Original Article. Division of Gastrointestinal and General Surgery, Department of Surgery, 2 Department of Radiation Medicine, 3
|
|
|
- Damon Wilkerson
- 5 years ago
- Views:
Transcription
1 Diseases of the Esophagus (2017) 30, 1 7 DOI: /dote/dox015 Original Article Neoadjuvant chemoradiotherapy with concurrent cisplatin/5-fluorouracil is associated with increased pathologic complete response and improved survival compared to carboplatin/paclitaxel in patients with locally advanced esophageal cancer K. R. Haisley, 1 K. D. Hart, 1 N. Nabavizadeh, 2 K. G. Bensch, 3 G. M. Vaccaro, 3 C. R. Thomas, Jr, 2 P. H Schipper, 4 J. G Hunter, 1 J. P. Dolan 1 1 Division of Gastrointestinal and General Surgery, Department of Surgery, 2 Department of Radiation Medicine, 3 Division of Medical Oncology, Department of Internal Medicine, and 4 Division of Cardiovascular and General Thoracic Surgery, Department of Surgery, Oregon Health and Science University, Portland, OR, USA SUMMARY. Trimodal therapy consisting of neoadjuvant chemoradiation followed by esophagectomy has become the standard of care in North America for locally advanced esophageal cancer. While cisplatin/5-fluorouracil has been a common concurrent chemotherapy regimen since the 1980s, its utilization has declined in recent years as the Chemoradiotherapy for Oesophageal Cancer Followed by Surgery Study (CROSS) trial regimen of carboplatin/paclitaxel has become widely adopted. The efficacy of the CROSS regimen compared to alternate chemotherapy choices, however, has rarely been evaluated when each is used as a component of a trimodal treatment approach. The aim of this study is to report our institutional experience with these two concurrent chemotherapy regimens at a specialized esophageal cancer center. We performed an Institutional Review Board-approved retrospective review of a prospectively maintained institutional foregut registry from a single National Cancer Institute-designated cancer center. Esophageal cancer patients who completed trimodal therapy with a chemotherapy regimen of either carboplatin/paclitaxel or cisplatin/5- fluorouracil were identified and divided into groups based on their chemotherapy regimens. Multivariable logistic regression was used to analyze pathologic complete response rates, while the Kaplan Meier and Cox proportional hazards models were utilized to evaluate recurrence-free and overall survival. Analytical models were adjusted for age, clinical stage, radiation dose, histologic subtype (adenocarcinoma vs. squamous cell carcinoma), and time interval from completion of neoadjuvant therapy to surgery. One hundred and forty-two patients treated between January of 2000 and July of 2015 were identified as meeting inclusion criteria. Of this group, 87 had received the CROSS regimen of carboplatin/paclitaxel, while 55 had completed cisplatin/5-fluorouracil. Multivariable analysis demonstrated that the cisplatin/5-fluorouracil.group had an increased odds of pathologic complete response (odds ratio = 2.68, 95% confidence interval, P = 0.032), as well as significantly improved recurrence-free survival (hazard ratio = 0.39, 95% confidence interval , P = 0.003) and overall survival (hazard ratio = 0.46, 95% confidence interval , P = 0.016), compared to the carboplatin/paclitaxel group. Concurrent chemotherapy with cisplatin/5-fluorouracil in locally advanced esophageal cancer is associated with higher rates of pathologic complete response and improved recurrence-free and overall survival compared to the CROSS regimen of carboplatin/paclitaxel. This suggests that, for select patients, alternate neoadjuvant chemotherapy approaches, such as cisplatin/5-fluorouracil, merit reconsideration as potential primary treatment choices in the management of this highly morbid disease. KEY WORDS:: carboplatin + paclitaxel, cisplatin + 5-fluorouracil, esophageal cancer, neoadjuvant chemotherapy, pathologic complete response. Address correspondence to: James Dolan, MD, MCR, 3181 SW Sam Jackson Park Road, Mailcode L223A, Portland, OR 97239, USA. dolanj@ohsu.edu Conflicts of interest: The authors declare that they have no conflict of interest. Funding Sources: None. C The Authors Published by Oxford University Press on behalf of International Society for Diseases of the Esophagus. All rights reserved. For permissions, please journals.permissions@oup.com 1
2 2 Diseases of the Esophagus INTRODUCTION Esophageal cancer is an increasingly prevalent disease that accounts for greater than 15,000 deaths in the United States every year. 1 Even early-stage cancers have been associated with five-year survival rates as low as 37%, with more advanced presentations having survival times measured in months. 1 The high morbidity and mortality associated with the diagnosis of esophageal cancer highlights the need to refine treatment strategies in order to better optimize outcomes. In recent years, some progress has been made with the addition of concurrent chemoradiation to the standard treatment protocol for esophageal cancers. This trimodal treatment approach, consisting of neoadjuvant chemotherapy and radiation followed by esophagectomy, has gained considerable favor since the publication of the Chemoradiotherapy for Oesophageal Cancer Followed by Surgery Study (CROSS) in This landmark trial demonstrated a markedly improved five-year survival rate in patients receiving trimodal therapy versus those having surgery alone. As a result, trimodal therapy has become the standard of care in North America for locally advanced esophageal cancer. To date, the efficacy of the CROSS chemotherapy regimen of carboplatin/paclitaxel has not been directly compared to alternate chemotherapy regimens when each is used as a component of a full trimodal treatment approach. 3 Our working hypothesis was that outcomes would not differ between the CROSS regimen and the conventional regimen utilized prior to this study. Hence, the primary aim of this study is to analyze our institutional experience, comparing the CROSS regimen of carboplatin/paclitaxel to a conventional regimen of cisplatin/5-fluorouracil, including only patients who underwent a trimodal treatment approach. METHODS Study design and participants We performed a retrospective review of a prospectively maintained esophageal disease registry from a single National Cancer Institute-designated cancer center under Institutional Review Board-approved (IRB#15198). We selected patients who had completed neoadjuvant chemoradiotherapy (CRT) followed by esophagectomy for documented esophageal cancer between January of 2000 and July of Preoperative tumor staging was performed using endoscopy, computed tomography (CT) scanning, and radiolabeled fluorodeoxyglucose whole body positron emission tomography. Each patient s case was discussed in detail at a biweekly esophageal care conference. Decisions regarding the type of chemotherapy administered were left to the discretion of the treating oncologist. Those patients who had received a chemotherapy regimen of either cisplatin/5-fluorouracil or carboplatin/paclitaxel were included in the study. Patients who received any other chemotherapy regimen, or who had missing or incomplete treatment data were excluded from further analysis. Patients were then divided into two groups based on their administered chemotherapy regimens, either carboplatin/paclitaxel or cisplatin/fluorouracil. Statistical analysis Demographic and clinical characteristics of patients included in the analysis were analyzed using descriptive statistics. Analytical models were adjusted for age, clinical stage, radiation dose, histologic subtype (adenocarcinoma vs. squamous cell carcinoma), and time interval from completion of neoadjuvant therapy to surgery. We utilized multivariable logistic regression to analyze pathologic complete response rates and the Kaplan Meier plots, as well as Cox proportional hazards models to analyze recurrence-free and overall survival designating the day of surgery as time zero. RESULTS Patient demographics Of the 529 patients in our esophageal diseases registry at the time of our query, 248 had completed trimodal therapy with a diagnosis of esophageal cancer. Twenty-six patients were excluded due to our inability to determine what specific chemotherapy regimen was administered. Seventy additional patients were removed from analysis due to having received any one of 27 unique chemotherapy regimens that were neither of the regimens under current review. These regimens ranged from single agent to quadruple agent, and were largely platinum based. No one of these alternate regimens was administered in more than eight cases. An additional 10 patients had other missing data variables that required their exclusion from the study. In total, 142 patients were identified who had undergone neoadjuvant CRT with one of the two regimens of interest. Fifty-five patients received cisplatin/5-fluorouracil, and the remaining 87 were given carboplatin/paclitaxel (Fig. 1). There was no significant difference between groups in terms of ethnicity, gender, tumor histology, or adjuvant therapies received (Table 1). In the carboplatin/paclitaxel group, the mean age at surgery was more advanced (65.6 vs. 60.4, P = 0.003), and median time between completion of neoadjuvant therapy and surgery was longer (64 vs. 56 days, P = 0.001). The cisplatin/5-fluorouracil group appeared to show a trend toward having higher stage cancers, though this did not reach statistical significance (P = 0.07).
3 Neoadjuvant CRT in esophageal cancer 3 overall in the cisplatin/5-fluorouracil group with a complete response rate of 33% compared to a rate of only 22% in the carboplatin/paclitaxel group, though this finding did not reach statistical significance on univariable analysis (P = 0.21). Under multivariable analysis correcting for age, histologic subtype, clinical stage, neoadjuvant radiation dose, and days between CRT and surgical resection, the cisplatin/5- fluorouracil group had a significantly increased odds of pathologic complete response (odds ratio 2.67, 95% confidence interval: , P = 0.032, Table 2). Fig. 1 Patient enrollment flowsheet. Pathologic complete response Overall, 37 patients (26%) achieved a pathologic complete response as determined by final pathology. There was a trend toward increased pathologic complete Survival On the Kaplan Meier analysis, median recurrencefree survival time (including recurrence at any site, both locoregional or metastatic) was higher among patients who received cisplatin/5-fluorouracil (median: 2.5 years) than among those who received carboplatin/paclitaxel (median: 1.25 years). Recurrence-free survival probabilities at one, two, and three years were higher in the cisplatin/5- fluorouracil group (70%, 53%, and 44%) than in Table 1 Demographic information for our patient cohort All patients Cisplatin/5-FU Carboplatin/paclitaxel P-value (n = 142) (n = 55) (n = 87) Age ± ± ± Gender Male 82% (117) 80% (44) 84% (73) Female 18% (25) 20% (11) 16% (14) Ethnicity Caucasian 98% (139) 96% (53) 99% (86) American Indian 1% (1) 0% (0) 1% (1) Asian 1% (1) 2% (1) 0% (0) Other 1% (1) 2% (1) 0% (0) Histologic subtype Adenocarcinoma 86% (122) 85% (47) 86% (75) SCC 14% (20) 15% (8) 14% (12) Clinical stage 1 2% (3) 2% (1) 2% (2) % (43) 27% (15) 33% (28) 3 62% (88) 60% (33) 64% (55) 4 5% (7) 11% (6) 1% (1) Radiation dose (cgy) 5040 (5000, 5040) 5040 (4770, 5040) 5040 (5000, 5040) Adjuvant chemotherapy Yes 5% (6) 4% (2) 5% (4) No 95% (124) 96% (52) 95% (72) Days from CRT to surgery 62 (52.25, 73.00) 56 (48.00, 69.00) 64 (56.00, 85.00) Pathologic node positivity No 58% (83) 69% (38) 52% (45) Yes 42% (59) 31% (17) 48% (42) Pathologic complete response Yes 26% (37) 33% (18) 22% (19) No 74% (105) 67% (37) 78% (68) Student s t-test (two-sided); Pearson s chi-squared test; Fisher s exact test; Wilcoxon rank-sum test with continuity correction. FU, fluorouracil; SCC, squamous cell carcinoma; x:x (x:x, x:x) indicates median and inter-quartile range; x±x indicates mean ± standard deviation.
4 4 Diseases of the Esophagus Table 2 Multivariable logistic regression exploring pathologic complete response Clinical variable OR (95% CI) P-value Cisplatin/5-fluorouracil (vs. carboplatin/paclitaxel) (1.086, 6.610) Age (per year) (0.980, 1.076) Stage III of IV (vs. I or II) (0.172,0.954) Squamous cell carcinoma (vs. adenocarcinoma) (0.550, 5.127) Days from ncrt to surgery (0.999, 1.001) Total radiation dose (0.999, 1.001) ncrt, neoadjuvant chemoradiotherapy. Fig. 2 Kaplan Meyer plot of (a) recurrence-free and (b) overall survival as a factor of chemotherapy regimen (shaded areas denote 95% confidence interval). the carboplatin/paclitaxel group (56%, 31%, and 31%) (Fig. 2a). Similarly, median overall survival time was higher among patients who received cisplatin/5-fluorouracil (6.8 years) than among those who received carboplatin/paclitaxel (1.8 years). Further, predicted overall survival probabilities at one, two, and three years were higher in the cisplatin/5-fluorouracil group (76%, 60%, and 52%) than in the carboplatin/paclitaxel group (69%, 36%, and 24%) (Fig. 2b).
5 Neoadjuvant CRT in esophageal cancer 5 Table 3 Multivariable Cox proportional Hazards model of overall and recurrence-free survival Clinical variable Overall survival Recurrence-free survival (n = 133) (n = 133) HR (95% CI) HR (95% CI) cisplatin/5-fluorouracil (vs. carboplatin/paclitaxel) (0.244,0.865) (0.209,0.727) Age (per year) (0.964,1.022) (0.269,1.497) Stage III of IV (vs. I or II) (0.935,3.323) (1.270,4.314) Squamous cell carcinoma (vs. adeno) (0.238,1.557) (0.269, 1.497) Days from ncrt to surgery (0.980,1.007) (0.977, 1.003) Total radiation dose (0.999,1.000) (0.999,1.000) P < 0.1. P < P < In a multivariable analysis, patients who received a neoadjuvant chemotherapy regimen of cisplatin/5- fluorouracil had significantly improved recurrencefree (hazard ratio: 0.39, 95% confidence interval: , P = 0.003) and overall survival (hazard ratio: 0.46, 95% confidence interval , P = 0.016), compared to the carboplatin/paclitaxel group (Table 3). DISCUSSION In this study, we have shown that concurrent chemotherapy with cisplatin/5-fluorouracil is associated with higher rates of pathologic complete response and improved recurrence-free and overall survival, compared to the widely utilized CROSS regimen of carboplatin/paclitaxel when each is used as a component of trimodal therapy for locally advanced esophageal cancer. The adoption of standardized trimodal therapy has resulted in significant improvements compared to surgery alone. 1 2,4 However, the question of which patients will most benefit from CRT 5 and which neoadjuvant chemotherapy regimen might be best for optimizing outcomes and survival remains unanswered. 6 While cisplatin/5-fluorouracil was previously a commonly utilized regimen, the CROSS regimen of carboplatin/paclitaxel has largely become the standard of therapy over the last five years. It is important to recognize that the use of carboplatin/paclitaxel in the CROSS trial, and its subsequent adoption nationwide, may have been more a reflection of institutional preference and tolerability, rather than a direct comparison of this regimen versus any other in terms of survival or oncologic outcomes. Since the publication of the CROSS trial and the rapid spread of the carboplatin/paclitaxel concurrent chemotherapy regimen, several authors have retrospectively evaluated its efficacy compared to alternate chemotherapy choices. A recent metaanalysis concluded that carboplatin/paclitaxel was the superior regimen, 3 while other authors have shown no difference between the two regimens in terms of survival. 7,8 Still others have shown finding similar to our study and suggest that carboplatin/paclitaxel might be associated with higher recurrence 9 and lower rates of pathologic complete response 10 than cisplatin/5-fluorouracil. Taken together, while each of these studies has certain limitations, the cumulative literature highlights the need for ongoing research in this field. The improved survival rates we and other authors have shown following completion of neoadjuvant CRT with cisplatin/5-fluorouracil certainly has biologic plausibility. Our findings may be a result of the increased rates of pathologic complete response (elimination of all detectable tumor from the surgical specimen) seen with this more aggressive regimen. 7,8,11 Several studies have demonstrated that pathologic complete response in esophageal cancer is associated with improved survival While the exact factors that predict or increase the likelihood of pathologic complete response remain an area of intense research, 13 these data support the idea that the choice of chemotherapy may significantly affect rates of response. As cisplatin/5-fluorouracil appears to be associated with higher rates of pathologic complete response in this study, it stands to reason that it may eliminate tumor more effectively than carboplatin/paclitaxel, thus reducing recurrences and improving survival. Comparing our results to those of the CROSS trial highlights the finding that our institution did not find equivalent survival rates to those published in the CROSS trial when using the regimen of carboplatin/paclitaxel (49 months in the CROSS versus only 21.7 months in our population). This may be due to our smaller sample size compared to the CROSS group as well as a larger proportion of squamous histology seen in the CROSS cohort. In addition, it is fairly well established that adenocarcinoma patients (86% of our patients vs. 75% of the CROSS patients) have lower rates of pcr and shorter median survivals. 2 In addition, our higher median age at surgery (65.6 years) compared to the CROSS patients (60 years) may have contributed to increased perioperative mortality. Finally, the higher doses of
6 6 Diseases of the Esophagus radiation used at our institution (50.4 Gy) compared to the published CROSS regimen of (41.4 Gy) may also contribute to increased toxicity and decreased survival. 17 It is worth mentioning that the tolerability profile of carboplatin/paclitaxel is generally considered to be superior to that of cisplatin/5-fluorouracil in terms of side effects and patient experience. While direct dosing and tolerability data could not be expressly collected in this study due to the disparate locations across a wide geographical area where our patients received their chemotherapy, other authors have demonstrated this to be the case. 7,8 It is also important to recognize that the better tolerability of the carboplatin/paclitaxel regimen may create a manner of selection bias such that weaker patients with more comorbidities are making it through neoadjuvant therapy who would have otherwise failed on the cisplatin/5fu regimen. Nonetheless, treatment decisions must be individualized, based on the patient s risk for complications from chemotherapy versus their risk of cancer spread or recurrence. In the era of personalized medicine, it will be interesting to address if stage, age, or other clinical factors might predict which patients would most benefit from one regimen over the other. More research will be required to determine definitively which patients might benefit from a more intensive chemotherapy regimen such as cisplatin/5- fluorouracil, versus those that will do well with a more tolerable regimen of carboplatin/paclitaxel. We recognize that there are a number of other limitations to this study. First, it is retrospective in nature. However, our data were conducted prospectively under a single institution with standardized protocols for staging, treatment, and specimen analysis. We are further limited by our relatively small sample size, with only 142 patients meeting criteria for inclusion. In addition, there is also almost certainly a temporal effect within our data, as the cisplatin/5-fluorouracil group was treated mostly between the years of 2000 and 2012, while the carboplatin/paclitaxel group was treated more recently. There have been other care pathway changes for our patients between these time periods that cannot be fully accounted for in our statistical modeling. This might include improved ICU care, implementation of our institutional esophagectomy pathway, and evolution of surgical technique and practice. Furthermore, intensity-modulated radiation therapy (IMRT) has seen increased utilization over-time, concurrent with carboplatin/paclitaxel use. 14 It is well known that thoracic irradiation can cause acute and chronic lung injury and absolute volume of the total lung spared from radiation doses greater than 5 Gy has been strongly associated with risk of postoperative pulmonary complications. 15 Compared to traditional, three-dimensional conformal radiotherapy techniques, the modulation of multiple beams inherent to IMRT exposes larger proportions of the bilateral lung to a low-dose bath of radiation. Given that a very large proportion of patients receiving carboplatin/paclitaxel were treated with IMRT it is difficult to remove this confounding variable in our analysis. At our institution, the total radiation dose was maintained at 50.4 Gy both before and after the transition a carboplatin/paclitaxel chemotherapy regimen rather than adopting the CROSS dosing of 41.4 Gy. This gives consistency to the radiation dosing between eras. Despite recent advancements, esophageal cancer remains a prevalent and deadly malignancy with an urgent need for further refined treatment strategies. Future studies evaluating the efficacy of various neoadjuvant approaches, such as the currently enrolling PROTECT trial, 16 as well as evaluation of different radiation doses and modalities 17 will be an integral part of improving outcomes of this highly morbid disease. Such research is vital to further elucidate the role of alternate neoadjuvant chemotherapy regimens in esophageal cancer. CONCLUSION In our patient population, concurrent chemotherapy with cisplatin/5-fluorouracil in locally advanced esophageal cancer is associated with higher rates of pathologic complete response and improved recurrence-free and OS, compared to the CROSS regimen of carboplatin/paclitaxel. These data suggest that alternate neoadjuvant concurrent chemotherapy approaches merit reconsideration as potential primary treatment options in the management of this disease. ACKNOWLEDGEMENTS We would like to acknowledge the contributions of Charlie Borzy, our Study Coordinator, as well as Hope Hardaker, our Database Manager. We additionally thank Mary Kwatkosky-Lawlor for her invaluable assistance with manuscript preparation, editing, and formatting. References 1 Walsh T N, Grennell M, Mansoor S, Kelly A. Neoadjuvant treatment of advanced stage esophageal adenocarcinoma increases survival. Dis Esophagus 2002; 15: Van Hagen P, Hulshof M, Van Lanschot J et al. Preoperative chemotherapy for esophageal or junctional cancer. N Engl J Med 2012; 366: Huang T C, Hsu C H, Lin C C, Tu Y K. Systematic review and network meta-analysis: neoadjuvant chemoradiotherapy for locoregional esophageal cancer. Jpn J Clin Oncol 2015; 45: Siddiqui F A, Atkins K M, Diggs B S, Thomas C R, Jr, Hunter J G, Dolan J P. Overall survival analysis of neoadjuvant
7 Neoadjuvant CRT in esophageal cancer 7 chemoradiotherapy and esophagectomy for esophageal cancer. J Gastrointest Oncol 2014; 5: Eil R, Diggs B S, Wang S J, Dolan J P, Hunter J G, Thomas C R. Nomogram for predicting the benefit of neoadjuvant chemoradiotherapy for patients with esophageal cancer: a SEER-Medicare analysis. Cancer 2014; 120: Adenis A, Mirabel X, Mariette C. Is preoperative chemoradiation with paclitaxel and carboplatin a new standard of treatment for esophageal cancer? Int J Radiat Oncol Biol Phys 2013; 86: Blom R L, Sosef M N, Nap M et al. Comparison of two neoadjuvant chemoradiotherapy regimens in patients with potentially curable esophageal carcinoma. Dis Esopahagus 2014; 27: Honing J, Smit J, Muijs C et al. A comparison of carboplatin with paclitaxel and cisplatinum with 5-fluorouracil in definitive chemoradiotherapy in esophageal cancer patients. Ann Oncol 2014; 25 (3): Thomay A A, Su S, Friedant A J et al. Freedom from recurrence after induction cisplatin/5-fu/rt versus carboplatin/paclitaxel/rt in patients with esophageal cancer (Abstract 126). J Clin Oncol 2014; 32 ( Suppl 3): pp Schellenberg D, Peixoto R, Lee A, Lim H J. A province-wide retrospective comparison of pathologic response and progressionfree survival in locally advanced esophagus cancer patients treated with either cisplatin-5fu(cf) or carboplatin-paclitaxel (CP) concurrent with radiation (XRT) with or without surgery (Abstract 107). J Clin Oncol 2014; 32( Suppl 3): pp Berger A C, Farma J, Scott W J et al. Complete response to neoadjuvant chemoradiotherapy in esophageal carcinoma is associated with significantly improved survival. J Clin Oncol 2005; 23: Donahue J M, Nichols F C, Li Z et al. Complete pathologic response after neoadjuvant chemoradiotherapy for esophageal cancer is associated with enhanced survival. Ann Thorac Surg 2009; 87: LinSH,WangJ,AllenPKet al. A nomogram that predicts pathologic complete response to neoadjuvant chemoradiation also predicts survival outcomes after definitive chemoradiation for esophageal cancer. J Gastrointest Oncol 2015; 6: Simpson D R, Lawson J D, Nath S K, Rose B S, Mundt A J, Mell L K. A survey of image-guided radiation therapy use in the United States. Cancer 2010; 116: Wang S L, Liao Z, Vaporciyan A A et al. Investigation of clinical and dosimetric factors associated with postoperative pulmonary complications in esophageal cancer patients treated with concurrent chemoradiotherapy followed by surgery. Int J Radiat Oncol Biol Phys 2006; 64: Messager M, Mirabel X, Tresch E et al. Preoperative chemoradiation with paclitaxel-carboplatin or with fluorouraciloxaliplatin-folinic acid (FOLFOX) for resectable esophageal and junctional cancer: the PROTECT-1402, randomized phase 2 trial. BMC Cancer 2016; 16: Nabavizadeh N, Shukla R, Elliott D A et al. Preoperative carboplatin and paclitaxel-based chemoradiotherapy for esophageal carcinoma: results of a modified CROSS regimen utilizing radiation doses greater than 41.4 Gy. Dis Esophagus 2016; 29:
Overall survival analysis of neoadjuvant chemoradiotherapy and esophagectomy for esophageal cancer
 Original Article Overall survival analysis of neoadjuvant chemoradiotherapy and esophagectomy for esophageal cancer Faisal A. Siddiqui 1, Katelyn M. Atkins 2, Brian S. Diggs 3, Charles R. Thomas Jr 1,
Original Article Overall survival analysis of neoadjuvant chemoradiotherapy and esophagectomy for esophageal cancer Faisal A. Siddiqui 1, Katelyn M. Atkins 2, Brian S. Diggs 3, Charles R. Thomas Jr 1,
The role of chemoradiotherapy in GE junction and gastric cancer. Karin Haustermans
 The role of chemoradiotherapy in GE junction and gastric cancer Karin Haustermans Overview Postoperative chemoradiotherapy Preoperative chemoradiotherapy Palliative radiation Technical aspects Overview
The role of chemoradiotherapy in GE junction and gastric cancer Karin Haustermans Overview Postoperative chemoradiotherapy Preoperative chemoradiotherapy Palliative radiation Technical aspects Overview
Original article. Department of Radiation Medicine, 2 Division of Medical Oncology, Department of Internal Medicine, 3
 Diseases of the Esophagus (2015), DOI: 10.1111/dote.12377 Original article Preoperative carboplatin and paclitaxel-based chemoradiotherapy for esophageal carcinoma: results of a modified CROSS regimen
Diseases of the Esophagus (2015), DOI: 10.1111/dote.12377 Original article Preoperative carboplatin and paclitaxel-based chemoradiotherapy for esophageal carcinoma: results of a modified CROSS regimen
Medicinae Doctoris. One university. Many futures.
 Medicinae Doctoris The Before and The After: Can chemotherapy revise the trajectory of gastric and esophageal cancers? Dr. David Dawe MD, FRCPC Medical Oncologist Assistant Professor Disclosures None All
Medicinae Doctoris The Before and The After: Can chemotherapy revise the trajectory of gastric and esophageal cancers? Dr. David Dawe MD, FRCPC Medical Oncologist Assistant Professor Disclosures None All
Münch et al. Radiation Oncology (2017) 12:182 DOI /s y
 Münch et al. Radiation Oncology (2017) 12:182 DOI 10.1186/s13014-017-0904-y RESEARCH Open Access Comparison of neoadjuvant chemoradiation with carboplatin/ paclitaxel or cisplatin/ 5-fluoruracil in patients
Münch et al. Radiation Oncology (2017) 12:182 DOI 10.1186/s13014-017-0904-y RESEARCH Open Access Comparison of neoadjuvant chemoradiation with carboplatin/ paclitaxel or cisplatin/ 5-fluoruracil in patients
Are we making progress? Marked reduction in operative morbidity and mortality
 Are we making progress? Surgical Progress Marked reduction in operative morbidity and mortality Introduction of Minimal-Access approaches for complex esophageal cancer resections Significantly better functional
Are we making progress? Surgical Progress Marked reduction in operative morbidity and mortality Introduction of Minimal-Access approaches for complex esophageal cancer resections Significantly better functional
Introduction ORIGINAL RESEARCH
 Cancer Medicine ORIGINAL RESEARCH Open Access The effect of radiation therapy in the treatment of adult soft tissue sarcomas of the extremities: a long- term community- based cancer center experience Jeffrey
Cancer Medicine ORIGINAL RESEARCH Open Access The effect of radiation therapy in the treatment of adult soft tissue sarcomas of the extremities: a long- term community- based cancer center experience Jeffrey
Updated Apr 2017 by Dr. Jenny Ko (Medical Oncologist, Abbotsford Cancer Centre)
 Local Esophageal Cancer Summary Updated Apr 2017 by Dr. Jenny Ko (Medical Oncologist, Abbotsford Cancer Centre) Reviewed by Dr. Yoo-Joung Ko (Medical Oncologist, Sunnybrook Odette Cancer Centre, University
Local Esophageal Cancer Summary Updated Apr 2017 by Dr. Jenny Ko (Medical Oncologist, Abbotsford Cancer Centre) Reviewed by Dr. Yoo-Joung Ko (Medical Oncologist, Sunnybrook Odette Cancer Centre, University
Advances in gastric cancer: How to approach localised disease?
 Advances in gastric cancer: How to approach localised disease? Andrés Cervantes Professor of Medicine Classical approach to localised gastric cancer Surgical resection Pathology assessment and estimation
Advances in gastric cancer: How to approach localised disease? Andrés Cervantes Professor of Medicine Classical approach to localised gastric cancer Surgical resection Pathology assessment and estimation
Characteristics and prognostic factors of synchronous multiple primary esophageal carcinoma: A report of 52 cases
 Thoracic Cancer ISSN 1759-7706 ORIGINAL ARTICLE Characteristics and prognostic factors of synchronous multiple primary esophageal carcinoma: A report of 52 cases Mei Li & Zhi-xiong Lin Department of Radiation
Thoracic Cancer ISSN 1759-7706 ORIGINAL ARTICLE Characteristics and prognostic factors of synchronous multiple primary esophageal carcinoma: A report of 52 cases Mei Li & Zhi-xiong Lin Department of Radiation
Tristate Lung Meeting 2014 Pro-Con Debate: Surgery has no role in the management of certain subsets of N2 disease
 Tristate Lung Meeting 2014 Pro-Con Debate: Surgery has no role in the management of certain subsets of N2 disease Jennifer E. Tseng, MD UFHealth Cancer Center-Orlando Health Sep 12, 2014 Background Approximately
Tristate Lung Meeting 2014 Pro-Con Debate: Surgery has no role in the management of certain subsets of N2 disease Jennifer E. Tseng, MD UFHealth Cancer Center-Orlando Health Sep 12, 2014 Background Approximately
Temporal Trends in Demographics and Overall Survival of Non Small-Cell Lung Cancer Patients at Moffitt Cancer Center From 1986 to 2008
 Special Report Temporal Trends in Demographics and Overall Survival of Non Small-Cell Lung Cancer Patients at Moffitt Cancer Center From 1986 to 2008 Matthew B. Schabath, PhD, Zachary J. Thompson, PhD,
Special Report Temporal Trends in Demographics and Overall Survival of Non Small-Cell Lung Cancer Patients at Moffitt Cancer Center From 1986 to 2008 Matthew B. Schabath, PhD, Zachary J. Thompson, PhD,
Author s response to reviews
 Author s response to reviews Title: Preoperative chemoradiation with paclitaxel-carboplatin or with fluorouracil-oxaliplatin - folinic acid (FOLFOX) for resectable esophageal and junctional Cancer: the
Author s response to reviews Title: Preoperative chemoradiation with paclitaxel-carboplatin or with fluorouracil-oxaliplatin - folinic acid (FOLFOX) for resectable esophageal and junctional Cancer: the
Accuracy of endoscopic ultrasound staging for T2N0 esophageal cancer: a national cancer database analysis
 Review Article Accuracy of endoscopic ultrasound staging for T2N0 esophageal cancer: a national cancer database analysis Ravi Shridhar 1, Jamie Huston 2, Kenneth L. Meredith 2 1 Department of Radiation
Review Article Accuracy of endoscopic ultrasound staging for T2N0 esophageal cancer: a national cancer database analysis Ravi Shridhar 1, Jamie Huston 2, Kenneth L. Meredith 2 1 Department of Radiation
Long term survival study of de-novo metastatic breast cancers with or without primary tumor resection
 Long term survival study of de-novo metastatic breast cancers with or without primary tumor resection Dr. Michael Co Division of Breast Surgery Queen Mary Hospital The University of Hong Kong Conflicts
Long term survival study of de-novo metastatic breast cancers with or without primary tumor resection Dr. Michael Co Division of Breast Surgery Queen Mary Hospital The University of Hong Kong Conflicts
Resectable locally advanced oesophagogastric cancer
 Resectable locally advanced oesophagogastric cancer Clinical Case Discussion Florian Lordick University Cancer Center Leipzig University Clinic Leipzig Leipzig, Germany esmo.org DISCLOSURES Honoraria for
Resectable locally advanced oesophagogastric cancer Clinical Case Discussion Florian Lordick University Cancer Center Leipzig University Clinic Leipzig Leipzig, Germany esmo.org DISCLOSURES Honoraria for
Research Article Survival Benefit of Adjuvant Radiation Therapy for Gastric Cancer following Gastrectomy and Extended Lymphadenectomy
 International Surgical Oncology Volume 2012, Article ID 307670, 7 pages doi:10.1155/2012/307670 Research Article Survival Benefit of Adjuvant Radiation Therapy for Gastric Cancer following Gastrectomy
International Surgical Oncology Volume 2012, Article ID 307670, 7 pages doi:10.1155/2012/307670 Research Article Survival Benefit of Adjuvant Radiation Therapy for Gastric Cancer following Gastrectomy
The following slides are provided as presented by the author during the live educa7onal ac7vity and are intended for reference purposes only.
 The following slides are provided as presented by the author during the live educa7onal ac7vity and are intended for reference purposes only. If you have any ques7ons, please contact Imedex via email at:
The following slides are provided as presented by the author during the live educa7onal ac7vity and are intended for reference purposes only. If you have any ques7ons, please contact Imedex via email at:
Introduction. Original Article
 Original Article A nomogram that predicts pathologic complete response to neoadjuvant chemoradiation also predicts survival outcomes after definitive chemoradiation for esophageal cancer Steven H. Lin
Original Article A nomogram that predicts pathologic complete response to neoadjuvant chemoradiation also predicts survival outcomes after definitive chemoradiation for esophageal cancer Steven H. Lin
RESEARCH ARTICLE. Kuanoon Boupaijit, Prapaporn Suprasert* Abstract. Introduction. Materials and Methods
 RESEARCH ARTICLE Survival Outcomes of Advanced and Recurrent Cervical Cancer Patients Treated with Chemotherapy: Experience of Northern Tertiary Care Hospital in Thailand Kuanoon Boupaijit, Prapaporn Suprasert*
RESEARCH ARTICLE Survival Outcomes of Advanced and Recurrent Cervical Cancer Patients Treated with Chemotherapy: Experience of Northern Tertiary Care Hospital in Thailand Kuanoon Boupaijit, Prapaporn Suprasert*
Single centre outcomes from definitive chemo-radiotherapy and single modality radiotherapy for locally advanced oesophageal cancer
 Original Article Single centre outcomes from definitive chemo-radiotherapy and single modality radiotherapy for locally advanced oesophageal cancer Ben Alexander Fulton 1, Joanna Gray 2, Alexander McDonald
Original Article Single centre outcomes from definitive chemo-radiotherapy and single modality radiotherapy for locally advanced oesophageal cancer Ben Alexander Fulton 1, Joanna Gray 2, Alexander McDonald
Outcome of rectal cancer after radiotherapy with a long or short waiting period before surgery, a descriptive clinical study
 Original Article Outcome of rectal cancer after radiotherapy with a long or short waiting period before surgery, a descriptive clinical study Elmer E. van Eeghen 1, Frank den Boer 2, Sandra D. Bakker 1,
Original Article Outcome of rectal cancer after radiotherapy with a long or short waiting period before surgery, a descriptive clinical study Elmer E. van Eeghen 1, Frank den Boer 2, Sandra D. Bakker 1,
After primary tumor treatment, 30% of patients with malignant
 ESTS METASTASECTOMY SUPPLEMENT Alberto Oliaro, MD, Pier L. Filosso, MD, Maria C. Bruna, MD, Claudio Mossetti, MD, and Enrico Ruffini, MD Abstract: After primary tumor treatment, 30% of patients with malignant
ESTS METASTASECTOMY SUPPLEMENT Alberto Oliaro, MD, Pier L. Filosso, MD, Maria C. Bruna, MD, Claudio Mossetti, MD, and Enrico Ruffini, MD Abstract: After primary tumor treatment, 30% of patients with malignant
Impact of esophageal cancer staging on overall survival and disease-free survival based on the 2010 AJCC classification by lymph nodes
 Journal of Radiation Research, 2013, 54, 307 314 doi: 10.1093/jrr/rrs096 Advance Access Publication 2 November 2012 Impact of esophageal cancer staging on overall survival and disease-free survival based
Journal of Radiation Research, 2013, 54, 307 314 doi: 10.1093/jrr/rrs096 Advance Access Publication 2 November 2012 Impact of esophageal cancer staging on overall survival and disease-free survival based
Gastroesophag Gastroesopha eal Junction Adenocarcinoma: What is the best adjuvant regimen? Michael G. G. H addock Haddock M.D.
 Gastroesophageal Junction Adenocarcinoma: What is the best adjuvant regimen? Michael G. Haddock M.D. Mayo Clinic Rochester, MN Locally Advanced GE Junction ACA CT S CT or CT S CT/RT Proposition Chemoradiation
Gastroesophageal Junction Adenocarcinoma: What is the best adjuvant regimen? Michael G. Haddock M.D. Mayo Clinic Rochester, MN Locally Advanced GE Junction ACA CT S CT or CT S CT/RT Proposition Chemoradiation
Research and Reviews Journal of Medical and Clinical Oncology
 Comparison and Prognostic Analysis of Elective Nodal Irradiation Using Definitive Radiotherapy versus Chemoradiotherapy for Treatment of Esophageal Cancer Keita M 1,2, Zhang Xueyuan 1, Deng Wenzhao 1,
Comparison and Prognostic Analysis of Elective Nodal Irradiation Using Definitive Radiotherapy versus Chemoradiotherapy for Treatment of Esophageal Cancer Keita M 1,2, Zhang Xueyuan 1, Deng Wenzhao 1,
A Proposed Strategy for Treatment of Superficial Carcinoma. in the Thoracic Esophagus Based on an Analysis. of Lymph Node Metastasis
 Kitakanto Med J 2002 ; 52 : 189-193 189 A Proposed Strategy for Treatment of Superficial Carcinoma in the Thoracic Esophagus Based on an Analysis of Lymph Node Metastasis Susumu Kawate,' Susumu Ohwada,'
Kitakanto Med J 2002 ; 52 : 189-193 189 A Proposed Strategy for Treatment of Superficial Carcinoma in the Thoracic Esophagus Based on an Analysis of Lymph Node Metastasis Susumu Kawate,' Susumu Ohwada,'
The following slides are provided as presented by the author during the live educa7onal ac7vity and are intended for reference purposes only.
 The following slides are provided as presented by the author during the live educa7onal ac7vity and are intended for reference purposes only. If you have any ques7ons, please contact Imedex via email at:
The following slides are provided as presented by the author during the live educa7onal ac7vity and are intended for reference purposes only. If you have any ques7ons, please contact Imedex via email at:
Surgical Management of Metastatic Colon Cancer: analysis of the Surveillance, Epidemiology and End Results (SEER) database
 Surgical Management of Metastatic Colon Cancer: analysis of the Surveillance, Epidemiology and End Results (SEER) database Hadi Khan, MD 1, Adam J. Olszewski, MD 2 and Ponnandai S. Somasundar, MD 1 1 Department
Surgical Management of Metastatic Colon Cancer: analysis of the Surveillance, Epidemiology and End Results (SEER) database Hadi Khan, MD 1, Adam J. Olszewski, MD 2 and Ponnandai S. Somasundar, MD 1 1 Department
Research Article Prognostic Factors in Advanced Non-Small-Cell Lung Cancer Patients: Patient Characteristics and Type of Chemotherapy
 SAGE-Hindawi Access to Research Lung Cancer International Volume 2011, Article ID 152125, 4 pages doi:10.4061/2011/152125 Research Article Prognostic Factors in Advanced Non-Small-Cell Lung Cancer Patients:
SAGE-Hindawi Access to Research Lung Cancer International Volume 2011, Article ID 152125, 4 pages doi:10.4061/2011/152125 Research Article Prognostic Factors in Advanced Non-Small-Cell Lung Cancer Patients:
Introduction. Methods
 Original Article Neoadjuvant vs. adjuvant treatment of Siewert type II gastroesophageal junction cancer: an analysis of data from the surveillance, epidemiology, and end results (SEER) registry Joseph
Original Article Neoadjuvant vs. adjuvant treatment of Siewert type II gastroesophageal junction cancer: an analysis of data from the surveillance, epidemiology, and end results (SEER) registry Joseph
Newly Diagnosed Cases Cancer Related Death NCI 2006 Data
 Multi-Disciplinary Management of Esophageal Cancer: Surgical and Medical Steps Forward Alarming Thoracic Twin Towers 200000 150000 UCSF UCD Thoracic Oncology Conference November 21, 2009 100000 50000 0
Multi-Disciplinary Management of Esophageal Cancer: Surgical and Medical Steps Forward Alarming Thoracic Twin Towers 200000 150000 UCSF UCD Thoracic Oncology Conference November 21, 2009 100000 50000 0
The CROSS road in neoadjuvant therapy for esophageal cancer: long-term results of CROSS trial
 Editorial The CROSS road in neoadjuvant therapy for esophageal cancer: long-term results of CROSS trial Ian Wong, Simon Law Division of Esophageal and Upper Gastrointestinal Surgery, Department of Surgery,
Editorial The CROSS road in neoadjuvant therapy for esophageal cancer: long-term results of CROSS trial Ian Wong, Simon Law Division of Esophageal and Upper Gastrointestinal Surgery, Department of Surgery,
17. Oesophagus. Upper gastrointestinal cancer
 110 17. Upper gastrointestinal cancer Oesophagus Radical treatment For patients with localised disease, the standard curative approach to treatment is either surgery + perioperative chemotherapy, surgery
110 17. Upper gastrointestinal cancer Oesophagus Radical treatment For patients with localised disease, the standard curative approach to treatment is either surgery + perioperative chemotherapy, surgery
Primary radio(chemo)therapy for esophageal cancer in elderly patients: are efficiency and toxicity comparable with younger patients?
 DOI 10.1186/s40001-017-0265-x European Journal of Medical Research RESEARCH Open Access Primary radio(chemo)therapy for esophageal cancer in elderly patients: are efficiency and toxicity comparable with
DOI 10.1186/s40001-017-0265-x European Journal of Medical Research RESEARCH Open Access Primary radio(chemo)therapy for esophageal cancer in elderly patients: are efficiency and toxicity comparable with
Management of Esophageal Cancer: Evidence Based Review of Current Guidelines. Madhuri Rao, MD PGY-5 SUNY Downstate Medical Center
 Management of Esophageal Cancer: Evidence Based Review of Current Guidelines Madhuri Rao, MD PGY-5 SUNY Downstate Medical Center Case Presentation 68 y/o male PMH: NIDDM, HTN, hyperlipidemia, CAD s/p stents,
Management of Esophageal Cancer: Evidence Based Review of Current Guidelines Madhuri Rao, MD PGY-5 SUNY Downstate Medical Center Case Presentation 68 y/o male PMH: NIDDM, HTN, hyperlipidemia, CAD s/p stents,
THE ROLE OF RADIATION THERAPY IN MANAGEMENT OF PANCREATIC ADENOCARCINOMA. TIMUR MITIN, MD, PhD
 THE ROLE OF RADIATION THERAPY IN MANAGEMENT OF PANCREATIC ADENOCARCINOMA TIMUR MITIN, MD, PhD RESECTABLE DISEASE MANAGEMENT: RESECTABLE DISEASE Resection offers the only possibility of long term survival
THE ROLE OF RADIATION THERAPY IN MANAGEMENT OF PANCREATIC ADENOCARCINOMA TIMUR MITIN, MD, PhD RESECTABLE DISEASE MANAGEMENT: RESECTABLE DISEASE Resection offers the only possibility of long term survival
Determining the optimal number of lymph nodes harvested during esophagectomy
 Original Article Determining the optimal number of lymph nodes harvested during esophagectomy Khaldoun Almhanna, Jill Weber, Ravi Shridhar, Sarah Hoffe, Jonathan Strosberg, Kenneth Meredith Department
Original Article Determining the optimal number of lymph nodes harvested during esophagectomy Khaldoun Almhanna, Jill Weber, Ravi Shridhar, Sarah Hoffe, Jonathan Strosberg, Kenneth Meredith Department
The prognosis for patients with esophageal cancer is poor.
 ORIGINAL ARTICLE A Phase II Study of Paclitaxel, Carboplatin, and Radiation with or without Surgery for Esophageal Cancer Henry Wang, MD, Janice Ryu, MD, David Gandara, MD, Richard J. Bold, MD, Shiro Urayama,
ORIGINAL ARTICLE A Phase II Study of Paclitaxel, Carboplatin, and Radiation with or without Surgery for Esophageal Cancer Henry Wang, MD, Janice Ryu, MD, David Gandara, MD, Richard J. Bold, MD, Shiro Urayama,
Management of Squamous Cell Cancer of the Esophagus: Surgery Should Follow Chemo + RT
 Management of Squamous Cell Cancer of the Esophagus: Surgery Should Follow Chemo + RT David H. Ilson, MD, PhD Gastrointestinal Oncology Service Memorial Sloan Kettering Cancer Center Disclosure Consulting
Management of Squamous Cell Cancer of the Esophagus: Surgery Should Follow Chemo + RT David H. Ilson, MD, PhD Gastrointestinal Oncology Service Memorial Sloan Kettering Cancer Center Disclosure Consulting
Outcome of nonsurgical treatment for locally advanced thymic tumors
 Original Article Outcome of nonsurgical treatment for locally advanced thymic tumors Chang-Lu Wang 1, Lan-Ting Gao 1, Chang-Xing Lv 1, Lei Zhu 2, Wen-Tao Fang 3 1 Department of Radiation Oncology, 2 Department
Original Article Outcome of nonsurgical treatment for locally advanced thymic tumors Chang-Lu Wang 1, Lan-Ting Gao 1, Chang-Xing Lv 1, Lei Zhu 2, Wen-Tao Fang 3 1 Department of Radiation Oncology, 2 Department
Adjuvant Chemotherapy for Rectal Cancer: Are we making progress?
 Adjuvant Chemotherapy for Rectal Cancer: Are we making progress? Hagen Kennecke, MD, MHA, FRCPC Division Of Medical Oncology British Columbia Cancer Agency October 25, 2008 Objectives Review milestones
Adjuvant Chemotherapy for Rectal Cancer: Are we making progress? Hagen Kennecke, MD, MHA, FRCPC Division Of Medical Oncology British Columbia Cancer Agency October 25, 2008 Objectives Review milestones
Update on Neoadjuvant Chemotherapy (NACT) in Cervical Cancer
 Update on Neoadjuvant Chemotherapy (NACT) in Cervical Cancer Nicoletta Colombo, MD University of Milan-Bicocca European Institute of Oncology Milan, Italy NACT in Cervical Cancer NACT Stage -IB2 -IIA>4cm
Update on Neoadjuvant Chemotherapy (NACT) in Cervical Cancer Nicoletta Colombo, MD University of Milan-Bicocca European Institute of Oncology Milan, Italy NACT in Cervical Cancer NACT Stage -IB2 -IIA>4cm
PERIOPERATIVE TREATMENT OF NON SMALL CELL LUNG CANCER. Virginie Westeel Chest Disease Department University Hospital Besançon, France
 PERIOPERATIVE TREATMENT OF NON SMALL CELL LUNG CANCER Virginie Westeel Chest Disease Department University Hospital Besançon, France LEARNING OBJECTIVES 1. To understand the potential of perioperative
PERIOPERATIVE TREATMENT OF NON SMALL CELL LUNG CANCER Virginie Westeel Chest Disease Department University Hospital Besançon, France LEARNING OBJECTIVES 1. To understand the potential of perioperative
Indeterminate Pulmonary Nodules in Patients with Colorectal Cancer
 Indeterminate Pulmonary Nodules in Patients with Colorectal Cancer Jai Sule 1, Kah Wai Cheong 2, Stella Bee 2, Bettina Lieske 2,3 1 Dept of Cardiothoracic and Vascular Surgery, University Surgical Cluster,
Indeterminate Pulmonary Nodules in Patients with Colorectal Cancer Jai Sule 1, Kah Wai Cheong 2, Stella Bee 2, Bettina Lieske 2,3 1 Dept of Cardiothoracic and Vascular Surgery, University Surgical Cluster,
Tratamiento Multidisciplinar de Estadios Localmente Avanzados en Cáncer de Pulmón
 Tratamiento Multidisciplinar de Estadios Localmente Avanzados en Cáncer de Pulmón Santiago Ponce Aix Servicio Oncología Médica Hospital Universitario 12 de Octubre Madrid Stage III: heterogenous disease
Tratamiento Multidisciplinar de Estadios Localmente Avanzados en Cáncer de Pulmón Santiago Ponce Aix Servicio Oncología Médica Hospital Universitario 12 de Octubre Madrid Stage III: heterogenous disease
Ratio of maximum standardized uptake value to primary tumor size is a prognostic factor in patients with advanced non-small cell lung cancer
 Original Article Ratio of maximum standardized uptake value to primary tumor size is a prognostic factor in patients with advanced non-small cell lung cancer Fangfang Chen 1 *, Yanwen Yao 2 *, Chunyan
Original Article Ratio of maximum standardized uptake value to primary tumor size is a prognostic factor in patients with advanced non-small cell lung cancer Fangfang Chen 1 *, Yanwen Yao 2 *, Chunyan
3/8/2014. Case Presentation. Primary Treatment of Anal Cancer. Anatomy. Overview. March 6, 2014
 Case Presentation Primary Treatment of Anal Cancer 65 year old female presents with perianal pain, lower GI bleeding, and anemia with Hb of 7. On exam 6 cm mass protruding through the anus with bulky R
Case Presentation Primary Treatment of Anal Cancer 65 year old female presents with perianal pain, lower GI bleeding, and anemia with Hb of 7. On exam 6 cm mass protruding through the anus with bulky R
Combined modality treatment for N2 disease
 Combined modality treatment for N2 disease Dr Clara Chan Consultant in Clinical Oncology 3 rd March 2017 Overview Background The evidence base Systemic treatment Radiotherapy Future directions/clinical
Combined modality treatment for N2 disease Dr Clara Chan Consultant in Clinical Oncology 3 rd March 2017 Overview Background The evidence base Systemic treatment Radiotherapy Future directions/clinical
Which Treatment Approach is Most Appropriate for Primary Therapy of Gastric Cancer: Neoadjuvant Chemotherapy
 Which Treatment Approach is Most Appropriate for Primary Therapy of Gastric Cancer: Neoadjuvant Chemotherapy Joseph Chao, M.D. Assistant Clinical Professor Department of Medical Oncology & Therapeutics
Which Treatment Approach is Most Appropriate for Primary Therapy of Gastric Cancer: Neoadjuvant Chemotherapy Joseph Chao, M.D. Assistant Clinical Professor Department of Medical Oncology & Therapeutics
Locoregional treatment Session Oral Abstract Presentation Saulo Brito Silva
 Locoregional treatment Session Oral Abstract Presentation Saulo Brito Silva Background Post-operative radiotherapy (PORT) improves disease free and overall suvivallin selected patients with breast cancer
Locoregional treatment Session Oral Abstract Presentation Saulo Brito Silva Background Post-operative radiotherapy (PORT) improves disease free and overall suvivallin selected patients with breast cancer
Surgical strategies in esophageal cancer
 Gastro-Conference Berlin 2005 October 1-2, 2005 Surgical strategies in esophageal cancer J. Rüdiger Siewert Department of Surgery, Klinikum rechts der Isar Technische Universität München Esophageal Cancer
Gastro-Conference Berlin 2005 October 1-2, 2005 Surgical strategies in esophageal cancer J. Rüdiger Siewert Department of Surgery, Klinikum rechts der Isar Technische Universität München Esophageal Cancer
Lung Cancer Epidemiology. AJCC Staging 6 th edition
 Surgery for stage IIIA NSCLC? Sometimes! Anne S. Tsao, M.D. Associate Professor Director, Mesothelioma Program Director, Thoracic Chemo-Radiation Program May 7, 2011 The University of Texas MD ANDERSON
Surgery for stage IIIA NSCLC? Sometimes! Anne S. Tsao, M.D. Associate Professor Director, Mesothelioma Program Director, Thoracic Chemo-Radiation Program May 7, 2011 The University of Texas MD ANDERSON
Towards a more personalized approach in the treatment of esophageal cancer focusing on predictive factors in response to chemoradiation Wang, Da
 University of Groningen Towards a more personalized approach in the treatment of esophageal cancer focusing on predictive factors in response to chemoradiation Wang, Da IMPORTANT NOTE: You are advised
University of Groningen Towards a more personalized approach in the treatment of esophageal cancer focusing on predictive factors in response to chemoradiation Wang, Da IMPORTANT NOTE: You are advised
Although esophagectomy remains the standard of care for esophageal
 Keresztes et al General Thoracic Surgery Preoperative chemotherapy for esophageal cancer with paclitaxel and carboplatin: Results of a phase II trial R. S. Keresztes, MD J. L. Port, MD M. W. Pasmantier,
Keresztes et al General Thoracic Surgery Preoperative chemotherapy for esophageal cancer with paclitaxel and carboplatin: Results of a phase II trial R. S. Keresztes, MD J. L. Port, MD M. W. Pasmantier,
Clinicopathologic and prognostic factors of young and elderly patients with esophageal adenocarcinoma: is there really a difference?
 Diseases of the Esophagus (2008) 21, 596 600 DOI: 10.1111/j.1442-2050.2008.00817.x Original article Clinicopathologic and prognostic factors of young and elderly patients with esophageal adenocarcinoma:
Diseases of the Esophagus (2008) 21, 596 600 DOI: 10.1111/j.1442-2050.2008.00817.x Original article Clinicopathologic and prognostic factors of young and elderly patients with esophageal adenocarcinoma:
Workshop LA RADIOTERAPIA DEI TUMORI RARI I TIMOMI : INDICAZIONI
 XXI CONGRESSO NAZIONALE AIRO Genova, 19-22 novembre 2011 Workshop LA RADIOTERAPIA DEI TUMORI RARI I TIMOMI : INDICAZIONI PIERA NAVARRIA Unità Operativa di Radioterapia e Radiochirurgia Humanitas Cancer
XXI CONGRESSO NAZIONALE AIRO Genova, 19-22 novembre 2011 Workshop LA RADIOTERAPIA DEI TUMORI RARI I TIMOMI : INDICAZIONI PIERA NAVARRIA Unità Operativa di Radioterapia e Radiochirurgia Humanitas Cancer
CONTROVERSIES IN THE PREOPERATIVE RADIOTHERAPEUTIC MANAGEMENT OF RESECTABLE ESOPHAGEAL CANCER
 SA-CME INFORMATION SA CME Information CONTROVERSIES IN THE PREOPERATIVE RADIOTHERAPEUTIC MANAGEMENT OF RESECTABLE ESOPHAGEAL CANCER Description This review examines the role of trimodality therapy in the
SA-CME INFORMATION SA CME Information CONTROVERSIES IN THE PREOPERATIVE RADIOTHERAPEUTIC MANAGEMENT OF RESECTABLE ESOPHAGEAL CANCER Description This review examines the role of trimodality therapy in the
Surgical resection improves survival in pancreatic cancer patients without vascular invasion- a population based study
 Original article Annals of Gastroenterology (2013) 26, 346-352 Surgical resection improves survival in pancreatic cancer patients without vascular invasion- a population based study Subhankar Chakraborty
Original article Annals of Gastroenterology (2013) 26, 346-352 Surgical resection improves survival in pancreatic cancer patients without vascular invasion- a population based study Subhankar Chakraborty
Radiation Therapy for Recurrent Esophageal Cancer after Surgery: Clinical Results and Prognostic Factors
 Radiation Therapy for Recurrent Esophageal Cancer after Surgery: Clinical Results and Prognostic Factors Yoshiyuki Shioyama 1, Katsumasa Nakamura 1, Saiji Ohga 1, Satoshi Nomoto 1, Tomonari Sasaki 1, Toshihiro
Radiation Therapy for Recurrent Esophageal Cancer after Surgery: Clinical Results and Prognostic Factors Yoshiyuki Shioyama 1, Katsumasa Nakamura 1, Saiji Ohga 1, Satoshi Nomoto 1, Tomonari Sasaki 1, Toshihiro
Surgical resection alone remains a worldwide standard for
 Original Article Influence of Preoperative Radiation Field on Postoperative Leak Rates in Esophageal Cancer Patients after Trimodality Therapy Aditya Juloori, BS,* Susan L. Tucker, PhD, Ritsuko Komaki,
Original Article Influence of Preoperative Radiation Field on Postoperative Leak Rates in Esophageal Cancer Patients after Trimodality Therapy Aditya Juloori, BS,* Susan L. Tucker, PhD, Ritsuko Komaki,
A phase II study of weekly paclitaxel and cisplatin followed by radical hysterectomy in stages IB2 and IIA2 cervical cancer AGOG14-001/TGOG1008
 A phase II study of weekly paclitaxel and cisplatin followed by radical hysterectomy in stages IB2 and IIA2 cervical cancer AGOG14-001/TGOG1008 NCT02432365 Chyong-Huey Lai, MD On behalf of Principal investigator
A phase II study of weekly paclitaxel and cisplatin followed by radical hysterectomy in stages IB2 and IIA2 cervical cancer AGOG14-001/TGOG1008 NCT02432365 Chyong-Huey Lai, MD On behalf of Principal investigator
Perioperative management of esophageal cancer
 Perioperative management of esophageal cancer Lucas Goense Perioperative management of esophageal cancer Lucas Goense Perioperative management of esophageal cancer PhD thesis, Utrecht University, The
Perioperative management of esophageal cancer Lucas Goense Perioperative management of esophageal cancer Lucas Goense Perioperative management of esophageal cancer PhD thesis, Utrecht University, The
Treatment outcomes and prognostic factors of gallbladder cancer patients after postoperative radiation therapy
 Korean J Hepatobiliary Pancreat Surg 2011;15:152-156 Original Article Treatment outcomes and prognostic factors of gallbladder cancer patients after postoperative radiation therapy Suzy Kim 1,#, Kyubo
Korean J Hepatobiliary Pancreat Surg 2011;15:152-156 Original Article Treatment outcomes and prognostic factors of gallbladder cancer patients after postoperative radiation therapy Suzy Kim 1,#, Kyubo
Accepted Manuscript. Early stage (ct2n0) esophageal cancer: should induction therapy be a standard? Michael Lanuti, MD
 Accepted Manuscript Early stage (ct2n0) esophageal cancer: should induction therapy be a standard? Michael Lanuti, MD PII: S0022-5223(18)30392-1 DOI: 10.1016/j.jtcvs.2018.02.029 Reference: YMTC 12608 To
Accepted Manuscript Early stage (ct2n0) esophageal cancer: should induction therapy be a standard? Michael Lanuti, MD PII: S0022-5223(18)30392-1 DOI: 10.1016/j.jtcvs.2018.02.029 Reference: YMTC 12608 To
Does the Timing of Esophagectomy After Chemoradiation Affect Outcome?
 ORIGINAL ARTICLES: SURGERY: The Annals of Thoracic Surgery CME Program is located online at http://cme.ctsnetjournals.org. To take the CME activity related to this article, you must have either an STS
ORIGINAL ARTICLES: SURGERY: The Annals of Thoracic Surgery CME Program is located online at http://cme.ctsnetjournals.org. To take the CME activity related to this article, you must have either an STS
Adjuvant and neoadjuvant chemotherapy for rectal cancer: Expensive but little gain
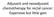 Adjuvant and neoadjuvant chemotherapy for rectal cancer: Expensive but little gain Outline The problem Adjuvant therapy Neoadjuvant therapy Options Conclusion The problem 30 years ago: Local recurrence
Adjuvant and neoadjuvant chemotherapy for rectal cancer: Expensive but little gain Outline The problem Adjuvant therapy Neoadjuvant therapy Options Conclusion The problem 30 years ago: Local recurrence
Survival benefit of surgery with radiotherapy vs surgery alone to patients with T2-3N0M0 stage esophageal adenocarcinoma
 /, Vol. 7, No. 16 Survival benefit of surgery with radiotherapy vs surgery alone to patients with T2-3N0M0 stage esophageal adenocarcinoma Yaqi Song 1,*, Guangzhou Tao 1, Qing Guo 3,*, Xi Yang 2,*, Hongcheng
/, Vol. 7, No. 16 Survival benefit of surgery with radiotherapy vs surgery alone to patients with T2-3N0M0 stage esophageal adenocarcinoma Yaqi Song 1,*, Guangzhou Tao 1, Qing Guo 3,*, Xi Yang 2,*, Hongcheng
Controversies in management of squamous esophageal cancer
 2015.06.12 12.47.48 Page 4(1) IS-1 Controversies in management of squamous esophageal cancer C S Pramesh Thoracic Surgery, Department of Surgical Oncology, Tata Memorial Centre, India In Asia, squamous
2015.06.12 12.47.48 Page 4(1) IS-1 Controversies in management of squamous esophageal cancer C S Pramesh Thoracic Surgery, Department of Surgical Oncology, Tata Memorial Centre, India In Asia, squamous
Clinicopathological Factors Affecting Distant Metastasis Following Loco-Regional Recurrence of breast cancer. Cheol Min Kang 2018/04/05
 Abstract No.: ABS-0075 Clinicopathological Factors Affecting Distant Metastasis Following Loco-Regional Recurrence of breast cancer 2018/04/05 Cheol Min Kang Department of surgery, University of Ulsan
Abstract No.: ABS-0075 Clinicopathological Factors Affecting Distant Metastasis Following Loco-Regional Recurrence of breast cancer 2018/04/05 Cheol Min Kang Department of surgery, University of Ulsan
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Abdominal drainage, after hepatic resection, 159 160 Ablation, radiofrequency, for hepatocellular carcinoma, 160 161 Adenocarcinoma, pancreatic.
Index Note: Page numbers of article titles are in boldface type. A Abdominal drainage, after hepatic resection, 159 160 Ablation, radiofrequency, for hepatocellular carcinoma, 160 161 Adenocarcinoma, pancreatic.
Mini J.Elnaggar M.D. Radiation Oncology Ochsner Medical Center 9/23/2016. Background
 Mini J.Elnaggar M.D. Radiation Oncology Ochsner Medical Center 9/23/2016 Background Mostly adenocarcinoma (scc possible, but treated like anal cancer) 39, 220 cases annually Primary treatment: surgery
Mini J.Elnaggar M.D. Radiation Oncology Ochsner Medical Center 9/23/2016 Background Mostly adenocarcinoma (scc possible, but treated like anal cancer) 39, 220 cases annually Primary treatment: surgery
Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers
 日大医誌 75 (1): 10 15 (2016) 10 Original Article Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers Naotaka Uchida 1), Yasuki Matsui 1), Takeshi Notsu 1) and Manabu
日大医誌 75 (1): 10 15 (2016) 10 Original Article Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers Naotaka Uchida 1), Yasuki Matsui 1), Takeshi Notsu 1) and Manabu
News Briefing: Treatment Considerations for Focused Populations
 News Briefing: Treatment Considerations for Focused Populations Moderator: Pranshu Mohindra, MD, University of Maryland, Baltimore Reirradiation of Thoracic Cancers with Intensity Modulated Proton Therapy
News Briefing: Treatment Considerations for Focused Populations Moderator: Pranshu Mohindra, MD, University of Maryland, Baltimore Reirradiation of Thoracic Cancers with Intensity Modulated Proton Therapy
CHAPTER 5 TUMOR SIZE DOES NOT PREDICT PATHOLOGICAL COMPLETE RESPONSE RATES AFTER PRE-OPERATIVE CHEMORADIOTHERAPY FOR NON-SMALL CELL LUNG CANCER
 TUMOR SIZE DOES NOT PREDICT PATHOLOGICAL COMPLETE RESPONSE RATES AFTER PRE-OPERATIVE CHEMORADIOTHERAPY FOR NON-SMALL CELL LUNG CANCER Cornelis G. Vos Max R. Dahele Chris Dickhoff Suresh Senan Erik Thunnissen
TUMOR SIZE DOES NOT PREDICT PATHOLOGICAL COMPLETE RESPONSE RATES AFTER PRE-OPERATIVE CHEMORADIOTHERAPY FOR NON-SMALL CELL LUNG CANCER Cornelis G. Vos Max R. Dahele Chris Dickhoff Suresh Senan Erik Thunnissen
The clinicopathological features and treatment modalities associated with survival of neuroendocrine cervical carcinoma in a Chinese population
 Zhang et al. BMC Cancer (2019) 19:22 https://doi.org/10.1186/s12885-018-5147-2 RESEARCH ARTICLE Open Access The clinicopathological features and treatment modalities associated with survival of neuroendocrine
Zhang et al. BMC Cancer (2019) 19:22 https://doi.org/10.1186/s12885-018-5147-2 RESEARCH ARTICLE Open Access The clinicopathological features and treatment modalities associated with survival of neuroendocrine
Aytul OZGEN 1, *, Mutlu HAYRAN 2 and Fatih KAHRAMAN 3 INTRODUCTION
 Journal of Radiation Research, 2012, 53, 916 922 doi: 10.1093/jrr/rrs056 Advance Access Publication 21 August 2012 Mean esophageal radiation dose is predictive of the grade of acute esophagitis in lung
Journal of Radiation Research, 2012, 53, 916 922 doi: 10.1093/jrr/rrs056 Advance Access Publication 21 August 2012 Mean esophageal radiation dose is predictive of the grade of acute esophagitis in lung
CHEMOTHERAPY FOLLOWED BY SURGERY VS. SURGERY ALONE FOR LOCALIZED ESOPHAGEAL CANCER
 CHEMOTHERAPY FOLLOWED BY VS. ALONE FOR LOCALIZED ESOPHAGEAL CANCER CHEMOTHERAPY FOLLOWED BY COMPARED WITH ALONE FOR LOCALIZED ESOPHAGEAL CANCER DAVID P. KELSEN, M.D., ROBERT GINSBERG, M.D., THOMAS F. PAJAK,
CHEMOTHERAPY FOLLOWED BY VS. ALONE FOR LOCALIZED ESOPHAGEAL CANCER CHEMOTHERAPY FOLLOWED BY COMPARED WITH ALONE FOR LOCALIZED ESOPHAGEAL CANCER DAVID P. KELSEN, M.D., ROBERT GINSBERG, M.D., THOMAS F. PAJAK,
WHO BENEFITS FROM ADJUVANT CHEMOTHERAPY RADIATION CHEMORADIATION? Dr. Paul Gardiner April 23, 2001 Discipline of Surgery Grand Rounds
 WHO BENEFITS FROM ADJUVANT CHEMOTHERAPY RADIATION CHEMORADIATION? Dr. Paul Gardiner April 23, 2001 Discipline of Surgery Grand Rounds LUNG Dr. Greenland ESOPHAGUS Dr. Gardiner ESOPHAGEAL CANCER 1200 new
WHO BENEFITS FROM ADJUVANT CHEMOTHERAPY RADIATION CHEMORADIATION? Dr. Paul Gardiner April 23, 2001 Discipline of Surgery Grand Rounds LUNG Dr. Greenland ESOPHAGUS Dr. Gardiner ESOPHAGEAL CANCER 1200 new
Lower lymph node yield following neoadjuvant therapy for rectal cancer has no clinical significance
 Original Article Lower lymph node yield following neoadjuvant therapy for rectal cancer has no clinical significance Dedrick Kok Hong Chan 1,2, Ker-Kan Tan 1,2 1 Division of Colorectal Surgery, University
Original Article Lower lymph node yield following neoadjuvant therapy for rectal cancer has no clinical significance Dedrick Kok Hong Chan 1,2, Ker-Kan Tan 1,2 1 Division of Colorectal Surgery, University
Updates on the Conflict of Postoperative Radiotherapy Impact on Survival of Young Women with Cancer Breast: A Retrospective Cohort Study
 International Journal of Medical Research & Health Sciences Available online at www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2017, 6(7): 14-18 I J M R
International Journal of Medical Research & Health Sciences Available online at www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2017, 6(7): 14-18 I J M R
Esophageal cancer located at the cervical and upper thoracic
 ORIGINAL ARTICLE Esophageal Cancer Located at the Neck and Upper Thorax Treated with Concurrent Chemoradiation: A Single- Institution Experience Shulian Wang, MD,* Zhongxing Liao, MD, Yuan Chen, MD, Joe
ORIGINAL ARTICLE Esophageal Cancer Located at the Neck and Upper Thorax Treated with Concurrent Chemoradiation: A Single- Institution Experience Shulian Wang, MD,* Zhongxing Liao, MD, Yuan Chen, MD, Joe
Insights into Thymic Epithelial Tumors: Radiation Therapy
 Insights into Thymic Epithelial Tumors: Radiation Therapy Charles R. Thomas, MD Professor and Chairman, Department of Radiation Medicine Professor, Department of Medicine, Division of Hematology/Medical
Insights into Thymic Epithelial Tumors: Radiation Therapy Charles R. Thomas, MD Professor and Chairman, Department of Radiation Medicine Professor, Department of Medicine, Division of Hematology/Medical
Concurrent chemoradiotherapy (CRT) followed by surgery
 Original Article Re-evaluating the Optimal Radiation Dose for Definitive Chemoradiotherapy for Esophageal Squamous Cell Carcinoma Liru He, MD,* Pamela K. Allen, PhD,* Adam Potter, PhD, Jingya Wang, MD,*
Original Article Re-evaluating the Optimal Radiation Dose for Definitive Chemoradiotherapy for Esophageal Squamous Cell Carcinoma Liru He, MD,* Pamela K. Allen, PhD,* Adam Potter, PhD, Jingya Wang, MD,*
NEOADJUVANT THERAPY IN CARCINOMA STOMACH. Dr Jyotirup Goswami Consultant Radiation Oncologist Narayana Superspeciality Hospital, Howrah
 NEOADJUVANT THERAPY IN CARCINOMA STOMACH Dr Jyotirup Goswami Consultant Radiation Oncologist Narayana Superspeciality Hospital, Howrah NEOADJUVANT THERAPY?! Few believers Limited evidence Many surgeons
NEOADJUVANT THERAPY IN CARCINOMA STOMACH Dr Jyotirup Goswami Consultant Radiation Oncologist Narayana Superspeciality Hospital, Howrah NEOADJUVANT THERAPY?! Few believers Limited evidence Many surgeons
Association of Age and Survival in Patients With Gastroesophageal Cancer Undergoing Surgery With or Without Preoperative Therapy
 Association of Age and Survival in Patients With Gastroesophageal Cancer Undergoing Surgery With or Without Preoperative Therapy Fadi Braiteh, MD 1 ; Arlene M. Correa, PhD 2 ; Wayne L. Hofstetter, MD 2
Association of Age and Survival in Patients With Gastroesophageal Cancer Undergoing Surgery With or Without Preoperative Therapy Fadi Braiteh, MD 1 ; Arlene M. Correa, PhD 2 ; Wayne L. Hofstetter, MD 2
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Ablative therapy, nonsurgical, for pulmonary metastases of soft tissue sarcoma, 279 280 Adipocytic tumors, atypical lipomatous tumor vs. well-differentiated
Note: Page numbers of article titles are in boldface type. A Ablative therapy, nonsurgical, for pulmonary metastases of soft tissue sarcoma, 279 280 Adipocytic tumors, atypical lipomatous tumor vs. well-differentiated
Nasopharyngeal Cancer:Role of Chemotherapy
 Nasopharyngeal Cancer:Role of Chemotherapy PANAGIOTIS KATSAOUNIS Medical Oncologist IASO GENERAL HOSPITAL Athens, 16/9/2017 2 nd Hellenic Multidisciplinary Conference on Head and Neck Cancer INTRODUCTION
Nasopharyngeal Cancer:Role of Chemotherapy PANAGIOTIS KATSAOUNIS Medical Oncologist IASO GENERAL HOSPITAL Athens, 16/9/2017 2 nd Hellenic Multidisciplinary Conference on Head and Neck Cancer INTRODUCTION
Is consolidation chemotherapy after concurrent chemo-radiotherapy beneficial for patients with locally advanced non-small cell lung cancer?
 Is consolidation chemotherapy after concurrent chemo-radiotherapy beneficial for patients with locally advanced non-small cell lung cancer? ~A pooled analysis of the literature~ Satomi Yamamoto 1, Kazuyuki
Is consolidation chemotherapy after concurrent chemo-radiotherapy beneficial for patients with locally advanced non-small cell lung cancer? ~A pooled analysis of the literature~ Satomi Yamamoto 1, Kazuyuki
Prognosis of esophageal squamous cell carcinoma patients with preoperative radiotherapy: Comparison of different cancer staging systems
 Thoracic Cancer ISSN 1759-7706 ORIGINAL ARTICLE Prognosis of esophageal squamous cell carcinoma patients with preoperative radiotherapy: Comparison of different cancer staging systems Qifeng Wang 1 *,
Thoracic Cancer ISSN 1759-7706 ORIGINAL ARTICLE Prognosis of esophageal squamous cell carcinoma patients with preoperative radiotherapy: Comparison of different cancer staging systems Qifeng Wang 1 *,
Case Scenario 1. The patient has now completed his neoadjuvant chemoradiation and has been cleared for surgery.
 Case Scenario 1 July 10, 2010 A 67-year-old male with squamous cell carcinoma of the mid thoracic esophagus presents for surgical resection. The patient has completed preoperative chemoradiation. This
Case Scenario 1 July 10, 2010 A 67-year-old male with squamous cell carcinoma of the mid thoracic esophagus presents for surgical resection. The patient has completed preoperative chemoradiation. This
Thymic neoplasms are the most common tumors of
 Thymic Carcinoma: A Multivariate Analysis of Factors Predictive of Survival in 290 Patients Benny Weksler, MD, Rajeev Dhupar, MD, MBA, Vishal Parikh, BS, Katie S. Nason, MD, MPH, Arjun Pennathur, MD, and
Thymic Carcinoma: A Multivariate Analysis of Factors Predictive of Survival in 290 Patients Benny Weksler, MD, Rajeev Dhupar, MD, MBA, Vishal Parikh, BS, Katie S. Nason, MD, MPH, Arjun Pennathur, MD, and
Log odds of positive lymph nodes is a novel prognostic indicator for advanced ESCC after surgical resection
 Original Article Log odds of positive lymph nodes is a novel prognostic indicator for advanced ESCC after surgical resection Mingjian Yang 1,2, Hongdian Zhang 1,2, Zhao Ma 1,2, Lei Gong 1,2, Chuangui Chen
Original Article Log odds of positive lymph nodes is a novel prognostic indicator for advanced ESCC after surgical resection Mingjian Yang 1,2, Hongdian Zhang 1,2, Zhao Ma 1,2, Lei Gong 1,2, Chuangui Chen
Nasopharyngeal Cancer/Multimodality Treatment
 Nasopharyngeal Cancer/Multimodality Treatment PANAGIOTIS KATSAOUNIS Medical Oncologist IASO GENERAL HOSPITAL Athens, 22/10/2016 1 st Hellenic Multidisciplinary Conference on Head and Neck Cancer INTRODUCTION
Nasopharyngeal Cancer/Multimodality Treatment PANAGIOTIS KATSAOUNIS Medical Oncologist IASO GENERAL HOSPITAL Athens, 22/10/2016 1 st Hellenic Multidisciplinary Conference on Head and Neck Cancer INTRODUCTION
UPDATE IN THE MANAGEMENT OF INVASIVE CERVICAL CANCER
 UPDATE IN THE MANAGEMENT OF INVASIVE CERVICAL CANCER Susan Davidson, MD Professor Department of Obstetrics and Gynecology Division of Gynecologic Oncology University of Colorado- Denver Anatomy Review
UPDATE IN THE MANAGEMENT OF INVASIVE CERVICAL CANCER Susan Davidson, MD Professor Department of Obstetrics and Gynecology Division of Gynecologic Oncology University of Colorado- Denver Anatomy Review
EFFICACY OF NECK DISSECTION FOR LOCOREGIONAL FAILURES VERSUS ISOLATED NODAL FAILURES IN NASOPHARYNGEAL CARCINOMA
 ORIGINAL ARTICLE EFFICACY OF NECK DISSECTION FOR LOCOREGIONAL FAILURES VERSUS ISOLATED NODAL FAILURES IN NASOPHARYNGEAL CARCINOMA Raymond King Yin Tsang, FRCSEd, Joseph Chun Kit Chung, MRCSEd, Yiu Wing
ORIGINAL ARTICLE EFFICACY OF NECK DISSECTION FOR LOCOREGIONAL FAILURES VERSUS ISOLATED NODAL FAILURES IN NASOPHARYNGEAL CARCINOMA Raymond King Yin Tsang, FRCSEd, Joseph Chun Kit Chung, MRCSEd, Yiu Wing
RESEARCH COMMUNICATION
 DOI:http://dx.doi.org/10.7314/APJCP.2012.13.1.199 RESEARCH COMMUNICATION Prognostic Significance of CYFRA21-1, CEA and Hemoglobin in Patients with Esophageal Squamous Cancer Undergoing Concurrent Chemoradiotherapy
DOI:http://dx.doi.org/10.7314/APJCP.2012.13.1.199 RESEARCH COMMUNICATION Prognostic Significance of CYFRA21-1, CEA and Hemoglobin in Patients with Esophageal Squamous Cancer Undergoing Concurrent Chemoradiotherapy
Extent of lymphadenectomy for esophageal squamous cell cancer: interpreting the post-hoc analysis of a randomized trial
 Accepted Manuscript Extent of lymphadenectomy for esophageal squamous cell cancer: interpreting the post-hoc analysis of a randomized trial Vaibhav Gupta, MD PII: S0022-5223(18)33169-6 DOI: https://doi.org/10.1016/j.jtcvs.2018.11.055
Accepted Manuscript Extent of lymphadenectomy for esophageal squamous cell cancer: interpreting the post-hoc analysis of a randomized trial Vaibhav Gupta, MD PII: S0022-5223(18)33169-6 DOI: https://doi.org/10.1016/j.jtcvs.2018.11.055
Analysis of the outcome of young age tongue squamous cell carcinoma
 Jeon et al. Maxillofacial Plastic and Reconstructive Surgery (2017) 39:41 DOI 10.1186/s40902-017-0139-8 Maxillofacial Plastic and Reconstructive Surgery RESEARCH Open Access Analysis of the outcome of
Jeon et al. Maxillofacial Plastic and Reconstructive Surgery (2017) 39:41 DOI 10.1186/s40902-017-0139-8 Maxillofacial Plastic and Reconstructive Surgery RESEARCH Open Access Analysis of the outcome of
Advances in radiotherapy for esophageal cancer
 Review Article Page 1 of 10 Advances in radiotherapy for esophageal cancer Wei Deng 1, Steven H. Lin 2 1 Department of Radiation Oncology, National Cancer Center/Cancer Hospital, Chinese Academy of Medical
Review Article Page 1 of 10 Advances in radiotherapy for esophageal cancer Wei Deng 1, Steven H. Lin 2 1 Department of Radiation Oncology, National Cancer Center/Cancer Hospital, Chinese Academy of Medical
