mark Attiah, MD, MS,
Diagnosis of Middle Cerebral Artery Occlusion with Transcranial Color-Coded Real-Time Sonography
 Diagnosis of Middle Cerebral Artery Occlusion with Transcranial Color-Coded Real-Time Sonography Kazumi Kimura, Yoichiro Hashimoto, Teruyuki Hirano, Makoto Uchino, and Masayuki Ando PURPOSE: To determine
Diagnosis of Middle Cerebral Artery Occlusion with Transcranial Color-Coded Real-Time Sonography Kazumi Kimura, Yoichiro Hashimoto, Teruyuki Hirano, Makoto Uchino, and Masayuki Ando PURPOSE: To determine
Imaging of Moya Moya Disease
 Abstract Imaging of Moya Moya Disease Pages with reference to book, From 181 To 185 Rashid Ahmed, Hurnera Ahsan ( Liaquat National Hospital, Karachi. ) Moya Moya disease is a rare disease causing occlusion
Abstract Imaging of Moya Moya Disease Pages with reference to book, From 181 To 185 Rashid Ahmed, Hurnera Ahsan ( Liaquat National Hospital, Karachi. ) Moya Moya disease is a rare disease causing occlusion
Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke
 Original Contribution Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke Abstract Introduction: Acute carotid artery occlusion carries
Original Contribution Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke Abstract Introduction: Acute carotid artery occlusion carries
Moyamoya disease (MMD) is a rare idiopathic occlusive
 Moyamoya Disease in Europeans Markus Kraemer, MD; Wilhelm Heienbrok, MD; Peter Berlit, MD Background and Purpose We describe the clinical, diagnostic, and outcome features of a cohort of white patients
Moyamoya Disease in Europeans Markus Kraemer, MD; Wilhelm Heienbrok, MD; Peter Berlit, MD Background and Purpose We describe the clinical, diagnostic, and outcome features of a cohort of white patients
Asymptomatic Moyamoya Disease: Literature Review and Ongoing AMORE Study
 REVIEW ARTICLE Neurol Med Chir (Tokyo) 55, 194 198, 2015 doi: 10.2176/nmc.ra.2014-0305 Online February 20, 2015 Asymptomatic Moyamoya Disease: Literature Review and Ongoing AMORE Study Satoshi Kuroda;
REVIEW ARTICLE Neurol Med Chir (Tokyo) 55, 194 198, 2015 doi: 10.2176/nmc.ra.2014-0305 Online February 20, 2015 Asymptomatic Moyamoya Disease: Literature Review and Ongoing AMORE Study Satoshi Kuroda;
Moyamoya disease. Critical Role of PDGFR-α in Angiogenesis through Indirect Bypass in Mouse Model of Moyamoya Disease.
 FPⅢ- Critical Role of PDGFR-α in Angiogenesis through Indirect Bypass in Mouse Model of Moyamoya Disease Tomohide Hayashi Departments of Neurosurgery, University of Toyama Background - is a unique cerebrovascular
FPⅢ- Critical Role of PDGFR-α in Angiogenesis through Indirect Bypass in Mouse Model of Moyamoya Disease Tomohide Hayashi Departments of Neurosurgery, University of Toyama Background - is a unique cerebrovascular
What Is an Arteriovenous malformation (AVM)?
 American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD
 Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
PTA 106 Unit 1 Lecture 3
 PTA 106 Unit 1 Lecture 3 The Basics Arteries: Carry blood away from the heart toward tissues. They typically have thicker vessels walls to handle increased pressure. Contain internal and external elastic
PTA 106 Unit 1 Lecture 3 The Basics Arteries: Carry blood away from the heart toward tissues. They typically have thicker vessels walls to handle increased pressure. Contain internal and external elastic
DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service
 M AY. 6. 2011 10:37 A M F D A - C D R H - O D E - P M O N O. 4147 P. 1 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration 10903 New Hampshire Avenue Document Control
M AY. 6. 2011 10:37 A M F D A - C D R H - O D E - P M O N O. 4147 P. 1 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration 10903 New Hampshire Avenue Document Control
Diagnostic and Therapeutic Consequences of Repeat Brain Imaging and Follow-up Vascular Imaging in Stroke Patients
 AJNR Am J Neuroradiol 0:7, January 999 Diagnostic and Therapeutic Consequences of Repeat Brain Imaging and Follow-up Vascular Imaging in Stroke Patients Birgit Ertl-Wagner, Tobias Brandt, Christina Seifart,
AJNR Am J Neuroradiol 0:7, January 999 Diagnostic and Therapeutic Consequences of Repeat Brain Imaging and Follow-up Vascular Imaging in Stroke Patients Birgit Ertl-Wagner, Tobias Brandt, Christina Seifart,
Tohoku J. Exp. Med., 2015, 236, Current Management of Moyamoya Disease 45
 Tohoku J. Exp. Med., 2015, 236, 45-53 Current Management of Moyamoya Disease 45 Invited Review Current Status of Revascularization Surgery for Moyamoya Disease: Special Consideration for Its Internal Carotid-External
Tohoku J. Exp. Med., 2015, 236, 45-53 Current Management of Moyamoya Disease 45 Invited Review Current Status of Revascularization Surgery for Moyamoya Disease: Special Consideration for Its Internal Carotid-External
Acute Complications of Sickle Cell Disease Case Study 5 year old girl with Hemoglobin SS, weakness and slurred speech
 Acute Complications of Sickle Cell Disease Case Study 5 year old girl with Hemoglobin SS, weakness and slurred speech Beatrice E. Gee, MD Medical Director, Sickle Cell and Hematology Program Children s
Acute Complications of Sickle Cell Disease Case Study 5 year old girl with Hemoglobin SS, weakness and slurred speech Beatrice E. Gee, MD Medical Director, Sickle Cell and Hematology Program Children s
UPSTATE Comprehensive Stroke Center. Neurosurgical Interventions Satish Krishnamurthy MD, MCh
 UPSTATE Comprehensive Stroke Center Neurosurgical Interventions Satish Krishnamurthy MD, MCh Regional cerebral blood flow is important Some essential facts Neurons are obligatory glucose users Under anerobic
UPSTATE Comprehensive Stroke Center Neurosurgical Interventions Satish Krishnamurthy MD, MCh Regional cerebral blood flow is important Some essential facts Neurons are obligatory glucose users Under anerobic
TRAUMATIC CAROTID &VERTEBRAL ARTERY INJURIES
 TRAUMATIC CAROTID &VERTEBRAL ARTERY INJURIES ALBERTO MAUD, MD ASSOCIATE PROFESSOR TEXAS TECH UNIVERSITY HEALTH SCIENCES CENTER EL PASO PAUL L. FOSTER SCHOOL OF MEDICINE 18TH ANNUAL RIO GRANDE TRAUMA 2017
TRAUMATIC CAROTID &VERTEBRAL ARTERY INJURIES ALBERTO MAUD, MD ASSOCIATE PROFESSOR TEXAS TECH UNIVERSITY HEALTH SCIENCES CENTER EL PASO PAUL L. FOSTER SCHOOL OF MEDICINE 18TH ANNUAL RIO GRANDE TRAUMA 2017
Lecture Outline: 1/5/14
 John P. Karis, MD Lecture Outline: Provide a clinical overview of stroke: Risk Prevention Diagnosis Intervention Illustrate how MRI is used in the diagnosis and management of stroke. Illustrate how competing
John P. Karis, MD Lecture Outline: Provide a clinical overview of stroke: Risk Prevention Diagnosis Intervention Illustrate how MRI is used in the diagnosis and management of stroke. Illustrate how competing
Subject Review. Moyamoya Disease: The Disorder and Surgical Treatment
 Subject Review Moyamoya Disease: The Disorder and Surgical Treatment KEISUKE UEKI, M.D.,* FREDRIC B. MEYER, M.D., AND JAMES F. MELLINGER, M.D. Objective: To discuss the clinical features of moyamoya disease,
Subject Review Moyamoya Disease: The Disorder and Surgical Treatment KEISUKE UEKI, M.D.,* FREDRIC B. MEYER, M.D., AND JAMES F. MELLINGER, M.D. Objective: To discuss the clinical features of moyamoya disease,
Effect of Surgery on the Long-Term Functional Outcome of Moyamoya Disease: A Meta-Analysis
 DOI: 10.5137/1019-5149.JTN.22598-18.3 Received: 14.01.2018 / Accepted: 06.04.2018 Published Online: 24.04.2018 Turk Neurosurg, 2018 Original Investigation Effect of Surgery on the Long-Term Functional
DOI: 10.5137/1019-5149.JTN.22598-18.3 Received: 14.01.2018 / Accepted: 06.04.2018 Published Online: 24.04.2018 Turk Neurosurg, 2018 Original Investigation Effect of Surgery on the Long-Term Functional
Surgical techniques and procedures for cerebrovascular surgery. Surgery for the AVF at the cranio-cervical junction and high cervical spine
 VS-1 Surgery for the AVF at the cranio-cervical junction and high cervical spine Hiroyuki Kinouchi University of Yamanashi, Department of Neurosurgery Dural AVFs have been recognized as common type of
VS-1 Surgery for the AVF at the cranio-cervical junction and high cervical spine Hiroyuki Kinouchi University of Yamanashi, Department of Neurosurgery Dural AVFs have been recognized as common type of
This quiz is being published on behalf of the Education Committee of the SNACC.
 Quiz 48 Cerebrovascular Atherosclerotic Disease Shobana Rajan, M.D. Associate Director of Neuroanesthesia, Vice Chair of Education, Allegheny Health Network. Quiz team; Suneeta Gollapudy M.D, Angele Marie
Quiz 48 Cerebrovascular Atherosclerotic Disease Shobana Rajan, M.D. Associate Director of Neuroanesthesia, Vice Chair of Education, Allegheny Health Network. Quiz team; Suneeta Gollapudy M.D, Angele Marie
Carotid Revascularization
 Options for Carotid Disease Carotid Revascularization Wayne Causey, MD 2 nd Year Vascular Surgery Fellow Best medical therapy, Carotid Endarterectomy, and Carotid Stenting Who benefits from best medical
Options for Carotid Disease Carotid Revascularization Wayne Causey, MD 2 nd Year Vascular Surgery Fellow Best medical therapy, Carotid Endarterectomy, and Carotid Stenting Who benefits from best medical
Vascular Malformations of the Brain: A Review of Imaging Features and Risks
 Vascular Malformations of the Brain: A Review of Imaging Features and Risks Comprehensive Neuroradiology: Best Practices October 27-30, 2016 Sudhakar R. Satti, MD Associate Director Neurointerventional
Vascular Malformations of the Brain: A Review of Imaging Features and Risks Comprehensive Neuroradiology: Best Practices October 27-30, 2016 Sudhakar R. Satti, MD Associate Director Neurointerventional
Intracranial vascular anastomosis using the microanastomotic system
 J Neurosurg 89:676 681, 1998 Intracranial vascular anastomosis using the microanastomotic system Technical note DAVID W. NEWELL, M.D., ANDREW T. DAILEY, M.D., AND STEPHEN L. SKIRBOLL, M.D. Department of
J Neurosurg 89:676 681, 1998 Intracranial vascular anastomosis using the microanastomotic system Technical note DAVID W. NEWELL, M.D., ANDREW T. DAILEY, M.D., AND STEPHEN L. SKIRBOLL, M.D. Department of
Department of Neurosurgery, Showa University School of Medicine; and 2 Tokyo Midtown Medical Center, Tokyo, Japan
 CLINICAL ARTICLE Detection rates and sites of unruptured intracranial aneurysms according to sex and age: an analysis of MR angiography based brain examinations of 4070 healthy Japanese adults Yohichi
CLINICAL ARTICLE Detection rates and sites of unruptured intracranial aneurysms according to sex and age: an analysis of MR angiography based brain examinations of 4070 healthy Japanese adults Yohichi
Oltre la terapia medica nelle dissezioni carotidee
 Oltre la terapia medica nelle dissezioni carotidee Rodolfo Pini Chirurgia Vascolare Università di bologna Alma Mater Studiorum Carotid and Vertebral Artery Dissection What we know from the literature Epidemiology
Oltre la terapia medica nelle dissezioni carotidee Rodolfo Pini Chirurgia Vascolare Università di bologna Alma Mater Studiorum Carotid and Vertebral Artery Dissection What we know from the literature Epidemiology
EXPERIMENTAL AND THERAPEUTIC MEDICINE 15: , 2018
 3570 Clinical and angiographic outcomes after combined direct and indirect bypass in adult patients with moyamoya disease: A retrospective study of 76 procedures JINBING ZHAO, HONGYI LIU, YUANJIE ZOU,
3570 Clinical and angiographic outcomes after combined direct and indirect bypass in adult patients with moyamoya disease: A retrospective study of 76 procedures JINBING ZHAO, HONGYI LIU, YUANJIE ZOU,
Vertebrobasilar Insufficiency
 Equilibrium Res Vol. (3) Vertebrobasilar Insufficiency Toshiaki Yamanaka Department of Otolaryngology-Head and Neck Surgery, Nara Medical University School of Medicine Vertebrobasilar insufficiency (VBI)
Equilibrium Res Vol. (3) Vertebrobasilar Insufficiency Toshiaki Yamanaka Department of Otolaryngology-Head and Neck Surgery, Nara Medical University School of Medicine Vertebrobasilar insufficiency (VBI)
Carotid Stenosis 1/24/2019. Review of Primary Studies. NASCET- Moderate stenosis. ACAS (Asymptomatic Carotid Atherosclerosis Study) NASCET
 Review of Primary Studies Carotid Stenosis NINDS National Institute of Neurological Disorders and Stroke 2 large studies to determine who would benefit from surgery NASCET North American Symptomatic Carotid
Review of Primary Studies Carotid Stenosis NINDS National Institute of Neurological Disorders and Stroke 2 large studies to determine who would benefit from surgery NASCET North American Symptomatic Carotid
GUIDELINE FOR RECOVERY ROOM MANAGEMENT OF PATIENTS AFTER CAROTID ENDARTERECTOMY
 GUIDELINE FOR RECOVERY ROOM MANAGEMENT OF PATIENTS AFTER CAROTID ENDARTERECTOMY Full Title of Guideline: Author (include email and role): Guideline for Recovery Room Management of Patients after Carotid
GUIDELINE FOR RECOVERY ROOM MANAGEMENT OF PATIENTS AFTER CAROTID ENDARTERECTOMY Full Title of Guideline: Author (include email and role): Guideline for Recovery Room Management of Patients after Carotid
Carotid Artery Disease How the Data Will Influence Management The Symptomatic vs. the Asymptomatic Patient
 Carotid Artery Disease How the 2014-2015 Data Will Influence Management The Symptomatic vs. the Asymptomatic Patient Christopher J. White, MD, MSCAI, FACC, FAHA, FESC Professor and Chair of Medicine Ochsner
Carotid Artery Disease How the 2014-2015 Data Will Influence Management The Symptomatic vs. the Asymptomatic Patient Christopher J. White, MD, MSCAI, FACC, FAHA, FESC Professor and Chair of Medicine Ochsner
Anastomosis of the superficial temporal artery to the distal anterior cerebral artery with interposed cephalic vein graft
 J Neurosurg 58~25-429, 1983 Anastomosis of the superficial temporal artery to the distal anterior cerebral artery with interposed cephalic vein graft Case report RYOJI ISHII, M.D., TETSUO KOIKE, M.D.,
J Neurosurg 58~25-429, 1983 Anastomosis of the superficial temporal artery to the distal anterior cerebral artery with interposed cephalic vein graft Case report RYOJI ISHII, M.D., TETSUO KOIKE, M.D.,
Comparison of Five Major Recent Endovascular Treatment Trials
 Comparison of Five Major Recent Endovascular Treatment Trials Sample size 500 # sites 70 (100 planned) 316 (500 planned) 196 (833 estimated) 206 (690 planned) 16 10 22 39 4 Treatment contrasts Baseline
Comparison of Five Major Recent Endovascular Treatment Trials Sample size 500 # sites 70 (100 planned) 316 (500 planned) 196 (833 estimated) 206 (690 planned) 16 10 22 39 4 Treatment contrasts Baseline
Post-op Carotid Complications A Nursing Perspective of What to Watch Out for
 Post-op Carotid Complications A Nursing Perspective of What to Watch Out for By Kariss Peterson, ARNP Swedish Medical Center Inpatient Neurology Team 1 Post-op Carotid Management Objectives Review the
Post-op Carotid Complications A Nursing Perspective of What to Watch Out for By Kariss Peterson, ARNP Swedish Medical Center Inpatient Neurology Team 1 Post-op Carotid Management Objectives Review the
Cerebral Hemodynamic Change in the Child and the Adult With Moyamoya Disease
 272 Cerebral Hemodynamic Change in the Child and the Adult With Moyamoya Disease Yasuo Kuwabara, MD, Yuichi Ichiya, MD, Makoto Otsuka, MD, Takashi Tahara, MD, Ranjan Gunasekera, MD, Kanehiro Hasuo, MD,
272 Cerebral Hemodynamic Change in the Child and the Adult With Moyamoya Disease Yasuo Kuwabara, MD, Yuichi Ichiya, MD, Makoto Otsuka, MD, Takashi Tahara, MD, Ranjan Gunasekera, MD, Kanehiro Hasuo, MD,
Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease
 Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease Michael R. Jaff, D.O., F.A.C.P., F.A.C.C. Assistant Professor of Medicine Harvard Medical School Director, Vascular Medicine
Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease Michael R. Jaff, D.O., F.A.C.P., F.A.C.C. Assistant Professor of Medicine Harvard Medical School Director, Vascular Medicine
Cardiac evaluation for the noncardiac. Nathaen Weitzel MD University of Colorado Denver Dept of Anesthesiology
 Cardiac evaluation for the noncardiac patient Nathaen Weitzel MD University of Colorado Denver Dept of Anesthesiology Objectives! Review ACC / AHA guidelines as updated for 2009! Discuss new recommendations
Cardiac evaluation for the noncardiac patient Nathaen Weitzel MD University of Colorado Denver Dept of Anesthesiology Objectives! Review ACC / AHA guidelines as updated for 2009! Discuss new recommendations
Extracranial-to-Intracranial Bypass Using Radial Artery Grafting for Complex Skull Base Tumors: Technical Note
 Extracranial-to-Intracranial Bypass Using Radial Artery Grafting for Complex Skull Base Tumors: Technical Note Saleem I. Abdulrauf, M.D., F.A.C.S. 1 ABSTRACT The management of complex skull base tumors
Extracranial-to-Intracranial Bypass Using Radial Artery Grafting for Complex Skull Base Tumors: Technical Note Saleem I. Abdulrauf, M.D., F.A.C.S. 1 ABSTRACT The management of complex skull base tumors
Corporate Medical Policy
 Corporate Medical Policy Endovascular Therapies for Extracranial Vertebral Artery Disease File Name: Origination: Last CAP Review: Next CAP Review: Last Review: endovascular_therapies_for_extracranial_vertebral_artery_disease
Corporate Medical Policy Endovascular Therapies for Extracranial Vertebral Artery Disease File Name: Origination: Last CAP Review: Next CAP Review: Last Review: endovascular_therapies_for_extracranial_vertebral_artery_disease
ESC Congress 2011 SIMULTANEOUS HYBRID REVASCULARIZATION OF CAROTID AND CORONARY DISEASE INITIAL RESULTS OF A NEW THERAPEUTIC APPROACH
 ESC Congress 2011 SIMULTANEOUS HYBRID REVASCULARIZATION OF CAROTID AND CORONARY DISEASE IN PATIENTS WITH ACUTE CORONARY SYNDROME: INITIAL RESULTS OF A NEW THERAPEUTIC APPROACH AUTHORS: Marta Ponte 1, RICARDO
ESC Congress 2011 SIMULTANEOUS HYBRID REVASCULARIZATION OF CAROTID AND CORONARY DISEASE IN PATIENTS WITH ACUTE CORONARY SYNDROME: INITIAL RESULTS OF A NEW THERAPEUTIC APPROACH AUTHORS: Marta Ponte 1, RICARDO
Cerebral hyperperfusion syndrome after carotid angioplasty
 case report Cerebral hyperperfusion syndrome after carotid angioplasty Zoran Miloševič 1, Bojana Žvan 2, Marjan Zaletel 2, Miloš Šurlan 1 1 Institute of Radiology, 2 University Neurology Clinic, University
case report Cerebral hyperperfusion syndrome after carotid angioplasty Zoran Miloševič 1, Bojana Žvan 2, Marjan Zaletel 2, Miloš Šurlan 1 1 Institute of Radiology, 2 University Neurology Clinic, University
Clinical Features and Subtypes of Ischemic Stroke Associated with Peripheral Arterial Disease
 Cronicon OPEN ACCESS EC NEUROLOGY Research Article Clinical Features and Subtypes of Ischemic Stroke Associated with Peripheral Arterial Disease Jin Ok Kim, Hyung-IL Kim, Jae Guk Kim, Hanna Choi, Sung-Yeon
Cronicon OPEN ACCESS EC NEUROLOGY Research Article Clinical Features and Subtypes of Ischemic Stroke Associated with Peripheral Arterial Disease Jin Ok Kim, Hyung-IL Kim, Jae Guk Kim, Hanna Choi, Sung-Yeon
CAROTID ARTERY ANGIOPLASTY
 CAROTID ARTERY ANGIOPLASTY Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical Coverage Guideline
CAROTID ARTERY ANGIOPLASTY Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical Coverage Guideline
Although moyamoya disease, a rare cerebrovascular occlusive
 Renal Artery Lesions in Patients With Moyamoya Disease Angiographic Findings Ichiro Yamada, MD; Yoshiro Himeno, MD; Yoshiharu Matsushima, MD; Hitoshi Shibuya, MD Background and Purpose Renal artery lesions
Renal Artery Lesions in Patients With Moyamoya Disease Angiographic Findings Ichiro Yamada, MD; Yoshiro Himeno, MD; Yoshiharu Matsushima, MD; Hitoshi Shibuya, MD Background and Purpose Renal artery lesions
Intracranial-to-intracranial vascular anastomosis created using a microanastomotic device for the treatment of distal middle cerebral artery aneurysms
 J Neurosurg 97:486 491, 2002 Intracranial-to-intracranial vascular anastomosis created using a microanastomotic device for the treatment of distal middle cerebral artery aneurysms Technical note DAVID
J Neurosurg 97:486 491, 2002 Intracranial-to-intracranial vascular anastomosis created using a microanastomotic device for the treatment of distal middle cerebral artery aneurysms Technical note DAVID
Redgrave JN, Coutts SB, Schulz UG et al. Systematic review of associations between the presence of acute ischemic lesions on
 6. Imaging in TIA 6.1 What type of brain imaging should be used in suspected TIA? 6.2 Which patients with suspected TIA should be referred for urgent brain imaging? Evidence Tables IMAG1: After TIA/minor
6. Imaging in TIA 6.1 What type of brain imaging should be used in suspected TIA? 6.2 Which patients with suspected TIA should be referred for urgent brain imaging? Evidence Tables IMAG1: After TIA/minor
CAROTID DEBATE High-Grade Asymptomatic Disease Should Be Repaired Selectively; Medical Management is NOT Enough
 Todd W GenslerMD April 28, 2018 CAROTID DEBATE High-Grade Asymptomatic Disease Should Be Repaired Selectively; Medical Management is NOT Enough DISCLOSURES I have no financial disclosures Presenter name
Todd W GenslerMD April 28, 2018 CAROTID DEBATE High-Grade Asymptomatic Disease Should Be Repaired Selectively; Medical Management is NOT Enough DISCLOSURES I have no financial disclosures Presenter name
